Monday, April 17, 2017
Printer Friendly Version in PDF Format (12 PDF pages)
National Research Summit on Care, Services and Supports for Persons with Dementia and their Caregivers
Progress to Date
Laura N. Gitlin and Katie Maslow
- SAVE THE DATE -
October 16-17, 2017
Natcher Building, NIH Campus
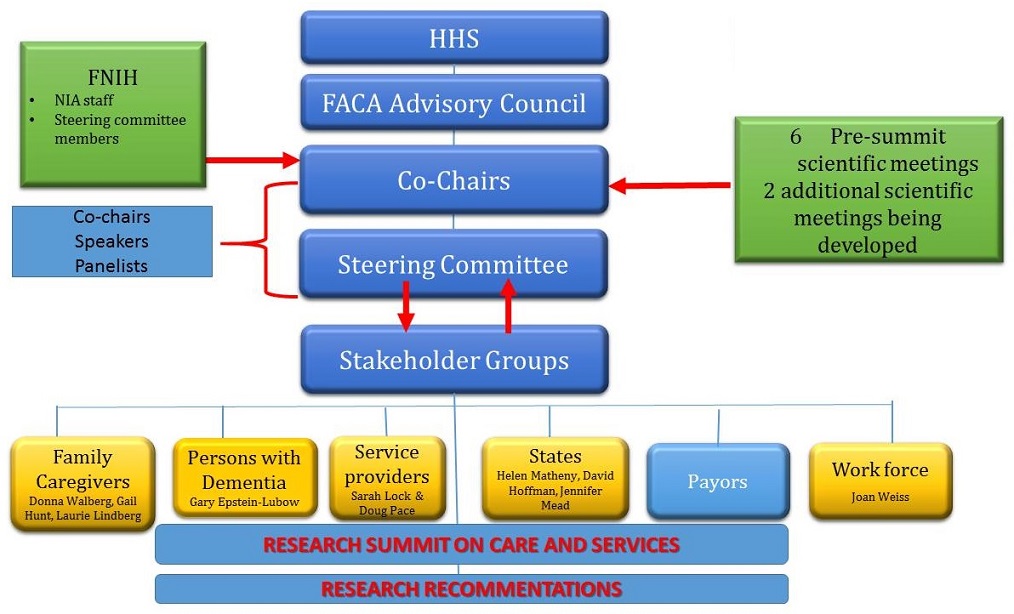 |
Steering Committee Members
- Two New Members who are persons with dementia and Co-Chairs of the Summit Persons with Dementia Stakeholder Group
- Lonni Schicker, EdD, MHSA, RN, retired nurse, associate professor, managed care professional, current member of the Alzheimer's Association 2016 National Early-Stage Advisory Group
- Teresa Webb, RN, former nurse, current Advisor, Association of Frontotemporal Degeneration, and founder, Frontotemporal Dementia Advocacy Resource Network
- Gary Epstein-Lubow, MD (Brown Univ.)
- Lori Frank, PhD (PCORI)
- Richard Hodes MD (NIA)
- Ian Kremer JD (LEAD)
- Shari Ling, MD (CMS)
- Sarah Lenz Lock JD (AARP)
- Helen Matheny, MS (West Virginia University)
- Lisa McGuire, PhD (CDC)
- Jennifer Mead, MPH (Oregon Dept. of HS)
- Linda Nichols, PhD. (VA Medical Center)
- Douglas Pace, NHA (Alzheimer's Association)
- Jane Tilly, DrPH (ACL)
- Lois A. Tully, PhD (NINR)
- Joan Weiss, PhD, RN (HRSA)
Co-chairs
- Laura N. Gitlin, PhD
- Katie Maslow, MSW
Executive Committee
- Ron Petersen MD, PhD. , (Mayo Clinic)
- Rohini Khillan, MPH (ASPE)
Summit Sessions and Co-chairs
2 days, 8 am to 4 pm, 6 main sessions
- Opening Plenary Sessions--setting the stage
- Ron Peterson, MD, Ph.D
- Maria Carrillo, Ph.D.
- Ken Langa, MD, Ph.D.
- Jennifer Manly, Ph.D.
- Maria Aranda, Ph.D.
- Session I: Research on Care Needs and Supportive Approaches for Persons with Dementia (Co-chairs: Richard Fortinsky, Ph.D., Ann Kolanowski, Ph.D.)
- Session II: Research on Supportive Approaches for Family and Other Caregivers (Co-chairs: Linda Teri, Ph.D, Lisa Fredman, Ph.D.)
- Session III: Involving Persons with Dementia and Family and Other Caregivers as Active Members of the Research Team to Identify Research Topics and Meaningful Outcomes (Co-Chairs: Mark Snowden, MD, M.P.H, Lee Jennings, MD, M.S.H.S.)
- Session IV: Research on Care Coordination and Care Management for Persons with Dementia and Family Caregivers (Co-chairs: David Reuben, MD., Vincent Mor, Ph.D.)
- Session V: Challenges in Involving Persons with Dementia as Study Participants in Research on Care and Services (Co-chairs: Darby Morhardt, Ph.D., David Bass, Ph.D.)
- Session VI: Research on Translation, Dissemination, Implementation, and Scaling Up of Effective Care, Services, and Supportive Approaches for Persons with Dementia and Family and Other Caregivers (Co-chairs: Chris Callahan, MD., Alan Stevens, Ph.D.)
- Cross-cutting chairs: Technology -- Dr. Czaja; Race/ethnicity/culture -- Dr. Hinton; Etiologies/disease stage -- Angela Taylor; Pending -- Women/gender
Stakeholder Group Activities
Stakeholder groups are charged with identifying problems, ideas, issues, and recommendations for the summit
- Persons with Dementia Stakeholder Group: 12 members, 2 meetings so far, meeting monthly by Zoom, facilitated by Alzheimer's Association Early- Stage Staff
- Family Caregiver Stakeholder Group: 12 members, may add a few, 1 meeting by phone so far
- Service Provider Stakeholder Group: 25 members, 2 meetings by phone so far, meeting monthly by phone; have a group listserve
- State Government Stakeholder Group, 2 calls by phone so far: one with State Dementia (ADSSP) Grantees with 9 states represented, and one with State Chronic Disease Directors in the Alzheimer's Interest Group with 9 states represented
- Payors Stakeholder Group: TBA
- Workforce Development Stakeholder Group: 10 members, 1 meeting by phone so far
Pre-Summit Activities
- Evidence for home-based dementia care -- systematic literature review and think tank (funded by BrightFocus Foundation, Drs. Lyketsos, Samus & team, Johns Hopkins University)
- Determinants of behavioral symptoms -- systematic literature review (Dr. Kolanowski and team, Penn State University)
- Diversity and Alzheimer's Disease Caregiving Conference, Race/ethnicity and caregiving (Dr. Meyer, University of California, Davis) May 2-3, 2017
- Caregiving and program research on caregiving of persons with intellectual disability and dementia practices (Dr. Tamar Heller, UIC, Working Group Chair) Meeting at Alzheimer's Association, Chicago, March 22, 2017
- 2015 Survey data on Family Caregivers of Persons with Dementia (National Alliance on Caregiving and Alzheimer's Association)
- Methodological considerations in research on dementia care and services (Dr. Frank, PCORI) June 7-8, 2017
- Two additional Pre-summits being organized:
- NIA -- Caregiver intervention workshop
- Alzheimer's Association -- Outcome measures
Sources of Research Recommendations
- Plenary Summit speakers
- Summit Session co-chairs, speakers, and panelists
- Summit Cross-cutting chairs
- Summit audience members
- Stakeholder groups
- Pre-Summit Activities
- Public listening sessions
- RTI background papers and issue briefs
Accelerating development, testing, and dissemination of Home-based Dementia Care
BrightFocus™ Foundation
Johns Hopkins Medicine
Members of the Consensus Panel
- Constantine G. Lyketsos, MD, MHS Johns Hopkins School of Medicine
- Quincy M Samus, PhD, MS Johns Hopkins School of Medicine
- Laura N. Gitlin, PhD Johns Hopkins School of Nursing
- Betty Smith Black, PhD EdS Johns Hopkins School of Medicine
- Christopher Callahan, M.D. Indiana University Center for Aging Research
- Deirdre Johnston, M.B.B.Ch., M.D. Johns Hopkins School of Medicine
- Michael Buckley BrightFocus Foundation
- Diane Bovenkamp, PhD BrightFocus Foundation
- Helen Kales, M.D. University of Michigan
- Nancy Hodgson, PhD, RN, FAAN Johns Hopkins School of Nursing
- Michele Karel, PhD, ABPP Veterans Administration Central Office
- Karen Davis, PhD Johns Hopkins Bloomberg School of Public Health
- Helen Kales, M.D. University of Michigan
- Michele Karel, PhD, ABPP Veterans Administration Central Office
- Shari M. Ling, M.D. Centers for Medicare and Medicaid Services
- John Jay Kenney, PhD. MD Department of Health & Human Services
- Maï Panchal, PhD. LECMA, AFi, and iSAO (France)
- Amber Willink, PhD Johns Hopkins Bloomberg School of Public Health
Core Recommendations
Need for development, evaluation and dissemination of:
- New models of long term care and support that centers around the home as the nexus of care from diagnosis to end of life, integrating medical, social, emotional, environmental and supportive care must be prioritized for ADRD into the future
- New payment models to support effective evidence-based home care practices and that stimulate and reward integration of care across acute and long-term care services needs further development and testing and policy reform.
- Preparation of a dementia competent workforce to offer a range of home-based care services is critically needed and could be supported by addressing key issues related to employee retention including increasing salaries, better supervision, more flexible, continuous and engaging training, creation of "credentialing" for skilled workers along with pathways for promotion, and rewarding high quality care.
- New and existing technologies to link families to care providers and share information more efficiently, monitor and promote home safety, monitor health and symptoms status, and deliver care strategies, care management, and treatments must be fully utilized, deployed, and tested.
- A national plan to address barriers to home-based dementia care including addressing the absence of a coherent national approach to payment for home based care, cultural factors, and lack of understanding of the long term value of home based dementia care,
- A major priority of the field should be effectively educating consumers and payers about the need and benefits of home based dementia care.
Personal, Interpersonal And Environmental Determinants Of Behavioral And Psychological Symptoms of Dementia
Council For The Advancement Of Nursing Science
September 15, 2016
The Team
- Ann Kolanowski PhD, RN, FAAN
- Marie Boltz PhD, RN, FAAN
- Beth Galik PhD, RN, FAAN
- Laura Gitlin PhD
- Helen Kales MD
- Barbara Resnick PhD, CRNP, FAAN
- Kimberly Van Haitsma PhD
- Amy C. Knehans MLIS, AHIP, Librarian
- Jane Sutterlin MEd, Instructional Designer
- Justine Sefcik, MS, RN
- Wen Liu PhD, RN
- Darina Petrosky RN, MN
- Lauren Massimo PhD, RN, CRNP
- Andrea Gilmore-Bykovskyi PhD, RN
- Margaret MacAndrew PhD, RN
- Glenna Brewster RN, PhD, CRNP
- Vycki Nalls GNP-BC CWS ACPHN
- Ying Ling Jao PhD, RN
- Naomi Duffort MSW
- Danny Scerpella BA
STATE OF THE ART REVIEW
DETERMINANTS OF AGITATION
- NEURODEGENERATION ASSOCIATED WITH DEMENTIA
- INCREASED VULNERABILITY TO STRESSORS
- PATIENT FACTORS
- Type of Dementia (2)
- Severity of Cognitive deficits (1)
- APOE (2)-mixed
- Age (2)- mixed
- Gender(2)- mixed
- Discomfort (1)
- Premorbid Personality (1)- SR weak evidence
- CARE GIVER FACTORS
- Communication (1)
- ENVIRONMENTAL FACTORS
- Tailored/Montessori activities (3)
- Acupressure (1)
- Aromatherapy (2)- lack of evidence
- Music (1)
- Therapeutic Touch (1)- lack of evidence
- Arousal Balance (1)
- PATIENT FACTORS
- AGITATION
Research Implications
- Significant methodological flaws in existing research:
- Need for well-characterized samples that meet criteria for dementia
- Need to focus inclusion criteria on those participants who exhibit targeted behavior
- No consensus as to how to define and operationalize BPSD
- Need for greater precision in defining and measuring target symptoms and their determinants.
- Wide variety of methods and measures for all behaviors- problem comparing across studies.
- BPSD cluster and can be "moving targets" over time. Reliance on cross-sectional data limiting
- Need more longitudinal data.
- Determinants of BPSD differ across individual symptoms- not all interventions will be equally effective.
- Interventions will need to be individualized.
- Consider using multiphase optimization strategy (MOST) and other adaptive designs when testing non-pharmacological interventions.
- Incorporating biomarkers and neuroimaging in study designs will help elucidate the mechanisms by which interventions produce their effects.
- Very little high quality research on effects of caregiver and environment on BPSD.
BPSD and National Plan to Address Alzheimer's Disease*
https://aspe.hhs.gov/report/national-plan-address-alzheimers-disease-2016-update
- Goal 1: Prevent and Effectively Treat Alzheimer's Disease and Related Dementia by 2025
- Early detection and treatment of BPSD may help slow disease progression
- Goal 2: Enhance Care Quality and Efficiency
- Detection and assessment with better measurement may improve care quality
- Goal 3: Expand Supports for People with Alzheimer's Disease and Related Dementia Their Families
- Providing caregiver education/support and tailoring to BPSD presentation may improve quality of life
- Goal 4: Enhance Public Awareness and Engagement
- Public education about BPSD may enhance earlier detection and treatment
- Goal 5: Improve Data to Track Progress
- Better identification and tracking of BPSD needed to evaluate disease impacts
- Better identification and tracking of BPSD needed to evaluate disease impacts
Time Line
- April - May: Identification of Speakers and Panelists:
- Co-chairs recommend speakers and panelists
- Katie and Laura review and have follow-up calls with co-chairs for each session to finalize recommended speakers and panelists
- Steering committee reviews recommended speakers and panelists
- Early May -- invitational letters will be sent to the recommended speakers and panelists
- April - NAPA website goes live
- May-June: Save the Date Card distributed
- June-July: Registration open
- April-Oct: Generation of recommendations
NEXT STEPS
- Katie and Laura continue to meet weekly and periodically with ASPE and NIA
- Selection of Summit session speakers and panelists
- Steering committee meets monthly
- Stakeholder groups meeting regularly
- Process for generating final set of research recommendations on day 3 of the Summit currently being developed
- With FNIH:
- Organization of press release and dissemination
- Fundraising
- Working timeline
- Working budget
April 17, 2017 -- Advisory Council Meeting #24
The meeting was held on Monday, April 17, 2017, in Washington, DC. The Advisory Council spent the majority of the April meeting considering recommendations made by each of the three subcommittees for updates to the 2017 National Plan. Afternoon presentations included a presentation on results from a research project on dementia care components, planning progress towards a Care and Services Summit, and federal workgroup updates. Material available from this meeting is listed below and is also available at https://aspe.hhs.gov/advisory-council-alzheimers-research-care-and-services-meetings#Apr2017.
Comments and questions, or alerts to broken links, should be sent to napa@hhs.gov.
General Information
-
Agenda -- [HTML Version] [PDF Version]
-
Meeting Announcement -- [HTML Version] [PDF Version]
-
Meeting Summary -- [HTML Version] [PDF Version]
-
Public Comments -- [HTML Version]
Handouts
-
LTSS Subcommittee 2017 Recommendations -- [HTML Version] [PDF Version]
Presentation Slides
-
2017 Research Subcommittee Recommendations -- [HTML Version] [PDF Version]
-
Alzheimer's and Related Dementias Research -- [HTML Version] [PDF Version]
-
Clinical Care Subcommittee Report -- [HTML Version] [PDF Version]
-
Clinical Services Subcommittee Federal Update -- [HTML Version] [PDF Version]
-
Examining Models of Dementia Care -- [HTML Version] [PDF Version]
-
Long Term Services and Supports Subcommittee Recommendations -- [HTML Version] [PDF Version]
-
Long-Term Services and Supports Committee Update -- [HTML Version] [PDF Version]
-
National Research Summit on Care, Services and Supports for Persons with Dementia and Their Caregivers Progress to Date -- [HTML Version] [PDF Version]
