Contents
- Introduction
- Overview of DSH Funding Policies
- What Is a Safety Net Hospital?
- How Should Financial Vulnerability Be Defined?
- Framework for Analyzing DSH Allocation Policies
- Hospital Data Set and Low-income Patient Variables
- Joint Distribution of DSH Payments under Current Policies
- Exploratory Analyses Using National HCUP Data
- Three State Analysis of Alternative DSH Policies
- Summary of Findings and Conclusions
Introduction
The Medicare and Medicaid programs distribute extra payments to hospitals that treat a disproportionate share of indigent patients. The disproportionate share hospital (DSH) payment policies differ substantially between the two programs and, under Medicaid, across states as well. Nevertheless, the general objectives of each program are the same: to support the hospitals that are crucial to the health care safety net, and to preserve access to these hospitals for the respective program's enrollees.
Medicare and Medicaid DSH payments represent an important source of hospital revenues. In federal fiscal year 1998, Medicare DSH payments totaled an estimated $4.8 billion and Medicaid DSH payments totaled $15.0 billion, of which $8.3 billion were federal funds. This represented almost seven percent of total hospital revenues from all sources in that year. Yet relatively little is known about the distribution of these payments and how well they are targeted toward financially vulnerable safety net hospitals.
State-reported information on Medicaid DSH payments to individual hospitals permits for the first time a national examination of the joint distribution of Medicare and Medicaid funds and how well the funds are targeted toward vulnerable safety net hospitals. This report provides the results of our analyses to: 1) examine the distribution of both Medicare and Medicaid DSH funds across hospitals, 2) assess alternative criteria that could be used to identify safety net hospitals, 3) develop measures of hospital financial vulnerability to identify those safety hospitals that are under most financial pressure, and 4) explore the extent to which alternative allocation policies to the current Medicare and Medicaid DSH payment mechanisms would improve the distribution of funds to those safety net hospitals that are most vulnerable.
Overview of DSH Funding Policies
Medicare DSH Policies
The Medicare DSH payment is an adjustment to the DRG payment for inpatient hospital services furnished by acute care hospitals. The adjustment is based on the hospitals disproportionate share patient percentage. This is the sum of:
- the percentage of the hospital's total Medicare patient days attributable to Medicare patients who also are federal Supplemental Security Income (SSI) beneficiaries (excluding state supplement only beneficiaries), and
- the percentage of the hospital's total patient days attributable to Medicaid beneficiaries (excluding Medicare beneficiaries).
The eligibility criteria and formulae for determining Medicare DSH payments have changed over time to include more hospitals and (except for the temporary reductions in the Balanced Budget Act of 1997 (BBA)) to provide more generous payment levels. As a result, the amount of these payments has grown considerably over the last decade. In fiscal year 1989, Medicare DSH payments were an estimated $1.1 billion. By 1992, payments had doubled to $2.2 billion, and they had more than doubled again by 1997.
The Centers for Medicare and Medicaid Services (CMS, formerly the Health Care Financing Administration) has generally maintained that the DSH adjustment is intended to cover only the higher costs associated with the care of Medicare beneficiaries in hospitals serving a disproportionate share of low-income patients. For example, when the prospective payment system for capital costs was implemented in FY1992, the DSH adjustment was established administratively based on the estimated effect of the disproportionate share of low- income patient percentage on total inpatient costs per case and has no minimum threshold (but is limited to urban hospitals with at least 100 beds). On the other hand, the Medicare Payment Advisory Commission (MedPAC) views the DSH adjustment as a policy adjustment independent of hospital cost that is intended to assure access to care for low-income Medicare beneficiaries and other poor people.
MedPAC has made several recommendations regarding the formula used to determine Medicare DSH payments (MedPAC 1998; MedPAC 1999, MedPAC 2001), including:
- The low-income share measure should reflect the costs of services provided to low-income patients in both inpatient and outpatient settings.
- In addition to Medicare SSI and Medicaid patients, the low-income share measure should include patients sponsored by other state and local indigent care programs and uninsured and underinsured patients represented by uncompensated care. This would eliminate disparities caused by differences in Medicaid eligibility rules across states.
- Medicare DSH payments should be concentrated among hospitals with the highest shares of low-income patients. A minimum threshold should be established below which a hospital receives no DSH payment but there should be no notch that would provide substantially different payments to hospitals just above and below the minimum threshold.
- To eliminate the disparity between the payments received by urban and rural hospitals with the same proportion of low-income patients, the same general approach for distributing Medicare DSH payments should apply to all PPS hospitals.
- The Secretary should collect the data necessary to implement a revised Medicare DSH payment mechanism.
Medicaid DSH Payments
In keeping with the federal/state partnership under Medicaid, states have considerable latitude in determining which hospitals are eligible for DSH payments and how those funds are distributed. The Medicaid law requires states to designate as disproportionate share hospitals all hospitals meeting one of the following criteria:
- a Medicaid inpatient utilization rate one standard deviation or more above the mean for all hospitals in the state, or
- a low-income utilization rate exceeding 25 percent.
In determining the amount of the DSH payment to eligible hospitals, states may use the Medicare formula or make an adjustment that increases proportionally with the hospital's low- income utilization rate. States may designate other hospitals as disproportionate share hospitals and separate formulae are allowed for different types of hospitals.
In the early 1990s, Medicaid DSH payments grew rapidly from less than $1 billion in FY 1989 to more than $17 billion in FY1992; however, the use of DSH by the states is highly uneven. A study by Ku and Coughlin (1995) found that Medicaid DSH and related programs help support uncompensated care, but that only a small share of these funds were available to cover the costs of uncompensated care because of intergovernmental transfers and the amounts retained by the states. In a later re-examination of this issue after legislation aimed at addressing this issue had taken effect, Coughlin, Ku, and Kim (2000) found that an increasing share of the DSH gains was paid to local public and private hospitals and less was retained by the states.
[ Go to Contents ]
What Is a Safety Net Hospital?
Federal policymakers, states and researchers have used a broad range of definitions to characterize safety net hospitals. While the definitions vary, a common theme is that safety net hospitals provide a disproportionate amount of care to vulnerable populations. Which hospitals are ultimately identified as safety net providers has important implications for evaluating whether DSH payments are well targeted: Is the purpose to help relieve hospitals financial burden of caring for low-income populations? Help hospitals in financial distress? Protect low- income Medicare and Medicaid beneficiaries access to care? Compensate hospitals for providing care to the uninsured? Help states and local governments in areas with high levels of need? Encourage selected hospital behavior such as providing special servicesteaching, emergency room care, trauma care and the like? Or, perhaps, the purpose is some combination of these. A summary of the key dimensions to describing a safety net hospital and how policymakers and researchers have defined safety net hospitals is provided in Table ES.1.
An important distinction of safety net hospitals is that they provide care to vulnerable populations. Unfortunately, there is no general agreement on which groups should be considered vulnerable. The Institute of Medicines recent report, Americas Health Care Safety Net, adopted a broad definition of vulnerable populationsincluding the uninsured, Medicaid and other vulnerable patients (IOM 2000). The other vulnerable groups included homeless persons, persons with HIV, substance abusers, and the mentally ill.
A major issue is whether low-income patients with insurance should be included in the definition of vulnerable (IOM, 2000). The principal argument for excluding low-income Medicare patients (i.e., those that are entitled to SSI) and Medicaid patients is that they have insurance and thus have access to the health care system. The uninsured, by definition, have no insurance, and generally have very limited ability to pay for their care. The arguments for counting Medicaid patients as a vulnerable population is that, despite having insurance, Medicaid patients have complex health care needs and often have trouble gaining access to health care services because of the historically low program payment rates. Further, their low- income and complex health care needs make them a vulnerable population. An alternative to an all-or-nothing policy would be to include shortfalls (the difference between the costs and the amounts received) from Medicaid and local indigent care programs.
Another distinguishing feature of safety net hospitals is that they provide a disproportionate amount of care to vulnerable populations. A key issue in quantifying the amount of care is whether it should be based on the volume of care provided to vulnerable populations or the uncompensated cost of that care. While the Medicare and Medicaid DSH programs identify a safety net hospital primarily on the volume of low-income patients it serves, another common strategy, especially in the research literature, is to designate safety net hospitals by their level of uncompensated care coststhat is, the costs of charity care and bad debt.
Another important issue is how to decide whether the care to vulnerable populations is disproportionate to that provided by other hospitals. Medicare uses a national benchmark while Medicaid compares hospitals to others in the same state. MedPAC recommends that a threshold be set so that between 50-60 percent of hospitals would qualify for Medicare DSH payments.
| Dimension | Research and Policy Definitions |
|---|---|
| Legal Mandate or Mission | Clinton Health Care Proposal: Legal mandate and in area of high need Gaskin and Hadley: Mandate or mission driven or high share of low- income discharges |
| Vulnerable Populations | Medicare DSH formula: Medicaid and Medicare/SSI recipients Basic Medicaid DSH formula: Three available options, which can be used separately or jointly Medicare DSH formula Medicaid recipients only or Low-income populations including Medicaid and indigent persons Medicaid DSH option: states free to establish own criteria for vulnerable populations IOM: uninsured, Medicaid, and other populations such as people with HIV or mental illness. |
| Disproportionate Amount of Care | Volume of care: Medicare DSH Formula: threshold volume of Medicaid and Medicare SSI patients depending upon selected hospital characteristics such as size and location Federal Medicaid DSH minimum standards: Hospitals Medicaid inpatient rate at least 1 S.D. above state mean Medicaid inpatient rates Hospitals low-income use rate (Medicaid and charity care patients(1)) >25% Many states pay DSH to other hospitals as well Costs of uncompensated care: Top 10% of hospitals providing most bad debt and charity care (Baxter and Mechanic 1997) Top 10% of hospitals with highest ratio of bad debt and charity care to operating expense (Fishman 1997) Ratio of hospitals uncompensated care to hospitals total costs >10% (Cunningham and Tu 1997) Type of care: Provision of certain types of services (e.g. ER, trauma, burn) as indication of safety net hospital |
| Level of Aggregation | National Hospital-type State Market level |
[ Go to Contents ]
How Should Financial Vulnerability Be Defined?
Developing and evaluating alternative methods for distributing Medicare and Medicaid DSH payments requires measures of the financial pressure faced by each safety net hospital. The measures serve two potential purposes. First, one or more of them could be used as an explicit factor in allocating funds to safety net hospitals. The measures most appropriate for this purpose would be those that are directly related to serving low-income populations such as shortfalls from Medicaid and local indigent care programs and/or uncompensated care. Second, more general measures such as a hospitals margin net of DSH payments can be used to evaluate how well the DSH allocation policy targets financially vulnerable safety net hospitals without being explicitly incorporated into the allocation formula. Comparing total margin net of DSH payments to total margin including DSH subsidies under alternative DSH allocation methodologies provides an indication of how a hospitals financial viability would be affected assuming no behavioral changes occur in the services it provides or in the revenues it receives from Medicaid and other payers.
[ Go to Contents ]
Framework for Analyzing DSH Allocation Policies
The literature concerning safety net hospitals and the current policies for Medicare and Medicaid DSH payments suggest a set of policy issues related to the distribution of DSH funds.
- To what extent should DSH funds be targeted on core safety net providers that are financially vulnerable? Should hospitals that are able to cover losses attributable to uncompensated care and Medicaid shortfalls receive subsidies? Some hospitals that provide a substantial volume of services to low- income patient populations are not financially vulnerable because they are able to generate sufficient revenue (in the absence of government subsidies) to cross-subsidize the cost of caring for low- income patients.
- How can the allocation policy be structured to maintain or enhance level of effort regarding Medicaid eligibility and reimbursement rates as well as programs to subsidize care provided to the uninsured?
- Should a threshold be used to target DSH payments on those hospitals that serve as core safety net hospitals? What are the implications for communities where caring for the uninsured is shared across hospitals relative to those where it is concentrated in a few hospitals?
Analytical Policy Questions
Underlying these major policy issues are empirical questions regarding the sensitivity of the allocations to different measures that could be used to define financially vulnerable safety net hospitals. These questions are important in understanding the impact the policy choices could have on the distribution of DSH funds to particular hospitals and identifying those choices where administrative preferences for readily available measures would have little effect on the distributions. In this report, we evaluated how different measures of financially vulnerable safety net hospitals would affect 1) the set of hospitals eligible to receive federal subsidies and 2) the distribution of funds among those hospitals. The analytical questions related to the distribution of DSH funds include:
- How sensitive is the allocation of DSH funds to different measures of vulnerable populations? Do measures that use only a subset of low-income patients (e.g. Medicaid patients) target the same hospitals as more inclusive measures?
- Is it feasible for the allocation formula to take into account both inpatient and outpatient services? How does this affect the relative distribution of DSH funds?
- Do measures based on the proportion of care furnished to low-income patients target a different set of hospitals than those based on the financial risk associated with serving low- income patients?
- Does a strategy such as a minimum threshold or sliding scale improve the relationship between a hospitals financial risk and the subsidy it would receive from a DSH fund?
Our exploratory analyses of alternative allocation policies are within the context of using a single federal DSH funding mechanism. By assuming there would be a new funding stream to support financially vulnerable safety net hospitals, there is no need to link the funds to services provided to Medicare and Medicaid beneficiaries and there is greater flexibility to address the identified shortcomings of the current system. Our baseline is current law Medicare payments and the federal share of Medicaid DSH payments.
The simulations included:
- a MedPAC-like approach that would distribute funds based on the hospitals proportion of low-income revenues and adjusted discharges(2);
- policies focused on the financial risk associated with serving Medicaid and self-pay patients (i.e., Medicaid shortfalls and uncompensated care costs).
To minimize issues related to whether higher costs are attributable to hospital inefficiency or justifiable differences in costs, the financial measures used in the allocation policies do not measure costs directly; rather, they express financial risk associated with serving poor people as a percentage of revenues or costs. In some allocation policies, we made adjustments for cost differences attributable to case mix and hospital wage levels.
[ Go to Contents ]
Hospital Data Set and Low-income Patient Variables
Ideally, all required data needed to evaluate the distribution of DSH funds would be available for all hospitals across the country for the same time period. Substantial information on individual hospital characteristics is available from national sources, including cost reports filed by Medicare participating providers. However, some utilization and financial data that are needed to measure hospital services to low-income populations (or at least the resources devoted to Medicaid patients and self-pay patients) are not directly available. Detailed inpatient utilization data on self-pay patients are available only for the 20 percent sample of hospitals from the 24 states included in the Agency for Healthcare Research and Qualitys Hospital Cost and Utilization Project (HCUP) database. Much of the needed information on revenues by payer and on uncompensated care is collected in the American Hospital Association (AHA)s Annual Survey, but confidentiality considerations preclude using that information for detailed exploratory analyses requiring hospital-level information. Thus, we supplemented the available national data with the HCUP national sample and detailed claims and financial data from three states: California, New York, and Wisconsin. The state financial data have detailed information by payer source on inpatient and outpatient gross revenues and on uncompensated care. In addition, we had access to 100% of their 1997 inpatient claims through HCUP.
Medicare DSH Payments: We drew on several public use files maintained by CMS to simulate Medicare FY1998 DSH payments and the payments that would have been made under FY2003 DSH payment assuming all other FY1998 payment parameters remained unchanged.
Medicaid DSH Payments: We relied primarily on the state reports submitted to CMS on FY 1998 DSH payments to individual hospitals. An issue is the extent to which the reported DSH funds represent new money to the hospitals. It is commonly recognized that the states often use the Medicaid DSH program not only to finance hospitals serving a disproportionately large share of low-income patients (the programs direct purpose), but also to secure additional federal funds for the state budget. To evaluate the effect of the program on the financial positions of hospitals, we needed to understand the underlying composition of total Medicaid DSH funds. We were limited in our analysis to information on new DSH for the three states for which we had comprehensive financial data.
Low-Income Patient Measures:
Claim-based Measures. These measures are based on the amount of care a hospital furnishes to low-income patients as measured through claims data, i.e. the proportion of days or discharges attributable to low-income patients. Inpatient claims data can also be used to measure the hospitals percentage of gross inpatient revenues attributable to low-income patients. Inpatient claim-based measures involve several assumptions:
- All utilization on the claim is attributed to the primary payer. For example, the measure is not sensitive to situations where Medicaid is secondary payer for part of an inpatient stay.
- Low-income patients utilize outpatient services in the same proportion as inpatient services. Low-income patients tend to have a relatively higher outpatient utilization rates than inpatient (because they have less access to community physicians).
Including self-pay and no-charge patients in the statistic implicitly assumes that no-charge patients are charity care and that self-pay patients represent low-income patients that are unable to pay for their care. We know that no-charge patients include those receiving courtesy and employee allowances and that the percentage of no-charge patients is likely to overestimate the percentage of charity care patients. Similarly, some self-pay patients are able to pay for some or all of their care (and some, such as wealthy foreign patients are able to pay full charges).
Utilization Measures Derived From Financial Data. Financial data can be used to measure the percentage of gross revenue attributable to low-income patients. These measures have several advantages over those derived from inpatient claims data.
- Secondary payers are accounted for (assuming the reporting is accurate).
- Both inpatient and outpatient volume are directly measured.
- Implicit recognition is given to differences in severity across the hospitals patient population.
Financial Risk Measures. Instead of measuring low-income patients utilization, financial data can also be used to measure the financial risk associated with serving low-income patients. In this report, we define financial risk in terms of shortfalls from Medicaid and local indigent care programs, bad debt, and uncompensated care. Under this definition, Medicare SSI patients and Medicaid patients to the extent the Medicaid payment covers the cost of their care do not contribute to financial risk.
[ Go to Contents ]
Joint Distribution of DSH Payments under Current Policies
Medicare DSH Payments
We estimate Medicare FY 1998 actual DSH payments at $4.83 billion. If the FY2003 DSH payment rules had been in effect and all other FY1998 payment parameters remained unchanged, payments would have been $358 million higher, or $5.18 billion. Consistent with the changes in the formula, most payment increases occurred among rural hospitals and small urban hospitals. Although rural hospitals provided 19% of total Medicare inpatient days, they received only 3.1% of the Medicare DSH payments. Under BIPA, the rural share of DSH payments will more than double to 7.2%.
Medicaid DSH Payments
Nationally, we found that the states reported $15 billion in DSH payments to hospitals, with about 23% of this amount paid to institutes for mental disease. The states with the largest DSH programs are California, New York, New Jersey, and Texas. Utilizing the estimates made by Coughlin et al. for FY 1997, we estimate that 11 states retained DSH funds: California, Connecticut, Georgia, Indiana, Kentucky, Massachusetts, Mississippi, Missouri, North Carolina, Rhode Island, and Texas. The amounts retained by the 11 states represented 15% of federal DSH payments. If we assume that only the federal share of DSH payments represents new money to facilities, new DSH payments would total $8.3 billion.
Distribution of Total DSH Payments
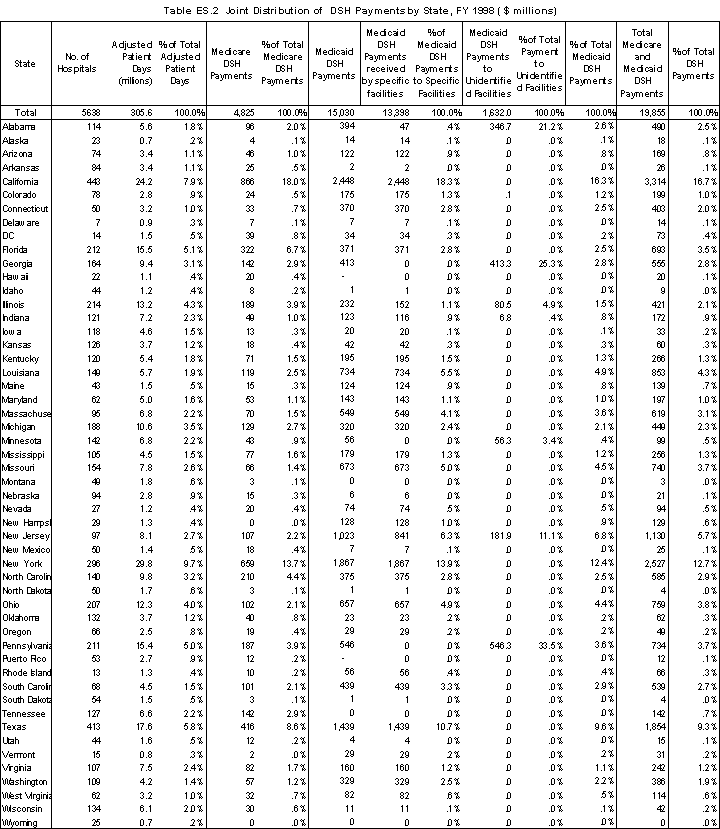
Five states together receive almost half of the total amount of DSH payments: California (16.7%), New York (12.7%), Texas (9.3%), New Jersey (5.7%), and Louisiana (4.3%). At the same time, these states have only 28% of the total adjusted patient days (7.9, 9.7, 5.8, 2.7, and 1.9 %, respectively) (Table ES.2).
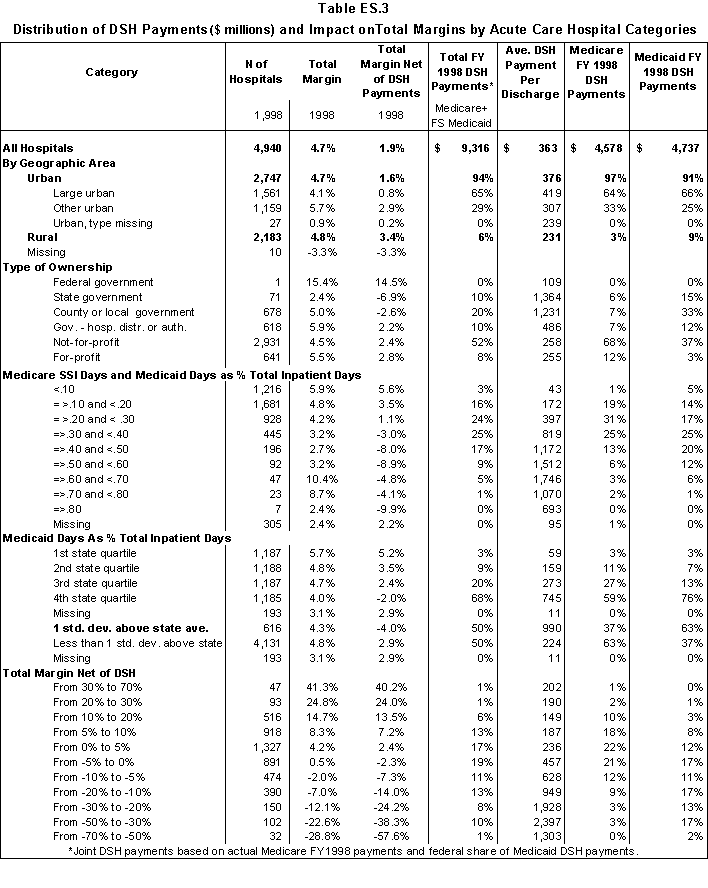
In Table ES.3, we summarize the distribution of DSH payments to the acute care hospitals in our analysis file by hospital characteristics. For the Medicaid component of the DSH payment, we have used only the federal share of DSH payments.
- Across all hospitals, the joint DSH payments raise total margins from 1.9% to 4.7%.
- State and county-owned hospitals receive 13% of Medicare DSH payments and 48% of Medicaid payments.
- Using Medicare SSI and Medicaid days as the measure of low-income patients, 50% of Medicare payments and 64% of Medicaid payments are to hospitals with at least 30% low- income patients. Except for the highest categories, the average DSH payment per discharge increases as the percentage of low-income patients increases.
- 37% of Medicare DSH payments and 63% of Medicaid payments are to hospitals with a Medicaid utilization rate that is above one standard deviation from the state average. The average DSH payment per discharge increases by hospital quartile (the first quartile is the lowest quartile of acute care hospitals in the state based on Medicaid utilization).
- Generally, the average DSH payment per discharge increases as hospital margins decline. The exceptions are the hospital classes with the highest and lowest margins.
- About 53% of Medicare DSH payments and 24% of Medicaid payments went to hospitals that had positive margins prior to taking DSH payments into account.
[ Go to Contents ]
Exploratory Analyses Using National HCUP Data
As noted earlier, data were not available that allowed us to examine alternative allocation policies with a national set of hospitals. Using the hospitals that are represented in the HCUP national sample that we were able to link with hospital-specific Medicaid DSH payments (100% inpatient claims from a 20% sample of hospitals in 15 states), we examined the relationship between key low-income patient measures that could be used in an allocation formula (e.g. proportion of days, discharges, and revenues and case-mix index including/excluding Medicare SSI patients). The degree of correlation between the measures can be used to predict whether the choice of the measure (utilization or revenue) used to describe hospitals low-income patients is likely to have a significant effect on the distribution of funds. We were able to evaluate only inpatient utilization and gross revenue low-income patient measures with the HCUP data. The HCUP does not have outpatient data or the uncompensated care data needed to measure financial risk.
There are several findings from our HCUP analysis that have import in designing a DSH allocation policy. First, in defining safety net hospitals, it appears that the choice of patient population to be included in the allocation statistic (e.g. with or without Medicare SSI beneficiaries) is more important than how care provided to those patients is quantified. It may not be administratively feasible to take into consideration all low- income patients. A hospitals proportion of low-income days is more highly correlated with its proportion of Medicaid days than either its proportion of Medicare SSI and Medicaid patients or its Medicare DSH patient percentage.
The different measures quantifying the amount of care provided to a low-income population (days, discharges, or charges) are highly correlated with each other. However, the choice could have implications for certain hospitals. Those with a high volume of Medicaid maternity cases or shorter than average length of stay (e.g. California hospitals) would benefit if discharges were used instead of days as the measure of the proportion of care provided to low-income patients.
Neither the current DSH allocation policies nor the alternatives that we examined target DSH payments to safety net hospitals in a way that is strongly correlated with net income.(3) However, the current DSH policies are more highly correlated than the alternatives that we examined. For example, the correlation between the joint DSH payments to safety net hospitals and their net income was -.48 compared to only -.17 for an allocation policy based on non-Medicare low-income patient days with a wage-index adjustment.
[ Go to Contents ]
Three State Analysis of Alternative DSH Policies
By linking inpatient claims and financial data for the hospitals in California, New York, and Wisconsin, we were able to:
- Trace the actual distribution of new Medicaid DSH payments.
- Assess how well the claims-generated measures of low-income patients correspond to measures generated from financial data (e.g. proportion of self-pay and no-charge patients relative to bad debt and uncompensated care costs); and,
- Compare how well the current and alternative DSH allocation policies target financially vulnerable safety net hospitals. In this regard, we were able to examine how funds might be redistributed across classes of hospitals, but because only three states were involved, we could not estimate the redistributions that might occur across states under the different alternatives.
The findings from the three state analysis indicate that an across-the-board assumption regarding new DSH funds such as that used in Table ES.3 is not borne out at the hospital level. In California, intergovernmental transfers from county-owned hospitals and the University of California clinics financed over 56 percent of total DSH payments; $936.3 million of $2,153.8 million reported in DSH payments were new DSH funds. In New York, the hospital inpatient assessment contributed 13% of the funds to support the indigent care pool, with the remaining coming from payer contributions; $1,169.5 of the $1,350.5 million in DSH payments received by New York hospitals was new money. All DSH funds received by Wisconsin hospitals were new ($11.2 million).
When we examined the relationship between financial risk as a percentage of operating expenses and the percentage of care provided to low-income patients (Table ES.4), we found only a modest correlation. Consistent with the HCUP findings, there was a stronger correlation between the low-income patient utilization and revenue measures.
| Ratio of FR to Operating Expenses | % Low-income days | % Low-income revenue | % Non-Medicare low-income days | % Non-Medicare low-income revenue | |
|---|---|---|---|---|---|
| MEAN | 0.077 | 0.256 | 0.246 | 0.210 | 0.212 |
| STD | 0.071 | 0.184 | 0.178 | 0.169 | 0.166 |
| N hospitals | 614 | 614 | 614 | 614 | 614 |
| Pearsons Correlation Coefficient** | |||||
| Ratio of FR to Operating Expenses | 1.000 | 0.567 | 0.591 | 0.560 | 0.579 |
| % Low-income days | 1.000 | 0.826 | 0.979 | 0.786 | |
| % Low-income revenue | 1.000 | 0.811 | 0.984 | ||
| % Non-Medicare low-income days | 1.000 | 0.803 | |||
| % Non-Medicare low-income revenue | 1.000 | ||||
| **all values p.0001 | |||||
Finally, we examined the relationship between the DSH allocations, financial risk and the hospitals income net of DSH. We expected to find a negative correlation between the hospitals ratio of revenues (net of DSH) to expenses and its ratio of financial risk to operating cost; that is, hospitals with high financial risk have more difficulty generating revenues to cover their expenses. While the correlation was in the expected direction, it was modest (-.407). The correlation was -.302 between the DSH funds a hospital receives under current Medicare and Medicaid policies and its ratio of revenues to expenses. When the analysis is limited to the 307 safety net hospitals in the three states (Table ES.5), the correlation between net income and current DSH funding policies is stronger for current DSH policies than alternative policies.
| Income net DSH ($ mill) | Financial risk ($ mill) | Joint DSH funds ($ mill) | Medicaid New DSH ($ mill) | Medicare DSH ($ mill) | Sim A ($ mill) | Sim B ($ mill) | Sim C ($ mill) | |
|---|---|---|---|---|---|---|---|---|
| MEAN | -8.351 | 12.025 | 8.568 | 4.752 | 3.816 | 8.917 | 8.349 | 8.265 |
| STD | 26.222 | 19.924 | 16.025 | 13.784 | 4.902 | 17.778 | 18.361 | 15.532 |
| N | 307 | 307 | 307 | 307 | 307 | 307 | 307 | 307 |
| Pearsons Correlation Coefficient** | ||||||||
| Income net DSH | 1.00 | -0.57 | -0.52 | -0.41 | -0.52 | -0.24 | -0.29 | -0.44 |
| Financial risk | 1.00 | 0.74 | 0.64 | 0.63 | 0.73 | 0.73 | 0.83 | |
| Joint DSH funds | 1.00 | 0.96 | 0.58 | 0.80 | 0.81 | 0.78 | ||
| New Medicaid funds | 1.00 | 0.31 | 0.79 | 0.81 | 0.77 | |||
| Current law Medicare funds | 1.00 | 0.40 | 0.35 | 0.40 | ||||
| Sim A: % Non-Medicare low-income days w/WI | 1.00 | 0.96 | 0.81 | |||||
| Sim B: % Non-Medicare low-income revenues | 1.00 | 0.85 | ||||||
| Sim C: Financial risk | 1.00 | |||||||
| ** All values p.0001 | ||||||||
The mean DSH payments reported in Table ES.5 pertain to safety net hospitals only, which are defined for purposes of this analysis as hospitals with at least 20 percent of their inpatient days attributable to low-income patients. The baseline used in the simulations totaled $2,748 billion across all three states. If all DSH funds had been distributed to safety net hospitals, a hospital would have received on average $8.951 million.(4) The difference between this amount and the mean payment in each simulation is accounted for by DSH funds distributed to hospitals with less than 20 percent of their inpatient days attributable to low-income patients. The differences between Simulation A and Simulation B highlight the differences between allocations based solely on inpatient care and allocations that take into account both inpatient and outpatient care. Including all care only slightly improves the targeting of DSH funds to financially vulnerable safety net hospitals. Simulation C allocates funds based on financial risk.
[ Go to Contents ]
Summary of Findings and Conclusions
Overall, we found that despite the known issues with the current Medicare and Medicaid DSH policies, the current distribution targets financially vulnerable safety net hospitals at least as well as the alternatives that we examined. The multiple Medicare formula and the flexibility of the Medicaid program may allow for better targeting than a single formula-driven allocation policy. Nevertheless, it is clear that there is room for improvement in the current policies and that further study is warranted. In particular, a multi-variate analysis of the factors affecting financial risk and financial viability is needed. Ideally, the analysis would involve a national database with information on each hospitals uncompensated care and shortfalls from Medicaid and local indigent care programs. Given the diversity of the Medicaid DSH program, a national database is needed to fully understand the potential impact of alternative allocation policies at both the national and market levels.
Criteria to Measure Care Provided to Low-Income Patients. We explored several types of criteria that could be used to identify safety net hospitals, including inpatient claims-based measures and measures derived from hospital financial data. Our analyses suggest that how the patient population (e.g., with or without Medicare SSI beneficiaries) is defined in the DSH allocation statistic is more important than how the care provided to those patients is quantified (e.g. days, discharges, revenues). Measures that included Medicare SSI beneficiaries along with all other low-income patients generally performed better than those that did not in targeting financially vulnerable hospitals.
The different measures quantifying the amount of inpatient care provided to a low-income population (days, discharges, or charges) are highly correlated. However, the choice could have implications for certain hospitals. Those which have a high volume of Medicaid maternity cases or shorter than average length of stay (e.g. California hospitals) would benefit if discharges were used instead of days as the measure of the proportion of care provided to low-income patients. The Medicare case mix index is not a good proxy for the hospitals low-income patient case mix. In the absence of data on the case mix of low-income patients, days or charges should be used instead of discharges as the allocation statistic.
From the financial data for the three states we were able to compare how a revenue statistic that includes both inpatient and outpatient care compares to one that includes inpatient care only. The correlation between low-income days and low-income total (inpatient and outpatient) revenues was .811, which indicates the choice of measure could have significant implications for some hospitals. The measure of the proportion of a hospitals gross revenues that is attributable to low-income patients was slightly more correlated with the hospitals ratio of financial risk to operating expenses (.591) than the other utilization measures. However, it is not clear from the correlation results that including all care significantly improves the targeting of DSH funds to financially vulnerable safety net hospitals. Also, the inclusion of outpatient care raises issues regarding subsidies to other ambulatory care providers. A policy that concentrates federal support for uncompensated care solely on hospitals may serve to discourage community providers from furnishing substantial amounts of care to indigent populations. It may also have implications for the relative generosity of Medicaid payments for services provided in hospital outpatient departments and clinics and in physician offices.
Evaluation of Alternative Allocation Policies. Neither the current DSH allocation policies nor the alternatives that we examined in the analysis target DSH payments in a way that is strongly correlated with net income. This is an issue that warrants further investigation and understanding. The different Medicare formulae and the Medicaid DSH programs flexibility may provide mechanisms to target financially vulnerable hospitals in a way that a single formula-driven allocation may not. Targeting financially vulnerable safety net hospitals may require taking into consideration more factors than the amount of care a hospital provides to low-income patients. A multi-variate analysis of the factors affecting a hospitals financial risk and its overall financial status using a broader set of hospitals could help identify additional factors that should be considered in an allocation policy.
Allocations based on the proportion of care provided to low-income patients (e.g. revenues) result in very different distributions than an allocation based on financial risk (Medicaid shortfalls, uncompensated care and bad debt). Financial risk, however, is not the same as financial viability (i.e., total margins net of DSH payments). Some hospitals with substantial financial risk also have positive margins. The simulations highlighted the need to clarify the policy goals for DSH funding. The key issue is the extent to which subsidies should be given to hospitals that serve low-income patients but do not incur financial risk or are able to cover their risk with other revenues. A closer examination of the hospitals with substantial gains or losses in moving from an allocation policy based on serving low-income patients to one based on incurring financial risk might help clarify the issues. This examination should consider the role of other federal subsidies such as the Medicare indirect teaching adjustment in explaining why some hospitals with substantial financial risk appear to be in a strong financial position.
Data Issues and Limitations. Examining the relationship between the financial status of hospitals and the distribution of DSH payments was a complex task. Particular areas where data issues became potentially problematic included:
- Matching hospitals across multiple data sources: Medicare cost reports, state DSH reports, AHA survey data, HCUP, and (in the case of California, New York and Wisconsin) state financial reports. The inclusion of Medicare provider numbers on the state DSH reports would facilitate matching hospitals with their DSH payments. Universal adoption of the uniform provider number would also help.
- For Medicaid DSH, the net gains to the hospital are more important than the reported DSH payments. CMS should give consideration to obtaining this information. It could be included in the state reports on DSH payments (in which case the information would be available for all hospitals) or it could be required as part of the Medicare cost report. Even knowing the net DSH payments to individual hospitals is not enough; it is also important to know how DSH payments (and any provider contributions) are handled in reporting Medicaid contractual allowances and patient revenues.
- The differences in state accounting and reporting practices made it difficult to determine Medicaid shortfalls and to take new DSH payments into account. The financial data for several public hospitals was problematic. It is important to understand how financing occurs for county-owned hospitals in terms of other intergovernmental transfers and deficit funding. An allocation based on financial measures would require uniform reporting by payer.
The snapshot approach of looking at one years data may not be sufficient for an adequate understanding of the financial implications of serving low-income patients. In California, the FY1998 payments included payments from the states fiscal year 1997 and thus overstated average DSH payments. The New York indigent care pool was in transition during FY1998 and additional changes were enacted in 2000. Wisconsins uncompensated care costs have increased 60 percent since 1997. Only the first-year impacts of the Balanced Budget Amendment are reflected in the FY1998 data. These considerations suggest that a multi-year study- perhaps with periodic updating- would be appropriate.
Even more troubling than using one years data is the lack of a national database that provides uniform information on the quantity of care provided to low-income patients and the financial risk associated with that care. The BBRA provision requiring the Secretary to collect through the Medicare cost report data on uncompensated costs should help. This provision is effective for cost reporting periods beginning on or after October 1, 2001.
Areas for Additional Research
Absent a national database with uncompensated care data and other information needed to develop measures of financial risk, three areas of investigation could be pursued that would provide valuable information related to federal support for hospitals that provide a disproportionate share of care to poor patients.
Update the analysis of the current distribution of DSH payments and expand the in-depth state analyses to include additional states that require hospitals to report uncompensated care information.
- Examine market-level issues related to DSH funding such as how the low-income patient burden shared by the hospitals within a market area and whether it varies by type of payer and type of service.
- Investigate the characteristics of hospitals with large indigent care loads that incur substantial financial risk yet are financially viable. This would include looking at the impact of state and local indigent care programs and other subsidies such as Medicares indirect teaching adjustment.
A national database is needed to fully understand the potential impact of alternative allocation policies at both the national and market levels. Having the national database would facilitate:
- A multi-variate analysis of the factors affecting a hospitals financial risk and its overall financial status using a broader set of hospitals could help identify additional factors that should be considered in an allocation policy.
- An evaluationof inter-state redistributions that would occur under alternative DSH financing policies, including the types of policies examined in this paper as well as additional ones that would take into account a states ability to finance indigent care and/or market-level factors.
[ Go to Contents ]
Endnotes
1. Low income use rate is the sum of two ratios. The first is the share of the hospitals total revenue for patient services that are paid by Medicaid or state/local subsidies. The second is the percent of total hospital charges for inpatient services accounted for by the net (of state and local subsidies for inpatient care) amount of charity care provided to inpatients.
2. The terms adjusted days and adjusted discharges refer to adjusting inpatient volume statistics to take into account outpatient services. To do so, the inpatient statistic is increased by the ratio of total patient revenues to inpatient revenues.
3. For this purpose, safety net hospitals were defined as acute care hospitals with at least 20 percent inpatient days attributable to low-income patients.
4. The baseline for the simulations was current law Medicare and the federal share of DSH payments.
