April 6, 2021
Link to Printer Friendly Version in PDF Format (11 PDF pages)
KEY POINTS
-
Approximately 1.6 million adults 65 years of age and over living in the United States may have trouble accessing the COVID-19 vaccine because they are homebound; 51% of these older adults face at least one additional barrier, such as living alone or lacking technology.
-
Nearly 15% of Hispanic older adults are homebound, compared to 7% of Black older adults, 5% of older adults who are American Indian, Asian, or Pacific Islander, and 3% of those who are White.
-
Just under half of homebound older adults are connected to assistance programs and services such as food stamps, Meals-on-Wheels, and in-home rehabilitative care; vaccinating homebound older adults could be facilitated through partnerships with these programs.
-
Almost all homebound older adults--96%--report having seen their doctor in the past year; working more closely with primary care providers and health centers may also benefit vaccination efforts.
BACKGROUND
Vaccinating older adults against COVID-19 is currently one of the United States' highest public health priorities; however, older adults who live in the community, particularly those that are homebound, face several challenges to accessing the COVID-19 vaccine. Many older adults who want the vaccine may miss the opportunity, because it is the responsibility of the individual to find, sign up for, travel to, and get their own vaccine. At present, the COVID-19 vaccine is predominantly scheduled online and offered at pharmacies and hospitals rather than through individual physicians or health centers, which is how older adults generally receive care.[1] Older adults may lack internet access, be unfamiliar with online scheduling, and lack transportation. Further these individuals may lack a social network that might assist in making online appointments or traveling to vaccination sites.[1, 2, 3] Older adults who are disproportionately impacted by COVID-19 are also individuals that may face additional challenges accessing the vaccine: older adults who are Black or Hispanic, and those who live in rural areas or low-income neighborhoods.[1, 2, 3]
Current vaccination efforts primarily allocate vaccines to various sites throughout communities, such as local long-term care facilities, health departments, hospitals, pharmacies, and federally qualified health centers.[4] Although engaging with these partners has expanded access for many, traveling to vaccine sites in the community remains a challenge for older adults who are homebound. The Centers for Medicare & Medicaid Services (CMS) define homebound as normally unable to leave home unassisted and for whom leaving the house would take considerable and taxing effort.[5] Research has consistently found that homebound individuals tend to have multiple health conditions, both chronic and acute, at higher rates than older adults who are not homebound. These older adults also have higher rates of depression and anxiety, feelings of depression without a clinical diagnosis, and probable dementia.[6, 7, 8] They have higher rates of hospitalization and emergency department utilization, and are more likely to rely on others for assistance with activities of daily living (ADLs) and household activities.[7, 8, 9] Homebound older adults are also likely to take more medications than other adults living in the community.[8] Homebound older adults have greater mortality than those who are not homebound, even after controlling for comorbidities and functioning.[7]
Reaching homebound individuals is challenging despite their high prioritization for the COVID-19 vaccine due to age or underlying medical conditions. However, homebound older adults are likely unable to get to a vaccination site, even with improved scheduling and transportation options.[1, 2, 10] The public health departments, health care systems, and pharmacies that currently administer vaccines face barriers to delivering these vaccines at home including vaccine handling and storage, transportation, and costs.[9] Home care and other community providers that are positioned to overcome these barriers do not currently have the access or authority to administer to the COVID-19 vaccine.[11] Although the Centers for Disease Control and Prevention (CDC) recently posted guidance on vaccinating homebound persons, individuals who are homebound have not been classified by the CDC as a discrete priority group or one that requires extra precautions.[12, 13, 14]
Given the vulnerability of this population, it is critical that policymakers determine the prevalence and characteristics of this population and develop interventions to target homebound older adults for vaccination efforts.
METHODS
We used the National Health and Aging Trends Study (NHATS) 2015 cohort survey data Round 5 to determine the size and characteristics of the homebound population. NHATS is a panel study that gathers information on an annual basis from a nationally representative sample of Medicare beneficiaries aged 65 and over in the contiguous United States (n=8,334). We used 2015 because it was the most recent round of NHATS representative of the 65+ population. NHATS respondents self-report on factors such as physical capacity, economic well-being, living arrangements, and social, physical, and technological environment. NHATS oversamples by age and for Black non-Hispanic individuals. We used survey design weights in all of our analyses.
Our study only included older adults who reported living in the community (n=7,070). We defined a person as homebound if the person stated that they rarely or never (≤1 day/week) went outside. This definition is consistent with previous studies that used NHATS to explore the homebound population.[12, 13]
We analyzed the demographics and socioeconomic characteristics of homebound older adults and compared to non-homebound individuals. These characteristics included: age; sex; race/ethnicity; mean annual income; and past month receipt of Social Security Income (SSI). We also analyzed the functional acuity of homebound older adults using NHATS mobility questions: "Do you require help going outside" and "How much difficulty do you have when leaving the house by yourself?". We classified older adults as having lower mobility limitations if they reported not requiring help going outside or experiencing no difficulty leaving the house alone; otherwise, respondents were classified as having higher mobility limitations. To better understand the difficulty and risk of accessing the COVID-19 vaccines among homebound older adults, we also determined the number of both chronic conditions and ADLs for which they required assistance. We also examined potential additional barriers to accessing COVID-19 vaccines, such as: living alone; size of social support network; metropolitan/non-metropolitan indicators; technological environment; use of transportation for medical care activities; and frequency of doctor visits (see Appendix 1 for more details).
Finally, we explored the rates of use of various assistance programs and in-home services, including: Meals-on-Wheels; food stamps and other food assistance; gas/energy assistance; and in-home rehabilitative services, which includes physical, occupational, and speech therapy.
FINDINGS
Of the NHATS participants residing in the community, who represent 39 million Medicare beneficiaries over 65 years of age, approximately 4% are categorized as homebound, representing 1.6 million people. Among homebound older adults, 27% are male and 73% female. The proportion of adults who are homebound increases with age.
Hispanic older adults are more likely to be homebound. Overall, Hispanic older adults are the most likely to be homebound (14.5%) and twice as likely as the next closest population of non-Hispanic Black older adults (7.3%). Non-Hispanic White older adults and American Indian, Asian, and Pacific Islander older adults both have comparably low rates (3.0% and 4.5% respectively) of being homebound. Across all race/ethnicity groups, the proportion of homebound older adults tends to increase with age, though there is some variation among American Indian, Asian, and Pacific Islander older adults.
| Figure 1. Distribution of Homebound Old Adults by Race/Ethnicity and Age |
|---|
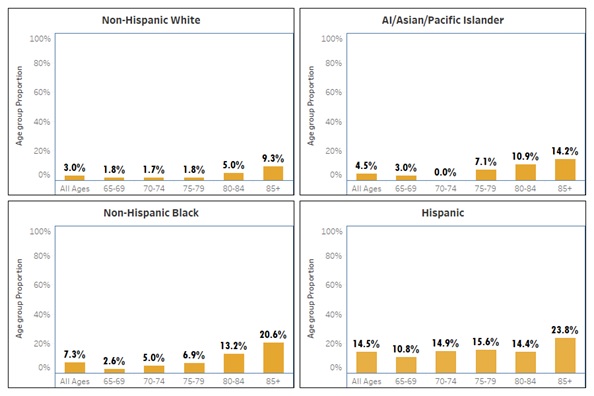 |
| SOURCE: NHATS 2015 (Round 5 Cohort). |
Homebound adults often have multiple chronic conditions that increase their risk for COVID-19. Nearly 80% of homebound older adults report having higher mobility limitations; that is, they need assistance or find it difficult to go outside. As can be found in the literature,[11, 12, 13, 14] homebound older adults often have at least one chronic condition, putting this population at risk for poor outcomes due to COVID-19.[15] Self-reported chronic conditions in this analysis include ever having a heart attack, heart disease, arthritis, osteoporosis, diabetes, lung disease, stroke, dementia, or cancer. More than 73% of all homebound older adults report having three or more chronic conditions, and fewer than 3% report having no chronic conditions.
| Figure 2. Distribution of Mobility Limitations and Number of Chronic Conditions Among Homebound Older Adults |
|---|
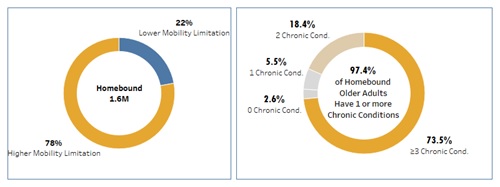 |
| SOURCE: NHATS 2015 (Round 5 Cohort). |
Majority of homebound older adults need assistance with daily living. Older adults who are homebound also frequently report receiving assistance for ADLs, which include eating, toileting, bathing, and dressing. The majority of homebound older adults (62.8%) report needing help with two or more ADLs. These functional limitations could pose further challenges for homebound older adults in attempting to access vaccination.
| Figure 3. Number of ADLs Assistance Received |
|---|
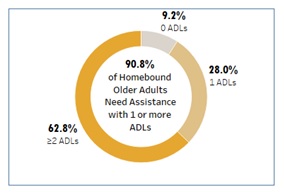 |
| SOURCE: NHATS 2015 (Round 5 Cohort). |
Half of homebound older adults have at least one barrier to accessing vaccines. Roughly a fifth of homebound older adults live alone or have one or no persons in their social network, suggesting some homebound older adults may face the additional vaccination barrier of having poor social support. Older adults in rural communities also report struggling to access the COVID-19 vaccine; the 18% of homebound older adults living in non-metro areas may therefore be harder to reach than their metro-residing counterparts. Similarly, 15% of homebound individuals report having no access to a computer, smartphone, or tablet, which would make online scheduling of a vaccination challenging for this group. Accessing transportation to medical appointments poses a challenge for 14% of homebound older adults.
Taken together, 51% of all homebound older adults, or 820,000 people, experience at least one potential barrier. In addition to being homebound, challenges to accessing the vaccine may be further exacerbated by these vulnerabilities. These barriers suggest that while most homebound older adults are capable of attending a medical appointment (about 96% report having seen their regular doctor in the past year), it is an extremely difficult task.
| Figure 4. Potential Barriers to Accessing COVID-19 Vaccines Among Homebound Older Adults |
|---|
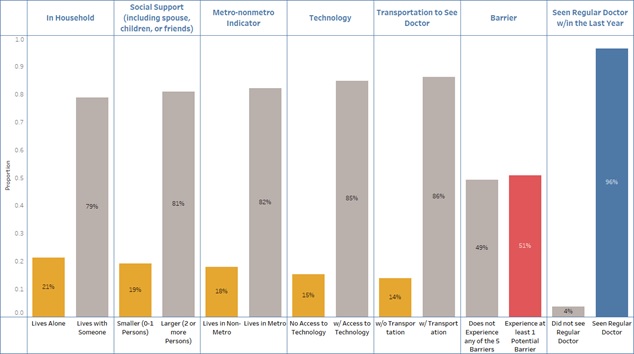 |
| SOURCE: NHATS 2015 (Round 5 Cohort). |
Homebound older adults have fewer economic resources. Homebound older adults tend to have much lower mean annual income than non-homebound individuals and are more likely to receive SSI in the past month.
| Figure 5. Economic Well-Being of Homebound Older Adults versus Non-Homebound Older Adults |
|---|
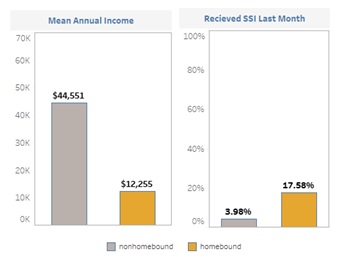 |
| SOURCE: NHATS 2015 (Round 5 Cohort). |
Nearly half of all homebound older adults receive assistance. Among homebound older adults living in the community, a total of 47% receives some form of assistance, including rehabilitative care, food stamps or other food assistance, Meals-on-Wheels, and gas/energy assistance. In-home rehabilitative care is the most common among homebound with higher mobility limitations at 27%, and 18% reported receiving food assistance including food stamps. Older adults who are homebound with lower mobility limitations report receiving food assistance to be most common (15%) while in-home rehabilitation is the least common assistance at roughly 2%. Meals-on-Wheels is also less common among the lower mobility limitation population (6%), as well as among higher mobility limitation individuals (12%). Just 9% of older adults report receiving gas or energy assistance. These finding suggests that while some older adults are already connected to services, the majority may require significant and tailored outreach to connect them with vaccination opportunities.
| Figure 6. Percentage of Homebound Older Adults Receiving Assistance or In-Home Rehabilitation | |||||
|---|---|---|---|---|---|
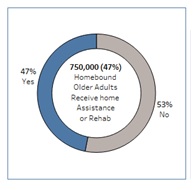 |
Among Homebound Individuals that Receive Assistance | ||||
| Program | Population Estimate | Homebound | Higher Mobility Limitation | Lower Mobility Limitation | |
| Receive Rehab at Home | 350,000 | 21.7% | 27.1% | 2.4% | |
| Food Stamps or Assistance | 300.000 | 17.6% | 18.3% | 15.0% | |
| Meals-on-Wheels | 160,000 | 10.4% | 11.5% | 6.4% | |
| Gas/Energy Assistance | 140,000 | 9.0% | 8.6% | 10.7% | |
| SOURCE: NHATS 2015 (Round 5 Cohort). | |||||
DISCUSSION
Homebound older adults are vulnerable to severe illness caused by COVID-19 due to their age and high rates of chronic conditions and are therefore likely to be included in current vaccine priority groups.[16] Despite this priority status, homebound older adults, particularly those with higher mobility limitations, may face significant barriers accessing the COVID-19 vaccine at sites in their community due to the need to travel to vaccination sites. This gap in the ongoing vaccination effort also risks exacerbating existing disparities seen in the COVID-19 pandemic itself based on age, race, and income. This is especially true for Hispanic older adults, who are much more likely to be homebound and also face high rates of hospitalization and death due to COVID-19.[17]
In order to serve homebound older adults, some in-home vaccination provision likely is necessary. In-home vaccination can be optimized through partnerships with home care providers and expanded engagement of primary care providers. Approximately 350,000 homebound older adults receive in-home rehabilitative services, which offers eligible vaccine providers a means to reaching this population. While NHATS does not provide data on receiving home and community-based services, roughly 4.5 million older adults use a home health agency, suggesting partnerships with home health agencies could also facilitate in-home vaccination provision.[18] Area Agencies on Aging, which often provide meal-delivery and case management services, could also provide information on homebound older adults living in the community who may require in-home vaccinations.[19] Given the findings on homebound older adults receiving assistance, partnering with Meals-on-Wheels and using data from federal food assistance programs could also provide insight into reaching these individuals. Leveraging these partnerships could provide either identification of individuals for outreach or an opportunity to vaccinate in-home by having an eligible provider accompany the meal or service delivery program to the homes of these older adults.
That said, since 53% of homebound older adults are not connected with services such as Meals-on-Wheels or in-home care, agencies and organizations involved in the vaccine efforts may need to increase outreach in their communities to ensure this population is aware of the vaccination options available. Better engaging primary care providers and health clinics could facilitate greater outreach and engagement with homebound older adults, since 96% of individuals report seeing their regular physician within the past year.
Some localities are already providing in-home vaccinations. For example, the Nevada Senior Services has been designated as a vaccine administrator. They are providing vaccinations first to active adult day center clients, followed by at-home program participants. In Maryland, certain counties are deploying emergency medical technicians to provide in-home vaccinations.[20] The Ventura County Area Agency on Aging relies on a strike team of public health nurses to vaccinate homebound individuals where they live.[21] However, efforts such as these are not yet widespread.
There is hope that vaccination efforts for homebound older adults will become easier to implement. The recent authorization of the Janssen's (Johnson & Johnson) single-dose vaccine, which has less challenging storage requirements, will provide new opportunities to deliver the vaccine in primary care, health clinic, and home environments, among other places, that are more accessible to homebound older adults.[22] Establishing a reliable infrastructure for vaccine delivery to this population is important to this round of vaccinations as well as any required future "booster shots". Increased attention to this population will help ensure that these vulnerable adults have the opportunity to be vaccinated against COVID-19.
APPENDIX 1. VARIABLES OF INTEREST
| Variables of interest | Description |
|---|---|
|
Demographics |
Includes age (65-69; 70-74; 75-79; 80-84; 85-89; 90+), sex (Male; Female), Race/Ethnicity (White; American Indian/Asian American/Pacific Islander; non-Hispanic Black; Hispanic) |
|
Homebound |
The person is classified as homebound if the person responded that they have rarely or never (≤1 day/week) gone outside in the past month. |
|
Mobility Limitation |
Among homebound individuals, the person is classified as having lower mobility limitation if the person reported they did not require help or that they experienced no difficulty going outside in the past month. Otherwise, the person is classified as having higher mobility limitation. |
|
Chronic Health Condition |
The person is defined as having chronic health condition if the person responded yes to ever having 1 or more of the following conditions: ever having a heart attack, heart disease, arthritis, osteoporosis, diabetes, lung disease, stroke, dementia, or cancer; the total number of chronic conditions for each person were then recorded. |
|
Activities of Daily Living (ADLs) |
The person is defined as requiring assistance with ADLs if the person responded yes to receiving assistance with 1 or more of the following activities: eating, toileting, dressing, and bathing; the total number of ADLs for each person were then recorded. |
|
Transportation |
The person is classified as not having transportation for medical care if the person responded that they have not driven, have not taken public transportation, have not taken a taxi, and were not driven by family or friends to see the doctor. |
|
In Household |
The person is classified as living alone if the person reported not residing with a spouse, children, or others. |
|
Social Support Network |
The person is defined as having a smaller social support network if the person reported having ≤1 person in social network, no spouse, ≤1 child, and no one to talk to. The person is defined as having a larger social support network if the person reported having ≥2 persons in their social network, a spouse, ≥2 children, and someone to talk to. |
|
Metropolitan/non-Metropolitan indicator |
Describes if the person lives in a metropolitan or non-metropolitan residence. |
|
Technological Environment |
The person is classified as lacking access to technology if the person reports having no working cellphone, does not own a computer or tablet, does not know how to use a computer or tablet online, and does not email or text. |
|
Doctor Visit |
The person is classified as not having seen the doctor if the person reports not having seen their regular doctor within the past year. |
|
Economic Well-Being |
Includes average annual income and receipt of SSI in past month. |
|
Type of Assistance Program Received |
Describes if the person receives at least 1 of the following: food stamps or other food assistance; rehabilitative care at home; Meals-on-Wheels; or gas/energy assistance. |
REFERENCES
-
Bergal J. (2021). Without a Ride, Many in Need Have No Shot at COVID-19 Vaccine. Accessed February 11, 2021 at https://www.pewtrusts.org/en/research-and-analysis/blogs/stateline/2021/02/01/without-a-ride-many-in-need-have-no-shot-at-covid-19-vaccine.
-
Graham J. (2021). Older Adults Without Family or Friends Lag in Race to Get Vaccines. Accessed February 11, 2021 at https://khn.org/news/article/older-adults-without-family-or-friends-lag-in-race-to-get-vaccines/.
-
Noguchi Y. (2021). Race Versus Time: Targeting Vaccine To The Most Vulnerable Is No Speedy Task. Accessed February 23, 2021 at https://www.npr.org/sections/health-shots/2021/02/23/969384904/race-versus-time-targeting-vaccine-to-the-most-vulnerable-is-no-speedy-task.
-
Centers for Disease Control and Prevention (CDC). (2021). How Vaccines Get to You. Accessed April 6, 2021 at https://www.cdc.gov/coronavirus/2019-ncov/vaccines/distributing.html.
-
Centers for Medicare & Medicaid Services (CMS). (2006). Glossary. Accessed February 24, 2021 at https://www.cms.gov/apps/glossary/search.asp?Term=homebound&Language=English.
-
Cheng J., Batten G., Cornwell T., Yao N. (2020). "A qualitative study of health-care experiences and challenges faced by ageing homebound adults." Health Expectations, 23(4), 934-942. doi: 10.1111/hex.13072.
-
Soones T., Federman A., Leff B., Siu A.L., Ornstein K. (2017). "Two-year mortality in homebound older adults: An analysis of the National Health and Aging Trends Study." Journal of the American Geriatrics Society, 65(1), 123-129. doi: 10.1111/jgs.14467.
-
Ornstein K.A., Leff B., Covinsky K.E., Ritchie C.S., Federman, A.D., Roberts L., Kelley A.S., Siu A.L., Szanton S.L. (2015). "Epidemiology of the homebound population in the United States." JAMA Internal Medicine, 175(5), 1180-1186. doi: 10.1001/jamainternmed.2015.1849.
-
Musich S., Wang S., Hawkins K., Yeh C. (2015). "Homebound older adults: Prevalence, characteristics, health care utilization and quality of care." Geriatric Nursing, 36(6), 445-450. doi: 10.1016/j.gerinurse.2015.06.013.
-
Graham J. (2021). Countless Homebound Patients Still Wait for Covid Vaccine Despite Seniors' Priority. Accessed February 23, 2021 at https://khn.org/news/article/countless-homebound-patients-still-wait-for-covid-vaccine-despite-seniors-priority/.
-
Pittman P., Westfall N., Ziemann M., Strasser J. (2021). "Who is Allowed to administer COVID-19 vaccines? The list is growing." Health Affairs Blog. doi: 10.1377/hblog20210303.890600.
-
Centers for Disease Control and Prevention (CDC). (2021). Vaccinating Homebound Persons With COVID-19 Vaccine. Accessed February 12, 2021 at https://www.cdc.gov/vaccines/covid-19/clinical-considerations/homebound-persons.html.
-
Centers for Disease Control and Prevention (CDC). (2021). COVID-19: CDC's COVID-19 Vaccine Rollout Recommendations. Accessed February 26, 2021 at https://www.cdc.gov/coronavirus/2019-ncov/vaccines/recommendations.html.
-
Centers for Disease Control and Prevention (CDC). (2021). COVID-19: Other People Who Need Extra Precautions. Accessed February 26, 2021 at https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/other-at-risk-populations.html.
-
Bosworth A., Finegold K., Samson L., Sheingold S., Tarazi W., Zuckerman R. (2021). Risk of Covid-19 Infection, Hospitalization, and Death in Fee-For-Service Medicare (Issue Brief). Washington, DC: Office of the Assistant Secretary for Planning and Evaluation, U.S. Department of Health and Human Services. Accessed April 2, 2021 at https://aspe.hhs.gov/sites/default/files/private/pdf/265271/risk-score-issue-brief.pdf.
-
Centers for Disease Control and Prevention (CDC). (2021). COVID-19: People with Certain Medical Conditions. Accessed February 26, 2021 at https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/people-with-medical-conditions.html.
-
Centers for Disease Control and Prevention (CDC). (2021). COVID-19: Hospitalization and Death by Race/Ethnicity. Accessed March 22, 2021 at https://www.cdc.gov/coronavirus/2019-ncov/covid-data/investigations-discovery/hospitalization-death-by-race-ethnicity.html.
-
Harris-Kojetin L., Sengupta M., Lendon J., Rome V., Valverde R., Caffrey C. (2019). Long-Term Care Providers and Services Users in the United States, 2015-2016. Washington, DC: National Center for Health Statistics, U.S. Department of Health and Human Services.
-
National Association of Area Agencies on Aging. (2021). Roles of Area Agencies on Aging in the Vaccination of Older Adults. Accessed March 2, 2021 at https://www.n4a.org/Files/AAA%20Roles%20in%20the%20Vaccination%20of%20Older%20Adults%202.9.21%20Final%20to%20Share.pdf.
-
Link G. "Re: Issue Brief on Barriers to Access for Homebound and Semi-homebound Older Adults." Received by authors February 22, 2021.
-
Long E. "Re: Ventura CA." Received by authors March 22, 2021.
-
Centers for Disease Control and Prevention (CDC). (2021). Janssen COVID-19 Vaccine (Johnson & Johnson): Transporting Vaccine for Vaccination Clinics Held at Satellite, Temporary, or Off-Site Locations. Accessed March 11, 2021 at https://www.cdc.gov/vaccines/covid-19/info-by-product/janssen/downloads/janssen-transportation-guidance.pdf.
U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES
Office of the Assistant Secretary for Planning and Evaluation
200 Independence Avenue SW, Mailstop 447D
Washington, D.C. 20201
For more ASPE briefs and other publications, visit: aspe.hhs.gov/reports
ABOUT THE AUTHORS
Emma Nye and Martin Blanco work in the Office of Behavioral Health, Disability, and Aging Policy in the Office of the Assistant Secretary for Planning and Evaluation
SUGGESTED CITATION
Nye, E., & Blanco, M. Characteristics of Homebound Older Adults: Potential Barriers to Accessing the COVID-19 Vaccine (Issue Brief). Washington, DC: Office of the Assistant Secretary for Planning and Evaluation, U.S. Department of Health and Human Services. April 6, 2021.
COPYRIGHT INFORMATION
All material appearing in this report is in the public domain and may be reproduced or copied without permission; citation as to source, however, is appreciated.
___________________________________
Subscribe to ASPE mailing list to receive email updates on new publications: aspe.hhs.gov/join-mailing-list
For general questions or general information about ASPE: aspe.hhs.gov/about
