Prepared by:
Stan Dorn, Sarah Minton, and Erika Huber
The Urban Institute
Under Task Order: HHSP23337026T
Integrating Health and Human Services Programs and Reaching Eligible Individuals Under the Affordable Care Act
Prepared for:
Alana Landey
Office of the Assistant Secretary for Planning and Evaluation, DHHS
Project 08800-026-00
This paper presents findings from case studies of selected state-level integration and coordination approaches under the ACA and identifies areas of notable success or potential which may be of interest to other states.
"Executive Summary
It is not easy to effectively integrate and coordinate the operation of multiple health and human services programs that serve overlapping populations, but such efforts can yield significant gains. When one program determines eligibility based on the work already done by another program, public agencies can save administrative costs and streamline enrollment and retention for consumers. When programs jointly develop and operate shared eligibility infrastructure, they can achieve gains together that no single program could accomplish alone. And when programs collaborate in reaching out to a shared client population, more consumers can receive benefits for which they qualify.
This work has grown increasingly important following the 2010 enactment of the Patient Protection and Affordable Care Act (Affordable Care Act or ACA). In three basic categories, states and private-sector organizations have achieved notable success.
- Streamlining eligibility for one program based on data linkages with another program.
- Louisiana renews children’s eligibility for Medicaid and the Children’s Health Insurance Program (CHIP) through data from other public agencies, whenever possible. More than 3 in 4 of renewals (76 percent) are based on data matches, without any need to contact families for additional information. Nearly all children (95.4 percent) have eligibility continue at renewal, and fewer than 1 percent lose coverage for procedural reasons.
- Louisiana and South Carolina have implemented Express Lane Eligibility (ELE) to provide children with Medicaid based on the income determinations of human services programs—especially the Supplemental Nutrition Assistance Program (SNAP). This initiative has covered more than 27,000 and 92,000 previously uninsured children in the two states, respectively. Mainly because of the many children who are automatically renewed based on their receipt of SNAP, each of these states achieved annual net savings of roughly $1 million and $1.6 million, respectively. Similar efforts are now beginning with adults as well, through targeted Medicaid enrollment strategies under the ACA.
- In many states, Combined Application Project (CAP) demonstrations provide SNAP to recipients of Supplemental Security Income (SSI) based largely or entirely on information these seniors and people with disabilities already furnished when they sought SSI in a CAP demonstration state. From 2000 to 2008, CAP states experienced a 48% increase in SNAP participation levels among 1-person SSI households, at a time when such households’ enrollment in other states saw little change. To simplify SNAP procedures, CAP demonstrations use standardized rather than individualized SNAP benefit amounts, or individually determined benefits reflecting standardized shelter costs, either of which can result in slightly different amounts of aid than if beneficiaries had gone through the full SNAP eligibility assessment process. However, although SNAP programs provide notice, few CAP participants know they can obtain an individualized eligibility determination, and perhaps additional benefits, by submitting a regular SNAP application.
- Coordinating administration of multiple programs. Through efforts that spanned the better part of a decade, Utah built an integrated system of electronic case records, rules engine, external data matching, on-line applications, and benefit payment that serves multiple health and human services programs. From 2008 to the system’s full implementation in 2010, the caseload capable of being managed by a single worker increased 53 percent. From 2009- 2010, caseloads rose by 12.3 percent as total operating costs fell by 9.6 percent.
- Coordinating outreach and enrollment.
- In implementing early Medicaid expansion under the Affordable Care Act, Minnesota enrolled eligible consumers through the “low-tech” strategies of (a) making a toll-free number available to hospital emergency rooms and (b) having state and local staff manually convert consumers from a prior state health program to Medicaid. The latter step was cumbersome and administratively costly, but these methods helped the state enroll 51,583 eligible consumers by the end of March 2011, the expansion’s first month. They represented 68% of all consumers who received coverage by the end of calendar year 2011.
- Single Stop USA, a non-profit organization, helps community college students and their families enroll into health and human services programs, while providing financial and legal counseling. At 17 sites in seven states, 18,000 students were counseled in 2012, of whom 29% received health and human services benefits averaging $5,400 per student— roughly the maximum Pell Grant for a low-income college student. More than half also received financial or legal counseling. It took hard work to integrate this initiative into existing community college culture, but most school leaders have grown highly supportive, investing much of the funding needed for ongoing program operation.
On the other hand, several initially promising strategies have not yet achieved major gains. Another Single Stop effort involved connecting low-income consumers to health coverage when they filed tax returns at volunteer tax preparation sites. This effort faced serious challenges, including difficulty obtaining the necessary investment of time and staff from pre-ACA health application assisters, the unwillingness of many consumers to invest the additional time needed to apply for health coverage after completing the tax preparation process, and limitations of volunteer tax preparer health knowledge that forced a cumbersome “hand-off” from tax preparer to health application assister. The ACA strengthens the logical nexus between health coverage and tax preparation, which will provide increased motivation to overcome these challenges.
As another example, referring consumers to programs for which they apparently qualify, rather than actually signing them up for assistance, has achieved little success. One randomized, controlled experiment involved the tax preparation firm H&R Block. When the firm used tax return data and interviews to complete and file SNAP application forms on behalf of low-income customers, 80 percent more applications were filed than with a control group that received only basic SNAP information and a blank SNAP form. By contrast, no statistically significant effects were observed, compared to the control group, when H&R Block completed SNAP forms, handed them to families, and explained where and how to file them. A similar H&R Block experiment involving applications for college student aid reached similar results.
Efforts to integrate and coordinate enrollment, retention, and eligibility determination for health and human services programs typically require considerable effort, and not all such efforts have proven successful. That said, many states, localities, and private-sector groups have achieved significant positive outcomes using strategies that appear capable of replication elsewhere.
Introduction
For many years, state and federal officials have grappled with the challenge of effectively integrating and coordinating the operation of multiple health and human services programs that serve overlapping populations. Such efforts can yield many gains. When one program determines eligibility based on the work already done by another program, it simplifies eligibility determination, lowering public-sector administrative costs while streamlining the enrollment and retention process for consumers. The latter goal is particularly important for low-wage, working families, as taking time off from work to seek public benefits can place employment at risk. A streamlined process removes barriers to accessing services, helping more eligible people obtain promised benefits in uncapped programs like Medicaid and the Supplemental Nutrition Assistance Program (SNAP). Agencies can lower administrative costs by jointly procuring or operating shared systems for eligibility and enrollment, thus benefiting from economies of scale and more highly-leveraged purchasing power. Multiple programs working together can develop administrative capacities beyond the reach of any single program operating alone. And when agencies benefit from one another’s work to assess the circumstances of low-income households, they can more easily detect ineligibility, safeguarding program integrity.
Many barriers stand in the way of fully realizing these opportunities. Depending on the circumstances, such barriers can include perceived or actual legal limitations on information sharing, differences between programs’ technical rules for defining such things as household size and income deductions, outdated information technology (IT) systems used for eligibility purposes, federal or state statutes that make integration or coordination difficult, competing demands for the staff time and other resources needed for innovation, and the absence of strong relationships between agencies that administer different programs.
The 2010 enactment of the Patient Protection and Affordable Care Act (Affordable Care Act or ACA) has sparked discussion of new possibilities for program integration and coordination. To implement the legislation’s vision of 21st-century, data-driven eligibility determination, the federal government has offered significant funding to help cover the cost of necessary modernization of IT for health coverage, which can also benefit human services programs. In states that implement the Affordable Care Act’s Medicaid expansion, more low-income people will qualify for insurance affordability programs (IAPs)—that is, Medicaid, the Children’s Health Insurance Program (CHIP), and subsidies for individual coverage in health insurance marketplaces—than for any other need-based program. If IAP beneficiaries apply for human services programs, the latter might achieve efficiency gains if they can leverage the work that health programs have already done to determine consumers’ eligibility. And programs like SNAP seeking to reach eligible nonparticipants could use IAP records to target outreach efforts and serve additional eligible households. At the same time, many uninsured consumers who will newly qualify for health coverage under the ACA already participate in human services programs. If IAPs could utilize case records from human services programs to streamline eligibility determination and enrollment into health coverage, many uninsured Americans could receive coverage without burdening social services offices with the manual processing of IAP applications.
In view of these possibilities, the Office of the Assistant Secretary for Planning and Evaluation of the U.S. Department of Health and Human Services (ASPE/HHS) initiated a study—Integrating Health and Human Services Programs and Reaching Eligible Individuals Under the Affordable Care Act—of which this paper is a part. Here, we describe examples of state, local, and private efforts to integrate and coordinate eligibility determination, enrollment, and retention. We focus on promising examples that other states, localities, and private organizations can adapt, replicate, and improve. Some of these practices were already under way prior to the ACA, and others began in response to the ACA.
We start by describing the methodology for this research, including how we selected our case studies and how we gathered evidence about each practice. Next, we describe case study results in three categories:
- Streamlining eligibility for one program based on data linkages with another program. We include programs that changed their eligibility rules so that, when consumers have already demonstrated eligibility for one program, they do not need to provide the same or similar information to qualify for a different program. We find that such innovations have both streamlined enrollment for consumers and reduced public-sector administrative costs.
- Coordinating administration of multiple programs. In this category, case study states use a single automated system to help determine eligibility for multiple programs. The resulting economies of scale have let multiple programs achieve administrative savings while implementing functions that no single program could easily achieve on its own.
- Coordinating outreach and enrollment. This category includes both public- and private-sector strategies to help consumers learn about and qualify for multiple services or benefits atthe same time.
These key results, challenges, and lessons learned from these case studies are summarized in Tables 1 and 2.
We conclude the body of the report by describing strategies of multi-program integration and coordination that initially appeared promising but that have not yet resulted in notable gains. We then present two appendices, the first of which briefly lists examples of other promising innovations that resource constraints prevented us from exploring in detail. We briefly describe those examples and suggest additional sources of information for the interested reader. Our second appendix lists members of this project’s Technical Working Group, who have provided invaluable guidance and assistance, both with this paper and other parts of the project.
Table 1. Summary of case study findings
| State/Organization | Practice | Key Results |
|---|---|---|
| Streamlining eligibility for one program based on data linkages with another program | ||
| Louisiana | Medicaid/CHIP renewal through multiple strategies, including data matching | More than 3 in 4 (76%) of Medicaid/CHIP children’s renewal is based on data; nearly all children (95.4%) have eligibility continue at renewal; <1% lose coverage for procedural reasons. |
| Louisiana | Express Lane Eligibility (ELE): children receive or renew Medicaid based on SNAP receipt unless parents opt out | During 2010, ELE provided Medicaid to approximately 18,000 uninsured children, representing a 3% total increase for Medicaid/CHIP children. ELE renews 20 percent of all Medicaid and CHIP children. Net administrative savings of roughly $1 million per year. |
| South Carolina | ELE: children receive or renew Medicaid based on SNAP or TANF receipt unless parents opt out | Medicaid provided to more than 92,000 uninsured children, increasing total enrollment by 15 percent. More than 276,000 children renewed through ELE. Net administrative savings of $1.6 million per year. |
| Food and Nutrition Service | SNAP/Supplemental Security Income (SSI) Combined Application Projects (CAPs): SSI recipients receive SNAP. SSI data establish (a) standardized benefits or (b) standardized shelter costs, which result in individually determined benefits. | From 2000 to 2008, CAP states experienced a 48% increase in SNAP participation levels among 1-person SSI households, while other states saw little change. |
| Coordinating administration of multiple programs | ||
| Utah | Automated electronic eligibility system: a combined system of electronic case records, rules engine, data match system, on-line applications, benefit payment system for multiple health and human services programs | From 2008 to 2010, the caseload that can be handled by a single worker rose by 53 percent. From 2009-2010, caseloads grew by 12.3 percent as total operating costs fell by 9.6 percent. |
| Coordinating outreach and enrollment | ||
| Minnesota | Enrollment into Medicaid expansion based on (a) toll-free number for hospital emergency rooms and (b) manual conversion of records from prior state health program | 51,583 indigent consumers enrolled by end of the first month, March 2011—68% of all consumers enrolled by the end of 2011. |
| Single Stop USA | Community organization helps community college students and their families enroll into health and human services programs, provides financial and legal counseling | 29% of counseled students received health and human services benefits in 2012, averaging $5,400 per student. More than half of students also received financial or legal counseling. |
Table 2. Summary of case study challenges and lessons learned
| State/Organization | Practice | Important Challenges and Lessons Learned |
|---|---|---|
| Streamlining eligibility for one program based on data linkages with another program | ||
| Louisiana | Medicaid/CHIP renewal through multiple strategies, including data matching | Continuing improvement possible. Requires significant work from state staff and meaningful involvement of front-line case workers in developing policy. |
| Louisiana | ELE: children receive or renew Medicaid based on SNAP receipt unless parents opt out | Considerable work, time, and patience needed from staff. Children who do not use their cards to access care typically do not renew coverage. |
| South Carolina | ELE: children receive or renew Medicaid based on SNAP or TANF receipt unless parents opt out | Separate agencies had to overcome differences in data collection methods. To address limited provider capacity, implemented ELE enrollment incrementally, by county. Caseworker confusion resulted from lack of training in advance of implementation. |
| Food and Nutrition Service | SNAP/SSI CAP: SSI recipients receive SNAP. SSI data establish (a) standardized benefits or (b) standardized shelter costs, which result in individually determined benefits. | Streamlined enrollment requires standardized benefits or shelter costs, which are sometimes different from levels that would result from normal SNAP processes. Despite notices, few CAP participants know they can obtain an individualized benefit determination by filing a regular SNAP application. |
| Coordinating administration of multiple programs | ||
| Utah | Automated electronic eligibility system: a combined system of electronic case records, rules engine, data match system, on-line applications, benefit payment system for multiple health and human services programs | Considerable time and effort required. State used consultants and vendors selectively and strategically. Rules engine hard to implement with policies that have ambiguities. Gradual “roll out,” with careful testing, avoided problems. No evidence of increased participation by eligible consumers. |
| Coordinating outreach and enrollment | ||
| Minnesota | Enrollment into Medicaid expansion based on (a) toll-free number for hospital emergency rooms and (b) manual conversion of records from prior state health program | Doing manual record conversion was administratively costly, as a trade-off for significant early enrollment before IT improvements were ready to implement. |
| Single Stop USA | Community organization helps community college students and families enroll into health and human services programs, provides financial and legal counseling | School staff needed to go beyond educational goals so students could have broader needs met. To overcome stigma associated with public benefits, services framed within the context of financial aid available to students. Organization had to learn to work within the college environment, requiring less aggressive approaches than in other environments. |
Methodology
Case study selection
The case selection process was a highly collaborative effort between Urban Institute staff and ASPE. We decided to seek practices that—
- Reduce the burden that consumers must shoulder to qualify for or retain benefits;
- Reduce agencies’ administrative costs for determining eligibility, at application and/or renewal;
- Reduce the proportion of denials and terminations that occur for procedural reasons, such as a consumer’s failure to provide requested information;
- Reduce (or at least not increase) delays before applicants’ eligibility is determined;
- Reduce (or at least not increase) the proportion of erroneous eligibility determinations; and
- Retain or strengthen programs’ targeting of eligibility and enrollment.
We looked for initiatives with a reasonable quality of evidence documenting fulfillment of one or more of these substantive criteria. However, many integration efforts are in their early stages, and others have not been evaluated to assess their impact at the desired level of precision. Particularly given that our research took place as states, localities, and private-sector organizations were developing their approaches to implementing the Affordable Care Act, we recognized that extensive, written evidence of outcomes, including formal evaluations or peer-reviewed publications, would not be available for some of the very interventions that may be especially important candidates for replication in 2014 and beyond. We accordingly decided to look for a blend of promising and emerging practices with a range of evidentiary support.
To find our case studies, we canvassed the published literature, both formal and “gray.” The latter effort included special attention to web sites that serve as the repository for multiple “best practices” at the state, local, and community level, such as websites maintained by the National Academy for State Health Policy (especially NASHP’s “State Refor(u)m” project), the State Coverage Initiatives Program of AcademyHealth, the National Governors Association Center for Best Practices, Enroll America, the National Conference of State Legislatures, the American Public Human Services Association, and the Coalition for Access and Opportunity.
We also consulted with experts who are tracking state, local, and private-sector activities in this area. They included Urban Institute staff monitoring state implementation of the ACA as part of work funded by the Robert Wood Johnson Foundation; staff of both the Urban Institute and the Center on Budget and Policy Priorities assisting in the Work Support Strategies Project funded by the Ford Foundation and other leading philanthropies; the members of the Technical Working Group for this project, who are identified in Appendix B; and other national experts. This led to a list of potential case studies, from which those profiled below were selected.
Case study development
We investigated written literature to learn about policy decisions, implementation details, and key results for case studies involving data-based renewals in Louisiana, Express Lane Eligibility in Louisiana and South Carolina, SNAP/SSI pilot projects, and Utah’s “eREP” initiative. For the remaining case studies—those involving Minnesota and Single Stop USA—the Urban Institute conducted five interviews with key informants. These interviews examined how each practice was developed, its operation, its results, key lessons learned, and additional sources of information relevant to understanding the practice and its effects. Interviews were conducted by telephone, using semi-structured discussion guides that were tailored to the characteristics of each practice and the information known to the study team before the interview.
First case study area: Streamlining eligibility determination for one program based on data linkages with another program
This first section focuses on practices that have shown progress in streamlining eligibility determination for one program based on data linkages with another program. This can take place across both health and non-health programs. Such strategies can involve, for example, “deeming” eligibility for one program based on decisions made by another program or using data matches from another program to facilitate enrollment or renewal. Creating a new eligibility category or process that overcomes methodological differences between programs can greatly reduce the amount of work required to determine eligibility. Programs can also lighten consumers’ loads, simplifying and shortening application or redetermination procedures while reducing state administrative burdens by taking into account information already received by other agencies. This has been a particularly appealing strategy in recent years, when caseloads in need-based programs rose as social services staffing levels remained flat or fell. This general approach has the further advantage of being able to take advantage of enhanced federal funding. So long as they are fully implemented by December 31, 2015, investments in eligibility systems that help Medicaid determine eligibility can qualify for 90 percent federal funding; even if those systems also help human services programs, the latter can be relieved of the obligation to share development costs, under a time-limited waiver of standard cost allocation rules.1
The practices highlighted in this category include Louisiana’s use of data matches for Medicaid and CHIP renewals, Louisiana and South Carolina’s “Express Lane Eligibility,” and the U.S. Department of Agriculture’s Food and Nutrition Service’s (FNS’s) SNAP/SSI combined application projects (CAPs). Most examples in this category involve adjustments to program eligibility rules. Those adjustments relieve government agencies of the need to request and process information from consumers about issues nearly identical to those already resolved by a different government agency.
Louisiana: Medicaid and CHIP program data matches to renew eligibility
Overview
Louisiana has been a national leader in streamlining eligibility determination for health coverage. A particularly promising set of practices involves renewing children’s health coverage, including a heavy emphasis on data matching with human services programs and other sources of information relevant to eligibility.
Description
Louisiana’s approach to renewal is part of the state’s broader approach to streamlined eligibility determination for children’s Medicaid and CHIP, which encompasses initial applications as well as renewal. That includes such measures as 12-month continuous eligibility; electronic case files; an integrated application and renewal process that combines Medicaid and CHIP; the absence of any asset tests; in-person interviews at the family’s option, rather than as a state requirement; electronic signatures; business process reengineering in social services offices; and the use of a “reasonable certainty” standard in determining eligibility.
At the same time, the state has compiled a track record of accuracy well above the national average in determining eligibility. Louisiana’s most recent federal payment error review, for example, found an eligibility error rate of 0.3 percent—less than one-tenth the national average.2 Put simply, Louisiana is a national leader in both streamlining eligibility determination and safeguarding program integrity.
With that as context, Louisiana’s approach to renewing children’s Medicaid and CHIP coverage begins by seeing whether available data establish a reasonable certainty of continued eligibility. For the vast majority of children in these programs—90 percent of Medicaid children and 84 percent of those receiving CHIP3—data matches allow continued coverage without families needing to provide any information. The state applies three steps in sequence:
- Administrative Renewal: The state’s eligibility system checks to see whether the child falls into a category where Administrative Renewal applies. In such cases, certain household characteristics, based on prior data mining of administrative records, make continued eligibility virtually certain. Examples include a child in a household with income that consists entirely of Social Security; a child whose caretaker’s income is excluded for purposes of determining eligibility; a child with a single parent whose income consists entirely of child support; and a child who has qualified for Medicaid or CHIP for at least three years and who lives in a household with income of less than $500 per month. In such cases, the state sends a notice of renewal that requires households to provide information about relevant changes in household circumstances. If households do not respond, coverage continues. Caseworkers are not involved, unless families report changed circumstances.
- Express Lane Eligibility (ELE): If a child cannot be renewed administratively, ELE may apply. When a data match shows that a Medicaid household consists entirely of children who receive SNAP benefits, all members of the household are automatically renewed via ELE, without any need for manual intervention by caseworkers or any requirement for families to report changes in household circumstances.
- “Ex Parte” Reviews: Unlike the above two steps, this one requires manual action by caseworkers. If a child cannot be renewed using Express Lane or Administrative Renewal procedures, caseworkers see whether “Ex Parte” renewal is possible. “Ex Parte” is a Latin phrase indicating that action is taken by one party without involvement from the other. In this context, caseworkers investigate available data sources to see whether a child’s eligibility can be established with reasonable certainty, based on a combination of SNAP and TANF records, wage and unemployment insurance information, eligibility and payment data for Social Security and SSI, private vendor information, child support enforcement agencies, and other records. Before implementing ELE, the state renewed about half of Medicaid and one-third of CHIP cases using ex parte review, which eliminates the need for families to provide information before their children’s coverage continues.
If the state is unable to renew a child’s eligibility using any of these three methods, the state seeks to obtain additional information by phone. Only if all else fails does the state send renewal forms to families, seeking written information to redetermine eligibility.
Louisiana has also implemented other policies to streamline renewals. Paper signatures are not required to renew eligibility. Families can renew their children’s coverage at any time, outside normally scheduled renewal dates. For example, even if a child is in the middle of a 12-month coverage period, a new period can immediately begin when another program gathers information that demonstrates income at Medicaid levels, or when a family contacts the Medicaid agency for a different reason and the agency learns that the child continues to qualify. Moreover, Louisiana does not require financial verification if income is believed to be at least 25 percent below the maximum level permitted for Medicaid eligibility.
Results
From October 2012 through September 2013, the most recent 12 months for which data are available, 76 percent of children’s renewals were based on data matches, either through ELE (20 percent), administrative renewal (36 percent), or ex parte renewal (20 percent) (fig. 1). Of the remainder, most (15 percent) were renewed by telephone. Only 4 percent of families whose children’s coverage was renewed had to complete and return paper forms to retain coverage.
Figure 1. Renewal methods for Louisiana children covered through Medicaid and CHIP: October 2012 through September 2013
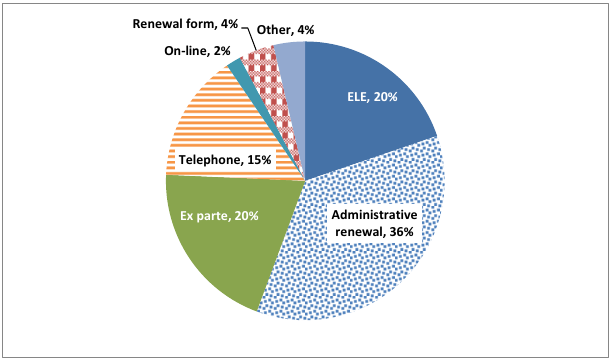
Source: Louisiana Department of Health and Hospitals 2013.
In 2008, when the state used administrative, ex parte, and telephonic renewal but not ELE, 19 in 20 children (95.4 percent) had their eligibility continued at renewal, with fewer than 1 percent losing coverage for procedural reasons.4 By contrast, in the nation as a whole, approximately 29 percent of Medicaid and CHIP children lost coverage at the time of their renewal, according to 2005 research, even though 44 percent of the children losing coverage remained eligible.5
Modeling conducted through the ELE Evaluation mandated by the Children’s Health Insurance Program Reauthorization Act of 2009 (CHIPRA) implied that adding ELE to the state’s previous arsenal of renewal strategies boosted the likelihood of Louisiana children retaining Medicaid continuously for 15 months by the small but statistically significant amount of roughly 2 percentage points.6 In part because of its work on renewals, Louisiana won CHIPRA performance bonus awards for three consecutive years, FY 2009-11.7
Challenges and lessons learned
Louisiana officials note that their approach is not static, and the state continues to make changes. They highlight that retention improvement is a continual process with significant potential for enhanced outcomes and greater efficiencies for both clients and program staff.
State officials believe that their approach to renewal has achieved administrative savings by substantially reducing the need for caseworker involvement. On the other hand, state officials report that the thoughtful and careful implementation of innovative reforms requires significant effort. That effort was aided by several years of support from the Robert Wood Johnson Foundation’s “Maximizing Enrollment” national program (“MaxEnroll”).
Louisiana typically involves, in addition to state officials, front-line caseworkers in helping shape the details of implementing innovative policies. The state often tests new approaches on a small scale before implementing them statewide. At the same time, an attitude of experimentation and willingness to make mistakes and learn from them is inculcated at all levels of the agency, from front-line caseworkers to leading state officials. This kind of agency culture has been critically important to the state’s success, and it may not be simple to replicate it elsewhere.
Louisiana: Express Lane Eligibility
Overview
A state practice that has gained much attention in discussions of integration and streamlining the enrollment processes of health and human services programs is ELE, discussed briefly above in connection with Louisiana’s renewal of children’s health coverage. A new option created by CHIPRA, ELE permits states to provide children with Medicaid or CHIP based on findings from other public agencies. Even if the other agency uses a methodology for determining eligibility—such as household definitions and income disregards—that differs from Medicaid and CHIP methodologies, the other agency’s findings can be used to qualify children for health coverage. This eliminates the need for the health program’s case workers to “cross-walk” information from the other agency’s case files to see how it fits into the slightly different rules used for health coverage. It also means that families are not required to provide additional information that may be needed to address minor differences in program rules.
“Deemed” eligibility, comparable to ELE, has long been used by many different programs across the country, which apply different names to the same basic concept. For example, pregnant women and infants automatically qualify as “adjunctively eligible” for the Special Supplemental Nutrition Program for Women, Infants, and Children (WIC) based on their receipt of Medicaid; children are “direct certified” as eligible for the National School Lunch Program (NSLP) based on their receipt of SNAP or Temporary Assistance for Needy Families (TANF); and through “categorical eligibility,” SNAP eligibility extends automatically to households in which every member receives Supplemental Security Income (SSI), TANF, or other cash assistance.
One option available to states implementing ELE is automatic enrollment, through which children can receive health coverage without filing standard Medicaid applications. Louisiana was the first state in the country to implement ELE auto-enrollment, and the second to implement ELE in any form. The Louisiana Department of Health and Hospitals (DHH) worked with the Department of Child and Family Services (DCFS), which administers SNAP, to implement an enrollment and renewal process that qualifies children as financially eligible for Medicaid based on data matches showing SNAP receipt.
Description
Louisiana applies ELE to both initial enrollment of previously uninsured children and to renewing coverage for Medicaid beneficiaries. SNAP findings about income, state residence, identity, and Social Security Number (SSN) are used to satisfy Medicaid eligibility requirements. The state matches records between the programs, based on identifying information such as name, SSN, and address. However, the SNAP program’s verification of a child’s citizenship or satisfactory immigration status is used to establish Medicaid eligibility only if the evidence meets standard Medicaid requirements. Otherwise, these non-financial requirements are verified through typical Medicaid procedures.
Much of the initial funding for development and implementation of this practice came from the above-described “MaxEnroll” program, which proved particularly important in funding necessary information technology (IT) improvements. Implementation of ELE also required coordination between two separate agencies: DHH (the agency responsible for Medicaid) and DCFS (the agency responsible for SNAP). State health officials met twice per week, spending months to plan implementation. Once the program was underway, DHH drafted and paid for all mailings to SNAP recipients, which reduced the cost and effort required of DCFS. DCFS supported ELE as helping meet the needs of the agencies’ shared low-income clientele while generating administrative savings for taxpayers.
Louisiana’s ELE implementation began in late 2009. DHH matched SNAP and Medicaid records to identify children who received SNAP but not Medicaid. To prevent duplicate enrollment, the state began by covering SNAP-recipient children who previously received Medicaid or CHIP but no longer participated. With other children, the state delayed enrollment until conducting further investigation to ensure that they weren’t actually receiving Medicaid but described differently in SNAP records—for example, with a nickname rather than a formal first name, or with an SSN or address that had several digits reversed.
The state sent letters to families whose children were in the group slated for initial enrollment. The letters explained that, if families did not “opt out,” their children could be enrolled in Medicaid, based on their receipt of SNAP. Less than one percent of the letters’ recipients opted out, and the state prepared to enroll the remainder into Medicaid.
Before the state could do so, however, clarification from CMS forced a change in direction. “Opting out” is sufficient to authorize data matching between SNAP records and Medicaid records, explained CMS officials, but enrolling children into Medicaid coverage requires 8affirmative consent from their parents, under the federal ELE statute. To meet this requirement, the state informed parents that it would send them Medicaid cards, and that using the cards to access care would signify affirmative consent to enrollment. CMS accepted this as meeting statutory requirements. In February 2010, Louisiana mailed Medicaid cards to more than 10,000 children who had qualified for Medicaid in December 2009 because of SNAP receipt.
The state also enrolled children into Medicaid based on monthly SNAP applications, starting in January 2010. For this ongoing, monthly process, parents could “opt-out” of data sharing on the SNAP application form. When those who did not opt out qualified for SNAP, their children’s identity was compared to records of current Medicaid enrollees. Children not participating in Medicaid were sent Medicaid cards, and their parents could complete the enrollment process by providing affirmative consent through using the cards to access care.
In November 2010, Louisiana began using ELE to renew coverage for all families whose Medicaid households consisted entirely of children with SNAP cases, regardless of how or when those children originally joined Medicaid. However, when it came time to renew the first group of automatically enrolled ELE children, the state experienced problems because of its IT system. Different renewal procedures applied to (a) ELE enrollees who had consented through card use and (b) those who had not yet used their cards. However, children’s utilization of services could be analyzed only by accessing the state’s claims payment system, which could not communicate with the state’s eligibility system. As a result, the expensive manual involvement of state staff was required for renewal.
To prevent this problem from recurring, state officials changed to a new consent policy that would permit renewal without any need to access data outside DHH’s eligibility system. Starting in January 2011, affirmative consent to enrollment was provided, not by using Medicaid cards to access care, but by checking a box on the SNAP form requesting Medicaid coverage. The check box was bolded, prominently placed at the top of the second page, and written in plain language, to maximize the chances that it would be read and understood.
Results
Louisiana’s use of ELE increased children’s Medicaid enrollment. During 2010, approximately 18,000 previously uninsured children joined Medicaid due to ELE. This represented a 3 percent increase in total children’s enrollment in Medicaid and CHIP, with ELE accounting for 28 percent of all new enrollees between February and July 2010. By November 2012, the total number of children enrolled through ELE reached 27,347.9
According to a state survey, the percentage of Medicaid-eligible children who lacked coverage fell from 5.3 percent in 2009 to 2.9 percent in 2011—the period that overlapped with ELE implementation.10 At that time, state officials did not implement any other policies that sought to increase participation among eligible children, and the percentage of uninsured increased among all other groups of low-income residents.11 As a result, state officials believe that ELE was responsible for these gains in children’s enrollment. Such gains were confirmed by the observations of community outreach groups as well as the different characteristics of ELE children compared to other Medicaid children. For example, in Louisiana, children age 7 or older are 22 percent more likely to be uninsured than are younger children. Yet 74 percent of ELE children were age 7 or older, compared to 57 percent of other Medicaid children.12
Enough time has passed to analyze the utilization levels that resulted from this streamlined enrollment method. A regression-adjusted model estimated that, during their first 12 months of coverage, 83 percent of children who auto-enrolled in Medicaid through ELE obtained services, compared to 88 percent of children who enrolled through non-ELE methods in Louisiana.13
Auto-enrolled ELE children in Louisiana were almost as likely to obtain some services as other children, but among the children who received care, ELE enrollees tended to use fewer services. For children who used any health care, regression-adjusted average costs for ELE children during their first 12 months were just 48 percent of the average amount for similar Louisiana children who enrolled using other methods.
Once the state changed its enrollment method to require parents to check an opt-in box on the SNAP application form, the average number of children enrolled via ELE as a result of monthly SNAP applications fell by 62 percent.14 This change did not result in a population more likely to use some rather than no services, however. The above-described regression-adjusted model estimated that, during their first 12 months of enrollment under the new “opt-in” check-box approach, 75 percent of ELE children used any services, compared to 83 percent who enrolled during the “consent through card use” method, and 88 percent who enrolled through non-ELE methods.15
As noted earlier, Louisiana’s use of ELE to renew children’s Medicaid coverage whenever all members of a Medicaid-enrolled household received SNAP allowed a substantial automation of renewals, with a small but statistically significant increase in the number of children receiving continuous coverage. Altogether, approximately 330,000 children had their Medicaid coverage renewed via ELE between November 2010 and November 2012. Primarily by automating the ongoing renewal of a sizable portion of the state’s Medicaid caseload, the state achieved roughly $1 million in net, annual administrative savings.
Challenges and lessons learned
State officials overcame several challenges. ELE implementation required considerable time and patience from state staff– especially with two different agencies administering Medicaid and SNAP. States with a single agency administering both programs would probably have had an easier time implementing this ELE approach. State policymakers also noted that they may have been able to move more quickly if a single project manager had the authority to make final decisions once issues were thoroughly explored by the interagency team.
Roughly half of the children initially enrolled via ELE saw their Medicaid coverage terminate in November of 2010. Most terminations involved children who never used their cards and whose parents did not consent to enrollment at renewal. But among the children whose parents had consented to enrollment by using their card, at least 92 percent retained Medicaid.
South Carolina: Express Lane Eligibility
Overview
As described above, ELE lets state Medicaid and CHIP programs enroll and renew children based on the findings of other public agencies. In 2011, South Carolina adopted ELE, qualifying children for Medicaid based on their receipt of SNAP or TANF. Unlike Louisiana, which started with enrollment, South Carolina began by using ELE for renewals. The state then extended ELE to enrollment in 2012, providing Medicaid to uninsured children who received SNAP or TANF.
Description
In South Carolina, children in low-income families with incomes up to 200 percent of the Federal Poverty Level (FPL) have long qualified for Medicaid. As of 2011, 19 percent of children in this income band were uninsured; only five states had a higher percentage of low-income children without coverage.16
“Churning” was also a common problem, with close to 140,000 children (roughly half of all enrolled children) losing coverage annually, and almost 90,000 of them returning to the program within the year, according to estimates from South Carolina’s Department of Health and Human Services (DHHS). Most children reapplied and rejoined the program within 2 months or less of termination. This churning raised administrative costs as staff members had to complete new eligibility determinations for children who, despite ongoing eligibility, exited and reentered the program. In addition to coverage rates and churning, the state’s program also faced challenges in paper processing and administrative burdens on staff and families.17
With a new governor taking office in 2011 and a new Medicaid director arriving from Louisiana, these problems received a fresh review. To address the administrative costs of churning, among other issues involving children’s health coverage, the state began planning to implement Express Lane Eligibility. As part of this process and before seeking approval from CMS, DHHS staff consulted with officials in Alabama, Louisiana, and Oregon, states that had previously adopted ELE, to learn more about the process and to identify the best strategies for South Carolina.18
In June 2011, South Carolina received CMS approval to implement ELE by qualifying children as financially eligible for Medicaid based on the income determinations of SNAP and TANF. South Carolina began using ELE to renew children’s coverage starting in July 2011. Data matches with the Department of Social Services (DSS) determine if children enrolled in Medicaid are part of an open TANF or SNAP case. If so, DHHS sends a letter to the family explaining that Medicaid has been automatically renewed. The family is not required to submit any additional information.19
Starting in September 2012, the state extended ELE to enroll children who had not previously received Medicaid. South Carolina compares TANF/SNAP records and Medicaid records to identify children who receive TANF or SNAP but not Medicaid. The state enrolls these children in Medicaid and sends their families a letter encouraging them to select a managed care plan. The letter lists a toll-free number that parents can call if they want to opt out of Medicaid coverage. The letter explains that those who neither opt out nor select a plan can use their Medicaid coverage to access fee-for-service care for their children, which constitutes consent to enrollment. Accessing care also triggers a new round of managed care selection, with a plan chosen by default if a family fails to select a plan within 90 days of seeking fee-for-service care.
Results
Between September 2012 and June 2013, more than 92,000 previously uncovered children enrolled in Medicaid through ELE in South Carolina.20 Compared to the state’s FY 2012 enrollment of 607,681 children,21 ELE enrollees represented a 15 percent increase in coverage.
Not enough time has passed to conduct the kind of utilization analysis described above for Louisiana ELE. However, state officials found that about one-third of children enrolled through ELE since September 2012 had used services as of May 2013, which was comparable to utilization levels among children enrolling through non-ELE methods.22
Between July 2011 and June 2013, more than 276,000 enrolled children had their coverage renewed through ELE. The combination of automated rather than manual renewal and greatly reduced churning were the main factors responsible for ELE yielding approximately $1.6 million in net annual administrative savings.23
South Carolina’s implementation of ELE helped the state receive a federal CHIPRA performance bonus for the first time in 2011, recognizing its implementation of various best practices specified in CHIPRA as well as increased Medicaid enrollment of eligible children. The bonus exceeded $2 million. The state received a second performance bonus in 2012.24
Challenges and lessons learned
The state had to overcome various challenges to implement ELE effectively. As with much interagency collaboration, South Carolina’s DHHS and DSS offices had to resolve differences in data collection methods before they could share information efficiently. DHHS also needed to decide how to handle cases that did not easily fit into the automated ELE process. For example, children who do not have Social Security Numbers create the potential for duplicate enrollment. DHHS decided to manually process these cases to see if the children appear in open SNAP and TANF cases.25
South Carolina also recognized potential limits in provider capacity when the state enrolled thousands of new children. The state accordingly decided to implement ELE for enrollment gradually by county, rather than immediately implementing ELE enrollment state-wide, as had been done for ELE renewal.26 Focus groups with parents of ELE-enrolled children indicated that their children enjoyed good access to Medicaid providers.27
An additional challenge resulted from state officials’ determination that staff training was unnecessary for ELE because of its automated nature. Caseworker confusion about ELE caused unnecessary manual editing in the ELE system in the early stages of the process. In retrospect, DHHS recognized that providing more information to staff prior to implementing ELE could have prevented this confusion.28
Using ELE best practices to strengthen ACA targeted enrollment
To cover the uninsured as part of ACA implementation, several states are now applying policies like ELE to both children and adults. In May 2013, CMS issued a State Health Official (SHO) letter that permits states to provide consumers with Medicaid based on their receipt of SNAP, using waivers under Social Security Act §1902(e)(14)(A) to bypass the normal requirement of individualized income determinations. States can qualify all or some SNAP recipients who meet Medicaid’s non-financial requirements. By October 2013, five states were approved for such waivers, including three that were also approved for similar waivers providing parents with Medicaid based on data from family members’ Medicaid and CHIP records. Four out of the 5 states began implementation before October 2013, enrolling nearly a quarter of a million people by November 15 (table 3).
Table 3. Results of targeted enrollment initiatives reported by 11/15/13
| State | Target group: SNAP recipients | Target group: People with family members enrolled in Medicaid or CHIP | Phone response accepted? | People sent mailings | Mailing response rate | People found eligible for Medicaid and enrolled |
|---|---|---|---|---|---|---|
| Arkansas | Y | 154,000 | 41% | 63,465 | ||
| Illinois | Y | 123,000 | 33% | 35,500 | ||
| Oregon | Y | Y | Y | 260,000 | 27% | 70,000 |
| West Virginia | Y | Y | Y | 118,000 | 46% | 54,100 |
| Total: | 655,000 | 34% | 223,065 | |||
Source: Manatt Health Solutions and the Kaiser Commission on Medicaid and the Uninsured, 2013. Note: total response rate is the average for all states, weighted based on the number of mailing recipients.
States implementing targeted enrollment can build on these early successes to incorporate lessons learned from ELE. Requiring consumers to respond to a mailing before they receive Medicaid greatly limits coverage gains. The initial response rates to mailings in Oregon, West Virginia, and Arkansas, for example, averaged 34 percent (table 3). Moreover, the most successful states, Arkansas and West Virginia, had state staff call every non-responsive mailing recipient to encourage form completion. States could likely cover many more consumers at much lower administrative cost if, as in South Carolina, (a) states enroll all targeted, eligible consumers not participating in Medicaid and (b) accessing fee-for-service care both gives consent to coverage and triggers mandatory managed care assignment.
Sources: “Facilitating Medicaid and CHIP Enrollment and Renewal in 2014,” Center for Medicare and Medicaid Services (CMS), Department of Health and Human Services (HHS), May 17, 2013.
http://www.medicaid.gov/Federal-Policy-Guidance/downloads/SHO-13-003.pdf; CMS. New State Medicaid & CHIP Targeted Enrollment Strategies (As of October 1, 2013) http://medicaid.gov/AffordableCareAct/Medicaid- Moving-Forward-2014/Targeted-Enrollment-Strategies/targeted-enrollment-strategies.html, downloaded 12/26/13;
Jocelyn Guyer, Tanya Schwartz and Samantha Artiga, Fast Track to Coverage: Facilitating Enrollment of Eligible People into the Medicaid Expansion, Manatt Health Solutions and the Kaiser Commission on Medicaid and the Uninsured, November 19, 2013, http://kaiserfamilyfoundation.files.wordpress.com/2013/11/8517-fast-trac....
SNAP/SSI Combined Application Projects
Overview
Combined Application Projects (CAPs) involve partnerships between the Social Security Administration (SSA), state agencies, and FNS that simplify the SNAP application process for SSI recipients who live alone or with a spouse who also receives SSI. CAPs utilize a SNAP law permitting households to be treated as categorically eligible for SNAP if all members receive SSI. CAP benefits can be based on the information already used to determine SSI eligibility, plus one or two additional questions, without any need to visit local SNAP offices.
Description
Low rates of SNAP participation among the elderly have posed a longstanding problem. In fiscal year 2010, SNAP served only 35 percent of eligible elderly persons—defined for SNAP purposes as people age 60 and older—compared with an overall participation rate of 75 percent among all SNAP-eligible consumers.29 Causes of non-participation identified in prior research include the perceived complexity of the application and enrollment process, transportation difficulties involved in reaching local SNAP offices, misunderstanding about available benefits, and stigma.30 To reach this population, FNS has long recognized the need for innovative enrollment and outreach strategies.
Since 1997, federal law has required SSA to give SSI applicants and recipients the opportunity to file a SNAP application while at the SSA office31. However, the process has not always worked seamlessly. For example, SSA case workers may not always obtain enough information to complete a SNAP application, due to differences in SNAP and SSI program requirements; or SSI might convey records to SNAP before verifying an applicant’s income. In either case, SNAP would need to follow-up with an elderly or disabled consumer to complete the application.
To improve this process, FNS (in collaboration with SSA) began authorizing state agency demonstrations for CAPs. By modestly “tweaking” the rules for determining SNAP benefits, these projects allow a significant simplification of the SNAP application process for SSI recipients who live alone or with a spouse who also receives SSI. These seniors and people with disabilities can qualify for SNAP based on the receipt of SSI by all household members, which establishes categorical eligibility. In such states, the SNAP application requires just one or two additional items of information. Benefit levels are standardized, often set at two or more values based on shelter expenses. FNS requires that, on average, participants applying through CAPs must receive benefits like those they would have received under the regular SNAP program, thus promoting both fairness and cost neutrality.
Standardizing benefits in this way allows a substantial simplification of application forms, since consumers are not required to provide the detailed information needed to establish precise benefit levels under standard SNAP rules. CAP participants are also exempt from the face-to-face interview usually required at SNAP offices. This exemption is helpful for SSI recipients, as the elderly and people with disabilities sometimes find it difficult to reach local social services offices. Recognizing that SSI recipients approved through CAP typically experience little income fluctuation,32 CAP households may have certification periods lasting 24, 36, or 48 months, reducing administrative and client burdens substantially compared to those experienced with SNAP’s normal 6- or 12-month certification periods.33 Operationally, SNAP programs can tap into information they already receive from SSA through an automated data exchange system, using that existing system for the additional purpose of identifying SSI recipients who have been approved for SNAP receipt and offering the CAP benefit to those not already approved. Such seniors and people with disabilities can begin receiving SNAP the month after they qualify for SSI if they applied with their SSI application. However, most CAP participants do not join SNAP through an application submitted at the SSA office, because the pool of people applying for SSI is small compared to the much larger pool already receiving SSI benefits.
As of 2013, 18 states were operating CAP demonstrations:34 Arizona, Florida, Kentucky, Louisiana, Maryland, Massachusetts, Michigan, Mississippi, New Jersey, New Mexico, New York, North Carolina, Pennsylvania, South Carolina, South Dakota, Texas, Virginia, and Washington. In most states, households receive a standard benefit, with the amount based on whether the state categorizes them as having “high” or “low” shelter expenses. In several states (including Florida, Massachusetts, New York, and Washington), the benefit calculation is a bit more complex. Households receive a SNAP benefit that is based on gross income, the standard deduction, a standard utility allowance (SUA), and standardized shelter expense. CAP participants receive no other SNAP income deductions.
Almost all states give CAP participants the opportunity to seek a fully individualized benefit determination, rather than a more standardized amount. In effect, someone making this choice opts out of CAP and into the regular SNAP program. A number of states give this option to all CAP recipients. Others limit this choice to consumers with shelter or medical expenses that exceed specified levels and thus are especially likely to receive larger SNAP benefits under regular procedures.
States take two basic approaches to CAPs. Through the “standard” model, all information needed by SNAP can be obtained during the SSA interview. For example, South Carolina, the first state to implement this model, asks SSI applicants to state whether average monthly shelter and utility expenses are in one of three specified ranges (less than $300, $301-$466, or more than $466). This information, which is not required for SSI purposes, determines which of several standardized SNAP benefit levels will apply. In addition, consumers must attest to living alone and receiving no earned income. SSA then transfers all data electronically to the SNAP program, which issues benefits without any further step required from the consumer or the state.
By contrast, the “modified” model does not feature SSA collecting CAP information. Instead, the State performs a data match to SSA data and captures the names and address information of SSI recipients who are not in the State’s SNAP records. SNAP then mails these consumers a highly simplified SNAP application form, encouraging them to enroll by completing and returning the form, free from the normal obligation to visit the SNAP office in person.
While beginning implementation of either model, states may convert existing SNAP beneficiaries to CAP if the CAP benefit is larger. They may also conduct outreach to households who already receive SSI but not SNAP. Such outreach consists of sending them either simplified SNAP/CAP application forms or electronic benefit transfer (EBT) cards pre-loaded with the smallest CAP benefit in their State. When the recipients use those cards, such use constitutes consent to enrollment into CAP.35 If the consumers respond to requests for information about shelter costs, their benefits can be increased to the appropriate CAP amounts.
Before using either model for a CAP waiver, states must obtain FNS approval. Standardized values that achieve cost neutrality are determined based on current SNAP-participating SSI-recipient households. Every 12 to 18 months, a CAP state must gather all the information necessary to perform a regular SNAP benefit calculation for a sample of CAP cases to determine if the CAP standardized values still meet cost neutrality requirements. If CAP benefits are not cost neutral, FNS and the State determine how to adjust CAP standardized benefits either up or down to establish cost neutrality. In addition, standardized CAP benefits must be changed to reflect cost-of-living (COLA) changes to SSI as well as SNAP COLAs, legislated changes, and any state changes to SNAP options.
SNAP benefits paid under a CAP waiver are subject to SNAP quality control reviews and potential inclusion in the state’s SNAP payment error rate. However, CAP cases are excluded if an erroneous CAP certification results from incorrect information from SSA regarding household composition or the beneficiary’s incorrect description of living arrangements on a simplified CAP application form. Although such cases do not count as a SNAP error, affected beneficiaries are removed from CAP and informed that they must file a standard SNAP application to continue receiving benefits.
Results
South Carolina began the first CAP in 1995. This state raised SNAP participation among SSI recipients from 38 percent in 1994 to 50 percent in 1998. During this same time period, SNAP participation among SSI recipients nationally decreased, from 42 percent to 38 percent. South Carolina’s efforts led to more than 8,500 seniors and people with disabilities receiving aid.36 The state also reported net administrative savings of approximately $575,000 per year.37
Overall, CAPs have achieved considerable success. According to a report by Mathematica Policy Research (MPR), 13 percent of all seniors receiving SNAP in fiscal year 2007 enrolled through a CAP. This percentage was even higher in some CAP states, including Florida (23 percent), New York (30 percent), and Mississippi (44 percent).38 Between fiscal years 2000 and 2007, the states that saw elderly participation increase by 100 percent or more had all implemented CAPs, expanded categorical eligibility, or took both steps.
Perhaps the clearest evidence of CAPs’ impact is the following. From fiscal year 2000 to fiscal year 2008, the average SNAP participation rate among 1-person SSI households in 12 states that implemented CAP rose from 26.4 percent to 39.1 percent—a 48 percent relative increase. At the same time, participation levels remained relatively flat for both (a) SSI-recipient households in non-CAP states (rising from 30.7 percent to 32.6 percent) and (b) non-SSI households in CAP states. Surveys report that most CAP participants are satisfied or very satisfied with the program, finding the enrollment process easy or very easy.39
Challenges and lessons learned
One key to CAPs’ simplification of the enrollment process is the replacement of individualized with more standardized benefit determinations. Although states seek to set the latter as close to the former as possible, some imprecision is inevitable. The presumptions underlying CAP are that most participants would trade a few dollars in benefits for a significantly simplified enrollment process, recognizing that CAP focuses on consumers who (a) were not otherwise participating in SNAP and (b) belong to a significantly underserved population.
Among 13 CAP projects that FNS analyzed in detail over multiple years, standardized benefits ranged from an average of $54 below fully individualized levels per case per month to $20 above those levels, with most states falling within $10 of fully individualized levels for most years.
Shelter costs were responsible for most cases in which CAP benefits were more than 20 percent below individualized levels. Using four standardized benefit levels, based exclusively on variations in shelter costs, appeared to be an effective approach to preventing significant variation.
The states that mailed EBT cards to all individuals identified as eligible reported the largest variation, with average shortfalls of more than $50, compared to what individuals could have received had they gone through the full SNAP eligibility determination process. To some degree, this comparison is more theoretical than real in that these CAP recipients previously were receiving no SNAP benefits at all. Further, the largest difference results from loading EBT cards with the lowest standardized CAP benefit for recipients who could instead qualify for a larger CAP standardized value by providing information about their shelter costs.40
A related concern involves the option for CAP enrollees to obtain a fully individualized benefit determination by submitting a normal SNAP application. Although all enrollees receive notices explaining that option, surveys show that the vast majority do not know about it.41
Each CAP takes significant time for the review, approval, and initiation of new CAPs. Some delays result from the effort required to coordinate with SSA. Other delays involve the time required for the state to clarify its CAP goals and establish its cost neutrality calculations and for FNS to review and recommend cost neutrality solutions. Some observers propose changing the SNAP statute to simplify and streamline the approval process,42 but under current law, states must work closely with FNS before implementing a CAP.
States pursuing CAP waivers must choose between standard and modified models. By eliminating the need for consumers to respond to a mailing, the standard model could increase participation more than the modified model. On the other hand, because of reduced need to build and test new data exchange mechanisms and develop other relationships between SSA and SNAP, the modified model may be easier to implement and may allow more rapid approval from FNS.
States pursuing CAP waivers must choose between standard and modified models. We are aware of no rigorous research that analyzes the impact of this difference on participation levels. However, some observers suggest that, by eliminating the need for consumers to respond to a mailing, the standard model could increase participation more than the modified model, but CAP participation is delayed until the SSI application is approved.43 On the other hand, because of reduced need to build and test new data exchange mechanisms and develop other relationships between SSA and SNAP, and because SSI has been approved, the modified model may be easier to implement and may allow more rapid approval from FNS, compared to the standard model.44
According to FNS, states that sent pre-loaded EBT cards to their entire outreach population and that implemented the standard model for new SSI applicants achieved the highest participation gains. However, such states also incurred relatively high administrative costs, enrolled consumers with relatively low utilization of SNAP benefits, and had the highest average shortfall in benefit levels, compared to those that would have resulted from the SNAP program’s normal benefit determination process.
Second case study area: Coordinating administration of multiple programs
This section focuses on the coordinated administration of multiple health and non-health programs. Such efforts can include synchronized redeterminations, through which information provided to renew eligibility for one program automatically reestablishes eligibility for other programs; coordinated systems of consumer communications that prevent multiple programs from sending redundant or conflicting messages to their common clients; and joint procurement or development of eligibility technology, including on-line application systems, electronic case records, eligibility data warehouses, enterprise service buses (which could include shared rules engines and data-matching hubs), upgraded automatic voice response systems, technology for interacting with customers’ mobile phones (including to permit customers to photograph pay stubs and other documentation and furnish such information over the internet), and similar steps that could potentially qualify for enhanced federal funding. As noted earlier, when such investments develop systems that benefit Medicaid along with human services programs and are completed by December 31, 2015, they can potentially qualify for 90 percent federal Medicaid funding, without a need for human services programs to share the development costs.45
As with the previously described strategies, the benefits of coordinated administration can be realized by both agency staff and clients. Clients of several programs can provide information once rather than multiple times, simplifying application and renewal procedures. Coordinated administration can also lessen burdens on caseworkers and reduce administrative costs—an appealing result during the recent economic slowdown, when caseloads increased and state-funded caseworker staffing levels remained stagnant or fell.
Here, we describe Utah’s automated eligibility determination system, which has achieved remarkable efficiencies serving multiple health and human services programs. Appendix A provides briefer summaries of other examples in this category.
Utah: Electronic Resource and Eligibility Product (eREP)
Overview
In 2010, Utah launched the Electronic Resource and Eligibility Product (eREP) system. The eREP system replaced the state’s 20-year-old eligibility system and was designed to both determine eligibility and issue benefits for more than 60 federal and state programs.46
Description
A 2001 review of Utah’s previous eligibility system found that it met only 52 percent of business needs, eligibility determinations varied based on the worker’s expertise, and the system provided no online access for customers.47 Other factors drove policymakers to revise the state’s eligibility system, including a prior history of inconsistent modernization efforts and economic downturns that led to both high caseload growth and reduced funding for eligibility staff.48
Beginning what turned out to be a nearly decade-long modernization effort, the state released a request for proposals for the new work in 2002. Utah’s Department of Workforce Services managed the eREP system’s development, in collaboration with the Department of Human Services, the Department of Health Services, and the State Department of Technology Services49.
The project’s initial development budget was $79 million. Several sources provided funding, with TANF reserve funds contributing $34 million to build the core system. Seventy-eight percent of the total funding for system development came from federal dollars, with the state paying the remaining 22 percent. By program, the federal government furnished 100 percent of TANF funds, 50 percent of SNAP dollars, and a combination of 50 percent and 90 percent funding of Medicaid costs, depending on the expenditure involved.50
The state developed and implemented the eREP system in three phases. The state’s contractor, IBM, carried out the first phase, which focused on TANF and the subsidized child care program. Utah state staff, rather than a contracting vendor, carried out phases 2 and 3. In all three phases, the state rolled out its updated eligibility procedures in one geographic area at a time.
In 2003, Utah began updating its eligibility and benefit processes, releasing several website and eligibility system updates. The first release involved the Utah Cares website, which gave the public information about different assistance programs.
Effective in 2004, the state implemented eFIND, a shared web-based system that health and human services programs use to verify information for eligibility determinations. Caseworkers use eFIND to gather information from 21 federal, state, and local databases, eliminating the need for workers to search each database individually. Data available through eFIND include, but are not limited to, SSA data, unemployment data, wage data, and SNAP qualification data. Individual consumers are required to provide documentation only for items that cannot be electronically verified through eFIND.
Over the next several years, the state built several new resources, including an online application and a customer directory. The state further developed the electronic eligibility system in 2007, issuing the first eREP benefits in 2008. The state finally released the full, modernized eligibility system, including the online application, customer directory, electronic policy, and resource and referral capabilities, in 2010.51
The eREP system incorporates a number of different functions and services to determine eligibility and manage benefits. An eligibility rules engine is the core of the system, facilitating eligibility determination across several programs. Eligibility rules for more than 60 programs let caseworkers use the system to efficiently and consistently determine benefit levels and eligibility for programs like Medicaid, CHIP, SNAP, TANF, and child care assistance.
A customer directory with information about more than 2.3 million people provides a single source of information that can be shared and updated across programs. When one program obtains information from or about a client, that information becomes immediately available to other programs. Such sharing of information across programs reduces the resources required to verify eligibility for each program. It also eliminates the need for consumers to provide the same information multiple times to different agencies.
In addition, the system also provides an integrated communication process for families. For example, if a family applies for multiple benefits, the family does not receive separate notices from different programs describing the applications’ outcomes. Instead, the state sends a single notice that identifies the programs for which the family qualified, identifies the programs for which the family was found ineligible, explains the reasons for such ineligibility, and describes the family’s rights to appeal any adverse determinations. Utah’s previously developed phone system, electronic data matching, and electronic case files were all interfaced with the new eREP system to provide a more seamless eligibility process.52
Under eREP, customers can enter information into the online application, which provides an authentication number to the customer, who then calls to speak with a caseworker. Once all information is entered, the system performs a check to determine the programs for which the individual may qualify. Face-to-face interviews are no longer needed to obtain benefits, but customers can meet with a caseworker, upon request.53
The implementation steps for eREP included training for state staff, conversion to the new system, assessment of operational impacts, and ongoing support for staff. Utah officials note that the training and support were important to ensure that staff learned the new system. The conversion step involved “translating” cases from the old system to the new system. Rather than convert all cases immediately, officials moved only those cases that were determined ready for the new system. Officials shifted work between different staff teams so that those being trained could take the time to learn the new system without affecting ongoing work.54
Table 4 outlines how various components of the eREP system were implemented over time.
Table 4. Timeline of eREP Implementation
| Date | Milestone |
|---|---|
| October 2003 | Utah Cares – resource and referral website for multiple programs |
| January 2004 | eFIND – data matching to external sources of verification |
| April 2004 | InfoSource – online resource for eligibility policies |
| February 2007 | Utah Helps – online application |
| October 2007 | Eligibility Module development – eligibility system, rules engine, benefit calculation, correspondence, case review, and case management Customer Directory – integrated customer data shared across multiple programs |
| August 2008 | Eligibility Pilot |
| October 2008 | First benefits issued through eREP |
| June 2009 | 5,000+ cases in eREP system |
| August 2009 | Human services programs fully integrated |
| October 2009 | Health programs fully integrated |
Results
For 2010, the first year eREP was fully operational, the caseload that could be handled by a single worker increased by 53 percent, compared to 2008. From 2009 to 2010, total caseloads increased by close to 19,000 cases, or 12.3 percent, while operational costs decreased by $7.3 million, or 9.6 percent.55
State officials describe the eREP system as increasing benefits access for customers, speeding decisions for eligibility, and improving accuracy in benefit determination.56 With eREP, 80 percent of applications are submitted online.57 The state reports improved workflow, with applications assigned based on program type and easily moved into different queues as needed.
Additionally, data security has been improved with the new system. The eREP system provides information to staff only as needed, limiting data access based on the specific jobs workers are assigned.58
The eREP system’s web-based interface allows for more efficient use of staff time. Much more intuitive than the state’s old system, the new interface uses drop-down options and “radio buttons.” By contrast, the previous system relied on staff knowing the correct codes to enter. This change both reduced the amount of necessary staff training and simplified ongoing operations.59
This new system’s most recent accomplishments built on the earlier results achieved by the state’s eFind system. The latter had reduced the average time needed to verify eligibility through multiple databases from 17 minutes to 3 minutes per case. While the eFIND system cost $2 million to build, the state estimated that eFind would result in $2.1 million in average savings each year due to a more efficient use of staff time.60
Challenges and lessons learned
Building the eREP system was a large project, involving many different programs and interfaces. Utah officials report that, as with many such projects, it was complex to integrate multiple systems. However, coordination and communication among state program staff and IT staff helped overcome these difficulties.
From a very early stage, Utah officials recognized the central importance of maximizing federal funding for IT development. As explained earlier, this ultimately involved drawing down federal dollars from three different programs, TANF, SNAP, and Medicaid. The proposal development and application process was complicated, especially with staff not completely familiar with all applicable procedures across multiple federal agencies. To address this challenge, the state hired an expert consultant to help prepare the documents needed to obtain federal funding.61
Utah officials cited working with outside vendors as another challenge. While the collaboration with IBM on phase 1 of the project was successful, state staff found that partnering with an outside vendor reduced their ability to nimbly modify the project’s scope of work. After assessing in-house expertise and determining that they had the necessary project-management and IT expertise, officials decided to bring the process in-house for phases 2 and 3, both to save money and to enhance the state’s flexibility. Officials cautioned that in moving the process in-house, they needed very clear goals and requirements to ensure that they did not continue to expand the scope of the project more than was needed.62
State staff also noted that building a rules engine can be difficult when existing policies leave room for interpretation. Officials were surprised to find that many of existing policies were confusing and difficult to follow. They expect to see improvement in this area over time, with a new system in place that enforces the disciple of requiring a precise and objective statement of decision rules.63
From initial planning and development in 2002 to the first benefits issued through eREP in 2009, the full release of the system in 2010, and expansions in 2011, the process for implementing eREP took nearly a decade. While counseling patience and realistic expectations about long time frames, officials also stress a countervailing need for clearly defined plans and goals, with a focus on outcomes, to keep ongoing state efforts on track.64
Other observers note that states are now positioned to pursue initiatives like Utah’s on a much more rapid time frame, for many reasons. States can learn from Utah’s experience; information technology has advanced considerably since 2002; eligibility systems and interagency collaboration are farther advanced than they were a decade ago; and as noted earlier, enhanced federal funding is currently available for IT investments in eligibility systems, allowing more rapid, short-term progress.65
Utah staff noted the importance of adequately testing new systems. The state used small batches of cases to see how information would interact in the new system. Rather than rolling out an entire system at once, the state staggered implementation, using a five- to six-month period to bring innovations live in one part of the state at a time. The state found this to be a useful approach that allowed the early identification and resolution of problems before statewide implementation.
Utah staff noted the importance of adequately testing new systems. Utah’s protocols included user, system, and production testing. The state used small batches of cases to see how information would interact in the new system. Rather than rolling out an entire system at once, the state staggered implementation, using a five- to six-month period to bring innovations live in one part of the state at a time. While this presented some challenges in terms of operating both the new and old system at the same time in different parts of Utah, the state found this to be a useful approach that allowed the early identification and resolution of problems before statewide implementation.66
Finally, documentation of favorable outcomes has focused on state efficiency gains. No evidence of which the authors are aware has shown increased receipt of benefits by eligible households.
Third case study area: Multi-program outreach and enrollment
This section focuses on practices that involve outreach and enrollment across multiple health and non-health programs. Examples include coordinated efforts to help individuals receive services from multiple programs or efforts to target beneficiaries of one program for outreach efforts from another program. Likewise, multi-program coordination may involve screening consumers for potential eligibility, educating them about available benefits, or helping consumers complete and submit applications. Outreach can also focus at particular locations, such as tax preparation sites that serve numerous low-income clients who qualify for many need-based programs or hospital emergency rooms with many uninsured who qualify for health coverage.
The coordination of outreach and enrollment across multiple programs can facilitate enrollment into one program by leveraging either: (a) the consumer contacts maintained by a different organization or agency; or (b) the consumer demand for a different service. By collaborating with outside organizations, a health or human services program may be able to reach eligible consumers while reducing outreach burdens on agency staff.
The practices highlighted in this category involve a Medicaid enrollment effort in Minnesota and multi-program enrollment conducted by Single Stop USA in community colleges across the country.
Minnesota: coordinated outreach and enrollment
Overview
In March 2011, Minnesota expanded Medicaid coverage to childless adults with incomes up to 75 percent FPL. This represented an “early expansion” of the ACA’s increased Medicaid eligibility for adults. To quickly enroll eligible consumers, the state used two primary strategies. First, the Minnesota Department of Health Services (DHS) collaborated with hospitals to enroll eligible uninsured patients who sought care in hospital emergency rooms (ERs). Via a DHS-operated toll-free line, hospital ER staff could initiate their patients’ enrollment into Medicaid. Second, DHS provided Medicaid to participants in the state’s former General Assistance Medical Coverage (GAMC) program. The state’s IT system was not ready to handle this conversion, so state and county staff did the necessary work manually.
Description
On January 5, 2011, in his first official act, incoming Governor Mark Dayton signed executive orders implementing Medicaid expansion in Minnesota to cover childless adults with incomes at or below 75 percent FPL, beginning on March 1, 2011.67 Among the adults newly qualifying for Medicaid coverage, many were already served by the state-funded GAMC program. Although that program already had 75 percent FPL as an upper eligibility limit, it had been severely cut back under the previous Governor and served only a small percentage of income-eligible consumers. Even fewer were covered by MinnesotaCare, a longstanding state program that offered more mainstream insurance (with limited hospital coverage) to childless adults up to 175 percent FPL. State officials believed that replacing these state-funded programs with federally-matched Medicaid would improve indigent residents’ access to care, cut financial losses experienced by Minnesota hospitals, and provide fiscal relief to the state budget.
To provide Medicaid both to these consumers and the uninsured who would become newly eligible, the state used two major strategies. The first involved coordination with Minnesota Hospital Association (MHA), which represents all but three hospitals in the state. DHS established a toll-free telephone line dedicated to hospital emergency rooms. ER staff could use this number to begin applications on behalf of uninsured patients. DHS would complete the application, enroll patients into coverage, and ensure that the hospital received reimbursement.
Both MHA and DHS communicated with hospitals via newsletters, email messages, and other channels. According to MHA officials, some hospitals were at first skeptical but rapidly became convinced of the reliability and value of this telephone resource. If DHS staff were not immediately available, hospitals could leave a message and would soon receive a return call. DHS staff provided knowledgeable, accessible assistance that eliminated the need for hospitals to refer patients to local social services offices for hospital staff to become Medicaid eligibility experts.
This telephonic connection helped when new patients who were uninsured sought emergency care. It also proved useful with uninsured or GAMC-covered patients who were well-known to hospitals. Before the March 1 start date of new Medicaid eligibility, many hospitals connected these “regulars” with DHS staff and enrolled them into Medicaid so that they were pre-qualified when new coverage began.
A second strategy provided Medicaid to consumers known to DHS based on their receipt of coverage through Minnesota’s previous state-funded health programs. This group included approximately 17,000-20,000 people GAMC recipients, approximately 35,000 people who had previously received GAMC coverage but left the program since changes made during the previous Administration, and a number of MinnesotaCare recipients with incomes at or below 75 percent FPL.
Officials recognized that the laborious and complex task of updating the Medicaid program’s 30-year-old computer system required a long time to accomplish. Rather than delay all the gains of expansion until the necessary IT investment was complete, DHS enrolled these consumers into Medicaid manually. The workload was divided between state and county eligibility staff, and many with other duties were reassigned to Medicaid enrollment. Case workers read information from the GAMC and MinnesotaCare case files and manually entered this into the Medicaid eligibility system, as if each individual were newly applying and qualifying for Medicaid. As with hospital-based enrollment of frequent ER visitors, this second strategy enrolled numerous eligible consumers before expanded eligibility began on March 1.
DHS also used more traditional outreach and enrollment strategies, including funding community-based organizations to provide public education and application assistance. The state streamlined application procedures for the new category of Medicaid coverage to eliminate questions about assets and income verification requirements officials viewed as redundant.
Results
By the end of March 2011, the first month of expanded Medicaid coverage, 51,853 individuals had been enrolled. The GAMC program supplied 45 percent of the new enrollees, and MinnesotaCare was responsible for 33 percent.68 This represented a very rapid start to a program that the previous Administration believed could not be implemented until final months of 2011, at the earliest. The first month’s enrollment in March comprised more than two-thirds (68 percent) of the total 75,982 consumers who enrolled into expanded Medicaid coverage by the end of calendar year 2011.69
Challenges and lesson learned
The state’s rapid success involved trade-offs. Because officials decided to enroll as many people as possible, as quickly as possible, state and county staff did a tremendous amount of work manually over a short period of time. This imposed administrative costs. Although staff expressed great enthusiasm for undertaking the work, some exhaustion and “burn-out” resulted.
Officials understood that they could have avoided these costs by delaying the start of enrollment until IT systems were ready. That would have impeded access to care for consumers and adequate reimbursement for hospitals for at least an additional six months. Or they could have asked consumers, rather than state staff, to complete the necessary paperwork to transition from GAMC or MinnesotaCare to Medicaid. The foreseeable result would have been that many would have failed to make the transition. Instead, DHS and counties chose to shoulder the burden themselves. Consumers and hospitals benefited greatly, but it came at a cost.
Single Stop USA: community college program
Overview
Single Stop USA is a nonprofit organization that provides assistance to individuals and families by helping them connect to benefits and services for which they are eligible. The organization began as a program under the Robin Hood Foundation in New York City. In 2007, Single Stop split off from the Foundation and became an independent, national organization.
Among its programs, Single Stop provides services for community college students and their families, including efforts to help them connect to various assistance programs. To this end, Single Stop started a pilot project in 2009 at Kingsborough Community College in New York City, providing comprehensive, integrated services to students. This project sought to increase graduation rates and reduce the hurdles students face in working, supporting families, and graduating from college. After achieving positive results in this pilot project, Single Stop expanded to other community colleges—expansion that continues today.
Description
Students attending community colleges often face financial and other hurdles to completing school. These challenges include balancing work and school priorities, managing finances, raising children, or supporting themselves and their families. In order to help students handle these challenges, Single Stop developed a program that provides a comprehensive approach to assisting students, beyond the support offered by colleges in the past. By providing multiple, integrated services at school sites, Single Stop, in partnership with the community colleges that house the program, can address many student needs by linking students and their families to multiple health and human services programs. Rather than focusing solely on educational financial assistance, narrowly defined as under traditional college student aid programs, Single Stop considers the student’s needs more broadly. The program assesses whether students qualify for different government assistance programs, provides legal assistance when needed, and furnishes financial counseling to help students and their families on limited budgets meet household needs.
Beginning with a single school in 2009, this program expanded to 17 colleges in seven states by 2012, helping more than 32,000 students receive more than $60 million in benefits and services.70 Single Stop continues to expand the number of community colleges it serves.
In its earliest form, the program relied on a community group to coordinate program activities. However, Single Stop’s process for selecting schools and administering the program has evolved over time. Single Stop now works with the Association of Community College Trustees to identify potential new sites and to foster relationships with school chancellors. Single Stop assesses each candidate school’s capacity to administer the program, readiness to make changes, and other key features of the local environment. This environmental scan determines, among other things, whether similar services are already being provided by other organizations, what public benefits are available in that particular state and locality, and the students’ need for services. If Single Stop and the school decide that the community college will act as a new site, they enter into a contract that requires the school to hire a site coordinator. Single Stop then works with local organizations and contracts with a financial advisor, legal counselor, and tax service provider. While the school directly hires the site coordinator, Single Stop provides initial staff training as well as ongoing training and support, with the goal of program institutionalization.71 Single Stop generally provides initial funding to cover the costs, with the schools contributing more funding over time and eventually paying most program costs. As colleges see the program achieving positive results, they often invest increasing amounts of their own resources to build capacity and raise these initiatives’ visibility. Because they are strongly embraced by college leadership, these programs become institutionalized as an ongoing part of college life, which increases students’ willingness to use the services they offer.
In practice, Single Stop typically begins its work with a student who is facing a particular challenge that is brought to the attention of school officials, such as a threatened eviction. It often becomes clear that the student’s struggles are not limited to that single “presenting issue.” A student experiencing one financial challenge often faces other challenges as well, such as food insecurity, debt and legal issues, or an inability to afford health care. Rather than just address the single “presenting” issue, Single Stop recognizes potential overlapping needs that cross many assistance programs. Students are often unaware of many available services and may not seek this information on their own. By educating students about these programs and helping them apply, Single Stop leads many students to obtain essential services for which they qualify.
Schools still commonly refer students to the Single Stop office when a specific financial issue arises. The Single Stop offices at the colleges are considered a part of the college, like other campus offices providing student services. Once students enter the Single Stop office, staff use the Benefit Enrollment Network (BEN), Single Stop’s online screening and eligibility determination tool, to collect the student’s information, quickly assess the student’s needs, and identify the benefits for which the student may qualify.
Staff then explain the different benefits for which the student appears to qualify. Whenever possible, the program helps the student apply electronically for benefits. If electronic applications are not possible—for example, because a certain program does not allow on-line applications—the site coordinator helps the student to apply in-person for benefits. Caseworkers make sure the students have all of the necessary forms, direct the student to the appropriate social services office, and in some cases even provide transportation. To facilitate this process, site coordinators often develop relationships with the local offices administering applicable benefit programs.72 In some cases, local social service agency staff visit the college to help students and their families enroll.
Much of Single Stop’s work, including the community college program, is funded through grants from the Robin Hood Foundation and other philanthropies. Single Stop also received two grants (the first for $1.1 million and the second for $1 million, with a match from the Community College of Philadelphia) from the White House’s Social Innovation Fund. Single Stop in turn provides grants to the program sites and seeks additional support from the host colleges and local community organizations. While philanthropic funding helps start the program at community college sites, the colleges themselves contribute significant funding, which grows over time.73
Results
Single Stop tracks benefit receipt by contacting students directly. If the agency cannot reach students to confirm benefit receipt, the agency assumes that no aid was obtained. Therefore, the outcomes reported by Single Stop and discussed here probably underestimate the number of students who receive assistance.
In 2012, Single Stop confirmed the receipt of public benefits by nearly 29 percent of the 18,000 students who were screened. The average value of the cash and noncash benefits received by each student was approximately $5,400—only slightly less than the maximum $5,550 Federal Pell Grant available to low-income students in 2011-2012.74 In addition to public benefits, a majority of the students served in Single Stop offices also received financial counseling, legal assistance, or help with tax preparation.75
From January 2010 to June 2012, Single Stop screened more than 36,000 students for benefits and services. During this period, Single Stop filed 24,508 federal income tax returns that provided students and their families with an estimated $36.4 million in refunds and tax credits. Single Stop enrolled 3,138 students and family members into health coverage, worth an estimated $23.7 million. Single Stop helped 3,502 students and family members receive $9.1 million in SNAP benefits, cash assistance enrollments totaled 653 ($2.2 million), Unemployment Insurance enrollments totaled 143 ($2 million), child care enrollments totaled 189 ($1.1 million), housing and utility assistance enrollments totaled 336 ($850,000), SSI/SSDI enrollments totaled 78 ($260,000), and WIC enrollments totaled 235 ($90,000).76
Challenges and lessons learned
Over time Single Stop has seen an increasing willingness on the part of community college personnel to partner with the program. Despite some initial reluctance to deviate from traditional educational roles, college officials have become increasingly aware of the challenges facing low-income students. A large and growing share of community college students are low-wage, working adults over age 25—often parents. These demographic factors have persuaded many community colleges to provide comprehensive services that can help students graduate. Perhaps because funding is growing more linked to graduation rates, community colleges appear increasingly willing to participate in programs like those operated by Single Stop.77
However, the program has had to overcome the stigma students often attach to receiving government assistance. Many students feel a responsibility to handle their financial struggles on their own. Single Stop has addressed this challenge by framing additional assistance as an extension of post-secondary-school financial aid, which can help students graduate and become self-sufficient.
Examples of practices that have not yet yielded significant gains
Here, we describe two practices that, at first, seemed promising, but have yet to yield significant levels of enrollment. The first involves Single Stop’s effort to pair health application assisters with nonprofit tax preparers. The second consists of efforts to refer consumers to benefit programs for which they apparently qualify without actually enrolling them.
Pairing volunteer tax preparers with health application assisters
Single Stop’s work connecting individuals to services and benefits is not limited to helping students at community colleges. Another initiative focuses on volunteer tax preparation sites in New York City. Single Stop funds nonprofit tax preparers so that, when their low-income clients file federal income tax returns to claim Earned Income Tax Credits (EITC), child tax credits, or other tax refunds, the clients can also obtain additional benefits or services for which they qualify. One such service is health coverage. As a small part of its overall program, Single Stop has encouraged some volunteer tax preparers to link their low-income clients with health application assisters, who enroll them into Medicaid or CHIP. In the past, “Facilitated Enrollers” (FE) in New York’s Medicaid and CHIP programs have most often been employed by health plans but sometimes consisted of the staff of community-based organizations.
While the practice varies by site, the consumer typically goes through the intake process and provides information that is entered into BEN, Single Stop’s screening tool, described above.78 The tax preparer helps the person with his or her taxes and then takes the person to the on-site facilitated enroller. The FE then helps the consumer apply for health coverage. In order to avoid potential criminal liability for sharing confidential tax information with FEs, the FE does not receive any tax information for the individual. Instead, the FE uses the BEN intake form as the basis for the health application. The FE asks additional questions of the individual as needed, then files an application for Medicaid and CHIP.
Many sites do not include a facilitated enroller, and even those with FEs have them available only at certain hours. If the FE is not present, the consumer can have his or her contact information shared, letting the FE reach out to the consumer after the tax preparation visit and enroll the consumer into health coverage.
This effort has been, in the words of one key informant, “great in theory, but a heavy lift” in practice. Only a minority of tax filers have been helped to apply for health coverage.
One challenge involves the temporary nature of tax preparation services. Tax preparers are often short-term volunteers without the expertise to do more than tax preparation. Also, tax preparation services are heavily concentrated in a relative short amount of time. More than 78 percent of returns that claim EITCs are filed before March 31.79 Linking tax preparers to organizations that already have health knowledge—that is, FEs—eliminates the need for tax preparers themselves to acquire that knowledge. However, shuttling clients from tax preparers to FEs in crowded quarters can create challenges, and it is easy for information to get lost in the process or for clients to get discouraged and leave.
A second challenge involves potential criminal liability for sharing tax information. As explained earlier, that issue was circumvented by using intake information, rather than tax information, to complete applications for health coverage. However, that “work around” makes the process much less efficient than the more automated procedures normally employed by Single Stop in other contexts.
A third challenge involves the “push back” Single Stop received when it first started encouraging tax preparers to help their clients qualify for non-tax benefits. Over the years, the organization’s tax preparers have grown increasingly receptive to providing more comprehensive services. Single Stop staff note that while there was a desire to help people, tax preparers were sometimes hesitant to take on additional tasks due to organizational issues related to the nature of tax preparation services, including the limited expertise and time of volunteer tax preparers.
Fourth, as indicated above, most FEs serving the state’s Medicaid and CHIP programs were health plan staff. When a community organization served as an FE, significantly above-average results were typically obtained, according to Single Stop officials. Such improved results could become more common under the ACA since New York’s Navigators and other health application assisters will mainly consist of mission-driven, community-based organizations.
Fifth, low-income people filing tax returns tend to be very focused on completing the tax filing process and obtaining refunds. Given the hectic atmosphere of nonprofit or volunteer tax preparation sites, consumers may be forced to wait before seeing the tax preparer, with whom consumers often have no prior relationship. Linking low-income tax filers to public benefits of any sort is not easy, and health coverage is no exception. After finally meeting with a tax specialist and obtaining a tax refund, many low-income people are not willing to spend the additional time needed to meet with a FE and enroll into health coverage.
Sixth, as indicated earlier, FEs did not have the staff needed to be present at tax filing sites whenever low-income consumers were seeking aid. In the majority of tax filing sites, FEs were never present on site. Even in sites where FEs were sometimes present, they would generally be available only part-time—typically between 10 am and 2 pm, and just two days per week.
FEs face a fundamental trade-off. To help the largest number of consumers, they need to be present when tax preparation sites are at their busiest. But it is at precisely such times when low-income consumers have the least willingness to wait the additional period of time that is often required to apply for health coverage.
The model of using “the tax filing moment” to jump-start enrollment into health coverage has substantial appeal. Many low- and moderate-income people who will qualify for health coverage in 2014 and beyond are motivated to file federal income tax returns, both to claim refunds and, in some cases, to comply with their legal duty to file. Further, filing tax returns is less stigmatized than applying for public benefits. On the other hand, successful partnerships between tax preparers and health application assisters are not always easy to develop.
National conversations among organizations providing nonprofit tax preparation services to low- and moderate-income consumers are increasingly exploring the nexus between health coverage and tax filing, according to Single Stop staff who are part of those discussions. The combination of tax-enforced penalties for failing to obtain coverage, tax credits to subsidize premiums in health insurance marketplaces, and the risks of tax reconciliation obligations if advance payment of such credits turn out to be excessive, all create a natural link between tax filing and applications for health coverage. The nonprofit tax preparation community has been expressing increased interest in helping low-income taxpayers obtain health coverage as part of tax filing.
Single Stop is now transitioning to the direct provision of tax preparation and health enrollment services on-site. Instead of the past bifurcated service delivery model, with volunteers furnishing tax preparation services and a FE helping consumers enroll into health coverage, Single Stop plans to provide both sets of services, with health application assistance supported through New York’s “Navigator” program. Notwithstanding past challenges, Single Stop’s leaders believe that combining free tax-preparation services with enrollment into health coverage offers enormous potential to provide health coverage for numerous low- and moderate-income uninsured. They are optimistic that additional resources will make it possible to surmount the obstacles this strategy has experienced to date.
Encouraging consumers to apply for benefits for which they may qualify
Repeated experience suggests that simple referrals may enroll no more than a minority of eligible consumers into benefits for which they qualify. For example, two randomized, controlled experiments analyzed H&R Block’s efforts to help taxpayers obtain various forms of assistance:
- When H&R Block used tax return data and interviews to complete and file SNAP application forms on behalf of families, the number of applications for aid was 80 percent higher than with the control group that received no assistance beyond basic SNAP information and blank SNAP application forms. By contrast, no statistically significant effects were observed, compared to the control group, when H&R Block filled out the forms, handed them to families, and explained where and how to file them.80
- When H&R Block used tax return data and interviews to complete and file college student aid forms on behalf of families, successfully filed applications for aid were 40 percent higher than in the control group that received only general information about college aid. By contrast, no statistically significant effects were observed when H&R Block gave the families written, personalized estimates of their likely eligibility for student aid, along with information about tuition costs at nearby colleges and instructions about completing the application process.81
In some cases, when agencies have gone beyond mere referrals to send application forms to potentially eligible consumers, relatively few people have enrolled. For example:
- In 2002 the Social Security Administration sent 16.4 million letters to low-income Medicare beneficiaries who were probably eligible, according to federal income data, for Medicare Savings Programs (MSP). The letters provided information about MSP, which pays some or all Medicare cost-sharing, depending on income. The letters also listed a phone number that could be called to enroll. Only 74,000 people—0.5 percent of letter recipients—enrolled in MSP as a result.82
- Since the late 2000s, Iowa and New Jersey have required taxpayers to indicate on state income tax returns whether their children have insurance coverage. In 2009, when parents in these states said that their children were uninsured, they were mailed application forms for health coverage, along with information about how to enroll. In Iowa, roughly 1 percent of parents filed application forms and sought coverage.83 New Jersey streamlined its already simple child health application—eliminating all income questions, for example—and mailed out approximately 172,000 simplified forms to parents who indicated that their children were uninsured, accompanying the mailer with a targeted media campaign; roughly 750 children enrolled—less than 0.5 percent of the children in these families.84
- More recently, several states have implemented ELE using enrollment processes that reached many fewer children than the ELE approaches described above for Louisiana and South Carolina. Iowa, Oregon, Maryland, and New Jersey each sent simplified health forms to families whose children received SNAP, participated in the National School Lunch Program, or potentially qualified for Medicaid or CHIP based on state income tax records. For children to receive ELE, families needed to complete these simplified forms by mail or phone. Many forms did not even ask about income. Typically, 5 percent or fewer of families who were sent such forms returned them. In the most successful ELE processes that required this step, just 13 percent of families returned the forms.85 More recent efforts at Medicaid targeted enrollment strategies have achieved much better results, as explained earlier, but the initial mailing response rates still averaged only 34 percent.
- Even asking consumers to complete a simple “opt-in” check-box can dramatically reduce participation levels. As explained earlier, when problems with the state’s information technology systems forced Louisiana’s ELE program to shift from its “consent through accessing care” policy to a new approach through which parents consented to enrollment by checking a box on the SNAP application form, the average number of children being enrolled via ELE as a result of monthly SNAP applications fell by 62 percent.86
This behavioral pattern is not unique to low-income people seeking public benefits. For example, similar patterns are observed with enrollment of many middle-income people into retirement savings accounts. In one classic example, roughly 33 percent of newly hired workers enroll in 401(k) accounts when their employer requires them to complete a form. In firms where such workers are enrolled unless they complete a form opting out, 90 percent participate.87
Another study, aptly titled, “$100 Bills on the Sidewalk,” analyzed seven companies that offered employer matches to worker contributions into 401(k) accounts. Workers over 591⁄2 years of age could obtain employer payments without cost; because of their age, such employees’ contributions could be withdrawn, immediately, without penalty. Nevertheless, at each of the seven firms, between 20 and 60 percent of eligible workers failed to claim their employers’ maximum matching contribution, with losses that could range as high as 6 percent of annual income. At the median firm, 31 percent left employer contributions unclaimed, averaging 2 percent of annual income.
Researchers implemented a careful education intervention that, among other things, had each worker calculate the amount of employer contributions that the worker was leaving unclaimed. Participation rates increased by just one-tenth of one percentage point, compared to a control group that received no educational intervention. Researchers concluded, “In this instance, providing better information did not lead to better choices.”88
Conclusion
Several themes emerge from almost every successful case study described above. For health and human services programs to effectively integrate and coordinate eligibility determination and enrollment, a great deal of work may be required. At the same time, a broad range of innovative strategies have increased eligible consumers’ participation levels in uncapped health and human services programs, lowered administrative costs in capped and uncapped programs alike, and increased the accuracy of eligibility determination.
About the authors and acknowledgments
The authors, Stan Dorn, Sarah Minton, and Erika Huber, are a Senior Fellow and Research Associates at the Urban Institute. They are grateful for the financial support provided by ASPE as well as the substantive guidance provided by their extraordinary project officer, Alana Landey in ASPE’s Office of Human Services Policy. This paper benefited from the thoughtful feedback from Brigette Courtot of the Urban Institute, for which the authors are grateful, as well as from members of this project’s Technical Working Group, listed in Appendix B. However, the views expressed in this report are solely those of the authors and may not reflect the views of ASPE, the Urban Institute or its trustees or funders, the individuals referenced above, or their affiliated organizations.
Appendix A. Additional promising or emerging practices
This appendix lists a number of promising or emerging practices that, due to resource limits, could not receive a detailed profile in the body of the report. The practices fall into the same three broad categories described above:
- Streamlining eligibility determination for one program based on data linkages with other programs;
- Coordinating administration of multiple programs; and
- Coordinating outreach and enrollment.
1. Streamlining eligibility determination for one program based on datalinkages with other programs
| Location and Programs | Practice | Additional Resources |
|---|---|---|
| Alabama – Medicaid and SNAP | The state implemented Express Lane Eligibility, qualifying children for Medicaid based on SNAP findings. | Kaiser Commission on Medicaid and the Uninsured. 2012. Secrets to Success: An Analysis of Four States at the Forefront of the Nation’s Gains in Children’s Health Coverage. http://www.kff.org/medicaid/upload/8273.pdf |
| Iowa – SSA and Health Programs | The state verifies citizenship for health programs using electronic data matches with SSA. This practice along with other initiatives has helped Iowa reduce the number of uninsured children by 19.4 percent between 2008 and 2010. | Kaiser Commission on Medicaid and the Uninsured. 2012. Secrets to Success: An Analysis of Four States at the Forefront of the Nation’s Gains in Children’s Health Coverage. http://www.kff.org/medicaid/upload/8273.pdf |
| Massachusetts – Health Care | Individuals were qualified for subsidies based on data matches with the state’s former free care program without having to complete applications. Approximately one out of every four newly insured individuals was found eligible due to data matches. | Dorn, Stan and Elizabeth Lower-Basch. 2012. Moving to 21st- Century Public Benefits: Emerging Options, Great Promise, and Key Challenges. Kaiser Family Foundation. http://www.clasp.org/admin/site/publications/files/Moving-to- 21st-Century-Public-Benefits.pdf |
| Massachusetts – SNAP and Children’s Health Care | Through an ELE waiver, the state uses SNAP findings to renew eligibility for both children and parents. | Kaiser Commission on Medicaid and the Uninsured. 2012. Secrets to Success: An Analysis of Four States at the Forefront of the Nation’s Gains in Children’s Health Coverage. http://www.kff.org/medicaid/upload/8273.pdf |
| New Jersey – Low Income Home Energy Assistance Program (LIHEAP) and Medicare | The state automatically provides LIHEAP to residents who qualify for the Medicare Part D Low-Income Subsidy (LIS). This program operates by means of data exchange among the LIHEAP program, the state’s Pharmaceutical Assistance to the Aged and Disabled (PAAD) program, and LIS. PAAD and LIS have income eligibility limits lower than for LIHEAP. Automatic enrollment raised the proportion of income-eligible elders enrolled in NJ’s LIHEAP, compared with other states. | Dieterle, Jim. 2011. Automatic Enrollment of New Jersey’s Low-Income Elderly and Disabled Households Into LIHEAP, MJ’s Universal Service Fund Program, and SNAP Application Assistance. Presentation for the National Energy and Utility Affordability Conference. AARP. http://www.energyandutilityconference.org/Assets/2011%20Co nference/2011%20Presentations/3D_Jim%20Dieterle.pdf |
| New Jersey – SNAP and Medicare | Building on New Jersey’s LIHEAP and Medicare Part D Automatic Enrollment, the state took advantage of the data matching potential with SNAP. County social services offices receive partially completed SNAP applications, on which they then follow up. | Dieterle, Jim. 2011. Automatic Enrollment of New Jersey’s Low-Income Elderly and Disabled Households Into LIHEAP, MJ’s Universal Service Fund Program, and SNAP Application Assistance. Presentation for the National Energy and Utility Affordability Conference. AARP. http://www.energyandutilityconference.org/Assets/2011%20Co nference/2011%20Presentations/3D_Jim%20Dieterle.pdf |
| Oregon – SNAP and Medicaid | The state implemented Express Lane Eligibility to use SNAP findings to establish children’s eligibility for Medicaid. The state’s Self-Sufficiency Modernization Project, an effort to provide online applications and automate eligibility decisions for all work supports programs, is ongoing. | Kaiser Commission on Medicaid and the Uninsured. 2012. Secrets to Success: An Analysis of Four States at the Forefront of the Nation’s Gains in Children’s Health Coverage. http://www.kff.org/medicaid/upload/8273.pdf |
| National – Medicare, Medicaid, and SSI | Medicare recipients who are identified through data matches as having received Medicaid or Supplemental Security Income in the previous year automatically qualify for Low-Income Subsidies for Medicare Part D prescription drug coverage. | Stan Dorn and Elizabeth Lower-Basch. 2012. Moving to 21st-Century Public Benefits: Emerging Options, Great Promise, and Key Challenges. Kaiser Family Foundation. http://www.clasp.org/admin/site/publications/files/Moving-to-21st-Centur... |
| National – WIC and Medicaid | WIC has used Medicaid participation to establish adjunct income eligibility since 1989. An individual is deemed adjunctively income eligible for participation in WIC if she or a qualifying family member (a pregnant woman or infant) is certified to receive Medicaid. | Food and Nutrition Services (FNS). http://www.fns.usda.gov/wic/howtoapply/eligibilityrequirements.htm; and 42 U.S.C. 1786, section 17(d)(2)(A). |
| National – NSLP and SNAP | Direct certification in the National School Lunch Program (NSLP) automatically qualifies students for free school meals, based on receipt of SNAP or TANF benefits, without the need for parents or guardians to submit a NSLP application and without any requirement to determine NSLP eligibility on other grounds. | Food and Nutrition Services (FNS). 2012. Direct Certification in the National School Lunch Program: State Implementation Progress School Year 2011-2012: Report to Congress. http://www.fns.usda.gov/ora/MENU/Published/CNP/FILES/DirectCert2012.pdf; and National School Lunch Program: Direct Certification Continuous Improvement Plans Required by the Healthy, Hunger-Free Kids Act of 2010. Federal Register Vol. 78, No. 36. http://www.fns.usda.gov/cnd/governance/regulations/2013-02-22_AE10.pdf |
| Selected States – NSLP and Medicaid | Pilot project to test direct certification in NSLP through which children automatically qualify for free school lunches based on Medicaid findings of income at or below 133 percent FPL, without any new NSLP application from parents and without any other eligibility determination by NSLP. Six states implementing as of 2012-2013. | Example of Illinois implementation: Nutrition and Wellness Programs Division, Illinois State Board of Education. Electronic Direct Certification with Medicaid Demonstration Pilot – SY2013-2014 Update. May 21, 2013. http://www.isbe.net/nutrition/dc-medicaid/edc-demo-pres052113.pdf Vivian Lees and Patricia von Reyn, FNS. The Road to 95%: What’s Ahead for Direct Certification. December 6, 2012 http://www.schoolnutrition.org/uploadedFiles/Presentations/ANC_2012_-_De... |
2. Coordinatingadministration of multiple programs
| Location and Programs | Practice | Additional Resources |
|---|---|---|
| Florida – SNAP and Medicaid | SNAP recipients are recertified at six month intervals. If income changes are reported at the time of the SNAP recertification and individuals are shown to qualify, a new 12-month Medicaid eligibility period begins. | Kellenberg, Rebecca, Sharon Silow-Carroll, Eileen Ellis, Esther Reagan, and Jennifer Edwards, Health Management Associates, personal communication. |
| Colorado – Health and Human Services Programs | The state’s Program Eligibility Application Kit (PEAK) is an online screening and application tool that screens applicants for multiple benefits. | Loprest, Pamela and Lindsay Giesen. 2013. Early Lessons from the Work Support Strategies Initiative. The Urban Institute. http://www.urban.org/publications/412790.html |
| Illinois – Medicaid and Human Services Programs | The state is developing a new eligibility system (using 90/10 Medicaid funding) and call centers for Medicaid as well as other human service programs, including TANF and SNAP. | Hahn, Heather, Olivia Golden, and Jessica Compton. 2013. Early Lessons from the Work Support Strategies Initiative: Illinois. The Urban Institute. http://www.urban.org/publications/412792.html |
| Kentucky – Health and Human Services Programs | The Kentucky Access, Accuracy and Accountability Project (KAAAP) includes electronic case files that are being implemented to enhance productivity, improve accuracy, and better program access; new system will replace the current eligibility system. | Rohacek, Monica and Lindsay Giesen. 2013. Early Lessons from the Work Support Strategies Initiative: Kentucky. The Urban Institute. http://www.urban.org/publications/412797.html |
| Massachusetts – Health Programs | A single application form is used for several health-related programs. All completed forms are processed by the Medicaid agency, with computer technology used to place people in the programs for which they qualify. | Stan Dorn and Elizabeth Lower-Basch. 2012. Moving to 21st- Century Public Benefits: Emerging Options, Great Promise, and Key Challenges. Kaiser Family Foundation. http://www.clasp.org/admin/site/publications/files/Moving-to- 21st-Century-Public-Benefits.pdf |
| Oregon – SNAP and Medicaid/CHIP | Policy workgroups closely aligned eligibility requirements for SNAP and the state’s child care assistance program. The application process for Medicaid/CHIP, especially for children, was simplified. | Kaiser Commission on Medicaid and the Uninsured. 2012. Secrets to Success: An Analysis of Four States at the Forefront of the Nation’s Gains in Children’s Health Coverage. http://www.kff.org/medicaid/upload/8273.pdf |
| Pennsylvania – Medicaid and CHIP | When children are denied benefits or become ineligible for Medicaid or CHIP because of income changes, their eligibility records are transferred electronically to and they automatically qualify for the other program. | Stan Dorn and Elizabeth Lower-Basch. 2012. Moving to 21st- Century Public Benefits: Emerging Options, Great Promise, and Key Challenges. Kaiser Family Foundation. http://www.clasp.org/admin/site/publications/files/Moving-to- 21st-Century-Public-Benefits.pdf |
| Rhode Island | The state is currently integrating its IT infrastructure for serving health and human services programs. | The Henry J. Kaiser Family Foundation. State Exchange Profiles: Rhode Island. July 26, 2013. http://kff.org/health- reform/state-profile/state-exchange-profiles-rhode-island/. |
| National – College Financial Aid and IRS | When applying for federal financial aid for college, applications can be prepopulated using IRS data from federal income tax forms. The IRS data fully verify relevant financial eligibility requirements. | Stan Dorn and Elizabeth Lower-Basch. 2012. Moving to 21st- Century Public Benefits: Emerging Options, Great Promise, and Key Challenges. Kaiser Family Foundation. http://www.clasp.org/admin/site/publications/files/Moving-to- 21st-Century-Public-Benefits.pdf |
3. Coordinatingoutreach and enrollment
| Location and Programs | Practice | Additional Resources |
|---|---|---|
| Iowa – Children’s Health Program | County public health agencies use outreach coordinators to work with schools, providers, other public health agencies, faith-based organizations, and other groups to conduct outreach for the children’s health program. Presumptive eligibility also allows the coordinators and other partners (such as school nurses and providers) to enroll children who appear eligible for the program. The children then receive care while full eligibility is being determined. | Kaiser Commission on Medicaid and the Uninsured. 2012. Secrets to Success: An Analysis of Four States at the Forefront of the Nation’s Gains in Children’s Health Coverage. http://www.kff.org/medicaid/upload/8273.pdf |
| Massachusetts – Health Programs | Hospitals, health centers, and other community partners help enroll children in the health program, using the online Virtual Gateway. The state both communicates with partners about new policies and receives feedback about emerging problems. As of FY 2010, more than 60 percent of successful applications were filed, not by consumers, but by these organizations acting on consumers’ behalf. | Kaiser Commission on Medicaid and the Uninsured. 2012. Secrets to Success: An Analysis of Four States at the Forefront of the Nation’s Gains in Children’s Health Coverage. http://www.kff.org/medicaid/upload/8273.pdf Commonwealth of Massachusetts. EOHHS Virtual Gateway: Health Insurance and Health Assistance Programs. September 2011. http://www.masshealthmtf.org/uploadedFiles/MassHealth_Training_Forum/Gate way%20Overview%209-8-2011.pdf. |
| Oregon – Children’sProgram Health | From 2009 to 2011, community-based organizations were given more than $3 million in grants to conduct outreach and help families apply for children’s health coverage. Sites worked with schools, other safety net program offices, and rural clinics to provide training. Coordinators also received a $75 payment for each application that led to at least one child being enrolled in the program. | Kaiser Commission on Medicaid and the Uninsured. 2012. Secrets to Success: An Analysis of Four States at the Forefront of the Nation’s Gains in Children’s Health Coverage. http://www.kff.org/medicaid/upload/8273.pdf |
| New York – Tax Credits and Child Support | An initiative provides employment services and tax credits to low-income noncustodial parents behind on their child support payments. | Sorensen, Elaine. 2011. New York Initiative Helps Fathers Increase their Earnings and Child Support Payments. The Urban Institute. http://www.urban.org/publications/412443.html |
| Rhode Island – LIHEAP and SNAP | LIHEAP applicants are asked if they want help paying for food, and if so, their application information is used to automatically prepopulate the SNAP application. | Stan Dorn and Elizabeth Lower-Basch. 2012. Moving to 21st-Century Public Benefits: Emerging Options, Great Promise, and Key Challenges. Kaiser Family Foundation. http://www.clasp.org/admin/site/publications/files/Moving-to-21st- Century-Public-Benefits.pdf |
| National - EITC | EITC Awareness Day is a one-day event that uses mainstream and social media to reach a broad audience of potentially eligible taxpayers. | IRS. 2013. EITC Awareness Day. http://www.eitc.irs.gov/ptoolkit/awarenessday/ |
Appendix B. Members of the Technical Working Group
Federal Officials
HHS
Susan Golonka, ACF/OFA
Vicki Turetsky (along with Jennifer Burnszynski), ACF/OCSE
Mark Fucello, ACF/OPRE
Rochelle Rollins, advisor to the Chief Medical Officer, ACF
Jeannie Chaffin, ACF/OCS
Suma Nair, HRSA/Bureau of Primary Care
Ben O’Dell and Lisa Carr, Center for Partnerships
Gregorio Hunt, OIEA
Elizabeth Hadley and Christie Peters, ASPE/Office of Health Policy
Donna Cohen Ross, CMS/CMCS
USDA/FNS
Kathryn Law, Office of Policy Support
SSA
Craig Streett, Office of Income Security Programs
State Officials
Louisiana
Ruth Kennedy, Medicaid director
Nongovernmental Members
Anita Light and Megan Lape, American Public Human Services Association
Catherine Hess, National Academy for State Health Policy
Helen Neuborne, Ford Foundation
Andy Hyman, Robert Wood Johnson Foundation
Elisabeth Mason, SingleStop USA (representing the Coalition for Access and Opportunity)
Meghan Wills, National Governors Association
Jennifer Sullivan, Enroll America
Steve Taylor, United Way
Notes
1 American Public Human Services Association (APHSA). A-87 Exception Toolkit for Human Service Agencies: Description of the Exception and Recommendations for Action. January 2014.
http://www.aphsa.org/content/APHSA/en/pathways/NWI.html.
2 CMS. “FY 2011 Louisiana Medicaid: Payment Error Rate Measurement (PERM) Cycle 3 Summary Report.” November 31, 2012. Available at: http://ccf.georgetown.edu/wp-content/uploads/2013/01/LA.Error_.Rates_.Su....
3 These estimates applied before the state implemented ELE, which further increased the state’s automation of renewals. Georgetown University Health Policy Institute. “The Louisiana Experience: Successful Steps to Improve Retention in Medicaid and SCHIP” February 2009.
http://www.maxenroll.org/files/maxenroll/resources/Louisiana%20Experienc....
4 Georgetown University Health Policy Institute. “The Louisiana Experience: Successful Steps to Improve Retention in Medicaid and SCHIP” February 2009.
http://www.maxenroll.org/files/maxenroll/resources/Louisiana%20Experienc...
5 Benjamin D. Sommers. “From Medicaid to Uninsured: Drop-Out among Children in Public Insurance Programs.”
Health Services Research 40, no. 1 (2005): 59–78..
6 Sheila Hoag, et al. “Final Findings.” CHIPRA Mandated Evaluation of Express Lane Eligibility. Mathematica Policy Research, Inc. 2013.
7 Kaiser Family Foundation. “CHIPRA Performance Bonus Awards, FY2009-FY2012.” Statehealthfacts.org.
Available at: http://kff.org/other/state-indicator/chipra-performance-bonuses/.
8 Social Security Act §1902(e)(13)(D)(i) [42 USC §1396a(e)(13)(D)(i)].
9 Hoag, et al., op cit.
10 Goidel, Kirby, Stephen Barnes, and Dek Terrell. “Louisiana’s Uninsured Population: A Report from the 2011 Louisiana Health Insurance Survey.” Baton Rouge: Louisiana State University Division of Economic Development and Public Policy Research Lab, January 2012. Available at:
http://dhh.louisiana.gov/assets/medicaid/LHIS/2011LHIS/LHIS_Layout_FINAL....
11 Dorn et al., 2012.
12 Dorn et al., 2012.
13 Colby, Maggie and Brenda Natzke. “Utilization of Services by ELE Enrollees.” CHIPRA Express Lane Eligibility Evaluation. Princeton, NJ: Mathematica Policy Research, 2013. To analyze the impact of ELE enrollment on utilization, researchers used a regression analysis to adjust the characteristics of ELE enrollees, in terms of age, gender, geography, and other factors, to fit the characteristics of Medicaid children enrolling through other methods.
14 Stan Dorn, Margaret Wilkinson, and Sarah Benatar. “Case Study of Louisiana’s Express Lane Eligibility: Final Report.” CHIPRA Express Lane Eligibility Evaluation. Washington, DC: Urban Institute 2013. August 2013.
15 Among children who did use services, average costs were slightly higher with the opt-in process: with the opt-in check box, ELE children who used services incurred costs that were 52 percent of average costs among non-ELE children who used services, compared to 48 percent of ELE children who enrolled under the earlier, opt-out, “consent through card use” process.
16 Edwards, Jennifer and Rebecca Kellenber. 2013. CHIPRA Express Lane Eligibility Evaluation: “Case Study of South Carolina’s Express Lane Eligibility Process.” Mathematica Policy Research; Hensley-Quinn, Mary Henderson, and Kimm Mooney. 2012. State Experiences with Express Lane Eligibility: Policy Considerations and Possibilities for the Future. State Health Reform Assistance Network. Robert Wood Johnson Foundation.
17 Supra, John. 2011. South Carolina’s Experience Implementing Express Lane Redeterminations. South Carolina Health and Human Services.; Iritani, Katherine. 2012. Medicaid and CHIP: Considerations for Express Lane Eligibility. Presentation to the U.S. Senate Committee on Finance. Presented December 5. GAO-13-178R. Government Accountability Office.
18 Edwards, op cit.
19 Edwards, op cit.
20 Hoag, et al., op cit.
21 Division of Policy and Research on Medicaid and Medicare at the University of South Carolina Institute for Families in Society, SC HealthViz, a project of the SC Department of Health and Human Services,
http://schealthviz.sc.edu/total-members-and-member-months#%7B%22path%22%..., downloaded 10/31/13.
22 Edwards, op cit.
23 Hoag, et al., op cit.
24 Hensley-Quinn, op cit.; National Academy for State Health Policy. 2012. South Carolina CHIP Fact Sheet.
http://nashp.org/sites/default/files/private/CHIP/2012/NASHP-2012-South-Carolina... Insure Kids Now. N.D. CHIPRA Performance Bonuses: A History. http://nashp.org/sites/default/files/private/CHIP/2012/NASHP-2012-South-Carolina-
CHIP-Fact-Sheet.pdf?q=files/CHIP/2012/NASHP-2012-South-Carolina-CHIP-Fact-Sheet.pdf.
25 Edwards, op cit.
26 Hoag, et al., op cit.
27 Edwards, op cit.
28 Hoag, op cit.
29 Esa Eslami, Joshua Leftin, and Mark Strayer. “Supplemental Nutrition Assistance Program Participation Rates: Fiscal Year 2010.” Mathematica Policy Research, Inc. December 2012.
http://www.fns.usda.gov/ora/menu/Published/snap/FILES/Participation/Tren....
30 See general discussion in Karen Cunnyngham, “Final Report.” State Trends in Supplemental Nutrition Assistance Program Eligibility and Participation Among Elderly Individuals. Sept. 28, 2010. Mathematica Policy Research, Inc. September 28, 2010. http://www.mathematica-mpr.com/publications/PDFs/nutrition/SNAP_elderly.pdf.
31 Food and Nutrition Service (FNS). “Combined Application Projects Guidance for States Developing Projects.”
March 2005. http://www.fns.usda.gov/snap/government/promising-practices/CAPsDevelopm...
32 Social Security Administration, Office of Retirement and Disability Policy. “The Food Stamp Program and Supplemental Security Income.” Social Security Bulletin Vol. 67 No. 4. 2007.
http://www.ssa.gov/policy/docs/ssb/v67n4/67n4p71.html
33 FNS. “Characteristics of Supplemental Nutrition Assistance Program Households: Fiscal Year 2011.” November 2012. http://www.fns.usda.gov/sites/default/files/private/2011Characteristics.pdf
34 FNS, 2013 Program Access Toolkit. March 2013.
35 Barbara Murphy. Combined Application Projects: An Analysis of their Impact on the Supplemental Nutrition Assistance Program. USDA Food and Nutrition Service, Sept. 2010 draft (Contract # AG‐3198‐D‐08‐0111).
36 FNS, March 2005.
37 Food Research and Action Center (FRAC). A Guide to the Supplemental Security Income/Food Stamp Program Combined Application Projects. January 2004.
38 Cunnyngham, Karen. “State Trends in Supplemental Nutrition Assistance Program Eligibility and Participation Among Elderly Individuals.” Mathematica Policy Research, Inc. September 28, 2010. http://www.mathematica-mpr.com/publications/PDFs/nutrition/SNAP_elderly.pdf
39 CAP states’ increase in participation levels among SSI recipients was apparently not a function of more general changes to their overall SNAP programs. Unlike in non-CAP programs, where the average participation level of SSI-recipient households, as a percentage of the total SNAP participation rate among all households, declined slightly from 2000 to 2008, it rose in CAP states by almost a third, from 45 to 58 percent. Murphy, op cit.
40 Murphy, op cit.
41 Murphy, op cit.
42 APHSA. Interoperable IT for Health and Human Service Programs. September 14, 2012.
43 FRAC, op cit.
44 FRAC, op cit.
45 APHSA 2014, op cit.
46 NASCIO Awards. 2011. Utah EREP: Enterprise Eligibility.
http://www.nascio.org/awards/nominations2011/2011/2011UT1-NASCIO%20eREP%....
47 Governing. 2010. Utah eREP: An Innovative and Cost-Effective Approach to Transform Social Services Delivery.
Webinar presented April 6. http://www.governing.com/events/webinars/Utah-eREP.html.
48 Erickson, Casey. 2012. Utah’s Eligibility System: Rebooting from the Ground Up. Presentation for the NASHP Annual State Health Policy Conference. Presented October 17. http://www.nashpconference.org/wp-content/uploads/2012/presentations/eri....
49 NASCIO, op cit.; Governing, op cit.; Erickson, op cit.
50 Governing, op cit.
51 Governing, op cit.; NASCIO, op cit.
52 Governing, op cit.; NASCIO, op cit.
53 Governing, op cit.
54 Governing, op cit.
55 Governing, op cit.; NASCIO, op cit.
56 Erickson, op cit.
57 Governing, op cit.
58 Governing, op cit.
59 Governing, op cit.
60 Manatt Health Solutions. Income Verification Product Evaluation. Memorandum to New York State Exchange Team, October 2011; Utah Department of Workforce Services. eFind. (undated)
http://www.insurekidsnow.gov/professionals/events/2011_conference/utah_d...
d_508.pdf.pdf.
61 Governing, op cit.
62 Governing, op cit.
63 Governing, op cit.
64 Erickson, op cit.
65 Megan Lape, APHSA, personal communication, 2013.
66 Governing, op cit.
67 Office of Governor Mark Dayton, “Governor Dayton Signs Executive Orders Implementing Medicaid Opt-In In First Act As Governor,” January 05, 2011, http://mn.gov/governor/newsroom/pressreleasedetail.jsp?id=102-9259.
68 Gibson, Karen. “Minnesota’s Early Medicaid Adult Expansion.” April 14, 2011.
http://www.shadac.org/files/shadac/publications/GibsonSlides_EarlyMedica.... The previous Legislature had authorized the Governor to take this action.
69 Kaiser Commission on Medicaid and the Uninsured, States Getting a Jump Start on Health Reform’s Medicaid Expansion, Apr 02, 2012, http://kff.org/health-reform/issue-brief/states-getting-a-jump-start-on-....
70 Goldrick-Rab, Sara, Katharine Broton, Christin Gates. 2013. Clearing the Path to a Brighter Future: Addressing Barriers to Community College Access and Success. University of Wisconsin. Prepared for the Association of Community College Trustees and Single Stop USA.
71 Kauff, Jacqueline, Emily Sama-Miller, Gretchen Rowe, Cicely Thomas, and Libby Makowsky. 2011. Promoting Public Benefits Access Through Web-Based Tools and Outreach. Final Report. Mathematica Policy Research.
72 Goldrick-Rab et al., op cit.
73 Kauff et al., op cit.; Goldrick-Rab et al., op cit.
74 U.S. Department of Education. Federal Pell Grant Program. http://www2.ed.gov/programs/fpg/index.html.
75 Goldrick-Rab et al., op cit.
76 Goldrick-Rab et al., op cit.
77 Goldrick-Rab et al., op cit.
78 Kauff, Jacqueline, Emily Sama-Miller, Gretchen Rowe, Cicely Thomas, and Libby Makowsky. 2011. Promoting Public Benefits Access Through Web-Based Tools and Outreach. Final Report. Mathematica Policy Research.
79 . During the average year in 2009-2011, 78.2 of all returns claiming EITC were filed by the end of the first calendar quarter. Authors’ calculation, IRS, Taxpayer Filing Attribute Report, op cit.
80 Diane Whitmore Schanzenbach. “Experimental Estimates of the Barriers to Food Stamp Enrollment.” Institute for Research on Poverty, Discussion Paper no. 1367-09. Sept. 2009.
81 Eric P. Bettinger, Bridget Terry Long, Philip Oreopoulos, and Lisa Sanbonmatsu, “The Role Of Simplification And Information In College Decisions: Results From The H&R Block FAFSA Experiment,” National Bureau of Economic Research Working Paper 15361 (September 2009). Bettinger and colleagues found that, among dependents, completing the form on behalf of the family raised the proportion submitting applications from 40.2 percent to 55.9 percent—a 40 percent relative increase. Among independent adults, the form completion intervention nearly tripled the likelihood of filing for student aid, raising the form submission rate from 13.8 percent to 39.5 percent.
82 Government Accountability Office, Medicare Savings Programs: Results of Social Security Administration’s 2002 Outreach to Low-Income Beneficiaries, GAO-04-363, March 2004. In the case of MSPs, sending notices increased the volume of phone calls, but few consumers managed to complete the enrollment process.
83 Brenda Freshour Johnston, Reaching Uninsured Children: Iowa’s Income Tax Return and CHIP Project, prepared by the Iowa Department of Human Services for the State Health Access Reform Evaluation project of the Robert Wood Johnson Foundation, with the State Health Access Data Assistance Center serving as national program office, August 2010.
84 John Guhl and Eliot Fishman, New Jersey Family Care: Express Lane Eligibility, State Coverage Initiatives Program National Conference, July 2009.
85 Hoag, et al., op cit.
86 Under the state’s prior approach, a family would check a box on the SNAP form to “opt out” of data sharing. The greatly reduced level of participation that resulted when the state changed from an “opt out” to an “opt in” approach is consistent with considerable behavioral research. See, e.g., Johnson, E.J., and D.G. Goldstein. “Defaults and Donation Decisions.” Transplantation. 78 (12): 1713-1716. December 27, 2004; Sunstein, C.R., and R. H. Thaler.
“Libertarian Paternalism is Not an Oxymoron.” The University of Chicago Law Review. 70 (4): 1159-1202. Fall 2003. Based on such research, the Centers for Disease Control and Prevention now recommend that, in almost all clinical settings, patients should be tested for HIV using “opt-out” regimens, through which they are tested unless they object. Branson BM, Handsfield HH, Lampe MA, Janssen RS, Taylor AW, Lyss SB, et al. “Revised recommendations for HIV testing of adults, adolescents, and pregnant women in health-care settings.” MMWR Recomm Rep. 2006;55(RR-14):1–17. See also Ari Bitnun, Susan M. King, Cheryl Arneson, Stanley E. Read. “Research Letter: Failure to prevent perinatal HIV infection.” CMAJ. 2002 April; 166(7): 904–905. Gayatri C.
Jayaraman, Jutta K. Preiksaitis, Bryce Larke. “Mandatory reporting of HIV infection and opt-out prenatal screening for HIV infection: effect on testing rates.” CMAJ. 2003 March; 168(6):679-82.
87 David Laibson, “Impatience and Savings,” National Bureau of Economic Research Reporter, Fall 2005, pp. 6-8.
88 James J. Choi, David Laibson, and Brigitte C. Madrian. $100 Bills on the Sidewalk: Suboptimal Investment in 401(K) Plans. NBER Working Paper 11554. August. 2005.
http://www.nber.org/papers/w11554.pdf?new_window=1.
