By: Mathematica Policy Research and The Cloudburst Group
Abstract
This study examined models of integration and coordination of housing assistance services and HIV care. The final report describes findings from a quantitative analysis of national HIV housing assistance data, and highlights from case studies conducted at four Integrated HIV/AIDS Housing Plan (IHHP) projects funded by the U.S. Department of Housing and Urban Development (HUD). Findings from this study offer insights about existing program models and the components that facilitate service integration to address both housing and health to improve outcomes among people living with HIV.
"executive summary
In the United States, it is estimated that more than 1.1 million people are infected with HIV/AIDS (Centers for Disease Control and Prevention [CDC] 2013). Data indicate that individuals with HIV infection suffer far greater housing instability and homelessness than the general population: an estimated one-third to one-half are homeless or at risk of becoming homeless (Rourke et al. 2010). People living with HIV/AIDS (PLWHA) who lack stable housing are more likely to delay entering HIV care and less likely to have access to regular care, to receive anti-retroviral therapy (ART), or to adhere to their HIV medication regimen (White House Office of National AIDS Policy 2010).
The two main sources of federal housing assistance targeted specifically to PLWHA are the Housing Opportunities for Persons With AIDS program (HOPWA), provided through the U.S. Department of Housing and Urban Development (HUD); and the Ryan White HIV/AIDS Program (RWP), provided through the Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS). HOPWA’s primary focus is on providing housing assistance and related support services to PLWHA and their families. RWP’s is to provide HIV treatment and care: grantees can spend only a portion of funds on support services (of which housing assistance is one type).
In 2010, the Obama administration created the country’s first National HIV/AIDS Strategy (NHAS), designed to reduce the number of new HIV infections, increase access to HIV care, optimize health outcomes for PLWHA, and reduce related disparities (White House Office of National AIDS Policy 2010). Recognizing the role of housing in the HIV epidemic, the NHAS identified ways to increase federal HIV housing supports. To address the NHAS goal of greater access to HIV care, in 2011, the HUD Office of HIV/AIDS Housing awarded seven competitive Integrated HIV/AIDS Housing Plan (IHHP) grants that were designed to integrate housing assistance with HIV care and other supports at the individual service and community planning levels.
In 2012, the HHS Office of the Assistant Secretary for Planning and Evaluation (ASPE) contracted with the Mathematica Policy Research/Cloudburst team to analyze current federal HIV housing assistance services and study best practices integrating HIV housing and health care services. This project includes a quantitative study of the costs, utilization, and outcomes of current federal HIV housing assistance services and a qualitative study of innovative IHHP programs integrating housing assistance with HIV care.
The quantitative analysis includes significant findings: (1) a direct comparison of 2010 HOPWA and RWP data; (2) a housing assistance analysis of 2010 RWP Services Report (RSR) data, (3) a feasibility assessment of a correlational study of HOPWA and RWP housing assistance and outcomes, and (4) national, state-level, and time trend analyses. The qualitative analysis documents key features of four IHHP sites, including their site characteristics, program models, and integration of HIV housing, health care, and other supports. These IHHP grants are unique in their efforts to integrate housing and HIV care at three levels: individual client services, organizational data systems, and community-level planning processes.
A. HIV Housing Analysis Findings
- The reported number of PLWHA in the United States in 2010 was 888,904.1 Almost 1 in 10 (81,100) were receiving HOPWA and/or RWP housing assistance.
- Because HOPWA and RWP serve different purposes, the proportion of funding targeted toward housing assistance was very different. Whereas two-thirds (67%) of HOPWA’s funding was used for housing assistance in 2010, a total of 3.2 percent of RWP funding was used for housing assistance.
- In general, the characteristics of participants served were similar across the two programs. HOPWA participants (which include family members) tended to be younger because HOPWA serves more families with children than RWP.
- In both programs, the majority of participants served were within the lowest poverty category (at or below 100% federal poverty level [FPL] for RWP and up to 30 percent of Area Median Income for HOPWA).
- Because HOPWA and RWP collect housing status data at different points of enrollment, it is not possible to compare housing status across the two programs prior to program entry. However, HOPWA reported that 13 percent of participants were homeless at entry.
- Although RWP housing status is measured “at the end of the reporting period” and not at program entry or exit, among RWP Clients receiving housing assistance, about one quarter (24%) were “temporarily or unstably housed,” compared to 14 percent that were not receiving RWP-funded housing assistance.
- Of the RWP clients receiving housing assistance, 5 percent were still “unstably housed” at the end of the reporting period. This emphasizes the importance of connecting RWP clients to long-term or permanent housing assistance through HOPWA, homeless Continuum of Care (CoC), or other mainstream public housing programs.
1 The reported number of PLWHA differs from the 1.1 million estimate of the total number of people in the U.S. with HIV/AIDS due to the status of names-based HIV surveillance systems in 2010.
B. HIV Housing Integration Study Findings
- The project studied four IHHP sites representing a range of service models and approaches: (1) the River Region Human Services (RRHS) FUSE project in Jacksonville, Florida; (2) the Frannie Peabody Center (FPC) statewide Maine IHHP project; (3) the Portland (Oregon) Housing Bureau (PHB) S4H project; and (4) the Albany Corporation for AIDS Research, Education, and Services (CARES) Foundations for Living (FFL) project in upstate New York.
- The four IHHP sites in this study have extensive experience providing HIV housing assistance and support services in collaboration with local partners. They have also been involved in community-level planning of homeless services through their participation and leadership of CoC planning processes and in RWP planning councils, task forces, and provider networks.
- The IHHP program models show a gradient of service integration (from most to least): (1) all four sites provide direct housing assistance; (2) all four sites fund “housing coordinator” positions; two sites contract them out; (3) two sites fund “employment coordinator” positions; both sites contract them out; and (4) no sites fund medical case management directly; all four sites collaborate with medical case managers funded by RWP.
- Program components that facilitate service integration include (1) in-depth screening of clients’ housing, health care, and other support service needs at intake; (2) development of individualized care plans for program clients tailored to their needs and circumstances; and (3) frequent in-person contact between housing coordinators, peer specialists, and clients and their medical providers and medical case managers.
- Two IHHP sites are also participating in a HRSA Special Project of National Significance addressing the coordination of housing and HIV care. In those medical home-focused programs, the sites are working with clients who are more medically needy and less likely than IHHP clients to become employed and mainstreamed into public housing.
- Recent funding restrictions at the federal, state, and local levels are limiting the grantees’ ability to fully realize their IHHP goals. Additional concerns include (1) the lack of affordable housing available; (2) uncertainty about the potential impact of the Affordable Care Act on RWP-funded services, notably medical case management; and (3) the need for HIV service providers to shift from simply securing HIV-specific benefits for their clients to helping clients move into mainstream housing and employment.
- Neither HUD’s Homeless Management Information System (HMIS) nor HRSA’s CAREWare data system has the comprehensive set of housing and health care data needed to evaluate the effectiveness of the IHHP grantees’ programs. All four sites are working on data system integration to address this problem.
- The IHHP grantees plan to bring together groups from public housing, homeless (CoC) grantees and service providers, city planning, RWP grantees, and AIDS service organizations to create community-wide IHHP plans, but note two challenges: (1) CoC and RWP grantees do not typically have a history of working together, and (2) some worried that HOPWA programs were historically marginalized in both CoC and RWP planning processes.
C. Opportunities for Improvement
This section offers ideas for how the service integration and data management of integrated housing and HIV care programs can be improved through further study and policy development.
- The IHHP sites should be revisited at the end of their grant cycle to see how they were able to develop an integrated planning process at the community level and what they have accomplished in terms of creating more integrated data systems.
- The potential impact of the Affordable Care Act on the linkage between HOPWA housing assistance and RWP case management programs could be significant. Monitoring and researching as Affordable Care Act coverage expansions are implemented in 2014 and beyond is warranted.
- The three-way model of housing assistance, employment services, and HIV care integration should be studied in more detail, and the model’s effectiveness evaluated as an alternate model of service integration.
- New demonstration projects pooling HOPWA and RWP resources into one integrated HIV housing and care program should be considered and researched as an alternate model bundling housing with health care.
- Adding client-level variables that are common to both HOPWA and RWP data systems, including variables that capture the assistance received from both programs, would allow better linkage of the programs’ databases and facilitate research examining the services received and resulting outcomes for participants served by both programs.
- Increased understanding of the differences between PLWHA who receive housing assistance and those who do not could help to inform and improve housing practices addressing the unique needs of these subgroups. It may also be valuable to explore state-level program differences in greater detail.
- The creation of new integrated CoC intake systems might involve developing new linkages among HMIS, CAREWare, and electronic health record data systems. This development should be monitored and studied to see what new data system forms result.
I. Introduction
In the United States, it is estimated that more than 1.1 million people are infected with HIV/AIDS (Centers for Disease Control and Prevention [CDC] 2013). Data indicate that individuals with HIV infection suffer far greater housing instability and homelessness than the general population: an estimated one-third to one-half are homeless or at risk of becoming homeless (Rourke et al. 2010). Homelessness and unstable housing are linked to higher risk of HIV infection, inadequate health care, poor health outcomes, and early death (National AIDS Housing Coalition 2007). People living with HIV/AIDS (PLWHA) who lack stable housing are more likely to delay entering HIV care and less likely to have access to regular care, to receive anti-retroviral therapy (ART), or to adhere to their HIV medication regimen (White House Office of National AIDS Policy 2010).
Unable to afford housing, some PLWHA turn to federal HIV programs for assistance. The two main sources of federal housing assistance targeted specifically for PLWHA are the Housing Opportunities for Persons With AIDS program (HOPWA), provided through the U.S. Department of Housing and Urban Development (HUD), and the Ryan White HIV/AIDS Program (RWP), provided through the Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS).
In 2010, the Obama administration created a National HIV/AIDS Strategy (NHAS), designed to reduce the number of new HIV infections, increase access to HIV care, optimize health outcomes for PLWHA, and reduce related disparities (White House Office of National AIDS Policy 2010). Recognizing the role of housing in the HIV epidemic, NHAS identified ways to increase federal HIV housing supports. HHS, designated as the lead agency for implementing federal activities under the NHAS, is responsible for monitoring national progress toward meeting its goals. To address the NHAS goal of greater access to HIV care, in 2011, the HUD Office of HIV/AIDS Housing awarded seven competitive Integrated HIV/AIDS Housing Plan (IHHP) grants that were designed to integrate housing assistance with HIV care and other supports at the individual-service and community planning levels.
In 2012, the HHS Office of the Assistant Secretary for Planning and Evaluation (ASPE) contracted with the Mathematica Policy Research/Cloudburst team to analyze current federal HIV housing assistance services and study best practices integrating HIV housing and health care services. This project includes a quantitative study of the costs, utilization, and outcomes of current federal HIV housing assistance, as well as a qualitative study of innovative HUD program models integrating housing assistance with HIV care. The overall goals of the project are (1) to review the current status of HIV housing programs; and (2) to document innovative, replicable program models integrating housing assistance with HIV health care.
A. Purpose of the Report
The purpose of this report is to present the findings from the project’s quantitative analysis of federal HIV housing programs and qualitative study of a set of IHHP grantees. The report aims to answer the following questions for each component:
Quantitative HIV Housing Analysis Research Questions:
- What is the prevalence and incidence of HIV/AIDS in the United States?
- What proportion of the HIV/AIDS population receives federal HIV housing assistance?
- What is the level of funding for federal HIV housing assistance?
- What federal HIV housing assistance services are provided?
- What are the characteristics of participants in federal HIV housing programs?
- What are the outcomes of federal HIV housing assistance programs?
- Can available federal data support an analysis of the association between housing assistance, enhanced housing status, increased access and retention in HIV care, and improved clinical outcomes?
Qualitative Study of Integrated HIV Housing Research Questions:
- What are best practices among HOPWA’s integrated HIV housing programs?
- How do these program models integrate housing and HIV care at the individual service, organizational data management, and community planning levels?
- How do these programs identify and enroll eligible people, assess their service needs, and integrate housing, HIV care, and other supports?
- How do these programs link housing and health care data in their organizational data systems?
- How is the planning and coordination of housing, HIV care, and other support services integrated at the community level?
- What approaches promote or hinder the integration of housing, HIV care, and other support services?
B. Information Sources and Study Methods
The quantitative study analyzed HUD and HRSA administrative data from HOPWA and RWP. In addition, the team obtained publicly available HIV surveillance data from the CDC and homeless services needs assessment and service data from the HUD Office of Special Needs Assistance Programs. The study team finalized a statistical analysis plan based on the study objectives and on the aggregate nature of the data available, and conducted descriptive analyses of each of the variables of interest and compiled state and national summaries. The team also compared HOPWA and RWP services (such as relative percentages of participants served by type of housing assistance, income level, or demographics). For HOPWA data, the average cost per person served by specific type of housing was also calculated. The analysis drew on information from multiple sources (See Appendix A for details):
- HOPWA Consolidated Annual Performance Evaluation Reports (CAPER) (2007-2010)
- HOPWA Annual Performance Reports (APR) (2007-2010)
- 2010 Annual Homeless Assessment Report (AHAR)
- Homeless Management Information System (HMIS) (2010)
- Ryan White Program Expenditure Reports (2007-2010)
- Ryan White Program Data Reports (RDR) (2007-2010)
- Ryan White Services Report (RSR) (2010)
The qualitative study selected program models drawn from HUD’s seven IHHP grantees in 2011. In May 2013, Mathematica and Cloudburst conducted in-person site visits to four of the seven sites: (1) the River Region Human Services (RRHS) FUSE project in Jacksonville, Florida; (2) the Frannie Peabody Center (FPC) statewide IHHP project; (3) the Portland (Oregon) Housing Bureau (PHB) S4H project; and (4) the Albany Corporation for AIDS Research, Education, and Services (CARES) Foundations for Living (FFL) project in upstate New York. The one-day in-person visits at each site included discussions with IHHP grantees, community partners, and RWP grantees and service providers. Interviews were conducted with IHHP grant administrators, local housing program directors, IHHP housing coordinators, RWP-funded medical case managers, local IHHP grant evaluators and data systems managers, and other local housing agencies involved in planning community-level housing. Appendix L contains the study’s site visit interview protocols.
The study collected information from the four IHHP grantees about three levels of activity: (1) the integration of program policies and practices at the client level; (2) efforts to integrate housing and health care data systems; and (3) community-level efforts to coordinate and align HIV housing, health care, and other support services. Site profiles were created using information gathered during the discussions and based on review of program documents, including grant applications, site reports, and APR data. The site profiles were systematically coded and analyzed to address the study’s research questions. The project also used a mixed-methods approach to integrate the quantitative and qualitative studies and findings. Early findings from the quantitative analysis were used to inform the selection of the four sites for the IHHP case studies and to inform site visit topics and questions. For example, in the site visits, we asked questions about the compatibility of the HOPWA and RWP data sets, based on challenges encountered in the quantitative analysis.
C. Organization of this Report
The rest of this report comprises three chapters. Chapter II presents the findings from the quantitative analysis, providing an overview of the HIV/AIDS epidemic and key features of HOPWA and RWP, including their funding, service utilization, and participant characteristics and outcomes. Chapter III presents the findings from the qualitative study, comparing the integration of housing and HIV care in four IHHP site program models, and focusing on their client services, data systems, and community planning processes. Chapter IV offers ideas for improving the integration of federal housing, HIV care, and other support services for PLWHA.
II. hiv housing Analysis
A quantitative analysis of federal housing assistance program data was conducted to understand and compare the scope of HIV housing assistance services funded by HOPWA and RWP, including the volume and types of services provided and the characteristics of the people receiving the assistance. The analysis also sought to compare the housing status and health outcomes of people who received housing assistance to those of people who did not. An additional goal was to explore the feasibility of conducting a correlational study of the relationship between individual housing assistance and health and housing outcomes.
The findings are significant in several ways. First, the analysis provides a direct comparison of 2010 program data available from HOPWA and RWP. Second, it provides the first public reporting of RSR housing assistance analyses. Third, it assesses the feasibility of conducting correlational studies of housing assistance and outcomes using HOPWA and RWP data. Last, where possible, findings are reported at both state and national levels to aid federal housing assistance planning and development.
A. Overview of HIV/AIDS Housing Assistance
Although HOPWA and RWP both provide housing assistance and support services to PLWHA, their missions differ. RWP’s overall goal is to provide HIV care and related services to people who are without sufficient health care coverage or the financial resources to cope with the disease on their own (U.S. Department of Health and Human Services, HIV/AIDS Bureau [HAB] 2013). Although RWP provides housing assistance as part of its portfolio of support services, current law requires that most RWP funds are used for core medical services, including outpatient ambulatory medical care, prescription HIV medications, and oral health care. In contrast, HOPWA is the only federal program dedicated to addressing the housing needs of PLWHA and their families (HUD 2013). Most, but not all, HOPWA funds are spent on housing assistance. The differences in the programs’ services are detailed below.
1. RWP Housing Assistance
RWP funds a range of medical and support services. The program’s core medical services encompass outpatient ambulatory health care, oral health care, early intervention services, home health care, home and community-based health services, hospice care, mental health services, medical nutrition therapy, medical case management, outpatient substance abuse services, health insurance premium and cost-sharing assistance, prescription medications, and local pharmaceutical assistance. RWP-funded support services include nonmedical case management, food bank/home delivered meals, health education/risk reduction, transportation services, psychosocial support, child care, pediatric development assessment, emergency financial assistance, housing services, legal services, linguistic services, outreach services, permanency services, rehabilitation services, respite services, residential substance abuse services, and treatment adherence counseling (HAB 2013). Under the Ryan White HIV/AIDS Treatment Extension Act of 2009, RWP Part A, B, and C grantees are required to expend at least 75 percent of their grant on core medical services, including anti-retroviral drugs (Federal Register 2013). The other 25 percent can be used to pay for support services, including housing assistance.
RWP-funded housing assistance provides short-term aid to support emergency, temporary, or transitional housing so that an individual or a family can gain or maintain health care. However, RWP housing funds cannot include direct cash transfers to recipients of services and cannot be used for mortgage payments. In addition, the housing assistance cannot be permanent and must be accompanied by a strategy to transition the individual or family to long-term, stable housing.2 The program can also fund housing referral services, including housing assessment, search, placement, advocacy services, and associated housing fees. RWP-funded housing may include housing with medical or support services (such as for residential treatment of substance abuse). RWP also funds Emergency Financial Assistance (EFA), which can provide one-time or short-term payments for emergency expenses related to utilities, housing, food, transportation, and medication. EFA was not included in these analyses, because it was not possible to separate out EFA expenditures and services from other types of financial assistance.
2 2012 Annual Ryan White HIV/AIDS Program Services Report Instruction Manual. Available at [http://hab.hrsa.gov/Manageyourgrant/Files/Rsrmanual.pdf].
2. HOPWA Housing Services
HOPWA also funds both housing and support services. Housing services include the acquisition, rehabilitation, or new construction of housing units; costs for facility operations; rental assistance; and short-term payments to prevent homelessness. HOPWA may also fund health care and mental health services, chemical dependency treatment, nutritional services, case management, assistance with daily living, and other support services. The HOPWA housing service categories used in this analysis include tenant-based rental assistance (TBRA); permanent housing facilities; transitional/short-term housing facilities; and short-term rent, mortgage, and utility (STRMU) assistance. Within HOPWA, the following housing-related services are eligible3:
- TBRA: This rental subsidy program helps low-income households gain access to affordable housing. TBRA vouchers are not tied to specific units, so tenants can move to a different unit without losing their assistance.
- Permanent Housing Facilities
- Operating subsidies pay for facility-based permanent housing expenses, including utilities, maintenance, equipment, insurance, security, furnishings, supplies, and salary for housing project (but not service delivery) staff.
- The program pays for the cost of leasing permanent housing units (scattered sites or entire buildings) that a nonprofit or public agency leases from a landlord and then subleases to program participants.
- HOPWA also pays for capital development projects, specifically for the acquisition, conversion, lease, repair, and rehabilitation of permanent housing facilities and the construction of Single Room Occupancy facilities and community residences dedicated to PLWHA.
- Transitional/Short-Term Facilities (Short-Term): This category includes short term supported housing facilities and transitional housing support that may also include provision of supportive services as part of an individualized plan to guide the client’s linkage to permanent housing.
- STRMU Assistance: This time-limited housing subsidy provides short-term payment of rental costs, mortgage payments, or utilities; designed to prevent homelessness and increase housing stability. Assistance can be provided for up to 21 weeks in any 52-week period.
HOPWA also funds Permanent Housing Placement services which are used to establish a household in a housing unit. However, Housing Placement service data were not included in these analyses because it was not possible to de-duplicate the number of households that received housing assistance services from the number of households that received housing placement services.
3 HOPWA Program: Consolidated Annual Performance and Evaluation Report. Available at [https://www.onecpd.info/resource/1011/hopwa-caper-form-hud-40110-d].
B. Prevalence and Incidence of HIV/AIDS
As mentioned in Chapter I, the number of PLWHA in the United States has grown steadily, from 188,968 in 19934> to more than 1.1 million in 2013, as more people with the disease live longer, while the number of new infections remains steady, at about 50,000 per year (Centers for Disease Control and Prevention [CDC] 1993 & 2013). CDC’s National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention (NCHHSTP) collects and compiles surveillance data for 55 states and territories (NCHHSTP 2013).5 This data-set provides a national picture of HIV/AIDS prevalence and incidence.6 Since 2008, the national incidence of new HIV diagnoses has decreased slightly, but the national prevalence of PLWHA has increased (Figure II.1).
Figure II.1. United States HIV/AIDS Prevalence and Incidence (per 100,000 population)
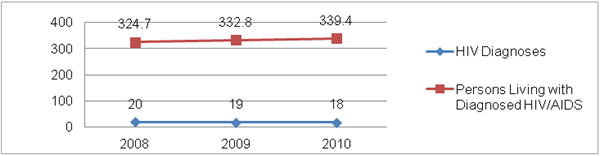
Source: CDC NCHHSTP Atlas [http://www.cdc.gov/nchhstp/atlas].
The most recent (2010) data from CDC show that the states with the most PLWHA aged 13 and older were New York (132,523), California (111,666), and Florida (94,897) (Appendix B). Most PLWHA are concentrated in a few states; two-thirds reside in just 10 states. In 2010, Washington, D.C., had both the highest prevalence of HIV/AIDS and the highest incidence of HIV diagnoses. Other states and territories have a high prevalence of HIV/AIDS (Florida, Maryland, New York) and an incidence of HIV diagnoses substantially above the national average – although well below the incidence of Washington, D.C. (Florida, Louisiana, Maryland, Virgin Islands; Table II.1).
Table II.1. States and Territories with Highest Incidence and Prevalence of HIV/AIDS, 2010
| States with Highest Incidence | Rate of HIV Diagnoses | States with Highest Prevalence | Rate of Persons Living with Diagnosed HIV/AIDS |
|---|---|---|---|
| District of Columbia | 172.8 | District of Columbia | 2,704.3 |
| Maryland | 38.3 | New York | 810.0 |
| U.S. Virgin Islands | 35.8 | U.S. Virgin Islands | 667.1 |
| Louisiana | 31.3 | Maryland | 632.9 |
| Florida | 30.5 | Florida | 592.7 |
Source: CDC NCHHSTP Atlas [http://www.cdc.gov/nchhstp/atlas]. Rates are per 100,000 people.
4 HIV/AIDS Surveillance Report from [http://www.cdc.gov/hiv/pdf/statistics_hivsur54.pdf].
5 NCHHSTP Atlas. Retrieved on March 7, 2013, from [http://www.cdc.gov/nchhstp/atlas/].
6 Data not available for 2007.
C. Proportion of HIV/AIDS Population Receiving Housing Assistance
Surveillance reports indicate there were 888,904 PLWHA in the United States in 2010. Of that total, we calculated that almost 1 in 10 (81,100) were receiving HOPWA or RWP housing assistance.7, 8 However, this assumes that no individual received housing services from both HOPWA and RWP in the same year; as a result the total number served is not unduplicated and may be overstated. The proportion of PLWHA receiving HOPWA or RWP housing services varied significantly by state.9 In Maine, for example, more than 40 percent of PLWHA received federal housing assistance in 2010, but in Arkansas, Kansas, New Jersey, and Virginia, 5 percent or less received housing assistance (see Appendix B).
People who are homeless in the United States have a higher rate of HIV/AIDS than the general population. According to HUD’s Annual Homeless Assessment Report (AHAR), on a single night in January 2010, 3.9 percent of the adult sheltered homeless population self-reported living with HIV/AIDS, roughly 10 times the percentage of the adult general population living with HIV/AIDS (about 0.37 percent).10 In addition to the 81,100 persons receiving housing services funded by HOPWA or RWP in 2010, an estimated 13,940 homeless people with HIV/AIDS and their families received Permanent Supportive Housing (PSH) services through HUD’s Continuum of Care (CoC) grant program (U.S. Department of Housing and Urban Development, 2010 Annual Homeless Assessment Report to Congress.).11 These Permanent Supportive Housing services are funded through the Shelter Plus Care (S+C) program and the Supportive Housing Program (SHP) under the CoC program. The CoC program is now a single grant program that includes the Supportive Housing program, the Shelter Plus Care program, and the Moderate Rehabilitation/Single Room Occupancy (SRO) program.12
Unfortunately, it is impossible to determine exactly how many PLWHA currently need housing assistance. HOPWA grantees provide an annual estimate of unmet housing needs, but they do not use a standard method for making their calculations.[13] In 2010, HOPWA grantees estimated that 191,809 HOPWA-eligible households had some form of unmet housing need at some point during the year.
7 The number 888,904 does not include American Samoa (2 people) or the Northern Mariana Islands (14).
8 Comprises 62,297 HIV-positive participants served by HOPWA and 18,803 served by RWP (3,049 of the 18,803 RWP participants had a “missing” or “unknown” HIV status).
9 State numbers reported are from the RWP Data Report (versus the RWP Services Report), which are not unduplicated across providers.
10 CDC. “Monitoring Selected National HIV Prevention and Care Objectives by Using HIV Surveillance Data—United States and 6 U.S.-Dependent Areas—2010.” HIV Surveillance Supplemental Report 2012; June 2012. Available at [http://www.cdc.gov/hiv/pdf/statistics_2010_HIV_Surveillance_Report_vol_17_no_3.pdf]. Percentage calculated using 2010 Census Data for total U.S. population in 2010 (308,745,538). Annual data for the percentage of PLWHA who are homeless are not available.
11 Permanent Supportive Housing funding is provided through the CoC Grant program via Shelter Plus Care (S+C) or the Supportive Housing Program (SHP).
12 These programs were consolidated under the HEARTH Act of 2009. The HEARTH Act was enacted after the 2010 AHAR was produced.
13 For HUD Consolidated Annual Performance Evaluation Report reporting methods, see [https://www.onecpd.info/resource/1011/hopwa-caper-form-hud-40110-d].
D. HOPWA and RWP Housing Expenditures
Unlike HOPWA, which focuses primarily on housing, most RWP funds are allocated to core medical services as required by law. In 2010, only 3.2 percent of total RWP Part A and Part B funds were spent on housing assistance. In contrast, two-thirds (67 percent) of HOPWA’s 2010 expenditures were allocated to housing (Figure II.2). In total housing program expenditures, in 2010, RWP’s Part A grants (to metropolitan areas) and Part B grants (to states) spent a total of $27,541,664 on housing assistance, compared to the $211,114,260 spent on housing services through HOPWA’s formula and competitive grants (Appendices C and D). While HOPWA’s housing assistance expenditures rose substantially between 2007 and 2010, RWP expenditures for housing services remained relatively constant over the same period (Figure II.3).
RWP housing program allocations vary across states. Eighteen states and territories that received Part A or B grant funding in 2010 spent nothing on housing assistance, while another six spent less than 0.5 percent of their funding on housing services (Appendix C).14 Only the Part A grantees in Massachusetts and Oregon spent 10 percent or more of their Part A grant on housing assistance. The states with the greatest share of Part B housing expenditures were Hawaii and Nebraska, which spent 19 and 13 percent of their Part B grants, respectively, on housing services. RWP housing policy limits the use of funding to short-term and emergency housing assistance. Due to the statutory limitation on RWP grantees’ spending on non-medical support services such as housing assistance, it is difficult to draw conclusions from these spending data about the actual level of need that exists.
Figure II.2. Distribution of HOPWA and RWP Expenditures in 2010
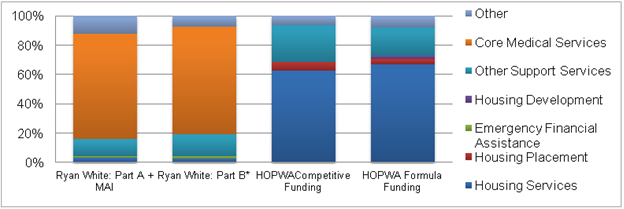
Source: HRSA Ryan White Expenditure Reports, Part A and Part B, 2010; HUD HOPWA formula grant Consolidated Annual Performance Evaluation Report (CAPER) and HUD HOPWA competitive grant Annual Performance Report (APR), 2010.
MAI = Minority AIDS Initiative.
* Part B includes only Consortia, State Direct Services, and Emerging Communities Expenditures.
HOPWA formula funds are awarded to eligible cities on behalf of their metropolitan areas and to eligible States. Under current law, to be eligible for awards, states must have more than 1,500 cumulative AIDS cases outside of eligible metropolitan statistical areas.15 The proportion of total HOPWA funds spent on housing services varied by state. Of the states with entitlement grant expenditures (reported through CAPER), 12 spent three-fourths (75 percent) or more of their reported total expenditures in 2010 on housing services, and 7 that received formula funding spent 44 percent or less of their grant on housing services. Of the states with competitive grant expenditures in 2010 (reported through APR), six spent three-fourths (75 percent) or more of their total expenditures on housing services, and four others spent 44 percent or less (Appendix C). States’ combined formula and competitive spending on housing services ranged from 8.6 to 56.2 percent of their total funds.16
In 2010, of the two-thirds of HOPWA funds that were spent on housing assistance, more than half (51 percent) were spent on TBRA (Figure II.4). Of the total HOPWA housing funds, one quarter (26 percent) was spent on permanent housing facilities. HOPWA housing assistance resources (including capital, leasing, and operating resources, permanent and transitional project-based assistance, and TBRA assistance) often leverage RWP resources for case management at the project level, allowing HOPWA resources to be focused on providing housing assistance.
Figure II.3. HOPWA and RWP Housing Assistance Expenditures
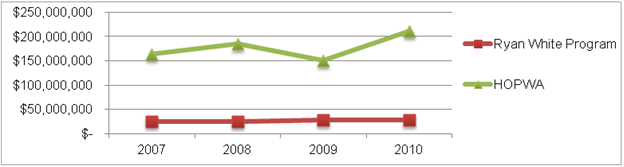
Source: HRSA Ryan White Expenditure Reports, 2007–2010; HUD HOPWA CAPER and APR data, 2007–2010.
Housing assistance services vary by cost, duration, and intensity; some are more short-term or temporary than others. Among the primary types of HOPWA housing (TBRA, PSH, short-term, and STRMU), the average cost of housing a family in permanent facilities with operating subsidies or leased units is comparatively high. In 2010, in housing facilities with operating subsidies or leased units, average permanent assistance costs per household were more than twice the average cost per household in transitional/short-term housing facilities (in part because the two programs cover different activities). Permanent housing facilities assistance also cost 30 percent more, on average, per household than TBRA. In contrast, STRMU assistance costs were far less per household: three to seven times less than other types of HOPWA housing assistance (Table II.2 and Appendix E).
Table II.2. Average Annual Cost per Household, by Type of HOPWA Housing Service
| HOPWA TBRA | HOPWA Permanent Housing Facilities | HOPWA Transitional/ Short-Term Facilities | HOPWA STRMU |
|---|---|---|---|
$5,584 | $7,303 | $3,255 | $930 |
Source: HUD HOPWA CAPER and APR data, 2010.
Figure II.4. Percentage of HOPWA Housing Expenditures, by Type
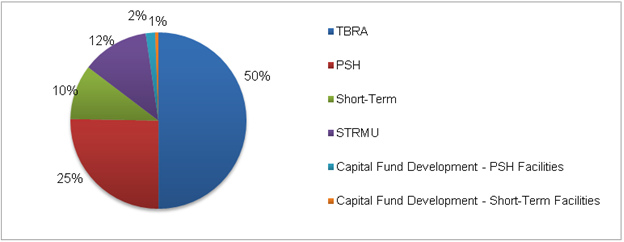
Source: HUD HOPWA CAPER and APR data, 2010.
14 Percentage expenditures were rounded to the nearest whole number, so this total includes states that spent less than 0.5 percent of their funds on housing.
15 Although HOPWA funds are awarded only to states, for the purposes of this report, the funds were aggregated at the state and national levels for comparison purposes.
16 Guam has 0 percent but received only $78,927 total funds. South Dakota has 0 percent, and North Dakota has 1 percent; however, this is because their data are reported under Montana. Montana has a percentage of 60.68, but that includes North and South Dakota and thus is inflated.
E. Housing Assistance Services
1. Services Provided
RWP is the largest federal program targeting core medical and support services specifically to PLWHA and their families. According to RDR, in 2010, RWP provided services to 556,175 people (including HIV-negative family members), of which 18,904 received housing assistance (Appendix A and Appendix F).17
Relatively few (3.4 percent) RWP clients received RWP-funded housing assistance in 2010.18 This proportion remained fairly steady between 2007 and 2010, with no significant change in the percentage of HIV-positive/indeterminate clients receiving housing assistance.19 In contrast, 57 percent of all RWP clients received outpatient ambulatory medical care, and 53 percent received medical case management services (Figure II.5). About 6 percent of RWP clients received some type of emergency financial assistance, which in some cases may have been used for short-term housing-related costs such as rent or utilities. Note that some unknown percentage of clients served by RWP also received housing assistance through HOPWA.
Figure II.5. Number of Ryan White Program Clients Served, by Type of Selected Service
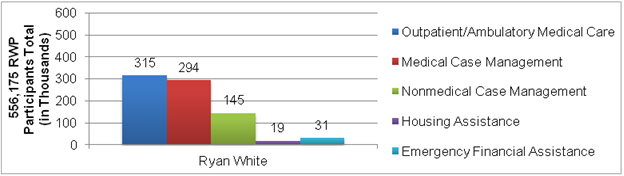
Source: HRSA Ryan White Program Services Report, 2010.
In 2010, HOPWA provided housing assistance to 61,268 households.20 There is no unduplicated count of the total number of HOPWA households who received assistance other than housing. Figure II.6 illustrates that of the 61,268 HOPWA households that received housing assistance in 2010, most (45 percent) received STRMU, the least expensive form of assistance (Table II.2), and 31 percent received TBRA, which makes up the largest percentage of HOPWA housing expenditures (Figure II.6).
Figure II.6. Distribution of HOPWA Housing Assistance Households, by Type of Assistance
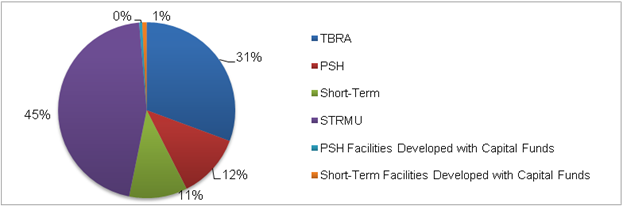
Source: HUD HOPWA CAPER and APR data, 2010.
17 This does not include households receiving Emergency Financial Assistance provided for housing-related costs. Housing services specifically include short-term emergency, temporary, and transitional housing assistance services to help participants access or remain in medical care, and housing referral services, including housing assessment, search, placement, and advocacy services, plus associated housing fees.
18 No more than 25 percent of Ryan White Funds can be used for support services, which include housing. There is an option for grantees to apply for a waiver of this spending requirement.
19 Comparison of 2007-2010 data was done using RDR data, which is not unduplicated across programs.
20 This does not include households receiving housing placement services.
2. Participant Demographics
In 2010, HOPWA and RWP clients receiving housing services were similar in gender, race, and ethnicity. Both groups were predominantly male, and half (50 percent) were African American (Appendices G and H). HOPWA participants tended to be younger than RWP clients; 19 percent of HOPWA participants were under age 18, and only 2 percent of RWP clients receiving housing were under age 20 (Appendix G).21 The demographics of RWP clients receiving housing assistance compared to those not receiving it were similar, with participants who did not receive it being slightly younger (35 percent under age 40 versus 28 percent).
Although income categories reported by the two programs are not the same, it is possible to compare the proportion of RWP clients and HOPWA households in the lowest income categories (Figures II.7 and II.8). Sixty-four percent of RWP clients receiving housing assistance were at or below 100 percent of FPL, compared to 74 percent of the HOPWA households who were below 30 percent of their area’s median income (AMI).22 This was slightly higher than the percentage of RWP clients not receiving housing (55 percent) who were at or below 100 percent of FPL.[23]
Figure II.7. Area Median Income of HOPWA Households
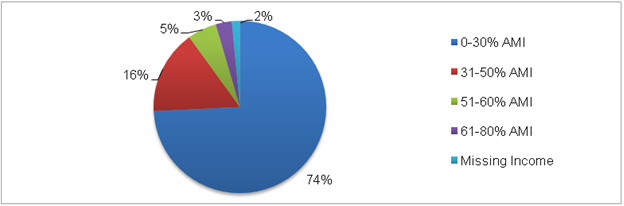
Source: HUD HOPWA CAPER and APR data, 2010.
Figure II.8. Percentage of Federal Poverty Level: RWP Clients
Source: HRSA Ryan White Program Services Report, 2010.
The proportion of HOPWA households and RWP HIV-positive/indeterminate clients served at the lowest income category differed across the states and between the two programs. The percentage of HOPWA households with incomes up to 30 percent of AMI varied from 15 percent (North Carolina) to 99 percent (District of Columbia). Nine states served more than 90 percent of all HOPWA households with incomes up to 30 percent AMI (Appendix I). The percentage of RWP HIV-positive/indeterminate clients at or below 100 percent of FPL ranged from 26 percent (in the Virgin Islands) to 83 percent (in Puerto Rico) (Appendix I).24
22 The poverty guidelines are established annually by HHS and are used as an eligibility criterion for many federal programs. The poverty level issued by HHS is based on the poverty thresholds used by the Census Bureau and is adjusted annually on the basis of the Consumer Price Index for All Urban Consumers (CPI-U). AMI is calculated by dividing the income distribution in the area into two groups, half having income above that amount, and half having income below it.
23 240,722 participants were at or below 100 percent of FPL, of 437,010 who did not receive a housing service and who reported income based on Ryan White Program Services Report Data, 2010.
24 State numbers reported are from the RWP Data Report (versus the RWP Services Report) and are not unduplicated across providers.
3. Participant Housing Status
Unfortunately, the analysis was not able to compare the two programs on the housing status of participants, because each program captures this differently. HOPWA reports on the prior living arrangements of HOPWA-eligible housing participants entering the program during the reporting year, and RWP reports on the housing/living arrangements of clients receiving services as of the end of the reporting period. In addition, HOPWA collects information on a wide range of prior living arrangements, whereas RWP classifies living arrangements as “stable/permanent,” “temporary, unstable,” or “unknown,” It is also challenging to make comparisons between the RWP categories of “temporary” and “unstable” and the HOPWA category of “homeless.” Therefore, we report housing status separately for the two programs.
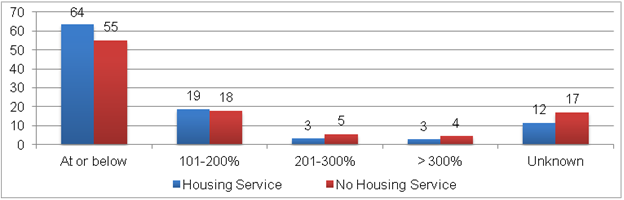
Housing Status of RWP Clients: Among RWP clients that did not receive housing assistance, relatively few (about 3 percent) reported their housing as “unstable” at the end of 2010 (Figure II.9).25, 26 This percentage was slightly higher when looking only at RWP clients who received a housing service (5 percent). In addition, 19 percent of clients receiving a housing service reported their housing status as temporary, compared to 11 percent of clients not receiving a housing service. There was a much higher percentage reporting an unknown or missing housing status among clients not receiving a housing service (18 percent).
Examination of RDR data on housing status shows there were no significant changes in this percentage over the four years examined (2007–2010).27 However, the percentage varied across states and territories (Appendix J). Four states (New Mexico, North Dakota, South Dakota, and West Virginia) served less than 5 percent of RWP HIV-positive/indeterminate clients in nonpermanent housing situations, whereas Guam, New York, Pennsylvania, and Wyoming each served more than 15 percent of HIV positive/indeterminate clients who were in nonpermanent housing.
Figure II.9. Housing Status/Living Arrangements of RWP Clients
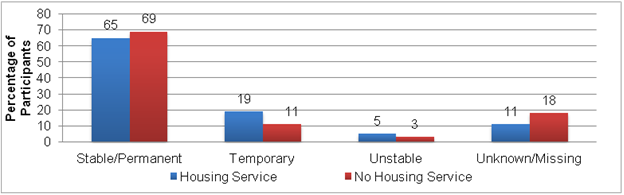
Source: HRSA Ryan White Program Services Report, 2010.
Housing Status of HOPWA Participants: Thirteen percent of HOPWA HIV-positive participants enrolling in housing services reported their prior living situation as homeless, defined as “a place not meant for human habitation, an emergency shelter, or transitional housing for homeless persons.” The most common prior living situation reported was “rented room or apartment of house.” Across states, the proportion of homeless status of the participants entering the HOPWA program varied. In five states (Idaho, Maine, New Hampshire, New Mexico, and Wyoming), no participants entered the program from a homeless living situation. In contrast, 44 percent of new participants in Puerto Rico were previously homeless; in two other states (Alabama and California), 20 percent of the new HOPWA participants were previously homeless (Appendix J).
25 “Unstable” includes participants who are homeless, as well as those living in transient or transitional housing. “Homeless” includes shelters, vehicles, the streets, or other places not intended as regular accommodations for living. “Transitional housing” includes any stable but temporary living arrangement, whether or not it is part of a formal program. “Homeless” is defined as having a prior living situation that includes a place not meant for human habitation, an emergency shelter, or transitional housing for homeless persons.
26 Housing status was not collected for 7,250 RWP participants; therefore, the percentage is calculated using the 548,925 participants for whom housing status was collected.
27 RDR data do not provide an unduplicated across programs.
4. Participant Health Characteristics
Unlike HOPWA, which does not report on participants’ health characteristics, RWP does report health data. Among RWP clients who received a housing service, about 40 percent were HIV positive but did not have AIDS, and 54 percent had CDC-diagnosed AIDS (Figure II.10). Of the clients receiving housing services, just over 1 percent were HIV-affected participants (including those who were HIV negative or whose status was unknown). In comparison, there was a slightly lower percentage of participants with CDC-diagnosed AIDS among RWP clients not receiving housing services (44 percent) and a slightly higher percentage with HIV, AIDS status unknown (10 percent).
Figure II.10. HIV Status of RWP Clients
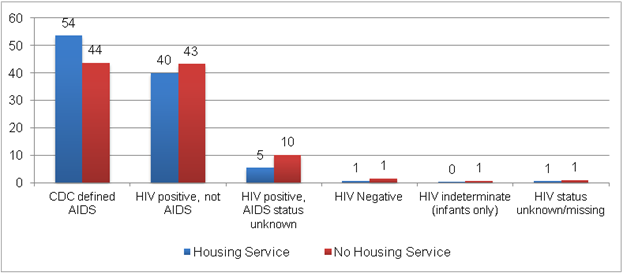
Source: HRSA Ryan White Program Services Report, 2010.
Sixteen percent of RWP clients receiving housing services reported having no insurance, and 46 percent reported having public insurance (Medicare, Medicaid, or other insurance) (Figure II.11). A higher percentage of RWP clients not receiving housing services did not have any insurance (22 percent), and a lower percentage reported having public insurance (38 percent).
Figure II.11. Insurance Status of RWP Clients
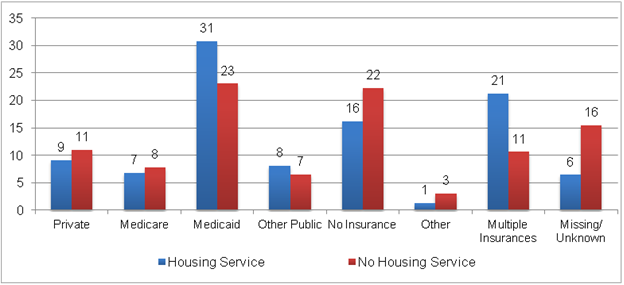
Source: HRSA Ryan White Program Services Report, 2010.
F. Housing Outcomes
Unlike RWP, which does not report the housing outcomes of program clients, HOPWA grantees do report on a number of outcomes. In 2010, reported outcomes included the household’s housing status at program exit and their access to care (defined as their connection to medical care and other types of support). At program exit, more than four-fifths (80 percent) of HOPWA households were successfully connected to housing, case management, primary care, medical insurance, or income sources (Table II.3).
Table II.3. Percentage of HOPWA Households Receiving Housing Assistance Who Achieved Outcomes
| Outcome | Percentage of Total Participants |
|---|---|
| Has a housing plan for maintaining or establishing ongoing housing | 93 |
| Has contact with a case manager as specified in individual service plan | 91 |
| Had contact with a primary health care provider | 87 |
| Has access and can maintain medical insurance/assistance | 86 |
| Successfully accessed or maintained income | 8 |
Source: HUD HOPWA CAPER and APR, 2010.
In 2010, only 6 percent of all HOPWA households receiving housing assistance exited to an unstable situation, defined as an “emergency shelter, jail, prison, disconnected, or unknown.” This proportion of unstable housing exits remained steady between 2007 and 2010). Three of the four types of housing assistance services have had relatively low rates of unstable housing exit (less than 5 percent); however, four times the percentage (20 percent) of the households residing in transitional/short-term facilities exited to unstable housing (1,415 households) (Figure II.12.)
Figure II.12. Exits to Unstable Housing, by Type of Housing Assistance
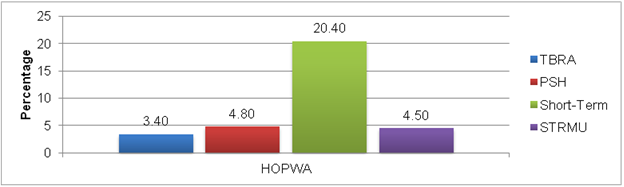
Source: HOPWA CAPER and APR, 2010.
The percentage of HOPWA households exiting to unstable housing varied widely across states, with one state (New Mexico) having no such exits in 2010 (Appendix K). Only four (California, Florida, Idaho, and South Carolina) had a percentage higher than 10 percent, with the highest (South Carolina) being 20 percent. Across states, HOPWA households also varied in their connection to primary care at exit, with a range of 13 to 100 percent (Appendix K). In eight states, 100 percent of HOPWA households reported having had contact with a primary care physician at program exit.28
28 Two states (New Jersey and Wyoming) had more than 100 percent because they reported more people receiving an outcome than total people.
1. Feasibility of Correlational Study
One of the original questions of the quantitative analysis was whether or not the available HOPWA and RWP data could support an analysis of the association between housing assistance, enhanced housing status, increased access and retention in HIV care, and improved clinical outcomes. Although RWP began collecting individual level data in 2010, before then, data were collected and reported at an aggregate level. All HOPWA data in this report are reported in aggregate. The lack of client-level data makes it difficult to examine any correlations between housing assistance and outcomes such as housing status, access to care or improved clinical outcomes. Although HOPWA does currently require grantees to report on participant outcomes, these outcomes are limited to housing status at exit from the program and are reported in aggregate across all participants. The lack of follow-up data for either program also makes it difficult to come to any conclusions about the intermediate and long-term impacts of HIV housing assistance.
G. Housing Data Analysis Summary
Based on the analysis of the national program data and CDC surveillance data, as many as 10 percent of the identified PLWHA in the United States and its territories are receiving some sort of housing assistance through RWP and/or HOPWA. Although there is no systematic way of assessing the extent of housing need among everyone with HIV/AIDS, it is clear from HUD’s CoC data that housing is a definite need for a subset of the HIV/AIDS population. The 2012 national homeless point-in-time count found that 3.9 percent of the homeless adults reported that they were living with HIV/AIDS. This is a much higher percentage than in the general population (less than 1 percent).
Because HOPWA and RWP serve different but complementary purposes, the proportions of funding they targeted toward housing assistance were very different. Whereas two-thirds (67 percent) of HOPWA’s funding was used for housing assistance, and 61,268 participants received housing assistance in 2010, 3.2 percent of RWP funding was used for housing assistance, and 18,904 participants received RWP-funded housing assistance that year. RWP’s primary focus is to provide HIV treatment and care, and grantees can spend only a portion of funds on support services (of which housing services is one type), whereas HOPWA’s focus is on providing housing assistance and related support services. Another key difference is that RWP assistance is targeted toward emergency and short-term housing, whereas HOPWA provides help with a range of short-term, long-term, and permanent housing.
In general, the characteristics of participants served were similar across the two programs. HOPWA participants (which include family members) tended to be younger, because HOPWA serves more families with children than RWP. Within both programs, the majority of participants served were within the lowest poverty category (at or below FPL for RWP and up to 30 percent of AMI for HOPWA). Because the two programs collect housing status at different points of enrollment (HOPWA collects it prior to program entry; RWP collects it as of last day of reporting period), it is impossible to compare housing status prior to program entry across the two programs. HOPWA reported that 13 percent of participants were homeless at program entry.
Although housing status was based on the end of the reporting period and not program exit, among RWP clients receiving housing assistance, about one quarter (24 percent) were temporarily or unstably housed, compared to 14 percent of RWP clients not receiving RWP-funded housing assistance. Note that RWP housing assistance is intended to be a short-term aid, not a long-term solution. However, the fact that 5 percent of the RWP clients receiving housing assistance were still unstably housed at the end of the reporting period emphasizes the importance of connecting RWP clients to long-term or permanent housing assistance through HOPWA, CoC, or other mainstream public housing programs.
HOPWA also collects client information about housing status at exit and reports it separately for different types of assistance. The percentage of participants exiting to homelessness was below 5 percent for all types of assistance except for short-term transitional facilities, which saw 20 percent exit to homelessness. This indicates that participants served with STRMU were much less likely to exit to homelessness compared to the short-term facilities.
III. Analysis of Integrated HIV Housing and CARE Services
In response to the NHAS request for greater access to HIV care, in 2011 the HUD Office of HIV/AIDS Housing awarded seven competitive Integrated HIV/AIDS Housing Plan (IHHP) grants designed to combine housing assistance with a community planning component.29 This chapter documents key features of the IHHP programs: their site characteristics, their program models, and details of their integration of HIV housing, health care, and other services.
While many HOWPA programs work closely with RWP providers to link housing with HIV care, these IHHP grants are unique in their integration of housing and HIV care at three levels: individual services, organizational data systems, and community-level planning processes. By documenting the program models, implementation processes, and integration challenges of these IHHP sites, we hope that lessons learned from this analysis can inform policy and program-planning discussions about how best to integrate these programs.
29 2011 Integrated HIV/AIDS Housing Plan Special Projects of National Significance Program Grantees. Accessed August 11, 2013, at [https://www.onecpd.info/hopwa/2011-ihhp-spns-program-grantees].
A. Overview of IHHP Grantees
The 2011 IHHP grants were intended to “combine housing support with a community planning component . . . to make community-wide system changes in service delivery for low-income HIV-positive individuals.” A diverse group of organizations received the grants. Located across the country, they target different populations and use different program models (Table III.1).
Mathematica and Cloudburst worked with ASPE and HUD staff to select four of the seven grantees as study sites: (1) the RRHS FUSE project in Jacksonville, Florida; (2) the FPC statewide Maine IHHP project; (3) the PHB S4H project; and (4) the Albany CARES FFL project in upstate New York (see Table III.1). Although all seven IHHP sites were identified as implementing best practices, this study could examine only four of the sites, a result of study constraints. Consequently, we selected sites that represented diversity in grantees’ (1) site characteristics and geographic scope, (2) project implementation status, (3) target populations, and (4) models of integration.30 Of particular interest were the statewide scope of the Maine IHHP project, the FUSE project’s targeting of African American families; and the program models of Portland’s S4H and CARES FFL projects linking housing assistance, HIV care, and employment services.
The four selected sites have extensive experience providing HIV housing assistance and support services in collaboration with local partners. They have also been involved in community-level planning of homeless services through their participation and leadership of CoC planning processes and their participation in RWP planning councils, task forces, and provider networks. Through the IHHP grants, the sites are exploring new forms of system integration at multiple levels. We provide a brief overview of each grantee and IHHP project below:
Table III.1. IHHP Grantee Characteristics
| Grantee Location | Program | Target Populations | IHHP Funding | Site Start Date | May 2013 Enrollment Status |
|---|---|---|---|---|---|
| City of Los Angeles, CA | CHISS | Homeless, at-risk of homelessness, and newly diagnosed or out of care | $1,375,000 | July 1, 2012 | Still enrolling 20/25 enrolled |
| River Region Human Services: Jacksonville, FL | FUSE | Homeless. Female heads of household with children less than 18 years old | $1,353,743 | November 1, 2011 | Full; 40 families and individuals enrolled |
| Frannie Peabody Health Center; Portland, ME | Maine IHHP | People with HIV/AIDS potentially eligible for public housing | $930,909 | January 1, 2012 | 90 enrolled |
| Justice Resource Institute; Boston, MA | Youth Housing Initiative | Homeless youth, court-involved persons, other vulnerable groups | $1,223,388 | January 1, 2012 | Full; 20 enrolled |
| Portland Housing Bureau; Portland, OR | S4H | Homeless or at risk of homelessness | $1,365,900 | January 1, 2012 | Full; 60 enrolled |
| Albany CARES; Albany, NY | FFL | People with HIV/AIDS interested in employment | $1,344,375 | January 1, 2012 | 20+ enrolled |
| City of Dallas, TX | Ex-offender and IHHP | Ex-offenders | $1,287,500 | January 1, 2012 | Full; 60 enrolled |
Source: Discussions with program staff and program data, Mathematica Policy Research, 2013.
CHISS = Collaborative for Housing Integrated with Supportive Services; FFL = Foundations for Living; FUSE = Forging Useful Systems to Empower Project; S4H = Springboard to Stability, Self-Sufficiency and Health Program.
30 For example, the Los Angeles site was excluded because it implemented later than the other sites, and the Dallas site was excluded because its housing and health care data systems were not integrated.
1. River Region Human Services: Forging Useful Systems to Empower Project
Established in 1979 as a nonprofit behavioral health organization with mental health counseling, RRHS’s mission is to “improve the quality of life for individuals and families in northeast Florida affected by substance abuse, mental illness, homelessness, HIV/AIDS, and other communicable diseases through outreach, prevention, treatment, and housing services.” The agency’s HIV services include outreach and linkage, HIV testing and referral, case management, and housing assistance. Notably, RRHS was part of a core group that created a national model for peer-based HIV outreach services, and is the northeast Florida trainer of peer specialists. RRHS received $1,353,743 to implement the FUSE project, which is designed to provide tenant-based rental assistance and coordinated linkages to support services for households headed by homeless PLWHA (primarily African American women and their children) in the Jacksonville, Florida, area. The project promotes stable housing, health outcomes, and client achievements toward self-sufficiency.
2. Frannie Peabody Center: Maine Integrated HIV/AIDS Housing Plan Project
FPC, a community-based organization headquartered in Portland, Maine, was formed in 2002 by the merger of two HIV/AIDS service providers. Currently the largest AIDS service organization in the state, FPC provides both prevention services for those at risk of HIV and direct services to HIV-positive individuals and their families. FPC’s four HOPWA grants fund permanent supportive housing services for PLWHA statewide. Though service provision varies somewhat by program, these HIV housing services offer a combination of supports through local community resources, including access to case management, volunteer assistance, life skills education and training, and medical care. FPC was awarded $930,909 for their Maine Integrated HIV/AIDS Housing Plan. The project coordinates with four local housing authorities across the state to integrate HOPWA clients into mainstream HUD housing. The project hopes to promote stable housing and improved health outcomes by providing people with the support and services they need to facilitate their transition to HUD Housing Choice Vouchers. FPC is the only IHHP grantee with a statewide client base.
3. Portland Housing Bureau: Springboard to Stability, Self-Sufficiency and Health Program
A department in Portland, Oregon’s municipal government, PHB manages a number of affordable housing development and assistance resources, including CoC funds, an Emergency Solutions grant, the city’s HOPWA formula grant, a Community Development Block Grant, HOME, and other state and local housing-related resources. To better serve its low-income and homeless residents, PBH and the Housing Authority of Portland (known as Home Forward) combined several emergency and short-term housing assistance programs into one pooled fund to provide a continuum of eviction prevention, rapid re-housing, and housing retention services for PLWHA and others who are homeless or at risk of homelessness. PHB was awarded $1,365,900 for its S4H Project. The S4H project builds upon a successful collaboration with Worksystems, a Portland-based nonprofit organization that designs and coordinates workforce development programs. In addition to providing housing assistance and linkages to health care and other supports, the S4H project will expand and adapt the Worksystems model for PLWHA. The project also builds on other long-standing, collaborative relationships between public housing, HOPWA, Ryan White Program Part A and B grantees, workforce providers, and state and local planning groups.
4. Albany CARES: Foundations for Living Project
Founded in the early 1990s, CARES began as an AIDS service organization, providing HOPWA rental assistance and Shelter-Plus Care housing services in the Albany area. Since then, the agency’s housing work has expanded to include community-level planning and administration of HUD’s CoC (homeless) services. CARES currently serves as the collaborative applicant for six CoCs in the Capital Region, coordinating their joint funding applications; acts as the HMIS administrator for CoC programs in 21 counties; and provides technical assistance to the City of Rochester’s HOPWA formula grant. CARES was awarded $1,344,375 to implement the FFL project, which provides permanent housing, linkages to medical care, employment services, and other supports, and supports comprehensive planning and coordination of HIV housing and CoC services in Albany and Rochester. CARES partners with project sponsors in both communities to provide local housing assistance and service coordination: the Albany Damien Center (ADC) and Catholic Charities Community Services (CCCS) in Rochester.
5. Factors Affecting Program Enrollment
Not all four sites chosen for in-depth study have currently met their enrollment targets (Table III.1). PHB’s S4H project was fully enrolled early on, aided by the Cascade AIDS Project’s (CAP) preexisting waiting list for other housing resources. In contrast, the other IHHP sites identified some challenges reaching and enrolling their clients. Although FUSE is fully enrolled, not all participants come from the program’s target population of women and their families. To fill the gap, RRHS has enrolled some people from other target groups. CARES reported several issues that have slowed program implementation and recruitment, including setup and administrative burden. After sensing some reluctance among local service providers and case managers to refer clients to employment services, staff conducted two days of employment orientation to shift their thinking about the value of employment for PLWHA.
Despite having enrolled 90 clients, FPC encountered a number of enrollment barriers, including finding clients that qualify for mainstream housing assistance through FPC’s four public housing authority partners; finding clients willing to leave their existing housing to move into public housing in another community; and ensuring that they are not initiating leases for IHHP clients that will not be able to sustain independent living when the IHHP grant ends. FPC staff felt that there have also been missed enrollment opportunities in other parts of the state, as not all AIDS service organizations are using the FPC screening/eligibility tool effectively, and statewide uptake of the tool has been slow. FPC also described difficulties serving the state’s refugee population with HIV/AIDS, as Maine will not provide Medicaid to immigrants who have lived in the United States for less than five years. Finally, the limited availability of rental housing across the state has made it harder for FPC to move eligible clients into the IHHP program.
B. IHHP Housing Assistance and Care Coordination Models
The 2011 Notice of Funding Availability for the HOPWA IHHP grants announced that funds were available for projects that addressed “(1) direct housing assistance and service delivery to low-income PLWHA and their families, including homeless individuals and families; and (2) comprehensive planning and coordination of local resources in meeting the housing and service needs of the population.” It specified that the grants would support the NHAS goals of reducing HIV infection, increasing access to care, and improving the health outcomes of PLWHA through “improved cross-agency planning [and] resource utilization and service integration among mainstream housing and HIV-related agencies and providers.” Finally, the notice stipulated that “grant applicants must commit to increasing coordination among local partners in providing housing as a base for access to services that target the needs of PLWHA and their families.”31
The four IHHP sites we studied are fulfilling these requirements, working with a range of community partners to provide direct housing assistance funded by HOPWA, with service coordination funded by their IHHP grants in collaboration with HIV medical case management funded by the RWP. In addition, they have developed and are starting to implement community-level integrated HIV housing planning efforts. Among the four IHHP sites, there is a gradient of service coordination in three areas: (1) direct housing assistance and housing service coordination, (2) coordination with employment services, and (3) linkage to HIV care through medical case management (See Figure III.1). In Figure III.1, the darkest oval represents the highest level of service coordination and collaboration. First, all four sites provide housing assistance (rental payments or housing units) directly to their clients. All four sites also fund “housing coordinator” positions, though two contract out that function. Second, of the four sites, only two fund “employment coordinator” positions, both contracted out. Third, the position of “medical case manager” is funded by none of the sites directly, but all four sites work closely and collaboratively with medical case managers funded by RWP to access medical case management for housing program participants.
Figure III.1. IHHP Service Components
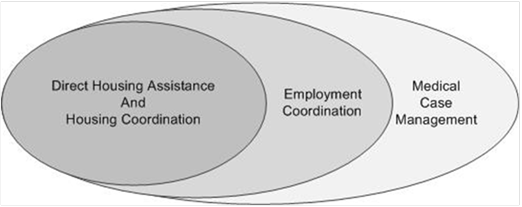
FPC is the only grantee providing direct housing assistance. The other three grantees (RRHS, CARES, and PHB) are contracting with project sponsors to carry out housing assistance activities. All four include housing coordination services in the programs: identifying, recruiting, and enrolling program participants; assessing clients’ service needs; and linking clients to support services. Of the four sites, two (RRHS and FPC) used their IHHP funding to hire internal staff to provide housing coordinator, case manager, and/or peer support functions. The other two (PHB and CARES) funded community partners to provide those services (See Table III.2).
The sites also differed in their approach to employment services. Two sites (PHB and CARES) are using their IHHP funds to build employment services into their program models. CARES used an evidenced-based “considering work” model; the CARES FFL project is working to create “a seamless collaborative team approach to service planning that includes service integration and coordination with health care and other support services (such as mental health and substance abuse treatment), with vocational rehabilitation, workforce development, and employment programs.” PHB is expanding the Worksystems model of employment and vocational rehabilitation services for PLWHA. In contrast, the other two sites (RRHS and FPC) are using their housing coordinators to assess the education, employment, and training needs of clients and refer them to appropriate services, but are not funding employment services directly through IHHP funds.
Table III.2. IHHP Program Models
| . | RRHS FUSE | FPC Maine IHHP | PBH S4H | CARES FFL |
|---|---|---|---|---|
| Program Goal(s) | FUSE goals: to increase access to affordable housing for families headed by homeless PLWHA; to coordinate housing, HIV care, and other services; to integrate housing and HIV data; and to coordinate community planning to leverage public housing for PLWHA | FPC goal: to increase statewide access to public housing for PLWHA, with linkages to HIV care maintained by local HIV medical case management services | PHB goal: to improve health outcomes for PLWHA by leveraging collaboration among HIV housing and service providers in Portland and surrounding counties, and by adapting the Home Forward model to offer workforce development services to PLWHA | FFL goals: to offer housing assistance and services to low-income PLWHA interested in employment; to link housing, HIV, and employment systems; and to improve comprehensive planning and coordination of local services to meet the needs of PLWHA |
| Primary Partners | Ability Housing (AH); and Health Planning Council of NE Florida | Maine State Housing; Bangor, Portland and Sanford Housing Authorities; Maine’s RWP Part B Grantee | Cascade AIDS Project (CAP); The Multnomah County Health Department (MCHD) Part A Grantee and Worksystems, Inc. | Albany Damien Center (ADC); Catholic Charities Community Services of Rochester (CCCS) |
| Staffing | The FUSE project funds three full-time staff: a program manager, a services coordinator, and a peer specialist, with part-time support from an evaluator and a database integration specialist | FPC funds an FT IHHP housing specialist and a portion of the program evaluator position, with in-kind assistance from FPC’s occupancy specialist and housing coordinator | PHB funds an FT housing case manager and FT employment specialist at CAP; a PT position at Worksystems; a PT BHP consultant working with the S4H evaluation and data collection; and some BHP project management time | The FFL program funds a program coordinator, FT employment coordinators at ADC and CCCS, a PT CCCS program developer; and in-kind rent assistance, HMIS, and evaluation services (CARES) |
| Program Model | RRHS leases units in two AH apartment complexes. FUSE service coordinator and peer specialist work on site to enroll families in FFL, assess their needs, provide peer support and transportation to, and coordinate with RW-funded medical case managers on HIV care issues | FPC offers TBRA, STRMU, and related support services to HOPWA-eligible clients, while working with local housing authorities to move them into mainstream public housing. Local providers or AIDS service organizations provide medical case management, linking PLWHA to medical care | PHB coordinates the data collection, evaluation, and funds services provided by key partners: rental and homelessness prevention assistance (CAP); housing and employment case management (CAP); and linkage to employment (Worksystems), and coordinates with HIV-related care (MCHD) | Region-wide, CARES facilitates CoC planning; administers the HMIS, and provides HOPWA-funded rental assistance; ADC and CCCS staff provide direct housing services, outreach, intake, housing and employment counseling, and HIV care coordination |
The fourth IHHP component is medical case management. All four sites also include linkages to HIV care in their program models, and their housing coordinators are working closely and collaboratively with medical case managers who are employed in local HIV clinics, supported by RWP funds. The details of these health care linkages are described in more detail in the next section.
31 Department of Housing and Urban Development [Docket No. FR -5500-N-13 Notice of Funding Availability for HUD’s Fiscal Year 2011 Housing Opportunities for Persons With AIDS. Accessed August 11, 2013, at [http://archives.hud.gov/funding/2011/hopwanofa.pdf].
1. HRSA Special Projects of National Significance
Two of the sites (RRHS and PHB) are also participating in a HRSA Special Project of National Significance (SPNS) that addresses the coordination of housing and HIV care. However, in those programs, the sites are working with client populations that are more medically needy than the IHHP clients and less likely to become employed and mainstreamed into public housing. In Florida, RRHS and its partner, Ability Housing, are working with the University of Florida CARES medical clinic, which is developing a medical home for people who are HIV positive or at high risk of HIV and who are homeless or in an unstable housing situation. UF CARES medical case managers refer their clients to RRHS for housing assistance, but do not fund housing services. An RRHS evaluator is assessing the interplay between the IHHP and HRSA SPNS projects in that site.
In Oregon, PHB’s partner, the Multnomah County Health Department (MCHD) also manages a HRSA SPNS site. That program connects homeless, multiply-diagnosed PLWHA with substance use disorders and/or mental illness to care through a medical home model. MCHD contracts with CAP, which has three network navigators who are part of the medical team at clinic and spend time at CAP. The navigators accompany participants to medical appointments and address any barriers to housing. The project does not focus on employment; its goals include getting participants into permanent housing, into appropriate mental health and substance abuse treatment, and into routine (non-emergency, non-acute) medical care.
2. Factors Affecting Implementation of IHHP Models
Recent funding restrictions at the federal, state, and local levels are limiting the ability of grantees to realize their IHHP program goals. All four sites noted the challenges of these budget uncertainties. In May 2013, HUD announced that several of its programs, including its CoC programs, would be cut by 5 percent overall as a result of federal sequestration. The IHHP sites reports that these cuts are beginning to “trickle down” to state and local housing authorities and other programs. In Maine, for example, one of FPC’s public housing partners, the Sanford Housing Authority, has already begun to reduce its housing vouchers through attrition, although this has not yet affected the Maine IHHP grant. In Oregon, PHB and its partners (CAP, Workforce Systems, and RWP Part B) are all planning budget reductions next year for between 5 and 8 percent of their total budgets.
Other concerns voiced by the IHHP sites include the lack of affordable mainstream housing available for their clients (FPC and CARES); uncertainty about the potential impact of the Affordable Care Act (health reform) on RWP-funded services, including medical case management (RRHS, PHB, and PHB); and the need for a paradigm shift among HIV providers away from simply securing benefits for their clients to helping them move into mainstream housing and employment (all four sites).
C. Integration of Individual Housing and Health Care Services
The IHHP notice stipulates that grantees should demonstrate “a concerted effort . . . to integrate and coordinate cross-cutting resources in providing a comprehensive approach to HIV/AIDS housing and support services.” The IHHP sites we visited created program models involving significant service coordination among housing, health care, and other support service coordinators. Key program components facilitated service integration: (1) in-depth screening of clients’ housing, health care, and other support service needs at intake; (2) development of individualized care plans tailored to the needs and circumstances of participants; and (3) frequent in-person contact between housing coordinators and peer specialists, clients, and medical providers (Table III.3).
Table III.3. Service Provision and Linkage to Care
| . | River Region Human Services | Frannie Peabody Health Center | Portland Housing Bureau | Albany CARES |
|---|---|---|---|---|
| Direct Housing Services | RRHS provides tenant-based rental assistance to FUSE clients and others | FPC provides tenant rental assistance and linkages to housing vouchers and public housing statewide | PHB provides short-term rental assistance: helping with eviction prevention, rapid re-housing, and housing retention | CARES provides tenant-based rental assistance and helps with clients’ transition to housing self-sufficiency |
| Service Coordination | FUSE service coordinator and peer specialist offer coordinated linkages and transportation to medical care and support services | FPC works with AIDS service organization (ASO) partners across the state to coordinate local case management with IHHP housing assistance | System-wide, PHB and local partners use common assessment form and “acuity scale” to rate and assess client need for housing, employment, and HIV medical care | Local partner sites (Albany and Rochester) offer both housing and employment service coordination, and closely collaborate with local medical providers |
| Health Care Linkage | Site uses a single health impact assessment tool to link to care. The FUSE service coordinator is a former RWP-funded medical case manager who works closely with the local medical case manager network | Local ASO partners coordinate referrals and engage with local health care providers. Integration of HIV housing and medical care is coordinated statewide by FPC staff | PBH coordinates all services, but linkages to medical care are made directly by partner organizations. Program has strong system connections to HIV care | New York state is moving to a Medicaid health home model for PLWHA CARES’ local partner organizations are providing linkages to medical providers and medical homes |
Source: Discussions with program staff and document review conducted by Mathematica Policy Research, 2013.
CoC = Continuum of Care; HOPWA = Housing Opportunities for Persons With AIDS; IHHP = Integrated HIV/AIDS Housing Plan; RWP = Ryan White HIV/AIDS Program.
Each program also uses an interdisciplinary team made up of internal staff and external partners with the technical knowledge, collaborative skills, and program experience to meet the multiple needs of the client population. All sites leverage existing staff resources, but they have used their IHHP grants to incorporate housing coordinator positions into their programs; such positions are deemed critical to the integration of care and housing services, which is achieved through the activities described below. Sites described using multidisciplinary teams and suggested frequent communication among core staff to help clients make and keep service appointments, address problems with rental payments and compliance with rental requirements, motivate clients to make and work toward long-term self-sufficiency goals, and handle crises that could disrupt clients’ housing stability and access to health care.
In addition, all four IHHP programs have developed policies and practices to facilitate care coordination. For example, RRHS employs an internal service coordinator/peer specialist team to maintain close personal contact with clients and with other agencies. FPC contracts with local partners to provide case management and care coordination. PHB uses a common client assessment form and “acuity scale” of clients’ housing and HIV needs. CARES uses service coordinators that offer comprehensive housing and employment service planning and collaborate closely with medical providers. Other site-specific service integration-related practices are summarized below.
RRHS FUSE staff use a program-specific intake form that is a modified version of the RRHS general housing program intake form. The FUSE form includes RWP-specific data elements, including CD4/viral load counts, Medicaid status, enrollment in RWP, and medical and provider history. At intake, FUSE staff also inquire about the client’s history of substance use and homelessness, criminal background, demographic information, income, and medications. Notably, the local CoC coalition task force is using the FUSE intake form as a model for the common intake and assessment form it is developing. If necessary, FUSE team members provide transportation and accompany clients to medical and other service appointments. The FUSE service coordinator also conducts home visits with each client at least monthly, and asks clients to provide their lab test results from each medical visit (every three to six months) to track their retention in care and clinical outcomes. The service coordinator also leverages his preexisting relationships with local medical providers and RWP medical case managers (he was previously a medical case manager himself), calling them once or twice a week to ask for verification of medical appointments and other information.
At intake, FPC staff also use a detailed screening form that is used in FPC housing programs and that FPC staff encourage AIDS service organization partners to use statewide. The screening tool is used to assess physical and mental health, oral health, financial assets, legal history, and transportation issues. The use of a universal screening form allows intake staff to ask clients about their long-term housing plans, beyond the three-year limit of the IHHP program. Physical and mental health status is assessed at intake and then annually, at a minimum. As part of the intake process, the case manager contacts the applicant’s health care providers; for some clients, the case manager may call the provider as often as once a week. The case manager also creates an individualized housing plan, linking the client to a range of medical and social services, such as the AIDS Drug Assistance Program (ADAP), RWP, Medicaid, SSI, TANF, and SNAP. At FPC, health care coordination includes setting appointments; ensuring that clients get to appointments; working with pharmacies to help clients refill prescriptions, ensuring that clients understand any medical jargon, and accompanying clients to appointments, if needed. Overall, FPC described a high level of integration between HIV housing and medical care.
PHB’s service partners, CAP and MCHD, use a “no wrong door” approach to intake. That is, they work closely together to integrate housing and care at the client level regardless of whether the initial point of contact by someone with HIV/AIDS is with the housing or the medical care system. CAP and MCHD conduct intake assessments independently. CAP collects clients’ demographic information and creates a profile in HMIS. CAP staff assess clients across a wide range of indicators, including housing stability/status, behavioral health (mental health, substance use, domestic violence), medical care, insurance, and risk indicators (unprotected sex and drug/alcohol use), then refer the client to the appropriate programs. MCHD also assesses clients’ housing needs upon intake, relies on CAP for support on most housing-related issues, but also refers clients to other non-HIV-specific housing resources in the community, as appropriate. MCHD and CAP informants reflected on the relative merits of their case management approaches. MCHD medical case managers could confer directly and immediately with clients and health care providers, offering rapid referral and care coordination; however, they have high case loads, which reduces their frequency of client contact. CAP staff work with lower case loads and a higher degree of flexibility and thus are able to accompany clients to appointments (with lawyers, landlords, or even health care providers) and facilitate assistance with overcoming a variety of barriers to care.
CARES is working to create a seamless collaborative team approach to integrate housing programs with (1) health care, (2) support services (e.g., HIV prevention, mental health, and substance abuse treatment), and (3) vocational rehabilitation and employment programs. Like PHB, CARES’ partner organizations, ADC and CCCS, use a similar in-depth intake and assessment process. Clients are referred to ADC or CCCS and assessed (using the same program assessment template) regarding their interest in employment, eligibility for HOPWA, and legal history. Clients are contacted at least once a month, but more frequently if required. Both ADC and CCCS conduct in-person visits at which they develop individualized service plans that address employment, improvement in health, and access to primary care. Clients are connected to housing, vocational training and employment services, and medical care depending on their needs and goals as detailed in their service plan. The case manager is in regular contact with medical providers to ensure that clients are complying with their recommended course of treatment and are attending primary care appointments. HIV-related documentation is also collected and includes viral loads and CD4 counts.
D. Integration of HMIS, HOPWA, and CAREWare Data Systems
The IHHP notice included several data collection and reporting requirements for the grantees. In addition to providing program-level HOPWA Annual Performance Reports each year, grantees are required to use HUD’s CoC HMIS or an “equivalent client-level information system” to support the planning and reporting activities of their projects. The notice says that “participation in client-level information systems will support community collaboration in providing services across federal HIV/AIDS programs on outcomes related to housing stability for PLWHA and will foster further federal agency collaborations.”
Housing and HIV care data integration can improve the performance of integrated HIV housing programs in multiple ways. At the service level, housing coordinators and HIV medical case managers can share client-specific information by “seeing” key data elements and case notes in the others’ systems. Having access to integrated client-level housing status, housing service use, and housing and health outcome data can help managers evaluate the effectiveness of their programs. Linking client counts across programs also enables more accurate planning at the community level. For these reasons, all four IHHP sites were eager to improve the integration of their local housing (HMIS) and HIV care (CAREWare) systems.
No federal client-level data systems currently include a comprehensive set of housing and health care variables that can monitor the performance and evaluate the housing and health outcomes of integrated housing services. Neither HUD’s HMIS nor HRSA’s CAREWare systems have the comprehensive set of housing and health care data needed to evaluate the effectiveness of the integrated HIV housing programs operated by the IHHP grantees. While the HMIS data system can track changes in housing status, it does not collect key client-level measures of health care access, use, and changes in clinical outcomes. Although CAREWare collects and reports client-level data on HIV status, health access, utilization and clinical outcomes, the data system does not collect baseline data on clients’ housing status and stability at intake, and thus cannot measure client-level change in housing status. As discussed in the quantitative analysis in Chapter II, it was not possible to combine the data across these two data systems to conduct these analyses.32
Because HMIS and CAREWare were developed separately, they are incompatible. In order to build a comprehensive data system appropriate for their programs, the IHHP grantees must select one system or the other (HMIS or CAREWare) as their base, and then customize that system to add their APR data and other missing data elements (Figure III.2). Three IHHP sites (RRHS, PHB, and CARES) are using locally adapted HMIS data systems to collect and report their IHHP data. The fourth site (FPC) is using their state’s CAREWare system for their IHHP program. Among the four sites, we found no direct linkages between local or state HMIS and CAREWare data systems (indicated by the dotted line in Figure III.2). The IHHP sites’ aggregated APRs were also insufficient to track the client-level data needed to manage their integrated programs. The sites needed to incorporate their aggregate HOPWA data into either of the two larger client-level data systems to manage their programs better. All four IHHP sites in this study are using their grants to improve the integration of the housing, HIV care, employment, and other program-specific data elements in their data systems. However, they are facing different challenges in their efforts (Table III.4). For example, while the RRHS program currently tracks client-level FUSE program data in their CoC HMIS database, the local RWP Part A grantee utilizes CAREWare. The two systems are currently separate, but RRHS is spearheading an effort to link HMIS and CAREWare databases to coordinate their services and minimize duplicate data entry. The linking of these systems will open lines of communication between the RWP case managers and the FUSE service coordinators, allowing each to view the others’ case notes and clients’ lab test results (for example, CD4 counts). This will not involve making changes to CAREWare but rather will create external bridges from HMIS to access CAREWare data. Although the site is working to link the two data systems, the Part A grantee is concerned about making functional changes to CAREWare to foster data interoperability.
Figure III.2. HMIS, CAREWare, and HOPWA APR Data Relationships
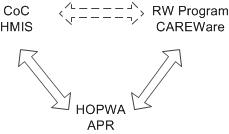
FPC case managers collect client-level data from HOPWA TBRA, PHP, and STRMU housing applications and housing plans, and measure clients’ housing stability at intake, at annual assessments, and during tenancy. They also collect qualitative information on clients’ sobriety and other characteristics to track the impact of housing stability on sobriety and other outcomes. Although FPC staff use the state’s CAREWare data system to input their HOPWA data, including their case notes, and report that CAREWare, at least in their state, limits their ability to share client-level data with other agencies. The state data system is set up so that FPC and partner agencies can see only program-level data, limiting the data’s utility. Although some demographic fields are shared, many HOPWA-specific health and housing benchmarks are available only at the service provider level. Both FPC and the state’s RWP Part B grant hope to modify their data systems in the near future, but the timing of these information technology (IT) projects may limit the opportunity for system integration. The state anticipates that its IT development process will take longer to complete than FPC’s.
As the lead agency for Multnomah County CoC, PHB manages the CoC’s HMIS data system and uses the system CoC, HOPWA, and RWP reporting. Using HMIS for collecting and reporting non-CoC programs (HOPWA and RWP) has been a challenge. The primary barrier for using HMIS systems for HOPWA data collection is the incompatibility between HOPWA data requirements and HUD’s formal HMIS data standards. Even though HOPWA and CoC programs share common data elements, there are incompatibilities, including differing eligible activity types and performance outcomes. Further, HOPWA reporting does not track data at the client level, and HMIS does not have many data elements tracking changes in health status.
There is also minimal client-level data sharing between PHB and its partners. PHB requires HMIS for reporting HOPWA services; MCHD clinics collect data through electronic health records but use the TOURS system for reporting (soon to be replaced by CAREWare); and the state’s RWP Part B grantee uses CAREWare. Although some RWP funds have been allocated to improve HMIS/CAREWare communicability, the federal sequestration and related state and local budget cuts have hampered this effort. Ultimately, the RWP grantee hopes to develop a data warehouse that would allow multiple users across systems to view common, real-time data.
Table III.4. Integration of Data Systems
| . | RRHS FUSE | FPC Maine IHHP | PBH S4H | Albany CARES FFL |
|---|---|---|---|---|
| Data Systems Used | RRHS collects FUSE client-level data in the CoC HMIS database. RWP Part A utilizes CAREWare | CAREWare is used to input HOPWA program data, including case notesFigure III.2. HMIS, CAREWare, and HOPWA APR Data Relationships | PHB utilizes the CoC HMIS data system. MCHD clinics use electronic health records but report through TOURS system and will soon move to CAREWare. Oregon uses CAREWare | CARES utilizes HMIS, as implemented by Foothold Technology (FT), which includes a customization module called Form Builder. Both ADC and CCCS use the same FT HMIS system |
| Data Sharing and Integration | Currently, CAREWare and HMIS are separate data systems. There is no data bridge between them. The FUSE program coordinator uses an Excel spreadsheet to record clients’ lab results, which are reported in the IHHP grant’s APR | HOPWA data are uploaded to CAREWare, but data sharing is limited because it is set up only for provider-level viewing. FPC also shares HOPWA data with some medical providers | MCHD and CAP had used a common health care and housing assessment tool in the past but now have only a few data elements in common. Only medical engagement data are shared by MCHD and CAP | CARES does not share its data system with other organizations. Currently, an external evaluation tracks health outcomes |
| Outcomes Measured | HMIS tracks housing placement and stability; access to case management and medical care; access to and maintenance of income; housing planning; and CD4 counts and viral loads | FPC tracks housing type at program entry and exit; homelessness history; housing stability based on HOPWA codes; medical care source information; medical insurance coverage; client income; employment; and some health outcomes | PBH tracks housing placement and stability; access to case management and medical care; access to and maintenance of income; housing planning; employment; and engagement with medical case manager | CARES tracks housing placement and stability; access to case management and medical care; access to and maintenance of income; housing planning; and health, wellness, and employment data. The FFL evaluation also tracks health care status, mental health status, substance use, prevention/risk behaviors, and employment status |
| Challenges | The CoC’s old HMIS system went off-line in December 2012, but the new HMIS system did not become operational at RRHS until May 2013. Over 200 paper notes created in the interim must be entered into HMIS | HOPWA-specific data elements in CAREWare are not maintained when the CAREWare system is upgraded on an annual basis. HOPWA-specific health and housing benchmarks are available only at the provider level | HOPWA data elements are incompatible with HMIS data standards, including differences in eligible activity types and performance outcomes. HOPWA reporting does not track client-level data; HMIS does not track key health status data | CARES opted not to provide evaluation data for FFL’s 2012 APR because of data quality issues, including inconsistencies in defining and recording some data elements due to FFL staff turnover |
| Future Planning | RRHS is spearheading an effort to link the new HMIS and CAREWare databases. This will coordinate services and minimize duplicate data entry. The RWP Part A grantee is not seeking full integration of the two systems | FPC seeks a new data system combining housing, case management, and HIV care data. Maine’s RWP Part B grantee also wants to replace CAREWare with a new system to meet state-specific needs. In the new system, there is potential for integrating housing and health care data | MCHD is transitioning to CAREWare from Tours. PHB and CAP are working together to export HMIS data into the Tours system and, eventually, into CAREWare | CARES is developing a common CoC intake and assessment model for housing, mental health, and other services. A new, integrated data system will be needed to manage this common assessment process |
As the CoC HMIS administrator in 21 counties, CARES has the staff capacity to modify its HMIS data system. CARES staff use an HMIS module called Form Builder to collect additional information on health, wellness, and employment at six-month intervals. An outside evaluation of the FFL program is also using HMIS to measure client progress. At an operational level, employment counselors at ADC and CCCS (the FFL program’s partner agencies) use the data system to track clients’ employment, income documentation, and compliance with their medical appointments. The staff record diagnostic information, such as CD4 counts, in their HMIS progress notes. CoCs will now be required to create and monitor a common client intake and assessment system, which will eventually require a new data system.
32 Though it is theoretically possible to conduct a correlation analysis for a subset of HOPWA and RWP clients enrolled in Medicaid. Such an analysis would exclude the impact of integrated housing services on uninsured clients—the bulk of HOPWA and RWP recipients.
E. Integration of Community Planning
The IHHP grants have many purposes. In addition to implementing innovative programs linking HIV housing assistance to medical care and other supports, grantees are expected to work at the community level to create integrated housing plans designed to improve the functioning and efficiency of the local HIV housing service delivery system. The community planning requirements were more prescriptive. Grantees had to develop and submit an integrated HIV housing plan that contained specific elements, including (1) a common vision or goal, (2) a list of planning team members, (3) a description of the community planning process, (4) an accounting of the systems changes planned to improve the delivery of housing and support services, (5) an assessment of the unmet housing and support service needs of the local HIV population, (6) an inventory of the local HIV service providers, and (7) a set of the outcomes expected from the community planning process. At the same time, the planning requirements were flexible, in terms of not prescribing how grantees were to go about the complex process of bringing together a wide range of stakeholders to jointly develop and implement a community-wide integrated housing and service plan. This flexibility recognized community-level differences in existing housing resources, planning structures, and relationships.
When we visited the IHHP grantees in May 2013, the four grantees had just finished writing and submitting their IHHP work plans. Some grantees were farther along than others in their planning, but all acknowledged that their top priority during the first year of the grant had been to get their programs up and running in order to maximize their programs’ enrollment. Some teams were also getting technical assistance from HUD to help with their community planning efforts.
The grantees discussed two common challenges in bringing disparate groups “to the table” to work together on the IHHPs. First, all four grantees had extensive experience with community planning, serving on numerous councils, task forces, provider networks, coalitions, and work groups, often acting as a link between homeless and HIV service groups. However, some of the CoC and RWP groups they worked with did not have a history of working together. Second, some IHHP grantees felt that HOPWA programs were historically marginalized in both CoC and RWP planning processes. Although RWP planning councils often identified housing as a high priority, few allocated funds for housing assistance on the assumption that HIV housing needs were already being addressed by HOPWA. Likewise, some CoCs also felt that because homeless PLWHA were already being served by HOPWA, there was no need to enroll them in CoC programs.
The IHHP grantees plan to use a variety of strategies to overcome these challenges and bring together groups from different sectors (public housing, homeless services, city planning, and HIV services) to create community-wide IHHP plans (see Table III.5).
- CARES plans to use its leverage as the lead “collaborative applicant” in six regional CoCs to roll up IHHP planning into a larger CoC planning process in which the six regional CoCs would develop integrated intake, assessment, and data systems.
- FPC plans to use its presence on state planning groups (on the state’s Balance of State CoC, and on statewide ADAP and RWP Part B advisory committees) and in community planning processes (assessing unmet HIV housing needs for the City of Portland’s Consolidated Plan and serving on Portland’s CoC) to create statewide collaboration supporting the development of community-based IHHPs.
- RRHS hired the Health Planning Council of NE Florida to conduct a regional health impact assessment of potential changes in housing, consolidated planning, and other community policies. RRHS plans to use this impact assessment process to start the IHHP planning process and to build stronger relationships among these groups.
- PBH and its S4H partners have a history of successful collaboration, and plan to use this collaborative approach to work with the RWP Part A planning council and with the City of Portland’s Consolidated and Action Planning process to create a local IHHP.
Table III.5. Integration of Community Planning
| . | RRHS FUSE | FPC Maine IHHP | PBH S4H | Albany CARES FFL |
|---|---|---|---|---|
| Community Plan | The project director will work with the FUSE planning team and other local stakeholders to develop the IHHP. The task will begin with a community health impact assessment conducted by the Health Policy Council of NE Florida. | FPC is active in state and local RWP and CoC planning efforts, and with housing authorities. As part of a statewide collaboration, the project will assist in developing a community model for an IHHP. | Site has a strong, active planning group, with larger systems-change efforts and CoC coordination. The group will develop the IHHP plan. | CARES will form a planning team to create IHHP’s implementation plan. CARES is not planning to create an IHHP-specific plan, but to roll IHHP planning up into a larger CoC planning process. |
Source: Discussions with program staff and document review conducted by Mathematica Policy Research, 2013.
CoC = Continuum of Care; HOPWA = Housing Opportunities for Persons With AIDS; IHHP = Integrated HIV/AIDS Housing Plan; RWP = Ryan White HIV/AIDS Program.
IV. Conclusions
The results of these analyses illustrate some key differences between the HOPWA and RWP programs that affect the integration of housing and HIV care. The findings also suggest the importance of exploring and capitalizing on the strengths of each program and identifying ways they can complement each other, rather than working to maximize the impact of each program in isolation. Exploring program models that focus on the integration of housing and medical care services—and on the integration of HOPWA and RWP data systems and community planning processes—may lead to more effective use of limited HIV program resources.
A. Service Integration Conclusions
This section summarizes the report’s service integration findings and offers ideas for how service integration can be improved through further study and policy development.
The IHHP program models show a gradient of service coordination and collaboration in three areas: (1) housing assistance and housing service coordination, (2) employment service coordination, and (3) medical case management. All four sites provide housing assistance, and all four fund housing coordinator positions, though two contract out that function to community partners. Two sites fund employment coordinator positions, but both are contracted out to community partners. All four sites provided medical case management through coordination with RWP-funded medical case managers.
However, all four IHHP sites are concerned about the potential impact of the Affordable Care Act private health insurance coverage expansions and Medicaid expansion on their clients’ future access to RWP-funded medical case managers. As a payer of last resort, RWP may not pay for duplicate services that are available through other sources. Sites expressed concern that RWP clients who enroll in Medicaid may lose their eligibility for RWP-funded case management. In Maine, for example, RWP’s Part B program recently lost most of its case management clients when it was determined that those services duplicated case management services covered by Medicaid.
- The potential impact of the Affordable Care Act on this HOPWA housing-RWP case management linkage could be significant, and is worth monitoring and researching during the roll out of the implementation of Affordable Care Act coverage expansions in 2014 and beyond.
This study also offered a unique opportunity to observe two different housing-HIV care service integration models operating at the same time in the same program site in two different IHHP locations (PHB and RRHS). In both locations, the IHHP model features a “housing first” approach that funds clients’ housing while reaching out to external medical case management and other support services. The HRSA medical home-based SPNS model in both sites addresses clients’ physical health, mental health, and substance abuse issues first, while reaching out to local HOPWA programs for potential housing assistance. Both programs are made somewhat vulnerable by not funding both housing and HIV care elements. IHHP clients have housing, but rely on medical case management available through their health insurance (i.e., Medicaid) or RWP; conversely, HRSA SPNS clients are housed in an HIV medical home, but HOPWA-funded housing assistance may not be available and the client is waitlisted for housing services.
- There is potentially a third option of service integration that encompasses and funds both housing and HIV care, so that client access to both services is guaranteed. It would be useful to study examples of this third option to understand how it compares to the IHHP “housing first” and HRSA “health care first” models.
Two of the IHHP grants are also adding employment coordination to their integrated housing service models. This is a potentially important service integration model that offers clients an opportunity to move into mainstream housing through employment. In these models, IHHP clients become more financially self-sufficient as they gain housing stability and improve their health. The IHHP sites are challenged, however, by employment service providers who were not familiar with the service needs of PLWHA and were somewhat reluctant to take them on as new clients.
- This three-way model of integration (housing, employment, and health care services) should be studied in more detail, and the model’s effectiveness evaluated.
The IHHP sites were studied early in their grant cycle, at the beginning of their second year of operation. As a result, the programs were not very far along in their community planning activities. The sites have developed First Year Implementation Strategies to bring together groups from public housing, homeless (CoC) services, city planning, and HIV (RWP) service organizations to create community-wide IHHP plans, but noted two challenges that they will have to overcome to succeed. First, local CoC and RWP groups have not typically had a history of working together. Second, some sites felt that the needs of their HOPWA clients had historically been marginalized in both local CoC and RWP planning processes.
- The IHHP sites should be revisited at the end of their grant cycle to see what they are able to accomplish in terms of developing integrated planning processes at the community level.
Finally, this study shows that PLWHA have complex housing needs that cannot always be solved through temporary, short-term assistance from RWP or HOPWA. Some PLWHA may need assistance from both programs to stabilize their housing on a long-term basis. Operationally, RWP planning councils should reconsider past decisions not to fund housing assistance.
- New demonstration projects that are designed to formally integrate HOPWA and RWP housing and HIV care components, or to pool HOPWA and RWP resources into one integrated program, should be considered and researched.
B. Data Systems Conclusions
This final section summarizes the report’s data system integration findings and offers ideas for how housing data systems can be improved through further study and policy development.
There were numerous challenges in analyzing the HOPWA and RWP housing services. The data were compiled from several different sources that did not have identical collection methods. Some variables were collected across both programs, but the variables were collected in different formats and on different timelines. Other variables were collected in one program but not the other, which made comparisons difficult. In addition, HOPWA data are collected at an aggregate level, whereas RWP data are collected at the client level as of 2010.
- Adding client-level variables that are common to both housing and HIV care programs, especially data variables that capture the assistance received from both programs, would allow linkage of the programs’ databases and facilitate research examining services received and outcomes for participants served by both types of programs.
The implementation of the RSR in 2010 allowed for a comparison of the housing status of RWP clients who received housing services to the status of those who did not. This is particularly helpful for understanding the subset of RWP clients who are receiving housing assistance. There was also a great deal of variation across states in almost all the analyses. Unfortunately, it is impossible to determine whether or not these differences in housing status existed prior to program enrollment or as a result of services received, since most RSR variables are reported “as of end of the reporting period.”
- Increased understanding of these subgroup differences could help to inform and improve RWP housing practices around the unique needs of clients with housing needs. It may also be valuable to explore state-level differences housing status in greater detail.
The qualitative analysis found that many factors affected the coordination and integration of the IHHP grantees’ HMIS, HOPWA, and CAREWare data systems. The owners of these systems need to have the capacity, funding, interest, and timing to work together to integrate their systems.
- It will be important to revisit the IHHP sites at the end of their three-year grant period to see what they have accomplished in developing more integrated data systems.
At the data systems level of integration, the development of common intake and assessment systems for HUD’s CoC programs creates an opportunity to enhance HMIS systems to accommodate a “no wrong door” approach to client intake, assessment, and service provision from any of three entry points through HOPWA, RWP, Medicaid, or other patient-centered medical home options.
- The creation of this new CoC intake system might involve developing new linkages among HMIS, CAREWare, and electronic health record data systems. This development should be monitored and studied.
references
Centers for Disease Control and Prevention. 1993 Centers for Disease Control and Prevention HIV/AIDS Surveillance Report, vol. 5, no. 4, 1994, pp. 1–33. Available at [http://www.cdc.gov/hiv/pdf/statistics_hivsur54.pdf]. Accessed August 2013.
Centers for Disease Control and Prevention. “Monitoring selected national HIV prevention and care objectives by using HIV surveillance data—United States and 6 U.S. dependent areas—2010.” HIV Surveillance Supplemental Report, 2012, vol. 17, no 3. Available at [http://www.cdc.gov/hiv/pdf/statistics_2010_HIV_Surveillance_Report_vol_17_no_3.pdf.]
Centers for Disease Control and Prevention. “National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention (NCHHSTP) Atlas.” 2013. Available at [http://www.cdc.gov/nchhstp/atlas/]. Accessed March 7, 2013.
Federal Register. “Ryan White HIV/AIDS Program Core Medical Services Waiver; Application Requirements: A Notice by the Health Resources and Services Administration on May 24, 2013.” 2013. Available at [https://www.federalregister.gov/articles/2013/05/24/2013-12354/ryan-white-hivaids-program-core-medical-services-waiver-application-requirements.] Accessed August 20, 2013.
National AIDS Housing Coalition. “Findings from the National Housing and HIV/AIDS” Research Summit Papers, 2007. Available at [http://www.aidschicago.org/pdf/2008/housing_summitIII_findings.pdf]. Accessed July 17, 2012.
Rourke, S.B., T. Tucker, L. Monette, et al. (2010). Positive spaces healthy places: Identifying those in greatest need three years later. Presented at the North American Housing and HIV/AIDS Research Summit V, Toronto, Ontario: June 2010.
U.S. Department of Health and Human Services, HIV/AIDS Bureau. “2012 Annual Ryan White HIV/AIDS Program Services Report Instruction Manual.” 2012. Available at [http://hab.hrsa.gov/Manageyourgrant/Files/Rsrmanual.Pdf]. Accessed August 2013.
U.S. Department of Health and Human Services, HIV/AIDS Bureau. “HRSA HIV/AIDS Programs: Technical Assistance.” 2013. Available at [http://hab.hrsa.gov]. Accessed August 20, 2013
U.S. Department of Health and Human Services, HIV/AIDS Bureau. “2013 Annual Ryan White HIV/AIDS Program Services Report (RSR) Instructional Manual.” 2013. Available at [https://careacttarget.org/content/ryan-white-hivaids-program-services-report-rsr-instruction-manual.] Accessed August 21, 2013.
U.S. Department of Housing and Urban Development. “The 2010 Annual Homeless Assessment Report to Congress.” 2011. Available at [https://www.onecpd.info/resources/documents/2010homelessassessmentreport.pdf]. Accessed August 2013.
U.S. Department of Housing and Urban Development. “Housing Opportunities for Persons With AIDS (HOPWA) Program: Consolidated Annual Performance and Evaluation Report (CAPER).” February 2011. Available at [https://www.onecpd.info/resource/1011/hopwa-caper-form-hud-40110-d/]. Accessed August 2013.
U.S. Department of Housing and Urban Development. “HUD HIV/AIDS Housing.” 2013. Available at [http://portal.hud.gov/hudportal/HUD?src=/program_offices/comm_planning/aidshousing]. Accessed August 20, 2013.
White House Office of National AIDS Policy. “National HIV/AIDS Strategy for the United States.” July 2010. Available at [http://www.whitehouse.gov/sites/default/files/private/uploads/NHAS.pdf]. Accessed July 14, 2012.
Appendix A
Description of Data sets and their limitations
A. Description of Data Sets
Ryan White HIV/AIDS Program, HRSA
The Ryan White HIV/AIDS Program is administered by the Health Resources and Services Administration (HRSA). The Ryan White Program provides a variety of services that cover the gaps in HIV care that are not provided by other resources.33
- Ryan White Expenditure Reports 2007–2010. Grantees submit expenditure reports to HRSA annually. Part A and Part B expenditure reports were used in this analysis.
- Ryan White Program Data Reports 2007–2010. The RDR is a program-level data report. All funded Ryan White grantees submitted an RDR data report annually until it was replaced by the RSR in 2011. Each grantee submits one RDR report, including data on services funded with any Ryan White funding. An important limitation of RDR data is that participant counts can be duplicated. Although each provider unduplicates participant counts, a participant can visit more than one provider.
- Ryan White Program Services Report 2010. The Ryan White HIV/AIDS Program Services Report (RSR) is a participant-level data-reporting system. All funded Ryan White grantees and providers must submit an RSR data report annually. The RSR data used for this analysis represent the first complete year of reporting. Therefore, there may be incomplete and inaccurate reporting from some providers.
33 About the Ryan White HIV/AIDS Program. Retrieved on March 7, 2013, from [http://hab.hrsa.gov/abouthab/aboutprogram.html].
1. Housing Opportunities for Persons with AIDS, HUD
The Housing Opportunities for Persons With AIDS program (HOPWA) is provided through the U.S. Department of Housing and Urban Development (HUD). HOPWA covers a variety of housing, social services, program planning and development costs.34
- HOPWA Consolidated Annual Performance Evaluation Report 2007–2010. The HOPWA Consolidated Annual Performance Evaluation Report (CAPER) is completed annually by formula grantees and provides information on expenditures, activities, and program accomplishments. Information collected and reported in CAPER represents activities carried out with HOPWA funds during the grantee’s operating year, including any funds subcontracted to providers.
- HOPWA Annual Performance Report 2007–2010. All HOPWA Competitive Program grantees submit an Annual Progress Report (APR) to HUD annually. The APR provides information on expenditures, activities, and program accomplishments. Information collected and reported in the APR represents activities carried out with HOPWA funds during the grantee’s operating year, including any funds subcontracted to providers. The information reported in the APR does not overlap with data reported by HOPWA Formula Program grantees (in CAPER).
34 Housing Opportunities for Persons With AIDS propgram. Retrieved on March 7, 2013, from [http://portal.hud.gov/hudportal/HUD?src=/program_offices/comm_planning/aidshousing/programs].
2. Homeless Continuum of Care Program, HUD
HUD’s CoC program is designed to promote community-wide planning to end homelessness, and it provides funding for efforts by nonprofit providers and state and local governments to quickly re-house homeless individuals and families. HUD sets specific community requirements regarding the collection of data on the met and unmet needs of homeless individuals and families in the geographic area covered by the CoC program.
- The 2010 Annual Homeless Assessment Report (AHAR)35 is an annual report to Congress on the extent and nature of homelessness; it contains data from several sources, including:
- Homeless Point-in-Time Count. Each Continuum is required to conduct a point-in-time count of the number of individuals and families experiencing homeless on a single night in the last week of January. The results of these counts are submitted to HUD at least every other year.
- Homeless Housing Inventory. Each Continuum is required to conduct an annual inventory of the number and type of emergency, transitional, and permanent supportive housing units targeted to individuals and families. The results of the inventories are submitted to HUD annually.
- Homeless Management Information System. HMIS data from participating communities report on the use of emergency shelter, transitional housing, and permanent supportive housing programs during the AHAR reporting period; these data are weighted to produce national estimates.
35 See [https://www.onecpd.info/resources/documents/2010HomelessAssessmentReport.pdf].
B. Limitations of Data and Analyses
Because data were compiled from several different sources that did not have identical collection methods, there are a number of considerations when examining the analyses:
- Ryan White Emergency Financial Assistance can be used for housing assistance; however, it was not included in these analyses because it was not possible to separate out the expenditures and clients for housing financial assistance versus other types of financial assistance.
- HOPWA Permanent Housing Placement (PHP) can also be used for short-term financial assistance with housing including costs associated with helping participants to establish permanent residences; however, it was not included in these analyses as housing assistance because it was not possible to de-duplicate households served with housing assistance and housing placement.
- The Ryan White Program Data Report collects aggregate data on individuals and reports these separately for HIV positive and HIV affected. In contrast, the Ryan White Program Services Report collects and reports data on an individual level, which allows for de-duplication across service providers.
- The Ryan White Program Services Report collects data on individual clients served which is then unduplicated across grantees. However, not all variables are reported for all clients, therefore the total number of participants used to calculate percentages is the total number of participants required to answer that specific question.
- HOPWA reports did not provide an unduplicated count of households served across types of services; therefore, unduplicated households receiving support services was used as a proxy for the total of unduplicated households served.
Some HOPWA grants cover more than one state and report in aggregate; therefore, it is not possible to separate expenditures or participants by state for those grantees. This is particularly problematic for Montana (which includes North Dakota and South Dakota) and the District of Columbia (which includes parts of Virginia and West Virginia).
Due to a midyear change in grant year, the City of Miami submitted two CAPERs in 2010 and was not able to deduplicate information across the two reports. Both reports are included in the analysis, so the results for Florida are slightly higher than they should be.
Appendix B
Receipt of Federal Housing Assistance Compared to HIV/AIDS Prevalence, 2010
Table B. Receipt of Federal Housing Assistance, by State
| State | Number of Persons Living with Diagnosed HIV/AIDS in 2010 | Number of Individuals with HIV/AIDS Who Received HOPWA Housing Subsidy Assistance | Number of Ryan White Program HIV-Positive/ Indeterminate Clients Who Received Housing Services | Total Number of HIV-Positive Individuals Receiving Housing Assistance | Percentage of HIV-Positive Individuals Receiving Housing Assistancea |
|---|---|---|---|---|---|
| Total | 888,904c | 62,297 | 28,506 | 90,803e | 10 |
| RSR | NA | NA | 18,803d | 81,100e | 9 |
| AK | 628 | 74 | 83 | 157 | 25 |
| AL | 11,539 | 555 | 265 | 820 | 7 |
| AR | 4,684 | 224 | 0 | 224 | 5 |
| AZ | 12,532 | 793 | 128 | 921 | 7 |
| CA | 111,666 | 7,255 | 4,309 | 11,564 | 10 |
| CO | 11,006 | 376 | 857 | 1,233 | 11 |
| CT | 10,822 | 377 | 666 | 1,043 | 10 |
| DCb | 14,359 | 1,269 | 50 | 1,319 | 9 |
| DE | 2,968 | 250 | 117 | 367 | 12 |
| FL | 94,897 | 9,425 | 1,030 | 10,455 | 11 |
| GA | 33,920 | 2,220 | 69 | 2,289 | 7 |
| GU | 87 | 0 | 0 | 0 | 0 |
| HI | 2,310 | 184 | 67 | 251 | 11 |
| IA | 1,722 | 109 | 17 | 126 | 7 |
| ID | 792 | 117 | 5 | 122 | 15 |
| IL | 31,884 | 2,488 | 647 | 3,135 | 10 |
| IN | 8,511 | 744 | 0 | 744 | 9 |
| KS | 2,696 | 144 | 0 | 144 | 5 |
| KY | 5,225 | 1,060 | 295 | 1,355 | 26 |
| LA | 16,892 | 2,481 | 634 | 3,115 | 18 |
| MA | 17,502 | 669 | 931 | 1,600 | 9 |
| MD | 30,558 | 1,072 | 953 | 2,025 | 7 |
| ME | 1,162 | 227 | 274 | 501 | 43 |
| MI | 13,961 | 555 | 748 | 1,303 | 9 |
| MN | 6,564 | 352 | 29 | 381 | 6 |
| MO | 11,087 | 1,155 | 550 | 1,705 | 15 |
| MS | 8,213 | 1,107 | 38 | 1,145 | 14 |
| MTb | 376 | 218 | 2 | 220 | 59 |
| NC | 24,476 | 3,045 | 844 | 3,889 | 16 |
| NDb | 185 | 0 | 7 | 7 | 4 |
| NE | 1,721 | 128 | 30 | 158 | 9 |
| NH | 1,152 | 201 | 0 | 201 | 17 |
| NJ | 35,860 | 1,373 | 423 | 1,796 | 5 |
| NM | 2,445 | 666 | 83 | 749 | 31 |
| NV | 6,894 | 412 | 124 | 536 | 8 |
| NY | 132,523 | 5,818 | 3,040 | 8,858 | 7 |
| OH | 17,146 | 1,453 | 834 | 2,287 | 13 |
| OK | 4,690 | 341 | 161 | 502 | 11 |
| OR | 5,130 | 374 | 659 | 1,033 | 20 |
| PA | 31,468 | 1,782 | 2,487 | 4,269 | 14 |
| PR | 18,129 | 1,614 | 424 | 2,038 | 11 |
| RI | 2,046 | 180 | 286 | 466 | 23 |
| SC | 14,044 | 951 | 2,296 | 3,247 | 23 |
| SDb | 443 | 0 | 1 | 1 | 0 |
| TN | 15,881 | 1,373 | 283 | 1,656 | 10 |
| TX | 64,498 | 4,392 | 2,227 | 6,619 | 10 |
| USVI | 589 | 42 | 0 | 42 | 7 |
| UT | 2,364 | 168 | 0 | 168 | 7 |
| VA | 20,721 | 721 | 109 | 830 | 4 |
| VT | 439 | 153 | 0 | 153 | 35 |
| WA | 10,732 | 653 | 662 | 1,315 | 12 |
| WI | 5,047 | 561 | 762 | 1,323 | 26 |
| WV | 1,476 | 369 | 0 | 369 | 25 |
| WY | 242 | 27 | 0 | 27 | 11 |
Source: CDC NCHHSTP Atlas [http://www.cdc.gov/nchhstp/atlas]; HRSA Ryan White Program RDR Report, 2010; HUD HOPWA CAPER and APR Reports, 2010; Bottom column is based on Ryan White Program Services Report, 2010.
a Percentage of number of PLWHA.
b Some HOPWA grants cover more than one state and report in aggregate. Therefore, it is not possible to separate expenditures or participants by state for those grantees. The most notable are Montana (which includes North Dakota and South Dakota) and the District of Columbia (which includes parts of Virginia and West Virginia).
c Total Number of Persons living with diagnosed HIV/AIDS in 2010 does not include American Samoa (2 people) or the Northern Mariana Islands (14 people).
d Unduplicated number of RWP clients receiving a housing service (includes HIV positive, indeterminate, and 3,049 clients who’s status was unknown/missing/not collected) based on 2010 RSR data. Number does not include 101 HIV negative clients who received a housing service.
e It is possible, but unlikely, that a person might receive housing services from both the HOPWA and Ryan White programs. More commonly, a person might receive housing assistance from HOPWA and other HIV-related services through the Ryan White Program.
