A Report to Congress on Substance Abuse and Child Protection
Department of Health and Human Services
Administration for Children and Families
Substance Abuse and Mental Health Services Administration
Office of the Assistant Secretary for Planning and Evaluation
"
Executive Summary
In a field where difficult decisions are made every day, child welfare workers face particular dilemmas when working with the extremely troubled families whose complex and multiple problems include both substance abuse and child maltreatment. Central to their challenge is that addiction to alcohol and other drugs can be a chronic, relapsing disorder and recovery can be a long term process. At the same time, children have an immediate need for safe and stable homes in which to grow up.
Substance abuse (including both licit and illicit drugs) can impair a parent's judgment and priorities, rendering the parent unable to provide the consistent care, supervision and guidance children need. For child welfare workers it is difficult to determine what level of functional improvement will enable a parent with substance abuse problems that have precipitated child maltreatment to retain or resume his or her parental role without jeopardizing a child's safety, particularly as relapse remains a significant possibility. With the implementation of the Adoption and Safe Families Act (ASFA, P.L. 105-89) and renewed emphasis on achieving permanency for children in the child welfare system, finding effective ways to address concurrent substance abuse and child maltreatment problems in families takes on renewed importance.
Section 405 of ASFA requires that the Secretary of Health and Human Services prepare a Report to Congress on substance abuse and child protection, describing: (1) the extent and scope of the problem of substance abuse in the child welfare population; (2) the types of services provided to this population; (3) the effectiveness of these services; and (4) recommendations for legislative changes that might be needed to improve service coordination. This document fulfills this legislative mandate. Although intended for Congress, the report will also be of interest to other national, State, and local policy makers concerned with the interrelationships between substance abuse and child maltreatment.
Understanding Addiction, Substance Abuse Treatment, and Recovery
Substance abuse is a major public health problem that affects millions of people and places enormous financial and social burdens on society. Addiction can be a chronic, life-threatening condition. Most people whose use has progressed to addiction cannot simply stop using alcohol or drugs, no matter how strong their inner resolve, without one or more courses of structured substance abuse treatment. Like virtually any other medical treatment, addiction treatment cannot guarantee lifelong health. Relapse, often part of the recovery process, is always possible. Even if a person never achieves perfect abstinence, addiction treatment can reduce the number and duration of relapses, minimize related problems such as crime and poor overall health, reduce the impact of parental addiction on children, and improve the individual's ability to function in daily life. Nearly one-third of substance abuse treatment clients achieve sustained abstinence from their first attempt at recovery. An additional one-third have a period of relapse episodes but eventually achieve long-term abstinence. The remaining third have chronic relapses that result in eventual death from complications of their addiction.
The Nature of Child Maltreatment
Child abuse and neglect is also a widespread problem in American society. Child maltreatment is commonly divided into four categories:
- physical abuse, characterized by physical injury resulting from beating, kicking, burning, or otherwise physically harming a child;
- neglect, which includes the failure to provide for the child's basic needs;
- sexual abuse, comprising a variety of sexual behaviors toward children; and
- emotional maltreatment, such as acts of commission or omission by the parents or other persons responsible for the child's care that have caused serious behavioral, cognitive, emotional or mental disorders.
The majority of all child protection reports (61 percent in 1996) involve the neglect of children. Neglect is especially predominant in child maltreatment reports in which the parent has a substance abuse problem.
Extent and Scope of the Problem
While parents abuse alcohol and other drugs at lower rates than do persons without children, 11 percent of U.S. children, 8.3 million, live with at least one parent who is either alcoholic or in need of treatment for the abuse of illicit drugs. Of these, 3.8 million live with a parent who is alcoholic, 2.1 million live with a parent whose primary problem is with illicit drugs, and 2.4 million live with a parent who abuses alcohol and illicit drugs in combination. These children are distributed relatively evenly across the childhood age span, although child welfare agencies are more likely to encounter younger children. While they have received the majority of attention, children prenatally exposed to drugs and alcohol represent only a small proportion of the children affected and potentially endangered by parental substance abuse.
Few of the children living with parents who have substance abuse problems come into contact with the child welfare system. Of children prenatally exposed to drugs, most studies find that approximately 10 to 20 percent enter foster care around the time of birth and that about a third do so within a few years. Others are cared for by relatives who may or may not have legal custody. Most remain in their parent(s)' care for all or most of their childhoods.
Parents who are alcoholic or are in need of treatment for the abuse of illicit drugs are demographically quite similar to the U.S. population as a whole. They are as likely to be fathers as mothers, although mothers with substance abuse problems are much more likely than fathers to be reported to child protective services. African American women with substance abuse problems are more likely to be involved with child welfare agencies than are similar women of other races. Many parents, especially mothers, who enter substance abuse treatment are motivated to do so out of concerns about their parenting and how their substance abuse is affecting their children.
For many children who are reported to the child welfare system, parental substance abuse is a critical factor. While figures vary for methodological reasons, most studies find that for between one-third and two-thirds of children involved with the child welfare system, parental substance abuse is a contributing problem (lower figures tend to involve child abuse reports and higher findings most often refer to children in foster care). Children with open child welfare cases whose parents have substance abuse problems are younger than other children in the child welfare system, are more likely to be the victims of severe and chronic neglect, are from families with more problems overall, and are more likely than other children to be placed in foster care rather than served while remaining at home. Once in foster care, children whose parents have substance abuse problems tend to remain in care for longer periods of time than other children.
The Complexity of Child and Family Needs
Families involved with the child welfare system are among the most troubled in our society. In maltreating families, child abuse and neglect are rarely the only issues. Even addiction, while among the most common of the co-occurring problems, is rarely the only serious problem. Mental illness is often present, as are domestic violence and HIV/AIDS. Most families involved with child welfare agencies have very low incomes, and inadequate or unsafe housing are very significant issues, particularly in urban areas. These difficulties combine in the lives of these families to produce extremely complex situations and relationships that are challenging to resolve. The presence of so many serious problems also implies that addressing the substance abuse alone is not likely to produce the changes in a family that are necessary to ensure a healthy family environment for a child. Unless the whole of a family's situation is addressed, substance abuse treatment is unlikely to be successful - and even if a parent achieves abstinence, the other issues present may continue to pose safety problems for the child.
No less complex than the problems of substance abusing parents are their children's needs. The two main research findings regarding children of parents with substance abuse problems are that (1) these children have poorer developmental outcomes (physical, intellectual, social and emotional) than other children, although generally in the low-normal range rather than severely impaired; and (2) they are at risk of substance abuse themselves. Prenatal abuse of alcohol appears to have more severe and long-lasting effects on development than do cocaine and other illicit drugs, including serious intellectual and behavioral consequences in many children. Babies who were prenatally exposed to cocaine or other drugs may experience a range of problems, however, including some that can be long-lasting and serious. These physical and mental deficits are not seen in infants to the overestimated extent that earlier expert warnings and media reports regarding "crack babies" had predicted . Most research finds that factors in the postnatal environment mediate prenatal factors. It is now recognized that the older a child gets, the more important the home environment is in predicting developmental outcome, including how the environment interacts with any direct effects of prenatal drug exposure.
The Context of Collaboration and Overcoming Barriers to Quality Service
While both the substance abuse treatment and the child welfare fields have the vision of healthy, functional families resulting from their interventions, in moving from the family's immediate situation to that end result, different perspectives and philosophies sometimes impede cooperation, engender mistrust, and can cause agencies to hamper one another's efforts and stymie progress. Several key differences in perspectives underlie the majority of misunderstandings and frustrations child welfare agencies and substance abuse treatment agencies feel toward one another. These include different definitions of who "the client" is; what outcomes are expected on what time lines; and potentially conflicting responses to setbacks. In addition, factors related to the legal and policy environments in which agencies operate set a context for joint activities and affect the willingness and ability of agencies to work together. These include State and Federal laws regarding child abuse and neglect and child welfare; the sense of crisis under which many child welfare agencies operate; chronic shortages of substance abuse treatment services, particularly services appropriate for women with young children; and confidentiality requirements of both fields that are often perceived as impediments to cooperation.
There are real and significant barriers to productive collaborations between child welfare and substance abuse agencies. But these differences can and must be accommodated. Doing so will require sustained efforts by Federal, State and local staff in the child welfare, substance abuse, and related fields throughout the nation - efforts to learn about one another, to understand one another, and to establish a shared set of expectations for each other and for clients.
Service Delivery Models — Approaches to Addressing Joint Substance Abuse and Child Maltreatment Problems
Addressing the problems of substance abuse and child maltreatment requires interventions at a variety of levels. Among the clear lessons that have emerged from the decades of effort by dedicated service providers in both fields are that there are no easy answers and that what works for one family will not necessarily work for another. It is only by working together that agencies are likely to make progress in serving these families well. Efforts to address the dual problems of substance abuse and child maltreatment must include the following:
Valuing Prevention. The maltreated children we serve now are at high risk of becoming the next generation of adults with addiction problems and/or the next generation of abusive or neglectful parents. An effective approach to addressing substance abuse among parents and its harmful effects on children must include a strong prevention component.
Strengthening Training and Identification Skills. A key factor in assuring that both substance abuse and child protection issues are addressed is making sure that workers are trained to identify both problems in families served. Training can improve the ability of workers to identify and intervene effectively with families.
Enhancing Risk Assessment, Needs Assessment, and Referral Capacity. Unless workers can appropriately identify risk to children, accurately assess client needs, refer clients to appropriate services in their communities, and evaluate clients' progress, treatment plans are likely to be based on inadequate, erroneous or useless information.
Increasing the Availability, Access and Appropriateness of Substance Abuse Treatment. Child welfare agencies consistently report difficulty obtaining substance abuse treatment for clients who need it, particularly programs that are designed to meet the specific needs of women with children. Until clients have access to quality substance abuse treatment services, it is unrealistic to expect significant improvement in problems surrounding their substance abuse.
Promoting Client Retention and the Effectiveness of Services. The experience of substance abuse treatment programs, particularly those geared toward parents and their children, demonstrates that many clients can and do improve their lives and many are able to resume their parenting roles. Service providers have discovered repeatedly, however, that it is extremely challenging to engage and retain these clients in treatment programs.
Improving Time Lines and Decision Making for Children. Among the key issues in improving child welfare services is ensuring that permanency decisions are made in keeping with a child's developmental time line. Common to the variety of innovations being developed in communities to improve outcomes for children in foster care are that efforts to resolve the issues which led to maltreatment must begin immediately; appropriate intervention plans are developed with the family's involvement and are monitored closely; and lack of progress or non-compliance with the treatment plan is dealt with swiftly.
Supporting Ongoing Recovery. One of the frustrations frequently expressed by professionals working with families with substance abuse and child maltreatment problems is that significant setbacks often occur after long strides have been made. While recovery is a lifelong process, most interventions are designed to be short term. For this population, however, short term interventions may not be sufficient and continuing care is critical.
While the substance abuse and child protection fields have a long way to go toward improving how they work together to serve their mutual clients, a great deal has been learned about what it takes to produce positive outcomes for these parents and children. Improved efforts across a wide spectrum of activities are needed throughout our nation. While no community has yet put in place an entirely satisfactory response network, the examples and research results described in this report demonstrate that there are solid indications of how outcomes can be improved at each stage of intervention.
Where Do We Go From Here?
There are significant roles for service providers, program administrators and policy makers at all levels in order to improve services and achieve better outcomes for families with substance abuse and child maltreatment problems. Chapter 8 discusses actions the U.S. Department of Health and Human Services (HHS) will take in several areas to improve service provision to families affected by both substance abuse and child maltreatment, and also challenges service providers in the field to take steps to better address families' needs.
Building Collaborative Working Relationships. HHS intends to lead the field toward improving communications and developing common ground between the child welfare and substance abuse treatment fields. Our activities will include: (1) conducting leadership meetings that will convene national and regional discussions among agency leaders, service providers, and consumers of our services to begin the process of working through our different perspectives to build common ground; (2) preparing informational materials regarding substance abuse screening and assessment tools that can be used in child protective services contexts, and child safety assessments that may be useful for substance abuse treatment providers; and (3) funding a series of small grants to States and communities that will support the planning and implementation of joint strategies for service delivery, staff development and training, treatment retention, relapse management and post-treatment support.
We challenge State and community leaders in the child welfare and substance abuse fields, in consultation with the juvenile and family courts, to initiate discussions on these issues within their own jurisdictions. Such discussions should focus on an analysis of the way in which these service systems and the court currently operate and interact with one another, and the impact of these operations on child safety and family functioning. These deliberations should also identify shared goals, gaps in service, and innovations applicable to their community that can improve the outcomes for children and families.
Assuring Timely Access to Comprehensive Substance Abuse Treatment Services. There are currently several important opportunities for States and local communities to expand substance abuse treatment for child welfare clients. Specific opportunities within the Substance Abuse Prevention and Treatment Block Grant, the Targeted Capacity Expansion Program, Medicaid, and the Temporary Assistance for Needy Families and Welfare to Work Programs are discussed in Chapter 8. The availability of new resources can promote the building of capacity at the State and local levels to provide services in ways that promote safety and permanency for children and sobriety for families. State and local leaders are urged to consider the variety of options available to address the substance abuse treatment needs of child welfare clients.
Improving Our Ability to Engage and Retain Clients in Care and to Support Ongoing Recovery. In order to assist service providers to implement effective strategies for these clients, the Administration for Children and Families (ACF), the Substance Abuse and Mental Health Administration (SAMHSA) and other partner agencies will: (1) expand our research in this area to build knowledge and develop effective program strategies; (2) utilize our technical assistance mechanisms to assure materials on effective approaches are available to the field; and (3) make particular efforts to work with the Court Improvement Projects to share information on effective programs, assessing treatment progress, and on the application of drug court methods to juvenile and family courts. We urge service providers to design programs with a recognition that recovery from addiction is an ongoing process and to structure services in ways that promote retention and provide relapse prevention services.
Enhancing Children's Services. As substance abuse treatment programs design services for parents, children's needs also must be addressed. For children in foster care, increased attention to children's healthy emotional, social, and cognitive development is needed. In addition, program models are needed to address the particularly high risk of substance abuse and other problematic behaviors among children in foster care. Among ACF's planned activities in this area are (1) highlighting opportunities to address substance abuse within the Independent Living Program; and (2) developing training materials for foster parents on working with the children they care for to prevent future substance abuse. In addition, in recent years SAMHSA has significantly expanded its attention to early childhood issues, particularly through the Starting Early Starting Smart Program, which, in conjunction with several partner agencies, funds a child-centered, family-focused, and community-based initiative designed to test the effectiveness of integrating behavioral health services with primary care and early childhood service settings for children age 0-7. SAMHSA's Center for Substance Abuse Prevention is also planning a new SAMHSA-wide effort focusing on outreach to the children of substance abuse treatment clients. We challenge State and local service providers to identify opportunities for prevention and treatment services for children who are in foster care and for those under protective supervision in their homes.
Filling Information Gaps. Gaps in our knowledge base must be addressed in the coming years to ensure programs and approaches are well grounded in research findings. A discussion of specific information gaps appear in Chapter 8. In order to address knowledge gaps, ACF has proposed that these substance abuse issues be the subject of the next annual Federal Forum on Child Abuse and Neglect Research, to take place in the Spring of 1999. In addition, the National Institutes of Health, in partnership with ACF, other HHS agencies and the Department of Justice, will soon issue a grant announcement soliciting research proposals addressing child neglect. It is expected that a number of the proposals will address alcohol and drug abuse as factors in child neglect. SAMHSA's Center for Substance abuse prevention is in the process of implementing two new Knowledge and Application programs, one aimed at children of substance abusing parents and the other aimed at parenting adolescents, which are designed to develop new knowledge about ways to improve substance abuse prevention with these populations.
Moving Forward, Together
The congressional request for a report on substance abuse and child protection has provided a unique opportunity for HHS to focus on the maltreatment of children where substance abuse is a contributing factor. This report documents what we know about substance abuse treatment and recovery and its relationship to maltreatment. It further documents both systemic and individual factors that contribute to or minimize our ability to protect children and assist families in recovery.
Families often come with serious problems to service systems which are fragmented, and as such limited in their ability to facilitate safety, permanency, and sobriety. The Adoption and Safe Families Act recognizes the importance of time to children and establishes an expectation of urgency in decision making regarding their welfare. The imperative for timely decisions for children and the time frames necessary for recovery should also create a sense of urgency for policy makers and service providers. Those of us who work in these fields must recognize the immediate need to eliminate barriers to effective treatment. This report sets the stage for a number of actions which can improve the nation's capacity to serve families whose children are at the greatest risk.
The challenge before us is substantial. However, we believe that there is a broad recognition of the issues we face and a willingness to make the changes necessary at all levels of government to reach our goal.
Endnotes
1 Due to space limitations, citations are not included in the Executive Summary. Full citations may be found in the main report.
Acknowledgments
This publication was developed jointly by the Administration for Children and Families, the Substance Abuse and Mental Health Services Administration, and the Office of the Assistant Secretary for Planning and Evaluation, in consultation with the National Institute on Drug Abuse, the National Institute on Alcohol Abuse and Alcoholism, and the Health Care Financing Administration.
Chapter 1. Introduction
In a field where difficult decisions are made every day, child welfare workers face particular dilemmas when working with the extremely troubled families whose complex and multiple problems include both substance abuse and child maltreatment.
Central to their challenge is that addiction to alcohol and other drugs can be a chronic, relapsing disorder and recovery can be a long term process. At the same time, children have an immediate need for safe and stable homes in which to grow up. Balancing these factors, as parents make sincere efforts to provide safe and loving homes for their children, represents a key challenge for the child welfare field and for judges making critical custody decisions.
Substance abuse (including both licit and illicit drugs) can impair a parent's judgment and priorities, rendering the parent unable to provide the consistent care, supervision, and guidance children need. For child welfare workers it is often difficult to determine what level of functional improvement will enable a parent with substance abuse problems to resume or retain his or her parental role without jeopardizing child safety, particularly as relapse remains a significant possibility. As child welfare workers address safety concerns, substance abuse treatment counselors work to ensure that the treatment process promotes recovery while addressing parents' concerns about their children's safety and their fear of losing their children to the child welfare system.
An important challenge facing both the child welfare and substance abuse fields is to take a comprehensive view of families' situations and to understand the contributions of various problematic behaviors to child maltreatment. The relationship between substance abuse and child welfare is complicated by the presence of other personal, health, environmental, social and economic factors. These factors, in many cases, contribute to the development of addiction and confound both the process of securing safe, stable homes for children and the treatment process. For this reason, although this report concentrates on the relationship between substance abuse and child maltreatment, it is important to note that all major family problems must be addressed to achieve substance abuse treatment success and child safety.
Many in the child welfare field have recognized for a number of years that substance abuse is central to child welfare issues (Child Welfare League of America North American Commission on Chemical Dependency, 1992). But with the implementation of the Adoption and Safe Families Act (ASFA, P.L. 105-89) and renewed emphasis on achieving permanency for children in the child welfare system, finding effective ways to address concurrent substance abuse and child maltreatment problems in families takes on renewed importance. As the Adoption and Safe Families Act was developed, the Congress debated potential Federal policies that would allow child welfare agencies and partners in the substance abuse treatment field to better address the needs of parents whose substance abuse problems rendered them unable to care for their children. After considerable debate on a variety of measures, Congress asked for more information. Section 405 of ASFA required that the Secretary of Health and Human Services (HHS) prepare a Report to Congress on Substance Abuse and Child Protection Services. In particular, the law required the Department to submit a report that:
"describes the extent and scope of the problem of substance abuse in the child welfare population, the types of services provided to such population, and the outcomes resulting from the provision of such services to such population. The report shall include recommendations for any legislation that may be needed to improve coordination in providing such services to such population."
This document fulfills this legislative mandate. Although intended for Congress, the report will also be of interest to other national, State, and local policy makers concerned with substance abuse and child maltreatment. Over the past year, staff from several agencies within HHS have worked together to gather information from the fields of child welfare and substance abuse prevention and treatment regarding the needs of families in which both substance abuse and child maltreatment are present. Along the way we have consulted with practitioners and researchers in both fields regarding their views of how efforts could be improved to better meet the needs of the children and families we serve. In conversations and focus groups we solicited input on several topics, including:
- What are the most important themes and messages that the report should address?
- What are the most significant problems in current relationships between child welfare agencies and substance abuse treatment agencies?
- What are the most important issues that agencies need to consider in establishing partnerships between substance abuse and child protection agencies?
- What are the most promising approaches to addressing concurrent substance abuse and child protection issues in families?
- What are the most important ways in which the Federal Government could assist in the improvement of practice in this area?
In conducting research for this report, it became clear that the child welfare and substance abuse fields have different definitions of "the client," different training and education which lead to different perspectives in defining families' problems, and often see each other as at fault when conflicts arise. Our professions have a long way to go in learning about one another, blending perspectives, and developing ways to work together more effectively. The lack of understanding, different and often conflicting frameworks and priorities, as well as a lack of communication and collaboration among the providers of care in the child welfare and substance abuse fields must be addressed if we are to better serve the children and families who most need our help.
Substance Abuse is a Critical Child Welfare Issue
Parental substance abuse, with its related physical and mental health problems and its social and economic facets, is a critical factor in many families who come to the attention of the child welfare system. While data will be discussed in detail in Chapter 4, it is clear that throughout the child welfare system, but especially with respect to children in foster care, alcohol and other drug abuse is recognized as a major contributing factor to child neglect and abuse and as one of the key barriers to family reunification. Parental substance abuse is among the factors that have fueled the rising number of abuse and neglect reports and has contributed to the rising number of children in foster care. It remains a key barrier to reunification for many of the children who reside in foster care for extended periods.
Because substance abuse is so often intertwined with a family's maltreatment of their children, the availability of effective, substance abuse treatment must become a priority for child welfare agencies seeking to address families' needs. When substance abuse treatment includes a well-coordinated service delivery system designed to address the variety of family needs, it does work for many families, allowing the addicted individual to regain control over his or her life and keep his or her family intact. Providing effective substance abuse treatment services will be discussed in Chapter 7. While child welfare agencies are rarely the providers of substance abuse treatment services, they must become knowledgeable about treatment and recovery (including its potential and limitations), should be active referral sources for treatment programs, and must be active partners in the treatment process.
Furthermore, while substance abuse treatment is often effective, appropriate, high quality treatment designed for parents, especially women with young children, is not easily available in many communities. Most providers are not prepared or equipped to address the complex physical, mental, social, and economic issues facing these women and their children. Moreover, they often lack the resources to provide the level of comprehensive, gender-specific care that is required. Even where such programs exist, child welfare agencies too often have not established effective links with treatment providers that facilitate referral and follow up. Until treatment access for child welfare system clients is ensured, it is difficult to argue that parents are being afforded the opportunity to address the barriers to successful family life. Child welfare agencies must become advocates in their communities for the establishment and provision of the types of services their clients need.
Even with adequate treatment services, not all substance abusing parents will be able to improve sufficiently to function in their parental roles. In order to make appropriate and realistic decisions about child safety, reunification, and family preservation, and termination of parental rights, increased attention must be given to appropriate assessment of the family's needs, to individualized treatment plans for these parents and their children, to the progress clients make in treatment, and to the length of time required in treatment to address major issues -- all of which relate to effective parenting. In addition, if new time lines are to be adhered to while providing realistic opportunities for recovery, it will be important to provide joint parent-child services that address parenting and other priority issues while working on recovery. Recovery is a lifetime journey, not an event. As a result, success in treatment is not likely to mean complete, permanent abstinence immediately, though progress in treatment can be observed and documented. Child welfare staff and judges, however, often do not know how to identify whether or not such progress is taking place, nor do they have the skills to determine the extent to which progress on substance abuse treatment goals is likely to translate to children's safety.
Timely Substance Abuse Services Are Key to Achieving Permanency for Children
Child welfare agencies throughout the U.S. have long recognized that every child needs a safe and permanent home, whether that home is with a birth parent, a relative, or an adoptive parent. The goal that permanency decisions be made promptly, while giving parents the opportunity and support to make the changes in their lives necessary to address safety concerns, has not been adequately realized. The Adoption and Safe Families Act of 1997 (ASFA) emphasizes timely decision making, requiring that permanency decisions be made on a 12-month time line, and requiring that agencies move to terminate parental rights once a child has been in foster care for 15 of the previous 22 months, unless there is a compelling reason not to initiate termination. These new time lines make it essential that agencies ensure that services for parents, including appropriate substance abuse treatment, be provided promptly.
For substance abuse treatment to be successful, the types, settings, and duration of treatment must be tailored to the individual client based on the severity of the addiction and other disorders that may exist. Even in the best situations, substance abuse treatment takes time and relapses are part of the recovery process, as with other diseases, particularly in the early stages of treatment. The new time lines provide sufficient opportunity for parents to take important steps into the recovery process, but only if treatment is available quickly. However, recovery is likely to be successful in the long term only if appropriate, quality substance abuse treatment services are provided promptly, and include aggressive outreach, retention, and monitoring as integral service components.
Collaboration Between Child Welfare and Substance Abuse Treatment Agencies is Challenging
The complexities within child welfare agencies and substance abuse treatment agencies, coupled with different perspectives and world views, make cooperation and collaboration between service systems difficult to establish and harder to maintain. But now more than ever, collaboration between these agencies is essential if families are to be given real opportunities for recovery and children are to have the chance to grow up in healthy family situations. As will be discussed more fully in Chapter 6, the differences between agencies are real and there are good and important reasons staff find it difficult to work together. Yet to the extent we let these differences block communication between agencies and prevent caseworkers and staff at all levels from working together, we cannot serve families effectively and we sabotage the goals both systems strive for: healthy, well-functioning families. Our clients come to us with needs for both substance abuse treatment and family intervention and are unlikely to succeed unless both are addressed.
Consider a typical case in which an addicted mother gives birth to a child who is soon taken into foster care. Handed a list of local treatment agencies (whose programs are likely to be full), the mother is told to "get clean" if she wants her child back, but is given little or no further assistance in securing treatment. Meanwhile, the child welfare agency places the child in a foster home with adoption potential. If the mother happens to be successful (without help from the child welfare agency), reunification is a possibility. If not, the child may be adopted relatively quickly. Many would consider this standard practice and adequate performance. Yet, while the child welfare agency may secure a permanent home for the child, the birth mother is likely to have received little or no treatment and thus may be reported again in 12 to 18 months with a new infant. The problem has not been solved, for either the mother or her children, often because inappropriate or very short-term treatment was the woman's only option. Unless we successfully intervene with the addicted parent (who may be a father rather than or in addition to a mother, although fewer addicted fathers are reported to child welfare agencies), we will never be able to make real progress. Improved collaboration, as well as understanding and responding to the need for high quality and appropriate treatment, are essential to these efforts.
Improved Practice and Outcomes are Possible and Essential
While effective collaboration between substance abuse and child welfare agencies is often difficult, it is possible and is the only way to address successfully the needs of the families we serve. Chapter 7 contains examples of efforts being made around the country to bring our disciplines closer together. While no easy recipe exists for putting together a comprehensive plan for addressing the problems of substance abusing families whose children suffer from maltreatment, effective pieces of the puzzle are in place in many communities. Our challenge is to learn from these efforts in order to build an effective system of care for families. While full solutions are not at hand, solid, practical next steps are clearly discernible.
Resource issues quickly arise whenever we discuss improving services for families. These issues are real and important. But we believe the issues faced in improving services for these families are not just about having additional treatment funding, but also about how we do business together. Changing the ways these systems relate to one another will do more to improve outcomes for these children and families than will simply spending significantly more money under current circumstances. Better use of current resources will allow agencies and communities to determine to what extent additional resources are needed and will demonstrate how such resources may be deployed most effectively.
Organization of the Report
The next two chapters of this report provide a brief overview of the nature of addiction, substance abuse treatment, and recovery (Chapter 2), and the nature of child maltreatment (Chapter 3). These are followed by information regarding the co-occurrence of these two serious problems (Chapter 4) and a discussion of the complexity of child and family needs (Chapter 5). The final three chapters of the report discuss overcoming barriers to collaboration (Chapter 6), provide examples of successful service delivery (Chapter 7), and lay out next steps for the Federal Government and our partners at the national, State, and local levels (Chapter 8). Three appendices provide information on Medicaid coverage of substance abuse treatment services, the Center for Substance Abuse Treatment's comprehensive treatment model for substance abusing women and their children, and current programs of the Department of Health and Human Services directed at substance abuse and child maltreatment.
Chapter 2. Understanding Addiction, Substance Abuse Treatment, and Recovery
Substance abuse is a major public health problem that affects millions of people and places enormous financial and social burdens on society. It destroys families, damages the economy, victimizes communities, and places extraordinary demands on the education, criminal justice, and social service systems. To understand the connections between substance abuse problems and the child welfare system, it is important that substance abuse and the medical, social, and economic problems that are associated with the use and misuse of alcohol and other drugs, as well as addiction to these drugs, be clearly understood.
The Spectrum of Substance Use, Abuse, and Addiction
The use of alcohol and other drugs is a multifaceted phenomenon, varying with the individual's level of use and the dysfunction he or she experiences as a result of his or her use. The range includes the following:
Drug experimentation
The use of alcohol or illicit drugs at any time for experimentation. While in and of itself experimentation may not appear to be abusive, even a single episode of experimentation can result in harm to self or to others. For example, the use of alcohol or other drugs at all during pregnancy could result in harm to the fetus, the experimental use of alcohol or other drugs while driving can result in harm to the user as well as others, or a child may be injured when left unsupervised while a parent is intoxicated. Also, if experimental use continues or serves as a gateway to additional use, as often it does, patterns of alcohol and other drug abuse may develop.
Social use of drugs
Use of any drug or combination of drugs in social situations, or for social reasons. If such social use causes any harm, physical or otherwise, to the user or others, it is also considered abuse. Social use of alcohol or other drugs often leads to further and elevated use.
Binge drinking
Heavy use of alcohol periodically. This can result in harm to the physical health of self and others, and negative behavioral consequences, which may result in bodily harm to self or others. For example, harm may be caused by heavy periodic use of alcohol or other drugs while pregnant, driving while intoxicated, or either neglecting or inflicting violence on self and others while under the influence. The National Household Survey on Drug Abuse defines binge alcohol use as drinking five or more drinks on the same occasion at least one day in the past 30 days.
Substance abuse
The characteristic feature of abuse is the presence of dysfunction related to the person's use of alcohol or other drugs. One standard definition (U.S. Department of Health and Human Services, Substance Abuse and Mental Health Services Administration [HHS/SAMHSA], 1994) describes it as "the use of a psychoactive drug to such an extent that its effects seriously interfere with health or occupational and social functioning." Abuse may or may not involve physiologic dependence or tolerance. For example, use of substances in weekend binge patterns may not involve physiologic dependence; however, it may have adverse affects on a person's and possibly others' lives. The Diagnostic and Statistical Manual of Mental Disorders (DSM-IV) produced by the American Psychiatric Association is used across the medical and mental health fields for diagnosing both substance abuse and mental health disorders. According to the DSM-IV, substance abuse is "a maladaptive pattern of substance use leading to clinically significant impairment or distress, as manifested by" a variety of possible symptoms of impairment. Neglect of children is specifically listed as a potential symptom of substance abuse (American Psychiatric Association, 1994).
Addiction or Chemical Dependency
With continued use, many persons' use or abuse of alcohol or other drugs becomes addiction, a disease in which the substances have caused changes in a person's body, mind, and behavior. As a result of this disease, addicted persons are unable to control their use of substances, despite the bad things that happen when they use them. Addiction may be a chronic, relapsing disorder and if the disease process progresses, recovery becomes more difficult. Chemical dependency occurs most frequently in those who have a family history of the disease. Chemical dependency may cause death if the person does not completely abstain from using alcohol and other mood-altering drugs (HHS/SAMHSA, 1996a). The DSM-IV distinguishes dependence from abuse primarily by the presence of more abuse symptoms (three or more rather than at least one), and the possible presence of tolerance (needing more of the substance for the same intoxicating effect) or withdrawal (physical symptoms when the substance is not used).
The American Society of Addiction Medicine describes drug dependence as having two possible components: 1) psychological dependence and 2) physical dependence. Psychological dependence centers on the user's need of a drug to reach a level of functioning or feeling of well-being. Due to the subjective nature of this term, it is not very useful in making a diagnosis. Physical dependence, however, refers to the issues of physiologic dependence, establishment of tolerance, and evidence of an abstinence syndrome or withdrawal upon cessation of alcohol or other drug use. Tolerance, dependence, and withdrawal develop differently depending on the particular substance (HHS/SAMHSA, 1994).
Myths and Facts About Addiction and Treatment
Myth:
Addiction is a bad habit, the result of moral weakness and overindulgence.
Fact:
Addiction can be a chronic, life-threatening condition, like atherosclerosis, hypertension or adult diabetes. Addiction has roots in genetic susceptibility, social circumstance, and personal behavior.
Myth:
If an addicted person has enough willpower, he or she can stop abusing alcohol or other drugs.
Fact:
Most people addicted to alcohol and other drugs cannot simply stop using them, no matter how strong their inner resolve. Most need one or more courses of structured substance abuse treatment to reduce or end their dependence on alcohol and/or other drugs.
Myth:
Many people relapse, so treatment obviously doesn't work.
Fact:
Like virtually any other medical treatment, addiction treatment cannot guarantee lifelong health, although nearly one-third of clients achieve abstinence from their first treatment attempt. Relapse, often a part of the recovery process, is always possible and treatable. Even if a person never achieves perfect abstinence, addiction treatment can reduce the number and duration of relapses, minimize related problems such as crime and poor overall health, reduce impact of parental addiction on children, improve the individual's and his or her family's ability to function in daily life, and strengthen the individual's ability to cope with the next temptation or craving. These improvements reduce the health, social, and economic costs of addiction.
Substance Abuse Treatment and Recovery
In order to understand the treatment that is needed for addiction, it is important to emphasize that medical experts today generally consider alcohol and other drug addiction to be a disease that, while treatable, is chronic and relapsing. Because dependency on alcohol and other drugs creates difficulties in one's physical, psychological, social, and economic functioning, treatment must be designed to address all of these areas. Addiction and its related problems can be treated successfully, but no single treatment works for all substances, nor for all substance abusers.
It is important to note that not all persons in recovery for substance abuse relapse. Nearly one-third achieve permanent abstinence from their first attempt at recovery. An additional one-third have brief periods of substance use but eventually achieve long-term abstinence, and one-third have chronic relapses that result in premature death from chemical addiction and related consequences. These statistics are consistent with the life-long recovery rates of any chronic lifestyle-related illness (HHS/SAMHSA, 1996a).
Substance abuse treatment refers to a broad range of activities or services, including identification of the problem (and engaging the individual in treatment); brief interventions; assessment of substance abuse and related problems including histories of various types of abuse; diagnosis of the problem(s); and treatment planning, including counseling, medical services, psychiatric services, psychological services, social services and follow-up for persons with alcohol or other drug problems (Institute of Medicine, 1990).
Substance abuse treatment may be based on one of several traditional approaches: the Medical Model which focuses on the recognition of addiction as a bio/psycho/social disease, the need for life-long abstinence, and the use of an ongoing recovery program to maintain abstinence; the Social Model which focuses more on the need for long-term abstinence and the need for self-help recovery groups to maintain sobriety; and the Behavioral Model which focuses more on diagnosis and treatment of other problems or conditions that can interfere with recovery (HHS/SAMHSA, 1996a). Many programs use a combination of some aspects of the various models in order to facilitate the most appropriate treatment for the individual and to give patients options. Others also include innovative non-traditional models of treatment such as acupuncture and traditional healing practices associated with specific cultural groups.
Treatment may occur in various settings, such as inpatient, hospital-based programs; short- and long-term residential programs; or outpatient programs; and may be augmented by self-help/12-step and other support groups. Treatment may also use a combination of therapies, such as pharmacological therapy to treat certain addictions (for example the use of methadone for heroin addiction or the use of antabuse to treat alcoholism); use of psychological therapy or counseling, education and social learning theories; and non-traditional healing methods such as acupuncture. Treatment may extend over the course of weeks, months, or years, depending on the severity of the problems and the level of burden created by clients' multiple disorders such as alcoholism, other drug addiction, HIV/AIDS, mental illness (especially depression), and serious physical illnesses. The type and intensity of treatment depend on the patient's psychological, physical, and social problems; the stage (or severity) and type of addiction; personality traits; and social skills before the onset of addiction (HHS/SAMHSA, 1996a).
The concepts of treatment and recovery are not one and the same. However, treatment is a very important part of the recovery process. When the formal treatment component (s) are completed, whether it be outpatient, inpatient or short- or long-term residential treatment, this is not the end for anyone with an addiction problem, much less for an addicted woman with children. Recovery is a lifelong process that takes place over time and often in specific stages. In addition to abstinence, recovery includes a full return to bio/psycho/social functioning (HHS/SAMHSA, 1996a).
One widely accepted model of recovery, known as the Developmental Model, identifies six stages that addicted individuals must undergo for long-term recovery:
- Transition, the period of time needed for the addicted individual to come to grips with the realization that safe use of alcohol or other drugs for them is not possible;
- Stabilization, during which the chemically dependent person experiences physical withdrawal and other medical problems and learns how to separate from people, places and things that promote substance abuse;
- Early recovery, when an individual faces the need to establish a chemical-free lifestyle and build relationships that support long-term recovery;
- Middle recovery, seen as time for the development of a balanced lifestyle where repairing past damage is important;
- Late recovery, during which the individual identifies and changes mistaken beliefs about oneself, others and the world that caused or promoted irrational thinking; and
- Maintenance, the lifelong process of continued growth, development, and managing routine life problems.
Recovery is very complex, is not exempt from vulnerabilities, and requires a long-term commitment. This important part of the treatment continuum must be taken into account in the design of training programs for providers of substance abuse treatment and those of child welfare services. The complexities of recovery must be understood as well as the compelling need to address the issues of children and addicted parents and other family members. It is often said in the recovery communities that the whole family is in recovery because many changes affecting the entire family system will necessarily occur as the recovering person embarks on this lifelong journey of well being. However, many programs do not include a specific focus on parenting and family dynamics.
With respect to women in particular, additional problems emerge in early recovery, including problems related to parenting, to trauma resulting from physical or sexual abuse, or to mental illness. Together with the model described above, a woman's recovery will only be successful to the extent that the other issues which precipitate or relate to the abuse of alcohol or other drugs are also ameliorated. That is to say, if a woman who is newly drug-free returns to a hostile, abusive environment, to high levels of stress in raising one or more children alone, to unsafe housing and insecurity in the employment arena, and with minimal resources for physical and mental health care and other basic needs, recovery will be difficult. Under such circumstances recovery will require ongoing counseling, attendance in self-help and other support groups and accessibility to other available resources. Child welfare workers must become aware of the implications and critical importance of these factors to overall treatment for women, in particular as they relate to identifying proper services for them and their children.
Understanding Relapse and Factors Associated with Relapse
Relapse is not an isolated event, but rather a process whereby an individual becomes dysfunctional or unable to cope with life in sobriety, and thus can no longer avoid using alcohol or other drugs. This process of becoming dysfunctional may lead to renewed alcohol or other drug use, physical or emotional collapse, or even suicide. The process is marked by predictable and identifiable warning signs that begin long before the return to use or collapse occurs. Progressively increased distress levels in any one of the problem areas — physical, psychological or social — can lead to physical or emotional collapse, resulting in relapse. These symptoms increase and intensify unless the individual returns to the use of alcohol or other drugs (HHS/SAMHSA, 1996a). One particular warning in early recovery occurs when a recovering person begins to seek out situations involving people who use alcohol or other drugs.
Given that addiction can be a chronic, progressive disorder often characterized by relapse, and given the fact that women who relapse may be in particular need of intensive treatment and continued support, the opportunity to reenter treatment must remain open. Continued relapse may point to a more serious disorder that was not initially diagnosed, such as post traumatic stress syndrome resulting from past sexual or physical abuse or current abuse. In order to address these and other issues in women's lives, such as stress connected with being a single parent, low income, being identified as a maltreating parent, and having few social resources, any or all of which may bring about relapse, separate attention to these issues is needed — attention that extends beyond the substance abuse treatment process. In order to prevent relapse, the client may have to continue addressing these issues for years after leaving treatment. Formal relapse prevention components that offer means for early detection of relapse and tools for intervention should be included in every treatment program.
Impact of Substance Abuse on the Individual, Family, and Community
Substance abuse affects and costs the individual, the family, and the community in significant, measurable ways including loss of productivity and unemployability; impairment in physical and mental health; reduced quality of life; increased crime; increased violence; abuse and neglect of children; dependence on non-familial support systems for survival; and expenses for treatment. The physical and mental health and social consequences of alcohol and other drug use by women can seriously affect their lives and those of their families (HHS/SAMHSA, 1997a). Not only are women, especially young women, beginning to close the gap between female and male consumption of alcohol and other drugs, they suffer earlier and more serious consequences. Women become intoxicated and addicted more quickly than men and develop related diseases earlier (National Center on Addiction and Substance Abuse, 1996). As will be described more fully in Chapter 5, children also bear the burden of biological and environmental consequences of parental substance abuse.
Chapter 3. The Nature of Child Maltreatment
Child abuse and neglect is a widespread problem in American society. A child of any age, sex, race, religion and socioeconomic background can fall victim to maltreatment, which may include both acts of commission and those of omission. Media stories tend to highlight the sensational aspects of child abuse and neglect: babies abandoned or killed by their mothers; toddlers beaten by their parents; school-aged children who are subjected to sexual abuse. While such stories attract tremendous interest and empathy for the victims, these accounts fail to reveal the complex interplay of factors that influence the origin and consequences of child maltreatment. In fact, we know that no single risk factor provides the overriding catalyst for child abuse and neglect. Multiple stresses and conditions are implicated in contributing to abusive or neglectful behavior (National Research Council, 1993). It is entirely appropriate to examine the relationship between child abuse and neglect and substance abuse, as we know that these problems are interrelated and affect many American families. We must understand the relationship between substance abuse and child maltreatment in order to maximize opportunities for successful intervention with troubled children and families.
Definitions
The first step in preventing and treating child abuse and neglect effectively is to reach a common understanding of the definition of the phenomenon and its causes. Unfortunately, the field lacks consistent definitions and faces difficulty in developing valid instruments to identify and assess maltreatment. The very nature of child maltreatment, which tends to co-exist with many other problems, including individual psychopathology, poverty, domestic violence and other forms of victimization, as well as substance abuse, makes it difficult to define it conclusively and isolate key factors in its causation (National Research Council, 1993). Despite the difficulty in determining its causes, there is some consensus on its definition. For working purposes, child maltreatment is commonly divided into four categories: (1) physical abuse; (2) neglect; (3) sexual abuse; and (4) emotional maltreatment. The Child Abuse Prevention and Treatment Act of 1996 (CAPTA, P.L. 104-235) contains definitions of child abuse and neglect and sexual abuse for purposes of interpreting the legislation. The law states, "the term 'child abuse and neglect' means, at a minimum, any recent act or failure to act on the part of a parent or caretaker, which results in death, serious physical or emotional harm, sexual abuse or exploitation, or an act or failure to act which presents an imminent risk of serious harm" (Section 111(2)).
Although it is difficult to isolate the causal factors of child maltreatment, much progress has been achieved by researchers and practitioners who study and work with abusive and neglectful families. Anecdotal assumptions have been refined to incorporate research findings about the nature of child maltreatment, the characteristics of individuals, families, neighborhoods, and social and cultural values that affect the presence or absence of abuse and neglect. The importance of the developmental level of the child has been recognized in studying the consequences of child maltreatment and in designing prevention and intervention programs. The relationship between experiences with child maltreatment and a broad range of health and behavioral disorders has been explored through longitudinal studies with increasingly larger samples (National Research Council, 1993).
The original notion of the nature of child maltreatment was univariate, centering on the portrait of "the battered child," and referring primarily to physical abuse perpetrated by a mentally unstable and cruel parent (National Research Council, 1993). The current perspective on the problem of child maltreatment is more ecological, encompassing not only a broader range of causes, both intrinsic and extrinsic to the individual, but also a wider continuum of types and severity of abuse. Each category covers a range of behaviors, and is not perfectly discrete from the others. Despite this, each category has become the focus of separate studies of incidence and prevalence, etiology, prevention, consequences, and treatment. These studies have led to the development of unique frameworks for each type of abuse, revealing certain similarities (such as the importance of developmental perspectives in considering the consequences of maltreatment), but also important differences (such as the predatory behavior associated with some forms of sexual abuse that do not appear with other forms of child maltreatment) (National Research Council, 1993).
Physical Abuse
Physical abuse is characterized by physical injury (for example, bruises and fractures), resulting from punching, beating, kicking, biting, burning or otherwise physically harming a child. Although the injury is not an accident, the parents or caretaker may not have intended to hurt the child. The injury may have resulted from too much discipline, physical punishment that is inappropriate to the child's age or condition, an unexpected loss of control in response to a child not meeting parental expectations, or poor coping skills on the part of the parent (DePanfilis and Salus, 1992). In 1996, 24 percent of confirmed child maltreatment reports involved physical abuse (U.S. Department of Health and Human Services, Children's Bureau [HHS/CB], 1998d).
The injury may be the result of a single episode or of repeated episodes and can range in severity from minor bruising to death. According to 1996 data collected under the auspices of the National Child Abuse and Neglect Data System (NCANDS), some 1,077 children died in the U.S. that year due to maltreatment, about half as a result of physical abuse and half as a result of neglect. Children younger than age 4 accounted for 76 percent of fatalities (HHS/CB, 1998d). Any injury resulting from physical punishment that requires medical treatment is considered outside the realm of normal disciplinary measures. A single bruise may be inflicted inadvertently; however, old and new bruises in combination, bruises on several areas of the face, or bruising in an infant suggest abuse. In addition, any punishment that involves hitting with a closed fist or an instrument, kicking, inflicting burns, or throwing the child is considered child abuse regardless of the severity of the injury sustained (DePanfilis and Salus, 1992).
Child Neglect
n the most general sense, child neglect is characterized by failure to provide for the child's basic needs, including food, clothing, shelter, supervision, and/or medical care. Neglect covers a range of behaviors and is difficult to define. It can be confounded by differences in cultural norms between families and the child protective service system, poverty, the current state of knowledge about what constitutes adequate care, and other factors. Further, its manifestations can derive from many causative or concurrent conditions. For example, abandonment of the child may stem from parental alcoholism, drug abuse, and/or depression. Inattention to dangerous, avoidable hazards in the home may stem from lack of knowledge, poverty, and/or apathy. A significant delay in obtaining medical treatment for illness or injury may be the result of lack of knowledge, lack of transportation, prohibitive costs, or other barriers to seeking medical services.
It is important to note that the majority of cases reported to the child protective services system, 61 percent according to 1996 NCANDS data, involve a primary allegation of neglect or emotional maltreatment, and that the majority of such cases occur in families with very low incomes. However, it is equally important to note that most impoverished families do not neglect their children, and provide strong, nurturing care for their children. Even among impoverished families, neglectful families tend to be the "poorest of the poor," often lacking adequate housing, health care and child care (National Research Council, 1993). As will be discussed in detail in Chapter 4, neglect is especially predominant in child maltreatment reports in which the parent has a substance abuse problem.
Neglect can be broken down into two types for purposes of discussion: physical and educational. (Emotional neglect will be covered in the discussion of emotional maltreatment). Physical neglect includes failure to provide or allow needed care in accordance with recommendations of a competent health care professional for a physical injury, illness, medical condition, or impairment (also called medical neglect); inadequate or nonexistent supervision of a child; chronically leaving a child with others who are not qualified to take care of him or her for days or weeks at a time; inattention to avoidable hazards in the home; inadequate nutrition, clothing, or hygiene, and other forms of reckless disregard of the child's safety and welfare, such as leaving a young child unattended in a motor vehicle. Educational neglect includes allowing or condoning chronic truancy; the failure to register or enroll a child in school; the refusal to allow or failure to obtain recommended remedial educational services, or neglect in obtaining or following through with treatment for a child's diagnosed learning disorder or other special education need (DePanfilis and Salus, 1992).
Sexual Abuse
Sexual abuse includes a wide variety of behaviors, including fondling a child's genitals, intercourse, rape, sodomy, exhibitionism, and commercial exploitation through prostitution or the production of pornographic materials. According to the Child Abuse Prevention and Treatment Act (CAPTA, section 111(4)), "the term 'sexual abuse' includes: (A) the employment, use, persuasion, inducement, enticement, or coercion of any child to engage in, or assist any other person to engage in, any sexually explicit conduct or simulation of such conduct for the purpose of producing a visual depiction of such conduct; or (B) the rape, and in cases of caretaker or inter-familial relationships, statutory rape, molestation, prostitution, or other form of sexual exploitation of children, or incest with children." Most State laws distinguish between sexual abuse and sexual assault. To be considered sexual abuse, these acts have to be committed by a person responsible for the care of the child (for example, a parent, baby-sitter, day care provider, or other person responsible for a child). Sexual assault is usually defined as sexual acts committed by a person who is not responsible for the care of the child.
Sexual abuse can involve varying degrees of violence and emotional trauma. The most commonly reported cases involve incest (sexual abuse occurring among nuclear family members), which most often occurs between father or stepfather and daughter. However, mother-son, father-son, mother-daughter, and brother-sister incest also occurs. Sexual abuse may also be committed by other relatives such as aunts, uncles, grandfathers, grandmothers, and cousins.
Emotional Maltreatment
Emotional maltreatment includes acts of commission or omission by the parents or other persons responsible for the child's care that have caused serious behavioral, cognitive, emotional, or mental disorders. This can include extreme or bizarre forms of punishment, such as torture or confinement of a child in a dark closet, or more subtle forms of abuse, such as belittling, scapegoating, or terrorizing a child.
Emotional abuse is the most difficult form of child maltreatment to identify. First, the effects of emotional maltreatment, such as lags in physical development, learning problems, and speech disorders are often evident in children who have not experienced emotional maltreatment. Second, the effects of emotional maltreatment may only become evident in later developmental stages of the child's life. Third, the behaviors of emotionally abused and emotionally disturbed children are often similar (DePanfilis and Salus, 1992).
There are some guidelines that can help distinguish an emotionally disturbed child from an emotionally maltreated one. The parents of an emotionally disturbed child generally recognize the existence of the problem and seek help, whereas the parents of an emotionally maltreated child often blame the child for the problems or ignore the existence of a problem. These parents often refuse offers of help and appear punitive and unconcerned about the child's welfare (DePanfilis and Salus, 1992).
Although any form of maltreatment may be found in isolation, they often occur in combination. Emotional maltreatment is almost always present when other forms of maltreatment are identified (DePanfilis and Salus, 1992).
Longer Term Effects of Abuse and Neglect
Beyond the immediate physical injuries children may suffer, child abuse and neglect can also have longer lasting impacts across the developmental spectrum. The effects of chronic neglect are especially significant for later social and emotional functioning. Individual child characteristics, such as temperament and intelligence, may mediate the effects of neglect and abuse. Problematic school performance is among the more common problems associated with child abuse and neglect, with neglected children most adversely affected. Neglect during early childhood has negative consequences for later social relationships, problem solving, and the ability to cope with new or stressful situations. Some abused or neglected children develop aggressive behavior patterns, while others become withdrawn. Children experiencing abuse or neglect are at risk for delinquency, violence and other self destructive behaviors as well as at risk for post-traumatic stress disorder, major depression disorder, and other diagnostic conditions (National Research Council, 1993).
Characteristics of Persons Who Maltreat Children
As noted above, it is difficult to isolate the factors that lead to abuse. It is also hard to classify the personality characteristics of abusers. Attempts to identify such characteristics have produced inconsistent and contradictory results, largely because many factors interact to produce the occurrence of child maltreatment (English, 1995). Maladaptive parenting can arise in a variety of ways, especially when a parent's behavioral characteristics or personal history, such as excessive anger, anxiety, impulsivity, depression, background of abuse, or poor coping skills, are exacerbated by such stresses as marital conflict, social isolation, unemployment, substance abuse, the disability of a child, lack of community support systems, and other violence in the environment. In general, several studies have found that abusive parents are more psychologically disturbed than non-abusive parents, though true psychosis is seen in only the most violent and abusive parents (English, 1995). The relationships among all these factors are not well understood in determining the origins of child maltreatment. It is important to be aware that what may be the cause of maltreatment in one family may not be the cause in another. Thus, it is important to use a holistic model in analyzing child abuse, examining the interplay of many conditions and circumstances, including those affecting the parents, the family, and the community, that combine to produce an abusive or non-abusive situation.
We know from the most recent NCANDS data (1996) that 77 percent of perpetrators of child maltreatment are parents, and an additional 11 percent are relatives of the victim. It is estimated that over 80 percent of all perpetrators are under age 40 and that almost two-thirds are female. An estimated three-quarters of neglect and medical neglect cases are associated with female perpetrators, while almost three-quarters of sexual abuse cases are associated with males.
The most consistent finding in the child abuse literature is that maltreating parents often report having been physically, sexually, or emotionally abused or neglected as children. Steele (1980) found that the presence of additional circumstances interacting with a prior history of abuse can increase the likelihood of abusive behavior, e.g., situational crisis, lack of social support, and a perception of the child as "unsatisfactory." However, it is incorrect to draw the conclusion that maltreated children all grow up to become maltreating parents. There are individuals who have not been abused as children who become abusive, as well as individuals who have been abused as children but do not subsequently abuse their own children. Some researchers have identified protective factors that seem to break the cycle of abuse. Parents with reported histories of abuse who do not abuse their own children are more likely to have (1) a better current social support system, including a supportive spouse; (2) a positive relationship with a significant adult in childhood or a positive experience with therapy as an adolescent or adult; (3) an ability to provide a clear account of their childhood abuse, with anger appropriately directed at the perpetrator, not at themselves (National Research Council, 1993).
Certain children are more physically and emotionally vulnerable than others to maltreatment. The child's age and physical, mental, emotional, and social development can greatly increase or decrease the likelihood of maltreatment, depending on the interactions of these characteristics with parental factors previously discussed. Younger children, due to their small size and development, are particularly vulnerable to certain forms of maltreatment. In addition, the child's behavior, such as chronic crying or unresponsiveness, can increase the likelihood of maltreatment, particularly if the parents have impulsivity problems and cannot empathize with the child. Children with disabilities are also at higher risk for abuse and neglect (National Research Council, 1993).
Prevention and Intervention in Child Maltreatment
It is now generally recognized that a community-wide approach to the prevention of child maltreatment is the most promising technique for reducing its incidence and prevalence. Since child maltreatment is such a multivariate phenomenon, the resources of many different professional disciplines, as well as the resources of neighborhoods and communities at large, must be enlisted in a coordinated fashion. Child abuse and neglect stem partially from broad socioeconomic difficulties, so a response is required by society in general. It is also a problem that is caused in part by psychosocial factors, which requires the intervention of many branches of the helping professions. The interactions between child, parent, and environmental factors in precipitating maltreatment further indicate the necessity of comprehensive approaches. In short, the most effective prevention and intervention strategies must be:
- Comprehensive, integrating the contributions of social service, legal, law enforcement, health, mental health and education professionals;
- Neighborhood-based, strengthening the neighborhood and community by encouraging and supporting local improvement efforts, including self-help programs, that make the environment more supportive of families and children;
- Child-centered, protecting the safety and personal integrity of children and giving primary attention to their best interests; and
- Family-focused, strengthening families, supporting and enhancing their functioning, providing intensive services when needed, and removing children when such action is appropriate (U.S. Advisory Board on Child Abuse and Neglect, 1993).
Some specific activities that characterize a comprehensive, ecologically-based model of prevention and intervention include:
Health Care Initiatives, such as prenatal and early childhood health care to improve pregnancy outcomes and health among new mothers and young children; home health visitors to provide support, education and community linkage for new parents; and support programs for parents of special-needs children to assist them with their unique problems.
Community-Based Initiatives, such as self-help and mutual aid groups like Parents Anonymous, which provide nonjudgmental support and assistance to troubled families; child care programs to reduce the stress for employed parents; programs that address the impact of lack of economic resources on children and families such as the lack of adequate shelter, nutrition and health care, and public education; and media campaigns to increase public knowledge and awareness about the importance of prevention of child abuse and neglect.
A good example of a community-based initiative founded on the principles of coordination and collaboration of related services is mandated by the Child Abuse Prevention and Treatment Act of 1996. Title II of the Act established the Community-Based Family Resource and Support Grants Program whose purpose is "to support State efforts to develop, operate, expand, and enhance a network of community-based, prevention-focused, family resource and support programs ... to foster an understanding, appreciation, and knowledge of diverse populations in order to be effective in preventing and treating child abuse and neglect."
Parent Education Programs,such as those geared toward young parents, first-time parents, and parents with young children, which provide training in developmental stages, behavioral expectations and alternative disciplinary techniques.
Workplace Initiatives, such as the provision of flexible work schedules to help families balance the demands of their work with parenthood; education and support programs on parenting; employer-supported child care; and liberal parental leave polices.
Family-Centered Welfare to Work Programs which provide family support services both pre- and post-employment.
Social Service Programs, such as parent aide programs to provide a supportive relationship for parents at risk of harming their children; crisis and emergency services to provide respite at times of crisis; alcohol, substance abuse and mental health treatment; treatment for abused children to prevent intergenerational abuse; comprehensive prevention programs to provide multi-disciplinary services and support to families at risk; and respite care for women experiencing domestic violence, or taking care of a disabled family member.
Prevention Programs in Schools, such as self-protection training for children; family life education to equip children and adolescents with skills for coping with family problems and to prepare them for their future roles as parents, and programs for children with special needs to help reduce the stress on families with a disabled child. These may also include child abuse/neglect prevention and intervention programs in the school or in other settings which specifically address the needs of children of substance abusing parents.
It is clear that while our understanding of the nature of child maltreatment has expanded greatly as a result of years of research, demonstration, and clinical observation, there is still much to be learned and determined about the etiology, prevention, and treatment of this complex problem. We have come to understand the extreme importance of a coordinated response to child maltreatment, one that incorporates a recognition of its relationship to a multiplicity of factors, both within and outside the family system. Substance abuse is certainly one of the most important of these factors.
As far back as 1989, Congress recognized the link between substance abuse and child maltreatment. That year the Child Abuse Prevention and Treatment Act was amended to establish the Emergency Child Abuse and Neglect Prevention Services Program. This legislation authorized the Secretary of the Department of Health and Human Services to establish "a grant program to make grants to eligible entities to enable such entities to provide services to children whose parents are substance abusers." No funds were authorized until fiscal year 1991, when approximately $18 million was made available for grants to prevent the maltreatment of the children of substance abusing parents through comprehensive, multi-disciplinary, coordinated services addressing the needs of these children and their families. Ninety-four grants were funded by the National Center on Child Abuse and Neglect in four sub-categories: comprehensive emergency services, public information and education, improvement of services to substance abuse-affected families, and multi-disciplinary/interdisciplinary training. Some excellent projects emerged from this effort, and many lessons affecting policy, planning and service delivery were learned. Results from these grants are discussed in Chapter 7. The program was later combined with several other discretionary grant programs into what has become the Community-Based Family Resource Program.
Chapter 4. The Extent and Scope of the Problem
The language authorizing this Report to Congress specifically required that we describe the extent and scope of the problem of substance abuse among families involved with the child welfare system. In this chapter we review data available from a variety of sources. The data available represent different and often conflicting numbers and patterns. These differences are largely the result of the differing methodologies by which they were obtained, differences in the populations studied, and differences in how the researchers defined both what represented a substance abuse "problem" and what threshold of conduct represented child maltreatment. In addition, the figures presented below examine the problem from a variety of standpoints: the prevalence of substance abuse among the child welfare population; the prevalence of child maltreatment and other parenting problems among substance abusing parents; and the prevalence of children residing in families with substance abuse problems, regardless of whether specific maltreatment issues have been identified.
Our basic conclusions are as follows:
- While parents, especially mothers, abuse alcohol and other drugs at lower rates than do persons without children, there are a great many children, 8.3 million, living with substance abusing parents (Huang et al, 1998). Few of these children come into contact with the child welfare system.
- Most studies find that for between one third and two-thirds of children involved with the child welfare system, parental substance abuse is a contributing factor. Lower figures tend to involve child abuse reports and higher findings most often refer to foster care. There are as many substance abusing fathers with children in their households as mothers (HHS/SAMHSA, 1997d), although mothers are far more likely to come to the attention of child protective services agencies.
- Substance abusing African American women are more likely to come to the attention of Child Protective Services agencies than are white or Hispanic women with substance abuse problems.
- Children prenatally exposed to drugs and alcohol represent only a small proportion of the children affected and potentially endangered by parental substance abuse.
- Both the abuse of alcohol and the abuse of illicit drugs are linked to child maltreatment. In many families, both alcohol and illicit drugs are abused simultaneously, making the two problems indistinguishable. Numerically, however, the problem-level use of alcohol is far more prevalent than illicit drug use. Binge drinkers (those who drink five or more drinks on the same occasion) outnumber cocaine users by 21 to 1 and outnumber heroin users 98 to 1 (HHS/SAMHSA, 1998c).
- Many parents, especially mothers, who enter substance abuse treatment are motivated to do so by concerns regarding their parenting and how their substance abuse is affecting their children (HHS/SAMHSA 1996b).
How many children live with substance abusing parents?
The child welfare system serves children who come to its attention as the result of abuse and neglect reports. These children, however, are a small fraction of those who live in households in which a parent has a serious alcohol or drug problem. Data from the 1996 National Household Survey on Drug Abuse (NHSDA) reveal that an estimated 8.3 million children in the United States, 11 percent of all children in the U.S., live in households in which at least one parent is either alcoholic or in need of substance abuse treatment.
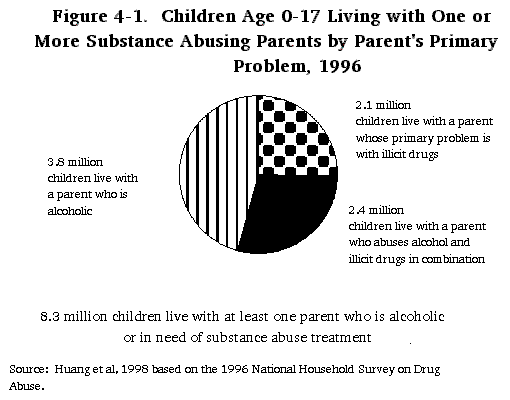
As shown in Figure 4-1, 2.1 million of these children live in families in which the predominant problem is illicit drugs; 3.8 million live in families in which the primary problem is alcohol, and 2.4 million of these children live with parents who abuse both alcohol and illicit drugs in combination. The children living in substance abusing households are evenly spread across the age spectrum, from infants to teenagers, as shown in Figure 4-2.
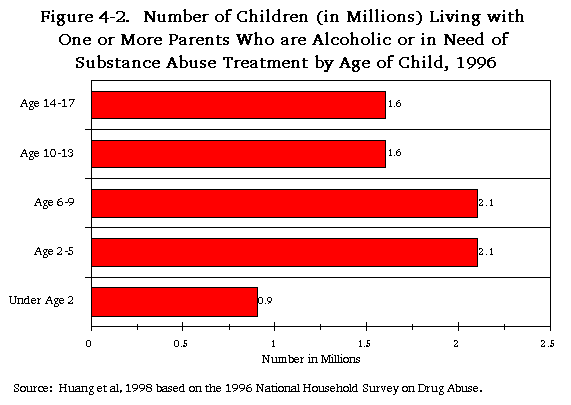
The substance abuser is the mother in about half these families, and the father in the other half. These figures include only those children residing with their parent(s) at the time of the survey and do not include children who had been removed to foster care (Huang et al, 1998). Figure 4.3 and Table 4-A illustrate the number of children living in families with varying levels of substance abuse problems.
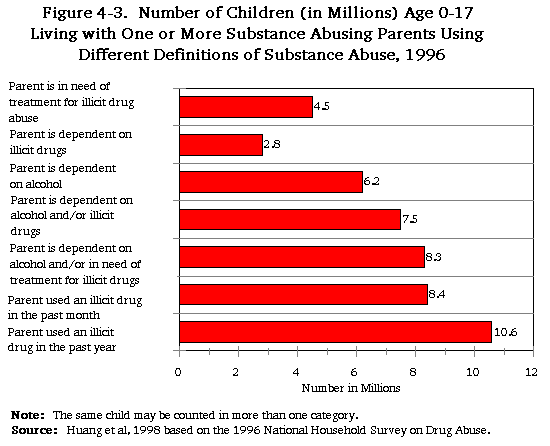
| Definition of Substance Abuse | Number of Children Less than or Equal to 17 Years Old Living With One or More Parents With This Level of Use (in millions) |
Percentage of Children Less than or Equal to 17 Years Old in the U.S. Population Living With One or More Parents With This Level of Use (in percent) |
|---|---|---|
| Parent is in need of treatment for illicit drug abuse | 4.5 | 6.0 |
| Parent is dependent on illicit drugs | 2.8 | 3.8 |
| Parent is dependent on alcohol | 6.2 | 8.3 |
| Parent is dependent on alcohol and/or illicit drugs | 7.5 | 10.0 |
| Parent is dependent on alcohol and/or in need of treatment for illicit drugs | 8.3 | 11.1 |
| Parent used an illicit drug in the past month | 8.4 | 11.2 |
| Parent used an illicit drug in the past year | 10.6 | 14.3 |
| 1 Includes biological, step, adoptive or foster children. 2 For definitions of dependence and "in need of treatment" used in this analysis, see Huang et al, 1998. Source: Huang et al, 1998, based on the 1996 National Household Survey on Drug Abuse. |
||
Additional data on the characteristics of alcohol and drug using parents from the 1994 and 1995 National Household Surveys on Drug Abuse reveal that there were an estimated 649,000 women and 645,000 men with problem levels of illicit drug use who were living with children younger than 18 years of age. Problem drug users living with children represent 30 percent of all women with this level of drug problem and 18 percent of such men (SAMHSA, 1997d). As shown in Table 4-B, parents with problem levels of drug use look remarkably like parents without such problems demographically, particularly with regard to race.
| Parents with Problem Drug Use | Parents without Problem Drug Use | |||
|---|---|---|---|---|
| Men | Women | Men | Women | |
| Age Group (Years) | ||||
| 18 - 25 | 12.2* | 18.7 | 5.5 | 11.8 |
| 26 - 34 | 43.0 | 41.9 | 28.2 | 32.8 |
| 35 and older | 44.8* | 39.9* | 66.3 | 55.3 |
| Total | 100.0 | 100.0 | 100.0 | 100.0 |
| Race/Ethnicity | ||||
| White | 64.9 | 71.7 | 73.0 | 68.2 |
| Black | 14.9* | 20.0 | 9.9 | 14.4 |
| Hispanic | 10.5* | 7.4* | 12.6 | 12.6 |
| Total | 90.3 | 99.1 | 95.5 | 95.22 |
| Education | ||||
| Less than high school | 33.0 | 28.3 | 17.0 | 17.1 |
| High school graduate | 44.3 | 40.2 | 31.0 | 34.5 |
| Some college | 12.9 | 21.3 | 21.3 | 25.1 |
| College graduate | 9.7 | 10.1 | 30.6 | 23.2 |
| Total | 100.0 | 100.0 | 100.0 | 100.0 |
| Current Employment Status | ||||
| Full-time | 74.9 | 31.3 | 81.5 | 45.7 |
| Part-time | 3.6 | 12.1 | 4.6 | 17.6 |
| Unemployed | 14.9 | 12.9 | 4.2 | 5.0 |
| Other | 6.5 | 43.6 | 9.6 | 31.7 |
| Total | 100.0 | 100.0 | 100.0 | 100.0 |
| Marital Status | ||||
| Married | 78.2 | 47.4 | 91.3 | 75.2 |
| Divorced or Separated | 11.3 | 31.4 | 4.9 | 12.5 |
| Never married | 10.1 | 21.1 | 3.0 | 9.7 |
| Total | 99.6 | 99.9 | 99.2 | 97.43 |
| Family Member Participated in Welfare Programs | ||||
| Yes | 19.8 | 40.9 | 5.9 | 12.3 |
| No | 80.2 | 59.1 | 94.1 | 87.7 |
| Total | 100.0 | 100.0 | 100.0 | 100.0 |
|
Footnotes: Source: U.S. Department of Health and Human Services, Substance Abuse and Mental Health Services Administration, Office of Applied Studies. National Household Survey on Drug Abuse, 1994-B, 1995. This table originally appeared in HHS/SAMHSA, 1997d, Substance Use Among Women in the United States. |
||||
Nearly three-quarters (72 percent) of problem drug using mothers and 65 percent of problem drug using fathers are white, 20 percent of these mothers and 15 percent of these fathers are black, and 10 percent of these fathers and 7.4 percent of these mothers are Hispanic. Figure 4-4 shows the racial/ethnic distribution of mothers with problem levels of illicit drug use.
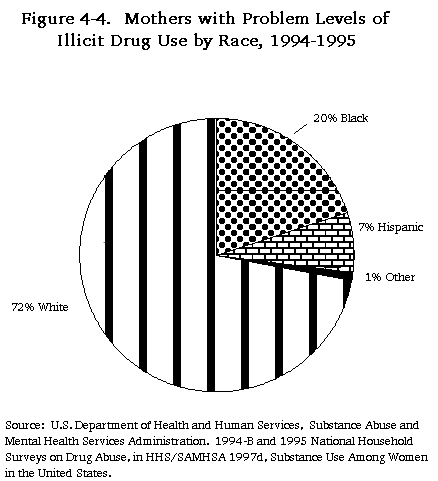
As a group, parents with substance abuse problems have somewhat less education, are somewhat less likely to be employed full time, and are much less likely to be married and much more likely to participate in welfare programs than are other parents. Seventy-five percent of fathers with substance abuse problems are employed full time, as are nearly one-third of such mothers.
Prenatal drug abuse has been a particular focus of media, policy and research attention. Some 221,000 infants (5.5 percent) are born each year prenatally exposed to illicit drugs. Most of these have been exposed to marijuana (2.9 percent or 119,000 children), while 1.1 percent (45,000) are exposed to cocaine and 1.5 percent (61,000) pregnant women used prescription medications during pregnancy without physician direction (U.S. Department of Health and Human Services, National Institute on Drug Abuse [HHS/NIDA], 1994). In addition, some 140,000 pregnant women (3.5 percent of all pregnant women) each year drink heavily, placing their children at risk for Fetal Alcohol Syndrome and Fetal Alcohol Effects (U.S. Department of Health and Human Services, Centers for Disease Control and Prevention [HHS/CDC], 1997). Figure 4-5 shows the number of women who use illicit drugs or drink heavily during pregnancy.
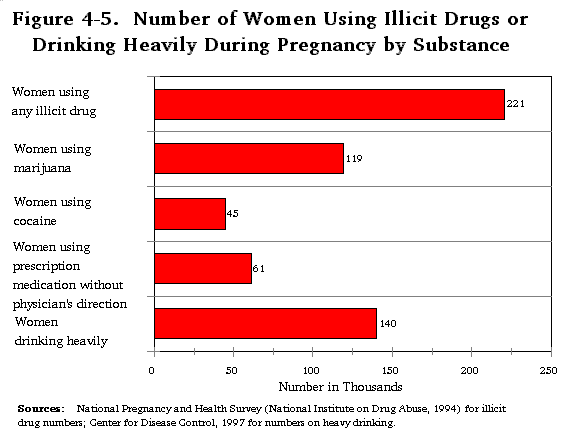
Table 4-C shows the numbers of women using illicit drugs by pregnancy and child rearing status. Substance abuse rates are considerably lower among women who have children in the home than among women who are not raising minor children, and pregnant women report lower substance use rates than non-pregnant women. Particularly notable, and encouraging, are the very low reported rate of binge drinking and of heavy drinking among pregnant women.
| INDEX | WOMAN'S PREGNANCY AND CHILD-REARING STATUS (NUMBER IN THOUSANDS) |
|||||||
|---|---|---|---|---|---|---|---|---|
| Pregnant | Raising Child(ren) <2 Years Old | All Children Are 2+ Years Old | No Children | |||||
| N | % | N | % | N | % | N | % | |
| Population N (thousands) |
2,400 | 100 | 7,500 | 100 | 25,000 | 100 | 26,000 | 100 |
| Any illicit drug | 59 | 2.5 | 385 | 5.5 | 981 | 4.1 | 2,579 | 10.4 |
| Any, excluding marijuana | 28 | 1.2 | 147 | 2.1 | 417 | 1.7 | 1,150 | 4.6 |
| Cocaine | 4 | 0.2 | 33 | 0.5 | 151 | 0.6 | 353 | 1.4 |
| Heroin | 4 | 0.2 | 5 | 0.1 | 19 | 0.1 | 41 | 0.2 |
| Binge drinking1 | 30 | 1.3 | 622 | 9.2 | 2,395 | 10.3 | 4,009 | 16.7 |
| Heavy drinking2 | 6 | 0.3 | 133 | 2.0 | 532 | 2.3 | 1,100 | 4.6 |
|
Footnotes: Source: Adapted from Preliminary Results from the 1997 National Household Survey on Drug Abuse (1998c), p. 94-95. Annual averages based on 1996 and 1997 samples. |
||||||||
With respect to drug use by pregnant women and by parents, African American women have higher rates of illicit drug use and particularly cocaine use than do white women (HHS/SAMHSA, 1997d). However, there are many more white women, including white pregnant women and white parents, who use illicit drugs than there are minority women in these categories who use illicit drugs (HHS/SAMHSA, 1998a). The number of African American women who use cocaine during pregnancy, (30,000 in 1992) far exceeds the number of white and Hispanic women who used that drug prenatally (HHS/NIDA, 1994). Studies have shown, however, that African American children prenatally exposed to illicit drugs are much more likely than white children to be both reported to child protective services (Chasnoff, 1989) and to be placed in foster care, even after taking into account factors such as the family's previous child welfare involvement, the physical health of the child, and other related factors (Neuspiel et al, 1993).
Rates of both alcohol and illicit drug abuse are even higher among Native Americans than among other ethnic groups in the U.S., although most national data on substance abuse have insufficient samples to separately analyze data for Native Americans (HHS/SAMHSA, 1998a).
Child welfare agencies tend to focus their attention on infants and very young children of substance abusers, particularly children who have been prenatally exposed to illicit drugs. But as Figure 4-2 illustrated, children of all ages reside in substance abusing families, and prenatally exposed infants represent a very small proportion of children in such households. These data also illustrate how closely intertwined and inseparable alcohol and illicit drug abuse are.
How many of the families involved with the child welfare system have substance abuse problems?
For decades child welfare staff have recognized that substance abuse is common in the families they serve (Fanshel, 1975). Studies have long shown that parents with substance abuse problems are more likely than other parents to maltreat their children (Famularo et al, 1986; Jaudes et al, 1995; Kelleher et al, 1994). The wide variety of figures cited in the literature, however, makes it difficult to sort out how the numbers fit together. Several issues drive the differences in the statistics:
- The point in the child welfare system being studied. Numbers differ depending on whether what is being counted is substance abuse among families with child abuse reports, open child welfare cases, or children in foster care. For the most part, substance abuse prevalence has been found to be greater the "deeper" into the system one looks (i.e. greater prevalence is found among parents of children in foster care than among parents of children reported to child protective services).
- How the study defines what counts as substance abuse. Numbers differ depending on whether the study counts any family suspected of substance abuse, families with clinically diagnosed conditions, parents who have tested positive for drugs, or some other threshold. Most studies include both alcohol and illicit drugs, but numbers are smaller if only illicit drug abuse is counted.
- How the information is collected. Studies surveying administrators about how many families in an agency's caseload have substance abuse problems routinely generate higher figures than do studies interviewing caseworkers about specific children or looking at case files to determine whether substance abuse is noted.
Despite these issues, it is clear that substance abuse is a significant factor in the lives of families served by the child welfare system.
Child Abuse Reports
In 1996, child protective services (CPS) agencies received more than 2 million reports of alleged child abuse and neglect involving more than 3 million children. CPS staff conducted approximately 1.6 million investigations of these reports and found evidence to substantiate that more than 970,000 children had been victims of child abuse and neglect that year. While a great many child abuse reports are received and investigated annually, studies show that most children recognized by community professionals as having experienced injury-causing child abuse or neglect (72 percent) had not been reported to (or, if reported, had not been investigated by) the local CPS agency (U.S. Department of Health and Human Services, National Center on Child Abuse and Neglect [HHS/NCCAN], 1996).
Most studies report that between one-third and two-thirds of substantiated child abuse and neglect reports involve substance abuse. Substance abuse is more likely to be a factor in reports regarding younger children, particularly infants, than older children. In addition, substance abuse is much more likely to be a factor in child neglect than in child abuse (Herskowitz et al, 1989; HHS/NCCAN 1993; Walker et al, 1991). In a recent survey of State child welfare administrators, the Child Welfare League of America (CWLA) found that at least 50 percent of substantiated child abuse and neglect reports involve parental abuse of alcohol or other drugs, and fully 80 percent of States reported that substance abuse and poverty are the top two issues contributing to abuse and neglect in their States (CWLA, 1998). The Indian Child Welfare Association estimates that 90 percent of Indian child welfare neglect cases and 60 percent of abuse cases involve families in which drinking or drug abuse is a major problem (Cross, 1997).
The National Child Abuse and Neglect Data System (NCANDS), operated by the Children's Bureau within HHS, compiles data voluntarily supplied by States regarding child abuse and neglect reports. In addition to aggregate data, a number of States (twelve in 1996) participate in the Detailed Case Data Component (DCDC) of the system which describes individual cases. Among the data elements in the DCDC, States are invited to report whether the parent or child has an alcohol or drug problem that contributed to the abuse or neglect report. Currently only two of the twelve States participating in the DCDC supply this information (New Jersey and South Carolina), and even in these States the information supplied appears to be incomplete. New Jersey reports that 20.3 percent of child abuse and neglect reports in 1996 involved caretaker drug abuse, and 7.3 percent involved caretaker alcohol abuse. South Carolina's figures were 10.9 percent caretaker alcohol abuse and 8.6 percent caretaker drug abuse. Each State also reports a handful of cases in which the child's alcohol or drug abuse were factors in the maltreatment allegation. In some cases these child drug abuse problems were in infants (presumably prenatally exposed), while in others the child in question was a teenager who was a drug user himself or herself. For the most part, the low substance abuse figures in NCANDS and some other tracking systems is related to the fact that agencies usually categorize cases by the type of maltreatment (e.g. physical neglect) rather than the reason(s) behind the maltreatment.
The 1993 Study of Child Maltreatment in Alcohol Abusing Families, based on a national probability sample of children with substantiated maltreatment reports, found that substance abuse was part of the presenting problem for 42 percent of children found to be victims of child abuse and neglect in 1989. Among the caretakers with substance abuse problems, alcohol was a problem substance for 77 percent, and, as shown in Figure 4-6, it was the primary (most harm-causing) substance for 64 percent. Cocaine was the primary problem substance for most of the rest (23 percent overall).
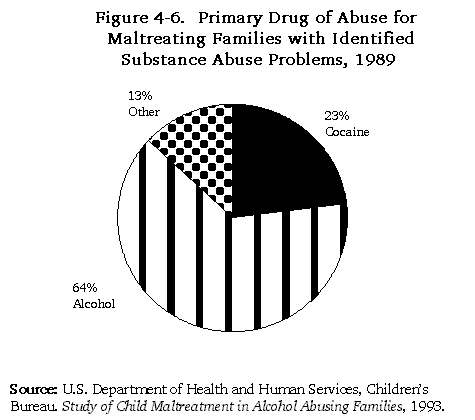
This study found that maltreatment cases involving alcohol and drugs had distinctive profiles (HHS/NCCAN, 1993). In particular:
- These cases involved younger children. Half of the cases in which a parent abused illicit drugs involved children under age 5, as compared to 29 percent in other cases. Alcohol-related cases were no more likely to involve preschoolers than other cases.
- Maltreatment cases involving illicit drug abuse had a distinctive profile in terms of the types of maltreatment involved. Drug-related cases were much more likely than others to involve physical neglect (46 percent of drug related cases versus 24 percent of others) and to have been based on a positive drug or alcohol toxicology (12 percent of drug-related cases versus 1 percent of others). Cases involving illicit drug abuse rarely involved sexual abuse (4 percent of drug-related cases versus 24 percent of non-drug-related cases) or physical abuse (13 percent of drug-related cases versus 32 percent of non-drug-related cases). Emotional abuse was reported in 20 percent of both drug and non-drug-related cases.
- Medical and hospital staff were important sources of CPS referrals of drug-related cases (accounting for 29 percent of these cases versus 9 percent of other cases), but not for alcohol-related cases. Mental health and substance abuse treatment staff were responsible for 7 percent of alcohol-related referrals but for fewer than 1 percent of the drug-related referrals.
- Both alcohol- and drug-related cases were more likely to result in foster care placements than other cases (nearly a third of cases involving substance abuse resulted in foster care, versus less than 20 percent of other cases).
In addition to national data and State reports to Federal information systems, several State-level reports contain data regarding substance abuse and child protection. In Illinois, where health professionals are required to report all substance exposed infants to child protective services, between 1985 and 1992 nearly 12,000 such reports were filed. Of these, 87 percent were indicated (similar to the "substantiated" category used by most States), and of indicated cases, 11 percent were taken into foster care immediately, while a total of 30 percent had child welfare cases opened. Many of these open cases involved children being served while remaining at home (Goerge and Harden, 1993). New York has reported that in 1990, 40 percent of substantiated child abuse reports involved a caretaker's drug abuse, and an additional 15 percent involved alcohol abuse (NYDSS 1992, cited in Magura et al, 1998). An early study in Massachusetts found that excessive alcohol or drug use was a factor in 64 percent of all substantiated child abuse and neglect reports and was even more common in reports of infants, where 89 percent were alcohol or drug related (Herskowitz et al, 1989).
Open Child Welfare Cases
If a child and family is to be monitored by or receive services from the child welfare system following an investigation, the child welfare agency opens a child welfare case with the family. About half the children with open child welfare cases are in foster care, while the other half receive services while remaining in their parents' care (HHS/CB, 1997). Most studies that look at children in the child welfare system look only at foster care rather than the broader population of children with open child welfare cases. The one recent national study that did look at a sample of open child welfare cases, the National Study of Protective, Preventive and Reunification Services Delivered to Children and Their Families, found parental substance abuse to be a problem in 26 percent of child welfare cases (see Figure 4-7).
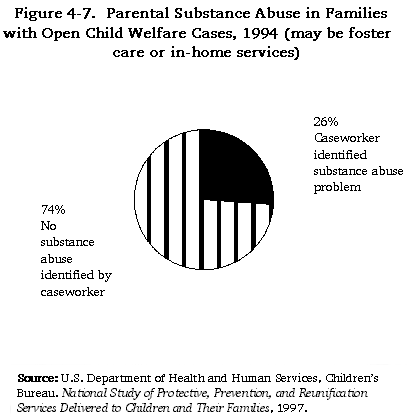
An additional 5 percent of cases involved a child's own substance abuse (HHS/CB, 1997). This study looked at a representative sample of cases nationally and interviewed the child's caseworker about the family and provided services. There may have been additional substance abuse than is reflected in these data, but if so the caseworker was unaware of it.
This study found that the typical open child welfare case in which there was a substance abusing caretaker involves a young child (median age 5 years at case opening) probably being served in foster care (54 percent). The family is somewhat likely to be from a large metropolitan area (42 percent) and from a neighborhood with safety problems (63 percent). The caretaker is very likely single (71 percent) almost certainly a mother (95 percent) and probably over age 30 (median age 31). The family is probably enrolled in one or more government assistance programs such as Medicaid, welfare or food stamps. The typical child has been in foster care for almost a year (median time in care, 11 months) (U.S. Department of Health and Human Services, unpublished tables produced for this report). As compared with maltreating families without identified substance abuse, families with substance abuse problems are much more likely to be from a large urban area and from a neighborhood with safety problems. Families with substance abuse problems are more likely on welfare, have child welfare cases opened at younger ages, are twice as likely to be in foster care, and have been in foster care an average of six months longer.
Foster Care Cases
Most lay persons equate child welfare with foster care, although only a small minority of families with substantiated or indicated child abuse or neglect complaints have children placed in foster care -- 16 percent in 1996 (HHS/CB, 1998d). The remainder either are served while remaining at home, or child welfare workers have determined that no services are necessary to keep the child safe (for instance if the perpetrator has left the home). Because foster care is provided to the most troubled families and provides the most intensive (and therefore most expensive) services to children, it is often the focus of public attention. Foster care is also the focus of Federal child welfare policy. There were approximately 520,000 children in foster care on March 31, 1998, a figure that has been rising steadily for a decade (Adoption and Foster Care Analysis and Reporting System, 1998).
The U.S. General Accounting Office (USGAO) in a recent report (USGAO, 1998) found that approximately two-thirds of foster care cases reviewed in urban counties in two States involved parental substance abuse (Figure 4-8).
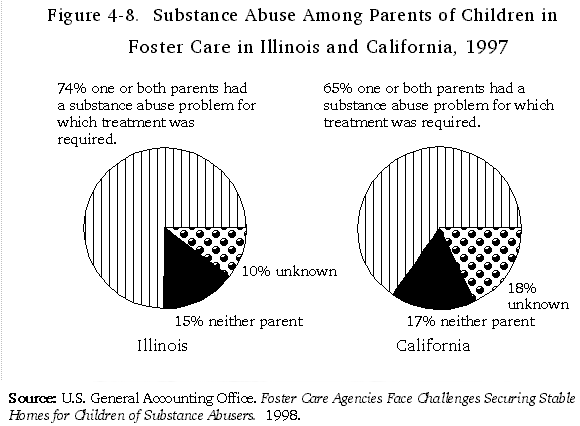
Substance abuse was noted in 65 percent of cases in California and 74 percent of cases in Illinois. The problem was usually abuse of cocaine or methamphetamine (Figure 4-9), was usually noted in the mother or in both parents of the child, and was in most cases a longstanding problem of at least 5 years duration.
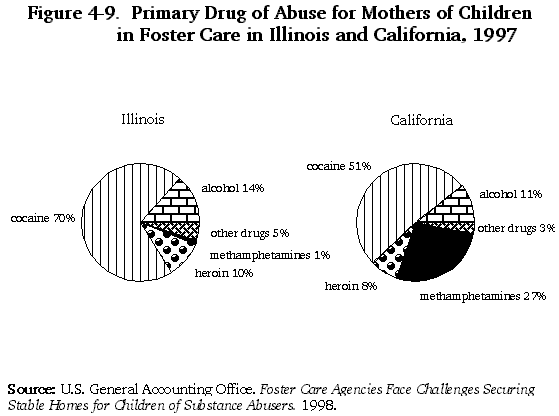
In 80 percent of substance abuse related cases, the child's entry into foster care was the result of severe neglect. In a related study conducted several years ago, the USGAO had found 78 percent of children in foster care had parents with substance abuse problems (USGAO, 1994). These figures have remained remarkably consistent, particularly in studies that look at cases in urban locations.
The Child Welfare League of America's 1998 survey on alcohol and drug issues found that only 8 States could provide information regarding the proportion of foster care cases involving alcohol or other drugs. Even if not able to report specific numbers of cases, States were asked to report whether the proportion of child welfare cases involving substance abuse was up or down in recent years. Thirteen of 47 States reported that more cases than in the past involved substance abuse (CWLA, 1998). The remaining states lacked information on trends in substance abuse in their caseloads.
In preparing this report, we reviewed data reported by States under the Adoption and Foster Care Analysis and Reporting System (AFCARS), a new reporting system under which States provide semi-annual information about all children in foster care or who have been adopted from the public child welfare system. While reporting under AFCARS is mandatory, these requirements are still in the implementation stage and not all States are yet reporting complete data. For the purposes of this report we analyzed data regarding children in care on March 31, 1998. Regarding substance abuse, AFCARS contains the following data elements for each child: yes/no fields indicating whether the parent had an alcohol problem that contributed to the child's placement; whether the parent had a drug problem that contributed to the child's placement; whether the child had an alcohol problem; and whether the child had a drug problem. Child alcohol and drug problems could represent either their own use of substances (primarily in adolescents) or a prenatal exposure to substances (seen in infants).
In the reporting period examined, only 32 States plus the District of Columbia reported any data in the four alcohol and drug fields, and many of these data are incomplete and under-reported. Reports of caretaker alcohol and/or drug problems ranged from less than 1 percent to 62 percent in the States reporting data for these elements (Figure 4-10).

Most of the large States, including New York and Illinois, were not yet reporting these data. We expect reporting for AFCARS to improve considerably over the next several reporting periods. As compared with many of the other required data elements, however, we expect information about substance abuse to be problematic for some time. Whereas elements such as the child's placement setting, case goal, or characteristics have long been part of States' own administrative data systems and transfer reasonably well to AFCARS, documentation of the problems that led to the child's foster care placement has not traditionally been included in automated child welfare information systems. Because reporting these items is not familiar to State and local agencies, it will take them longer to report these data reliably. In addition, it will be difficult to make cross-state comparisons because States may use varying thresholds to decide when substance abuse "contributes" to the foster care placement. Some States may be reporting only drug exposed infants under these data elements, while others report any case in which substance abuse is either part of the allegation or is documented. In States where at least some alcohol and drug data are being reported in AFCARS, there was no consistent pattern regarding either child and family characteristics or the child's experiences in the child welfare system. In most States, substance abuse-related cases looked quite similar to other cases, although under-reporting of substance abuse could have diluted any differences which might exist.
A few smaller studies in particular localities have also examined parental substance abuse as a factor in families with children in foster care. Walker and her colleagues in a study of children in foster care in 1986 found that substance abuse was noted in the case files for 18 - 52 percent of African American children in foster care, varying by city. In general, just over one-third of the children in foster care in New York, Miami, Seattle, Detroit and Houston had a parent with a substance abuse problem that was mentioned in the case file (Walker, et al, 1991; Walker et al, 1994).
While most analyses of data regarding children in foster care look at individual children rather than sibling groups, we must also recognize that many children in foster care are from larger families. Recent analyses of data from California find that of 1,600 newborns entering foster care in that State because of neglect or abandonment, nearly 60 percent had siblings already in care, totaling over 2,500 siblings (Barth, 1997).
How many families with substance abuse problems have contact with the child welfare system?
As discussed above, there are approximately 1.3 million parents with problem levels of illicit drug use (and many more alcoholic parents) who are living with children younger than age 18. These figures do not include children in foster care (because children in foster care are not living in their parents' households and are thus not picked up in a household survey). Most alcohol and drug using parents do not come into contact with the child welfare system, although they are more likely to do so than other parents. HHS's 1993 Study of Child Maltreatment in Alcohol Abusing Families reported that child maltreatment was three times as likely in alcohol abusing families compared with non alcohol abusing families. It also found that once child maltreatment was substantiated, children in alcohol or drug abusing families were more likely to enter foster care than were children in other maltreating families (30 percent versus 17 percent). Where child welfare cases were opened, 97 percent of cases involving drug abuse and 87 percent of cases involving alcohol abuse were closed within four months, indicating that the child welfare agency was satisfied that the safety issues had been resolved (HHS/NCCAN, 1993).
Other researchers found that child abuse occurred in 27 percent of families with an alcoholic parent and 19 percent of families with an opiate addicted parent. Serious neglect occurred in nearly a third of both alcoholic and opiate addicted families, and children in all families with an alcoholic or drug addicted parent experienced some degree of neglect (Black and Meyer, 1980).
The Maternal Lifestyles Study, a longitudinal study following 1,400 cocaine and/or opiate exposed children and a matched comparison sample in several cities, found that 42 percent of the drug exposed infants were reported to child protective services at the time of the child's birth. Reporting rates varied substantially among study sites depending on the State reporting policies. Of the drug exposed children, 82 percent were living with the biological mother at the time of hospital discharge and virtually all of those were still living with the mother at one month of age. Of the children not discharged to the mother, at one month of age 13 percent were back in the mother's care, 32 percent were in the care of relatives, 41 percent were in non-relative foster care, and 14 percent were in some other living arrangement (Maza et al, 1998).
The Center for Substance Abuse Treatment, within SAMHSA, is currently evaluating a grant initiative to provide residential substance abuse treatment for pregnant women and women with children. Early data show that about one-fifth of women in these programs were referred to treatment by a child welfare agency, probably because of issues related to child abuse or neglect. Far more had children living in foster care. Overall, 40 percent of women in the programs had at least one child living primarily in foster care during the 30 days prior to admission. Crack cocaine, methamphetamine, and alcohol were the most common drugs of abuse for these clients (Dowell and Roberts, 1998).
Studies of women in particular substance abuse treatment programs also show high rates of child welfare system involvement. Kearney reports that in a sample of heavy cocaine users, 69 percent had lost or given up custody of a child at some time (Kearney, 1994). Evaluators of a program in Arizona report that 33 percent of clients were involved with child protective services at the time of admission, although only 11 percent admitted to being the aggressor in a violent incident toward their children (Steven and Arbiter, 1995). A residential treatment center for women with children reports that only 37 percent of women enrolling in the program had custody of a child at intake (indicating that most clients' children were either in foster care or with relatives) (Wobie, 1997). And Brindis reports from another treatment program that for the mothers entering the program she studied, of the parents' youngest child under three years old, 43 percent were living with the mother, 19 percent lived with relatives, and 38 percent lived in foster care or other living situations outside the family (Brindis et al, 1997). The high rates of child welfare system involvement in these studies is in part due to the target client populations of these treatment programs and the recruitment techniques used.
Other studies have shown high protective service needs among families with substance abuse problems (Kelley, 1992). For instance, one study found that teachers have reported a need for protective services three times more often for children being raised by someone with an addiction than for other children (Hayes and Emshoff, 1993).
How are families with substance abuse problems different from other child welfare clients?
Few studies directly compare child welfare clients with substance abuse problems to other child welfare clients. Analyses of the Children's Bureau's National Study of Protective, Preventive and Reunification Services conducted expressly for this report found significant differences between child welfare clients with substance abuse problems and other clients of the child welfare system. This study was based on a national sample of children with open child welfare cases in 1994 (for the report's previously published findings and a full description of the study's methodology, see HHS/CB, 1997). The 26 percent of families with identified substance abuse problems were significantly more troubled than other families in the child welfare system as measured by the frequency with which substance abuse problems were seen in tandem with a variety of other family problems. As shown in Figure 4-11, alcohol was the primary drug abused by 25 percent of substance abusing families in the child welfare system, illicit drugs were the problem for 40 percent, and in 35 percent both alcohol and drugs were abused.
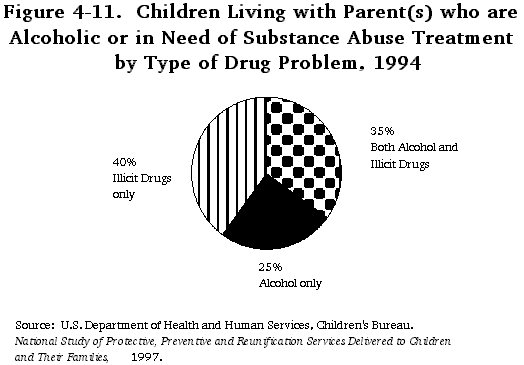
Children from substance abusing households were much more likely than others to be served in foster care rather than in the home (54 percent in foster care versus 23 percent of children in non-substance abuse cases), spent longer periods of time in foster care than other children (median 11 months versus 5 months for others in foster care) and were less likely to have left foster care within a year than other children (55 percent versus 70 percent). Families with substance abuse problems were equally likely to be white or African American (47 percent), while only 6 percent were Hispanic.
Children in foster care from families with substance abuse problems were more likely than others to have a case plan of adoption (9 percent versus 3 percent) and were less likely to have a case plan of emancipation or independent living (3 percent versus 11 percent), both likely linked in part to having entered care at younger ages and being younger at the time of the study (i.e. a two-year-old is more likely than a 16-year-old to have an adoption case plan, while a 16-year old is more likely to have a plan of emancipation). Substance abusing families and others were equally likely to have a case plan goal of reunification (54 percent versus 56 percent). Children from substance abusing families were an average of 5 years old at the time of case opening, versus average age 7 for other children.
The services most commonly offered to substance abusing parents were employment training (82 percent), substance abuse treatment (70 percent), parenting training (59 percent), psychological assessment (22 percent) or household management services (22 percent). As shown in Figure 4-12, far fewer actually received the offered services -- in the case of substance abuse treatment approximately half of families with identified substance abuse problems received any substance abuse treatment services. In 23 percent of cases, substance abuse treatment services were offered but not provided, and services were not offered to another 23 percent of cases.
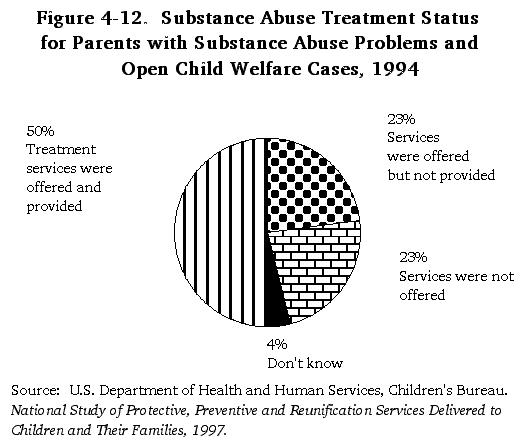
"Offered" services might not be delivered for a variety of reasons including clients' refusal, mismatches between available services and client needs, or ineffective referral processes. Although many of these women have multiple drug-exposed children, only 8 percent were offered family planning services. Chapter 7 includes additional information on the substance abuse treatment status of parents.
Substance abusing families were more likely than others to have had multiple caseworkers while involved with the child welfare system. Only 35 percent of families with substance abuse problems had a single caseworker, versus 59 percent of other families, and 41 percent had three or more caseworkers (versus 21 percent). This is likely due in part to the fact that cases involving substance abuse were open for longer periods of time, making multiple caseworkers more likely.
Another study, this one focusing on African American children in foster care, also found that families with substance abuse problems had more problems overall than other families, were more likely than other families to be neglectful rather than abusive, and children from these families entered care younger and stayed in care longer than other children in foster care (Walker et al, 1991; Walker et al, 1994). Researchers looking at children reported to child protective services in one California county found that 35 percent of such children were not removed from the home; 29 percent were removed from the home on an emergency basis but were returned to the parent's custody within a few days; 12 percent were removed but returned home within 18 months; and 24 percent were removed and were not expected to return home (Sagatun-Edwards et al, 1995). Ellwood and colleagues (1993) found that 25 percent of drug-exposed infants born to women on Medicaid spent most of their first two years of life in foster care, while the remainder continued in their families' care.
How are families with child maltreatment problems different from other substance abuse treatment clients?
Data from SAMHSA's evaluation of grant initiatives to provide residential substance abuse treatment for pregnant women and women with children indicate that female substance abuse treatment clients who have ever had children removed from the home by child protective services tend to be older than other clients, have more children, and have more other problems such as having been homeless and unemployed, than do other clients entering these substance abuse treatment programs (Dowell and Roberts, 1998).
Among substance abuse treatment clients who are parents, child custody issues are a major reason for treatment entry. In the National Treatment Improvement Evaluation Study (NTIES), 44 percent of female clients with children under 18 (and 15 percent of male clients with such children) reported that they entered substance abuse treatment in order to keep and/or regain custody of their children (Figure 4-13).
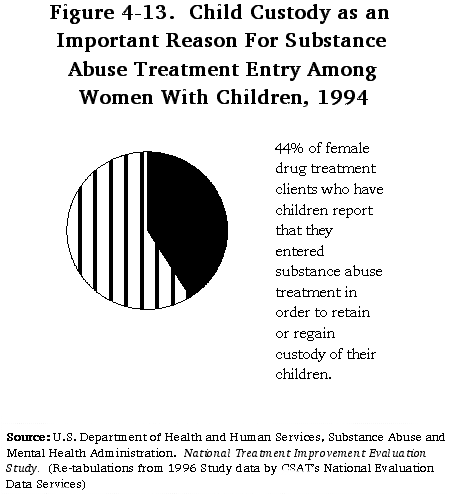
Of female clients who entered treatment within a year of their most recent birth, two-thirds did so because of custody concerns and 86 percent of these women had already lost custody of this child (HHS/SAMHSA, 1996). Findings from a California study of substance abuse treatment outcomes further confirm that parenting and custody issues are an important motivation for treatment entry (Gerstein et al, 1997).
Child Abuse as a Precursor to Substance Abuse
The child welfare system most commonly perceives substance abuse as causing abuse or neglect of children. However, research is also beginning to show that child abuse, particularly sexual abuse, is a common precursor of substance abuse (Dembo et al, 1997; National Research Council, 1993). The early initiation of substance use is a risk factor for addiction, and may in part represent a child's attempts to escape the unresolved emotional trauma of abuse or neglect (National Research Council, 1993). This suggests the need for improved attention to the emotional health of children in foster care, and to the need for substance abuse prevention activities focused on children involved with the child welfare system. Without intervention, the child victims we seek to protect today may become the next generation of abusive or neglectful parents.
McCauley and colleagues (1997) found that women with a history of childhood physical or sexual abuse were nearly 5 times more likely to be current users of street drugs and over twice as likely to have a history of alcohol abuse than were other women. In addition, a study of alcohol and other drug dependent persons in Iowa found that a third of dependent persons reported physical abuse as children (as compared with 11 percent in the general population), and 13 percent reported sexual abuse as children (compared with 6.3 percent in the general population) (Lutz et al, 1995).
Discussion
Figures regarding the extent to which abusive and neglectful families also have substance abuse problems, and vice versa, are complex and confusing. While specific studies vary considerably for methodological and other reasons, the bottom line is that a very significant portion of the child welfare caseload involves families with substance abuse disorders. But these are far from the only problems these families face. In addition, we must recognize that while substance abuse impairs parental functioning and has negative impacts on children, most substance abusing parents do not engage in behaviors that rise to the child protective services definitions of abuse or neglect. In addition, it is clear that alcohol as well as illicit drugs may place children at risk, and that parental substance abuse is a problem for children of all ages.
Chapter 5. The Complexity of Child and Family Needs
Families involved with the child welfare system are among the most troubled in our society. The child welfare system serves as the final safety net, when no other public or private institution has been able to address a family's problems successfully. It is expected to meet the family's needs and assure a permanent, safe environment for the child, either at home with the biological family or elsewhere. But even if the child welfare agency, in a particularly egregious case, responds by moving a child out of the family quickly and on to an adoptive home, unless the parents' problems are addressed, the family is likely to remain unhealthy and may reappear at a future date, with another child identified as at-risk.
In maltreating families, maltreatment is rarely the only issue. Even addiction, while among the most common co-occurring problems, is rarely the only significant one. Serious mental illness may be present, particularly among substance abusing women. Domestic violence and HIV/AIDS are also critical factors in the lives of some families. Poverty is pervasive, and inadequate or unsafe housing are very significant problems, particularly in urban areas. These serious difficulties combine in the lives of these families to produce extremely complex and dysfunctional situations and relationships that are difficult to resolve. The presence of so many serious issues also implies that addressing the substance abuse alone is not likely to produce the changes in a family that are necessary to ensure a healthy environment for a child. Unless the whole of a family's situation is addressed, substance abuse treatment is unlikely to be successful -- and even if a parent achieves abstinence, the other issues present may continue to pose safety problems for the child(ren).
The National Research Council of the Institute of Medicine, in its comprehensive volume Understanding Child Abuse and Neglect (1993), cautions against viewing substance abuse as a monolithic cause of child maltreatment. The panel notes that substance abuse and child maltreatment are "often complicated by the presence of other social and economic variables ... that confound the analysis of the contributing role of drugs themselves. At this time the literature on substance abuse and child maltreatment is not well ... developed" (National Research Council, 1993, p. 19). Mental illness, health problems, past childhood abuse and domestic violence are examples of these other variables.
Co-Occurring Health and Social Factors
Particularly among women, mental illness and substance abuse are often intertwined. Over one third of females with problem drug use have experienced a major depressive episode in the past year, and 45 percent have experienced at least one of several mental health problems including panic attacks and anxiety disorders. These rates are more than double those for men with similar levels of substance use (HHS/SAMHSA, 1997d). Chavkin and her colleagues (1993) found that most crack cocaine using women reported psychiatric symptoms, and nearly a third had histories of psychiatric medication or hospitalization. Half reported having been sexually abused as children. Merikangas and Stevens (1998) present a comprehensive review of the literature on psychiatric comorbidity in women with substance use disorders. It has been hypothesized that for many women with both substance abuse and other affective disorders, drug use may in part represent self-medication, that is, drugs are being used to alleviate psychiatric symptoms (Dackis and Gold, 1992). To the extent this is the case, abstinence alone will not solve the problem. If the underlying psychiatric problem is not addressed, the factors causing the drug problem have not gone away (at least in part) and relapse is likely to result. Dually diagnosed clients (those with both substance abuse and other mental illnesses) are known to have higher relapse rates than other clients (HHS/SAMHSA, 1994). Diagnosis of co-occurring mental and addictive disorders can be difficult but is extremely important for effective treatment and recovery. Because alcohol and drug abuse may mask other symptoms, it is often several months into sobriety before additional diagnoses can be made.
The nation's AIDS epidemic is also closely intertwined with problems of substance abuse. Two thirds of AIDS cases among women are the result of either intravenous drug use or sexual relations with an intravenous drug user (Selwyn and Gorevitch, 1998). Women with substance abuse problems are more likely both to have high risk sexual partners and to have multiple sexual partners than are women without such problems. The vast majority of women diagnosed with HIV or AIDS are between the ages of 15 and 44 (the childbearing years). Many of these women have children who may be born with HIV themselves, or are likely to be orphaned as their mothers succumb to the disease, although prenatal HIV treatments have reduced mother-infant transmission rates substantially. Between 72,000 and 125,000 U.S. children are expected to be orphaned because of parents' AIDS by the year 2000 (Levine and Stein, 1994). Women are likely to be diagnosed with HIV or AIDS at later stages than are men and are less likely to receive health care for their infections (Selwyn and Gorevitch, 1998).
The relationship between domestic violence and substance abuse is well documented (HHS/SAMHSA, 1997b) and recent consensus panels held by SAMHSA conclude that "failure to address domestic violence issues interferes with treatment effectiveness and contributes to relapse" (HHS/SAMHSA, 1997b, page 5). In up to 70 percent of all incidents of domestic violence, the victim, the batterer, or both, had been drinking. Women who are alcoholics are more likely to have been beaten than non-alcoholics and are more likely to have partners who also drink heavily. Miller (1998) reports that 88 percent of women in a drug treatment program for women had experienced severe partner violence in their lifetimes, and 26 percent had experienced such violence in the past six months. The most common forms of severe partner violence were being hit with a fist, beaten up, hit with an object, or choked. Women in substance abuse treatment had much higher rates of partner violence than women in comparative community samples -- often 2, 3, or 4 times higher depending on the specific type of violence. In these women, substance abuse may be related to victimization either because alcohol and drugs are used as a general coping mechanism, or to deal with post traumatic stress disorder resulting from the violence (Miller et al, 1997).
Women with substance abuse problems are frequently involved with men who are also substance abusers. In fact, women are often introduced to substance abuse by male partners. These men may feel threatened by their partners' efforts to get clean and may actively or tacitly undermine the goals of her treatment. A woman's efforts to separate from an abusive partner during recovery may also place her at risk for further violence. Treatment programs which fail to recognize this dynamic may inadvertently contribute to escalating violence. Child welfare agencies, too, must acknowledge these risks and recognize potential danger to the mother, as well as the children, as they intervene with families.
Women who abuse alcohol and other drugs have often been the victims of violent crimes, either as children or adults. According to several research studies, between 41 percent and 74 percent of women in treatment for alcohol and other drugs reported being childhood or adult victims of sexual abuse, including incest (Wilsnak, 1991). A number of researchers have found significantly higher proportions of histories of sexual and/or physical abuse among women in treatment as opposed to comparison groups of women (Bergman et al, 1989).
Preliminary data from a cross-site evaluation of demonstration grants funded by SAMHSA's Center for Substance Abuse Treatment finds that 76 percent of clients in treatment programs for women with children report a personal history of abuse, neglect or trauma. About a fourth report physical abuse by a parent, a third report emotional or psychological abuse by a parent, and slightly over 10 percent report sexual abuse by a parent. Many more report physical, emotional or sexual abuse by a non-parent (over three-quarters report physical and emotional abuse and about one-half report sexual abuse). Clearly, many of these women have experienced severe stress which may affect their basic abilities to function socially and emotionally and especially as a parent. (Dowell and Roberts, 1998)
Finally, substance abuse is also related to increased involvement of women in the criminal justice system. Sales of illicit drugs and drug use have contributed to the enormous 386 percent rise in the female prison population between 1980 and in 1994 (Wilsnack, 1995). The average percent of arrested women who tested positive for drugs in 20 cities in 1996 was 64 percent (U.S. Department of Justice, National Institute of Justice, 1997).
Substance Abuse and Parenting
The complexity of these families often makes it difficult for child protective services workers to determine the extent to which substance abuse presents a risk to children. Again, it is important to recognize that not all those who abuse or are dependent on alcohol or other drugs abuse or neglect their children, and that danger to a child may or may not be the direct result of a parent's substance abuse. Child welfare workers struggle with trying to evaluate the role of substance abuse in the dynamics of a given family and what a child is experiencing. In many cases, while a parent's substance use may impair his or her parenting ability, these parenting deficiencies do not rise to the level of neglect or abuse at which a child welfare agency would intervene.
Substance abuse has profound effects on parental disciplinary choices and child rearing styles. Research has shown that parents with substance abuse problems employ less effective discipline than other parents (Tarter et al, 1993). Research through taped clinical observations have shown that drug abusing parents are very limited in their ability to attend to their children's emotional and social cues and to respond appropriately (Hans, 1995). As a consequence, substance abusing parents can overreact with harsh discipline or neglectful child support leading to the higher levels of child abuse and neglect in substance abusing parents (Kumpfer & Bayes, 1995). They also tend to be poor role models for the use of alcohol and drugs and effective conflict resolution and family management skills (Kumpfer, 1987). However, research also demonstrates that substance abusing parents, whether in treatment or not in treatment, can be taught through therapeutic child play and behavioral parent training to be more empathetic and effective parents. Through these family interventions child abuse and neglect and harsh and ineffective discipline can be decreased, while also decreasing the child's emotional and behavioral risk factors for later substance abuse and other adolescent problems (Egeland & Erickson, 1990; Kumpfer, Molgaard & Spoth, 1996; Kumpfer & Alvarado, 1995, 1998; Kumpfer, Williams & Baxley, 1997, Kumpfer, 1999).
Kearney and colleagues (1994) studied the parental attitudes and behaviors of drug dependent mothers. They found that these women felt a strong responsibility toward their children and were quite proud of them. Studying how these mothers try, unsuccessfully, to balance their addictions with their parenting responsibilities, they found that "the basic problem crack cocaine presented to mothers was its drain on their attentiveness, their financial resources and their efforts to be appropriate role models for their children" (p. 354). Hawley and colleagues (1995) also found that motherhood was often the only legitimate social role valued by drug dependent women and that most women in treatment were very concerned about how their substance abuse had affected their children - indeed such concern was a powerful treatment motivation. Catalano and associates (1999) have found that providing a parenting program to parents while in drug treatment, in fact, also reduces relapse after treatment. Because of the importance of being a good parent, offering effective parenting programs during outpatient or inpatient residential treatment improves recruitment, retention and outcomes for parents and children in addition to reducing relapse.
Effective Parenting and Family Interventions for Substance Abusers
Over the past twenty years, a number of behavioral parent training, family skills training, family therapy and family support programs have been found effective in improving behavioral and emotional outcomes for both parents and children (Ashery et al, 1999; Kumpfer & Alder, in press) and with children from diverse cultures (Kumpfer & Alvarado, 1995). Over 50 effective, research-based models of parenting interventions have been identified by SAMHSA/CSAP in their expert review of the family-based intervention research literature (SAMHSA/CSAP, 1998). The Office of Juvenile Justice and Delinquency Prevention (OJJDP) also conducted two expert reviews over the past then years of their Strengthening Families Initiative and have identified 34 model parenting and family programs which are being disseminated though conferences, training of trainers, technical assistance and mini-grants. For a review of these programs see Kumpfer and Alvarado (1998), or program descriptions on their web site: www.strengtheningfamilies.org.
A number of these parenting interventions have been specifically tested in federally-funded research projects with drug abusing parents. For instance, the Strengthening Families Program for substance abusing parents has been fount to significantly improve the parent's parenting skills, parenting self-efficacy, depression, stress and drug, while also improving the children's emotional and behavioral status (Kumpfer, Molgaard, & Spoth, 1996). This program has been culturally adapted for different ethnic populations and field tested with similar positive results with five different investigators. A version for rural families has been developed and found effective in reducing alcohol use (Spoth & Redmond, 1996; Spoth, Redmond & Lepper in press).
Despite these positive research findings, few substance abuse treatment programs offer these or other research-based and effective parenting programs to their clients. A great gap exists between scientifically valid prevention and treatment programs and the commercially marketed but untested programs being implemented by practitioners. To improve the dissemination and adoption of science-based parenting and family support interventions, SAMHSA's Center for Substance Abuse Prevention is investing $10 million in grants to over 100 communities to select, implement and evaluate their choice of over 50 research-based models.
Children of Substance Abusers
No less complex than the problems of substance abusing parents are their children's needs. A large research literature exists from epidemiological, family, adoption and twin studies concerning the genetic and environmental risks that put these children at higher risk for a variety of problems (Kumpfer, 1987; Tarter & Messich, 1997; Johnson and Leff, in press). Whether because of in utero exposure to stressors including tobacco, alcohol, or drugs, or to genetic and environmental family risks, children of substance abusers are more frequently described by their parents as being hyperactive and as having difficult temperaments. Clinical studies do not find these children to have significantly more diagnosable attention deficit disorder, but simply to be more active and have a high energy level. McMahon and Luthar (1998) report in a review of developmental issues in children of substance abusers that the two main research findings regarding such children are (1) that they have poorer developmental outcomes (physical, intellectual, social and emotional) than other children, although generally in the low-normal range rather than severely impaired; and (2) they are at risk of substance abuse themselves.
Evidence is increasing that children of substance abusers are at elevated risk for developing substance use disorders at young ages due to familial and genetic factors. Merikangas, Stolar, and their colleagues (1998) report an 8-fold increased risk of drug disorders among relatives of 299 individuals with drug disorders. These findings were reinforced in a second generation study of the children of these drug dependent research subjects (Merikangas, Dierker, et al., 1998). The strongest link was found between substance disorders in offspring (mean age 12 years) with parental substance abuse although the link for psychopathology, particularly anxiety disorders, was similar. Risks of this magnitude place a family history of drug disorder as one of the most potent risk factors for the development of the child and the child's development of drug disorders at an early age. These findings suggest that substance prevention and intervention programs should target offspring of parents with substance use disorders. In fact, children of alcohol and drug abusing parents are at the highest risk of any children for later drug use and other adolescent behavioral health and mental health problems. Research also suggests that some children of substance abusers, like other children of dysfunctional parents, can develop special resilience skills with appropriate adult support (Johnson & Leff in press; Kumpfer, Walker & Richardson, in press).
A number of good literature reviews have been published regarding developmental issues in children prenatally and environmentally exposed to substance abuse (Harden, 1998; Pagliaro and Pagliaro, 1997; Carta et al, 1997). Generally, most research finds that factors in the postnatal environment mediate prenatal factors. It is now recognized that the older a child gets, the more important the home environment is in predicting developmental outcomes, including how the environment interacts with any direct effects of prenatal drug exposure. Women who use drugs during pregnancy are at risk for delivering premature and low birth weight babies. Alcohol appears to have more profound and long-lasting effects on development than do cocaine and other illicit drugs, including serious intellectual and behavioral consequences in many children.
SAMHSA's Center for Mental Health services has found, through an evaluation of its Comprehensive Community Mental Health Services Program for Children and Their Families, that children's mental health problems are closely intertwined with parents' substance abuse, child maltreatment, and other forms of family violence. These grantees serve children with serious emotional disturbances. Evaluation results reveal that over 60 percent of families have had a history of substance abuse, and over half of the families had a history of family violence. Almost one-fourth of children were reported to have been sexually abused prior to entering services, 20 percent of children were reported to have used alcohol and drugs, and 59 percent of children served were described by their caregivers as having one or more risk factors including: physical abuse, sexual abuse, previous psychiatric hospitalization, sexual abusiveness, suicide attempts, drug and alcohol use, and a history of running away (HHS/SAMHSA, 1999).
Babies whose mothers drink alcohol during pregnancy can be born with Fetal Alcohol Syndrome (FAS) or alcohol-related birth disorders. FAS is among the leading known causes of mental retardation in the United States. Infants born with FAS have difficulties with coordination, speech and hearing impairments, and heart defects. Research indicates that there is no known safe level of alcohol consumption during pregnancy, although FAS and related problems are more likely with heavy consumption of alcohol, particularly binge drinking. According to the National Organization on Fetal Alcohol Syndrome, at least 5,000 infants are born with FAS annually and another 50,000 infants demonstrate symptoms of alcohol-related birth disorders (National Organization on Fetal Alcohol Syndrome, no date).
Consumption of illicit drugs during pregnancy also may harm the fetus and may have long-term effects on children. Babies who were prenatally exposed to cocaine or other drugs may experience a range of problems, including some that can be long-lasting and serious. However, these physical and mental deficits are not seen in infants to the extent that earlier expert warnings and media reports regarding "crack babies" had predicted (HHS/NIDA, 1994).
Some researchers have found that more subtle developmental problems, particularly in language skills, can be observed in prenatally drug-exposed children as they age. A recent meta-analysis combining results from eight studies finds that cocaine-exposed infants have, on average, IQ scores that are 3.26 points lower than other children. While the effects of cocaine exposure on IQ were small, medium sized differences (defined as those in which cocaine exposed children's scores were lower than those of other children by between 0.5 and 0.75 standard deviations) were found in receptive and expressive language functioning (Lester et al, 1998). Although the developmental effects are subtle, special education to prevent these children from failing in the school environment could cost up to $352 million per year according to the Brown University analysis.
How much of children's presenting developmental difficulties are due to prenatal injury versus postnatal deprivation continues to be a matter of some debate. In their review, Bernstein and Hans (1994) conclude that it may be the number and persistent nature of threats that best predicts developmental outcomes. That is, more risk factors in place for longer periods in a child's life are most likely to have long lasting and serious negative consequences.
Implications for Intervention
Given the multi-problem nature of these clients and their families, it is no wonder that programs serving them find it difficult to meet their needs. Indeed, most evaluations of programs serving parenting substance abusers report that it is difficult to identify these women, it is difficult to engage them in services, and it is difficult to retain them in treatment. Women who are in need of treatment often do not seek it due to the social stigma of using alcohol and other drugs. Denial of her problem on the part of the woman and her family, as well as the fear of losing her partner, is another significant barrier to treatment for a substance abusing women. However, many of the grantees operating programs developed under SAMSHA's women's and children's programs have developed substance abuse treatment programs that are sensitive to the needs of women and children and have been successful in recruiting and retaining them in treatment. Programs have shown particular success if they have
- Removed barriers to attendance by allowing the women to come into treatment with their children;
- Provided therapeutic child care, children's skills training and substance abuse education for the children to simultaneously address their emotional and behavioral problems; and
- Provide parent training and parent support services to improve the women's feelings about being a more effective mother and her actions to accomplish these goals.
The physical and mental health consequences of alcohol and other drug use for women are often different in nature and degree from those of men, as is the etiology of alcohol and other drug use. Often women arrive at substance abuse treatment later in the progression of the disease than do men. These factors require both different approaches to treatment of the drug use itself and to treatment of the consequences of use.
SAMHSA's Center for Substance Abuse Treatment has developed a model for women's substance abuse treatment services (U.S. Department of Health and Human Services, Substance Abuse and Mental Health Administration, Center for Substance Abuse Treatment [HHS/SAMHSA], 1994) which recommends a series of 17 components that are critical for substance abuse treatment for women. The model recommends that all services planned and developed must be age appropriate, culturally relevant and gender-specific for the different populations of women and their children. The components range from substance abuse counseling to obstetrical and gynecological services, and parenting counseling through housing and legal services. These components are implemented through:
- Carefully monitored proactive case management approaches which are an integral part of the treatment process, beginning with intake procedures and following through with continuing care;
- Materials that address the multiple needs of the women;
- Counseling and educational processes that address therapeutic needs and life skills services;
- Involvement of the family and other care givers in the recovery process; and
- A focus on effective discharge planning methods, including creative arrangements for shared housing and relapse prevention services.
A detailed description of this model appears as Appendix B.
Working with parents and children together is generally more effective than working with children only, particularly if the children have conduct problems (Dishion & Andrews, 1995). However, a number of children of alcohol and drug abusers programs have been developed to work directly with these children primarily through educational and support groups offered through schools, community agencies, or faith-based organizations. Research suggests that these children need to be informed about their potential genetic, biological, cognitive and emotional risk factors. School-based programs such as the CASPAR program and the New York-based Student Assistance Services program (HHS/SAMHSA, 1993, HHS/SAMHSA, in press) have demonstrated significant reductions in risk factors and improved social competencies and effective problem solving skills. Services like these could be used effectively in substance abuse treatment programs to produce educational and behavioral change and ultimately reduce the risks these children face for later drug use.
Addressing families' multiple needs is a critical factor in the successful engagement and retention of clients in substance abuse treatment and related services. Often a family's basic needs (such as those for food, shelter, and safety) are so pressing that they must be addressed before a parent has the ability to focus on his or her addiction. Further, a crisis in any single area of their lives may cause a client to relapse and/or drop out of treatment. If a treatment program does not or cannot help the client to address what he or she defines as the family's most significant problem(s), the client is likely to view the program as irrelevant. Efforts to coordinate treatment with other systems are also vital to treatment engagement and retention. These program design issues will be discussed further in Chapter 7.
Chapter 6. The Context of Collaboration and Overcoming Barriers to Quality Service
It becomes obvious to observers of interactions between service providers in the child welfare and substance abuse treatment fields that in most instances, agencies do not work well together and that truly collaborative relationships are rare. This chapter will explore why this is so often the case. Substance abuse treatment agencies and child welfare agencies both have the vision of healthy, functional families resulting from their interventions. In moving from the family's immediate situation to that end result, however, very different perspectives and philosophies may impede cooperation, causing agencies to mistrust each other, hamper one another's efforts, and stymie progress.
Several key differences in perspective underlie the majority of misunderstandings and frustrations child welfare agencies and substance abuse treatment agencies feel toward one another (Feig, 1998; Young et al, 1998). These include: different definitions of "the client," what outcomes are expected on what time lines, and how best to respond to setbacks. In addition, interagency collaborations do not happen in a vacuum. Factors related to the legal and policy environments in which agencies operate set a context for joint activities and affect the willingness and ability of agencies to work together. For the substance abuse and child protection fields, these factors include the following:
- State and Federal laws and policies regarding child abuse reporting, foster care, permanency planning, and termination of parental rights, including new time lines for decision making set forth in the Adoption and Safe Families Act.
- The sense of crisis under which many child welfare agencies operate.
- Chronic shortages of substance abuse treatment services, particularly services appropriate for women with young children.
- Confidentiality requirements of both fields that are often perceived as impediments to cooperation.
Client Identification
For many substance abuse treatment programs, the adult is the primary client and the one around whom services revolve. The adult's relationship with the drug is the focus of the clinical intervention, and everything else in the client's life is of secondary importance. While family relationships and other life issues are assessed, they are not the principal focus and may be de-emphasized until at least several months into the treatment process, if the client remains with the program that long. While parents may discuss their children in group therapy sessions, most treatment programs do not consider children and other family members to be clients, do not include them in therapeutic activities, and may not know whether the client even has children or whether child protective services is involved with the family, unless the client raises the issue or the child welfare agency was the client's referral source.
For many parenting women who enter substance abuse treatment, however, concerns about their parenting and the effects of their substance abuse on their children are key reasons why they enter treatment in the first place (HHS/SAMHSA, 1996b; Gerstein et al, 1997). Unless these issues are addressed, the women may not be getting what they seek from treatment. This may contribute to high drop out rates for women in treatment programs that are not specifically designed to assess and treat these and related critical issues. Lack of attention to family issues also frustrates child welfare workers who may have referred the parent for substance abuse treatment in the first place, but do not see improved parenting and child safety as a consequence of the substance abuse agency's treatment plan.
For child welfare agencies, the child is the focus of activity, and the entire family is usually defined as the client. A variety of services may be offered to the family, with the intent of assuring the child's safety, within the family if possible. But when a choice must be made in balancing children's needs and parents' needs, the mandates of child welfare agencies demand that the children must come first.
With both agencies viewing themselves as the primary service provider, differences may arise around who the client is, what service goals are selected, who is responsible for assuring that outcomes are achieved, what information gets shared and with whom, and myriad other day-to-day issues around working with clients.
Defining Outcomes and Success
Substance abuse and child welfare agencies have different views of what represents a successful outcome and what they seek to achieve. Most substance abuse treatment outcome studies focus on the extent to which treatment results in decreased alcohol and drug use, decreased criminal behavior, and decreased need for and utilization of health care services. Very few measure child- and family-related outcomes unless they are programs specifically designed for women and their children, of which there are few. By these definitions, treatment may be successful even when child safety issues remain and may be unsuccessful even if child welfare goals have been met. Similarly, for a child welfare agency, the child's safety, well-being and ensuring he or she has a permanent family situation in which to grow up are the primary goals. These may be met either within the family of origin or by identifying a substitute. But success may be achieved at a cost of separating a child permanently from his or her biological parents. Further complicating the situation, custody decisions are made by family court judges who may hold yet another set of expectations for clients and may seek additional evidence of success.
As staff begin to work together more closely, child welfare and substance abuse agencies should talk through these issues, both institutionally and also on a case-by-case basis, seeking common ground regarding their definition of the client, mutual expectations for the client and for each other as the case develops. Establishing joint case goals for clients may also prove helpful, particularly identifying interim goals that will allow both agencies to determine, together, the extent to which progress is being made. Such discussion on joint goals may lead to broader interagency agreements on working together. Involving judges in setting expectations may also help assure key players are all in agreement.
Balancing Competing Time Lines
Families involved with the child welfare and substance abuse treatment systems, and who are often involved with other service providers as well, face a variety of time constraints that may be at odds with one another and that may frustrate interagency cooperation. These time lines have been referred to as "the four clocks" (Young et al, 1998) and include:
Child welfare mandates for decisions regarding permanent placements for children who are in foster care. Federal child welfare law now requires that permanency hearings to determine the long term plan for a child be held within 12 months of a child's entry into foster care, and that a petition to terminate parental rights be filed after a child has resided in foster care for 15 of 22 months, unless there is compelling reason not to do so, or other specific circumstances exist, such as that the child is in the care of a relative or the family has not received planned services.
The pace of recovery from addiction. Addiction is a complex illness and multiple treatment attempts over a period of time may be required before significant improvement is seen. Relapse is common, particularly in the early stages of recovery. The long term needed for recovery for many women with multiple problems may conflict with shorter time lines associated with child welfare decision making.
Time limits associated with welfare receipt. Some parents in substance abuse treatment are welfare recipients and subject to Federal and State work requirements and time limits on cash assistance. The majority of female parents in publicly funded substance abuse treatment programs, for example, are welfare recipients (64 percent according to one study of California treatment clients) (Gerstein et al, 1997). As these clients reach their time limits and can no longer depend on welfare income, or are required to participate in extensive work activities, treatment programs will need increasingly to accommodate clients' other activities.
Children's developmental time line. Children grow up quickly and need consistent parental attention. While several months or years is a short period to parents and service providers, to a child that time is essential developmentally. A child cannot be put on hold during a parent's addiction and recovery without serious developmental consequences. Children's developmental time frames are the rationale for speedy child welfare mandates discussed above.
The differences in perspective between a substance abuse treatment program's attention to the relatively long time frames of addiction and recovery and the child welfare agency's shorter time line to be attentive to children's developmental need for permanency and statutory time lines for service delivery, further sets the stage for difficult interagency relationships.
Child Protection Laws and Policies
State laws regarding child abuse reporting, foster care and termination of parental rights set a tone for the consideration of substance abuse as a factor in child protection decisions. Mandatory child abuse reporting laws identify who must report suspected child abuse or neglect and under what circumstances. Most State child abuse and neglect reporting laws do not explicitly mention substance abuse, but rather speak to physical abuse, sexual abuse, and neglect. Generally these laws focus on parental behaviors toward children rather than potential conditions that may precipitate those behaviors.
Each of the seven state laws that did mention substance abuse as of the end of 1996, (California, Illinois, Iowa, Minnesota, Missouri, Oklahoma, and Utah) pertain only to infants prenatally exposed to drugs. None of these reporting laws mention substance abuse beyond pregnancy (HHS/NCCAN, 1997b; HHS/NCCAN, 1998c) and most refer only to illicit drugs, not alcohol. Most of these State child abuse reporting laws require that health professionals make mandatory child abuse reports regarding all infants who are known to be drug exposed at birth. Minnesota's law includes considerable detail regarding the conduct of drug tests. The Illinois law requires a report to the public health agency rather than the child protection agency. California's law specifies that a positive toxicology is not in and of itself sufficient grounds for a child protection report, but requires that an assessment of the parent be conducted, and requires a child protection report if the assessment determines there is danger for the child.
These laws seek to bring particular children at risk of abuse and neglect to the attention of child protection agencies. They also serve to emphasize prenatal exposure to illicit drugs rather than the longer-term risks (arguably more significant to a child's development) of living with a potentially neglectful or abusive substance abusing caretaker. This factor can impede a substance abusing pregnant or post partum woman from seeking health care or substance abuse treatment for fear that admitting a problem will lead to the loss of her child(ren).
In addition to child abuse reporting laws, substance abuse is sometimes mentioned in the statutory criteria for termination of parental rights, particularly laws regarding when expedited adoptions are appropriate. Several States have expedited adoption laws that mention substance abuse, but observers have noted that existing laws include significant flaws (Hardin and Lancour, 1996) which may include: the degree of substance abuse that might lead to termination of parental rights is not specified; unsuccessful treatment attempts need not be demonstrated; and harm to the child need not be shown. Some States' termination of parental rights statutes contain language describing when a parent's continued substance abuse may be considered grounds for terminating parental rights and how many treatment attempts constitute reasonable efforts to facilitate reunification (USGAO, 1998; HHS/NCCAN, 1997a).
As noted above, the Adoption and Safe Families Act (ASFA), passed in November of 1997, requires that decisions regarding permanency for children who enter foster care are to be made within 12 months of a child's entry into care. This requirement creates a context of urgency around the provision of services to families with children in foster care that put special strains on the usual and customary course of substance abuse treatment plans. Communities have very limited time frames within which to offer reunification services (including substance abuse treatment, as needed) before alternative plans must be made for the child. And parents have the same limited time frames within which to demonstrate their readiness to provide a safe home environment for their children. These factors also make it critically important that child welfare workers be able to judge accurately whether a parent is making sufficient progress in his or her rehabilitation program to reasonably expect the child could be returned to the parent within 12 months or shortly thereafter.
The Impact of Perpetual Crisis in the Child Welfare Field
Child welfare staff make complex decisions daily regarding child safety that fundamentally affect the lives of children and families. These decisions are made in an environment of "zero tolerance" for error, in which a worker's error may become tomorrow's headline accusing an agency of overlooking "obvious" peril for a child. The constant possibility of harm to a child following a decision that the child is not at immediate risk, or following reunification with a parent who has improved, makes workers cautious about withdrawing from the lives of families. Child welfare professionals know that if a child is harmed following reunification with a parent who relapses, it is the child welfare agency, not the substance abuse treatment agency, that will be blamed by the media and politicians. In this environment of high visibility in the case of error, workers are often also faced with large caseloads that make it extremely difficult to adequately attend to families' complex situations. This combination of factors may produce a crisis orientation in which only the most pressing situations are addressed and other families' needs are given only cursory attention.
An environment of perpetual crisis also manifests its impact in high burnout and turnover rates among child welfare staff, making it difficult to assure continuity and therefore quality casework. Workers become frustrated because services for families are in critically short supply and many are not within the caseworker's authority to provide. The result is that too often families receive whatever services are available rather than those that may be most appropriate for their needs. These frustrations are particularly evident when a client's key problem is substance abuse and the child welfare agency does not itself have the authority to access or pay for substance abuse treatment services. In addition, the courts become frustrated by the apparent disconnect between clients' needs and delivered services - and it is the child welfare staff who tend to bear the brunt of this frustration. Families, however, face the loss of their children when termination of parental rights actions are initiated in the absence of appropriate, accessible services.
Chronic Shortages of Substance Abuse Treatment
Another contextual issue that must be considered in any discussion of addressing problems related to substance abuse is that substance abuse treatment, particularly treatment tailored to the needs of women and parents, is in chronically short supply. As illustrated in Figure 6-1, approximately 37 percent of problem drug users who are mothers with children under 18 years of age reported receiving some form of substance abuse treatment in 1994-95, significantly fewer than the 48 percent of male parents with substance abuse problems in treatment (HHS/SAMHSA, 1997d).
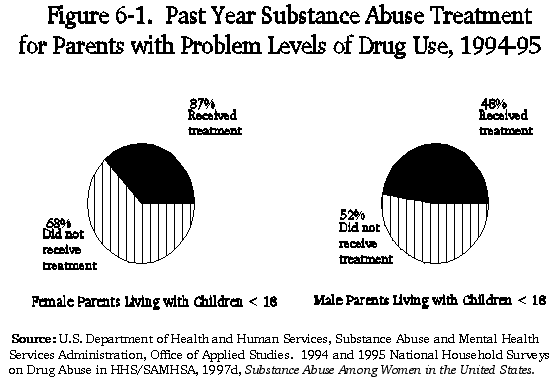
Table 6-A shows trends in the demographics of substance abuse treatment clients 1980-1992. Women make up less than a third of substance abuse treatment clients, up only slightly between 1980 and 1992. The population of persons in treatment closely resembles the age and racial/ethnic distribution of the population of parents in need of treatment (presented in chapter 4, Table 4-B), but differs significantly from the population of parents with substance abuse problems who are clients of child welfare agencies in gender (child welfare clients are predominantly women), and race (minority and especially African American women are over represented in the child welfare system).
| CLIENT CHARACTERISTICS | Percent of Active Substance Abuse Treatment Clients on Survey Reference Date | |
|---|---|---|
| 1980 | 1992 | |
| Substance of Abuse Alcohol only Alcohol and illicit drugs Illicit drugs only |
- - - |
37 38 25 |
| Age 12-20 21-44 45+ |
15.7 61.7 22.5 |
10.1 75.2 14.6 |
| Race/Ethnicity White, non-Hispanic Black, non-Hispanic Hispanic Other |
62.7 20.6 13.4 3.3 |
59.8 21.6 14.6 2.1 |
| Gender Men Women |
74.8 25.2 |
71.1 28.9 |
| Source: HHS/SAMHSA, Overview of the National Drug and Alcoholism Treatment Unit Survey (NDATUS): 1992 and 1980-1992 (Advance Report Number 9), January 1995. | ||
Table 6-B shows the prevalence of substance abuse treatment by type of treatment and demographic group. As shown, an estimated 3.3 million Americans, 1.5 percent of the population age 12 and older, reported receiving some form of drug and/or alcohol treatment in 1995. The number reporting any form of substance abuse treatment was only slightly higher than the number reporting treatment for alcohol abuse (3.3 million versus 3.0 million), which suggests that the great majority of substance abuse treatment clients (upwards of 90 percent) sought treatment partly or wholly for problems with alcohol.
Additional information on substance abuse treatment supply and demand are available from State and local sources. The National Association of State Alcohol and Drug Abuse Directors (NASADAD) reports that in on a given day in 1997 there were nearly 52,000 persons on substance abuse treatment waiting lists maintained by State agencies (NASADAD, 1997). Further, only 10 percent of child welfare agencies report that they can find substance abuse treatment programs for most of the clients who need it within 30 days (Child Welfare League of America, 1998). Although not everyone who receives treatment will recover, and not all those who need it will enter a treatment program even if one is available, without treatment few of those who are as severely impaired by substance abuse as are many child welfare clients will be able to address their addictions successfully and become better functioning parents.
| Demographic Group | DRUG ABUSE TREATMENT | ALCOHOL ABUSE TREATMENT | ANY SUBSTANCE ABUSE TREATMENT | |||||
|---|---|---|---|---|---|---|---|---|
| N (1000s) |
Percent Receiving Treatment in Past Year | N as Percent of Past-Month Any-Drug Users | N (1000s) |
Percent Receiving Treatment in Past Year | N as Percent of Past-Month Binge1 Drinkers | N (1000s) |
Percent Receiving Treatment in Past Year | |
| Total | 2,363 | 1.1 | 13 | 3,426 | 1.6 | 9 | 3,713 | 1.7 |
| Age Group 12-17 18-25 26-34 35+ |
203 500 569 1,154 |
0.9 1.8 1.6 0.9 |
10 6 18 17 |
180 667 922 1,667 |
0.8 2.4 2.6 1.3 |
16 4 12 10 |
248 723 958 1,795 |
1.4 1.6 2.9 1.2 |
| Race/Ethnicity White Black Hispanic |
1,764 407 146 |
1.1 1.7 0.7 |
13 10 15 |
2,726 457 208 |
1.7 1.4 1.0 |
9 8 6 |
2,886 505 250 |
1.6 1.4 1.1 |
| Gender Male Female |
1,544 778 |
1.5 0.7 |
12 14 |
2,367 1,111 |
2.3 1.0 |
9 10 |
2,470 1,322 |
2.2 0.9 |
|
1 5 or more drinks on the same occasion 1 or more days in the past 30 days. Source: Adapted from HHS/SAMHSA, National Household Survey on Drug Abuse, Main Findings, 1996 (1998) p. 160. |
||||||||
While women's specific treatment needs are slowly being recognized, recent drug treatment data demonstrate that over the past decade there have been significant declines in the delivery of a variety of services provided in conjunction with substance abuse treatment. For instance, only 8.3 percent of patients in outpatient, drug free treatment programs (through which most persons are treated for substance abuse) had received any family services (such as parenting classes or family therapy) during the first three months of treatment according to a 1990 survey. A similar study a decade earlier had found much more comprehensive service delivery. In the earlier study, nearly 43 percent of outpatient clients reported receiving family services. Clients of long term residential programs and short term inpatient programs were somewhat more likely to receive family services, but even in the most service intensive modalities fewer than 40 percent of clients received these services (Figure 6-2).
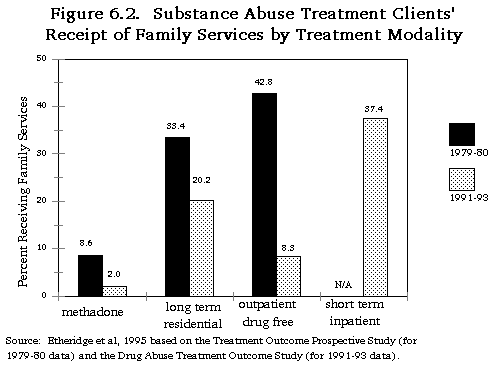
Similar declines were reported in the provision of medical, psychological, legal, educational, vocational and financial services. Declines were marked in all modalities but were especially severe in outpatient programs, where fewer than 10 percent received any ancillary services other than medical treatment, and over 60 percent received no services beyond basic substance abuse counseling (Etheridge et al, 1995). Pressures from managed care may be responsible for some of the decline in comprehensive services. The shortages of substance abuse treatment, particularly treatment with services designed specifically for women with children, mean that treatment programs do not feel the need to develop new referral sources such as child welfare agencies - their programs are full without seeking new clients. Despite increased Federal substance abuse treatment funding over the last decade, funds to develop additional treatment capacity have not caught up with the need.
Confidentiality Issues
Confidentiality has long been central to both the substance abuse treatment and child welfare fields. Both fields recognize a need to guard clients' rights to privacy and shield clients from outside scrutiny while they address the problems which led them to service providers' attention. Confidentiality is especially important in both these fields because stigma may cause clients to avoid needed services if, as a consequence of receiving assistance, their problems become known to others in the community. In the substance abuse field, confidentiality is governed by Federal law (42 U.S.C. § 290dd-2) and regulations (42 C.F.R., Part 2) that dictate under what limited circumstances information about the client's treatment may be disclosed with and without the client's consent.
In child welfare, confidentiality is governed by State laws and regulations that conform to the Federal child abuse and neglect and child welfare statutory and regulatory standards. Title IV-E of the Social Security Act requires that States provide safeguards to restrict the use and/or disclosure of information regarding children receiving title IV-E foster care and adoption assistance (section 471(a)(8)). Further, in accordance with 45 C.F.R. 1355.30(p)(3), records maintained under titles IV-B and IV-E are subject to the confidentiality provisions in 45 C.F.R. 205.50. Those provisions restrict the release or use of information to certain persons or agencies that require the information for specified purposes. The Child Abuse Prevention and Treatment Act (CAPTA) further requires that States preserve the confidentiality of all child abuse and neglect reports and records; however, it allows information to be shared in certain circumstances, for purposes related to child abuse and neglect intervention (section 106(b)(2)(A)(v)). The only exception to those restrictions is the CAPTA provision which requires that States allow for public disclosure in cases of child abuse or neglect that result in the death or near death of a child (section 106(b)(2)(A)(vi)). Authorized recipients of information under titles IV-B, IV-E and CAPTA are in turn subject to the same confidentiality standards as the child welfare or child protective services agency that released it.
While there are excellent reasons to guard clients' confidentiality, there are also important reasons for sharing information among programs that are working together to serve clients. These include the need to assure full assessment and understanding of client needs, progress and case goals among varied service providers; the need to assure that agencies do not work at cross purposes, accidentally making conflicting demands of clients or undermining each other's efforts; and the desire to make an efficient use of resources, avoiding a duplication of efforts.
When child welfare and substance abuse treatment agencies begin to work together, confidentiality issues arise quickly. One or the other agency will often claim that the information needed by the other "can't" be shared. Most often, it is the Federal substance abuse confidentiality rules which are said to prevent collaboration. Experts on both sides point out, however, that existing Federal confidentiality guidelines incorporate mechanisms for appropriate information sharing to take place - but agencies at the local level tend not to incorporate them into their daily activities. For instance, Qualified Service Organization Agreements (QSOAs) may be established between a substance abuse agency and other organizations that provide services to the program and its clients (HHS/SAMHSA, 1997c). The regulations specifically mention agencies that provide "services to prevent or treat child abuse and neglect" as being among those with whom QSOAs may be established in order to facilitate services to the client. Under a QSOA, information about clients may be disclosed between the two agencies without the individual consent of each client (although both agencies remain bound by rules about re-disclosing information outside the agreement). In addition, if child welfare agencies routinely requested written parental consent for the release of substance abuse treatment records early in the life of a case, many parents might readily consent. Since the child welfare agency remains bound by prohibitions against redisclosure (again, unless consent is provided), they should be able to receive critical information from the treatment provider about the parent's participation and progress. However, few child welfare and substance abuse agencies have entered into QSOAs. Nor does it seem that many child welfare agencies have procedures in place to routinely request consent from clients early in the case.
Agencies that want to cooperate have been able to establish working relationships within the rules to provide child welfare agencies with updates regarding clients' progress in treatment and to ensure that treatment agencies are partners in efforts to achieve child safety. During our consultation process we heard reports of excellent working relationships from a number of treatment agencies and child welfare agencies, which use each other's expertise to work as a team on behalf of the family. These relationships take time to build and maintain, however, while staff learn about each other, gain an understanding of each other's role, constraints, and bottom line imperatives, gain confidence and trust in one another, and put in place policies and procedures governing the sharing of information and preventing redisclosure of confidential information.
Dealing with Setbacks
As has been noted previously, most substance abuse treatment clients will suffer relapses, no matter how great their resolve to stop using alcohol and other drugs. Unfortunately, however, there are not reliable ways of predicting which clients will be successful. Relapse does not necessarily indicate treatment failure. It may instead be an indication that the treatment plan has not adequately addressed important issues, and in addition may present a therapeutic opportunity to teach the client that controlled use of substances is not possible. Given that most clients will relapse, the questions for service providers become (a) how to prevent relapses to the maximum extent; and (b) how to respond to relapses in order to minimize their duration and consequences for the individual, his or her family, and the community.
While the substance abuse treatment community views relapse as a part of the recovery process, relapse makes it extremely difficult for child welfare professionals to determine whether the client is making appropriate progress in treatment. Even if progress is recognized, it remains hard to determine accurately whether that progress is sufficient to assure children's safety. To a child welfare professional, relapse indicates that the client's behavior is likely to be unpredictable and that neglect of children's needs is a significant possibility.
Responses to setbacks may cause tension between service agencies. A brief relapse may be taken by child welfare officials as evidence of treatment failure, even if the parent makes efforts to assure adequate supervision of children during relapse, for instance by taking children to a relative. On the other hand, a substance abuse professional is likely to view a brief relapse during which child safety precautions are taken as a significant step forward for a severely addicted client who has not before achieved significant sobriety. Further, if the relapse is more than brief, child welfare staff are likely to conclude alternative permanency options for the child should be pursued. Yet foreclosing the possibility of regaining custody may further undermine the client's motivation for treatment.
It is important that steps be taken to keep clients engaged in the treatment process following a relapse. Child welfare time lines, as discussed above, do not allow for a "hands off" attitude in which treatment providers wait for clients to become "treatment ready." If clients cannot be made treatment ready quickly, child welfare agencies and courts must expeditiously make alternative permanency decisions for children. Child welfare and substance abuse treatment staff must become better at utilizing parental concern for children to engage and re-engage families in treatment.
While tensions on these issues are inevitable, there are a number of steps which might be taken by child welfare and substance abuse agencies to build common ground regarding appropriate relapse planning and response. These include articulating more clearly the demonstrable signs of treatment progress that child welfare agencies and courts can use to inform child welfare decisions; assuring that substance abuse treatment programs and child welfare agencies discuss with clients safety planning for children in the event of relapse; and establishing policies regarding under what circumstances the substance abuse treatment agency should notify the child welfare caseworker of a relapse (assuming a QSOA is in place, the client has provided consent for information exchange, or the situation warrants a formal child protective services report). Similarly, substance abuse treatment agencies are likely to be more willing to discuss clients' relapses if there is a consistent pattern of child welfare system response they can anticipate.
Striving Toward Improved Service Delivery — Together
There are real and significant barriers to productive collaborations between child welfare and substance abuse agencies. The differences in perspectives and traditional methods of functioning are real. But for agencies that truly want to work together to improve services to clients, these differences can and must be accommodated. Doing so will require sustained efforts by staff in agencies in communities throughout the nation — efforts to learn about one another, to understand one another, and to establish a shared set of expectations for each other and for clients.
Chapter 7. Service Delivery Models: Approaches to Addressing Joint Substance Abuse and Child Maltreatment Problems
Addressing the problems of substance abuse and child maltreatment requires intervention at a variety of levels. Among the clear lessons that have emerged in the decades of effort by dedicated service providers in both fields is that there are no easy answers and that what works for one family will not necessarily work for another. Flexibility and comprehensiveness are key, and, particularly when dealing with these multi-problem clients, collaborative working relationships across agencies are essential.
A variety of documents have been written about building interagency collaborative relationships, generally (e.g., Melaville et al, 1993; Mattessich & Monsey, 1992; Gardner, in press) and specifically to address substance abuse and child maltreatment in families (Young, Gardner and Dennis, 1998; Jones and Hutchins, 1993). Collaborative working relationships are important for several reasons: (1) they enable service providers to meet a broader range of family needs; (2) they allow agencies to better coordinate their efforts and ensure that they neither overwhelm families with requirements nor impose conflicting demands; and (3) they enable a more efficient use of limited resources and prevent inefficient parallel program development. Effective teamwork is difficult to achieve, however, and harder to sustain. But it is only by working together that our agencies are likely to make progress in serving these children and families well. No single agency can provide all the supports these families need, nor does any agency alone have the knowledge or authority upon which to make informed decisions about the strengths and needs of the family as a unit, parents and children.
The sections below describe interventions for families with substance abuse and child maltreatment issues across a spectrum of care, and, to the extent information is available, describe what is known about the effectiveness of interventions. Generally, however, information on the effectiveness of interventions to address child maltreatment is sparse. Few studies of child maltreatment interventions directly address the particular issue of substance abuse. Similarly, few evaluations of substance abuse interventions directly address child maltreatment. Nonetheless, below we describe what we know about:
- Valuing Prevention
- Strengthening Training and Identification Skills
- Enhancing Risk Assessment, Needs Assessment, and Referral Capacity
- Increasing the Availability, Access and Appropriateness of Substance Abuse Treatment
- Promoting Client Retention and the Effectiveness of Services
- Improving Time Lines and Decision Making for Children
- Supporting Ongoing Recovery
Valuing Prevention
An effective, comprehensive approach to addressing substance abuse among parents and its harmful effects on children must include a strong prevention component. The maltreated children we serve now are at high risk of becoming the next generation of adults with addiction problems and/or the next generation of abusive and neglectful parents whose family, legal, and health problems will have to be addressed. Of the population being served in SAMHSA's program of Comprehensive Mental Health Services for Children with Serious Emotional Disturbances, 60 percent of the children are from homes in which at least one parent has been identified as having a substance abuse problem. This strongly suggests the need for early intervention services for children of parents with substance abuse and related problems.
Research regarding substance abuse prevention has developed significantly in recent years, and has begun to demonstrate clear lessons for program developers (Office of Technology Assessment, 1994; HHS/NIDA, 1997). Among these lessons are that: (1) interventions need to be directed at clearly defined target populations, and (2) must address the specific risk and protective factors associated with substance abuse. Too often, broad based prevention programs fail to incorporate these and other lessons learned through research.
SAMHSA's Starting Early Starting Smart projects are leading efforts to produce new institutional approaches to collaboration in social services programs. These projects are designed to generate new empirical knowledge about the effectiveness of integrating substance abuse prevention, substance abuse treatment and mental health services for children aged zero to seven and their families. Grantees are integrating these behavioral health services into early child care settings such as day care facilities and Head Start Centers. Starting Early Starting Smart programs will create partnerships among community service providers in various fields to better meet the needs of young children.
Child abuse prevention research is much less well developed than research on substance abuse prevention. Few maltreatment prevention programs have been designed with a clear theoretical framework regarding risk and protective factors that ultimately lead to reduced abuse or neglect. Until the early 1990s, prevention models focused almost exclusively on parental behaviors such as excessive physical discipline. While some existing programs have been able to demonstrate some changes in parental knowledge and attitudes, they have not been shown conclusively to reduce abuse. In addition, relatively little is known about child neglect, which is the principal issue in cases where substance abuse is significant. As the National Research Council noted in 1993, "in designing preventive interventions, researchers have given very little attention to interactions among multiple variables in the determination of risk status for subsequent maltreatment" (National Research Council, 1993). A key challenge in research regarding prevention programs in both substance abuse and child protection has been the difficulty in measuring behavior that does not occur. While the crux of prevention lies in avoiding negative outcomes, decreases in what are relatively rare behaviors even among high risk groups is difficult, particularly when these behaviors are ones the subject is likely to hide.
Children of substance abusing parents generally, and children in foster care particularly, possess, almost by definition, many of the risk factors and few of the identified protective factors associated with a host of negative outcomes. For instance, children exposed to severe substance abuse in the home often experience mental, emotional, and developmental problems, as well as severe trauma, which may result from physical or sexual abuse or chronic neglect. These children are among the populations at highest risk of developing substance abuse disorders, including addictions. Despite their high risk, few efforts have been made to target children and youth in foster care specifically for substance abuse prevention activities. In most communities, substance abuse prevention is not viewed as a function of the child welfare agency, even for the children in their care. "They'll get that in school" is the typical reaction to the subject, although few school-based prevention programs are equipped to deal with the personal and family experiences with alcohol and drug abuse and child abuse or neglect that children in foster care bring to standard drug education programs.
Reducing the emotional trauma experienced by children in foster care or who are living in abusive or neglectful families and/or with substance abusing caretakers is a significant approach to preventing substance abuse among these children as they grow up. If substance use is in part a means of self medication to dull emotional pain and avoid trauma, it is only by providing other ways of addressing these needs that destructive behaviors, including future substance abuse, will be avoided. An argument growing in prominence is that providing therapeutic services for children in the context of a parent's substance abuse treatment program provides a significant opportunity to prevent future maladaptive behaviors in these children (Kumpfer, 1998; McMahon and Luthar, 1998).
Strengthening Training and Identification Skills
A key factor in assuring that both substance abuse and child protection issues are addressed is making sure that workers are trained to look for and identify both problems in families served. Yet neither child welfare nor substance abuse pre-service training typically includes information on the other field (Dore et al, 1995). A variety of studies have shown that training for child welfare staff includes inadequate information on substance abuse and case planning skills to use with these families (Gregoire 1994; Tracy 1994). Indeed, one study found that social workers failed to correctly identify and respond to clients' alcohol problems in 83 percent of cases (Kagel, 1987). The 1993 Study of Child Maltreatment in Alcohol Abusing families found that only 21 percent of caretakers of maltreated children received a substance abuse assessment by an alcohol or drug abuse professional (HHS/NCCAN, 1993). If we do not accurately identify these problems, we are unlikely to adequately assess or treat them. Routine screening and identification systems have the potential to improve services provision. For instance, recent HCFA demonstrations to improve medicaid-provided services to pregnant substance abusing women found that systematic screening and identification raised service enrollment rates (Howell et al, 1998). Too often, however, CPS staff do not ask about or follow up on potential substance abuse, and substance abuse treatment providers have a similar stance toward child maltreatment.
Several studies have been identified that address substance abuse training and identification issues for child welfare staff. It appears that less attention has been devoted to assisting substance abuse treatment staff to recognize child safety issues. Many treatment programs have policies about reporting suspected abuse and neglect, but aside from treatment programs specializing in treating women with children, usually little attention is paid to training staff on how to recognize abuse and neglect, the effects it has on children, or how to intervene beyond making a child protective services report. Many of the substance abuse treatment programs that provide residential treatment for women with their children or outpatient programs that have on-site services for children have paid more attention to these issues, but they are few and far between.
Training can improve the ability of workers to identify and intervene with families. For instance, Gregoire (1994) found that following a seven-hour training on substance abuse issues, child welfare workers showed an increased awareness of the connection between alcohol and other drug abuse and child maltreatment. In addition, workers' aversion to engaging clients with alcohol and drug problems decreased. As a recent Child Welfare League of America publication points out, "the prerequisite to a serious commitment on training is a recognition that the great majority of workers in the child welfare system and in the treatment agencies do not know enough about the 'other side' to work effectively across systems" (Young et al, 1998, p. 18).
Both the Administration for Children and Families (ACF) and the Substance Abuse and Mental Health Services Administration (SAMHSA) have recognized the need to improve training on these crossover issues. In 1994, the National Center on Child Abuse and Neglect (NCCAN) issued a widely-used manual on protecting children in substance abusing families (HHS/NCCAN, 1994), and will soon complete a substance abuse training curriculum developed as a result of several communities' activities under Federal demonstration grants during the early 1990s. SAMHSA's Center for Substance Abuse Treatment is also in the process of developing a manual for treatment programs on the implications of child abuse for substance abuse treatment programs. In our discussions with grantees working on both sides of this issue, we were told repeatedly that joint training is an important key to effective collaboration. Until local staff in both fields have opportunities to learn about the other's discipline and to interact constructively with respect to families' needs, they will find it difficult to meet expectations for positive outcomes. Appendix C describes existing Federal child welfare and substance abuse treatment services and research programs, and Chapter 8 will discuss additional steps toward addressing these issues.
One community that has taken seriously the importance of training on these and related issues is Sacramento County, California. Since 1993, the county's Department of Health and Human Services has developed an extensive, three-level training effort for its employees in order to provide child welfare workers and their partners in related agencies the knowledge and skills necessary to identify and intervene with substance abusing families. Topics in the basic level of training include, among others, the awareness that alcoholism and drug dependence are diseases; the effectiveness of different modalities of treatment for different clients; the relevance of client measures of functioning in addition to abstinence; and an awareness of the phases of recovery as measures of parents' readiness for child custody. Staff undergoing additional levels of training may be certified in administering the substance abuse screening instrument used in the county, and become skilled at making assessment-based referrals to the nine treatment options available in the county. Sacramento County has struggled to implement consistent processes to identify substance abuse problems in maltreating parents so that appropriate interventions may be provided. The county's efforts are described in more detail in the recent volume Responding to Alcohol and other Drug Problems in Child Welfare (Young, Gardner & Dennis, 1998).
In 1991, NCCAN funded 25 grants to develop and implement multi-disciplinary training programs on substance abuse and child maltreatment (HHS/NCCAN, 1995b). Evaluations of these efforts indicate that trainees:
- developed an increased awareness and understanding of substance abuse related child abuse and neglect;
- became more accurate in their identification of substance abuse and child abuse in families;
- improved their assessment skills;
- developed a better understanding of the services and resources that were available in their communities and appropriate for these families; and
- reduced frustration levels with other services providers as they gained a better understanding of their mandates and roles.
Process evaluations of these efforts also revealed a number of lessons. These grantees found that success required: that professionals from various disciplines be involved early in the development of training; that needs assessments were essential in assuring curricula addressed the needs of their target populations. In addition, evaluations indicated that outreach and recruitment of potential trainees is extremely difficult because professionals in these fields have to meet numerous time commitments and are likely to be skeptical about the quality and value of additional training. Successful projects involved both management and line staff in training and used a variety of training strategies emphasizing interactive methods.
Enhancing Risk Assessment, Needs Assessment, and Referral Capacity
Unless workers can appropriately identify risk to children, accurately assess client needs, refer clients to appropriate services in their communities, and evaluate clients' progress, treatment plans are likely to be based on inadequate, erroneous, or useless information. Yet many child protection risk assessments barely mention substance abuse (Dore et al, 1995). The Child Welfare League of America recently found that 18 of 47 child protection risk assessment protocols reviewed did not address parental drug abuse, 19 did not address parental alcohol abuse and 35 did not include items about a child's potential substance abuse (CWLA, 1998).
There is further evidence that even when the issue does appear on forms, workers may be uncomfortable asking about it. An NCCAN-funded study entitled Casework Decision-Making in CPS, based on the risk assessment model utilized in Washington State and interviews with workers there, found that substance abuse is one of the three risk factors most likely to be rated as "insufficient information to assess." One explanation offered by the study's principal investigator is that workers are often questioned in court as to their qualifications to make substance abuse assessments and because most are not certified assessors, they tend to rate that factor as "insufficient information to assess" unless they have clear evidence of such a problem. Washington State now requires workers to order a substance abuse evaluation in the absence of clear, sufficient information (English, 1998).
An important set of innovations regarding assessment and referral of maltreating parents to substance abuse services is occurring in the State of Delaware under a Federal demonstration project. Under normal circumstances, Federal foster care funding under title IV-E of the Social Security Act may be used only for foster care maintenance payments on behalf of eligible children in foster care as well as for expenses related to the administration of foster care. Delaware requested and has received a demonstration waiver allowing the State to use some of these funds for a system of substance abuse assessment and referral. This system provides for staff from the substance abuse agency to be located in child welfare offices to do substance abuse assessments and to identify appropriate substance abuse treatment resources for those parents who need them. While the project has not yet been operating long enough for thorough evaluation, initial results show that the demonstration is improving the engagement of clients in substance abuse treatment services. Indications so far are that foster care costs for families participating in the demonstration will be significantly reduced in comparison to the control group (Lockwood, 1998). The State of New Hampshire will begin a similar demonstration soon, to further test the efficacy of using substance abuse assessment and referral staff in a child welfare agency.
Outstationing substance abuse staff to child welfare agencies is also occurring in other communities using more standard financing mechanisms, most often using State or Federal substance abuse treatment funds. Such co-location allows more timely and accurate substance abuse assessments than might otherwise be available to a child welfare agency. Another alternative is for a child welfare agency to arrange with local substance abuse services providers to set aside several assessment appointments per week (based on the child welfare agency's typical need) that are designated as the slots for parents whose children have just been placed in foster care or on whom child abuse or neglect complaints have just been substantiated. In this way, long waiting lists for assessments can be avoided for these parents in crisis, and the child welfare agency can quickly determine what substance abuse services should be included in a family's service plan.
Key to making appropriate service referrals is knowing the treatment providers in the local community and the services they offer. Social service agencies are now a relatively minor source of referrals to alcohol and other drug treatment facilities. One recent study revealed that in 1996, 7.2 percent of referrals to alcohol and drug programs were from welfare and social service agencies, including child welfare (Horgan & Levine, in press). As ongoing working relationships are established, it is essential that substance abuse treatment providers understand what the child welfare agency is expecting treatment to accomplish, and that, in turn, the child welfare agency understands what substance abuse treatment can provide. To the extent that these expectations are not entirely compatible initially, ongoing discussions may be needed.
As child welfare agencies become more active sources of substance abuse treatment referrals, a number of administrative procedures may be necessary to facilitate the ongoing exchange of information about joint clients. For instance, establishing processes to get consent from the client at the time of referral for the sharing of treatment information between the child welfare and substance abuse agency can avoid considerable frustration and delays later on when the child welfare agency wants information regarding the results of an evaluation or the client's progress in treatment. In most cases child welfare clients are willing to sign release of information forms because they are eager to cooperate in order to retain or regain custody of children. Establishing Qualified Service Organization Agreements (QSOAs) between service providers is another way of assuring that information can be shared on behalf of clients within the scope of Federal drug treatment confidentiality guidelines. As discussed in chapter 6, under a QSOA, in certain circumstances client-specific information may be shared between the substance abuse treatment agency and another agency providing services to the program and its clients without the consent of individual clients.
In many communities, substance abuse treatment providers routinely provide biweekly or monthly progress reports on clients to their referral sources. Child welfare agencies may wish to work out such arrangements with their treatment agency partners to assure that they have timely and up-to-date information upon which to base case decisions. Agreeing ahead of time on formats and content for such updates may also help assure the usefulness of information exchanged.
Increasing the Availability, Access, and Appropriateness of Substance Abuse Treatment for Families
Child welfare agencies consistently report difficulty obtaining substance abuse treatment for clients who need it, particularly programs that are designed to meet the specific needs of women with children. The Child Welfare League of America reports that agencies can obtain timely treatment for only one-third of clients who need it, and only 10 percent of agencies report being able to find treatment within a month for most who need it. Also disturbing is the fact that many agencies report being unaware of whether treatment is available in their communities (CWLA, 1998). Until clients have access to treatment services it is unrealistic to expect significant improvement in problems surrounding their substance abuse.
Often a family crisis, such as a child protective services intervention, is the catalyst needed to prompt a substance abusing parent to seek treatment. The resolve of an addicted person is often short lived, however, and unless treatment is available promptly the opportunity for intervention may be lost. This is another issue on which different views of a problem may create misunderstanding between substance abuse and child welfare agencies. If, for instance, half of a child welfare agency's referred clients cannot locate treatment or are placed on long waiting lists which fail to result in services, the child welfare agency may very well consider those clients as treatment failures. The substance abuse agency, however, is likely to argue that they should not be held responsible for the "failure" of a client who has never entered their program or received a service. In addition, some treatment programs are reluctant to accept clients who may not be entering treatment voluntarily. Regardless, the reality is that the substance abuse has not been addressed and the client's problems continue.
Nationally there is a shortage in all varieties of publicly funded substance abuse treatment opportunities for those in need. As noted in Chapter 4, only 37 percent of mothers with problem levels of drug use who are living with children under age 18 and 48 percent of such fathers received treatment services in the past year (SAMHSA, 1997d). In addition, substance abuse patterns vary greatly regionally and locally. This fact, coupled with the significant gap between available treatment capacity and current demand, often impedes the ability of the existing treatment system to respond quickly to changing needs. Within States, the needs of a variety of treatment-seeking populations must be balanced. Competing demands for services for criminal justice clients, HIV+ clients, and others under conditions of service scarcity often result in unpredictable and inconsistent funding for treatment programs and force treatment providers to constantly pursue new funding streams rather than concentrate on the provision of quality services.
In addition to the general problem of treatment availability, programs addressing parents' needs are in particular shortage. The fact that parents, and in particular, mothers, have specific needs in treatment that most programs do not address has been widely observed (HHS/CSAT, 1994; Magura, 1998; Grella, 1997). These needs may include child care, services to address parenting stress, economic and educational issues, reproductive health care services, psychological services, domestic violence services and more. These services are generally not as applicable to male substance abuse treatment clients, but are essential for effective women's services.
Many comprehensive substance abuse treatment programs for women are the result of Federal grant initiatives from either the Substance Abuse and Mental Health Services Administration or the Administration for Children and Families, and most have very small client loads (Allen & Larson, 1998). As demonstration projects and new Federal funds have become less available, it is unclear the extent to which these programs will survive with other funding sources. Few States have extensive networks of substance abuse treatment programs geared toward women and children, and child welfare agencies spend little money to acquire substance abuse treatment for families. The Child Welfare League of America's recent survey found that nearly half of States report spending no child welfare money at all on substance abuse treatment; the most active State spent 2 percent of its child welfare funds for this purpose (Child Welfare League of America, 1998). When States were asked to identify the funding sources used for treatment for child welfare clients, State alcohol and drug agencies were such a minor funding source that they ended up in a category entitled "other," combined with a variety of funding sources that did not merit their own categories.
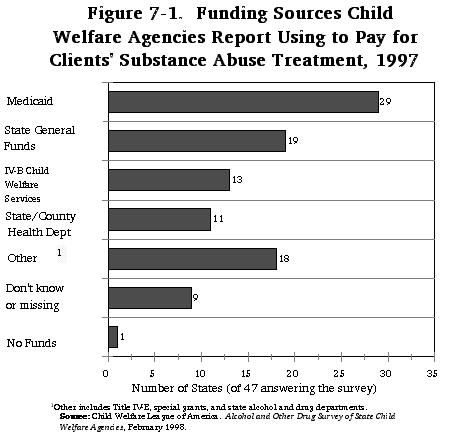
As Figure 7-1 illustrates, Medicaid is the funding source most often used by child welfare agencies to obtain treatment for clients. Indeed, a majority of States cover substance abuse services through mandatory and optional Medicaid service benefits. Medicaid coverage for substance abuse treatment is described at more length in Appendix A. States are increasingly submitting State plan amendments to cover substance abuse services, both for children and adults, primarily using the optional rehabilitation benefit, because of its flexibility.
During our consultation process, a number of experts pointed out that a significant limitation in Medicaid's coverage of substance abuse treatment services is the prohibition on payments to certain facilities classified as institutions for mental diseases (IMDs). As currently defined, an IMD is any facility of more than 16 beds that specializes in psychiatric care. This includes most residential substance abuse treatment programs. Thus, for clients aged 22 - 64 whose payment source is Medicaid, the IMD exclusion significantly limits access to the more intensive models of substance abuse treatment, which are often indicated for the most severely addicted clients.
The IMD exclusion, which dates back to the 1950s, applies to Alcohol, Drug Abuse, and Mental Health (ADM) inpatient facilities. Since the general trend in the total system has been to outpatient or partial care since 1972, the IMD policy now limits Medicaid payment for a smaller proportion of total ADM services today than it did in years past. The IMD statutory definition that exempts facilities of under 17 beds should further reduce this proportion. The two types of inpatient facilities most clearly meeting the IMD criteria are State and county mental hospitals, and private psychiatric hospitals.
Despite the IMD exclusion, a number of States and localities have found ways, within the existing rules, to make residential-like substance abuse treatment services eligible for Medicaid reimbursement. Exhibit 7-A describes a number of these methods which may be used to expand treatment access.
Exhibit 7-A:
State Methods Used to Ease the Effect of the Institutions for Mental Diseases (IMD) Exclusion
Many States looked to the following methods as a way to address treatment access and lessen the effect of the IMD exclusion in order to provide substance abuse services to their Medicaid population.
Size Limits. Psychiatric hospitals and psychiatric nursing facilities that have fewer than 17 beds are not IMD's and are not subject to the exclusion. Patients in facilities, such as many substance abuse treatment facilities, continue to be Medicaid funded for covered services if the facility has fewer than 17 beds. Larger facilities are being legally divided into a number of smaller facilities with fewer than 17 beds each.
Mergers. Psychiatric hospitals are merging with general hospitals that are somewhat larger so that the resulting entity is not an IMD, but a general hospital with a large psychiatric "wing." This type of merger can be accomplished largely via legal paperwork and seems to be an increasingly popular way to negate IMD status. If a psychiatric hospital is larger than the general hospital, a portion of the psychiatric hospital that is smaller than the general hospital merges with the general hospital — or just uses a general hospital for all psychiatric care.
During the 1990s, five States (MD, MA, NY, SC and WA) expanded services for pregnant substance abusing women using Medicaid waivers initiated as demonstration projects. The demonstrations varied widely, but included the following components:
- Outreach to pregnant substance abusers;
- Screening for substance abuse and assessment of the severity of substance abuse;
- Case management to link women with appropriate services, including prenatal care and substance abuse treatment;
- Expanded Medicaid coverage for substance abuse treatment and an enriched package of support services provided during treatment; and
- Efforts to better integrate the prenatal care and substance abuse treatment system.
Most States chose to modify and enhance existing substance abuse treatment programs; none developed entirely new programs. Howell and colleagues (1988) have described the projects in detail. Each site had significant difficulty engaging clients in program services. The experiences of these projects may be a source of insight for others considering service expansions. The significant differences in program designs across States made the detection of cross-site results difficult.
Some States have begun to address treatment access issues by building networks of treatment programs, sometimes with services specifically designed for women and parents. In Missouri, for instance, the State has invested in a series of programs called the Comprehensive Substance Abuse Treatment and Rehabilitation program (CSTAR). CSTAR is a flexible model emphasizing community-based service provision in an intensive outpatient model, beginning with programming seven days per week, ten hours per day that tapers off as recovery is established. Case management, family therapy and co-dependency counseling are among the components included in addition to more traditional substance abuse counseling. Child care and supported housing are also available. Using this model the State treats approximately 2,000 women and over 6,000 children annually and has achieved good recovery rates and satisfaction ratings from clients (Jordon, 1997).
Eight States have also begun using some of their funding under the Promoting Safe and Stable Families Program (formerly the Family Preservation and Support Program), authorized under title IV-B, subpart 2 of the Social Security Act, to pay for substance abuse assessment and treatment services for some clients. While substance abuse services are among the relatively minor uses of these funds (in contrast, thirty States support parent skills training, 23 States support respite care and 17 support recreation programs using these funds), such services are a growing category of State spending under this program (Kaye and Ensign, 1998). These funds are a flexible source of funds States use to serve families, primarily those at risk of child abuse or neglect.
Another opportunity for States to expand treatment access is through Child Welfare Demonstration Waivers. These demonstrations are intended to allow States the flexibility to try alternative means of addressing the child welfare needs of families through use of existing foster care and related funding streams for activities that are not usually allowable under titles IV-E and IV-B of the Social Security Act. The announcement to States soliciting applications for the Fiscal Year 1998 and Fiscal Year 1999 application cycles have included a Federal priority for addressing the substance abuse treatment needs of families in the child welfare system. Among the initial ten States receiving Child Welfare Demonstration Waivers, only one (Delaware, described above in the section on assessment and referral) identified itself as intending to address the problem of substance abuse and its relationship to child maltreatment. Among the Fiscal Year 1998 demonstrations, one addresses substance abuse as its main focus (New Hampshire) and one more includes it as a sub-focus (Kansas). The remainder address it only indirectly. States may wish to look toward the use of this demonstration waiver mechanism in the future as they seek innovative ways of addressing substance abuse in families where child maltreatment occurs. The Department of Health and Human Services has the statutory authority to grant additional waiver demonstrations, up to ten per fiscal year. Demonstrations may last up to five years (although under some circumstances they may be extended), must be cost-neutral to Federal child welfare programs over five years (that is, they must cost no more to these programs than would be spent under current law, although funds may be spent in alternative ways), and must have strong evaluations.
Promoting Client Retention and the Effectiveness of Services
Closely related to access and appropriateness of treatment are retention and effectiveness. Substance abuse treatment has been found to be effective for many people in both the short and long terms as well as cost effective for taxpayers and society. Outcomes for substance abuse treatment are closely linked to clients' length of stay and treatment completion. Typically, the longer the client is in treatment, the better the outcomes. Generally, few positive long term outcomes are seen unless the client is in treatment for at least three months (Hubbard et al, 1989). Treatment may still be cost effective for shorter treatment episodes and for persons who do not maintain long term abstinence, (because of reduced crime, health care and other such costs while the person is in treatment and afterwards) but it is less likely that short stays produce long-term behavior change.
Effectiveness studies of substance abuse treatment programs consistently find positive outcomes, including reduced alcohol and other drug use, reduced criminal activity, improved health outcomes and improved employment and earnings. For instance, the National Treatment Improvement Evaluation Study (NTIES), an examination of 4,400 clients who received treatment services in 1993-94 in programs funded at least in part by SAMHSA's Center for Substance Abuse Treatment, found that one-year post-treatment abstinence rates for 495 women seeking to regain or retain custody of children were highest for cocaine users (70-71 percent for powdered cocaine users and 52-62 percent for crack cocaine users) and were lowest for those who sought treatment primarily for alcohol problems (only 26-37 percent of these clients remained abstinent throughout the year after treatment). Figure 7-2 shows one-year abstinence rates by treatment modality for female clients seeking to regain custody of children.
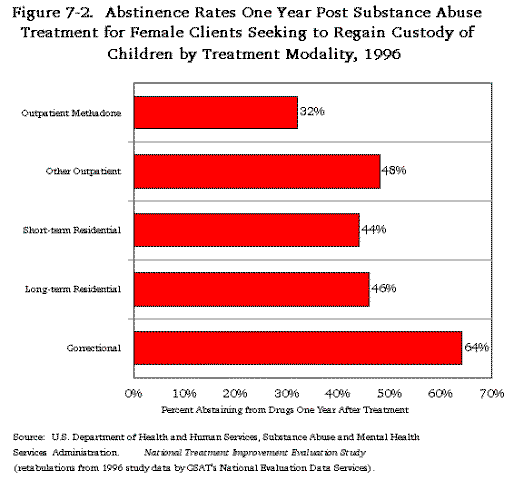
Figure 7-3 shows this data by primary drug of abuse.
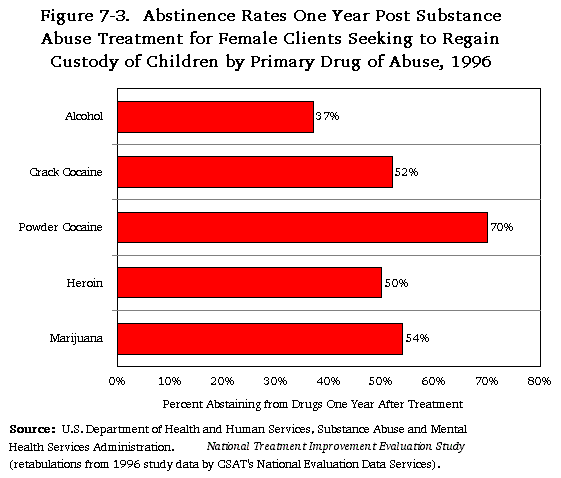
Further, in addition to outcomes related to abstinence, women in these treatment programs showed improvements in other dimensions. These included reduced crime and violence, increases in employment, and reduced mental health concerns. For instance, among women seeking to regain child custody, the prevalence of prostitution declined from 54 percent in the year before substance abuse treatment to 17 percent in the year after treatment. The study found that in this population, outcomes for outpatient treatment programs were generally similar to those for residential programs (Burgdorf, 1998).
Family and child custody outcomes appear to have improved for some NTIES clients following treatment, as shown in Table 7-A, although the relationship between treatment outcome and child custody outcomes was not strong. Of female clients seeking to regain custody of children and remaining abstinent in the year post-treatment, 39 percent were living with more children after treatment than at admission. Of female clients seeking to regain custody but who had negative outcomes, 26 percent were living with more children post-treatment. Overall, 32 percent of the female clients who sought to regain custody of their children reported living with more children after treatment than before. It seems likely that many of these were living with additional children because of successful reunification efforts (Burgdorf, 1998).
| CLIENT MOTIVATION FOR SUBSTANCE ABUSE TREATMENT, GENDER, AND TREATMENT OUTCOME | NUMBER OF CLIENTS |
POST-TREATMENT CHANGE IN NUMBER OF CHILDREN (row percent) |
||
|---|---|---|---|---|
| FEWER | SAME | MORE | ||
| Clients seeking to regain custody Women: Positive outcome (abstinent) Negative outcome (not abstinent) Men: Positive outcome (abstinent) Negative outcome (not abstinent) |
185 210 162 213 |
12 15 12 17 |
49 59 67 66 |
39 26 20 16 |
| Clients seeking to retain custody Women: Positive outcome (abstinent) Negative outcome (not abstinent) Men: Positive outcome (abstinent) Negative outcome (not abstinent) |
44 56 39 39 |
20 29 54 44 |
70 48 41 51 |
9 23 5 5 |
| Source: U.S. Department of Health and Human Services, Substance Abuse and Mental Health Services Administration. National Treatment Improvement Evaluation Study, (re-tabulations of 1996 study data by CSAT's National Evaluation Data Services). | ||||
NTIES clients who were motivated to enter substance abuse treatment by a desire to maintain custody of their children were more successful. Of these clients, 51 percent of the male clients and 75 percent of the women reported no reduction, post-substance abuse treatment, in the number of children they were raising. For male clients seeking to retain or regain custody there was essentially no relationship between treatment outcome and whether or not a client was living with their children.
Child welfare outcomes are rarely measured by substance abuse treatment programs, but early results from SAMHSA grantees operating substance abuse treatment programs targeting women with children report that 75 percent of their clients who successfully completed treatment remained drug free; 46 percent obtained employment following treatment; and 65 percent of clients' children in foster care were reunited with their families (HHS/SAMHSA, 1995).
Recently released findings from the Services Research Outcome Study (SROS), a five-year follow up of over 1,800 substance abuse treatment clients discharged from treatment in 1989-1990, show that substance abuse declined substantially in the five years after treatment (Figure 7-4).
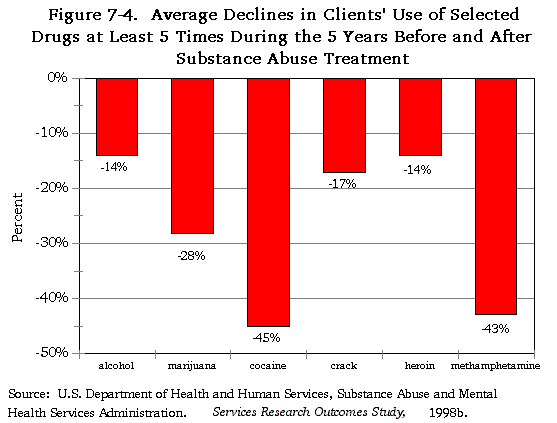
A minority of clients were abstinent, or nearly so, for a full five years after treatment. Women consistently had greater declines in drug use than did men (Figure 7-5).
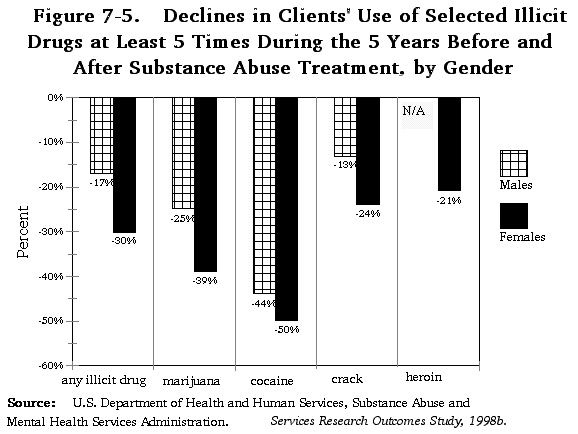
The number of clients who reported having lost custody of children declined by 30 percent five years after treatment as compared with the five years before treatment (HHS/SAMHSA, 1998b), indicating that many had been reunited with absent children during this period.
A variety of individual evaluations of women's treatment programs have also found positive outcomes. A study of PAR Village, a residential substance abuse treatment program for women and children in Florida, found positive outcomes such as reduced alcohol and drug use and reduced criminal behavior. Success rates of over 80 percent were reported for those who completed treatment (Hughes, 1994). A therapeutic community program in Arizona reports that 77 percent of treatment completers had at least one of their children living with them 6 to 12 months post treatment, as compared with 52 percent of treatment dropouts (Stevens and Arbiter, 1995).
While many treatment clients show improvements in a variety of areas, abstinence and other positive outcomes are not universal by any means, and improved outcomes are needed in several areas. In particular, substance abuse treatment programs are known for high drop out rates that typically run upwards of 50 percent and may approach 80 percent in some instances. A recent report from the U.S. General Accounting Office (USGAO, 1998) found that of substance abusing parents whose children have been in foster care at least one year in Illinois and California, most had either never entered substance abuse treatment (42 percent in Illinois and 40 percent in California) or had dropped out of treatment (34 percent in Illinois and 40 percent in California). Fewer than 20 percent in each State had completed treatment or were currently enrolled in a treatment program (Figure 7-6).
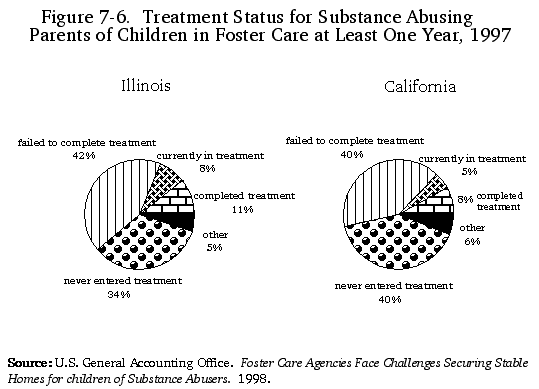
Along similar lines, Wobie and colleagues (1997) report a 38 percent completion rate for women entering a residential treatment program for mothers with infants. Connecticut's Project SAFE reports that only 30 percent of clients assessed as needing treatment and referred to treatment programs actually enroll (Sheehan and Libby, 1998). Zlotnick (1996) reports dropout rates ranging from 52 percent to 78 percent. And Stranz and Welch (1995) report that 45 percent of their sample of mostly CPS-referred clients completed an intensive day treatment program for women with children - not ideal, but more than double the 21 percent completion rate for participants in a traditional outpatient program that served as their comparison group. Famularo and colleagues (1989) found that 80 percent of parents failed to comply with substance abuse treatment ordered by courts in order to retain or regain child custody, and fewer than 10 percent of parents attended at least two-thirds of treatment sessions. Clients addicted to alcohol and illicit drugs were equally non-compliant. When looking at substance abuse treatment outcome studies it is important to understand the base group for whom outcomes are being reported. Often outcomes are reported only for those who complete the full course of treatment. Alternatively, data may be reported for all clients referred to treatment, even those who may have participated for as short a time as one day.
In large part because of such high drop out rates, the effectiveness of treatment is often challenged, particularly in the child welfare community. In what are reasonably typical responses, an Ohio study found that substance abuse treatment was judged "not very effective" by more than half (53 percent) of child welfare caseworkers. An additional 21 percent rated it as "somewhat effective," 14 percent said it was "adequate" and 12 percent thought treatment was "very effective" (The Public Child Services Association of Ohio, 1995).
Research suggests that providing child development, health care and other services to children of drug abusers promotes improved treatment outcomes for parents, including longer treatment stays (Stevens et al, 1989) and reduced frequency of relapse (Kumpfer, 1998). The provision of child care has similarly been shown to improve treatment retention (Beckman and Amaro, 1986) and its lack has been shown to be a treatment barrier (Brown, 1992). Studies of parent-oriented treatment programs also find improvements in family functioning. Olsen (1995) found that a majority of mothers participating in a comprehensive, multi-agency collaborative treatment program made steady progress on goals related to substance abuse. Families also showed improvements in housing, mental health, knowledge of child development and other related issues. Magura and colleagues (1998), looking at intensive family treatment programs in New York City, found positive outcomes on many indicators, although not on foster care reunification rates. Liddle and Dakof (1995) review the literature on the use of family therapy in drug treatment and conclude that several models of family intervention show promise as a means to engage and retain clients in treatment, reduce drug use and improve family functioning. Research has also shown that parenting programs can improve parenting knowledge, attitudes, and practice of women with substance abuse problems (Camp and Finkelstein, 1997; Black et al, 1994).
Evaluations of programs funded in the early 1990s by the National Center on Child Abuse and Neglect to provide services to substance abusing families with child maltreatment issues documented a number of positive outcomes. For instance, a number of projects were successful in getting parents to enter and remain in substance abuse treatment. Some grantees achieved higher rates of treatment completion and longer periods of abstinence than had previously been attained. Also reported were more effective discipline techniques among parents; better understanding of and response to meeting children's needs; more nurturing behaviors toward the children and less use of corporal punishment; and improved communications between parents and children. Projects noted that while there were families who showed little or no progress, there were also many families who became committed to recovery and healthy parenting. For these clients, programs became a lifeline and parents often became strongly attached both to project staff and to other clients who became a social support network to replace the unhealthy networks developed while immersed in the drug culture (HHS/NCCAN, 1995a).
In Illinois, Project SAFE and its successor, the Illinois Treatment Expansion Initiative, have for a number of years, worked hard to engage child welfare clients in substance abuse treatment services (USGAO, 1998). Project staff have found that intensive, persistent outreach services are essential to engaging this client population in treatment. Their efforts seem to have paid off. Outcomes for initial clients included 81 percent treatment completion rates, with 51 percent of clients judged as having good or excellent prognosis. More than half of clients' children in foster care (54 percent) had been reunified with their parents (White, 1995). Others have also found that effective outreach is essential with this population (HHS/NCCAN, 1995b).
The experience of substance abuse treatment programs, particularly those geared towards parents and their children, demonstrates that many clients can and do improve their lives and many are able to resume their parenting roles. Service providers have discovered repeatedly, however, that these clients are extremely difficult to engage and to retain in treatment programs. However, programs geared specifically to the needs of women and their children and with highly trained outreach and treatment staff are more likely to get and keep women in treatment. We must do a significantly better job in this regard if treatment progress is to be made within the time frames mandated by the Adoption and Safe Families Act. Improving access to family services, psychological treatment, and other wrap-around services that have declined in recent years (Etheridge et al, 1995) may improve retention rates. Closer collaboration with child welfare agencies may also be helpful in this regard.
Improving Time Lines and Decision Making for Children
Among the key issues in improving child welfare services is ensuring that permanency decisions are made in keeping with a child's developmental time line. Children should not have to wait indefinitely for a permanent home, be that with their biological parents or in an alternate home with adoptive parents or relatives. The pace of casework, court procedures, and appeals has often meant, however, that children are left in limbo far too long. By the time many of them find permanent homes, they have spent much of their childhoods and developmental years in temporary living situations.
Among the goals of the Adoption and Safe Families Act is to speed decision making regarding permanent homes for children and avoid such delays. Rather than only making administrative machinery work faster, many communities are trying also to work smarter. Innovations being tried include using the leverage of child protective services involvement to require treatment participation, adapting criminal drug court models to the family court, and concurrent planning. Concurrent permanency planning is an alternative to the traditional sequential case planning process, in which, at the same time services are being provided to achieve family reunification, alternative permanency options for the child are also being explored in the event that the child cannot be safely returned to the biological parent(s). The goal is to expedite the permanency process for those children who may linger in foster care.
Common to the variety of innovations being developed in communities to improve outcomes for children in foster care are that:
- efforts to resolve the issues which led to maltreatment must begin immediately;
- clients should receive up-front, clear disclosure regarding the consequences of a lack of participation or progress;
- appropriate intervention plans are developed with the family's involvement and are closely monitored; and
- lack of progress or non-compliance is dealt with swiftly.
Whether initiated from the child welfare agency or the court, the notion of mandating treatment and closely monitoring compliance and outcomes is a relatively new concept in child welfare. Social services generally, and reunification services specifically, have traditionally been offered on a voluntary basis. As noted above, however, purely voluntary models have not resulted in high completion rates. In response, particularly in light of data showing that treatment completion is higher among clients whose participation is mandated by the criminal justice system (Collins et al, 1983; Haller et al, 1993), some child welfare agencies began asking their family court judges to mandate treatment for some clients.
Pressure from a child welfare agency can be helpful for treatment retention. Carten (1996) reports that interviews with women who successfully completed a substance abuse treatment program in New York City often said that "although they initially experienced their CPS referral as intrusive and unfair ... the ever-present threat that their children would be placed in foster care provided the external pressure to continue in drug treatment." Similar information is reported from a Rhode Island program (Caldwell, 1998) that found most of its clients entered treatment primarily because of child welfare mandates and indicate that most clients would not have stayed in treatment without them. Indeed, this program reports that most of those who dropped out did so shortly after such a treatment mandate ended. A downside of mandatory treatment efforts, and particularly programs that seem to punitively jail women for refusing treatment, is that potential clients are more likely to hide from service systems, possibly placing children at greater risk.
In 1992, the National Council of Juvenile and Family Court Judges issued its Protocol for Making Reasonable Efforts to Preserve Families in Drug-Related Dependency Cases. The protocol suggests factors judges should consider in making custody and permanency decisions regarding child protection cases involving substance abuse, suggests services that should be made available to families as part of "reasonable efforts," and discusses opportunities for judicial leadership. Juvenile and family courts can provide initiative in mobilizing resources for families coming before them and monitoring agencies' activities and families' progress to assure the best possible outcomes for children.
Building upon the notion of treatment mandates is the swiftly growing innovation of drug courts. Now common in the criminal court system, the use of treatment mandates with intensive follow-up procedures and strict sanctions for noncompliance is now being tried in several family court settings around the nation. When used in criminal cases, drug courts have been found consistently to achieve much better treatment retention rates; substantially reduced drug use and criminal behavior during the participation periods; and, to a lesser but still significant extent, reduced criminal behavior following program participation (Belenko, 1998). Drug courts are designed to improve the court's handling of cases involving substance abuse by providing:
- immediate intervention and continuous supervision of the family's progress;
- development of a treatment and rehabilitation program, usually administered by the court or its designee;
- judicial oversight and coordination of treatment and rehabilitation services to provide accountability and reduce duplication of effort;
- immediate judicial response to family needs and to episodes of noncompliance; and
- judicial leadership in bringing together community agencies to achieve the drug court's goals.
Family drug courts were operational in only six jurisdictions nationally as of January 1998, but are expected to proliferate quickly. Extensive information regarding these programs is available in a recent Department of Justice publication, Juvenile and Family Drug Courts: A Profile of Program Characteristics and Implementation Issues (Office of Justice Programs Drug Court Clearinghouse and Technical Assistance Project at American University, 1998), and several family drug court programs are profiled in a recent publication of the National Center on Addiction and Substance Abuse at Columbia University (1999).
Concurrent Planning is a casework approach that has recently become popular as a tool to improve the timely achievement of permanency for children. Traditionally, case workers have been taught to work diligently toward the singular goal of family reunification. Only after a year or more of unsuccessful efforts could other permanency options (such as adoption) be considered. Adoption planning from scratch could then take additional years, further prolonging uncertainty for the child. Concurrent planning instead emphasizes working toward reunification while at the same time establishing one or more "back up" permanency plans to be implemented if reunification proves unlikely. By considering a variety of permanency alternatives from the start and by engaging parents and other family members more effectively in early discussions of children's needs and permanency options, children's lives can be stabilized more quickly, in keeping with children's developmental time frames.
Concurrent planning provides the opportunity and the challenge for caseworkers and families to realistically face the problem(s) which prompted the child's removal, collaborate in planning interventions and following through on treatment, within the much more stringent time lines detailed in ASFA. Agencies and families must honestly acknowledge the external constraints of the new time lines, which imply a new type of accountability.
Supporting Recovery
One of the frustrations frequently expressed by professionals working with families with substance abuse and child maltreatment problems is that significant setbacks often occur after long strides have been made, particularly in the weeks immediately following discharge. During our consultation process, we heard from a number of sources comments such as, "we can get these clients clean and sober. It's the longer term, after we step back, that's the problem." Families often lack the ongoing support structures, formal and informal, that make sustained recovery possible. Especially important in ongoing recovery efforts are that the client learns the skills to create drug-free leisure time effectively after treatment and socialize without intoxicants.
Recovery is a lifelong process, but the substance abuse treatment field has come to view chronic relapse as a preventable part of the recovery process (HHS/SAMHSA, 1996a). There are predictable causes of relapse during each stage of recovery. For instance, during early recovery (described in Chapter 2 and which encompasses the first year to two years of sobriety), it is the lack of effective social and recovery skills needed to build a sobriety-based lifestyle that is the major cause of relapse. By understanding these issues and teaching clients the skills they need to successfully overcome them, substance abuse treatment programs can reduce relapse rates. Child welfare agencies can also assist in this process by recognizing how their actions regarding custody, visitation and other family issues affect the recovery process. Without needed support, even positive actions like the return of custody can undermine recovery.
Most of our interventions with families are designed to be short term. Indeed, the main Federal child welfare program directed at these problems was for years called the Emergency Services Program, calling forth images of short term interventions which grantees subsequently found completely inadequate to address the complex family situations confronting them. One of the most common themes in grantees' progress reports and process evaluation results was that intervention periods needed to be much longer than grantees anticipated (HHS/NCCAN, 1995b). Grantees of ACF's Abandoned Infants Assistance program, intended to prevent the abandonment of drug-exposed and/or HIV+ infants, as well as SAMHSA grantees serving these clients, had similar experiences, often extending their intervention periods beyond their initial expectations.
Continuing care for this population is critical. Without it, relapse rates are high, even after long periods of sobriety while in treatment. It is at this point in treatment that the need for safe, affordable and sober housing is especially critical. Also, because issues related to substance abuse, such as a client's possible history of sexual abuse or incest, may go beyond the scope of substance abuse treatment, ongoing efforts to address such issues may need to continue long after leaving formal substance abuse treatment. For recovery to be successful, treatment counselors must help the client identify stressful areas in her life and learn to locate and use resources to deal with the stress.
Some have suggested that we may need to rethink the short term way in which we conceptualize child welfare interventions and instead provide longer term interventions for at least some families. The current movement toward two-track child protective services systems with many families receiving non-coercive, community-based support may be an opportunity to provide such longer-term services. Post placement support services, provided after a child returns home in order to assure the success of reunification, can also play this role. Such services may also be developed and implemented using the Promoting Safe and Stable Families Program (formerly the Family Preservation and Family Support Program) administered by the Children's Bureau. However they are provided, services of this sort can help assure child safety and family stability on a more ongoing basis and prevent the need either for initial foster care placements or for the re-entry of children into foster care following reunification.
Building a Stronger Continuum of Interventions
Specialized services for female substance abusers, particularly those who are parents, is a relatively new concept in substance abuse treatment, one which has developed considerably over the past decade. During that time as well, the child welfare field has come to recognize that substance abuse is among the most pressing problems facing families who neglect or abuse their children. While these fields have a long way to go in improving how they work together to serve their mutual clients, we have learned a great deal about what it takes to produce positive outcomes for these parents and children. Improved efforts across a wide spectrum of activities from prevention through aftercare are needed in States and communities across our nation. While we do not believe that any of us yet has put in place an entirely satisfactory network of interventions, the examples and research results described above demonstrate that we have solid indications of how outcomes can be improved at each stage of intervention. Strengthened partnerships between child welfare and substance abuse professionals are key to many of these innovations.
Chapter 8. Where Do We Go From Here? Directions and Next Steps for Federal, State, and Local Efforts
By listening to partners, reviewing what has been learned through decades of research in both the child welfare and alcohol and drug fields, and conducting additional focused analyses of the data collected by HHS, the agencies involved in producing this report have begun to understand the complex interactions among substance abuse, child maltreatment, and other problems within families, and among the service providers and policy makers in these and related fields who struggle to make a difference in the lives of children and families. Available information indicates that while the nation is a long way from having in place an effective, smoothly functioning service network to address these issues, there are clear indications of how services must be refocused in order to generate better outcomes: safety, stability and improved developmental outcomes for children; healthier, sober, and more productive parents; and better-functioning families.
Nationally and in many States and communities, mutual lack of knowledge, understanding, and trust creates barriers that hinder effective collaboration between child welfare and substance abuse treatment agencies and professionals, as well as with other services systems and judges and court personnel. These barriers ultimately prevent effective service delivery to families with substance abuse and related problems, further placing their children at risk, or preventing their healing. The most critical problem is the scarcity in many communities of available, appropriate services designed to address the multiple problems these clients face. The preceding chapters have detailed the parameters of the problem and have explored isolated promising efforts in communities across the nation. This chapter suggests steps that might be taken to improve the situation more broadly. It is important to note that there is not currently a consensus in the field as to how to solve these problems effectively. Yet finding common ground is imperative if these fields are to "do right" by the families who are clients of both systems. To the extent that the differences between the child welfare and substance abuse treatment fields prevent collaboration and quality service delivery, service systems will continue to fail these families.
While the Congress has asked Federal agencies within the U.S. Department of Health and Human Services to prepare this Report to Congress, much of the difficult work of building effective collaboration between these fields must happen at the local and State levels. In discussions with practitioners, their national associations and advocates, several themes emerged regarding steps the Federal Government could take that would assist agencies to improve their working relationships and ultimately the services delivered to families. A number of these are discussed below. It must be acknowledged, however, that neither the child welfare system nor the substance abuse treatment system is nationally operated, and while the Federal government provides significant funding and related structure to both fields, the day-to-day relationships which ultimately determine effective service provision are primarily local. Therefore it is not sufficient to discuss what the Federal government should do to address these issues. There are significant roles for service providers, program administrators and policy makers at all levels, from front line social workers and treatment counselors to agency administrators, political leaders and judges at the community and State levels as well as in Federal agencies.
With the implementation of the Adoption and Safe Families Act, child welfare agencies are required under most circumstances to make decisions about permanent living arrangements for children within 12 to 15 months of the time they enter foster care. Equally, agencies are required to make reasonable efforts to prevent foster care placement and reunify families, so long as children can be kept safe. It is hard to argue that these reasonable efforts for a substance abusing parent do not include substance abuse treatment. Yet it is clear that case plans for many parents of children in foster care do not include substance abuse assessment and, as needed, treatment, even when substance abuse is identified or suspected. Even if a case plan requires a parent to attend substance abuse treatment, in many instances there is not an available treatment slot in a program with services designed for women and parents, or outreach and engagement efforts are insufficient to secure clients' participation. Finally, it is clear that substance abuse is rarely the only serious problem in families whose children are neglected or abused and it cannot be expected that abstinence alone will produce healthy, functioning families.
While discussions of improving the situation usually focus on funding, addressing the problem is not just an issue of funding. Rather, service providers on both sides of the divide, child welfare and substance abuse treatment, must change how they do business, and especially how they deal with each other. As McMahon and Luthar (1998, p. 147) recently observed, "regardless of how difficult the clients might be and how easy it may be to blame them when things do not go well, provider-provider interaction is often the critical and rarely acknowledged factor in many of our service delivery failures."
Below, five topics are described on which important actions must occur in order to improve outcomes for these vulnerable children and families. Strengthening both fields' activities on these issues will improve the ability of front line staff to achieve, whenever possible within a reasonable time frame, safe and well-functioning families, and, when family preservation or reunification is not possible, other permanent living arrangements for children. Whether or not the children can return home, there must be a continuing commitment to parents' recovery as well as to the well being of their children. No agency can be complacent or claim that the burden of action is solely on another system or another level of government. Progress is possible only if approaches are adapted at all points in the process to focus, in a collaborative manner, on achieving client outcomes.
Building Collaborative Working Relationships
The first step toward improved services and ultimately better outcomes for these families is to begin working together more effectively. Partnerships are essential for progress. No single agency's services are adequate. Until agencies work together to assist families move toward healthy lifestyles, they risk an expensive and futile tug of war in which families are torn apart between conflicting imperatives as staff argue over whose problem it is. In order to build relationships successfully that can address the complex needs of substance abusing parents with children in the child welfare system, ongoing interdisciplinary training is required as well as training in effective parenting, family support and family skills training models. Cross disciplinary training is a powerful vehicle for sharing values, skills and knowledge. Such training is necessary to reach the common goals implicit in partnership building.
HHS intends to lead the field toward improving communications and developing common ground between the child welfare and substance abuse treatment fields. We began by sponsoring, through ACF's Child Maltreatment Resource Center, a conference in June of 1998 focusing on the nexus between these fields and models of collaborative professional activities. In addition, we are increasing the collaborative activity between ACF and SAMHSA, as well as with NIDA, NIAAA and HCFA, beginning with the production of this report. We expect further joint activities among these agencies over the next several years, including:
- Developing a framework for cross system collaboration and conducting leadership meetings that will convene national and regional discussions among agency leaders, service providers, and consumers of our services to begin the process of working through our different perspectives to build common ground.
- Preparing and disseminating information regarding substance abuse screening and assessment tools that can be used in child protective services contexts, and child safety assessments that may be useful for substance abuse treatment providers.
- Funding a series of small grants to States and communities that will support the planning and implementation of joint strategies for service delivery, staff development and training in effective parenting and family interventions, treatment retention, relapse management and post-treatment support.
- Exploring ways in which improved interagency cooperation can result in more effective substance abuse assessment and treatment referrals.
We challenge State and community leaders in the child welfare and substance abuse fields, in consultation with the juvenile and family courts, to initiate discussions on these issues within their own jurisdictions. These discussions should focus on an analysis of the way in which these service systems and the court currently operate and interact with one another, and the impact of these operations on child safety and family functioning. These deliberations should also identify shared goals, gaps in service, and innovations applicable to their community that can improve the outcomes for children and families.
Assuring Timely Access to Comprehensive Substance Abuse Treatment Services
Parents must be provided with opportunities for treatment and recovery. Addiction is a treatable disease. With high quality care, many addicted parents can and will take control over their lives, enter recovery, and provide safe and loving homes for their children. Unfortunately, however, few of the parents who come to the attention of the child welfare system ever receive such care.
There are currently several important opportunities for States and local communities to expand substance abuse treatment for child welfare clients.
The Fiscal Year 1999 appropriations includes a significant increase in substance abuse treatment funding, particularly an increase of $225 million over last year's funding level for the Substance Abuse Prevention and Treatment Block Grant, the Federal block grant to States that provides funds for substance abuse prevention and treatment services.
Treatment for women with children was last year and will again this year be a priority population for applications under SAMHSA's Targeted Capacity Expansion Program. This program allows State and local government agencies to apply for funds to enhance treatment capacity for populations for which local treatment capacity is insufficient. In Fiscal Year 1999, a total of $55 million will be available for the program, and $110 million has been requested for this program in the President's Budget for Fiscal Year 2000, doubling the size of the program with a significant investment of new resources. SAMHSA's Center for Substance Abuse Treatment (CSAT) will also continue to support a number of long-term residential substance abuse treatment programs for women with children that enable women to bring their infants and children into treatment with them.
Further opportunities for States and local governments to improve treatment for parents include making increased use of Medicaid to fund substance abuse treatment services. Many child welfare clients are Medicaid-eligible. As described in Appendix A, most substance abuse treatment services for adults, with the exception of services provided in large residential facilities, can be paid for under Medicaid. A number of States have expanded their provision of substance abuse treatment services through Medicaid in recent years, and additional States may wish to consider this option as a way of expanding treatment capacity.
Finally, many substance abuse services could be paid for under the Temporary Assistance For Needy Families (TANF) and Welfare-to-Work Programs. Many families with substance abuse problems who come to the attention of the child welfare system are families receiving welfare benefits. If these parents' substance abuse problems are interfering with their ability to care for their children, it is likely that the substance abuse is also compromising employment. States and counties may wish to consider writing substance abuse treatment services into these clients' employment plans. Under these circumstances, TANF funds, and funds under the Welfare-to-Work program, could be used for non-medical aspects of substance abuse treatment, if such treatment is not otherwise available to the participant. Non-medical services include services performed by those not in the medical profession such as counselors, technicians, social workers and those services not provided in a hospital or clinic. The Welfare-to-Work Program, operated by the U.S. Department of Labor and implemented through local Private Industry Councils (PICs) and/or State and local Workforce Investment Boards (WIBs), specifically targets individuals who require substance abuse treatment for employment and allows non-medical substance abuse treatment as an allowable activity under job retention and support services.
State and local leaders are urged to consider these options as they plan to address the treatment needs of child welfare clients. It is essential that communities provide substance abuse treatment services to these clients so as to allow as many parents as possible to establish sobriety and provide safe homes for their children. The availability of new resources can promote the building of capacity at the state and local levels to provide services in ways that promote safety and permanency for children and sobriety for families. If the utilization of these resources can be shaped in a collaborative way that builds on the knowledge and expertise of both systems and the needs of families, the stage can be set for more effective use of future resources.
Improving Our Ability to Engage and Retain Clients in Care and to Support Ongoing Recovery
Assuring adequate treatment capacity is not sufficient to produce significant changes in families' behavior unless clients engage in the recovery process and stick with programs long enough for learning to occur and behavior to change. Too often, clients fall through gaps between agencies before intervention begins, as relapses occur, and after treatment programs end. A clear lesson shown by research is that engagement and retention is an extremely difficult process with this client population. It is precisely during these transition periods that contact with clients is likely to be lost, and with it the opportunity for constructive intervention.
In order to assist service providers to implement effective engagement and retention strategies, ACF and SAMHSA, with other agency partners, will:
- Expand our research in this area to build knowledge and develop effective program strategies.
- Utilize our technical assistance mechanisms to assure materials on effective approaches are available to the field. In ACF this will include updating materials on substance abuse and child welfare that are available through its clearinghouse and resource centers. In addition, materials will be developed for the field regarding assessing progress in treatment and on decision making for families of children in foster care. SAMHSA/CSAT is also exploring the development of a technical assistance publication or publications for use by child protective services agencies that will answer questions about substance abuse treatment services.
- The Children's Bureau within ACF will make particular efforts to work with the Court Improvement Projects (State grantees working to improve courts' capacity to deal with dependency proceedings) to share information on effective programs, assessing treatment progress, and on the application of drug court methods to juvenile and family courts.
- SAMHSA/CSAT will continue to focus on increasing opportunities for family reunification and improved child safety though the Family Drug Court Program. Since 1997, SAMHSA/CSAT has funded this pilot program to evaluate the use of family drug courts as a strategy for reducing the cost and trauma that result from foster care in neglect and abuse cases.
We encourage child welfare and substance abuse treatment providers at the local level to design programs with a recognition that the recovery from addiction is an ongoing process that is characterized by the risk of relapse and that clients are prone to dropping out of treatment. To mediate against the likelihood of these events and to respond to them, services need to be structured in ways that promote retention and provide relapse prevention and supportive services.
Enhancing Children's Services
As substance abuse treatment programs design services for parents, children's needs must also be addressed. Services for infants and children are designed to foster healthy development, linking primary health care, prenatal, hospital inpatient and postnatal care, and mental health and social services. Activities and services may be provided for the children either on-site or through linkages with other appropriate and qualified community service providers. Whenever possible these services should include extensive joint parent-child activities focused on improving substance abusing parents' ability to avoid emotional or physical abuse and neglect. These include interventions such as therapeutic play, family skills training or family therapy. For children in foster care, increased attention to children's healthy emotional, social and cognitive development is needed. In addition, program models are needed to address the particularly high risk of substance abuse and other risky behaviors among children in foster care. A family history of drug disorder is one of the most potent risk factors for the development of the child and the child's development of drug disorders at an early age. This suggests that substance abuse prevention and intervention programs should target offspring of parents with substance use disorders.
ACF intends to focus new attention on issues of preventive services. These activities will include:
- Highlighting opportunities to address substance abuse within the Independent Living Program.
- Developing training materials for foster parents on working with the children they care for to prevent future substance abuse.
- Focusing attention on substance abuse issues within the Community Based Family Resource and Support (CBRFS) Program (Title II of the Child Abuse Prevention and Treatment Act), which provides services in every State for the prevention of child abuse and neglect and coordinates a Statewide network of family resource services. Agencies supported by the CBFRS Program offer a variety of training programs that help all parents reduce stress, teach basic child development and parenting skills, and support adults in creating safe and stable environments for their children.
SAMHSA has in recent years significantly expanded its attention to early childhood issues. These efforts include:
- SAMHSA's three Centers in collaboration with the Health Resources and Services Administration, The Administration for Children and Families, the Department of Education, the National Institutes of Health and the Casey Family Program support the Starting Early Starting Smart (SESS) Program which is a child-centered, family-focused, and community-based initiative designed to test the effectiveness of integrating behavioral health services within primary care and early childhood service settings for children age 0 - 7.
- SAMHSA's Center for Substance Abuse Prevention (CSAP) has funded 15 community sites for three years to field test effective, research-based models of prevention interventions for children of substance abusers from diverse cultural populations. Some of these children and their older siblings are already in the child welfare system due to neglect and/or abuse or from the need for temporary placement while their mothers are in treatment.
We challenge State and local service providers to identify opportunities for prevention and treatment services for children who are in foster care and for those under protective supervision in their own homes. Efforts should be made to work with prevention service providers to identify maltreated children as a priority for such services.
Filling Information Gaps
Our fields' understanding of the interrelated issues of substance abuse and child maltreatment has progressed significantly over the past decade. Research and demonstration programs sponsored by SAMHSA, ACF, NIDA and NIAAA have been instrumental in exploring these issues and testing intervention approaches. For instance, CSAT's demonstration programs for women with children have helped build model substance abuse treatment programs that also serve children and which provide parenting training to treatment clients. While our understanding of these issues has improved, it has also become clear that significant gaps in the knowledge base remain. These gaps must be addressed in the coming years to ensure programs and approaches are well grounded in research findings.
As noted above, there are significant gaps in knowledge about the interrelationships among substance abuse, child maltreatment, and related problems. The discussion below describes a number of the gaps that became clear as we developed this report.
Regarding the extent and scope of the problem, much better information is available nationally on the prevalence and severity of substance abuse among child welfare clients than there is about the prevalence and severity of child welfare and parenting issues in families with substance abuse problems. In the child welfare system, the new Adoption and Foster Care Analysis and Reporting System (AFCARS) will soon provide more accurate information nationally about the extent to which substance abuse has contributed to children's placement in foster care. There is currently no data being collected through Federal substance abuse data systems, however, about clients' children. The National Household Survey on Drug Abuse does collect information about whether respondents have children in their households, although in depth analysis of this information is not often conducted.
That these clients have complex needs has become a familiar refrain among service providers in both the substance abuse and the child protection systems, and it is the truth. However, while many sources list a multitude of problems often affecting these clients, there exists little information on the relationships between various needs, and virtually no information on causal relationships among co-existing problems. In addition, there is considerably more information on the small population of infants prenatally exposed to illicit drugs and alcohol than on the much larger population of children living in households with ongoing alcohol and illicit drug abuse.
Barriers to service are a common subject of research, often as evaluators try to determine why programs have been unsuccessful in meeting their goals. Programs in the substance abuse and child welfare fields often list many of the same barriers to service, generally relating to the complexity of child and family needs. Less has been written, however, about cross-system efforts to address barriers, their results, and why such efforts have been difficult to establish and maintain.
For some years now, communities have sought approaches to addressing the joint problems of substance abuse and child maltreatment. But while there is considerable information about single system approaches, there are only a few studies documenting cross-system approaches to these problems. Most of those that do exist were conducted under the auspices of demonstration grants initiated by the Administration for Children and Families or the Substance Abuse and Mental Health Services Administration. State- and community-generated activities have not generally been evaluated. In addition, while these grantees have learned a great deal about developing and implementing comprehensive services for these families, what has been produced thus far are a series of consensus-based "lessons learned" and "promising strategies." To date there is little effectiveness data to guide practice in this area.
In order to address knowledge gaps,
- ACF has proposed that these issues be the subject of the next annual Federal Forum on Child Abuse and Neglect Research, to take place in the Spring of 1999. ACF will urge the variety of research agencies within HHS and elsewhere in the Federal Government to consider these issues as they formulate their future research agendas.
- The National Institutes of Health, in partnership with ACF, other HHS agencies and the Department of Justice, will soon issue a grant announcement soliciting research proposals addressing child neglect. It is expected that a number of the proposals will address alcohol and drug abuse as factors in child neglect. Studies and research are needed on the links between physical and sexual abuse and substance abuse. In addition, studies of co-occurring and/or predisposing factors to substance abuse and child maltreatment, such as mental disorders, are urgently needed. While our knowledge base is quite thin, it nonetheless is clear that successful intervention with substance abuse and child maltreatment will necessitate treatment of such comorbid conditions as mental disorders.
- SAMHSA's Center for Substance Abuse Prevention (CSAP) has two new Knowledge Development and Application (KDA) programs, Children of Substance-Abusing Parents (COSAPs) and Initiatives on Welfare Reform and Substance Abuse Prevention for Parenting Adolescents (Parenting Adolescents), which are designed to develop new knowledge about ways to improve the prevention of substance abuse aimed at children of substance abusing parents or parenting teens. The knowledge generated from the SAMHSA KDA grants will be used to work with State and local governments as well as providers, families, and consumers to improve or develop comprehensive systems of care which address the issues of substance abuse and child welfare.
- SAMHSA's/CSAP has implemented a new Family Strengthening cross-site grantee program in over 100 communities across the country in order to increase our knowledge about how to better disseminate research-based models currently available and how to convince practitioners in the field to adopt models that have proven effective and to adapt them to diverse populations.
- The National Association of Children of Alcoholics has conducted a call for program submissions from the field to determine what types of prevention services are being provided to children of substance abusing parents in schools, treatment and youth program settings. SAMHSA/CSAP will support the analysis of these prevention programs to determine those that are the most cost-beneficial and promote their adoption with block grant and local prevention funding.
Researchers in the substance abuse field are urged to consider parenting issues as they develop research on the consequences of substance abuse and the effects of substance abuse treatment. Similarly, child maltreatment researchers are urged to consider the role of substance abuse in the dynamics of maltreating families.
Other Activities Across Action Areas
Several ongoing activities cut across the service areas described above. These activities will involve efforts to work across fields to improve the capacity of child welfare and substance abuse agencies to work together and serve families effectively. They include:
Technical Assistance and Training Activities. In the coming year, ACF will be examining its child welfare technical assistance strategy. The current cooperative agreements for five Child Welfare Resource Centers will be expiring, and new resource centers or other technical assistance mechanisms will be put in place to continue our efforts to assist the field in adapting to child welfare challenges. As this strategy is developed, ACF intends to assure that substance abuse issues are given adequate attention and that technical assistance providers have expertise to assist agencies in developing improved procedures for addressing families' complex needs. ACF will also be considering the need to develop specific resource materials on targeted topics such as confidentiality issues; establishing effective procedures for making substance abuse assessments and treatment referrals; using non-traditional resources for the purchase of substance abuse services; and judging progress in substance abuse treatment. ACF also expects to produce a series of "promising practices" documents highlighting emerging models of serving these families in a collaborative fashion.
In Fiscal Year 1997, ACF funded 11 Child Welfare Training Grants to schools of social work to develop competency-based interdisciplinary training curricula and training plans to enhance and strengthen the capacity of child welfare workers to respond to the complex family problems of child abuse and neglect resulting from substance abuse, mental illness and domestic violence. These three-year grants will soon be completed. The National Clearinghouse on Child Abuse and Neglect Information will disseminate information regarding the availability of training materials resulting from these projects.
SAMHSA's technical assistance is provided primarily through 14 Addiction Technology Transfer Centers (ATTCs) located throughout the United States. Among the goals of the ATTCs is the cultivation of an interdisciplinary consortium of health care and related professionals to address effective approaches to substance abuse treatment and recovery. As part of these efforts, fostering collaboration between child welfare and substance abuse treatment agencies has been and will continue to be an ongoing focus of the ATTCs. In addition, SAMHSA's Center for Substance Abuse Treatment also funds a number of grant programs involving substance abuse treatment for women and children and provides technical assistance on child welfare issues to these grantees.
Child Welfare Demonstration Waivers. As noted in Chapter 7, HHS has the authority to grant demonstration waivers of legal and regulatory provisions of Federal child welfare programs (especially the Title IV-E Foster Care and Adoption Assistance programs) in order to allow States to test innovative child welfare service models. As was the case last year, the Department will again this year give priority consideration to demonstration approaches designed to improve the child welfare system's response to families with substance abuse problems. ACF encourages States to consider whether such demonstration waivers would be helpful to the implementation of improved service approaches.
To date, 18 States have received approval for demonstration projects which aim to improve child welfare outcomes through:
- subsidized guardianship programs;
- more flexible use of foster care funds;
- fixed-cost funding arrangements;
- increasing the availability of services for specific sub-populations of children or families;
- efforts to increase adoption opportunities for children for whom reunification is unlikely.
As discussed in Chapter 7, two States are using demonstration waivers to provide specialized services for caretakers with substance abuse problems.
Moving Forward, Together
The congressional request for a report on substance abuse and child protection has provided a unique opportunity for HHS to focus on the maltreatment of children where substance abuse is a contributing factor. This report documents what we know about substance abuse treatment and recovery and its relationship to maltreatment. It further documents both systemic and individual factors that contribute to or minimize our ability to protect children and assist families in the recovery process.
Families often come with serious problems to service systems which are fragmented, and as such are limited in their ability to facilitate safety, permanency and sobriety. The Adoption and Safe Families Act recognizes the importance of time to children and establishes an expectation of urgency in decision making regarding their welfare. The imperative for timely decisions for children and the time frames necessary for recovery should also create a sense of urgency for policy makers and providers of service. Those of us who work in the areas of substance abuse and child welfare services must recognize the immediate need to eliminate barriers to effective treatment. This report sets the stage for a number of actions which can improve the nation's capacity to serve families whose children are at the greatest risk.
By embarking on efforts to collaborate toward better outcomes for families and children and to increase service providers' understanding, identification, and responsiveness to the dual problems of maltreatment and substance abuse, we will not only enable families to address their own issues, but will improve our systemic ability to prevent and treat addictions that compromise children's care.
The challenge before us is substantial. However, we believe that there is a broad recognition of the issues we face and a willingness to make the changes necessary at all levels of government to reach our goal.
References
Allen, M., & Larson, J. (1998). Healing the Whole Family. Washington, DC: Children's Defense Fund.
American Psychiatric Association (1994). Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV), Washington, DC: American Psychiatric Association, 181-183.
Ashery, R., Robertson, E., & Kumfer, K.L. (Eds.)(1999). Drug Abuse Prevention Through Family Interventions. NIDA Research Monograph #177. Rockville, MD: DHHS, National Institute on Drug Abuse. NIH Publication No. 97-4135.
Barth, R. (1997). Substance Abuse and Child Welfare: Problems and Proposals. Testimony before the U.S. House of Representatives, Committee on Ways and Means, Subcommittee on Human Resources, 28 October 1997.
Bays, J. (1990). Substance abuse and child abuse: Impact of addiction on the child. Pediatric Clinics of North America, 37(4), 881-904.
Beckman, L., & Amaro, H. (1986). Personal and social differences faced by females and males entering alcoholism treatment. Journal of Studies on Alcohol, 47, 135-145.
Belenko, S. (1998). Research on drug courts: A critical review. National Drug Court Institute Review 1(1).
Bergman, G., Larrson, G., & Brismar, B. Battered wives and female alcoholics: A Comparative Social and Psychiatric Study. Journal of Advanced Nursing, 14, 727-734.
Bernstein, V., & Hans, S. (1994). Predicting the developmental outcome of two-year-old children born exposed to methadone: Impact of social-environmental risk factors. Journal of Clinical Child Psychology, 23, 349-359.
Black, R., & Mayer, J. (1980). Parents with special problems: Alcoholism and opiate addiction. Child Abuse and Neglect, 4:45.
Black, M., Nair, P., Kight, C., Wachtel, R., Roby, P., & Schuler, M. (1994). Parenting and early development among children of drug-abusing women: effects of home intervention. Pediatrics, 94(4), 440-448.
Brindis, C., Berkowitz, G., & Clayson, Z. (1997). Options for Recovery: promoting perinatal drug and alcohol recovery, child health and family stability. In B. Bullington and C. McNeece (Eds.), Journal of Drug Issues, 27(3), 607-624.
Brown, E. (1992). Program and staff characteristics in successful treatment. In M. Kilbey & K. Asghar (Eds.), Methodological Issues in Epidemiological, Prevention and Treatment Research on Drug-Exposed Women and Their Children, Research Monograph #117. Rockville, Maryland: U.S. Department of Health and Human Services, National Institute on Drug Abuse.
Burgdorf, K. (1998). Secondary analysis of data from the National Treatment Improvement Evaluation Study. Unpublished raw data.
Caldwell, D. (1998). Does the child welfare system "facilitate" drug treatment? A client's perspective. The Source, 8(2). Berkeley, CA: Abandoned Infants Assistance Resource Center.
Camp, J., & Finkelstein, N. (1997). Parenting training for women in residential substance abuse treatment - results of a demonstration project. Journal of Substance Abuse Treatment, 14(5), 411-422.
Carta, J., McConnell, S., McEvoy, M., Greenwood, C., Atwater, J., Baggett, K., & Williams, R. (1997). Developmental outcomes associated with in utero exposure to alcohol and other drugs. In M. Haack (Ed.), Drug Dependent Mothers and Their Children: Issues in Public Policy and Public Health. New York: Springer.
Carten, A. (1996). Mothers in recovery: rebuilding families in the aftermath of addiction. Social Work, 41(2), 214-223.
Catalano, R.F. (1999). In Ashery, R., Robertson, E., & Kumfer, K.L. (Eds.)(1999). Drug Abuse Prevention Through Family Interventions. NIDA Research Monograph #177. Rockville, MD: DHHS, National Institute on Drug Abuse. NIH Publication No. 97-4135.
Catalano, R.F., Haggerty, K., Gainey, R., & Hoppe, M. (submitted). The effects of parenting training and case management on parents in methadone treatment: Immediate posttreatment effects. Journal of the American Medical Association.
Chasnoff, I. (1989). Class found no barrier to drug use in pregnancy. Presentation to the annual meeting of the American Academy of Pediatrics in Chicago. Reported in Pediatric News, 23, 1.
Chavkin, W., Paone, D., Friedmann, P., & Wilets, I. (1993). Psychiatric histories of drug using mothers: Treatment implications. Journal of Substance Abuse Treatment, 10(5), 445-448.
Child Welfare League of America. (1998). Alcohol and Other Drug Survey of State Child Welfare Agencies. Washington, DC: Child Welfare League of America.
Child Welfare League of America North American Commission on Chemical Dependency. (1992). Children at the Front: A Different View of the War on Alcohol and Drugs. Washington, DC: The Child Welfare League of America.
Collins J., & Allison M. (1983). Legal coercion and retention in drug abuse treatment. Hospital and Community Psychiatry, 34(12), 1145-1149.
Cross, T. (1997). Heritage and Helping. A Model Curriculum for Indian Child Welfare Practice. Portland: Indian Child Welfare Association.
Dackis, C., & Gold, M. (1992). "Psychiatric Hospitals for Treatment of Dual Diagnosis." In J. Lowinson & P. Ruiz (Eds.), Substance Abuse: A Comprehensive Textbook. Baltimore: Williams and Wilkins, 467-485.
Dembo, R., Dertke, M., LaVoie, L., Borders, S., Washburn, M., & Schmeidler, J. (1997). Physical abuse, sexual victimization and illicit drug use: A structural analysis among high risk adolescents. Journal of Adolescence, 10, 13.
DePanfilis, D., and Salus, M. (1992). A Coordinated Response to Child Abuse and Neglect: A Basic Manual. Washington, DC: National Center on Child Abuse and Neglect.
Dishion, T.J., & Andrews, D.W. (1995). Preventing escalation in problem behaviors with high-risk young adolescents: Immediate and 1-year outcomes. Journal of Consulting and Clinical Psychology 63:538-548.
Dore M., Doris J., & Wright, P. (1995). Identifying substance abuse in maltreating families: a child welfare challenge. Child Abuse and Neglect, 19(5), 531-543.
Dowell, K., and Roberts, T. (1998). Preliminary findings from the cross-site evaluation of the Center for Substance Abuse Treatment's Residential Women and Children and Pregnant and Postpartum Women Programs. Unpublished raw data.
Egeland, B., & Erickson, M.F. (1990). Rising above the past: Strategies for helping new mothers break the cycle of abuse and neglect. Zero to Three 11(2): 29-35.
Ellwood, M., Adams, E., Crown, W., & Dodds, S. (1993). An Exploratory Analysis of the Medicaid Expenditures of Substance Exposed Children Under 2 Years of Age in California. Washington, DC: U.S. Department of Health and Human Services, Office of the Assistant Secretary for Planning and Evaluation.
Emshoff, J. (in press). Prevention intervention strategies for children of alcoholics. Pediatrics.
English, D. (1995). The Navy Risk Assessment Model on Child Maltreatment and Domestic Violence: A Review of the Research Literature. Washington, DC: Bureau of Naval Personnel, Family Advocacy Program.
________. (1998). Final Report, NCCAN grant #90CA-1563, Caseworker Decision Making in CPS.
Ensign, K. & Kaye, E. (1998). Analysis of States' FY97 Annual Progress and Services Reports. Presented to the Family Preservation Program Implementation Study Technical Work Group Meeting, Washington, D.C., April 16, 1998.
Etheridge, R., Craddock, S., Dunteman, G., & Hubbard, R. (1995). Treatment services in two national studies of community-based drug abuse treatment programs. Journal of Substance Abuse, 7, 9-26.
Famularo, R., Kinsderff, R., Bunshaft, D. (1989). Parental compliance to court ordered treatment interventions in cases of child maltreatment. Child Abuse and Neglect 13:1507.
Famularo, R., Stone, K., Barnum, R., & Wharton, R. (1986). Alcoholism and severe child maltreatment. American Journal of Orthopsychiatry, 56(3), 482-485.
Fanshel, D. (1975). Parental failure and consequences for children: The drug abusing mother whose children are in foster care. American Journal of Public Health, 65(6), 604-612.
Feig, L. (1998). Understanding the problem: the gap between substance abuse programs and child welfare services. In R. Hampton, V. Senatore & T. Gullotta (Eds.), Substance Abuse, Family Violence, and Child Welfare: Bridging Perspectives. Thousand Oaks, CA: Sage.
Gardner, S. (in press). Beyond Collaboration to Results. Phoenix: Arizona State University Press.
Gerstein, D., Johnson, R., Larison, C., Harwood, H., & Fountain, D. (1997). Alcohol and Drug Abuse Treatment for Parents and Welfare Recipients: Outcomes, Benefits and Costs. Washington, DC: U.S. Department of Health and Human Services, Office of the Assistant Secretary for Planning and Evaluation.
Goerge, R., & Harden, A. (1993). The Impact of Substance Affected Infants on Child Protection Services and Substitute Care Caseloads: 1985-1992. Springfield, IL: Illinois Department of Children and Family Services.
Gregoire, T. (1994). Assessing the benefits and increasing the utility of addiction training for public child welfare workers: a pilot study. Child Welfare, 73(1), 69-81.
Grella, C. (1997). Services for prenatal women with substance abuse and mental health disorders: The unmet need. Journal of Psychoactive Drugs, 29(1), 67-77.
Haller, D., Elswick, R., Dawson, K., Knisely, J., & Schnoll, S. (1993). Retention in treatment of perinatal substance abusers. In L. Harris (Ed.), Problems of Drug Dependence, 1992: Proceedings of the 54th Annual Scientific Meeting, The College on Problems of Drug Dependence, Inc. NIDA Research Monograph 132. Rockville, MD: National Institute on Drug Abuse.
Hans, S. (1995). Diagnosis in etiologic and epidemiologic studies. In C. Jones & M. De La Rosa (Eds.) NIDA Technical Review: Methodological Issues: Etiology and Consequences of Drug Abuse Among Women. Rockville, MD: National Institute on Drug Abuse.
Harden, B. (1998). Building bridges for children: addressing the consequences of exposure to drugs and to the child welfare system. In R. Hampton, V. Senatore, & T. Gullotta (Eds), Substance Abuse, Family Violence, and Child Welfare: Bridging Perspectives. Thousand Oaks, CA: Sage.
Hardin, M., & Lancour, R. (1996). Early Termination of Parental Rights: Developing Appropriate Statutory Grounds. Washington, D.C.: American Bar Association Center on Children and the Law.
Hawley, T., Halle, T., Drasin, R., & Thomas, N. (1995). Children of addicted mothers: Effects of the "crack epidemic" on the caregiving environment and the development of preschoolers. American Journal of Orthopsychiatry, 65, 364-379.
Hayes, H., & Emshoff, J. (1993). In R. Hampton, T. Gullotta, G. Adams, & E. Potter (Eds.), Issues in Children's and Families' Lives, Vol. 1, Family Violence: Prevention and Treatment. Newbury Park, CA: Sage, 281-310.
Herskowitz, J., Seck, M., & Fogg, C. (1989). Substance Abuse and Family Violence. Boston: Massachusetts Department of Social Services, Research, Evaluation and Planning Unit.
Horgan, C., & Levine, H. (in press). The substance abuse treatment system: what does it look like and whom does it serve? In Bridging the Gap Between Practice and Research: Forging Partnerships with Community-Based Drug and Alcohol Treatment.
Howell, E., Thornton, C., Heiser, N., Chasnott, I., Hill, I., Schwalberg, R., & Zimmerman, B. (1998). Pregnant Women and Substance Abuse: Testing Approaches to a Complex Problem. Princeton, NJ: Mathematica Policy Research, Inc.
Huang, L., Cerbone, F., & Gfroerer, J. (1998). Children at risk because of parental substance abuse. In Substance Abuse and Mental Health Administration, Office of Applied Studies, Analyses of Substance Abuse and Treatment Need Issues (Analytic Series A-7). Rockville, MD: U.S. Department of Health and Human Services, Substance Abuse and Mental Health Services Administration.
Hubbard, R., Marsden, M., Rachal, J., Harwood, H., Cavanaugh, E., & Ginzburg, H. (1989). Drug Abuse Treatment: A National Study of Treatment Effectiveness. Chapel Hill: The University of North Carolina Press.
Hughes, P. (1994). Operation PAR: Therapeutic community research for substance abusing women and their children. Paper presented at a National Institute on Drug Abuse technical Review, Palm Beach Florida, June 18-19.
Institute of Medicine (1990). Broadening the Base of Treatment for Alcohol Problems. Washington, DC: National Academy of Sciences.
Jaudes, P., Ekwo, E., & Van Voorhis, J. (1995). Association of drug abuse and child abuse. Child Abuse and Neglect, 19(9),1065-1075.
Jones, V., & Hutchins, E. (1993). Finding Common Ground: A Call for Collaboration. Arlington, VA: National Center for Education in Maternal and Child Health.
Jordon, L. (1997). Bridging the public policy/public health gap: Organizing multiple agencies to deliver coordinated services. In M.Haack, M. (Ed.), Drug Dependent Mothers and Their Children: Issues in Public Policy and Public Health. New York: Springer.
Kagel, J. (1987). Secondary prevention of substance abuse. Social Work, 32, (5), 446-448.
Kearney, M., Murphy, S., & Rosenbaum, M. (1994). Mothering on crack: A grounded theory analysis. Social Science and Medicine, 38, 351-361.
Kelleher, K., Chaffin, M., Hollenberg, J., & Fischer, E. (1994). Alcohol and drug disorders among physically abusive and neglectful parents in a community-based sample. American Journal of Public Health 84, (10), 1586-1590.
Kelley, S. (1992). Parenting stress and child maltreatment in drug-exposed children. Child Abuse and Neglect, 16, 317-328.
Kumpfer, K.L. (1998). Links between prevention and treatment for drug-abusing women and their children. In C. Wetherington, & A. Roman (Eds.), Drug Addiction Research and the Health of Women. Washington, DC: National Institute on Drug Abuse.
Kumpfer, K.L. (1999). Selective prevention interventions: The Strengthening Families Program. In R. Ashery, E. Robertson & K.L. Kumpfer (Eds.) Drug Abuse Prevention Through Family Interventions Rockville, MD: National Institute on Drug Abuse.
Kumpfer, K.L. & Alder, S. (in press). Effective family interventions for the prevention of problems in youth. American Psychologist. Special issue on Prevention.
Kumpfer, K.L. & Alvarado, R. (1995). Strengthening families to prevent drug use in multi-ethnic youth. In G. Botwin, S. Schinke, & M. Orlandi (Eds.) Drug Abuse Prevention With Multi-Ethnic Youth: 253-292. Newbury Park, CA: Sage Publications.
Kumpfer, K.L. & Alvarado, R. (1998). Effective Family Strengthening Interventions. Juvenile Justice Bulletin, Family Strengthening Series, November 1998. Available through Juvenile Justice Clearinghouse, Aspen Systems.
Kumpfer, K.L. & Bayes, J. (1995). Child abuse and drugs. In J.H. Jaffe (Ed.) The Encyclopedia of Drugs and Alcohol. Vol. 1, pp. 217-222. New York: Simon & Shuster.
Kumpfer, K.L., Molgaard, V., & Spoth, R., (1996). The Strengthening Families Program for prevention of delinquency and drug use in special populations. In R. Peters, & R.J. McMahon (Eds.), Childhood Disorders, Substance Abuse and Delinquency: Prevention and Early Intervention Approaches. Newbury Park, CA: Sage Publications.
Kumpfer, K.L., Walker, R., & Richardson (in press). Resilience in children of alcoholics. Journal of Substance Use and Abuse.
Kumpfer, K.L., Williams, M.K., & Baxley, G. (1997). Selective Prevention for Children of Substance Abusing Parents: The Strengthening Families Program, Resource Manual. Silver Spring, MD: National Institute on Drug Abuse, Technology Transfer Program.
Kumpfer, K.L., Alexander, J., McDonald, L, & Olds, D. (1999). Family-focused substance abuse prevention: What has been learned from other fields. In R. Ashery, E. Robertson, & K.L. Kumpfer, (Eds). Drug Abuse Prevention Through Family Intervention. NIDA Research Monograph #177, Rockville, MD: DHHS, National Institute on Drug Abuse.
Lester, B., LaGasse, L., & Seifer, R. (1998). Cocaine exposure and children: The meaning of subtle effects. Science, 282:633-634.
Levine, C., & Stein, L. (1994). Orphans of the HIV Epidemic: Unmet Needs in Six Cities. New York: The Orphan Project.
The Lewin Group. (1997). State Profiles on Public-Sector managed Behavioral Health Care and Other Reforms. Washington, DC: Substance Abuse and Mental Health Services Administration.
Lockwood, D. (June, 1998). Title IV-E Waiver Multidisciplinary Team Treatment Project, Semi-annual evaluation Report. Delaware: Department of Services to Children, Youth and Families.
Lutz, G., Kramer, R., Crew, B., Lantz, G., & Turner, T. (1995). Iowa 1993 Adult Household Survey of Substance Use and Treatment Needs. Des Moines, Iowa: Iowa Department of Public Health, Division of Substance Abuse and Health Promotion.
Magura, S., Laudet, A., Kangy, S., & Whitney, S. (1998). Effectiveness of comprehensive services for crack-dependent mothers with newborns and young children. New York: National Development and Research Institutes.
Mattessich, P. & Monsey, B. (1992). Collaboration: What Makes it Work. St. Paul, MN: Amherst H. Wilder Foundation.
Maza, P., Wright, L., Bauer, C., Shankaran, S., Bada, H., Lester, B., Krause-Steinrauf, H., Smeriglio, V., Bowler, A., & Katsikiotis, V. (1998). Maternal Lifestyles Study (MLS) Caretaking environment and stability of substance exposed infants at one month corrected age. Annals of the New York Academy of Sciences, 846, 358-61.
McCauley, J., Kern, D., Kolodner, K., Dill, L., Schroeder, A., DeChant, H., Ryden, J., Derogatis, L., & Bass, E. (1997). Clinical characteristics of women with a history of childhood abuse. Journal of the American Medical Association, 277, 1362-1368.
McMahon, T., & Luthar, S. (1998). Bridging the gap for children as their parents enter substance abuse treatment. In R. Hampton, V. Senatore & T. Gullotta (Eds.), Substance Abuse, Family Violence, and Child Welfare: Bridging Perspectives. Thousand Oaks, CA: Sage.
Melaville, A., Blank, M., & Asayesh, G. (1993). Together We Can. Washington, DC: U.S. Government Printing Office.
Merikangas, K.R., Dierker, L., & Szatmari, P. (1998) ,Psychopathology among offspring of parents with substance abuse and/or anxiety: A high-risk study. Journal of Child Psychology and Psychiatry, 39(5):711-720.
Merikangas, K., & Stevens, D. (1998). Substance abuse among women: Familial factors and comorbidity. In C. Wetherington & A. Roman (Eds.), Drug Addiction Research and the Health of Women. Washington, DC: National Institute on Drug Abuse.
Merikangas, K.R., Stolar, M., Stevens, D.E., Goulet, J., Preisig, M., Fenton, B., Zhang, H., O'Malley, S., & Rounsaville, B.J., (1998). Familial transmission of substance use disorders. Archives of General Psychiatry, 55:973-979.
Miller, B. (1998). Partner violence experiences and women's drug use: Exploring the connection. In C. Wetherington & A. Roman (Eds.), Drug Addiction Research and the Health of Women. Washington, DC: National Institute on Drug Abuse.
Miller, B., Maguin, E., & Downs, W. (1997). Alcohol, drugs and violence in children's lives. In M. Galante (Ed.), Recent Developments in Alcoholism, Volume 13: Alcohol and Violence. New York: Plenum.
National Association of State Alcohol and Drug Abuse Directors. (1997). "Estimated Number of Individuals Needing Treatment." Washington, DC: National Association of State Alcohol and Drug Abuse Directors.
The National Center on Addiction and Substance Abuse at Columbia University (1996). Substance Abuse and the American Woman. New York, NY: The National Center of Addiction and Substance Abuse.
The National Center on Addiction and Substance Abuse at Columbia University (1999). No Safe Haven: Children of Substance Abusing Parents. New York, NY: The National Center of Addiction and Substance Abuse.
National Council of Juvenile and Family Court Judges (1992). Protocol for Making Reasonable Efforts to Preserve Families in Drug-Related Cases. Reno, NV: National Council of Juvenile and Family Court Judges.
National Organization of Fetal Alcohol Syndrome. Fetal Alcohol Fact Sheet. (http://www.nofas.org/stats.htm).
National Research Council Panel on Research on Child Abuse and Neglect (1993). Understanding Child Abuse and Neglect. Washington, DC: National Academy.
Neuspiel, D., Zingman, T., Templeton, B., DiStabile, P., & Drucker, E. (1993). Custody of Cocaine-Exposed Newborns: Determinants of Discharge Decisions. American Journal of Public Health, 83(12), 1726-1729.
Office of Justice Programs Drug Court Clearinghouse and Technical Assistance Project at American University. (1998a). Juvenile and Family Drug Courts: An Overview. Washington, DC: U.S. Department of Justice, Office of Justice Programs, Drug Courts Program Office.
________. (1998b). Juvenile and Family Drug Courts: Profile of Program Characteristics and Implementation issues. Washington, DC: U.S. Department of Justice, Office of Justice Programs, Drug Courts Program Office.
Office of Technology Assessment. (1994). Technologies for Understanding and Preventing Substance Abuse and Addiction. Washington, DC: Congress of the United States.
Olsen, L. (1995). Services for substance affected families: the project connect experience. Child and Adolescent Social Work Journal, 12(3), 183-195.
Pagliaro, A., & Pagliaro, L. (1997). Teratogenic effects of in utero exposure to alcohol and other abusable psychotropics. In M. Haack (Ed.), Drug Dependent Mothers and Their Children: Issues in Public Policy and Public Health. New York: Springer.
Potocky, M., & McDonald, T. (1996). Evaluating the effectiveness of family preservation services for the families of drug exposed infants: a pilot study. Research in Social Work Practice, 6(4), 524-535.
The Public Children Services Association of Ohio. (1995). Ohio Needs Assessment Report. Columbus, OH: The Public Children Services Association of Ohio.
Resnik, H., Gardner, S., & Rogers, C. (1998). Child welfare and substance abuse: premises, programs and policies. In R.Hampton, V. Senatore, & T. Gullotta (Eds.), Substance Abuse, Family Violence, and Child Welfare: Bridging Perspectives. Thousand Oaks, CA: Sage.
Sagatun-Edwards I., Saylor C., & Shifflett B. (1995). Drug exposed infants in the social welfare system and juvenile court. Child Abuse and Neglect, 19(1), 83-91.
Selwyn, P., & Gorevitch, M. (1998). HIV infection in women: Implications for Drug Abuse Treatment and Research. In C. Wetherington & A. Roman (Eds.), Drug Addiction Research and the Health of Women. Washington, DC: National Institute on Drug Abuse.
Sheehan, J., & Libby, B. (1998). Project SAFE Substance Abuse Family Evaluation. Presentation at Between Two Worlds - Child Maltreatment and Substance Abuse Conference, June 22-24.
Spoth, R., & Redmond, C. (1996). Illustrating a framework for prevention research. In R. Peter, & R.J. McMahon (Eds.) Childhood Disorders, Substance Abuse and Delinquency: Prevention and Early Intervention Approaches. Newbury Park, CA: Sage Publications.
Spoth, R., Redmond, C., & Lepper, H. (in press). Alcohol initiation outcomes of universal family-focused preventive interventions: One- and two-year follow-ups of a controlled study. Journal of Studies on Alcohol, Special NIAAA Issue.
Steele, B. (1980). Psychodynamic factors in child abuse. In C. Kempe & R. Helfer (Eds.), The Battered Child. Chicago: University of Chicago Press.
Stevens, S., & Arbiter, N. (1995). A therapeutic community for substance abusing pregnant women and women with children: process and outcome. Journal of Psychoactive Drugs, 27(1), 49-56.
Stevens, S., Arbiter, N., & McGrath, R. (1994). Women and children: Therapeutic community substance abuse treatment and outcome findings. In G. De Leon (Ed.), Therapeutic Communities for Special Populations in Special Settings. New York: Greenwood.
Strantz, I., & Welch, S. (1995). Postpartum women in outpatient drug abuse treatment: Correlates of retention/completion. Journal of Psychoactive Drugs, 27(4), 357-373.
Tarter, R., Blackson, T., Martin, C., Loeber, R., & Moss, H. (1993). Characteristics and correlates of child discipline practices in substance abuse and normal families. American Journal on Addictions, 2(1):18-25.
Tracy, E. (1994). Maternal substance abuse: protecting the child, preserving the family. Social Work, 39(5), 534-540.
U.S. Advisory Board on Child Abuse and Neglect. (1993). Neighbors Helping Neighbors: A New National Strategy for the Protection of Children. Washington, DC, U.S. Government Printing Office.
U.S. Department of Health and Human Services, Center for Substance Abuse Prevention (1998). Family-centered Approaches to Prevent Substance Abuse Among Children and Adolescents: A Guideline. Rockville, MD: Center for Substance Abuse Prevention.
U.S. Department of Health and Human Services, Center for Substance Abuse Prevention (1993). Signs of Effectiveness in Preventing Alcohol and Other Drug Problems. Rockville, MD: Center for Substance Abuse Prevention.
________. (1994). Practical Approaches in the Treatment of Women Who Abuse Alcohol and Other Drugs. Rockville, MD: Center for Substance Abuse Treatment.
________. (in press). Exemplary Models from the High Risk Youth Grantee Program. Rockville, MD: Center for Substance Abuse Treatment.
U.S. Department of Health and Human Services, Centers for Disease Control and Prevention. (1997). Facts About Fetal Alcohol Syndrome. Atlanta, Georgia: Centers for Disease Control and Prevention.
U.S. Department of Health and Human Services, Children's Bureau (1997). National Study of Protective, Preventive and Reunification Services Delivered to Children and Their Families. Washington, DC: U.S. Government Printing Office.
________. (1998a). Child Abuse and Neglect State Statutes Series, Volume VI, Number 38, Termination of Parental Rights: Grounds for Termination. Washington, DC: HHS Children's Bureau.
________. (1998b). Child Abuse and Neglect State Statutes Series, Volume I, Number 8, Special Reporting Procedures: Drug-Exposed Infants. Washington, DC: HHS Children's Bureau.
________. (1998c). Child Abuse and Neglect State Statutes Series, Volume I, Number 1, Definitions of Child Abuse and Neglect. Washington, DC: HHS Children's Bureau.
________. (1998d). Child Maltreatment 1996: Reports from the States to the National Child Abuse and Neglect Data System. Washington, DC: U.S. Government Printing Office.
U.S. Department of Health and Human Services, National Center on Child Abuse and Neglect. (1993). A Report To Congress: Study of Child Maltreatment in Alcohol Abusing Families. Washington, DC: HHS National Center on Child Abuse and Neglect.
________. (1994). Protecting Children in Substance Abusing Families. Washington, DC: HHS National Center on Child Abuse and Neglect.
________. (1995a). Descriptive Analysis of Projects to Improve Services to Substance Abuse-Affected Families. Washington, DC: National Center on Child Abuse and Neglect.
________. (1995b). Descriptive Analysis of Multidisciplinary/Interdisciplinary Training Projects. Washington, DC: National Center on Child Abuse and Neglect.
________. (1996). Third National Incidence Study of Child Abuse and Neglect. Washington, DC: U.S. Government Printing Office.
U.S. Department of Health and Human Services, National Institutes of Health, National Institute on Drug Abuse (1994). Outcomes of children of substance abusers. In NIDA Second National Conference on Drug Research and Practice: An Alliance for the 21st Century: Conference Highlights. Rockville, MD: HHS National Institutes of Health.
________. (1996). National Pregnancy and Health Survey. Rockville, MD: U.S. Department of Health and Human Services, National Institutes of Health.
________. (1997). Preventing Drug Use Among Children and Adolescents. Rockville, MD: U.S. Department of Health and Human Services, National Institutes of Health.
U.S. Department of Health and Human Services, Substance Abuse and Mental Health Services Administration (1993). CSAT Comprehensive Treatment Model for Alcohol and Other Drug Abusing Women and their Children. Rockville, MD: HHS Substance Abuse and Mental Health Administration.
________. (1994). CSAT Treatment Improvement Protocol #9: Assessment and Treatment of Patients with Co-existing Mental Illness and Alcohol and Other Drug Abuse. Rockville, MD: HHS Substance Abuse and Mental Health Services Administration.
________. (1995). Producing Results ... A Report to the Nation, 1995 Rockville, MD: Substance Abuse and Mental Health Services Administration.
________. (1996a). CSAT Technical Assistance Publication #19: Counselors' Manual on Relapse Prevention with Chemically Dependent Criminal Offenders. Rockville, MD, DC: HHS Substance Abuse and Mental Health Services Administration.
________. (1996b). The National Treatment Improvement Evaluation Study. Rockville, MD: HHS Substance Abuse and Mental Health Services Administration.
________. (1997a), CSAT Pregnant and Postpartum Women's Program Report to Congress. Rockville, MD: HHS Substance Abuse and Mental Health Services Administration.
________. (1997b). CSAT Treatment Improvement Protocol #25: Substance Abuse Treatment and Domestic Violence. Rockville, MD: HHS Substance abuse and Mental Health Services Administration.
________. (1997c). Confidentiality of Patient Records for Alcohol and Other Drug Treatment. Rockville, MD: HHS Substance Abuse and Mental Health Services Administration.
________. (1997d). Substance Use Among Women in the United States. Rockville, MD: HHS Substance Abuse and Mental Health Services Administration.
________. (1998a). Prevalence of Substance Abuse Among Racial and Ethnic Subgroups in the United States, 1991-1993. Rockville, MD: HHS Substance Abuse and Mental Health Services Administration.
________. (1998b). Services Research Outcomes Study. Rockville, MD: HHS Substance Abuse and Mental Health Services Administration.
________. (1998c). Preliminary Results from the 1997 National Household Survey on Drug Abuse. Rockville, MD: HHS Substance Abuse and Mental Health Services Administration.
________. (1999). 1998 Annual Report to Congress on the Evaluation of the Comprehensive Community Mental Health Services for Children and Their Families Program. (SAMHSA/CMHS unpublished draft manuscript. Rockville, MD: HHS Substance Abuse and Mental Health Services Administration.
U.S. Department of Justice, National Institute of Justice (1997). Drug Use Forecasting 1996: Annual Report on Adult and Juvenile Arrestees. Washington, DC: National Institute of Justice, 21-46.
U.S. General Accounting Office (1994). Foster Care: Prenatal Drug Abuse has an Alarming Impact on Young Children. Washington, DC: U.S. General Accounting Office.
________. (1998). Foster Care Agencies Face Challenges Securing Stable Homes for Children of Substance Abusers. Washington, DC: U.S. General Accounting Office.
Walker, C., Zangrillo, P., & Smith J. (1991). Parental Drug Abuse and African American Children in Foster Care: Issues and Study Findings. Washington, DC: U.S. Department of Health and Human Services, Office of the Assistant Secretary for Planning and Evaluation.
________. (1994). Parental drug abuse and African American children in foster care. In R. Barth, J. Berrick, & N. Gilbert (Eds.), Child Welfare Research Review. New York: Columbia University Press, 109-122.
White, W. (1995). Project SAFE Program Handbook: Revised Edition. Bloomington, IL: Lighthouse Institute.
Wilsnack, S. (1984). Drinking, Sexuality, and Sexual Dysfunction. In Wilsnack & Beckman, (Eds.), Alcohol Problems in Women: Antecedents, Consequences and Intervention. New York: Guilford.
________. (1995). Alcohol Use and Alcohol Problems in Women. In A. Stanton and S. Gallant (Eds.), The Psychology of Women's Health. American Psychological Association.
Wobie, K., Davis-Eyler, F., Conlon, M., Clarke, L., & Behnke, (1997). Women and children in residential treatment: outcomes for mothers and their infants. In B. Bullington and C. McNeece (Eds.), Journal of Drug Issues, 27(3), 585-606.
Young, N., & Gardner, S. (1998). Children at the crossroads. Public Welfare, Winter 1998, 56(1), 3-10.
Young, N., Gardner, S., & Dennis, K. (1998). Responding to Alcohol and Other Drug Problems in Child Welfare: Weaving Together Policy and Practice. Washington, DC: CWLA Press.
Zlotnick, C., Franchino, K., St. Clair, N., Cox, K., & St. John, M. (1996). The impact of outpatient drug services on abstinence among pregnant and parenting women. Journal of Substance Abuse Treatment, 13(3), 195-202.
Appendix A. Medicaid Services for Substance Abuse Treatment
Under Medicaid, States are required to provide a series of mandatory services, and may, should they so choose, provide an additional series of optional services. States define the details of what is provided under both the mandatory and optional services and may place limits on these services. Substance abuse treatment may be offered in a variety of forms under several mandatory or optional benefits.
Mandatory Medicaid Services
States may fund substance abuse treatment in many forms through the mandatory benefits required by the Health Care Financing Administration. Those benefits that are most relevant for substance abuse treatment include:
Inpatient hospital services - services available at general hospitals, including psychiatric units of general hospitals.
Outpatient hospital services - services available through outpatient departments of general hospitals or of psychiatric hospitals qualified to participate in Medicaid.
Rural health clinic (RHC) services - services at special clinics in rural areas in States permitting RHC's;
Early and periodic screening, diagnosis and treatment (EPSDT) services - regularly scheduled screening examinations to determine the presence of developmental disorders or chronic conditions for beneficiaries under age 21;
Nursing Facility services - services in licensed nursing homes for people over age 21;
Home Health services - care provided in the home, including part-time nursing services of a home health aide, and medical supplies and equipment used in the home; and at least one of the following optional home services: physical therapy, occupational therapy, speech pathology, and audiology services for individuals over age 21;
Physician services - services of physicians, including psychiatrists.
Optional Services
Optional services allow States to tailor their Medicaid programs to meet specific State objectives. States have chosen to use coverage for optional services in varied ways to support substance abuse services. Optional services that are particularly relevant include clinic services, rehabilitation services, other practitioners services, therapy services, prescribed drugs, personal care services, transportation services, case management services, inpatient psychiatric services for under age 21, and IMD services for over age 65.
Options available under Medicaid allow States to support many of the elements of substance abuse services that have been demonstrated to be cost-effective alternatives to inpatient care. This is most clearly the case for outpatient alcohol and drug treatment, which can be provided as clinic or rehabilitative services. In addition, other optional services, such as services of psychologists and psychiatric social workers, occupational therapy, personal care, transportation, and targeted case management, can be used to support such programs.
Additionally, States may provide home and community-based waiver services to individuals who would otherwise be institutionalized. These services are designed to maintain persons in their communities. They may include those, such as respite care, that are not normally available under the Medicaid program or to other enrollees within the State.
Medicaid Managed Care Programs (1)
Increasingly, States are using managed care programs for their Medicaid populations. Managed care is emerging as the principal means for financing and delivering physical and behavioral health care services under Medicaid (Lewin Group, 1997). As of the spring of 1997, a number of things could be said about substance abuse services in Medicaid managed care programs. These include:
- 33 States and the District of Columbia had Medicaid managed care waivers implemented or approved that included some form of behavioral health services: Alabama, Arizona, California, Colorado, Connecticut, Delaware, the District of Columbia, Florida, Hawaii, Iowa, Kansas, Kentucky, Maryland, Massachusetts, Michigan, Minnesota, Missouri, Montana, Nebraska, North Carolina, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, South Dakota, Tennessee, Texas, Utah, Virginia, Vermont, Washington, and Wisconsin. Fourteen of these States and the District provide behavioral health services through Section 1115 waivers. Twenty-two of these States and the District do so using Section 1915(b) waivers. (There is some overlap among these two groups.)
- 30 of these 33 States and the District had the same or a greater scope of mental health and/or substance abuse benefits under the waivers, compared to their fee-for-service systems.
- 13 States and the District of Columbia covered substance abuse services under approved or implemented Section 1115 waivers: Alabama, Arizona, Delaware, Hawaii, Maryland, Massachusetts, Minnesota, Ohio, Oklahoma, Oregon, Rhode Island, Tennessee, and Vermont.
- 14 States and the District of Columbia covered substance abuse services under approved or implemented Section 1915(b) waivers: Connecticut, Iowa, Kansas, Kentucky, Massachusetts, Michigan, Minnesota, Missouri, Nebraska, North Carolina, Pennsylvania, South Dakota, Texas, and Wisconsin.
- The following States specifically listed children for whom adoption assistance or foster care maintenance payments are made among their targeted populations for Medicaid managed behavioral health care waivers: Arizona, Florida, Illinois, New Mexico, North Carolina, Ohio, Oregon, Pennsylvania, and Utah (inpatient services only). Some other States include these children under broad populations covered under Medicaid managed behavioral health care waivers.
1. Information in this section is derived from The Lewin Group (1997). State Profiles on Public-Sector managed Behavioral Health Care and Other Reforms. Washington, DC: Substance Abuse and Mental Health Services Administration.
Appendix B. Center for Substance Abuse Treatment Comprehensive Treatment Model for Alcohol and Other Drug Abusing Women and Their Children
The purpose of this model is to foster the development of state-of-the-art recovery for women with alcohol and other drug dependence and to foster the healthy development of the children of substance-abusing women. The model is a guide that can be adapted by communities and used to build comprehensive programs over time. The goal of alcohol and other drug treatment is to support a woman's journey to a healthy lifestyle for herself, and for her family whenever possible. Because alcohol and drug dependent women tend to have few economic and social resources, comprehensive treatment is extremely important. The purpose of comprehensive treatment is to address a woman's substance abuse in the context of her health and her relationship to family, community, and society. This relationship is influenced by gender, culture, race and ethnicity, social class, sexual orientation, and age.
Treatment that addresses the full range of a woman's needs is associated with increasing abstinence and improvement in other measures of recovery, including parenting skills and overall emotional health. Treatment that addresses alcohol and other drug abuse only may well fail and contribute to a higher potential for relapse.
Confidentiality and informed consent, as well as the establishment of universal precautions against spread of communicable diseases, are essential throughout all aspects of treatment.
Although this treatment model has been designed specifically for women and their families, many components apply to men as well.
I. Program Structure and Administration
- Development of joint cooperation among substance abuse agencies, schools, courts, probation, health and mental health providers, job training programs, and human service agencies. Creation of an inventory of local, State, and Federal resources available to the treatment program.
- Establishment of an advisory body to assist the treatment program in collaborating with other resources and organizations, and to advocate on behalf of the program. This body should reflect the cultural and socioeconomic diversity of the women and include recovering persons as well as community leaders. Training and support are necessary.
- Cross training of staff in collaborating organizations should foster the development of an integrated continuum of care for each woman in treatment and must address differences in philosophy, experience, and style of various disciplines.
- Staffing should include individuals who are culturally competent and sensitive to and knowledgeable about treating substance abusing women.
- Substance abuse treatment in correctional facilities should be delivered by trained and certified personnel.
- Staff training should encompass the guidelines generated in CSAT's TIPs that relate specifically to Perinatal Substance Abuse.
- Clinicians and program managers should participate in staff training. Such training should lead to understanding the impact of psychological and psychiatric disorders, incest, physical and sexual abuse and their impact on recovery, and readiness for treatment, family dysfunction, multi-addiction, and the importance of flexible treatment approaches.
II. Clinical Interventions and Other Services
Intake Screening and Comprehensive Health Assessment
- Admission priority must be given to women who are known to be pregnant, HIV-positive or who have AIDS, and/or TB. Pregnant/postpartum women should be immediately referred for obstetrical care. (See TIPs.) Immediate referrals must be made if the program cannot provide appropriate care for these women. Documentation of referrals and admissions is essential.
- Assessments for possible pregnancy, HIV status and exposure to and/or existence of TB should begin immediately.
- Same-day intake services should be offered whenever possible.
- Assessment may occur over a period of time. A complete health assessment must be conducted, and must include a physical examination, psychosocial (including psychiatric assessment where indicated), as well as an assessment of a woman's reproductive, oral, and nutritional health status.
- Other assessments must include a substance abuse history; physical, emotional, and sexual abuse history (past and present); educational level and intellectual functioning; work history; family assessment; current living situation and childcare responsibilities; and racial/cultural/ethnic factors that are relevant to treatment. There should be an assessment of patient eligibility (and subsequent registration) for Medicaid, Medicare, SSI, public assistance, and other health and human service benefits.
- An individualized treatment plan, including a plan for relapse prevention and continuing care, must be developed in collaboration with each woman entering treatment.
Medical Interventions
- Medical assessments and subsequent care should be provided through arrangements with healthcare facilities accessible to individuals in the community or on-site, and should include the provision of preventive and primary medical care (including prenatal care, if appropriate); medical or medically supervised detoxification services, where clinically indicated; linkage to psychiatric care; provision of or established referral linkages as needed for acute medical care; testing and treatment for hepatitis, tuberculosis, HIV and HIV disease, sexually transmitted diseases, anemia and malnutrition, hypertension, diabetes, cancer, liver disorders, eating disorders, gynecological problems, dental and vision problems, and poor hygiene. It is preferable to have a healthcare professional available to consult directly with the program.
- Women's Health Services. Preconceptional care should be provided either on-site or through referral, for nutrition, family planning, and general gynecological services to those women deemed appropriate.
- Pharmacotherapy intervention should be provided on an as-needed basis and should include provision of, or established referral linkages, for concomitant assessment and monitoring by qualified medical or psychiatric staff. Interventions should promote equal access to treatment for all women based on assessment of their ability to participate in treatment.
- Urine testing should be used where clinically appropriate, and should be conducted on an initial and random basis. (See TIPs.) The program should follow informed consent guidelines responsive to State reporting requirements, if applicable.
- Infant and Child Health Services. Infant and child health services should be provided either on-site or through referral and should include the following: primary and acute healthcare for infants and children, including immunizations, nutrition services (including assessment for WIC eligibility), and a developmental assessment by qualified personnel. For treatment programs without medical personnel on-site, a back-up medical plan that identifies a protocol for pediatric emergencies must be in place.
- Early Intervention Services. Access to an age-appropriate, comprehensive developmental assessment by qualified personnel, including an assessment of learning and developmental disabilities, should be provided to all children, beginning at birth. On-site provision of, or referral to, early intervention and remedial programs, and linkages with State Individuals with Disabilities Education Act (IDEA) should be encouraged.
- Home-Based Support. Public health nursing and/or social work visits should be provided to high-risk postpartum women and their infants, especially to new mothers and those who are discharged within 24 hours after delivery. Linkages and referrals should be established with home care agencies.
- Counseling for HIV-positive/AIDS Patients. The program must provide for pre- and post-test counseling for HIV-positive/AIDS patients as well as individual counseling and support groups. Staff should be properly trained to intervene on behalf of those who are HIV-seropositive, whether symptomatic or asymptomatic. Appropriate care for HIV-positive children must also be assured.
Linkages and Collaboration
- Appropriate linkages to local, State, and Federal programs must be maintained for those services not provided on-site.
- Linkages with outreach, outpatient, and residential programs should be maintained as a means to assure appropriate matching of women to substance abuse treatment. Similarly, linkages with parental/child programs (e.g., Head Start) should be encouraged.
- Support should be offered with the criminal justice system where appropriate, and should include intervention with juvenile or adult justice authorities, TASC (or related case management/tracking systems), Legal Aid, and/or Bureau of Indian Affairs. Access to needed legal services should be provided if not available through Legal Aid, probation, immigration, child welfare, foster care, and legal service.
Substance Abuse Counseling and Psychological Counseling
Substance abuse education and counseling, psychological counseling (where appropriate), and other therapeutic activities should be provided by practitioners who are licensed or certified to provide these services and matched in competency to the populations served.
Services should be offered in the context of families and relationships, including individual/group/family therapy. Counseling for partners and fathers of babies should be promoted/provided at critical times throughout treatment.
Counseling should address low self-esteem; race and ethnicity issues; gender-specific issues; family of origin relationships; attachment to unhealthy interpersonal relationships; interpersonal violence, including incest, rape, and other abuse; eating disorders; sexuality; parenting issues; grief related to loss of alcohol and other drugs, children, family, partner, work, and appearance; creating a support system that may or may not include family and/or partner; developing a vision for the future and creating a life plan; and therapeutic recreational activities for women alone and with their children.
Parenting Education. Counseling, including information on child development, child safety, injury prevention, and child abuse prevention should be provided. Parenting education should be integrated with substance abuse counseling in order to be recovery-oriented. A woman's family of origin issues that affect parenting should be addressed in a way that supports rather than compromises her stage of recovery.
Relapse prevention should be a discrete component or phase of each woman's recovery plan.
Flexibility and creativity should be stressed in the use and timing of therapeutic approaches. Accusatory, judgmental, and humiliation techniques are inappropriate and have not been proven to be effective.
Health Education and Prevention Activities
- Health education and prevention activities should include HIV/AIDS education; the physiology and transmission of sexually transmitted diseases; reproductive health; understanding female sexuality; preconception care; prenatal education; child birth education; childhood safety and injury prevention; physical and sexual abuse education and prevention; and nutrition, and smoking cessation classes, especially for pregnant women; and general health education.
Life Skills Education. Life skills education should be offered and should cover practical life skills such as parenting (where appropriate); vocational evaluation, financial management, negotiating access to services, stress management and coping skills; and personal image building.
Educational Training and Remediation Services
- Educational training and remediation services should be provided, with on-site provision of or case-managed linkages to local education/GED programs and other remediation issues identified at intake.
- English language competency and literacy assessment programs should be facilitated.
- Job counseling and training should be provided, if possible, via case managed/coordinated linkages to community programs.
Transportation. Transportation to programs is needed to access treatment and related community services.
Housing. Access to safe, drug-free housing throughout treatment is all-important.
Childcare Services. Age-appropriate care of infants and children should be provided at treatment facilities using a developmental model. Respite care should also be available. If space or licensing requirements prohibit on-site care, contractual arrangements with local licensed childcare providers should be provided.
Continuing Care. Continuing Care should be provided, planned for, and should include sustained and frequent interaction with recovering individuals who have graduated from the intensive or primary phase of treatment.
- Provision should be made for graduate re-admission to more intensive forms of therapy in cases where relapse has occurred.
- As women complete the intensive phase of treatment and move into the community, the effects of domestic violence, rape, and childhood sexual abuse must be addressed over time. A plan for "safety" must be developed.
- Socioeconomic issues (e.g., jobs/educational deficits) require long-term remedies and must be included in relapse prevention planning.
- Public assistance and housing must be addressed in the continuing care plan.
- Ongoing transportation assistance must be provided for attendance at self-help groups (AA, NA, and other support meetings).
- Continuing provision of primary healthcare services and medical assistance as needed for women and children.
Appendix C. Key Federal Programs Funding Substance Abuse and Child Welfare Services and Research
Substance Abuse Treatment Funding
Nationally, mental health, alcohol, and drug abuse treatment expenditures were $79.3 billion, or 8.1 percent of the $942.7 billion in total health care expenditures in 1996, with $12.6 billion spent on treatment for alcohol and other drug abuse (AOD). This represents a 10 percent decrease from 1986, when mental health, alcohol, and drug treatment expenditures were 9.0 percent of national health expenditures.
Since 1986, the average annual growth rate for all health care expenditures has been 8.3 percent, while the average annual growth rate of expenditures for alcohol and other drug abuse diagnoses has been 7.0 percent.
Public funding for substance abuse treatment grew from 53 percent of total substance abuse expenditures in 1986 to 63 percent in 1996. This was countered by a decreasing share of expenditures paid out-of-pocket, while private insurance payments remained relatively constant during this period.
Federal dollars, including the Federal portion of Medicaid, Medicare, DOD, VA, and the Substance Abuse Prevention and Treatment (SAPT) Block Grant, paid for 31 percent of national expenditures on AOD treatment in 1996. State and local contributions to AOD treatment expenditures were approximately equivalent at 31.5 percent.
SAMHSA's Center for Substance Abuse Treatment (CSAT) is the lead Federal Agency for substance abuse treatment, with responsibility for management of the $1.4 billion SAPT Block Grant. The SAPT Block Grant is is the cornerstone of the States' substance abuse programs, accounting for about 40% of the public funds expended for treatment and prevention. This is a formula-driven grant, and it includes several mandatory distributions and set-asides for allocations made to the States:
- 35% must be used for ALCOHOL prevention and treatment activities;
- 35% must be used for OTHER DRUG prevention and treatment activities;
- 20% must be used for prevention activities (estimated at $262 million for 1998);
- 2% - 5% must be spent on AIDS-related drug abuse programs in States with AIDS case rate of 10 per 100,000 population (reported at $53 million for latest year available);
- States must spend from their allocation an amount "equal to fiscal year 1994 spending levels" on programs for pregnant women and women with dependent children (reported at $195 million for latest year available); and,
- up to 5% of a State's allocation may be used for State administration (maximum of approximately $62 million in 1998).
Federal funding for public treatment facilities, as reported on the block grant applications, ranges from 11%-84% of all funding being used for substance abuse treatment.
In 1997, nineteen States received the majority of their funding for support of substance abuse treatment services from the SAPT Block Grant.
Over 7,000 Community Based Organizations (CBOs) receive SAPT Block Grant funding.
It is estimated that the FY 1998 SAPT Block Grant funding supported treatment for approximately 300,000 drug-abusing persons. While estimates for the number of persons served who only abuse alcohol are not available, it can be estimated that approximately $500 million of the total SAPT Block Grant must be spent on alcohol prevention and treatment programs.
CSAT's other primary funding category, the Knowledge Development and Application Program, provides support for a wide variety of grants to States and other treatment entities in an effort to continually improve the quality of services, implement best practices, and expand service capacity. For example, in 1998, this initiative provided continuation funding of approximately $82 million for current programs, such as Residential Treatment for Women and Children, Starting Early Starting Smart (SESS) jointly funded by CSAP and CMHS, Supplemental awards for Children's Services, Criminal Justice, Managed Care and Vulnerable Populations, Wrap Around Services, Recovery Networks, Target Cities, Rural Remote and Culturally Distinct, Addiction Technology Centers, and others. CSAT also provided funding for the following new programs in 1998:
- $23.7 million for forty-one Targeted Capacity Expansion grants, which focus on providing a clinically appropriate range of services, reducing service gaps and reducing drug use and abuse by under-served populations. Approximately 35% of the grants that were awarded are targeted to addicted women and their children.
- $8.5 million for fifteen Women and Violence grants (jointly funded with CSAP and CMHS) for studies targeting women, age 18 and above, with co-occurring disorders, who have histories of physical and/or sexual abuse. If the targeted women are mothers, their dependent children will also be included.
- $3.7 million for nineteen Recovery Community Support Program (RCSP) grants to State, provider, and community-based organizations for enhancing development of substance abuse treatment programs in 15 States.
- $3 million for eight Methamphetamine Treatment Program grants to test replicability and cost-effectiveness of specific non-residential programs for treatment of methamphetamine abuse. This program will contribute to the development of knowledge on methamphetamine treatment and will help support needed treatment in communities impacted by increasing methamphetamine addiction.
- Approximately $4.4 million for other new grant support in FY 98 knowledge development activities that include women, such as those targeted to Adolescents, Elderly, and Substance Abusing Women Eligible for Temporary Assistance to Needy Families.
Child Welfare Funding
With an annual budget of nearly $5 billion, the Children's Bureau works with State and local agencies to develop programs to assist America's children and their families.
The Children's Bureau administers nine state grant programs and six discretionary grant programs. The state grant programs have their own legislatively mandated matching requirements and formulas for allocation and all require that the funds go to and be administered only by the State child welfare agency or, in some programs, Indian Tribes or Tribal organizations. The State agency can have agreements and contracts with other public agencies and with private agencies for provision of appropriate services. In the discretionary programs, the Administration for Children and Families policy requires a match from the grantees for all discretionary grant projects other than research.
The vast majority of Federal child welfare funding is spent on Title IV-E Foster Care and Adoption Assistance payments to States (described below). Most of the remainder goes to States in the form of the Child Welfare Services Block Grant (Title IV-B part 1) and the Promoting Safe and Stable Families (Title IV-B part 2) formula grant program. Several small discretionary grant programs, described below, provide demonstration funds to State and local agencies and other organizations for innovative child welfare activities.
State Grant Programs
The Title IV-E Foster Care program provides funds to States to assist with: the costs of foster care maintenance for eligible children; administrative costs to manage the program; and training for staff, for foster parents and for private agency staff. The purpose of the program is to help States provide proper care for children who need placement outside their homes, in a foster family home or an institution. Nearly $4 billion will be spent for these purposes in FY1999.
The Title IV-E Adoption Assistance Program provides funds to States to assist in paying maintenance costs for adopted children (AFDC or SSI eligible) with special needs, e.g., children who are older or handicapped. Funds are also used for the administrative costs of managing the program and training staff. The goal of this program is to facilitate the placement of hard to place children in permanent adoptive homes and thus prevent long, inappropriate stays in foster care. This program is expected to provide approximately $869 million to States in FY1999.
The Independent Living Program provides services to foster children who are 16 years or older to help them to make the transition to independent living by helping them earn a high school diploma or receive vocational training, receive training in daily living skills such as budgeting, locating housing, career planning and job finding; or otherwise make the transition to independent living. $70 million will be spent on the Independent Living program in FY1999.
The Safe and Stable Families Program (formerly called the Family Preservation and Support Services Program) encourages and enables "each State to develop and establish, or expand, and to operate a program of family preservation services and community based family support services." Family preservation services typically are activities to assist families in crisis, often families where a child is at imminent risk of being placed in out-of-home care because of abuse and/or neglect. Family support services are primarily preventive activities with the aim of increasing the ability of families to successfully nurture their children, most often provided at the local level by community-based organizations. This program will in FY1999 provide $275 million to States for these efforts.
The Child Welfare Services Program helps State public welfare agencies improve their child welfare services with the goal of keeping families together. State services include preventive intervention, so that, if possible, children will not have to be removed from their homes; services to develop alternative placements like foster care or adoption if children cannot remain at home; and reunification so that children can return home if at all possible. The funding level for this program has been stable at $292 million for a number of years.
Basic State Grants provide assistance in developing, strengthening, and implementing child abuse and neglect prevention and treatment programs. Eligible states must have established the following: a mandatory reporting law; procedures for the prompt investigation of reports; provisions to provide emergency services to protect reported children; provisions for immunity from prosecution for reporters; an assurance that a guardian ad litem is appointed in judicial proceedings to represent and protect the rights and best interests of the child; a system of preventive and treatment services and related multi-disciplinary programs and services; and a process in which reports and records are kept confidential and in which unauthorized disclosure is a criminal offense. States must also have programs and/or procedures in place to respond to reports of medical neglect, including instances of withholding medically indicated treatment from disabled infants with life threatening conditions. In FY1999, $21 million will be awarded participating States and Territories.
Community-Based Family Resource Program Grants are provided to States to develop and implement, or expand and enhance, a comprehensive, statewide system of community-based family resource services. To receive these funds, states must have established or maintained a trust fund or other funding mechanism that pools Federal, state, and private funds and makes them available for child abuse and neglect prevention and family resource programs. In FY1999, participating jurisdictions will receive grants totaling $33 million.
Children's Justice Act Programs help States to develop, establish, and operate programs designed to improve the investigation and prosecution of child abuse and neglect cases, particularly cases of child sexual abuse and exploitation, in a manner which reduces additional trauma to the child; and to improve the handling of cases of suspected child abuse or neglect related fatalities. Funds for this program are allocated from the Department of Justice's Victims of Crime Fund. FY1999 grants will total $8.5 million.
Discretionary Grant Programs
The Adoption Opportunities Program eliminates barriers to adoption and helps to find permanent families for children who would benefit by adoption, particularly children with special needs. The five major program areas, as mandated by the legislation, are: (1) the development and implementation of a national adoption and foster care data gathering and analysis system; (2) the development and implementation of a national adoption information exchange system; (3) the development and implementation of an adoption training and technical assistance program; (4) increasing the placements in adoptive families of minority children who are in foster care and have the goal of adoption with a special emphasis on recruitment of minority families; and (5) post-legal adoption services for families who have adopted children with special needs. A total of $25 million will be distributed through this program in FY1999.
The Child Welfare Training Program upgrades the skills and qualifications of child welfare workers through their participation, full-time or part-time, in programs focused specifically on child welfare services. Discretionary grants are awarded to public and private non-profit institutions of higher learning to develop and improve education/training programs and resources for child welfare service providers. The FY1999 funding level for these activities is $7 million.
The Child Welfare Research and Demonstration Program strengthens the family as the primary agent responsible for the developmental needs of children and youth. The Administration for Children, Youth and Families funds research, demonstration, dissemination, utilization and technical assistance activities in four basic areas: child welfare, child care, youth development, and child and family development. The resources budgeted for these four areas address the needs and problems confronting some of the most vulnerable children and families in the country: children in foster care, children in need of adoptive homes, children from poor families who require child care, and vulnerable youth who are runaways or homeless. No funds have been appropriated for this program since Fiscal Year 1995.
The Abandoned Infants Assistance Program is intended for development, implementation and operation of projects to demonstrate how to (1) prevent abandonment; (2) identify and address needs of abandoned infants, especially those with AIDS; (3) assist these children to reside with their natural families if possible, or in foster care; (4) recruit, train and retain foster parents; (5) carry out residential care programs for abandoned children and children with AIDS; (6) establish programs of respite care for families and foster families; (7)recruit and train health and social services personnel to work with families, foster families and residential care staff. Grants are made to public and nonprofit private entities. This program has enjoyed stable funding of $12.25 million per year for a number of years.
The Child Abuse Prevention & Treatment Act Research and Demonstration Projects are funds which support research on the causes, prevention, and treatment of child abuse and neglect; demonstration programs to identify the best means of preventing maltreatment and treating troubled families; and the development and implementation of training programs. Grants for these projects are provided nationwide on a competitive basis to state and local agencies and organizations. Projects have focused on every aspect of the prevention, identification, investigation, and treatment of child abuse and neglect. In FY 1999, approximately $14.2 million in discretionary funds will be awarded to support new and continuing research and demonstration grants, as well as evaluation, technical assistance and information dissemination activities.
Alcohol and Other Drug Research
The National Institute on Drug Abuse (NIDA) and the National Institute on Alcoholism and Alcohol Abuse (NIAAA) each conduct research on a variety of substance abuse topics, including basic research and studies of epidemiological, clinical, prevention, and services aspects of alcohol and illicit drug abuse and addiction.
Among NIDA's activities is a program of research on the health and development of children whose parents abuse illicit drugs. This effort is based on the following principles. Parental substance abuse had the potential to influence the development and the health of infants and children in many ways, via direct effects (e.g., prenatal drug exposure, postnatal passive drug exposure) and via indirect effects associated with drug abuse. Some of these indirect effect may be very specific (e.g., transmission of HIV from mother to infant) and some may be complexly interwoven (e.g., violence in the home and community and dysfunctional parenting associated with substance abuse). Outcomes of interest range from fetal development to infant and child developmental functioning, to vulnerability to drug abuse among these children and adolescents.
NIAAA supports a range of research on the etiology, prevention and treatment of alcohol-related family problems through two programs: one addressing alcohol-related violence, the other focusing on child development and family dynamics in alcohol-abusing families. Studies address both the direct and indirect effects of alcohol on developmental processes and on outcomes ranging from fetal alcohol syndrome to heightened vulnerability to alcohol-related problems over the life course.
