September 2018
Printer Friendly Version in PDF Format (7 PDF pages)
ABSTRACT
This brief describes findings from the ASPE chartbook "Older Adults with Dementia and Their Caregivers: Key Indicators from the National Health and Aging Trends Study".
DISCLAIMER: The opinions and views expressed in this report are those of the authors. They do not necessarily reflect the views of the Department of Health and Human Services, the contractor or any other funding organization.
Dementias, including Alzheimer's disease, frontotemporal, Lewy body, mixed, and vascular dementias, are conditions that affect the health and well-being of the United States population, especially among older adults. As the United States population ages, the prevalence of dementia is expected to grow, placing an increasing burden on people with the condition and their families, as well as the health and long-term care systems.
Using nationally representative data from the 2015 National Health and Aging Trends Study (NHATS) and the National Study on Caregiving (NSOC), we examined the national profile of older adults living in community settings with dementia and their informal caregivers. In 2015, sociodemographic groups were disproportionately affected by dementia. Individuals with the condition received more and different types of care than their peers without dementia. In addition, the amount and burden of informal caregiving was significantly greater for caregivers of people with dementia.
A detailed book of charts displaying the characteristics of the population of people with dementia and their caregivers is available at https://aspe.hhs.gov/basic-report/older-adults-dementia-and-their-caregivers-key-indicators-national-health-and-aging-trends-study.
KEY FINDINGS
More than half (63%) of older adults with dementia were 80 years old and older. The prevalence of dementia among older adults increased with age, from 2% among adults aged 65-69 to 33% among adults aged 90 and older. Despite the similar prevalence of dementia across both genders at all ages, there were more women living with dementia (1.8 million) than men (1.5 million), likely due to differential mortality.
Across all age groups, non-Hispanic Whites were least likely to have dementia, although disparities were greater at older ages. From 65-74, the prevalence of dementia was 2% among non-Hispanic Whites, 5% among non-Hispanic Blacks, 7% among non-Hispanic people of other races, and 3% among Hispanics. Over age 85, the prevalence was much higher among non-Hispanic people of other races (43%), non-Hispanic Blacks (38%), and Hispanics (35%) than among non-Hispanic Whites (22%).
| Dementia was more prevalent among older adults who:
|
Older adults with less than a high school education are significantly more likely to have dementia than older adults with more education. This difference is most pronounced at the younger ages (65-74), but persists across age groups.
| FIGURE 1. Dementia Prevalence by Educational Attainment and Age |
|---|
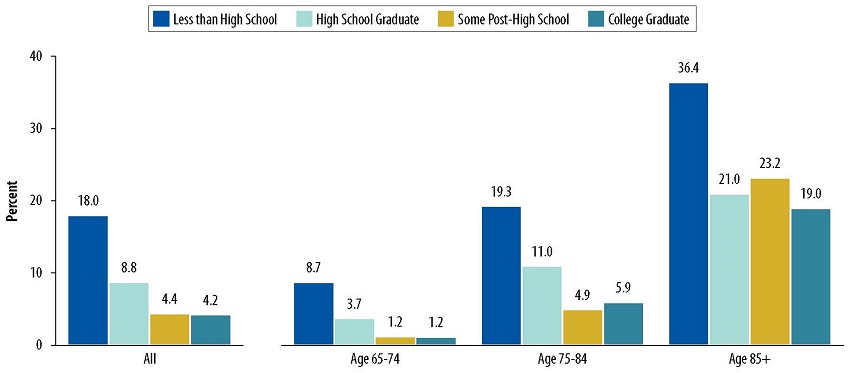 |
| SOURCE: Analyses of 2015 NHATS data conducted by RTI International, 2017. NOTE: For the purposes of the chartbook, only individuals who met the criteria for the NHATS dementia classification (Kasper et al., 2013) of probable dementia were considered to have dementia. This was a conservative definition, because individuals with mild cognitive impairment or those with early stages of dementia (i.e., individuals with possible dementia) are likely to be classified as not having dementia. The estimates presented in the chart were based on older adults living in community settings. Older adults living in nursing homes were excluded. |
People with dementia also have more chronic health conditions and higher rates of depression. Fifty-nine percent of older adults with dementia reported three or more chronic health conditions, compared to 43% of older adults without dementia. Older adults with dementia are four times more likely to report depressive symptoms (24%) than those without dementia (6%).
| FIGURE 2. Distribution of Chronic Conditions among Older Adults with and without Dementia |
|---|
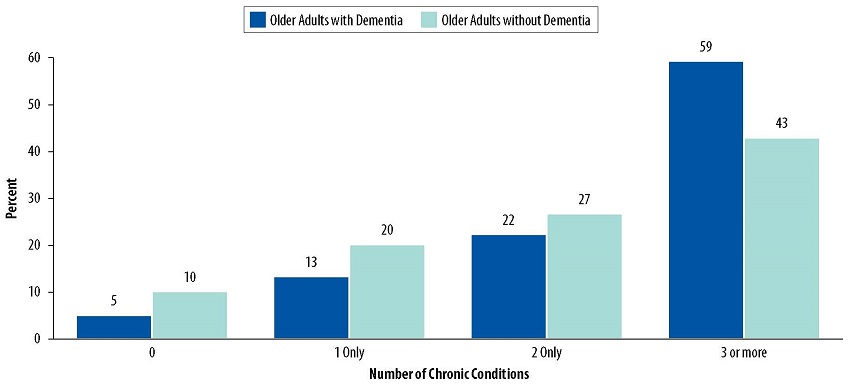 |
| SOURCE: Analyses of 2015 NHATS data conducted by RTI International, 2017. NOTE: Dementia was not included in the list of chronic conditions examined. The chronic conditions examined included heart attack, heart disease including angina or congestive heart failure, hypertension, arthritis including osteoarthritis and rheumatoid arthritis, osteoporosis, diabetes, lung disease, stroke, and cancer. For the purposes of the chartbook, only individuals who met the criteria for the NHATS dementia classification (Kasper et al., 2013) of probable dementia were considered to have dementia. This was a conservative definition, because individuals with mild cognitive impairment or those with early stages of dementia (i.e., individuals with possible dementia) are likely to be classified as not having dementia. The estimates presented in the chart were based on older adults living in community settings. Older adults living in nursing homes were excluded. |
Much higher rates of self-care, mobility, and household activity limitations are reported by people with dementia (88%) compared to those without dementia (43%). Although the prevalence of these limitations increased with age among those with and without dementia, older adults with dementia had consistently higher prevalence of limitations. Assistance with two or more self-care or mobility activities was reported by 64% of people with dementia, but only 19% of people without dementia. Similarly, people with dementia (12%) were much less likely than those without dementia (57%) to need no assistance.
As a result, nearly all (95%) older adults with dementia received some sort of assistance with these activities. Most (63%) rely on unpaid help exclusively, followed by a combination of paid and unpaid assistance (26%), and paid assistance exclusively (5%). Older adults with dementia received more than twice as many total hours of paid and unpaid care per month as those without dementia.
| FIGURE 3. Amount of Care Received by Older Adults, by Dementia Status |
|---|
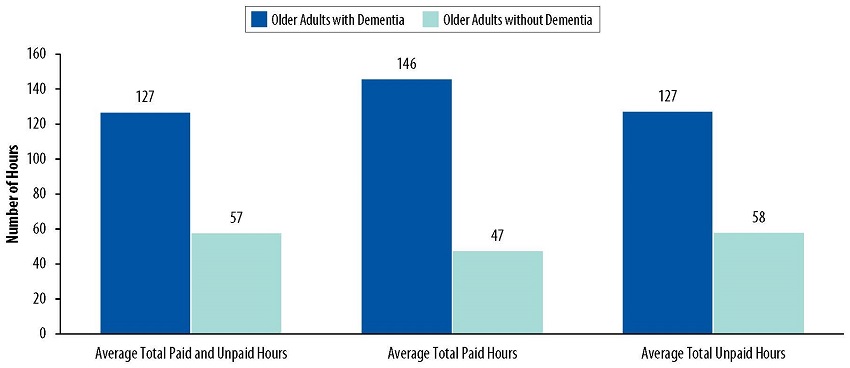 |
| SOURCE: Analyses of 2015 NHATS data conducted by RTI International, 2017. NOTE: For the purposes of the chartbook, only individuals who met the criteria for the NHATS dementia classification (Kasper et al., 2013) of probable dementia were considered to have dementia. This was a conservative definition, because individuals with mild cognitive impairment or those with early stages of dementia (i.e., individuals with possible dementia) are likely to be classified as not having dementia. The estimates presented in the chart were based on older adults living in community settings. Older adults living in nursing homes were excluded. Only adults receiving more than 1 hour of care in the previous month were included in these analyses. |
An estimated 21.6 million informal caregivers provided care to older adults living in community settings. Older adults with dementia have more caregivers than people without dementia. Although approximately 8% of older adults living in community settings had dementia, 27% of all informal caregivers provided care to them, which accounts for an estimated 5.7 million informal caregivers. Most older adults with dementia (70%) received assistance from two or more caregivers, while most (53%) of older adults without dementia have none or one caregiver.
The vast majority (66%) of caregivers of people with dementia were female. More than half (53%) were between the ages of 45 and 64. Children are more likely than spouses to be caregivers of people with dementia.
However, while more daughters provided care to older adults with dementia than spouses (34% vs. 14%, respectively), on average, spouses provided more hours of care per month than daughters (164 hours vs. 124 hours, respectively).
| FIGURE 4. Distribution of Informal Caregivers' Relationship to Older Adults with and without Dementia |
|---|
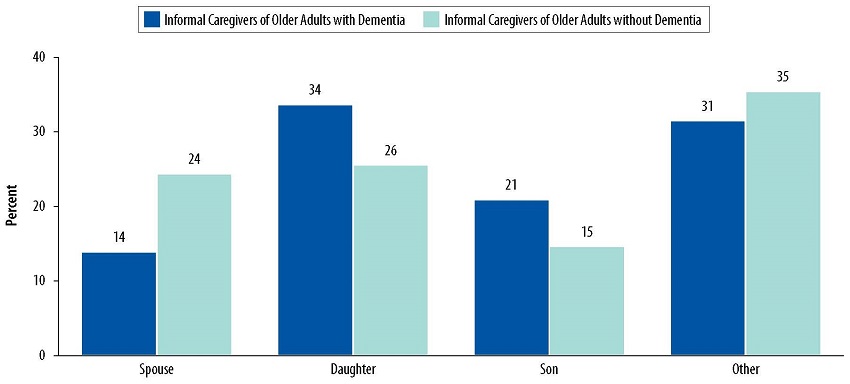 |
| SOURCE: Analyses of 2015 NHATS and NSOC data conducted by RTI International, 2017. NOTE: The percentages may not add up to exactly 100 due to rounding. For the purposes of the chartbook, only individuals who met the criteria for the NHATS dementia classification (Kasper et al., 2013) of probable dementia were considered to have dementia. This was a conservative definition, because individuals with mild cognitive impairment or those with early stages of dementia (i.e., individuals with possible dementia) are likely to be classified as not having dementia. The estimates presented in the chart were based on older adults living in community settings. Older adults living in nursing homes were excluded. |
The vast majority (90%) of informal caregivers of older adults with dementia reported substantial positive impacts of caregiving, but 44% also reported substantial negative aspects such as having more things than they could handle and not having time to themselves. Overall, informal caregivers assisting older adults with dementia experienced twice as much work productivity loss compared to informal caregivers assisting older adults without dementia (approximately 4.2% vs. 2.3%, respectively).
Nearly all (95%) informal caregivers of older adults with dementia received some support themselves. The three most commonly reported types of support were support from family and friends, such as having family or friends to talk to; having family or friends help with caring for older adults; and having family or friends help with activities.
REFERENCES
Chi W., E. Graf, L. Hughes, J. Hastie, G. Khatutsky, S. Shuman, E.A. Jessup, S. Karon, & H. Lamont. (2017). Community-Dwelling Older Adults with Dementia and Their Caregivers: Key Indicators from the National Health and Aging Trends Study. Washington, DC: U.S. Department of Health and Human Services. https://aspe.hhs.gov/basic-report/community-dwelling-older-adults-dementia-and-their-caregivers-key-indicators-national-health-and-aging-trends-study
Kasper J.D., V.A. Freedman, & B. Spillman. (2013). Classification of Persons by Dementia Status in the National Health and Aging Trends Study. Technical Paper #5. Baltimore, MD: Johns Hopkins University School of Public Health. http://www.nhats.org.
Analyses of Disability, Aging and Long-Term Care Policy and Data
This report was prepared under contract #HHSP233201600021I between the U.S. Department of Health and Human Services (HHS), Office of Disability, Aging and Long-Term Care Policy (DALTCP) and RTI International. For additional information about this subject, you can visit the DALTCP home page at http://aspe.hhs.gov/office-disability-aging-and-long-term-care-policy-daltcp or contact the ASPE Project Officer, Helen Lamont, at HHS/ASPE/DALTCP, Room 424E, H.H. Humphrey Building, 200 Independence Avenue, SW, Washington, DC 20201. Her e-mail address is: Helen.Lamont@hhs.gov.
Reports Available
A Profile of Older Adults with Dementia and their Caregivers Issue Brief
- HTML Version: https://aspe.hhs.gov/basic-report/profile-older-adults-dementia-and-their-caregivers-issue-brief
- PDF Version: https://aspe.hhs.gov/pdf-report/profile-older-adults-dementia-and-their-caregivers-issue-brief
Community-Dwelling Older Adults with Dementia and Their Caregivers: Key Indicators from the National Health and Aging Trends Study
- HTML Version: https://aspe.hhs.gov/basic-report/community-dwelling-older-adults-dementia-and-their-caregivers-key-indicators-national-health-and-aging-trends-study
- PDF Version: https://aspe.hhs.gov/pdf-report/community-dwelling-older-adults-dementia-and-their-caregivers-key-indicators-national-health-and-aging-trends-study
