Potential Impacts of Minimum Wage Increases on Nursing Homes: Issue Brief
Michael Lepore, PhD; Ian Livingstone, PhD; David Naden, MA; and Zhanlian Feng, Ph.D.
RTI International
June 2020
Printer Friendly Version in PDF Format (5 PDF pages)
ABSTRACT
Nursing homes employ large proportions of their workforce at the minimum wage. This project sought to understand the potential impacts of federal minimum wage increases on nursing staff hours and labor costs of nursing homes. We found that an increase of the federal minimum wage would result in large proportions of nursing assistants gaining a wage increase, thereby increasing direct labor costs to nursing homes. These results are based on national estimates.
This brief was prepared under contract #HHSP233201600021I between HHS's ASPE/DALTCP and RTI International. For additional information about this subject, you can visit the DALTCP home page at https://aspe.hhs.gov/office-disability-aging-and-long-term-care-policy-daltcp or contact the ASPE Project Officers at HHS/ASPE/DALTCP, Room 424E, H.H. Humphrey Building, 200 Independence Avenue, S.W., Washington, D.C. 20201; Iara.Oliveira@hhs.gov, Marie.Squillace@hhs.gov.
DISCLAIMER: The opinions and views expressed in this brief are those of the authors. They do not reflect the views of the Department of Health and Human Services, the contractor or any other funding organization. This brief was completed and submitted in December 2019.
Summary
Nursing homes employ large proportions of their workforce at the minimum wage. This project sought to understand the potential impacts of federal minimum wage increases on nursing staff hours and labor costs of nursing homes. We found that an increase of the federal minimum wage would result in large proportions of nursing assistants (NAs) gaining a wage increase, thereby increasing direct labor costs to nursing homes. These results are based on national estimates.
Background
The need for long-term care (LTC) services to help individuals perform routine activities of daily living has increased substantially at the national level.[1] One of the challenges for meeting the growing LTC need is maintaining a sufficient workforce as providers in the LTC industry, including nursing homes, employ large proportions of their workforce at the minimum wage.
On January 16, 2019, the U.S. Congress introduced H.R.582, the Raise the Wage Act--a bill to increase the federal minimum wage to $15 per hour. We are unaware of any recent research assessing how increases to the federal minimum wage may impact nursing home providers. This project sought to understand the impacts of potential federal minimum wage increases on nurse staffing and labor costs in nursing homes.
Study Methods
The study used publicly available data from the Bureau of Labor Statistics (BLS), U.S. Department of Labor (DOL), and the Centers for Medicare & Medicaid Services (CMS), January 1, 2017-December 31, 2017. The BLS data include information about staff pay in nursing homes, DOL data include state minimum wage levels, and the CMS Payroll-Based Journal system provides data on hours worked by nursing home employees. The study population included 15,330 Medicare and/or Medicaid-participating nursing homes from every state and the District of Columbia.
Two nurse staffing pattern variables were used: the average number of facility hours worked and hours per resident day (HPRD) among registered nurse (RN), licensed practical nurse (LPN), and NA occupations. Two wage variables were also used: state average wage levels for each nursing occupation (RN, LPN, and NA) and state minimum wage levels. State average wage levels and average number of facility hours worked were used to explore the relationship between wages and staffing patterns at the state level and state minimum wage levels and HPRD were used to explore the relationship at the nursing home level.
Additionally, we estimated the impacts of potential minimum wage increases to $10, $12, and $15 per hour, including the proportion of nursing occupation workers who would be affected, the average increase in wages and direct labor costs per nursing occupation, and the costs of the increases as a proportion of total direct labor costs were estimated, separately, for RNs, LPNs, and NAs, nationally and across select states whose minimum wage levels differ: California ($10.00), New York ($9.70), Florida ($8.10), Texas ($7.25), Arizona ($10.00), and Arkansas ($8.50).
Limitations
This study was limited to state-level minimum and average wage data, and did not account for any state-level factors, such as state policies, regulations, or market dynamics that might impact nursing home wages or hours. Our analyses also assumed full-time employment, and thus may overestimate the financial impact of minimum wage increases.
Findings
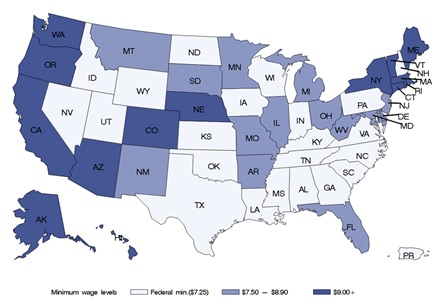
Approximately 44% of nursing homes are in states that use the federal minimum hourly wage level of $7.25, 28% are in states with a minimum hourly wage between $7.50 and $8.90, and 28% are in states with a minimum hourly wage of $9.00 or more (Figure 1).
Nursing Home Staffing
We found positive relationships between wages and staffing levels for RNs and NAs in nursing homes. On average, RNs and NAs in states with higher minimum wage levels worked more HPRD than RNs and NAs in states that use the federal minimum wage level of $7.25. For LPNs, we found a negative association, showing fewer HPRD in states with a higher minimum wage.
| Compared with RNs in states with the $7.25 federal minimum wage, RNs in states with higher minimum wage levels at $7.50 to $8.90 and $9.00+ averaged 5 and 8 minutes more of work per resident day, respectively. Nursing assistants had similar patterns as RNs, with 5-9 minutes more of work per resident day in states with higher wage levels. LPNs worked an average of 5 minutes per resident day fewer in states with higher wage levels. |
Nursing Home Labor Costs
Overall, the impacts on nursing homes of raising the federal minimum wage would be almost completely restricted to increases in wages among NAs, since most of this workforce earn at or close to the federal minimum wage. The effect on the LPN workforce was negligible.
| Increasing the federal minimum wage would increase total direct labor costs (wages and payroll taxes) in nursing homes by about $72.6 million if set to $10, approximately $600 million if set to $12, and more than $2.5 billion if set to $15. |
We found that increasing the minimum wage to $10 would require average hourly wage increases of about $0.55 for 12% of NAs; increasing it to $12 would require an hourly wage increases of $1.44 for 38% of NAs; and increasing it to $15 would require an hourly wage increases of $3.03 for 76% of NAs. LPNs would only be affected if hourly wage increased to $15, requiring very small hourly wage increases of $0.04 for 1% of LPNs.
| FIGURE 1. States by Minimum Wage Categories, 2017 |
|---|
 |
Conclusion
This study provides foundational insights into potential impacts of federal minimum wage increases on nursing home staffing and labor costs across states and by nursing occupation. Select state findings are also reported, highlighting substantial cross-state differences.
To better understand the relationships between wages and hours in nursing homes, additional research that takes into account key state-level policy and market factors is needed.
Endnotes
-
Favreault, M., Dey, J. (2015). Long-Term Services and Supports for Older Americans: Risks and Financing. Research Brief for the Office of the Assistant Secretary for Planning and Evaluation. Retrieved from https://aspe.hhs.gov/basic-report/long-term-services-and-supports-older-americans-risks-and-financing-research-brief.
ANALYSES OF DISABILITY, AGING AND LONG-TERM CARE POLICY AND DATA: MINIMUM WAGE
This brief was prepared under contract #HHSP233201600021I between HHS's ASPE/DALTCP and RTI International. For additional information about this subject, you can visit the DALTCP home page at https://aspe.hhs.gov/office-disability-aging-and-long-term-care-policy-daltcp or contact the ASPE Project Officers at HHS/ASPE/DALTCP, Room 424E, H.H. Humphrey Building, 200 Independence Avenue, S.W., Washington, D.C. 20201; Iara.Oliveira@hhs.gov, Marie.Squillace@hhs.gov.
Reports Available
Impacts of Minimum Wage Increases on Nursing Homes: Final Report
- HTML version: https://aspe.hhs.gov/basic-report/impacts-minimum-wage-increases-nursing-homes-final-report
- PDF version: https://aspe.hhs.gov/pdf-report/impacts-minimum-wage-increases-nursing-homes-final-report
Potential Impacts of Minimum Wage Increases on Nursing Homes: Issue Brief
- HTML version: https://aspe.hhs.gov/basic-report/potential-impacts-minimum-wage-increases-nursing-homes-issue-brief
- PDF version: https://aspe.hhs.gov/pdf-report/potential-impacts-minimum-wage-increases-nursing-homes-issue-brief
