Friday, July 30, 2018
Printer Friendly Version in PDF Format (7 PDF pages)
Clinical Services Federal Update
Terri Postma, MD
National Partnership to Improve Dementia Care in Nursing Homes
- The National Partnership to Improve Dementia Care in Nursing Homes is committed to improving the quality of care for individuals with dementia living in nursing homes with a mission to deliver health care that is person-centered, comprehensive and interdisciplinary with a specific focus on protecting residents from being prescribed antipsychotic medications unless there is a valid, clinical indication and a systematic process to evaluate each individual's need
- CMS is tracking the progress of the National Partnership by reviewing publicly reported measures -- the official measure of the Partnership is the percentage of long-stay nursing home residents who are receiving an antipsychotic medication, excluding those residents diagnosed with schizophrenia, Huntington's Disease or Tourette's Syndrome
Information at: https://www.cms.gov/Medicare/Provider-Enrollment-and-Certification/SurveyCertificationGenInfo/National-Partnership-to-Improve-Dementia-Care-in-Nursing-Homes.html
Strategy 2.D
National Partnership to Improve Dementia Care in Nursing Homes
| Quarterly Prevalence of Antipsychotic Use for Long-Stay Nursing Home Residents 2011Q2 to 2017Q4 |
|---|
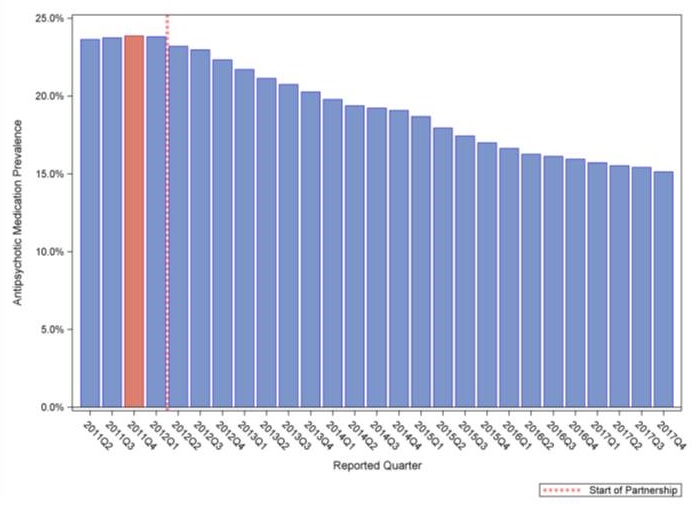 |
| Source: CMS Quality Measure, based on MDS 3.0 data. For more information, see the MDS 3.0 Quality Measures Users Manual |
Quarterly Prevalence of Antipsychotic Use for Long-Stay Nursing Home Residents, CMS Regions
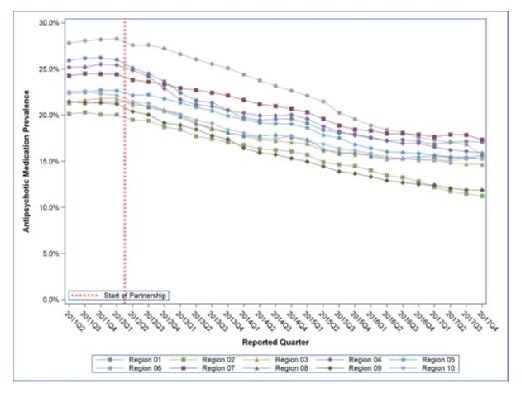 |
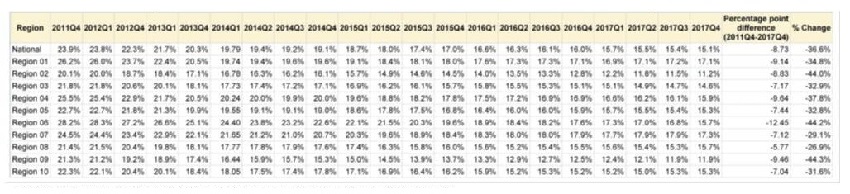 |
| Source: CMS Quality Measure, based on MDS 3.0 data. For more information, see the MDS 3.0 Quality Measures Users Manual |
Comprehensive Primary Care Final Report, Plus Infographics
- In May CMS released the final report from the independent evaluation of the CPC demonstration that was accompanied by an article in Health Affairs
- Results showed participating practices engaged in substantial, challenging transformation and improved how they delivered care, reducing Medicare beneficiaries' hospitalizations and ED visits; however, savings to Medicare were not sufficient to cover total care management fee payments
- CPC+ also released two infographics summarizing progress in the first year with a CPC+ Medicare Payments Calendar Year highlights that and highlight Medicare's investment in CPC+ practices through care management fees and incentive payments/reconciliation
Information at: https://innovation.cms.gov/initiatives/Comprehensive-Primary-Care-Initiative/
Strategy 2.E
Medicare 2019 Payment and Policy Changes for Nursing Homes
- In April CMS issued a proposed rule, CMS-1696-P, outlining 2019 Medicare payment updates and proposed quality program changes for nursing homes
- The proposed Patient-Driven Payment Model (PDPM) will replace the Resource Utilization Group system used to categorize Medicare Part A residents into various payment groups based on their level of need and would reduce the number of payment group combinations by 80%, use more standardized items for payment calculations and greatly simplify providers' paperwork
- The proposal would also allow rehabilitation physicians to conduct some meetings without being physically in the room and remove some burdensome admission documentation requirements
- The 2.4% market basket increase is slated to go into effect 10/1, the PDPM one year later
- The comment period closed in June
Strategy 2.F
Calendar Year (CY) 2019 Medicare Physician Fee Schedule (PFS) Proposed Rule
- Documentation Requirements and Payment for Evaluation and Management (E/M) Visits & Advancing Virtual Care
- See the Physician Fee Schedule website at: https://www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/PhysicianFeeSched/index.html
- The comment period will close on September 10, 2018
Medicare Supplemental Benefits
- In April CMS released guidance to the Medicare Advantage Organizations to help offer additional services to beneficiaries with multiple chronic conditions, and the social factors outside the reach of traditional medicine that can contribute to them
- The supplemental benefits are home and community-based services such as wheelchair ramps, transportation to doctor's offices and home-delivered meals
- Beginning in 2019, CMS is expanding the definition of "primarily health related" to consider an item or service if it is used to diagnose, compensate for physical impairments, acts to ameliorate the functional/psychological impact of injuries or health conditions, or reduces avoidable emergency and healthcare utilization. A supplemental benefit is not primarily health related under the previous or new definition if it is an item or service that is solely or primarily used for cosmetic, comfort, general use, or social determinant purposes
- Additional guidance will be released associated with the CHRONIC Care Act of 2017
Strategy 2.G
Home Health Proposed Payment Rules
- In July CMS issued a proposed rule, CMS-1689-P, outlining 2019 Medicare payment updates and quality reporting changes for home health agencies
- It continues a shift in Medicare payments from volume to value that focuses on the patient's condition and resulting care needs rather than on the amount of care provided
- The proposed rule would also modernize Medicare through innovations in home health, meaningful quality measure reporting, reduced paperwork, and reduced administrative costs
- The rule also includes the cost of remote patient monitoring on the Medicare cost report form, so home health agencies can better adopt emerging technology and promote quality care in Medicare.
- CMS will accept comments until August 31, 2018 and the proposed rule can be downloaded from the Federal Register at: https://www.federalregister.gov/public-inspection
Strategy 2.F
VA Geriatric Scholars Program
- A workforce development program to integrate geriatrics into primary care practices
- Longitudinal, multi-modal continuing education program for healthcare professions:
- Intensive education, clinical practicum experiences, self-paced learning through webinars and on-line learning communities, demonstration of knowledge through quality improvement projects
- Focus on rural VA clinics; outreach to rural Indian Health Service clinics
- Funded by VA Offices of Rural Health and Geriatrics/Extended Care
- Collaboration of 12 VA Geriatric Research, Education and Clinical Centers (GRECC), in partnership with VA Employee Education System (EES), academic affiliates and HRSA-funded Geriatric Workforce Education Programs (GWEP)
VA Geriatric Scholars Program Updates
- Geriatric Scholars Program Clinical Practicum with focus on dementia at the following VA GRECCs in Quarter 3: Madison, New England, Palo Alto, Puget Sound.
- Geriatric Scholars Program Webinars to support the Geriatric Scholars Toolkit:
- Dementia and Rehabilitation, June 19, 2018
- GRECC Connect Webinars for VA Staff with specific focus on dementia:
- Overview of Dementia 4/16/2018
- Pain Assessment and Management with Dementia 5/10/2018
- Ethics in Dementia 5/25/2018
- Modifiable Risks Factors for Dementia 6/8/2018
VA Geriatric Scholars Rural Interdisciplinary Team Training (RITT) Updates
- Geriatric Scholars Program Rural Interdisciplinary Team Training (RITT) in care of older Veterans. On-site training for rural community-based outpatient clinic staff on teamwork in care of older adults; recognition of geriatric syndromes, "red flags," functional impairments including dementia.
- Geriatric Scholars Program RITT in care of older Veterans held in:
- Salisbury, NC April 3, 2018
- Wilmington, NC May 30, 2018
- Southern New Mexico Healthcare System, June 12, 13, 2018
- Hot Springs, AR, June 22, 2017
- Conway, AR, June 29, 2018
- For IHS and Tribal partners in:
- Rosebud, SD 5/31/2018
- California Area Annual Best Practice Conference May 23, 2018 (booth to promote RITT)
REACH in Indian Country
- For the Indian Health Service:
- The program has been extended for another year through January 2019 with the continued support of the Rx Foundation. Implementation began in February 2015, with 47 Communities as of December 2016
- Website Developed https://www.uthsc.edu/prevmed/memphis-caregiver-center/index.php
- Brochure developed and posted on website: https://www.uthsc.edu/prevmed/documents/reach/reach-indian-country-brochure.pdf
- Implementation in 50 Tribal communities by February 2018
- In addition, HRSA-funded GWEP programs have formed a coalition that will provide training for IHS and Tribal health programs serving American Indians and Alaska Natives with dementia, using Banner Alzheimer's Institute training materials, in Alaska, Arizona, California, North Carolina, and Wyoming.
