ADVISORY COUNCIL ON ALZHEIMER'S RESEARCH, CARE, AND SERVICES
Monday, May 3, 2021
Printer Friendly Version in PDF Format (6 PDF pages)
Approaches to Improving Dementia Diagnosis in Diverse Communities
Kate Possin, PhD
John Douglas French Foundation Endowed Professor
Associate Professor in Residence
Memory and Aging Center
University of California San Francisco
Outline
- Racial and ethnic disparities in dementia diagnosis
- Consortium for the Detection of Cognitive Impairment, including Dementia (DetectCID)
- Approaches to link PCP diagnosis with quality care
Disclosures
- Research funding from Quest Diagnostics
- Consulting fees from ClearView Health Partners and Vanguard
- Grants from NIA, NINDS, Global Brain Health Institute, Administration for Community Living, Rainwater Foundation
Racial/ethnic disparities in timeliness of dementia diagnosis
- 10,472 California Medicare beneficiaries with incident MCI or all-cause dementia diagnoses
- Timeliness: incident MCI vs. all-cause dementia diagnosis
- 23% of non-Hispanic White beneficiaries were first diagnosed at the MCI stage
- versus
- 18% of Hispanics beneficiaries
- 16% of Black beneficiaries
- 12% of Asian beneficiaries
Tsoy et al., 2021, JAMA Neurology
Racial/ethnic disparities in comprehensiveness of diagnostic work-up for dementia
- Comprehensiveness: specialist (e.g., neurology, geriatrics) evaluation, laboratory tests (B12, TSH), and neuroimaging (CT, MRI)
- Asian and Hispanic beneficiaries residing in highly disadvantaged neighborhoods were less likely to receive a comprehensive evaluation
- 10% of non-Hispanic White beneficiaries received all 3 recommended elements of diagnostic evaluation
- versus
- 5% of Hispanic beneficiaries
- 2% of Black beneficiaries
- 2% of Asian beneficiaries
Tsoy et al., 2021, JAMA Neurology
The Consortium for Detecting Cognitive Impairment, Including Dementia
- RFA-NS-17-012 PURPOSE: Address the unmet need to detect cognitive impairment, including dementia, in large & diverse U.S. populations seen everyday clinical settings, including in health disparities populations, when a patient, relative, or care provider indicates concern. Clinical paradigms should utilize tools that are simple to use, standardized, ideally take < 5 minutes to administer in primary care, and must provide turnkey follow-up recommendations.
- Project Scientist: Rod Corriveau
- Program Official: Claudia Moy / Rebecca Hommer
- Advisory Board: David Knopman, Katie Maslow, Terri Postma
- Ideal Outcome: Validated paradigms that are ready for large scale use in primary care and other everyday clinical settings.
Research on detecting CID was a high priority recommendation at the ADRD Summit 2016 & 2019
- Multiple Etiology Dementia Session 2019
- Recommendation 1 -- Priority 1. Detect whether cognitive impairment is objectively present when a patient, care partner or clinician reports cognitive, behavioral or functional changes (3- 7 y).
- Please see full recommendations here: https://www.ninds.nih.gov/sites/default/files/2019_adrd_summit_recommendations_508c.pdf
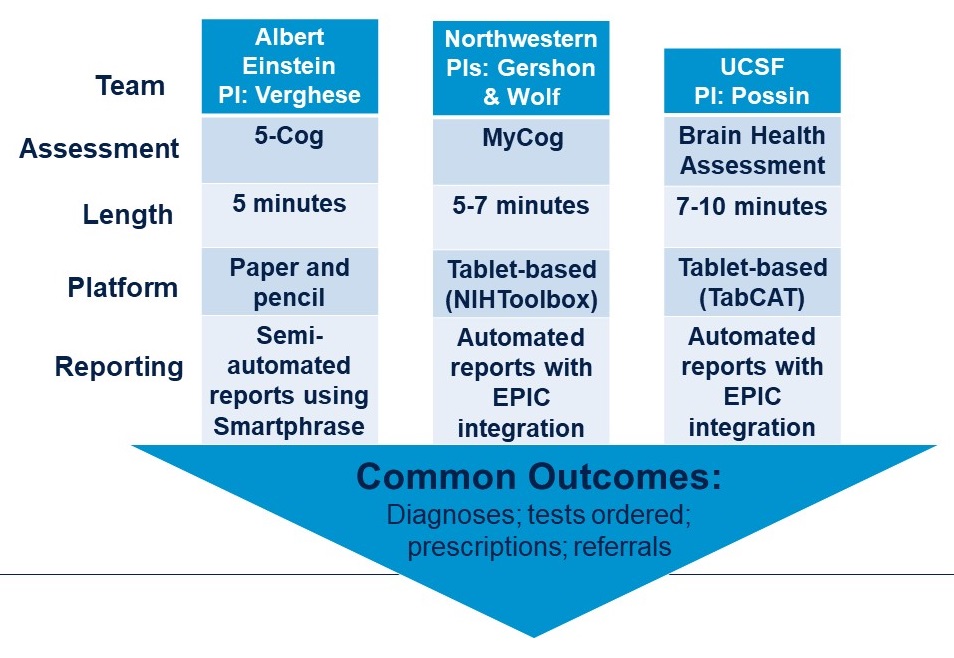 |
How to improve the detection of CID in primary care
- Engage primary care as partners in design
- Results must be easy to access in the EHR
- Diagnosis must be linked to better care
- Paradigms must address the needs of the increasingly diverse older adult population
- Paradigms should be flexible to include care partners, but must not require them
Primary Care Workflow for Detecting CID
- The biggest unmet challenge is linking the detection of CID with better care that supports the patient, care partner, and PCP
- patient, informant, clinician observation
- Cognitive test administered to detect CI
- PCP reviews results
- PCP discloses findings, continues workup, and provides care
Linking PCP diagnosis with better care
- Brain Health Consultation
- Conducted by dementia nurse with patient and care partner following PCP diagnosis
- Call is 30-60 minutes
- Needs assessment
- Questions answered and basic education about the condition given
- Resources offered and referrals facilitated
- Findings and next steps documented in the EMR for the PCP
Linking PCP diagnosis with better care
- The Care Ecosystem is telephone-based care navigation for dementia designed to supplement primary care, from diagnosis until end-of-life
- Over 12-months, in comparison to the usual care group, the dementia care navigation:
- Improved caregiver well-being
- Improved patient quality of life
- Reduced emergency room visits
