Catherine Hawes, Ph.D. and Charles D. Phillips, Ph.D., M.P.H.
Texas A&M University System Health Science Center
Miriam Rose, M.Ed.
Myers Research Institute
"This report was prepared under contracts #HHS-100-94-0024 and HHS-100-98-0013 between the U.S. Department of Health and Human Services, Office of the Assistant Secretary for Planning and Evaluation, Office of Disability, Aging, and Long-Term Care Policy (ASPE) and Research Triangle Institute. In addition to ASPE, other support for the study, A National Study of Assisted Living for the Frail Elderly, has been provided by the American Association of Retired Persons, the Alzheimer's Association and the National Institute on Aging. For additional information about the study, you may visit the DALTCP home page at http://aspe.hhs.gov/daltcp/home.shtml or contact the ASPE Project Officer, Pamela Doty, at DHHS/ASPE/DALTCP, H.H. Humphrey Building, Room 424E, 200 Independence Avenue, SW, Washington, DC 20201. Her e-mail address is: Pamela.Doty@hhs.gov.
I. INTRODUCTION AND STUDY BACKGROUND
This summary combines information from final reports based on data collected in a series of surveys conducted in a national probability sample of assisted living facilities (ALFs). These data were collected as part of a study, "A National Study of Assisted Living for the Frail Elderly," funded by the U.S. Department of Health and Human Services (HHS), Office of the Assistant Secretary for Planning and Evaluation (ASPE). Additional support for the study was provided by American Association of Retired Persons (AARP), the Administration on Aging (AoA), the National Institute on Aging (NIA), and the Alzheimers Association.
| This paper summarizes the findings presented in four project reports:
|
This overall summary has five sections, four of which have appeared as portions of separate project reports.
-
The first section presents the overall study goals and design.
-
Section II presents data on a nationally representative sample of ALFs and provides a basic description of the industry.
-
Section III summarizes information on a subset of these facilities. This subset is comprised of the group of ALFs that seemed most likely to embody the philosophical tenets of assisted living. Thus, the ALFs studied in this part of the project were restricted to those that offered either a relatively high level of services or a relatively high privacy environment. In these high privacy or high service ALFs, all the administrators and a random sample of staff and residents were interviewed in-person. In Section III summarizes information on a subset of these facilities. This subset is comprised of the group of AL
-
Section IV of this report describes residents who were interviewed in the high privacy or high service facilities but left those ALFs within an average of six months of that original interview. It focuses on the reasons for their exit or discharge and the characteristics of ALFs associated with earlier discharges.
-
Section V presents an examination of the facility characteristics associated with differences on key issues, such as the ability of residents to age in place, affordability for lower income elderly, willingness to meet residents personal care needs, and, more generally, the degree to which the facility exhibits elements reflecting the philosophy of assisted living.
A. What is Assisted Living
Assisted living means different things to different people, but there is general agreement on the key aspects of what constitutes assisted living. For example, one commonly accepted definition has been offered by Kane and Wilson (1993):
Any residential group program that is not licensed as a nursing home, that provides personal care to persons with need for assistance in daily living, and that can respond to unscheduled needs for assistance.
The key philosophical principles or tenets that distinguish assisted living are:
|
A similar but more expansive definition was specified by the Assisted Living Quality Coalition. This coalition is a group representing consumer groups (the Alzheimers Association and AARP) and provider associations (the American Association of Homes and Services for the Aging [AAHSA], the Assisted Living Federation of America [ALFA], the American Seniors Housing Association, and the American Health Care Association [AHCA]/National Center for Assisted Living [NCAL]). According to the Coalition, an assisted living setting is:
A congregate residential setting that provides or coordinates personal services, 24-hour supervision and assistance (scheduled and unscheduled), activities, and health related services; designed to minimize the need to move; designed to accommodate individual residents changing needs and preferences; designed to maximize residents dignity, autonomy, privacy, independence, and safety; and designed to encourage family and community involvement.
| Philosophically, assisted living represents a promising new model of residential long-term care, one that blurs the sharp and invidious distinction between receiving long-term care in one's own home and in an "institution." |
There is substantial agreement among provider and consumer groups about the key elements of the assisted living philosophy. Moreover, some, like the Assisted Living Quality Coalition, argue that some of these elements or principles distinguish it from other types of long-term care. There is less agreement on the degree to which the current industry embodies those principles. Determining this is one of the study goals.
B. Overall ASPE Study Goals
The overall purpose of the study was to learn about the role ALFs play in providing a residential setting and supportive long-term care services for the frail elderly. As part of this process, we reviewed the literature on assisted living, conducted focus group interviews with residents and families to help define the meaning of quality in assisted living, interviewed developers, and examined and reported on state regulation and financing for assisted living in surveys in 1994, 1996 and 1998. Reports on these project activities continue to be available from ASPE and can either be ordered from ASPE or downloaded from ASPEs Internet site. (The address for both is shown on the inside of the front cover of this Executive Summary.)
| Even if some facilities embody the key tenets of assisted living's philosophical model, that is, policies emphasizing autonomy, dignity, and service flexibility that facilitate maximum independence and aging in place, the degree to which this model predominates in the industry is unknown. |
In addition, the project involved substantial collection of primary data in ALFs. The specific objectives of the studys primary data collection on ALFs were to:
-
Determine the size of the assisted living industry;
-
Describe the basic characteristics of the assisted living industry, particularly in terms of philosophy, services, accommodations, staff and basic price;
-
Describe the residents in assisted living;
-
Examine the extent to which the supply of ALFs embodied the key philosophical tenets of assisted living; and
-
Examine the effect of key ALF service and environmental characteristics on such issues as price and the ability of residents to age in place.
C. Overall Study Methods
The individual reports discussed in this Final Report (which are all available from ASPE) have extensive research methods sections that provide relevant detail. The discussion of study methods here provides a general overview, emphasizing the sampling strategy and is intended to allow readers to better understand the results discussed in this summary.
In order to obtain generalizable results, the project staff implemented a complex, multi-stage sampling design. At the first stage, project staff selected a random sample of 60 geographic areas across the nation, known as first-stage sampling units (FSUs). These 60 FSUs were comprised of 1,086 counties in 34 states. At the second stage of sampling, staff selected a sample of facilities in those FSUs.1
The sample design called for selection of a set of geographic areas or FSUs prior to selecting the facility sample for several reasons. First, in order to conduct the survey, staff had to construct a listing of ALFs. There is no national list that is comprehensive and exhaustive. Moreover, definitions of assisted living vary across the states. In some states, there are no limits on the types of facilities that may call themselves assisted living or advertise that they provide assisted living, regardless of the kind of services and accommodations they provide. Further, some states did not have a licensure category known as assisted living or included all types of residential care facilities in the category called assisted living (Mollica and Snow, 1996; Mollica, 1998).2 As a result, the study could not rely on state licensure lists to provide a comprehensive and exhaustive listing of ALFs. Some places meeting study criteria would have been missed, while other facilities licensed under the category of assisted living might not have met more commonly understood definitions of assisted living.
Lists from established trade associations were also insufficient as a sampling frame. First, while there are multiple trade associations, their combined membership accounts for an unknown proportion of the total number of ALFs in operation. Second,ALFA merged with the association that represented board and care homes (i.e., the National Association of Residential Care Facilities). As a result, the membership of ALFA was expected to include both ALFs and places that were more traditionally thought of as board and care homes, some of which would meet study criteria and some which might not.
Finally, the study could not rely solely on retirement directories or local advertisements, since they appeared to have differing definitions (or no criteria) for what should be classified as assisted living. Similarly, in many localities, there were no restrictions on the kinds of places that could call themselves assisted living.
As a result, a crucial aspect of the sampling design was the development of an enumeration strategy that would enable selection of a nationally representative sample of ALFs. However, because of the extensive level of effort involved, creating a comprehensive list at the national level (i.e., in each of the >3,000 counties in the country) would have been prohibitively expensive for this project. Thus, project staff decided to select a random sample of geographic areas across the country in which to enumerate an exhaustive list of facilities.3 This involved a two-stage enumeration and screening process to provide comprehensive coverage of the target population of ALFs.
Creating a List or National Sampling Frame of ALFs
In order to create a list or sampling frame of ALFs, project staff first had to define the relevant study population. These were the criteria used to determine whether a place was eligible for inclusion in the study. As noted, the definition of assisted living varied across the country. Thus, to define assisted living for this study, project staff specified selected features about which there was general agreement among industry and consumer groups that the feature was characteristic of assisted living.
Eligibility Criteria
To be eligible for this study, a facility had to serve a mainly elderly population. In addition, a facility had to have more than 10 beds.
There were several reasons for the size restriction. We expected that few small facilities would meet the study criteria related to services provided and population served. A 1993 survey funded by HHS/ASPE examined board and care homes in ten states (Hawes et al., 1995b). Two-thirds of the licensed board and care homes had 10 or fewer beds. Few of those facilities identified themselves as assisted living or provided personal assistance with two or more activities of daily living (ADLs). In addition, none of the states that had specific licensure categories known as assisted living had actually granted a license to an ALF that had fewer than 11 beds. As a result, project staff expected that few small facilities (i.e., <10 beds) would meet the service-related criteria. In addition, small homes tended to have significant numbers of non-elderly residents; they were more likely to have residents with mental retardation, developmental disabilities, and persistent and serious mental illness.
In addition to the two eligibility criteria based on population served (i.e., elderly) and size (i.e., >10 beds), the facility had to describe or represent itself as being an ALF or it had to be a place that offered at least a basic level of services thought to be consistent with assisted living. Those services were:
- 24-hour staff oversight;
- Housekeeping;
- At least 2 meals a day; and
- Personal assistance, defined as help with at least two of the following: medications, bathing, or dressing.
| ELIGIBILITY CRITERIA To be eligible for the study, a facility had to:
AND Either
OR
|
Additional details on the selection of the FSUs can be found in the full report on the results of a telephone survey of administrators of a national probability sample of ALFs. What is important to know is that the 60 FSUs were randomly selected, with higher selection probabilities for those FSUs anticipated to contain larger numbers of expected ALFs. These FSUs consisted of 1,086 counties in 34 states. They contained 40 percent of the U.S. population aged 65 and older and 43 percent of the initial sample frame of expected ALFs.
Source of Listings of Candidate ALFs
The next task, which was completed in September 1997, was to create a comprehensive list of candidate ALFs in each of the 60 FSUs. This involved the collection of multiple lists of places that described themselves as ALFs and other places that appeared to meet the studys eligibility criteria. For each FSU, project staff obtained data from the following:
-
ALFAs 1997 list of members.
-
AHCAs National Center on Assisted Living 1997 list of assisted living members.
-
AAHSAs 1997 list of assisted living members.
-
The 1997 HCIA Directory of Retirement Facilities (DRF, 1997).
-
State licensure agency lists for 1997 for all types of residential care facilities that had 11 or more beds.
-
Listings and advertisements of assisted living, residential care, and retirement facilities from telephone book yellow pages.
-
State directories of local ALFA members, in those states in which the state affiliate of ALFA had one.
-
Local retirement directories and Internet listings of facilities.4
| Among the 18,298 places on the combined list of candidates:
Among the remaining 10,720 candidates:
|
After collecting these multiple lists, project staff spent considerable effort making sure they were in one of the 60 FSUs5 and creating an unduplicated list.6
From all these sources, for the 60 FSUs, an unduplicated total of 18,298 candidate facilities were listed. Project staff then eliminated known ineligibles based on size. Project staff found that among the 18,298 candidates 7,578 places (41 percent) were ineligible because they had 10 or fewer beds. The degree to which such small facilities might otherwise have met study criteria (e.g., be a self-described ALF or provide the required services) is unknown.
Selecting the Sample for the Telephone Screening and Survey
The next task was to select a sample of facilities from the remaining 10,720 candidates on the combined listing (e.g., after eliminating the 7,578 places with 10 or fewer beds).
In selecting the sample to be screened by telephone, project staff oversampled the larger facilities (>51 beds) in order to increase the likelihood of encountering ALFs offering a high level of services. This was based on an earlier study of residential care that found that larger facilities were more likely to have nurse staffing and to offer more services (Hawes et al., 1995a and 1995b). Thus, project staffs assumption at this stage was that larger facilities would have greater capacity to offer more services. Further, this approach would improve the sampling efficiency at later stages (i.e., when the resident sample was selected, since most residents lived in large ALFs). This oversampling did not affect final estimates about the prevalence of various types of ALFs (including various sizes), since data were weighted to account for the oversampling.7 From this list of 10,720 potential candidate facilities, project staff selected a stratified (by size), random sample of 2,945 facilities for the telephone survey.
The administrators of a sample of these candidate facilities were then surveyed by telephone during 1998. If the candidate facility met the study eligibility criteria specified in a set of screening questions, then the administrator was asked to respond to questions about the facility, its size, occupancy, accommodations, services, price and basic admission and discharge criteria. A total of 1,251 facilities was contacted, found to be eligible, and interviewed. These interviews were the basis for the first project report, and data from these interviews were also used in subsequent reports.
Our second report presents data from a series of in-person and telephone interviews with administrators, staff, residents and family members in a subset of these eligible 1,251 facilities. The subset of ALFs involved in this data collection represented that group of ALFs that offered a mix of services and privacy thought to approximate most closely key aspects of the philosophy of assisted living.
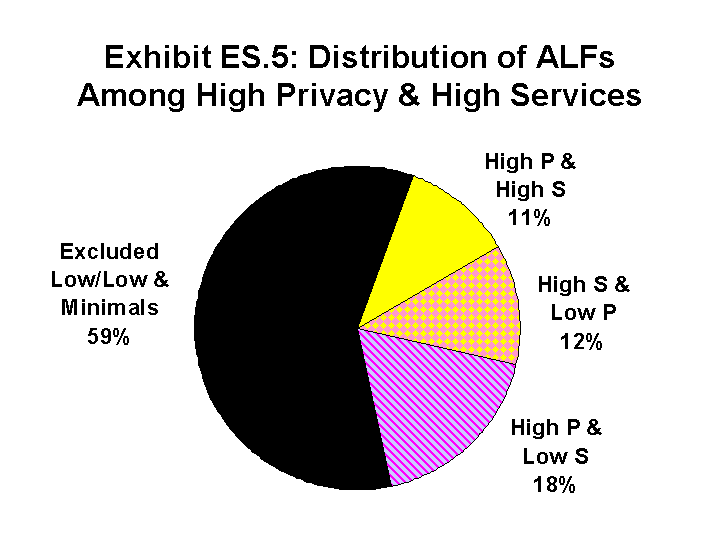
To identify this subset of ALFs, the facilities in the original sample were divided into groups, based on the level of privacy (i.e., high, low or minimal) and the level of service (i.e., high, low or minimal) that they provided. An explanation of the way in which these groups were defined is discussed in detail in Report 1 ("Results of a National Survey of Facilities") and Report 2 ("High Service or High Privacy Assisted Living Facilities, Their Residents and Staff") of this report. Facilities that offered either minimal services or minimal privacy were combined with the ALFs that provided a combination of low services and low privacy. These ALFs were excluded from any on-site data collection. Facilities in three of these groups (i.e., high service & high privacy, high service & low privacy, low service & high privacy) were chosen for further study through site visits that included more detailed data collection. The site visits included interviews with facility administrators, staff, residents, and family members, as well as a walk-through evaluation of the facility environment. The 300 facilities involved in the site visits represented a population of 4,383 ALFs across the nation -- or all those that met the definition of a facility that offered either high services or high privacy.
| TABLE ES.1: Distribution of ALFs Nationwide and Those Included in Site Visits | ||
|---|---|---|
| High Services | Low Services | |
| High Privacy | 11% of all ALFs Included | 18% of all ALFs Included |
| Low Privacy | 12% of all ALFs Included | 59% of all ALFs EXCLUDED |
II. RESULTS OF A NATIONAL SURVEY OF FACILITIES
This section presents a summary of data from a telephone survey of the administrators from a national sample of ALFs across the country. These facilities were selected from a national probability sample of all facilities that met the criteria for inclusion in the study. Thus, the findings are representative of the industry as a whole at the time of the survey in early 1998. As such, they represent the first empirical data on the characteristics of the assisted living industry nationwide based on a representative national sample of facilities.
| This section of the report presents the results of a telephone screening of a list of 2,945 places identified as "likely" ALFs and a more extensive survey of a group of 1,251 of those places that met study eligibility criteria. These 1,251 ALFs constituted a nationally representative sample of ALFs. |
A. Study Purpose
The overall purpose of the study was to learn about the role ALFs play in providing a residential setting and supportive long-term care services to the elderly. The specific objectives of this telephone survey were to:
-
Determine the size and nature of the supply of ALFs;
-
Describe the basic characteristics of the assisted living industry particularly in terms of the services, accommodations and basic price;
-
Begin examining the extent to which the existing supply of facilities embodies the key philosophical tenets of assisted living; and
-
Identify facilities for subsequent, more extensive data collection.
B. Results
This section summarizes the findings on key aspects of the assisted living industry nationwide.
Size of the Assisted Living Industry
There were an estimated 11,459 ALFs nationwide, with approximately 611,300 beds and 521,500 residents, as of the beginning of 1998.
General Characteristics of the Assisted Living Industry
The average number of beds or ALF size was 53 beds; 67 percent of the ALFs had 11-50 beds; 21 percent had 51-100 beds; and 12 percent had more than 100 beds. Facility occupancy averaged 84 percent. The average length of time the ALFs had been in business was 15 years, but slightly more than half (58 percent) of the ALFs had been in business for 10 years or less. About one-third (32 percent) had been in business no more than 5 years.
 |
Accommodations
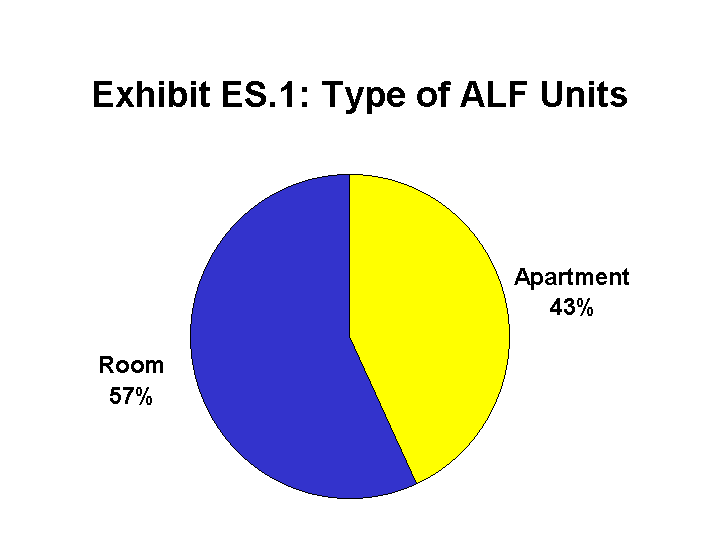
Unit Type. A bedroom was the dominant type of resident unit (57 percent) in ALFs; 43 percent of the units were apartments. The most common type of room was a private room with a full bathroom (42 percent of all single rooms). The most common type of apartment was a one-bedroom, single occupancy apartment (41 percent).
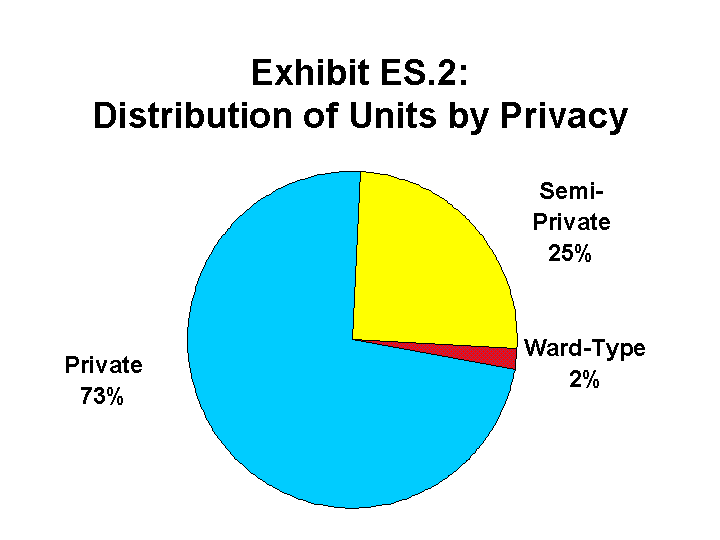 |
Privacy. Most ALFs offered consumers a range of options in terms of private or shared accommodations. Only 27 percent of the facilities had all-private accommodations. A plurality of ALFs (45 percent) had a mix of private and shared units. Slightly more than one-fourth of the ALF administrators (28 percent) reported that the facility had at least one bedroom shared by three or more residents. Although ALFs offered residents a range of options, 73 percent of all resident units were private. Twenty-five percent of the units were semi-private, that is, shared by two unrelated persons. Two percent of resident units were in ward-type rooms that housed three or more unrelated persons.
Bathrooms. While nearly three-quarters (73 percent) of the rooms or apartments were private, less than two-thirds (62 percent) of the units offered a private full bathroom (i.e., toilet, sink and shower or tub). An additional 6 percent of the units had a private half bath (i.e., toilet and sink). However, one-third (33 percent) of all ALF units required the resident to share a full bathroom.
Services and Nurse Staffing
General Services. Nearly all facilities provided or arranged 24-hour staff, three meals a day, and housekeeping. More than 90 percent of the ALF administrators also reported that the facility provided medication reminders and assistance with bathing and dressing; 88 percent of the ALFs provided or arranged central storage of drugs or assistance with administration of medications.
Nurse Staffing. Almost three-quarters of the ALFS (71 percent) had a licensed nurse, either a registered nurse (RN) or licensed vocational nurse (LVN), working on staff full or part-time. Slightly more than half the ALFs (55 percent) reported having an RN on staff either full or part-time. Forty percent of the ALFs reported having a full-time RN on staff.
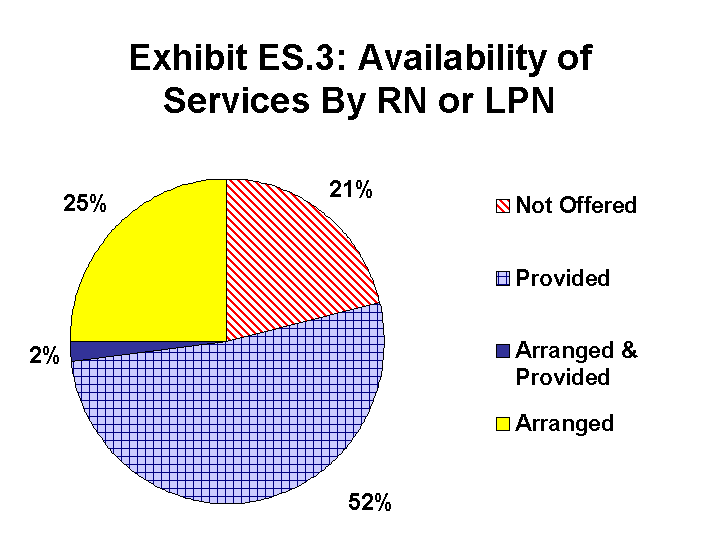 |
Providing or Arranging Services. Administrators were also asked whether the facility provided services with their own staff or arranged with an outside agency for the provision of the service. With the exception of therapies, if an ALF offered a service, such as help with bathing, dressing, and managing medications, most provided it with their own staff. About half (52 percent) of the facilities provided some care or monitoring by a licensed nurse (RN or LPN) with their own staff, and one-quarter (25 percent) arranged for nursing care with an agency. However, one in five ALF administrators (21 percent) reported that the facility did not arrange or provide any care or monitoring by a licensed nurse.
Admission and Retention Policies
Most ALFs reported a willingness to admit residents with moderate physical limitations, such as using a wheelchair (71 percent) or needing help with locomotion (62 percent) (i.e., walking or using a wheelchair or cart). However, fewer than half the ALFs (44 percent) were willing to admit residents who needed assistance with transfers (i.e., in or out of bed, a chair or wheelchair). Administrators also reported that fewer than half the ALFs (47 percent) would admit a resident with moderate to severe cognitive impairment.8
Facilities also had criteria about the retention of residents with certain types of conditions or problems, although, as with admission policies, many facilities had idiosyncratic policies (see footnote #8). Nearly one-third of the administrators (31 percent) reported that the ALF would not retain a resident who used a wheelchair (or that it depends), and 38 percent would discharge a resident who needed assistance with locomotion. More than half (55 percent) of the ALFs would not retain a resident with moderate to severe cognitive impairment, and 76 percent not retain residents with behavioral symptoms (e.g., wandering). Seventy-two percent of the ALFs would not retain a resident who needed nursing care for more than 14 days.
Resident Characteristics
ALF administrators estimated that about 24 percent of their residents received help with three or more ADLs, such as bathing, dressing, and locomotion. They estimated that about one-third of the residents (34 percent) had moderate to severe cognitive impairment.
Different Models of Assisted Living
The information provided by administrators identified two significant variations among the ALFs that are worth noting. One group of ALFs identified or described themselves as ALFs. Another much smaller group provided the same basic services but identified themselves by some other designation, such as adult congregate living, residential care, or community residential facility. Another significant variation was between ALFs that were free-standing and ALFs located on a campus that offered multiple levels of care. Such multi-level campuses typically housed an ALF and a nursing home or some other type of residential care, such as congregate apartments or independent living facilities.
Self-Described ALFs. Seven out of ten (72 percent) of the administrators represented or described the facility as being an assisted living facility or residence. Twenty-eight percent of the administrators did not describe the facility as assisted living; however, the facility still met study eligibility criteria. Despite the differences in how the administrators characterized the facilities, the two groups of facilities were remarkably similar in terms of their size, the services they offered, their nurse staffing, most admission and retention criteria, and the basic characteristics of their residents. Self-described ALFs, however, tended to have lower occupancy rates, had been in business for a shorter period of time, were more likely to offer apartments and private units, and were more likely to admit and retain residents who used a wheelchair or received help with locomotion. They also tended, on average, to have higher monthly prices.
Free-Standing ALFs Compared to ALFs Located on a Multi-Level Campus. The majority of ALFs (55 percent) were free-standing, while 45 percent were located on a campus housing multiple facilities or residential settings offering different levels of care. ALFs on a multi-level campus had higher occupancy rates and tended to have higher monthly prices than free-standing ALFs. They were also more likely to have private units and apartments and to provide or arrange more services for residents, most notably nursing care and therapies. ALFs on multi-level campuses also tended to have higher levels of nurse staffing than free-standing ALFs. In addition, they were more likely to admit and retain residents who needed nursing care and residents who used a wheelchair. Despite this, the administrators did not report having a heavier care resident case mix than the free-standing ALFs.
Categorization of ALFs by Combined Levels of Service and Privacy. Any attempt to understand assisted living and its role in providing long-term care to the frail elderly is hindered by the lack of a common definition of assisted living. Currently, places known as ALFs differ widely in ownership, auspice, size, services, staffing, accommodations, and price. Thus, analyzing data on facilities and reaching conclusions about assisted living as a whole involves comparing apples to oranges. As a result, project staff developed a classification that divided the universe of ALFs into distinct categories or types of facilities, representing their mix of services and privacy. The four types the study identified represent reasonably homogeneous groups of facilities. Moreover, the data revealed significant differences among groups.
Definitions of high, low and minimal privacy. High privacy meant that at least 80 percent of the resident units were private. A total of 31 percent of the facilities met this definition of high privacy. Twenty-eight percent of the ALFs offered minimal privacy because they had one or more rooms that housed at least three residents. The remainder of the ALFs (41 percent) fell between these two types of facilities in a low privacy category.
Definitions of high, low and minimal services. High services was defined as having a full-time RN on staff and providing nursing care, as needed, with facility staff, as well as providing help with at least two ADLs, 24-hour staff, housekeeping, and at least two meals a day. Thirty-one percent of the ALFs met this criterion. Five percent of the ALFs did not offer help with even two ADLs and were thus defined as providing minimal services. The remaining ALFs (65 percent)9 were categorized as low service, although some that did not provide nursing care with their own staff were willing to arrange a higher level of services through an outside provider, such as a home health agency.10
Combining the mix of services and privacy revealed four basic types. The first type of ALF combined facilities in the minimal group of ALFs (i.e., the 32 percent with either minimal privacy or minimal services) and facilities offering low privacy and low service (i.e., 27 percent of the ALFs). The facilities classified as minimal had either at least one room shared by three or more unrelated individuals (i.e., minimal privacy) or did not provide basic services, such as assistance with ADLs (i.e., minimal services).
| TABLE ES.2: Distribution of ALFs by Categories | |
|---|---|
| Category | National Estimate |
| 1a. Low Privacy & Low Service | 27% |
| 1b. Minimal Privacy or Service | 32% |
| 2. High Privacy & Low Service | 18% |
| 3. High Service & Low Privacy | 12% |
| 4. High Privacy & High Service | 11% |
The combined low/minimal privacy and services group was the most common type of ALF, comprising 59 percent of all the ALFs. This type of ALF cannot be easily distinguished from the traditional concept of board and care homes. A significant proportion of resident rooms were shared rather than private, and such facilities offered little beyond assistance with medications, bathing, or dressing. In two of five (41 percent) ALFs described by this model, there was at least one room shared by three or more people. ALFs of this type not only represented the majority of all ALFs nationwide, they also constituted 58 percent of all the facilities that described themselves as assisted living.
Another ALF type offered a high degree of privacy in accommodations but low services, a sort of cruise ship model of assisted living. In this type of ALF, more than 80 percent of the accommodations were private. However, these facilities would have had a difficult time helping residents age in place, since they had no RN on staff and most were unwilling or unable to provide or arrange any nursing care for residents. Only 19 percent of the ALFs in this model would provide or arrange nursing care and retain a resident who needed such care. This ALF type comprised 18 percent of all ALFs nationwide.
A third type of ALF was one described as high service/low privacy. In such facilities, two-thirds of the accommodations were in single rooms rather than apartments, and fewer than 80 percent of the rooms were private. However, all such facilities had a full-time RN on staff. About half (53 percent) of the ALFs of this type were willing to provide or arrange nursing care, as needed, and retain residents who needed such care. This was also the type of ALF that had the most expansive admission and retention criteria and the highest resident acuity. For example, such facilities were more likely to retain residents who needed assistance with transfers and to retain residents who needed nursing care. Compared to the other ALF types, the high service/low privacy type also had a much higher proportion (35 percent) of residents who received assistance with three or more ADLs, such as help with locomotion or using the toilet, as well as bathing and dressing. An estimated 12 percent of the ALFs across the country were in this category.
A fourth type of ALF offered high service and high privacy. Only 11 percent of all ALFs fell into this category. While resident accommodations were almost evenly split between rooms and apartments, nearly all of the accommodations were private. In addition, 41 percent of the high service/high privacy ALFs offered to arrange or provide nursing care and retain residents who needed such care. All had an RN on staff.
Price of Assisted Living
There were many variations in pricing structure among the ALFs nationwide. Some ALFs had a single monthly price for what they defined as basic services and accommodations. Other ALFs had multiple rates, varying with either the type of accommodation or the service package provided to the resident.
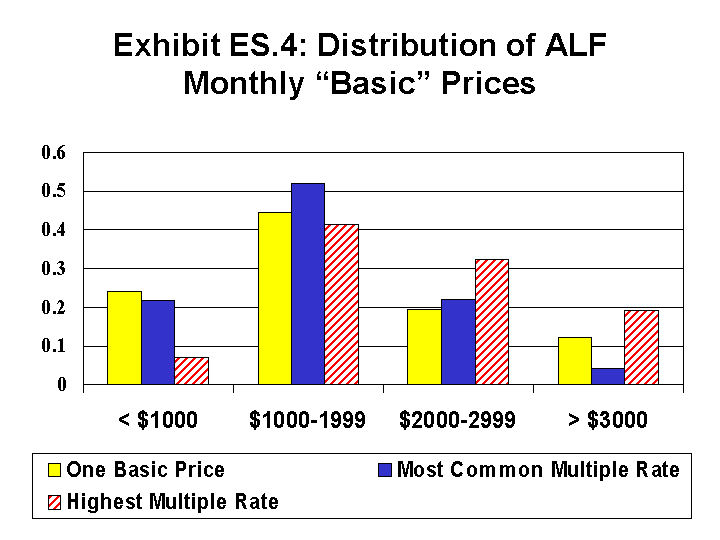 |
The most common monthly price was between $1000 and $1999 for both facilities with a single rate (i.e., 45 percent were in this range) and for facilities with multiple rates (i.e., the range covered the most common rate for 52 percent of the ALFs). Thus, the most common basic price was between $12,000 and $24,000 per year. However, it is important to note that the average price was depressed by the presence of a very large number of ALFs (59 percent) that offered minimal or low privacy and services. The most common base price for facilities that offered multiple rates was just over $22,000 per year for the high service/low privacy ALFs and $23,000 for the high service/high privacy ALFs. For the high privacy/low service ALFs, the most common basic annual rate was slightly more than $22,000 when one combines single rate and multiple rate facilities.
These rates are striking for two reasons. First, in many ALFs, they do not cover all services. Residents often pay extra for such services as medication administration, transportation, and any assistance with ADLs or nursing care above the minimum covered by the basic rate of a facility.
Second, the rates are largely out of reach for most low-income older persons and unaffordable for many moderate-income elderly unless they are supplementing their income with additional funds generated by disposal of their assets. According to data from the U.S. Bureau of the Census,11 40 percent of persons aged 75 and older had incomes in 1997 of less than $10,000 per year. Eighty-four percent of persons aged 75 and older had incomes of less than $25,000 per year in 1997. This would make the average high service ALF or the average high privacy ALF unaffordable for the vast majority of older persons, particularly since they must also pay for other basic needs (e.g., supplemental insurance, out-of-pocket spending on health care and medications, clothing).12
C. Conclusions
What is Assisted Living?
Any attempt to understand assisted living and its role in providing long-term care to the frail elderly is hindered by the lack of a common definition of assisted living. Places known as ALFs differed widely in ownership, auspice, size, and philosophy. Indeed, the results of this national survey identified four different types of ALFs within the industry that had very different patterns with respect to accommodations, services, staffing, policies on admission and retention of residents, and price. Some of these types, such as those offering high privacy and high service, appeared to be consistent with the philosophy of assisted living. Other types, such as the low-minimal privacy and service types were much closer to the traditional concept of domiciliary care or board and care, with few services and relatively little privacy.
| "Assisted living is known by dozens of different terms throughout the country. ...The multitude of names for assisted living reflects the diversity of services offered in the cloudy nexus between retirement housing and skilled nursing care." Hodlewsky, National Center for Assisted Living, 1998 |
Does the Environment of ALFs Match the Philosophy of Assisted Living?
The answer to this question is mixed. On the one hand, residents of ALFs had considerably more privacy and choice than residents of most nursing homes and the majority of board and care homes. On the other hand, there was significant variability within the assisted living industry, and a substantial segment of the industry provided environments that did not appear consistent with the environmental aspects of the assisted living philosophy.
Do ALF Services Match the Philosophy of Assisted Living?
The ability of ALFs to meet health-related unscheduled needs of residents is still an open question -- in part because of facility policies (e.g., on nurse staffing and retention criteria or discharge policies) and in part because of potential constraints imposed by state licensure regulations.
Can ALF Residents Age in Place?
The answer depends on ones concept of aging in place. For example, in most ALFs, a resident could move from relative independence (e.g., needing or wanting only meal preparation, housekeeping, and staff that can respond to emergencies) to a more complex stage at which the resident needed help with bathing, dressing, and managing medications and used a wheelchair to get around. If this span or change in needs were the definition of aging in place, then the admission and retention policies of ALFs suggest they were willing to allow residents to age in place.
On the other hand, if aging in place meant that the average consumer could select an ALF and reasonably expect to live there to the end of his or her life, regardless of changes in health or physical and cognitive functioning, then the answer must be no. In most ALFs, a resident whose functional limitations necessitated help with transfers or whose cognitive impairment progressed from mild to moderate or severe or who exhibited behavioral symptoms would be discharged from the facility. The same is true for a resident who needed nursing care for more than two weeks.
Thus, there is a limitation in terms of the ability of ALF residents to age in place.
Is Assisted Living Affordable for Low and Moderate Income Older Persons?
Assisted living was largely not affordable for moderate and low-income persons aged 75 or older unless they disposed of their assets and spent them down to supplement their income. Further, to the degree that some ALFs were affordable for low and moderate-income older persons, they were more likely to be ALFs categorized as low service and low privacy facilities.
| National Study of Assisted Living for the Frail Elderly: Results of a National Survey of Facilities AUTHORS: Catherine Hawes, Miriam Rose and Charles D. Phillips DATE: December 14, 1999 AVAILABLE ONLINE: Executive Summary (http://aspe.hhs.gov/daltcp/reports/facreses.htm) Full Report (http://aspe.hhs.gov/daltcp/reports/facres.htm) |
III. ASSISTED LIVING RESIDENTS, STAFF AND FACILITIES: DATA FROM A NATIONAL SAMPLE OF HIGH PRIVACY OR HIGH SERVICE ALFS
A. Background
The most rapidly growing form of senior housing in recent years has been a form of supportive housing or residential long-term care known as assisted living. This growth has been a response to several factors, including the aging of the population, the preferences of the elderly for settings other than nursing homes, the availability of private financing for development and construction of ALFs, and public policies aimed at containing use of nursing homes.
| This report presents data on 41% of the ALFs nationwide and on the residents and staff in those facilities. These are the facilities among all ALFs that offer the highest levels of services and privacy. |
ASPE has a long-standing interest in the ability of residential and community-based service providers to meet the needs of the elderly and people with disabilities. As a result, ASPE has funded several studies of residential long-term care, including this first national study of ALFs for the frail elderly. ASPEs interest in assisted living and its ability to meet the needs of the frail elderly has been heightened during the study by a series of reports and a Congressional hearing that raised concerns about quality and consumer protection in assisted living (U.S. General Accounting Office, 1997 and 1999).
 |
This section also presents data collected on facilities. It reports data on a nationally representative sample of residents and staff in ALFs classified as providing the highest levels of services or privacy. These facilities comprise about two-fifths (41 percent) of the places calling themselves assisted living and were selected for more extensive and in-depth data collection because they seemed to most effectively exhibit key elements of the philosophy of assisted living.
B. The Results
ALF Residents
The residents in the high privacy or high service ALFs were largely white, widowed females, who were quite elderly. More than one-half of the residents were 85 years of age or older. ALF residents were relatively well-educated; 45 percent had completed at least some college. They were also relatively affluent. Most entered assisted living from their own home or apartment (70 percent) and made the decision with help from someone else (90 percent), almost always their adult children. However, one-quarter of residents indicated that they had little or no control over the decision to enter a facility.
| Residents in ALFs Offering High Services or High Privacy
|
Over one-quarter (27 percent) of the residents suffered from moderate or severe cognitive impairment, one-half of residents (51 percent) received assistance with bathing, and one-fifth of residents received assistance in some other ADL. The overwhelming majority (77 percent), however, received help with their medications, and many residents used assistive devices, especially to help with ambulation or locomotion. Almost one-third (32 percent) experienced urinary incontinence. Two-fifths of the residents considered themselves in only fair or poor health, and, in the year prior to their interview, they used inpatient hospital services at rates much higher than the general population.
Residents were relatively satisfied with the attitudes of staff and how staff treated them (e.g., with respect and affection), although some residents (i.e., between 12 percent and 26 percent) who received help with ADLs reported some problems with unmet needs. Overall, however, residents greatest points of concerns about staff were related to inadequate staffing levels and high staff turnover. There was also some concern about the adequacy of activities. Residents were split almost evenly in their perceptions of the availability of activities they enjoyed and on the availability of transportation to events they might enjoy. One of the more unsettling findings concerning activities was that almost three-fifths of the residents (59 percent) indicated that ALF staff never or only sometimes asked them about their activity preferences.
Assisted living residents in ALFs classified as providing high services or high privacy were almost equally likely to be found in accommodations consisting of a full apartment or only a bedroom. The majority (81 percent) had a private living space or shared it with a related individual; however, nearly one-third of the residents did not have a private full bathroom. Most residents (i.e., more than three-quarters) also had other types of autonomy over their environment, such as ability to lock their doors, furnish their apartments and arrange the furniture as they wished, and control the temperature in their room or apartment. Only about half, however, had a refrigerator and only about one-third had personal space for cooking. Most had access to key supportive devices, such as call buttons and safety railings in the bathroom.
| Residents' Perceptions About ALFs Offering High Services or High Privacy
|
When they needed temporary nursing care, they were most likely to receive it from the facility staff; however, one-third of the residents who needed such care were either discharged to a hospital or nursing home or, with help from family members, arranged for home health services themselves. Finally, less than one-third of the residents reported being informed by the facility about the discharge and retention policies. Despite this, the vast majority of residents expected to be able to stay in the facility for as long as they wished.
Staff in High Privacy or High Service ALFs
The project investigated facility staffs knowledge of the appropriate response in a variety of situations involving relatively common health problems among frail older persons. In many instances, the vast majority of staff were aware of the proper response to specific situations, including most medication management issues. On the other hand, a significant number of staff members were poorly informed about antipsychotic drugs and some issues related to the care of individuals with dementia. More troubling, the majority of staff members were almost completely unaware of what constitutes normal aging. Given the goal of enabling residents to age in place and the advanced age of current residents, these results are particularly disquieting. Poor training and knowledge in these areas may in the future become more and more troublesome and risky, both for providers and residents, since many of the conditions staff identified as a normal part of aging were potentially treatable and reversible.
| Staff in ALFs Offering High Services or High Privacy
|
Most staff in the high privacy or high service ALFs reported relatively high levels of satisfaction or positive attitudes toward their working conditions. Two areas, however, were a concern for most staff. The first was their pay level, which usually ranged from between $5 and $9 per hour for personal care attendants. They also expressed dissatisfaction with what they viewed as limited possibilities for advancement.
| The median ratio of direct care staff to residents was 1:14 in high service or high privacy ALFs; however, these staff, particularly the personal care assistants typically were responsible for tasks such as laundry, housekeeping, and meal service, in addition to direct resident care. |
Personal care staff did not report their workload as overly heavy, and the median number of residents for whom they cared was fourteen.13 In a nursing home this level of staffing would cause concern for some experts. However, as discussed above, the ALF residents were not as impaired as nursing home residents. At the same time, the survey demonstrated that most direct care staff in ALFs also had responsibility for a variety of tasks in addition to direct resident care, including housekeeping, laundry, and meal service. This complicates any attempt to evaluate the adequacy of staffing levels or compare them to those in other settings.
Walk-Through Observations
The observers judgments about the physical plant in ALFs indicated that these settings were largely well-maintained, clean, relatively homelike settings for the frail elderly with a wide range of social and recreational resources. Most were in suburban areas, and nearly half (46 percent) were single story buildings.
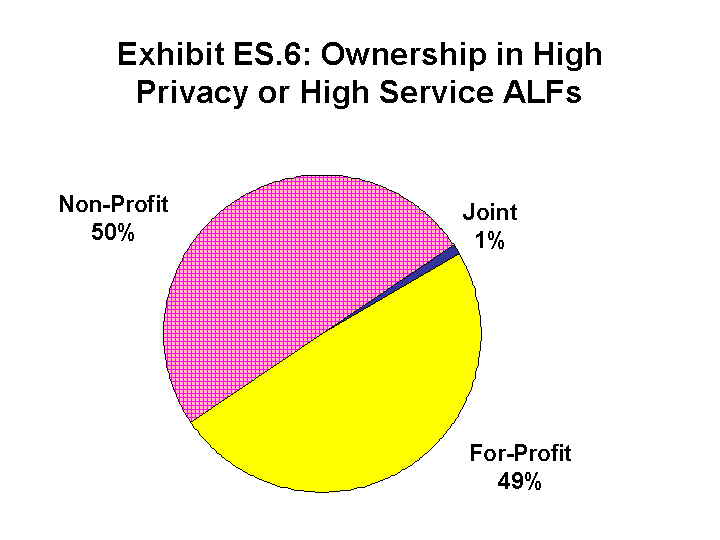
Facilities, Administrators, and Staffing
ALFs were almost equally likely to be operated by for-profit as by not-for-profit entities. However, the vast majority (79 percent) of organizations that owned or operated the high service or high privacy ALFs were involved in the operation of other types of supportive housing for the elderly, such as nursing homes and congregate apartments. Almost two-thirds (64 percent) of the not-for-profit ALFs, for example, were located on a multi-level campus that housed various types of supportive housing for the elderly, including a nursing home. Indeed, nearly half (49 percent) the owners of all of the high service or high privacy ALFs owned or operated nursing homes, and nearly half (46 percent) of these ALFs were part of a multi-facility system or chain of ALFs.
Facilities showed some variation in the level of functional limitations and cognitive status among their residents. In most ALFs, relatively few residents had significant functional limitations and care needs. In most ALFs, assistance with medications was the only area in which they reported most residents needing and receiving help. However, approximately 15 percent of ALFs seemed to have a substantial proportion of residents with somewhat heavier physical care needs, such as need for help with transfers and other middle-range and late-loss ADLs. Administrators also reported fairly high turnover rates among residents, with an average annual rate of 41 percent of the residents each year.
 |
Staffing across facilities varied considerably. On first shift, one-quarter of the ALFs had direct care staff to resident ratios of 8-to-1 or lower, and another quarter had ratios of 16-to-1 or greater. While staffing ratios varied considerably, there was some consistency across ALFs in the types of staff used. For example, the sampled ALFs that were site-visited almost universally utilized some licensed nursing services. Staff turnover was lowest among licensed nursing staff, but administrators estimated that roughly one-quarter of all direct care staff turnover during the course of a year.
| High Privacy or High Service Facilities
|
The most common monthly charge for living in an ALF was approximately $1,800. However, because of the diversity among ALFs in what was included in that base rate, one is not quite sure what that sum purchased. For example, relatively few facilities (36 percent) provided temporary nursing care as part of their base monthly rate, while a substantial majority (80 percent) provided planned recreational activities. For those residents who exhausted their funds paying at this level, many facilities were willing to accept payments from alternative sources (e.g., charity, Supplemental Security Income, Medicaid). Policy in a substantial proportion of facilities (45 percent), however, simply called for the discharge of those who exhausted their private financial resources.
C. Conclusions
There are a number of policy issues surrounding the emergence and growth of assisted living and its ability to help meet the long-term care needs of the elderly and disabled. This report begins to address some of these by focusing on only those facilities that seem to most closely embody the philosophical tenets of assisted living. Thus, the report describes the facilities that offer either high privacy or high services -- or both -- and their policies and practices, particularly with respect to services, policies on autonomy and resident control, and staffing. Further, this report describes the characteristics of the residents and their perceptions about the care they receive and the environment of the facilities in which they live. In providing this descriptive data, we begin to address questions about the role and performance of ALFs and their place in the constellation of long-term care services. We also attempt to relate the descriptive data to the central study questions about whether ALFs embody the principles of assisted living and whether the needs of residents are being met. We also note that even in this special subgroup of ALFs, there is tremendous variability.
| High Service or High Privacy Assisted Living Facilities, Their Residents and Staff: Results from a National Survey AUTHORS: Catherine Hawes, Charles D. Phillips and Miriam Rose DATE: November 2000 AVAILABLE ONLINE: Executive Summary (http://aspe.hhs.gov/daltcp/reports/hshpes.htm) Full Report (http://aspe.hhs.gov/daltcp/reports/hshp.htm) |
IV. RESIDENTS LEAVING ASSISTED LIVING: RESULTS FROM A NATIONAL SURVEY OF HIGH SERVICE AND HIGH PRIVACY ALFS
A. Background
This section provides information on departures from assisted living, the reasons for departure, and those resident and facility characteristics that affected the likelihood of various resident outcomes associated with departure. The report focuses on a nationally representative sample of ALFs in 1998 that offered either a relatively high level of services or a relatively high level of privacy or both high services and high privacy. This special group of ALFs represents 41 percent of places calling themselves assisted living facilities.
| This report describes residents discharged from high service and high privacy ALFs during the six months following their initial interview. It focuses on their reasons for leaving and examines differences in ALFs associated with differences in discharge. |
B. Results
Our best estimates from this national sample indicate that in 1998 approximately 24 percent of residents left an ALF over the course of 12 months. The results indicate that roughly one-third of the residents who left a study ALF between baseline and follow-up (roughly 8 percent of all residents on a yearly basis) either died in the ALF or elsewhere prior to follow-up contact. Most of the remainder who left went to a nursing home or some other residential care setting (e.g., another ALF or personal care home). On an annualized basis, 8 percent of all residents went to a nursing home and 4 percent of all residents moved to some other residential care setting. The need for more care was the most commonly cited reason by respondents for leaving an ALF. Very few (9 percent) of the respondents indicated that they or their family member left the original ALF because they could no longer afford to remain in the facility.
| We estimated that roughly one-quarter of ALF residents left their facility over 12 months. The most common reason given for leaving an ALF was the need for more care. Those who left a study ALF were most likely to have died or entered a nursing home. |
This research also provided some previously unavailable information on the characteristics of residents and facilities that affect individuals exit from an ALF. In the multi-variate analyses that controlled for both individual and also facility characteristics, older age and marital status were associated with a residents increased likelihood of death prior to follow-up. Although only a small percentage of ALF residents were married, they were twice as likely as unmarried residents to die prior to the follow-up interview. The only individual characteristic or resident-level variable that affected an individuals likelihood of entering a nursing home was the residents cognitive status. Residents who had moderate to severe cognitive impairment were more likely to enter a nursing home.
| Both individual-level and facility-level factors determined where residents went when they left their ALF. Residents in ALFs without a full-time RN involved in direct care were twice as likely to leave their ALF and go to a nursing home or some other care setting than were similar residents in ALFs that had a full-time RN. Residents in not-for-profit ALFs were significantly less likely than similar residents in for-profit ALFs to move to a different ALF or other residential care facility. |
In the multi-variate models, facility characteristics also had an impact. No facility characteristics had a significant impact on a residents likelihood of death. However, residence in a for-profit ALF was highly associated with movement into another residential care setting other than a nursing home. Also, residing in an ALF with a full-time RN who provided care to residents reduced a residents likelihood of going to a nursing home or to some other setting by roughly half.
These results have a number of relatively interesting policy implications. For policy-makers interested in developing an assisted living industry that can delay nursing home use, creating incentives for facilities to provide a higher level of service could be productive. However, such a policy stance would mean encouraging the development of higher cost ALFs. Yet how to develop ALFs that are affordable for individuals with low or moderate income is also a significant issue. In addition, if higher cost ALFs are encouraged, then the specific amount of delay in nursing home use (i.e., the number of person months) that results from these increased costs become a critical parameter for policy discussions. In addition, one must consider any additional home health, ambulatory care, medications, or acute care use that are required during the delay and might have been avoided by earlier placement in a nursing home.
For consumers intent on avoiding or delaying nursing home placement, seeking out ALFs that have full-time RNs and provide nursing care with their in-house staff may represent a good choice in an ALF. Also, for consumers interested in aging in place, being in a facility with a full-time RN active in direct care may significantly reduce the likelihood that one will move to some other ALF or another care setting other than a nursing home.14
Most people entering an ALF are not as disabled as those entering a nursing home. This means that the choice to enter an ALF with a full-time RN active in direct care may only be important to more impaired residents or to residents over the course of time as they age in place. Thus, many consumers might end up paying at the front-end for services that will only be important to them later, if they stay in the same facility.
One must also remember that this analysis focused on facilities that chose at a specific point in the evolution of the industry to have a full-time RN and provide direct care with in-house nursing staff. These services seem to have had a direct impact on resident outcomes. However, the effect of these services in facilities that add them as a marketing tool, in response to a reimbursement incentive, or because of regulatory mandates may differ from the effects we observed in ALFs that voluntarily chose their particular staffing and service pattern.
The finding that cognitive impairment has such an important impact on discharge to a nursing home may also have substantial policy implications. To the degree that the industry is encouraged to care for more severely cognitively impaired residents, then savings in nursing home costs may accrue. However, the industrys ability to provide appropriate care to this population is unproven. Moreover, the overall effect on total long-term care costs cannot be predicted.
As the discussion above indicates, the policy issues here are complex, and our knowledge base is limited. This is, after all, a single study. Even though it is based on a nationally representative sample of higher service or higher privacy ALFs, an appropriate measure of caution should be used when considering these results in the policy-making process.
| Residents Leaving Assisted Living: Descriptive and Analytic Results From a National Survey AUTHORS: Charles D. Phillips, Catherine Hawes, Kathleen Spry and Miriam Rose DATE: June 2000 AVAILABLE ONLINE: Executive Summary (http://aspe.hhs.gov/daltcp/reports/alresdes.htm) Full Report (http://aspe.hhs.gov/daltcp/reports/alresid.htm) |
V. THE EFFECT OF DIFFERENCES IN FACILITY CHARACTERISTICS ON THE PERFORMANCE AND POLICIES OF ALFS
A. Background
This section seeks to address the final question proposed for the ASPE study -- whether different ALF characteristics, particularly differences in services and the environment (i.e., privacy) -- have an effect on such important issues as environmental autonomy, unmet care needs, the ability of residents to age in place, and affordability. This report represents an initial step aimed at understanding the effects of various facility characteristics on how well ALFs may meet the needs of different residents. Comparisons were made on a number of facility characteristics related to the philosophy of assisted living and their ability and willingness to meet resident needs and desires. The comparisons involved the effect of the mix of privacy and services in facilities. In this section, we briefly review the findings about differences among facility types based on the telephone interviews with administrators in a national sample of all ALFs. However, the most detailed information was collected during the site visits that excluded the low service/low privacy facilities. Thus, the analysis concentrates on the observed differences among the high service or high privacy ALFs included in the site visits.
| This section of the report examines the effect of facility characteristics on key issues, such as unmet care needs, environmental autonomy, the ability of the facility to meet scheduled and unscheduled needs, and affordability. It briefly summarizes the effects among all ALFs but concentrates on differences among the ALFs that offer high services or high privacy. |
B. Results
Differences Based on Data From All ALFs
Previous reports, such as the initial telephone interviews with administrators demonstrated that there were differences between ALFs in terms of such characteristics as their affiliation, environment, staffing, and policies on admission and retention. For example, ALFs differed in both the proportion of private units and the proportion of apartments. The ALFs offering high privacy, both those that offered high services and those that provided low services, had higher proportions of resident units that were apartments than did the low privacy/low service ALFs.
There was also significant variation among different types of ALFs on staffing. By definition, ALFs providing high services had a full-time RN on staff. What is striking is the level of difference between these ALFS and those offering low services. Among both types of ALFs offering low service (i.e., low service/high privacy ALFs and low service/low privacy ALFs), only about one-third had a full or part-time RN on staff. By definition, all (100 percent) of the high service ALFs had a full-time RN on staff. Similarly, three-quarters of the high service ALFs also had an LPN on staff, while among the low service ALFs, half or fewer had an LPN on staff.
Administrators reports about their admission and retention policies also revealed significant diversity among different types of ALFs. Facilities offering a combination of high services with low privacy had the most expansive admission and retention policies, while the low service/high privacy ALFs had the most restrictive admission and retention policies. For example, both types of low service ALFs were less likely to admit or retain residents who needed any nursing care or monitoring, even temporarily. However, the high privacy/low service ALFs had the most restrictive retention policies. They were less likely to admit or retain residents with behavioral symptoms, urinary incontinence, or moderate to severe cognitive impairment, or who needed help with transfers.
The interviews with administrators also revealed that the low service/low privacy facilities, which comprised a significant proportion of all ALFs nationwide (i.e., 26.9 percent), were unlike the other ALFs on key dimensions. They were significantly less likely to offer private accommodations or apartments (with only 17 percent apartments and 83 percent rooms). They were significantly less likely to have any type of nurse staffing and also less likely to admit or retain residents who needed nursing care. Finally, their basic monthly price in multi-rate facilities was significantly lower than the average price across the industry as a whole.
Differences Among ALFs That Provided High Services or High Privacy
Resident Case Mix and Hospital Use. The analyses conducted of data from the site visits to those facilities that offered high privacy or high services (or both) also revealed some differences in the distribution of resident characteristics and care needs across the three types of ALFs. ALFs classified as low privacy/high service served a resident population with significantly higher levels of cognitive impairment than one would expect, given the distribution in the ALF resident population as a whole. More that one-third (36 percent) of the residents in the high service/low privacy facilities had moderate or severe cognitive impairment, in comparison to only about one-quarter in the high privacy/high service and high privacy/low service ALFs. There were no statistically significant differences across the three facility types in the proportion of residents needing ADL assistance. The low privacy/high service facilities did serve a population with a somewhat higher proportion of individuals who needed help with two or more ADLs; however the difference was not statistically significant. Similarly, residents in ALFs offering the combination of high privacy and low service did have somewhat higher hospitalization rates than the whole population (i.e., 37 percent vs. 32 percent), although the difference was not statistically significant.15
Facility Effects on Resident Discharges and Exits from ALFs. The data on resident discharges from assisted living also revealed significant differences among facilities. Residents in the low service ALFs, which did not have a full-time RN and did not offer nursing care with their own staff, were twice as likely to enter a nursing home between baseline and follow-up.16
In addition, the analysis demonstrated that residence in a for-profit ALF was highly associated with movement into another residential care facility. Since the most common reason for leaving a facility was the need for more care, this finding suggests that the for-profit sector of the industry may be less committed to, or capable of, meeting the increasing needs of residents.
Facility Characteristics and the Philosophy of Assisted Living. We also examined a series of indicators associated with the philosophy of assisted living. These included aspects of privacy and environmental autonomy; service-related features, such as the willingness of the facility to meet scheduled and unscheduled needs and resident reports of unmet needs for assistance; the ability of residents to age in place, based on retention policies; and affordability.
High Privacy/Low Service vs. High Privacy/High Service. There were few statistically significant differences between the two groups of facilities that offered high privacy but provided differing levels of service (i.e., high privacy/high service and high privacy/low service). The only significant difference between such facilities came in a service-related indicator -- their willingness to meet residents unscheduled care needs. Scheduled care needs are those that can be performed at set times, such as receiving medications and bathing. Unscheduled needs are those that arise more randomly throughout the day, such as the need for assistance using the toilet. Analysis demonstrated that the high privacy/high service ALFs were significantly more willing than high privacy/low service ALFs to meet individual residents needs for assistance in toileting, locomotion, and transfer.
The analysis based on information provided by administrators in the telephone survey also suggested that these high privacy/low service facilities had much more restrictive admission and discharge policies. In general, they were less willing to admit or retain residents with moderate to severe cognitive impairment, residents who needed any nursing care or monitoring (even temporary), residents with behavioral symptoms or urinary incontinence, or those who needed help with transfers.
High Service/Low Privacy vs. High Service/High Privacy. The two groups of ALFs that offered high service but differed on privacy exhibited statistically significant differences for two of the six indicators. These differences were, as one would expect, in the areas of privacy and environmental autonomy. The high privacy/high service ALFs offered more private resident accommodations and more of the environmental features associated with autonomy (e.g., ability to control the temperature in the room or apartment, access to personal applicances for cooking, a refrigerator in the residents unit, and the ability to lock the door of the room or apartment.
| TABLE ES.3: Summary of Differences Based on Facility Types | |||
|---|---|---|---|
| Performance Indicator | Comparisons Among Facility Types | ||
| Low Privacy/ High Service vs. High Privacy/ Low Service | Low Privacy/ High Service vs. High Privacy/ High Service | High Privacy/ Low Service vs. High Privacy/ High Service | |
| Privacy | Significant Difference | Significant Difference | |
| Environmental Autonomy | Significant Difference | ||
| Unmet Personal Care Needs | Significant Difference | ||
| Affordability for Low Income Elderly | |||
| Retention Policies | Significant Difference | ||
| Meet Scheduled and Unscheduled Needs | Significant Difference | ||
| Significant Difference = statistically significant at p>.01 | |||
Low Privacy/High Service vs. High Privacy/Low Service. Comparisons between ALFs that differed in both privacy and services also exhibited significant differences in privacy, unmet need for assistance, and policies on retention. As one might expect, residents in ALFs classified as high privacy had significantly greater environmental autonomy. Higher service ALFs had more liberal retention policies and were less likely to have residents with unmet care needs, compared to ALFs that offered high privacy but lower services.
C. Conclusions
These results indicate that significant differences in policies and performance exist between groups of facilities categorized on the basis of different combinations of service and privacy levels. They respond differently to residents needs and preferences and embody, to varying degrees, key elements of the philosophy of assisted living. Some features seem to have a fairly direct effect. For example, ALFs with higher levels of privacy tend to offer residents both greater privacy and greater levels of autonomy. However, the effect of facility characteristics is more complex when multiple characteristics (i.e., service and privacy) are considered. Moreover, some features will increase one desirable performance indicator (e.g., environmental autonomy) and decrease another (e.g., affordability). Perhaps the most significant finding, however, is that no one model or type of ALF appeared to maximize ALF performance across all or even most of the indicators. Thus, at present, the results provide only limited guidance for policy.
It is important to note the limitations of this analysis. First, this array of performance indicators is limited in scope. Moreover, the basic classification system for ALFs is restricted in scope, and there may be a variety of other facility classification schemes that could work equally well with these and other indicators. The task for future analyses is to develop a wider range of indicators of residents needs and preferences and more sensitive facility classification schemes that might provide more comprehensive and consistent differentiation among these indicators.
These findings -- and their necessarily limited nature -- present policy-makers and consumers with significant challenges. For consumers, the multiplicity of models of assisted living and the differential effects of key features on facility performance mean that consumers must seek and consider substantial, diverse information when selecting from among a group of facilities. For policy-makers it seems clear that they must not consider the effect of individual features but instead take into account their combined effects when setting standards for licensure or certification (e.g., for participation in Medicaid waiver programs).
| Differences Among Services and Policies in High Privacy or High Service Assisted Living Facilities AUTHORS: Charles D. Phillips, Catherine Hawes and Miriam Rose DATE: November 2000 AVAILABLE ONLINE: Full Report (http://aspe.hhs.gov/daltcp/reports/alfdiff.htm) |
REFERENCES
DRF. (1997). The Directory of Retirement Facilities -- 1997. Baltimore, MD: HCIA, Inc.
General Accounting Office, U.S. Congress. (1997). Consumer protection and quality of care issues in assisted living. Washington, DC: U.S. Government Printing Office.
General Accounting Office, U.S. Congress. (1999). Assisted living: Quality-of-care and consumer protection issues in four states. Report to Congressional Requesters.
Hawes, C., Mor, V., Wildfire, J., Lux, L., Green, R., Iannacchione, V., & Phillips, C. (1995a). Executive summary: Analysis of the effects of regulation on the quality of care in board and care homes. Research Triangle Park, NC: Research Triangle Institute. [http://aspe.hhs.gov/daltcp/reports/care.pdf]
Hawes, C., Wildfire, J., Mor, V., Wilcox, V., Spore, D., Iannacchione, V., Lux, L., Green, R., Greene, A., & Phillips, C. (1995b). A description of board and care facilities, operators and residents: Analysis of the effect of regulation on the quality of care in board and care. Research Triangle Park, NC: Research Triangle Institute. [http://aspe.hhs.gov/daltcp/reports/bcdesces.htm]
Hodlewsky, R. T. (1998). Facts and trends: 1998 -- The assisted living sourcebook. Washington, DC: National Center for Assisted Living, American Health Care Association.
Kane, R. A., & Wilson, K. B. (1993). Assisted living in the United States: A new paradigm for residential care for frail older persons? Washington, DC: American Association of Retired Persons.
Mollica, R. (1998). State assisted living policy: 1998. Portland, ME: National Academy for State Health Policy. [http://aspe.hhs.gov/daltcp/reports/98states.htm] [http://aspe.hhs.gov/daltcp/reports/98state.htm]
Mollica, R., & Snow, K. (1996). State assisted living policy: 1996. Portland, ME: National Academy for State Health Policy. [http://aspe.hhs.gov/daltcp/reports/96states.htm]
NOTES
-
The third stage involved selection of the resident and staff samples for in-person interviews.
-
Nearly half the states lacked a licensure category known as “assisted living” or classified such facilities together with traditional “board and care” homes during the period in which we attempted to enumerate a list of ALFs.
-
The second reason for first selecting a limited number of geographic areas as FSUs was that it facilitated cost-effective data collection on-site in sample facilities, a subsequent data collection task.
-
For example, the California Association of Homes and Services for the Aging posted a statewide list of places offering housing with supportive services.
-
Some sources, such as most state licensure lists, identified the county, while other lists (e.g., telephone book yellow pages) did not.
-
This was particularly complex because of the large number of multi-facility systems that might list only the administrative office address in a particular city for all the facilities on the list for an FSU. In addition, we found high prevalence of multi-level campus settings that often housed two or more places that met study eligibility criteria. For example, Menorah Park Center for Senior Living has two different residential settings (i.e., Stone Gardens Assisted Living and The R.H. Myers Congregate Apartments) that met study eligibility criteria, although only one self-identifies as assisted living. Both are on the same campus and are listed at the same address.
-
Facility candidates with unknown size were undersampled to improve the cost-effectiveness of the telephone screening. The fact that they appeared, for the most part, on only one list, suggested that they were small and less likely to meet study eligibility criteria. And indeed, only 8 percent of the places with unknown size were found to be eligible during the telephone screening and survey. Again, weighting the final sample adjusted for this undersampling and generated valid estimates about the universe of ALFs.
-
Many facilities had idiosyncratic policies about admission and retention. That is, the administrators responded “it depends” when asked about whether the facility would admit or retain residents with a specified condition. For example, 33 percent of the administrators responded “it depends” when asked whether they would admit a resident with moderate to severe cognitive impairment. One-third (33 percent) reported that “it depends” when asked whether they would retain a resident with moderate to severe cognitive impairment. When the “it depends” response was given, it was counted as a “no” since residents and families could not rely on either admission or retention in such instances.
-
Numbers may not total 100 percent due to rounding.
-
The differences between facilities that had a full-time RN and provided nursing care with their own staff and those that did not have a full-time RN on staff but were willing to provide or arrange nursing care are discussed at greater length in the report on discharged residents.
-
U.S. Bureau of the Census, published data from the 1998 Current Population Survey, “Money Income in the United States, 1997” (series P60-200), Table 8, Income Distribution of Older Persons, 1997.
-
This is based on estimates of annual income. More people could afford assisted living for some period of time by selling their assets, such as a family home, and using those funds to pay the monthly charges for assisted living. Alternatively, families could supplement the income available to the elderly, although this is rare for most community-dwelling elders.
-
These data come from the staff interviews, and nearly all the staff interviewed worked the day shift. Information on staffing by shift appears in the full report.
-
Some “unmeasured” facility characteristic that is very highly correlated with our service measure (i.e., a full-time RN who does direct care) may be driving this relationship, either wholly or partially. However, this relationship does not appear when one uses other service measures, so any unobserved variable must be correlated with this specific measure and not with overall RN staffing, aide staffing, the willingness to arrange for RN care, or simply having an RN on staff. Such a characteristic is relatively hard to conceive of, so the authors’ best judgment, until other evidence is provided, is that the observed relationship is driven by the measured characteristic -- the presence of a full-time RN providing direct care.
-
In these earlier analyses, for all comparisons involving the various facility types, the statistical significance of the prevalence in each type of facility was compared with that in the population as a whole, using a series of logistic regressions in which the independent variables were the facility types. Later analyses specifically compared the three facility types with each other.
-
The effect of this service or staffing variable did not vary depending on the specific characteristics of the resident. For example, no significant interaction was observed between this service indicator and a resident’s level of cognitive impairment.
