Judith Wooldridge, Mathematica Policy Research, Inc.
Ian Hill, The Urban Institute ,
Mary Harrington, Mathematica Policy Research, Inc. ,
Genevieve Kenney, The Urban Institute ,
Corinna Hawkes, The Urban Institute ,
Jennifer Haley, The Urban Institute
with assistance from
Hilary Bellamy, Health Systems Research, Inc. ,
Renee Schwalberg, Health Systems Research, Inc.
Submitted to:
Department of Health and Human Services
Office of the Assistant Secretary for Planning and Evaluation
200 Independence Avenue S.W.
Washington, DC 20201
Submitted by:
Mathematica Policy Research, Inc.
P.O. Box 2393
Princeton, NJ 08543-2393
(609) 799-3535 and
The Urban Institute
2100 M Street, NW
Washington, DC 20037
Project Director: Judith Wooldridge
"Executive Summary
In 1997, Congress passed legislation creating the State Children’s Health Insurance Program (SCHIP), the first major federally funded health program to be established since Medicare and Medicaid were enacted in 1965. SCHIP, authorized by a new Title XXI in the Social Security Act, was designed to extend health insurance to approximately 40 percent of the then-estimated 10 million uninsured children. The SCHIP legislation offered states the option to expand Medicaid, create a separate program, or undertake a combination of both. The separate program option provides states with broad flexibility to adopt many design features of private health insurance, such as premiums, cost-sharing, and mainstream benefit packages.
In the Balanced Budget Refinement Act of 1999, Congress mandated that the Department of Health and Human Services (DHHS) conduct an evaluation of ten states’ SCHIP programs, and further directed that a wide range of issues be addressed, including, among others, SCHIP enrollment and disenrollment dynamics, the impact of SCHIP and Medicaid enrollment practices on enrollment of children, and coordination between SCHIP and Medicaid. The mandate also required surveys of the target population—enrollees, disenrollees, and children who are eligible for but not enrolled in SCHIP. The evaluation began in January 2000, under the guidance of the DHHS’ Office of the Assistant Secretary for Planning and Evaluation (ASPE). This Report to Congress is the first from the evaluation and is based on information collected during 2001. Final results from the surveys and additional findings from the evaluation will be available in the final Report to Congress in 2004.
This report draws primarily on findings from case studies in six of the ten states selected for the evaluation, whose early experiences implementing SCHIP have been examined closely: California, Colorado, Louisiana, Missouri, New York, and Texas (Hill et al. 2002). Case study respondents interviewed in the case studies included state officials, advocates, plan staff, and providers. Also, to assess the program from the perspective of the low-income families whose children SCHIP targets, the report draws heavily on findings from focus groups conducted with parents of low-income children who (1) are enrolled in SCHIP and/or Medicaid, (2) are disenrolled from SCHIP and/or Medicaid, (3) would be eligible for SCHIP except that they are privately insured, and (4) who are eligible for public coverage but not enrolled (Bellamy et al. 2002). The findings from these qualitative studies are supplemented by analyses of awareness of and perceptions about SCHIP and Medicaid among low-income uninsured families nationwide, based on preliminary data collected using the State and Local Area Integrated Telephone Survey (SLAITS) (Kenney et al. 2002). The report also includes an analysis of retention and enrollment turnover using SCHIP administrative data from three states. Finally, the report draws on an ASPE-sponsored study of three states (New Jersey, Rhode Island, and Wisconsin) that have introduced coverage for parents under Title XXI (Kaye, Wysen, and Pernice 2001).
The nearly five years since the creation of the State Children’s Health Insurance Program (SCHIP) have witnessed substantial growth in publicly funded health systems for children. All states implemented Title XXI initiatives over this period (one-third solely through expansions of Medicaid, and two-thirds by creating separate programs, either alone or in combination with Medicaid expansions). These programs have increased the national average income eligibility threshold for subsidized coverage of children nearly twofold, to 214 percent of the federal poverty level (FPL). In fiscal year (FY) 2002, 5.3 million children were insured by SCHIP at some time during the year (CMS 2003).
The trends in the six states discussed in this report mirror the overall national trends closely. Except for Texas, the states studied had implemented the major portion of their SCHIP expansions within roughly one year of passage of the SCHIP law. Four states chose to create separate programs, while two expanded coverage of children through Medicaid. The average income eligibility threshold for children now stands at 231 percent of FPL in the six study states—slightly above the national average. Because the six study states include the three largest SCHIP programs in the nation, enrollment in these states makes up a large share of national total enrollment; indeed, in FY 2002, over 2.6 million children were covered by SCHIP in the six study states. (CMS 2002).
Based on the analyses conducted for this first Report to Congress, the following sections highlight SCHIP’s successes as well as the challenges that face the program. The data available for this interim report suggest that states have learned much about how to design and operate a successful children’s health insurance program, that they acted quickly to implement their programs and have accomplished much since the program began. At the same time, the analyses reveal disparities and problems that remain to be addressed if the program is going to more fully realize its potential to cover and improve the care and health of uninsured children. The final Report to Congress will provide additional, more rigorous analyses of the issues covered in this report; it is also expected to shed light on emerging new questions concerning SCHIP and Medicaid and low-income children.
Successes
High Enrollee Satisfaction. State officials and advocates responding to case study interviews report that families are satisfied with SCHIP. Focus group participants with children enrolled in SCHIP and Medicaid bear out these reports. Families like the low price, the range of benefits, and the access to providers that the programs offer. While these findings must be considered preliminary, the survey of parents in ten states, whose findings will be reported in the final Report to Congress, will provide richer and more detailed information about enrollee satisfaction.
Millions of Low-Income Children Enrolled. The flexibility afforded by Title XXI allowed states to adopt the program designs that best met their needs. Some states elected Medicaid expansions both as a means of extending Medicaid’s broad coverage to more children and because it was administratively efficient. Others chose separate programs in order to use features of private insurance, and sometimes to avoid saddling the new program with longstanding negative associations that many had with Medicaid. Regardless of their program choice, however, most states enjoyed strong support for implementing a SCHIP program.
States began implementing their SCHIP programs soon after the law was passed, and enrollment has grown continuously ever since. By the end of 1998, about 1 million children had been enrolled (CMS, 2002). Enrollment grew steadily so that by FY 2002, 5.3 million children were covered under the program at some time during the year—a 15 percent increase over the numbers enrolled in FY 2001. The growth from year to year was fueled both by increases in the number of states operating a program (all but two states had programs up and running by the second anniversary of SCHIP’s enactment) and by aggressive outreach to and simpler enrollment processes for families with eligible children. While quantitative evidence is scant, state officials who were interviewed in the study states indicate that Medicaid enrollment has increased as a result of SCHIP outreach.
Streamlined Program Entry. Nearly all states developed simple application and enrollment processes for their separate SCHIP programs. Aspects of typical SCHIP application processes include short, joint applications for SCHIP and Medicaid, mail-in application options, and telephone-based or local hands-on application assistance. Few use an asset test (a common feature of Medicaid applications in the past for families and children on welfare), and many have 12-month continuous eligibility periods and require only minimal documentation to prove eligibility. State officials believe that these features have been crucial to their successful enrollment of children in SCHIP.
Some of the design features of SCHIP have spilled over to Medicaid. For example, due to reforms in California and Texas, children can now apply for Medicaid, too, by mail, and documentation requirements have been reduced. To the extent that such reforms make Medicaid and SCHIP more alike, coordination and family transitions between the two programs become smoother. The cumulative effect of the streamlining has been a “reinvention” of public health insurance—a replacement of the old welfare-style program with a more accessible, consumer- driven program.
Strategic Outreach. Based on their experience, states have continued to adopt new outreach strategies for SCHIP that they expect to be more effective. While the early emphasis in outreach was on statewide mass media campaigns to establish an identity for the new programs, community-based efforts have since played an increasingly important role. Community-based outreach, often conducted by local organizations and trusted community groups, is often used to target hard-to-reach families and subpopulations.
Broad and Affordable Benefits. Medicaid benefits are usually more comprehensive than benefits covered under separate state SCHIP programs. But SCHIP programs, too, offer broad benefits that were consistently described as much broader than benefits offered in private health insurance. Case study respondents and focus group participants said SCHIP benefits met the needs of the vast majority of children.
Many states require modest cost-sharing, including premiums, enrollment fees, and co- payments in their separate SCHIP programs. According to case study respondents interviewed for this study, as well as most focus group participants, families consider the cost-sharing reasonable and not overly burdensome, financially. Also, many of those interviewed support the cost-sharing requirements in SCHIP because they believe that they encourage “pride of ownership” and appropriate use of services. An additional reason that states have included cost- sharing is to discourage families with private insurance coverage from disenrolling from that coverage and substituting public coverage. However, the impacts of premiums on SCHIP participation will be rigorously assessed later in this study.
Apparent Good Access to Care. Overall, access to care under SCHIP was described by case study respondents as good, especially in urban areas. In large part, this was attributed to states’ widespread use of managed care arrangements, which have reportedly helped increase both the supply of participating providers and the number of children with a “medical home.” Where Medicaid programs use service delivery arrangements similar to those used by SCHIP—most often in urban areas—access to care for Medicaid enrollees was also described as good.
Positive Attitudes toward SCHIP and Medicaid. The steady growth in SCHIP enrollment confirms that the programs are successful in providing coverage to low-income children. Families want and will enroll their children in affordable health insurance. Analyses of low- income families’ knowledge of and attitudes toward SCHIP and Medicaid showed that fully 82 percent of low-income uninsured children whose parents had heard of either Medicaid or SCHIP, or both, say they would enroll their children if told they were eligible. In addition, 88 percent of parents of low-income, uninsured children who have been enrolled in Medicaid in the past have positive views about enrolling their children again (Kenney et al. 2002).
Although awareness of SCHIP among low-income families still lags behind awareness of Medicaid (55 percent versus 87 percent in early 2001)—as might be expected given that SCHIP is relatively new—awareness of the program appears to be increasing over time among low- income families with uninsured children. Widespread interest in enrolling their children among parents who had heard of Medicaid and SCHIP, suggests that improving awareness of the programs and understanding of eligibility rules could lead to further increases in enrollment.
Ongoing Support. Support for SCHIP has been strong and steady since the program’s inception. The enhanced federal match for SCHIP made it popular with the states, and states have been using their tobacco settlement dollars and general appropriations to fund their portion of the program. Despite the softening economy, most state officials we interviewed pointed to broad-based support for the program and predicted a positive future.
Challenges
Gaps in Outreach and Awareness. States beginning to implement their SCHIP programs faced the challenge of reaching out to a large and diverse population of low-income families with uninsured children, who may never have been enrolled in a public assistance program. Outreach has not been uniformly effective across states or across subpopulations, and more work is needed to increase program awareness and understanding of SCHIP and Medicaid program rules among families, regardless of race, ethnicity, or age of children.
Among low-income families with uninsured children, those least aware of SCHIP are Hispanic families interviewed in Spanish and the very poorest families (that is, those below 50 percent of the poverty level). Many low-income parents with uninsured children, though they are aware of Medicaid and SCHIP, do not believe that their children are eligible. Confusion about who is eligible is most common among parents of Hispanic children interviewed in Spanish, parents of white children, parents of older children, and parents of children in families with higher incomes.
Application Process Widely Perceived as Difficult. Fewer than half of all low-income uninsured children whose parents had, in 2001, heard of at least one of the two programs have parents who view the Medicaid and SCHIP application processes as easy. Negative perceptions are more widespread for the Medicaid program than for SCHIP (32 versus 22 percent). This result is not surprising given that the application process for Medicaid is not typically as easy as it is for SCHIP. (Focus group participants also reported negative experiences in the past with Medicaid applications.) Less-educated parents and those interviewed in Spanish more often reported difficulties with the application process. Thus, making the application process for the programs easier and more accessible to parents from diverse ethnic backgrounds and educational levels remains as a program challenge.
More Coordination Needed. SCHIP and Medicaid together offer the potential for seamless coverage so that children whose family’s income changes can move between the programs without disruption, and families with children in both programs need not navigate two distinct systems. However, coordination has not yet been perfected in states that operate separate SCHIP programs. While separate programs appear to enjoy high levels of support, case study respondents in states with such programs reported that coordinating SCHIP and Medicaid poses significant challenges. These challenges stem from differences between the two programs’ eligibility rules, administrative structures, and delivery systems. Even minor discrepancies in eligibility policy between the two programs can complicate the “screen-and-enroll” procedures, required by law to place children into the program for which they are eligible. Likewise, focus group participants found differences between the programs to be confusing.
Understanding Why Children Leave the Program. As state programs mature, an emerging challenge is tracking the retention and disenrollment of eligible children and understanding the reasons for disenrollment of eligible children. No one yet knows what “reasonable” rates of retention or disenrollment are, and the availability and quality of data on the reasons for disenrollment are limited. Although disenrollment might appropriately result from changes in employment, income, access to employer-sponsored insurance, or other factors, there is a concern among state officials interviewed in the case studies that administrative barriers (for example, redetermination procedures) and confusion among parents of enrolled children are significant causes of disenrollment. This concern is replicated in the statements of some focus group participants who reported that they had not intended to disenroll their children, but did not realize what the renewal process entailed.
Lingering Resistance to Medicaid. Despite the positive views about Medicaid among many families whose children have been enrolled in the program, Medicaid is not always viewed so positively. Providers have often been reluctant to accept Medicaid patients, mostly because of low Medicaid payment rates in the past. Some families are reluctant to enroll in Medicaid; their reasons include past difficulties applying, the stigma arising from Medicaid’s longstanding linkage to the welfare program, and the concern among immigrant families that receipt of Medicaid could jeopardize their immigration status or their efforts to obtain citizenship. These perceptions were reportedly one of the factors that led some states to choose separate SCHIP programs rather than Medicaid expansions.
Gaps in Access. Despite the broad benefits offered by Medicaid and SCHIP, early success enrolling health plans and providers into SCHIP networks, and reported good access to primary and preventive care, focus group participants and case study respondents indicate that families still have difficulty obtaining some covered benefits, particularly dental and certain specialists’ services.
Access in rural areas is reported to be more limited than in urban areas. Some states have responded to the limited number of providers in rural areas and provider rejection of capitated managed care by introducing “exclusive provider organizations,” which recruit and extend to families an identified network of primary care physicians for their children.
Maintaining Provider Payment Levels. Most states employ capitated managed care for the majority of their SCHIP enrollees. Lacking an alternative basis for setting capitation rates, state officials have typically paid health plans participating in SCHIP the same (or nearly the same) rates they pay under Medicaid. Likewise, health plans have most often elected to pay their providers according to the fee schedules they use in Medicaid. In states where providers view these rates as unfairly low, case study respondents were concerned about reduced provider participation and potential reductions in access to care.
Emerging Issues
The challenges identified earlier are likely to remain central for the foreseeable future. But new issues are also emerging: case study respondents in the six states under study indicated that family coverage under SCHIP is a topic of growing interest. While some states have already obtained approval for such programs, an increase in the number of states proposing both these arrangements and other, new approaches is likely in light of the flexibility recently offered under CMS’ Health Insurance Flexibility and Accountability (HIFA) initiative. The impact of these programs on the number of low-income, uninsured individuals and also on the profile of the Medicaid and SCHIP programs, will along with operational issues, be of great interest.
Summary
The evidence to date suggests that SCHIP is a successful program. It is popular among legislators, families, advocates, and providers alike. As long as state funds remain available, the future of the program appears secure.
Knowledge of the program among eligible low-income families is widespread and growing, due in part to aggressive mass-media and community-based outreach (though some families have been more difficult to reach than others). Enrolling in SCHIP is easier than enrolling in Medicaid, as a result of the more straightforward eligibility rules and application methods adopted by states; but Medicaid enrollment is getting easier too, as SCHIP approaches spill over into this program.
Families’ access to primary care, once they are enrolled, is judged by case study respondents, including state officials, advocates, plans and providers, to be good, though they raised concerns about the adequacy of access to dental care and specialists’ services.
While the analyses completed for this first report on the Congressionally mandated evaluation of SCHIP have yielded substantial information, major aspects of the study that are still in progress are expected to enrich the evaluation of the program greatly. The surveys of the target population, the entire body of ten state case studies, and the survey of all SCHIP administrators will provide data critical to understanding enrollment and disenrollment behavior and its determinants, the relationships among utilization, enrollee characteristics and program design, and the context in which programs were conceived and operate. These study components will also illuminate SCHIP enrollees’ access to care, their satisfaction, and whether they substitute SCHIP for private coverage. The final Report to Congress on the SCHIP evaluation, to be submitted in 2004, will present the findings on this broad spectrum of policy issues.
References
Bellamy, Hilary, Renee Schwalberg, Dorothy Borzsak, Jennifer Dunbar, Christopher Botsko, Jamie Hart, Michael Perry, and Adrianne Dulio. “Findings From The State Children’s Health Insurance Program Focus Group Study.” Washington, DC: Health Systems Research, January 2002.
Centers for Medicare & Medicaid Services (CMS). “The State Children’s Health Insurance Program Preliminary Annual Enrollment Report for Fiscal Year 2002.” Added January 31, 2003. Website: [http://www.cms.hhs.gov/schip/schip02.pdf]
Hill, Ian, Mary Harrington, and Corinna Hawkes. “Congressionally Mandated Evaluation of the State Children’s Health Insurance Program: Interim Cross-cutting Report on the Findings from Six State Site Visits.” Princeton, NJ: Mathematica Policy Research, Inc., November 25, 2002.
Kaye, Neva, Kirsten Wysen, and Cynthia Pernice. “SCHIP Family Coverage in Three States: A Report on the Early Experiences of New Jersey, Rhode Island, and Wisconsin.” Report prepared for the Assistant Secretary of Planning and Evaluation, DHHS. Washington DC: George Washington University. December 2001.
Kenney, Genevieve, Jennifer Haley, and Stephen Blumberg. “Awareness and Perceptions of Medicaid and SCHIP Programs Among Low-Income Families with Uninsured Children: Findings from Early 2001.” Draft Report submitted to OASPE. Washington, DC: The Urban Institute, November 8, 2002.
Part 1: Background
I. A Brief History of Schip
A. Introduction
The creation of the State Children's Health Insurance Program (SCHIP) in 1997 was a landmark event in American social history. The program substantially broadened the role of public health insurance for children living near poverty, illuminating wide popular support for ensuring coverage for the most vulnerable in American society. Not since Medicare and Medicaid were established in 1965 had the Congress enacted such a large, subsidized health insurance program. Designed to provide health insurance coverage for many of our nation's low-income uninsured children, the SCHIP legislation enjoyed enthusiastic support in all quarters. Universal concern for low-income children, the availability of federal surpluses, and successful compromises converged to make this historic achievement possible.
B. Statutory Framework
SCHIP was created as Title XXI of the Social Security Act by the Balanced Budget Act of 1997, which was signed into law in August 1997. Congress appropriated approximately $40 billion for the program's first ten years (fiscal years [FY]1998 through 2007). The funds were allotted to the states based on a formula that considers, primarily, the number of all low-income children and the number of low-income uninsured children residing in each state. It also includes a factor for each state's health care costs relative to the others'. To encourage states to implement this program, the federal match for SCHIP expenditures was enhanced relative to Medicaid: each state's share was set at 70 percent of its Medicaid (Title XIX) share. Under the law, states may cover uninsured children in families with income under 200 percent of the federal poverty level (FPL), and up to higher income levels in states that already provide extensive coverage under Medicaid.
The SCHIP legislation gave states three broad options for program design. A state could choose to expand its Medicaid program, develop a separate program, or implement a combination of both. By law, Medicaid expansion programs under SCHIP are subject to all the requirements of Title XIX, but raise the income eligibility thresholds. In particular, these programs establish an entitlement for all children who meet the eligibility criteria, and eligibility must comply with the Title XIX requirements for comparability and statewideness. In addition, states that expand Medicaid under SCHIP must cover the same broad benefits offered under Medicaid and use the Medicaid service delivery network, and may not impose cost-sharing. (Medicaid expansions established under a Section 1115 demonstration may require cost-sharing for children if a waiver of the prohibition against cost-sharing has been obtained.)
By contrast, the option for separate, non-Medicaid SCHIP programs permits states to adopt programs that more closely resemble private insurance. Separate child health programs do not establish an entitlement for children. Moreover, states electing this option have considerable flexibility in defining eligibility. Another important eligibility-related difference between Medicaid and separate child health programs concerns other insurance coverage. Whereas insurance status is irrelevant to eligibility for Medicaid (i.e., insured individuals can still qualify for Medicaid if they meet the eligibility criteria), SCHIP explicitly excludes insured children. Further, to discourage parents from substituting SCHIP for their children's existing private insurance, states with separate programs may impose waiting periods on children who have or who recently dropped their private health insurance. Except when using waiver authority, states with Medicaid expansion programs may not impose waiting periods.
Although subject to statutory standards for benefit packages, states with separate child health programs can provide benefits less broad than Medicaid's and more like coverage offered in the private sector. All the states with separate programs have adopted broad benefit packages, though usually not as comprehensive as Medicaid's. States with separate child health programs may also impose premiums and cost-sharing, and many do. Some have developed service delivery networks different from those serving Medicaid, and managed care is more widespread in SCHIP than in Medicaid.
C. Program Implementation
By December 1999, all states, territories, and the District of Columbia had received federal approval to expand coverage under SCHIP (CMS 2002a). States launched their SCHIP programs at different times. Most states started enrolling children during 1998; however, a few began as early as October 1997, and a few did not start until 1999. By March 2002, 16 states were operating separate programs, 21 were operating Medicaid expansion programs, and 19 were operating combination programs (CMS 2002b). State programs have evolved steadily; one indication of this dynamism is that, by March 2002, 106 state plan amendments had been submitted to and approved by DHHS and seven more were under review.
D. Enrollment Trends
The states have enrolled large numbers of children and enrollment has grown rapidly from year to year. During FY 2002, 5.3 million children were enrolled in SCHIP for at least part of the year, (CMS 2003). Before that, enrollment (i.e., number of children enrolled at some point in the year) grew from 1.0 million in calendar 1998, to 2.0 million in FY 1999, and, further, to 3.3 million in FY 2000. Enrollment has grown most rapidly in separate programs. The proportion of children in SCHIP who were enrolled in separate programs rose from 65 percent in FY 1999 to 74 percent in FY 2001. 1 In part, this growth reflects an increase in the number of states that operate separate programs, whether alone or in combination with a Medicaid expansion program.
1. In one third of the states operating both types of programs, the Medicaid portion of the SCHIP initiative represents less than 10 percent of the enrollment, whereas in just over one third, the Medicaid portion is more than half. CMS op. cit.
E. Delivery Systems
Many of the states have chosen to deliver services to their SCHIP children through capitated managed care plans. Most states developed experience in managed care contracting after its rapid adoption in their Medicaid programs during the 1990's. However, in rural and other areas where managed care penetration is limited or non-existent, alternative delivery systems are used. In these cases, a mix of primary care case management and fee-for-service arrangements is common.
F. What Is Known?
Based on steadily rising enrollment in SCHIP and the recently reported decline in the number of uninsured children, from 9.9 million (13.9 percent) in 1997 to 7.8 million (10.8 percent) in 2001, 2 we know SCHIP has succeeded in expanding health insurance coverage among children. However, three years after SCHIP was enacted, when this evaluation got underway, understanding of the mechanisms that produced this overall result was still limited. While the need for information and analysis to guide federal and state policy was great and growing, little systematic analysis of the implications of states' program choices had been conducted. Although a body of literature on the program is emerging, knowledge is still limited about a host of important issues across the states and at the national level. For example, the reasons why some parents enroll their children and others do not, and the factors associated with disenrollment are still unclear. Likewise, knowledge about children's access to care and use of SCHIP benefits is limited, as is information about their parent's satisfaction with the care they receive. The impact of cost-sharing on utilization and satisfaction has been little studied. Empirical evidence to inform the debate about "crowd-out"--the substitution of SCHIP for private coverage also remains limited and equivocal.
Recognizing the importance of improving our knowledge about these issues and others, Congress appropriated $10 million for a comprehensive evaluation of SCHIP. The scope and purpose of this congressionally mandated evaluation are described in the next chapter.
2. Table 1.1, Family Care Component of 1997-2001 NHIS.
[ www.cdc.gov/nchs/about/major/nhis/released200207/table01_1.htm]
II. The Congressionally Mandated Evaluation
This report to Congress summarizes the findings to date stemming from the Congressionally mandated study of SCHIP. The study, to be completed in three years, had been underway for only one year when this report was prepared. Therefore, this first report presents interim findings from data collected and analyzed early in the study, and it focuses primarily on the implementation of SCHIP and its effects on state, contractor, health care provider, and family experiences.
The report has two parts. Part 1 provides background about SCHIP and the mandated evaluation, including the evaluation design. Part 2 presents interim findings from the study. Appendix A displays the legislation mandating the study. Appendix B includes tables displaying the composition of the 51 focus groups. Appendix C describes further analyses that will be conducted under this evaluation and the final report to Congress in which they will be presented.
This chapter begins by providing an overview of the congressional mandate to evaluate SCHIP. This is followed by a description of how the evaluation "blueprint," laid out in the statutory language, was translated into a concrete research strategy and evaluation design. In the process, the broad policy concerns and specific research questions this evaluation addresses are reviewed.
A. The Congressional Mandate
Congress mandated in the Balanced Budget Refinement Act of 1999 that the Secretary of the Department of Health and Human Services (DHHS) conduct an independent study of the State Children's Health Insurance Program. The legislation articulates the range of issues that the evaluation is to investigate, as well as some of the methods to be used. Congress specifically directed that the evaluation:
- Identify enrollment barriers and the key elements of effective and ineffective outreach and enrollment practices in both SCHIP and Medicaid (under Title XIX), including practices that successfully enroll hard-to-reach populations.
- Assess the extent to which state Medicaid eligibility procedures are a barrier to enrollment of children in Medicaid.
- Assess the extent to which coordination between Medicaid and SCHIP (or lack thereof) affects enrollment of children in both programs.
- Determine the effect of cost-sharing on use of services, enrollment and retention in the program.
- Identify and assess causes of disenrollment, such as switching to private coverage, failure to pay premiums, and barriers in the redetermination process.
The mandate also stipulated the following study parameters:
- Include ten states.
- Select states that reflect geographic and urban/rural representation, diverse approaches to program design, and large proportion of all low-income uninsured children in the United States.
- Survey enrollees and disenrollees and collect information about why many eligible children are not enrolled.
- Report to Congress due December 31, 2001. 3
3. As described in the section on evaluation design (see page 15), ASPE required substantial additional time to carry out the required study, and renegotiated the due date for the report with Congressional staff. After all the research components have been completed, a final report will be submitted to Congress in 2004.
B. Development of the Evaluation Plan
The congressional mandate was broad in scope, and to fulfill it required that a complex set of activities be organized and implemented rapidly. The Office of the Assistant Secretary for Planning and Evaluation (ASPE) in the Department of Health and Human Services (DHHS) was assigned responsibility for the evaluation. The task of translating Congress' comprehensive mandate into a responsive and manageable evaluation plan was challenging. To carry it out, ASPE consulted widely with policy experts and researchers, with the aim of producing a robust specification of the questions the evaluation should address and thorough consideration of methodological issues. This consultation also enabled ASPE to devise a strategy that: built on existing research efforts to the extent possible; avoided duplication of other work; and maximized the potential of the evaluation to add to our knowledge about SCHIP and Medicaid.
Federal and state policymakers and researchers both within and outside the government participated in these early planning efforts and discussions, which formed the basis for ASPE's decisions about the evaluation design and methods. A multi-faceted research strategy ultimately emerged that, while addressing the broad range of issues articulated in the mandate, also met the need for results in the near term. The three-year evaluation project has numerous research components that include both qualitative and quantitative approaches and that bring data and information from multiple sources--including states, health care providers, families, and other interested parties--to bear. While time, resource and legislative constraints necessitated this somewhat complex strategy, the design is expected to produce a uniquely rich assessment of the program.
The evaluation plan ASPE developed included three contractual components: (1) an overall study of the issues identified in the legislative mandate, but focused primarily in ten states; (2) a focus group study in nine states during 2001; and (3) special studies on issues of immediate policy interest, such as the experience of states providing family coverage under SCHIP. Although conducted under separate contracts, the findings from the three different components will be fully integrated by the investigators under the contract for the overall study. 4, 5, 6, 7
The central focus of the overall study is states' programmatic and policy choices and their implications. Data and information for this study will come from three sources: (1) in-depth case studies of ten states; (2) a nationally representative survey, in the same ten states, of parents of SCHIP enrollees and disenrollees, and, in two of the states, of parents of Medicaid enrollees and disenrollees; and (3) a survey of SCHIP administrators in all 50 states, the District of Columbia, and the five U.S. territories. The study will also draw on a national survey of awareness and perceptions of Medicaid and SCHIP among low-income families with uninsured children, using the State and Local Area Integrated Telephone Survey (SLAITS), as well as states' SCHIP and Medicaid administrative files. Finally, as indicated earlier, the overall study will incorporate the findings from the focus group study and the studies of special topics. These data sources are described in Chapter III as part of the discussion on the evaluation design.
4. The contract for the overall study was awarded to Mathematica Policy Research, Inc. (MPR), under contract number HHS-100-01-00002. MPR subcontracted with The Urban Institute and The MayaTech Corporation. The contract began on December 22, 2000, and will end in October 2004.
5. This is the second study of SCHIP to be mandated by Congress. In the legislation creating SCHIP (the Balanced Budget Act of 1997), Congress had already mandated that DHHS submit a report to Congress by December 31, 2001, based on mandated state evaluations. Recognizing this statutory requirement--as well as the need for a more detailed assessment of the performance of the SCHIP programs--the Centers for Medicare & Medicaid Services (CMS), which administers SCHIP, contracted for an evaluation.
The CMS evaluation also is being conducted by MPR (contract number 500-96-0016 [03]). That evaluation is reviewing the literature on the effects of SCHIP; drawing on state data to examine SCHIP enrollment, expenditures, and service use; synthesizing information on program performance from the state evaluations and annual reports; and examining outreach and enrollment processes in eight states using site visits and focus groups. In addition, the study will review trends in the number of uninsured children before and after SCHIP implementation, using data from the Current Population Survey (CPS).
6. Health Systems Research, Inc. (HSR) conducted the focus group study for ASPE (Bellamy et al. 2002).
7. George Washington University and the National Academy for State Health Policy conducted the family coverage study for ASPE (Kaye, Wysen, and Pernice 2001)
C. Evaluation Topics and Research Questions
ASPE identified eight distinct areas of inquiry contained in the evaluation mandate, as follows: (1) SCHIP program choices; (2) outreach and barriers to enrollment; (3) enrollment and retention in SCHIP; (4) enrollment trends; (5) SCHIP's relationship to Title XIX and private insurance; (6) impact of SCHIP on the uninsured; (7) premiums and cost-sharing; and (8) access to care, utilization, and satisfaction with care. These topics reflect key aspects of SCHIP programs and their impacts. Table 1 displays the data sources that are used to explore each of them, and the subsequent narrative identifies the primary questions associated with each topic.
| Evaluation Topics | Survey of Target Population | State Case Studies | Survey of Program Administrators | Program Data | Focus Groups | SLAITS Survey | Special Studies |
|---|---|---|---|---|---|---|---|
| 1. SCHIP Program Choices | P | P | S | ||||
| 2. Outreach and Barriers to Enrollment | P | S | S | S | P | ||
| 3. Enrollment and Retention in SCHIP | P | S | P | S | S | ||
| 4. Enrollment Trends | S | P | |||||
| 5. SCHIP's Relationship to Title XIX and Private Insurance | P | P | P | S | S | ||
| 6. Impact of SCHIP on the Uninsured | S | P | |||||
| 7. Premiums and Cost Sharing | P | S | S | S | S | ||
| 8. Access to Care, Utilization, and Satisfaction | P | S | S |
Note: P indicates primary source for addressing topic; S indicates a secondary source for addressing topic.
Topic: 1. SCHIP Program Choices. A detailed understanding of the context in which states designed and operate their SCHIP programs is essential to critically assess the SCHIP implementation experience. Knowledge about states' program design choices is necessary in order to explore how different choices bear on such key outcomes as enrollment trends, access, and enrollee satisfaction. Program design choices cover many matters, including (among others): outreach, enrollment and retention strategies, benefit design, delivery systems and payment arrangements, cost-sharing policies, anti-crowd-out measures, and state financing.
The key question to be addressed under this evaluation topic is:
- What are the state characteristics and/or other factors that most influence the design and implementation of SCHIP?
Topics: 2. Outreach and Barriers to Enrollment; 3. Enrollment and Retention in SCHIP; and 4. Enrollment Trends. Perhaps because SCHIP enrollment has grown continuously from year to year, our understanding of the barriers to enrollment and retention and the turnover and churning behind the total enrollment numbers remains limited. For example, the reasons why families enroll and disenroll their children are not well understood. Furthermore, we know little about families' experience with the coordination (or lack thereof) between Medicaid and SCHIP, which is important because of the need for easy transitions between the two programs for low-income families.
Key questions to be addressed under these topics include:
- What are the trends in SCHIP and Medicaid enrollment? How do they relate to program design choices?
- What are the barriers to enrollment in SCHIP and Medicaid?
- Is there a relationship between utilization and enrollment and retention in the program?
- How does the extent of coordination between Medicaid and SCHIP affect disenrollment of eligible children?
- Why do some eligible families enroll in SCHIP while others do not?
- What policies reduce disenrollment of eligible children?
- Why do eligible children disenroll? How likely are they to reenroll?
Topics: 5. SCHIP's Relationship to Title XIX (Medicaid) and Private Insurance; and 6. Impact of SCHIP on the Uninsured. Little is known about the most recent insurance status of children before they enroll in SCHIP, or about their insurance status following disenrollment. Understanding the role SCHIP plays in the larger scheme of insurance dynamics among low-income children and families is an important evaluation issue, and may help federal and state policymakers guide the program's future effectively and strategically.
Key questions under these topics include:
- What types of health insurance coverage, if any, do children have before they enroll in SCHIP and after they leave?
- What is the transition between Medicaid and SCHIP like for children?
- To what extent does SCHIP enroll children who would otherwise be uninsured, versus children who would otherwise have other coverage, especially private coverage?
Topic: 7. Premiums and Cost-Sharing. Many states have introduced premiums and cost sharing in their programs, and the effects of these program choices on beneficiaries is a subject of keen interest. The two key questions are:
- Does cost-sharing affect enrollment in SCHIP?
- What is the effect of cost-sharing on use of services?
Topic: 8. Access to Care, Utilization, and Satisfaction with Care. The purpose of SCHIP and Medicaid is to improve access to health care by providing health insurance. Policy makers and program officials need to know whether the programs are improving access to care, satisfaction, and appropriate utilization and what the chief determinants of these outcomes are.
Key questions to be addressed within this topic include:
- Do parents of children enrolled in SCHIP and Medicaid report adequate access to care? What is the utilization profile of these children? Are there essential services their parents believe are not available? How satisfied are parents with SCHIP and Medicaid?
- Does enrollment in SCHIP and Medicaid lead to increased access to care? What is the impact of enrollment in SCHIP and Medicaid on utilization and satisfaction with care?
III. Evaluation Design
This chapter describes the design of each of the evaluation components and explains how these components, together, will yield a rich and integrated evaluation of SCHIP. The study will provide both a profile of the program at the national level and state-specific analyses. Further, it will explore whether and how important program outcomes vary by subpopulation.
The time frame that Congress provided for a report on the evaluation could not be met, given the scope and requirements of the evaluation mandate. Indeed, significant aspects of the required work--in particular, the enrollee survey and related analyses--were infeasible in the time frame allowed. Consequently, following consultation with Congressional staff, ASPE developed a research strategy that would enable the Secretary to provide a preliminary report on the full range of issues specified in the mandate early on, and a final report on findings at the end of the three-year-long evaluation. To illustrate, this first report's description and analysis of states' program choices and their outcomes are based on the first six of the ten case studies completed for the evaluation. The analysis of program perceptions, attitudes and experiences among families whose children are eligible for Medicaid and SCHIP is based on: (1) a focus group study including 51 diverse focus groups across nine states and (2) preliminary data from a 50-state survey of parents of low-income, uninsured children. These efforts provide valuable new information for this first report. However, a richer and more rigorous quantitative analysis will be available for the final report, based on all ten of the state case studies, a nationally representative survey of enrollees and disenrollees in all ten of those states, and the final data files from the survey of parents of eligible-but-uninsured children.
A. Overview of Design Activities
Designing the evaluation required specifying the research questions in detail, selecting the ten evaluation states and gaining their cooperation, designing the primary data collection approaches, and defining the analytic approaches to be used to address the questions. A ten-member technical advisory group of researchers and policy experts convened by the contractor, along with a departmental advisory group convened by ASPE, reviewed the draft evaluation design. The input from these groups was incorporated in a final design report (Wooldridge et al. 2001).
The first year of the congressionally mandated study of SCHIP was devoted primarily to case study and focus group data collection and analysis, and to other study components that would provide usable information for this report. Also during the first year, the contractor designed the mandated survey of SCHIP enrollees and disenrollees and worked with the states to collect the enrollment records needed both to conduct the survey and to analyze enrollment and disenrollment patterns.
This chapter begins by describing the activities related to the study components whose findings are included in this report to Congress:
- Selection of ten study states (Section B)
- Case study design and implementation (Section C)
- Focus group study design and implementation (Section D)
- SLAITS analysis (Section E)
- Special Studies (Section F)
The chapter continues with a discussion of the design of the remaining study components, which will generate findings that will be reported in a final, comprehensive report to Congress. Those components are:
- Analysis of state enrollment data (Section G)
- Survey of SCHIP and Medicaid enrollees and disenrollees and survey of state program administrators (Section H)
B. Selecting States and Gaining Their Cooperation
Ten states were selected for this study in accordance with the legislative requirements. These ten states capture: (1) a high proportion of low-income uninsured children in the United States; (2) wide geographic (including urban/rural) representation, and (3) diverse approaches to program design. The selection process began with a list of 25 states, prepared by ASPE based on a wide array of factors, including the size of the SCHIP and Medicaid populations, the number of low-income uninsured children, representation of important subpopulations, program design features, maturity of program, and state data capability. 8 In addition, priority was given to selecting states from among the nine states included in the focus group study that was also a part of ASPE's evaluation. Based on a nonprobability, replicable protocol, ten states were selected: California, Colorado, Florida, Illinois, Louisiana, Missouri, New Jersey, New York, North Carolina, and Texas. 9 These ten states fulfill the legislatively specified selection criteria:
- They include more than half (56 percent) of the target population of uninsured children with family income under 200 percent of the federal poverty level.
- They include approximately 1.3 million of the children who were enrolled in SCHIP during at least part of the second quarter of federal fiscal year 2000, or about 53 percent of such children nationwide (Rosenbach et al. 2001).
- All four Census regions are represented. Four of the ten states are in the South, and there are two states each in the other three regions (Northeast, Midwest, and West).
- They include two states whose SCHIP programs are an expansion of their Medicaid programs, six states whose SCHIP programs are separate programs only, and two states with combination programs.
To capture additional diversity, other program design features were monitored and taken into consideration:
- Income eligibility thresholds: Three of the ten selected states have an income threshold of 250 percent or more of the federal poverty level.
- Medicaid waivers: Four of the states, including one of the two with a Medicaid expansion-only program, had approved or pending Medicaid Section 1115 demonstrations.
Finally, six of the ten states were among those included in the focus group study: California, Colorado, Florida, Missouri, New York, and Texas.
The states were keenly interested in the study. When approached about participating, all states agreed to cooperate with the evaluation contractor to provide access to state staff and to provide program enrollment data needed for the study, and all signed memoranda of understanding to do so. By the end of 2001, most of the states had supplied both test data and the enrollment data required for drawing the first sample wave of the survey of SCHIP enrollees and disenrollees. The two states selected for a survey of Medicaid enrollees and disenrollees--California and North Carolina--had by March 2002 signed memoranda of understanding to provide the necessary Medicaid enrollment data.10
8. The 25 states from which the 10 were chosen were: Alabama, Arizona, California, Colorado, Florida, Georgia, Illinois, Indiana, Kansas, Kentucky, Louisiana, Maryland, Massachusetts, Michigan, Missouri, New Jersey, New York, North Carolina, Ohio, Oregon, Pennsylvania, South Carolina, Texas, Utah, and Virginia.
9. The statistical information used for state selection (and reported here) was the most recent available at the time of selection in early 2001. Note that Arizona was originally selected; but, because it was unable to participate, Colorado was selected as its replacement.
10. The states are being paid to provide the data for the evaluation. Therefore, the contractor has entered into subcontracts with each state or its contractor to supply the data.
C. Designing and Implementing the Case Studies
Case studies of the ten selected states were designed and conducted in 2001 to develop an understanding of why states designed their children's health insurance programs as they did, the challenges and issues states faced during implementation, the perceived and measurable effects of states' efforts, and the continuing evolution of SCHIP programs. These case studies provide critical background for interpreting findings from other analyses conducted under this evaluation.
The first step was to collect and review information about the case study states. Protocols for semi-structured interviews with policymakers, advocates, providers and other key state and local staff were developed, and visits to each state were arranged. Between June 2001 and October 2001, the evaluation team visited six of the ten study states: California, Colorado, Louisiana, Missouri, New York, and Texas. The team spent a full week in each state. Team members conducted interviews with between 40 and 50 state and local officials, including SCHIP and Medicaid administrators and their staff, state legislators and their staff, officials from the governor's office, state public health officials, provider associations, health plan associations, and private sector vendors under contract with the states to perform various administrative functions. In selected localities in each state, the team interviewed providers, child and family advocates, health plan officials, local Medicaid eligibility workers, outreach workers, and community-based application assisters. These 40 to 50 individuals in each state are described throughout the report as "case study respondents." Based on the information gathered during the site visits, detailed state-specific, case study reports were developed.
The site visit protocols included questions on the following topics:
- Outreach and program awareness
- Eligibility standards and policies designed to foster enrollment and retention
- Policies intended to avoid the substitution of SCHIP for private insurance coverage
- The benefits packages offered to SCHIP enrollees
- The service delivery system, service use, and access
- Cost-sharing
- Family coverage and premium assistance programs
- Financing and the fiscal outlook
- Coordination between Medicaid and SCHIP
Each case study report synthesized the information collected. The case study reports from the first six states were the primary source for an interim cross-cutting report (Hill, Harrington and Hawkes 2002), from which Part 2 of this report (study findings) draws heavily.
D. Focus Group Study Design
As indicated earlier, the survey of enrollees and disenrollees, which will be the principal source of data and analysis on families' experience of SCHIP and Medicaid, could not be fielded in time to meet the due date for the report to Congress. To provide preliminary information on this subject for this report, ASPE contracted for a focus group study, which was conducted during the summer of 2001. Focus groups were held in nine states, of which the six marked with asterisks are also included in the overall ten-state study: California*, Colorado*, Florida*, Georgia, Maryland, Missouri*, New York*, Ohio, and Texas*. A total of 51 focus groups was convened with parents of SCHIP and Medicaid enrollees and disenrollees and with parents of low-income uninsured and privately insured children. Nineteen focus groups included parents of children enrolled in SCHIP and Medicaid; 14 groups included parents of children who had disenrolled from one of the two programs; 13 groups included the parents of eligible but not enrolled low-income children; and five focus groups were with the parents of privately insured children in low-income families. Ethnicity, race, and language spoken at home were also factors used to define the focus groups, so as to capture the experience of important subpopulations. In total, 367 parents participated. 11 These parents are described throughout the report as focus group participants. Appendix B shows the distribution of focus groups by the insurance status of the child and other selection criteria.
The focus groups addressed the following key topics: parents' perceptions of the SCHIP and Medicaid programs; barriers to enrolling children in SCHIP and Medicaid; family attitudes toward and experience of cost-sharing (premiums and copayments) in SCHIP; access to services, benefits used; parents' experiences with private insurance; the effect of outreach efforts and messages on parents' awareness and understanding of the programs; and parents' attitudes toward enrolling their children.
To organize and synthesize the information collected, transcripts from the focus groups were coded uniformly using software, designed for analyzing qualitative data, that allows all passages related to a specific theme to be retrieved for synthesis and comparison across groups. The study findings, reported in full in Bellamy et al. (2002), are incorporated in Part 2 of this report.
It should be noted that the findings from focus groups represent only the views of those individuals who participated in the focus groups and thus cannot be generalized to the broader population. While recognizing the limitations of this study methodology, ASPE believed it was important to include the beneficiary perspective in this first report on the evaluation. The quantitative analyses of the enrollee and disenrollee survey data and SLAITS data will explore in more detail and with greater rigor the issues raised by the focus groups.
11. The contractor worked with the states to identify enrolled and disenrolled families and with local groups to identify privately-insured and eligible but not enrolled families. Community agencies such as community health centers and women, infants, and children (WIC) programs also were a supplemental source of families.
E. State and Local Area Integrated Telephone Survey (Slaits) Analysis
The State and Local Integrated Telephone Survey (SLAITS) is a sampling and survey mechanism, developed by the National Center for Health Statistics of the Centers for Disease Control and Prevention (CDC). The Health and Resources Services Administration (HRSA) of the DHHS is currently using SLAITS to study the prevalence and experience of children with special health care needs. ASPE determined that the large number of households that had to be sampled to identify special needs children for the HRSA study made the survey an ideal source for identifying low-income households with uninsured children. By adding to the HRSA survey a Low-Income Uninsured Supplement, information could be gathered that was needed to address Congress' interest in the reasons many eligible children are not enrolled in Medicaid and SCHIP.
This survey is the largest to date that addresses barriers to enrollment in Medicaid and SCHIP. The survey, which was still in the field at the time this report was being prepared, will ultimately provide detailed data on an average of 200 low-income uninsured children in each state, for a total of nearly 10,000 nationwide. 12
For this first evaluation report, the National Center for Health Statistics developed a preliminary data file and preliminary sample weights. An analysis of these preliminary data is included in Part 2 of this report, in Chapter VII (on families' awareness and perceptions of SCHIP and Medicaid). The analysis focuses on the awareness of SCHIP and Medicaid among parents of low-income uninsured children, their beliefs about their children's eligibility for these programs, their perceptions of SCHIP and Medicaid application processes, their experiences in these programs, and their attitudes toward enrolling their children. An analysis of the complete survey supplement will be conducted later in the study and included in the final report to Congress.
12. SLAITS is a random digit dial survey of households that uses computer-assisted telephone interviewing methods.
F. Special Studies
To gather information on specific policy or program topics that were not covered by the overall study, or that emerge in the course of the evaluation, ASPE plans to conduct several targeted studies. In this report to Congress, ASPE has included findings from a special study on family coverage. Other special studies will be conducted for the final report to Congress.
The family coverage study analyzed family coverage policies in three states--New Jersey, Rhode Island, and Wisconsin--that received demonstration authority to cover families, not just children, under Title XXI. The focus of the study was on program design, enrollment, the effect on the private health insurance market, and the impact on children's insurance coverage. The study was based on visits to the three states, during which interviews were conducted with state SCHIP staff, staff of managed care organizations, child health advocates and parents, employers, state insurance agency staff, legislators, and governors' health policy advisors. The information gathered through these interviews and a literature review is presented in full in a report to ASPE (Kaye, Wysen, and Pernice 2001). The findings are incorporated in Part 2 of this report in Chapter XIV (on family coverage).
G. Enrollment Data
State SCHIP and Medicaid enrollment data are key sources of data for this evaluation. First, they are being used to select the sample for the survey of enrollees and disenrollees. Second, these data are being analyzed to cast light on program enrollment, disenrollment, retention patterns and movement between the two programs. Enrollment data will be used to describe the SCHIP population--how many children are enrolled, the characteristics of these children, how many children are disenrolled and their characteristics, and net growth in program enrollment. A second focus of analysis is the redetermination process and its outcomes. Finally, the states' administrative data will be matched with data from the enrollee and disenrollee survey, providing a rich source for understanding the relationships and dynamics that underlie program entry and exit of members of the study sample.
In the course of the initial data acquisition for survey sampling, sufficient data were acquired from three of the states (Louisiana, New Jersey, and Texas) to permit preliminary analyses of both retention and reenrollment of children who were previously enrolled (Moreno and Black 2001). Findings from this analysis are described in Part 2 of the report, in Chapter IX (on eligibility redetermination and retention). Later in the study, the program data will be matched to the data from the survey of SCHIP enrollees and disenrollees to conduct an extensive analysis of enrollment patterns, duration of enrollment, reasons for exit, and reenrollment for members of the survey sample.
H. Survey Design and Analysis
1. Survey of SCHIP and Medicaid Enrollees and Disenrollees
A unique feature of this evaluation is a telephone survey of SCHIP enrollees and recent disenrollees in ten states, and of Medicaid enrollees and recent disenrollees in two of the ten. This survey will permit the first systematic look across states of the characteristics of the SCHIP population, as well as an assessment of the effects of particular program features on the enrollment experience, experience in the SCHIP program, and reasons for disenrollment. The survey, which will be fielded during 2002 and early 2003 and analyzed during 2003, will collect information from approximately 21,000 children across the ten study states.
The survey instrument was designed to address the detailed evaluation questions spelled out in the design report. To the extent possible, it draws heavily on valid and reliable questions from existing surveys. 13
The survey asks about:
- Insurance status before enrollment
- Insurance status since disenrollment
- The enrollment process
- Reasons for enrolling and disenrolling
- Access to care, service use, and satisfaction
- Demographic characteristics
The survey targets three distinct groups of children: (1) those who enrolled recently, (2)those who have been enrolled for five or more months, and (3) those who disenrolled recently. By targeting children in these distinct groups, the survey will gather data on questions that are salient for each group. 14 For example, the parents of recent enrollees--for whom the experience of enrollment is fresh--will be asked how easy it is to enroll, while the parents of disenrollees--for whom leaving is recent--will be asked why their child left the program.
The analysis of the survey of SCHIP enrollees and disenrollees will provide new descriptive information about program participation behavior and enrollment dynamics--why families enroll and disenroll from SCHIP and Medicaid; coverage transitions (that is, among SCHIP, Medicaid, private coverage and periods without insurance); SCHIP's role as a transitional versus longer-term source of insurance; whether public health insurance programs substitute for private coverage; and access to care, service use and satisfaction with SCHIP and Medicaid. The analysis will also estimate whether SCHIP leads to improvements in access to care, service use, and satisfaction.
13. Surveys from which the SCHIP survey drew are: SLAITS, the National Study of America's Families (NSAF), the Medical Expenditure Panel Study (MEPS), the National Health Insurance Study (NHIS), the Community Tracking Study (CTS), the Medicaid CAHPS, the Studies of Section 1115 Medicaid Demonstrations conducted in five states by MPR and in four states by the Urban Institute, and Kaiser Family Foundation Medicaid surveys on barriers to enrollment. In addition, we looked at the set of common questions developed by researchers participating in the Child Health Insurance Research Initiative (CHIRI) and questionnaires developed by Peter Szilagyi and his coworkers for a longitudinal study of SCHIP enrollees in four geographic regions of New York State.
14. Recent enrollees are defined as those who have been enrolled one month or less at the time the sample frame was constructed. Longer-term enrollees are those enrolled five or more months. Recent disenrollees were disenrolled at the time of sample frame construction but were enrolled in the preceding month (In all three cases, however, by the time the sample member is surveyed, additional time will have passed).
2. Survey of State Program Administrators
To provide a national context for the intensive analysis of the ten study states, the evaluation also includes a survey of the SCHIP program administrators in all 50 states, the District of Columbia, and the five territories. This telephone survey, which will collect information about program design and evolution, will take place in 2003; the analysis, summarizing national trends, will be completed during 2003. In addition to providing basic descriptive information on program design features, the findings will be organized around three topics: (1) reasons why children's health insurance programs are designed as they are; (2) accomplishments and challenges to date, for example, with respect to outreach and enrollment, design of delivery systems and provider networks, and administration of premium and cost-sharing provisions; and (3) pressing new issues requiring attention in the near term.
Part 2: Findings
IV. Introduction to Findings
The findings presented in this report are based on several studies. First, the findings draw extensively on the case studies of six of the ten study states and the focus group study included in the overall evaluation. Preliminary, quantitative analyses of state administrative data and SLAITS data contributed additional findings. Finally, a special study of family coverage is the source of findings on that subject. Table 2 shows, for each evaluation topic covered by a chapter of this report, which studies contributed to the findings. Table 3 shows which states each of the studies included. Next follow chapters devoted to key evaluation topics. We begin with outreach (Chapter VI), awareness of SCHIP and Medicaid among low-income families (Chapter VII), eligibility and enrollment (Chapter VIII), and eligibility redetermination and retention (Chapter IX). We move on to discuss program benefits (Chapter X), service delivery systems, access and utilization (Chapter XI), and cost sharing (Chapter XII). We then present chapters on crowd-out (Chapter XIII), family coverage and premium assistance programs (Chapter XIV), financing and fiscal outlook (Chapter XV), and the coordination of SCHIP and Medicaid in the states with separate programs (Chapter XVI). A chapter summarizing the study findings and drawing conclusions completes Part 2.
| Chapter/Topic | Data Source | ||||
|---|---|---|---|---|---|
| Case Studies | Focus Group Study | SLAITS Analysis | Program Data Analysis | Family Coverage Study | |
| V. Overview of SCHIP Programs in Six of the Ten Study States | x | ||||
| VI. Outreach | x | x | |||
| VII. Awareness of SCHIP and Medicaid Among Low-Income Families | x | x | |||
| VIII. Eligibility and Enrollment | x | x | |||
| IX. Eligibility Redetermination and Retention | x | x | x | ||
| X. Benefits | x | x | |||
| XI. Service Delivery Systems, Access and Utilization | x | x | |||
| XII. Cost Sharing | x | x | |||
| XIII. Crowd-Out | x | x | |||
| XIV. Family Coverage and Premium Assistance Programs | x | x | |||
| XV. Financing and Fiscal Outlook | x | ||||
| XVI. Coordination of SCHIP and Medicaid in States with Separate Programs | x | x | |||
| States Included in Each Study | Data Source | ||||
|---|---|---|---|---|---|
| Case Studies | Focus Group Study | SLAITS Analysis | Program Data Analysis | Family Coverage Study | |
| All states | x | ||||
| California | x | x | |||
| Colorado | x | x | |||
| Florida | a | x | |||
| Georgia | x | ||||
| Illinois | a | ||||
| Louisiana | x | x | |||
| Maryland | x | ||||
| Missouri | x | x | |||
| New Jersey | a | x | x | ||
| New York | x | x | |||
| North Carolina | a | ||||
| Ohio | x | ||||
| Rhode Island | x | ||||
| Texas | x | x | x | ||
| Wisconsin | x | ||||
aFlorida, Illinois, New Jersey, and North Carolina are included in the evaluation, but case studies of these states will not be completed until after this report has been finalized. Findings from these four case studies will be included in the final Report to Congress.
V. Overview of Schip Programs in Six of the Ten Study States
Because this report draws heavily on data from six case studies conducted in time to be included in the report, we present background on these states in this chapter. The six states are: California, Colorado, Louisiana, Missouri, New York, and Texas. The findings from the case studies are presented in greater detail in Hill, Harrington, and Hawkes (2002).
Four of the six case study states responded promptly when Title XXI was enacted in the Balanced Budget Act of 1997 (BBA). Within four months of the August 1997 passage of the BBA, California, Colorado, Missouri, and New York had submitted SCHIP plans to the Health Care Financing Administration(now known as Centers for Medicare and Medicaid Services(CMS)) (HCFA(now known as CMS)); 15 by April 1998, each of these states except Missouri had implemented its program. 16 Texas and Louisiana submitted their initial state plans in April and July 1998, respectively, and both implemented at least the initial phases of their SCHIP initiatives during 1998 (see Table 4). The timing of the study states' responses to the SCHIP legislation fairly closely reflects the national pattern: within six months of the SCHIP legislation's passage, 18 states had submitted plans to CMS and four had been approved; by the first anniversary of the law, 48 states had submitted plans, and 41 had received federal approval; by early 2000, every state and the District of Columbia had approved plans in place. 17, 18, 19 Title
XXI originally called for all states to have approved plans by September 30, 1998. Congress extended this deadline to September 30, 1999.
| Dates of Approved Submission | |||||
|---|---|---|---|---|---|
| State | Program Name | Program Type | Submitted | Approved | Implemented |
| California | Healthy Families | Combination | 11/19/97 | 3/24/98 | 3/1/98 (Medicaid expansion) 7/1/98 (Separate program) |
| Colorado | Child Health Plan Plus | Separate | 10/14/97 | 2/18/98 | 4/22/98 |
| Louisiana | LaCHIP | Medicaid | 7/31/98 | 10/20/98 | 11/1/98 |
| Missouri | MC+ for Kids | Medicaid | 9/2/97 | 4/29/98 | 7/1/98 children 2/1/99 parents |
| New York | Child Health Plus | Combination | 11/5/97 | 4/1/98 | 4/15/98 |
| Texas | TexCare | Combination | 4/1/98 6/23/99 |
6/15/98 11/8/99 |
7/1/98 (Medicaid expansion) 4/3/00 (Separate program) |
Sources:
Centers for Medicare & Medicaid Services (CMS), California Title XXI Program Fact Sheet. CMS Web site http://cms.hhs.gov/schip/chpfsca.pdf ]
Centers for Medicare & Medicaid Services (CMS), Colorado Title XXI Program Fact Sheet. CMS Web site http://cms.hhs.gov/schip/chpfsco.asp]
Centers for Medicare & Medicaid Services (CMS), Louisiana Title XXI Program Fact Sheet. CMS Web site http://cms.hhs.gov/schip/chpafsla.asp]
Centers for Medicare & Medicaid Services (CMS), "Missouri Title XXI state Plan Summary Fact Sheet." Web site http://www.hcfa.gov/init/chpfsmo.htm ] Missouri Statewide Health Reform Demonstration Fact Sheet. Web site [http://cms.hhs.gov/schip/chpfsmo.pdf] The State Of Missouri 1915(b) Program. Web site [http://www.hcfa.gov/medicaid/1915b/mo03fs.htm]
Centers for Medicare & Medicaid Services (CMS), New York Title XXI Program Fact Sheet. CMS Web site http://cms.hhs.gov/schip/chpfsny.pdf] New York Governor's Press Office, Child Health Plus Expansion Means Healthier Kids, Press Release, June 18, 1998. Department of Health and Human Services, "HHS Approves Changes in New York SCHIP Program" HHS News, July 12, 2001.
Centers for Medicare and Medicaid Services (CMS), Texas Title XXI Program Fact Sheet. CMS Web site [http://cms.hhs.gov/schip/chpfstx.pdf]
Title XXI provides states with three options for expanding coverage under SCHIP: (1)expanding Medicaid, (2) creating a new insurance program separate from Medicaid, or (3)implementing a combination of the two. Our six study states include examples of each approach, illustrating both that states' made different choices based on the variables and considerations facing them, and that the statutory options, rather than a "one-size-fits-all" authority suited the diversity of state circumstances. Louisiana and Missouri enacted Medicaid expansions; Colorado created a separate program; and California, New York, and Texas each chose to adopt combination approaches. 20 This distribution of program types is similar to that seen nationally--16 states, or roughly one-third of the 50 states and the District of Columbia, implemented Medicaid expansions under SCHIP; whereas 35 states, roughly two-thirds, have created separate programs, either alone or in combination with Medicaid expansions. 21
As illustrated in Table 5, the maximum income eligibility thresholds ultimately adopted by the study states vary considerably--from 185 percent of the federal poverty level (FPL) in Colorado, to 300 percent of the FPL in Missouri. Before SCHIP, the average income threshold for children in all six states was 119 percent of the FPL. After SCHIP, the average income threshold increased to 231 percent of the FPL, an increase of 112 percentage points. 22 This increase is somewhat higher than the increase across all 50 states and the District of Columbia--nationally, the average income threshold for children was 121 percent of poverty before SCHIP, and 214 percent after SCHIP, an increase of 93 percentage points. 23
The three states with the most low-income uninsured children in the nation during the period 1997 to 1999 (California, New York, and Texas) are among the six study states. The other three states were above the mean on this measure. Uninsured children comprised between 22 percent
| Income Eligibility Levels | ||||||||
|---|---|---|---|---|---|---|---|---|
| Infants | Ages 1 to 6 | Ages 6 to 15 | Ages 15 to 19 | |||||
| State | Medicaid Expansion % |
Separate Program % |
Medicaid Expansion % |
Separate Program % |
Medicaid Expansion % |
Separate Program % |
Medicaid Expansion % |
Separate Program % |
| California | N.A.a | 201 to 250 | N.A. a | 134 to 250 | N.A. a | 101 to 250 | 86 to 100 | 101 to 250 |
| Colorado | N.A.b | 134 to 185 | N.A. b | 134 to 185 | N.A. b | 101 to 185 | N.A. b | 38 to 185 |
| Louisiana | 134 to 200 | N.A. c | 134 to 200 | N.A. c | 101 to 200 | N.A. c | 11 to 200 | N.A. c |
| Missouri | 186 to 300 | N.A. c | 134 to 300 | N.A. c | 101 to 300 | N.A. c | 101 to 300 | N.A. c |
| New York | N.A. | 186 to 250 | N.A. | 134 to 250 | N.A. | 101 to 250 | 88 to 100d | 101 to 250 |
| Texas | N.A.a | 186 to 200 | N.A. a | 134 to 200 | N.A. a | 101 to 200 | 19 to 100 | 101 to 200 |
Notes:
Income less than the lower-income eligibility band represent the Medicaid standards for children in effect March 31, 1997.
N.A. = not applicable.
aIn California and Texas, children under 16 years in Medicaid were already covered to 100 percent of the FPL; the
Medicaid expansion under SCHIP does not apply.
bIn Colorado, there is no Medicaid expansion.
cLouisiana and Missouri do not operate a separate children's health insurance program.
dAn expansion up to 133 percent has been approved but will not be implemented until April 2002.
Sources:
Centers for Medicare & Medicaid Services (CMS), California Title XXI Program Fact Sheet. CMS Web site [http://cms.hhs.gov/schip/chpfsca.pdf] State of California. State Child Health Plan under Title XXI of the Social Security Act: California's Healthy Families program. November 18, 1997 Web site [http://www.dhs.cahwnet.gov/org/Director/healthy_families/stplan.pdf]
Donna Cohen Ross and Laura Cox, Making It Simple: CHIP Income Eligibility Guidelines and Enrollment procedures: Findings from a 50-State Survey. Kaiser Commission on Medicaid and the Uninsured, October 2000.
Centers for Medicare & Medicaid Services (CMS), "Eligibility Standards in the 50 States and District of Columbia," January 2001.
Louisiana Department of Health and Hospitals (DHH), Annual Report of State Children's Health Insurance Plans Under Title XXI of the Social Security Act, 2000, March 22, 2001.
Centers for Medicare & Medicaid Services (CMS), "Eligibility Standards in the 50 States and District of Columbia (01/01/01)."
Louisiana DHH, "More Children Now Eligible for Health Insurance," January 9, 2001.
State of Missouri, Department of Social Services, Missouri's Children Health Insurance Program Evaluation." Submitted to the Health Care Financing Administration, March 31, 2000.
American Academy of Pediatrics, Improving Access to Children's Health Insurance in New York. AAP: 2000 Web site: [http://www.aap.org/advocacy/chi2/ny.pdf]
Centers for Medicare & Medicaid Services (CMS), Texas Title XXI Program Fact Sheet. CMS Web site [http://cms.hhs.gov/schip/chpfstx.pdf]
(New York) and 38 percent (Texas) of all low-income children in five of the six states, all figures close to or above the national average of 25 percent. 24 Because of the large numbers of low- income children and the high percentages of low-income children without insurance before SCHIP, the study states also have above-average numbers of children enrolled in SCHIP. Indeed, the study states include the three states with the largest SCHIP enrollment in the nation--again, New York, California, and Texas--with approximately 480,000, 476,000, and 433,000 children participating, respectively, as of September 2001. 25 The remaining three states had far smaller programs--Missouri (approximately 76,000 children); Louisiana (56,000 children); and Colorado (37,000 children)--but each still fell above the national median of 20,389 children.26
15. In 2001, the agency was renamed the Centers for Medicare & Medicaid Services (CMS). To avoid confusion, all further references to the agency in this report are to CMS, regardless of whether the agency was named HCFA(now known as CMS) or CMS in the period under discussion.
16. New York had an existing state children's health insurance program in place before passage of Title XXI, and recognized in Title XXI.
17. Ian Hill, "Charting New Courses for Children's Health Insurance," Policy and Practice, vol. 58, no. 4, December 2000.
18. Frank Ullman, Ian Hill, and Ruth Almeida, CHIP: A Look at Emerging Programs Washington, DC: The Urban Institute, September 1999.
19. Centers for Medicare & Medicaid Services, Web site: [www.cms.hhs.gov/schip/]
20. On October 1, 2002, all of these programs will become "separate" state child health programs, (with the possible exception of New York due to recent federal approval of an additional Medicaid expansion), as opposed to "combination" programs, as the federal mandate for phasing in poverty-level Medicaid coverage of children under age 19 born after September 30, 1983 will be complete. Thus, these states' initial Title XXI efforts, which accelerated the phase-in of Medicaid coverage for children between the ages 15 and 19 living in families with incomes below poverty, will be subsumed within Title XIX, as of October 2002.
21. Centers for Medicare & Medicaid Services, Web site [http://cms.hhs.gov/schip/]
22. Average income eligibility thresholds for children were generated by determining the income eligibility threshold for children of all ages up to age 19, summing the income thresholds, then dividing by 19.
23. Frank Ullman, Ian Hill, and Ruth Almeida, CHIP: A Look at Emerging Programs, Washington, DC: The Urban Institute, September 1999.
24. Catherine Hoffman and Mary Pohl, Health Insurance Coverage in America: 1999 Data Update. Washington, DC: The Kaiser Commission on Medicaid and the Uninsured, December 2000. These data were not available for Missouri.
25. Drawn from SCHIP administrative data and information provided by Marilyn Ellwood from the CMS sponsored study of SCHIP.
26. Vernon K. Smith, CHIP Program Enrollment: December 2000. Kaiser Commission on Medicaid and the Uninsured: September 2001.
VI. Outreach
Highlights of Findings
- Outreach strategies for separate state programs typically consist of state-wide media campaigns to increase public awareness and community-based efforts to reach hard-to-reach families
- Medicaid expansion states rely primarily on community-based outreach strategies
- Community-based outreach workers play an important role by helping families complete SCHIP applications
- Outreach efforts need to address public charge-related fears among immigrants
A. Background and Policy Development
The initiation of a new health insurance program required publicity to ensure that eligible families would learn of it and apply on behalf of their children. States implementing SCHIP were required by Title XXI to describe their outreach strategies in their SCHIP plans. To ensure that program funds pay primarily for health care, Title XXI prohibits states from spending more than 10 percent of their SCHIP expenditures on administrative activities, including outreach.
B. Outreach Strategies
Like states across the country, every state in our study undertook unprecedented levels of outreach for SCHIP. 27 All the states adopted strategies for making families aware of the new coverage, the importance of health insurance for children, and the availability of assistance in enrolling their children. After assessing their alternatives, most states decided to mount broad, statewide marketing efforts, to create a strong brand identity for their programs, and also to support more targeted, community-based efforts designed to "reach in" to harder-to-reach communities and families. To encourage SCHIP enrollment--the primary objective of outreach--most states also offered application assistance. Their strategies are described in Table 6.
| Statewide Marketing | Community-Based Marketing | |||||||
|---|---|---|---|---|---|---|---|---|
| State | New Name | TV And/Or Radio | Print Materials | Health Plans | Hotline | Web Site | Grants/ Contracts with CBOs | CBOs Involved with Application Assistance |
| California | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ |
| Colorado | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ |
| Louisiana | ✓ | ✓b | ✓ | ✓ | ✓ | a | ||
| Missouri | ✓ | ✓ | ✓ | ✓ | ✓ | a | ||
| New York | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ |
| Texas | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ |
Notes: CBO = community based organization.
aLocal and county government organizations receive free printed materials and actively market SCHIP and Medicaid; indeed, this is the core outreach strategy in these states. There are no contracts, however, with community-based organizations
bLouisiana uses radio advertising in a limited number of urban markets.
Source: Information obtained during site visits.
1. Statewide Marketing Efforts
All the study states adopted similar strategies to market SCHIP to families with uninsured children. They created program names with positive images or brand identities, launched television and radio advertising campaigns, posted and distributed promotional print materials, worked with health plans to promote SCHIP and/or Medicaid, established toll-free information hotlines, and created program information Web sites. For example:
- Program Names. States created new and appealing names for their programs, such as Healthy Families (California), Child Health Plan Plus (Colorado), LaCHIP (Louisiana), and TexCare (Texas). State officials described these program names as "not sounding like government programs." In Louisiana, LaCHIP was described as part of the state's effort to "forge a new identity" for its Medicaid program.
Missouri set out to build on the name recognition the state had established for the Medicaid program's managed care initiative, MC+.The State called its SCHIP effort MC+ for Kids. (Reportedly, this name has confused consumers in those parts of the state without managed care.)
- Television and Radio Advertising. In California, Colorado, New York, and Texas the principal outreach component consisted of television and radio advertising, broadcast either statewide or to particular neighborhoods and/or ethnic markets. 28 State officials in these four states described the goals for such marketing as (1) creating a strong identity and promoting name recognition for SCHIP, (2) raising families' awareness of the program and of the importance of health insurance for children, and (3) persuading parents to enroll their children in SCHIP. State campaigns embraced broad slogans, including "Growing Up Healthy" (New York) and "A Healthier Tomorrow Starts Today" (California), and, in TV advertising, used bright colors and images of diverse children to promote their programs. In New York, the governor was featured prominently in several TV ads, urging parents to enroll their children in Child Health Plus.
Mass media outreach was less extensive in Louisiana and Missouri, the two states in the study with Medicaid expansions. Historically, Medicaid programs have not conducted extensive marketing and outreach campaigns. This may help to explain why case study respondents in these two states reported less support for the high-profile marketing of Medicaid.
- Printed Materials. In every study state, printed materials were a core medium of SCHIP outreach and marketing. Colorful, attractive application forms, brochures, posters, and fact sheets were designed and distributed to schools, health departments, WIC clinics, hospitals, Head Start and preschool programs, child care agencies, churches, and other community-based organizations. Billboards often were placed in communities where many families are uninsured.
Attempts were made to target specific racial and ethnic groups. In every state, program applications were printed in English and Spanish; in most states, Spanish-language brochures and posters were also available. In California, state officials found their new Fotonovelas--comic book-style magazines presenting stories about families needing health care and insurance for their children--to be an effective vehicle for promoting SCHIP to Hispanic families.
- Working with Health Plans. To varying extents, five of the six study states used managed care health plans as partners in SCHIP outreach. State officials indicated that they wished to take advantage of plans' marketing expertise but were also mindful of the need to minimize the potential for marketing abuses. For the most part, states have enlisted health plans' assistance, while continuing to carefully regulate the ways in which plans can participate. In California, Colorado, Missouri, and New York, for example, plans must submit all television, radio, and printed marketing materials to the state for review and approval before use. The plans may publicize SCHIP and Medicaid and their role as providers in these programs, but their logos typically must be less prominent than those of the state programs they are promoting. Plans may not contact potential enrollees directly, discuss health plan choice or enrollment in their promotions, or imply that they are the program or the only plan providing care under the program. Some focus group participants were confused between the program and the plan: For example, at the focus groups, participants frequently confused their plan name and the SCHIP program name, and many parents did not know the names of the plans their children were enrolled in.
- Toll-Free Telephone Hotlines. Every study state established one or more toll-free information hotlines that are mentioned prominently in television, radio, and print advertisements. Hotline operations have mostly been contracted out to vendors, whose multi-lingual staffs field questions from callers. Texas originally intended for hotline staff to take applications over the phone, but a heavy volume of calls precluded this from happening often.
- Web sites. Every study state created a program Web site. These Web sites were usually designed for consumers, providing electronic versions of brochures, fact sheets, and, in California, Louisiana, Missouri, and Texas, program applications. Some Web sites also were designed to serve the needs of policymakers, state and local program managers, and researchers; in California, Colorado, New York, and Texas, the Web sites include detailed information on policies and procedures, as well as program data.
2. Community-Based Outreach
Community-based outreach complemented statewide media marketing in California, Colorado, New York, and Texas; in Louisiana and Missouri, it was the main outreach strategy. Whereas statewide outreach was viewed as a means of raising awareness and boosting SCHIP name recognition, community-based outreach was viewed as a way to tell families about the importance of coverage, explain program eligibility rules and application procedures, and correct misconceptions about SCHIP and Medicaid. Often, community-based outreach was seen as the only way states could reach such populations as ethnic minorities, working families with no prior experience with public programs, and immigrant families afraid of becoming a public charge. The states funded a broad array of local organizations to provide community-based outreach, in the hope that "trusted voices" in the community would reach parents and encourage them to enroll their children. It is important to note that these groups were charged with assisting families in completing program applications, and that they were trained to do so. State-specific examples of community-based outreach follow:
- California used two strategies to fund community-level outreach and enrollment assistance. First, outreach contracts were extended to community-based organizations (CBOs) across the state, such as community collaboratives and school-based organizations, to enable them to hire staff to engage in community-wide education, partnership-building with other organizations, and door-to-door and telephone outreach and enrollment assistance. Second, the state trained nearly 24,000 individuals, affiliated with 3,600 "enrollment entities," to serve as Certified Application Assistors who seek out families with uninsured children and enroll them in Healthy Families and/or Medi-Cal in return for a $50 finder's fee per completed application.
- Colorado's outreach and enrollment contractor has networked with local partners, including schools, hospitals, community health centers, local health departments, local social services agencies, and WIC clinics to distribute program materials and promote SCHIP to the families they serve. After training, 82 of these sites were certified as Satellite Eligibility Determination sites to assist families in completing Child Health Plan Plus applications.
- Each of Louisiana's nine Department of Health and Hospitals (DHH) regional offices was asked to develop an outreach plan for its region. Each office has marketed LaCHIP aggressively by distributing applications and brochures through schools and health fairs, outstationing eligibility staff at hospitals and other health care providers, placing articles in local newspapers and contacting and promoting SCHIP with employers, among other strategies. DHH's most ambitious effort was back-to-school campaigns in 1999, 2000, and 2001, in concert with the state Department of Education, the National School Lunch Program, and the state Covering Kids initiative (funded by the Robert Wood Johnson Foundation).
- Missouri distributed program materials, posters, brochures, and applications to local schools, social services offices, hospitals and health centers, health department clinics, and a range of community-based organizations. The state also trained 3,000 individuals to serve as "ambassadors" for MC+ for Kids, spreading the word to community-based organization staff, clients, and others in the community. Finally, piggybacking on an existing initiative, Medicaid officials integrated SCHIP promotional efforts with the activities of eight Community Partnerships, multi-agency consortia charged with addressing the needs of children in such areas as health, mental health, public safety, and juvenile justice.
- In New York, since the inception of Child Health Plus, managed care health plans have marketed the program and enrolled children. More recently, the state launched its Facilitated Enrollment initiative, which gave grants to 32 "lead agencies," representing county health departments, county social services departments, perinatal networks, hospital associations, rural health networks, and senior citizen centers--to develop partnerships with "literally hundreds" of other local organizations to reach out to families and assist them to enroll in SCHIP and Medicaid.
- Texas implemented a regional procurement process that permitted its eight regional Health and Human Services Commission offices to solicit proposals and award contracts to support local outreach and application assistance. In all, 50 community-based organizations received contracts, including community action agencies, county health departments, faith-based charities, health provider groups, hospital partnerships, and other grassroots organizations. Typically, these community-based organizations have networked with other organizations in their communities, training them in TexCare eligibility rules and application procedures and organizing regional outreach and enrollment.
Frequently, community-level outreach efforts were complemented by state support for Medicaid outreach, using funds provided in the Personal Responsibility and Work Opportunity Reconciliation Act of 1996 (PRWORA) specifically for costs attributable to the delinkage of Medicaid from welfare. Most states distributed these funds to county departments of social services, to be used to inform former welfare recipients of the availability of continued Medicaid coverage for them and their children. Louisiana, for example, used PRWORA fundsto distribute LaCHIPmaterials to families enrolled in the Food Stamp Program. In California, the Los Angeles County Department of Social Services partnered with community organizations to publicize Healthy Families/Medi-Cal for Children, and outstationed eligibility workers at hospitals and clinics throughout the county, under its Child Medicaid Enrollment Project.
27. Ian Hill, "Charting New Courses for Children's Health Insurance," Policy and Practice, vol. 58, no. 4, December 2000.
28. In one other state, Louisiana, radio ads were broadcast only in selected, urban markets.
C. Implementation Experiences
Combining statewide media marketing and local community-based outreach was considered a fruitful approach. Case study respondents in four states--California, Colorado, New York, and Texas--considered the two approaches to be complementary. They suggested that broader marketing got families' attention, sparked initial interest in SCHIP, and built "brand recognition" over the long run, while community-based efforts using "trusted voices" from the neighborhood provided the crucial ingredient needed to contact families directly, discuss details of the program, answer questions and clarify misconceptions, and assist families in completing their program applications. Toll-free hotlines were seen as a critical back-up to broader marketing, providing families with a means of obtaining further information about the program. In the two states with Medicaid expansion programs (Louisiana and Missouri), state and local officials wished there was a more prominent mass-media component to their states' strategies. Although they believed that their community-based efforts were highly effective, at the same time, they felt that informing families of the program, in the absence of a broader media effort to raise awareness, posed a significant challenge.
The qualitative findings from the focus groups that follow give a flavor of the views of participants in the SCHIP program. However, since they do not represent a statistically selected sample, their representativeness is clearly limited. The focus groups suggest that awareness of Medicaid comes mainly from experience with the program or through word of mouth. By contrast, the focus groups suggest that awareness of SCHIP comes through mass media:
"I saw a poster, there was a billboard up on Sligh Avenue. It said 'If you need insurance for your kids….' over the railroad track. (I said to my friend) I keep seeing that number, let me take it down and call them. That's how I got it." (Tampa, Florida)"Television. When Pataki started talking about it. That's how I heard about it." (Buffalo, New York)
"I heard it on the radio. I was looking for insurance for my kids, or for all three of us, and couldn't find anything and I heard this and I thought, 'Oh well, I might as well call and they'll tell me it was too much money or whatever.' And I called." (San Jose, California)
Several states reported that their marketing approach had become more targeted over time. Input from consumer focus groups and marketing consultants helped them refine their advertising messages. In both Texas and California, for example, messages included in initial campaigns were described as "too generic" and "limited." However, second-generation SCHIP advertising replaced earlier vague references to "affordable coverage" with the actual dollar costs of premiums, described the benefits in greater detail, provided testimonials from satisfied parents, and, in California, gave clearer statements about children being eligible regardless of citizenship status or participation in "welfare." In Colorado, officials avoided such phrases as "health care for low-income children," which might repel working families. Participants in the focus groups supported the emphasis on explicit, concrete messages, regardless of the medium. They indicated that the most important messages to include in marketing are:
- Applying is simple and convenient
- Insurance is low-cost or no-cost (with details of the costs)
- Coverage offers many benefits
- Working families are eligible (with details on who is eligible)
To increase enrollment, several states targeted particular racial and ethnic groups. California described how it placed advertisements on numerous Spanish-speaking radio stations in various markets across the state; and Texas incorporated into some of its radio and TV ads the well-known Hispanic nursery rhyme sung by mothers to their sick children--"Sana Sana." Participants in evaluation focus groups agreed that strategies such as these would be successful. They suggested using TV, radio, and newspapers in both English and other prominent local languages to reach eligible families. In addition, focus group participants in cities in several of the states suggested placing ads in bus and train stations, as well as on buses and trains. For example, "TV doesn't have but a couple of seconds, and half the time you're in the kitchen or something. The bus, you're sitting there and looking." (SCHIP enrollee, Kansas City, Missouri). Finally, focus group participants recommended reaching out to eligible families in all the places they go in their daily lives, such as health care providers, pharmacies, community centers, grocery stores, fast-food restaurants, shops and post offices, schools, and places of worship.
Among the study states, New York makes the greatest use of health plans as marketing partners.State officials are convinced that health plans play a crucial role in promoting Child Health Plus and boosting program enrollment. They are confident that the state can ensure appropriate marketing by health plans. Although New York continues to review and approve all plan promotional materials, health plans are encouraged to market the program; they may also assist families in completing applications for SCHIP and Medicaid, however, they may not contact families who have not called them. Other states, however, limit the extent to which health plans may assist families with information and enrollment. Such policies frustrated some health plan officials who were eager to become more involved, and who believe that state officials are missing an opportunity to capitalize on health plans' marketing expertise.
States reported having less success with certain outreach strategies. For example, officials in both Colorado and Louisiana said that distributing program brochures, flyers, and applications at health fairs, community events, and open houses at schools resulted in little interest or sustained followup by parents. In California, local outreach agencies were surprised to learn that some of the organizations they had viewed as "obvious partners" resisted getting involved. Reportedly, both WIC agencies and faith-based organizations often were not interested in participating inHealthy Families outreach. For these groups, as well as many schools and school districts, persistence by outreach workers in educating key personnel such as school principals, nurses and administrators may be required to forge successful outreach partnerships.
States with separate state programs also reported that marketing SCHIP alongside Medicaid poses challenges. According to state and local officials in California, Colorado, New York, and Texas, some parents resist enrolling their uninsured children in Medicaid because of negative prior experiences with the program's enrollment process and/or an association of Medicaid with welfare and poverty; these impressions were borne out in the focus group discussions with working families. Parents' negative perceptions of Medicaid stemming from these associations were reported to limit the effectiveness of state and local efforts to promote health insurance more broadly; even as they were favorably disposed toward SCHIP, parents were "turned-off" by the idea of Medicaid. Notably, once they have navigated the system and successfully enrolled in Medicaid, families are generally happy; it is the experience of applying and being screened for eligibility that is considered to be unpleasant. In Colorado and Texas, concerns about stigma have persuaded community organizations to market SCHIP without mentioning Medicaid. "We can get our foot in the door with SCHIP, and then talk about Medicaid when we have to," was a sentiment expressed by outreach staff in these community-based organizations. In California, where all promotional materials display the joint logo, Healthy Families/Medi-Cal for Children, strategies are more mixed. Some community-based organizations and health plans market the programs jointly, while others avoid mentioning Medi-Cal, in order not to lose families' interest. Although advocates understood these dynamics, they took the view that outreach for health insurance should promote SCHIP and Medicaid jointly. Reflecting this perspective, officials of one health plan said they marketed both programs together because "…what we are marketing is health insurance, not Healthy Families." Of note, the focus group participants generally distinguished SCHIP (both separate and Medicaid expansion programs) from Medicaid, suggesting that even when marketed jointly, outreach workers had managed to educate families about the differing nature of the two programs.
Another factor frequently mentioned as a barrier to successful outreach was the widespread fear among immigrant families that participation in SCHIP could jeopardize their (and their children's) residency or citizenship by making them a "public charge." This issue is particularly salient in California and Texas. Also, because some illegal immigrant parents of citizen children also believe that information written on the application form will be passed to the Immigration and Naturalization Service (INS), they are resistant to outreach. It is noteworthy, however, that community-based workers reported that families tended to be considerably less fearful of public charge implications and the INS in relation to SCHIP compared to Medicaid, simply because they perceive SCHIP more as a private health-insurance program, whereas Medicaid is clearly viewed as a government program. Outreach staff have worked hard to overcome the misconception that receipt of Medicaid (except long-term care) or SCHIP is counted when determining public charge status in immigration proceedings. (29)
At the time that state officials were interviewed, support for the programs appeared strong; officials in most states were optimistic that SCHIP outreach to promote recruitment and retention would be sustained. Four of the six study states were satisfied with the amount of funding they had devoted to outreach to date. Only one state, Colorado, told us that the 10 percent federal cap on administrative spending had significantly constrained its outreach efforts.
29. The welfare reform legislation enacted in 1996 included provisions that altogether banned immigrants who arrived in the United States after August 22, 1996, from receiving Medicaid and other federal means-tested public benefits for a period of five years from the time of their entry. However, in many families, some members--those who arrived on or before August 22, 1996 and those who were born in the U.S. and are, thus, citizens--may be eligible for Medicaid even though others in the family are excluded. Although guidance issued by the Immigration and Naturalization Service (INS) has clarified that receipt of Medicaid (except long-term care) and SCHIP is not counted when determining "public charge" status in immigration proceedings, fear persists among immigrant families that Medicaid participation by some members might undermine the renewal of a "green card" or prevent a green card-holder who goes abroad from re-entering the U.S. These fears--which arose from well-publicized incidents in the 1990s of INS officials wrongly requiring green card-holders who were returning to the U.S. to reimburse the government for services received in Medicaid as a condition of reentry--may continue to affect enrollment decisions by immigrant families.
VII. Awareness of SCHIP and Medicaid Among Low-Income Families
Highlights of Findings
- Low-income families value health insurance
- Families are generally satisfied with SCHIP and Medicaid
- Awareness of SCHIP continues to grow but is still not as high as awareness of Medicaid
- Low-income families express widespread interest in enrolling their children in SCHIP or Medicaid
- Knowledge and enrollment barriers for SCHIP and Medicaid still exist for low-income families
If families are to enroll their children in SCHIP and Medicaid, they need both to be aware of the programs and to perceive that these programs offer a valuable benefit. Changing direction somewhat from previous chapters, this chapter offers the perspective of families whose children are targeted by Medicaid or SCHIP. Drawing on findings from focus groups conducted in 2001 with a broad range of low-income families and from preliminary data from the SLAITS National Survey of Children with Special Health Care Needs (CSHCN), 30 this chapter presents information on families' knowledge and perceptions of these programs.
Program activities to increase Medicaid/SCHIP participation among eligible children are successful if the families of eligible children know both that the programs exist and that their children are eligible; value the coverage the programs offer; and consider the coverage worth the time and effort spent in enrolling their children in the programs. Medicaid and SCHIP programs are now enrolling about two-thirds of the children eligible to participate who would otherwise be uninsured (Dubay, Kenney, and Haley 2002). This success shows that program outreach activities are reaching the majority of the children they are targeting. The other side of the same coin, however, is that about one-third of eligible children do not participate for reasons that are not yet fully understood. Gaining their participation is crucial to reducing child uninsurance rates.
30. For information on the data and methods for the survey, see van Dyck et al. (2002) and Kenney et al. (2002).
A. perceptions of the value of ScHIP and Medicaid
Low-income parents participating in focus groups across the country have wide-ranging concerns about their children's education, safety, and health, including health insurance coverage. All these concerns, they say, contribute to their placing a high value on health insurance. Families who participated in focus groups were those interested enough in insurance to attend a focus group, and thus may not represent all low-income families. However, their response was powerful and was consistent across families with different types of insurance coverage (that is, private insurance, Medicaid, SCHIP, and uninsured), different racial and ethnic groups, geographic locations, and primary language (Spanish, English, and other languages).
Focus group participants cited several advantages of having health insurance for their children. In particular, they mentioned freedom from worry about the high cost of a major injury or illness, the ability to take their children for preventive care and to treat acute conditions early, and access to private-sector health care providers and a wide range of benefits. The value families placed on health insurance stemmed from concerns about their children's health and their ability to pay for medical care. Although they used different languages and different words to describe it, the "peace of mind" that comes with health insurance coverage was an important benefit and source of comfort to many parents. For example:
"If you have insurance you don't have to worry about where you are going to get the money to take your child to the doctor or to the emergency room. You just make the appointment and you know you can pay the co-payment. You don't have to worry about it. You don't have to just give them Tylenol and hope it doesn't get any worse. It's just easier money-wise when you have insurance." (San Antonio, Texas)
Many parents in focus groups also believed that having health insurance improved their children's access to care; that is, they reported that their children receive services they otherwise would not, or that they receive better or more timely care, when they are insured. For example:
". . . I believe one of my major benefits for my son will be that he can have one doctor. When you go to health clinics or go to Highland or Acute Care or whatever you see a different doctor each time and no one really knows your case." (Oakland, California)
In addition to their appreciation of the value of health insurance, parents of children enrolled in Medicaid and SCHIP appreciated the coverage and services they received specifically through these programs. In general, families expressed high levels of satisfaction with the benefits, providers, and services available to them under both Medicaid and SCHIP. In many cases, families reported that the range of benefits covered by these programs exceeded their expectations; services that parents were particularly grateful to have covered included prescription drugs, dental care, and vision care. In addition, focus group participants frequently cited the quality of their children's physicians as a source of satisfaction. Finally, a major attraction of Medicaid was that it is free for children; many parents likewise cited the low cost of SCHIP coverage as a significant advantage:
"Like my 20 month old. They go to the doctor every time you turn around. And a lot of it is just well visits and...immunizations, but...if you actually go and try to pay for something like that it's like $100-$150 just for one visit...that's a lot of money. And insurance, whether you're paying for it yourself, the full premium or whatever, it pays for itself just that first two years." (Tampa, Florida)
B. Awareness and Perceptions of Medicaid and SCHIP Among Low-Income Families with Uninsured Children
1. Background and Policy Issues
Despite the value low-income families seem to place on health insurance and the apparent satisfaction with Medicaid and SCHIP of parents who have enrolled their children, some families with low-income children do not enroll them in these programs. Understanding the factors that contribute to this seeming contradiction is key to further improvements in program outreach and enrollment strategies. Therefore, this chapter turns from opinions about health insurance expressed in focus groups conducted with families who have a broad spectrum of experience with these programs, to nationally representative survey data from early 2001 on program awareness levels and perceptions among low-income families with uninsured children whom states had not managed to enroll.
2. The National Picture
a. Program Awareness
In early 2001, almost all (91 percent) low-income uninsured children had parents who had heard of either Medicaid or the separate SCHIP program in their state. Awareness of Medicaid, at 87 percent, is much more common than of SCHIP, at 55 percent (see Figure 1). 31 As SCHIP programs mature, however, awareness of them has been growing. For example, awareness of SCHIP programs in existence in 1999 was 10 to 15 percentage points higher by early 2001 than it was in 1999. 32 And SCHIP programs launched at least 18 months prior to the fielding of the SLAITS survey were recognized by twice as many of the relevant respondents as more recently launched programs were.
Figure 1: Awareness of Medical and Separate SCHIP Programs
Early 2001
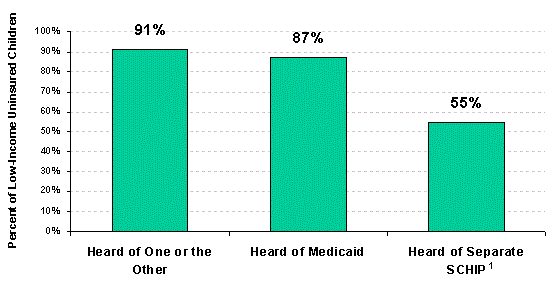
Sourse Urban Institute tabulations of SLAITS National Survey of CSHCN, Preliminary Data File.
Notes: 1. Defined for those in states with separate SCHIP programs with different names than Medicaid programs: Alabama, Arizona, California, Colorado, Delaware, Florida, Georgia, Illinois, Iowa, Kansas, Kentucky, Maine, Michigan, Mississippi, Montana, Nevada, New Hampshire, New Jersey, New York, North Carolina, North Dakota, Oregon, Pennsylvania, Texas, Utah, Virginia, Washington, West Virginia, and Wyoming.
b. Interest in Enrolling in Medicaid/SCHIP
The vast majority of respondents say they would enroll their children if told they were eligible. For example, among low-income uninsured children whose parents know of at least one of the programs, more than four out of five have parents who say they would enroll their child if told that the child was eligible (see Figure 2). Twelve percent have parents who say they would not enroll their uninsured child, and 6 percent have parents who do not know whether or not they would enroll their child. The stated interest in enrolling children in both programs is high, at over 75 percent; but it appears to be somewhat higher for SCHIP than for Medicaid. Among the low-income uninsured children whose parents had heard only of Medicaid, 77 percent had parents who said they would enroll their child if told they were eligible; among those whose parents had heard of both programs, 85 percent had parents who said they would enroll their child; and among the small number whose parents had heard only of SCHIP, 89 percent had parents who said they would enroll their child.
Figure 2: Perceptions of Eligibility for and Attitudes Toward Enrolling in Medicaid/SCHIP Programs
Early 2001
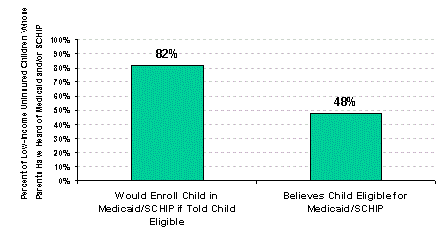
Source: Urban Institute tabulations of SLAITS National Survey of CSHCN, Preliminary Data File.
Furthermore, almost all parents whose children have been enrolled in either Medicaid or SCHIP previously have positive views about enrolling their children again. Nearly 9 out of 10, for example, say they would enroll or reenroll their child if told the child was eligible. And interest in enrolling children is similar among families whose children have previously been enrolled in Medicaid and families whose children have previously been enrolled in SCHIP. Eighty-eight percent of low-income uninsured children previously enrolled in Medicaid have parents who say they would enroll their child in Medicaid/SCHIP if told they were eligible, compared with 89 percent for previous SCHIP enrollees. The interest in enrollment is consistent with high levels of satisfaction with Medicaid and SCHIP reported by parents in focus groups who had experiences with the programs, as discussed above. The challenge of converting this expressed interest into actual Medicaid and SCHIP enrollment remains, however.
c. Beliefs about Eligibility
In spite of widespread program awareness and expressed willingness to enroll, the majority of parents with low-income uninsured children still do not understand that their children are eligible for coverage. According to the most recent estimates (Dubay, Haley, and Kenney 2002), 84 percent of all low-income, uninsured children actually qualify for coverage under Medicaid or SCHIP. But the parents of just under half of the low-income uninsured children whose parents have heard of either Medicaid or SCHIP believe that their child is eligible (see Figure 2). The rest of the parents either believe their child is not eligible (22 percent of children) or do not know (29 percent).
Older children are more likely than younger children to have parents who do not believe they are eligible. Specifically, school-age children (ages 6 to 12, and 13 to 17) are considerably less likely to have parents who think their child is eligible for coverage, than are preschool children (under age 6)--even though all children below a state's income eligibility threshold are eligible for coverage regardless of age (Ullman et al. 1999). 33 These findings strongly suggest that many parents of uninsured children are confused about Medicaid and SCHIP eligibility policies, and are unaware that eligibility is not a function of age.
d. Perceptions of Medicaid and SCHIP Application Processes
Many low-income parents with uninsured children who have heard of Medicaid and SCHIP programs have fairly positive views overall about both the Medicaid and SCHIP application processes. Still, a substantial minority has negative views, and a sizable group has no view at all. In addition, beliefs about the Medicaid process seem to be both more negative, and more intensely negative, compared to beliefs about SCHIP. For example, more parents say that applying for Medicaid is difficult than do so for SCHIP; in addition, parents are more likely to say that applying for Medicaid is very difficult as opposed to somewhat difficult. Among low-income uninsured children whose parents have heard of Medicaid, half have parents who believe it is very or somewhat easy to apply for Medicaid, a third have parents who believe it is somewhat or very difficult, and 15 percent have parents who do not know. In comparison, among the low-income, uninsured children whose parents have heard of the SCHIP program in their state, half have parents who believe it is very or somewhat easy to apply for SCHIP, 22 percent have parents who believe it is very or somewhat difficult, and 24 percent have parents who do not know.
Combining perceptions about the Medicaid and SCHIP application processes into a single indicator clarifies overall perceptions of the application processes. As measured by this indicator, 45 percent of all low-income uninsured children whose parents have heard of at least one of the two programs have parents who see the application processes as easy. This, however, leaves more than half (55 percent) with parents who either think the process is difficult or have too little information to form a view--strongly suggesting that the application processes themselves still constitute a potential barrier to enrollment.
It is encouraging that families who are the most familiar with the processes (that is, those whose children have had prior experiences with Medicaid and SCHIP) have significantly more positive views about the application processes and are much less likely to say they do not know how difficult or easy the processes are, compared to those with no prior experience. For example, about 60 percent of low income uninsured children with prior Medicaid experience had parents who thought the Medicaid application process was easy, while just 37 percent of those with no prior Medicaid experience believed this. Five percent of those with prior Medicaid experience had parents who did not know how easy/difficult the process was, compared with 31 percent of those with no prior Medicaid experience. At the same time, however, those with prior experience are just as likely as those with no prior experience to have negative perceptions of the process--for example, about a third of each group believed the Medicaid application process was difficult.
e. Potential Barriers to Enrollment
The discussion so far has identified several potential barriers to enrollment. Table 7 pulls this information together and categorizes children into five groups based upon the type of barrier their parents reported: lack of knowledge about the programs; problems with the enrollment system; both lack of knowledge and problems with the enrollment system; lack of interest; and no barriers identified. Nearly two-thirds (65 percent) of low-income uninsured children have parents who indicate a knowledge barrier (25 percent), an enrollment system barrier (20 percent), or both (20 percent). Thus, a large group of children appear not to be enrolled because their families lack information about the existence of the programs, their eligibility rules, and/or their enrollment processes; or because they have negative perceptions of those processes.
| Type of Barrier | Percentage of Children |
|---|---|
| Knowledge Barriers Only | 25 |
| Not heard of either program (9 percent) | |
| Heard of at least one program, would enroll child, see application process as easy, but confused about eligibility (16 percent) | |
| Enrollment System Barriers Only | 20 |
| Heard of at least one program, would enroll child, not confused about eligibility, but do not see application process as easy (20 percent) | |
| Both Knowledge and Enrollment System Barriers | 20 |
| Heard of at least one program, would enroll child, confused about eligibility, and do not see application process as easy (20 percent) | |
| Lack of Interest Barriers | 16 |
| Heard of at least one program, would not enroll child (10 percent) | |
| Heard of at least one program, do not know if would enroll child (6 percent) | |
| No Barriers Identified | 19 |
| Heard of at least one program, would enroll child, not confused about eligibility, see application process as easy (19 percent) | |
| Total | 100 |
| Source: Urban Institute tabulations of SLAITS National Survey of CSHCN, 2001 Preliminary Data File. |
Only 16 percent indicate a lack of interest in enrolling. Those who say they would not enroll their child give various reasons for their unwillingness. But the most common reasons are: unwillingness to accept welfare or not wanting to be in a public program; no need for insurance for their child; and time-consuming application processes. Other data indicate that the children of parents who report not needing or wanting insurance tend to be in better health and have fewer unmet needs than other low-income uninsured children (Kenney and Haley 2001).34
Parents of the remaining 19 percent of children indicate no identifiable barrier related to enrolling in Medicaid or SCHIP. These families may be in transition in or out of the workforce, they may have applied for the programs and be awaiting a determination, or they may simply have not applied even though they intend to. Understanding more about this significant group is a key to states' efforts to facilitate program enrollment.
31. Knowledge of SCHIP programs was analyzed for the states with separate SCHIP programs in 2000/2001, with different names than Medicaid programs.
32. According to the National Survey of America's Families (NSAF), 47 percent of low-income uninsured children had parents who had heard of the separate SCHIP program in the 25 states with separate SCHIP programs in 1999 (Kenney et al. 2001). When we reexamined awareness of separate SCHIP programs in those same states in 2001, using the SLAITS, we found that 62 percent of the low-income uninsured children had parents who had heard of these programs. In contrast, we found virtually no difference in the proportion of low-income uninsured children whose parents had heard of Medicaid in these two years, using the two surveys.
33. However, whether the child is eligible for Medicaid or SCHIP does vary by age in some states.
34. Analysis from the 1999 National Survey of America's Families (NSAF).
3. Subgroup Differences
a. Differences by Income and Education
Awareness of both Medicaid and SCHIP programs appears to increase with income. For uninsured children in the very poorest income group--at or below 50 percent of the federal poverty level (FPL)--18 percent had parents who had not heard of Medicaid, while 53 percent had parents who had not heard of the SCHIP program in their state. At the same time, interest in enrolling appears highest (at 91 percent) among these poorest families (see Figure 3). Considerable levels of misperception about eligibility were found across the income spectrum, with misconceptions more common among higher-income families (Figure 3). The trends are similar when the data are stratified by level of parents' education; that is, less highly educated parents are less aware of the programs than more educated parents but are more willing to enroll their uninsured children. Parents' education also seems to be associated with how the application processes are perceived. Less educated parents are more likely to perceive the application processes as difficult and less likely to view them as easy. These patterns are not surprising, considering that low levels of education are associated with illiteracy and numerous related problems.
Figure 3: Perceptions of Eligibility for and Attitudes Toward Enrolling in Medicaid/SCHIP Programs, by Household Income
Early 2001
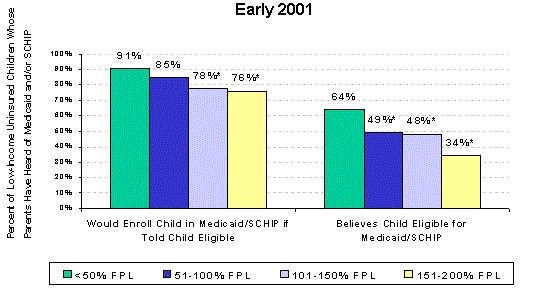 Source: Urban Institute tabulations of SLAITS National Survey of CSHCN, Preliminary Data File.*Indicates group is significantly different from the <50% FPL group at the 0.05 level.
Source: Urban Institute tabulations of SLAITS National Survey of CSHCN, Preliminary Data File.*Indicates group is significantly different from the <50% FPL group at the 0.05 level.
b. Differences by Race, Ethnicity and Language 35
Awareness of Medicaid and SCHIP programs varies widely by race, ethnicity and language group. Low-income uninsured Hispanic children whose parents were interviewed in Spanish are the least likely to have parents who have heard of Medicaid and/or SCHIP, and believe the application processes are easy. Specifically, the parents of these children are 20 percentage points less likely to have heard of SCHIP, and 15 to 20 percentage points more likely to believe that the Medicaid application process is difficult. At least three-quarters of the low-income uninsured children in every race and ethnicity group have parents who say they would enroll their uninsured child in Medicaid or SCHIP if they were told that their child was eligible. However, interest in enrolling children in Medicaid and SCHIP is about 10 to 15 percentage points lower for white children, compared to Hispanic children and black children; in addition, white children are the least likely to have parents who believe they are eligible for coverage.
That the lowest levels of basic awareness, and the most negative perceptions of the application processes, were found among parents who were interviewed in Spanish suggests the need to develop outreach strategies targeted to the Hispanic community, particularly in states with large numbers of uninsured children in this ethnic group. 36
Indeed, focus groups of Hispanic families in California, Florida, and Texas voiced concerns that they were not being targeted effectively by SCHIP outreach efforts and that more materials needed to be developed in Spanish.
35. As described in Kenney et al. (2002), we examined four subgroups of children categorized by their race/ethnicity and the language in which the interview was conducted. The four mutually exclusive groups are: non-Hispanic white (referred to as "white"), non-Hispanic black (referred to as "black"), Hispanic/Spanish language interview, and Hispanic/English language interview. No separate estimates are presented for children of other races because of size and representativeness concerns about these subsamples in this preliminary data set.
36. In 2002, HHS launched an effort to provide information booklets to Spanish-speaking parents whose children may be eligible for coverage through the State Children's Health Insurance Program and Medicaid. The booklets, written in Spanish and English on alternating pages, explain the importance of having health insurance and address common questions about program eligibility. State agencies and other organizations can use the bilingual booklets in their efforts to reach eligible children in the Hispanic community.
VIII. Eligibility and Enrollment
Highlights of Findings
- States have simple application processes for SCHIP
- Many of SCHIP's enrollment processes have been adopted in Medicaid, but barriers to Medicaid enrollment remain
- Medicaid is still associated with welfare in many parents' minds, and this perception is a barrier to enrollment
A. Background and Policy Development
With the explicit goal of expanding health insurance coverage for children, Title XXI brought the implicit charge to states to undertake strategies that would facilitate children's enrollment into the program. Indeed, during each state's SCHIP design phase, officials focused considerable attention on making enrollment simple and devising streamlined enrollment procedures. Their goals were to make it easy for eligible families to enroll and to reach SCHIP enrollment targets on schedule. In addition, states are required by federal law to have "screen and enroll" procedures in place, to ensure that only those eligible for SCHIP are actually enrolled in SCHIP, while those eligible for Medicaid are identified and enrolled in that program.
The states' goal was to make the application process simple. States designed SCHIP application processes to make it easy for families to sign up. Adopting streamlined procedures was one way separate programs tried to model themselves after private insurance. In the two Medicaid expansion programs studied, too, considerable support emerged for simplifying existing eligibility determination procedures. In Missouri, for example, a user-friendly enrollment system was seen as crucial to attracting higher-income families typically unfamiliar with government programs.
All of the study states have embraced the idea that families should be able to get help applying for SCHIP or Medicaid. The states have introduced both telephone-based and in-person assistance in communities throughout their states, and modified a variety of eligibility requirements, such as removing assets tests and reducing the amount of documentation families must provide in support of their applications. Still, while many of the simple procedures adopted under SCHIP have "spilled over" to Medicaid policy, coordination of SCHIP and Medicaid in states with separate programs remains a challenge.
B. Program and Policy Characteristics
Eligibility Policies and Enrollment Processes
Simple Applications. The study states have adopted a variety of policies aimed at keeping the SCHIP application process simple (see Table 8). Specifically, every state has developed a joint application form for its SCHIP and Medicaid programs (ranging from one to eight pages), and none of them requires a face-to-face interview with an eligibility worker; families can apply for SCHIP by mail. In addition, to keep enrollment simple, five of the six states do not use an assets test in SCHIP. One of the states--New York--has adopted (but not yet implemented) presumptive eligibility for SCHIP applicants. 37
Another aspect of simple applications is minimal documentation requirements (see Table 9). Four study states do not require families to verify children's ages; four do not require them to document state residency; three do not require them to verify income the state has disregarded; three do not require families to verify their immigrant status; and none of the study states requires families to submit verification of their children's social security numbers. In the one state (Missouri) that applies an assets test for SCHIP, families do not have to submit documentation. All six study states, however, require that applicants submit verification of income (Missouri initially permitted families to self-declare their income).
Most states have simplified Medicaid application rules and procedures since the implementation of SCHIP. However, the Medicaid application process typically remains more difficult than the process for SCHIP (see Table 8). For example, Medicaid programs have been less likely than SCHIP programs in the same states to minimize verification requirements (Table 9). Medicaid programs in the study states often require applicants to submit verification of income deductions, assets, children's ages, residency, immigration status, and social security numbers--requirements they do not impose on SCHIP applicants. Further, only two of the six study states have eliminated assets tests for Medicaid, compared to five for SCHIP.
Continuous Eligibility and Retroactive Eligibility Policies. Four of the six study states extend 12-month continuous eligibility to children in their SCHIP programs. 38 Only three of the six states do so for children in their Medicaid programs (Texas extends 12-month continuous eligibility in its SCHIP program but 6-month continuous eligibility in its Medicaid program). Medicaid is required by law to make eligibility retroactive to 90 days prior to the date
| State | Simplification Strategies | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Joint Application | No Face-to-Face Interview | Dropped Assets Test | 12-Month Continuous Eligibility | Presumptive Eligibility | Retroactive Eligibility | ||||||
| (Length) a | SCHIP | Medicaid b | SCHIP | Medicaidb | SCHIP | Medicaid b | SCHIP | Medicaid b | SCHIP | Medicaidb,c | |
| California | ✓(4) | ✓ | ✓ | ✓ | ✓ | ✓ | d | ✓ | |||
| Colorado | ✓(8) | ✓ | ✓ | ✓ | ✓ | ✓d | ✓ | ||||
| Louisiana | ✓(2) | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓c | ✓ | ||
| Missouri | ✓(2) | ✓ | ✓ | ✓ | |||||||
| New York | ✓(2) | ✓ | ✓ | ✓ | e | ✓ | ✓ | f | ✓ | ||
| Texas | ✓(2) | ✓ | g | ✓ | ✓ | ✓h | ✓ | ||||
Sources:
Centers for Medicare & Medicaid Services (CMS), Framework For State Evaluation of Children's Health Insurance Plans Under Title XXI of the Social Security Act, 1999: California, March 2000. Web site http://cms.hhs.gov/schip/caeval98.pdf]
Kaiser Commission on Medicaid and the Uninsured. Comparison of Medi-Cal and Healthy Families Programs in California, October 2000.
Centers for Medicare & Medicaid Services (CMS), Annual Report of State Children's Health Insurance Plans Under Title XXI of the Social Security Act: Colorado, November 2000.
Centers for Medicare & Medicaid Services (CMS), "Application and Enrollment Simplification Profiles: Medicaid for Children and SCHIP";
Centers for Medicare & Medicaid Services (CMS), Framework for Annual Report of State Children's Health Insurance Plans Under Title XXI of the Social Security Act: New York State, November 2000. CMS Web site [http://cms.hhs.gov/schip/charny99.pdf]
Centers for Medicare & Medicaid Services (CMS), Framework For State Evaluation Of Children's Health Insurance Plans Under Title XXI of the Social Security Act, 1999: Texas, March 2000. Web site [http://cms.hhs.gov/schip/txeval98.pdf]
Notes:
aThe numbers of pages in the application form are shown in the table. The application package includes instructions of varying length.
bChildren's programs under Title XIX.
cRetroactive to up to three months prior to date of application.
dMedicaid policy requires retroactive coverage to date of application in many cases.
eNew York has a 12-month redetermination cycle.
fPresumptive eligibility for children was approved in the 1998 New York Health Care Reform Act, but it has not been implemented.
gTexas has since taken action to allow children (but not adults) to apply for Medicaid without a face-to-face interview.
hContinuous eligibility under Medicaid in Texas is for 6 months, not 12.
| Verification Requirements | ||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
State |
Income | Deductions | Assets | Age | State Residency | Immigration | SSNe | |||||||
| SCHIP | Medicaidc | SCHIP | Medicaidc | SCHIP | Medicaidc | ✓ | ✓ | SCHIP | Medicaidc | SCHIP | Medicaidc | SCHIP | Medicaidc | |
|
California |
Net | Net | ✓ | ✓ | NA | ✓ | ✓ | ✓ | ✓ | ✓ | ||||
|
Colorado |
Net | Net | ✓ | NA | ✓ | ✓ | ✓ | |||||||
|
Louisiana |
Net | Net | ✓ | ✓ | NA | NA | a | a | ✓b | ✓b | ||||
|
Missouri |
Gross | Net | NA | ✓ | ✓ | ✓ | a | a | ✓b | ✓b | a | a | ||
|
New York |
Grossd | Net | NA | ✓ | NA | NA | ✓ | ✓ | ✓ | ✓ | NA | ✓ | ||
|
Texas |
Net | Net | ✓ | ✓ | NA | ✓ | ✓ | ✓ | ✓ | |||||
Notes: SSN = social security number.
Blank indicates that self-declaration is sufficient.
NA = not applicable.
aVerified using state databases.
bFor applicants who are noncitizens.
cChildren's programs under Title XIX.
dSelf-declaration of income is permitted as a last resort, when no income verification can be provided.
eNote that this refers to the verification of the SSN. NA indicates that the SSN is not required.
Sources: Donna Cohen Ross and Laura Cox, Making It Simple: CHIP Income Eligibility Guidelines and Enrollment procedures: Findings from a 50-State Survey.Kaiser Commission on Medicaid & the Uninsured, October 2000.
Centers for Medicare & Medicaid Services (CMS), Framework For State Evaluation Of Children's Health Insurance Plans Under Title XXI of the Social Security Act, 1999: California. March 2000. Web site [http://www.hcfa.gov/init/caeval98.pdf]
Kaiser Commission on Medicaid and the Uninsured. Comparison of Medi-Cal and Healthy Families Programs in California, October 2000.
Annual Report of State Children's Health Insurance Plans Under Title XXI of the Social Security Act: Colorado November 2000.
Centers for Medicare & Medicaid Services (CMS), Application and Enrollment Simplification Profiles: Medicaid for Children and SCHIP.
Centers for Medicare & Medicaid Services (CMS), Framework for Annual Report of State Children's Health Insurance Plans Under Title XXI of the Social Security Act: New York State, November 2000. CMS Web site http://www.hcfa.gov/init/charny99.pdf ]
Centers for Medicare & Medicaid Services (CMS), Framework For State Evaluation Of Children's Health Insurance Plans Under Title XXI of the Social Security Act, 1999: Texas, March 2000.Web site [http://www.hcfa.gov/init/txeval98.pdf]
| Avenue of Submission | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| State | Mail-In Applicationa | Community-Based Enrollment | Phone Applicationb | Internet Applicationb | County Social Services | |||||
| SCHIP | Medicaid c | SCHIP | Medicaid c | SCHIP | Medicaid c | SCHIP | Medicaid c | SCHIP | Medicaid c | |
| California | ✓ | ✓ | ✓ | ✓ | ✓d | ✓ | ✓ | |||
| Colorado | ✓ | ✓ | ✓ | ✓ | ✓e | ✓ | ✓ | |||
| Missouri | ✓ | ✓ | ✓f | ✓ f | ✓ | ✓ | ||||
| Louisiana | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ||||
| New York | ✓g | ✓ | ✓ | ✓ | ✓ | |||||
| Texas | ✓ | h | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ||
Notes:
aTherefore, no face-to-face interview is required.
bSignature required either electronically or as a hard copy.
cChildren's programs under Title XIX.
dCurrently in a pilot phase. Soon to be introduced on a county-by-county basis.
eCurrently under development.
fPhone center staff fill out the application during the phone call, but then mail it to the family for a signature. The family then mails the signed application back to the phone center for final processing.
gA face-to-face interview is required for children referred to Medicaid, but it can be conducted by a facilitated enroller rather than a social services worker.
hTexas now allows mail in applications to Medicaid for children (but not adults).
Source: Information obtained during each site visit.
of application. SCHIP programs, like private insurance, for the most part begin coverage after an application has been approved, or as of the application date. 39
Enrollment Procedures. Children in the study states can enroll in SCHIP and Medicaid in many ways. These methods, displayed in Table 10, are summarized below:
- Mail. All six study states accept mailed-in SCHIP applications. They adopted this policy to make it easier for parents to apply and to avoid any resistance that might arise from requirements to meet with an eligibility worker in a social services agency. Although five states permit mail-in applications to be used for both SCHIP and Medicaid, New York requires a face-to-face interview for those children who apply for, or are referred to, Medicaid. 40
- Community-Based Application Assistance. Five states have introduced community-based help for families completing program applications, as discussed extensively in Chapter VI, which describes states' outreach activities.
- Telephone Assistance. Two states can take applications by telephone. Missouri has established seven regional telephone application assistance centers. The state's outreach materials display a toll-free hotline number. Phone center staff can take an applicant's personal information over the phone, make a preliminary eligibility determination based on that information, and then mail the application to the parent for a signature. Alternatively, phone center staff can just mail parents a blank application. Texas has a similar system; however, its hotline staff typically mail applications to families, rather than completing applications over the phone, due to a high volume of calls.
- Internet. Three states are exploring using the Internet to facilitate SCHIP and Medicaid enrollment. California and Texas have pilot-tested Internet-based applications and are introducing their systems in selected counties. California's Certified Application Assistors and Outreach Contractors initially will use the Health-E Application to help families apply. Texas' "E-Z App" will be directly available to consumers for them to complete their applications online. Although Colorado has been designing a similar program since the program began, it is not yet in use.
- County Departments of Social Services. Finally, in all six study states, families can apply for SCHIP coverage at county welfare offices or with eligibility staff outstationed at public clinic and hospital sites. In states with separate programs, families applying in this way typically complete the longer Medicaid (or multiprogram) application and eligibility is reviewed for the entire family. This process can lead to referrals to SCHIP for children in families with incomes or assets above Medicaid limits. The county staff we interviewed stated that they infrequently help families complete SCHIP application forms; instead, they refer families to SCHIP but also may give them a SCHIP application form. In states with Medicaid expansions, of course, county social services agencies review applications for both SCHIP and Medicaid eligibility.
Screen-and-Enroll Procedures. To ensure that children eligible for Medicaid are enrolled in Medicaid rather than SCHIP, states must review every SCHIP application for Medicaid eligibility before covering any child under SCHIP. In the two study states with Medicaid expansion programs, Louisiana and Missouri, screen-and-enroll is relatively simple; social services staff in county offices, phone centers, and application centers review all applications and determine which program each child is eligible for.
In the four states with separate programs, screen-and-enroll procedures have proven complex. This occurs primarily because county social services agencies retain responsibility for Medicaid, while a different entity is responsible for determining SCHIP eligibility. Thus, states needed to develop mechanisms for transferring applications back and forth between these entities. In California, Colorado, and Texas, vendors act as "single points of entry" into SCHIP and Medicaid; all applications in these states are mailed to the vendors, who then conduct screen-and-enroll reviews. The vendors process SCHIP-eligible applications but transfer to county social services offices in the child's county of residence applications for those children who appear to be Medicaid-eligible. In New York, no single point of entry exists; instead, "Facilitated Enrollers" and their "lead agencies" conduct screen-and-enroll and make referrals to county social services offices.
37. Presumptive eligibility policies permit designated local agencies and providers to deem someone "presumptively eligible," based on information provided by the applicant. Services may then be provided (and will be paid for) for these applicants during the time period, until the state completes its official eligibility determination.
38. Neither Missouri nor New York guarantees continuous coverage for 12 months in the SCHIP program, although both states redetermine eligibility every 12 months. During that period, families must notify the state of any changes in income or family structure that could affect their eligibility status.
39. Of the two Medicaid expansion programs in the study, Missouri, under its Section 1115 Medicaid demonstration, provides no retroactive coverage to Title XXI enrollees.
40. In New York, a qualified "Facilitated Enroller" can conduct the face-to-face interview, rather than a county social services worker.
C.Implementation Experiences
1. Eligibility Policies and Enrollment Procedures
State and local officials and advocates interviewed in the case studies recognized that SCHIP enrollment had been made simple in important and beneficial ways. Many parents participating in the focus groups were in agreement; they found the application and document requirements simple and manageable. In addition, those who chose to mail in their applications appreciated the convenience of that mechanism, as well as being spared a trip to the social services office:
"It was a legal-size paper and there was a column for your information and whoever you wanted to put on the insurance and then there was a thing for your income and that was pretty much it and then you signed it." (Tampa, Florida)"All they needed was proof of my income. And everything was laid out and they had a number you could call for help with the application. It was a booklet by the time I got it. It looked like a lot but it wasn't a lot." (San Jose, California)
It has been widely noted that Medicaid is adopting some SCHIP application features. In every study state, SCHIP either stimulated the creation of shorter, simpler "joint" application forms or it reinforced existing simplification efforts. In California, simple strategies adopted by the separate SCHIP program--for example, permitting applications to be mailed in, imposing no assets tests, minimizing verification requirements, and guaranteeing 12 months of continuous eligibility--were also adopted by the Medicaid program with the goal of aligning the rules of the two programs (even though these policies had been resisted by the state for Medicaid for years before SCHIP was created). Also, in Texas, much more stringent eligibility rules for Medicaid than for SCHIP spurred support for passage of a Medicaid simplification bill. Beginning in late 2001, Texas' Medicaid eligibility rules were brought into closer alignment with those of SCHIP--with an assets test persisting as the only key difference between the programs. Case study respondents in the study states predicted that such simplification progress would eventually greatly benefit families whose children enroll in Medicaid. Notwithstanding claims of simplification, focus group participants who had applied for Medicaid in New York, California and Colorado (which have separate SCHIP programs) seemed to think the process was very onerous.
More subtly, but equally important, case study respondents indicated that SCHIP may also be promoting changes in the culture and operations of traditional welfare programs. In both Louisiana and Missouri, efforts already underway to delink Medicaid from welfare eligibility systems were expanded after Title XXI, in an effort to create more consumer-friendly systems. And in each state with a separate program, the social services system was working hard to facilitate families' access to coverage, as opposed to discouraging it. Especially in high-density population centers such as Los Angeles County and the boroughs of New York City, local eligibility staff made such observations as: "…we've had a real culture shift here. No longer are we supposed to keep everybody out; we're supposed to help them get in!" Yet, some focus group participants still reported problems with rude and unhelpful eligibility workers.
Despite the streamlining of children's enrollment and the spillover effects noted by case study respondents, they reported that many SCHIP and Medicaid eligibility system issues still need to be addressed:
- While SCHIP and Medicaid eligibility have been greatly simplified, differences in the rules and procedures of the two programs persist in several states with separate programs, causing confusion among families and difficulties with application processing. As detailed above, states have simplified their eligibility rules and procedures for Medicaid, but they are not as simple as in SCHIP. The effects of the differences were clear to many study informants at the state and local levels--confusion among families and more complex administration, especially with regard to the screen-and-enroll function.
- Even with simplified forms, reduced verification requirements, and the widespread availability of application assistance for parents, many parents are confused about eligibility and many submit incomplete applications. Often, this was blamed on continued differences between SCHIP and Medicaid rules, which result in unnecessarily long joint applications (that must take into account the rules of both programs) and confuse parents. For advocates, in particular, this was evidence that SCHIP and Medicaid application procedures were still "too complex." Reported rates of "incompletes" varied from 70 percent in California to 35 percent in Texas. Interestingly (and, perhaps, discouragingly), case study respondents in California and Louisiana reported that incomplete rates are no lower among parents who received application assistance. Both California and Texas were hopeful that their Internet-based applications would significantly increase families' rates of submitting complete applications.
Low-income focus group participants often were confused about eligibility rules. Some eligible families thought they made too much money to qualify, or felt that it was not right that someone in their income bracket should qualify for a government program. Other families assumed that they wouldn't qualify for SCHIP because of experience with or assumptions about Medicaid:
"I always thought medical assistance was the medical side of welfare." (Maryland)
- In states with separate programs, screen-and-enroll procedures were described as complex and confusing for families. Families' confusion was attributed once again to differences between SCHIP and Medicaid rules that frequently require that eligibility be determined twice. The most prominent problems surrounded the logistics of sharing information between "single point of entry" vendors and county departments of social services. Depending on where an application is initiated, screen-and-enroll may require vendors to "deem" or refer applications to their social services counterparts, or vice versa. Due to differing eligibility rules (and confusion over how rules for one program may or may not apply to the other), applications are often sent back and forth between vendors and social services offices several times. Several social services staff described the vendor in California as "a black hole" because of its inability to track the status of applications. Colorado enrollers were concerned that many children referred to Medicaid were "falling through the cracks"--because the state did not have a system for tracking applications. Case study respondents viewed the vendor in Texas more favorably because this vendor can track applications (by bar codes) and electronically transfer "images" of applications to county offices.
In addition to screen and enroll problems, families in focus groups reported not always being told about the availability of SCHIP when they were denied Medicaid. Although families in focus groups in Georgia and Colorado report that caseworkers told them about the availability of another program, families in other states where focus groups were held said that caseworkers had not told them about SCHIP. Participants mentioned finding out about SCHIP from friends and from TV.
- Community groups sometimes criticized retroactive "finder's fees" as an ineffective way to pay community-based application assistors.Despite considerable praise voiced for community-based application assistance efforts, those states that pay agencies retroactive finder's fees for successfully enrolled children (California, Colorado, and Louisiana) tended to be criticized by community groups. Fees vary from $12 in Colorado to $50 in California. Regardless of the fee level, community-based organizations in each of these states reported that fees did not cover the time and costs involved in assisting families with applications. Furthermore, satisfaction was undermined in California by slow payment by the state's vendor. Not surprisingly, community groups tended to prefer grants or contracts to support application assistance activities. In particular, they praised up-front funding because it enabled them to add capacity by hiring new staff.
- State eligibility data systems also were criticized by case study respondents for their inability to track applications through the process and report precise figures on SCHIP and Medicaid eligibility outcomes. While every state strongly believed that Medicaid enrollment of children had increased as a result of SCHIP outreach and enrollment efforts, the states in our sample could not quantify this claim with precise program data.
- Changes in culture, approach, and attitudes in county social services departments have occurred in many localities, but many counties have been "slow to give up their welfare mentality and practices." Case study respondents in California, Colorado, New York, and Texas spoke of the wide variation in practices between counties, with some cooperating with community application assistors and others seemingly resentful that other groups were determining eligibility. They also noted instances where counties' actual eligibility-review procedures differed, despite uniform state policy. These problems contributed to difficulties with screen-and-enroll and perpetuated some families' negative feelings toward Medicaid. Moreover, some focus group respondents pointed out that a welfare mentality persists. Many parents stated that they felt hostility and condescension from the social services workers and some felt that they were discriminated against based on their race, ethnicity, or gender:
"I think they should treat people like they're people and with a little bit of more respect. Like I said before, if you don't need these services you certainly wouldn't put yourself out to go down there and take the treatment." (Cleveland, Ohio)
Case study respondents reported that family resistance to Medicaid was strong in several states and believed that it was undermining states' efforts to achieve high enrollment in public insurance programs. However, it is not clear how common resistance to Medicaid is, since very few low-income families with uninsured children say that they would not enroll their child in Medicaid if told their child was eligible. Moreover, as demonstrated in the next section, in the six states examined here, Medicaid enrollment by children dwarfs SCHIP enrollment, which suggests that many families overcome whatever resistance they may have felt toward Medicaid. Case study respondents indicated that some of the resistance stems from prior negative enrollment experiences at county welfare offices--advocates and others noted families feeling "…intimidated by local DSS offices," and of being "treated rudely." The focus groups strongly supported this point. Families with experience with the Medicaid program were particularly critical of eligibility staff at social services agencies. "I think the people who work in that office should be conscientious about that they are helping people who truly need it." (Miami, Florida, translated from Spanish)
Family resistance to Medicaid was manifest most clearly during screen-and-enroll activities. In California, New York, and Texas, we repeatedly heard that families were attracted to SCHIP's promise of health coverage for children, but did not want to participate if their children were found to be Medicaid-eligible. Local enrollers reported that "…families have begged us to stay on SCHIP and even offered to pay premiums to do so."
Community-based enrollers have had mixed success in persuading these families to sign their children up for Medicaid. In New York, Facilitated Enrollers reported they were able to convince the majority of the families with whom they worked to follow through with Medicaid enrollment for their children. (This may be related to the fact that fears of public charge seem to have largely dissipated, due in part to New York's decision to use state funds to cover immigrant and noncitizen children in Child Health Plus.)The challenge was, however, far greater in California and Texas. One Application Assistor in California noted "…I lose 90 percent of the children that I find Medicaid-eligible…they simply walk away." The fact that 43 percent of parents check the box on the Healthy Families/Medi-Cal for Children application form indicating that they do not want their application forwarded to DSS was described as further evidence of Medicaid welfare stigma, and of the fact that the fear of public charge has been "very slow to fade." In Texas, case study respondents stated that only 25 percent of families referred to Medicaid ultimately enroll in the program.
2.Enrollment
As a result of the outreach and enrollment procedures discussed above, the six study states enrolled more than 1.5 million SCHIP enrollees by September 2001 (see Table 11). 41 Most of these enrollees were in California, New York, and Texas, which have the three largest programs in the nation, each with between 400,000 and 500,000 children enrolled. The states with smaller populations--Colorado, Louisiana, and Missouri--had enrolled fewer than 100,000 children. In every state, SCHIP enrollment is dwarfed by that of Medicaid (for children).
| State | SCHIP Enrollment (2001)a | Medicaid b Child Enrollment (FFY2000) |
|---|---|---|
| California | 475,795 | 3,243,667 |
| Colorado | 36,536 | 196,695 |
| Louisiana | 63,046 | 450,806 |
| Missouri | 75,856 | 432,899 |
| New York | 479,973 | 1,510,433 |
| Texas | 432,745 | 1,612,401 |
| Total | 1,563,951 | 7,446,901 |
Notes:
aPoint-in-time data for the most recent month available, which is September 2001 for all states.
bChildren's programs under Title XIX. Children under age 19 ever enrolled during federal fiscal year 2000.
Source: SCHIP enrollment figures: State administrative data; Medicaid: Kaiser Family Foundation. State Health Facts Online. Medicaid enrollment figures: Rosenbach et al. 2002.
Enrollment in the study states grew significantly during the first three years of SCHIP, as seen in Figure 4, but trend lines vary across the states. Whereas California, Colorado, Louisiana, and Missouri experienced fairly steady growth, Texas' enrollment increased dramatically with the implementation of its Phase 2 TexCare program in April 2000; and New York's enrollment recently began to decline as a result of low renewal rates (see Chapter IX). Figure 5 illustrates the percentages of their goals that states have enrolled. 42 Target attainment varies widely from a high of 101 percent in Texas, to a low of 53 percent in Colorado; California, Louisiana, Missouri, and New York each enrolled 68 percent or more of their target populations of children, as of late 2001.
FIGURE 4: SCHIP ENROLLMENT TRENDS FOR THE STUDY STATES
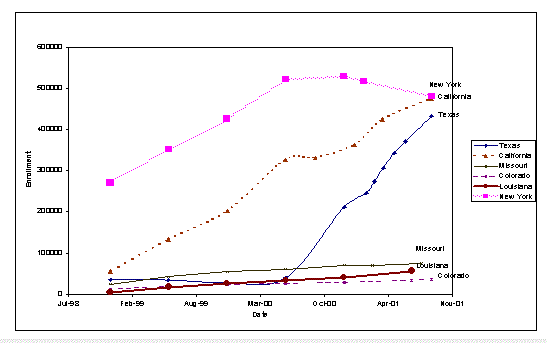
SOURCE: Centers for Medicare and Medicaid Services (CMS), “State Children’s Health Insurance Program (SCHIP) Aggregate Enrollment Statistics for the 50 States and the District of
Columbia for Federal Fiscal Years (FFY) 2000 and 1999.”
Web site [http://cms.hhs.gov/schip/fy99-00.pdf]
Vernon K. Smith, “CHIP Program Enrollment: December 2000,” Kaiser Commission on Medicaid and the Uninsured, September 2001.
Colorado Department of Health Care Policy and Financing (HCPF)
Louisiana Department of Health and Hospitals, Medicaid Division
Managed Risk Medical Insurance Board. Health Families Program Enrollment History. Web site [http://www.mrmib.ca.gov/MRMIB/HFP/HFPRptHG.html]
Missouri Department of Medical Services
Web site [http://www.dss.state.mo.us/mcplus/index.htm]
New York State Department of Health.
Web site [http://www.health.state.ny.us/nysdoh/chplus/index.htm]
Texas Department of Health Services. Cumulative DHS CHIP Status Report (Updated Weekly): CHIP Enrollment and Referrals, September 04, 2001. TexCare Partnership Web site: [http://www.hhsc.state.tx.us/chip/DHSrpt.pdf]
FIGURE 5: SCHIP ENROLLMENT TRENDS AS A PERCENTAGE OF THE TARGET FIGURE FOR EACH STATE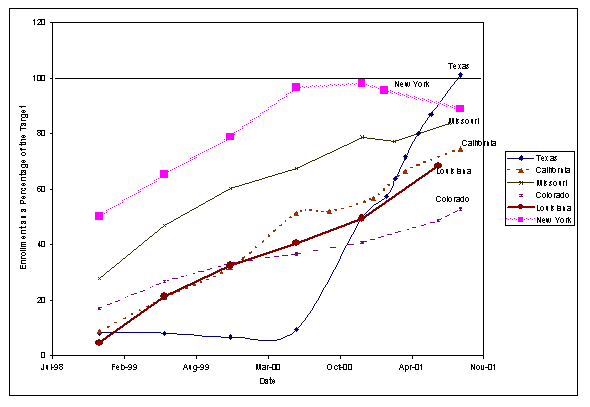 SOURCE: See Sources Figure 4.
SOURCE: See Sources Figure 4.
Most state officials were highly satisfied with their enrollment success. They were pleased with the simpler enrollment systems, as well as the success of outreach in building strong program recognition and persuading large numbers of families to enroll their children. Community-based application assistors, working in a variety of settings, appear to be an important ingredient in achieving high enrollment. Satisfaction varied among other case study respondents, both across the study states and within each state. Comments from case study respondents in the states that used application assistance the most (those with separate programs) include the following:
- In California, state officials, advocates, and local-level enrollers consistently believed that the state had improved after a shaky start. The launch of Healthy Families was marred by the state's use of a 28-page form, which was universally criticized as unworkable. By early 1999, state officials, working closely with advocates and other interested groups, had developed a simpler, four-page form and designated its vendor, EDS, as the "single point of entry" for all applications. These improvements helped increase enrollment, beginning in late 1999. The case study respondents also pointed to steady expansion and growth in funding for application assistance as crucial to reaching hard-to-reach groups and improving the state's enrollment of Hispanic children, who now comprise roughly 70 percent of all enrollees, commensurate with the representation of low-income Hispanic children.
- In New York, state officials believe that it takes time to increase enrollment. They had an advantage over most states in building SCHIP on a state-funded initiative that had been in place for six years before SCHIP enactment. Most case study respondents felt that health plans had been successful partners in outreach and enrollment. With careful oversight and monitoring by the state, these plans had aggressively identified and enrolled eligible children. With the addition of Facilitated Enrollment in mid-2000, New York appears to have improved its screen-and-enroll capability.
- In Texas, enrollment grew rapidly beginning in April 2000, coincident with the launch of its separate program, TexCare. While some criticized the state's slow start, which left many thousands of children uninsured during its two-year planning phase, within 18 months of start-up, Texas' enrollment had reached nearly the level of enrollment in California and New York. State officials attribute this success to two years of careful planning of outreach and enrollment strategies that drew heavily on the input of consumers, advocates, and other groups interested in expanding insurance coverage for children, as well as on observations of strategies that had worked in other states.
- In Colorado, case study respondents believed that enrollment growth could have been greater. While they viewed the SCHIP eligibility process as dramatically simplified, they also cited factors that had suppressed enrollment, including a complicated joint application form (recently revised and improved), inconsistencies in SCHIP and Medicaid rules, sometimes problematic relationships between SCHIP and county social services agencies, and a premium structure that may have induced consumer resistance to the program, especially in light of the state's existing low-cost Indigent Care Program (see Chapter XII which discusses cost sharing).
41. Table 11 presents the latest point-in-time enrollment estimates for Medicaid and SCHIP.
42. These targets do not represent the total number of low-income uninsured children eligible for SCHIP in each state; also, states employed different assumptions to set these targets. The targets do, however, reflect policymakers' program goals and are the benchmarks against which they judged whether they were achieving their goals.
IX. Eligibility Redetermination and Retention
Highlights of Findings
- Retention of eligible children has emerged as a concern and priority for many states
A. Background and Policy Development
Though states made early headway in enrolling eligible children into SCHIP, anecdotal evidence emerged as early as mid-1999 that many SCHIP enrollees were losing eligibility, or disenrolling, at the end of their initial period of coverage. It became clear during this study that states had not necessarily anticipated this issue; they had, after all, focused much of their attention on getting their programs up and running and on facilitating initial enrollment. They devoted less time to thinking about retention rates or policies to simplify children's renewal of coverage. However, three years into the program, the study states had realized that the challenge of keeping eligible children covered required their attention, and they were beginning to adapt the measures that had proved so successful for initial eligibility determination and apply them to redetermination procedures.
In addressing retention, state officials recognized that they could not easily define what an "appropriate" or "ideal" rate of retention for SCHIP enrollees might be. Rather, it is apparent that the SCHIP population is a dynamic one in which parents of enrollees move in and out of employment, and in and out of employer-sponsored health insurance coverage. Therefore, some attrition in the program is appropriate--as families obtain private coverage through new jobs, lose jobs (and income) and become Medicaid eligible, move out of state, or their children reach age 19. Some causes of disenrollment, however, are inappropriate; these include administratively complex redetermination procedures, and parental confusion regarding the steps they must take to retain their children's coverage in SCHIP and/or Medicaid. The lack of current germane research also contributes to the uncertainty about appropriate retention rates and strategies. In March 2002, the National Academy for State Health Policy published findings from a telephone survey of parents in seven states and focus groups in three of the states (Pernice et al. 2002). This study showed that two-thirds of the children who were disenrolled either had private coverage or had parents who believed they were no longer eligible.
B. Program and Policy Characteristics
SCHIP eligibility redetermination processes were similar in five of the six study states. Four states offer 12-month continuous eligibility, and one follows a 12-month redetermination cycle under SCHIP (Table 8). The redetermination process begins when computer-generated letters are mailed to parents (usually at the beginning of their child's 10th month of eligibility), notifying them that it is time to renew their child's coverage and (usually) enclosing a blank application form. Parents are asked to complete the form and submit it, along with selected documentation. Reminder notices usually are sent out in Month 11 to nonresponding families. In addition, vendor, state, county, community-based organization, or, in some states, health plan marketing staff, make several attempts to contact families (by phone or mail) before the child's coverage period ends. Applications received by the due date are reviewed for continued eligibility (and referred to Medicaid if family income has dipped to Medicaid-eligible levels). Children are disenrolled if their parents do not submit complete applications.
In Missouri, state officials described county social services offices as "chronically understaffed"; therefore, eligibility redetermination (formally on a 12-month cycle) is not conducted on schedule. Rather, staff prioritize redeterminations, focusing first on families in which changes are known to have occurred (for example, adolescents aging out of the program), and on families more likely to experience a change in income or family circumstances (including families in lower-income groups and those with certain types of jobs). Meanwhile, children's enrollment continues until staff have time to redetermine their eligibility.
Although states have streamlined the SCHIP renewal process, the renewal process is not as simple as the initial application process (Table 12). In every study state, SCHIP renewal can be completed by mail. California and Texas have streamlined their processes the most; vendors in these states produce preprinted renewal applications based on information from the previous application. Parents are asked only to indicate changes and to submit verification for any items that have changed. Louisiana officials reported that they had recently developed a shorter and simpler renewal form for LaCHIP that they believe will be easier for families to complete.
As was the case with initial application procedures, states' SCHIP eligibility redetermination rules and procedures were often simpler than those used for Medicaid. First, SCHIP redetermination forms are often shorter and less complex than those for Medicaid. Second, while all states permit SCHIP renewals to be completed by mail, New York requires in-person interviews for Medicaid redeterminations. (Texas has a similar requirement for adults.) Third, no states preprint their renewal applications for Medicaid. Most commonly, in states with separate programs, Medicaid programs require verification of family income, children's ages, social security numbers, residence, and immigration status--while SCHIP requires only verification of income, unless other items have changed.
| Procedure | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| State | Mail-In Redetermination | Pre-Printed Form | Same Form As Application | Income Verification Requireda | Other Verification Required | |||||
| SCHIP | Medicaid | SCHIP | Medicaid | SCHIP | Medicaid | SCHIP | Medicaid | SCHIP | Medicaid | |
| California | ✓ | ✓ | ✓ | ✓ | a | a | ✓ | |||
| Colorado | ✓ | ✓ | ✓ | ✓ | ✓ | |||||
| Missouri | ✓ | ✓ | ✓ | |||||||
| Louisiana | ✓ | ✓ | ✓ | |||||||
| New York | ✓ | ✓ | ✓ | ✓ | a | ✓ | ||||
| Texas | ✓ | b | ✓ | ✓ | a | a | ✓ | |||
Source: Information obtained during each site visit.
aVerification required only if circumstances have changed.
bTexas now allows mail-in redetermination for children, but not adults, in its Medicaid program, as a result of recent simplification.
C. Implementation Experiences
Children may be disenrolled from SCHIP for three types of reasons: (1) they do not fulfill administrative requirements, such as paying premiums or completing a renewal application, (2)they are no longer eligible (for example, because of the child's age or changes in the family's income), or (3) they obtain private insurance. In the six study states, all of which, as a practical matter, allow children to be enrolled for 12 months without their eligibility being redetermined, the only disenrollment that would be expected before 12 months would be for children who do not meet administrative requirements, such as paying premiums, or who obtain private health insurance. At the 12-month point, when eligibility is redetermined, it would be reasonable to expect more children to be disenrolled because they are no longer eligible. The states have focused on the rates of re-enrollment at 12 months as a marker of retention. In a preliminary analysis of retention rates during the first year in two study states, Moreno and Black (2001) found that up to 6 months after enrollment, very few children had been disenrolled in Louisiana and Texas (94 percent still enrolled) and there was little change in Texas 9 months after enrollment (92 percent still enrolled). 43 Thus the states' focus on factors leading to disenrollment at redetermination time seems appropriate.
According to the focus groups, most parents with SCHIP experience viewed the process of reenrollment in SCHIP as simple and straightforward (although these participants are the ones who re-enrolled successfully):
"Unless your address changes or your marital status, or if you have more kids. There are boxes and you mark yes or you mark no, it is simple." (Buffalo, New York)"When your card is about to run out, they'll send you something in the mail and you fill it out, which is very convenient." (Salisbury, Maryland)
In some states, including Florida, the process was simple enough that parents of program participants were barely aware they had to reapply, while in other states they said the process required minimal effort.
The focus group study reported that parents whose children were reenrolled in Medicaid were more likely to have experienced difficulty with the reenrollment process than were parents whose children were reenrolled in SCHIP. For example:
"They mail [the forms] to you, so you fill them out and then take them back in. Once you get there then you have to go through the whole computer with her to ask the different questions. These questions are already on the papers, and then she asks all the questions in the computer, and then they ask stupid stuff like, 'Do you have farm equipment?'" (Atlanta, Georgia)"I work 45 to 50 hours a week so I don't have much time to do anything. That's the reason he doesn't have coverage now, because I couldn't take time off work to go recertify." (Rochester, New York)
Challenges associated with SCHIP eligibility renewal and retention remain, however. In three of the study states--Colorado, Louisiana, and New York--SCHIP children's renewal rates had begun to attract the attention of state officials. State officials in Colorado reported disenrollment rates of approximately 40 percent. In Louisiana, state officials were equally concerned about lower-than-expected numbers of children renewing their coverage. In New York, state and local officials reported that they were "losing children at redetermination faster than we can sign them up." These observations are consistent with recent declines in total enrollment in New York (recall Figure 4) attributed by state officials to retention problems. Between 25 and 50 percent of children coming up for renewal in New York were disenrolled (it varies by health plan). Plans that had redeployed much of their marketing staffs to focus on eligibility redetermination and had made aggressive attempts to contact families were achieving renewal rates of 75 percent.
In two of the other study states, there is less information about renewal rates. In California, data systems cannot report routinely on the outcomes of eligibility renewals; thus, a precise retention figure was unavailable. 44 In Texas, officials had had little experience with eligibility renewal at the time of our visit, since TexCare's Phase 2 was only 14 months old. A preliminary analysis of enrollment records fount that, 12 months after enrolling, 65 percent of children remained enrolled in TexCare--yielding a disenrollment rate of 35 percent (Moreno and Black 2001).
State officials suggested reasons why children were disenrolled at redetermination, but had limited data. The limited data indicate that nearly as many children lose SCHIP eligibility at redetermination because they never complete the renewal process, as lose coverage because they are found to be no longer eligible for the program. For example, in Colorado, state officials estimated that roughly 40 percent of children who lose coverage at redetermination do so because their renewal applications are either never submitted or are submitted incomplete. In California, state data systems were unable to generate precise reasons for children being disenrolled, but officials estimated that two-thirds of children are disenrolled for "potentially avoidable reasons," including the state never receiving renewal applications from families and nonpayment of premiums. In Texas, the one state with findings (from a preliminary analysis of state enrollment records for which 12 months of information for each enrollee was analyzed), failure to pay premiums or to meet other administrative requirements related to eligibility renewal at 12 months represents a more common reason for exits than ineligibility does (Moreno and Black 2001). The parents of some children who are disenrolled do not renew SCHIP because they have gained access to private coverage--a positive outcome--but case study respondents in several states believed that this was not a major reason for children being disenrolled.
Again, findings from the focus group study provide insights into why children were disenrolled from Medicaid or SCHIP when they were still eligible for coverage. In most cases, parents had not made a deliberate decision to stop participating as a result of dissatisfaction with the programs or because they decided they did not need insurance. In fact, much of the disenrollment discussed by focus group participants represents what is referred to as "churning," the temporary exit of children from a program. The three main reasons for disenrollment that focus group participants noted are: (1) lack of knowledge about the reenrollment process and the consequences of not reapplying; (2) (for Medicaid eligible children) the time, cost, and stigma associated with visiting social services offices and providing the documentation required to re-apply; and (3) problems resulting from different program requirements for Medicaid and SCHIP. Less frequently cited reasons included failure to pay premiums.
Preliminary analyses of SCHIP retention and reenrollment patterns using program data, including the reasons for exiting the program, revealed important differences across a number of key sociodemographic characteristics of children and their families. For instance, in Louisiana, African American children are less likely to remain enrolled in LaCHIP than Hispanic or White children, even after controlling for income (Moreno and Black 2001). These findings suggest that reenrollment and retention policies might need to be targeted to specific groups of children. For instance, state efforts to follow up children who do not return their reapplication forms may need to take into account language and other cultural differences across racial and ethnic groups.
Survey data will be available to clarify the reasons why children are disenrolled. The survey of children who were disenrolled that took place during 2002 and 2003 asked the reasons why the children were disenrolled. The analysis of these reasons for disenrollment will provide the first really detailed information coded uniformly across a large number of states.
43. Nine months of data were not available for Louisiana.
44. State officials recently analyzed their data and found that for every 100 children who enroll in Healthy Families, 76 remain on the program one year later--an apparent retention rate of 76 percent.
X. Benefits
Highlights of Findings
- Separate state programs have comprehensive benefit packages that appear to be meeting the needs of enrolled children
- Limited dental benefits appear to be a problem in some states
A. Background and Policy Development
States with Medicaid expansion programs must use their Medicaid benefit package for SCHIP. States with separate programs have greater flexibility, although they still must ensure that the SCHIP benefit package meets, or exceeds, the minimum coverage parameters outlined in Title XXI legislation, by adopting one of the following options:
- Benchmark coverage equivalent to the standard Blue Cross/Blue Shield PPO option of the Federal Employees' Health Benefit Program (FEHBP), the State Employee Health Benefit Plan, or coverage offered by the HMO with the largest commercial enrollment in the state
- Coverage that is equivalent actuarially to any of the above benchmarks (and that meets coverage requirements specified in Title XXI)
- Grandfathered coverage provided through pre-SCHIP state programs (offered only to Florida, New York, and Pennsylvania)
- Other coverage approved by the Secretary
Upon passage of Title XXI, one of the most persuasive arguments among advocates in support of adopting Medicaid expansions under SCHIP was that Medicaid extends to children the broadest possible benefits coverage and virtually open-ended protection against any illness. 45 The Omnibus Budget Reconciliation Act of 1989 (OBRA 89) strengthened Medicaid's Early and Periodic Screening, Diagnosis, and Treatment (EPSDT) provisions by defining them more clearly and, most important, by requiring states to provide, rather than simply arrange for:
"…such other necessary health care, diagnostic services, treatment, and other measures described in [the list of covered services] to correct or ameliorate defects and physical and mental illnesses and conditions discovered by the screening services, whether or not such services are covered under the state plan."
At least on paper, therefore, the OBRA 89 provisions gave Medicaid-eligible children coverage for any medically necessary service. Some referred to Medicaid's comprehensive coverage as the "gold standard."
Those debating whether to design SCHIP as a Medicaid expansion or as a separate state program looked closely at benefit packages. Some states saw Medicaid's broad coverage for low-income children as a good thing, while others viewed it as "too generous," preferring coverage that would more closely resemble private insurance options. Benefits issues influenced the debates greatly in Louisiana, one of the two Medicaid expansion states, where concerns about the adequacy of available private plans for children with special healthcare needs figured importantly.
To varying degrees, all four study states with separate state programs (California, Colorado, New York, and Texas) sought to make the SCHIP benefit package similar to commercial ones rather than designing packages like Medicaid's. In California and Colorado, there were also concerns that the SCHIP benefit package should be no more comprehensive than the packages available to state employees and people covered by the typical private insurance plan.
In New York and Texas, pre-existing state programs for children influenced the design of the benefit packages. The fact that New York's pre-SCHIP benefits package was given "grandfather" approval reinforced its decision to operate a separate program. On the other hand, the pre-existing program in Texas, which had a limited benefit package, helped pave the way for a more comprehensive SCHIP package. 46 In Texas, providers and advocates for children with special health care needs pushed for enhancements to the benchmark to provide adequately for these children.
45. Ian Hill, "Charting New Courses for Children's Health Insurance," Policy and Practice, vol. 58, no. 4, December 2000.
46. Texas Healthy Kids Program was a public-private partnership that had enrolled 15,000 low-income children.
B. Program and Policy Characteristics
All four states with separate programs enhanced the benchmarks they used as models for SCHIP. In California and Texas, the benchmark consisted of the state employee health benefits plans. Colorado has a benchmark-equivalent package based on the Colorado Standard and Basic Health Benefit Plans for small employers 47 and New York started with the package used in its preexisting, state-only Child Health Plusprogram. New York made the greatest number of enhancements to its plan. Features of the benefit packages adopted by the four separate state programs are summarized in Tables 13 through 15. The most common enhancements (made by three states) were the addition of vision and substance-abuse treatment services. Two states added coverage for mental health and durable medical equipment, while individual states added coverage for dental, hearing, orthodontia, and therapy services, as well as over-the-counter drugs. California added retroactive coverage for screening EPSDT services provided to children whose doctors refer them to SCHIP and who are found eligible for SCHIP.
Medicaid, in essence, provides children with coverage for any service considered medically necessary, whereas coverage in the four separate state programs is not as extensive. Nevertheless, a review of the benefits packages in these four study states reveals that they are quite comprehensive. As shown in Table 14, the few services excluded were also often excluded from private insurance packages. The most common exclusions from the SCHIP package are coverage for care in intermediate-care facilities for the mentally retarded, and residential substance-abuse treatment services (each one not covered by three states). Other services excluded by more than one state are orthodontia, care in nursing facilities, over-the-counter medications, personal care services, and non-emergency transportation. In addition, New York excludes hospice care and emergency transportation, while Texas excludes family planning services. 48 Colorado is one of only two states in the nation that excluded preventive dental services from its SCHIP package; but the state added these services in 2002.
Separate SCHIP programs limit the amount of coverage provided for some services. All four of the separate programs in the study placed limits on restorative dental care, durable medical equipment and medical supplies, and mental health services; three of the four placed limits on preventive dental, therapy, and outpatient substance abuse services (Table 15). 49 While some service limits affect a wide range of children, most of the limitations have a much greater potential to affect children with special health care needs. Colorado's child health program, for example, limits coverage for durable medical equipment to $2,000 per year, which is less than half the cost of the typical power wheelchair covered by Medicare. With its Title V program, Colorado's children's health insurance program is developing a strategy to address the needs of children with special health care needs.
| Services Added | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| State (benchmark plan) | Vision | Dental | Hearing | OT, PT, ST | Substance Abuse Treatment | Mental Health Treatment | Over-the-Counter Medication | Durable Medical Equipment/ Medical Supplies | Other |
| California (SEHBP) | c+ | c | c | c | c | c | c | c | EPSDTa CSHCN servicesb |
| Colorado (Standard plan for small employer market) | c+ | nc | c | c | c+ | c | nc | c+ | |
| New York (GrandfatheredChild Health Plus program) | c+ | c+ | c+ | c | c+ | c+ | c+ | c+ | |
| Texas (SEHBP) | c | c | c | c+ | c+ | c+ | nc | c | |
Notes: SEHBP = State Employee Health Benefit Plan; OT = Occupational therapy; PT = physical therapy; ST = speech therapy; CSHCN = children with special health care needs; EPSDT = Early Periodic Screening, Diagnosis, and Treatment.
aCalifornia's SCHIP program provides retroactive coverage of EPSDT screening services provided to children referred to and found eligible for SCHIP.
bAdditional services for children with special health care needs are provided through the Title V/California Children's Services (CCS) program, as they are under the state's Medicaid program.
c+ = Service added beyond benchmark coverage
c = Covered under benchmark
nc = Not covered
| Services Excluded | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| State | Preventive Dental | Orthodontia | Family Planning Contraceptive Services | Long-Term Care | Over-the-Counter Medication | Personal Care | Substance Abuse Treatment | Transportation | Case Management |
| CA | c | nc | c | ICF/MR | c | nc | Residential | c | c |
| CO | nc | c | c | ICF/MR | nc | nc | Residential | Non-emergency | c |
| NY | c | nc | c | ICF/MR Nursing facility Hospice care |
c | c | c | Emergency Non-emergency |
nc |
| TX | c | c | nc | Nursing facility | nc | c | Residential Inpatient | c | c |
Notes: ICF/MR = Intermediate care facility for the mentally retarded.
c = Covered
nc = Not covered
| Service Limits | |||||||
|---|---|---|---|---|---|---|---|
| State | Prescription Drugs | Preventive Dental | Restorative Dental | Medical Supplies/ DME | OT, PT, ST | Substance-Abuse Treatment | Mental Health Treatment |
| CA | Varying limits | Varying limits | Varying limits | Covers diabetic supplies; no coverage for therapeutic footwear | 60 days | Detoxification services and 20 visits for outpatient | 30 days for inpatient; 20 visits for outpatient |
| CO | Unlimited | Not covereda | Not covered | $2,000 limit; diabetic supplies not covered | 30 visits | Unlimited for inpatient; 20 visits for outpatient | 45 days for inpatient; 20 visits for outpatient |
| NY | Varying limits | Varying limits | Varying limits | Covers only commodes, walkers, diabetic supplies, and wheelchairs | Short-term PT and OT | 30 days for inpatient; 60 visits for outpatient | 30 days for inpatient; 60 visits for outpatient |
| TX | Unlimited | Varying limits | $300 limit | $20,000 limit; diabetic supplies not counted against cap | Unlimited | 14 days for detoxification and crisis stabilization; 60 days for partial hospitalization; 12- week limit for rehabilitation | 45 days for inpatient; 60 visits for outpatient |
Notes: Information on limits for some services was taken from Hill, Lutzky, and Schwalberg, "Are We Responding to Their Needs? States' Early Experiences Serving Children with Special Health Care Needs Under SCHIP," Washington DC: The Urban Institute, May 2001.
DME = Durable Medical Equipment; OT = Occupational therapy; PT = physical therapy; ST = speech therapy.
aColorado has since added a dental benefit to its SCHIP program.
47. As implemented, the Colorado plan exceeds the actuarial value of all Title XXI benchmarks in the state.
48. Study informants described the omission of emergency transportation services in New York as an oversight; efforts were underway at the time of our site visit to add this service to the SCHIP benefit package.
49. As noted, Colorado excluded preventive dental care entirely at the time of the site visit, but has since added such a benefit.
C. Implementation Experiences
Case study respondents in all six study states consider the SCHIP benefit packages good or, in some cases, comprehensive; moreover, the parents participating in focus groups in nine states were, for the most part, satisfied with coverage. Furthermore, SCHIP coverage across the six case study states was consistently described as at least as good as, and often considerably better than, private insurance. While coverage in the two Medicaid expansion programs obviously is considered much broader than private insurance, this same opinion was often held of separate programs. In California and Texas, for example, case study respondents noted that dental, hearing, and vision services are better under SCHIP than in most private insurance options (and that SCHIP has less onerous cost sharing). In Texas, also, SCHIP coverage is considered better than private options for behavioral health and physical, speech, and occupational therapies. The SCHIP package in Colorado is well-regarded (especially after the state added dental coverage) because it is comparable to packages offered by local employers.
Across the six states, case study respondents, including child advocates, identified few children who needed care that was not covered; and state officials have received few complaints from families about coverage limits. The most notable complaints lodged against a state's coverage were found in Colorado, where case study respondents reported that the initial lack of coverage for preventive dental care was a problem. New York plans to address the major gap in its benefit package--emergency transportation--by adding coverage in the near future.
Parents in the focus groups concurred with the case study respondents with respect to the limitations in dental coverage in SCHIP. At the same time, complaints about dental coverage were also common among those whose children are enrolled in Medicaid or have private insurance. Although children frequently used preventive dental services, many parents lamented the number of dental care procedures that are considered cosmetic and not covered by SCHIP. SCHIP parents in the focus groups also commented on the limitations in the coverage of vision services and prescription drugs. Other parents, though not as often as SCHIP parents, also voiced complaints, about their limited choice of vision care providers and suppliers, the frequency with which they can exercise their child's vision benefit, and the poor quality and limited choice of eyeglass frames. In addition, some parents voiced frustration about limitations on drugs covered by the program.
Nevertheless, with these exceptions, parents who participated in the focus groups were happy with the benefits their children received in Medicaid and SCHIP. In contrast, privately insured parents in the focus groups commented on the lack of coverage for preventive services for their children.
XI. Service Delivery Systems, Access and Utilization
Highlights of Findings
- Managed care is the cornerstone of SCHIP delivery systems in most of the study states
- Access is generally described as "good;" however, access to dental care, specialist care, and access in rural areas where there are provider shortages, are more problematic
- Rates paid to managed care health plans in SCHIP appear to be similar to rates paid to managed care health plans in Medicaid, and have been mostly well received by health plans
- Rates paid to physicians in SCHIP are also similar to Medicaid's, which is causing a provider backlash in many states
A. Background and Policy Development
The increase in managed care arrangements in this country's health systems are well- documented. Today, nationally, more than half of all privately insured persons receive their care through risk-based (capitated, pre-paid) managed care arrangements. For Medicaid, managed care penetration is similar--just under 46 percent of all Medicaid beneficiaries are covered by managed care in the average state. 50
Consistent with the extensive use of risk-based managed care in the United States today, five of the six study states set out to make managed care the cornerstone of their SCHIP delivery systems. 51 California, Colorado, Missouri, and New York each launched their programs with the goal of implementing risk-based managed care statewide for SCHIP; in Texas, policymakers acknowledged that managed care implementation would not be possible in many rural areas, but committed to using prepaid arrangements as extensively as possible. State officials embraced managed care for several reasons. First, managed care was described as an efficient way to leverage limited SCHIP dollars. Second, it was viewed as a vehicle for improving delivery systems for low-income children. Third, it was seen as a means of modeling delivery arrangements on those found in private insurance markets. Finally, in some states, managed care offered an opportunity to test new approaches for delivering care that were not feasible within the larger Medicaid program.
Existing service-delivery arrangements, including those in the Medicaid programs, greatly influenced the nature of SCHIP delivery systems in all six states. Missouri built on the managed care delivery system it had launched successfully several years earlier, in counties in the state's more populated east-west corridor. In California, Colorado, New York, and Texas, state officials sought to align SCHIP and Medicaid delivery systems whenever possible, while also extending managed care to a larger number of counties, including rural ones.
Louisiana was exceptional among the study states in that it has experienced minimal managed care penetration in both the private and Medicaid markets and, thus, could not consider using risk-based arrangements for SCHIP. Rather, at the time of our visit, the state had implemented a Primary Care Case Management system in 20 of the state's 64 parishes, and plans called for expanding this system statewide by 2004.
50. This percentage excludes people enrolled in primary care case management. With these people, the percentage in managed care is almost 56 percent. Centers for Medicare & Medicaid Services. "Medicaid Managed Care State Enrollment as of June 30, 2000." http://cms.hhs.gov/medicaid/managedcare/mmcss00.asp
51. Managed care here is generally defined as prepaid, capitated arrangements, as in the model of Health Maintenance Organizations. It does not include managed fee-for-service models such as Primary Care Case Management systems.
B. Program and Policy Characteristics
Every state except Louisiana has implemented mandatory, risk-based managed care arrangements for SCHIP in at least the more populated urban areas of the state (Table 16). In
| Proportion of State Covered by Mandatory Risk-Based Managed Care Arrangements | ||||||
|---|---|---|---|---|---|---|
| State | Number of Counties in State | Number of Counties with Mandatory Risk-Based Managed Care Arrangements in SCHIP | Number of Counties with Mandatory Risk-Based Managed Care Arrangements in Medicaid | |||
| CA | 58 | 43 | 22 | |||
| CO | 63 | 38 | 38 | |||
| NY | 62 | 61 | 14 | |||
| TX | 254 | 84 | In 50 urban counties, enrollees must select an HMO or PCCM | |||
| LA | 64 | None | None | |||
| MO | 115 | 37 | 37 | |||
| Proportion of Program Participants in Mandatory Risk-Based Managed Care Arrangements | ||||||
| SCHIP | Medicaid | |||||
| CA | Nearly 100% | 52% a | ||||
| CO | Roughly 66% | Roughly 40%b | ||||
| NY | Nearly 100% | 25% b | ||||
| TX | 58% | 32% b | ||||
| LA | None (6-7% in PCCM) | None | ||||
| MO | 58% | 41-44% c | ||||
| Number of Capitated Managed Care Plans Serving Program Enrollees | ||||||
| SCHIP | Medicaid | Both SCHIP and Medicaid | ||||
| CA | 26 | 26 | 22 | |||
| CO | 6 | 5d | 5 d | |||
| NY | 30 | 30 | 28 | |||
| TX | 12 | 12 | 6 | |||
| LA | None | None | N.A. | |||
| MO | 9 | 9 | 9 | |||
| Special Arrangements in Rural Areas | ||||||
| SCHIP | Medicaid | |||||
| CA | EPO | FFS | ||||
| CO | EPO | PCCM | ||||
| NY | PCCM (one county) | FFS | ||||
| TX | EPO | PCCM | ||||
| LA | Limited PCCM; FFS | Limited PCCM; FFS | ||||
| MO | FFS | FFS | ||||
| Populations and Services Carved Out from Managed Care | ||||||
| CSHCN/SSI | Behavioral Health | Dental | Prescription Drugs | Other Services | ||
| CA | SCHIP and Medicaid | |||||
| CO | ||||||
| NY | Medicaid | Medicaid (option) | Medicaid (option) | |||
| TX | Medicaid | Medicaid | SCHIP and Medicaid | SCHIP and Medicaid | ||
| LA | N.A. | N.A. | N.A. | N.A. | N.A. | |
| MO | SCHIP and Medicaid | SCHIP and Medicaide | ||||
Notes: CSHCN = Children with special health care needs; EPO = Exclusive provider organization; SSI = supplemental security income; N.A. = Not applicable; PCCM = Primary care case management.
a "Medi-Cal Managed Care," Medi-Cal Facts, No. 8. Oakland, CA: the Medi-Cal Policy Institute, March 2000.
bSeptember 2001 GAO report, Medicaid and SCHIP: States' Enrollment and Payment Policies Can Affect Children's Access to Care.
cFrom the State of Missouri Department of Social Services, Division of Medical Services. As of June 2001, pregnant women, children, and their caregivers covered under the state's section 1915(b) managed care program.
dAlthough Colorado requires all SCHIP plans to participate in Medicaid, one of the SCHIP plans meets the Medicaid participation requirement indirectly through another SCHIP/Medicaid plan, of which they are part owner. The two plans share the same provider network; under SCHIP, the parent plan manages care directly, while under Medicaid, care is managed through its subsidiary plan. eIndividualized Education Plan (IEP) and Individualized Family Service Plan (IFSP) services, environmental lead assessments, bone marrow and organ transplants, protease inhibitors, sexual assault and child abuse assessments, and abortion services.
Source: State program officials.
New York, such arrangements are being used in all but one rural, upstate county; and in California, such arrangements are in place in all but 15 rural counties. Thus, in both New York and California, nearly all SCHIP participants are enrolled in risk-based managed care. In Colorado, Missouri, and Texas, managed care participation rates are closer to 60 percent, because such arrangements are not available in many rural areas within these states.
States typically build on managed care arrangements already in place for Medicaid, although, in most of the study states, managed care's reach is more extensive in SCHIP than in Medicaid. In New York, three times as many counties and an equally large proportion of participants are enrolled in risk-based managed care for SCHIP, compared to Medicaid. In California and Texas, mandatory risk-based arrangements operate in many more counties for SCHIP than for Medicaid, and the proportion of program participants enrolled in risk-based arrangements under SCHIP is twice as high as that under Medicaid. In Colorado, Medicaid and SCHIP operate managed care in a similar number of counties, and there is nearly full alignment among health plans participating in SCHIP and Medicaid, although the proportion of program participants enrolled in managed care is slightly greater in SCHIP than in Medicaid. Managed care is the same for SCHIP and Medicaid enrollees in Missouri, because as a Medicaid expansion program the same delivery system serves both groups.
In the five states with risk-based managed care, most plans participate in both Medicaid and SCHIP. When the same plans participate, families find it easier to make a transition from one program to the other. In three states, plan participation is the same (Colorado and Missouri) or nearly the same (New York) across the two programs. The SCHIP authorizing legislation in Colorado specifically requires that plans participating in SCHIP also participate in Medicaid, a provision that has helped ensure alignment between the two programs. 52 In New York, the only difference between the two programs is that one large New York City plan participates in SCHIP but not in Medicaid.
More plans in California and Texas participate in only one of the two programs. Although, in California, the same number of plans participate in Medicaid and SCHIP, eight plans (four per program) participate in one program, but not the other; and managed care systems differ considerably across the two programs. Moreover, in California, SCHIP operates managed care in many more counties than Medicaid does; also, whereas contracts with plans are statewide for SCHIP, Medicaid managed care systems and contracting arrangements are county-based.
In part because SCHIP is more streamlined and utilizes managed care throughout the state, California was able to secure SCHIP contracts with three large commercial insurers that participate in Medicaid, either in selected counties only, or that do not participate in Medicaid at all. Case study respondents in California noted that these "mainstream" health plans are very popular among families because they offer broad provider networks throughout the state. Enrollees switching from SCHIP to Medicaid, however, might not have access to the same plans and providers. Lack of alignment between SCHIP and Medicaid managed care plans is perhaps greater in Texas than in other states. There, only 6 of the 12 plans participating in Medicaid have submitted bids to participate in SCHIP. The networks of these six plans, along with six others that do not participate in Medicaid, are dominated by traditional safety net providers. In Texas, plans with larger commercial enrollment typically did not bid on SCHIP because they deemed it not profitable. Some of these plans with experience in Medicaid saw SCHIP as merely "more of the same."
Although a few states have contracted with mainstream commercial insurers in SCHIP, managed care enrollment in three of the five study states with risk-based managed care programs is concentrated in plans with strong links to traditional safety net providers. SCHIP managed care enrollment in Texas is exclusively in these types of plans. In New York, 70 percent of SCHIP enrollment is with plans that participate only in Medicaid or SCHIP; safety net providers play a large role in the provider networks for these plans. Roughly half of SCHIP managed care enrollment in Colorado is with a plan formed by community health centers and safety net hospitals. In Missouri and California, a larger share of SCHIP managed care enrollment is in plans with significant commercial enrollment.
Medicaid and SCHIP delivery systems typically are similar in urban areas, where both programs operate managed care arrangements. In geographic areas where delivery system features vary, provider participation in SCHIP is considered comparable to--and, in some cases, better than--participation in Medicaid. Case study respondents described SCHIP's more extensive use of managed care as giving participants in some areas access to a larger and/or better selection of providers--because either the program's image was more appealing to providers or payments were better.
In rural areas, the case studies found distinct differences between the SCHIP and Medicaid delivery systems. New models for delivering care in rural areas have emerged in the SCHIP programs of several states--California, Colorado, and Texas each operate a form of exclusive provider organization (EPO) in rural communities. 53 In California and Colorado, access to providers reportedly is better in areas with these organized networks than it is under Medicaid fee-for-service arrangements, both because SCHIP has attracted more providers, and because the programs are able to provide families with a list of participating doctors from whom to select a primary care physician, rather than leaving families to find a physician willing to accept Medicaid. California recently launched a program to stimulate innovative delivery models in rural areas. Meanwhile, health plans and providers have competed to obtain special funding to develop and test new approaches for serving the populations of Alaska Natives, American Indians, and forestry, fishery, and migrant workers. Some ideas being explored for bringing specialty care to rural areas are longer clinic hours and the use of mobile vans and telemedicine.
In the study states, carve-outs are less common in SCHIP than they are in Medicaid; that is, states have tended to include all (or more) populations and services within the managed care contracts with health plans. However, California's SCHIP contracts exclude services for children with qualifying special health care needs, and plans refer these children to county-based specialty health and mental health systems in which providers are paid directly by the state on a fee-for-service basis. Health plan contracts in Missouri include carve-outs for some behavioral health care services and a few other specialized services for both SCHIP and Medicaid enrollees (listed in Table 16). In Texas, SCHIP and Medicaid contracts exclude dental care and prescription drugs while Medicaid contracts also exclude behavioral health services (all such covered services and paid for by the state using fee-for-service payment). In New York, SCHIP contracts with health plans include the full scope of benefits, whereas the state's Medicaid contracts in New York exclude children with special health care needs on SSI; plans have the option to provide dental care and prescription drugs.
Dental care arrangements differ across the study states. As with other services, dental care more often is included in managed care arrangements in SCHIP than in Medicaid. Under SCHIP in New York and Missouri, health plans are responsible for dental care (although plans typically subcontract with dental managed care organizations to meet this obligation). In California's SCHIP program, the state contracts directly with five managed dental care plans to provide coverage to SCHIP enrollees. Texas had hoped to secure contracts with dental plans; but when none applied they carved this care out of health plan contracts and pay for this care directly on a fee-for-service basis.
Under SCHIP, several states negotiate payment rates individually with health plans (California, Missouri, and New York); others set payment rates based on historic Medicaid data (Colorado and Texas). Because SCHIP is a relatively new program, most states used Medicaid cost and utilization data to set or evaluate health plan capitation rates. As plans have gained experience serving SCHIP enrollees, some states have begun using actual cost data from plans to reassess rates when contracts are renegotiated. It is difficult to compare SCHIP and Medicaid plan payment rates directly since the programs cover different population groups and different services. Health plan officials interviewed for the study reported that, generally, after adjusting for population and service differences, capitation rates were roughly comparable for Medicaid and SCHIP in Colorado and Texas, and slightly higher under SCHIP than Medicaid in New York and California. Plans in California and New York also noted that the process they undergo in responding to and negotiating contracts with the state is more streamlined in SCHIP than in Medicaid.
SCHIP provider payments are similar to Medicaid provider payments, regardless of the payment arrangements (which vary widely within and across states). 54 Some fee-for-service rates and provider capitation payments under SCHIP are tied to existing Medicaid fee schedules, while others are enhanced by health plans in order to increase provider participation. Many providers in managed care arrangements are paid at levels comparable to those of Medicaid. According to state officials, provider payment rates in fee-for-service regions are the same for SCHIP and Medicaid in Texas; but they tend to be slightly higher for SCHIP in California, Colorado, and New York.
52. One of the six SCHIP plans in Colorado is able to meet its Medicaid participation requirement through its affiliation with another plan.
53. In Colorado, the network began before SCHIP to serve mainly rural areas; but it has since become statewide. Under SCHIP, network providers also serve as primary care providers for SCHIP participants until the managed care plan enrollment process is complete.
54. Some health plans pay providers on a capitated basis, whereas others pay fee-for-service rates. Health plans most often use capitation arrangements for routine primary care, but pay fee-for-service rates for specialty and ancillary services. Some plans, however, offer partial-risk contracts or restrict capitation to urban and/or larger-volume providers. Outside managed care areas, providers usually are paid on a fee-for-service basis; but, in some EPO regions, providers receive a capitation payment for primary care and care-coordination services.
C. Implementation Experiences
The findings presented here on states' implementation experiences with regard to access and service use are qualitative in nature; they are based on comments by case study respondents, focus group participants, and other sources. Ideally, assessments of service use and access to care should be conducted using quantitative data. In years 2 and 3 of this Congressionally mandated evaluation, such empirical data will be gathered and analyzed, and more definitive analyses of use and access will be presented.
Case study respondents described access to care under SCHIP as good, especially in urban areas. This was attributed largely to the widespread use of managed care, which reportedly has helped increase the number of participating providers, as well as children with a designated source of primary care. Also, it appears that most parents of Medicaid or SCHIP enrollees had a choice of managed care plans in which they could enroll their children, as reported by nearly all focus group participants with Medicaid or SCHIP experience. 55 Case study respondents in California and Missouri characterized access as better in managed care regions of the state (even those with long-standing provider shortages) than in fee-for-service regions. In some states, health plans have influenced state legislatures to approve rate increases for health plans and providers under Medicaid; this, in turn, has helped states and plans recruit more providers to SCHIP and Medicaid. Where Medicaid programs use managed care arrangements similar to those used by SCHIP--mostly, urban areas--access to care also was described as good for Medicaid enrollees.
Nevertheless, case study respondents did report challenges retaining plans and providers in the program. A few health plans quit both the SCHIP and Medicaid programs because payment rates were too low. In addition, physicians in some areas are dropping out of the programs--some because of low payment rates, and some because they do not like managed care. Provider resistance to managed care was cited as contributing to access problems in the more rural regions of Colorado, Missouri, and Texas. In several states, providers participating in Medicaid and SCHIP reportedly limit the number of people they serve, thus limiting access even in more densely populated urban regions. In the two states with behavioral health carve-outs (California and Missouri), problems sometimes surfaced with care coordination across the different systems.
Over time, Medicaid programs in many states have experienced problems with provider participation, either due to shortages of providers in certain regions (such as rural areas) or because of provider unwillingness to accept Medicaid patients into their practices (for example, due to perceived low rates of payment). This was a problem before states introduced managed care, and it has not been resolved by the use of managed care, with the exception of improved access to primary care. SCHIP programs have not been immune to this circumstance, and provider shortages and limited provider participation were cited as problems in rural areas of the study states (more so than in urban areas), especially in areas with a limited managed care infrastructure. In Louisiana, some rural providers have stopped participating in Medicaid and SCHIP because payments are low and because rates have fluctuated in recent years. Provider shortages and low participation rates were described as a problem in many rural regions of Colorado, Missouri, and Texas. Still, as mentioned earlier, California, Colorado, and Texas have used SCHIP to implement managed care models in rural areas that reportedly have improved access compared with the fee-for-service delivery systems used by Medicaid. Rural residents who participated in the consumer focus group study were well aware of the limited access to providers in rural areas, regardless of the type of children's insurance. Finally, the focus group study identified access to specialists as another problem. Getting referrals to specialists often requires lengthy waiting periods. Finding specialists and scheduling appointments is no easy task, either, according to most parents who participated in the focus group study. Often, the intervention of a child's pediatrician or other medical professionals can facilitate these matters.
Long-standing shortages of certain services (especially pediatric, psychiatric, and orthopedic ones) remain under both SCHIP and Medicaid. Informants in several study states noted concerns about access to dental care; shortages of dentists willing to treat Medicaid and SCHIP patients are a major concern in Louisiana and Missouri and in the rural areas of New York. Notably, though, case study respondents reported that managed care has improved access to dental care in California and in the urban areas of New York.
Most SCHIP plans interviewed in the case studies seemed satisfied with their capitation rates, although some noted that rates were too low when they first contracted with the program. Significant concerns about health plan payment rates did surface in Texas, however, where SCHIP payments (based on historic Medicaid costs) reportedly do not reflect the costs of serving children with special health care needs. Because other states have experienced lower or comparable service use rates under SCHIP than under Medicaid, capitation payments currently appear to be adequate to cover the costs of serving SCHIP enrollees. Several health plans in California and New York noted that they were "doing quite well," given enrollees' low service use.
In nearly every state, however, physicians complained about payment levels under both SCHIP and Medicaid. Providers in several states noted that the rates they receive from health plans (in managed care regions) and from the state (in fee-for-service regions) under SCHIP are "just as bad" as those of Medicaid. As one provider put it, basing SCHIP rates on those of Medicaid "was the wrong place to start." Although SCHIP has increased fees in some states, many providers reported that SCHIP and Medicaid payments still do not cover their overhead costs. Low payment levels have reportedly contributed to serious provider shortages in parts of Colorado, Louisiana, Missouri, and Texas. Indeed, some families who participated in the focus group study reported losing access to doctors who decided that accepting patients covered by certain health plans was not in their best interest.
Several case study respondents in Texas suggested that low payments, combined with high enrollment, have raised concerns about access to care. Case study respondents in other states expressed concerns that, without substantial increases in provider payments, access under SCHIP may erode. Some parents in the focus groups reported being treated poorly or at least differently from other families in the physician's office because of their children's insurance coverage.
Alongside access and payment, utilization rates of SCHIP enrollees emerged as a perplexing issue in some of the study states. There is conflicting evidence about whether service use differs between SCHIP enrollees and Medicaid enrollees. The two states with Medicaid expansion programs had examined utilization rates and found that these programs had largely comparable services for SCHIP and Medicaid enrollees--with the exception that Louisiana reported that SCHIP enrollees use fewer emergency room and inpatient hospital services than Medicaid enrollees. 56 Health plans in California and New York reported that SCHIP enrollees use fewer services than Medicaid enrollees. In Texas, however, plans reported that SCHIP enrollees are using more services than Medicaid enrollees; they attributed this both to pent-up demand and to the fact that SCHIP enrolls children with special health care needs (who use a lot of services) into managed care while such children are largely in fee-for-service arrangements under Medicaid.
55. Parents would have liked more information to help them select their children's plans and providers.
56. In Missouri, state officials also reported that service use in both programs has been greater than expected, especially the use of prescription drugs.
XII. Cost Sharing
Highlights of Findings
- States with separate programs have made extensive use of cost sharing under SCHIP, but premiums and copayments are typically considered to be "affordable"
- Cost sharing does not appear to be a barrier to enrollment or service use
A. Background and Policy Development
States with Medicaid expansion programs must follow Medicaid's cost-sharing rules, which generally prohibit cost sharing for services provided to children, except under special waiver authority. 57 States with separate programs, however, may impose cost sharing as long as it meets federal requirements. Specifically, the following rules apply: (1) cost sharing for children below 150 percent of the FPL is limited to the nominal levels specified in Medicaid regulations; (2) the cumulative, annual cost sharing incurred under SCHIP for the children in any one family may not exceed five percent of the family's annual income; (3) copayments may not be imposed on well-baby or well-child care or related preventive and diagnostic services; and (4) families with lower incomes may not be charged more than families with higher incomes.58 Because cost sharing is relatively new in publicly funded health insurance programs for low-income families, there is great interest in the approaches that states have adopted, as well as how these approaches affect enrollment, utilization, retention, and other outcomes.
According to the majority of people interviewed in the five study states that use it, cost sharing was considered an important and positive program element. (These were the four states with separate SCHIP programs and Missouri, which was permitted to include cost sharing under its Section 1115 demonstration. 59) Officials in the four states with separate programs believed that cost sharing modeled on private insurance provided a "bridge" to help families make the transition from public to private coverage. In Colorado, New York, and Texas the emphasis on making SCHIP look like private insurance was seen as a way to promote SCHIP as health insurance, rather than as welfare. There was strong sentiment in Missouri, New York, and Texas that higher-income families should contribute to the cost of coverage. Finally, to varying degrees, cost-sharing proponents in each state believed that cost sharing would promote personal responsibility and reinforce the value of health care coverage.
57. Nominal cost sharing is permitted for children who qualify under Medicaid's medically needy provisions.
58. In addition, American Indians and Alaska Natives are exempt from cost sharing.
59. Although state leaders in Missouri originally had planned an expansion that would not include cost sharing, they became convinced early in the design phase that to get legislative approval they needed cost sharing, particularly given the high income threshold proposed for SCHIP (up to 300 percent of the FPL).
B. Program and Policy Characteristics
States employed four types of cost-sharing policies: (1) annual enrollment fees; (2) monthly premiums; (3) copayments; and (4) deductibles (Table 17). States vary in the income thresholds at which they apply cost-sharing requirements, the amounts of enrollment fees, premiums, copayments, and deductibles, and the administrative rules governing the payment process, including policies on non-payment of cost sharing. Most states have modified their policies since they began.
Colorado and Texas currently charge an annual enrollment fee and four states (California, Missouri, New York, and Texas) require families to pay monthly premiums. This cost sharing begins at different income levels across the states. Only two of the study states require cost sharing of families whose income is between 100 and 150 percent of the FPL: California charges families in this income range a monthly premium, while Texas charges a $15 annual enrollment fee (see Table 17).
Colorado charges an annual enrollment fee for families above 150 percent of the FPL, New York requires families with incomes above 160 percent of the FPL to pay premiums, and Missouri requires families with incomes above 225 percent of the FPL to pay premiums. According to state officials, the different policies lead to varying proportions of enrolled families who are subject to premiums or enrollment fees: from 100 percent in California, to 40 percent in New York, 25 percent in Texas, and 5 percent in Missouri. 60, 61
Missouri changed its premium program significantly in July 2001. It changed monthly premium levels from a fixed $80 per family to a sliding fee ranging from $55 to $218, depending on income and family size. As a result, the highest premium payments are now close to the full cost of coverage under the state employee health benefit plan, as required by the state's authorizing legislation. Importantly, families are required to pay premiums only if their income is above 225 percent of the federal poverty level.
Three states (California, New York, and Texas) require initial payments to be submitted along with the application, as a condition of eligibility. Colorado and Missouri wait until after eligibility has been determined to invoice families for the annual fee or initial premium payment;
| A. ENROLLMENT FEES AND PREMIUMS | ||||||
|---|---|---|---|---|---|---|
| Annual Enrollment Fees | Premiums | |||||
| Annual Enrollment Fee? | Amount of Annual Enrollment Fee | Any Premiums? | Premium Amounts | Conditions Attached to Payment of Premiums? | ||
| Grace Period | Black Out Period | |||||
| California | No | -- | Yes | <150% FPL: 1 child: $4; $7a 2 children: $8; $14a 151-250% FPL: |
60 days | 6 months |
| Colorado | Yes | <150% FPL: $0
151-185% FPL: |
Nob | -- | -- | -- |
| Louisianac | No | -- | No | -- | -- | -- |
| Missouri | No | -- | Yes | <225% FPL: $0
226-300% FPL: $55-218; |
90 days | 6 monthsd |
| New York | No | -- | Yes | <160% FPL: $0
161-222%: 223-250%: >250%: Full premium |
30 days | None |
| Texas | Yes | <150% FPL: $15
>150% FPL: $ 0 |
Yes | <150% FPL: $0
151-185%: $15/family 186-200%: $18/family |
60-90 days | 3 months |
TABLE 17 (continued)
| B. COPAYMENTS AND DEDUCTIBLES | ||||||
|---|---|---|---|---|---|---|
| Any Copayments? | Emergency Room Visits Copay Amount |
Medical Office Visits Copay Amount |
Prescription Drugs Copay Amount |
Any Deductibles? | Deductible Amount | |
| California | Yes | All incomes: $5e | All incomes: $5e | All incomes: $5f | No | -- |
| Colorado | Yes | <100% FPL: $0
101-150%: $5 151-185%: $15 |
<100% FPL: $0
101-150%: $2 151-185%: $5 |
<100% FPL: $0
101-150%: $1 151-185% $3-5 |
No | -- |
| Louisiana | No | -- | -- | -- | No | -- |
| Missouri | Yes | $0 | <185% FPL: $0
186-225%: $5 226-300%: $10 |
<225% FPL: $0
226-300%: $9 |
No | -- |
| New York | No | -- | -- | -- | No | -- |
| Texas | Yes | <150% FPL: $5
151-185%: $25 186-200%: $35 ($100 annual family cap) |
<150% FPL: $2
151-185%: $5 186-200%: $10 |
<150% FPL: $1-2
>150% FPL: |
Yes | <150% FPL: $0
186-200% FPL: |
Notes:
N.A. = not applicable.
Blackout period = length of time following disenrollment that a participant must wait before they are allowed to reenroll in the program.
aLower amount is for families who opt to participate in a Community Provider Plan (which involves safety net providers).
bPremiums were eliminated and replaced by enrollment fees in October 2000.
cAs a Medicaid expansion state without a Section 1115 demonstration, Louisiana could not require cost-sharing.
dAs of August 2001, the state had not yet acted on this provision to disenroll any family for nonpayment of premiums.
eBefore July 1, 2001, the premium was $80 per family
fUp to $250 annual limit (excluding vision and dental).
gTexas has since dropped the deductible.
enrollment takes effect when payment is received. Both California and Texas allow families to pay premiums in advance for multiple months; but only California provides an incentive to do so--families paying for three months in advance get their fourth month of coverage free. Also, to facilitate premium payment, California allows families to make their premium payments at any Rite Aid drugstore.
Every study state with a premium offers a grace period of 30 to 90 days before families are disenrolled for nonpayment. To strengthen its ability to take action against families who fail to pay, Missouri received approval from CMS in January 1999 to disenroll families after four or more instances of nonpayment. To date, however, the state has taken no action to disenroll any families using this authority.
With the exception of New York, families disenrolled for nonpayment may not reenroll during a "blackout" period ranging from three to six months. In New York, families may reenroll at any time. New York's policy has raised concerns about potential adverse selection; some health plan officials in the state believe that some families avoid paying monthly premiums when their children are healthy, and allow their coverage to lapse until their children need care.
Four states impose copayments on selected services. Copayment amounts vary but are comparable, or lower than, copayments imposed by private insurers. Except for emergency room copayments in Texas ($25 or $35 for families in the higher-income groups), copayment amounts typically are no more than $5 or $10 per visit or prescription (Table 17). California imposes a $5 copayment for each type of service and for families in all income groups. Similarly, all families in Texas must make copayments, although lower-income families pay less than others. Colorado and Missouri base copayments on family income but exempt the lowest-income families. Providers are expected to collect copayments at the point of service. Whether or not health plans deduct copayment amounts from the fees they pay providers varies from plan to plan and from state to state. In no state that requires copayments may providers deny service for refusal to pay and some providers are reported to write off copayments as "a cost of doing business." New York eliminated copayments when it introduced premiums during the conversion of its state-funded program to SCHIP.
Texas is the only state in the nation that incorporated a deductible in its SCHIP program. Families with incomes above 185 percent FPL had to meet an annual deductible of $200 for inpatient hospital care and $50 for outpatient care. Texas since dropped the deductible.
60. New York is the only state among the six study states that allows families to buy coverage by paying the full cost. Families with incomes above 250 percent FPL may purchase coverage at an average cost of $115 per month per family.
61. Colorado revised its cost-sharing policies in January 2001. Before this revision, all enrollees with family incomes above 100 percent of the FPL, 72 percent of families with enrolled children, were subject to monthly premiums. Beginning in January 2001, children with family incomes above 150 percent of the FPL, 30 percent of families with enrolled children, were subject to an annual enrollment fee (Colorado Department of Health Care Policy and Financing 2000).
C. Implementation Experiences
The qualitative findings from the focus groups that follow give a flavor of the views of participants in the SCHIP program. However, since they do not represent a statistically selected sample, their representativeness is clearly limited. In the final report to Congress in 2004, results of surveys of enrollees and disenrollees will provide quantitative evidence about the effects of cost sharing on SCHIP enrollment and service use.
In states that require a premium or enrollment fee, most case study respondents (including child advocates) reported that they have not heard that cost sharing poses a barrier to enrollment. They reported that premium amounts are considered reasonable and that, compared with the cost of alternative private-sector options, premium levels adopted by most states appear to be quite affordable. Front-line staff in Texas had heard families describe the premium as "too good to be true," and "the deal of the century." Furthermore, premium requirements were often described as making the program more appealing to some families. As an informant in one state put it, "I think that if we had made this program free, families would have probably been more skeptical of it, or dismissed it as welfare."
Few focus group participants viewed premiums as a positive attribute of SCHIP, but few considered them burdensome. For example, "It's the lowest check I write the whole month," and "Oh it's a blessing to have this kind of coverage for 15 bucks" (Fort Pierce, Florida). (It is important to note that these findings reflect the opinions of parents who have chosen to participate in SCHIP; they do not tell us how parents who have not enrolled their children view the affordability of premiums.) From the families' perspective, the main problem with premiums was logistical--it was hard to remember to pay premiums every month (hence, some consumers disliked state policies to disenroll children whose parents missed payments). The practical implications of such disenrollment--gaps in coverage and/or "churning" as children lost, and then regained coverage--were widely viewed by focus group participants as negative outcomes of these circumstances.
Privately insured, low-income families in the focus group study had much larger financial payments than SCHIP participants--and some resent both that they have to pay such high premiums and that families in SCHIP do not.
Some case study respondents in Missouri believe that the state's premium could be a barrier to enrollment, although premiums apply only to families with incomes above 225 percent of the FPL. (Focus group participants in Kansas City, Missouri who make premium payments spoke of the challenge of monitoring their incomes closely to avoid jumping to the next tier of payments or above the eligibility level.) Premium amounts are higher in Missouri than in any of the other study states, and they have recently been increased. Since the inception of the program, however, enrollment in this eligibility group has been low, so it is not clear whether the small number of enrollees in this segment of the program (five percent of total enrollment) indicates that premiums are less affordable, that families are not aware of the program, or that the need for the program is less among families at these higher-income levels. The buy-in premium component in New York--which also has a higher premium ($115) and applies to families with incomes above 250 percent of the FPL--also constitutes a small part (two percent) of total SCHIP enrollment in that state.
Colorado experienced problems with its premium program and ultimately dropped it. The state initially required all families to pay premiums, including those with incomes between 100 percent and 150 percent of the FPL (a lower threshold than the one used by most states). Unlike most other states, however, Colorado's program did not penalize families for nonpayment of premiums. Delinquency rates escalated over time; and eventually, the state comptroller threatened to send overdue accounts to collection agents. Public opinion of the program then dropped, and with it, enrollment. Ultimately, the state abandoned the premium program and replaced it with an annual enrollment fee that did not apply to families with incomes under 150 percent of the FPL. Some months later, enrollment growth rates returned to earlier levels. The availability of free or low-cost care through a well-known indigent care program operating in the most populous regions of the state seems to have influenced families' perceptions of whether SCHIP offered a "good deal," especially for families in the lowest-income groups.
In all states, case study respondents reported that copayments are considered reasonable, that families are happy to make copayments, and that this type of cost sharing does not reduce the use of services--views that were echoed by focus group participants. Case study respondents in several states noted that higher copayment amounts, especially for emergency room care, may in fact reduce inappropriate emergency room use. While it was not widespread, case study respondents noted that some families do not meet their copayment obligations. This seemed to happen more often in areas where families are accustomed to accessing free care through programs for the medically indigent. Providers had varying views of unpaid copayments. While some reported that they absorbed the cost when copayments were not paid, providers in one state saw this as a reason to limit their SCHIP caseload. In several states, case study respondents noted that providers with a tradition of providing charity care often resist collecting copayments.
A consistent finding across the study states was that cost sharing is not considered a "revenue maker." State officials reported that premium programs cost more to administer than they bring in given the low value of the premiums compared with cost of monthly invoicing, payment processing, and reminder systems. Costs may decrease as states explore using payroll deduction systems, quarterly or semiannual billing cycles with incentives, and other ways of reducing administrative costs. Despite the administrative costs, however, states find cost sharing beneficial because of the positive image it engenders for the program among participants, politicians, and the general public.
XIII. Crowd-Out
Highlights of Findings
- Study states have made widespread use of waiting periods to deter crowd-out
- Anecdotal evidence, while limited, suggests that crowd-out is not occurring frequently
A. Background and Policy Development
When designing their SCHIP programs, policymakers were concerned that government-sponsored health insurance would be substituted for existing employer-based coverage--a phenomenon known as "crowd-out." The key strategy that states considered for limiting such substitution was to impose a waiting period during which children had to be uninsured before they could be eligible for SCHIP. While many policymakers viewed this strategy as necessary to discourage parents from dropping their children's private insurance and joining SCHIP, others feared that it might erect a barrier for families who could not afford the premiums they paid for private insurance, or for children who need more comprehensive health coverage, or that it could lead to temporary spells of uninsurance. This conflict generated considerable debate in five of the six study states and ultimately led to a variety of policies to prevent crowd-out. In Missouri, the program's high income threshold generated concerns about crowd-out that resulted in inclusion of a waiting period for the Medicaid expansion program. 62 In Texas, too, a 3-month waiting period was established. Legislators and officials in California, Colorado, and Louisiana, after debate, also eventually included waiting periods in their children's health insurance programs to limit crowd-out.
Only in New York were legislators less concerned about crowd-out. Substitution had not surfaced as a problem during the previous six years the state was running its state-funded Child Health Plus program. Nevertheless, CMS officials were concerned that crowd-out might occur, especially among families with incomes above 200 percent of poverty. Therefore, CMS required the state to monitor crowd-out and implement a waiting period should crowd-out exceed a threshold of eight percent over any nine-month period. Louisiana, on the other hand, dropped its waiting period in January 2001, after CMS issued a new SCHIP rule that clarified the Medicaid rule that precludes states with Medicaid expansion SCHIP programs from imposing waiting periods.
62. Waiting periods are not allowed in Medicaid, but Missouri received a waiver of this provision in its Section 1115 demonstration.
B. Program and Policy Characteristics
Five of the six study states chose waiting periods as the primary strategy to deter crowd-out (Table 18). California also wrote into its statute the possibility of increasing the waiting period from three to six months if significant crowd-out occurred. At the same time, state officials established exceptions to the waiting periods in the following circumstances:
- In all the states with waiting periods: when a child's loss of insurance is involuntary, due to parents' loss of employment, a change to employment that does not offer dependent coverage, or expiration of COBRA coverage
- In three of the states: when a child is "underinsured," that is the insurance the child has is either very expensive or very limited in scope:
- In California, children who have been covered by individual, rather than group, policies- In Colorado, children whose parents are responsible for paying more than 50 percent of the premium costs for employer-sponsored coverage
- In Texas, children whose parents are paying premiums that exceed 10 percent of total family income
States instituted other measures to deter crowd-out and to reinforce the waiting period (Table 18), including: monitoring (New York only), asking questions about current and prior insurance on the application form, verifying other insurance, requiring applicants to get price quotes from private insurers, imposing obligations on employers in order to deter employer-driven crowd-out, imposing cost-sharing requirements, and having a benefits package similar to private insurance. 63
| State | Waiting Period (Number Indicates Length in Months) | Monitoring | Application Question(s) | Verifying Insurance Status Against a Database of Private Coverage/Price Quotes | Cost Sharing | Imposing Obligations on Employers and/or Insurers |
|---|---|---|---|---|---|---|
| California | 3 | ✓ | ✓ | ✓ | ||
| Colorado | 3 | ✓ | ✓ | |||
| Louisiana | a | ✓ | ||||
| Missouri | 6 | ✓ | ✓ | ✓ | ||
| New York | - | ✓ | ✓ | ✓ | ||
| Texas | 3 | ✓ | ||||
| Number of States Using Policy | 4 | 1 | 6 | 1 | 4 | 1 |
aLouisiana had a waiting period but dropped it.
All six study states included questions on the application form about the status of applicants' health insurance. This is considered an anti-crowd-out strategy because parents who state that their children have been covered by insurance within the waiting period are automatically denied, and states believe that the questions deter families from dropping coverage. The questions are similar in every state, asking whether the child already has health insurance, if the child has had coverage in the past three or six months, if the child has lost this coverage and, if so, why. To satisfy CMS's requirement, New York also asks parents applying for Child Health Plus detailed questions that allow the state to monitor crowd-out. 64
Four states impose cost-sharing provisions (especially premiums) as an anti-crowd-out measure to make SCHIP more like private insurance and make a switch less advantageous. Officials in these states believe that cost sharing poses an economic disincentive for families considering substituting SCHIP for private insurance. (Cost sharing is discussed in Chapter XII.)
Two states adopted unusual strategies to deter crowd-out. Missouri verifies the health insurance status of the applicant against a private coverage database, a provision aimed at enforcing the waiting period. Also, applicants who fall within the higher, premium-paying income group (226 to 300 percent of poverty) must obtain and provide price quotes from two private insurers for the cost of dependent coverage, to ensure that lower-cost alternatives for coverage do not exist. Families with access to what could be deemed "affordable" coverage, (those who obtain quotes for less than $290 per month) may not enroll in SCHIP. 65
California has adopted a strategy aimed at deterring employers from directly encouraging families to enroll their children in SCHIP. Insurance agents and insurance companies may not refer their insureds' dependents to Healthy Families if they already have employer-sponsored coverage. Employers are also prohibited from changing the extent and price of their coverage in a way that might encourage employees to switch to Healthy Families.
63. A. Westpfahl Lutzky and I. Hill, "Has the Jury Reached a Verdict? States' Early Experiences with Crowd-Out Under SCHIP," The Urban Institute, June 2001.
64. The state tabulates (1) the number of children who have had health insurance in the previous six months; (2) of those, the number that had this insurance through an employer; (3) the numbers of those who dropped that insurance for any of the following reasons: (a) the employer discontinued offering dependent coverage or is no longer contributing toward a premium for dependent coverage; (b) the premium was increased beyond a level that was affordable to the family and: (i) Child Health Plus was judged to be a more affordable alternative, (ii) Child Health Plus' benefits were judged to be better, or (iii) the parent was no longer working for the employer who offered health insurance. (A. Westpfahl and I. Hill, "Has the Jury Reached a Verdict? States' Early Experiences with Crowd-Out Under SCHIP." The Urban Institute, June 2001.)
65. The affordability threshold is adjusted periodically.
C. Implementation Experiences
Perceptions about the extent of crowd-out varied across the study states and by case study respondents. However, with the exception of Louisiana, most state officials, legislative staff, and advocates were not concerned about crowd-out and did not perceive consumer- or employer-based crowd-out as occurring at significant levels.
New York was the only state able to substantiate its assessment of the extent of crowd-out with data. 66 Parents of between four and six percent of children enrolled in Child Health Plus indicated that they had held private health insurance coverage within the six months preceding their application for SCHIP but had dropped it voluntarily. In the four states with waiting periods, between 1 and 5 percent of children applying for SCHIP were denied coverage because they had private insurance during the waiting period. 67
In these states, officials tended to use these figures to indicate the low potential for crowd-out since the numbers actually represent "prevented" crowd-out cases.
Most case study respondents believe that waiting periods may deter crowd-out because families are unwilling to allow their children to go without health insurance for three to six months while waiting to obtain SCHIP; state and local officials reported that they actively discouraged parents from taking this step. Most staff assisting parents to apply stated that they discouraged applicants from dropping their children's private insurance. In New York, which has no waiting period, enrollers warned applicants that if families were found to be dropping private coverage, a waiting period might be introduced.
Louisiana is the one state in the study where some case study respondents believed that it is not uncommon for families with private dependent coverage to drop it to qualify for LaCHIP. According to eligibility workers in New Orleans, the number of children whose parents dropped private insurance for them increased after the SCHIP waiting period was dropped. One application assistor said that, among the families she has helped, as many as one in five had dropped coverage in order to apply for LaCHIP. Application assistors indicated, too, that many children who are denied coverage because they have existing coverage drop the coverage and reapply. Case study respondents cited prohibitively expensive employer-sponsored coverage as the driving force behind this trend.
Despite the widespread perception that rates of crowd-out were low in the other five states, staff assisting parents with applications reported anecdotes about crowd-out at the local level. They reported that high (or rising) insurance costs was the most common reason families gave for dropping private insurance. In addition, case study respondents believed that crowd-out is an issue to monitor in the future.
Many families in the focus groups indicated that they had tried to obtain insurance for their children through their employers, but that when private insurance was unaffordable or otherwise unavailable, many turned to Medicaid and SCHIP as an alternative source of coverage. The study also reveals that some parents who previously had private insurance for their children enrolled them in public programs either because they wanted to save money or because they wanted the better benefit package public programs offer. Some families did not understand the purpose of the waiting period.
Case study respondents viewed as "equitable and fair" the exemptions from waiting periods that were implemented in three states to allow children covered by high-cost policies to switch to broader, less expensive coverage under SCHIP. The impact of the exemptions on enrollment was not clear in California or Colorado; but, in Texas, "literally thousands" of families were reported to be qualifying for coverage under the "10 percent of income" exception.
66. The data obtained from monitoring are subject to applicants' accuracy in self reporting previous coverage.
67. There are no current data for Louisiana, in part, because the application questions do not necessarily reveal whether families dropped coverage before they applied. When the waiting period was in place, prevented crowd-out cases reportedly were 1 percent.
XIV. Family Coverage and Premium Assistance Programs
Highlights of Findings
- States have an interest in extending coverage to parents because they believe it would be an effective way of enrolling more children in SCHIP
- The size of states' allotments is a key factor in whether states feel they can pursue family coverage
- States think that the federal rules for premium assistance programs are too restrictive and few have used this option
A. Background and Policy Development
Some states expressed interest early on in adopting strategies that would allow them to cover low-income parents as well as children under SCHIP, or that would allow them to leverage employer-based and other insurance packages available to some families by subsidizing the cost of such coverage. Although CMS did not allow parent coverage waivers during the program's first two years, the agency issued guidance in July 2000 that clarified the conditions under which it would grant approval of state applications to test such strategies. Different rules govern applications for premium assistance programs. The initial regulations governing premium assistance programs reportedly posed barriers for many states.
At the time this report was prepared, eight states nationally had been given approval to cover low-income parents under SCHIP (California, Arizona, Illinois, Minnesota, New Jersey, Oregon, Rhode Island, and Wisconsin), and seven states had received approval to use SCHIP funds to support premium assistance programs (Maryland, Massachusetts, Mississippi, New Jersey, Virginia, Wisconsin, and Wyoming) (Rosenbach et al. 2002).
In 2001, the Administration formulated a new approach for states seeking to obtain Section 1115 waivers for Medicaid and SCHIP--the Health Insurance Flexibility and Accountability (HIFA) demonstration initiative. Federal officials expect that states will, in the future, use HIFA authority when requesting SCHIP waivers to expand health insurance coverage to low income parents and/or create premium assistance programs. The primary goal of the HIFA demonstration initiative is to encourage new comprehensive state approaches to increase the number of low-income individuals who have health insurance coverage, without increasing resources spent on Medicaid and SCHIP. HIFA encourages innovative programs that coordinate public and private health insurance coverage options. HIFA provides for a simpler demonstration application process for states that commit to reducing the number of people without health insurance. (Of the states authorized to cover parents (Arizona, California, Illinois, New Jersey, and New Mexico), Arizona, Illinois, and Oregon have taken advantage of the initiative.)
B. Family Coverage
Before HIFA, states desiring parental coverage waivers under SCHIP had to demonstrate that they covered children up to 200 percent of the FPL, that they enrolled children statewide without a waiting list, adequately promoted enrollment and retention of children in SCHIP and Medicaid, and that coverage expansions to parents would make lower-income parents eligible for coverage prior to making higher-income parents eligible. 68 Also, since no additional funds were provided to finance expansions to parents, states with separate state programs had to ensure that the cost of covering children and parents does not exceed the state's SCHIP allotment. 69 The states in this study implemented their family coverage programs before HIFA was established.
68. Lisa Dubay and Genevieve Kenney, "Covering Parents Through Medicaid and SCHIP: Potential Benefits to Low-Income Parents and Children," Washington, DC: The Urban Institute, October 2001.
69. When a Medicaid expansion program expands coverage to parents under SCHIP, these parents may use Title XIX funds when the SCHIP allotment runs out and receive federal funds at the regular Medicaid matching rate.
1. Experiences with Family Coverage in the Study States
Although none of the six study states had SCHIP programs for parents in place at the time of our site visits, CMS approved California's Section 1115 demonstration application to expand SCHIP coverage to parents in January 2002. California submitted its application to CMS in December 2000, requesting approval to use SCHIP funds to cover parents of SCHIP-enrolled children with incomes between 100 and 200 percent of the FPL, as well as parents with incomes below 100 percent of the FPL who do not qualify for Medicaid because of excess assets.70 In Louisiana, the Governor has signed legislation authorizing the Medicaid agency to seek approval to use SCHIP funds to cover parents with family incomes under 100 percent of the FPL (mostly parents of children covered under Title XIX) and pregnant women with incomes between 185 percent and 200 percent of the FPL. Louisiana also needs approval from its legislature for enrollment targets and its plan for covering the state's share of the expansion costs.
In both states, similar reasons were given by state officials for pursuing the coverage expansions for parents:
- First, it was believed that parents of Medicaid- and SCHIP-eligible children would be more likely to enroll their children if coverage also was available to them.
- Second, it was felt that when parents themselves are covered, they are more likely to seek appropriate care for their children.
- The expansion to parents would allow the state to access a greater portion of its federal SCHIP allotment.
- In Louisiana, the expansion for pregnant women was also seen as a way to reduce future program costs by preventing poor birth outcomes and childhood disabilities.
Two other study states, Missouri and New York, had already covered some low-income parents under their Section 1115 Medicaid demonstrations. Missouri sought approval to cover parents under SCHIP when it submitted its SCHIP plan in 1997; but when that request was denied, the state revised the proposal to cover parents under Title XIX. New York's Title XIX parental coverage program was approved in June 2001. In neither state does the target population covered under the demonstrations include the parents of SCHIP-eligible children, because the income thresholds are lower for the Medicaid demonstrations than they are for SCHIP. 71 At the time of the visits, neither state thought it would be feasible to extend coverage to parents under SCHIP; New York cannot do so because it has spent its full Title XXI allotment, and Missouri does not have the financial capacity to support additional expansions at this time.
One challenge that states with parent coverage face is minimizing confusion about the different SCHIP rules governing eligibility for children and parents. In Missouri, for example, different SCHIP income thresholds for parents and children have confused families and front-line eligibility staff, adding to the difficulties for outreach and enrollment staff. California anticipates similar problems, since the income threshold for its parent coverage component will be lower than the threshold for children (200 versus 250 percent of the FPL).
70. Medicaid already covered parents under 100 percent of the FPL under a Section 1931(b) waiver.
71. Missouri's program, however, includes a small number of parents of SCHIP-eligible children.
2. Experiences with Family Coverage in New Jersey, Rhode Island, and Wisconsin
On January 18, 2001, CMS authorized three states to extend SCHIP coverage to parents: New Jersey, Rhode Island, and Wisconsin. All three states had begun covering adults under Medicaid before their SCHIP waivers were approved. Both New Jersey and Rhode Island did so under Section 1931 of the Social Security Act, while Wisconsin did so under a Section 1115 Medicaid demonstration. According to a recent report on the early experiences of these three states prepared as part of ASPE's evaluation of SCHIP (Kaye et al. 2001), the early experience in these three states suggest that:
- States believe that family coverage is an effective way to cover children
- Employers, parents, health plans, and providers strongly support family coverage
- These programs appear not to have crowded out the private market
Enrollment of children increased rapidly in all three states when they expanded their programs to include parents of Medicaid and SCHIP eligible children. It is not possible to identify how much of the increase in enrollment was due exclusively to family coverage, as opposed to other factors, such as increased outreach efforts, streamlined enrollment, and, in Rhode Island, erosion of the private insurance market. All three states reported that the greatest enrollment growth was among children. In many of these cases, the children (but not the parents) could have been eligible for Medicaid before family coverage was implemented. In other words, even though some children in many of these families were eligible for Medicaid, it appears that the families did not apply for coverage for their children until the parents also could be covered. Due to a short program history, the study could not examine SCHIP family coverage's effect on retention of children in the program. However, some anecdotal evidence suggests that family coverage has encouraged appropriate utilization among enrolled children. Moreover, providers felt that family coverage not only increased children's enrollment in the program, but also improved the parents' health and knowledge about health care, thus enabling them to better care for their children.
All employers, staff from health plans and providers, and parents interviewed in the three states supported family coverage. Employers praised the program as a way to provide coverage to low-income families who do not have access to employer-sponsored coverage and/or to help families in transition from welfare to work. Parents were overwhelmingly positive about family coverage.
Any expansion of publicly funded insurance coverage raises the possibility that public coverage will crowd out private coverage; family coverage is no exception. Nevertheless, there is little evidence that crowd-out occurred. Stakeholders in New Jersey and Wisconsin felt that the crowd-out prevention provisions of the SCHIP program (such as waiting periods) and insurance laws (that require employers to offer health insurance to all qualified employees) played a role in preventing crowd-out. A good economy and low unemployment also contributed to preventing crowd-out. Rhode Island has experienced a distinct problem. In the past few years, two of the four commercial insurance carriers providing employer coverage withdrew from the state. Premiums in the remaining two commercial plans increased significantly. As a result of the plan withdrawals and the premium increases, people dropped private coverage and some enrolled in RIteCare (the SCHIP program). There is insufficient information to determine what portion of the increase is attributable to which factors. Those interviewed, however, expressed the view that the existence of RIteCare did not contribute to either the withdrawals or premium increases, but it did provide an important safety net for many people who probably would otherwise not have been able to obtain health insurance coverage.
A major concern among health plans was the higher cost of serving SCHIP parents compared with Medicaid parents. They reported that SCHIP parents were likely to be older than adults in Medicaid and more likely to have chronic diseases. To address these concerns, Rhode Island and Wisconsin raised their capitation rates to plans and instituted risk sharing. New Jersey already had risk sharing in place at the time of program expansion.
C. Premium Assistance Programs
The purpose of a premium assistance program is to leverage available employer-sponsored and other private health insurance for children or families. To operate a premium assistance program, states must demonstrate that program costs will not exceed the costs the state would incur if it were to provide direct insurance coverage. The initial SCHIP regulations limited premium assistance to situations in which the employer contributed at least 60 percent of the cost of the premium. Additionally, the benefit package offered through the private insurance must be at least as comprehensive as the package the state provides to SCHIP participants. States must also require waiting periods in the premium assistance program to prevent the substitution of public for private coverage, which would happen if employers reduced or eliminated their premium contributions, or families opted to drop dependent coverage with an employer to enroll their children in SCHIP.
In response to complaints from many states that the initial proposed regulations were too limiting, final rules issued by CMS in January 2001 eliminated the minimum percentage-contribution language from the final SCHIP regulation (as many states argued, the employer contribution must still be significant for the cost effectiveness standard to be met), allowed states to establish "reasonable" exceptions to the waiting period, and clarified how states can meet the benefit package standards when employer benefit packages do not comply with the SCHIP statute.
Among the six study states, Colorado originally envisioned a second phase to its SCHIP program, which would include a premium assistance component. The state explored the idea further during 2000, but concluded that federal rules would make implementation of the program infeasible. Texas also has expressed some interest in a SCHIP premium assistance program (they already have a premium assistance program in Medicaid). In summer 2001, the state legislature gave the SCHIP agency authority to explore this option and the state is considering a HIFA waiver for premium assistance. To date, no other study state has added a premium-assistance component to its SCHIP program.
XV. Financing and Fiscal Outlook
Highlights of Findings
- During the early years of SCHIP, states had little difficulty financing their share of SCHIP spending
- SCHIP's fiscal outlook is positive in most states because support remains strong
A. Policy Development and Program Characteristics
The legislation that established SCHIP made available approximately $40 billion in federal funds to states for fiscal years 1998 through 2007. From FY 1998 to FY 2001, states had access to slightly more than $4 billion per year. 72 (States were allowed to spend a given year's fiscal funds over the 3-year period.) State allotments are derived from a formula based primarily on two factors: (1) the number of low-income, uninsured children in the state, and (2) the number of low-income children in the state. Health care costs in the state relative to those of other states are also part of the allotment formula. States that exceed their allotment in the 3-year period of availability may draw on other states' unspent allotments. 73
Because the criteria for state selection for the evaluation favored larger states, the allotments available to the six study states, shown in Table 19, tended to be larger than the national median. Due to the large estimates of uninsured children in California, Texas, and New York, these states received the first, second, and fourth largest allotments in the country; Louisiana received the tenth largest amount. Colorado and Missouri received allotment amounts close to the national median. Altogether, the six study states received 44.2 percent of the total federal funds allocated for SCHIP.
States receive an enhanced Federal Medical Assistance Percentage (FMAP) for SCHIP relative to the FMAP provided under Medicaid. 74 Thus, from the start, SCHIP has been a financially attractive program for the states. As shown in Table 20, SCHIP federal matching rates for the six study states ranged from 65 to 79.4 percent.
| State | FFY | Federal Allotment | Expenditures | Expenditures as % of Allotment | Redistributed Allocations |
|---|---|---|---|---|---|
| California | 1998 | $854.6 | $2.0 | 0% | |
| 1999 | $850.6 | $67.7 | 8% | ||
| 2000 | $765.5 | $187.3 | 25% | 0 | |
| 2001 | $704.9 | $311.4 | 44% | 0 | |
| Colorado | 1998 | $41.8 | $ 1.0 | 2% | |
| 1999 | $41.6 | $ 9.0 | 22% | ||
| 2000 | $46.9 | $13.9 | 30% | 0 | |
| 2001 | $44.6 | $20.9 | 47% | 0 | |
| Louisiana | 1998 | $101.7 | |||
| 1999 | $101.3 | $10.4 | 10% | ||
| 2000 | $91.1 | $25.3 | 28% | 0 | |
| 2001 | $82.0 | $39.7 | 48% | 0 | |
| Missouri | 1998 | $51.7 | $9.2 | ||
| 1999 | $51.4 | $19.7 | 38% | $61.8 | |
| 2000 | $58.0 | $41.2 | 71% | $9.2 | |
| 2001 | $65.5 | $52.3 | 80% | $9.2 | |
| New York | 1998 | $255.6 | $50.1 | 20% | $197.5 |
| 1999 | $254.4 | $239.4 | 94% | $129.8 | |
| 2000 | $286.8 | $401.0 | 140% | $434.9 | |
| 2001 | $322.0 | $343.8 | 107% | $197.5 | |
| Texas | 1998 | $561.3 | $1.3 | 0% | |
| 1999 | $558.7 | $38.5 | 7% | ||
| 2000 | $502.8 | $41.5 | 8% | 0 | |
| 2001 | $452.5 | $264.0 | 58% | 0 |
Notes: The percentages of 1999 and 2000 allotments spent do not take into account redistributed amounts; states have several options as to when they use these funds.
FFY 2002 federal allotments were as follows: California: $704.9; Colorado: $44.6; Louisiana: $82.0; Missouri: $65.5; New York: $322.0; Texas: $452.5 (Federal Register Notice, January 22, 2001.)
SCHIP = State Children's Health Insurance Program (Title XXI); FFY = federal fiscal year.
Source: Centers for Medicare & Medicaid Services (CMS), Memo from Center for Medicaid and State Operations to State, January 25, 2000; Federal Register Notice, June 21, 2001; Kenney et al., Three Years into SCHIP: What States Are and Are Not Spending, The Urban Institute, September 2000. CMS provided figures for 2000 and 2001 to authors.
| State | Federal Matching Rate for Medicaid (FY 2002) | Enhanced Federal Matching Rate for SCHIP (FY 2002) | Sources of State Matching SCHIP Share |
|---|---|---|---|
| California | 51.40% | 65.98% | State appropriations |
| Colorado | 50.00% | 65.00% | State appropriations |
| Louisiana | 70.30% | 79.21% | Until 1999, foundation grants and school board funds. Since then, tobacco settlement funds and state appropriations |
| Missouri | 61.06% | 72.74% | State appropriations and, since 2001, tobacco settlement funds |
| New York | 50.00% | 65.00% | State appropriations |
| Texas | 60.17% | 72.12% | Tobacco settlement funds |
Source: Federal Register, vol. 65, no. 223, November 17, 2000.
State expenditures under SCHIP are matched with federal funds. To obtain this federal match, the study states used primarily two sources for funding--state appropriations and tobacco settlement funds (Table 20). Five states use general state appropriation monies; three draw on tobacco settlement funds, and some use both. The tobacco settlement in Texas--the largest in the nation--was the only source used to fundTexCare each year.
72. The President's budget for FY 2003 would extend the availability of FY 1998, FY 1999 and FY 2000 SCHIP funds until the end of FY 2006.
73. Cited in Kenney et al., Three Years into SCHIP: What States Are and Are Not Spending. The Urban Institute, September 2000.
74. Specifically, the state share of SCHIP costs was established at 70 percent of what states pay under Medicaid.
B. Implementation Experiences
SCHIP spending patterns varied across the six study states. As in 10 other states in the nation, Missouri and New York had spent their full FFY 1998 federal allotment by the end of the 3-year spending period for the funds (Table 20); on this basis, they qualified for additional distributions from the pool of funds unexpended in the other 38 states. New York received the largest redistribution of FFY 1998 funds (nearly $435 million), while Missouri received more than $9 million. The remaining four states pose a sharp contrast. Colorado spent 57 percent of its FFY 1998 allotment, the median percentage nationwide; whereas spending in California, Louisiana, and Texas, was far below the national median percentage.
State officials in Missouri and New York attributed their high spending levels to high rates of enrollment. Notably, too, both states had programs ready to start immediately after obtaining SCHIP funds--a Medicaid expansion program in Missouri and a pre-existing separate state children's program in New York. Missouri also cited high per capita costs and large increases in prescription drug costs as factors associated with its high level of spending. In neither case, however, did the high spending lead to a state fiscal crisis or to a cap on enrollment. Missouri came closest to a shortfall of state matching funds as a result of a unique constraint known as the "Hancock Amendment," which precludes state revenues from increasing at a higher rate than personal income growth, unless taxpayers agree to a tax increase. A funding problem was averted for FFY 2001, when the state received approval to use tobacco settlement funds to meet the shortfall. New York officials interviewed in the case study were concerned about a shortfall because they believed that they had received an inadequate federal allotment. The large amount New York received from redistributed allocations was sufficient to avert a shortfall in total funding.
According to case study respondents, the relatively low spending in the remaining states resulted from four factors: (1) overestimates of eligible, uninsured children in calculating the federal allotment; (2) lower than average per capita expenditures under SCHIP than the federal allotment anticipated; (3) late program starts; and (4) low-income eligibility thresholds that limited the number of children who qualified.
In California, state officials interviewed for the case study believed that the federal estimate of uninsured, low-income children overstated the number who would qualify for SCHIP by neglecting to account for those who would qualify for Medicaid, resulting in an inflated allotment. This was the major reason cited by state officials for their "underspending." Officials in California also cited lower per capita expenditures under SCHIP than they had expected. In Louisiana, low spending was attributed to two factors. First, LaCHIP was not implemented until the end of 1998, with only two small Medicaid expansions--first, to 133 percent, then to 150 percent of the FPL; and, second, it did not raise the eligibility level to 200 percent until the beginning of 2001. A late start was also the cause of low spending rates in Texas--that state's separate program component did not begin until April 2001, and the first two years saw negligible spending on behalf of children covered by the limited Medicaid "placeholder" expansion.
The views of state officials and legislators on the fiscal outlook for SCHIP--which were obtained during the summer of 2001, a period before the full impact of the economic recession was felt in most states--ranged from "very positive" to "uncertain." Most of the opinions concerned the prospects for state financing and tended to be correlated with legislative and gubernatorial support for the program.
XVI. Coordination of Schip and Medicaid in States with Separate Programs
Highlights of Findings
- States with separate programs still face challenges coordinating Medicaid and SCHIP, especially with regard to enrollment
A fundamental feature of Title XXI is that it gave states a choice regarding how they could expand children's health coverage. As discussed earlier in this report, roughly one-third of the states elected to expand through Medicaid, while two-thirds chose to create separate programs, either alone or in combination with smaller Medicaid expansions. 75 For those states expanding Medicaid, coordination between Title XXI and Title XIX was not an issue--the two programs, by definition, were integrated. However, states creating separate programs were required to coordinate SCHIP and Medicaid coverage and operations, and the numerous challenges involved with coordinating these two, sometimes very different, programs quickly became apparent. In many states, families may have children in both programs. In fact, SCHIP and Medicaid coordination has been difficult in the four study states that created separate programs (California, Colorado, New York, and Texas). Coordination issues have arisen mostly with regard to three program areas:
- Enrollment and retention
- Outreach and marketing
- Service delivery and access
Ideally, the policies and practices of Medicaid and separate SCHIP programs should be aligned so that children receive seamless coverage and consumers should not easily be able to detect differences between the two programs. However, many states adopted separate program expansions under Title XXI specifically in order that the SCHIP programbe different from Medicaid and to test new models for enrollment, service delivery, and cost sharing, among other program areas. Dissimilar rules and policies can confuse families and affect them negatively if enrollment is not efficient or coordinated, and gaps materialize in coverage and care.
This section discusses SCHIP and Medicaid coordination, drawing on findings presented in earlier chapters of the report and highlighting both innovative strategies for improving coordination and problems that may affect beneficiaries' ability to access services.
75. This trend is seen both nationally, and in our sample of ten states.
A. Enrollment and Retention
Lack of coordination between separate SCHIP programs and Medicaid programs affected families most seriously in the program areas of enrollment and retention. As discussed in Chapter VIII, the study states, like those across the nation, have introduced simple eligibility rules and enrollment procedures under SCHIP. Consistently, the study states employ joint SCHIP/Medicaid application forms; permit applications to be submitted by mail; apply no assets test in the SCHIP eligibility process; extend 12 months of continuous eligibility to children; and, to varying extents, require little documentation from parents submitting applications for their children. However, the study states had done much less to simplify their Medicaid rules and procedures or their SCHIP eligibility redetermination rules. The lack of alignment in eligibility and enrollment procedures was described as very confusing for families, sometimes resulting in inappropriate interruptions or losses of coverage, and was observed as presenting the most challenging administrative and coordination problems for states.
At enrollment, differing program rules sometimes resulted in joint application forms that were longer than necessary for SCHIP, since they had to reflect the rules and requirements for both SCHIP and Medicaid. During the federally required "screen-and-enroll" process, differing rules essentially required families to apply for coverage twice. Reportedly, families were often confused when, after they submitted applications for SCHIP, they were later contacted and told that their children were being considered for Medicaid and that they needed either to submit more information and verification to the state or county, or appear for a face-to-face interview.
One of the more prominent coordination problems concerns the logistics of information sharing between "single point of entry" vendors (under contract to determine SCHIP eligibility) and county social services departments (which maintain responsibility for Medicaid eligibility determination). Many case study respondents noted problems related to the "deeming" of applications, back and forth, between SCHIP vendors (who had received applications for children who appeared Medicaid-eligible) and county social services agencies (who had screened applicants who appeared SCHIP-eligible), and that the two entities interpreted program eligibility rules differently. Moreover, these entities often had severe problems tracking the status of applications moving between them. Ultimately, these problems had serious implications for families: in one state applications were described as falling into "a black hole" once they were submitted to the single point of entry; and, in several states, advocates feared that many families were falling through the cracks.
"After I got pregnant with my son, I enrolled in Healthy Start a second time. They covered us through my pregnancy and then they did one of these switcheroos to the Medicaid and needed multiple types of paperwork--car titles and bills and some back paychecks that I was unable to receive from the companies. So they discontinued my coverage and since that point in time my children either have health insurance through their father when he is employed, or they have no insurance when he is unemployed." (Suburban Cleveland, Ohio)
Coordination problems at redetermination were analogous to those that occurred during initial enrollment. For example, SCHIP and Medicaid programs often use different forms for redetermining eligibility, and impose different requirements on families concerning the submission of information and documentation. Families experienced the problems that can arise when two sets of rules apply when screen-and-enroll procedures at renewal time resulted in their applications being referred from SCHIP to Medicaid, or vice versa. Once again, if a child enrolled in one program was found at redetermination to be eligible for the other program, it often meant that parents had to complete additional steps, submit additional information, and, sometimes, appear for a face-to-face interview. If parents failed to abide by any of these additional requirements, their child or children might be disenrolled from coverage. The focus group study indicated that states are more likely to refer to Medicaid children whose family income drops below the SCHIP minimum than they are to refer to SCHIP children whose family income rises above the Medicaid maximum. Even in states that make an effort to make transitions smooth, families may face difficulties:
"My son has been bounced around from Medicaid to Child Health Plus to Medicaid to Child Health Plus so many times, I didn't even know what he was on until I got the phone call [to participate in the focus group] and said, 'Oh. Okay.' I had no idea and to this day I'm still getting bills from when they dropped and changed and I don't know who to call. I don't know what he had at that time." (Buffalo, New York)
On a more positive note, it appeared that several states have improved coordination of SCHIP and Medicaid enrollment over time, and that many of the most egregious problems could be attributed to start-up confusion and administrative "glitches." In California, state officials were working with their vendor to design improved tracking mechanisms and, in Texas, the electronic transmission of applications and documentation between the vendor and county social services agencies appeared to smooth screen and enroll efforts. In addition, case study respondents noted that community-based application assistors played a key role in alleviating parents' stress and confusion by helping families negotiate the sometimes confusing procedures, and by supporting families when coordination problems arose between vendors and county agencies.
B. Outreach and Marketing
State outreach efforts also gave rise to coordination issues which contributed to families' confusion over the identities, requirements, and relationships between SCHIP and Medicaid. As discussed in Chapter VI, the four study states with separate programs designed marketing campaigns to promote public awareness of SCHIP, while also implementing ambitious community-based initiatives to recruit "hard-to-reach" families with uninsured children at the local level. The programs were given catchy sounding names--Healthy Families, Child Health Plus, TexCare, etc.--and marketing campaigns presented positive and colorful images of healthy mothers, infants, and children, using upbeat slogans like "Growing Up Healthy," and "A Healthier Tomorrow Starts Today." Print materials distributed to community-based organizations reproduced these images, logos, and slogans.
Importantly, however, three of the four study states did not prominently promote Medicaid in their marketing materials; only California'sHealthy Families/Medi-Cal for Children campaign explicitly placed Medicaid on an equal footing with SCHIP. In Texas, the TexCare Partnership was created as an "umbrella" identity through which SCHIP and Medicaid could be promoted, but the Medicaid connection is not prominently advertised. For years, New York kept the identities of Child Health Plus and Medicaid separate, and the same is true for Colorado.
According to case study respondents interviewed for this study, these arrangements arose for a variety of reasons. Some state officials noted that Medicaid was not aggressively promoted for fear of "turning off" families who might hold negative opinions of Medicaid, either because of previous negative experiences with the Medicaid enrollment process or, among immigrant Hispanic families, who feared that Medicaid enrollment may adversely affect their or their child's ability to obtain citizenship. In Colorado and Texas, community-based application assistors defended the marketing emphasis on SCHIP, noting that they could use SCHIP to begin a conversation about health insurance coverage and then talk about Medicaid when appropriate. In California, staff of some (but not all) health plans and community-based organizations noted that they tend to market Healthy Families and avoid directly discussing Medi-Cal, for fear of losing families. Notably, officials in every state with a separate program were quick to point out that they believed their SCHIP campaigns effectively promoted enrollment in both programs, largely because of their use of joint applications. By responding to an advertisement or flyer and calling a program hotline, families can request and receive a joint SCHIP/Medicaid program application and, upon completing it, obtain either SCHIP or Medicaid coverage for their child/children.
State and local officials who we interviewed for the study had mixed opinions about the appropriateness of single-program marketing. Some were pragmatic, believing that the states would attract more families by promoting a new and "baggage-free" product, while taking comfort in the likelihood that these efforts would also succeed in reaching families with Medicaid-eligible children. Other case study respondents, however, disagreed with this approach, suggesting that it promoted SCHIP in a very positive light, while ignoring Medicaid; these respondents consistently believed that the much larger Medicaid program should be promoted equally.
The ultimate impact that these marketing messages have had on families is unclear. It was reported that some parents were confused (and sometimes angry) when they responded to SCHIP advertising, submitted a program application, and then learned that they were being reviewed for Medicaid eligibility. Some parents in the focus groups did not understand and did not like having their children switched from SCHIP to Medicaid.
New York offers an example of how marketing efforts might evolve in the future. There, after maintaining totally separate identities for Child Health Plus and Medicaid for years, the state renamed Medicaid Child Health Plus "A," while the SCHIP program assumed the name Child Health Plus "B." As a result, New York officials hoped that Medicaid would accrue all the positive benefits of SCHIP marketing, and that the two programs would begin to be perceived by consumers as one. Many advocates and other study participants in most of the states supported this approach. The case study respondents commonly expressed that, ultimately, states should promote "health insurance," and not "SCHIP" or "Medicaid."
C. Service Delivery and Access
The third program area where coordination between SCHIP and Medicaid is crucial for children is service delivery. The extent to which SCHIP and Medicaid delivery systems are aligned is a significant aspect of coordination between the two programs, that largely determines whether children receive seamless and integrated health care. In cases where SCHIP and Medicaid programs in a given state share the same (or at least similar) provider networks, children are more likely to receive continuous care from the same provider regardless of which program is paying the bills. If the opposite is true and SCHIP and Medicaid programs use significantly different networks, then children and families may be much more likely to experience disruptions in their relationships with caregivers and their continuity of care. This issue is especially important for "mixed coverage" families (that is, those with children covered by each of the programs), who might face the prospect of having different children enrolled in different health plans, receiving care from different providers.
As discussed in Chapter XI, most of the study states set out to make managed care the foundation of their SCHIP delivery systems. 76 Among the four states with separate programs, state officials explicitly sought to align SCHIP and Medicaid delivery systems to the greatest extent possible, while also expanding the use of managed care arrangements to a larger number of counties, including rural ones. Yet, in only half of these states did these efforts result in closely aligned systems of care for beneficiaries of the two programs, as described below. In two of the four states with separate programs, SCHIP and Medicaid systems were quite well coordinated; the vast majority of managed care health plans participated in both programs, and delivery arrangements in urban areas, in particular, were quite consistent. In Colorado, the state's authorizing legislation required that plans participating in SCHIP must also participate in Medicaid. In New York, the only difference between the two programs is that one large New York City plan participates in SCHIP but not Medicaid. In California and Texas, however, differences in plan participation across the two programs were more pronounced. Both states operate managed care arrangements in considerably more counties under SCHIP than Medicaid, and in Texas, only half of the health plans that participate in Medicaid also participate in SCHIP.
In all four states, there were more distinct differences between SCHIP and Medicaid service delivery in rural areas. SCHIP programs in California, Colorado, and Texas each operate some form of exclusive provider organization (EPO) with an organized network of participating physicians in their rural regions, while Medicaid programs operate traditional fee-for-service systems.
Despite the remaining differences between SCHIP and Medicaid service delivery networks, it appears that state efforts to achieve SCHIP and Medicaid alignment have fostered relatively coordinated service delivery in most areas of the study states, according to state and local officials, providers, and advocates. When the same plans participate in both programs, case study respondents informed us that families have a much easier time making the transition from one program to the other as family income or circumstances change. We also heard from advocates and local application assistors that families care most about being able to retain their relationships with particular physicians when they switch programs, rather than with particular health plans. On this score, it was reported that close alignment between SCHIP and Medicaid plans, and the provider networks in those plans, had led to consistent access and continued relationships with providers for most families. In Texas, the state with the most distinct SCHIP and Medicaid systems, the fact that SCHIP health plans are dominated by traditional safety net providers, and that Medicaid enrollment is concentrated in these plans as well, meant that families moving from one program to the other most often have had the same choices of plans and providers.
In the rural areas of the six states, however, more coordination problems related to service delivery were reported. As discussed in Chapter XI, the SCHIP programs in California, Colorado, and Texas use EPOs in rural areas, as a strategy to increase the numbers of physicians available to SCHIP enrollees and, in turn, improved children's access to primary care providers. However, continued reliance on traditional fee-for-service systems in Medicaid in these states has resulted in limited numbers of providers who are willing to participate in the program. Thus, when families switch programs in these regions, they face a greater likelihood of confronting disruptions in service delivery.
76. Louisiana is the only state of the first six we visited whose SCHIP program relies primarily on fee-for-service delivery and payment arrangements.
XVII. Conclusions
SCHIP is a program that allows the states to offer unparalleled new coverage to children using both existing Medicaid systems and alternative insurance models that reflect private sector delivery systems. States have acted quickly to implement the programs and have had many early successes, though they have also had to overcome challenges and new issues are becoming apparent as the programs mature.
A. Successes
High Enrollee Satisfaction.State officials and advocates responding to case study interviews report that families are satisfied with SCHIP. Focus group participants with children enrolled in SCHIP and Medicaid bear out these reports. Families like the low price, the range of benefits, and the access to providers that the programs offer. While these findings must be considered preliminary, the survey of parents in ten states, whose findings will be reported in the final Report to Congress, will provide richer and more detailed information about enrollee satisfaction.
Millions of Low-Income Children Enrolled. The flexibility afforded by Title XXI allowed states to adopt the program designs that best met their needs. Some states elected Medicaid expansions both as a means of extending Medicaid's broad coverage to more children and because it was administratively efficient. Others chose separate programs in order to use features of private insurance, and sometimes to avoid saddling the new program with longstanding negative associations that many had with Medicaid. Regardless of their program choice, however, most states enjoyed strong support for implementing a SCHIP program.
States began implementing their SCHIP programs soon after the law was passed, and enrollment has grown continuously ever since. By the end of 1998, about 1 million children had been enrolled (CMS, 2002). Enrollment grew steadily so that by FY 2002, 5.3 million children were covered under the program at some time during the year--a 15 percent increase over the numbers enrolled in FY 2001. The growth from year to year was fueled both by increases in the number of states operating a program (all but two states had programs up and running by the second anniversary of SCHIP's enactment) and by aggressive outreach to and simpler enrollment processes for families with eligible children. While quantitative evidence is scant, state officials who were interviewed in the study states indicate that Medicaid enrollment has increased as a result of SCHIP outreach.
Streamlined Program Entry.Nearly all states developed simple application and enrollment processes for their separate SCHIP programs. Aspects of typical SCHIP application processes include short, joint applications for SCHIP and Medicaid, mail-in application options, and telephone-based or local hands-on application assistance. Few use an asset test (a common feature of Medicaid applications in the past for families and children on welfare), and many have 12-month continuous eligibility periods and require only minimal documentation to prove eligibility. State officials believe that these features have been crucial to their successful enrollment of children in SCHIP.
Some of the design features of SCHIP have spilled over to Medicaid. For example, due to reforms in California and Texas, children can now apply for Medicaid, too, by mail, and documentation requirements have been reduced. To the extent that such reforms make Medicaid and SCHIP more alike, coordination and family transitions between the two programs become smoother. The cumulative effect of the streamlining has been a "reinvention" of public health insurance--a replacement of the old welfare-style program with a more accessible, consumer-driven program.
Strategic Outreach.Based on their experience, states have continued to adopt new outreach strategies for SCHIP that they expect to be more effective. While the early emphasis in outreach was on statewide mass media campaigns to establish an identity for the new programs, community-based efforts have since played an increasingly important role. Community-based outreach, often conducted by local organizations and trusted community groups, is often used to target hard-to-reach families and subpopulations.
Broad and Affordable Benefits.Medicaid benefits are usually more comprehensive than benefits covered under separate state SCHIP programs. But SCHIP programs, too, offer broad benefits that were consistently described as much broader than benefits offered in private health insurance. Case study respondents and focus group participants said SCHIP benefits met the needs of the vast majority of children.
Many states require modest cost-sharing, including premiums, enrollment fees, and co-payments in their separate SCHIP programs. According to case study respondents interviewed for this study, as well as most focus group participants, families consider the cost-sharing reasonable and not overly burdensome, financially. Also, many of those interviewed support the cost-sharing requirements in SCHIP because they believe that they encourage "pride of ownership" and appropriate use of services. An additional reason that states have included cost-sharing is to discourage families with private insurance coverage from disenrolling from that coverage and substituting public coverage. However, the impacts of premiums on SCHIP participation will be rigorously assessed later in this study.
Apparent Good Access to Care. Overall, access to care under SCHIP was described by case study respondents as good, especially in urban areas. In large part, this was attributed to states' widespread use of managed care arrangements, which have reportedly helped increase both the supply of participating providers and the number of children with a "medical home." Where Medicaid programs use service delivery arrangements similar to those used by SCHIP--most often in urban areas--access to care for Medicaid enrollees was also described as good.
Positive Attitudes toward SCHIP and Medicaid.The steady growth in SCHIP enrollment confirms that the programs are successful in providing coverage for low-income children. Families want to and will enroll their children in affordable health insurance. Analyses of low-income families' knowledge and attitudes toward SCHIP and Medicaid showed that fully 82 percent of low-income uninsured children whose parents had heard of either Medicaid or SCHIP, or both, say they would enroll their children if told they were eligible. In addition, 88 percent of parents of low-income, uninsured children who have been enrolled in Medicaid in the past have positive views about enrolling their children again (Kenney et al. 2002).
Although awareness of SCHIP among low-income families still lags behind awareness of Medicaid (55 percent versus 87 percent in early 2001)--as might be expected given that SCHIP is relatively new--awareness of the program appears to be increasing over time among low-income families with uninsured children. Widespread interest in enrolling their children among parents who had heard of Medicaid and SCHIP, suggests that improving awareness of the programs and understanding of eligibility rules could lead to further increases in enrollment.
Ongoing Support. Support for SCHIP has been strong and steady since the program's inception. The enhanced federal match for SCHIP made it popular with the states, and states have been using their tobacco settlement dollars and general appropriations to fund their portion of the program. Despite the softening economy, most state officials we interviewed pointed to broad-based support for the program and predicted a positive future.
B. Challenges
Gaps in Outreach and Awareness.States beginning to implement their SCHIP programs faced the challenge of reaching out to a large and diverse population of low-income families with uninsured children, who may never have been enrolled in a public assistance program. Outreach has not been uniformly effective across states or across subpopulations, and more work is needed to increase program awareness and understanding of SCHIP and Medicaid program rules among families, regardless of race, ethnicity, or age of children.
Among low-income families with uninsured children, those least aware of SCHIP are Hispanic families interviewed in Spanish and the very poorest families (that is, those below 50 percent of the poverty level). Many low-income parents with uninsured children, though they are aware of Medicaid and SCHIP, do not believe that their children are eligible. Confusion about who is eligible is most common among parents of Hispanic children interviewed in Spanish, parents of white children, parents of older children, and parents of children in families with higher incomes.
Application Process Widely Perceived as Difficult.Fewer than half of all low-income uninsured children whose parents had, in 2001, heard of at least one of the two programs have parents who view the Medicaid and SCHIP application processes as easy. Negative perceptions are more widespread for the Medicaid program than for SCHIP (32 versus 22 percent). This result is consistent with focus group participants' comments comparing Medicaid and SCHIP application processes. (Focus group participants also reported negative experiences in the past with Medicaid applications.) Less-educated parents and those interviewed in Spanish more often reported difficulties with the application process. Thus, making the application process for the programs easier and more accessible to parents from diverse ethnic backgrounds and educational levels remains as a program challenge.
More Coordination Needed.SCHIP and Medicaid together offer the potential for seamless coverage so that children whose family's income changes can move between the programs without disruption, and families with children in both programs need not navigate two distinct systems. However, coordination has not yet been perfected in states that operate separate SCHIP programs. While separate programs appear to enjoy high levels of support, case study respondents in states with such programs reported that coordinating SCHIP and Medicaid poses significant challenges. These challenges stem from differences between the two programs' eligibility rules, administrative structures, and delivery systems. Even minor discrepancies in eligibility policy between the two programs can complicate the "screen-and-enroll" procedures, required by law to place children into the program for which they are eligible. Likewise, focus group participants found differences between the programs to be confusing.
Understanding Why Children Leave the Program. As state programs mature, an emerging challenge is tracking the retention and disenrollment of eligible children and understanding the reasons for disenrollment of eligible children. No one yet knows what "reasonable" rates of retention or disenrollment are, and the availability and quality of data on the reasons for disenrollment are limited. Although disenrollment might appropriately result from changes in employment, income, access to employer-sponsored insurance, or other factors, there is a concern among state officials interviewed in the case studies that administrative barriers (for example, redetermination procedures) and confusion among parents of enrolled children are significant causes of disenrollment. This concern was also found in the statements of some focus group participants who reported that they had not intended to disenroll their children, but did not realize what the renewal process entailed.
Lingering Resistance to Medicaid. Despite the positive views about Medicaid among many families whose children have been enrolled in the program, Medicaid is not always viewed so positively. Providers have often been reluctant to accept Medicaid patients, mostly because of low Medicaid payment rates in the past. Some families are reluctant to enroll in Medicaid; their reasons include past difficulties applying, the stigma arising from Medicaid's longstanding linkage to the welfare program, and the concern among immigrant families that receipt of Medicaid could jeopardize their immigration status or their efforts to obtain citizenship. These perceptions were reportedly one of the factors that led some states to choose separate SCHIP programs rather than Medicaid expansions.
Gaps in Access.Despite the broad benefits offered by Medicaid and SCHIP, early success enrolling health plans and providers into SCHIP networks, and reported good access to primary and preventive care, focus group participants and case study respondents indicate that families still have difficulty obtaining some covered benefits, particularly dental and certain specialists' services.
Access in rural areas is reported to be more limited than in urban areas. Some states have responded to the limited number of providers in rural areas and provider rejection of capitated managed care by introducing "exclusive provider organizations," which recruit and extend to families an identified network of primary care physicians for their children.
Maintaining Provider Payment Levels. Most states employ capitated managed care for the majority of their SCHIP enrollees. Lacking an alternative basis for setting capitation rates, state officials have typically paid health plans participating in SCHIP the same (or nearly the same) rates they pay under Medicaid. Likewise, health plans have most often elected to pay their providers according to the fee schedules they use in Medicaid. In states where providers view these rates as unfairly low, case study respondents were concerned about reduced provider participation and potential reductions in access to care.
C. Emerging Issues
The challenges identified earlier are likely to remain central for the foreseeable future. But new issues are also emerging: case study respondents in the six states under study indicated that family coverage under SCHIP is a topic of growing interest. While some states have already obtained approval for such programs, an increase in the number of states proposing both these arrangements and other, new approaches is likely in light of the flexibility recently offered under CMS' Health Insurance Flexibility and Accountability (HIFA) initiative. The impact of these programs on the number of low-income, uninsured individuals and also on the profile of the Medicaid and SCHIP programs will, along with operational issues, be of great interest.
References
American Academy of Pediatrics. Improving Access to Children's Health Insurance in New York. AAP: 2000 Web site: [http://www.aap.org/advocacy/chi2/ny.pdf]
Bellamy, Hilary, Renee Schwalberg, Dorothy Borzsak, Jennifer Dunbar, Christopher Botsko, Jamie Hart, Michael Perry, and Adrianne Dulio. "Findings From The State Children's Health Insurance Program Focus Group Study." Washington, DC: Health Systems Research, January 2002.
Centers for Medicare & Medicaid Services. Web site [http://www.cms.hhs.gov/]
Centers for Medicare & Medicaid Services (CMS). "Application and Enrollment Simplification Profiles: Medicaid for Children and SCHIP."Centers for Medicare & Medicaid Services (CMS). "Eligibility Standards in the 50 States and District of Columbia," January 2001.
Centers for Medicare & Medicaid Services (CMS). Memo from Center for Medicaid and State Operations to State, January 25, 2000.
Centers for Medicare and Medicaid Services (CMS), "State Children's Health Insurance Program (SCHIP) Aggregate Enrollment Statistics for the 50 States and the District of Columbia for Federal Fiscal Years (FFY) 2000 and 1999." Website: [http://www.cms.hhs.gov/schip/fy99-00.pdf]
Centers for Medicare & Medicaid Services (CMS). "The State Children's Health Insurance Program Preliminary Annual Enrollment Report for Fiscal Year 2002." Added January 31, 2003. Website: [http://www.cms.hhs.gov/schip/schip02.pdf]
Centers for Medicare & Medicaid Services (CMS).
California:
California Title XXI Program Fact Sheet. CMS Web site [http://www.cms.hhs.gov/schip/chpfsca.pdf]
State Child Health Plan under Title XXI of the Social Security Act: California's Healthy Families program. November 18, 1997 Web site [http://www.dhs.cahwnet.gov/org/Director/healthy_families/stplan.pdf]
Framework For State Evaluation of Children's Health Insurance Plans Under Title XXI of the Social Security Act, 1999: California, March 2000. Web site [http://www.cms.hhs.gov/schip/caeval98.pdf]
Colorado:
Colorado Department of Health Care Policy and Financing. "Children's Basic Health Plan Cost-Sharing." Position Paper. Denver, CO: October 1, 2000.
Colorado Title XXI Program Fact Sheet.
CMS Web site [http://www.cms.hhs.gov/schip/chpfsco.asp]
"Annual Report of State Children's Health Insurance Plans Under Title XXI of the Social Security Act." November 2000.
CMS Web site [http://www.cms.hhs.gov/schip/charco99.pdf]
Louisiana:
Louisiana Title XXI Program Fact Sheet.
CMS Web site [http://www.cms.hhs.gov/schip/chpafsla.asp]
Missouri:
"Missouri Title XXI state Plan Summary Fact Sheet."
Web site [http://www.cms.hhs.gov/schip/chpfsmo.pdf]
Missouri Statewide Health Reform Demonstration Fact Sheet.
Web site [http://www.cms.hhs.gov/medicaid/1115/mofact.pdf]
The State Of Missouri 1915(b) Program.
Web site [http://www.cms.hhs.gov/medicaid/1915b/momcpfs.pdf]
New York:
New York Title XXI Program Fact Sheet.
CMS Web site [http://www.cms.hhs.gov/schip/chpfsny.pdf]
New York Governor's Press Office. Child Health Plus Expansion Means Healthier Kids, Press Release, June 18, 1998.
Department of Health and Human Services. "HHS Approves Changes in New York SCHIP Program" HHS News, July 12, 2001.
Framework for Annual Report of State Children's Health Insurance Plans Under Title XXI of the Social Security Act: New York State, November 2000.
CMS Web site [http://www.cms.hhs.gov/schip/charny99.pdf]
Texas:
Texas Title XXI Program Fact Sheet.
CMS Web site [http://www.cms.hhs.gov/schip/chpfstx.pdf]
Framework For State Evaluation Of Children's Health Insurance Plans Under Title XXI of the Social Security Act, 1999: Texas, March 2000.
Web site [http://www.cms.hhs.gov/schip/txeval98.pdf]
CMS. The State Children's Heath Insurance Program Annual Enrollment Report Federal Fiscal Year 2001. Dated February 6, 2002. [http://www.cms.hhs.gov/schip/schip01.pdf]. Accessed: March 17, 2002a.
CMS. State Children's Health Insurance Program State Activity Map.
[http://www.cms.hhs.gov/schip/chip-map.asp]. Accessed: March 17, 2002b.
Cohen Ross, Donna, and Laura Cox. "Making It Simple: CHIP Income Eligibility Guidelines and Enrollment procedures: Findings from a 50-State Survey." Kaiser Commission on Medicaid and the Uninsured, October 2000.
Colorado Department of Health Care Policy and Financing (HCPF)
Dubay, Lisa, Jennifer Haley, and Genevieve Kenney. "Children's Eligibility for Medicaid and SCHIP: A View from 2000." Assessing the New Federalism Policy Brief B-41. Washington, D.C.: Urban Institute, January 2002.
Dubay, Lisa, John Holahan, and Genevieve Kenney. "Which Children Are Still Uninsured, and Why?" In The Future of Children, forthcoming.
Dubay, Lisa, and Genevieve Kenney. "Covering Parents Through Medicaid and SCHIP: Potential Benefits to Low-Income Parents and Children," Washington, DC: The Urban Institute, October 2001.
Dubay, Lisa, Genevieve Kenney, and Jennifer Haley. "Children's Participation in Medicaid and SCHIP Early in the SCHIP Era." In Assessing the New Federalism Policy Brief B-40. Washington, DC: The Urban Institute, March 2002.
Dubay, Lisa, Genevieve Kenney, and Stephen Zuckerman. "Extending Medicaid to Parents: An Incremental Strategy for Reducing the Number of Uninsured." Assessing the New Federalism Policy Brief B-20. Washington, D.C.: Urban Institute, June 2000.
Federal Register. Notice, June 21, 2001.
Federal Register, vol. 65, no. 36, February 23, 2000.
General Accounting Office. "Medicaid and SCHIP: States' Enrollment and Payment Policies Can Affect Children's Access to Care." September 2001.
Hill, Ian. "Charting New Courses for Children's Health Insurance," Policy and Practice, vol. 58, no. 4, December 2000.
Hill, Ian, Mary Harrington, and Corinna Hawkes. "Congressionally Mandated Evaluation of the State Children's Health Insurance Program: Interim Cross-Cutting Report on the Findings from Six State Site Visits." Report prepared by The Urban Institute and Mathematica Policy Research, Inc., November 25, 2002.
Hoffman, Catherine, and Mary Pohl. "Health Insurance Coverage in America: 1999 Data Update." Washington, DC: The Kaiser Commission on Medicaid and the Uninsured, December 2000.
Kaiser Commission on Medicaid and the Uninsured. "Comparison of Medi-Cal and Healthy Families Programs in California," October 2000.
Kaye, Neva, Kirsten Wysen, and Cynthia Pernice. "SCHIP Family Coverage in Three States: A Report on the Early Experiences of New Jersey, Rhode Island, and Wisconsin." Report prepared for the Assistant Secretary of Planning and Evaluation, DHHS. Washington DC: George Washington University. December 2001.
Kenney, Genevieve and Lisa Dubay. "Awareness of and Beliefs About Medicaid and SCHIP Programs: Findings from Early 2001."
Kenney, Genevieve, and Jennifer Haley. "Why Aren't More Uninsured Children Enrolled in Medicaid or SCHIP?" In Assessing the New Federalism Policy Brief B-35. Washington, DC: The Urban Institute, 2001.
Kenney, Genevieve, Jennifer Haley, and Stephen Blumberg. "Awareness and Perceptions of Medicaid and SCHIP Programs Among Low-Income Families with Uninsured Children: Findings from Early 2001." Draft report submitted to OASPE. Washington, DC: The Urban Institute, November 8, 2002.
Kenney, Genevieve, Jennifer Haley, and Lisa Dubay. May 2001. "How Familiar Are Low-Income Parents With Medicaid and SCHIP?"Assessing the New Federalism Policy Brief No. B-34. Washington, D.C.: The Urban Institute.
Kenney, Genevieve, Frank Ullman, and Alan Weil. "Three Years into SCHIP: What States Are and Are Not Spending." The Urban Institute, September 2000.
Louisiana Department of Health and Hospitals, Medicaid Division
Managed Risk Medical Insurance Board. Health Families Program Enrollment History. Website [http://www.mrmib.ca.gov/MRMIB/HFP/HFPRptHG.html]
Missouri Department of Medical Services
Medi-Cal Policy Institute. "Medi-Cal Managed Care," Medi-Cal Facts, No. 8. Oakland, CA, March 2000.
Moreno, Lorenzo, and William Black. "Congressionally Mandated Evaluation of the State Children's Health Insurance Program: Retention and Reenrollment in Three States. Draft Report." Princeton, NJ: Mathematica Policy Research, Inc., December 7, 2001.
National Governors' Association. State Children's Health Insurance Program Plan Summaries. California S-CHIP Plan Summary. Web site [http://www.nga.org/cda/files/CASCHIP.pdf]
National Survey of America's Families (NSAF). 1999.
New York State Department of Health, Web site [http://www.health.state.ny.us/nysdoh/chplus/index.htm]
Pernice, C., T. Riley, M. Perry, and S. Kannel. Why Eligible Children Lose or Leave SCHIP: Findings from a Comprehensive Study of Retention and Disenrollment. National Academy of State Health Policy. February 2002.
Rosenbach, Margo, Marilyn Ellwood, John Czajka, Carol Irvin, Wendy Coupe, and Brian Quinn. "Implementation of the State Children's Health Insurance Program: Momentum is Increasing After a Modest Start: First Annual Report." Cambridge, MA: Mathematica Policy Research, Inc., January 2001.
Rosenbach, Margo, Marilyn Ellwood, John Czajka, Carol Irvin, Angela Merrill, Cheryl Young, Wendy Coupe, and Brian Quinn. "Evaluation of the State Children's Health Insurance Program: Background Report to Congress: Final Report." Cambridge, MA: Mathematica Policy Research, Inc., 2001.
Smith, Vernon, David Rousseau, and Jocelyn Guyer, "CHIP Program Enrollment: December 2000," Washington, DC: The Kaiser Commission on Medicaid and the Uninsured, September 2001.
State and Local Area Integrated Telephone Survey. 2001 Preliminary Data File.
State of Colorado. "Annual Report of State Children's Health Insurance Plans Under Title XXI of the Social Security Act," November 2000.
State of Louisiana Department of Health and Hospitals (DHH). "Annual Report of State Children's Health Insurance Plans Under Title XXI of the Social Security Act, 2000." March 22, 2001.
State of Louisiana DHH, "More Children Now Eligible for Health Insurance," January 9, 2001.
State of Missouri, Department of Social Services. "Missouri's Children Health Insurance Program Evaluation." Submitted to the Health Care Financing Administration, March 31, 2000.
Texas Department of Health Services. Cumulative DHS CHIP Status Report (Updated Weekly): CHIP Enrollment and Referrals, September 04, 2001. TexCare Partnership Web site: [http://www.hhsc.state.tx.us/chip/DHSrpt.pdf]
Ullman, Frank, Ian Hill, and Ruth Almeida. "CHIP: A Look at Emerging Programs." Washington, DC: The Urban Institute, September 1999.
Ullman, Frank, Ian Hill, and Ruth Almeida. "CHIP: A Look at Emerging State Programs." Assessing the New Federalism Policy Brief No. A-35. Washington, DC: The Urban Institute, September 1999.
Van Dyck, Peter C., Merle McPherson, Bonnie B. Strickland, Kerry Nesseler, Stephen J. Blumberg, Marcie L. Cynamon, and Paul W. Newacheck. "The National Survey of Children with Special Health Care Needs." Ambulatory Pediatrics, vol. 2, no. 1, 2002, pp. 29-37.
Weil, Alan. "The New Children's Health Insurance Program: Should States Expand Medicaid?" Washington, DC: The Urban Institute, Issue Brief Series A, no. A-13, October 1997.
Westpfahl Lutzky, Amy, and Ian Hill "Has the Jury Reached a Verdict? States' Early Experiences with Crowd-Out Under SCHIP," The Urban Institute, June 2001.
Wooldridge, Judith, Brenda Cox, Mary Harrington, Lorenzo Moreno, Christopher Trenholm, Welmoet van Kammen, Will Black, Nancy Fasciano, Amy Zambrowski, Lisa Dubay, Genevieve Kenney, Ian Hill, Ruth Almeida, Jennifer Haley, Amy Westpfahl-Lutsky, Jamie Chriqui. "Design Report: Congressionally Mandated Evaluation of the State Children's Health Insurance Program: Final Report." Report prepared by Mathematica Policy Research, Inc., The Urban Institute, and The MayaTech Corporation, November 30, 2001.
Appendices
A. Enabling Legislation for the SCHIP Evaluation
ENABLING LEGISLATION FOR THE SCHIP EVALUATION H.R.3426
Medicare, Medicaid, and SCHIP Balanced Budget Refinement Act of 1999
(Introduced in the House)
SEC. 703. IMPROVED DATA COLLECTION AND EVALUATIONS OF THE STATE CHILDREN’S HEALTH INSURANCE PROGRAM.
(b) FEDERAL EVALUATION, OF STATE CHILDREN'S HEALTH INSURANCE PROGRAMS-
Section 2108 (42 U.S.C. 1397hh) is amended by adding at the end the following:
(c) FEDERAL EVALUATION
(1) IN GENERAL- The Secretary, directly or through contracts or interagency agreements, shall conduct an independent evaluation of 10 States with approved child health plans.
(2) SELECTION OF STATES- In selecting States for the evaluation conducted under this subsection the Secretary shall choose 10 States that utilize diverse approaches to providing child health assistance, represent various geographic areas (including a mix of rural and urban areas) and contain a significant portion of uncovered children.
(3) MATTERS INCLUDED- In addition to the elements described in subsection (b)(1). the evaluation conducted under this subsection shall include each of the following:
- Surveys of the target population (enrollees, disenrollees, and individuals eligible for but not enrolled in the program under this title).
- Evaluation of effective and ineffective outreach and enrollment practices with respect to children (for both the program under this title and the Medicaid program under title XIX), and identification of enrollment barriers and key elements of effective outreach and enrollment practices, including practices that have successfully enrolled hard-to-reach populations such as children who are eligible for medical assistance under title XIX but have not been enrolled previously in the Medicaid program under that title.
- Evaluation of the extent to which State Medicaid eligibility practices and procedures under the Medicaid program under title XIX are a barrier to the enrollment of children under that program and the extent to which coordination (or lack of coordination) between that program and the program under this title affects the enrollment of children under both programs.
- An assessment of the effect of cost-sharing on utilization, enrollment, and coverage retention.
- Evaluation of disenrollment or other retention issues, such as switching to private coverage, failure to pay premiums, or barriers in the recertification process.
(4) SUBMISSION TO CONGRESS- Not later than December 31, 2001, the Secretary shall submit to Congress the results of the evaluation conducted under this subsection.
(5) FUNDING- Out of any money in the Treasury of the United States not otherwise appropriated, there are appropriated $10,000,000 for fiscal year 2000 for the purpose of conducting the evaluation authorized under this subsection. Amounts appropriated under this paragraph shall remain available for expenditure through fiscal year 2002.
B. Focus Group Summary Tables
TABLE B.1 SUMMARY OF FOCUS GROUPS BY TARGET AUDIENCE AND BY STATE
| State | Target Audiences | Total | |||
|---|---|---|---|---|---|
| Eligible but not enrolled | Enrolled | Disenrolled | Privately Insured | ||
| Medicaid Expansion Programs | |||||
| Maryland | 2 | 1 | 1 | 1 | 5 |
| Missouri | 2 | 2 | 1 | 1 | 6 |
| Ohio | 1 | 2 | 1 | 1 | 5 |
| Separate State Programs | |||||
| Colorado | 1 | 3 | 2 | 1 | 7 |
| Georgia | 1 | 2 | 2 | 5 | |
| Combination Programs | |||||
| California | 2 | 4 | 2 | 1 | 9 |
| Florida | 1 | 1 | 2 | 4 | |
| New York | 1 | 2 | 2 | 5 | |
| Texas | 2 | 2 | 1 | 5 | |
| Total | 13 | 19 | 14 | 5 | 51 |
Source:Bellamy, Hilary, Renee Schwalberg, Dorothy Borzsak, Jennifer Dunbar, Christopher Botsko, Jamie Hart, Michael Perry, and Adrianne Dulio. “Findings From The State Children’s Health Insurance Program Focus Group Study.” Washington, DC: Health Systems Research, January 2002.
aMaryland implemented a separate SCHIP program in July 2001, making it a State that has adopted a combination SCHIP program design. However, due to the recent implementation date of the Maryland SSP, the State was considered a Medicaid expansion program for this study.
TABLE B.2 SUMMARY OF FOCUS GROUPS BY TARGET AUDIENCE AND RACE AND GEOGRAPHIC LOCATION
| Enrolled | Disenrolled | ||||||
|---|---|---|---|---|---|---|---|
| Eligible | Medicaid | Separate State Program | Medicaid | Separate State Program | Privately Insured | Total | |
| Race/Ethnicity | |||||||
| White | 1 | 2 | 1 | 1 | 2 | 2 | 9 |
| Black | 2 | 1 | 1 | 2 | 1 | 7 | |
| Hispanic | 2 | 3 | 1 | 2 | 1 | 9 | |
| Asian | 1 | 1 | 2 | ||||
| American Indian | 1 | 1 | 2 | ||||
| Mixed | 6 | 4 | 4 | 3 | 3 | 2 | 22 |
| Total | 13 | 12 | 7 | 8 | 6 | 5 | 51 |
| Geography | |||||||
| Urban | 9 | 6 | 3 | 4 | 2 | 2 | 26 |
| Suburban/Small City | 2 | 2 | 3 | 1 | 2 | 2 | 12 |
| Rural | 2 | 4 | 1 | 3 | 2 | 1 | 13 |
| Total | 13 | 12 | 7 | 8 | 6 | 5 | 51 |
Source: Bellamy, Hilary, Renee Schwalberg, Dorothy Borzsak, Jennifer Dunbar, Christopher Botsko, Jamie Hart, Michael Perry, and Adrianne Dulio. “Findings From The State Children’s Health Insurance Program Focus Group Study.” Washington, DC: Health Systems Research, January 2002.
C. Final Report to Congress
At the end of the study period, Congress will receive a comprehensive report on SCHIP, which addresses all the issues laid out in the legislation that mandated the evaluation. The report will encompass all research activities that take place under the study, as well as those conducted through a series of smaller, related ASPE-sponsored studies. The report will present findings of the four major analyses: (1) state context and SCHIP program design; (2) SCHIP enrollment and disenrollment; (3) links between SCHIP and Medicaid, uninsurance, and private coverage; and (4) SCHIP access, service use, and satisfaction. In addition, the report will address the major similarities and differences between the SCHIP and Medicaid populations.
The first analysis—on state context and program design—will examine the key contextual factors and design elements that define SCHIP programs and their program experience (enrollment, access, service use, and so on). The analysis draws on several qualitative sources, as displayed in Table B.1 by research question. The two most important sources are the case studies in the 10 study states and the survey of SCHIP administrators in all states and territories. In addition, several external studies—most notably, the focus group study—provide further insight into SCHIP program design and consumer experience.
The remaining three analyses explore the program experiences of SCHIP enrollees and disenrollees (see the lower panels of Table B.1). Each analysis relies on quantitative data, although the qualitative data provide important contextual information for interpreting results. The most important data source for these analyses is the survey of SCHIP enrollees and disenrollees across the 10 study states. Additional sources include the SLAITS survey of
TABLE B.1: SUMMARY OF QUESTIONS TO BE ADDRESSED IN THE FINAL REPORT TO CONGRESS
| Qualitative Data Sources | Quantitative Data Sources | ||||||
|---|---|---|---|---|---|---|---|
| Research Questions | Case Studies | Program Administrator Survey | External Studies | Survey of SCHIP Enrollees | Survey of SCHIP Disenrollees | State Eligibility/ Enrollment Data | SLAITS |
| State Context and Program Design | |||||||
| What are the key state characteristics influencing the development, implementation, or efficacy of SCHIP; and what are the specific design features of each state’s program? | Main | Main | ü | ||||
| Why did states design SCHIP programs as they did? What factors drove the adoption of various policies and models among states, given the flexibility afforded by Title XXI? | Main | Main | ü | ||||
| What are the perceived linkages (from state officials, program participants, policymakers, and other stakeholders) between individual mediating factors and various programmatic goals and outcomes? | Main | Main | ü | ||||
| Enrollment and Disenrollment | |||||||
| Why do some eligible families enroll in SCHIP, while others do not; and what policies are effective in reducing the share who are eligible- but-uninsured? | ü | ü | Main | ü | ü | Main | |
| Why do some eligible-enrolled families disenroll from SCHIP, while others do not; and what policies are effective in reducing the share of eligible enrollees who disenroll and become uninsured? | ü | ü | Main | Main | ü | ||
| What are the reasons for SCHIP disenrollment, and how likely are families to reenroll? | ü | ü | Main | ü | |||
| Links Between SCHIP, Uninsurance, Medicaid, and Private Coverage | |||||||
| What type of insurance coverage do SCHIP enrollees have prior to entering SCHIP and after leaving SCHIP? | Main | Main | ü | ||||
| To what extent does the SCHIP program draw from those who would otherwise be uninsured or substitute for private or Medicaid coverage? | ü | ü | Main | ü | |||
| Access, Service Use, and Satisfaction | |||||||
| What kind of access to care, service use, and satisfaction with care do SCHIP enrollees experience under SCHIP? | ü | ü | Main | ü | |||
| To what extent does SCHIP lead to improvements in access to care, service use, and satisfaction with care for children who enroll? | ü | ü | Main | ü | |||
| Main = the primary source used for analyzing this question. ü = a supplementary source used for analyzing this question. |
|||||||
low-income uninsured children, and the SCHIP program and enrollment files in each of the 10 study states.
A parallel analysis of the Medicaid program (not shown in Table B.1) will focus on these same three policy areas—namely, Medicaid enrollment and disenrollment, interactions between Medicaid and other types of coverage (and noncoverage), and the access to care, service use, and satisfaction of Medicaid recipients. This analysis will rely almost entirely on the survey Medicaid enrollees and disenrollees in 2 of the 10 study states, described previously.
By the time Congress receives the final report, the findings from these analyses will already have been presented in interim evaluation reports. The final report to Congress will synthesize findings from these reports in a concise, comprehensive review of key findings and conclusions.
