The Mental Health of Vulnerable Youth and their Transition to Adulthood: Examining the Role of the Child Welfare, Juvenile Justice, and Runaway/Homeless Systems
August 2009
Additional information regarding this study can be obtained from the Federal Project Officers: Flavio Menascé (202-260-0384, Flavio.Menasce@hhs.gov), and Lisa Trivits (202-205-5750, Lisa.Trivits@hhs.gov).
The Research Brief is available on the Internet at:http://aspe.hhs.gov/hsp/09/YouthMentalHealth/Services/rb.shtml
Printer friendly version in PDF format (22 pages)Free PDF reader 
Contents
- Introduction
- Key Research Questions
- Methodology
- Analysis
- Key Findings
- Question 1: What percentage of youth have contact with multiple service systems?
- Question 2: What is the mental health status of youth who come into contact with service systems or who are at risk of having contact with service systems as they transition to adulthood?
- Question 3: How does the mental health of youth affect their experience as they transition to adulthood?
- Question 4: Do youth who have contact with service systems have different outcomes as they transition to adulthood, compared to youth at low risk for contact?
- Question 5: For youth, does involvement with any public service system increase the likelihood of receiving mental health services?
- Question 6: Does involvement in multiple public service systems increase the likelihood of receiving mental health services?
- Conclusion
Introduction
Adolescence and the transition to adulthood is a period marked by significant changes and new challenges. This transition is difficult for many adolescents as research has shown that approximately five to seven percent of young people fail to successfully transition to independent adulthood by the age of 25.
There is also still much to be learned about the mental health of adolescents as they transition into adulthood. For many adolescents, the presence of mental health disorders makes the successful transition to adulthood even more difficult. Youth who do not successfully transition impose significant social costs on society through criminal activity, loss of productivity, and the increased use of expensive social services. Despite the significance and prevalence of this issue, policymakers and researchers have not been particularly attentive to this population of young people as they transition to adulthood.
A population of particular interest is youth who have had contact with service systems. These youth tend to experience negative outcomes, such as behavior problems and academic failure. This study has as a particular focus on the mental health of vulnerable youth who have been in contact with service systems, including child welfare, juvenile justice, and runaway and homeless programs. Although these service systems are not generally viewed as mental health programs, many children and adolescents who have come in contact with these services either require, or have obtained mental health services through them.
This vulnerable population is a small group of adolescents who are hard to serve and who, without the proper intervention, may experience negative outcomes during adolescence and the transition to adulthood. Compounding this issue is the fact that many of these youth are being served by multiple service systems in largely uncoordinated systems of care. As a result, success in school and the workforce, the ability to achieve a supportive, independent living situation, and obtaining continuity of care for mental health needs during the transition to adulthood are particularly challenging.
[ Go to Contents ]
Key Research Questions
This study considered six key research questions.
- What percentage of youth have contact with multiple service systems (i.e., child welfare, juvenile justice, and homeless/runaway service systems)?
- What is the mental health status of youth who came into contact with service systems or who were at risk of having contact with service systems prior to age 18 as they transition to adulthood? (This is in comparison to the mental health of youth without contact.)
- How does the mental health of youth affect their experience as they transition to adulthood?
- Do youth who have contact with service systems have different outcomes as they transition to adulthood, compared to youth at low risk for contact? (Here, outcomes refer to typical experiences which young adults go through as they enter early adulthood, such as maintaining employment, being in school, or obtaining a credit card.)
- Does involvement with any public service system increase the likelihood of receiving mental health services?
- Does involvement in multiple public service systems increase the likelihood of receiving mental health services?
[ Go to Contents ]
Methodology
Data Source
Data for this project come from the National Longitudinal Study of Adolescent Health (Add Health). The Add Health is a nationally representative study that was designed to examine the causes of health-related behaviors of adolescents in grade 7 through 12 and their outcomes in young adulthood (Udry, 2003). More specifically, the Add Health was designed to enable researchers to examine how social contexts, including families, peers, schools, neighborhoods, and communities, influence the health and risk behaviors of youth as well as their subsequent outcomes during their transition to adulthood (Harris et al., 2003).
A sample of 80 high schools and 52 middle schools across the United States was selected using systematic sampling methods and stratification to ensure that the sample was representative of U.S. schools with respect to U.S. region, urbanicity, school size, school type, and ethnicity (Harris et al., 2003). Study participants were interviewed in three Waves from 1996 to 2002. Wave 1 occurred in 1994, when youth were in grades 7 through 12. Wave 2, occurring in 1996, included all study participants except those who were in 12th grade at Wave 1. Wave 3 included all participants interviewed at Wave 1, and took place in 2001-2002 when study participants were between the ages of 18 and 26 years of age.
Given the complex sampling design of the Add Health, the analytic sample for this current study was limited to participants who completed an interview at Waves 1 and 3 and who have a valid population weight for these Waves. Based on these criteria, the number of Wave 1 respondents lost to follow-up was 4,600. Therefore, the Full Sample includes the Wave 1 - Wave 3 sample (N=14,322). Limiting the data in this manner allows for weighted estimates of the associations of interest, capitalizing on the representativeness of the data.
Differences in demographic characteristics, mental health characteristics, and contact with the social service and juvenile justice systems were examined between the analytic sample and those lost to follow-up. Slightly more males, Hispanic and non-Hispanic Black respondents, youth who were living with a single parent or only one biological parent, and those who are foreign born were more likely to be lost to follow-up at Wave 3, as were respondents whose parents had a high school diploma or less, or who lived below the poverty line. It is important to note, however, that the vast majority (98%) of vulnerable youth who had come in contact with a social service or juvenile justice system was followed-up over time, and few differences were found in the mental health characteristics between those in the analytic sample and individuals lost to follow-up.
Defining Contact with Service Systems
Although there are numerous systems with which vulnerable youth may come in contact, this study utilized three sources of service system contact: child welfare services (CWS), the juvenile justice system, and homeless shelters/group homes. Each construct is described briefly below.
- Child Welfare Services: Adolescents were considered to have contact with child welfare services if they lived with a foster parent or were removed from their home by child protective services (CPS) prior to age 18.
- The Juvenile Justice System: Adolescents were considered to have contact with the juvenile justice system if they were arrested prior to age 18.
- Homeless Shelters/Group Homes: Adolescents were considered to have contact with these services if they reported staying in either a homeless shelter or group home at any point prior to the Wave 3 interview.
Sample Distribution by Level of Risk
Our sample can be divided into three levels of risk of coming into contact with the service systems described above:
- System contact (n=1,380)
- Youth with actual system contact made up 9.6% of the full sample.
- At-risk, but no contact (n=5,013)
- Youth at risk of coming into contact with service systems, but who did not have contact, made up 35.0% of the full sample.
- This includes youth who did not have contact with any service system, but did meet the at-risk criteria for at least one service system. For example, a youth at risk for child welfare contact may have been investigated by social services, but was not removed from the home. A youth at risk for juvenile justice system contact may have committed an illegal act, but was not arrested. Finally, a youth at risk for coming into contact with a homeless shelter or group home may have run away from home, but did not actually have contact with a homeless shelter or group home.
- Low risk and no contact (n=7,929)
- Youth at low risk of coming into contact with service systems, but who did not have contact, made up 55.4% of the full sample.
- This includes all other youth who did not have contact with any service system and were not at risk for contact, as defined above.
Measuring Contact with Service Systems
Youths contact with the service systems was measured in three different ways: a dichotomous measure of contact, a summary measure of the total number of system contacts, and a three-level variable examining the type of system contact. Each is described in more detail below.
- Any System Contact: Adolescents were considered to have any system contact if they met the contact criteria for any of the service systems. This is a dichotomous measure (yes/no) of those who had any service system contact.
- Number of System Contacts: This is a summary measure, ranging from 0 contacts to 2 or more contacts, that indicates the number of service systems youth had contact with.
- Type of System Contact: This was a 3-level variable looking at the type of system contact youth had, identified as child welfare services, juvenile justice system, or homeless shelters/group homes. It is important to note, however, that this measure is not mutually exclusive because youth could have been involved with more than one service system.
Type of Contact by Level of Risk
Here we describe the breakdown of each type of service system by level of risk. As mentioned previously, the full sample can be divided into three levels of risk: 1) System contact; 2) At-risk, but no contact; and 3) Low risk and no contact. Additionally, the three service systems examined in this study are child welfare services, juvenile justice system, and homeless shelter/group homes.
Child Welfare Services
- System contact (n=480; 3.1%)
- At-risk, but no contact (n=622; 4.3%)
- Youth whose families were investigated by social services, but that were not removed from the home.
- Low risk and no contact (n=13,220; 92.3%)
- Youth whose families were not investigated by social services.
Juvenile Justice
- System contact (n=608; 5.1%)
- At-risk, but no contact (n=4,811; 33.6%)
- Youth who reported committing at least one illegal act at Waves 1 or 2, but were not arrested.
- Low risk and no contact (n=8,903; 62.2%)
- Youth who did not commit an illegal act.
Homeless Shelter/Group Home
- System contact (n=493; 3.7%)
- At-risk, but no contact (n=2,135; 14.9%)
- Youth who reported running away from home, but did not have contact with a homeless shelter or group home.
- Low risk and no contact (n=11,694; 81.7%)
- Youth who did not report running away from home or residing in a homeless shelter or group home.
Defining Mental Health Issues of Adolescents and Young Adults
This study utilized information on five mental health issues particularly relevant to the population of vulnerable youth, and available within the Add Health dataset. These include: depressive symptoms, suicide ideation and attempts, delinquency (as an approximation of conduct disorder), alcohol use, and illicit drug use. All measures of mental health were drawn from Wave 3 of the survey. Depressive symptoms were measured using the CES-D depressive symptom scale, asking youth to report about symptoms over the last twelve months. Suicide ideation and attempts were measured by asking youth whether they had thought about committing suicide and, if so, whether they had made a suicide attempt. Delinquency was used here as an approximation of conduct disorder and was measured by asking youth to report on 9 items related to stealing, selling drugs, and trespassing on private property. Alcohol use and illicit drug use (including marijuana) were measured based on the extent to which they interfered with activities of daily life. For this study, depressive symptoms and suicide ideation and attempts were combined to create a single indicator of depressive symptoms.
Defining Mental Health Service Utilization
We examined the utilization of two types of mental health services: psychological or emotional counseling; and drug or alcohol abuse treatment. At each Wave youth were asked to report whether they had received psychological or emotional counseling, and at Wave 3 youth were asked whether they had spent a day in a facility for treatment of a mental illness. In addition, at each Wave youth were asked whether they had been involved in a drug or alcohol abuse treatment program, and at Wave 3 youth were asked specifically about involvement in a 12-step recovery group or program.
[ Go to Contents ]
Analysis
Profile Analyses for the Full Sample
This study used latent class analysis (LCA) in Mplus to examine mental health profiles among our sample. LCA places individuals with similar mental health characteristics into homogeneous groups, or profiles. Indicators included depressive symptoms, alcohol interference, drug interference, and delinquency, all of which were obtained at Wave 3, when youth were ages 18-26. We used dichotomous measures reporting any vs. none.
In the analyses of the full sample, LCA resulted in the creation of five profiles of mental health and related behaviors for youth during the transition to adulthood:
- Non-troubled youth;
- Depressed youth;
- Depressed and Delinquent Plus youth;
- Alcohol Interference youth; and
- Troubled youth.
Below we describe the analyses of the 5-profile solution for the Any vs. None mental health and related behaviors variables for the full sample. Figure 1 graphically displays the profiles of the mental health and related behaviors for the full sample.
Figure 1.Five-class profile analyses for youth exhibiting any vs. none of the mental health and related behaviors by most likely class membership Profiles of Mental Well-being in Full Sample
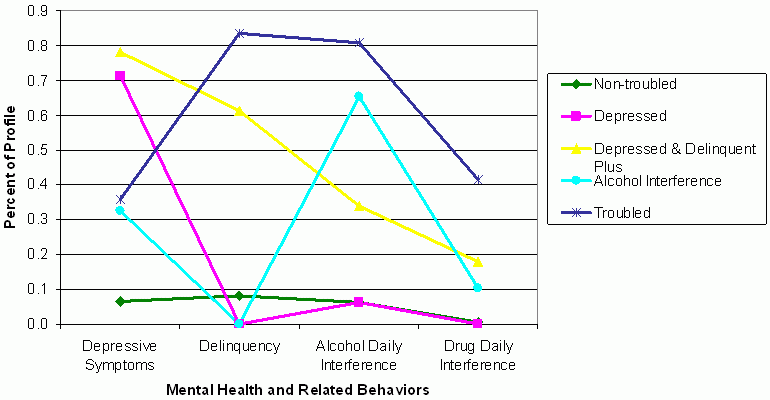
Non-troubled youth are represented by the green line along the bottom of the figure. Non-troubled youth comprised 31.7% of the sample and consisted of youth who were, on average, not experiencing depressive symptoms, and not engaging in delinquent or life-interfering substance use. Depressed youth are represented by the pink line. Depressed youth made up 23.8% of the sample and consisted of youth who were, on average, exhibiting depressive symptoms (71.2%), but had no other major issues. Depressed and Delinquent Plus youth are represented by the yellow line. Depressed and Delinquent Plus youth comprised 11.1% of the sample and consisted of youth who were, on average, exhibiting depressive symptoms (78.2%), were engaging in delinquent behaviors (61.4%), and reported daily interference from alcohol (33.9%) and drugs (18.0%). Since some of these youth also reported daily interference from alcohol and drugs, they are called Depressed and Delinquent Plus. Alcohol interference youth are represented by the teal line. Alcohol Interference youth comprised 17.6% of the sample and consisted of youth who were, on average, reporting alcohol daily interference (65.3%) and about a third reported depressive symptoms (32.5%). Troubled youth are represented by the dark blue line and were elevated on all four dimensions. Troubled youth comprised 15.7% of the sample and consisted of youth who, on average, were exhibiting depressive symptoms (35.8%), delinquent behaviors (83.4%), and reported daily interference from alcohol (80.8%) and drugs (41.5%).
The table below provides another way of visualizing the probabilities of mental health and related behaviors of the five profiles in the full sample.
| Non-Troubled Youth | Depressed Youth | Depressed & Delinquent Plus Youth | Alcohol Interference Youth | Troubled Youth | |
| Percent of Sample | 31.7% | 23.8% | 11.1% | 17.6% | 15.7% |
| Size | N=3,815 | N=2,863 | N=1,337 | N=2,115 | N=1,892 |
| Mental Health and Related Behaviors | % | % | % | % | % |
| Depressive Symptoms | 6.5% | 71.2% | 78.2% | 32.5% | 35.8% |
| Delinquency | 8.1% | 0.0% | 61.4% | 0.0% | 83.4% |
| Alcohol Daily Interference | 6.1% | 6.1% | 33.9% | 65.3% | 80.8% |
| Drug Daily Interference | 0.5% | 0.0% | 18.0% | 10.3% | 41.5% |
Profile Analyses for the Service System Sample
Using the same indicators of mental health and related behaviors, we also ran latent class analysis (LCA) on the service system sample alone. This sample includes youth who have had contact with a service system (N=1,380). LCA resulted in the creation of four profiles of mental health and related behaviors for youth during the transition to adulthood:
- Depressed youth;
- Depressed and Delinquent Plus youth;
- Alcohol Interference and Depressed youth; and
- Troubled youth.
It is important to note that a Non-Troubled profile did not emerge in the service system only sample. Below we describe the analyses of the 4-profile solution for the Any vs. None mental health and related behaviors variables for the service system sample. Figure 2 graphically displays the profiles of the mental health and related behaviors for the service system sample.
Figure 2.Four-class profile analyses for youth exhibiting any vs. none of the mental health and related behaviors by most likely class membershipProfiles of Mental Well-Being in Service System Sample
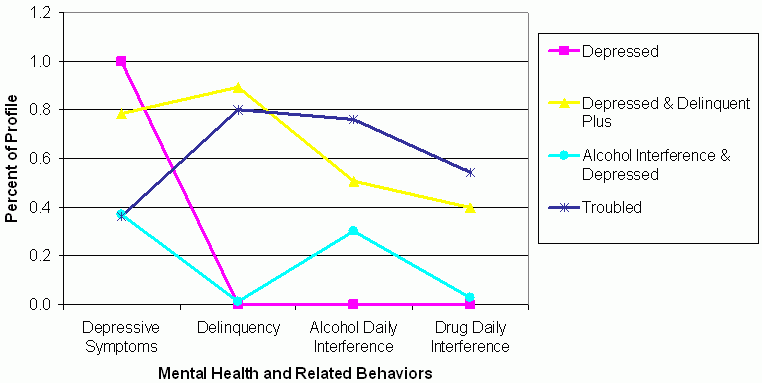
Depressed youth are represented by the pink line. Depressed youth comprised 8.0% of the sample and included youth who were, on average, exhibiting depressive symptoms (100.0%), and no other behaviors. Depressed and Delinquent Plus youth are represented by the yellow line. Depressed and Delinquent Plus youth comprised 30.7% of the sample and consisted of youth who were, on average, exhibiting depressive symptoms (78.6%), were engaging in delinquent behaviors (89.3%), and reported daily interference from alcohol (50.7%) and drugs (39.9%). Since some of these youth also reported daily interference from alcohol and drugs, they are called Depressed and Delinquent Plus. Alcohol Interference and Depressed youth are represented by the teal line. Alcohol Interference and Depressed youth comprised 34.9% of the sample and consisted of youth who were, on average, reporting alcohol daily interference (30.4%) and depressive symptoms (37.1%). Troubled youth are represented by the dark blue line and were elevated on all four dimensions. Troubled youth comprised 26.3% of the sample and consisted of youth who, on average, were exhibiting depressive symptoms (36.1%), delinquent behaviors (80.2%), and reported daily interference from alcohol (76.2%) and drugs (54.3%).
The table below provides another way of visualizing the probabilities of mental health and related behaviors of the four profiles in the service system sample.
| Depressed Youth | Depressed & Delinquent Plus Youth | Alcohol Interference & Depressed Youth | Troubled Youth | |
| Percent of Sample | 8.0% | 30.7% | 34.9% | 26.3% |
| Size | N=85 | N=325 | N=370 | N=279 |
| Mental Health and Related Behaviors | % | % | % | % |
| Depressive Symptoms | 100.0% | 78.6% | 37.1% | 36.1% |
| Delinquency | 0.0% | 89.3% | 1.3% | 80.2% |
| Alcohol Daily Interference | 0.0% | 50.7% | 30.4% | 76.2% |
| Drug Daily Interference | 0.0% | 39.9% | 2.9% | 54.3% |
Profile Analyses for the Combined Service System and At-risk Sample
Finally, we conducted profile analyses for a subgroup comprised of both the service system and at-risk samples. These analyses enabled us to examine the mental health profiles of a group of more vulnerable youth relative to the full sample. Using the same indicators of mental health and related behaviors, we ran latent class analysis (LCA) on the combined service system and at-risk sample. This sample includes youth who have had contact with a service system and those at-risk for contact, N=6,393. LCA resulted in the creation of five profiles of mental health and related behaviors for youth during the transition to adulthood:
- Depressed and Delinquent youth;
- Depressed and Delinquent Plus youth;
- Depressed youth with Alcohol Interference;
- Alcohol Interference youth; and
- Troubled youth.
It is important to note that a Non-Troubled profile did not emerge in the combined service system and at-risk sample and that a new profile, Depressed and Delinquent youth, emerged. Furthermore, with this sample, two profiles emerge that have a high likelihood of experiencing multiple issues: the Troubled profile and the Depressed and Delinquent Plus profiles. Although the percent of youth experiencing each mental health issue in the Depressed and Delinquent Plus is as high or higher than the Troubled youth, the profile names remain consistent with the profile patterns from the previous samples in order to maintain consistency.
Below we describe the analyses of the 5-profile solution for the Any vs. None mental health and related behaviors variables for the service system and at-risk sample. Figure 3 graphically displays the profiles of the mental health and related behaviors for the combined service system and at-risk sample. In examining the service system only sample and the combined service system and at-risk sample, we found a similar pattern from the full sample. The profile patterns hold true or similar across the three different samples.
Figure 3.Five-class profile analyses for youth exhibiting any vs. none of the mental health and related behaviors by most likely class membershipProfiles of Mental Well-Being in Combined Service System and At-Risk Sample
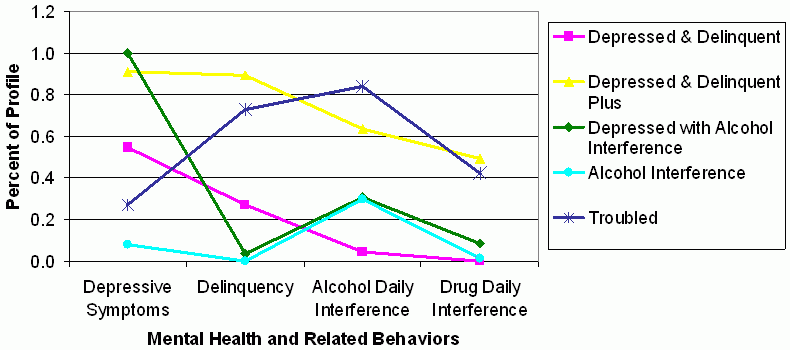
Depressed and Delinquent youth are represented by the pink line. Depressed and Delinquent youth comprised 21.5% of the sample and included youth who were, on average, exhibiting depressive symptoms (54.7%), delinquent behaviors (27.0%), and a small percentage reported alcohol daily interference (4.6%). Depressed and Delinquent Plus youth are represented by the yellow line. Depressed and Delinquent Plus youth comprised 14.7% of the sample and consisted of youth who were, on average, exhibiting depressive symptoms (91.0%), were engaging in delinquent behaviors (89.4%), and reported daily interference from alcohol (63.7%) and drugs (49.4%). Since some of these youth also reported daily interference from alcohol and drugs, they are called Depressed and Delinquent Plus. Depressed youth with Alcohol Interference are represented by the green line. Depressed youth with Alcohol Interference comprised 13.0% of the sample and consisted of youth who were, on average, reporting depressive symptoms (100.0%) and alcohol daily interference (30.7%). Alcohol Interference youth are represented by the teal line. Alcohol Interference youth comprised 25.0% of the sample and consisted of youth who were, on average, reporting daily interference from alcohol (29.9%), and only a minor amount reported depressive symptoms (7.8%). Troubled youth are represented by the dark blue line and were elevated on all four dimensions. Troubled youth comprised 25.8% of the sample and consisted of youth who, on average, were exhibiting depressive symptoms (27.1%), delinquent behaviors (73.1%), and reported daily interference from alcohol (83.9%) and drugs (42.1%).
The table below provides another way of visualizing the probabilities of mental health and related behaviors of the five profiles in the combined service system and at-risk sample.
| Depressed & Delinquent Youth | Depressed & Delinquent Plus Youth | Depressed Youth with Alcohol Interference | Alcohol Interference Youth | Troubled Youth | |
| Percent of Sample | 21.5% | 14.7% | 13.0% | 25.0% | 25.8% |
| Size | N=1,137 | N=776 | N=689 | N=1,322 | N=1,365 |
| Mental Health and Related Behaviors | % | % | % | % | % |
| Depressive Symptoms | 54.7% | 91.0% | 100.0% | 7.8% | 27.1% |
| Delinquency | 27.0% | 89.4% | 3.5% | 0.1% | 73.1% |
| Alcohol Daily Interference | 4.6% | 63.7% | 30.7% | 29.9% | 83.9% |
| Drug Daily Interference | 0.0% | 49.4% | 8.3% | 1.3% | 42.1% |
Additional Analyses
In addition to the profile analyses, we also conducted multivariate regression models to examine the concurrent relationship between the mental health profiles at Wave 3 with young adult outcomes at Wave 3, such as disconnection (i.e., not in school and not employed), receipt of public assistance, and credit card debt. We ran these multivariate regression models predicting to young adult outcomes with the full sample, service system sample, and the combined service system and at-risk sample. In addition, we examined the longitudinal relationship between these young adult outcomes and service system contact. All multivariate models included a detailed set of covariates including adolescent characteristics, family environment, peer influence and support, school environment, and county environment.
[ Go to Contents ]
Key Findings
Below, we review the key findings from the study. More detailed information and further results will be available in the technical report. In order to facilitate discussion of the key findings, it is helpful to refer back to the six key research questions presented on page 2.
Question 1: What percentage of youth have contact with multiple service systems?
Finding: Only 10% of the full sample had any contact with a service system. Of the youth who had any contact with a service system, roughly one in five had involvement with multiple service systems (i.e., two or more contacts). See Table 4 below.
| Frequency, (%) | |
| Full Sample | N=14,322 |
| Any System Contact | |
| Yes | 1,380 (10.2%) |
| No | 13,000 (89.8%) |
| Number of System Contacts | |
| 0 | 13,000 (89.8%) |
| 1 | 1,099 (8.2%) |
| 2+ | 281 (2.0%) |
Question 2: What is the mental health status of youth who come into contact with service systems or who are at risk of having contact with service systems as they transition to adulthood?
Findings: Based on the full sample, we found that youth who had contact with a service system compared to those youth who were at low-risk for contact were more likely to be in the Troubled youth profile, the Alcohol Interference youth profiles, the Depressed and Delinquent Plus youth profile, and the Depressed youth profile than in the Non-troubled youth profile. In addition, youth who were at-risk for contact with a service system compared to those youth who were at low-risk for contact were more likely to be in the Troubled youth profile, the Alcohol Interference youth profile, and the Depressed and Delinquent Plus youth profile than in the Non-troubled youth profile. See Table 5 below.
| Non-Troubled Youth | Depressed Youth | Depressed & Delinquent Plus Youth | Alcohol Interference Youth | Troubled Youth | |
| Percent of Sample | 31.7% | 23.8% | 11.1% | 17.6% | 15.7% |
| Size | N=3,815 | N=2,863 | N=1,337 | N=2,115 | N=1,892 |
| Service System Contact | % | % | % | % | % |
| Service System Contact | 8.6% | 20.0% * | 21.2% *** | 12.5% ** | 37.8% *** |
| At-risk for Contact | 19.1% | 18.3% | 12.6% *** | 21.1% ** | 28.9% *** |
| Note: Significance testing compared the non-troubled profile to the other mental health profiles. *p.05, **p.01, ***p.001 | |||||
Question 3: How does the mental health of youth affect their experience as they transition to adulthood?
Findings: Youth with poorer mental health during the transition to adulthood faced difficulty on other young adult experiences. The following tables present results from the full sample, though it is important to note that the findings from the service system sample and the combined service system and at-risk sample were very similar. For example, Depressed youth were 30% more likely to be disconnected (i.e., not in school and not employed) than Non-Troubled youth during the transition to adulthood. See Table 6 below.
| Full Sample N=14,322 | ||
| Profile Classification | OR | |
| Non-troubled youth | ref. | |
| Depressed youth | 1.3 | *** |
| Depressed and Delinquent Plus youth | 1.2 | |
| Alcohol Interference youth | 0.9 | |
| Troubled youth | 1.1 | |
| OR=odds ratio*p.05, **p.01, ***p.001 | ||
In addition, Depressed youth were 40% more likely to receive public assistance than Non-Troubled youth during the transition to adulthood. In contrast, Alcohol Interference youth and Troubled youth were 40% less likely to receive public assistance than Non-Troubled youth. See Table 7 below.
| Full Sample N=14,322 | ||
| Profile Classification | OR | |
| Non-troubled youth | ref. | |
| Depressed youth | 1.4 | * |
| Depressed and Delinquent Plus youth | 1.3 | |
| Alcohol Interference youth | 0.6 | * |
| Troubled youth | 0.6 | ** |
| OR=odds ratio*p.05, **p.01, ***p.001 | ||
Depressed and Delinquent Plus youth, Alcohol Interference youth, and Troubled youth reported more sexual partners than Non-Troubled youth. Therefore, mental health was related to the number of sexual partners, whereas contact with service systems was not. See Table 8 below.
| Full SampleN=14,322 | |||
| Profile Classification | B | SE | |
| Non-troubled youth | ref. | ref. | |
| Depressed youth | 0.0 | (0.1) | |
| Depressed and Delinquent Plus youth | 0.8 | *** | (0.2) |
| Alcohol Interference youth | 0.5 | *** | (0.2) |
| Troubled youth | 1.1 | *** | (0.1) |
| B=Beta, SE=standard error *p.05, **p.01, ***p.001 | |||
In addition, Alcohol Interference youth were 30% more likely than the Non-Troubled youth to have a credit card and debt. Depressed youth and Troubled youth were, respectively, 20% and 30% less likely to have a credit card and no debt than the Non-Troubled youth. In addition, the Depressed and Delinquent Plus youth were 30% less likely to have a credit card and debt than the Non-Troubled youth. See Table 9 below.
| Full Sample N=14,322 | No credit card, no debt | No credit card, has debt | Credit card, no debt | Credit card, has debt | ||
| Profile Classification | OR | OR | OR | OR | ||
| Non-troubled youth | ref. | ref. | ref. | ref. | ||
| Depressed youth | ref. | 0.8 | 0.8 | * | 0.9 | |
| Depressed and Delinquent Plus youth | ref. | 1.1 | 0.8 | 0.7 | * | |
| Alcohol Interference youth | ref. | 1.0 | 1.0 | 1.3 | ** | |
| Troubled youth | ref. | 1.1 | 0.7 | ** | 1.0 | |
| OR=odds ratio *p.05, **p.01, ***p.001 | ||||||
Question 4: Do youth who have contact with service systems have different outcomes as they transition to adulthood, compared to youth at low risk for contact?
Findings from the Full Sample: Those youth in contact with a public service system had harder experiences when transitioning to adulthood than those youth at low risk for contact. Tables 10 through 17 present results from the full sample, the service system sample, and the combined service system and at-risk sample. For example, youth who had been in contact with a service system were 80% more likely to be disconnected than youth at low risk for contact. Similarly, youth who were at-risk for contact, but had not had contact with a service system were 30% more likely to be disconnected than youth at low risk for contact. See Table 10 below.
| Full Sample N=14,322 | ||
| Service System Contact | OR | |
| Service System Contact | 1.8 | *** |
| At-risk for Contact | 1.3 | * |
| Low Risk for Contact | ref. | |
| OR=odds ratio *p.05, **p.01, ***p.001 | ||
In addition, youth who had been in contact with a service system were twice as likely to receive public assistance as youth at low risk for contact. See Table 11 below.
| Full Sample N=14,322 | ||
| Service System Contact | OR | |
| Service System Contact | 2.0 | *** |
| At-risk for Contact | 1.3 | |
| Low Risk for Contact | ref. | |
| OR=odds ratio *p.05, **p.01, ***p.001 | ||
Youth who had contact with a service system were 30% less likely to have a credit card, regardless of debt, compared to youth who were at low risk for contact with the service systems. See Table 12 below.
| Full Sample N=14,322 | No credit card, no debt | No credit card, has debt | Credit card, no debt | Credit card, has debt | ||
| Service System Contact | OR | OR | OR | OR | ||
| Service System Contact | ref. | 0.9 | 0.7 | * | 0.7 | *** |
| At-risk for Contact | ref. | 0.9 | 0.9 | 0.9 | ||
| Low Risk for Contact | ref. | ref. | ref. | ref. | ||
| OR=odds ratio *p.05, **p.01, ***p.001 | ||||||
Findings from the Service System Sample: Youth who had one contact with a service system were 60% more likely to attain a high school diploma than youth who had two or more contacts. See Table 13 below.
| Service System Sample N=1,380 | ||
| Service System Contact | OR | |
| One Contact with a Service System | 1.6 | * |
| Two or More Contacts with Service Systems | ref. | |
| OR=odds ratio *p.05, **p.01, ***p.001 | ||
In addition, youth who had one contact with a service system were 70% more likely to have attained a high school diploma and be in post-secondary school than youth who had two or more contacts. This outcome refers to those students who attained a high school diploma and are now enrolled in post-secondary school, such as college, vocational training, or trade school. See Table 14 below.
| Service System Sample N=1,380 | ||
| Service System Contact | OR | |
| One Contact with a Service System | 1.7 | ** |
| Two or More Contacts with Service Systems | ref. | |
| OR=odds ratio *p.05, **p.01, ***p.001 | ||
Findings from the Combined Service System and At-risk Sample: Youth who had not had contact with a service system and youth with one contact were 150% and 60%, respectively, more likely to attain a high school diploma than youth who had two or more contacts. See Table 15 below.
| Combined Service System & At-Risk Sample N=6,393 | ||
| Service System Contact | OR | |
| No Contact with Service Systems | 2.5 | *** |
| One Contact with Service Systems | 1.6 | * |
| Two or More Contacts with Service Systems | ref. | |
| OR=odds ratio *p.05, **p.01, ***p.001 | ||
In addition, youth who had not had contact with a service system and youth with one contact were 100% and 60%, respectively, more likely to attain a high school diploma and be in post-secondary school than youth who had two or more contacts. This outcome is referring to those students who attained a high school diploma and are now enrolled in post-secondary school, such as college, vocational training, or trade school. See Table 16 below.
| Combined Service System & At-Risk Sample N=6,393 | ||
| Service System Contact | OR | |
| No Contact with Service Systems | 2.0 | ** |
| One Contact with Service Systems | 1.6 | * |
| Two or More Contacts with Service Systems | ref. | |
| OR=odds ratio *p.05, **p.01, ***p.001 | ||
In addition, youth who had not had contact with a service system were 40% less likely to be disconnected than youth who had two or more contacts. See Table 17 below.
| Combined Service System & At-Risk Sample N=6,393 | ||
| Service System Contact | OR | |
| No Contact with Service Systems | 0.6 | ** |
| One Contact with Service Systems | 0.8 | |
| Two or More Contacts with Service Systems | ref. | |
| OR=odds ratio *p.05, **p.01, ***p.001 | ||
Question 5: For youth, does involvement with any public service system increase the likelihood of receiving mental health services?
Findings: Adolescents who had any service system contact were significantly more likely to report receiving counseling, with 13.4% reporting counseling in the 12 months prior to Wave 3. Of the youth at-risk for service system contact, 7.2% reported receiving counseling at Wave 3, while youth at low risk had the lowest rates of counseling at 6.6% at Wave 3. It is not known from these analyses whether youth who had a mental health need were more likely to receive counseling.
Youth who reported spending at least one day in a mental health facility varied greatly by level of service system contact. Over 7.0% of youth who had any contact with a service system reported spending a day in a mental health facility compared to 2.0% of those at-risk and close to 1.0% of those at low risk. Similar patterns are seen for drug abuse treatment and whether the youth was currently attending a 12-step program. When examined by service system contact, 7.0% of youth who had any service system contact reported undergoing treatment, compared to 3.2% of those at-risk, and 1.7% of those at low risk. See Table 18 below.
| Service System Contact N=1,380 | At-risk for Contact N=5,013 | Low Risk for Contact N=7,929 | |
| Characteristics | Frequency (%) | Frequency (%) | Frequency (%) |
| Psychological/emotional Counseling, Wave 3 | |||
| Yes | 185 (13.4%) | 363 (7.2%) | 462 (6.6%) |
| Ever spent a day in a mental health facility, Wave 3 | |||
| Yes | 101 (7.3%) | 98 (2.0%) | 78 (0.9%) |
| Drug/alcohol abuse treatment, Wave 3 | |||
| Yes | 117 (7.0%) | 129 (3.2%) | 113 (1.7%) |
| Currently attending a 12-step program, Wave 3 | |||
| Yes | 100 (7.3%) | 115 (2.2%) | 67 (0.8%) |
Question 6: Does involvement in multiple public service systems increase the likelihood of receiving mental health services?
Findings: Youth who had contact with multiple public service systems were more likely to have ever received mental health services in the four categories we investigated (i.e., (1) receiving psychological/emotional counseling, (2) having spent a day in a mental health facility, (3) receiving drug/alcohol abuse treatment, and (4) currently attending a 12-step program). The proportion of individuals receiving mental health services also increased as the number of service system contacts increased. See Table 19 below.
| No Contact N=12,942 | 1 Contact N=1,099 | 2+ Contacts N=281 | |
| Characteristics | Frequency (%) | Frequency (%) | Frequency (%) |
| Psychological/emotional Counseling, Wave 3 | |||
| Yes | 825 (6.8%) | 141 (12.7%) | 44 (16.4%) |
| Ever spent a day in a mental health facility, Wave 3 | |||
| Yes | 176 (1.3%) | 65 (6.5%) | 36 (10.3%) |
| Drug/alcohol abuse treatment, Wave 3 | |||
| Yes | 242 (2.3%) | 82 (5.5%) | 35 (13.2%) |
| Currently attending a 12-step program, Wave 3 | |||
| Yes | 182 (1.3%) | 76 (6.3%) | 24 (11.4%) |
[ Go to Contents ]
Conclusion
Summary of Key Findings and Implications
This study found that only a small proportion of the full sample, approximately 10%, had contact with at least one service system. In addition, youth who were in contact with service systems were more likely to report having ever received mental health services; yet, these youth had poor mental health. In fact, the Non-troubled mental health and related behaviors profile did not emerge for either the service system sample or the combined service system and at-risk sample. This suggests that enhanced mental health services may help these at-risk youth.
Youth who had contact with multiple service systems did not experience better outcomes related to the transition to adulthood. This suggests that communication and information sharing across service systems may improve the services that these youth receive. Information on the dosage and quality of the services youth receive is needed to better understand why these youth have poor outcomes. In addition, more research and longitudinal data is needed to examine the pathways through which services system contact may influence young adult outcomes.
There is also a sizable group of youth who are at risk for contact but have not been in contact with one of the service systems (about 35% of the full sample). These youth experienced poor mental health and poor outcomes during the transition to adulthood. Therefore, better screening procedures may help to identify and to provide assistance to these at risk youth.
Strengths and Limitations
This study has multiple strengths and limitations. One strength is that the study utilized a nationally representative sample of adolescents to examine the mental health of adolescents during the transition to adulthood. By using a nationally representative sample of adolescents, we were able to compare the mental health of youth who had contact with a service system with the mental health of youth who were designated at risk for contact with a service system, as well as youth who were at low risk for contact with a service system. A second strength of this study is that we examined the naturally occurring patterns of mental health and related behaviors (i.e., depressive symptoms, conduct, and drug and alcohol life interference) of youth during the transition to adulthood. Most of the previous research has examined each mental health domain in isolation. A third strength of the study is that we examined the relationship between service system contact and multiple outcomes during the transition to adulthood, net of a host of socio-demographic, family, school, and community characteristics.
Two key limitations of the study are that the measures of service system contact are self-reported and retrospective. It is possible that adolescents may under report their contact with a service system. For instance, youth who have been removed from their home by child welfare, but placed with a family member may not report that they have had contact with the child welfare system.
In addition, many of the measures of service system contact collected information on whether the adolescent had ever had involvement with the system. To create the measures of service system contact, we utilized information from all three rounds of data. As such, we were not able to determine the direction of causality. For instance, we found an association between service system contact and the use of mental health services. However, since both measures captured information across the rounds, we do not know if increased service system contact helped to gain access to mental health services or if being in mental health services initiated contact with a service system.
Furthermore, the measures of service system contact in this study do not capture the intensity or number of contacts the youth had with each system. For instance, a youth who only had contact with the child welfare system once was coded the same as a youth who may have had contact with the child welfare system multiple times. Capturing this level of contact was not possible within this dataset. In addition, we were not able to capture the nature of the contacts with the service system. Specifically, we could not measure anything about the quality of services that the youth received from the service systems.
Directions for Future Research
Listed below are directions for future research that may help to expand upon the findings discussed in this study of the mental health of vulnerable youth as they transition to adulthood. The analyses should be carried forward to Wave 4 of the Add Health in order to examine longer term effects of service system contact. In addition, the use of evidence-based practices, meaning practices based on methods that are shown to be effective, should be examined in order to enhance youth development for this population. For instance, several studies have demonstrated that practices such as long term mentors and engaging youth in program development and delivery enhance outcomes for at-risk youth.
Furthermore, we should explore how to identify a sequence of programs that are developmentally appropriate for this at-risk population as they age. The needs of these youth differ depending on their age. More work is needed to explore how to provide developmentally appropriate supports for each age group. For instance, school age children need social-emotional and homework support, whereas youth during the transition to adulthood need employment and social-network support.
Effective interventions for vulnerable youth with large effect sizes also need to be identified. Research based on experimental evaluations has demonstrated effective interventions for adolescents with large effect sizes such as Multidimensional Treatment Foster Care and Multisystemic Therapy (Child Trends, 2003, 2004). For instance, Multidimensional Treatment Foster Care has shown to decrease rates of incarceration, arrests, and drug use among adolescent youth with severe criminal behaviors by providing them with the skills and structure to modify their behavior (Child Trends, 2004). In addition, Multisystemic Therapy has shown to improve family correlates of antisocial behavior and decrease post-treatment criminal activity in a population of serious juvenile delinquents by incorporating youths families into an action-oriented and present-focused therapeutic method (Child Trends, 2003). Although these programs have shown to be effective, it is important to remember that they are based on small samples and that larger, nationally representative samples should be evaluated. Finally, more research is needed to develop and identify effective interventions to improve outcomes for vulnerable youth as they transition to adulthood.
References
Child Trends. (2003). Multisystemic therapy. In LINKS: Guide to Effective Programs for Children and Youth. Washington, DC: Child Trends.
Child Trends. (2004). Multidimensional Treatment Foster Care. In LINKS: Guide to Effective Programs for Children and Youth. Washington, DC: Child Trends.
Harris, K. M., Florey, F., Tabor, J., Bearman, P. S., Jones, J., & Udry, J. R. (2003). The National Longitudinal Study of Adolescent Health: Research Design [WWW document]. Retrieved June 20, 2007, from http://www.cpc.unc.edu/projects/addhealth/design
Udry, J. R. (2003). The National Longitudinal Study of Adolescent Health (Add Health), Waves I & II, 1994-1996; Wave III, 2001-2002 [machine-readable data file and documentation]. Chapel Hill, NC: Carolina Population Center, University of North Carolina at Chapel Hill.
[ Go to Contents ]
