|
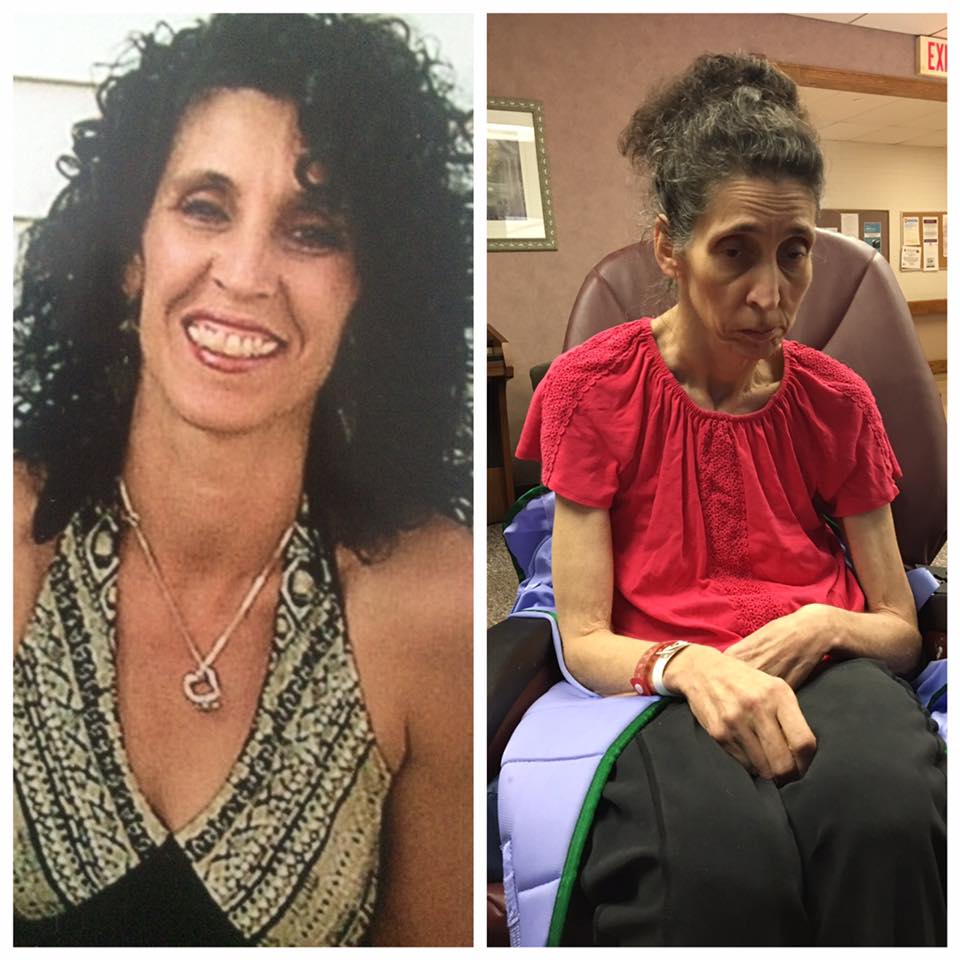
My husband, Jack and I met and fell in love in 1987. He had served in the Marines and worked construction before we met but spent most of his life working in the field of caregiving. The final years he was able to work he was a CNA and activities assistant at a care facility and took wonderful care of elderly and dementia patients.
Jack was a loving, funny and kind man but eventually excessive drinking made him very depressed. He went to alcohol rehab three times in his late 40's and in 2009, the year he turned 50, a counselor convinced us to live a part until he fully recovered. He lived in a clean and sober house and went back to college earning straight A's and an AAS degree. He set up a routine including going to an early meeting, walking for miles each day and calling me each morning and evening.
When he moved back home, he was different but I assumed it was because he was sober and we'd been living apart. I decided to just be happy he was sober, content and healthy. I now see the beginnings of bvFTD in his behaviors and changes, even many years earlier.
January of 2015, at 56, he wasn't working, had quit going to school and was watching TV and sleeping a lot. Some of his behaviors reminded me of when he was drinking but I was sure he wasn't. One day he bought $500 of frozen meat from a door-to-door salesman (which now I know is common behavior for someone bvFTD but at the time I was mad and so confused). By summer I told him he had to get a job or move out. He got a job but was let go after first day. That weekend I drove him 200 miles to stay with friends until he could get his life back on track.
The next three weeks it became clear to his good friends there was something very wrong. He wasn't his old friendly, funny self. The final straw was his car being towed because he ran out of gas and walked away leaving it in the middle of a busy road. I asked his friend to get him on a shuttle to come home.
I insisted on going with him to see his doctor. Jack had been going to the same GP for 12 years but hadn't been in a few years. Jack said he was fine but I told his doctor some of what was going on including the car being towed. He ordered blood tests and CT scan. When we walked out his doctor called me back to say this isn't him, I don't know what's wrong but I'm going to find out, hang in there with him. Then said he was afraid it was a tumor on his frontal lobe.
A week after the CT was an MRI. His doctor pulled up the results as we sat there and said this isn't good. That's when we first heard of FTD. He printed out pages explaining it and after Jack walked out said he'd call me over the weekend. He later said the loss on MRI was striking. On the way home my husband said, that's rather disturbing what he said about my frontal lobe disappearing but I don't have dementia, my memory is really good. I agreed.
That night after Jack went to bed at his new normal time of 7pm, I stayed up late reading online about FTD. I was scared by what I read and also relieved in a way to find an explanation for the odd behaviors and frustrating personality changes. From that day forward the anger and frustration I'd felt towards him in the past year disappeared. The next day he started taking low dose of Paxil and we had the nicest day in a long time. I think in a way he was also relieved to have an idea why things were getting difficult for him. I'm thankful he had no interest in reading about the illness.
Jack's GP said he'd only seen FTD once before in his 20 some years of being a doctor. He explained it would need to be confirmed through a neuropsych eval and a neurologist exam. He also gave me great advice like that I should let his family know right away, see an elder care attorney and apply for SSDI. He said some people with FTD get angry and agitated but Jack might just stay easy going, he was living in the moment. He also told me that he may only have two years to live and suggested trying to show him the best time possible and live life to fullest possible.
I'm not sure the neurologist we saw had met anyone with FTD before. The first 15 minutes of the first visit he seemed like he didn't really see anything wrong with my husband. Then my husband went to the bathroom so I was able to tell him some of the most concerning behaviors. When Jack returned he paced the little room and answered a few more questions with answers that didn't make as much sense. I think the neurologist started seeing behavior I had been seeing. Later we changed to a neurologist at Virginia Mason who specializes in FTD.
We managed to get in for a neuropsych eval within a month due to a cancelation. My husband only lasted one of the two hours before telling him he was done. The neuropsychologist told me afterwards that in a short, casual conversation with Jack he wouldn't have guessed many issues but the test confirmed the major deficiencies and FTD.
I took his doctor's advice to live life to the fullest. Soon after diagnosis we made a trip to the coast and a couple months later flew across country to see his family. We also went to concerts and festivals in the spring and summer. I had worry and stress during trips and outings with my husband but I'm thankful we did those things while we could and it was worth it for the good moments. I know how fortunate I am that my husband stayed sweet and easy going, that we had an excellent doctor and supportive family and friends.
Thankfully in addition to helpful information on the AFTD website I also found the FTD spouse facebook group. There I learned how to deal with the new normal of my husband not wanting to brush his teeth, shave, shower, change clothes, the heartbreak when it was time for depends and the other sad stages that followed. It was from the amazing people in that group I learned his muscle twitches sounded like beginning signs of ALS so we went back to Virginia Mason for testing. In September 2016, my husband was diagnosed with ALS. I believe both illnesses were caused by his time in the Marines stationed at Camp Lejeune when the water was toxic. I also know Jack was so proud of his service and didn't regret the time he spent in the USMC.
On the evening of December 29, 2016, fifteen months after bvFTD diagnosis, I called 911 because he was having trouble breathing. I gave the EMTs his advance directive paperwork but asked that they take him to the hospital. When I arrived at ER I asked them to remove the intubation. I was able to lay down next to him and he slept peacefully for a couple hours. He even woke one last time and pulled me in for a kiss. He passed away about 15 minutes later. I always used to think ALS was the worst disease but now I agree with others who have said ALS actually saved their loved one from the devastating and heartbreaking end stages of FTD. I miss him so much. I'm forever grateful for all the years we had including the last 15 months after diagnosis.
|