Final Report Presented to:
Lynn Nonnemaker
DHHS/OS/ASPE
Presented by:
NORC at the University of Chicago
1350 Connecticut Ave, NW, Suite 500
Washington, DC 20036
(202) 223-6040
Executive Summary
Purpose: This report assesses effects of a variety of refinements to the current Sustainable Growth Rate (SGR) Medicare physician payment update process. A spreadsheet model of the SGR process was developed to examine changes in conversion factors (CFs) and program spending in response to changes in the SGR process, including changes to the SGR formula and changes in the formation and composition of target spending.
Background: Medicare allowed charges increased from a total of just under $45 billion in 1996 to almost $82 billion in 2004, a 51 percent increase. While spending on evaluation and management (E&M) services and procedures remained at about 40 percent of total Part B spending, E&M spending as a share of SGR physician services increased from about 45 percent to 48 percent. In 2004, expenditures for procedures accounted for about 30 percent of total SGR physician spending, and imaging spending accounted for about 17 percent.
Examination of spending trends over time reveals that changes in intensity – defined as changes in utilization of services or procedures that are not attributable to program size or price – vary over time and by type of service. Intensity estimates for E&M during the 2000-2004 period averaged about 3.7 percent per year, less than the intensity value for all SGR services combined, 5.5 percent. By contrast, imaging procedure intensity averaged over 10 percent per year. Intensity of major procedures (including major surgical procedures that require over-night hospitalization) declined slightly during 2002-2004 by about one-half of one percent per year on average. Intensity for all other procedures (including minor procedures, endoscopies, and eye procedures) increased an average of 7.1 percent per year.
The shift away from utilization of major procedures is also revealed from the perspective of site-of-service. About 62 percent of charges were for services provided in office settings in 2004, whereas services provided in inpatient settings accounted for about 20 percent of Part B allowed charges by physicians. The share of charges for services provided to inpatients declined by about a third between 1996 and 2004. The shift of services to the office setting is not strictly due to increases in the provision of E&M services. In 2004, for every dollar of E&M care provided in an inpatient setting, $2.60 of E&M care was provided in other settings. But the ratio for non-E&M care was even larger. Over four times as many allowed charges under Part B were for non-E&M services and procedures provided in non-inpatient settings than in inpatient settings.
While spending patterns vary by type of service, physician payment updates under the current SGR process are based on trends in total spending. The SGR process consists of three formulas – formulas for the CF, Update Adjustment Factor (UAF), and SGR, the rate used to calculate the spending target from the target for the previous year. The SGR is based on changes in Gross Domestic Product, practice costs, and the number of Medicare beneficiaries who participate in Part B fee-for-service Medicare. The CF is calculated from the rate at which the costs of medical practice change each year and the UAF, a reward/penalty for under-/over-spending in past years. The UAF is set based on the difference between target and actual spending during the previous year, and the difference between target and actual spending levels, cumulated over time. Under the SGR process, a floor of -7 percent constrains the amount by which the payment update can be reduced by the UAF each year.
A serious flaw with the SGR process is that recent payment updates have been negative, meaning that the CF used to calculate payment changes over time and associated Medicare payment rates should have declined. Concerns that reductions in Medicare payments could negatively impact access to care under the Medicare program, however, have resulted in recent Congressional intervention and subsequent revisions to payment updates.
Methods: A spreadsheet model was constructed for use in examining changes to the SGR payment formula. The model was first constructed to ensure that its outputs – CFs and spending – were consistent with past experience. The model was then extended to cover the period 2007-2014. Data used to construct the model were from various sources compiled by the Center for Medicare and Medicaid Services (CMS), including preliminary and final rules published in the Federal Register, information published in the 2006 Medicare Trustees’ Report, and information available for downloading from the CMS website.
The model was constructed for study of the separate contribution of certain types of services on the conversion factor and program spending, and for study of refinements to the SGR formula as currently constructed. Thus, modeling required estimates of various components of physician spending used to calculate the payment update. Predictions on the level and composition of spending on physician services that enter the SGR process were not available from CMS publications. Physician/Supplier Procedure Summary Master File (PSPSMF) data (from CMS) for years 1996-2004 were used to study spending for groups of services, e.g., E&M services, imaging procedures, and the remainder of non-E&M services that affect calculation of the SGR update. Spending shares for these groups of services were calculated from the PSPSMF data and used to estimate spending by service group for the years 2005-2013.
The spreadsheet model was used to study effects of two fundamental types of revisions to the SGR process. First, effects of changes in various attributes of the SGR formula were studied. Attributes of interest included: the Medicare Economic Index (MEI), effects of not adjusting the index for economy-wide changes in productivity; and the design of the UAF, effects of changing the UAF floor and the severity of penalties on over-spending in the previous year and cumulated over time.
Second, effects of several changes in the definition of target spending were studied. Effects of increases in the SGR were examined. Spending projections suggest that spending will continue to exceed target spending. An increase in the size of targets, e.g., to reflect a strengthening of preferences for more health care spending by program beneficiaries over time, should by definition reduce the size of future payment update reductions.
Another refinement of interest is target-rebasing. Under the current SGR process, the spending target has been updated since the late-1990s and the UAF penalizes providers for the cumulated difference between actual and target spending levels since that time. With rebasing, target spending would be reset for the year 2006, thereby affecting calculation of updates beginning with the 2007 update. Providers would no longer be held accountable for over-spending that has been accumulating for a number of years. The method of rebasing studied here is to simply set target spending to actual spending for 2006; under this option, the accumulation of over-/under-spending amounts would begin in 2007.
An attribute of target spending also addressed in this report is the composition of spending that is used by the SGR process in the setting of UAF penalties/rewards. At present, the UAF is calculated using the total of provider spending on physician services, laboratory tests, and drugs. Some policymakers and providers have expressed concerns that providers who are affected by updates under the Medicare Fee Schedule have less control over drug and lab prices, and therefore spending, than over prices for physician services. In fact, baseline drug and lab spending components of SGR spending are expected to increase more rapidly than physician spending in the near future. Perhaps physician service updates should not be based on drug and lab spending. In this analysis, effects of deleting drug and lab spending from the update process are studied.
Findings: An important caveat of this study is that no behavioral responses, on the part of any agents affected by the update process, including providers, Medicare beneficiaries, and Congress, have been incorporated into the structure of the update model. Thus, no behavioral responses to changes in updates affect simulated effects on future updates and program spending.
In spite of this caveat, a model of the SGR process is a useful source of information on relative magnitudes of effects of changes in the current update process. Effects of the payment reform options addressed in this report may be summarized from the perspective of an update continuum. Under the current SGR process, negative payment updates (declining CFs) are expected through 2014. The UAF formula would penalize over-spending, a consequence of expected total SGR spending levels in excess of target spending levels (bottom, Table ES-1). At the opposite end of the update continuum is the cost approach, under which the update would be based only on the expected rate of increase in the costs of practice (as measured by the MEI). The average CF under the cost approach would exceed the average under baseline by 20 percent between 2007 and 2010, and by 60 percent between 2011 and 2014 (top, Table ES-1). The difference in total program spending between these two extremes is large – about $190 billion, or 27 percent of baseline spending during 2007-2013.
|
2007-'10 |
2011-'14 |
|||||
|---|---|---|---|---|---|---|
|
Model |
CF (Range) |
Average |
Spending |
CF (Range) |
Average |
Spending** |
| Cost |
$40.13 |
2.2 |
$468.5 |
$43.58 |
2.2 |
$433.2 |
|
($38.88-41.34) |
|
($42.17-45.06) |
|
|||
| Baseline |
$33.52 |
-5.0 |
$403.4 |
$27.23 |
-5.0 |
$308.5 |
|
($36.16-30.93) |
($29.34-25.21) |
|||||
| Notes: Baseline results are based on CFs predicted for years 2007-2014. Cost model CFs were predicted from the SGR model by basing updates only on the MEI and ‘other’ factors used by CMS; i.e., the UAF is not used in calculating the update for the cost model. CFs and percent changes are arithmetic averages over the period of interest. The CF range refers to the values at the beginning and end of the period. Spending is total SGR spending during the period. *Target spending amounts rebased to 2006 spending. **Spending estimates are for years 2011-2013. | ||||||
The update options that are the focus of this report are positioned within the update continuum bounded by the cost and baseline approaches. Each offers smaller update reductions than the current SGR process, but at a price – higher spending than baseline, but lower spending than under the cost approach.
Refinements to the SGR Formulas. The payment update under the current SGR process is calculated as the rate at which the cost of practicing medicine (measured by the MEI) is expected to change, adjusted for past over-/under-spending (measured by the UAF). Under the current update process, the MEI is adjusted for changes in physician productivity over time. Because the MEI is not net of the price effects of improvements in human productivity, the rationale for including the productivity adjustment is to offset the increase in medical care prices that reflect advances in productivity. Critics of the productivity adjustment argue that the productivity adjustment factor is an inadequate proxy for productivity by physicians. Elimination of the productivity adjustment would increase the value of the MEI. Simulation results confirm that eliminating the productivity adjustment would increase CFs in the future relative to baseline, but these increases would not be enough to result in positive updates in the near future (Model 2, Table ES-2). Spending for 2006-2013 associated with this refinement would increase by about 3 percent relative to baseline.
The driver of future negative payment updates is the UAF, which penalizes providers for over-spending. Its rationale is cost-containment. Through the UAF, CFs are adjusted to help the Medicare program recover a portion of spending in excess of targets. Simulations indicate that the UAF during years 2007-2013 is expected to be less than the floor, meaning that the UAF itself would contribute -7 percent to the payment update.
|
2007-'10 |
2011-'14 |
||||||
|---|---|---|---|---|---|---|---|
|
Model |
CF |
Average |
Spending |
CF |
Average |
Spending* |
Spending |
| (1) Current process (baseline) |
$33.52 |
-5.0 |
$403.4 |
$27.23 |
-5.0 |
$308.5 |
1.00 |
| (2) revised MEI |
$34.25 |
-4.1 |
$410.5 |
$28.81 |
-4.1 |
$320.8 |
1.03 |
| (3) revised UAF |
$34.31 |
-4.0 |
$411.2 |
$30.20 |
-2.2 |
$329.5 |
1.04 |
| (4) 0-update floor |
$37.84 |
-0.1 |
$446.0 |
$37.82 |
0.0 |
$390.0 |
1.17 |
| Notes: Estimates in this table are from Tables 8a, 8b, 10, 11a, and 11b. Model (1) estimates are for the current SGR process. Model (2) estimates are from the baseline model, but after eliminating the productivity adjustment from the MEI. Model (3) estimates were obtained from the baseline model after revising the UAF; revisions include elimination of the cumulated over-/under-spending term from the UAF, and reduction in the penalty/reward for spending during the previous year by 50 percent. Model (4) estimates were obtained from the baseline model, but after modifying the floor of the UAF to offset the MEI each year, such that the revised floor is 0. CFs and percent changes are arithmetic averages over the period of interest. Spending is total SGR spending during the period. The Spending Ratio is the ratio of estimated total spending associated with the model to estimated total spending under baseline, Model (1). *Spending estimates are for years 2011-2013. | |||||||
Expected future reductions in CFs could be mitigated with changes in the structure of the UAF. One policy option is to reduce the size of the UAF penalty by eliminating the penalty associated with cumulated over-spending and simultaneously cutting the penalty associated with over-spending in the previous year. Elimination of the cumulated spending term and a reduction in the penalty/reward associated with over-/under-spending by 50 percent would also help reduce the magnitude of payment reductions, especially after 2010 when the average annual percent change in the update would be -2.2 percent (compared to -5 percent under baseline) (Model 3, Table ES-2).
Yet another option is to alter the floor of the UAF, essentially ensuring that negative updates do not occur. Under this 0-update floor, the floor is calculated such that the penalty associated with over-spending is only so large as to offset the MEI’s positive impact on payment changes. At worst, this floor would result in a zero update. Simulations indicate that CFs would be stable in the near future, as in most years the 0-update floor would be effective. Spending for 2006-2013 under this option would increase by 17 percent relative to baseline.
Refinements to Target Spending. A challenge posed by most of the studied changes to the SGR formula is that payment updates would generally decline (albeit not by as much as under baseline) or fail to increase in the future. Thus, some Congressional intervention would be likely with these refinements. Several studied refinements to target spending would yield larger payment updates in the future, but with increased spending.
The model was used to examine effects of an increased SGR, increased by about one-third to adjust for the tendency for error in estimating past values of the SGR and to account for tastes favoring more health care. This change, however, would have no effect on future CFs and on program spending through 2013 because increases in target spending are not large enough to offset expected spending increases.
With target rebasing (so that the 2007 update is calculated by setting the target for 2006 to the level of actual spending in 2006), CFs would decline from 2008 to 2012 but exceed baseline levels due to an initial update increase for 2007 (Model 1 in Table ES-3). Spending would be higher than under baseline by 6 percent during 2007-2010. The CF would begin to increase by 2013, contributing to a 12 percent increase in spending over baseline during 2011-2013.
|
2007-'10 |
2011-'14 |
||||||
|---|---|---|---|---|---|---|---|
|
Model |
CF |
Average |
Spending |
CF |
Average |
Spending* |
Spending, |
|
Rebased Spending |
|||||||
| (1) basic model |
$36.24 |
-3.0 |
$429.6 |
$32.47 |
-0.6 |
$345.4 |
1.09 |
| (2) less drug and lab spending |
$36.68 |
-2.2 |
$434.0 |
$35.19 |
1.0 |
$366.0 |
1.12 |
| (3) with revised SGRs |
$38.29 |
0.1 |
$450.2 |
$41.61 |
4.0 |
$413.3 |
1.21 |
| (4) with revised UAF |
$38.78 |
0.6 |
$455.0 |
$41.60 |
3.2 |
$414.7 |
1.22 |
| Notes: Estimates in this table are from Tables 13a, 13b, 14a, 14b, 15a, 15b, 16a, 16b. Model (1) estimates are with rebased spending. Model (2) estimates are with rebased spending, after deleting drug and lab spending from SGR spending. Model (3) estimates were obtained with revisions to SGR values used in Model (2), and Model (4) estimates were obtained by eliminating the cumulated over-/under-spending term from the UAF in Model (3). Rebased means that in calculating the CF for 2007, the target for 2006 is estimated spending for 2006, and initial cumulated actual and target spending amounts are set to total estimated 2006 spending; the SGR formula was then applied for years 2007-2014. CFs and percent changes are arithmetic averages over the period of interest. Spending is total SGR spending during the period. The Spending Ratio is the ratio of estimated total spending associated with the model to estimated total baseline spending under the current SGR process ($711.9 billion). *Spending estimates are for years 2011-2013. | |||||||
The spreadsheet model was used to examine a variety of refinements to the rebased version of the update process, each of which helps to mitigate future update reductions. If CFs were derived after rebasing and eliminating lab and drug spending from the CF calculations, CFs would decline between 2008 and 2010, as with simple rebasing, but CF levels would be higher without than when drug and lab spending are included (Model 2 in Table ES-3). Total spending would increase as a consequence. Spending would be 3 percent higher than with rebasing only, and 12 percent higher than is expected under the current SGR process.
Effects of sequentially implementing several refinements after excluding spending for drugs and laboratory tests in the rebased SGR model were also studied. These included increases in SGR values and eliminating the cumulated over-/under-spending portion of the UAF. Conversion factors tend to increase with each additional refinement, albeit at varying rates. And each refinement, successively imposed, would increase program spending. An increase in SGRs after eliminating lab and drug spending would increase the average CF in the near future, but add 21 percent to baseline spending (Model 3 in Table ES-3). Subsequent revision to the UAF would increase the average CF somewhat between 2007 and 2010, and increase spending relative to baseline by 22 percent (Model 4, Table ES-3).
Conclusions: Reforms of the SGR update process that appear to hold the most promise are those involving changes in the definition of target spending, including rebasing of spending targets, changes in the definition of target spending, and changes in the rates at which targets increase after rebasing. How best to fix the SGR process requires that policymakers agree on how to balance concerns over the benefits of avoiding future Congressional intervention and increases in program spending.
1.0 Purpose and Overview
There has been considerable recent interest in revising the Sustainable Growth Rate (SGR) process of updating payments to physicians and other providers under the Medicare program. Researchers at the Centers for Medicare & Medicaid Studies (CMS) and with the U.S. Government Accountability Office (GAO) have studied the implications of basing the payment update solely on estimates of the prices of inputs used by practitioners and implications of several other changes in the SGR formula.1 The objective of this study is to evaluate various revisions to the current SGR physician payment update methodology with a focus on changes to attributes of the SGR process that might be implemented in the short-run. For example, short-run “fixes” of interest include: “increasing” the update floor to reduce the size of annual payment reductions in response to over-spending, and increasing the rate used to set spending targets, e.g., to account for new, cost-increasing but quality-enhancing technologies.
The next section provides a context for this study, including a description of trends in spending for services and procedures affected by the SGR process. The current SGR process is described and several criticisms of the process are noted. Section 3.0 describes the analytic approach and structure of the spreadsheet model of the SGR process. A brief description of how spending predictions for future years were obtained is provided in Section 3.0, and more details are provided in the Appendix.
Results are presented in Sections 4.0 and 5.0. Several criteria are used to assess each refinement to the SGR process. Primary criteria include the extent to which the refinement contains program spending, and the extent to which the refinement would affect stable, sustainable payment updates. In this context, sustainability refers to the extent to which updates do not change dramatically from year to year and can stand alone, i.e., will not likely require Congressional intervention out of concerns that access to care by beneficiaries will be compromised. A summary and discussion of implications comprise Section 6.0.
2.0 Background
2.1 Spending Trends
Medicare allowed charges increased from a total of just under $45 billion in 1996 to almost $82 billion in 2004, a 51 percent increase (Figure 1)2. Most of this spending was for physician services included in spending estimates used in the SGR payment update process. If spending on chemotherapy and other drugs and on lab tests are subtracted from spending, ‘SGR physician’ spending in 1996 and 2004 was about $40 billion and $68 billion, respectively.
While spending on E&M services and procedures remained at about 40 percent of total Part B spending ($18 billion in 1996, and $33 billion in 2004), E&M spending as a share of SGR physician services increased from about 45 percent to 48 percent. In 2004, expenditures for procedures (major and other, over $20 billion) accounted for about 30 percent of total SGR physician spending, and imaging spending accounted for about 17 percent ($12 billion). Over time, the proportion of SGR physician spending for procedures declined from 34 to 30 percent, whereas the share of spending on imaging procedures increased from 12 to 17 percent.
Figure 1. Medicare Allowed Charges by Type of Service, 1996-2004
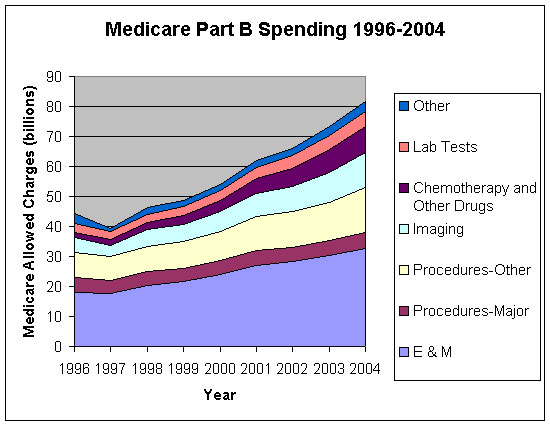
Source: NORC examination of PSPSMFs
2.1.1 Per Beneficiary Spending
On a per beneficiary basis, SGR spending increased from $1,371 in 1996 to $2,376 in 2004 – a total of 73 percent (61 percent of spending if drugs and lab tests are excluded) (Table 1). It is clear that growth in spending varies by type of service from one year to the next, as changes in price (as measured by the update), impact most types of services under Medicare uniformly. In recent years, growth in per beneficiary spending for E&M services has lagged behind growth for non-E&M services. Between 2000 and 2004, average annual growth in spending per capita on E&M services was about 5.3 percent. By contrast, expenditures on non-E&M services grew at an average annual rate of about 10.3 percent. The fastest growing portion of spending (from among those groups of services listed) was for chemotherapy and other drugs. Drug spending increased at an average annual rate of about 19.6 percent (versus an average rate of 8.2 percent for all services during the same time period).
|
1996 |
1997 |
1998 |
1999 |
2000 |
2001 |
2002 |
2003 |
2004 |
|
|---|---|---|---|---|---|---|---|---|---|
|
Spending per Medical Enrollee (Part B, FFS) |
|||||||||
| Total |
1371 |
1240 |
1493 |
1577 |
1737 |
1932 |
2004 |
2158 |
2376 |
| E&M |
550 |
560 |
656 |
698 |
770 |
840 |
855 |
889 |
946 |
| Non-E&M |
821 |
680 |
837 |
879 |
968 |
1092 |
1149 |
1269 |
1429 |
| Procedures-Major |
157 |
136 |
149 |
147 |
150 |
155 |
148 |
150 |
157 |
| Procedures-Minor |
262 |
250 |
271 |
286 |
314 |
352 |
359 |
376 |
438 |
| Imaging |
151 |
115 |
177 |
188 |
210 |
245 |
254 |
297 |
341 |
| Chemotherapy and Other Drugs |
52 |
68 |
77 |
97 |
121 |
151 |
186 |
225 |
247 |
| Lab Tests |
89 |
84 |
92 |
96 |
105 |
114 |
124 |
131 |
143 |
| Other |
110 |
27 |
72 |
65 |
67 |
75 |
78 |
90 |
103 |
| Source: NORC examination of PSPSMFs. | |||||||||
2.1.2 Decomposing Spending Growth
Some of the changes in spending displayed in Figure 1 are due to changes in price and changes in the number of Medicare beneficiaries over time. Year-to-year changes in total spending were decomposed into changes attributable to price, the number of traditional fee-for-service Part B program beneficiaries, and intensity – changes in utilization of services or procedures that were not attributable to program size or price. Data suggest that intensity varies over time, and by service type. Intensity estimates for E&M during the 2000-2004 period averaged about 3.7 percent per year, less than the intensity value for all SGR services combined, 5.5 percent. By contrast, imaging procedure intensity averaged 11.2 percent per year (Table 2).
Real growth in utilization has been away from major procedures, toward minor and ambulatory procedures. Intensity of major procedures (including major surgical procedures that require over-night hospitalization) declined slightly during 2002-2004 by about one-half of 1 percent per year on average. Intensity for all other procedures (including minor procedures, endoscopies, and eye procedures) increased an average of 7.1 percent per year. In 1996, spending on major procedures accounted for about 37 percent of spending on all procedures. By 2004, the major procedure share had declined to 26 percent. Intensity for other (non-major) procedures during 2000-2004 exceeded intensity for SGR services by about 29 percent.
|
|
Intensity |
|||
|---|---|---|---|---|
| Percent Share of Allowed Charges |
Average Annual |
|||
|
Service Group |
1996-97 |
2003-04 |
1996-2000 |
2000-04 |
|
All Services |
100.0 |
100.0 |
3.5 |
6.5 |
|
E&M |
42.7 |
40.5 |
5.7 |
3.7 |
|
Office Visits |
16.9 |
16.7 |
7.2 |
4.5 |
|
Hospital Visits |
12.5 |
9.5 |
2.2 |
1.6 |
|
ER Visits |
2.7 |
2.3 |
4.2 |
3.4 |
|
Home & Nursing Home Visits |
2.3 |
1.9 |
3.2 |
3.5 |
|
Specialty Visits |
2.7 |
5.1 |
12.9 |
5.3 |
|
Consultations |
5.6 |
5.0 |
4.5 |
4.2 |
|
Non-E&M |
57.3 |
59.5 |
2.1 |
8.6 |
|
Major Procedures |
11.2 |
6.8 |
-3.7 |
-0.4 |
|
Other Procedures |
19.6 |
17.9 |
1.7 |
7.1 |
|
Imaging |
10.1 |
14.1 |
8.7 |
11.2 |
|
Chemotherapy and Other Drugs |
4.6 |
10.4 |
20.0 |
18.0 |
|
Lab Tests |
6.6 |
6.0 |
1.4 |
6.5 |
|
Other |
5.1 |
4.3 |
17.1 |
9.8 |
|
Note: E&M refers to evaluation and management services. Intensity is calculated as percent change in spending after controlling for changes in price and number of fee-for-service beneficiaries. Source: NORC analysis of Physician/Supplier Procedure Summary MasterFile data, 1996-2004. |
||||
During the period from 1996-2004, growth in utilization was rapid for the chemotherapy and other drugs category of services. Rapid increases in the utilization of imaging procedures are observed during this period, as well. Utilization of both standard and advanced procedures exceeded increases for the average service during 1996-2000 and 2000-2004 (Table 3).
| Service Group | Percent Share of Allowed Charges 1996-97 | Percent Share of Allowed Charges 2003-04 | Intensity: Average Annual Percent Change 1996-2000 | Intensity: Average Annual Percent Change 2000-04 |
|---|---|---|---|---|
| All Procedures | 30.8 | 24.7 | -0.2 | 4.9 |
| Major, Cardiovascular Procedures | 4.6 | 2.9 | -0.2 | -3 |
| Major, Orthopedic Procedures | 2.9 | 1.8 | -3.8 | 1.8 |
| Ambulatory Procedures | 3.2 | 3.2 | 4.4 | 4.5 |
| Oncology Procedures | 1.9 | 2.3 | 4.4 | 14.8 |
| All Imaging | 10.1 | 14.1 | 8.7 | 11.2 |
| Standard Imaging | 4.5 | 5.2 | 3.9 | 10.8 |
| Echograhy, other than heart imaging | 1.2 | 1.5 | 12.6 | 7.1 |
| Advanced, MRI imaging | 1.3 | 2.5 | 14.6 | 16.4 |
| Chemotherapy and Other Drugs | 4.6 | 10.4 | 20 | 18 |
|
Note: Intensity is calculated as percent change in spending after controlling for changes in price and number of fee-for-service beneficiaries. Source: NORC analysis of Physician/Supplier Procedure Summary MasterFile data, 1996-2004. |
||||
The shift away from utilization of major procedures is also revealed from the perspective of where services are obtained. About 62 percent of charges were for services provided in office settings in 2004, whereas services provided to inpatients accounted for about 20 percent of Part B allowed charges by physicians (Table 4). The share of charges for services provided to inpatients declined by about a third between 1996 and 2004. The shift of services to the office setting is not strictly due to increases in the provisions of E&M services. In 2004, the ratio of allowed charges for E&M services provided in non-inpatient to inpatient settings was 2.6 – for every dollar of E&M care provided in an inpatient setting, $2.60 of E&M care was provided in other settings (Table 5). But the ratio for non-E&M care was even larger. Over four times as many allowed charges under Part B were for non-E&M services and procedures, less spending for drugs and lab, provided in non-inpatient settings than in in-patient settings.
| 1996 | 2000 | 2004 | |
|---|---|---|---|
| Total Allowed Charges (billions) |
44.5 |
54.0 |
81.8 |
|
Percent Distribution |
|||
| Office |
47.3 |
55.0 |
62.3 |
|
Outpatient |
14.2 |
12.9 |
11.1 |
|
Inpatient |
30.3 |
25.3 |
19.8 |
|
Other |
8.3 |
6.9 |
6.8 |
| Source: NORC analysis of Physician/Supplier Procedure Summary MasterFile data, 1996, 2000, 2004. | |||
The rapid growth in spending for chemotherapy and other drugs is cited as a reason for revising the SGR process used to update Medicare physician payments over time.3 One rationale is that physicians have less control over drug spending than over spending on services and procedures provided in their offices. A similar argument might be used for services and procedures provided by allied health personnel. If spending on services provided by the latter is rapidly increasing, an argument for removing this spending from the SGR process is that the physician update should not reflect this trend. In 2000, spending for services provided by allied health practitioners totaled $3.2 billion, less than 6 percent of total spending (Table 6). By 2004, spending for allied health services had grown to $5.9 billion, over 7 percent of total spending. Spending has grown relatively more rapidly, however, for services provided by nurses and physician assistants, professionals who are often under the direct employ of physicians.
|
1996 |
2000 |
2004 |
|
|---|---|---|---|
| All Services |
5.5 |
7.8 |
11.0 |
|
E&M |
1.8 |
2.2 |
2.6 |
|
Non-E&M |
1.9 |
2.8 |
4.2 |
|
Lab Tests |
12.5 |
15.4 |
18.9 |
|
Note: refers to evaluation and management services. Source: NORC analysis of Physician/Supplier Procedure Summary MasterFile data, 1996, 2000, 2004. |
|||
|
|
Spending |
Average Annual Intensity, |
|||
|---|---|---|---|---|---|
|
Specialty |
2000 |
Share |
2004 |
Share |
|
| Non-Allied Health Specialties |
50.88 |
94.2 |
75.86 |
92.8 |
6.1 |
| All Allied Health |
3.16 |
5.8 |
5.90 |
7.2 |
12.3 |
|
Nurses/Physician Assistants |
0.29 |
0.5 |
0.95 |
1.2 |
29.2 |
|
Other Allied Health Professionals |
2.86 |
5.3 |
4.95 |
6.0 |
10.2 |
| All Providers |
54.04 |
100.0 |
81.77 |
100.0 |
9.2 |
|
Note: Intensity is calculated as percent change in spending after controlling for changes in price and number of fee-for-service beneficiaries. Source: NORC analysis of Physician/Supplier Procedure Summary MasterFile data, 2000-2004. |
|||||
2.2 Physician Payment Policy
2.2.1 History
Over time, a variety of policy measures designed to help contain costs has been incorporated into the Medicare program. But policymakers have also demonstrated concerns with maintaining efficiencies and not introducing policies with incentives that distort the health care system and lead to undesirable distributional outcomes. Prospective payment systems have been implemented to help contain costs and eliminate inefficiencies of previous payment systems based not on relative costs, but on historical charge patterns. These systems revolutionized how Medicare payments for hospital care and physician services are determined, and more recently how payments for home health care, nursing home care, and hospital outpatient services are determined.
Under the Medicare Fee Schedule (MFS), each service is assigned its relative value unit (RVU), a measure of resources used to produce the service. A conversion factor (CF) was used to convert RVUs to dollar payment amounts. Payments were updated over time by updating the CF. When the MFS was first implemented, payment updates were determined by the Volume Performance Standard (VPS) process. VPS was designed so that if the volume of services grew beyond a target amount (with adjustments for factors such as the effect of changes in laws and regulations), the annual update to the physician fee schedule would be less than the rate of inflation, and vice versa if volume grew more slowly than the target. Under the VPS system, the Secretary of Health and Human Services established a target rate of growth in the volume of physician services. The conceptual design of the VPS system was that physician payments would be reduced if service volume rose too rapidly to adequately control program cost, giving the physician community as a whole an incentive to avoid increasing services to compensate for any payment changes. The performance measure setting process took several factors into account, including growth and productivity of the economy at large, and changes in laws and regulations affecting the Medicare program. Initially, a single performance standard and update were employed. For several years in the mid-1990’s, separate targets were used to produce separate updates for medical and surgical services, and then for E&M services.
The VPS system contained costs reasonably well for the first several years, but over time it exhibited a degree of instability that was projected to lead to wide swings in updates from one year to the next. In addition, some criticized the VPS system for failing to set strong incentives for individual physicians to modify their own behavior. An individual physician’s impact on program spending is minimal, and it was difficult, therefore, to convince physicians to take actions that would have collective consequences on the annual update. Furthermore, the use of multiple updates over time distorted relative values, defeating the purpose of the resource-based MFS. This happened because resource content across services is measured by differences in the service’s relative values. Payment for a service is calculated by multiplying the service’s relative value by the conversion factor. If there is more than one conversion factor, payment will vary by both resource content and the conversion factor used to calculate the payment.
2.2.2. The SGR Process
The VPS was replaced with the SGR process, following passage of the Balanced Budget Act of 1997. As was VPS, the SGR process was designed to allow for increases in Medicare payments while ensuring that growth in aggregate spending would be contained.4 Unlike the VPS when it was replaced, the SGR system produces a single update.
Figure 2. Calculating the SGR for the CY 2006 Physician Payment Update
For CY 2006:
2005 Conversion Factor: $37.8972
MEI Factor: 1.0290
Update Adjustment Factor (UAF) By formula: 0.9300
Other Adjustments (Laws and Regulations): 0.9985
Total Update Factor (= MEI x UAF x Other): 0.9555
2006 Conversion Factor: $ 36.2121
2006 Conversion Factor after Congressional intervention: $37.8972
CMS, Office of the Actuary, “Estimated Sustainable Growth Rate and Conversion Factor, for Medicare Payments to Physicians in 2002,” http://www.hcfa.gov/pubforms/actuary/sgr, March 19, 2001.
The payment update calculation updates the MFS CF annually. The update reflects changes in the cost of providing care, the update adjustment factor (UAF), and other adjustments (Figure 2). The cost of providing care is measured by the MEI. The UAF adjusts for previous over-/under-spending relative to targets set in previous years. Other adjustments include adjustments to payments deemed necessary or required by CMS, e.g., to implement fixes in the resource-based relative value scale in a budget-neutral fashion.
Conceptually, the SGR5 may be viewed as the rate at which physician expenditures under Medicare should increase, ‘should’ referring to CMS’s interpretation of the intent of Congress, which in turn represents—in some sense—society’s statement of how many additional real dollars are to be targeted to cover per capita medical expenses of the elderly. In actuality, and in the context of program cost containment, the SGR process intends to allow for increases in Medicare payments, but at rates that ensure that growth in aggregate Medicare spending will be contained. The numerical value of the SGR is determined by how the economy at large is growing, as measured by changes in per capita Gross Domestic Product (GDP), the total number of Part B fee-for-service beneficiaries, the cost of producing services covered by the Medicare Fee Schedule, and laws and regulations governing the Medicare program (bottom frame, Figure 2).
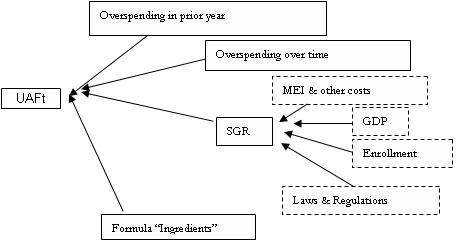
A key part of the SGR process is the UAF. The UAF, defined by formula, penalizes/rewards providers for over-/under-spending. This is the portion of the SGR process that has given rise to recent declines in the payment update. There are two parts to the formula, which can be written as follows:
UAFt = { 0.75 * [ (targett-1 – actualt-1) / actualt-1 ] }
+ { 0.33 * [ (targetc – actualc) / (actualt-1 * SGRt) ] }
where
targett-1 is target spending for year t-1;
actualt-1 is actual spending;
targetc is the sum of previous years’ targets (back through part of 1996); and
actualc is the sum of previous years’ actual spending.
The first part of the formula accounts for over-/under-spending in the prior year (year t-1). Over-/under-spending is expressed as a fraction of spending for the year. The second part of the formula accounts for cumulated over-/under-spending. The denominator of the cumulated spending term is spending during the previous year, updated by the current year’s SGR – a measure of next year’s target spending. Thus, the second term expresses cumulated spending as a fraction of what spending is expected next year if the target is met. Because the SGR enters the UAF formula, the UAF indirectly depends on those factors that influence the value of the SGR (Figure 2). The UAF formula’s ‘ingredients’ include the weights attached to the previous and cumulated spending terms (currently, set at 0.75 and 0.33, respectively). Currently, the UAF has floor and ceiling values that limit its effects: the floor is -0.07 and ceiling is 0.03, a maximum penalty of 7 percent and a maximum reward of 3 percent.
Using calculation of the CF for 2006 as an example of how the SGR process works, the cost of practice factor (measured by MEI as fraction plus 1) was 1.029, indicating that the cost of providing services increased by 2.9 percent over the previous year. The UAF, 0.9300, means that over-spending in the previous and prior years contributed to a reduction of 7 percent in the CF relative to CY 2005. In 2005, spending exceeded the target by about $13 billion (target and actual spending were $80.4 and $93.3 billion, respectively), about 14 percent of 2005 spending. Cumulated spending exceeded the cumulated target by $30.7 billion (cumulated spending and target amounts were $611.8 and $642.5 billion, respectively), and cumulated overspending was about 32 percent of 2005 spending updated by the SGR. The value of the UAF, after applying the formula weights, was -0.21, considerably below the floor of -0.07. Thus, the UAF is 1-0.07, or 0.9300. The impacts of other adjustments reduced the CF (relative to CY 2005) by another 0.15 percent, so the corresponding factor is 0.9985 (1-0.15). The CF for CY 2006 was to be the product of the CF for CY 2005, multiplied by the set of factors in Figure 1:
CF2006 = $37.8972 * 1.029 * 0.9300 * 0.9985
= $37.8972 x 0.9555
= $36.2121
In other words, the update would be a 4.5 percent reduction in payment, from $37.90 to $36.21 per relative value unit of service. Congress intervened, however, defining the update to be 0, so CF2006 remained as in CY 2005.
2.2.3 Criticisms of the SGR Process
Advocates for SGR reform cite significant flaws with the current process. First, recent updates have been large and negative, a consequence of over-spending. A string of negative updates has pressured Congress to intervene legislatively, as large and widespread changes in provider behavior are necessary to overcome the negative impacts on payment updates from the terms of the UAF. The SGR process as legislated is not sustainable. As demonstrated below, the update calculated by the original formula has been consistently negative during the last several years and is expected to remain so into the future. Congressional intervention may be needed annually until the process is changed.
A second flaw is that the target-setting mechanism may not accurately measure desired growth. Some providers argue that the process does not allow for enough growth to accommodate changes in technology. For example, some argue that GDP, as the measure of allowance for spending growth, is too low and thus not representative of society’s value of health care relative to other goods and services in the economy. Some policymakers argue that certain types of services should be exempt from inclusion in the target setting process. For example, expenditures on certain types of drugs are included, even though physicians have little control over drug pricing. Others argue that the target should be applied only to services that are responsible for the fastest spending growth, e.g., due to overuse or incentives based on MFS relative values that are not correct measures of resource composition.
Another set of criticisms has been directed at the presuppositions that target mechanisms implemented at the national level (such as the formula currently in use) generate incentives that will successfully alter behavior of individual providers, and that providers will overlook incentives on individual behavior and practice in a manner that benefits all physicians. The update process’ lack of transparency makes it difficult for providers and policymakers to understand how behavior might be affected to help contain costs.
3.0 Modeling the SGR Process
3.1 Methods
Analysis of the SGR process might be helpful in setting the stage for refinements that can be implemented to overcome current flaws resulting from the formula, as well as suggesting longer run changes that might be considered for more substantive changes to the payment update process in the future. A spreadsheet model of the SGR process was constructed. First, rules underlying payment updates announced by CMS were reviewed and data used to calculate these updates were compiled. CMS’s calculations of annual updates that are implemented in January of each year are generally based on data available to CMS no later than November of the previous year (e.g., rules defining the update for CY 2006 were published in the Federal Register in November, 2005) and updated the following month as described via memoranda available from the CMS website.6
Second, a spreadsheet version of the update process was developed. The model consists of three SGR formulas for each year, covering the years 2000-2014 (described in Figure 2). One formula calculates the SGR from data on the costs of practice and changes in GDP and Medicare enrollment. The second formula calculates the UAF from data on target and actual spending from prior years. The third formula calculates the update for the year, using results from the first two formulas.
Outputs of the three-formula model include the payment update and CF for the year. The CF is then used to estimate spending for the year (which appears in the UAF formula for the following year’s CF). For example, the update for 2007 is based in part on the SGR for 2007 and the UAF for 2007. The latter is determined by comparing actual and target spending for 2006. When the model is used to study effects of a hypothetical change in the formula, for example, and the simulated CF for year t differs from the CF under baseline assumptions, this different CF is used to adjust baseline spending for that year upwards/downwards to reflect the higher/lower CF produced by the model. The spreadsheet model is designed to cumulate actual and target spending amounts over time, amounts that are carried forward into the formulas used to calculate updates and spending for subsequent years. Spending estimates from the model (and presented below) are tabulated separately for SGR physician services (sometimes by type of service, depending on the option under study), for spending on lab and drugs combined, and in total.
Application of the SGR formulas over time is complicated by the fact that data items used to calculate updates are subject to change over time. Thus, for example, the estimate of spending for 2005 that was used to calculate the CF for 2006 may change in late 2006 and again in later years. Updated spending estimates are used in calculating the spending amounts that enter the formula for the CF for 2007 and beyond, but not to retroactively change the 2006 update. In a similar fashion, details of the payment update for 2003 were published in the Federal Register on December 21, 2002. CMS revised these estimates in February 2003, and again in November 2004 and November 2005. Revisions cannot be used to retroactively change values of updates affecting payment levels of previous years, but are made to data used in future applications of the formula. Adjustment factors have been developed to ensure that estimates of spending obtained from the model reflect adjustments in data made each year by CMS.7
Simulation of payment updates for future years is of more interest from a policy perspective than what payments would have been. Data items required to estimate updates for these years, of course, are not known and had to be predicted. Predicted levels of future spending are required by the SGR formula, as well as predictions for Part B enrollment, the cost of inputs faced by physicians, the measure of physician productivity (used to adjust cost changes measured by the MEI), and the fee index used to estimate the SGR factor (that is used, in turn, to estimate the spending target). Analysts with CMS’s Office of the Actuary predict future spending for the three categories of services that enter the SGR formula: most physician services, certain lab procedures, and selected physician-administered drugs physician services. These are estimated separately and summed to obtain annual estimates of total SGR spending for use in calculating future payment updates. Information on the rates of per beneficiary growth in the three spending components and total SGR spending over time (from the 2006 Trustees Report) was used to estimate dollar spending streams for the SGR physician, lab, and drug components of spending and for total spending as described in the Appendix.8 These baseline spending estimates are adjusted by the spreadsheet model as updates depart from baseline values.
One of the challenges confronting Medicare payment policymakers is that changes in payments may alter behavior in unanticipated ways and in ways counter to program goals. Traditional economic theory suggests that physicians will shift toward supplying services with relatively higher prices and away from services that generate lower payments. This is the theory, for example, that supports policymakers seeking to increase payments for primary care services believed to be under-utilized. It is also the theory that underlies arguments by physicians’ associations that payment reductions will threaten access to services (presumably because the supply of those services will be reduced). This view implies that there is unmet demand for services that are reimbursed more generously (e.g., services covered by some private insurers), and that labor supplied by physicians is not easily augmentable in the short-run, but shifted toward those services with higher prices. An alternative theory, however, suggests that physicians seek to maintain a target level of income, and simply increase the number of services provided when payment per unit of service declines. Under this perspective, reductions in price result in volume increases, not decreases. This perspective implies that there is unmet demand (or demand can be generated) for services for which payment has declined, and that physicians seek to maintain their income levels by providing more of those services for which payments have declined.
The evolution of Medicare physician payment policy reflects both theories. Efforts to increase use of primary care services by increasing payments for these services reflect perspectives of traditional economics, as do efforts to limit spending with reductions in the CF. By contrast, the target income theory of behavior is asserted when policymakers argue that spending estimates include a behavioral offset to correct for the belief that volume will increase if payment declines. 9 Solid evidence on the direction and magnitude of provider responses to payment changes is lacking, in part because of difficulties in attributing changes in behavior to payment changes when many other (non-price) factors are also changing. Given the challenges of estimating provider response to payment changes, the spreadsheet model of the SGR process used to examine effects of changes in CFs and spending does not include adjustment for behavioral effects predicated on changes in payment levels. No behavioral responses, on the part of any agents affected by the update process -- including providers, Medicare beneficiaries, and Congress -- have been incorporated into the structure of the spreadsheet model and predicted effects on updates and program spending. This also means that future estimates derived from the model are based on the assumption that Congress will not intervene in the future, despite the fact that Congress has intervened in recent years.
3.2 Current Law Baseline
On the surface, study of the SGR payment process is straightforward. The process can be described as a recursive model, consisting of a set of algebraic relationships that are linked over time. This view, however, is somewhat naïve, as noted above. Changes in data alter future but not past values of SGR process relationships, and predictions of updates for future years are subject to uncertainties. Application of the process’ relationships is straightforward at each point in time, but data in each year’s calculations are subject to change in future years. CMS incorporates these changes into calculations over time (e.g., the accumulation of actual and target spending as spending data change and components of the SGR change), but payment updates cannot be changed retroactively. For example, changes in estimated SGR expenditures for 2004 due to more complete data for 2004 in 2006 can be factored into future calculations using the formula, but are not used to change the update paid to physicians for work performed in 2005, even though the update would have differed had full information been available when the 2005 update was calculated. Projected values of the update for future years require projections on various components of spending that enter the SGR calculations.
The primary baseline against which changes to the SGR mechanism will be analyzed below is the SGR process under current law. Payment updates and spending estimates are displayed in Tables 7a and 7b. SGR values beginning in 2005 are subject to change, as are other data items used to calculate the update (see Figure 2) beginning in 2007.
The conversion factor for CY 2000 was about $36.61, an increase of over 5 percent relative to the average conversion factor (CF) implemented (under VPS) for 1999 (Table 7a). Part of this increase reflected spending during 1999 that did not exceed the target for that year. The CF for 2001 increased by 4.5 percent. During 2001, however, actual SGR spending exceeded target spending (by $7.0 billion), a consequence of which was that the CF for CY 2002 declined by 5.4 percent. Even though over-spending continued through 2002, the CF increased for CY 2003 because the MEI more than offset the UAF penalty for spending through 2002.
| Update Year (t) |
SGR |
CFt |
Percent |
|---|---|---|---|
|
2000 |
1.021 |
36.61 |
5.42 |
|
2001 |
1.056 |
38.26 |
4.49 |
|
2002 |
1.056 |
36.20 |
-5.38 |
|
2003 |
1.075 |
36.79 |
1.62 |
|
2004 |
1.074 |
37.34 |
1.50 |
|
2005 |
1.043 |
37.90 |
1.50 |
|
2006 |
1.017 |
37.90 |
0.00 |
|
2007 |
1.007 |
36.16 |
-4.58 |
|
2008 |
1.039 |
34.37 |
-4.96 |
|
2009 |
1.035 |
32.63 |
-5.05 |
|
2010 |
1.029 |
30.93 |
-5.23 |
|
2011 |
1.034 |
29.34 |
-5.14 |
|
2012 |
1.042 |
27.86 |
-5.05 |
|
2013 |
1.045 |
26.50 |
-4.86 |
|
2014 |
1.039 |
25.21 |
-4.86 |
| Notes: SGR values through 2006 are those used by CMS to calculate CFs as implemented, and are from the Federal Registers that document the payment update process (see Appendix). Values for 2007-2014 are calculated using the SGR formula and various data sources noted in the text. Values in italics are subject to change. CF values for 2007-2014 are estimated. | |||
During the years 2003-2005, actual spending exceeded target levels. (Over-spending amounts used to estimate corresponding CFs for years 2004-2006 were $6 billion, $8 billion, and $13 billion.) For each of these three years, the UAF was negative and the factor’s magnitude exceeded 7 percent each year. These UAFs activated the floor of the UAF to -7 percent. Conversion factors for the years 2004-2006 (based on spending during 2003 through 2005, respectively) would have declined, had not Congress intervened. Rather than payment reductions of 4.5 percent and 4.3 percent for 2004 and 2005, Congressional intervention propped updates at 1.5 percent for these years. Rules for CY 2006 published in November 2005 called for a payment reduction of about 4.5 percent, but Congressional action negated the payment reduction, keeping the CF for 2006 at the 2005 level.
Application of the current SGR process is expected to lead to continued declines in the CF from 2007 through 2014. For each of these years, the UAF is expected to exceed 7 percent in magnitude, which triggers the implementation of the UAF floor (-7 percent). The model predicts over-spending (spending in excess of target levels) for years 2006-2013, during which time the UAF is -7 percent each year. The SGR model predicts that by the end of 2013, total spending will exceed target spending since 1996 by about $117 billion.
Baseline spending between 2006 and 2010 is expected to be about $501 billion, more than 80 percent for physician services and the remainder for laboratory and drug spending that are currently part of total SGR spending (Table 7b). Total spending for years 2000 through 2013 is expected to exceed $1,264 billion.
|
Period |
Physician |
Lab and |
Total |
|---|---|---|---|
|
2000-2005 |
380.4 |
74.6 |
455.0 |
|
2006-2010 |
401.8 |
99.0 |
500.8 |
|
2011-2013 |
228.1 |
80.3 |
308.5 |
|
Total |
1010.4 |
253.9 |
$1,264.3 |
| Note: Spending estimates were derived using CFs displayed in Table 7a, adjusted for data corrections reported by CMS in various Federal Registers. | |||
4.0 Potential Refinements of the SGR
4.1 Changes in the Measure of the Costs of Practice
The MEI is a fixed-weight input price index reflecting average annual changes in prices for inputs required to produce physician services, namely the physician’s own time and practice expense. The MEI is an important ingredient in the SGR process, affecting payment updates in two ways (Figure 2). The measure is used directly in the calculation of CFs. The MEI is also used as a measure in the calculation of the fee component of the SGR (which, in turn, is used to calculate target spending levels).
Under the current SGR formula, the MEI is adjusted for changes in physician productivity over time using a 10-year moving average of a measure of economy-wide multifactor productivity. Because the MEI is not net of the price effects of improvements in human productivity, for example, the rationale for including the productivity adjustment is to offset the increase in medical care prices that reflect advances in productivity. Critics of the productivity adjustment argue that the productivity adjustment factor is an inadequate proxy measure of physician productivity. The measure may be deficient, because it is an economy-wide measure, reflecting input prices for many different types of markets, including non-service markets that differ from health care markets.
Elimination of the productivity adjustment increases the value the MEI. A larger MEI has a direct effect on the size of the update because the product of the MEI factor and UAF is the main determinant of the payment update (Figure 2 above). But as noted, a larger MEI also increases the size of the SGR. This increase affects the payment update in two ways: an increased SGR lowers the size of the prior year penalty in the UAF (as the SGR is in the denominator of the cumulated spending term), and increases the size of spending targets in future years. The combination of effects of changes in the MEI is positive: payment updates should increase with the MEI.
|
Baseline |
Revised MEI |
|||||||
|---|---|---|---|---|---|---|---|---|
|
Update |
SGR |
MEI |
CFt |
Percent |
SGR |
MEI |
CFt |
Percent |
|
2000 |
1.021 |
1.024 |
36.61 |
5.42 |
1.029 |
1.033 |
36.61 |
5.42 |
|
2001 |
1.056 |
1.021 |
38.26 |
4.49 |
1.070 |
1.035 |
38.26 |
4.49 |
|
2002 |
1.056 |
1.026 |
36.20 |
-5.38 |
1.070 |
1.041 |
36.20 |
-5.38 |
|
2003 |
1.075 |
1.030 |
36.79 |
1.62 |
1.081 |
1.038 |
36.79 |
1.62 |
|
2004 |
1.074 |
1.029 |
37.34 |
1.50 |
1.082 |
1.038 |
37.34 |
1.50 |
|
2005 |
1.043 |
1.031 |
37.90 |
1.50 |
1.046 |
1.040 |
37.90 |
1.50 |
|
2006 |
1.017 |
1.029 |
37.90 |
0.00 |
1.025 |
1.038 |
37.90 |
0.00 |
|
2007 |
1.007 |
1.026 |
36.16 |
-4.58 |
1.015 |
1.035 |
36.48 |
-3.75 |
|
2008 |
1.039 |
1.024 |
34.37 |
-4.96 |
1.048 |
1.033 |
34.97 |
-4.12 |
|
2009 |
1.035 |
1.021 |
32.63 |
-5.05 |
1.044 |
1.030 |
33.50 |
-4.21 |
|
2010 |
1.029 |
1.019 |
30.93 |
-5.23 |
1.039 |
1.028 |
32.03 |
-4.40 |
|
2011 |
1.034 |
1.020 |
29.34 |
-5.14 |
1.043 |
1.029 |
30.65 |
-4.30 |
|
2012 |
1.042 |
1.021 |
27.86 |
-5.05 |
1.051 |
1.030 |
29.36 |
-4.21 |
|
2013 |
1.045 |
1.023 |
26.50 |
-4.86 |
1.054 |
1.032 |
28.18 |
-4.02 |
|
2014 |
1.039 |
1.023 |
25.21 |
-4.86 |
1.048 |
1.032 |
27.04 |
-4.02 |
| Notes: Baseline estimates are as in Table 3a; baseline values of the MEI are from Global Insight, Inc. (see Appendix). Revised MEI values are undjusted for productivity; values through 2006 are from various Federal Registers documenting CFs. Productivity adjustments for 2007-2014 are assumed to be 0.9 percent per year based on data from the Bureau of Labor Statistics (see Appendix). SGRs were recalculated using the unadjusted MEIs through 2006; from 2007-2014, the MEI is assumed to be the fee component used to calculate the SGR. Baseline data items in italics subject to change. | ||||||||
To simulate effects of eliminating the productivity adjustment, an unchanging productivity adjustment factor of 0.9 percent from 2007 through 2014 was assumed. This is the value of the productivity adjustment factor used to calculate the adjusted MEI in 2004 and 2005. (The value used for 2006 was 1.0.)10 The CF for 2006 would have been $39.85, 5 percent larger that its current value of $37.90. Compared to baseline, conversion factors under the simulation would be larger and decline at slightly slower rates through 2014 (Table 8a). Expected spending with increases in the MEI would by about 1 percent larger than under baseline between 2006 and 2010, and 4 percent larger for 2011 through 2013 (Table 8b).
|
Baseline (billions) |
With Revised MEI (billions) |
|||||
|---|---|---|---|---|---|---|
|
Period |
Physician |
Lab and |
Total |
Physician |
Lab and |
Total |
|
2000-2005 |
380.4 |
74.6 |
455.0 |
380.4 |
74.6 |
455.0 |
|
2006-2010 |
401.8 |
99.0 |
500.8 |
409.0 |
99.0 |
507.9 |
|
2011-2013 |
228.1 |
80.3 |
308.5 |
240.4 |
80.3 |
320.8 |
| Total |
1010.4 |
253.9 |
$1,264.3 |
1029.8 |
253.9 |
$1,283.7 |
| Note: Spending estimates were derived using CFs displayed in Table 8a, adjusted for data corrections routinely reported by CMS. | ||||||
4.2 Changes in the Design of the UAF
As indicated in the summary discussion of the current SGR update process, the magnitude of the UAF is a key determinant of the size of Medicare payment updates. Without the UAF portion of the SGR process, payments would be updated using the MEI. The UAF is the means by which the update process recovers over-spending.
The UAF used to calculate the CF for year t consists of two parts – a reward/penalty for under-/over-spending during the previous year, and the accumulation of under-/over-spending through the previous year. The previous-year component is calculated from the amount of under-/over-spending for the previous year as a percent of total spending for the year. Thus, for example, the previous-year component of the UAF for 2007 is over-spending during 2006 as a percent of 2006 spending. Using data from Table 9, the previous-year term is
(target spending - actual spending) / actual spending
= ($81.7 b – $97.4 b) / $97.4 b
= - 0.161.
Thus, over-spending is about 16 percent of actual spending for 2006.
| Calendar Year |
Baseline Spending | UAF and Components | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Target | Actual | Over-Spending | Previous Year |
Cumu- lated |
Total | Effective | ||||
|
$ |
% |
$ |
% |
$ |
% Actual |
|||||
|
2000 |
56.6 |
8.6 |
55.1 |
9.0 |
-1.5 |
-2.7 |
0.02 |
0.02 |
0.04 |
0.03 |
|
2001 |
59.3 |
4.8 |
66.3 |
20.3 |
7.0 |
10.6 |
-0.08 |
0.01 |
-0.07 |
-0.07 |
| 2002 |
67.6 |
14.0 |
69.1 |
4.2 |
1.5 |
2.2 |
-0.02 |
0.01 |
-0.01 |
-0.01 |
| 2003 |
71.7 |
6.1 |
77.8 |
12.6 |
6.1 |
7.8 |
-0.06 |
-0.03 |
-0.09 |
-0.07 |
|
2004 |
77.1 |
7.5 |
84.9 |
9.1 |
7.8 |
9.2 |
-0.07 |
-0.05 |
-0.12 |
-0.07 |
| 2005 |
80.4 |
4.3 |
93.3 |
9.9 |
12.9 |
13.8 |
-0.10 |
-0.11 |
-0.21 |
-0.07 |
| 2006 |
81.7 |
1.6 |
97.4 |
4.4 |
15.7 |
16.1 |
-0.12 |
-0.16 |
-0.28 |
-0.07 |
|
2007 |
82.3 |
0.7 |
98.3 |
0.9 |
16.0 |
16.3 |
-0.12 |
-0.20 |
-0.33 |
-0.07 |
|
2008 |
85.5 |
3.9 |
100.3 |
2.0 |
14.8 |
14.8 |
-0.11 |
-0.25 |
-0.36 |
-0.07 |
|
2009 |
88.5 |
3.5 |
102.3 |
2.0 |
13.9 |
13.5 |
-0.10 |
-0.29 |
-0.39 |
-0.07 |
|
2010 |
91.0 |
2.9 |
102.4 |
0.1 |
11.4 |
11.1 |
-0.08 |
-0.32 |
-0.41 |
-0.07 |
|
2011 |
94.1 |
3.4 |
102.2 |
-0.2 |
8.1 |
7.9 |
-0.06 |
-0.35 |
-0.41 |
-0.07 |
|
2012 |
98.1 |
4.2 |
102.8 |
0.5 |
4.7 |
4.6 |
-0.03 |
-0.36 |
-0.39 |
-0.07 |
|
2013 |
102.5 |
4.5 |
103.5 |
0.7 |
1.0 |
0.9 |
-0.01 |
-0.36 |
-0.37 |
-0.07 |
| Notes: Over-spending is the difference between actual and target spending levels. The Previous Year UAF component is calculated by multiplying over-spending as a fraction of actual spending by the fraction, 0.75; the Cumulated component is calculated as cumulated target spending less cumulated actual spending, divided by actual spending updated by the SGR, multiplyed by the fraction, 0.33. The total UAF is the sum of the Previous Year and Cumulated fractions. The Effective UAF is the value of the total UAF used to calculate the update -- the value of the UAF after applying the floor or ceiling, -0.07 or 0.03. | ||||||||||
The portion of the UAF that measures the accumulation of over-/under-spending (hereafter, the “cumulated spending” component) is calculated as the difference between cumulated target and actual spending, as a percent of next year’s spending under “good behavior” – current year spending, increased by the value of the SGR that will be used to calculate target spending for the following year. For 2006, the cumulated spending component of the UAF is
(cumulated target spending - accumulated actual spending) / (actual spending * SGR factor)
= ($693.6 b – $741.0 b) / ($97.4 b * 1.007)
= - 0.483.
Thus, cumulated over-spending is about 48 percent of expected spending for 2007. The total value of the UAF for 2006 is calculated as the sum of the previous-year and accumulation components, after weighting the former by 0.75 and the latter by 0.33, the UAF for 2006 is (-0.161 x 0.75) + (-0.483 x 0.33) = (-0.12) + (-0.16) = -0.28 (the total UAF value in Table 9). As -0.28 is less than the floor (-0.07), the floor becomes the effective UAF for 2006, and is used to calculate the update for CY 2007. It is clear from Table 9 that the UAF for spending during years 2007-2013 is expected to be less than the floor. During these years, actual spending will exceed target spending, the UAF value will be its floor value, and CFs will continue to decline as UAFs more than offset the MEI.
The size of expected future reductions in CFs can be reduced with changes in the structure of the UAF. In the remainder of this section, effects of changes in UAF floor and relative importance of the previous-year and cumulated spending terms of the UAF are explored.
4.2.1 The UAF Floor
An option that retains some cost-containment incentives but does not lead to negative payment updates is to set the UAF floor such that the largest over-spending penalty would completely offset the MEI. Under this option, the floor is a negative percent that would be just large enough in magnitude to offset the MEI, producing a 0-percent update. The formula used to calculate the CF for year t is as follows:
(1) CFt = CFt-1 * (1+MEIt) * (1+UAFt) * (1+OTHERt),
where MEIt is the MEI fraction for year t, e.g., 0.029 (2.9 percent), UAFt is the UAF fraction, and OTHERt is the fractional change in the CF attributed to other factors by CMS. The OTHER factor is determined by CMS, and reflects effects of laws and regulations; if this factor is ignored (assumed to equal 0) as it is under baseline for years beyond 2008, formula (1) becomes
CFt = CFt-1 * (1+MEIt) * (1+UAFt).
The update is 0 when the CF is unchanged, CFt=CFt-1. This occurs when
(1+MEIt) * (1+UAFt) = 1.
If it is assumed that the MEI is always a positive fraction – that costs faced by providers increase each year – then the 0-update floor is algebraically determined as the value of the UAF given by UAFft,
(2) UAFft = -MEIt/(1+MEIt).
In other words, if the UAF floor is calculated each year using equation (2), the floor for the year is a negative fraction that at worst, offsets the MEI, and results in a 0, not negative, update.
The SGR model was used to examine effects of adoption of the 0-update floor. Intuitively, this 0-update floor would become binding whenever the -7 percent floor becomes binding. The CF would decline from $37.90 in 2007 to $37.82 in 2008. The CF would remain at this value through 2014. Thus, between 2006 and 2014, the CF would decline by less than 0.3 percent (from $37.90 to $37.82), whereas the baseline CF is expected to decline by 34 percent (from $37.90 to $25.21) during the same period. Spending implications of the 0-update floor beginning in 2007 are significant. The “price” of payment stability between 2006 and 2013 is a 15 percent increase in spending relative to baseline, a 10 percent increase in total spending for the period, 2000-2013 (Table 10).
| Baseline (billions) | With 0-Update Floor (billions) | Spending Ratio |
|||||
|---|---|---|---|---|---|---|---|
| Period | Physician | Lab and Drug |
Total | Physician | Lab and Drug |
Total | |
|
2000-2005 |
380.4 |
74.6 |
455.0 |
380.4 |
74.6 |
455.0 |
1.00 |
|
2006-2010 |
401.8 |
99.0 |
500.8 |
444.4 |
99.0 |
543.4 |
1.08 |
|
2011-2013 |
228.1 |
80.3 |
308.5 |
309.6 |
80.3 |
390.0 |
1.26 |
|
Total |
1010.4 |
253.9 |
$1,264.3 |
1134.5 |
253.9 |
$1,388.3 |
1.10 |
| Notes: 0-Update Floor estimates are based on CFs derived by modifying the floor of the UAF to offset the MEI each year, such that the revised floor is a 0-update. The Spending Ratio is the ratio of spending under the 0-floor and baseline spending. | |||||||
4.2.2 The Size of the UAF Penalty
In addition to changes in the UAF penalty floor, the size of the UAF penalty for over-spending can be reduced by lowering the weights applied to the measures of over-spending in the previous year and cumulated spending. A rationale for the cumulated spending term of the UAF is that CFs can be adjusted to help the Medicare program recover a portion of spending in excess of targets. On the other hand, it may take years for the program to recover over-spending, even during a time when contemporaneous spending is less than the target.
One way of placing relatively more emphasis on recent practice behavior is to eliminate the cumulated spending term of the UAF.11 Implementing this change beginning in 2007, however, would have little impact. The CF would not change from its baseline level until 2012 because even without the cumulative component of the UAF, the previous year over-spending penalty is large enough to trigger the -7 percent floor (see Table 9). As expected, spending from 2006-2013 would increase, but by only 1 percent over baseline.
Another policy option is to reduce the size of the penalty levied against previous year spending. Effects of simultaneously eliminating the cumulative term of the UAF and reducing the magnitude of the penalty for prior year over-spending by one-half were studied using the model.12 With these changes, the CF for 2007 would decline from its 2006 level by less than under baseline (a decline of 3.6 percent vs. 4.6 percent under baseline, Table 11a). For 2008-2014, the CF would continue its descent, but at slower rates than under baseline. Spending with these changes, of course, would exceed baseline spending by 4 percent during 2006-2013, 2 percent during 2000-2013 (Table 11b).
|
Baseline |
With Revised UAF Spending Weights |
||||||||
|---|---|---|---|---|---|---|---|---|---|
|
Update |
SGR |
Weight |
Weight on |
CFt |
Percent Change |
Weight on |
Weight on |
CFt |
Percent |
|
2000 |
1.021 |
0.75 |
0.33 |
36.61 |
5.42 |
0.75 |
0.33 |
36.61 |
5.42 |
|
2001 |
1.056 |
0.75 |
0.33 |
38.26 |
4.49 |
0.75 |
0.33 |
38.26 |
4.49 |
|
2002 |
1.056 |
0.75 |
0.33 |
36.20 |
-5.38 |
0.75 |
0.33 |
36.20 |
-5.38 |
|
2003 |
1.075 |
0.75 |
0.33 |
36.79 |
1.62 |
0.75 |
0.33 |
36.79 |
1.62 |
|
2004 |
1.074 |
0.75 |
0.33 |
37.34 |
1.50 |
0.75 |
0.33 |
37.34 |
1.50 |
|
2005 |
1.043 |
0.75 |
0.33 |
37.90 |
1.50 |
0.75 |
0.33 |
37.90 |
1.50 |
|
2006 |
1.017 |
0.75 |
0.33 |
37.90 |
0.00 |
0.75 |
0.33 |
37.90 |
0.00 |
|
2007 |
1.007 |
0.75 |
0.33 |
36.16 |
-4.58 |
0.38 |
0.00 |
36.53 |
-3.60 |
|
2008 |
1.039 |
0.75 |
0.33 |
34.37 |
-4.96 |
0.38 |
0.00 |
34.95 |
-4.33 |
|
2009 |
1.035 |
0.75 |
0.33 |
32.63 |
-5.05 |
0.38 |
0.00 |
33.55 |
-4.00 |
|
2010 |
1.029 |
0.75 |
0.33 |
30.93 |
-5.23 |
0.38 |
0.00 |
32.21 |
-3.99 |
|
2011 |
1.034 |
0.75 |
0.33 |
29.34 |
-5.14 |
0.38 |
0.00 |
31.14 |
-3.32 |
|
2012 |
1.042 |
0.75 |
0.33 |
27.86 |
-5.05 |
0.38 |
0.00 |
30.36 |
-2.51 |
|
2013 |
1.045 |
0.75 |
0.33 |
26.50 |
-4.86 |
0.38 |
0.00 |
29.84 |
-1.73 |
|
2014 |
1.039 |
0.75 |
0.33 |
25.21 |
-4.86 |
0.38 |
0.00 |
29.47 |
-1.22 |
|
30.20 |
-2.19 |
||||||||
| Notes: Simulation estimates are based on revisions to the UAF beginning in 2007. Revisions include deleting the portion of the UAF that penalizes/rewards providers for cumulative over-/under-spending, and cutting the weight on the previous-year over-/under-spending by 50 percent, to 0.375. Baseline data in italics are subject to change. | |||||||||
|
Baseline (billions) |
With Revised UAF |
Spending Ratio |
||||||
|---|---|---|---|---|---|---|---|---|
|
Period |
Physician |
Lab and |
Total |
Physician |
Lab and |
Total |
||
|
2000-2005 |
380.4 |
74.6 |
455.0 |
380.4 |
74.6 |
455.0 |
1.00 |
|
|
2006-2010 |
401.8 |
99.0 |
500.8 |
409.6 |
99.0 |
508.6 |
1.02 |
|
|
2011-2013 |
228.1 |
80.3 |
308.5 |
249.1 |
80.3 |
329.5 |
1.07 |
|
|
Total |
1010.4 |
253.9 |
$1,264.3 |
1039.2 |
253.9 |
$1,293.1 |
1.02 |
|
| Notes: Spending estimates were derived using CFs displayed in Table 11a, adjusted for data corrections routinely reported by CMS. The Spending Ratio is the ratio of simulated to baseline spending. | ||||||||
5.0 Changes in Target-Setting Processes
Changes in the UAF formula can be used to change the size of penalties/rewards associated with over-/under-spending, which in turn changes the rate at which provider payments would change year to year. An alternative approach is to alter the way in which target spending is defined or the composition of spending that is counted towards target spending. Changes in the size of the target or its composition may change over-/under-spending and its accumulation, thereby changing the UAF and the payment update. Two refinements are described in this section. The first is a change in the SGR, the rate at which the spending target is calculated; the second is a change in the composition of SGR spending – elimination of drug and lab spending from the payment update process.
5.1 Effects of Changes in SGR Values
A fundamental explanation for payment update declines that have been recently experienced and are likely in the near future without significant changes to the SGR process is that spending increases faster than target spending levels. This over-spending determines the penalty of the UAF, which can more than offset the MEI when the update is calculated. One policy option is to simply revise the SGR. Recall that the SGR is calculated from data that measure changes in costs facing providers (in part, the MEI measure), changes in per capita GDP, changes in enrollment in the Medicare fee-for-service program, and changes precipitated by laws and regulations. The GDP measure is a proxy for real increases in utilization that presumably track beneficiary tastes. An increased societal preference for health care spending for the elderly might be factored into the update process by changing the GDP measure to “GDP plus.”
Increasing the size of the SGR component that measures real increases in utilization is one means of recognizing that the elderly should receive benefits from cost-increasing, quality-enhancing technologies without penalizing providers. An increase in the SGR is also a means of adjusting the spending target to reflect increases in utilization associated with new technologies and increases in utilization that have been hypothesized to accompany shifts over time from inpatient-based care to care delivered in the office and other settings.
The model was used to examine effects of an increase in the SGR. Two changes were made to baseline SGR values, beginning in 2007. First, baseline SGR values were adjusted to reflect the tendency for error in estimating past values. CMS updates the SGR value for each year with new information several times after its use in calculating the payment update. A comparison of SGR ‘baseline’ values used to implement the SGR (‘baseline’ values in Table 12) with their corrected values for the recent five year period, 2001-2005 (‘corrected’ values in Table 12), indicates that the average updated SGR increased by about 9.4 percent. Thus, baseline SGR values beginning in 2007 were adjusted by increasing each by 9.4 percent (‘adjustments’ in Table 12 are 9.4 percent of ‘baseline’ values). ‘Adjusted baseline’ SGR values are displayed in Table 12, calculated as the sum of the baseline value and its adjustment for years 2007-2014.
|
SGR (Percent) |
|||||
|---|---|---|---|---|---|
| Update Year |
Baseline |
Corrected |
Adjustment |
Adjusted |
Revised |
|
2000 |
2.10 |
7.30 |
5.20 |
na |
na |
|
2001 |
5.60 |
4.30 |
-1.30 |
na |
na |
|
2002 |
5.60 |
8.10 |
2.50 |
na |
na |
|
2003 |
7.50 |
7.30 |
-0.20 |
na |
na |
|
2004 |
7.40 |
8.10 |
0.70 |
na |
na |
|
2005 |
4.30 |
5.10 |
0.80 |
na |
na |
|
2006 |
1.70 |
1.70 |
0.00 |
na |
na |
|
2007 |
0.70 |
na |
0.07 |
0.77 |
1.77 |
|
2008 |
3.90 |
na |
0.37 |
4.27 |
5.27 |
|
2009 |
3.50 |
na |
0.33 |
3.83 |
4.83 |
|
2010 |
2.90 |
na |
0.27 |
3.17 |
4.17 |
|
2011 |
3.40 |
na |
0.32 |
3.72 |
4.72 |
|
2012 |
4.20 |
na |
0.39 |
4.59 |
5.59 |
|
2013 |
4.50 |
na |
0.42 |
4.92 |
5.92 |
|
2014 |
3.90 |
na |
0.37 |
4.27 |
5.27 |
| Notes: Baseline SGRs were used to calculate baseline CFs (e.g., displayed in Table 3a); values in italics are subject to change. Corrected values are the most recent revisions to baseline values subsequently published in Federal Registers based on updated data. Adjustments through 2006 are differences between Corrected and Baseline values; Adjustments from 2007 through 2014 were calculated as 9.4 percent of corresponding Baseline values. The Adjustment percentage, 9.4 percent, is the average percent difference between Corrected and Baseline values for the years 2001-2005. The Adjusted Baseline is the sum of Baseline and Adjustment values for years 2007-2014, and the Revised Baseline is the sum of the Adjusted Baseline and 1 percent. | |||||
Second, the SGR was increased beginning in 2007 by a single percentage point. This hypothetical increase was specified as a means of accounting for an increase in preferences for health care. (Under the current formula, the percent change in GDP, a determinant of the SGR, is a proxy measure of trends in preferences.) The ‘revised baseline’ values in Table 12 for 2007-2014 are the sum of 1 percent and the ‘adjusted baseline’ value for each year.
Changes in the SGR to the revised values in Table 12 for years 2007-2014 are relatively large, averaging about 37 percent between the years 2008 and 2014 (the 2007 SGR would increase by a factor of 2.5). Nevertheless, these revisions would have no effect on future CFs and on program spending through 2013. The reason is that increases in target spending are simply not large enough to offset expected spending increases. For example, the 2007 spending target would increase from $82.3 to $84.2 billion, while projected spending is $98.3 billion. The UAF penalty for over-spending would increase from -0.33 to -0.30, which is still well below the 7 percent UAF floor. The UAF is not expected to rise above the floor in the near future, even with the SGR increases in Table 12.
5.2 Rebasing Target Spending
The current SGR process was implemented with an initial target level based on actual spending levels in the late 1990s. Since that time, each year’s target has been increased using the SGR. Over time, the rate of spending has increased and the cumulated difference between annual actual and target spending levels has grown rapidly. Effects of these trends are evident from the lack of update effects associated with relatively large increases in target spending beginning in 2007 (described in the previous section).
An SGR refinement is to “restart” the target. An important policy question is how target spending should be re-defined. Recall that the UAF under the current SGR process is based on comparisons of actual and target spending, as follows:
UAFt = { 0.75 * [ (targett-1 – actualt-1) / actualt-1 ] }
+ { 0.33 * [ (targetc – actualc) / (actualt-1 * SGRt) ] }.
Target spending for year t-1 is the target for year t-2, updated using the SGR for year t-1, and cumulated spending and target spending are based on levels dating back to the late 1990s. The simplest revised target mechanism is to rebase the SGR formula -- that is, reset the target so that payment incentives are more realistically in line with current spending goals. There may be more support among providers for conscientious control over spending if payment changes are more directly tied to current behavior.
The project team rebased the SGR process, beginning with data used to calculate the CF for 2007. Target non-E&M spending for 2006 was reset to actual non-E&M 2006 spending, and cumulated actual and target spending levels were reset to the 2006 actual spending level in the formula for calculating the UAF for the 2007 update. In other words,
UAF2007 = { 0.75 * [ (target2006 – actual2006) / actual2006 ] }
+ { 0.33 * [ (target2006 – actual2006) / (actual2006 * SGR2007) ] }
And when the 2006 target is reset to actual spending for 2006,
UAF2007 = { 0.75 * [ (actual2006 – actual2006) / actual2006 ] }
+ { 0.33 * [ (actual2006 – actual2006) / (actual2006 * SGR2007) ] }
= { 0.75 * [ (0) / actual2006 ] } + { 0.33 * [ (0) / (actual2006 * SGR2007) ] }
= 0.
In other words, this simple re-definition of target spending would eliminate the UAF penalty for 2007, but re-start cumulated spending for the calculation of CFs for the years 2008-2014.
|
Current Law |
Rebased |
||||
|---|---|---|---|---|---|
|
Update |
SGR |
CFt |
Percent |
CFt |
Percent |
|
2007 |
1.007 |
36.16 |
-4.58 |
38.88 |
2.60 |
|
2008 |
1.039 |
34.37 |
-4.96 |
37.19 |
-4.36 |
|
2009 |
1.035 |
32.63 |
-5.05 |
35.35 |
-4.95 |
|
2010 |
1.029 |
30.93 |
-5.23 |
33.55 |
-5.08 |
|
2011 |
1.034 |
29.34 |
-5.14 |
32.51 |
-3.10 |
|
2012 |
1.042 |
27.86 |
-5.05 |
32.23 |
-0.87 |
|
2013 |
1.045 |
26.50 |
-4.86 |
32.39 |
0.50 |
|
2014 |
1.039 |
25.21 |
-4.86 |
32.74 |
1.08 |
| Notes: Baseline estimates are as in Table 7a; baseline data in italics subject to change. Rebased estimates were calculated using the SGR formula, but with actual and target spending amounts 'rebased' to 2006. Rebased means that in calculating the CF for 2007, the target for 2006 is estimated spending for 2006, and initial cumulated actual and target spending amounts are set to total estimated 2006 spending. The SGR formula was then applied for years 2007-2014. | |||||
Effects of rebasing are summarized in Tables 13a and 13b. Rebasing would increase the CF for 2007 by 2.6 percent (Table 13a). Conversion factors would decline from 2008 to 2012, but continue to exceed baseline levels due to the initial increase for 2007 and smaller declines relative to baseline during 2008-2013. Spending would be higher than under baseline by 6 percent during 2007-2010 (Table 13b). The CF would begin to increase in 2013, contributing to a 12 percent increase in spending over baseline during the 2011-2013 period.
5.3 Elimination of Drug and Lab Spending from the SGR
An argument raised by some providers and critics of the SGR process is that the payment update should not be based on events beyond control of providers. An example is spending for drugs and lab tests. These components of SGR spending are less within the control of providers than services and procedures routinely provided under the MFS. Drug and lab test prices are not subject to the same controls as under the MFS. Physicians write prescriptions, but have little control over drug pricing.
|
Baseline (billions) |
Rebased (billions) |
Spending |
|||||
|---|---|---|---|---|---|---|---|
| Period |
Physician |
Lab and |
Total |
Physician |
Lab and |
Total |
|
|
2007-2010 |
321.3 |
82.2 |
403.4 |
347.4 |
82.2 |
429.6 |
1.06 |
|
2011-2013 |
228.1 |
80.3 |
308.5 |
265.0 |
80.3 |
345.4 |
1.12 |
|
Total |
549.4 |
162.5 |
$711.9 |
612.4 |
162.5 |
$774.9 |
1.09 |
| Notes: Spending estimates were derived using CFs displayed in Table 13a, adjusted for data corrections routinely reported by CMS. The Spending Ratio is the ratio of rebased to baseline spending. | |||||||
In fact, baseline drug and lab spending components of SGR spending are expected to increase more rapidly than physician spending in the near future. The average annual rate of increase in total baseline physician spending between 2006 and 2013 is -1.6 percent, whereas the increase for the total of drug and lab spending is 7.4 percent per year during this time period (calculated from Appendix Table A1).
The rebased version of the model was used to examine the effects of deleting drug and lab spending from SGR spending beginning in 2007. In this application of the rebased model, the UAF for 2007 was calculated by comparing actual SGR physician spending (e.g., total SGR spending less spending on drugs and lab tests) to target spending, defined as SGR physician spending in 2006, and CFs were calculated using SGR physician spending only for 2008-2014.
|
Rebased |
Less Drug and Lab |
||||
|---|---|---|---|---|---|
|
Update |
SGR |
CFt |
Percent |
CFt |
Percent |
|
2007 |
1.007 |
38.88 |
2.60 |
38.88 |
2.60 |
|
2008 |
1.039 |
37.19 |
-4.36 |
37.27 |
-4.15 |
|
2009 |
1.035 |
35.35 |
-4.95 |
35.87 |
-3.74 |
|
2010 |
1.029 |
33.55 |
-5.08 |
34.69 |
-3.31 |
|
2011 |
1.034 |
32.51 |
-3.10 |
34.41 |
-0.81 |
|
2012 |
1.042 |
32.23 |
-0.87 |
34.81 |
1.17 |
|
2013 |
1.045 |
32.39 |
0.50 |
35.44 |
1.80 |
|
2014 |
1.039 |
32.74 |
1.08 |
36.10 |
1.88 |
| Notes: Rebased estimates are as in Table 13a; baseline data in italics subject to change. Estimates on right side are derived by deleting drug and lab spending from SGR spending and rebasing so that actual and target spending levels exclude drug and lab spending. Rebased means that in calculating the CF for 2007, the target for 2006 is estimated spending for 2006, and initial cumulated actual and target spending amounts are set to total estimated 2006 spending. The SGR formula was then applied for years 2007-2014. | |||||
Conversion factors would decline between 2008 and 2011 with elimination of drug and lab spending as with simple rebasing (left side of Table 14a), but CF levels would be higher without than when drug and lab spending are counted in the UAF. In 2010, for example, the CF would be $34.69 without lab and drug spending, $33.55 with simple rebasing (Table 14a), and $30.93 under the current SGR process (Table 7a).
Total spending would increase as a consequence of rebasing after eliminating re-defining SGR spending. Spending would be 3 percent higher than with rebasing only, and 12 percent higher than is expected under the current SGR process (Tables 14b and 13b).
|
Rebased (billions) |
Less Drug and |
Spending |
|||||
|---|---|---|---|---|---|---|---|
|
Period |
Physician |
Lab and |
Total |
Physician |
Lab and |
Total |
|
|
2007-2010 |
347.4 |
82.2 |
429.6 |
351.8 |
82.2 |
434.0 |
1.01 |
|
2011-2013 |
265.0 |
80.3 |
345.4 |
285.7 |
80.3 |
366.0 |
1.06 |
|
Total |
612.4 |
162.5 |
$774.9 |
637.5 |
162.5 |
$800.0 |
1.03 |
| Notes: Spending estimates were derived using CFs displayed in Table 14a, adjusted for data corrections routinely reported by CMS. The Spending Ratio is the ratio of spending without drug and lab spending included, to baseline rebased spending. | |||||||
5.4 Additional Refinements
Refinements to the SGR process that have been discussed above can be considered simultaneously. Tables 15a and 15b document effects on CFs of sequentially imposing two refinements on the rebased model with drug and lab spending excluded from SGR spending: use of the higher SGR values (displayed in Table 12), e.g., to accommodate desire for higher target spending; and elimination of the cumulated spending portion of the UAF, e.g., to reduce effects of past behavior on the update.
An increase in the SGR in addition to elimination of drug and lab spending would increase CFs because higher spending targets reduce levels of over-spending and make it easier for providers to achieve update increases. With larger SGRs, the CF in 2010 would be $38.03 (Table 15a) versus $34.69 (Table 14a). When the cumulated spending portion of the UAF is then eliminated, rates at which CFs fall would be reduced because the penalty of over-spending is lessened (Table 15b), which would increase CFs even more through 2010.
|
Rebased |
Less Lab and Drug |
|||||
|---|---|---|---|---|---|---|
|
Update |
SGR |
CFt |
Percent |
SGR |
CFt |
Percent |
|
2007 |
1.007 |
38.88 |
2.60 |
1.018 |
38.88 |
2.60 |
|
2008 |
1.039 |
37.19 |
-4.36 |
1.053 |
38.22 |
-1.70 |
|
2009 |
1.035 |
35.35 |
-4.95 |
1.048 |
38.05 |
-0.45 |
|
2010 |
1.029 |
33.55 |
-5.08 |
1.042 |
38.03 |
-0.05 |
|
2011 |
1.034 |
32.51 |
-3.10 |
1.047 |
38.90 |
2.30 |
|
2012 |
1.042 |
32.23 |
-0.87 |
1.056 |
40.54 |
4.20 |
|
2013 |
1.045 |
32.39 |
0.50 |
1.059 |
42.47 |
4.77 |
|
2014 |
1.039 |
32.74 |
1.08 |
1.053 |
44.53 |
4.83 |
| Notes: Rebased estimates on left side are as in Table 13a; baseline data in italics subject to change. Estimates on right side were derived by (1) rebasing after deleting drug and lab spending from SGR spending, and (2) using SGR values that were revised to reflect CMS's revision experience and increased by 1 percentage point (values displayed in Table 12). Rebased means that in calculating the CF for 2007, the target for 2006 is estimated spending for 2006, and initial cumulated actual and target spending amounts are set to total estimated 2006 spending; the SGR formula was then applied for years 2007-2014. | ||||||
At the same time, relative rates of increase in CFs would be reduced because cumulated under-spending does not occur when the cumulated spending portion of the UAF is eliminated. The latter would occur during 2011-2014 (Table 15b versus 15a).
Each refinement would increase program spending. Spending with rebased targets would be $774.9 billion between 2007 and 2013 (v. $711.9 billion under baseline). During this period, elimination of drug and lab spending from total SGR spending would increase program spending by $25.1 billion ($800.0-$774.9 billion, Table 14b). Increases in the SGR would increase spending by an additional $63.5 billion ($863.5-$800.0 billion, Table 16a). Elimination of the cumulated spending portion of the UAF would increase spending by another $6.4 billion ($869.9-$863.5 billion, Table 16b).
|
Rebased |
Less Lab and Drug Spending, |
|||||||
|---|---|---|---|---|---|---|---|---|
|
Update |
SGR |
Cumulated |
CFt |
Percent |
SGR |
Cumulated |
CFt |
Percent |
|
2007 |
1.007 |
0.33 |
38.88 |
2.60 |
1.018 |
0.00 |
38.88 |
2.60 |
|
2008 |
1.039 |
0.33 |
37.19 |
-4.36 |
1.053 |
0.00 |
38.67 |
-0.56 |
|
2009 |
1.035 |
0.33 |
35.35 |
-4.95 |
1.048 |
0.00 |
38.75 |
0.21 |
|
2010 |
1.029 |
0.33 |
33.55 |
-5.08 |
1.042 |
0.00 |
38.82 |
0.18 |
|
2011 |
1.034 |
0.33 |
32.51 |
-3.10 |
1.047 |
0.00 |
39.49 |
1.72 |
|
2012 |
1.042 |
0.33 |
32.23 |
-0.87 |
1.056 |
0.00 |
40.71 |
3.09 |
|
2013 |
1.045 |
0.33 |
32.39 |
0.50 |
1.059 |
0.00 |
42.24 |
3.76 |
|
2014 |
1.039 |
0.33 |
32.74 |
1.08 |
1.053 |
0.00 |
43.96 |
4.07 |
| Notes: Rebased estimates on left side are as in Table 13a; baseline data in italics subject to change. Estimates on right side were derived by (1) rebasing after deleting drug and lab spending from SGR spending, (2) using SGR values that were revised to reflect CMS's revision experience and increased by 1 percentage point (values displayed in Table 12), and (3) eliminating the cumulated spending term from the UAF. Rebased means that in calculating the CF for 2007, the target for 2006 is estimated spending for 2006, and initial cumulated actual and target spending amounts are set to total estimated 2006 spending; the SGR formula was then applied for years 2007-2014. | ||||||||
|
Rebased (billions) |
Less Lab and Drug |
||||||
|---|---|---|---|---|---|---|---|
|
Period |
Physician |
Lab and |
Total |
Physician |
Lab and |
Total |
Spending |
|
2007-2010 |
347.4 |
82.2 |
429.6 |
368.0 |
82.2 |
450.2 |
1.05 |
|
2011-2013 |
265.0 |
80.3 |
345.4 |
333.0 |
80.3 |
413.3 |
1.20 |
|
Total |
612.4 |
162.5 |
$774.9 |
701.0 |
162.5 |
$863.5 |
1.11 |
| Notes: See notes, Table 15a. Spending estimates were derived using CFs displayed in Table 15a. The Spending Ratio is the ratio of spending with revisions (right side) to baseline rebased spending (left side). | |||||||
|
Rebased (billions) |
Less Lab and Drug |
|
|||||
|---|---|---|---|---|---|---|---|
|
Period |
Physician |
Lab and |
Total |
Physician |
Lab and |
Total |
Spending Ratio |
|
2007-2010 |
347.4 |
82.2 |
429.6 |
372.8 |
82.2 |
455.0 |
1.06 |
|
2011-2013 |
265.0 |
80.3 |
345.4 |
334.3 |
80.3 |
414.7 |
1.20 |
|
Total |
612.4 |
162.5 |
$774.9 |
707.2 |
162.5 |
$869.7 |
1.12 |
| Notes: See notes, Table 15b. Spending estimates were derived using CFs displayed in Table 15b. The Spending Ratio is the ratio of spending with revisions (right side) to baseline rebased spending (left side). | |||||||
6.0 Discussion
The primary objective of this report has been to evaluate revisions to the current SGR physician payment update methodology with a focus on refinements to attributes of the SGR process and changes in the definition of target spending. A spreadsheet model of the current SGR process was constructed for comparative study of effects of changes in the current payment update process. The basic building blocks of these modeling efforts include data from the past, and data that were used to project future spending patterns. Outputs of the modeling effort include estimated payment updates and associated levels of program spending.
It is important to emphasize that interpretation of results of these modeling efforts is subject to two important caveats. First, no behavioral responses on the part of any agents affected by the update process, including providers, Medicare beneficiaries, and Congress, have been incorporated into the structure of the spreadsheet model. Thus, no behavioral responses to increased or decreased updates affect the model’s predicted effects on updates and program spending. A consequence is that if volume is expected on net to increase in response to large reductions in CFs, spending effects reported above should best be interpreted as lower-bounds. In the same way, no behavioral responses to changes in CFs by program beneficiaries or Congress has been assumed other than those already built into data from CMS that have been used to construct the SGR process model. Second, results reflect various assumptions. Whenever possible, data from CMS have been used and these reflect study by the CMS Office of the Actuary. Examples include how the number of Medicare beneficiaries is expected to change in the future and trends in per beneficiary utilization in total SGR services.
In spite of these caveats, use of the model in examining effects of refinements in the SGR process is helpful. Modeling is a source of information on relative magnitudes of effects stemming from different refinements and combinations of refinements, and helps the user understand what drives the SGR process. Key findings from this work may be seen from the perspective offered by Table 17, which displays CFs and spending estimates for future years corresponding to two main SGR approaches: ‘cost’, and the current approach. Under the current SGR approach, negative updates are expected, CFs would be relatively low (absent Congressional intervention assumptions), and spending is relatively low. The UAF formula will continue to penalize over-spending, a consequence of expected total SGR spending levels in excess of target spending levels. At the opposite end of the continuum, updates would be based strictly on the expected rate of increase in the costs of practice (as measured by the MEI) under the cost approach, with no payment rewards/penalties (in fact, estimates are produced using the current SGR formula and eliminating UAF rewards and penalties). Average CFs under the cost approach would exceed CFs under baseline by 20 percent between 2007 and 2010, and by 60 percent between 2011 and 2014. The difference in total program spending between these two extremes is large – over $190 billion, or 26 percent of baseline spending during 2007-2013.
|
2007-'10 |
2011-'14 |
|||||
|---|---|---|---|---|---|---|
|
Model |
CF (Range) |
Average |
Spending |
CF (Range) |
Average |
Spending** |
| Cost |
$40.13 |
2.2 |
$468.5 |
$43.58 |
2.2 |
$433.2 |
|
($38.88-41.34) |
|
($42.17-45.06) |
|
|||
| Rebased Spending* |
$36.24 |
-3.0 |
$429.6 |
$32.47 |
-0.6 |
$345.4 |
|
($38.88-33.55) |
($32.51-32.74) |
|||||
| Baseline |
$33.52 |
-5.0 |
$403.4 |
$27.23 |
-5.0 |
$308.5 |
|
($36.16-30.93) |
($29.34-25.21) |
|||||
| Notes: Baseline results are based on CFs predicted for years 2007-2014. Cost model CFs were predicted from the SGR model by basing updates only on the MEI and ‘other’ factors used by CMS; i.e., the UAF is not used in calculating the update for the cost model. Remaining estimates in this table are from Tables 13a and 13b. CFs and percent changes are arithmetic averages over the period of interest. The CF range refers to the values at the beginning and end of the period. Spending is total SGR spending during the period. *Target spending amounts rebased to 2006 spending. **Spending estimates are for years 2011-2013. | ||||||
A number of refinements to the current process were considered in this report, each motivated by the importance of identifying changes that would reduce the need for yearly Congressional intervention in response to formula-driven reductions in Medicare payments. Fundamental challenges are that spending in the near future, at least, is expected to be in excess of spending targets as currently defined, and that the downward pressure on payment updates is increasing with the accumulation of over-spending over time, given the design of the SGR. The primary policy goal, of course, is to identify refinements to the update process that would eliminate or reduce the magnitude of payment reductions but without large increases in spending.
Each of the refinements considered in this report could be summarized by adding a row between the cost and current payment update approaches in Table 17. CFs for these reforms would exceed baseline levels in the near future, but would be less costly than under the cost model. Reforms that appear to hold the most promise are those involving changes in the definition of target spending, including rebasing the spending target (beginning in 2007), in combination with the elimination of drug and lab spending from SGR. Under the current SGR approach, the average percent change in CFs between 2007 and 2010 is expected to be -5 percent without Congressional intervention. With rebasing as defined in this study, the average reduction in CFs during 2007-2010 would be -3.0. With simultaneous elimination of lab and drug spending from SGR spending and increases in the SGR (as specified in this study, e.g., to reflect increased preferences for spending on health care), payment updates would increase by 2010 without Congressional intervention. While these approaches would preserve means of recovering at least a portion of over-spending, program spending would increase but by less than if the cost model were adopted. The price of less Congressional intervention with CFs obtained with rebasing, elimination of drug and lab spending, and revised SGRs would be 4 percent less than under the cost model, and 12 percent more than under the status quo between 2007 and 2010. So long as spending continues to increase at expected rates, identifying how best to fix the SGR update process requires that policymakers balance benefits of less future Congressional intervention with the costs of increases in program spending.
Appendix. SGR Spending Predictions
Data Sources. Implementation of the SGR process requires that CMS use the most current information at its disposal to estimate components of the SGR formula, including spending, and components that are used to calculate the SGR (which in turn, are used to calculate annual target spending and cumulated target spending). As noted in the text, CMS uses current data to re-estimate data items used to calculate the update.
A number of data sources were used in construction on the SGR simulation model. These are listed below:
- Various versions of the Federal Register document calculation of Medicare payment updates over time, and data from these volumes were used in attempts to replicate updates and spending estimates that define the current law baseline:
- Update for 1997: Vol. 61, No. 227, Tuesday, November 22, 1996
- Update for 1998: Vol. 62, No. 211, Friday, October 31, 1997
- Update for 1999: Vol. 63, No. 211, Monday, November 2, 1998
- Update for 2000: Vol. 64, No. 211, Tuesday, November 2, 1999
- Update for 2001: Vol. 65, No. 212, Wednesday, November 1, 2000
- Update for 2002: Vol. 66, No. 212, Thursday, November 1, 2001
- Update for 2003: Vol. 67, No. 251, Tuesday, December 31, 2002 and Vol. 68, No. 40, Friday, February 28, 2003
- Update for 2004: Vol. 68, No. 216, Friday, November 7, 2003
- Update for 2005: Vol. 69, No. 219, Monday, November 15, 2004
- Update for 2006: Vol. 70, No. 223, Monday, November 21, 2005
- Preliminary information in support of the Update for 2007 is from M. Kent Clemens, “Estimated Sustainable Growth Rate and Conversion Factor, for Medicare Payments to Physicians in 2007,” downloaded from http://www.cms.hhs.gov/SustainableGRatesConFact/Downloads/sgr2007p.pdf
- First quarter values of the MEI for years 2008-2014 from Global Insight, Inc., downloaded from http://www.cms.hhs.gov/MedicareProgramRatesStats/downloads/mktbskt-economic-index.pdf.
- Number of fee-for-service Medicare beneficiaries for years 2008-2014 (Table III.A3) and components of increases in total allowed charges (Table IV.B1), from 2006 Annual Report of the Boards of Trustees of the Federal Hospital Insurance and Federal Supplementary Medical Insurance Trust Funds (the 2006 Trustees Report).
- GDP data are from The Budget and Economic Outlook: An Update. Congressional Budget Office. 15 Aug 2005, http://www.cbo.gov/showdoc.cfm?index=1824&sequence=0
- 1995-1999 population estimates are from the US Census Bureau, http://www.census.gov/popest/archives/EST90INTERCENSAL/US-EST90INT-01.html.
- Population for 2000 and projections for 2004-2014 are from the US Census Bureau, http://www.census.gov/population/projections/DownldFile1.xls
- Multifactor Productivity Index values, private non-farm business, from the US Bureau of Labor Statistics, http:data.bls.gov/PDQ/servlet/SurveyOutputServlet.
Spending. Modeling for this project requires spending projections, and the application of corrections that adjust projections to obtain values actually used by CMS when updates were calculated. This portion of the Appendix describes how baseline spending estimates were obtained.
Modeling needs included spending estimates by type of service. Thus, total SGR spending was decomposed into spending for physician services and for the total of drug and lab spending. Then, SGR-physician spending was be decomposed into spending by type of service: E&M, all non-E&M, and the imaging and ‘other service’ components of spending on non-E&M services. Adjustment factors were then applied to SGR spending components to ensure that by-year and cumulative spending amounts matched those reported by CMS.
Step 1. Predict physician, lab, and drug spending components of total SGR spending. The year 2002 was used as the ‘anchor’ year. Total SGR spending for 2002 was divided into its physician, drug, and lab components: data from the Federal Register indicated that 83.5 percent of SGR spending was for physician services, 8.5 percent was for drug spending, and 8.0 percent for lab spending (Vol. 67, December 31, 2002). Data from the 2006 Trustees’ Report were then used to predict physician, lab, and drug spending amounts both forward and back in time. Predictions began from 2002, obtained using data on yearly percentage changes in physician spending per beneficiary and the number of Medicare fee-for-service beneficiaries. Similar calculations were used to estimate drug and lab spending over time. Spending predictions are displayed in Table A1.
Step 2. Decompose total physician spending (for each year) into spending by type of service. For years 1999-2004, data from the Physician/Supplier Procedure Summary Master Files (PSPSMFs), obtained from CMS, were used to estimate the fraction of physician spending on each service group of interest.13 Predicted spending shares are displayed in Table A1; corresponding dollar amounts are displayed in Table A2.
|
Calendar |
Predicted SGR Spending (billions) |
Percent Decomposition of SGR |
|||||
|---|---|---|---|---|---|---|---|
|
Physician |
Drug |
Lab |
E&M |
Non-E&M |
Imaging |
"Other" |
|
|
1996 |
42.21 |
2.73 |
5.25 |
0.45 |
0.55 |
0.12 |
0.43 |
|
1997 |
42.76 |
3.06 |
4.87 |
0.51 |
0.49 |
0.11 |
0.38 |
|
1998 |
43.84 |
3.30 |
4.32 |
0.50 |
0.50 |
0.13 |
0.37 |
|
1999 |
45.27 |
3.63 |
4.29 |
0.50 |
0.50 |
0.14 |
0.36 |
|
2000 |
50.05 |
4.18 |
4.66 |
0.51 |
0.49 |
0.14 |
0.35 |
|
2001 |
56.59 |
5.01 |
5.15 |
0.50 |
0.50 |
0.15 |
0.35 |
|
2002 |
59.20 |
6.03 |
5.67 |
0.50 |
0.50 |
0.15 |
0.35 |
|
2003 |
64.57 |
7.21 |
6.24 |
0.49 |
0.51 |
0.16 |
0.34 |
|
2004 |
72.11 |
7.89 |
6.82 |
0.48 |
0.52 |
0.17 |
0.35 |
|
2005 |
79.19 |
8.38 |
7.53 |
0.46 |
0.54 |
0.18 |
0.36 |
|
2006 |
83.63 |
9.46 |
7.99 |
0.45 |
0.55 |
0.18 |
0.36 |
|
2007 |
80.13 |
10.11 |
8.09 |
0.45 |
0.55 |
0.19 |
0.35 |
|
2008 |
80.69 |
11.19 |
8.45 |
0.44 |
0.56 |
0.20 |
0.36 |
|
2009 |
81.01 |
12.34 |
8.98 |
0.43 |
0.57 |
0.21 |
0.36 |
|
2010 |
79.44 |
13.49 |
9.52 |
0.43 |
0.57 |
0.22 |
0.35 |
|
2011 |
77.47 |
14.73 |
10.04 |
0.43 |
0.57 |
0.24 |
0.33 |
|
2012 |
76.03 |
16.08 |
10.66 |
0.44 |
0.56 |
0.25 |
0.31 |
|
2013 |
74.65 |
17.48 |
11.34 |
0.44 |
0.56 |
0.27 |
0.29 |
| Notes: Predicted spending amounts are estimated using data from the 2006 Trustees' Report. Shares are based on spending reported in the 1996-2004 Physician/Supplier Procedure Summary Master Files. | |||||||
For years 2005-2013, the composition of SGR physician spending could not be observed, but was predicted (predicted shares and corresponding amounts are in italics in Tables A1 and A2). Data from CMS include annual percent changes in Medicare price (reflecting its current law baseline, past and future) and annual percent changes in the number of program beneficiaries. Data for 1996-2004 were used to decompose estimates of changes in physician spending into portions attributable to changes in price, changes in the number of fee-for-service beneficiaries, and intensity – residual changes in utilization that underlie changes in total spending, but not attributable to changes in price and the number of program beneficiaries.
Intensity estimates for 2005-2013 are based on assumptions from values estimated for 2000-2004 (appearing in italics in Table A2). Intensity values for E&M spending for years 2005-2013 were assumed to be the average for years 2000-2004, 3.7 percent per year. E&M spending estimates were calculated based on this assumption. The remainder of predicted physician dollars was for non-E&M services. Dollar spending amounts for non-E&M were estimated, from which non-E&M intensity values were calculated algebraically.
Similarly, the 2000-2004 average intensity of 10 percent for imaging was assumed for years 2005-2013. Using imaging and E&M intensity assumptions, corresponding dollar spending amounts were estimated. The latter were subtracted from total predicted physician spending to obtain total spending for ‘other’ services. Intensity values for this latter group of other services were calculated algebraically.
Step 3. Adjust spending amounts for use in modeling. Spending amounts in Tables A1 and A2 are baseline spending amounts that are used as inputs of the spreadsheet payment update model. Amounts for years 2000-2006 are corrected to yield values used by CMS when payment updates were calculated. Baseline SGR physician spending amounts are adjusted when simulated CFs differ from baseline values.
| Calendar Year |
Predicted SGR Physician Spending (billions) |
Predicted Dollar Decomposition of SGR Physician Spending (billions) |
Factors | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
|
Intensity |
|
Number of Beneficiaries |
|||||||||
| E&M |
Non-E&M |
Imaging |
"Other" |
E&M |
Imaging |
"Other" |
Non E&M |
Price |
|||
|
1996 |
42.21 |
18.89 |
23.32 |
5.17 |
18.16 |
NA |
NA |
NA |
NA |
1.008 |
0.985 |
|
1997 |
42.76 |
22.02 |
20.74 |
4.51 |
16.23 |
1.185 |
0.888 |
0.909 |
0.904 |
1.006 |
0.978 |
|
1998 |
43.84 |
21.72 |
22.12 |
5.84 |
16.27 |
0.981 |
1.288 |
0.997 |
1.060 |
1.028 |
0.978 |
|
1999 |
45.27 |
22.82 |
22.45 |
6.15 |
16.29 |
1.030 |
1.033 |
0.982 |
0.995 |
1.026 |
0.994 |
|
2000 |
50.05 |
25.49 |
24.55 |
6.97 |
17.59 |
1.046 |
1.060 |
1.010 |
1.024 |
1.059 |
1.009 |
|
2001 |
56.59 |
28.53 |
28.06 |
8.33 |
19.74 |
1.031 |
1.101 |
1.034 |
1.053 |
1.053 |
1.031 |
|
2002 |
59.20 |
29.87 |
29.33 |
8.88 |
20.44 |
1.063 |
1.083 |
1.051 |
1.061 |
0.958 |
1.029 |
|
2003 |
64.57 |
31.85 |
32.72 |
10.64 |
22.08 |
1.022 |
1.148 |
1.035 |
1.069 |
1.014 |
1.029 |
|
2004 |
72.11 |
34.36 |
37.75 |
12.39 |
25.36 |
1.025 |
1.106 |
1.091 |
1.096 |
1.038 |
1.014 |
|
2005 |
79.19 |
36.49 |
42.69 |
13.95 |
28.74 |
1.037 |
1.100 |
1.107 |
1.105 |
1.021 |
1.003 |
|
2006 |
83.63 |
37.82 |
45.81 |
15.33 |
30.48 |
1.037 |
1.100 |
1.061 |
1.074 |
1.002 |
0.997 |
|
2007 |
80.13 |
36.32 |
43.80 |
15.61 |
28.20 |
1.037 |
1.100 |
0.999 |
1.033 |
0.934 |
0.991 |
|
2008 |
80.69 |
35.69 |
45.00 |
16.26 |
28.74 |
1.037 |
1.100 |
1.076 |
1.084 |
0.953 |
0.994 |
|
2009 |
81.01 |
35.07 |
45.94 |
16.94 |
29.01 |
1.037 |
1.100 |
1.065 |
1.078 |
0.953 |
0.994 |
|
2010 |
79.44 |
34.40 |
45.03 |
17.61 |
27.42 |
1.037 |
1.100 |
0.999 |
1.036 |
0.953 |
0.993 |
|
2011 |
77.47 |
33.70 |
43.77 |
18.29 |
25.48 |
1.037 |
1.100 |
0.984 |
1.029 |
0.950 |
0.994 |
|
2012 |
76.03 |
33.25 |
42.77 |
19.13 |
23.64 |
1.037 |
1.100 |
0.975 |
1.027 |
0.951 |
1.000 |
|
2013 |
74.65 |
32.83 |
41.82 |
20.03 |
21.80 |
1.037 |
1.100 |
0.969 |
1.027 |
0.950 |
1.002 |
| Notes: A factor is percent change expressed as a fraction, plus 1; e.g., the factor 1.021 corresponds to a 2.1 percentage increase over the previous year. E&M spending, non-E&M spending, and non-E&M intensity factors in italics are based on the assumption that E&M intensity is 3.7 percent for years 2005-2013. Imaging spending, and "other" spending and intensity values in italics are based on the assumption that E&M intensity is 3.7 percent and imaging intensity is 10 percent for years 2005-2013. Factors measuring price and number of beneficiaries are from the 2006 Medicare Trustees' Report; the price factor is based on percents reported as "Modified Physician Updates," p. 135. Spending decomposition is based on data from the 1996-2004 Physician/Supplier Procedure Summary Master Files. | |||||||||||
Footnotes
1 E.g., GAO, Medicare Physician Payments: Concerns about Spending Target System Prompt Interest in Considering Reforms.Washington GAO, Report #GAO-05-85, October 2004.
2 Data presented in this section are based on NORC’s analysis of allowed charges from the Physician/Supplier Procedure Summary Master Files (PSPSMFs) for years 1996-2004. These files and their use in SGR modeling are described in more detail below.
3 Utilization of chemotherapy and other drugs reflected in Tables 2 and 3 is only a portion of the drug spending included in the drug component of the SGR process, but its relatively rapid growth applies to the total, not just to the portion reflected in Tables 2 and 3.
4 CMS, Office of the Actuary, “Estimated Sustainable Growth Rate and Conversion Factor, for Medicare Payments to Physicians in 2002,” http://www.hcfa.gov/pubforms/actuary/sgr, March 19, 2001.
5 The SGR “process” refers to the entire update process. By contrast, the SGR is the factor used to compute spending targets, a part of the SGR process.
6 E.g., CMS, Estimated Sustainable Growth Rate and Conversion Factor for Medicare Payments to Physicians in 2006, December 21, 2005.
7 Two types of adjustments have been incorporated into the model. The first adjusts for year-to-year changes in actual and target spending that are used to determine the year’s payment update. The second adjusts for changes in total program spending based on the most recent data available from the Federal Register through late 2006 and in the 2006 Trustee’s Report (CMS, 2006 Annual Report of the Boards of Trustees of the Federal Hospital Insurance and Federal Supplementary Medical Insurance Trust Funds). This latter adjustment is embodied in total, cumulated spending estimates that are reported in tables describing hypothetical changes to the SGR process compared to spending under current law.
8 The model produced for this study was designed to also study the use of the SGR framework in estimating updates by type of service (Analysis of the Exemption of E&M Services on Alternative Spending Targets for Medicare Physician Payments, Final Report presented to DHHS/OS/ASPE, October 2006). Thus, modeling required estimates of various components of SGR physician spending. Predictions of the level and composition of spending on physician services included in SGR spending were not available from CMS publications. Instead, data from the PSPSMFs for years 1996-2004 were used to study spending for groups of services, e.g., E&M services, imaging procedures, and the remainder of non-E&M services that affect calculation of the SGR update. Spending shares for these groups of services were calculated and used to estimate spending by service group for the years 2005-2013. How predictions were obtained is summarized in the Appendix.
9 A recent citation of both theories and their relevance to current policy is on p. 79, of the Medicare Payment Advisory Commission’s (MedPAC’s) Report to the Congress: Increasing the Value of Medicare (MedPAC: Washington, DC), June 2006.
10 The primary determinant of the fee component of the SGR is the MEI, but the fee component also depends on measures of changes in drug and lab spending. In this analysis, it has been assumed that fee component of the SGR is the MEI for years 2008-2014.
11 The weight for the accumulation component was set to 0 (instead of 0.33) to examine the effect of removing the cumulative component of the UAF.
12 The previous-year weight was reduced from 0.750 to 0.375.
13 The PSPSMFs include data from all Medicare Part B Carriers. Each annual file represents procedure-specific billing data for physician/supplier services rendered to beneficiaries during the calendar year (e.g., 2004) and processed through June of the following year (e.g., June 30, 2005). Services included in the PSPSMFs that are included in spending used to calculate the physician update each year were identified using separate data files for 1998-2004, obtained from the CMS website. The latter files identify services and procedures (including special services, e.g., J-codes for drugs) covered under Medicare Part B in each calendar year. These files contain an indicator identifying whether spending for a service was included in the SGR calculation for a given year. The SGR indicator was added to the PSPSMF data. For services rendered during 1996 and 1997, the SGR indicator from the 1998 list was used. Certain types of services (e.g., some outpatient lab services) are not included in the PSPSMF data but are included in the SGR calculation. Thus, expenditure estimates are somewhat less than total annual expenditures used in the calculation of payment updates. But differences are small. For example, total physician spending for 2000 from the PSPSMF is $47.0 billion, whereas CMS’s estimate used in calculating the 2001 CF was $46.8 billion.
