RTI International
September 15, 2017
Printer Friendly Version in PDF Format (70 PDF pages)
ABSTRACT
Access to services, particularly behavioral health and substance use disorder (SUD) treatment services, is challenging in rural and other underserved areas. Some of the reasons for these challenges include lack of specialty providers and local primary care providers without experience in behavioral health treatment as well as concerns over stigma and lack of privacy for individuals from smaller communities. Telehealth can ease these challenges and support behavioral health, specifically SUD treatment, in a variety of ways, including direct patient care, patient engagement, and provider education. This is particularly relevant for the growing opioid epidemic, which has profoundly affected rural areas.
DISCLAIMER: The opinions and views expressed in this report are those of the authors. They do not necessarily reflect the views of the Department of Health and Human Services, the contractor or any other funding organization.
TABLE OF CONTENTS
1. INTRODUCTION AND BACKGROUND
1.1. Key Objectives
2.1. Data Collection
2.2. Data Analysis
3. RESULTS
3.1. Implementation and Use
3.2. Financing and Sustainability
3.3. Impact
4. DISCUSSION
APPENDICES
- APPENDIX A: Discussion Guide
- APPENDIX B: Site Briefs
LIST OF EXHIBITS
LIST OF TABLES
- TABLE 1: Literature Review Search Terms
- TABLE 2: Stakeholder Organizations and Perspectives Represented
- TABLE 3: States and Roles in Discussions
- TABLE 4: Modes of Telehealth by Site
- TABLE 5: Summary of Telehealth Modes and Behavioral Health Service Delivery Methods
- TABLE 6: Reimbursement for Telehealth Services, by Payer Type
ACRONYMS
The following acronyms are mentioned in this report and/or appendices.
| ACO | Accountable Care Organization |
|---|---|
| AHRQ | HHS Agency for Healthcare Research and Quality |
| ASPE | HHS Office of the Assistant Secretary for Planning and Evaluation |
| ATA | American Telemedicine Association |
| CAH | Critical Access Hospital |
| CEU | Continuing Education Unit |
| CFR | Code of Federal Regulation |
| CMHC | Community Mental Health Center |
| CMS | HHS Centers for Medicare & Medicaid Services |
| CPT | Current Procedural Terminology |
| DATA 2000 | Drug Addiction Treatment Act of 2000 |
| DBT | Dialectical Behavioral Therapy |
| DEA | Drug Enforcement Agency |
| ECHO | Extension for Community Healthcare Outcomes |
| ED | Emergency Department |
| EMCMHC | Eastern Montana Community Mental Health Center |
| FFS | Fee-For-Service |
| FQHC | Federally Qualified Health Center |
| HCIA | Health Care Innovation Award |
| HCPCS | Healthcare Common Procedure Coding System |
| HERA | Health Evaluation and Referral Assistant |
| HHS | U.S. Department of Health and Human Services |
| HIPAA | Health Insurance Portability and Accountability Act |
| HPSA | Health Professional Shortage Care |
| IT | Information Technology |
| MACRA | Medicare Access and CHIP Reauthorization Act |
| MAT | Medication-Assisted Treatment |
| NFAR ATTC | National Frontier and Rural Addiction Technology Transfer Center |
| NP | Nurse Practitioner |
| OAT | Opioid Addiction Treatment |
| OUD | Opioid Use Disorder |
| PA | Physician Assistant |
| PCAT | Psychiatry Consultation and Telepsychiatry |
| PCP | Primary Care Provider |
| PCSS-MAT | Providers' Clinical Support System for Medication Assisted Treatment |
| RTI | Research Triangle Institute |
| SAMHSA | HHS Substance Abuse and Mental Health Services Administration |
| SBIRT | Screening, Brief Intervention, and Referral to Treatment |
| SUD | Substance Use Disorder |
EXECUTIVE SUMMARY
Access to services, particularly behavioral health and substance use disorder (SUD) treatment services, is challenging in rural and other underserved areas. Some of the reasons for these challenges include lack of specialty providers and local primary care providers (PCPs) without experience in behavioral health treatment, as well as concerns over stigma and lack of privacy for individuals from smaller communities.
Telehealth can ease these challenges and support behavioral health, specifically SUD treatment, in a variety of ways, including direct patient care, patient engagement, and provider education. This is particularly relevant for the growing opioid epidemic, which has profoundly affected rural areas.
The U.S. Department of Health and Human Services Office of the Assistant Secretary for Planning and Evaluation sought to understand how telehealth is used to support behavioral health and SUDs, with a particular focus on implications for medication-assisted treatment for opioid use disorders. The intent was to understand telehealth implementation and use, financing and sustainability, and impact in the field. The results of this work can be used to inform future policy and practice.
RTI International conducted an environmental scan and site visits with participants in the field. The environmental scan consisted of a targeted literature review and discussions with key leaders. The scan informed site visits with participants with a range of telehealth experiences across the country. The team identified a diverse set of participants, including clinical staff, administrators, telehealth coordinators, and information technology staff. We analyzed research notes to extract themes from participant experiences to answer the study questions.
We found that telehealth is used in a variety of ways for provider-to-patient and provider-to-provider interactions. Provider-to-patient interactions included real-time live video, remote monitoring, and asynchronous communication. Provider-to-provider interactions included education and consultation.
Organizations varied in how they implemented telehealth services and the services they offered. Common themes arose in implementation, such as planning for both technical and organizational impacts of telehealth, the importance of leadership support, and tailoring programs to community needs. Financing and sustainability themes included inconsistent interpretation of policies about delivering telehealth services, which influenced which services organizations chose to implement. Funding telehealth was accomplished through a variety of methods, such as grants and demonstration programs, and reimbursement varied by payer. Telehealth affected behavioral health services by providing improved access to different types of services, such as specialty services and translation, and extending delivery of services.
1. INTRODUCTION AND BACKGROUND
Access and availability of health care in rural areas is challenging in the United States, particularly for behavioral health, including substance use disorder (SUD) treatment. The recent rise of opioid use and misuse and its associated overdose epidemic requires specialized care that is not necessarily available in these areas. Telehealth can improve access to treatment for SUDs, including opioid use disorders (OUDs), through new approaches that use technology to expand virtual access to the behavioral health workforce and the services it provides, particularly in under-resourced rural areas (Bashshur, Shannon, Bashshur, & Yellowlees, 2016; Benavides-Vaello, Strode, & Sheeran, 2013; Nelson & Bui, 2010; University of New Mexico, 2016). For example, in areas with few behavioral health providers, telehealth can be used to expand the provider care team to include geographically dispersed specialists who work with a local provider in addressing the patient's health care and psychosocial needs related to their SUD. The uses of telehealth may include direct care, provider-to-provider communication, and electronic data exchanges, as well as electronic data collection and dissemination. This is important for medication-assisted treatment (MAT) of OUDs, which requires a specialized skill set that may not be available in the primary care setting.
To overcome some of the policy issues and challenges associated with telehealth, innovative strategies and policies at both the federal and state levels are being implemented in varying degrees. For example, the U.S. Department of Health and Human Services (HHS) Centers for Medicare & Medicaid Services (CMS) is testing a more expansive use of telehealth through its Next Generation Accountable Care Organization (ACO) Model Telehealth Waiver. Current Medicare payment regulations limit payment for telehealth services to rural Health Professional Shortage Areas (HPSAs) and CMS-defined telehealth originating sites. These originating sites are where the patient is physically located. They include the offices of physicians or practitioners, hospitals, critical access hospitals (CAHs), rural health clinics, and federally qualified health centers (FQHCs); hospital-based or CAH-based renal dialysis centers (including satellites); skilled nursing facilities; and community mental health centers (CMHCs). Distant sites are where the provider delivering services is located. The Next Generation ACO Telehealth Waiver eliminates the requirement that the originating site be one of the above locations and the rural HPSA requirement, allowing Next Generation ACO beneficiaries to receive telehealth services in their home, whether they are in a rural area or not. Eighteen ACOs are participating in this demonstration.
The Medicare Improvements for Patients and Providers Act of 2008 authorized CMS to conduct demonstrations to test various reimbursement strategies to aid frontier CAHs. To that end, CMS and the Health Resources and Services Administration (HRSA) are testing the effect of changing payment models for telehealth in the CAH setting through the Frontier Community Health Integration Project Demonstration, which aims to improve access to and integration of care in frontier communities. The act defines frontier communities as those located in a state where the majority of counties have six or fewer residents per square mile. Applications for the demonstration were accepted from CAHs in Alaska, Montana, Nevada, North Dakota, and Wyoming (Medicare Improvements for Patients and Providers Act of 2008). Participating CAH telemedicine originating sites are paid 101% of cost for providing telehealth services instead of the fixed fee in an effort to promote provision of telehealth services.
The Medicare Access and CHIP Reauthorization Act (MACRA) of 2015 also encourages use of telehealth by lifting all restrictions that would otherwise exist under fee-for-service (FFS) and allowing physicians to use telehealth services where appropriate. For example, MACRA allows the Medicare Shared Savings Program to recognize telehealth services, such as for care coordination, as a clinical practice improvement activity, one of four components required to qualify for incentive payments. This allows physicians and other practitioners who coordinate care using telehealth to receive incentives even when direct reimbursement may not be available.
Changes in behavioral health care supported by telehealth are occurring in multiple areas, including access to care, care delivery, and payment structures. Several barriers to using telehealth within behavioral health care may exist; for example, funding mechanisms, start-up costs, licensing requirements, credentialing/privileging technological requirements (e.g., integration, standards), broadband connectivity, and workforce training needs (Office of the Assistant Secretary for Planning and Evaluation [ASPE], 2016; Benavides-Vaello et al., 2013; Hilty, Cobb, Neufeld, Bourgeois, & Yellowlees, 2008; Larsen, Farmer, Weaver, Young, & Tarassenko, 2012). To fully take advantage of the opportunities that telehealth presents for behavioral health, organizations are implementing policies and innovative programs to overcome some of these challenges. However, more needs to be done to understand the opportunities and barriers for telehealth in behavioral health.
1.1. Key Objectives
As telehealth continues to expand, more information is needed about how it can be used to identify and manage behavioral health conditions. We also must understand key factors that may affect implementation and sustainability. Specifically, information is needed to better understand how direct service providers can effectively implement and maintain telehealth in their practices to better reach individuals with behavioral health disorders and serve their patients. This report was developed to help fill this gap by collecting and synthesizing information from the field as presented in literature and reports, as well as discussions with experts and those with field experience. The primary focus for this effort was providers who deliver treatment for SUDs, in particular MAT, with support from telehealth.
The study addressed research questions in three key areas: implementation and use, financing and sustainability, and impact.
-
Implementation and Use:
-
What is actually being implemented, how is it being implemented, who does it reach, and how does it compare with what was intended?
-
What are the best practices, barriers, and facilitators in using telehealth to identify and manage behavioral health disorders?
-
How is telehealth being used to support provider-to-provider communication?
-
How does choice of telehealth modality affect barriers, facilitators, and costs?
-
What strategies and solutions have providers used to overcome barriers?
-
-
Financing and Sustainability:
-
How are telehealth services reimbursed generally and for behavioral health disorders?
-
Does reimbursement for telehealth for behavioral health disorders differ from reimbursement available for medical or surgical services?
-
How does reimbursement for behavioral health services delivered via telehealth differ across payers (e.g., Medicaid, Medicare, private insurance)?
-
What payment models support the use of telehealth?
-
-
Impact:
-
How can telehealth affect access to behavioral health services, especially MAT in rural primary care settings?
-
How can telehealth affect delivery of behavioral health services, including provider-to-provider communication?
-
To answer these research questions, the study used qualitative data collection and analysis methods that supported the three interrelated research areas. This report presents the findings from this study and contains the following sections: Data and Methods (Section 2), Results (Section 3), and Discussion (Section 4).
2. DATA AND METHODS
2.1. Data Collection
Data collection consisted of an environmental scan, discussions with key stakeholders, and discussions with selected providers that occurred by telephone and during in-person site visits. The objective of the environmental scan was to understand the state of telehealth for behavioral health from literature and key stakeholders. The objective of the provider discussions was to learn from on-the-ground experiences of those who administer and use telehealth in the field. Below, we describe each activity in detail.
2.1.1. Environmental Scan
The environmental scan included two main components: reviewing published and unpublished literature and conducting discussions with key policy and research leaders in the field.
Review of Relevant Literature
The first step of the environmental scan was a literature review that identified and synthesized reliable findings from peer-reviewed journals; gray literature; issue briefs; federal, state, and local government reports; conference proceedings and presentations; and unpublished materials on the use of telehealth for behavioral health disorders, with a focus on more recent literature (past 10 years). To conduct the literature review, we developed a list of keywords (presented in Table 1) that were the most relevant for the study questions. The team used RTI's Master's in Library Science-trained librarians to provide input on the keywords and assist in searches. The RTI team obtained relevant articles for review and analysis.
| TABLE 1. Literature Review Search Terms | |||
|---|---|---|---|
| Modality | Service | Location | Coverage |
| Telehealth | Behavioral health | Rural | Insurance |
| Telemedicine | Substance abuse | FQHC | Medicaid |
| eTherapy | Substance use | Primary care | Medicare |
| eHealth | Mental health | Federally qualified health center | Co-pay |
| Mobile health | Medication-assisted therapy | Remote | Co-insurance |
| mHealth | Medication-assisted treatment | Health Professional Shortage Area | |
| Telemonitoring | MAT | Medically underserved area | |
| Tele* | Opioid | Rural health services | |
| Opiate | Medical home | ||
| Drug therapy | Accountable care organization | ||
| ACO | |||
Discussions with Key Informants
To supplement the findings from the literature review, we conducted unstructured discussions via telephone with key stakeholders who were selected to represent the following perspectives:
-
Researchers
-
Health care providers or administrators in rural primary care practices (providers)
-
MAT providers
-
Health insurance executives (insurers)
-
Policy makers
The RTI team also developed a semi-structured discussion guide (presented in Appendix A) to support the discussions that covered the key research questions. The guide was customized to the unique perspectives of each selected stakeholder. For each discussion, a note taker joined the lead facilitator on the phone to capture detailed notes on the discussion occurring between the facilitator and the key informant. Each discussion lasted approximately 1 hour. To verify the accuracy of the notes, we requested permission from participants to audio record the discussions and used the recording as needed to validate notes. Once the facilitator and note taker validated the notes, the audio recordings were destroyed. Verified notes included a summary of key themes identified by the facilitator and note taker before being made available for analysis. Table 2 lists stakeholder organizations and the perspective they represented. The study process, including these discussions, was reviewed by RTI's Institutional Review Board. As part of the discussion, the facilitator explained the objectives of the study to the discussant as well as their rights as a participant. Each discussant was assured confidentiality and that their responses would not be directly attributed to them.
| TABLE 2. Stakeholder Organizations and Perspectives Represented | |
|---|---|
| Organization | Perspective Represented |
| American Telemedicine Association | Policy Maker |
| Anthem Blue Cross and Blue Shield | Insurer |
| Maine Rural Health Research Center | Researcher (2) |
| National Telehealth Policy Resource Center | Policy Maker |
| University of Colorado | MAT Provider/Researcher |
| University of New Mexico | Provider/Researcher (2) |
| University of Virginia Center for Telehealth | Provider/Researcher |
2.1.2. Provider Discussions
To support the findings from the environmental scan and gain additional perspective from provider organizations in the field, we conducted discussions with staff from a handful of selected provider organizations. We developed separate discussion guides for these discussions that were informed by the environmental scan and research questions. Each discussion guide was customized for the discussant's perspective, with probing subquestions to address the unique perspective of their dissimilar roles.
Potential provider sites for discussion recruitment were identified based on the findings of the environmental scan and review of relevant professional organization rosters. From this potential list, nine provider sites were selected based on several criteria, including the following:
-
Experience with telehealth for behavioral health.
-
Experience with telehealth for MAT.
-
Geography (rural vs. urban).
-
Type of telehealth in use (provider-to-provider or provider-to-patient).
-
Type of behavioral health services provided.
In conducting these discussions, we followed a similar approach used for the environmental scan discussions. Specifically, these discussions were conducted by one lead facilitator and one note taker. The note taker also audio recorded the discussion with permission from the participant and used the recording to verify notes. We assured discussants that we would protect their confidentiality and not attribute any responses directly to them. Once the facilitator and note taker verified the notes, the audio recordings were destroyed. Each discussion lasted approximately 1 hour.
Table 3 outlines the states in which provider discussions were conducted and the roles represented by each participant. In total, we held discussions with 19 staff across multiple roles within the nine provider sites; however, no more than nine staff within a single role were included. It should be noted that the Montana and New York discussions were conducted in person as part of a site visit, and all other discussions were conducted via telephone.
| TABLE 3. States and Roles in Discussions | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Role | MT | NY | CA | GA | MD | NC | NM | WA | WV |
| Administrator | x | x | x | x | x | ||||
| Provider | x | x | x | x | x | ||||
| Telehealth Coordinator | x | x | x | ||||||
| Technical Staff | x | ||||||||
The in-person site visits included more participants (seven for Montana and three for New York), as the team met with multiple staff across roles during the visit. The remaining provider sites each had one discussion, except for New Mexico, where we spoke with two providers who participated in TeleECHO: one who provided education and guidance through the program, and one who received the education and guidance.
In addition to seeking diversity in roles, we also sought diversity in the types of telehealth services provided, including provider-to-patient, provider-to-provider, or both. Table 4 presents the types of telehealth modalities used by provider site location.
| TABLE 4. Modes of Telehealth by Site | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Mode | MT | NY | CA | GA | MD | NC | NM | WA | WV |
| Provider-to-Patient | x | x | x | x | x | x | x | x | |
| Provider-to-Provider | x | x | x | x | |||||
As shown, five sites used telehealth for provider-to-patient interactions only, one site used telehealth for provider-to-provider interactions only, and three sites used telehealth services for both.
2.2. Data Analysis
Data were analyzed using qualitative analytic methods. Results from the literature review portion of the environmental scan were analyzed by manual review. Qualitative data from key informant discussions were analyzed using thematic analysis of the documented data. The team analyzed these data based on the key themes associated with each research question. Data were grouped and analyzed to identify themes, associated vignettes, and relevant quotes. Team members reviewed common themes and added subthemes as appropriate.
3. RESULTS
The results of the literature review and the discussions with key stakeholders are presented by the primary research question topics: implementation and use, financing and sustainability, and impact. We also highlight innovative programs and approaches to the use of telehealth identified in the literature and based on discussions with key stakeholders.
3.1. Implementation and Use
3.1.1. How and what is actually being implemented, who does it reach, and how does it compare with what was intended?
Four different telehealth approaches (modes) are described in the August 2016 Report to Congress: E-health and Telemedicine (ASPE, 2016): live video (synchronous), store and forward (asynchronous), remote patient monitoring, and mobile health. (See Exhibit 1 for descriptions.) All of these modes are used in some way to support behavioral health services, patients, providers, or care delivery models. To better understand how and what is actually being implemented, Table 5 summarizes the modes used to support specific behavioral health services. As shown and described in more detail below, live video was the most common mode and used across a variety of services. Less common was the use of store and forward, remote patient monitoring, or mobile health. Stakeholders and providers who participated in discussions indicated both live video and remote patient monitoring are used to support provider-to-patient visits for behavioral health. Other less intensive modes included telephone follow-up and use of online tools and resources for providers. Behavioral health services for which these modes were used include:
-
Patient visits with their providers.
-
Group therapy sessions.
-
Consultations between providers.
-
Integrated care team approaches.
-
Follow-up care and monitoring.
-
Dissemination of educational and other resources for providers, patients, or the community.
| EXHIBIT 1. Telehealth Modes |
|---|
|
| SOURCE: ASPE, 2016. |
| TABLE 5.Summary of Telehealth Modes and Behavioral Health Service Delivery Methods | |||||||
|---|---|---|---|---|---|---|---|
| Telehealth Mode | Provider-to-Patient Visit | Group Therapy Session | Provider-to-Provider Consultation | Integrated Care Team | Education: Provider-to-Provider or Community | Follow-Up Care and Monitoring | Connect Individual to Resources |
| Live Video | X | X | X | X | X (Provider-to-Provider) | ||
| Store and Forward | X | ||||||
| Remote Patient Monitoring | X | ||||||
| Mobile Health | X | ||||||
| Othera | X (Community) | X | |||||
| |||||||
Live Video (Synchronous)
The most common method for delivering telehealth uses live video to connect providers to patients or providers to providers via videoconferencing technology. Findings from the discussions and published literature reveal that several behavioral health care delivery models are supported through live video, including patient visits and encounters, group therapy, integrated care team consultation, and provider-to-provider consultation and education. For example, at one provider site videoconferencing is primarily used for patient-to-provider visits, but the equipment is also used for provider-to-provider consultation and education, as well as integrated care team consultation. Even the dentists associated with the site are encouraged to complete opioid awareness training and become competent with telehealth tools to enhance their effectiveness as part of the care team.
Patient Visit and Encounter
Live video (or other two-way communication such as e-mail, text, or telephone) is being used by providers to support contact between a patient and provider, allowing an individual to connect virtually with a clinician and receive basic medical care or consultation (MedPAC, 2016). With this approach, the individual initiates the digital visit through a website or application and provides clinical information about their symptoms. The extent to which telehealth can be used in this way is still being explored. For example, the use of live video to support behavioral health-related patient visits or encounters is being implemented in different settings in which professionals with specialized expertise are not readily available or patients cannot easily access services because of the distance needed to travel. In primary care settings, telehealth is used to provide a patient with direct access to behavioral health specialists and psychiatry for evaluation, assessment, or treatment. In one example, providers connected directly with community schools in the state (not another health care provider). The schools are equipped with a videoconferencing unit to reach a target population and provide specialty services (Nelson & Bui, 2010). Hospital emergency departments (EDs) and inpatient units were also found to use live video to connect patients with behavioral health specialists (Hilty, Ferrer, Parish, Johnston, Callahan, & Yellowlees, 2013; Hilty, Nesbitt, Kuenneth, Cruz, & Hales, 2007). Provider sites report that telehealth has been an effective way to obtain specialty care that would not normally be available on site.
Several stakeholders and providers reported positive results and feedback from patients and staff who used live video for behavioral health patient visits and encounters. When asked about MAT services delivered via live video, providers relayed anecdotal information and a belief that it could be occurring on a limited basis. Among the provider sites participating in this study, three reported use of telehealth to deliver patient visits and encounters for MAT. The MAT telehealth services provided by these sites varied, but, depending on the site, could include assessment, therapy and other psychosocial services, prescribing, and medication management. The basic model of telehealth used in the direct delivery of MAT services includes a patient at the originating site (e.g., PCP office, health department, school) and the MAT provider at the distant site. Patient and provider are connected via live video. The patient is supported by a health care professional at the originating site and, possibly, a telehealth coordinator. At the distant site, the MAT provider may also be supported by a telehealth coordinator. An identified barrier to the use of telehealth for MAT is the lack of awareness and the comfort level of PCPs with regard to using medication therapy for treatment of a patient's OUD. As awareness grows, discussants perceived that telehealth for MAT could increase as well.
One health system included in the discussions established and maintains a telehealth network that includes an integrated delivery system of CAHs, clinics, CMHCs, and other facilities located in multiple communities in a multistate region. In the network, interactive videoconferencing is used to deliver medical and behavioral health services to the region. Telehealth visits are scheduled and conducted at the clinical site in rooms equipped with videoconferencing equipment and facilitated or monitored by a staff member. The network also provides telehealth visits to EDs. One hospital has a behavioral health specialist available to other EDs in the network and uses a mobile cart equipped with videoconferencing equipment for the telehealth visit or consultation.
Another provider site uses live video not just for patient visits but to deliver intensive outpatient services, including group therapy sessions. This CMHC uses telehealth to deliver group therapy for early recovery skills, relapse prevention, family education, and moral recognition therapy. Group therapy sessions are scheduled at multiple clinical sites in their network, patients arrive at the clinical site for their scheduled therapy session, a therapeutic aide is available at each site and monitors the session, and live video connects the clinical sites to the group therapy clinician or facilitator. Using live video for this type of therapy has increased access to this type of care for individuals in rural and frontier communities who would otherwise have difficulty attending sessions because of distance.
Provider-to-Provider Communication
Telehealth is commonly used to support communication among geographically dispersed providers. For example, integrated care models, such as patient-centered medical homes and ACOs, can use telehealth to bring together care teams to plan and coordinate care, including behavioral health care, for high-risk and target populations. The teams may include one or more case managers, the PCP, specialists, community service providers, and the patient or their family member. Telehealth is used to connect team members across locations--particularly those locations that are relatively isolated--for cases that would benefit from direct communication and care coordination (Rosenberg, 2012).
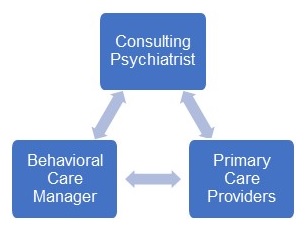
While early implementation of ACOs lagged in the integration of behavioral health in primary care, Next Generation and Medicaid ACOs and other state programs have included a focus on both behavioral health integration and telehealth (Lewis, 2014; Richards, 2015). For example, one stakeholder provided psychiatric consultation and telepsychiatry as part of an integrated care team that supports state programs related to behavioral health integration programs. In this model, telehealth allows a behavioral health care manager to work directly with a patient's PCP and to consult with a psychiatrist (see Exhibit 2). The psychiatrist gives advice to a care manager during the check-in and is available for direct patient treatment as needed, including via telehealth. The integrated care team uses standardized test scores and other tools to identify patients for the program. Patients who have severe symptoms or are not meeting their treatment goals are typical candidates.
| EXHIBIT 2. Integrated Care Team Members |
|---|
 |
Among the provider sites participating in this study, most used live video to facilitate provider-to-provider communication related to MAT. This telehealth model for MAT includes consultations related to MAT between a local health professional (e.g., a PCP) who provides the direct care delivery, and a distant MAT specialist who provides guidance and specialized knowledge of MAT and OUDs. This mechanism is also used in educating non-specialists on OUD and MAT issues.
Two additional approaches use live video to support provider-to-provider communication, including provider-to-provider consultations that connect physicians and clinicians to specialized behavioral health experts, and provider-to-provider education that is used for training, mentoring, and sharing resources. The literature described two approaches for provider-to-provider consultation via telehealth. With one approach, the patient is present when a clinician connects to a consultant via live video. With the second, the patient is not present for the consultation between clinicians (MedPAC, 2016). Several stakeholders and providers participating in the discussions use live video to support provider-to-provider consultation when specialized services are not available on site. For example, provider-to-provider consultations are offered to hospitals and ED clinicians who are seeking advice or a second opinion on a patient's behavioral health issues. In some cases providers may also book time during a specialist's regularly scheduled telehealth hours. As discussants described, this enables providers to review several cases during one session and allows the opportunity to educate PCPs.
| "It's [telehealth] a way for us to educate our providers, and now they're just sending the specialists the more difficult cases. They've seen enough conversations that they're more comfortable treating some of the patients. That's our return on investment." |
Providers also use telehealth to connect for education, mentoring, and resource sharing. This model often involves a specialist consulting with a PCP or hosting educational sessions for multiple providers. One such program is Project ECHO (Extension for Community Healthcare Outcomes), which encourages physicians to identify specialty areas critical to their patients, invest in equipment that operates without high-bandwidth use, and join educational webinars on relevant topics (Warner, Montenegro, Stroup, Kinney, & Kirchhoff, 2014). The organization offers continuing education units (CEUs) to providers who complete coursework with ECHO (American Medical Association, 2016). ECHO has expanded to include physicians across the United States and supports new telehealth initiatives.
A new ECHO specialty program for Opioid Addiction Treatment (OAT) launched in January 2017 (University of New Mexico, 2016). Clinicians (e.g., PCPs, community health workers, counselors, social workers, and psychologists) connect with specialists to review and discuss de-identified cases; obtain OUD treatment training, including management of naloxone/buprenorphine and injectable naltrexone; and access tools and resources. One provider reported that they host a biweekly OAT ECHO clinic via videoconference. More than 25 providers from across the region regularly participate in the sessions. The site reported positive results and perceived that participants find value in ongoing participation. Because the OAT ECHO clinic is relatively new, data are still being collected on effectiveness and reach.
Another example is the Providers' Clinical Support System for Medication Assisted Treatment (PCSS-MAT) whose development was supported through HHS Substance Abuse and Mental Health Services Administration (SAMHSA) grants. PCSS-MAT provides online education opportunities to providers through an electronic repository of training materials and educational resources and maintains a virtual provider mentoring program ( http://pcssmat.org/ ).
| "The PCPs just want a few questions answered. When they're just looking for an opinion, this [asynchronous data sharing] is much more efficient and effective than traveling to see them. ... They send that recording to the psychiatrist, and then the psychiatrist can ping them back. It's more straightforward for scheduling, and the PCPs want to manage [the patients] anyway. Or for something like chronic illness, it's helpful to do a store and forward every 6 months to reassure the PCP that they're doing their best or offer other [treatment] options." |
Store and Forward Data Transmission (Asynchronous)
Store and forward involves one health care provider transferring shared patient information to another clinician using e-mail or another communication tool used to share video or photographs/images (MedPAC, 2016). Many examples identified in the literature focused on specialty areas such as radiology or dermatology rather than behavioral health. However, a discussant provided an example of asynchronous data sharing of audio files where PCPs sent recordings from challenging cases, and the behavioral health specialist sent back advice to reassure the PCP or offer other treatment options. In this way, the specialist could act as a consultant on a patient's care team, support the PCP as they managed the patient's care, and avoid investing unneeded resources in scheduling and supporting a meeting.
Remote Patient Monitoring
Health care organizations are using remote patient monitoring for target populations and conditions. For example, Intermountain Healthcare is working on obtaining data through an individual's personal electronic devices (e.g., mobile devices or smartphones, tablets, or laptops) for remote monitoring of chronic obstructive pulmonary disease, motion, and wellness in their cardiovascular and diabetes pilot programs (Larkin, 2016). A stakeholder also described an application available for personal electronic devices that supports remote patient monitoring for chronic condition management, including behavioral health. For behavioral health services, the application is used to supplement in-person and telehealth patient visits. As an example, the stakeholder described how telehealth can be used in conjunction with Dialectical Behavior Therapy (DBT). For DBT, the patient can maintain a diary in the application to track their mental and emotional status throughout the day. The diary is submitted through the application to the psychologist, who can monitor and use the information to augment the patient's visits. Telehealth allows providers to check the patient's progress more frequently and access a reliable record during appointments to support clinical decisions.
Mobile Health
The remote patient monitoring application and patient-directed digital consultation previously described are examples of using mobile health tools to collect and share patient information. Other examples relate to the availability of targeted information on behavioral health and SUD treatment for individuals and patients to access.
SAMHSA, for example, has published an online resource available across multiple platforms to help providers and patients navigate OUD treatment. Through several modules, the easily accessible intervention covers motivations for opioid use cessation, options for MAT, advantages to various treatment methods, and recommendations for approaching support networks (SAMHSA, nd). The system is accessible to individuals through mobile devices, such as a tablet, and functions by providing a screening for tobacco, alcohol, and drug misuse. Another tailored intervention, the Health Evaluation and Referral Assistant (HERA), translates the commonly used Screening, Brief Intervention, and Referral to Treatment (SBIRT) practice into a dynamic, electronic-based program. After completion, it provides the individuals with a brief feedback sheet, and the system can fax this information to a SUD treatment provider matched with the individual based on demographic information (Boudreaux, Abar, Baumann, & Grissom, 2013). Patients can be referred to HERA under a wide range of circumstances, including during treatment in an ED.
Other Methods
In addition to the telehealth modes and examples described previously, other methods identified from the literature review have a relationship to MAT or follow-up care after a telehealth visit. Several pilot programs use telephone follow-up to educate patients, assess treatment progression, provide interventions, or support behavior change goals. One program provides telephone support to supplement OUD treatment, using specially trained staff who regularly check in with patients. The telephone intervention is used in the first 3 months of treatment to provide education, assistance navigating resources, and personal support (Ruetsch, Tkacz, McPherson, & Cacciola, 2012). Another program uses virtual care navigators to follow up with patients who have recently accessed telepsychiatry and provides an avenue to help patients with appointment scheduling and feedback (Johnston & Yellowlees, 2016). A managed care organization funded a pilot telebehavioral health initiative program focused on diabetes treatment; however, program coordinators calling patients also reported fielding questions about comorbid disorders, including opioid misuse. Coordinators were able to provide patients with timely feedback and support them in their goals of behavioral change (Kahn et al., 2009). Finally, some sites described integrating home health visits into their telehealth programs. These visits could be used to lend additional support to patients, give providers insights into the patient's environment, or review complex medication regimens.
| "It takes less time to send an RN out with video capabilities than have a patient bring in their bag of medicines and forget that one on the cabinet every time. We do so much with patients in their homes as well, we just want to incorporate it [telehealth]." |
Several programs have been developed in the past few years to foster collaboration and increase awareness of education and resources available for telehealth within behavioral health care communities. For example, the National Frontier and Rural Addiction Technology Transfer Center (NFAR ATTC) Network hosts an annual conference to spread telehealth awareness and best practices. The American Telemedicine Association (ATA) has established a website that offers resources and guidance to providers interested in implementing telehealth interventions. And the TeleMental Health Institute provides online training and certification programs for providers, with a focus on mental and behavioral health (https://telehealth.org).
Telehealth is most commonly used through live video to support the direct delivery of behavioral health care services and provider-to-provider communication. The use of other telehealth modes in behavioral health implementation is less common. However, emerging studies as well as providers' observations suggest that telehealth has a positive impact on behavioral health care delivery for patients with limited access to specialty services due to their location or travel distance. Stakeholders and providers in this study reported interest in expanding their programs. While telehealth awareness is growing anecdotally, strategies may be needed to reach target clinicians (like PCPs) with training and implementation approaches for using telehealth to better serve their patient populations, especially in OUD treatment.
Implications for MAT
|
3.1.2. What are the best practices, barriers, and facilitators in using telehealth to identify and manage behavioral health disorders?
Best Practices
As telehealth use has grown, some best practices have been formalized and disseminated in the form of handbooks or guidelines. Some of these resources offer broad guidance; for example, the United Kingdom's National Health Service released a guide on telehealth capabilities aimed at garnering support from public officials (National Health Services, 2016). Other telehealth best practices are tailored to specific treatment programs, such as the desire to provide rapid access to MAT and frequent contact with support systems for OUD treatment (Knopf, 2013). In one discussion, a stakeholder described a new telehealth guide for MAT providers, slated for publication in fall 2017, that presents strategies for effectively using telehealth to treat behavioral health disorders.
Although best practices are still evolving within the field of behavioral health, there are three key areas in which best practices are emerging: planning and implementation, patient privacy, and meeting both the patient's and provider's needs.
Detailed Planning
One of the best practices frequently noted in the literature and in discussions is the need for detailed planning prior to implementation. Planning should begin with an early assessment of the needs of the community and the capability of telehealth to address any gaps or issues (California Telehealth Resource Center, 2014). Factors such as the existing technology available, how technology might be adapted for future programs, and quality assurance should all be considered and addressed early on (Perry, 2016). In addition, it is recommended that physicians and other staff consider how telehealth will be worked into their daily practice. This includes identifying what information will be transmitted over which electronic platform--for example, how patients will contact the provider and how the provider will consult with colleagues (Gagnon, Duplantie, Fortin, & Landry, 2006). As providers described, planning involves carefully thinking through how background information and laboratory results will be collected, what assistance is needed from the originating site during a telehealth session, how malpractice insurance covers the service, where to place equipment in a clinic, and the experience of staff members. Providers discussed the need for in-person experience with treatments like MAT before telehealth is used. As described, this traditional care experience allows providers a frame of reference for the standard of care when using telehealth. One site finalized its process of organizing key staff and installing technology with test calls between sites without patients. These calls gave the sites the opportunity to run through emergency scenarios and troubleshoot camera arrangements for glare or distracting backgrounds, such as a window behind the care provider. In addition, telehealth providers advise developing a system for managing non-urgent requests, such as for a new appointment, received via telehealth (Tofighi, Grossman, Sherman, Nunes, & Lee, 2016).
Things to consider in planning:
|
Discussants noted that strong communication between originating sites (where the patient is located) and distant sites (where the provider delivering services is located) during the planning phase is crucial. Interdisciplinary coordination between sites, including discussions among program coordinators and providers, was identified as a critical step for planning success. On a basic level, this communication can help sites establish procedures, define roles, and streamline clinical operations. Physicians, other clinical staff, and coordinators can receive telehealth training and practice with the equipment before seeing patients. In addition, this provides an opportunity to build trust and buy-in between the sites. Key stakeholders often described the difficulty physicians have "letting go" of their patients and trusting originating site staff to complete examinations or follow up. Sustained contact during planning can increase distant providers' confidence in the originating site staff. At one site, a nurse practitioner (NP) functioned as the clinical coordinator. At the beginning of each telehealth program, she would visit the distant site, discuss their processes, and observe the operation of the site for a day to ensure their systems could be integrated.
| "I don't think there's anything about the [treatment] process that's different. It differs because of the specialty and treatment. I think you have to teach the basics about providing MAT. We're one of the few medical schools that actually does that. We have a pretty active addiction program. We do psychiatric treatment for 6 months in the first year. We teach them how to do MAT. I don't think it makes a big difference for MAT. The difference in treatment is just getting used to not being in the same room." |
Contributing to planning may also improve buy-in among originating site staff who feel involved in the process. After the planning phase, coordinators at originating and distant sites maintain communication in many robust telehealth programs. As described, their roles in scheduling, relaying laboratory results, and following up with providers and patients heavily influence the strength of a program.
Ensuring Privacy
Data from the literature and discussions highlight the need for providers to establish mechanisms to protect patient privacy when using telehealth. Some mechanisms and policies deal with communication, such as only one provider at a practice communicating with a patient via text messaging. Other mechanisms are more technology focused, such as use of password protection or other security measures on either end of a platform. Still other measures are aimed at preventing individuals other than the patient from accessing private health information from a patient's device (Tofighi et al., 2016). For videoconferencing, ensuring individuals who are present are involved with the patient's care is an important consideration (Paing, Weller, Welsh, Foster, Birnkrant, & Weller, 2009). As one site described, patients may lose trust when individuals other than the physician appear on camera during a session. Even if a physician uses headphones and a privacy screen protector, patients are not always aware of these precautions and may be uncomfortable with seeing other people on the screen. The same may be true if a patient sees other individuals through a window and assumes the physician's display is visible. Confidentiality protections for behavioral health records are addressed by the Health Insurance Portability and Accountability Act (HIPAA) and 42 CFR Part 2, but there are no specific requirements for telehealth. Organizations must take both technical and process factors into account when planning and implementing telehealth to protect patient privacy.
One provider described their process for obtaining informed consent for using telehealth. In the early implementation of their program, they found that patients did not have clear expectations for their telehealth appointments. In some cases, the nature of the appointment was miscommunicated, patients anticipated an in-person meeting, and they found the telehealth equipment unsettling during their initial appointment. In other instances, patients expressed concerns about the privacy of the platform. The provider found that explaining the nature of the appointment beforehand, allowing the patients to see the equipment before using it, and explaining consent forms helped alleviate anxieties and gain buy-in from the patient.
| "We [telehealth originating site] learned from that [original experiences with patient education on telehealth]. Now we tell [the patients] what we're going to do, take them into the room, show them what it's going to look like, and point out that we will be around the corner. That's all we needed to do." |
Tailoring Technology for Patient and Provider Needs
There are several technologies used to support telehealth, including videoconferencing, text messaging, and portals. Regardless of the technical platform, many studies suggest that efforts should be made to tailor technology use for patients and providers. One example of this is updating online patient questionnaires with questions that screen patients for key issues and allowing them to skip further questions that do not apply to their circumstances. For example, if a patient indicates that he or she does not smoke at the beginning of a questionnaire, an electronic questionnaire could be programmed not to probe for the frequency of tobacco use or age of first use (Graham, Tomcavage, Salek, Sciandra, Davis, & Stewart, 2012).
Another example is allowing physicians to request telepresenters at the originating site with skills relevant to their practice, as is the case at several of the provider sites in this study. Telepresenters are health care professionals at the originating site who may remain in the exam room with patients during their telehealth sessions and provide support. They can be a range of professionals, from medical assistants to registered nurses, and they can provide services from behavioral health support to a physical exam.
Interacting with patients over technology may require a cultural competency and understanding of visual cues or communication styles from providers, which differs from traditional in-person encounters (Newman, Bidargaddi, & Schrader, 2016). Several providers described the importance of cultural competency training when working in rural areas with populations that may have few resources and speak a range of languages. Education-based programs for providers may also be tailored to their experience and scope of practice, such as the ECHO program for OUD treatment education, which focuses units on the unique contributions physicians, social workers, and psychiatrists can make to treatment (University of New Mexico, 2016). In addition, key stakeholders from Project ECHO indicated that even with the specific units tailored to different disciplines, there is also a focus on how to work across disciplines to coordinate patient care.
Telehealth may require different approaches to tailoring for referrals. Some experts argue that typical referral networks must be used to minimize harmful competition among health care providers, and others maintain that reliance on a typical referral network stunts the growth of telehealth and the number of people it can effectively impact (Gagnon et al., 2006; Kraetschmer, Deber, Dick, & Jennett, 2009). Careful planning, visualization of how telehealth will function in the clinical setting, and clear communication have consistently been identified as elements that allow programs to start with a strong foundation for success.
Implications for MAT
|
Barriers and Facilitators
Patient Factors
Telehealth reach is influenced by individuals' access to technology, knowledge of the resources available, and willingness to interact with the technology. For example, Schmeida and McNeal (2007) found that older, low-income individuals were likely to search for Medicare and Medicaid information online while young, highly educated, and wealthy individuals were more likely to use the Internet in general. Patients with more than a high school education who are seeing a physician with training in telehealth were more likely to use telehealth services when offered (Lowery, Bronstein, Benton, & Fletcher, 2014). For OUD treatment, computer-based treatments have been shown to be more effective for patients who are employed, highly anxious, or ambivalent about continuing substance use (Kim, 2015).
Beyond patient demographics, other factors may influence use and effectiveness of telehealth. In a clinical trial of a remote SBIRT implemented in an ED setting, researchers found several factors that could hinder use, including complications with provider engagement, delays in warm handoffs to remote behavioral health interventions, and disruptions from other individuals (e.g., other medical staff or family members). Feedback and acceptance ratings from participants, however, were generally favorable, and the study ultimately concluded that a remote SBIRT application held great promise (Boudreaux, Haskins, Harralson, & Bernstein, 2015). Similarly, discussants in this study reported that patients often appreciated the opportunity to use telehealth once they were educated about it. One program reported that individuals from the community were incentivized to change providers in order to use telehealth to access services that were not available locally. When patient buy-in is not immediate, some sites described engaging patients in their care through skill building and support as critical to improving outcomes. Patient experience and acceptance with technology, coupled with organizational support of telehealth, influenced patients' willingness to use the technology for treatment.
Provider Factors
Telehealth uptake and reach is also influenced by provider factors such as training and technology acceptance. One pilot study found that after 10 months, only two of 12 rural providers were using telehealth methods for which they trained. The physicians cited difficulty with the infrastructure needed to implement telehealth as a key barrier (SAMHSA, 2016). Several programs reported that providers and other staff often have more difficulty than patients adjusting to telehealth. One discussant described planning a telehealth link with a local hospital to enable provider communication and translation services. Although the equipment and processes were established, staff at the hospital did not use the equipment or integrate it into their workflow.
| "The doctor has to be willing to adjust their workflow and accommodate this new way of seeing patients. If the doctor is the champion of the system, they will get it. Those are the ones that are driving it and adopting the technology." |
Some initiatives have found that providers may also be wary of becoming credentialed at facilities they plan to serve only through telehealth. Other providers cited concern about being able to provide quality care using telehealth. Another provider concern mentioned by discussants was difficulty fitting telehealth into clinical and administrative workflows. Some sites described reframing telehealth as another tool in the physician's or other staff member's toolkit when faced with resistance, but it was necessary for these programs to continuously work to ensure staff buy-in.
| "They [rural providers] are very intimidated by medication-assisted treatment for opioid addiction. For one, it was always done in methadone clinics, so it was far away and you didn't have to worry about it, which was nice. Now, it's a part of your clinic, and I think people are very intimidated now. So the telehealth [provider] can mentor people when they are sole providers and they have no one else to talk to; it can be helpful to have that person there." |
MAT Considerations
Use of telehealth for MAT is not as prevalent as telehealth in other behavioral health services due to some unique considerations. Prescribing medications electronically for MAT, particularly controlled substances such as buprenorphine, was cited by discussants as a significant barrier to using telehealth for direct provider-to-patient interactions. Key stakeholders noted during discussions that they felt that the Ryan Haight Online Pharmacy Consumer Protection Act, by modifying the Controlled Substances Act, made it more difficult for telehealth providers to e-prescribe controlled substances. The Ryan Haight Act does not specifically prohibit telemedicine, but it requires that patients being prescribed controlled substances be treated by, and physically located in, a hospital or clinic registered under Section 303(f) of the Controlled Substances Act. In some cases, a patient's remote location may not have this registration, even though the telehealth provider may be registered under Section 303(f). This requirement of the Ryan Haight Act has caused some concern for key stakeholders about how to make MAT available to patients. To prescribe and dispense buprenorphine requires even further certification of providers under the Drug Addiction Treatment Act of 2000 (DATA 2000), which requires them to complete an 8-hour training to qualify for a waiver. In addition, midlevel staff who have not traditionally been able to prescribe for MAT are now being integrated into programs through an expanded waiver program to varying degrees. As one site described, these providers may need to familiarize themselves with MAT before using it via telehealth. However, key stakeholders involved in tele-MAT did report that telehealth allows for more frequent check-ins with patients and communication between providers. These check-ins and communication are particularly beneficial and may facilitate successful treatment.
Implications for MAT
|
3.1.3. How is telehealth being used to support provider-to-provider communication?
Telehealth is being used to support provider-to-provider communication in several ways, including clinical support, education, and administrative services. Through provider-to-provider communication, telehealth supports interaction between PCPs and geographically dispersed care specialists (e.g., addiction specialists and counselors). Discussants described the benefit of using telehealth broadly, including in multiple service lines and administrative work such as staff meetings. The continuous use of technology encourages interacting with colleagues while increasing familiarity with the technology. Some telehealth organizations, such as the ATA, maintain directories of their members, allowing practitioners the opportunity to communicate with their peers (ATA, 2016). The NFAR ATTC even holds an annual summit for telehealth training during which providers can interact in person (NFAR ATTC, 2015). Discussants noted the importance of integrating midlevel staff into the telehealth team. Physician assistants (PAs) and NPs have traditionally been very involved in ECHO-style programs, as key stakeholders and providers described. On a basic level, this communication can help sites establish procedures, define roles, and streamline clinical operations to allow the distant and originating sites to operate as a team.
Specialist and Primary Care Communication
Many stakeholders described telehealth's ability to connect specialty providers and PCPs as its greatest strength. One stakeholder noted many of the geographic areas in which telehealth is provided simply do not have specialists available, and PCPs are tasked with providing the full range of needed services. The addition of telehealth specialty providers greatly reduces initial visit wait times for patients seeking mental health services in rural clinics by making addi-tional providers available. In one model, the remote specialist providers can more quickly perform initial diagnostic assessments and help plan for ongoing medication maintenance (Johnston & Yellowlees, 2016). Remote specialists also often give recommendations to the PCPs and their on-site behavioral health managers on how to continue care for patients in the 3-4 months between telehealth appointments with the specialist. Several providers described similar models that support increased communication between primary and specialty providers. PCPs may even schedule time with a specialist to discuss several patients, as one specialist provider described. Some studies have shown that with a great need for services, especially in rural areas, ongoing coordination of services can still be challenging, with some telehealth educational services being scheduled as far as a year in advance because of demand (Kraetschmer et al., 2009).
| "I just think this notion of a community of practice where clinicians that share interests continue to talk to each other is important. I don't think we've done a lot of evaluation of that. ... If we could build a community with PCPs that can have one person with SUD expertise, one person who knows rheumatology, etc., I think building that community would build us up so much more and enrich them." |
Careful allocation of distant and originating provider resources was described as a strategy for using telehealth for effective and timely treatment. The ECHO model is one approach that addresses this issue by educating practitioners. It aims to increase the knowledge base in specialty areas to minimize coverage gaps in communities (American Medical Association, 2016). In ECHO's OAT program, specialist teams associated with an academic "hub" are connected with physicians, midlevel practitioners, social workers, and any additional members of a primary care team. While the local community providers who make up the "spokes" of the program can connect with any of the five hubs that have been established across the United States, they are encouraged to attend training at their regional location. Interacting with regional hubs connects practitioners with local resources and colleagues, enriching their experience and ability to treat (University of New Mexico, 2016).
Rural Providers
When providers and patients in rural areas engage in telehealth, they may practice it differently than their urban or suburban counterparts. Compared with suburban providers, rural PCPs with access to telehealth consultation request less help with diagnoses or altering established care plans, but they request more assistance with creating new treatment plans. They are also more likely to attend consultations rather than receiving a fax with the details of the appointment afterward (Hilty et al., 2007). Attending consultations may allow these rural providers an opportunity to learn from the specialist and be more involved in their patients' care.
| "Our doctors can talk to each other through telehealth, and they can do curbside consults. They can build relationships through that and build their skills. Then we can retain them." |
For some rural provider sites, telehealth is used as a tool to recruit and retain providers by offering them access to further education and a community of other providers. One site indicated, "You have to use creative models to recruit and maintain providers." As explained in the literature, connecting rural providers with other practitioners may alleviate feelings of isolation (Gagnon et al., 2006). Telehealth also allows programs to tap into a wider workforce. As one site noted, there are few rural health residencies compared to the number of physicians needed to serve large rural areas. Telehealth may help distribute resources to these rural areas, although one site noted that it can be difficult to find specialists with time in their schedules to assess telehealth patients.
Initiatives are more likely to have an impact on care outcomes and facilitate access to care when physician engagement and buy-in are achieved. Although technology can occasionally be a barrier, it often allows for more convenient access to treatment at home or at an established community center. There have even been documented cases of communities seeking the inclusion of telehealth and identifying resources that could allow access. In rural Alabama, for example, a community organized a child telepsychiatry program around the distance learning equipment available at the county technical high school. Active community members reached out to clarify Medicaid reimbursement and to request services from the University of Alabama Department of Psychiatry. Their program now provides weekly services to children with a range of diagnoses (Merrell & Doarn, 2013).
Implications for MAT
|
3.1.4. How does choice of telehealth modality affect barriers, facilitators, and costs?
Technology Investment
Equipment needs, maintenance, and costs vary across telehealth modalities. In many models, videoconferencing tools play a prominent role. Although the exact brand and specifications for technology vary according to program, best practice minimums for the amount of bandwidth and quality of technology used have been established. Often, quality videoconferencing can use at a minimum 384 Kbps of bandwidth (McGinty, Saeed, Simmons, & Yildirim, 2006), which can be a challenge when introduced into the 1.5 Mbps environment providers traditionally use (California Telehealth Resource Center, 2014). In this situation, a videoconference using a fair portion of the network may have quality issues such as lag or skipping. High network use may also interfere with other staff members' work. Current industry standards recommend that small physician practices and rural health clinics establish minimum bandwidths of 10 Mbps and hospitals use 100 Mbps to allow for electronic health records, videoconferencing, and other technological interventions (Federal Communication Commission, 2010). As one provider emphasized, the quality of the video connection relies primarily on bandwidth or cellular speed specifications and secondarily on videoconferencing technology.
| "First, you want to get your bandwidth working appropriately. You can get the best equipment ever and it won't work without the appropriate bandwidth." |
Technical aspects to protecting patient privacy include the use of a virtual private network or a virtual local area network. The use of Internet Protocol networks with enhanced security is often an attractive option because they use existing infrastructure and can be considered sunk costs without additional up-front investment in infrastructure (McGinty et al., 2006). Other elements, such as a high-megapixel camera, microphones, speakers, and monitors, can also use the existing infrastructure to minimize costs. Intermountain Healthcare, for example, uses the televisions already installed in each patient room to act as monitors. Physicians may also make use of their desktops and existing computers to sustain a telehealth practice (Perry, 2016). Often, physicians described arranging two monitors with their telehealth equipment, allowing them to chart and speak to patients simultaneously. At the end of a conference, providers can then immediately send their notes to the originating site for review. Distant sites generally described a preference for using their desktop computers to conduct telehealth visits, as this allows for easier scheduling and coordination than sharing telehealth equipment with other providers. Some platforms can also be used through mobile devices such as tablets or smartphones. Key stakeholders even suggested that some patients and providers can use FaceTime and Skype for services. Clarifying expectations and optimizing technology use can present a challenge to emerging programs as they balance privacy and quality requirements with ease of access.
| "It's virtually limitless the ways people can connect. So, we use the ... videoconferencing platform to have people connect simultaneously, and then people can just call in if they don't have access to a computer or Internet." |
Models that do not use videoconferencing have very different technology needs. For mobile-based programs that guide self-assessments or link patients with information or providers, accessibility to a computer, smartphone, or telephone is often critical. For some programs, a series of phone calls is necessary to maintain contact or progress through a treatment plan. In these instances, reliable contact information and access to technology is critical to success (Kim, Michalopoulos, Kwong, Warren, & Manno, 2013). As one stakeholder described, providers may use mobile applications to offer patients resources or encourage them to complete regular assessments that can be reviewed during appointments. It is important to note that some patients or providers may struggle with the emerging technology and require assistance to become proficient in using it (Larkin, 2016). Associations such as the ATA and the TeleMental Health Institute may provide some training or resources for providers incorporating new equipment, but these resources are not likely to reach patients.
Impact on Programs
Several telehealth modalities can be easily adapted to facilitate patient access to support networks during their treatment. In these cases, the modality is a facilitator. In 2013, a practice in West Virginia reported using telemedicine to refine its protocol of rapid access to buprenorphine and frequent meetings to treat OUD by allowing patients to contact physicians and support networks via videoconferencing (Knopf, 2013). The Tofighi et al. (2016) case study of an at-home induction into a buprenorphine treatment program described a similar strategy, with a young man being inducted into treatment and gaining rapid access to his physician through text messaging during business hours. In this example, the patient felt comfortable reaching out to his provider when experiencing issues with maintaining his buprenorphine supply and sobriety. The provider could adapt the care plan to address the patient's concerns and help him continue with treatment (Tofighi et al., 2016).
Stakeholders and provider sites described similar successes using videoconferencing, text messages, and telephone contact to foster support networks. Care coordinators at several sites used telehealth to connect with patients between appointments and address their concerns. At one site, group therapy sessions for individuals in rural areas were hosted via telehealth. At another site, community health workers made home visits and used telehealth applications to give providers a view of the patient's environment. As one participant noted, "You need a provider, equipment, and people to grease the wheels and make everything work."
There may be challenges in widespread adoption of mobile interventions to help treat individuals with OUDs. Tofighi and colleagues noted that although patients express interest in using text messaging to contact their providers, they also have a high rate of cell phone turnover and experienced difficulty reaching providers through an established telephone hotline (Tofighi, Grossman, Buirkle, McNeely, Gourevitch, & Lee, 2015). Additional studies have found that in programs that frequently use the telephone, lack of stable contact information may make it difficult for patients to be reached or successfully enrolled (Kahn et al., 2009). Guarino, Acosta, Marsch, Xie, and Aponte-Melendez (2016), however, found that mobile phone turnover was limited in a trial where 25 OUD treatment patients were given phones during treatment. While research on the feasibility of telehealth interventions for MAT is mixed, additional research has examined the potential impact of telehealth on treatment. One study that followed 100 patients completing either in-person or telepsychiatry MAT programs found that there was no statistically significant difference in outcomes between the programs. Both groups were able to supplement their program with regular drug screenings and achieved similar rates of 30 and 90 days of abstinence (Zheng et al., 2017).
Implications for MAT
|
3.1.5. What strategies and solutions have providers used to overcome barriers?
Providers have taken several approaches to address barriers related to patient and provider buy-in, the complexity of coordination, and telehealth treatment limitations. Provider and patient engagement was addressed in several ways. Thorough planning for integration into a typical clinic workday can help support efficiency and reduce interruption to workflow, both of which are critical to physician buy-in and the ultimate success of initiatives (Gagnon et al., 2006). As provider sites identified, frequent use and interaction with reliable telepresenters can increase provider comfort and engagement. Careful planning, however, can be thwarted by poor technology access or low technology competency in the population served (Muench, nd).
Common barriers include
|
Key stakeholders emphasized the need to establish clear expectations with patients by explaining the program and showing them any telehealth equipment before their appointment. Understanding the role of telehealth in their care and the alternatives, such as traveling to the area where a specialist practices, may increase patient buy-in. In addition, studies have shown that while patients often express interest in using telehealth in their care, interruptions and other issues using the technology represent common barriers (Boudreaux et al., 2015; Tofighi et al., 2016).
| "You have to have somebody whose job it is to grow the business and work with partners. Many rural places have no IT expert at all. The technology and the organization is overwhelming. They need assistance to develop the services that they want." |
Introducing patients and providers to the telehealth program may be included in the role of a telehealth coordinator, which many key stakeholders and provider sites highlighted as a solution to the complex logistical needs of telehealth programs involving patients and providers. Coordinators often schedule appointments for patients at the originating site and ensure that the appointment time is communicated with the distant site provider. They may manage the setup of telehealth technology before the appointment or the induction of a patient into a mobile application or text-based program. They often coordinate any tests needed for the appointment, such as urine drug screenings for MAT. As a program progresses, coordinators may also be tasked with monitoring the wearing of telehealth equipment or identifying other areas in which telehealth could be used. The addition of a focused telehealth coordinator to a program can mitigate many issues related to coordination and planning, as provider sites described.
Discussions with key stakeholders and provider sites revealed several strategies for addressing providers' challenges in prescribing using telehealth. In many cases, physicians at the distant site worked closely with the PCP or other providers at the originating site. Providers at distant and originating sites indicated that providers who were engaged in discussions around MAT and treatment courses with a specialist or experienced physician felt more comfortable prescribing medications such as methadone, buprenorphine, and buprenorphine with naloxone (suboxone). ECHO programs also capitalize on the impact of physician-physician collaboration to guide practitioners through MAT. As one individual involved in the ECHO program described, "They have the skills; they're just not confident in implementing [MAT]." After providers develop self-efficacy, they may be able to continue treating patients with SUDs without such close collaboration.
In addition to the providers participating in this study, other treatment centers and initiatives have already scaled up telehealth application from clinical trials. Tarzana Treatment Centers, for example, use telehealth to support treatment for adolescents with SUDs. Tarzana also uses telehealth to provide additional clinical support for individuals in inpatient treatment and to supplement the available outpatient treatment sessions (Tarzana Treatment Centers, 2014).
Several new efforts to include telehealth in opioid treatment are supported by the HHS Agency for Healthcare Research and Quality (AHRQ) and the Health Care Innovation Awards (HCIAs). AHRQ is supporting three demonstrations in Colorado, Oklahoma, and Pennsylvania that will attempt to train rural PCPs in OUD treatment. Their model includes collaboration with Project ECHO for specialty training (Whitman, 2016). The eight HCIA-funded initiatives that include telehealth are under way throughout the country and include different forms of technology. Five of the programs champion the development of electronic health records that allow providers to share records, notes, and care plans for patients. Other HCIA initiatives support the use of mobile phone applications that allow patient and provider contact, self-evaluation mobile applications, prescriber recommendation tools, and online case management platforms (Ireys, 2014). Two of the providers in this study maintain telehealth programs with broad scopes ranging from Hepatitis C and HIV to substance use and psychiatric treatment. They described learning more with each program that was implemented and building on their previous experience. As these initiatives progress, they will likely provide a wealth of information about the effectiveness of telebehavioral health interventions and guidance to emerging programs.
| "I know about MAT. ... The Ryan Haight Act was passed as an attempt to be helpful, and it excludes telemedicine from that. The DEA has been slow to change that. I personally don't prescribe any controlled substances over telemedicine. I wouldn't do it, and I wouldn't tell anyone else to do it." |
Prescribing medications in the context of MAT is a significant barrier to using telehealth for direct provider-to-patient interactions. Key stakeholders noted during discussions that they felt that the Ryan Haight Online Pharmacy Consumer Protection Act, by modifying the Controlled Substances Act, placed challenges on the ability of telehealth providers to prescribe controlled substances. The Ryan Haight Act does allow for telemedicine, but it also requires that patients being prescribed controlled substances must be treated by, and physically located in, a hospital or clinic registered under Section 303(f) of the Controlled Substances Act. In some cases, a patient's remote location may not have this registration, even though the telehealth provider may be registered under Section 303(f). This requirement of the Ryan Haight Act has caused some concern for key stakeholders about how to make MAT available to patients.
| "Ryan Haight is the big one. Every conference we go to, they [other providers at the conference] talk about that need for a face-to-face before we prescribe with telemedicine. That always comes up, and it's a major barrier." |
During discussions with providers, the most referenced barrier to using telehealth for MAT continued to be the Ryan Haight Act. Most providers interpreted the act as prohibiting using telemedicine to prescribe controlled substances for MAT. Several providers noted having specific conversations with the Drug Enforcement Agency (DEA) about these limitations, which include a requirement that a provider cannot use telemedicine to prescribe medications without seeing the patient in person every 2 years. The ATA is proposing modifying the Ryan Haight Act to better align with the need of telehealth providers to deliver MAT.
Implications for MAT
|
3.2. Financing and Sustainability
3.2.1. How are telehealth services reimbursed generally and for behavioral health disorders?
One of the key challenges of using telehealth is the financing of services by Medicare, Medicaid, and private payers. Each of these payment sources comes with a unique set of requirements around the types of services that will be covered, the location and setting, and the types of providers. A summary of telehealth coverage by payer type is provided in Table 6.
| "I am a believer in telemedicine, and I think it works, but the reimbursement is a problem." "I have spent 20 years doing telehealth, so this is my 2 cents on what works. To me the funding is the biggest thing." |
| TABLE 6. Reimbursement for Telehealth Services, by Payer Type | |||||
|---|---|---|---|---|---|
| Payer | Reimburses for | Types of Behavioral Health Services Covered | Requirements | ||
| Telehealth? | Medical/Surgical Services via Telehealth? | Behavioral Health via Telehealth? | |||
| Medicare | Yes | Yes | Yes | Included: Mental health services, medication management, SUD assessment, diagnosis, and brief interventions Excluded: Psychiatric diagnostic interviews or medical evaluation/ management services | Originating site in rural HPSA; limitations on eligible providers |
| Medicaid | Yes; in 48 states and DC (excludes CT and RI) | Yes; in 48 states and DC (excludes CT and RI) | Yes; in 48 states and DC (excludes CT and RI) | No noted specific inclusions or exclusions | 24 states and DC have no restric-tions on location and setting; 15 of these states also place no restrictions on the type of provider |
| Private payer | Dependent on payer | Dependent on payer | Dependent on payer | Dependent on payer | 23 states and DC require private payers to have full parity with respect to telehealth services |
Medicare
The Balanced Budget Act of 1997 established FFS payment for Medicare telehealth services that provided payment for services to the remote service provider and a small facility fee to the originating site where the patient is located (ASPE, 2016). The act limited eligible originating sites only to those in a rural HPSA in a rural census tract (CMS, 2016). Eligible providers from remote sites include physicians, NPs, PAs, nurse-midwives, clinical nurse specialists, certified registered nurse anesthetists, registered dietitians, and nutrition professionals. Clinical psychologists and clinical social workers may also provide telehealth services. However, they may not bill for psychiatric diagnostic interview examinations with medical services or medical evaluation and management services under Medicare. Medicare covers a limited number of telehealth services, but many are related to mental health services, from initial assessment and diagnostic visits to therapy and medication management. Alcohol and SUD services are more limited, primarily focusing on assessment, diagnosis, and brief interventions (CMS, 2016).
Medicare requires that Medicare Advantage Plans provide coverage for the same telehealth services as in the FFS system. In addition, Medicare Advantage Plans have the option to cover additional telehealth services as supplemental benefits to their beneficiaries (ASPE, 2016). The Anthem Medicare Advantage Plan offers telehealth benefits through its LiveHealth Online system in 48 out of 50 states (Anthem Blue Cross Blue Shield, 2016). Beneficiaries can access general medical and psychological services through the system.
When discussing Medicare reimbursement for telehealth services, providers reiterated the limitations of providing reimbursement only for telehealth services provided by rural HPSAs in a rural census tract. Providers identified the need for behavioral health services in nursing homes, whose patients have limitations on mobility outside of the home yet are often not located in rural areas. They also noted that some individuals with psychiatric-related disabilities may not be able to leave their homes for treatment even if they live in an urban area because of the nature of their disability. In those cases, telehealth may be a good option to provide care within their home.
Medicaid
Although Medicare coverage of telehealth could be characterized as limited but consistent, coverage of telehealth services by Medicaid and private payers could be characterized as highly variable and ever changing by state (Thomas & Capistrant, 2015). Medicaid provides some level of telehealth coverage in 48 states and the District of Columbia, with only Connecticut and Rhode Island not providing any coverage for telehealth services. Unlike Medicare, which restricts the coverage to patients receiving services at a provider located in an HPSA, Medicaid in 24 states and the District of Columbia places no restrictions on the location and setting in which patients receive telehealth services. Fifteen of these states also place no restrictions on the type of health care provider delivering services via telehealth.
When it comes to behavioral health, all 48 states providing Medicaid coverage for telehealth services include some form of coverage and reimbursement for mental health provided via telemedicine videoconferencing. It is common for states to allow physicians who are psychiatrists, advanced practice nurses with clinical specialties, and psychologists to provide telehealth services for behavioral health issues. Many states also allow licensed clinical social workers or licensed professional counselors to provide services. However, only New Mexico, Oklahoma, Virginia, West Virginia, and Wyoming specify coverage for telemedicine when provided by an SUD or addiction specialist (Thomas & Capistrant, 2015).
Private Payers
Limited information is available on the coverage of telehealth services by private payers. Many private payers consider information on their coverage of services to be proprietary, so it is not often publicly available. To assess the potential impact of private payer coverage for telehealth services, we can look at the state-level policies governing private payers. Twenty-three states and the District of Columbia have policies requiring their private payers to have full parity with respect to telehealth services, meaning that private payers must provide coverage and reimbursement for telemedicine-provided services comparable to that of in-person services (Thomas & Capistrant, 2015). Additional research in private payer coverage for telehealth services is underway at the Center for Connected Health Policy ( http://www.telehealthpolicy.us/). Under a Milbank Memorial Fund grant, researchers at the center reviewed in detail private payer policies by state and conducted interviews with private payers to identify additional information on coverage and reimbursement of telehealth services. The results of this study are under review and are expected to be released in 2017.
Implications for MAT
|
3.2.2. Does reimbursement for telehealth for behavioral health disorders differ from reimbursement available for medical or surgical services?
Reimbursement for telehealth for behavioral health disorders does not significantly differ from reimbursement for medical/surgical services because of parity laws. However, several discussants noted that coverage for telehealth for behavioral health services was better than telehealth for medical or surgical services because of the nature of behavioral health services. Medical or surgical services often require specialized remote instruments such as stethoscopes to provide services over telehealth, whereas most behavioral health services are focused on speaking with patients. One discussant even noted that Medicaid in their state did not allow for reimbursement for telehealth medical services but did for telehealth behavioral services.
Implications for MAT
|
3.2.3. How does reimbursement for behavioral health services delivered via telehealth differ across payers?
Medicare, Medicaid, and private payer coverage of behavioral health services differ with their approaches to reimbursement for behavioral telehealth services. Discussants found Medicare to be the most restrictive, with requirements for the location, setting, and types of providers who could deliver services. Most discussants noted that one of the key factors affecting Medicaid and private payer reimbursement was parity. Most states had parity in coverage and payment, so telehealth visits were reimbursed at the same rate as in-person visits. The greatest challenge for reimbursement for telehealth services with private payers is that existing contracts between private payers and providers often did not include the telehealth GT modifier as covered for Current Procedural Terminology (CPT) or Healthcare Common Procedure Coding System (HCPCS) codes. Although a small change, it often resulted in larger contract renegotiation efforts between private payers and providers.
| "We've had to go renegotiate health system contracts with all of our insurers. I don't know if you've seen these contracts, but they're terrifying. They go down to the level of detail of only paying for certain codes. We wanted to add GT modifiers [required by CPT to denote telehealth services] for telehealth, and they had to renegotiate the whole thing to get those included. We had to do it from scratch to include telemedicine. ... And that's how they get out of paying for this." |
Implications for MAT
|
3.2.4. What payment models support use of telehealth?
Fee-For-Service versus Value-Based Purchasing
Several discussants noted specific challenges in reimbursement using an FFS model for telehealth for behavioral health services. In an FFS model, providers are reimbursed per service provided. Therefore, the incentive for providers is to focus on the quantity rather than the quality of services provided. With telehealth and lack of in-person contact, discussants expressed concern that some providers may move through assessments or services as quickly as possible to get to the next patient without focusing on how comprehensive or tailored the services should be to meet the patient's needs. Several providers suggested that moving toward value-based purchasing may help address some of these concerns.
Some organizations working under a value-based purchasing model, such as FQHCs and Indian Health Service sites, have established contracts that purchase blocks of time with specialty providers such as psychiatrists to provide telehealth services to their patients. For example, under these contracts, a psychiatrist may be contracted to provide up to 4 hours of telehealth services per week at a specific rate per hour for an FQHC. The FQHC can then use that time to support whatever patient needs it has that week. The FQHC takes on the risk associated with how paying the psychiatrist to be available for services factors into the overall FQHC payment rate for their patients (Kraetschmer et al., 2009).
The MACRA of 2015 included several telehealth provisions that are expected to affect the coverage and reimbursement for Medicare telehealth services (ASPE, 2016). The legislation includes the "use of remote monitoring or telehealth" as one of the services for which physicians or other providers would be reimbursed at a higher rate to encourage the coordination of care for their patients. MACRA also allows for physicians or providers participating in advanced alternative payment models to provide a variety of modalities of telehealth (i.e., not restricted to live videoconferencing) to patients without restrictions on the location of the patient or provider (i.e., no longer limited to HPSA locations).
Coverage of Telehealth Provider Training
The primary focus of telehealth financing has been on reimbursing direct services from remote providers to patients. However, one of the most promising telehealth approaches is the use of telehealth to connect providers with training, expertise, and/or certification in areas that are relevant to the patients they are treating. For example, Project ECHO links expert specialist teams at an academic "hub" with providers in local communities--the "spokes" of the model. These local providers participate in weekly TeleECHO clinics, which are like virtual grand rounds, combined with mentoring and patient case presentations. One of the challenges affecting provider participation in these types of telehealth activities is the lack of funding for the time providers spend attending and participating in these activities. Strategies that Project ECHO has used to address this concern include holding TeleECHO clinics at typical lunchtimes for the local providers and offering CEUs as an incentive for the providers to participate (American Medical Association, 2016; University of New Mexico, 2016). In some cases, Project ECHO participation is covered by grant funding or included as time to be covered by the provider organization under employment contracts with their providers. Although these efforts may be effective in some cases, some providers may still choose not to take advantage of telehealth training in the absence of specific reimbursement for their time.
Provider sites in this study that use a TeleECHO approach noted that they started off with grant funding to start their programs, which helped them purchase equipment and defray administrative costs associated with start-up. Providers noted that the costs associated with these programs are relatively low compared to the impact of helping clinicians provide better services to their patients. One provider even noted that their organization felt that using telehealth helped them better meet the needs of their patients; therefore, their organization commits funds every year to cover the administrative costs of its telehealth programs.
Implications for MAT
|
3.3. Impact
The literature identifies access to and delivery of behavioral health services in rural and underserved areas as an ongoing challenge. Among the specific issues affecting access and delivery in rural areas are a lack of providers to deliver services, ongoing stigma around behavioral health services, and lack of perceived privacy (i.e., being recognized in a small community) (Taylor, Symonette, & Singleton, 2009). Research has suggested that telehealth can be used to overcome these barriers so that behavioral health services can be made available and used in underserved areas (Riding-Malon & Werth, 2014).
| "There's a stigma with mental health. Having technology integrated into that system can help. It's like FaceTime with HIPAA compliance and everything. That takes away the stigma for mental health services, especially for those that need it more. Having a patient adopt the platform can open up their willingness to access mental health services when they need them. We're looking for ways to help with other representative groups." |
3.3.1. How can telehealth affect access to behavioral health services--especially MAT--in rural primary care settings?
Telehealth services can improve access to behavioral health services, especially in rural communities, in several ways. Access can be improved by providing patients direct contact with specialty providers in rural communities, serving difficult to reach populations, reducing wait times to obtain services, increasing access to services in other languages, and providing services confidentially.
Without telehealth, providers in the study indicated that patients must travel or wait for a rotating provider to come to their area on a limited basis. As one participant noted, "If I think about the issues, it's that there are limited providers. The supply ... is limited. Behavioral health providers are limited. How do you tap into the people you have without traveling and make it more efficient?" In addition, in many rural areas access to care in languages other than English is not available because of lack of providers. Through telehealth, patients can leverage bilingual services at distant providers.
| "If you read about the [opioid] epidemic, every national and state organization talks about improving access. I think telehealth is a simple way to do it. There are impediments to doing it, but it makes sense. You have to have a diverse model. We can't take care of everyone. ... There has to be a diverse program. Also, you can use it to train and do consultations with physicians that may not feel as comfortable with it [MAT]. That's huge for expanding access. |
An example of increased access is Inova, which is a health system that provides care in Northern Virginia and the District of Columbia. Inova introduced a 24-hour psychiatric consultation service that connects ED patients with psychologists and psychiatrists via teleconferencing. Inova also has piloted a program in eight PCP offices that allows patients to access walk-in psychiatric services. Through this program, PCPs who recommend psychiatric care for their patients can connect them virtually to behavioral health providers capable of assessing the patient and recommending a course of treatment. As the program expands, Inova hopes to alleviate the stigma of physically attending a psychiatric walk-in clinic in addition to barriers such as distance to a clinic (Bowman, 2016).
Another example is Open Door, a program that began telehealth services in 1990 and is currently funded by the California Healthcare Foundation to support telehealth use in its nine community health centers and a range of rural sites in California. These sites can access specialists through the program's Telehealth and Visiting Specialist Center, which provides specialists in Eureka, California, with videoconferencing units capable of connecting with remote sites. Rather than operating solely from EDs or PCP offices, the "spokes," or remote sites of this program, have expanded to include community schools to allow for consistent pediatric care and other specialists' offices to allow for learning and collaboration (California Health Care Foundation, 2016).
Telehealth also can afford access to populations that are traditionally difficult to reach. For example, one provider site used telehealth to provide continuity of care to migrant farmworkers when they were in different states for part of the year. The site reported anecdotally that outcomes were improved for those workers compared to workers who did not receive continued care through telehealth. In another program, telehealth was used to provide services in correctional and juvenile treatment facilities. The program reported a reduction in cost (primarily due to the reduced need for secure transport to services) and shorter patient wait time (Paing et al., 2009).
Telehealth also can help decrease service wait times by reducing patients' or care teams' transportation requirements, which can affect scheduling of services. For example, some sites, as part of their traditional care approach, provided a clinical team escort for the patient when visiting distant providers. Thus, the site had to coordinate distant provider availability, patient availability, and escort or transportation availability. With telehealth, traveling to the distant provider was not necessary. One site noted that "we've cut the wait time from 6 months to 3 weeks" because telehealth afforded increased availability to get appointments with a specialist since travel requirements were removed.
| Implications for MAT Telehealth for MAT promotes:
|
3.3.2. How can telehealth affect delivery of behavioral health services, including provider-to-provider communication?
Telehealth has implications for care delivery and may affect multiple areas within the care continuum. Care delivery is affected through provider-to-provider mechanisms such as consultations, training, and remote supervision (Riding-Malon & Werth, 2014) as well as direct patient interactions and patient engagement. Remote providers can collaborate with local providers to coordinate care and develop and execute an integrated care approach, thereby improving care coordination and augmenting existing service offerings.
Telehealth can be used to:
|
Provider Education
Provider education is one use of telehealth that can affect delivery. Several participants noted using telehealth for formal and informal provider-to-provider education. Formal education included case conferences and presentation of materials about best practices. Informal education included consultation about cases. Participants indicated that sharing provider education and knowledge made local providers feel more confident about delivering new services because "providers always have the option to call someone in the room for help." This is particularly important in the rural setting, where clinics may be smaller and providers do not have the opportunity for "water cooler" conversations with their peers to ask questions or review cases informally.
Care Coordination
Discussants noted that telehealth is a mechanism to improve care coordination, particularly for coordination between specialists and PCPs. One participant indicated that "in primary care, using telehealth there can be more of a clear, whole approach to building care. They come in to see their specialist [using telehealth], but they also get to see their PCP and build that relationship." In other models, a team-based approach can be used to engage specialists, PCPs, and other members of the care team. One participant described a telehealth program where a care manager supported the PCP by attending frequent consultations with a psychiatrist, relaying their recommendations, and working with the PCP to amend treatment plans.
In another example of care coordination, the Tarzana Treatment Centers use telehealth so that the first off-site outpatient visit occurs on site at their residential facility prior to the patient's residential discharge. This establishes the provider-patient relationship. The center found that treatment was not delayed in this case, and it allowed establishment of rapport and facilitated coordination between inpatient and outpatient settings (Tarzana Treatment Centers, 2014).
Patient Engagement
Telehealth facilitates patient engagement and education. Patients can meet with their provider and related ancillary providers through telehealth and receive patient education materials at their local site. If patients have questions about the materials after the telehealth visit is over, they are already in a primary care setting with individuals who can provide guidance about the materials. In addition, patients can use telehealth to receive education.
Telehealth can also assist patients in connecting to programs that may not be available locally, such as programs that help individuals returning to the community from the criminal justice system. For example, telehealth may be used within the courts to deliver educational information on treatment approaches. This allows efficient delivery of educational material for individuals across several locations.
Telehealth also facilitates engagement when dealing with migrant populations. One provider indicated that the migrant individuals in their area had developed trust with their site and did not feel comfortable going to a provider at their new location. The site used telehealth to facilitate a virtual meeting between the patient and the distant provider before the patient moved. They also used telehealth to facilitate a handoff of care between the two providers. The site found that this increased the likelihood of the patient's visiting the new provider and improved coordination of care.
Expand Service Offerings
Provider sites use telehealth to augment existing services. For example, one site that uses telehealth in tandem with an app for patients to submit diaries has seen an increase in diaries submitted. It noted that this was because of "convenience and patient demand" so that sites can be "more relevant to patients." Another example of augmenting existing services is to provide services locally that are not traditionally available. Several sites referenced behavioral health workforce shortages in the rural setting and stated that telehealth is key to providing services in shortage areas.
At Intermountain Healthcare, telehealth is used to enhance delivery of services through remote monitoring (Congdon, 2013). In this way, expertise available at the main hospital through intensive care unit, crisis, and stroke services can be shared with remote hospitals. This includes providing remote monitoring and provider-to-provider consultation on care. Intermountain can use existing technology in these high-care rooms for monitoring with minimal additional technology (e.g., technology enabled crash carts, microphones, and cameras with indicators for when the room was being monitored).
Quality
Although telehealth has been shown to improve access to and delivery of behavioral health services, it is important to also consider whether is the services delivered are of comparable quality to similar services if they were provided in person. Telehealth can help overcome issues of distant providers not being able to engage with local resources or focusing on assessments. An effectiveness review of telemental health in 2013 by Hilty and colleagues found that telemental health is effective for diagnosis and assessment across many populations (e.g., adult, child, geriatric, and ethnic) and for disorders in many settings (e.g., emergency, home health), and appears to be comparable with in-person care (Hilty et al., 2013). A recent review by AHRQ found that a large volume of research reported that telehealth interventions produced positive results when used in the clinical areas of chronic conditions and behavioral health, and when telehealth is used for providing communication or counseling and monitoring or management (Totten et al., 2016). These review articles suggest that using telehealth for behavioral health services provides quality similar to in-person services.
| "I think the miracle and wonder is that telehealth allows you to share resources electronically rather than moving people. The quality of care is excellent, and it saves time and energy and allows for more frequent and follow-up care." |
Frequency of Services
Several discussants noted that telehealth helps patients work around stigma to receive services, thereby increasing frequency of visits. In smaller communities, it may be difficult for participants to go to an office known for providing behavioral health services because people may not want to be seen in the waiting room or have their car seen there. By providing telehealth in a primary care office, a patient's presence in the office does not reflect a particular health condition or service offering. Several participants indicated that patients told them this was a significant factor in their receiving ongoing care. Anecdotally, providers noted improvements in quality as a result.
Implications for MAT
|
4. DISCUSSION
The continued epidemic of prescription opioid misuse and heroin use and its associated overdose epidemic has put increased strain on an already overloaded health care system. It is often noted that the size of the health workforce is insufficient to meet the current and increasing demand for behavioral health services. Shortages are particularly felt within rural communities (Baldwin et al., 2006; Cramer, Nienaber, Helget, & Agrawal, 2006; MacDowell, Glasser, Fitts, Nielsen, & Hunsaker, 2010). Telehealth has the power to connect patients, providers, and staff who are geographically dispersed, and this approach may help expand patients' access to SUD treatment services, including MAT for OUDs. In assessing the use of telehealth within the field of behavioral health, there are several important issues to consider, some of which are specific to behavioral health while others apply when using telehealth across health conditions and/or health sectors.
In implementing telehealth, information from discussants and the literature indicate that planning is essential, including both technical and non-technical aspects. For example, some sites may find the cost of technology burdensome. However, if technology, including bandwidth and equipment, does not meet the minimum standard, that can have repercussions for the quality of the telehealth interaction. In addition to technical aspects, planning includes incorporating telehealth into the workflow of organizations, ensuring sufficient trained staffing, and planning for when things go wrong. This involves staff time for coordinating telehealth services and for providing training, troubleshooting, and technical support.
For ongoing delivery and sustainability, discussants noted that one of the key challenges of using telehealth is financing. Telehealth services vary in terms of how and what is funded. Variation in reimbursement occurs across payers and states. Most states allow for reimbursement of some behavioral health services delivered via telehealth either through Medicare, Medicaid, or private payer; however, each payment source within a state comes with its own unique set of requirements around the types of services that will be covered, the location and setting, and the types of providers. Almost half of the states require private payers to have full parity among medical/surgical and behavioral health care with respect to telehealth services. Yet, although telehealth may be covered, reimbursement rates may be lower than similar services provided in person to the patient (Campbell, Miele, Nunes, McCrimmon, & Ghitza, 2012; Rose, Skelly, Badger, Naylor, & Helzer, 2012). In addition, funding typically does not cover remote provider training. Reimbursement options to cover remote training on using MAT need to be identified to support this low-cost/high-impact approach. Despite these issues, there appears to be significant support for the reimbursement of behavioral health services via telehealth, which could serve as a basis for the reimbursement of telehealth for MAT.
In addition, interpretation of policies such as the Ryan Haight Act and the DATA 2000 guides the use of telehealth for MAT and influences the models that are implemented. For example, multiple discussants believed that the Ryan Haight Act, by modifying the Controlled Substances Act, placed specific restrictions on the ability of telehealth providers to prescribe controlled substances. The Ryan Haight Act does allow for telemedicine under the applicable parameters of current law, which requires that patients being prescribed controlled substances be treated by, and physically located in, a hospital or clinic registered under Section 303(f) of the Controlled Substances Act. In some cases, a patient's remote location does not have this registration even though the telehealth provider may be registered under Section 303(f). This requirement has caused some concern about how to make MAT available to patients with OUDs. Lack of understanding among providers regarding certain policies and regulations may create unintended barriers to telehealth implementation for MAT.
Telehealth has effects on delivery, access, and quality of services. Those who did use telehealth found that it increased availability of services, with little detriment to delivery despite the mode. Participants did not note significant quality changes. Recent studies in the literature support these findings; however, more work is needed to further explore the effect of telehealth on behavioral health care for patients, especially patients with OUDs.
The findings from this study suggest that use of telehealth can greatly improve access to and delivery of behavioral health services, including MAT, but this potential has not yet been realized. Several barriers in its use need to be addressed, including funding mechanisms, licensing requirements, credentialing/privileging technological requirements (e.g., integration, standards), and workforce training needs (Hilty et al., 2008; Larson et al.,2012; Benavides-Vaello et al., 2013; ASPE, 2016). In addition, challenges may arise regarding provider and staff buy-in for telehealth use and lack of guidance around interpretation of policies governing telehealth services. These findings point to the need for more formalized guidance from policy makers, funders, and implementers of telehealth. Overall, results from this study show that policies and innovative programs are being implemented to overcome some of these challenges, but more needs to be done to understand the opportunities and barriers for telehealth in behavioral health.
| Implications for MAT Implementation and Use
|
Financing and Sustainability
|
Impact
|
REFERENCES
American Medical Association. (2016). Adopting the ECHO model™ (Extension for Community Healthcare Outcomes)--STEPS Forward. Retrieved from https://www.stepsforward.org/modules/project-echo.
American Telemedicine Association (ATA). (2016). Website. Retrieved December, 2016, from http://learn.americantelemed.org/diweb/start/.
Anthem Blue Cross Blue Shield. (2016). Website. Retrieved from https://www.livehealthonline.com/availability.
Baldwin, L.M., Patanian, M.M., Larson, E.H., Lishner, D.M., Mauksch, L.B., Katon, W.J., Walker, E., & Hart, L.G. (2006). Modeling the mental health workforce in Washington State: using state licensing data to examine provider supply in rural and urban areas. Journal of Rural Health, 22(1), 50-58. http://onlinelibrary.wiley.com/doi/10.1111/j.1748-0361.2006.00003.x/abstract.
Bashshur, R.L., Shannon, G.W., Bashshur, N., & Yellowlees, P.M. (2016). The empirical evidence for telemedicine interventions in mental disorders.Telemedicine Journal and E-Health, 22(2), 87-113. http://dx.doi.org/10.1089/tmj.2015.0206.
Benavides-Vaello, S., Strode, A., & Sheeran, B.C. (2013). Using technology in the delivery of mental health and substance abuse treatment in rural communities: A review. Journal of Behavioral Health Services & Research, 40(1), 111-120. https://link.springer.com/article/10.1007%2Fs11414-012-9299-6.
Boudreaux, E.D., Abar, B., Baumann, B.M., & Grissom, G. (2013). A randomized clinical trial of the Health Evaluation and Referral Assistant (HERA): Research methods. Contemporary Clinical Trials, 35(2), 87-96. http://dx.doi.org/10.1016/j.cct.2013.04.010.
Boudreaux, E.D., Haskins, B., Harralson, T., & Bernstein, E. (2015). The remote brief intervention and referral to treatment model: Development, functionality, acceptability, and feasibility. Drug and Alcohol Dependence, 155, 236-242. http://dx.doi.org/10.1016/j.drugalcdep.2015.07.014.
Bowman, D. (2016). ATA16: Telehealth helps Inova improve care access for stroke, behavioral health patients. Retrieved November 2016 from http://www.fiercehealthcare.com/it/ata16-telehealth-helps-inova-improve-care-access-for-stroke-behavioral-health-patients.
California Health Care Foundation. (2016). Implementation of telehealth in community clinics. Retrieved November 2016 from http://www.chcf.org/publications/2010/11/implementation-telehealth-community-clinics.
California Telehealth Resource Center. (2014). The CTRC Telehealth Program Developer Kit. Retrieved from http://www.telehealthresourcecenter.org/sites/main/files/file-attachments/complete-program-developer-kit-2014-web1.pdf.
Campbell, A.N., Miele, G.M., Nunes, E.V., McCrimmon, S., & Ghitza, U.E. (2012). Web-based, psychosocial treatment for substance use disorders in community treatment settings. Psychological Services, 9(2), 212-214. http://dx.doi.org/10.1037/a0025968.
Centers for Medicare & Medicaid Services (CMS). (2016). Telehealth services: Rural health series. Retrieved from https://www.cms.gov/Outreach-and-Education/Medicare-Learning-Network-MLN/MLNProducts/downloads/TelehealthSrvcsfctsht.pdf.
Congdon, K. (2013). Intermountain's telehealth triumph. Retrieved from https://www.healthitoutcomes.com/doc/intermountain-s-telehealth-triumph-0001.
Cramer, M., Nienaber, J., Helget, P., & Agrawal, S. (2006). Comparative analysis of urban and rural nursing workforce shortages in Nebraska hospitals. Policy, Politics, and Nursing Practice, 7(4), 248-260. http://dx.doi.org/10.1177/1527154406296481.
Federal Communication Commission. (2010). Health care broadband in America: Early analysis and a path forward. Retrieved from http://download.broadband.gov/plan/fcc-omnibus-broadband-initiative-%28….
Gagnon, M.P., Duplantie, J., Fortin, J.P., & Landry, R. (2006). Implementing telehealth to support medical practice in rural/remote regions: What are the conditions for success? Implementation Science, 1(1), 1.
Graham, J., Tomcavage, J., Salek, D., Sciandra, J., Davis, D.E., & Stewart, W.F. (2012). Postdischarge monitoring using interactive voice response system reduces 30-day readmission rates in a case-managed Medicare population. Medical Care, 50(1), 50-57. http://dx.doi.org/10.1097/MLR.0b013e318229433e.
Guarino, H., Acosta, M., Marsch, L.A., Xie, H., & Aponte-Melendez, Y. (2016). A mixed-methods evaluation of the feasibility, acceptability, and preliminary efficacy of a mobile intervention for methadone maintenance clients. Psychology of Addictive Behaviors, 30(1), 1-11. http://dx.doi.org/10.1037/adb0000128.
Hilty, D.M., Cobb, H.C., Neufeld, J.D., Bourgeois, J.A., & Yellowlees, P.M. (2008). Telepsychiatry reduces geographic physician disparity in rural settings, but is it financially feasible because of reimbursement? Psychiatric Clinics of North America, 31(1), 85-94. http://dx.doi.org/10.1016/j.psc.2007.11.010.
Hilty, D.M., Ferrer, D.C., Parish, M.B., Johnston, B., Callahan, E.J., & Yellowlees, P.M. (2013). The effectiveness of telemental health: A 2013 review. Telemedicine and E-Health, 19(6), 444-454.ss. http://dx.doi.org/10.1089/tmj.2013.0075.
Hilty, D.M., Nesbitt, T.S., Kuenneth, C.A., Cruz, G.M., & Hales, R.E. (2007, Spring). Rural versus suburban primary care needs, utilization, and satisfaction with telepsychiatric consultation. Journal of Rural Health, 23(2), 163-165. http://dx.doi.org/10.1111/j.1748-0361.2007.00084.x.
Ireys, H. (2014). Evaluating the HCIA--Behavioral Health/Substance Abuse Awards: First Annual Report. Retrieved from https://www.mathematica-mpr.com/our-publications-and-findings/publications/evaluating-the-hcia-behavioral-healthsubstance-abuse-awards-first-annual-report.
Johnston, B., & Yellowlees, P. (2016). Telepsychiatry consultations in primary care coordinated by virtual care navigators. Psychiatric Services, 67(1), 142-142. http://dx.doi.org/10.1176/appi.ps.660905.
Kahn, L.S., Fox, C.H., Carrington, J., Desai, U., Bartlett, D.P., Lyle, H., & Kowalski, M. (2009). Telephonic nurse case management for patients with diabetes and mental illnesses: A qualitative perspective. Chronic Illness, 5(4), 257-267. http://dx.doi.org/10.1177/1742395309350229.
Kim, S.E., Michalopoulos, C., Kwong, R.M., Warren, A., & Manno, M.S. (2013). Telephone care management's effectiveness in coordinating care for Medicaid beneficiaries in managed care: A randomized controlled study. Health Services Research, 48(5), 1730-1749. http://dx.doi.org/10.1111/1475-6773.12060.
Kim, S.J., Marsch, L.A., Guarino, H., Acosta, M.C., & Aponte-Melendez, Y. (2015). Predictors of outcome from computer-based treatment for substance use disorders: Results from a randomized clinical trial. Drug and Alcohol Dependence, 15(7), 174-178. http://dx.doi.org/10.1016/j.drugalcdep.2015.09.019.
Knopf, A. (2013). Buprenorphine by telemedicine: Reaching rural West Virginia patients. Alcoholism & Drug Abuse Weekly, 25(41), 3-4.
Kraetschmer, N.M., Deber, R.B., Dick, P., & Jennett, P. (2009). Telehealth as gatekeeper: Policy implications for geography and scope of services. Telemedicine and E-Health, 15(7), 655-663. http://dx.doi.org/10.1089/tmj.2009.0004.
Larkin, T. (2016). Rural Project Summary: Intermountain Healthcare Telehealth Services. Retrieved November 2016 from https://www.ruralhealthinfo.org/community-health/project-examples/925.
Larsen, M.E., Farmer, A., Weaver, A., Young, A., & Tarassenko, L. (2012). Mobile Health for Drug Dose Optimization. Proceedings of the Proceedings of the Annual International Conference of the IEEE Engineering in Medicine and Biology Society, pp. 1540-1543.
Lewis, V.A., Colla, C.A., Tierney, K., Van Critters, A.D., Fisher, A.S., and Meara, E. (2014). Few ACOs pursue innovative models that integrate care for mental illness and substance abuse with primary care. Health Affairs, 22(10), 1808-1816 http://dx.doi.org/10.1377/hlthaff.2014.0353.
Lowery, C.L., Bronstein, J.M., Benton, T.L., & Fletcher, D.A. (2014). Distributing medical expertise: The evolution and impact of telemedicine in Arkansas. Health Affairs, 33(2), 235-243. http://dx.doi.org/10.1377/hlthaff.2013.1001.
MacDowell, M., Glasser, M., Fitts, M., Nielsen, K., & Hunsaker, M. (2010). A national view of rural health workforce issues in the USA. Rural Remote Health, 10(3), 1531.
McGinty, K.L., Saeed, S.A., Simmons, S.C., & Yildirim, Y. (2006). Telepsychiatry and e-mental health services: Potential for improving access to mental health care. Psychiatric Quarterly, 77(4), 335-342. https://link.springer.com/article/10.1007%2Fs11126-006-9019-6.
MedPAC. (2016). Telehealth Services and the Medicare Program. Report to the Congress: Medicare and the Health Care Delivery System.
Merrell, R.C., & Doarn, C.R. (2013). Tales of telemedicine-Telepsychiatry at work. Telemedicine and E-Health, 19(4), 233-234. http://dx.doi.org/10.1089/tmj.2013.9995.
Muench, F. (nd). Technology Based Interventions for Substance Users: Promises and Pitfalls of Integration into Clinical Care. Retrieved from http://www.nfarattc.org/wp-content/uploads/2016/08/Frederick-Muench.pdf.
National Frontier and Rural Addiction Technology Transfer Center (NFAR ATTC). (2015). National Frontier and Rural ATTC: Home. Retrieved from http://www.nfarattc.org/.
National Health Services. (2016). Technology Enabled Care Services. Retrieved November 2016 from https://www.england.nhs.uk/ourwork/qual-clin-lead/tecs/.
Nelson, E.L., & Bui, T. (2010). Rural telepsychology services for children and adolescents. Journal of Clinical Psychology, 66(5), 490-501. http://dx.doi.org/10.1002/jclp.20682.
Newman, L., Bidargaddi, N., & Schrader, G. (2016). Service providers' experiences of using a telehealth network 12 months after digitisation of a large Australian rural mental health service. International Journal of Medical Informatics, 94, 8-20. http://dx.doi.org/10.1016/j.ijmedinf.2016.05.006.
Office of the Assistant Secretary for Planning and Evaluation (ASPE). (2016). Report to Congress: E-health and Telemedicine. Retrieved from https://aspe.hhs.gov/sites/default/files/pdf/206751/TelemedicineE-HealthReport.pdf.
Paing, W.W., Weller, R.A., Welsh, B., Foster, T., Birnkrant, J.M., & Weller, E.B. (2009). Telemedicine in children and adolescents. Current Psychiatry Reports, 11(2), 114-119.
Perry, V. (2016). Recorded Webinar: Telehealth at Intermountain Healthcare | Sirius Computer Solutions. Retrieved from http://www.siriuscom.com/2016/09/recorded-webinar-telehealth-intermountain-healthcare/.
Richards, D. (2015). Behavioral telehealth key for ACO success. Healthcare IT News. Retrieved from http://www.healthcareitnews.com/news/behavioral-telehealth-key-aco-success.
Riding-Malon, R., & Werth, J.L. (2014). Psychological practice in rural settings: At the cutting edge. Professional Psychology-Research and Practice, 45(2), 85-91. http://dx.doi.org/10.1037/a0036172.
Rose, G.L., Skelly, J.M., Badger, G.J., Naylor, M.R., & Helzer, J.E. (2012). Interactive voice response for relapse prevention following cognitive-behavioral therapy for alcohol use disorders: A pilot study. Psychological Services, 9(2), 174-184. http://dx.doi.org/10.1037/a0027606.
Rosenberg, C.N., Peele, P., Keyser, D., McAnallen, S., & Holder, D. (2012). Results from a patient-centered medical home pilot at UPMC health plan hold lessons for broader adoption of the model. Health Affairs, 31, 2423-2431. http://dx.doi.org/10.1377/hlthaff.2011.1002.
Ruetsch, C., Tkacz, J., McPherson, T.L., & Cacciola, J. (2012). The effect of telephonic patient support on treatment for opioid dependence: Outcomes at one year follow-up. Addictive Behaviors, 37(5), 686-689. http://dx.doi.org/10.1016/j.addbeh.2012.01.013.
Substance Abuse and Mental Health Services Administration (SAMHSA). (2016). Rural behavioral health: Telehealth challenges and opportunities. In Brief, 9(2).
Substance Abuse and Mental Health Services Administration (SAMHSA). (nd). Decisions in Recovery: Treatment for Opioid Use Disorder. Washington, DC: HHS Substance Abuse and Mental Health Services Administration. Retrieved from http://archive.samhsa.gov/MAT-Decisions-in-Recovery/Default.aspx.
Schmeida, M., & McNeal, R. (2007). The telehealth divide: Disparities in searching public health information online. Journal of Health Care for the Poor and Underserved, 18(3), 637-647. http://dx.doi.org/10.1353/hpu.2007.0068.
Tarzana Treatment Centers. (2014). Tarzana Treatment Centers Telehealth Program. Retrieved November 2016 from https://www.tarzanatc.org/tarzana-treatment-centers-telehealth-program/.
Taylor, E., Symonette, E., & Singleton, E. (2009). Considerations for the Provision of E-therapy. Rockville, MD: HHS Substance Abuse and Mental Health Services Administration.
Thomas, L., & Capistrant, G. (2015). State Telemedicine Gaps Analysis. Retrieved from http://cdn2.hubspot.net/hubfs/1775981/omada-pdf/50-state-telemedicine-gaps-analysis---coverage-and-reimbursement.pdf?t=1461875181706.
Tofighi, B., Grossman, E., Buirkle, E., McNeely, J., Gourevitch, M., & Lee, J.D. (2015). Mobile phone use patterns and preferences in safety net office-based buprenorphine patients. Journal of Addiction Medicine, 9(3), 217-221. http://dx.doi.org/10.1097/ADM.0000000000000121.
Tofighi, B., Grossman, E., Sherman, S., Nunes, E.V., & Lee, J.D. (2016). Mobile phone messaging during unobserved "home" induction to buprenorphine. Journal of Addiction Medicine, 10(5), 309-313. http://dx.doi.org/10.1097/ADM.0000000000000198.
Totten, A.M., Womack, D.M., Eden, K.B., McDonagh, M.S., Griffin, J.C., Grusing, S., & Hersh, W.R. (2016). Telehealth: Mapping the Evidence for Patient Outcomes From Systematic Reviews [Internet]. Rockville, MD: Agency for Healthcare Research and Quality. Technical Briefs, No. 26. Findings. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK379312/.
University of New Mexico. (2016). Project ECHO: A Revolution in Medical Education and Care Delivery. Retrieved December 29, 2016, from https://echo.unm.edu/ .
Warner, E.L., Montenegro, R.E., Stroup, A., Kinney, A.Y., & Kirchhoff, A.C. (2014). Health care concerns of rural childhood cancer survivors. Journal of Health Care for the Poor and Underserved, 25(2), 901-912. http://dx.doi.org/10.1353/hpu.2014.0095.
Whitman, E. (2016). Building a lifeline for rural addicts. Modern Healthcare, 46(40), 18.
Zheng, W., Nickasch, M., Lander, L., Wen, S., Xiao, M., Marshalek, P., Dix, E., & Sullivan, C. (2017). Treatment outcome comparison between telepsychiatry and face-to-face buprenorphine medication-assisted treatment for opioid use disorder: A 2-year retrospective data analysis. Journal of Addiction Medicine, 11(2), 138-144.
APPENDIX A. DISCUSSION GUIDE
| ASPE Telehealth Key Stakeholder Discussion Guide | |||
|---|---|---|---|
| Discussion Lead: | Note Taker: | ||
| Key Stakeholder: | Organization: | ||
| Date/Time of Discussion: | |||
Purpose: The purpose of this discussion is to gather different perspectives on the key issues related to telehealth use for behavioral health care. These discussions will provide each key informant an opportunity to identify what they believe are the key factors and reimbursement issues affecting the use of telehealth for behavioral health care.
Introduction and Consent to Audio Record
Thank you for making time to speak with us today. As we explained in our e-mail, we are independent researchers from RTI International who are contracted with the HHS Office of the Assistant Secretary for Planning and Evaluation (ASPE) to better understand how providers can successfully implement and maintain telehealth for behavioral health disorders in their practices. A particular focus of this project is to understand how telehealth can facilitate access to medication-assisted therapy (MAT) for opioid use disorders in rural primary care settings. To support these goals, we are conducting discussions with key stakeholders to gather different perspectives on the issues related to telehealth use for behavioral health care. Given your position in the field, we are interested in your perspectives, and there are no right or wrong answers. (Introduce team members and briefly describe qualifications/background and roles during the discussion.)
We expect that our conversation will take about 1 hour. Participation in this discussion is voluntary. If you do not wish to participate or answer any specific questions, please let us know.
Finally, we would like to audio record our conversation to ensure that our notes from today are complete. Although we are taking detailed notes, the audio recording will help verify our discussion notes. We will not share the recording outside of this team, and it will be deleted when the project is complete.
Do we have your permission to record this discussion?
Do you have any questions about what I have explained?
Note to RTI staff:
-
If yes, start audio recording.
-
Begin discussion.
Introduction and Background
1. Could you please tell us your name, title, and a little bit about your role with [Insert Organization]?
Implementation--For Providers: Rural PCPs and MAT Providers
2. How is your organization currently using telehealth to identify and manage behavioral health conditions?
-
Is your use of telehealth different for different behavioral health services? If so, how?
3. How is telehealth being used?
-
Provider-to-provider?
-
Provider-to-patient?
-
Synchronous vs. asynchronous?
4. What type(s) of technology are you using?
-
How has the technology been working?
-
What has been working well? What would you change?
5. What populations are served using telehealth? Has the population you are serving changed since introducing the use of telehealth? If so, how?
Implementation--For Researchers
6. Could you describe some of the research you have been involved in with respect to telehealth and behavioral health services?
7. How are the organizations you have studied using telehealth to identify and manage behavioral health conditions?
-
Is their use of telehealth different for different behavioral health services? If so, how?
8. How is telehealth being used by these organizations?
-
Provider-to-provider?
-
Provider-to-patient?
-
Synchronous vs. asynchronous?
9. What type of technology are they using?
-
How has the technology been working?
-
What has been working well? What would you change?
10. What populations are they serving using telehealth? Has the population they are serving changed since introducing the use of telehealth? If so, how?
Financing and Sustainability--Ask of all key informants
11. How are telehealth services reimbursed generally and for behavioral health disorders?
12. Does reimbursement for telehealth for behavioral health disorders differ from reimbursement available for medical/surgical services?
13. How does reimbursement for behavioral health services delivered via telehealth differ across payers (e.g., Medicaid, Medicare, private insurance)?
14. What payment models support the use of telehealth?
Barriers and Facilitators--Ask of all key informants
Note to RTI Staff: For Researcher respondents, the questions below are most likely in relation to research studies with which they have been involved.
15. What barriers have you experienced in implementing telehealth for behavioral health conditions? What strategies/solutions have been used to overcome those barriers?
16. What factors have facilitated the use of telehealth for behavioral conditions?
-
Implementation factors?
-
Financing and reimbursement factors?
17. Are there best practices you have identified in using telehealth to identify and manage behavioral health disorders? If so, please describe.
Impact--Ask of all key informants
18. What do you perceive as the impact(s) of telehealth on access to behavioral health services?
-
Has the impact differed for those providing MAT in rural primary care settings?
19. What do you perceive as the impact(s) of telehealth on the delivery of behavioral health services?
Conclusions and Next Steps
20. Is there anything else you think we should know about the use of telehealth for behavioral health services that we have not asked about today?
If we have any questions after today's discussion, may we contact you to follow up? Thank you so much for taking the time to speak with us today! We appreciate you sharing your perspective on this important issue.
APPENDIX B. SITE BRIEFS
New York
Finger Lakes Community Health is a FQHC with nine sites in upstate New York. The population is diverse, including those native to upstate New York and migrant workers who do not speak English. Thus, the needs of the community are diverse.
The site uses telehealth for a variety of purposes within and outside the organization. These uses include provider-to-provider education, administrative meetings, and provider-to-patient services. Within-organization uses connect the nine locations. Extra-organizational uses provide access to services and specialists in Rochester and Syracuse, New York, that are not locally available.
The site is not using telehealth for MAT. Its MAT provider left, and it is in the process of training a new provider on MAT generally. Once those processes are in place, the site intends to use telehealth to support MAT within the organization.
Montana
Billings Clinic is an integrated delivery network serving individuals in Montana, Wyoming, and the western Dakotas. The main campus is in Billings, Montana, and includes a hospital, Level II emergency and trauma center, cancer center, surgery center, Level III neonatal intensive care unit, and a large multispecialty group practice with more than 50 specialties. In addition to the main campus, three branch clinics are in Billings, and six primary care specialty clinics are in cities across Montana and Wyoming. In addition, Billings Clinic manages 11 CAHs and maintains the Eastern Montana Telemedicine Network.
Billings Clinic uses telehealth to deliver 30 specialty services (e.g., oncology, cardiology, nephrology, mental health) over its telemedicine network. The Eastern Montana Telemedicine Network supports 28 sites, including Billings Clinic and other community providers across the four-state region. The sites include a variety of providers such as hospitals, clinics, and CMHCs. The area served by the network consists of rural and frontier communities where access to specialty services is challenging. Specialty populations served include Native Americans, veterans, aging adults, and individuals with low socioeconomic status. Although MAT is not specifically called out as a behavioral health service provided via telehealth at this time, it is possible that some mental health providers were offering services that may include MAT.
Billings Clinic receives grant funding to host and lead a biweekly OAT ECHO clinic, which provides free training on OAT to providers, primary care teams, community health workers, counselors, social workers, and psychologists. The clinic uses case studies, training on topics such as management of naloxone/buprenorphine and injectable naltrexone, and access to a virtual learning community for guidelines, tools, and resources. Each clinic typically has more than 25 participating sites joining via videoconference.
The Eastern Montana Community Mental Health Center (EMCMHC) provides comprehensive mental health and SUD treatment services in 17 counties in the eastern Montana region. They offer a variety of outpatient mental health and SUD programs, including a group home and residential treatment program. EMCMHC is a member of the Eastern Montana Telehealth Network. Telehealth is used to support various programs, including patient assessment, individual therapy, group therapy, and specialty programs such as a Driving Under the Influence school mandated by the courts. EMCMHC accepts a variety of insurances and has special programs available for limited-income clients. Services are provided to those in need of treatment regardless of ability to pay.
California
The California discussion included a psychiatrist who delivered both provider-to-patient and provider-to-provider services within a university-based health system and Indian Health Service primary care clinics. Both systems purchased blocks of time from the psychiatrist that they could use to meet the needs of their clinics. Sometimes that was providing direct services to individuals with needs ranging from schizophrenia to depression to SUD using web-based videoconferencing. Other times, PCPs would use the time to reach out to the psychiatrist to get advice on treating patients, including how to adjust medications.
Georgia
The Georgia site included discussions about telehealth across states. A remote patient monitoring platform was used in a variety of ways. The primary uses of the platform were for primary care, with some behavioral health services. Telehealth is not used to establish care, but to provide ongoing monitoring and support for existing care. For example, some patients used telehealth to submit DBT diaries and discuss them with their provider. The site cited reimbursement and licensure as key barriers for telehealth.
Maryland
The Maryland site uses telehealth to provide provider-to-patient psychiatric services, including MAT. Maryland has both rural and urban areas in the same state. Telehealth is used to link prescribing providers who are not co-located with counselors. Counselors prescreen patients prior to referring them for telehealth services. There are telehealth coordinators at both the sending and receiving sites who manage documentation, coordinate care with patients, and ensure that necessary orders and follow-up care are in place. At the remote site, the coordinators also work with counselors and patients to facilitate lab tests and make sure the results are in the chart.
North Carolina
The North Carolina Statewide Telepsychiatry Program connects 80 or more hospital EDs across the State of North Carolina to provide psychiatric assessments and consultations to patients linked using telemedicine technologies in these EDs. In addition, the North Carolina Hospital Association provides support for MobileMed, which provides in-home medication management services to patients. Most support is for psychiatric medication management, but up to 80% of patients may also have co-occurring SUD. At this time, management of SUD medications is not occurring within the program.
New Mexico
The New Mexico site was a community health center, providing medical and dental care to the underserved people of Santa Fe, New Mexico. A NP in the clinic participates in Project ECHO to receive support in providing MAT to her patients. The provider uses Project ECHO as an opportunity for mentorship with more experienced behavioral health providers on how to treat her panel of approximately 60 buprenorphine patients.
Washington
The University of Washington Integrated Care Training Program/Psychiatry Consultation and Telepsychiatry (PCAT) offers a variety of programs to support the behavioral health needs of communities across the state and region. PCAT offers three types of telehealth service programs: provider-to-provider consultation, integrated care consultation, and direct patient care. They are also piloting the use of remote monitoring. Those who partner with PCAT are able to reduce the burden of recruiting, credentialing, supervising, and monitoring psychiatric consultants.
West Virginia
Telehealth is used in a variety of ways in West Virginia and was supported through the West Virginia Telehealth Alliance, which has since been disbanded. Telehealth is used for a number of services such as behavioral health, neurology, and dermatology. As grant funding and other opportunities arose, telehealth services were added to the portfolio. Services are provided in both academic and non-academic settings throughout the state. In addition, the site uses telehealth to deliver provider-to-provider training to support a variety of services, including MAT. One of the academic medical centers in West Virginia includes telehealth as part of its training programs in psychiatry and neurology, which both increases access to services through provider-to-patient interactions and provides training to physicians through provider-to-provider interactions.
USING TELEHEALTH TO IDENTIFY AND MANAGE MENTAL HEALTH AND SUBSTANCE USE DISORDER CONDITIONS IN RURAL AREAS
This report was prepared under contract #HHSP233201600021I between the U.S. Department of Health and Human Services (HHS), Office of Disability, Aging and Long-Term Care Policy (DALTCP) and Research Triangle Institute. For additional information about this subject, you can visit the DALTCP home page at http://aspe.hhs.gov/office-disability-aging-and-long-term-care-policy-daltcp or contact the ASPE Project Officers, Joel Dubenitz and Laurel Fuller, at HHS/ASPE/DALTCP, Room 424E, H.H. Humphrey Building, 200 Independence Avenue, S.W., Washington, D.C. 20201; Joel.Dubenitz@hhs.gov, Laurel.Fuller@hhs.gov.
Reports Available
Using Telehealth to Identify and Manage Mental Health and Substance Use Disorder Conditions in Rural Areas
- HTML https://aspe.hhs.gov/basic-report/using-telehealth-identify-and-manage-health-and-substance-use-disorder-conditions-rural-areas
- PDF https://aspe.hhs.gov/pdf-report/using-telehealth-identify-and-manage-health-and-substance-use-disorder-conditions-rural-areas
Using Telehealth to Support Opioid Use Disorder Treatment Issue Brief
