Friday, January 26, 2018
Printer Friendly Version in PDF Format (10 PDF pages)
CLINICAL SUBCOMMITTE UPDATE
Shari Ling, MD
2017 Measures Under Consideration (MUC) List
- In December CMS released the annual MUC list
- MUC17-258 seeks to measure resident satisfaction with nursing home care
- Collecting this information is important to understand preferences, help people choose a facility, and assist facilities in improving quality of care
- The measure calculates the percentage of residents discharged in a six-month time period from a SNF within 100 days of admission who are satisfied
- The measure is based on the CoreQ: Short Stay Discharge questionnaire that utilizes four items: 1. In recommending this facility to your friends and family, how would you rate it overall? (Poor, Average, Good, Very Good, or Excellent) 2. Overall, how would you rate the staff? 3. How would you rate the care you receive? 4. How would you rate how well your discharge needs were met?
(Strategy 2.D)
Information at: https://www.cms.gov/Medicare/Quality-Initiatives-Patient-Assessment-Instruments/QualityMeasures/Pre-Rule-Making.html
Integrated Care Resource Center
- In December CMS's Medicare-Medicaid Coordination Office (MMCO) sponsored a Webinar on Interdisciplinary Care Teams for Older Adults, the fifth session of a five-part series from the "2017 Geriatric-Competent Care Webinar Series"
- The session covered the Role of an Interdisciplinary Care Team, Strategies for Implementing Care Teams , Successful Clinical Care, and Interdisciplinary Care Team Perspective of a Care-Recipient
- MMCO also has three new resource guides intended to support providers and health plans serving older adults with dementia and their caregivers
- These two resource guides, one created for caregivers and the other for healthcare professionals, include training and toolkits, fact sheets, publications, and information resources from various organizations and health plans, and are aimed at dementia care
(Strategy 2.D)
Information at: https://www.resourcesforintegratedcare.com/GeriatricCompetentCare/2017_GCC_Webinar_Series/ICT and https://resourcesforintegratedcare.com/GeriatricCompetentCare/2017_GCC_Resource_Guides/Dementia
Medicare Advantage Value-Based Insurance Design (VBID) Model for 2019
- In November CMS announced several updates to the Medicare (VBID) Model for 2019 that encourage customized benefit designs and flexibilities
- VBID can address the specific health needs of certain beneficiaries including people with dementia under Medicare Advantage to allow additional plan variety and options, reduced cost sharing for customized benefits, and different cost-sharing
- Beginning in 2019 VBID will expand to an additional 15 new states for a total of 25 states, allow Chronic Condition Special Needs Plans to participate, and allow participants to propose their own systems or methods for identifying eligible enrollees
- Applications from Medicare Advantage Organizations are due today (1/26)
(Strategy 2.E)
Information at: https://innovation.cms.gov/initiatives/VBID/
Comprehensive Primary Care Plus (CPC+)
- Five-year model and two rounds of participants, launched in January 2018
- Two tracks with incremental payment options and care delivery expectations
- 18 regions
- 2,989 primary care practices and over 13,000 practitioners supporting over 1.8 million Medicare beneficiaries
- 62 payer partners, including 8 State Medicaid Agencies
- National + regional learning communities
(Strategy 2.E)
Information at: https://innovation.cms.gov/initiatives/comprehensive-primary-care-plus
 |
| Track 1 | Track 2 | |
|---|---|---|
| Care Management Fee | $15 average | $28 average; including$100 to support patients with complex needs
|
| Performance Based Incentive Payment | $2.50 opportunity | $4.00 opportunity |
| FFS Payment Redesign | N/A (Medicare FFS only) | Hybrid payment: upfront Comprehensive Primary Care Payments + reduced FFS |
| *all payments in per beneficiary per month (PBPM) terms | ||
Community-Based Care Transitions (CCTP) Model Final Report
- In November CMS posted the CCTP model report
- CCTP was authorized to operate for five years to test improving care transitions from the hospital to other settings and reducing readmissions for high-risk Medicare beneficiaries (including some people with dementia), and ended in January 2017
- The final evaluation report found that CCTP did not have hospital-wide impacts on readmissions or expenditures for all FFS beneficiaries at partner hospitals, and that receiving CCTP services was associated with lower readmissions and expenditures for beneficiaries served
- The report's conclusion suggests that future models must recognize the importance of understanding the population that is at risk for readmission within the community to identify how to best address their needs, and that multiple strategies are warranted
(Strategy 2.F)
Information at: https://downloads.cms.gov/files/cmmi/cctp-final-eval-rpt.pdf
Chronic Care Management (CCM) Service Update
- In 2015, CMS introduced a CCM service to improve the benefit primary care for Medicare beneficiaries and enhance continuity of care, coordination, and care planning
- 665,000 beneficiaries received CCM services in the first 2 years; most lived in the South and had poor health status and received CCM services as needed, not monthly
- The co-pay is 20%, so about 8 dollars are the beneficiary's responsibility, but most either have MediGap or Medicaid to cover the co-pay
- 16,238 providers billed for a total of $101.4 million in CCM fees, most were primary care physicians
- Both beneficiaries and providers indicated generation satisfaction with the CCM service
Coverage to Care Roadmap to Behavioral Health
- This fall CMS's Office of Minority Health, working with the Substance Abuse and Mental Health Services Administration, issued the Roadmap as a companion guide to the Coverage to Care Roadmap to Better Care and a Healthier You
- This consumer-facing resource offers important information to help people connect to mental health services, walking through 8 Steps to offer information specific to topics like finding a behavioral health provider, defining behavioral health terms, receiving services, and following up on care, and it also links to other HHS resources.
- Many people with dementia also have depression
(Strategy 3.D)
Information at: https://www.cms.gov/About-CMS/Agency-Information/OMH/equity-initiatives/from-coverage-to-care.html
National Partnership to Improve Dementia Care in Nursing Homes Update 2017, Quarter 2
Decrease of 35 % to a national prevalence of 15.5 %
 |
(Strategy 3.D)
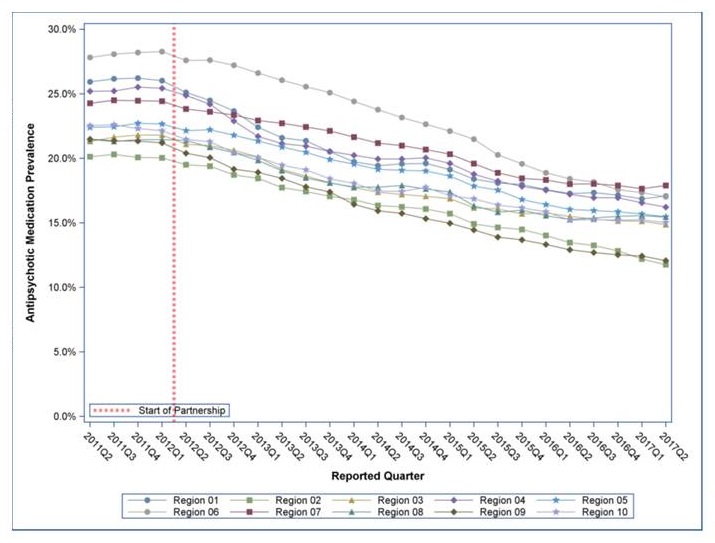
National Partnership to Improve Dementia Care in Nursing Homes Regional Data 2017 Q2
Two regions and several states had increases; CMS is exploring why including examining nursing homes with high rates
 |
National Partnership to Improve Dementia Care in Nursing Homes - 2018
- Nursing homes with low rates of antipsychotic medication use are encouraged to continue their efforts and maintain their success
- Nursing homes with high rates are to work to decrease antipsychotic medication use by 15 percent for long-stay residents by the end of 2019
- These are nursing homes that remain above the national average and have had little change in their antipsychotic medication utilization rates
Focused Dementia Care Survey Updates
- In November 2015, CMS released Survey & Certification Memo 16-06 (SC Letter 16-04), that included tools that were utilized for the Focused Dementia Care Survey process to help nursing homes assess their unique practices in providing resident care
- The tools have been updated and current versions have been added to the National Partnership website
- The Focused Dementia Care Survey process is separate from the standard survey process, as are the revised tools
- The new Dementia Care Critical Element Pathway (Form CMS-20133) was developed using principles from the Focused Dementia Care Survey process
(Strategy 2.D)
Information at: https://www.cms.gov/Medicare/Provider-Enrollment-and-Certification/SurveyCertificationGenInfo/National-Partnership-to-Improve-Dementia-Care-in-Nursing-Homes.html
More Partnership Activities for 2018
- Collaboration with State Dementia Care Coalitions, CMS Regional Offices, and State Survey Agencies
- Comprehensive focus on poor performing nursing homes
- Revision of "Hand in Hand" training series
- Data tracking and distribution
- Federal Civil Monetary Payment fund initiative
- Medicare Learning Network national provider calls
- The Focused Dementia Care Surveys continue and CMS is doing more Schizophrenia Surveys to monitor the increase in Schizophrenia diagnoses in nursing home residents; CMS also held an MLN call on appropriate diagnosis of Schizophrenia in June, 2017
(Strategy 3.D)
Information at: https://www.cms.gov/Medicare/Provider-Enrollment-and-Certification/SurveyCertificationGenInfo/National-Partnership-to-Improve-Dementia-Care-in-Nursing-Homes.html
Health Resources Services Administration Accomplishments
- Caregiving curriculum
- With federal partners and public stakeholders, HRSA created the Alzheimer's Disease and Related Dementias Caregiving Training Curriculum to provide training for the primary care workforce and caregivers about dementia care.
- The curriculum consists of 11 modules (4 modules to assist providers in understanding and addressing caregiver needs and 7 modules to help family and other caregivers of persons living with dementia take care of their own health and understand and cope with the challenges of caregiving.
- Each of the modules that constitute the curriculum can be accessed at
Psychotropic Drug Safety Initiative (PDSI)
- U.S. Dept. Veterans Affairs (VA) system-wide psychopharmacology quality improvement (QI) program that improves medication prescribing practices based on evidence & clinical practice standards
- Collaboration across multiple Veterans Health Administration (VHA) program offices and initiatives
- PDSI supports facility-level QI through quarterly quality metrics, clinical decision support tools, QI technical assistance, and a virtual learning collaborative with educational resources
- Phase 2 (October 2015 - June 2017): Focus was to improve psychopharmacologic prescribing practices for older Veterans (age 75+) in both the outpatient and VHA Community Living Center care settings (VHA nursing homes)
- Each facility prioritized at least one of 14 metrics representing indicators of quality prescribing identified as national priorities, including metrics addressing psychopharmacologic prescribing for Veterans with dementia
Positive Impact on Veterans With dementia
- By the end of PDSI Phase 2
- Over 5,700 fewer Veterans with dementia received a prescription for benzodiazepines
- 29% reduction in outpatient settings
- 25% reduction in VHA CLC settings
- Over 1,400 fewer Veterans with dementia received a prescription for antipsychotics
- 8% reduction in outpatient settings
- 11.5% reduction in VHA CLC settings
- Over 5,700 fewer Veterans with dementia received a prescription for benzodiazepines
For more information on PDSI, please contact Ilse.Wiechers@va.gov
VA GERIATRIC SCHOLARS PROGRAM
- A workforce development program to integrate geriatrics into primary care practices
- Longitudinal, multi-modal continuing education program for healthcare professions:
- Intensive education, clinical practicum experiences, self-paced learning through webinars and on-line learning communities, demonstration of knowledge through quality improvement projects
- Focus on rural VA clinics; outreach to rural Indian Health Service clinics
- Funded by VA Offices of Rural Health and Geriatrics/Extended Care
- Collaboration of 12 Geriatric Research, Education and Clinical Centers (GRECC), in partnership with VA Employee Education System (EES), academic affiliates and HRSA-funded Geriatric Workforce Education Programs (GWEP)
2018 quarter 1 VA Geriatric Scholars Dementia Education and Resources
- Rural Interdisciplinary Team Training for Tohono O'Odham Nation 11/29/2017
- On-site training for all clinic staff on teamwork in care of older adults; recognition of geriatric syndromes and "red flags," including dementia.. Staff from VA Office of Tribal Government Affairs identified opportunities to coordinate care between VA and IHS for Veterans who are eligible for both healthcare organizations. The program was also conducted in partnership with the UCLA and Arizona GWEPs.
- Webinars for VA Staff:
- Gaps in Primary Care for Dementia: Lessons Learned and Filling Gaps 11/9/2017
- Intimacy and Dementia Symposium 10/27/2017
- Behavioral Approaches to Managing Challenging Situations in Patients with Dementia 10/4/2017
- Geriatric Scholars Toolkits:
- Dementia http://www.gerischolars.org/course/view.php?id=29
- Cognitive Impairment, Memory Loss and Dementia http://www.gerischolars.org/course/view.php?id=2
QUESTIONS-DISCUSSION
Contact: Shari Ling - shari.ling@cms.gov
January 26, 2018 -- Advisory Council Meeting #27
The meeting was held on Friday, January 26, 2018, in Washington, DC. The Research Subcommittee took charge of this meeting's theme, focusing on the process from targets to treatments. The Council heard speakers on the preclinical pipeline, the clinical trial pipeline, and the industry perspective. The meeting also included discussion of a driver diagram to guide the Council's future work, updates and a report from the October Care Summit, and federal workgroup updates. Material available from this meeting is listed below and at https://aspe.hhs.gov/advisory-council-alzheimers-research-care-and-services-meetings#Jan2018.
Comments and questions, or alerts to broken links, should be sent to napa@hhs.gov.
General Information
-
Agenda -- [HTML Version] [PDF Version]
-
Meeting Announcement -- [HTML Version] [PDF Version]
-
Meeting Summary -- [HTML Version] [PDF Version]
-
Public Comments -- [HTML Version]
Handouts
-
Care Summit Report Themes -- [PDF Version]
-
NAPA Driver Diagram Draft Examples -- [PDF Version]
-
Outline for Care Summit Final Report -- [PDF Version]
Presentation Slides
-
AbbVie's R&D Vision for Alzheimer's Disease -- [HTML Version] [PDF Version]
-
Care Summit Report -- [HTML Version] [PDF Version]
-
Clinical Subcommittee Update -- [HTML Version] [PDF Version]
-
Initiatives, Partnerships and Collaboration to Help Patients with the Highest Unmet Need: Dominantly Inherited Alzheimer's Disease Trials Unit (DIAN-TU) as a Case Example -- [HTML Version] [PDF Version]
-
Long-Term Services and Supports Committee Update -- [HTML Version] [PDF Version]
-
NAPA Driver Diagram -- [HTML Version] [PDF Version]
-
Overview of the Clinical Trial Pipeline for AD -- [HTML Version] [PDF Version]
-
Overview on NIA Preclinical Pipeline -- [HTML Version] [PDF Version]
-
Participating in an Alzheimer's Clinical Study: Perspectives on Involvement of a Person Living with Dementia and Her Study Partner -- [HTML Version] [PDF Version]
-
Progress Since October -- [HTML Version] [PDF Version]
-
Research Progress on Alzheimer's Disease and Related Dementias -- [HTML Version] [PDF Version]
-
Research Subcommittee Agenda: The Journey from Targets to Treatments -- [HTML Version] [PDF Version]
