Final Report
Lynn Quincy
Patricia Collins
Kristin Andrews
Christal Stone
Submitted to:
ASPE/HHS
200 Independence Ave., S.W.
Washington, DC 20201
Project Officer:
Donald Cox
Submitted by:
Mathematica Policy Research, Inc.
600 Maryland Ave., S.W., Suite 550
Washington, DC 20024-2512
Telephone: (202) 484-9220
Facsimile: (202) 863-1763
Project Director:>Deborah Chollet
Acknowledgments
This report was prepared by Mathematica Policy Research, Inc., under contract number 233-02-0086 for the Assistant Secretary of Planning and Evaluation (ASPE), U.S. Department of Health and Human Services. Donald Cox and Donald Oellerich served as project officers for this report. We gratefully acknowledge their support of this study.
Many individuals contributed to this report. Lynn Quincy is the primary author of the report. She received significant research and writing assistance from Kristin Andrews, Patricia Collins, Elizabeth Seif, Christal Stone, and Kia Alston. Deborah Chollet, Mary Harrington and Chris Trenholm provided expert advice. Debra Lipson reviewed the report and made useful suggestions that improved the quality of the report. Amanda Bernhardt led the editorial team and Donna Dorsey provided production assistance.
Although we gratefully acknowledge the input of these individuals, the authors alone are responsible for any errors or omissions in the report. Any opinions expressed in this report are those of the study participants and authors and do not necessarily reflect the views of the U.S. Department of Health and Human Services.
Finally, and most importantly, the study authors acknowledge the program directors, enrollment counselors, brokers, community advocates and others who agreed to participate in this study. Participants’ willingness to share their time, expertise, and program experience is very much appreciated. We have received permission to list these individuals below in alphabetical order by the program with which they are associated. Our thanks to:
Access Health
- Jeff Fortenbacher, Executive Director, AccessHealth
Adult Basic
- Steve Fera, Vice President, Government and Social Mission programs, Independence Blue Cross
- George Hoover, Deputy Commissioner, Children’s Health Insurance Program and adultBasic Programs, Pennsylvania Insurance Department
- Ed Naugle, Division Chief of Operations Support, Pennsylvania Insurance Department
- John Mancano, Director of Special Programs, Independence Blue Cross
- Melissa Van Benthuysen, Team Leader, Policy Studies, Inc.
Alliance Family Care
- Ingrid Lamirault, CEO, Alameda Alliance for Health
- Nina Marayuma, Director, Business Planning and Regulatory Affairs and Compliance Officer, On Lok
- Luella Penserga, Project Director, Alameda County Access to Care Collaborative
AR Health Networks
- Dan Adams, Project/Program Director, Department of Human Services, Division of Medical Services
- Suzanne McCarthy, Founding Senior Associate, Arkansas Center for Health Improvement
- John Ryan, CEO, NovaSys Health
- Kevin Ryan, Executive Director, Arkansas Center for Health Improvement
- Dwane Tankersley, Vice President Sales and Marketing, NovaSys Health
Brooklyn Health Works
- Joseph (J.C.) Cohen, CFEd® Employee Benefit Services
- Jim Cosares, Broker, JIMCO Associates, Inc.
- Mark Kessler, Vice President, Membership & Member Services, Business Council of New York State
- Dean Mohs, Executive Director of Brooklyn Healthworks, Brooklyn Chamber of Commerce
- Family Health Insurance Assistance Program
- Craig Kuhn, Program Manager, Family Health Insurance Assistance Program
- John Gridley, President, First Choice Health Insurance, Inc.
- Ann Gridley, Secretary/Treasurer, First Choice Health Insurance, Inc.
- Mark Jungvirt, Marketing Manager, State of Oregon, Office of Private Health Partnerships
FOCUS
- Rick Kronick, Professor and Chief, Division of Health Care Sciences, Department of Family and Preventive Medicine, University of California, San Diego
Health Advantage
- Kim Harper, VP of Human Resources and Public Affairs, Wishard Health Services
- Rhonda Peterson, Financial Counselor, Raphael Health Center
- Susan Jo Thomas, Director, Health Advantage
Health Choice
- Michael D. Grundy, Executive Director, HealthChoice of Michigan
- Lorenzo Lopez, Deputy Director, Wayne County Patient Care Management System
- Artiss White, Department Manager PCMS and HealthChoice, Wayne County Patient Care Management
Healthy San Francisco
- Lindsey Angelats, Senior Health Program Planner, San Francisco Department of Public Health
- Tangerine Brigham, Deputy Director of Health, Director of Healthy San Francisco, San Francisco Department of Public Health
- Danice Cook, Health Program Planner, San Francisco Department of Public Health
- Michael Drennan, Director of Primary Care Division, Community Oriented Primary Care
- Robert Menezes, Director of Marketing & Communications, San Francisco Health Plan, San Francisco Department of Public Health
- Marcelina Ogbu, COO of DPH clinics, Community Health Programs, San Francisco Department of Public Health
- Jenine Smith, Supervisor, Enrollment Unit, San Francisco Department of Public Health
Hinds County Health Alliance
- Dr. Aaron Shirley, Board of Directors, Jackson Medical Mall
- Primus Wheeler, Executive Director, Jackson Medical Mall Foundation
Ingham Health Plan
- Dr. Jaeson Fournier, Deputy Health Officer, Ingham County Health Department
- Joan Nelson, Director, Allen Neighborhood Center
- Robin Reynolds, Executive Director, Ingham Health Plan Corporation
- Dr. Dean Sienko, Health Officer/Medical Director, Ingham County Health Department
Insure Montana
- Howard Bouma, Sales Executive, Northern Montana Insurance Services
- Tim Garden, MBA, Insurance Producer, Western States Insurance
- Erin McGowan, Legislative/Health Policy Advisor, State Auditor’s Office
- Jill Sark, Director, Insure Montana Program, State Auditor's Office
- Insure Oklahoma/O-EPIC IP Plan and Employer Sponsored Insurance Plan
(many, but not all, discussants responded to questions about both plans) - Nicole Altobello, Operations Supervisor, Oklahoma Insurance Department
- David Blatt, Director of Policy, Oklahoma Policy Institute
- Regena Carlson, Insure Oklahoma Supervisor, EDS Call Center
- Mike Fogarty, CEO, Oklahoma Health Care Authority
- Nico Gomez, Director of Communication Services, Oklahoma Insurance Department
- Buffy Heater, Manager of Planning & Development, Oklahoma Insurance Department
- Jo Kilgore, Public Information Manager, Oklahoma Insurance Department
- Craig Knutson, Chief of Staff, Oklahoma Insurance Department
- Tyler LaReau, Broker, LaReau & Associates, Inc.
- Matt Lucas, Director, Insure Oklahoma
- Scott Mack, EDS Account Executive
- Lynn Mitchell, Medicaid Director, Oklahoma Insurance Department
- Melissa Pratt, Outreach Supervisor, Oklahoma Insurance Department
- Becky Pasternik-Ikard, State Medicaid Chief Operations Officer, Oklahoma Health Care Authority
- Dot Rhyne, General Manager, Griffin Marketing Solutions
- Matthew Robison, Vice President of Small Business and Workforce Development, State Chamber
- Kathy Sercel, Griffin Communications’ Subject Matter Expert for Insure Oklahoma (through August 2008)
Jax Care
- Rhonda Davis Poirier, President & CEO, JaxCare, Inc.
Primary Care Network
- David Ostrom, Assistant Deputy, Utah Department of Workforce Services
- Amanda Sok, Medical Program Specialist, Utah Department of Workforce Services
- Sheila Walsh-McDonald, Health Care Advocate, Salt Lake Community Action Program
- Heidi Weaver, Primary Care Network Program Manager, Utah Department of Health
Sac Advantage
- Jim Hunt, Chairman, Board of SacAdvantage
- John Ramey, Executive Director, Local Health Plans of California
- Garry Maisel, President and CEO, Western Health Advantage
RiteShare
- Deborah Florio, Administrator, Center for Child and Family Health, Medicaid Division, RI Department of Human Services
- Linda Katz, Director of Policy, The Poverty Institute
- Gayle Wentworth, Benefits Specialist, Westerly Hospital
Utah Premium Partnership/Covered at Work
- Heidi Weaver, Utah Premium Partnership Program Manager, Utah Department of Health
- Colleen Mellor, Employee Benefits Specialist, Strategic Employee Benefit Services
- Sheila Walsh-McDonald, Health Care Advocate, Salt Lake Community Action Program
Contents
Chapter
There Is Inadequate Knowledge to Guide Program Designers
A Broad Spectrum of Partnerships Is Key for Creating Awareness That Leads to Enrollment
Applicants Need A High Level of Insurance Counseling and Application Assistance
Program Officials Need to Manage Expectations and Avoid Negative Perceptions
Additional Research Is Needed to Quantify the Role of Nonprice Design Features in Enrollment
- Why This Study Is Needed
- Study Approach
- Programs Included in the Study
- Report Structure and Preview of Findings
- Successful Strategies Common to All Programs
- Findings Specific to the Coverage Approach
- Brokered Access to Subsidized Care
- Program Background and Enrollment Experience to Date
- Key Findings
- Program Awareness
- Program Comprehension
- Program Appeal
- Benefit Design/Provider Network
- Premium Subsidy Structure
- Enrollment Process/Eligibility Criteria
- Stigma
- Program Permanence
- Subsidized Nongroup Coverage for Adults
- Program Background
- Key Findings
- Program Awareness
- Program Comprehension
- Program Appeal
- Benefit Design/Provider Network
- Premium Subsidy Structure
- Enrollment Process/Eligibility Criteria
- Stigma
- Program Permanence
- Premium Subsidies for Workers
- Background and Enrollment Experience
- Unique Features of Medicaid- and SCHIP-Financed Programs
- Key Findings
- Program Awareness
- Program Comprehension
- Program Appeal
- Benefit Design/Provider Network
- Premium Subsidy Structure
- Enrollment Process/Eligibility Criteria
- Stigma
- Program Permanence
- Premium Assistance for Nongroup vs. Group Coverage
- Premium Subsidies for Employers and Workers
- Program Background
- Sole Proprietors Are a Special Case
- Key Findings
- Program Awareness
- Program Comprehension
- Program Appeal
- Benefit Design/Provider Network
- Enrollment Process/Eligibility Criteria
- Stigma
- Program Permanence
- How Can Programs Get Brokers on Board?
- Conclusions
- Successful Strategies Common to All Programs
- Program Awareness
- Program Comprehension
- Program Appeal
- Ease of Application
- Findings Specific to Program Types
- Gaining Small-Firm Participation Requires a Very Appealing Design
- Subsidized Programs That Target Adults Directly Have an Easier Time Attracting Enrollment
- Premium Assistance Programs Face Enrollment Challenges
- Varying Perceptions of Demand Among the Target Population
- More Research Needed to Guide Program Designers
- Recommended Next Steps
- Study Methodology
- Programs Included in the Study
- Logic Model Used to Frame the Analysis
- Approach to Literature Review
- Approach to Stakeholder Discussions
- Data Analysis and Synthesis
- Quotes in the Report
- A Review of SCHIP Literature
- Background
- Nonprice Factors Affecting Children’s Enrollment
- Program Awareness
- Program Comprehension
- Program Appeal
- Collateral Enrollment into Other Coverage Programs
Executive Summary
T he rising number of uninsured individuals in the United States is of concern to policymakers at the federal, state, and local levels. Fueled by private foundations and the federal government, state and local policymakers have developed a wide variety of programs designed to expand coverage for the uninsured. These programs have met with varying degrees of success with respect to enrolling their target population, but the program features that determine enrollment success are not well understood.
Researchers generally agree that substantial subsidies are needed to entice the uninsured to take up coverage. However, program experience shows that large subsidies may not attract the desired level of enrollment if other program features are unappealing. To date, the impact of nonprice program features, such as outreach and marketing, insurance counseling to help eligible firms or individuals understand the program, the appeal of benefit design, and ease of the application process, have been only lightly examined. Without better information, program administrators are handicapped in their efforts to design programs that effectively and efficiently enroll their target populations.
Recognizing the significant work already conducted on the determinants of children’s enrollment, Mathematica Policy Research focused this study on the nonprice program features that influence the enrollment of nonelderly adults into voluntary state and local programs that subsidize coverage or care. Reflecting the limited state of research in this area, our approach to the study question included two phases. Phase 1 was a literature review to assess the current state of knowledge regarding the impact of nonprice design features on enrollment. Information gathered from this literature was used to inform Phase 2: discussions with 67 program directors and other key informants from 17 subsidized coverage programs across the country.
In structuring this study, we postulated that enrollment is the result of three sequential steps:
- The target audience for a program is aware of the initiative.
- Once aware, the target audience comprehends the information that they receive about the program.
- Their understanding of the program leads the target audience to find the program appealing at the price at which it is offered. This step is defined broadly to encompass the appeal of all features of the program. For example, not only must the coverage have appeal, but also the applicant cannot find the enrollment process too difficult or onerous.

To the best of our knowledge, this is the first study to focus exclusively on the nonprice design features that influence take-up of subsidized coverage programs for nonelderly adults. At the highest level, this study finds that nonprice program features strongly affect enrollment. Other key findings from the study are listed below and a summary of findings by type of coverage approach (see side bar) is included as table ES.1.
There Is Inadequate Knowledge to Guide Program Designers
This study confirms that policymakers and program designers lack the information needed to accurately predict the level and pace of enrollment, based on different program features. Specifically, they do not know how different outreach approaches, benefit designs or application processes affect enrollment levels. Many program designers significantly overestimated enrollment in their programs, while others significantly underestimated enrollment. The ability to accurately gauge the strength of a response to a new subsidized coverage program is an essential component of the program’s success and duration, and critical to keeping costs in line with allocated funds, and to managing political and public expectations.
Outreach Is Critical
Study participants widely agreed that programs must be proactive to create awareness that results in enrollment. Even programs that almost “sell themselves” due to their appealing design require some awareness raising activities on the part of program officials. As a general rule, targeted, decentralized, community-based, in-person outreach approaches were deemed effective in creating awareness that leads to enrollment. Other effective methods varied depending on the coverage approach used (Table ES.1). Mass media, on the other hand, was viewed as ineffective when used in isolation. Mass or local media can be effective in creating awareness that leads to enrollment if used in conjunction with other outreach methods as it reinforces the message.
A Broad Spectrum of Partnerships Is Key for Creating Awareness That Leads to Enrollment
Discussants from all types of programs agreed that enrollment rates will be higher if a broad spectrum of “partners” favors the program and promotes it. The correct set of partners will depend on the program type. For brokered access to care, involving community clinics and trusted representatives in each community may be key. For small employer programs, involving insurance agents or brokers and the state department of insurance may be the correct partners.
These partnerships were consistently identified as the most effective way to create program awareness. Discussants speculated that when potential enrollees view these partners as a trusted source that instantly increases the coverage program’s credibility. These partners can also play a critical role by providing application assistance and insurance counseling (next topic). A successful method for engaging prospective partners is to include them in the program’s design phase.
Applicants Need A High Level of Insurance Counseling and Application Assistance
Discussants from all program types noted pervasive confusion among program applicants, particularly with respect to 1) insurance concepts, 2) program income eligibility criteria and 3) required documentation. Discussants were united in their belief that the availability of insurance counseling and application assistance was critical to completing the enrollment process. Other strategies, such as simplifying the application process and removing technical terms/jargon, were noted as desirable or even critical in the case of employer programs, but appeared to be insufficient in and of themselves. Addressing these three areas of confusion were characterized as extremely time consuming for enrollment counselors and others. We were surprised by the absence of studies or discussant opinions with respect to new strategies that would effectively reduce applicants’ confusion around these issues in order to enroll them more cost-effectively.
Program Officials Need to Manage Expectations and Avoid Negative Perceptions
Informal, word-of-mouth advertising is widely believed to have a tremendous influence on enrollment. Discussants pointed out that surmounting poor public perceptions of a program (for example, time consuming enrollment process; concerns about program permanence or funding; or fear that personal information might be turned over to immigration officials) is much more difficult than properly managing expectations in the first place. While program officials have only limited control over word-of-mouth, it is critical that they anticipate areas of confusion and tailor the outreach message and materials to ensure that accurate information about the program is circulated. One promising technique for averting negative impressions is to test market the messages and enrollment systems with a small group initially.
Programs That Target Adults Directly Attract Enrollment Much More Easily Than Programs That Involve Employers
This study found that the relative importance of nonprice features in terms of enrollment depends on the type of subsidized coverage program (see side bar above). Programs that seek to attract small, nonoffering employers as participants must be designed so that the benefit structure, enrollment processes, eligibility criteria and other features have strong appeal to several audiences (firm owners, workers and in many cases brokers). These programs must do everything right and still be prepared to enroll just a portion of the eligible population.
In contrast, programs marketed directly to adults can contain many unappealing features yet still attract significant enrollment if the premiums are very low, the target population is aware of the program and application assistance is available. When these nongroup programs feature more substantial premiums, a carefully crafted outreach strategy and benefit design may become more important.
Programs that provide premium assistance for employer coverage (but do not subsidize the employer's premium share) appear to face some unique enrollment challenges. This coverage approach faces some inherent limitations, particularly due to the limited and often unpredictable number of workers who are both income-eligible and have access to qualifying employer coverage. Complex eligibility criteria and applicant’s difficulties understanding insurance concepts combine to preclude significant enrollment. Premium assistance "opt out" programs (as opposed to mandatory programs) face significant challenges in identifying and directing their outreach efforts to potentially interested employers and workers. Identifying successful enrollment strategies in the face of these limitations proved difficult, but included involving brokers in outreach and educational efforts and creating less restrictive enrollment periods.
Table ES.1 provides additional detail on the study’s key findings by program type using the organizing principles of our study. In other words, we present the nonprice program features that appear to influence enrollment by the type of intermediate outcome: awareness, comprehension or appeal.
Additional Research Is Needed to Quantify the Role of Nonprice Design Features in Enrollment
Our study confirms that nonprice program features strongly affect enrollment. However, the existing literature and our discussions with program stakeholders exploit only a small fraction of extant program knowledge. There are many other state and local coverage initiatives that could increase our understanding of the determinants of adult enrollment in subsidized coverage programs. Furthermore, the qualitative approach used by this study suggests the need for complementary research that attempts to quantify the relative importance of the nonprice enrollment determinants. Additional research around this topic will better enable policymakers and program designers to evaluate alternative designs and to set and achieve enrollment targets. The national drive for new approaches to health coverage suggests that information on the nonprice determinants of enrollment, in both high demand and low demand settings, will be needed soon.
| Coverage Approach | ||||
|---|---|---|---|---|
| Brokered Access to Subsidized Care | Subsidized Nongroup Coverage for Adults | Premium Subsidies for Workers | Premium Subsidies for Employers and Workers | |
| Key Enrollment Messages |
|
|
|
|
| Creating Awareness that Leads to Enrollment |
|
|
|
|
| Role of Program Comprehension |
|
|
|
|
| Appealing Enrollment Processes |
|
|
|
|
| Appealing Eligibility Criteria |
|
|
|
|
| Reducing Stigma | All discussants believed stigma to be a real phenomenon that can deter enrollment. Successful strategies that minimize this effect include having higher income eligibility criteria, charging premiums and co-pays (however, modest) and other measures that make the coverage as similar to commercial coverage as possible. | |||
| Appealing Benefit Designs/Provider Networks |
|
|
|
|
Chapter I
Why This Study Is Needed
The rising number of uninsured individuals in the United States is an issue of increasing concern to policymakers at the federal, state, and local levels. The Institute of Medicine (IOM) has issued a series of reports detailing the effects of uninsurance on individuals, families, communities, and society. These include poorer health, reduced quality of life, lower worker productivity, and the broader societal burden of financing uncompensated care (IOM 2003).
Fueled by private foundations and the federal government, state and local policymakers have developed a wide variety of programs designed to expand coverage for the uninsured. These programs have met with varying degrees of success with respect to enrolling their target population, but the program features that determine enrollment success are not well understood.
Researchers generally agree that substantial subsidies are needed to induce the uninsured to take-up coverage, since low- to middle-income individuals targeted by these programs cannot afford private insurance premiums. However, program experience demonstrates that large subsidies may be insufficient if other program features are unattractive. Policymakers seeking to provide coverage to uninsured adults will find little guidance in the literature regarding the enrollment impact of nonprice program features such as benefit design and the ease of the application process.
Mathematica Policy Research conducted this study for the U.S. Department of Health and Human Services to address this gap, focusing on the role of nonprice design and implementation features in determining enrollment. Nonprice program features include outreach methods used to create awareness, the simplicity or complexity of program eligibility rules and the structure of the premium subsidy, the attractiveness of the benefits and the provider network, and the ease or difficulty of the application process. To the best of our knowledge, this is the first study to focus exclusively on the nonprice design features that affect take-up of subsidized coverage by nonelderly adults.
Study Approach
This study was conducted in two phases. Phase 1 was a literature review of the current state of knowledge on the impact of nonprice design features on enrollment. Information gathered from this literature was used to inform Phase 2—discussions with 67 program directors and other key informants from subsidized coverage programs across the country including in-depth discussions around 17 programs. (A complete list of the study participants and their affiliation is available in the acknowledgements section; Appendix A contains a full description of our study methods.)
This study makes use of a framework or logic model to structure the analysis. It postulates that enrollment is the result of three, sequential steps:
- The target audience for a program is aware of the initiative.
- Once aware, the target audience comprehends the information that they receive about the program.
- Their understanding of the program leads the target audience to find the program appealing at the price at which it is offered. This step is defined broadly to encompass the appeal of all features of the program. For example, not only must the coverage have appeal, but also the applicant cannot find the enrollment process too difficult or onerous.
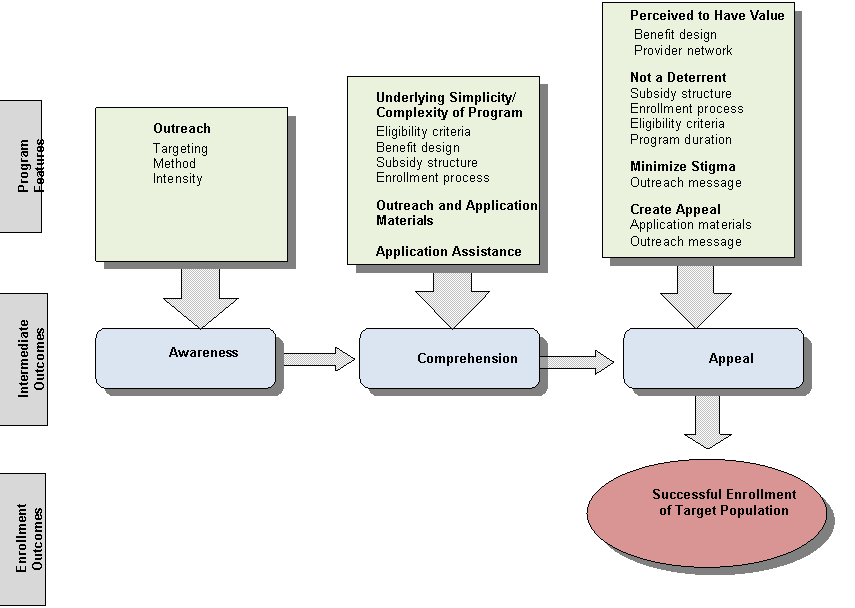
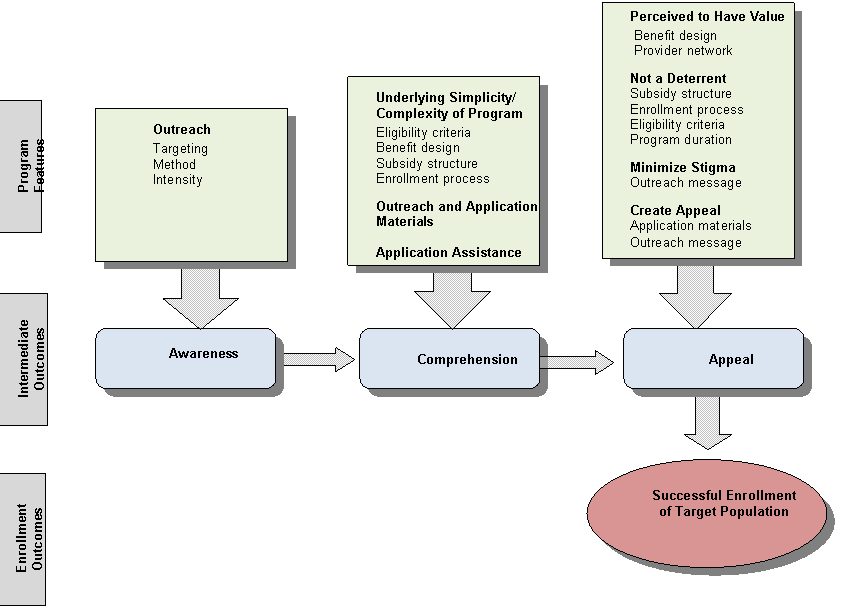
In the literature review and in discussions with stakeholders, we examined how the program’s design and implementation features influenced enrollment via these three intermediate outcomes of awareness, comprehension and appeal. For example, we explored how the feature “outreach methods” created awareness that ultimately led to enrollment in the program. Figure I.1 depicts this logic model.
Programs Included in the Study
Recognizing that there has been significant work on the determinants of children’s enrollment, this study focuses on voluntary state and local programs that subsidize coverage or care for nonelderly adults. Specifically, we examine the determinants of enrollment within four broad coverage approaches:
- Brokered Access to Subsidized Care. Programs that offer access to subsidized medical services but are not true health coverage. These programs use safety net providers but also coordinate care in some way (such as the creation of a “medical home”) and include the concept of membership or enrollment.
- Subsidized, Nongroup Coverage for Adults. Programs that subsidize nongroup coverage purchased directly by adults.
- Premium Subsidies for Workers. Programs that subsidize just the worker’s share of the premium for employer-based coverage. Typically, the worker must have an offer of coverage from their employer and the employer’s share is not subsidized.
- Premium Subsidies for Employers and Workers. Programs that subsidize both the employer and worker’s premium shares for group coverage.
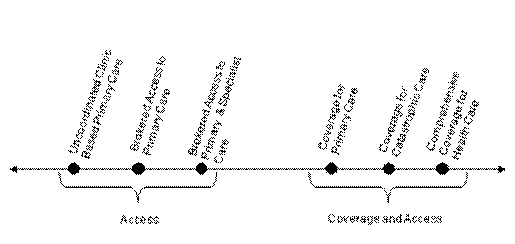
Not all programs reviewed for this report fall cleanly into one of these four types. For example, Access Health in Muskegon, Michigan closely resembles health insurance coverage, but it is not a licensed insurance product. Conversely, there are some products which have very limited benefits yet are licensed insurance products. In general, the variety of subsidized health coverage/care programs around the country can be thought of as a continuum, with uncoordinated safety-net care on one end, and comprehensive health coverage on the other. Somewhere in the middle are programs that broker access to subsidized care, comprehensive products that are not insurance (like Access Health), and some insurance programs that feature a very limited set of benefits (Figure I.1).
Figure I.1. A Continuum of Health Care and Health Coverage Options
Report Structure and Preview of Findings
To make the study findings more useful to policymakers, we first present findings for each of the four program types. Chapters II through V, respectively, describe how nonprice program features appear to affect enrollment in brokered access programs, subsidized nongroup insurance programs, programs that subsidize worker premiums, and programs that subsidize premiums for both employer and workers. In each chapter, findings are organized around the three key factors that trigger enrollment: awareness, comprehension and appeal.
Chapter VI synthesizes key findings across the four program types, noting the remaining gaps in understanding how program features may affect enrollment. As an aid to the reader, we preview those key findings here:
Successful Strategies Common to All Programs
- Using outreach to create awareness is critical, even for very appealing programs.
- Outreach will be most effective if done by a “trusted source.” When information is received from a trusted source, the information has more credibility and the potential enrollee is more likely to act on the information. The appropriate trusted source varies by community and coverage approach.
- By comparison, marketing through mass media is not effective when used alone. Media can be useful if it reinforces the information learned from the trusted source.
- Word-of-mouth can have a powerful effect on enrollment, either positive or negative. To facilitate positive word-of-mouth, programs should ensure that accurate and complete information about the program is in circulation, particularly with respect to eligibility information. Program designers should also manage expectations and use a phase-in enrollment strategy so they can fine-tune as needed.
- One-on-one application assistance and insurance counseling was critical for all programs. Discussants noted pervasive comprehension gaps among applicants, particularly with respect to insurance concepts and program income eligibility criteria. Simply ensuring that materials were written at a lower reading level and in languages other than English was insufficient to overcome the comprehension issues.
- Discussants believed stigma was a real phenomenon with the potential to deter enrollment. However, stigma can be readily minimized by making the program resemble commercial coverage (for example, by having insurance cards), operating the program out of offices that are not associated with welfare or Medicaid, and other methods.
Findings Specific to the Coverage Approach
- As described in Chapter V, gaining small-firm participation in programs that subsidize premiums for employers as well as workers is very difficult. Program designers must make their program very appealing to both firm owners and brokers and must use brokers to help market the product.
- In contrast, programs that provide coverage directly to adults, brokered access to care, and subsidized nongroup coverage for adults can attract enrollment even if they have unappealing benefit structures and cumbersome application processes. It is critical, however, that these programs create awareness and provide application assistance coupled with insurance counseling as described above (see Chapters II and III).
- Programs that provide premium subsidies for workers face unique enrollment challenges. As described in Chapter IV, targeting outreach to the eligible population is difficult. Program eligibility criteria are often very complex and difficult to convey. Two successful strategies identified by discussants included using brokers for outreach and creating less restrictive enrollment periods.
It is our hope that this report will aid policymakers considering different coverage approaches. We remind readers that the study is essentially qualitative. It relies on our discussions with program officials and other key stakeholders as well as a review of studies that are also qualitative (making use of focus group data, program reports, and occasionally enrollee surveys). While study authors and program officials believe that these design features may encourage enrollment, we are unable to establish positive causation. Rigorous, cross-program comparisons have not been conducted, and the observations that follow may derive from just one study or program.
Figure I.2. Nonprice Factors Affecting Enrollment Into Subsidized Health Coverage or Care Programs
Chapter II
Brokered Access to Subsidized Care
For reasons that range from insufficient funding to difficulties building political support, not all communities are able to offer subsidized health coverage to their uninsured residents. As a compromise, some communities have instituted programs that attempt to rationalize the care delivered through the safety net system.1 These programs generally involve membership or enrollment and the use of safety net providers within a managed care model. Consistent with earlier research, we call these “brokered access” programs (Taylor et al. 2006).
This chapter presents findings from discussions with individuals associated with three brokered access to care programs: Ingham Health Plan in Michigan (specifically Plan B), Healthy San Francisco in California, and Health Advantage in Indiana.2,3 Each of these programs has unique characteristics and serves a distinct population (see Appendix B). The discussants’ insights often reflected differences across the three programs, particularly with regard to specific strategies to address the needs of their enrollees.
Our findings also suggest some common experiences among brokered access to care programs in each area (awareness, comprehension, and appeal). Program designers and policy makers who seek more general, overarching information on factors affecting enrollment in brokered access to care programs may find these “lessons learned” in common of particular interest.
Program Background and Enrollment Experience to Date
Brokered access to care programs seek to reduce uncompensated care and to replace the use of expensive inpatient and emergency department care with primary care (Taylor et al. 2006). Several studies have found that these programs are successful in their objectives and have saved their communities money (Silow-Carroll 2001).
Brokered access programs do not provide insurance (although their members may not be aware of the distinction). Because they do not involve insurance, these programs are able to avoid state insurance regulations, minimum reserve requirements, and reporting requirements—and consequently may be easier to implement. This model also allows the community to continue receiving federal and state funds to support charity care, which can be critical for the programs’ viability (Katz 2008).
Programs that provide brokered access to care are as varied as the communities that sponsor them. Some common activities undertaken by managed safety net providers include efforts to better coordinate care by centralizing some administrative functions, and introducing managed care elements, such as primary care case management or medical homes. These programs may be administered through a local department of health, such as Healthy San Francisco, or by a provider, such as in Bexar County, Texas, where the University Hospital System runs Care Link. Their hallmark is that they coordinate care for patients, although, as indicated in Figure I.1 (Chapter 1) they may vary in whether they provide access to primary or specialty services.
Enrollment in some of these programs is quite large, and in some cases accounts for a large percentage of the uninsured population (Table II.1). For example, Health Advantage served more than 52,000 enrollees in 2008. In 2002, Ingham Health Plan accounted for an estimated 50 percent of the county’s uninsured population (Mack et al. 2006); Ingham Health Plan representatives indicated that the actual percentage may have been (and currently is) higher.
| Program | Eligibility Criteria | Enrollment
|
|---|---|---|
| Source: Appendix B. SMaximum allowed at current funding levels. Maximum allowed at current funding levels. Former enrollees in the state medical plan are also eligible. | ||
| CareLink (1997), | Uninsured county residents, without access to public coverage, with incomes below 300% of the FPL | 50,000 to 55,000a |
| Care Partners (2001), | Uninsured county residents with incomes up to 175% of FPL | 1,000b |
| Health Advantage (1997), | Uninsured county residents who do not qualify for other government assistance, with incomes up to 200% of FPL | Over 52,000 |
| Healthy San Francisco (2007), | Uninsured city residents, without access to public coverage, with incomes below 300% of FPL (regardless of employment or immigration status or pre-existing conditions) | 24,868 |
| Ingham Health Plan (1998), | Uninsured county residents, without access to public coverage, with incomes below 250% FPL, (regardless of immigration status)c | 17,000 |
Key Findings
Many people who enroll in brokered access to subsidized care programs have immediate medical needs requiring attention, and encouraging people to enroll before a medical need arises is a challenge for these programs.4 Discussants believed that some factors may help attract early enrollment:
- Common reasons for enrollment in brokered access to care programs are the affordability, accessibility, and convenience of these programs. Those who enroll in brokered access to care programs have very limited, if any, alternative ways to access health care services.
- Discussants emphasized the attraction of being part of a structured, organized system of care as a key factor attracting enrollment. Enrollees appreciate having a medical home, continuity of care, and help in navigating the health care system.
- Enrollees’ lack of comprehension of the features of brokered access to care programs was a pervasive concern. Programs adopt various strategies to address language or cultural barriers to understanding health care concepts (for example, co-pays, specialty versus primary care services).
- Discussants reported that having a medical ID card is appealing to enrollees, as it lends the program the feel of traditional insurance. However, having a membership card may also create a degree of confusion, as it leads some enrollees to believe brokered access to care programs is equivalent to health insurance.
- Prescription drug coverage is a very attractive feature that discussants believe attracts enrollment.
- The enrollment process was facilitated through use of enrollment counselors, preparation of enrollees so they know what to expect when the process begins, providing multiple points of entry to the program (for example, at clinical sites, neighborhood centers, etcetera), and the use of electronic enrollment systems.
- There was no consensus on whether cost sharing has a positive or negative effect on enrollment. For instance, one discussant noted that co-pays and premiums can be deterrents, but can also help convince enrollees of the worth of the care they are receiving.
- Discussants report little use of formal marketing campaigns. Outreach to enhance enrollment in brokered access to care programs depends heavily on community relationships and partnerships. Discussants emphasized the importance of grassroots, community-level outreach to enroll hard-to-reach individuals.
- Stigma was not a common concern in brokered access to care programs. In one program, stigma was mentioned as an initial barrier to enrollment, but it decreased over time as the program grew in size and popularity.
Program Awareness
Several discussants confirmed a finding in the literature that brokered access to care programs often conduct very limited marketing (Silow-Carroll 2001). Small program budgets and high demand for services commonly forced the programs to strike a balance between making qualified enrollees aware of the program and being inundated with applicants, some of whom already have health insurance.
Indeed, multiple discussants reported that formal marketing campaigns could have hurt, rather than helped, their programs. One discussant noted the importance of a slow phase-in to avoid having to turn people away, which might have deterred future applicants. Several other discussants noted that they shied away from a formal marketing campaign because they did not want their program to appear more attractive than other coverage programs.
Despite concerns about aggressive marketing, most of our discussants reported conducting active outreach at a more grassroots level. All worked with other community-based organizations to spread awareness. They reported community partnerships and face-to-face contact with potential enrollees as particularly effective in enrolling more hard-to-reach, vulnerable populations. As one discussant noted:
I would say we are pervasively present in the community and in the minds of individuals who work in the social service fields…. Someone will be aware of what is available and will be able to help you. But this has all happened over time and is not related to one marketing campaign.
Discussions with one program, the Ingham Health Plan revealed the importance of navigators—community members who go door-to-door to spread awareness and increase enrollment among hard-to-reach populations. Navigators offer advice and resources on many types of social services, including but not limited to the health care program. This particular program has used navigators employed by a local neighborhood networking center in five annual neighborhood door-to-door sweeps. In the warm months, they may knock on as many as 1,200 doors. Crucially, navigators are empowered to enroll people in Ingham Health Plan on their doorsteps using PDAs or paper applications. Because navigators are familiar faces in the communities, they “connect better with their neighborhood than [a conventional plan representative] would.”
Using PDAs or paper applications, navigators have the ability to take the applicant’s information on the spot, enabling them to convert awareness directly into enrollment and avoid the pitfalls of a multi-step enrollment process (Mack et al. 2006)5. Ingham Health Plan’s campaign resulted in a significant increase in enrollment during the program’s early years.
Discussants from Health Advantage and Healthy San Francisco also indicated that community outreach and partnerships are effective ways to contact hard-to-reach populations. Health Advantage shares materials at ethnic fairs, health fairs, and neighborhood association meetings. Its online application process (Ind-e-App) allows outreach workers to enroll people anywhere with an internet connection, including “soup kitchens, halfway houses, post-incarceration houses, and shelters.” Similarly, Healthy San Francisco program leaders talk to “every type of [community] group possible,” offering information about the program to San Francisco’s “tight-knit” interconnected social service programs.
Community outreach can be successfully augmented by referrals from the local emergency room. Discussants noted that a local public hospital emergency room contacts Health Advantage if a patient presents frequently for routine primary care. Health Advantage contacts these patients to invite them to enroll in the program. In addition, financial advisors in the local public hospital present Health Advantage as an option to patients seeking care.6
Finally, many discussants cited word-of-mouth as an important factor in developing awareness and enrollment, especially in communities with many new immigrants. Some expressed concern about whether information conveyed by word-of-mouth is accurate and conveys the program in a positive light.
Program Comprehension
Discussants reported widespread comprehension difficulties among their applicants and enrollees. In some cases these comprehension difficulties reflected language or cultural barriers; in other cases a lack of familiarity with insurance concepts.7
Discussants shared many strategies for assisting for non-native English speakers. For instance, Ingham Health Plan publishes its program materials in Spanish, reflecting the prevalence of this language in the community it serves. In addition, Ingham employs Spanish speakers on its outreach team and works with a clinic that targets the Spanish-speaking population.
Healthy San Francisco addresses language barriers in its community by printing all brochures in English, Spanish and Chinese, and enrollment counselors speak Spanish, Cantonese, Vietnamese, and Mandarin. The program operates an information hotline: by dialing 311, a caller can be automatically transferred to a language system to speak one’s native language. The program also makes an effort to connect each enrollee to a medical home with providers who speak the enrollee’s language.
Despite these programs’ efforts to eliminate language barriers, several discussants reported that comprehension issues were still a matter of concern. Cultural differences go beyond language differences and may affect enrollment. For example, applicants who do not have a tradition of insurance coverage in their birth-country may have difficulty with the concept. As one discussant stated:
Speaking to a culture is an issue. Unless we can have people who are experts in all cultures, it is hard to make sure a person fully understands the program.
Finally, several discussants noted that enrollees are often unfamiliar with concepts such as co-pays, premiums, and having a medical home as their point of access to services. Moreover, it is unclear whether enrollees understand that brokered access to subsidized care is not equivalent to traditional health insurance coverage.8 Discussants commented that the effect of comprehension difficulties on enrollment is difficult to assess. However, it is important to note that these areas of potential confusion may affect enrollees’ experiences in brokered access to subsidized care programs.
Program Appeal
The major appeal of brokered access to subsidized care programs is rooted in their promise of affordable care for individuals with few, if any, other options for health coverage or health care. While some specific aspects of brokered access programs may affect their appeal, the negative features of these programs were not viewed as major deterrents to enrollment.
Benefit Design/Provider Network
Discussants noted that perceived inadequacies with respect to benefits or providers did not deter enrollment. While discussants from all three programs reported some complaints from enrollees about lack of certain types of coverage, such as dental, discussants added that there is a strong appeal to having even basic coverage. However, several discussants reported having some prescription drug coverage as a major selling point for enrollees, who recognize that brokered access programs provide benefits above and beyond typical services offered by free clinics. As one discussant stated:
In the past, [enrollees] have always been able to get cheap or free primary care at clinics, but [if] by enrolling…[they] also get pharmaceutical benefits, [then] the program saves them money.
It was less clear whether assignment of a provider (versus allowing enrollees to choose their provider) affects enrollment. Discussants in one program believed that assigning enrollees to a specific provider helped to eliminate access barriers. In contrast, discussants in another program reported that offering enrollees a choice of providers was a popular feature. These differences of opinion may reflect the different populations that brokered access programs serve. Some programs serve populations that may have established relationships with providers and wish to maintain these relationships. Others work with populations who may have no established provider and find it difficult to find one—so that assignment to a provider would be viewed as a valuable service.
Several discussants acknowledged that lack of access to providers could be an issue for enrollees, although this did not appear to deter enrollment. For example, in one program access to specialty care is limited due to specialists’ concerns that the program does not cover inpatient care. Many specialists refuse to treat patients in this program, rather than confront the moral and financial quandary that would arise if their patient would need inpatient care.
Discussants mentioned several aspects of their programs’ benefit design and provider networks that might attract enrollment—prominently including dental care. However, some discussants stressed that their program’s mission was not to provide comprehensive benefits. Rather, it is to be a last resort for the uninsured. As one discussant stated:
Some people want us to pay for Viagra, implants, surgery…but there has to be a limit as to what the government pays for.
Some were concerned that brokered access programs not be more attractive than Medicaid, so that individuals would not drop their current coverage to enroll in this program.
All three programs included modest cost-sharing at point of service. Discussants’ views on whether co-pays enhance or deter enrollment were mixed. Some discussants felt that cost-sharing is prohibitively expensive for low-income enrollees. Others felt that cost-sharing allowed enrollees to believe they are receiving higher-quality care because it is not free. For instance, one discussant stated:
There is appeal to the co-pays. We hear story after story of people who didn’t pay their co-pay and then will come back the next day and pay us.
However, another discussant in the same program stated:
Some people think that because they have zero income, how can they pay a co-pay?
Other discussants clearly saw both sides of the issue and were undecided. For instance, one discussant stated that co-pays (and premiums) could act as deterrents. However, she added:
On the other hand, if people feel like something is free, people don’t feel like they are receiving the best care, so in a way, maybe it would be bad to take away the co-pay.
While discussants did not provide consensus on this issue, several discussants agreed that clinic and program staff were more resistant to charging co-pays than enrollees were in paying them. As one discussant noted:
Clinics complained that their clients were too poor and that now the clinics might be targets for crime [since there would be money on site]. But once we made the collection mandatory, the clinics’ complaints subsided.
Premium Subsidy Structure
Few brokered access programs charge premiums (or their near equivalent, enrollment or participation fees). Only one of the three study programs charged a sliding–scale participation fee that varied with income.9 For the same reasons as those given above for point-of-service cost-sharing, discussants’ views on whether premiums enhance or deter enrollment were mixed. Our literature review revealed a similar ambiguity. Several studies note that charging even minor enrollment fees deters enrollment for some populations, yet may attract other enrollees because it makes the coverage seem less like a hand-out (Mack et al. 2006; Minyard et al. 2007).
Enrollment Process/Eligibility Criteria
Discussants were unable to attribute enrollment trends directly to the ease or difficulty of the enrollment process. However, they pointed to several program practices that they believed greatly eased the enrollment process: (1) providing assistance, such as enrollment counselors, to guide enrollees through the process; (2) preparing enrollees beforehand so they know what to expect during the enrollment process; (3) providing multiple points of entry into the program; and (4) using electronic enrollment whenever possible.10
Discussants from all three brokered access programs reported the value of employing enrollment counselors and others to assist with the enrollment process. Such assistance helps to overcome comprehension barriers. In addition to answering questions, checking documentation, and guiding enrollees through the application process, enrollment counselors are able to solve problems that could otherwise impede enrollment. For instance, one discussant reported:
We make it easy. If a patient comes in and hasn’t worked for two years and is homeless, then we can use verification from a shelter and fast-track the application easily…. As a counselor, you don’t want to ask for too much information because then people won’t want to apply.
If the application system is linked to other social welfare programs, enrollment counselors are able to enroll eligible individuals (and other eligible family members) in multiple programs. Enrollment counselors also play an important role in ensuring that applications are complete, speeding enrollment of applicants who otherwise might be delayed by an incomplete application. A discussant from Healthy San Francisco explained that 98 percent of unassisted applications were incomplete.
Discussants also emphasized the importance of preparing enrollees for the process before they attempt to enroll. This included communicating information about the forms of documentation needed, where the enrollee must go to complete an application, and how much time the process would take. As one discussant stated:
I would find it intrusive and strange if I were asked all these questions and needed to show these documents. So we want to prepare people. It doesn’t mean that people don’t forget to bring these documents, but we do what we can to make the process go faster.
Several discussants observed that providing multiple points of entry into the program facilitated enrollment. For example, the Ingham Health Plan’s navigators can enroll eligible individuals on their doorsteps using PDA’s, but people can also enroll at neighborhood centers, primary care sites, or via telephone. Health Advantage uses the Ind-e-App system for enrollment, screening for multiple programs so that individuals seeking other services may discover they also are eligible for Health Advantage (or vice versa).11 Primary care sites also use Ind-e-App and can enroll patients on-site. Finally, Healthy San Francisco allows enrollment at primary care sites, San Francisco General Hospital, and a centralized enrollment unit at the Department of Public Health.
Finally, discussants mentioned that electronic application systems can be of significant value in helping eligible individuals and families to access needed services. Electronic applications are immediately transferable to other social service agencies (with enrollees’ knowledge and permission). Finally, programs can use the electronic information provided by applicants to identify neighborhoods that they may not be reaching.
Stigma
In one of the three brokered access programs in this study, discussants uniformly acknowledged that stigma could be a barrier to enrollment but generally downplayed its potential effects. One discussant reported the program is occasionally associated with welfare, which “affects enrollment a little bit.” Another discussant stated the program faced stigma primarily in the first few years of existence, but this perception seems to have decreased with time, as enrollment has increased. A third discussant noted that “overcoming stigma is difficult” but was unclear about how big a factor stigma was in deterring enrollment into the program. With respect to the other programs, discussants stated they had encountered no perceptions of stigma.
Recognizing the potential for stigma, discussants listed several ways that the programs had attempted to avoid or to counter stigma, including:
- Asking for “contributions” or co-pays so that the program “does not seem like Medicaid”
- Using membership cards, which lend the program an air of a traditional coverage program—although it may also lead enrollees to confuse the program with insurance coverage
- Reducing barriers to entry—for instance, making the enrollment process more streamlined and asking for information just once per year, distancing the program from traditional social welfare programs
Program Permanence
While program officials may be concerned about the permanence of their programs due to funding issues, eligible individuals may react to a perception of impermanence by enrolling sooner. For example, discussants reported that during the pilot phase of Healthy San Francisco, “people thought they better sign up now because they don’t know how long the program will last.” However, this sense of urgency has since passed. In contrast, one discussant believed that people would be hesitant to enroll in a short-term program, and that program permanence was important for enrollment.
Chapter III
Subsidized Nongroup Coverage for Adults
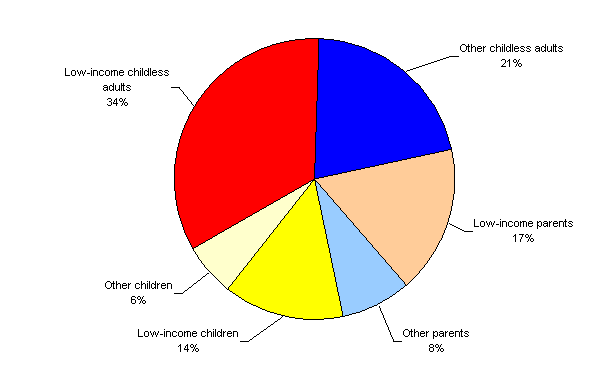
In most states, traditional public coverage options for adults, particularly childless adults, are more limited than those for children.12 Additionally, many lower-income adults do not have access to coverage from an employer. These nonelderly adults (ages 19–64) are thus more likely to be uninsured than children or the elderly. Nationally, uninsured adults account for 80 percent of the uninsured population under age 65 (Figure III.1). Among adults, uninsured adults without dependent children at home are twice as prevalent as uninsured adults with dependent children at home.
In response to high uninsured rates among low-income adults, states and communities have implemented various subsidized coverage approaches that target them directly, with no employer involvement. Demand for this type of coverage is high, and these programs tend to fill their available slots quickly.
This chapter focuses on subsidized nongroup coverage programs for adults. In addition to reviewing the literature, we spoke to program directors and other discussants in five programs: adultBasic in Pennsylvania; Alliance Family Care in Alameda County, California; the Family Health Insurance Assistance Program (FHIAP) in Oregon, the individual plan component of Insure Oklahoma; and Utah’s Primary Care Network (PCN).13,14 Despite sharing a common purpose, each of these programs has unique characteristics, serves a somewhat different community, and has developed specific strategies to meet their enrollees’ needs. Below, we summarize the lessons learned on outreach techniques and program features that efficiently attract enrollment.
Figure III.1. Distribution of the Nonelderly Uninsured, by Age and Income, 2006
Note: “Low-income” refers to uninsured persons with family incomes below 200 percent of FPL.
Program Background
At least 22 states offer subsidized nongroup coverage to low-income adults with incomes above the federal poverty level (FPL), although only 18 states also make that coverage available to adults without dependent children at home (Table III.1). Almost a third of the uninsured population are adults above 200 percent of FPL (Figure III.1) but, as the table indicates, very few states have subsidized, nongroup coverage options for this group. While many states offer subsidized coverage to nonelderly, nondisabled, nonpregnant adults with very low incomes, this chapter focuses on coverage programs that are offered to childless adults as well as parents and that include options for uninsured adults above FPL.
| Offer to at Least Some Adults in the Indicated Income Range (income as a percent of FPL) | Adults with Dependent Children | Other Adults |
|---|---|---|
| 100%–200% | 22 | 18 |
| 200%–300% | 4 | 3 |
| Notes: Includes six programs that have closed enrollment. Includes programs that provide coverage directly (such as RiteCare) as well as those that provide premium subsidies for nongroup coverage (such as Oregon’s FHIAP). Source: Klein and Schwartz 2008; Kaiser State Health Facts (Income Eligibility for Parents Applying for Medicaid by Annual Income as a Percent of federal poverty level (FPL), 2008, accessed 11/12/2008); and Appendix B. | ||
Many of the programs offering coverage to adults (including childless adults) operate under Medicaid or State Children’s Health Insurance Program (SCHIP) waivers, which may involve complex eligibility requirements. For example, Utah’s PCN operates under a Medicaid 1115 waiver. Eligibility for the program is restricted to uninsured legal residents without access to other forms of public coverage or affordable employer coverage. In addition, the program may not enroll more than a certain ratio of childless enrollees to parent enrollees, sometimes leading the program to have open enrollment only for parents.15
Various federal provisions governing the Medicaid and SCHIP programs as well as limits on state sources of funding often force these programs to cap enrollment so as not to exceed available funds.16 Table III.2 shows selected features for selected programs, most with capped enrollment, that subsidize coverage for adults.
The combination of high-demand, affordable premiums and capped enrollment means that these programs tend to fill their available slots quickly (see Appendix B). 17 On the other hand, slots can fill more slowly than expected in subsidized programs with higher premiums, such as Healthy New York (Kilbreth 2006).
| Program Name | Maximum | Monthly Premium Share After Subsidy | Enrolled as Individuals or Sole Proprietorsa | Is Program Enrollment Capped? | No. of Individuals or Sole Proprietors on Waiting List |
|---|---|---|---|---|---|
| State- or Locality-Funded Only | |||||
| adultBasic Pennsylvania | 200% | $35 | 53,534 | Yes | 95,649 |
| Alliance Family Careb Alameda County, CA
| 300% | $20–$120 | 7,300 | Yes | 2,500 |
| DirigoChoice Maine
| 300%c | Sliding-scale subsidies | 10,700 | Yesd | e |
| Healthy New York New York | 250% | $230 (average) | 101,795 | No | n.a. |
| Medicaid- or SCHIP-Funded | |||||
| Family Health Insurance Assistance Program (FHIAP) Oregon
| 185% | Sliding-scale subsidies | 10,680 | Yes | 25,000 |
| Family Health Plus New York
| 100% / 150% (childless/ parents) | $0 | 509,091 | No | n.a. |
| Insure Oklahoma—individual plan
| 200% | $0–$69 | 2,923 | No | n.a. |
| New Mexico State Coverage Insurance
| 200% | $0–$110 | 3,000 | No | n.a. |
| Primary Care Network Utah
| 150% | $50 annual enrollment fee | 20,120 | Yes | n.a. |
| Source: See Appendix B a Several of these programs, such as DirigoChoice, also allow small employers to participate, but small employer enrollment is not included in this table. See Chapter V for a discussion of this group. Enrollment does include unsubsidized nongroup enrollees, where such enrollment is permitted. b Program operated from 2001 to 2005; enrollment is as of 2003. c Families at all income levels may enroll in DirigoChoice, but those with incomes higher than 300 percent FPL are not eligible for a premium subsidy. Most DirigoChoice individual enrollees are eligible for the highest subsidy level. d Individual (nongroup) enrollment in DirigoChoice was capped during 2005, the program’s first year of operation. The cap was lifted in 2006 and then reinstituted in 2007 when individual enrollment constituted 50 percent of the DirigoChoice member mix. e Wait list size not found. n.a. = not applicable. | |||||
Key Findings
Many programs that subsidize nongroup coverage for nonelderly adults charge no premiums or very low premiums. Very affordable premiums—along with high need among the target population—may overcome some unappealing program features (for example, lengthy applications) that might otherwise deter enrollment. However, the presence of enrollment caps in many of the programs also suggests that a broader test of enrollment strategies has yet to be conducted. Indeed, several stakeholders acknowledged that they were unsure who might comprise a “hard-to-reach” segment of their target population.
Program directors and other discussants offered valuable lessons on efficient outreach techniques and program features that attract enrollment:
- Affordability and the absence of other coverage options are the most important reasons that adults enroll in this type of subsidized coverage program. All discussants believed that their target populations were widely aware of the need for coverage and felt anxious about how vulnerable they were without coverage. They disputed the common perception that uninsured adults are primarily “young invincibles” who are difficult to enroll.
- Creating awareness of the product is important. No matter how attractive the program is, eligible adults cannot apply if they are not aware of it.
- Fostering partnerships with trusted community representatives (with support from program outreach coordinators) is effective in creating awareness that leads to enrollment. On the other hand, mass media, while effective, may not be necessary for programs with limited enrollment slots.
- States and communities have identified diverse ways to target outreach successfully, reflecting important differences in the populations they are trying to reach.
- Applicants need multiple points of access to the program because of differences in Internet access, need for assistance in completing an application, and concerns about stigma.
- Despite efforts to simplify the application process, many applicants need assistance in completing an application. Some need help learning how to access services or understand insurance concepts. Programs should be prepared to furnish that substantial assistance and can work with community partners to create more options for assistance.
- Many program features that were characterized as “unappealing” by discussants (e.g., limited benefits, a complex application, welfare stigma, a required face-to-face interview) did not discourage people from enrolling when premiums are very low.
The research literature, while limited, supports these lessons offered by discussants but offers one important addition: when adult coverage programs feature higher premiums, program designers must pay more rigorous attention to the outreach and implementation features that attract enrollment. For example, Healthy New York (featuring substantial but subsidized premiums) only enrolled about 15,000 individuals and sole proprietors in the first two years despite a media campaign, a website, a 1-800 number, and some informal outreach to community groups (Lewin 2003). In contrast, New York’s heavily subsidized Family Health Plus program enrolled 400,000 (half of the eligible population) after two years of operation. As discussed below, Healthy New York took a number of steps to boost enrollment in subsequent years.
Program directors agreed that they were not armed with sufficient information to predict the demand for their program and were often surprised by (and in some cases unprepared for) the high number of applications. To help increase understanding of program features that attract enrollment, we offer our detailed findings below.
Program Awareness
All discussants believed that outreach was necessary to enroll adults in nongroup coverage programs. Certain outreach approaches (such as local media and grassroots outreach to trusted community partners) appeared to be more effective than others.
While demand was uniformly high for subsidized coverage programs that targeted adults, this demand translated into enrollment only if the target population was aware of the program. For example, the individual plan component of Insure Oklahoma had not been widely promoted and had fairly low initial enrollment (approximately 3,000 after 18 months). In contrast, Utah’s PCN, which features more limited benefits and a lower threshold for income eligibility, did carry out a significant outreach effort and enrolled 3,000 adults in two months. PCN reached its enrollment cap of approximately 18,000 adults after a year of operation.18
Research done in connection with the SCHIP evaluation effort (Appendix C) distinguished between general awareness and awareness that results in enrollment. Discussants identified local media and grassroots outreach to trusted community partners as particularly effective in creating the kind of awareness that leads to enrollment. These trusted community partners could be local health clinics, advocates working in the community, or informal leaders in an ethnic neighborhood.
Discussants cautioned that it takes work to partner with community organizations effectively. In one program, poor information about income eligibility requirements led to negative feelings among community advocates during the program’s early years. Several states made “mini-grants” available to encourage local community organizations to promote the programs. One discussant characterized the attributes that lead the community to trust the local clinic:
At our clinics, most of the staff are from the community. They are bilingual and ethnically similar to the patient. The clinics also don’t have government names.
Discussants believed that hearing about the program from multiple sources creates awareness that is more likely to lead to enrollment (e.g., hearing about the program on local radio as well as from people at the barber shop).19 As one discussant noted:
It takes a couple of touches. He needs to see the product a few times and hear about it from a few different people, and then the light bulb will finally go on.
Most discussants told us that word-of-mouth was the most effective means of creating awareness that leads to enrollment. Word-of-mouth is typically a personal referral from a trusted source who shares similarities with the listener (for example, ethnically similar, in the same neighborhood, with a similar job or economic circumstances). Program designers can promote word-of-mouth by tailoring outreach messages and materials to ensure that accurate information about the program is circulated. Conversely, word-of-mouth can deter enrollment if negative information about the program begins to spread. One discussant noted that surmounting poor public perceptions of a program was much more difficult than properly managing public expectations in the first place.
A few discussants speculated on how word-of-mouth leads to enrollment. Several suggested that the importance of word-of-mouth outreach may vary depending on the strength of community social ties. For example, word-of-mouth was believed to have worked very effectively in a tight-knit Russian immigrant community. Another discussant speculated that young African American men were hard to enroll because their communities lacked mutual trust and a tendency to share information.20
States and communities have identified many ways to target outreach with apparent success. Several programs target adults with a family member who is already enrolled in coverage (typically a Medicaid or SCHIP child). If there is good coordination between the Medicaid/SCHIP agencies and the program serving adults, eligible parents can be efficiently targeted for mailings or when their children receive services. In some cases, the potential enrollee may have already visited the enrollment location for other reasons. For example, the enrollment location may serve as an entry point for social services already being used by the potential enrollee (food stamps, etc). In some programs, clinics can enroll uninsured patients when they come in for services. Discussants noted that providers (typically safety-net clinics but sometimes hospitals) are generally motivated to enroll patients if their reimbursement goes up.
While the research literature generally supports our discussants’ contention that outreach is effective and necessary, we found no studies that rigorously examined the effectiveness of alternative outreach methods in programs that offer subsidized nongroup coverage to adults. Nevertheless, the research literature suggests that some targeting approaches that discussants did not mention may be effective. These include providing information through school lunch forms (Rhode Island) or children’s SCHIP enrollment forms (New Jersey) and identifying eligible residents through state tax returns (New Jersey). Other approaches include using information for residents enrolled in government programs to identify eligible people, such as SCHIP in New Jersey or the Food Stamp Program in Wisconsin (Howell et al. 2002).
The literature suggests that the outreach may be more important for programs featuring higher premiums (Bowe 2005). For example, individual enrollment in Healthy New York was modest for the first two years of operation despite a media campaign, a website, a toll-free number, and informal outreach to community groups (Lewin Group 2003). Participating health plans viewed the state advertising campaign for Healthy New York as a key to increasing enrollment. In its third year, Healthy New York was able to significantly boost enrollment by stepping up its media campaign and increasing the amount of the reinsurance subsidy, effectively lowering the premium cost by 17 percent (Lewin Group 2003).
Program data from later years of Healthy New York suggest that outreach effectiveness may change over time. According to call logs, in the early years of program operation, callers were more likely to cite all types of outreach, including mass media, when asked how they heard about the program. In later years, “family and friends” were by far the most common method by which individuals and sole proprietors learned about the program (EP&P Consulting 2008).21
Program Comprehension
Discussants routinely noted that applicants have difficulty with certain aspects of the application process, particularly understanding eligibility criteria and the requirements for documenting income. In addition, many applicants are unfamiliar with certain insurance concepts and had difficulty understanding which services were covered or that referrals from primary care providers were needed to see a specialist.
Discussants characterized insurance counseling and application assistance as time-consuming but critical to the enrollment process.22 For example, discussants variously mentioned:
People don’t understand how insurance works…probably about 30 to 40 percent of our time is spent educating people about insurance.
Our agents spend more time trying to explain to people how insurance works than signing them up for coverage.
For a lot of these people, the idea of a checking account is foreign. We explain that they must pay their bills and pay the full amount listed on the bill, as opposed to just sending in what they can.
Besides application assistance, discussants described various program approaches designed to minimize comprehension issues, such as writing materials at the sixth-grade (or lower) reading level, preparing materials in diverse languages, and simplifying the enrollment application.
However, such efforts may be insufficient. Discussants from one program spoke of pervasive literacy issues. Many applicants to the programs were illiterate in their own, non-English native language. One small immigrant population had no written language:
I just saw a prescription that showed a moon with a taped pill and a sun with a different taped pill. This way, the patient was sure to take the correct medicine.
When literacy concerns are so pervasive, merely translating program documents into other languages may not overcome comprehension difficulties. Enrollment staff often must still read the materials aloud for the applicant and explain them. “The burden completely falls on the staff,” declared one discussant.
If a subsidized coverage program is modeled on coverage already being used by the target population, discussants reported that it was easier for applicants to understand the program features and how to apply. For example, Alliance Family Care was intentionally modeled on an existing, widely used coverage program for children, and discussants reported few concerns about the target population’s ability to understand the program. In contrast, Utah’s PCN is different from other subsidized coverage programs in the state. Utah conducted mandatory orientation sessions for PCN enrollees during which staff explained not only the PCN but also the other two Medicaid programs—traditional Medicaid and nontraditional Medicaid. The study notes that orientation staff had difficulty overcoming confusion among the program enrollees. Many enrollees had difficulty understanding the multiple programs, particularly if they had family members in more than one program (Oppenheimer et al. 2006).
Discussants agreed about the need for application assistance and the underlying literacy issues that contribute to that need. However, we were unable to find any studies that rigorously explored the comprehension difficulties facing low-income uninsured adults seeking coverage. Similarly, our discussants did not seem to have detailed information about the nature and cause of comprehension difficulties or possible solutions beyond one-on-one assistance. Existing program information systems did not appear to collect detailed information on applicants’ ability to comprehend program structure, eligibility, or the enrollment process.
Program Appeal
Discussants widely agreed that affordable coverage of any kind has tremendous appeal to uninsured adults without other coverage options. As one stakeholder put it, “Groups that never had access to ESI [employer-sponsored insurance] feel they have no options.”
Discussants felt that they understood the program features that appealed to applicants as well as the features that enrollees disliked, such as limited benefits or lengthy applications. Yet, they observed strong enrollment despite unappealing features, noting that the “lion’s share” of eligible adults are not deterred.
Benefit Design/Provider Network
Discussants noted, not surprisingly, that applicants desired comprehensive coverage with low, affordable cost-sharing. Nonetheless, even with significant benefit limitations, the programs still experienced strong enrollment.23 However, one discussant speculated that an unappealing provider network could deter enrollment.
Many discussants cited commercial coverage (or coverage that feels like commercial coverage) as very appealing. One discussant mentioned having an insurance card (specifically, from a commercial carrier) as very attractive.24
Discussants were careful to note that one feature common in nongroup private coverage, pre-existing condition exclusions, did not appeal to applicants. Instead, the absence of pre-existing condition exclusions (in four of the five programs) had tremendous appeal. As one discussant noted:
With private nongroup coverage, they get a quote but no coverage for like a year. With our program, they don’t have to wait.
Program officials in Alameda County’s Alliance Family Care noted that “oral health care is one of the things that draws families to the program” (W.K. Kellogg Foundation 2002). However, to address funding shortages, the oral health benefit was later dropped from the coverage package with no perceptible effect on enrollment. This may be because the program offered many other highly attractive features, including multilingual providers (or interpreters) and providers with evening office hours.
Premium Subsidy Structure
Four of the programs had very low premiums or no premiums at all. Consequently, the discussants had little evidence that particular subsidy structures either attracted or deterred enrollment (apart from the amount of the net premium).
When premiums are charged, a few studies suggest that the premium subsidy methods may affect enrollment. Maine’s DirigoChoice program sends premium subsidy amounts to an electronic benefits transfer (EBT) debit card supplied to the enrollee. Balances on the card can be used to make purchases at locations that accept the card or used for cash withdrawals at certain banks and credit unions. An early survey of individual and employee disenrollees from the DirigoChoice program after one year found a few respondents who specifically cited the reimbursement process in their decision to disenroll (Anderson and Bowe 2006). These former enrollees believed the EBT card to be a cumbersome means of reimbursing enrollees. The study cited one informant who considered the program but did not enroll because she associated this reimbursement method with welfare stigma. Oregon’s FHIAP uses another possible approach: billing nongroup participants for just their portion of the premium. The program then combines the enrollee’s portion with the state subsidy and pays the carrier.
The SCHIP literature (Appendix C) suggests that an annual premium payment option may prevent enrollees from becoming disenrolled due to nonpayment of a monthly premium (Ryan 2005). Monthly payments were perceived by some enrollees to be a burden and were administratively costly to the program. Utah’s PCN program collects their “enrollment fee” annually, but discussants did not report whether this frequency helped enrollment.
Enrollment Process/Eligibility Criteria
Many discussants readily admitted that certain elements of the application process were unappealing or difficult to complete, which can deter enrollment. Discussants were acutely aware of the extensive assistance needed to complete applications but generally lacked precise information about how many applications were never completed and for what reasons. The literature review includes many studies that acknowledge the appeal of a simple and nondemeaning enrollment process, but none link this feature directly to enrollment outcomes.
Invariably, discussants told us that applicants needed help completing the application process, even in cases where the application was characterized as “simple.” If the process had multiple steps, completion rates were especially low. A discussant referring to a program with multiple enrollment steps estimated that 50 percent of applicants who completed the initial application steps didn’t complete the last step (although this estimate may include applicants who were ultimately deemed ineligible). Discussants associated the need for enrollment assistance with comprehension difficulties (as described above) but also felt that applicants “don’t read what they are given.”
None of the programs had the information systems necessary to assess enrollment barriers in the application process. Many discussants told us that they didn’t know how many people requested applications but failed to complete the application process. Because these programs easily filled their available slots, they had little incentive to investigate why some applications were not completed.
Nonetheless, discussants and some of the literature did point to certain enrollment practices that may appeal to their target population:
- Provide multiple access points (Internet, phone, in person). Discussants noted that different methods appeal to different types of applicants, some of whom prefer the anonymity of an online or paper application and some of whom need the application assistance available by phone or in person.
- Keep the application as short and simple as possible and use “plain language.”
- Provide community-based enrollment counselors in minority communities where distrust of and miscommunication with the government and medical community are common (Friedsam et al. 2003).
- Make the enrollment process a one-step process (or as few steps as possible).
- Coordinate with other coverage programs to make coverage of the whole family part of a one-step enrollment process–even if family members are enrolling in different programs.
The Alliance Family Care program is an example of a program that included many of these features. Alliance Family Care coordinated with other social service agencies to create a “No Wrong Door” enrollment process in 2001. After this process began, approval rates increased from 59 percent to 83 percent, processing time decreased, and clients reported that they were more satisfied with the experience (Zahn et al. 2003). Under “No Wrong Door,” patients could enroll in the Alliance Family Care program at community health centers where they seek services as well as at other community sites. One discussant noted that community health centers serve as important outreach vehicles for the program because they are trusted by immigrant families who would normally be reluctant to enroll because of concerns about immigration status (Silow-Carroll 2001). Applicants also received one-on-one assistance to apply for coverage for everyone in the family, regardless of payer source.
Enrollment processes with multiple application steps are unappealing and may deter enrollment. For example, residents who call the DirigoChoice toll-free number cannot be enrolled directly—they must be referred to a licensed insurance seller. Applicants for DirigoChoice subsidies must also submit application forms to Anthem (for coverage) as well as to the Dirigo Health Agency (for premium subsidies). In one study, some stakeholders believed this was a barrier to enrollment by individuals (Lipson et al. 2007).25
Many enrollment complexities stem from a program’s underlying eligibility requirements. Not surprisingly, broad, clear eligibility criteria can have tremendous appeal to applicants. For adults in families, being able to enroll the whole family—both parents and children as well as immigrant and citizen family members—has appeal. Some low-income families are of mixed immigration status, meaning that some family members may be eligible for public Medicaid/SCHIP coverage while others are ineligible. Alliance Family Care was open to these otherwise ineligible family members (documented or not). The program also offered coverage that was already familiar to these families as it resembled the Medicaid benefit package. Alliance Family Care successfully enrolled this sometimes hard-to-reach population and achieved a retention rate that exceeded 97 percent (Zahn et al. 2003).26
Stigma
Discussants believed that welfare stigma was a real phenomenon that may deter enrollment. However, most felt that their program had taken steps to successfully minimize stigma. They identified several factors that help reduce stigma:
- Multiple access points (paper, Internet, phone, in person). Online and mail-in applications are more anonymous. For one discussant, a key outreach message was to reassure applicants that they would not have to apply at the welfare office.
- The “trappings” of private coverage. The program should feature an insurance card (that does not look like the Medicaid card), a booklet, and a “brand” that doesn’t have government connotations. Housing the program in a different branch of government (for example, the state department of insurance) instead of the Medicaid agency also helped with this perception.
- Program duration. To a minor extent, discussants felt that the longer a program had been in operation, the less stigma was associated with it.
Focus groups conducted for one program found that the target population wanted straightforward information. If the program featured a government subsidy, then it should say so. One discussant speculated that preference might be somewhat unique to their state.
In one study that examined Utah’s PCN, state officials and advocates reported that some individuals may not have enrolled because of stigma associated with the Medicaid program, particularly individuals in small communities (Office of Health Care Statistics 2004). As a rule, however, perceived stigma and its impact on enrollment has not been studied in these programs.
Program Permanence
Only a few programs that we studied had a reputation for having a limited duration. Discussants in this limited sample suggested that lack of permanence did not deter enrollment. One discussant noted:
People saw [the program] as a stepping stone until they got coverage through their employer. The impermanence definitely didn’t deter enrollment.
In one program, stakeholders noted that the use of preventive services was very high as the program reached the end of its scheduled duration.
Chapter IV
Premium Subsidies for Workers
An estimated 20 percent of uninsured workers have an employer offer of coverage available to them but choose not to enroll (Table IV.1). In this chapter, we discuss programs that target these low-income workers by subsidizing the worker’s share of the group premium, often termed premium assistance programs.27 Such programs do not directly subsidize the employer’s share and are not explicitly intended to encourage new offers of employer coverage.
Employer coverage has many features that may appeal to prospective enrollees, such as the convenience of making premium payments via payroll deduction, having all family members on the same plan, and having the same type of coverage as “everybody else.” But eligible workers often don’t enroll in their employer’s coverage because they can’t afford their share of the premium. By subsidizing the worker’s share of the premium, premium assistance programs capture the premium contribution of the employer as a valuable source of financing. In many cases, these initiatives can leverage Medicaid and/or SCHIP financing as well.
This chapter presents findings from discussions with individuals associated with three premium assistance programs: Family Health Insurance Assistance Program (FHIAP) in Oregon,28RIte Share in Rhode Island, and Utah’s Premium Partnership (UPP). Each program has unique characteristics and serves a distinct community (see Appendix B). We also present relevant findings from our literature review.
| Percent of All Uninsured Workers | |
|---|---|
| Employer offers; worker is eligible | 20% |
| Employer offers; worker is not eligibl e | 17% |
| Employer does not offer | 64% |
| Source: Garrett 2004. Note: Table excludes uninsured, self-employed workers. | |
Background and Enrollment Experience
Programs that subsidize the worker’s share of a group premium can be distinguished by whether they operate as (1) premium assistance programs receiving SCHIP match, (2) Health Insurance Premium Payment (HIPP) Programs receiving Medicaid match, or (3) solely state-funded programs.29 Table IV.2 shows this program typology. As we discuss below, programs financed using SCHIP or Medicaid must comply with Centers for Medicare & Medicaid (CMS) rules. These rules influence the eligibility requirements and enrollment processes of these programs.
| Eligible for Federal Match | Eligible Coverage | Sample Programs |
|---|---|---|
| Note: For additional information on these programs, please see Appendix B. | ||
| Medicaid match (HIPP program) | Most employer coverage qualifies | Rhode Island’s RIte Share |
| Mixture of Medicaid/SCHIP | Most employer coverage qualifies | Oregon’s FHIAP (2002–present) |
| Other financing sources | Most employer coverage qualifies | Oregon’s FHIAP (prior to 2002) |
| Subsidy can only be used for specific coverage | Maine’s DirigoChoice program | |
Two unique aspects of Maine’s DirigoChoice program bear mention. First, DirigoChoice is a rare example of a premium assistance program that does not benefit from federal Medicaid or SCHIP match.30 Second, and more important, firms must choose to offer the DirigoChoice coverage for their low-income workers to benefit from the premium subsidies. In other words, premium assistance is not available for other types of employer coverage. This level of employer effort means that the enrollment lessons from this program differ from many others discussed in this chapter and, in fact, relate to the next chapter, which discusses attracting employer participation in coverage programs.
To date, far fewer employers have participated in DirigoChoice than expected. Employer survey data for DirigoChoice suggest that most small firms opted not to enroll in the coverage due to the cost of the program (Lipson et al. 2007). A few nonoffering employers cited a lack of demand among their workforce, a topic that is explored to a greater extent in the next chapter. When employers do offer the coverage, workers participate at high rates, with about 3,400 small firm workers enrolled in early 2008 (Appendix B).
Unique Features of Medicaid- and SCHIP-Financed Programs
Many Medicaid- and SCHIP-financed premium subsidy programs target children, although adults in the family may be covered incidentally under the family policy purchased to cover the child.31 In several states, however, premium assistance is directly available to adults, and these programs are the focus of this chapter. Table IV.3 shows the recent enrollment levels of selected plans that are offered to adults. Altogether, about 20 states operate some form of Medicaid or SCHIP premium assistance program that includes coverage for adults, with enrollment numbers ranging from 61 individuals in the smallest program to more than 30,000 in the largest (Belnap and Schwartz 2007). Overall, however, premium assistance enrollees constitute less than 1 percent of total enrollment in Medicaid and SCHIP (Shirk and Ryan 2006).
Several studies attribute low enrollment to requirements associated with receiving SCHIP or Medicaid matching funds—for example, verifying citizenship (Volpel et al. 2007). Depending on the type of premium assistance program a state has, there may be other restrictions on the design and administration of the program. Unless a waiver has been granted, CMS requires program designers to evaluate available benefit packages and calculate cost-effectiveness.32 Some states have had trouble completing this cost-effectiveness calculation due to difficulty obtaining a description of the applicant’s employer health plan. Even when health plan information is available, the coverage may fail these tests, further curtailing the pool of workers who could benefit from such a program. Other potential requirements include a six-month waiting period to prevent crowd-out, a predetermined employer contribution, a minimum benefit package, and a ceiling on a family’s out-of-pocket costs (Westpfahl, Lutzky and Hill 2003).
| State (year initiated) | Maximum Income Eligibility for Parents/Childless Adults | Maximum Income Eligibility for | Enrollment |
|---|---|---|---|
| Source: Appendix B; Belnap and Schwartz 2007. Note: Programs in states such as Massachusetts, Arkansas, Oklahoma, and New Mexico are covered in the next chapter of this report since they also offer subsidies to employers. Programs that provide premium assistance to cover children only (although the worker may be covered incidentally) are not included. a As noted in Chapter III, another 10,700 enrollees use FHIAP to subsidize nongroup coverage. Beginning in 2002, applicants were required to use their premium subsidy for employer coverage if such coverage was available to them. b In Idaho, enrollment into qualifying coverage is mandatory for parents and optional for children. NA = Not available to childless adults. | |||
| Programs with Mandatory Enrollment | |||
| Rhode Island (2007) | 185% / NA | 250% | 7,190 |
| Wisconsin (1999) | 185% / NA | 200% | 1,691 |
| New Jersey (2001) | 200% / NA | — | 770 |
| Oregon (2008) | 185% / 185% | 185% | 5,993a |
| Idaho (2005)b | 185% / 185% | 185% | 456 |
| Programs with Voluntary Enrollment | |||
| Illinois (2002) | 185% / NA | 200% | 6,005 |
| Nevada (2006) | 200% / NA | — | — |
| Utah (2006) | 150% / 150% | — | 570 |
Medicaid- and SCHIP-financed programs can be further distinguished by whether they are mandatory or “opt-out” programs. Mandatory programs require public coverage applicants to enroll in employer coverage when the coverage meets certain standards. Opt-out programs allow the applicant to choose between direct public coverage or premium subsidies for employer coverage. For mandatory programs, states typically continue to provide the full range of Medicaid or SCHIP benefits—either through a “wraparound” benefit provided by the state or by ensuring that the private coverage meets benefit and cost-sharing standards. In opt-out programs, families may not be receiving the full Medicaid/SCHIP benefits package; as such, these programs must operate under a Section 1115 waiver from the federal government.
A few states stand out as having higher enrollment than others. About 7,000 individuals are enrolled in Rhode Island’s RIte Share program, representing 3 percent of the state’s total Medicaid enrollment. RIte Share attributes its higher-than-average enrollment to a number of design modifications. After initially experiencing low enrollment rates, Rhode Island (1) made it mandatory to enroll in qualifying employer coverage, when available; (2) made it possible for those who are eligible for RIte Share to enroll before the employer’s open enrollment period; (3) relaxed its criteria for qualifying employer plans; and (4) implemented an information system that used various state data sources to identify potential participants. In many states, the income eligibility range is much broader for children than for adults, making it more likely that children will have access to employer coverage.
Key Findings
To date, the majority of premium assistance programs have failed to fulfill policymakers’ expectations, sometimes enrolling just a few workers and dependents (Alker 2008). Nonetheless, interest in this coverage approach remains high. Our discussants shared their ideas for maximizing enrollment in premium assistance programs:
- Brokers strongly influence worker enrollment by playing many needed roles, including raising awareness of the program among employers and workers, educating applicants about insurance concepts and cost-sharing responsibilities, and assisting with the application process. Brokers are a “trusted source” of information. Focusing program outreach efforts on brokers, as opposed to employers and workers, may be the most effective means of generating awareness that leads to enrollment.
- Employers are also an important influence on worker awareness and enrollment. However, leveraging this influence can be difficult as not all employers are willing participants. Discussants also recommend minimize the employer’s role in program administration.
- Applicants have difficulty understanding insurance concepts and cost-sharing requirements, especially those who have limited experience with commercial insurance. Significant resources are required to explain the program and complete the application process.
- Many low-income workers who qualify for employer-sponsored insurance earn wages that are slightly higher than most eligibility rules allow. To increase group market participation, most discussants recommended increasing income eligibility requirements to 200 or 300 percent of FPL.
- Open enrollment restrictions make it difficult for workers to enroll in the programs. Some states have laws that require eligibility for medical assistance to be a qualifying event; thus, enrollment into an employer health plan can take place at any time. Such laws do not directly benefit eligible workers in self-insured businesses who are exempt under the Employee Retirement Income Security Act (ERISA).
- The presence or even threat of a waitlist may deter the support of brokers and employers, the two key groups that influence worker enrollment. However, as in Oregon’s FHIAP, a waitlist may motivate workers to submit their names for future participation.
Discussants confirmed that they lack reliable approaches for estimating enrollment. This is not entirely due to a lack of familiarity with the program features that promote enrollment. The discussants and our review of the literature reveal that it is also due to difficulty estimating the size of the eligible population. This difficulty stems from the myriad requirements for eligibility and uncertainty about how many low-income workers qualify to participate in their employer’s insurance plan (Williams 2003; Westpfahl Lutzky and Hill 2003).
Using the framework of our logic model, we next present our detailed findings with respect to the program features that influence enrollment among the eligible population.
Program Awareness
Awareness of premium assistance programs is often very low among the target population. In part, this is due to the fact that many premium assistance and HIPP programs are not actively marketed. Programs that require mandatory enrollment do not typically conduct outreach specific to premium assistance because applicants are screened for eligibility as part of their general application for Medicaid or SCHIP coverage. Oregon’s FHIAP does not actively market when all available slots have been filled. When considering options for their 2002 waiver for FHIAP, Oregon recommended that states be allowed to limit their outreach efforts so as not to exceed the state’s ability to provide services (Office for Oregon Health Plan Policy and Research 2001).
It is more common for “opt-in” programs to conduct outreach. These efforts including direct mailings, television and radio advertisements, informational brochures in health care settings and eligibility offices, and attendance at community events.
Discussants identified three key groups that influence enrollment of workers: employers, brokers, and enrollment counselors.
Employers play an important role in worker awareness and enrollment in these programs, given their responsibility for administering health insurance, selecting qualified plans, determining premium contributions, and providing required benefit information. To create program awareness among employers, several discussants recommended reaching employers through brokers, chambers of commerce, and business associations as opposed to contacting employers directly. Discussants believed that these sources had more creditability with employers and hence, increased the likelihood of employer participation. Nonetheless, several studies show that it can be difficult to secure employer cooperation. Early experiences in Rhode Island illustrate the difficulty they had getting employers to participate in the RIte Share program. In the first eight months, they only enrolled 100 businesses and 275 individuals compared to 2,200 individuals the year after they made worker participation mandatory regardless of employer cooperation. One discussant stated:
Some employers were good Samaritans who felt a responsibility to cover their folks, but for the most part, employers don’t want to participate because it would cost them more money.
Utah’s program (UPP) also received pushback from employers. Discussants felt that employers were concerned about the impact on their insurance’s experience rating, overall costs, and perceptions of unequal treatment of workers, yet they shared a belief in the value of an insured workforce.
Brokers can play an important role in raising awareness among employers with whom they work in selecting and purchasing group coverage. Program directors described brokers as “critical,” “ambassadors,” and “our number one asset.” After an employer has selected a group plan, brokers can help identify qualified workers and assist them in enrolling in the program.
Program staff can take a number of steps to reach and motivate brokers, including offering trainings and free continuing education credits for their license renewal. They can also place articles in insurance broker association newsletters, target newly licensed brokers using lists from the state Insurance Department, keep referral lists of trained brokers, and pay small fees for denied applicants to compensate brokers’ time. Unfortunately, our discussions made clear that many brokers are not aware of these programs nor are they necessarily interested in promoting them. Several discussants felt that a strong, compelling message could be marketed to brokers, such as the additional commissions, new business, and increased customer loyalty associated with promoting the program. Another discussant noted that awareness and interest in well-designed premium assistance programs is likely to naturally increase over time.
Enrollment counselors play similar roles in educating and assisting with the application process, but they focus on the applicant rather than the employer. At some state eligibility offices, enrollment counselors screen and inform applicants about premium assistance programs when they are determined ineligible for traditional Medicaid. They also help educate enrollees about how the program works. In addition, enrollment counselors work in the community and at hospitals and clinics to inform and enroll potential applicants. Two states studied have referral mechanisms to help connect interested applicants to community organizations or brokers in their area to assist with the application process.
Program staff can also target workers directly, although such efforts are not as effective as targeting employers and brokers. Discussants recommended two approaches to targeting workers: (1) partnering with community organizations and community leaders and (2) coordinating with other programs that serve workers. Strategies used include contacting individuals denied for traditional Medicaid, providing a single application for multiple government assistance programs, offering online applications, placing enrollment counselors in health care settings, and developing information systems that collect employment and income information.
Our discussants did not recommend targeting workers directly through mass media campaigns or direct mailings. One reason to avoid mass media campaigns is the difficulty in creating an effective message given the complex eligibility rules. For example, Rhode Island conducted an early marketing campaign consisting of information sessions with insurers, brokers, employers, and advocates, along with radio and television advertisements. But despite these efforts, an evaluation revealed that some enrollees and employers were still confused about how the program is structured and who is eligible (Williams 2003).
Program Comprehension
Brokers and enrollment counselors from the opt-out programs noted the significant amount of time spent educating employers and workers about the program as part of the enrollment decision. One broker stated:
The education piece of the program is huge. There is a lot of hand-holding, and much of our time is spent helping people become familiar with the system.
Brokers noted a lack of knowledge about insurance concepts and cost-sharing requirements, particularly among those who had limited experience with commercial insurance. Similarly, a study that included interviews with officials at several programs found that there was a general lack of understanding about health insurance among prospective enrollees. A large part of the enrollment process consisted of educating potential enrollees about the role and value of health insurance (Volpel et al. 2007).
Program staff can help to alleviate comprehension difficulties by offering wraparound coverage. For example, the mandatory RIte Share program tries to provide seamless wraparound coverage with the traditional Medicaid program. Discussants noted that seamlessness was made possible because many providers in Rhode Island accepted both commercial and Medicaid patients, allowing them to bill Medicaid for co-payments and deductibles.
Discussants also identified misunderstandings about eligibility rules and enrollment procedures as another common difficulty. As noted in a study of RIte Share’s early experiences, enrollees and employers were confused about how the program is structured and who is eligible, despite extensive outreach efforts (Williams 2003).
The lack of comprehension among applicants about insurance concepts or program details may not deter enrollment if applicants have access to enrollment counselors or brokers. One program official felt that, because of pent-up demand and lack of access to commercial coverage, applicants had an incentive to work with counselors and brokers to better understand how premium assistance programs work.
Program Appeal
Discussants agreed that access to commercial coverage for the entire family had significant appeal among enrollees. On the other hand, many programs are limited in their ability to make the enrollment process more appealing, as certain requirements, such as federal requirements for citizenship, must be maintained. Unfortunately, discussants did not have a clear sense of the impact of unappealing program features on enrollment.
Benefit Design/Provider Network
Discussants widely believed that commercial coverage, in particularly the provider networks associated with commercial coverage, is very appealing to applicants. One discussant believed that access to commercial health insurance was the number one feature attracting people to enroll. Compared to public coverage, discussants believed that employer coverage is preferred by low-income workers because it is “the same coverage that everybody else has.”
Several discussants mentioned that the lowest-income workers may still not be able to afford their employer’s insurance even with the subsidy due to point-of-service cost-sharing requirements (in programs that don’t feature a wraparound). However, we found no studies that methodically examine whether these requirements—typically associated with employer-based coverage—deterred enrollment into premium assistance programs.
Premium Subsidy Structure
In most of the HIPP and premium assistance programs, states pay premium subsidies directly to enrollees. All states except Oregon pay participants prospectively. Additional administrative duties may be required of enrollees. For example, to monitor continued enrollment, Wisconsin requires applicants to submit monthly pay stubs. We found no studies that linked these processes to enrollment, nor did our discussants identify an enrollment impact. However, it is important to note that nonpayment of premiums—once enrolled—is often cited as the reason for disenrollment.
Enrollment Process/Eligibility Criteria
Several discussants recommended broadening income eligibility criteria to increase take-up. Low-income workers who qualify for employer-sponsored insurance tend to have slightly higher wages than most eligibility rules allow. To increase group market participation, most discussants recommended increasing the income eligibility limit to 200–300 percent of the FPL.
Discussants noted that workers, employers, and brokers were put off by crowd-out provisions, which require enrollees to be uninsured for a specified length of time. This is seen as punishment for low-income families who have “done the right thing” and incurred the financial burden of enrolling in coverage. One discussant was worried that families were dropping coverage for the required amount of time in order to qualify for premium assistance.
Discussants did not identify complex enrollment processes as a major barrier but did recognize that many more applications are started than finished. They also noted that collecting the necessary documentation can be difficult for some enrollees.
In contrast, several studies found that complex enrollment processes—reflecting complex eligibility criteria—can be a key barrier to participation by workers, and sometimes employers. Wisconsin’s Premium Assistance program historically had very low enrollment. One analysis found that almost 50,000 employer information forms, corresponding to an equal number of applicants, were returned to the state. From these, only 109 families were determined eligible and 32 families actually enrolled in the program. The low proportion of enrollees was attributed to a variety of reasons, including applicants who were no longer employed at the firm, were ineligible for the coverage, or had employer coverage that did not meet the state’s requirements.33 The state subsequently made changes to its policies—such as reducing the minimum employer contribution to 40 percent (from 60 percent)—to increase take-up (Williams 2003). An early survey of disenrollees from the DirigoChoice program found that about one-quarter of small-firm workers cited “administrative hassles” as their reason for voluntarily leaving the program (program cost was the most common reason). Overall, however, a fairly small number of individuals (14 percent) disenrolled after just under one year of program operation (Anderson and Bowe 2006).
According to our literature review and many of the discussants, states that devote significant resources to employer education, recruitment, and relationship-building have more success with their premium assistance programs over time (Shirk and Ryan 2006). In many of these programs, the employer role is minimal but cannot be eliminated completely. In SCHIP and Medicaid premium assistance programs, employers must provide a description of coverage to ascertain benefit adequacy. But a 2003 study noted that employers failed to respond to requests for information about 25 percent of the time (Williams 2003). ERISA (see sidebar) precludes states from requiring employers to share health plan information; however, good working relationships with employers can encourage voluntary compliance with this step.

Rhode Island’s RIte Share program is an example of a program that minimized the employer’s role and afterwards experienced an increase in take-up. At inception, Rhode Island paid the enrollee’s premium directly to his or her employer, who then paid the premium to the health plan. While this process minimized cash-flow issues for the worker, employers perceived it as administratively challenging. In late 2001, the state began to reimburse workers directly for the family’s share of the coverage costs, taking the burden off the employer. As a result, employer participation increased dramatically. Between January and June 2002, enrollment jumped from 275 to more than 2,000 (Shirk and Ryan 2006). The state also created new information systems to track employer health plan information, minimizing the need to collect such information from employers.34 Oregon’s FHIAP circumvents this issue by requiring applicants to obtain health plan information from their employers and submit this information as part of the program application. By law, employers must respond to requests for information that come from workers (Williams 2003).
Illinois’s premium assistance approach allows it to avoid several administratively complex requirements. This program allows participating parents and children to move freely between the premium assistance and direct public coverage programs. This design obviated the costly administrative tasks of setting minimum standards for employer-based insurance, auditing employer health plans to ensure that they meet those standards, and providing wraparound coverage for services not covered under the employer plan. The result, however, is only minimal enrollment in the premium assistance program.
Brokers and enrollment counselors play a vital role in assisting workers with the application process. As discussed previously, such assistance is critical to overcoming the difficulty that applicants have in understanding the application materials, the enrollment process, and the program structure. In Rhode Island, “resource counselors” are contracted by the state to serve in emergency rooms and other provider sites to inform and assist eligible uninsured patients.
Discussants also noted that restrictive enrollment periods can limit enrollment. Almost all employer coverage programs feature annual open enrollment periods. Except for certain qualifying events (such as the birth of a child), workers cannot generally enroll at other times of year. Some states have enacted laws that make eligibility for Medicaid or SCHIP a qualifying event so that eligible workers and their dependents can enroll outside the annual open enrollment period. One state official identified this as one of the most important features that has helped increase enrollment in the program. As of July 2007, Utah has made eligibility for medical assistance a qualifying event. Discussants were optimistic that this, along with several other recent changes, would boost enrollment. However, this strategy does not aid workers whose employers are self-insured and hence exempt under ERISA (Shirk and Ryan 2006).
Requiring an in-person visit to the state benefits office is unappealing to many workers. Instead, discussants told us it was preferable to have multiple avenues for enrollment, including online applications, clinic enrollment sites, and applications that screen eligibility for multiple state benefit programs.
Stigma
Our premium assistance discussants did not identify stigma as an enrollment deterrent. The use of commercial coverage helps counteract negative perceptions about these programs, especially among former enrollees in traditional Medicaid. Some programs have income guidelines that are more generous than traditional Medicaid guidelines for adults, which helps disassociate the program from Medicaid. An early survey of disenrollees from the DirigoChoice program found that fewer than 10 percent listed “don’t like public/social programs” as the reason for disenrollment (Anderson and Bowe 2006).
Program Permanence
Discussants told us that the presence or even threat of a waitlist may deter the support of brokers and employers—two key groups that influence the enrollment of workers. At least one discussant noted that the longer a program is in existence, the greater its acceptance among brokers and employers. Discussants also noted that program permanence is less of a concern for workers. In fact, as in the case of Oregon’s FHIAP, a waitlist may motivate workers to submit their name for future participation.
Premium Assistance for Nongroup vs. Group Coverage
The experience of the Oregon FHIAP suggests that premium assistance for commercial nongroup coverage may be more attractive than premium assistance for employer coverage. Before 2002, Oregon permitted individuals to choose whether to apply their subsidy to nongroup or group coverage. In 2002, as part of Oregon’s CMS waiver, enrollment in qualifying employer coverage became mandatory. As Table IV.4 shows, the share of employer enrollment more than doubled. The 2003 enrollment numbers suggest that more than 20 percent of enrollees had access to employer group coverage but opted for nongroup.
| Percent Distribution by Type of Coverage | |||
|---|---|---|---|
| Year | Nongroupa | Group | |
| Source: Appendix B. a Includes sole proprietors. * Enrollment capped. | |||
| 2000 (pre-2002 waiver) | 82 | 18 | |
| 2003 (post-2002 waiver) | 58* | 42 | |
| 2008 (latest enrollment) | 64* | 36* | |
Chapter V
Premium Subsidies for Employers and Workers
It is well established that the vast majority of the uninsured are either workers or members of a family with a worker. Yet most uninsured workers do not have access to an employer offer of coverage and can not benefit from the premium assistance programs described in the previous chapter. In response, many states and communities have developed programs designed to increase the prevalence of employer offers of coverage, generally by offering an employer premium subsidy in conjunction with premium subsidies for workers. Such programs are generally, but not always, restricted to nonoffering employers.
We held discussions with six such programs: ARHealthNetworks in Arkansas, Brooklyn Healthworks in New York, Health Choice in Michigan, InsureMontana, the employer plan in the Insure Oklahoma program, and the recently closed SacAdvantage program in Sacramento County, California. Each of these programs has many unique characteristics (see Appendix B) and our discussants’ views yield important insights with respect to the specific strategies that help enroll this hard-to-reach population.
As our discussants and selected other case studies reveal, the complexities of crafting a subsidized coverage program are amplified when an employer subsidy is introduced. In addition to the design decisions needed to attract workers, such programs need to also attract employers, and in some cases, brokers. Extensive and differently targeted outreach must be conducted. Compared to other coverage approaches, program designs are more complex. For example, employer eligibility criteria must be established, as well as minimum standards for employer premium contributions and employee participation.
Program Background
Compared to programs that target individuals directly, programs that target small, nonoffering employers find it difficult to realize significant enrollment. Researcher Beth Kilbreth contrasted the experience of four programs featuring both individual and employer coverage options and found that
the experience of all four programs makes clear that in voluntary enrollment initiatives, response is much greater from individuals and families than from small businesses. While substantial discounts attract some small business participation, the take-up is relatively modest in relation to the number of small businesses without health benefit plans (Kilbreth 2006).
Similarly, Jaxcare, Small Business Health Insurance (NY) and SacAdvantage programs all featured substantial subsidies yet experienced much lower than expected enrollment for several years.35 Several researchers have suggested that even large premium subsidies do not result in a significant increase in employer offers of health coverage (Hadley and Reschovsky 2002; Kronick and Olsen 2006). Some studies suggest that not only cost but a lack of worker demand is an important factor in employers’ decision not to offer coverage (McLaughlin and Zellers 1992). Kronick and Olsen (2006) suggest one reason for low demand—the fact that uninsured workers, while numerous, are not concentrated in great numbers in individual nonoffering firms. In other words, a given nonoffering firm may have just one uninsured worker, along with several workers with coverage from sources outside the firm, such as a spouse.
Many discussants and at least one study concluded that there is a core set of nonoffering employers that will not offer coverage regardless of the subsidy that accompanies it (Belloff and Fox 2006). Employer surveys suggest that 10 to 30 percent of nonoffering small employers would not voluntarily participate in subsidized coverage programs like those described in this chapter (Seninger 2006).
Nonetheless, a large number of nonoffering employers may be willing to participate in a subsidized coverage program if the program is structured correctly. Neuschler and Curtis looked at the experience of three programs (FOCUS, Access Health, and HealthChoice) and speculated that
many small employers with mostly low-wage workers will offer health insurance if they feel the amount they must contribute is affordable and predictable and will remain so over time, if their contribution reduces the costs their workers face, if their workers can afford what they are asked to contribute, and if the coverage source is reliable and sustainable and minimizes the employer’s administrative burden (Neuschler and Curtis 2003).
Table V.1 contains recent enrollment experience for some sample programs. The table also highlights the very small size of the typical firm that chooses to enroll.
| Program | Firm Eligibility Criteria | Worker Eligibility Criteria | Enrollment of Small Group Workersa | Average Firm Size of Enrolled Firms |
|---|---|---|---|---|
| Source: Appendix B a Some programs permit other populations, such as individuals without access to employer coverage, to enroll. Only enrollment through participating firms is reported in this table. JaxCare, FOCUS and SacAdvantage are no longer operating. b Enrollment is/was capped. c Insure Montana also offers a tax credit to offering small employers who are struggling with their premium payments. We do not include this program component in our discussion, as there is no subsidy to employees. d Massachusetts operates two programs. The Insurance Partnership provides premium subsidies to employers for their low-income workers. The Family Assistance program provides premium subsidies to low-income workers. | ||||
| Access Health Muskegon County, MI | Nonoffering, businesses with a median wage of less than $11.50 per hour | Uninsured and ineligible for public programs | 1,100 | Most have fewer than six employees |
| AR Health Networks Arkansas | Nonoffering, 2-500 employees, at least 1 employee qualifies for premium subsidies | All workers can enroll but only those 200% of FPL are eligible for premium subsidies | 4,700 | Most have fewer than six employees |
| Brooklyn Health Works Brooklyn, NY | Nonoffering, 2-50 employees, 30% of whom earn no more than $38,000 | All workers in eligible firms can enroll | 1,500 | Most have fewer than six employees |
| FOCUS San Diego, CA | Nonoffering, 2-50 employees | Uninsured workers with income 300% of FPL | 1,700b | “Very small” |
| Health Choice Wayne County, MI | Nonoffering, 50% of qualified employees earn less than $14.50 per hour, at least 2 employees qualify for subsidies | All workers employed | 4,450 | ”Very small” |
| Healthy New York New YorkState | Nonoffering, 2-50 employees, 30% of whom earn no more than $36,500; half of eligible employees must enroll | All workers in eligible firms can enroll | 43,500 | 75% have fewer than six employees |
| Insure Montana (Purchasing Pool Program)c Montana | Nonoffering, 2-9 employees, all employees earn less than $75,000 (excludes owner) | Full-time employees unless employer extends coverage to all employees working 20-30 hours per week | 4,000b | “Very small” |
| Insure Oklahoma Oklahoma | 2-50 employees | Income 200% FPL and not enrolled in other public coverage | 8,760 | Most have 3-4 employees |
| JaxCare Duval County, FL | At least 3 employees | Uninsured county residents with income | 1,380 | Unknown |
| Mass Health Family Assistance/Insurance Partnershipd Massachusetts | 1-50 full time employees; contributes 50% to premiums, and provides insurance benefits approved by MassHealth | Children or adults with household incomes | 20,000 | 88% have fewer than six employees |
| Sac Advantage Sacramento County, California | Nonoffering, 2-50 employees | Uninsured for last 3 months and with income 300% FPL | 666 | Unknown |
| State Coverage Insurance New Mexico | Nonoffering, 1-50 employees | Uninsured with income | 9,200b | 9 employees |
Sole Proprietors Are a Special Case
Subsidized coverage programs that target small firms vary in their treatment of sole proprietors (self-employed firm owners with no employees). Many exclude sole proprietors from their subsidized coverage programs due to fears of adverse selection. Others include them but may limit their enrollment to annual periods of open enrollment. Some studies suggest that sole proprietors often participate in subsidized coverage initiatives at high rates (Mitchell 2002; Taylor and Forland 2003). This population typically suffers from high rates of uninsurance and may have a strong desire for coverage.36 As such, it may be easier to attract the participation of sole-proprietors in subsidized coverage initiatives than is indicated by the responses of small firms more generally. In the discussion that follows, the findings with respect to the program features that attract small firm participation apply to groups of two or more workers.
| Percent Distribution by Type of Enrollee | |||
|---|---|---|---|
| Program Name | Individual | Sole Proprietor | Small Business |
| Source: Appendix B. a While the DirigoChoice program does not provide employer premium subsidies, we include this program because the division of enrollment by enrollee type is so similar to other programs. b Program has a waiting list. c These 2001 figures for Massachusetts are based on the distribution of employers not individuals. n.a = not applicable. | |||
| DirigoChoice in Mainea | 38b | 26 | 35 |
| Massachusetts Family Assistancec | n.a. | 66 | 34 |
| Healthy New York | 59 | 19 | 22 |
Key Findings
The study participants provided a rich body of information regarding the key strategies that successfully enroll small firms and their workers. Their most important observations were:
- Affordability is critical but not sufficient to enroll small employers.
- Outreach to the employer, not the employee, is critical.
- Brokers are critical for reaching and enrolling small employers. They play a key role in every step of the enrollment process--creating awareness, comprehension and appeal.
- Programs need to actively partner with brokers in order to secure their participation. Programs should use a compelling message (emphasizing the program as an opportunity for brokers to serve their community, earn extra commissions, and establish a client relationship that may lead to the sale of other insurance products) and provide training and support.
- Programs should supplement broker involvement with a combination of other, effective outreach methods (using a single method is insufficient) and tailored the outreach to the local community. Outreach methods deemed effective by our discussants include grassroots outreach approaches, maintaining an Internet presence (as many small business owners searching online for insurance), visible support from a politician (creates awareness and lends credibility), and direct mailings.
- Local media can raise awareness about the program, but to create enrollment it must be combined with other outreach methods. Mass media was not generally considered important for creating awareness that results in enrollment.
- Word-of-mouth is an extremely important mechanism by which firm owners hear about the program and ultimately enroll. Programs can facilitate word-of-mouth recommendations by offering a cash incentive for referrals and by managing public expectations about the program.
- A strong, well-regarded provider network was noted as an important factor in employers’ decisions to enroll in the program. Firm owners prefer benefits that look like “real insurance” and don’t feature excessively high deductibles.
- Determining eligibility for the program at the firm level and not the employee level so that all employees can participate.
- Application assistance and other services are crucial to getting firms enrolled and keeping them enrolled. Brokers, program representatives, and marketing representatives do a lot of "hand-holding" and give a lot of personal attention to small business owners, as they do not have HR staff or the time to perform these functions themselves.
- Simplicity of the enrollment process (application and eligibility requirements) can be a deciding factor in terms of whether or not a small business will enroll.
Using the framework of our logic model, we present our detailed findings below.
Program Awareness
Our discussants emphasized that in order to generate awareness that leads to enrollment targeting employers, not employees, is key. Employers should be reached using a combination of outreach methods in order to generate awareness that leads to enrollment. Effective outreach methods to employers include: using brokers to advertise and sell the program, facilitating word-of-mouth advertising, grassroots outreach efforts37, getting a recognized politician to promote the program, direct mailings to eligible businesses, and an informative and easy-to-understand website. In each case, these approaches need to be tailored to the local community. Supplementing these methods with paid or free local media can help boost awareness about the program, but rarely compels people to enroll when used on its own.
Overwhelmingly, our discussants emphasized the importance of brokers in creating program awareness, specifically awareness that resulted in enrollment. Brokers are critical because they are skilled at reaching and selling insurance to small business owners. Three of our study programs did not initially reach out to brokers and saw low enrollment. When the brokers came on board, enrollment increased rapidly in all three programs- so much so that in two of the programs, subsidy funding was depleted. Not only do brokers know how to reach small business owners who might not yet be seeking insurance, but they are a source that employers turn to when searching for insurance. Many brokers did their own marketing by inviting small business owners to a presentation at a local chamber of commerce or other community organization, which allowed business owners to ask questions. Other brokers reach out to and meet one-on-one with small business owners whom they may already have as clients for other types of insurance.
Because brokers can facilitate the entire enrollment process, the awareness that they generate is likely to lead to enrollment. Brokers increase comprehension of all aspects of the program by explaining the benefit design, provider network, enrollment process, and subsidy structure to employees and by giving them the opportunity to ask questions. For these reasons, niche brokers—those who deal exclusively with a certain ethnic population—are particularly effective at reaching and enrolling small business owners who are otherwise hard to reach. These business owners often do not speak English and are unfamiliar with insurance concepts. Niche brokers can reach out to these business owners, explain insurance to them in a way that they can understand culturally, and also fill out applications for them, minimizing language barriers. In one program, over half of program enrollment came from niche brokers serving the Russian community.
While not typically suggested by our discussants, it does appear that other entities can successfully take on the functions typically preformed by brokers. The one program that did not use brokers (as the program is not true insurance but instead contracts with providers for services) used marketing representatives from each of the participating providers instead. These representatives performed similar functions and services and generated about half of the program’s monthly enrollment of small firms. In other programs, program staff took on some of these functions to alleviate burden on the brokers and improve customer service.
Discussants emphasized that outreach approaches for creating awareness that leads to enrollment should be tailored to the community. As an example, in California, a program that has a large Arabic population worked with the Arabic Chamber of Commerce to get the word out about the program. As a result, a large proportion of this program’s enrollees are Arabic small business owners. Another program hired a private firm to conduct focus group research to figure out what type of message would be appealing to that particular community, and began using that message in its outreach.38 The program felt that the tailoring of its outreach message to the community through focus group research greatly enhanced enrollment, and that they should have done it sooner.
Discussants emphasized that successful outreach to small employers uses a combination of methods. Employers need the reinforcement of hearing about the program from multiple sources and it makes the job of the broker easier. Discussants suggested combining the use of brokers with word-of-mouth advertising, political endorsements, grassroots outreach efforts, and a website that is informative and easy to understand.
Discussants agreed that word-of-mouth advertising (that is, enrollees telling their fellow business owners about the program) is effective in creating awareness that leads to enrollment. The person referring by word-of-mouth is usually a trusted source, increasing the credibility of the endorsement. Programs are limited in their ability to spur word of mouth advertising. One program offers a cash incentive to businesses that refer others, and approximately one-third of the program’s monthly enrollment comes from these referrals. Two other programs are considering implementing this incentive, while other programs encourage enrollees to voluntarily spread the word to other business owners in an attempt to spur word-of mouth advertising. Programs can also prevent negative messages about the program from spreading by word-of-mouth by properly managing public expectations. One program was advised by its brokers not to launch a mass media campaign as part of the roll out. The brokers reasoned that an untested program might not meet the expectations created by the large media campaign and the resulting distrust of the program would make it difficult to enroll eligible firms.
Obtaining the endorsement of a politician (governor, insurance commissioner, county executive, etcetera) was found to be extremely beneficial in creating awareness that leads to enrollment. Not only did the politician's promotion increase awareness of the program, but as a trusted source, it also lent credibility to the program, which compelled people to enroll.
Grassroots outreach was found by all discussants to have a greater impact on awareness that leads to enrollment compared with paid mass media. Grassroots outreach involves working with local, trusted community organizations (such as chambers of commerce, associations, churches, and other organizations that have a presence in the community) to spread the word about the program, for example by inviting small business owners to attend local meetings and presentations to learn more about the program. Programs often used listservs from chambers of commerce or ads on local radio stations or newspapers to invite business owners out to these meetings.
Half of our programs noted that they get significant enrollment from people who found out about the program from an internet search, therefore it is important to have a program website that is informative and easy to understand. One program also created website banners advertising the program (with a link to the program website) that chambers of commerce or other organizations could add to their websites.
All six programs used direct mailings to eligible businesses to let them know about the program and that they are eligible. Of these, five noted that this method was very effective at increasing awareness that led people to call to find out more about the program. The remaining program did not see much effect, speculating that small business owners will not read the letter, throwing it out as junk mail.
Free media—that is, getting reporters interested in the program so they will write a story about it—was found to be one of the most cost-effective methods of marketing. However, it can be risky because the program cannot control how it will be portrayed. For a program that does not have a marketing budget, these articles (if they portray the program positively) can be as effective, or more effective, than paid media, as they are seen as more objective than paid advertising and lend credibility to the program. Other cost-effective methods include encouraging word-of-mouth advertising, having an informative, easy-to-understand website, and e-newsletters.
Discussants agreed that paid local media, including newspaper and radio advertising, was less effective compared with word-of-mouth advertising or grassroots outreach. However, programs also noted that local media can boost awareness and can be effective in increasing enrollment when used in combination with other outreach methods. When used in combination with other methods, three programs noted enrollment spiked after starting a radio campaign. Insure Oklahoma experienced an 81 percent increase in enrollment after the launch of a major media campaign (Oklahoma Healthcare Authority 2008).
In contrast to local media, mass media was generally not used by our study programs. Our literature review generally supports these observations. One program (the Arizona Health Care Group) found that targeting small employers using a major direct marketing campaign that included television and other media advertising was not very successful. They concluded that small businesses purchase insurance almost exclusively through brokers (Silow-Carroll et al. 2001). Volpel and colleagues also encountered a program that termed mass media not a good investment (Volpel et al. 2007).
The one program did conduct a successful ($1 million) media campaign but did not rely solely on conventional advertising methods. Instead, it used a well-known and trusted news reporter to feature news stories about the program and to feed information about the program to other reporters. The marketing campaign also featured radio and TV infomercials, but one program discussant said that repetition of these ads was required in order to have success, noting “you have to pound in the message about health care (seven times) before they pay attention.” Program discussants noted that the campaign had a strong effect on awareness that led to enrollment, as their call centers receive a much higher volume of calls when advertisements are run or the campaign has more activity, and enrollment in the program increased 81 percent once the campaign began. However, the program has learned to prepare their call centers in advance to make sure they have enough staff and resources on hand. Initially, they were not prepared and didn’t have enough staff, phone lines, or fax machines and many callers were receiving busy signals.
Outreach should feature a compelling and quickly assimilated message. Our discussants recommended the following messages: (1) the coverage is affordable (2) make the program sound as commercial as possible (avoid sounding like a government program), and (3) emphasize the name of the program and (4) the phone number to call for more information. Within these general guidelines, it is important to tailor the message to the local community. For example, in Oklahoma, focus groups showed that people prefer a direct message about the program compared with a creative one. As an example, program information is straightforward about the source and size of subsidy component of the program. Brokers reported that “scare tactics” can be effective messages; reminding business owners that if they don’t have insurance and incurred some large medical costs they could find themselves in a lot of debt, as well as emphasizing the affordability and value of the program (that it was a good deal for the business owner).
While less common, some programs do target their outreach to workers. An extensive media campaign in Massachusetts is believed to have accelerated the participation of employers in the Insurance Partnership program.39 The campaign was conducted in both English and Spanish, and targeted workers rather than employers (Mitchell and Osber 2002). The authors observe that six months after the campaign was launched, firm participation had increased eightfold (to 1,311 firms). Fifteen months later, enrollment had nearly tripled again, to 3,500 firms.
Discussants generally found that workers will usually sign up for subsidized coverage programs offered by their employer, as this type of coverage is usually very attractive to them. One program frequently gets calls from workers asking how they can get their employer to sign up for the program. This program leverages this employee interest by allowing them to send their employer an anonymous email asking them to enroll in the program through the program website.
Employer-based health insurance is not universally attractive to employees, however. Several programs were familiar with firm owners who said their employees preferred an equivalent raise instead of the health insurance. For example, in the Insure Oklahoma program discussants were familiar with employees who said that they would rather have an extra $40 in their pocket rather than the coverage.
Program Comprehension
Many discussants noted that comprehension of the program, including understanding the enrollment process, benefit design, cost to enroll, and eligibility criteria are important to enrollment. Comprehension of the application and enrollment process was most commonly noted as important. Even programs that had greatly simplified their design features emphasized that it was still necessary to explain things to small business owners and provide enrollment assistance. As one broker noted:
I just can’t imagine the employer getting the application package and filling it out themselves, even though there are instructions. They don’t want to do it or don’t understand it.
Brokers play a key role in helping potential employers and employees understand the benefit design, eligibility requirements, provider network, and subsidy structure of the program. Discussants described this broker role as critical and strongly linked this activity to increased enrollment, although noting that in some cases, program staff can also play this insurance counseling role. In the words of one broker on his role in the enrollment process:
Once they decide to enroll in [the subsidized coverage], I sit down one-on-one with groups. I prearrange a meeting with the business owner—this is very important. I’ll sit with the employees and their spouses and we’ll discuss the coverage. They each get a brochure describing the coverage, benefits, and rules of the plan. They address questions to me. It’s critical for me to explain what they have. I highlight the benefit package that they’ll receive from the employer and really explain the coverage. They go away very happy. If not, they have my card to call me and I’ll answer their questions.
To perform this role, brokers themselves must be able to understand the application process and program. Holding information presentations for brokers and aligning the application as closely as possible with the standard small group application with which brokers are familiar, are vital in this regard. In some states, brokers receive continuing education credits for attending these training sessions. One program initially started off with an application process similar to Medicaid, but the brokers were not familiar with it and did not understand it, so they did not want to enroll people in the program. Switching to a standard form with which brokers were familiar increased their willingness to sell the plan and increased enrollment.
Discussants recommended making the application and enrollment process as simple as possible, even if this means eliminating things like checking for Medicaid Eligibility or eliminating pages of medical history. For programs that target small employers, it seems especially true that a complex application will deter enrollment. Discussants speculated that this was due in part to unwillingness of employers to take on a new administrative burden but other factors may be at work. Program designers are not widely aware of the exact reading level of target population. Nonetheless, about half of the programs made sure reading materials were at a 6th grade level and eliminated or minimized legal jargon so- that materials were written in “plain English.” Discussants from several programs believed this increased understanding of the program materials.
Similarly, some discussants recommended simplifying the underlying eligibility features of the program, and another noted that making the subsidy structure simple promotes enrollment. Two programs simplified their benefit design by offering fewer choices, which increased enrollment. Finally, Insure Oklahoma program noted that using a program name that is easy to remember and accurately conveys what the program is about is important to enrollment. The program was formerly called O-EPIC and focus group research found that no one recognized or understood the O-EPIC name, which prompted the name change.
About half of the programs studied decided not to make materials available in languages other than English. In some cases, this was due to the fact that program designers believed there was not a significant non-English speaking population among the eligible population. One program that did translate materials into other languages said that this was not nearly as effective as explaining the benefit structure, subsidy structure, and program to the small business owners in-person, in their own language and in cultural terms that they could understand. Several program emphasized that niche brokers can be especially affective in increasing comprehension among the ethnic populations they work with.
Program Appeal
In general, employer-based coverage was noted as attractive to employees because it is commercial coverage that is the same as what their co-workers have. However, discussants agreed that it is important for the benefit design to be attractive to the firm owner in order to secure firm participation in the program. In fact, almost all aspects of the program (eligibility criteria, enrollment process, provider networks, etcetera) had to appeal to firm owners in order garner participation.
Benefit Design/Provider Network
Discussants from all programs agreed that the program’s benefit design influences enrollment. As one broker said, “It is important for the benefits to be as strong as possible.” Two broker discussants said, respectively, that a $1000 or a $1500 deductible was critical to enrollment, as is a design that does not include huge co-payments for hospital or doctor visits. One program that initially included very large hospital co-pays found that this was a big deterrent to enrollment (BHW). When hospital co-pays were reduced, the program saw increased enrollment. As one discussant said:
Co-pays [must not be] extravagant—someone with insurance does not want a $100 co-pay in the benefit structure. If someone gets sick, [he or she] can afford to go to the doctor and pay the co-pay.
In addition, offering at least some first-dollar coverage for preventative services or office visits (such as two free office visits per year) is also a draw. Several programs mentioned that adding vision, dental, and prescription drug coverage (which many programs added via riders) was a less expensive alternative to incorporating these benefits into the benefit plan. Such riders often were what sold the plan to a smaller employer. One program, which does not exclude pre-existing conditions from coverage under the plan, noted that this was a big reason why small employers enroll; in other commercial plans, these conditions would either be excluded or the coverage very expensive as a result. Other features were noted as attractive to enrollees, but were not necessarily critical to enrollment. For example, not requiring a referral to see a specialist was noted as very attractive to the small business owner, for whom taking the time to see a primary care physician first means a loss of work time during the day.
While comprehensive coverage has great appeal to this population, it is important to note that Arkansas’s ARHealthNetworks program features a fairly limited benefit has nonetheless enrolled a significant number of small firms. Similarly, another program excluded chiropractic services, substance abuse services, and mental health services from coverage, but discussants agreed that they were able to sell around these exclusions such that they did not negatively deter enrollment.
Five of the six programs noted that having a strong, far-reaching provider network that is highly regarded in the target community is either critical or helpful to enrollment. Four of these programs noted that their provider network fulfilled these criteria and had therefore increased enrollment, while the other program, which had a smaller network, noted that it would like to increase the number of participating providers in order increase enrollment. Brooklyn Healthworks, which started with a small provider network, switched to a larger, well-recognized network and saw enrollment soar. Using a recognized commercial carrier is attractive not only because people are confident that they can find a provider they like, but also because it reduces stigma. In contrast, one program, which featured a more limited provider network, said that its limited network was not a deterrent to enrollment, in particular because the providers included in the plan are easy to access in terms of not having to wait to receive services and people are mainly concerned that they will be able to access services in their town or hospital.
Enrollment Process/Eligibility Criteria
All programs mentioned that the services that either program representatives or brokers provide to small business owners are crucial to getting them enrolled and keeping them enrolled.
Brokers increase the appeal of the enrollment process by facilitating enrollment. Brokers, program representatives, and marketing representatives do a lot of hand-holding and give a lot of personal attention to small business owners, including traveling to the business location, helping employees fill out their applications, filling out and submitting the application for the small business owner, answering questions, and acting as an advocate for the employer to the insurance company. Five of the 6 programs felt this customer service provided by brokers, marketing representatives, or the program staff was one of the main things that promotes and maintains enrollment, as these services are not typical of large insurance companies.
Since small businesses rarely have any HR staff, this function is critical to small business owners who don’t have the time or inclination to perform these functions themselves. A common response from brokers was:
I enroll new groups because I do everything for them. Every month I talk to them, submit their invoices, etc. We really hold the worker’s hand, especially with the online application.
Enrolling through a broker also increases the appeal of the program by reducing stigma related to the enrollment process, as business owners are enrolling in the program through a private entity rather than a government welfare office. Brokers also increase the appeal of the plan itself by really selling and conveying enthusiasm about the strengths of the plan, while also presenting any limitations of the plan in a straightforward way. As one broker noted:
Small employers have no idea what they’re buying and have to be convinced to buy the program to begin with. That takes a personal sales relationship through brokers to make that happen.
Finally, many small business owners who are eligible for subsidized coverage believe that they are not, and the broker can dispel this myth.
Eligibility criteria can affect enrollment both by dictating the overall size of the eligible population and by affecting the appeal of the program. Programs noted the key eligibility feature that increases enrollment is to determine eligibility at the firm level rather than the employee level. This is because in the small employer market, getting health insurance is a group decision, and the employers want a health plan that all of their employees are eligible for. As one broker noted:
[A] lot of [nonoffering] employers have three or four employees, and they say, “Let’s get some health insurance.” And they are looking at this and saying, “But the receptionist can’t participate because she was previously on Medicaid.” Then they say, “We’re not going to do it because we want to get insurance that everyone can get.” At the very small business level, health insurance is really a group decision, made collectively.
One program said that allowing independent contractors and part-time employees to enroll can be the tipping point for small businesses to enroll.40 Employers like that they can give coverage to their contract workers without having to pay anything toward it (this program does not have a minimum employer contribution).
Reducing or eliminating crowd-out provisions (that is, requirements that an employer not offer coverage for a certain period of time prior to enrolling in the subsidized coverage) is also beneficial to enrollment. As an intermediate measure, shortening the length of time an employer must not have offered insurance was cited as beneficial to enrollment.
Another eligibility requirement that can be unappealing is very low income eligibility criteria. Two programs noted that if the income limits are not generous enough, this causes people to associate the program with welfare.
Finally, the one program that did not require a minimum employer contribution noted that this was very appealing to small employers, as they could choose not to contribute to part-time employees if they wished. Interestingly, this program said that most employers contribute a lot more than 50 percent anyway. Conversely, in programs that required a minimum 50 percent contribution, employers usually contributed just 50 percent (as this “minimum” is interpreted as a “suggested” contribution).
Stigma
All but one program acknowledged that stigma was a consideration in designing their program, implying that stigma is something that can impact enrollment in subsidized programs. Discussants noted that programs can do a lot to prevent stigma. Stigma was rarely present because of the government subsidy itself, but rather, whether the program has a government feel to it, or is perceived by potential enrollees as closely associated with the government or welfare. Programs that offer premium subsidies for employers and workers are already at an advantage in terms of combating stigma, as several programs noted that offering the subsidy only to those who are working negates the perception of welfare.
Most discussants felt that their program features or marketing methods prevented enrollees from perceiving stigma or associating the program with welfare such that it did not deter enrollment. Programs avoided stigma by forming a partnerships with private entities to administer, sell, or promote the program (for example, using private brokers or marketing representatives, a third-party administrator, commercial carriers and plans) and giving the program a private name and feel. Cost-sharing also reduces stigma, particularly requiring the workers and/or employer to pay a premium.
The fact that the program is for people who are working also reduces stigma, which gives programs that offer premium subsidies for employers and workers a natural advantage in reducing stigma. One program said that they avoid emphasizing the government subsidy in their outreach but instead emphasized that the program is affordable. However, another program found through focus groups that enrollees in their particular community like a straightforward message about the program, including that there is a subsidy involved. Another program removed the term “poverty level” from its promotional materials and instead listed income eligibility in dollar terms. One program felt that since it did not have any cap on business revenue, it showed employers that the program is not just for “poor” businesses.
Some discussants felt stigma might be a problem, and one program felt a perception of stigma might have affected enrollment. Reasons noted for this possible stigma included that the application process checked for Medicaid eligibility, the program had low income limits, or because the program had a “government feel” or the program was closely tied with state. Brokers involved with two programs were also wary of a program tied with the government, so these programs were careful to minimize the government subsidy in their marketing to brokers, and instead emphasized the program's commercial qualities to both brokers and potential enrollees. One discussant also said that they tried to reduce stigma by emphasizing the personal, customer service that enrollees don’t typically get with a large insurance company—regarding stigma affecting enrollment, “it’s all in how you market it.”
Program Permanence
All programs said that program permanence is a concern for small employers and in some cases, for brokers. However, only half of programs felt that concern about program permanence was a deterrent to enrollment. Furthermore, discussants suggested several factors that can mitigate concern program permanence. The first is program duration. Two programs felt that the longer they had been around, the less concern there was among potential enrollees that the program would end. One broker noted that after the program had been around three years, it gained legitimacy in the eyes of the broker community, despite a fixed level of funding. The second is the appeal of other program features, including price, benefit design, and provider network, which if strong enough, outweigh concerns about program permanence. Brokers or program representatives also helped overcame potential enrollees’ concerns about program permanence by reassuring them that there was a lot of political support for the program and/or that it had the backing of a government entity, and also letting them know that funding was guaranteed through a certain date. Offering employers at least a two-year contract for the insurance and subsidy was noted by one program to alleviate fears of program permanence.
Although ties to the government can increase stigma, two programs (HealthChoice, O-EPIC) said that the government backing lent it credibility and stability. Some discussants emphasized that a program operating out of the state department of insurance was not the same as a program operating out of the department of health and welfare. However, enrollees in another program were concerned that because it was a government program, it could more easily go away.
How Can Programs Get Brokers on Board?
As noted above, discussants overwhelmingly pointed to brokers (or broker-like agents) as playing a critical hand-holding, marketing, and educational role that successfully enrolls small firms in subsidized coverage initiatives. As such, program officials must “sell” the program to brokers first in order to secure their participation.
To reach brokers, our discussants recommended starting with a compelling message that emphasized the salability of the program, the opportunity to serve the community and the ability to earn competitive commissions. Discussants also noted that in many cases, the target population represents new markets for these brokers and an opportunity to sell of other insurance products (such as life insurance). Another compelling message to brokers, as implied by one of our broker discussants, is that selling the subsidized coverage was cost-effective in terms of time spent by the broker, because although more up-front time was required of the broker, the employers stay with the plan for a long time (since there is no cheaper alternative), during which the broker receives the monthly commission without having to spend much additional time (depending on the commission structure). Conversely, small group commercial plans usually see big rate increases every year, prompting small groups to want the broker to shop for a cheaper plan, necessitating more time spent for the broker if they want to keep their client.
All programs that used brokers eventually paid commission rates (between 4 and 6 percent on the full, unsubsidized price of the plan) to be competitive with commissions offered by other commercial plans. All programs using brokers noted that this was important to getting brokers to sell the program. One program that did not offer competitive commissions at the start had a difficult time getting brokers’ attention. When the program started paying competitive commissions, brokers were ready to get on board and sell the program.
As important as commissions are, they are not sufficient to get brokers “on board.” Brokers can’t sell the program if they don’t know about it, and will be less likely to sell it if they don’t understand how the program works or if the application process is too foreign to them or too lengthy.
One program solicited broker input during the design stage of the program. Once the program design is in place, programs must establish relationships with brokers and market the program to them so that they understand how it works and how it will benefit them. Several programs have offered broker training sessions, and sometimes these session can be used to satisfy broker continuing education requirements. For example, one program initially used a statewide carrier that did not reach out to brokers in a particular county. When the program switched to a local carrier that had an established relationship with brokers in that county, and was very good at marketing to them, enrollment took off. This program set up meetings with brokers and used an outreach message emphasizing the program as an opportunity for brokers to give back to their community (community service), as well as earn commissions.
One program started off with an application process that was lengthy and foreign to brokers (similar to a Medicaid application), which brokers didn’t want to deal with. Switching to a standard small group market application with which brokers were accustomed greatly increased the appeal of the enrollment process and therefore increased the brokers’ willingness to sell the plan.
Discussants from two of our programs noted that only 10 percent or 20 percent of brokers are “really good brokers”, that is, willing and motivated to sell the plan. These programs leveraged these brokers by referring businesses that contacted the program office to them, increasing their chances of enrollment.
Anecdotal evidence suggests that not involving brokers in selling the program can actually be detrimental to enrollment. Brokers saw this program as competing with the insurance products they were trying to sell, so would speak negatively of the program. A negative perception of the program then spread by word-of-mouth among the target population of small business owners. The program had a very difficult time combating this negative perception, and enrollment suffered.
Chapter VI
Conclusions
The findings from our study confirm that nonprice program features affect enrollment. Specifically, discussants from all four coverage approaches agreed that certain nonprice program features were especially helpful for creating program awareness, comprehension, and appeal that led to enrollment. Further, the enrollment experience of several programs in this study indicate that efficiently enrolling significant numbers of adults into subsidized coverage programs is an achievable goal.41
In this final chapter, we compare our study findings across the four program types. This exercise identified some themes and lessons common in all program types. But it also confirmed that each coverage approach faces unique enrollment challenges and the outreach tactics, enrollment processes, and coverage design must be customized to attract efficiently enrollment. Research gaps remain, however, and we conclude with some suggestions for further research into the factors that influence nonelderly adult enrollment into subsidized coverage programs.
Successful Strategies Common to All Programs
Discussants from all four program types offered universal lessons about the program design and implementation features that attract enrollment. These include the importance of creating awareness of the program, getting trusted members of the community to deliver the message, avoiding stigma-inducing terms and application procedures, and providing application assistance and insurance counseling.
Program Awareness
Study participants widely agreed that programs must be proactive in creating awareness that results in enrollment. Even programs that almost “sell themselves” due to their appealing design require some marketing on the part of program officials. As a general rule, targeted, decentralized, community-based, in-person outreach approaches were deemed effective in creating awareness that led to enrollment. Discussants speculated that, with this type of outreach, potential enrollees hear about the program from a trusted source, which instantly increases the program’s credibility in ways that more generic marketing cannot accomplish. For similar reasons, discussants believed that word-of-mouth advertising was extremely important in developing awareness that leads to enrollment.
The program staff we spoke with employed various strategies to partner with trusted, community-based resources. The type of partner (clinic, community advocate, broker, etc.) varied depending on the type of program and the target audience.
Word-of-mouth advertising can be effective in creating awareness, but influencing or controlling it can be difficult. Many discussants emphasized that program officials must tailor the outreach message and materials to ensure that people are circulating accurate information about the program. Some discussants pointed out that surmounting poor public perceptions of a program is much more difficult than properly managing expectations in the first place. Poor public perceptions arise if enrollment systems cannot handle an unexpectedly large influx of applicants when the program begins or after a big marketing campaign. People also may develop negative feelings toward the program if there is confusion or incorrect expectations about who is eligible.
Discussants offered several suggestions for averting these issues. One promising technique is to test messages and enrollment systems with a small group initially. Some discussants also mentioned the need to balance politicians’ tendency to oversell the program’s potential; to do this, program staff should provide information about the enrollment levels that can be supported with the financing available for each program year. Discussants also recommended using a mix of outreach methods since potential applicants are more likely to enroll if they hear about the program from more than one source. However, discussants did not all agree on the best mix of methods within or across programs. While they believed that local media is effective in creating awareness, local media is not always necessary if limited program slots are available. In addition, studies and discussants were inconclusive on the impact and importance of broadly targeted mass media campaigns.
Program Comprehension
Discussants from all program types noted pervasive comprehension gaps among program applicants, particularly regarding insurance concepts and income eligibility criteria for the program. Discussants widely believed that providing insurance counseling is critical, in part because of these comprehension difficulties. They noted other strategies as desirable or even critical, such as simplifying the application process and removing technical terms and jargon, but these strategies appeared to be insufficient when used alone.
Discussants emphasized the significant time investment needed on the part of program representatives, brokers, and others to explain insurance concepts, the program’s income eligibility criteria, and required documentation. Difficulty understanding a program’s eligibility criteria concerned our discussants because individuals may fail to enroll if they erroneously believe that they are not eligible, a phenomenon also observed in the literature.
In light of concerns about comprehension difficulties consuming staff resources and possible underenrollment in the program, we were surprised that programs seemed to devote so little attention to new strategies that would reduce these problems. Similarly, program comprehension topics received the lightest treatment in our review of the literature. A few studies reinforced our discussants’ views that educating potential enrollees about the role and value of health insurance was a central part of the enrollment process. However, we found no studies that methodically measured comprehension difficulties among the target population for these programs or examined linkages to enrollment.
Program Appeal
Across all program types, discussants agreed on the key program features that appeal to enrollees. These include offering coverage that resembles private insurance, avoiding terms and application approaches that may create stigma, and providing a convenient and simple application process. However, the programs in our study were rarely able to implement coverage containing all the desired features; simplifying the application process was the most difficult to achieve. As discussed in the next section, the impact of unappealing features on enrollment varied by type of program.
Appealing Coverage
Comprehensive coverage, commercial provider networks, and low point-of-service cost-sharing are very appealing program features, according to almost all discussants.42 Discussants emphasized that coverage that resembles private insurance (with an insurance card, a booklet, and a nongovernmental name) had tremendous appeal because it is similar to the coverage that “everybody else has.” Other features universally noted as appealing include:
- No exclusions for pre-existing conditions
- Point-of-service cost-sharing in the form of co-payments rather than other forms (coinsurance, deductibles) because the enrollee’s financial risk is more predictable
- A provider networks that includes physicians and other providers who speak the applicant’s language (for those whose first language is not English)
- Coverage for the whole family, rather than just children or just the adult worker in the family (for applicants with spouses or children)
Stigma
Across all program types, discussants believed that welfare stigma was a real phenomenon that could deter enrollment. Neither the discussants nor the studies in our literature review rigorously contrasted the various forms of stigma. These include traditional welfare stigma (program is a government handout for poor people), application-related stigma (demeaning or intrusive application process), and provider stigma (providers treat program participants differently than privately insured patients).43 However, strategies mentioned by discussants seem to suggest that they were trying to avoid all three types of stigma. Most discussants felt that their program had taken steps to successfully minimize stigma by designing programs to look and feel like commercial coverage. However, discussants found it more difficult to minimize stigma during the application process due to the inherently intrusive nature of this process.
Ease of Application
Many discussants confirmed our findings from the SCHIP literature—that the convenience and simplicity of the application process plays an important role in program enrollment. An inconvenient and unappealing application process can be an especially strong deterrent in programs that have an employer role.
To make the application process more appealing, discussants recommended providing several entry points and integrating the outreach and application process so that applicants can apply “on the spot.” Making applications simpler and more user-friendly also has great appeal to the target population. The impact of these strategies on enrollment is uncertain, however, as applicants to almost all programs typically faced applications that could not be completed without extensive insurance counseling and application assistance from brokers, enrollment counselors, or others. It appears that this assistance is critical to completing the application process and that other steps (such as simplification) may be desirable but insufficient.
The complexity of the application process reflects to some degree the program’s underlying eligibility criteria. Because subsidized coverage programs typically target low-income residents, it’s necessary to collect income information from applicants. Almost all program designers faced a difficult trade-off between having an “ideal” application process (convenient, understandable, and nonintrusive) and program target effectiveness (maximizing enrollment of the targeted group – typically the low-income uninsured). Asking for income information is inherently intrusive; however, discussants identified some practices that minimized the intrusiveness, such as using existing information systems to validate income or allowing self-declaration of income. Similarly, anti-crowd-out provisions may dictate questions about eligibility for employer coverage or public coverage. The studies we reviewed provided little guidance on structuring or evaluating the trade-offs between simplifying the application process to encourage enrollment and the target effectiveness.
Findings Specific to Program Types
In comparing discussants’ views across program types, we found some critical differences in the relative importance of the design and implementation features that attract enrollment. Discussants also had surprising differences in their perception of the target population.
Gaining Small-Firm Participation Requires a Very Appealing Design
Both the literature and the discussants suggest that substantial premium subsidies are necessary but insufficient to attract enrollment by nonoffering employers in small firms. To attract enrollment, these programs must be designed so that every feature, including the benefit structure, enrollment processes, and eligibility criteria, are very appealing to several audiences: firm owners, workers, and often brokers. Program designers cannot overlook any dimension of the program in the planning stages, and well-targeted, sustained outreach, coupled with insurance counseling, is critical. For example, an otherwise well-designed program may still fail to attract significant enrollment if not all workers in a small firm are eligible. Similarly, if the coverage does not appeal to the firm owner, participation may be modest even if all other program dimensions are appealing.
Subsidized Programs That Target Adults Directly Have an Easier Time Attracting Enrollment
Compared with programs that target employers, programs that market directly to adults can offer less comprehensive benefits and have less attractive enrollment processes and still attract significant enrollment. This is especially true if the premiums are very low, the target population is aware of the program, and application assistance is available.
Premium Assistance Programs Face Enrollment Challenges
Premium assistance programs face some unique challenges in attracting enrollment. Some of these challenges are inherent and not easily surmounted by the program designer. Nationally, only about 20 percent of uninsured workers have access to an employer offer of coverage for which they are eligible (Garret 2004). The prevalence of Medicaid and SCHIP as funding sources often entails complex, multipart eligibility criteria and fairly low income eligibility levels—further limiting the size of the eligible population. Discussants reported that teasing out successful enrollment strategies in the face of these limitations proved difficult. Strategies included involving brokers in outreach and educational efforts and creating less restrictive enrollment periods. Discussants strongly recommended broadening income eligibility criteria, as they believed that many uninsured workers could meet the program’s other eligibility criteria and were having difficulty affording their employer’s coverage, despite their slightly higher incomes.
Varying Perceptions of Demand Among the Target Population
Discussants had very different perceptions of the demand for coverage across the four program types. Discussants for the brokered access and nongroup coverage programs widely emphasized the tremendous demand for coverage among their target populations. Often, they discounted the notion of “young invincibles” who do not want health coverage even when the cost is very low. Yet stakeholders for the employer subsidy programs reported that one of their enrollment barriers was the fact that many workers preferred higher wages over paying premiums of $40 a month. There is some overlap between these two target populations (as many uninsured adults work in small, nonoffering firms). Therefore, it is difficult to know how to reconcile these competing views.
Recognition of non-English speakers in the target population also varied widely between program types. In the brokered access and nongroup coverage programs, most discussants were aware of the non-English speakers in their target population, had strong views on the effectiveness of specific program features and outreach strategies for this population, and actively sought to enroll eligible non-English speakers. In contrast, discussants in the employer-based programs were often unsure how many non-English speakers were present in their target population and did not have strong views on the need for or effectiveness of enrollment strategies to attract this population. A few discussants from employer programs were aware of instances in which specific brokers successfully enrolled businesses within their ethnic community, but in only one case was this a purposeful enrollment strategy.44
More Research Needed to Guide Program Designers
Our study findings strongly suggest that nonprice program features affect enrollment but that additional research is needed to better quantify these determinants. Policymakers and program designers currently lack guidance on how to evaluate alternative designs and how to set and achieve enrollment targets. There is uncertainty about how alternative approaches to outreach, benefit designs, or application processes affect enrollment levels. In their initial stages, many program designers significantly overestimated enrollment in their programs, while others significantly underestimated take-up of the coverage.
Our review of the literature revealed little in the way of rigorous evaluations that relate program design and implementation features to enrollment levels in programs targeting uninsured, nonelderly adults. In part, this stems from the fact that subsidized coverage initiatives for nonelderly adults have not been evaluated to the degree associated with SCHIP and other children’s public coverage programs (see Appendix C) or even supplemental coverage options for the Medicare-eligible population.45
Because of the dearth of relevant literature, this study relied heavily on the rich body of information gleaned from our discussants. However, the discussants were hampered by the near-absence of measurement systems that relate nonprice design and implementation features to enrollment. Information systems that are missing include formal feedback systems that gauge the effectiveness of outreach strategies, the prevalence and characteristics of uncompleted applications, and a detailed picture of the eligible but unenrolled population. Discussants shared many apparently successful enrollment strategies (for example, a niche broker who brings in many enrollees from an ethnic community), but they often lacked the resources to better understand and replicate these successes. In addition, they were often unable to disseminate successful strategies to programs in other states.
Several areas investigated by this study were inconclusive. For example, in each program type, discussants gave inconsistent responses about the enrollment impact of charging nominal premiums or point-of-service co-payments. Many discussants believed these payments were attractive to applicants because they distinguish the program from Medicaid coverage. Discussants speculated that program participants felt the coverage had value because they were paying for it and that providers would treat them better if they paid for services. Other discussants felt that there was a segment of the eligible population (with very low income) who could not afford these payments; thus, the payments were an enrollment deterrent. Likely both views are accurate, as evidenced by occasions in which one stakeholder held both views.
Additional research is also needed to better understand and address the underlying sources of widespread comprehension difficulties among applicants. Furthermore, additional research is needed to understand the implementation and design features that are necessary to attract enrollment in a voluntary nongroup coverage program featuring more substantial (but still subsidized) premiums. Finally, attracting enrollment into premium assistance programs, especially opt-out programs, continues to be challenging for states. In particular, it is difficult to minimize the administrative role of the employer while also leveraging the employer’s influence on enrollment.
Several other areas merit additional investigation. Discussants cited many successful examples of partnering with trusted community partners, but program designers may need additional guidance to choose from among the various recommendations. Researchers should also investigate ways to minimize the intrusiveness of income verification procedures and reduce applicants’ confusion about these procedures. A few programs are using third-party verification procedures or allowing self-declaration of income, but the effectiveness of these promising approaches has not been rigorously studied or widely emulated.
Recommended Next Steps
The national drive for new approaches to health coverage suggests that more information is needed on the nonprice determinants of enrollment, in both high-demand and low-demand settings. Our literature review and discussions with program stakeholders exploited a small fraction of extant program knowledge. To aid policymakers at the federal, state, and local levels, significant additional research and knowledge dissemination are needed to better understand the relative importance of nonprice program features.
Based on our experience with this study, we recommend new qualitative studies that include additional subsidized coverage programs and more diverse stakeholders. In particular, researchers may find it useful to include stakeholders closer to the enrollee decision-making process as well as focus groups of eligible residents who are not enrolled. To quantify the importance of these design and implementation features, program officials and researchers must roll out changes to enrollment processes or other program features in a controlled fashion so that they can be evaluated to better understand their enrollment impact. To facilitate such investigations, a concerted effort must be made to improve the informational feedback systems of these subsidized coverage programs.
References
Access to Benefits Coalition, National Council on Aging. “Pathways to Success: Meeting the Challenge of Enrolling Medicare Beneficiaries with Limited Incomes.” June 24, 2005.
Adams, J. M. “San Francisco Launches Universal Health Care.” Chicago Tribune, September 18, 2007.
Aizer, A. “Low Take-Up in Medicaid: Does Outreach Matter and for Whom?” American Economic Review, vol. 93, no. 2, 2003, pp. 238-241.
Alexander, G. “Annual Report on the Department of Human Services' Implementation of Programs to Address Uninsurance among Rhode Islanders.” Rhode Island: Permanent Joint Committee on Health Care Oversight, 2008.
Alker, J. “Premium Assistance Programs: How Are They Financed and Do States Save Money.” Washington, DC: Kaiser Family Foundation, 2005.
Alker, Joan. “Choosing Premium Assistance: What Does State Experience Tell Us?” Kaiser Commission on Medicaid and the Uninsured. [Avaiable at http://www.kff.org/medicaid/upload/7782.pdf]. May 2008
Anderson, N., and T. Bowe. “Understanding Disenrollment from DirigoChoice: Results of a Survey and Telephone Interviews with Former Members of Maine's State-Sponsored Health Insurance Program. Draft Report Prepared for the Dirigo Health Agency and the Governor's Office of Health Policy and Finance.” Portland, ME: University of Southern Maine, Muskie School of Public Service, 2006.
Artiga, Samantha, D. Rousseau, B. Lyons, S. Smith, and D. Gaylin. “Can States Stretch The Medicaid Dollar Without Passing The Buck? Lessons from Utah.” Health Affairs, vol. 25, no. 2, 2006, pp. 532-540.
Bansak, C. and S. Raphael. “The Effects of State Policy Design Features on Take-Up and Crowd-Out Rates for the State Children's Health Insurance Program.” Journal of Policy Analysis & Management, vol. 26, no. 1, 2007, pp. 149-175.
Belloff, D. and K. Fox. “Design and Enrollment in Premium Support Programs for Low Income Populations: State Interviews and New Jersey Data Simulations.” New Jersey: State of New Jersey Department of Human Services, Rutgers Center for State Health Policy, 2006.
Belnap, D. and S. Schwartz. “Premium Assistance.” Portland, ME: National Academy for State Health Policy, October 2007.
Bowe, T. “DirigoChoice Member Survey: A Snapshot of the Program's Early Adopters.” Portland, ME: Institute for Health Policy, Muskie School of Public Service, University of Southern Maine, 2005.
Brown, L. “Impermanent Politics: The Hillsborough County Health Care Plan and Community Innovation for the Uninsured.” Health Affairs, vol. 25, no. 3, 2006, pp. 162-172.
Brown, L. D., and B. Stevens. “Charge of the Right Brigade? Communities, Coverage, and Care for the Uninsured.” Health Affairs, vol. 25, no. 3, May 1 2006, pp. 150-161.
Christensen, M. “Wayne County, Mich., Small-Business Health Plan Tries to Regroup.” Knight Ridder Tribune, May 18, 2004.
Cohen, R., and T. Wolfe. “Implementing New York’s Family Health Plus Program: Lessons From Other States.” New York, NY: The Commonwealth Fund, November 2001.
Dorn, S. “Health Coverage Tax Credits in North Carolina: Heroic Efforts, Modest Results.” Washington, DC: Economic and Social Research Institute, 2004.
Dorn, S. “How Well do Health Coverage Tax Credits Help Displaced Workers Obtain Health Care?” Testimony before the Committee on Education and Labor, Congress of the United States and U.S. House of Representatives, 2007.
Dorn, S. “Millions of Low-Income Americans Can’t Get Medicaid: What Can Be Done?” Washington, DC: AARP Public Policy Institute, 2008.
Dorn, S., J. Varon, and F. Pervez. “Limited Take-Up of Health Coverage Tax Credits: A Challenge to Future Tax Credit Design.” Report No. 869. New York, NY: Commonwealth Fund, October 2005.
Dorn, Stan, and Jack Meyer. “Pennsylvania: A Case Study in Childless Adult Coverage.” Washington, DC: Economic and Social Research Institute, 2004.
Dubay, Lisa, and Genevieve Kenney. “Expanding Public Health Insurance to Parents: Effects on Children's Coverage Under Medicaid.” Health Services Research, vol. 38, no. 5, 2003, pp. 1283-1302.
Dunkelberg, A. “Simplified Eligibility for Children's Medicaid in Texas: A Status Report at Nine Months.” Washington, DC: Kaiser Commission on Medicaid and the Uninsured, 2003.
EP&P Consulting, Inc. “2007 Annual Report on Healthy NY.” New York: State of New York Insurance Department, 2008.
EP&P Consulting, Inc. “Report on the Healthy NY Program 2004.” New York: State of New York Insurance Department, 2004.
Espeseth, A. H., and R. Riportella. “Wisconsin's Recent BadgerCare Enrollment Decline: How Administrative Rules Can Set Off Unanticipated Change.” The Journal of Ambulatory Care Management, vol. 29, no. 4, 2006, pp. 300-309.
Ettner, S. L. “Medicaid Participation Among the Eligible Elderly.” Journal of Policy Analysis & Management, vol. 16, 1997, pp. 237-255.
Flores, Glenn, Milagros Abreu, Christine E. Chaisson, Alan Meyers, Ramesh C. Sachdeva, Harriet Fernandez, Patricia Francisco, Beatriz Diaz, Ana Milena Diaz, and Iris Santos-Guerrero. “A Randomized, Controlled Trial of the Effectiveness of Community-Based Case Management in Insuring Uninsured Latino Children.” Pediatrics, vol. 116, no. 6, December 2005, pp. 1433-1441.
Frates, J., J. Diringer, and L. Hogan. “Models and Momentum for Insuring Low-Income, Undocumented Immigrant Children in California.” Health Affairs, vol. 22, no. 1, 2003, pp. 259-263.
Friedsam, D., G. Haug, M. Rust, and A. Lake. “Tribal Benefits Counseling Program: Expanding Health Care Opportunities for Tribal Members.” American Journal of Public Health, vol. 93, no. 10, 2003, pp. 1634-1636.
Fronstin, P., and J. Lee. “A Community Expands Access to Health Care: The Case of Access Health in Michigan.” Health Affairs (Project Hope), vol. 24, no. 3, May-June 2005, pp. 858-863
Garnick, D. W., A. M. Hendricks, K. E. Thorpe, J. P. Newhouse, K. Donelan, and R. J. Blendon. “How Well Do Americans Understand Their Health Coverage?” Health Affairs, vol. 12, no. 3, fall 1993, pp. 204-212.
Garrett B. “Employer-Sponsored Health Insurance Coverage: Sponsorship, Eligibility, and Participation Patterns in 2001.” Menlo Park, CA: Kaiser Commission on Medicaid and the Uninsured, July 2004.
Glied, S. “Lessons from SCHIP.” Health Services Research, vol. 42, no. 4, 2007, pp. 1439-1442.
Grantmakers In Health. “Improving Health Access in Communities: Lessons for Effective Grantmaking.” Washington, DC: Grantmakers In Health, February 2005.
Hadley, J., and J. D. Reschovsky. “Small Firms' Demand for Health Insurance: The Decision to Offer Insurance.” Inquiry: A Journal of Medical Care Organization, Provision and Financing, vol. 39, no. 2, summer 2002, pp. 118-137.
Helms, W. D., A. K. Gauthier, and D. M. Campion. “Mending the Flaws in the Small-Group Market.” Health Affairs, vol. 11, no. 2, summer 1992, pp. 7-27.
Hendryx, M., M. Ahern, N. Lovrich, and A. McCurdy. “Access to Health Care and Community Social Capital.” Health Services Research, vol. 37, 2002, pp. 87–103.
Hill, I., and A. W. Lutzky. “Getting in, Not Getting in, and Why: Understanding SCHIP Enrollment.” Washington, DC: Urban Institute, 2003.
Hill, I., B. Courtot and E. Wada. “A Healthy Start for the Los Angeles Healthy Kids Program.” Washington, DC: Urban Institute, 2005.
Hoffman, C., A., Carbaugh, and A. Cook. “Health Insurance Coverage in America: 2003 Data Update.” Washington, DC: Kaiser Commission on Medicaid and the Uninsured, 2004.
Holahan, D., and E. Hubert. “Lessons from States with Self-Declaration of Income Policies.” Report No. 148. New York, NY: United Hospital Fund, 2004.
Howell, E., Ruth Almieda, Lisa Dubay, and Genevieve Kenney. “Early Experience with Covering Uninsured Parents Under SCHIP.” Washington, DC: Urban Institute, 2002.
Howell, Embry, Christopher Trenholm, Kathy Gifford, and Bridget Lavin. “Case Study of Virginia: Exploring Medicaid and SCHIP Enrollment Trends and Their Links to Policy and Practice. Final Report.” Mathematica Policy Research, Inc., The Urban Institute; Health Management Associates, 2006.
Institute of Medicine. A Shared Destiny: Community Effects of Uninsurance. Washington, DC: National Academies Press, 2003.
Institute of Medicine. Health Literacy: A Prescription to End Confusion. Washington, DC: National Academy Press, 2004.
Irvin, Carol, Nancy Fasciano, and Margo Rosenbach. “SCHIP in Ohio: Evolution and Outlook for the Future.” Mathematica Policy Research, Inc., 2004.
Katz, M. H. “Golden Gate to Health Care for All? San Francisco’s New Universal Access Program.” The New England Journal of Medicine, vol. 358, no. 4, January 2008, pp. 327-329.
Kenney, G., and D. I. Chang. “The State Children's Health Insurance Program: Successes, Shortcomings, and Challenges.” Health Affairs, vol. 23, no. 5, 2004, pp. 51.
Ketsche, Patricia, E., K. Adams, Karen Minyard, and Rebecca Kellenberg. “The Stigma of Public Programs: Does a Separate S-CHIP Program Reduce It?” Journal of Policy Analysis & Management, vol. 26, no. 4, fall 2007, pp. 775-789.
Kilbreth, E. “Comparing the DirigoChoice Program Experience with Other State Initiatives Targeted to Small Business and Individuals.” Portland, ME: University of Southern Maine, Edmund S. Muskie School of Public Service, Institute for Health Policy, August 2006.
Kincheloe, J., J. Frates, and E. R. Brown. “Determinants of Children's Participation in California's Medicaid and SCHIP Programs.” Health Services Research, vol. 42, no. 2, April 2007, pp. 847-866.
Klein, K., and S. Schwartz. “State Efforts to Cover Low-Income Adults Without Children.” State Health Policy Monitor, vol. 2, issue 3, September 2008, pp. 1–12.
Kronebusch, K., and B. Elbel. “Enrolling Children in Public Insurance: SCHIP, Medicaid, and State Implementation.” Journal of Health Politics, Policy, and Law, vol. 29, no. 3, June 2004, pp. 451-489.
Kronick, R. “Is Small Business the Key to Insuring More Californians?” Oakland, CA: California HealthCare Foundation, 2005.
Kronick, R., and L. C. Olsen. “A Needle in a Haystack? Uninsured Workers in Small Businesses That Do Not Offer Coverage.” Health Services Research, vol. 41, no. 1, February 2006, pp. 40-57.
Kronick, R., L. C. Olsen, and T. P. Gilmer. “The Response of Small Businesses to Variation in the Price of Health Insurance: Results from a Randomized Controlled Trial.” Medical Care Research and Review, vol. 65, no. 2, April 2008, pp. 187-206.
Ku, L., and M. Broaddus. “The Importance of Family-Based Insurance Expansions: New Research Findings About State Health Reforms.” Washington, DC: Center on Budget and Policy Priorities, 2000.
Kullgren, J., and C. McLaughlin. “Beyond Affordability: The Impact of Nonfinancial Barriers on Access for Uninsured Adults,” unpublished manuscript.
Lewin Group in partnership with Empire Health Advisors. “Report on Healthy NY Program 2003.” New York: State of New York Insurance Department, December 31, 2003.
Lipson, D. J., J. M. Verdier, and L. Quincy. “Leading the Way? Maine’s Initial Experience in Expanding Coverage through Dirigo Health Reforms.” Commonwealth Foundation, Robert Wood Johnson Foundation, Mathematica Policy Research, 2007.
Littlepage, M. K. “Jaxcare Mid-Point Report.” Jacksonville, FL: The Jacksonville Community Forums on Health Care and the Uninsured, April 3, 2006.
Lo Sasso, A. T., and B. Meyer. “The Health Care Safety Net and Crowd-Out of Private Health Insurance,” unpublished manuscript, May 2004.
Long, S. H., and M. S. Marquis. “Low-Wage Workers and Health Insurance Coverage: Can Policymakers Target Them Through Their Employers?” Inquiry, vol. 38, no. 3, fall 2001, pp. 331-337.
Mack, M., R. Uken, and J. Powers. “People Improving the Community's Health: Community Health Workers as Agents of Change.” Journal of Health Care for the Poor and Underserved, vol. 17, no. 1 suppl, February 2006, pp. 16-25.
Mann, C. “Reaching Uninsured Children Through Medicaid: If You Build It Right, They Will Come.” Washington, DC: Kaiser Commission on Medicaid and the Uninsured, 2002.
McLaughlin, C. G., and W. K. Zellers. “The Shortcomings of Voluntarism in the Small-Group Insurance Market.” Health Affairs, vol. 11, no. 2, summer 1992, pp. 28-40.
Minyard, K., D. J. Chollet, L. Felland, L. Lonergan, C. Parker, T. Anderson-Smith, C. Lacson, and J. Wong. “Lessons from Local Access Initiatives: Context, Sustainability, and Replication. Findings from a Study of Five States.” Working paper. Atlanta, GA: Georgia Health Policy Center, 2005.
Minyard, Karen, Deborah Chollet, Laurie Felland, Lindsey Lonergan, Chris Parker, Tina Anderson-Smith, Claudia Lacson, and Jaclyn Wong. “Lessons from Local Access Initiatives: Contributions and Challenges.” The Commonwealth Fund, August 2007.
Mitchell, J. B., and D. S. Osber. “Using Medicaid/SCHIP to Insure Working Families: The Massachusetts Experience.” Health Care Financing Review, vol. 23, no. 3, 2002, pp. 35-45.
Mitchell, J. B., S. G. Haber, and S. Hoover. “Premium Subsidy Programs: Who Enrolls, and How Do They Fare?” Health Affairs, vol. 24, no. 5, 2005, pp. 1344-1355.
Nakashian, M. “Increasing Health Insurance Coverage at the Local Level: The Communities in Charge Program.” In RWJF Anthology: To Improve Health and Health Care Volume X, edited by S. L. Isaacs and J. R. Knickman. San Francisco, CA: Jossey-Bass, 2006.
Neuschler, E., and R. Curtis. “Premium Assistance: What Works? What Doesn’t?” Washington DC: Institute for Health Policy Solutions, 2003.
Nicholson-Crotty, S. “The Impact of Program Design on Enrollment in State Children's Health Insurance Programs.” Policy Studies Journal, vol. 35, no. 1, 2007, pp. 23-35.
Office for Oregon Health Plan Policy and Research. “SCHIP Funding for Employer-Sponsored Insurance: Federal Issues and Barriers Encountered.” February 2001.
Office of Health Care Statistics. “Utah Primary Care Network Disenrollment Report.” Salt Lake City, UT: Utah Department of Health, 2004.
Oklahoma Health Care Authority. “Insure Oklahoma Enrollment Climbs 81 Percent.” Oklahoma City, OK: Oklahoma Health Care Authority, 2008.
“One-e-App Helps Keep Healthy San Francisco Healthy.” Oakland, CA: California HealthCare Foundation, 2007.
Oppenheimer, C., A. Jaszczak, S. Goldman, D. Gaylin, S. Artiga, and D. Rousseau. “A Case Study of the Utah Primary Care Network Waiver: Insights into its Development, Design, & Implementation.” Washington, DC: Kaiser Family Foundation, 2006.
Ormond, C., and S. Gerrish. “Opportunities and Challenges: Improving Access and Health Outcomes through the CarePartners Program.” Portland, ME: MaineHealth Access Foundation, 2006.
Paasche-Orlow, M. K., R. M. Parker, J. A. Gazmararian, L. T. Nielsen-Bohlman, and R. R. Rudd. “The Prevalence of Limited Health Literacy.” Journal of General Internal Medicine, vol. 20, no. 2, 2005, pp. 175-184.
Perry, M. “Marketing Medicaid and CHIP: A Study of State Advertising Campaigns.” Washington, DC: Kaiser Commission on Medicaid and the Uninsured, 2000.
Remler, D. K., and S. A. Glied. “What Other Programs Can Teach Us: Increasing Participation in Health Insurance Programs.” American Journal of Public Health, vol. 93, no. 1, January 2003, pp. 67-74.
Rosenbach, M., C. Irvin, A. Merrill, S. Shulman, J. Czajka, C. Trenholm, S. Williams, S. S. Limpa-Amara, and A. Katz. “National Evaluation of the State Children’s Health Insurance Program: A Decade of Expanding Coverage and Improving.” Cambridge, MA: Mathematica Policy Research, Inc., September 2007.
Rosenbach, M., M. Ellwood, J. Czajka, C. Irvin, C. Young, W. Conroy, B. Quinn, and M. Kell. “Implementation of the State Children’s Health Insurance Program: Synthesis of State Evaluations.” Cambridge, MA: Mathematica Policy Research, Inc., March 2003.
Rosenberg, S. N. “Lessons from a Small Business Health Insurance Demonstration Project.” Report No. 149. New York, NY: The Commonwealth Fund, 2002.
Ryan, J. “Local Coverage Initiatives Solution or Band-Aid for the Uninsured?” Washington, DC: National Health Policy Forum, 2005.
Shirk, C., and J. Ryan. “Premium Assistance in Medicaid and SCHIP: Ace in the Hole or House of Cards?” Washington, DC: National Health Policy Forum, July 2006.
Silow-Carroll, S. “Community-Based Health Plans for the Uninsured: Expanding Access, Enhancing Dignity.” Battle Creek, MI: WK Kellogg Foundation, 2001.
Silow-Carroll, S. “New York: A Case Study in Childless Adult Coverage: State Report.” Washington, DC: Economic and Social Research Institute, 2004.
Silow-Carroll, S., E. K. Waldman, and J. A. Meyer. “Expanding Employment-Based Health Coverage: Lessons from Six State and Local Programs.” New York, NY: The Commonwealth Fund, 2001.
Silow-Carroll, S., S. E. Anthony, and J. A. Meyer. “State and Local Initiatives to Enhance Health Coverage for the Working Uninsured.” New York, NY: The Commonwealth Fund, 2000.
Silow-Carroll, S., T. Alteras, and H. Sacks. “Community-Based Health Coverage Programs: Models and Lessons.” Battle Creek, MI: WK Kellogg Foundation, 2004.
Sparer, M. “Health Policy for Low-Income People in Arizona.” Washington, DC: Urban Institute, 1999.
Spencer, A. “Covering California’s Kids: Multi-Pronged Approach Yields Impressive Results.” State Health Notes, 2006.
State Coverage Initiatives. “Profiles in Coverage: New Mexico State Coverage Insurance.” Available at [www.statecoverage.net/nmcoverageprofile.pdf]. 2005.
Seninger, Steve. “2006 Employer Survey on Health Insurance in Montana.” Montana Business Quarterly, winter 2006.
Stuber, J. P., K. A. Maloy, S. Rosenbaum, and K. C. Jones. “Beyond Stigma: What Barriers Actually Affect the Decisions of Low-Income Families to Enroll in Medicaid?” Washington, DC: George Washington University Medical Center, School of Public Health and Health Services, 2000.
Sullivan, Jennifer, Ian Hill, and Christopher Trenholm. “Case Study of California: Exploring Medicaid and SCHIP Enrollment Trends and Their Links to Policy and Practice. Final Report.” Mathematica Policy Research, Inc.; The Urban Institute; Health Management Associates, 2006.
Taras, H. L., M. L. Zuniga de Nuncio, and E. Pizzola. “Assessing an Intensive School-Based Assistance Program to Enroll Uninsured Children.” Journal of School Health, vol. 72, no. 7, Sep 2002, pp. 273-277.
Task Force on Access to Health Care in Texas. “Code Red: The Critical Condition of Health Care in Texas.” Texas: Task Force on Access to Health Care in Texas, 2008.
Taylor, E. F., C. G. McLaughlin, A. W. Warren, and P. H. Song. “Who Enrolls in Community-Based Programs for the Uninsured, and Why Do They Stay?” Health Affairs, vol. 25, no. 3, May-June 2006, pp. 183-191.
Taylor, E. F., J. T. Kullgren, and C. G. McLaughlin. “Who Enrolls in a Program for Parents of Publicly Insured Children?” Health Affairs, 2003.
Taylor, E. F., P. Cunningham, and K. McKenzie. “Community Approaches to Providing Care for the Uninsured.” Health Affairs, vol. 25, no. 3, May-June 2006, pp. 173-182.
Taylor, L., and Rafe Forland. “Coverage of Uninsured Workers in Small Firms: The Significance of Self-Employment among Firm Owners.” Washington, DC: Institute for Health Policy Solutions, 2003.
Taylor, L. “Using Premium Assistance to Expand Coverage Through Small Firms Appendix.” Washington, DC: Institute for Health Policy Solutions, 2004.
The National Institute for Health Care Management Research and Educational Foundation. “Understanding the Uninsured: Tailoring Policy Solutions for Different Subpopulations.” Washington, DC: National Institute for Health Care Management Research and Educational Foundation, April 2008.
The National Institute for Health Care Management Research and Educational Foundation. “The Uninsured: A Study of Health Plan Initiatives and the Lessons Learned.” Washington, DC: National Institute for Health Care Management Research and Educational Foundation, March 2003.
U.S. Government Accountability Office. “Medicaid: Three States' Experiences in Employer-Based Health Insurance.” Report No. GAO/HEHS-97-159. Washington, DC: United States General Accounting Office, 1997.
Volpel, A., A. Mikow, and T. Eberly. “Marketing State Insurance Coverage Programs: Experiences from Four States.” AcademyHealth, November 2007.
W. K. Kellogg Foundation. “Community Voices: Alameda County.” Available at [http://www.wkkf.org/default.aspx?tabid=102&CID=7&CatID=7&ItemID=70204&N…]. 2002.
Walls, J., B. Lavin, Kathy Gifford, and C. Trenholm. “Case Study of Arkansas: Exploring Medicaid and SCHIP Enrollment Trends and Their Links to Policy and Practice. Final Report Submitted to the Robert Wood Johnson Foundation.” Mathematica Policy Research, Inc., The Urban Institute, Health Management Associates, July 2006.
Weiss, B. D., J. S. Blanchard, D. L. McGee, G. Hart, B. Warren, M. Burgoon, and K. J. Smith. “Illiteracy Among Medicaid Recipients and its Relationship to Health Care Costs.” Journal of Health Care for the Poor and Underserved, vol. 5, no. 2, 1994, pp. 99-111.
Westpfahl Lutzky, Amy, and Ian Hill. “Premium Assistance Programs under SCHIP: Not for the Faint of Heart?” Urban Institute, Occasional Paper Number 65, 2003.
Williams, C. “A Snapshot of State Experience Implementing Premium Assistance Programs.” Portland, ME: National Academy for State Health Policy, 2003.
Wolfe, B. L., and S. Scrivner. “The Devil May Be in the Details: How the Characteristics of SCHIP Programs Affect Take-Up.” Journal of Policy Analysis & Management, vol. 24, no. 3, 2003, pp. 499-522.
Wooldridge, J. “Congressionally Mandated Evaluation of the State Children's Health Insurance Program: Final Report to Congress.” Princeton, NJ: Mathematica Policy Research, Inc., 2005.
Zahn, D., S. Hirota, J. Garcia, and M. J. Ro. “Alliance Family Care—Filling the Gap in Health Coverage.” American Journal of Public Health, vol. 93, no. 11, 2003, pp. 1797-1799.
Zambrana, R. E., and O. Carter-Pokras. “Improving Health Insurance Coverage for Latino Children: A Review of Barriers, Challenges and State Strategies.” Journal of the National Medical Association, vol. 96, no. 4, April 2004, pp. 508-523.
Appendix A
Study Methodology
Mathematica Policy Research, Inc. (MPR) conducted this study for the Office of the Assistant Secretary of Planning and Evaluation in the U.S. Department of Health and Human Services to identify nonprice program features that contribute to the successful enrollment of the program’s target population.46 Reflecting the limited state of research on this topic, our approach to the study question included two phases. Phase 1 was a literature review of the current state of knowledge on the impact of nonprice design features on enrollment. Information gathered from this literature was used to inform Phase 2—discussions with program directors and other key informants from 17 subsidized coverage programs across the country.
This study is qualitative in design. Guided by the concept of triangulation to validate findings, MPR included a variety of perspectives in selecting programs and stakeholder participants for the study. Nonetheless, the opinions expressed in the findings represent a limited number of viewpoints. Similarly, most of the studies reviewed for this report were qualitative in nature and reflected the views of a small group of individuals. As such, we cannot say with certainty whether our study findings can be generalized to all subsidized health coverage programs. Despite this limitation, we believe the combined evidence from the literature review and discussions with program representatives yields valuable information that will help focus future research on the determinants of enrollment. Further, these study findings may immediately help program administrators and policymakers design programs that successfully and predictably attract their target populations.
Programs Included in the Study
Reflecting the fact that many high-quality studies have already examined the determinants of children’s enrollment (see Appendix C), this study is restricted to voluntary state and local programs that subsidize care or coverage for non-elderly adults, although some programs also provide coverage to children. To make our findings more useful and accessible to policymakers, we structured our study around four focal program types. They represent different approaches to expanding access to subsidized coverage or care:
- Brokered Access to Subsidized Care. Programs that offer access to subsidized medical services but are not true health coverage. These programs use safety net providers but also coordinate care in some way (such as a managed care model), may function as a “medical home,” and include the concept of membership or enrollment.
- Subsidized, Nongroup Coverage for Adults. Programs that subsidize nongroup coverage purchased directly by adults.
- Premium Subsidies for Workers. Programs that subsidize the worker’s share of the premium for employer-based coverage. Subsidy may extend to worker’s dependents covered under an employer-sponsored family policy, but the employer’s share of the premium is not directly subsidized.
- Premium Subsidies for Employers and Workers. Programs that subsidize both the employer and worker’s premium shares for group coverage.
Not all programs reviewed for this study fall cleanly into one of these four categories. For example, Access Health in Muskegon, Michigan, closely resembles health insurance coverage but is not, in fact, a licensed insurance product. As shown in Appendix B, in the case of this program (and a few others), we believe this is not a meaningful distinction from the perspective of the beneficiary, and thus have included such products in “Premium Subsidies for Employers and Workers.”
Logic Model Used to Frame the Analysis
This study makes use of a framework or logic model to structure the analysis. This logic model hypothesizes how various nonprice program design and implementation features influence program enrollment via three intermediate outcomes: awareness, comprehension, and appeal.
The logic model is based on the premise that program premiums (post-subsidy) and the characteristics of the target population are controlled for, recognizing that these factors have a significant impact on enrollment. Within a given premium range and target population, the model then postulates that enrollment is the result of a program’s nonprice design and implementation features. These include outreach method, intensity, targeting and message; benefit design; the underlying simplicity or complexity of the program (particularly related to the eligibility criteria, the benefits design, the subsidy structure, and the application materials and process); and the perceived value of the benefits design, such as minimizing stigma and creating appeal.
These features influence enrollment via three intermediate outcomes: awareness, comprehension, and appeal.
- Awareness refers to whether the target population knows that the program exists. Our study looked at how the program’s outreach methods, intensity, and targeting (successfully getting the message in front of its intended audience) influenced program awareness. In particular, we focus on awareness that resulted in enrollment.
- Comprehension refers to whether or not the target population understands the eligibility criteria for the program, its costs and benefits, and the actions necessary to apply for enrollment. Comprehension is contingent upon program awareness. Program design features that may influence comprehension include the underlying complexity (or simplicity) of the benefit design, the subsidy structure, and the enrollment process. Comprehension may also be facilitated by outreach materials written at an appropriate grade level for the target population and available in appropriate languages, and by the availability of application assistance.
- Appeal is contingent upon awareness and comprehension and is key to successful enrollment. For the program to be appealing, the benefits design and the provider network must appear to have value. The premium subsidy structure, the mechanism by which enrollees receive the premium subsidy, must not be a deterrent to enrollment. Similarly, the application process and the eligibility criteria should not deter enrollees. Our study also examined how outreach messages and application materials could be crafted to promote program appeal.
The detailed logic model is depicted in Figure A.1.
In developing this model, we carefully reviewed the SCHIP research findings described in Appendix C, examining a total of 34 studies. We also reviewed a large study that examined reasons for lower than expected take-up of the federal Health Coverage Tax Credit (HCTC) enacted in 2003 (Dorn 2007; Dorn et al. 2005). Finally, we consulted a study by Remler and Glied (2003) who reviewed a large number of peer-reviewed studies examining a broad range of programs (from Medicaid and Medicare to food stamps to 401(k) plans), and comprehensively examined the determinants of enrollment in social benefit programs.
Figure A.1. Nonprice Factors Affecting Enrollment Into Subsidized Health Coverage or Care Programs
Approach to Literature Review
In Phase 1, we reviewed the literature on studies assessing nonprice design and implementation features that encouraged or impeded the enrollment of various programs’ target populations.
To identify potential studies, we searched the MEDLINE database, using both PubMed and OVID with key words such as “community health services,” “heath coverage,” “medically uninsured,” and “health services accessibility.” We also performed more general searches such as “health or health care” in combination with “access,” “subsidy,” “take-up,” or“program participation.” Realizing these programs are relatively new and that few have undergone rigorous evaluations to assess their effectiveness (particularly with respect to nonprice design features), we also used our key words to search Google Scholar, an online resource that includes publications from research organizations, professional societies, and academic publishers (sometimes referred to as the “grey literature”). We did not apply strict criteria with respect to study design but did cast a broad net that included enrollee surveys and informed speculation by program officials. Finally, we reviewed the reference lists of relevant studies to identify additional studies.
Generally, we limited the results to studies published in 1996 (when SCHIP was enacted) or later. The review was further limited to studies that had an abstract available through PubMed or OVID. Ultimately, several additional studies were included as seminal. Studies that did not address nonprice design features (i.e., studies that focused solely on issues such as financing, provider networks, managed care elements, or harnessing local support for a program) were deemed outside the scope of this review.
This review was completed in April of 2008 and this report may not reference studies published since that time.
We identified approximately 46 studies or articles that contained findings on at least one nonprice design feature of a subsidized coverage initiative affecting enrollment of the target population (Table A.1). All of these studies were descriptive in nature.
| Program Type | Number of Studies Reviewed |
|---|---|
| Brokered access to subsidized care | 13 |
| Subsidized, nongroup coverage for adults | 23 |
| Premium subsidies for workers | 14 |
| Premium subsidies for employers and workers | 20 |
| Total* | 46 |
*Numbers do not sum because many studies addressed more than one type of coverage program.
Approach to Stakeholder Discussions
In Phase 2, our goal was to gather a variety of stakeholders’ perspectives on nonprice features that influence enrollment in subsidized health coverage programs. In all, we held 67 discussions with stakeholders representing 17 different programs.
Programs were selected purposively in order to achieve multiple aims. First, we included several programs representing each of the four focal types discussed above. This made it possible to conduct analyses both within and across program types. Within each program type, the objective was to achieve geographic diversity in the selection of programs. In addition, selected programs had a range of experiences and lengths of operation to help us gain an understanding of programs that have achieved their enrollment goals as well as those still working toward these goals.
We spoke with a variety of stakeholders in order to incorporate a wide variety of perspectives, ranging from the views held by program implementers during the design phase to views of “on-the-ground” enrollment counselors and providers after implementation. A complete list of program directors, outreach specialists, enrollment counselors, community advocates, health care providers, brokers, and others who participated in this study is included in the acknowledgments section of the report. Including an array of stakeholders also allowed us to validate findings by comparing responses across discussants who played different roles in the same program.
To encourage frank discussion, we told our discussants that we would not attribute specific comments or observations to him or her in our final report. However, we received permission from all discussants to list their names and affiliations in the acknowledgements section of the report.
We asked our study participants open-ended questions about their views on the program features that encouraged or deterred enrollment. We also used our logic model structure to probe for additional insights. For example, if a discussant did not volunteer any enrollment insights about the program’s application, we would pose a specific follow-up question. If the response was not clear on this point, we might probe further to understand if the application was difficult to understand, unappealing, or both.
Most discussions were held over the telephone, with one MPR team member leading the discussion and another taking detailed notes. We also conducted four site visits to gain more in-depth knowledge of a representative sample of our programs. Team members collaboratively reviewed discussion notes for accuracy and contacted discussants to clarify lingering questions and unclear points.
Data Analysis and Synthesis
We used a systematic approach to the analysis and synthesis of our discussants’ views. Specifically, we imported the notes into the ATLAS.ti system and used the software’s coding and query functions to rearrange and categorize their views by type of program and other characteristics. We also examined responses by program type and respondent type. Within-program type analysis allowed for the assessment of nonprice program features influencing enrollment that are specific to that particular type of program. Across-type analysis allowed us to identify both common themes and important differences in findings across program types.
The final steps in our analysis were interpretation of the data (noting strong consensus as well as conflicting findings), a synthesis of the literature review findings and the discussants views, and analysis to extract the relevant implications for program design, research, and policy. Reflecting the thinness of the relevant literature, we relied heavily on the rich body of information gleaned from our discussants in crafting this report. These informants provided many insights but (indirectly) they also yielded important information about gaps in current systems for tracking and understanding enrollment determinants.
Quotes in the Report
We have included several quotes in the report, both to give the reader a flavor of the discussants’ views and to provide context for our findings. In keeping with our policy of anonymity for discussants, quotes are not attributed to specific individuals. The discussions were not transcribed from recordings and it is possible that the quote was not captured verbatim in our notes. However, we are confident these quotes accurately capture the sentiment of the discussion, based on careful review of notes by all team members present during the discussion, and verification of any unclear points with the discussant.
Appendix B
Program descriptions
Access Health, Muskegon County, Michigan
adultBasic, Pennsylvania
Alliance Family Care, Alameda County, California
ARHealthNetworks, Arkansas
Brooklyn Healthworks, Brooklyn, New York
CareLink, Bexar County, Texas
CarePartners, Southern Maine
Covered at Work, Utah
DirigoChoice, Maine
Family Health Plus, New York
FHIAP (Family Health Insurance Assistance Program), Oregon
FOCUS (Family Obtainable Coverage for Uninsured San Diegans), San Diego, California
Health Advantage, Marion County, Indiana
HealthChoice, Wayne County, Michigan
Healthy New York, New York
Healthy San Francisco, San Francisco, California
Hillsborough County Health Care, Hillsborough County, Florida
Hinds County Health Alliance, Hinds County, Mississippi
Ingham Health Plan, Ingham, Michigan
Insurance Partnership, Massachusetts
InsureMontana, Montana
Insure Oklahoma/O-EPIC IP, Oklahoma
Insure Oklahoma/O-EPIC ESI, Oklahoma
JaxCare, Duval County, Florida
Oregon Health Plan, Oregon
Primary Care Network, Utah
RIte Share, Rhode Island
SacAdvantage, Sacramento County, California
Small Business Health Insurance (SBHI), New York
State Coverage Insurance (SCI), New Mexico
Utah Premium Partnership, Utah
(2001-2005)
| Program Feature | Description | |
|---|---|---|
| Sources | (1) http://www.allhealth.org/BriefingMaterials/localcoverageinitiatives-298… (2) http://www.coderedtexas.org/files/Appendix_D.pdf (3) Fronstin, et al. 2005 (4) http://www.hrsa.gov/stateinsurance/michigan.htm (5) http://www.access-health.org/?page=howaccesshealthworks (6) Personal Communication with Jeff Fortenbacher 7/10/08. | |
| Overview | Premium Subsidies for Employers and Workers This long-running three-share program has received national attention, serving as the model for other programs in Michigan and for several pieces of federal legislation. (1) As the name suggests, employers, workers, and the county each pay one third of the cost of coverage. | |
| Target Population | Non-offering Muskegon businesses of 2 or more workers. The median hourly wage of the workers must be $11.50 or less. Seasonal, contract, and temporary employees, as well as employees who have other insurance, are not eligible for the coverage. (1) | |
| Enrollment | 2008: 325 - firms 1,100 - covered lives (6)The program seeks to enroll up to 3,000 full- or part-time working uninsured individuals and up to 500 small to medium-size businesses in Muskegon County, which is about 22% of the uninsured population. (2) Muskegon county had about 13,700 working uninsured in 2004. (1) The majority (88%) of enrolled firms had five or fewer employees. (4) | |
| Outreach | Outreach efforts have targeted restaurants, day-care centers, hair salons, and other small businesses. A professional sales staff markets the product to eligible businesses. (1) | |
| Enrollment Process | Businesses may contact Access Health by phone or email to request an application or learn more about eligibility (5). As part of the enrollment process, families are screened for eligibility for Healthy Kids (Medicaid) and MIChild (SCHIP) programs for the children. (1) | |
| Coverage | The benefit package includes local physician services, inpatient hospitalization, outpatient services, emergency care, behavioral health care, prescription drugs, diagnostic laboratory and x-rays, home health, and hospice care. There is no preexisting condition exclusion. The program is not a licensed insurance product and does not cover services outside the county. The program also offers a premium discount if enrolled members meet with a health coach and attend health and wellness classes (5). All enrollees face modest cost-sharing for services such as $7 copayment for each office visit. (1) | |
| Premiums and Subsidy Structure | Employers, workers, and the program each pay roughly a third of the approximately $150 monthly premium. The full premium is somewhat below market due to the exclusion of care outside the county and certain tertiary services as well as the fact that physicians donate 10 percent of their fee to the program. (4) Close coordination with existing safety-net programs also minimizes premium by ensuring that Access Health is “payor-of-last-resort.” | |
| Funding | The community share (Access Health) is made up of a combination of local government, community, and foundation funds, as well as federal disproportionate share hospital (DSH) funds. (1) | |
| Contact | Jeff Fortenbacher, Executive Director | Phone: (231) 728-5180 x104 |
FPL = federal poverty level
| Program Feature | Description | |
|---|---|---|
| Sources | (1) http://www.ins.state.pa.us/ins/cwp/view.asp?a=1278&q=527068 (2)http://www.ins.state.pa.us/ins/lib/ins/chip_ab/2007_Adultbasic_Annual_R… | |
| Overview | Subsidized, Nongroup Coverage for Adults AdultBasic, subsidized coverage for adults, was the single largest component of Governor Ridge’s Health Investment Insurance Act of 2001. (1) | |
| Target Population | Uninsured adults (ages 19-64), with family incomes below 200% FPL. Must be residents of Pennsylvania and be US citizens or legal aliens. Must be ineligible for other public coverage (Medicaid eligibility for all adults in PA is limited to those with family incomes below 61% FPL). (1) | |
| Enrollment | 2007: 53,534 total enrollees Enrollment began July 2002 and 6,000 adults enrolled in the first month. Within six months, 50,000 had enrolled and the state instituted a waiting list, which reached 127,000 names at its peak. (1) In December 2007, 95,649 individuals were on the waiting list. The state receives about 5,000 applications for adultBasic a month. (2) | |
| Outreach | In the early months, print media and radio advertisements were used to promot e the program. Currently the state conducts little outreach because enrollment is capped. However, the Department of Insurance continues to work with community service partners to share information about adultBasic. (2) | |
| Enrollment Process | Applications for enrollment are available from adultBasic contractors, by calling toll-free number (1-800-G0-BASIC) and on-line. In light of the cap on enrollment, applicants to the program may be referred to other sources of healthcare (e.g., Medicaid, Federally Qualified Health Centers, etc.). (2) | |
| Coverage | adultBasic offers basic benefits, including: preventive care, physician services (including specialists), laboratory tests including x-ray, in-patient hospitalization, out-patient hospital services, and emergency care. Pharmacy is not covered. There are no pre-existing condition exclusions. Enrollees pay modest co-pays. (1/2) | |
| Premiums and Subsidy Structure | Enrollees pay a premium of $35 per month. Eligible adults on the waiting list can buy-in to the program by paying full-cost (approximately $300 per month). (1/2) | |
| Funding | Funding for this program comes from a portion of Pennsylvania’s Tobacco Settlement funds (estimated to be approximately $400 million a year). (1) Three of the four Pennsylvania Blues insurance companies also contribute money to adultBasic through the Community Health Reinvestment clause. | |
| Contact | George Hoover, Deputy Commissioner Pennsylvania Insurance Department 1326 Strawberry Square Harrisburg, PA 17120 | Phone: (717) 346 1366 |
| Program Feature | Description | |
|---|---|---|
| Sources | (1) Taylor et al. 2003 (2) Powerpoint by Luella J. Penserga, “Alliance Family Care Health Care Coverage for Low-Income Immigrant Families.” http://www.wkkf.org/DesktopModules/WKF.00_DmaSupport/ViewDoc.aspx?Langu… (3) Zahn et al. 2003 (4) http://alamedaalliance.org/ | |
| Overview | Subsidized, Nongroup Coverage for Adults Alliance Family Care was a coverage product for uninsured family members of Alliance Health enrollees. The program was administered by Alameda Alliance for Health, a not-for-profit health maintenance organization in Alameda County, California. | |
| Target Population | Uninsured residents, ages 0-64, with household incomes below 300% FPL, with a family member enrolled in the Alliance health care system. Citizenship was not a requirement. (1) | |
| Enrollment | 2003: ~7,300, wait list 2,500 (2) The program successfully enrolled families of mixed immigration status who are often reluctant to participate in public coverage programs. (3) | |
| Outreach | Little formal marketing. In order to effectively target the immigrant population, outreach relied heavily on community-based agencies that had established trusting relationships with these county residents. (5) Outreach was also conducted at sites of care. (1) Because families typically had a child already enrolled in Medi-Cal (California’s Medicaid program), other family members—eligible for Family Care—could be readily identified. | |
| Enrollment Process | Clinic-based enrollment counselors provided one-on-one assistance with the application process. Information was collected on all family members who were screened for other health coverage options and benefits such as food stamps. Increased coordination across benefit programs over time made the enrollment process more efficient. Application processing time was reduced from 45 days to 7-15 days. (3) | |
| Coverage | Benefits included physician care, inpatient and outpatient hospital care, laboratory services and prescription drugs. (1) The coverage was modeled on the benefit package for the Medicaid program so families only have to learn to navigate one system. Members paid a $10 co-pay for non-preventive services. | |
| Premiums and Subsidy Structure | Individuals pay premiums ranging from $20-$120 per month, depending on age. (1) | |
| Funding | Funded with the Alliance's reserve fund, the California Endowment, the California HealthCare Foundation and some tobacco settlement money from the state. (1) | |
| Contact | Ingrid Lamirault Alameda, California 94502 | Phone: (510) 747-4500 |
| Program Feature | Description | |
|---|---|---|
| Sources | (1) http://www.arhealthnetworks.com/ | |
| Overview | Premium Subsidies for Employers and Workers The AR Health Networks program offers low-cost coverage featuring a limited set of benefits to qualified small businesses with eligible uninsured employees. Novasys Health, in its capacity as third party administrator (TPA), supplies administrative services, a provider network, the broker network, and oversees marketing efforts. The program was formerly known as the Arkansas Safety-Net Benefit. (1) | |
| Target Population | Employers: 2-500 employees, not have offered health coverage in last 12 months, and at least one employee who qualifies for the premium subsidy. Workers: all workers in firm working more than 30 hours a week must be offered coverage. To qualify for the subsidized premium: family income of 200% of FPL or less; not be eligible for coverage through the Arkansas State and School Health Plan; live in Arkansas; age 19-64; U.S. citizen. All subsidy eligible workers of participating businesses must enroll, unless they can provide evidence of other insurance coverage. (1) | |
| Enrollment | Jan 2008: 2,448 workers and spouses, including 250 unsubsidized (4) Per their HIFA waiver, enrollment will occur in two phases. Phase I (years one and two) is capped at 15,000 adults. Phase II (begins in year three) will target approximately 35,000 additional adults. (2) Enrollment is evenly divided between parents and childless adults. (4) | |
| Outreach | Website, media coverage, and other efforts are overseen by the TPA, NovaSys Health, responsible for marketing and outreach. (2) | |
| Enrollment Process | Employer groups in ARHealthNetworks enroll in coverage through a dedicated agent or an independent broker appointed by NovaSys Health. Employers can search for an appointed broker in their area on the www.arhealthnetworks.com website. (3) | |
| Coverage | The limited benefit plan includes six clinician visits, seven hospital days, two outpatient procedures/ER visits per year, and two prescriptions per month. Services received outside of the network are not covered, even in cases of emergency. After a $100 deductible, the plan has a 15% co-insurance, $1000 maximum out-of-pocket on select services, and $100,000 maximum annual benefit. (1) | |
| Premiums and Subsidy Structure | Effective 9/1/2008: Total participant cost is $25 per month for each worker at 200% or less of FPL and $200 premium per month for each worker over 200% FPL. (1) Employers may ask employees to pay some of the premium cost as long as they meet the requirement that 100 percent of subsidy-eligible workers participate. The state and federal government subsidize the remainder of the premium cost. (1) | |
| Funding | The subsidy is funded by state tobacco settlement funds and federal Medicaid (childless workers) and SCHIP (parent workers) match through a HIFA waiver. (1) | |
| Contact | Dan Adams Project/Program DirectorDepartment of Human ServicesDivision of Medical Services | |
| Program Feature | Description | |
|---|---|---|
| Sources | (1) http://www.ibrooklyn.com/site/chamberdirect/brooklyn_healthworks (4) http://www.rwjf.org/files/publications/books/2007/AnthologyX_CH04.pdf (6) http://www.nyshealthfoundation.org/content/grant/detail/638 | |
| Overview | Premium Subsidies for Employers and Workers A low-cost, comprehensive health insurance plan for non-offering small businesses. The program experienced mild take-up before programmatic changes in 2005 boosted enrollment significantly. Brooklyn HealthWorks builds on the success of Healthy NY by providing additional premium subsidies and offering a plan that eliminates hospital co-payments. (2) The program is administered by the Brooklyn Chamber of Commerce in partnership with the New York State Department of Insurance. In 2008, local officials announced plans to expand the program to Queens, Manhattan, and ultimately citywide, with funding support from the city. (5) | |
| Target Population | Employers: located in Brooklyn; 2-50 workers; 30% of employees must earn $38,000 or less per year (adjusted every July 1); must not have provided comprehensive coverage during the past 12 months (or contributed less than $75 per month per worker). Workers: All workers employed more than 20 hours per week are eligible and must be offered the coverage. Part-time and temporary workers may also be offered coverage. At least 50% of eligible workers must enroll (coverage through another source counts towards 50%). Unlike Healthy NY and other small group plans, businesses may provide Brooklyn HealthWorks coverage to independent contractors (1099 employees) who work at least 20 hours per week and also cover traditional (W-2) workers. (2) | |
| Enrollment | 2005: 55 (18 businesses) (3) Employers attributed the initial low level of interest to the program’s small provider network. In August 2005, Brooklyn HealthWorks added GHI’s large tri-state network of doctors, specialists, and hospitals and eliminated the need for referrals to see in-network doctors and specialists. (4) Fluctuations in funding necessitated an enrollment cap in March of 2006 and a waiting list of more than 200 businesses developed. (7) Permanent State funding was secured in August 2006 and the enrollment cap was lifted. | |
| Outreach | Plan quotes are available directly from HealthWorks, through licensed brokers, and online using HealthConnect. Brokers are paid 4% commissions. Additional outreach occurs through established relationships with community organizations and a marketing campaign that includes newspaper, radio, and direct mail advertisement.(1) | |
| Enrollment Process | Employers send application and supporting documentation to Brooklyn HealthWorks. (1) | |
| Coverage | Comprehensive medical plan with prescription drug coverage up to $3,000 per calendar year. Co-payments between $10 and $500. Two plan options: “Total” and “Max”. “Max” eliminates 3 large co-pays. (1) | |
| Premium and Subsidy Structure | Two subsidies: State provides a reinsurance subsidy through Healthy NY, and HealthWorks subsidizes the premium further by 19%. Premiums for individual coverage range from $221 (“Total” plan) to $234 (“Max” plan). (1) Unlike Healthy NY, Brooklyn HealthWorks does not establish a minimum employer premium contribution. Nonetheless, most employers pay 80-100%. (3) | |
| Funding | 2008: $1.5 million in State funding; $100,000 grant from the New York State Health Foundation. (4) | |
| Contact | Dean Mohs 25 Elm Place, Suite 200 Brooklyn, NY 11201 | Phone: (718) 943-3882 |
| Program Feature | Description | |
|---|---|---|
| Sources | (1) http://www.coderedtexas.org/files/Appendix_D.pdf (2) Program Website: http://www.universityhealthsystem.com/carelink/default.shtml (3) An Assessment of the Safety Net in San Antonio, Texas: http://urgentmatters.org/media/file/aboutProject_reports_Final_SanAnton… | |
| Overview | Brokered Access to Subsidized Care Carelink is the Bexar County ’ indigent care program--a financial assistance plan with managed care features. The program uses a provider network that includes medical school and private practice physicians, pays providers on a fee-for-service basis, and collects payments from the family over an extended period of time. An integrated patient record system has also been developed allowing for a system-wide quality assurance program. (1) | |
| Target Population | Uninsured County residents with family income below 300% FPL. (2) | |
| Enrollment | Enrollment stands at approximately 50,000 to 55,000 (maximum enrollment that can be funded at current funding levels.) (3) | |
| Outreach | ||
| Enrollment Process | Families apply for enrollment at the main CareLink office or at one of the seven ambulatory centers or FQHC sites. If a family member is determined to be potentially eligible for Medicaid or CHIP, a 60-day enrollment period into CareLink is allowed during which the individual must apply to the Medicaid and/or CHIP program or face being kicked out of the program. (1) | |
| Coverage | Available services are comprehensive and include comprehensive array of primary, preventive, specialty, and inpatient services. Care is provided by University Health System, San Antonio’s primary safety net provider. (4) Cost-sharing varies with income with no costs for those below 75% of FPL. | |
| Premiums and Subsidy Structure | There is no premium cost for those with incomes at or below 75% of the FPL. Enrollees with income above 75% of the FPL make monthly payments based on family size and income. These amounts area based on the maximum family liability concept, or the amount a family can be expected to contribute based on their income. (1) | |
| Funding | A county hospital district tax levy, equaling 25 cents per $100 valuation, is the primary funding source. Medicaid DSH funds are also used to help fill the funding gap in health care delivery. The annual budget/revenue is currently about $95 million. Annual collections from enrollees are around $11 million. (1) | |
| Contact | ||
| Program Feature | Description | |
|---|---|---|
| Sources | (1) Brown and Stevens 2006 (2) http://www.carepartnersmaine.org/ (3) Taylor et al. 2005 (4) Ormond et al. 2006 (5) Taylor et al. 2006 | |
| Overview | Brokered Access to Subsidized Care In Portland, mainstream institutions created a plan, CarePartners, which reorganized the delivery system to expand care for the uninsured. The partners included MaineHealth (an integrated nonprofit hospital system that served three-fourths of the state’s population), affiliated hospitals in three counties, Anthem BlueCross (which supplied claims management at no cost), and more than 900 primary care and specialty practices. Providers delivered uncompensated care to a limited number of uninsured patients via primary care “medical homes,” office-based specialty care, and hospitalization when needed. (1) | |
| Target Population | Residents in one of the 3 eligible areas who are uninsured and have a household income of less than 175% FPL. (2) | |
| Enrollment | 2004: 1,000 enrollees Enrollment is capped at this level due to funding constraints. (3/4) | |
| Outreach | ||
| Enrollment Process | Eligibility screening process also checks to see if applicant is eligible for MaineCare. | |
| Coverage | Copays ranging from $5-$25. (2) | |
| Premiums and Subsidy Structure | Premiums are fully subsidized. (2) | |
| Funding | Health care for CarePartners enrollees is provided through the donated in-kind services of physicians and hospitals. The local health system (Maine-Health) also provides substantial funding for administrative and support services (such as staff salaries). The program has received a HRSA CAP grant and grants from local foundations. (5) | |
| Contact | ||
| Program Feature | Description | |
|---|---|---|
| Sources | (1) http://www.kff.org/medicaid/loader.cfm?url=/commonspot/security/getfile… | |
| Overview | Premium Subsidies for Workers This premium assistance program was part of the state’s Primary Care Network Medicaid 1115 demonstration waiver. Due to low enrollment, it was replaced by Utah's Premium Partnership for Health Insurance (UPP) program in November 2006. (1) | |
| Target Population | Uninsured workers with an offer of health insurance who are citizens or legal residents, and whose premium share exceeds five percent of total household monthly income with an income up to 150% of FPL. Employer must contribute at least 50 percent of the premium. (1) | |
| Enrollment | May 2004: 55 adults Enrollment is capped at 6,000 due to funding limits. (3) Very low enrollment was attributed to subsidy amounts that were too low. (4) | |
| Outreach | The program was promoted to the Utah Association of Health Underwriters. Mailings were sent to community organizations and government agencies. Postcards were mailed to CHIP families and outreach representatives attended health fairs and community events. (5) | |
| Enrollment Process | Due to limited employer open enrollment periods, interested applicants needed to apply about 30 days before open enrollment. (3) Used a different application from the Primary Care Network. | |
| Coverage | The employer coverage was not subject to any minimum service coverage requirements other than what the state law requires of all insurers. (1) | |
| Premiums and Subsidy Structure | Retrospectively paid premium subsidies of $50 per month for one person (the estimated market value of the PCN benefit package) or $100 per family. Beginning in the third year, this amount decreased by 20% a year with no subsidies after five years. (2) In addition, enrollees paid a $50 enrollment fee (5) | |
| Funding | Received federal Medicaid match under a Medicaid 1115 demonstration waiver. (1) | |
| Contact | Heidi Weaver, Program Manager | Phone: (801) 538-6806 |
| Program Feature | Description | |
|---|---|---|
| Sources | (1) http://www.dirigohealth.maine.gov/dhlp02.html (2) Lipson et al. 2007 (3) Deborah Chollet Testimony before the Appropriations Committee 3/5/08: http://www.mathematica-mpr.com/publications/pdfs/Chollet_Testimony_0305… | |
| Overview | Premium Subsidies for Workers’ Group Coverage and Subsidized, Nongroup Coverage for Adults The DirigoChoice subsidized coverage offering is part of a broad strategy (DirigoHealth) to lower health care costs, increase access to health care, and ensure high quality health care in Maine. (1) | |
| Target Population | Applicants must fall into one of three eligibility categories: Small Employers: 2 to 50 employees, with a 75% participation rate among eligible workers; Households with incomes below 300% FPL qualify for sliding scale subsidies. (1) | |
| Enrollment | 2008: Individuals – 6,800, Sole Proprietors – 3,900, Small Group – 3,400 (3) Individual (non-employer) enrollment in Dirigo was capped during 2005, the program’s first year of operation. The cap was lifted in 2006 and then reinstituted again in 2007 when individuals constituted 50% of the DirigoChoice member mix. (2) | |
| Outreach | DirigoChoice was advertised in TV and print and received significant media coverage. A targeted outreach campaign featuring one-on-one assistance was directed to home care workers. (2/4) | |
| Enrollment Process | As a licensed insurance product, only brokers or insurance agents can complete the sale of the DirigoChoice coverage. Applicants who call the program’s toll-free number cannot be enrolled—they must be referred to a licensed insurance seller. Applicants for subsidies need to complete a second application submitted to the Dirigo Health Agency. Subsidy level is unknown when applying for coverage. | |
| Coverage | Comprehensive coverage with an emphasis on preventive care. Cost-sharing slides with income for enrollees below 300% FPL. | |
| Premiums and Subsidy Structure | Below 100% FPL: Small group enrollees and individuals are fully subsidized. Between 100% and 300% of FPL: premiums slide with income. Above 300% FPL: No premium subsidies At incomes below 300% of FPL, sole-proprietors are eligible for premium subsidies for the employee’s share of the premium but must pay the employer’s share (2). | |
| Funding | Program designers initially intended to fund DirigoChoice through employer and enrollee contributions and two innovative, largely untested mechanisms. The first mechanism was the Savings Offset Payment (SOP), which was designed to capture 1) savings from reduced bad debt and charity care as a consequence of expanded health coverage, and 2) savings from the Dirigo Health plan’s other cost control initiatives. The second mechanism was to claim federal Medicaid matching funds on employer premium contributions for DirigoChoice enrollees eligible for the state Medicaid program. These two sources of funding did not generate expected revenues and the state is looking at new alternatives. (2) | |
| Contact | Karynlee Harrington 53 State House Station August, Maine 04333 (1) | Phone: (207) 287-9900 Fax: (207) 287-9922 Email: DHA@Maine.gov |
| Program Feature | Description | |
|---|---|---|
| Sources | (1) Silow-Carroll, S. 2004 (2) Program Website: http://www.health.state.ny.us/nysdoh/fhplus/what_is_fhp.htm (3) New York Stat Monthly Medicaid Managed Care Enrollment Report March 2008: http://www.health.state.ny.us/health_care/managed_care/reports/enrollme… | |
| Overview | Subsidized, Nongroup Coverage for Adults Family Health Plus, legislated by the Health Care Reform Act (HCRA) of 2000, is a managed care program for low-income adults implemented as an expansion of Medicaid coverage. (1) | |
| Target Population | Family Health Plus is available to adults aged 19 to 64, income below 100% FPL (single adults or couples without children), or income below 150% FPL (parents) who are residents of New York State, United States citizens or fall under one of many immigration categories. Adults with access to ESI may be eligible for help to pay for premiums, deductibles, coinsurance and co-payments through the Family health Plus Premium Assistance program. (1/2) | |
| Enrollment | 2004: 407,536 total (148,746 childless adults) (1) 2008: 518,189 total (199,456 childless adults) (3) | |
| Outreach | Growth during 2003-2004 is attributable, in part, to a major outreach and education campaign organized by the State, including television ads, a website (although there is no on-line application), and facilitated enrollment by community based organizations (HMOs, hospitals, lead agencies, others) (1) | |
| Enrollment Process | Applications for the FHP as well as regular Medicaid are accepted through local social services districts, as well as enrollment facilitators within communities available at convenient times for working families and individuals. These facilitators assist individuals in completing a combined and streamlined application for various public programs. The facilitators also help the applicant select a participating plan and a primary care physician. Household members are encouraged, but not required, to participate in the same plan as other FHP, Child Health Plus (CHP) or Medicaid managed care family members. Recertification is on an annual basis and entails an in-person or a mail-in process, with enrollment facilitators available to provide assistance. (1) | |
| Coverage | Family Health Plus provides comprehensive coverage, including prevention, primary care, hospitalization, prescriptions and other services. There are no co-payments or other types of cost sharing. (2) | |
| Premiums and Subsidy Structure | Coverage is fully subsidized. There are no premiums. (2) | |
| Funding | Family Health Plus is an expansion of Medicaid and receives federal match. | |
| Contact | ||
| Program Feature | Description | |
|---|---|---|
| Sources | (1) Program Website: http://www.oregon.gov/OPHP/FHIAP/index.shtml | |
| Overview | Premium Subsidies for Worker's Group Coverage and Nongroup Coverage The FHIAP program provides premium subsidies to individuals and families to pay for employer-sponsored insurance or to buy individual (non-group) health plans if insurance is not available through an employer. This program is the only large example of a coverage approach that provides direct premium subsidies for commercial non-group products. (1) | |
| Target Population | Eligible individuals must be uninsured for at least six months or leaving the Oregon Health Plan (OHP); live in Oregon; be a US citizen or qualified non-citizen; have less than $10,000 in savings; and have a family income less than 185% FPL. (1) Effective June 1, 2008, applicants for non-group premium subsidies must have family incomes above 85% FPL. (3) | |
| Enrollment | 2007: 5,000 group lives, 10,700 individual lives Waiting list: 7,000 group, 25,000 individual (estimated to be a 1.5 to 2 year wait) (1) Applicants with access to qualified employer-sponsored coverage must enroll in their employer coverage if there is an employer contribution. To accommodate a funding reduction, FHIAP reduced enrollment by approximately 4000 adult members. Effective June 1, 2008, FHIAP non-group members below 85% federal poverty level (FPL) had to chose to either self pay their insurance premium or transfer to the Oregon Health Plan for a minimum of six months.(3) | |
| Outreach | At the outset, the State deployed three-member teams to educate stakeholders and insurance agents in local communities about the program. These teams held eighty three-hour training sessions for agents throughout the state. Applicants who call the program’s 1-888 number are referred to these trained agents, who receive a commission from the carrier upon enrollment. Oregon has also used presentations, focus groups, direct mailings, and articles in local publications to inform employers about the program. Outreach was scaled back as funding limits were reached. (2) | |
| Enrollment Process | Applicants call a 1-888 number or use the website to get onto the waiting list to receive an application. When there is space in the program, they are mailed an application packet. Once they have been determined eligible and receive an approval letter from FHIAP, they then apply for group or individual insurance coverage. (1) | |
| Coverage | Qualifying coverage must be actuarially equivalent to a FHIAP benchmark. The benefits will vary with the insurance plan being subsidized but are generally comprehensive. Enrollees are responsible for co-pays and deductibles. (1) Individual deductibles can range up to $500 per year. (4) | |
| Premiums and Subsidy Structure | FHIAP pays from 50 percent to 95 percent of the premium depending on income and family size. Enrollees in the non-group market are billed by FHIAP each month for their portion of the premium. The State then combines the enrollee’s portion with the subsidy and pays the carrier. Group enrollees have the employee’s full share withheld from their paycheck and are then reimbursed for subsidy amount, provided the enrollee submits verification that the premium is being withheld (such as a paystub). (4) | |
| Funding | Originally, the program was state funded. From 2002 to 2007, it received federal funding from both Medicaid and (SCHIP). However, effective 11/2007, the federal government prohibited FHIAP adults from receiving SCHIP match. (Some FHIAP children are still funded through SCHIP.) | |
| Contact | Craig Kuhn Program Manager, FHIAP | Phone: (503) 378-6032 |
| Program Feature | Description | |
|---|---|---|
| Sources | (1) Taylor 2004 | |
| Overview | Premium Subsidies for Employers and Workers The program was developed as a partnership between the Alliance Healthcare Foundation and Sharp Health Plan. The California Healthcare Foundation sponsored a comprehensive evaluation of the program providing researchers with a substantial body of data. (1) | |
| Target Population | Employers: 2-50 employees in San Diego who had not offered health insurance in the previous year. Workers: uninsured for the prior year and income of less than 300% of FPL. (Higher-income workers are not eligible for the coverage even at unsubsidized rates although they could enroll in other Sharp Health plan products). (1) | |
| Enrollment | June 2000: 216 Firms Program filled all available subsidy slots and instituted a waiting list. To stretch limited grant funds, in its third year of operation, eligible children were moved to public programs. (1) An evaluation estimated that 20 percent of eligible businesses purchased the coverage. (2) | |
| Outreach | A media campaign, targeting key local business organizations, and enrollee referrals were characterized as successful outreach efforts. A separate effort included two mailings to firm owners and two phone contacts. (2) Some brokers worked pro bono to promote the product. | |
| Enrollment Process | ||
| Coverage | A comprehensive, commercial benefit design, including physician office visits for a $5 copay (1) | |
| Premiums and Subsidy Structure | Employers paid about 20 percent of the estimated total (unsubsidized) premium. Workers’s paid 1 percent to 4 percent of their monthly household income. | |
| Funding | Together, employer and employee contributions covered approximately 47 percent of the full cost of the plan. In addition, total premiums (before subsidy) were below market (about 75 percent of the cost of standard commercial premiums) reflecting: brokers worked pro bono, providers accepted reduced reimbursement, and Sharp Health Plan donated significant administrative costs.(1) | |
| Contact | ||
| Program Feature | Description | |
|---|---|---|
| Sources | (1) Program Website: http://www.wishard.edu/health-advantage.html (2) History and Overview of the Health Advantage Program: http://www.hhcorp.org/PDF/adv_history_overview.pdf (3) http://www.coderedtexas.org/files/Appendix_D.pdf (4) Taylor et al. 2006 (5) http://www.naco.org/content/ContentGroups/Programs_and_Projects/Health_… | |
| Overview | Brokered Access to Subsidized Care Health Advantage (formerly known as Wishard Advantage) is a managed care program providing high quality, seamless medical care to low-income and uninsured residents of Marion county, IN. Program goals include improving the overall quality of health care in Marion County, effectively coordinating and managing patient care, strengthening doctor/patient relationships, decreasing inappropriate emergency room use and producing reliable data to guide future decision-making. (1) | |
| Target Population | All Marion county residents with incomes below 200% FPL who do not qualify for other government assistance. (1) | |
| Enrollment | 2004: 47,486 enrollees. (2) 2008: Over 52,000 enrollees. (1) Over two-thirds are minorities, and approximately one-fifth of members are Hispanic. (2) | |
| Outreach | With enrollment at high levels, there is little formal outreach. Many members learn about the program through word of mouth or when they seek care at a clinic or an emergency room. (6) | |
| Enrollment Process | In 2002, Health Advantage streamlined its application system with the Ind-e-App system. This system screens for multiple programs at once which serves to increase patient enrollment into other government programs. Patients can be enrolled at clinics and other sites of care. (2) | |
| Coverage | Services, accessible only through network providers, include routine exams and sports physicals, immunizations, GYN care, referrals to specialty care, lab and X-ray services, prescribed medicine, emergency and inpatient services. Upon enrollment, members receive a personalized membership card, 24-hour access to a nurse on-call hotline and other service components found in typical commercial insurance plans. (2) Program is not insurance coverage although members receive a membership card. | |
| Premiums and Subsidy Structure | There are no monthly premiums or membership fees. For members with incomes below 150% FPL there are also no “fixed patient responsibilities” (similar to a co-pay). Members with incomes from 150%-200% FPL pay a “fixed patient responsibility” on a sliding scale. (3) | |
| Funding | The project receives grants from foundations (CAP grant), DSH money ($20 million), and money from the city and county property taxes ($56 million). (4/5) | |
| Contact | Susan Jo Thomas, Director Health Advantage 2951 E 38th Street Indianapolis, IN 46218 | Phone: (317) 221-3163 Fax: (317) 221-2008 |
| Program Feature | Description | |
|---|---|---|
| Sources | (1) http://waynecountyhealthchoice.org/index.html | |
| Overview | Premium Subsidies for Employers and Workers HealthChoice is one of the longest-running “three-share” programs for small employers in the US. An overarching program, also called HealthChoice, includes four other components: the Young Adult Program, the Tempro program for part-time and temporary workers, and the indigent “BasiCare” program, and a dental assistance program (1). | |
| Target Population | Employers: 100% of the company’s business is based in Wayne County; 50% of workforce earns less than $14.50 per hour; has not have offered insurance in the prior three months; and at least two workers must qualify for the subsidy. (1,6) Workers: must be ineligible for public coverage, work at least 20 hours a week, and anticipate working for at least the next five months. At employer’s option, family coverage may be offered. (1) | |
| Enrollment | 2006: 3,700 (3) By December 31, 2008, the program seeks to achieve an enrollment of 5,000 (7). | |
| Outreach | Information is distributed at health fairs, in radio and television advertisements, and some direct marketing is funded by the program. Each health plan employs sales staff to target small and midsized businesses. (5) | |
| Enrollment Process | Administrative support, enrollment, eligibility, and outreach services are provided by the Patient Care Management System, a management corporation created by the Wayne County Executive and Wayne County Board of Commissioners. (8) | |
| Coverage | While not a licensed insurance product, HealthChoice provides a comprehensive, capitated package of services, including primary and specialist care, inpatient, outpatient, diagnostic, and prescription drug coverage. Co-payments vary based on the services rendered.(1) | |
| Premiums and Subsidy Structure | Designed as a three-share program, one-third of premium from the employer, employee, and the subsidy. (1) Employees pay as little as $58 a month for premiums. | |
| Funding | HealthChoice (and several other programs that serve the uninsured in Wayne County) are funded by partner Wayne County hospitals who contract with Metro Health Services to provide an array of health care programs and services for low-income individuals. The services that are supported with these funds help reduce uncompensated care at the hospitals and reduce the use of hospital emergency rooms for routine health care. These initiatives are also part of the community benefit provided by the hospitals (7) | |
| Contact | Michael Grundy 640 Temple Detroit, MI 48201 | Phone: (313) 833-3430 |
| Program Feature | Description |
|---|---|
| Sources | (1) EP&P Consulting, Inc. 2008 (2) http://www.commonwealthfund.org/innovations/innovations_show.htm?doc_id… (3) Lewin Group 2003 (4) EP&P Consulting, Inc. 2004 |
| Overview | Premium Subsidies for Workers’ Group Coverage and Subsidized, Nongroup Coverage for Adults The Healthy New York program is one of the few state insurance programs to rely on “stop-loss” reimbursement payments to health plans as its subsidy mechanism. (1) |
| Target Population | Sole proprietors and individuals: Low-income (less than 250% FPL), uninsured and underinsured New York state residents who were employed within the past 12 months. If currently employed, the employer must not provide comprehensive health insurance. (1/2) Employers: Non-offering firms, firms offering limited benefits, or firms contributing less than $50 per month in New York state where 30% of their employees earn less than $36,500 per year. All workers in qualifying firms are eligible to purchase coverage. (1) |
| Enrollment | 2003: 39,661 total – 23,234 individuals, 8,250 sole proprietors, and 8,177 small business. (3) 2004: 71,778 total – 42,052 individuals, 13,778 sole proprietors, and 15,948 small business. (4) 2007: 145,198 total – 78,465 individuals, 23,237 sole proprietors, and 43,496 small group workers. (1) Three-quarters of participating small employers have five employees or less. (1) |
| Outreach | Until 2007, Healthy New York used mass media and worked with community groups and various state agencies to create program awareness. (6) In 2006, most callers reported hearing about Healthy NY from the television; however, in 2007 television ranked third behind family or friends and the internet. (1) |
| Enrollment Process | In a 2007 survey of sole proprietors and individuals, 66% were satisfied with the enrollment process. (1) |
| Coverage | Coverage is available from one of 17 health plans. Employers contribute at least 50% of the premiums. Individuals pay the rest of the reduced premium. The premium is reduced because the State of New York makes “stop-loss” reimbursement payments to health plans that cover 90 percent of all claims between $5,000 and $75,000 per enrollee. (1/2) |
| Premiums and Subsidy Structure | Because the subsidy is paid via the reinsurance feature, subsidy payments are “invisible” to enrollees. The reinsurance feature is estimated to reduce premiums by 30% compared to other HMOs currently offering health plans. The average monthly individual premium is $230. (1) |
| Funding | Health Care Reform Act (HCRA) set aside $219 million for the program. The funds came partially from the tobacco settlement and increased cigarette tax. (5) |
| Contact | Phone: (518) 474-4567 |
| Program Feature | Description | |
|---|---|---|
| Sources | (1) For more on ERISA and ESR, see http://www.ncsl.org/programs/health/healthysanfran.htm (4) Personal communication from Brigham, 7/22/08 | |
| Overview | Brokered Access to Subsidized Care This ambitious program seeks to provide comprehensive health care to all of the city’s uninsured adults. (An earlier effort provided coverage to nearly all children.) A companion program, separate from HSF is the Employer Spending Requirement (ESR). Under this requirement, certain employers must use one of several methods to contribute towards health care for their employees. One method includes payment into HSF. The ESR has been challenged on ERISA grounds. (1) On 1/9/08, the requirement was allowed to go forward while the lawsuit was under review by Ninth Circuit Appeals Court. | |
| Target Population | Currently, uninsured city residents up to 300% of FPL are eligible, regardless of employment, immigration status or pre-existing conditions, if ineligible for existing public coverage programs. Eligibility will be expanded to uninsured city residents at higher income levels based on current enrollment and the decision in the ESR lawsuit. (2) | |
| Enrollment | July 2008: 24,868 participants The initial phase-in (launched in July 2007 at two Chinatown health centers) targeted the uninsured with incomes at or below the poverty line. HSF then expanded to all 27 health center sites in September 2007. Uninsured residents with incomes up to 300% FPL became eligible for the program in January 2008 (3). | |
| Outreach | There is little formal marketing. The City’s 3-1-1 system provides information on the program and directs people to various enrollment sites throughout the city. (4). | |
| Enrollment Process | Members may enroll when they seek services through primary care centers, San Francisco General Hospital or a centralized enrollment unit at the Department of Public Health. During the application process, clients’ eligibility for federal and state coverage programs (such as Medicaid) is first determined. Those enrolled in HSF choose a primary care medical home from among 14 public and 13 private non-profit clinics. (2) | |
| Coverage | Inpatient and outpatient care, tertiary subspecialty care, prescription coverage, laboratory services, durable medical equipment coverage, and treatment for mental illnesses and substance abuse. (Cosmetic procedures, dental services, fertility treatments, organ transplantation, vision care, and long-term care are excluded.) Care is only provided in the city limits and the program is not considered insurance. All enrollees face modest cost-sharing for services. Clinic visits range from $10 to $20 for those whose income is above 100% FPL. (2) | |
| Premiums and Subsidy Structure | Quarterly participation fee slides with income ($60 for those with income 101%-200% FPL; $675 for those above 500% FPL). Participants with incomes below poverty do not pay a participation fee (3). | |
| Funding | Public funding for indigent care, enrollee participation fees and fees paid by employers who select the program to meet their Employer Spending Requirement. (2) The City received additional federal funds over a three-year period to support the program. | |
| Contact | Tangerine Brigham Director of Healthy San Francisco San Francisco Department of Public Health 101 Grove Street, Room 103 San Francisco, CA 94102 | Phone: (415) 554-2779 Fax: (415) 554-2811 |
| Program Feature | Description | |
|---|---|---|
| Sources | (1) Program Website: http://www.hillsboroughcounty.org/hss/hhcprogram/ (2) Hillsborough HealthCare Program Study Committee Subcommittee 2005 Report: http://www.hillsboroughcounty.org/hss/hhcprogram/resources/publications… (3) http://www.cjaonline.net/Communities/FL_Hillsborough.htm | |
| Overview | Subsidized, Nongroup Coverage for Adults Hillsborough HealthCare is a comprehensive managed care program for Hillsborough County residents with limited income and assets who do not qualify for other health care coverage, including Medicare and Medicaid. (1) | |
| Target Population | Uninsured county resident, with a household income below 100% FPL. Applicants must not qualify for other government insurance plans such as Medicaid and Medicare. (1) | |
| Enrollment | 2005: 21,977 people “served” during the year. A report estimated that 38% of the eligible population was served by this program. (2) | |
| Outreach | ||
| Enrollment Process | Individuals enroll at enrollment sites with case managers. A person can download the forms in advance from the website to speed up the process. (1) | |
| Coverage | Hillsborough HealthCare covers primary and specialty care, inpatient and outpatient treatment, pharmaceuticals, and other services that are "medically necessary." Members are responsible for small copayments. (1) | |
| Premiums and Subsidy Structure | The premiums are fully subsidized. | |
| Funding | 1/2 cent sales tax by the county, along with $26.8 million per year in property taxes (as mandated by the State to fund indigent care). 1/2 cent sales tax reduced to 1/4 cent in 1998. (3) | |
| Contact | Toni Beddingfield Phone: (813) 301-7346 | |
| Program Feature | Description | |
|---|---|---|
| Sources | (1) Brown and Stevens 2006 (2) http://www.communitiesincharge.org/Documents/PhaseII%20PressRelease/Jac… | |
| Overview | Brokered Access to Subsidized Care The program sought to provide uninsured residents with access to comprehensive health care through a community-based, integrated delivery system by facilitating referral to a "medical home.” The centerpiece of the plan was the ER ReDirect Program. This program tried to shift non-urgent Emergency Department use to less expensive and more clinically appropriate primary care providers at The Jackson Medical Mall and other county providers. (1/2) | |
| Target Population | 45,000 uninsured in Hinds County , Mississippi. (3) | |
| Enrollment | Total referred clients 6,500. (3) Of the first 6,000 referrals to the Alliance through the ER ReDirect Program, just 20-25% made an appointment for primary care at the medical mall. (2) | |
| Outreach | The four major hospitals and health systems agreed to refer non-urgent ED users to the medical mall. The Metropolitan Council of Churches also provided more outreach regarding Alliance services to the uninsured. The local press and television stations agreed to promote this program during "Covering the Uninsured Week" in March 2003. The Alliance also believed that the business community would support their effort. (2) | |
| Enrollment Process | The ER ReDirect Program identified uninsured individuals seeking routine care in the county’s Emergency Departments. After being seen and treated, patients are then advised by a hospital case manager of the 7 primary care community-based facilities that they could use to link to a PCP, providing access to a medical home, and continuity of care. The Hinds County Health Alliance staff was available to assist clients in securing an appointment at one of the network primary care sites. (2) However, almost half of the ED patients gave incorrect addresses or phone numbers, leaving Alliance staff unable to contact them about referrals. (1) | |
| Coverage | The program focused on primary care, as well as providing extra services like a mobile phone system to prevent missed appointments, transportation to appointments, a discount prescription drug program, and disease management. (1) | |
| Premiums and Subsidy Structure | No enrollment fees were charged. | |
| Funding | The Hinds County Health Alliance was initially founded by the RWJF Communities in Charge Project and then received subsequent founding by HRSA. Two of the major participating hospitals and the United Way of the Capitol Area committed $100,000 or $300,000 respectively for 2004 to continue the work of the Alliance. (2/3) | |
| Contact | Dr. Aaron Shirley Board of Directors Jackson Medical Mall P.O. Box 11508 Jackson, MS 39283 Phone: (601) 982-0673 | |
| Program Feature | Description | |
|---|---|---|
| Sources | (1) Silow-Carroll 2001 (3) www.rwjf.org/reports/grr/031797.htm (4) www.ippsr.msu.edu/Documents/Forums/2007/Pulse_Story.pdf (5) www.communityvoices.org/Community.aspx?ID=10 (6) www.communityhealthplans.org/ihp/healthplans.asp?plan=ingham | |
| Overview | Brokered Access to Subsidized Care The Ingham Health Plan, specifically Plan B, provides access to primary care services for low-income, uninsured county residents. In addition to Plan B, Ingham Health Plan includes two other plans: 1) a Medicaid 1115 waiver program for adults with incomes less than 50 percent of the FPL (called Plan A) and 2) the Ingham County Advantage Program, which is a private insurance product that targets small businesses. | |
| Target Population | Plan B: Uninsured county residents between 50% to 250% of FPL. Immigration is not an eligibility factor. (2) | |
| Enrollment | 2000: 10,000 (estimated to be one-third of the uninsured population) (2) 2002: 15,821 (estimated to be fifty-seven percent of the uninsured population) (3) 2008: 17,000 (7) | |
| Outreach | In general, marketing is limited. Outreach has been conducted by Michigan State University, by local hospital systems, and by community centers. (2/7) A successful grass roots outreach campaign was also conducted by the Grass Roots Outreach Project and it helped to enroll an additional 2,340 of the county’s hard to reach population in 2007. (5/7) | |
| Enrollment Process | Members may enroll when they seek services through a primary care centers or by calling a local telephone number. Community outreach workers also may help to enroll members through their neighborhood centers. (2) | |
| Coverage | Program provides access to primary and specialty care, prescription drugs, and other services but does not pay for inpatient hospitalization. (2) All individuals face modest cost-sharing requirements. (2) | |
| Premiums and Subsidy Structure | Enrollees do not pay premiums; product is fully subsidized. (2) | |
| Funding | Ingham Health Plan receives per member per month state assistance and a hospital grant. (7) | |
| Contact | Robin Reynolds,Program Director Ingham Health Plan P.O. Box 30125 Lansing, MI 48909 Phone: (517) 887-4359 | |
| Program Feature | Description | |
|---|---|---|
| Sources | (1) http://www.insurancepartnership.org/who/index.asp (2) http://www.mass.gov/Eeohhs2/docs/masshealth/el2006/el-148.pdf (3) http://www.utexas.edu/lbj/faculty/warner/uninsured/papers/sec2_apph.pdf (4) http://www.ncsl.org/programs/health/buyin03.htm (5) http://www.mass.gov/Eeohhs2/docs/masshealth/research/1115_2006_dem_waiv… (6) http://www.urban.org/UploadedPDF/310794_OP-65.pdf (7) http://www.mass.gov/?pageID=eohhs2terminal&L=5&L0=Home&L1=Consumer&L2= (8) Mitchell et al. 2002 | |
| Overview | Premium Subsidies for Employers and Workers The Massachusetts Insurance Partnership provides premium subsidies for small employers offering coverage. The program also provides premium assistance for eligible families to help pay the cost of qualifying employer-sponsored health insurance (formerly called the MassHealth Family Assistance program). (1) | |
| Target Population | Employers: must have less than 50 full-time workers, contribute at least 50% to the worker’s premium, and provide a specified basic set of benefits. Sole-proprietors are eligible. (1) Workers: Massachusetts residents between 19 and 65 years of age, income of 300% or less FPL, not eligible for MassHealth Standard or MassHealth CommonHealth, have access to cost effective coverage, work for a qualified employer, or are self-employed. (Income eligibility levels were raised from 200% as part of the 2006 reforms). Six month crowd out provisions apply for applicants with incomes between 200% and 300% FPL. (2) Individuals employed by a large employer (>50) may receive premium assistance for eligible children. (2) | |
| Enrollment | 1999: 7,000 (3) 88% of participating firms have fewer than six employees (8) | |
| Outreach | Included mailings to insurance brokers and insurance companies, contacts with Chambers of Commerce, radio announcements, television commercials, mailings to nonprofit organizations with fewer than 50 employees, calls to small businesses by regional representatives, telephone cold calls followed with literature mailings to interested employers, print media, and billboard advertisements. (6) | |
| Enrollment Process | Process has been characterized as administratively complex. (6) MassHealth primarily identifies participants through the joint Medicaid and SCHIP application. After an initial review to determine which state program an applicant is eligible for and whether they have access to private insurance coverage, an independent check of insurance availability is conducted. Then a private vendor conducts the health insurance investigation process about benefit package, employer contribution level, and the premium determination and cost-effectiveness test. The entire process must be complete within 60 days. (6) The other route for obtaining premium assistance is through the Insurance Partnership program for MassHealth eligible members who have access to insurance through a small employer. | |
| Coverage | Benefits vary by employer coverage, but qualifying plans must meet a basic benchmark. The MassHealth agency pays co-payments, coinsurance, and deductibles for children eligible for premium assistance provided the expense was incurred as the result of a well-child visit, or the policyholder’s annualized out-of-pocket costs exceed five percent of the family group’s gross income. (2) | |
| Premiums and Subsidy Structure | Employers contribute 50% of premiums, workers contribute monthly fees based on a sliding scale for incomes above 150% FPL. Monthly fees range from $12 to $28 per child with a family maximum between $36 and $84. For employed adults and their spouses who do not have children and with incomes over 100% FPL, the monthly fee is $27 per adult. (2) Insurance Partnership fees are higher for families with incomes between 200% and 300% FPL. (7) The state’s maximum contribution amount is based on the cost of the publicly offered MassHealth insurance premium. Employer-sponsored insurance premium costs over the maximum are the responsibility of the worker. (2) The MassHealth Family Assistance Program employs two methods of paying subsidies. The state can either make direct payments to the family or the state can employ intermediaries to remit subsidies to employers. (3) | |
| Funding | Employers, workers, Medicaid, SCHIP, and other state funds. (6) | |
| Contact | ||
| Program Feature | Description | |
|---|---|---|
| Sources | (1) http://www.insuremontana.org/ | |
| Overview | Premium Subsidies for Employers and Workers Insure Montana is designed to assist small businesses with the cost of health insurance, whether they have provided health insurance previously or not. Small business that currently offer health insurance receive refundable tax credits and non-offering small businesses can participate in a small business health care purchasing pool and receive assistance with premiums. (1) | |
| Target Population | For both programs, eligible employers must have 2-9 workers, all earning less than $75,000 a year in wages (excluding the owner). Eligible workers must work full-time (30+ hours per week), unless the business owners opt to include part-time employees working 20-30 hours per week. Currently, sole proprietors and contract/1099 workers are ineligible. (4) - To join the purchasing pool and receive premium assistance, employers must not have offered insurance for the past 24 months. Seventy-five percent of eligible workers must enroll in the coverage. | |
| Enrollment | July 2008: 711 businesses (4,029 covered individuals) received the tax credit ; 47 businesses on waitlist 747 businesses (3,986 covered individuals) were in the purchasing pool and received premium | |
| Outreach | At program inception, letters were sent to potentially eligible small businesses informing them about the program. (4) Program features a comprehensive website. (1) An employer survey conducted in Montana after about one year of program operations found that about half of apparently eligible small employers had heard about the program. (3) | |
| Enrollment Process | Employers apply to Insure Montana for eligibility determination and placement on the wait list. Insure Montana sends enrollment packets to an employer when they may enroll. Employers have 30 days to complete the health applications and premium assistance applications. (1) | |
| Coverage | Two comprehensive plans offered by Blue Cross Blue Shield: “Premier” and “Standard”. Both include dental, prescriptions, and preventative services. Vision coverage is not available. “Standard” plan has higher deductibles. (2) | |
| Premiums and Subsidy Structure | Purchasing pool/ premium assistance participants: Employers are required to contribute 50% of the total premium cost, and state reimburses 50% of the employer contribution on a monthly basis (called an employer incentive payment). After premium incentive, the net employer payment is 25% of the total premium cost. Workers pay 50% of their premium cost, and are reimbursed 20% to 90% of this cost by the state (called a worker assistance payment). Employers may choose to contribute greater than 50% of the employee’s premium, but the monthly incentive payment they receive will not increase. (4) Premiums in the purchasing pool are experience rated. Tax credits: To qualify, an employer must pay at least half of the cost of insurance. Additional tax credits are available when an employer pays insurance premiums for spouse or dependents. (1) | |
| Funding | Employer and worker premium contributions; subsidies are provided through state funds ($13 million for program’s first two years, $20 million for following two years), and revenue from a $1 per pack cigarette tax. (2) | |
| Contact | Jill Sark, Program Director 840 Helena Avenue Helena, MT 59601 | Phone: (406) 444-2406 |
| Program Feature | Description | |
|---|---|---|
| Sources | (1) http://www.oepic.ok.gov | |
| Overview | Subsidized, Nongroup Coverage for Adults Insure Oklahoma!/O-EPIC Individual Plan (IP) is designed to be a safety net for eligible people, who cannot access group health care coverage through their employer, by providing them with affordable access to a limited SoonerCare (Medicaid) benefits package. (1) | |
| Target Population | Eligible enrollees must be a U.S. citizen or qualified alien, ages 19-64, 200% or less FPL (expanded from 185% FPL in November 2007), resident of Oklahoma, and not enrolled in Medicaid or Medicare. The Insure Oklahoma/O-EPIC IP eligible population includes: 1) self-employed individuals not eligible for small group health coverage; 2) workers at small businesses not eligible to participate in their employer's health plan or whose employer does not offer a Qualified Health Plan; 3) temporarily unemployed individuals, who are eligible to receive benefits from the OK Employment Security Commission; and 4) and working adults with a disability who work for any size employer and have a ticket to work. (1) The IP plan has a crowd-out provision, so employers must not have dropped coverage within the previous six months. (2) | |
| Enrollment | 2008: 2,923 IP (Total ESI and IP is 11,684) (5) Funding available for 40,000 adults in combined ESI and IP programs. Current goal is to enroll 25,000. (2) | |
| Outreach | There is a comprehensive website. Brochures are distributed to providers and community partners. IP is not actively promoted, but referrals are made if someone is not eligible for the ESI program. | |
| Enrollment Process | Online or paper application procedure. Approved applications are cross-checked with OK Employment Security Commission. A telephone help-line exists to help with questions and selection of a Primary Care Provider. (1) | |
| Coverage | IP offers a limited version of the SoonerCare (Medicaid) benefit package and uses Medicaid service providers. (1) The IP benefit package includes office visits, emergency care, inpatient and outpatient hospital benefits, pharmacy, X-rays, maternity care, durable medical equipment, etc. Some SoonerCare excluded services include dental, vision, emergency transportation, nursing home care, hospice, and transplants. There are no pre-existing condition exclusions and an overall lifetime benefit of $1 million. (1) Co-pays are required for some services, ranging between $5 and $50. | |
| Premiums and Subsidy Structure | The Insure Oklahoma/O-EPIC IP premiums are based on a sliding scale of income ranging between $0 and $69. The premium is approximately 4% of the annual household income (1). Members are sent invoices monthly for payment to the State. (1) | |
| Funding | Funded by federal matching Medicaid funds through a HIFA waiver, dedicated state tobacco tax funds, and individual premiums. (1) | |
| Contact | Matt Lucas, Director | |
| Sources | (1) http://www.oepic.ok.gov | |
| Program Feature | Description | |
|---|---|---|
| Overview | Premium Subsidies for Employers and Workers Insure Oklahoma/O-EPIC Employer Sponsored Insurance (ESI) is designed to assist lower income, small business workers and their spouses with health insurance premiums. The state also launched the Insure Oklahoma/O-EPIC Individual Plan (IP) in January 2007 for qualified Oklahomans who do not have access to employer-sponsored insurance. (1) | |
| Target Population | Employers: Oklahoma businesses with 50 or fewer employees. Legislation was signed in June 2007 that would increase the size of employers to 250 or fewer workers and increase income eligibility to 250% FPL. These changes are dependent on CMS approval. (3) | |
| Enrollment | 2006: 1,200 (2) Funding available for 40,000 adults in combined ESI and IP programs. Current goal is to enroll 25,000. (2) | |
| Outreach | Includes mailings, presentations, brown bag luncheons, continuing education classes for agents, and community events. There is also a comprehensive website. Insurance agents are used heavily to market the product and assist with questions and purchasing. Program officials worked closely with the Oklahoma Insurance Department (OID) to implement and promote the program. OID also employs Agent Partners to provide education and support to current insurance agents as well as travel throughout the state to recruit new agents. There is also an Agent Partner through Electronic Data Systems (EDS) our third party agent. (2) A statewide media campaign was launched in mid-October 2007 and is attributed with contributing to an 81% enrollment increase. (5) | |
| Enrollment Process | On-line and paper application procedure. Small businesses must apply to receive approval of their health plan. Application materials for potential enrollees are sent to the employer, which must be completed and approved by the worker. The State contracts with a call center to assist with questions and application. Agents also assist with the application process. Worker’s approved applications are cross-checked with the OK Employment Security Commission. (1) | |
| Coverage | Benefits vary depending on what is offered by the employer sponsored insurance plan. A stipulated minimum benefit package must cover hospital, physician, lab, x-ray, and pharmacy services. Plans must have a $3000 out of pocket maximum, $50 office visit co-payment maximum, and $500 pharmacy annual deductible maximum. (1) | |
| Premiums and Subsidy Structure | An employer must contribute a minimum of 25% of premium costs and the worker must contribute up to 15% of premium costs. (1) The state subsidizes 60% of health insurance premium for qualified workers and 85% for their spouses, up to $240 per member per month. (2) Employers must send the monthly health plan invoice to Insure Oklahoma, who then will pay the premium subsidy to the employer monthly. The employer sends the full payment to the insurance company. (1) | |
| Funding | Funded by federal matching Medicaid funds through a HIFA waiver, dedicated state tobacco tax funds, and individual and employer premiums. (1) | |
| Contact | Matt Lucas, Director | |
| Program Feature | Description | |
|---|---|---|
| Sources | (1) http://www.jaxcare.org/ | |
| Overview | Self-Insured Coverage Program for Employers and their Uninsured Workers JaxCare is a public/private partnership whose mission is to increase access to health care for lower-income, working, uninsured residents of Duval County for the purpose of improving overall community health, containing health care costs, and enhancing the economic foundation and social well being of the community. (1) Funding shortages caused the program to close in June 2008. | |
| Target Population | Employers: Any Duval county employer with at least 3 employees and at least one eligible worker. Workers: Must be uninsured county residents up to 200% of FPL (and their spouses) working for a participating Duval county employer. Must not be eligible for public coverage. (1) Qualified part-time and 1099 contract workers are eligible. (4) Children are not covered under JaxCare because Florida KidCare, the state’s health coverage program for low-income children, covers children in this income range. (3) | |
| Enrollment | 2005: 413 | |
| Outreach | Initially, JaxCare did not have a marketing plan. The organization viewed itself as a community service provider and not as being in the business of selling coverage. Experiencing low enrollment, JaxCare initially contracted with one insurance agent to sell the program to business owners, and then in December 2004, JaxCare moved its marketing efforts in-house and began actively marketing the product. (2) In December 2005, JaxCare began paying a one-time 15% commission to insurance agents for each JaxCare enrollee. (4) | |
| Enrollment Process | Once an eligible business chooses to participate, employees, who pass an initial, 5-question screening, submit applications. A JaxCare enrollment specialist then comes to the business to complete the enrollment process for qualified workers and to provide an orientation about the program. JaxCare enrollment specialists will also help employees determine if their children are eligible for Florida KidCare, and help them apply for enrollment in that program. Employees must pay a $15 administration fee. (3) | |
| Coverage | Comprehensive, managed care health plan using hospital-anchored provider networks. $5-$100 co-pays. (1) | |
| Premiums and Subsidy Structure | Employer pays $50 per month per member. Employee pays $15 per month. The city and hospitals cover 75% of the costs of the plan and foundations and premium revenues cover the remaining 25% of health plan costs. (1) | |
| Funding | There are five primary revenue streams for JaxCare: premiums and fees charged to members and employers; City of Jacksonville funding; donated health care; federal grants; and private grants and donations. The JaxCare program was initially developed through a RWJF Communities in Charge grant. (2) | |
| Contact | Rhonda Davis Poirier, Dr.P.H. 580 West 8th Street Tower II-9th Floor Jacksonville, FL 32209 | Phone: (904) 244-9270 |
| Program Feature | Description | |
|---|---|---|
| Sources | (1) http://www.orsilc.org/DHS/healthplan/data_pubs/ohpoverview0706.pdf | |
| Overview | Subsidized, Nongroup Coverage for Adults The Oregon Health Plan is Oregon’s Medicaid program. After receiving a HIFA waiver in 2002, the program made significant changes and broaden the broadened the eligible population to include childless adults. The basic Medicaid package was renamed OHP Plus and a new package to cover adults not previously eligible was created, OHP Standard. This description focuses on OHP Standard for adults. | |
| Target Population | Age 19-64, uninsured, US citizen or meets immigration requirements, Oregon resident, with household income below 100% FPL. (2) | |
| Enrollment | Funding limitations have capped enrollment at approximately 24,000. | |
| Outreach | ||
| Enrollment Process | ||
| Coverage | Compared to OHP Plus, OHP Standard has a leaner set of benefits and includes co-pays. (2) | |
| Premiums and Subsidy Structure | $9 to $20 per month premiums | |
| Funding | In 2002, the state received both an 1115 and a HIFA waiver to amend and expand the OHP (the state's existing 1115 waiver) and to create the second iteration of the Oregon Health Plan (OHP Standard). (2) | |
| Contact | ||
| Program Feature | Description | |
|---|---|---|
| Sources | (1) Program Website: http://health.utah.gov/pcn/index.html (2) Oppenhiemer et al. 2006 (3) Artiga et al. 2006 (4) http://www.hrsa.gov/stateinsurance/utah.htm | |
| Overview | Subsidized, Nongroup Coverage for Adults Utah was the first state to use reductions in benefits and increases in cost-sharing for existing beneficiaries to finance a limited benefit for an expansion group. (5) | |
| Target Population | U.S. citizens or legal residents, ages 19-64, with a household income below 150% FPL, uninsured for more than 6 months and do not qualify for any other health insurance. (1/2) | |
| Enrollment | July 2003: 15,835 enrollees (49% parents; 51% childless adults) July 2008: 17,391 enrollees (68% parents; 32% childless adults) Enrollment is capped due to funding limits. At the capped level, the program is estimated to reach about 16% of its target population. (3) Program does not maintain a waiting list. Because childless adults are more expensive to enroll than parents and in order to achieve budget neutrality under the 1115 budget neutrality formula, PCN has procedures to enroll more parents than childless adults and often only opens enrollment to parents. (4) | |
| Outreach | Initially, some marketing efforts were made to dispel any stigma associated with enrolling in a public program but outreach was limited. (3/6). Because enrollment caps were reached in 2003, outreach is conducted only during open enrollment periods using the website and radio, by informing organized advocacy groups, and through targeted mailings. If enrollment is only open to parents, limited outreach is done such as posting information in the Department of Workforce Services Office and updating the PCN website. (5) | |
| Enrollment Process | Utahans apply through the Department of Workforce Services (DWS) using a variety of access points including the internet, paper, fax, and in person at DWS offices. Applicants are first screened for Medicaid and then screened for several other programs. CHIP, PCN, and the Utah Premium Partnership program all use the same 3-page application. If found eligible, they are then required to pay their enrollment fee. Enrollees then receive a PCN card. They must renew their membership after 12 months. Materials are available in English and Spanish. (5) | |
| Coverage | The coverage is a limited, primary care benefit (including some dental) using existing Medicaid providers. PCN does not cover specialty care or hospital care. Enrollees face minimal co-pays. Pre-existing conditions are not excluded (within the covered services) (1) | |
| Premiums and Subsidy Structure | Enrollees are charged an annual enrollment fee that varies with income: 150%-50% FPL: $50; 50%-0% FPL: $15-$25. (1) | |
| Funding | The program operates under an 1115 waiver and is funded with state funds and federal Medicaid match. (4) | |
| Contact | Heidi Weaver | Phone: (801) 538-6806 |
| Program Feature | Description | |
|---|---|---|
| Sources | (1) http://www.ritecare.ri.gov/documents/reports_publications/RS%20Savings%…% | |
| Overview | Premium Subsidies for Workers RIte Share is a premium assistance program meant to support RIte Care-eligible families obtain or maintain access to Department of Human Services-approved, cost-effective employer-sponsored health insurance and utilize public dollars in the most responsible way. (1, 2) | |
| Target Population | Parents and/or their children that would ordinarily qualify for RIte Care (Medicaid) that have access to DHS-approved, cost effective employer-sponsored insurance. Eligibility is based on income: 185% FPL adults, 250% FPL children and pregnant women. (1) The 2009 budget has cuts to adults that would lower their income eligibility from 185% FPL to 175% FPL effective October 2008. (2) | |
| Enrollment | 2001: 275 (3) Currently, about one third of enrollees are adults and two thirds are children. (2) | |
| Outreach | Initially, the strategy was to focus on employer “participation.” Early marketing strategies included information sessions with insurers, brokers, employers, and advocates along with radio and television advertisements. (5) In January 2002, RIteShare became mandatory for RIte Care members whether or not their employer “participated.” Per State policy, enrollment in RIte Share is a condition of Medical Assistance eligibility when required by the State. Currently, minimal marketing or outreach takes place since the state identifies which applicants may qualify for RIteShare. (2) | |
| Enrollment Process | There is one application for RIte Care/RIte Share that is used to determine which applicants may qualify for RIteShare. A database of employer insurance status of qualified, cost-effective plans is checked. Staff also follow-up with potential enrollees based on nightly downloads of state database information. If necessary, the enrollee must collect information from their employers that is entered into the state’s cost effectiveness calculator. If the plan is approved, staff send a letter notifying who in the family must enroll in the employer-sponsored plan. The state also conducts a quarterly data match comparing state-required commercial insurance carrier enrollment lists to the Medicaid member list. Anyone identified as having both commercial coverage and RIte Care is transitioned from RIte Care to RIte Share. (This includes children who have coverage through the non-custodial parent.) (2) | |
| Coverage | Qualified plans must meet a benchmark and be determined to be cost effective. RIte Share will pay for wrap-around coverage and co-payments for RIte Care-eligible individuals if they visit a physician that accepts Medicaid. (1) | |
| Premiums and Subsidy Structure | Initially, “participating” employers received subsidy payments from the state after reducing the payroll deduction for a member. After RIteShare became mandatory, the subsidy payment was made directly to families on a prospective basis. (3) The subsidy is the balance of any monthly cost share premium the family may have based on their income. The 2009 budget has increased the monthly cost share premium for RIte Care/RIte Share eligibles over 150% FPL from 3-4% of their income to 5% and introduced new cost sharing for those RIte Care/RIte Share eligibles between 133% and 150% FPL. (2) | |
| Funding | State and federal Medicaid funds. | |
| Contact | Deborah Florio, Administrator | |
| Program Feature | Description | |
|---|---|---|
| Sources | (1) http://www.sacdhhs.com/article.asp?ContentID=920 (2) Taylor 2004 (3) http://www.westernhealth.com/prospect/downloads/WHA_SacAdv_Brochure.pdf (4) Phone discussion with Gary Maisel, 9/11/2008 (5) http://www.californiahealthline.org/articles/2008/5/6/Funding-Questions… (6) http://www.bizjournals.com/sacramento/stories/2006/08/21/story4.html | |
| Overview | Premium Subsidies for Employers and Workers This program provides premium subsidies for small employers and their lower-income employees in Sacramento County. Originally, the subsidies could be used for any coverage was purchased through Kaiser, Western Health Advantage, or PacAdvantage (a small employer purchasing cooperative in California). When PacAdvantage closed 12/31/2006, Western Health Advantage became the sole HMO carrier for SacAdvantage. SacAdvantage is slated to close at the end of fiscal year 2008 when funding will end. (7) | |
| Target Population | Employers: • based in Sacramento County Workers: work full time, have no insurance (and must not have been covered by employer-sponsored insurance for at least 3 months) and are not eligible for any other government healthcare program. Income must be under 300% of FPL. Employees not meeting this criteria can purchase the coverage without premium subsidies. (3) | |
| Enrollment | 2006: 313 employees at less than 50 companies (6) In 2004, SacAdvantage staff estimated that approximately 100 businesses and 500 uninsured individuals would enroll in the program (2). | |
| Outreach | Initially, SacAdvantage was marketed through PacAdvantage. In 2006, enrollment increased when Western Health Advantage took over as the sole carrier of the program and began to market the plan through its broker network. (7) | |
| Enrollment Process | Brokers identify small businesses that may be eligible for SacAdvantage and inform them about the product. The application contains two parts, one which must be filled out by the employer, the other by the employee. The broker then sends the completed application to Western Health Advantage, which qualifies the group based on eligibility criteria and then determines each employee’s subsidy level based on income. (4) | |
| Coverage | Coverage is comprehensive. Initially, insurance riders were available for dental and vision coverage (unsubsidized) – a benefit that many SacAdvantage participants took advantage of. (2) | |
| Premiums and Subsidy Structure | The employer and the worker split the portion of the premium that is not subsidized. The subsidy amount ranges from 40% to 65% of the premium. Under PacAdvantage, the premium subsidy depended on the employee’s age, income, and coverage tier. Under Western Health Advantage, the premium subsidy is based on employee’s income. (1) Hence, the premium amounts vary depending on the employee’s characteristics. Initially, the subsidy was tied to PacAdvantage’s lowest-cost HMO in the county. (5) | |
| Funding | Funds from Tobacco Litigation trust fund and a 2003 $700,000 federal appropriation. (2) Current funding will exhausted at the end of fiscal year 2008. (7) | |
| Contact | Jim Hunt, Chairman of the board of SacAdvantage | Phone: 916-244-1945 |
| Program Feature | Description | |
|---|---|---|
| Sources | (1) Rosenberg 2002 (2) The National Institute for Health Care Management Research and Educational Foundation 2003 | |
| Overview | Premium Subsidies for Employers and Workers Prior to implementation, program officials conducted extensive market research to evaluate the potential market and product design. Research revealed that owners wanted to legitimize their businesses, increase employee retention, and decrease sick time. (2) | |
| Target Population | Small businesses with 2 to 50 employees located in sections of the Bronx, Brooklyn, Manhattan, and Queens (1) | |
| Enrollment | 2000: 53 businesses Low participation caused the program to stop taking new enrollees in October of 2001. (1) The goal of SBHI was to enroll 3,000 lives. (Total eligible lives were estimated to be 100,000.) More than half of the enrollees had no coverage prior to SBHI. (2). | |
| Outreach | Marketed channels included direct mail, media, letters to brokers, lunch with community leaders, and print advertising. To address the city’s large Spanish speaking population, SBHI materials were printed in both English and Spanish. Program worked with only a few brokers who were hand-selected due to their involvement with the community. Commissions were smaller than they would have been for conventional products. (2) Program officials later concluded that more resources should have been devoted to marketing. | |
| Enrollment Process | ||
| Coverage | Market research reveals that employers were interested in plans with emergency room coverage and open access. The plan featured comprehensive coverage with copayments for selected services. (2) The provider network was limited. | |
| Premiums and Subsidy Structure | Market research revealed that plans with monthly premiums of $100 were appealing. The premiums were 50% less than comparable plans in the market area, and a single coverage after subsidy was about $100. | |
| Funding | ||
| Contact | ||
| Program Feature | Description | |
|---|---|---|
| Sources | (1) http://www.statecoverage.net/newmexicoprofile.htm | |
| Overview | Premium Subsidies for Employers and Workers, and Subsidized, Nongroup Coverage for Adults SCI is a component of the Insure New Mexico! initiative. SCI permits individuals to enroll through their employer or as individuals (at a higher cost). (1) | |
| Target Population | Employer: non-offering, with 50 or fewer eligible employees | |
| Enrollment | Aug 2006: 4,837 enrollees; 97 percent of these as individuals without employer sponsors (3) | |
| Outreach | Outreach was incorporated as part of Insure New Mexico! campaign which included visits to local chambers of commerce and organizations, mailings, and special outreach efforts to parents of SCHIP children. NMSCI brokers are also being used. (1) | |
| Enrollment Process | Employers apply for SCI participation through the MCOs who make the eligibility determination using state provided guidelines. | |
| Coverage | Benefits are similar to a comprehensive commercial plan with a $100,000 annual benefit limit. Copayments slide with income (1) | |
| Premiums and Subsidy Structure | Employer pays a portion ($0 to $75) of the monthly premium, the employee pays a portion ($0 to $35) of the monthly premium, and the state and federal government pays the remainder. Enrollees under 100 percent of FPL pay nothing. (1) Individuals not affiliated with an employer pay the $75 employer premium in addition to the employee premium. (1) | |
| Funding | Implemented under a HIFA waiver, the program uses unspent SCHIP funds as well as workers and employer premium contributions. (1) | |
| Contact | ||
| Program Feature | Description | |
|---|---|---|
| Sources | (1) Program Website: http://health.utah.gov/upp/ | |
| Overview | Premium Subsidies for Workers In 2006, after very low enrollment in a predecessor program (Covered at Work), the state began the Utah Premium Partnership (UPP) which featured (a) larger subsidies and (b) subsidies for child dependents. (1) | |
| Target Population | Uninsured workers with an offer of health insurance who are citizens or legal residents, and whose premium share exceeds five percent of total household income, and their uninsured, citizen or legal resident dependent children. (1) Income guidelines are higher for children (200% FPL) than for adults (150% FPL). Compared to the former Covered at Work program, the addition of coverage for children is thought to be attractive because it is easier to cover the entire family. (2) | |
| Enrollment | July 2008: 221 adults and 349 children (almost all adults are parents) The program provides funding for up to 1,000 adults. (1) | |
| Outreach | Outreach efforts include radio and TV ads, inserts in SCHIP premium notices and utility bills, community events, and other methods. The Utah Department of Health conducts a continuing education course for brokers that explains and promotes UPP. (5) However, a Department of Health survey found that 88% of Utahans had not heard about the Utah Premium Partnership (UPP) program. (3) In 2008, the state passed a bill to increase marketing of UPP (HB364) through schools and other means. Grants will be available for community organizations to help enroll Utahans in Medicaid, CHIP, and UPP. (3) | |
| Enrollment Process | Uses the same application as the Primary Care Network and CHIP with plans to combine with the Medicaid application. Employers must fill out a one-page form. Due to limited employer open enrollment periods, interested applicants initially need to apply about 30 days before open enrollment. 2008 legislation made UPP eligibility a qualifying life event (like having a baby, getting married, or having a divorce) which should alleviate the limitations of open enrollment periods for non-self-insured firms. (4) Brokers will often assist with the application process although they do not receive reimbursement from the Utah Department of Health (but typically receive commission from the insurance carrier for the policy). Materials are available in Spanish and English. | |
| Coverage | Qualifying employee coverage is subject to minimum service coverage requirements with the employer’s health plan. This includes physician visits, hospital inpatient services, pharmacy, well-child exams and child immunizations. The in-network deductible must be $1000 or less per person and the lifetime maximum must be at least $1,000,000. Qualifying plans pay at least 70% of an in-network inpatient stay (after the deductible) and the employer pays at least 50% of the premium for the primary insured individual. (6) Enrollees are responsible for any cost-sharing. (2) | |
| Premiums and Subsidy Structure | Workers make their monthly payment to their employer’s health plan and the program then reimburses the worker up to $150 per adult and up to $100 per child (based on the least expensive, qualifying plan the employer offers). (1) | |
| Funding | The UPP program draws federal Medicaid matching funds under the Primary Care Network waiver. (2) | |
| Contact | Heidi Weaver, Program Manager | Phone: (801) 538-6806 |
Appendix C
A Review of SCHIP Literature
This appendix acknowledges and summarizes a significant body of research that has yielded a good understanding of the determinants of children’s enrollment into State Children’s Health Insurance Programs (SCHIP). Given that the children’s Medicaid and SCHIP programs feature zero or very low premiums and cost sharing, studies of these programs usefully isolate the nonprice features that affect enrollment.
This rich SCHIP literature strongly influenced the development of our initial logic model (see Appendix A) and the formulation of the discussion topic guidelines for our stakeholder discussions. Our review of both the non-elderly adult coverage and subsidized children’s coverage literature found little direct evidence for or against the transferability of the SCHIP enrollment lessons to coverage approaches that target adults. Nonetheless, we note that parents almost always make the enrollment decisions for their children, suggesting that at least some of the findings might be transferable to programs that target parents, if not all adults.
The literature reviewed here includes 34 studies that examined SCHIP or closely related coverage expansions for children. Unlike the adult coverage literature review, these evaluations of children’s coverage include both qualitative and quantitative analyses. Overall, these evaluations found that mere expansion of eligibility is not sufficient to increase enrollment of eligible uninsured children in public health coverage programs. States also need to conduct extensive outreach and remove enrollment barriers, such as complex application procedures, to ensure robust take-up.
Background
Federal funding under the Balanced Budget Amendment of 1997 gave states the opportunity to expand Medicaid coverage to or create a separate coverage program for uninsured children under the age of 19 as part of SCHIP. The magnitude of the SCHIP initiative and the flexibility accorded the states in designing their programs resulted in a wealth of evaluations. As Glied (2007) notes:
SCHIP’s impact has come about because its design optimally encouraged states to act as laboratories of policy design. The design has been a springboard for health policy observers and health services researchers, equipped with relevant and timely data and innovative methods, to learn lessons that can be applied to much broader (and costlier) expansions.
Nonprice Factors Affecting Children’s Enrollment
Below we summarize some of the key studies that examined the determinants of children’s enrollment in subsidized public coverage programs using the steps in our logic model (awareness, comprehension, and appeal). As noted above, these programs feature zero or very low premiums and cost sharing, allowing researchers to readily isolate the nonprice features that affect enrollment.
Program Awareness
The literature found both outreach intensity and outreach method to be important factors contributing to enrollment. More intensive outreach (measured by either dollars spent per eligible child or the number of outreach activities undertaken by a state) was a significant predictor of SCHIP enrollment. Not all outreach methods are equally effective, however. Mass media campaigns, such as statewide television or radio advertisements, billboards, and posters, though successful in increasing program awareness, were least effective in stimulating enrollment. Furthermore, when a community develops a negative first impression of a program (for example, through word of a cumbersome enrollment process) against a backdrop of media campaigns designed to increase awareness of the program, the unfavorable impressions interact with the promotional efforts and hamper enrollment. The most effective outreach methods were decentralized, community-based, or in-person approaches, such as partnering with established community organizations and schools. We found few studies that examined the effect of the outreach message on enrollment.
Outreach Intensity
- Two multivariate studies showed that outreach measurably and significantly increased enrollment. A study of California Medicaid and SCHIP enrollment found that each additional dollar spent on outreach (excluding media) per eligible child significantly increased the odds of enrollment in Medicaid by 6 percentage points (p0.08) and significantly increased the odds of enrollment in SCHIP by 7 percentage points (p0.05). Conversely, money spent on media campaigns tended to decrease enrollment in SCHIP for each additional dollar spent (Kincheloe et al. 2007). Nicholson-Crotty found that states’ comprehensiveness of outreach activities, defined as number of outreach activities used in an individual state divided by the total number of outreach activities used by all states, is positively and significantly associated with the proportion of eligible children enrolled in the SCHIP program (p 0.001) (Nicholson-Crotty 2007). Several other case studies provided additional support for the impact of outreach intensity on enrollment, but their study designs did not allow the authors to definitively attribute the enrollment increases conclusively to outreach. For example, a major overhaul of Virginia’s SCHIP program, including intensified statewide outreach, raised awareness of the remodeled SCHIP program and coincided with a sustained rise in SCHIP enrollment (Howell 2006). Conversely, California found the effect of outreach to be “reversible”; the state reduced outreach intensity for its SCHIP program in 2002 (by eliminating all community- and school-based outreach contracts and its mass media campaign) and experienced stagnating or declining enrollment (Sullivan et al. 2006).
- Importantly, certain populations may need more resource-intensive outreach efforts. For instance, an evaluation of California community-based child health programs showed that a variety of outreach and enrollment activities were crucial to serving and enrolling the target population of Latino children (Frates et al. 2003). More intensive outreach is necessary to overcome the several enrollment barriers faced by Latinos, particularly procedural barriers to enrollment, language and cultural barriers, and lack of clarification on eligibility for children of noncitizen parents (Zambrana and Carter-Pokras 2004).
Outreach Method
- One comprehensive SCHIP evaluation, which analyzed participant survey data, found that it was health care providers, public agencies, and families and friends who most influenced families to decide to enroll their children in SCHIP. Although television advertisements or radio announcements about SCHIP were seen or heard by many families, the various types of communications were rarely the factors that influenced parents to enroll their children (Wooldridge 2005).
- Six studies noted that conducting outreach through community partners or in-person local outreach was an effective outreach method (Flores et al. 2005; Frates et al. 2003; Hill et al. 2005; Rosenbach et al. 2003; Rosenbach et al. 2007; Sullivan et al. 2006). Community outreach was particularly effective for enrolling Latino children, specifically by partnering with trusted community sources that subsequently made referrals to SCHIP. Effective outreach methods for Latino children included soliciting referrals through trusted sources, working with community organizations that serve immigrant children (such as migrant education and Head Start programs, schools, and community providers), developing a short, simple application form, providing personal assistance in applicants’ languages, and actively helping families enroll eligible children in public programs (Frates et al. 2003). One randomized controlled trial showed that community-based case managers are more effective than traditional Medicaid/SCHIP outreach and enrollment methods in enrolling uninsured Latino children (Flores et al. 2005).
- The literature generally shows that mass media campaigns, though effective at increasing awareness of programs, are not effective in terms of increasing children’s Medicaid and SCHIP enrollment. One comprehensive SCHIP evaluation found that mass media approaches, including direct mail, signs and posters, public transportation advertisements, and billboards, proved to be the least effective outreach activities (Rosenbach et al. 2003). In addition, state experience with outreach led most states away from mass media campaigns (and toward other types of approaches discussed above) as they gained program experience (Rosenbach et al. 2007), suggesting that these types of outreach strategies may have limited or short-term effectiveness. One multivariate analysis showed that media expenditures per eligible child in California were associated with decreased SCHIP take-up. For every additional dollar per eligible child in the Designated Market Area (DMA) that was spent on media, the odds of enrollment decreased among the SCHIP population by 9 percentage points (p .05), though the decline was smaller and not significant among the Medicaid population. Initial rumors of cumbersome enrollment procedures for a new program (in this case, SCHIP), coupled with a heightened awareness of the program through media exposure, reduced take-up; for an established program such as Medicaid, however, the effect was much smaller (Kincheloe et al. 2007).
- Researchers noted that most states initially mounted mass media campaigns for SCHIP outreach and then partnered with a wide range of state and local organizations. Over time, however, most states shifted resources away from mass media campaigns and focused on building partnerships with community-based organizations in order to access to “hard-to-reach” populations (Rosenbach et al. 2007), suggesting either that earlier methods were not succeeding or that later waves of enrollees require different methods.
- Seven studies found that school-based outreach was an effective outreach method (Frates et al. 2003; Hill et al. 2005; Howell et. al 2006; Irvin et al. 2004; Rosenbach et al. 2003; Rosenbach et al. 2007; Taras et al. 2002). For example, distributing enrollment brochures with the National School Lunch Program application was effective in enrolling children in SCHIP in Ohio (Irvin et al. 2004). In addition, contacting parents through schools, educating them about health insurance programs and preventive care, and helping them with insurance applications proved useful in locating large numbers of uninsured children who were unreachable via other outreach methods (Taras et al. 2002). Back-to-school campaigns in Kentucky, Ohio, and Virginia coincided with spikes in enrollment, although it was not possible to tease out the effects of these campaigns from those of other concurrent programmatic changes (Howell et al. 2006; Rosenbach et al. 2007).
Outreach Message
- An evaluation of state marketing campaigns found that the main message used by states to promote their program was that SCHIP/Medicaid is affordable health coverage for uninsured children of working families (Perry 2000). Previous focus group research with parents suggested that the message has much appeal. Parents of uninsured children say that they worry about their children and feel vulnerable without coverage.47
- As noted, one study found that initial rumors of cumbersome enrollment procedures for a new SCHIP program may have deterred enrollment (Kincheloe et al. 2007), suggesting there is a role for the outreach messages in combating negative perceptions about the program. In this case, perhaps the outreach messages could have emphasized ease of enrollment.
Program Comprehension
We found very few studies that examined the role of comprehension on program enrollment. A few studies indirectly suggested that program comprehension has an effect on program enrollment, particularly when families erroneously believe that their children are ineligible for a program because of income or immigration status and thus do not enroll or, conversely, when application assistance helps families understand the program’s eligibility requirements, thereby leading to an increase in enrollment.
- A survey of the parents of children dually eligible for Oregon’s public coverage plan (Oregon Health Plan) and the state’s premium subsidy program (FHIAP) asked FHIAP enrollees why they chose premium assistance instead of public coverage (which offers more generous coverage).48 Almost all respondents reported that they were aware of the public coverage option, but about half reported that they did not think that their child was eligible (Mitchell et al. 2005). The study did not investigate whether the gap in knowledge about the program’s eligibility requirements resulted from an ineffective outreach message or other reasons.
- One study found that community-based application assistance significantly improves take-up of Medicaid coverage, especially among Hispanics and Asians. The author suggested that “process costs” were important barriers to the use of public programs and that such costs were greater for those with language barriers and immigration concerns (Aizer 2003). The author did not directly address comprehension, but the study findings are consistent with comprehension difficulties.
- An outreach message believed to have a notable effect on enrollment of Latino children in Healthy Kids coverage (a privately funded SCHIP expansion program in California) emphasized that any child may sign up for coverage regardless of immigration status (Spencer 2006). While the research did not rigorously assess the extent to which enrollment may be attributed to the outreach message, the program’s rapid enrollment increase and the fact that the majority of enrolled children are indeed Latino suggest that the strategy was effective, particularly given the reported difficulties in reaching the Latino population. The targeted message may have “headed off” potentially erroneous understanding of program eligibility (Spencer 2006).
We found no evidence that SCHIP’s premium or cost-sharing structure posed a comprehension barrier to enrollment. When premiums or co-payments are charged, they are small and fixed, making it easy for the participant to understand and predict his or her financial responsibility. It is possible that the comprehensiveness of the SCHIP benefit design and simplicity of its cost-sharing arrangements minimize any enrollment barriers related to comprehension of the benefit and subsidy structure.
Program Appeal
The literature reviewed below examined program appeal from several perspectives. Several studies showed that a convenient enrollment process, featuring enrollment assistance and simplified applications, significantly increased SCHIP enrollment. In contrast, we found the literature inconsistent with regard to whether stigma reduced take-up of SCHIP and uncovered only limited evidence that attractive benefits encourage enrollment.
Enrollment Process
According to survey data, a major reason for under-enrollment is that families find enrollment procedures too complex. In a multivariate analysis, Stuber found that people who perceived Medicaid forms as long and complicated were 1.8 times less likely to enroll in Medicaid, all else equal (Stuber et al. 2000). The study demonstrated that increased enrollment depends in large measure on reduced barriers to enrollment. The literature examined both state efforts to remove barriers (such as offering telephone-based application assistance and setting up enrollment outstations) and state policy features designed to remove barriers (such as the elimination of asset tests and waiting periods). Here, we focus on the former where the following were found to be effective: (1) a simplified and shortened Enrollment Process, (2) a telephone line for answering applicant questions, (3) application support, and (4) a family-friendly website.
Several studies found that application simplification increased enrollment, particularly among immigrant and Latino populations with low literacy and/or language barriers.
- Dunkelberg (2003) reported a 30 percent increase in the number of children enrolled in Medicaid in Texas after the state simplified enrollment for children. Texas did not simplify enrollment for parents; over the same period, the number of enrolled parents rose by just 6 percent. An evaluation of Ohio’s SCHIP attributed the state’s successful enrollment in part to a shortened, two-page application (Irvin et al. 2004).
- For the Latino population, one study found that short, simple application forms and in-person application assistance in the applicants’ languages was particularly helpful for enrollment (Frates et al. 2003).
Another multivariate analysis found that allowing self-declaration of income was another simplification method that increased the probability of enrollment, by 3.5 percentage points (p0.05) (Kronebusch and Elbel 2004). Holahan found that, with the appropriate third-party verification procedures, it is possible to simplify the Enrollment Process by allowing self-declaration of income without increasing eligibility error rates (Holahan and Hubert 2004). Ohio ran a pilot tested allowing participants to self-report income; though the pilot was a success (only 2 percent of those self-declaring were ultimately deemed ineligible), political considerations prevented statewide implementation of the change (Irvin et al. 2004).
Joint applications for Medicaid-SCHIP (sometimes called a “No Wrong Door” policy) increased take-up, particularly during the renewal process (which, according to one multivariate analysis, increased the probability of take-up by 5.5 to 7.5 percentage points) (p0.05) (Bansak and Raphael 2007). A case study of Virginia’s SCHIP also found that implementation of a joint application for Medicaid/SCHIP coincided with increased enrollment in fall 2002 (Howell 2006).
Despite the success of most simplification efforts, mail-in and telephone applications appear to have no effect on enrollment levels when other policy and demographic characteristics are taken into account (Kronebusch and Elbel 2004). Similarly, another study noted that elimination of the face-to-face interview did not increase or decrease enrollment (Wolfe and Scrivner 2003). As noted, mail-in applications had a much higher denial rate compared with in-person applications. Mail-in applications tended toward incomplete information or errors, which in-person enrollment counselors can address (Hill and Lutzky 2003).
According to several studies, the provision of application assistance in the form of toll-free telephone numbers and a family-oriented and informative website was significantly associated with increased take-up among eligible children.
- Among SCHIP-eligible children, telephone application assistance increased take-up by 5 percentage points (p0.05) and availability of a family-friendly website by 2 percentage points (p0.01) (Wolfe and Scrivner 2003).
- Two studies found that community-based application assistance significantly improved take-up of Medicaid coverage, especially among Hispanic and Asian populations. Aizer (2003) reported that access to bilingual application assistants increased new monthly Medicaid enrollment among Hispanic and Asian children by, respectively, an average 4.6 and 6 percent relative to other children in the same neighborhood. Similarly, Flores et al. (2005) conducted a randomized controlled trial of Latino children in which treatment group patients benefited from the involvement of a case manager in providing information on Medicaid/SCHIP eligibility, application assistance, and liaison services; at the same time, control group patients received usual Medicaid/SCHIP outreach and enrollment. The study showed that children assigned to the treatment group had eight times the odds of enrolling in Medicaid/SCHIP.
Attractiveness of Benefit Design
One study found that the benefit packages of SCHIP-like child health expansion programs were attractive to enrollees, and one of the studies concluded that this influenced enrollment (Frates et al. 2003; Hill et al. 2005). Both studies also found that dental benefits were one of the most attractive features of the benefit package. Frates found dental benefits to be a strong enrollment incentive in the CalKids, Family Care, and Kaiser subsidized products and Hill et. al found that dental benefits or were one of the two most-used services of the program.49
Stigma
The evidence of the effect of stigma associated with Medicaid is mixed, partially because many authors fail to define stigma clearly; moreover, stigma poses measurement difficulties. Stuber and colleagues, however, developed a useful framework for understanding the role of stigma by characterizing Medicaid-related stigma into different types: (1) the traditional notion of “welfare stigma,” meaning that people enrolling in welfare or other public assistance programs will see themselves or society’s view of them in negative terms because they need public assistance; (2) application-related stigma, or the fear that the Enrollment Process will be demeaning or ask intrusive or unfair questions; and (3) provider stigma, whereby providers will treat Medicaid patients worse than privately insured patients. In a multivariate analysis of survey data to assess the impact of the three types of stigma on enrollment, the researchers found that, while 50 percent of respondents perceived some form of stigma associated with Medicaid, traditional “welfare stigma” did not significantly affect the probability of Medicaid/SCHIP enrollment. Instead, application-related stigma and provider stigma, as well as other types of barriers such as lengthy application procedures, were the significant causal factors affecting enrollment. Those perceiving application-related stigma were 2.2 times more likely to be eligible but not enrolled; those perceiving provider stigma were 1.7 times more likely to be eligible but not enrolled. Welfare stigma, perceived by just 11 percent of the sample, was not significantly associated with odds of enrollment (Stuber et al. 2000). Other studies analyzed stigma in a less specific and rigorous way. Mann et al. (2002) made the case that it is not the stigma associated with Medicaid itself but rather the enrollment barriers that have historically hampered Medicaid take-up; the authors, however, did not test their hypothesis.
As evidenced by state efforts to reduce the effects of stigma, states perceive stigma as an issue affecting the attractiveness of the program (Irvin et al. 2004). Several studies support this contention:50
- Some of Georgia’s Medicaid-enrolled children carry a card similar to the state’s SCHIP card rather than carrying a Medicaid card. A recent study found that these participants were more satisfied with the treatment they received and perceived a better attitude on the part of providers compared with those who carry a Medicaid card, indicating that programmatic identity contributes substantially to differential care experience (Ketsche et al. 2007).
- Ohio sought to decouple the stigma associated with Medicaid from SCHIP by not mentioning Medicaid in its outreach materials. State program officials reported complaints from parents who thought that they were enrolling in a non–Medicaid public program but then felt deceived when they received a Medicaid card in the mail, reinforcing suspicions that stigma indeed reduced program attractiveness (Irvin et al. 2004).
- In their efforts to reduce stigma, Ohio, Arkansas, Texas, and other states have eliminated the requirement for face-to-face interviews and allow mail-in applications; in Texas, the change coincided with a large increase in enrollment. One study found that mail-in application option made the Enrollment Process more acceptable to families and led to a higher volume of applications. Although mail-in applications generated a higher percentage of denials associated with incomplete information, state officials generally agreed that the trade-off was worthwhile (Hill and Lutzky 2003; Irvin et al. 2004).
- Other states have attempted to destigmatize their Medicaid or SCHIP programs through “branding.” For example, Arkansas sought to reduce the perceived stigma associated with traditional Medicaid by coupling it with the SCHIP Medicaid expansion under the combined name ARKids (Walls et al. 2006).
Collateral Enrollment into Other Coverage Programs
Several studies found that successful enrollment of one target population can have spillover enrollment effects for other programs or populations. For example, SCHIP outreach tended to increase enrollment of Medicaid-eligible children. The offer of parental coverage can also increase enrollment of children. Reasons included the appeal of programs that cover the whole family (regardless of age or immigration status) and increased ability to refer applicants across programs.
Availability of Parental Coverage
Programs that cover the whole family have greater appeal than do programs targeting either children or parents. The primary reason is that decisions to apply for health insurance are usually made at the family level, generally by the parents. When deciding to enroll, families must weigh the cost of applying (time taken off from work to apply, out-of- pocket expenses) against the benefits of health coverage. Coverage is more appealing if the whole family can be covered with a single application, increasing the probability that the family will apply (Ku and Broaddus 2000). Some states have used Section 1115 waivers to extend SCHIP benefits to parents of SCHIP-eligible children, and the review of all five studies of such expansions found the expansions to be somewhat to very effective for enrolling children (Ku and Broaddus 2000; Dubay and Kenney 2003; Bansak and Raphael 2007; Espeseth and Riportella 2006; Espeseth and Riportella 2006; Wolfe and Scrivner 2003). For example, one study showed that participation rates of children in states with expanded programs (those in which parents of Medicaid-eligible children are eligible for public health insurance coverage) were 20 percentage points higher compared with children in states lacking expanded programs (Dubay and Kenney 2003). The study also examined enrollment in Massachusetts before and after it expanded eligibility to parents and found that enrollment of eligible children increased by 14 percentage points following the expansion. One recent multivariate analysis found that extending benefits to parents led to an increase in take-up of 8 to 11 percentage points (p0.05) (Bansak and Raphael 2007). Another multivariate analysis showed smaller, nonsignificant gains; offering SCHIP coverage to parents was associated with a nonsignificant increase of about 2 percentage points in the probability of SCHIP take-up by children (Wolfe and Scrivner 2003).
Availability of Coverage for Recent Immigrants
Expanding coverage to residents ineligible for SCHIP due to income or immigration status can often increase SCHIP enrollment, especially when such programs are set up to cross-refer applicants. One multivariate analysis examined the extent to which the presence of county-sponsored SCHIP expansion programs in California affected Medicaid and SCHIP enrollment (Kincheloe et al. 2007). These SCHIP expansion programs extend coverage to children whose family income or immigration status makes them ineligible for SCHIP or Medicaid. The study found that children who lived in counties with a county-sponsored SCHIP expansion were almost three times as likely to be enrolled in Medi-Cal versus children from counties without such a program (p>.06) and 17 percent more likely to be enrolled in SCHIP (nonsignificant). The authors concluded that the difference in enrollment rates likely results from increased referrals from children applying for the expansion program who are in fact Medicaid- or SCHIP-eligible. However, children of immigrant parents with permanent resident status were less likely to enroll in Medi-Cal than children of citizen parents.
1 The safety net loosely refers to federally qualified community health centers, free clinics, public hospitals and other sources of care accessed by the low-income, uninsured population. Clinic charges are usually nominal and slide with income.
2 We also conducted two discussions with representatives from Hinds County Health Alliance in Mississippi. Due to lack of additional discussants available in Hinds County, we do not include results of these discussions in this chapter.
3 In addition to Plan B, a brokered access to care program, Ingham Health Plan includes two other plans: 1) a Medicaid 1115 waiver program for adults with incomes less than 50 percent of the FPL (called Plan A) and 2) the Ingham County Advantage Program, which is a private insurance product that targets small businesses.
4 In programs with high take-up, the enrolled population may have average health care needs. The majority of enrollees in Ingham Health Plan are young, fairly healthy, and are not excessive users of health care resources (Silow-Carroll 2001).
5 Ingham Health Plan has dedicated appointment slots for new members to ensure that members begin using primary care services instead of the emergency room. Navigators can make these initial appointments for members at the time that they enroll them in the program.
6 This approach is not always successful. For instance, the Hinds County Health Alliance in Mississippi attempted to divert Emergency Department patients to primary care clinics. However, almost half of the Emergency Department patients gave incorrect addresses or phone numbers, leaving Alliance staff unable to contact them about referrals (Brown and Stevens 2006).
7 While these programs are not technical insurance coverage, they typically borrow many concepts from insurance. For example, instead of a premium, members may pay a membership fee or participation fee. Instead of a copay, they may face a point of service fee.
8 This finding comports with previous research that found enrollees in Ingham Health Plan believed they were enrolled in health coverage because they had a membership card (Silow-Carroll 2001).
9 Healthy San Francisco; members with incomes below poverty level do not pay this fee. As Katz reported, this is expected to attract some people whohave refrained from seeking care because they refuse to accept “charity care” (2008).
10 In contrast, testing for public program eligibility appears to impede enrollment in some cases: For example, the enrollment process for CarePartners in Maine was described by one observer as being a deterrent. “This process began with proof that they did not qualify for Medicaid, a time-consuming and stigmatizing determination that some uninsured people declined to pursue” (Brown and Stevens 2006). Similarly, if a CareLink applicant is determined to be potentially eligible for Medicaid or CHIP, the individual must apply to the Medicaid and/or CHIP program prior to the end of a 60-day temporary enrollment period into CareLink (Task Force on Access to Health Care in Texas 2008).
11Ind-e-App is a browser-based system that assists with entitlement program application generation, eligibility determination, on-line provider selection, verification document management, workflow management, disposition tracking and report generation. This integrated system is designed to improve customer service, increase application accuracy, increase financial counselor accountability, expedite enrollment, prompt receipt of Medicaid reimbursements and provide reliable data regarding the indigent population of Marion County.
12 More than half of all poor uninsured people are adults who are not categorically eligible for Medicaid. (Dorn 2008). Medicaid covers adults only if they fit within federally defined eligibility categories—that is, they must be pregnant, caring for dependent children, severely disabled, or age 65 or older. Section 1115 of the Social Security Act permits the secretary of the Department of Health and Human Services (HHS) to waive this prohibition. However, few states use such waivers because, under federal “budget neutrality” rules, waivers give no additional federal money to defray the cost of covering more people.
13 Oregon’s FHIAP features premium subsidies for both group and nongroup coverage. This chapter focuses on findings specific to premium subsidies for non-group coverage. Chapter IV addresses premium subsidies for group coverage.
14 Alliance Family Care in Alameda County, California, closed in 2005 (see Appendix B).
15 This is mostly driven by federal budget neutrality calculations. In the 1115 budget neutrality formula, childless adult member months do not count in the denominator even though their health care costs are in the numerator (www.hrsa.gov/stateinsurance/utah.htm).
16 Demonstrations set up as 1115 waivers must be “budget neutral.” In other words, the costs of covering the “expansion population” must be offset by other programmatic changes in Medicaid. A limited ability to make offsetting cuts in other Medicaid programs means that states must often cap enrollment of these expansion populations. Similarly, SCHIP state funding caps limit federal funding available to SCHIP populations.
17 We are aware of just one program, the Premium Support Program in Arizona, which was heavily subsidized and had lower-than-expected enrollment in its early years (Sparer 1999).
18 Personal communication from H. Weaver, August 14, 2008.
19 Several discussants noted that mass media, while effective, may not be necessary if only a limited number of program slots need to be filled.
20 One discussant cited the limited body of research in the area of community “social capital” and its effect on access to health insurance information. Social capital is the level of community connectedness and strength of social networks, as manifested in civic participation, trust in neighbors, and a sense of belonging (Hendryx et al. 2002). Communities with high levels of social capital may disseminate information about social services, including health coverage programs, more efficiently and the phenomenon of “word-of-mouth” may play a more critical role. Conversely, word-of-mouth may be less critical in communities with low levels of social capital.
21 In 2007, 16 percent of callers cited television as how they had heard about the program—despite the fact that Healthy New York stopped running its television advertisement campaign in 2007. This suggests that the media campaign made a lasting impression (EP&P Consulting 2008).
22 In all five programs, applicants had access to enrollment assistance from program staff and community partners.
23 For example, Utah’s PCN features extremely limited primary care benefits and no coverage for hospital or specialty care. One case study reported that some eligible adults did not enroll because they did not perceive the PCN’s benefits to be worth the $50 annual enrollment fee. A disenrollment survey conducted after one year of operation found that 26 percent of former beneficiaries reported that they disenrolled from the program because it failed to meet their health care needs; 62 percent of this group reported that PCN did not offer needed services (Office of Health Care Statistics 2004). Nonetheless, the program reached its enrollment cap of 19,000 adults (an estimated 16 percent of the eligible population) after a little more than one year of operation (see Appendix B). This suggests that the limited benefit design did not overly deter enrollment.
24 Some of the literature reinforces this view. An analysis of Oregon’s FHIAP found that many children eligible for the state’s public coverage plan (Oregon Health Plan, the state’s SCHIP plan) instead enrolled in FHIAP, which provides a subsidy for group and nongroup private coverage. When FHIAP families were asked why they chose FHIAP instead of SCHIP, 16 percent cited a preference for private rather than public insurance coverage, and an equal number cited a desire to cover the entire family (Mitchell et al. 2005). The study did not directly ask if people preferred private coverage because of stigma associated with public coverage.
25 The same study included a survey of Maine employers (enrolled and not enrolled), and very few reported that this dual application was a barrier to enrollment by their workers.
26 In contrast, many coverage programs for those with low income experience significant “churning.” Utah’s PCN, for example, found that 27 percent of enrollees left the program during July through September 2003 (Office of Health Care Statistics 2004).
27 To increase readability, the term worker (as opposed to employee) is used in this discussion. This is intended to include the worker’s dependents when other family members are also eligible for subsidized coverage.
28 Oregon’s FHIAP features premium subsidies for both group and nongroup coverage. We briefly contrast these two variations at the end of this chapter but otherwise focus on findings specific to premium subsidies for group coverage.
29 States have been operating HIPP programs since 1990. Premium assistance was included in the SCHIP statute in 1997. States can also use Medicaid 1115 waiver authority to request waivers from many of the federal Medicaid and SCHIP requirements. A CMS initiative that began in 2001 was designed to encourage the use of these waivers to expand coverage under premium assistance programs. The 2005 Deficit Reduction Act prohibits CMS from approving new §1115 waivers that use SCHIP funding to cover childless adults, although adult parents can continue to be covered.
30 Small-group enrollees who are dually eligible for MaineCare (the state’s Medicaid program) and DirigoChoice are eligible for federal match, but the program has few dual enrollees.
31 These programs appear to have low uptake in part because they cover only children—as opposed to whole families—within a narrow band of eligibility. Rhode Island found that premium assistance was cost-effective much more frequently for families with incomes below 185 percent of FPL, where both parents and children are eligible, than for families with incomes above 185 percent of FPL, where only children are eligible. Similarly, Maryland’s program, which covered only children between 200 and 300 percent of FPL, enrolled slightly fewer than 200 children (Shirk and Ryan 2006).
32 In the program’s early years, CMS also required a minimum employer contribution of 60 percent. In 2001, CMS relaxed this requirement, and now states must merely set a minimum contribution level for employers.
33 One study suggested that policies designed to enroll residents into public coverage quickly and easily may make employers less forthcoming about the details of their own coverage. Such policies may therefore reduce the potential reach of premium assistance (Neuschler and Curtis 2003).
34 At the same time, the state made enrollment in employer coverage mandatory for those who are eligible, although overall enrollment in public coverage remained voluntary.
35 Low levels of enrollment in subsidized coverage programs targeting small employers have been observed over a substantial period of time. In the late 1980s, the Robert Wood Johnson Foundation sponsored 10 projects that either developed new insurance products or subsidized existing products under their Health Care for the Uninsured Program. Despite premium reductions averaging between 25 and 50 percent, most programs never reached even 10 percent of their target market. The reluctance of small employers to participate was attributed mainly to fears of increased labor costs and the administrative burden associated with a benefit for a small number of workers (Helms et al. 1992).
36 In most states, sole proprietors purchase coverage in the nongroup market. A few states, including New York, Massachusetts and Maine, allow sole proprietors to purchase coverage in the small group market. In 2007, Massachusetts combined their small group and nongroup health insurance markets as part of a larger set of health reform measures, including an individual mandate.
37 “Grassroots” outreach approaches include working with local, trusted community organizations (such as chambers of commerce, associations, churches, and other organizations that have a presence in the community) to spread the word about the program, for example by inviting small business owners to attend local meetings and presentations to learn more about the program.
38 Interestingly, the effective message for this community involved some straightforward discussion of the government subsidies available for coverage. Feedback from other discussants suggests this is not always the best message to emphasize.
39 The Insurance Partnership program is the component of the Family Assistance program that subsidizes employers (see Appendix B). As Table V.2 reports, two-thirds of firm participants are sole-proprietors.
40 Independent contractors are also referred to as “1099” employees as IRS form 1099-MISC is used to pay for their services, instead of W-2 form.
41 As one program observer noted, “Our experience in Alameda County demonstrates that offering an affordable, comprehensive family coverage product and transforming the enrollment process means that families will not only enroll but stay enrolled” (Zahn 2003).
42 Reflecting great underlying need, a few previous studies and some discussants suggested that dental benefits are a particularly attractive component of comprehensive coverage, a finding echoed by the SCHIP studies. Dental benefits may also be a cost-effective addition to some programs. Service use data from Ingham Health Plan suggest that many emergency room visits by enrollees were instigated by oral health conditions. At the time of the study, this program did not cover oral health (Silow-Carroll 2001).
43 See Appendix C for more discussion of these forms of stigma.
44 Certain states, such as Montana, may have few non-English speakers among their eligible population.
45 A recent and promising exception is State Health Access Reform & Evaluation (SHARE), a four-year Robert Wood Johnson Foundation initiative that supports the systematic evaluation of state health care reform activities. The goal is to help state policymakers identify approaches to health reform that are suited to their state by assembling evidence from diverse reform approaches. The Robert Wood Johnson Foundation’s Communities in Charge initiative (2000–2004) and the W. K. Kellogg Foundation’s Community Voices program (1998–present) generated significant literature on community-based programs, but the studies were descriptive in nature and did not rigorously extract the lessons that would inform our study (Grantmakers in Health 2005).
46 There are many other ways to measure the success of a subsidized health coverage program, such as its duration or ability to meet other program objectives. Further, there are myriad program features (e.g., broad local/state political or community support) that contribute to program success (broadly defined). This study is restricted to program features that have a direct bearing on the decision to participate by an individual or employer.
47 However, later focus group research showed that some parents felt that the advertisements lacked important information, such as program facts, costs, and a toll-free telephone number for more information. However appealing the messages were, the advertisements were missing key content necessary to spur enrollment.
48 See Appendix B for more information on Oregon’s Family Health Insurance Assistance Program.
49 Another study, which conducted key informant interviews with providers, found that dental care was one of the two most widely used program benefits, reinforcing the notion of its appeal to participants.
50 A SCHIP program separate from Medicaid was often associated with higher take-up than combined programs, although one study showed that it is the features associated with separate SCHIP programs and the higher amount of money typically spent on outreach that drive the higher take-up of separate SCHIP programs, not the separation of SCHIP from Medicaid per se.