Acknowledgments
The Work Group recognizes the contributions of presenters at the July, 2002 Listening Session including: Virginia Harmon, Deputy Director for Quality Management, Department of Community Health, Michigan; Charles Kieffer, Coordinator, Homeless Programs, State Housing Development Authority, Michigan; Robert Hess, Deputy Managing Director for Special Needs Housing, City of Philadelphia; DiAnn Koehl, Executive Director, Midland Fair Haven, Midland Texas; Heidi Nelson, Executive Director, Chicago Health Outreach; Ralph Forquera, Executive Director, Seattle Indian Health Board; and Philip Mangano, Executive Director, Interagency Council on Homelessness.
Work Group members are grateful to the staff and clients of Unity Health Care Inc., Washington, DC. Mr. Jose Aponte generously arranged two visits for the Subcommittee and the presentations about their work with homeless persons were most informative.
Chapter 1: The Approach
Background
Each year, approximately one percent of the U.S. population, some two to three million individuals, experiences a night of homelessness that puts them in contact with a homeless assistance provider. The estimate is conservative — it does not include those affected by natural disasters, nor those who do not contact a homeless assistance provider, e.g., who may be taken in by a friend or spend the night in a car.
The circumstances that cause homelessness for two to three million Americans are varied. However, research conducted since the late 1980's shows that interactions among the supply of affordable housing, poverty, and disability account for most of the precipitating factors. Among poor persons, the risk of a night of homelessness is far higher than for the general population. Somewhere between four to six percent of the poor experience homelessness annually. Most of these experiences are short-term and the individuals exit homelessness with minimal assistance and generally are not seen again.
But the subgroup that tends to be the most visible is a group of about 200,000 people who experience homelessness on a protracted or repeated basis. On any given night, this group will represent almost half of those who are homeless. This subgroup has been identified as the chronically or long term homeless. There is increasing consensus that we can take actions that will reduce and end this level of chronic homelessness.
Exploring Solutions
Beginning in March, 2001, the Secretary's office initiated several activities to improve the Department of Health and Human Services' (HHS) response to the services needed by persons experiencing homelessness.
- Secretary Tommy Thompson met with Secretary Mel Martinez of the Department of Housing and Urban Development (HUD) and Secretary Thompson committed his Department to a collaboration that capitalized on the expertise of HHS in service delivery and of HUD in housing.
- HHS staff initiated regular, informal discussions with HUD and Department of Veterans Affairs (VA) staff to understand the programs and opportunities that could be involved in a collaboration.
- HHS, HUD and VA staff explored goals and activities of mutual interest and recommended to leadership that collaboration was best achieved by adopting a specific and targeted focus on the issue of long term and repeated homelessness.
- Discussions with the HHS Operating Divisions were held to determine what options they saw to make their programs more accessible to homeless persons.
- Budget formulations and other administrative scenarios within HHS were considered.
- An ambitious partnership with States was initiated that acknowledged the role of State agencies in setting the priorities for using HHS assistance. The Secretary sent all Governors an invitation to participate in the partnership. Beginning in November 2001, a series of Policy Academies for State and Local Policymakers was begun. Thirty-six States applied to participate in the first of these, knowing that only eight could be accommodated.
Throughout these explorations, a leading concern was for HHS-assisted services to be more accessible to eligible homeless persons being placed in HUD-supported housing. Interdepartmental discussions had clearly identified new emphases that were making it increasingly important for applications for HUD's homelessness assistance to demonstrate the use of mainstream HHS treatment services to assist chronically homeless people. By summer's end, it was clear that the complexity of HHS' structure and program variety obviated a simple linear plan, i.e., one that involved an easily introduced change that expanded opportunities for access by homeless individuals.
The final development of significance came in the release of the Administration's budget for fiscal year 2003. President George W. Bush endorsed as goal of his administration ending chronic homelessness in a decade.
The Secretary's Work Group on Ending Chronic Homelessness
At the start of calendar year 2002, Secretary Thompson established the Secretary's Work Group on Ending Chronic Homelessness. He asked Deputy Secretary Claude Allen to lead the Work Group in a comprehensive review of the Department's relevant programs. The Work Group was to report recommendations for a Department-wide approach that would contribute to the Administration's goal of ending chronic homelessness and improve HHS' ability to assist persons experiencing chronic homelessness.
Representation on the Secretary's Work Group On Ending Chronic Homelessness:
|
The action simultaneously addressed two needs:
- First, it brought the relevant HHS agencies into a collaboration to formulate a Department-wide strategy that addressed the multiple needs of this subgroup.
- Second, by focusing on chronic homelessness, it established a compelling link to themes that had been articulated by the White House, HUD and VA on this same issue.
On February 28, 2002, Deputy Secretary Allen convened the first meeting of the Secretary's Work Group on Ending Chronic Homelessness. Representatives were chosen by agency administrators for their knowledge of agency programs and their ability to represent the agency authoritatively (Appendix A). Mr. Allen itemized charges to the Work Group members and offered a plan of approach to undertake four tasks:
- Define the population that experiences chronic homelessness and itemize their service needs.
- Analyze the response of relevant HHS mainstream assistance programs to the itemized service needs.
- Specify outcomes and objectives that would improve the response of these mainstream programs to long term and repeated homelessness.
- Offer actions the agencies could take that would improve access to and coordination of services that would contribute to reducing and ending chronic homelessness.
Charge to the Work Group:
|
An Interagency Subcommittee was formed immediately (Appendix B) and charged with pursuing each of the four tasks. The Subcommittee met formally over a dozen times and held numerous informal meetings to analyze data, formulate recommendations, and edit written work.
To accomplish its work, the Subcommittee:
- Reviewed epidemiological and services research literature that documented what is known about those who experience long term and repeated homelessness and about treatments, services, and supports that are effective with these persons. This material is summarized in Chapter 2.
- Developed, administered and tabulated a service inventory for eight relevant mainstream HHS programs. The inventory sought not only to understand the administrative features of each program, but their specific response to the services needed by persons experiencing chronic homelessness. The findings are summarized in Chapter 3.
- Summarized what was learned from the inventory in the areas of
- a) administrative characteristics of the programs;
- b) regulatory or program design barriers to services identified by program officials;
- c) service coverage offered by relevant programs, including what was known about current access by homeless persons; and
- d) opportunities or concerns that program officials identified for improved access by chronically homeless persons.
- Convened a Listening Session on July 16 to benefit from the experiences of States, municipalities, and providers who had struggled with weaving together a comprehensive set of funding sources to address the complexities of chronic homelessness. Six presenters, including the executive director of the U.S. Interagency Council on Homelessness spoke to Work Group and Subcommittee members about their experiences, with particular attention to the use of HHS assistance to provide treatments and services responsive to chronic homelessness.
- Based on the above processes, the Subcommittee identified objectives under each of its charges that could position HHS to be more responsive to the issue of chronic homelessness. Numerous options were itemized that could contribute to implementing the objectives, with an emphasis on short term steps HHS could take that would support the Administration's goal of ending chronic homelessness. The Work Group selected and refined these options and developed goals and strategies for a comprehensive Department plan. The Work Group recommendations are presented in Chapter 5.
Throughout the process, the Deputy Secretary's office provided critical guidance and support for the completion of the tasks. Work Group members were kept informed via a series of progress reports that summarized progress and next steps and by their representatives on the Interagency Subcommittee.
Chapter 2: Defining Chronic Homelessness and Understanding Treatment and Support Needs
What is Chronic Homelessness?
The first attempts to describe the current generation of homeless persons were based on survey methods. The surveys were conducted during a specific time period, e.g, the month of February, and used a convenience sample, e.g., going to soup kitchens or providers that specifically assist homeless individuals. Survey methods are the source for a commonly cited figure for homelessness in the United States, viz., 600,000 persons are homeless on any given night. Survey approaches continue to be used and are a legitimate, valuable tool for understanding the prevalence of a condition, such as chronic homelessness, and for understanding the characteristics of those experiencing that condition.
As homeless assistance matured, information system technologies were introduced into many homelessness assistance settings. Administrative systems made another method of population description possible — one that described the users of homeless assistance over a long period of time rather than a snapshot in time. Longitudinal analyses of the service users confirmed important distinctions among homeless persons that had first been noted by the Institute of Medicine in 1988. Specifically, the group is not homogeneous and three important subgroups regularly appear:(1)
- temporarily homeless — persons who experience only one spell of homelessness, usually short, and who are not seen again by the homeless assistance system;
- episodically homeless — those who use the system with intermittent frequency, but usually for short periods; and
- chronically homeless — those with a protracted homeless experience, often a year or longer, or whose spells in the homeless assistance system are both frequent and long.
These subgroups emerge from actual utilization patterns in numerous cities and show relatively similar distributions: Approximately 80 percent of users are temporarily homeless, 10 percent are episodic, and 10 percent are chronic.
Applying the 10 percent estimate to the number of persons who are homeless annually results in a figure of approximately 200,000 individuals annually who will be chronically homeless.(2) The Department believes that by linking affordable housing with treatment and support services, substantial and permanent reductions in the occurrence of chronic homelessness are achievable.
What Characteristics Are Associated with Chronic Homelessness?
While chronic homelessness may be identifiable by a pattern of homeless duration, other facts associated with this subgroup add to our understanding.
- Disability: The presence of a disabling condition is almost universal in the population. These conditions involve serious health conditions, substance abuse, and psychiatric illnesses. The prevalence of a disabling condition runs as high as 85 percent having one of more of these chronic problems. In contrast, data from mid-1990's indicate approximately 12 percent of working-age persons have a moderate to severe disability. Disability is a highly relevant factor where services are concerned since certain kinds of disability are an eligibility portal for many HHS assistance programs.
- Heavy Use of Services: Persons experiencing chronic homelessness are heavy users of the homeless assistance system and of other health and social services. Although they constitute 10 percent of the users of homeless shelter assistance, they consume fully 50 percent of the days of shelter provided by that system.
In addition, analyses in New York City indicate that use of expensive emergency room visits, uncompensated care, and involvement with the criminal justice system among the chronically homeless represent significant costs to local, State, and Federal programs. The analysis tracked the service costs attributable to a cohort of chronically homeless persons before and after their placement in permanent supportive housing. The following New York data were provided at the July 18, 2002 meeting of the U.S. Interagency Council on Homelessness and show the changes in annual health care costs for the 2 years after a person was placed in housing compared to the annual costs incurred for the 2 years preceding housing placement. For health care, the data clearly show placement in supportive housing is associated with overall reductions in health care costs.
Psychiatric hospital $8,260 Municipal hospital 1,771 Medicaid-Inpatient 3,787 Medicaid-Outpatient 2,657 Annual savings (per person) $11,161 - Engagement with Treatments: More than a decade of research has shown that persons experiencing chronic homelessness frequently exhibit a pattern of being disconnected from conventional community life. Many have limited support systems, reflected in most being single adults with weak family connections. Many are from ethnic and racial minorities and research also shows they may be reluctant to interact with systems they do not understand or which do not understand them. Many have past experiences with mainstream services that did not effectively address their needs or prevent them from falling into homelessness. These characteristics contribute to the long or repetitive patterns of homelessness they exhibit. They also reflect why re-engaging a chronically homeless person with treatments can be challenging.
- Multiple Problems: Chronically homeless individuals fall within the subset of persons who present a complex set of multi-problem challenges to service providers. Like frail elders with complex medical conditions, HIV patients with psychiatric and substance abuse issues, or a TANF client with domestic violence or counseling needs, the service needs of chronically homeless people outstrip the in-house competencies of most providers.
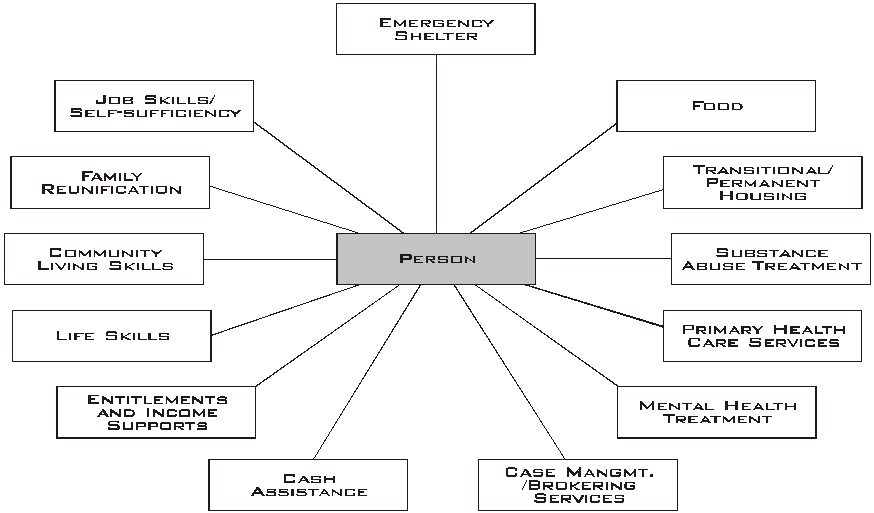
The Needs of a Chronically Homeless Person Cross Many Service System Boundaries.
In addition to the issues noted above, extreme poverty, poor job skills, lack of education, and negative childhood experiences are common features of chronic homelessness. The figure above, first used in the briefing material to the Work Group, describes the array of complex service needs associated with chronic homelessness.
- Fragmented Systems: Both practice and research have shown that the chronically homeless person is most likely to face a service system that is fragmented and providers who are not able to summon the flexible or comprehensive set of treatments and services the person needs. For providers to be effective with such individuals, they must either become uniquely specialized or piece together an informal system of referrals and service collaborations with other providers to ensure access to at least some of the needed services. The homeless shelter system, in dealing with daily demands that routinely exceed capacity, typically is not able to reshape itself along either of these tracks. Without services that address the multi-problem nature of long term and repeated homelessness, multi-problem clients rarely progress out of the system.
What Treatments and Services Are Effective?
Responding to the needs of people who experience chronic homelessness poses significant challenges. Their needs include a broad range of services, from food, clothing and emergency shelter to treatment and income support, and cross many service systems.
However none of these services are as effective without safe, affordable housing. Years of federal demonstration programs and the experience of community and faith-based providers have shown what is effective in preventing and ending homelessness among people who have serious health and behavioral health disorders. Implementing evidence-based and promising practices is essential for a comprehensive, integrated service system that effectively reduces chronic homelessness.
The following services and treatment needs are organized into core and supportive services. The core services include those that are needed to move people from the streets into housing and to stabilize their conditions. The supportive services include those that are needed to reintegrate people into the community, such as with jobs, education and socialization. The full definitions for each of the services are presented in Appendix C. Appendix D lists representative published citations of the effectiveness for each service.
Core Services
- Information and Referral
- Outreach and Engagement
- Health Related and Home Health Services, Including HIV/AIDS
- Alcohol and Drug Abuse Services
- Mental Health and Counseling Services
- Inpatient Services
- Supportive Case Management Services
- Intensive Case Management Services
- Income Management and Support
- Residential Treatment Services
- Discharge Planning
Supportive Services:
- Life Skills Services
- Child Care Services
- Education and Training Services
- Employment Services
- Legal Services
- Transportation Services
To be effective, these services must be accessible and provided in a coordinated and flexible manner. This includes the option of being offered in non-office based settings (e.g., on the street or in shelters) and during non-standard operating hours, being able to increase or decrease service levels to accommodate changing needs over time, and keeping case files open even during periods of inactivity so that eligibility does not have to be re-established when an individual is ready to engage or re-engage.
Providers need the flexibility to operate with a "no wrong door, no reject" policy, meaning that services are made available to individuals no matter where they enter the system and whether or not they are willing to accept specific interventions that may be indicated. In addition, strategies such as co-location of services not typically offered under the same roof can help reduce fragmentation and increase access to services.
| HHS, HUD, and VA have agreed on the characteristics of persons experiencing chronic homelessness and use the following definition in their collaborations:
An unaccompanied homeless individual with a disabling condition who has either been continuously homeless for a year or has had at least four (4) episodes of homelessness in the past three (3) years. |
Why the Definition of Chronic Homelessness and the List of Treatments Are Relevant to HHS Assistance Programs
There are at least three reasons why understanding who experiences chronic homelessness and what treatments and services are effective is relevant to the HHS programs designed to assist poor and disabled persons.
First, these mainstream programs are extremely likely to have had substantial contact with these individuals prior to their becoming chronically homeless. Research studies show that persons experiencing chronic homelessness have long and extensive histories of involvement with the publicly-funded treatment system before their period of long term homelessness. These service experiences seemingly did little to prevent their slide into a pattern of long term homelessness.
No mainstream program wants to waste an investment it has made in helping clients make gains. Falling out of treatment and into a pattern of long term homelessness represents a set back to gains the client experienced from treatment and services. In addition to concerns about the efficient use of resources, this experience may mean the person is wary of re-engaging with the types of providers that were not attentive to his or her risk of becoming homeless.
Second, their homeless status does not mean that chronically homeless persons are no longer using mainstream service resources. As noted above, they are heavy users of services, often expensive inpatient and emergency room services, unguided by a comprehensive treatment plan. Mainstream programs continue to absorb at least some of the costs for these expensive and ad hoc treatments.
Third, the levels of disability and poverty that characterize persons experiencing chronic homelessness make them likely to be eligible for a number of the HHS mainstream programs. The fact that they are unsheltered should not restrict them from benefitting from this assistance, but their homelessness often presents so many challenges that access to these benefits is not ideal. If HHS can craft approaches that improve their access to mainstream HHS service programs, contributing to a reduction in chronic homelessness, these same approaches should work for other eligible homeless individuals. These approaches might, thereby, provide solutions for addressing homelessness among families or youth.
HHS recognizes that the characteristics of chronic homelessness are primarily conceptual. They help to distinguish a population that presents service providers with unique demands and unique opportunities. The characteristics are an assortment of various problems and eligibility criteria that are relevant to many of the assistance programs supported by the Department. The characteristics reinforce the multiple treatment needs suggested in the earlier figure, but they do not have the rigor or uniqueness to suggest a singular eligibility group.
Instead, chronic homelessness — as a group of individuals with multiple service needs — overlaps with the types of beneficiaries and services of many of the HHS mainstream programs. This overlap suggests the appropriateness of response by the mainstream.
The access chronically homeless persons have to the mainstream programs and the ability of these programs to deliver the needed treatments and services consumed significant attention prior to the development of recommendations. The results of this examination are presented in the following chapter.
1. Institute of Medicine. Homelessness, Health, and Human Needs: Committee on Health Care for Homeless People. National Academy Press, Washington, DC, 1988
2. Metraux, Stephen, Dennis P. Culhane, Stacy Raphael, Matthew White, Carol Pearson, Eric Hirsch, Patricia Ferrell, Steve Rice, Barbara Ritter, & J. Stephen Cleghorn. "Assessing Homeless Population Size through the Use of Emergency and Transitional Shelter Services in 1998: Results from the Analysis of Administrative Data in Nine US Jurisdictions." Public Health Reports 2001; 116: 344-352.
Chapter 3: How HHS Mainstream Service Programs Align With the Treatments and Services That Address Chronic Homelessness
Mainstream HHS Service Delivery Programs
In 1999, the General Accounting Office (GAO) examined the extent to which Federal programs designed to assist low income and disabled persons responded to homelessness.(1) The report identified up to 50 programs in eight Departments and Agencies that provided relevant assistance. Almost one-third of these programs were specifically targeted to homeless persons (16 of the 50)(2), while the balance constitute some of the largest and best known of the Federal assistance programs such as Food Stamps, Medicaid, Public Housing, and Supplemental Security Income. Collectively, these programs serve millions of individuals. The report referred to these as non-targeted programs, but the phrase 'mainstream programs' has been widely used to embrace them.
GAO identified 12 relevant mainstream programs in HHS. The Work Group took these 12 programs as a starting point to explore improved access, coordination, and prevention activities related to chronic homelessness. Three were eliminated as being less applicable to chronic homelessness. Specifically, Head Start, the State Children's Health Insurance Program, and the Maternal and Child Health Services Block Grant were dropped from further consideration because they were not likely to address single, disabled, poor adults who primarily make up the chronically homeless population. Two others were collapsed into one program, based on advice from the Health Resources and Services Administration which administers them. Specifically, Migrant Health Centers were not treated as a separate program as GAO had done, but were subsumed within the Consolidated Community Health Centers cluster. This left 8 mainstream programs as the focus of the Work Group.(3)
Mainstream HHS Programs Selected for Their Relevance to Chronic Homelessness:
|
Are HHS Mainstream Programs Responsive to Chronic Homelessness?
Each of the eight programs was asked to provide responses for the following information:
- Coverage of each core and supportive service.
- Access to the service by homeless and chronically homeless persons.
- Concerns or opportunities program officials noted that might influence the applicability of the program to chronic homelessness.
- Administrative features of each program that might affect the ability of the program to respond to chronic homelessness.
All of these circumstances were integrated into an inventory that was completed by each of 8 mainstream programs. The compilation and review of these service inventory responses was carefully reviewed and contributed substantially to the Work Group's recommendations. In addition, experiences shared by States, municipalities, and providers in the Listening Session and lessons from a site visit to a homeless health care clinic by members of the Interagency Subcommittee members were considered.
Findings
1) Availability of Core and Supportive Services
Each program was asked to indicate for each core and supportive service whether that service was required or optional (e.g., could be selected from a menu of options; offered at State's discretion). Several findings are noteworthy.
As these programs have been authorized, there is substantial flexibility in the services that can be supported. Four of the 8 programs give the State discretion in selecting what services will be supported. The others feature both required and optional services that the State, city or community-based recipient may offer. Therefore, in administering these 8 programs, there is considerable opportunity for the State or grant recipient to tailor service responses to the unique circumstances of the service beneficiaries. These opportunities extend to including the services the identified in the previous chapter as effective in helping people break a cycle of chronic homelessness. (See insert and Table 1.)
In all of the programs, there are also restrictions on offering certain services. The most common exclusion was on support for inpatient care. Only Medicaid is authorized to provide inpatient services.
The only core service to be offered in all 8 programs was information and referral, but outreach, supportive case management and substance abuse services are available from at least 7 of the 8 programs.
| Information and Referral | 8 |
| Outreach and Engagement | 7 |
| Alcohol and Drug Abuse Services | 7 |
| Supportive Case Management Services | 7 |
| Health Related and Home Health Services, Including HIV/AIDS | 6 |
| Intensive Case Management Services | 6 |
| Discharge Planning | 6 |
| Mental Health and Counseling Services | 5 |
| Residential Treatment Services | 5 |
| Income Management and Support | 4 |
| Inpatient Services | 1 |
Three of the 8 programs can support 10 of the 11 core services (inpatient coverage is excluded in each): TANF, Ryan White titles, and the Community Mental Health Services Block Grant. However, these programs also serve the most highly specified target groups — by family status or diagnosis. They may be accessible only by certain persons who are chronically homeless.
None of the 8 programs offers all of the core and supportive services. This fact contributes to the frequently cited complaint of community and faith-based providers that they must juggle multiple funding sources to sustain a program that provides comprehensive services to their clients. For example, in one northeastern state, an average homeless shelter uses 17 sources of Federal support and 5 State sources to compile the array of services needed by its clients.(4)
This factor also has implications for homeless people. They are most likely to encounter providers who are not able to offer the comprehensive set of services. Negotiating such fragmentation is especially challenging for a person dealing with impairments.
For supportive services, coverage appears to be somewhat better. Five of the 8 programs cover all of the supportive services. Transportation, primarily as it relates to accessing treatments and services, is covered by all 8 programs. However, as Table 1 shows, variability in coverage remains a pattern and it reinforces the fragmentation issue noted above.
| Transportation | 8 |
| Education and Training | 6 |
| Life Skills | 6 |
| Child Care | 6 |
| Employment Services | 6 |
| Legal Assistance | 5 |
2) Use of Available Services by Chronically Homeless Persons
Two inventory questions are relevant here.
- In describing the administrative features of each program, program officials indicated whether homelessness was mentioned as a circumstance that received consideration in the program. One program — the Community Services Block Grant — reported this to be the case.
- In addition, officials were asked if factors that characterize chronic homelessness — a disabling condition or the pattern of homelessness — would affect a person's eligibility for the program. Two of the programs — Medicaid and the Mental Health Block Grant — indicated that a disabling condition would be critical for program eligibility. No programs indicated that a pattern of long term or repeated homelessness presented a barrier to accessing a service, nor would it suggest that a priority consideration for access to one of the mainstream programs be given.
Thus, while the majority of the programs do not identify homelessness as a circumstance for consideration, the characteristics of chronic homelessness appear to create few barriers for access to these services.
For each core and supportive service, the inventory also asked whether persons experiencing chronic homelessness used the service and if data were available on the extent of use. Since homelessness was generally not identified as a circumstance for consideration for receipt of services by these programs, it is not surprising that their administrative systems would not flag homelessness or former homelessness as a characteristics on which data could be tabulated.
Consistent with the observations in the 1999 GAO report — which found that mainstream, non-targeted programs could not document access by homeless persons — 70 percent of the inventory responses about service use by homeless persons are unknowns. The programs report that they have no data to inform them about access. Thirty percent of the responses are positive, indicating homeless persons do use the service. But officials were not able to provide hard data on utilization.(5)
Clearly, it is a challenge for HHS to provide a baseline to demonstrate current access to mainstream services by persons experiencing long-term homelessness. The challenge will have to be addressed in any Department attempt to document that efforts to reduce the prevalence of chronic homelessness or end it are successful.
3) Concerns and Opportunities
To benefit from the insights of program officials about the relevance of their program to addressing chronic homelessness, the program officials were invited to offer observations about concerns or opportunities in five areas:
- Regulation or administrative issues (e.g., flexibility and limitations in designing service content, role of States in designing program, eligibility specifications, opportunities to apply for waivers or expansions, legal/civil rights concerns)
- Patterns of funding (e.g., how traditions influence fund distribution toward new issues, services, client groups, or groups of providers)
- Capacity issues (e.g., resource trends in the Program, treatment gaps, models of effective interventions, competencies of provider staff)
- Fragmentation of services (e.g., degree of specialization by service or funding, program culture on client referral and linkage, prevalence of one-stop service approaches, integration of providers into HUD's continuum of care planning processes)
- Priorities, incentives and motivations (e.g., priority placed on addressing homelessness in the Program, emphasis on cost containment, emphasis placed on the underserved, nature of the performance that is incentivized)
Several of these areas yielded information from program officials that was even more clearly expressed in the July 2002 Listening Session with States, municipalities and providers.
- Funding Silos: Each of the 8 mainstream programs was created to respond to a unique need or population and its implementation is most often driven by its authorization. The consequence of this evolution is an assortment of assistance programs covering health and social services, and administered by a variety of State and local entities. The administering entities are not required to assemble these programs into a coherent pattern that might result in an improved response to the overlapping, multiple needs of the targeted populations. In addition, the administering entities may find that the authorizations for these programs make such a coordinated approach difficult.
The problem is often captured by the phrase "funding silos." The implications are not unique for homelessness. For example, in discussions of TANF reauthorization in June, 2002, both the Administration and the House of Representatives included provisions that addressed the impact of such silos on serving needy families. Specifically, it was proposed that States receive flexible authority to build integrated service delivery systems for TANF families involving as many as nine separate assistance programs.
Fragmented funding led to the following issues for chronic homelessness:
- Coordination Issues: Funding silos mean that Federal assistance moves to different agencies within State government, sometimes going directly to the community level. There is no requirement for coordination across these programs. One multi-State report summarized this as:
"...the federal government thinks about policy in terms of specific programs and categorical funding streams... States, on the other hand, increasingly think about how a coherent and seamless service delivery system might better assist disadvantaged [persons]."(6)
While States and community organizations are required to submit applications and plans when seeking HHS assistance, it has been several decades since HHS required any degree of joint planning or coordination across the assistance programs it supports. Thus, a State's TANF plan may discuss the State's plan to address substance abuse among eligible families. But there is no requirement that the State plan show a relationship to the assistance offered by the State under its Substance Abuse Prevention and Treatment Block Grant, nor demonstrate consultation and collaboration with the State's substance abuse administration.
The proposal noted above to give States authority for flexibility under TANF reauthorization was intended to address this difficulty by mandating close coordination among the programs it would cover. Another relevant parallel is the success HUD has had requiring that its applicants demonstrate a rational plan for the range of assistance HUD offers: A consolidated plan for all HUD assistance is required. In addition, HUD requires communities to develop a coherent, prioritized approach for the homeless assistance that HUD offers. This 'continuum of care' plan is a well-known homelessness planning strategy in over 400 communities in the U.S.
- Eligibility Gaps: For chronically homeless clients, particular those with multiple diagnoses, funding silos mean they may be eligible for some of the services they need from one program, but not be able to secure the remainder of their services because they are not eligible under the rules of those other programs.
The most telling example of this involves homeless persons with substance use disorders and co-occurring psychiatric and primary health care problems. They may have access to limited substance abuse treatments supported by the Substance Abuse Prevention and Treatment Block Grant. But, they may find that they do not meet eligibility criteria for receipt of Medicaid coverage, nor qualify as having a serious and persistent mental illness for access to services supported by the Community Mental Health Services Block Grant.
Such problems in accessing services reimbursed by other funding sources are not uncommon. The Listening Session further underscored the obstacles States, municipalities and providers face in using multiple funding sources to address the multi-problem nature of chronic homelessness.
- Flexibility: Many service providers have learned to live with funding silos and pursue funding from multiple assistance programs to be able to offer comprehensive services to their clients. But they report that they are challenged in trying to work flexibly across these silos.
- Privacy provisions may mean that information in client records is not accessible across programs serving the same clients.
- Audit teams have different rules and visit at different times so that providers are continually making adjustments to comply with each new visit.
- Cost allocation rules governing Federal funds require that States and providers which are using multiple funding sources to serve a client group must establish a reasonable methodology for how much of each funding source will be used. One basis for reasonable allocation is the size of the benefitting population. Cost allocation rules may mean that the relatively low representation of chronic homelessness (or the absence of a priority to identify such consumers) in a large mainstream caseload restricts the resources that providers may be able to devote to this group.
- Adjusting or securing service funding to match a client's need for treatment and support as the client moves out of homelessness may be so difficult that gaps in services occur and jeopardize progress. One example of this involves clients losing a case manager at each stage of progress that requires them to shift to a different provider or service reimbursement source. At the Listening Session, one representative noted clients who had worked with more than a dozen case managers as they exited homelessness.
- Lastly, attempts at collaboration with other providers, including those who offer housing, are often considered overhead — a cost of doing business. In cash-strapped human services programs, this can become a disincentive to engage in planning for seamless service delivery systems.
Capacity Issues: The capacity of the programs to respond to chronic homelessness was expressed in several forms.
- Funding: Program officials uniformly expressed that resources were finite and their application to particular population groups was usually a priority left to the State or provider. There is considerable variety in the scale of funding and how extensively each program is relied on as a source of service dollars. Some, such as Medicaid, come with a requirement for matching funds that requires substantial investment of a State's own funds. Any expansion of programs has implications for the program partners that have to be considered carefully.
Funding trends also varied in the 8 programs. In a few, such as the Social Services Block Grant, the trend line has been down. In others, such as the Community Health Centers, Administration and Congressional interest has led to current and promised future expansion.
Under any of these funding conditions, HHS does not mandate what the State or grantee must do. The Department's approach has been to encourage States and community-based grantees to capitalize on existing flexibility, issue letters of guidance, offer technical assistance, and promulgate evidence-based practices. The recommendations to the Department are consistent with this approach.
- Staffing: An important aspect of quality of services is the availability and qualifications of staff to deliver health and social services. Program officials reported staffing shortages that led to waiting lists and high case loads under existing service demands. They voiced that working with chronically homeless groups would present substantial challenges to mainstream systems because of the multi-problem nature of this group, current workloads, and staff readiness to work with such a clientele.
Many mainstream staff are not prepared to provide the outreach and engagement services to chronically homeless persons who have not yet re-engaged with treatment services. In addition to the fact that these services often occur out-of-office, reimbursement practices associated with managed care may limit the extensiveness or intensiveness of these services.
When staff do work with such clients, they may not be prepared to modify some of their clinical practices for a clientele whose lack of a stable residence makes a treatment regimen impossible — the classic example is prescribing a refrigerated medication. As clients change from homeless to housed, mainstream staff may not be sufficient or prepared to provide needed services in non-office based settings, such as the client's home, or deliver services that are critical to the person's successful placement, e.g., helping a client gain skills at budgeting or working a microwave.
- Knowledge and Technology: HHS has invested uniquely in research that demonstrates effective, evidence-based treatments and supports for persons experiencing chronic homelessness. Outside of the homeless-specific service delivery system, these findings and service models are not widely known, practiced, or reimbursed. Consequently, homeless-specific providers frequently report that the mainstream programs in their cities often direct homeless persons to their systems because of concerns about service reimbursement or not knowing what to do with such clients. For mainstream providers to be more receptive to this group of clients, much needs to be done to convey what is known about effective treatment and to encourage action.
Another concern relates to the technology of administrative information systems. Such systems provide documentation of treatment for billing, linking a client's records over time, and program accountability. As noted previously, mainstream program officials were not able to provide data to demonstrate their programs served chronically homeless persons. Providers could benefit from guidance in identifying how a treatment plan for a person with long term or repeated homelessness is formulated, implemented, documented, and assessed. A consequence of such capacity would be in supporting the establishment and documentation of performance measures on homelessness.
Finally, an important area is privacy and civil rights issues. Expediting coordination of services across multiple providers has to be balanced with protections of civil rights (e.g., commitment statutes), privacy, and significant challenges to how information can be better linked. The goal of ensuring access to needed services should be enhanced while giving careful consideration to protecting each client's rights.
Implications of the Findings
The findings presented above represent a consolidation of statements, tabulations, or observations accumulated during several months of information seeking. Few of the findings are unique to any one service program; they tended to cover concerns and opportunities involving multiple programs and agencies. The next chapter briefly describes the processes used to distill the accumulated information and to develop recommendations for a comprehensive approach for the Department.
| Services Provided —
HHS Mainstream Assistance Programs |
CORE SERVICES | SUPPORTIVE SERVICES | ||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Out- reach |
Primary Health Care | Alcohol & Drug Abuse Services | Mental Health & Counsel- ing Services |
In- patient Services |
Suppor- tive Case Mgt |
Intensive/ ACT Case Mgt |
I & R | Income Mgmt & Support | Resi- dential Treat- ment |
Dis- charge Planning |
No. of Core Services Offered | Life Skills | Child Care | Educa- tion & Train- ing |
Employ- ment Services |
Legal | Trans- portation |
No. of Suppor- tive Services Offered |
||
| Community Mental Health Services Block Grant (CMHSBG) | X | X | X | X | X | X | X | X | X | X | 10 | X | X | X | X | X | X | 6 | ||
| Community Services Block Grant (CSBG) | X | X | X | X | 4 | X | X | X | X | X | 5 | |||||||||
| Consolidated Community Health Centers (CHCs) | (b) | X(c) | (d) | (d) | (b) | (b) | X | X(e) | X(f) | 4 | X(g) | X(h) | 2 | |||||||
| Medicaid k | X(l) | X(m) | X(n) | X(o) | X | X(p) | X(q) | X(r) | (s) | X | 9 | X(t) | X(u) | X(v) | 3 | |||||
| Ryan White Act | X | X | X | X | X | X | X | X | X | X | 10 | X | X | X | X | X | X | 6 | ||
| Social Service Block Grant (SSBG) | X | X | X | X | X | X | X | X | 8 | X | X | X | X | X | X | 6 | ||||
| Substance Abuse Prevention & Treatment Block Grant | X | X | X | X | X | X | X | 7 | X | X | X | 3 | ||||||||
| Temporary Assistance for Needy Families (TANF) | X(w) | X(x) | X(x) | X(w) | X(w) | X(w) | X | X(w) | X(w) | 10 | X(w) | X(w) | X(w) | X(w) | X(w) | X(w) | 6 | |||
| No. of Programs Offering Service | 7 | 6 | 7 | 5 | 1 | 7 | 6 | 8 | 4 | 5 | 6 | 6 | 6 | 6 | 6 | 5 | 8 | |||
| Notes: (a) Services provided refers to those that are required, eligible or covered in each program. (b) A supplemental service available to some but not all centers. (c) In-home services not a requirement of the program. (d) Mental health service include services of a psychiatrist, psychologist, & other appropriate mental health professionals. These services are supplemental; most centers do not have extensive mental health services. (e Through referrals to other providers. (f) Patients are followed in the hospital either directly with privileges or through appropriate referral mechanisms. (g) Limited to health education (h) Transportation, as needed for adequate patient care. Residents of catchment area served by the Center with special difficulties of access to services provided by the Center may receive such services. (I) Outreach & engagement are required in Head Start, but are not specific to homeless persons. (j) Not used. (k) All provided Medicaid services are State administered and limited in amount, duration, and scope. (l) As administrative expense (50 percent match). (m) Physician, outpatient hospital, home health for persons eligible for nursing facility services, rural health clinic services, lab & x-ray, FQHC services. Eligible/covered include clinic, optometrist/eyeglasses, prescribed drugs, prosthetic devices, dental. (n) Eligibility requires meeting categorical requirements other than substance abuse. (o) If physician service or in-patient hospital. Eligible/covered: prescription drugs & additional services under a waiver program. (p) State option (q) Service may be created using State plan option(s). (r) May be part of case management services or service provided by managed care organizations. (s) If inpatient hospital, nursing facility, intermediate care facility for mental retardation, or psychiatric residential treatment facility for persons under 21 years of age. (t) Particularly under a waiver program. (u) Specialized therapies only (e.g., occupational, speech, & physical). (v) May be covered to receive medical care as program or administrative costs by a state. (w) State option, but families are the clients, not individuals. (x) Service must be non-medical in nature. |
||||||||||||||||||||
1. General Accounting Office. "Homelessness: Coordination and Evaluation of Programs Are Essential." GAO/RCED-99-49. Wash, DC: 1999.
2. HHS is responsible for five programs specifically targeted to homeless persons. Three of these were acknowledged in the GAO report:
- Health Care for the Homeless, providing primary care services to homeless persons;
- Runaway and Homeless Youth programs, providing street outreach, transitional living, and basic service centers for this population; and
- Projects for Assistance in Transition from Homelessness, assisting States to provide a variety of services to homeless persons with serious psychiatric problems.
HHS is also responsible for a Federal Surplus Real Property program that transfers surplus Federal land and buildings to organizations that use it to provide homeless assistance. Since the latter program was not a direct service program, it was not included in the 1999 GAO study. Finally, in 2001, HHS added its newest targeted program: Cooperative Agreements for the Development of Comprehensive Drug and Alcohol Treatment for Systems for Homeless Persons, stressing service delivery to those with substance use problems. All of these programs emphasize service responses to homelessness and cumulatively report assisting more than 600,000 homeless persons annually. In this report, the emphasis was on the contribution the non-targeted HHS programs can make to reducing and ending chronic homelessness. The Department acknowledges the vital contributions the targeted programs are already making in addressing chronic homelessness and the de facto role they will play in a comprehensive approach.
3. This is not meant to convey that other HHS assistance programs are not relevant or applicable to chronic homelessness. The selection of these eight was consistent with expectations established by the earlier GAO study and provided a diverse sample of HHS programs for consideration.
4. Personal communication to W. Leginski from L. Hatton, May 2002.
5. The authorization for some of these mainstream programs may restrict whether the Department can obtain specific data on homelessness. Only the Community Health Centers reported data for the service of primary health care, indicating that the service was provided to 80,000 homeless persons.
6. "Eliminating the Silos" January 2002. The Midwest Welfare Peer Assistance Network: Madison, WI. p. 2.
Chapter 4: How The Plan Was Developed
Addressing the Charge
The overall charge to the Work Group was to develop and recommend a comprehensive approach for how the Department could contribute to the Administration's goal of ending chronic homelessness in a decade. The approach had to be responsive to three(1) components of the original charge. Each of these components has been restated as a separate charge addressed by the plan.
- To improve access for persons experiencing chronic homelessness — 'determine what actions can be taken to expand access to treatments and supports for chronically homeless persons.'
- To improve service coordination — 'identify partnerships at the federal, national, state, and local levels to improve coordinated service delivery.'
- To prevent additional chronic homelessness — 'identify and address the risks of homelessness faced by current service participants' and 'provide treatments and supports that contribute to housing stability.'
The Administration's goal to end to chronic homelessness in a decade has been incorporated into the charge by offering both short term recommendations, reflecting actions for the next two years, as and recommendations that would allow the Department to evolve and adapt throughout the decade.
The Structure of the Plan
A comprehensive plan for HHS on chronic homelessness should demonstrate parallels to the HHS strategic plan to permit its possible consolidation into the HHS strategic plan. Therefore, the Work Group has used the components of the HHS strategic plan — mission, goals, objectives, and strategies — to structure its recommendations.
The mission and goals are readily derived from the overall charge and the three component charges noted above. Within each of the three goals, the Work Group formulated objectives — statements that are unique to each goal and articulate what the Department might try to accomplish. They have been stated with a long-term focus, but could be modified based on experience or policy.
For each set of goals and objectives, strategies that implement the goal and its objectives have also been listed. These strategies have a shorter time frame: It is generally the Work Group's expectation that they would be focused on during the next two years.
While the time frame for these strategies may be short term, the actions they reflect are founded on the relatively well-defined repertoire of responses that the Department and its programs must work within. The Department's repertoire is summarized in the themes noted in the insert. One of more or these themes characterizes each of the strategies for action stated in the next chapter.
Recurring Themes for Opportunities Where HHS May Take Action:
|
Action steps typically constitute the next component of a plan. However, since each of these strategies will need to be considered by the divisions of the Department that are responsible for the relevant program, action steps are not offered in this report. The final level of the plan presents examples. For each strategy, brief examples of how the strategy might be implemented have been developed. The examples apply either to specific operating divisions within HHS or may have broader Departmental application. The examples are illustrative; their viability under Department authority or regulation has not yet been vetted.
As the strategies are explored by the divisions that make up HHS, the examples may fall away or undergo substantial modification. Actions by Department and its components will be based on careful consideration of each of the following:
- Authority
- Resources, staffing, and program applicability
- Time frame for accomplishment
- Cost to the State or grantee
- Internal consistency
- The best sequence for implementation
Feasibility of Recommendations
The Work Group was further assisted in developing its goals and strategies by program officials from the eight mainstream programs identified in Chapter 2. The officials were invited to review an extensive listing of potential recommendations and, using a standard response protocol, to identify:
- The program's current implementation of any activity related to the recommendation;
- What HHS agencies should be involved if the recommendation were to move to the implementation stage;
- If there were cost implications to the program, States, or grantees; and
- If new legislation or regulation would be required.
The responses of the program officials were considered before shaping final suggestions. The desire was to ensure a mix of challenges, rather than a set of recommendations that might be too complex to be attempted or a set that was so elementary that it reflected actions that had already been taken in the programs.
The result of all of the processes described above is presented in the next chapter.
1. A charge to the work group also called for establishing monitoring and evaluation benchmarks. The absence of data to inform the Department about a baseline suggested considerable developmental work would be needed before empirical benchmarks could be established. The plan includes a recommendation for this work.
Chapter 5: A Formal Statement of the HHS Comprehensive Plan to End Chronic Homelessness
Formal Statement (1)
Mission: To end chronic homelessness in a decade.
Goals:
- Goal 1.
Improve access to treatments and supports- Objective:
Expand the capacity of HHS programs to assist persons experiencing chronic homelessness. - Strategies that Help Homeless People
- Develop approaches in relevant programs to strengthen outreach and engagement activities that will facilitate enrollment in treatment and service programs of individuals who are chronically homeless.
Examples:
- Encourage mainstream programs that support outreach and case management to identify chronically homeless persons as potentially eligible candidates for these services. Where appropriate, pursue new funding to expand services such as increased outreach, increased case management/enrollment assistance, or ombudsman programs for homeless persons that will advocate for service access.
- Investigate approaches that expedite eligibility processes (such as reducing or simplifying documentation requirements, and/or use out- stationing where applicable) or advances in technology and communications that expedite the exchange and processing of information, including rural areas or where providers are distant from clinic sites and Disability Determination Offices.
- Implement approaches in relevant programs that facilitate prompt eligibility review for persons identified as chronically homeless or at risk of becoming chronically homeless.
Examples:
- Relevant Operating Divisions could establish an interagency agreement with the Social Security Administration (SSA) to provide cross training for people working with homeless individuals on appropriate medical documentation needed to determine disability.
- SSA should be encouraged to designate appropriate contacts in Disability Determination Service offices who would work with individuals serving as homeless ombudsmen in HHS programs to identify barriers to eligibility and work collaboratively to rectify them.
- Promote the inclusion of homeless shelters among the entities conducting eligibility and enrollment functions for mainstream programs.
- Explore ways to maintain periods of program eligibility and/or avoid loss of coverage for individuals who are chronically homeless.
Example:
- Encourage States to "suspend" and not "terminate" Medicaid eligibility for individuals who are institutionalized so that the individuals do not have to initiate the application process over again upon their release.
- Develop approaches in relevant programs to strengthen outreach and engagement activities that will facilitate enrollment in treatment and service programs of individuals who are chronically homeless.
- Strategies to Give Service Providers Tools, Training or Technical Assistance
- Develop toolkits and blueprints that describe exemplary outreach, enrollment, and service delivery approaches for persons experiencing chronic homelessness, disseminate them and support their use in in-service training.
Examples:
- Develop interagency agreements between relevant Operating Divisions (e.g., the Centers for Medicare & Medicaid Services, the Health Resources and Services Administration, Substance Abuse and Mental Health Services Administration, etc) and the U.S. Department of Housing and Urban Development (HUD) to develop tools that explain the basic eligibility requirements for mainstream programs and health and social service resources available to homeless persons. These tools should be designed for use by both individuals who are homeless and providers/persons who assist them.
- SAMHSA is developing a blueprint on ending chronic homelessness.
- Provide training and technical assistance for mainstream service providers on steps that can be taken to end chronic homelessness.
Examples:
- Repeat the "We Can Do This" training conference (SAMHSA's 2001 training on ending chronic homelessness among persons with behavioral health problems) on a biennial basis and emphasize the participation of mainstream service providers as sponsors and presenters to encourage the inclusion of chronically homeless persons in their activities.
- Identify annual meetings of homeless-specific grantees (e.g., annual Health Care for the Homeless Conference) and of associations representing mainstream programs (e.g., meetings of the American Public Human Services Association) and capitalize on opportunities to present approaches to improving access for persons experiencing chronic homelessness.
- Promote the availability of technical assistance documents on services and policy issues related to chronic homelessness via internet access, distribution at relevant meetings, and to academic settings offering instruction on the issue of homelessness.
- Support the homeless-specific service providers assisted by HHS in developing and establishing administrative arrangements with mainstream providers to ensure that their homeless clients can effectively use the mainstream programs for which they are eligible.
Example:
- Develop program guidance showcasing exemplary practices, based on actual experiences, that demonstrates how effective collaboration can be achieved between the homeless-specific service system, including faith and community-based providers, and the mainstream system. These exemplary practices may include co-location arrangements, financial agreements between two systems, restructuring, and/or skill-specialization agreements that recognize the differences in the systems to work with clients at various stages of readiness to benefit from mainstream services.
- Establish a formal program of training for providers of services to persons experiencing chronic homelessness.
Example:
- Fund an expansion of the existing training centers in HRSA's Bureau of Health Professions to provide intensive training on providing effective services, outreach and care to persons who are chronically homeless. Training could extend beyond mainstream providers to include opportunities for formerly homeless persons to become providers. A training certificate for specific skill sets acquired in training (e.g., outreach worker) or for completing the overall curriculum could be awarded as an indication of the quality of the training process.
- Provide technical assistance to States through State Policy Academies to develop and implement State-specific action plans to identify and address chronic homelessness.
Example:
- Expand the Policy Academy on Chronic Homelessness from an event that reaches a limited number of States to an opportunity for all States willing to implement an action plan to end chronic homelessness in their State. Provide participating States with up to one year of intensive technical assistance to achieve a break-through in policy direction.
- Develop toolkits and blueprints that describe exemplary outreach, enrollment, and service delivery approaches for persons experiencing chronic homelessness, disseminate them and support their use in in-service training.
- Strategies that Involve New or Realigned Funding
- As mainstream programs formulate future budgets or experience budget growth, set priorities for a sharpened focus on addressing chronic homelessness.
Examples:
- a) In developing budget submissions for future years, relevant mainstream programs should reflect the Department's goal of reducing chronic homelessness by including activities that will support the goal.
- b) Direct a percentage of the growth in the community health care center funding to services to chronic homelessness.
- c) Relevant block grant programs should actively examine how their programs can contribute to the Department's and Administration's goal of ending chronic homelessness, including the feasibility of legislative proposals that identify the inclusion of homelessness or establishing priorities for the use of any increased funding for the program.
- As mainstream programs formulate future budgets or experience budget growth, set priorities for a sharpened focus on addressing chronic homelessness.
- Strategies for Accountability
- Establish a work group under the HHS Data Council that will investigate the feasibility of developing quality measures and/or performance measure(s) that can be reported by States and grantees to reflect the access of chronically homeless persons to mainstream assistance programs. Where appropriate and feasible, the measures should be uniform across these assistance programs. The work group should identify implementation issues, the frequency of reporting, and how requested reporting might vary across the different types of assistance programs to provide the Department with a baseline and ability to monitor changes over time.
Examples:
- SAMHSA has developed the following "core client outcome measure" for its discretionary programs, which may be applicable to other mainstream programs:
- Number of clients who are homeless (i.e. no fixed address, includes shelters) at admission to a treatment setting and at six months post-admission.
- In annual reports or grant/project reports, require State and local grantees to provide timely information, e.g. no less then every two years, describing how program activities have assisted homeless persons.
- HUD allows applicants for homeless grants to request funding to develop homeless management information systems (HMIS) that can provide HUD with annual performance data. These HMIS approaches could be examined as a possible source of information on the use of HHS assistance to address chronic homelessness.
- SAMHSA has developed the following "core client outcome measure" for its discretionary programs, which may be applicable to other mainstream programs:
- Establish a work group under the HHS Data Council that will investigate the feasibility of developing quality measures and/or performance measure(s) that can be reported by States and grantees to reflect the access of chronically homeless persons to mainstream assistance programs. Where appropriate and feasible, the measures should be uniform across these assistance programs. The work group should identify implementation issues, the frequency of reporting, and how requested reporting might vary across the different types of assistance programs to provide the Department with a baseline and ability to monitor changes over time.
- Objective:
- Goal 2.
Improve coordination at Federal, State, and local levels- Objectives
Develop a framework for promoting collaboration in providing services to persons experiencing chronic homelessness at Federal, State, and local levels.Use the Interagency Council on Homelessness and other interagency mechanisms to coordinate planning, programmatic activities, and evaluation that address chronic homelessness efforts in HHS with HUD, VA, and other relevant Departments.
- Strategies to Promote Collaboration
- Promote and incentivize coordination between all mainstream and homeless-specific HHS funding sources that address chronic homelessness.
Examples:
- Where appropriate, add a new section to applications requesting funding for mainstream assistance that requires the applicants to demonstrate how the assistance will be used in concert with other HHS support to form an integrated safety net for poor and disabled individuals and families. Require that they articulate outcomes associated with the coordination and that they have an infrastructure in place to operationalize and manage this coordination.
- Develop an incentive program in which States submitting block grant applications that demonstrate a coordinated set of activities to address services to homeless people (including those who are chronically homeless) across mainstream programs are eligible for a partial bonus payment up front, with the balance of the bonus based on their achievement of a performance goal they set-e.g., number of chronically homeless people receiving comprehensive support in housing.
- Provide incentives for States and localities to coordinate HHS-assisted services and housing for persons experiencing long-term homelessness.
Examples:
- Permit applicants to use grant funds to support interagency collaborations that address chronic homelessness, including expenses for FTEs associated with partnership activities, incentive funds, flexible fund reserves, contributions to HUD continuum of care activities, etc.
- In competitive applications for services (such as community health centers, some Ryan White programs, SAMHSA's Grants for the Benefit of Homeless Individuals), give bonus points to applicants willing to address chronic homelessness via partnerships with other types of providers, notably housing providers.
- Permit States and communities to experiment with various approaches to creating a coordinated, comprehensive system of services to address chronic homelessness (e.g., establish an infrastructure that supports coordination, have flexibility in the use of funds, forge systemic relationships between providers for effective client referral, conduct cross-system training) and introduce new service technologies (e.g., assertive case management models, critical time intervention approaches). This might be done as pilot projects, under existing authorities, such as the recent Medicare+Choice arrangements with preferred provider organizations.
- Permit flexibility in paying for services delivered to individuals experiencing chronic homelessness, particularly involving services from different funding streams.
Examples:
- Explore the authority for appropriate grantees to designate a percentage amount of an award that can be used flexibly and to assist in providing timely, comprehensive services to a person who is chronically homeless, e.g., to secure a critical service that is only available from another provider.
- Allow States to blend a small portion of funds from multiple, relevant HHS assistance programs to target homelessness. The Listening Session presenters referred to the application of this concept to homelessness as a 'mini-waiver.' This could be done through a multi-program waiver or through relief from cost allocation rules for this portion of the funds. One large-scale version of this was attempted with the flexible authorities proposed in legislation reauthorizing the Temporary Assistance for Needy Families program. The intent of such flexible waivers and authorities is a relaxation of rules would be to permit States to experiment with adaptive uses of these assistance programs to respond comprehensively and flexibly to the needs of poor and disabled clients. Persons experiencing chronic homelessness should be included in this consideration.
- Develop a pilot program that covers multiple mainstream programs and allows funds to be pooled for a specific purpose. For example, multiple systems could contribute resources to pay for continuity of case management. As the chronically homeless client progresses from homeless-to-housed or receives services from different systems, the case manager would remain constant, ensure consistency of a treatment plan, and be empowered to work with each system.
- Promote and incentivize coordination between all mainstream and homeless-specific HHS funding sources that address chronic homelessness.
- Strategies to Improve Coordination
- Establish an ongoing body within HHS to identify, monitor, and coordinate Departmental activities to address services to eligible persons experiencing homelessness, including those with long term and repeated patterns of homelessness, and coordinate these efforts with other Federal agencies.
Example:
- Charge and rename the Secretary's Work Group on Ending Chronic Homelessness to serve in this capacity. Subcommittees of the Work Group could address and advise on specific facets such as chronic homelessness or homelessness among families with children. The Work Group could also ensure that the activities undertaken by the Department are periodically assessed and adjusted to achieve long-term outcomes, e.g., ending chronic homelessness.
- Establish an ongoing body within HHS to identify, monitor, and coordinate Departmental activities to address services to eligible persons experiencing homelessness, including those with long term and repeated patterns of homelessness, and coordinate these efforts with other Federal agencies.
- Objectives
- Goal 3
Prevent additional chronic homelessness- Objectives:
Promote programs and policies designed to ensure that persons returning to the community from institutional or other sheltered settings (including foster care) do not become homeless.Promote programs and policies that address the service and housing needs of persons identified as at-risk of housing loss who are currently participating in HHS assisted mainstream programs.
- Strategies to Reduce the Incidence of Homelessness
- Identify both the risk and protective factors for homelessness and preventive interventions that could be used to identify and prevent homelessness among persons at risk.
Examples:
- The Research Coordination Council could be requested to examine how HHS can synthesize, sponsor or conduct epidemiological and health services research on protective and risk factors for homelessness and to identify preventive interventions that could be provided in health care and human services settings that are effective at preventing at-risk clients from entering a pattern of residential instability that could result in chronic homelessness. A dissemination plan should be an integral part of a department plan.
- NIH or AHRQ could sponsor investigator-initiated research to examine the organization, effectiveness, and cost of such preventive interventions. In addition, NIH or ASPE could also fund a contract for a 'meta-analysis' of existing research and evaluation studies on the histories of persons experiencing long-term homelessness to determine what is known about identifiable risk factors for chronic homelessness. Alternatively, this could be done by stimulating investigator initiated research in NIH that explores these factors and then applies them retrospectively to shelter data bases and assesses their predictive ability. The risk factors could then be promulgated as 'markers of concern' to mainstream providers so that current clients with these characteristics might have housing stability issues included in their treatment plans.
- Identify and promote the use of effective, evidence-based homelessness prevention interventions, ranging from family strengthening and high-risk youth programs to specific interventions such as discharge planning, Assertive Community Treatment (ACT) and Critical Time Intervention (CTI). Develop and disseminate guidelines for these interventions in order to reduce the incidence of individuals being placed in emergency shelter or other fragile residential circumstances.
Examples:
- HRSA has recently supported a grantee to disseminate discharge-planning guidance via the Internet. The applicability of this homelessness prevention strategy could be reinforced via in-service training, letters of guidance, and other dissemination approaches.
- Conduct replicability studies of ACT and CTI and provide models and guidelines for their use in community based settings, as well as their applicability to effective discharge planning.
- Identify both the risk and protective factors for homelessness and preventive interventions that could be used to identify and prevent homelessness among persons at risk.
- Objectives:
An Alternate Listing
The above approach organizes the goals and strategies under each of the original charges to the Work Group. Such an approach demonstrates the responsiveness of the Work Group to each charge, but is not the only way of presenting HHS' comprehensive approach. This alternative listing may also prove useful. Three restated goals describe the HHS plan to end chronic homelessness:
- Help eligible, chronically homeless persons receive health and social services;
- Empower our State and community partners to improve their response to the needs of homeless people; and
- Work to prevent new episodes of homelessness within the HHS clientele.
The strategies listed previously can be aligned with each of these restated goals to present a comprehensive approach. They are briefly paraphrased and aligned with one of the above goals:
Help eligible, chronically homeless individuals receive health and social services
- Strengthen outreach and engagement activities
- Improve the eligibility review process
- Explore ways to maintain program eligibility
- Improve the transition of clients from homeless-specific programs to mainstream service providers
Empower our State and community partners to improve their response to people experiencing chronic homelessness.
- Use State Policy Academies to help States develop specific action plans to respond to chronic homelessness
- Permit flexibility in paying for services that respond to the needs of persons with multiple problems
- Reward coordination across HHS assistance programs to address the multiple problems of chronically homeless people
- Provide incentives for States and localities to coordinate services and housing
- Develop, disseminate and use toolkits and blueprints to strengthen outreach, enrollment, and service delivery
- Provide training and technical assistance on chronic homelessness to mainstream service providers
- Establish a formal program of training on chronic homelessness
- Address chronic homelessness in the formulation of future HHS budgets or in priorities for using a portion of expanded resources
- Develop an approach for baseline data, performance measurement, and the measurement of reduced chronic homelessness within HHS
- Establish an ongoing oversight body within HHS to direct and monitor the plan
Work to prevent new episodes of homelessness within the HHS clientele
- Identify risk and protective factors to prevent future episodes of chronic homelessness
- Promote the use of effective, evidence-based homelessness prevention interventions
Closing Considerations
These recommendations form a basis for the programs of HHS to explore ways in which their actions can contribute to the Administration's goal of ending chronic homelessness. They are neither prescriptive nor exhaustive of the possibilities for programs. However, in recognizing that categorical program approaches have limits in responding to the needs of a multi-problem clientele, the Work Group explicitly avoided recommendations that create additional programs or funding streams. Success is not measured exclusively by the existence of a program, but from the accumulation of operations supported by:
- a program mission;
- a management structure to carry out the mission;
- policies that guide operations;
- funding and incentives for the activities of the program;
- technical assistance to ensure credible and accountable activities; and
- outcomes that demonstrate the success of the above.
The Work Group believes the Administration's goal of ending chronic homelessness combined with the recommendations offered above accumulate to provide these six supports. Their interaction will guarantee the Department's success.
1. It is assumed throughout this document that no strategies will be implemented without seeking and attaining all relevant legislative and/or regulatory changes needed to ensure that all programs within HHS continue to operate within their given authority and mission. It is also assumed that, to the extent the strategies seek to impose any requirements on applicants as conditions of given awards, before doing so, programs will confirm that their authorizing authority and program/administrative regulations permit such imposition of conditions. It is further assumed that no proposals will be implemented without resolving any inherent budget implications.
Appendix A: Membership of the Secretary’s Work Group on Ending Chronic Homelessness
CHAIR |
|
|---|---|
| Claude Allen Deputy Secretary, DHHS Room 606-G 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 690-6133 Fax: (202) 690-7755 |
|
Immediate Office of the Secretary |
|
| Willis Morris Senior Advisor to the Deputy Secretary Room 614-G 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 690-6133 Fax: (202) 690-7755 |
Cynthia Kenny Policy Coordinator, Office of the Executive Secretariat, Room 629H 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 205-9162 Fax: (202) |
|
Administration for Children and Families |
|
| Clarence Carter Director, Office of Community Services Aerospace Building - 5th Floor 901 D St, S.W. Washington D.C., 20447 Ph: (202) 401-9333 Fax: (202) 401-4694 |
|
|
Administration on Aging |
|
| Edwin Walker Director, Center for Wellness and Community-Based Services. Room 4733, Cohen Building 330 Independence Avenue, S.W. Washington, D.C., 20201 Ph: (202) 619-0011 Fax: (202) 260-1012 |
|
|
Centers for Medicare & Medicaid Services |
|
| Timothy Trysla Policy Advisor, Office of the Administrator Room 314-G 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 690-6726 Fax: (202) 690-6262 |
|
|
Health Resources and Services Administration |
|
| Lyman Van Nostrand Acting Director, Office of Policy and Evaluation Room 14-45 5600 Fishers Lane Rockville, Maryland 20857 Ph: (301) 443-1891 Fax: (301) 443-0007 |
|
|
Substance Abuse and Mental Health Services Administration |
|
| Gail Hutchings Senior Advisor to the Administrator Room 12-105 5600 Fishers Lane Rockville, Maryland 20857 Ph: (301) 443-4795 Fax: (301) 443-0284 |
|
|
Office of the Assistant Secretary for Budget, Technology, and Finance |
|
| Kathlene Heuer Deputy Assistant Secretary for Performance and Planning Room 524G 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 690-6061 Fax: (202) 690-5405 |
Alternate: Kerry Weems Deputy Assistant Secretary for Budget Room 503H 200 Independence Avenue Washington D.C. 20201 Ph: (202) 690-7393 Fax: (202) 690-6896 |
|
Office of the Assistant Secretary for Legislation |
|
| Barbara Pisaro Clark Senior Legislative Analyst, Human Services Room 411-H 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 690-6311 Fax: (202) 690-8425 |
|
|
Office of the Assistant Secretary for Planning and Evaluation |
|
| Don Winstead Deputy Assistant Secretary, Human Services Policy Room 404E-2 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 690-7409 Fax: (202) 690-6562 |
|
|
Office of the Secretary |
|
| Robert Keith Office of General Counsel Room 411-D 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 690-8005 Fax: (202) 690-7320 |
James Mason Intergovernmental Affairs Humphrey Building, Room 614-E 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 401-5639 Fax: (202) 690-5672 |
|
Staff |
|
| Peggy Halpern Policy Analyst, Human Services Policy, ASPE Room 424E.11 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 260-0285 Fax: (202) 690-6562 |
Walter Leginski Senior Advisor on Homelessness Human Services Policy, ASPE Room 426F.6 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 260-0384 Fax: (202) 690-6562 |
Appendix B: Membership of the Interagency Subcommittee of the Secretary’s Work Group
| Immediate Office of the Secretary | |
| Willis Morris Senior Advisor to the Deputy Secretary Room 614-G 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 690-6133 Fax: (202) 690-7755 |
Cynthia Kenny Policy Coordinator, Office of the Executive Secretariat, Room 629H 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 205-9162 Fax: (202) 205-2135 |
|
Administration for Children and Families |
|
| Beverly Bunn Staff Assistant for Marriage Education Office of the Assistant Secretary 6th Floor-West 901 D St, S.W. Washington D.C., 20447 Ph: (202) 401-5240 and 401-9207 Fax: (202) 401-5770 |
|
| Administration on Aging | |
|---|---|
| Sherri Clark Program Specialist Room 4747 330 Independence Avenue, SW Washington, DC 20201 Ph: (202) 619-3955 Fax: (202) 260-1012 |
|
| Centers for Medicare & Medicaid Services | |
| Glenn Stanton Deputy Director Disabled and Elderly Health Program Group Center for Medicaid and State Operations Rm S2-14-26 7500 Security Blvd Baltimore, MD 21244-1850 Ph: (410) 786-6768 Fax: (410)786-9004 |
Susan McNally Director, Medicaid Group Office of Legislation Room 331H 200 Independence Ave, S.W. Washington, DC 20201 Ph: (202 ) 690-7762 Fax: (202) 690-8168 |
| CMS Alternate: Gina Clemons Rm S2-17-04 Ph: (410) 786-9644 Fax: (410) 786-9004 |
CMS Alternate: Sue Clain Room 341H Ph: (202) 690-8226 Fax: (202) 690-8168 |
| Health Resources and Services Administration | |
| Lynnette S. Araki Office of Policy and Evaluation Room 14-45 5600 Fishers Lane Rockville, Maryland 20857 Ph: (301) 443-6204 Fax: (301) 443-0007 |
Jean Hochron Chief, Health Care for the Homeless Branch Bureau of Primary Health Care Room 9-6D2 4350 East West Highway Bethesda, MD 20814 Ph: (301)594-4437 Fax: (301)594-2470 |
|
Indian Health Service |
|
| James F. Cussen Director, Urban Indian Health Programs Room 200 810 Thompson Ave. Rockville, MD 20857 Ph: (301) 443-4680 Fax: (301) 443- 8446 |
|
|
Substance Abuse and Mental Health Services Administration |
|
| Gail Hutchings Acting Director, Center for Mental Health Services Room 17-99 5600 Fishers Lane Rockville, Maryland 20857 Ph: (301) 443-0001 Fax: (301) 443-1563 |
Winnie Mitchell Team Leader, Office of Policy and Planning, SAMHSA Rm. 12C-05 5600 Fishers Lane Rockville, MD 20857 Ph: (301) 443-2324 Fax: (301)443-1450 |
| Frances Randolph Chief (Acting), Homeless Programs Branch Center for Mental Health Services Room 11C-05 5600 Fishers Lane Rockville, MD 20857 Phone: (301)443-3706 Fax: (301)443-0561 |
|
| Office of the Assistant Secretary for Budget, Technology, and Finance | |
| Nick Burbank Room 503H 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 690-7846 Fax: (202) 690-6896 |
|
| Office of the Assistant Secretary for Legislation | |
| Barbara Pisaro Clark Senior Legislative Analyst, Human Services Room 411-H 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 690-6311 Fax: (202) 690-8425 |
Sharon Clarkin Associate Director of Health Legislation Room 409-H 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 690-7450 Fax: (202) 690-8425 |
| ASL Alternate Jessamy Taylor Ph: (202) 690-7627 Fax: (202) 690-8425 |
|
|
Office of the Assistant Secretary for Planning and Evaluation |
|
| Peggy Halpern Policy Analyst, Human Services Policy, ASPE Room 424E.11 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 260-0285 Fax: (202) 690-6562 |
Walter Leginski Senior Advisor on Homelessness Human Services Policy, ASPE Room 426F.6 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 260-0384 Fax: (202) 690-6562 |
|
Office of General Counsel |
|
| Robert Keith Office of General Counsel Room 411-D 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 690-8005 Fax: (202) 690-7320 |
Catherine Hess Office of General Counsel Room 411-D 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 690-8005 Fax: (202) 690-7320 |
|
Office of the Secretary |
|
| Jim Mason Senior Advisor to the Director Intergovernmental Affairs Room 614-E 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 401-5639 Fax: (202)690-5672 |
|
|
Office of Women's Health |
|
| Frances Ashe-Goins Deputy Director and Director-Division of Policy and Program Development Office of Women's Health Room 728E 200 Independence Avenue S.W. Washington D.C., 20201 Ph: (202) 690-6373 Fax: (202) 401-4005 |
OWH Alternate Jeannine Greenfield Room 718F Ph: (202) 401-9545 Fax: (202) 401-4005 |
Appendix C: Definitions of Treatments and Services for People Who Experience Chronic Homelessness
The following services and treatment needs are organized into core and supportive services: The core services include those that are needed to transition people from the streets into housing and to stabilize their conditions. The supportive services include those that are needed to reintegrate people into the community, such as with jobs, education and socialization.
CORE SERVICES:
- Information and Referral. Individuals who are homeless need to be able to access appropriate services and supports when they enter into the service system. Information and referral services are those services or activities designed to provide information about services provided by public and private service providers and a brief assessment of client needs (but not diagnosis and evaluation) to facilitate appropriate referral to these community resources.
- Outreach and Engagement. Outreach services include extending services or help in order to develop a relationship of trust and engage homeless persons into treatment and service programs; to provide basic materials, such as meals, blankets, or clothes, to homeless persons; or to publicize the availability of various types of assistance such as emergency shelter or food programs that are available to a homeless person. Outreach services may take place in a variety of settings, including public places, meal programs, shelters, drop-in centers, or health care facilities.(i)
- Health Related and Home Health Services, Including HIV/AIDS. People who experience homelessness need access to a range of comprehensive services that respond to their complex and multiple health care needs. Health related and home health services are those in-home or out-of-home services or activities that provide direct treatments or are designed to assist individuals and families to attain and maintain a favorable condition of health. Component services and activities may include providing an analysis or assessment of an individual's health problems and the development of a treatment plan; assisting individuals to identify and understand their health needs; providing directly or assisting individuals to locate, provide or secure, and utilize appropriate medical treatment, preventive medical care, and health maintenance services, including in-home health services and emergency medical services; provision of appropriate medication; and providing follow-up services as needed. HIV/AIDS services include HIV/AIDS primary and secondary prevention services, HIV/AIDS counseling and testing, primary care, provision of HIV/AIDS anti-retrovirals and other medications, rehabilitative, and supportive services for persons affected and infected with HIV.
- Alcohol and Drug Abuse Services. Effective approaches for providing substance abuse treatment to people who are homeless include those activities primarily designed to prevent, deter, reduce, or eliminate substance abuse or addictive behaviors. Component substance abuse services or activities may include a comprehensive range of personal and family counseling methods, early interventions, methadone treatment for opiate abusers, or detoxification treatment for alcohol and other drug abusers. Treatment services may include intake and assessment; treatment matching and planning; behavioral therapy and counseling appropriate to the client and the severity of the problem; substance abuse toxicology and screening; clinical and case management; outcome evaluation; pharmacotherapies; and self-help and peer support activities.(ii) Services may be provided in outpatient settings and alternative living arrangements such as institutional settings and community-based halfway houses.
- Mental Health and Counseling Services. People who are homeless must have access to a full range of mental health and counseling services. This includes those services and activities that apply therapeutic processes to personal, family, situational, or occupational problems in order to bring about a positive resolution of the problem or improved individual or family functioning or circumstances. Problem areas may include family and marital relationships, parent-child problems, bereavement, or symptom management. Component services may include crisis interventions; individual supportive therapy, family or group therapy sessions; the prescription of psychotropic medications or explanations about the use and management of medications; and combinations of therapeutic approaches to address multiple problems. Access to coordinated treatment for co-occurring mental health and substance use disorders is also necessary and superior to other approaches for reducing alcohol and drug use, homelessness, and the severity of mental health symptoms among people with co-occurring disorders.(iii)
- Inpatient Services. Inpatient services are those medical, psychiatric, or substance abuse treatment services that are provided for acute conditions on a time-limited basis in a licensed setting that provides 24-hour care by licensed and qualified staff. Such services are an important component of the full-range of comprehensive services needed to help stabilize and prepare people who experience chronic homelessness for housing.
- Case Management: Supportive Services. Supportive case management services are services or activities for the arrangement, coordination, monitoring, and delivery of services to meet the needs of individuals and families who experience homelessness. Component services and activities may include individual service plan development; counseling; monitoring, developing, securing, and coordinating services; monitoring and evaluating client progress; and assuring that clients' rights are protected.
- Case Management: Clinical, Intensive, or Assertive Community Treatment Models. These are service-delivery models that are effective in providing comprehensive community-based treatment and services to people who are homeless. Using a multidisciplinary staff, treatment and services are provided on a continuous/long-term basis, and in the community rather than an office.(iv)
- Income Management and Support. Individuals who experience chronic homelessness are often entitled to income support and cash assistance. Many require services to help secure these entitlements including assistance being referred and making it to appointments with benefits specialists, completing application forms, and compiling medical and other records that will support the individual's application for assistance or disability insurance.(v) Individuals may also need a representative payee or other designee to help manage the income they receive from entitlements.
- Residential Treatment Services. While people who experience chronic homelessness ultimately need permanent housing with flexible supports, residential treatment services provide short-term residential care, respite, and comprehensive treatment and services for children or adults whose problems are so severe or are such that they cannot be cared for at home or in foster care and need the specialized services provided by specialized facilities. Component services and activities delivered during the short-term residential stay may include diagnosis and evaluation; medical treatments; alcohol and drug detoxification services; psychiatric services; individual, family, and group therapy and counseling; remedial education and GED preparation; vocational or pre-vocational training; training in activities of daily living; supervised recreational and social activities; case management; transportation; and referral to and utilization of other services.
- Discharge Planning. Discharge planning help prevent chronic homelessness by preparing people residing in hospitals, shelters or jails for return or re-entry to the community by linking them with community treatment, housing and supports. Ideally, such planning begins upon entry to an institution, is ready to be implemented upon discharge, involves input from the individual, and includes time-limited, intensive supports during the transition from hospitals, shelters or jails to community-based services.(vi) Ensuring the availability of stable housing at time of discharge is critical, as people often lose their housing while in institutions.
SUPPORTIVE SERVICES:
- Life Skills Services. Life skills services provide critical life management skills that may never have been learned or have been lost during the course of mental illness, substance use, and homelessness. They are targeted to assist the individual to function independently in the community and make the transition from homelessness to stable housing. Component life skill training includes the budgeting of resources and money management, household management, conflict management, shopping for food and needed items, nutrition, the use of public transportation, parent training, time management and social skills development.
- Child Care Services. Child care services for children (including infants, pre-schoolers, and school age children) are services or activities provided in a setting that meets applicable standards of state and local law, in a center or in a home, for a portion of a 24-hour day. Component services or activities may include a comprehensive and coordinated set of appropriate developmental activities for children, recreation, meals and snacks, transportation, health support services, social service counseling for parents, and plan development.
- Education and Training Services. People who experience homelessness often need education and training services designed to improve the knowledge, daily living, or social skills needed to reintegrate into the community. Services may include instruction or training in, but are not limited to, such issues as consumer education, health education, education to prevent substance abuse, community protection and safety education, literacy education, English as a second language, and General Educational Development (GED), job skills training and employment skills. Component services or activities may include screening, assessment and testing; individual or group instruction; tutoring; provision of books, supplies and instructional material; counseling; and referral to community resources.
- Employment Services. Employment services or activities that assist individuals in securing employment; acquiring or learning skills that promote opportunities for employment, advancement, and increased earning potential; and in retaining a job often help people who are homeless acquire or regain a valued role in society. Component services or activities may include employment screening, assessment, or testing; structured job skills and job seeking skills; specialized therapy (occupational, speech, physical); special training and tutoring, including literacy training and pre-vocational training; provision of books, supplies and instructional material; counseling or job coaching; transportation; and referral to community resources.
- Legal Services. Legal services are those services or activities provided by a lawyer or other person(s) under the supervision of a lawyer to assist individuals in seeking or obtaining legal help in civil matters such as housing, divorce, child support, guardianship, paternity, and legal separation. Component services or activities may include receiving and preparing cases for trial, provision of legal advice, representation at hearings, and counseling.(vii)
- Transportation Services. Transportation services are those services or activities that provide, arrange or pay for the travel of individuals in order to access treatment, medical care, services, or employment. Component services or activities may include special travel arrangements such as special modes of transportation and personnel to accompany or assist individuals or families to utilize transportation.
i Morse, G.A., et al. (1996). Outreach to homeless mentally ill people: Conceptual and clinical considerations. Community Mental Health Journal 32(3): 261-274. Witheridge, T.F. (1991). The active ingredients of assertive outreach. New Directions for Mental Health Services 52: 47-64.
ii Oakley, D. and Dennis, D. (1996). Orwin, R.G., Mogren, R.G., Jacobs, M.L., Sonnefeld, L.J. (1999) Retention of homeless clients in substance abuse treatment: Findings from the National Institute on Alcohol Abuse and Alcoholism Cooperative Agreement Program. Journal of Substance Abuse Treatment 17(1-2): 45-66. Sosin, M.R., Bruni, M., Reidy, M. (1995) Paths and impacts in the Progressive Independence Model: A homelessness and substance abuse intervention in Chicago. Journal of Addictive Diseases 14(4): 1-20. Cox, G.B., Walker, D., Freng, S.A., Short, B.A., Meijer, L, Gilchrist, L. (1998) Outcome of a controlled trial of the effectiveness of intensive case management for chronic public inebriates. Journal of Studies on Alcohol 59(5): 523-532. Stahler, G.J., Stimmel, B. (eds.) (1996) The Effectiveness of Social Interventions for Homeless Substance Abusers. Binghamton, NY: The Haworth Press, Inc. Tommasello, A.C., Myers, C.P., Gillis, L., Treherne, L.L., Plumhoff, M. (1999) Effectiveness of outreach to homeless substance abusers. Evaluation and Program Planning 22(3): 295-303.
iii Carey, K.B. (1996). Treatment of co-occurring substance abuse and major mental illness. New Directions for Mental Health Services 70:19-31. Drake, R.E., et al. (1998). Review of integrated mental health and substance abuse treatment for patients with dual disorders. Schizophrenia Bulletin 24(4): 589-608.
iv Morse, G. (1999). A review of case management for people who are homeless: Implications for practice, policy, and research. In Fosburg, L.B., Dennis, D.L. (eds.) Practical Lessons: The 1998 National Symposium on Homelessness Research. Delmar, NY: National Resource Center on Homelessness and Mental Illness. Ziguras, S.J., Stuart, G.W. (2000). A meta-analysis of the effectiveness of mental health case management over 20 years. Psychiatric Services 51(11): 1410-1421.
v Rosen, J., et al. (2001)
vi Shinn, M., Baumohl, J. (1999) Rethinking the prevention of homelessness. In Fosburg, L.B., Dennis, D.L. (eds.), Practical Lessons. Washington, DC: HHS & HUD. Interagency Council on the Homeless (1999) Exemplary Practices in Discharge Planning. Washington, DC: Interagency Council on the Homeless. Susser, E., Valencia, E., Conover, S., et al. (1997) Preventing recurrent homelessness among mentally ill men. American Journal of Public Health 87(2): 256-262.
vii Federal Task Force on Homelessness and Severe Mental Illness. (1992)
Appendix D: Citations for Research/Evaluation Findings on Effective Treatments and Services for People Who Experience Chronic Homelessness (1)
Core Services
- Outreach and Engagement
Bybee, D., Mowbray, C.T., Cohen, E.H. (1995). Evaluation of a homeless mentally ill outreach program: Differential short-term effects. Evaluation and Program Planning 18(1): 13-24.
Lam, J.A., Rosenheck, R. (1999). Street outreach for homeless persons with serious mental illness: Is it effective? Medical Care 37(9): 894-907.
Morse, G.A., et al. (1996). Outreach to homeless mentally ill people: Conceptual and clinical considerations. Community Mental Health Journal 32(3): 261-274.
Tsemberis, S., Elfenbein, C. (1999). A perspective on voluntary and involuntary outreach services for the homeless mentally ill. New Directions for Mental Health Services 82: 9-19.
Witheridge, T.F. (1991). The active ingredients of assertive outreach. New Directions for Mental Health Services 52: 47-64.
- Primary Health Care
McMurray-Avila, M. (2001) Organizing Health Services for Homeless People: A Practical Guide. Nashville, TN: National Health Care for the Homeless Council, Inc.
McMurray-Avila, M., Gelberg, L., and Breakey, W.R., (1999) Balancing act: Clinical practices that respond to the needs of homeless people. In Fosburg, L., and Dennis, D. (eds.). Practical Lessons: The 1998 National Symposium on Homelessness Research. Washington, DC: HUD and HHS.
Song, J.Y. (1999) HIV/AIDS and Homelessness: Recommendations for Clinical Practice and Public Policy. Nashville, TN: National Health Care for the Homeless Council, HCH Clinicians' Network.
- Alcohol and Drug Abuse Services
Cox, G.B., Walker, D., Freng, S.A., Short, B.A., Meijer, L, Gilchrist, L. (1998) Outcome of a controlled trial of the effectiveness of intensive case management for chronic public inebriates. Journal of Studies on Alcohol 59(5): 523-532.
Oakley, D.A., Dennis, D.L. (1996) Responding to the needs of homeless people with alcohol, drug, and/or mental disorders. In Baumohl, J. (ed.), Homelessness In America. Phoenix, AZ: Oryx Press, 179-186.
Orwin, R.G., Mogren, R.G., Jacobs, M.L., Sonnefeld, L.J. (1999) Retention of homeless clients in substance abuse treatment: Findings from the National Institute on Alcohol Abuse and Alcoholism Cooperative Agreement Program. Journal of Substance Abuse Treatment 17(1-2): 45-66.
Sosin, M.R., Bruni, M., Reidy, M. (1995) Paths and impacts in the Progressive Independence Model: A homelessness and substance abuse intervention in Chicago. Journal of Addictive Diseases 14(4): 1-20.
Stahler, G.J., Stimmel, B. (eds.) (1996) The Effectiveness of Social Interventions for Homeless Substance Abusers. Binghamton, NY: The Haworth Press, Inc.
Tommasello, A.C., Myers, C.P., Gillis, L., Treherne, L.L., Plumhoff, M. (1999) Effectiveness of outreach to homeless substance abusers. Evaluation and Program Planning 22(3): 295-303.
Zerger, S. (2002) Substance Abuse Treatment: What Works for Homeless People?: A Review of the Literature. Nashville, TN: National Health Care for the Homeless Council.
- Mental Health and Counseling Services
Breakey, W.R. (1992) Mental health services for homeless people. In Robertson, M.J., and Greenblatt, M. (eds.) Homelessness: A National Perspective. New York, NY: Plenum Press.
Carey, K.B. (1996) Treatment of co-occurring substance abuse and major mental illness. New Directions for Mental Health Services 70:19-31.
Drake, R.E., et al. (1998) Review of integrated mental health and substance abuse treatment for patients with dual disorders. Schizophrenia Bulletin 24(4): 589-608.
Federal Task Force on Homelessness and Severe Mental Illness. (1992) Outcasts on Main Street. Washington, DC: Interagency Council on the Homeless.
Susser, E., Goldfinger, S., White, A. (1990) Some clinical approaches to the homeless mentally ill. Community Mental Health Journal 26(5): 463-480.
- Inpatient Services
Federal Task Force on Homelessness and Severe Mental Illness. (1992) Outcasts on Main Street. Washington, DC: Interagency Council on the Homeless.
McMurray-Avila, M. (2001) Organizing Health Services for Homeless People: A Practical Guide. Nashville, TN: National Health Care for the Homeless Council, Inc.
McMurray-Avila, M., Gelberg, L., and Breakey, W.R., (1999) Balancing act: Clinical practices that respond to the needs of homeless people. In Fosburg, L., and Dennis, D. (eds.). Practical Lessons: The 1998 National Symposium on Homelessness Research. Washington, DC: HUD and HHS.
- Supportive Case Management
Morse, G. (1999). A review of case management for people who are homeless: Implications for practice, policy, and research. In Fosburg, L.B., Dennis, D.L. (eds.) Practical Lessons: The 1998 National Symposium on Homelessness Research. Delmar, NY: National Resource Center on Homelessness and Mental Illness.
Rog, D.J., Holupka, C.S., McCombs-Thirnton, K.L., Brito, M.C., Hambrick, R. (1996) Case management in practice: Lessons from the evaluation of the RWJ/HUD Homeless Families Program. Journal of Prevention and Intervention in the Community 15(2): 67-82.
- Clinical/Intensive/ACT Model Case Management
Lehman, A.F., et al. (1997). A randomized trial of Assertive Community Treatment for homeless persons with severe mental illness. Archives of General Psychiatry 54: 1038-1043.
Meisler, N., Blankertz, L., Santos, A.B., McKay, C. (1997). Impact of Assertive Community Treatment on homeless persons with co-occurring severe psychiatric and substance use disorders. Community Mental Health Journal 33(2): 113-122.
Morse, G. (1999). A review of case management for people who are homeless: Implications for practice, policy, and research. In Fosburg, L.B., Dennis, D.L. (eds.) Practical Lessons: The 1998 National Symposium on Homelessness Research. Delmar, NY: National Resource Center on Homelessness and Mental Illness.
Rosenheck, R., Dennis, D. (2001). Assertive Community Treatment for homeless persons with severe mental illness. Archives of General Psychiatry 58(11): 1073-1080.
Ziguras, S.J., Stuart, G.W. (2000). A meta-analysis of the effectiveness of mental health case management over 20 years. Psychiatric Services 51(11): 1410-1421.
- Information and Referral
Federal Task Force on Homelessness and Severe Mental Illness. (1992) Outcasts on Main Street. Washington, DC: Interagency Council on the Homeless.
McMurray-Avila, M. (2001) Organizing Health Services for Homeless People: A Practical Guide. Nashville, TN: National Health Care for the Homeless Council, Inc.
Morse, G. (1999). A review of case management for people who are homeless: Implications for practice, policy, and research. In Fosburg, L.B., Dennis, D.L. (eds.) Practical Lessons: The 1998 National Symposium on Homelessness Research. Delmar, NY: National Resource Center on Homelessness and Mental Illness.
- Coordinated Treatment/Services
Beyond Shelter. (1998). The "Housing First" Program for Homeless Families: Methodology Manual. Los Angeles, CA: Beyond Shelter, Inc.
Culhane, DP, Metraux, S, Hadley, T., (2001) The New York/New York Agreement Cost Study: The Impact of Supportive Housing on Services Use for Homeless Mentally Ill Individuals. New York: Corporation for Supportive Housing.
Davis, G., Johnson, G., Mayberg, S. (2002). Effectiveness of Integrated Services for Homeless Adults with Serious Mental Illness. Sacramento, CA: California Department of Mental Health.
Dennis, D.L., Steadman, H.J., Cocozza, J.J. (2000). The impact of federal systems integration initiatives on services for mentally ill homeless persons. Mental Health Services Research 2(3): 164-174.
Lipton, F.R., Siegel, C., Hanningan, A., Samuels, J., and Baker, S., (2000) Tenure in supportive housing for homeless persons with severe mental illness. Psychiatric Services 51(4): 479-486.
Proscio, T. (2000). Supportive Housing and Its Impact on the Public Health Crisis of Homelessness. New York, NY: Corporation for Supportive Housing
Rosenheck, R., et al. (1998). Service system integration, access to services, and housing outcomes in a program for homeless persons with severe mental illness. American Journal of Public Health 88(11): 1610-1615.
Tsemberis, S., and Eisenberg, R.F. (2000) Pathways to housing: Supported housing for street-dwelling homeless individuals with psychiatric disabilities. Psychiatric Services 51(4): 487-493.
- Income Support/Cash Assistance
Rosen, J., Hoey, R. and Steed, T. (2001) Food stamps and SSI benefits: Removing access barriers for homeless people. Clearinghouse Review 34: 679-696.
Rosenheck, R., Frisman, L., Kasprow, W. (1999) Improving access to disability benefits among homeless persons with mental illness: An agency-specific approach to services integration. American Journal of Public Health 89(4): 524-528.
- Residential Treatment Services
Goldfinger, S.M. (1990) Homelessness and schizophrenia: A psychosocial approach. In Herz, M.I., Keith, S.J., and Docherty, J.P. (eds.) Handbook of Schizophrenia, Psychosocial Treatment of Schizophrenia 4. Elsevier Science Publishers.
McMurray-Avila, M. (2001) Organizing Health Services for Homeless People: A Practical Guide. Nashville, TN: National Health Care for the Homeless Council, Inc.
Stecher, B.M., Andrews, C.A. , et al. (1994) Implementation of residential and nonresidential treatment for the dually diagnosed homeless. Evaluation Review 18(6): 689-717.
- Discharge Planning
Commonwealth of Massachusetts Executive Office for Administration and Finance. (2000). Moving Beyond Serving the Homeless to Preventing Homelessness. Boston, MA: Commonwealth of Massachusetts Executive Office for Administration and Finance.
Substance Abuse and Mental Health Services Administration. (1997). Exemplary Practices in Discharge Planning. Rockville, MD: Substance Abuse and Mental Health Services Administration, U.S. Department of Health and Human Services.
Massachusetts Housing and Shelter Alliance. (2002). Essential Tools for Discharge Planning. Nashville, TN: National Health Care for the Homeless Council.
Susser, E., Valencia, E., Conover, S., Felix, A., Tsai, W., Wyatt, R.J. (1997) Preventing recurrent homelessness among mentally ill men: A "critical time" intervention after discharge from a shelter. American Journal of Public Health 87(2): 256-262.
Supportive Services
- Life Skills Services
Shern, D.L., Tsemberis, S., Anthony, W., Lovell, A.M., Richmond, L., Felton, C.J., Winarski, J., Cohen, M. (2000) Serving street-dwelling individuals with psychiatric disabilities: outcomes of a psychiatric rehabilitation clinical trial. American Journal of Public Health 90(12): 1873-1878.
- Child Care
DiBlasio, F.A., Belcher, J.R. (1992) Keeping homeless families together: Examining their needs. Children and Youth Services Review 14: 427-438.
Murrell, N.L., Scherzer, T., Ryan, M., Frappier, N., Abrams, A., Roberts, C. (2000) The AfterCare Project: An intervention for homeless childbearing families. Family and Community Health 23(3): 17-27.
- Education, Training and Employment Services
Bennett, G., Shane, P., Tutunjian, B., Perl, H.I. (1992) Job Training and Employment Services for Homeless Persons with Alcohol and Other Drug Problems. Rockville, MD: U.S. Department of Health and Human Services.
Cook, J., Pickett-Schenk, S., Grey, D., Banghart, M., Rosenheck, R.A., Randolph, F. (2001) Vocational outcomes among formerly homeless persons with severe mental illness in the ACCESS program. Psychiatric Services 52(8): 1075-1080.
Shaheen, G., Mikloucich, F., Dennis, D. (eds). (2001) Work as a Priority: A Resource for Employing People Who Have a Serious Mental Illness and Who Are Homeless. Rockville, MD: Center for Mental Health Services.
Trutko, J.W., Barnow, B.S., Kessler-Beck, S., et al. (1997) Employment and Training for America's Homeless: Final Report of The Job Training for the Homeless Demonstration Program. Washington, DC: U.S. Department of Labor.
U.S. Department of Labor. (1997) Employment and Training for America's Homeless: Best Practices Guide. Washington, DC: U.S. Department of Labor.
- Legal Services
Blasi, G.L. (1992) The role of legal aid organizations in helping homeless people. In Jahiel, R.I. (ed.), Homelessness: A Prevention-Oriented Approach. Baltimore, MD: The Johns Hopkins University Press.
Moxley, D.P., Freddolino, P.P. (1991) Needs of homeless people coping with psychiatric problems: Findings from an innovative advocacy project. Health and Social Work 16(1): 19-26.
- Transportation Services
Acosta, O., Toro, P.A. (2000) Let's ask homeless people themselves: A needs assessment based on a probability sample of adults. American Journal of Community Psychology 28(3): 343-366.
1. Compiled for SAMHSA and HRSA by Policy Research Associates, Inc., Delmar, NY, July 2002
