Prepared by:
Adil Moiduddin
Jonathan Moore
Prepared for:
Office of the Assistant Secretary for Planning and Evaluation (ASPE)
U.S. Department of Health and Human Services (HHS)
| This report was produced under the direction of Caroline Taplin and Dale Hitchcock, Project Officers, Office of the Assistant Secretary for Planning and Evaluation (ASPE), Office of Science and Data Policy. The findings and conclusions of this report are those of the authors and do not necessarily represent the views of ASPE or HHS. |
Introduction and Objectives
NORC at the University of Chicago is pleased to present this white paper entitled “The Underserved and Health Information Technology: Issues and Opportunities” for the Assistant Secretary for Planning and Evaluation (ASPE) at the U.S. Department of Health and Human Services (HHS). Due to recent advances in technology and greater attention to problems associated with quality and efficiency of health care delivery, we see new opportunities to improve the health and health care for underserved Americans through the use of emerging information technologies.
President George W. Bush announced an Executive Order in 2004 prioritizing the adoption and use of health information technology (health IT) by patients and providers as well as the use of secure health information exchange (HIE) to improve the quality, safety, effectiveness and efficiency of health care delivery in the United States, and creating the Office of the National Coordinator for Health IT (ONC). Several agencies within HHS including the Health Resources and Services Administration (HRSA), the Indian Health Service (IHS), the Office of Minority Health (OMH), the Agency for Healthcare Research and Quality (AHRQ), the Centers for Medicare and Medicaid Services (CMS), the Office of Disease Prevention and Health Promotion (ODPHP), ASPE and others had been working on programs and policies to assure that the nation’s most vulnerable Americans are not left behind as the health care sector moves to adopt a more automated information driven approach to promoting health and preventing and treating illness. More recently several States have joined in these activities by sponsoring their own programs to encourage health IT adoption.
This purpose of this paper is to summarize a selected set of programs, policies and research findings that demonstrate both the potential for health IT to improve health and health care to underserved Americans as well as the challenges and barriers facing effective use of these technologies. We will attempt to cover an array of technologies including electronic health records (EHRs), e-Prescribing (eRx), chronic disease registries and clinical decision support systems (CDS) by health care providers predominantly serving the underserved. Additionally, we will examine technologies such as personal health records (PHRs), messaging and reminder systems, patient kiosks and other technologies that are “patient facing” where the theory is that IT can empower patients to take more control over their own health information and health care.
Finally, we will provide summary conclusions regarding what is known and yet to be understood regarding use of health IT among the underserved and highlight areas where further programmatic, policy or research activities sponsored by the federal government or others may be important. We begin with a brief discussion on health and health care challenges facing underserved Americans.
Why Focus on the Underserved?
While there is no single, universally accepted definition of the underserved, for the purpose of this paper, we characterize this population simply as those living in the United States who do not have adequate access to health care services. They share one or more of these characteristics: they may be poor; uninsured; have limited English language proficiency and/or lack familiarity with the health care delivery system; or live in locations where providers are not readily available to meet their needs. Members of ethnic and racial minority groups are not by definition “underserved”, but are disproportionately found among their numbers. Disparities in health status and access to health care that leave these populations worse off relative to others have been well documented by HHS over the last fifteen years.
Of the diverse set of groups represented among the underserved, perhaps disparities in health and health care of racial and ethnic minorities have been most thoroughly documented. Recently the Commonwealth Fund released a chart book analyzing data on the status of racial and ethnic minorities in the United States (available at http://www.commonwealthfund.org/publications). This effort compliments the primary federal government publication on health disparities, the “National Healthcare Disparities Report”, released annually by AHRQ with the last release for 2007 occurring in February of this year (available at http://www.ahrq.gov/qual/qrdr07.htm).
Product or Functionality
Description
Electronic Health Record (EHR)
An electronic record of health-related information on an individual that conforms to nationally recognized interoperability standards and that can be created, managed, and consulted by authorized clinicians and staff across more than one health care organization.
Electronic Medical Record (EMR)
An electronic record of health-related information on an individual that can be created, gathered, managed, and consulted by authorized clinicians and staff within one health care organization.
e-Prescribing (eRx)
Enables a physician to transmit a prescription electronically to the patient’s choice of pharmacy. It also enables physicians and pharmacies to obtain information about the patient’s eligibility and medication history from drug plans. Often comes with built in alerts for drug-drug, drug-allergy and drug-disease interactions.
Personal Health Records
An electronic record of health-related information on an individual that conforms to nationally recognized interoperability standards and that can be drawn from multiple sources while being managed, shared, and controlled by the individual.
Computerized Physician Order Entry (CPOE)
Refers to a computer-based system of ordering medications and often other tests. Physicians directly enter orders into a computer system that can have varying levels of sophistication. Basic CPOE ensures standardized, legible, complete orders, and thus primarily reduces errors due to poor handwriting and ambiguous abbreviations.
Clinical Decision Support (CDS)
Any system designed to improve clinical decision making related to diagnostic or therapeutic processes of care. CDS addresses activities ranging from the selection of drugs (e.g., the optimal antibiotic choice given specific microbiologic data) or diagnostic tests to detailed support for optimal drug dosing and support for resolving diagnostic dilemmas. Often incorporated as part of CPOE or EMR/EHR systems.
Disease Registries
A database feature that includes key clinical data on a subset of chronically ill patients for the purpose of tracking their condition and managing treatment.
In other cases, health IT enables providers and patients to access information that they otherwise would not be able to access. Exhibit 1 above outlines some basic definitions of health IT applications. Implemented properly, these technologies can create tremendous efficiencies and improvements in health and health care by providing “the right information to the right person at the right time”. This results in benefits such as greater adherence to evidenced based guidelines for screenings and vaccinations, better patient compliance with treatment instructions, reductions in medication errors and improved patient education.
As noted above, specific technologies that are most commonly referred to as health IT include electronic health records (EHRs) and personal health records (PHRs), the former being the systems used by providers to electronically record and maintain patient demographic information and information on activities, diagnoses and orders associated with a clinical episode, and the latter being an application for use by patients to access and update information related to their own health and health care or that of a family member or loved one. One key distinction between EHRs and PHRs lies in defining the locus of usage and control. EHRs are controlled and used primarily by the provider whereas PHRs are used and controlled by patients and their surrogates.
Additional applications include functionalities that may be considered add-ons to these core concepts, including clinical decision support (CDS) which in the context of an EHR would provide patient specific information on an appropriate course of treatment based on clinical effectiveness research; issue alerts if an order entered by the clinician is counter-indicated based on the patient’s profile; or provide reminders regarding the need to order specific interventions such as screenings, vaccinations, blood tests or foot exams.
In addition to PHRs, other health IT applications aimed at patients include health kiosks, where patients could obtain information on health conditions or access to information on their own health and health care using publicly available computer terminals set up within the community. These may also include messaging systems that allow transmission of reminders, information to guide healthful behavior, or even direct communication with providers through email or short message service (SMS) messaging accessed via cell phones or personal digital assistants (PDAs). In a 2006 report entitled, “Expanding the Reach and Impact of Consumer e-Health Tools”, the Office of Disease Prevention and Health Promotion at HHS identified a series of functions that might be considered some of the key potential benefits to patients using health IT. These functions included provision of health information to patients in a searchable format to help with researching treatment options; support for behavior modification and self management of a healthy lifestyle; access to online communities for interacting with others on health issues; and functions that allow joint management and tracking of treatment involving online collaboration between patients and clinicians.
Provider Objectives
Activities Enabled by Health IT
- Provide Access to the Uninsured
- Deliver Evidence-based Care
- Actively Manage Chronic Illnesses
- Improve Patient Safety
- Improve Care Coordination
- Maximize 3rd Party Reimbursement
- Report to Funding Agencies
- Reduce Administrative Costs
- Electronic referral to specialty care
- Track eligibility for Medicaid
- Track care delivered and outcomes
- Generate reminders at point of care
- Prescribe drugs electronically with built in
formulary data and interaction warnings - Automate patient follow-up
- Access to patient records online
- Bill electronically
- Generate custom reports
It should be noted that existing research on EHR adoption nationally shows relatively low rates of adoption, with estimates ranging from 4 percent for adoption of a fully functional EHR to 17 percent for any form of EHR using consensus based definitions.Exhibit 3: Overview of Kentucky Community Tracking database
Note: solid lines indicate data transfer; dotted lines indicate referral or other case management contact.
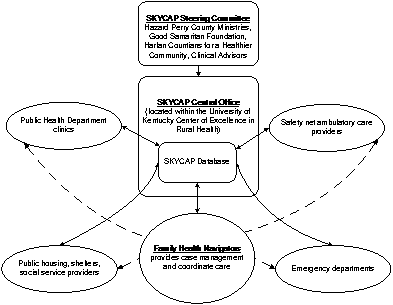
This graphic illustrates the flow of data in and out of the SKYCAP Central Office and its community data base. Data come from and go to 1) Public Health Department clinics, 2) safety net ambulatory care providers, 3) emergency departments and 4) social service providers, public housing and shelters. In addition, family health navigators, who provide case management and care coordination, make referrals to these four types of entities and also provide data to and receive data from the community data base.
Issues Facing Use of Health IT in the Underserved
The preceding discussion demonstrates that while the underserved and their providers are in very early stages of making use of health IT, there are a wide range of attractive opportunities and at least several good examples of effective use of health IT to improve the health and health care of the underserved. The discussion of specific examples also illustrates some of the challenges inherent in making the benefits of health IT available for the underserved. While stakeholders responsible for using health IT to improve care to the underserved must also contend with significant challenges associated with the design, adoption, implementation and use of health IT generally, we focus for the following pages on those issues and challenges which are specific to the context of addressing the needs of the underserved.
Issues for Provider Facing Health IT
Providers who disproportionately care for the underserved often face different circumstances and barriers in effectively providing care. Some of these challenges reappear in implementing health IT among providers working with the underserved. For example, community health centers often work with patients who have complex mental and physical health needs.http://www.ahrq.gov/qual/nhdr07/slides/dr07slides.htm
