The full report is available as PDF only
Presented to:
Assistant Secretary for Planning and Evaluation
U.S. Department of Health and Human Services
200 Independence Ave., SW
Washington, DC 20201
Presented by:
National Opinion Research Center (NORC)
at the University of Chicago
4350 East West Highway, Suite 800
Bethesda, MD 20814
301-634-9300
301-634-9301 (fax)
This report reviews important lessons learned from the experience of network-enabled health IT adoption among federally funded health centers. It reviews challenges and opportunities associated with adoption of health IT, perceived costs and benefits and the experiences of providers working to leverage health IT to improve quality and efficiency of care. It also addresses the nature of support and technical assistance required at various stages of health IT adoption and the role networks have played in addressing those needs among federally funded health centers.
The report focuses on areas that represent challenges and opportunities for officials responsible for implementing the Health Information Technology for Economic and Clinical Health Act (HITECH) provisions designed to provide additional reimbursement and technical assistance resources to motivate meaningful use of health IT among all providers in the United States. To inform the report, several site visits were conducted between August 2008 and April 2009. The site visits included discussions with leadership and staff from nine health center networks, over 30 federally funded health centers and over 100 individuals across all organizations.
Material contained in this publication is in the public domain and may be reproduced, fully or partially, without permission of the Federal Government. The courtesy of attribution is requested. The recommended citation follows:
Office of Science and Data Policy, ASPE(2010) Assessment of Health IT and Data Exchange in Safety Net Providers Final Report.
Washington, DC: U.S. Department of Health and Human Services, Office of the Assistant Secretary for Planning and Evaluation.
Alliance of Chicago
Introduction
NORC at the University of Chicago (NORC) is pleased to present this report detailing findings from our recent site visit to Chicago, IL for the "Assessment of Health IT and Data Exchange in Safety Net Providers," a project sponsored by the Office of the Assistant Secretary for Planning and Evaluation (ASPE) at the U.S. Department of Health and Human Services (HHS). ASPE is conducting this project in close collaboration with the Health Resources and Services Administration (HRSA). Our report synthesizes findings from our first of six site visits examining Electronic Health Record (EHR) implementation among health center networks. The current report focuses on discussions held with staff and members of the Alliance of Chicago Health Centers (hereafter referred to as "the Alliance"). In a separate report, we summarize findings from discussions with Access Community Health Network, another large Federally Qualified Health Center (FQHC) organization implementing health IT in Chicago.
The meetings summarized below took place on August 18-21, 2008. Prior to arriving on site in Chicago our team conducted initial telephone and email discussions to coordinate logistics and provide basic information on the agenda and topics to be covered in the in-person meetings. We conducted a total of 12 meetings with over 15 participants representing the Alliance's network and health center staff. Site visits took place at the Alliance's headquarters on the north side of Chicago as well as with members of its four regional health centers: Erie Family Health Center, Heartland Health Outreach, Howard Brown Health Center and Near North Health Service Corporation. Telephone and in-person meetings were conducted using open-ended discussion agendas that provided a consistent structure to each exchange while allowing sufficient flexibility to capture all relevant information from participants. For each scheduled site visit discussion, the NORC team prepared materials that highlighted outstanding questions to address during the meeting.
We begin summarizing findings from the site visit by providing an overview of the Alliance, including a description of its history, governance and organizational structure, key services and functions, involvement with health IT and future trajectory. We then focus on specific aspects of an EHR implementation conducted by the Alliance, including the process used to facilitate EHR adoption among member health centers; enablers and success factors for EHR implementation; challenges and barriers facing health centers adopting EHRs via the Alliance and the impact of EHR implementation on health centers, their clients and staff as well as health IT topics such as lab interfaces, e-prescribing (eRx), health information exchange (HIE), use of standards in the Alliance implementations and sustainability.
We end the report with a series of conclusions regarding our findings and initial conclusions for policy makers, program officials, health centers, health center networks and other stakeholders. Because this is one of several site visit reports that will be produced, we will present a more definitive and comprehensive set of conclusions and lessons learned as part of the final report for the project, which will synthesize and summarize findings across each of the sites.
Overview of the Alliance
The Alliance of Chicago Health Care Network is a non-profit member organization providing services to FQHCs. The Alliance primarily serves and is governed by four of its original member health centers located on the north side of Chicago. These four institutions serve as operating partners in what Alliance leadership refers to as "a joint venture of four independent organizations with the desire and ability to work together on building common infrastructure to improve service delivery and health status."
Annually, the Alliance's core health centers serve 100,000 clients, making over 340,000 service encounters across 32 different service delivery sites. While each of the four member health centers differs in terms of the specific populations served and the scope of services offered, they share a common commitment to delivering high quality health care and social services efficiently to improve the quality of life for vulnerable, uninsured and minority communities in Chicago.
In addition, the Alliance has prioritized expanding its membership to produce economies of scale that would allow them to continue their EHR implementation without external grant support. Rather than restrict themselves to expansion within the city, the Alliance has been building relationships and working towards establishing service level agreements (SLAs) with health centers throughout the nation that have a similar orientation and goals as the core membership. We provide more details on this expansion and second tier of members later in the report.
Exhibit 1 below is a map of main Alliance sites (representing four of the original member health centers and seven total sites) taken from a presentation regularly delivered by Alliance leadership.
Exhibit 1: Map of Core Alliance Health Centers
Network history and purpose. While the Alliance was incorporated as a legal entity in 1997, its origins trace back to the early 1990's when a group of Medical Directors from health centers based on the North Side of Chicago began meeting to discuss their clinical and administrative responsibilities and share challenges and lessons from their experience. While it was a larger group of Medical Directors that met, ultimately four health centers agreed to form the Alliance. These four (Erie Family Health Center, Heartland Health Outreach, Howard Brown Health Center and Near North Health Service Corporation) each enjoyed a long history of serving their communities on the north side of Chicago and enjoyed a large client base and solid reputations on their own. Still, they believed that changes in the health care delivery and payment system warranted an organization like the Alliance that could help them achieve economies of scale, collaborate and share information for the benefit of the communities they serve. A primary source of initial funding for the Alliance was the Integrated Service Delivery Initiative (ISDI) grant program administered by HRSA's Bureau of Primary Health Care (BPHC). The objectives for the Alliance identified as part of that exercise included: managed care readiness and contracting, joint clinical services, health education, marketing, mental health, purchasing and finance and human resources.
After formalizing their association as the Alliance, Medical Directors and leadership from the four core health center members continued to meet and share lessons learned. Originally, there was a belief that Medicaid managed care in the state would transform the manner in which health centers were reimbursed and perhaps require health centers to form their own health plan. While this did not happen, there were ample opportunities for collaboration, particularly in setting quality goals and establishing quality improvement practices. In 2001 the Alliance shifted focus. That year the Alliance became incorporated as a limited liability company (LLC) and became increasingly focused on providing IT applications and services to its members as an important mechanism for achieving the network's goals around quality and administrative efficiency. Exhibit 2 below outlines key events in the history of the Alliance and their movement towards focusing on using EHRs to achieve Quality Improvement (QI) goals.
Exhibit 2: Alliance History, Key Events
| Year | Event |
|---|---|
| 1997 | Four original health centers convene to form Alliance |
| 2001 | Alliance incorporated as a limited liability company Restructures, re-focuses on health IT |
| 2003 | Alliance obtains Integrated Communications Technology (ICT) grant from HRSA, BPHC to initiate EHR system |
| 2004 | Alliance obtains Agency for Health Research and Quality (AHRQ) implementation grant to develop clinical data warehouse, develop quality metrics and evaluate |
| 2006 | Initial EHR, data warehouse go-live for core Alliance health centers in Chicago |
| 2007 | Alliance obtains HRSA High Impact Grant to expand network presence, move toward self-funding |
| 2008 | Planned go-lives for initial non-core sites in North Carolina, San Francisco and Michigan |
In describing this focus on IT, Alliance and health center leadership cite several factors. First, the Alliance was moving toward efforts to measure improvements in safety, quality and consistency of care and it was determined that EHR supported by a data warehouse was an important tool for achieving these goals. Second, a perceived increase in competition among health centers in Chicago led some to want to differentiate themselves through IT. Third, there were increasing incentives under Medicaid to have tight documentation of care delivery costs and charges to optimize payments under a prospective payment system. And fourth, they noted that there were an increasing number of grants sponsored by HRSA and others that sought to encourage networked computing on the part of health centers.
They decided to pursue a group EMR application rather than practice management, in part because Alliance priorities were driven by Medical Directors more than others and, in part, because it seemed unlikely that Alliance members would be able to agree on the details of how to switch over to a common practice management platform. The effort to pursue an EMR began in earnest following the AHRQ grant that the Alliance received in September 2004. The network engaged in planning and procurement activities through 2006 when they made their first "go-live" at the main site at Near North Health Services Corporation. Since then, the network has continued to support go-lives at member sites throughout Chicago with the last site scheduled to go-live by June of 2009. Network and health center discussants report that for any given site the planning period takes between six and nine months and the process for getting fully up to speed and making substantial use of the EMR functionality takes an additional three to six months post go-live. During this period the EMR implementation requires substantial focus (approximately one quarter to one half time) from several individuals: an Alliance Implementation Specialist, a dedicated trainer, center Medical Directors, QI specialists and site IT leaders.
Characteristics of core members. As noted above, each of the four health centers is a FQHC, but they differ on key dimensions, including the communities they serve, the range of services they provide, the number of care delivery sites and their overall size. We focus here on describing these health centers as they are the health centers represented on the Alliance's Board of Managers, the chief decision making body governing the Alliance.
Erie Family Health Center (29,998 clients served in 2007) has existed for over 50 years. Erie serves a primarily Hispanic population (87 percent) and has a strong emphasis on providing bilingual care. Erie's patients are primarily female and live below the federal poverty level. Erie maintains eight primary care sites, all situated on Chicago's North Side. While the demographics of the neighborhoods where these sites are located have shifted over the 50 year history of the organization, Erie continues to be known as a key provider for Chicago's Hispanic community and many of their clients commute long distances to receive care.
The Heartland Alliance is comprised of two separate but related FQHCs that serve nearly 20,000 clients annually. The Heartland Alliance also includes an agency focused on housing issues as well as an advocacy and human rights organization. The organization's health care focus includes primary care, dental care and mental health care offered across approximately one dozen sites mostly located on the far northwest side of the city.
Howard Brown Health Center (6,284 clients served in 2007) is the leading provider for Chicago's lesbian, gay, bisexual and transgender (LGBT) community. Howard Brown provides comprehensive care to the LGBT community including social and educational services. The center runs two sites primarily dedicated to primary health care and mental health services.
Near North Health Service Corporation (34,926 clients served in 2007) serves the impoverished and uninsured residents of Chicago's Near North region. More than half of Near North's patients are uninsured (51 percent) and the remainder are covered by either Medicaid or Medicare. The center runs five health centers. Each location provides comprehensive primary care services and major sites also provide dental and mental health care.
Organization, staffing and governance. The Alliance is primarily staffed by individuals who have worked at one or more of the four original health centers. Fred Rachman, the Alliance's Chief Executive Officer (CEO) and Chief Medical Officer (CMO) has served as a clinical leader at several Chicago-based health centers including Howard Brown Health Center and Erie Family Health Center. Andrew Hamilton who serves as the Director of Operations and Clinical Informaticist for the Alliance has served as the Director of Patient Care Services for Howard Brown Health Center. Furthermore, many of the Alliance's Implementation Specialists, quality improvement managers and other staff have experience working in one of the four core health centers. In total, the Alliance employs approximately 10 individuals for full or part time for a total of approximately 8 full time equivalents (FTEs). The Alliance noted that the total number of staff and FTEs can differ depending on the number of implementations and planning activities happening at a given time and that their plan for expansion will require them to quickly bring on more staff in key areas.
Although the network shies away from direct outreach, the Alliance's leadership goes out to speak at many meetings and encourages health centers around the country to learn more about their activities and consider joining. In the most recent phase of the Alliance's development expansion is a particular emphasis because of the need to achieve economies of scale that would enable their EHR implementation program to achieve self-sufficiency.
The Alliance members are split into two groups. The first group consists of the four original Chicago based health centers that signed an operational agreement and jointly administer and govern the LLC. Other members are not part of the LLC but have contracted with the Alliance and have service level agreements (SLAs) in place through which they access the Alliance's health IT services. Unlike the core members, members with SLAs do not pay annual dues; instead they pay for the services provided by the Alliance. The Alliance is working to expand their SLA partners, which currently include FQHCs and nurse managed health centers in Michigan, North Carolina and Northern California. Currently, there are four health centers that are SLA-based members of the Alliance and several others that are in the process of becoming members.
The Alliance's governance structure is made up of executive staff, Finance Directors and Chief Medical Officers from the four original health centers. The network staff includes Fred Rachman, Chief Medical Officer (CMO) and Chief Executive Officer (CEO), Andrew Hamilton, Director of Operations and Clinical Informaticist, Jerry Lassa, Director of Performance Excellence and other staff including an Implementation and a Business Operations Manager. Several committees support and coordinate the Alliance's work. These include the Clinicians' Committee, IT Steering Committee, Behavioral Health Committee and the Finance Committee.
The Board of Mangers has ultimate governance responsibility for the Alliance and consists of leadership staff from each of the four original health centers. The second tier of governance includes operations leads from each health center and is led by the Alliance's Director of Operations and Clinical Informatics. The third body with governance responsibility is the EHR Systems Users' Board, which includes representation from all health centers that are part of the Alliance and informs the activities of the Board of Managers and the Operations Group. This group often sets priorities for enhancements to the EHR.
Services and functions. Since 2001, the Alliance has primarily provided IT applications and QI support for member health centers. The Alliance worked with staff from health centers to define requirements and set up a contract with General Electric (GE) to use the Centricity EMR product, customize the product to meet functionality requirements at the network and health center level, deploy the application, set up appropriate interfaces with laboratory providers, maintain a data warehouse housing clinical indicators and to provide reports to health centers allowing them to track quality and efficiency of care.
There are several health centers that are also working with the Alliance to move their practice management platform from a pre-existing system to one that is offered by GE and is seamless with Centricity. While Alliance members did make a decision early on to focus initially on EMR implementation rather than practice management, as the implementation has evolved and the network has gained the trust of member health centers, there is increasing interest among members in switching to a network-supported practice management solution that is seamless with Centricity.
While the Alliance has always facilitated collaboration among member health center Medical Directors on quality, the recent addition of a network-wide QI Director has allowed the Alliance to take a more hands on approach to assist health centers in incorporating a culture of quality and promoting adherence to evidence-based practice guidelines. In particular, the Alliance's QI Director has begun working with Medical Directors and health center leaders on developing ways to link provider compensation and rewards to EMR-generated metrics and evaluating the impact of clinical decision support and disease management functionality on provider behavior. The Alliance also serves as the gatekeeper for matters concerning GE's Centricity, providing an important tier of application and systems support.
Future direction. While the Alliance has undergone tremendous changes and made important accomplishments over the last decade, the network continues to work towards expanding its reach. Given the emphasis on self-financing and sustainability of health center networks beyond the period when they are supported by dedicated grants, the Alliance has been working towards increasing the number of EHR users to allow for greater economies of scale. They are planning an approximately five fold growth in the total number of EHR users over the next two to three years. They also have longer term development plans that include adoption of personal health records, eRx, health information exchange (HIE) and other technologies designed to improve quality.
Health IT at the Alliance
Given that EHR implementation is a major focus of the Alliance and is central to the purpose of our broader project, in this section, we summarize findings from our meetings on the motivation and approach for health IT adoption in general and EHR implementation in particular. We provide this overview as a precursor to a more detailed discussion on enablers, barriers and impact of health IT adoption in subsequent sections.
EHR implementation process. The Alliance's standardized rollout occurs in three phases: pre-implementation phase, implementation and full functionality. The rollout process begins with the designation of an Implementation Team including staff from the health center and an Implementation Specialist from the Alliance. Because of the need for heavy involvement from staff at the health center and because these staff have limited time away from clinical and administrative responsibilities, the planning and roll-out for an implementation often takes place over a series of months with long weekly meetings serving as the central management vehicle to map out tasks and responsibilities and develop a site specific Implementation Plan.
Among the first tasks is conducting a comprehensive review of clinical workflow. This process helps the team identify areas for improvements and allows the center to use the implementation to address overall efficiency objectives. The workflow assessment also sets a benchmark so that health centers can look back after the rollout and see how changes in workflow facilitated by the EMR either improves or does not improve efficiency.
Drawing partially on the workflow assessment, the Implementation Team develops a set of requirements for the roll-out. While core system requirements were worked out on the Alliance level with input from all Medical Directors, there are always some changes to settings, menus and interfaces based on the specific needs at the health center level. The need for health center or even site level customizations may be driven by characteristics of the population being served, the suite of services offered by the site or workflow limitations that are driven by the space and appointment schedule of the site.
Staff at the health center are introduced to the EHR over a series of meetings where basic concepts are laid out and staff at all levels that will actively use the application have an opportunity to contribute to customizations and ask questions regarding the impact of the system on their work processes and responsibilities. All forms of communication ranging from emails to lunch time meetings have been used to make sure that staff are aware that change to their work process is coming, allowing them to prepare for the change and get questions answered up front. Some centers also indicated that they posted signs and provided flyers for patients, so they would also be prepared to see clinicians interacting with computers in the exam room. Training occurs in the weeks immediately prior to implementation. The Alliance typically requires 16 hours of training for all users and has established separate curricula for all types of users.
Before implementation there is often a "dress rehearsal" where the center closes and simulates implementation for part of a day. Implementation Specialists from the Alliance remain on site throughout the rollout's first few weeks of implementation. In some of the health centers "super users" were assigned to receive advanced training so that in the future these users could answer day-to-day end user questions. Super users serve an important part in ensuring that clinicians can ask questions and receive timely answers from a colleague, they also serve as clinician champions and it is envisioned that they will play a leadership role in evaluating the use of the EMR over time. It should be noted that the super user role is sometimes formally assigned; alternatively, super users can be clinical staff (often nurses) that take it upon themselves to engage in the implementation process. While the implementation process varies from center to center and site to site, the steps outlined above were fairly consistently reported across the four centers we visited. Currently, the Alliance is live with the Centricity product in all four health centers and is supporting approximately 325 clinician users.
Motivation for health IT adoption. All of the health centers in the Alliance provided relatively consistent answers to the question regarding their motivation for adopting health IT and their answers also confirmed g. the vision for increased quality, transparency, safety and efficiency of care outlined by Alliance leadership. We provide detail on specific thoughts offered by meeting participants below.
Quality of care. Almost all participants explained that improving the quality of health care delivery and outcomes was their primary motivator for adopting health IT. Many health centers look to analyze patient clinical data using nationally recognized quality measures and benchmarks between centers as well as national standards. Multiple participants indicated the need to strive for greater consistency and adherence to guidelines for care to patients with chronic conditions such as HIV and diabetes. Also, many participants wanted to be able to proactively identify adverse drug interactions. The FQHC Medical Directors and leadership discussed the benefits of advanced reporting and dashboard functionality that the Alliance had customized within the Centricity System. A key metric for the Alliance has been monitoring the extent to which this dashboard is being used. They are finding that in the initial months following go-live, dashboard reports are primarily used to establish use of the system and answer questions such as, "Do all patients who should have an electronic record based on practice management data, actually have a record?" and "Are forms being used for structured documentation of care to specific populations?" The Alliance reports that some health centers, specifically those that implemented early, are just now at the point of being able to identify baseline levels of clinical indicators for key populations and consequently look at how the baseline has changed with increased use of EMR functionality. We provide more details on impacts observed to date later in this report. Although still in early stages, discussants indicated that having center and provider level reports on quality and efficiency metrics encourages and rewards quality improvement and will continue to do so over time. Several participants also mentioned opportunities to conduct research in the area of disparities using the clinical data warehouse application.
Administrative efficiency. Participants also cited administrative efficiency as a rationale for adopting health IT. In particular, they sought to eliminate the burden associated with locating charts and providing visit summaries for referrals. Though we did not learn of efforts to document or measure these improvements formally, discussants did provide some anecdotal information. One discussant commented that the system has "revolutionized the role of the nurse." By this she meant that workflow analysis done before the EMR implementation had dramatically improved old processes that had required more onerous verbal coordination and exchange of paper documents. For example, where intake may have previously required several conversations and exchange of paper records between front office staff, medical assistants and nurse practitioners, to verify that specific information had been collected, the process of planning for and using the EMR helped to streamline this coordination. Through this process health centers had the opportunity to reevaluate each step of key processes, such as patient intake, history and physical, clinical evaluation, vital signs monitoring and close out to assure that the appropriate individual conducts the appropriate activity in the appropriate order. In some health centers this has increased the level of involvement of medical assistants and allowed clinicians to be more focused on direct care delivery. Some health centers, particularly those that have implemented the GE Centricity system for both practice management and EHR, mentioned efficiencies in complying with the HRSA Uniform Data System reports required for all FQHCs and other funder reporting requirements.
QI support. The Alliance staff has worked with GE to incorporate key decision support and QI elements into the EHR application being implemented in their health centers. In particular, they created a format where health center providers can continue to focus on chronic disease treatment by designing special disease management screens for patients with diabetes, heart disease or other chronic illnesses. These screens list required preventive and treatment services, such as specific blood tests or exams, the last record that each of these services were provided, the associated clinical data, evidence-based guidelines and normal ranges for each clinical indicator and decision support flags in red font for services that are "due" based on the guidelines. While providers are not required to go to and use the disease management screens at the point of care, the approach does support disease-specific quality initiatives, such as the Health Disparities Collaboratives and allows health centers to actively manage specific groups of patients. Exhibit 3 below shows an example of a disease management screen for diabetes. Data from the EHR are also maintained in a data warehouse that supports the advanced quality reporting feature described below.
Exhibit 3 below shows an example of a disease management screen for diabetes.
Exhibit 3: Alliance EHR Disease Management Screen
Reporting using the EHR. Because the Alliance was able to work with GE to establish a clinical data warehouse populated using clinical data from each EHR implementation, they are able to produce a variety of reports that track utilization and outcomes at the network, center, site and provider level. While there is a level of basic reporting that can be conducted directly from a given center's EHR, more complex reporting is conducted using the clinical data warehouse where de-identified utilization and outcomes data are maintained.
The Alliance built and designed the warehouse reports in close collaboration with Medical Directors and other clinical leaders. Because of the design of the EHR application itself, there are also opportunities for Medical Directors and staff to develop and run their own reports, though most of the Medical Directors reported that their staff are only beginning to learn how to generate reports and then use the data effectively. Many Medical Directors noted that sharing data on quality with clinicians is an important part of establishing a culture of quality and that over time they looked forward to using the reports to create incentives for quality improvement.
Alliance staff noted that in addition to diabetes there are ten other areas where formal quality measures have been established, along with forms in the EMR and reports generated out of the data warehouse. For each of these efforts, the metrics were identified through consultation with the American Medical Association and National Quality Forum as well as peer reviewed literature and HRSA-wide quality reporting targets. Other focus areas of quality for the Alliance include depression, smoking cessation, well child care and other clinical priority areas identified by the Medical Directors.
Exhibit 4 below provides an example of a quality report generated by the data warehouse for diabetic patients. The report shown is for the Alliance as a whole, but the same report can be generated at the center and provider level. The report demonstrates how the EHR and data warehouse can be used to support the Health Disparities Collaborative.
Exhibit 4: Example Diabetes Report
Process for enhancements. Although the EHR implementation at Alliance sites is relatively recent, they have a robust process in place for users to communicate with each other; share lessons learned and suggest recommended enhancements to the Alliance. Mechanisms for this communication include regular meetings of the users group and a user's portal for online collaboration. Because the Users' Committee is a formalized part of the Alliance governance, their concerns are usually prioritized by the Board of Managers and the Operations Committee. The Alliance reported using a transparent process for analyzing requests for enhancements based on the level of importance and the level of difficulty and costs. For several areas, including eRx (discussed below), desired enhancements are not available through GE Centricity. In order to expedite and facilitate health center focused enhancements to the core GE product, several Alliance staff are active in the user community for all GE Centricity customers.
Enablers and Success Factors
In this section we review enablers and success factors facilitating EHR implementation described by health center and network respondents.
Network culture and dynamics. The organizational culture of the four FQHCs that make up the Alliance has played a critical role in the Alliance's success in its initial launch of the EMR solution as well as in its current efforts to offer the EMR as a hosted service to other safety net providers around the country. The four FQHCs that operate the Alliance have worked together for over 12 years on Alliance-related efforts. They share strong professional relationships and a consensus-based approach to decision making. In addition, the staff at the Alliance all previously (and in one case currently) worked at one or more of the Alliance's individual FQHCs in provider, management and quality assurance roles. As a result, the Alliance's staff all have deep understanding of the on-the-ground realities of day-to-day operation of these specific health centers. One key player at the Alliance noted that the network was only able to successfully implement its solution because there was a good alignment of leadership at all of the FQHCs and external funding to support the initial implementation that all became available at the same time.
Federal grant support. The staff at the Alliance feel that ongoing support from HRSA and other funders is crucial for establishing the Alliance's health IT infrastructure and would also be crucial for ongoing operations. In particular, respondents noted that the labor costs for Alliance staff have been almost fully funded through grants from HRSA and AHRQ, without these grants this entire implementation effort would not have gotten off the ground. In addition to financial support, there were also examples of technical assistance, AHRQ and its resource center provided extremely critical guidance that played a key role in helping establish the capacity to provide a centrally administered EHR application to a range of sites. Finally, there is evidence that federal grants have served as a catalyst to motivate the EMR vendor to take a stronger role in the implementation of the EMR at FQHCs.
In the absence of knowledge that this funding will continue, the Alliance has developed an aggressive business model that calls for it to bring on more health centers onto its platform. However, should the Alliance fall short in this effort, it will not be able to internally fund its ongoing health IT needs based on current expenditure levels. On the other hand, if the Alliance succeeds in this effort, the additional health centers that sign up with the Alliance may eventually create a "profit," which can be used to lower the annual fees paid by the four core FQHCs or create additional funding for other Alliance-sponsored activities.
Expertise and experience. The staff discussed several different factors related to staff expertise, which they felt were crucial to success in their implementation. The Alliance has carefully used outside consultants for a range of tasks, including development of a long-term business plan, an interim Chief Technology Officer who was able to design a cost-effective technical architecture for the overall GE solution, informatics IT consulting on an as-needed basis and the long-term "rental" of a part time CIO for one of the FQHCs from a health IT consulting firm. The Alliance staff also noted that the network model allowed health centers to retain staff that would otherwise move on to different opportunities by giving them an opportunity to expand their skills by working at the network level. The Alliance created an Implementation Specialist role that has proven to be very successful in their experience. This position serves a range of IT lifecycle roles in the planning, training, rollout and ongoing support of all of the health centers. Finally, the Alliance is able to access deep product skills by establishing a close and collaborative relationship with the EMR vendor, which improves the ability to obtain timely product support and has a strong say in providing guidance on future product enhancements.
Deployment success factors. In developing the IT implementation process outlined above, the Alliance made a number of decisions regarding how to work best with the each health center. During the interviews several key success factors were identified in the rollout strategy. One of the key decisions was about which existing patient data should be moved forward from their "legacy" formats into the new system prior to the system going live. This, in essence, is the data that the providers would see for the patients the very first time (and every subsequent time) that they entered the patient's electronic chart. Two specific types of data were mentioned in the interviews, the patients' paper charts and the results of the patients' prior laboratory tests.
While the Alliance and its FQHCs had initially planned to scan at least a subset of their paper records, eventually a decision was made not to scan these charts. Instead, each site focused during the pre-implementation phase on developing a robust "minimum data set" for each patient on a paper "cover sheet." This information was validated with patients in a pre-deployment clinic visit and was then preloaded into the system by non-clinical staff before the system was first launched. In retrospect all involved felt that loading the old paper records would have been a distraction from the electronic system and would not have been useful based on how rarely the paper records were reviewed for reference post-launch.
Historical laboratory data results were felt to be much more useful in the EMR context. This data was already considered to be of consistently higher quality than the paper charts, since it was already electronic and structured (i.e., specific values in specific fields) as opposed to unstructured (i.e., handwritten free text on pages of essentially blank paper).
The Alliance and the FQHCs made the decision to import existing laboratory results data into each patient's record and make these data look essentially no different than if they had been ordered directly through the EMR. These data, unlike the paper charts, are frequently referenced by clinicians. Another key element of the success of the deployment was the strong focus that the Alliance and the FQHCs placed on developing super users and extensive "grass roots" expertise at the site and FQHC level. Additionally, the network had super users handle all interactions with the Implementation Specialist staff at the Alliance.
Role of workflow assessments. The usefulness of the workflow analysis was also cited as a key success factor in the implementation. Every site invested extensive effort to document and understand the current workflows and then to map these workflows to the EMR system (even when the staff found it to be an arduous process). As noted above, some sites used this as an opportunity to redesign some workflows and ended up substantially redesigning their operations, including allowing non-clinical staff to play a greater role in non-technical aspects of managing a patient visit. Some health centers also found the workflow assessment to be valuable as a check of the appropriateness of their processes. For example, one site noted that their process for intake often took place in the hallways of their facility, which could have resulted in a series of problems with respect to regulatory compliance and was not consistent with best practices or their organizational policy. Other health centers did not attempt workflow redesign at the same time as the initial documentation. In both cases the staff felt that the due diligence involved in this step was a key enabler to a successful implementation.
Impact of EMR. While Alliance health centers are still in early stages of EMR use, some have reported rates of provision of preventive services such as vaccinations and the number of patients who are developing and reporting self management goals. It was clear from the discussions that Medical Directors are just now getting familiar with the quality reports that are being generated on a regular basis and looking at the quality and change in quality at the provider and center level. Many of the Medical Directors noted that they were anticipating important benefits in the ability to track manage and improve the quality of their services. In particular, Medical Directors noted that they would be interested in using provider specific data to set incentives and set performance goals for each of their providers.
Medical Directors also felt that EHRs would allow them to compete more effectively for clinical talent by attracting and retaining residents and doctors who had been trained to practice medicine with only electronic records or who had already switched from paper to electronic environments in past positions. Finally, a few discussants noted the basic public relations value of having electronic-only sites in that the EHR would contribute to a perception of a high quality of care among patients, the general public and potential local funders.
Challenges and Opportunities
This section includes a discussion of areas where the Alliance has made important progress, but where some aspects of their experience demonstrate barriers and challenges to making the most out of their health IT activities.
Technical infrastructure. One infrastructure-related challenge that was mentioned by some participants was related to a decision early on to equip some clinical workstations with a thin client desktop, as opposed to a full desktop PC. When this decision was made at two of the early adopting sites, the sites experienced poor performance with using the thin client workstations, this caused both reduced productivity and increasing user frustration. However, according to the network, this issue was diagnosed as being an issue having to do with the software and not thin client set up. The only other infrastructure issue that was mentioned was the productivity loss created by a lack of a single sign-on to workstations and applications. (This, in turn, is caused by limitations in the currently implemented version of the EMR product.) It is unclear whether "single sign" on would result in significant productivity improvement, however, our discussions suggested that having this feature would improve perceived system efficiency. Network leadership notes that some infrastructure issues that arise are inherent to the challenge of delivering centrally hosted applications through different health centers that have different network attributes.
Resistance to changes in workflow. One important change in workflow that is typically required by EMR adoption is a different approach to charting. During planning and implementation phases the Alliance noted some important differences in charting practices across member health centers. Using the older paper based systems health centers differed in the extent to which they promoted a culture of charting immediately following the patient encounter verses maximizing clinic time to see patients and charting during non-clinic hours. Use of an EMR typically requires enhanced charting at the point of care or immediately following the encounter. One health center reported having difficulty regaining their normal volume of patients because of difficulties with charting during or immediately following a visit.
This center may have been a less attractive candidate for a quality-driven EMR implementation, since other prerequisites for EMR implementation (e.g., sufficient time for an "EMR-proficient" physician to finish charting) were not in place at the time of implementation. In addition, this health center reported greater problems with the EMR user interface relative to other centers.
Cost and sustainability. As with many health centers and networks, the Alliance operates on what it considers to be a very "lean" budget, approximately $2.2 million annually. It was clear from our visit that the staff at the Alliance work extensive hours, in some cases more than twice what would be considered full time. It is not clear if this level of work is sustainable over a long-term or what level of revenue will be required to reduce the number of requirements put on staff at the Alliance. Most of the health center respondents noted that they were concerned about whether the Alliance would be able to continue providing the same level of service as they look to expand, given that current staff seems to be stretched. Also, while most health centers that participated in the discussions indicated they understood the rationale behind plans to expand EMR users supported by the Alliance, some also indicated that if the Alliance was not facing an imperative to be self sufficient, they may be more likely to ask the Alliance to take on a broader role in coordinating administrative and billing functions to achieve even more economies of scale among the core Chicago members.
Training. While extensive effort was put into training in both the laboratory and in real-clinic simulations, some discussants felt that the "big bang" approach to rolling out all EMR functionality at one time in a single site was less than optimal. Some noted that they would have preferred to rotate through a site that was using EMR for a period of time before having to adopt it in their home site. One unsolved challenge to date has been the ability to find a training approach to ongoing "advanced/special topics" training for the system that staff will consistently devote the time to attend. It has been much easier to accomplish initial training efforts than to find a way to help the users continue to find ways to gain ever increasing value from the vast functionality of the system.
HIE and use of standards. While the staff at the Alliance expressed great optimism and interest in participating in a comprehensive, standards-based HIE mechanism, such as a state-wide Regional Health Information Organization (RHIO) or a loose affiliation for data sharing among ambulatory and acute care safety net providers in the Chicago area, to date, broader efforts to achieve local or regional HIE in Chicago have been stalled. The Alliance's Director of Operations and Clinical Informaticist noted that he is very active with the Health IT Standards Panel (HITSP) and is a member of standards development organizations (SDOs) and is optimistic that standards based exchange will occur in the region with the Alliance playing the role of leader.
The only significant RHIO-type activity undertaken by the Alliance has been in relation to a major hospital system that shares many patients with the Alliance. That hospital system is currently planning the implementation of an internal HIE, designed to let its disparate clinical IT systems share data with each other. At the urging of the Alliance, this hospital system is considering designing this HIE so that it could be opened up to external providers such as local FQHCs in the future. However, this effort is moving very slowly due to a lack of seed funding to perform the initial strategic and operational planning. Notably, we did not find evidence that health centers exchange data with each other; this is primarily due to the fact that these health centers offer parallel services to different niches within Chicago's undeserved population. To date, the Alliance has been involved in other more localized efforts, such as the bi-directional exchange of vaccination data with a state registry as well as use of lab interfaces described below.
Lab interfaces. In the context of their EMR implementation the Alliance has begun to engage in one form of HIE. Their EMR implementations involve the establishment of a bi-directional interface with clinical laboratories that serve their member health centers in Chicago. These interfaces, which support both lab ordering and integration of results with the EMR, are critical for the use of EHRs for quality improvement.
The Alliance reports that setting up interfaces with various laboratories has proven difficult due to the use of proprietary product based interfaces rather than universal standards being used by both the EMR and the clinical laboratories and the lack of commercially available interfaces that work without significant customization. Because each health center may work with several distinct laboratories, the need to create one to one interfaces between each health center, health center sites and the laboratory creates a substantial technical and administrative burden that gets considerably higher as the Alliance seeks to expand beyond Chicago.
The demands associated with monitoring interfaces once the interfaces were put into place are also considerable, as relatively minor changes in process at the laboratory side can result in orders not being received or results not being delivered or being delivered incorrectly. Every problematic transmission of laboratory results represents an often crucial piece that must be manually handled; this delays the EMR, the provider and the patient from acting on those results. Additionally, the Alliance reports that for each interface in use, on average problems arise once every other month.
E-prescribing (eRx). Notably, eRx was not an initial component of Alliance's EMR implementation. The imperative to pursue eRx increased earlier this year due to new state requirements that will require the use of tamper proof prescription paper for the transmission of prescriptions to pharmacies or, alternatively, e-prescribing. Alliance and health center staff cited the desire to move to eRx using the Centricity system to avoid the cost of tamper-proof prescriptions. However, they noted that the vendor was not able to provide this functionality in the required timeframe. In follow, up exchanges, the network has indicated that they ultimately worked with a vendor to come up with a plain paper solution to the tamper proof paper issue and that it is still not clear that the benefits of pursuing eRx outweigh the costs at this time.
Value of the data warehouse. Network staff noted that the decision to develop and employ a data warehouse was largely driven by the complex reporting requirements necessary to support quality improvement in a health center environment. The various dashboard reports referenced above are generated through the data warehouse. Although health centers are able to run reports out of their local EMR database, most indicated that they rely on the Alliance to generate reports coming from the data warehouse for tracking key performance metrics. In particular, the data warehouse allows for aggregation of data for the purpose of making baseline comparisons across health centers. In addition, discussants noted that that the data warehouse allows for more efficient analysis of specific populations as would be possible through registries. While there was substantial cost associated with designing and implementing the data warehouse, the network noted that GE was supportive of the effort. Similarly, there are some costs associated with managing the data warehouse, but most discussants referenced the data warehouse itself or its functionality as a key benefit of the Alliance's activities to date.
Supporting long-distance implementations. As noted above, beginning in 2007 the Alliance began increasing the number of health center members and provider users who are able to access EMR through their arrangement with the GE Centricity. Network staff note that they are still early in the process of supporting EMR implementations outside of Chicago. While they acknowledge the challenges associated with managing implementations from a distance, the Alliance notes that they have implemented measures to mitigate these challenges. First, they do not actively sell their services, but instead provide information to prospective members and then spend a fair amount of time evaluating prospective members to ensure that they share a basic philosophy around implementation and quality. They have also worked to employ staff that are close to the implementation site and have brought key staff from long distance members to Chicago. Still, the network acknowledges that there are unanswered questions regarding how best to integrate the SLA members and what level of integration is realistic.
Sustainability outlook. The Alliance leadership has initiated a sustainability plan. As part of this effort they contracted with an independent consulting and law firm to develop a business plan that would allow for sustainability. This business plan highlighted the need to achieve greater economies of scale to ensure that, in the absence of grant revenues, they could keep membership dues and user fees at a level that would continue to be affordable to safety net providers. The Alliance has specific goals with respect to growth in terms of members and users. While they have developed members and potential members to stay on track with their objectives to date, they note that the level of growth that they are looking for will require substantial increase in staffing at the network level.
Preliminary Conclusions
We conclude with some brief preliminary conclusions and areas for future inquiry that will inform overall conclusions for our final report.
Long-term staffing and sustainability. It is important to note that the initial development and ongoing management of the Alliance has involved a significant investment of time from a wide range of clinical, financial, administrative and IT staff at each of the core FQHCs. All of this time was invested in the Alliance, in addition to all of the time staff from these FQHCs spent performing their existing "day jobs." While the level of time invested in the Alliance has decreased since the EMR solution has gone live, the Alliance still depends on this external investment of "free" resources in order to perform its ongoing work.
Network focus. One interesting issue that surfaced in the interviews is the inherent tension between the Alliance serving as a consortium-type resource organization for the four core FQHCs and the Alliance serving as a hosted solution service provider for the additional SLA provider clinics. The additional clients provide funds to support the EMR implementation for Alliance members and expand the base of customers that support the entire Alliance staff.
On the other hand, by focusing on solutions that can be resold to other provider clinics, the Alliance and its owner FQHCs are not able to devote additional "mindshare" to the provision of other types of shared services that they could offer, such as other types of administrative software, human resource management, pooled purchasing and facility management. It remains to be seen to what extent the Alliance and its owners choose and are able to successfully expand the scope of the Alliance to include these and other types of services.
Research and innovation. One feature of this site visit that was not as evident in the site visits conducted three years ago is the interest of network leadership in capturing clinical data and using it to conduct research. Meeting participants were eager not only to use the clinical data warehouse to publish the impact of EHRs on the quality of care, but also to use these data to develop requirements and assess needs that could be addressed using different applications, such as different forms of personal health records (PHRs) and other technologies that could enable patients to take charge of their own health and health care.
Providing services remotely. While several health center networks have begun to provide extensive services to health centers that are geographically removed from their core sites, the process for broadening their reach beyond their core geographic area will also differ because each network employs different model. Alliance staff continuously made the point that their EHR implementation process was very "hands on" and focused on workflow assessment, improvement and development of a quality focus in each site rather than simply providing access to the EHR software.
They are cognizant that not all health centers are appropriate for joining the Alliance as their needs to be some agreement among the health center and network in the philosophy underlying their activities. They also noted that their approach requires extensive travel for network staff to remote locations. It will be instructive to note how this model evolves or is adapted as the network rapidly ramps up its membership as well as how the approach that is used by the Alliance differs from other networks that have expanded geographically.
[1] Taken from PowerPoint Presentation forwarded by Fred Rachman on 10/1/2008
[2] Taken from PowerPoint Presentation forwarded by Fred Rachman on 10/1/2008
[3] Taken from PowerPoint Presentation forwarded by Fred Rachman on 10/1/2008
Access Community Health Network
Introduction and Methods
NORC at the University of Chicago (NORC) is pleased to present this report detailing findings from our site visit to Access Community Health Network (“Access”) for “Assessment of Health IT and Data Exchange in Safety Net Providers.” NORC conducted this site visit under contract with the Office of the Assistant Secretary for Planning and Evaluation (ASPE) at the U.S. Department of Health and Human Services (HHS). The Health Resources and Services Administration ( HRSA) works in conjunction with ASPE to guide activities under this project. This report is one of several site visit reports for the project. NORC researchers visited four Access sites and met with network leaders at Access’s central administrative office in August of 2008. We conducted a total of six meetings including 12 discussants. Notes taken during these visits along with various background and administrative information made available by Access constitute the primary data sources for this report.
History and Background
Access is a single federally qualified health center (FQHC), comprised of 51 individual sites. The Access service area spans from downtown Chicago to large portions of the city’s south and west sides and suburban DuPage County. Their total service area encompasses 1,700 square miles. Although Access is a single health center, Access claims that its annual patient volume (around 217,000 individuals for the current year) is the most for any health center in the country. Access’s primary care visit volume (600,000 visits), employee base (800 individuals: 230 board certified and board eligible physicians and midlevel providers, 300 RNs, licensed clinical social workers, medical assistants, case managers and outreach workers) also stand out as exceptional among FQHCs.
Figure 1 shows how the Sinai Family Health Centers span across several regions of the Chicago metropolitan area.
Figure 1: Access Community Health Network Service Area
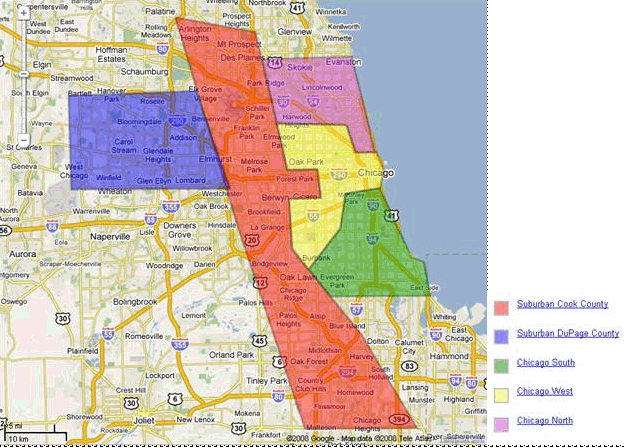
Access began as Sinai Family Health Centers, an entity that brought together a small group of ambulatory clinics established and operated by Mount Sinai Hospital on Chicago’s west side. These centers were originally designated federally qualified health center (FQHC) “look-alikes.” In the early 1990’s Sinai Family Health Centers won a small grant and used it to establish compliance with Section 330 requirements, thereby making it eligible for designation as an FQHC look-alike. Sinai Family Health Centers’ senior leadership team coalesced in 1994 and the organization’s first CEO stayed with the network until 2000.
In 2003, Sinai Family Health Centers was formally spun off from Sinai Health System and took on the name Access Community Health Network. Since then, Access has acquired many health centers across Chicago and its suburbs. These sites span several regions across the Chicago metropolitan area as shown in Figure 1 above. Like other health centers, Access serves a disproportionate number of racial and ethnic minorities (94 percent of their patients in a given year), individuals on Medicaid (nearly half of all patients) and the uninsured (over 20 percent of patients). Overall, Access estimates that it serves approximately 10 percent of all uninsured individuals in the Chicago area.
Access differs from many other CHCs taking part in this study because it is a single federally qualified health center, not a health center controlled network (HCCN), composed of multiple FQHCs. Access resembles an HCCN in that it has many sites, serving many communities. In many cases, health centers have joined Access after having been an independent FQHC. Access is also different in its historical relationship with Sinai Health System’s hospital and it’s reliance on the hospital to support its IT function for several years. While there have been some benefits to working with Sinai, as the health center has expanded to areas well beyond the service range for Sinai, its relationship with Sinai on IT issues in particular has become less important and, the need to establish a their own suite of IT applications and hosting capabilities has become apparent.
Access provides a variety of services geared toward individual and family care. Most Access sites offer standard primary care services as well as disease management, outreach and health education. Access sees specialty care as a significant gap for many underserved patients and is seeking to address the problem by expanding capacity in various specialties. Some Access centers offer specialty care such as dental care, obstetrics and gynecology, dermatology, HIV care, psychiatry and nephrology. Access has created one clinic solely devoted to specialty care and maintains strong ties with local hospitals to ensure that their patients can obtain access to necessary providers. Access works with state social service agencies to screen and enroll patients in Medicaid and the state’s SCHIP program, “All Kids.” Many Access sites include enrollment specialists expressly for this outreach function.
Governance
Access is governed by a twenty-member board of directors. A majority of board members are patients, and the current board chair, vice chair and secretary are all patient representatives. This governance structure creates a direct link between the network’s senior leadership team and the patients Access serves. The senior leadership team is composed of the CEO, Medical Director, Chief Financial Officer, CIO/Process Improvement Officer, Vice President of Human Resources, and the Vice President for Strategy, Planning and External Affairs.
This senior leadership team works directly with clinical and management leaders split across the organization’s eight regions. Each region is directed by a regional medical director and a regional manager who also serve as clinic-level leaders for one of the clinics within their region. Given this organizational model, our site visit included meetings with the network’s chief information officer and medical director as well as regional medical directors and managers from four of the eight regions.
Overall Approach to IT
Access is in the midst of implementing a long term strategic plan for IT which includes upgrading a variety of key systems that serve the network including the practice management system, data warehouse and enterprise resource management software. The timeline for these and other IT projects is provided as Figure 2. Access also recently completed an upgrade of its computing infrastructure to accommodate these new applications. These activities have been led by Steven Glass who serves as the Chief Information Officer (CIO) and Performance Improvement Officer for the network. Access notes that the integration of the IT and performance improvement functions can help optimize translation of technology use to quality improvement.
Access network leaders stressed the importance of their historic financial commitment to health IT. In recent years, Access has devoted 3-5 percent of its roughly $97 million operating budget to IT. While in the past much of this expenditure went to support services acquired from Mount Sinai, Access has recently decided to take the same resources and apply them to upgrades and new applications to support its mission.
At the time of NORC’s visit, Access had concluded an intensive requirements development and vendor selection process. Having chosen Epic as its EMR and practice management (PM) vendor, Access is set to begin phased staff training and implementation across its sites.
Figure 2 provides a timeline for Access in the midst of implementing a long term strategic plan for IT which includes upgrading a variety of key systems that serve the network including the practice management system, data warehouse and enterprise resource management software.
Figure 2: Access IT Milestones
Source: Glass & Miller, 2008
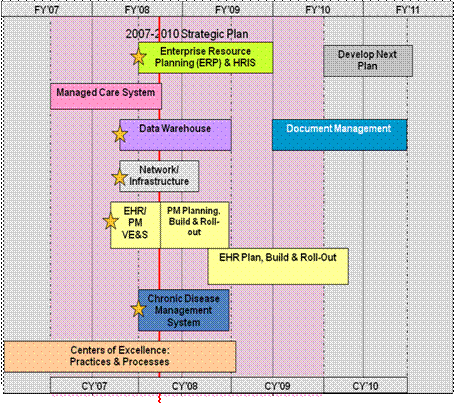
Key Findings
We organize our presentation of findings from this site visit around key themes for the overall study including the current state of IT use and quality improvement; motivation for health IT adoption; enablers and barriers to health IT adoption and sustainability of health IT investments.
Current uses of IT at Access
Currently, Access relies on the Meditech practice management system hosted by the Sinai Health System (the network first implemented Meditech in 1987). In addition to serving the usual practice management functions such as scheduling and billing, this system houses and maintains patients’ basic clinical data and is able to share data between individual Access clinics and specialty and emergency providers at Sinai. Meditech also has a communication module that is used by Access providers as an alternative to email (administrative staff rely on MS Outlook). Notably, Meditech does not allow appointment scheduling across Access sites.
As part of developing an IT strategic plan, Access concluded that Meditech should be replaced both because it had limited functionality and because it was inefficient for a network of Access’s size. In the last several years, network leaders have acquainted themselves with the EMR market, various vendors and the experiences of other health center networks with them. The Access senior management team narrowed the initial field of EMR vendors to five. Criteria for making the selection included the desirability of a single application for practice management and EMR, robust clinical decision support capabilities and the ability to track specific quality measures.
In 2008, network leaders asked regional managers and regional medical directors to assist in selecting a vendor for both a new EMR and PM system from among the five finalists. Those involved formed committees based on specific needs and concerns and attended demonstrations of the five finalists. The final determination to move forward with a contract with Epic was made in mid-year 2008. Since the vendor selection process concluded, regional leaders have reached out to their staff to help build buy-in.
At the time of the site visit, network leaders had begun discussing developing an arrangement with the Oregon Community Health Information Network (OCHIN) to provide FQHC-specific training and data management services. In addition to the OCHIN arrangement, Access negotiated contracts to migrate data from legacy systems and paper systems to the new Epic system. These negotiations have stalled and created delays for the OCHIN-led training and implementation effort. Training of super users was set to begin in August, with practice management implementation beginning in select centers weeks after. EMR implementation would begin in January 2009 with a goal of full implementation in 10 centers by the end of the fiscal year and an overall goal to complete implementation over a 24-month period. While the network remained hopeful that this timeline would remain intact, they acknowledged that contracting issues could create delays that would prevent them from adhering to the original timeline above.
Motivation for IT adoption on the health center and network level 7
We found that health centers and network staff had differed somewhat in their motivation for adopting a new health IT system. Overall, comments regarding motivation on the health center and regional level fell into two categories: those commenting on negative aspects of the current system and those articulating anticipated benefits of switching to Epic.
Problems with existing systems. Some leaders saw inefficiencies in the existing system. Access’s regional managers (charged with managing a cluster of health centers’ administrative operations) repeatedly noted that Meditech did not meet their practice management needs. Primary problems included: a cumbersome navigation system, a steep learning curve (particularly detrimental given high turnover in front-end positions at Access) and general system slowness. Meditech’s slowness often results in excessive wait times for patients registering and checking in. Some managers indicated that this can create bottlenecks, forcing providers to wait for patients as they register. Others noted that Meditech does not allow scheduling across Access sites. This is a significant barrier given that many Access providers rotate across various centers within a close geographic area. These concerns contributed to a general belief that Meditech does not meet Access’s IT needs, especially relating to practice management tasks. In addition to management concerns, comparing Meditech with other, newer EMR systems made it clear to Access network and clinic-level staff that Meditech did not have comparable clinical functionality. While these clinical functions did not push the network away from Meditech in the same way that practice management concerns did, they combined to motivate the network to consider other options. Additional detail on such clinical functions is described below. The problems with Meditech, on both the operations and clinical sides, emerged as the primary justification for the switch to Epic among regional leaders.
Clinic level management. Many discussants expressed hope that Epic could add value in certain areas of management operations and clinical practice. With respect to operations, comments focused primarily on internal operations and financing issues. Some discussants mentioned the possibility that Epic could help improve communications internally. It was noted that clinical and operations staff often use different forms of communication under the Meditech system, with physicians relying primarily on the MOX (Magic Office) messaging system within Meditech and administrative staff using Microsoft Outlook for email. Some staff noted that having one system for all functions would consolidate communication systems and help bring together the operations and clinical staff at all levels.
One physician noted that Epic could help to allocate resources between Access sites in a more efficient manner. With Epic, regional managers will be able to monitor patient flow in real time, allowing them to shift staff and other resources more effectively. Another discussant indicated that scheduling would be more efficient under the new system, noting that patients would not need to schedule follow-up appointments to refill prescriptions. Others mentioned basic benefits such as moving away from illegible patient logs and reducing the number of lost charts.
Access staff also saw a potential to increase their patient throughput with Epic. Some spoke specifically about the potential to increase patient volume, especially after the first few weeks of implementation. Others thought that improved wait times would help to keep patient flow moving more efficiently. One discussant expressed hope that moving to Epic would help Access secure reimbursement faster. While details relating to how data would be exchanged with payers and the state were not discussed, the potential to increase reimbursement speed could be a significant benefit and motivator for networks such as Access that rely heavily on Medicaid payment.
Using data better. As noted above, Access touts its commitment to using data and quality metrics to drive operations. Metrics used by Access fall into four categories: patients/customers, employees, financial and quality & patient safety. Currently, data to support these metrics are generated through Meditech, as well as manual data entry conducted at the site level. The primary motivating factor for health IT adoption articulated at the network and clinic level was the promise of allowing center staff to more efficiently generate data for metrics and make more effective use of these data at all levels within the organization. Some Access staff members specifically mentioned the ability to more easily extract and use clinical and administrative data as a possible benefit. One discussant mentioned the ability to improve data exchange efforts both internally and with external partners, including academic medical centers, health systems, labs and pharmacies. Physicians with academic and research appointments in local hospitals focused on the potential to use aggregated Access EMR data for population-based health research. One discussant mentioned how difficult it had been to pull data for research under Meditech. Others discussed efficiencies related to data in a broader sense. The potential to manage a higher quantity of medical images and to automate exchange of data with labs were both were mentioned by discussants. While some Access sites have experience with e-prescribing through a PocketScript pilot, regional leaders at these centers noted connectivity problems (causing delays for providers) and high costs related to the effort. Network officials have not yet implemented e-prescribing through Epic, but moving toward a more integrated health IT solution such as Epic represents an opportunity to transition away from standalone systems and update infrastructure to accommodate more robust data exchange applications. Access plans to pursue a SureScripts interface in the coming months, although network leaders anticipate that creating an interface would take five months and indicated that they would not allow the e-prescribing module to delay the wider EMR implementation. In this way, Access staff felt that Epic could tangibly improve the utility, accessibility and efficiency of clinical information.
A tool for improved quality of care. Network leaders view health IT applications as tools that can support QI initiatives rather than drive the QI initiatives. Access leaders indicated that they have effectively used their existing Meditech system and a manual process to track quality measures established by their Medical Director and based on evidence-based guidelines for years. At the clinic level, these measures include compliance with recommended pain assessments and screening, “do not use” abbreviation guidelines and medication management protocols. At the regional level, metrics include the percentage of bonded diabetic patients with HbA1c < 7, up to date childhood immunizations at 24-months and regional HEDIS indicators. Unlike other FQHCs that we have met with for this project, Access staff indicated that they are currently able to track measures on a site and provider level and have used this reporting process as a way to reward sites and clinicians based on performance. Although they anticipate clinical improvements with Epic through use of clinical decision support, better coordination and increased efficiency, they also acknowledged that special efforts will be required to re-create the quality improvement culture in the context of an EMR. While network leaders acknowledge that the EMR will change quality improvement initiatives to a degree, they also indicated that the metrics they use are not unique and would be accessible under Epic. It may take time to develop a coherent QI strategy under Epic, but Access believes that the EMR will allow them to do more in this area, potentially reassigning staff who had abstracted charts to areas such as health informatics and epidemiology.
While they plan on taking advantage of point of care decision support tools over time, Access clinician leadership emphasizes that providers are likely to make the same clinical decisions that they would have made without Epic, but that they will spend less time trying to locate and verify the data they need to make those decisions.
An opportunity to realize new efficiencies. Network officials signaled the possibility of realizing efficiencies at the practice level, particularly with respect to relationships to ancillary care providers like laboratories. For example, as a part of its clinic acquisition process, Access network leaders allow new clinics to maintain relationships with their previous laboratories. Network officials see this as a workable concession to help make the transition into Access a bit smoother. Over the years, this policy has resulted in Access working with 14 different lab providers, creating inefficiencies that network officials would like to address using Epic. Network officials indicated that the Epic implementation could provide a justification for streamlining and reducing the number of lab providers. The onerous process of creating 14 different lab interfaces could provide a reasonable rationale for reversing the open-ended lab provider policy.
Network officials also noted potential administrative benefits. Access’s Medical Director explained their reasoning this way, “We have a growing cost per visit. I see efficiencies we can gain through the electronic system.” For example, under Meditech 33% of visits to Access resulted in lab orders. Each order comes back at different times creating coordination and organizational inefficiencies which are exacerbated by the multitude of lab partners (14 total). Moving to an EMR will allow for greater organization and tracking of returned lab results and because so many visits go to labs, network officials and regional mangers anticipate that this increased efficiency will significantly reduce the cost per visit. The cost per visit represented a significant metric for many of the clinic sites NORC visited and framing the decision in these terms may have been persuasive for some staff. Reducing the cost per visit is also a relatively unthreatening goal for Access staff, as many recognized the growing importance of payment and uncertainty surrounding future Medicaid reimbursement policy.
Finally, Access leadership sees health IT advancement as an essential cost of doing business in the future. The network’s CIO put it this way, “In the future, EMRs will be like oxygen.” Overall, Access sees the EMR as a tool that will empower them to transform centers, both administratively and clinically.
Key factors related to health IT adoption
In the next several paragraphs we outline specific barriers and enablers to health IT adoption articulated by discussants. We note that some factors represent both enablers and barriers to adoption.
Buy-in among regional managers. According to regional and network level discussants, the vast majority of Access staff supported the move to Epic. A number of regional medical directors spoke eloquently about the potential for health IT to help them provide care more efficiently and effectively. Staff members who were less enthusiastic about the new system recognized the importance of the switch to the network generally, with one regional leader saying, “In an organization this size, you need to trust the senior management.” Some regional leaders remained uneasy about the amount spent on information technology generally. Having been exposed to the costs of health IT through an e-prescribing pilot, one regional leader remained unconvinced that the network’s commitment to health IT was worth it. While this opinion was not widely held at the regional level, it does represent a certain level of difficulty in securing buy-in throughout a network of Access’s size.
Clinician buy-in. Despite general support for EMRs across the organization, Access also confronts typical physician buy-in challenges often associated with EMR adoption. Access physicians are generally less computer-literate than other staff. This is a concern for network and regional staff, but one that they hope will be addressed through tiered training and peer-to-peer support. Some physicians remain skeptical of the new system’s potential to increase patient volume. One physician noted that another local health system in the area, Northwestern Memorial, saw a significant decrease in patient volume following their EMR implementation and that reality caused him concern. Others were more optimistic, even suggesting that patient volume could increase after the first week of implementation. Access has established a strict 60-day adoption policy for its providers with financial penalties associated with not using the EMR. Network officials anticipate that this will lead a small number of providers (roughly two out of a total of around 250) to retire within a few years of implementation, although network leaders have taken steps to provide intensive computer and EMR-specific training for willing staff who may feel uncomfortable with the new system. More than anything, network leaders feel that attitude, not age is the most important consideration in building buy-in among providers.
Relationship to Sinai Health System. Access’s relationship with Sinai Health System represents both an opportunity and challenge for the network. Having been formed out of Sinai’s outpatient clinic system, Access relies on Sinai to provide specialty care for many of its patients and many Access providers are affiliated with Sinai. In addition to close operational ties, Access relies on Sinai for technical support and has shared the Meditech information system with them. The transfer of patient clinical information between Access and Sinai represents a significant benefit to Access’s current IT configuration and any changes to it required Access to consider its partnership with this hospital. Network officials asked Sinai leaders about switching to a new system far in advance of the switch, and again more recently. Sinai officials considered moving to a new system, but decided on both occasions to continue to use Meditech. Access values the connection with Sinai and its ability to provide continuous care for patients, but ultimately network officials decided that it needed to adopt an EMR and move away from the Meditech system.
Relationships with other health systems. Although switching to the Epic system may bring some disadvantages with respect to integration with Sinai, Access is hopeful that adoption of an advanced, standards-based EMR will allow them to more effectively share data and coordinate care with other provider systems in the area. They particularly hope to leverage relationships with academic medical centers and ambulatory specialty care providers that are also adopting Epic or similar systems. Network leaders indicated that local academic medical centers and community hospitals have expressed interest in exchanging data with ambulatory care centers such as Access, although no clear precedent for this kind of relationship exists in the Chicago area.
Federal grant support. HRSA’s financial support is an important asset to Access in pursuing HIT. Nearly half of Access’ total projected costs are covered by the HRSA “high impact” grant award. This award amounts to a significant enabler for Access in terms of start-up costs. Without this infusion of capital, Access would have to borrow significantly or postpone implementation until additional capital could be made available.
Staff expertise. Expertise and experience also represent enablers for Access’s implementation efforts. Partly due to its large size, Access has more IT resources than many other health centers. Glass directs a department of roughly five full time equivalents devoted to both health IT and quality improvement. Dedicated staff in these areas amounts to a luxury not available to other networks. Integration of quality improvement and IT has allowed Access to map existing performance metrics to health IT implementation.
Roll out process. Access chose to implement their PM and EMR systems separately, along slightly different timelines. Both systems are set to roll out in phases across Access’ 51 sites, depending on site size. Sites with medium levels of patient volume will implement new systems first, with smaller and larger centers following. According to Access, this will allow the network to learn from the experiences of medium-sized clinics without interference from the idiosyncratic concerns typical of their very small and very large clinics.
Access’s contractor charged with scanning paper records and migrating data to the new system has delayed the contracting process, forcing the involvement of legal representatives. This issue has slowed Access down by about a month and may force future delays. Due to the contracting delay, OCHIN has not been able to move forward with training sessions for the first group of staff super users. this way, external entities and influences can greatly affect any and all aspect of PM and EMR rollouts.
Communication across the network. Partly due to the contracting delays and partly due to internal communication issues, staff members were not clear on the current timeline for implementation. Some expressed doubts that Access would be able to maintain its planned timeline (implementing PM at all sites and EMR at 10 sites by end of FY ’09), although many seemed undeterred by current difficulties, citing trust in senior management to lead this effort. Network leaders conceded that greater attention to internal communication regarding the selection, training and implementation timelines would have also helped the network overcome a certain level of uncertainty and anxiousness among staff members.
Site-level computing. Infrastructure emerged as an issue in some cases but not others. Some clinics reported no problems with their computing. Other regional leaders complained that too many computers were devoted to single uses, such as reporting for specific grants. Having single use computers artificially inflates reports of IT infrastructure and regional leaders noted that these computers can crowd already congested clinics. Many regional leaders expressed concern about the technical support provided through Sinai Health System and others noted that current bandwidth levels would not allow them to efficiently work with web-based clinical tools (e.g. e-prescribing systems). Under Access’s current IT structure and usage, printers play an integral role in center operations. In a particularly extreme case, one regional manager noted that it took two business days for Sinai’s tech support staff to repair a single printer. Network leaders note that these issues will be addressed as the organization moves towards an IT model more independent of Sinai.
Cost of implementation. Interestingly, cost was not mentioned as a significant barrier by Access network officials. Although the network relies on HRSA support for much of the initial investment, Access was not deterred by the usually prohibitive ongoing costs associated with EMRs broadly and Epic in particular. As stated previously, Access made a commitment to invest in information technology at rates in line with industry standards. This commitment to IT, often in the face of financial barriers, has prepared Access both financially and psychologically for the investment required to move toward a robust PM and EMR system. Steven Glass noted that Access had been investing 3-4 percent of operational costs annually in health IT. His estimates suggested that roughly 3-5 percent would be required for any of the systems under serious consideration during the selection process, including Epic. Network leaders also noted that Epic would provide additional services including a new financial and HR system, adding to the value of the network’s investment in Epic.
Training. Access has not yet begun training staff on the Epic system, but network officials hope to begin PM training in the near future. Training will occur in phases, with regional leaders and super users training first and other staff (including operations/front desk staff) following, based on their comfort level and abilities. EMR training will begin with an online demonstration, then there will be on-site training, followed by support during the final “go live.” Network staff anticipate more problems with the EMR training than the PM training because physicians will be involved. They feel that front desk staff are less reticent to change and more familiar with the internet and computers. Access has agreed to contract with OCHIN to conduct trainings on EPIC, specific to FQHC sites. Staff members also mentioned a model exam room that would allow providers to experiment with the new EMR system during the on site training.
Connectivity, workflow and interoperability. In 2007, Access initiated an e-prescribing pilot through PocketScript in a number of sites. Access staff had a number of problems accessing the web-based system and integrating e-prescribing into their daily work. One regional medical director noted that it could take her up to three minutes to fill a single prescription through PocketScript, valuable time in a provider's day. Additionally, the SureScripts pharmacy data intermediary which is an essential partner for eRx with retail pharmacies may not be immediately interoperable with the new Epic system. Network leaders plan to implement a SureScripts interface, but concede that it will take several months to develop and test it.
Sustainability and Financing
As noted above, Access network and regional staff seemed to be confident that they are prepared to make the financial commitment necessary to sustain effective use of EMR. In part, this is due to its size and its ability to realize efficiencies of scale in both start-up and maintenance phases of implementation and use. Return on investment is less certain in Access’s view. Estimates offered by the network remain relatively conservative in terms of savings accrued from the new system, with most savings coming from new efficiencies such as repurposed facilities and decreased costs associated with paper charts. Many staff raised concerns that it may slow down their clinics and limit patient throughput (although others disagreed, arguing that patient volume would return to 80% within a week of go live). One discussant noted that the real savings from the new system will benefit not Access or its centers, but payers who will see reduced costs without significant investments. Some regional managers noted that centers would save on office supplies and network estimates point toward increased revenue from converting chart rooms to exam rooms. Others simply reiterated the connection to Access’s overall mission, asserting that Epic will make Access centers more efficient and increase their ability to provide quality care generally to their patients. While many remain nervous about the new system’s potential impact on centers’ bottom lines, regional leaders expressed confidence that network leaders had adequately considered the financial implications of the move and that their staff would be able to adjust quickly to the new system.
Conclusions
We end with a series of conclusions regarding the relationship of findings from this site visit to broader project objectives.
Dynamics and savings from a consolidated approach (i.e. Access vs. a health center controlled network). Access offers a distinct organizational and management model, characterized by a centralized leadership team and regional managers to address both the administrative and clinical concerns of daily operation across the network’s 51 sites. While regions within Access’ organization maintain some autonomy and contribute to decision making through formalized channels (i.e. topical working committees), significant authority in areas such as health information technology and strategy are left to the network’s central leadership team. This structure differs markedly from the health center controlled network (HCCN) model that brings together independent health centers (often with multiple sites) for a handful of enumerated functions and services. HCCNs may have a board of directors and centralized staff, but they do not perform similarly comprehensive function for their members.
Challenges with buy-in. While decision making regarding technology has been rolled up to the network in Access’s model, buy-in among center leaders and staff cannot be assumed. Some staff were apprehensive about the financial investment being made by the network for technology, indicating a not entirely successful buy-in campaign. In this way, delegating decision making to network leaders represents a clear economy of scale, yet other considerations like buy-in become more difficult to achieve.
EMR as a tool. Both network leaders and regional leaders emphasized that moving toward a new PM system and EMR would not change the care they provide in a fundamental way. Access has experience with a limited EMR (Meditech) and some providers have already adjusted to consulting a computer application in providing care. More importantly, the EMR was framed as a tool for providers not as a revolutionary quality improvement initiative. While quality improvement may prove to be a beneficial side effect of moving toward an EMR, the stated reason for moving toward an EMR was to empower providers to more efficiently do the work they are currently doing. Access leaders also noted that the network has an entrenched culture and structure devoted to quality improvement (e.g. variable provider compensation based on quality metrics). The EMR is just one element of that value structure, not the linchpin or starting point. Additionally, staff see the EMR as a tool for finding information quicker. This will allow them to comply with various reporting requirements in a more efficient manner.
Influence of external partners in vendor selection. Access had a number of considerations in their vendor selection process. Interestingly, the attitudes and EMR adoption of neighboring academic medical centers played an important role in the selection process. Access has a historic relationship with Sinai Health System, a local community hospital. While the network’s movement away from Sinai’s Meditech system will limit its ability to exchange data with the hospital, Access sees Epic as a way of creating new partnerships and exchange agreements in the future. In their view, most hospitals in the area have chosen either Epic, Cerner or McKesson. Making lab exchanges more efficient and exchanging data with other local hospitals such as academic medical centers makes Epic an appealing choice for Access.
Community Partners HealthNet
Introduction
NORC at the University of Chicago is pleased to present this draft site visit report outlining findings from our site visit to community-based health centers that are members of Community Partners HealthNet ( CPH) a federally funded health center controlled network (HCCN) based in eastern North Carolina. NORC conducted this site visit under contract with the Assistant Secretary for Planning and Evaluation ( ASPE) at the United States Department of Health and Human Services as part of our project entitled Assessment of Health IT and Data Exchange in Safety Net Providers. Meetings with four health centers as well as network leadership were conducted the week of October 13th 2008.
This report summarizes findings from this site visit as they relate to the major themes to be explored in the project including the opportunities, challenges and barriers associated with adoption of health IT generally and clinical health IT applications in particular as well as the use of standards-based exchange of health information. Wherever possible we draw on comments made during meetings with clinical leaders, executive leadership and IT specialists to understand the perceived, anticipated or actual impact of health IT on the quality efficiency and effectiveness of health care delivery. We present our findings in four sections. First we present information on the background and history of CPH and the health centers we visited as part of the study and their current status with respect to health IT adoption. We then outline their experience with adopting and using health IT, providing details on specific applications including EHRs and practice management systems, and their motivation for adopting health IT. A third section discusses challenges and enablers to effective use of health IT. Finally, we end with summary conclusions and additional questions to be addressed in subsequent site visits and as part of the final report for the project.
Background and Methods
Community Partners HealthNet ( CPH) is a non-profit organization that provides information technology and administrative services to ambulatory care safety net health centers in eastern North Carolina. The network is based in Snow Hill, North Carolina approximately 80 miles southeast of the Raleigh-Durham area. The majority of its members are located in the area between Snow Hill and the South Carolina border in the eastern part of the state including Greene County Community Health Center located in Snow Hill itself, Kinston Community Health Center located 30 miles due south of Snow Hill, Steadman-Wade Health Center located in the very small town of Wade located southwest of Snow Hill on Interstate 95 and Robeson Healthcare Corporation also located off Interstate 95 close to the South Carolina border.
While these health centers serve a population typical of other health centers in the nation, namely a disproportionate share of Medicaid and uninsured individuals, they each have specific characteristics. Because many of these health centers are located in small towns or rural areas where they are one of a limited set of ambulatory care providers and where the population is older than in urban areas, these health centers see more Medicare patients than many health centers. Also, Robeson is unique in that it is located near large Indian reservations in the southern part of the State. In addition to serving the American Indian population, some Robeson sites serve a large number of African Americans, stemming from the distribution of racial/ethnic groups in Robeson’s service area.
CPH was founded and incorporated in 1999 and was initially meant to help health centers adapt to Medicaid managed care. While Medicaid managed care did not become a reality in the state, several of the original partners, maintained the organization to provide assistance on administrative and information technology (IT) needs. The organization began by collaborating on a joint project around Y2K compliance and continued to build a shared infrastructure for providing practice management services. To do this, the network leveraged a series of HRSA network grants including the Integrated Communications Technology (ICT) grant and the Integrated Service Delivery Networks (IDSN) grant.
Around 2001, the network began looking into options for electronic medical records (EMRs) and opted to learn more about an application called Cliniflow that was developed by an Israeli firm. In 2002, the network entered into a contractual relationship with the vendor, which subsequently changed its name to MicroMD and was purchased by Henry Schein, Inc. Greene County Health Care began use of the MicroMD EMR product in 2004, Steadman-Wade began implementation and use two years later, Kinston implemented in August 2007 and Robeson went live at all of its sites in January 2008.
CPH indicates that it operates largely as an application service provider (ASP) and hosting service for its member health centers. Health center members pay annual membership dues which are currently $15,000/year as well as additional fees based on the number of users at each health center to help cover the costs of licensing software and support services. In addition to the EMR product, CPH also supported implementation of the MicroMD practice management system as well as the Dentrix dental record system which are also products owned and supported by Henry Schein, Inc. The network also developed and supports the use of a data warehouse that regularly compiles and stores data from all the applications it supports and allows health centers to access reports on utilization and efficiency metrics drawn from each of these systems.
As part of its hosting function, CPH supports all of the issues associated with HIPAA compliance of electronically-stored patient data, backs-up data from these applications, supports training and implementation of the applications at each health center site, works out connectivity issues with the sites and acts as a convener of users to allow for discussion and resolution of common issues. CPH also provides direct technical support to users for the MicroMD EMR system: however, staff members note that direct technical support for the MicroMD Practice Management system and Dentrix dental record application are provided directly by Henry Schein.
Figure 1 below provides an illustration of the network configuration and applications provided to various members. As depicted below, Community Partners HealthNet centrally maintains servers housing its data warehouse, applications ( EMR, PM and dental) and Citrix which serves as a “Metaframe” across which the health centers can access these applications. Connectivity to most health centers is maintained through the Internet, the exception being Greene County Healthcare which, due to its proximity to the network, has a dedicated fiber optic connection. CPH is also connected, via the Internet, to an off-site facility where servers replicating the three production servers are housed and updated nightly as back-up.
Figure 1: Network Configuration at Community Partners HealthNet
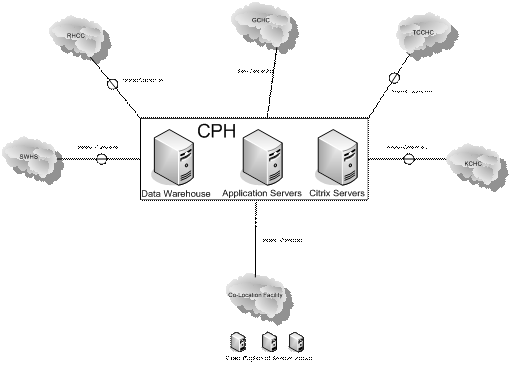
As with the other site visits conducted under this project, NORC staff travelled to North Carolina to meet in person with staff from CPH including their Executive CEO, Doug Smith as well as executive, clinical and IT leaders from member health centers. In addition to discussing topics related to EMR implementation and impact, we asked discussants to describe their motivation for health IT adoption and their experiences, positive and negative, in working in the network framework to support health IT adoption and maintenance. We also asked networks and health centers to comment on the sustainability of their health IT initiatives and expected financial returns from their IT investments.
Key Findings from Site Visit
In this section we summarize responses from discussants as they relate to key themes of the site visit described above. We begin by discussing motivation for health IT adoption by health centers at the network and health center level.
Motivation for Health IT Adoption
Overall, health centers and network discussants provided similar responses on topics related to their motivation for pursuing health IT and, in particular, pursuing health IT in the context of a network. We highlight these responses below.
Opportunity, resources. Most discussants highlighted the high cost of establishing and maintaining their IT infrastructure and the computer applications necessary for successfully fulfilling their mission as health centers on a day to day basis. The need for additional resources beyond those that could be reasonably dedicated by the health centers themselves became increasingly evident as the health centers looked to tackle complex issues such as Y2K preparation, HIPAA compliance and evaluation and contracting with vendors.
Documenting and standardizing clinical practice. Health centers also noted that they were looking forward to use of EMRs as a means for better clinical documentation and standardization of clinical practices, particularly those related to caring for high priority populations such as individuals with chronic illnesses. One medical director in particular noted being very impressed by an original demonstration of Cliniflow conducted for CPH in 2002. He instantly became convinced that use of the application would dramatically improve documentation and the ability for each health center to develop templates and reminders that would create a consistent level of clinical quality within each center.
Billing and revenue. While most health center respondents did not believe that use of EMRs was increasing their revenue and in some cases, health centers noted substantial dips in revenue particularly in early stages of adoption, some did note that they believed at the start that better documentation of clinical practice could lead to more accurate documentation and billing to Medicare and private payers. While most health centers predominantly treat the uninsured and Medicaid populations, we found that some more rural sites within North Carolina treated a larger number of Medicare and privately insured patients than health centers in urban areas, largely because the limited options for receiving primary care in their region. The health centers we visited in North Carolina indicated that between 10 and 30 percent of their patients has some form of outpatient Medicare (Part B or Medicare Advantage). Health centers in relatively rural areas typically had a higher Medicare payer share than those closer to population centers.
Better reporting and quality improvement. Finally, health centers indicated that one of the most important reasons for adopting health IT including EMRs was the ability to effectively track care, report on care delivery processes and outcomes and use information from these activities to create new incentives to improve care.
Barriers and Success Factors
Discussants provided substantial detail on their experience working with the network, implementing and using health IT applications including practice management and EMRs. In this section, we summarize these experiences in the context of barriers and success factors associated with health IT adoption and use. We note that, as in prior site visits, several areas highlighted below may be considered to be both barriers and success factors in different respects.
Timeline for implementation. Some health centers indicated that the implementation timelines that they pursued for implementation of EMR and PM systems are sometimes unrealistically compressed. One health center indicated that in order to prevent complications from having data for one grant year in two systems, they set up a plan to cut over to a new EMR and PM system in January of 2008. CPH was able to negotiate with Henry Schein to purchase licenses and rights to implement the MicroMD practice management application across a series of health centers in the Fall of 2007. While health centers saw advantages to moving to MicroMD over their legacy practice management systems, most of which were inadequate, some discussants indicated that the implementation process was far too fast.
Training and support. CPH employed one trainer two support individuals using accepted approaches including “train the trainer.” Some health centers indicted the need for more support. As an example, one health center noted that staff did not receive an agenda ahead of the planned training session and that they did not receive guidance on how best to set up forms and templates. Discussants also noted limited capacity to provide support in general and that there were many questions that remained unanswered or are not answered in a timely manner.
Some expressed frustration that the support model for the EMR, which requires members to go directly to CPH, was different than the support model for practice management, where CPH is involved in coordination but not directly responsible. These discussants felt that it would be better if they were able to go directly to the vendor for all support concerns. Numerous respondents indicated that CPH staff was not always prepared or able to handle their questions. However, several noted that their biggest problems relate to connectivity losses which can be a result of an individual providers’ internet connection. Other areas of concern included the lack of use of common EMR templates across health center users and difficulty re-creating reports following software upgrades.
Expertise at the health center level. Network leadership noted that some frustrations related to connectivity and user support may be due to the lack of IT expertise and experience at the health center level. They note that many calls coming in to user support are for basic connectivity and problems with software use that are best handled through a more robust IT staffing at the center site itself. They estimate that up to two thirds of the problems related have to do with basic errors with the use of computers or connectivity and hardware problems that are the responsibility of the health centers.
Governance and collaboration. While network officials indicated that CPH is governed by a board of directors that is made of member health centers, some health centers were not aware of the extent to which they had leverage over the direction and operations of CPH and indicated they were not sure when or how often the board met to provide oversight.
Some mentioned that the focus at the network level seemed to be geared toward meeting the requirements of Greene County Healthcare whose leadership overlaps with that of CPH. Health center officials also indicated some concern regarding the strength of the collaboration across CPH members. Discussants partially attributed both turnover and distances between members health centers for the lack of a robust exchange of lessons learned and best practices across the consortium. Interestingly, not all health centers we spoke with indicated that they know that they have a seat on the Board of Directors overseeing CPH.
Relationship with Henry Schein. Health centers indicated both advantages and disadvantages to working with Henry Schein products. Most understood the value of having a relationship with a single vendor for practice management and EMR. However, some also noted the fact that these are three separate applications (EMR, PM and dental) that require external interfaces to pass data. Network leadership noted that Henry Schein is currently working on integrating the practice management and EMR application to operate as a single application by integrating the databases associated with the two applications.
Laboratory interfaces. As part of its EMR implementation CPH supported the establishment of bi-directional interfaces between clinical laboratories providing laboratory tests to member health centers and the MicroMD EMR products being employed. While health centers indicated that the lab interface was an important functionality that improved the efficiency of ordering and receiving results, they indicated that the implementation of the interface proved problematic because it does not allow automated reconciliation between the tests orders and results. This leaves health centers unable to confirm that all tests result in valid reports back from the laboratory without a separate reconciliation process. That additional reconciliation process requires staff to print out each requisition ordered via the EMR and each result reported back through the interface and manually verify that a result was received for each test.
Efficiency. Health centers noted that EMRs have helped improve their clinical documentation, but that they have also resulted in a decrease in the number of patients seen by a health center in a given period following EMR implementation. They noted that at the start of implementation, productivity is reduced on average by half. Even after a year of use, they still experience a decrease in productivity relative to their pre-EMR state. Additionally, after operations return to “normal” and all providers are fully trained in use of the application, health centers note that the increased focus on documentation occasioned by use of the EMR results in lower productivity overall.
Staff turnover. Health centers also noted challenges associated with turnover at the health center level among leadership and clinicians. One health center NORC visited experienced a near complete turnover of leadership including Executive Director and Medical Director in the midst of planned conversion to the EMR, leaving the new team feeling not well equipped to manage the implementation. In other cases, health centers noted the challenges associated with training new providers in use of the EMR as they come on board in the period following implementation and initial training.
Retaining talent at the network and health center level. Health centers noted the limited capacity for training, implementation and support of health IT applications at the network level. They noted that financial considerations and difficulty in recruiting and retaining staff could contribute to these issues. In particular, health centers gave the example of a programmer who had been employed by the network who was skilled at creating and running custom reports from the CPH data warehouse based on health center requirements who left the network when her spouse switched jobs and moved to Durham. The health centers and the network both acknowledged that hiring and retaining high caliber professionals in the network has presented challenges. Network leadership also noted similar or potentially greater problems recruiting and retaining IT talent at the health center level.
Lack of standard use of templates and forms for quality improvement. One shortcoming of CPH that was acknowledged by both network leadership and health centers was the lack of dedicated network-level clinical leadership to provide additional resources and support for quality improvement efforts tied to the EMR at the health center level. In particular, health centers noted that there were a number of customizations and templates and clinical reminders that they have designed and implemented individually and that there was relatively little guidance provided by network leadership regarding appropriate use of templates. For example, one health center noted that they had implemented a reminder in their pediatrics department to prompt providers treating patients with asthma to consult the patient’s asthma action plan.
While health center leaders could not gauge providers’ receptiveness to clinical decision support functionalities such as this, it is important to note that some within CPH have taken steps toward integration of QI efforts into the new health IT environment. Beyond this, network leadership indicated that while the central goal of EMR implementation is quality improvement, they have not been provided adequate resources to support clinical improvement efforts across their members. The network also noted a general philosophy of EMR use that suggests that use of an EMR is optimized when individual sites and providers are able to develop customizations and use forms that meet their particular needs.
Support for billing issues. Discussants at health centers noted some important challenges with respect to billing from the MicroMD practice management system for which the network and Henry Schein have not posed adequate solutions. One in particular relates to problems with entry of multiple types of primary payers which is a common requirement for health centers, as there may be different primary payers for their patients depending on the type of service being provided (e.g., the dental care primary payer could be different that primary payer for medical care). One health center indicated that they were not aware of a solution for this issue other than to generate offline claims. Another health center noted that there is an unreasonable lag in working with Henry Schein, CPH and the billing clearinghouse employed by Henry Schein to trouble shoot and resolve problems with unpaid claims. The example provided was of a claim where the non-payment was due to a simple inversion of a key number, but the issue took the clearinghouse and Henry Schein over six weeks to identify.
Network infrastructure. Despite the challenges and barriers described above, health centers universally acknowledged the importance of the network as a means to achieve substantial economies of scale and provide for a stable hosting and back-up environment. Most acknowledged that they would likely not have implemented EMR without the assistance of the network and that, while they experience challenges with use of the EMR, they believe that their health centers have and will benefit from EMR adoption. This is primarily due to the perceived potential for EMR to facilitate quality improvement and the increasing imperative among funders and others to demonstrate improvements in care using EMR-based reports and analysis.
Data warehouse. Most health centers noted that they found the data warehouse concept employed by the network to represent a useful approach to aggregating data and allowing for detailed analysis. They indicated that the data warehouse was a rich resource with potential for sophisticated use as part of reporting and QI. While the data warehouse contains significant amounts of clinical data (especially for Greene County Health Care, the first center to implement the EHR) use up until this point has been limited to populating center specific reports generated out of the warehouses’ Cognos reporting software and not a network-wide quality improvement or benchmarking initiative. Even so, this is a significant improvement for CPH members.
One center noted that reporting was nearly impossible before the EMR and data warehouse, indicating that their reports had included little to no actual clinical data. Additionally, this center’s peer review process benefited enormously from the increased accessibility of provider-level data. Health center leaders noted that they target a number of key measures with the primary measure of interest rotating each month. While one center described utilization of clinical data for quality improvement, health center leaders across CPH’s membership also noted some issues associated with use of the data warehouse.
These included difficulty obtaining accurate reports that are well formatted and documented now that the former lead programmer is no longer an employee of the network and difficulty importing existing data into the current SQL database Network leadership notes that health centers are often not in a position to identify what they need by way of reporting in a timely fashion and that many health centers cannot put aside the funds necessary to support substantial reporting to be conducted on a short turn around basis by the network.
Sustainability and Impact
Of the health centers we spoke with, two had implemented EMRs in the last year and were not in a position to discuss broader impact of EMR use beyond the challenges and productivity losses associated with the first year of EMR implementation. The two health centers that have had substantial experience with use of the EMR, Greene County and Steadman-Wade noted that use of the EMR and the data warehouse has enhanced their ability to track care and measure improvement over time.
Greene County indicated that they have been able to achieve sustained improvements in the quality of care provided to chronically ill patients. They cite steady improvements in process measures such as the rate of follow up for diabetic patients in the form of routine testing and clinically recommended examinations (e.g. foot exams). They also indicated improvements in the percentage of patients who regularly receive HbA1c tests as well as the number of diabetic patients whose HbA1c values are “under control.” Greene County has also been able to use the data warehouse to conduct research demonstrating clinical impact and is in the process of publishing findings.
Steadman-Wade health center indicated a slightly less positive picture regarding clinical impact. While the medical director at this center indicated that they were able to observe improvements in key clinical indicators over time, he also noted that these gains were regularly lost because of high turnover among providers and the challenges associated with getting new providers up to speed on effective use of the EMR. This medical director was also among those who noted that a more standardized approach to forms and templates at the network level may help individual centers achieve and measure more consistent improvements in quality over time. The network noted that they have encouraged the medical directors to take the lead, but that health centers have had difficulty finding the time to coordinate on these issues.
Financially, most health center discussants did not believe that they had seen returns or savings equaling their investment in health IT and did not believe that they would. Network discussants emphasized that while there may be savings in some areas, the EMR initiative was largely motivated by quality improvement and not an understanding that costs would be recouped through revenue gains or savings. Health centers noted that use of EMRs would likely represent a “cost of doing business” in their view and that effective use of health IT could improve revenues over time by putting the individual health centers and networks in better position to pursue grants from federal and state government as well as foundations.
Finally, network discussants did not have a clear picture of how they will remain sustainable over time. While CPH did have some members outside their region and, particularly, in rural areas, they were not as aggressive as some networks were in using expansion as a means to achieve sustainability. Network staff did indicate that part of their approach has been to maintain a skeleton staff at the network level to keep labor costs under control. They acknowledge that this approach limits their capacity to serve as a comprehensive resource for health center members particularly as related to providing direct support for QI initiatives, noting that the network serves primarily as an ASP at this point.
They felt that the federal grants meant to support networks did not provide sufficient funds to help achieve their primary goal of improving quality of care and that, in some cases, health centers were not able to contribute resources necessary to support a network-wide QI function. Rather, in their view, these funds provided the resources necessary only to build infrastructure, provide applications and assist with implementation. In the case of CPH, federal funds had been used primarily for software, set-up, implementation and initial training. Membership dues go to pay for support costs, contracting with the vendor and products and services they use outside the basic implementation including additional interfaces, templates or special reports.
Conclusions
We end with a series of preliminary conclusions based on our discussion of findings above. We note that these conclusions are based only on the discussions conducted as part of the North Carolina site visit and that these observations will be consolidated with findings and conclusions from other site visits to establish findings and conclusions for the overall study.
Impact on productivity has been negative except in Greene County. Some EMR adopters anticipate short term reductions in productivity followed by a return to capacity and perhaps even improved productivity over time. Most respondents in North Carolina indicated that even when all providers are fully trained, the EMR still contributed to productivity losses because of increased documentation requirements facing providers.
Health center networks face competing priorities. In summarizing the enablers and challenges associated with health IT adoption in the health center network context, discussants highlighted the important differences in skill set required to support the varied functions that health center networks are expected to fulfill. They also pointed to the resulting need for a varied staffing model that includes individuals with IT infrastructure, support and training backgrounds as well as clinical quality improvement specialist, overall administrators and grant writers. While some individuals may have the skill set to allow them to meet more than one of these needs, it is rare to be able to adequately capture all of these skills in a small group of individuals. CPH’s current staffing model, which includes a total of four FTEs, may not be sufficient to adequately address all of these needs.
De-centralized approach to customization has advantages and disadvantages. We note in our findings that CPH has not been asked by health centers to standardize work flow, forms or templates to be used by health centers implementing the MicroMD EMR to meet regularly (see not above) Instead, it allows health centers and even individual providers to customize their own forms and views and establish a flow and documentation approach that works best for them. This philosophy has the obvious advantages of allowing individuals flexibility and not requiring the network itself to convene clinical leaders to achieve consensus on complex issues. At the same time, it does not allow for the establishment of a common approach to QI and collaboration across health centers and it can lead to problems with using reports of aggregate data from across health centers for the purpose of benchmarking.
For example, if each health center is using different forms to enter common data, developing aggregate reports would require complex queries where comparable data is drawn from different fields in the data warehouse. This level of complexity leads to the potential for error and raises the cost associated with use of the data warehouse for cross-center comparisons or aggregate estimates. Because health centers and individuals are free to create their own forms and use different fields in idiosyncratic ways, reports run out of the EMR or data warehouse must be reviewed thoroughly by the users and programmers to ensure that data are being pulled from appropriate fields for each health center and provider.
Sustainability approach uncertain and relies on keeping scope limited. CPH was up front in indicating that it did not have a clear sense of its long term sustainability beyond plans to leverage additional grant opportunities as they became available. Network leaders were clear that they were interested in seeing how grant opportunities evolve over the next several years given the change in administration. To date its approach to maintaining financial viability has been to keep staff relatively small and to generally stay focused on IT support, vendor contracting and infrastructure rather than employ the network in active, “hands on” quality and process improvement initiatives.
Health Choice Network (Utah and New Mexico)
Introduction
The National Opinion Research Center (NORC) is pleased to present this report detailing findings from our recent site visits to Utah and New Mexico for the “Assessment of Health IT and Data Exchange in Safety Net Providers.” NORC conducted this site visit under contract with the Office of the Assistant Secretary for Planning and Evaluation (ASPE) at the U.S. Department of Health and Human Services (HHS). The Health Resources and Services Administration (HRSA) worked in conjunction with ASPE to guide activities under this project.
This report summarizes the experience of health centers working with the Health Choice Network (HCN) in implementing electronic medical records (EMR) and other IT applications and services. Although, HCN is headquartered in Southern Florida, our site visit focused on HCN members that are located in Utah and New Mexico –Utah Health Choice Network (UHCN), New Mexico Health Choice Network (NMHCN) and their member centers. This design allows us to look into the challenges and opportunities facing rural health centers as well as the effectiveness of networks working with member health centers that are not located in the network’s home region. The report is organized as follows:
Site Visit Methods and Background. In this section we review our methods for conducing site visits and briefly describe the centers we visited. We also summarize the history, size, mission and core functions of HCN overall.
Key Findings from Utah and New Mexico. In this section we summarize findings that relate to the key themes of inquiry for the project. Specifically, we describe health centers’ motivation for joining HCN and adopting EMRs, the extent to which they are using EMRs currently, challenges and benefits of working with HCN, the extent of their involvement in health information exchange (HIE), the impact of the EMR on quality improvement or cost of care and related topics.
Future Directions for the National Network. In this section we highlight findings from discussions with HCN leadership both in South Florida and in the two regional networks we visited, Utah and New Mexico. These discussions examine the future direction of HCN and how that direction will impact HCN member health centers. HCN operates in 10 states with member centers in Florida, Arkansas, Iowa, Kansas Missouri, Nebraska, New York, New Mexico, Utah and Hawaii.
Conclusions. Finally, we end the report with a set of preliminary conclusions of relevance to program officials, policy makers and other stakeholders.
Site Visit Methods and Background
As with other site visits conducted for this project, preparation for the visit began approximately one month prior to the in-person meetings with initial telephone conversations with HCN national leadership and the Executive Directors of UHCN and NMHCN. These three initial conversations were conducted to share the aims of the site visit, obtain agreement from leadership to participate in the site visit, discuss potential discussants for the in-person meetings and set a date for the in-person meetings. Following these initial telephone conversations, we revised background materials, developed detailed agendas for each meeting and set appointments with clinical, administrative and IT leadership from across HCN member health centers in Utah and New Mexico.
The site visits themselves took place on the week of November 10th 2008. We deployed one team of three NORC staff to New Mexico to conduct in-person meetings with three health centers as well as NMHCN President David Roddy and a second team to Utah to conduct in person meetings with three health centers as well as UHCN Managing Director Chris Viavant. For each meeting, we prepared materials that outlined our preliminary knowledge of the discussant organization and highlighted outstanding questions to address during the in-person discussion. Having multiple team members at each meeting allowed us to have some individuals dedicated to taking notes and documenting the content from the meeting while others focused on assuring that the goals of each meeting were being addressed through engagement with the participants. Finally, after concluding the site visit, we conducted two additional lengthy telephone meetings with HCN National Executive Director Kevin Kearns and Chief Information Officer (CIO) Alex Romillo to follow-up on some of the findings from health center discussions and explore priorities and future direction for the national network. Exhibit 1 below lists the various discussants that participated in the site visit from HCN National, UHCN and NMHCN.
Exhibit 1: Site Visit Discussants
| Health Choice Network, National Leadership | |||
|---|---|---|---|
| President and CEO: Kevin Kearns Senior VP and Chief Information Officer: Alex Romillo | HCN National | ||
| Health Choice Network, Utah | |||
| Managing Director: Chris Viavant | Utah HCN | ||
| Executive Director: Allan Ainsworth IT Director: Godo Delgado | Wasatch Homeless Health Care | ||
| Executive Director: Mary Winter Medical Director: Kim Macfarlane | Green River Medical Center | ||
| Executive Director: Yvonne Jennson, Medical Director: Virginia Wheeler | Carbon Medical Services | ||
| Health Choice Network, New Mexico | |||
| President and CEO: David Roddy | New Mexico HCN | ||
| Chief Executive Officer: Harriet Brandstetter Chief Operations Officer: Martin Lopez Chief Information Officer: Daniel J. Guevara | La Clinica de Familia | ||
| Executive Director: Mary Alice Garay Chief Financial Officer: Mary Rooker | Ben Archer Community Health Center | ||
Chief Executive: Officer Seferino Montaño, Chief Financial: Officer: Steven Connelly | La Casa Family Health Center | ||
Health Choice Network Background
HCN was founded in 1994, by a group of four health centers in South Florida. The founding health centers, Economic Opportunity Family Health Center, Community Health of South Dade, Helen B. Bentley Family Health Center and Camillus Health Center are all based in Miami-Dade County and a fifth health center; Family Health Centers of Southwest Florida based in Fort Meyers joined the network in 1996. These health centers came together to look for opportunities for achieving administrative efficiencies and economies of scale through collaboration and joint purchasing. Like many health center networks, they were also motivated by the potential to form a health center-based managed care organization.
Eventually a sister organization, Atlantic Care, was developed to address the managed care issue, but members decided that the most important role for the core-HCN organization was coordination on information systems and billing. In addition, there was interest among medical directors in regularly meeting and coordinating on a single approach to achieving clinical quality improvement.
Overall role for the network. Consistent with the theme of coordination around information systems and billing, around 1997, HCN decided to adopt a model they refer to as an integrated delivery system. Although each member health center continued to operate as a separate 501c(3) organization with their own individual grant as a federally qualified health center, they agreed to join together to hire a common chief financial officer (CFO) and chief information officer (CIO) and fully consolidate all computing through a single network operation. The initial senior executive who played both of these roles, Kevin Kearns, continues to lead the network (although Alex Romillo took on the CIO role in 2004).
Under this arrangement; and leveraging HRSA grants such as the Shared Integrated Management Information Systems (SIMIS), the Integrated Service Delivery Initiative (ISDI) and the Healthy Communities Access Program (HCAP); HCN adopted an integrated accounting application, a single practice management system through Medical Manager and initiated a single, central billing office in 2001. Each member health center supported the network through payment of an annual fee and paid additional, transaction fees for making use of the central billing office and consulting services. HCN received approximately 800,000 dollars in grant support from HRSA for these activities. HRSA’s contribution accounted for roughly 30 percent of the infrastructure with the remaining support coming from member dues. HCN runs on an operating budget of close to 12 million dollars annually, 4 percent of which comes from federal grants. The rest is accounted by 28 percent from membership dues, 40 percent from contributions from foundations, 20 percent from HMOs, 2 percent from state grants and those grants designated by HCN as “other” comprise the rest.
In order to achieve further economies of scale, HCN maintains a basic IT infrastructure for their members including maintenance of a data center with redundancy and recovery capabilities. HCN also works with member health centers to assure adequate connectivity to their applications and data.
Supporting EMRs and Quality Improvement. HCN’s initial effort to implement EMRs was guided by medical directors of member health centers led largely by Dr. St. Anthony Amofah, Medical Director at Helen B. Bentley. In seeking to systematize care and encourage use of consistent templates, the medical directors began discussions about EMRs with Kearns and other network officials around 1999. HCN began offering Medical Manager’s OmniDoc EMR to health centers in 2002.
Out of the box, OmniDoc offered a set of basic functions for maintaining a medical record and for e-prescribing, but the Medical Directors invested a great deal of time in developing diagnosis specific templates and automated reminders to facilitate QI and add some clinical decision making components to the EMR. Decisions regarding the configuration of the EMR and ongoing enhancements are made by HCN’s clinical committee made up of the medical directors from across the networks. Almost eight years after initiating EMR implementation, HCN has over 500 custom-configured templates which have allowed them to transform OmniDoc into a health center-centric EMR product.
After having used OmniDoc for several years, the clinical committee, still led by Dr. Amofah, started looking for an EMR to meet more sophisticated requirements around condition specific templates, registry-type functionality, clinical decision support and reporting on specific quality metrics. After considering their options, HCN decided to shift from Medical Manager's OmniDoc product to a combined practice management/EMR solution known as Intergy developed by Sage Health (by this time Sage Health had purchased Medical Manager). The network is currently planning for migration from OmniDoc to Intergy and all new implementations, including several that recently took place in Utah, are to the Intergy practice management/EMR application.
HCN has sought to closely link its EMR and quality improvement efforts. In addition to supporting EMR applications, HCN also supports disease management and reporting applications such as Patient Electronic Care System (PECS) and Practice Analytics. As described above, the clinical committee is responsible for defining all requirements for and enhancements to the EMR system and for defining requirements for a set of quality-related reports that are distributed to all health centers using EMRs supported by HCN on a monthly basis. Initially, the committee’s focus was on automating quality reports for those measures mandated by HRSA related to specific funding opportunities. While some HCN members such as the original founding members have been able to work together on quality improvement beyond the establishment of common reports, HCN currently does not provide more advanced quality improvement services outside of Florida. HCN recommends that these activities get coordinated at the state network level.
An expanding, evolving model. Between the years of 2000 and 2006, HCN staff led EMR and practice management implementation efforts in several health centers with dozens of sites, initially in Florida but eventually spreading out to satellite sites in Utah, New Mexico, New York, Michigan, Hawaii and beyond. This expansion is motivated primarily in an effort to expand their customer base, achieve greater economies of scale and limit their reliance on federal grants. Expansion brought about the need to create new membership options for health centers that sought a certain level of service from HCN. For example, HCN organized membership options for those health centers that wanted to access the Medical Manager practice management application, but were not prepared to join in the fully integrated model with a single CFO and use of centralized billing.
HCN employs 122 full time employees (FTEs) or their equivalent. Twenty of which reside in Fort Myer Florida, all other Florida employees work in Miami and 9 work within the states they serve. Out of those located centrally in Florida 1 or 2 staff are dedicated to each of the states to lead training and technical efforts. HCN has 49 members in its IT staff, 34 in centralized billing, 10 in finance, 10 who work in managed care/clinical/doctors, 8 in development and the remaining staff contribute in a support role such as administrative.
Governance. Maintaining an effective governance model has proven to be a challenge to HCN in recent years. In earlier years, leadership from the original health center members constituted the network’s Board of Directors, the body that is ultimately responsible for key decisions and the overall direction of the network. While the five original members retain more votes on the board than newer members, the model up to this point has been to add one member to the board with each additional health center or regional health center network that joins HCN. This has resulted in a board of over 30 members currently.
In addition to the board, many decisions are made at the committee level and separate committees have been set up to address IT infrastructure, managed care (now spun off as Atlantic Care), clinical care and finance. As with the overall board, in order to provide all members a voice, every health center is allowed to have staff on each committee.
Recently, HCN has also announced a plan to move towards a more streamlined board and committee structure that puts greater voting and decision making authority in the hands of health centers that are “fully integrated” with the network. These are primarily those health centers that are using HCN as their single CIO and CFO and that have fully adopted EMR and practice management software supported by the network. Over time, this will reduce the number of individuals that have a definitive say in key decisions such as those regarding EMR templates, assessment of new vendors or establishment of new HCN services. While other health centers will continue to be able to join HCN and purchase services, they will not have direct input into the direction of the network. This change in governance approach is consistent with the overall future direction for the network that is described near the end of this report.
Relationship with Utah and New Mexico. HCN’s relationship with health centers outside of Florida dates back to 2000 when they began discussions with the Primary Care Association and Integrated Services Network of health centers in New Mexico. Members of this existing organization created NMHCN as a means to leverage the existing HCN infrastructure and provide the practice management and EMR applications to their six member health centers. Today, NMHCN has been a part of HCN for approximately four years, enjoys a seat on the HCN Board of Directors and is considered a “fully integrated” partner with HCN.
In 2002, HCN established a similar relationship with a Utah based association of health centers known as the Association for Utah Community Health (AUCH). A subset of AUCH member centers formed UHCN which also is considered a “fully integrated” member with a seat on the board. Although HCN continues to expand to additional states, network leaders indicated that Utah and New Mexico offer the most comprehensive picture to date of HCN’s experience working outside Florida and of the interaction between state-based networks such as UHCN and NMHCN with the national network.
In subsequent sections of this report, we outline the experiences of health centers in Utah and New Mexico with implementation and use of HCN services and applications including EMR and practice management systems. We then return to the topic of HCN organization and functions to discuss the future direction of the network as articulated by the network's national leadership team.
Key Findings: Utah Health Choice Network
As noted above, one arm of our site visit focused on HCN’s presence in Utah. UHCN dates back to 2002 and since 2004 has provided health centers in Utah access to HCN services including networked practice management and EMR systems.
We conducted four total meetings on site in Utah, three with health center leaders mainly in the Northern and Eastern parts of the state starting in Salt Lake City and stretching out to rural mining communities of East Carbon and Green River. The Salt Lake City health center, Wasatch Homeless Health Care, Inc. (WHHC) is a health care for the homeless (HCH) program grantee that treats approximately 6,000 patients annually, totaling over 25,000 visits. WHHC provides primary care as well as extensive case management and outreach. The center also provides specialty services of particular importance to homeless populations including mental health, dental and dermatology services. Like many HCH grantees WHHC relies extensively on volunteer physicians.
Green River Medical Center (GRMC) is located in a town of approximately 1,000 individuals in Eastern Utah. In 2007, GRMC served approximately 1,000 patients in over 2,985 encounters. In addition to providing comprehensive primary medical care services, the health center offers radiology and dental care services, and serves as an emergency medical services provider and triage point for motorists who are injured on nearby U.S. Route 70, the major freeway going through Eastern Utah. Finally, we visited Carbon Medical Services Association (CMSA) located in two sites, one in East Carbon, UT and another in Helper, UT. Both locations are small mining towns also in the Eastern part of the State. Although CMSA sees the fewest patients of the health centers visited, they offer a similar set of services as GRMC. CMSA also provides pharmacy services for multiple counties as they have a pharmacist who fills prescriptions in multiple counties using a tele-pharmacy system.
As part of these meetings, we explored health center leaders' motivations for joining HCN and adopting EMRs, their experience with EMR implementation and use, the impact of the EMR on their practice and their overall experience (e.g. challenges and opportunities) working with a network based in a different part of the country. Although a limited number of health centers in Utah took part in the initial EMR roll-out of OmniDoc, the UHCN centers that we visited have recently adopted the newer, Intergy application that combines practice management and EMR functionality.
Motivations for Health IT Adoption and Network Participation
Health centers in Utah cited the ability to benefit from economies of scale and coordinate among each other as their primary motivation for creating UHCN. All UHCN health centers had an existing relationship through AUCH and noted that vendors and suppliers of IT services, including practice management software vendors, offered very different pricing plans to different health centers. They also noted wide variations in their ability to maintain IT staff and obtain the necessary level of service and support.
Finally, health centers noticed that they were unable to provide a consistent set of data on utilization and cost to their state Medicaid agency. Under Medicaid rules in Utah, the state was able to negotiate individually with each health center on cost-based reimbursement formulas. Because they lacked common systems and consistent data, AUCH members could not share information on costs with each other, eliminating any collective leverage that they may have had with the state and their ability to demonstrate inconsistency in the state’s application of rules from health center to health center.
Noting potential inefficiencies and unfairness in this situation and building on the example of NMHCN, several health center members of AUCH approached Kevin Kearns to discuss the potential of setting up UHCN. Although they had considered other networks, the Utah group believed that their immediate focus on achieving economies of scale with core IT applications and establishing a common baseline for cost accounting, lent itself to involvement in HCN. The Florida-based network which focused on IT infrastructure, support, billing and finance and served as a networked provider of an established practice management application seemed like a logical fit. Overall, the three health center leaders that we spoke with indicated that their engagement with HCN had borne the intended benefits, particularly with regard to practice management, billing and the ability to establish consistent reporting of accounts. Discussants in Utah felt that by virtue of HCN’s experience expanding outside of its state of origin, HCN would have cultivated the adaptive skills needed to face unique challenges that a network unfamiliar with Utah’s payer environment would encounter. Utah has a unique payer environment due to its small population and because the payer scene is largely dominated by Intermountain Healthcare, which is comprised of 21 hospitals and more than 150 clinics in Utah and southeastern Idaho. While the motivation for joining HCN overall was clear and consistent, health centers in Utah did vary considerably in their level of enthusiasm for adopting EMRs. The most enthusiasm for EMRs was voiced by the one urban health centers we visited, WHHC, which noted that as a health care for the homeless in Salt Lake City they saw so many patients with long, complicated medical charts, that having an electronic replacement for the paper record would substantially reduce time and work associated with finding a specific piece of clinical information in a timely fashion.
Other health centers had recently adopted EMRs at the time of our visit and had differing views on their expectations. Executive Directors at both East Carbon and Green River indicated that they anticipated improvements in efficiency of clinical operations and that they felt that moving towards EMRs was an inevitable result of progress in their field. However, one of the providers we spoke with in East Carbon, heavily resisted the idea that having EMRs substantially improved her ability to deliver health care now or in the future. In this case it was the executive director who had led the effort to implement the EMR. Leaders of the Green River health center expressed the belief that EMRs could improve the quality and efficiency of care, but also noted problems with the manner in which EMRs had been implemented at that site.
EMR Implementation, Opportunities and Challenges
Implementation of the Intergy combined practice management/EMR application in UHCN health centers has created interesting opportunities and challenges. As noted above, the ability of the network to build enthusiasm for EMR implementation among providers was highly variable. In addition, respondents noted that a handful of UHCN sites, not among those we visited, decided to skip the Intergy implementation having decided that another EMR vendor, eClinicalWorks, would better meet the needs of their organization. The health centers that eventually moved to adopt Intergy, expressed mixed feelings regarding the quality of the implementation and the system itself. They also ended expressed different opinions regarding the level of customization support provided through HCN. Each of these themes is reviewed below.
Laying the groundwork for EMRs. One of the greatest benefits of HCN membership according to administrative leadership at all three health centers was the standardized way in which HCN helps health centers to prepare their IT infrastructure for EMR adoption and to assure a consistent level of service from vendors. Health centers that were UHCN members reported that they would not have access to the expertise or staff capacity to investigate different practice management and EMR products or research and execute necessary upgrades to their computing and connectivity environment without the support of HCN. Still, they noted important differences in their ability to comply with HCN guidelines prior to implementation of specific applications such as EMRs. For example, HCN’s implementation approach includes a period of documentation and assessment of clinical workflow followed by a re-configuration of workflow to achieve gains through EMR implementation.
One health center was able to take this process very seriously and, in the end, was extremely pleased with changes they made as a result of workflow assessment (some of which had nothing to do with EMRs per se). In this case, the workflow assessment showed that the practice of scheduling prioritized appointments over walk-ins was inefficient. Under the appointment system, sometimes both providers and patients would be waiting for scheduled clients that were late or no-shows. That health center moved to a complete “walk-in” system to better meet the needs of a population (the homeless) with inconsistent access to transportation or the means to keep appointments. Additionally, WHHC's patients often face acute health care needs that are properly handled promptly in an outpatient setting (e.g., a worsening skin condition or wounds that require care).
Other health centers did not feel they had the time and expertise to effectively document their workflow, let alone assess it and make appropriate changes. These centers were smaller, had fewer resources and had a less clear vision of what they wanted from an EMR. In addition, they found that HCN made some challenging assumptions with respect to health centers’ ability to re-configure workflow, such as the ability to assign a physician extender to record some basic clinical information and conduct intake using the EMRs. Rural sites in particular did not always have access to staff that would allow for these changes.
Another area that posed a challenge for health centers prior to implementation relates to the guidance that they scan all prior medical records going back one year into the electronic chart prior to going live. The health centers we visited did not have enough staff to efficiently scan all prior records and have only been able to scan prior records incrementally. WHHC noted that they have made a special effort to manually enter lab values from the old paper chart directly into the medical record because they feel it is important to be able to pull up the last set of lab values rather than having to pull up a scanned version of the full chart. They have done very limited scanning, opting instead to selectively enter historical lab values from the paper charts into the EMR as patients are seen.
Finally, HCN makes specific assumptions regarding the need for reliable connectivity for EMR adoption that are relatively stringent relative to practice management. The rationale for robust and reliable connectivity for EMRs is clear as down time makes it impossible to access clinical information and treat patients. Still, we found that not all rural health centers were able to afford the recommended form of connectivity, T1 lines, and were using less reliable forms of connectivity such as frame relays and DSL. This may have contributed to some complaints from the rural health centers regarding system down time with their EMRs.
Rolling out the EMR to clinicians. Each health center discussed the HCN EMR rollout to clinicians as occurring in two phases: an initial education and orientation phase which took place over the course of several weeks, primarily via WebEx, and a second in-person training phase which took place over the course of several days and coincided with the official rollout of the application. While this approach was generally seen as adequate, it was clear that some clinicians had an easier time adopting the EMR than others.
For example, while WHHC discussants indicated that the training was intense, sometimes going up to 16 hours in a day and requiring the health center to shut its doors to patients for two days, they believed that they were able to effectively use the EMR basically right away and were able to return to full productivity within a few weeks of implementation. Also, WHHC leadership noted that a commitment on its part to educate clinicians regarding the rationale for adopting EHRs, separate from the training offered by HCN, led to faster adoption and greater receptivity on the part of providers.
Clinicians at CMSA and GRMC did not express frustration at the training and roll-out approach per se, but they did indicate a higher level of discomfort with using the system. One provider, a nurse practitioner in her 70’s, felt that there were no computerized clinical features that could improve care, that the process of documentation took her longer because of the EMR and that use of the EMR required her to stay late in order to enter data in the system. She noted that there was not an adequate level of responsiveness from the network to assuage her concerns regarding the usability of the software.
Another clinician indicated that the system for designing and implementing customized forms did not work well for rural health care providers who need different kinds of forms than the core-HCN health centers in Miami (e.g., forms to evaluate patients coming in after automobile accidents). Discussants were unclear as to whether these types of issues could be addressed through better training, although they did note that there could be improvements in the process for creating new forms and for customization.
These comments reflected both natural apprehension of EMRs as well as some perceived lack of responsiveness to the needs of rural providers using EMRs.
EMR functions. All three health centers employed a similar level of functionality through Intergy. Specifically, they had access to the basic EMR and practice management application including the ability to document patient encounters, use population-specific forms pertaining to individuals with chronic illness or patients with specific symptoms. They also had some form of e-prescribing, either electronic fax transmission of prescriptions to retail pharmacies or direct messaging of prescriptions to in-house pharmacy systems (both WHHC and CMSA maintain in-house pharmacies) and bi-directional exchange of lab data. Finally, they have access to a series of standardized reports on utilization and expenses from the practice management database, provided on a monthly basis by HCN, and to separate reporting modules that allow them to run health center level reports on quality of care outcomes.
Practical issues in EMR use. Health centers reported that they were able to actively use the lab interface and e-prescribing functionality without a problem. They also noted that the monthly reports provided by HCN were useful, primarily to track productivity and utilization rather than report on clinical outcomes. Clinicians noted that they were still in the process of working with HCN to adjust their clinical templates, clinical reports and reminders to meet their specific needs and that their staff was still working on being able to document all aspects of a visit comprehensively and appropriately using the EMR. There seemed to be greater demand for templates that were organized based on a patient’s chief complaint in rural areas, compared to the disease and diagnosis based templates that were developed by the clinical committee in Florida.
Others felt that the clinical committee as a whole and the subcommittee that deals with forms in particular, was largely oriented to the needs of the Florida HCN members who were able to attend the meetings in person and that, consequently, the forms were not particularly well-suited to the population served in rural Utah, including a disproportionate share of elderly individuals and accident victims. Still, one health center, WHHC did note some improvements in processes that would improve quality over time; those findings are detailed in a subsequent section of the report.
Finally, there were some uses of technology at the rural Utah health centers that had pre-dated EMR implementation and were not yet integrated into Intergy. For example, they noted that because health centers in rural areas are often the only location where X-rays can be performed and there are very few radiologists in close proximity, having a robust picture archive and communications system (PACS) is critical to assure efficient transmission of images and timely assessments. Currently, the PACS applications being used at both CMSA and GRMC are not interfaced with Intergy and, although there was a plan to create this interface, the health centers reported that this effort had been delayed. In addition, they note that the Intergy EMR and the telepharmacy system are not integrated. This telepharmacy system, used by health centers in Eastern Utah, allows pharmacy orders to be placed by clinicians in location A, approved and “filled” by a pharmacist in location B and then dispensed back in location A using a machine that automatically packages with the correct dosage and medication based on the pharmacists direction. This system allows the pharmaceutical dispensary at location A to be staffed by a surrogate such as a medical assistant rather than a pharmacist or provider.
Quality Improvement and Return on Investment
Because they are relatively early in their use of EMRs, health centers were unable to provide solid evidence of quality improvement as a result of EMR implementation. However, staff at WHHC did note a number of process improvements such as more detailed and complete documentation and the ability to track medications and laboratory results electronically that they felt were bound to improve quality over time. WHHC felt that in their environment, where individuals with complex health care needs are seen sporadically by a myriad of clinicians both paid and volunteer, having a complete, well-documented and legibly presented medical record in electronic format was crucial to providing good care efficiently.
WHHC noted that they have done some studies of care efficiency and patient satisfaction pre and post EMR adoption and found improvements in both areas, however, they were quick to point out that there were other changes that happened concomitant with EMR adoption (re-configuration of the center and the move to a “walk in” model) that could have also contributed to these improvements. Other health centers did not express the same level of optimism regarding the potential for EMRs to improve quality within the current HCN environment. This was either because they had not bought into the benefits of using EMRs in general or had not bought into HCN’s approach to develop EMR based QI tools through its clinical committee. The model for enhancing QI benefits of EMR suggested by HCN, the formation of a state-specific organization of medical directors to develop EMR-based tools for Utah was met with skepticism on the part of medical directors who were already apprehensive regarding the benefits of the EMR. The WHHC medical director has tried to organize other UHCN leaders using Intergy, but there has not been enthusiasm for coordinating around this task partially due to the perception that each health center has its own unique QI needs, the differences in the populations they serve and the long distance between centers.
Key Findings: New Mexico Health Choice Network
In this section we examine findings from meetings with New Mexico Health Choice Network and three of its member centers. NMHC’s predecessor organization was formed by a group of New Mexico Health Centers that came together in the late 1980s and early 1990s to create alliance with the goal of developing an HMO. New Mexico HCN has six member health centers across the state, with a total of 49 sites and 107,895 patients in 2006, the vast majority of whom are uninsured or on Medicaid. NORC visited three New Mexico HCN member centers in the southern portion of the state: La Clinica de Familia, Ben Archer Community Health Center and La Casa Family Health Center.
La Clinica is located in Las Cruces, a city of roughly 90,000 people situated roughly 40 miles from the New Mexico/Texas/Mexico border. La Clinica served 12,477 patients in 2007, 83 percent of whom were of Hispanic descent. La Clinica is both a community health center and a migrant health center, spanning nine medical center sites and 4 dental sites in southern New Mexico. To best meet its patients’ needs, La Clinica offers bilingual care programs and Early Head Start opportunities. Ben Archer is headquartered in the remote village of Hatch, 40 miles northwest of La Cruces. Ben Archer includes seven sites (including a migrant health center) and served 31,399 patients in 2007. Forty-five percent of Ben Archer’s patients were reported to be best served in a language other than English. Because of the rural and dispersed nature of Ben Archer’s health centers, some low-income patients qualify for highly-subsidized transportation services to and from health center locations. After visiting Ben Archer, NORC traveled roughly 280 miles northeast of Las Cruces to Portales, a city of roughly 12,000 people. Located approximately 30 miles from New Mexico’s eastern border with Texas, La Casa includes four health centers (expansion to a fifth site is underway) and served 12,477 patients in 2007. Because of La Casa’s relatively remote location, the center strives to provide “the most comprehensive care in the area,” including pediatrics, women’s health, internal medicine and diabetes support. In addition to meeting with health center leaders, NORC met with New Mexico HCN CEO David Roddy in Mesilla, located just south of Las Cruces.
The health centers NORC visited in New Mexico had vastly different levels of experience and satisfaction with health IT through HCN, ranging from positive and supportive to noncommittal and unsatisfied La Clinica has not implemented an EMR to date, and is “months away” from implementing the Intergy EMR/PM system. La Clinica is one of the six founding health center members of the New Mexico Integrated Services Network (ISN) and maintains an “amicable and supportive” relationship with HCN in Florida. Ben Archer has not implemented an EMR and center leaders hope to be among the last in New Mexico to implement the Intergy suite. Ben Archer staff expressed high levels of frustration with the return on their monthly contributions to HCN and New Mexico HCN, although they remained hopeful that the overall value proposition would improve under the new EMR/PM system. The third health center NORC visited, La Casa, implemented the OmniDoc EMR at all of its sites in 2006. La Casa’s CEO serves on the HCN Board of Directors and maintains close ties with HCN, but La Casa did not seem reliant on HCN, having taken steps to build up its own IT support resources, independent of NMHCN and HCN generally. While only La Casa had implemented an EMR, all three centers NORC visited had implemented the Medical Manager practice management system. Our conversations in New Mexico focused on health centers’ motivations for joining HCN and their overall experience working with HCN for the last few years.
Motivations for Health IT Adoption and Joining A Network
In 1999, David Roddy began conversations with HCN about possibly expanding operations to include an existing network of health centers in New Mexico. Roddy, whose background is in finance, had worked at the National Association for Community Health Centers (NACHC) and at the time directed the New Mexico Primary Care Association and Integrated Services Network (ISN). This confederation of New Mexico health centers understood the importance of improving their approach to IT with the help of a larger organization and actively began researching a shared practice management application. As the New Mexico clinics began looking into the software vendor market, they met with Kevin Kearns from Health Choice Network (HCN) in Florida and this eventually led to the establishment of an HCN New Mexico headed by Roddy.
A number of factors led the New Mexico clinics to formally affiliate their network with HCN and subsequently rename their network New Mexico Health Choice Network (NMHCN). First, they were impressed with the staff and accomplishments of HCN, specifically the software functionality and support service provided to their members. Second, New Mexico was impressed with HCN’s relationship with Medical Manager, a product that rated highly in their assessment of the practice management market.
Finally, more than just becoming customers of HCN, they were offered the opportunity to make a strategic alliance with HCN that involved New Mexico staff joining the HCN Board of Directors and working committees. In their eyes, this relationship offered the New Mexico network an opportunity to help set the direction for HCN overall. HCN’s approach involved regularly scheduled visits to New Mexico by members of the HCN team in Florida. These visits were intended to help ensure close ongoing contact with the satellite network and to build trust based in large part on personal relationships.
As HCN continued to expand its national customer base, New Mexico HCN and its member centers have continued to play an integrated role, both as a customer of HCN’s services and as a leader in the organization. In 2007, New Mexico HCN members’ contributions to HCN accounted for two percent of HCN’s total budget of approximately 22 million annually.
At the health center level, motivations for health IT adoption varied. Improving quality of care was cited as an original motivating factor, especially for tracking measures such as hemoglobin A1Cs among diabetic patients. Health centers leaders also enumerated specific situations and processes requiring data that the EMR would ideally improve, including internal peer review processes and increasingly frequent data requests from payers. One health center thought that the EMR would improve competitiveness both among patients and prospective employees. Other motivations included improved integration of currently standalone processes, the ability to track patient across health centers and improved protections against malpractice claims due to illegible records.
Current IT Capacity and HCN’s Role
NMHCN provides various services for its members including managing the contracts with HCN that provide health centers access to practice management and other network functions. Some health centers noted more success than others in working with the NMHCN to handle problems with HCN in Florida, including delays in changing reports, general unresponsiveness, occasional outages in Florida that affect New Mexico members, overwhelmed HCN Florida staff and the notion that Florida staff were not well versed in New Mexico billing issues. NMHCN also provides finance and billing consulting services to the individual health centers to help them better manage their finances. In addition, the network convenes a local billing committee to share experiences and address issues that HCN employees in Florida are ill equipped to handle. Finally, several New Mexico health centers also access the Dentrix dental health record application through HCN.
As noted above, only one of the health centers in New Mexico has implemented an EMR through HCN and this health center, La Casa, is using the OmniDoc product. While the other health centers in New Mexico are not currently using EMRs, they have adopted other types of clinical applications. For example, La Clinica uses two reporting packages, Practice Analytics and DART (data analysis and reporting tool) to facilitate reporting on quality of care and practice performance.
La Clinica also uses an innovative scheduling system taking advantage of a Voice over Internet Protocol (VoIP) based call center. Under this configuration, patients from La Clinica’s 13 medical and dental sites call a centralized telephone line to schedule appointments. La Clinica’s ten call center workers handle roughly 70 percent of incoming calls and direct patients to the most appropriate care setting. La Clinica’s call center workers not only schedule appointments for their own clinics, but also for other clinics as a fee-based service. La Clinica is currently starting to plan their implementation of the Intergy EMR with HCN. Implementation remains several months away, but La Clinica will most likely be the first New Mexico HCN center on the new system. La Clinica will most likely implement Intergy at four sites initially. They indicated that financial constraints are the only reason they are not implementing across all of their sites at the same time.
La Clinica has a fairly extensive IT team, composed of a CIO, a network manager and five technicians, three of whom are focused on hardware and two of whom are focused on software. In addition, an HCN IT employee who provides application training statewide to the network is based at La Clinica. The health center is also in the process of expanding IT staff, partially in anticipation of the increased demands the center expects to place on IT staff as a result of the EMR implementation and post-implementation usage.
Ben Archer Health Center also uses a number of different information systems to manage its operations. In addition to the Medical Manager practice management system, they also use the Practice Analytics reporting software as well as the PECS software package for chronic disease management (e.g. diabetes and heart disease). All of these software packages are hosted by HCN. In addition, Ben Archer currently uses the Veterans Administration’s VISTA EMR system at one site where they are contracted to provide services for the VA. They also have other information systems such as a pharmacy management system. While Ben Archer has access to several electronic systems through HCN, they reported significant problems (detailed below) and are not currently pursuing an EMR through the network.
Of the three health centers that we visited, La Casa is the most mature and stable in terms of its health IT capacity and usage. They currently use Medical Manager for practice management, and have used OmniDoc as their EMR solution for the last two years. As a result, their clinical operations are now completely digital. Provide.rs use wireless lifebooks at the point of care and exam rooms are fitted with computer terminals. Additionally, some lab orders and results are exchanged electronically through a LabCorp interface. While La Casa has benefited significantly from their involvement with HCN, they rely primarily on their own IT staff to train other staff and support their EMR product.
Health Center Experience with Health IT
Health centers in New Mexico reported a range of experiences with IT in general and their relationship with HCN in particular. Overall, while each health center reported some issues with HCN’s timeliness in responding to support and billing issues, they did, by and large, indicate that the relationship with HCN has been worthwhile. Two of the health centers are ready to move forward with the new iteration of HCN’s Intergy practice management and EMR software offering and expressed enthusiasm for working with the health center on IT infrastructure issues.
Of the three health centers that NORC spoke to in NM, the staff at Ben Archer are by far the least satisfied with the relationship with HCN. Since their implementation of Medical Manager, they have had persistent problems including fundamental issues such as not being able to use the product adequately for billing and overall connectivity. It should be noted that while other health centers did raise issues about their experiences with HCN, they felt that they had the adequate staff to work with HCN to resolve billing problems over time. Some noted that Ben Archer may not have adequate in-house IT capacity to gain the most benefit from their relationship with HCN and effectively make use of networked applications. Another discussant noted that Ben Archer and HCN made a decision regarding entry of historical billing data into Medical Manager that has proven to be the source of many of their issues.
Ben Archer was convinced to convert their transaction histories in the move to Medical Manager. This is notable because Ben Archer was not an initial implementation site. While this has caused significant difficulties for Ben Archer and created substantial unexpected costs, it seems that Ben Archer was the only New Mexico site to experience this problem. Fellow New Mexico centers NORC spoke with were undeterred by Ben Archer’s negative experience. Leaders at Ben Archer also noted that the relative value for what their center is getting from HCN remains low at this point. The center pays $100,000 out of their roughly $20 million operating budget to HCN. Health center leaders at Ben Archer noted that they were close to leaving the network to pursue eClinicalWorks, but were convinced to stay with HCN after considering the Intergy product. Ben Archer’s leaders indicated that tremendous cost of supporting an EMR without the resources of a network led them to stay with HCN.
The staff at La Clinica highlighted the relationship with HCN as essential to their success as an organization. In addition to having access to applications such as Dentrix and Medical Manager, they appreciate having access to a deep pool of expertise in HCN’s staff and trust that HCN officials in Florida have a relative good understanding of their needs. While the team at La Clinica noted that their relationship with New Mexico HCN and HCN is far from perfect, it has been a solid partnership that has taken them much farther than they could have ever accomplished on their own. La Clinica has a relatively robust IT support structure, with a full time IT director as well as an additional IT support role which is currently unfilled. They rely on HCN for vendor selection, training and general accounting assistance and were hopeful that the network could develop centralized billing mechanisms in the future.
La Casa is the only health center in New Mexico HCN to have implemented an EMR. La Casa implemented OmniDoc in 2006, originally with the help of HCN. The health center adhered to the network’s generic rollout procedures, implementing an electronic prescription writing module first. Eventually, the health center migrated 90 percent of its patient records onto OmniDoc, excluding only those who had not visited in the clinic in the previous decade. Moving forward, La Casa plans to add every new patient to the EMR system. La Casa is currently planning to convert their EMR system from OmniDoc to Intergy in the spring of 2009. Health center leaders indicated that they would prefer to be the first site to implement Intergy and that their staff members were entirely bought into the EMR and would not revert to paper charts if given the choice. While La Casa was generally satisfied with HCN, they noted that their success is in large part due to the high caliber of their staff (particularly in IT) and that they had begun teaching HCN about reporting techniques. Additionally, health center leaders expressed some frustration in efforts to exchange data with other providers in the state and concluded that providers feel that patient data belongs to them and not individual patients.
Quality Improvement and Return on Investment
As only one New Mexico HCN center has implemented an EMR, most of our discussion on returns related to improvements in administrative operations, billing and organizational efficiency. La Clinica and La Casa noted improvements in these areas and attributed the improvements to their relationship with HCN, while leaders at Ben Archer found that their operations had generally become more costly and less efficient. Generally, health centers emphasized that by taking part in this network, they have been able to benefit from economies of scale, as well as funding that HCN has been able to obtain separately and make available to its customer health centers. Leaders at La Casa indicated that having clearer diagnostic information, better coding and decreased liability from illegible records and fewer lost records produced significant savings for the center, although they noted that ROI for an EMR is inherently difficult as costs and savings are shifted from certain areas to others.
Despite their overall satisfaction with HCN, many discussants noted that recent reductions in federal grants have placed a significant strain on HCN’s ability to provide timely and active support for its current customers while it also focuses on the acquisition and launch of new customers. Some also noted that HCN had suffered from turnover among their staff, which reduced the deep institutional knowledge necessary to provide high-quality support to the NM health centers. One health center felt that the network was so overstretched in its attempt to achieve sustainability that it was only able to address relatively superficial concerns, such as distributing applications and not more substantive attempts to tie health IT to quality improvement. As a result, the perception of the value provided to health centers by HCN, though still strong, has eroded somewhat.
New Mexico health centers have not experienced significant benefit from their relationship with HCN with respect to quality improvement. La Casa, the center that has implemented an EMR, has largely continued its QI program using the PECS disease management software and has only recently made plans to move away from PECS, towards an EMR-based system to track quality of care. Health centers noted that they make use of monthly reports provided by HCN as a way to compare metrics across centers, but also noted that these reports include very limited clinical data.
As in New Mexico, Utah health centers found it difficult to collaborate on a State-level to address QI and organizational performance issues. Roddy indicated that there was not enough funding at the state or national level within HCN to do robust quality improvement. Additionally, health centers have proven to be less interested in sending clinical leaders to the network to discuss quality initiatives, limiting New Mexico HCN’s ability to capitalize on the diverse and complimentary experiences of its member centers.
Future Direction for Health Choice Network
As noted early in this report, our site visit activities culminated with two 90-minute calls with HCN's national leadership. The bulk of these conversations centered around HCN’s ongoing strategic planning and partnership process which is designed to lead it to a position of longer term financial sustainability independent of federal funding. HCN is also focused on a re-organization that would consolidate decision making authority in the hands of “fully integrated” health center members. There are several key components HCN’s strategic planning process and we summarize some of these below.
Creation of a for-profit subsidiary. HCN’s charter as a non-profit organization calls for it to provide support for health centers specifically. They have purposefully avoided offering services to for-profit providers such as private primary care practices that have approached them over the years.
However, HCN believes that its experience and organizational assets could lend themselves to providing services to private practices. By pursuing this market through a for-profit subsidiary of HCN, the organization could establish a revenue stream to support its non-profit core business and help it achieve even greater economies of scale. HCN leadership indicated that they are considering this option seriously.
Creation of “HCN Florida”. Currently, HCN is involved in multiple services, some of which are targeted to all of HCN’s customers nationally, and others of which are only targeted to the HCN health centers in Florida. The nationally-targeted services primarily consist of the “fully integrated” and hosted offering discussed above. Examples of the Florida-only activities include a cancer prevention initiative and a managed care network. In addition, findings from our site visit suggest that the QI-focused activities of the clinical committee primarily address the wants and needs of Florida members. Since HCN is now much more heavily focused on outreach outside of Florida and since a nationwide network of FHQCs is now buying into HCN, the model of a single HCN providing both types of services is beginning to seem somewhat outdated. HCN may decide to separate the current HCN into a “HCN National,” focused on the delivery of IT and financial services on a nationwide basis, and “HCN Florida,” responsible for leading Florida-specific activities.
New strategic partnerships. Over the last year, HCN has entered into discussions with outside organizations that might be interested in taking a financial stake in its organization.
In this model, an organization such as a private foundation would provide a large infusion of capital into HCN, in return for an ownership stake in the organization. Also, for the first time, individual FHQCs outside of Florida have both become customers and taken an ownership stake in the organization. This model encourages HCN to continue with its nationwide expansion by adding new board members who are very focused on the success for this effort.
Conclusions
As part of this site visit we attempted to establish findings related to the experience of health centers’ with EMR adoption and specifically look at the motivation and experiences of health centers that work with a network that is headquartered in a different part of the country. Overall, we found that health centers in Utah and New Mexico did experience the benefits that had motivated their decisions to join HCN.
Discussants appreciated a variety of features of their EMR and PM systems, including remote access to medical records, the ability to send and receive records electronically, increasingly efficiently production of reports and interfaces with labs and e prescribing. We also found that some health centers faced challenges using HCN services due to inadequate connectivity and difficulty in getting the customizations necessary for rural providers. Finally, in conversations with HCN's national leaders, we learned of new direction for the overall organization as they look to re-organize and achieve sustainability in the near future. We highlight several key conclusions below.
Challenges Facing QI Activities. Overall we found that HCN was able to adequately support health centers’ needs relating to implementation and support for practice management. Although health centers reported varying levels of satisfaction, most health centers in Utah and New Mexico believed that they had received the level of service and value from its practice management application that they had signed up for when they joined HCN. However, for QI support, we found that health centers in New Mexico and Utah felt removed from HCN’s clinical committee and improvement efforts underway in Florida.
Health centers in New Mexico and Utah were also compromised in their ability to re-create the Florida environment which encouraged collaboration on QI issues in states where there were greater distances between health centers and greater variation in patient population and focus. In some cases, these health centers did not have a high level of expectation for collaborative QI support. Also, it was difficult to use the EMR tool for active QI if they had to work with HCN’s clinical committee in Florida to make changes to EMR templates.
While in South Florida, one medical director at a health center was able to coordinate medical director colleagues at other health centers and develop a detailed set of requirements and forms for the EMR, even very motivated medical directors in New Mexico and Utah were not able to achieve a similar level of enthusiasm and willingness to collaborate within their own State.
More integration, more benefit. Our findings generally support the idea that health centers that health centers that are most integrated within the HCN system report deriving the most benefit. Being fully integrated means adopting HCN-hosted PM and EMR software and allowing HCN to serve in the CIO role for the health center. Full integration also means a health center taking an active role in the management of HCN through its board, and in the ongoing development of HCN’s products and services through its various working committees.
While several of the health centers in New Mexico and Utah are considered “fully integrated” from an application and service uptake perspective, we found some distance-related limitations in their ability to participate actively in some committees. In addition, we found that HCN national’s ability to maintain a tight level of integration and coordination is increasingly compromised as they grow larger.
Scalability and continuity are issues. While health centers working with HCN from Utah and New Mexico were positive overall on their involvement with the HCN network, they did express some concerns regarding the HCN’s ability to provide a consistent level of service over time. They have noted that applications are not always configured to meet the requirements of non-Florida sites that the committees may not adequately prioritize their needs and that sometimes essential fixes, such as mandatory changes to billing screens, take longer than is ideal.
Impetus to be self-sustaining may result in organizational changes. If HCN is successful in achieving outside funding through foundation partnerships or other sources, their orientation may change over time. Up until now, HCN has been focused on delivering on the goals of their federal grant sponsors as well as the needs of their health center customers. There has been a relatively close alignment between these two objectives given that both the health centers and HCN are funded through HRSA. Their primary strategy for achieving self-sufficiency has been through expansion to other health centers. If HCN or other networks move to a privately funded model, there may be less alignment between network funders and network customers over time.
Council of Community Clinics
Introduction and Methods
NORC at the University of Chicago (NORC) is pleased to present this report detailing findings from our site visit to San Diego, CA for "Assessment of Health IT and Data Exchange in Safety Net Providers," a project sponsored by the Office of the Assistant Secretary for Planning and Evaluation ( ASPE) at the U.S. Department of Health and Human Services ( HHS). ASPE is conducting this project in close collaboration with the Health Resources and Services Administration ( HRSA). This report synthesizes findings from our fourth of six site visits examining implementation of health IT applications among health center networks. The site visit to San Diego included a series of discussions held with staff and members of the Community Clinics Health Network (CCHN), a subsidiary of the Council of Community Clinics in San Diego, CA.
The discussions summarized below took place in person at the CCHN and individual health center sites on November 18-19th, 2008. Prior to arriving on site in San Diego our team conducted initial telephone and email discussions to coordinate logistics and provide basic information on the agenda and topics to be covered in the in-person meetings. We conducted a total of eight meetings. Site visits took place at CCC's headquarters and at five member health centers: Vista Community Clinic, Neighborhood Healthcare, Operation Samahan, San Ysidro Health Center and La Maestra Community Health Care. NORC also met with the Physicians' Council of CCHN, CCHN staff and a regional HIE group called Connecting for Care. Meetings were conducted using agendas that provided a consistent structure to each exchange while allowing sufficient flexibility to address all relevant information from participants. For each scheduled site visit discussion, the NORC team prepared materials that highlighted topics to address during the meeting.
We begin summarizing findings from the site visit by providing an overview of CCHN, including a description of its history, governance, key services and functions, involvement with health IT and overall budget. We then focus on specific aspects of health IT adoption by CCHN members including motivations, enablers and barriers as they relate to health IT. We also describe areas where participating health centers note specific costs and benefits associated with health IT adoption.
We end the report with a series of conclusions regarding our findings and initial conclusions for policy makers, program officials, health centers, health center networks and other stakeholders. Because this is one of several site visit reports that will be produced, we will present a more definitive and comprehensive set of conclusions and lessons learned as part of the final report for the project, which will synthesize and summarize findings across each of the sites.
Background
As noted above, though the focus of our site visit was CCHN, this network is a subsidiary of a long standing council of safety net providers in San Diego. This entity, the Council of Community Clinics ( CCC) was founded in 1977 by local community health centers to take advantage of economies of scale and to advocate for the interests of their patient base. Since that time, the CCC has expanded to offer its members a variety of services through three organizational units all operating under the CCC umbrella (the third unit is Council Connections, an organization devoted to group purchasing). Unlike other networks we have visited, a relatively large number of CCC's 16 member health centers started out as independent safety net clinics and have only recently become Section 330-funded health centers. CCC is governed by a board of directors, composed of its member health centers' Executive Directors. The core CCC organization handles advocacy and fund development; a subsidiary unit called "Council Connections" provides a group purchasing vehicle for non IT products and services.
CCHN is a second subsidiary unit to CCC. CCHN provides software acquisition and hosting, quality of care and disease management programs and other related IT and quality of care services. CCHN has over 30 participating health centers and is governed by a nine-member board of directors. CCHN board of directors members occupy a number of positions in their home health centers, ranging from chief executive officers to program managers. We provide more detail on CCHN services below and in the remainder of the report we refer to CCHN by name or as "the network".
Network services and functions. CCHN offers a specific set of services around quality improvement, disease management, consulting, project management and hosting software. These services include conducting quality of care audits and reporting on behalf of health centers, developing RFPs and providing vendor selection support for software acquisitions, negotiating and supporting enforcement of agreements between health centers and vendors, and, increasingly, serving as a central hosting and technical support site for numerous applications used by health centers for clinical initiatives.
CCHN members pay a small amount in membership fees (Five percent of CCHN's total revenue) which allows them to help define these service offerings through direct input. They can then purchase specific "canned" services from the network through an a la carte schedule. In addition to a Board of Directors comprised of Executive Directors from all member health centers, CCHN convenes two subgroups representing their key constituents among the health center staff. There is a Physicians' Council comprised of Medical Directors and the CIO (Chief Information Officer) Council. In addition to helping shape the service offerings and priorities of the network, these two groups offer members a chance to learn from each others' experiences.
The network indicates that the Physicians' Council performs the following functions: setting quality and patient health improvement priorities, partnering with other innovative health center organizations and overseeing clinical improvement and disease management programs. The CIO Council provides a forum to share best practices and meet with health IT vendors. In addition to convening these groups and providing the types of services described above, CCHN offers grant writing services and opportunities for the network and its members and in some cases has served as a "network grantee" for funding that flows through them to the health centers. We describe some of the core CCHN functions that are central to this study below.
Support for key applications such as EHRs and registries. As noted above a key role for CCHN is helping its members navigate the software acquisition, adoption and use process, particularly as it relates to clinical applications. In doing so, CCHN works with a range of health center applications and approaches to IT and looks for ways to facilitate learning across the various models employed with member health centers and facilitate adoption of best practices in the acquisition and use of software. Table 1 below provides a summary of the current software environment as it relates to practice management systems, electronic health records and other clinical applications in CCHN health centers we visited as well as their plans for moving forward with new software acquisitions.
In the past year, CCHN has helped to facilitate EHR selection for its members. In selecting vendors, members considered service capability, integration with clinics' practice management systems and overall expense. While the network serves as a conduit between vendors and health center members, the network has concluded that no single solution will satisfy the needs of all of its members. Currently, CCHN hosts eClinicalWorks and supports NextGen, Practice Partner and Epic. In addition to supporting these EHRs, CCHN also supports disease management and reporting software such as the Patient Electronic Care System ( PECS) and i2iTracks and has begun implementation of a stand-alone e-Prescribing system on a pilot basis at two health centers. i2i Tracks is a chronic disease and preventive health management system that allows providers to track groups of patients, such as diabetic or asthmatic patients. I2iTracks resembles an EHR in that it provides direct access to patient data for providers, but it differs in that it does not include an entire patient record. I2iTracks can interface with EHRs and other systems to facilitate disease reporting. CCHN members hope to use i2iTracks to improve quality without having to make a commitment to a full EHR.
Table 1: Software Environment at Select CCHN Health Centers
| Health Center | Current or Legacy | Planned (Go live date) |
|---|---|---|
| Vista Community Clinic Federally-Funded Health Center with 5 sites and 188,000 visits / year | Used Script and Mysis for practice management (PM) and disease management. | Switched to integrated PM/EHR NextGen - went live in July 2007 |
| Neighborhood Healthcare Federally-Funded Health Center with 10 sites and 221,000 visits / year | Have used both Sage (old Medical Manager) and HealthPro for PM with PECSPlanning to switch to a combined PM/EHR either Epic or eCW - their goal is to do this in 2009 | |
| Operation Samahan Federally-Funded Health Center look alike with 2 sites and 40,000 visits / year | MegaWest for PM | Implemented open source ClearHealth application for PM in 2007, planning to integrate with a ClearHealth EHR in late 2008/early 2009. |
| San Ysidro Federally-Funded Health Center w. 10 sites and 250,000 visits / year | MegaWest for PM, Dentrix for dental EHR, i2iTracks for reporting, they have one site running an EHR | Planning to switch to a combined PM/EHR at all sites but has not yet made a selection. |
| La Maestra Federally-Funded Health Center w. 3 sites and 65,000 visits / year | MegaWest, Dentrix, i2iTracks | Planning to switch to a combined PM/EHR at all sites but have not yet made a selection. |
A number of CCHN member health centers have implemented MegaWest practice management software. While CCHN currently does not support practice management applications, they are working with health centers that are looking to migrate to a new comprehensive PM/EHR system to be hosted by CCHCN. Importantly, CCHN "support" of an application can include serving as a direct provider of day-to-day technical support or as a conduit between the health centers and the vendor support staff, it can also include development of interfaces across applications and with outside providers such as clinical laboratories.
Support for quality improvement and reporting. In addition to supporting acquisition and use of clinical IT applications, CHCN plays a role in helping health centers improve quality of care. This support includes CHCN-organized chart audits to produce summaries of performance and progress on the part of health centers in specific areas such as delivery of preventive and diagnostic care or management of chronic illness. CHCN works with health centers to support reporting on quality measures as now required under UDS[2] and in building interfaces to public health resources such as county and state immunization registries. Finally, CHCN is a network grantee for the Tools for Quality program which is a California Health Care Foundation (CHCF) program that provides resources for health centers to implement and use i2iTracks in their organizations. In its role in Tools for Quality, CHCN is helping their own member health centers with implementation and interface set up, but also convening learning sessions for all CHCF Tools grantees in Southern California.
Looking towards health information exchange. As in other parts of the country, safety net involvement in regional health information exchange efforts in Southern California is relatively modest. Outside of exchange of clinical laboratory results and some limited eRx and connectivity to immunization registries, there is not a lot of formal exchange taking place. CHCN is beginning to establish a vision for safety net provider engagement in HIE including establishing a clinical data warehouse and applications allowing access to inpatient and ED records and to records from different ambulatory care sites. CCHN convenes local safety net providers, including its member centers, to form a group called Connecting for Care. This group has existed in multiple forms over the last several years, having initially focused on telemedicine. They are now hoping to mobilize multiple partners in the area to move towards establishing a health information organization to govern exchange of health care data among safety net providers in San Diego.
CCHN budget. CCHN's most recent annual budget was $3.5 million, out of CCC's annual budget of roughly $10 million. Network leaders estimate that roughly five percent of the network's revenues come from membership fees, while grants account for the majority of revenues. Fees for services also contribute to CCHN's overall revenue. Grants typically cover startup costs for new initiatives. Most grants come from private foundations while HRSA and other federal grants provide important financial support as well. In some cases, the network will expand its services or expand to a new geographic area without a clear source of grant support to do so.
Motivation for Health IT adoption
In this section, we will detail a number of key themes emerging from our discussions with staff from CCHN and the health centers we visited as they relate to their interest and motivation to adopt health IT.[3] Interestingly, unlike other health center network models we have observed, CCHN has not taken on the task of forging consensus among member health centers around pursuing a consistent approach to health IT adoption in the form of specific applications and adoption timeframes. Instead, CCHN has focused on understanding and addressing the needs and motivations of individual health centers and building a broad set of capabilities and flexible hosting options to addressing a range of needs.
Need to upgrade existing applications. One of the primary motivating factors for many health center members who are looking into adopting new health IT applications is dissatisfaction with their current practice management system. Centers noted ongoing dissatisfaction with their ability to use their practice management applications to efficiently address basic health center needs around grant reporting (e.g., UDS) and Medicaid billing. Some health centers had switched practice management applications somewhat quickly in response to Y2K system concerns and were later surprised to learn their practice management system could not fully meet HIPAA requirements could not facilitate quick, accurate reporting. Also, given that many Federally-Funded Health Centers in San Diego achieved status as Section 330 funded entities since 2002, many of these acquired their practice management system prior to being subject to the reporting requirements that come with federal funding.
EHRs seen as the wave of the future. Health centers we spoke with agreed that adoption of EHRs would be essentially a requirement in the near future. They noted their interest in pursuing new funding opportunities through the federal government and that many of those new funding opportunities focused on use of EHRs to improve quality and efficiency of care. They also noted an increasing preference among clinicians they are recruiting to work in a setting where they are using EHRs rather than relying on paper-based clinical record keeping and that regardless of whether they require EHR adoption, increasingly reporting requirements from federal grants required the aggregation of clinical data that could be facilitated by EHRs or other clinical applications. In particular, several health centers noted the requirement to report on clinical measures as part of UDS as being a motivator for EHR adoption.
Facilitating quality improvement. Both health center and network respondents discussed the potential for EHRs and other clinical applications to improve quality. Some of the health centers we spoke with were looking forward to implementing i2iTracks as an interim measure prior to EHRs and as an application that could ultimately compliment an EMR. Some noted the difficulties in keeping existing registries up to date and difficulties due to the lack of available customer support for the PECS software originally promoted for registry development and quality management. CHCN staff noted that most member centers were moving to implement i2iTracks and that once i2iTracks is fully implemented they would have greater capacity to do more quality of care review and benchmarking across the network in a more comprehensive, timelier and far less costly manner.
Motivation and interest in specific applications varied. We should note that although there was some enthusiasm around i2iTracks, there was also a diversity of opinion regarding whether i2iTracks as a stand-alone system was the best choice. One health center that had customized and implemented an open source integrated practice management and EHR solution, felt that it would be more effective to have disease registry functionality built into their EHR itself and is working towards that goal. Another health center noted that i2iTracks could help on quality, but believed that it alone would not address quality of care and improve reimbursement the more accurate coding in the manner that an EHR might.
Enablers and Barriers to Health IT adoption
NORC's discussions with CCHN and its members produced a number of findings related to overall enablers and barriers to health IT adoption.
Network culture, dynamics. Discussants noted that CCHN's efforts to leverage its influence as a group and work directly with vendors on behalf of its members amounts to a significant enabler for health IT adoption. In particular, health centers noted the importance of having a trusted source of knowledge on vendors and access to experts who could translate specifications and infrastructure requirements for adoption of a particular software application into the practical terms of costs, resources and time required for successfully adopting that application.
They also appreciated the network's help in negotiating with vendors and helping hold vendors accountable to the terms of agreements following the purchase of a system. Most of the health centers we visited agreed that they would not be able to afford similar IT leadership within their organizations. Finally, while the health centers we spoke with were not always on board with every network initiative, they genuinely appreciated the ability to interact with other health center colleagues on use of IT for quality improvement.
Grant support. Grant support was also an important enabler for CCHN members. Health centers in the San Diego area and the network itself rely heavily on grants for new initiatives. Grant writers employed by health center members play an active role in CCHN's funding committee and the network ensures that health centers have agreed to apply for specific grants before moving forward with them. In addition to the i2i Tracks grant described above, CCC is currently benefiting from a HRSA e-prescribing grant that has allowed the network to expand an existing pilot program. The Los Angeles Department of Health Services contracts with CCC to provide support to its health centers. CCC is also contracted by San Diego County for project work. Additionally, CCHN brings centers together as a network to apply for network-only grants. While these grants offer useful and significant revenues for CCHN, some noted that they occasionally create collaboratives that centers would never pursue absent grant requirements. These health centers find that grant requirements may encourage collaboratives that do not make sense in that the requirements could force them to work with health centers that are far less advanced in terms of health IT.
Health center members also rely on grants for covering startup costs, standalone applications such as i2iTracks, implementations at individual health centers and staff training. For obvious reasons grants are primarily seen as an enabler of health IT adoption, however some San Diego respondents noted down sides to grant-funded adoption of health IT. One health center that had purchased a practice management system jointly with other health centers as part of a HRSA grant awarded several years ago noted that grant funds have been useful for initial costs, but ongoing maintenance costs of their practice management system, had proven unsustainable. Additionally, grants have a significant impact on the timing of EMR implementation, with some grants forcing health centers to implement along a strict timeline. Another health center noted that two percent of their Section 330 grant went directly to health information technology expenses.
Finding the right people. Some health centers reported that IT professionals with experience in working with related applications were particularly helpful in implementing new EHR systems. A number of health centers indicated that in preparing for the adoption of EHRs, they had shifted from having a lower skill level technical support staff member to an information technology director with analytic skills. One member health center relied heavily on the experiences of their medical director who had worked with a NextGen EHR in a previous setting. The medical director's experience proved useful to the health center in navigating the EHR marketplace and to the wider network through the Physicians' Council. Health centers also benefited from the experience and expertise offered by CCHN. In some cases, the network was able to help health centers with information technology needs without charging service fees. Some discussants noted that their experience with older practice management systems made them more aware of their information technology needs and the importance of specific concerns such as integrating various information systems.
Cost. Cost was not a significant barrier for many of the health center members NORC visited. This is partly attributable to the fact that most health centers had opted to implement i2iTracks and had not moved to implement an EHR. The fact that CCHN had been successful in securing grant funding for a number of initiatives may have also helped to reduce costs for health center members.
In a broader sense, some health centers were optimistic that their eventual implementation of an EHR would not be devastatingly costly. One health center explained their justification for pursuing a new EMR/PM system, saying, "It's costing us more by not doing this." This health center leader felt that they would benefit greatly from increased efficiencies, fewer lost charts and better data accessibility. Further, she felt it might be possible to repurpose billing rooms and potentially reassign staff currently working in the billing department. Health centers that had been using the MegaWest system pointed out that the ongoing maintenance costs associated with that system were prohibitive. Some saw the prospect of moving toward a new integrated EHR/PM system as a way to reduce ongoing costs over their current MegaWest configuration.
Operation Samahan, a member center located near the United States/Mexico border pursued an open source PM/EHR solution called ClearHealth to avoid costs associated with other EHRs. This center's billing and IT director outsourced much of the development of the application to various programmers around the world and the center claims they have been able to keep costs low. As with most open source efforts, however, the true costs are hard to measure given that researching, implementing and managing development in an open source environment requires a very knowledgeable, motivated individual (in this case a very motivated computer science major who happened to be working at the health center's billing department) and if such an individual is not available to the health center by serendipity, finding and paying for such a person may be cost prohibitive.
Workflow and Training. The site visit to San Diego offered us really only one opportunity to discuss a recent EHR implementation in a health center. Vista Health Center implemented a new NextGen EHR product in 2007 and discovered several unanticipated challenges from having to support specialized training for providers with no prior computer knowledge at all to re-designing basic processes including patient intake, history and physical exam administration and prescribing. The costs associated with these challenges were hard to quantify, but ultimately the health center experienced a greater than 10 percent productivity loss that is ongoing over a year after implementation.
Returns, Sustainability and Financing
CCHN and its members offered insights into financing models and returns on investment during our conversations with them. Because many of the health centers in San Diego are new to relying on federal grants, these health centers have potential private sector donors and use these contacts to support IT investments. Health centers noted that local foundations such as Tides offered important financial support for Health IT initiatives. Most health centers' payer mixes were heavily weighted toward Medicaid (MediCal) which offers some enhanced reimbursement for use of health IT by Federally-Funded Health Centers through scope of service adjustments to the base payment formulas.
Health centers noted the importance of creating economies of scale through their affiliation with CCHN. As one health center leader put it, "we need economies of scale; we can't do it on our own." CCHN, along with CCC, offer important opportunities to take advantage of group purchasing discounts and certain IT consulting services that may be out of reach if provided by other service providers.
Return on investment was not frequently mentioned in health center leaders' discussion of EMR systems. One health center pointed to patient safety as a potential area for return on investment, but generally felt that there was "no reason to measure ROI." Another center indicated that implementing an EMR had slowed them down considerably and that payers had not increased reimbursements for using an EMR (aside from minor adjustments to MediCal reimbursement). This severely limited this center's ability to produce a return on their investment and, more broadly, justify expanding their limited EMR implementation.
CCHN members are notable in that they have implemented different applications and information systems along different timelines. Some health centers can describe evidence of changes in quality of care, efficiency and provider satisfaction. For instance, the health center that implemented NextGen reported that they had reached 90 percent compliance with some clinical guidelines after implementation, including greater adherence to recommended frequency of conducting foot exams for diabetic patients.
Another center looking toward implementation of i2iTracks and an EHR listed provider satisfaction and recruitment efforts as primary motivators for pursuing more robust health IT applications. At the network level, CCHN is looking to digitize the chart review process that currently occurs by hand. Currently, many member health centers look to CCHN to perform continuous quality improvement functions, such as chart reviews. Moving to an electronic system could help streamline and enrich the network's quality offerings.
The one health center that has recently moved to an EHR noted that it had seen a measurable improvement in meeting quality targets since implementation. After a year of having used NextGen, this center is now meeting 90 percent of its process metrics in diabetes (e.g., compliance with foot exams and HbA1c test) and has improved metrics in other areas. While there is limited anecdotal evidence about increases in quality of care, health centers noted that costs and efficiency had not improved measurably. California allows for limited MediCal reimbursement based on quality reporting and improvement, but health centers report that such payments are not large enough to motivate health IT adoption. (Again, note that this was pre Recovery and Reinvestment funding).
Conclusions
We conclude with some brief preliminary conclusions and areas for future inquiry that will inform overall conclusions for our final report.
The technical service organization model. CCHN is an interesting network model in that it is relatively distributed with no centralized approach to practice management, administration and billing, yet still manages to be very engaged with working with and across health centers on IT and quality improvement priorities. The network thinks of itself as a technical services organization ( TSO) with a small fee for entry into the network and then a highly modularized approach to purchasing additional services. While this is a relatively new model for health centers, there are several networks that seem to be moving in this direction especially within California.
Pros and cons of a distributed model. Network discussants articulated a coherent rationale for making sure that they stay flexible to meet the needs of their member health centers. Ultimately, there is a realization that unless grants require them to explicitly, health centers will tend to arrive at different conclusions regarding the suite of clinical and billing applications that best suits their purpose. This is consistent with the reality that while similar in many respects each health center has its unique organizational history, administrative practices, clinician staffing, populations served and services provided beyond primary medical care.
While hosting multiple EHR products and supporting health centers as IT consultants when they use applications that are not managed centrally at the network, makes some processes (e.g., quality benchmarking across health centers) more challenging, it may also open the door for these networks to break new ground in terms of use of content standards and consistent use of different EHR products to produce comparable reports. Having this expertise, could, in turn position networks to serve as key conduits for community and regional HIE.
Adjusting to ARRA. Finally, throughout this report we note that this site visit was conducted prior to the American Recovery and Reinvestment Act of 2009. As a result, several of the factors creating motivation or lack of motivation for EHR adoption cited here have become overwhelmed by the financial incentives that will be available through Medicare and, in particular, Medicaid for providers engaging in meaningful use of EHRs. We will explore implications of ARRA for the findings from this site visit and others as part of our final report for the project which will integrate findings across all of the site visits.
Appendix A: CCC Organization Structure

[1] PECS is the Patient Electronic Care System, an electronic disease registry system originally used by the Bureau of Primary Health Care's Health Disparities Collaboratives.
[2] UDS is the Uniform Data System, a core set of data reported by HRSA-funded health centers used to review the operation and performance of health centers.
[3] It is important to note that this site visit took place prior to enactment of the American Recovery and Reinvestment Act of 2009 and the new incentives around health IT adoption created by that legislation.
District of Columbia Primary Care Association
Introduction
NORC at the University of Chicago (NORC) is pleased to present this report detailing findings from our meeting with the District of Columbia Primary Care Association (DCPCA) for “Assessment of Health IT and Data Exchange in Safety Net Providers.” NORC conducted this meeting under contract with the Office of the Assistant Secretary for Planning and Evaluation ( ASPE) at the U.S. Department of Health and Human Services ( HHS). The Health Resources and Services Administration ( HRSA) works in conjunction with ASPE to guide activities under this project. This report is one of a number of white papers produced for the project.
The purpose of the meeting was to explore the experience of DCPCA and its member health centers and clinics during the implementation of the eClinicalWorks (eCW) electronic medical record ( EMR) in six provider member organizations across the District. DCPCA received a substantial grant from the Washington, DC government to implement electronic health records (EHRs) among a number of its members. While we have investigated a number of consortia based EHR implementation projects under the current task order, DC offers a unique opportunity to look at an effort funded primarily by municipal government and managed through a local primary care association.
NORC convened a panel of DCPCA members at the Association’s offices in downtown Washington, DC on January 14th, 2009. There were 10 participants, spanning three of the providers involved in the EHR implementation and including clinical, administrative and IT staff. Jim Costello, IT Program Manager at DCPCA also participated actively in the meeting. Adil Moiduddin and Dan Gaylin of NORC led the conversation, with two NORC staff taking notes. Federal partners from both ASPE and HRSA as well as representatives from Cumberland Consulting (DCPCA’s partner) joined the panel as observers. The conversation lasted roughly three hours, with one 10-minute break. NORC conducted a one-hour follow-up meeting with Jim Costello of DCPCA over the phone to address issues not covered during the January meeting.
This report will provide background information on DCPCA and summarize the meeting. The first section will detail the history of DCPCA and background of their involvement with HIT. Following this, there is an explanation of DCPCA’s EHR implementation process, detailing motivations, planning, training and roll-out. We then discuss future direction for the Association in health IT including plans around HIE, strategies for long term sustainability and project financing both at inception and over time. We end with some conclusions on the meeting.
DCPCA and the EHR Project
The District of Columbia Primary Care Association (DCPCA) was founded in 1996, in an effort to promote primary care and support health centers and free clinics in the community. Before DCPCA’s inception, the District did not have any coordinated effort to support primary care and community health centers through an association. In the years since its founding, DCPCA has focused on initiatives to enroll more health center patients in Medicaid, increase the use of the medical home model in DC and various efforts around increasing civic engagement and communication among local stakeholders. Currently, DCPCA focuses on capital improvements and physical expansions among its members (especially in wards seven and eight), improving quality of care and increasing efficiency, particularly through the use of health information technology. DCPCA also serves as an advocate for its members, particularly on the issue of local Medicaid reimbursement rates.
DCPCA currently has 14 health care provider members and a number of organizational member partners. While the association focuses on health center operations, its members vary greatly in the services they provide, with some focusing almost exclusively on health care and others specializing in securing food and clothing or providing other social services. Consequently, not all DCPCA members are federally-funded health centers, with some receiving little to no federal funds. DCPCA is governed by an eleven-member board of directors. Some of the member provider organizations are represented on the board of directors, although most are not. DCPCA has a staff of 29 regular employees, supported by interns and volunteers. The Association’s overall budget in 2008 was reportedly $20 million.
EHR Project Background. Between 2004 and 2005, DCPCA staff recognized an interest among its members in adopting an electronic health record (EHR). Most member clinics expressed some level of interest and some providers serving at DCPCA members had experience working with EHRs either at Veterans Administration hospitals or other sites. Overall, however, providers were discouraged by the high costs, lack of support for initial investments and questions about ongoing maintenance and sustainability. Despite these concerns, the Association recognized a certain level of need and interest among its members and DCPCA’s CEO Sharon Bakersville, lobbied the DC Department of Health to provide funding. These efforts culminated in a $5M grant from the DC government to implement a combined practice management system (PMS) and EHR. After being funded, DCPCA brought together 14 interested health centers to determine which centers would be most interested in implementing first, serving as “early adopters.” Six clinics volunteered: Bread for the City, Family and Medical Counseling Service, Inc. La Clínica del Pueblo, Mary’s Center for Maternal and Child Care, SOME (So Others Might Eat) and Whitman-Walker Clinic.
Motivations. Health center representatives expressed a number of motivating factors that led to their participation in the DCPCA PMS/EHR initiative. Most felt that the new system would improve continuity of care and communication within their health centers. One health center felt that the EHR would help them consolidate patient records. Before implementing the PMS/EHR, this center maintained separate paper records for individuals across the center’s departments. This fragmented system hindered development efforts as visiting funders would often note problems in the area of communication and collaboration across departments. Others hoped that the PMS/EHR would improve communication between staff that perform different functions within a center, particularly between providers and front desk staff. Some noted the amount of time they spend tracking down paper records and the prospect of running reports more easily. Others explained that the availability of grant funds served as a motivating factor in itself, citing limited capital and aging existing IT infrastructures at their centers. DCPCA staff supported this explanation in discussing their motivating factors, explaining that they observed inefficiencies and deficiencies in member centers’ infrastructures leading them to pursue an EHR despite some uncertainty among members. Still, others expressed a belief that “EHRs are the future” while some said that moving toward an EHR represented an effort to increase collection rates for reimbursement.
Adoption and Implementation
We break up discussion of DCPCA’s EHR adoption experience into several phases articulated by the DCPCA project leadership: planning, training, data transfer and implementation.
Planning. DCPCA partnered with Cumberland Consulting throughout the training and implementation process. At the earliest stages, Cumberland did an assessment of the six participating clinics’ infrastructures focusing on hardware, software, connectivity, building set up and other relevant parameters. Participants noted that process and workflow at the sites were not assessed at this stage, although they were assessed later as part of product customization.
Following the initial assessment, all of the clinics came together to develop user and functional requirements for a PMS/EHR system. That list of requirements became the request for proposals (RFP) that was sent to vendors. The participating clinics continued to meet at DCPCA throughout the planning process to discuss what reports and summary data would be useful outputs. Member centers noted that Cumberland Consulting’s role early in the project, even before vendor selection to guide discussion leading up to and including functional requirements, was very useful as it provided an outside perspective and seeded some consensus around the benefits of collaborating and finding common needs across sites.
From the initial stage of assessing needs, DCPCA narrowed the field of vendors to a smaller group. As the list of vendors shortened, health centers were encouraged to bring staff to view the finalists, eClinicalWorks (eCW) and Centricity. There was a final discussion of the pros and cons of both finalists and then one representative from each member health center voted to select a vendor. In voting, members considered the following criteria in particular: user friendliness, the details of training processes, Spanish language functionality (particularly for those with differing levels of education and computer literacy), the experience of other health centers with these vendors and the ability of the product to support the needs of all center users including front office, back office, case managers and providers. While member center representatives expressed doubts that one EHR could fulfill all their requirements, they indicated that both finalists represented a marked improvement over their previous systems, citing an inability to capture simple demographic information like ethnicity before implementing the EHR. DCPCA members selected eCW and chose to implement it using both standard desktop PCs and tablet PCs.
Functionality, customization and implementation planning. Once eCW had been selected, Cumberland Consulting worked closely with staff across implementation sites to understand their clinical workflow and processes and develop a set of customizations of the basic eCW software that would meet requirements across providers. Discussants noted that given the differences in services and operations, this proved to be a challenge and they had to find ways to make the same software usable for a variety of workflows. For example, one clinic’s workflow involved shorter and higher intensity patient encounters where detailed documentation had to be done after the visit rather than during the visit as would be considered the usual optimal use of the application.
In addition, in the initial implementation, DCPCA noted that there were not sufficient funds or time to make effective use of all the functionality available through eCW including clinical reminders. They were able to make use of basic forms for specific types of clinical as well as different patient panels (e.g., diabetics), but that the development of disease and assessment specific forms needs to continue as the clinics learn more about how to operate in an EHR environment. The initial implementation included automation of laboratory interfaces with the EHR and three health centers are making use of the e-Prescribing (eRx) functionality built into eCW while another three continue to rely on in house pharmacies.
Training. Participants noted that training was particularly important in their eyes because of the high levels of staff turnover at their centers. Super users, primarily clinicians from various health centers, were trained first with trainings on the PMS preceding EHR training by two months in some cases. Having more experienced super users on hand during general staff training proved helpful. Super users asked questions of staff and assisted trainers when necessary. Despite this, training was not entirely successful at first, as some staff members needed more individual attention from the trainers. One participant noted that staff would leave the training, and when the trainers would come back, the staff would have forgotten everything that had been covered previously. Others suggested that trainings occur a bit later in the process, roughly a month before go live, rather than soon after selection. Some health center representatives added that trainings were not particularly interactive and that combining workflow exercises with eCW trainings would have helped staff apply trainings to their everyday work. One participant suggested using old (de-identified) patient notes during trainings to make them more useful.
Some changes were made to the original trainings, with eCW trainers tying their trainings to specific tasks and DCPCA assisting when possible. While member center representatives agreed that the more tailored trainings were an improvement, some felt that Cumberland Consulting would have been better suited to conduct the trainings than the vendor because of their familiarity with center processes. Alongside the eCW trainings, DCPCA organized after-hours training for staff unfamiliar with basic computer use and email. In addition to initial training, some groups attended “refresher courses” to provide additional training opportunities.
Members noted that while helpful, these types of supplementary trainings amounted to a big time investment. Some participants expressed concerns about ongoing training, indicating that that the initial training had been successful but ongoing training sessions have not been discussed and could amount to a significant time and resource burden, with providers presumably training constantly rotating public health service corps members and other volunteers. Others suggested that web seminars conducted by the vendor had not proved helpful, particularly in moving beyond the basics of EHR usage. In discussing EHR implementation, one participant noted that more comprehensive trainings would have been helpful but that members did not know exactly what they wanted or could ask of the system. One participant noted that front desk staff would need to be well-trained in the future, saying “They are doing more than just checking in patients.”
Data transfer. In moving toward eCW, member centers’ patient demographic information was transferred from existing systems. After review by health center providers, select clinical information was entered manually “as if they were new patients.” Participants noted that providers were very concerned about condensing patient information from the paper record to the EHR. While some noted that this process was not as time consuming and difficult as they had imagined, others indicated that the process was as difficult and lengthy as they had expected. One participant noted that not all data were entered manually and that the center needed to enlist the help of volunteers to scan hundreds of patient records.
Implementation. Directly following the initial migration of data, staff did not begin entering encounters, instead starting with basic patient scheduling. Some participants noted that this helped staff adjust to the new system gradually. Health centers generally extended appointment times and reduced overall patient throughput during implementation. DCPCA recommended a 50 percent reduction in patient appointments, but many felt that such a large reduction was unrealistic. The exact strategy in reducing patient appointments was left to the discretion of member health center leaders.
One participant noted that increasing access to the system (via trainings or some other means) might have improved implementation. This health center continued to use parallel systems concurrently beyond the initial training and go live period. Others pointed to the important role played by super users. They indicated that while these staff are integral to a successful implementation, health centers should expect that the super users will experience reduced productivity for a longer period of time than other staff. Super users spent significant amounts of time addressing colleagues’ needs in the absence of actual trainers and support personnel. Similarly, some felt that Cumberland Consulting should have been asked to stay to help with implementation for a longer period of time, particularly to support super users. One super user explained, saying “After the consulting group left… there were times I didn’t do work for a couple days. I had my own questions as well [as addressing other staff members’ question].”
Some participants noted specific issues encountered by staff during implementation. For one health center, attaching a funding source to every encounter has proven problematic. Linking funding sources (whether that be a health plan, Medicaid or a grant program) often requires several attempts and identifying encounters that lack funding sources takes additional time. One participant noted that users must remember funding sources when switching between relevant screens in the system. Others noted that staff remain frustrated with the system’s performance, particularly its speed, propensity to log users off or freeze and difficulty scheduling specific providers for specific appointment times.
While a number of panel participants expressed frustration with attaching funding sources to encounters under eCW, others felt that this requirement motivates providers to “work for their money,” knowing that their income comes from specific funders. Others noted that eCW’s ability to suggest coding levels helped providers to reconsider documentation in some cases. One participant suggested that eCW has helped their clinic track spending on specific groups such as Ryan White grant patients.
Many health center representatives indicated that they had not begun using all of eCW’s features, particularly relating to automation and reminders. One health center noted that reminders for preventive medicine are always “in the back of their mind,” but they have yet to implement them. Some health centers have begun using alerts. One center has begun tracking missed appointments using eCW, taking action after three consecutive missed appointments.
Staff satisfaction. Staff have voiced varying levels of satisfaction with eCW. Some have complained that things are not easy to see in the EHR. Others have indicated that eCW has been somewhat disappointing, noting “everyone says the system could do things, but what it ended up being didn’t help me to do my job better. There were things we thought would help that didn’t.” Other participants indicated that providers appreciate being able to see what they have and have not done in a single place and the system encourages writing notes effectively after each visit. They also indicated that some providers see the EHR as a customizable tool. While greater transparency offered benefits for some (primarily managers), others noted that having productivity numbers available on the EHR makes some providers uncomfortable.
One area where there were particular concerns was with eRx. The eCW eRx solution used by DCPCA members relies in part on faxing and this has proven problematic for DCPCA members engaged in eRx, with some faxes not transmitting successfully. Others noted success with eRx saying that under the previous system it would take a full 24 hours to process and send a prescription. This process takes approximately 1.5 minutes under the new system. One participant noted increases in patient safety as well, especially in identifying drug interactions. Having an EHR has negatively affected the health centers that chose not to implement eRx because they had their own pharmacies. These centers have experienced increased costs in integrating eCW into their existing pharmacy and prescribing processes.
Another area of concern is related not to the clinical application but to billing. Some discussants felt that eCW has caused a number of problems for members in billing for services. Some health centers noted that they had seen more denials than expected under eCW, as a result of supposedly invalid insurance or inadequate follow-up. These denials have decreased revenues and increased workloads for billing staff. DCPCA is investigating these problems.
Financial implications. Some noted direct financial implications of moving toward eCW. Requiring that all procedures be linked to a payer, including vaccinations, has improved reimbursement for at least one center. Services that previously went uncompensated are now being linked to a payer. Others said that third party reimbursement had increased, but that other factors like decreased grant funding, increased demand on billing staff to follow-up with payers, and greater demands on IT support staff generally had increased costs. In discussing the increased IT needs, one participant noted, “Our IT person on staff had to increase their time in the clinic because of eCW. It won’t decrease now, it’s a daily need.” One participant noted that having greater access to financial data had amounted to a motivating factor for his center to pursue payment, saying “You know how much money you are leaving on the table. From that point of view, it’s a motivator. Every duck has to be in a row.” It should be noted that almost all comments related to financial benefits at this early stage referred to the practice management application rather than the EHR.
Future Directions
In this section we outline next steps beyond implementation involved in the DCPCA’s engagement with member health care providers on health IT.
Current health information exchange. DCPCA has not begun sharing EHR data across health centers at this point, although health center representatives indicated that such sharing would be useful. In working with other health centers, members still need to submit requests for patient records in paper. The new PMS/EHR has led to new information sharing in other areas though. Participants noted that eCW has facilitated easier prescriptions refills and lab refills (although one participant noted difficulty tying ordered labs to funding sources). Members also expressed some concern about maintaining compliance with HIPAA.
Quality improvement. DCPCA’s quality improvement (QI) initiatives are still in the beginning stages of development. One health center, Whitman-Walker Clinic, reports that it has begun using eCW for quality, but most other centers are just beginning to consider how to use the EHR to improve quality. Participants noted that having the EHR has served as a type of motivation for developing QI initiatives. In their view, the EHR has forced them to pay attention to data quality for things like reporting. Having spent resources to develop clean data sets, these centers see the additional cost of pursuing more formal quality improvement initiatives as low. The existence of additional health center data has also led DCPCA to pursue a central quality improvement program. One health center agreed that having additional data made QI a possibility, but felt that additional training would be needed to capitalize on the opportunity.
Future directions. DCPCA plans to expand its PMS/EHR initiative to all of the health centers in DC. It is their hope that such an expansion will help to control costs for individual health center participants. Additionally, DCPCA is moving forward with a RHIO (regional health information organization). The DC government has provided $6 million in grant support to help develop the RHIO. DCPCA hopes that the RHIO will help to expand the utility of the EHR, providing health centers with a more complete picture of patients’ care, particularly in hospital settings. Participating hospitals include: Washington Hospital Center, Georgetown University Medical Center, Howard University Hospital and Providence Hospital. DCPCA is also developing resources to increase members’ use of functionality available in eCW. This may take the form of another staff member devoted to the PMS/EHR initiative. Both DCPCA member representatives and staff indicated that they had more or less mastered the basics of using eCW, but felt frustrated that they could not make use of more of the system’s available functionality.
Enablers to health IT adoption
This section will detail key factors that have both helped and hindered DCPCA in its PM/EHR implementation process.
DCPCA leadership. While DCPCA’s approach differs somewhat from more unified health center controlled networks and individual FQHCs, the organization’s leadership amounts to a significant enabler for its members. DCPCA made efforts to standardize the approach to health IT adoption among its members, although some variation was permitted. Members saw the importance of a shared approach for data elements such as appointment types. In cases such as this one, member centers agreed on the type of appointment to build into eCW and the way to store appointment data. At the same time, differences in the intervals between appointments were permitted.
Even when differences persisted, having DCPCA as a forum to discuss differences across health centers and their needs proved useful in developing a shared system. For example, one health center does not bill for homeless patients, but others might. Being able to discuss the implications of differences like this was an important enabler to adoption for DCPCA members. Additionally, health centers noted that they had neither the time nor the staff to pursue and implement an EHR on their own. Members looked to DCPCA for expertise and strategic thinking. Health center staff felt pressed to find the time needed for things like vendor selection, planning, training and implementation. Having to handle grant applications, software installation and data management would have completely overwhelmed member centers’ staffs.
Grant support. While some participants decided to pursue an EHR after being presented with a grant opportunity, the DC government’s support also served as a general enabler for success for DCPCA members. Participants noted on numerous occasions that they would not have been able to implement an EHR without the District’s grant money. DCPCA staff supported this characterization, indicating that health centers did not need to provide significant support for the initial costs associated with eCW. The grant covered hardware costs such as PCs, tablet PCs, scanners and printers. The only start-up costs not covered by the grant were things like improving internet access for member centers (i.e. going from a DSL connection to T1). While the DC government grant covered nearly all initial costs, member centers now pay all of the ongoing costs through fees to DCPCA (eCW invoices DCPCA).
Consultant support. Consultants also provided valuable support for DCPCA and its members. They assisted in vendor selection, adapting eCW to members’ needs, data collection and overall strategy. Participants expressed appreciation for this support, while also noting some minor difficulties. One participant indicated that Cumberland’s schedule for adoption prevented them from asking questions at some stages. Others simply wished that representatives from Cumberland Consulting had been available for longer periods of time or had transitioned away from their support role in a more seamless way. Despite these issues, members seemed to view Cumberland Consulting in the same way they discussed DCPCA’s support: not perfect but still essential.
Challenges in Health IT Adoption
While some key factors helped DCPCA and its members to effectively implement a new PMS/EHR system, other aspects presented challenges.
Staff expertise/learning curve. Staff presented a number of challenges for DCPCA members. Participants noted low levels of computer literacy among some staff as the primary personnel challenge. Some employees had trouble with basic tasks such as opening technical support tickets and using computers and the internet for work tasks (rather than entertainment). Other staff members simply could not perform computer-related tasks in a timely manner. Some providers had trouble adjusting to the constraints of an EHR, having been able to write “what they want” on the paper record. Others relied on administrative staff to enter things from the paper chart into the EHR. Some health center representatives at our meeting discussed the specific needs of their administrative support staff, indicating that requirements that staff reflect patients demographically and a predominance of Spanish-speaking staff at another center presented challenges in vendor selection, training and implementation.
Needs of non-medical staff and specialty providers. DCPCA member centers expressed some frustration with eCW’s inability to address the needs of non-medical staff and specialty providers. Not all members are FQHCs or lookalikes (e.g., some are free clinics) and some had no existing practice management system. Also, DCPCA member centers provide other services including determination of benefit eligibility, WIC, case management, social work and behavioral health. Because eCW serves as the patient record for these centers, staff in non-medical divisions often find themselves accessing patient medical information unnecessarily, compromising patient privacy. One participant explained, saying, “Every time a case worker goes in, all of their history of medications is there. But that kind of extensive data is not necessary for securing bus tokens and other unrelated social services.”
Additionally, non-medical staff and specialty providers have expressed frustration with eCW’s inability to adapt to meet their own needs. For example, behavioral health providers at one center were unable to create a solution within eCW to track patients’ progress on 90-day treatment plans. These plans amount to a significant aspect of care for behavioral health patients, yet no clear functionality exists or has been created to incorporate plan progress data in eCW. Behavioral health providers have also had trouble scheduling individual providers for group treatment sessions.
Others indicated that eCW does not generally reflect the interconnectedness of medical and social service functions within centers. Staff working in other areas such as WIC and public benefits have had difficulty working with eCW, continuing to rely on standalone applications in some cases. One participant summarized saying, “Our staff are frustrated because eCW is really medical software.” While the medical focus of eCW has presented challenges for DCPCA members, panel participants suggested that staff in non-medical positions and specialty providers have not entirely rejected eCW. One participant noted, “Our case management and social work staff are living with it, but they are not entirely happy with it.”
Vendor support. Some participants noted difficulty in working with eCW throughout the implementation process. One health center representative indicated that the vendor had not been helpful in general, while others pointed specifically to the trainings conducted by eCW staff as problematic. Those who found eCW trainings lacking were glad to have the Cumberland Consulting available for additional trainings. One participant recognized deficiencies in working with eCW, but put them in a broader context, saying “In the whole scheme of EHRs, any vendor goes in there to make money, and they started out making these for hospitals. CHCs are unique because we provide free care. We have so many funding sources, each with their own requirements, and data fields are dependent on those requirements. There is no EHR out there that could meet all of our needs.”
Reporting functionality. Reporting was often raised by participants as a key difficulty in working with eCW. Participants noted difficulties in accessing reports on financial data, HIV positive patients and labs ordered. Generally, health center staff have found the reporting functionalities within eCW to be lacking in terms of user friendliness. Some attributed difficulties to a lack of experience and expertise on the part of health center staff and leadership, pointing to additional training as a possible solution. Others felt that eCW simply, “wasn’t good at reporting.” These participants pointed to difficulties scrubbing data and problems encountered by auditors and reviewers in working with eCW reports. DCPCA has taken steps to address some of these issues, hiring an additional staff person to build customized reports for things like Title X family planning funding.
Costs, Benefits and Sustainability
This section will provide an overview of financial commitments made by the DC government, DCPCA and its members. Returns on these investments and discussions of longer-term sustainability are also summarized.
Overview of approximate costs. The table below provides a summary of estimated costs of implementation as reported by DCPCA for an implementation involving approximately 1,100 users of both practice management and EHR. Notably, the soft costs associated with planning, implementation and training constituted $3.25M of the almost $5M in initial costs. Much of this cost went to consulting and professional services provided by DCPCA, Cumberland Consulting and eCW.
| Costs | Paid by | |
|---|---|---|
| Training (1,000-1,200 various staff) | $250,000 | DCPCA, with DC grant |
| Hardware | $1 million | DCPCA, with DC grant |
| Licensing | $650,000 | DCPCA, with DC grant |
| Planning | $500,000 | DCPCA, with DC grant |
| Implementation (including consultants) | $2.5 million | DCPCA, with DC grant |
| Total ongoing costs per year | $250,000 | Member centers (some goes to DCPCA for ongoing support) |
Return on investment. Health center representatives explained how implementing eCW has affected their finances and the types of returns they expect on their HIT investments. Some centers pointed to the requirement that all procedures be linked to a funding source, indicating that having such a requirement has changed their center’s business model and increased third party reimbursement significantly. Some participants noted efficiencies, with one representative indicating that documentation, which previously took providers 30 minutes, takes 10 minutes under eCW.
Another participant noted that electronic billing and eRx had increased efficiency at their clinic. Other participants were less sanguine, saying that necessary interactions and exchanges with non-electronic entities had limited increases in efficiency. Some indicated that anticipated savings in staffing had not been realized, saying, “We got rid of medical records people, but there’s still a huge need… You don’t need less people; they’re just doing different things. We overtaxed staff in making those changes.” Other participants noted that expected revenue increases and savings had not materialized, but remained hopeful that given more time savings and revenues would increase. DCPCA members have also experienced increased costs after implementing eCW. Health centers reported significant decreases in provider productivity, especially during training periods. Additionally, some centers have had to increase funding for IT support staff. One participant expressed skepticism in the overall sustainability of the DCPCA plan, saying, “These are costs that didn’t exist before, there is an increased cost going forward.”
DCPCA staff predicted that, over time, increased patient throughput, not staffing reductions, would cover the costs of eCW for its members. Additionally, DCPCA hopes to expand their EHR initiative to all health centers in DC. In their view, such an expansion would help to increase economies of scale and diminish individual centers’ ongoing costs.
Conclusions
Overall the findings from the meeting mirror some of the findings we have achieved on site visits to health center controlled networks for another part of the current project with training, implementation and converting to new billing processes being the principal challenges and areas of concern in the initial stages of an EHR implementation. DCPCA’s ability to provide more detailed cost information as it relates to their implementation allows us to demonstrate the importance of what are often called soft costs (non-hardware or software costs) in relation to the overall cost of implementation.
The DCPCA experience also demonstrates some of the challenges faced by primary care associations with very little prior involvement in IT to ramp up staff and work with members to create a successful implementation. One ongoing theme throughout the meeting was that having been through systems implementation with DCPCA and other providers, there is a much greater appreciation of each others “day to day lives” and a sense that over time this will lead to better coordination across the safety net in DC and more success with cross provider initiatives.
Another theme that ran across the meeting was a general sense of optimism that the eCW implementation, as supported by DCPCA, would lead to improvements over time. Most tangible improvements related to practice management functionality and billing in particular with providers that had previously not billed at all or comprehensively finding benefits from being able to track services and charges. As it relates to EHRs, even the discussants that reported having the greatest difficulty with implementation expressed the sense that EHRs are an essential means for doing their work at this time, did not see going back to paper as an option and felt that there would be tangible benefits to the new environment that would manifest over time.
San Francisco Community Clinic Consortium
Introduction
NORC at the University of Chicago is pleased to provide this site visit report from our recent visit to health centers and safety net health clinics in San Francisco, CA. This site visit was conducted as part of “Assessment of Health IT and Data Exchange in Safety Net Providers” a project sponsored by the Office of the Assistant Secretary for Planning and Evaluation ( ASPE) at the U.S. Department of Health and Human Services ( HHS). ASPE is conducting this project in close collaboration with the Health Resources and Services Administration ( HRSA).
As with other site visit reports produced as part of this project, we begin by presenting background information on health centers in San Francisco with a specific focus on clinics associated a network, the San Francisco Community Clinics Consortium (SFCCC). We then describe major health IT and data exchange activities taking place among safety net providers in the city and elaborate on opportunities and challenges associated with those activities. We end with a set of conclusions and issues to consider when drafting our final report.
Background on San Francisco and SFCCC
Eight community health centers founded SFCCC as a non-profit 501(c)(3) organization in 1987 to pursue a dual mission: to advocate for local community health center patients and reduce operating costs for centers through group purchasing. Since its start, SFCCC’s mission has expanded. According to its current mission statement, the consortium “develops programs and advocates for policies that increase access to community-based primary care for all San Franciscans, targeting the uninsured and underserved.”
Increasingly, SFCCC has focused on helping health centers access and leverage IT tools to improve their ability to coordinate care and improve quality. Among the IT initiatives that SFCCC supports in some form or another are the Lifetime Clinical Record (LCR) housed by the San Francisco Department of Public Health ( DPH), an eReferral system built through the LCR, an installation of i2iTracks chronic disease management system ( CDMS) and other initiatives. Beyond the initiatives supported directly through SFCCC, we also provide information on IT initiatives that are being pursued on an individual basis by clinics that are part of the consortium.
SFCCC employs 28 full time staff and 22 AmeriCorps VISTA volunteers and includes ten health centers or clinics (some are not FQHCs). SFCCC has established strong partnerships with the SF Department of Public Health ( DPH) as well as the major safety net hospital in San Francisco, SF General. The consortium serves an administrative role as the institutional grantee for the Ryan White Care Act and for the Health Care for the Homeless (HCH) program, subcontracting with eight partner health centers and the Department of Public Health. They also run a workforce development program, continuous quality improvement programs and disaster planning initiatives, and provide development, public relations, a policy program, some advocacy and lobbying at all levels of government. In total, SFCCC members serve roughly 65,000 patients each year and combined revenues exceed $33 million annually.
In general, SFCCC serves as a convener and forum for brainstorming for its members, creating ties between members through its work. Priorities for the consortium change across years. For example, the consortium focused on an eReferrals last year, but has since moved on to focus on supporting Healthy San Francisco, a county-wide program to manage information on eligibility and enrollment in public insurance or health care subsidization options. Other areas of involvement include quality improvement, technical assistance and EHR planning.
Exhibit 1 depicts how SFCCC is governed by a 10-member board (with two additional members emeriti). Board members are the Executive Directors (or equivalent) of the consortium’s 10 member health care providers. SFCCC members are diverse. Three members are Section 330 Health Centers, four are FQHC lookalikes, two are free clinics and one is an Indian Health Service Clinic. A number of these centers receive funding as faith-based initiatives. Others serve very specific populations such as lesbians and transgender individuals. In most cases, differences among members manifest themselves in different eligibility requirements and funding sources.
Exhibit 1: SFCCC Membership and Governance Model
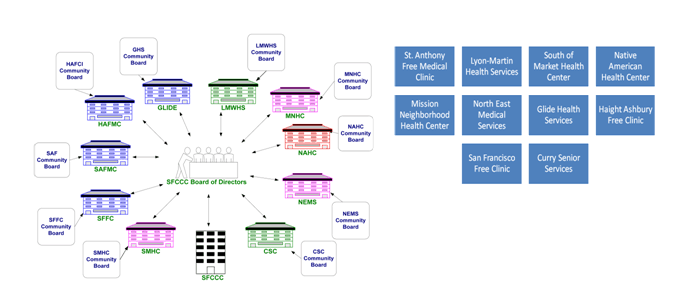
Governance and Membership
As depicted in Exhibit 1, SFCCC is governed by a 10-member board (with two additional members emeriti). Board members are the Executive Directors (or equivalent) of the consortium’s 10 member health care providers. SFCCC members are diverse. Three members are Section 330 Health Centers, four are FQHC lookalikes, two are free clinics and one is an Indian Health Service Clinic. A number of these centers receive funding as faith-based initiatives. Others serve very specific populations such as lesbians and transgender individuals. In most cases, differences among members manifest themselves in different eligibility requirements and funding sources.
NORC visited three SFCCC member health centers: Glide Health Services, South of Market Health Center and Lyon-Martin Health Services. Glide Health Services was founded in 1997 as a partnership between the Glide Foundation (a local faith-based organization), the University of California San Francisco School of Nursing and Catholic Healthcare West/Saint Francis Medical Center (a local hospital). Glide is a nurse practitioner-managed primary health care teaching clinic serving roughly 6,000 patients each year. Glide largely serves homeless patients and patients with HIV/AIDS and serves as the health care service provider for HRSA HCH and Ryan White Care Act grants that are administered by SFCCC.
South of Market Health Center is a health center, serving the South of Market and Tenderloin neighborhoods. Founded in 1973, South of Market has grown to provide comprehensive dental care and primary care at two health center sites. The center serves roughly 5,000 patients annually, 60 percent of whom are homeless and uninsured. Roughly 40 percent of the centers funding comes from the federal government while the remaining 60 percent comes from third party payers and Medi-Cal reimbursement. Overall 73 percent of SMHC patients are uninsured, 17 percent are on Medi-Cal and 10 percent are Medicare beneficiaries.
Lyon-Martin Health Services was founded in 1979 by volunteers who saw a need for a provider to meet the needs of lesbians who had experienced discrimination in other health care settings. Originally a research project sponsored by UCSF and San Francisco General Hospital, Lyon-Martin services roughly 2,400 patients, 80-90 percent of whom are uninsured. Services include primary care, behavioral health, gynecology services, services for HIV positive women and services for transgender individuals. The center employs a medical director (another physician sees patients on a volunteer basis), a physician’s assistant, four medical assistants, four front desk workers, and various other staff. The center’s budget totals roughly $1 million, split into three roughly equal parts: government funding, reimbursement and development.
IT Functions Supported by SFCCC
San Francisco City (and county) is a particularly interesting case study to learn about health IT and the safety net. Aside from SFCCC members, a number of other organizations provide care for the underserved in San Francisco. Section 17000 of the California state code mandates that counties provide care for indigent residents. Thus, the SF DPH runs individual safety net health care sites around the city. Other providers, including Magic Johnson Clinics, also provide for the underserved in the area. Outside of primary care, San Francisco General Hospital (“General”) provides inpatient care for many of the underserved in the area.
As noted above, SFCCC works in close collaboration with other entities in the city on IT issues. Though many of the systems efforts originate through SF DPH, SFCCC serves as a primary driver for health IT in San Francisco and among its members. In addition, SFCCC facilitates quality improvement initiatives, provides support services in the areas of IT technical assistance and advocacy and helps secure grant funds for its members. SFCCC hosts and supports a number of IT applications, each with a specific use and purpose. Exhibit 2 below presents major IT community-wide applications currently being employed by safety net health centers in San Francisco.
Exhibit 2: Community-Wide Health IT Applications
Other applications are specific to health center members. These include the HIV/AIDS patient registry for Ryan White Patients (CareWare), Preventing Heart Attacks and Stroke Everyday (PHASE) registry sponsored by Kaiser Permanente and other population specific applications. Most clinics and health centers also have electronic practice management systems (PMS) and some have adopted electronic health records (EHRs). EHRs currently in use include: NextGen (at North East Medical Services) and Centricity (joint EHR/PMS at Glide Health Services). SFCCC PMS applications include HealthPro (South of Market Health Center) and Misys (Lyon-Martin Health Services).
Key Findings from Discussions with Health Centers and Consortium
SFCCC differs from some of the other site visit networks in that it has facilitated health IT implementation and planning, but does not host EHRs or PM systems. Instead, SFCCC has promoted quality and efficiency improvement tools such as eReferrals, i2iTracks and greater access to existing systems like DPH’s Siemens Lifetime Clinical Record (LCR). SFCCC also works in conjunction with city and county officials on the use of applications such as One-e-App as part of Healthy San Francisco. Several factors led health centers to pursue i2iTracks, including the fact that more were joining disease collaboratives, more health centers were planning to do quality improvement at the center level and centers were looking to have data to compare themselves to national standards.
Health centers also articulated a number of motivations for pursuing IT including their existing systems and EHRs. Glide Health Services is one of a minority of SFCCC members that has implemented an EHR. In describing their motivation, health center leaders indicated that they had always been early adopters and that impending pay for performance changes require access to data through an EHR. South of Market Health Center is waiting to pursue an EHR until they move into a new clinic facility. Lyon-Martin Health Services has not implemented an EHR, but indicated that patient recruitment could be affected by not having an EHR in the future. Lyon-Martin’s Executive Director sees an EHR as a way to improve reporting and would most likely stay with their existing PM system rather than adopting a joint EHR/PMS to reduce costs. Finally, health centers did cite new incentives for EHR adoption as a result of the American Recovery and Reinvestment Act (ARRA) though they acknowledged a limited understanding of the nature of those incentives at the time of our site visit.
Motivation at the network level
SFCCC indicated that its IT initiatives are based on needs articulated by member clinics. For example, SFCCC members had difficulty accessing and reading specialty provider reports and progress notes. That led to increased cooperation and eventual access to the LCR and the implementation of eReferral. The LCR serves as a single, primary care record for all care received at DPH clinics and at SF General Hospital. Access to this record by SFCCC clinics provided those clinics access to laboratory results, discharge summaries, visits outcomes, and information on visits to DPH clinics.
In addition, SFCCC leaders saw a need for disease registry software after the retirement of CDEMS and PECS. SFCCC leaders cite reporting mandates from the Accelerating Quality Improvement through Collaboration (AQIC) initiative in California, HRSA Uniform Data System (UDS), California’s Office of State Health Planning and Development (OSHPD) and HRSA/BPHC along with increased attention to network-wide reporting in SFCCC’s strategic plan as reasons for pursuing i2i Tracks at the consortium level. i2i Tracks is a chronic disease management system tool that uses interfaces to generate registries and reports to track care and improve quality for specific panels of patients. SFCCC saw i2i Tracks as necessary to fill in where EHRs were lacking. Specifically, SFCCC envisioned i2i Tracks as a point of care tool for specific groups of patients (e.g. diabetics) in centers that could handle changes in workflow and as a reporting tool to make better use of aggregate data in EHR systems without having to rely on ad hoc reports.
Current Status of IT Use
The applications described above vary in spread and use across SFCCC clinics. Individual health center characteristics contribute to differing levels of health IT use. For instance, one center is waiting to implement an EMR/PMS until it moves to a new location. Some health centers are involved with external funders and care for specific patient groups, leading them to use various health information systems. While implementation and usage differ across health centers, information on current use of each of these applications (and the programs they are affiliated with) is provided below.
One-e-App. One-e-App is a web-based application used by safety net clinics and health centers to determine eligibility for and enroll patients in Healthy San Francisco, a county-program to subsidize health care for low income residents of San Francisco. As of March, 2009 One-e-App could also be used to determine eligibility for and enroll patients in Medi-Cal. One-e-App includes a one way interface with the State Department of Human Services to submit Medi-Cal applications. Once submitted applications are reviewed by state employees and a final eligibility determination is made within 45 days. Healthy San Francisco eligibility is more direct and certified application agents (CAAs) receive eligibility decisions within ten seconds via the One-e-App website.
In determining eligibility, One-e-App collects demographic information such as family size, address and income. These data are transmitted to the vendor host in Sacramento (the Center to Promote Health Care Access) that stores the data in separate databases by county. Counties across California use One-e-App to determine eligibility for and enroll residents in public health care insurance programs SFCCC member centers have hired additional front desk staff to work as application agents for Healthy San Francisco, using the One-e-App application. In some cases, the county has funded these positions, but in most cases health centers provide funding for application agents. Some centers have made changes to their health centers’ physical layout to ensure some privacy for application agents and patients discussing income and other potentially sensitive topics. Technical support for One-e-App comes from a number of resources including DPH, the San Francisco Health Plan, the Center and individual health centers themselves.
While health centers understood and valued One-e-App as a resource, they did note some missed opportunities associated with using it. For example, the application is not interfaced with health center applications and reports from the One-e-App database are not available or accessible to SFCCC clinics. Several individuals noted that because it is increasingly used as a way to check eligibility for low income San Franciscans, One-e-App has come to represent a “safety net” master patient index that, if integrated with the LCR and EHR databases, could serve a critical role in facilitating health information exchange.
LCR/Invision. As noted above, SF DPH maintains its own electronic Lifetime Clinical Record (LCR). The LCR is hosted in Pennsylvania by Siemens and operates on their Invision platform. DPH implemented the LCR as its primary record over 20 years ago. Today, various partners including local hospitals, health centers, the Department of Housing and the county jail system have access to the LCR. In the time since its inception, the LCR has come to serve as a shared, but limited, medical record between San Francisco General, DPH health centers and SFCCC health centers. The LCR houses patient data including registration information, lab, pharmacy, radiology and diagnostic data.
While DPH regulation requires their clinics to use the LCR to comprehensively record care delivery, SFCCC health centers use the LCR in a far more limited manner. SFCCC health center providers have the ability to add progress notes to the LCR, create LCR identification numbers (“B numbers”) for SFCCC patients and access specialty provider progress notes. In some cases, SFCCC health centers task AmeriCorps VISTA volunteers with entering patient information into the LCR. Some centers have moved to integrate the LCR into their operations, changing their patient ID numbers to reflect the “B numbers” used in the LCR system. The LCR does not interface with other systems, including One-e-App, practice management systems and EHRs. This is because the LCR was meant to serve DPH’s needs and has only come to accommodate external viewing and editing after lengthy negotiations between UCSF, the city attorney and others. The LCR does, however, interface with the SFCCC installation of i2i Tracks described below.
i2i Tracks. Many SFCCC members have implemented a disease registry program called i2i Tracks. They initially obtained access to the system through a grant sponsored by Kaiser Permanente. I2i Tracks is a population health management tool used to track care processes and outcomes for patients with specific diseases and conditions. SFCCC members all have access to i2i Tracks, but not all of them use it. Those that do, use the program to track patients with diabetes, cardiovascular disease, asthma and hepatitis C. Some plan to expand their usage to other conditions including chronic pain and HIV.
Typically, i2i Tracks is installed at a health center and is populated through interfaces with laboratory and practice management systems being used at that health center. Because the Kaiser Permanente grant did not allow for individual health centers to obtain their own i2i Tracks license, the application is centrally administered by SFCCC and is populated through the LCR. While this is a cost effective approach and could allow for comparisons across health centers and benchmarking at a community level, it does raise important workflow challenges.
First, because SFCCC sites are not required to use the LCR to enter data on visits or procedures, many of them are doing so for the first time in order to take advantage of i2i Tracks. Over the last year, SFCCC has put considerable effort into establishing consistent coding and data entry practices across SFCCC clinics so that data entered into the LCR appropriate for tracking in i2i. Because considerable new data entry is required, there has been extensive use of Vista and AmeriCorps volunteers to assist with these activities.
SFCCC centers have used i2i Tracks to varying degrees. Most see i2i Tracks as a useful tool for population health management, especially its reporting features. Some centers staple printouts from i2i Tracks into their paper patient records and use additional copies to educate patients about their health status. Additionally, some centers use the “to do list” section of patient printouts to direct medical assistants and future patient visits. This has proven successful in at least one case, with center leaders indicating that under i2i “things just get done.”
While i2i Tracks has proven useful for SFCCC members, some changes have been made to the product. For instance, some additional fields have been pulled over from the LCR and SFCCC has successfully lobbied the vendor to create patient summary reports for i2i Tracks. Additionally, some centers have recoded certain data elements (including making dummy codes) to improve reporting including diabetes, asthma and homelessness. Using i2i Tracks at the point of care has proven problematic as some providers come to see i2i Tracks as an EMR, though it is much more limited in functionality and purpose. A central challenge for SFCCC’s quality team has been to work with member clinics to enter data into the LCR in a manner that would allow their full panel of diabetic patients to be tracked in i2i. the graphic below demonstrates the progress they have achieved over the last year and the varying abilities of different clinics to achieve the 100 pct objective over a specific timeframe.
Exhibit 3 is a diagram depicting the tracking of Diabetics using i2i Tracks in San Francisco from May 2007 and May 2008. The markets targeted are South of Market, San Francisco Free Clinic, St. Anthony's, Native American, Mission, Lyon-Martin, Glide and Curry.
Exhibit 3: Tracking Diabetics using i2i Tracks in San Francisco[1]
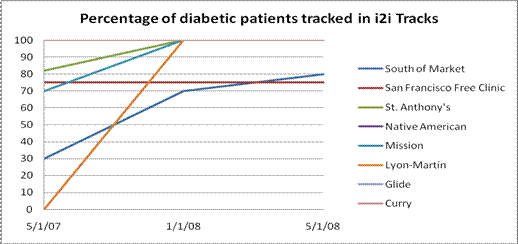
Note: Clinics that achieve 100% remained at that level through May 2008 [SFCCC, please confirm]
eReferral. The eReferral application currently in use by SFCCC clinics was created by a physician at a San Francisco specialty clinic roughly five years ago to improve communication between health centers and specialty clinics. SFCCC staff describe it as a basic email application “dropped on top of” the LCR that allows SFCCC clinicians to transmit orders for specific patients to area specialists electronically. Providers access eReferral through the LCR and use it for a number of procedures and referrals, including breast evaluations, cardiology, colonoscopies, endocrinology, gastroenterology, neurology, neurosurgery, neurotrauma, orthopedic surgery, podiatry, MRIs, respite care, rheumatology, sleep studies, urology and home health. Providers can send their interpretations of tests and initial findings via eReferral as well. Providers have seen a marked improvement over the previous system of faxing referrals. The application also sends reminders to specialists for overdue referrals and includes decision support to alert SFCCC clinicians of potentially inappropriate referrals.
Exhibit 4 is a graph chart depicting the effects of eReferrals on Key Measures. The variables are Time spent submitting, Access for urgent issues, Wait time for new appt, Access for non-urgent referrals, Guiding pre-visit work up, Ability to track referrals. Based on a scale of 0 to 100%. The green shows Better, the orange showing No difference and white depicting worse.
Exhibit 4: Effect of eReferrals on Key Measures
Electronic health records. Some SFCCC health centers have implemented EHRs, while the majority has not. NEMS is migrating to NextGen and Glide Health Services has been paperless on Centricity since September 2008. In most cases, however, health centers are waiting to either see which products the San Francisco safety net coalesces around or to move to new facilities. Glide Health Services has worked with the Alliance of Chicago to implement Centricity. They used nursing students to preload data into the system in June and July of 2008. Since implementing, Glide has experienced significant reporting difficulties, most notably in counting homeless patients on their UDS report.
In addressing this problem, Glide sought the advice of the Alliance of Chicago rather than SFCCC as the Consortium does not provide support for the GE system. In working with the Alliance, Glide realized that updates to the system had caused patients that were homeless only part of the year to not be listed as homeless at all. This type of error could have drastic consequences for a health center like Glide that relies on accurate reporting for specific patient groups to maintain grant funding.
Other health centers that have not implemented EHRs are looking to SFCCC and other area providers for guidance. South of Market Health Center is in the midst of planning and constructing a new clinic facility. They are 18 months from completion and hope to include EHR requirements in the physical design and layout of the facility. Lyon-Martin Health Services is a relatively small health center. They have left the possibility of going to an EHR open in a recent move to a new PMS, but are unsure if they would be able to support an EHR given their small size and limited resources.
Practice management system. Similarly, SFCCC centers have chosen various PMS applications. Glide Health Services uses a joint Centricity EHR/PMS. South of Market uses HealthPro from Sage, having recently updated from HealthPro Legacy to HealthPro Excel. Lyon-Martin used a 2007 grant from the California State Treasurer to implement Allscripts (Misys) Tiger and install computers with the PMS in every exam room. Because some patients are not in the LCR and Lyon-Martin does not have an EHR, the center relies on the PMS for certain functions like reminders and reporting. As with EHRs, SFCCC has not decided to support any one PMS application.
Findings: HIE and Interfaces
The Consortium’s many partners and applications have led to a concerted effort to link systems and partners whenever possible. SFCCC and DPH have been funded by organizations like the Tides Foundation Community Clinic Initiative, Kaiser Permanente, federal programs and others to maintain connectivity between systems. I2i Tracks which is hosted at SFCCC gets demographic and diagnostic data from the LCR. This one-way interface only allows updates to demographic data from the LCR. Lab data are also dropped into i2iTracks through a real-time HL7 lab interface with all SF General labs and public health labs that have numeric results. Another interface between additional external data sources and i2i is in development. One SFCCC health center characterized i2i Tracks as a “form of health exchange” and called it a good idea.
Labs are also fed into the LCR, from private clinical labs as well as DPH and San Francisco General. An OpenLink data aggregator maintained by the county unduplicates data, matches data to individual patients and feeds that into the LCR. Despite this, the LCR remains a relatively closed system from the perspective of some SFCCC clinics. SFCCC members expressed some frustration with not being able to interface their practice management systems or One-e-App with the LCR. One-e-App transfers non-health related demographic and eligibility information between SFCCC centers and the State Department of Human Services by way of the Center to Promote Health Care Access in Sacramento. While most SFCCC centers have been able to exchange lab data with San Francisco General, others have existing relationships with other lab providers that are not at that point.
For example, Glide Health Services relies on St. Francis Medical Center for their patients’ labs. St. Francis is part of Catholic Health Care West which uses a Perot Systems application. They have worked to develop an HL7 interface with Glide, but budget constraints have delayed that effort. Others use Quest Care360 to access lab results in a web-based system that is not integrated with any of their own applications. In the future, SFCCC and its members hope to expand upon its HIE efforts. Currently, SFCCC is looking to create a fiber optic network for the safety net in San Francisco to address connectivity issues and connect safety net providers more directly. Others have expressed interest in e-prescribing and generally increasing access to other providers’ information systems.
Enablers and Barriers to Health IT Adoption
In this section we review specific barriers and enablers to health IT adoption and information exchange among safety net providers in San Francisco. We begin with enablers.
Funding. SFCCC and its members have benefited enormously from private funding sources, primarily foundations, in the acquisition of IT systems. Funders include: Kaiser Permanente, Tides Foundation, California Endowment Foundation, CalRHIO (funded by Blue Shield of California Foundation), California Wellness Foundation, California Pacific Medical Center, St. Luke’s Hospital and Foundation, San Francisco Foundation, Cisco, Wells Fargo, McKesson, Chiron and various other foundations. These grants have been integral in bringing new applications to SFCCC and its members and facilitating ongoing collaboration with DPH, the state Medi-Cal office, UCSF and the San Francisco Health Plan.
SFCCC leadership. SFCCC has also provided valuable leadership on key health IT issues for its members. Their advocacy efforts have shaped policy at all levels of government and have proven especially successful when collaborating with other CHC networks in the state [NEED EXAMPLES]. They have also been able to pull SFCCC members together to address common issues, including health IT. While the consortium has had a relatively limited role in directing individual centers’ health IT decisions, they have offered specific applications like i2i Tracks and eReferrals and will continue to facilitate discussions about more shared applications (including the possibility of an EHR) in the future. SFCCC also offers staff resources to its members to handle issues like continuous quality improvement and technical support. These are functions that may be too expensive for some centers to devote full FTEs to. This has proven especially helpful for health centers that have little experience or capacity in the area of health IT.
DPH collaboration/ Healthy San Francisco impetus. Ongoing collaboration between SFCCC and DPH, especially around Healthy San Francisco has made for successful health IT adoption. In the past, DPH and SFCCC saw each other as separate entities. DPH had no compelling reason to be interested in SFCCC centers. With SFCCC’s help, member centers now have read and write access to DPH’s LCR system. Use of i2i Tracks has cemented this collaboration. Finally, by serving as an active partner with the State on Healthy San Francisco and One-e-App, SFCCC has forged a strong bond with the Medi-Cal office as well. Without these successful collaborations, health IT efforts would be more fragmented and less useful for SFCCC members.
Despite the enablers listed above, a number of barriers have prevented SFCCC and its members from further health IT adoption. While SFCCC has exerted leadership and found common funding opportunities for its members, SFCCC health centers have also pursued many opportunities on their own. For example, SFCCC centers use 10 different practice management systems, making the prospect of moving toward a shared EHR all the more difficult.
Varied center missions. While they occupy the same general space, SFCCC centers’ missions and patient populations differ widely. This has become a point of contention in standardizing data elements across health centers and with other partners. For example, Lyon-Martin may need to list transgendered individuals on their systems, but other health centers or partners may not see the need to build in this functionality. These kinds of individual needs and the fact that many SFCCC members are not FQHCs make shared health IT more difficult.
Infrastructure Problems. One of the biggest barriers for SFCCC members involved connectivity and infrastructure problems. The LCR system was built on a network architecture over 20 years ago that was intended for use only by DPH and was not meant to handle large data files. SFCCC noted that the LCR in its current form had exceeded electrical capacity at its server farm, signaling significant overuse. Health centers visited by NORC had problems accessing the LCR and were often booted from it.
In addition, health centers adopting EHRs, such as Glide, are finding that their connectivity and physical environment is not conducive to adopting advanced IT applications. Infrastructure problems have slowed the system to a high degree, causing extensive frustration among Glide staff members. Also, SFCCC leadership acknowledged that connectivity through traditional means is difficult in San Francisco due to extensive Internet traffic and an aging infrastructure. They noted that they are working on securing funding to establish a new fiber optic network dedicated to safety net health care computing in the city.
Anticipated and unanticipated costs of implementation and participation in community programs. As in many other cases, cost remains a significant barrier for SFCCC centers both in terms of adoption of their own systems and for participation in community-wide initiatives. Glide Health Services, which has implemented Centricity, indicated that they had seen large drops in productivity resulting in higher costs of care reported in their UDS. Additionally, Glide has had to train volunteers and many nursing students on the system, amounting to a significant investment of time and increasing the number of necessary licenses for the center beyond what they had originally anticipated. SFCCC centers have also experienced increased costs in working with Healthy San Francisco and One-e-App. While these centers are reimbursed for care provided to Healthy San Francisco patients, One-e-App eligibility workers are generally funded by individual health centers. South of Market and Lyon-Martin both cited costs as one of the primary reasons they had not already implemented EHRs.
Duplication. While SFCCC members enjoy access to various information systems, using these systems can be frustrating in some cases. Many SFCCC health center leaders explained that there is little communication between the LCR, centers’ practice management systems and EHRs, i2i Tracks and One-e-App. This means that information could be different for a single patient between these systems (e.g. outdated address or vaccination records) and health center staff must often take it upon themselves to reenter the same data in 3-4 different systems. Signing in to each of these systems and ensuring adequate access to computer terminals can also be time consuming and difficult. Some mentioned an OpenLink data aggregator to sort through duplicate data, but in many cases data reconciliation becomes the responsibility of SFCCC members and staff. Without rigorous efforts in this area, health IT systems could become inaccurate, resulting in lower provider trust and usage.
Conclusions
As usual, we end this report with conclusions from this site visit that may relate to broader themes to be explored in this project.
Chronic disease management system v. EHRs. SFCCC members have generally not implemented EHRs and many of them have looked to other applications to perform the functions typically done by an EHR. i2i Tracks specifically has filled in gaps for SFCCC members, with its progress note functionality, population health management tools and patient printouts. Still, some providers have had their appetites whetted for health IT with their initial use of i2i Tracks, the LCR and practice management systems. Some providers are looking for an application to use at the point of care to tell them about the patient in front of them. Still, i2i Tracks may be a cost effective solution, especially for small centers like Lyon-Martin that cater to a very specific population.
Multiple sources of funding create opportunities and challenges. Respondents in San Francisco were quick to cite the many generous funding opportunities that are available to them through corporations, charitable foundations and local government. We did notice less of a reliance on federal funding in California relative to other site visits. However, we also noted that multiple sources of funding are sometimes in competition with each other to fund similar interventions and that there is potential for systems based initiatives to get established in parallel rather than in conjunction with other similar efforts.
For example, the i2i Tracks implementation being sponsored by the Community Clinics Initiative in Alameda County and elsewhere in the state, would have allowed SFCCC sites the ability to implement i2i at the health center-level, however they were not eligible for that program because they already had access to i2i (albeit not at a health center level) through a Kaiser Permanente grant to SFCCC. Also, even government sponsored efforts such as LCR and One-e-App are not usually integrated or interfaced effectively.
A single network’s reach is limited in some cities. Although SFCCC has an impressive reach in San Francisco, it is clear that its members make up one pocket of a very complex safety net with a range of institutional relationships. The site visit to San Francisco illustrates the complexity of the safety net in some cities and the inability of a single consortium or network to serve as an umbrella for all safety net IT efforts. SFCCC’s approach has been to work collaboratively with any provider that requires assistance and look for ways to leverage advances made by others such as the DPH in furthering their mission. This does result in some confusing relationships and overlapping responsibilities, but is ultimately seen as a reality of supporting safety net initiatives in this setting.
Very difficult to understand costs and benefits. Perhaps because of the multiple sources of charitable funding and perhaps because many of them are not accustomed to reporting on operations as FQHCs, the clinics that we visited in San Francisco were not able to give us a solid understanding of their total spending on health IT initiatives or the returns they were expecting. In terms of QI returns from IT, most providers we spoke with were focused on process outcomes such as increasing the number of individuals tracked as part of their disease specific registries and establishing baseline data on process measures relevant to key populations such as diabetics. Providers were able to comment on the improvements afforded by access to the LCR, eReferral and One-e-App systems, but these benefits focused on improved efficiency and convenience in accessing necessary information rather than clinical improvements.
[1] Diagram provided by SFCCC in Spring of 2009.
[2] Diagram provided by SFCCC in Spring of 2009.
Community Health Center Network
Introduction
The National Opinion Research Center (NORC) is pleased to present this report detailing findings from our recent site visit to Alameda County, California for the “Assessment of Health IT and Data Exchange in Safety Net Providers.” NORC conducted this site visit under contract with the Office of the Assistant Secretary for Planning and Evaluation (ASPE) at the U.S. Department of Health and Human Services (HHS). The Health Resources and Services Administration (HRSA) worked in conjunction with ASPE to guide activities under this project.
This report summarizes the experience of health centers working with the Community Health Center Network (CHCN) to use and maintain a range of systems for administration and quality improvement. While in the Bay Area we also visited the San Francisco Community Clinic Consortium (SFCCC) and findings from that visit are detailed in a separate report.
The report is organized as follows:
Background and Methods. This section provides a profile of CHCN and the three member health centers we met with during our visit. These centers include Tri-City Health, LifeLong Medical Care and Axis Community Health. In additional, an overview of the methods used to organize and conduct this site visit can be found in this section.
Network Level Findings. This section provides an introduction to the portfolio of services that CHCN provides and a look into their activities surrounding their applications. These applications include an automated disease registry system called i2i Tracks, an application for managed health care operations called EZ-Cap, and a county-level eligibility screening program called One-E-App, various practice management systems (PMS), e-referral system, a case management system known as Altruista and clinical data access with the local safety net hospitals.
Health Center Level Findings. This section looks at the health IT applications being used at each health center for administrative and clinical quality improvement (QI) and the role CHCN plays in supporting each.
EHRs and the Future of CHCN. This section provides some preliminary conclusions from the site visit relating to the function of CHN, health center experiences and future directions, particularly in light of a new emphasis on EHR adoption following passage of the American Recovery and Reconstruction Act of 2009 (ARRA).
Background and Methods
As with other site visits conducted for this project, preparation for the visit began approximately one month prior to the in-person meetings with initial telephone conversations with CHCN leadership. These initial conversations were conducted to share the aims of the site visit, obtain agreement from network leadership to participate in the site visit, discuss potential discussants for the in-person meetings and set a date for the in-person meetings. Following these initial telephone conversations, we revised background materials, developed detailed agendas for each meeting and set appointments with clinical, administrative and IT leadership from across CHCN member health centers in and nearby Alameda County.
The site visits themselves took place on the week of March 9, 2009. We deployed one two-person team to conduct meetings with three health centers as well as CHCN’s executive staff. For each meeting, we prepared materials that outlined our preliminary knowledge of the discussant organization and highlighted outstanding questions to address during the in-person discussion. Having two team members at each meeting allowed us to have one individual dedicated to taking notes and documenting the content from the meeting while the other focused on assuring that the goals of each meeting were being addressed through engagement with the participants. Finally, after concluding the site visit, we conducted an additional telephone meeting with CHCN’s CEO, Ralph Silber, to follow-up on some of the findings from the health center discussions and explore priorities and future direction for the network.
CHCN Network Profile. The Community Health Center Network of Alameda County, CA was formed in 1996, largely response to rapid expansion of managed care in California. CHCN was established out of the Alameda Health Consortium (AHC), an entity that serves as a primary care association for Alameda County. The network’s seven member clinics came together and formed CHCN in order to facilitate their member clinics’ participation in California’s safety net managed care system.
To serve its primary purpose, CHCN began operations as a managed care management services organization or MSO establishing “at risk” contracts on behalf of member health centers with three MediCal health maintenance organizations (HMOs). The network still maintains these contracts and offers managed care services including all claims adjudication, capitation distribution, membership reports, quality improvement, utilization management, financial and encounter data reporting and HMO contracting for its member health centers. To facilitate reporting, CHCN maintains a data warehouse that holds claims, labs, pharmacy, and hospital visit data for all of CHCN’s managed care patients as well as outpatient claims and clinical laboratory data for all patients seen by CHCN’s member clinics.
After building capacity to operate functions associated with a typical MSO, CHCN began offering practice management, business operations, quality improvement and information systems in response to the needs of network members. For example, CHCN employs a network-wide medical director who coordinates chronic disease management programs focusing on diabetes, asthma, and cardiovascular health. In the QI role, CHCN led its member health centers in an effort to apply for a Tides Foundation grant and to implement i2i Tracks. CHCN is also implementing for its managed care patients, an advanced case management system using an application called Altruista. Increasingly, CHCN plans to create and support options for health center adoption of electronic health records (EHRs).
CHCN member health centers include: Asian Health Services, Axis Community Health, La Clinica de La Raza, LifeLong Medical Care, Native American Health Center, Tiburcio Vasquez Health Center, and Tri-City Health Center. As of July 2009, West Oakland Health Council has joined CHCN. These health centers provide services in more than 29 locations throughout the East Bay. CHCN centers are located in a range of settings from urban (Oakland, Berkley) to suburban (Fremont) and “small city” locations (Pleasanton). The NORC team visited three CHCN health centers, LifeLong Medical Care, Axis Community Health and Tri-City Health Center, located in Berkley, Pleasanton and Fremont respectively.
CHCN’s health centers provide medical care to a diverse population and use over 25 different languages in delivering health care and outreach services. Combined, CHCN’s health centers serve 164,717 patients with 647,055 annual encounters. These visits include over 400,000 general medical visits, over 36,000 prenatal visits and just fewer than 55,000 dental visits each year. The vast majority of their patients are uninsured or on Medicare, Medicaid or CHIP. Approximately 40 percent of patients seen in CHCN centers report to be of Hispanic ethnicity, 20 percent each report to be African American and Asian Pacific Islander and 4 percent Native American7.
Tri-City Health Center Profile. In the early 1970’s Tri-City Health Center (TCHC) first opened as a women's health clinic, offering family planning health services and pregnancy counseling. They have had section 330 funding for nearly (if they opened in the 70’s) 40 years and over the last couple of years have almost tripled in size. TCHC serves a 150 square mile radius in Southern Alameda County. In 2007 TCHC’s clinics provided services for over 19,000 patients with more than 70,000 yearly visits. Seventy-seven percent of their patients are below the poverty level, and 67% of patients who visit the clinic are uninsured. Overall they serve a relatively young population with only 3 to 5 percent seeking geriatric care.
In addition to primary care, TCHC offers some specialty care programs including dental services for all ages. They also maintain an HIV treatment facility that is the second largest in the area and provide a range of social support and wellness services to complement their healthcare program. Their management structure includes a board of directors, an executive director, quality director, chief financial officer, development director, medical director, chief operating officer, human resources director and chief information officer.
LifeLong Medical Profile. LifeLong Medical Care was formed in 1996 as a merger between two clinics with deep community roots in Berkeley. One clinic had focused on care for older Americans and another focused on pre-natal care for low income women. Since the merger, they have grown to include five medical clinics, a dental clinic, an adult day health center for elders with complex care needs and a supportive housing program for formerly homeless adults.
Their mission is to provide health and social service programs to improve access to care for the underserved and improve population health. LifeLong provides primary care, mental health and case management programs. LifeLong is known as the primary safety net provider of medical services to the uninsured and those with complex health needs and due to its origins cares for a greater elderly population than its counterparts. Lifelong concentrates its activities in Berkley where 5 of its sites are located. Outside of Berkley Lifelong has sites in Oakland, Albany and Emeryville. In 2007, LifeLong provided approximately 115,000 primary care visits to over 18,000 people.
Typical of many health centers, LifeLong is managed by a Board of Directors and directly led by an executive director, chief financial officer and chief medical officer. They also have a QI director and IT director. LifeLong employs 100 full time equivalents (FTEs) providing care as licensed medical providers. Their IT department employs six FTEs. Overall they employ about 430 staff members at about 340 FTEs. Their QI department includes a clinical measures committee, a chronic care management committee and a clinical planning committee. These committees are comprised of the medical director other clinicians and the QI director and are staffed by three FTE AmeriCorps volunteers.
Axis Health Services Profile. Axis Community Health began in 1972 in Pleasanton, CA as a health center for low income children in far eastern Alameda County who had no other access to health care. Over the past thirty years Axis has grown to include medical care for all ages. They have added mental health counseling services, addiction recovery programs, court-ordered courses, a WIC nutrition program, and school and community-based health education services. A week prior to NORC’s visit to the Bay Area Axis received word that they will become a federally funded health center beginning immediately as part of ARRA infrastructure funding.
Axis’ patients come from a large geographical area. Because they are the only safety net provider in their region, they receive all of the uninsured patients and Medicaid patients in their service area of about 108 square miles. They have four sites, one exclusively for nutrition services, one focused only on behavioral health and two others that provide medical and mental health services. To meet new requirements for being funded by HRSA, Axis reported needing to increase their business by approximately 40 percent.
Axis employs a staff of 60 FTEs that include physicians, nurses, mental health professionals, drug and alcohol counselors, registered dieticians, health educators and a variety of support personnel. Axis also has an intern program for post-master's level mental health professionals. Their staff provides services in a variety of languages. At the executive level they employ a chief executive officer, medical director, chief financial officer, development director and IT director.
Network Level Findings
In discussions on their role in the area of information systems, CHCN emphasizes QI activities and seeks to find the optimal intersection of QI and IT. CHCN’s role has included providing assistance to the selection, contracting and implementation of day to day applications such as practice management systems (PMS’) being used at health centers and automated interfaces with clinical laboratories. They currently play a particularly active role in the ongoing installations of i2i Tracks for chronic disease management in their member health centers. They also maintain an application called EZ-Cap which is used for the network’s Medicaid managed care and CHIP patients, together which are approximately 20-30% of each clinic’s patient population. EZ-Cap processes member eligibility, claims, payments, tracks detailed data on utilization, and supplies reports and analyses on managed care patients. Finally, they help coordinate the use of the county hospital based e-referral system, and a system which connects their health centers to county hospital inpatient, emergency, and specialty care clinical information.
CHCN does not host any of the applications utilized by member health centers. However, CHCN’s data warehouse pools data from a variety of applications including all encounter data from health center PMS systems, and all lab results; hospital, pharmacy and ED claims for managed care patients, and (very soon) i2i Tracks. In the sections below we highlight CHCN's role as it relates to each of these information tools.
i2i Tracks. i2i Tracks is a chronic disease management application that pulls data from existing health center systems such as PMS’ as well as clinical laboratories to establish panels of patients with specific characteristics and tracks care delivery and clinical results variables associated with each panel. It serves the function that registries such as PECS and CV DEMS, which function as chronic disease database applications that track quality of care using a system of computer and paper based tracking tools and act as a tool for providers at the point-of-care. But i2i uses automated interfaces instead of manual data entry and analysis as a means to define panels, track measures, and act as a point of care tool. i2i provides advanced functionality such as the ability to define new panels “on the fly” and integrate with mail merges to generate reminder mailings or telephone calls with a subset of patients.
Upon our meeting with CHCN four of their centers had begun the process of implementing i2i. The grant from Tides is covering approximately half of the full cost of the i2i implementation in these health centers. CHCN’s role in the i2i Tracks project includes assistance in contracting and project managing the implementation with local clinic teams. This role has involved convening a learning community with others in the Alameda County to share “best practices’ in the implementation and use of the i2iTracks systems. All the major safety net providers, including the county medical center have adopted i2iTracks. Moreover, CHCN has helped their health centers standardize definitions for chronic conditions. For example, in order to examine diabetes across the entire universe of health centers came to agreement on shared indicators such as frequency of testing for A1C levels as well as how to define and code basic measures such as height, weight and blood pressure.
CHCN is also helping health centers adjust documentation practices to support robust use of i2i Tracks. For example, because there is a greater need for consistent and comprehensive documentation of intake information including chief complaint, some health centers are working with their medical assistants to re-work their process for entering these data into PMS’. Specifically, CHCN has helped “re-work” centers’ intake and billing forms that are used by health center staff to improve data quality. They have also worked with health centers to assure that clinicians and coders record care processes such as “conduct of foot exams” that are sometimes overlooked in documentation.
Given the incentives laid out in ARRA, it is likely that member health centers will look to implement EHRs in the near future. CHCN is assisting their health centers to monitor and prepare for ARRA incentives and EHRs. In the event that a selected EHR will not be able to meet meaningful use standards, i2i could be interfaced with the EHR, and operate as a parallel system using PMS and lab interfaces.
EZ-Cap. CHCN uses EZ-Cap software, a well established tool for MSOs to receive, store and manage encounter data from health centers, inpatient providers and Emergency Departments (EDs). EZ-Cap also tracks data on services provided by clinical laboratories, pharmacies and specialty care providers to CHCN health center patients enrolled in the contracted health plans. Although EZ-Cap’s primary function is to process claims and generate reports required by Medicaid HMOs, it also provides an important source of data for a data warehouse maintained by CHCN that houses data for all patients treated in CHCN clinics.
One-E-App. One-E-App is a web based application adopted by the State of California and its county governments to verify eligibility for a variety of state and locally administered insurance programs. The implementation of One-E-App varies from county to county and therefore the entities for which eligibility is being verified differ. In Alameda County, any provider can use One-E-App to check the Medicaid or CHIP eligibility of a patient using a web-based interface that uses state government data to assess eligibility. There is no direct relationship between One-E-App and CHCN’s data warehouse or individual health center PMS. CHCN helped define and implement the system, and coordinate ongoing assistance for the member health centers to use and access the application.
Merritt and Other PMS'. As noted above CHCN does not host PMS’ for use by member health centers. However, CHCN does help centers maintain their PMS’ by providing guidance for managing vendor relations and providing legal support for contract negotiation. CHCN played a pivotal role in brokering a deal to acquire Merritt, a practice management system (PMS), that four of their health centers use and helps host that system at La Clinica de La Raza. In addition, CHCN played an important role in brokering a deal between Axis Health and NextGen. We provide more details on PMS use among CHCN health centers in the subsequent section of this report.
E referral and Hospital Interface. Increasingly, CHCN has been moving towards adoption of functionality designed to facilitate coordination of care between ambulatory and inpatient settings. They found that there was substantial demand among their health centers to access ED and inpatient hospitalization records of their patients, particularly from Alameda County Medical Center, the primary safety net hospital in their area. In response, CHCN helped negotiate and establish a web-based virtual private network (VPN) connection that allows the clinicians to access hospital systems to view inpatient, ED, and specialty consult records.
Originally hospitals refused to give access privileges to staff other than medical doctors, over time they extended access to nurses and the medical assistants. There are other issues with the current system which is the inability to print and the multiple layers of passwords needed to access the application. CHCN and the hospitals are working together to choose IT upgrades for improving this connection.
CHCN has also helped establish a separate Alameda County Medical Center e-referral web portal known as Reftrack. The hospital’s Reftrack system allows health centers to access a separate bi-directional referral system which allows clinicians to submit and look at referrals to and from hospital-based specialists and add notes to documents. Guidelines and reminder prompts for specific types of referrals pop up when entering a referral. Notifications such as whether a referral request has been booked for appointment or the patient has canceled, are sent securely by email to the submitting provider.
Originally hospitals refused to give access privileges to staff other than medical doctors, over time they extended access to nurses and the medical assistants. CHCN and the hospitals are working together to choose IT upgrades for improving this connection. CHCN reported occasional issues with printing, referrals and with the time and energy that goes into receiving an alert via email and then having to track the patient and report back to the physician. In addition to Alameda County Medical Center, Sutter Medical Center and Children’s Hospital of Oakland also participate in this hospital interface and e referral program.
Altruista Case Management and Data Warehouse. As previously outlined, CHCN works with a variety of IT applications and data from those applications is extracted and pooled within their data warehouse. These data are collected from health center PMS’, i2i Tracks, EZ-Cap, hospital systems and laboratories. The data warehouse currently supports a series of QI reports that are generated by CHCN and discussed on a monthly basis by medical directors and QI directors from across the network.
To optimize use of these data, and to help managed the patients who could most benefit from coordinated care, CHCN will implement a new web-based case management system, Altruista. When we met with CHCN their implementation was forthcoming. CHCN is looking to Altruista to extract patient level data from their EZ-Cap system and data warehouse to track patient care. The following anecdote was given to us as a case in which Altruista would be of service.
“A week ago I was reviewing the case for a patient seeing many specialists. As I was reviewing his case I learned that he was admitted to the hospital following a visit to a health center. This guy had a metastasized fracture. I realized that once he is ejected from the hospital then there would be no one to coordinate all the other help he would need like all the equipment such as a wheelchair and other loose ends and everything else that he will need in the days to come. I realized I didn’t have a tool to alert the outreach staff at health center to reach out.”
CHCN intends to use Altruista as a way to alert providers in the cases where synchronization between health care delivery services and outreach services is required. This may be done through automated alerts generated through the use of algorithms that are being designed by Altruista and CHCN or through the identification and tracking of panels of patients with a combination of complex health care and social service needs.
A few weeks following our site visit we followed up with CHCN on their progress with Altruista. At that point they had data coming into Altruista and they were “playing around” with the software. So far the system was in use only for managed care patients. They were enthusiastic about the upcoming case management of all of their patients, but noted that this stage of the project would require generating an enterprise master patient index (EMPI) to link the diverse data sources. An EMPI would provide the means to quickly associate any particular event to a unique patient.
In the future, CHCN thinks that Altruista will be able to look at hospital visits, watch for frequency of re-admittance, ensure that patients make it to their follow up visits following hospital discharge, monitor compliance with prescriptions (i.e., track whether a prescription was picked up) and confirm that that appropriate equipment was purchased by individuals with special needs. They also anticipate that since Altruista is available over the Internet, it can extend the service to the hospitals so that an ER doctor can reconcile key information such as medication history at the point of care.
Health Center Level Findings
In this section we describe key findings from our discussions with health centers both in the context of their use of health IT broadly and in terms of their association with CHCN. To frame our discussion of health center specific experiences with health IT we present Table 1 below. The table lists health IT tools used by each of the centers visited by NORC. These applications include chronic disease registries, hospital and e-referral interfaces, PMS’, an eligibility verification application (One-E-App) and lab interfaces. Additionally this table shows the i2i Tracks go-live dates per health center visited.
Table 1: Health Center Health IT
| Health Center | Applications | New Software | i2i Tracks Go-Live |
|---|---|---|---|
| LifeLong Medical Care | Merritt PMS, Hospital and eReferral Interface, One-E-App Disease Registry diabetes, cardiovascular Merritt module diabetes cardiovascular registry module Merritt eReferral Module Lab interface | i2i Tracks | April 29, 2009 |
| Tri-City Health Center | Merritt PMS, Hospital and eReferral Interface, One-E-App and Diabetes Registry Merritt diabetes and cardiovascular registry module Lab interface | i2i Tracks | June 22, 2009 |
| Axis Community Health | Next Gen PMS, Hospital and eReferral Interface One-E-App Diabetes spreadsheet (used as registry) Lab interface | i2i Tracks | March 18, 2009 |
Health Center Experience with CHCN
Health centers we visited expressed satisfaction with the CHCN network and its services. They did, however, share some information on the limitations of specific applications that CHCN helps them use. The staff at Axis Health told the NORC team that there were activities that would have been insurmountable without the help of their network. They particularly noted CHCN’s very important support for their QI activities such as helping with the acquisition of i2i Tracks and with fielding and analyzing a patient satisfaction survey that has been used regularly by the health center.
They also indicated that CHCN was a great help when obtaining NextGen as their PMS noting that they “could not be as agile without CHCN.” Specifically they felt as though they would have been less successful in negotiating with vendors and visiting centers that have implemented products they themselves were considering. Lastly, the executive team at Axis told us that having the ability to share best practices from other clinics and avoid pitfalls due to shared experience was invaluable to their center. These themes were echoed at the other centers we visited.
At the time of our visit LifeLong was undergoing their i2i Tracks implementation which was scheduled to be completed the following week. They thought that the center by center implementation approach would allow CHCN to incorporate improvements and lessons learned along the way. The executive staff at LifeLong spoke well of their QI efforts facilitated through CHCN, such as the establishment of QI measures across the network’s health centers and the overall ability to see another center perform better and to incorporate strategies that will enhance LifeLong’s performance.
The executive staff at LifeLong noted that there are advantages to acting outside of a network and that there is a tradeoff for network participation, namely the speed of decision making. They explained their need for consensus among members has perhaps prevented them from having an EHR to date. They also noted that the i2i implementation helped put them in a far better position to implement an EHR because of the work they did on workflow redesign and coding.
i2i Tracks experience and anticipated experience. While they were still early in the implementation cycle, we were able to have conversations with health centers regarding their expectations and anticipated uses of the software. Health centers expressed enthusiasm for the ability to specify and pull data on different patient panels depending on their own priorities or depending on varying reporting requirements that come from funders. They also all noted that the ability to more precisely define panels could feed into their efforts to conduct effective outreach to these groups. Finally, they were also very interested in being able to benchmark their performance to other health centers.
Health centers did express some apprehension about their capacity to use the tool effectively. i2i Tracks provides a two day intensive training but there was concern voiced at some centers regarding turnover at their center and the potential cost of conducting ongoing training to accommodate that turnover. One strategy to address this concern will be the establishment of super-users or clinical champions responsible for conducting the bulk of the direct support to new staff learning to use the application. There was also a broad concern that the tool would be so popular that they would need more licenses than they currently have.
From an implementation perspective, there was confidence at all the centers we visited that i2i Tracks would be able to interface with their labs systems. Axis explained that i2i Tracks had previously created successful interfaces with all the leading PMS software products, including their PMS, NextGen. The same sentiments were shared at the two centers we visited that use Merritt. At LifeLong i2i Tracks is being interfaced with Merritt and concurrently they are working to interface i2i Tracks with the second of their two clinical labs. Currently they have an interface with Labcorp and in the near future they will also interface with Quest.
Much of the health centers’ enthusiasm for i2i Tracks stemmed from their sense that i2i Tracks represented a better and faster way to do QI reporting and information by gathering data on activities that already take place. For example, each health center we spoke with had a pre-existing registry or set of registries that were interfaced in a rudimentary fashion with their practice management system. This situation is notably different than those where the adoption of a new QI application leads to the need to find time and resources to move forward with a set of activities that did not take place prior to the system.
Experience with Practice Management. Four of CHCN’s members use a proprietary system called Merritt as their PMS. The other three centers in the network use HealthPro, Centricity and NextGen. The NORC team met with two centers using Merritt (LifeLong and Tri-City) and one center using Next Gen (Axis). According to staff at Tri-City, Merritt is a small customized proprietary practice management system. Merritt was described as “not the prettiest of PMSs” though it does perform certain functions well and is very useful for generating HIPAA transactions and supporting electronic billing and the necessary reporting for variety of health programs. Health centers also were pleased with the level of customization allowed by the application.
The move to Merritt was precipitated by a grant from the Tides Foundation that came from Y2K funding. At the time the PMS being used was Opus, which was a Merritt predecessor. The Merritt system is hosted by La Clinica de La Raza because La Clinica was the original health center that had installed Merritt and had customized its use for over 15 years. CHCN had developed a formal business plan and contract to establish a collaborative among the health centers, La Clinica, and Merritt Software. The Merritt system is physically hosted at La Clinica with separate databases for each health center. So, the Merritt-using health centers rely on at La Clinica for implementing customizations and for help getting the system back online or when users get locked out of the system. A Merritt users group is convened among the four health centers to share experience. Also general coordination and support by the CHCN network is included in the broad set of benefits health centers get from their affiliation with CHCN.
Axis Health, which decided to go in a different direction with their PMS, believes that their recent move to NextGen will help them implement new technologies like an EMR and i2i Tracks. Axis went live with NextGen in April of 2008 and reports having very limited experience with creating customized reports out of the system to date. Both NextGen and Merritt users noted some frustration that One-E-App is not interfaced directly with their practice management system and noted that One-E-App is often too cumbersome to use as it can take up to 45 minutes to check eligibility on an individual. All health centers noted that their next step in terms of EMR adoption would likely also affect the direction they go with PMS. The two health centers using Merritt noted that they were likely to move to a joint EMR/PMS product.
Hospital Interface and Electronic Referral. Health centers spoke favorably of CHCN’s role in helping them connect to hospitals. The executive staff at LifeLong explained that prior to the CHCN-facilitated interface, they had a very clunky connection to the County Medical Center but that CHCN is responsible for streamlining that connection, and further improvements are underway. At LifeLong the providers can use the web-based VPN into the hospital system and they are working out standard processes for when to use this connection. Health centers did note some frustration because of the access being limited to licensed providers. However, there was an indication that access would be made available to medical assistants in the near future.
There are some important differences in the way each health center uses or would like to use the VPN connections to hospitals. Some health centers rely on these connections primarily to facilitate referrals to hospital-based facilities for radiology, specialty care or other procedures and then accessing summary reports on the results of these interventions. Others focus on the benefits of being able to look up patient hospitalizations and or ED visits and print that information out prior to a medical visit.
Costs and Returns of Quality Improvement and IT. While none of the health centers we visited in Alameda County had implemented EHRs, there were still some important findings related to health IT investments and returns. Even prior to the i2i effort, health centers in Alameda County report having interfaces between their PMS’ and clinical laboratories as well as advanced registries that have facilitated active QI.
In each of the sites discussants were asked to describe returns on investment from their QI efforts and in particular those efforts involving IT. Though there were no reported financial returns health centers reported very important improvements over the last several years in terms of compliance with process measures such as regular LDL and HbAIc screenings for hypertensives and diabetics. LifeLong health center reports that they have been able to virtually eliminate differences in some treatment patterns (though not clinical indicators) across different racial and ethnic groups. We found that the health centers we visited had more dedicated QI team staff than health centers in other networks, in part through extensive use of AmeriCorps volunteers. We also found that health centers often had one or more FTE dedicated only to measuring and reporting on quality as opposed to the practice at many centers of making a very busy practicing clinician in charge of QI.
The health centers we spoke with indicated that IT and QI staffing represent a relatively small portion of their budget, between 5 and 6 percent in most cases. Health center administrators we spoke with discussed their decision to move forward with i2i Tracks rather than an EHR in economic terms. Most estimated that the software costs alone would have been close to 75 to 100 percent greater. Also, they noted that, as with any clinical implementation, the “soft” costs would constitute the largest portion of overall implementation expenses.
One health center estimated that $300,000 would be spent on licenses and interfaces for i2i Tracks (half of which they would pay for and the other half of which would come from the Tides grant), but that another $500,000 would be spent on staff time in planning, workflow redesign, training and other activities. They noted that this ratio of soft costs to licenses and hardware costs is even greater in EHR implementation, which means that EHR implementations extract a huge toll on the staff as well as the budget of a health center. Still, every health center acknowledged that they are actively reviewing EHR options in light of the Recovery Act incentives. We discuss this in greater detail below.
EHR and the Future Direction of CHCN
Prior to ARRA, conclusions from this site visit would have highlighted opportunities for health centers and networks to support real QI efforts using health IT that falls short of an EHR. The rationale for forgoing EHRs was made on two basic premises. First, there was agreement among CHCN and health centers that EHRs were not sufficiently advanced to allow for a cost-effective approach to implementation that would yield quality of care benefits in the medium term and that the costs both human and financial would be overwhelming. There was also the argument that having i2i Tracks would provide a basis from which health centers could move to EHRs and whet the appetite of clinicians for use of information systems to improve the delivery of care.
Given the recent legislation however, we end this report by discussing future direction of CHCN in light of ARRA incentives. While they are still confident that the decision to move forward with i2i Tracks will be useful, there is an increasing imperative to make sure that each health center and the network have a plan for adoption of an application that will allow them to engage in “meaningful .use” of a “certified EHR”, however those phrases are ultimately defined.
As noted in our report CHCN does not currently host any applications that are used for day to day operations at health centers. There is some discussion of the possibility of CHCN serving in a support, planning and consulting role. They would help each health center make a decision on EHRs that works for them, but also assure that the vendors selected can ultimately interface with the data warehouse set up by CHCN and other systems.
Health centers are also exploring the possibility of signing on to other networks that have hosted EHR solutions such as OCHIN, HCN, the Alliance of Chicago Health Centers or others. While this approach may work in terms of getting access to an EHR quickly, findings from our other site visits suggest that the training, workflow assessment and planning portions of an EHR implementation are made more difficult by distance and that use of EHRs for QI is a long term struggle that is also hampered to a degree by distance. They key question for CHCN moving forward may be if they can adopt a model where members look to their local network (CHCN) for vendor selection, implementation support and advanced reporting and data integration, while joining a separate, non-local network to access an EHR.
Boston HealthNet
Introduction
The National Opinion Research Center (NORC) is pleased to present this report detailing findings from our site visit to Boston HealthNet in Boston, Massachusetts for the “Assessment of Health IT and Data Exchange in Safety Net Providers.” NORC conducted this site visit under contract with the Office of the Assistant Secretary for Planning and Evaluation ( ASPE) at the U.S. Department of Health and Human Services ( HHS). The Health Resources and Services Administration (HRSA) worked in conjunction with ASPE to guide activities under this project.
This report summarizes the experience of health centers members working with Boston HealthNet (BHN) to use and maintain a range of systems for administration and quality improvement including a centrally administered and hosted electronic health record (EHR). In addition to examining the experiences of BHN and its member health centers, this report discusses the role of Boston Medical Center ( BMC) in network level and health center level activities.
Background and Methods
In accordance with our previous site visits, preparation for this visit began approximately one month prior to the in-person meetings. Initial contact with BHN leadership was made by telephone. These initial conversations were conducted to share the aims of the site visit, obtain agreement from network leadership to participate in the site visit, discuss potential discussants for the in-person meetings and set a date for the in-person meetings. Following these initial telephone conversations we revised background materials, developed detailed agendas for each meeting and set appointments with clinical, administrative and IT leadership from across BHN member health centers.
The site visits took place on the week of April 13, 2009. Two teams of two were deployed to conduct meetings with five health centers as well as BHN and BMC executive staff. For each meeting, we prepared materials that outlined our preliminary knowledge of the discussants’ organization and highlighted outstanding questions to address during the in-person meeting. Having a minimum of two team members at each meeting allowed us to have at least one individual dedicated to taking notes and documenting the content from the meeting while the other focused on assuring that the goals of each meeting were being addressed through engagement with the participants.
Boston HealthNet Profile
Boston HealthNet (BHN) was established in 1995 to create an integrated health care delivery system among its members. This network quickly became a major focus of the public debate around Mayor Thomas M. Menino’s plans to merge its two hospital partners, Boston City Hospital and Boston University Medical Center Hospital. The creation of the Boston HealthNet as a partnership between the newly merged hospital, Boston Medical Center, and the health centers was often cited as an essential element in protecting the public mission of Boston City Hospital in the new merged institution. The network’s partners are Boston Medical Center (BMC), Boston University School of Medicine (BUSM) and 15 community health centers (CHCs). Boston HealthNet has become the largest community health care networks in Boston serving the city’s underserved and working class neighborhoods.
BHN is located on the BMC campus and has numerous ties to the hospital’s executive staff and resources. The impact of this relationship between the BHN health centers and BMC is seen in the number of initiatives and programs within the network. Sixteen BMC specialty departments provide an average of 105 sessions per week at the BHN CHCs. Additionally, the network’s Inpatient Rounder System brings together physicians from the health centers and the BMC Department of Family Medicine to care for patients from these sites while they are in the hospital, thereby, facilitating continuity of care.
Five of the BHN CHCs are also on the BMC license. A Joint Commission working group consisting of administrators from BMC and the BMC licensed health centers was formed to prepare these CHCs for the Joint Commission surveys and meets monthly. The Joint Commission working group has developed collaborations in laboratory medicine and infection control. All BMC licensed health center laboratories are now under the single direction of one Medical Director with the help of a Laboratory Outreach Coordinator, and infection control practitioners assist with the coordination of infection control at the hospital licensed health centers. Other key initiatives among the BHN CHCs and BMC include shuttle services from the health centers to BMC, residency training and group purchasing. In addition, BHN draws upon a variety of BMC’s IT resources, some of which are entirely dedicated to the network. These resources are essential to BHN’s IT portfolio, which focuses on a centrally hosted EHR and a broader health information exchange (HIE) to connect all the entities within the BHN network.
BHN CHCs serve a diverse population of patients. These centers are Codman Square Health Center, Dorchester House Multi-Service Center, East Boston Neighborhood Health Center, Geiger-Gibson Community Health Center, Greater Roslindale Medical and Dental Center, Harvard Street Neighborhood Health Center, Boston Health Care for the Homeless Program, Manet Community Health Center, Mattapan Community Health Center, Neponset Health Center, Roxbury Comprehensive Community Health Center, South Boston Community Health Center, South End Community Health Center, Upham's Corner Health Center and Whittier Street Health Center.
Health Center Profiles
The NORC team met with staff from the following five BHN’s health centers: Boston Health Care for the Homeless Program, East Boston Neighborhood Health Center, South Boston Community Health Center, Dorchester House Multi-Service Center and Codman Square Health Center. In addition to meeting with health center staff the NORC team met with a staff member from a joint enterprise between Codman Square and Dorchester House known as DotWell.
Many of BHN federally qualified health centers (FQHCs) have historic roots in their communities, some dating back to over a century. As a result there is diversity in services and size of the health centers due to the evolving needs of the communities they serve. The table below illustrates the relative sizes of these organizations.
| Community Health Center | Number of Employees | Total FTE | Physician FTE |
|---|---|---|---|
| East Boston Neighborhood Health Center | 770 | 628 | 42.63 |
| Boston Healthcare for the Homeless Program | 362 | 248 | 15 |
| Dorchester House Multi-Service Center | 205 | 195.4 | 9.9 |
| Codman Square Health Center | 180 | 166.44 | 13.42 |
| South Boston Community Health Center | 174 | 141.2 | 14.5 |
The five health centers visited span over five of Boston’s distinct neighborhoods. As a result these centers are unique to their surroundings. The following map shows the main heath center campus for each of the centers that were represented in our meetings.
Image 1 shows the five health centers visited span over five of Boston’s distinct neighborhoods. As a result these centers are unique to their surroundings. The following map shows the main heath center campus for each of the centers that were represented in our meetings.
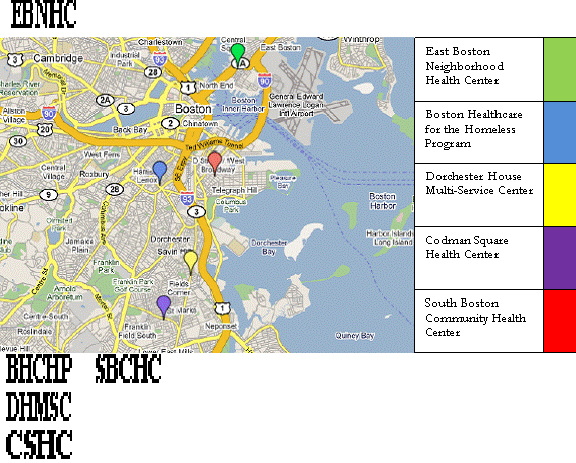
South Boston Community Health Center Profile. South Boston Community Health Center (SBCHC) originated in 1972 with the mission of providing care to their entire South Boston community. Today, South Boston provides nearly 60,000 visits a year to almost half of the neighborhoods residents and is the primary source of health services in the community. The neighborhood demographics of South Boston have shifted over time. While still a predominately white Irish Catholic population, there has been an increased number of Hispanic and African American residents. In addition, South Boston has a large population of Albanians accounting for 15 percent of the community’s population. SBCHC provides a full suite of medical services including a cancer survivor clinic, behavioral health services, full laboratory and radiological services as well as community services including arts programs for youth and financial counseling.
East Boston Neighborhood Community Health Center Profile. East Boston Neighborhood Health Center (EBNHC) was established in the 1960’s to address the need for care in a geographically disparate region of Boston. Today, EBNHC has grown to care for more than 300,000 patient visits per year -more than any other ambulatory care center in New England, delivers 1,000 babies annually and provides care to the vast majority of East Boston’s children. Other medical services that EBNHC provides include a 24 hour emergency room and an on-site pharmacy. Originally, East Boston served a primarily Italian-American population. Since its inception, various immigrant populations have passed through the area and today the neighborhood is multicultural. Although the community is multicultural the majority of EBNHC’s patient population is Hispanic.
Boston Healthcare for the Homeless Program Profile. In 1984 The Robert Wood Johnson Foundation and the Pew Charitable Trust collaborated in developing a pilot that would eventually be called “Boston Health Care for the Homeless Program (BHCHP)." BHCHP serves more than 11,000 patients with more than 72,000 outpatient medical, dental and mental health visits across its 80 sites throughout Boston. These sites include two hospital locations, BMC and Massachusetts General, and a 104 bed medical respite center for patients that do not meet the threshold of being admitted to the hospital but need an environment conducive to recovery.
BHCHP provides a comprehensive set of services to its population, including an outreach van, motel services, a behavioral health department, a pharmacy, 24 hour medical respite care for homeless adults as well as a full range of primary care and dental services. The patient cohort is diverse and reflects the demographics of the city’s homeless population. Forty-two percent (42%) are white non-Hispanic, while Hispanic and African American patients combined make up roughly 50% of patients seen.
Codman Square Health Center Profile. Codman Square Health Center (CSHC) was founded in 1979 with the broad mission to improve the quality of life in the Codman Square community, a neighborhood within Dorchester. CSHC records more than 90,000 patient visits annually and provides primary medical care as well as non-medical services such as continuing education, fitness, youth programs and financial services. Eighty-five percent (85%) of Codman Square’s patient population are African Americans, with a far smaller Haitian and Hispanic population. Many of Codman Square’s initiatives are held in collaboration with Dorchester House Multi-Services Center. A number of these shared initiatives are managed through DotWell, a joint venture between the two centers.
Dorchester House Multi-Services Center Profile. Dorchester House Multi-Services Center (DHMSC) has provided its community with services for over a century. Originally a settlement house by the name of “Gordon House,” in 1909 the Commonwealth of Massachusetts incorporated the institution giving it the name “Dorchester House.” Its original mission sought to provide library and educational services as well as to conduct charitable acts and social meetings. In the mid 70’s a health center was built on the grounds and given its current name of “ Dorchester House Multi-Services Center.”
DHMSC provides approximately 70,000 patient visits a year. More than 60% of DHMSC patients are African American and Asian. The center offers a wide array of medical and non-medical services in addition to its in-house diagnostic services, including radiology and full-service laboratory, as well as a host of community services programs. As outlined before, Dorchester House and Codman Square collaborate on numerous projects, including a shared venture, DotWell.
DotWell Profile. DotWell is a joint venture between Codman Square and Dorchester House that serves both centers with IT support, quality improvement, public advocacy and financial management. The partnership originated in 1998 and was designed to be a cost efficient way to share management and other services. These services include IT support, data storage and management of shared software applications. DotWell utilizes shared resources from CSHC and DHMSC and employs 50 full time staff. DotWell provides shared IT services between the two organizations as well as a single place to manage and execute joint public health and community programs such as a health van, HIV outreach, diabetes services and Social Capital Inc. a Dorchester community engagement service.
Network Level Findings
As noted above, BHN emerged as an organization during the 1990’s merger of Boston University Medical Center and Boston City Hospital. The network is governed by a Board of Directors comprised of executive leadership from ten of the health centers (10 primary partners) in the Boston area, BMC and the BUSM. Each of the10 CHCs has one vote on the Boston HealthNet Board, BMC has three and BUSM has one. The remaining five CHCs are secondary partners due to their affiliations with other hospitals. These secondary partners take part in BHN programs and do not sit on BHN’s Board.
The health centers and BMC leadership recognize the reciprocal nature of benefits each gets from the partnership. In addition to the IT function, the BHN committees, including the Community Health Automated Record Technology (CHART) Working Group, BHN Human Resource Directors, BHN Chief Financial Officers Forum, BHN Research Subcommittee, and BHN Clinical Committee, meet regularly to examine issues of common concern to its partners.
In the paragraphs below we outline key aspects of our discussions with staff from the network, CHCs and BMC. We include a discussion of the IT functions that have been the focus of the network throughout its history.
Building trust. In the initial stages of the merger, there was some anxiety among health centers that the new BMC organization would absorb all the Medicaid business through its ambulatory care and outpatient clinics. There was also concern that the hospital would want to acquire the existing health centers that had significant existing market share. This represented a substantial concern to health centers that were firmly rooted in their communities, provided a special mix of services to meet the needs of their patients and, in some cases, had been in the community for several decades. In late 1994, eight community health centers, Boston University Medical Center Hospital and Boston City Hospital began discussions regarding the development of a community health care network in Boston to preserve the mission of Boston City Hospital and to foster collaboration among the entities. As a result, when BMC was formed, the hospital reserved several seats on its board of directors for representatives of the health centers. As such, there is Board reciprocity, with health centers being a part of BMC governance and BMC being a part of the network’s governance.
BMC actively solicited health center participation in a network under the BHN umbrella. They sold this as an opportunity to build economies of scale and leverage the unique level of resources available through the new hospital organization. While discussants reported that it took over a year to address trust issues, after a series of retreats and meetings there was an increasing understanding among the health centers that BHN offered opportunities and that there was an interest on the part of the new BMC in collaboration rather than acquisition. There continues to be some apprehension among sharing data across health centers within the city, which still do see themselves as competitors in some sense, but IT opportunities offered through the network continue to facilitate collaboration and understanding even at the health center to health center level.
Initial grant funding. At the baseline for BHN’s IT activities in the late 1990’s, most Boston health centers existed at a fairly rudimentary level of IT adoption. DotWell had a slightly more sophisticated IT structure than most of the other sites but lacked an EHR. The one exception was the East Boston Neighborhood Health Center whose experiences are detailed in the next section. While most health centers had some form of billing and practice management applications, only one health center had invested in an EMR and it had relatively limited connectivity to the main safety net hospital, Boston City Hospital. The connectivity that existed between Boston City Hospital and individual health centers was mediated through barely used terminals in some health center sites that allowed providers to look up whether a given patient had registered as an inpatient or in the ED as well as the location and time of the visit. These terminals were often not operational.
In 2001, the network approached a philanthropic foundation in Boston to fund an electronic health record (EHR) project. The foundation asked the network to supply a proposal to support EHR adoption among member health centers. Many respondents indicated that establishment of the network and the tight relationship with BMC motivated the foundation to make such an offer. Even still, BHN executives were surprised when their proposal was funded in full, initiating a $5.9 million project. The initiation of this grant program and the relationships formed between individual health centers, the network and BMC as a result, solidified the organizational commitment and collaboration and provided a substantial “test case” to determine how each health center could continue to operate independently even with a significant dependency on the network and hospital which hosts the EHR application.
EMR Implementation Approach. From the beginning of the EHR project, later named the Community Health Automated Record Technology (CHART) Project, all stakeholders understood that the health centers would rely extensively on the expertise and experience of IT resources at BMC. A committee of individuals from the network, BMC and the BHN health centers came together to identify requirements and needs, develop an RFP and assess EHR vendors. Based largely on the expertise from BMC’s IT team, BHN selected the GE Logician system as their EHR and began an implementation regimen across 8 out of the 10 primary BHN health center members.
The Logician implementation took place between 2002 and 2004. Numerous work groups support the CHART Project. Initially, the Boston HealthNet CHART Working Group, a sub-group of the BHN Board of Directors, met monthly to discuss “big picture” issues related to the CHART Project such as implementation, budgeting, planning, and resource allocation. Now that these eight health centers are using Centricity, the Working Group continues to meet monthly to address developmental issues, customization and to evaluate and prioritize future CHART projects.
Ongoing Maintenance. The CHART Working Group continues to operate today and is a primary aggregator of follow-up needs and initiatives to be pursued by BHN from an IT perspective. The Working Group is chaired by the Chief Executive Officer of Dorchester House Multi-Service Center and is focused on carrying out the goals and objectives of the BHN IT strategic plan and leveraging hospital systems for the benefit of the overall network. For example, while the CHART Working Group does work on making adjustments to standardized forms, the baseline version these forms were taken from the Internal Medicine outpatient clinics of BMC. Most health center level respondents noted that even when they are working to create custom forms for their own use, they are more likely to look to BMC than the vendor for support in the design and creation of these forms. BMC continues to host the EHR application and is the main point of contact for connecting with the GE vendor.
Connectivity across providers. One of the obvious benefits of vertical collaboration between ambulatory and inpatient providers on IT is the opportunity to achieve greater connectivity and coordination of care. As noted above, prior to BHN, some health centers in Boston had a less than reliable mainframe connection to Boston City Hospital that informed them if a patient had been recently discharged from an inpatient floor or had visited the Emergency Room. When the mainframes worked appropriately, this system still required the health center to then contact the hospital separately to receive information on the nature of the visit. Following the establishment of BHN, T1 lines were set up between each member health center and the new BMC network. Using these T1 lines, health centers were able to access ED or inpatient records on a patient through a read-only Citrix connection. This model allowed health center staff to view and print information about their patients that were seen at BMC and obtain some clinical data relevant to that visit. Later, BMC’s Information Technology Services Department launched myBMC.org, a program that facilitates secure access to BMC’s clinical applications to qualified staff within Boston HealthNet’s network. Providers who want access apply for a security token. Once they receive this token, they can connect to BMC’s clinical applications from work, home or wherever a computer and a version of Internet Explorer are available.
In addition, BMC helped established an external Laboratory Information System (LIS) environment using Antek’s Labdaq for the health centers. In combination with BMC’s interface engine, this environment provides a connection between the EHR and clinical laboratories used by health centers – either commercial laboratories such as Quest or, in some cases, BMC hospital laboratories. The LIS mediated interface functions for both lab orders and results reporting.
Finally, through the work of the CHART Working Group and ongoing work with GE, BHN recently implemented automated routing of prescription requests to pharmacies through the e-Rx feature included in the EHR package. Prior to this initiative, pharmacy orders were entered electronically through the EHR. This form of e-Rx provided the benefit of automated checks of medication history and interaction warnings based on prescriptions previously entered in the EHR. Although prescriptions were entered electronically under the prior system, routing to the pharmacy occurred via fax with a medical assistant printing out the form and faxing it over to the appropriate pharmacy. As currently implemented, pharmacy orders are routed electronically either to a BMC pharmacy or to a number of retail pharmacy chains used by individual health centers. Most health centers reported significant efficiencies as a result of the addition of electronic routing to the e-Rx functionality. We note however, that like most e-Rx implementation, many of the functionalities that require connectivity to payer databases and advanced use of standards such as checking a payer-based medication history at the time of prescribing or requesting prior authorization at the point of care are not currently in place at BHN.
Future directions for HIE. For several years, BHN has been working on opportunities to leverage vertical exchange of data within their network. Earlier in the decade, the network was a recipient of a three-year, $382,000 HRSA Bureau of Primary Health Care (BPHC) Integrated Delivery System Development Initiative (ISDI) grant that supported improving communication and access to BMC Clinics by developing a template in the electronic medical record. BHN also took part in a national demonstration project funded by HRSA to establish a community-wide record locator service (RLS) established and maintained by the Massachusetts Health Data Consortium. Both BMC and the health centers found relatively little value from use of the application deployed as part of the pilot because it offered only a static view into a limited set of data on new patients presenting at the hospital or in health centers. BHN and BMC officials noted that the use of the application deployed in the pilot effort dropped off following its completion because of its limited usefulness and usability.
In 2007, BHN was awarded a three-year grant from HRSA Office of Health Information Technology (OHIT) to implement a network wide clinical information exchange or CIE. This clinical information exchange project, named CHART-Plus, integrates the Centricity EMR of nine BHN health centers with that of BMC allowing BHN clinicians to view patients’ clinical information aggregated from separate EMRs across the network. The information is displayed within the clinician’s local EMR, providing real-time access to clinical. While the initial focus of the grant was sharing laboratory results across Centricity installation, the project evolved in 2008 to include medication lists, problem lists, allergies and laboratory results. The CIE will potentially establish a single master patient index (MPI) across the network that will allow linkages across records from multiple provider data sources in a single data repository that can be queried when a new patient presents in the Emergency Department, in a health center or needs to be admitted quickly and in an unplanned manner. One main benefit is to allow providers to view baseline clinical assessment directly from their local EMR for a patient that has been seen elsewhere in the network. Clinicians find this especially useful when trying to obtain a complete treatment and medication history.
The goal of the CIE is to capture and exchange a full continuity of care document (CCD) message for any patient that has been seen by a provider at BMC or any of the BHN sites. The CCD will include medications, allergies, laboratory results and problem lists going back to the patients’ initial visit to a BHN site and updated with each visit.
In addition to exchanging clinical information, the CIE serves as the platform that will allow health centers to make automated referrals of patients to BMC specialty clinics and electronically access assessments and test results conducted during those specialty referrals. The network’s eReferral Project, a one-year grant from HRSA OHIT, will make it possible for the CHCs to schedule appointments electronically, submit required clinical information to the specialist, receive electronic information about the referral, track patients no-show rates and receive return specialist reports through the local EMR or by opening a web-based practice portal. The objective of the eReferral Project is to eliminate most of the inefficiencies inherent in the current referral process and to enhance the quality and continuity of patient care. The gains in quality improvement of this project will be assessed by observing metrics around colon cancer screening and cardiac diagnostic testing as well as tracking the no show rates.
BHN and BMC leadership noted that in collaboration with GE, they have developed an approach to present the CIE clinical summary to a clinician. They note that each provider must still maintain their own single, comprehensive medical chart on a given patient and that it is not feasible to have automatic updates to ambulatory charts based on procedures or tests conducted in an inpatient setting. At the moment they are working on a user interface that presents the clinical summary information for each patient presented on a separate “tab” within the local EMR. Providers would then have the ability to update their native provider record with more up to date information from the CCD either manually or automatically. At the time of our site visit in April 2009, BHN and BMC officials indicated that two health centers were planning on going live with a demonstration version of the CIE and roll-out is planned for the remaining sites in the coming months.
While still being piloted, all the health centers we spoke with, including East Boston Neighborhood Health Center which operates using an entirely different EHR platform, were very enthusiastic about the initiation of the CIE project, which is unlike state-wide or community-wide efforts, there would be more functionality would be limited and where the focus would not be on their specific patient population. The CHCs were quick to point out potential benefits of an HIE grounded in the major safety net hospital and connected to all health centers and safety net clinics with significant capacity to exchange data (e.g., the full CCD not just an indication of a visit). They were particularly excited about the ability to access information on procedures and test results more efficiently and more easily refer patients to specialists and access assessments from those specialists.
Quality improvement initiatives at the network level. While there is active collaboration between BMC and health centers and across health centers as it relates to the IT components of the EHR as well as operational functions such as human resources, financial planning and Joint Commission accreditation, we found limited coordination across health centers on quality improvement initiatives. BHN staff from BMC and BHN’s CHCs have collaborated on the development of a network-wide Ambulatory Standards of Practice, which focus on increasing access and the coordination of services to patients and improving communication to providers. BHN staff noted that the CHART Working Group offered some standard forms such as a diabetes form that was used by many health centers. Historically, QI projects are discussed and presented at both the BHN Clinical Committee and Board meetings. BHN officials noted that most health centers develop their own registries and customize reports for their own site.
With the recent award of the two HRSA funded HIT projects, BHN has begun to work toward a network-wide Continuous Quality Improvement (CQI) initiative. The participating health centers have integrated the CIE and eReferral measures into their existing CQI programs. The projects will also initiate network-wide standards setting and performance measurement for patients with diabetes and heart disease as well as for cardiac diagnostic testing and colon cancer screening. A QI subcommittee has been established and is meeting monthly to discuss the integration of CHART-Plus QI and eReferral measures into their health centers overall QI goals. BHN is also planning a network-wide QI program based on the needs of the CHCs.
As described in the health center findings section below, several health centers have challenges using the EHR for quality improvement purposes. We describe anecdotal observation of improvements in quality in the section below.
Discussants noted that one approach to network level QI initiatives was pursued earlier in the decade through a Healthy Community Action Program (HCAP) grant that made use of common diabetes templates being used across many health centers to generate a series of reports on diabetes measures that were shared on a regular basis with medical directors at participating health centers. Although this was a centerpiece of BHN’s quality improvement programs at one time, at the time of the current site visit they noted that this was one of many attempts to use the EHR to more formally establish QI programs on a network level and it was lost after the grant period, though it should be noted that an HCAP diabetes template is still in use at several of the sites. Use of the diabetes template populates the flow sheets with current data and future templates. They note that the current strategy of establishing an MPI and a comprehensive data warehouse as part of the CIE initiative will produce better more sustainable opportunities for network wide QI initiatives.
Health Center Level Findings
In addition to extensive discussions with BHN and BMC leadership, we met with staff from five BHN partner health centers. Four of these health centers, Codman Square, Dorchester House, South Boston Health Center and Boston Health Care for the Homeless Program adopted the Centricity EHR supported through the BHN grant that is hosted at BMC. The fifth health center, East Boston, also had deployed an EHR, Epic, but conducted this implementation independently in the late 1990’s. In the paragraphs below we highlight key findings from our discussions with these health centers including opportunities and challenges presented by their use of EHRs, unmet needs and their vision for the future.
Sub-network collaborations and large health centers. We found that in Boston, as in other markets where there is a network presence, there are additional, sub-network collaborations across institutions where a high level of trust has been built over time. One example is the DotWell partnership, a small non-profit that jointly manages some administrative functions for Codman Square Health Center and Dorchester House Multi-Service Center. While each health center continues to maintain a separate board and institutional status, they have, over the last several years come together for the purposes of joint purchasing and administration. The extent of the collaboration has waxed and waned at different periods and is currently focused on IT staff and purchasing which is currently combined.
The large health center model. Some of the key findings from this site visit came from discussions with leadership at East Boston Neighborhood Health Center which had initiated an EHR program working with Epic prior to BHN’s purchase of Centricity and has continued to be an Epic user. East Boston was in a good position relative to other health centers in Boston to go it alone largely because of their size and level of sophistication. With over 300,000 patient visits annually, well over 500,000 encounters and 600 clinicians spanning a range of subspecialties, the health center is the largest in New England and offers a wider array of services than any other health center in Boston.
Unlike the health centers using the Centricity software, East Boston indicated that, from the beginning, they were able to use Epic’s reporting and analytic functions to support their participation in QI programs such as the health disparities collaboratives (HDCs), replacing their existing PECSYS and CV-DEMS registries [1]. Because most of EBNHC prescriptions are routed through an in-house pharmacy, they also were able to adopt end-to-end e-Rx at a fairly early stage in their implementation and were able to roll-out EHR into specialty clinics such as pediatrics and OB-GYN as well as special facilities such as their 24-hour emergency department. Finally, there is some sense that they were able to get a better original deal from Epic because they adopted very early and were Epic’s first health center customer. EBNHC reports spending around $6 M in 1998 for their original purchase of licenses and implementation services including training and installation and that this original roll-out included most of their 600 clinician users, which BHN claims represents a lower cost per user than many of the other sites where we were able to get this information.
Challenges with using EHR for QI. The challenges articulated by many health centers in Boston, particularly those that accessed Centricity through BHN, was the difficulty in finding dedicated clinical staff to work closely with the BMC IT team to optimize the use of the EHR from the perspective of quality or clinical efficiency. There were both limitations on the extent to which health centers could offer staff to engage and the extent to which BMC had the resources to accommodate health center needs. For example, many of the BHN health centers continue to use CV-DEMS or PECSYS with manual data entry even following the Centricity implementation because they lacked the resources and expertise to develop custom screens to assure capture of all necessary variables in a structured manner at the point of care and were unable to create the reports necessary to effectively use the data that was captured. While BMC reports having approximately 2 IT FTEs dedicated to working with the health center EHR hosting, maintenance and support, there seemed to be relatively limited resources that regularly go into working with health centers to design and implement new EHR screens and design new reports. They noted that a priority for the CHCs and BMC is to configure the clinical forms developed in Centricity by BMC specifically for use by the CHCs.
Some medical directors noted that they were skeptical of the ability of the Centricity system as currently configured at each site to help them assess quality because of the variation in which data is entered in the system from health center to health center and provider to provider and the difficulty in enforcing a single approach to using the EHR to consistently capture the same data in the same place in the same way. They also noted extensive and complicated issues with defining appropriate populations and denominators to support key measures, noting for example, that there was no easy way to exclude a patient from being included in assessment for legitimate, but uncommon reasons (e.g., the lack of a dental visit may not be an issue for an individual with no teeth). They also noted that some of the measures they would like to assess, such as frequency of foot exams for diabetic patients, are typically very poorly documented regardless of whether the provider is using an EHR or a paper chart.
IT staffing model. One area where East Boston demonstrated success where other health centers indicated frustration was their ability to achieve synergies between their IT staff and their clinical staff both on designing and implementing ongoing enhancements that make the EHR easier to use and in terms of helping create reports and functions that allow the EHR to support QI. While East Boston reports having a relatively lean IT operation, fewer than 10 employees to support a health center with multiple sites and functions and over 600 EHR users, they are more of a driver of change and improvement within the health center than a typical health center IT department.
The CIO at East Boston is a former IT consultant who brings a focus on business process re-engineering. He noted that he typically hires business analysts into the IT department that often have little or no clinical or IT background, but are smart, capable and computer savvy individuals he can train to use MS Visio to document current processes in the health center, work with clinical and administrative staff to re-design those process and configure Epic or other software applications to meet the requirements of the new, optimized design. These staff, some of which comprise a dedicated “clinical applications team” work closely with clinicians in some cases doing extensive shadowing and observation of the workflow in a given area in order to achieve a solid understanding of the needs, frustrations and priorities of the clinicians and support staff.
East Boston also noted that they always have a dedicated member of the clinical applications team that was a former clinician at the health center and can represent that perspective directly during discussions and planning around adaptation of the technical design and play the role of clinician champion when new features are rolled out. Over the years, East Boston reports using these types of processes to design new functionality such as the clinical lab ordering and reporting modules that work with interfaces to Quest and other laboratories as well as in working with their medical director to set up alerts within the EMR. They indicated that the need for alerts is driven by problems or areas for improvement that are prioritized by the clinical committee.
Use of EHRs for panel management and quality reporting. Again, unlike other health centers East Boston indicated extensive use of their Epic package to define panels of patients, design screens to consistently capture key information on those patients and track that information over time. In addition to using Epic from the start to support their participation in the Health Disparities Collaborative in diabetes, they also report using reporting and analytic functions in Epic to track immunization rates and to track information about basic preventive care and screenings for their general population. They note that when a new area is identified by clinical leadership as needing to be tracked more effectively, they convene a meeting of the clinical applications team and key clinicians in the relevant departments and go through both the workflow that would support better capture of data or capture of new data as well as the existing “screen” where data would be entered. They are able to review several options for changing the screen or workflow and discuss how the new tools and processes should be adapted to the appropriate clinics.
Benefits of the EHR .Interestingly, the BHN health centers using Centricity did report extensive benefits following the adoption of their EHR. Although they acknowledge that they face limitations in terms of their ability to use the tool to track quality, they point to benefits in efficiency and work flow that they believe have improved care. Although they acknowledge that forms are being used inconsistently, most did indicate that their measures of quality, even if they are based on manually entered registries, have improved since adopting EHRs and they attribute this to an increased focus on documentation, the use of some alerts and in some cases, health center and provider report cards.
By far, however, the benefit that the Centricity health centers described were the ability to accomplish their tasks without having to find and access patient charts, the efficiency of being able to route prescriptions without printing and faxing and the general conveniences with having adopted an EHR. All the clinicians we spoke with indicated that there was very little remaining “dissent” regarding the use of EHRs and in fact, having EHRs served as a good recruiting tool. The convenience issues were particularly important for the Boston Health Care for the Homeless Program. The staff explained that they had been able to work with BMC to use small laptops and tablets in their mobile vans and satellite clinics to wirelessly access patient records which greatly facilitated their ability to deliver and document care and health status among Boston’s homeless.
East Boston Neighborhood Health Center was able to make more specific claims than others regarding quality improvement. They indicated that they had seen a significant improvement in the number of diabetics that are receiving HbA1cs on a regular basis as well as the numbers of patients that have their HbA1c values. They indicated that in 2005 they had over 2,000 patients with HbA1c’s over 8.5 and that, tracked as a panel, the average HbA1c for this group has decreased to 7.5 currently. They attribute this to their focus on translating their panel identification and tracking work to case management.
They note that they do not view registries and databases for analysis but as lists of patients that are the target for specific types of outreach via phone or mail. For example, outreach workers monitor the high risk diabetes group identified above and send out regular reminders for the need to have HbA1c tests conducted and, in the case of those who are out of control, having intensive visits with nurse diabetes case managers to review the need to modify their therapy, diet or exercise regimen.
Costs associated with the EHR. Not surprisingly, no health centers described a positive relationship between financial costs and benefits associated with EHR use. By and large, health centers described costs in the range of $500 to $1,000 per year per user as the average cost of renewing licenses, adding functionality, training new employees in the system and upgrades. Importantly, the extent of these costs vary from year to year and do not include the periodic upgrades of hardware that are sometimes seen as more important for health centers that are using EHRs and those that only use computers for billing and administrative purposes.
East Boston Neighborhood Health Center also noted that following adoption of EHR their clinicians were working harder to document care they receive and that the time required to document care typically increases as they add new features, forms and alerts to their base EHR application. They emphasized their sense improving quality through EHRs requires more focus, attention and time on the part of clinicians and that there is no way around this reality. They also noted that since adopting EHRs they have conducted a far more extensive set of outreach activities and employed more individuals in this function which typically is not reimbursed.
They did not feel that there was potential for ROI through increased throughput that allows the same number of clinicians to treat and document more patients in a given amount of time. They did seem to indicate, however, that effective use of EHRs could lead to more visits overall and the need to expand their health center because the enhanced ability to follow-up with patients leads to more frequent and more extensive visits. They also indicated that their use of EHR to track care to patients and re-design workflow has led to an increase in the use of mid-level clinicians to help manage and counsel patients and that the numbers of nurses, nurse practitioners and physician assistants they employ has increased relative to the number of physicians.
Conclusions
There are several important conclusions that we draw from our site visit to Boston. First, there is some confirmation of the assumed value of vertical integration for a variety of reasons outlined below. In addition, we see continued evidence of the challenges inherent in using EHRs for QI initiatives such as those that focus on following and tracking care to patients with specific conditions. Finally, we see support for the value of a functionality-rich version of HIE focused on safety net providers in urban areas. We describe each of these concepts in greater detail below.
Benefits of vertical integration. Aside from the considerable economies of scale that are achieved when health centers form networks, this site visit demonstrates a couple of the specific benefits associated with a vertical integration between a safety net hospital and health centers in a given market. First, discussions with health centers and BMC indicate that having the hospital on board was essential to helping mediate trust and competition issues that are natural among health centers in the same market. The fact that all Boston HealthNet health centers had something to gain from collaboration with BMC and BMC gained from collaboration with these health centers made it more likely for the health centers themselves to work together. In addition, BMC’s contribution of IT staff and expertise were the primary drivers of the Centricity EHR initiative and many indicate that it would have been unlikely to have received a grant for EHR implementation absent the participation of the hospital.
Demand for a safety net HIE. Discussions in Boston suggest considerable demand for a safety net focused HIE that is based in BMC. While there are significant challenges associated with working with GE Centricity to design and implement an application that will work well for health centers and meet basic needs, there does seem to be a commitment from BMC to invest in a more robust program of HIE with health centers moving forward. One challenge will be the cost associated with integrating East Boston Health Center.
East Boston, like the other health centers, is very eager to participate but is wary of the costs associated with getting Epic to participate in the exchange. They also indicate that Epic is currently not capable of or willing to generate the full CCD message for patients included in their EHR databases so significant work would have to go into compiling generic HL7 messages into the CCD format for inclusion in the CIE warehouse being contemplated by BMC. Not surprisingly, the greatest demand for the CIE is coming from health centers that want greater connectivity to specialty providers and a better view into the care delivered in inpatient settings and ED’s where there is high demand for instant access to basic information such as blood type, allergies and medications for patients that walk in unexpectedly due to an acute event.
The costs of meaningful use. As policy makers begin to add more substance to topics surrounding the definition of meaningful use of EHRs for the purpose of determining eligibility for payment incentives, health centers in Boston offer a prime example of the challenges and opportunities inherent in using EHRs for systematic quality reporting and improvement, the value of exchanging data and the investment and costs inherent in successfully improving quality through an EHR.
The East Boston example demonstrates that using an EHR to accurately track patient populations requires more work on the part of providers, sophisticated design of workflow and reporting templates and a more substantial outreach function. In other words, there are a number of important costs that go well beyond the cost of a successful EHR implementation. The example of health centers using Centricity demonstrates that providers can achieve successful adoption and recognize convenience benefits of using the EHR especially as it relates to connectivity with labs and pharmacies with a baseline level of investment. However, it also shows that an entirely different level of commitment, investment and focus is needed to use EHRs to replicate the role that registries play in traditional QI models that use panel-based approaches to manage chronic illness.
[1] PECSYS and CV-DEMS registries are chronic disease registries used to track and manage targeted population with chronic illnesses.
