Prepared by:
Lynne M. Fender, Project Director
Melissa Panagides-Busch
Rhoda Schulzinger
American Institutes for Research
Acknowledgements
The Office of the Assistant Secretary for Planning and Evaluation (ASPE) and the American Institutes for Research are extremely grateful to all of the staff in the governors’ offices, executive and legislative branch offices, and advocacy organizations who generously gave of the time, information, and insights that made this report possible. Further, the American Institutes for Research staff gratefully acknowledge the ongoing consultation and review of this report by Ms. Cheryl Austein-Casnoff, formerly Director of Public Health Policy in ASPE and currently Deputy Director of the Children’s Health Insurance Program in the Health Care Financing Administration(now known as Centers for Medicare and Medicaid Services(CMS)), and Ms. Caroline Taplin, Acting Director of Public Health Policy in ASPE.
Chapter I: Early Implementation of the Child Health Insurance Program
Background
Research has demonstrated that children with health insurance coverage have greater access to medical care than those without coverage. On average, those with health insurance visit doctors more frequently than those without coverage. A 1993 survey, for example, found that of all children who had no physician visits in the past year, 39 percent were uninsured compared to 20 percent of children with private coverage. (See Exhibit 1.) Children with health insurance coverage pay fewer visits to the emergency room in an average year than those without coverage. Those with health insurance develop fewer chronic illnesses, and those they do develop are treated more successfully than the chronic illnesses of uninsured children.
Parents report that children with health insurance are able to obtain regular primary and preventive care. With the help of proper preventive care, including immunizations and regular check-ups, it is possible to identify children’s problems as they occur, treat them as early as possible and avoid unnecessary complications. A common adage among health policy analysts, researchers, and service providers is, "Children are not little adults."
Recent trends in health insurance coverage have not been kind to the nation’s children. The Census Bureau estimates that at least 10.7 million children lacked health insurance coverage in 1997, up from 9.8 million in 1995.1 The proportion of all children with no health insurance increased from 13.8 percent in 1995 to 15 percent in 1997. The proportion of poor children with no health insurance rose to nearly 24 percent in 1997, from 21.4 percent in 1995.2
The Medicaid program, begun in 1965, was designed to cover the health care costs of children and families in poor and near-poor households. For children, Medicaid, which includes Early and Periodic Screening, Diagnosis and Treatment (EPSDT) Program provides comprehensive benefits including preventive, primary, developmental and long-term care services to eligible children. Under current Federal law, States must cover all children up to age six with family incomes up to 133 percent Federal poverty level (FPL) and children age six and older and born after September 30, 1983, with family incomes at or under 100 percent FPL. Under this provision, States must phase in coverage one year at a time so that by September 2002, all children under age 19 living below poverty will be eligible.
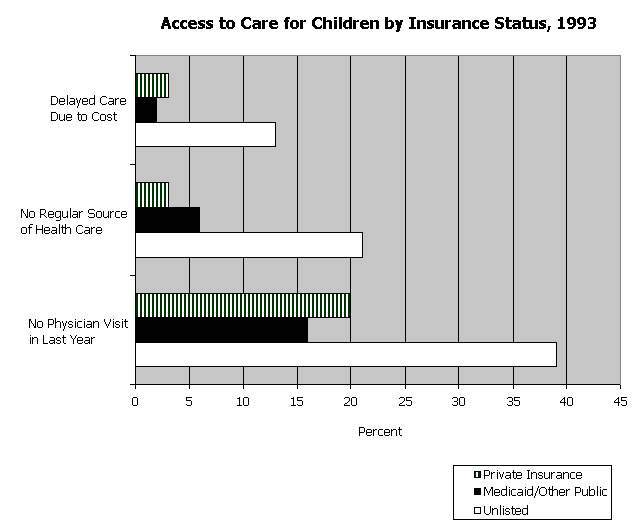 |
Source: National Center for Health Statistics, 1997. Kaiser/Commonwealth Survey, 1997. |
States have flexibility to extend Medicaid coverage beyond the Federal requirements and a number have done so.
However, even when there is expanded coverage, States have consistently fallen short of enrolling all children who qualify for Medicaid. The American Hospital Association estimates that as many as 4.3 million of the nation’s 10.7 million uninsured children may be eligible for but not enrolled in Medicaid.3 Reasons for the gap include inadequate marketing and outreach by State public assistance offices, families unaware of their eligibility, and families reluctant to apply because of the stigma they associate with Medicaid — a government assistance program too much like welfare. Recently, the gap in coverage between those eligible and those enrolled has increased even more.
One segment of the population that, historically, has been enrolled in Medicaid is families on welfare. Until recent changes, families with children who were receiving cash payments from the most prominent welfare program — Aid to Families with Dependent Children — were automatically eligible for Medicaid. The new welfare law, the Personal Responsibility and Work Opportunity Reconciliation Act of 1996, separated Medicaid and welfare eligibility for the first time. Now families losing eligibility for cash assistance may continue to qualify for Medicaid under other eligibility categories. States are required to make a separate determination about Medicaid eligibility when a family no longer qualifies for cash assistance. However, many parents do not know about the possibility of continued Medicaid and workers often fail to provide them with appropriate information about their potential ongoing eligibility.
To help reduce the number of uninsured children and to increase their access to medical care Congress established, in 1997, a new Children’s Health Insurance Program (CHIP) as Title XXI of the Social Security Act. Intended to supplement — not supplant — Medicaid, CHIP is designed to find and enroll "targeted low-income children" whose family income puts them above the Medicaid eligibility threshold, but below an income level that makes private health insurance premiums affordable. A targeted low-income child is one whose family income does not qualify for Medicaid, but is lower than 200 percent of the FPL — approximately $32,000 for a family of four, in 1998.4
The statute clearly requires States to first screen every child for Medicaid eligibility before determining eligibility for CHIP. In this way, Congress sought to ensure that every child is enrolled in the correct program and that CHIP would help increase the number of insured children across the nation.
Key Requirements for CHIP
The law allows States to provide children’s health insurance in one of three ways: 1) by developing a State-initiated plan for children’s health insurance; 2) by expanding current State Medicaid provisions to incorporate more uninsured non-Medicaid children; or 3) a combination of both. The law further lays out options for the benefits package of CHIP programs in States choosing to implement a State-initiated program. Those States must provide benefits equivalent to one of the following: benchmark coverage (i.e., the standard Blue Cross/Blue Shield Preferred Provider Option, the health plan that is provided for State employees, or the HMO plan with the largest enrollment in the State); benchmark-equivalent coverage (any other health plan that is equivalent to the benchmark plans); existing comprehensive State-based coverage (coverage that already exists in another Statewide program in Florida, Pennsylvania and New York); or other coverage approved by the Secretary of HHS.
States are required to submit, for approval by the Secretary of HHS, a detailed plan of the proposed CHIP program. States need to include the following information in their State Plans:
- Type of program (State-initiated, Medicaid expansion, or a combination);
- Overview of current coverage for children and how the new plan will be integrated;
- Eligibility requirements and enrollment procedures;
- Outreach strategies to make the public aware of the new program;
- Cooperation between the program and other public and private insurance programs;
- A description of cost-sharing, (such as premiums, co-payments, and deductibles to be charged to families);
- Performance goals and measures;
- Procedures for data collection, assessment, reporting, and evaluation of the program; and
- Outline of the budget.
The law provides for higher Federal matching funds to States for CHIP than the regular Medicaid program. Because of this "enhanced matching rate" for CHIP, additional provisions were added to ensure that Medicaid eligible children are enrolled in Medicaid and not CHIP, and that CHIP coverage does not substitute for private coverage. These potential substitutions of coverage are called "crowd-out." See the sections in this chapter on Federal/State Financing and Crowd-out Prevention for additional details on the statutory requirements and HCFA(now known as CMS) guidance to States.
The Study
The Assistant Secretary for Planning and Evaluation(ASPE) in the Office of the Secretary, U.S. Department of Health and Human Services(HHS) commissioned the American Institutes for Research to conduct this study — intended to be one of the earliest studies of CHIP implementation.
Purpose
ASPE commissioned in the spring of 1998 a study of the early implementation of CHIP. The study was designed to understand and document the decisions in six States regarding the:ASPE intends the resulting report and the information collected about different State practices to be shared with other States, particularly those that might not be as far along in their own implementation.
- planning process;
- key factors affecting the program design in their initial plans submitted to HHS;
- CHIP program design as a separate State-initiated program, a Medicaid expansion, or a combination;
- choice of income eligibility levels;
- parameters of State-initiated health insurance programs implemented prior to CHIP; and
- implementation of specific features of their CHIP programs during the early months.
Issues Selected
ASPE staff chose, for its first study of CHIP, to focus on three issues of particular interest to them and the Health Care Financing Administration(now known as Centers for Medicare and Medicaid Services(CMS)) (HCFA(now known as CMS)), the agency administering the CHIP program. These issues are the States’ efforts to:
- conduct marketing and outreach activities;
- implement strategies to mitigate against the possibility of publicly-provided insurance substituting for private insurance (commonly called "crowd-out"); and
- collect data to evaluate their CHIP programs.
The methods utilized for this study emphasized site visits to selected States, and in-depth interviews with gubernatorial, executive agency, legislative, and advocacy organization staff. The information presented in this report, unless otherwise noted, reflects data and opinions presented by each State’s officials. AIR staff supplemented the interviews with reviews of relevant research on children’s health insurance and access to care, State Plans, State design papers, outreach materials, applications and enrollment packets, and available State research reports. Staff also interviewed national experts on children’s health, insurance coverage, welfare and Medicaid from the Center for Law and Social Policy, Institute for Health Policy Solutions, National Conference of State Legislatures, and National Governors’ Association. State visits were conducted between September 1998 and January 1999.
The product of those interviews and reviews are individual State case studies of the early implementation of CHIP. The case studies generally reflect conditions in the fall and winter of 1998/99, except in Colorado where significant changes occurred later that warranted inclusion in that State’s case study. All case study drafts were thoroughly reviewed for accuracy by State officials and advocacy staff who were interviewed.
States Selected
Selection of States to be the subjects of site visits and case studies was a group effort. In June 1998, ASPE convened an informal working group of representatives from their own office and from other divisions in HHS including HCFA(now known as CMS), the Health Resources and Services Administration, Agency for Health Care Policy and Research, and Administration for Children and Families.
The group determined that they would select States from among those with plans approved by HCFA(now known as CMS), as of June, 1998, that represented a mix along the following dimensions:
- CHIP separate State-initiated CHIP program vs. Medicaid-expansion, or a combination;
- Income eligibility level selected for CHIP;
- Those with and without pre-CHIP State health insurance programs for low-income families;
- Geographic distribution; and
- Demographic mix of the population.
Additional criteria for selection were that a State be far enough along in implementation (at least six months) that they have experiences to report, that there is evidence they have (or have plans to collect) data for evaluation, and that they subsequently indicate a willingness to participate in the study.
Based on these criteria, the working group chose the following States for inclusion in the study:
- Colorado
- Massachusetts
- New York
- Ohio
- Oregon
- South Carolina
However, by the time the site visit was scheduled in South Carolina, the Governor had lost his re-election and it was difficult for the outgoing staff to participate. To replace South Carolina with another southern State, Alabama was chosen. Exhibit 2 displays selected characteristics of the six States and their CHIP programs.
Organization of the Report
Chapter I is a cross-case analysis of early implementation in the six study States. It opens with an analysis of common themes and contrasts in the States’ legislative history and implementation of children’s health insurance, Federal/state financing of the programs, and key players in the administration of CHIP. The remaining sections focus on analysis of outreach activities, crowd-out prevention strategies, and data collection and evaluation methods.
Chapters II — VII are devoted to an in-depth case study of each State. Each case study is organized in the following manner:
- History and Implementation
- Federal and State Financing
- Current Enrollment
- Key Factors in the State’s Implementation
- Outreach
- Crowd-Out Prevention
- Data Collection and Evaluation
Featured in the section on outreach is advice the State officials chose to share with other States. Where available, the individual case studies provide Web addresses for other States to access outreach materials, application forms, research studies, and other reports.
HISTORY AND IMPLEMENTATION
A history of pre-CHIP programs in most of these States helped smooth enactment of conforming legislation. Since five of the States were poised to expand health insurance for low-income children at the time that Title XXI passed, it made it easier to quickly conform with Title XXI provisions. In all six States, implementation of CHIP was smoothed by broad-based advisory boards of private and public officials, gradual expansion of coverage, and targeted outreach to known pools of CHIP-eligible children who were already enrolled in State-funded (pre-CHIP) public health insurance programs.
| Precedence was helpful. Five States had a history of State-initiated programs to provide public insurance or direct services for uninsured, low-income children. Those States were able to build on existing administrative structures, outreach, enrollment practices, and provider networks. |
- Colorado’s history dates back to 1983:
- The Colorado Indigent Care Program served poor, non-Medicaid residents of all ages through direct services by physicians and other fee-for-service providers who agreed to participate. The program focused on rural areas where residents were especially under-served and included outpatient and inpatient services.
- The Colorado Child Health Plan (1990) originally provided free insurance for outpatient and preventive services to children under age nine in families with incomes below 185 percent of poverty.
- Massachusetts’ history dates back at least to 1993.
- The Children’s Medical Security Plan was created to serve uninsured children. Over time, its age and income eligibility criteria expanded to cover children up to age 19 living in families ineligible for Medicaid.
- The Insurance Reimbursement Program was proposed to offer tax credits to businesses covering 50 percent of the insurance costs for employees with incomes below 200 percent FPL. This proposal was later modified several times and it now provides direct subsidy payments to families through the Premium Assistance Program.
- New York’s history dates back to 1990 with a program to provide primary, preventive care to non-Medicaid-eligible children under age 13. The program subsequently expanded by adding children one year older each year until children up to age 15 were covered.
- Oregon obtained a landmark Section 1115 waiver in 1993 to ration care in its Medicaid program, Oregon Health Plan. The waiver allowed the State to expand eligibility to persons who would not have otherwise qualified for Medicaid coverage.
| Timing was critical. Five States were poised to expand coverage for more uninsured, low-income children when Title XXI passed. This facilitated their efforts to comply with the new Federal requirements for Title XXI and allowed them to quickly initiate CHIP. |
- One State Legislature had just approved expanding the Healthy Start Medicaid program. Officials were ready to submit two amendments to their Medicaid State Plan and quickly prepared a CHIP State Plan. (Ohio)
- Another State Legislature passed a law further expanding Medicaid eligibility from 133 percent to 150 percent FPL for children through age 18. (Massachusetts)
- One State Legislature was poised to approve a Section 1115 waiver request to HCFA(now known as CMS), expanding their pre-CHIP health insurance program for low-income, uninsured children to include inpatient and mental health services. This was, coincidentally, a big step in complying with XXI requirements. (Colorado)
- Yet another State Legislature had just approved moving Medicaid eligibility from 100 percent for children under age six to 170 percent for children through age 12. After Title XXI passed, the Emergency Board (which takes action when the legislature is out of session) quickly approved expanding the age eligibility to age 18 and redirected State matching funds from the planned Medicaid expansion to CHIP. (Oregon)
- A State wanted to expand its Child Health Plus program so Title XXI provided additional funds. State legislation was passed to enhance the existing program and to ensure its compliance with Federal requirements. (New York)
- Finally, one State Legislature was meeting for a special budget session just after Title XXI passed so CHIP was added to its agenda. (Alabama)
| Bipartisanship prevailed. Interviews with legislative and executive officials testify to the bipartisanship that is a hallmark of both pre-CHIP and CHIP enabling legislation. Officials reported that "doing good things for children’s health" is endorsed by both parties in all States. |
| Finding State matching funds was easier in some States than others. The strong fiscal condition of some States, and their attendant budget surpluses helped. In two States, statutory limitations on expenditure growth capped funding. In two States, increased tobacco taxes provided additional revenues for children’s health. |
- One State Legislature was already in a special budget session and the gubernatorial race created a climate to discuss "What is best for Alabama’s uninsured children?" This facilitated consensus and a Joint Resolution passed authorizing $5 million for the initial State match. (Alabama)
- Two State Legislatures raised tobacco taxes, earmarking the projected receipts for children’s health initiatives. (Massachusetts and Oregon)
- One State Legislature had already given the State Medicaid agency approval to expand their Medicaid program. When Title XXI was passed, the funds were already in place and the State was able to go ahead with the expansion and take advantage of the enhanced match. (Ohio)
- Two States face statutory limits on annual spending increases that limited CHIP funding. (Colorado and Oregon) In one of these States, the program also relies on private funding sources to supplement State appropriations. (Colorado)
| States’ experience with Medicaid played a role in the debates in two State Legislatures. |
- One State Legislature chose the Department of Public Health, rather than the Medicaid agency, to administer its CHIP program. At the time, the Medicaid agency was facing a serious shortfall and historically, the agency has little support among legislators, health care providers, and child advocates. (Alabama)
- Another State Legislature was concerned about an earlier time when the Medicaid costs escalated. At that time, the legislature voted to drop the Medicaid program and while the governor vetoed the bill, legislators had continued concern about the program’s impact on the State’s statutory annual limit on spending increases. For this reason, a Medicaid expansion was never considered as an option for the State’s CHIP program. (Colorado)
| Advisory groups helped some States secure buy-in from a wide group of interested stakeholders. Through a variety of mechanisms, private sector CEOs, physicians, family representatives, and executive agency officials helped design programs and built broad support among Governors, legislators, advocates, and other stakeholders. |
- A Children’s Health Insurance Program Commission helped plan a new State program. Chaired by the State Health Officer, Commission membership included State legislators, executive agency staff, and non-profit representatives. The commission received help from an Advisory Council comprised of stakeholders from a variety of constituencies. (Alabama)
- One State convened a Policy Board that receives input from design teams and work groups on specific issues. The Policy Board includes the CEOs of Kaiser Permanente, Blue Cross/Blue Shield, the State branch of the country’s largest private retirement fund, the State American Academy of Pediatrics chapter, Valley-Wide Health Services, a pediatrician from University Hospital (who played a key role in Colorado’s earlier State children’s health insurance programs), and the executive directors of four State agencies. The Board also includes a parent whose children are enrolled in the Colorado Children’s Health Program. The Board recommends policy on eligibility, benefits, cost sharing, managing HMO contracts, reporting and evaluation, and quality assurance. Design teams and work groups, with staff from several State agencies, report to the Policy Board. (Colorado)
- One Governor created a Task Force of 17 members representing health care providers, consumer advocates, businesses, State representatives, public health agencies and private health care plans. The Task Force met ten times during a five month period to develop recommendations for the Governor on Phase II — the expansion of CHIP to 200 percent FPL. (Ohio)
- A State Health Council was created by the State Legislature to recommend policy for the State Medicaid program and, later, CHIP. The Council consists of nine members of the public appointed by the Governor. (Oregon)
| Children’s advocacy organizations in all six States substantially influenced the planning and implementation of CHIP. They helped influence the design of benefit packages, advocated for low or no cost-sharing by families (premiums and co-payments), collaborated on outreach strategies and, in some cases, encouraged States to collect specific types of data. |
| Implementation is proceeding in phases in all six States. Some are first expanding their State-initiated programs and expanding Medicaid later while others are doing the reverse. Most States, but not all, are planning an employer buy-in program for a later phase. |
- Two States are expanding Medicaid during Phase I. (Alabama and Ohio) One has already implemented a separate State program in Phase II and is considering a Phase III to enhance benefits for children with special health care needs through a CHIP Plus program. (Alabama)
- One State’s Phase I expands its State-initiated Colorado Child Health Program (CCHP) into CHP+ while working to resolve issues to implement an employer buy-in program in Phase II. No Medicaid expansion is planned. (Colorado)
- Another State simultaneously expanded Medicaid eligibility and its State-initiated program (Children’s Medical Security Plan) in the summer of 1998. The Premium Assistance Program (subsidizing employer premiums) was to begin in January 1999, starting with companies having less than ten employees and later expanding to cover employers with less than fifty employees. (Massachusetts)
- One State expanded its State-initiated program (CHPlus) first, beginning in January 1999. Later, the income eligibility will increase for Medicaid. (New York)
- One State’s Phase I expanded Medicaid to cover eligible children up to 150 percent FPL and Phase II awaits legislative approval of Task Force recommendations to cover children up to 200 percent FPL. Phase II, although not a Medicaid expansion, plans to use the Medicaid (HealthyStart) infrastructure to administer the new program. (Ohio)
- Another State’s Phase I implemented a Medicaid "look-alike" program, adding teenagers up to 170 percent FPL. Phase II-A will try to link the look-alike program with an existing State-initiated premium subsidy program. In a potential Phase II-B, the State would request a waiver to work with its only State Health Insurance Purchasing Cooperative to encourage small employers to offer health insurance with help from State premium subsidies. Phase III may have a waiver request to reimburse community-based clinics for direct services to children who are difficult to reach with CHIP. (Oregon)
Title XXI of the Social Security Act authorizes $24 billion over five years for CHIP with specific allocations to each State.5 The formula for allocating funds is based on each State’s share of the nation’s low-income uninsured children in families with income below 200 percent of the Federal poverty level (FPL), adjusted for a geographic health care cost factor for each State. Federal matching contributions are called the "Enhanced FMAP."
The Enhanced FMAP for a State for a fiscal year is "equal to the Federal medical assistance percentage (i.e., the State’s Federal Medicaid matching rate6) increased by 30 percent of the difference between its regular Federal Medicaid matching rate and 100 percent; but in no case shall the enhanced FMAP for a State exceed 85 percent. Thus, the Federal contribution to total expenditures is higher in CHIP, vis-a-vis the State contribution, than it is in Medicaid. For example, a State that pays 50 percent of its Medicaid costs (with the Federal government paying the other 50 percent) has an enhanced Federal match of 65 percent and is responsible for 35 percent of the new CHIP costs.7
| None of the six States have drawn down their full Federal allocation of matching funds in the first year. |
First, some States designed limited "placeholder" plans that are starting small. In addition, as is common with all new Federal public assistance programs, these States need time to fully implement CHIP. Considerable staff time and attention is required to plan, analyze data for program design, obtain State legislatures’ approval, obtain Federal approval of official State Plans, design procedures and forms, select or expand on outreach strategies, collaborate with other public agencies and private organizations, and initiate or modify media campaigns. Implementing a new program must necessarily begin slowly, to allow time to test and redesign along the way, before full operation is feasible.
As a result, none of the six States are enrolling all eligible children or expending their full allotment of Federal funds in the first year. Even States with fully matured pre-CHIP health insurance programs cannot become fully operational in the first year or two. It has taken time for media campaigns and other marketing and outreach to succeed. States are, however, making concerted efforts to locate traditionally hard-to-reach populations, such as ethnic minorities and families living in rural areas.
Exhibit 3 portrays the allocation of Federal matching funds and State matching rates.
Exhibit 3
Federal/State Financing FY98
Funds Allocated | Matching Rate | |
| Alabama | $85.6 million | 21 percent |
| Colorado | $42 million | 34 percent |
| Massachusetts | $45 million | 35 percent |
| New York | $257 million | 35 percent |
| Ohio | $116 million | 29 percent |
| Oregon | $40 million | 27 percent |
Title XXI granted States considerable discretion to decide which agencies will oversee program administration, including outreach, eligibility determination, final enrollment, monitoring crowd-out, and collecting data for evaluation.
| CHIP implementation and administration in the six States reflects a rich mosaic of State agency partnerships and collaboration with other State and county agencies, community organizations, advocates, and the private sector. Many States also rely on different types of advisory groups to recommend policies, program design, and phased expansions. |
The individual case studies reveal the broad array of State agencies, county agencies, community organizations, advocacy groups and private sector organizations involved in design, administration, outreach, crowd-out prevention and data collection for evaluation.
- Alabama
- Lead agency: Department of Public Health
- Key collaborators: State Medicaid Agency, State Employees Insurance Board, Department of Education, Children’s Hospital, State Hospital Association, Children’s Rehabilitation Services, State Medical Association
- Colorado
- Lead agency: Department of Health Care Policy and Financing
- Key collaborators: Foundation for Children and Families (since replaced by a private, non-profit contractor), Department of Public Health and Environment, Division of Insurance, Community Health Network
- Massachusetts
- Lead agency: Department of Health
- Key collaborators: Department of Public Health, Area Health Education Center, Department of Transitional Assistance, Department of Education, Office of Child Care Services
- New York
- Lead agency: Department of Health
- Key collaborators: New York Health Plan Association, Unemployment Insurance Division, Child Support Enforcement Office, Department of Education
- Ohio
- Lead agency: Department of Human Services
- Key collaborators: 88 county agencies or non-profit organizations in those counties, Department of Health, Governor’s Ohio Family and Children First Council, Bureau for Children with Medical Handicaps, Child Care Centers, Medical and School Nurse Associations
- Oregon
- Lead agency: Office of Medical Assistance Program
- Key collaborators: Insurance Pool Governing Board, Office for Oregon Health Plan Policy and Research, 924 "community partners" representing a wide variety of State and local agencies and service providers
Title XXI requires each State plan to describe its efforts to identify and enroll all uncovered children who are eligible to participate in public health insurance programs. By law, enhanced Federal matching funds for spending on administration (direct services, administration, and outreach and data evaluation) cannot exceed ten percent of the State’s benefit expenditures. This limit may be waived by the Secretary, allowing the State to use more than ten percent for direct services, if these services are considered to be cost-effective. For States choosing to expand Medicaid, once they reach the ten percent limit for CHIP, they may only claim the regular Federal match rate for administrative expenditures.
HCFA(now known as CMS) stresses the importance of making enrollment as easy and accessible as possible for parents and communities. In a letter to State Health Officials, dated January 23, 1998, HCFA(now known as CMS) addressed the topic of outreach. For more information on HCFA(now known as CMS)’s outreach directives, see http://www.hcfa.gov/init/children.htm and click on Letters to State Officials as well as Frequently Asked Questions and Answers.
| All six States combined Statewide and community outreach efforts. The result is a wide mixture of arrangements between public and private agencies as well as non-profit organizations and for-profit companies. Some outreach services are performed through contracts with the State’s lead CHIP agency and some are in-kind donations. |
- A State Department of Health coordinates the Statewide media campaign, but contracts local efforts to a "community outreach coordinator" who staffs a toll-free hotline for families and conducts a wide array of activities in communities. The private managed care plans actually enroll eligible children. (New York)
- A Department of Human Services maintains a toll-free Statewide Consumer Hotline and works with many State agencies to disseminate information to providers and families while individual counties develop and implement their own customized outreach plans. (Ohio)
- One lead State agency built upon existing relationships among other public agencies and private organizations to reach families as quickly as possible. Efforts were made to educate a wide variety of child-serving providers and specific professional audiences about the new program and mailings were sent to all public school districts. (Alabama)
- Another State agency combines outreach for both CHIP and its State-funded children’s health insurance program and offers training seminars to a variety of participants, including private insurance agents, who have contact with uninsured families. (Oregon)
- A non-profit organization, under contract to the CHIP lead agency, conducts selected outreach activities. Its key feature is the use of Satellite Eligibility Determination sites in community locations where families can enroll immediately. Several sites now have the capacity to process applications through an electronic connection with the lead agency’s central database; the Network plans to expand this capacity, which is expected to increase enrollments significantly. (Colorado)
- A State agency focused on moving children from a State-funded program into CHIP while local community groups received special grants from the State to help enroll hard-to-reach populations. (Massachusetts)
| States conduct aggressive outreach when they have the fiscal resources to enroll all the children who apply. While some States can market CHIP to "find every eligible child," others must target the children they can enroll given the State’s fiscal constraints. |
- Four States’ CHIP lead agencies have aggressive, multi-pronged marketing and outreach campaigns to find eligible children and enroll them. (Alabama, Massachusetts, New York and Ohio)
- Two other States’ agencies have been more cautious about their outreach because their budgets limit the number of children they can enroll. In these States, other agencies organized CHIP outreach initiatives as part of their promotional efforts for other public children’s health programs. (Colorado and Oregon)
| States used the existing pool of children already enrolled in public health insurance programs to target their efforts to reach newly-eligible children. |
- Where Medicaid expansion is part of CHIP, staff sent mailings to households where some children are already covered by Medicaid to notify older siblings that they may now qualify. (Alabama and Massachusetts)
- Where there are existing State-funded programs, staff directed marketing campaigns at this known pool of children enrolled in them, to encourage parents to convert their children to CHIP. (Colorado, Massachusetts and Oregon)
A Seamless Health Care System for Children
State officials recognize the need to design an insurance system for lower income children that can accommodate changes in family circumstances that affect program eligibility. It is not uncommon for children’s eligibility to fluctuate between Medicaid, CHIP, private insurance, and/or State-funded programs when employment, family income, or other circumstances change. All six States have taken steps to ensure that children have the continuity of health care that they need.
| States simplified application forms and eligibility determination processes for multiple programs. |
- All States developed a simplified, integrated application that is used for both the CHIP and Medicaid programs.
- Two States use the same application for the Special Supplemental Food Program for Women, Infants and Children (WIC). (New York and Ohio)
- One State’s application also enrolls children for Children and Family Health Services and Bureau for Children with Medical Handicaps. (Ohio)
- Four States allow families to mail in their CHIP applications so there is no need to go to a government office. (Alabama, Massachusetts, Ohio and Oregon)
- Five States provide a Statewide toll-free telephone number for families to call where trained personnel help them complete applications. Three of them mail applications to families to sign, attach necessary documentation, and return by mail for processing. (Ohio, Oregon and Alabama, where families receive a postage-paid envelope to return the signed application.)
- In one State, information from the integrated application is entered, and an automated decision tree places the children in the appropriate public health insurance program depending on the family income and insurance status. After qualifying, families get an information package in the mail to select a managed care plan. (Massachusetts)
- To expedite enrollment in Phase I, a new simplified Medicaid application was developed to add CHIP-eligible teenagers living in families where other children are already enrolled. (Alabama)
| States offer presumptive and continuing eligibility to help ensure the continuity of health care. |
- Four States (all but Alabama and Colorado) offer variations on presumptive eligibility during the time it takes the State to process applications.
- All States offer continuing eligibility. Oregon and Ohio provide it for six months while the others offer it for 12 months.
Collaboration Among Public and Private Agencies
All six States are organizing creative collaborations to market CHIP to eligible families. The CHIP lead agencies have entered into innovative public-private partnerships and are also forging new relationships with other State agencies, private organizations and provider networks.
| CHIP lead agencies created new public-private partnerships to help market the program and to enroll eligible children by contracting with non-profit or for-profit organizations. |
- In two States, a second State agency, under contract to the lead agency, helps administer CHIP. In one of those States, a State Employees Insurance Board serves as the enrollment broker. SEIB has experience managing another health benefit program in the State so it was well-positioned to help with CHIP. SEIB hired and trained staff to answer questions and take applications over a Statewide toll-free telephone number. (Alabama) In a second State, the Insurance Pool Governing Board, which administers several other health insurance subsidy programs for low-income individuals, has taken responsibility for marketing, evaluation, and outreach to children in families likely to be CHIP-eligible. (Oregon)
- An actuarial analysis firm, under contract to the CHIP lead agency, provided assistance when the State designed the RFP for private vendors and helped assess bids that were received after it was issued. The firm had previous experience working in the State’s insurance market and was also familiar with child health insurance programs in other States. (Alabama)
- A community outreach coordinator, under contract to the lead agency, attends local events across the State and organizes a variety of activities to educate the public about children’s health insurance programs. Numerous promotional materials are used as part of the public education effort: bumper stickers, Frisbees, refrigerator magnets, and sun visors. The outreach coordinator also staffs a Statewide toll-free number for families to call for information about available benefit programs. Families select a health plan for their children and the plan enrolls them. All participating plans must submit a marketing and enrollment plan to the Department of Health for review and approval prior to implementation. (New York)
- A foundation, and later a private, non-profit organization, under contract to the State oversight agency, administers the CHIP program. Its staff conducts marketing, handles customer services, processes applications, finalizes enrollment, develops the management information system, analyzes data on outreach, and also maintains the provider network. (Colorado)
| CHIP lead agencies coordinated outreach with a variety of State agencies to reach large numbers of potentially eligible children. |
- The collaborating agency staff sent notices to food stamp recipients and the State Medicaid agency placed inserts about children’s health insurance programs in Medicaid denial notices (Oregon)
- The Department of Transitional Assistance provides the Division of Medical Assistance with lists of families recently terminated from the time-limited welfare program. DMA notifies these families about their continued eligibility for Medicaid, which they often do not know about. (Massachusetts)
- A lead agency mailed information to 85,000 WIC households inviting them to call the Consumer Hotline and/or apply for public children’s health insurance programs, which generated a tremendous response. (Ohio)
| State Education departments and local school districts are critical outreach partners. |
- All school superintendents received an informational mailing about the program that also described available outreach materials. At the local level, the outreach coordinator arranged for materials to go home with students, including with report cards. (New York)
- Immediately after Phase II began, all school-age children received a program brochure and application with a self-addressed stamped envelope to return to the enrollment broker. Over 750,000 applications were distributed. (Alabama)
- The Department of Education and Office of Child Care Services play major roles in the State’s annual school-based outreach effort to provide information through every public and private school and every child care program in the State. (Massachusetts)
- Thousands of applications and brochures were sent to school district contacts. Program staff report that nearly one-third of callers to a Statewide phone bank report hearing about CHIP from their children’s school. Orientation sessions were held in school districts identified as having a large percent of children enrolled in the school lunch program. (Colorado)
| CHIP lead agencies coordinated outreach with other State health agencies, especially when CHIP includes expanding Medicaid. |
- One lead agency worked with the medical assistance agency to mail notices to all 300,000 Medicaid households and all 10,000 Medicaid managed care providers. Brochures were distributed widely, especially to outstationed Medicaid workers who are placed in county health departments, hospitals, clinics and community health centers. These outstationed workers are electronically connected to the State Medicaid computer system to expedite the eligibility process. (Alabama)
- CHIP outreach was incorporated into on-going efforts by public health nurses to educate families about other child health initiatives. (Colorado)
- Two States’ lead agencies mounted a major effort to move thousands of children enrolled in the State-funded children’s health insurance program into the CHIP. Families received letters, with an application, that explained their potential eligibility for the new program and described its advantages. In one of these States, families who did not respond to the letter were personally contacted by specially trained college students who made calls at night or over the weekends when families were most likely at home. (Massachusetts) In the other State, families that did not respond to the mailing or did not agree to switch programs were permitted to maintain their enrollment in the old program for one year beyond their enrollment date. (Colorado)
| CHIP lead agencies relied heavily on a wide variety of child-serving providers, including health professionals. |
- Two free, live satellite video conferences were produced by the CHIP lead agency. They were available for viewing at county health departments and other facilities with satellite downlinks in multiple sites on two different dates. Copies were also distributed to those who could not attend the live broadcast. The video was viewed by educators and school guidance counselors; social workers; hospital staffs; different medical professionals; child care providers; social service workers; and clergy. The lead agency also produced videos for five special professional audiences who see potentially eligible children. (Alabama)
- Agency staff conducted more than 100 training seminars at a variety of locations where uninsured families are most likely to visit or live. Seminars last half a day and are well attended by a variety of "community partners" who have contact with uninsured families. Community partners include representatives from State agencies; community action agencies; WIC programs; school districts; service agencies for homeless families, and youth shelters. Over 900 private insurance agents also attended. (Oregon)
- A CHIP lead agency sent a mailing to nearly 12,000 licensed home-based and center-based child care facilities to inform both families and child care providers who may not have health insurance for their children. (Ohio)
- A non-profit organization (the Children’s Health Network) conducts outreach through Satellite Eligibility Determination sites. These 36 sites (and nine more are planned) are located in various community settings, such as school-based health clinics and community health centers, where eligibility is determined immediately. Five sites process applications through a computer link to a central database, and by late 1999, half the sites will have the computer link. To educate child-serving professionals, training sessions were held in local communities to teach participants how to help families complete the application. Over 800 people participated including: public school nurses, social workers and psychologists; EPSDT workers, Family Resource Center and Head Start staff, and school-based health center staff. (Colorado)
- The Community Partnerships Initiative was developed by the CHIP lead agency to identify and disseminate information and applications through key community stakeholders. Partners included school nurses, municipal skating rink directors, librarians, summer camp directors, public housing directors, civic and neighborhood association leaders and others. (Massachusetts)
- In three States, CHIP lead agency staff worked closely with different medical associations by offering seminars to explain the program, sending informational packets and using their newsletters. A Children’s Hospital provided information through its Sports Medicine Clinic to reach uninsured teenagers. It also reviewed its records to identify all uninsured children seen over the past 18 months and sent them letters explaining the new program along with an application package. (Alabama, Massachusetts, Ohio)
| Some CHIP lead agencies target outreach for children with special health care needs. |
- One lead agency is coordinating discussions among the appropriate agencies to develop CHIP/Phase III, to address the special needs of children with disabilities and chronic health conditions. The State Children’s Rehabilitation Services (CRS) identified children in its program who are uninsured and contacted their families to explain the new program. CRS pays CHIP premiums and co-payments for children in its Children with Special Health Care Needs program, because it is more cost-effective to provide this primary and preventive care than to face the higher specialty costs that may later be incurred. With the projected savings due to ALL KIDS and CHIP coverage, CRS reintroduced services to these children that were previously eliminated because of funding cutbacks. (Alabama)
- Another State added questions to the application, expressly designed to refer children with special health care needs to that program and to the Supplemental Security Income (SSI) program. (Colorado)
- One Bureau for Children with Medical Handicaps sent informational mailings to families already enrolled in BCMH families as well as those now applying or having a re-certification. The mailing explained CHIP and directed the families to call the Consumer Hotline to begin the enrollment process. (Ohio)
Marketing to Hard-to-Reach Populations
All States expressed concern about locating under-served populations and recognized the need to customize strategies for different cultural and ethnic populations.
| States recognize the need for local groups to conduct outreach in their own communities, in order to customize marketing approaches and materials to discrete hard-to-reach populations. |
- Three State agencies in one State contribute funds to support a competitive mini-grant program. The program targets organizations that have successfully demonstrated their ability to serve their communities, especially hard-to-reach families who would not otherwise have health insurance coverage. The mini-grant program awarded grants to 52 organizations last year. The grants, which range from $5,000-$20,000, were awarded to community health centers, housing groups, child care agencies, immigrant and refugee service programs, and hospital community programs. Mini-grant recipients attend monthly regional Health Access Networks, along with other health-related community groups, to meet with local and State public agency staff to share information and develop linkages to facilitate outreach. (Massachusetts)
- One State is developing a "facilitated enrollment" process to assist families applying for Medicaid or CHIP. Community workers will help families through the application process by screening them for the appropriate program, completing the application, collecting required documentation and submitting the application to the appropriate organization for eligibility determination. The goal is to recruit facilitators who work in a variety of community settings (e.g., child care, social services, schools) and who speak different languages, among the diverse populations. (New York)
| States recognize the need to provide accessible information for bilingual families. |
- A simplified, unified application will soon be available in English and Spanish. (Ohio)
- Staff developed brochures, posters, enrollment packets and benefit booklets in Spanish and English. They plan to expand and enhance a toll-free Family Health Line to add Russian and Southeast Asian languages to the current Spanish and English translation capabilities. (Colorado)
- The League of Community Health Centers promoted child and family health insurance enrollment through an English/Spanish poster campaign. (Massachusetts)
| States recognize that certain populations need more individual attention. |
- Staff met with fishing families in eight coastal communities to inform them about the public children’s health insurance programs. In addition, they attended conferences for two Native American tribes and held Rural Health Forums across the State. (Oregon)
- Staff consulted Native American tribal representatives about how to best inform families about public health insurance. Tribal members want to develop fact sheets for health care providers to explain specific cultural beliefs about health that affect how certain medical conditions are prevented or treated. (Alabama)
- Staff held a series of Statewide meetings with Latino community leaders to increase awareness about the availability of public health insurance and develop effective outreach and marketing strategies for Latino neighborhoods. (Massachusetts)
- Public health nurses go door-to-door in trailer parks and many of them reach deeply into rural parts of the State. (Colorado)
- One CHIP lead agency sent a mailing to approximately 13,000 individuals affiliated with the State Council of Churches. They also worked with the Commission on Minority Health to notify many minority clergy about the program. (Ohio)
| All States use print and electronic media as part of their public education, especially to reach families living in rural areas and those who rely on their own ethnic newspapers or radio/television stations. |
- A public relations firm, under contract, was hired to generate continuous media coverage for the CHIP program. The firm is expected to develop newsworthy stories about participating families, providers and prepare press releases to cultivate and maintain interest in the program. Ads were placed on 40 Hispanic radio stations(Colorado) and a Public Service Announcement was developed for a Latino television station. (Massachusetts).
- A media event was held on the steps of the State Capitol when the new State program began. It was broadcast to eight sites around the State where press conferences, hosted by members of the State Hospital Association, were held to promote CHIP in the local community. (Alabama)
- One Department of Health runs a major Statewide media campaign. State officials believe radio and television ads were most effective because they reach large segments of the general population. (New York)
- Public service announcements were developed for a Latino television station. (Massachusetts)
- Most States ran television and radio ads, prepared news releases and camera-ready copy for newspapers.
| States are using different funding sources to cover their outreach expenses. |
- One State allocated most of the Medicaid eligibility outreach funds, available through the Temporary Assistance for Needy Families (TANF) block grant, to counties based on the number of their potentially eligible Medicaid individuals. To receive the outreach funds, county stakeholders (e.g., local Department of Health, country departments of human services, advocacy organizations) had to develop an outreach plan through a collaborative process. Counties were also required to provide matching funds. (Ohio)
- Two State agencies in one State allocated funds for the mini-grant program designed to find hard-to-reach families. These funds are a mixture of Medicaid, Title XXI and TANF block grant dollars. (Massachusetts)
- Using Title XXI funds, the State will significantly supplement its outreach budget to fund facilitated enrollment in local communities across the State. (New York)
| States are allocating outreach funds for a variety of activities or program-related expenses. |
- Half the States expect to exceed the ten percent cap on enhanced matching funds for administration because of outreach expenditures. (Alabama, Colorado, and Oregon) Colorado projects those expenditures will reach 16 percent of total expenditures in the first year, for outreach and other administrative costs.
- Most outreach funds were spent to print and distribute date-stamped application forms and to provide training for community partners around the State. (Oregon)
- Most outreach funds were spent to print 1.5 million program brochures, applications and return envelopes with postage paid. The agency made a conscious decision to use an attractive color brochure that makes the CHIP program look different from a typical government program. (Alabama)
- In one State, the primary expenditure for outreach is the contract with a private, non-profit organization (formerly a foundation). In addition, a $75,000 grant for outreach was awarded to the Children’s Health Network from the Federal Health Resources and Services Administration. (Colorado)
Woodwork Effect
Some agency officials and legislators worry that vigorous outreach for public insurance programs will draw more eligible individuals "out of the woodwork" than originally projected, and drive costs beyond anticipated levels.
| Many States are using CHIP to surface children eligible for Medicaid, as well as CHIP. Some are concerned about the effect of CHIP outreach on Medicaid growth. Still others are concerned about exceeding initial target enrollments for CHIP, itself. |
- State agency staff in two States worry about creating more demand for CHIP than they can respond to and having to start waiting lists. They are also concerned that CHIP outreach will locate more children who are Medicaid-eligible, which will significantly increase State costs. (Oregon) In another State, there was similar concern during the first seven months of implementation, but that concern has abated since enrollments are falling short of the target. Staff in both public and private agencies disagree about whether aggressive outreach will produce CHIP waiting lists. Although the State budget limits how many children can enroll, some staff believe that the cost sharing requirements deter enough families so that target enrollment numbers are not likely to be reached. (Colorado)
- As a result of outreach efforts for the non-Medicaid CHIP program, applications for Medicaid soared. Although Medicaid staff anticipated that CHIP outreach would increase enrollment, the agency was surprised by how quickly families responded and how large a backlog of applications it created. (Alabama)
- CHIP lead agency staff, by design, planned a Medicaid waiver demonstration project to attract many families who were previously eligible for, but not enrolled, in Medicaid. They estimate that two of every three families applying this past year fall into that category and hope that CHIP outreach will have the same effect. (Massachusetts)
- State officials recognize that a woodwork effect may result from its aggressive efforts to identify uninsured children who may qualify for CHIP or Medicaid. They want to encourage eligible children to enroll in Medicaid by reducing its stigma and making the application process more convenient for the family through a newly facilitated enrollment process. (New York)
Congress has a longstanding concern about whether Federally subsidized health insurance programs unintentionally encourage families to substitute free or low-cost public insurance for their existing private health coverage. In addition, Congress is concerned that the increased availability of public insurance through CHIP may encourage companies to drop coverage for their employees or dependents. This concern about whether public insurance will substitute for private coverage is commonly referred to as "crowd-out." Congress is also concerned about another potential form of crowd-out — that States may substitute CHIP coverage for Medicaid coverage in the face of the enhanced Federal matching rate for CHIP. With the passage of Title XXI, Congress expressly directed States to guard against crowd-out and, where necessary, adopt measures to prevent it.
Employee crowd-out occurs when families drop employer-provided insurance coverage altogether, or disenroll their children in the dependent portion of that coverage, in order to enroll them in public insurance. It may also occur with families already enrolled in public health insurance who obtain a job with employer-provided dependent coverage, but do not switch their children to that coverage.
Employer crowd-out occurs when employers cease offering health insurance, or cease offering dependent coverage, because they believe the children could be enrolled in public insurance plans. It may also occur where employers might otherwise offer health insurance with dependent coverage (especially new businesses) were it not for their awareness of public health insurance available for children.
Some State officials believe that employee crowd-out is not a genuine concern, at least until the income eligibility levels for public insurance reach at least twice the Federal poverty level. Officials often point to a study in Minnesota8 that documented little to no crowd-out.9 Others believe that some small amount of crowd-out is a price the nation should be willing to pay in exchange for providing low-income children with health insurance that provides access to medical care.
According to the Institute for Health Policy Solutions, little is known about what policies effectively reduce crowd-out. Only a handful of States have State-only programs that pre-date CHIP and offer comprehensive health benefits coverage for children in families with incomes up to 200 percent of poverty. Even fewer have implemented direct measures intended to reduce crowd-out. Further, no empirical evaluations have been conducted of programs that have adopted these measures.10
There has been no research on employer crowd-out. There is, however, a national trend towards reducing employer-provided health insurance — a trend that has not yet been correlated with growth in public insurance programs for low-income children. This trend is evident in all of the case study States, except Oregon.
"Title XXI requires that every State Plan include a description of procedures to ensure that the insurance provided by CHIP does not substitute for coverage under (private) group health plans." Policy options identified by States to mitigate or prevent crowd-out include:
- Setting the income eligibility level (percentage of Federal Poverty Level) low enough so as to attract families unlikely to have been covered by employer insurance;
- Adopting waiting periods before families previously covered by employer insurance can qualify;
- Adopting cost-sharing provisions using premiums and/or co-payments for families with higher incomes, to mirror the private/employer insurance market;
- Imposing lock-out periods on families failing to pay their premiums;
- Subsidizing the families’ premiums, called employer buy-in, for employer-provided dependent coverage, under certain circumstances approved by HCFA(now known as CMS).11
In States with CHIP Medicaid expansions, Title XXI requires that a State: must assure that it will coordinate its program with other public and private programs; may not make its Medicaid eligibility requirements stricter (to crowd children out of Medicaid and into CHIP to claim the enhanced matching rate) than those already in place on June 1, 1997; and must screen CHIP applicants for Medicaid eligibility and enroll them in the latter, if eligible.
On February 13, 1998, HCFA(now known as CMS) issued guidance for States intending to use CHIP funds to subsidize employer-sponsored group plans. They must develop provisions for their plan that are equivalent to the following:
- ensure that coverage is targeted to children whose families were previously unable to afford dependent coverage — Children cannot qualify for subsidies through an employer sponsored group health plan if the family had coverage for them within the previous six months. States can require a longer period of uninsurance, but no longer than 12 months. Exceptions are allowed if the prior coverage was involuntarily terminated. Newborns who are not covered by dependent coverage would not be subject to any such waiting period.
- discourage employers from lowering existing contributions for dependent coverage—States can only provide subsidies to purchase dependent coverage through employer-sponsored group health plans when the employer contributes at least 60 percent of the cost of family coverage, the median employer contribution nationwide. HCFA(now known as CMS) will consider a somewhat lower level if states have additional provisions to limit employers’ ability to lower contribution levels.
- ensure that providing child health coverage through employer-sponsored group health plans is cost effective and that the state is not inappropriately subsidizing coverage for adults in a family—States cannot pay more for a child enrolled in an employer-sponsored group health plan than what it would spend if the child was enrolled in a separate CHIP plan or Medicaid.
- promote cost effectiveness—Families electing to receive child health assistance through an employer-sponsored group health plan must apply for the full premium contribution available from the employer.
- demonstrate cost effectiveness—States must collect information and conduct an evaluation that examines the substitution (if any) that has occurred under the program and the effect of these provisions on access to the program.
| The six case-study States adopted a variety of policy options to prevent employee crowd-out. Some State officials dismiss employee crowd-out as a problem, especially where a pre-CHIP program was operating that showed no evidence of crowd-out. They adopted one or two policies, nevertheless, because the statute requires it. One State is taking a wait-and-see policy. Other State officials are concerned about employee crowd-out and adopted multiple policies to prevent it. |
| Some officials were sanguine about employee crowd-out, but genuinely concerned about employer crowd-out. One State is subsidizing employers’ premiums with the goal of sustaining employer-provided health insurance for children and attracting more small employers into the employer-provided insurance market. |
- One State expressly pegged its CHIP income eligibility level at 185 percent FPL in an effort to avoid crowd-out. This FPL level is also used for the State’s pre-CHIP health insurance program where officials do not believe that any crowd-out has occurred. (Colorado)
- In another State, some concern about crowd-out affected the decision to cap the CHIP program at 250 percent FPL. (New York)
- The other States did not cite the FPL level as a crowd-out prevention strategy. Two States are simply expanding Medicaid to older children for Phase I (Alabama and Ohio). Another State moderately raised the FPL level for CHIP/Medicaid so employee crowd-out in families with moderate income is not viewed as an issue. (Alabama)
Waiting Periods
Waiting periods are policies that require families currently enrolled in, or who recently dropped, employer coverage to have no coverage for some months before their children qualify for CHIP. Waiting periods are sometimes also called "look-back periods." Some States have raised equity concerns about waiting periods: should the waiting period for eligibility apply to families currently or recently insured or should it also apply to those with access to employer coverage that chose not to enroll?
| Four States use waiting periods as an explicit strategy to prevent employee crowd-out. They only apply the waiting periods to children currently or recently insured by employers. (Alabama, Colorado, Ohio (Phase II), Oregon) Three States use a three-month waiting period (Alabama, Colorado and Ohio) while another uses six months. (Oregon) |
One State currently has no waiting period, but is monitoring quarterly information. If evidence shows that CHIP is substituting for private coverage in excess of eight percent, then the State will impose a six month waiting period. (New York)
In two States, the equity issue was debated.
- One State chose to apply it only to the currently or recently insured because policymakers determined it would be too complex to assess the potential availability and affordability of workplace health insurance for families. (Colorado)
- In the other State, the discussion among State agency officials, a policy council, and advocacy organizations was particularly contentious because the proposed waiting period was six months. However, a small majority prevailed and the six month waiting period is not imposed on families who have access to, but never enrolled in, employer insurance programs. The decision was made for reasons similar to those in Colorado. (Oregon)
| Four States impose premiums on families at graduated levels depending on family income (Alabama, Colorado, Massachusetts, New York). Two of these States also require co-payments. |
A Task Force planning Phase II/CHIP recommended that the legislature impose both premiums and co-payments. The issue will be debated as part of the legislature’s biennial budget for State fiscal years 2000 and 2001. (Ohio) See Exhibit 4 for cost-sharing levels.
Lock-out Periods
When States use premiums as a crowd-out prevention strategy, they may impose lockout periods as a sanction against families who fail to pay their premiums. A lockout is a period of time when children are excluded from coverage, or disenrolled by the administering agency, for an arrearage in premium payments.
Two States impose lockout periods.
- Families who fail to pay receive three written notices and a 30-day grace period. Continued failure to pay excludes the children from CHIP for six months. (Colorado)
- Families who are in arrears for two months are locked out of CHIP for one year. There are, however, special hardship provisions. (Massachusetts)
Alabama has no lockout period, but children cannot re-enroll for a new year if premium payments are not current.
Employer Buy-in
Title XXI permits States, under certain circumstances, to "buy in" to employer insurance, by subsidizing employee premiums.
| Among the six States, three have or are planning a program to help employees buy in to employer insurance by subsidizing their premiums. One State’s program is operating while two others are planning pilot programs later in their CHIP implementation. |
- In one State, officials believe that employer and employee subsidies offer the most effective way to discourage further erosion of employer-sponsored health insurance. Under a Medicaid waiver, the State’s Insurance Reimbursement Program (IRP) provides premium assistance payments for families (and individuals) with incomes below 200 percent FPL. The IRP also offers incentive payments for small employers who provide insurance to lower income employees and pay at least half the premium cost. The program will begin with companies of less than ten employees and expand to those with less than 50 employees. (Massachusetts)
Two States want to pilot programs with a purchasing cooperative of employers.
- In one State, officials are working with HCFA(now known as CMS) to develop an employer buy-in program. In December 1998 they were developing a "white paper" raising the issues and questions that must be answered in order to select program features. The current plan would pilot the program with a purchasing cooperative of employers who offer a standardized benefit package. (Colorado)
- In another State, officials may request HCFA(now known as CMS)’s permission, in a Phase II Plan Amendment, to pilot an employer buy-in program. They would work with the State’s only health insurance purchasing cooperative to market CHIP to employers for eligible families who are not enrolled in their employer’s plan. (Oregon)
In order to insure that State programs are effective and are reaching the intended populations, States need to collect information and report back to the Federal government on their progress. Evaluations for States with approved plans are due to the Secretary by March 31, 2000. The evaluation will include (but is not limited to) discussion of: the effectiveness of the program in reducing the number of uninsured children in the State; the characteristics of the population being served; quality of services; coordination with other public and private health care programs; analysis of changes that may affect access to coverage; and recommendations for improving the program.
In addition, States must submit annual reports every January. On a quarterly basis, States must report expenditure data to support their claims for federal matching funds and financial/statistical data for program monitoring and evaluation purposes. States are required to collect data in the following areas:
- Expenditures;
- Number of children enrolled by age group;
- Number of children by income categories;
- Baseline estimate of the number of uninsured children in the State.
| The six case study States are now refining their CHIP data collection and evaluation efforts. Several States reported that their efforts initially focussed on establishing the program and the requisite administrative infrastructures so they are only now turning their attention to data collection and evaluation. Several States recommended that data collection and evaluation efforts be planned in the initial program planning. This was often something that they were not able to do due to the quick turnaround in launching their CHIP programs. |
Data Used for Program Design
All six States are collecting and reporting the required data. However, baseline estimates of the number of uninsured in the State will be difficult for some States to obtain.
| The sample size used by CPS is considered too small to accurately estimate the number of uninsured in most states. In some cases CPS data were used in conjunction with other data collection to provide more precise estimates. In other cases, estimates were achieved through State-sponsored surveys. |
- The lead agency in one State and a University are collecting data on the number of uninsured in the State. Regional estimates on the number of uninsured are being compiled using data already available from surveys conducted by the agency, the University, and the Urban Institute. (Massachusetts)
- One State is estimating the number of uninsured by using CPS data to project county estimates of uninsured, taking a three year average of the 1995, 96, and 97 March supplement to CPS. (Colorado)
- One State contracted with a private consulting firm to study the number of potentially eligible individuals. Using CPS data, a model was created to estimate the number of potentially eligible individuals under 150 percent FPL. (Ohio)
- By using data collected in a State population survey, one State developed estimates of the number of uninsured adolescents, which bolstered the case for expanding public health insurance to children through age 18. (Oregon)
- A State Legislature mandated a study of uninsured individuals to provide estimates of the uninsured at the sub-state level. (New York)
| During the planning phase, States relied on data from a variety of sources to make decisions about program design. |
- One State relied on data from a study of uncompensated care as well as a separate study designed to compare various approaches to cover uninsured working families. (Massachusetts)
- A study that compared the quality of care and utilization of the earlier State-funded children’s health plan to Medicaid and private health insurance was used to advocate for certain features of the current CHIP program (Colorado).
- One State used Statewide forums to gather qualitative information about community priorities while planning their CHIP Medicaid expansion. After the expansion, forums were used again to get feedback on expanding eligibility to children to 200 percent FPL in Phase II. (Ohio)
- Findings from a study of health insurance in 13 States, which included both a household and employer survey, were used to recommend the six month waiting period in CHIP for those who are already insured. (Oregon)
| CHIP lead agencies contracted with private actuarial companies to help establish reimbursement rates for the program. (Alabama, Colorado, Ohio) |
Data Used for Program Evaluation
| States added questions to their CHIP applications or to existing surveys to collect specific information about the CHIP program. |
- In order to analyze the effect of the six-month waiting period on potential CHIP eligibles, agency officials will analyze special items that were added to the CHIP application form. (Oregon)
- Questions designed to measure crowd-out were added to one State’s application. If evidence emerges that CHIP is substituting for private health coverage in excess of eight percent, then the State will impose a six month waiting period. (New York)
- One State added questions on the joint CHIP/Medicaid application to identify if children are successfully referred to the Health Care Program for Children with Special Needs and SSI. (Colorado)
- Questions were added to the CDC Behavioral Risk Factor Survey and a State Health Survey to collect data specific to CHIP. (Alabama, Ohio)
| CHIP lead agencies are monitoring outreach through toll-free hotlines used by families to apply. |
- Phone bank operators ask how applicants heard about the program and report the information back to those responsible for outreach. Agency personnel can often quickly assess the impact of high-visibility outreach campaigns through hotline usage. (Colorado, Ohio) Collaborating agency staff analyze reservation cards and applications and conduct surveys to gauge the success of discrete outreach activities. (Oregon)
| States are measuring quality of care by collecting claims and encounter data as well as consumer satisfaction surveys. |
- One State receives performance data from the participating health plans. The information describes the population served, utilization, quality, access, and consumer satisfaction. (New York)
- One State Medicaid agency provides claims information to a company that will format the data so that the lead agency can evaluate enrollment, claims and encounter data as well as quality measures (HEDIS) (Alabama).
- The claims system in one State captures which services are provided by managed care organizations across the State. The Medicaid agency can then match encounter data to eligibility files to examine access and quality measures for specific populations. (Massachusetts)
- One State is expanding efforts to measure the quality of care to include CHIP. The State is studying client satisfaction surveys, and analyzing HEDIS data on utilization, access, and quality. (Colorado)
- One State is evaluating the quality of care provided by CHIP by reviewing medical records, conducting consumer satisfaction surveys, and analyzing claims data against standardized quality measures. (Ohio)
- One State is using a Consumer Assessment of Health Care Survey to collect information about access to and experience with quality of care. The survey, in English and Spanish, is mailed directly to individuals to complete. (Massachusetts)
- One State CHIP lead agency receives monthly reports from its community outreach coordinator. These reports have demographic information and also indicate how families heard about CHIP so the agency can evaluate its outreach strategies. (New York)
| Three States are conducting their own population surveys in order to gather comprehensive information about health care, monitor health care trends, and evaluate the impact of changes in health care. |
- One State has surveyed 16,261 households with questions on various aspects of health care including insurance coverage, health care utilization, and income level. Where appropriate, the 20 minute phone survey included questions about a child in the household. The State department of Health took the lead on the survey but collaborated with various State agencies and a University to develop the survey instrument. Certain geographical areas and subgroups were over sampled to provide better estimates. Counties in the State were invited to purchase additional surveys. The State Department of Health is providing some analysis to the counties but is also making the data available to the counties to conduct further analysis. (Ohio)
- One State has developed a population survey that has been administered every two years since 1994. The survey includes 5,000 households of approximately 14,000 individuals. The survey includes questions about employer-sponsored insurance, and current health insurance coverage. Agency staff plan to analyze the CHIP penetration rate from the survey results. They also plan to use data from the population survey and a State-sponsored survey of employers, as well as questions on the Medicaid/CHIP application, to analyze employee crowd-out. (Oregon)
- One State is currently designing a comprehensive study of uninsured individuals that will be fielded in November 1999. (Massachusetts)
The foregoing analysis focuses on one point in time in the early implementation of CHIP in only six States. That time is the late fall or early winter of 1998/99. In the process of sending draft case studies back to the States for review and fact-checking, some changes in policy and practice were revealed in a couple of States. Since that time and the publication of this report, there are likely to have been changes in the other States, as well.
This report describes briefly the history of child health insurance programs prior to CHIP in the six States, the locus of administration and collaboration with other public and private administrative entities, and federal/state financing, then focuses the remainder of attention on outreach strategies, crowd-out prevention policies, and data collection and analysis plans.
The cross-case analyses in this report, and the case studies from which the analyses draw, are based on six States that are not necessarily representative of all the States. Nevertheless, these States were selected from those approved as of June 1998, to represent a mix of program options (state-initiated program vs. Medicaid-expansion, or a combination), income eligibility levels, existence of pre-CHIP State health insurance programs, geographic distribution of the States, and demographic mix of the population. As such, their policies, practices and experiences are likely to be found in many other States. Thus, some general conclusions can be drawn from these States about the early implementation of CHIP.
States are moving aggressively in the variety, scope, and intensity of their marketing and outreach campaigns to find and enroll both children eligible for but not enrolled in Medicaid, and enroll them in Medicaid, and children eligible for CHIP. The campaigns are both broad-based and targeted to find children among traditionally hard-to-reach families. Statewide mailings and media campaigns are supplemented with targeted outreach to families in deeply rural areas of the States, ethnic minorities, children of foreign-born parents, Native American children, and families known to be traditionally resistant to enroll in government programs. And the most significant feature of States’ outreach strategies appears to be the broad collaboration with other public and private agencies and organizations.
Crowd-out is not universally embraced as a problem. This is especially the case in the five States with pre-CHIP health insurance programs for low-income children, where staff assert that no credible evidence of crowd-out emerged. Moreover, advocacy organization staff and other researchers note that the adoption of crowd-out prevention policies (e.g., waiting periods and cost-sharing) may thwart the very policy for which Congress adopted CHIP — reduction in the numbers of low-income, uninsured children in the United States. Nevertheless, five States adopted at least preliminary crowd-out prevention methods. The sixth State is taking a wait-and-see approach, carefully monitoring for the potential emergence of crowd-out, and planning to adopt prevention methods if it exceeds a threshold level.
Finally, data collection for the evaluation of CHIP’s outcomes is nascent. For the most part, States took quick advantage of the availability of Title XXI funding to expedite planning, program design, operational decisions, State Plan submittal and approval, and to vigorously undertake outreach, application processing, and enrollment. At the time of the State visits for this study, data collection was beginning. Perhaps the most developed data collection and analysis activities are those in the two States that have population surveys that include questions on health insurance coverage and access to care. But those surveys are not specific to CHIP, as they were initiated at least one year prior to CHIP implementation.
1 - American Hospital Association, Campaign for Coverage: A Community Health Challenge, Washington, DC. SPring 1998.
2 - U.S. Bureau of the Census, March 1996, 1998 Current Population Survey.
3 - American Hospital Association, Campaign for Coverage: A Community Health Challenge, Washington, DC. SPring 1998.
4 - States are permitted flexibility to set lower or, in some cases, higher income eligibility levels.
5 - Total allocations are approximately $4.3 billion for FY 1998-2001, decreasing to $3.2 billion for FY 2002-2004, and rising again through 2007.
6 - Medicaid matching rates vary by State. See Exhibit 3 for the six States' matching rates.
7 - Ullman, F., Bruen, B., and Holihan, J., The State Children's Health Insurance Program: A Look at the Numbers, The Urban Institute, Washington, DC, March 1998.
8 - Private Market Crowd Out and Minnesota Care: Evidence to Date, Minnesota Department of Human Services, July 1998, p. 4.
9 - Other researchers caution that Minnesota's experience is not a good case in point. The State adopted extraordinary crowd-out prevention policies that no other State has so far adopted. For example, applicants are not eligible if (1) they now have access to or had access to employer-subsidized insurance during the 18 months prior to applying or (2) had any health insurance in the four months prior to applying.
10 - Hearn, Jean, Coordinating Children's Coverage Expansions with Employer-Sponsored Coverage, Institute for Health Policy Solutions, Washington, DC, March 1998.
11 - February Letter HCFA(now known as CMS).
Chapter II: Chip in Alabama
History and Implementation
Alabama had no separate children’s health insurance program prior to implementation of CHIP. However, the state legislature moved quickly to take advantage of the new Federal legislation, recognizing that it provided a new opportunity to expand health coverage for uninsured children.
At the time CHIP was authorized, there were significant political dynamics in Alabama. The State Legislature was in a special session because the Governor had vetoed the state budget; and the Lieutenant Governor was running against the incumbent Governor. CHIP became a major campaign issue because the candidates had different ideas about the urgency of applying for the new Federal funds for children’s health insurance. The Republican Governor wanted to wait before deciding how to proceed, but the state legislature (with a Democratic majority, led by the Lieutenant Governor) wanted to proceed immediately.
The end result was that the legislature passed a Joint Resolution establishing a Children’s Health Insurance Program Commission to plan the program and authorized $5 million for the program over the Governor’s objection. The Commission was chaired by the State Health Officer, who runs the Department of Public Health (DPH). That agency was given authority to use the appropriation to begin planning CHIP. The decision to name DPH as the lead agency reflects several political and fiscal factors. At the time, the Medicaid agency was facing very serious budget overruns, as well as the potential loss of additional revenue under new Federal rules, and the agency had little support among the legislature, provider community, or child advocates.
The Commission, working with a broad-based Advisory Council and DPH, developed a two phase program that both expands Medicaid and also implements a new state children’s health insurance program.
Alabama was the first in the country to have its CHIP plan approved on January 30, 1998 and began implementation February 1, 1998. It is also the first state to have a major expansion approved through a Plan Amendment to HCFA(now known as CMS). The expansion, approved August 18, 1998, authorized implementation of ALL KIDS on September 1, 1998. Alabama has two phases for its CHIP program:
- Phase I: Expands Title XIX Medicaid program (SOBRA) to extend coverage for children ages 15-18 under 100% FPL. This phase was implemented in February 1998. Previously, Medicaid only covered children from birth to age five, up to 133% FPL and children through age 14 up to 100% FPL.
- Phase II: Creates ALL KIDS, a new separate state program to cover children under age 19 in families with incomes up to 200% FPL who are not eligible for Medicaid. This phase was implemented in September 1998, with coverage effective October 1, 1998.
- Its benefits are the same as those offered by the HMO with the largest commercial enrollment in state.
- Its coverage is available through Blue Cross/Blue Shield statewide and the family can select any ALL KIDS provider from their network. In one region of the state, a second insurer, Prime Health, is available.
- Premiums are only charged for children living in families whose incomes are above 150 percent FPL. To date, 68 percent of the children are eligible for no-fee coverage.
- It emphasizes providing primary and preventive care to previously uninsured children through a "medical home" that can ensure regular health care.
When the RFP was first issued for private insurers to bid for the ALL KIDS contract, DPH realized that it was too expensive to select a fully insured model where the vendor bears the risk. Consequently, DPH selected a self-insured model and the agency bears the risk for children enrolled in ALL KIDS. The plan costs between $6.32 and $7.77 per member per month depending on the number of children enrolled.
Several state agencies have already begun discussing a possible Phase III to enhance benefits for children with special health care needs through a CHIP Plus program; they hope to submit a second plan amendment to HCFA(now known as CMS) in 1999.
Federal State Financing
Alabama’s Title XXI allocation of Federal funds in the first year was up to $85 million. Its state matching rate is 21 percent and it state match is $23.4 million.
- For the Phase I Medicaid expansion, the state is targeting to enroll up to 17,000 children and by February 1999 had enrolled almost 11,000 teenagers.
- For Phase II, they are targeting to enroll 20,000 children in ALL KIDS during the first year and in its first three months, enrolled just over 13,000 children. The state legislature budgeted funds to cover 20,000 children and the Department of Public Health will ask for additional funds if enrollment exceeds the current target. The program is averaging 800 applications each week. One day in October 1998, ALL KIDS received 6,000 applications. The surge in applications was probably a function of an outreach campaign that mailed applications to all public schools in the state (see Exhibit 1).
Key Factors in Alabama’s Implementation
- Timing was critical. The legislature was meeting for a special budget session during the month after Title XXI was authorized so CHIP was added to its agenda quickly.
- The political climate was right. State politics, especially the gubernatorial race, created a climate where people wanted to discuss "What is best for Alabama’s uninsured children?"
- A lengthy legislative debate was avoided. By appointing the Children’s Health Insurance Program Commission, instead, the Commission — comprised of state legislators, executive agency staff, and non-profit representatives — met to discuss major policy decisions.
- Stakeholder involvement proved useful. The Commission received extensive help from a broad-based Advisory Council that provided a mechanism for stakeholders from a variety of constituencies to share their expertise, opinions and recommendations. See page Appendix 1 for a list of entities represented on the Council.
- ALL KIDS (the new separate children’s health insurance program) was placed in a state agency—the Department of Public Health—that does not report to the Governor. The State Health Officer, who runs DPH, is appointed by and reports to the State Committee of Public Health, which is the governing board of DPH. Final decisions about program design and operation were made by DPH staff after the Commission discussions.
- Phased implementation was a sound approach. The Commission, Advisory Council, state agency personnel and advocates all believed it was important to provide access to good primary care with reasonable in- and outpatient benefits for children who were previously uninsured. The logical first step, given the basic needs of the uninsured population, was to expand Medicaid for teenagers and plan a new state program as the second phase.
- Commission members discussed whether establishing a new state program might create a two-tiered system by providing more resources for a program serving higher income children than what Medicaid-eligible children receive. However, they concluded that to raise the level of care for all low-income children, it was wiser to invest in a new children’s health insurance rather than an existing program with a problematic history. Members believed that a new public-private partnership between DPH and the private insurance industry could provide primary and preventive care and help establish a "medical home" for these children.
State Approach
The original intent was to have both statewide efforts and local partnerships to implement both the Medicaid expansion and ALL KIDS. Since there were only a few months to get enrollment started, DPH and Medicaid focused on reaching a large number of families across the state.
Phase I outreach included:
- Mailing notices to all 300,000 Medicaid households, where uncovered teenagers might reside, and all 10,000 Medicaid providers.
- Distributing 150,000 brochures to a variety of service providers including: out-stationed Medicaid workers; public health workers; county human resources workers; family services centers; primary health care centers and hospitals; advocacy and professional organizations; educational professionals (school systems, principals and guidance counselors); and appropriate professional groups at statewide meetings (social workers, pediatricians).
Outreach in Phase II is broader.
- Building upon existing relationships among other public agencies and private organizations, the Department of Public Health used a "shot gun approach" to reach as many families as possible through: a statewide media campaign; satellite teleconference for a wide variety of child-serving providers; videotapes for specific professional audiences; and mailed applications to all public school districts to distribute to students.
- DPH distributed posters and information through schools, health and human service agencies, medical providers and their associations and community-based organizations.
- Public service ads were provided to newspapers and radio stations.
As a result of these initial efforts, the volume of applications for Medicaid increased tremendously, especially during outreach for Phase II, the ALL KIDS program.
Key Players and Administration
Several state agencies as well as private organizations play important roles in outreach.
- Department of Public Health (DPH)
- Medicaid Agency
- State Employees Insurance Board (SEIB), under contract to DPH, performs all eligibility determinations, enrollment work and premium collections for ALL KIDS. SEIB was established by the State Legislature in 1965 to provide a health insurance plan for state employees, but its role has expanded in recent years.
- Medicaid out-stationed workers
- Numerous collaborations with other state agencies and private organizations (described below)
Collaboration with Other Agencies and Organizations on Outreach
State Medicaid Agency
- For CHIP Phase I (expanding Medicaid for teenagers), additional eligibility workers were hired and trained to process applications and certify children for either Title XXI, or if eligible but not enrolled, for Medicaid. There are 119 out-stationed workers serving the 67 counties who are placed in county health departments, hospitals, clinics, and community health centers. Out- stationed workers are all electronically connected to the state Medicaid computer system to expedite the eligibility process.
- The capacity of the Medicaid toll-free information number was expanded. There was a state hiring freeze so women inmates from a pre-work release program were trained to answer the telephones and provide information about Medicaid and Title XXI.
- In Phase I, Medicaid staff believed it was most cost-effective to focus its outreach to families already enrolled because it assumed that many new eligible teenagers were members of families where younger children are already receiving Medicaid. Using its mailing lists, the agency sent information to all current recipients and providers and all children received a brochure about Phase I expansion at their annual review. To expedite enrollment, a new simplified Medicaid application was developed to add CHIP-eligible teenagers living in families where children are already enrolled.
Other State Agencies
- The Superintendent of the Department of Education was very supportive of CHIP. Immediately after the Phase II began, mailings were sent to all 129 school systems across the state so that virtually all school-age children received a program brochure and application with a self-addressed stamped envelope to return to SEIB. Over 750,000 applications were distributed.
Private Organizations
- During Phase II, Children’s Hospital provided information through its Sports Medicine Clinic, its toll-free 800 telephone number, and its financial counselors who help families plan payment of medical expenses. It also distributed applications at United Way agencies and provided information through its community contacts. The hospital identified all the self-pay/uninsured children seen by the hospital over the last 18 months (about 9,000 children for either out- or inpatient services). It sent a letter explaining the new program along with an application package and a self-addressed return envelope to the Department of Public Health.
- The State Hospital Association sent two informational packages to all 120 members that explained the program and described how hospitals could help educate families about the new program.
- Children’s Rehabilitation Services used its computer records to identify, among its population of families with children who have special health care needs, those who lack insurance; they discovered it was approximately 19 percent of the 14,000 children they serve. CRS then contacted these families to explain CHIP, especially for their teenagers who may now qualify for Medicaid. Applications were available in the 15 CRS offices across the state and staff were educated about CHIP so they could explain it to families.
- The State Medical Association paid the costs of printing 500 ALL KIDS t-shirts. The t-shirts were distributed to CHIP commission members, Medical Association members, the CHIP Advisory Council, children and others who attended the kick-off to promote ALL Kids in the community. The t-shirts are also used as door prizes at meetings where CHIP presentations were made.
Media Activities
When the State Plan was first approved, there was a joint press conference with the Medicaid Commissioner, the Department of Public Health’s State Health Officer, and CHIP Commission members. A second media event was held at the State Capitol when ALL KIDS (Phase II) began. The Capitol event was broadcast to eight local press conferences across the state hosted by members of the Hospital Association. The local press conferences followed the 20-minute State Capitol kick-off, with presentations by local dignitaries, in order to personalize and promote CHIP for the local TV market.
Additional media activities included distributing:
- news releases and camera-ready materials for newspapers;
- radio spots; and
- articles published in health care provider newsletters (e.g., State Medical and Hospital Associations).
Provider Outreach
Two free, live satellite video conferences (45 minutes) were produced by DPH, which has its own sophisticated television studio and recording facility. They were available for viewing at county health departments and other facilities with satellite downlinks in multiple sites on two different dates. For those who could not attend the live broadcast, copies of the conference were made on video and distributed to a wide range of service providers including: educators and school guidance counselors; social workers; hospital staffs including nurses and other clinical personnel; dental staff; pediatricians/family practitioners; pharmacists; child care providers; social service personnel; clergy; and others who help parents complete ALL KIDS applications.
The Department of Public Health also produced videos for five special professional audiences who serve children potentially eligible for ALL KIDS. The videos target pediatricians, family practitioners, dentists, pharmacists and emergency room doctors.
Creating a Seamless Health Care System for Eligible Children
Presumptive Eligibility
Alabama does not have presumptive eligibility for Medicaid for ALL KIDS.
Continuing eligibility
Alabama Medicaid changed its internal data systems to ensure 12 months of continuous eligibility for all children. ALL KIDS provides continuous coverage for one year before re-determining eligibility, unless the child reaches the age of 19.
Simplified Application and Eligibility Decisions
- ALL KIDS has no income verification because the Department of Public Health did not want to create unnecessary barriers for families. The Department of Revenue will audit a sample of tax returns to check the income reported to each agency; if there is evidence of excessive under-reporting of income to ALL KIDS, then DPH will consider imposing more stringent policies.
- Medicaid and ALL KIDS have a joint application. Eligibility questions for ALL KIDS were added to the existing Medicaid application. Since the state ALL KIDS and Medicaid offices are located only two blocks apart, employees can manually transfer eligibility application forms from one agency to the other.
- ALL KIDS has a 1-888 enrollment telephone line that is staffed, under contract, by employees of the State Employees Insurance Board. Specially-trained staff answer questions and take applications over the telephone, although the families must send certain documents to finalize the process. Twice a week, approved application data is transmitted to Blue Cross/Blue Shield to begin a child’s coverage.
Funding for Outreach
DPH used the bulk of its outreach budget to print 1.5 million program brochures, applications and return envelopes with postage paid. The agency made a conscious decision to use an attractive color brochure that makes ALL KIDS look different from a typical government program.
Expenses for outreach activities were minimized by asking other state agencies to use their existing contacts with lower income families. Many expenses were covered through in-kind contributions from non-governmental organizations that worked with DPH and Medicaid to help locate potentially eligible children and young people.
DPH decided to use its administrative funds to hire consultants to provide expertise that was not available within the agency. Through these contracts, the agency obtained actuarial information, project management services and an enrollment broker. The three consultant arrangements are:
- William A. Mercer — an acturial analysis firm — estimated the population of potential eligibles; helped design the RFP for private vendors and assessed bids after it was issued; and provided actuarial information when DPH negotiated ALL KIDS benefits. Having worked in Alabama before, Mercer knew the state’s insurance market and was also familiar with child health insurance programs in other states. The firm also helped plan outreach and marketing activities and will help evaluate the program.
- Draper Associates—a project management and professional services firm—managed the technical administrative details while providing timelines and accountability checks for the implementation schedule. This allowed DPH staff to focus on developing policy and taking the actions necessary for implementation of ALL Kids.
- The State Employees Insurance Board (SEIB) serves as the enrollment broker. The Department of Public Health hired SEIB, which manages and designs a health benefit program for its 100,000 members, to run the ALL KIDS program. SEIB staff has experience negotiating with insurance companies and administering an insurance plan. SEIB hired and trained staff to run the ALL KIDS enrollment process through its toll-free telephone number. Senior SEIB staff provide assistance when DPH negotiates with insurance vendors about benefits. SEIB receives $500,000 each year for its services.
Marketing to Hard-to-Reach Populations
- The Department of Public Health has consulted with local Native American representatives. The Poarch Band of Creek Indians wants to train its own outreach workers and provide information through monthly newsletters distributed to each household and through schools and PTA meetings. Members want to develop fact sheets for health care providers explaining tribal beliefs about health that affect prevention and treatment of medical conditions. For example, tribe members do not eat meat during the summer so health professionals should not prescribe more red meat when children are anemic at that time of year.
Woodwork Effect
As a result of Phase II outreach efforts, applications for Medicaid soared. Among the 25,000 Phase II applications received, half were referred to the Medicaid agency. Prior to Title XXI, in January 1998 there were about 162,000 children enrolled in Alabama’s Medicaid program. By June 1998, the numbers had increased to about 180,000 and six months later, to about 190,000. Although Medicaid staff anticipated that CHIP outreach would increase their enrollment, the agency was surprised by how quickly families responded and how large a backlog of applications it caused.
Potential Future Outreach
DPH is considering additional outreach strategies. These include:
- Use child-related programs such as: child care agencies; MCH clinics; WIC clinics; community health centers; Indian Health Services; school nurse programs; school counselor programs; and other social service agencies.
- Develop local partnerships and establish one major point of contact in each county, allowing each county to select the responsible individual and agency performing this role.
- Run more public service announcements on radio and television during the next phase of ALL KIDS outreach.
- Continue existing contacts with child service and health providers and schools, but target outreach for younger children through child care agencies.
- Organize hospitals to inform families when children are born and target parents of newborns, especially their first children.
Advice for Other States on Outreach
- Establish a strong program identity so families are attracted to enroll their children.
- Establish a sufficient infrastructure—either within a state agency or contractor—that can sustain an organized recruitment and enrollment campaign and respond to resulting program inquiries.
- Identify one or two key people in each geographical area to maintain on-going outreach activities.
- Inquire whether the Postal Service loans its executives to help local non-profit organizations as it does in some places around the country. In one small town, a Postmistress helped organize outreach activities that was very successful because she knew everyone in town.
- Develop easy-to-understand information about the children’s health insurance program.
- Send program information to both the medical office/clinic administrators as well as the administrative office managers and staff who file insurance claims. They often have direct contact with families and can explain the benefits of the new program.
State’s Response
Alabama has a multi-strategy approach to the issue of crowd-out although there is some doubt about whether it is a real threat given the state’s low average family income. The state believes the following mechanisms will help reduce crowd-out:
- A joint application for Medicaid Title XIX and ALL KIDS Title XXI so that children found eligible for Medicaid are referred for enrollment in that program.
- A question on the joint application about whether the applicant has insurance coverage or has had it in the last three months.
- A requirement that applicants sign a statement giving DPH the authority to verify the information presented on the application.
- A three month waiting period for ALL KIDS for families who currently have or voluntarily dropped health insurance coverage. ALL KIDS sends enrollment information electronically to Blue Cross/Blue Shield to check if the child is insured or recently dropped coverage. This is easy to check because "the Blues" cover over 80 percent of those who have health insurance in Alabama. The plan is to include additional insurance vendors in a master patient index of private health coverage by April 1999.
- Premiums for families whose incomes are above 150 percent FPL. Since the ALL KIDS benefits are similar to the standard benefits in private plans available to most employees, requiring premiums further reduces any incentive to drop employer-based dependent coverage.
- The Alabama Child Caring Foundation for uninsured children who are not eligible for Medicaid or ALL KIDS due to access to insurance, immigrant status, and income. Blue Cross/Blue Shield runs this program; there are currently 20,000-30,000 children enrolled who pay a $240 premium each year for a very limited benefit package.
- No premiums for families with incomes under 150 percent FPL.
- Families above 150 percent FPL pay an annual premium of $50/child or $60/child if premiums are paid in ten monthly installments. A Family’s total premium cannot exceed three times the selected annual payment method, (i.e., only $150 with annual premium payment or $180 with installment payments). Coupon books are sent to enrolled children by SEIB and premiums can be paid through state banks.
- Children’s Rehabilitation Services pays any premiums or co-payments for families in its Children with Special Health Care Needs program. The agency projected potential savings of $750,000, annually, due to ALL KIDS and CHIP coverage for children served by CRS for whom drugs, surgery or other medical services will now be covered by CHIP, rather than CRS. CRS used these savings to reintroduce cardiac care services that were previously eliminated because of funding limitations. Families can now request reimbursement for lodging, transportation and medical care expenses when their children need specialized cardiac treatment.
Lock-out Periods
There is no lock-out period, but children cannot re-enroll at the end of a year unless premium payments are current.
- Families above 150 percent FPL have a $5 co-payment for inpatient hospital stays, physician office visits, emergency room visits where the patient is not admitted, urgent care services, confinement for inpatient chemical dependency, and dental services. Prescription drugs cost $3 for brand names and $1 for generics.
- DPH is not worried about family cost sharing exceeding the statutory cap of five percent of annual income, because the premiums and co-payments are so low that few families are likely to exceed the $500 annual limit on out-of-pocket expenses or the percent-of-income limit.
- Nevertheless, families are informed about the $500 limit through ALL KIDS brochures and by social service agencies. Families are encouraged to keep receipts for all co-payments and premiums in a "shoe box," so if they reach the maximum, they have the necessary documentation to stop cost-sharing and reclaim occasional over-payments of co-payments or premiums.
Employer Buy-In
No program is planned at this time to subsidize premiums for employer-provided insurance.
Alabama has no existing system to identify the total number of uninsured children, which presented a major challenge while planning the two phases of CHIP. While it is too soon to have any meaningful data, DPH is laying the groundwork to track the State Plan’s performance measures. For the data collection work, DPH staff will have assistance from Advisory Council members, SEIB (which has statewide Blue Cross/Blue Shield claims data and will have Medicaid claims data) and outreach partners (which have utilization data by zip code).
Program Design Data
To help plan Phase I (Medicaid expansion for teenagers), Medicaid staff estimated the number of young people in the age range statewide who would qualify through the CHIP/Medicaid expansion and then subtracted the number of children who were already enrolled. This calculation produced a very rough estimate of the number of young people who could enroll. The staff factored in some reduction in that number based on the assumption that not all eligible teenagers would respond. Using this estimate, the Medicaid agency predicted that 20,000 would enroll in CHIP/Medicaid.
- The CHIP Commission filed its first report with the State Legislature in January 1998 and will file its second in March 1999.
- SEIB has an information system in place through its existing computer software that provides financial expenditures, demographics and encounter data. This information is provided monthly after claims are adjudicated.
- The Medicaid agency gives its claims information to a company under contract to SEIB that will put it in a format for DPH to evaluate enrollment, claims encounter data and HEDIS measures.
- The Department of Public Health plans to work with the University of Alabama at Birmingham (UAB) School of Public Health to develop a mechanism to assess the quality and appropriateness of care provided through ALL KIDS. The state wants to use both process and outcome measures for this assessment. Among the items to track may be the following:
- Do children have a "medical home"?
- Are children receiving appropriately scheduled well-child examinations?
- Are children immunized at the appropriate times?
- Is non-trauma emergency room use decreasing?
- How are referrals made?
- Are specialty care and related services provided?
- What are the patterns of prescription drug use?
- The state also may use other data that provides general indicators of child health and well-being such as: immunization registry (after fully operational); adolescent pregnancy rate; health care utilization patterns; and results of mandatory child death reviews. These data will come from other public health initiatives.
Other Data Collection Methods
Other DPH data collection mechanisms include the following:
- Consumer and provider satisfaction surveys; and
- A Center for Disease Control survey called the Behavioral Risk Factor Survey. Alabama officials have added ten questions about CHIP to this existing survey and are distributing it to 4,000 families.
Ten Percent Cap on Administrative Expenses
The Department of Public Health realizes that its costs may exceed the legislated cap on administrative expenses eligible for the Federal match. The agency will reallocate or request additional state funds to cover the administrative expenses, if necessary. The agency will also carry forward into future years of CHIP reimbursement, CHIP start-up expenses.
Some individuals interviewed expressed concern that this cap is too restrictive, especially in a state that is organizing a new program that requires a substantial investment for start-up expenses.
DPH did much of its initial outreach by collaborating with other state agencies and private organizations. This approach provided the flexibility to use administrative funds to hire outside experts to help plan and administer ALL KIDS.
Web Sites for More Information
For additional information, visit their web site:
http://www.alapubhealth.org/chip/index.htm.
Appendix 1: Advisory Council Membership
Alabama Medicaid Agency
Alabama Department of Public Health
Children’s Health Systems
Alabama Arise
Family Health Care Corporation (a Federally qualified health center)
University of South Alabama, Children’s and Women’s Clinic
Alabama Department of Rehabilitation
Alabama Department of Human Resources
Alabama Department of Education
Prime Health
Alabama Child Caring Foundation
Alabama Department of Mental Health and Mental Retardation
Alabama Hospital Association
Alabama Primary Health Care Association
Alabama Department of Industrial Relations
Medical Association of the State of Alabama
Alabama Dental Association
Alabama Psychological Association
Alabama Chapter of the American Academy of Pediatrics
Alabama Academy of Family Physicians
American Academy of Pediatrics — Alabama Chapter
Blue Cross Blue Shield
Children’s First
Family Voices
Health Maintenance Organization Association
Legislative Fiscal Office
Legislative Reference Service
University of Alabama at Birmingham
United Health Care
Voices for Alabama’s Children
State Employee’s Insurance Board
State Insurance Department
Poarch Band Creek Indians
Chapter III: Chip in Colorado
History and Implementation
The state legislature has authorized health insurance programs for low-income Colorado children for more than a decade. However, the legislature has not appropriated much general fund money to support the programs. The reluctance to appropriate state funds reflects two political realities in Colorado. First, there is a statutory limit on annual revenue and spending increases. Second, there is skepticism among legislators and segments of the public toward government-run programs. Both realities have led to legislative mandates to privatize child health insurance programs as much as possible. The legislature reinforced privatization for the state’s CHIP program.
Pre-Title XXI
- The Colorado Indigent Care Program (CICP) began in 1983 to serve poor, non-Medicaid residents of all ages. This is not an insurance program, but a system for reimbursing participating physicians and other fee-for-service providers a portion of their costs for serving indigent uninsured individuals.
- Legislation passed in 1990 that established the first insurance program for low-income, non-Medicaid children, the Colorado Child Health Plan (CCHP). CCHP provided outpatient and preventive services to children age nine and under in families with incomes below 185 percent of poverty. Services were focused in rural areas where there were few or no community health centers. The law stipulated that CHP be financed with "gifts, grants, and donations." The legislature, reflecting its skepticism about government-run, public assistance programs, authorized CHP in the higher education budget, to be administered by the University of Colorado Health Sciences Center. Claims processing, referral authorization, and card production were donated by HMO Colorado, a subsidiary of Blue Cross/Blue Shield of Colorado.
- The legislature, in 1993, authorized but did not appropriate funds for expansion of CCHP to cover children through age 13.
- During the 1996 legislative session, a bi-partisan group of legislators requested that the Joint Budget Committee appropriate funds for CCHP. The committee balked, then relented, and appropriated $1 million in what is described as a "one-time-only-and-don’t-come-back" appropriation for CCHP. This occurred during a period when Colorado was $100 million overspent in its Medicaid program and costs were escalating 20 percent annually.
- That year, the legislature voted to drop out of the Medicaid program, but Governor Romer vetoed the legislation.
- In the 1997 session, legislators considered:
- Eliminating the indigent care program (CICP);
- Requesting a waiver of some Medicaid rules from HCFA(now known as CMS);
- Using some Medicaid funds to reimburse schools for health services;
- Expanding CCHP statewide and raising the age limit from 13 to 17;
- Submitting a Section 1115 waiver to HCFA(now known as CMS) to obtain a higher match and create the Children’s Basic Health Plan (CBHP) with comprehensive coverage that would include inpatient and mental health coverage.
- At the same time, a bill was introduced to control rising Medicaid costs by enrolling many Medicaid recipients in HMOs. The bill projected Medicaid savings that would help fund the CBHP.
- Simultaneously, Congress passed Title XXI so the legislature dropped the waiver idea in favor of submitting a State Plan for a CHIP program.
This chronology occurred in an environment of statutory limits on annual revenue and spending growth. The statutes index revenue and spending growth to population plus inflation, which has amounted to a limit of roughly 6 percent, annually, over the past several years. One statute requires excess revenues above 6 percent to be returned to the taxpayers in a rebate, unless they vote in a referendum to spend some of it. The limit cannot apply to growth in federal entitlement programs like Medicaid. When Medicaid is experiencing runaway growth, as it was during the early 1990s, legislators must appropriate state matching funds to it. This restricts their ability to fund discretionary programs.
Title XXI
Colorado was one of the earliest states to receive federal approval of their Title XXI State Plan and the first to receive approval for a non-Medicaid program. The plan builds upon the existing Colorado Child Health Plan. The new program, Child Health Plan Plus (CHP+) offers a more comprehensive set of health care benefits to children that includes inpatient hospital services, extends eligibility to older children up to age 19, and expands to residents in all 63 counties.
When Title XXI passed in August 1997, with funding to become available in October, Colorado still had another year before its CCHP expansions were to take effect. So the legislature passed a fast track bill to correct the following discontinuities between CCHP and Title XXI:
- Make inpatient coverage effective in July 1998.
- Clarify that children through age 18 would be eligible.
- Extend the sunset date of CCHP from July 1998 to July 1999.
- Establish cost-sharing provisions for CHIP/CHP+.
- Offer an option to children already enrolled in CCHP to remain there (without inpatient, mental health, and other services) until their certification period expires, or to enroll in CHP+ with cost-sharing. New applicants are enrolled in CHP+.
Phase I of CHIP/CHP+ began in April 1998 and included the following features:
- It continued the income eligibility cutoff of the predecessor CCHP program, covering children up to age 19 living in families with incomes up to185 percent FPL.
- It established an asset test which limits the dollar value of non-income resources available to applicants, such as a car, to $45001. Since the asset test in Medicaid is $1500, staff recognize that many children in families with incomes considerably below 100 percent FPL who are found ineligible for Medicaid (on asset grounds) will be eligible for CHP+.
- Officials set a target to enroll no more than 25,000 children by June, 1999.
- Day-to-day program administration — such as outreach, application processing, and enrollment — would be conducted by a private foundation, under contract to the state Department of Health Care Policy and Financing, the oversight agency.2
- Other agencies and organizations actively participate in outreach.
- The majority of CHP+ enrollees receive services through HMOs. Since the provider networks offered by the plans in many counties were found inadequate to serve enrollees’ needs, HMOs currently serve 29 of the 63 counties. However, this represents about sixty percent of the enrollees and about 80 percent of children eligible for CHP+ throughout the state.
In Phase II the state plans to pilot an employer buy-in program.
- Colorado’s Title XXI allocation of Federal funds in the first year was up to $42 million.
- The state matching rate is 34 percent.
- State matching funds of $7.2 million consist of a legislative appropriation from the general fund; an intergovernmental transfer from University Hospital (stipulated in state legislation); donations from the Blue Cross/Blue Shield Foundation and other businesses; an allocation of a portion of the state’s disproportionate share fees that would have gone to hospitals; and a legislative, one-time appropriation.
- While counties in Colorado are required to fund part of the state match in other public assistance programs, like welfare, they are not required to do so for CHIP.
- The state estimates there are 180,000 uninsured children, of whom approximately 75,000 live in families with incomes less than 185 percent FPL.
- HCPF estimates there were 25,000 low-income children eligible for Medicaid who were not enrolled.
- In November, HCPF estimated they had enrolled 12,000 in CHP+ toward their target of 25,000 by June 1999. Staff estimated there were another 3,000 applications in the pipeline, awaiting eligibility determination.
- Following enactment of CHP+ there were 14,000 children enrolled in the predecessor CCHP, all of whom were eligible to roll over into CHP+. The families of these children received letters informing them of the new program and encouraging them to switch over. At the time of the first mailing, 40 percent of the families had responded; 79 percent of them — representing all premium levels — agreed to move into the new program when it became available.
- Children in families that did not respond to the mailing, or did not agree to switch, were permitted to maintain their eligibility in the old program for one year beyond their enrollment date. As of March 1998, all new applicants to the program were required to enroll in CHP+ and all enrollment periods for existing CHP cases will terminate in March 1999.
Key Factors for Colorado’s Implementation
Many circumstances facilitated the authorization and implementation of CHIP in Colorado. Statutory limits on revenue increases, which constrain the growth of programs, served to temper enrollments during early CHIP implementation.
- Precedence was helpful. A nine-year history of expanding eligibility in state-initiated health insurance programs for low-income children created a conducive atmosphere for consideration of CHIP.
- Timing was critical. On the eve of Title XXI passage, the state legislature authorized submission of an 1115 waiver to HCFA(now known as CMS), so it was an easy step to modify the waiver provisions to comply with Title XXI requirements. The waiver request already included expansion of the earlier state program to include inpatient and mental health services, which was a big step toward complying with Title XXI requirements.
- Existing public-private partnerships facilitated implementation. State initiated children’s health insurance programs already relied heavily on public-private partnerships. The presence of Foundation staff who had managed outreach and enrollment for the state program made it easy to continue the Foundation’s management of CHIP/CHP+.
- One man’s tireless efforts on behalf of uninsured Colorado children facilitated legislative debate, as well as implementation. A pediatrician at the University of Colorado Health Sciences Center began advocating for the various health insurance programs in 1992, and testified on CHIP/CHP+, as well. He understood how the pieces would fit together. Under his direction, the University already had 3300 contracts in place with fee-for-service providers. This enabled CHP+ to get underway immediately while enrollees were selecting managed care plans.
- A Policy Board, design teams, and work groups helped ensure buy-in by a wide array of private, as well as, public stakeholders.
State Approach
Faced with statutory constraints on funding for CHIP/CHP+ and the capped enrollment target in the first year, attitudes toward outreach were initially mixed. Although there was interest in reaching out to the maximum number of children, there was concern about "being too successful" and creating waiting lists. As one person explained the trepidation: "Can we serve them if they come?" As it has recently become clear that total enrollment would not exceed 25,000 during the first fiscal year, state officials expressed renewed interest in more vigorous marketing and outreach.
Key Players and Administration
A Policy Board recommended overall CHP+ policy. Two state agencies and a private foundation played a direct role in early CHP+ administration, and there is collaboration with a third state agency and another private organization.
- The Policy Board recommended policies on: coordinating CHP+ eligibility with Medicaid; designing the benefits package and cost sharing schedules; managing HMO, University, and systems information contracts; reporting and program evaluation; and quality assurance. Members included the CEOs of Kaiser-Permanente, Blue Cross/Blue Shield, past president of Colorado’s chapter of the American Academy of Pediatrics, the state manager of the nation’s largest private retirement fund, a representative from a benefits consulting firm, the pediatrician from University Hospital who has been instrumental in passage of various children’s health insurance initiatives, Executive Director of Valley-Wide Health Services, and the Executive Directors of four state agencies (Health Care Policy and Financing; Department of Public Health and Environment; Education; and Human Services).
- The Department of Health Care Policy and Financing (HCPF) is the oversight agency for CHP+. Legislative staff and some executive branch staff observed that the Legislature envisioned little more than "the banking function" for HCPF. In fact, they administer contracts with the foundation, managed care organizations, the information systems vendor, and also manage the quality assurance reporting.
- Foundation for Children and Families — under contract to HCPF — conducted marketing and outreach, handled customer service, processed applications and determined eligibility, and finalized enrollment of eligible children in CHP+. (The Foundation was recently replaced by a private, non-profit contractor). With a staff of 20, Foundation staff performed those functions and the "rating" function that determines income and assigns children’s families to the appropriate premium group. Foundation staff also developed and managed the information system and analyzed data to evaluate their outreach strategies. They administered the provider network in non-HMO counties.
- Department of Public Health and Environment, maternal and child health staff help market CHP+, as part of their public health nurses’ marketing and outreach activities for other child health initiatives.
- Colorado Division of Insurance staff, in collaboration with HCPF staff, are analyzing the complexities of employer buy-in, and will develop plans for a pilot test for Phase II. During the design phase, Division staff advised the Policy Board about benefits and cost-sharing provisions of CHP+.
- Community Health Network staff operate community health centers, of which some are Satellite Eligibility Determination (SED) sites for CHP+, as well as outreach sites for Medicaid and the Indigent Care Program. More centers will be trained as SED sites this year.
Administration
HCPF contracted for outreach and enrollment functions to the Foundation for Children and Families.3
- The Foundation designed and implemented a marketing plan that includes:
- community outreach;
- public relations;
- media activities;
- a phone bank;
- distribution of materials;
- outreach to schools; and
- materials development.
- Community Outreach. Orientation sessions were held with groups of public school nurses, social workers and psychologists, EPSDT workers, Family Resource Center personnel, community health center staff, Head Start staff, public health staff, and school-based health center staff. A few child support enforcement workers have also attended, and the number of Head Start attendees was on the rise. Sessions were held in 24 school districts identified as having 30 percent or more of the children in the school-lunch program.
- Public Relations. The Bawman Group, a public relations consultant, has a contract to generate continuous media coverage. The contract is for $2500 per month for three - six months. The firm’s responsibility is to network with media to cultivate an interest in CHP+ coverage, develop newsworthy stories about CHP+ participating families, providers, and enrollment projects, and write press releases and telemarketing scripts.
- Media Activities. Airtime for TV ads was purchased for two blocks of time during the fall and early winter. The Colorado Broadcasters Association ran PSAs in the fall. Several staff reported that ads during the Jerry Springer show — a daytime TV talk show — generated the largest number of telephone inquiries.
- Phone Bank. A 1-800 Family Health Line phone bank at Department of Public Health and Environment receives and tracks calls generated from advertising. The phone line is linked to the National Governors’ Association 1-800 CHIP information phone line. Staff of the phone bank record the source of referral (i.e., where the caller heard about CHP+), and send out application and enrollment information. If the caller is inquiring about CHP+, they are referred to the CHP+ special 1-800 line. If the caller lives close enough to a SED site, they are referred there. If the caller is inquiring about Medicaid, they are referred to their local Department of Social Services office.
- Distribution of Materials. CHP+ outreach materials are distributed at community training sessions, in response to bulk requests from community agencies, and to individuals who call. Visitors to a Website can request materials. The Website address is http://www.cchp.org. Materials consist of applications, brochures and posters.
- Outreach to Schools. Many thousands of applications and brochures are sent to contacts in Colorado’s school districts. As a result, staff report that nearly one-third of callers to the marketing phone bank report they heard about CHP+ from their school.
- Materials development. Staff have developed the brochures, posters, enrollment packets, and benefits booklets in Spanish as well as English, as well as a five-minute informational video. A second version of the video was produced without reference to HMOs for use in areas of the state where no HMO contracts are in place.
Collaboration with Other Agencies and Organizations on Outreach
Several other agencies and organizations conduct outreach for CHP+:
- Department of Public Health and Environment;
- Colorado Community Health Network;
- Facilities and individual providers participating in the Colorado Indigent Care Program.
The Foundation, Department of Public Health and Environment, and Health Network have worked closely together with HCPF. The main feature of Colorado’s outreach is marketing through community-based direct service workers.
The Department of Public Health and Environment houses the Early Periodic Screening, Diagnosis, and Treatment (EPSDT) program in their Title V agency administering maternal and child health programs. DPHE contracts with the 63 county public health agencies, who hire case managers backed up by public health nurses.
- DPHE develops policies and strategies on outreach for all child health programs, including CHP+. These policies and strategies, with a special focus on access to care and special needs children, are communicated to the case managers and public health nurses in the 63 counties. The nurses actually conduct outreach with families and other community groups.
- The Colorado Covering Kids Coalition, comprised of a diverse group of state and local partners and led by DPHE, is conducting additional outreach interventions with a grant from the Robert Wood Johnson Foundation for a "Covering Kids Initiative."
Colorado Community Health Network works under contract to HCPF to conduct selected outreach activities. The Health Network works with the State Primary Care Association, whose members operate 85 primary care clinics for the uninsured (including 20 school-based sites). The Primary Care Association receives 80 percent of its funding from the federal Health Resources and Services Administration (HRSA) in HHS. The Community Health Network has a grant from HRSA for CHP+ and Medicaid outreach.
- The Network’s key outreach feature is its Satellite Eligibility Determination (SED)sites. SEDs are located at school-based health clinics and community health centers, county social service departments, family resource centers and hospitals where eligibility can be determined immediately. In the fall of 1998 36 sites were accepting CCHP and CHP+ applications, and another nine are expected by the summer of 1999. Five sites process applications via an Internet hookup to a central SQL server database. With the HRSA grant, the Health Network plans to purchase additional software and hardware to expand the Internet connection to half the sites by the end of 1999. This additional capacity is expected to greatly increase enrollments.
- Under a "Covering Kids Initiative" awarded by the Robert Wood Johnson Foundation, the state and its private sector partners plan to develop and implement model outreach and enrollment initiatives statewide and in three designated Colorado counties.
Finally, Colorado Indigent Care Program providers, many of whom are community health centers, received information about CHP+ and are encouraging their families to apply.
- Some CICP facilities, working with Foundation staff, helped with mass mailings to CICP participants about the availability and advantages of CHP+. The CHP+ legislation calls for moving all CICP children into CHP+. But some staff observed that at least three factors could deter that. One is the relatively high premiums imposed on families whose incomes place them above the poverty level. The second is the 25,000-child cap on targeted enrollments in CHP+. The third is a three month lock-out period (to be implemented) imposed on families who fail to pay their CHP+ premiums. Those families will continue to use CICP providers while they are locked out of CHP+.
Creating a Seamless Health Care System for Eligible Children
Presumptive Eligibility
Colorado does not offer presumptive eligibility to children applying for CHP+, but there was provisional eligibility. Once an application was received, the child was made provisionally eligible during the approximately 60 days it took to process the application and make a final determination.
- Staff in local sites, such as SED sites, took applications, entered data in the SQL server database via Internet, and conferred provisional eligibility. The file was transferred to Denver for final determination; verification that the applicant is not on or eligible for Medicaid; verification of immigration status; Quality Control checks; and verification of assets and income.
- During the provisional eligibility period, the child was in a "fee-for-service", state contracted provider system until final eligibility was determined and the child was moved into managed care.4 Staff were concerned about the impact on benefit costs of covering children with fee-for-service for up to 60 days, and feared that provisional eligibility may be eliminated. In fact, the Policy Board recently directed the cessation of this practice.5
Continuing Eligibility
CHP+ children, once certified and enrolled, enjoy a 12 month continuous eligibility period before re-certification must occur.
Simplified Application and Eligibility Decisions
- HCPF consolidated and simplified the application form for Medicaid and CHP+. The form is four pages with a fifth page of rights and responsibilities. Department of Public Health and Environment staff added seven questions designed to identify and facilitate referral of children with special health care needs both to SSI and the state’s Health Care Program for Children with Special Needs. The application also asks "How did you hear about CHP+ and/or Medicaid?"
- HCPF believes the simplified, integrated, four-page application form has significantly improved the application process. They intend to collaborate with other agencies to make even more improvements this year.
- HCFP is spending approximately one-third of its administrative funds on outreach for Medicaid and CHP+. Because outreach for both programs is combined, they cannot estimate a separate amount for CHP+ outreach.
- The maternal and child health staff in DPHE is piggybacking CHP+ outreach on outreach it already conducts for other child health insurance programs, so cannot disaggregate the costs.
- The Covering Kids Initiative grant provides $1 million over three years for outreach on Medicaid and CHP+. Half must be allocated to the state’s local partners.
- Colorado Community Health Network has a grant of $75,000 from HRSA for CHP+ and Medicaid outreach. In addition, Medicaid reimburses the Network $12.65 for each application processed by outstationed Medicaid sites, and CHP+ reimburses $10.00 for each application processed electronically at SED sites.
Marketing to Hard-to-Reach Populations
- With the large proportion of Hispanics in Colorado’s population, virtually all outreach materials are produced in Spanish and English.
- Newspaper ads were purchased in three-week blocks in rural newspapers.
- DPHE placed ads on 40 Hispanic radio stations across the state.
- Some public health nurses go door to door in trailer parks, and many nurses reach deeply into rural areas.
Woodwork Effect
Staff in both public and private agencies noted the dilemma they faced near the end of 1998 over engaging in too aggressive an outreach campaign that may create more demand for CHP+ than the budget permits them to meet. This would create waiting lists. On the other hand, others felt that the cost sharing requirements of CHP+ would deter enough families from enrolling their children that the target enrollment numbers might not be met in the first year. In the spring of 1999, staff recognized they were falling short of their enrollment targets.
Still others were more concerned that CHP+ outreach would surface more Medicaid-eligibles and drive up Medicaid costs. The legislature is particularly sensitive to this scenario, given the painful experience of the early 1990s. To date, at least 2500 children have been referred to Medicaid since July 1998, but HCPF is unable to estimate the number of children who enrolled. It is likely that enrollments in Medicaid would be larger were it not for the low asset test in Colorado’s Medicaid program. Since a family with a car worth $1500 may be ineligible for Medicaid, staff believe that many of these families will have incomes below the FPL and be eligible for CHP+, with its asset limit of $4500.
Potential Future Outreach
Colorado’s plans for future outreach include:
- Conduct more person-to-person outreach with trusted individuals visiting individual families; initiate a training program for this outreach and enrollment strategy;
- Develop a single consolidated application and simplified enrollment process for Medicaid, CHP+, CICP, and the Health Care Program for Children with Special Needs. The application would be produced in several languages, and the enrollment system would allow mail-in applications;
- Expand and enhance a central 1-800 Family Health Line to operate 12 hours daily, seven days a week, adding Russian and Southeast Asian languages to the current Spanish and English translation capabilities.
- Public health nurses are a key asset for outreach. Colorado’s public health nurses have served tirelessly as the front line of outreach to eligible families at the county and local levels, encouraging enrollment at immunization and well-child clinics, promoting the program throughout their county, and persuading doctors to participate in the program.
- One-on-one assistance to apply for CHP+ is the most effective way to enroll children in the program.
- Community-designed outreach and enrollment is critical. People at the local level know best how and where to enroll eligible children in their own community. Colorado invited communities with over 30 percent of school children enrolled in the school meal program to develop community-based enrollment projects. Each project assembled a collaboration of local organizations and agencies, including the local Medicaid agencies, community health centers, schools, and family resources centers, to design their own enrollment plan.
- Colorado’s CHP+ staff have a policy to treat all callers, families, intermediaries and providers with respect and dignity. This has gone a long way to promote the success of the program. Families all over the state know that they can count on CHP+ staff to listen to their concerns and respond courteously and with caring.
State’s Response
The state legislature, Policy Board, and departmental officials were seriously concerned about crowd-out. Their concerns influenced the choice of FPL eligibility level for CHP+, the benefits package, adoption of waiting periods, premiums and co-payments, and investigation of an employer buy-in program.
FPL Eligibility Level
The legislature was apprised of the research from Minnesota and elsewhere that seemed to document that crowd-out does not occur at least until a health insurance program’s eligibility levels reach 200 percent of the federal poverty level. To be cautious, they chose to leave the FPL level for CHP+ at the same 185 percent as it was in the earlier state program.
- The working group which designed benefits and eligibility, with representatives from HMOs, providers, and other businesses, grappled with whether and what to add to the benefits package to make it richer than the old CCHP. They recognized trade-offs between making the benefits rich enough to equate with the Medicaid benefits package, or conserving on benefits in order to cover more children.
- The legislature wanted the plan to be based on basic and standard plan benefits in the commercial arena. They adopted a package that includes mental health, substance abuse, a $50 annual benefit for eyeglasses, but no dental.
Waiting Periods
As an explicit employee crowd-out measure, the legislation states that children are ineligible who are covered under an employer plan with at least a 50 percent employer contribution to premiums during the three months before application. There was some discussion about whether to impose this wait also on families who had access to employer coverage but opted not to enroll. A consensus developed that it was too complex to assess availability to, and affordability of, employer insurance coverage.
Premiums
The state charges monthly premiums as follows:
- Families below 100 percent FPL, no premiums;
- Families at 100-149 percent FPL, $9 per child, $15 per family maximum;
- Families at 150-169 percent FPL, $15 per child, $25 family maximum;
- Families at 170-185 percent FPL, $20 per child, $30 family maximum;
- Families above 185 percent FPL will pay full premiums. This provision is not yet operational, so no decision has been made on what the full premium will be.
Advocates and even some state officials fear these premiums are too high and deter enrollment in CHP+. They point to the forty-percent response rate to letters sent to families with children enrolled in CCHP, inviting them to convert to CHP+. They also point to the high number of families remaining in the free Colorado Indigent Care Program. Finally, some worry about the "cliff effect" — where one extra dollar of income or assets makes a family ineligible for Medicaid, but unable to afford the premiums in CHP+.
Lock-out Periods
Colorado has developed a policy, to be implemented, wherein families failing to pay premiums will be given three written notices and a 90-day grace period. If they still fail to pay, the children will be excluded from coverage for 90 days.
Co-Payments
Families with incomes above 100 percent of poverty in CHP+ face different co-payment schedules depending on whether they earn 100-150 percent FPL or 151-185 percent. Generally, physician visits, clinic services, vision care, occupational, physical and speech therapy, mental health and substance abuse treatment services are either $2 or $5, respectively. Prescriptions cost $1 or $3, respectively, for generic drugs, but $5 for brand names. Officials are less worried about any deterrent effect on enrollment from the co-payments than they are the premiums.
Employer Buy-In
Colorado officials in the Division of Insurance’s Office of Policy and Research are working with HCPF to develop an employer buy-in program. In November 1998, staff were developing a "white paper" raising the issues to consider and questions that need to be answered to help select program features. The paper was to be presented to the Policy Board in December, 1998. Among the issues and questions they were considering:
- In accord with HCFA(now known as CMS) requirements, how can the state "bulk up" the benefits in employer-provided plans to be benchmark equivalent? Should the state purchase wrap-around coverage for benefits not included in an employer plan?
- Can the state pay employers a certain amount per family per month to "buy up" benefits for children to a benchmark-equivalent level, when there are approximately 2400 different plans operating in Colorado?
- How should the state accommodate employer plan coverage that includes co-payments that are higher than those in CHP+?
- How can the state avoid having children in families working at very low incomes receiving more generous benefits at a lower cost with CHP+ than children in low-to-middle income families who have less generous employer coverage?
- How can the state accommodate the HCFA(now known as CMS) requirement that children must lack insurance for six months before they can be eligible for an employer buy-in? This seems particularly inequitable for families who do not enroll immediately upon the onset of their employment, whom the employers will lock out of coverage until the next open enrollment period.
- How can an employer buy-in program be marketed through employees, not employers, to avoid employer crowd-out?
Colorado plans to conduct a pilot test of employer buy-in, to test the most appropriate responses to these and other questions. They are looking into piloting the program with a purchasing cooperative of employers that offer a standardized benefit package.
State policymakers and agency staff relied on a variety of data to design their program, and plan to collect data from other sources to evaluate outreach, crowd-out, cross-program referrals, and cost-sharing.
- An independent actuarial consulting firm (Leif Associates, Inc.) conducted actuarial and claims analysis to help the state design a benefits package. The analysis considered both children who would have to stay in fee-for-service coverage (approximately one-fifth of the state’s children) and those who would be covered by managed care.
- The University of Colorado Health Sciences Center’s Department of Health Outcomes conducted a study comparing the earlier CCHP program to Medicaid and private health insurance on measures of quality of care and utilization. They looked at preventive care services (e.g., immunizations), care for acute illness, and care for children with asthma, the most common chronic illness of childhood. The results were used to advocate for certain features of the benefits package. The results can be found in, Colorado Child Health Plan Annual Report, The University of Colorado Health Sciences Center, March 1, 1998.
- To measure how well the state improves the health status of children — especially with the availability of preventive and early primary treatment — Plans must submit independently audited HEDIS data. Where possible, HCPF will obtain these data for the state-contracted provider network (fee-for-service) as well. HCPF will use the data to measure success in reaching performance goals regarding immunizations and well-child visits.
- The state also plans to analyze questions on the joint Medicaid/CHP+ application related to children with special needs, to track what proportion of applicants are children successfully referred to the Health Care Program for Children with Special Needs and SSI.
- To measure how much the proportion of uninsured children is reduced, the state will analyze CPS data. Baseline numbers of uninsured children will be calculated from a three-year average of the 1995, ‘96, and ‘97 March supplement to the CPS. New estimates of uninsured children will be calculated as more current data become available and will be used to compare trends from year to year. The CPS data has been used by analysts at the American Academy of Pediatrics (Colorado) and the Foundation to project county estimates of uninsured children. State analysts are concerned about accurately estimating the baseline since the proportion of employers providing coverage was already on the decline (i.e., employment in sectors that traditionally do not provide employer coverage was on the rise) prior to CHP+.
- The Robert Wood Johnson Covering Kids grant includes funds for technical assistance to better estimate the numbers of uninsured children.
- To assess how to reduce the financial barriers to affordable health care, clients who disenroll once their 12 months of eligibility have expired will be asked to explain why they are leaving. Responses will be tabulated. In addition, responses to a question on the application form, "How much would you be willing to pay for health insurance for your children?" will be analyzed and the results used to reassess the premium levels.
- To measure the effectiveness of certain outreach strategies over others, staff will analyze responses to the phone bank operators’ inquiry: "Where did you hear about CHP+?" This analysis may alter next spring’s marketing campaign.
- To measure employer crowd-out, analysts will obtain from CPS a three-year average estimate of the proportion of children under 185 percent FPL covered under an employer-based plan. They hope to devise a methodology that accounts for decreases due to increasing health care costs or a downturn in the economy. They expect to supplement this with Labor Department data on insurance coverage. This task will be challenging. For example, if a large company in Colorado has only ten percent of its employees earning under 185 FPL, and it drops dependent coverage from the firm’s Plan, it is unlikely to be attributable to CHP+. But when does attribution become credible? Is it at 20 percent or 40 percent of the company workforce earning under 185 percent FPL?
- To measure employee crowd-out, analysts hope to study responses to questions on the application about current and recent employer health coverage. They want to develop a methodology to follow applicants denied CHP+ eligibility due to current or recent employer coverage (last three months), to determine whether they drop coverage, or whether they take up other coverage. They may interview a sample of families whose children are denied.
- Numerous efforts are underway to measure quality in managed care. These efforts were originally intended to analyze quality of care for Medicaid recipients, but will apply to CHP+ recipients in the same managed care plans, as well. Examples include studies of continuity of client access to appropriate care; client satisfaction surveys; and collection of HEDIS data on utilization, access, and quality.
State officials cited several challenges to implementation. Staff turnover in HCPF and the few FTEs the legislature authorized to administer CHP+ slowed implementation. Delays were attributed to the time spent writing an RFP and evaluating proposals for a contract to the new private, non-profit organization conducting day-to-day administration. More delays were attributed to the time Foundation staff spent responding to the RFP, and transitioning to the private, non-profit organization.
Some officials stated that, in retrospect, it might have been easier to get a brand new program off the ground than to transition from CCHP to CHP+. The most pressing administrative barrier they face is the ten percent cap on federal match for administrative expenses.
Ten Percent Cap on Administrative Expenses
By November 1998, Colorado estimated their administrative expenses had already reached 17 percent of total expenses for CHP+, with recent projections that it might average 16 percent. In a report to the legislature in 1998, HCPF stated that they projected health care costs of $14.3 million (net premiums) and $3.3 million in administrative expenses, with federal reimbursement of the latter expected to be $1.4 million. The difference of $1.8 million must be paid with state-only funds.
Officials pointed to various causes for their high administrative costs, including: the transition costs from a previous to new state program; expanding to inpatient coverage; and developing a new automated, rules-based eligibility determination system (Colorado Benefits Management System) that will include CHP+ and other public assistance programs. One official said that the ten percent cap must cover fifty percent of what Colorado is trying to do.
Other Challenges
Funding limitations and a consequent enrollment cap initially tempered what might otherwise have been vigorous outreach and enrollment efforts. However, more recent projections of enrollment suggest that CHP+ might fall short of its target, so outreach has become more aggressive.
Moreover, staff turnover in HCPF and legislative authorization for only 3.5 positions to implement CHP+ are reported to have been a barrier to implementation.
Finally, staff believe the integration of the Application Form has improved the process for Medicaid but hindered the process for CHP+. This is because Medicaid rules require collection of information to determine "blood lines" and establish "the Medicaid budget unit", a requirement that is unnecessary for CHP+.
Web Sites for More Information
www.cdphe.state.co.us/cdphehom.html
1 - For example, if the net asset value of the family vehicle exceeds $4500, the excess is treated as additional family income.
2 - Since the time of the site visit for this case study, the foundation has been replaced by a private, non-profit contractor.
3 - The Foundation has been replaced, since the site visit, by Child Health Advocates—a private, non-profit organization. To ensure continuity of operations, the new contractor hired most of the Child Health Plan staff from the Foundation for Children and Families.
4 - State contracts with a primary care provider network provide for no risk-shifting to the providers.
5 - The processing time has recently been reduced from 60 days to 15 days.
Chapter IV: Chip in Massachusetts
History and Implementation
Pre-Title XXI
Massachusetts has a long and active history of state initiatives to expand health coverage for the uninsured. Prior to the Title XXI legislation, the State Legislature had already created a separate children’s health insurance program, expanded Medicaid eligibility through a waiver and explored ways to subsidize employer-sponsored insurance. As a result of these initiatives, Massachusetts’ presents a unique Title XXI program. An abbreviated history follows which helps explain certain elements of the state’s Title XXI program:
- The Children’s Medical Security Plan (CMSP) began in 1993 to serve uninsured children. Over time, its age and income eligibility criteria expanded to cover children up to age 19, living in families who were not eligible for Medicaid. The CMSP provides basic primary care to children, with a very limited benefits package.
- The state submitted a request for a Medicaid waiver in 1994 to expand program eligibility, simplify eligibility rules, and create an Insurance Reimbursement Program (IRP) to help subsidize employer-sponsored insurance. The original idea was to offer tax credits to businesses covering 50 percent of the insurance costs for their employees with incomes under 200 percent FPL. A Study Commission convened to discuss the waiver. The Commission included administration officials, legislators, and representatives of the public. Although there was consensus about simplifying Medicaid and expanding eligibility up to 133 percent FPL, there was disagreement about whether tax credits to employers would reduce the number of uninsured. Part of the debate focused on the plan to finance a portion of the waiver demonstration from the Uncompensated Care Pool, which was then funded by an assessment on hospitals. The concern was the extent to which using the Pool to cover the subsidy costs would deplete funding available to help uninsured hospital patients.
- During the legislative discussion in 1996 to approve the state’s Medicaid waiver request, it was decided to fund the state’s share of the expansion costs through an increase in the tobacco tax and to convene an IRP Study Commission. The State Legislature approved:
- expanding Medicaid for families (among others) up to 133 percent FPL and for those under 12 up to 200 percent FPL;
- creating a senior pharmacy fund; and
- expanding eligibility for CMSP to age 18.
- Governor Weld vetoed the legislation because it raised taxes and had no IRP, but the legislature overrode the veto. The tobacco tax idea inspired Senator Kennedy to use the same financing approach in the Federal Child Health Insurance Program legislative proposal.
- The new Governor proposed and the State Legislature approved legislation in 1997 that further expanded Medicaid (renamed as MassHealth) to children with family incomes below 200 percent FPL. An Uncompensated Care Commission convened to discuss how to finance the Pool. The Commission recommended changing the Pool financing so that the IRP became a direct cash subsidy only for small businesses (under 50 workers) that provide employer-sponsored insurance for employees with family incomes under 200 percent poverty.
Title XXI
After the Federal legislation passed, the State Legislature and Governor approved a combination CHIP plan with several components, that include:
- Expanding Medicaid (MassHealth Standard) coverage for uninsured children through the age of 18 from the previous level of 133 percent FPL to 150 percent FPL.
- Providing a new program for uninsured children between 150-200 percent FPL (MassHealth Family Assistance). This program, based on a modification of the IRP, requires children in families where employer-provided coverage is available, to enroll in that coverage.
- Limiting eligibility for the state-funded Children’s Medical Security Plan to children who are ineligible for MassHealth programs, including non-qualified aliens who are ineligible for Federal benefits.
- Providing limited (60 days) presumptive MassHealth eligibility for children while verification of income and other information is obtained.
- Expanding MassHealth coverage for pregnant women from 185 percent FPL to 200 percent FPL to create a continuum of care for all low-income children beginning with comprehensive pre-natal care.
As a result of the state expansions and legislation implementing Title XXI, lower income women and children under age 19 are insured through one of three programs depending on their health status and family income:
- Children through age 18 with family incomes under 150 percent FPL are eligible for MassHealth Standard through either Medicaid or Title XXI. They have access to full Medicaid coverage and no premiums are charged.
- Children with disabilities through age 18 with family incomes between 150-200 percent FPL who are ineligible for the standard program qualify for MassHealth CommonHealth. This fee-for-service program provides all Medicaid services.
- Non-disabled children through age 18 with family incomes between 150-200 percent FPL are eligible for MassHealth Family Assistance. Children are placed in one of two components, depending on their insurance status:
- if they are uninsured, they receive coverage directly from the state; or
- if they have access to or are enrolled in private insurance, they receive premium assistance.
Both charge a $10/child per month premium with a family cap of $30 per month.
- Pregnant women with family incomes up to 200 percent FPL are eligible for MassHealth Prenatal. They have access to MassHealth Standard coverage. (See Exhibit 1, MassHealth Expansions.)
Insert Exhibit I Here
Federal/State Financing
Massachusetts’ Title XXI allocation of Federal funds in the first year was up to $43 million. The state matching rate is 35 percent, funded through a tobacco tax so no new state appropriation is required. The state is projecting they will spend $6.7 million in state matching funds.
- MassHealth Standard enrolled about 15,000 children as of November 1998.
- MassHealth Family Assistance covered about 28,500 children of whom:
- Direct Coverage paid for about 12,500 children
- Premium Assistance enrolled about 16,000 children
The Division of Medical Assistance projects that within one or two years there will be 37,100 children covered through Title XXI in MassHealth Standard. Some percentage of these children were previously enrolled in the state-funded health insurance program (Children’s Medical Security Plan), but are now eligible for Title XXI coverage. No data are available to indicate the number of children now eligible for Premium Assistance who already have private insurance.
Key Factors in Massachusetts Implementation
- Precedent was key. Massachusetts has a long history of expanding public health insurance for children dating back several administrations, so the political climate was very supportive of additional expansions.
- Outreach funds were already available. The State Legislature had already appropriated state funds to conduct outreach to locate more children eligible under state expansions.
- Provider collaboration was essential. The Division of Medical Assistance was already working with providers to serve more children eligible under state expansions.
- Automation helped. For the state expansions, an automated eligibility "decision tree" was developed which was easily modified to accommodate additional children eligible under Title XXI.
- A known pool of eligible children was tapped. There was already a large pool of CHIP-eligible children in the state-funded program, Children’s Medical Security Plan. To enroll this group, the Department of Public Health was able to transfer their cases to the Division of Medical Assistance, which was less labor intensive than organizing a statewide outreach campaign to locate uninsured children.
- Good data were useful. The Division of Medical Assistance already had some initial baseline data about the number of uninsured children in the state. These data were not dependent on CPS estimates, so it will be possible to measure enrollment changes in the different children’s health insurance programs now available.
State Approach
Massachusetts has a multi-pronged outreach approach involving both community-based and statewide activities. While the statewide agency efforts are significant, a creative feature of Massachusetts’ approach to involving communities and finding hard-to-reach populations is their mini-grant program (described in detail on page 13).
Key Players and Administration
- Division of Medical Assistance (DMA) — the Medicaid agency — formerly part of the Department of Public Welfare, that administers MassHealth.
- Department of Public Health (DPH) — the Maternal and Child Health agency (Title V) that administers the Children’s Medical Security Plan (the state-funded children’s health insurance program).
- Area Health Education Center/Community Partners — A private, non-profit organization that supports a mini-grant program to find hard-to-reach populations.
Collaboration with Other Agencies and Organizations
State Agencies
- Department of Public Health (DPH). There was a major effort undertaken to move 20,000-30,000 children enrolled in the Children’s Medical Security Program into MassHealth as they became income eligible for a better benefit package in CHIP. DPH sent a letter to all these families explaining their potential eligibility for MassHealth, describing the advantages and enclosing the MassHealth application form to complete and return.
- The Department of Transitional Assistance provides the Division of Medical Assistance with lists of families recently terminated from the time-limited welfare program. These families are often unaware of their continued eligibility for MassHealth, so DMA notifies them of their continued eligibility.
- The Department of Education and Office of Child Care Services play major roles in the distribution of material for the state’s annual school-based outreach effort.
- The University of Massachusetts at Worcester administers half of the mini-grants, with the Department of Public Health administering the other half.
Community Efforts
- School-based outreach. This effort was developed by the Division of Medical Assistance to disseminate information through every public and private school, and every child care program in the state.
- Area Health Education Center (AHEC) coordinates the Health Access Networks, which provides an infrastructure of support for the mini-grant program. The 52 mini-grant organizations and many others who attend the Health Access Networks make up the bulk of community-based activity on outreach and enrollment in the state. (Additional detail is provided on page 14.)
- Coaches Campaign. Organized by five teenagers in the Boston area, this effort was supported by Health Care for All, a statewide health care advocacy organization. The campaign wants to "spread the word that no one should be left on the sidelines." The brochure explains that there are six health insurance options that teenagers should explore with their families before deciding which is best for them. The brochure slogan says: "There are many worthy opponents. Health insurance shouldn’t be one of them."
- The Community Partnerships Initiative was developed by DMA to identify and disseminate information and applications through key community stakeholders. Stakeholders included school nurses, municipal skating rink directors, librarians, summer camp directors, public housing heads, civic and neighborhood association leaders, and others.
- The Targeted Cities Initiative was developed by the Executive Office of Health and Human Services and involved working with municipal governments to highlight MassHealth and enroll uninsured children and families.
- DMA held a series of statewide meetings with Latino community leaders in an effort to increase awareness about MassHealth availability and develop effective outreach and marketing strategies to Latino neighborhoods.
Provider Outreach
- The State Hospital Association promoted the American Hospital Association’s Campaign for Coverage using press events, posters, brochures, mailings, and buttons to generate publicity.
- The Massachusetts Medical Society sponsored a statewide series of ten free seminars called "What are the Health Care Options for Massachusetts’ Uninsured"? Physicians and office staff who receive inquires from families about health insurance were encouraged to attend. The same seminar was offered twice, at 4 PM and 6 PM, with a light dinner in between as an incentive to attend.
- The Massachusetts League of Community Health Centers recently promoted child and family health insurance enrollment through an English/Spanish poster campaign.
- The state chapter of American Academy of Pediatrics and DMA are sponsoring Children’s Health Care Access Seminars to familiarize pediatricians and their office staff with MassHealth. The effort includes a take-back-to-your-office kit that contains enrollment applications, a "What to do" instruction card, posters, brochures, rolodex cards, a list of community mini-grant programs, and a MassHealth outreach worker contact.
Media
- DMA held several press events and disseminated subsequent news stories with particular attention to weekly and ethnic publications.
- The agency arranged for two PSAs to be developed by a Boston radio station with the highest 18 to 34-year-old audience demographics.
- The agency worked with a Latino television station and Univision affiliate to develop three PSAs.
- DMA is currently working with an advertising agency (pro bono) to finalize an FY2000 public awareness and enrollment campaign.
Creating a Seamless Health Care System for Eligible Children
Presumptive Eligibility
Children have presumptive eligibility in MassHealth for up to 60 days while verification of income and other information is obtained.
To determine eligibility for one of the two MassHealth Family Assistance programs, the state contracted with a health insurance identification vendor, Public Consulting Group of Boston. This company investigates applicant families with incomes between 150-200 percent FPL to check the status of their access to employer health insurance, which determines which type of coverage the children receive. Enrollment of the children while these investigations are pending is time-limited for another 60 days, during which they are covered by fee-for-service. However:
- If families already have insurance, their children are not eligible for 60-day fee-for-service benefits;
- If families have potential access to employer health insurance, their children are enrolled in direct coverage on a fee-for-service basis.
Continuing Eligibility
Children who are eligible for Title XXI will have their eligibility re-determined at least once annually, unless reported changes in family circumstances (income, number of children) trigger an earlier review.
Simplified Application and Eligibility Decisions
There is a single application for MassHealth (including CHIP) and CMSP, called the Medical Benefit Request (MBR). The MBR goes to the Division of Medical Assistance which uses a computerized "decision tree" that automatically assigns children to the appropriate program, depending on their family income and whether they have access to employer health insurance.
Working together, the Division of Medical Assistance and Department of Public Health reduced the application to four pages with supplements for additional questions in four areas: health insurance status; injury, illness or disability; absent parent1; and immigrant status.
Families can enroll by calling a toll-free number or visiting one of the four MassHealth enrollment centers across the state. After qualifying, the family receives an information package in the mail to select its provider. The number of choices varies statewide, but in general families may have a choice among six managed care organizations or the state-contracted Primary Care Clinicians Program.
Funding for Outreach
Even before Title XXI passed, the State Legislature appropriated $1.5 million to conduct outreach to find children who were eligible under its own pre-CHIP expansion plan. No additional funding was allocated for CHIP outreach.
The Division of Medical Assistance and Department of Public Health allocated $647,000 for a mini-grant program that is designed to find hard-to-reach families. Some of this funding will be charged to Title XIX, to Title XXI, and to the TANF block grant for federal reimbursement.
Marketing to Hard-to-Reach Populations
The Mini-Grant Program is jointly administered by three agencies and has two components: (1) to conduct outreach activities and enroll eligible children and families, and (2) to create innovative programs to alleviate pressure on the Uncompensated Care Pool which serves children who are ineligible for MassHealth.
The Mini-Grant Program is a direct outgrowth of discussions among staff of the three agencies — Division of Medical Assistance, Health Care Finance and Policy, and Department of Health — seeking a more coordinated approach to multi-layered outreach on health insurance programs. It is supported by an organization in the western part of the state that has worked for years to establish and expand community health centers. The Area Health Education Center (AHEC) has a contract with the state Division of Medical Assistance to convene Health Access Network meetings for mini-grantees and others. AHEC convenes regional Health Access Networks monthly in five areas of the state. Attended by a wide range of health-related community groups together with local and state public agency staff, participants share "best practices" for outreach and discuss policy and program developments. They also develop linkages and relationships to facilitate outreach. Finally, the Networks afford an opportunity for the community groups to provide feedback to state agencies about how to expand enrollment and decrease unnecessary emergency room use.
The mini-grants are designed for organizations that have successfully demonstrated their ability to serve their communities, especially hard-to-reach families who would not otherwise be found. In 1998, 52 community-based organizations received grants of $5,000-$20,000. Grantees include:
- community health centers;
- local organizations serving specific populations (e.g., Latino, Vietnamese, Portuguese, Hispanic, Cambodian);
- community coalitions;
- housing groups;
- child care agencies;
- mental health agencies;
- visiting nurses associations;
- immigrant and refugee service organizations;
- multi-service centers; and
- hospital community programs.
Examples of strategies used by mini-grant programs to provide information about children’s health insurance include:
- holding a Saturday raffle for a chain saw at the town dump to attract fathers;
- using billboards that show pictures of the local outreach workers in rural communities where many families know and trust each other;
- placing announcements on cable television;
- canvassing homeless shelters;
- attaching stickers about health insurance to applications for school-sponsored sports teams.
There is widespread support for the Mini-Grant Program among the state agencies, local organizations and health care advocates who all concur that it provides the most effective way to locate hard-to-reach populations.
AHEC produced a free guide, Health Access Tips: Making Outreach Work, based on ideas used by community groups in MA and elsewhere. The guide is available at AHEC’s Web site, http://www.ahecpartners.org/resources or by calling (413)253-4283.
Woodwork Effect
DMA staff assert that all of their planning for the Medicaid waiver demonstration was designed to cause a woodwork effect. They hoped to attract many families who were previously eligible for but not enrolled in Medicaid. They estimate that two of every three families applying this past year fall into that category, and they hope that CHIP outreach will cause the same woodwork effect.
Advice for Other States on Outreach
- Working with providers produces the greatest impact on increasing initial enrollment. First, staff must convey to providers that "it’s good for them to inform patients about the program." Providers see a lot of uninsured families, from whom they may never receive payment for services. Once you point out the benefit to providers, you get buy-in from them, and you will begin to see a dramatic surge in applications. Of course, providers cannot help with families that do not see doctors.
- To reach the maximum number of children, state administering agencies need as many partners as they can establish partnerships with — other state agencies, providers, community groups, Universities, and private non-profits.
State’s Response
Under state legislation, the Division of Medical Assistance can provide premium assistance to maximize the use of employer-sponsored health insurance. To prevent crowd-out and encourage employer-based coverage, the Division funds premium assistance payments to employees and incentive payments to employers by using a combination of Federal revenue available through its Medicaid waiver and Title XXI. Massachusetts has the first approved State Plan in the country that subsidizes private health insurance for workers who cannot afford employer-based insurance.
State officials believe that its premium assistance plan (authorized through its Insurance Reimbursement Program) is the best defense against crowd-out among both currently uninsured families and the increasing numbers who might drop coverage because of rising costs. Indeed, they point to the goal of "horizontal equity" as the most compelling reason for trying to help everyone at a given income level, insured and uninsured alike. Thus, the premium assistance plan is designed to prevent families from canceling their employer-based coverage, especially families with children who are eligible through state and Title XXI expansions who may already have private insurance. However, state officials additionally support using public funds to provide coverage for families who are already insured because they believe that the state’s long term goal is to encourage the private insurance market to serve lower income families.
There was political debate over the size of the financial contribution to require from families through their premium payments. The State Legislature approved a compromise between DMA and the advocates that limits monthly premiums to $10 per child up to a maximum of $30 per family when the family income is between 150-200 percent FPL.
Some debate continues within Massachusetts about the state’s premium assistance plan, though it should be noted that HCFA(now known as CMS) has approved the plan. Among the issues that are raised by advocates and others are the following:
- Should the state be permitted to establish different benchmarks for benefits, one for children enrolled in the MassHealth Family Assistance premium assistance component (funded through the state’s Medicaid authority and state legislation) and one for children enrolled in the MassHealth Family Assistance direct coverage (funded through Title XXI)? State officials believe it is permissible to have different benefits for the premium assistance component, which offers fewer benefits. Advocates maintain that Title XXI establishes a Federal floor for children’s health benefits (as a condition for federal reimbursement). Children affected by this disagreement are those with incomes between 150-200 percent FPL who are enrolled in one of two Family Assistance programs depending on their access to private insurance (MassHealth Family Plan, Title XXI benefits, if no access; Mass Health Premium Assistance Plan, if have access).
- Does the premium assistance plan itself promote crowd-out by using public dollars to help subsidize the cost of private health coverage for insured children? State officials maintain that the answer is, "Yes, precisely for horizontal equity reasons." They believe that by accepting a certain amount of crowd-out up front, they dampen future crowd-out.
- Will the premium assistance plan significantly increase the number of insured children or will it instead offer subsidized coverage for children who are already insured? Again, state officials respond that subsidizing coverage for insured children is part of their program design, to maintain equity.
- Has the state structured the different types of family plans in a way that can ensure continuous coverage for children, as family circumstances alter that affect their eligibility status? For example, consider these situations:
- What happens to a child’s existing coverage when a parent changes jobs and suddenly has access or loses access to private insurance?
- What happens when a parent loses a job and the family income decreases?
- What happens when another sibling is born or adopted and the family size changes but income does not?
Premiums
The imposition of premiums for the MassHealth Family Assistance Plan is a direct response to crowd-out concerns and horizontal equity. State officials believe that premiums place the public program on a more equal footing with employer-provided coverage.
- MassHealth Family Plan (Title XXI program). The family pays a $10 per child premium monthly and receives comprehensive benefits similar to, but not equal to, Medicaid (prescriptions drugs are included but not long term care or transportation). Families may choose among any managed care plans available in Medicaid, or the Primary Care Clinicians Program. Federal law requires that the out-of-pocket expenses for premiums and co-payments must be capped at five percent of the family’s annual income. This group — often called the "shoebox" children — must keep track of their expenses to avoid exceeding the five percent cap. (Note: Children who were previously enrolled in the state health insurance program who are now eligible for this coverage do not pay premiums.)
- MassHealth Premium Assistance Plan. The family pays a $10 per child premium monthly and the state subsidizes employee and employer coverage through its Insurance Reimbursement Program, authorized by its Medicaid waiver. This plan is different than Title XXI in that the minimum benefit package is lower. The state cannot claim the enhanced match through Title XXI for these children who were previously insured, because Federal law does not allow states to assist currently insured families.
Lock-out Periods
DMA officials do not characterize their policy and practice as a lock-out period. However, if a family’s premium payments are in arrears for two months, they will generally be terminated from coverage. If that family returns to re-enroll, they may request that a repayment plan be worked out for them. There are special hardship provisions, as well.
Co-payments
If a child is enrolled in the Family Assistance Plan direct coverage component, there are no co-payments. If a child is enrolled in the Family Assistance Plan premium assistance component, there may be co-payments depending on family income, and the co-payments are included in the calculation of the aggregate five percent cap on out-of-pocket costs.
A Health Care Kit was prepared — to remedy the need for shoeboxes — that helps eligible families track their out-of-pocket expenses and send all receipts to the Division of Medical Assistance. After meeting the cap, DMA will notify the family so that when the next medical bill arrives, the family can forward it to the agency for payment or the provider can bill DMA directly. Families will receive a letter to show providers that the family must no longer be charged co-payments. Alternatively, the provider can access the Recipient Eligibility Verification System (through the child’s Social Security number) to check if the family has reached its cap.
Employer Buy-In
Massachusetts officials believe that employer and employee subsidies offer the most effective way to discourage further erosion of employer-sponsored health insurance. Through its Medicaid waiver, the state has the authority to implement an Insurance Reimbursement Program to provide:
- premium assistance payments for families (and individuals) with incomes below 200 percent FPL; and
- incentive payments for small employers providing insurance to lower income employees.
For Employees
Families participating in the subsidy program are served using Federal funds available from the state’s Medicaid waiver. When the employer pays at least 50 percent of the cost, the state believes it is more economical to purchase family coverage; this is also less disruptive for families because it allows all family members to use the same providers. Families in this program do not have the same benefits or protections given to Title XXI families:
- Children are covered through the standard small group plan where benefits can vary (e.g., some lack prescription drugs, dental or other services) from Title XXI benefits.
Data from the Division of Medical Assistance indicates that by October 1998, 150 children were enrolled in the premium assistance component and another 2,000 were awaiting their insurance investigations. The investigations determine who already had insurance and was eligible for this program versus those who were uninsured and would be placed in the MassHealth Family Assistance Plan (Title XXI).
For Employers
The employer subsidy program began phase-in in January 1999 and includes employers paying at least 50 percent of the insurance premium costs for lower income employees.
- The program will begin with employers who have less than ten employees and later will expand to companies with less than 50 employees. Small businesses were targeted for the program because they are the fastest growing group of employers and the state wants to encourage them to offer employee health benefits.
- The program will provide subsidies of $400-$1,000 for small businesses.
The program is funded by the Uncompensated Care Pool, federal funds, tobacco tax revenues, and general fund dollars.
Data for Program Design
- A special commission conducted a study of uncompensated care in the state. It was delivered to the State Legislature in February 1997. The report is briefly described on the Web site of the Division of Health Care Finance and Policy, www.magnet.state.ma.us/dhcfp, and is available in full, hard copy, from the Division.
- A survey on the number of uninsured in the state was conducted by the Division of Health Care Finance and Policy and the University of Massachusetts, Survey Research division. This survey was designed to have a larger sample than, and improve on the scope of, the Current Population Survey.
- The Division of Health Care Finance and Policy conducted a study to compare various approaches to covering working families who are uninsured. This report was filed with the State Legislature in April 1998, and is available from the Division only in hard copy.
- The University of Massachusetts is helping the Division of Medical Assistance (DMA) collect baseline data about the number of uninsured individuals. One method is through a state survey of 3,600 families that asks "Are you uninsured today?" to compare responses to earlier work done by CPS and the Urban Institute. No report is available at this time.
- The second method will supplement this information by developing more targeted, regional baseline estimates. DMA has commissioned the University to compare results from the 3 surveys — the Urban Institute’s, the University’s, and the University Survey Research division’s — to compile better forward-looking projections on regional uninsured rates.
- The Division of Health Care Finance and Policy reported on an independent evaluation of the effectiveness of all MassHealth Programs in March 1998 and a second report is due March 2000. A hard-copy report is available from the Division.
- HCF&P will conduct a comprehensive survey of uninsured individuals by November 1999.
- To monitor outreach, DMA will track enrollment data by zip code, primary language, outreach site, and mini-grant recipient to monitor where and with what populations outreach efforts should be modified.
- To monitor the new, simplified application process, DMA will track the number of applications filed, number approved, number denied, number needing further verification and the decision turnaround time. This study will also examine the success of presumptive eligibility and whether families submit necessary verification or lose coverage because they fail to do so.
- To monitor the new Premium Assistance Plan, DMA will track the number of children receiving this new coverage and whether they already had private insurance, as well as how many plans meet the benchmark package of benefits. It will also track the impact of premiums and whether they contribute to families’ disenrollment.
- To monitor quality of care, DMA can collect data from its claims system showing what services are provided by managed care organizations across the state. This allows the Medicaid agency to match encounter data with eligibility files to examine access and quality measures for specific subpopulations (e.g., number of visits to specialists; screening rates; well-child visits; inpatient and outpatient visits; and number of children with specific diagnoses).
- DMA will monitor the employer assistance plan once there are enough small employers subscribed so that the data is meaningful.
- Consumer Assessment of Health Care Survey (CAHCS). The survey will include information about consumers’ access to and experience with quality of care. It is mailed directly to individuals (in English and Spanish) to determine their experiences over six months. The state is testing ways to determine how to ensure the highest response rate by combining mailings and telephone follow-ups and possibly some face-to-face interviews.
- Child and Adolescent Health Measurement Advisory Panel. Massachusetts is one state participating in this national initiative that is trying to determine how to measure certain health issues such as getting healthier, staying healthy and living with chronic illness. The state will pilot a survey of adolescents to determine how to ensure an adequate response rate.
- A Robert Wood Johnson Foundation grant will be used to evaluate all of Massachusetts’ health care expansions that use either state or Federal funds. So far, the state is working under a planning grant, and will apply for the next phase.
- As the state begins to implement both its employee and employer subsidies, state staff anticipate a challenging change to their outreach strategies. With subsidies, outreach becomes more of a workplace activity. This will require the state or the contractor running the subsidy program (Public Consulting Group of Boston) to work with personnel offices and companies across the state to ensure program enrollment. This type of outreach is very different than strategies historically associated with finding lower income families who may be eligible for public services.
1 - These questions are designed to pursue medical support enforcement. federal law requires that custodial parents receiving child support services from a public child support agency, must report the non-custodial parent's employer (if known). The child support agency must determine whether the non-custodial parent has employer-provided health insurance available at "reasonable cost," that could cover his/her children. If so, he/she must enroll the child.
Chapter V: Chip in New York
History and Implementation
The Title XXI program expands access to an existing state Child Health Plus (CHPlus) program, a partnership between the state and private insurers with the state subsidizing private coverage for enrollees. The Title XXI program will also support expanded Medicaid eligibility in New York.
Pre-Title XXI
The Child Health Plus (CHPlus) Program was established in 1990, with a $20 million state appropriation, to provide primary, preventive care for low-income children under age 13. For six years, the program slowly expanded age eligibility as additional funding became available. By 1996, CHPlus covered children up to age 15 with a state annual appropriation of $73 million.
In 1996, Governor Pataki proposed to expand the program significantly by raising eligibility through age 18, adding inpatient care, and increasing annual funding. The Legislature approved authorizations to increase to $207 million by 1999, and also approved $1 million specifically for outreach activities. As a result of these changes, CHPlus grew to serve over 140,000 children under the age of 19 with family incomes up to 185 percent FPL, before Title XXI was enacted.
State Compliance with Title XXI
With the passage of Title XXI, additional funds were made available for children’s health insurance initiatives. New York’s State Plan, submitted to the Health Care Financing Administration(now known as Centers for Medicare and Medicaid Services(CMS)) (HCFA(now known as CMS)) in November 1997, became effective April 15, 1998. Legislation was enacted in 1998 which enhanced the program, and ensured that CHPlus was in compliance with the Federal requirements.
New York was one of three states in which existing children's health coverage benefit packages were "grandfathered" into the CHIP legislation, along with Florida and Pennsylvania.
Title XXI
In 1998, the Governor and both chambers of the State Legislature wanted to expand publicly funded children’s health insurance. A political compromise between the Governor, the Republican Senate and the Democratic Assembly resulted in new state legislation that significantly expanded eligibility for CHPlus and Medicaid, effective January 1999. Initially, these changes will:
- Allow children under age 19 with family incomes up to 230 percent FPL (rising to 250 percent in July 2000) to qualify for CHPlus;
- Allow all children under age 19 with family incomes up to 100 FPL to qualify for Medicaid; and
- provide 12 months of continuous Medicaid eligibility for all children under age 19.
Later, Medicaid eligibility will expand to children ages 6-19 whose net income is less than 133 percent FPL when one of the following two events occurs:
- The state secures the necessary Federal approval to enroll children in a managed care program; or
- The Commissioner of Health certifies that at least 50 percent of the persons eligible to enroll under a managed care program through a Federal waiver are enrolled.
Presumptive eligibility for Medicaid will begin when the eligibility expands (see Exhibit 1).
- New York’s Title XXI allocation of Federal funds in its first year was up to $256 million.
- The state contribution is $205 million funded through the health care initiative pool approved in 1996 by the legislature in its Health Care Reform Act that expires in 1999.
- New York’s state match for Medicaid is 50 percent. The state normally imposes a local Medicaid matching requirement with 25 percent paid by the counties and the remaining paid by the state. There was unanimous agreement among state officials to pay the local share for children who qualify for Medicaid under the expansion (i.e., over six and under 19 up to 133 percent FPL). However, the state will not pay the local cost if the children were previously eligible, but not enrolled.
Insert Exhibit 1 Here
Current Enrollment
In 1997, 3,000 children a month were enrolled in CHPlus. Enrollment has been steadily increasing, with the monthly average now about 9,000 children. In New York State, there were 281,000 children receiving public health insurance as of February 1, 1999.
The state will soon establish a community-based infrastructure for applications for children’s health insurance programs (both Medicaid and CHPlus). Referred to as "facilitated enrollment", trained individuals will be stationed in community settings to help families apply for children’s health insurance; facilitate completion of the application; and forward the application to the appropriate program for eligibility determination. (The new enrollment process is described in more detail below.)
Key Factors in New York Implementation
- Phased expansion was helpful. By starting small with its state-funded program (CHPlus), New York could adapt its program as eligibility and funding expanded. State officials felt prepared to plan further modifications and expansions when the Federal Title XXI funds became available.
- Stakeholder support strengthened the foundation. CHPlus is very popular among all stakeholders. Families like it because they consider it a private insurance program that does not have the stigma of Medicaid. Insurance companies and the Business Council like it because they consider it an effective partnership between the public and private sectors benefiting low-income children and their families.
- Bipartisanship prevailed. Republicans and Democrats were prepared to allocate state funds to expand access to children’s health services, including the need to support outreach to locate potentially-eligible uninsured children.
- Policy discussions about how to expand CHPlus with the new Federal funds were bipartisan, and conducted independent of state budget negotiations.
State Approach
Various public and private agencies share responsibility for various outreach, marketing and enrollment activities. Their outreach activities are targeted to locate lower income children who are eligible for either Medicaid or CHPlus. The different agencies include:
- A community outreach contractor, selected through a competitive RFP process, who manages outreach and marketing.
- Participating private plans distribute marketing materials and enroll applicants.
- Local social services and health agencies help establish linkages with schools and community-based organizations.
- The Department of Health coordinates a statewide media campaign.
Key Players and Administration
- The New York Health Plan Association is the community outreach contractor.
- There are 27 managed care organizations participating across the state although Empire Blue Cross/Blue Shield covers about one-half of all the children eligible for CHPlus.
- County social services and health agencies conduct final enrollment.
- State Department of Health provides overall administration.
Title XXI
The Governor wanted an aggressive outreach strategy that is tailored for local communities. Advocacy organizations, health plans and consumers helped design a new approach called "facilitated enrollment" to assist families to apply for either Medicaid or CHPlus. The facilitated enrollment provides community-based workers to assist families in completing an application for CHPlus or Medicaid and WIC. Located where families are already receiving services, such as child care centers or schools, facilitated enrollers screen the family for the appropriate program, help complete the application, collect the required documentation, and transmit the completed application to the appropriate program.
State officials believe that the new outreach and enrollment infrastructure will help ensure that children are properly placed in CHPlus or Medicaid, depending on their eligibility. Another major goal is to locate multi-lingual community-based workers to interview potentially eligible families in the enormous range of ethnic populations in the state, especially in New York City. Specific language in the recent state legislation details how the facilitated enrollment process should operate.
The new approach was motivated, in part, by a desire to remove some of the stigma families report feeling when applying for Medicaid. For many years, because of a longstanding concern about possible fraud and abuse, state law has required face-to-face interviews of Medicaid applicants in local Department of Social Services (DSS) offices where families also apply for welfare. Under the new procedure, after the face-to-face interview in a community setting, the paperwork will be transmitted by mail or in person by the facilitated enroller to the local DSS office for the final eligibility decision. Federal law requires that eligibility determination be conducted by the Medicaid agency.
The initial phase of facilitated enrollment includes:
- The Department of Health recently issued a $10 million RFP to develop and implement the process.
- Two non-profit child advocacy groups have implemented "facilitated enrollment" programs and are testing the use of the single application for CHPlus, Medicaid and WIC. One project partners community-based organizations, community members and local students in an outreach and enrollment initiative in several neighborhoods in northern Manhattan. This group provides application assistance and developed an extensive booklet of information to use as a tool for this process. Another group obtained private foundation funding to train a network of child care workers in New York City to conduct family interviews. A model training curriculum was developed, including information to share with parents about establishing a schedule for well-child visits and learning about the developmental stages of childhood. It is anticipated that this group will obtain parent satisfaction information regarding the facilitated enrollment process
Collaboration with Other Agencies and Organizations
State Agencies
- The Unemployment Insurance Division in the Department of Labor distributed program information.
- The Office of Child Support Enforcement in the Department of Social Services distributed information.
- The Department of Education sent a mailing to all school superintendents informing them about CHPlus and the availability of promotional materials to distribute through their individual school systems. On an individual district basis, the outreach coordinator arranged for program materials to be distributed at various points in the school year such as information that accompanied student report cards. A statewide informational mailing was sent to school nurses regarding the program and the availability of outreach materials.
Private Organizations
The Department of Health first contracted with the New York Health Plan Association as its community outreach coordinator in 1997. The Association represents the CHPlus program in a wide variety of venues across the state.
The initial funds for its $250,000 annual contract were provided through the health care initiative pool when the legislature approved expansions for CHPlus in 1996. Under its contract, which expires in December 1999, the coordinator:
- works with the State Perinatal Association to provide information at the regional level to providers and families;
- staffs the toll-free number that families call to discuss available programs and benefits and to request enrollment information; and
- conducts a wide array of outreach activities in local communities.
Families do not enroll through the outreach coordinator’s toll-free number. Families call the number to request the enrollment package which lists the approved managed care organizations in their area. Applications for CHPlus are handled by each participating MCO. This will continue on a voluntary basis as facilitated enrollment is implemented.
The community outreach coordinator attends local events across the state and organizes a variety of activities to educate the public about available children’s health insurance programs. Strategies include:
- Attending health fairs and community gatherings, sometimes with a van and a 20 foot tall blimp. At these events, bumper stickers, Frisbees, refrigerator magnets and sun visors are distributed to encourage interest in the program along with informational brochures.
- Making presentations at schools and through different faith communities;
- Arranging with McDonald’s to put CHPlus information on its tray placements; and
- Arranging with utility companies to include bill stuffers about CHPlus in its monthly statements mailed to households.
The Department of Health meets monthly with the outreach coordinator to review progress and tailor outreach strategies as necessary.
Media
- The Department of Health maintains responsibility for a major statewide media campaign that relies heavily on radio and television advertising. Agency officials believe that radio ads were most effective because they could be tailored for specific audiences. For example, the state developed public health messages about specific prevalent childhood conditions, such as asthma, and then followed it with an announcement about CHPlus to tell families how to call for more information.
- Highway billboards are placed prominently across the state to advertise CHPlus to state residents.
Provider Outreach
The managed care organizations that participate in CHPlus have the responsibility to enroll families and to market the program in their service areas. They must submit a marketing and enrollment plan detailing all of their activities to the Department of Health for review and approval prior to implementation. The MCOs are permitted to distribute marketing materials in any public meetings or gathering places, but may not distribute information door-to-door or offer any incentives, either cash or in-kind.
Creating a Seamless Health Care System for Eligible Children
Presumptive Eligibility
- Children have presumptive eligibility in CHPlus for 60 days while documentation is collected to establish whether they qualify for Medicaid or CHPlus. This provision was effective January 1, 1999.
Continuing Eligibility
- Starting January 1, 1999, children receive continued Medicaid eligibility for one year.
- The state requires an annual recertification of eligibility by the anniversary date of the child’s enrollment. Children who qualify for Medicaid are not eligible for CHPlus and their information is forwarded to Medicaid, if parental consent is obtained to do so. Previously, children could receive coverage through CHPlus even if they also qualified for Medicaid, but this is no longer possible under Federal law. Title XXI funds cannot be used to cover Medicaid-eligible children.
Simplified Application and Eligibility Decisions
- There is one integrated application form that includes eligibility for Medicaid, CHPlus and the Special Supplemental Food Program for Women, Infants and Children (WIC) Program.
- The current outreach budget is $3.5 million.
- Using Title XXI funds, the state will significantly increase this budget by funding facilitated enrollment across the state. A $10 million RFP was recently issued for this process.
Marketing to Hard-to-Reach Populations
State officials believe that New York’s very visible, on-going statewide media activities reach large segments of the general population, especially through television and radio. However, some advertisements were modified to use for different ethnic newspapers.
State officials acknowledge that groups require different marketing approaches. This is extremely challenging in New York State with its wide variety of populations.
Woodwork Effect
State officials recognize that a "woodwork" effect may result from its aggressive outreach efforts so they factored this into their fiscal projections for their Medicaid costs.
A larger concern among state officials is whether the state’s successful outreach efforts identify uninsured children whose families are reluctant to enroll in Medicaid. To help encourage eligible children to enroll in Medicaid, state officials want to reduce the program’s stigma and make the application process more convenient for the family. They hope that the facilitated enrollment process that uses trained workers to interview families in friendly community settings will help accomplish this. State officials are working to ensure that all children in CHPlus who are Medicaid eligible are moved to the Medicaid program as appropriate and that the continuity of health care is maintained.
Advice for Other States on Outreach
- Air public service announcements for children’s health insurance program after public health message about a specific condition (e.g., asthma) to capture more attention among television or radio audience.
- Families report radio announcements are their most frequent source of information.
- Convene monthly meetings with outreach coordinator to check enrollment data and to obtain feedback on different outreach strategies.
- Take a broad-based approach in the types of mass media used. Some types of media may be more effective in particular geographic regions or specific community environments.
- Disseminate informational materials in creative ways where people have easy access. For example, CHPlus brochures were displayed together with traveler information pamphlets in rest areas along the New York State Thruway.
- Educate other public agencies and local governments about the program. These entities can function as an important avenue of informal outreach their specific consumers.
Employer
State officials believe that a previous evaluation of the CHPlus program demonstrated that crowd-out did not occur — employers did not drop coverage for employees as the program expanded.
Employee
In New York, employers who offer insurance are statutorily required to meet minimum benefit standards defined by the State Insurance Commissioner for a particular type of insurance benefit. For example, Major Medical coverage has a minimum standard of benefits that must be included to be classified as Major Medical. Thus, officials believe there is little incentive for people to prefer the publicly-funded program benefits. On the other hand, there is some concern about families who cannot afford the cost of private insurance for their children. At a public hearing, a mother whose employer offered no premium assistance spoke about having to drop her child’s private insurance when the $200 monthly cost to cover both of them doubled. She enrolled her child in CHPlus and was able to keep her own coverage for the same $200.
State’s Response
To comply with Federal requirements to monitor crowd-out, state officials will continue to analyze its potential emergence through two mechanisms. They are evaluating:
- The proportion of children covered under an employer-based plan for evidence of possible employer or employee crowd-out, using the Current Population Survey as a base; and
- Responses to specific questions added to the single application formto ensure that families are not dropping employer-based coverage to enroll their children in CHPlus.
These questions will also help track the number of children who have access to employer-based coverage and verify that children enrolling in CHPlus are uninsured. The questions developed to track possible crowd-out are:
- Is the parent or responsible adult a public employee with access to family coverage by a state health benefits plan, and is the public agency paying all or part of the cost of the health care benefits coverage?
- Have your children been covered by health insurance, other than CHPlus, in the past six months?
- Was your prior insurance through an employer?
- Why was your prior insurance stopped? (Check only one)
- Employer discontinued offering this benefit or is no longer contributing toward premium for your children but continued the benefit for working parent.
- Premium was increased beyond what you could afford.
- Child Health Plus is a less expensive insurance.
- Child Health Plus insurance benefits are better.
- You are no longer working for employer who offered insurance.
Since the MCOs actually enroll children, they will collect and submit the information about crowd-out on a quarterly basis to the Department starting April 15, 1999.
- The state currently imposes no waiting period for children to become eligible for CHPlus. However, the Department of Health will assess quarterly the information submitted by MCOs from the application’s crowd-out questions. If evidence emerges that CHPlus is substituting for private health coverage in excess of eight percent, then the state will impose a six month waiting period.
FPL Eligibility Levels
Some concern about crowd-out did affect the Governor’s interest to cap the program at 250 percent FPL. After much negotiation between the Governor and the Legislature, the final eligibility criteria were selected:
- For CHPlus, children under age 19 with family incomes at or below 230 percent FPL rising to 250 percent by July 2000.
- For Medicaid, children under age 19 with family incomes below 100 percent FPL. This will later expand to cover children ages 6-19 whose net income is less than 133 percent FPL, after the state secures the necessary Federal Medicaid waiver or the Commissioner certifies that at least 50 percent of the population now eligible for Medicaid managed care is enrolled in that program.
- Families in CHPlus with incomes below 160 percent FPL make no premium contribution.
- Families with incomes between 160 percent-222 percent FPL pay $9 per month for each eligible child, capped at $27 per family.
- Families with income between 223 percent-230 percent FPL pay $15 per month for each eligible child, capped at $45 per family.
- Families of any income can purchase CHPlus for about $1,000 a year per child.
When families submit their CHPlus applications to their providers, they are placed in the appropriate premium contribution group and the managed care organization bills the state for the difference between the premium and the required contribution.
- Previous co-payment requirements for prescription drugs, physician office visits, and emergency room use were eliminated after January 1, 1999.
Employer Buy-In
Small businesses and sole proprietors may apply for financial assistance from the state to purchase health insurance through the Small Business Health Insurance Partnership Program. Through the program, the state subsidizes up to 45 percent of the employers’ cost of health insurance. Businesses that have fewer than 50 employees and have not provided health insurance benefits to any employee in the past year can participate.
To be eligible, employees must work at least 20 hours per week. Employees may not pay any more than ten percent of the premiums, at the discretion of the employer.
Data is collected on an on-going basis for analysis by program staff. Insurers submit statistics on enrollment, disenrollment, and other aspects of the program on a regular basis. Outreach activities are also reported monthly, including information on the volume and region where program materials were disseminated, as well as data on the telephone information lines.
- There are no current data about the number of uninsured children in the state below the statewide level projected in the CPS data. State officials and policy makers recognized that they disagreed about what methodology to use to establish the baseline data about uninsured children. To address this problem, the legislature mandated a study of uninsured individuals which will be conducted by either the Department of Health or contracted to an outside organization. There is no specific due date for the report.
- For CHPlus enrollment data, the Department of Health (DOH) reviews monthly reports from the community outreach coordinator. These reports also have demographic information about the children (e.g., age and family income) and how families learned about the program so DOH can evaluate the different outreach strategies.
- For Medicaid enrollment, the Department of Social Services district offices use the Medicaid Budget Logic system to make eligibility decisions.
- For performance data, participating private insurers must submit certain information annually to the Department of Health. If insurers do not submit these data, they are sanctioned. The information required from plans about the CHPlus population includes:
- Membership (by age, sex and payer; enrollment by county)
- Utilization (by condition and type of service; disenrollment rates)
- Quality (prenatal care; well child care visits in first year of life; adolescent well child care visits; HIV education; substance abuse counseling; immunizations; mental health follow-up)
- Access and member satisfaction (utilization of primary care providers; availability of scheduled service and emergency medical care).
- The Department of Health will monitor the facilitated enrollment process to identify and eliminate remaining barriers to enrollment.
Other Data Collection Methods
There are currently no identifying numbers for children enrolled in CHPlus. To help cross-link the Medicaid and CHPlus populations, state officials are exploring the feasibility of using a SmartCard to record a child’s eligibility information and possibly, even medical information.
Ten Percent Cap on Administrative Expenses
The Department of Health does not believe that the ten percent cap provides sufficient funding for outreach activities and for presumptive eligibility. The state is committed to enrolling eligible children, and these two activities are essential to successful enrollment.
Other Challenges
Officials pointed out several other challenges.
- Administration officials and the advocacy community anticipate a challenge to maintaining continuous coverage for children who must now switch from CHPlus into Medicaid. Part of the challenge is administrative, but some of it reflects the reluctance of families to enroll in Medicaid because of the required face-to-face interview at the welfare office. The facilitated enrollment program is designed to ease movement of children between the two public programs.
- Maintaining the "seamless" connection between CHPlus and Medicaid will be important for children moving back and forth between the two public health insurance programs when their employment status and family income fluctuates.
- The goal is to have the same local managed care organizations serve both Medicaid and CHPlus children, but when this is not possible, the continuity of health care may be disrupted for some children.
- Managed care organizations report some access to care problems, especially in rural areas, where they are unable to meet the needs of enrolled children, especially for mental health and dental problems.
- There is some concern about providing health insurance coverage to more higher income children through CHPlus than the number of lower income children who gain access to Medicaid.
- Management Information Systems specialists maintain that correcting all Y2K computer problems must take precedence over any requests to modify software or add data elements to evaluate CHPlus.
Chapter VI: Chip in Ohio
History and Implementation
Ohio’s Medicaid program for children, called Healthy Start, is administered by the Ohio Department of Human Services (ODHS). When Title XXI was enacted, the state agency already had the necessary statutory and spending authority to expand Healthy Start.
After Congress passed Title XXI, Ohio submitted two amendments to its Medicaid State Plan as well as a CHIP Plan. Using Title XXI to cover uninsured children and Title XIX1 to provide wraparound services for under-insured children, Ohio developed a more comprehensive health insurance system. Since the State Legislature had already given ODHS statutory authority to expand Medicaid, there was little legislative debate on CHIP’s first phase. (See Figure 1).
Figure 1: Children Ineligible for
for CHIP2 Pass through for a Title XIX Eligibility Determination
When children who are under 150 percent FPL apply for health insurance, ODHS checks to determine if they have had access to private health coverage. All children who meet program eligibility and get coverage through Healthy Start are tracked and coded differently depending on their insurance status:
- Children who have no coverage qualify for CHIP and the state receives a 70 percent match from Title XXI.
- Children who now have or had access to private insurance qualify for Healthy Start and the state receives a 60 percent match from Medicaid.
- By using a Combined Programs Application (CPA), the distinction between CHIP and Healthy Start is invisible to families. The benefits packages are the same and so are the providers. Medicaid contracts with licensed private sector managed care plans in all major urban areas of the state. Consequently, many Healthy Start children receive their care through a private health insurance plan and even have the same membership cards.
Ohio is implementing its CHIP program in phases:
- Phase I: Healthy Start/CHIP covers children ages 0-18 up to 150 percent FPL. See Exhibit 1: Ohio Medicaid expansion. Prior to the expansion, Ohio’s Healthy Start covered children ages 0-5 up to 133 percent FPL; and ages 6-14 up to 100 percent FPL. There was no Healthy Start for children ages 15-19. That age group could only get coverage if they were in a family that received cash assistance or if they were eligible by virtue of a disability.
- Ohio is a highly industrialized and unionized state in which many families with incomes under 150 percent FPL have access to employer-provided health care coverage. Since a child does not have to be uninsured to be eligible for Healthy Start, (an insured child would be covered under Medicaid), underinsured children can enroll. The number of underinsured people in Ohio is likely to be high because of the existence of coverage in low wage jobs. The availability of wrap around insurance for a limited benefit package can be very helpful to many families.
- Phase II: The Governor created a Task Force in January 1998 to study how to expand CHIP to 200 percent FPL. The Task Force had 17 members representing health care providers, consumer advocates, businesses, state representatives, public health agencies and private health care plans. They met ten times from February-June 1998 and then submitted recommendations to the Governor.
- The Task Force’s recommendations included: an expansion of program eligibility to 200 percent FPL; minimal cost-sharing expenses for families; and a 90-day enrollment waiting period. It was also recommended that ODHS administer Phase II to utilize existing Healthy Start and CHIP administrative structures and service delivery arrangements. Final decisions about expansion will be debated as part of the legislature’s biennial budget for state fiscal years 2000 and 2001.
- State officials estimate that 40,000 children will be eligible for the Healthy Start/Phase II, but believe that only 50 percent of that population will actually enroll.
- In addition to sharing providers, it is likely that the benefit package offered to Phase II enrollees will closely resemble the Healthy Start benefits. However, families who enroll their children in the expanded Phase II will likely pay co-payments for the same services that children under 150 percent FPL will receive free. The amounts of co-payments, as well as other details, remain undetermined.
- ODHS officials already had contracts with managed care plans to serve families and children covered by Medicaid. When the Healthy Start expansion group was added, ODHS’ contracted actuary, Deloitte and Touche helped ODHS revisit the rates to reflect the new population.
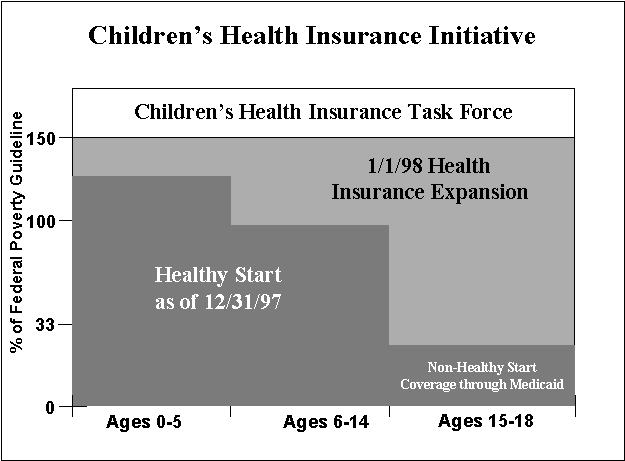
- Ohio’s Title XXI allocation of Federal funds in the first year was $115 million.
- The state match rate is 29 percent.
- The state share will be $8.8 million.
- Between January and December 1998, 85,257 children were enrolled for the Healthy Start expansion and CHIP program. By June 1999, the maximum number of children enrolled is expected to be 133,000. Approximately 67 percent of eligible children in December 1998 entered the CHIP program (i.e., they previously had no health insurance).
- To date, 13 private plans participate in Healthy Start and CHIP. Among Ohio’s 88 counties, 16 are covered by managed care and nearly 60 percent of the current Healthy Start population are located in those counties. Each provider is required to submit utilization, encounter and quality assurance data to the state.
Key Factors for Ohio’s Implementation
- The Medicaid expansion sped implementation. Because Ohio chose to do a Medicaid expansion, they were able to use existing administrative structures and service delivery arrangements to minimize administrative costs of CHIP and combine outreach efforts.
- Timing was helpful. When Title XXI was enacted, the Department of Human Services already had legislative authority to expand Medicaid so they were able to establish the first phase of the program quickly and efficiently.
- Applications by phone accelerated enrollments. Ohio offers a toll-free consumer hotline with evening and weekend hours to make it easy for families to get information about Healthy Start and CHIP and apply by phone.
- Welfare reform fund facilitated county outreach. Ohio allocated most of its enhanced Federal matching funds available under the Personal Responsibility and Work Opportunity Reconciliation Act (PRWORA) to counties in order to generate community-specific outreach. PRWORA funds target those at risk of loosing or not gaining Medicaid coverage, which includes children potentially eligible for Healthy Start.
- Mail-in applications helped parents. Ohio uses a simplified two-page Healthy Start application that can be mailed in so parents do not have to apply at a government office.
State Approach
Ohio combines state and community-level outreach strategies. The 88 counties in the state have the opportunity to develop customized outreach plans while state-level efforts are also underway.
Key Players and Administration
- Ohio Department of Human Services (ODHS)
- Local community efforts involving advocates, county commissioners, departments of health, and providers.
Ohio Department of Human Services
- Families and service providers can call a Consumer Hotline (1-800-324-8680) to receive information about Healthy Start that includes brochures, posters, and cards with the hotline number on them. The hotline operators facilitate enrollment by completing applications and mailing them to applicants for signatures. Applicants sign the form, attach the necessary documentation, and return the application by mail to ODHS.
- ODHS is working with many state agencies to disseminate information about Healthy Start. State agencies that have requested information about Healthy Start from ODHS include: Department of Mental Health; Department of Education; Bureau of Employment Services; Child Support Enforcement Agencies; Department of Alcohol & Drug Addiction Services; Department of Health; and the Ohio Minority Commission.
- The Department is also reaching out to non-profit organizations. Some of the organizations that have received information from ODHS include: Planned Parenthood and Family Planning Agencies; Head Start Association; North American Indian Cultural Centers; Salvation Army; and Urban Appalachian Council.
- ODHS received a grant from HCFA(now known as CMS) to purchase television time to run paid Healthy Start advertisements.
- In the first nine months of the Healthy Start expansion, ODHS partnered with a variety of statewide and local agencies to provide information about the expansion and to encourage families to call the hotline.
- ODHS markets Healthy Start, directly, and encourages consumers to use the statewide consumer hotline as a resource for information and application assistance. Within this work, ODHS is sensitive to the fact that local outreach plans have also created marketing strategies and support structures for applicants. Attempts are made to have complimentary activities and messages—but duplication is sometimes inevitable.
- The Ohio Child Health Coalition recommended that the state organize both media and school-based campaigns to complement the counties’ efforts to help ensure more consistency. The Coalition is comprised of the following organizations: Association of Ohio’s Children’s Hospitals; Children’s Defense Fund-Ohio; Franciscan Health Partnership Program; Ohio Primary Care Association; Ohio Public Health Association; and the Universal Health Care Action Network of Ohio.
- ODHS state-level activities include conducting large mailings to targeted populations; overseeing community-level outreach efforts; conducting tailor-made presentations; providing information to interested groups, and participating in local level health fairs and community events.
- The ODHS is looking into enhancing the current Medicaid Web site to include outreach information.
County Outreach
In order to obtain Federal funds for county-level outreach, counties were required to submit outreach plans to the state for approval.
- In FY 1998, 61 county plans were submitted and approved. An additional 11 counties submitted plans for FY 1999.
- The Department reviewed the plans to ensure that they reflect local needs, but allowed communities to develop their own customized Healthy Start outreach strategies.
- The lead agency for outreach varies among counties (e.g., local Department of Health, county departments of human services, advocacy organizations or organizations contracted to provide outreach).
- Some local outreach efforts include:
- Many counties have hotline numbers where people can request an application for Healthy Start. Some counties have coordinated with each other to share responsibility to operate the hotline numbers.
- Some counties have contracted with non-profit organizations, providers, or health organizations to conduct outreach by providing application assistance, collecting applications, running information lines/hotlines, providing follow-up assistance to get needed verifications, and developing grassroots campaigns.
- Given the amount of local control, some communities have selected different program names, logos and informational telephone numbers. Advocates and some state staff believe it can be confusing for families who hear about different local health insurance programs that may all be Healthy Start. To address these concerns, some advocates have suggested that the state develop certain basic guidelines to ensure uniformity among communities for the program name, logo, and information telephone numbers.
Collaboration with Other Agencies
Ohio Family and Children First Council
- The OFCF Council is a Governor’s initiative to create local councils of child and family-serving agencies to coordinate activities for families and children. ODHS partnered with the Council to disseminate information about the Healthy Start expansion.
Department of Health
- WIC clinics’ staff members received information about the Medicaid expansion and CHIP. ODHS sent a direct mailing to 85,000 WIC households inviting them to call the Consumer Hotline and/or apply for Healthy Start or CHIP. Using its database, the Department targeted families that would probably be eligible. It was estimated that the mailing reached 100,000 children and the Consumer Hotline reported a tremendous response to it.
Bureau for Children with Medical Handicaps
- The Bureau for Children with Medical Handicaps (BCMH), the state agency serving children with special health care needs, is requiring its families who are at or below 185 percent FPL to apply for Healthy Start. A one-time informational mailing was sent to approximately 5,000 current BCMH families who were directed to call the Consumer Hotline. BCMH is now sending information about Healthy Start to families who are enrolling or being re-certified for BCMH enrollment.
Child Care Centers
- ODHS sent a mailing to nearly 12,000 licensed home-based and center-based childcare facilities to inform both families and child care providers who may not have health insurance for their children.
Provider Associations
- ODHS attended over 20 medical association meetings to provide information about the expansion. Many statewide providers published articles about the expansion in their association newsletters, including: Medical Association; Hospital Association; Dental Association; Ambulance Association; and Association of Medical Equipment Suppliers. Presentations were also made to the State Medical Care Advisory Board.
- The School Nurse Association invited ODHS to participate in four regional conferences to share information and materials. These presentations prompted many requests to the hotline for written materials to use in schools.
Ohio Churches
- Working with the Commission on Minority Health, ODHS notified many minority clergy about the Healthy Start expansion.
- ODHS sent a mailing to approximately 13,000 individuals affiliated with the Ohio Council of Churches.
Creating a Seamless Health Care System for Eligible Children
Presumptive Eligibility
Ohio offers presumptive eligibility only for newborns born to women already covered by Healthy Start. Ohio does have retroactive coverage for people eligible in the previous three months, but it does not begin until eligibility has been established.
Continuing Eligibility
Ohio has a six month re-determination cycle. However, significant changes in family income or household composition that occur must be reported, and may therefore affect eligibility.
Simplified Application and Eligibility Decisions
- Ohio uses a Combined Programs Application (CPA) to enroll children for Healthy Start, WIC, BCMH, and Children and Family Health Services (CFHS). The CPA, created in 1989, was revised in 1991 to be more "user-friendly". The next revision is expected in the summer of 1999. The application will be two pages long and will be available in Spanish and English.
- Ohio does not require a face-to-face interview for eligibility determination for Healthy Start. The application can be mailed to the county department of human services for processing.
- Prior to Title XXI, Ohio had decided to access Federal matching funds for Medicaid eligibility outreach under the Temporary Assistance for Needy Families (TANF) block grant of the Personal Responsibility and Work Opportunity Reconciliation Act. The state made almost all of the $16.1 million available to counties based on the number of their potentially eligible Medicaid recipients. Approximately $20 million of combined Federal and local funding is available for FY 1998 activities and comparable funding is available for FY 1999.
- To receive the funds, county commissioners had to develop an outreach plan through a collaborative process with all the community stakeholders, ensuring that the plans reflect the wishes of the community. Counties were also required to provide the necessary matching funds. In some counties, the match was raised through a collaborative public-private arrangement.
- Build evaluation into outreach activities. Any evaluations should be based both on outcomes (caseload impact) and other measures (e.g., public perception).
- Create a statewide name and logo for the program even if counties or municipalities are primarily responsible for conducting outreach.
- Encourage and fund local outreach efforts that complement the statewide strategy but are tailored to the specific community.
State’s Response
- Crowd-out is not an issue for CHIP/Phase I because children with access to health insurance that meet the income requirements are still eligible for the expansion via Title XIX.
- Crowd-out is expected to be an issue during Phase II. The primary strategy recommended by the Task Force is to impose a 90-day waiting period. In its report, the Task Force wrote: "This period is designed to discourage a family from dropping their existing child coverage in favor of the CHIP Phase II plan, by ensuring that the family will be exposed to a period of financial risk before the coverage would begin."
- Other recommended strategies to address the problem are:
- impose some cost sharing for the CHIP plan through an annual non-refundable premium and targeted co-payments;
- develop measures and mechanisms to monitor crowd-out; and
- use an Advisory Board as a forum to monitor crowd-out.
- The State Legislature may debate these and other Task Force recommendations of Phase II during the development of the SFY 2000/2001 biennial budget.
Employer Buy-In
Ohio has no provision for an employer buy-in program at this time.
Data for Program Design
- ODHS and the Ohio Department of Health (DOH) wanted to assess the impact of expanding Medicaid even before Title XXI. As part of the planning for the Title XIX expansion, ODHS contracted with a private consulting firm (The Lewin Group) to study the number of potentially eligible individuals. Using CPS data, an estimation model was created to convert the uninsured rate into a monthly number that was used to estimate the number of potentially eligible individuals under 150 percent FPL. The study estimated that 290,000 children were potentially eligible, but researchers believed that only 133,000 would actually enroll. State officials used these figures to budget for and plan the Title XIX expansion.
- During planning for the SFY 98/99 biennial budget, ODHS and Lewin conducted a series of public forums for input about Medicaid program priorities. Forum participants identified expanding Medicaid coverage for children as one of their highest priorities.
- Additional forums were conducted in the fall of 1997 to receive input from interested parties about the option of covering children up to 200 percent FPL through CHIP. The Task Force considered comments from these forums when they developed recommendations for the expansion.
- ODHS uses data from its Medicaid Management Information System (MMIS) and Client Registration Information System (CRIS-E) to monitor characteristics of its Medicaid population. ODHS data staff use MMIS claims data to analyze utilization and to monitor performance measures. They use CRIS-E to analyze demographics and caseload trends.
- Healthy Start and other programs are evaluated through the efforts of the Office of Medicaid Health Care Quality Program that assesses quality against standardized quality measures. Examples of activities include: medical record review; consumer satisfaction surveys; feedback to health plans and providers regarding their performance; feedback to consumers in the form of consumer guides; and communication to the public about important findings. Questions are now being added to various instruments to collect data specific to the Healthy Start expansion.
- For its quality measurement work, ODHS faces certain challenges including how to obtain clinical records from providers; how to improve encounter data submitted by managed care plans; and how to stay current with state-of-the-art quality measurements for medical care.
- Ohio is now evaluating its outreach efforts funded through PRWORA Medicaid outreach by determining what was actually done for outreach and comparing it to what was planned. They are also looking at best practices, evaluation results, and comparing outreach activities and spending to caseload trends.
Ohio Family Health Survey
- The State Legislature created the Ohio Health Data Center in 1993 to collect, analyze and disseminate health care information. A critical component of the Data Center’s mission is the Ohio Family Health Survey that will provide baseline measures for health status, health coverage, satisfaction with coverage, utilization of services, and access to care. The survey will help assess existing health care trends, monitor impacts of changes in the health care marketplace, and evaluate the impact of health care reforms to provide information to the State Legislature for their health policy decisions. The first survey was fielded in January-August 1998. The Data Center plan to repeat the survey in 2001.
- The Health Survey will also collect information about the uninsured and underinsured to better understand why families lack insurance. State officials believe that national surveys do not sample enough Ohioans to provide the information that they need.
- The survey instrument was developed by a committee with representatives from different state agencies (DOH, Medicaid and Mental Health) and the Ohio State University. Survey questions were developed using a variety of sources including SF12, Physical and Mental Health Summary Scales, the National Health Interview Survey, the Current Population Survey, and the Behavioral Risk Factor Surveillance System. Detailed information about the survey and a list of information collected in the survey is included in Appendix 1.
- The sample size was 16,261 households, where one randomly selected adult was interviewed in each home. If children were members of the selected adult’s family, then an adult family member was asked questions about a randomly selected child. The income levels for the survey sample were determined by poverty level. Among the children interviewed, there were 703 living with families reporting income at 150-200 percent FPL. Of the 5,788 children surveyed 648 were reported as receiving Medicaid.
- Among the issues related to CHIP that the survey addresses are:
- Where is a person employed compared to how do they receive insurance coverage?
- How do Medicaid recipients compare to non-Medicaid recipients in their ability to access health care and insurance?
- How long have individuals had health insurance?
- When were individuals last uninsured?
- Why did families who may be eligible for Medicaid not apply for Medicaid?
- If a non-Medicaid family below 200 percent FPL applies for Medicaid, what happens to their application?
- The survey measures access to health care and insurance. It asks individuals with insurance about their satisfaction with the ability to choose a doctor, benefits, ability to get emergency care, out of pocket costs, and the ability to see a specialist. Non-Medicaid recipients with other coverage were asked whether their plans included mental health services, dental care, vision services, hearing services, or prescriptions. They also were asked how much they pay for coverage. Workers were asked whether their employer offered insurance. All respondents were asked about their health care utilization, usual source of care, quality of the services they received, and unmet health care needs. Uninsured respondents were asked why they were uninsured and what kinds of problems they had as a result of being uninsured.
- Certain geographical area and subgroups were over-sampled to obtain sufficient data for point estimates. Oversampled areas and subgroups were: Appalachian counties (5 counties); rural farm regions (5 counties); metropolitan areas (9 counties); African Americans; Hispanics; Asian/Pacific Islanders; suburban commuters (3 counties).
- DOH’s initial sample was 12,400 households, but other state agencies and counties were invited to purchase additional surveys. Cuyahoga County, for example, paid to add an extra 1,000 households in its county to the sample. Some counties used their TANF dollars to augment the number of households in their counties’ sample. To encourage counties to purchase additional household surveys, DOH offered to generate county sampling frames and is providing the results in cross-tabulations. The data will be made available to counties that want to conduct additional analysis.
- The 20-minute telephone survey was conducted in two phases. During Phase 1 (January-May 1998), a few questions were inadvertently skipped for some respondents, so surveyors attempted to re-contact those participants between June and August. This second phase also included additional interviews to meet minimum sample size requirements for African-Americans in several counties, along with newly purchased surveys for five counties. Participants who wanted more information about the survey were encouraged to call the DOH 1-800 number.
- DOH was the primary contractor for the survey. They issued a RFP and the Gallup Organization won the bid to conduct the survey. The cost of the survey is hard to calculate since there were several contributors. The state contribution from ODH and the ODHS was approximately $800,000, not including ODH and ODHS staff time spent on the project or the costs borne by the six county organizations that purchased additional surveys.
- A methodology report and a clean database were due to the Data Center by the end of 1998. The first analytical report will present a series of tables by various categories such as insurance status by gender, race, and income. Subsequent reports are expected to include uninsured rates by county and a profile of the number of Medicaid eligible children insured by Medicaid, insured by other plans and uninsured.
- DOH plans to repeat the survey in three years to see how health care has changed and want to provide the data to universities and other interested researchers to encourage further research.
Web Sites for More Information
For additional information visit their web site:
Ohio Family Health Survey
Health Services Research and Quality Unit, Health Care Date Center, Office of Policy and Planning, Ohio Department of Health
Background
The General Assembly created the Ohio Health Care Data Center (Data Center) in House Bill 478. It was signed into law in January 1993. The Data Center exists to collect, analyze, and disseminate health care information. This survey is a critical component to the Data Center’s mission. The Data Center has requirements to determine the number of uninsured and underinsured persons in Ohio at the state and county level. It also has other mandates that require good health care information. The survey should provide this required baseline and descriptive information.
Additional impetus for this survey is the Administration’s needs for good information by which to make health care policy decision. In the past several years the pace of marketplace health care reforms has quickened. Moreover, discussions in Washington suggest that significant changes will occur in the administration of public health care programs, as well as the passage of some incremental health care reforms. Finally, the state is also looking at reworking how it administers public health care programs and regulates the private health care system.
These changes will produce intended and unintended consequences. However, without good baseline information, policy makers will be without an effective way to determine these changes. They will be unable to evaluate claims that individuals or groups raise about continuing needs, problems, or solutions. Therefore, the survey serves the purpose of providing Ohio with needed baseline data for monitoring the health care system.
Finally, Ohio’s Medicaid system is facing potentially significant changes. The Medicaid program needs good information about how its population and its system compare to others. This survey will provide the first comprehensive set of data to allow for such a comparison.
Purpose of the Survey
Development of baseline measures of health status, health coverage satisfaction with coverage, utilization of services, and access to care to allow for assessing existing health care trends, monitoring of the impacts of changes in the health care marketplace, and evaluating the impact of health care reforms.
Analysis on specific questions about Ohio’s uninsured population such as the estimated number of uninsured person in Ohio and by country, the reasons for being uninsured, the health status of the uninsured, the health care utilization of uninsured person, the existing costs of serving the uninsured, and the estimated level of unmet need;
Refinement and validation of estimates regarding the number of uninsured and underinsured persons in Ohio at the State and county level from state or national-level data and development of a mechanism for regular updates of this information.
Comparisons of the health status, access to care, utilization of service, and unmet health need patterns between the Medicaid, uninsured, and the commercially insured populations in Ohio;
Assessment of differences in these measures: health status, health coverage, unmet need, satisfaction with coverage, and with different health status levels;
Assessment of the relationship between behavioral risk factors and health care utilization, health care costs, and general health;
Measurement of the extent of movement and reason for a change in coverage source to another in the past year, whether from one employer-based plan to another, from uninsured to insured or vice versa, from Medicaid to insured or uninsured or vice versa.
Sources of Survey Questions
Many of the questions used on the survey were obtained from recognized sources. For example we are using the SF21 (Physical and Mental Health Summary Scales), modified National Health Interview Survey questions for utilization, Census questions for insurance status and demographics including industry and size of employer, and questions from the Behavioral Risk Factor Surveillance System, for lifestyle factors.
Information that will be collected with the questions (* information only collected for adults)
Insurance Coverage
- Type and source of current insurance coverage
- Medicaid
Medicare
Employer/Union
Self-insured
Military or Veterans
Other - Previous type and source of insurance coverage if change in status during past 12 months
- Insurance coverage of specific benefits
- Medications
Dental care
Vision services
Hearing services
Mental health services - Cost of insurance premium (employer/union based or self-insured)
- Number of weeks covered in past 12 months
- Change in type of insurance coverage in past 12 months
- Reasons for lack of insurance in past 12 months
- For currently uninsured last time had coverage
- Medicaid past or present, length of coverage
Satisfaction with health care coverage
- Ability to choose doctor
- Benefits covered
- Ability to get emergency medical care
- How much they have to pay for medical services
Utilization of health care services and satisfaction with used services
- Physician visits
- Emergency room visits
- Outpatient surgery
- Hospital admissions
- Dental visits
- Pap test*
- Mammogram*
- Physical exam or well baby check-up (children only)
Access to care
- Usual source of care
- Ability to see a specialist
Health status
- Overall health status
- Functional status*
- Mental health status*
- Chronic conditions
- Activities of daily living (ADL) for 65 and over*
Personnel behaviors
- Cigarette smoking (current, former, never)*
- Physical activity*
- Height and weight
Unmet health care needs
- While uninsured
- Major medical costs
Delayed or avoided getting care
Had problems getting care they needed - Listing of problems getting health care such as medical, mental, or dental care. Respondent ask to include medications, equipment and supplies
Financial Burden
- How much family had to pay for medical care in past year (out of pocket costs)
Demographics
- Age
- Race
- Gender
- Hispanic Origin
- Employment (Industry, Class or worker, Size of employer, Hours work per week)*
- Family size
- Family income
- Martial status*
- County of Residence
- County of work (for policy holder)*
- Zip code
- Educational attainment*
Sample Size
The sample size is 12,400 households. One randomly selected adult will be interviewed from each household. If there are children residing in the household who are members of the selected adult’s family a child will be randomly selected. Information will be collected for 12,400 adults and approximately 4,100 children.
Over Sampling
Certain geographical areas and subgroups of the population will be over sampled to provide sufficient sample size for point estimates to be reasonably accurate. The areas and the subgroups are as follows:
- Appalachian Region (5 counties)
- (Adams, Belmont, Clermont, Jackson, Morgan)
- Rural Farm Region (5 counties)
- (Ashtabula, Dark, Huron, Logan, Putnam)
- Inner City Areas
- (Census tracks where proportion of population below the poverty level is 20% or greater)
- Industrial Regions
- (Proportion of persons 16 years and over employed in manufacturing industries is 30% or greater)
- Metropolitan Areas (9 counties)
- (Butler, Cuyahoga, Franklin, Lorain, Lucas, Hamilton, Montgomery, Summit, Stark)
- African Americans
- Hispanics
- Asian/Pacific Islanders
- Suburban Commuters (3 counties)
- (Clark, Delaware, Lake)
- Medicaid recipients
- Uninsured persons
Who is conducting the Survey?
The Gallup Organization of Princeton, New Jersey obtained the contract to conduct the survey through an RFP using State Purchasing.
Who else is participating?
The Department of Human Services, Medicaid Policy Section (Lorin Ranbom) participated in the development of the RFP, selection of The Gallup Organization, development of the survey instrument, and is paying for part of the survey.
A Health Economist for the Ohio State University, in the School of Public Health (Gil Nestel) has assisted in the development of the survey and analysis of the results.
For additional information contact:
Dave Dorsky (614) 728-4738
Mary Plummer (614) 728-9579
1 - Title XIX is pre-CHIP Medicaid.
2 - Children with insurance
Chapter VII: Chip in Oregon
History and Implementation
The history of health insurance (especially Medicaid) for low-income children in Oregon established a context for implementation of CHIP in Oregon. The state has the only Medicaid program in the country that openly rations medical treatments for its recipients (i.e., the legislature annually sets priorities on allowable treatments) yet allows more categories of individuals to be eligible for Medicaid than do other states. The numbers and proportions of uninsured residents has declined in Oregon, contrary to national trends, so crowd-out is less of a worry there. The legislature meets every other year, and was not in session when Title XXI money became available to states, so the legislature has not yet played a role in policy decisions around CHIP. Moreover, Oregon had established precedence for publicly-funded insurance programs to cover the uninsured, beyond Medicaid — precedence that made it easier to embrace CHIP.
Pre-Title XXI
- The origins and history of CHIP evolved in the context of a landmark Section 1115 demonstration, approved by HCFA(now known as CMS) in 1993, and called the Oregon Health Plan (OHP). Under the Plan, a panel of six consumers and five physicians meets to prioritize health services. The legislature then "draws the line" on the priority list to determine, based on available funding, those treatments that will be covered and those that fall below the line and will not be covered by Medicaid.
- The concept was intended to "ration care, not people," so the demonstration also authorizes expanding Medicaid eligibility to persons who are not otherwise categorically eligible, such as childless single adults, and makes eligibility contingent only on income.
- According to legislative staff, the eligibility expansions have added 120,000 people to OHP/Medicaid rolls, and resulted in costs of $285 million. The caseload and cost increases set the stage for legislators’ distress about Medicaid.
- In November 1996, the voters passed an increase in the tobacco tax to support and expand the Oregon Health Plan.
- When the legislature met the next year, it faced additional revenues available from projected tobacco tax proceeds. At that time OHP/Medicaid covered most children and adults up to 100 percent FPL, except children age six and under and pregnant women were covered up to 133 percent FPL. The legislature authorized expansion of coverage for children under age 12 in families earning up to 170 FPL. This would have added 25,000 children to OHP/Medicaid.
Title XXI
- After the legislature adjourned, Title XXI money became available. The Emergency Board, which takes required actions when the legislature is out of session, refinanced funds from Title XIX to create matching funds for Title XXI, and approved the addition of children ages 12 — 18 under OHP. The combined expansions of eligibility to children ages 6 — 12 and 12 — 18 were projected to add 15,000 — 17,000 children to OHP. The legislative session during the winter and spring of 1999 will be the first opportunity for legislators to consider and examine CHIP.
At the time of the CHIP appropriation and its addition to OHP/Medicaid, Oregon had three other health insurance programs.
- The Family Health Insurance Assistance Program (FHIAP) provides state-only funds to subsidize Oregonians who are unable to afford health insurance and have been uninsured for at least six months. The subsidies pay between 70 — 95 percent of the family share of premiums for health insurance plans offered by employers. Members must pay the unsubsidized portion of their share of the premium cost, as well as the usual co-payments and deductibles of the private insurance market. [A brochure and chart depicting monthly income eligibility levels by premium subsidy level are available at http://www.ipgb.state.or.us.]
- The Oregon Medical Insurance Pool (OMIP), provides coverage to individuals denied individual health insurance because of a pre-existing medical condition. OMIP is not a low-cost insurance program1 but FHIAP subsidies can be applied to any of the four insurance plans offered through OMIP. Pricing varies by age and geographic location.
- The Insurance Pool Governing Board (IPGB), offers a variety of group insurance plans at affordable prices to the self-employed and small businesses with no more than 25 employees.
Oregon is implementing CHIP in phases:
- Phase I: An OHP/Medicaid "Look-Alike" was implemented in July 1998, which allows income eligibility up to 170 percent FPL for children through age 18. Children under 100 percent FPL are eligible for Medicaid, except for children under age 6, who are eligible up to 133 percent FPL. The asset test in CHIP and Medicaid is $5,000 regardless of family income2.
- Phase II - A: FHIAP, also implemented in July, 1998, will be linked as much as possible to CHIP. The state intends to submit a Plan Amendment to HCFA(now known as CMS) for this phase and target implementation for May 1999. The Amendment will seek HCFA(now known as CMS) approval of FHIAP benefit plans to be qualified under Title XXI.
- In his FY99/01 budget, the Governor has included assumptions about covering certain children in FHIAP with CHIP funds. These children would only be eligible for CHIP funding where the FHIAP plans meet benchmark coverage, either Kaiser or the state employees’ package.
- Oregon will request permission (where cost effective) to allow any children and their families enrolled in a qualified HMO with a 50 percent employer contribution to enroll in FHIAP, if the cost would not exceed what it would have cost to cover the children only with Medicaid. The state projects that this scenario will add 7,000 individuals to FHIAP, of which 1,000 will be CHIP children.
- Phase II — B: The state may also submit an amendment to conduct a pilot test with the state’s only Health Insurance Purchasing Cooperative (HIPC), called Associated Oregon Industries. The pilot would market CHIP coverage through the HIPC, offering to small employers the opportunity for subsidies to enroll uninsured employees in a health insurance plan. In effect, they would say to employers, "If you’ve got employees with children who are uninsured, it’s probably because the insurance is not affordable. We’ll make it affordable by offering them subsidies." The state would run the pilot test for two years, and evaluate the results. Associated Oregon Industries would use a third party to administer the plan.
- Phase III: After implementing Phases I and II, the state would seek a waiver from HCFA(now known as CMS) to allow reimbursement of direct services by safety net clinics (school-based, hospital-based, community-based) to supplement Oregon’s insurance programs. State officials estimate that, even with their variety of publicly-funded insurance programs, they may never enroll more than 80 percent of eligible children. They believe there is a cadre of children who are very difficult to reach and enroll, or may never enroll, for reasons that include:
- Parents think CHIP is stigmatizing because it is a government program;
- Families live in rural areas and either have a healthy suspicion about government programs or are simply "anti-government";
- Families are immigrants who arrived after August 1996.3 Many of these families already use Federally Qualified Health Centers, migrant clinics, and other community and hospital clinics.
-
State officials would like to use CHIP funds to reimburse clinics for this care. In particular, state staff pointed to a robust cadre of school-based clinics funded by the Robert Wood Johnson Foundation. The goal is to get uninsured, low-income children into this clinic care until they are enrolled in an insurance program. The Title XXI statute permits states to use only their 10 percent administrative funds for direct services. But Oregon officials said that their waiver request to HCFA(now known as CMS) will make the point that they have followed the statutory recipe, and still have uninsured, non-Medicaid eligible children, demonstrating the need to move beyond the insurance model.
- Oregon’s Title XXI allocation of Federal funds in the first year was up to $39 million. The state matching rate is 27 percent. State officials estimate they are spending $6 million in state matching funds.4
- Oregon has a statutory cap on revenue expenditure increases. If revenue collections exceed the end of session forecast by more than two percent, the excess must be returned to the taxpayers. The forecasts are done in May of the odd years. Thus, Oregon never accumulates General Fund revenue surpluses, although the Legislature does set aside $25-35 million as an emergency fund for all of state government for the two-year period. As a result, large programs like the Oregon Health Plan have no "safety net" in the event of a budget overrun. To gain maximum legislative support for CHIP, the Medicaid agency guaranteed that the program would not run a budget deficit. Thus, the state chose to implement CHIP as a "stand-alone" Title XXI program so that enrollment could be capped. One official noted that to keep faith with the legislature, they have sized CHIP to stay within the Medicaid expansion dollars originally authorized by the 1997 legislature.
Current Enrollment
Oregon officials point proudly to a decade-long decline in the proportions of uninsured Oregonians. They estimate that in 1989 there were 450,000 of 2.7 million residents uninsured (about 18 percent); 22 percent of all children were uninsured. In 1998, they estimate that 345,000 of 3.2 million residents (about 11 percent) were uninsured; nine percent of all children were uninsured. CHIP has helped continue that trend.
- For the Phase I Medicaid look-alike, Oregon had enrolled 10,200 children by January, 1999, and is targeting to enroll 17,000 — 18,000 children by spring of 1999. They enroll 300-400 children each week. Staff closely monitor applications in the pipeline to ensure they will not exceed the target enrollment. When the number of enrolled plus applications in the pipeline estimated to be eligible exceed the target, OMAP will be forced to close the pipeline for a few months until sufficient attrition occurs. People who apply when the program is closed and who appear to be eligible will be given priority notification when it reopens.
- For Phase II, where CHIP/Oregon Health Plan and FHIAP become linked, the state expects to add another 7,000 individuals of which 1,000 will be CHIP children.
- For Phase III, under a prospective waiver that would permit use of CHIP dollars for the provision of direct services, the state expects to pay for health care for an unknown additional number of children whose families did not enroll in the publicly funded insurance market (OHP/Medicaid, FHIAP or CHIP).
Key Factors for Oregon’s Implementation
Several circumstances and factors were critical to implementation of CHIP.
- Timing was critical. Since the legislature was not meeting when Title XXI money became available, the Emergency Board approved, quickly, reprogramming of some tobacco tax funds as matching funds for CHIP. One legislative staff observed that was literally a one-line item in a two-inch-thick budget book.
- Finding the state matching funds was relatively easy. The Department of Human Resources had already earmarked projected tobacco tax revenues to expand Medicaid to add children ages 6 — 12 under 170 percent FPL. These funds were designated as state matching funds for CHIP and children age 13-18 were added.
- Data helped seal the case. The Oregon Health Council, a policy advisory body to the Governor and legislature, presented survey data documenting the large proportions of uninsured adolescents in the prospective CHIP population. These data bolstered the case for expanding eligibility through age 18.
- Precedence was helpful. The state has a history of "breaking the mold" with government programs, in particular its Medicaid waiver demonstration that established the Oregon Health Plan. And they already had three other programs aimed at helping disadvantaged, uninsured individuals obtain health insurance.
- Crowd-out was not evident. Unlike national trends in the opposite direction, Oregon was experiencing growth in employer-provided health insurance coverage.
State Approach
Oregon’s Office of Medical Assistance Programs (OMAP), administering agency for CHIP, must balance its interest in outreach with fiscal constraints limiting the numbers of eligible children they are targeting to enroll this year. A second agency, the Insurance Pool Governing Board, has assumed a large part of the responsibility for outreach on CHIP while it simultaneously conducts outreach for the Family Health Insurance Assistance Program (FHIAP). FHIAP was designed prior to CHIP, but implemented at the same time. Outreach efforts both for FHIAP and CHIP are very proactive.
Key Players and Administration
Two agencies administer outreach for CHIP, with a third agency establishing CHIP policy and conducting research.
- The Oregon Department of Human Resources houses OMAP, which administers CHIP and Medicaid. DHR characterizes their CHIP program as a Medicaid look-alike program. Both programs operate under the moniker of the Oregon Health Plan. Outreach activities undertaken on behalf of Medicaid over the past several years now also double as outreach activities under CHIP.
- The Insurance Pool Governing Board, which administers several other health insurance subsidy programs for disadvantaged individuals, has taken responsibility for marketing, education, and outreach to children in families likely to be eligible for CHIP. Outreach activities for CHIP are most closely linked to similar activities for FHIAP. FHIAP offers state funds for three levels of income-conditioned subsidies to individuals unable to afford health insurance (usually available from their employers) who have been uninsured for six months.
- The Office for Oregon Health Plan Policy and Research was established by and reports to the legislature. They are responsible for policy oversight, research, furthering the goals of the OHP, collecting health data, and being staff support to the:
- Oregon Health Council, which recommends policy for OHP/Medicaid and CHIP;
- Health Resources Commission, which oversees a process for deciding on the allocation of medical technologies in Oregon;
- Health Services Commission, which prioritizes medical services for OHP/Medicaid.
Collaboration with Other Agencies and Organizations on Outreach
State officials strive for a seamless system of health care between CHIP and FHIAP so the Medicaid agency and Insurance Pool Governing Board strive simultaneously to locate children eligible for either program.
State Medicaid Agency
- OMAP’s outreach methods include a simplified, integrated application form both for OHP/Medicaid and for CHIP. The form itself is four pages, on a double-sided fold-over with large print and ample white space for families to record the information. It is accompanied by an equally clear set of information and instructions that includes:
- How to apply for OHP;
- Why Social Security Numbers are needed5;
- Your Health Insurance Rights and responsibilities;
- The significance of the date-stamped application and the 30-day limit on returning the form;
- Income guidelines and family size for eligibility;
- Other health resources for you and your family;
- Who to call about each of the other programs;
- A one-page explanation of managed care;
- Who might have to pay premiums and how much;
- Special rules for victims of domestic violence; and
- When insurance coverage will begin.
- All applicants are screened first for Medicaid and then CHIP. Agency staff estimate there are 50,000 — 60,000 eligibles of all ages not enrolled in Medicaid. The joint application for these two programs does not cover FHIAP because officials did not want to ask FHIAP applicants about non-custodial parents’ availability of health insurance for their children — a Federal requirement under OHP/Medicaid. However, anyone applying for Medicaid and CHIP who is found ineligible for those programs is referred to FHIAP; and FHIAP applicants are informed about OHP/Medicaid and CHIP.
- The agency offers a 1-800 phone number to call to receive date-stamped applications and an information packet.
- The agency has established a variety of sites where people can pick up date-stamped applications, including:
- Hospitals;
- Clinics;
- WIC Centers;
- FHQCs;
- Rural Clinics;
- Tribal Clinics;
- All county public health centers; and
- Welfare offices.
- The OMAP provides date-stamped applications with a 30-day return deadline to ensure that providers will be paid. While insurance plans may not distribute date-stamped applications, providers may do so. A substance abuse treatment center, for example, can hand out an application to an adolescent and begin treatment right away. Center staff encourage families to send it in within 30 days, which provides some assurance that the center will be reimbursed for treatment provided during the retroactive eligibility period.
Other State Agencies
Insurance Pool Governing Board staff are conducting the largest outreach effort on behalf of the FHIAP and CHIP programs. These efforts involve other state and local agencies, called community partners, as well as non-profit organizations.
- Staff conducted more than 100 training seminars since April 1998 at a variety of locations where uninsured families are most likely to visit or live. Seminars last a half a day, and are aimed at a variety of participants who come in contact with the uninsured. Seminars have been held in 28 cities in all parts of the state. Among participants were 953 insurance agents.
- 924 "community partners" have participated. Community partners include:
- Adult and Family Services;
- Disabled Services agencies;
- Employment Department;
- Vocational Rehabilitation Division;
- Education Department;
- WIC programs;
- Department of Consumer and Business Services;
- County and Public Health Departments;
- Head Start and Healthy Start programs;
- Mental Health agencies and clinics;
- Community Action Agencies;
- Jefferson and Beaverton School Districts;
- Legal Aid staff;
- Information and Referral agencies;
- Providers, hospitals, and health centers;
- Homeless and youth shelters and service agencies.
- Board staff mailed 45,000 notices to food stamps recipients and placed inserts in Medicaid denial notices;
- They put up posters at various locations in the seminar communities. Posters have removable stickers with the FHIAP 1-800 phone number, so families could pull them off and take them home.
- Staff at all of the seminars distributed a tri-fold brochure on FHIAP and CHIP that includes answers to simple questions:
- What is FHIAP?
- Do I Qualify?
- How Does FHIAP Work?
- How Do I Figure My Income Level?
- What Are My Other Options?
- What’s My Next Step?
Board staff noted that approximately 37 percent of FHIAP enrollees are eligible for CHIP but are remaining in FHIAP because the parents are willing to pay something to stay in what they perceive as a private program. FHIAP staff have surveyed families of children in FHIAP and asked why they did not enroll their children in CHIP. The most frequent response is that CHIP is a free government program while FHIAP is not perceived as a government program.
Media Activities
A radio news release, NewsNet, was aired for stations to use in late September. News releases were distributed to local newspapers in June and September, one month before and after the program began.
Creating a Seamless Health Care System for Eligible Children
Presumptive Eligibility
- Oregon does not offer presumptive eligibility to children applying for CHIP because state Medicaid officials assumed they would have to fund it with their capped administrative funds.
- Retroactive eligibility is provided through date-stamped applications at a variety of locations. The application has clear instructions alerting the family to return it within 30 days to ensure eligibility back to the date of application.
Continuing Eligibility
CHIP children, once certified and enrolled, enjoy a six month continuing eligibility period before re-certification must occur.
Simplified Application and Eligibility Decisions
- OMAP believes the simplified, integrated, four-page application form for Medicaid and CHIP makes the application process very easy for both programs. They have tried to make the accompanying instructions to families equally clear.
- They offer one-to-two-week turnaround time on eligibility and enrollment decisions to those applicants who return the date-stamped applications within 30 days of acquiring them.
- The entire application process can be completed by mail, with no need for the family to come to an office.
- OMAP reports spending only a small amount of its administrative funds on outreach. Officials feel they must conserve most of their administrative funds for management and operational activities. The fiscal constraints on the number of children they are targeting to enroll this year makes them cautious about too aggressive an outreach campaign. They do not wish to create unrealistic expectations among uninsured families about the capacity of CHIP to enroll children.
- Most of the outreach funds were spent on printing and distribution of the date-stamped application forms, and training of the workers in the various hospitals, clinics and other sites where CHIP information and applications are available.
- The Insurance Pool Governing Board has a $1 million appropriation for the biennium to conduct outreach for FHIAP. Since outreach targets both FHIAP and CHIP eligible families combined, staff cannot estimate a separate portion that is spent on CHIP.
Marketing to Hard-to-Reach Populations
- FHIAP staff participated in five Rural Health Forums held across the state, and made presentations at 21 other conferences. These included:
- Oregon Health Action Campaign Annual Conference;
- Small Business Fair;
- Commission on Children and Families;
- Chinook Winds Casino and Confederated Tribes;
- Chambers of Commerce.
- They held meetings with Oregon Fishing Families in eight coastal communities to promote CHIP and FHIAP.
- Staff designed and disseminated information about CHIP and FHIAP that included a special barbers and hairdressers board brochure (22,000); they mailed marketing materials in English and Spanish to Head Start Centers, the Oregon Association of Hospitals and Health Systems, Disproportionate Share teaching hospitals, school nurses and school-based clinics, industry associations, county commissioners, and Rotaries.
Woodwork Effect
Several officials in Oregon noted the tension that may result if the state does so much outreach that they create more demand for CHIP than they can respond to, and have to form waiting lists. More budget-related concern was expressed, however, that CHIP outreach will cause Medicaid eligibles to "come out of the woodwork" and drive up OHP/Medicaid costs. Since the CHIP program was implemented, in July 1998, the number of children covered by OHP/Medicaid has increased by 3,000.
- A potential source of outreach funds for CHIP is the $300,000 annual grant for the next three years from the Robert Wood Johnson Foundation for their Covering Kids initiative. OMAP staff hope to use the funds to target outreach on homeless youth in Portland, a high uninsured area in Eastern Oregon, and two areas in southern Oregon with high proportions of Hispanics.
- Capitalize on other state health insurance programs’ outreach efforts for CHIP outreach. This can conserve CHIP administrative funds for real administrative expenses such as application processing and enrollment and computer systems enhancements.
- Monitor the number of applications in the pipeline, awaiting eligibility decisions, if enrollment targets are limited by budgetary constraints to avoid exceeding the targets and claims budget.
- Customize outreach efforts for the hard-to-reach populations in your particular state. In Oregon, these include fishing families and Native American tribes.
- Outreach should focus on populations with disproportionately high numbers of uninsured. In Oregon, those are Hispanics and rural residents.
- Reach out to private insurance agents and a broad group of community partners to publicize CHIP.
State’s Response
Some historical information is helpful to understanding state decisions about crowd-out prevention strategies.
- The State Legislature enacted an employer mandate statute in 1989, requiring all employers in the state to provide health insurance for their employees, or pay into an insurance fund. The statute was intended to take effect in January of 1994, was subsequently deferred by the legislature — first to July of 1995 for all affected employers, and then to March, 1997 for businesses with 26 or more employees and to January, 1998 for businesses with 25 or fewer employees.
- The mandate expired without ever being implemented.
- Simultaneous with enactment of the employer mandate, legislation passed to expand Medicaid to all below 100 FPL, and develop a benefit package based on a prioritized list of services. The expansion was based on the assumption that the impending employer-provided insurance mandate would cover most of those above poverty. Although the employer mandate expired, employer-based coverage is on the rise in Oregon. The Governor has cautioned that the state move deliberately with CHIP expansions, so as not to reverse the trend of rising employer coverage.
Waiting Period
- As an explicit employee crowd-out measure, The Oregon Health Council recommended and OMAP adopted a six month waiting period for children in families who dropped insurance or are currently insured. This was a contentious issue between staff of the Council, OMAP, the Insurance Pool Governing Board, and advocates. Since the Legislature was not in session, they have not yet expressed opinions on the topic. Council staff want at least six months of solid data on impacts, before considering a recommendation to shorten or eliminate this waiting period.
- The waiting period was contentious and resulted in a split vote. The contention arose around the "equity issue" — whether the waiting period would apply only to those insured or also to those with access to employer-provided insurance who have not enrolled. A small majority voted to limit the waiting period only to those who are already insured.
- Some Council members and staff felt that one of CHIP’s big challenges would be the inequity between families who made the sacrifice and paid premiums for employer-provided insurance, thus rendering them ineligible for CHIP for six months, and those who did not and were immediately eligible.
- Others believed that crowd-out would be extremely unlikely to occur so long as there was a six month waiting period, because the projected eligible population for CHIP will be so small among the number of families covered by private insurance. There are 1.9 million Oregonians with private insurance coverage, so those officials think that a small program like CHIP that may serve 15,000-20,000 children is unlikely to contribute to crowd-out.
- Under Phase II, Oregon is requesting HCFA(now known as CMS) approval to use CHIP funds in the private sector group market to subsidize employer coverage for the whole family. Officials are looking beyond the notion of using a "shoebox" approach to calculating when a family reaches the five percent limit on out-of-pocket expenses. They are searching for actuarial alternatives for estimating at what points different types of families are likely to hit the limit.
Employer Crowd-Out
- State officials are more concerned about employer crowd-out than employee crowd-out. They fear the propensity is high for employers to drop dependent coverage in the face of CHIP and FHIAP’s availability, calling this "push out."
- With CHIP’s free coverage for children, and employers’ far larger share of FHIAP premiums than a family’s share of premiums, officials worry that employers will stop contributing to dependent coverage.
- Health Council staff have not determined how to measure "push out" but are giving it considerable thought.
- There are no premiums charged for children in CHIP. However, families in FHIAP pay 5, 10, or 30 percent of their premium costs in the FHIAP program. Under the state’s proposal for Phase II, enrolling families in FHIAP but funding eligible children in those families with Title XXI funds (where cost-effective), it is not clear whether the state will continue exempting the children’s portion of the premium costs.
- Since there are no CHIP premiums, there are no disenrollment penalties for failure to pay.
- Under the Phase II plan, the state will establish policies about whether children funded with Title XXI in FHIAP face a lock-out period, if their families fail to pay a premium.
- CHIP children currently do not make co-payments for health services.
- Under Phase IIB, the state may request permission from HCFA(now known as CMS) to conduct a pilot test of employer buy-in, subsidizing employee premiums for employer coverage. They would work with the state’s only health insurance purchasing cooperative — Associated Oregon Industries — to market CHIP coverage to employers for eligible families not enrolled in their employer’s plan. The state is committed to conducting an evaluation.
The State Legislature created the Oregon Health Plan Policy and Research office to conduct planning research and evaluation on the Oregon Health Plan, including Medicaid and, now, CHIP. The legislature requests specific studies and OHPPR reports during the interim or two years later, when the legislature reconvenes. OHPPR has a staff of 20 and an annual budget between $700,000 and $800,000.
Staff usually design and conduct their own surveys of providers, plans, and families, although they occasionally contract out to a local survey specialist. Staff also can initiate studies if they obtain a foundation grant (e.g., from the Robert Wood Johnson Foundation).
OHPPR plans to analyze data from a variety of sources to assess CHIP. There is speculation that the Legislature will be most interested in research on crowd-out, while the advocates are most interested in research on the impact of the six month waiting period.
- In 1993, the RAND Corporation and Mathematica Policy Research conducted a study of health insurance in 13 states, of which Oregon was one, which included a household survey and employer survey. In 1997, they conducted a follow-up. The data (available in a report to be published in late 1999) helped Oregon officials study the potential for crowd-out and led the Council staff to recommend the six month waiting period for those insured.
- Staff in OHPPR and FHIAP worked with the Urban Institute and the RAND Corporation on the best approaches to analyze CHIP. The combined staff have developed an evaluation plan that will be part of the Phase II Plan Amendment they will send to HCFA(now known as CMS).
- The Oregon Population Survey, the most significant effort underway, is a data collection and research response to the Oregon Healthy People initiative. The survey includes questions about employer-sponsored insurance, and about the coverage families have in place. [To view data from the ’94 and ’96 OPS, see www.govinfo.kerr. orst.edu.] Since the CPS sample size for Oregon is too small to accurately estimate the numbers of uninsured at anything other than the statewide level, their own Oregon Population Survey has been a more useful source of statewide data.
- OPS surveys include 5,000 households of approximately 14,000 individuals, every other year. "The Uninsured in Oregon 1997" reports on the 1996 results. The next report is available in March 1999 on 1998 results, at www.govinfo.kerr.orst.edu.
- Staff will analyze the penetration rates in OHP/Medicaid and CHIP from OPS. However, they recognize these data can mask the distinction between insurance coverage and access to care. Oregon officials believe that the state has one of the highest rates of alternative medicine usage in the country, with very little of it covered by traditional health insurance plans. While officials estimate that the penetration rate in Medicaid and CHIP could climb into the high seventy percent range, the coverage of alternative treatments and services used by enrollees could remain low. On the other hand, chiropracty has recently been added to coverage by many insurers in the state, and other alternative medical treatments are being considered for coverage.
- Staff also plan to analyze the effect of the six month waiting period on potential CHIP eligibles. They cannot use OPS for this analysis, as it was last fielded only a month or two following implementation of CHIP. Instead, they will analyze special items on the combined Medicaid/CHIP application form, and an accompanying, one-page Medical Resource Report. The items include:
- List anyone who can get health insurance through an employer or absent parent.
- List anyone who has health insurance now. Do not include anyone covered by OHP only.
- List anyone who had health insurance any time in the last six months. Do not include any time that you were covered by OHP only. Include the month and year your coverage ended.
- Researchers will merge data on how many children were turned down for CHIP due to the waiting period with data from the 1998 Population Survey, and calculate the average period of uninsurance. This should provide guidance on whether they can roll back the waiting period.
- Other data is available from a monthly Wage Survey conducted by the Department of Employment. Each month they routinely survey a different occupation code among Standard Industrial Classification(SIC) codes, so that after three years they have covered all occupation codes in the state, and begin the cycle again. Questions asked of employers and employees include those relating to the availability of health insurance coverage, and how much the employer and employee pay of the premiums. The sample size is 150 businesses per occupation. Data from the Wage Survey will be merged with data from OPS and from the Medicaid/CHIP application form to analyze employee crowd-out.
- Council staff also plan analysis of employer crowd-out, but have left a "place-saver" in the evaluation plan until they determine precisely how they will measure this. They may survey a sample of families with children enrolling in CHIP and enrolling in FHIAP to assess what insurance coverage they lost before enrolling in CHIP or FHIAP. Both programs require six months without insurance prior to enrollment.
- FHIAP staff will analyze reservation cards and applications for FHIAP and CHIP to assess the success of discrete outreach activities. The objective is to gauge why they are not succeeding with certain groups and modify their outreach efforts, accordingly. They will continue to survey FHIAP families about why they do not enroll their eligible children in CHIP, to share this information with OMAP and the Council. Reports and other resources about FHIAP and CHIP are available at http://www.ipgb.state.or.us.
Ten Percent Cap on Administrative Expenses
- Staff on the Oregon Health Council believe the cap on Federal match for administrative expenses will impede OMAP’s outreach activities during Phase I and II. Those funds must be conserved for real administrative functions, like processing applications and enrolling CHIP children. Council staff expressed concern that OMAP will need to hire more people for those functions and to re-determine eligibility and upgrade their computer systems. They appreciate, therefore, the funding available to IPGB for simultaneous outreach for FHIAP and CHIP.
- Council staff believe the cap will cause a more serious impediment during Phase III, when they hope to gain HCFA(now known as CMS)’s permission to fund direct services with CHIP money. They acknowledge that HCFA(now known as CMS) has indicated it may grant waivers permitting more than ten percent spending on administrative costs for outreach and payment for direct services.
Web Sites for More Information
For additional information, visit a web site at:
1 - Though not an insurance program, OMIP is funded in part through pro rata assessments on health insurance carriers.
2 - Assets are non-income resources available to an applicant family, such as a car. A family with a car worth more than $5,000.00 is ineligible for CHIP or Medicaid.
3 - Federal law makes immigrants arriving after August 1996 ineligible for most public assistance benefits.
4 - This is not state General Fund revenue, but revenue from state tobacco taxes.
5 - Social security numbers and copies of social security cards are required "for you and anyone you are applying for."
