Prepared for the Office of the Assistant Secretary for Planning and Evaluation
Conference on Prescription Drug Costs and Pricing
August 8-9, 2000
By
Cindy Parks Thomas Ph.D.
Grant Ritter Ph.D.
Schneider Institute for Health Policy
Brandeis University Heller Graduate School
Final - Prepared 8/31/00
Introduction/Overview
Recent increases in prescription drug expenditures have been attributed to various factors: more people using medications; higher utilization of medications per person; and a changing drug mix from older medications to new, more expensive classes of medications (Barents, 1999; Express-Scripts, 2000; Schneider Institute for Health Policy, 2000; Merck-Medco, 2000). Most analyses study the growth of medication use and changing drug mix by measuring aggregate changes. However, in order to understand how treatment strategies evolve, it is necessary to follow individuals over time and observe changing use patterns as new medications are introduced.
This study uses prescription claims data to examine the dynamics of medication use over time in a fixed population. In this way, we can identify the users of the new and increasingly prescribed medications. We can also examine the extent to which the growth of these medication classes represents substitution from older medications or greater numbers of people being brought into treatment. In the present study, we examined medications used in the treatment of three conditions -- gastrointestinal conditions, arthritis and other musculo-skeletal problems, and elevated cholesterol. These diagnoses account for 22 percent of 1999 prescription drug expenditures in our data, and include some of the fastest growing individual medications in terms of use and expenditures. In combination, they reveal several of the dynamics that are contributing to dramatic expenditure increases for prescription drugs.
Background: Disease categories/Medication classes chosen for analysis
The study began by ranking all prescription medications according to contribution to overall 1999 expenditure and 1996-1999 expenditure growth. Choice of specific disease category for examination was to be based on several factors. Obviously, we wanted to capture those disease groups that contributed most to the large growth in medication use in the past few years. We also wanted to select groups that would tell different stories and illustrate different important aspects of expenditure growth and treatment changes over time. In the end, three disease categories were selected: gastrointestinal disorders, arthritis, and hyperlipidemia (elevated cholesterol). We briefly describe some background for each group studied, in terms of the market, the science of treatment, and the technology available.
Gastrointestinal Medications
Commonly treated gastrointestinal disorders include gastritis, gastroesophageal reflux disease (GERD, or mild, moderate or severe heartburn), and peptic ulcer disease (PUD). The same medications can be used to treat each, although dosages may differ. The most common of these conditions is GERD, estimated to affect 60 million Americans at least once a month.
In the past two decades, treatment of these disorders has been vastly affected by the availability of acid suppression agents (H2 receptor antagonists, or H2RAs) medications in the 1970’s, followed by their generic replacements, and by a new generation of medications in the 1990’s. When first introduced in 1977, H2RAs such as Tagamet® and Zantac® (approved in 1983) represented an improvement in heartburn and ulcer treatment over palliative therapy for mild or moderate symptoms, or surgery for severe conditions. The H2RA medication class achieved sustained market growth for years after its introduction (Berndt et al, 1997). According to the American College of Gastroenterology (ACG), H2RA’s are still preferred for initial treatment of mild GERD. Since the early 1990’s, several H2RAs have gone off patent and are available in less expensive generic form. As well, they have been available over the counter (OTC) in lower strength forms since 1995.
In 1989, a new class of medications, the proton pump inhibitors (PPIs), was introduced for treatment of gastrointestinal disease. PPIs suppress acid more effectively and work faster than do H2RAs. First approved in 1991 for treatment of peptic ulcer disease and for severe GERD not responding to H2RA therapy, several PPI’s, Prilosec, Prevacid and Aciphex, are now marketed for GERD. PPIs were initially recommended for short term use. However, more recently, they have been recommended for longer term therapy where indicated (DeVault et al, 1999).
Since their introduction, PPI’s have captured a large portion of the market, and are now among the highest selling medications of all categories (by expenditure share). Due to the introduction of PPIs, which can cost several times more than generic H2RAs, the cost of medication per prescription for gastointestinal disease is increasing among the fastest of any therapeutic category.
It is still the case that H2RAs are considered effective for mild heartburn, although in more severe or chronic cases, PPIs can be more effective. The most recent ACG clinical guidelines for treatment of GERD recommend that physicians use either step-up therapy (begin with H2RAs and move to PPIs if necessary), or begin with PPI therapy and then step down to H2RAs as symptoms abate) (DeVault et al, 1999). An important question in relation to expenditures is how often physicians use the step-up clinical approach (usually less costly) or prescribe PPIs as the first drug of choice regardless of the severity of the disease.
Pain relief medications for arthritis and other chronic conditions (NSAID Class)
The largest class of prescription medications for pain relief is the nonsteroidal anti-inflammatory drugs (NSAIDs). These medications have been available since the 1970’s. The NSAIDs are used to treat primarily two distinct conditions: osteoarthritis (OA), which affects over half of the elderly population; and rheumatoid arthritis (RA), which affects a much smaller group. NSAIDs have fewer side effects than salicylates (most commonly aspirin), which were previously the medications routinely used to treat osteoarthritis. The NSAIDS consist of several subclasses; people respond differently to different subclasses of these medications, so it is not unusual to find individuals switching between different NSAIDs. NSAIDS are prescription medications at higher doses, and are available OTC at lower doses. Various brands as well as generic versions are available, sold as prescription and OTC.
A major disadvantage of the NSAID class is its side effect profile. NSAIDs inhibit cycloxygenase-1, an enzyme that protects the lining of the stomach. This contributes to GI symptoms, ranging from mild upset to severe ulcerations. Studies examining the incidence of these symptoms have found that approximately 20-30 percent of the population taking NSAIDs may develop mild GI symptoms (Simon et al, 1999); fewer than five percent develop more severe problems such as symptomatic complicated ulcers (Silverstein et al, 1995; Langman et al, 1999). In extreme cases, hospitalization is required for treatment of GI bleeding.
In 1999, a new class of NSAIDs, the cyclooxegenase-2 enzyme blocker agents (Cox-2s), was approved. They selectively block Cox-2 enzymes and protect the stomach lining, resulting in an improved side effect profile limiting (but not eliminating) the GI distress common to NSAIDs. Two Cox-2 medications are currently available: Celebrex® and Vioxx®. These medications pose less risk of ulcerations to the GI tract, but have not been shown to be more effective in arthritis pain relief than NSAIDS (Peterson and Cryer, 1999). Thus, at the present time, they may represent an improved therapy only for the percentage of NSAID users who are prone to serious GI problems. However, there is controversy about the proportion of NSAID users that would benefit from taking Cox-2s.
Cox-2 medications can cost approximately $3-4 per day for therapy (Average Wholesale Price), approximately four to five times as much as generic NSAIDs. When launched on the market in January 1999, Celebrex had the fastest growth rate in expenditures of any medication to that point. The sales growth rate was even faster for Vioxx after its introduction in June 1999. Recently, Cox-2’s were found to be effective in treatment of familial colonic polyps (Steinbach et al, 2000), an additional indication that may further increase sales.
Antihyperlipidemics
An estimated twenty percent of the adult U.S. population has hyperlipidemia, or cholesterol levels considered above normal (American Heart Association, 2000). Medications to treat high cholesterol include HMG-COa Reductase Inhibitors that interrupt the formation of cholesterol (statins) and other agents that reduce cholesterol formation or absorption into the blood. Because of the increased effectiveness of statins, and a relative low side effect profile associated with their use, they are much more commonly used than are other cholesterol reducing medications.
Statins are not new to the market. The first was approved in the 1980’s. However, due to recent efforts to screen and treat cholesterol over the past several years, the population on statins has been growing. Statin use is chronic; a dose should be taken each day, and generally on a long term basis. In 1993, guidelines for treatment of high cholesterol were revised to include use of statins and expanding the proportion of people for whom treatment is indicated (NHLBI, 1993). Some research suggests that hyperlipidemia is still an undertreated disease, and a larger proportion of the public might benefit from both screening and treatment with medications (Cleeman and Lenfant, 1998). As such, in spite of its rapid growth, this class of medication may represent an underused therapy.
Six statins are currently on the market.1 The dominant market leader is Lipitor®. While this is a category in which there is some price competition among brands, overall expenditures for statins in the aggregate have been growing rapidly due to increased utilization. Recently, the makers of two major statins, Pravachol® and Mevacor®, applied for FDA approval to move their products to OTC status. As of the present time, an FDA advisory committee has recommended against approving the first one, Mevacor®, for OTC.
Methods
Data:
Data for the study were provided by PCS Health Systems, Inc., a major pharmaceutical benefits management firm (PBM) that manages prescription drug benefits for approximately 50 million covered members at any given point in time. The PCS covered population is comprised of largely employed enrollees and their families with a broad range of benefit designs, including the pharmacy component for many managed care organizations. From all PCS prescription drug claims for the years 1996-1999, all claims for hundreds of carrier groups were selected. This selection was made based on: stability as a PCS client over time; and general availability of good denominator data that included age and gender of covered individuals and their dependents. This provides the advantage of having actual demographic data to work with and an accurate denominator, rather than using a multiplier that is often applied to members that purchase family coverage. From these data, we selected all persons who were continuously enrolled in PCS between the years 1996 and 1999, and for whom demographic data were available. The resulting sample population was approximately 1.3 million covered lives, with an age distribution in 1996 roughly reflecting the U.S. population. An analysis of prices for the medications within the classes discussed here is included in a paper by DiMasi being presented at this conference.
Method of analysis:
Claims counts for all relevant medications within each disease category were used to construct person-level analytic files for our cohort. To identify which persons were eligible in each disease category, we chose the following definitions of disease treatment medications, and identified all persons who used any of these medications for the study year (separately for each diagnosis):
Figure 1: Medication Categories for Study
|
Disease Treatment Category | Medication Classifications | Medications Included |
| Gastrointestinal Disease | H2 Receptor Antagonist (H2RA) | All prescription H2RAs – brand and generic (e.g. Tagamet®, Zantac®, cimetidine, etc.) |
|
| Proton Pump Inhibitor (PPI) | Prilosec®, Prevacid® |
|
| Other (antibiotics, anticholinergics, coating agents, etc.) | sucralfate, pro-banthene, etc. |
| Arthritis and pain relief | Nonsteroidal Anti-inflammatory Drug (NSAID) | All prescription NSAIDS – brand and generic (e.g. ibuprofen, Motrin®, naproxen) |
|
| Cox-2 Inhibitor | Celebrex®, Vioxx® |
| High Cholesterol | Statins | Lipitor®, Zocor®, Pravachol®, Mevacor®, Lescol®, Baycol® |
|
| Other antihyperlipidemics | Niacin, gemfibrozil, etc. |
Within each category, we summarized the claims data for each medication to obtain cost and prevalence estimates. In addition, we analyzed particular questions of interest within each therapeutic category. For instance, for PPIs and Cox-2 medications (which represent additions to the market), we identified all users of medications in 1999 and looked back one year to see if they were previously on other prescription medications for the same condition, or began therapy with introduction of the new medication. Also, for PPIs (which were originally approved for short-term use and now often used on a chronic basis), we examined duration of therapy by identifying the length of discrete episodes using a Kaplan-Meier estimate to adjust for truncation. For antilipid agents, we looked at the prevalence of use within our population, as well as consistency of use, or compliance.
Results
All three categories of medications showed a large increase in expenditures between 1996 and 1999. Figure 2 shows the increase in percent of users and overall cost for the continuously enrolled sample of 1.3 million for the three study categories.
Figure 2
|
| Users as % of cohort 1996 | Users as % of cohort 1999 | Annual % change | $ per enrollee per year 1996 | $ per enrollee per year 1999 | Annual % change |
| Gastrointestinal | 8.3 | 10.0 | 6.1 | 26.71 | 39.74 | 14.2 |
| Antiarthritics | 14.0 | 16.8 | 6.3 | 9.82 | 14.92 | 15.0 |
|
Anti- hyperlipidemics
| 3.9 | 7.3 | 23.8 | 16.70 | 39.14 | 32.8
|
Figure 3 decomposes the increased annual cost per enrollee into three components: price, utilization, and their interactions.2
Figure 3

Gastrointestinal (GI) Medications Claims 1996 and 1999
Figures 2 and 3 show that while each of the individual categories shown grew significantly in terms of use and expenditures (the growth for antihyperlipidemics appears higher because it is a smaller category in the base year than the others), the relative contribution of price versus quantity differs across categories. For instance, the majority of growth in expenditures for antihyperlipidemics is due to an increased number of prescriptions per enrollee, indicating a combination of more people being treated and more prescriptions per person being treated. On the other hand, the increasing cost per prescription for antiarthritics accounts for a large proportion of growth in per enrollee expenditures for the class, due to the emergence of medications that are many times the cost of older ones. The following sections of the paper describe what has happened within these classes to contribute to the different growth patterns.
Gastrointestinal Disease
Figure 4 shows the growth in users and claims for gastrointestinal medications between 1996 and 1999.
Figure 4
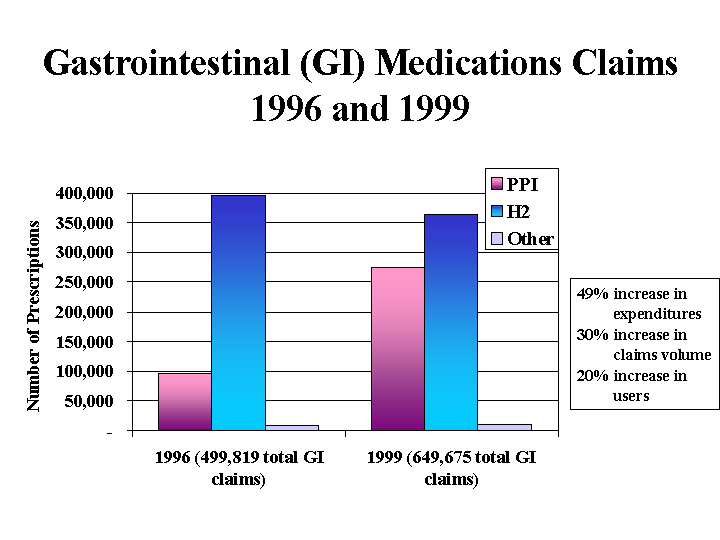
As Figure 4 indicates, claims for all GI medications increased by 30 percent over three years, with a 20 percent increase in users during that time. While both H2RA and PPIs are used for similar conditions, it appears that PPIs have not substituted for the earlier medications. Claims for prescription H2RAs decreased modestly (some users may have gone to OTC purchases as well as switched to PPIs) while PPI medication use increased far more significantly in the same time period. Overall, expenditures for the therapeutic class increased by 49 percent during the time period.
Regarding the contribution to expenditures, PPIs went from 19 percent of claims and 43 percent of GI dollars in 1996 to 43 percent of claims and 74 percent of expenditures for GI medications in 1999. On average, PPIs in our data cost approximately $3-4 per day for therapy. Brand name H2RAs are nearly expensive for therapy as the PPIs, but generic H2RAs cost less than a dollar a day.
Further analyses show that users of newly introduced medications are distributed across several categories. They include: 1) people initially taking H2RAs for the same conditions and began taking PPIs; 2) people taking no medications prior to PPIs because the condition was new, or symptoms were not severe enough to warrant medical treatment; and 3) people taking OTC medications prior to PPI use such as H2RAs or antacids. Understanding who were the users of PPIs allows us to determine whether the introduction of PPIs brought new users into the system (perhaps the effect of increased demand and increased use stimulated by direct to consumer advertising), or whether they served as a substitute for H2RAs. To examine this, we identified users of PPIs in 1999 and looked back one year to see whether they were on GI prescription medications previous to PPIs (Figure 5).
Figure 5

The majority of PPI users (55 percent) show no claims for any GI medications prior to their use of PPI medications. Approximately 40 percent of PPI users switched from a prior H2RA medication, with eight percent using both medications concurrently (potentially inappropriate use). It is impossible from claims data to determine what proportion of the 55 percent of “new to class” users of PPIs self treated with OTC H2RAs. However, whether these people took OTC medications or none at all prior to PPIs, PPIs were the first physician- prescribed medication for the condition. These results therefore indicate that the availability of PPIs has expanded considerably the population with gastrointestinal disorders treated with prescription medications.
We also examined PPI use by length of episode of therapy. As noted earlier, while initially approved for short term use (up to 12 weeks), PPIs are now being used on a chronic basis. Our data indicate the extent to which this is occurring, and suggest how medications originally indicated (and priced) for one regimen can lead to greater use and expenditures. Figure 6 shows the duration of episodes of use of PPIs in 1999. An episode is defined as use of therapy with no inferred interruption of 60 days or more. That is, if an individual begins using a PPI for some duration, there must be the indication of 60 days of no therapy for the episode to end and a new one to begin. The duration of the episode is the period from the first prescription to the last plus the days supply in the last.
Figure 6
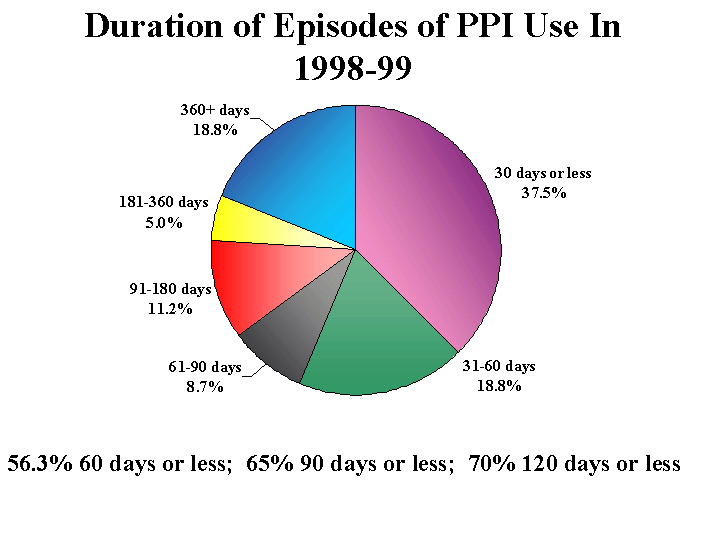
Over half of the episodes of PPI use in 1998 - 1999 are less than eight weeks, and one fourth of episodes are more than six months. Considering the recent American College of Gastroenterology (ACG) guidelines for treatment of GI disease, extended use does not necessarily indicate inappropriate care. However, this does indicate that PPIs are being prescribed for longer periods than originally approved, and provides another reason that the PPIs and the GI medications as a whole are among the fastest growing and widest selling of all medications.
NSAIDS and Cox-2 medications
Figure 7 shows a similar pattern in claims growth as to that seen in the GI medications -- new medications rapidly gaining in market share, older medications increasing in use as well, and more users in the class in its entirety.
Figure 7

Between 1996 and 1999, expenditures for the NSAID class, including Cox-2 medications, increased by 50 percent. Because Cox-2 medications were only available for part of FY 1999, the true impact of Celebrex and Vioxx in terms of market share is difficult to discern from this table. For the entire FY 1999, however, 11 percent of the total year’s claims and 28 percent of expenditures for the NSAID class were attributed to Cox-2 medications. This is of course due to the greater cost per prescription of Cox-2s. In the final month of the study, September 1999, the two Cox-2 medications accounted for 23 percent of NSAID claims, and 48% of expenditures for the therapeutic class.
Our annual data indicate that in only three-fourths of a year since their introduction, Cox-2 medications were already prescribed for fourteen percent of NSAID users, either alone or in combination with the older medications. A fourteen percent rate in so short a time confirms how quickly new medications can gain market share, when there is an obvious demand.
Figure 8 shows how users of Cox-2 medications were distributed according to prior use, and the extent to which these medications substituted for other NSAIDs. Again, for all people on Cox-2 medications, we looked back one year to determine if there were any claims for prescription NSAIDs.
Figure 8

Similar to the pattern that was seen with GI medications, over half of users of Cox-2 medications had no claims for NSAIDS in 1998 or 1999 prior to their Cox-2 use. Again, a small proportion of users filled prescriptions for both medications simultaneously, or switched back and forth. It appears that rather than take the more cost efficient ‘step-up’ approach of prescribing older NSAID medications and seeing whether they lead to undesired side effects, many physicians are immediately prescribing the newer, more expensive Cox-2 medications for patients with newly diagnosed arthritic conditions.
Cholesterol reducing medications (Statins)
Cholesterol lowering medications also experienced rapid growth in utilization between 1996 and 1999 (Figure 9). Number of users approximately doubled (with claims more than doubling), contributing in large part to the 134 percent growth in expenditures for the therapeutic category.
Figure 9

Because the statins were on the market prior to the study period, the growth within this class does not reflect the appearance of new medications between 1996 and 1999. Rather, it reflects the fact that more individuals were taking statins. In addition, the number of prescriptions per user increased over time from 5.9 to 6.3 per year.3 In the population we studied, by 1999, nearly ten percent of the adult population in our sample was taking cholesterol reducing medications. While the prevalence of hyperlipidemia is estimated to be higher among U.S. adults (approximately 20 percent), this discrepancy can not be considered “underutilizaton.” Because initial treatment of hyperlipidemia involves diet and other lifestyle changes, it is likely that not all people with high cholesterol are being treated with medication at any one time.
Since many clinical experts assert that statins may be an underutilized therapy for persons with cardiovascular disease, we also examined how consistently medications within this class are being used once the therapy is prescribed. To be fully effective, statins must be taken consistently over time. This means for claims analysis purposes, that once an individual begins a course of statins, the quantity purchased should include a daily dose or its equivalent for every day after the prescription was initiated. Appropriate switching may take place across statins and between statins and other cholesterol lowering medications as levels are adjusted. In order to look at adherence to treatment, we examined 1999 claims for all antihyperlipidemics and looked at the consistency of use once therapy was started (Figure 10).
Figure 10
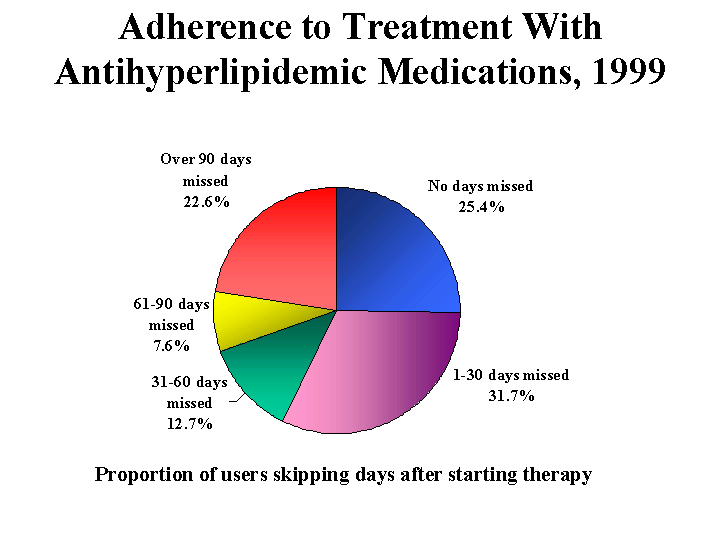
We found that nearly half of people being treated for high cholesterol were missing more than 30 days of therapy during the remainder of the year following initial treatment. These findings are essentially the same as that of 1996. To some extent, missing days of statin use may be appropriate. For instance, an individual may discontinue the medication for any medically indicated reason or because of side effects. Also, that person may not purchase the medications because of hospitalization. However, such a large proportion of days missed probably indicates that some users may be underutilizing these medications in spite of the rapid growth of the class as a whole.
Discussion
We observe certain patterns common to all the therapeutic categories studied. These include: leveling off of use of some older drugs, which are to some extent, but not completely, being replaced by new classes of medications; and increased numbers of people being treated as new medications enter the market. Our results regarding expenditure growth in the disease categories studied are consistent generally with PBM industry reports and research papers (Express Scripts, 2000; Merck-Medco, 2000; Dubois et al, 2000). In some cases, we differ from earlier research. For instance, our data show higher overall expenditure growth for cholesterol-lowering agents, and higher impact of cost versus volume for several medication classes than that of Dubois and Associates. This may be due to details of the analysis, selection of different study years in a very dynamic market, and our use of a continuously enrolled cohort.
As more medications are introduced, we can assume that the pattern of partial substitution of newer more effective drugs will continue to occur. For instance, during the next year, the patent on Prilosec (the first PPI) will expire, freeing the market for generic products. However, a second generation PPI, Nexium®, is expected to be available by 2001 and will likely offset to some extent the potential savings from generic forms of Prilosec. In effect, as soon as a generic medication is on the market, new and improved medications are also entering the market as higher cost brands. The same may hold true for other classes studied here. For instance, a new “superstatin” (ZD-4522) is in the pipeline that is reported to be more effective than those currently available. Regarding other classes of medication, the utilization growth patterns for the therapeutic categories shown in this paper are for the most part consistent with the rapid growth in prescriptions shown in a recent case study of the antidepressant class (Foote and Etheridge, 2000).
The rapid growth in utilization and expenditures for prescription drugs has both positive and negative implications. For instance, in an effort to increase the market for antihyperlipidemics, drug manufacturers engaged in aggressive advertising, resulting in many new people in treatment who might not otherwise have been. The growth in use of cholesterol lowering medications can be considered a benefit to public health, considering the evidence regarding the association of high cholesterol and cardiac disease. However, the cost implications are dramatic. Understanding the extent to which the appropriate medications are used by the population most at risk and in an effective manner is the next step in understanding the impact of prescription drugs on the health care system.
It is clear that disease management has progressed significantly as a result of new pharmaceutical technology. The market dynamics of these and other health care innovations are important, as well as the degree to which medications can offset use of other medical services. Further research on these data will identify particular patterns by age and link other medical services with pharmaceutical use.
References
American Heart Association (AHA) (2000). Cholesterol Statistics. www.americanheart.org.
Barents Group (1999). Factors Affecting the Growth of Prescription Drug Expenditures. National Institute of Health Care Management Research and Educational Foundation, Washington DC.
Berndt E, LT Bui, DH Lucking-Reiley, GL Urban (1997). “The Roles of Marketing, Product Quality, and Price Competition in the Growth and Composition of the U.S. Antiulcer Drug Industry” Chapter 7 in Timothy Bresnahan and Robert J. Gordon, eds., The Economics of New Goods, Chicago: University of Chicago Press for the National Bureau of Economic Research, 1997.
Cleeman JI and C Lenfant (1998). “The National Cholesterol Education Program – Progress and Prospects.” Journal of the American Medical Association 280(24):2099-2104.
DeVault KR, D O Castell, et al (June 1999). “Updated Guidelines for the Diagnostics and Treatment of Gastroesophageal Reflux Disease.” American Journal of Gastroenterology 94(6):1434-1442.
Dubois RW, AJ Chawla, CA Neslusan et al (2000). “Explaining Drug Spending Trends: Does Perception Match Reality?” Health Affairs 19(2):231-239.
Express-Scripts (2000). 1999 Drug Trend Report. www.express-scripts.com.
Foote S and L Etheridge (2000). Increasing Use of New Prescription Drugs: A Case Study” Health Affairs 19(4):165-170.
Langman MJ, DM Jensen, DJ Watson et al (1999). “Adverse Upper Gastrointestinal Effects of Rofecoxib Compared With NDAIDS.” Journal of the American Medical Association 282(2):1929-1933.
Merck-Medco (2000). Managing Pharmacy Benefit Costs www.merckmedco.com.
National Heart Lung and Blood Institute (NHLBI) (1993). www.nhlbi.nih.gov
Peterson WL and B Cryer (1999). “Cox-1 Sparing NSAIDS – Is the Enthusiasm Justified?” Journal of the American Medical Association 282(20):1961-1963.
Schneider Institute for Health Policy (2000). Factors Driving Prescription Drug Expenditure Increases. Unpublished data.
Silverstein FE, DY Graham, JR Senior et al (1995). “Misoprostol Reduced Serious Complications in Patients with Rheumatoid Artritis Receiving Nonsteroidal Antiinflammatory Drugs.” Annals of Internal Medicine 123:241-249.
Simon et al (1999). “Anti-inflammatory and Upper Gastrointestinal Effects of Celocoxib in Rheumatoid Arthritis: A Randomized Controlled Trial.” Journal of the American Medical Association 282(20):1921-1928.
Steinbach G, PM Lynch, RKS Phillips et al (2000). “The Effect of Celecoxib, a Cycloxegenase-2 Inhibitor, in Familial Adenomatous Polyposis.” The New England Journal of Medicine 342(26):1946-1952.
(1) These include: Lipitor® (with an overwhelming market share); Pravachol®; Mevacor®; Zocor®; Baycol®; Lescol®.
Footnotes
(2) The interaction is defined as the portion of the overall effect, usually small, that is left over after the direct effects of price and volume are taken into account.
(3) The number of prescriptions per user in this preliminary analysis is unadjusted for number of days supply per prescription.
