Printer Friendly Version in PDF Format (75 PDF pages)
ABSTRACT
This study conducted exploratory analyses to develop a better understanding of community-admitted Medicare home health patients, including whether there have been any differential trends between community-admitted and post-acute care (PAC) patients over time and what their patterns of care tell us about the underlying reasons for the community-admitted increased numbers. The findings indicate that there are many important differences between patients based on the length of their home health care use, not just based on their source of admission, and that the source of admission may be a more important differentiator among patients who use home health care for longer periods. The study also found that use of the home health care benefit is changing--use of home health aide care has declined and use of physical therapy services has increased, even for longer periods of care.
This report was prepared under contract #HHSP233201600017I between HHS's ASPE/DALTCP and Mathematica Policy Research. For additional information about this subject, you can visit the DALTCP home page at https://aspe.hhs.gov/office-disability-aging-and-long-term-care-policy-daltcp or contact the ASPE Project Officer, Judith Dey, at HHS/ASPE/DALTCP, Room 424E, H.H. Humphrey Building, 200 Independence Avenue, S.W., Washington, D.C. 20201. Her e-mail address is: Judith.Dey@hhs.gov.
DISCLAIMER: The opinions and views expressed in this report are those of the authors. They do not reflect the views of the Department of Health and Human Services, the contractor or any other funding organization. This report was completed and submitted on November 14, 2017.
TABLE OF CONTENTS
I. INTRODUCTION
II. PROJECT OBJECTIVES AND APPROACH
III. RESULTS
A. Trends in Community-Admitted and PAC Home Health Users Over Time
B. Cross-Sectional Comparison of Home Health Users
IV. LIMITATIONS
A. Summary
B. Discussion
APPENDICES
- APPENDIX A: Research Questions, Data, and Methods
- APPENDIX B: Comparison of Logical Groups of Home Health Users
- APPENDIX C: Utilization Patterns and Costs of Home Health Users
- APPENDIX D: Correlation between Utilization Patterns and Types of Home Health Use
- APPENDIX E: Growth in Community-Admitted Home Health Users
LIST OF FIGURES
- FIGURE II.1: Logical Groups of Home Health Users
- FIGURE III.1: Trends in the Number of Community-Admitted and PAC Patients
- FIGURE III.2: Trends in Congregate Residence among Community-Admitted and PAC Patients
- FIGURE III.3: Trends in Dual Eligibility Status among Community-Admitted and PAC Patients
- FIGURE III.4: Trends in HCC Scores among Community-Admitted and PAC Patients
- FIGURE III.5: Trends in For-Profit Ownership of HHAs Serving Community-Admitted and PAC Patients
- FIGURE III.6: Trends in the Percentage of Patients in Fraud and Abuse States among Community-Admitted and PAC Patients
- FIGURE III.7: Trends in Average Number of Aide Visits Per Episode Per Year among Community-Admitted and PAC Patients
- FIGURE III.8: Trends in Average Number of Therapy Visits Per Episode Per Year among Community-Admitted and PAC Patients
- FIGURE III.9: Trends in the Proportion of Community-Admitted and PAC Patients with At Least 3Episodes Who had Physical Therapy Use in the Third or Later Episode
- FIGURE III.10: Breakdown of PAC Users by Short-Term and Long-Term Use
- FIGURE III.11: Breakdown of Community-Admitted Users by Short-Term and Long-Term Use
- FIGURE III.12: HCC Scores among PAC and Community-Admitted Users
- FIGURE III.13: Home Health Visits in the First Episodes of the Home Health Spell among PAC and Community-Admitted Users
- FIGURE III.14: Acute Hospitalization within 120 Days of the Start of the Spell among PAC and Community-Admitted Users
- FIGURE III.15: SNF Admission within 120 Days of the Start of the Spell among PAC and Community-Admitted Users
- FIGURE III.16: Mortality within 120 Days of the Start of the Spell among PAC and Community-Admitted Users
- FIGURE III.17: Dual Eligibility Status among PAC and Community-Admitted Users
- FIGURE III.18: Living Arrangement among PAC and Community-Admitted Users
- FIGURE III.19: Agency Ownership of HHAs Serving PAC and Community-Admitted Users
- FIGURE III.20: Residence in a State with Fraud and Abuse among PAC and Community-Admitted Users
- FIGURE III.21: Breakdown of Long-Term Community-Admitted Users by the Type of Home Health Use
- FIGURE III.22: Living Arrangement among Long-Term Community-Admitted Users by Type of Home Health Use
- FIGURE III.23: Proportion of Patients with No or Any Aide Services among Long-Term Community-Admitted Users, by Dual Eligibility Status and State LTSS Ranking
- FIGURE III.24: Hospital and SNF Admissions within 120 Days of the Start of the Spell among Long-Term Community-Admitted Users
- FIGURE A.1: Identifying Logical Groups of Home Health Users
- FIGURE A.2: Analysis Period for Utilization and Costs
LIST OF TABLES
- TABLE III.1: Top 10 States for PAC and Community-Admitted Home Health Use per 100,000 Age 65 and Older
- TABLE B.1: Characteristics of PAC and Community-Admitted Home Health Spells
- TABLE C.1: Utilization Patterns and Costs for Home Health Spells
- TABLE D.1: Correlation between Type of Home Health User and Hospitalizations, SNF Admissions, and Mortality
- TABLE D.2: Correlation between Type of Home Health User and Number of Hospitalizations and SNF Admissions
- TABLE E.1: Yearly Characteristics of PAC and Community-Admitted Home Health Users
- TABLE E.2: Yearly Characteristics of PAC and Community-Admitted Dually Eligible Home Health Users
ACRONYMS
The following acronyms are mentioned in this report and/or appendices.
| ADL | Activity of Daily Living |
|---|---|
| ARF | Area Resource File |
| CA | Community-Admitted |
| CHF | Congestive Heart Failure |
| CI | Confidence Interval |
| CME | Common Medicare Environment |
| CMS | Centers for Medicare & Medicaid Services |
| COPD | Chronic Obstructive Pulmonary Disease |
| FFS | Fee-For-Service |
| HCBS | Home and Community-Based Services |
| HCC | Hierarchical Condition Category |
| HHA | Home Health Agency |
| HHGM | Home Health Groupings Model |
| LTAC | Long-Term Acute Care |
| LTSS | Long-Term Services and Supports |
| MedPAC | Medicare Payment Advisory Commission |
| OASIS | Outcome and Assessment Information Set |
| OR | Odds Ratio |
| PAC | Post-Acute Care |
| POS | Provider of Services |
| PPS | Prospective Payment System |
| RAP | Request for Anticipated Payment |
| SNF | Skilled Nursing Facility |
EXECUTIVE SUMMARY
A substantial proportion of growth in Medicare home health care over the past 15 years has been driven by patients who are admitted to home health care directly from the community, rather than from an acute care or post-acute care (PAC) setting. The purpose of this study was to develop a better understanding of the characteristics of community-admitted Medicare home health care patients, how these patients use care, and what their patterns of care tell us about the underlying reasons for their increased numbers. We also focused on understanding the role of home health as a substitute for long-term services and supports (LTSS).
To address the study objectives, we used the U.S. Department of Health and Human Services Centers for Medicare & Medicaid Services DataLink file, which contains episode-level information for all Medicare home health care patients from October 1, 2000, to June 30, 2014.[1] We conducted two sets of analyses, using alternative definitions of community-admitted patients. First, to examine trends in community-admitted patients, we classified patients as community-admitted or PAC in each calendar year from January 1, 2002, until December 31, 2013, based on whether the majority of their episodes in a particular calendar year were community-admitted or PAC episodes. This approach allowed us to include in the analysis all patients who received care in a given year, regardless of when they actually entered Medicare home health care. We then compared trends over time for the two groups of patients. Second, we identified a cross-sectional sample of home health care users who had at least one episode of care between January 1, 2013, and December 31, 2013, and had a spell of care (that is, care without interruption) starting no earlier than January 1, 2011, and no later than December 31, 2013.[2] For this analysis, we defined community-admitted and PAC patients based on whether they had an inpatient or PAC stay in the 14 days before their home health care spell began. This allowed us to explore whether the patient's point of entry into home health care was related to patient characteristics. After defining the source of admission, we further defined logical groups of home health care users based on the length of the patient's spell (one episode [short-term] versus two or more episodes [long-term]) and type of service use (no use of aide services versus any use of aide services and high or low use of skilled services). We then compared the patient-level and geographic characteristics of the groups.
The results from our trend analysis show that there was large growth in community-admitted patients from 2002 to 2010, and much smaller growth from 2010 to 2013. There are two trends that may also be related to this growth. First, the proportion of community-admitted patients entering home health care in states with a history of fraud and abuse grew dramatically over time. Second, therapy use in later episodes of a home health care spell increased substantially among community-admitted patients from 2002 to 2010, then leveled off after 2010.
Our cross-sectional analysis showed that the increase in community-admitted patients has been mostly driven by an increase in the number of episodes per patient. When we focused on the initial source of entry into the system, we found differences between community-admitted and PAC patients based on where they lived and the type of agencies they received care from. However, the length of spell affected the patterns of care more than source of admission. Patients who had fewer episodes were very similar to one another in terms of health status and utilization, whether they were admitted from the community or from an acute care or PAC facility. Patients who had more episodes were more similar to one another in terms of health status, home health care utilization, and the use of other acute care and PAC than to short-term patients with the same source of admission. This is not to say that source of admission did not matter, especially for home health users with many episodes. There were greater differences between the PAC and community-admitted long-term care patients than there were between the PAC and community-admitted short-term care patients.
To understand whether these differences could possibly indicate substitution between LTSS and home health, we examined the patterns of care of long-term community-admitted patients, focusing on type of service use, whether patients lived in congregate living facilities, or entered care from states with poorer LTSS systems. We found limited evidence that the growth in community-admitted patients was related to the growth in individuals living in congregate living facilities, nor an increased use of aide services associated with the community-admitted patients or those admitted from states with poor LTSS systems. There was substantial growth in community-admitted patients in states with a past history of fraud and abuse, suggesting that the growth could be related to fraud issues.
The findings indicate that there are many important differences between patients based on the length of their home health care use, not just based on their source of admission, and that the source of admission may be a more important differentiator among patients who use home health care for longer periods. We also found that use of the home health care benefit is changing--use of home health aide care has declined and use of physical therapy services has increased, even for longer periods of care. Future research should focus on better understanding the increase in long-term home health care users.
I. INTRODUCTION
During the last 15 years, there has been dramatic growth in the use of the Medicare home health benefit, with much of the growth driven by patients who are admitted directly from the community rather than from an acute or post-acute care (PAC) setting. The Medicare home health benefit was originally intended for patients to receive extended care in a less expensive setting than a hospital or PAC facility. It covered care only for patients who were hospitalized within 30 days prior to the start of care. In 1980 the benefit was extended to allow patients to be admitted directly to home health care from the community. By allowing beneficiaries who did not have a previous hospitalization to receive Medicare home health care, beneficiaries may be receiving home health services for an acute care need that is minimal while benefiting from personal support services, which would shift some costs for long-term services and supports (LTSS) to Medicare. However, the Medicare home health benefit may also complement LTSS by providing necessary skilled services to ill beneficiaries in their homes.
In 2015, total Medicare spending for home health care was $18.1 billion, which covered 6.6 million episodes for 3.5 million users (MedPAC 2017). The Medicare Payment Advisory Commission (MedPAC) found a 115 percent increase from 2001 to 2013 in episodes not preceded by a hospitalization compared to a 25 percent increase in episodes preceded by a hospitalization or other PAC stay during the same period (MedPAC 2016). This research also found some important differences between the two types of home health users, including a larger share of dually eligible beneficiaries and higher numbers of visits from home health aides among community-admitted users. Many factors could contribute to the differential growth in community-admitted home health patients:
-
Changes in patients' characteristics or needs. Increases in the numbers of adults in the oldest age groups and with certain types of chronic diseases or conditions could affect the demand for home health among Medicare beneficiaries. For example, the growth in the reported number of patients with Alzheimer's disease might mean that more patients need home health to help manage their health conditions. In addition, these patients could be more likely to be community-admitted users.
-
Changes in providers' payments. Over the years, the U.S. Department of Health and Human Services Centers for Medicare & Medicaid Services (CMS) adjusted home health episode payments, which made some types of patients more financially attractive to home health agencies (HHAs) and other types of patients less so. As a result, HHAs might cherry-pick certain types of patients or drive demand among patients who produce higher margins.
-
Changes in program administration. CMS has also made changes to home health program administration and clarified its coverage policy. Some changes might affect the availability of care more for community-admitted patients than for PAC-admitted patients. For example, in response to a 2010 court case, CMS clarified that the Medicare program covers skilled services in order to maintain or slow the decline in functioning for those who are not expected to improve their functioning (Pear 2010; CMS 2013). Therefore, more patients who need maintenance therapy might be admitted from the community. Other changes in the administration of the home health program include differential program implementation standards by Medicare Administrative Contractors and fraud and abuse enforcement.
-
Changes in environmental factors. Many changes in the medical and LTSS system could contribute to the differential growth in home health patients. For example, the shift to Medicaid community-based care has moved many patients from nursing homes to the community. Such patients could be more likely to require skilled care. There has also been a substantial increase in assisted living as another residential option on the spectrum from institutions to home. Assisted living facilities might be using home health services as a supplement to or substitute for services that should be part of the assisted living care package, which typically includes personal care services and nursing care. The growth in community-admitted patients might in part be driven by the growth in assisted living residents. Another environmental factor that could be changing the types of home health users is the increase in hospital observation stays (in lieu of hospital admissions) and the decrease in hospital readmissions, which could reduce the number of PAC-admitted patients. Even if patients can be diverted from an inpatient admission through a hospital observation stay, they might still have a need for home health services, which could be contributing to the growth in community-admitted patients. In addition, skilled nursing facility (SNF) stays are not Medicare reimbursable after a hospital observation stay, which could result in more beneficiaries using the home health benefit in lieu of the SNF benefit.
-
Changes in providers' practices. Providers continuously look for ways to improve care and their bottom lines, which can lead to approaches to care that are more beneficial for chronically ill patients and can motivate a greater number of physicians to order home health care for such beneficiaries. In addition, changes to payment policy and program administration create incentives that might lead to changes in providers' practices. For example, changes to the payment policy regarding therapy, such as new thresholds implemented in 2008, could lead to increases in therapy use, and new regulations about certification and recertification of the plan of care, such as the statutory regulations put in place in 2010, could lead to changes in the mix of home health patients or the number of episodes per patient.
This study will improve our understanding of community-admitted Medicare home health patients by observing differences in patient characteristics and other trends relative to the PAC-admitted patients.
II. PROJECT OBJECTIVES AND APPROACH
The purpose of this study was to develop a better understanding of the characteristics of community-admitted Medicare home health patients, how these patients use care, and what their patterns of care tell us about the underlying reasons for their increased numbers. We also focused on understanding the role of home health as a substitute for LTSS. To address the project objectives, we used the CMS DataLink file, which contains episode-level information for all Medicare home health patients from October 1, 2000, to June 30, 2014.[3] We conducted two separate sets of analyses, with alternative definitions of community-admitted patients.
To examine trends in community-admitted and PAC patients, we used a 20 percent random sample of all Medicare fee-for-service (FFS) home health users age 65 and older from January 1, 2002, until December 31, 2013. We classified patients for each calendar year in which they used Medicare home health, based on whether the majority of their episodes in a particular calendar year were community-admitted or PAC episodes. We compared characteristics of community-admitted and PAC home health users in each calendar year and examined trends over time to determine if there were any differential patterns for the two groups of patients. (The data, sample, and approach are described in greater detail in Appendix A. Appendix E contains the detailed output.)
In addition to comparing trends over time, we conducted a cross-sectional analysis to compare community-admitted and PAC patients. For this analysis, we used a 20 percent random sample of all Medicare FFS home health users age 65 and older who had at least one episode of care between January 1, 2013, and December 31, 2013, with spells of care starting no earlier than January 1, 2011, and no later than December 31, 2013.[4] We defined community-admitted and PAC patients based on whether or not they had an inpatient or post-acute stay in the 14 days prior to the start of their home health spell. After defining the source of admission (community versus PAC), we further defined logical groups of home health users based on a patient's length of the spell and type of service use (Figure II.1). Although a primary focus of this study was the source of admission, it was important to examine the length of use for these two groups because MedPAC found that an increase in the number of episodes per patient has been a key driver of the increase in community admissions. In addition, one of the key objectives of this study was to better understand whether the Medicare home health benefit was being used more for acute care or long-term care, which is not necessarily connected to the source of admission. Specifically, many beneficiaries could enter home health from the community and use care for only a short period of time in ways that are similar to beneficiaries who enter care directly from an inpatient or post-acute setting. Without distinguishing between short-term and long-term users of home health, these differences would not be apparent. We defined short-term patients as those with one episode in their spell (in care for 60 days or less) and long-term patients as those with two or more episodes in their spell (in care for 61 days or more). To better understand whether certain groups of beneficiaries might be using home health as a substitute for other LTSS, we also defined patients by their type of service use, including no use of aide services versus any use of aide services and high or low use of skilled services. After categorizing patients, we compared patient-level and geographic characteristics between the groups. (We include a detailed description of the data, sample, and approach in Appendix A. Appendices B, C, and D include details on the output.)
| FIGURE II.1. Logical Groups of Home Health Users |
|---|
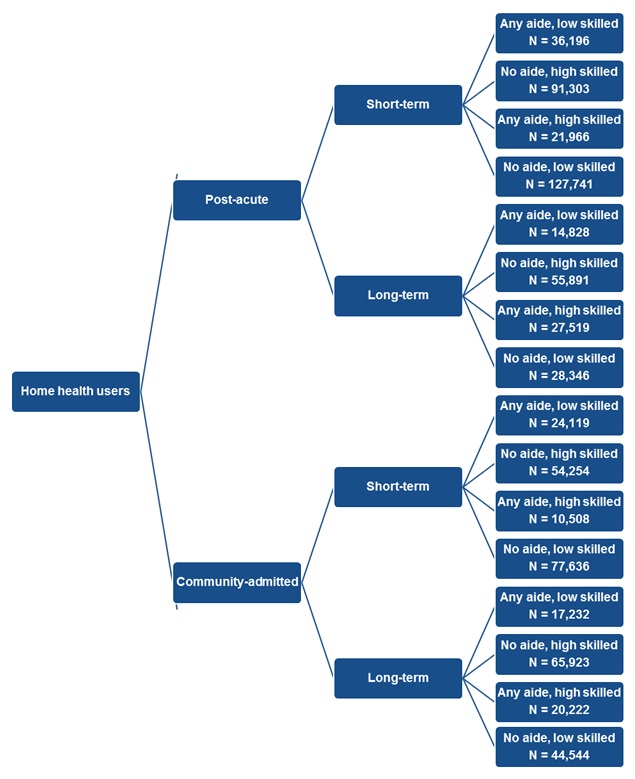 |
| NOTE: The sample includes a 20% random sample of all Medicare FFS home health users age 65 and older who used home health services between January 1, 2013, and December 31, 2013, and who had spells starting no earlier than January 1, 2011, and no later than December 31, 2013. Aide use refers to home health aide and medical social service use. Skilled use refers to therapy and skilled nursing use. Appendix A includes the details of how these groups were defined. |
III. RESULTS
A. Trends in Community-Admitted and PAC Home Health Users Over Time
Similar to MedPAC's findings, we found that the number of community-admitted patients increased dramatically over the period of our analysis--from 882,285 in 2002 to 1,509,070 in 2013, a 71 percent increase (Figure III.1). The growth was greater for these patients from 2002 to 2010, after which it slowed. The number of PAC patients increased slightly over the period, from 1,419,805 in 2002 to 1,469,615 in 2013, a 3.5 percent increase. A number of changes to the Medicare home health benefit were implemented in 2010, including adding payment safeguards to improve enrollment and reduce fraud, and these changes might have contributed to the slower growth in community-admitted patients after 2010.
The numbers from our analysis reflect only the total number of unique patients in each year, so the growth observed for the community-admitted patients does not account for the growth in the number of episodes per patient--which increased substantially over the period, particularly among community-admitted patients. MedPAC found that although the total growth in community-admitted episodes from 2001 to 2013 was 115 percent, most of the growth was driven by growth in subsequent episodes, rather than first episodes (MedPAC 2016).
| FIGURE III.1. Trends in the Number of Community-Admitted and PAC Patients |
|---|
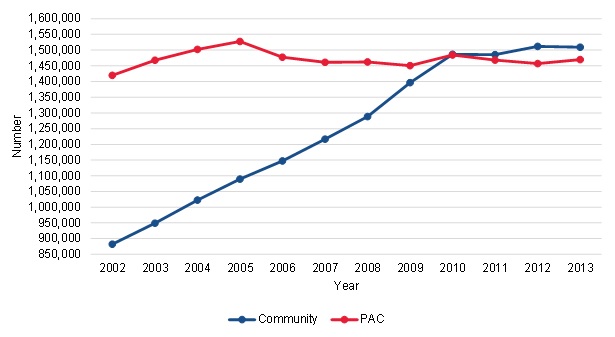 |
| SOURCE: National estimates based on Mathematica analysis of a 20% sample of the CMS DataLink file, from January 1, 2002, to December 31, 2013. |
To help us understand potential sources of growth in community-admitted patients, we examined patient-level and state-level characteristics and patterns of care over time for PAC and community-admitted patients, with a focus on trends from 2002 to 2013.
Slightly higher growth in congregate residence among community-admitted patients suggests that increased use of assisted living facilities is not a major contributor to the growth in community-admissions. The growth of assisted living facilities could result in an increase in frail older adults living in the community rather than in nursing homes (Harris-Kojetin et al. 2016). This could lead to an increase in community-admitted home health patients over time if more patients with skilled needs are living in community settings. In addition to an increase in frail individuals living in community settings, assisted living facilities themselves could impact community admissions. For example, staff at assisted living facilities might be better at identifying skilled care needs and getting access to home health services, or they might encourage home health to provide care that otherwise would be provided by the facility. We found that over the entire period from 2002 to 2013, higher proportions of community-admitted patients lived in a congregate setting compared with PAC patients (Figure III.2). The proportion of community-admitted patients in congregate settings increased slightly over time, while the proportion of PAC patients in congregate settings remained relatively steady. Specifically, in 2002, about 12 percent of community-admitted patients lived in a congregate setting. By 2013, about 14 percent lived in a congregate setting, a 16 percent increase over the period. Among the PAC patients, about 6 percent lived in a congregate setting throughout the period. Although there was a slight increase among community-admitted patients living in congregate residences, the trend does not suggest that this was a large contributor to the growth in community-admitted patients over the time period.
| FIGURE III.2. Trends in Congregate Residence among CA and PAC Patients |
|---|
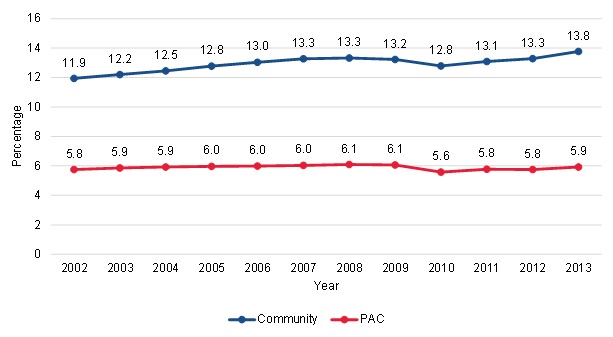 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, from January 1, 2002, to December 31, 2013. NOTE: The documentation of living arrangement changed in 2010 with the switch from OASIS-B to OASIS-C. |
Slightly higher growth in dual eligibles among community-admitted patients also suggests that changes in Medicaid is not a major contributor to the growth in community-admitted patients. Over the past few years, the Medicaid program has emphasized providing community-based long-term care services (Ng et al. 2013). As with assisted living facilities, this could result in more dual eligibles receiving skilled care services in the home under the Medicare benefit, as more duals would be in their homes rather than institutions. At the same time, there could be differential changes in the proportion of dual eligible patients if the Medicare home health benefit is being used as a substitute for other types of long-term care for duals. Overall, the proportion of dually eligible beneficiaries was consistently higher among community-admitted patients in all years. In addition, there was slightly higher growth in the proportion of dual eligibles among the community-admitted patients over time (Figure III.3). In 2002, 26 percent of community-admitted patients and 15 percent of PAC patients were dually eligible. In 2013, 31 percent of community-admitted patients and 16 percent of PAC patients were dually eligible, for an 18 percent increase among community-admitted patients and a 7 percent increase among PAC patients over the period. The slightly higher growth in dual eligibles among community-admitted patients does not appear to be a large contributor to the overall growth in community-admitted patients.
| FIGURE III.3. Trends in Dual Eligibility Status among Community-Admitted and PAC Patients |
|---|
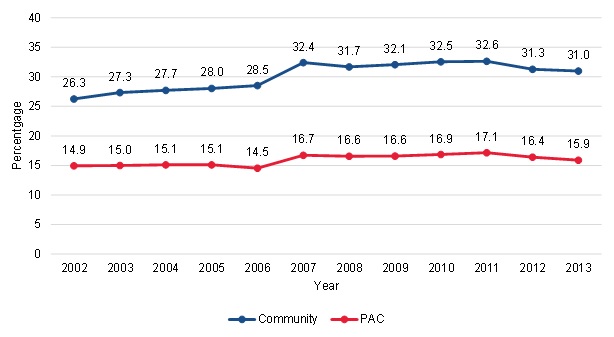 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, from January 1, 2002, to December 31, 2013. NOTE: The variables available in the DataLink file to determine dual eligibility status changed in 2007. |
Similar trends in health status and cognitive function for community-admitted and PAC patients suggest that these factors did not contribute to the growth in community-admitted users. Changes in the numbers of community-admitted and PAC patients could reflect changes in the health status of the two types of patients over time. Specifically, with the shift from institutional to community settings, there could be an increase in community-admitted patients due to relatively sicker individuals staying in the community and requiring home health services. If this were the case, we would expect to observe greater increases in acuity among the community-admitted patients relative to the PAC patients. From 2004, the first year for which we could assess hierarchical condition category (HCC) scores,[5] to 2013, the community-admitted patients had consistently higher HCC scores than PAC patients (Figure III.4). In 2004, community-admitted patients had an average score of 1.95 and PAC patients had an average score of 1.64. The average HCC score increased for both groups of patients, with relatively similar trends over the period for both groups. By 2013, community-admitted patients had an average score of 2.04, a 5 percent increase from 2002 to 2013, while PAC patients had an average score of 1.78, a 9 percent increase over the period. Likewise, the community-admitted group was more cognitively impaired over the entire time period. However, both groups became more cognitively impaired over time and had comparable trends. These trends do not suggest that differential health status or cognitive functioning had a large influence on the growth of community-admitted patients.
| FIGURE III.4. Trends in HCC Scores among Community-Admitted and PAC Patients |
|---|
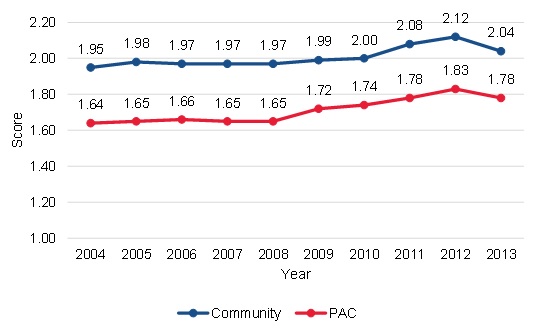 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, from January 1, 2002, to December 31, 2013. NOTE: 2004 was the first year that HCC scores were included on the DataLink file. |
Slightly higher growth in for-profit share among PAC patients indicates that changes in for-profit HHA practices was not a major contributor to the growth in community-admitted patients. There were also some differences in levels and trends of several provider and geographic characteristics between community-admitted and PAC patients. We examined the trends in the proportion of community-admitted and PAC patients served by for-profit HHAs because the share of these agencies has grown over time, and they might be more aggressive about admitting community patients, especially if for-profit agencies find them more financially advantageous. We found that higher proportions of community-admitted patients received care from a for-profit HHA compared to PAC patients (Figure III.5). The community-admitted patients had slightly higher growth in the proportion of patients served by for-profit HHAs up to 2009--from 45.9 percent in 2002 to 71.5 percent in 2009, for a growth rate of 56 percent. This compared with a 52 percent increase in the proportion of PAC patients served by for-profit agencies from 2002 to 2009. After 2009, the trend among community-admitted patients leveled off. By 2013, 72.8 percent of community-admitted patients were served by for-profit agencies, for a total growth rate of 59 percent from 2002 to 2013. The proportion of PAC patients served by for-profit HHAs grew steadily over time and continued to increase slightly even after the growth for community-admitted patients had leveled off--from 31.2 percent of patients in 2002 to 51.8 percent of patients in 2013, for a total growth rate of 66 percent. Although a higher proportion of community-admitted patients were served by for-profit agencies, the trends over time do not suggest that changes in practices at for-profit agencies have contributed to the large differential growth in community-admitted and PAC patients because the growth was relatively similar for the two groups of patients.
| FIGURE III.5. Trends in For-Profit Ownership of HHAs Serving Community-Admitted and PAC Patients |
|---|
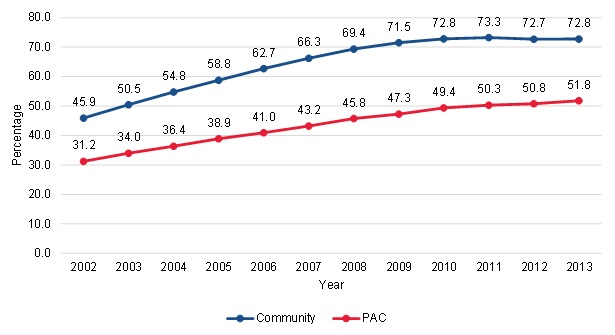 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, from January 1, 2002, to December 31, 2013. |
Substantial growth in community-admitted patients in states with a past history of fraud and abuse indicates that potentially fraudulent practices might have been a contributor to the growth in community-admitted patients. One concern is that fraud may be contributing to the growth in community-admitted patients, as it may be easier to obtain a certification for a plan of care for a person who lives in the community, rather than attempting to obtain one for a patient as they leave the hospital. The proportion of community-admitted and PAC patients who lived in states with a past history of Medicare home health fraud and abuse[6] was similar at the beginning of the period (26.0 percent and 24.1 percent in 2002, respectively). However, the proportion of PAC patients in these states decreased slightly over time (to 22.8 percent in 2013) while the proportion of community-admitted patients in these states increased up to 2010 (to 38.5 percent) and then decreased slightly (to 35.7 percent in 2013) (Figure III.6). These patterns reflect a 5.4 percent decline among PAC patients and a 37.3 percent growth rate among community-admitted patients from 2002 to 2013. The increase in the proportion of community-admitted patients in the states with fraud and abuse issues suggests that potentially fraudulent practices might have contributed to the growth in these patients over time. Some overarching policy changes were implemented to the Medicare home health benefit in 2010, including putting caps on outlier payments and adding payment safeguards to reduce fraud. The combination of these changes might have contributed to some of the declines observed from 2010 to 2013, even before more recent antifraud efforts were implemented in these states.
| FIGURE III.6. Trends in the Percentage of Patients in Fraud and Abuse States among Community-Admitted and PAC Patients |
|---|
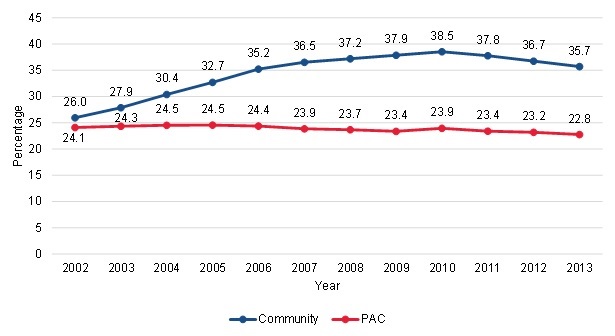 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, from January 1, 2002, to December 31, 2013. |
Growth in community-admitted patients in counties with high numbers of HHAs suggests that competition among HHAs might have contributed to higher numbers of community-admitted patients. We also considered whether there are more community-admitted patients in areas where there is more competition--it may be that agencies will aggressively seek out more patients in areas where competition makes it challenging to obtain referrals. We found higher proportions of community-admitted patients than PAC patients living in counties with high numbers of HHAs. Over time, the proportion of patients in these counties increased for community-admitted patients from 29.7 percent in 2002 to 34.1 percent in 2013 (a 14.8 percent growth rate), while the proportion decreased for PAC patients from 20.9 percent in 2002 to 17.5 percent in 2013 (a 16.3 percent decline). These patterns indicate that there could be induced demand among community-admitted patients or that areas with greater competition are more aggressive about seeking outpatients in the community.
| FIGURE III.7. Trends in Average Number of Aide Visits Per Episode Per Year among Community-Admitted and PAC Patients |
|---|
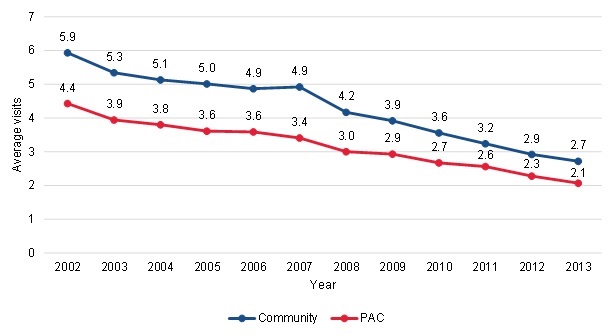 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, from January 1, 2002, to December 31, 2013. |
Similar declines in aide visits per episode for community-admitted and PAC patients suggests that substitution of aide for other care has not been a contributor to the growth in community-admitted patients. There is some concern that the growth in community-admitted patients has been driven by an increase in patients using Medicare home health services as a substitute for other LTSS. Since home health aide care is the primary service that overlaps between Medicare home health and LTSS, if providing more long-term care is underlying the growth in community-admitted patients, we would expect to observe different changes in home health aide utilization among the community-admitted patients relative to the PAC users. That is, we would expect to see a higher rate of increase, or a slower rate of decline. We found that the average number of home health aide visits per episode per year declined over time for both community-admitted and PAC patients (Figure III.7), with the use declining more rapidly for the community-admitted patients. In 2002, the community-admitted patients had an average of 5.9 aide visits per episode and the PAC patients had an average of 4.4 aide visits per episode, an average difference of 1.5 visits. By 2013, the community-admitted patients had an average of 2.7 aide visits per episode and the PAC patients had an average of 2.1 aide visits per episode, an average difference of 0.6 visits. This resulted in a 54.2 percent decline in the average number of aide visits among community-admitted patients and a 52.3 percent decline among PAC patients. The average number of skilled nursing visits per episode per year showed a similar pattern, with both groups declining over time and the differences between the two groups declining.
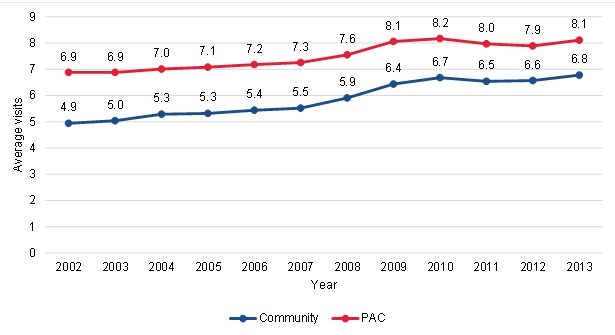
| FIGURE III.8. Trends in Average Number of Therapy Visits Per Episode Per Year among Community-Admitted and PAC Patients |
|---|
 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, from January 1, 2002, to December 31, 2013. |
Higher growth in therapy visits per episode among community-admitted patients suggests that financial incentives in the payment system might be a contributor to the growth in community-admitted patients. Incentives in the home health payment policy regarding the use of therapy might have made certain patients more financially attractive, resulting in differential patterns over time for community-admitted and PAC patients. The average number of therapy visits per episode per year has increased over time for both community-admitted and PAC patients (Figure III.8). PAC patients had more therapy visits on average than community-admitted patients in all years, but the difference between the two groups declined over time. In 2002, PAC patients had an average of 6.9 therapy visits per episode and community-admitted patients had an average of 4.9 therapy visits per episode, an average difference of 2.0 visits per episode. By 2013, PAC patients had an average of 8.1 therapy visits per episode and community-admitted patients had an average of 6.8 therapy visits per episode, an average difference of 1.3 visits per episode. This resulted in a 17.4 percent growth rate among PAC patients and a 38.8 percent growth rate among community-admitted patients. The increases in therapy use among all patients likely reflects inherent payment incentives in the prospective payment system (PPS) for providing therapy, as well as increasing acuity among home health patients. Some of the specific changes to the payment system for therapy can be observed in the data. In 2008, CMS refined the home health PPS, including changes for therapy visits. Until 2008, the PPS used a ten-therapy threshold for payment, and updates in 2008 implemented therapy thresholds at six, 14, and 20 visits, which could have contributed to the increase after 2008.
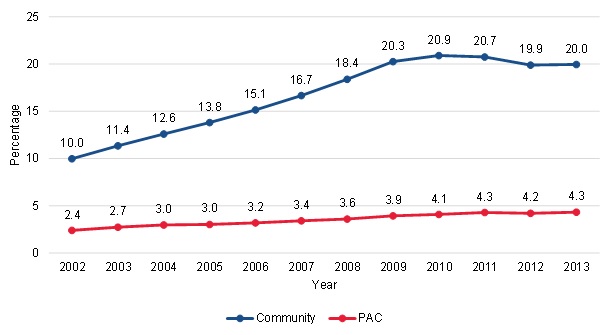
Higher growth in physical therapy use in later episodes of care among community-admitted patients suggests that financial incentives to provide therapy might be a contributor to the growth in community-admitted patients. Prior to 2010, some stakeholders in the Medicare system misinterpreted the Medicare home health standard and required patients to improve their functioning or health status in order to continue receiving home health care. After court decisions in 2010, CMS provided clarification that Medicare home health covers skilled care services when a beneficiary needs such care in order to maintain function or to prevent or slow decline or deterioration.[7] Therefore, we expected that we might observe an increase in maintenance therapy after the 2010 court decisions, and this might have contributed to the increase in community-admitted patients. The proportion of patients with physical therapy use in later episodes of a spell, which would indicate maintenance therapy, was higher for the community-admitted patients (Figure III.9). Among community-admitted patients, the proportion of patients with physical therapy use in Episode 3 or later increased from 10.0 percent in 2002 to 20.9 percent in 2010. The proportion declined slightly after 2010 to 20.0 percent in 2013, for an overall growth rate of 100 percent from 2002 to 2013. For PAC patients, the proportion of patients with physical therapy use in Episode 3 or later increased slightly over the period, from 2.4 percent in 2002 to 4.3 percent in 2013, for an overall growth rate of 79.2 percent from 2002 to 2013. Thus, we found that maintenance therapy decreased slightly among community-admitted patients after 2010, while it increased slightly after 2010 then leveled off among PAC patients--indicating that physical therapy care patterns did not markedly change shortly after clarification from the court decisions. However, these patterns show increases in physical therapy in later episodes of care in years prior to the court decision, suggesting that HHAs were already shifting to more maintenance care and that there were important changes in the use of the benefit occurring among long-term home health patients over the period. As shown in Figure III.4, there were small increases in HCC scores over the period, with slightly higher increases among PAC patients, which does not suggest that these patterns in therapy use among community-admitted patients are driven by large changes in acuity. It is possible that these patterns could be related to a shift to substituting therapy for other services because of the payment incentives to provide more therapy, or an increase in the number of physical therapists available to serve the Medicare population.
| FIGURE III.9. Trends in the Proportion of Community-Admitted and PAC Patients with At Least 3 Episodes Who had Physical Therapy Use in the Third or Later Episode |
|---|
 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, from January 1, 2002, to December 31, 2013. |
Similar trends among dual eligible beneficiaries as found for the full sample indicates that substitution of care has not been a large contributor to the growth in community-admitted patients. When we examined visit trends among the two groups of patients in the dual eligible subsample, we found similar patterns for the average number of home health visits across all types as we found for the full patient sample over time. There were no distinct patterns in home health aide visits among dual eligibles. Similarly, we found that, although higher proportions of dually eligible community-admitted patients lived in states with lower Medicaid expenditures for home and community-based services (HCBS) versus institutional care, there were not large, differential shifts over time for community-admitted patients versus PAC patients that would suggest that states were increasingly using the Medicare home health benefit to substitute for Medicaid LTSS.
Summary of trends. Overall, community-admitted and PAC patients had relatively similar patterns over time for many characteristics. However, a few characteristics had notable differences. Specifically, there was a substantial increase of community-admitted patients living in states targeted for fraud and abuse issues, which suggests either that fraudulent admissions are more likely for patients in community settings or that there is a relationship between the fraudulent admissions and the length of home health care. There was also a large growth in therapy visits overall, and in later episodes of a spell, among community-admitted patients--indicating that there might be important differences between long-term and short-term patients, which suggests a need to further explore the length of home health spells among different groups of patients to determine how the source of admission interacts with the length of home health use.
B. Cross-Sectional Comparison of Home Health Users
In addition to comparing trends over time, we conducted a cross-sectional analysis to compare community-admitted and PAC patients. For this analysis, we defined patients based on the source of admission at the start of their spell of care, rather than within each calendar year, as we did to analyze trends. Because patients can use home health for many years, the classification of a patient in a particular calendar year is impacted by both the source of admission of each of his or her episodes, and the number of episodes he or she has in that year. Defining patients at the start of their spell of care explicitly focuses the analysis on the interaction of the source of admission and length of use, so that we can better understand whether there differences between patients due to whether they entered care from the community or an acute or post-acute setting, and whether they are a short-term or long-term user.
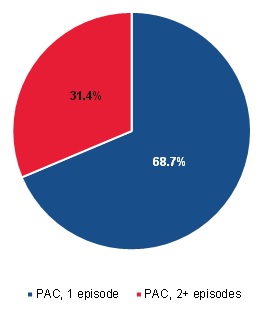
| FIGURE III.10. Breakdown of PAC Users by Short-Term and Long-Term Use |
|---|
 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, with home health use between January 1, 2013, and December 31, 2013 and spells starting no earlier than January 1, 2011, and no later than December 31, 2013. |
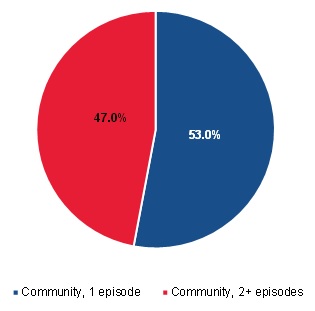
As described previously, MedPAC identified that a substantial component of the growth in community-admitted home health users was due to the increase in users who received multiple episodes of care. As Figure III.10 and Figure III.11 show, in our analysis only 31 percent of PAC users had more than one 60-day episode during their spell, whereas 47 percent of community-admitted patients did. Furthermore, we found that 30 percent of the beneficiaries who started their spell as PAC users were reclassified as community-admitted users when their spell spanned multiple calendar years. Because there is such a confounding relationship between length of care and classification as a community-admitted patient, we examined the differences between PAC and community-admitted patients for those who had only one episode and those with multiple episodes.
| FIGURE III.11. Breakdown of Community-Admitted Users by Short-Term and Long-Term Use |
|---|
 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, with home health use between January 1, 2013, and December 31, 2013 and spells starting no earlier than January 1, 2011, and no later than December 31, 2013. |
1. Patients with similar lengths of home health use have comparable characteristics regardless of their admission source, but there are greater differences for patients with multiple episodes of care.
Several of the patient clinical and functional characteristics, as well as the patterns of home health use and other acute and post-acute use, indicate that the groups defined by length of use are similar to each other, regardless of the source of admission. That is, the short-term PAC and community-admitted users (with one episode in their spell) and the long-term PAC and community-admitted users (with two or more episodes in their spell) are more similar to each other across some factors than the users only defined by the source of admission (PAC versus community-admitted).
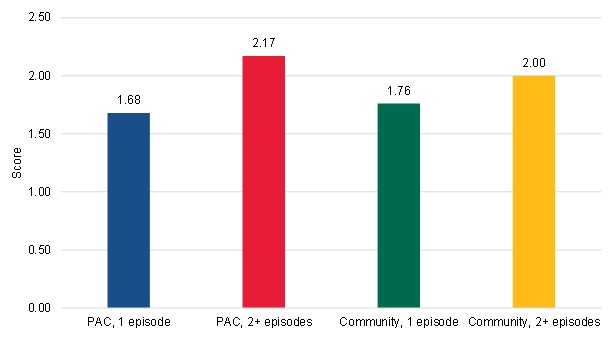
For instance, the long-term PAC and long-term community-admitted users had greater clinical severity, as reflected by higher HCC scores, than their short-term counterparts (Figure III.12). The long-term PAC users had the greatest clinical severity at the start of their spell, with an average HCC score of 2.17, followed by the long-term community-admitted users with an average HCC score of 2.00. The short-term users had much lower HCC scores than the long-term users. The short-term community-admitted users had an average HCC score of 1.76, while the short-term PAC users had the lowest average scores at 1.68. The larger difference in clinical severity between the two groups of PAC patients compared with the two groups of community-admitted patients likely reflects the fact that fewer PAC patients have a second episode of home health and only do if they are very sick, while more community-admitted patients tend to have longer spells of home health (Figure III.10 and Figure III.11).
| FIGURE III.12. HCC Scores among PAC and Community-Admitted Users |
|---|
 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, with home health use between January 1, 2013, and December 31, 2013 and spells starting no earlier than January 1, 2011, and no later than December 31, 2013. |
The long-term PAC and community-admitted users had higher rates than the short-term users of several chronic conditions, including chronic obstructive pulmonary disease (COPD), congestive heart failure (CHF), diabetes, and stroke. The long-term users were also slightly more functionally impaired at the start of their spell, as indicated by slightly higher activity of daily living (ADL) function scores than the two short-term groups. The long-term PAC users had an average ADL score of 13.9 (on a scale of 0-35, with higher scores indicating greater impairment) and the long-term community-admitted users had an average ADL score of 13.2. Among the short-term users, the community-admitted patients had an average score of 12.7, while the PAC patients had an average score of 12.4.
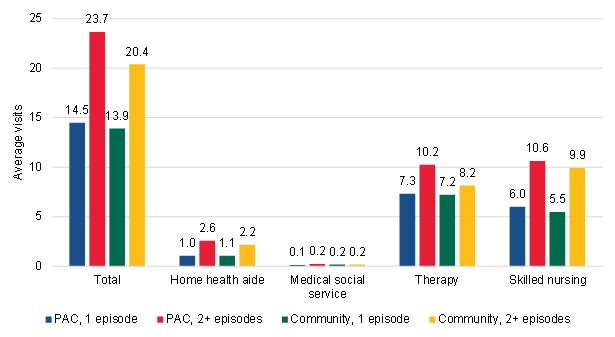
Patients who received multiple episodes of care had similar patterns of home health use, although that became more evident over time. The short-term PAC and community-admitted users and the long-term PAC and community-admitted users were more similar to each other based on home health service use in the first episode of the spell than the groups just based on source of admission (Figure III.13). The long-term PAC users had the highest average number of visits in the first episode, with an average of 23.7 total visits--which likely reflected their greater clinical severity than the other groups of users. The long-term community-admitted users had the next-highest home health use, with an average of about 20.4 total visits in the first episode of the spell. On average, the long-term PAC users had more of all types of visits in the first episode compared with the long-term community-admitted users, but the largest difference in visit types was for therapy visits (10.2 for the long-term PAC users versus 8.2 for the long-term community-admitted users). The short-term PAC and community-admitted users had fewer visits than the long-term users in the first episode of the spell, with the short-term PAC users having an average of 14.5 total visits and the short-term community-admitted users having an average of 13.9 total visits. The breakdown of visits was similar between the two short-term groups, except for slightly higher skilled nursing visits among the short-term PAC group compared with the short-term community-admitted group.
The patterns of home health visits became more similar for the two long-term groups in the second and third episodes, compared with the breakdown in the first episode. (By definition, the short-term users had only one episode.) Specifically, the average number of visits decreased from 23.7 to 16.7 from Episode 1 to Episode 2 for the long-term PAC users and from 20.4 to 16.4 from Episode 1 to Episode 2 for the long-term community-admitted users. The average number of visits increased slightly for both long-term groups in Episode 3 compared with Episode 2 for the patients who had at least three episodes in their spell. The largest change in visit types for both groups was due to decreases in therapy visits in subsequent episodes. Skilled nursing visits declined slightly from Episode 1 to Episodes 2 and 3, but the declines were not as great as the declines for therapy visits. Home health aide and medical social service visits were relatively steady from early to later episodes of the spell for the two groups.
These results suggest that in terms of home health utilization, short-term users and long-term users have much more in common than PAC and community-admitted patients. The users who are more clinically complex and functionally impaired when they enter home health have greater numbers of home health visits in the first episode, regardless of whether they are admitted as a PAC or community user. And although there were greater differences between the two groups of long-term patients than between the two groups of short-term patients, the patterns of home health use and visit types become more similar over time for long-term users, so the source of admission became less relevant as beneficiaries continued to use home health for a long period. The important differences between patients based on the length of their home health use implies that the concerns about the growth of community-admitted patients needs to take into account the number of episodes for a patient, as it is the long-term patients that have different characteristics and utilization patterns.
Overall, our findings for home health utilization are consistent with findings reported in the 2018 home health proposed rule. The findings presented in the proposed rule found that community-admitted patients have lower resource use than PAC patients, and early episodes are more resource intensive than late episodes (CMS 2017). However, there are differences between our results and the results presented in the proposed rule. The analyses in the proposed rule that examined resource use based on the source of admission reported resource use in 30-day increments that were independent of one another, and separate analyses in the proposed rule examined resource use in 30-day increments for early and late episodes of care. For our analyses, we examined utilization using 60-day episodes, taking into account both the source of admission and length of use at the same time. Our analyses indicate that the source of admission and timing interact with one another, so it is important to consider both of these factors together when examining home health patients. However, it is important to note that although the analyses separately examined source of admission and the timing of the episode, the proposed payment approach from CMS allows for an interaction between source of admission and the number of episodes, which would be the direction suggested by this research.
| FIGURE III.13. Home Health Visits in the First Episodes of the Home Health Spell among PAC and Community-Admitted Users |
|---|
 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, with home health use between January 1, 2013, and December 31, 2013 and spells starting no earlier than January 1, 2011, and no later than December 31, 2013. |
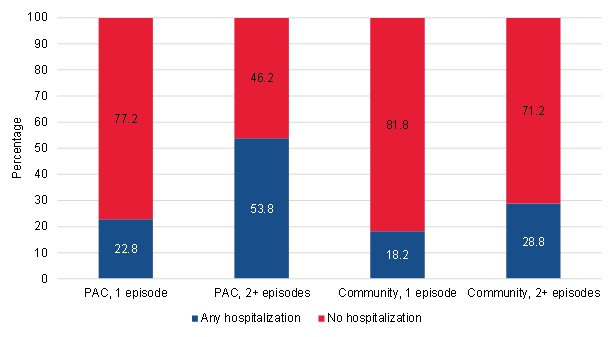
Similar to the relative ranking of the groups of patients in terms of home health utilization, the long-term PAC users had the highest acute hospital use during the 120 days after the start of their spell, with approximately 54 percent of beneficiaries in this group having at least one acute hospital stay in the 120-day period (Figure III.14). Nearly two times as many beneficiaries in the long-term PAC group had an acute hospital stay than the next-highest group of acute hospital users--the long-term community-admitted group, in which approximately 29 percent of beneficiaries had an acute hospital stay. Just as the patterns of home health use indicated, these utilization patterns likely reflect that the long-term PAC patients are sicker and more clinically complex, which would result in the greater likelihood of an acute hospital admission. The short-term users had lower use of acute hospitals. About 23 percent of short-term PAC users had an acute hospital admission and 18 percent of short-term community-admitted users had an acute hospital admission. Both groups of PAC users (the short-term and long-term users) had relatively more expensive acute stays than the community-admitted users when they had a stay.
| FIGURE III.14. Acute Hospitalization within 120 Days of the Start of the Spell among PAC and Community-Admitted Users |
|---|
 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, with home health use between January 1, 2013, and December 31, 2013 and spells starting no earlier than January 1, 2011, and no later than December 31, 2013. |
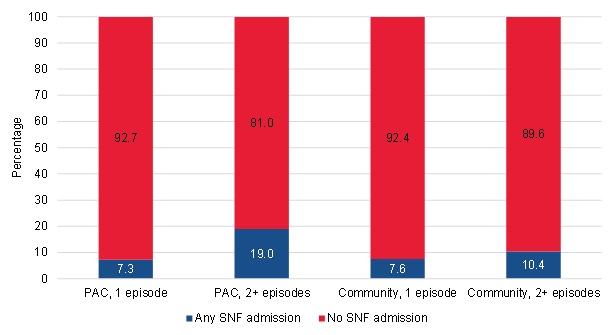
Long-term acute care (LTAC) and rehabilitation hospital admissions were less common. However, similar patterns held for these inpatient settings, with long-term PAC users using these settings the most. The long-term PAC users also had the most frequent SNF use, with 19 percent of beneficiaries in this group entering a SNF within 120 days of the start of their home health spell (Figure III.15). The long-term community-admitted users had the next-highest SNF use, with 10 percent of beneficiaries in this group entering a SNF within 120 days of the start of their home health spell. About 7-8 percent of short-term users entered a SNF within 120 days of the start of the home health spell.
| FIGURE III.15. SNF Admission within 120 Days of the Start of the Spell among PAC and Community-Admitted Users |
|---|
 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, with home health use between January 1, 2013, and December 31, 2013 and spells starting no earlier than January 1, 2011, and no later than December 31, 2013. |
Both the short-term PAC users and short-term community-admitted users had higher mortality than the long-term users, with approximately 9 percent of beneficiaries in either of these groups dying within the 120 days of the start of their spell (Figure III.16). This compared to about 2-4 percent of beneficiaries in either the long-term PAC or long-term community-admitted groups dying within 120 days of the start of their spell. The higher mortality rates for short-term users implies that some beneficiaries in these groups might have been short-term users because they died prior to having additional home health episodes.
The regression results for inpatient and SNF use were generally consistent with these descriptive results. When we examined the probability of any inpatient admission (including acute, LTAC, and rehabilitation) within 120 days of the start of a spell, we found that after controlling for patient characteristics (including the HCC risk score, chronic conditions, and physical and cognitive functioning) the long-term PAC and community-admitted users had significantly higher odds of an admission (compared to the reference group of short-term PAC users). The long-term PAC and community-admitted users also had significantly higher odds of a SNF admission. Overall, the long-term PAC users had the highest odds of any type of admission. These results suggest that multiple episodes of home health use did not prevent greater use of other acute and post-acute care.
| FIGURE III.16. Mortality within 120 Days of the Start of the Spell among PAC and Community-Admitted Users |
|---|
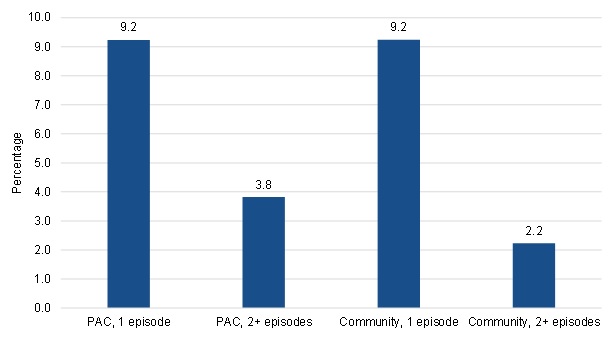 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, with home health use between January 1, 2013, and December 31, 2013 and spells starting no earlier than January 1, 2011, and no later than December 31, 2013. |
Taken together, these results show that the short-term PAC and community-admitted users are very similar to each other, despite their differing sources of admission. Although the long-term users are similar to each other across many characteristics, including the patterns of home health visits, the long-term PAC users are more clinically complex and have greater use of inpatient and SNF care. These findings indicate that there is an important relationship between the source of admission and length of use, and the source of admission itself is not the primary differentiator between patients. The 2018 home health proposed rule would include the source of admission as part of the new Home Health Groupings Model (HHGM), given findings that have demonstrated lower resource use among community-admitted patients (CMS 2017). In addition, the HHGM would include the timing of the episode, since early episodes have been found to be more resource intensive than late episodes. Our analyses support these findings; specifically, our analyses indicate that both the source of admission and timing are key factors that impact utilization, and both factors need to be considered.
2. PAC and community-admitted patients differ based on where they live and the agencies they receive care from.
We did not find meaningful differences for many of the patient-level demographic and health status characteristics that we compared between the groups of PAC and community-admitted users. However, two characteristics showed notable differences for PAC users versus community-admitted users: (1) dual eligibility status; and (2) living arrangement.
Specifically, the proportion of beneficiaries who were dually eligible for Medicare and Medicaid was higher among the community-admitted users compared with the PAC users, with the highest proportion among the long-term community-admitted users (Figure III.17). About 36 percent of community-admitted users who had two or more episodes in their spell were dually eligible, compared with about 22 percent of the PAC long-term users. Among short-term users, about 28 percent of community-admitted users were dually eligible compared with about 15 percent of PAC users.
| FIGURE III.17. Dual Eligibility Status among PAC and Community-Admitted Users |
|---|
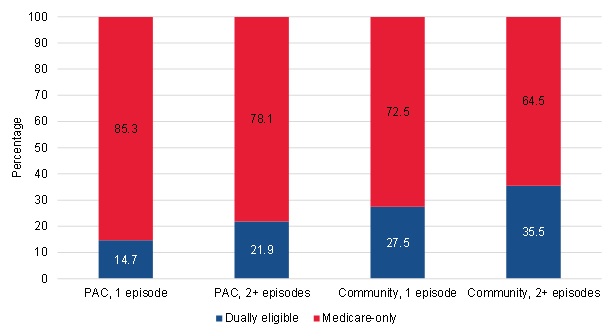 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, with home health use between January 1, 2013, and December 31, 2013 and spells starting no earlier than January 1, 2011, and no later than December 31, 2013. |
Community-admitted users were slightly more likely to live alone, but they were less likely to live with another person in their home relative to PAC users (Figure III.18). The difference between the community-admitted and PAC users is notable for the proportion living in a congregate setting (which includes assisted living facilities). About 15 percent of the short-term or long-term community-admitted users live in a congregate setting compared with 6 percent of short-term PAC users and 8 percent of long-term PAC users. Providers often find it easier and less costly to serve multiple patients at a single location. If beneficiaries in congregate settings receive more primary care directly in these facilities than beneficiaries who live at home and must visit a physician's office, the beneficiaries in congregate settings might be more likely to get certified for home health directly from the community. Staff in congregate settings might also be more proactive about seeking out home health for beneficiaries who need it.
| FIGURE III.18. Living Arrangement among PAC and Community-Admitted Users |
|---|
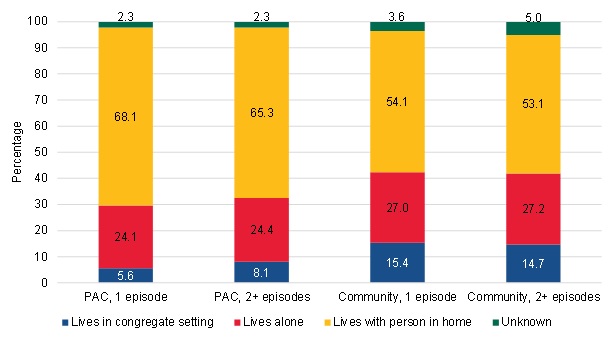 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, with home health use between January 1, 2013, and December 31, 2013 and spells starting no earlier than January 1, 2011, and no later than December 31, 2013. |
PAC and community-admitted patients also had important differences in terms of the ownership of the HHAs from which they received care and residence in a state with a previous history of fraud and abuse issues. Large differences exist in the proportions of beneficiaries in each group served by for-profit HHAs (Figure III.19). The short-term PAC users had the lowest proportion served by for-profit agencies (49 percent), followed by the long-term PAC users (64 percent), the short-term community-admitted users (65 percent), and the long-term community-admitted users (80 percent). It is possible that long-term community-admitted users have higher margins that make them particularly sought-after by for-profit agencies. Some of the differences in the proportions of patients served by for-profit agencies might also be driven by referral patterns or marketing by for-profit agencies.
| FIGURE III.19. Agency Ownership of HHAs Serving PAC and Community-Admitted Users |
|---|
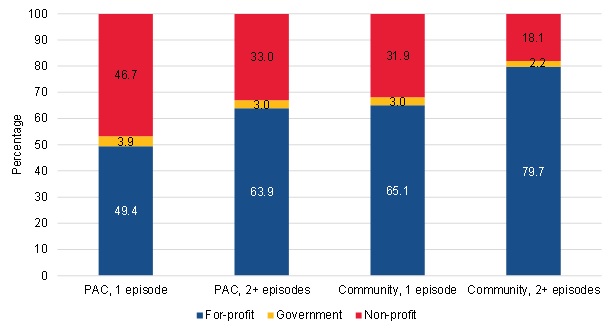 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, with home health use between January 1, 2013, and December 31, 2013 and spells starting no earlier than January 1, 2011, and no later than December 31, 2013. |
Community-admitted users were more likely to live in a state that had a past history of documented fraud and abuse (Figure III.20). Approximately 42 percent of the long-term community-admitted users lived in one of the four states (Florida, Illinois, Michigan, and Texas) currently being targeted by CMS for fraud and abuse issues, compared with only 22 percent of the short-term PAC users who lived in one of these states. Similar proportions of long-term PAC users and short-term community-admitted users (28 percent and 31 percent, respectively) lived in one of the four states with fraud and abuse.
| FIGURE III.20. Residence in a State with Fraud and Abuse among PAC and Community-Admitted Users |
|---|
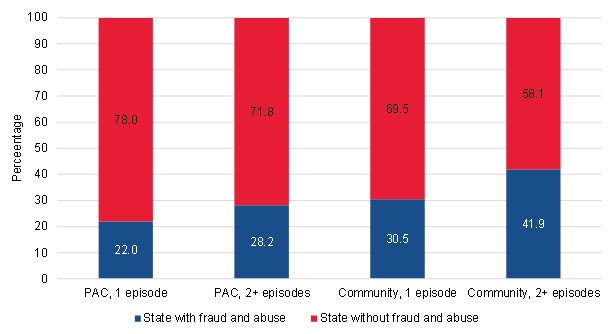 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, with home health use between January 1, 2013, and December 31, 2013 and spells starting no earlier than January 1, 2011, and no later than December 31, 2013. NOTE: States with documented fraud and abuse issues during the period of the analysis include Florida, Illinois, Michigan, and Texas. |
When we broke down the number of PAC and community-admitted patients per 100,000 age 65 and older by state, we found that there were some important geographic differences between PAC and community-admitted users. Among PAC users, the states with the highest numbers of users included a mix of states from the Northeast and the Southeast, with Mississippi ranking at the top of the list (Table III.1). No states in the Midwest or West were among the group with the highest rates of PAC use. Four of the highest states for community-admitted use (Georgia, Kentucky, Mississippi, and Vermont) were also among the top ten for PAC use, suggesting that there are certain states that have relatively high use of all types of home health services. Of the six states that differed between the two groups, four were flagged for fraud and abuse issues (Florida, Illinois, Michigan, and Texas).
Within the context of the LTSS system, the states with the highest community-admitted use were slightly poorer performing LTSS states.[8] None of the highest performing LTSS states (Minnesota, Oregon, and Washington) were among those with the highest PAC or community use. The community-admitted patients were more frequently entering Medicare home health in states with relatively poorer LTSS systems and with documented fraud and abuse.
| TABLE III.1. Top 10 States for PAC and Community-Admitted Home Health Use per 100,000 Age 65 and Older | ||
|---|---|---|
| Rank | PAC Use | Community-Admitted Use |
| 1 | Mississippi | Mississippi |
| 2 | Massachusetts | Illinois |
| 3 | Vermont | Florida |
| 4 | Virginia | Texas |
| 5 | Delaware | Louisiana |
| 6 | Kentucky | Oklahoma |
| 7 | Maine | Kentucky |
| 8 | Maryland | Michigan |
| 9 | New Hampshire | Vermont |
| 10 | Georgia | Georgia |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, with home health use between January 1, 2013, and December 31, 2013 and spells starting no earlier than January 1, 2011, and no later than December 31, 2013. | ||
Overall, the findings from the patient-level characteristics suggest that while some patient factors might be contributing to the differences in the numbers of PAC and community-admitted patients, they are unlikely to be the primary drivers of the large differences between the two types of patients. However, provider or geographic characteristics appear to be important factors that are contributing to the number of community-admitted patients.
3. Patterns of care alone provide little evidence to support the hypothesis that home health is being used as a substitute for LTSS.
The Medicare home health benefit is an acute care benefit, and a beneficiary can only receive personal care services if the beneficiary has a skilled care need. One concern about long-term community-admitted patients is that they may receive Medicare home health services as a substitute for LTSS. That is, patients who need personal care services can be admitted from the community with little skilled care needs and use the benefit to obtain the personal care that they need. If this is the case, then we might expect to observe community-admitted patients receiving low levels of skilled care services but high levels of home health aide use, although the payment system may create disincentives for these patterns. On the other hand, patients who need personal care may be those who are able to remain in their home because they get their personal care needs met by other sources (such as assisted living services), and their providers may be more aware of and knowledgeable about obtaining the skilled care that Medicare home health provides. Unfortunately, in our data, we do not observe LTSS use (except in the case of assisted living), so we cannot identify when care is complementary. We found that among long-term community-admitted users there were few patients that had patterns of care that were consistent with the theory that home health was being used as a substitute for LTSS if use of aides is the metric. The proportion of patients who used any aide care and little skilled care was only 12 percent of users (Figure III.21). Most of the long-term community-admitted users were beneficiaries who received no aide care and had high skilled care use (45 percent of the long-term community-admitted user group) or beneficiaries who used no aide and a relatively low amount of skilled care services (30 percent of the long-term community-admitted user group). The remaining 14 percent of beneficiaries in this group used an aide and a relatively large amount of skilled services. However, this does not suggest that Medicare home health is never being used to substitute for LTSS; but rather, as measured by aide services, it is not a major contributor. It is still possible that other service types may substitute for LTSS, though Medicare rules require that skilled providers provide skilled services.
| FIGURE III.21. Breakdown of Long-Term Community-Admitted Users by the Type of Home Health Use |
|---|
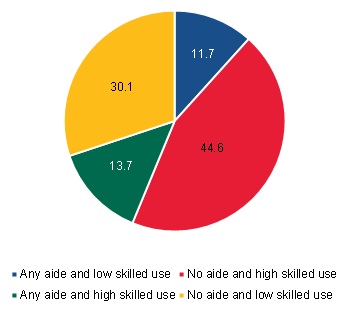 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, with home health use between January 1, 2013, and December 31, 2013 and spells starting no earlier than January 1, 2011, and no later than December 31, 2013. NOTE: Aide use refers to home health aide and medical social service use. Skilled use refers to therapy and skilled nursing use. Appendix A includes the details of how these groups were defined. |
To investigate further, we examined the Medicare home health patterns of two groups of beneficiaries: (1) those who lived in congregate living facilities; and (2) those who were dually eligible beneficiaries and who resided in states with good LTSS systems.[9] We found that very few beneficiaries who lived in congregate facilities have patterns of care that include high use of home health aide services and low skilled services--only 4 percent (Figure III.22). Rather, the vast majority had patterns of care that included a relatively high use of skilled services. In contrast, patients who lived alone or at home were more likely to have a care pattern that included aide services; however, they were still a minority of the patients overall. About 14 percent of the patients who lived alone and 12 percent of those who lived with another individual used home health aide services and few skilled services.
| FIGURE III.22. Living Arrangement among Long-Term Community-Admitted Users by Type of Home Health Use |
|---|
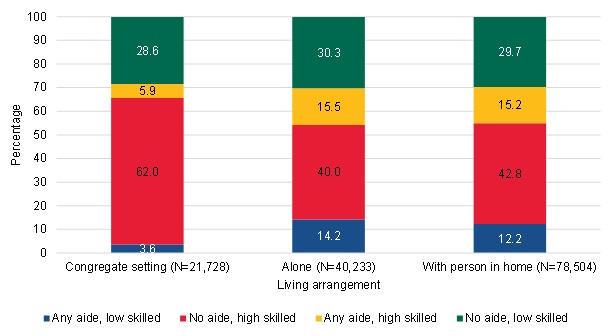 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, with home health use between January 1, 2013, and December 31, 2013 and spells starting no earlier than January 1, 2011, and no later than December 31, 2013. NOTE: Aide use refers to home health aide and medical social service use. Skilled use refers to therapy and skilled nursing use. Appendix A includes the details of how these groups were defined. |
Among duals who lived in states with good LTSS systems,[10] we found that they were slightly more likely to have a pattern of care that included home health aide services compared to states where the LTSS systems were weaker (Figure III.23). We would expect the opposite if Medicare home health was being used to substitute for LTSS--that is, we would expect more beneficiaries with home health aide care in states that have poor LTSS systems because some portion of those individuals would likely not have access to personal care services. We do not observe that pattern.
Another way to think about the role that Medicare home health is playing is to examine what acute care services long-term community-admitted patients' use. If patients receive aide care without much skilled care, it suggests that these patients may mostly need personal care services and not skilled care services. We would expect that these patients would have lower measures of acuity, as well as less utilization of acute care services after they have been admitted to Medicare home health.
| FIGURE III.23. Proportion of Patients with No or Any Aide Services among Long-Term Community-Admitted Users, by Dual Eligibility Status and State LTSS Ranking |
|---|
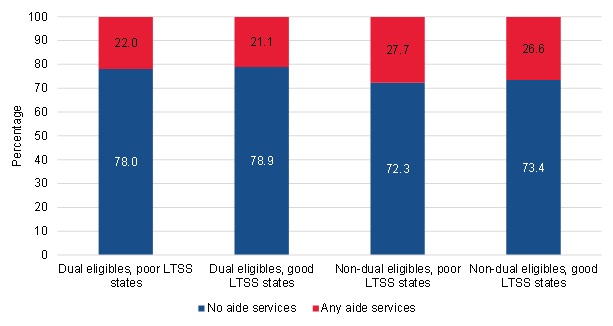 |
| SOURCE: Mathematica analysis of a 20% sample of the CMS DataLink file, with home health use between January 1, 2013, and December 31, 2013 and spells starting no earlier than January 1, 2011, and no later than December 31, 2013. NOTE: Aide use refers to home health aide and medical social service. The "no aide services" category includes patients with low and high skilled service use and the "any aide services" category includes patients with low and high skilled service use. Poor LTSS states refer to states in the third or bottom quartile of LTSS ranking based on the AARP 2014 State LTSS Scorecard quartile ranking. Good LTSS states in the second or top quartile. Appendix A includes more details about these groups. |
We found little difference in the HCC score of patients with different home health utilization patterns. Most of the scores were fairly similar to one another (data not shown). Among the long-term community-admitted group, those who used home health aide services and a relatively higher amount of skilled care had the highest HCC score (2.08), followed by those that used no aide and a relatively high level of skilled care (2.02). Those who used no aide services and relatively low skilled care did have the lowest HCC score (1.94), but it was not materially different from the others.
Furthermore, in terms of inpatient utilization after the start of home health care, we found that those who used aide services but not a lot of skilled care had slightly more admissions to acute care hospitals, SNFs, and other institutional providers (Figure III.24). This suggests one potential explanation for their low skilled care use--that is, these patients may be cycling in and out of home care, which results in lower skilled care over the course of their episode. Again, this pattern is not consistent with the theory that Medicare home health among community-admitted patients is being used to substitute for LTSS, although it does offer a potential reason why we may observe the low skilled care use.
| FIGURE III.24. Hospital and SNF Admissions within 120 Days of the Start of the Spell among Long-Term Community-Admitted Users |
|---|
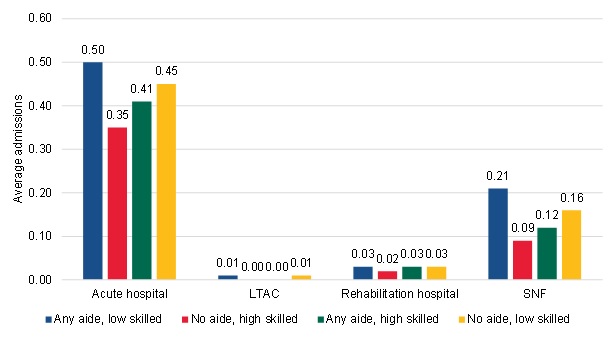 |
| SOURCE: National estimates based on Mathematica analysis of a 20% sample of the CMS DataLink file, from January 1, 2002, to December 31, 2013. NOTE: Aide use refers to home health aide and medical social service use. Skilled use refers to therapy and skilled nursing use. Appendix A includes the details of how these groups were defined. |
IV. LIMITATIONS
Although these analyses provide important descriptive information about different types of home health users, there are some limitations to note. Because our analyses relied on observational data, we were unable to draw conclusions about what is truly appropriate use of the home health benefit across the groups. Likewise, we were unable to draw any causal conclusions about the growth among certain beneficiaries. The care patterns could be indicators of other underlying issues, such as changes in provider payments or system-level changes, but we were unable to examine every factor that could drive the patterns of use. That is, we did not build a dynamic model of care for this analysis, instead we offer observations.
For these analyses, we had to measure beneficiaries at a particular point in time. However, home health patients are a dynamic group. Patients' care needs and other factors change over time, but we were unable to draw any conclusions about how the care patterns interact with a particular beneficiary's changing needs.
Although we descriptively analyzed indicators of the state-level LTSS system, we could not draw any conclusions about beneficiary-level LTSS use because we did not have any data about individual Medicaid or other LTSS use.
V. SUMMARY AND DISCUSSION
A. Summary
When we examined trends in community-admitted and PAC patients over time, we found that, although some of the growth in community-admitted patients was driven by new patients, a large portion of the growth was driven by increases in the number of patients with multiple episodes, who became community-admitted patients as they continued to use home health over many years. We found that the growth in community-admitted patients was greatest from 2002 to 2010 (69 percent), with much lower growth from 2010 to 2013 (2 percent).
Community-admitted and PAC patients had different average characteristics, but the trends in many of their characteristics were relatively similar over the study period. For instance, the number of aide visits per episode decreased at similar rates among community-admitted and PAC patients from 2002 to 2013. The share of patients served by for-profit agencies increased among both groups of patients, with slightly greater increases for the PAC patients during the study period. There was slightly higher growth among the community-admitted group for the proportion living in a congregate setting and the proportion of dual eligibles, but relatively similar trends in health status for the two groups.
Despite only small differences in trends for most characteristics, there were a few notable patterns of growth for the community-admitted patients. Specifically, there were substantial increases in the proportion of community-admitted patients entering home health from states with fraud and abuse issues, although these trends leveled off in later years of the analysis (2010-2013), suggesting that potentially fraudulent practices might have contributed to the growth in community-admitted patients. The community-admitted patients had greater increases in therapy visits per episode, and there were substantial increases in physical therapy use in later episodes of care among the community-admitted patients from 2002 to 2010, with much smaller growth among the PAC patients over the same time period. These trends imply that the use of the home health benefit has changed, with a greater focus on therapy among community-admitted patients.
Many of the patterns that we observed among the community-admitted patients reflected large growth up until 2010, with a leveling off or decrease after 2010. A number of changes in the home health benefit were implemented in 2010, including: (1) applying caps on outlier payments; (2) implementing the Outcome and Assessment Information Set-C (OASIS-C) and new quality measures; (3) requiring OASIS submission as a condition for payment; (4) removing payments for OASIS submissions for a significant change in condition; (5) implementing payment safeguards such as provisions related to agencies changing ownership status; and (6) statutory regulations for physician certification and recertification of the home health plan of care. These new provisions and safeguards that were implemented 2010 appear to have had a larger effect on the trends among community-admitted patients than among PAC patients. Multiple reasons are likely to have contributed to this effect, including that the new regulations made it more challenging to admit a patient from the community, the community-admitted patients may not have been as financially attractive to agencies, or there may have been more fraudulent use among the community-admitted patients prior to 2010. Similar to our findings, MedPAC has also reported that there have been declines in the number of episodes since 2011, with most of the decline concentrated in Florida, Illinois, Louisiana, Tennessee, and Texas. MedPAC concluded that a potential slowing in the demand for home health, declines in the supply of HHAs, and actions to address fraud and abuse have likely contributed to the declines (MedPAC 2016).
When we dug deeper into community-admitted versus PAC patients using a cross-sectional approach, we found that both groups had many similar average characteristics, there were a few differences in terms of the types of patients who are community-admitted, where they live, and which agencies they receive care from. Specifically, community-admitted patients were more likely to be dually eligible, more likely to live in a congregate setting, more likely to receive care from a for-profit HHA, and more likely to live in a state with fraud and abuse issues or poorer LTSS systems.
However, our findings also suggest that length of use is an important factor. We found that short-term users were very similar regardless of the source of admission. Specifically, both the short-term PAC and community-admitted patients were less clinically severe and functionally impaired and had fewer home health visits than the long-term patients. The PAC and community-admitted patients who needed more than one episode of care had poorer health status and relatively similar patterns of home health use. The two groups of short-term patients had relatively similar use of other acute and post-acute care. Both long-term PAC and community-admitted patients had higher use of other acute and post-acute care than the short-term patients within the first several months of the start of their home health spells. Even though long-term patients had greater use of other services, we also found that long-term PAC patients had much higher use of other acute and post-acute use than the long-term community-admitted patients, even after controlling for health and functional status. This suggests that there are larger differences between the long-term patients than between the short-term patients. The PAC and community-admitted long-term users became increasingly similar in terms of home health utilization as their home health spells progressed. These findings indicate that there are many important differences between patients based on the length of their home health use, not just based on their source of admission; and that the source of admission may be a more important differentiator among those that use home health for a longer period of time.
Since the long-term community-admitted patients had some different characteristics, the concern would be that community-admitted patients may be using the benefit for LTSS. Only a minority of the long-term community-admitted patients used home health aide services, which suggests that while some patients might receive services under the Medicare benefit in order to meet personal care needs, it does not appear to be a large issue. However, the evidence was mixed, since there were higher proportions of community-admitted patients entering care from states with fraud and abuse issues and states with relatively poorer LTSS systems, indicating that patients in certain states might be substituting services. It is also not clear whether some patients might be substituting skilled services for LTSS, although we note that Medicare rules do not allow for skilled providers to provide non-skilled care, so it is less likely that this is an issue.
B. Discussion
The purpose of this study was to explore the patterns of care of community-admitted home health patients. We found that the length of home health spells is a critical factor that is driving a substantial portion of the observed increase in "community" admissions. We also found that the use of the home health benefit is changing--the use of home health aide care has declined, and the use of physical therapy services has increased, even for longer periods of care.
Future research should focus on better understanding the phenomenon of the increase in long-term home health users, including the environmental and patient factors that could be leading to the increases in these patients and the patterns of other Medicare and LTSS utilization among these patients over time.
REFERENCES
Centers for Medicare & Medicaid Services (CMS). (2013) "Jimmo Settlement." Available at https://www.cms.gov/Center/Special-Topic/Jimmo-Center.html. Accessed September 28, 2017.
Centers for Medicare & Medicaid Services (CMS). (n.d.) "Reports and Evaluations." Available at https://www.medicaid.gov/medicaid/ltss/reports-and-evaluations/index.html. Accessed April 19, 2017.
Centers for Medicare & Medicaid Services (CMS). (2017) "CMS-1672-P." Federal Register, Proposed Rules, 82(144), July 2017.
Harris-Kojetin L, Sengupta M, Park-Lee E, et al. (2016) "Long-Term Care Providers and Services Users in the United States: Data from the National Study of Long-Term Care Providers, 2013-2014." Hyattsville, MD: National Center for Health Statistics, Vital and Health Statistics, 3(38), 2016.
Medicare Payment Advisory Commission (MedPAC). (2016) "Report to the Congress: Medicare Payment Policy." Washington, DC: MedPAC.
Medicare Payment Advisory Commission (MedPAC). (2017) "Report to the Congress: Medicare Payment Policy." Washington, DC: MedPAC.
Ng T, Harrington C, Musumeci M, & Ubri P. (2016) "Medicaid Home and Community-Based Services Programs: 2013 Data Update." Accessed at: http://kff.org/medicaid/report/medicaid-home-and-community-based-services-programs-2013-data-update/.
Pear R. (2010) "Medicare Standards Are Too Strict, 2 Courts Find." New York Times, A21, November 1, 2010.
Reinhard SC, Kassner E, Houser A, Ujvari K, Mollica R, & Hendrickson L. (2014) "Raising Expectations: A State Scorecard on Long-Term Services and Supports for Older Adults, People with Physical Disabilities, and Family Caregivers." Washington, DC: AARP, the Commonwealth Fund, and the SCAN Foundation.
APPENDIX A. RESEARCH QUESTIONS, DATA, AND METHODS
I. PROJECT OBJECTIVES AND KEY RESEARCH QUESTIONS
The purpose of this study was to develop a better understanding of the characteristics of community-admitted Medicare home health patients, how these patients use care, and what their patterns of care tell us about the underlying reasons for their increased numbers. We also focused on understanding how community-admitted patients might be interacting with the LTSS system. Specifically, we examined the following research questions:
-
How do community-admitted users of the home health benefit compare with PAC-admitted users?
-
What are the utilization patterns and Medicare costs over time across all settings of care of community-admitted users, and how do these differ from PAC-admitted users?
-
Is there correlation between utilization patterns and types of community-admitted users? Is there geographic variation by type of user?
-
What do the utilization patterns suggest about the causes of the growth in admissions of community-admitted users?
II. DATA SOURCES
A. DataLink File
The primary data source for the analyses was the CMS DataLink file. This file contains episode-level information for all Medicare home health patients from October 1, 2000, to June 2014 based on linked data from home health claims, inpatient hospital and SNF claims, the OASIS, Common Medicare Environment (CME), Area Resource File (ARF), Provider of Services (POS) file, Medicare Enrollment file, Low-Income Beneficiary file, and the Medicare risk model.
For these analyses, we used a 20 percent random sample of home health users from the DataLink file. Appendix A.III details our approach for defining the sample, characteristics, and outcomes to address the research questions.
B. Other Data Sources
To help us interpret findings and better understand the policy context of the patterns of use, we used other state-level information from publicly available data sources to supplement the DataLink file.
1. LTSS Indicators
To understand the results about the use of the Medicare home health benefit and the broader LTSS system, including the geographic distribution of the different types of home health users, we used data reflecting the quality of the state LTSS system. The AARP State Scorecard on Long-Term Services and Supports for Older Adults, People with Physical Disabilities, and Family Caregivers ranks state LTSS performance in five dimensions: (1) affordability and access; (2) choice of setting and provider; (3) quality of life and quality of care; (4) support for family caregivers; and (5) effective transitions. States are then ranked across the dimensions and organized into quartiles reflecting their summary rankings (Reinhard et al. 2014). We classified each state based on its 2014 Scorecard quartile ranking (top, second, third, or bottom) and merged this information to our sample of home health patients in the DataLink file by the beneficiary's state of residence.
We also used the historical Medicaid LTSS state expenditure data tables from 2002 to 2013 that include information about state Medicaid HCBS expenditures as a percentage of total state Medicaid LTSS expenditures (CMS n.d.). We categorized states into quartiles (top, second, third, or bottom) based on the percentage of expenditures for HCBS for each year. We merged this information to our sample of home health patients in the DataLink file by the beneficiary's state of residence and examined patterns among dually eligible beneficiaries.
2. Fraud and Abuse Indicators
CMS has documented aberrant patterns of utilization and potential fraud and abuse in the Medicare home health program and has implemented antifraud measures in states where this is a particular concern. Because the observed patterns of use among community-admitted patients might be related to these fraud and abuse issues, we examined whether there has been marked growth in community-admitted patients in states where there is known fraud and abuse. Specifically, there has been documented aberrant utilization in Florida, Illinois, Michigan, and Texas, and there are currently moratoria on HHAs in these states (MedPAC 2017).[11] We compared beneficiaries in these four states with fraud and abuse issues to beneficiaries in all other states to determine if growth in community-admitted patients might be related to fraud and abuse.
III. METHODS
A. Sample
1. Sample for Research Questions 1-3
To address Research Questions 1-3, the sample included all home health users during the period January 1, 2013, until December 31, 2013. Specifically, we used the episode from and through dates to determine all episodes that spanned 2013, even if the episode started prior to, or ended after, 2013. After identifying the relevant 2013 home health episodes, we identified the start of the home health spell for the 2013 episodes. We used the rule, consistent with the rule used in DataLink, that if there were fewer than 60 days between episodes, we called them consecutive episodes (and therefore part of the same spell); if more than 60 days, we called them distinct spells. Based on this identification, our sample included all home health spells where at least one episode occurred during the period from January 1, 2013, until December 31, 2013. The unit of analysis to address Research Questions 1-3 was a home health spell.
We made several exclusions for the Research Questions 1-3 sample. We limited the sample to beneficiaries age 65 or older at the start of the home health spell and to those who were not enrolled in managed care at any time during the spell. We dropped episodes with zero payments or zero covered services of any type, as well as episodes where a request for anticipated payment (RAP) claim was submitted but no final claim. We also dropped entire spells if the first episode in the spell had zero payments or zero covered services, or if a RAP claim was submitted but no final claim. Last, we dropped all spells that started prior to 2011 to limit the analyses to users who started care closer to the time period of interest.
After applying all sample limitations, we defined logical groups of home health users based on the source of admission, length of use, and type of use. We did so in three steps. First, we determined the source of admission based on whether the beneficiary had any covered days for part of an acute hospital, long-term hospital, rehabilitation hospital, or SNF stay in the 14 days before the home health spell started. If the beneficiary had any stay in the 14 days prior to the spell, the spell was defined as a PAC spell; otherwise, the spell was defined as a community-admitted spell.
Second, we counted the number of episodes in each home health spell and examined the distribution among all spells in the sample to determine a relevant cutoff for the length of use. We wanted to examine the length of use because it was not clear that the source of admission was the chief factor that would indicate whether the home health benefit is being used for acute or long-term care, and this was one of the policy questions of interest in this study. Specifically, many beneficiaries could enter home health from the community and use care for only a short period of time in ways that are similar to the beneficiaries entering care directly from an inpatient or post-acute setting. Without distinguishing between short-term and long-term users of home health, these differences would not be apparent. Among the sample, the median number of episodes in a spell was 1, so we used a cutoff of one episode or two or more episodes to stratify the PAC and community-admitted spells by length of use. We refer to the users with one episode as short-term users and users with two or more episodes as long-term users.
Finally, we counted the number of visits by type (skilled nursing, therapy, aide, and medical social services) in the first episode of each spell and examined the distribution among all spells in the sample to determine relevant cutoffs for the type of use. We were interested in further defining spells by the type of use to better understand if certain groups of beneficiaries might be using home health as a substitute for other LTSS or a complement to other acute services. We wanted to choose thresholds to categorize four distinct groups based on use: (1) high aide services and low skilled services; (2) high skilled services and low aide services; (3) high aide services and high skilled services; and (4) low aide services and low skilled services.
After examining the distributions, we used a cutoff of one aide and medical social service visits and 18 or fewer skilled nursing and therapy visits to define the any aide services and low skilled services group. We used a cutoff of no aide and medical social service visits and 13 or more skilled nursing and therapy visits to define the no aide services and high skilled services group. We used a cutoff of one aide and medical social service visits and 19 or more skilled nursing and therapy visits to define the any aide services and high skilled services group. We used a cutoff of no aide and medical social service visits and 12 or fewer skilled nursing and therapy visits to define the no aide services and low skilled services group. This classification resulted in 16 groups of home health users:
-
PAC user, one episode, any aide services and low skilled services.
-
PAC user, one episode, no aide services and high skilled services.
-
PAC user, one episode, any aide services and high skilled services.
-
PAC user, one episode, no aide services and low skilled services.
-
PAC user, two or more episodes, any aide services and low skilled services.
-
PAC user, two or more episodes, no aide services and high skilled services.
-
PAC user, two or more episodes, any aide services and high skilled services.
-
PAC user, two or more episodes, no aide services and low skilled service.
-
Community-admitted user, one episode, any aide services and low skilled services.
-
Community-admitted user, one episode, no aide services and high skilled services.
-
Community-admitted user, one episode, any aide services and high skilled services.
-
Community-admitted user, one episode, no aide services and low skilled services.
-
Community-admitted user, two or more episodes, any aide services and low skilled services.
-
Community-admitted user, two or more episodes, no aide services and high skilled services.
-
Community-admitted user, two or more episodes, any aide services and high skilled services.
-
Community-admitted user, two or more episodes, no aide services and low skilled service.
For comparison purposes, we also defined the spells by the source of admission and length of use but not by the breakdown of visit types. These four additional groups included: (1) PAC user one episode (consisting of spells in groups 1-4 from above); (2) PAC user two or more episodes (consisting of spells in groups 5-8 from above); (3) community-admitted user one episode (consisting of spells in groups 9-12 from above); and (4) community-admitted user two or more episodes (consisting of spell in groups 13-16 from above). Figure A.1 illustrates the steps for grouping home health patients for Research Questions 1-3 and Appendix Table B.1 includes samples sizes for each group.
| FIGURE A.1. Identifying Logical Groups of Home Health Users |
|---|
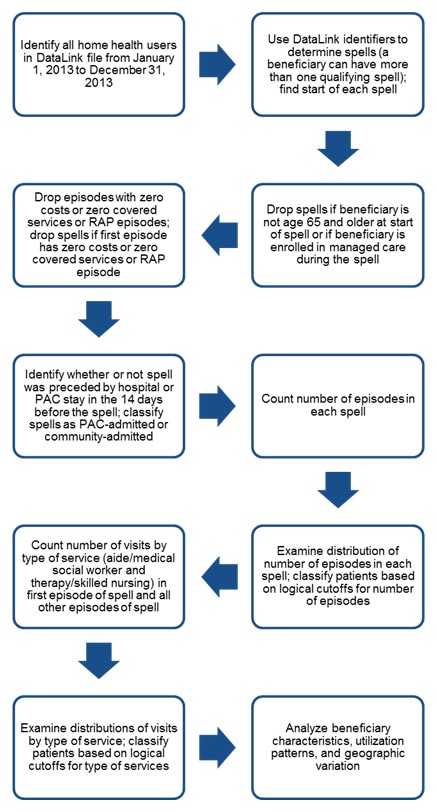 |
2. Sample for Research Question 4
Instead of focusing on home health spells as the unit of observation for Research Question 4, like we did for Research Questions 1-3, we wanted to focus on a beneficiary-year unit of observation to be able to examine growth in community-admitted patients over time. Using spells as the unit of analysis complicates the analysis of trends in the number of community admissions because we would have to attribute home health care spells to a particular year when many spells, in fact, span multiple calendar years. Measuring growth in the number of admissions using the same approach we used for Research Questions 1-3 would not adequately account for home health users with long spells, and we would not be able to accurately assess trends over time.
Therefore, to address Research Question 4 about the growth in community-admitted patients, we used data for all home health episodes that began on or after January 1, 2002, until December 31, 2013. After identifying the relevant episodes during the period, the next step was to apply a number of sample limitations. We limited the episodes during the analysis period to those where the beneficiary was age 65 or older at the start of the episode and not enrolled in managed care at any time during the episode. We dropped episodes with zero payments or zero covered services of any type, as well as episodes where a RAP claim was submitted but no final claim.
To define groups of post-acute and community-admitted patients, we identified the start year of each episode and classified each episode as a PAC admission or community admission. If the beneficiary had any covered days for part of an acute hospital, long-term hospital, rehabilitation hospital, or SNF stay in the 14 days before the home health episode started, the episode was classified as a PAC episode; otherwise, the episode was classified as a community-admitted episode. Next, we counted the number of episodes of each type (community-admitted and PAC) in each calendar year for a beneficiary and classified each beneficiary based on the type of the majority of their episodes in the calendar year. This approach was consistent with the approach that MedPAC used to examine the characteristics of community-admitted home health patients (MedPAC 2016). In the event of a tie (for example, a beneficiary with one PAC episode and one community-admitted episode in a calendar year), we classified the beneficiary based on the admission type of the first episode that started in the calendar year. This resulted in a beneficiary-year unit of observation. With this approach, a beneficiary could have a different classification type in different calendar years.
B. Approach
1. Comparison of Logical Groups of Home Health Users
To address Research Question 1, we compared the groups of home health users described above in Appendix A.III.A.1 across a number of sociodemographic and clinical characteristics defined at the beginning of the home health spell. This enabled us to determine if there were meaningful differences between patients defined by the source of admission, length of home health use, and type of home health use in terms of characteristics such as clinical severity, living arrangement, or agency ownership type.
The sociodemographic characteristics included age, sex, race and ethnicity, and dual eligibility status as defined from the Medicare enrollment file and CME.
We analyzed clinical severity indicated by the HCC score, as well as a number of diagnoses or conditions flagged in the HCC algorithm. These diagnoses or conditions included cancer, COPD, diabetes, disability, CHF, hip fracture, major depression or bipolar disorder, multiple sclerosis, schizophrenia, and stroke.
We classified a beneficiary's living arrangement as living alone, living in the home with another person, or living in a congregate setting based on the designation of the patient's living situation from the OASIS assessment at the beginning of the spell. We evaluated ADLs performance and cognitive functioning between the groups at the beginning of the spell. The ADL functioning score ranged from 0 to 35, based on performance from the OASIS assessment in grooming, ability to dress upper body, ability to dress lower body, bathing, toilet transferring, transferring, ambulation/locomotion, and feeding or eating. Cognitive functioning was measured as a five-category variable based on the OASIS assessment indicating alert/oriented, requires prompting, requires assistance, requires considerable assistance, or totally dependent.
We used the beneficiary's county of residence and variables from the ARF to determine residence in a rural area based on the rural/urban continuum codes, or a primary care health shortage area. The state LTSS ranking and whether there is a past history of Medicare home health fraud and abuse in the state of residence was examined based on the data sources described in Appendix A.II.B. We also compared the proportion of beneficiaries being served by non-profit, for-profit, or government HHAs based on the ownership type that was indicated for the HHA from the POS file. Detailed output is included in Appendix B.
2. Utilization Patterns and Costs of Home Health Users
To address Research Question 2, we examined the types of services used under the Medicare home health benefit, as well as the use of other acute and post-acute services, to better understand the extent to which beneficiaries are transitioning across various care settings.
For home health utilization and costs, we analyzed the first, second, and third episode of each spell separately. We analyzed the total number of visits, as well as the breakdown for home health aide; medical social service; therapy (physical, occupational, and speech); and skilled nursing visits for the first, second, and third episodes in the spell. We also examined the total costs of home health for the first three episodes in the spell.
For the analysis of other acute and post-acute utilization and costs, we examined a 120-day period after the start of the spell. Given the rules for defining home health spells, a beneficiary could have more than one spell that spans the sample analysis period (January 1, 2013, to December 31, 2013). The 120-day period after the start of each spell clearly defined the analysis period for examining other utilization and costs for home health users with more than one spell and for users with one versus many episodes in a spell so that there was no overlap in the utilization analysis periods across spells or episodes. For example, a beneficiary with two spells of home health use exactly 61 days apart (using the rules for defining spells) would not have any overlap in the counts of other acute and post-acute utilization between the two home health spells using the 120-day analysis period (Figure A.2).[12]
| FIGURE A.2. Analysis Period for Utilization and Costs |
|---|
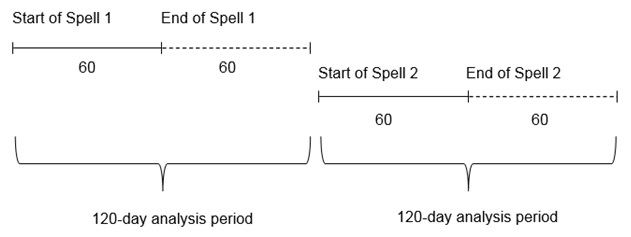 |
We examined the number and costs of acute, long-term care and rehabilitation hospitalizations, and SNF admissions within 120 days of the start of the home health spell. We also analyzed mortality within 120 days of the start of the spell. We include detailed results in Appendix C.
3. Correlation between Utilization Patterns and Types of Home Health Use
For Research Question 3, we used regression models to determine whether there was an association between being a particular type of home health user and a beneficiary's hospital and SNF use. We descriptively examined the patterns of use among the groups for Research Question 2, but the results from the regression models allowed us to control for potential confounders to better understand whether certain types of home health use are related to higher or lower use of other acute and post-acute services.
We used logistic regression models to compare the probability of experiencing a hospitalization or SNF admission or dying within 120 days after the start of a home health spell between the groups of community-admitted and PAC users, controlling for patients' characteristics. This is represented by Equation 1:
| (1) | 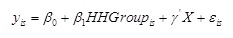 |
where yis is the dichotomous outcome for beneficiary iduring spell s indicating whether the beneficiary had a hospitalization, a SNF admission, or died within 120 days of the start of spell s. We examined each outcome using separate regression models. HHGroupis is the home health group for beneficiary i during spell s. We controlled for beneficiaries' characteristics, including age, sex, race and ethnicity, dual eligibility status, living arrangement, state of residence, HCC risk score, ADL functioning, and cognitive functioning, which are represented by vector X. We also examined the count of hospitalizations and of SNF admissions within 120 days after the start of a home health spell, controlling for beneficiaries' characteristics, using zero-inflated negative binomial models due to the large number of beneficiaries with no admissions. Appendix D includes detailed results from these models.
In addition to the regression analyses for acute and post-acute utilization, we examined geographic variation in the groups of community-admitted and PAC patients to gain insight into how regional and market factors drive patterns of home health use. To do so, we counted the number of spells for each of the 16 groups separately at the county-level, and again at the state-level. Next, we standardized the counts based on 20 percent of the population of adults age 65 and older within the county, or state. We adjusted by 20 percent to account for the 20 percent sample of home health users. Last, we ranked the top counties, and states, for each home health group and examined the patterns across groups. We also produced the same output for the four additional groups of home health users defined by source of admission and length of use, as well as for groups defined solely by the source of admission (PAC or community-admitted). We used the categorization of state LTSS systems and states with fraud and abuse issues to help interpret the findings.
4. Growth in Community-Admitted Home Health Users
To address Research Question 4, we compared characteristics of PAC and community-admitted home health users in each calendar year and examined trends over time. The sociodemographic characteristics included age, sex, race and ethnicity, and dual eligibility status as defined from the Medicare enrollment file and CME.
We analyzed clinical severity indicated by the HCC score and indicators for cancer, COPD, diabetes, disability, CHF, hip fracture, major depression or bipolar disorder, multiple sclerosis, schizophrenia, and stroke.
We used information from the first OASIS start of care or resumption of care assessment within the calendar year (or looked back to the most recent one in the previous calendar year). We classified a beneficiary's living arrangement as living alone, living in the home with another person, or living in a congregate setting based on the designation of the patient's living situation.[13] We evaluated ADL performance and cognitive functioning between the groups at the beginning of the spell. The ADL functioning score was based on performance from the OASIS assessment in grooming, ability to dress upper body, ability to dress lower body, bathing, toilet transferring, transferring, ambulation/locomotion, and feeding or eating.[14] Cognitive functioning was measured as a five-category variable based on the OASIS assessment indicating alert/oriented, requires prompting, requires assistance, requires considerable assistance, or totally dependent.
We used the beneficiary's county of residence and variables from the ARF to determine residence in a rural area based on the rural/urban continuum codes, or a primary care health shortage area. The state LTSS ranking and whether there is known Medicare fraud and abuse in the state of residence was examined based on the data sources described in Appendix A.II.B. We counted the number of HHAs per 100,000 population ages 65 and older in the county and used the 75th percentile cutoff to flag areas with a high number of HHAs located in the area. We then created an indicator for beneficiaries residing in the counties with a high number of HHAs.
We counted the number of visit types (aide, medical social service, therapy, and skilled nursing) for all episodes within a calendar year to determine whether certain visit types were increasing over time. We flagged beneficiaries who were using physical therapy in episode three or later to examine whether maintenance therapy increased after the court decision in 2010. We also compared the proportion of beneficiaries being served by non-profit, for-profit, or government HHAs based on the ownership type that was indicated for the HHA from the POS file.
In addition to examining patterns among all PAC and community-admitted users over the period 2002-2013, we also separately analyzed patterns among dually eligible beneficiaries. Specifically, we focused on the ranking for the state Medicaid LTSS system to determine if there were distinct patterns of use over time among dually eligible beneficiaries who lived in states with lower Medicaid LTSS. We also examined the visit types for dually eligible beneficiaries over time. Detailed results are included in Appendix E
APPENDIX B. COMPARISON OF LOGICAL GROUPS OF HOME HEALTH USERS
| TABLE B.1. Characteristics of PAC and Community-Admitted (CA) Home Health Spells | ||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| PAC user, 1 episode | PAC user, 2 or more episodes | CA user, 1 episode | CA user, 2 or more episodes | |||||||||||||||||
| 1 | 2 | 3 | 4 | 5 | 1 | 2 | 3 | 4 | 5 | 1 | 2 | 3 | 4 | 5 | 1 | 2 | 3 | 4 | 5 | |
| Number of spells | 36,196 | 91,303 | 21,966 | 127,741 | 277,206 | 14,828 | 55,891 | 27,519 | 28,346 | 126,584 | 24,119 | 54,254 | 10,508 | 77,636 | 166,517 | 17,232 | 65,923 | 20,222 | 44,544 | 147,921 |
| Number of beneficiaries | 35,656 | 89,437 | 21,692 | 125,170 | 265,925 | 14,734 | 55,134 | 27,208 | 28,137 | 123,420 | 23,700 | 50,432 | 10,370 | 75,365 | 155,329 | 16,962 | 63,040 | 19,883 | 42,665 | 138,460 |
| Sociodemographic characteristics | ||||||||||||||||||||
| Age (years) | 80.1 | 78.8 | 80.7 | 77.6 | 78.6 | 79.9 | 79.8 | 80.2 | 78.7 | 79.7 | 81.5 | 81.2 | 81.9 | 80.8 | 81.1 | 80.8 | 80.9 | 80.9 | 80.0 | 80.6 |
| Sex | ||||||||||||||||||||
| Female (%) | 66.7 | 61.5 | 67.1 | 57.3 | 60.7 | 66.3 | 61.2 | 65.1 | 59.8 | 62.3 | 68.2 | 66.8 | 68.6 | 64.8 | 66.2 | 69.3 | 66.2 | 68.2 | 65.4 | 66.6 |
| Male (%) | 33.3 | 38.5 | 32.9 | 42.7 | 39.3 | 33.7 | 38.8 | 34.9 | 40.2 | 37.7 | 31.9 | 33.2 | 31.4 | 35.2 | 33.8 | 30.7 | 33.82 | 31.8 | 34.6 | 33.4 |
| Race/ethnicity | ||||||||||||||||||||
| Asian (%) | 1.8 | 1.3 | 1.4 | 1.4 | 1.4 | 1.7 | 1.2 | 1.1 | 1.5 | 1.3 | 2.7 | 2.3 | 1.9 | 3.1 | 2.7 | 2.2 | 2.2 | 1.5 | 3.0 | 2.3 |
| Black (%) | 10.2 | 7.6 | 10.0 | 7.1 | 7.9 | 13.5 | 9.6 | 11.7 | 11.1 | 10.9 | 11.4 | 9.4 | 11.7 | 9.8 | 10.0 | 18.2 | 13.5 | 14.3 | 19.9 | 16.1 |
| Hispanic (%) | 2.0 | 1.5 | 1.4 | 1.3 | 1.4 | 2.4 | 2.0 | 1.9 | 2.1 | 2.1 | 3.3 | 9.1 | 2.2 | 3.4 | 5.1 | 3.6 | 6.4 | 3.2 | 5.2 | 5.3 |
| North American Native (%) | 0.3 | 0.3 | 0. | 0.3 | 0.3 | 0.4 | 0.3 | 0.5 | 0.4 | 0.4 | 0.3 | 0.3 | 0.4 | 0.3 | 0.3 | 0.5 | 0.3 | 0.4 | 0.5 | 0.4 |
| Other (%) | 1.1 | 0.9 | 1.0 | 1.1 | 1.0 | 0.9 | 0.8 | 0.9 | 1.0 | 0.9 | 1.1 | 1.2 | 1.0 | 1.3 | 1.2 | 1.0 | 1.1 | 1.0 | 1.2 | 1.1 |
| Unknown (%) | 0.3 | 0.3 | 0.2 | 0.4 | 0.3 | 0.2 | 0.2 | 0.2 | 0.2 | 0.2 | 0.4 | 0.5 | 0.3 | 0.4 | 0.4 | 0.3 | 0.5 | 0.3 | 0.3 | 0.4 |
| White (%) | 84.3 | 88.2 | 85.7 | 88.5 | 87.6 | 80.9 | 85.8 | 83.8 | 83.7 | 84.3 | 80.8 | 77.2 | 82.6 | 81.8 | 80.2 | 74.4 | 76.0 | 79.2 | 69.9 | 74.4 |
| Dual eligibility status | ||||||||||||||||||||
| Dually eligible (%) | 20.6 | 13.4 | 16.9 | 13.6 | 14.7 | 26.5 | 20.6 | 21.2 | 22.7 | 21.9 | 27.1 | 32.2 | 23.2 | 25.0 | 27.5 | 32.8 | 36.0 | 28.4 | 39.2 | 35.5 |
| Non-dually eligible (%) | 79.5 | 86.6 | 83.1 | 86.5 | 85.3 | 73.5 | 79.4 | 78.8 | 77.3 | 78.1 | 72.9 | 67.8 | 76.8 | 75.0 | 72.5 | 67.2 | 64.0 | 71.6 | 60.8 | 64.5 |
| Living arrangement | ||||||||||||||||||||
| Living alone (%) | 32.9 | 20.9 | 29.1 | 23.0 | 24.1 | 31.4 | 21.2 | 26.8 | 24.7 | 24.4 | 35.1 | 24.0 | 32.9 | 25.9 | 27.0 | 33.2 | 24.4 | 30.9 | 27.4 | 27.2 |
| Lives with another person in home (%) | 62.3 | 68.9 | 65.1 | 69.7 | 68.1 | 63.2 | 64.6 | 67.1 | 66.0 | 65.3 | 57.7 | 51.6 | 58.8 | 54.0 | 54.1 | 55.6 | 51.0 | 59.2 | 52.4 | 53.2 |
| Lives in congregate situation (%) | 2.5 | 8.2 | 3.6 | 5.0 | 5.6 | 2.9 | 12.0 | 4.0 | 6.9 | 8.1 | 3.7 | 20.7 | 5.5 | 16.6 | 15.4 | 4.5 | 20.4 | 6.3 | 13.9 | 14.7 |
| Unknown (%) | 2.4 | 2.2 | 2.1 | 2.4 | 2.3 | 2.5 | 2.2 | 2.1 | 2.3 | 2.3 | 3.5 | 3.7 | 2.9 | 3.6 | 3.6 | 6.7 | 4.2 | 3.6 | 6.3 | 5.0 |
| Lives in rural area (%) | 16.0 | 14.2 | 13.9 | 14.8 | 14.7 | 17.3 | 17.3 | 17.2 | 16.3 | 17.1 | 15.5 | 11.3 | 14.5 | 13.5 | 13.1 | 18.7 | 14.0 | 17.0 | 15.2 | 15.3 |
| County of residence is primary care health shortage area | ||||||||||||||||||||
| Some of county (%) | 58.2 | 57.6 | 60.9 | 57.0 | 57.7 | 57.2 | 56.4 | 56.6 | 56.1 | 56.5 | 58.2 | 62.8 | 60.8 | 56.6 | 59.1 | 52.6 | 54.5 | 55.7 | 48.4 | 52.6 |
| All of county (%) | 31.0 | 32.2 | 29.5 | 32.8 | 32.1 | 32.9 | 33.6 | 33.3 | 34.7 | 33.7 | 32.9 | 29.6 | 30.0 | 35.3 | 32.8 | 38.8 | 37.9 | 34.9 | 44.9 | 39.7 |
| None of county (%) | 10.7 | 10.2 | 9.5 | 10.2 | 10.2 | 9.8 | 10.0 | 10.1 | 9.2 | 9.8 | 8.8 | 7.6 | 9.2 | 8.1 | 8.1 | 8.5 | 7.6 | 9.4 | 6.6 | 7.7 |
| Unknown (%) | 0.1 | 0.0 | 0.0 | 0.1 | 0.0 | 0.1 | 0.1 | 0.0 | 0.1 | 0.1 | 0.1 | 0.0 | 0.0 | 0.1 | 0.1 | 0.1 | 0.1 | 0.1 | 0.1 | 0.1 |
| State LTSS ranking | ||||||||||||||||||||
| Top quartile (%) | 20.6 | 14.5 | 15.7 | 19.1 | 17.5 | 17.5 | 12.5 | 12.7 | 15.5 | 13.8 | 23.2 | 15.4 | 17.3 | 21.2 | 19.4 | 15.3 | 13.8 | 12.7 | 13.8 | 13.8 |
| 2nd quartile (%) | 30.0 | 25.5 | 27.1 | 27.1 | 27.0 | 25.9 | 21.3 | 20.6 | 24.0 | 22.3 | 23.7 | 18.1 | 21.7 | 21.9 | 20.9 | 19.2 | 17.6 | 17.5 | 23.4 | 19.5 |
| 3rd quartile (%) | 25.9 | 26.8 | 26.2 | 26.7 | 26.6 | 28.1 | 29.4 | 29.6 | 29.0 | 29.2 | 25.5 | 23.1 | 26.1 | 25.9 | 24.9 | 32.7 | 30.7 | 31.2 | 33.5 | 31.8 |
| Bottom quartile (%) | 23.3 | 33.0 | 30.8 | 26.8 | 28.7 | 28.3 | 36.6 | 37.0 | 31.4 | 34.6 | 27.3 | 43.1 | 34.8 | 30.6 | 34.4 | 32.6 | 37.7 | 38.5 | 29.1 | 34.6 |
| Unknown (%) | 0.2 | 0.2 | 0.2 | 0.2 | 0.2 | 0.2 | 0.2 | 0.2 | 0.1 | 0.2 | 0.2 | 0.4 | 0.2 | 0.4 | 0.4 | 0.2 | 0.2 | 0.1 | 0.3 | 0.2 |
| Lives in state with Medicare home health fraud and abuse (%) | 16.1 | 26.8 | 21.4 | 20.3 | 22.0 | 21.5 | 30.9 | 28.2 | 26.4 | 28.2 | 19.5 | 40.1 | 23.3 | 28.1 | 30.5 | 32.5 | 44.9 | 33.3 | 45.2 | 41.9 |
| Diagnoses or conditions | ||||||||||||||||||||
| Cancer (%) | 17.2 | 16.0 | 15.9 | 16.9 | 16.6 | 16.8 | 16.7 | 15.8 | 18.2 | 16.8 | 15.1 | 13.1 | 13.6 | 14.8 | 14.2 | 13.8 | 12.9 | 13.6 | 13.6 | 13.3 |
| COPD (%) | 24.9 | 21.1 | 23.8 | 21.2 | 21.9 | 31.0 | 28.1 | 27.8 | 29.6 | 28.7 | 20.6 | 20.7 | 20.0 | 19.4 | 20.1 | 24.5 | 23.7 | 23.9 | 24.4 | 24.0 |
| Diabetes (%) | 33.8 | 32.7 | 36.3 | 30.9 | 32.3 | 40.6 | 39.8 | 40.9 | 38.7 | 39.9 | 33.0 | 33.9 | 35.0 | 32.2 | 33.0 | 38.8 | 39.7 | 40.3 | 40.2 | 39.8 |
| Disabled (%) | 1.2 | 1.5 | 1.0 | 1.9 | 1.6 | 1.5 | 1.2 | 1.1 | 1.6 | 1.3 | 1.0 | 1.1 | 1.0 | 1.3 | 1.2 | 1.2 | 1.3 | 1.3 | 1.5 | 1.4 |
| Heart failure (%) | 26.4 | 23.4 | 27.3 | 21.4 | 23.2 | 34.2 | 33.1 | 33.4 | 32.7 | 33.2 | 22.4 | 22.8 | 24.0 | 22.0 | 22.5 | 27.7 | 28.2 | 29.3 | 28.0 | 28.2 |
| Hip fracture (%) | 3.3 | 3.3 | 4.2 | 2.2 | 2.9 | 3.5 | 3.9 | 4.5 | 3.1 | 3.8 | 2.8 | 3.4 | 3.6 | 2.8 | 3.1 | 3.1 | 3.7 | 4.0 | 2.7 | 3.4 |
| Major depression or bipolar disorder (%) | 6.2 | 4.9 | 6.1 | 4.4 | 5.0 | 7.7 | 6.2 | 6.4 | 6.3 | 6.5 | 6.8 | 8.7 | 7.2 | 6.5 | 7.3 | 7.2 | 8.4 | 7.6 | 6.8 | 7.7 |
| Multiple sclerosis (%) | 0.4 | 0.3 | 0.5 | 0.3 | 0.3 | 0.6 | 0.5 | 0.6 | 0.4 | 0.5 | 0.5 | 0.5 | 0.7 | 0.5 | 0.5 | 0.6 | 0.6 | 0.8 | 0.6 | 0.6 |
| Schizophrenia (%) | 0.7 | 0.4 | 0.6 | 0.5 | 0.5 | 0.9 | 0.7 | 0.7 | 0.8 | 0.8 | 0.9 | 1.4 | 0.9 | 1.0 | 1.1 | 1.1 | 1.4 | 1.0 | 1.5 | 1.3 |
| Stroke (%) | 6.6 | 6.1 | 8.6 | 4.9 | 5.8 | 8.4 | 8.2 | 9.5 | 7.2 | 8.3 | 7.2 | 8.0 | 9.2 | 6.5 | 7.2 | 8.1 | 8.8 | 9.6 | 7.3 | 8.4 |
| Clinical severity | ||||||||||||||||||||
| HCC risk score | 1.87 | 1.67 | 1.91 | 1.59 | 1.68 | 2.22 | 2.15 | 2.20 | 2.13 | 2.17 | 1.78 | 1.78 | 1.84 | 1.72 | 1.76 | 1.98 | 2.02 | 2.08 | 1.94 | 2.00 |
| ADL functioning | ||||||||||||||||||||
| Score 0-35a | 13.6 | 12.9 | 15.0 | 11.3 | 12.4 | 14.1 | 13.9 | 15.9 | 12.1 | 13.9 | 13.9 | 13.0 | 15.0 | 11.9 | 12.7 | 13.8 | 13.3 | 15.3 | 11.9 | 13.2 |
| Cognitive functioning | ||||||||||||||||||||
| Alert/oriented (%) | 48.9 | 59.2 | 45.5 | 65.3 | 59.6 | 44.3 | 48.7 | 42.4 | 54.8 | 48.2 | 37.8 | 44.1 | 38.1 | 48.5 | 44.9 | 34.8 | 38.7 | 36.6 | 39.1 | 38.1 |
| Requires prompting (%) | 32.5 | 28.4 | 35.8 | 23.9 | 27.5 | 36.0 | 35.4 | 37.7 | 31.4 | 35.1 | 34.1 | 35.6 | 37.1 | 30.5 | 33.1 | 36.5 | 39.5 | 38.6 | 38.0 | 38.6 |
| Requires assistance (%) | 11.6 | 8.0 | 12.4 | 6.1 | 7.9 | 12.3 | 10.4 | 13.3 | 8.4 | 10.8 | 16.1 | 11.9 | 15.8 | 11.4 | 12.5 | 14.8 | 13.0 | 15.7 | 11.7 | 13.2 |
| Requires considerable assistance (%) | 3.8 | 2.0 | 3.6 | 1.9 | 2.3 | 3.9 | 2.8 | 3.9 | 2.4 | 3.1 | 6.8 | 4.0 | 5.3 | 4.8 | 4.8 | 5.6 | 3.8 | 4.7 | 3.8 | 4.2 |
| Totally dependent (%) | 0.8 | 0.3 | 0.6 | 0.4 | 0.5 | 1.0 | 0.6 | 0.6 | 0.7 | 0.7 | 1.7 | 0.7 | 0.8 | 1.3 | 1.1 | 1.6 | 0.9 | 0.8 | 1.1 | 1.0 |
| Unknown (%) | 2.4 | 2.2 | 2.1 | 2.4 | 2.3 | 2.5 | 2.2 | 2.1 | 2.3 | 2.3 | 3.5 | 3.7 | 2.9 | 3.6 | 3.6 | 6.7 | 4.2 | 3.6 | 6.3 | 5.0 |
| Agency characteristics | ||||||||||||||||||||
| Ownership | ||||||||||||||||||||
| For-profit (%) | 41.5 | 58.8 | 54.6 | 44.0 | 49.4 | 52.6 | 69.6 | 67.9 | 54.8 | 63.9 | 52.1 | 75.9 | 62.3 | 62.0 | 65.1 | 70.1 | 84.0 | 76.9 | 78.4 | 79.7 |
| Government (%) | 4.7 | 3.3 | 3.4 | 4.1 | 3.9 | 4.1 | 2.6 | 2.9 | 3.5 | 3.0 | 3.9 | 2.1 | 3.1 | 3.2 | 3.0 | 3.7 | 1.6 | 2.5 | 2.3 | 2.2 |
| Non-profit (%) | 53.8 | 37.9 | 42.0 | 51.9 | 46.7 | 43.4 | 27.8 | 29.1 | 41.7 | 33.0 | 44.0 | 21.9 | 34.6 | 34.8 | 31.9 | 26.2 | 14.4 | 20.7 | 19.3 | 18.1 |
| SOURCE: Mathematica analysis of 20% sample of CMS DataLink File with home health use during January 1, 2013, to December 31, 2013, and spells starting no earlier than January 1, 2011, and no later than December 31, 2013. NOTE: Percentages might not add up to 100 due to rounding. 1 = Any aide or medical social services and low therapy or skilled nursing services. 2 = No aide or medical social services and high therapy or skilled nursing services. 3 = Any aide or medical social services and high therapy or skilled nursing services. 4 = No aide or medical social services and low therapy or skilled nursing services. 5 = All beneficiaries in groups 1-4.
|
||||||||||||||||||||
APPENDIX C. UTILIZATION PATTERNS AND COSTS OF HOME HEALTH USERS
| TABLE C.1. Utilization Patterns and Costs for Home Health Spells | ||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| PAC user, one episode | PAC user, two or more episodes | Community-admitted user, one episode | Community-admitted user,two or more episodes | |||||||||||||||||
| 1 | 2 | 3 | 4 | 5 | 1 | 2 | 3 | 4 | 5 | 1 | 2 | 3 | 4 | 5 | 1 | 2 | 3 | 4 | 5 | |
| Number of home health visits in Episode 1 | ||||||||||||||||||||
| Total | 15.6 | 19.6 | 33.9 | 7.2 | 14.5 | 18.1 | 25.0 | 40.7 | 7.5 | 23.7 | 15.4 | 19.3 | 33.6 | 7.0 | 13.9 | 19.8 | 23.2 | 39.0 | 8.1 | 20.4 |
| Home health aide | 3.8 | 0.0 | 6.9 | 0.0 | 1.0 | 5.4 | 0.0 | 8.9 | 0.0 | 2.6 | 4.2 | 0.0 | 7.1 | 0.0 | 1.1 | 7.6 | 0.0 | 9.3 | 0.0 | 2.2 |
| Medical social services | 0.6 | 0.0 | 0.6 | 0.0 | 0.1 | 0.6 | 0.0 | 0.7 | 0.0 | 0.2 | 0.8 | 0.0 | 0.8 | 0.0 | 0.2 | 0.7 | 0.0 | 0.8 | 0.0 | 0.2 |
| Therapy | 5.4 | 11.6 | 16.2 | 3.3 | 7.3 | 4.5 | 12.4 | 17.2 | 2.2 | 10.2 | 5.0 | 12.3 | 15.9 | 3.2 | 7.2 | 3.7 | 11.5 | 15.8 | 1.6 | 8.2 |
| Skilled Nursing | 5.8 | 8.0 | 10.2 | 3.9 | 6.0 | 7.5 | 12.6 | 13.9 | 5.3 | 10.6 | 5.5 | 7.0 | 9.8 | 3.8 | 5.5 | 7.9 | 11.7 | 13.1 | 6.6 | 9.9 |
| Number of home health visits in Episode 2 | ||||||||||||||||||||
| Total | n.a. | n.a. | n.a. | n.a. | n.a. | 18.6 | 14.9 | 22.5 | 13.7 | 16.7 | n.a. | n.a. | n.a. | n.a. | n.a. | 19.7 | 16.0 | 24.1 | 12.2 | 16.4 |
| Home health aide | n.a. | n.a. | n.a. | n.a. | n.a. | 4.9 | 0.3 | 6.0 | 0.7 | 2.2 | n.a. | n.a. | n.a. | n.a. | n.a. | 7.2 | 0.3 | 7.2 | 0.5 | 2.1 |
| Medical social services | n.a. | n.a. | n.a. | n.a. | n.a. | 0.3 | 0.1 | 0.2 | 0.1 | 0.1 | n.a. | n.a. | n.a. | n.a. | n.a. | 0.2 | 0.1 | 0.2 | 0.1 | 0.1 |
| Therapy | n.a. | n.a. | n.a. | n.a. | n.a. | 5.7 | 6.0 | 7.4 | 5.4 | 6.1 | n.a. | n.a. | n.a. | n.a. | n.a. | 4.7 | 6.5 | 7.4 | 4.0 | 5.7 |
| Skilled Nursing | n.a. | n.a. | n.a. | n.a. | n.a. | 7.7 | 8.6 | 8.9 | 7.5 | 8.3 | n.a. | n.a. | n.a. | n.a. | n.a. | 7.6 | 9.2 | 9.2 | 7.6 | 8.5 |
| Number of home health visits in Episode 3 | ||||||||||||||||||||
| Total | n.a. | n.a. | n.a. | n.a. | n.a. | 18.6 | 15.5 | 22.7 | 13.1 | 17.2 | n.a. | n.a. | n.a. | n.a. | n.a. | 19.9 | 16.7 | 24.2 | 11.8 | 16.7 |
| Home health aide | n.a. | n.a. | n.a. | n.a. | n.a. | 5.8 | 0.6 | 6.6 | 1.0 | 2.7 | n.a. | n.a. | n.a. | n.a. | n.a. | 8.1 | 0.6 | 7.6 | 0.7 | 2.5 |
| Medical social services | n.a. | n.a. | n.a. | n.a. | n.a. | 0.2 | 0.1 | 0.2 | 0.1 | 0.1 | n.a. | n.a. | n.a. | n.a. | n.a. | 0.2 | 0.1 | 0.2 | 0.1 | 0.1 |
| Therapy | n.a. | n.a. | n.a. | n.a. | n.a. | 4.5 | 5.1 | 6.3 | 4.0 | 5.1 | n.a. | n.a. | n.a. | n.a. | n.a. | 3.6 | 5.8 | 6.3 | 3.0 | 4.8 |
| Skilled Nursing | n.a. | n.a. | n.a. | n.a. | n.a. | 8.2 | 9.7 | 9.7 | 8.1 | 9.2 | n.a. | n.a. | n.a. | n.a. | n.a. | 8.1 | 10.2 | 10.1 | 8.0 | 9.3 |
| Total home health costs | ||||||||||||||||||||
| Episode 1 ($) | 2,720 | 3,597 | 4,483 | 2,024 | 2,828 | 2,371 | 3,749 | 4,585 | 1,644 | 3,298 | 2,631 | 3,781 | 4,365 | 2,016 | 2,828 | 2,379 | 3,722 | 4,373 | 1,914 | 3,110 |
| Episode 2 ($) | n.a. | n.a. | n.a. | n.a. | n.a. | 2,731 | 2,695 | 3,005 | 2,539 | 2,732 | n.a. | n.a. | n.a. | n.a. | n.a. | 2,604 | 2,909 | 3,028 | 2,429 | 2,745 |
| Episode 3 ($) | n.a. | n.a. | n.a. | n.a. | n.a. | 2,442 | 2,525 | 2,781 | 2,243 | 2,525 | n.a. | n.a. | n.a. | n.a. | n.a. | 2,301 | 2,729 | 2,804 | 2,119 | 2,507 |
| Number of acute hospital admissionsa | 0.4 | 0.3 | 0.4 | 0.3 | 0.3 | 1.1 | 0.8 | 0.7 | 1.2 | 0.9 | 0.3 | 0.2 | 0.3 | 0.3 | 0.2 | 0.5 | 0.4 | 0.4 | 0.5 | 0.4 |
| Proportion with an acute hospital admissiona (%) | 28.6 | 20.1 | 25.3 | 22.6 | 22.8 | 62.8 | 48.7 | 45.2 | 67.7 | 53.8 | 23.2 | 15.0 | 20.2 | 18.6 | 18.2 | 34.4 | 25.8 | 29.7 | 30.9 | 28.8 |
| Acute hospital costsa ($) | 17,162 | 14,105 | 14,406 | 16,661 | 15,803 | 18,127 | 15,496 | 14,360 | 19,279 | 16,712 | 13,922 | 12,319 | 12,458 | 13,737 | 13,300 | 12,888 | 11,515 | 11,515 | 13,497 | 12,345 |
| Number of LTAC admissionsa | 0.01 | 0.00 | 0.01 | 0.01 | 0.01 | 0.02 | 0.01 | 0.01 | 0.02 | 0.01 | 0.01 | 0.00 | 0.00 | 0.00 | 0.00 | 0.01 | 0.00 | 0.00 | 0.01 | 0.01 |
| Proportion with an LTAC admissiona (%) | 0.7 | 0.3 | 0.5 | 0.5 | 0.5 | 1.5 | 0.9 | 0.9 | 1.8 | 1.2 | 0.5 | 0.3 | 0.3 | 0.5 | 0.4 | 0.6 | 0.4 | 0.5 | 0.6 | 0.5 |
| LTAC costsa ($) | 34,384 | 36,727 | 34,714 | 35,858 | 35,646 | 34,543 | 32,033 | 34,439 | 34,921 | 33,846 | 34,174 | 32,675 | 34,727 | 36,112 | 34,910 | 31,100 | 33,263 | 34,794 | 32,768 | 32,959 |
| Number of rehab hospital admissionsa | 0.01 | 0.01 | 0.01 | 0.01 | 0.01 | 0.05 | 0.04 | 0.04 | 0.06 | 0.04 | 0.01 | 0.01 | 0.01 | 0.01 | 0.01 | 0.03 | 0.02 | 0.03 | 0.03 | 0.03 |
| Proportion with a rehab hospital admissiona (%) | 1.2 | 0.8 | 1.4 | 0.8 | 0.9 | 4.6 | 3.4 | 3.8 | 5.0 | 4.0 | 1.1 | 0.7 | 1.2 | 0.8 | 0.8 | 3.2 | 1.9 | 2.9 | 2.5 | 2.4 |
| Rehab hospital costsa ($) | 18,414 | 18,339 | 19,447 | 18,203 | 18,433 | 20,386 | 19,674 | 20,097 | 19,980 | 19,944 | 18,545 | 18,497 | 18,277 | 18,643 | 18,550 | 19,546 | 19,292 | 19,567 | 19,622 | 19,483 |
| Number of SNF admissionsa | 0.17 | 0.07 | 0.11 | 0.10 | 0.10 | 0.42 | 0.16 | 0.16 | 0.38 | 0.24 | 0.16 | 0.07 | 0.13 | 0.10 | 0.10 | 0.21 | 0.09 | 0.12 | 0.16 | 0.13 |
| Proportion with a SNF admissiona (%) | 12.2 | 5.2 | 9.1 | 7.0 | 7.3 | 31.8 | 13.4 | 13.8 | 28.1 | 19.0 | 11.7 | 5.4 | 9.7 | 7.5 | 7.6 | 16.7 | 7.5 | 9.9 | 12.5 | 10.4 |
| SNF costsa ($) | 14,063 | 13,412 | 14,364 | 13,410 | 13,648 | 13,738 | 11,371 | 12,245 | 13,763 | 12,769 | 17,269 | 17,118 | 18,080 | 16,552 | 16,967 | 15,594 | 13,410 | 13,879 | 15,277 | 14,554 |
| Mortalitya | 16.0 | 5.6 | 8.9 | 10.0 | 9.2 | 4.8 | 3.3 | 3.4 | 4.7 | 3.8 | 14.7 | 5.3 | 8.5 | 10.4 | 9.2 | 2.7 | 1.9 | 2.6 | 2.3 | 2.2 |
| SOURCE: Mathematica analysis of 20% sample of CMS DataLink File with home health use during January 1, 2013, to December 31, 2013, and spells starting no earlier than January 1, 2011, and no later than December 31, 2013. 1 = Any aide or medical social services and low therapy or skilled nursing services. 2 = No aide or medical social services and high therapy or skilled nursing services. 3 = Any aide or medical social services and high therapy or skilled nursing services. 4 = No aide or medical social services and low therapy or skilled nursing services. 5 = All beneficiaries in groups 1-4.
|
||||||||||||||||||||
APPENDIX D. CORRELATION BETWEEN UTILIZATION PATTERNS AND TYPES OF HOME HEALTH USE
| TABLE D.1. Correlation between Type of Home Health User and Hospitalizations,SNF Admissions, and Mortality | ||||||
|---|---|---|---|---|---|---|
| Hospitalization | SNF Admission | Mortality | ||||
| OR | 95% CI | OR | 95% CI | OR | 95% CI | |
| Home health group | ||||||
| PAC one episode, type 1 (ref) | ||||||
| PAC one episode, type 2 | 0.656 | 0.637-0.675 | 0.428 | 0.409-0.447 | 0.314 | 0.301-0.328 |
| PAC one episode, type 3 | 0.826 | 0.794-0.859 | 0.670 | 0.633-0.710 | 0.425 | 0.401-0.450 |
| PAC one episode, type 4 | 0.782 | 0.761-0.804 | 0.629 | 0.604-0.654 | 0.724 | 0.698-0.751 |
| PAC two or more episodes, type 1 | 4.306 | 4.129-4.491 | 3.498 | 3.332-3.672 | 0.220 | 0.202-0.240 |
| PAC two or more episodes, type 2 | 2.411 | 2.340-2.484 | 1.149 | 1.102-1.197 | 0.141 | 0.133-0.149 |
| PAC two or more episodes, type 3 | 2.055 | 1.985-2.127 | 1.132 | 1.079-1.188 | 0.127 | 0.118-0.137 |
| PAC two or more episodes, type 4 | 5.555 | 5.362-5.754 | 3.151 | 3.020-3.288 | 0.250 | 0.234-0.266 |
| CA one episode, type 1 | 0.809 | 0.778-0.841 | 0.968 | 0.919-1.019 | 0.877 | 0.835-0.921 |
| CA one episode, type 2 | 0.495 | 0.478-0.512 | 0.433 | 0.411-0.455 | 0.292 | 0.278-0.307 |
| CA one episode, type 3 | 0.647 | 0.613-0.683 | 0.722 | 0.671-0.777 | 0.407 | 0.376-0.440 |
| CA one episode, type 4 | 0.634 | 0.615-0.654 | 0.632 | 0.606-0.660 | 0.661 | 0.635-0.688 |
| CA two or more episodes, type 1 | 1.525 | 1.464-1.589 | 1.667 | 1.580-1.758 | 0.133 | 0.121-0.148 |
| CA two or more episodes, type 2 | 0.982 | 0.952-1.013 | 0.645 | 0.616-0.675 | 0.093 | 0.087-0.099 |
| CA two or more episodes, type 3 | 1.142 | 1.097-1.188 | 0.817 | 0.771-0.866 | 0.106 | 0.097-0.117 |
| CA two or more episodes, type 4 | 1.370 | 1.326-1.415 | 1.296 | 1.239-1.355 | 0.134 | 0.124-0.144 |
| Sociodemographic characteristics | ||||||
| Age | ||||||
| 65-74 (ref) | ||||||
| 75-84 | 0.972 | 0.959-0.986 | 1.313 | 1.285-1.343 | 1.130 | 1.100-1.160 |
| 85-94 | 0.978 | 0.963-0.994 | 1.532 | 1.496-1.568 | 1.437 | 1.397-1.478 |
| 95 and older | 0.985 | 0.953-1.019 | 1.449 | 1.383-1.519 | 2.109 | 2.007-2.215 |
| Sex | ||||||
| Male (ref) | ||||||
| Female | 0.884 | 0.873-0.894 | 0.989 | 0.972-1.006 | 0.663 | 0.650-0.677 |
| Race/ethnicity | ||||||
| White (ref) | ||||||
| Asian | 0.769 | 0.733-0.806 | 0.620 | 0.574-0.671 | 0.838 | 0.770-0.911 |
| Black | 0.933 | 0.915-0.951 | 0.757 | 0.734-0.780 | 0.855 | 0.824-0.887 |
| Hispanic | 0.741 | 0.714-0.769 | 0.487 | 0.454-0.521 | 0.718 | 0.665-0.776 |
| North American Native | 1.111 | 1.009-1.223 | 0.864 | 0.738-1.011 | 1.152 | 0.974-1.362 |
| Other | 0.843 | 0.795-0.893 | 0.654 | 0.594-0.721 | 0.856 | 0.771-0.951 |
| Unknown | 0.731 | 0.657-0.814 | 0.578 | 0.476-0.703 | 0.774 | 0.630-0.951 |
| Dual eligibility status | ||||||
| Non-dually eligible (ref) | ||||||
| Dually eligible | 0.874 | 0.861-0.887 | 0.877 | 0.858-0.897 | 0.788 | 0.766-0.811 |
| Living arrangement | ||||||
| Lives alone (ref) | ||||||
| Lives with another person in home | 1.055 | 1.041-1.070 | 0.772 | 0.757-0.787 | 1.138 | 1.109-1.168 |
| Lives in congregate situation | 1.058 | 1.035-1.082 | 0.977 | 0.948-1.006 | 1.293 | 1.244-1.343 |
| Diagnoses or conditions | ||||||
| Cancer | 1.078 | 1.061-1.095 | 0.986 | 0.964-1.009 | 1.634 | 1.594-1.674 |
| COPD | 1.201 | 1.185-1.218 | 1.084 | 1.063-1.106 | 1.275 | 1.245-1.306 |
| Diabetes | 1.027 | 1.015-1.040 | 1.065 | 1.046-1.084 | 0.863 | 0.844-0.882 |
| Disabled | 1.147 | 1.093-1.205 | 1.001 | 0.920-1.090 | 1.096 | 0.991-1.212 |
| Heart failure | 1.174 | 1.157-1.192 | 1.096 | 1.073-1.119 | 1.191 | 1.161-1.221 |
| Hip fracture | 0.799 | 0.774-0.824 | 0.971 | 0.930-1.013 | 0.701 | 0.663-0.742 |
| Major depression or bipolar disorder | 0.944 | 0.922-0.966 | 1.096 | 1.061-1.131 | 0.635 | 0.606-0.666 |
| Multiple sclerosis | 0.776 | 0.715-0.842 | 0.986 | 0.880-1.105 | 0.468 | 0.390-0.561 |
| Schizophrenia | 0.964 | 0.908-1.023 | 1.130 | 1.038-1.230 | 0.598 | 0.524-0.682 |
| Stroke | 0.946 | 0.926-0.966 | 1.051 | 1.020-1.082 | 0.716 | 0.688-0.744 |
| Clinical severity | ||||||
| HCC risk score | 1.213 | 1.206-1.220 | 1.126 | 1.117-1.134 | 1.227 | 1.217-1.237 |
| ADL functioning | ||||||
| Score 0-35a | 1.015 | 1.014-1.016 | 1.023 | 1.021-1.025 | 1.084 | 1.082-1.086 |
| Cognitive functioning | ||||||
| Alert/oriented (ref) | ||||||
| Requires prompting | 1.040 | 1.027-1.054 | 1.185 | 1.163-1.207 | 1.211 | 1.183-1.240 |
| Requires assistance | 1.086 | 1.065-1.108 | 1.263 | 1.229-1.297 | 1.306 | 1.265-1.349 |
| Requires considerable assistance | 1.083 | 1.048-1.118 | 1.077 | 1.030-1.126 | 1.530 | 1.461-1.601 |
| Totally dependent | 0.849 | 0.795-0.907 | 0.557 | 0.501-0.620 | 1.483 | 1.369-1.606 |
| SOURCE: Mathematica analysis of 20% sample of CMS DataLink File with home health use during January 1, 2013, to December 31, 2013, and spells starting no earlier than January 1, 2011, and no later than December 31, 2013. NOTE: The models include a fixed effect for state of residence and a fixed effect for the year the spell started. Type 1 = Any aide or medical social services and low therapy or skilled nursing services. Type 2 = No aide or medical social services and high therapy or skilled nursing services. Type 3 = Any aide or medical social services and high therapy or skilled nursing services. Type 4 = No aide or medical social services and low therapy or skilled nursing services.
|
||||||
| TABLE D.2. Correlation between Type of Home Health User and Number of Hospitalizations and SNF Admissions | ||||
|---|---|---|---|---|
| Hospitalizations | SNF Admissions | |||
| Estimate | Standard Error | Estimate | Standard Error | |
| Intercept | -0.6965 | 0.0835 | -1.0255 | 0.1439 |
| Home health group | ||||
| PAC one episode, type 1 (ref) | ||||
| PAC one episode, type 2 | -0.2427 | 0.0174 | -0.4357 | 0.0390 |
| PAC one episode, type 3 | -0.1894 | 0.0235 | -0.6020 | 0.0506 |
| PAC one episode, type 4 | -0.0294 | 0.0157 | 0.0560 | 0.0313 |
| PAC two or more episodes, type 1 | 0.4774 | 0.0167 | 0.0581 | 0.0324 |
| PAC two or more episodes, type 2 | 0.2006 | 0.0154 | -0.7411 | 0.0323 |
| PAC two or more episodes, type 3 | 0.1756 | 0.0172 | -0.8229 | 0.0357 |
| PAC two or more episodes, type 4 | 0.5493 | 0.0155 | 0.0590 | 0.0310 |
| CA one episode, type 1 | -0.1133 | 0.0236 | -0.1342 | 0.0418 |
| CA one episode, type 2 | -0.3032 | 0.0224 | -0.4242 | 0.0466 |
| CA one episode, type 3 | -0.3027 | 0.0368 | -0.3545 | 0.0659 |
| CA one episode, type 4 | -0.1539 | 0.0184 | -0.1263 | 0.0353 |
| CA two or more episodes, type 1 | 0.0992 | 0.0215 | -0.4073 | 0.0381 |
| CA two or more episodes, type 2 | -0.1063 | 0.0174 | -1.0638 | 0.0382 |
| CA two or more episodes, type 3 | -0.0987 | 0..0221 | -0.9843 | 0.0448 |
| CA two or more episodes, type 4 | 0.1218 | 0.0177 | -0.5631 | 0.0356 |
| Sociodemographic characteristics | ||||
| Age | ||||
| 65-74 (ref) | ||||
| 75-84 | -0.1132 | 0.0065 | 0.1027 | 0.0144 |
| 85-94 | -0.2255 | 0.0074 | 0.1030 | 0.0166 |
| 95 and older | -0.3822 | 0.0172 | -0.1169 | 0.0308 |
| Sex | ||||
| Male (ref) | ||||
| Female | -0.0327 | 0.0055 | 0.0031 | 0.0105 |
| Race/ethnicity | ||||
| White (ref) | ||||
| Asian | -0.0005 | 0.0245 | -0.2647 | 0.0531 |
| Black | 0.0282 | 0.0088 | -0.2527 | 0.0183 |
| Hispanic | -0.0222 | 0.0194 | -0.4195 | 0.0483 |
| North American Native | -0.0073 | 0.0442 | -0.1275 | 0.0937 |
| Other | -0.0404 | 0.0281 | -0.3474 | 0.0613 |
| Unknown | -0.0927 | 0.0584 | -0.2119 | 0.1398 |
| Dual eligibility status | ||||
| Non-dually eligible (ref) | ||||
| Dually eligible | -0.0274 | 0.0069 | -0.2158 | 0.0136 |
| Living arrangement | ||||
| Lives alone (ref) | ||||
| Lives with another person in home | 0.0477 | 0.0065 | -0.1174 | 0.0125 |
| Lives in congregate situation | -0.1273 | 0.0109 | -0.1916 | 0.0186 |
| Diagnoses or conditions | ||||
| Cancer | 0.0225 | 0.0070 | -0.0212 | 0.0138 |
| COPD | 0.0777 | 0.0062 | 0.0283 | 0.0120 |
| Diabetes | 0.0369 | 0.0057 | 0.0320 | 0.0109 |
| Disabled | 0.0718 | 0.0230 | -0.1070 | 0.0533 |
| Heart failure | 0.0875 | 0.0065 | 0.0579 | 0.0124 |
| Hip fracture | -0.1066 | 0.0143 | 0.0156 | 0.0252 |
| Major depression or bipolar disorder | -0.0103 | 0.0103 | 0.0803 | 0.0190 |
| Multiple sclerosis | -0.0912 | 0.0372 | -0.0482 | 0.0680 |
| Schizophrenia | -0.0159 | 0.0274 | -0.0263 | 0.0507 |
| Stroke | -0.0214 | 0.0094 | 0.0100 | 0.0175 |
| Clinical severity | ||||
| HCC risk score | 0.0568 | 0.0022 | 0.0326 | 0.0051 |
| ADL functioning | ||||
| Score 0-35a | 0.0029 | 0.0005 | 0.0036 | 0.0012 |
| Cognitive functioning | ||||
| Alert/oriented (ref) | ||||
| Requires prompting | -0.0334 | 0.0060 | 0.0026 | 0.0117 |
| Requires assistance | -0.0864 | 0.0093 | -0.0389 | 0.0169 |
| Requires considerable assistance | -0.1880 | 0.0156 | -0.2608 | 0.0279 |
| Totally dependent | -0.3734 | 0.0328 | -0.8293 | 0.0705 |
| SOURCE: Mathematica analysis of 20% sample of CMS DataLink File with home health use during January 1, 2013, to December 31, 2013, and spells starting no earlier than January 1, 2011, and no later than December 31, 2013. NOTE: The models include a fixed effect for state of residence and a fixed effect for the year the spell started. Type 1 = Any aide or medical social services and low therapy or skilled nursing services. Type 2 = No aide or medical social services and high therapy or skilled nursing services. Type 3 = Any aide or medical social services and high therapy or skilled nursing services. Type 4 = No aide or medical social services and low therapy or skilled nursing services.
|
||||
APPENDIX E. GROWTH IN COMMUNITY-ADMITTED HOME HEALTH USERS
| TABLE E.1. Yearly Characteristics of PAC and Community-Admitted Home Health Users | ||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 2002 | 2003 | 2004 | 2005 | 2006 | 2007 | 2008 | 2009 | 2010 | 2011 | 2012 | 2013 | |||||||||||||
| CA | PAC | CA | PAC | CA | PAC | CA | PAC | CA | PAC | CA | PAC | CA | PAC | CA | PAC | CA | PAC | CA | PAC | CA | PAC | CA | PAC | |
| Total number | 176,457 | 283,961 | 189,805 | 293,534 | 204,462 | 300,438 | 217,836 | 305,456 | 229,436 | 295,448 | 243,334 | 292,195 | 257,719 | 292,464 | 279,250 | 290,084 | 297,285 | 296,853 | 297,039 | 293,667 | 302,319 | 291,402 | 301,814 | 293,923 |
| Sociodemographic characteristics | ||||||||||||||||||||||||
| Age (years) | 80.5 | 78.6 | 80.5 | 78.6 | 80.4 | 78.6 | 80.5 | 78.7 | 80.5 | 78.7 | 80.5 | 78.8 | 80.6 | 78.8 | 80.6 | 78.8 | 80.6 | 78.8 | 80.6 | 78.9 | 80.6 | 78.8 | 80.7 | 78.6 |
| Sex | ||||||||||||||||||||||||
| Female (%) | 68.2 | 63.5 | 68.1 | 63.3 | 67.7 | 63.3 | 67.9 | 63.0 | 67.8 | 62.9 | 67.7 | 62.7 | 67.3 | 62.6 | 67.3 | 62.4 | 66.9 | 62.0 | 66.6 | 61.9 | 66.3 | 61.5 | 66.0 | 60.7 |
| Male (%) | 31.8 | 36.6 | 31.9 | 36.7 | 32.3 | 36.7 | 32.1 | 37.0 | 32.2 | 37.1 | 32.3 | 37.3 | 32.7 | 37.4 | 32.7 | 37.6 | 33.2 | 38.0 | 33.4 | 38.1 | 33.7 | 38.5 | 34.0 | 39.3 |
| Race/ethnicity | ||||||||||||||||||||||||
| Asian (%) | 1.8 | 0.9 | 2.0 | 0.9 | 1.8 | 0.9 | 1.7 | 1.0 | 1.8 | 1.1 | 1.8 | 1.1 | 1.9 | 1.2 | 2.0 | 1.2 | 2.0 | 1.3 | 2.1 | 1.3 | 2.1 | 1.4 | 2.2 | 1.4 |
| Black (%) | 12.9 | 8.8 | 13.2 | 8.7 | 13.8 | 8.7 | 14.1 | 8.5 | 14.2 | 8.3 | 14.0 | 8.0 | 13.9 | 8.0 | 14.2 | 8.0 | 14.3 | 8.3 | 14.2 | 8.3 | 13.6 | 8.3 | 13.3 | 8.4 |
| Hispanic (%) | 3.4 | 1.9 | 3.7 | 1.9 | 4.1 | 1.9 | 4.2 | 1.8 | 4.5 | 1.7 | 4.7 | 1.6 | 4.7 | 1.6 | 4.8 | 1.6 | 5.0 | 1.6 | 5.0 | 1.7 | 4.7 | 1.6 | 4.6 | 1.5 |
| North American Native (%) | 0.4 | 0.3 | 0.4 | 0.3 | 0.4 | 0.3 | 0.4 | 0.3 | 0.4 | 0.3 | 0.4 | 0.3 | 0.4 | 0.3 | 0.4 | 0.3 | 0.5 | 0.3 | 0.4 | 0.3 | 0.4 | 0.3 | 0.4 | 0.3 |
| Other (%) | 0.8 | 0.5 | 0.9 | 0.6 | 0.8 | 0.6 | 0.8 | 0.7 | 0.8 | 0.7 | 0.9 | 0.7 | 0.9 | 0.8 | 1.0 | 0.8 | 1.0 | 0.9 | 1.0 | 0.9 | 1.1 | 1.0 | 1.1 | 1.0 |
| Unknown (%) | 0.3 | 0.2 | 0.3 | 0.2 | 0.2 | 0.2 | 0.2 | 0.1 | 0.2 | 0.1 | 0.2 | 0.1 | 0.2 | 0.1 | 0.2 | 0.1 | 0.2 | 0.1 | 0.2 | 0.2 | 0.3 | 0.2 | 0.4 | 0.3 |
| White (%) | 80.3 | 87.5 | 79.6 | 87.5 | 78.9 | 87.4 | 78.6 | 87.5 | 78.2 | 87.9 | 78.0 | 88.1 | 78.1 | 88.0 | 77.5 | 87.9 | 77.0 | 87.4 | 77.1 | 87.3 | 77.8 | 87.2 | 78.1 | 87.0 |
| Dual eligibility statusa | ||||||||||||||||||||||||
| Dually eligible (%) | 26.3 | 14.9 | 27.3 | 15.0 | 27.7 | 15.1 | 28.0 | 15.1 | 28.5 | 14.5 | 32.4 | 16.7 | 31.7 | 16.6 | 32.1 | 16.6 | 32.5 | 16.9 | 32.6 | 17.1 | 31.3 | 16.4 | 31.0 | 15.9 |
| Non-dually eligible (%) | 73.7 | 85.1 | 72.7 | 85.0 | 72.3 | 84.9 | 72.0 | 84.9 | 71.5 | 85.5 | 67.6 | 83.3 | 68.3 | 83.4 | 67.9 | 83.4 | 67.5 | 83.2 | 67.4 | 82.9 | 68.7 | 83.6 | 69.0 | 84.1 |
| Living arrangementb | ||||||||||||||||||||||||
| Living alone (%) | 27.2 | 27.1 | 27.1 | 26.7 | 27.3 | 26.3 | 27.1 | 26.1 | 27.0 | 26.1 | 26.9 | 25.7 | 26.7 | 25.5 | 26.8 | 25.4 | 27.1 | 25.3 | 26.6 | 25.0 | 26.5 | 24.8 | 26.3 | 24.4 |
| Lives with another person in home (%) | 54.4 | 63.9 | 54.1 | 64.6 | 54.4 | 65.5 | 54.5 | 66.0 | 54.1 | 66.0 | 53.8 | 66.5 | 53.8 | 66.7 | 53.8 | 66.9 | 53.8 | 67.4 | 54.4 | 67.9 | 54.7 | 68.3 | 54.9 | 68.5 |
| Lives in congregate situation (%) | 11.9 | 5.8 | 12.2 | 5.9 | 12.5 | 5.9 | 12.8 | 6.0 | 13.0 | 6.0 | 13.3 | 6.0 | 13.3 | 6.1 | 13.2 | 6.1 | 12.8 | 5.6 | 13.1 | 5.8 | 13.3 | 5.8 | 13.8 | 5.9 |
| Unknown (%) | 6.5 | 3.3 | 6.6 | 2.9 | 5.9 | 2.2 | 5.7 | 2.0 | 5.9 | 1.9 | 6.0 | 1.8 | 6.3 | 1.7 | 6.3 | 1.6 | 6.4 | 1.7 | 5.9 | 1.3 | 5.5 | 1.1 | 5.1 | 1.2 |
| Lives in rural area (%) | 19.8 | 17.2 | 19.0 | 16.8 | 18.8 | 16.5 | 18.7 | 16.5 | 18.5 | 16.5 | 18.0 | 16.3 | 17.6 | 16.0 | 17.3 | 15.7 | 17.0 | 15.4 | 16.8 | 15.1 | 16.6 | 15.1 | 16.1 | 15.0 |
| County of residence is primary care health shortage area | ||||||||||||||||||||||||
| Some of county (%) | 56.1 | 58.0 | 55.7 | 57.9 | 55.5 | 57.4 | 55.4 | 57.9 | 54.8 | 57.5 | 54.8 | 57.6 | 54.8 | 57.8 | 54.7 | 57.3 | 54.8 | 57.6 | 54.5 | 57.2 | 55.1 | 57.4 | 55.2 | 57.5 |
| All of county (%) | 35.6 | 33.1 | 35.9 | 32.7 | 36.1 | 33.1 | 36.5 | 32.6 | 37.2 | 32.8 | 37.3 | 32.7 | 37.2 | 32.6 | 37.2 | 32.7 | 37.2 | 32.4 | 37.3 | 32.6 | 36.6 | 32.5 | 36.5 | 32.3 |
| None of county (%) | 8.2 | 8.9 | 8.4 | 9.3 | 8.3 | 9.5 | 8.1 | 9.5 | 8.0 | 9.7 | 7.8 | 9.7 | 7.9 | 9.6 | 8.1 | 10.0 | 8.0 | 10.0 | 8.1 | 10.1 | 8.2 | 10.0 | 8.3 | 10.1 |
| Unknown (%) | 0.1 | 0.1 | 0.1 | 0.0 | 0.0 | 0.0 | 0.1 | 0.0 | 0.1 | 0.0 | 0.1 | 0.0 | 0.1 | 0.0 | 0.1 | 0.0 | 0.1 | 0.0 | 0.1 | 0.0 | 0.1 | 0.0 | 0.1 | 0.0 |
| State LTSS ranking | ||||||||||||||||||||||||
| Top quartile (%) | 16.9 | 16.1 | 16.5 | 16.0 | 15.2 | 15.7 | 14.4 | 15.7 | 13.8 | 16.0 | 13.5 | 15.9 | 13.3 | 16.4 | 13.0 | 16.6 | 13.1 | 16.4 | 13.7 | 16.6 | 14.5 | 16.8 | 15.4 | 17.0 |
| 2nd quartile (%) | 19.2 | 24.5 | 18.9 | 24.6 | 18.5 | 25.0 | 18.1 | 25.0 | 17.8 | 25.3 | 17.4 | 25.5 | 17.7 | 25.8 | 17.9 | 25.9 | 18.1 | 25.9 | 18.3 | 26.1 | 18.9 | 26.3 | 19.3 | 26.3 |
| 3rd quartile (%) | 30.1 | 26.9 | 30.8 | 27.0 | 32.3 | 26.9 | 33.6 | 27.0 | 35.0 | 27.4 | 34.7 | 27.0 | 34.6 | 26.8 | 34.3 | 26.7 | 33.7 | 27.4 | 32.9 | 27.0 | 32.0 | 27.0 | 30.9 | 26.7 |
| Bottom quartile (%) | 32.1 | 31.8 | 32.2 | 31.7 | 32.6 | 31.8 | 32.7 | 31.8 | 32.8 | 31.1 | 33.8 | 31.3 | 34.0 | 30.8 | 34.4 | 30.6 | 34.7 | 30.2 | 34.7 | 30.1 | 34.3 | 29.8 | 34.2 | 29.8 |
| Unknown (%) | 1.8 | 0.8 | 1.6 | 0.7 | 1.4 | 0.6 | 1.2 | 0.5 | 0.7 | 0.3 | 0.5 | 0.3 | 0.5 | 0.3 | 0.4 | 0.2 | 0.4 | 0.2 | 0.3 | 0.2 | 0.3 | 0.2 | 0.3 | 0.2 |
| Lives in state with Medicare home health fraud and abuse (%) | 26.0 | 24.1 | 27.9 | 24.3 | 30.4 | 24.5 | 32.7 | 24.5 | 35.2 | 24.4 | 36.5 | 23.9 | 37.2 | 23.7 | 37.9 | 23.4 | 38.5 | 23.9 | 37.8 | 23.4 | 36.7 | 23.2 | 35.7 | 22.8 |
| Lives in area with extremely high number of HHAs per 100,000 people ages 65 and older (%) | 29.7 | 20.9 | 28.5 | 19.0 | 31.3 | 19.3 | 32.5 | 19.1 | 34.3 | 18.6 | 35.7 | 18.6 | 35.6 | 18.1 | 34.5 | 16.5 | 36.5 | 17.8 | 36.1 | 17.9 | 34.9 | 17.8 | 34.1 | 17.5 |
| Home health episode characteristics | ||||||||||||||||||||||||
| Number of aide visits per episode | 5.9 | 4.4 | 5.3 | 3.9 | 5.1 | 3.8 | 5.0 | 3.6 | 4.9 | 3.6 | 4.9 | 3.4 | 4.2 | 3.0 | 3.9 | 2.9 | 3.6 | 2.7 | 3.2 | 2.6 | 2.9 | 2.3 | 2.7 | 2.1 |
| Number of medical social service visits per episode | 0.2 | 0.2 | 0.2 | 0.2 | 0.2 | 0.2 | 0.2 | 0.2 | 0.2 | 0.2 | 0.1 | 0.2 | 0.1 | 0.2 | 0.1 | 0.2 | 0.1 | 0.2 | 0.1 | 0.2 | 0.1 | 0.2 | 0.1 | 0.2 |
| Number of therapy visits per episode | 4.9 | 6.9 | 5.0 | 6.9 | 5.3 | 7.0 | 5.3 | 7.1 | 5.4 | 7.2 | 5.5 | 7.3 | 5.9 | 7.6 | 6.4 | 8.1 | 6.7 | 8.2 | 6.5 | 8.0 | 6.6 | 7.9 | 6.8 | 8.1 |
| Number of skilled nursing visits per episode | 11.5 | 10.2 | 11.2 | 9.7 | 11.0 | 9.7 | 11.1 | 9.5 | 11.3 | 9.5 | 11.6 | 9.3 | 11.4 | 9.2 | 11.2 | 9.2 | 10.2 | 9.0 | 9.8 | 8.9 | 9.6 | 8.8 | 9.4 | 8.6 |
| High physical therapy use (%) | 10.0 | 2.4 | 11.4 | 2.7 | 12.6 | 3.0 | 13.8 | 3.0 | 15.1 | 3.2 | 16.7 | 3.4 | 18.4 | 3.6 | 20.3 | 3.9 | 20.9 | 4.1 | 20.7 | 4.3 | 19.9 | 4.2 | 20.0 | 4.3 |
| Diagnoses or conditions | ||||||||||||||||||||||||
| Cancer (%) | n.a. | n.a. | n.a. | n.a. | 14.4 | 16.1 | 14.4 | 16.3 | 14.5 | 16.7 | 14.2 | 16.5 | 14.4 | 16.7 | 14.4 | 16.9 | 14.5 | 16.9 | 14.4 | 17.1 | 14.6 | 17.2 | 14.8 | 17.1 |
| COPD (%) | n.a. | n.a. | n.a. | n.a. | 24.4 | 24.5 | 24.5 | 24.5 | 25.1 | 24.8 | 23.7 | 22.9 | 23.7 | 23.1 | 24.1 | 23.1 | 24.3 | 23.0 | 24.5 | 23.4 | 24.9 | 23.6 | 24.7 | 23.7 |
| Diabetes (%) | n.a. | n.a. | n.a. | n.a. | 33.3 | 29.0 | 34.1 | 29.5 | 34.9 | 30.2 | 36.1 | 31.1 | 37.1 | 31.6 | 37.8 | 32.4 | 38.0 | 32.8 | 38.3 | 33.3 | 38.8 | 33.7 | 38.6 | 33.9 |
| Disabled (%) | n.a. | n.a. | n.a. | n.a. | 0.9 | 1.1 | 0.9 | 1.1 | 1.0 | 1.1 | 1.1 | 1.2 | 1.1 | 1.2 | 1.1 | 1.2 | 1.0 | 1.2 | 1.1 | 1.3 | 1.3 | 1.5 | 1.2 | 1.5 |
| Heart failure (%) | n.a. | n.a. | n.a. | n.a. | 31.3 | 27.5 | 31.1 | 27.1 | 31.1 | 27.1 | 30.7 | 26.2 | 30.4 | 26.2 | 30.4 | 26.0 | 30.1 | 25.9 | 30.1 | 26.1 | 30.0 | 25.9 | 29.5 | 25.8 |
| Hip fracture (%) | n.a. | n.a. | n.a. | n.a. | 4.4 | 3.5 | 4.3 | 3.5 | 4.3 | 3.5 | 4.1 | 3.4 | 4.1 | 3.3 | 4.0 | 3.4 | 3.9 | 3.3 | 3.8 | 3.3 | 3.8 | 3.3 | 3.8 | 3.2 |
| Major depression or bipolar disorder (%) | n.a. | n.a. | n.a. | n.a. | 5.5 | 3.9 | 5.6 | 3.9 | 5.7 | 4.0 | 6.0 | 4.1 | 6.2 | 4.3 | 6.5 | 4.5 | 6.8 | 4.6 | 7.1 | 5.0 | 7.3 | 5.1 | 7.6 | 5.3 |
| Multiple sclerosis (%) | n.a. | n.a. | n.a. | n.a. | 0.7 | 0.3 | 0.7 | 0.3 | 0.7 | 0.3 | 0.6 | 0.3 | 0.6 | 0.3 | 0.6 | 0.3 | 0.6 | 0.3 | 0.7 | 0.3 | 0.7 | 0.3 | 0.7 | 0.4 |
| Schizophrenia (%) | n.a. | n.a. | n.a. | n.a. | 1.0 | 0.5 | 1.0 | 0.5 | 1.0 | 0.5 | 1.0 | 0.5 | 1.0 | 0.5 | 1.1 | 0.5 | 1.1 | 0.5 | 1.2 | 0.5 | 1.2 | 0.5 | 1.2 | 0.6 |
| Stroke (%) | n.a. | n.a. | n.a. | n.a. | 11.8 | 8.3 | 11.6 | 8.1 | 11.0 | 7.8 | 9.7 | 6.8 | 9.5 | 6.7 | 9.4 | 6.7 | 9.0 | 6.5 | 8.8 | 6.4 | 8.8 | 6.4 | 8.6 | 6.5 |
| Clinical severity | ||||||||||||||||||||||||
| HCC risk score | n.a. | n.a. | n.a. | n.a. | 2.0 | 1.6 | 2.0 | 1.7 | 2.0 | 1.7 | 2.0 | 1.7 | 2.0 | 1.7 | 2.0 | 1.7 | 2.0 | 1.7 | 2.1 | 1.8 | 2.1 | 1.8 | 2.0 | 1.8 |
| ADL functioning | ||||||||||||||||||||||||
| Score 0-35c | 10.1 | 8.4 | 10.0 | 8.5 | 9.9 | 8.6 | 9.9 | 8.7 | 10.1 | 9.0 | 10.3 | 9.3 | 10.6 | 9.6 | 10.8 | 10.0 | 11.7 | 11.1 | 12.4 | 11.7 | 12.9 | 12.2 | 13.4 | 12.7 |
| Cognitive functioning | ||||||||||||||||||||||||
| Alert/oriented (%) | 49.9 | 68.4 | 49.4 | 68.3 | 49.5 | 68.0 | 49.3 | 67.3 | 48.0 | 66.4 | 46.8 | 65.3 | 45.7 | 64.4 | 45.0 | 63.7 | 43.7 | 62.1 | 43.1 | 60.6 | 42.3 | 59.4 | 41.2 | 58.5 |
| Requires prompting (%) | 25.8 | 19.1 | 26.8 | 19.6 | 27.5 | 20.5 | 27.9 | 21.3 | 29.1 | 21.9 | 30.1 | 22.9 | 30.8 | 23.7 | 31.4 | 24.3 | 32.4 | 25.5 | 33.3 | 27.0 | 34.5 | 28.2 | 35.5 | 29.1 |
| Requires assistance (%) | 10.7 | 6.3 | 10.5 | 6.4 | 10.8 | 6.5 | 10.8 | 6.7 | 11.2 | 6.9 | 11.4 | 7.1 | 11.6 | 7.3 | 11.8 | 7.5 | 12.0 | 7.8 | 12.2 | 8.2 | 12.3 | 8.3 | 12.8 | 8.4 |
| Requires considerable assistance (%) | 4.8 | 2.3 | 4.6 | 2.2 | 4.5 | 2.2 | 4.5 | 2.2 | 4.3 | 2.2 | 4.3 | 2.3 | 4.4 | 2.3 | 4.3 | 2.3 | 4.3 | 2.4 | 4.3 | 2.5 | 4.3 | 2.4 | 4.4 | 2.4 |
| Totally dependent (%) | 2.3 | 0.8 | 2.1 | 0.7 | 1.9 | 0.7 | 1.8 | 0.7 | 1.6 | 0.6 | 1.4 | 0.5 | 1.3 | 0.5 | 1.2 | 0.5 | 1.2 | 0.5 | 1.2 | 0.5 | 1.1 | 0.5 | 1.1 | 0.5 |
| Unknown (%) | 6.5 | 3.3 | 6.6 | 2.9 | 5.9 | 2.2 | 5.7 | 2.0 | 5.9 | 1.9 | 6.0 | 1.8 | 6.3 | 1.7 | 6.3 | 1.6 | 6.4 | 1.7 | 5.9 | 1.3 | 5.5 | 1.1 | 5.1 | 1.2 |
| Agency characteristics | ||||||||||||||||||||||||
| Ownership | ||||||||||||||||||||||||
| For-profit (%) | 45.9 | 31.2 | 50.5 | 34.0 | 54.8 | 36.4 | 58.8 | 38.9 | 62.7 | 41.0 | 66.3 | 43.2 | 69.4 | 45.8 | 71.5 | 47.3 | 72.8 | 49.4 | 73.3 | 50.3 | 72.7 | 50.8 | 72.8 | 51.8 |
| Government (%) | 7.0 | 7.2 | 6.2 | 6.8 | 5.7 | 6.4 | 5.1 | 6.0 | 4.6 | 5.8 | 4.2 | 5.6 | 3.9 | 5.4 | 3.4 | 4.9 | 3.0 | 4.5 | 2.9 | 4.2 | 2.9 | 4.0 | 2.7 | 3.7 |
| Non-profit (%) | 47.1 | 61.5 | 43.3 | 59.3 | 39.5 | 57.2 | 36.2 | 55.1 | 32.7 | 53.3 | 29.5 | 51.2 | 26.8 | 48.9 | 25.1 | 47.8 | 24.2 | 46.2 | 23.8 | 45.5 | 24.4 | 45.2 | 24.5 | 44.5 |
| SOURCE: Mathematica analysis of 20% sample of CMS DataLink File from January 1, 2002, to December 31, 2013. NOTE: Percentages might not add up to 100 due to rounding.
|
||||||||||||||||||||||||
| TABLE E.2. Yearly Characteristics of PAC and Community-Admitted Dually Eligible Home Health Users | ||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 2002 | 2003 | 2004 | 2005 | 2006 | 2007 | 2008 | 2009 | 2010 | 2011 | 2012 | 2013 | |||||||||||||
| CA | PAC | CA | PAC | CA | PAC | CA | PAC | CA | PAC | CA | PAC | CA | PAC | CA | PAC | CA | PAC | CA | PAC | CA | PAC | CA | PAC | |
| State Medicaid LTSS system performance | ||||||||||||||||||||||||
| Top quartile (%) | 8.1 | 9.1 | 5.5 | 6.5 | 10.5 | 12.8 | 17.7 | 18.7 | 16.9 | 20.1 | 20.6 | 29.5 | 16.1 | 21.4 | 15.1 | 20.2 | 17.4 | 23.5 | 18.1 | 23.1 | 19.4 | 23.8 | 20.6 | 24.1 |
| 2nd quartile (%) | 48.9 | 40.8 | 51.0 | 44.0 | 41.7 | 33.8 | 33.8 | 28.8 | 34.2 | 28.2 | 32.5 | 22.3 | 36.4 | 28.6 | 33.4 | 28.3 | 29.0 | 26.3 | 28.3 | 26.4 | 27.1 | 27.8 | 29.9 | 31.0 |
| 3rd quartile (%) | 19.8 | 23.9 | 19.4 | 24.1 | 21.6 | 26.4 | 27.3 | 29.5 | 26.5 | 29.4 | 21.1 | 20.6 | 18.3 | 19.9 | 14.9 | 16.5 | 12.4 | 14.7 | 20.6 | 21.0 | 19.3 | 18.2 | 17.9 | 16.8 |
| Bottom quartile (%) | 23.1 | 26.1 | 24.0 | 25.3 | 26.1 | 27.0 | 21.1 | 22.9 | 22.4 | 22.3 | 25.8 | 27.5 | 29.1 | 30.0 | 36.6 | 35.0 | 41.1 | 35.5 | 32.9 | 29.5 | 34.1 | 30.1 | 31.6 | 28.0 |
| Unknown (%) | 0.1 | 0.1 | 0.1 | 0.1 | 0.1 | 0.1 | 0.1 | 0.1 | 0.1 | 0.0 | 0.1 | 0.1 | 0.1 | 0.1 | 0.0 | 0.0 | 0.0 | 0.0 | 0.0 | 0.1 | 0.0 | 0.0 | 0.0 | 0.1 |
| Home health episode characteristics | ||||||||||||||||||||||||
| Number of aide visits per episode | 5.9 | 4.6 | 5.4 | 4.0 | 5.4 | 4.2 | 5.4 | 4.2 | 5.5 | 4.5 | 6.1 | 4.5 | 4.7 | 3.8 | 4.2 | 3.6 | 3.5 | 3.3 | 3.2 | 3.2 | 2.9 | 2.9 | 2.8 | 2.5 |
| Number of medical social service visits per episode | 0.2 | 0.3 | 0.2 | 0.2 | 0.2 | 0.2 | 0.2 | 0.2 | 0.1 | 0.2 | 0.1 | 0.2 | 0.1 | 0.2 | 0.1 | 0.2 | 0.1 | 0.2 | 0.1 | 0.2 | 0.2 | 0.2 | 0.1 | 0.2 |
| Number of therapy visits per episode | 3.8 | 5.4 | 3.8 | 5.6 | 4.1 | 5.8 | 4.1 | 5.7 | 4.3 | 5.9 | 4.4 | 5.9 | 4.7 | 6.3 | 5.1 | 6.6 | 5.4 | 6.7 | 5.3 | 6.6 | 5.4 | 6.5 | 5.6 | 6.8 |
| Number of skilled nursing visits per episode | 13.4 | 10.9 | 13.4 | 10.6 | 13.2 | 10.6 | 13.9 | 10.4 | 14.0 | 10.5 | 14.5 | 10.2 | 14.3 | 10.2 | 14.1 | 10.2 | 11.7 | 9.5 | 11.1 | 9.5 | 10.8 | 9.3 | 10.4 | 9.1 |
| SOURCE: Mathematica analysis of 20% sample of CMS DataLink File from January 1, 2002, to December 31, 2013. NOTE: Percentages might not add up to 100 due to rounding. |
||||||||||||||||||||||||
NOTES
-
An episode is a 60-day period of home health care.
-
Medicare pays for home health care services in 60-day periods, which are called episodes of care. For this study, if there were fewer than 60 days between episodes of care, we called them consecutive episodes (and therefore part of the same spell of care); if there were more than 60 days between episodes, we called them distinct spells of care.
-
An episode is a 60-day period of home health care.
-
Medicare pays for home health care services in 60-day periods, which are called episodes of care. For this study, if there were fewer than 60 days between episodes of care, we called them consecutive episodes (and therefore part of the same spell of care); if there were more than 60 days between episodes, we called them distinct spells of care.
-
The HCC score is produced based on patient age, sex, reason for Medicare eligibility, Medicaid eligibility, and medical conditions that are expected to impact medical costs. As part of the construction of the score, the model also produces indicator variables for medical conditions. The HCC model is a payment model used by CMS for risk adjustment in the Medicare Advantage Program.
-
As described in greater detail in Appendix A, these states include Florida, Illinois, Michigan, and Texas.
-
Under the Jimmo Settlement Agreement in January 2013, CMS clarified the Medicare coverage of skilled nursing and skilled therapy services in the SNF, Home Health, and Outpatient Therapy settings. If all other coverage criteria are met, Medicare covers skilled nursing care and skilled therapy services when a beneficiary needs skilled care in order to maintain function or to prevent or slow decline or deterioration.
-
To determine state LTSS performance, we used the 2014 AARP State Scorecard on Long-Term Services and Supports for Older Adults, People with Physical Disabilities, and Family Caregivers (Reinhard et al. 2014). This Scorecard ranks state LTSS performance in five dimensions, as well as across the five dimensions. States are then organized into quartiles reflecting their summary rankings. Poorer performing LTSS states were those classified in the third or bottom summary quartile, while good LTSS states were those classified in the top or second quartile.
-
Poor LTSS states refer to states in the third or bottom quartile of LTSS ranking based on the AARP 2014 State LTSS Scorecard quartile ranking (Reinhard et al. 2014). Good LTSS states refer to states in the second or top quartile.
-
Poor LTSS states refer to states in the third or bottom quartile of LTSS ranking based on the AARP 2014 State LTSS Scorecard quartile ranking (Reinhard et al. 2014). Good LTSS states refer to states in the second or top quartile.
-
CMS has also launched a pre-claims review process, or prior authorization, in Florida, Illinois, Massachusetts, Michigan, and Texas. This process began in Illinois in August 2016 and in Florida in April 2017, and it will be implemented in the other three states in the future.
-
It is possible to have some overlap in the 120-day analysis periods in a case in which a beneficiary has one spell that ends in fewer than 60 days and has another spell that begins 61 days after the end of the first spell.
-
The variables capturing living arrangement changed in 2010 with the switch from OASIS-B to OASIS-C, so we had to crosswalk the categories of living arrangement to account for the change. It is possible that there were minor differences in how some beneficiaries were categorized, depending on the time period of their home health use.
-
The ADL functioning score ranges from 0-33 for years 2002-2009 and 0-35 for years 2010-2013, corresponding to the change from OASIS-B to OASIS-C in the response options for two items that make up the ADL functioning score.
