December 2020
Link to Printer Friendly Version in PDF Format (12 PDF pages)
ABSTRACT: Policymakers and care providers all over the world recognize that the risk of infection and of death from COVID-19 increases with age and among individuals with pre-existing conditions, especially diabetes and heart disease. Because many younger adults and children with physical or intellectual disabilities also have these and other medical conditions, they are also at higher risk of becoming seriously ill and dying from COVID-19 infections. Most highly developed countries as well as some countries with emerging economies are tracking rates of infection and deaths from COVID-19 among high-risk subsets of their populations. Due to the concern over infection rates in congregate settings, as of October 2020 most of the focus has been on rates of infection and death in residential long-term care (LTC) facilities serving the elderly (persons 65 and older) exclusively or predominantly. However, despite the dearth of comparable statistics about rates of COVID-19 infections and deaths among LTC users not residing in nursing homes or related residential care facilities, the available evidence suggests that COVID-19 infection rates are likely to be lower among the elderly and people of all ages with disabilities and chronic medical conditions who reside and receive assistance "at home." In this brief, we summarize the available data and literature on the cross-national impact of COVID-19 in LTC settings as of October 2020 and the changes in reported death rates since June 2020.
This brief was prepared through intramural research by the U.S. Department of Health and Human Services, Office of the Assistant Secretary for Planning and Evaluation, Office of Behavioral Health, Disability, and Aging Policy. For additional information about this subject, visit the BHDAP home page at https://aspe.hhs.gov/bhdap or contact the authors at HHS/ASPE/BHDAP, Room 424E, H.H. Humphrey Building, 200 Independence Avenue, S.W., Washington, D.C. 20201; Pamela.Doty@hhs.gov, Martin.Blanco@hhs.gov.
DISCLAIMER: The opinions and views expressed in this brief are those of the authors. They do not reflect the views of the Department of Health and Human Services, the contractor or any other funding organization. This brief was completed and submitted on November 17, 2020.
Introduction
Policymakers and care providers all over the world recognize that the risk of infection and of death from the Coronavirus 2019 (COVID-19) increases with age and among individuals with pre-existing conditions, especially diabetes and heart disease. Because many younger adults and children with physical or intellectual disabilities also have these and other medical conditions, they are also at higher risk of becoming seriously ill and dying from COVID-19 infections. Most highly developed countries as well as some countries with emerging economies are tracking rates of infection and deaths from COVID-19 among high-risk subsets of their populations. Due to the concern over infection rates in congregate settings, to date (October 2020) most of the focus has been on rates of infection and death in residential long-term care (LTC) facilities serving the elderly (persons 65 and older) exclusively or predominantly. However, despite the dearth of comparable statistics about rates of COVID-19 infections and deaths among LTC users not residing in nursing homes or related residential care facilities, the available evidence suggests that COVID-19 infection rates are likely to be lower among the elderly and people of all ages with disabilities and chronic medical conditions who reside and receive assistance "at home." In this brief, we summarize the available data and literature on the cross-national impact of COVID-19 in LTC settings as of October 2020 and the changes in reported death rates since June 2020.
Cross-National Comparative COVID-19 Infection/Death Rates among Nursing Home Residents as a Percentage of Total COVID-19 Deaths
Countries differ in how they collect and analyze data about COVID-19 infection and death rates among residents of LTC facilities. In addition, countries employ different terminology for their LTC facilities. Many countries distinguish between more and less "medicalized" LTC facilities (similar to the distinction made in the United States (U.S.) between "nursing homes" and "assisted living"). The comparative statistics cited here (unless otherwise noted) are from International Long-term Care Policy Network (ILPN) reports (Comas-Herrera et al., 2020a, 2020b), which are updated periodically on the ILPN COVID-19 website at the London School of Economics. Because countries use many different terms to characterize residential LTC settings that primarily provide care to older adults aged 65+, the ILPN refers to these facilities as "care homes." This brief refers to "care homes" when referencing ILPN reports and otherwise employs the term LTC facilities.
The following methodological differences in reporting COVID-19 cases and deaths also somewhat hamper comparability of reported figures.
-
Whether deaths are included only if there had been a positive COVID-19 test versus the inclusion of "probable" COVID-19 cases (those with symptoms but no test prior to death).
-
Whether counts include only deaths of residents occurring in nursing homes or also deaths in hospitals of persons normally residing in nursing homes.
-
Whether "excess deaths" among nursing home residents (those exceeding the number for a previous time period such as the same month the previous year) are attributed to COVID-19.
It is also worth noting that the U.S. compared to most other highly developed countries (with the exception of Italy and Japan among the G-7) has lower rates of care home use among older adults. Accordingly, U.S. care home residents are likely more severely disabled on average compared to care home residents in countries with higher rates of residential care use per 1,000 adults aged 65 and older. An OECD report (2020) suggests that the higher rate of COVID-19 deaths in France compared to other OECD member countries may be attributable to higher rates of residence in LTC facilities among older adults in France compared to those other countries.
Researchers affiliated with the London School of Economics' ILPN have been analyzing reports of COVID-19 infections and deaths of residents of LTC facilities or in LTC facilities based on statistics -- primarily official statistics -- from 26 countries. ILPN researchers update their analyses periodically. This brief relies on the published reports dated June 26 (Comas-Herrera et al., 2020a) and October 14 (Comas-Herrera et al., 2020b). These analyses indicate that, insofar as comparative data can be standardized, the rate of COVID-19 deaths of care home residents as a percentage of all COVID-19 deaths cross-nationally remained similar in both time periods: 47% in the June report and 46% in October (based on 21 countries' reports of deaths of individuals with confirmed cases of COVID-19).
Unlike most of the data sources for countries included in the ILPN report, the U.S. statistics that the report references are not based entirely on official U.S. government statistics. The estimates reported in both the June and October 2020 reports are extrapolations from Centers for Medicare & Medicaid Services (CMS) statistics and other private sources, including data collected by the Kaiser Family Foundation (KFF), the Atlantic newsmagazine, and Johns Hopkins University. The definition of U.S. "LTC facilities" that the KFF uses includes not only nursing homes but assisted living and related residential elder care facilities (which may be labeled "personal care" homes, "residential care" homes or something else depending on state regulatory requirements). This makes the U.S. numbers on "care homes" comparable to the data for the other countries since it includes both nursing homes and assisted living. Some state-specific statistics also report COVID-19 deaths associated with adult day care centers, although most of these closed early in the pandemic. However, it is important to bear in mind that the U.S. data initially included "confirmed" cases only, although, as of October, the U.S. statistic reported included both confirmed and probable COVID-19 deaths.
In June, among nine countries that counted only confirmed cases, Slovenia had the highest percentage (81%) of care home residents among all COVID-19 deaths. The U.S. had the second highest percentage of care home residents among all COVID-19 deaths (45%). Among other countries reporting only "confirmed" COVID-19 deaths, the percentages of nursing home residents among all decedents were 8% in Singapore, 24% in Hungary, 28% in Australia, 32% in Israel, 34% in Austria and South Korea, 35% in Denmark, and 39% in Germany. Germany included care homes in a broader category of "communal residences" that included homes for younger people with disabilities, homeless shelters, housing, including detention centers, for asylum seekers and other refugees, some of whom awaited repatriation, and prisons. As a result, Germany's statistic may be artificially low.
| FIGURE 1. Number of Care Home Resident Deaths as % of all COVID-19 Deaths by Country and Approach to Measuring Deaths (June 2020) |
|---|
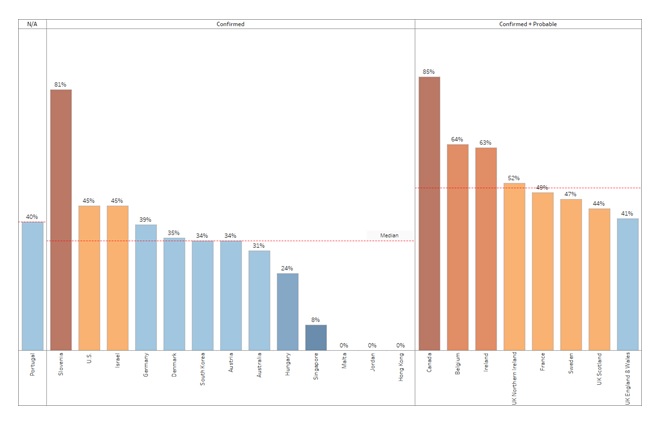 |
| SOURCE: Comas-Herrera, et al. June 2020. Mortality Associated with COVID-19 Outbreaks in Care Homes; Early International Evidence. NOTE: This figure shows the number of care home resident deaths as a percent of all COVID-19 deaths by country. This figure also shows the differences in reported deaths based on the approach to measuring deaths. Portugal does not have reports published however, the Government of Portugal released to the media the number of deaths in nursing homes. Norway, Finland, Spain, and New Zealand did not have data on number of care home resident deaths as a percent of all COVID-19 deaths by country. |
In countries that reported both confirmed and probable COVID-19 deaths, residents of care facilities generally accounted for higher percentages of total COVID-19 deaths compared to countries reporting only confirmed cases. In June (Figure 1), Canada reported the highest percentage of nursing home residents among total COVID-19 confirmed and probable deaths (85%) and England/Wales the lowest (41%). Percentages of nursing home residents among total confirmed and probable COVID-19 deaths were 43% in Northern Ireland, 44% in Scotland, 47% in Sweden, 49% in France, 63% in Ireland, and 64% in Belgium.
As of October, the U.S. had joined the countries reporting both confirmed and probable COVID-19 deaths and reported 41% of all COVID-19 deaths being of care home residents. Among countries reporting deaths among confirmed cases only and countries reporting deaths among confirmed and probable cases, Canada again reported the highest rate (80%), followed by Spain (63%), Belgium (61%), Sweden (46%), France (46%), the United Kingdom (U.K.; 44%), and Germany (39%). South Korea, which reported only confirmed COVID-19 deaths had the lowest rate among developed countries (8%).
| FIGURE 2. Number of Care Home Resident Deaths Attributed to COVID-19 as % of all Care Home Residents/Beds (October 2020) |
|---|
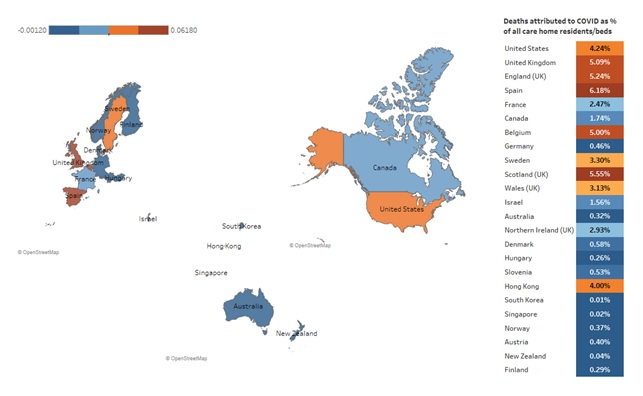 |
| NOTE: This heat map highlights the differences in deaths attributed to COVID as a percent of all care home residents/beds (October 2020). Includes countries reporting confirmed cases only and those reporting both confirmed and probable cases. |
In their October report, the ILPN researchers suggested that a different measure -- the percentages of COVID-19 resident deaths among all care facility residents -- may be a more useful measure of the relative impact across different countries of COVID-19 on care facilities. In June, COVID-19 deaths as a percentage of care home residents ranged from a low of 0.4% in New Zealand to a high of 6.1% in Spain. In October (Figure 2), the ILPN authors reported that the share of all care home residents whose death was linked to COVID-19 ranged from 0.01% in South Korea to over 4% (which would mean that over one in 25 care home resident deaths was linked to COVID-19, in Spain (6.18%), the U.K. (5.09%), Belgium (5%) and the U.S. (4.24%). The proportion of COVID-19 deaths among all care home residents was found to be highly correlated to the percentage of COVID-19 deaths in the population living outside care homes.
Only England has reported detailed statistics on the ethnicity of care home residents who died from COVID-19, reporting that death rates of nursing home residents were disproportionately higher among Black and Asian residents compared to White residents, and the highest death rate was among residents of Bangladeshi origin (Booth, 2020).
Explaining the Variation in Infection and Death Rates in LTC Facilities Cross-Nationally
ILPN researchers have been reluctant to offer potential explanations as to why COVID-19 infection and death rates among LTC residents as a percentage of all COVID-19 infections and deaths have varied so greatly. According to Davson et al., (2020) not enough information is available to do so and they do not want to encourage premature conclusions that could turn out later to be mistaken. A study by the Canadian Institute for Health Information (CIHI) published in June 2020 analyzed OECD statistics on reported COVID-19 infection and death rates. The authors suggest that countries that implemented specific, mandatory prevention measures targeted to the LTC sector at the same time as their stay-at-home orders and closure of public places had fewer COVID-19 infections and deaths in the LTC sector. These prevention methods included immediate infection control measures such as broad LTC testing and training, isolation wards to manage clusters and additional supports for LTC workers such as hazard pay, surge staffing, specialized teams and personal protective equipment (PPE) had fewer infections and deaths in LTC facilities. The countries that implemented the greatest number of such policies and had lower rates of COVID-19 infections and deaths in LTC facilities include Austria and Australia. Conversely, countries that did not implement many of these preventive policies early in the pandemic (e.g., Canada, the U.S., France, the U.K., and Spain) experienced comparatively higher rates of COVID-19 infections and deaths in LTC facilities.
Canadian Prime Minister Justin Trudeau responded to the CIHI report finding that Canada's percentage of COVID-19 deaths in LTC facilities was twice as high as the average of other highly developed countries. He told reporters at a news conference outside his home in Ottawa: "I think one of the things that is very clear is our current system of supporting seniors across this country has not worked." The Canadian LTC system compared to that of other economically advanced countries, including the U.S., is exceptionally de-centralized. Trudeau stated: "It is a provincial responsibility. So it is them that ... have failed to support our seniors ... What this recent report has shown, and quite frankly what this pandemic has shown from the very beginning, is that the job isn't being adequately done in long-term care centres across the country." He went on to say, "We will continue to work with the premiers on ensuring that our long-term care centres are properly supported, whether that's by bringing in national standards, whether that's by extra funding, whether that's by looking at the Canada Health Act." A CBC reporter covering the press conference interpreted Trudeau's comments as suggesting that the federal government might decide to take a larger role in financing and regulating LTC (Tunney, 2020).
Compared to other countries, Denmark experienced low infection and mortality rates from COVID-19, including in care homes, although one-third of COVID-19 deaths were of care home residents. A report published on the ILPN website in May identified a number of factors that the authors believe contributed to the relative success of Denmark in preventing and containing infections and deaths in care homes (Rostgaard, 2020). Many are the same as those highlighted in the Canadian report. These protective factors included:
-
A quick lock-down of the country.
-
A de-centralized and integrative approach to LTC. That is, municipalities are responsible for both LTC and medical care for frail elderly outside of hospitals. (Although the Canadian report questioned the wisdom of de-centralization of responsibility, Canada is a much larger country compared to Denmark and de-centralization to municipalities is different from de-centralization to large provinces).
-
Relatively few and large municipalities (98 in total) which ensures a more effective and coordinated approach.
-
Political attentiveness to and broad public support for LTC.
-
Due to de-institutionalization, care for frail older people more often provided in the home.
-
Care provided by formally employed and well-trained staff.
-
The majority of nursing homes are public and modern in providing private rooms/apartments.
However, the authors also cited several factors that may have interfered with containment of the virus. These included:
-
A testing strategy that changed a number of times and did not initially consider the need to test nursing home residents and staff.
-
PPE was initially prioritized for the health care sector, so municipal care providers had to find alternative ways to secure protection.
-
Guidelines regarding the use of PPE in the nursing home sector have also been inconsistent.
A report by researchers in New Zealand credits widespread testing and aggressive contact tracing both in the population at large and in LTC facilities with enabling New Zealand to control the spread of COVID-19 much more effectively than has been the case in many other countries (Ma'u, 2020). Austria has long relied heavily on migrant labor to staff the LTC sector and policies allowing the emergency importation of additional migrant workers to provide care both in facilities and at home may have helped maintain adequate staffing levels. Migrant workers are tested for COVID-19 prior to entering the country via special transport and are also quarantined for 14 days before beginning to work. They may not travel freely back and forth to their home countries (e.g., job sharing and alternating bi-weekly shifts) as previously permitted. Migrant workers are also being offered financial incentives to remain in Austria until after the pandemic has ended -- although not necessarily to immigrate permanently to Austria (Dawson et al., 2020). However, this policy of high reliance on migrant labor has also been criticized, especially in view of the risks to migrant workers and the high levels of emotional stress they have reportedly experienced (Dawson et al., 2020; Schmidt et al. 2020).
COVID-19 cases and death rates in nursing facilities were much lower in Japan compared to Western European countries. Japanese health officials and other health experts interviewed for a Washington Post article looking to draw lessons from Japan's experience mentioned that hygiene standards were already quite high (e.g., frequent handwashing) and infection control policies had already been prioritized in Japanese facilities to protect residents against risks posed to disabled older adults by influenza and norovirus which were known to spread readily in such settings. They also mentioned the lower rates of certain pre-existing conditions found to be associated with severe and fatal COVID-19 infections -- in particular, diabetes and obesity -- among Japanese elderly compared to elderly in the U.S. and other Western countries. However, Japan has also had community transmission rates for COVID-19 much lower than those of most countries, especially those not in Asia or in the Southern Pacific. (Denyer & Kashiwagi, 2020).
David Grabowski (2020) summarized the findings of U.S. studies carried out by researchers at Harvard University and elsewhere. Using data from 30 states, they found that nursing homes reporting at least one COVID-19 case early in the pandemic tended to be bigger, more urban, and had a higher share of African American residents. Facility characteristics found to be unrelated or only very weakly related included: quality scores on the CMS Nursing Home Compare 5-Star Quality Rating Index, having a prior infection control violation on inspection reports, for-profit (rather than non-profit or public) ownership, being part of a nursing home chain, and having a high proportion of Medicaid residents. The researchers concluded that individual facilities were seldom to blame for having COVID-19 cases. Preventing COVID-19 in nursing homes is a system level problem in need of system level solutions. Suggested solutions included: systematic COVID-19 testing for LTC facility staff and residents, PPE and infection control, workforce support policies (e.g., paid sick leave, hazard pay and bonuses), investment in home care alternatives, transparency for families and other stakeholders, and post-acute preparedness (e.g., testing everyone leaving hospitals, creating specialized COVID-only settings).
Infection and Death Rates among Older People with Dementia
Another cross-national ILPN report (Suarez-Gonzalez et al., 2020), focused specifically on infection and death rates among older people with dementia. Data were collected from nine countries: the U.K., Spain, Ireland, Italy, Australia, the U.S., India, Kenya and Brazil. The share of deaths related to COVID-19 of people with dementia in care homes ranged from 29% to 75%. However, national level data were only available from three countries of the U.K. (England, Wales, and Scotland) and from Italy. Death rates of people in care homes with dementia ranged from 19% in Italy, to 25% in England and Wales, and 31% in Scotland. Differences in data collection and reporting systems, often within countries, greatly hampered cross-national comparisons of COVID-related death rates among care facility residents with dementia. The authors expressed concern that "the basic human rights of people with dementia may have been compromised during the pandemic. These rights include access to intensive care units, hospital admissions, health care and palliative care. The controversial ban on visits (including spouses and care partners) to care homes across the world, have kept people with dementia detached from essential affective bonds and provision of family care for many months. There is now a pressing need and also an opportunity for innovation, looking at new ways of providing services such as allowing visits to care homes and access to health care."
Infection and Death Rates among Users of Publicly-Funded Non-institutional Care
Few countries appear to be tracking COVID-19 deaths among people with LTC needs living outside of institutional settings. Australia and Sweden are rare exceptions. In Australia, as of May 18 only three of 99 COVID-19 deaths had occurred among recipients receiving publicly-funded services delivered in their own homes, whereas 29% of all COVID-19 deaths were of care home residents (Low, 2020). In Sweden, as of July 22, 47 % of all COVID-19 deaths in Sweden were of care home residents and an additional 25% were of publicly-funded home care recipients. Thus, a total of 72% of all COVID-19 deaths in Sweden were of LTC users. LTC users who died represented 3.1% of all care home residents and 0.8% of all home care users (Szebehely, 2020).
In the U.S., published statistics on death rates among elderly LTC users by setting are available for only one state, Minnesota. According to cumulative totals on May 30, 2020, older people in LTC facilities accounted for over four-fifths of total COVID-19 deaths: 56% of total deaths were in nursing facilities, 22% were in assisted living facilities, 3% were in memory centers, and only 19% were in community settings (Arling & Arling, 2020).
Policy Responses Undertaken in Various Countries to Control the Spread of COVID-19 in the Long-Term Care Sector
According to the Dawson et al. (2020) research:
-
A number of countries have closed adult day care centers on the assumption that lack of social distancing in such settings would promote spread of the virus (China, Germany, Italy, South Korea) and Germany has also closed respite centers.
-
However, some countries have expanded bed capacity in residential care facilities (Austria, Italy) or redeployed home care workers to care facilities (Germany).
-
Most countries have faced worker shortages and have taken various steps to recruit more workers:
-
Germany now allows volunteers and family to be hired and reimbursed the same hourly wages as home care agency workers under the LTC insurance program for up to 3 months. Anyone with health credentials who had left the health care field are being encouraged to volunteer and may be freed up without penalty from other jobs
-
South Korea will pay volunteers and family at regular agency aide hourly wage rates after 2 hours of training.
-
Brazil is seeking to recruit 400,000 volunteer home care workers.
-
Ireland has also launched a national campaign to recruit volunteer care workers.
-
England launched a media campaign to recruit 20,000 social care workers within 3 months. Individuals who agree to work can be paid and those workers furloughed from other jobs and currently receiving 80% pay from those jobs can continue to receive this income without penalty while also being paid to provide social care (in home or in facility).
-
England is offering life insurance that will pay out £60,000 to families of care workers who die from COVID-19. Those who are infected and cannot work will continue to receive 80% pay and their sick leave has been increased. They are also eligible for other tax preferences.
-
Wales is offering £500 bonuses to care workers and has increased the minimum wage.
-
Scotland has increased pay for care workers by 3.3%.
-
Austria is recruiting migrant care workers from Bulgaria and Romania. Their transportation, accommodations, testing is covered, and they are paid while in quarantine awaiting test results. They also receive a bonus (one-time 500 euros) if they agree to remain in Austria. Some regional governments offer monthly bonuses to migrant care workers.
-
Several countries are offering pay incentives and other incentives to recruit care workers from within the country. In Germany, two states are offering one-time recruitment bonuses, minimum wage increases, and additional sick leave. Australia is offering after tax bonuses of $800 Australian dollars quarterly for up to two quarters for home care workers.
-
Additional LTC delivery system and regulatory changes include:
-
Germany has suspended quality assessments for care recipients in residential care and at home.
-
The Netherlands is only providing formal home care to individuals with high (essential) care needs and no family caregivers. Up to two informal caregivers are exempt from stay-at-home restrictions to provide care.
-
Hong Kong has reduced non-essential services, giving providers more flexibility.
-
Several countries have replaced reusable with disposable containers for meals-on-wheels deliveries (Australia, Hong Kong).
-
Australia has increased funding for home delivered meals and grocery shopping.
-
A number of countries are prioritizing continuity of care and using telephonic, video, online mechanisms for social supports to counter the adverse effects of social isolation and loneliness.
Conclusion
A review of the available literature and data as of October 2020, shows that the impact of COVID-19 on LTC populations residing in congregate settings has been significant across most countries, with a high percentage of the total deaths from COVID-19. The specific country data is difficult to compare based on different definitions, and because some countries use confirmed COVID-19 cases, whereas other use confirmed and probable cases. There was great variation across countries no matter which measure they used. However, across 21 countries, including those reporting deaths only among confirmed cases and those reporting deaths among probable as well as confirmed cases, the average percentage of care home resident deaths of all reported COVID-19 deaths was nearly the same in October (46%) as it had been in June (47%). Among nursing home residents, cross-national death rates again varied greatly, but some countries reported much higher death rates compared to others. As of October 2020, over one in 25 care home residents were reported to have died of COVID-19 in five countries: Belgium, Ireland, Spain, the U.K. and the U.S. Less is known about the impact of COVID-19 for populations receiving LTC outside of congregate settings, but preliminary reports indicate that the rates of infection and death are much less than in institutional settings. Countries have tried a number of policy responses to serve this high-risk population including attempts to deliver more LTC in the community, as well as efforts to address LTC worker shortages. LTC populations, particularly in congregate settings, will be an important group for countries to focus on as they address the COVID-19 pandemic.
Sources
Arling, Greg, & Priscilla Arling. 2020 (July). The COVID-19 Long-Term Care Situation in the state of Minnesota. Available at https://ltccovid.org/2020/07/27/new-report-the-covid-19-long-term-care-situation-in-the-state-of-minnesota-usa/.
Booth, Robert. 2020 (June). BAME Care Home residents in England more likely to die of COVID-19. The Guardian. "BAME" is an acronym for Black, Asian, Minority Ethnicities. Statistics cited are from the Care Quality Commission and also from the English Department of Health and the Office for National Statistics, Institute for Fiscal Studies. Available at https://www.theguardian.com/world/2020/jun/17/bame-care-home-residents-in-uk-more-likely-to-die-of-covid-19.
Canadian Institute for Health Insurance (CIHI). 2020 (June). Pandemic Experience in the Long-Term Care Sector: How Does Canada Compare with Other Countries? CIHI Snapshot. Available at https://www.cihi.ca/sites/default/files/document/covid-19-rapid-response-long-term-care-snapshot-en.pdf?emktg_lang=en&emktg_order=1.
Comas-Herrera, Adelina, Joseba Zalakain, Charles Litwin, Amy T. Hsu, Elizabeth Lemmon, David Henderson, & Jose-Luis Fernandez. 2020a (June). Mortality Associated with COVID-19 Outbreaks in Care Homes; Early International Evidence. London School of Economics, International Long-term Care Policy Network. Available at https://ltccovid.org/wp-content/uploads/2020/06/Mortality-associated-with-COVID-among-people-who-use-long-term-care-26-June-1.pdf.
Comas-Herrera, Adelina, Joseba Zalakain, Elizabeth Lemmon, David Henderson, Charles Litwin, Amy T. Hsu, Andrea E. Schmidt, Greg Arling, & Jose-Luis Fernandez. 2020 (October). Mortality Associated with COVID-19 in Care Homes: International Evidence. London School of Economics, International Long-term Care Policy Network. Available at https://ltccovid.org/wp-content/uploads/2020/10/Mortality-associated-with-COVID-among-people-living-in-care-homes-14-October-2020-3.pdf.
Dawson, Walter D., Elizabeth C. Ashcroft, Klara Lorenz-Dant, & Adelina Comas-Herrera. 2020 (May). Mitigating the Impact of the COVID-19 Outbreak: A Review of International Measures to Support Community-Based Care. London School of Economics, International Long-term Care Policy Network. Available at https://ltccovid.org/wp-content/uploads/2020/06/Community-Based-Care-Report-19-May.pdf.
Denyer, Simon, & Akiko Kashiwagi. 2020 (August). Japan has the world's oldest population. Yet it dodged a coronavirus crisis at elder care facilities. Washington Post. Available at https://www.washingtonpost.com/world/asia_pacific/japan-coronavirus-elderly-death-rate/2020/08/29/f30f3ca8-e2da-11ea-82d8-5e55d47e90ca_story.html.
Grabowski, David. 2020 (June). COVID-19 and Nursing Homes. Online webinar presentation to the Long-Term Care Discussion Group. Available at http://www.ltcdiscussiongroup.org/archives_182_1008427804.pdf.
Low, Lee-Fay. 2020 (April). The Long-Term Care COVID-19 Situation in Australia. London School of Economics, International Long-term Care Policy Network. Available at https://ltccovid.org/wp-content/uploads/2020/04/Australia-LTC-COVID19-situation-24-April-2020.pdf.
Ma'u, Etuini, Jackie Robinson, Gary Cheung, & Sarah Cullum. 2020 (June). COVID-Related Deaths in LTC in Aotearora New Zealand: Brief Report. London School of Economics, International Long-term Care Policy Network. Available at https://ltccovid.org/2020/06/23/covid-related-deaths-in-ltc-in-aotearoa-new-zealand-brief-report/.
OECD. 2020 (June). Workforce and Safety in Long-term Care during the Coronavirus Pandemic. Available at https://read.oecd-ilibrary.org/view/?ref=134_134521-x99q1iutux&title=Workforce-and-Safety-in-Long-Term-Care-during-the-COVID-19-pandemic.
Rostgaard, Tine. 2020 (May). The COVID-19 Long-Term Care Situation in Denmark. London School of Economics, International Long-term Care Policy Network. Available at https://ltccovid.org/wp-content/uploads/2020/05/The-COVID-19-Long-Term-Care-situation-in-Denmark-29-May-2020.pdf.
Schmidt, Andrea E., Kai Leichsenring, Heidemarie Staflinger, Charles Litwin, & Annette Bauer. 2020 (April). The Impact of COVID-19 on Users and Providers of Long-Term Care Services in Austria. London School of Economics, International Long-term Care Policy Network. Available at https://ltccovid.org/2020/04/16/the-impact-of-covid-19-on-users-and-providers-of-long-term-care-services-in-austria/.
Suarez-Gonzalez, Aida, Gill Livingston, Lee-Fay Low, Suzanne Cahill, Niamh Hennelly, Walter D. Dawson, Wendy Weidner, Martina Bocchetta, Cleusa P. Ferri, Jordi A Matias-Guiu, Suvarna Alladi, Christine Wayua Musyimi, & Adelina Comas-Herrera. 2020 (August). Impact and Mortality of COVID-19 on People Living with Dementia: Cross-Country Report. London School of Economics, International Long-term Care Policy Network. Available at https://ltccovid.org/2020/08/19/impact-and-mortality-of-covid-19-on-people-living-with-dementia-cross-country-report/.
Szebehely, Marta. 2020 (July). The Impact of COVID-19 on Long-Term Care in Sweden. London School of Economics, International Long-term Care Policy Network. Available at https://ltccovid.org/wp-content/uploads/2020/07/The-COVID-19-Long-Term-Care-situation-in-Sweden-22-July-2020-1.pdf.
Tunney, Catharine. 2020 (June). Provinces "failed to support seniors" Trudeau says following release of troubling new pandemic study. CBC News. Available at https://www.cbc.ca/news/politics/long-term-care-challenge-1.5626841.
