Monday, January 28, 2019
Printer Friendly Version in PDF Format (11 PDF pages)
CLINICAL SUBCOMMITTE UPDATE
Health Resources and Services Administration
- Notice of Funding Opportunities
- Geriatrics Workforce Enhancement Program
- Geriatrics Academic Career Awards Program
- Alzheimer’s Disease and Related Dementia Curriculum
- https://bhw.hrsa.gov/grants/geriatrics/alzheimers-curriculum
- Continuing Education for Physicians, Nurses, Allied Health Professionals, Health Educators, and for Module 14 Pharmacists
CDC: New Continuing Education Course: Brain Health
- Learning Outcomes:
- Explain-review brain health terminology
- Define and describe risk factors associated with age related cognitive decline, mild cognitive impairment, and dementia
- Summarize lifestyle medicine management strategies, including hypertension management, that may decrease risk
- Continuing Education:
- 1.0 CME/MOC education activity is available through ACPM's learning platform
- Cost:
- Learners can create a free login account and take the course at no cost
- Brain Health Course
U.S. Dept. Veterans Affairs Updates
Marianne Shaughnessy, PhD, CRNP
Susan G. Cooley, PhD
VA Office of Rural HealthDementia-Related Projects Funded for FY2019
- https://www.ruralhealth.va.gov
- VA Video Connect: Facilitate social worker support of rural Veterans' caregivers via video connection and other in-home technology
- Assessment of Caregiver Support for Rural Veteran Caregiver Dyads: Assess impact of current caregiver support programs for rural Veterans with special needs such as dementia; identify service gaps
- Caregiver Videos: Videos to educate, empower caregivers for Veterans with dementia
- Health & Independent Living for Rural Veterans with Disabilities: Analysis of services available and used by rural Veterans who require assistance for independent living, including those with dementia
- Improving Access to Geriatric Care in Rural Areas/Geriatric Research, Education, and Clinical Center (GRECC) Connect: National dissemination project to support providers caring for rural Veterans with geriatric syndromes, significantly those with dementia
- Geriatric Scholars: National dissemination program to address needs of rural Veterans by educating and supporting innovation of rural providers concerning geriatric needs including dementia.
VA Geriatric Scholars FY2019 Plans Initiated Dementia Education and Resources
- Geriatric Scholars Program core course in geriatric medicine and gerontology:
- Denver, May 20-22, 2019
- Los Angeles, September 11-15, 2019
- New York, September 9-13, 2019
- Wisconsin, September 23-27, 2019
- Geriatric Scholars Program Clinical Practicum with focus on dementia at the following GRECCs:
- Madison Geriatric Research, Education, and Clinical Center (GRECC), July 2019; August 2019; September, 2019
- Palo Alto GRECC, May 2019
- Puget Sound GRECC, April 2019, May 2019
- Geriatric Scholars Program Advance Scholar courses:
- American Geriatrics Society (AGS)/Portland, May 1-4, 2019
- Leadership and Management/Los Angeles, August, 2019
- Geriatric Scholars Program Rural Interdisciplinary Team Training in care of older Veterans
- Funded for 20 on-site training for all clinic staff on teamwork in care of older adults; recognition of geriatric syndromes, "red flags," functional impairments including dementia. All trainings have been updated to include the Rural Caregiver Resource Center and opportunities for Resources for Enhancing All Caregivers Health (REACH) training.
- Geriatric Scholars Program Rural Interdisciplinary Team Training in care of elders for Indian Health Service (IHS)
- Funded for 6 on-site training for all clinic staff on teamwork in care of older adults; recognition of geriatric syndromes, "red flags," functional impairments including dementia .
- GRECC Connect Webinars for VA Staff with specific focus on cognitive impairment, dementia:
- An Approach to Palliative and End-of-Life care for Dementia (Thomas Caprio) January 11, 2019
REACH VA Caregiver Support Intervention Updates
- National Program to Provide Resources for Enhancing All Caregivers Health (REACH) VA to Caregivers of Veterans
- Funded by VA Office of Rural Health and Caregiver Support Program
- At the end of FY18, 1225 staff at 282 VA sites (hospitals, clinics) had been trained in REACH VA
- At the end of FY18, the Memphis Caregiver Center had delivered REACH VA to 591 caregivers across the country
- Pilot enhancement to curriculum: REACH training
- The Caregiver Center, funded by the Caregiver Support Program, is being included in the VA Geriatric Scholars Program Rural Interdisciplinary Team Training (RITT) training. The goal is to identify, train, and certify staff from rural facilities to deliver the REACH (Resources for Enhancing All Caregivers Health) and Telephone Support Group programs. The Caregiver Center will provide all materials for staff and Caregivers.
- To date, no RITT attendees have been enrolled in the REACH VA training.
- For Indian Health Service/Administration on Community Living:
- REACH into Indian Country was a three year project funded by the Rx Foundation to implement the REACH caregiver support intervention for American Indian/Alaska Native caregivers of individuals with dementia.
- Going forward, there is a mechanism in place for ongoing training through the University of Tennessee Health Science Center (UTHSC) Caregiver Center.
VA "Hand-in-Hand" Dementia Training Preliminary Summary
- Roll-out of Centers for Medicare & Medicaid Services (CMS) "Hand-in-Hand" Dementia Training Program in VA Community Living Centers (CLCs), formerly known as VA nursing home care units, has been completed
- Data on implementation collected July 2015-Sept 2017
- 54 (40%) of VA CLCs across the national VA health care system reported using Hand-in-Hand training in their CLCs on a routine basis
- Classroom-based modules and new online instructional modules are now available for VA staff use
- VA Talent Management System allows for knowledge post-tests, learner evaluation and attendance tracking
- Summary report describing implementation and evaluation will be shared with National Alzheimer's Project Act (NAPA) Advisory Council later this year
VA Dementia Projections FY2019-FY2033Available Online
- Current VA statistical projections of dementia prevalence & incidence among Veterans are available online at https://www.va.gov/GERIATRICS/GEC_Data_Reports.asp
- Includes summary of projections for FY2019 compared with FY2033
- Separate projections for all Veterans; Veterans enrolled in VA health care system (enrollees); and Veterans who use VA health care system (VA patients)
- Based on national prevalence rates for dementia applied to Veteran population estimates
- Source: VA Office of Policy & Planning, Projections of Prevalence and Incidence of Dementias FY14-FY33; Sept. 2013
CMS Update
2019 Medicare Physician Fee Schedule (PFS)
- On Nov. 1 CMS released a final rule for the 2019 PFS, effective January 1, 2019 that includes:
- Improved telehealth coverage that permits providers to bill separately for virtual communications, including whether an in-person patient visit is needed, and review photos/videos
- Expansion of provider types in the Merit-based Incentive Payment System for physical therapists, occupational therapists, clinical psychologists, and registered dietitians or nutrition professionals
- Streamlined evaluation and management (E/M) visit coding that in 2021 collapses levels 2-4 into one to pay a single rate and maintains the level 5 code that accounts for care provided to the most complex patients, with a new "extended visit" add-on code for use with E/M level 2- 4 visits to account for additional resources when practitioners need to spend extended time with the patient.
- (Strategy 2.B) Information at: https://www.cms.gov/medicare/medicare-fee-for-service-payment/physicianfeesched/
Medicare Home Health Improvements
- In October CMS announced changes to the home health payment system that include introduction of remote payment monitoring technology and updated payments through a new case mix system called the Patient-Driven Groupings Model (PDGM)
- The PDGM puts the focus on patient needs rather than volume of care, and relies more heavily on the individual's characteristics
- The cost of remote patient monitoring can now be reported by home health agencies as allowable costs on the Medicare cost report form, fostering the adoption of emerging technologies by home health agencies and data sharing between patients, caregivers and providers
- (Strategy 2.F) Information at: https://s3.amazonaws.com/public-inspection.federalregister.gov/2018-24145.pdf
Medicaid Dually Eligible Guidance
- In December CMS sent a State Medicaid Director Letter outlining "Ten Opportunities to Better Serve Individuals Dually Eligible for Medicaid and Medicare"
- The letter highlighted opportunities to streamline care through dual-eligible special needs plans, Programs for All-Inclusive Care for the Elderly, the use of streamlined Medicare claims data, and improved opportunities for use of Medicare data for program integrity purposes
- The letter is here: https://www.medicaid.gov/federal-policy-guidance/downloads/smd18012.pdf
- (Strategy 2.H)
2018 Measures Under Consideration (MUC) List
- In December CMS released the annual MUC list
- MUC18-757 Annual Wellness Assessment: Preventive Care seeks to examine the percentage of patients 65 years of age and older with a Medicare Annual Wellness Visit who received age and sex-appropriate preventive services, including a depression screen
- Several other measures proposed for certain programs propose to examine the transfer of health information to the new provider, when patients travel from setting to setting, including information regarding medications
- (Strategy 2.D) Information at: https://www.cms.gov/Medicare/Quality-Initiatives-Patient-Assessment-Instruments/QualityMeasures/Downloads/Measures-under-Consideration-List-for-2018.pdf
Eligible Clinician Cognitive Impairment Related Electronic Clinical Quality Measures
- Documentation of a Health Care Partner for Patients with Dementia or Mild Cognitive Impairment
- Measure assesses whether clinicians are collecting contact information for a health care partner
- Measure's development began around 2013
- Strong clinician, patient, and caregiver support
- Practices not collecting data needed for measure calculation
- Restarted development in 2018
- Conducted a literature review, met with the work group, and initiated test site recruitment
- Still strong support for the measure
- Practices moving towards collecting necessary data, but measure still currently not feasible
- (Strategy 2.D)
- Cognitive Impairment Assessment Among Older Adults (75 Years and Older)
- Measure assesses whether clinicians are assessing patients aged 75 years and older for cognitive impairment
- Measure's development began around 2013
- Testing found measure to be feasible, reliable, and valid
- Strong clinician, patient, and caregiver support of the measure
- Restarted development in 2018
- Add a follow-up component for patients who screen positive
- Conducted a literature review and met with the work group
- Exploring the inclusion of the follow-up component: completing a follow-up appointment, conducting an additional assessment, or providing a referral to a specialist for additional evaluation
Medicare Shared Savings Program (MSSP) Final Rule
- In December CMS issued a final rule for MSSP called "Pathways to Success" that redesigns participation options to encourage Accountable Care Organizations (ACOs) to transition to performance based risk quickly and address additional tools and flexibilities in the areas of new beneficiary incentives, telehealth services, and beneficiary assignment methodology
- Examples in the rule of incentives that an ACO could make available include "electronic systems that alert family caregivers when a family member with dementia wanders away from home," and vouchers for disease-specific self-management, meals programs, "apps," wellness programs, etc.
- (Strategy 2.E) Information at: https://s3.amazonaws.com/public-inspection.federalregister.gov/2018-27981.pdf
Updates to Value-Based Insurance Design (VBID) Model
- CMS recently announced enhancements to the VBID model for 2020 that include:
- Allowing plans to provide reduced cost sharing and additional benefits to enrollees in a more targeted fashion such as customization based on chronic condition, socioeconomic status, or both, and benefits not primarily related to health care, such as transportation;
- Bolstering the rewards and incentives programs that plans can offer beneficiaries to take steps to improve their health, permitting plans to offer higher value individual rewards than were previously allowed; and
- Increasing access to telehealth services by allowing plans to use access to telehealth services instead of in-person visits, as long as an in-person option remains
- Beginning in the 2021 plan year, the VBID model will also test allowing Medicare Advantage plans to offer Medicare's hospice benefit, a change designed to increase access to hospice services and facilitate better coordination between a beneficiary's hospice providers and other clinicians
- Information at: https://innovation.cms.gov/initiatives/part-d-payment-modernization-model/
Nursing Home Oversight and Safety Improvements
- In November CMS announced changes to nursing home oversight to improve transparency and assure that facilities are staffed adequately to provide high-quality care
- These include sharing data with states when potential issues arise regarding staffing levels and the availability of onsite registered nurses, clarifying how facilities should report hours and deduct time for staff meal breaks, and providing facilities with new tools to help ensure their resident census is accurate
- (Strategy 3.D) For more on payroll based journal (PBJ) staffing: https://www.cms.gov/Medicare/Provider-Enrollment-and-Certification/SurveyCertificationGenInfo/Policy-and-Memos-to-States-and-Regions-Items/QSO18-17-NH.html?DLPage=1&DLEntries=10&DLFilter=payroll&DLSort=3&DLSortDir=descending
National Partnership to Improve Dementia Care in Nursing Homes: Update
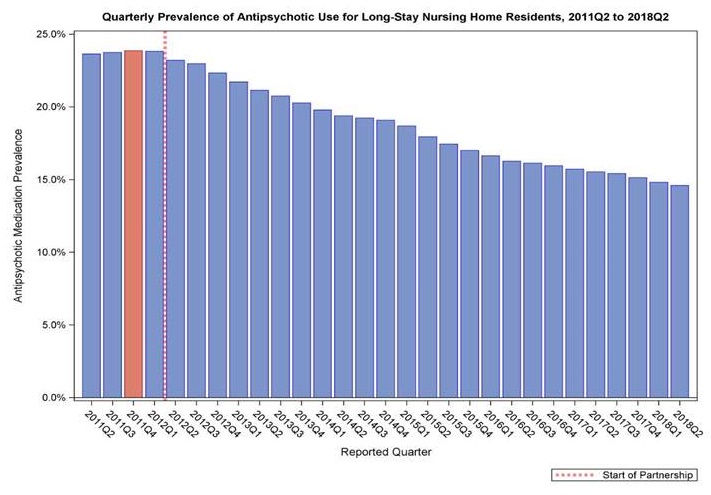 |
| Decrease of 38.9 percent to a national prevalence of 14.6 percent in Quarter 2, 2018. (Strategy 3.D) SOURCE: CMS Quality Measure, based on MDS 3.0 data. For more information, see the MDS 3.0 Quality Measures Users Manual. |
Medicare Learning Network - Dementia Care & Psychotropic Medication Tracking Tool
- Will be held Tuesday March 12, 2019, 1:30 - 3:00 PM Eastern Time
- Expected to provide insight on the the Dementia Care & Psychotropic Medication Tracking Tool, a free, publicly available electronic tool that facilitates a structured approach to tracking preference-based care and psychotropic medication use among residents living with dementia
- To register go to: https://blh.ier.intercall.com/details/f7dde2ecc6a54bebafca0ce5504b439a
- (Strategy 2.D)
