*This concept paper presents the views of the author alone and not those of the US Department of Health and Human Services nor those of the Urban Institute, its trustees, or its sponsors. It has benefitted from comments by Randy Bovbjerg and by ASPE staff on earlier drafts, as well as from conversations with Nicole Tapay at Georgetown University (formerly at NAIC) and Mary Beth Sankewitz of NAIC and Gretchen Babcock of the Blue Cross and Blue Shield Association. The author retains all responsibility for errors and ambiguities.
Elements of Insurance Market Decisions 6
- Types of licenses 7
- Indemnity 7
HMOs 8 Blues 10 PPOs 12 Non-profit 12 Product market Segments 13
- Group 13
Individual 16 Specific insurance products 17 Geographic markets 20 Analytic model of insurer market decisions 26
- Strategic Choices 26
Tradeoffs Among Choices 32 Constraints 35 Assessing and Monitoring Health Insurers' Strategic Choices 37
Preface
Pursuant to a delivery order (contract No.HHS-100-95-0021) from the Assistant Secretary for Planning and Evaluation (ASPE) in the Department of Health and Human Services, the Urban Institute undertook to produce this concept paper. The purposes of the task order and the paper are to provide ASPE with a framework for analyzing evolving insurer behavior, to identify potential data sources and data needs for further empirical work, and to provide ASPE staff with an accessible resource document that can facilitate better understanding of evolving health insurance markets.
This broad scope and general purpose limit the usefulness of extensive citations. Rather, some generally accepted "stylized facts" about health and insurance markets are presented as if in the common domain. Interested policy makers and researchers may want to consult other sources for more depth on specific issues. In particular, Vaughan and Vaughan (1996) offer a recent treatment of the financial theory of health insurance. Klein (1995) provides a very informatiave discussion of health insurance regulation from a regulator's point of view. GAO (1993) offers one of the few assessments of state regulatory capabilities. Blumberg and Nichols (1996) analyze recent state reforms for individual and small group markets. Marsteller et al (1996) presents a survey of state regulation of selective contracting by managed care organizations.
The American health care delivery and financing systems are being transformed, mostly by market forces, but also by piecemeal federal and state reforms. Private sector managed care growth and public sector payment reforms (e.g., Medicare's PPS, capitation for Medicaid enrollees) have revolutionized health care delivery patterns, reversing decades-long trends in utilization patterns, as well as growth rates of per capita costs and provider incomes. This revolution, coupled with insurance reform legislation and the increasing tendency of employers to self-insure, has accelerated the rate of decline in traditional indemnity plans' share of the overall health insurance market. This has led insurers to withdraw from certain markets, states, and the industry as a whole, but it also spawned a counter-revolution in product offerings and marketing strategies by traditional insurers, as well as entry by new types of managed care firms who are providing insurance services.
Understanding insurer strategies is important to policy analysis for at least two reasons. First, insurers themselves are often regulated entities, and the Health Insurance Portability and Accountability Act(1) makes that regulation partially federal for the first time. Thus the federal government now has a direct regulatory interest in understanding how insurers are likely to respond to specific constraints on their behavior in different environments.
Second, insurer responses to changing market and regulatory conditions affect both providers' and patients' opportunities and outcomes. In some ways the new economics of health service provision make insurer decisions the logical starting point of health market analyses, for they can easily become constraints to which providers and patients must react. These constraints span a wide range from incentive contracts to even more blunt utilization management techniques. This is a far cry from the mostly passive, "financial middleman" role health insurers played for much of the 20th century. Thus for traditional reasons of quality assurance in the provision of health services and for new and evolving consumer protection reasons, policy makers have a compelling interest in being able to anticipate insurer incentives, reactions and behavior so as to devise optimal ways of achieving policy goals.
This paper will provide a conceptual framework to interpret and assess evolutions in insurer strategies. It will describe the functions that health insurers perform, the various products they might offer, and the geographic market considerations that affect insurer location decisions. After describing these elements of the insurance market from an insurer's perspective, I then take up the paper's main purpose, to develop a simple model of insurer behavior than can illustrate the tradeoffs among multiple objectives caused by technological and market constraints. Finally, the paper concludes with a list of research questions and data development ideas for monitoring the performance of health insurance markets that is consistent with the model.
The primary role which health insurers play is that of financial risk bearing: in exchange for premium payments, they promise to pay or otherwise provide for the specified health care needs of an enrolled group of people. The profitability of any contract of this nature is inherently uncertain. A necessary but not sufficient condition for profitability is for the ex ante premium paid to exceed the ex post medical costs of the average person in the group. The strong desire to avoid financial risk, i.e., risk aversion, is what creates the willingness on the part of individuals and groups to pay a bit more than expected health care costs in order to shift the risk to insurers. Still, after the fact, insurers may discover they have priced the insurance product too low, and preparation for dealing with the financial consequences of this contingency is the essence of risk bearing. Unfortunate contingencies are met through reserves previously set aside and through changes in future pricing and other business practices.
There are three component steps of pricing the risky dimensions of the insurance contract:
(1) estimating the expected costs of a particular benefit package -- services covered and specific co-payment obligations --- for a standardized population most like the proposed group or individual, assuming the benchmark (local) delivery system; and (2) adjusting that estimate for health status particularities or recent health expenditure experience of the group or individual in question; and (3) estimating the cost savings that are achievable through the particular provider network (including any out-of-network options) proposed for the specific contract.
The first two components, estimating the health benefits paid of the prospectively insured group or individual, are central to the underwriting process, wherein the insurer evaluates whether they want to sell an insurance contract to this particular group/individual and if so, at what price. Actuarial science is conbined with business judgment in this traditional health insurance process.
Estimated cost savings from selective contracting with specific networks or providers is a new feature of the insurance business, applicable only to insurers selling managed care products. This component entails assessing provider practice styles, selecting providers for inclusion, negotiating price and incentive contracts with providers, and managing the provider network to accomplish utilization, quality, and savings goals. Thus, this dimension of setting the price of an insurance contract involved both an actuarial calculation -- estimating the utilization and cost implications of specific network restrictions on this particular insured population -- and a business management function, in which the insurer acts as an agent for plan payors and subscribers vis a vis providers in negotiting these same restrictions.
Before any risk is transferred however the insurance contract must first be sold. Selling functions include informing salespersons, often independent insurance agents, as well as potential enrollees directly about the insurer and the contract options it wants to make available. Agents are typically paid on commission, which are higher for new business than repeat business. These selling or marketing costs can be substantial on a per person basis, especially for individual and small group products.
Finally, after the risk contract is sold, it must be administered. This role includes setting up enrollment procedures, educating enrollees about required claims documentation, and claims processing functions so that providers and enrollees get paid or reimbursed. Again, these functions are costly, and while not the same as risk bearing, are essential to the implementation of any health insurance arrangement.
Algebraically, a premium can be summarized as follows. Let E[c] represent expected health care costs, per person, of a particular insurance contract. The difference between the premium (P) and E[c] is called the "load" or "loading factor," (L). Writing L as a percentage of expected medical costs, premiums are often summarized in an expression like P = (1+L)E[c]. The components of L are the selling (s), underwriting (u), network management (m) and contract administration (a) costs, per subscriber, PLUS a risk factor, (r), that reflects the insurer's assessment of the likely variance of health care costs from the expectation or average, premium taxes (t) [where applicable] and profits (). In general, P = (1+s+u+m+a+r+t+)E[c]. The larger the group, the smaller is r, and given the significant economies of scale in selling, managing networks, and administering contracts, the smaller are s, m, anda as well. Finally, because r declines with group size by the law of large numbers, u declines with group size as well.(2)
Figure 1 depicts these premium elements in rough proportions.
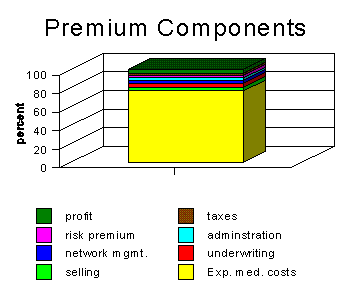
Algebraically, a premium can be summarized as follows. Let E[c] represent expected health care costs, per person, of a particular insurance contract. The difference between the premium (P) and E[c] is called the "load" or "loading factor," (L). Writing L as a percentage of expected medical costs, premiums are often summarized in an expression like P = (1+L)E[c]. The components of L are the selling (s), underwriting (u), network management (m) and contract administration (a) costs, per subscriber, PLUS a risk factor, (r), that reflects the insurer's assessment of the likely variance of health care costs from the expectation or average. In general, P = (1+s+u+m+a+r)E[c]. The larger the group, the smaller is r, and given the significant economies of scale in selling, managing networks, and administering contracts, the smaller ares, m, and a as well. Finally, because r declines with group size by the law of large numbers, u declines with group size as well.(3)
III. Elements of Insurance Market Decisions
Insurance markets and insurer behavior have many interrelated dimensions. This section describes four of the most important: types of licenses insurers may hold, product market segments insurers might target, specific types of insurance products insurers might offer, and geographic market conditions that insurers find favorable or unfavorable. Clarifying what is at stake when insurers decide among these elements will facilitate our discussion of the analytic model of insurer tradeoffs developed in Section IV.
A. Types of insurance licenses
Business entities are typically granted licenses by states to sell health insurance products of a certain type, depending on the nature of the financial risk that is borne by the licensee, the degree of the financial risk that is shifted to providers, and the nature of restrictions on provider access that are placed on enrollees. The name, exact type, and scope of license varies by state. For the purposes of this paper, I focus on three generic types of licenses: indemnity, Blue Cross and Blue Shield (Blues), and health maintenance organizations (HMOs). Which license(s) business entities hold determines to some extent the range of product offerings that entity can make, and thus their flexibility to compete. In a changing marketplace, flexibility is a natural asset, and thus the real or perceived strictures of particular licenses are increasingly contentious matters of policy debate.(4)
Indemnity. What is commonly referred to as indemnity insurance(5) may be sold through accident and health, life and disability, disability, life and casualty, or health insurance licenses. These licensing statutes are typically broad, allowing indemnity insurers to write a wide variety of insurance contracts or health insurance "plans." In some states, this includes contracts with provider network restrictions, very like PPO and some HMO plans. Typically, though, indemnity contracts are primarily financial, specifying services and types of providers covered (though not which providers) along with copayment and documentation requirements.
One major difference between indemnity licenses and others is in the nature of the entity that bears the financial risk. In the case of the indemnity insurance contract, it is the commercial (or for-profit) insurer who suffers financial losses if premiums paid turn out to be lower than the costs of reimbursing enrollees and paying providers for covered services, plus the full costs of selling, underwriting, and administering the product. It is for this contingency that insurers keep reserves and states enforce solvency requirements.
Despite the general looseness of indemnity statutes, indemnity licensees tend to focus on risk selection and marketing rather than advanced managed care techniques. If large enough they will certainly negotiate provider price discounts, but that is not a feasible option for most of them. Their path to profit tends to lie in selecting good risks and charging experience rated premiums with large load factors, not in offering specific provider networks with particular delivery styles. They are the health insurance licensees who are least supportive of insurance market reforms since the reforms tend to hamper or outlaw their traditional risk selection techniques. Many indemnity insurers consider these techniques to be necessary for survival in a competitive and voluntary insurance market.
HMOs. HMO licenses, by contrast with indemnity, are granted for much more specific contracts. They typically require pre-payment for health care and a guarantee that the licensed entity will deliver the medically necessary services. The "pre-payment" is analytically equivalent to a premium for indemnity insurance, but the promise by the licensee to provide the necessary care distinguishes HMOs from indemnity insurers. The entity that bears financial risk in this case is the same organization that provides the health services. Precisely because the insurer in this case can deliver the services, solvency requirements are typically set lower for HMOs than for indemnity insurers. The assumption is that HMOs are health care providers first and insurers second, and that HMOs can therefore make good on the promise to deliver appropriate care with less financial risk than third party payor insurance companies. This notion of HMOs as health care providers first and insurers second also explains why in some states HMOs are at least partially regulated by departments of health. Today, 33 states have two or more agencies involved in the regulation of managed care entities.(6)
The 1973 federal HMO Act places restrictions on the type of health insurance contracts that may be written by HMOs that want the designation "federally qualified."(7) They must use modified community rating when setting their premiums and they may impose no more than "nominal" cost sharing (less than 20% on average, no more than 50% for any specific service). In addition, 90% of health services must be provided under contract or by employees. Most state HMO licensing statutes are structured similarly, though no state requires federally qualified status as a condition of licensure. However, state HMO acts typically do not allow POS contracts to be written without additional state law, for this puts HMOs squarely in the business of being a third party payor, i.e., providing indemnity insurance. Indemnity insurance is presumed to require higher solvency standards than HMOs have been held to historically.
The effects of restrictions like making it difficult to write POS contracts will be discussed in more detail in Section IV. For now it is sufficient to point out that HMO licensees, whether they run staff/group, network, IPA or mixed type models primarily, tend to focus on their care delivery system more than do indemnity insurers. The full gamut of managed care techniques are employed by some HMOs, and both prohibitions on POS offerings and mandated POS options, along with other restrictions on their care management techniques like any willing provider laws, restrict their ability to pursue their preferred strategies to profit or surplus in a competitive market.
Blues. The third important type of health insurance license is for Blues plans, sometimes called hospital and medical service organizations or health care service contractors. These were the first health insurance plans in the U.S., organized in each state (and in some cases, in counties) as non-profit corporations,(8) sometimes as mutual organizations,(9) around and by provider groups (Blue Cross for hospitals and Blue Shield for physicians). Regulation of the Blues in most states stems from enabling legislation which is unique to the Blues and typically exempts them from some requirements imposed on commercial plans (e.g., initial capital requirements and premium taxes) but also imposes certain other requirements (e.g., open enrollment or insurer of last resort). "Last resort" requirements have been relaxed over time as states passed various insurance reforms and created high risk pools, though seven states' Blues plans still voluntarily offer an open enrollment period to all individuals. Blues' enabling laws often establish rate approval and "fair payment to provider" requirements. These requirements, though subject to judicial appeal, are generally not imposed o have turned with some vigor to managed care. Nationwide in 1995 Blues plans had 8 million HMO enrollees, 3 million in POS plans, and 19 million PPO subscribers. This represents almost half of collective Blues' enrollment.(11)
Blues plans were once near monopolies in many areas of the country. They also historically practiced community rating. As their market share declined, primarily from commercial insurers offering particular groups lower experience rated premiums and from larger firms moving to self-insurance, Blues were left with deteriorating risk pools and increasing community rated premiums, which only made it easier for commercial indemnity insurers and new HMOs to "cherry pick" good health risks from the Blues. Blues then fled unilateral community rating and other "community benefit" requirements in their original legislation as a survival strategy. As this transition occurred, along with insurance reforms that made it unnecessary for most states to require Blues to maintain "last resort" products, it became increasingly clear that many Blues plans were practically indistinguishable from commercial insurers. As the enrollment data cited above make clear, Blues plans use their unique licensing statutes to offer the full range of products in the market today.
PPOs. Twenty-six states have PPO-enabling legislation, largely passed to resolve the uncertainly about whether limited networks could operate under existing insurance laws in the 1980s. The concern was that "freedom of choice" provisions in existing statutes prohibited insurance policies from requiring that the health service be rendered by a specific person.(12) A few states today consider PPOs to require separate licensure and regulations, though most risk-bearing PPO products are issued by commercial insurers, HMOs, or Blues plans. Non-risk-bearing preferred provider networks (which may call themselves PPOs even though they do not sell PPO insurance contracts) typically serve self-insured (ERISA) plans outside the purview of state insurance regulations. Minnesota has Integrated Service Network legislation and Iowa licenses physician-hospitals organizations (PHOs) separately. A few states also have separate licenses for limited pre-paid health service organizations (e.g., dental). By and large, though, the vast majority of the important entities selling health insurance and bearing financial risk hold one or more of an indemnity, an HMO, or a Blues type of license.
Nonprofit status. Although not a separate category of health insurance license, nonprofit corporate status does have certain specific consequences for health-related entities. Many HMOs and all Blues plans were originally organized as non-profit organizations. Nonprofit status is granted separately by state and federal authorities. It typically confers exemption from corporate income and premium taxes, as well as local property taxes, in exchange for community benefits (e.g., open enrollment or community rating) which may be specified in statute, regulation, or in agreements with regulators. Nonprofits today account for 30% of HMOs and roughly 40% of HMO enrollees. About 10% of Blues plans are for-profit, though a larger number have for-profit subsidiaries (usually an HMO).
As commercial insurers came to play larger roles in providing health insurance, their complaints about the Blues' competitive advantages escalated, and the Blues' lost their federal tax exemption in 1986. The omnibus federal tax reform law passed that year did give them one tax deduction on the excess of 25% of claims and expenses over beginning year surplus, as a continued inducement to remain a Blue and continue providing insurance to small and high-risk groups and individuals. This deduction is lost if they drop high-risk coverage or convert to for-profit, but not if they convert to mutual company status. In order to convert, plans must secure the approval of their state's attorney general or insurance regulator. Conversion to for-profit status has generated considerable controversy beyond the scope of this paper.(13)
B. Product Market Segments
Group insurance. By far the most common product is group health insurance, most often sold to a single employment-based group. Other groups who purchase health insurance are union, professional association, multiple-employer, and religious. In the group setting, a single policy called a master contract is issued to the group policyholder to cover a group of individuals who have a defined relationship (other than insurance) to the policyholder, such as employee-employer, member-union, and debtor-creditor.
Insurers have long been comfortable selling to groups that were formed for a purpose other than to purchase health insurance, for these groups are expected to have a regular distribution of health risks (i.e., many healthy, few sick). This is more true the larger the group, however, for the law of large numbers guarantees that the variance of any group's health expenditure distribution is inversely related to the size of the group. Since any large groups' health expenditure distribution is highly skewed (typically 10% of the people account for 70% of the expenditures in a given year), this consideration is paramount, and is a large part of the reason that insurance is sold at lower premiums for large groups, ceteris paribus. The "risk" component (r in section II) of the loading factor is minimal or zero for large groups.
The group health insurance market has two distinct segments: (1) the small group market, the boundaries of which are defined by state law; (2) the medium and large group market. This second segment itself is divided into those employers that self-insure and those that purchase insurance from a risk-bearing entity (indemnity, Blue, or HMO). If self-insured, employers' health benefits are protected from state regulation by the federal law called ERISA (Employee Retirement Income Security Act). Consequently, their health plans are sometimes called "ERISA plans."
The self-insured often buy stop-loss insurance, a commercial product sometimes called re-insurance, that allows them to shift some of the risk back to insurance companies.(14) These self-insured employers are actually partially insured for health insurance, but in many descriptions they are often lumped with those who buy no stop-loss (high risk) insurance at all, since they do bear non-trivial financial risk from health insurance claims as a firm, and since they do share ERISA's exemption from state law. Employers that purchase health insurance are called "fully insured," since they shift all financial risk of high medical claims to the insurer, to whom they (and their employees) pay premiums.
The small group market is typically comprised of employers with 2-49 employees. Since they are so small, the expected variance of their health expenditures and the financial risk to them of self-insuring is very high, and thus they usually prefer to purchase insurance from an insurer or HMO, even though they pay more for the same coverage than larger firms. There is some evidence that increasing numbers of small firms are self-insuring and buying reinsurance.(15) Medium and large firms could self-insure more feasibly than small firms, and many do.
The NAIC has recommended that limits be placed on how high the individual and aggregate deductibles in stop-loss policies must be to merit the term "self-insured" and the resultant federal ERISA exemption.(16) The higher the deductibles, the greater the risk borne by the self-insured employer. The actual extent to which self-insured employers are buying very low deductible stop-loss policies and thus circumventing local insurance regulations while remaining for all practical purposes fully insured is not known. It was considered a serious enough problem or risk, however, for the NAIC to develop and adopt a model act to deal with the issue.
Section IV presents a more detailed discussion of insurer strategies, but it is worth making clear now that for these two medium/large market segments, the choices are, roughly: (a) sell a fully insured product; and (b) administer the self-insured plan for the employer. This latter set of services is sometimes called third party administration, and the entity which performs the services is known as a third party administrator or TPA. Ordinarily, the TPA is paid a fraction of claims to process them and to administer the plan for enrollees. This payment is functionally similar to a loading factor, the difference between expected medical claims costs and premium charged. In a competitive equilibrium for large firms with negligible variance in expenditures, the insurance "load" is equal to the average economic cost of selling, administering, and underwriting the health plan, per person, for that particular group of enrollees.(17) So, in a sense, being a TPA just removes the financial risk from the insurer's calculus. On the other hand, not bearing the risk reduces the potential reward, and competition for TPA contracts can be fierce. Over half of all self-insured employers purchase TPA services. HMOs also offer this service to self-insured employers, but they tend to call it ASO (administrative services only).
The self-insured employer is essentially engaged in a classic "make or buy" calculation. It can pay premiums to an insurer, in which case both the risk bearing and the administrative services are bought. It can completely self-insure and administer its own health plan, in which case the firm "makes" its own health insurance, i.e., bears all risk and incurs all administrative costs. Or, it can bear the financial risk while purchasing the TPA services. Finally, it can buy stop-loss and TPA services, in which case the employer is merely bearing a portion of the financial risk. This is the most common situation for self-insured employers.
Individual insurance. This product line is sold to individuals. Marketing and administrative costs are much higher, per person, than in group settings. Furthermore, because the potential for adverse selection is so much greater in the individual market, resources devoted to medical underwriting are much greater per person than in the group market. These costs increase the premium, all other things equal. While the problems with individual insurance markets are in many cases much worse than the problems faced by small groups, states have been relatively reluctant to pass legislation reforming this market, primarily because the transfer of economic well-being to the currently sick from insurers and the currently insured is so much greater than in the case of small group reforms. Also, most privately insured non-elderly individuals get their insurance through a group (about 90%), so the constituency favoring individual market reform is not as large. A widespread impression today is that more insurers serve group markets than individual markets, but there are no systematic data collected to verify this. In any event an important point is that the absolute number of insurers may be less important than the range of alternative products actually available.
C. Insurance products
There are five broad types of private health insurance products which insurers may choose to offer in the market segments described above: (1) indemnity, or free choice of provider fee-for-service; (2) PPO (preferred provider organization), fee-for-service with strong financial incentives to use a particular group of providers (sometimes called a "network"); (3) EPO (exclusive provider organization), a PPO with no reimbursement for out-of-network providers; (4) HMO (health maintenance organization), pre-paid health care (usually with modest copays) from a particular group of providers; and (5) POS (point-of-service), an HMO with an out-of-network option that entails higher copays. There are many, many variants of each type of product, with different covered services, provider arrangements, and enrollee copayment obligations.
Until the 1980s, there were only indemnity and HMO products.(18) Prior to then, it was common for insurance licensees to specialize in one type of product. Today, competitive pressures have led to indemnity and Blues licensees offering PPOs and sometimes HMOs, just as some HMO licensees now offer POS options (which look to patients very like PPO products with provider choice) and even indemnity products. Most health insurance entities want to be able to offer employer groups "one stop shopping" for all their health insurance and health care needs.
This is especially true in the market for large firms. Firms that decide they want to be self-insured, largely to avoid state regulation, cannot purchase fully insured products and retain their ERISA exemption. Thus, for example, HMOs cannot sell them their standard risk-bearing contract. However, an HMO could provide claims processing through an ASO, and in addition, it could provide fee-for-service medicine to the self-insured's enrollees, in effect, turning the HMO network into a "rental PPO." To recognize this reality, some states now require annual reports to distinguish between premiums written and premiums earned, the latter including fee-for-service payments plus premium revenue (e.g., Washington).(19)
Similarly, an indemnity licensee cannot sell the self-insured firm a full-risk product, but it too can sell TPA services (and PPO services if it has a network arrangement with providers). The rise of self-insurance has thus created market forces that allow networks of providers (sometimes called provider sponsored networks or PSNs) to bypass insurance license holders, i.e., risk bearers, altogether and to contract directly with health care purchasers. An interesting evolutionary twist is that PSNs are now asking for the right to bear financial risk without having to become health insurance licensees with all the solvency and regulatory oversight that usually entails. In effect, they want to compete with indemnity insurers on risk bearing and TPA services, and with HMOs on service delivery and ASO services. Calls for a level regulatory/competitive playing fields now come from all quadrants of the health insurance universe. Predictably, however, "level" is often in the eye of the beholder (and petitioner).
Public or public-related products. The major public insurance products which private insurers sell are Medicaid and Medicare managed care products and administrative services for Champus/VA/DoD. Medicare supplemental insurance (Medigap) is a private product, bought both by individuals and by employers on individual's behalf, but the conditions of its sale are so directly affected by what Congress does with the basic Medicare benefit package that it is best thought of in tandem with the public program. In addition, federal law regulates the types of Medigap policies that may be sold and other marketing rules.
Many states are moving their non-institutionalized Medicaid populations into capitated managed care as fast as possible. Medicare risk contracts are also growing rapidly, and they have been capitated since 1986. With few exceptions in the public sector, however, premiums are based on formulae or administrative fiat, not competitive bidding, and thus they sometimes encourage and sometimes discourage entry into this market. An entity does not have to be an HMO licensee to compete for Medicaid managed care contracts, but state Medicaid agencies and the U.S. Health Care Financing Administration (HCFA(now known as CMS)) have their own requirements that must be satisfied.
D. Geographic Markets
Factors that affect the relative attractiveness of particular geographicregions or states for health insurance are discussed in isolation for clarity, but they obviously interact to affect any final entry or exit decision. For example, highly favorable economic conditions can counterbalance unattractive regulatory regimes, and vice versa.
Economic Conditions. The economic conditions favorable to private health insurance are high employment and per capita income. The larger the employment base, the greater the likelihood of selling group health insurance products. Given a large employment base, the higher the per capita income, the higher the wages of the workers and thus the more likely they will be willing and have the opportunity to take some of their compensation in health benefits. Given an employment base and per capita income, the greater the relative preponderance of small and medium sized firms, the greater the likelihood that employers will be interested in purchasing insurance rather than self-insuring. No data base exists which counts licensees or products and enrollees by type of licensee or product, so it is impossible at present to test the quantitative significance of these logical assertions.
Regulatory structures. The distribution of random techniques and medical underwriting to select healthy groups and individuals and then offering insurance at lower than average prices (i.e., the Blues' community rate) that were more consistent with the particular group's claims experience. This left the Blues with less healthy groups and individuals, and in a classic adverse selection spiral, they had to raise their community rates to cover the now higher average cost of their deteriorating pool. This in turn increased the attractiveness of the commercial indemnity insurers' offers to other employment-based groups. Unilateral community rating, even by the largest single insurer, cannot withstand aggressive experience rating by all or most of its competitors.
At the same time, unfavorably rated groups were harmed by experience rating competition siphoning off the healthiest groups. They found insurance to be increasingly unaffordable or unavailable. Large groups self-insured to avoid premium sprials and state regulation, but small groups remained vulnerable. Thus, the pressure for health insurance reform came on behalf of small groups and individuals.
Forty-six states have passed and implemented some type of small group health insurance market reforms since 1990, and twenty-four have reformed the individual market in at least one dimension as well. Predictably, the laws vary considerably, but by July 1, 1997 guaranteed issue and renewal for groups will be the law of the land, and some kind of modified community rating requirements for the small group market are in place in forty-four states. Thus, after the Blues' community rating genie was let out of the bag, most states tried to re-impose some pooling of health risks across small groups, and some have tried to do so in the individual market as well.
It is a truism that any binding regulation costs someone something. In the case of rating restrictions and guaranteed issue or renewal, the health care costs of the unhealthy are somewhat subsidized by the currently insured healthy. If insurers' total revenue falls due to the aggregate loss of business from higher average premiums, insurers themselves may bear some of these costs as well. Thus, ceteris paribus, states with tighter rating and issue restrictions are less attractive to commercial indemnity firms who prefer to pursue strategies of risk selection. Again, there is no publicly available data base that would permit a tracking of exit and entry over time in various product lines, but states which have pursued reforms have had indemnity carriers pull out of either the small group or individual market (e.g., Washington, Kentucky, California, New York).
While insurance reforms, especially rating and issue reforms, make it harder for risk selection strategies to work, they also confer relative advantages to HMOs that wanted to community rate anyway (perhaps to maintain federally qualified status or nonprofit status). Thus, states with aggressive reforms may be more attractive to entities which pursue these kinds of strategies. The surprising growth in managed care enrollment among small groups may be somewhat due to this sort of phenomenon.(20)
Competitive conditions. Three major interrelated dimensions of the competitive environment affect the profitability and attractiveness of different types health insurance: health plan competition, health provider competition, and organized purchasing activity.
Health plan competition. In the absence of managed care, health plan competition is mostly about selection. That is to say, most competitors want to find and offer low prices to healthy groups while avoiding unhealthy groups and individuals. Insurers compete with each other for healthy groups by offering lower loads. Thus, a competitive market with no managed care will observe relatively low loading factors or high medical loss ratios (i.e., premiums will be closer to claims or medical expenses, on average).
With managed care, premium price competition gets even more serious, for not only lower loads but managed care savings can lower net premium prices offered to groups. Increasingly, though, quality is also important to buyers. In the absence of systematically available and accepted data on quality of care, choice of provider is considered to be a proxy for quality of care by some enrollees and payors.(21) This is one way indemnity plans and looser PPOs or HMOs with POS options can survive and still command higher premiums than tightly limited staff model HMOs. Risk selection is still relevant, however, and part of the difference between indemnity, PPO and HMO prices is driven by the favorable selection tightly managed HMOs apparently attract.(22)
Health provider competition. Risk-bearing entities which sell insurance purchase inputs, the most expensive of which by far are health services. Thus the underlying state of competition in health service markets will very much affect the nature of health insurance plan competition. Inpatient hospital spending is the largest single component of health care costs, so that market is the single most important, but physician markets are vitally important, too.
Historically, at least in medium and large cities, both physician and hospital markets were unconcentrated and competition was atomistic if not always aggressive on price. The revolution in delivery patterns that has created and exposed excess capacity in these markets, along with selective contracting among managed care entities, has intensified price competition at the provider level. This excess capacity and price competition has helped managed care plans gain market share much faster than they would have been able to otherwise. In response to this, over time, physicians have joined larger and larger groups, and hospitals have merged or formed affiliations with each other and with physician groups, largely for the purpose of increasing their bargaining power vis a vis managed care plans. Indemnity insurers by and large have been too small to share in many of the price discounts being offered by providers. Thus, these developments serve HMOs better than indemnity plans. To the extent these provider consolidations have been proactive and effective, they may have raised health service prices or at least stemmed the rate of decline.
Excess capacity in health services markets has helped to moderate premium increases lately, especially in markets with high managed care penetration. These patterns are not uniform, and excess capacity in hospital markets does not per se guarantee excess capacity in specialist physician service markets, thought the two would appear to be correlated. The longer this excess capacity lasts, the more advantaged managed care plans will be vis a vis indemnity plans. While it is true that political constraints often prevent hospital markets from adjusting rapidly, this excess capacity is unlikely to persist forever. As the excess capacity disappears, managed care plans' relative bargaining power will decline and plans that stress quality in their marketing, e.g., indemnity plans and PPOs, will likely do relatively better in that marketplace. Whether than means higher health insurance premium (and health service price) inflation will return then remains to be seen, and probably depends upon relative market shares of different types of health plans and provider organizations at the time the excess capacity disappears. .
Organized purchasing. Organized purchasing activity is relatively new, but it is spreading throughout both public and private sectors. On the public side, purchasing pools for state employees' plans and Medicaid managed care bureaus are leading the way, with HCFA(now known as CMS) gearing up for a more aggressive market-oriented purchasing for Medicare in the near future. On the private side, some organized purchasing cooperatives have implemented many of the tenets of managed competition, and over 100 private health insurance purchasing coalitions have taken more modest but still promising steps toward value based purchasing strategies.(23)
Value based purchasing means getting one's money's worth. It is impossible to evaluate "worth" in health markets without substantial process and outcome quality reporting requirements being imposed on plans, and in turn, on providers. Large organized purchasers are doing so, especially state employee plans, Medicaid agencies, and some employer coalitions. These requirements change local markets in two ways. First, plans unable or unwilling to comply drop out of the market. This often chases away indemnity or loosely managed HMO licensees. Second, competition orients itself around price and the quality measures that are required to be reported. The old adage, be careful what you ask for, is relevant. We do not know at present how indicative of true overall quality are the HEDIS and HEDIS-like measures that are reported. We do know that plans will endeavor to do well on criteria that are made available to the public.
Public buyers can report both quality and price data, and in doing so can affect the nature of health plan competition throughout the local market in two ways. Provider discounts made available to some purchasers are harder to hide. No one likes to pay "retail" anymore if it is common knowledge that someone else has obtained serious discounts. In addition, health plan and provider quality information that is reported to Medicaid, to state purchasing pools, or to large employer coalitions can hardly be said to be nonexistent and unavailable to all others. All organized purchasing and information-centered developments favor health plans with good information systems, and many insurers are investing in these today. Increasing the role of published information is most threatening to traditional indemnity plans without information systems or quality monitoring strategies.
IV. Analytic Model of Insurer Market Decisions
The standard method for constructing an economic or optimization model of insurer behavior would be to specify the objectives (e.g., profit maximization, growth), identify the operable constraints (e.g., regulations, competition), derive possible equilibria (e.g., which products sold at what prices) and discuss the intuition behind them. This paper could do that, though formal notation and mathematics should be kept to a minimum in a concept paper. It may be more useful for the overall purposes of this paper, however, to simply draw on the elements of insurance markets already described and work through the set of strategic choices and constraints faced by today's insurers, and from that process infer a set of criteria by which to judge specific observable choices. This is the approach taken in this paper.
A. Strategic Choices
Table 1 summarizes the five strategic choices which every health insurer must make in today's market.
1. Select a product strategy
Specialization:
Indemnity based: loose PPO + TPA HMO based: HMO + ASO
Diversification:
Indemnity + PPO + TPA + HMO HMO + POS + PPO for self-insured + Indemnity
2. Select a provider integration strategy
Employees or full risk partners Contractual relations, partial risk only
3. Select license(s)
Indemnity HMO
4. Select specific product(s)
5. Select prices for specific products
******************************************************************************
1. Regulations
2. Economic Structure
3. Provider market organization
4. Competitive Culture
History Agents
Select a product strategy. The basic choices here are specialization or diversification. While posed as starkly divergent for illustrative purposes, in reality the choices lie along a continuum. Both indemnity and HMO firms might reasonably conclude they will achieve the best financial performance if they specialize in what they do best. For indemnity firms, this is pricing and marketing fee-for-service contracts, as well as negotiating fee-schedules and discounts with established and relatively large groups of providers, avoiding detailed utilization management. For HMOs, what they do best is utilization management and clinical integration, so as to maximize the use of cost-effective health care through capitated contracts and other financial and managerial incentives or controls. Either could add TPA or ASO contracts for self-insured clients to their base and still maintain the essence of a specialization strategy. A specialization strategy is consistent with one of two beliefs an insurer might hold about the future: either the type of plan it is now will be dominant, or this particular firm's best chance of long run survival is to concentrate on being an exemplary representative of its type.
Diversification is a more risk averse strategy. In the familiar tradeoff depicted in Figure 2, greater return goes only to those who take the greater risk. Diversification in our context this

would represent, among other things, insurers enabling themselves to offer all kinds of products from pure indemnity to closed panel HMOs. This would necessarily reduce an insurer's ability to focus in a few areas, and thus organizational and managerial limits would likely prevent maximum efficiencies from being realized. At the same time, since no one knows which types of health plans will become the most popular in the long run, a diversification strategy hedges risk in that whichever health plan form becomes dominant, the diversified firm will share in that growth. Not as greatly as it would have if all its investment resources had been devoted to perfecting that particular form, however, and thus the risk-return contour in Figure 2 is upward sloping.
Select a provider integration strategy. This is particularly important for the long run. Again, there are two broad choices. Either providers are going to be full partners and share risk with insurers, i.e., the owners of risk-bearing firms, or their relationships with insurers will be merely contractual and entail at most only partial risk sharing. The full risk sharing strategy will enable insurer and provider groups to deal with the special challenges of self-insured firms and organized buyers as a team with incentives aligned, but it will also dissipate some of the rewards from selective contracting and risk bearing that aggressive insurers could perhaps obtain on their own. A major risk of the incomplete risk sharing strategy is that provider groups will accelerate formation of their own networks which are capable of direct contracting and even accepting full capitation risk. It is not clear whether this development will lead to a viable "third way" between indemnity insurers and HMOs, but it is clear that some provider groups are determined to try it. Whether providers and insurers generally end up as collaborators or competitors may depend in no small measure on the relationships insurers form with providers in the next few years.
Information system decisions may well be at the heart of this choice and outcome. To the extent that buyers demand more sophisticated process and outcome information, then insurers and providers who collaborate to devise and invest in effective systems will do well. At the same time, the cost involved may preclude most provider groups from going it alone without an insurer partner. The more important objective information becomes to health plan selection, the more collaborative one can expect insurers and providers to be.
Select license(s). The first choice dictates the technical strategy here. If diversification is the strategy, depending on the particular state, one or two (or more) licenses may be necessary to enable the insurer to pursue a true diversification strategy. This strategy may be pursued with subsidiaries, merger, or pure product expansion. Different solvency and reporting requirements make this strategy potentially costly, and this could deter some competition from being engendered.
Select product(s). It appears that very few health insurers, even those with specialization strategies, are pursuing "one product" strategies. Even the most committed indemnity firms are developing high deductible/MSA products as well as PPO and TPA arrangements they can market. Except for medical underwriting costs (which can be cut easily enough), the equilibrium TPA payment will be equivalent to the equilibrium loading factor previously earned, with some risk, from selling fully insured products. So, in the long run, there is no reason for indemnity insurers to avoid this large and growing market. It is not risk bearing, but it is in the purview of traditional functions insurers provide. In addition, as case management and cost containment strategies are increasingly adopted by self-insured firms, TPAs can take on some of these care or network management functions that could reap a return as well. Of course, risk sharing between the self-insured firm and the TPA jeopardizes the ERISA exemption, so these evolving contracts will be watched carefully.
Similarly, HMOs are evolving to meet the demands of a heterogeneous marketplace, adding POS options (where legal) as well as ASO and rental PPO arrangements for self-insured firms and even indemnity products to become the "one-stop shop" for large firms who want to offer choice to their enrollees. There is some anecdotal evidence that large, long-time self-insured firms are starting to offer one fully insured product, typically an HMO, along with their self-insured options (e.g., Boeing). In the long run, an employer's "make or buy" decision for all these products will depend on who is best at controlling costs and providing demonstrable quality. Fully integrated HMOs may be uniquely situated to "win" this kind of competition for that kind of employer.
But that is not the only kind of employer or group insurance market. Small employers cannot offer choice; they will choose one product from one insurer, unless they are in an organized purchasing cooperative. In the latter case, employees or employers will choose from the products of many insurers. If cooperatives becomes the dominant way small groups and individuals purchase health insurance, this may actually slow current trends toward product diversification in health insurance. Single insurance entities could never be the "one stop shop" in such cases anyway, and thus it may be unprofitable to devote resources to developing products that are likely to be inferior in some ways to similar ones produced by specialist insurers. Thus, while the large firm market has engendered forces which encourage product line diversification by insurers, the small firm market, even or especially the organized small group market, provides countervailing incentives. Since roughly ½ of all workers work in establishments with fewer than 100 workers, these countervailing forces may be roughly offsetting, which means that different insurance product strategies may both be successful in the long run.
Select prices for specific products. While this is the variable economic theory focuses on because it is a fundamental indicator of competitive performance, pricing strategy alone is somewhat anticlimactic after all the other strategic decisions have been made. Despite the recent focus on cost containment, buyers today are increasingly clearly interested inthree dimensions of health insurance: price, technical quality of care, and choice of provider.(24) Evidence of this is manifest in state legislatures, where over 400 bills purporting to regulate some aspect of managed care restrictions on access to providers or case management techniques were introduced in the first half of 1996 alone.(25) It is also clear from what organized purchasers are putting in their RFPs.(26) The relative growth of PPOs and HMOs with POS options vs. staff model/closed panel HMOs over the last 10 years is a manifestation of the market demand for choice of provider. Employers do respond to surveys that price is the number one consideration.(27) But relative emphasis on cost is also consistent that with the belief that quality among medical providers is uniformly high, and that unless cost growth is brought under control, no level of quality is affordable.
B. Tradeoffs Among Choices
The perceived tradeoffs (willingness to trade one for the other) among these dimensions vary across the population, and the technically feasible slopes of these tradeoffs vary across different health insurance organizations. Figure 3 is a graphical model that can illustrate these tradeoffs.
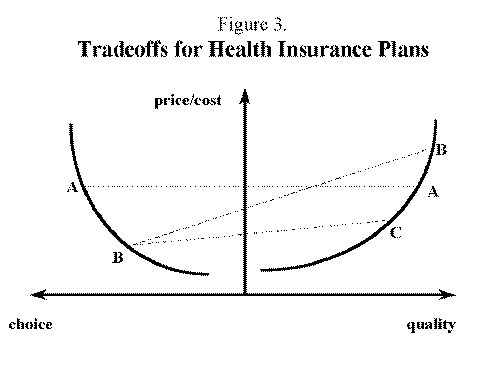
The three axes of Figure 3 represent the dimensions of a health insurance plan which consumers are presumed to care most about. The vertical axis is labeled price/cost because the relation between these two is not hard and fast. The cost of providing health care services at a given level of quality for a particular population can map into a higher or lower price (premium) depending on the load or cost (including profit) of providing the necessary non-health services attendant to health insurance plans. Load competition between TPAs, ASOs, HMOs, indemnity insurers, and self-insured firms' health benefits management units themselves will determine the markup in equilibrium.
The horizontal axis measures increasing quality of care to the right and increasing choice of provider to the left. There is a curved, parabolic line in each quadrant to represent technologically feasible contours of the relations between quality, choice, and price/cost. On the right hand side, the curved line is derived from an assumption that providing higher quality services costs more, and on the left hand side, the curved line reflects an assumption that providing greater choice of provider leads to higher costs since plans cannot trade volume promised for health service price concessions, and since larger provider networks are more difficult to control with particular utilization management techniques.
The straight dotted lines labeled AA, BB, and BC represent the net result of health plans' five different strategic choices outlined above. They can be thought of as "health plan contours," the tradeoffs among the dimensions available to specific insurer entities or specific products of larger risk-bearing entities. AA might be a loose PPO with most but not all local providers in the network and with high but not the very highest achievable level of quality delivered, on average. (More choice of provider opens up the plan to mediocre providers over which the PPO has relatively little control). BB is a small, tightly managed HMO with very high quality providers, perhaps organized around an academic health center or teaching hospital, and BC is a closed panel HMO with lower than average quality providers. The intersection of the health plan contours and the vertical axis reveals the premium at which these plans might be offered for sale to a particular group.(28) The PPO costs the most, the "high quality" HMO is next, and the "budget" HMO is the least expensive. Which plan the group selects, or how the members of the group sort themselves among the plans if they are offered all three by their employer or purchasing coalition, depends upon the individually and collectively expressed willingness to pay for choice and quality. The distributions of these willingnesses to pay is unknown at the moment, and given the powerful filtering role that employers play in mediating between insurer offers to plans actually offered to workers, it may be impossible to discern what the true underlying distributions are.
In addition, the measurement of quality is hardly fully objective at this point. Given this uncertainty, it is not surprising that the overall product diversification strategy is a popular one for insurers, since the more lines you have to offer people the greater the likelihood that at least some of your lines will cross the vertical axis at or near relevant willingnesses to pay for your choice and quality combinations. Ergo regulatory restrictions on particular combinations for specific licensees (or non-licensees) are strongly opposed among would-be insurers. They literally could be preventing or at least making it more costly for the insurer to offer specific products that might do very well in the marketplace. I discuss those constraints in a bit more detail and context below.
C. Constraints: Intervening and Environmental Factors.
State insurance regulations are among the most important constraints operable upon insurers. Some states require an HMO or PPO license for serious provider access restrictions to be imposed in health insurance contracts, and these requirements in turn trigger a level of oversight by health departments or other entities that evaluate network adequacy and quality. Complying with these oversight requirements is costly, though it is impossible to tell at the moment how much more burdensome state reporting requirements are than internal reporting and monitoring standards the insurer qua managed care entity would impose upon itself in order to compete successfully in the marketplace.
Community rating regulations reduce the ability to use experience rating and thus disadvantage indemnity license holders without a tightly managed care product that can offer reduced costs through utilization management. At the same time, the willingness to pay extra for choice and perceived quality could still be greater for many buyers than the cost savings managed care plans have heretofore passed along. To date there has been no systematic evidence presented that states with tighter rating restrictions have fewer indemnity plans than states with looser restrictions, or that the availability of certain products has been compromised beyond what the market is doing on its own. So, while some regulations raise costs and others constrain strategies, it is not clear at present how seriously they jeopardize, rather than strengthen, competitive pressures in the insurance market overall.
Any willing provider, freedom of choice, or mandated POS legislation can make it more difficult to manage the care delivered by a health plan.(29) Legislation banning financial incentive contracts with providers and other attempts to shift the balance of bargaining power back to providers and away from health plans would perhaps shift the stylized health plan contours upward even more, for the most efficient strategies for delivering quality and choice would be foreclosed.
The local economic structure -- distributions of employers by firm size and industry --
determines a large part of the market for health insurance. The larger the percentage of the workforce in large multi-state businesses, the greater the likelihood that self-insurance is very important, and therefore TPA and ASO products are more likely to be prominent.
Finally, the local competitive culture and history can effectively constrain health plan competition and thus health insurer behavior. Relative dominance by the Blues, the evolution of the local Blue plan(s), the existence, history and perception of managed care, provider supplies and the extent of provider (both hospital and physician) consolidation, the reactions of agents to health market evolutions will all shape the price and supply parameters that most health plans face.
Agents in particular may be the key to small group market equilibria, for health insurance is often described by insurance professionals as a product that is sold and not bought. Important as health insurance is, small employers have bigger worries, and they appear to trust their agents to sort out health insurance options for them. Agents tend to sell small businesses more than just health insurance, and they therefore have more credibility with small business owners than relative strangers trying to explain new health insurance options alone. Thus, insurers who want to target this market ignore agents' interests at their peril, at least in the current environment. Anecdotal evidence suggests that the best way to get agents to market your product is to pay market rate commissions. Organized buyers who tried to pay less have not been satisfied with how their products have sold.(30)
V. Assessing Health Insurers' Strategic Choices
It is not possible at the present time to derive general normative statements about which strategies are best for society as a whole, and thus which ones that policy should encourage or discourage. Returning to the heuristic model of Figure 3, one can imagine the health insurance market place as "spider's web" of health plan contour lines. In the abstract, a relatively dense web with a wide span, i.e., with widely varying quality, choice, and price dimensions, would seem to be ideal, for then all possible consumer preferences in that three-dimensional space could be accommodated.
It is important to keep in mind, however, that dense webs could result from either a large number of insurers pursuing specialization strategies or a small number of insurers pursuing diversification strategies. In essence, the question comes down to, are health care consumers better served if the health plan market evolves into something more like breakfast cereals (with a few purveyors of many, many brands) or more like restaurants (with many purveyors of relatively few brands each)? While economic science has made some progress in defining and answering this question ever more precisely, a general empirical or even theoretical answer is not feasible yet, for ultimately it depends on both the distributions of consumer preferences in this (at least) three-dimensional product space and the equilibrium cost and price implications of alternative production configurations. In the case of health insurance, given the crucial role that employers play in defining the options that workers see, it may be very difficult to discern the underlying distributions accurately. And the ultimate price consequences of the recent revolution in health care delivery patterns are very far from being settled. Not to mention that outpatient quality measurement is in its infancy.
In the absence of definitive science and empirical fact to guide us, then, the practical policy maker falls back to relative risk analysis and a monitoring strategy. A useful question may be, on the margin, would a particular policy action increase or reduce the density or span of the local health plan contour web that most workers actually face? This question may be easier to answer than the global one of, is the local web optimally dense, though policy analysis will always require that fundamentally normative judgments be made about the desirability or tolerableness of the current state of the world.
Unfortunately, data that would permit informed normative judgments about the current state of the world for health insurance markets are not generally collected or reported. The NAIC is working on database construction, but many state insurance departments do not require sufficiently detailed reports to support first-rate policy analysis at the present time. To some degree, this lack of data reflects political opposition to more detailed regulatory oversight, and new data collection initiatives must be mindful of these realities and constraints. At the same time, there are some bits of information that are currently reported that could be disseminated in a more systematic way, and there is a compelling reason to open up a dialogue with state insurance departments and legislatures to encourage or require data collection to support reasonable policy analysis and to avoid doing more harm than good through ill-informed public policy.
In concluding this concept paper, I outline four concrete monitoring steps that would improve the ongoing analysis of health insurance markets.
Step One: Measure changes in the relative density of the health plan contour "web" that most workers actually have access to. This is less abstract than it may appear. While insurance departments do not generally produce annual reports to make this easy, almost all require insurers to file policy forms for each different type of contract offered for sale. Thus, within state insurance departments (and other relevant departments that regulate insurers from time to time, e.g., the Commerce Department in Minnesota, the Department of Corporations in California), information exists about how many insurers and fully-insured products are offered to group and individual markets. ASPE/DHHS could survey the relevant state departments and institutionalize the reporting of these data.
Since the policy forms are filed, the types of network restrictions (choice) could be abstracted, much like hospital discharge forms are abstracted by private vendors, and reported in this same survey as well. Detailed abstraction of the policy forms could be expensive, but low-cost versions of this information in conjunction with the basic product market counts discussed above would add tremendous value to any policy-relevant appraisal of the current state of the world.
Collection of quality data, e.g., HEDIS 3.0, is not institionalized anywhere, and they have never been required of indemnity plans nor most PPOs. This is the greatest challenge to all health insurance policy makers as we enter the 21st Century. At the same time, there is sufficient political interest in quality measurement and reporting at the moment that this may be a most propitious time to invest in developing recommendations about quality reporting that could assist in characterizing the range of health plan options available to Americans. HEDIS 3.0 would seem to be a reasonable place to start the conversation.
While waiting for HEDIS/Godot, however, one practical local solution is to watch which plans the perceived "highest" quality providers affiliate with, and what kind of strategy they pursue generally. If they are available through all plans, then one may infer that quality is more nearly homogeneous across plans. If they are in only a few networks, however, then the quality differential among plans is probably greater. This information is trackable in individual states by knowledgeable observers, e.g., local departments of health, which could in turn be surveyed by ASPE.
Finally, there is the thorny issue of the disconnect between the choices available in the market as a whole, as filed with the insurance departments, and the choices that most workers actually face. This can only be resolved with periodic employer and employee surveys, but MEPS and NEHIS, if continued as planned, may be reasonably adequate for this purpose, especially if budgeted sample sizes permit state-specific estimates at least every 3-5 years.
Step Two: Track premiums and loading factors.
Historically, state insurance departments' primary function was to measure and assure the financial solvency of insurers. To perform this function, they must evaluate data that can be interpreted as premiums and medical expenses per covered life. Insurers must have this by product line, thought states do not always demand that it be reported in that level of detail. At a minimum, though, average load across product lines is computable from what the insurers report now. As long as health is separated from other lines the insurers might have (like disability income or life insurance), this would add considerable value to an analysis of market performance. Ideally, states would begin to require insurers to report implicit loads by health product line. The eight states with minimum loss ratios in the individual market currently do this. HMOs who want Medicare risk contracts report something close to this concept to HCFA(now known as CMS), and both Interstudy and AAHP surveys collect HMO-wide loads as well.
Step Three: Monitor the self-insured market as well. While there are reporting requirements to the Department of Labor for ERISA plans, we learned during health reform that reported premium equivalents are widely believed to be seriously inaccurate. Purchased stop-loss insurance as well as TPA/ASO services are corporate income tax-deductible, so records of them must be maintained, and could therefore be easily added to ERISA reporting requirements. Quality of care and choice of provider within ERISA plans also merit scrutiny, but many self-insured employers have been leaders in HEDIS development, so perhaps the urgency is less here than in the medium and small group commercial market. At the same time, while quality is on the table this year through the Presidential commission co-chaired by Secretary Shalala, it makes sense to expand the inquiry to self-funded plans in addition to those regulated by the states.
Step Four: Watch Organized Buyers. They may or may not be the future, but some private and public sector entities have taken impressive steps toward value based purchasing and filling in their health plan contour web with price-quality-choice options they want for their enrollees. State employee plans, state Medicaid agencies, large employer coalitions, and purchasing cooperatives for small employers have all exercised their ability to demand more accountability from health insurers and have been fairly successful in getting it. All health insurance purchasers would do well to consider emulation strategies that fit their particular circumstances.
American Association of Health Plans. HMO and PPO Industry Profile. Washington, DC (1995-1996 edition.).
Butler, P. "Public Oversight of Managed Care Entities: Issues for State Policymakers." draft paper prepared for the National Governors' Association. (March 1996).
BCBSA Internet World Wide Web page, http://www.bluecares.com/blue/about/blue_roots.html (1997).
Claxton, G, Feder J, Shactman D, and Altman S. "Converting From Nonprofit to For-Profit," Health Affairs v. 16 # 2 (March/April 1997).
Group Health Association of America. HMO Industry Profile. Washington, DC (1992 edition).
Hellinger, F. "Selection Bias in HMOs and PPOs: A Review of the Evidence," Inquiry v. 32 # 2 (Summer 1995), pp. 135-142.
Horvath J and Snow K. "Emerging Challenges in State Regulation of Managed Care: Report on a Survey of Agency Regulation of Prepaid Managed Care Entities." National Academy for State Health Policy monograph (August 1996).
Jensen G, and Morrisey, M. "Managed Care and the Small Group Market," paper presented to the American Enterprise Institute conference, Managed Care and Changing Health Care Markets, April 10, 1997.
McNerney, W. "Big Question for the Blues: Where to from here?" Inquiry, 33(2) (Summer 1996). pp. 110-117
Marsteller, J, Bovbjerg RB, Nichols LM. "State Policy Options for Nonprofit Conversion," February 1997.
Marsteller, J, Bovbjerg RB, Nichols LM. "Managed Care and the Resurgence of Selective Contracting Restrictions," Journal of Health Politics, Policy, and Law (forthcoming).
Meyer, J, Silow-Caroll S, Tillman I, and Rybowski L. "Employer Coalition Initiatives in Health Care Purchasing, Volumes I and II." Economic and Social Research Institute monographs. (February 1996 and September 1996).
Meyer J, Naughton D, and Perry M. "Assessing Business Attitudes on Health Care." Economic and Social Research Monographs (October 1996).
Rolph E, Ginsburg P, and Hosek S. "Regulation of Preferred Provider Arrangements," Health Affairs v. 6 #3 (Fall 1987).
1. PL 104-191, popularly known as Kassebaum-Kennedy.
2. For example, proof of insurability (e.g., health questionnaire, medical examination) is generally not required for group enrollees whereas it is almost always required (where legal) for individual insurance applicants. Again, the reason is that groups formed for purposes other than purchasing insurance provide natural pooling mechanisms that protect the insurer against adverse selection.
3. For example, proof of insurability (e.g., health questionnaire, medical examination) is generally not required for group enrollees whereas it is almost always required (where legal) for individual insurance applicants. Again, the reason is that groups formed for purposes other than purchasing insurance provide natural pooling mechanisms that protect the insurer against adverse selection.
4. Part of the motivation behind federal efforts to encourage provider sponsored networks (PSNs) through Medicare reform legislation is to enable providers to offer insurance products without having to bother with state regulations that are perceived to hamper their ability to compete with established HMOs.
5. Payment or reimbursement after the fact for services rendered, traditionally without restrictions on which licensed providers deliver the services. Most Blues plans reimburse providers, whereas most commercial indemnity plans reimburse subscribers after they pay the providers.
7. Originally, federally qualified HMOs benefitted from dual-choice requirements (employers of a certain size, if they offered health insurance at all, had to offer a federally qualified HMO to their workers) and from start-up grants and loans. Today, the advantages of being federally qualified are less clear, and may be mostly in marketing a symbol of approval. Federally qualified status is NOT required to write Medicare or Medicaid contracts, for example. It is possible that the federal HMO Act may preempt state any willing provider laws, but this has not been tested in the courts (Butler, 1996). The percentage of HMOs that are federally qualified has remained slightly above 52% since 1988, while the percentage of enrollees in federally qualified HMOs has remained about 70% over the same period (GHAA 1992; AAHP 1996).
9. A mutual insurance company is one in which the members are both the insurers and the insured. Shares are held exclusively by members to whom profits are distributed as dividends in proportion to the premiums the members paid the company. Since Blues mutuals were organized as nonprofits, if there was any "profit" left after all operations including community benefit actions were undertaken, it is/was distributed to enrollees/subscribers as premium rebates.
10. A short history of the Blues is contained on the Blue Cross Blue Sheild Association web page at http://www.bluecares.com/blue/about/blue_roots.html.
13. Claxton et al, (1997), Marsteller et al (1997).
14. The term "re-insurance" derives from the practice of insurance companies, especially small ones or with small specific product lines, insuring themselves against potential losses on their primary contracts by purchasing insurance. Thus, the primary insurance contract is "re-insured." Some firms specialize in selling reinsurance to primary insurers, but they are beyond the scope of this paper.
15. Jensen and Morrisey, (1997).
16. Through its "Stop Loss Insurance Model Act," 1996.
17. The concept of economic cost includes a normal or competitive profit.
18. Blues plans had "participating providers" who had agreed to accept their discounted fee schedule. This is like an EPO product, but the vast majority of providers did participate, so de facto provider choice was usually unlimited.
19. "Premiums written" means premiums received in exchange for fully insured products.
20. Jensen and Morrisey (1997).
21. The implicit assumption appears to be that as long as choice of provider is an option, if a medical condition is serious enough, then the "best" providers could surely be found and engaged. This does not mean that the front-line network of a POS or a PPO is perceived to be higher quality, per se. Whether these perceptions of choice as quality are more in employees' or employers/payors' eyes does not matter at the moment. In the absence of good quality data, they are operable in insurance markets on the demand side. Availability of accepted quality data may very well reduce the perceived need for absolute provider choice, as long as there is an opportunity for second opinions and provider switching within plans' networks. We are a long way from widely accepted quality data, however.
24. I subsume copayment liabilities (deductibles, coinsurance, stop-loss limits) as a sub-dimension of price: the level of generosity or comprehensiveness is presumed to be given.
25. America Health Line, 5/20/96.
26. See the RFPs of the Pacific Business Group on Health, Minnesota Buyers Action Group, the St. Louis Business Group on Health, CALPERS, and the Washington State Health Care Authority, and the Washington Department of Social and Health Services (re: Medicaid) for examples of informed buyers who are interested in quality and provider choice for all enrollees in addition to price. These entities span private and public employers as well as Medicaid.
27. Meyer, Naughton, and Perry (1996).
28. All lines would shift if the demographic composition of the group in question changed. We focus on the set of tradeoffs facing a single insured group without loss of generality.
30. Witness the California HIPCs decision to pay agents considerably higher commissions in the coming plan year than they have to date. Until this, agents had financial incentives to recommend non-HIPC plans.
