U.S. Department of Health and Human Services
A Descriptive Analysis of Patterns of Informal and Formal Caregiving among Privately Insured and Non-Privately Insured Disabled Elders Living in the Community
LifePlans, Inc.
April 1999
PDF Version: http://aspe.hhs.gov/daltcp/reports/ifpattrn.pdf (67 PDF pages)
This report was prepared under contract between the U.S. Department of Health and Human Services (HHS), Office of Disability, Aging and Long-Term Care Policy (DALTCP) and LifePlans, Inc. For additional information about this subject, you can visit the DALTCP home page at http://aspe.hhs.gov/_/office_specific/daltcp.cfm or contact the ASPE Project Officer, Pamela Doty, at HHS/ASPE/DALTCP, Room 424E, H.H. Humphrey Building, 200 Independence Avenue, S.W., Washington, D.C. 20201. Her e-mail address is: Pamela.Doty@hhs.gov.
TABLE OF CONTENTS
- I. BACKGROUND
- II. PURPOSE
- III. METHOD
- A. Sample
- B. Data
- C. Response Rates and Ultimate Analytic Samples
- IV. FINDINGS
- A. Profiling Privately Insured Claimants
- B. Examining the Relationship between Claimant Profiles and HIPAA Benefit Eligibility Triggers
- C. Use of Formal and Informal Care Services Among Privately Insured Claimants
- D. Benefits Paid Under Insurance Contracts and Insurance Policy Designs
- E. Claimant Satisfaction with Insurance Policy and Insurance Company
- F. Impact of Private Long Term Care Insurance
- G. Levels of Met and Unmet Need
- H. Comparing Privately Insured and Non-Privately Insured Community-Dwelling Disabled Elders
- APPENDIX 1: QUALITATIVE DESCRIPTION OF FOUR FAMILIES USING THEIR LTC BENEFITS
- LIST OF FIGURES
- FIGURE 1: Self Assessment of Health Status
- FIGURE 2: Functional Status of Claimants: ADL Limitations
- FIGURE 3: Functional Status of Claimants: IADL Limitations
- FIGURE 4: Cognitive Status of Claimants
- FIGURE 5: Proportion of Claimants Meeting HIPAA Disability Triggers at Time of Interview
- FIGURE 6: Availability of Informal Support Among Claimants
- FIGURE 7: Providers of Formal Care
- FIGURE 8: Average Weekly Hours of Informal & Formal Care
- FIGURE 9: Provided ADL and IADL Compared to Available Weekly Hours of Formal Support
- FIGURE 10: Average Monthly Benefit Payments for Claimants and for Beneficiaries of Medicaid Waiver Programs
- FIGURE 11: Amount of Time Claimants Have Been Receiving Benefits
- FIGURE 12: Level of Satisfaction with Long Term Care Insurance Policy
- FIGURE 13: Ease of Filing Benefits
- FIGURE 14: Presence of Disagreements Between Claimants and Insurance Company
- FIGURE 15: Actions Insurer Might Have Taken to Help Claimants
- FIGURE 16: Satisfaction with Amount of Home Care Coverage Chosen at time of Policy Purchase
- FIGURE 17: Claimants' Perceptions about Impact of Not Having LTC Insurance Policy
- FIGURE 18: Informal Caregivers' Perceptions about Impact of Claimants' Policy
- FIGURE 19: How care has changed for those Reporting that they have Changed the Type of Care they Provide
- FIGURE 20: Caregivers Assessment as to whether Presence of Insurance Benefits Has Reduced Stress
- FIGURE 21: Whether in Absence of Policy Institutional Care would be Sought
- FIGURE 22: Which Institutional Alternatives would be Sought in Absence of Policy
- FIGURE 23: Met, Unmet and Undermet ADL and IADL Needs
- FIGURE 24: Relationship Between ADL Loss and Unmet and Undermet ADL Need
- FIGURE 25: Differences in Socio-demographic Characteristics Of Disabled Elders by Insurance Status
- FIGURE 26: Functional Status of Claimants by Insurance Profile
- FIGURE 27: Cognitive Status by Insurance Profile
- FIGURE 28: Aggregate Disability Profile by Insurance Status
- FIGURE 29: Types of Care Received by Insurance Status
- FIGURE 30: Providers of Informal Support by Insurance Status
- FIGURE 31: Providers of Formal Care by Insurance Status
- FIGURE 32: Weekly Hours of Informal & Formal Care by Insurance Status
- FIGURE 33: Payment Source for Home Care Services by Insurance Status
- LIST OF TABLES
- TABLE 1: Sample Size and Response Rates by Company
- TABLE 2: Socio-Demographic Characteristics of Privately Insured Home Care Claimants and all Elders Age 65 and Over
- TABLE 3: Comparison of Individuals Who Did and Did Not Meet HIPAA Benefit Eligibility Requirements at the Time of Interview
- TABLE 4: Policy Design Features for Home Care Coverage
ACKNOWLEDGEMENTS
This research could not have been completed without the assistance and guidance of many individuals both inside and outside of the long-term care insurance industry. We would like to gratefully acknowledge the assistance provided by Robert Glowacki, Carolyn Eickenberg, and Sharon O'Dell from Aegon, Roy Christianson and David Rogers from American Travellers, Ray Nelson and Leslie Peters from Bankers Life & Casualty, Carol McBrayer, Melissa Stinson, Steve French and Richard Garner from CNA Insurance, Dan Nitz from Fortis Long-Term Care, Roger Desjardins, Mary Katz and Armando Leiva from G.E. Capital Assurance, Linda Berg-Maney and Peter Bokjov from John Hancock, and Bonnie Davis and Jim DuEst from Unum. All of these individuals devoted a significant amount of time to assure that the sample of home care claimants was representative, that data from administrative systems was uniform and accurate, and that the fieldwork could be completed successfully. We are grateful for their patience and good cheer during the entire research process.
The project's technical advisory group included Susan Morisato, FSA, Bankers Life & Casualty, Bob Yee, FSA, of G.E. Capital Assurance, Christopher Murtaugh, Ph.D., Center for Home Care Policy and Research, Vicki Freeman, Ph.D., Rand Corporation, Randy Brown, Ph.D. Mathematica Policy Research, Inc., Brenda Spillman, Ph.D., Agency for Health Care Policy & Research, Nancy Miller, Ph.D., and Health Care Financing Administration. Along with Dr. Laurence Branch of Duke University, the committee provided critical input into the initial design of the project and its sampling strategy.
Many individuals helped in the interpretation of study findings, provided important input into the final report, or assisted in refining certain analyses. We would like to thank Sue Morisato, FSA, Bankers Life & Casualty, Beth Jackson, Ph.D, Medstat, Christine Bishop, Ph.D., Brandeis University, Maurice Weinrobe, Ph.D., Clark University, Bart Munson, FSA, Munson & Associates, Jim Robinson, FSA, University of Wisconsin, and Robyn Stone, Ph.D, International Longevity Center. Their constructive comments and criticisms helped to greatly strengthen the report.
Finally, we greatly appreciate the patience, guidance, and advice of our two project officers and financial sponsors: Pam Doty, Ph.D. at the Office of the Assistant Secretary for Aging, Disability and Long-Term Care of the Department of Health and Human Services and Penny Feldman, Ph.D. of the Robert Wood Johnson Foundation Home Care Research Initiative. Their unwavering support and encouragement enabled us to overcome many of the hurdles presented by a study of this magnitude.
Of course the contents of this report are the sole responsibility of its authors. Any errors are their own.
EXECUTIVE SUMMARY
The demand for long-term healthcare services is rising rapidly in direct proportion to the growing population of Americans who require help with personal care and other daily functional tasks. Long-term care (LTC) expenditures now account for almost 12 percent of total personal health expenditures -- a threefold increase since 1960 -- leaving large numbers of elderly Americans vulnerable to catastrophic expenditures that can rapidly deplete their income and life savings.
At the same time, a series of government actions signal the federal government's continuing desire for individuals to accept personal responsibility for planning and paying for their long-term care needs. Limited public funding for long-term care expenses, coupled with tax incentives for individuals and companies to obtain private LTC policies, has once again heated up sales in the burgeoning private long-term care insurance market.
But does private LTC insurance represent a "good buy?" While there is a growing body of knowledge about who buys LTC policies and why, there has been no systematic study of the effectiveness of such policies. On an industry-wide basis, no one knows how benefits are being used, whether claimants feel they are getting good value for the premiums they pay, and whether the patterns of formal (paid) and informal (unpaid) service use differ for LTC insurance claimants compared to similarly disabled persons without LTC policies.
This research was designed to answer these questions. It was also designed to provide basic socio-demographic and service utilization profiles for disabled private LTC insurance policyholders, and to compare such data and findings to the experiences of non-insured disabled community-dwelling elders. Finally, we set out to discuss the implications of such findings on the service delivery system as well as on the design of private and public LTC programs and policies.
We did this by interviewing about 700 community-dwelling long-term care insurance claimants receiving benefits under their policies. We also interviewed their informal caregivers. Key findings of the study are presented below.
The Profile of Community-Dwelling Long-Term Care Insurance Claimants
-
Privately insured disabled policyholders are more likely to be older, widowed, and less likely to have children living nearby than are elders in the general population.
-
Long-term care insurance benefits are well targeted. The vast majority of recipients (79%) has significant dependencies in activities of daily living (ADLs) -- on average 3.3 dependencies -- or is cognitively impaired (32% of the sample).
-
Those who at the time of the interview did not meet HIPAA benefit eligibility triggers -- about 15% of the sample -- were either eligible at the time that they applied for benefits or were likely to become eligible in the very near future. This group is very frail and has few informal supports.
Use of Formal and Informal Care Services Among Privately Insured Claimants
-
About one-in-four claimants relies solely on formal (paid) services for their care.
-
Home health aides provide most of the formal care given to claimants. Two-in-three claimants receive care from this type of service provider.
-
On average, claimants receive 59 hours of care a week. Insurance pays for an average of 36 hours per week, which is equal to about 60% of the total care received.
-
Formal caregivers split their time fairly evenly between ADL and instrumental activities of daily living (IADLs) whereas informal caregivers are more likely to be providing greater amounts of IADL and less ADL assistance.
-
Formal service providers spent 44 hours in the homes of claimants of which 36 hours were spent on ADL and IADL assistance. About 18% of the time was spent on non-ADL/IADL activities.
Benefits paid under Insurance Contracts and Insurance Policy Designs
-
For more than 70% of claimants, insurance pays all of the costs of care.
-
The average monthly insurance benefit paid to claimants is $1,527. This compares to an average public insurance benefit (i.e. Medicaid waiver) for home care of $450.
-
As of the interview date, the average claimant had been in claim for about 13 months and had received $18,000 in benefits. This amount represents less than 20% of total available insurance benefits.
-
The typical coverage for home care reimburses up to $80 in daily costs for a period of about four years.
-
One-third of claimants has some form of inflation protection.
Claimant Satisfaction with Insurance Policy and Insurance Company
-
The vast majority of claimants (86%) is satisfied with their policy and most (75%) had no difficulty understanding what their policy covered. Most (70%) found it easy to file a claim. About 19% felt that the company could have provided additional customer support and more information about how to use benefits.
-
Claimants with a disability policy design were the most likely to be very satisfied with their insurance policy.
-
About 90% of all individuals filing claims had no disagreements with their insurance companies or had a disagreement that was resolved satisfactorily.
-
While most claimants felt they had purchased enough home care coverage (75%), the rest (25%) wished they had purchased more.
Impact of Private Long-Term Care Insurance on Claimants and Informal Caregivers
-
About 60% of claimants indicated that without their policy they would not be able to afford their current level of services and would have to consume fewer hours of paid care. Many also indicated that without their policy benefits, they would have to rely more on informal supports.
-
About half of all claimants and informal caregivers indicated that without private insurance, they would have to seek institutional alternatives -- nursing home care or assisted living facilities.
-
The presence of insurance benefits has not significantly reduced the level of informal care received by claimants. Roughly two-in-three informal caregivers have not reduced the level of care that they provide with half maintaining the same level of care. This finding suggests that for most informal caregivers, insurance financed formal care is not a perfect substitute for informal care.
-
Where formal care does substitute for informal care, the substitution is selective; that is, the formal care financed by insurance benefits may substitute for the care provided by adult children but not necessarily for the care provided by a spouse.
-
About two in three informal caregivers indicate that the presence of private insurance benefits has reduced their level of stress.
Levels of Met and Unmet Need
-
The majority of claimants do not report unmet (82%) or undermet (77%) needs. Yet for those who do, the principle contributing factors are service availability, scheduling, continuity and coordination of caregivers, claimant preference and the quality of caregivers.
-
While long-term care insurance is succeeding in bringing formal caregivers into the homes of disabled elders, in some cases the services of these providers are either not being utilized by claimants or are not being supplied to the claimant.
-
Claimants with multiple caregivers report greater levels of undermet need. This suggests that clearly delineated lines of responsibility may be particularly important in assuring that needs are adequately met.
Comparing Privately Insured and Non-Privately Insured Community-Dwelling Disabled Elders1
-
Compared to those without private insurance, disabled elders with private insurance are more likely to live alone and less likely to have children living nearby. They are also four times more likely to have some college education, eight times more likely to have incomes greater than $30,000 and are overwhelmingly white.
-
The prevalence of physical impairments (i.e. ADL limitations) is much greater among the privately insured than among the non-privately insured; on the other hand, cognitive impairment is much more prevalent among non-insured disabled elders.
-
About 90% of the non-privately insured rely on some level of informal care compared with 77% of the privately insured.
-
The privately insured are roughly five times more likely to rely exclusively on formal care than are those without private insurance. This finding supports the hypothesis that private insurance may be used to compensate for a lack of available informal support.
-
The majority (70%) of individuals with private LTC insurance primarily uses unskilled services such as home health aides and homemaker services, whereas among the non-insured disabled, nursing care remains the most prevalent Medicare funded home care service.
-
The privately insured receive 14 hours more per week of assistance than do the non-privately insured. Much of this is attributable to the receipt of formal services.
-
Very few of the privately insured use Medicare as a payment source for home care services. By contrast, roughly 30% of non-privately insured disabled elders use Medicare as a payment source.
Clearly, LTC insurance benefits are well targeted; they serve those truly dependent on on-going care. The vast majority of claimants is satisfied with their policies, understand their coverage and find it easy to file claims. Because of their LTC benefits, substantial numbers of disabled elderly individuals can remain at home instead of being forced to seek institutional care. Moreover, the availability of LTC benefits reduces stress among informal caregivers and decreases usage of Medicare to fund home health care expenses. Finally, for insured individuals, formal care may substitute for some, but not most informal care, and the two systems appear to be working together to better meet the needs of claimants. Expansion in the private market is likely to lead to reductions in public expenditures on long-term care and the insurance is likely to continue to help disabled individuals remain in their homes at the same time as it maintains and enhances the resiliency of informal support networks.
I. BACKGROUND
The population of Americans who require or are at risk of requiring help with personal care and other daily functional tasks is growing rapidly. This is primarily due to the growth rate of the elderly population -- especially those aged 85 and older. The proportion of the elderly requiring personal assistance ranges from 9 percent of those aged 65 to 69 to well over 50 percent of those age 85 and over (U.S. Census Bureau, 1998). Projections are that between 1990 and 2000 alone, the U.S. population aged 65 and older will grow by 12 percent, and the population aged 85 and older by 50 percent. This population growth among persons at high risk of disability cannot help but create a rising demand for long-term care (LTC) services.
Long-term care expenditures (i.e. expenditures on nursing homes and related facilities, in-home registered nurse and home health aide visits, and other home and community based services) now account for almost twelve percent of total personal health expenditures -- a three-fold increase since 1960. Among people aged 65 and older, long-term care expenditures account for 28 percent of personal health expenditures (21 percent for nursing home services and 7 percent for home and community-based care). This percentage is especially noteworthy given that only one-in-four older Americans with functional disabilities reside in nursing homes and related facilities. Among disabled elders who continue to reside in the community, two-thirds use no (paid) formal long-term care services at all, relying exclusively on the informal help provided by family, friends, and neighbors.
Those elders who do require formal long-term care are likely to have to rely on out-of-pocket payments. While Medicare finances 55 percent of the acute medical expenditures of older Americans, its LTC coverage is limited, covering just 18 percent of their long-term care expenditures. By contrast, out-of-pocket spending, which represents only 14 percent of medical care expenditures for the elderly, accounts for 42 percent of their long-term care expenditures. Medicaid finances a much greater share of long-term care services than acute care expenditures for persons aged 65 and older (35 percent as compared to 4 percent). But elders with long-term care needs who are not cash assistance (SSI) eligible can only access Medicaid by "spending-down" -- that is, by first using up nearly all of their income and assets to pay for care.
As of 1997, the average private pay daily rate for nursing home care was $125 and the average nursing home cost approximately $50,000 per year (AARP, 1998). The average charge for a skilled nursing visit from a registered nurse employed by a Medicare certified home health agency was $88 and the average charge for a home health aide visit was $58. (AARP, 1997). The high cost of formal long-term care services coupled with the continued reliance on out-of-pocket payments to cover these costs leaves those elderly needing long-term care potentially vulnerable to catastrophic expenditures that can rapidly deplete their income and life savings.
Historically, exposure to catastrophic cost risks of this nature has stimulated demand for private insurance, expanded public financing -- or both. Over the past decade, the potential of private long-term care insurance to become a significant source of financing for formal long-term care services has been much debated (See: Cohen et al, 1987; Rivlin and Wiener, 1988; Friedland, 1990; Families USA, 1993; Crown, Capitman, and Leutz, 1992). Many experts in long-term care have recommended expansion of public financing for both nursing home care and home and community-based services or, at a minimum, the latter. (Rivlin and Wiener, 1988; Wiener, Illston, Hanley, 1994).
President Clinton's 1993-94 health reform proposals attempted to expand public financing for long-term care. They included a joint federal/state sponsored program that would have funded home and community-based long-term care services for both middle-income and low-income elderly with severe disabilities. For the foreseeable future, however, there appears to be little prospect of Congress enacting legislation along these lines. Indeed, during 1995 and 1996, it seemed highly possible that even the availability of Medicaid's means-tested financing for long-term care might soon be cut back.
Recent actions suggest that the federal government has now shifted much of its focus to private insurance to help address the long-term care problem. Despite the partisan discord that has characterized congressional debate about Medicare/ Medicaid financing in recent years, agreement was finally reached on steps to increase access to private insurance for long-term care. The Health Insurance Portability and Accountability Act (HIPAA a.k.a. the "Kennedy-Kassebaum" legislation) that President Clinton signed into law in August 1996 included tax incentives for the purchase of long-term care insurance for both individual and employer-sponsored groups.
The granting of tax-favored treatment-- whether for charitable contributions, mortgage interest deduction, retirement savings, health insurance -- and, now, long-term care insurance -- is one way that the federal government encourages and rewards taxpayers for voluntarily engaging in behaviors that are socially responsible; i.e., that benefit not just individuals but society as a whole. Accordingly, financial columnist Jane Bryant Quinn counseled babyboomers to "...prick up your ears at the message behind the new LTC laws. The government wants you to plan on paying more toward your own late-age expenses. If you don't, you'll have to pay more taxes to keep the public programs afloat." (Aging: The End Game, Newsweek, September 30, 1996:53)
Among other things, the "Kennedy-Kassebaum" legislation grants private long-term care insurance tax status on par with acute medical insurance. This means that individuals with tax-qualified private long-term care insurance policies will be able to include private long-term care insurance premiums with other deductible medical expenses and will not be subject to income tax on benefits paid out under qualified long-term care policies. Most observers believe that this legislation is likely to stimulate sales of private long-term care insurance policies in coming years.
Finally, in his 1999 state of the union message, the President recommended that a new long-term care insurance program be established for federal employees. Moreover, in recognition of the financial burden imposed by informal caregiving, the President also recommended that a tax credit of up to $1,000 per year be available to those caring for disabled relatives. With these actions, the federal government is continuing to signal its desire that individuals accept personal responsibility for planning and paying for their long-term care needs.
Prior to 1985, the private long-term care insurance market barely existed. Indeed, the insurance industry was slow to respond because many industry experts questioned whether the need for long-term care could be considered an "insurable event." By the end of 1998, however, more than 5 million LTC policies had been sold (HIAA,1998). In the late 1980s and early 1990s, private long-term care insurance sales grew by more than 20 percent per year. These slowed temporarily during 1993-1994, when legislation based on President Clinton's health reform plan was under consideration by Congress and seemed to have a serious chance of being enacted. Since the demise of the health reform effort, however, private long-term care insurance sales have rebounded. The individual market is now growing rapidly, as is the employer group market. This suggests that more and more elderly and middle-aged Americans are becoming aware of their future risk of requiring long-term care services as a result of conditions and disabilities that become more prevalent at older ages. These "persons at risk" and their families are also realizing that coverage of these services by Medicare and other public programs is quite limited -- and is likely to remain so for the foreseeable future.
Questions remain, however, about whether private long-term care insurance represents a "good buy." Proponents of private long-term care insurance argue that purchase is the only viable alternative to out-of-pocket spending or reliance on informal family caregiving for elders with incomes and assets above the means-tested eligibility levels for most publicly-funded long-term care service coverage. Critics question both the affordability of private long-term care insurance to the target market of middle-aged and "young-old" individuals and the value of the product to those who do purchase it.
Given anticipated changes in Federal policy with respect to Medicare and Medicaid,2 as well as recent tax clarifications for long-term care insurance, it is likely that the market will continue to expand. Yet, while there is a growing body of knowledge about who buys policies and what motivates them to do so (HIAA, 1992 & 1995), there has been no systematic study of individuals who are receiving benefits under their long-term care insurance policies. On an industry-wide basis, no one knows how benefits are being used, whether claimants feel they are getting good value for their premiums, and whether patterns of formal and informal service use differ for long-term care insurance claimants compared to similarly disabled persons without insurance.
As the market for LTC insurance continues to grow, a number of key questions about claimants emerge. These include (but are not limited to):
-
In what ways do patterns of formal and informal caregiving differ in the presence of long-term care insurance?
-
Are claimants satisfied with their insurance?
-
How are long-term care insurance benefits affecting claimants' lives as well as those of their primary informal caregivers?
-
Is there a relationship between the types of policies that claimants have and their use of formal and informal care, their level of satisfaction, and the presence of any reported unmet or undermet need?
Obtaining answers to these questions is important from a public policy and regulatory standpoint. Because the vast majority of LTC policies now cover significant amounts of home and community-based care, their proliferation in the market will have financial and service delivery implications for both the formal and informal care networks. This necessarily will affect the level and mix of publicly funded long-term care services. In the absence of "hard data" about the experience of claimants, it is difficult to develop targeted regulatory and consumer protection strategies related to claims issues. Finally, if state and Federal governments wish to encourage development of this market, it is important that there be adequate information about how the product is performing from the perspective of claimants and their families. This will assist the government in assessing the future potential of this type of insurance.
Such information is also of interest to private insurers, who are trying to increase the market for long-term care insurance, and actuaries who are responsible for pricing long-term care insurance products. An important assumption used in the premium pricing decision relates to the mix of formal and informal care that will occur when an individual goes into claim status. Often, the only information available to actuaries on a national basis is derived from uninsured experience among the general population of disabled elders (e.g. 1982, 1984 and 1989 National Long-Term Care Surveys). Information from these surveys may not accurately represent experience in an insured context. Thus, it is important to determine whether, and in what ways, patterns of formal and informal care delivery differ in the presence of long-term care insurance. This has implications for the way policies are designed, priced, and marketed.
II. PURPOSE
The purpose of this research is to provide basic descriptive statistics on disabled private LTC insurance policyholders, who have accessed long-term care benefits in the community and to compare such data and findings to non-insured disabled community-dwelling elders.3 We intend to:
- provide detailed descriptive information on the socio-demographic and service utilization profile of disabled claimants receiving home and community-based care benefits under their LTC insurance policies;
- characterize the level and mix of informal and formal support among disabled claimants and compare this to a nationally representative sample of non-privately insured disabled elders living in the community;
- identify factors associated with observed differences between the insured and non-insured groups in relation to the utilization of home care;
- measure caregiver effort on behalf of home care claimants and compare this to caregiver effort for disabled non-privately insured elders living in the community;
- evaluate claimant and caregiver perceptions regarding the value of their LTC policy and estimate the extent of unmet and undermet need; and
- discuss the implications of findings on the service delivery system as well as on the design of private and public LTC policies and programs.
III. METHOD
A. Sample
The project relied on the development of four analytic samples. These included:
- insured community dwelling disabled elders who are accessing benefits under their LTC insurance policy (Home Care Claimants);
- the informal caregivers of privately insured claimants (Informal Caregivers);
- a subset of LTC policyholders living in the community who are disabled, but not accessing benefits under their LTC insurance policy (Policyholders); and
- a subset of moderately disabled Medicare beneficiaries living in the community who do not have private insurance for long-term care (1994 NLTCS sample).
Home Care Claimants
To be included in the claimant sample, individual claimants had to meet the following criteria:
- They had to be age 65 and over;
- They had to be classified as an active claim with at least one payment for home/community-based services;
- They had to have a policy that covered both nursing home care and home and community-based services; and,
- They had to be living in the community and not in an institution.
We asked each company to provide its total universe of claimants who met these criteria. We focused on individuals with "dual-coverage" policies, rather than on those with policies covering only institutional care, because roughly 80% of all policies currently selling in the market cover services in at least these two modalities. By doing so, we could assure that study findings would be applicable in the future as well as in the present.
Together, these eight companies provided a home care claimant block of 1,599 eligible individuals. Of these, 750 were removed from the study, leaving a "qualified" sample totaling 849 claimants, of whom 82% or 697 participated in the study. Most of those removed were either no longer receiving services at the time of the interview, were deceased, no longer had their policy, did not meet the age criteria, or could not be reached after repeated call attempts.
Informal Caregivers
We asked home care claimants to identify their primary informal caregiver. This was done by asking the claimant to indicate who helped them the most with their everyday activities but did not receive monetary payment for doing so. The proportion of the claimant population with at least one informal caregiver was 77% or 538 claimants. Of the 461 that we reached by telephone, 424 or 91% participated in the study.
Long-Term Care Insurance Policyholders
We interviewed by telephone 670 policyholders (randomly selected from non-claimants) to identify the proportion of individual policyholders who may be disabled (i.e. have two or more limitations in activities of daily living (ADLs) or are cognitively impaired) and yet are not accessing their insurance benefits. We achieved a 95% response rate for this sample. Because the proportion of disabled non-claiming policyholders was so small, (4 cases) we did not draw a sample from every company but rather, from only four of the eight participating companies.4
The 1994 National Long-Term Care Sample
The 1994 National Long-Term Care Survey (NLTCS) was designed to collect data about the health and function of the Medicare beneficiary population age 65 and older. The questions were meant to identify persons who had certain disabilities or health problems lasting three months or longer. In general, individuals who completed a comprehensive community survey were those who had at least one chronic limitation in either an instrumental activity of daily living (IADL) or in an activity of daily living (ADL). The total 1994 NLTCS sample consisted of 4,167 individuals.
Only sub-sets of the claimant sample and the NLTCS sample are used when we make comparisons between the privately insured (claimant sample) and the non-privately insured (NLTCS sample). In fact, only those individuals who had at least two ADL limitations out of six ADLs5or who were cognitively impaired or who had a primary cognitive diagnosis like Dementia or Alzheimer's disease were included in comparative analyses. These are criteria that mirror the benefit eligibility criteria commonly used in private LTC insurance policies.6 By holding the minimum disability threshold constant and limiting our analysis to this sub-sample of disabled individuals, we can then make direct comparisons between the privately insured sample (i.e. insurance claimants) and the non-privately insured sample (i.e. modified 1994 NLTCS sample). After applying these criteria, the total sample size of the 1994 NLTCS sub-sample was 1,357.
B. Data
Sources of Information
Eight of the largest long-term care insurance companies in the U.S. participated in the study and contributed a sample of claimants residing in the community. These companies also provided data from their administrative and claim systems to supplement information collected directly from claimants. Finally, claimants identified their primary informal (unpaid) caregiver so that they too could be interviewed.7
The participating companies included: (1) Aegon; (2) American Travellers; (3) Bankers Life and Casualty; (4) CNA Insurance; (5) Fortis Long-Term Care; (6) G.E. Capital Assurance; (7) John Hancock; and (8) UNUM. Together their claimant blocks represent more than 80% of all open home health care claims and nursing home claims.8 These companies also represent diverse market segments and policy designs, and employ differing underwriting and claims management strategies.
In addition to the information provided by the LTC insurance industry, we analyzed information from the 1994 National Long-Term Care Survey (1994 NLTCS).9 These data allowed us to make comparisons between privately insured and non-privately insured disabled elders living in the community. Questions on the claimant survey were designed to mirror those on the 1994 NLTCS; this assured that accurate comparisons between the privately insured and non-privately insured samples could be made.
Data Collection
Data from all privately insured home care claimants was gathered via in-person interviews conducted by trained nurses and social workers with at least two years of geriatric experience. Each interviewer underwent comprehensive training to assure inter-rater reliability. Information garnered from these interviews was then linked to policy design and claim information generated from the administrative systems of the participating insurance companies. In 15% of the cases, we conducted phone interviews with claimants who either could not or were not willing to be interviewed in their homes. We collected information from informal caregivers and from policyholders who were not making claims on their policy via telephone interviews. All fieldwork was completed between November 1997 and February 1999. It is important to note that each completed survey underwent a detailed quality review by home-office staff. In some cases, surveys had to be returned to the field either because certain data elements were not complete or because of the presence of clinical discrepancies.
C. Response Rates and Ultimate Analytic Samples
Table 1 displays the response rates for the claimant and informal caregiver samples who were located and contacted. As shown, we achieved high response rates for these analytic samples. The lowest response rate for a particular company was 78%, the highest was 92%. There was little variation across companies in the response rates of informal caregivers. Finally, (although not shown in the table), roughly 95% of all policyholders located and contacted agreed to participate in the very short phone screen survey.
| TABLE 1: Sample Size and Response Rates by Company | ||||
| Company | Privately Insured Sample | Informal Caregivers of Privately Insured Sample | ||
| Analytic Sample | Response Rate | Analytic Sample | Response Rate | |
| Company 1 | 54 | 91% | 39 | 88% |
| Company 2 | 96 | 79% | 44 | 85% |
| Company 3 | 65 | 80% | 48 | 94% |
| Company 4 | 108 | 78% | 56 | 92% |
| Company 5 | 48 | 87% | 24 | 83% |
| Company 6 | 156 | 79% | 97 | 96% |
| Company 7 | 78 | 92% | 55 | 95% |
| Company 8 | 93 | 82% | 61 | 95% |
| TOTAL | 697 | 82% | 424 | 92% |
| SOURCE: 1999 National Claimant Study. NOTE: These are the response rates among individuals who were successfully located and contacted. Even when we classify those who could not be located/contacted as "non-responders', the response rates among claimants is greater than 72% and among informal caregivers the rate is closer to 82%. | ||||
IV. FINDINGS
A. Profiling Privately Insured Claimants
Demographic Characteristics
The table below compares the demographic profile of privately insured claimants with a sample of elders -- able-bodied and disabled seniors alike -- age 65 and over.
| TABLE 2: Socio-Demographic Characteristics of Privately Insured Home Care Claimants and all Elders Age 65 and Over | ||
| Socio-Demographic Characteristics | All Privately-Insured Home Care Claimants | All Elders Age 65 and Over1,2 |
| Average Age | (n=686) | |
| 79 years | 75 years | |
| 65-69 | 5% | 32% |
| 70-74 | 18% | 23% |
| 75-79 | 28% | 19% |
| 80-84 | 28% | 15% |
| 85+ | 21% | 11% |
| Gender | (n=693) | |
| Male | 32% | 31% |
| Female | 68% | 69% |
| Marital Status | (n=693) | |
| Never married | 4% | 4% |
| Married | 46% | 55% |
| Divorced/separated | 5% | 7% |
| Widowed | 45% | 34% |
| Any children within 25 miles | (n=695) | |
| Yes | 54% | 69% |
| No | 46% | 31% |
| Education Level | (n=691) | |
| Less than High School Graduate | 10% | 33%3 |
| High School Graduate | 25% | 35% |
| Technical/Trade/Business/Some College | 28% | 17% |
| College Graduate | 37% | 15% |
| Race | (n=695) | |
| White (not Hispanic) | 97% | 85% |
| Non-White | 3% | 15% |
| Living Arrangement | (n=694) | |
| Alone | 34% | 34% |
| With spouse | 44% | 53% |
| With relative | 11% | 13% |
| Other | 11% | --- |
| Total Income | (n=492) | |
| $30,000 | 52% | 65% |
| >$30,000 | 48% | 35% |
| Total Income | (n=432) | |
| Less than $10,500 | 7% | 19%4 |
| $10,501-$19,999 | 22% | 28% |
| $20,000-$30,000 | 28% | 19% |
| $30,001-$39,999 | 13% | 11% |
| $40,000-$49,999 | 9% | 8% |
| $50,000-$74,999 | 11% | 8% |
| >75,000 | 10% | 8% |
| Estimated Current Value of Home | (n=431) | |
| Less than $50,000 | 7% | 25%5 |
| $50,000-$99,999 | 28% | 37% |
| $100,000-$149,999 | 19% | 18% |
| $150,000-$199,999 | 13% | 10% |
| $200,000-$249,999 | 11% | 4% |
| >$250,000 | 22% | 7% |
| ||
In general, privately insured claimants are more likely to be older and widowed than are elders in the general population. They are also less likely to have children living nearby. Long-term care insurance claimants are wealthier than their counterparts in the general population; they are 1.4 times more likely to have incomes greater than $30,000 than are elders in the general population. They also have significantly greater housing assets.
Health Status
Respondents were asked a number of questions relating to their health status. The figure below illustrates how claimants assessed their health status at the time of the in-person interview.
| FIGURE 1: Self Assessment of Health Status |
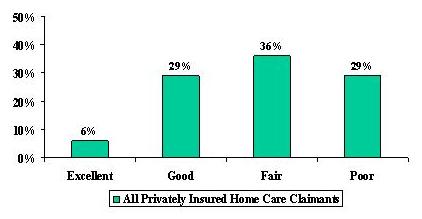 |
| SOURCE: 1999 National Claimant Study (n=688). |
Disability Status
The next three figures illustrate the extent of disability among privately insured claimants. Disability is measured in three ways: (1) the number of limitations in activities of daily living; (2) whether or not someone is cognitively impaired as measured by their score on the Short Portable Mental Status Questionnaire, and (3) whether or not an individual has a cognitive diagnosis such as Alzheimer's disease or other dementia.
Most currently available LTC policies require an individual have at least two ADL limitations or be cognitively impaired in order to qualify for benefits. All tax-qualified policies have such a requirement. Older and non-tax qualified policies do, however, enable an individual to access benefits if LTC services were deemed by a physician to be "medically necessary". As shown in Figure 2, 79% of current claimants have two or more ADL limitations. The average number of ADL limitations is 3.3. Not shown in the diagram is the fact that among the eight participating companies, the average number of ADL limitations ranged from 2.8 to 3.9.10
| FIGURE 2: Functional Status of Claimants: ADL Limitations |
| SOURCE: 1999 National Claimant Study (n=695). NOTE: The Activities of Daily Living measured include bathing, dressing, toileting, transferring, continence and feeding. |
Another measure of one's functional capacity is ability to perform IADLs. These higher order activities must also be performed as part of independent living. Such activities typically include shopping, laundry, light housework, outdoor mobility, managing medications, managing money, getting to places out of walking distance, and meal preparation. Loss in these activities is usually a precursor to loss of ADL function. Figure 3 shows that most, if not all, claimants require assistance with almost all of these activities.
| FIGURE 3: Functional Status of Claimants: IADL Limitaions |
| SOURCE: 1999 National Claimant Study (n=646). NOTE: The Instrumental Activities of Daily Living measured include shopping, laundry, light housework, outdoor mobility, managing medications, managing money, getting to places out of walking distance, and meal preparation. |
Figure 4 displays the claimant sample by cognitive status. In total, 32% of claimants are cognitively impaired. Roughly 29% have 4 or more errors on the Short Portable Mental Status Questionnaire (SPMSQ), this indicating moderate to severe cognitive impairment.11 An additional 3% has a cognitive diagnosis of Alzheimer's disease or other dementia.
Because companies use different underwriting techniques to identify individuals who may be at high risk for becoming cognitively impaired, there is a great deal of variation between companies in the cognitive status of claimants. The proportion of claimants with cognitive impairment ranges between 23% to 48%.12 Some companies conduct more intensive in-person assessments during the policy application process, while others rely exclusively on medical records or phone interviews. Clearly, some companies are more successful than others at identifying the risk of cognitive claims. Also, policy designs and claims adjudication procedures may lead to variability in the number of claimants with cognitive impairment.
| FIGURE 4: Cognitive Status of Claimants |
| SOURCE: 1999 National Claimant Study (n=556). NOTE: Cognitive impairment is present when an individual has 4 or more errors on the SPMSQ or a cognitive diagnosis such as Alzheimer's or dementia. |
B. Examining the Relationship between Claimant Profiles and HIPAA Benefit Eligibility Triggers
In the HIPAA (i.e. Kennedy-Kassebaum) legislation, long-term care insurance policies are tax qualified if access to benefits is limited to (1) individuals with at least 2 ADL limitations or (2) individuals who are moderately or severely cognitive impaired. Figure 5 shows that 85% of claimants met this definition of eligibility at the time of the in-person interview. Fifteen percent of claimants were neither impaired in at least two ADLs nor were cognitively impaired.
Not shown is the fact that there is significant variation across insurance companies: from a low of 5% to a high of 28% who, at the time of the in-person interview, did not meet HIPAA benefit-eligibility triggers.13
| FIGURE 5: Proportion of Claimants Meeting HIPAA Benefit Triggers at Time of Interview |
| SOURCE: 1999 National Claimant Study (n=695). NOTE: To meet HIPAA triggers, one must be disabled in at least 2 ADLs or be cognitively impaired. An ADL disability results when an individual requires either stand-by, cueing or hands-on assistance to perform an activity. Cognitive impairment is measured by the SPMSQ (i.e. 4+ errors) or by the presence of a cognitive diagnosis. |
Given that about one-in-seven claimants were neither functionally nor cognitively impaired as defined by HIPAA, an important question arises: Who are these people and why are they receiving insurance benefits? As shown in Table 3, compared to the 85% of claimants who did meet HIPAA triggers these 15% were older, more likely to live alone, less likely to be married and less likely to have available informal supports. Moreover, the majority had one ADL impairment and most also had multiple IADL impairments. Finally, 32% required assistance managing medications. An examination of claims payment data reveals that the average claims dollars spent per month on those not meeting HIPAA benefit eligibility triggers was $1,100 compared to $1,760 for those who did meet the triggers.
The data clearly indicate that these claimants are frail, disabled and in need of long-term care services. Either they met the HIPAA triggers at the time that they applied for insurance benefits or are fast on their way to becoming eligible. Given that insurers typically reassess home health care claimants at two to three month intervals, it is not surprising that some individuals improved and were therefore not HIPAA eligible at the time of our interview.
| TABLE 3: Comparison of Individuals Who Did and Did Not Meet HIPAA Benefit Eligibility Requirements at the Time of Interview | ||
| Characteristic | Claimants Meeting HIPAA Requirements | Claimants Not Meeting HIPAA Requirements |
| Average Age | (n=577) | (n=109) |
| 79** | 81 | |
| Gender | (n=583) | (n=110) |
| Male | 35%*** | 20% |
| Female | 65% | 80% |
| Living Arrangement | (n=584) | (n=110) |
| Alone | 29%*** | 61% |
| With someone | 71% | 39% |
| Marital Status | (n=583) | (n=110) |
| Married | 49%** | 34% |
| Unmarried | 51% | 66% |
| Informal Caregivers | (n=585) | (n=110) |
| None | 23%** | 41% |
| At least one | 77% | 59% |
| ADL Limitations | (n=585) | (n=110) |
| 0 | 2%*** | 39% |
| 1 | 5% | 61% |
| 2 or more | 93% | 0% |
| IADL Limitations | (n=543) | (n=106) |
| 0-5 | 7%*** | 43% |
| 6-7 | 31% | 30% |
| 8 | 62% | 27% |
| Need Assistance Managing Medications | (n=553) | (n=107) |
| 80% | 32% | |
| SOURCE: 1999 National Claimant Study. *** differences significant at the .001 level ** differences significant at the .05 level | ||
C. Use of Formal and Informal Care Services Among Privately Insured Claimants
It is well known that most long-term care is provided informally by family members, typically spouses, daughters and daughters-in-laws. Data presented thus far suggests that many privately insured claimants live alone and do not have children living nearby. Thus, many may view their LTC policy as compensating for the lack of informal (unpaid) support, especially single policyholders. Even for those with informal supports, the policy may be enabling them to decrease reliance on such support -- an important motivator for initial purchase (Cohen and Kumar, 1996).
As Figure 6 below shows, 23% of claimants rely solely on formal (paid) services for their care. In fact, as will be shown subsequently, privately insured claimants are about six times more likely to rely exclusively on formal care than are non-privately insured disabled elders living in the community.
| FIGURE 6: Availability of Informal Support Among Claimants |
| SOURCE: 1999 National Claimant Study (n=695). |
Unlike the acute care population, the long-term care population is characterized by its use of and dependence on personal care services provided by paraprofessionals. These include home health aide services, homemaker and companion services, and personal care aides. Figure 7 shows that home health aides provide most of the formal care given to claimants; two-in-three claimants receive care from this type of service provider. Noteworthy is the fact that relatively few claimants are receiving services provided by nurses. This suggests that, for the most part, long-term care insurance is not paying for skilled nursing services.14
| FIGURE 7: Providers of Formal Care |
| SOURCE: 1999 National Claimant Study (n=695). |
Given the functional and cognitive profile of these claimants, it is clear that they require a great deal of stand-by or hands-on assistance to perform the ADLs. Moreover, to continue living independently in the community, they also need assistance with more complicated tasks like shopping for groceries, preparing meals, doing light housework, and more (IADLs). Figure 8 shows that on average, these individuals receive 59 hours of such care a week -- roughly 8 hours a day of assistance. Insurance pays for about 35 hours per week or 5 hours per day of care, about 60% of the total care received by claimants.
An analysis of the data reveals that formal caregivers split their assistance fairly evenly between ADL and IADL activities. On the other hand, informal caregivers generally provide greater amounts of IADL assistance and less ADL assistance; 1.3 hours per day are devoted to ADL assistance compared to 2 hours per day for IADL activities. Not shown is the fact that roughly 10% of the sample receives round the clock care -- 24 hours per day seven days a week -- most of it stand-by assistance.
By obtaining the service schedules of formal providers, we determined how many hours per week they were spending in the homes of claimants. Figure 8 focused on the number of hours of ADL and IADL assistance that was provided to claimants. The claimant provided this information. Figure 9 shows the relationship between the number of care hours provided and the number of hours available (i.e. the number of hours that formal service providers were in the homes of claimants). As shown on the page that follows, over the course of a week, formal service providers spent an average of 44 hours in the homes of claimants of which 36 hours were spent on ADL and IADL assistance. This suggests that about 8 hours a week, or about 18% of the time, were spent on non-ADL/IADL activities.
| FIGURE 8: Average Weekly Hours of Informal and Formal Care |
| SOURCE: 1999 National Claimant Study (n=692). |
This is an important finding. As will be shown in a subsequent section, a sizeable minority of claimants indicates that they have unmet or undermet ADL and IADL needs. In other words, some claimants believe that they are not getting enough of the care that they think they need. This data suggests that the problem might not be that caregivers don't spend enough time with these claimants, but rather that they don't spend the right kind of time with them.
| FIGURE 9: Provided ADL and IADL Care Compared to Available Weekly Hours of Formal Support |
| SOURCE: 1999 National Claimant Study (n=692). |
D. Benefits paid under Insurance Contracts and Insurance Policy Designs
Clearly, claimants are receiving a substantial number of hours of assistance from formal caregivers. Much of this care is paid for by insurance benefits. In fact, for more than 70% of claimants, insurance pays all of the costs of care. Figure 10 shows that the average monthly insurance benefit paid to claimants is $1,527. How does this compare to the primary public payer of home and community-based care for disabled elders -- the Medicaid waiver program? As shown, the Medicaid waiver program pays an average of about $450 per month for care.15 This suggests that for every dollar spent on disabled elders in the waiver program, about three and one-half dollars are spent on disabled long-term care insurance claimants.16
Not shown in the diagram is the fact that as of the interview date, this sample of claimants had already used an average of $18,000 in insurance benefits per person. Given that most of these individuals have policies covering up to about four years of care at around $80 per day -- about $112,000 in available benefits -- these individuals have thus far used up less than 20% of their benefits. (See Table 4). The range in monthly benefit payments across the companies is from a low of $768 to a high of $2,200.
| FIGURE 10: Average Monthly Benefit Payments for Claimants and for Beneficiaries of Medicaid Waiver Programs |
| SOURCE: 1999 National Claimant Study (n=605). |
Most have been in claim for about 13 months (See distribution in Figure 11). About 30% have been receiving benefits for more than a year-and-a-half while another 20% have been receiving benefits for less than six months.Not shown is the fact that the average amount of time between policy purchase and first claim is three years.
| FIGURE 11: Amount of Time Claimants have been Receiving Benefits |
| SOURCE: 1999 National Claimant Study (n=611). |
Table 4 summarizes the typical home care policy design features of this study's claimants. In general, there are three types of benefit designs:
-
Indemnity model, which pays a fixed level benefit when an individual becomes disabled and long-term care expenses are incurred. The payment may be larger or smaller than the actual cost of services and bears no direct relationship to such expenses.
-
Reimbursement model, which reimburses costs of covered services for eligible individuals up to a maximum daily amount. In this model, insurance benefits are directly related to the incurred long-term care costs.
-
Disability model, which pays benefits directly to the insured when the individual becomes disabled, whether or not long-term care expenses are incurred. The insured has the freedom to spend the disability payment on whatever services he/she deems appropriate.
The most conservative -- although from a claims standpoint less predictable -- of these policy designs is the reimbursement model. Almost all of the home care benefits in the policies held by these claimants are paid on a reimbursement basis (86%). About 10% of claimants access benefits through a disability policy design.
The average daily benefit for home care coverage in the sample is $80. Given that most of the visits are home health aides, which typically cost less than $60 per visit, this represents a more than adequate daily reimbursement. It is also noteworthy that 34% of the claimants have policies that include some level of inflation protection. About 40% are eligible to receive over $100 per day in benefits for reimbursed home care benefits.
Finally, more than half of the claimants have policies that cover the equivalent of daily care for a three-year period. Among the Medicare home health population, fewer than 20% actually spend more than two years receiving home health care services.17 Thus, the duration of care covered by these policies will likely capture the duration of use for most of these individuals.
| TABLE 4: Policy Design Features for Home Care Coverage | |
| Policy Design Feature | Distribution |
| Home Care Payment Method | |
| Reimbursement | 86% |
| Indemnity | 4% |
| Disability | 10% |
| Home Care Daily Benefit Amount | |
| $50 | 26% |
| $51 to $74 | 17% |
| $75 to $99 | 19% |
| $100 to $124 | 31% |
| $125 or greater | 7% |
| Average | $80 |
| Home Care Duration | |
| 1 year | 10% |
| 2 year | 28% |
| 3 year | 17% |
| 4 year | 11% |
| 5 year | 6% |
| 6 year | 6% |
| Lifetime Coverage | 22% |
| Average | 4.4 Years |
| Elimination Period | |
| 0 day | 26% |
| 1-10 days | 23% |
| 11-20 days | 13% |
| 30-50 days | 7% |
| 60-90 days | 8% |
| 100 day | 23% |
| Average | 38 days |
| Percent with Inflation Protection | 34% |
| SOURCE: 1999 National Claimant Study (n=624). | |
Although about half of the policies held by this sample of claimants have very low elimination periods (i.e. less than 20 days), most policies now selling on the market have longer elimination periods. Through policy design changes, insurers are trying to target benefits to individuals with chronic, rather than post-acute and short-term, care needs.
E. Claimant Satisfaction with Insurance Policy and Insurance Company
The average age of individuals who purchase private long-term care insurance is 68 years. Yet, the average age of claimants is closer to age 80. This means that most current long-term care insurance policyholders can expect to hold their policy for 10 or more years before they might actually need to access benefits.18 During this premium payment period, the primary "benefit" of a policy is psychic in nature: individuals derive utility from knowing that the certain premium they pay reduces the uncertainty and ultimate financial risk they might face in the absence of a policy. The extent to which policyholders are satisfied with this "psychic benefit" is difficult to gauge. A way to more concretely evaluate consumer satisfaction is to interview individuals who require benefits under their policy. In the sections that follow, we focus on satisfaction from two perspectives: (1) that of the claimant and (2) that of the primary informal caregiver.
We asked claimants a series of questions related to general satisfaction with their insurance policy as well as with various insurer claims management practices. The results are summarized in Figure 12. The vast majority of claimants (86%) is satisfied with their policy; slightly less than two-in-three are very satisfied with their policy. Individuals with disability payment policies tended to be more satisfied than were those with other policy designs.19 The level of daily benefit or duration of coverage did not affect levels of satisfaction.
| FIGURE 12: Level of Satisfaction with Long-Term Care Insurance Policy |
| SOURCE: 1999 National Claimant Study (n=687). |
Given the relatively complex nature of long-term care insurance contracts, an issue of concern to consumer groups and the industry alike is whether or not claimants actually understand what they are buying. Claimants were asked whether they had any problems understanding what was and was not covered by their policy. The vast majority (75%) had no difficulty understanding what their policy covered; the other 25% had some difficulty. Those with disability policy designs were less likely to indicate a problem understanding their coverage. It follows that insurers must continue to work with agents and policyholders to minimize and confusion and false expectations that could arise at claim time.
Most long-term care insurance policies reimburse expenses incurred for direct service costs, or pay a flat benefit when service costs are incurred. This means that bills must be sent to the insurer in order to process a claim.20 One might imagine that such a process could be cumbersome, especially for policyholders suffering from dementia or other cognitive ailments.
We asked claimants whether it was difficult for them to file their claim and obtain benefits. Figure 13 shows that most individuals (70%) found the process to be easy. On the other hand, close to one-in-three claimants did find the process to be somewhat difficult. Across the companies, between 55% and 80% found the claims filing process to be easy.21 Again, this finding suggests that insurers should continue to refine and simplify their claims handling procedures.
| FIGURE 13: Ease of Filing Benefits |
| SOURCE: 1999 National Claimant Study (n=666). |
We then asked claimants if they had had any disagreements with the insurance company over their coverage, and whether such disagreements were resolved to their satisfaction. Figure 14 shows that 90% of all individuals filing claims had either no disagreements with their insurance companies or had a disagreement(s) that was resolved satisfactorily. About 10% of claimants felt their disagreement was not resolved satisfactorily.
Again, the findings varied greatly from company to company. The proportion of claimants who indicated that they had a disagreement with the insurer at claim time ranged by company from a low of 8% to a high of 30%.22
| FIGURE 14: Presence of Disagreements between Claimants and Insurance Company |
| SOURCE: 1999 National Claimant Study (n=680). |
Finally, claimants responded to a question about actions that their insurance company might have taken but didn't, to help them when they needed benefits. This was an open-ended question. As shown on the next page, about three in four respondents felt there was nothing else that the insurance company should have done. Nineteen percent felt that the company could have provided additional customer support, claims processing, and more advice about the policy itself.
An important issue is whether or not, at the time of initial policy purchase, individuals buy enough benefits to cover their costs of care. We asked claimants whether they believed they purchased enough home care coverage, and whether there were additional services they thought they needed but that were not covered by their policy. Figure 16 indicates that about three in four claimants felt that they had purchased enough home care coverage. In terms of the additional services that they wanted, slightly less than 10% indicated they wished their policy covered transportation and certain equipment and supplies. Another 12% provided a general answer of "more coverage". Many of these respondents also wished that their policy covered a greater proportion of care costs.
| FIGURE 15: Actions Insurer might have Taken to Help Claimants |
| SOURCE: 1999 National Claimant Study (n=695). |
Not surprisingly, those who are satisfied with their coverage amount tended to have higher daily benefit amounts -- $83 compared to $73.23 No other policy design parameter proved to be significantly related to this dimension of satisfaction.
| FIGURE 16: Satisfaction with Amount of Home Care Coverage Chosen at Time of Policy Purchase |
| SOURCE: 1999 National Claimant Study (n=678). |
F. Impact of Private Long-Term Care Insurance on Claimants and Informal Caregivers24
We asked claimants and informal caregivers a series of questions to gauge their perceptions about how having a long-term care insurance policy has influenced both the level and type of care received (for claimants) and provided (by informal caregivers). Figure 17 displays the responses of claimants to three questions:
-
In the absence of their policy, would they be able to afford the amount of care that they currently receive?
-
In the absence of their insurance, would they receive fewer hours of paid care?
-
In the absence of their insurance, would they have to rely more on family, friends or other volunteers to provide assistance?
| FIGURE 17: Claimants Perceptions about Impact of Not Having LTC Insurance Policy |
| SOURCE: 1999 National Claimant Study (n=675). |
For claimants, the greatest impact of receiving insurance benefits is on their level of paid care; only 40% indicate that in the absence of their policy they would be able to afford their current level of services. About 57% thought that they would have to consume fewer hours of paid care. Thus, from their perspective, the lack of insurance would result in greater levels of unmet or undermet need. About half of the claimants indicated that they would have to rely more on informal supports. It is unclear from these data alone whether such informal supports would be able to compensate for the loss associated with lower levels of formal (paid) care.
We asked a similar, although more detailed, set of questions to informal caregivers.25 We inquired as to whether:
- they provide more, less or the same amount of care given that insurance benefits are being paid to the claimant;
- in the absence of the claimant's policy would they provide more, less or the same amount of care as they currently provide; and
- in the presence of policy benefits, the nature of the care they provide has changed, and if so, how.
Figure 18 shows that in the presence of insurance benefits, roughly two-in-three informal caregivers have not reduced the level of care that they provide. In fact, half of the caregivers have not changed the amount of care they provide at all. This finding suggests that for most informal caregivers, formal care does not substitute for informal care. With that said, however, the picture is not crystal clear: about one-in three did indicate that they now provide less informal care. Among all caregivers, a slight majority (52%) indicated that if the policy were not paying benefits they would increase the level of informal care that they provide.
| FIGURE 18: Informal Caregivers Perceptions about Impact of Claimants Policy |
| SOURCE: Analysis of 1998 informal caregiver data (n=415 informal caregivers). |
It is also noteworthy that 15% informal caregivers suggested that they provide more informal care now that insurance benefits are being received and more formal care provided. This may reflect the fact that the situation of the claimant may have deteriorated since the onset of benefit payments so that the informal caregiver has had to increase the amount of care they provide. It may also be the case that the presence of insurance to finance formal care has enabled them to provide more care rather than less. This suggests that in some instances, formal care may be a complementary rather than substitute service for informal caregiving.
We asked informal caregivers whether the presence of insurance benefits has changed the nature of the care that they provide. Most (72%), indicated that it had not. For those informal caregivers who indicated that they had changed the type of care that they provide, most show a reduction in ADL and IADL assistance and an increase in companionship services (See Figure 19).
| FIGURE 19: How Care has Changed for Those Reporting That They Have Changed the Type of Care They Provide |
| SOURCE: Analysis of 1998 informal caregiver data (n=415 informal caregivers). |
Figure 20 shows that, for about two-in-three informal caregivers, stress has decreased since the person they are caring for began receiving insurance benefits. This is not surprising since one would expect that, as an individual has more caregivers to provide assistance, the "stress" associated with providing care by a single individual would decline.
One would have thought that the need to monitor formal caregivers or to interact with the insurer as well as with providers might have led to increased stress among many informal caregivers. Such is not the case. Only 4% of informal caregivers indicate that the presence of insurance actually increased stress levels. Finally, one-quarter of informal caregivers indicate that the insurance had no effect on their stress level. Additional analysis reveals that the caregivers least affected (in terms of stress levels) by the presence of insurance are predominately male.
| FIGURE 20: Caregivers Assessment as to Whether Presence of Insurance Benefits has Reduced Stress |
| SOURCE: Analysis of 1998 informal caregiver data (n=416 informal caregivers). |
A great deal of research has focused on whether the use of formal home care services delays or prevents the use of costly institutional care like nursing home care (See: Weissert, 1985; Weissert et al, 1988; Garber & MaCurdy, 1989; Shapiro and Tate, 1989 Green et al, 1993; Wolf, 1997; Kane 1998.) Most of this research suggests that, unless very carefully targeted, home care rarely prevents someone from using nursing home care. Instead, there is a growing consensus that home care serves a distinct population that differs in relevant respects from the nursing home population. Yet, the decision to seek institutional care is a complicated one involving a myriad of factors, many of which cannot be adequately captured even by the most sophisticated multivariate modeling.
Because this is such an important issue, we decided to approach it from a somewhat different perspective. Rather than model the characteristics of individuals to determine potential overlap with the nursing home population, we focus on potential service-seeking behaviors. In other words, in our survey of home care claimants, we asked both the claimant and the informal caregiver whether or not, in the absence of the insurance policy, the disabled claimant would be able to remain living at home. This provides an indication of whether or not the individual would be able to continue living independently in the community. Figure 21 shows that among both claimants and informal caregivers, about half indicated that in the absence of the private insurance, they would have to seek institutional alternatives.
An important question is whether or not there is agreement between the claimant and his/her informal caregiver. Our analysis suggests that in 31% of the cases, both the claimant and their informal caregiver agreed that institutional alternatives would be needed in the absence of a policy. In 18% of the cases the informal caregiver felt that the claimant would need institutional care and the claimant disagreed, whereas in 9% the claimant felt they would need institutional care and the informal caregiver disagreed. Thus, it appears that at a minimum somewhere between 30% and 50% of claimants would likely need to seriously examine institutional alternatives in the absence of their insurance benefits.
| FIGURE 21: Whether in Absence of Policy Institutional Care would be Sought |
| SOURCE: Analysis of 1998 claimant and informal caregiver data (n=643 claimants; n=416 informal caregivers). |
As shown in Figure 22, among claimants who thought that they could not remain in the community without their insurance benefits, roughly half said they would need to enter a nursing home and another half indicated they would move to an assisted living facility. Thus, it appears that receipt of these insurance benefits is equally likely to suppress the demand for assisted living services as it is for nursing home care.
| FIGURE 22: Which Institutional Alternatives Would be Sought in Absence of Policy |
| SOURCE: Analysis of 1998 informal claimants data (n=297 claimants). |
G. Levels of Met and Unmet Need
Much of the current research on long-term care is focused on characterizing the disabled population, identifying the type and level of services needed and used, and estimating public and private expenditures on care. Given the development of both longitudinal and cross-sectional databases, researchers have also tracked trends in disability rates and service use over time. Yet, there has been almost no examination of how well disabled individuals actually function in the community. With the recent increase in home care providers and both public and private spending on home care, one might assume that the current structure of the health care finance and delivery system is adequately responding to the care needs of disabled elders living at home. However, this may not be the case. In the section that follows, we examine whether or not claimants perceive their needs to be met by the formal and informal service system. We focus on whether needs are Unmet or Undermet. These are defined as follows:
- An Unmet Need is present when a claimant receives no ADL or IADL assistance but feels that they could use help;
- An Undermet Need is present when a claimant receives assistance performing a particular activity but indicates that they could use more help or believes that they had to wait too long to receive the help.
The presence of a reported Unmet Need may reflect individuals' lack of comfort performing a particular ADL, their unwillingness to use available care, or their inability to access the type of care that they want or need. It may also reflect the lack of responsiveness of the formal service system to client needs.
In contrast, the presence of an Undermet need may reflect the fact that caregivers are not available in a timely manner. This can result from scheduling difficulties or because, once in the home, caregivers are not providing the care when it is needed. Additionally, it may be that caregivers do not provide an adequate level of care either because of quality or coordination issues.
Figure 23 shows that for the vast majority of claimants, their needs are being met by the service system. In total, 35% of claimants report an unmet or undermet need in at least one ADL or IADL activity. Many of these same individuals also report that their policy is not meeting their current care needs.
| FIGURE 23: Met, Unmet and Undermet ADL and IADL Needs |
| SOURCE: 1999 National Claimant Study (n=695 claimants). |
The most commonly reported unmet need is in toileting. This makes sense given the highly personal nature of the activity and a general reluctance among individuals to ask for assistance, even when they do not feel fully confident on their own. The ADL with the highest level of reported Undermet need was bathing. This again is not surprising given the complexity of the activity and the greater chance for mismatch between service schedules and claimant preferences. Finally, those most likely to report unmet or undermet needs are unmarried women and individuals with multiple caregivers.
| FIGURE 24: Relationship Between ADL Loss and Unmet and Undermet ADL Need |
| SOURCE: 1999 National Claimant Study (n=695). Differences are significant at the .001 level. |
Figure 24 shows the relationship between the number of ADL limitations and the proportion reporting unmet and undermet needs. As the number of ADL limitations increases, the probability of reporting an unmet need declines. Put another way, the more disabled are getting their needs met. Regarding undermet needs, the exact opposite pattern emerges: those with greater disability also report more undermet need. This may reflect the difficulty of scheduling multiple caregivers who also have to provide service to individuals with multiple needs.
The presence of unmet and undermet need gives rise to a key question: Are caregivers present in the homes of claimants long enough to meet their needs? A review of service schedules reveals that, on average, those reporting unmet ADL needs receive 12 hours a week of formal ADL care in spite of the fact that caregivers are present in their homes for up to 30 hours a week. Put simply, care is available but not being fully utilized or provided.
A somewhat different picture emerges for those reporting undermet ADL needs. Here individuals who receive more hours of ADL assistance are also more likely to report greater undermet need. This is particularly true for individuals who rely more on informal rather than formal caregivers.26 This suggests that when multiple caregivers are involved in the care of an individual, clearly delineated lines of responsibility may be particularly important in assuring that needs are met. One implication of these findings is that training informal caregivers may better prepare them to respond to the multiple needs of their disabled care receivers.
Finally, policy design parameters such as daily benefit amount, duration of coverage, or inflation protection did not influence whether or not an individual reported unmet or undermet needs. The disability policy design was, however, associated with lower levels of reported unmet and undermet need.27
Clearly, long-term care insurance is succeeding in bringing formal caregivers into the homes of disabled elders, allowing many to remain in the community. Many rely solely on the insurance to provide access to care. The majority of claimants do not report unmet or undermet needs. Yet problems with service availability, scheduling, continuity and coordination of caregivers, claimant preference and the quality of caregivers all contribute to a sizeable minority reporting unmet and undermet needs.
H. Comparing Privately Insured and Non-Privately Insured Community-Dwelling Disabled Elders
Socio-Demographic Characteristics
A primary purpose of this study is to compare privately insured disabled elders, most of whom receive benefits under their LTC policies, to disabled elders who do not have private insurance protection. Information on this latter group is available from the 1994 NLTCS. But the criterion for inclusion in the 1994 NLTCS, a limitation in one or more IADLs or ADLs, is more liberal than the criteria for inclusion in the privately insured claimant sample -- service use among individuals with two or more ADL limitations or cognitive impairment. To enable meaningful, direct comparisons of the two populations, we need to make the two samples roughly comparable. We do this by applying the same minimum disability threshold to both the 1994 NLTCS and the 1998 privately insured sample and by including in the claimant sample policyholders who may be disabled in two or more ADLs or may be cognitively impaired but not yet making a claim on their policy.
The criteria that are applied to individuals in both samples include being:
- disabled in at least two out of six activities of daily living that require some level of human assistance;28or
- cognitively impaired as measured by the Short Portable Mental Status Questionnaire (SPMSQ);29or
- diagnosed with dementia or Alzheimer's disease.
| FIGURE 25: Differences in Socio-Demographic Characteristics of Disabled Elders by Insurance Status |
| SOURCE: 1999 National Claimant Study (n=583). For income, n=483. 1994 NLTCS data (n=1357). For education variable, n=1276 in NLTCS. NOTE: Differences are significant at the .05 level. |
Once these minimum disability selection criteria are applied, the samples can then be compared one to the other on all dimensions related to formal and informal service use. All subsequent analyses are based on sub-samples that reflect this underlying minimum disability threshold. The NLTCS sub-sample is comprised of 1357 individuals (out of 4,167) and the claimant sub-sample is comprised of 581 individuals (out of 691). Figure 25 shows the major differences between the socio-demographic profile of privately insured and non-privately insured disabled elders.
Clearly, there are stark differences between the two groups on some variables but there are also similarities on others. For example, both groups are primarily female (66%), are roughly the same age (mean of 79 years) and currently not married -- 52% of the privately insured and 56% of the non-privately insured. Disabled elders with private insurance are more likely to live alone and not have children living nearby. They are also four times more likely to have some college education, eight times more likely to have incomes greater than $30,000, and are overwhelmingly white. Because the privately insured are less likely to have children or potential caregivers living with them or nearby, it is likely that they may view future LTC policy benefits as compensation for the unavailability of informal supports.
Disability Status
The common measures of functional status -- ADLs and IADLs -- are used to compare the functional status of the two samples (See Figure 26 below). As shown, the privately insured sample has more functional limitations than does the non-privately insured sample: 3.8 ADL and 7.3 IADL limitations compared to an average of 2.8 ADL and 5.8 IADL limitations. Not shown in the figure is the fact that these privately insured individuals have been ADL dependent for an average of about 2 years, whereas the non-insured individuals have been ADL dependent for closer to 3 years.
| FIGURE 26: Functional Status by Insurance Profile |
| SOURCE: 1999 National Claimant Study (n=587 and 1994 NLTCS data (n=1357). NOTE: Differences are significant at the .001 level. |
Although not shown in the figure, the privately insured not only have a greater number of ADL dependencies, but also require more intensive care. In general there are two types of care to compensate for ADL dependency: (1) cueing or stand-by assistance and (2) hands-on assistance. Our analysis showed that for the most common ADL losses (e.g. bathing and dressing), the privately insured sample needs much greater hands-on assistance than does the non-privately insured sample. This suggests a higher level of need among the privately insured.
The biggest difference in disability between the two populations relates to cognitive impairment. As shown in Figure 27, disabled individuals without private insurance are about 1.4 times more likely to be cognitively impaired than are those with private insurance. In fact, the median number of SPMSQ errors for the privately insured sample is 2.0, whereas for the non-privately insured sample, the figure is 4.0.
| FIGURE 27: Cognitive Status by Insurance Profile |
| SOURCE: 1999 National Claimant Study (n=456) and 1994 NLTCS data (n=1357). NOTE: Differences are significant at the .001 level. |
To complete the disability profile, we segmented each group according to whether they were exclusively physically disabled (i.e. ADL impaired), cognitively disabled (i.e. SPMSQ score and cognitive-related diagnosis), or both. Figure 28 summarizes results.
The differences are striking. The privately insured are much more likely to be physically impaired, while the non-insured are much more likely to suffer cognitive impairment. These findings suggest that either:
- Those with private insurance who are cognitively impaired are less likely to be observed in the community because they have fewer available supports to care for them; or,
- the underwriting screens that individuals must pass before being issued a policy identify individuals who may be at future high risk for cognitive impairment. Therefore, the selection effect reduces the prevalence of cognitive impairment among the insured population.
| FIGURE 28: Aggregate Disability Profile by Insurance Status |
| SOURCE: 1999 National Claimant Study (n=456) and 1994 NLTCS data. This is based on the sample of individuals for which complete SPMSQ data was available. NOTE: Differences are significant at the .001 level. |
Use of Informal and Formal Care
Figure 29 shows that 89% of the non-privately insured rely on some level of informal care compared with 79% of the privately insured. Moreover, the privately insured are five times more likely to rely exclusively on formal care than those without private insurance. This finding supports the hypothesis that private insurance is used to compensate for a lack of available informal support or replace informal care provided by certain types of caregivers such as children or non-relatives (See Figure 30)
| FIGURE 29: Types of Care Received by Insurance Status |
| SOURCE: 1999 National Claimant Study (n=587) and 1994 NLTCS data (n=1357). NOTE: The less than 1% relying on informal help only are the few policyholders who are disabled but not making a claim on their policy. |
Not shown is the fact that the privately insured also have more caregivers: 2.7 as compared to 2.1 for the non-privately insured. The relative lack of informal caregivers for the privately insured sample is more than made up for by the presence of multiple formal caregivers.
Figure 30 below shows the relationship of the primary informal caregiver to the disabled individual. The primary informal caregiver is defined as the individual who helps the person the most with their ADL and IADL activities. Typically this is the individual who spends the greatest amount of time helping the disabled individual with ADLs.
| FIGURE 30: Providers of Informal Support by Insurance Status |
| SOURCE: 1999 National Claimant Study (n=461) and 1994 NLTCS data (n=1209). NOTE: Differences are significant at the .05 level. |
It is striking to note that even though the proportion of married individuals in the two samples is similar, the majority of informal caregivers for the privately insured are spouses, whereas for the non-privately insured relatives other than a spouse provide the bulk of care. Still, spouses represent the single largest category of informal caregiver for both groups. This finding suggests that where formal care does substitute for informal care, the substitution is selective; that is, it appears as if the formal care financed by insurance benefits may substitute for the care provided by adult children but not necessarily for the care provided by a spouse. This accords with previous research indicating that a primary motivation for the purchase of private LTC insurance is to "avoid being a burden on family members" (Cohen and Kumar, 1995). Data here suggests that the family members focused on are adult children, typically daughters and daughters-in-law.
Both public and private insurance programs are designed to pay for a variety of services in the community, including home health aide services, nursing care, personal care attendants, and homemakers. While most private LTC insurance covers all these services, public programs may be somewhat more restrictive. It is important to note that for the non-privately insured, the only specific home care utilization information available in the 1994 NLTCS is for Medicare-reimbursed services. We do not have information about specific services that are funded by Medicaid or are purchased privately. We do know, however, the payment sources for all formal care service. This information will be reported below.
Figure 31 shows that the majority (70%) of individuals with private LTC insurance uses unskilled services, such as home health aides and homemaker services. In contrast, among the non-insured disabled, skilled nursing services remain the most prevalent form of Medicare-funded service.30 Taken together, these findings suggest that a greater proportion of the privately insured population is accessing more skilled service. Such services may be designed to address post-acute and recuperative care needs, in addition to any chronic-care needs.
| FIGURE 31: Providers of Formal Care by Insurance Status |
| SOURCE: 1999 National Claimant Study (n=587) and 1994 NLTCS data (n=1357). |
Figure 32 shows the average number of hours of ADL and IADL assistance provided to privately and non-privately insured disabled individuals. A number of important points can be gleaned from this figure. First, the privately insured disabled population receives an average of 2 hours more per day of ADL and IADL assistance than does the disabled population without private insurance. Much of this is attributable to the receipt of formal services. It also reflects the fact that the privately insured sample is somewhat more disabled. Second, while about 63% of all ADL assistance to the privately insured is provided by formal caregivers, the figure is only 30% for the non-privately insured. Finally, the non-insured population is much less likely to use formal caregivers for IADLs; in fact informal caregivers provide 80% of IADL assistance to the non-privately insured whereas only 45% of IADL assistance is provided informally to those with private insurance.
| FIGURE 32: Weekly Hours of Informal and Formal Care by Insurance Status |
| SOURCE: 1999 National Claimant Study (n=587) and 1994 NLTCS data (n=1357). NOTE: Differences are significant at the .05 level. |
Payment Sources for Formal Care
While we cannot discern payment sources for each particular home care service for the two samples, we can identify the payment source for formal care as a whole and thereby compare the distribution of payment sources for home care services. As a starting point, it is important to remember that virtually all individuals in the privately insured sample have LTC policies, and the majority (more than 70%) do not pay anything out-of-pocket for formal care services. We found that Medicare is not a particularly important payment source for the privately insured, in contrast to the non-privately insured where roughly 30% of disabled elders use Medicare as a payment source for home care services (Figure 33).31
Medicaid payments play no role in financing the long-term care needs of the privately insured population. This is not surprising given the income profile of this population. A small percentage of the insured population does use additional insurance -- primarily Medicare Supplement policies -- to pay for certain types of home care services. In particular, it appears that such insurance is used to pay for the costs of nursing services.
| FIGURE 33: Payment Sources for Home Care Services by Insurance Status |
| SOURCE: 1999 National Claimant Study (n=586) and 1994 NLTCS data (n=1357). |
Finally, although they all had LTC policies, about 9% of the privately insured were unsure of how their services were being paid for. In most of these cases, the disabled individuals were receiving money management assistance from their primary caregiver.
V. SUMMARY AND IMPLICATIONS
Without question, the presence of long-term care insurance has increased the amount of hands-on and stand-by ADL and IADL assistance to disabled claimants. For many, the ability to access formal care services through their long-term care policies is what enables them to remain at home. This is because a disproportionate number of claimants have no available informal support services. Even among claimants with informal supports, the availability of insurance benefits has not led to a "breakdown" in informal caregiving by primary caregivers. On the contrary, most primary informal caregivers have not decreased the amount of care that they provide to their disabled relatives. For those who have, they indicate that they are now able to spend time "just being together" rather than providing direct services. This most likely reflects the type of relationship that existed prior to the claimant becoming disabled. Not surprisingly, informal caregivers overwhelmingly supported the proposition that having long-term care insurance pay for formal care has reduced the stress associated with informal caregiving. Taken together, these findings suggest that in the private insurance context, formal care may substitute for some, but not most informal care, and that the two systems appear to be working in tandem to meet the needs of claimants.
About half of claimants and informal caregivers indicated that in the absence of insurance benefits, institutional alternatives would likely be sought. Typically, claimants felt that they would have to enter an assisted living facility or a nursing home if they could no longer access their benefits. This is a particularly important finding and suggests that as more individuals purchase policies, the demand for institutional care may be delayed or actually diminished. From the point of view of companies marketing these products, the policies are doing what they are supposed to: enabling people to live independently in their homes for as long as possible. The challenge is to assure that the formal service system is able to respond to the growing demand for services.
Findings also suggest that while having private insurance has enabled claimants to receive care in their homes, problems exist with the way that it is being delivered and used. Put simply, it appears that, even with insurance, disabled claimants are reluctant to ask for help with specific -- and often more personal -- activities of daily living. Thus, formal caregivers may be in the homes of disabled claimants who refuse to ask for help, even when they feel it is needed. Alternatively, it is important to note that it is extremely difficult to monitor what actually happens when these caregivers, most of whom are paraprofessionals, work with disabled elders. Data suggests that some of these caregivers are not providing services to respond to specific types of claimant needs, even as other needs are being met.
When multiple formal and informal caregivers are involved in the care of a claimant, issues related to undermet need are more likely to arise. This can occur because of a lack of coordination of service schedules or because of unclear lines of responsibility between caregivers. Moreover, in some cases it is difficult to coordinate the service schedules of providers with the care expectations of claimants. Finally, in some cases, the actual care provided by formal and informal providers may not be perceived to be adequate by the claimant.
These issues all suggest that claimants could benefit from care coordination or care management services. Over the past few years, more policies do cover such services. In some cases, the insurance company pays for them as an administrative expense. In other cases, the cost of these services is charged to the policyholder's benefit account. Either way, there is a growing recognition that working with and navigating the formal service delivery system presents unique challenges to disabled claimants and their families. As insurers begin to differentiate themselves on a customer-service rather than product basis, it will become increasingly important to work with families to coordinate and manage the formal and informal service delivery system.
Another implication relates to actual policy design. Most policies have maximum daily limits on benefits. However, given the nature of service schedules, it is possible that an individual incurs no or low expenses on certain days and relatively high expenses on other days. In some cases, these expenses may exceed the established daily benefit cap. To accommodate the reality of variable service schedules, insurers may want to move away from daily benefit caps or budgets, toward weekly or monthly benefit budgets. A number of insurers are already experimenting with this promising approach. Results from this study suggest that as more companies begin to move in this direction, the reported amount of undermet need should decline.
The overwhelming majority of claimants are satisfied with their policy and with their interaction with the insurance company. Given that most companies are only beginning to gain experience in managing claims, this is a particularly positive finding. Still, there was a sizeable minority of claimants who felt that the insurance companies could be doing more on their behalf. In particular there was a sense among some that companies needed to improve customer service, provide more advice about how to use policy benefits,32 and process claims more efficiently. Also, companies need to continue to invest in their technological capacities to assure that claims processing can occur rapidly and accurately.
Roughly one-third of claimants felt that they had not purchased enough home care benefits. Given that most policies cover three to four years of care, and the average claimant has been receiving benefits for slightly more than a year, this deficiency is related to the daily benefit amount chosen at the time of purchase. While this does not represent an inherent flaw in insurance policy design, it does suggest that these claimants may not have had enough information on the actual costs of care that they might incur. (The issue is not related to affordability. Income level was not related to whether or not claimants' felt that they had purchased enough home care coverage.) This finding may also be a response to the actual effect of voluntary coinsurance. The implication is that additional consumer education is needed to assure that at the time of purchase, individuals have an understanding of the relationship between benefit amounts and costs of care.
Long-term care insurance benefits are well targeted. The vast majority of individuals has significant ADL dependencies or is cognitively impaired. More than half has over four ADL limitations. Even those, who at the time of the interview, did not meet HIPAA benefit eligibility triggers were either eligible at the time that they applied for benefits or were likely to become eligible in the very near future. Compared to other claimants, those not meeting HIPAA triggers are older and much less likely to have informal supports available. Most also have at least one ADL limitation and multiple IADL limitations including an inability to manage medications. Their profile characterizes what most professionals would consider to be a "long-term care eligible" population.
Given the fact that even among chronically disabled elders there is a great deal of change in functioning over time, it is not surprising that a "snapshot" reveals some individuals who are not HIPAA eligible. Insurers conduct reassessments of home care claimants only intermittently. Moreover, few if any of these individuals appeared to be perpetrating fraud; the need for assistance was present in almost all cases. Finally, some of the claimants may be benefit eligible from "grandfathered" policies that include medical necessity as a benefit trigger. Thus, it appears that while not perfect, the HIPAA triggers are indeed targeting benefits to the appropriate individuals. From a consumer protection standpoint, the standardization of benefit triggers and resultant reduction in consumer confusion must be weighed against the fact that any trigger will, at the margin, exclude some small number of individuals who need services.
The population of claimants differs in many important respects from the non-privately insured disabled population. Even so, there are a number of observations about patterns of formal and informal support among claimants that do have public policy implications. First, there is a very low rate of Medicare home health usage among the privately insured. Second, individuals with disability policy designs were more satisfied with their insurance and had fewer reported unmet and undermet needs. At the very least this suggests that programs designed to enhance consumer autonomy may be particularly effective in meeting client need. Finally, the lack of consumer fraud suggests that it is possible to establish measurable benefit triggers that most individuals can understand and adhere to. The notion that privately insured disabled elders are eager to access their insurance benefits and use them as quickly as possible is not borne out by the data; most claimants are not using their maximum daily benefit amount on home care. Together the combination of benefit design parameters (e.g. benefit caps and limits) and consumer preferences (i.e. desire to use both informal and formal care for personal care activities) assures that in the privately insured context moral hazard is minimized.
As the market continues to grow and mature, a new wave of claimants will begin to access benefits. Given the changes in the service delivery system as well as the innovations in policy designs, new patterns of service utilization will likely emerge. Still, some facets of these patterns will remain the same. Expansion in the private market is likely to lead to reductions in public expenditures on long-term care and the insurance is likely to continue to help disabled individuals remain in their homes at the same time as it maintains and enhances the resiliency of informal support networks.
NOTES
-
To be included in the comparison sample, the privately insured and non-privately insured had to meet a minimum disability threshold of at least two of six ADL limitations or be cognitively impaired.
-
There has been a growing trend toward trying to capitate Medicaid.
-
A companion study is being completed with privately insured claimants residing in nursing homes and in assisted living facilities.
-
These disabled "non-claimants" are included in the sample only in comparative analyses with the 1994 National Long-Term Care Survey.
-
An individual is considered to be dependent in an ADL if he/she requires stand-by or hands-on assistance to perform the particular activity.
-
In fact, more than 90% of policies currently being sold in the market use these benefit trigger definitions. This is in part driven by the fact that in order to be tax qualified, a long-term care insurance contract must employ these standardized benefit triggers.
-
The primary informal caregiver is the one identified by the claimant as the one who provides the most ADL and IADL assistance.
-
It is important to note that only in recent years has the volume of home health care claims grown significantly. For the most part, few carriers have garnered significant experience on home health care claims.
-
For more detail on the sampling frame of the 1994 National Long-Term Care Survey see Manton et al, (1997). Chronic Disability Trends in Elderly United States populations: 1982-1994. Procedures of the National Academy of Science, Volume 94 Pages 2593-2598, March 1997.
-
These differences across companies were statistically significant at the .05 level.
-
This is typically the "cut-off" point that is used in public and private insurance program to define an individual as being cognitively impaired.
-
There is a statistically significant difference across companies in the proportion of claimants with cognitive diagnoses. The differences are significant at the .10 level.
-
Note that these differences across companies were statistically significant at the .05 level.
-
It is important to note that because we are taking a cross-sectional sample, we are less likely to observe very short claims, that is, those that may be more post-acute in nature. Thus, there may be more claimants who receive benefits for post-acute care -- nursing care -- than what is suggested by this sample.
-
Personal Communication with Pamela Doty, Office of the Assistant Secretary for Planning and Evaluation, Office of Disability, Aging and Long-Term Care. February 11, 1999.
-
This assumes that private insurance benefits have not been exhausted.
-
For more information on Medicare home health care utilization see Leon et al. (1997). Understanding the Growth in Medicare's Home Health Expenditures. The Kaiser Medicare Policy Project, the Henry J. Kaiser Family Foundation.
-
Note that in this study the average amount of time claimants held their policies was 3 years. Thus, compared to the average age of current purchasers, the claimant cohort studied here represents "older" buyers.
-
Differences were statistically significant at the .001 level.
-
An exception is disability policies.
-
These differences across companies were significant at the .10 level.
-
These differences between companies were significant at the .05 level.
-
These differences across companies were statistically significant at the .05 level.
-
For additional information on the role played by private LTC insurance in the care of disabled elders and their families, see Appendix 1 which summarizes the experience of four individuals in the sample. These qualitative descriptions or "vignettes" are meant to provide contextual information for the quantitative findings presented in this section.
-
Note that a separate companion report entitled "Informal Caregivers for Disabled Elders with Long-Term Care Insurance: Their Characteristics and Behaviors" provides more detailed information on these issues.
-
Differences are significant at the .05 level.
-
Differences were significant at the .05 level.
-
The ADL activities include bathing, dressing, toileting, transferring, continence management, and feeding. A disability is present if an individual requires stand-by, cueing, or hands-on assistance.
-
Having 4 or more errors on the SPMSQ.
-
It is important to note that among the non-privately insured, in order to access Medicare funding for unskilled services, individuals must also be under the care and supervision of a skilled nurse. Thus, it may be that many of these individuals are not receiving hands-on nursing care.
-
For more detailed information on the use of Medicare home health services among chronically disabled elders see Jackson, B. and Doty, P. (1999). Medicare Home Health Services 1989-1994: Patterns of Benefit Use Among Chronically Disabled Elders. Office of the Assistant Secretary for Planning and Evaluation, Division of Aging, Disability and Long-Term Care Policy, U.S. Department of Health and Human Services, Washington, D.C. [http://aspe.hhs.gov/daltcp/reports/medhhs.htm]
-
Some of the newer policy design changes that incorporate greater care management as well as information and referral services may assist claimants in the effective use of benefits.
REFERENCES
AARP (1998). Medicaid and Long-Term Care for Older People. AARP Public Policy Institute, Washington, D.C.
AARP (1997). Out-of-Pocket Health Spending by Medicare Beneficiaries Age 65 and Older: 1997 Projections. AARP Public Policy Institute, Washington, D.C.
Cohen, M. and Kumar, N. (1996). "The Changing Face of Long-Term Care Insurance in 1994: Profiles and Innovations in a Dynamic Market. Inquiry.
Cohen, M, Tell, E. Greenberg, J. and Wallack, S. (1987). The Financial Capacity of the Elderly to Insure for Long-Term Care. The Gerontologist, Volume 27.
Crown, W. Leutz, W. and Capitman, J. (1992). Economic Rationality: The Market for Private Long-Term Care Insurance, and the Role for Public Policy. The Gerontologist, Vol. 32.
Friedland, R. (1990). Facing the Costs of Long-Term Care. Washington, D.C: Employee Benefit Research Council.
Garber, A.B. and MaCurdy, T. (1989). Predicting Nursing Home Utilization among the High Risk Elderly. National Bureau of Economic Research. Cambridge Massachusetts.
Greene, V., Lovely, M., Ondrich, J. (1993). The Cost-Effectiveness of Community Services in a Frail Elderly Population. The Gerontologist, Volume 33, No. 2.
Health Insurance Association of America (1998). Term Care Insurance in 1996: Research Findings, Washington, D.C.
Health Insurance Association of America (1995). Term Care Insurance in 1994: Profiles and Innovations in a Dynamic Market, Washington, D.C.
Health Insurance Association of America (1992). Who Buys Long-Term Care Insurance? Washington, D.C.
Jackson, B. and Doty, P. (1999). Medicare Home Health Services 1989-1994: Patterns of Benefit Use Among Chronically Disabled Elders. Office of the Assistant Secretary for Planning and Evaluation, Division of Aging, Disability and Long-Term Care Policy, U.S. Department of Health and Human Services, Washington, D.C. [http://aspe.hhs.gov/daltcp/reports/medhhs.htm]
Kane, R. (1998). Examining the Efficiency of Home Care. Unpublished manuscript submitted to the Home Care Research Initiative, University of Minnesota.
Leon, J. Neuman, P. and Parente, S. (1997). Understanding the Growth in Medicare's Home Health Expenditures. The Kaiser Medicare Policy Project, The Henry J. Kaiser Family Foundation.
Rivlin, A, Wiener, J. Hanley, R. and Spence, D. (1988). Caring for the Disabled Elderly: Who will Pay? Washington, D.C. Brookings Institution.
Shapiro, E. and Tate, R.B. (1988). Who is Really at Risk of Institutionalization. The Gerontologist, Volume 28.
United States Department of Commerce, Bureau of the Census: Statistical Abstract of the United States, 1994.
United States Department of Commerce, Bureau of the Census: Money Income in the United States: 1997. Washington, D.C..
United States Department of Commerce, Bureau of the Census: Educational Attainment in the United States: March 1998 Washington, D.C.
Weissert, W. (1985). Seven Reasons why it is so Difficult to Make Home and Community-Based Care Cost Effective. Health Services Research, 20.
Weissert, W. and Cready C. (1989). Toward a Model for Improved Targeting of Aged at Risk of Institutionalization. Health Services Research, 24.
Wiener, J. Illston, L. and Hanley, R. (1994). Sharing the Burden: Strategies for Public and Private Long-term Care Insurance Washington: Brookings Institution.
Wolf, D. (1997). Efficiency in the Allocation and Targeting of Community-Based Long-Term Care Resources. Unpublished manuscript submitted to the Home Care Research Initiative. Syracuse University.
APPENDIX 1: QUALITATIVE DESCRIPTION OF FOUR FAMILIES USING THEIR LTC BENEFITS
Case #1: Mr. and Mrs. Adams
Before Mr. Adams, age 77, had a stroke and developed severe knee problems, he and his wife were living comfortably in retirement. Due to his deteriorating health, the family quickly sold their business and decided to drastically change their living situation. The couple now lives in a small first floor apartment in a suburb of Boston.
Both Mr. and Mrs. Adams were present for the in-person interview. Though Mr. Adams passed the mental status questionnaire, he did become quite confused during the interview. His ADL limitations were bathing, dressing, transferring, toileting and continence. He also needed assistance in all IADLs.
Paid help is in the home each night for nine hours so that Mrs. Adams, age 74, can get some sleep. Mr. Adams is a fairly large man and his wife, who is quite small, takes care of the majority of his needs during the day. A cleaning person also comes in weekly to do housework and laundry.
Both husband and wife state they are satisfied with the policy but need additional help. They can't afford help during the day and state they desperately need it. It appears that long-term care insurance benefits make the difference in Mr. Adams' ability to remain at home. It is a much needed supplement to, rather than a replacement for, informal care-giving. Mrs. Adams stated that they would not be able to afford the amount of paid care they are currently receiving and Mr. Adams would need to seek assisted living care if they did not have the long-term care insurance benefit.
I then spoke privately with Mrs. Adams about how she is coping with the situation. Though they have six children, five of which are close by, she refuses to accept help from them stating they have their own lives and children to take care of. Mrs. Adams stated that she is doing "all right, but I'm very tired". Even with the help during the night she estimated that her sleep is interrupted five times each night. Mrs. Adams stated that it doesn't really matter how she feels because he is her husband and needs the help. She actually stated it is better this way than if it was her that was ill because she doesn't think he would be able to take care of both of them. Mrs. Adams did say that privacy is an issue, as the only time Mrs. Adams gets to herself is when she does weekly grocery shopping.
While discussing the role of the long-term care insurance benefits, Mrs. Adams said that having it in place definitely decreases the amount of stress and emotional difficulty she has with providing care for her husband. Though she stated that the amount of care she provides has increased since the benefits began, Mrs. Adams explained that while the paid help remains the same, over time her husband's health continues to worsen and she must compensate with more assistance.
In summary, Mr. and Mrs. Adams are very glad to have their long-term care benefits. Though Mrs. Adams still does a large amount of the care giving, the paid help is the supplement needed to keep the couple living in their own home.
Case #2: Mrs. Collins and her daughter-in-law, Jane
Mrs. Collins is an 81-year-old widow with one son and daughter-in-law who live fifty miles away. Mrs. Collins suffers from dementia and was, therefore, unable to participate in the interview. This interview was conducted over the phone with her daughter-in-law, Jane.
Jane describes her mother-in-law as a person who refuses to acknowledge any physical limitations. Because of this, Mrs. Collins refuses to use a much-needed walker as well as physical assistance with most ADLs. For example, Mrs. Collins insists on dressing herself. She usually puts on soiled clothes that are inappropriate for the time of year. The only activity of daily living with which she allows help is bathing. She does require and accepts help with all IADLs.
Mrs. Collins receives the majority of her help from a personal care attendant, five hours per day, seven days per week. Jane helps mostly with outdoor mobility, going places outside walking distance and money management.
Jane explains that the family is satisfied with the policy and found the claim process very easy. The concern is that Mrs. Collins needs twenty-four hour supervision and the family can't afford it. She states when the family bought the policy (on Mrs. Collins' behalf) they were looking for what they could afford to pay in monthly premiums rather than investigating the potential price of home care.
Currently benefits pay for 35 hours of care per week. Though Jane is concerned about the need for more care she states Mrs. Collins would not be able to afford the amount of care she is currently receiving if she did not have her long-term care benefits. If this care was not in place, Jane states she is certain her mother-in-law would be placed in an assisted living facility.
I then spoke with Jane about the impact this situation is having on her life. Jane is a fifty-five year old woman who works as an office manager. She has had to miss work without pay in the past in order to care for her mother-in-law. Just recently, she was out for two weeks. Though Jane states caring for her mother-in-law is hard on her emotionally, she doesn't feel that it impacts her health or time with her family. In fact, she states that having the insurance benefits in place allows her to spend less time on daily activities for Mrs. Collins and allows for more time just to visit with her.
As we concluded our interview, Jane stated that if they hadn't invested in the long-term care insurance her mother-in-law would probably have to move into their home while they looked for an appropriate placement. She explains that at this point she is grateful that they don't have to do that, but is concerned for the future as Mrs. Collins' health continues to deteriorate.
Case #3: Mr. and Mrs. Baker and their son, Edward
Mr. and Mrs. Baker (ages 81 and 73) are husband and wife, both receiving home care benefits. Mr. Baker has been diagnosed with Alzheimer's disease and Mrs. Baker has cancer. Their son, Edward (age 37) was present for both interviews and moved in with his parents in 1996 to oversee their care. Both Mr. and Mrs. Baker need assistance in most ADLs and all IADLs. The husband receives six hours of help five days per week from a home health aid, while his wife receives eight hours of help six days per week.
Edward was able to separate his two parents' experiences in regards to both the care he provides for each of them as well as interactions with the insurance company. Though he has experienced some difficulty with his mother's policy, Edward reports an easier time with his father's.
The son first talked about his father. Edward estimated that he spends about twenty-eight hours each week caring for his father. The interaction with the insurance company on his father's behalf has been a positive experience. Though he stated it was somewhat difficult to obtain benefits, there had been no disagreements or difficulties with his father's coverage. It is clear from his son's responses, that Mr. Baker needs more care and supervision in comparison to his wife. Edward states that his father would receive less hours of paid care and would have to seek institutional living if not for the insurance benefits.
Edward then spoke of his mother. He estimated helping her 25 hours per week. When asked about his dealings with the long-term care insurance company on her behalf, Edward explained that though it was very easy to file a claim, it was somewhat difficult to obtain benefits. He stated he has had difficulty with customer service and there are previous disagreements that have yet to be resolved to his satisfaction. Edward voiced that even without long-term care benefits he would be able to attend to his mother's needs in the home, with the acknowledgement that he would need more help from family, friends and volunteers.
Edward and I then talked about how caring for both of his parents impacted his life. It was clear that Edward's job had been impacted significantly by his parents' illness. As an insurance broker, he usually works forty hours per week. Edward explained that he would very much like to work more hours but he can't due to his parents' needs. He also reports missing hours of work at a time, without pay, when emergencies arise. Edward constantly has to rearrange his schedule and reported even having to quit and turn down jobs because of his responsibility for his parents. His care-giving schedule has also kept him from looking for employment.
With all of these responsibilities, Edward reported that helping his parents did not bother him, nor was it hard on him emotionally. He did not feel that these added responsibilities effected his personal life, free time or privacy, though he does have to give them almost his constant attention, even when he, himself, is ill.
Case #4: Mrs. Goldman (Non-HIPAA disabled claimant)
Mrs. Goldman is an eighty-four year-old woman living on her own with no informal caregivers available. Her main reason for needing long-term care is cardiac problems, but she is also recovering from a stroke.
Mrs. Goldman stated that she is in fair health. She reported being independent with all ADLs but has an unmet need for help with bathing. Mrs. Goldman receives help with housework, laundry, meal preparation, grocery shopping and outdoor mobility but states she needs more help. She talked about only one care giver, a paid personal care attendant. This person helps with IADLs in the home three days per week for four hours each day.
We then talked about the role of long-term care insurance in Mrs. Goldman's situation. She reported that long-term care insurance benefits pay for all of the care she is currently receiving. Mrs. Goldman stated she was certain that she would not be able to afford the care she receives if not for her insurance benefits. Though unsure of where she would go, Mrs. Goldman explained she would have to move out of her own home and seek the assistance of family, friends or volunteers if she did not have the long-term care policy.
Finally, Mrs. Goldman explained that she was somewhat satisfied with her policy, but suggested she would have liked the insurance company to help her when she had to fill out the initial claims paperwork. Overall, this claimant reported to be satisfied with the claims process and the amount of coverage she chose.
To obtain a printed copy of this report, send the full report title and your mailing information to:
U.S. Department of Health and Human ServicesOffice of Disability, Aging and Long-Term Care PolicyRoom 424E, H.H. Humphrey Building200 Independence Avenue, S.W.Washington, D.C. 20201FAX: 202-401-7733Email: webmaster.DALTCP@hhs.gov
RETURN TO:
Office of Disability, Aging and Long-Term Care Policy (DALTCP) Home [http://aspe.hhs.gov/_/office_specific/daltcp.cfm]Assistant Secretary for Planning and Evaluation (ASPE) Home [http://aspe.hhs.gov]U.S. Department of Health and Human Services Home [http://www.hhs.gov]
ASSESSMENT OF HOME CARE AND NURSING HOME/ASSISTED LIVING FACILITY BENEFITS USED BY HOLDERS OF PRIVATE LONG-TERM CARE INSURANCE
Other Reports Available
A Descriptive Analysis of Patterns of Informal and Formal Caregiving among Privately Insured and Non-Privately Insured Disabled Elders Living in the Community Executive Summary http://aspe.hhs.gov/daltcp/reports/ifpattes.htm HTML http://aspe.hhs.gov/daltcp/reports/ifpattrn.htm PDF http://aspe.hhs.gov/daltcp/reports/ifpattrn.pdf
Informal Caregivers of Disabled Elders with Long-Term Care Insurance Executive Summary http://aspe.hhs.gov/daltcp/reports/icdeltes.htm HTML http://aspe.hhs.gov/daltcp/reports/icdeltci.htm PDF http://aspe.hhs.gov/daltcp/reports/icdeltci.pdf
Multivariate Analysis of Patterns of Informal and Formal Caregiving among Privately Insured and Non-Privately Insured Disabled Elders Living in the Community Executive Summary http://aspe.hhs.gov/daltcp/reports/2000/multanes.htm HTML http://aspe.hhs.gov/daltcp/reports/2000/multanal.htm PDF http://aspe.hhs.gov/daltcp/reports/2000/multanal.pdf
The Use of Nursing Home and Assisted Living Facilities Among Privately Insured and Non-Privately Insured Disabled Elders Executive Summary http://aspe.hhs.gov/daltcp/reports/2000/nhalfues.htm HTML http://aspe.hhs.gov/daltcp/reports/2000/nhalfuse.htm PDF http://aspe.hhs.gov/daltcp/reports/2000/nhalfuse.pdf
