Contents
- Data and Methods
- Results
- Policy Implications
- Areas for Future Research
- Limitations of This Study
- Conclusion
Children in foster care are of special interest to policymakers because they are a particularly vulnerable population. Many of these children have physical, emotional, or developmental problems, frequently stemming from abuse or neglect, substance abuse by their mothers during pregnancy and beyond, or their own substance abuse. Yet, little is known about the health-related characteristics of children in foster care, such as their health status, health care utilization, and Medicaid expenditures. Existing data provide only a limited snapshot, due to incomplete and inconsistent reporting across states. Ongoing concerns, however, about the adequacy of health care services for children in foster care make such information essential, especially with the increasing role of managed care organizations in providing health care to this vulnerable population. This study was funded by the Office of the Assistant Secretary for Planning and Evaluation in the Department of Health and Human Services to inform policymakers of the health care experience of children in foster care who are enrolled in Medicaid, including their demographic characteristics, diagnosed health conditions, and patterns of health care utilization and expenditures.
DATA AND METHODS
The data source for this study is the State Medicaid Research Files (SMRF), a series of analytic files containing Medicaid eligibility and claims data. Mathematica Policy Research, Inc. obtained SMRF data from three states for two years. The study period for California and Florida was 1994-1995, and for Pennsylvania, 1993-1994 (the most recent years of data for each state). The criteria used to select these states included: (1) the availability of Medicaid claims and enrollment data in the SMRF files; (2) the ability to identify foster care children in the SMRF files; (3) an identifiable foster care population of at least 10,000 children; (4) the degree to which children were enrolled in Medicaid managed care; and (5) variation in features of state foster care systems. The study population was comprised of children under age 19 with a foster care placement during the year. The three comparison groups included children under age 19 who received adoption assistance, Aid to Families with Dependent Children (AFDC), or Supplemental Security Income (SSI) benefits due to disability.
RESULTS
Foster Children in Medicaid: Disproportionate Expenditures
Children in foster care accounted for a disproportionate share of Medicaid expenditures, relative to their share of Medicaid enrollment.
- Children in foster care comprised between 1.1 and 3.3 percent of the children enrolled in Medicaid in 1994, but accounted for 3.6 to 7.8 percent of Medicaid expenditures.
- Children receiving SSI used a larger share of resources than children in foster care, while AFDC children used far fewer resources than their share of enrollment would suggest. Children receiving SSI benefits made up 2 to 5 percent of the enrolled population, but were responsible for 15 to 27 percent of total expenditures. Children receiving AFDC comprised the largest share of children (51 to 58 percent), but represented a smaller share of expenditures (38 to 50 percent).
Medicaid Eligibility Dynamics: Discontinuities in Coverage
Research has shown that continuous health insurance coverage year-round is related to improved access to care. Children in foster care had less continuous Medicaid coverage than children receiving SSI benefits and those in families receiving adoption assistance.
- About 7 in 10 foster care children were enrolled continuously in Medicaid for all of 1994.
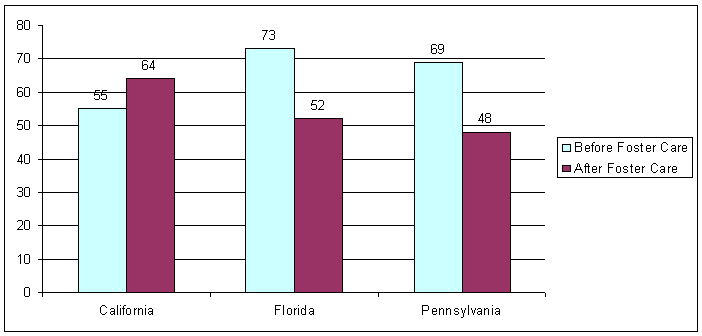
- Although the majority of children were enrolled in Medicaid prior to entering foster care, when they left foster care, one-third to one-half were not enrolled in Medicaid the month after their foster care eligibility ceased (Figure 1). In all three states, significant numbers of children lost Medicaid in the month they left foster care. Only in California were more children enrolled in Medicaid after foster care than were enrolled before they entered care.
- Children receiving SSI or adoption assistance had more continuous Medicaid coverage than children in foster care (80 to 90 percent of these groups were covered for the entire year). In general, continuity of Medicaid coverage among foster care children was similar to that among AFDC children, except in Florida, where turnover among AFDC children was much higher (only 56 percent were enrolled the full year).
Diagnosed Health Conditions: High Rates of Mental Health and Substance Abuse Conditions
Children in foster care were more likely than other groups of Medicaid children to have a mental health or substance abuse condition either alone or in combination with a physical condition (Figure 2). They had a higher likelihood of comorbidities than AFDC and adoption assistance children, but were less likely than SSI children to have multiple diagnoses.
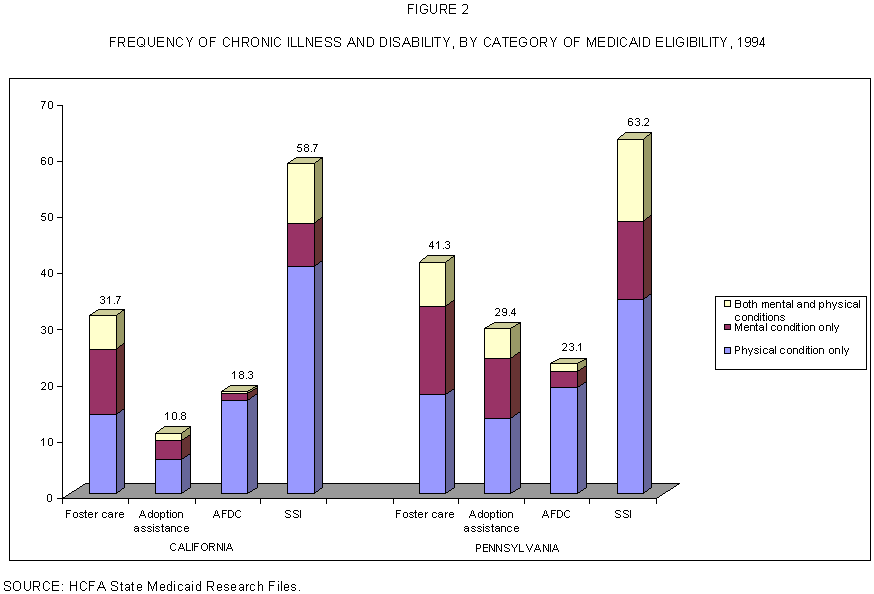
- We used the Chronic Illness and Disability Payment System (CDPS) to identify children with physical or mental conditions, based on diagnoses on Medicaid claims data. These data were not available for Florida, since diagnoses were not listed on outpatient claims.
- About one in three foster care children in California had a CDPS condition (32 percent) versus two in five in Pennsylvania (41 percent). The most common conditions in the foster care population were mental conditions (18 percent in California; 24 percent in Pennsylvania). The most common physical conditions were those associated with the central nervous system (5 percent) and pulmonary conditions (6.5 percent).
- SSI children were more likely than foster care children to have a CDPS condition recorded in the claims. This was entirely due to a higher rate of physical conditions among SSI children; the rate of physical conditions was two to three times higher among SSI children than among foster care children. On the other hand, the rate of mental conditions was slightly higher among foster care children.
- AFDC children were less likely than foster care children to have a CDPS condition, on the order of about one-half the rate. This was entirely due to lower rates of mental health conditions.
- Children receiving adoption assistance were less likely than foster care children to have a CDPS condition (11 percent in California; 29 percent in Pennsylvania). This could be a function of either the risk selection in the adoption process (that is, healthier children are adopted) or the more stable risk profile of children who have been in adoptive families for several years.
Utilization of Health Care Services: Considerable State Variation and Inadequate Preventive Care
There was considerable variation across states in health care utilization patterns. In general, foster care children in California were less likely to receive health care services than those in the other two states.
- Over 80 percent of the foster care children in Florida and Pennsylvania had at least one provider visit in 1994, compared to 65 percent in California (Figure 3). Foster care children in California also were less likely than AFDC and SSI children to see a provider during the year. In the other two states, foster care children were more likely to see a provider than the AFDC population, but only in Florida were they also more likely than the SSI population to see a provider during the year.
Figure 3
Percentage of Children in Foster Care Receiving Selected Types of Health Care, 1994
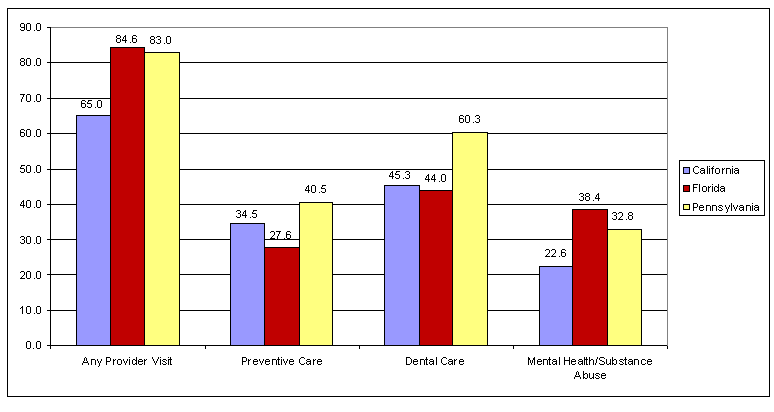
- The likelihood that foster care children received a preventive check-up during 1994 ranged from 28 percent in Florida to 41 percent in Pennsylvania. In California and Pennsylvania, foster care children were more likely than other Medicaid children to have a preventive check-up during the year. Nevertheless, many foster care children did not receive routine check-ups during the year, despite the recommendations for an annual physical and mental health assessment each year (CWLA 1988). In addition, very few received an assessment during the first two months of a foster care placement, according to Medicaid claims records. Interestingly, early assessments were received more often by children with no prior Medicaid coverage, suggesting that providers were more likely to perform assessments on those who were newly enrolled in Medicaid.
- Foster care children were far more likely to receive dental care than other groups of Medicaid children. Sixty percent of foster care children in Pennsylvania and 44-45 percent in California and Florida had at least one dental visit in 1994, compared to 28-38 percent of the AFDC population and 31-35 percent of the SSI population.
- The likelihood of foster care children receiving mental health or substance abuse treatment services varied substantially across states, from 23 percent in California to 38 percent in Florida (Figure 3). Foster care children were more likely than other groups of Medicaid children including those receiving SSI to receive mental health or substance abuse services. Most received treatment on an outpatient basis. The average number of outpatient visits per user varied widely, from 6 visits in California, to 18 in Florida, and 22 in Pennsylvania.
Level of Medicaid Expenditures: Wide Variations Among States
Average Medicaid expenditures varied widely across states, and were lowest in California, consistent with the findings on lower utilization in California. In general, expenditures were highest for the SSI population and second-highest for foster care children.
- Average monthly Medicaid expenditures for foster care children ranged more than twofold from $154 in California to $375 in Florida, with Pennsylvania averaging $293. Medicaid spending for foster care children was two or more times higher than the average for all Medicaid children (Figure 4). Average monthly Medicaid expenditures for SSI children were between four and seven times the level of those for all Medicaid children. Medicaid expenditures for AFDC children were well below the average for all Medicaid children.
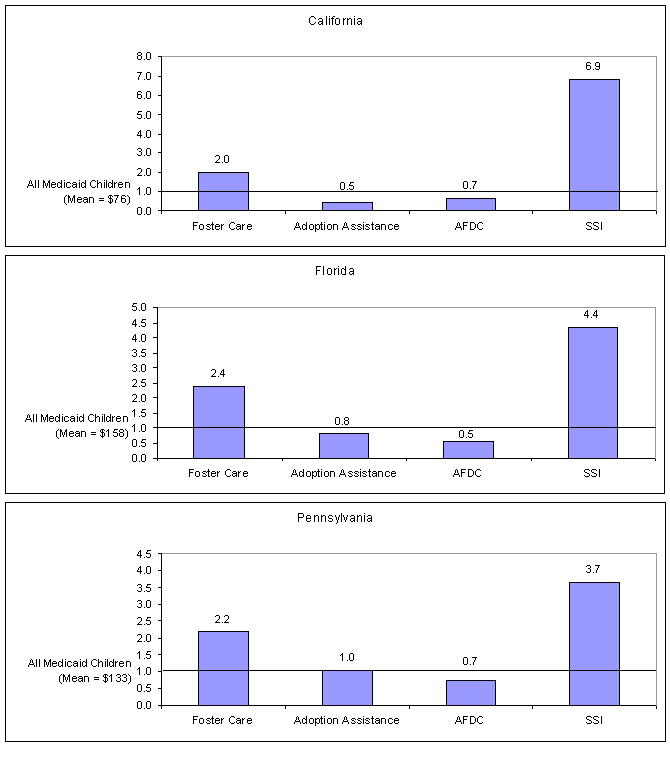
- Infants in foster care had by far the highest average monthly expenditures, driven primarily by high inpatient costs.
- Spending also varied by health condition. Compared to spending for foster care children with no CDPS condition, spending was 10 to 12 times higher for those with both physical and mental conditions, and 5 to 7 times higher for those with either a physical or mental condition.
POLICY IMPLICATIONS
These findings have important implications for policy and practice to improve the delivery of health care services to children in foster care, especially in the changing health care environment. Four main implications can be drawn from this study:
- Continuity of coverage. Discontinuities of health insurance coverage can have an adverse effect on access to care. Policymakers should focus on ways to improve continuity of health insurance coverage among children in foster care.
- Utilization of Medicaid as a source of funding. States have considerable flexibility in how they use Medicaid to pay for services for children in foster care. Medicaid can fund a comprehensive continuum of care, ranging from screening and assessment to follow-up treatment and ongoing therapies. Evidence of state-level variation in Medicaid expenditures suggests that states differ in the use of Medicaid to serve children in foster care.
- Coordination of care. The low level of compliance with screening and assessment protocols underscores the importance of care coordination as a vehicle for overcoming structural barriers to care, especially fragmentation between the child welfare and health care systems. A broad-based concept of care coordination is especially relevant for foster care families, whose needs may involve multiple systems of care, such as public health, child welfare, mental health, schools, and juvenile justice.
- Structure of managed care systems. This study has highlighted the special needs of the foster care population, especially the need for behavioral healthcare services. Because children in foster care represent only 1 to 3 percent of the child Medicaid population, policymakers may lose sight of their needs when designing programs for the larger and more visible Medicaid populations. Payment mechanisms (such as risk adjustment or risk corridors), provider networks, benefit packages (especially coverage of mental health services), and provider education all need to be designed with the special needs of the foster care population in mind.
AREAS FOR FUTURE RESEARCH
Like all research studies, this one raised questions that could be addressed in future studies.
- State-level variation. What accounts for the significant variation in diagnoses, utilization, and expenditure patterns across states? This study has taken a first step to document differences across states. Further research is required to explain the differences. Possible factors include: the role of child welfare and health agencies in coordinating and advocating for health care services for children in foster care; the role of the courts in mandating health care for children in foster care; characteristics of state programs (such as the use of health passports, level of staff caseload, availability of transportation services); variations in the Medicaid benefit package; availability of providers to serve the population; provider knowledge concerning services needed by the population; generosity of reimbursement rates; differences in casemix; and level of stigma about accessing services.
- Extent of unmet need. We cannot tell from claims data whether variations in the level of utilization are due to overutilization in some groups or underutilization in others. Without external benchmarks against which to evaluate patterns of care, together with more detailed clinical assessments, we cannot tell whether lower rates of utilization are indicative of access barriers or simply lower health care needs. To gain a better understanding of unmet needs in the foster care population, policymakers and researchers might consider performing a medical records review or conducting a survey of foster care families and caseworkers.
LIMITATIONS OF THIS STUDY
Although this study has shed light on patterns of diagnoses, utilization, and expenditures for children in foster care, the reader should note that the generalizability of the results may be limited for several reasons:
- The data are for three states. Although this is an improvement over previous studies that focused on a single state, the results cannot be generalized to all states or to the nation as a whole. The value of using multiple states is that it demonstrates the extent of variation and can provide useful comparisons to other states.
- The data were from the mid-1990s. These were the most-recently-available data for this study, but more recent data clearly would be desirable to ascertain whether certain patterns have changed.
- The analyses of diagnosed conditions, expenditures, and utilization exclude children enrolled in managed care. The SMRF did not gather encounter data for capitated services, which results in an undercounting of services received by children enrolled in managed care.. To the extent that there are systematic differences in the utilization patterns among children in foster care who are enrolled in managed care, these will not be captured in the analysis.
Readers should also be aware of some of the limitations of using SMRF for research purposes. First, there is no provider specialty on the SMRF file, which precluded us from looking at continuity of care or specialty referral patterns. Second, not all states report such basic data as diagnoses, but to our knowledge there is no central database that indicates which SMRF files contain which data elements and to what degree of completeness. Third, states often use state specific procedure codes, but the definitions are not uniformly available to researchers. Fourth, states differ in the way they code type-of-service categories, especially for mental health services. Fifth, the SMRF file contains only a single eligibility category each month, hampering our efforts to identify children receiving SSI benefits who were placed in foster care. Sixth, it is unclear whether the date of foster care placement on the eligibility file is accurate. This affects all analyses of pre- and post-placement utilization.
CONCLUSION
As increasing attention is focused on the health care needs of children in foster care, there is considerable interest in developing performance measures to track the effectiveness of child welfare services. This study has provided examples of how utilization and expenditure measures can be operationalized using Medicaid data. Additional analyses, based on more recent data, would be useful to determine how children in foster care are faring in the new millennium whether they are receiving more continuous coverage and more comprehensive care as a result of state efforts to improve health care for the foster care population.
