Monday, April 29, 2019
Printer Friendly Version in PDF Format (6 PDF pages)
Innovations in the Delivery of Dementia Care in a rapidly evolving health care landscape
Brent Forester, MD, MSc
Chief, Division of Geriatric Psychiatry, McLean Hospital
Medical Director, Behavioral Health and Evaluation & Research
Partners Population Health, Partners HealthCare
Associate Professor of Psychiatry,
Harvard Medical School
Disclosures
- Grants and Research Support Last 12 months:
- National Institute of Aging
- Rogers Family Foundation, Spier Family Foundation
- Eli Lilly, Biogen
- Consulting: Eli Lilly, Biogen
The Facts on Early Diagnosis and Disclosure
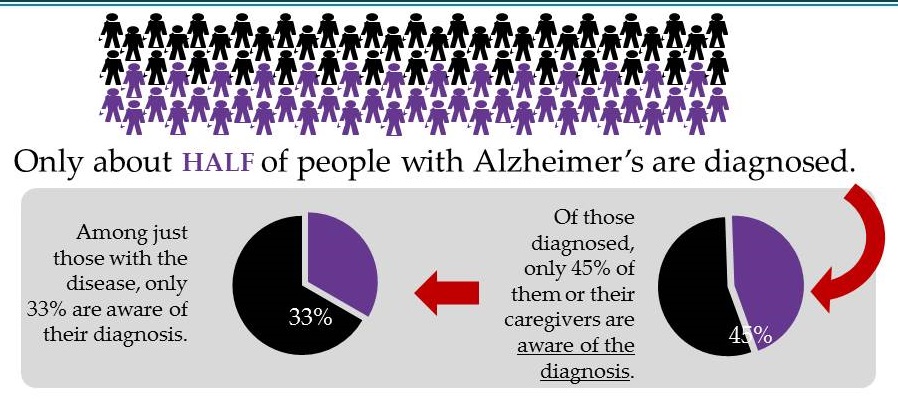 |
| >80% of medical care for dementia occurs in general medical setting Medicare reimbursement for dementia care planning: CPT Code 99483 Alzheimer's Association, 2018, Facts and Figures |
Health Care System Transformation
- Yesterday's Health Care
- Care built around the institution
- Payments incentivize more care
- Responsible for immediate outcome
- Grudging acceptance of cost
- Today's Health Care
- Care built around the patient
- Payments incentivize better care
- Responsible for ongoing health
- Unable to sustain cost burden
Partners Accountable Care Organizations
Our contracts 7 years in...
- Partners currently manages ~650,000 lives in various accountable care relationships.
- 41% of our primary care lives are part of our risk contracts
| COMMERCIAL | MEDICAID | SELF-INSURED | MEDICARE |
|---|---|---|---|
| Alternative Quality Contract (AQC) | MassHealth ACO | Partners Plus | Next Generation ACO |
| ~350k Covered Lives | ~100k Covered Lives | ~100k Covered Lives | ~100k Covered Lives |
| Younger population; specialists critical to management | Population with significant disability, mental health, and/or substance use challenges | Commercial population, but Partners at full risk for cost and quality | Elderly population; care management central to trend management |
| Massachusetts Blue Cross Blue Shield Neighborhood Health Plan Harvard Pilgrim HealthCare Tufts Health Plan |
Centers for Medicare & Medicaid Services MassHealth |
Partners HealthCare | Centers for Medicare & Medicaid Services |
Partners Memory Care Initiative
Needs Assessment
| Barriers to providing optimal patient care |
|---|
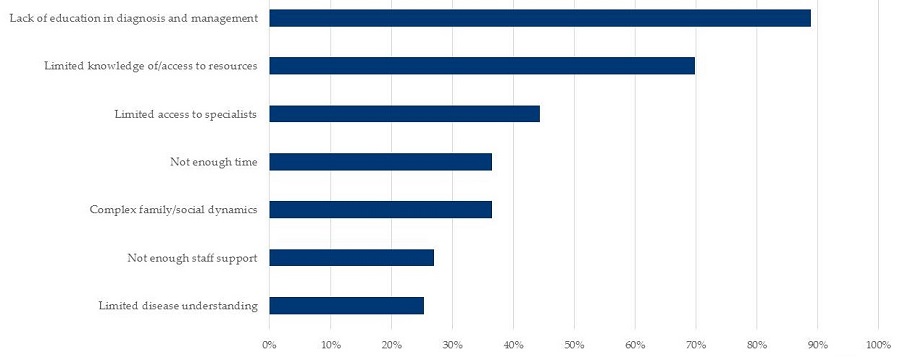 |
| Other identified challenges: | Opportunities: |
|---|---|
|
|
Goals & Objectives
- Primary program goal:
- "To deliver high quality care for individuals with cognitive impairment by facilitating evidence-based assessment and treatment in the primary care setting, over the full illness trajectory, and for both patient and caregiver"
- Specific aims:
- Support & train PCPs
- Improve patient health outcomes
- Improve caregiver health status
- Reduce total healthcare costs
Program Parameters
- Collaborative Dementia Care:
- Establish care team which collaborates with PCP to provide:
- Timely & regular patient assessment & severity stratification
- Assistance with diagnosis, disclosure, and difficult conversations
- Care planning
- Medication management
- Caregiver support
- Connection to specialties (neurology, geri psych) and other PHM programs (Collaborative Care, iCMP)
- Connection to community resources
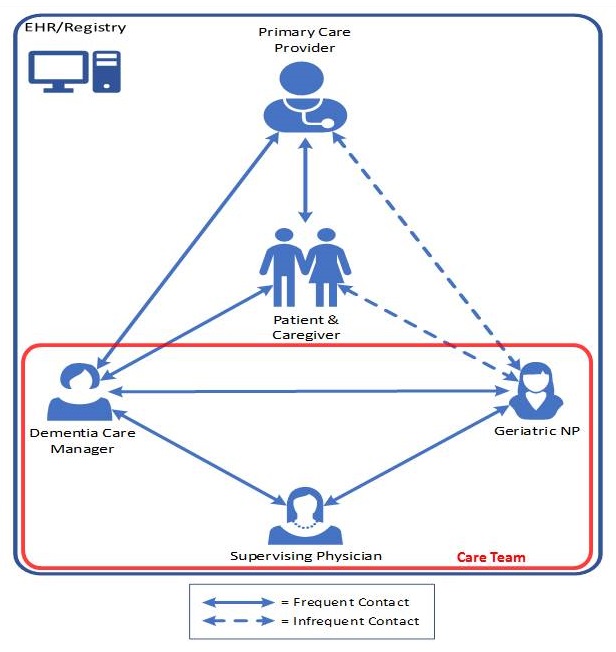 |
Full List of Objectives
- Improved assessment
- Increase rate of diagnosis for (true positive) cases of dementia
- Improve rate of disclosure of diagnosis to patient/caregiver
- Improved disease management
- Improve rate of advanced care planning
- Increased numbers of serious illness conversations
- Improved rate of medication review. Leading to:
- Decrease in number of harmful medications prescribed (i.e. deprescribing)
- Increase in number of evidence-based medications for dementia prescribed
- Improved access to specialty care and community resources
- PCP training
- Improve PCP knowledge of and comfort with managing dementia, esp. behavioral symptoms
- Health outcomes
- Reduction in caregiver stress and depression symptoms
- Improvement in patient health outcomes: depression, quality of life, behavioral & psychological symptoms of dementia (significant improvement in cognitive status not expected, but will be measured)
- Reduced healthcare system utilization: decreased number of ED visits and Inpatient days
- Costs
- Decreased Total Medical Expenditure (TME)
Partners eCare: Interdisciplinary Patient Plan of Care (IPPOC)
- Chronic Condition Management
- Problem: Memory Impairment
- Patient Goals:
- Adhere to medication regime
- Adapt to lifestyle changes and restrictions
- Participate in social and family activities
- Patient identified goal
- Tasks:
- Care Management regular follow up
- Address psychosocial issues relating to memory impairment
- Custom Intervention / Task
- Consider referral to Dementia Care Coordinator- Alzheimer's Association
- Patient Goals:
