Prologue
We are facing an asthma epidemic. Through newspaper stories and personal experiences, we hear more about asthma every day. A child at school has an asthma attack in the classroom. The radio reports an air pollution alert, warning anyone with breathing problems to stay indoors. The local school board debates a policy on students carrying inhaler medications. Stories of asthma are all around us.
The statistics support these impressions. From 1980 to 1996, the number of Americans with asthma more than doubled, to almost fifteen million, with children under five years old experiencing the highest rate of increase. Reasons for these increasing rates are unclear. Yet even if rates were to stop increasing, asthma would remain an enormous public health problem. Not only does it keep children in fear and pain – it keeps them out of school. In every classroom with 30 children, there are likely to be at least two with asthma. That adds up to over 10 million school days lost to asthma each year. And the problem is not limited to children. Asthma is the leading work-related lung disease. Moreover, the disease kills over 5,000 Americans and results in half a million hospitalizations every year. As serious as asthma is, it doesn’t strike evenly. Minorities and the poor are hit especially hard.
To confront this challenge, I called for a special asthma initiative in the Department of Health and Human Services. In response, the agencies of the Department worked together to assess current efforts on asthma and to develop a set of priorities for the future. This strategy identifies urgent needs for research to uncover the causes of the asthma epidemic and develop ways to prevent the disease from occurring. The strategy describes priority public health actions needed to eliminate the disparities in the burden of asthma and to reduce the impacts on all who suffer with the disease.
The success of efforts to combat asthma will depend on the joint efforts of many – providers of medical care, university researchers, non-governmental and community-based organizations, professional societies, insurance and pharmaceutical companies, other businesses, federal, state, local and tribal government agencies, and people with asthma and their families. This strategy describes the role of the Department of Health and Human Services. Others have equally important roles, and we must all work together in concerted action against asthma.
Executive Summary
Asthma: Epidemic of a Chronic Disease
Asthma is a chronic inflammatory disease of the airways. From 1980 to 1996, the number of Americans afflicted with asthma more than doubled to almost 15 million, with children under five years old experiencing the highest rate of increase. The steady rise in the prevalence of asthma constitutes an epidemic, which by all indications is continuing. Even if rates were to stabilize, asthma would continue to be a profound public health problem, responsible for 9 million visits to health care providers per year, over 1.8 million emergency room visits per year, and over 460 thousand hospitalizations per year. The burden of this chronic disease is felt everyday at the individual level, whether it's a frightening asthma attack or the constant vigilance and adherence to treatment plans required to keep it under control. In addition, there are disparities in the burden of asthma. Although asthma affects Americans of all ages, races, and ethnic groups, low-income and minority (1) populations experience substantially higher rates of fatalities, hospital admissions and emergency room visits due to asthma.
Asthma is a common chronic disease of childhood, affecting an estimated 4.4 million children. Asthma is one of the leading causes of school absenteeism, accounting for over 10 million missed school days annually. Symptoms not severe enough to require a visit to the emergency room or to a physician can still substantially impair quality of life. Asthma results in many lost nights of sleep and disruption of family and caregiver routines, and restricted activities. It is the leading work-related lung disease; and recent evidence suggests that, in some regions, as much as 20 percent of adult onset asthma may be work related. Taking care of asthma is expensive and imposes financial burdens on patients and their families, including lost work days and income, as well as lost job opportunity. In 1990, the annual cost of asthma to the U.S. economy was estimated to be $6.2 billion, with the majority of the expense attributed to medical care. A 1998 analysis using different methods estimated the cost of asthma in 1996 to be over $11 billion per year.
Critical breakthroughs in science in the last decade have generated a body of information that, when effectively used to guide care of patients, enables most people with asthma to live fully active lives. The National Asthma Education and Prevention Program (NAEPP), sponsored by the National Heart, Lung and Blood Institute (NHLBI), developed Guidelines for the Diagnosis and Management of Asthma ("Guidelines"), which translate the scientific findings into recommendations for patient care (see Appendix C). When the Guidelines are followed, health care providers, caregivers, and patients with asthma work together to control the disease. Appropriate medical care, monitoring of symptoms and objective measures of lung function, along with environmental control measures to reduce exposures to allergens and other asthma triggers (all described in the Guidelines), can substantially reduce the frequency and severity of asthma attacks.
Yet, many patients remain ill because of a complex interplay of factors. One impediment is that many patients are still not being treated or educated according to the Guidelines; another is patients' lack of access to quality medical care or resources to obtain sufficient medications or equipment. For example, a recent study found that one out of five children in Baltimore, MD and Washington, DC were receiving the wrong or no treatment for asthma. Even with high quality care, some cases of asthma are particularly difficult to control; and medications cause adverse side effects in some people. Moreover, lack of timely surveillance data (2) at the State and local levels impedes planning of intervention efforts. Finally, research results have not yet identified or demonstrated how to prevent asthma from occurring in the first place. The genetic basis of susceptibility to asthma and the biologic mechanisms that explain the interaction of susceptibility and environmental exposures are not well understood.
An array of activities -- promoting effective implementation of the Guidelines, ensuring access to quality medical care, enhancing surveillance and intensifying research across the spectrum from molecular biology to health services delivery -- implemented at an accelerated pace-- holds great promise for reducing the burden of asthma and reversing the steady increase in rates.
DHHS Capacity to Address Asthma
The Department of Health and Human Services (DHHS) conducts and supports research, public health practice (3), and health services delivery to address the growing problem of asthma. In fiscal year (FY) 1999, DHHS invested $145 million in asthma research. DHHS-supported grantees have been responsible for many of the scientific breakthroughs that helped shape the Guidelines. In fiscal year 1999, relatively few dollars (less than $10 million) were spent on public health practice for asthma. With those funds, the Department supported partnerships that are discovering new ways to increase dissemination and use of information by communities, health care providers, patients and their families. DHHS spends much more on direct delivery of medical care; for example, estimates of Medicaid and Medicare expenditures for treatment of asthma exceed one billion dollars per year. DHHS also funds research to improve the quality of health care received by individuals with asthma and could expand its evaluation of asthma care.
Secretary's Initiative on Asthma
In the fall of l997, DHHS convened a high-level workgroup to assess the most urgent needs and opportunities for tackling the growing problem of asthma (Appendices A and B). Shortly there-after, the President's Task Force on Environmental Health Risks and Safety Risks to Children, co-chaired by Secretary Shalala and Environmental Protection Agency Administrator Browner, decided to take immediate action across the government to address the environmental aspects of childhood asthma (Appendix D). At the Secretary's request, the DHHS workgroup developed a Department-wide strategy encompassing all age groups affected by asthma and the many factors, in addition to environment, influencing this disease. The DHHS initiative is closely coordinated with the activities of the President's Task Force. From FY 1999 to FY 2000, DHHS discretionary spending on asthma increased from $157 million to $183 million.
Four Priorities for Investment
This DHHS strategy includes four priority areas for investment over the next five years. The priorities are:
- Determine the causes of asthma and develop interventions to prevent its onset.
- Reduce the burden for people living with asthma.
- Eliminate the disproportionate burden of asthma in minority populations and those living in poverty.
- Track the disease and assess the effectiveness of asthma intervention programs.
This strategy is designed to help achieve the national Healthy People goals for asthma (See Table 1). The strategy envisions close coordination between DHHS initiatives and activities led by professional societies, universities, non-governmental and community-based organizations, providers of medical care, businesses, and other federal, state, local, and tribal government agencies in pursuit of progress in these areas over the next five years.
My asthma attacks are very different depending on whether they are exercise-induced or triggered by an allergen or irritant. When I'm running, I get hints of an asthma attack when the rhythm of my breathing starts to change. After that, the real struggle to breathe starts. I feel like I'm fighting with some unknown force for each breath. Sometimes, I feel like the air comes into my mouth but will not go down into my lungs, and all the breathing is in vain. Other times, it feels like all the air is coming into my lungs, but nothing is coming out. My lungs feel as if they're going to explode. I'm lightheaded and weak. My whole upper body gets tense and I feel frightened and panicked which makes things worse. Attacks not caused by athletics seem to come on more gradually but also feel like I'm not getting enough air with each breath. It's a full body workout to take each breath. My chest tightens up a lot and it either feels like I have 1,000 pounds of bricks on my chest or that someone has their hands on my lungs and is squeezing with all their might."
-An eighteen year old asthma sufferer
"My son has had chronic asthma since he was 18 months old. That means we ask the same questions again and again: Did you do your second puff [i.e., medication]? Did you rinse your mouth? Have we packed the nebulizer? Do we have the prescription for the medication on hand? It means his dad and I stay watchful because every season brings its own danger: pollen in the spring, heat and air pollution in the summer, leaf mold in the fall, and infection in the winter. It means that everyday events like soccer practice, visits with friends who have cats, and even hay rides require vigilance. Most of all, it means a cough is not just a cough. It can be the first cough in a long day and night punctuated every 10 seconds with another sharp little cough.
One of the hardest things about being a parent of a child with chronic asthma has been to acknowledge to myself that asthma, for my son, is chronic. It is not a temporary thing. Another difficult thing has been to deal with the symptoms and treatment of his asthma without making him feel different. And finally, the emotions are hard too. Not just the niggling fear but also, the surprising anger -- Why do some doctors seem to know so little about prevention and asthma management?"
-A young mother
Overview
Epidemic of a Chronic Disease
The Growing Problem of Asthma
Asthma is a chronic inflammatory lung disease characterized by recurrent episodes of breathlessness, wheezing, coughing, and chest tightness, termed exacerbations. The severity of exacerbations can range from mild to life threatening. Exacerbations can be triggered by exposures and conditions such as: respiratory infections, house dust mites, cockroaches, animal dander, mold, pollen, cold air, exercise, stress, tobacco smoke and indoor and outdoor air pollutants . Both the frequency and severity of asthma symptoms can be reduced by using medications and reducing exposure to environmental triggers.
Ongoing preventive management is needed for patients with persistent asthma, even when mild. Learning how to manage asthma as a chronic disease is a major challenge for patients, as well as for health care providers and others involved in asthma care.
An epidemic of asthma is underway in the United States. The number of people with asthma has more than doubled in the past 15 years. Even if rates were to stabilize, asthma would continue to be a profound public health problem.
For the past 15 years, an epidemic of asthma has been underway in the United States. The steady rise in the prevalence of asthma constitutes an epidemic, which by all indications is continuing. Even if rates were to stabilize, asthma would continue to be a profound public health problem. It is a potentially fatal, chronic disease responsible for over 1.8 million emergency room visits per year, over 460 thousand hospitalizations per year and over five thousand deaths per year (4). Although the burden asthma affects Americans of all ages, races and ethnic groups, recent data indicate that children, low-income and minority (4) populations have been most severely affected. (5)
Figure 1. Estimated average annual number of persons with self-reported asthma during the preceding 12 months by age group, United States, National Health Interview Survey, 1980-1994.
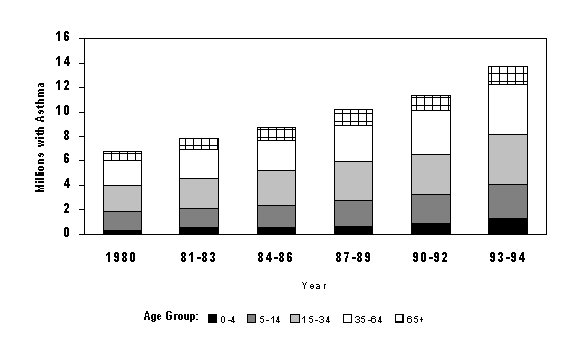
Source: Morbidity and Mortality Weekly Report, Vol. 47, No. SS-1, April 24, 1998.
National survey data - the responses of randomly selected US residents when asked whether they had symptoms of physician-diagnosed asthma in the previous 12 months -- indicate that the number of people with asthma in the United States has more than doubled in the past 15 years (see figure 1). In 1980, 6.8 million Americans had asthma. By 1996, the number had risen to 14.6 million (5). Rates of asthma are increasing in all age groups, among both men and women, and across all racial and ethnic groups (4) (see figure 2). Total deaths from asthma have also risen, from a low of 1,674 in 1977, to 5,637 in 1995 (4) (see figure 3).
Asthma is a common chronic disease of childhood, affecting an estimated 4.4 million children (6). In the United States, the prevalence of asthma is slightly higher in boys than in girls under age 18. Asthma is more common in school-aged children than in preschool-aged children or adults. However, the most rapid increase in cases of asthma are occurring in children under five years old, with rates increasing over 160 percent between 1980 and 1994 (4).
Figure 2. Estimated average annual rate of self-reported asthma during the preceding 12 months by age group, United States, National Health Interview Survey, 1980-1994.
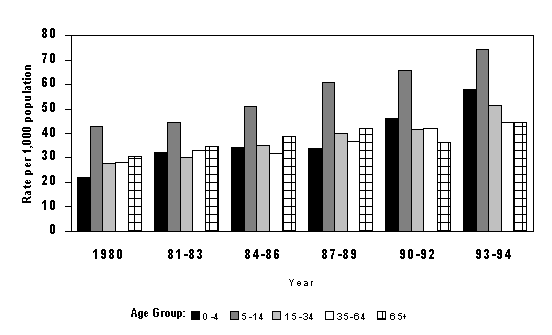
Source: Morbidity and Mortality Weekly Report, Vol. 47, No. SS-1, April 24, 1998.
Asthma remains a common problem in adults, reflecting the persistence of childhood asthma and the new cases that develop in adulthood . Among adults, women of all races suffer greater asthma mortality and morbidity than men. Occupational asthma, or the new onset of asthma due to conditions at the workplace , has become the most common occupational lung disease (7, 8, 9, 10, 11). Recent studies in the U.S. have found that in working adults, 6 to 21 percent of new onset asthma is attributable to occupational asthma (12, 13, 14). Depending on the type and intensity of work exposures, the frequency of occupational asthma may be very high in some industrial settings (e.g., about 25 percent in one group of platinum-refinery workers); in other industries, only sporadic cases may be reported (15).
Figure 3. Average number of deaths with asthma as the underlying cause of death diagnosis, by age group, United States, Underlying Cause of Death dataset, 1960-1995.
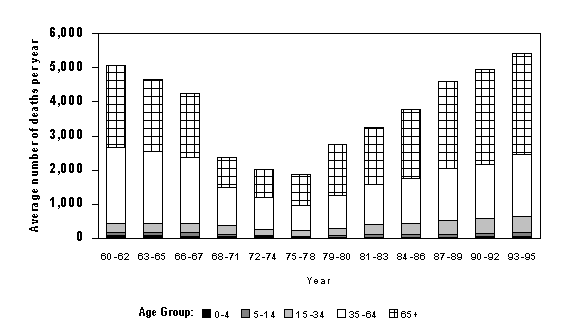
Source: Morbidity and Mortality Weekly Report, Vol. 47, No. SS-1, April 24, 1998.
Disproportionate Burden of Asthma Among Minority Groups and Those Living in Poverty
In the most recent years for which data are available, African Americans were slightly more likely to have asthma than were whites, with prevalence rates of 58.8 per 1,000 population and 50.8 per 1,000 respectively (4). However, it is disturbing to note that African Americans are much more likely to die from asthma than whites (4) . From 1993 through 1995, the death rate from asthma in African Americans of 38.5 per million was over twice the rate of 15.1 per million in white Americans (4) (see figure 4). Among children, the disparity was even greater: African American children were over four times as likely to die from asthma as were white American children (16). In the Northeast, Hispanics had a death rate of 34 per million (17).
Although asthma affects Americans of all ages, races, and ethnic groups, low-income and minority populations experience substantially higher rates of fatalities, hospital admissions, and emergency room visits due to asthma.
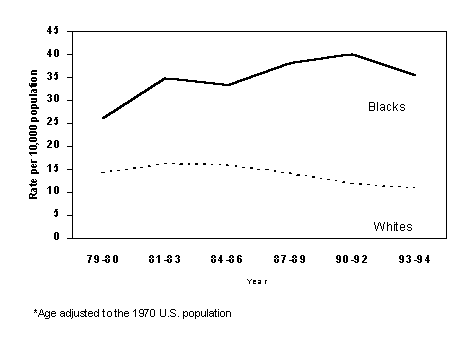
Figure 4. Rates of death with asthma as the underlying cause of death diagnosis, by race, United States, Underlying Cause of Death dataset, 1979-1995.
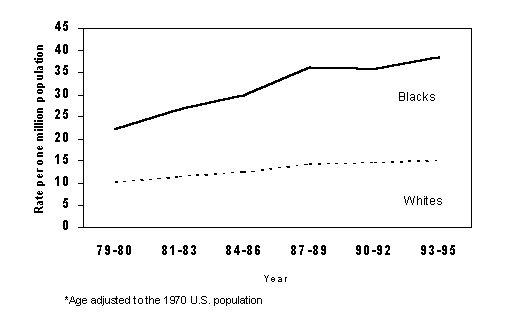
Source: Morbidity and Mortality Weekly Report, Vol. 47, No. SS-1, April 24, 1998.
Hospitalizations and emergency room visits for asthma demonstrate the disparity in the impact of asthma among different racial and ethnic groups. African Americans have an annual rate of hospitalization of 35.5 per 10,000, nearly four times that for whites (10.9 per 10,000) (see figure 5). African Americans are approximately five times more likely than white Americans to seek care for asthma at an emergency room (4) .
Studies examining the link between socioeconomic status and asthma confirm that the impacts of asthma are greatest on low income populations (18, 19, 20, 21). For example, in the U.S. in 1996, pediatric hospitalizations for asthma were estimated to be five times higher for children in lower income families (22). The National Cooperative Inner-City Asthma study demonstrated that over 50% of study participants, who were poor children living in inner cities, found it difficult to get follow-up asthma care. Among those with severe asthma, less than half were using anti-inflammatory medication (23, 24).
Figure 5. Estimated average rates of hospitalization for asthma as the first-listed diagnosis, by race, United States, National Hospital Discharge Survey, 1979-1994.
Source: Morbidity and Mortality Weekly Report, Vol. 47, No. SS-1, April 24, 1998.
Health Impairment from Asthma Not Fully Captured by Hospital or Emergency Room Visits
These measures -- rates of death, hospitalization, and emergency room visits -- give an incomplete picture of the true burden of asthma in the United States. Asthma symptoms that are not severe enough to require a visit to an emergency room can still be severe enough to restrict activities and affect quality of life . Asthma is responsible for 10 million physician office visits and 134 million days of restricted activities per year (4, 25). Children with asthma miss over 10 million school days annually, making asthma one of the leading causes of school absenteeism (26). Asthma in children also accounts for many lost nights of sleep, disrupts family and caregiver routines, including lost work days. Asthma in adults, including occupational asthma, has consequences of lost work time, job loss, disability and premature death (23, 27).
Data Tracking Asthma are Insufficient
Public health officials need to understand changes in rates of disease in different locations or populations in order to target health services and public health programs where they are most needed, to help evaluate the success of intervention efforts, and to provide clues about risk factors. At the present time, surveillance of asthma -- the systematic collection, evaluation and dissemination of data to track the occurrence and severity of the disease -- is limited to analyses of ongoing surveys and data systems on health events such as mortality, hospitalization, and outpatient visits. These data are typically several years out of date when they become available, and only provide national estimates. With the exception of recent work in several states to examine hospitalization and emergency room visits for asthma, data that would allow comparisons among states or cities are available only for deaths due to asthma.
Cost of Asthma to the U.S. Economy: Eleven Billion Dollars Annually
Estimating the costs of asthma is one way to measure its health burden. In 1990, the cost of asthma to the U.S. economy was estimated to be $6.2 billion, with the majority attributed to direct medical expenses, such as hospitalization, physician and nursing care, and medication (27). In 1998, the National Heart, Lung and Blood Institute (NHLBI) estimated that the annual costs of asthma were $11.3 billion per year. This estimate includes $7.5 billion in direct medical expenses and $3.8 billion in indirect expenses, such as lost workdays for adults with asthma and lifetime earnings lost due to mortality from asthma (28).
The Science of Asthma
Over the past 15 years, biomedical research has produced major advances in the understanding of asthma. Prior to this period the role of inflammatory mechanisms in asthma was not understood. Asthma is now known to be a disease of airway inflammation resulting from a complex interplay between environmental exposures and genetic and other host factors. Left untreated, inflammation may lead to irreversible changes in lung structure, called airway remodeling. Together, t hese findings have changed medical treatment and environmental management of asthma.
"Through scientific advances, much of the severe morbidity and mortality from asthma can now be prevented."
- Claude Lenfant, M.D., Director, National Heart, Lung, and Blood Institute
Based on an improved understanding of asthma, inhaled anti-inflammatory medications have become the mainstay of preventive medical management for patients with persistent asthma. Development of new medications to treat and prevent the symptoms of asthma based on new insights into the cellular mechanisms of inflammation will offer options to tailor therapy to the individual patient and, minimize the possibilities of side effects.
In addition to improvements in medical therapy, better monitoring techniques now permit objective measures of lung function that are simple tools for patients and physicians to use in assessing asthma severity and monitoring changes in the disease. In a disease like asthma, which varies considerably over time, and where changes in lung function can occur before symptoms develop, objective measures provide essential information for making decisions about adjusting medications.
The Causes of Asthma and of the Asthma Epidemic Are Not Well Understood
Although the causes of the increasing rates of asthma over the past 15 years are not known, the most likely reason is an interaction between environmental and genetic factors. Atopy, the genetically inherited susceptibility to become allergic, is the most important predictor of a person developing asthma (29). A substantial research effort is underway to identify the genes responsible for susceptibility to asthma. Since the genetic make-up of the population changes slowly, genetic susceptibility alone cannot be responsible for the epidemic of asthma which has occurred in the United States over the past 15 years. Further work is needed to clarify how genetic susceptibility and environmental exposures interact to cause asthma.
Many studies have demonstrated that exposure to indoor allergens and environmental tobacco smoke are risk factors for more severe asthma (30, 31, 32, 33). Some studies suggest that indoor allergen exposure is a risk factor for the initial onset of asthma (34, 35, 36). People now spend more time indoors, thus increasing exposure to indoor allergens and pollutants. In its recent review of the current scientific literature, the Institute of Medicine (IOM) drew several conclusions about the role of numerous indoor air exposures and the initial development of asthma (37). The findings were ranked according to the level of evidence linking any of the exposures to the onset of asthma. IOM emphasized that a particular agent may be associated with the development of asthma, but that does not mean it is the sole factor determining whether an individual will develop the illness. The IOM Committee found that exposure to house dust mite allergen can STYLE="text-decoration: underline">cause the development of asthma in susceptible children. The Committee also determined that exposure to environmental tobacco smoke is ssociated with the development of asthma in younger children. Maternal smoking during pregnancy was suggested to have a stronger adverse affect than exposure after birth. In addition, limited or suggestive evidence was found by the IOM for associations between cockroach allergen exposure or respiratory syncytial virus (RSV) infection and the development of asthma in infants. Both factors have been the subject of active research during the past few years and efforts currently underway may help shed greater light on their potential role in asthma development .
Other possible, but less well studied, factors that may affect the development of asthma include exposures that stimulate the immune system. One hypothesis is that certain infections in early life may block the allergic immune response and thereby protect against asthma (38, 39, 40, 41). Other factors have been postulated to cause asthma, including the diet during the prenatal period and early infancy (42) and obesity in adolescents and adults (43, 44). Such hypotheses remain controversial, and more research is clearly needed to understand the remarkable rise in asthma and the causes of the disease.
The Environment, Indoors and Outdoors, Can Exacerbate Asthma
While much remains to be learned about the causes of asthma, many studies have identified factors that exacerbate asthma in those who already have the illness (33, 45, 46, 47, 48, 49, 50). Asthma exacerbations or "attacks" involve the onset or worsening of symptoms (e.g., some combination of shortness of breath, cough, wheezing, and chest tightness). Reducing exposure to certain allergens has been shown not only to reduce asthma symptoms and the need for medication, but also, in some studies, to improve lung function (37, 48).
The IOM report drew several conclusions about the role of specific indoor exposures in the exacerbation of asthma. The IOM committee found sufficient evidence to conclude that expo-sure to allergens produced by cats, cockroaches, and house dust mites, causes exacerbations of asthma in sensitized individuals (i.e., those who are allergic to these substances). In addition, the committee found sufficient evidence that environmental tobacco smoke causes exacerbations of asthma in pre-school-aged children (see Appendix H for executive summary of the IOM report).
People with asthma, both children and adults, can be particularly sensitive to outdoor air pollution. Common air pollutants (also known as "ambient air pollutants") such as ozone, sulfur dioxide, and particulate matter, are known to be respiratory irritants and can contribute to an exacerbation of asthma symptoms. Air pollution also might act synergistically with other environmental factors to worsen asthma (51). For example, diesel exhaust particulates, by markedly increasing the capacity to produce IgE antibodies, may enhance responsiveness to allergens (52). Also , some evidence suggests that exposure to ozone can enhance a person's responsiveness to inhaled allergens (53, 54).
Workplace Exposures Can Aggravate or Cause Asthma
In persons with asthma resulting from workplace exposure, clear relationships have been identified between the level of exposure to specific chemicals and allergens and rates of sensi-tization and symptoms (55). Over 250 agents encountered at work can cause asthma, including isocyanates, wood dusts, anhydrides, dyes, formaldehyde, metals, latex, and enzymes (56). For example, even brief exposure to more than 20 parts per billion of isocyanates is considered hazardous ; isocyanates are widely used in many countries and are responsible for the most common form of occupational asthma. Many patients suffer chronic disease even after they are removed from an occupational exposure situation. However, early diagnosis and early removal from exposure increases the likelihood of recovery (56). Since workers are exposed to a wide range of possible causative agents, often at elevated exposure levels, the occupational setting offers a significant opportunity for research on asthma causes and triggers. Such research could prove to be a useful model for understanding how environmental exposures to certain chemicals and allergens might contribute to the development of asthma.
Knowledge Exists to Successfully Manage Asthma in Most Patients
Advances in the scientific understanding of the underlying mechanisms of asthma have led to treatment that can significantly improve the health of asthma patients. The Guidelines for the Diagnosis and Management of Asthma ("Guidelines") -- developed by experts convened by the National Institutes of Health (NIH) and updated in 1997 - recommend four strategies for managing asthma that substantially reduce the frequency and severity of asthma attacks (57, 58). The Guidelines emphasize: 1) assessment and monitoring of symptoms; 2) control of environmental factors to limit exposure to allergens and other triggers; 3) use of appropriate medication; and 4) education of the patient and family in asthma care. These recommendations promote a fundamentally new understanding of asthma and its treatment by emphasizing the role of inflammation in disease development, noting the importance of objective monitoring of lung function, and stressing the need to establish partnerships between patients and health care providers through patient education (see Appendix C for a summary of the 1997 Guidelines). In 1999, the Guidelines were adapted into an easily referenced pediatric document, Pediatric Asthma: Promoting Best Practice - Guide for Managing Asthma in Children (59). The Guidelines remain the world's most comprehensive, up-to-date source of information on asthma diagnosis and management. By f ollowing the recommendations , most people with asthma should be able to lead an active life, with their asthma well-controlled.
The benchmark publication by the National Heart, Lung, and Blood Institute, Guidelines for the Diagnosis and Management of Asthma, translates advances in scientific understanding into practical strategies for asthma care.
The Challenge of Asthma
Rates of asthma as well as the burden of this chronic disease are increasing, despite important advances in research. This paradox raises two distinct issues: the increase in asthma over the last 15 years, and the continuing hardships for those who already have the disease.
Why are rates of asthma increasing? Why is the burden of asthma still so great?
If there have been breakthroughs in understanding the mechanisms of the disease, why are rates of asthma increasing? One key reason is that the cause of the asthma epidemic in the United States, which is also affecting most industrialized countries, is not known. Further research is needed to clarify the genetic basis of susceptibility to asthma, and the biologic mechanisms that explain the interactions of susceptibility and other factors, such as environmental exposures, that lead to asthma. While this basic research requires additional emphasis, we also need to proceed with testing possible approaches to prevent asthma based hypotheses derived from basic and epidemiological studies. Both basic research and prevention trials can help identify promising strategies to prevent the disease from occurring in the first place.
If the tools exist to manage asthma more effectively, why is the burden of asthma still so great ? Although progress has been achieved in professional and patient education in the past decade, and research has shown that effective medical management and patient education reduces the use of emergency services and improves quality of life, many health care professionals and people with asthma are not making use of the Guidelines (60, 61, 62, 63). Various outstanding programs supported by federal and private funds have helped foster needed changes in medical practice and patient behavior, but these need to be evaluated in a greater variety of settings and implemented on a larger scale in order to have national impact. Populations and neighborhoods experiencing the greatest burden of disease often lack access to high quality medical care, including adequate education about asthma manag e ment and sufficient medications and equipment (24, 62, 64). Poor housing and environmental conditions make it difficult to control exposures that worsen asthma . In addition, lack of asthma surveillance at the State and local levels hampers public health efforts to direct quality health care toward the most severely affected populations.
In summary, we have made progress but we are not yet close to understanding the causes of the asthma epidemic nor to providing optimal care. In the meantime, we need to 1) improve the availability of quality asthma care, especially to underserved populations, which is feasible and can be done by a coordinated effort; and 2) increase research efforts to deal with chronic persistent asthma and to prevent the onset of the disease.
DHHS Capacity to Address Asthma
The Department of Health and Human Services (DHHS) has a broad mandate to advance the health and welfare of Americans (see box), and has a significant role to play in addressing the asthma epidemic. DHHS' areas of responsibility for asthma include research, public health, and health services delivery.
In Fiscal Year 1999, the Department of Health and Human Services (DHHS) invest ed $ 145 million in research on asthma. DHHS is uniquely positioned to enhance the scientific knowledge required to prevent the onset of asthma and to improve the quality of life for millions of asthma patients and their families. DHHS-supported grantees have been responsible for many of the scientific breakthroughs that helped shape the Guidelines.
Relatively few DHHS dollars - under $10 million - were spent on public health practice for asthma. Public health practice activities are those that facilitate the work of the medical community and others to prevent disease, reduce the severity of symptoms and improve the quality of medical care. The role of government in public health includes: 1) the systematic collection and analysis of health information; 2) the development of goals and priorities based on scientific knowledge and measures to achieve them; 3) taking action through public education, advocacy, negotiation, and mobilization of resources; and 4) evaluation to determine whether policy goals are achieved (3).
The Department has supported -- and could substantially expand -- partnerships and model programs that are discovering new ways to increase dissemination and use of information about how to manage asthma to communities, health care providers, patients and their families. It continues to evaluate methods that are most effective in translating important research findings into clinical practice to improve the quality of care. DHHS could expand its evaluation of asthma care, as well as its efforts to track the disease, to more fully ensure that appropriate and timely interventions are routinely provided, particularly to those in greatest need. Several DHHS agencies have undertaken activities in this area, while others have the capacity for public health practice activities on asthma but have not yet made substantial investments. Expanded collaboration at the local level will facilitate progress in eliminating asthma-related disparities. (Appendix E describes in detail the asthma-related activities of DHHS agencies.)
Mission of the Department of Health and Human Services
The mission of DHHS is to enhance the health and well-being of Americans by providing for effective health and human services and by fostering strong, sustained advances in the sciences underlying medicine, public health, and social services. DHHS' six strategic goals are:
- Reduce the major threats to the health and productivity of all Americans.
- Improve the economic and social well-being of individuals, families, and communities in the United States.
- Improve access to health services and ensure the integrity of the nation's health entitlement and safety net programs.
- Improve the quality of health care and human services.
- Improve the nation's public health systems.
- Strengthen the nation's health sciences research enterprise and enhance its productivity.
The great majority of DHHS expenditures for asthma are for direct delivery of health services. Estimates of Medicaid and Medicare expenditures for treatment of asthma exceed one billion dollars per year (65). Thousands of people receive care for their asthma at DHHS-funded health centers and hospitals, but estimates of expenditures on asthma alone are impossible because costs are covered by large block grants that support comprehensive primary care, not disease-specific programs .
For two decades, the U.S. Public Health Service has used Healthy People reports to set specific national objectives for health, to organize concerted action among the public health and private sectors to meet them, and to provide indicators for monitoring progress (22). National goals for improving asthma health outcomes have been established as part of the Healthy People initiative. In the first report, Healthy People 2000 had three objectives specifically relevant to asthma: reduce hospitalizations, reduce activity restriction, and increase the proportion of people with asthma who receive formal patient education. Results of a mid-course evaluation of progress toward Healthy People 2000 goals for asthma were disappointing . For example, by 1996, there was no progress toward eliminating disparities in hospitalization rates for African-Americans and other non-whites compared to whites (66). New goals for asthma for 2010 -- with a special focus on eliminating disparities -- include numerical targets for reducing hospitalizations, reducing emergency room visits, and reducing the proportion of people with asthma who experience activity limitations (see Table 1 and Appendix G). The challenge of accelerating progress and achieving the goals set for 2010 is substantial, but the foundation for doing so is well established.
Secretary's Initiative on Asthma
In the fall of 1997, DHHS Secretary Donna Shalala called for an initiative to tackle the growing problem of asthma. Shortly thereafter, the President's Task Force on Environmental Health Risks and Safety Risks to Children, which Secretary Shalala co-chairs with Environmental Protection Agency (EPA) Administrator Carol Browner, began to address the environmental influences on childhood asthma. In April, 1998, the Secretary's Science Advisor (the Deputy Assistant Secretary for Science Policy) convened a DHHS workgroup to help guide a Department- wide initiative on all aspects of asthma, including the environment and asthma in children. The DHHS workgroup developed a draft strategic plan (Action Against Asthma, March 22, 1999) and solicited public comment. The draft plan was revised in response to the comments received, and this final strategy is the result. For the first year of the strategy, DHHS discretionary funding for asthma increased from $157 million in FY 1999 to $183 million in FY 2000.
This strategy is designed to help achieve the national Healthy People goals for asthma. Over the next five years, this strategy will guide the development of budget proposals of DHHS agencies. Annually, budget proposals from each agency will be evaluated to ensure that they address the priority areas identified in this plan. Representatives from DHHS agencies will continue to coordinate and collaborate on key asthma programs. The agencies will assess progress in addressing the priorities of this strategy and contributions to achieving the Healthy People goals. The agencies will also continue to reach out to external constituencies to convey information on DHHS efforts and to receive advice on future directions.
The strategy envisions close coordination between DHHS initiatives and activities led by professional societies, universities, non-governmental and community-based organizations, providers of medical care, businesses, and other federal, state, local and tribal government agencies in pursuit of progress in these areas over the next five years (see Appendix F for a description of asthma programs outside of DHHS). A primary forum for coordination of education and public health programs with these entities is the National Asthma Education and Prevention Program (see Appendix F for a list of member organizations).
Table 1. Healthy People 2010: National Goals for Asthma
Healthy People 2010 is designed to achieve two over-arching goals: 1) to increase quality and years of life, and 2) to eliminate health disparities. Progress toward the goals will be monitored through specific objectives in 28 focus areas. Respiratory diseases, including asthma, are covered in Focus Area #24. The asthma objectives are:
24.1 Reduce asthma deaths | 1998 (baseline) | 2010 Target |
|---|---|---|
| Rate per million | ||
| a. Children under age 5 years | 1.7 | 1.0 |
| b. Children aged 5 to 14 years | 3.2 | 1.0 |
| c. Adolescents and adults aged 15 to 34 years | 5.9 | 3.0 |
| d. Adults aged 35 to 64 years | 17.0 | 9.0 |
| e. Adults aged 65 years and older | 87.5 | 60.0 |
| 24.2 Reduce hospitalizations for asthma | 1998 (baseline) | 2010 Target |
| Rate per 10,000 | ||
| a. Children under age 5 years | 60.9 | 25 |
| b. Children and adults aged 5 to 64 years | 13.8 | 8 |
| c. Adults aged 65 years and older | 19.3 | 10 |
| 24.3 Reduce hospital emergency department visits for asthma | 1995-97 (baseline) | 2010 Target |
| Rate per 10,000 | ||
| a. Children under age 5 years | 150.0 | 80 |
| b. Children and adults aged 5 to 64 years | 71.1 | 50 |
| c. Adults aged 65 years and older | 29.5 | 15 |
24.4 Reduce activity limitations among persons with asthma 24.5 (Developmental) Reduce the number of school or work days missed by persons with asthma due to asthma. 24.6 Increase the proportion of persons with asthma who receive formal patient education, including information about community and self-help resources, as an essential part of the management of their condition. 24.7 (Developmental) Increase the proportion of persons with asthma who receive appropriate asthma care according to the NAEPP guidelines. 24.8 (Developmental) Establish in at least 15 States a surveillance system for tracking asthma death, illness, disability, impact of occupational and environmental factors on asthma, access to medical care, and asthma management. (See Appendix G for additional data and data sources for these objectives.) | ||
As described in the following chapters, the priority areas for investment over the next five years are:
- Determine the causes of asthma and develop interventions to prevent its onset .
- Reduce the burden for people living with asthma.
- Eliminate the disproportionate health burden of asthma in minority populations and those living in poverty.
- Track the disease and assess the effectiveness of asthma programs.
The remainder of this strategic plan expands on these priorities. For each, it provides examples of current and relevant DHHS-supported activity to illustrate the breadth and depth of work underway, as well as the most urgent needs for additional investment. The plan concludes with detailed recommendations for activities to be undertaken in each priority area over the next five years. The recommendations represent the most urgent needs to control asthma and the DHHS' capacity to address those needs.
Priorities for Investment Over the Next Five Years
Priority Area 1: Determine the Causes of Asthma and Develop Interventions to Prevent Its Onset
Research has not yet identified or demonstrated how to prevent the onset of asthma. Research to prevent asthma in individual patients or in high risk populations is known as "primary prevention" research. It includes both research to understand the causes of asthma and testing strategies to prevent its occurrence. This research is critical to discovering the reasons for the current epidemic of asthma.
Current DHHS Activities: Primary Prevention Research
NIH sponsors the majority of primary prevention research funded by DHHS. The Centers for Disease Control and Prevention (CDC) also undertakes work in this area. Relevant research focuses on the natural history of the disease, risk factors, genetics, and the basic mechanisms and pathogenesis of asthma. An example of the research on the natural history of asthma is exploring the hypothesis that infection with respiratory viruses in early life, such as respiratory syncytial virus, may predispose an individual to an increased risk of asthma. In contrast, certain other infections in early life may block the immune response to allergens and thereby decrease the risk of asthma (37, 38, 39). In addition, research on risk factors includes examining the potential role of environmental and occupational exposures in the onset of asthma.
A major portion of NIH asthma-related research is devoted to enhancing understanding of pathogenesis and basic mechanisms of asthma. This work covers a range of issues relating to cellular and molecular-level events in asthma that cause the lung to become injured and repaired. It will help explain why asthma persists for many years, as well as why asthma is severe in some patients and not in others. The National Heart, Lung and Blood Institute (NHLBI), the National Institute for Allergy and Infectious Diseases (NIAID), and the National Institute of Environmental Health Sciences (NIEHS) support investigations of the immune system and asthma that may lead to prevention of the allergic inflammatory process. NIEHS is also studying other strategies for primary prevention of asthma, including how exposures to environmental agents modify the immune system, which may affect the early sensitization events preceding the onset of asthma.
Genetics Research
NIH is investing significantly in research on gene-environment interactions, including a genome-wide search to identify genes that confer susceptibility to asthma.
Family clustering of asthma and allergy suggests a genetic basis for asthma. However, since the genetic background of the population changes only slowly with the succession of generations, it is most likely that the rising trend in asthma in the last 15 years relates to environmental factors interacting with genetic susceptibility. Therefore, a major focus of research at several NIH institutes is on STYLE="text-decoration: underline">gene-environment interactions, and includes a genome-wide search as part of the Environmental Genome Project to identify genes that confer susceptibility to asthma. Early findings confirm that multiple genes may be involved . Defining how genetic and environmental factors interact to predispose certain individuals to asthma holds a key to prevention strategies for the disease.
Urgent Needs: Primary Prevention Research
DHHS will increase attention to three areas that show particular promise for uncovering clues to the onset of the disease, and will expand testing of innovative prevention strategies . (Many of these topics are also relevant to two other priority areas: reducing the burden of asthma and eliminating disparities in the impact of the disease on minority populations and the poor.)
Improve understanding of early life origins of asthma. While research on various aspects of the origins of asthma is already underway, further examination is needed of the potential for early life events to cause asthma, such as pre- and post-natal exposures to viral infections, allergens, tobacco smoke, and elements of the maternal and infant diet.
High levels of airborne allergen exposure in infancy have been shown to enhance the likelihood of sensitization and the development of asthma in childhood (34, 35, 37, 67). However, the immune mechanisms associated with the effects of allergens in infancy are not known and must be investigated. Another high priority need is the development of immunologic and clinical markers of asthma in infancy and early childhood among children of distinct genetic backgrounds.
Study gene-environment interactions and links to characteristics of asthma. As genes associated with asthma are defined, it will be important to establish their function, particularly how they regulate the disease process. Since genetic factors can also interact with environmental factors, understanding these links in the development of airway inflammation is another priority need. Recent data suggest that certain characteristics of asthma (e.g., whether it is exercise-induced, nocturnal, has persistent symptoms or episodic but severe attacks) are associated with specific genetic, immunologic and environmental factors (68). Examining these further could have significant implications for the prevention and treatment of asthma in individuals and in genetically distinct populations.
Investigate adult onset of asthma. Allergens may play an important role in some adults with asthma who did not exhibit the disease in childhood . In other adults with asthma , allergies are not detected; the mechanisms of "intrinsic" asthma are not well-understood. Additional research is needed on adult-onset asthma in areas such as: asthma during pregnancy, during menopause (especially in those on hormone replacement therapy), and in the elderly who have confounding medical complications. Another need is to characterize the conditions under which occupational asthma develops, including assessment of exposure-response relationships, so that prevention strategies can be developed.
Test strategies for prevention. Intervention trials are needed to test hypotheses of how to prevent asthma, even while work on understanding the basic mechanisms is proceeding. Tests of prevention strategies for those at high risk of developing asthma could include investigating whether eliminating various exposures during early life or providing pharmacologic treatments can delay or prevent the onset of the disease. Another promising strategy is to block the allergic immune response in susceptible individuals, for example by induction of immune tolerance (6) , thus preventing asthma from ever developing. Identifying interventions to prevent asthma is the most promising approach to ending the epidemic of asthma.
Priority Area 2: Reduce the Burden of Asthma for People with the Disease
Widespread use of the Guidelines is essential for reducing fatalities, emergency room visits and hospital stays, and for improving day to day quality of life for people with asthma (58). Despite the existence of the Guidelines, a substantial gap remains between their recommendations and the actual practices of many clinicians, people with asthma, and their families. Expanded investment in two areas can help close this gap: 1) promot ing widespread use of current scientific knowledge through public health activities , and 2) encouraging research to continually improve means of managing asthma.
Promote Wider Use of Current Knowledge to Diagnose and Manage Asthma: Public Health Actions
All segments of the health community have vital roles to play in improving the management of asthma. Medical professional societies can promote the use of best practices by their members and improve patient education. State and local health departments can sponsor education programs to promote improvements in managing asthma by health care providers, patients, families and the broader community. At the local level, coalitions among health care providers, public health planners, managed care organizations, school personnel, housing and environmental officials, and community outreach workers can promote improved asthma care in their community.
Current DHHS Activities: Promote Wider Use of Current Knowledge to Diagnose and Manage Asthma
DHHS support s an array of public health activities designed to promote broad dissemination and application of scientific knowledge to improve the diagnosis and management of asthma. These activities includ e clinician education and the promotion of improved quality in health care delivery, family and patient education, facilitation of community-based asthma programs and public education, and support for public health activities at the state level .
NHBLI supports clinician education through the translation of research on asthma into clinical practice guidelines and practical health education materials and tools. The first set of the Guidelines was widely distributed to physicians, medical schools and other health professionals and organizations, as well as to asthma patients. To promote broad use by other key health care professionals, targeted companion documents were developed for nurses, emergency department personnel, pharmacists, and school personnel. NHLBI also produced specialized reports on asthma during pregnancy, asthma in the elderly and asthma in minority children.
Research to Improve Quality of Care
The Agency for Healthcare Research and Quality is investigating whether several approaches to improve the quality of asthma care are effective in helping clinicians better manage the disease in accordance with the Guidelines.
Several programs are conducting research designed to understand which strategies are most effective in promoting the actual implementation of the Guidelines by health care providers. The Agency for Healthcare Research and Quality (AHRQ) has supported research on the factors that cause providers to not use the Guidelines. AHRQ is sponsoring several research projects to assess whether specific quality improvement approaches, being implemented in various clinical settings, are effective in helping clinicians better manage childhood and adult asthma in accordance with the Guidelines. Cost-effectiveness is being examined in several studies which are also testing health outcome measures such as symptom-free days to identify how treatments affect children's daily lives.
NHLBI sponsors a wide range of education and outreach activities through the National Asthma Education and Prevention Program (NAEPP), which is guided by a Coordinating Committee composed of diverse public and private sector organizations (7) . These groups have worked together and in partnerships with other organizations on outreach activities. Examples include: a national conference on "Managing Asthma in Managed Care;" a school-based asthma education program (implemented in partnership with EPA and the American Lung Association); and a bilingual asthma awareness program ("Sesame Street: A is for Asthma") with the Children's Television Workshop. The NAEPP has explored how best to convey strategies for asthma management not only to patients, but also to clinicians, family members, school personnel and caregivers.
Asthma Management Model System
The National Asthma Education and Prevention Program designed a model web-based system to improve the diagnosis and management of asthma. The site provides virtually all the scientific literature on chronic asthma that has ever been published, as well as practical information for clinicians, patients, and public health professionals. See www.nhlbi.nih.gov.
The National Institute of Nursing Research (NINR) evaluates the effectiveness of routine education in a clinic setting reinforced by nurse home visits which include a computer-based asthma instructional program on self-management. Another NINR program is instructing parents and caretakers to learn signs of pending asthma attacks in children living in rural areas. NIAID- and NHLBI-sponsored Demonstration and Education projects focus on improving management of asthma in under-served areas. The Inner-City Asthma study, (described more fully in the following section on research), has evaluated the impact of various types of outreach and education, including intervention with an asthma counselor tailored to the needs of each family.
Recently, DHHS has expanded efforts to address asthma in community settings, including collaborat ion with community-based coalitions that directly address asthma in a comprehensive manner at the local level. These coalitions are composed of community groups, health care providers, and other private and public sector organizations to foster better quality of care for asthma sufferers. For example, the NAEPP facilitates collaborative activities at the local level, has established a consortium of over 40 coalitions, and maintains an Asthma Coalition Exchange on the NHLBI website. CDC's National Center for Environmental Health has worked with DHHS Region IV and seventeen other organizations on a public health program known as "ZAP Asthma," a collaborative program to reduce the adverse impacts of asthma in the Atlanta Empowerment Zone neighborhoods.
NHLBI supports the development of model programs for improving asthma management in the school setting. NHLBI has also sponsored a number of media campaigns to promote asthma awareness among the general public and to encourage undiagnosed patients to seek care.
In communities where people might be exposed to hazardous substances in the environment, the Agency for Toxic Substances and Disease Registry (ATSDR) recommends actions for safeguarding people's health. The agency has made such recommendations at sites where exposures to substances known or suspected to exacerbate asthma have occurred. It has also supported general health education and promotion activities, including continuing medical education for physicians on the relationship between asthma and the environment.
To protect workers, the National Institute for Occupational Safety and Health (NIOSH) develops and recommends criteria for preventing disease (including asthma) and hazardous conditions in the workplace; the recommendations are transmitted to the U.S. Department of Labor for use in promulgating legal standards. Additionally, NIOSH issues alerts that urgently request assistance from workers, employers, and safety and health professionals in preventing, solving, and controlling newly identified occupational hazards. For example, alerts have been issued on asthma in animal handlers, and asthma from exposure to diisocyanate and natural rubber latex.
To support asthma programs at the state level, in late 1997, CDC established a network of asthma contacts that includes officials from every state, the District of Columbia, two city health departments and two territorial health departments. CDC supports the network through a series of activities, including sponsoring monthly teleconferences and annual meetings, working to identify and document scientifically proved intervention programs, identifying state laws that affect persons with asthma, and drafting model language for asthma to be used by state agencies in writing Medicaid contracts.
DHHS regions have also been involved in collaborative efforts on asthma . For example, in Region I (New England), DHHS, EPA, and the Department of Housing and Urban Development are convening a summit meeting of federal and state public health, environmental, and housing officials to develop a joint strategy to reduce the burden of asthma in New England. Region II (New York, New Jersey and Puerto Rico) awarded grants to the New York and New Jersey State Health Departments to develop community-based partnerships to focus on asthma. Region III (Philadelphia) co-sponsored a conference with EPA and Johns Hopkins University - involving health care providers, health educators, community health advocacy groups, managed care organizations, and others - to begin developing an asthma strategy for the mid-Atlantic region (See Appendix E for additional programs supported by DHHS regions).
Urgent Needs: Promote Wider Use of Current Knowledge to Diagnose and Manage Asthma
Help health care providers practice up-to-date asthma care. Recent evidence indicates that many health care providers do not follow the Guidelines for the diagnosis (8) and management of asthma (61, 62, 63, 69) . Failure to follow clinical guidelines stems in part from factors related to knowledge, attitudes and behavior (70), so multiple approaches will be needed to see improvements. Proactive approaches appear to be the most promising, and include educational outreach visits, interactive educational meetings, and consistent reminders integrated into medical care routines (71, 72, 73). As an example, one asthma study reported that an interactive seminar for physicians resulted in improvements in the prescribing and communications behavior of physicians, more favorable patient responses to physician's actions, and reductions in health care utilization (74). DHHS must expand and sustain partnerships with state and local health agencies, medical professional societies, and other organizations to sponsor education and outreach programs to improve the quality of asthma care available to patients with asthma. Such programs need to be developed for particular settings, and those that have demonstrated effectiveness in both changing health care practices and improving health outcomes need to be expanded.
Educate patients and their families. Asthma management often requires behavioral changes and vigilance on the part of people with asthma. This includes paying careful attention to respiratory symptoms and adhering to complex treatment regimens, which can be difficult for many asthma patients, including young children and the elderly, and for families and caregivers with multiple demands and stresses. To promote adherence to treatment recommendations, patients and their families need to be full participants in the development of the asthma management plan, and health care providers should seek to understand and address factors that can affect adherence. Additionally, some model programs promoting self-management of asthma have resulted in dramatic improvements in functional status and improved school performance for children. Moreover, they have achieved substantial cost reductions, in some cases up to 50 percent, by cutting hospitalizations and acute care visits (75, 76, 77). DHHS, working with state and local health agencies and other organizations, must increase and sustain support for effective and culturally-competent approaches that teach patients and families to control asthma, enhance their ability to communicate with health care providers about asthma, and help sustain progress in managing this chronic disease.
Evaluate and address organizational barriers to quality care for asthma. Creating and evaluating cost-effective methods for ensuring implementation of the Guidelines by so many people in so many settings demands continued research. In addition to evaluating education and outreach programs (as indicated in the preceding paragraphs), research should address how other aspects of the health care system affect asthma care. For example, time constraints and payment policies can affect the amount of time a health care provider can spend educating patients. In addition, insurance plans may not reimburse families for equipment used in administering asthma medications (e.g., spacers).
A number of managed care organizations and other types of comprehensive health care organizations are implementing disease management programs for asthma. Disease management is "a systematic, population-based approach to identify persons at risk, intervene with specific programs of care, and measure clinical and other outcomes" (78). In one model of disease management, specialized teams work within a health care organization to assist primary care physicians in treating chronic illnesses (79). In another type of program, services are provided through contracts with disease management companies, which stratify patients according to their costs of care, and then target services accordingly (80). Such approaches warrant testing and evaluation to assess their impact on health outcomes, physician practices, and cost-effectiveness.
Expand asthma control activities in community settings. The environment outside the home is beyond the patient's control, and others in those settings may not be trained to recognize symptoms, help support asthma management, or handle an emergency. Apartment buildings and rental housing also create circumstances where the environment inside the home may be out of an individual's control. DHHS must work with state and local health agencies and others to intensify efforts to promote ongoing asthma education in schools, workplaces, public housing, child care and youth programs, job training programs, and other community institutions. This will include outreach to school personnel, workplace supervisors, housing officials, and others, to provide information and to help identify institutional policies that may hamper effective asthma management. For example, o verly rigid policies resulting in inadequate access to and use of medication in school often unnecessarily disrupt classroom learning and make it difficult for children to achieve optimal management of their asthma. In addition to educating people with whom a patient comes into contact and generally expanding public awareness, public health programs should highlight the need to reduce levels of irritants (e.g., environmental tobacco smoke and some air pollutants) and allergens outside of the home environment and otherwise make it easier for patients to follow their treatment plans. DHHS must also increase support for public education campaigns to enhance public awareness about asthma as a serious disease and appropriate asthma management techniques.
Sustain support for State and local public health action. DHHS will seek to equip state health departments, through a grant program, to promote asthma education, prevention, and public health outreach activities in local communities. Activities will target the urgent needs described above and the public health programs described in Priority Area III, including clinician education programs, patient and family education, and training for school personnel. By working with public health and environmental agencies at all levels, as well as organizations outside of the government, scientific advances can be made available to all patients.
Discover and Develop Improved Means of Managing Asthma: Research
While work proceeds to implement state-of-the-art science through public health programs, further research is required to answer remaining questions about asthma care and to explore new ways of improving quality of life for people with asthma. "Secondary prevention" research is designed to identify methods to reduce illness in those who have asthma, but is not directed at preventing the primary onset of the disease.
Current DHHS Activities: Secondary Prevention Research
Discovery of the role that inflammation and allergic sensitization play in asthma led to the development of several new approaches for treating asthma. For example, inhaled corticosteroids reverse the inflammatory process, prevent or reduce severity of symptoms, and reduce emergency room visits, hospitalizations, and deaths due to asthma. Also, two new classes of drugs aimed at reducing asthma severity by inhibiting the inflammatory process have recently been developed - antileukotrienes and anti-IgE therapy.
Managing Childhood Asthma
NHLBI's Childhood Asthma Management Program, a multi-center clinical trial with over 1,000 children enrolled, will provide critical information about the long-term effects and safety of three key therapies for childhood asthma.
NHLBI devotes substantial resources to clinical trials evaluating and assessing treatment strategies. Multiple research investigations are underway to examine the impact and safety of medications at different stages of children's development (e.g., possible effects on bone growth and eye complications later in life) and to discover the best treatment options for children who have different genetic backgrounds or environmental exposures. NHLBI's Childhood Asthma Management Program supports a major multi-center trial to examine and compare the long-term effects of asthma medications on the course of the disease, lung growth and development, and overall physical and psychosocial development of 5-12 year old children. A new Pediatric Clinical Research Network has been established by NHLBI to evaluate clinical asthma treatments, especially in infants and young children. The Asthma and Pregnancy Trial, sponsored jointly by NHLBI and the National Institute of Child Health and Development (NICHD), examines the impact of asthma medication use and effective asthma control on perinatal outcome.
The National Cooperative Inner City Asthma Study, supported by NIAID since 1991, represents an effort to reduce asthma morbidity in inner-city, predominantly African-American and Hispanic children. The present study, funded by NIAID and NIEHS, tests the effect ivenes s of a comprehensive environmental intervention to reduce levels of indoor allergens such as cockroach, house dust mite and mold, and of environmental tobacco smoke, on asthma morbidity . Also , through a collaborative effort with the U.S. Environmental Protection Agency, a study will evaluate the impact of indoor and outdoor air pollutants on asthma among inner-city children.
The National Institute for Occupational Safety and Health (NIOSH) of the Centers for Disease Control and Prevention (CDC) examines environmental control issues in the workplace. NIOSH conducts studies evaluating the incidence, risk factors, and natural history of asthma in groups of workers employed in settings where substances recognized to exacerbate asthma are present. Exposures of current interest include: health care (natural rubber latex used in medical gloves), aluminum production , wood products manufacturing, and the indoor environmental quality of schools and offices . NIOSH has recently embarked on a multi-center trial to prevent latex sensitization in health care workers.
As the Guidelines assert, regular and effective monitoring of symptoms can help both health care professionals and patients gauge the severity of an asthma attack and react accordingly. NHLBI supports investigations examining the relative merits of different approaches to peak flow or symptom monitoring for guiding day-to-day therapeutic decisions. NINR is testing ways to promote children's use of home peak flow meters. In addition to approving safe and effective drugs for treating asthma, the Food and Drug Administration (FDA) approves medical devices such as peak flow meters and spirometers, as well as serologic tests used in allergy testing.
Urgent Needs: Secondary Prevention Research
Improve understanding of what makes asthma persistent and severe. Some patients, especially those with severe asthma, may have active inflammatory disease without apparent external triggers. Further, some patients may experience long-term, irreversible changes in the lungs. These permanent structural changes (known as airway remodeling) may contribute to the persistence of the disease, often lasting for many years or a lifetime. The mechanisms that induce these irreversible changes, and the methods to prevent them, are largely unknown. Identifying them will lead to effective therapies.
Develop improved means of controlling triggers of asthma and the allergic response to them. Recent research has shown that both the exposure and the allergic immune response to certain indoor allergens are responsible for many exacerbations of asthma. Present methods for modulation of the allergic immune response and for control of levels of certain allergens are of uncertain and possibly limited clinical benefit for asthma. Moreover, some allergens and other agents (in particular, cockroach and mold allergen, and respiratory viruses) are extremely difficult to control. There is a need to identify optimal and cost-effective methods for reducing levels of these asthma triggers in homes, schools and workplaces and for basic research to develop new approaches to modulate the human immune response to those allergens relevant to asthma. Other high priorities include work to identify as yet unknown triggers of asthma and optimal, cost-effective methods for reducing allergen levels.
Investigate the relationship between outdoor air pollutants and asthma. Several ambient air pollutants are known to be respiratory irritants and can exacerbate asthma symptoms (e.g., ozone, sulfur dioxide)(51). DHHS must accelerate efforts to better understand the cellular and molecular mechanisms by which air pollutants perturb the normal functioning of cells, tissues, and organs. In addition to refining understanding of the role of air pollutants in exacerbating asthma, this research will help determine whether they are implicated in the initial onset of the disease. Moreover, some pollutants may act synergistically with other environmental factors to worsen asthma.
Investigate variations in patient response to asthma medications. Not all patients respond favorably or in the same way to the same medications, and some patients experience adverse side effects from asthma medications. P atients would benefit from the development of both new treatments and the means for tailoring therapeutic approaches to the specific genetic and clinical characteristics of the individual's asthma.
Establish causes and risk factors of asthma fatalities. Asthma fatalities should be investigated to identify specific risk factors and to enhance understanding of how events lead to fatal disease. This information can lead to ways to improve patient management and prevent fatalities .
Develop non-invasive methods for diagnosis and disease monitoring. Asthma can be especially difficult to diagnose, monitor, and study in infants, young children, and the elderly. Therefore, new technologies -- such as imaging or biochemical markers of inflammation, and patterns of gene activation - are needed to detect disease and monitor disease progression, particularly in these vulnerable populations.
Expand research on asthma in pregnancy. Work has just begun on evaluating how infants are affected by asthma severity in the mother. Research is particularly needed on women whose asthma is difficult to control, and whose medication could have adverse side effects on the fetus.
Priority Area 3: Eliminate the Disproportionate Burden of Asthma in Minority Populations and Those Living in Poverty
Low income populations and minorities experience disproportionately higher morbidity and mortality due to asthma. The reasons for these disparities are not clearly understood, but where poverty is present they are probably due to an interaction of factors including: lack of access to quality medical care, high levels of exposure to environmental allergens and irritants, language barriers, and lack of financial resources and social support to manage the disease effectively on a long-term basis.
African American and Hispanic children appear to be at especially high risk of not receiving adequate preventive treatment for asthma attacks. Several studies have documented inappropriate treatment for asthma among inner-city children with asthma (64, 81, 82, 83). For example, an analysis of preschool children hospitalized for asthma found that only seven percent of African Americans and two percent of Hispanics, compared with 21 percent of white children, were prescribed routine medication to prevent future asthma exacerbations (82). A recent study of elementary school children in Baltimore, MD and Washington, DC, found that inner-city children with asthma frequently are undermedicated, using the wrong medication, or none at all despite daily symptoms, frequent school absences, and emergency room visits for asthma. More than 80 percent of those who did take regular medication did not use anti-inflammatory drugs (64) .
Inner-city children and their parents often live in highly challenging, difficult environments. Families often face economic uncertainty and live in homes or apartments with poor ventilation and high allergen levels. Children in these settings frequently have multiple caretakers for their asthma and little continuity of health care (84) . A study of Hispanic families in San Diego found that parents who speak only Spanish have significantly more misconceptions about asthma than English-speaking Hispanic parents (85). Although not as well studied, children with asthma from rural America also face multiple barriers that adversely affect their health including extensive poverty, geographic barriers to health care, less health insurance and poor access to health care providers (86).
Current DHHS Activities: Eliminating Disparities
The asthma objectives for Healthy People 2010 emphasize the need to reduce the disproportionate impact of asthma on minorities, particularly with regard to asthma death rates and hospitalization rates. Several DHHS agencies support public health programs designed to meet the needs of individuals and families in poverty. The NAEPP supports several such programs, and CDC's Z AP Asthma and other Regional programs described earlier have a particular focus on improving the lives of inner-city children. The Administration for Children and Families' (ACF's) Head Start program offers comprehensive early childhood education, nutrition, and health and social services, along with strong parent involvement, to low-income children nationwide. Caring for children with asthma is addressed in two important training guides used by Head Start front line staff, management teams, and parents. The Office of Minority Health (OMH) supports the "Minority Health Asthma Attack Avoidance Education Program," which is designed to increase awareness of asthma triggers and ensure appropriate referral to medical care.
The majority of DHHS funds dedicated to asthma provide direct health services to underserved populations. The Medicaid program administered by HCFA reimbursed costs of asthma care for over one million low income patients in 1995 (65). The Health Resources and Services Administration (HRSA) -supported Health Centers and the National Health Service Corps programs aim to increase access to comprehensive primary and preventive health care and to improve the health status of underserved and vulnerable populations. Comprehensive primary care services in Health Centers include the treatment of asthma; in 1998, patient visits for asthma exceeded 600,000 (87). The Indian Health Service (IHS) delivers health care to American Indians and Alaska Natives. In addition to providing asthma treatment as part of standard care, IHS has helped to establish several specialty clinics focused on asthma.
HRSA is also working with non-governmental institutes (co-sponsored and endorsed by the NAEPP) to develop and apply an innovative model to accelerate improved asthma care. The care model uses five basic elements to improve care: 1) collaboration between the health system and community organizations and agencies, 2) patient/family self-management, 3) support to enable clinicians to use guidelines in their every day work, 4) practice re-design, and 5) information systems to track individual patients as well as assess the health of the asthma patient population in the medical practice. HRSA and other organizations are supporting a number of community health centers in adopting this model of care, which involves a 12-14 month training program for health center teams.
Inner-City Asthma Study
The NIAID-sponsored National Cooperative Inner-City Asthma Study found that empowering families to increase their asthma self-management skills and to improve their interactions with the primary care physician were important ways to improve quality of care and reduce asthma symptoms. An asthma counselor helped not only with asthma education, but with problem solving tailored to the families' needs. Improvement in health continued at the same level during the second year of the program when the asthma counselor was no longer involved (84).
Various DHHS agencies and institutes conduct research to better understand the impact of asthma on vulnerable populations. NIEHS and NIAID sponsor research on community-based strategies to reduce exposures that trigger asthma in economically disadvantaged and/or underserved populations as in their National Cooperative Inner-City Asthma Study. Six of the eight NIEHS/EPA/CDC- sponsored Centers for Children's Environmental Health and Disease Prevention Research have projects focusing on asthma in under-served populations. NHLBI and NIAID support genetics research that is revealing that multiple genes may be involved in asthma, and early findings indicate that they may vary among ethnic/racial groups. The NIH Office of Research on Minority Health and NHLBI are also supporting a study of Genetics of Asthma in Hispanics. NHLBI and NINR sponsor research on the effectiveness of asthma education and self-management programs, targeting African Americans and Mexican Americans in both urban and rural areas.
Several DHHS agencies conduct research and evaluations to assess and improve both access to, and quality of asthma care. The Agency for Healthcare Research and Quality (AHRQ) supports research designed to measure and improve the quality of health care, reduce its cost, and broaden access to essential services . HRSA collaborates with AHRQ on the development of health center practice-based research networks. One of these projects is focused on asthma and involves epidemiologic investigations, clinical outcome studies, and intervention trials. HCFA conducts research on the use of services and expenditures for asthma care provided to its Medicare and Medicaid beneficiaries. Specific work includes examining the quality of asthma care - using the Guidelines - provided to Medicaid eligible children. NHLBI and NIAID support demonstration and education research to develop innovative, culturally-sensitive approaches to teaching asthma management strategies to African-American and Hispanic children and their families.
Urgent Needs: Eliminating Disparities
If we are to make progress in eliminating disparities, it is critical to investigate why these disparities exist. While the "Urgent Needs" described in the previous sections will help to address the disproportionately high impact of asthma on minority and low-income populations, more focused efforts are also needed. DHHS will seek a substantial expansion of public health programs to eliminate the disproportionate burden. The Department will accelerate research directed at the reasons for disparities and the means to reduce these impacts . Four key priorities include:
Promote wider use of current knowledge to diagnose and manage asthma, focusing on minority and low income populations. Programs that help health care providers practice up-to-date asthma care, educate patients and their families, expand asthma control activities beyond the home, -- all need to be targeted toward special population groups hardest hit by asthma. In doing so, such programs need to address the unique circumstances of the particular community. A high priority is to implement education programs that take into account the complexities of poverty, language barriers, and cultural sensitivities.
Improve access to quality care. DHHS agencies must work in public/private partnerships to address the barriers to quality asthma care and provide ongoing, comprehensive, quality health services for asthma. Such services would be based in the community and would encourage active participation of families, while addressing their cultural needs. A policy of collaboration at the local level and coordination of services among community providers (including health, environmental, and housing services) are important ingredients for success.
Expand research on asthma in special population groups. While data indicate greater hospitalizations and deaths from asthma among population groups such as Hispanics and African Americans (4, 88), additional research is needed to understand the reasons for these higher rates. For example, research is needed to understand if these disparities are due to more severe disease in these populations or to differences in health care practices and access to care, or a combination of both. One research priority is distinguishing the roles of environmental, socio-economic, cultural and genetic factors in contributing to asthma severity. Genetics research will help explain different risks for severe asthma and differences in response to asthma treatments. This can help identify new therapeutic approaches. Exposures to environmental allergens and pollutants may be greater for some population groups, particularly in the inner city. Research is needed to design interventions that could reduce asthma severity by addressing these environmental factors. In addition, some Hispanic populations appear to have a markedly elevated risk for developing asthma. Environmental, genetic and cultural factors need to be examined to understand why these differences occur. Finally, as prevention strategies for asthma are developed and tested, their effectiveness in different population groups should be a special focus for evaluation.
Investigate access to care and evaluate quality. Another priority is to better understand the degree to which individuals in poverty, particularly children, have access to care and whether the quality of that care is sufficient. Recent studies reveal that traditional measures of access (e.g., insurance coverage and source of routine care) may not reflect the realities affecting poor health outcomes for asthma. The National Cooperative Inner-City Asthma Study reported that 92 percent of children in the study were covered by insurance, and nearly three quarters were covered by Medicaid. While most families reported a usual source of routine care (neighborhood or hospital clinic), more than 50% of respondents found it difficult to get follow-up care. Quality of care was deficient and participants were unlikely to have continuity between usual sources of routine (follow-up) and acute care (23). Further studies are needed to uncover the barriers to improved health, including: access to quality and continuous care and access to prescription medication and delivery devices. Analyses must continue to evaluate the impact of managed care on delivery of health services and health outcomes.
Priority Area 4: Track the Disease and Assess the Effectiveness of Asthma Programs
Current DHHS Activities: Tracking the Disease
Surveillance - the systematic collection, evaluation, and dissemination of data used to track the occurrence and severity of particular diseases - is critical to research and public health practice. Combined with studies in large groups of people, surveillance results can identify populations with particularly high or low prevalence, and can shed light on factors influencing the develop-ment of asthma. Surveillance data can help identify high risk populations and risk factors to inform the design and implementation of interventions suitable for a particular community. Finally, state and local health agencies can use surveillance information to assess the impact of public health programs or environmental controls.
Surveillance for Asthma
National estimates for asthma are developed from ongoing general health surveys. CDC is collaborating with NIH and EPA to sponsor more localized surveillance activities in four states and two major cities.
Current surveillance for asthma provides national estimates, but cannot provide state or local level data on asthma. The national estimates are derived from ongoing health surveys (9) and data systems dealing with health events such as mortality, hospitalization, emergency room visits, and outpatient visits. Th is information does not reveal the detailed picture of how asthma varies from one location to another-information greatly needed for an effective public health response. Fewer than 10 states have conducted asthma prevalence surveys (89). Surveillance for occupational asthma is also limited. Since1987, NIOSH has provided funding to several state health departments to pilot case-based surveillance for selected occupational health conditions, including asthma. Currently, four states are conducting surveillance and preventive intervention programs for occupational asthma (90). In Fiscal Year 1999, NIH, CDC and EPA took an initial step toward addressing these limitations. They initiated a collaborative project to define ongoing surveillance activities and their utility in asthma control efforts. The activities were undertaken in four states and two city health departments.
Urgent Need: Tracking the Disease
Establish coordinated and systematic local, state and national systems for asthma surveillance. Timely data on asthma at the state and local level are needed to support the design of effective public health interventions . Such data are critical to finding answers to the troubling question, "Why is asthma prevalence rising?" Better data will also enable us to target populations in significant need of public health intervention, and to assess the geographic, ethnic, and gender differences in asthma morbidity and mortality . Furthermore, information about other aspects of the burden of asthma would be useful in designing interventions, including the quality of care or the severity of illness. Finally, surveillance data are needed to determine whether or not public health programs are succeeding in reducing the impacts of asthma.
Existing state-based surveys should be expanded to include questions related to asthma diagnosis, severity, management techniques, and suspected environmental and household risk factors. Also, DHHS could provide additional assistance to states to use existing data more effectively. In many cases, information is not analyzed or made accessible to those who plan asthma interventions. Finally, new systems of surveillance should be developed to gather additional information on locations with particularly elevated rates of asthma. One potential area for model surveillance in both urban and rural settings is in emergency rooms, where many children with asthma receive care for an acute episode, but fail to receive follow-up care. In addition, strategies to determine the incidence of asthma, at least in defined geographic areas, are needed.
Current DHHS Activities: Evaluations of Asthma Programs (10)
Evaluations of public health programs and health services addressing asthma can speed progress towards widespread establishment of programs that allow people with asthma to live fully active lives. Many of the major public health and health services programs sponsored by DHHS have evaluation components to determine whether they are effective. The NAEPP and HRSA's Health Centers, for example, include evaluation elements to prompt shifts when programs are not meeting their goals, and to make possible replication of successful projects and components. AHRQ is developing new measures to help evaluate systematic improvements in quality of care. Valid, sensitive measures allow investigators to reliably identify those interventions that lead to real improvements. Recently AHRQ and NAEPP helped develop a new measure of quality care to track the use of anti-inflammatory medications. This measure will be used in the most recent version of the Health Plan Employer Data and Information Set (HEDIS 2000), a system widely used to evaluate the quality of health plans.
Research aimed at developing effective public health programs by definition provides evaluative information that helps determine what kinds of interventions work. For example, the Inner-City Asthma Study investigates not only the impact on asthma severity of reducing exposure to allergens and receiving proper medical care, but also the role of physician education and feedback in supporting the management of asthma.
Urgent Needs: Evaluation of Asthma Programs
Evaluate public health and health services interventions. Disseminate results. While some programs that educate patients and families about asthma management have been rigorously evaluated, most local and regional asthma coalition efforts that mobilize the broader community have not. To rapidly extend primary care and public health programs so that large numbers of asthma patients receive quality care, public health practitioners need to understand the characteristics of successful programs implemented in a variety of settings. Strengthening three aspects of evaluation could enhance the knowledge base about how to cost-effectively scale up public health programs and ensure that they significantly reduce rates of morbidity and mortality from asthma.
First, there is a need for appropriate tools to evaluate the effectiveness of asthma intervention strategies. Second, there is a need to build in an evaluation component, and sufficient funding to support it, to all public health programs that address asthma (11).
Third, there is a need to disseminate evaluations of asthma programs and encourage the use of such evaluations in designing and funding programs. Evaluation analyses combined with relevant research findings will help delineate determinants of success and failure in reducing the burden of asthma.
Conclusion
This document describes an ambitious strategy for tackling asthma over the next five years. A concerted effort along these lines could identify strategies to reduce rates of asthma and could significantly improve asthma management for children, minorities and the poor. Now is the time to take full advantage of the discoveries of the last ten years in asthma research.
Highest priorities for additional investment are to: 1) accelerate the pace of research to understand the causes of asthma and test prevention strategies ; 2) reduce the burden for people with the disease through expansion of public health programs and research; 3) eliminate the disproportionate burden of asthma in minority populations and those living in poverty; and, 4) enhance surveillance and evaluation efforts in order to better target populations in need, and improve public health programs.
In Fiscal Year 2000 , DHHS is spending over $180 million on asthma research and public health programs, up approximately 16 percent from the previous year . This provides a strong base for further investments over the longer term -- investments that promise substantial gains in reducing the incidence, prevalence, severity, and social and economic burdens of this chronic disease.
Table 2. Action Against Asthma - Urgent Needs Top Priorities for Investment
| 1. Determine the Causes of Asthma and Develop Interventions to Prevent Its Onset Improve understanding of early life origins of asthma 2. Reduce the Burden of Asthma for People with the Disease Promote wider use of current knowledge to diagnose and manage asthma: public health actions Help health care providers practice up-to-date asthma care Discover and develop improved means of managing asthma: research Improve understanding of what makes asthma persistent and severe | Investigate variations in patient response to asthma medications 3. Eliminate the Disproportionate Burden of Asthma in Minority Populations and those Living in Poverty Promote wider use of current knowledge to diagnose and manage asthma, focusing on minority and low income populations 4. Track the Disease and Assess Effectiveness of Asthma Programs Establish coordinated and systematic local, state and national systems for asthma surveillance. |
Specific Recommendations
This five year strategy for DHHS, Action Against Asthma, was developed by the Department's asthma experts, along with input from public comment. The following specific recommendations address the four priority areas of the five-year strategy. With each recommendation, the agency with primary responsibility for implementation is identified. However, many recommendations require work and coordination among many agencies within the Department and, in these cases, multiple agencies are listed. The majority of the specific recommendations were developed near the time of the first year of the strategy-fiscal year 2000. However, as science continues to produce new findings, new recommendations will continue to emerge.
Priority Area 1: Determine the Causes of Asthma and Develop Interventions to Prevent its Onset
Improve Understanding of the Early Life Origins of Asthma
Determine how early life events, such as features of the mother's or child's diet, exposures in utero or in early infancy to allergens and environmental pollutants, tobacco smoke, or respiratory infections cause children to develop asthma (NIH).
Identify immunologic and clinical markers in infancy and early childhood among children of distinct genetic backgrounds. Determine the utility of these markers as predictors of the onset of asthma or of responsiveness to primary prevention therapy (NIH).
Study Gene-Environment Interactions and Links to Characteristics of Asthma
Identify different clinical characteristics (e.g., exercise induced, nocturnal, persistent symptoms, etc.) of asthma associated with different genetic, physiologic, immunologic and environmental factors (NIH).
Examine the processes involved in asthma, such as understanding: 1) airway biology, 2) role of genetic and environmental factors in the development of airway inflammation, 3) genetic factors underlying atopy (inherited susceptibility to become allergic) or bronchial hyper-responsiveness, and 4) genetic regulation of the immune inflammatory response relevant to asthma (NIH).
Investigate Adult Onset of Asthma
Study the mechanisms of adult onset asthma, including the development of asthma in women and its relationship to hormonal changes, and asthma in the elderly who are likely to have confounding medical complications. In the elderly, study the interaction of asthma medications with medications for other chronic conditions ( HCFA, NIH).
Seek to more fully elucidate asthma mechanisms, patterns of responses, and risk factors for work-related asthma (CDC, NIH).
Test Strategies for Prevention
Assess the effectiveness of allergen avoidance in preventing allergen sensitization and in reducing asthma prevalence among children from low-income families (NIH).
Conduct clinical trials using new immune approaches, in conjunction with optimized environmental control, to test their effectiveness in preventing the onset of asthma and allergic diseases (NIH).
Evaluate the efficacy of early pharmacologic treatment in reducing the onset of asthma in children (NIH).
Priority Area 2: Reduce the Burden of Asthma for People With the Disease
Promote Wider Use of Current Knowledge to Diagnose and Manage Asthma: Public Health Actions
Help Health Care Providers Practice Up-to-date Asthma Care, and Educate Patients and Their Families
To accelerate widespread use of the Guidelines and to increase self-management skills of families and parents, develop partnerships with State health officials, community coalitions, professional societies, public and private health care purchasers, health plans, patients and others (AHRQ, CDC, HCFA, NIH).
Working in partnership within and outside the Federal Government, develop and evaluate improved models and programs that can advance widespread use of the Guidelines by health care providers and patients (AHRQ, CDC, NIH).
Evaluate and Address Organizational Barriers to Quality Care for Asthma
Evaluate innovative and cost-effective methods promoting adoption of the Guidelines, with analysis focused on organizational factors that may drive provider and patient behavior (AHRQ, HRSA, NIH) .
Work with managed care and other health care organizations, and with State health officials, to accelerate widespread adoption of the Guidelines (HCFA, NIH, CDC ).
Extend Asthma Control Activities in Community Settings
Integrate asthma control activities into existing systems such as schools, public housing, child care, youth programs, workplaces, job training programs, and other community institutions (CDC, NIH).
Expand the capacity of school-based health centers to help promote and sustain improved health and environmental policies in schools (HRSA) .
Establish programs involving asthma management, education and awareness at the local school level to help monitor and control the physical environment, promote self-management, help identify students with asthma, train school staff, and establish action plans for handling asthma episodes (CDC, NIH).
Increase support for public education campaigns to enhance public awareness about asthma as a serious disease and appropriate asthma management techniques (NIH, CDC).
Sustain Support for State and Local Public Health Action
Provide grants to State health departments to ensure that effective asthma education, prevention, and public health outreach activities in local communities are developed and sustained (CDC, HCFA, NIH).
Discover and Develop Improved Means of Managing Asthma: Research
Improve Understanding of What Makes Asthma Persistent and Severe
Support basic research on the mechanisms underlying the chronic nature of asthma and the role of airway remodeling and repair in determining the persistence and severity of asthma (NIH).
Develop Improved Means of Controlling Triggers of Asthma and Allergic Responses
Develop new immunologic approaches to reduce allergic responses to indoor allergens responsible for asthma exacerbations. Conduct clinical trials using new immune approaches, in conjunction with optimized environmental control to test effectiveness in treating asthma and allergic diseases (this recommendation is also applicable to preventing the onset of disease) (NIH).
Identify optimal and cost-effective methods to reduce levels of cockroach and other allergens (NIH).
Investigate the Relationship Between Air Pollutants and Asthma
Analyze pollutant-allergen effects on immune responses in animal models and preclinical studies and better understand the mechanisms by which air pollutants contribute to, and mediate, asthma (NIH).
Identify the relative importance and potential synergistic effects of toxic air pollutants on asthma in population-based studies (ATSDR).
Develop and refine methods for medical and environmental monitoring for workplace asthma (CDC).
Investigate Variations in Patient Response to Asthma Medications
Study , in different population groups, the relationship of inherited characteristics of asthma, the severity of an individual's asthma, and the individual's response to medications. Develop appropriate tools to identify the best treatment options for patients based on these characteristics (NIH).
Establish Causes and Risk Factors of Asthma Fatalities
Establish a registry of fatal asthma to permit identification of specific risk factors and mechanisms of fatal and near fatal asthma. This research would provide a scientific basis for change in patient management to reduce the risk of asthma fatality (NIH, CDC).
Develop Non-invasive Methods for Diagnosis and Disease Monitoring
Research is needed to develop non-invasive methods such as imaging or biochemical markers of inflammation for detecting disease and monitoring disease progression. Surrogate markers for asthma in infants, young children and the elderly will also be included (NIH).
Expand Research on Asthma in Pregnancy
Examine the impacts of asthma during pregnancy and the effectiveness of specific treatment regimens on perinatal outcome (NIH).
Follow-up mothers and children currently enrolled in observational studies of asthma during pregnancy through the Maternal-Fetal Medicine Units network. Continue longitudinal observations to: compare asthma in non-pregnancy with prior pregnancy, and subsequent pregnancy in the same individuals; assess risk of development of asthma in study children and their siblings; investigate biomarkers of disease; and, measure environmental factors which may contribute to asthma during pregnancy (NIH).
Priority Area 3: Eliminate the Disproportionate Health Burden of Asthma in Minority Populations and Those Living in Poverty
Promote Wider Use of Current Knowledge to Diagnose and Manage Asthma, Focusing on Minority and Low Income Populations
Focus comprehensive public health initiatives (previously described) on underserved populations, taking into account unique circumstances of the community (ACF, CDC, HRSA, IHS, NIH).
Make culturally and linguistically appropriate information on asthma widely available (CDC, NIH, HRSA) .
Train Head Start staff in asthma management techniques by expanding existing programs on "Sustaining a Healthy Environment" and "Caring for Children with Chronic Illnesses" (ACF) .
Improve Access to Quality Care
Award grants to state and local agencies or organizations to develop and expand effective strategies for reducing the adverse effects of asthma by expanding access to high-quality health care. Key features include: use of the Guidelines; consistent and ongoing comprehensive care; adequate financing for services, medications and medical supplies that help control asthma; coordination of services among community providers; and active participation of families in the provision of culturally competent, family-centered, community-based services (HRSA).
Test the effectiveness of quality improvement strategies such as disease management (through grants and technical assistance to States), in reducing the frequency and severity of asthma attacks among children insured by Medicaid and the Children's Health Insurance Program (HCFA, HRSA, AHRQ) .
Expand Research on Asthma in Special Population Groups
Distinguish the roles of environmental, socio-economic and socio-cultural factors in asthma severity from those of genetically-based differences. For inner-city populations exposed to higher levels of environmental allergens and pollutants, design and evaluate interventions to reduce asthma severity. Investigate variations in responses to asthma medications (ATSDR, NIH).
Examine the prevalence and impacts of asthma on American Indians (IHS, NIH).
Examine the differences in asthma prevalence among people of different origins in order to provide insights on risk factors contributing to higher prevalence rates (NIH).
Investigate Access to Quality Care and Evaluate Quality
Develop and evaluate new models for delivering quality asthma care to patients most at risk for asthma related illness and death ( AHRQ , NIH, HRSA, HCFA).
Evaluate the utilization and expenditure patterns associated with asthma among low-income individuals covered under Medicaid, State Children's Health Insurance Program (SCHIP), and Medicare. Evaluate access to care and its barriers, the process and quality of care, and the outcomes of care for asthma (HCFA, AHRQ). Times">
Examine the health impact of managed care practices and policies on those with asthma insured under Medicaid and SCHIP (HCFA, AHRQ, HRSA).
Evaluate the roles of poverty, race and ethnicity in the use of emergency room services and hospitalization rates and in the quality of care received for asthma (CDC, NIH, AHRQ).
Priority Area 4: Track the Disease and Assess the Effectiveness of Asthma Programs
Establish Coordinated and Systematic Local, State and National Systems for Asthma Surveillance
Conduct surveys to determine the prevalence of asthma, the quality of asthma management and the quality of life for people with asthma (CDC).
Examine mortality and hospitalization data at the local level to allow for immediate investigation of deaths from asthma, and for rapid assessment of reasons behind changing rates of morbidity (CDC).
Develop supplementary data systems to gather additional information in locations with particularly elevated rates of asthma prevalence or other measures of the burden of the disease (CDC).
Develop model emergency department surveillance systems to identify characteristics of persons without access to quality care or with exceptionally severe disease (CDC).
Evaluate Public Health and Health Services Interventions, and Disseminate Results
Develop and utilize appropriate tools to evaluate the cost-effectiveness of various intervention and asthma management strategies ( AHRQ , HRSA, NIH)
Incorporate and adequately fund appropriate evaluation mechanisms into all asthma intervention programs (ACF, CDC, HCFA, HRSA, IHS, NIH)
Evaluate local and regional asthma coalition efforts ( AHRQ , NIH)
Widely disseminate the results of evaluations of asthma programs (ACF, AHRQ, CDC, HCFA, HRSA, IHS, NIH).
References
1. Thacker SB, Berkelman RL. Surveillance of medical technologies. Journal of Public Health Policy 1986; 7:363-377.
2. Teutsch SM, Churchill RE. Principles and Practice of Public Health Surveillance New York: Oxford University Press, 1994:3.
3. Institute of Medicine. The Future of Public Health. Washington, D.C.: National Academy Press, 1988.
4. Mannino DM, Homa DM, Pertowski CA, et al. Surveillance for asthma - United States, 1960-1995. Mortality and Morbidity Weekly Report 1998; 477 (No. SS-1):1-27.
5. National Center for Health Statistics, National Health Interview Survey 1996.
6. Adams PF, Marano MA. Current estimates from the National Health Interview Survey 1994. Vital Health Statistics 1995; 10:94.
7. National Institute for Occupational Safety and Health. Work-Related Lung Disease Surveillance Report-1994. DHHS (NIOSH) Publication No. 94-120, 1994.
8. Provencher S, Labreche FP, De Guire L. Physician based surveillance system for occupational respiratory diseases: the experience of PROPULSE, Quebec, Canada. Occupational & Environmental Medicine 1997; 54(4):272-6 .
9. Tarlo SM, Banks D, Liss G, Broder I. Outcome determinants for isocyanate induced occupational asthma among compensation claimants. Occupational & Environmental Medicine 1997; 54:756-61 .
10. Gannon PF, Burge PS. The SHIELD scheme in the West Midlands Region, United Kingdom. Midland Thoracic Society Research Group. British Journal of Industrial Medicine 1993; 50(9):791-6.
11. Cullen MR, Cherniack MG, Rosenstock L. Occupational medicine (1). [Review] New England Journal of Medicine 322(9):594-601, 1990 .
12. Milton DK, Solomon GM, Rosiello RA, Herrick RF. Risk and incidence of asthma attributable to occupational exposure among HMO members. American Journal of Industrial Medicine 1998 Jan; 33 (1): 1-10.
13. Timmer S, Rosenmann K. Occurrence of occupational asthma. Chest 1993; 104:816-20.
14. Blanc PD, Cisternas M, Smith S, Yelin E. Occupational asthma in a community-based survey of adult asthma. Chest 1996; 109(3 Suppl):56S-57S.
15. Venables KM, Chan-Yeung M. Occupational asthma. Lancet 1997 May; 349:1465-1469.
16. National Center for Health Statistics. Underlying cause of death dataset. 1996.
17. Homa DM, Mannino DM, Lara M. Asthma mortality in US Hispanics of Mexican, Puerto Rican, and Cuban heritage, 1990-1995. American Journal of Respiratory and Critical Care Medicine 2000 Feb; 161(2 Pt 1):504-509.
18. Halfon MD and Newacheck PW. Childhood asthma and poverty: differential impacts on utilization of health services. Pediatrics 1993; 91(1):56-61.
19. St. Peter RF, Newacheck PW, Halfon N. Access to care for poor children: separate and unequal? Journal of the American Medical Association 1992; 267(20):2760-2764.
20. Macdonald SC, Bensley LS, VanEenwyk J, Simmons KW. Self-Reported asthma in adults and proxy-reported asthma in children-Washington, 1997-1998. Morbidity and Mortality Weekly Report October 15, 1999; 48(40):918-919.
21. Corn B, Hamrung G., Ellis A. et al., Patterns of asthma death and near-death in an inner-city tertiary care teaching hospital. Journal of Asthma 1995; 32(6):405-12.
22. U.S. Dept. of Health and Human Services. Healthy People 2010 (Conference Edition, in Two Volumes). Washington DC: January 2000, p. 1-25.
23. Kattan M, Mitchell H, Eggleston P, et al. Characteristics of inner-city children with asthma: the National Cooperative Inner-City Asthma Study. Pediatric Pulmonology 1997: 24: 253-262.
24. Crain EF, Kercsmar C, Weiss KB, Mitchell H, Lynn H. Reported difficulties in access to quality care for children with asthma in the inner city. Archives of Pediatric and Adolescent Medicine 1998; 152(4):333-9.
25. National Center for Health Statistics. Current estimates from the National Health Interview Survey, 1990-92. National Center for Health Statistics. Vital and Health Statistics 1997: Series 10(194).
26. Taylor WR, Newachek PW. Impact of childhood asthma on health. Pediatrics 1992; 90: 657-662.
27. Weiss KB, Gergen PG, Hodgson TA. An economic evaluation of asthma in the United States. New England Journal of Medicine 1992 March 26; (13):862-6.
28. National Institutes of Health / National Heart, Lung and Blood Institute. Morbidity and Mortality:1998 Chartbook on Cardiovascular, Lung and Blood Diseases. October 1998.
29. Hopkin JM. Mechanisms of enhanced prevalence of asthma and atopy in developed countries. Current Opinion in Immunology 1997; 9:788-92.
30. Rosenstreich DL, Eggleston P, Kattan M, et al. The role of cockroach allergy and exposure to cockroach allergen in causing morbidity among inner-city children with asthma. New England Journal of Medicine 1997; 336:1356-1363.
31. Platts-Mills TA and Carter MC. Asthma and indoor exposure to allergens. New England Journal of Medicine 1997; 336:1382-1384.
32. Custovic A, Simpson A, Chapman MD, Woodcock A. Allergen avoidance in the treatment of asthma and atopic disorders. Thorax 1998; 53: 63-72.
33. Gergen PJ, Fower JA, Maurer KR, et al. The burden of environmental tobacco smoke exposure on the respiratory health of children 2 months through 5 years of age in the United States: Third National Health and Nutrition Examination Survey. Pediatrics 1998; 101(2):e8.
34. Hide DW, Matthews S., Tariq S,. Arshad SH.. Allergen avoidance in infancy and allergy at 4 years of age. Allergy 51(2):89-93, 1996.
35. Holt PG. Programming for responsiveness to environmental antigens that trigger allergic respiratory disease in adulthood is initiated during the perinatal period. Environmental Health Perspectives 1998; 106 Suppl 3: 795-800.
36. Coultas DB and Samet JM. "Epidemiology and Natural History of Asthma" in Tinkelman D and Naspitz CK (Eds.) Childhood Asthma. New York: Marcel Dekker, 1993:71-114.
37. Institute of Medicine. Clearing the Air: Asthma and Indoor Air Exposures. Washington, DC: National Academy Press, January 2000.
38. Shaheen SO, Aaby P, Hall AJ, et al. Measles and atopy in Guinea-Bissau. The Lancet 1996; 347:1792-1797.
39. Matricardi PM, Riondino S, Fortini M, Ferrigno L, Rapicetta M, Bonini S. Exposure to foodborne and/or fecal microbes versus airborne viruses in relation to atopy and allergic asthma: epidemiology study. British Medical Journal 2000; 320:412-417.
40. Bodner C, Godden D, Seaton A. Family size, childhood infections and atopic diseases. The Aberdeen WHEASE Group. Thorax 1998; 53:28-32.
41. Shirakawa T, Enomoto T, Shimazu S, Hopkin JM. The inverse association between tuberculin responses and atopic disorder. Science 1997; 275(5296):77-79.
42. Weiss ST. Diet as a risk factor for asthma. Ciba Foundation Symposium 1997; 206:244-257.
43. Gennuso J,. Epstein LH, Paluch RA, Cerny F. The relationship between asthma and obesity in urban minority children and adolescents. Archives of Pediatric Adolescent Medicine 1998; 152:1197-1200.
44. Camargo CA, Weiss ST, Zhang S, Willett WC, Speizer FE. Prospective study of body mass index, weight change, and risk of adult-onset asthma in women. Archives of Internal Medicine 1999 Nov; 159:2582-2588.
45. Warner AM, Bjorksten B, Munir AK, Moller C, Schou C, Kjellman NI. Childhood asthma and exposure to indoor allergens: low mite levels are associated with sensitivity. Pediatric Allergy & Immunology 1996; 7:61-67.
46. Platts-Mills TA, Sporik RB, Chapman MD, Heymann PW. The role of domestic allergens. Ciba Foundation Symposium 1997; 206:173-185.
47. Halonen M, Stern DA, Wright AL, Taussig LM, Martinez FD. Alternaria as a major allergen for asthma in children raised in a desert environment. American Journal of Respiratory & Critical Care Medicine 1997; 155:1356-1361.
48. Durham SR. Allergen avoidance measures. British Thoracic Society. Respiratory Medicine 1996; 90:441-445.
49. Chen Y, Rennie DC, Dosman JA. Influence of environmental tobacco smoke on asthma in nonallergic and allergic children. Epidemiology 1996; 7:536-539.
50. Samet JM. Asthma and the environment: do environmental factors affect the incidence and prognosis of asthma? Toxicology Letters 1995; 82/83:33-38.
51. Koren HS. Association between criteria air pollutants and asthma. Environmental Health Perspectives 1995; 103(suppl 6):235-242.
52. Nel AE, Diaz-Sanchez D, Ng D, Hiura T, Saxon A. Enhancement of allergic inflammation by the interaction between diesel exhaust particles and the immune system. J Allergy Clin Immunol 1998 Oct; 102(4 Pt 1):539-54.
53. Koren HS. Environmental risk factors in atopic asthma. International Archives of Allergy and Immunology 1997; 113:65-68.
54. Gordon T. and Fine J. Contribution of ambient air pollution to allergic asthma. Toxicology and Ecotoxicology News 1997; 4:20-24.
55. Bernstein DI. Allergic reactions to workplace allergens. Journal of American Medical Association 1997; 278:1907-1913.
56. Chan-Yeung M, Malo JL. Occupational Asthma (Review). New England Journal of Medicine 1995; 333(2):107-112.
57. National Asthma Education and Prevention Program (NAEPP), Expert Panel Report: Guidelines for the Diagnosis and Management of Asthma Bethesda, MD. National Institutes of Health. National Heart, Lung, and Blood Institute, NIH Publication No. 91-3042, 1991.
58. National Asthma Education and Prevention Program (NAEPP), Expert Panel Report 2: Guidelines for the Diagnosis and Management of Asthma Bethesda, MD. National Institutes of Health. National Heart, Lung, and Blood Institute, NIH Publication No. 97-4051, 1997.
59. American Academy of Allergy, Asthma, and Immunology. Pediatric Asthma: Promoting Best Practice - Guide for Managing Asthma in Children. 1999:1-139.
60. Clark NM, Feldman CH, Evans D, Levison MJ, Wasilewski Y, Mellins RB. The impact of health education on frequency and cost of health care use by low income children with asthma. Journal of Allergy and Clinical Immunology 1986; 78:108-115.
61. Goodman DC, Lozano P, Stukel TA, Chang C, and Hecht J. Has asthma medication use in children become more frequent, more appropriate, or both? Pediatrics 1999 Aug; 104(2):187-194.
62. Warman KL, Silver EJ, McCourt MP, Stein REK. How does home management of asthma exacerbations by parent of inner-city children differ from NHLBI recommendations? Pediatrics, 1999 Feb; 103(2): 422-427.
63. Laumann JM, Bjornson DC. Comparing asthma treatment with guidelines. Annals of Pharmacotherapy 1998 Dec; 32(12):1290-1294.
64. Eggleston PA, Malveaux FJ, Butz AM, Huss K, Thompson L, Kolodner K, Rand CS. Medications used by children with asthma living in the inner city. Pediatrics 1998; 101:349-354.
65. Health Care Financing Administration (HCFA) 1995, 1996, 1998. Estimate of expenditures and recipients extrapolated from unpublished data in HCFA's State Medicaid Research Files (1995) and HCFA's MEDPAR files (1996) and from the 1998 Data Compendium, Department of Health and Human Services, Health Care Financing Administration, Office of Strategic Planning, Research and Evaluation Group, Division of Beneficiary Studies. August 1998. The SMRF and MEDPAR data bases are maintained at the HCFA Data Center, Rockville, MD.
66. National Center for Health Statistics. Healthy People 2000 Review: 1998-1999. Department of Health and Human Services, Publication No. (PHS)99-1256. 1999: 119.
67. Sporik R, Hogate ST, Platts-Mills TA, Cogswell, JJ. Exposure to house-dust mite allergen and the development of asthma in childhood: A prospective study. The New England Journal of Medicine 1990; 323: 502-507.
68. Liggett DA and Meyers DA, editors. The Genetics of Asthma. 1996 New York: Marcel Dekker.
69. Meng YY, Kwan-Moon L, Berkbigler D, Halbert RJ, Legorreta AP. Compliance with US asthma management guidelines and specialty care: a regional variation or national concern? Journal of Evaluation in Clinical Practice 1999 May; 5(2):213-221.
70. Cabana MD, Rand CS, Powe NR, et al. Why don't physicians follow clinical practice guidelines? (Review) Journal of American Medical Association 1999; 282:1458-1465.
71. Greco PJ, Eisenberg JM. Changing physicians' practices. New England Journal of Medicine 1993; 329(17):1271-1273.
72. Grimshaw JM, and Thomson MA. What have new efforts to change professional practice achieved? J Royal Society Medicine 1998 ; 91 Suppl 35:20-25.
73. Bero LA, Grilli R, Grimshaw JM, et al. Closing the gap between research and practice: an overview of systematic reviews of interventions to promote implementation of research findings. British Medical Journal 1998; 317:465-468.
74. Clark NM, Gong M, Schork MA, et al. Impact of Education for Physicians on Patient Outcomes. Pediatrics 1998; 101:831-836.
75. Lewis CE, Rachelefsky G, Lewis MA, de la Sota A, Kaplan M. A randomized trial of asthma care training for kids. Pediatrics 1984; 74(4):478-486.
76. Greineder DK, Loane KC, Parks P. Reduction in resource utilization by an asthma outreach program. Archives of Pediatric Adolescent Medicine 1995; 149(4):415-420.
77. Sullivan S, Elixhauser A., Buist AS, Luce BR, Eisenberg J, Weiss KB. National Asthma Education and Prevention Program Working Group report on the cost-effectiveness of asthma care. American Journal of Respiratory and Critical Care Medicine 1996; 154: S84-S95.
78. Epstein RS, Sherwood LM. From outcomes research to disease management: a guide for the perplexed. Ann Intern Med 1996:124:832-7.
79. Bodenheimer T. Sounding board: disease management - promises and pitfalls. New England Journal of Medicine 1999:340(3)1202-1205.
80. Homer CJ. Asthma disease management (editorial). New England Journal of Medicine 1997:337(20)1461-1463.
81. Homer CJ, Szilagyi P, Rodewald L. et al. Does quality of care affect rates of hospitalization for childhood asthma? Pediatrics 1996; 98:18-23.
82. Finkelstein JA, Brown RW, Schneider LC, et al. Quality of care for preschool children with asthma: the role of social factors and practice. Pediatrics 1995; 95:389-394.
83. Evans D, Mellins R, Lobach K, et al. Improving care for minority children with asthma: professional education in public health clinics. Pediatrics 1997; 99(2):157-164.
84. Evans III R, Gergen PJ, Mitchell H, et al. A randomized clinical trial to reduce asthma morbidity among inner-city children. Pediatrics 1999 September; 135(3):332-338.
85. Gutierrez A, Rosas A, Wilson NW. Effect of Language on Parental Understanding About Asthma in Hispanic Children. Pediatric Asthma, Allergy, and Immunology 1992; 6(1):61-66.
86. Schwartz DA. Etiology and Pathogenesis of airway disease in children and adults from rural communities. Environmental Health Perspectives 1999; 107(Sup3):393-401.
87. Health Resources and Services Administration (HRSA), Bureau of Primary Health Care, Uniform Data System: 1999 Report.
88. DePalo VA, Mayo PH, Friedman P, et al. Demographic influences on asthma hospital admission rates in New York City. Chest 1994; 106(2): 447-451.
89. Centers for Disease Control and Prevention. Forecasted state-specific estimates of self-reported asthma prevalence--United States, 1998. Mortality and Morbidity Weekly Report 1998; 47:1022-1025.
90. Jajosky RA, Harrison R, Reinisch F, et al. Surveillance of work-related asthma in selected US states using surveillance guidelines for state health departments - California, Massachusetts, Michigan, and New Jersey, 1993-1995. Morbidity and Mortality Weekly Report 1999; 48(SS-3):1-20.
Notes
1. The term "minority" as used in the rest of this paper refers to "racial and ethnic minority."
2. Surveillance is the ongoing systematic collection, analysis, and interpretation of outcome-specific data for use in the planning, implementation and evaluation of public health practice (1). A surveillance system includes the functional capacity for data collection and analysis as well as the timely dissemination of these data to persons who can undertake effective prevention and control activities (2). Public health officials use surveillance to understand changes in rates of disease in different locations or populations, to help evaluate medical care and public health programs, and to identify clues about risk factors.
3. Public health practice activities are those that facilitate the work of the medical community and others to prevent illness, reduce the severity of symptoms, and improve the quality of medical care. The role of government in public health includes: 1) the systematic collection and analysis of health information; 2) the development of goals and priorities based on scientific knowledge and measures to achieve them; 3) taking action through public education, advocacy, negotiation, and mobilization of resources; and 4) evaluation to determine whether policy goals are achieved (3) .
4. The term "minority" as used in the rest of this paper refers to "racial and ethnic minority."
5. Although national data do not provide the resolution necessary to identify particular geographic areas hardest hit by the asthma epidemic, surveys undertaken in a number of large cities in the United States indicate that the prevalence and severity of asthma are greatest in the medically underserved, inner city. A large proportion of inner-city families are insured through Medicaid .
6. Tolerance is an immune state that can be induced, and that results in long term blocking of immune responses. Tolerance induction has recently been shown to be very promising for blocking immune responses leading to rejection of organs after transplantation.
7. Coordinating Committee member organizations are listed in Appendix F.
8. Recurrent episodes of cough and wheezing are almost always due to asthma in both children and adults. However, children are often diagnosed with bronchitis , bronchiolitis, or pneumonia, even though the signs and symptoms are most compatible with asthma (58) .
9. Many of these surveys are carried out by CDC's National Center for Health Statistics (NCHS). State-based surveillance supported by the National Institute for Occupational Safety and Health has been used to identify high risk industries, occupations and substances .
10. A number of current activities and urgent needs related to the evaluation of asthma programs were described in Priority Area II and are not repeated here.
11. Elements of such evaluations might include: whether an intervention program has an impact on reducing the health burden of asthma and to what degree; whether the activities themselves work as planned, such as whether the intended audience is reached, whether they understand what was taught, and whether they modify behavior as a result; whether the processes used to implement the activity are effective and sustainable over the long-term; and whether the intervention or activity is cost-effective.
Appendices
Appendix A: Agencies Participating in the HHS Asthma Workgroup
Administration for Children and Families
Administration for Children, Youth, and Families
Child Care Bureau
Head Start Bureau
Agency for Healthcare Research and Quality
Agency for Toxic Substances and Disease Registry
Division of Health Studies
Centers for Disease Control and Prevention
Division of Adolescent and School Health
National Center for Environmental Health
National Center for Health Statistics
National Institute for Occupational Safety & Health
Department of Health and Human Services Regional Offices
Region I
Region II
Region V
Food and Drug Administration
Center for Biologic Evaluation and Research
Center for Drug Evaluation and Research
Health Care Financing Administration
Center for Medicaid and State Operations
Office of Strategic Planning
Health Resources and Services Administration
Office of the Administrator
Bureau of Primary Health Care
Maternal and Child Health Bureau
Indian Health Service
Albuquerque Area
Office of Health Programs
National Institutes of Health
National Heart, Lung, and Blood Institute
National Institute on Aging
National Institute of Allergy and Infectious Diseases
National Institute of Child Health and Human Development
National Institute of Environmental Health Sciences
National Institute of Mental Health
National Institute of Nursing Research
Office of the Secretary
Office of the Assistant Secretary for Management and Budget
Office of Budget
Office of the Assistant Secretary for Planning and Evaluation
Office of Science Policy
Office of Health Policy
Office of Program Systems
Office of Public Health and Science
Office of Disease Prevention and Health Promotion
Office of Minority Health
Office of Women's Health
Appendix B: Participants in the DHHS Asthma Workgroup
Altamese Arnold, | M. Beth Benedict, Dr.P.H. |
Capt. Barbara Braden, R.N., M.S. | Robin Brocato, M.H.S. |
Olivia Carter-Pokras, Ph.D. | Marsha Davenport, M.D., M.P.H. |
Denise Dougherty, Ph.D. | Robinson Fulwood, M.S.P.H. |
James Gatz | Peter Gergen, M.D., M.P.H |
Mitchell Goldstein | Roger Gollub, M.D. |
Alison E. Greene | Rosemarie Hakim, Ph.D. |
Michael J. Hodgson, M.D., M.P.H. | Polly Hoppin, Sc.D. |
Moniquin Huggins | Suzanne Hurd, Ph.D. |
Richard Jackson, M.D., M.P.H. | Lynn Jenkins, M.A. |
John K. Jenkins, M.D. | Mirielle Kanda, M.D., M.P.H. |
Stacey Katz, M.P.H. | Woodie Kessel M.D., M.P.H. |
Ellen Kohl | Claude Lenfant, M.D. |
George Malindzak, Ph.D. | Merle G. McPherson, Ph.D. |
Robert J. Meyer, M.D. | Peter Muehrer, Ph.D. |
Janet Muckenthaler | Amy Nevel, M.P.H. |
Sheila Newton, Ph.D. | Michele Palmer |
Eileen S. Parish, M.D. | Dalton G. Paxman, Ph.D |
Jerry Phelps | Marshall Plaut, M.D. |
Andre Premen | William F. Raub, Ph.D. |
Stephen Redd, M.D. | Gail Robarge, M.S. |
William A. Robinson, M.D., M.P.H. | Hannah Rosenthal |
Daniel Rotrosen, M.D. | Jonelle Rowe, M.D. |
Diana Schmidt | Hilary Sigmon, Ph.D., R.N. |
Lisa Simpson, M.B., B.Ch. | Stanley Slater, M.D. |
Les Smith, Ph.D. | Lynn Squire |
David Stevens, M.D., F.A.A.F.P. | Virginia Taggart, M.P.H. |
Paul Turkeltaub, M.D. | Mary Vernon, M.D., M.P.H. |
Diane Wagener, Ph.D. | Mary White, Sc.D. |
Sumner Yaffe, M.D. | Francis A. Zampiello, M.D. |
Darryl Zeldin, M.D. | Phyllis Zucker |
Appendix C: Summary of the Guidelines for the Diagnosis and Management of Asthma
Experts convened by the National Asthma Education and Prevention Program coordinated by the National Heart, Lung and Blood Institute (NHLBI) of the National Institutes of Health (NIH) recently assessed the pertinent scientific literature and offered recommendations for managing asthma. Their report, Expert Panel Report 2: Guidelines for the Diagnosis and Management of Asthma updates the first expert panel report published in 1991. It identifies four disease-management strategies and details guidelines for implementation that will keep asthma under control and greatly improve the quality of life for people with the disease. The four strategies include: measures of assessment and monitoring, control of factors contributing to asthma severity, pharmacologic therapy, and education for a partnership in asthma care. These are briefly summarized below. The complete Guidelines are available at www.nhlbi.gov.
Component 1:
Measures of Assessment and Monitoring
Initial Assessment and Diagnosis of Asthma
Making the correct diagnosis of asthma is extremely important. Clinical judgment is required because signs and symptoms vary widely from patient to patient as well as within each patient over time. To establish the diagnosis of asthma, the clinician must determine that:
- Episodic symptoms of airflow obstruction are present.
- Airflow obstruction is at least partially reversible
- Alternative diagnoses are excluded.
Asthma severity classifications reflect the clinical manifestations of asthma. They are: mild intermittent, mild persistent, moderate persistent, and severe persistent. The Panel emphasizes that patients at any level of severity can have mild, moderate, or severe exacerbations.
Periodic Assessment and Monitoring
To establish whether the goals of asthma therapy have been achieved, ongoing monitoring and periodic assessment are needed. The goals of asthma therapy are to:
- Prevent chronic and troublesome symptoms
- Maintain (near) normal pulmonary function
- Maintain normal activity levels (including exercise and other physical activity)
- Prevent recurrent exacerbations of asthma and minimize the need for emergency department visits of hospitalizations
- Provide optimal pharmacotherapy (i.e., medication) with minimal or no adverse effects
- Meet patients' and families' expectations of and satisfaction with asthma care
Several types of monitoring are recommended: signs and symptoms, pulmonary function, quality of life/functional status, history of asthma exacerbations, medication, and patient-provider communication and patient satisfaction.
The Panel recommends that patients, especially those with moderate-to-severe persistent asthma or a history of severe exacerbations, be given a written action plan based on signs and symptoms and/or peak expiratory flow. Daily peak flow monitoring is recommended for patients with moderate-to-severe persistent asthma. In addition, the Panel states that any patient who develops severe exacerbations may benefit from peak flow monitoring.
Component 2:
Control of Factors Contributing to Asthma Severity
Exposure of sensitive patients to inhalant allergens has been shown to increase airway inflammation, airway hyperresponsiveness, asthma symptoms, need for medication, and death due to asthma. Substantially reducing exposures significantly reduces these outcomes. Environmental tobacco smoke is a major precipitant of asthma symptoms in children, increases symptoms and the need for medications, and reduces lung function in adults. Increased air pollution levels of respirable particulates, ozone, sulfur dioxide and nitrogen dioxide have been reported to precipitate asthma symptoms and increase emergency department visits and hospitalizations for asthma. In addition to irritants (e.g., tobacco smoke and pollutants) and occupational exposures, reducing exposure to allergens may be required for successful long-term management of asthma. Examples of inhalant allergens include: animal allergens, house-dust mites, cockroach allergens, indoor fungi (molds) and outdoor allergens. Other factors that can contribute to asthma severity include rhinitis and sinusitis, gastroesophageal reflux, some medications, and viral respiratory infections.
Component 3:
Pharmacologic Therapy
The updated Guidelines offer an extensive discussion of the pharamcologic management of patients at all levels of asthma severity. It is noted that asthma pharmacotherapy should be instituted in conjunction with environmental control measures to factors known to increase the patient's asthma symptoms.
A stepwise approach to pharmacologic therapy is recommended, with the type and amount of medication dictated by asthma severity. The updated Guidelines continue to emphasize that persistent asthma requires daily long-term therapy in addition to appropriate medications to manage the asthma exacerbations. Medications are classified into two general classes: long-term-control medications to achieve and maintain control of persistent asthma and quick-relief medications to treat symptoms and exacerbations.
Observations into the basic mechanisms of asthma have had a tremendous influence on therapy. Because inflammation is considered an early and persistent component of asthma, therapy for persistsent asthma must be directed toward long-term suppression of inflammation. Thus the most effective medications for long-term control are those shown to have anti-inflammatory effects. For example, early intervention with inhaled corticosteroids can improve asthma control and normalize lung function, and preliminary studies suggest that it may prevent irreversible airway injury. The updated guidelines also include discussion of the management of asthma in infants and young children that incorporates recent studies on wheezing in early childhood. Another addition is discussions of long-term-control medications that have become available since 1991.
Component 4:
Education for a Partnership in Asthma Care
Education for an active partnership with patients remains the cornerstone of asthma management and should be carried out by health care providers delivering asthma care. Education should start at the time of asthma diagnosis and be integrated into every step of clinical asthma care. Asthma self-management education should be tailored to the needs of each patient, maintaining a sensitivity to cultural beliefs and practices, and involving family members, particularly for pediatric and elderly patients. New emphasis is placed on evaluating outcomes in terms of patient perceptions of improvement, especially quality of life and the ability to engage in usual activities. Health care providers need to systematically teach and frequently review with patients how to manage and control their asthma. Patients also should be provided with and taught to use a written daily self-management plan and an action plan for exacerbations. It is especially important to give a written action plan to patients with moderate-to-severe persistent asthma or a history of severe exacerbations. Appropriate patients should also receive a daily asthma diary. Adherence should be encouraged by promoting open communication; individualizing, reviewing, and adjusting plans as needed; emphasizing goals and outcomes; and encouraging family involvement.
Appendix D: Asthma and the Environment
About the President’s Task Force on Environmental Health Risks and Safety Risks to Children
In recognition of the growing body of scientific information demonstrating that America’s children suffer disproportionately from environmental health risks and safety risks, President Clinton issued Executive Order 13045 on April 21, 1997, directing each Federal Agency to make it a high priority to identify, assess, and address those risks. In issuing this order, the President also created the Task Force on Environmental Health Risks and Safety Risks to Children, co-chaired by Donna Shalala, Secretary of the Department of Health and Human Services, and Carol M. Browner, Administrator of the Environmental Protection Agency. The Task Force was charged with recommending strategies for protecting children’s environmental health and safety. Two subcommittees were established in the Executive Order to carry out this directive: a subcommittee directed to review and foster public access to federal government sponsored research on environmental health and safety risks to children, and a subcommittee directed to identify priority public outreach activities related to protecting children’s environmental health and safety.
In April 1998, the Task Force identified four priority areas for immediate attention: childhood asthma, unintentional injuries, developmental disorders, and childhood cancer. The Task Force created and charged the Asthma Priority Area Workgroup, co-chaired by EPA and DHHS, with reviewing current Federal efforts to address the many facets of the issue and, most importantly, to make appropriate recommendations for action by the Federal government. This strategy is the result of that effort.
Executive Summary
An epidemic of asthma is occurring in the United States. While the epidemic affects people of all ages, children are particularly affected. Nearly 1 in 13 school-aged children has asthma, and the percentage of children with asthma (i.e., prevalence rate) is rising more rapidly in preschool-aged children than in any other age group.
There is no national system to collect data from states specifically on asthma, although several states are developing systems to collect such data. Although national data do not provide the resolution necessary to identify particular geographic areas hardest hit by the asthma epidemic, surveys undertaken in a number of large cities in the United States indicate that the prevalence and severity of asthma are greatest in the large, urban inner cities.
Asthma is one of the leading causes of school absenteeism, accounting for over 10 million missed school days per year. Asthma also accounts for many nights of interrupted sleep, limitation of activity, and disruptions of family and care-giver routines. Asthma symptoms that are not severe enough to require a visit to an emergency room or to a physician can still be severe enough to prevent a child with asthma from living a fully active life.
In 1990, the cost of asthma to the U.S. economy was estimated to be $6.2 billion, with the majority of the expense attributed to direct medical expenses. A 1996 analysis found the cost of asthma to be $14 billion, indicating a rapidly increasing financial burden. These estimates, which are not limited to the costs of childhood asthma, indicate that the direct medical costs of asthma account for between 1% and 3% of all health care expenditures in the United States.
Asthma is a particularly important disease to consider in the context of environmental hazards to which children are exposed. Children breathe more air, eat more food, and drink more liquid in proportion to their body weight than do adults, and their developing respiratory, immunological, and digestive systems may be more susceptible to environmental exposures than those of adults. In a typical day, children may be exposed to a wide array of environmental agents at home, in day
care centers, schools and while playing outdoors. There is substantial evidence that environmental exposures, including viruses and allergens, play a major role in triggering asthma symptoms. Indoor airborne allergens include those from house dust mites, cockroaches, mold and animal dander. In addition, exposure to environmental tobacco smoke (ETS), also known as secondhand smoke, has been shown to be a major determinant of asthma symptoms. Elevated levels of outdoor air pollutants, particularly ozone and exposure to outdoor allergens (e.g. pollens, molds), are associated with increased symptoms and an increased risk of emergency department visits for asthma, as well.
In addition, environmental factors such as airborne allergens and environmental tobacco smoke may play a major role in the onset of asthma. Other pollutants may also play a role, although the scientific data are inadequate to offer firm conclusions. Genetic predisposition is the strongest known risk factor for developing asthma, but the rapidly rising number of cases of childhood asthma cannot be solely genetic because the genetic composition of the population changes slowly. Rather, some interaction between genetic predisposition and environmental exposures, and possibly other factors such as diet, increased body weight, or lack of exercise are likely to be responsible for the increase. Further work is essential to clarify how genetic susceptibility and environmental exposures interact to cause asthma.
Reducing exposures of children with asthma to airborne allergens and pollutants will reduce the health burden of asthma and significantly improve their quality of life. It is not yet certain, but it is possible that reducing the exposure of infants and young children at risk of developing asthma may prevent its onset. Environmental control methods and asthma treatments are available now that can help children and their families control asthma and lead healthy, active lives. Yet not all children have access to these measures. Too many children miss school, limit their physical activity, and are seriously ill because of asthma. A child ill with asthma also has an impact on the entire family.
This strategy, prepared by the Task Force, is aimed at developing a further understanding of the role of environmental factors associated with the:
- onset of asthma; and
- triggers of asthma attacks
The efforts of the Task Force resulted in four recommendations for Federal action for addressing childhood asthma, which are presented in this strategy. The strategy also sets forth guiding principles that were used to develop the four recommendations.
Guiding Principles
Federal agency actions can provide leadership and direction in reducing environmental risks to protect
children who have asthma or are at risk of developing it. Recommendations for action put forward
in this initiative are predicated on the principles that federal action must have:
- A focus on efforts to eliminate the disproportionate impact of asthma in minority populations and those living in poverty.
- An emphasis on partnerships and community based programs.
- A commitment to setting measurable and consistent goals for childhood asthma under the Healthy People 2010 program.
- An investment in evaluation to identify those strategies that are most effective in reducing the burden of asthma so that they may be replicated.
Recommendations
Research
Strengthen and accelerate focused research into the environmental factors that cause or worsen childhood asthma.
- PStrengthen and accelerate research into the environmental factors that may contribute to the onset of asthma in children.
- PExpand and accelerate research to develop and evaluate environmental strategies that will improve the quality of life of people with asthma.
Public Health Programs
Implement public health programs that foster improved use of current scientific knowledge to reduce environmental exposures to prevent and reduce the severity of symptoms for those with asthma.
- Promote clinician and patient implementation of national guidelines for reducing environmental risks that worsen asthma.
- Expand support for state and local public health action.
- Reduce children’s exposure to environmental tobacco smoke and other indoor triggers in their homes.
- Establish school based asthma programs that help reduce or eliminate allergens and irritants and that promote student’s self management of asthma and full participation in school activities.
- Continue to reduce outdoor air pollution.
Surveillance
Establish a coordinated, integrated, and systematic nationwide asthma surveillance system for collecting and analyzing health outcome and risk factor data at the state, regional and local levels.
Disproportionate Impact on the Poor and Minorities
Identify the reasons for and eliminate the disproportionate burden of asthma among different racial and ethnic groups and those living in poverty.
- Improve asthma management for children within the medicaid program.
Members of the President’s Task Force on Environmental Health Risks and Safety Risks to Children
Honorable Donna E. Shalala
Co-chair
Secretary
Department of Health and Human Services
Honorable Carol M. Browner
Co-chair
Administrator
Environmental Protection Agency
Honorable Alexis Herman
Secretary
Department of Labor
Honorable Janet Reno
Attorney General
Department of Justice
Honorable Andrew Cuomo
Secretary
Department of Housing and Urban
Development
Honorable Bill Richardson
Secretary
Department of Energy
Honorable Richard Riley
Secretary
Department of Education
Honorable Dan Glickman
Secretary
Department of Agriculture
Honorable Rodney Slater
Secretary
Department of Transportation
Honorable Jacob J. Lew, Director
Office of Management and Budget
Honorable George Frampton, Acting Chair
Council on Environmental Quality
Honorable Ann Brown
Chairman
Consumer Product Safety Commission
Honorable Janet Yellen
Chair
Council of Economic Advisors
Honorable Neal Lane, Director
Office of Science and Technology Policy
Honorable Gene Sperling
Assistant to the President for Economic
Policy
Honorable Bruce Reed
Assistant to the President for Domestic
Policy
Asthma Priority Area Workgroup Members
Stephen Redd, MD (Co-chair)
National Center for Environmental Health
Centers for Disease Control and Prevention
Robert Axelrad (Co-chair)
Office of Children’s Health Protection
Environmental Protection Agency
Mary White, Sc.D
Division of Health Studies
Agency for Toxic Substances and Disease
Registry
John Talbott
Office of Building Technologies
Department of Energy
Ron Ashford
Department of Housing and Urban
Development
Warren Friedman, Ph.D, CIH
Office of Lead Hazard Control
Department of Housing and Urban
Development
Tracey Mitchell
Indoor Environments Division
Environmental Protection Agency
Marshall Plaut, M.D.
National Institute of Allergy and Infectious
Diseases
National Institutes of Health
Jerry Phelps
National Institute of Environmental Health
Sciences
National Institutes of Health
Virginia Taggart, M.P.H.
National Heart, Lung, and Blood Institute
National Institutes of Health
Hillel Koren, Ph.D.
National Health and Environmental Effects
Laboratory
Office of Research and Development
Environmental Protection Agency
Caroline Freeman
Occupational Safety and Health Administration
Department of Labor
George Malindzak, Ph.D
National Institute of Environmental Health
Sciences
National Institutes of Health
Lucas Neas, Ph.D
National Health and Environmental Effects
Laboratory
Office of Research and Development
Environmental Protection Agency
Edward Chu
Office of Children’s Health Protection
Environmental Protection Agency
Marilyn Wind
Consumer Product Safety Commission
Stacey Katz
Office of Science Policy
Department of Health and Human Services
Polly Hoppin, Sc.D
Office of Science Policy
Department of Health and Human Services
Introduction
The Growing Problem of Asthma in Children
Asthma is a chronic inflammatory lung disease characterized by recurrent episodes of breathlessness, wheezing, coughing, and chest tightness; these episodes are also known as exacerbations or attacks. The severity of exacerbations can range from mild to life threatening. Both the frequency and severity of asthma symptoms can be reduced by the use of medications and by reducing exposure to the environmental triggers of asthma attacks.
For the past 15 years, an epidemic of asthma has occurred in the United States. By all indications, this epidemic is continuing. Although asthma has become a major public health problem affecting Americans of all ages, races and ethnic groups, children have been particularly severely affected.
National survey data indicate that the number of children with asthma in the United States has more than doubled in the past 15 years. In 1980, 2.3 million American children had asthma. In 1995, the most recent year for which data are available, the number of affected children had risen to 5.5 million. Based on these trends, it is estimated that in 1998 more than 6 million children in the United States have asthma. Prevalence rates of asthma are highest in boys and are increasing in both boys and girls, and in all race and ethnic groups. The prevalence of asthma in children under age 18 is 7.3%. The most rapid increase has occurred in children under 5 years old, with rates increasing over 160% over the past 15 years.
The number of deaths attributed to asthma in children has also increased. In 1977, 84 deaths in children 18 and younger were recorded; the number of deaths has risen to 280 in 1995, a more than 3-fold increase. Although the death rate due to asthma has increased in all racial and ethnic groups, minority populations experience a disproportionately higher death rate from asthma. In 1995, the death rate from asthma in African-American children, 11.5 per million, was over four times the rate in white American children, 2.6 per million. The higher death rates among African-American children are especially troubling.
The number of hospitalizations and emergency room visits for asthma have increased in all population groups. Asthma accounts for one-third of all pediatric emergency room visits and is the fourth most common cause for physician office visits. The variation in the impact of asthma across racial and ethnic groups is significant. African-American children have an annual rate of hospitalization of 74 per 10,000, over 3 times that for white children, 21 per 10,000. In addition, African-American children are approximately 4 times more likely than white children to seek care at an emergency room. In short, African-American children have a slightly higher risk of getting asthma, but have a much higher risk of hospitalization or death due to the disease.
At the present time, surveillance for asthma in children is limited to analyses of ongoing surveys and data systems on health events such as mortality, hospitalization, and outpatient visits. Other than for African Americans, such information is extremely limited for most ethnic groups. There is no national system to collect data from states specifically on asthma, although several states are developing systems to collect such data. Although national data do not provide the resolution necessary to identify particular geographic areas hardest hit by the asthma epidemic, surveys undertaken in a number of large cities in the United States indicate that the prevalence and severity of asthma are greatest in the large, urban inner cities. These measures, particularly for death, hospitalization, and emergency room visits, give an incomplete picture of the true burden of asthma in the United States. For example, one follow-up study of children with asthma in inner city areas found a nearly 10 times higher likelihood of a child suffering symptoms of asthma on a given day than visiting an emergency room. Asthma is one of the leading causes of school absenteeism, accounting for over 10 million missed school days per year. Asthma also accounts for many nights of interrupted sleep, limitation of activity, and disruptions of family and care-giver routines. Asthma symptoms that are not severe enough to require a visit to an emergency room or to a physician can still be severe enough to prevent a child with asthma from living a fully active life.
Estimating the costs of asthma is an indirect way to measure its health burden. In 1990, the cost of asthma to the U.S. economy was estimated to be $6.2 billion (Weiss, 1992), with the majority of the expense attributed to direct medical expenses. A 1996 analysis (Farquhar, et al, 1998) found the cost of asthma to be $14 billion, indicating a rapidly increasing financial burden. These estimates indicate that the direct medical costs of asthma for all ages account for between 1% and 3% of all health care expenditures in the United States.
What We Know About Childhood Asthma
Over the past 15 years, there have been major advances in the scientific understanding of asthma. Asthma is now known to be a disease of airway inflammation resulting from a complex interplay between environmental exposures and genetic and other factors. This has implications for the medical treatment and for the environmental management of asthma.
In contrast to the limited understanding of the relationship of environmental exposures to the onset of asthma, the environmental triggers of asthma attacks for children with asthma have become increasingly well characterized. House dust mites, cockroaches, mold and animal dander have been identified as the principal allergens that trigger asthma symptoms. Reducing exposure to these allergens has been shown not only to reduce asthma symptoms and the need for medication, but also to improve lung function. Environmental tobacco smoke is an important irritant that can trigger an asthma episode and possibly worsen the effects of allergens. Upper respiratory viral infections are also recognized as important triggers for asthma episodes.
Children with asthma have long been recognized as particularly sensitive to outdoor air pollution. Many common air pollutants, such as ozone, sulfur dioxide, and particulate matter are respiratory irritants and can exacerbate asthma. Air pollution also might act synergistically with other environmental factors to worsen asthma. For example, some evidence suggests that exposure to ozone can enhance a person’s responsiveness to inhaled allergens. Whether long term exposure to these pollutants can actually contribute to the development of asthma is not known. To date, little research has examined the role of other hazardous air pollutants (e.g., metals and volatile chemicals) in the development or exacerbation of asthma, although this is an issue of increasing public concern. In addition to improved understanding of appropriate environmental management of asthma, the medical management of asthma has changed significantly. Inhaled anti-inflammatory medications have become the mainstay of medical management to prevent asthma episodes and lessen chronic symptoms of asthma. In addition, improvements in monitoring techniques now permit objective measures of lung function that are easy for patients and physicians to use in assessing asthma severity and monitoring changes in the disease. In a disease like asthma that varies considerably over time and where changes in lung function can occur before symptoms develop, these objective measures are essential tools for making management decisions.
As a result of these advances, the medical and environmental management of asthma is better defined and the knowledge exists to manage asthma better than ever before. One especially important finding is that patient education has been documented to be cost effective. Teaching patients and their families specific management skills improves asthma management, reduces the use of emergency services, and improves quality of life. This is particularly important for asthma management, since the environmental management of asthma requires knowledge of asthma triggers and specific actions that can be undertaken to reduce exposure to these triggers. The treatment goal for almost all individuals with asthma should be for that person to lead a life unrestricted because of asthma.
Reducing exposure to environmental allergens and pollutants will reduce the frequency and severity of attacks for children with asthma, reduce their need for medicine, and improve their lung function. Children are exposed to many environmental agents that could trigger asthma attacks. For example, 25% of children in America live in areas that regularly exceed EPA limits for ozone. Approximately 29% of households still permit exposure of children to secondhand smoke in the home on a regular basis and exposure to environmental tobacco smoke is so widespread that approximately 88% of all children have some level of documented exposure (Pirkle, 1996). A high proportion of children living in the inner city are exposed to high levels of cockroach antigen.
Why Has Asthma Reached Epidemic Proportions in Children?
The causes of the increasing rate of asthma over the past 15 years and the particular role that environmental exposures play are not known, but there are some clues. Atopy, the genetically inherited susceptibility to become allergic, is the most important predictor of a child developing asthma. A substantial research effort is underway to identify the genes that are responsible for susceptibility to asthma. Because the genetic make-up of the population changes slowly, genetic susceptibility alone cannot be responsible for the epidemic of asthma that has occurred in the United States over the past 15 years. Further work is essential to clarify how genetic susceptibility and environmental exposures interact to cause asthma. Factors such as the intensity of environmental exposure and the age of the person being exposed are likely to be important.
Exposure to allergens found indoors is a strong risk factor for developing asthma. Children are spending increasing amounts of time indoors, thus increasing their exposure to indoor allergens.
The environmental exposures most strongly suspected of causing asthma to develop include environmental tobacco smoke and allergens such as house dust mites, cockroaches, mold, and animal dander. Exposures that stimulate the immune system may also be significant, such as diet during the prenatal period and early infancy, the pattern of respiratory infections early in life, and even decreasing rates of exercise have all been suggested as risk factors for the development of asthma.
Scope of the Strategy
This strategy is about protecting children from the environmental risk factors that make their asthma worse. Environmental action may also help prevent asthma. To accomplish this goal, the environmental aspects of asthma must be considered in the context of other aspects of asthma prevention and management, such as access to quality medical care and efforts to understand the disproportionate health impact of asthma among minority populations. Childhood asthma is a multi-factorial disease, and efforts to improve its management and to prevent it will require multi-dimensional, multi-disciplinary efforts that must occur simultaneously. This Asthma and the Environment strategy focuses on improving the environment in which children with asthma live, learn, play and work. Environmental action, along with medical care, will help children with asthma live productive, active lives and may spare future generations of children from the disease altogether. The Task Force has prepared the following four goals to be accomplished in the next ten years, guided by the vision that in the 21st century, every child in America will live, learn, work, and play in environments that do not cause or worsen asthma.
Goals of the Asthma and the Environment Strategy
By the year 2005, the number of households in which Children are regularly exposed to secondhand smoke Will be reduced to 15%.1
By the year 2010, asthma hospitalization rates in children Will have fallen to no more than 10 hospitalizations per 10,000 people.2 (healthy people 2010 draft)
By the year 2010, emergency department visits will be Reduced to no more than 46 per 10,000 people.3 (healthy people 2010 draft)
By the year 2010, no more than 10% of children with Asthma will experience activity limitations.4 (healthy people 2010 draft)
1 Baseline: 29% in 1994. Source: Biennial Radon and ETS Survey of the Conference of Radiation Control Program Directors and EPA.
2 Baseline: Hospitalization rate per 10,000 population in 1993-94: 18 for total population; 50 for children 0-4 yrs of age and 18 for children 5-14 yrs. Source: Healthy People 2010 Draft
3 Baseline: Emergency room visits 71 per 10,000 population for total population in 1992-94; 121 for children 0-4 yrs of age and 81 for children 5-14 yrs. Source: Healthy People 2010 Draft
4 Baseline: Activity limitation for persons with asthma; 22 percent for overall population in 1992-94. No children-specific data available. Source: Healthy People 2010 Draft
Vision for the 21st Century
Every child in America will live, learn, work, and play in environments that do not cause or worsen asthma.
Guiding Principles
Federal agency actions can provide leadership and direction in reducing environmental risks to protect children who have asthma or are at risk of developing it. Recommendations put forward in this strategy are predicated on the principles that federal action must have:
1. A focus on efforts to better understand and eliminate the disproportionate impact of asthma in minority populations and those living in poverty.
Poor and minority children are much more likely than white, non-Hispanic children to visit an emergency room, to be hospitalized, or to die from asthma, although the rising prevalence of asthma has affected all populations. The reasons for this disparity are not known, although environmental exposures and limited access to quality medical care may all play a role.
The focus on eliminating disparities across racial and ethnic groups has to be considered in all efforts to prevent asthma and its health impact; however, because of the importance of this issue the Task Force has included a specific recommendation in this strategy to examine, understand, and ultimately eliminate disparities.
2. An emphasis on partnerships and community based programs.
A successful effort to reduce childhood asthma will depend in part on the level of success achieved in enlisting all sectors of society in efforts to implement effective programs to prevent and manage the disease. Federal agencies have already forged effective partnerships with many health and professional organizations, corporations, and foundations to conduct training, educate health care providers and the public, and to implement a wide range of prevention activities at the national, state, and local levels.
Expanded partnerships both within government and between government and the private sector are needed. With increasing knowledge about the primary causes of asthma and triggers of asthma attacks, the challenge for the 21st century will be to integrate new research findings into effective environmental, medical and educational programs. Partnerships will be critical to implementing this broad vision of asthma control. In particular, community-based programs should integrate asthma control activities into existing systems such as schools, child care, youth programs, workplaces, primary health, and job training programs.
3. A commitment to setting measurable and consistent goals for childhood asthma under the Healthy People 2010 program.
Health objectives are now being developed for the year 2010 and represent a significant revision of the goals set for the year 2000. These objectives will set the nation’s health agenda for increasing years of healthy life and reducing disparities among the entire American population. Draft objectives currently encompass an expanded set of asthma-related objectives for improved clinical management as well as a series of environmental objectives addressing known asthma triggers such as indoor allergens, secondhand smoke and outdoor air pollution. The goals embodied in the final Healthy People 2010 document will serve as the tools to measure progress towards control of asthma.
4. Investment in evaluation of programs to identify those strategies that are most effective in reducing the burden of asthma so that they may be replicated.
Asthma intervention programs and related activities need to be fully evaluated to determine those techniques which are successful and should be replicated. Evaluation should be incorporated in the planning of all programs and should include:
- identification of desired health outcomes of the program;
- measurement of effectiveness of the intervention activities and processes used to implement them;
- identification of unforseen obstacles;
- assessment of the cost-effectiveness of the program;
- a prediction of long term sustainability of the program.
Recommendations
1. Research
Strengthen and accelerate focused research into the environmental factors that cause or worsen childhood asthma.
Expand Research Into the Environmental Factors That Contribute to the Onset of Asthma in Children.
Though progress has been made in understanding what causes asthma, there is currently insufficient scientific information to establish specific guidelines and recommendations for public health practices to prevent the onset of asthma in children (i.e. primary prevention).
In order to establish primary prevention guidelines, the top priority for research is to determine the causes of asthma in children and particularly the role of the environment. To understand what causes asthma, research must identify the basic cellular and molecular mechanisms that cause airway inflammation and sensitization and, in particular, the interaction of environmental exposures and genetic susceptibility. In addition, clinical and epidemiologic studies are needed to examine the relationship between environmental exposures and the onset of asthma.
Because of promising preliminary work on the relationship of indoor allergens and asthma onset, as well as the much greater proportion of time that children spend indoors, greater emphasis on examining the relationship of indoor exposures to the development of asthma is warranted. Exposures to high levels of allergens in the indoor environment have been shown in some studies to be associated with the subsequent development of asthma. However, few studies have examined the importance, by geography, of particular allergens. In studies evaluating the role of indoor allergens on exacerbations of asthma, different allergens, such as those associated with cockroaches, dust mites, and mold, have been implicated in different cities. This suggests that different allergens can exacerbate asthma, and that different allergens may be capable of inducing the new onset of asthma.
1. Research
Strengthen and accelerate focused research into the environmental factors that cause or worsen childhood asthma.
Expand Research Into the Environmental Factors That Contribute to the Onset of Asthma in Children.
Though progress has been made in understanding what causes asthma, there is currently insufficient scientific information to establish specific guidelines and recommendations for public health practices to prevent the onset of asthma in children (i.e. primary prevention).
In order to establish primary prevention guidelines, the top priority for research is to determine the causes of asthma in children and particularly the role of the environment. To understand what causes asthma, research must identify the basic cellular and molecular mechanisms that cause airway inflammation and sensitization and, in particular, the interaction of environmental exposures and genetic susceptibility. In addition, clinical and epidemiologic studies are needed to examine the relationship between environmental exposures and the onset of asthma.
Because of promising preliminary work on the relationship of indoor allergens and asthma onset, as well as the much greater proportion of time that children spend indoors, greater emphasis on examining the relationship of indoor exposures to the development of asthma is warranted. Exposures to high levels of allergens in the indoor environment have been shown in some studies to be associated with the subsequent development of asthma. However, few studies have examined the importance, by geography, of particular allergens. In studies evaluating the role of indoor allergens on exacerbations of asthma, different allergens, such as those associated with cockroaches, dust mites, and mold, have been implicated in different cities. This suggests that different allergens can exacerbate asthma, and that different allergens may be capable of inducing the new onset of asthma.
In one study (Hyde, et al, 1997) avoiding exposure to dust mite and food allergens early in life was found to reduce the risk of developing asthma in the first year of life. However, this effect was not statistically significant at 2 to 4 years of age. Whether such allergen avoidance strategies are feasible and effective in reducing the development of asthma is not known. The complex interactions between outdoor air pollutants and allergens and the development of asthma have not been adequately evaluated. Some epidemiologic studies have suggested a relationship between exposure to volatile organic compounds and prevalence rates of childhood asthma. Because adult-onset asthma is known to be associated with occupational exposures to volatile organic compounds including formaldehyde, ethylene oxide, and isocyanates, further work to assess the possible etiologic role of specific pollutants in childhood asthma is appropriate.
Expand and Accelerate Research To Develop and Evaluate Environmental Strategies That Will Improve the Quality of Life for Children with Asthma.
It is well established that inhaled allergens and irritants and outdoor pollutants provoke asthma symptoms. Research is needed to identify if other environmental exposures are significant. Further, the relative importance of various exposures is not well understood. Cost effective strategies for reducing exposures are not well developed.
Patient education strategies in certain populations have profound impacts on reducing the frequency and severity of exacerbations and improving the quality of life for children. But many of these programs are not responsive to the cultural, ethnic, and economic diversity of the American population. Innovative strategies are urgently needed for reaching a wide range of children and their families, for tailoring recommendations for reducing environmental exposures to their needs, and for providing support to follow the recommendations.
2. Programs to Improve Public Health
Implement public health programs that improve use of scientific knowledge to prevent and reduce the severity of asthma symptoms by reducing environmental exposures.
Promote Clinician and Patient Implementation of National Guidelines for Reducing Environmental Risks That Worsen Asthma.
Despite uncertainty about the causes of the increase in asthma prevalence rates, much can and should be done to prevent severe illness and death from asthma and improve the quality of life of persons with asthma. Experts convened by the National Asthma Education and Prevention Program (NAEPP) coordinated by the National Institutes of Health (NIH) have reviewed the scientific literature and produced guidelines for managing asthma. These include specific recommendations for controlling environmental factors that contribute to asthma severity.
While there is consensus that NAEPP guidelines define the best diagnosis and management practices for asthma, dissemination of the guidelines must be expanded and adoption improved. Many clinicians do not include advice about environmental control in their patient education. Among families who do receive recommendations, adherence is generally low. Asthma is highly variable, and families need help establishing priorities for environmental control measures that will be suitable for their individual child’s asthma and their family circumstances. Effective public health programs can provide this education and support.
For children without access to quality health care, appropriate instruction on the environmental triggers of asthma is impossible or severely limited. Emergency rooms or urgent care facilities may serve as the only source of primary care for such children. These settings should be recruited to provide the kind of education and links to chronic disease management services that are essential to reducing the severity and frequency of asthma attacks.
Expand Support for State and Local Public Health Action.
Recent advances in the treatment of asthma and in identifying the environmental triggers of asthma attacks make it possible to control and prevent symptoms at a level unheard of just ten years ago. But these gains have not been realized by many of our children. Public health agencies have a critical role in helping to reduce environmental factors affecting asthma and the human and financial toll of the disease. These programs should include the following components:
(1) Education and training
(2) Asthma surveillance
(3) Coalitions for prevention
Reduce Children’s Exposure to Environmental Tobacco Smoke and Other Indoor Triggers in Their Homes.
Secondhand tobacco smoke and indoor allergens are major contributors to the incidence of wheezing in young children and play a significant role in the number and severity of asthma attacks. Reducing smoking in homes with young children will improve the health status of the estimated 2 million children with asthma who are exposed to secondhand smoke. In addition, exposure to allergens such as cockroach, house dust mite, mold, and animal dander causes many attacks of asthma that are preventable.
Establish School Based Asthma Programs in Every Community.
The educational system is a critical component of effective efforts to reduce illness due to asthma in children. Programs will be implemented in schools to assure a healthy physical environment at the school and to promote improved self-management of asthma through education.
Continue to Reduce Outdoor air Pollution
The U.S. EPA set national ambient air quality standards (NAAQS) for six air pollutants in 1971, in part based on evidence of associations between air pollutants such as ozone, particulate matter, and sulfur dioxide and asthma. Since that time substantial new epidemiological evidence has been published supporting the association between levels of ozone and particulate matter and increased hospitalization for respiratory causes, such as childhood asthma. In 1997, NAAQS for both ozone and particulate matter were strengthened to improve the protection afforded by these standards and to help reduce the risk of ambient exposures that aggravate asthma in children.
Federal, State, local, and private sector efforts to implement the original NAAQS resulted in substantial improvements in air quality, yet notable problems remain. Following the 1990 Clean Air Act Amendments, efforts were expanded to improve nationwide air quality and reduce related health effects. In conjunction with the strengthening of the ozone and particulate matter NAAQS, EPA has taken steps to integrate implementation measures for these pollutants and to improve the effectiveness of control programs. EPA has also taken steps to inform the public about air pollution that may affect children.
3. Surveillance
Establish a coordinated nationwide asthma surveillance system for collecting and analyzing health outcome and risk factor data at the state, regional and local levels.
Current national surveillance permits tracking of asthma prevalence, asthma physician office visits, asthma emergency room visits, asthma hospitalizations and asthma mortality at a national level and in four geographic regions (i.e., Northeast, Midwest, South, and West) through surveys conducted by the National Center for Health Statistics. Surveillance information on asthma, with the exception of mortality data, are not available at the state or local level. This information is needed to identify high risk populations and environmental risk factors of relevance to particular communities and to design and implement interventions that will be most suitable for, and therefore most likely to succeed, in that community. State and local health agencies also need this information to evaluate the impact of local sources of air pollution on childhood asthma in specific communities. A significantly enhanced and expanded surveillance program will be essential to study issues related to race and gender differences in asthma morbidity and mortality among children, identify gaps in providing comprehensive care, and monitor trends in asthma morbidity and mortality at the community level.
4. Disproportionate Impacts on the Poor and Minorities
Identify the reasons for and eliminate the disproportionate burden of asthma among different racial and ethnic groups and those living in poverty.
Poor and minority children are disproportionately affected by asthma, which has reached epidemic proportions in many American inner cities. Prevalence rates vary only by a few percentage points among different race and ethnic groups, yet emergency room use, hospitalization, and mortality rates vary 3- to 4-fold. Understanding the factors that contribute to the disproportionate impact of asthma on minority and lower income populations is the critical first step to reducing and eventually eliminating the disparities between rich and poor, minority and non-minority children. Such factors may include differing intensities of environmental exposures, such as exposure to cockroach antigen and access to and quality of care, among others.
Improve Asthma Management for Children Within the Medicaid Program.
Disease management combines prevention, intensive attention to treatment and patient compliance, and guidance for self-care. This concept has considerable promise for reducing the frequency and severity of asthma attacks. Integrating an asthma disease management initiative within the fee-for-service component of Medicaid would demonstrate the efficacy of this approach in improving children’s health.
Appendix E: Summary of Existing DHHS Programs
The Administration for Children and Families (ACF) is responsible for federal programs which promote the economic and social well-being of families, children, individuals, and communities. Through its Federal leadership, ACF sees: families and individuals empowered to increase their own economic independence and productivity; strong, healthy , supportive communities having a positive impact on the quality of life and the development of children; partnerships with individuals, front-line service providers, communities, American Indian tribes, Native communities, states, and Congress that enable solutions which transcend traditional agency boundaries; services planned, reformed, and integrated to improve needed access; and a strong commitment to working with people with developmental disabilities, refugees, and migrants to address their needs, strengths and abilities.
Administration For Children, Youth and Families -- Head Start
The Head Start Program offers comprehensive early childhood education, nutrition, health and social services, along with a strong parent involvement focus, to low-income children nationwide. The overall goal of the program is to bring about a greater degree of social competence in preschool children from low-income families. The recently funded Early Head Start initiative extends services to families with pregnant women, infants and toddlers. Asthma is addressed as part of this comprehensive program though educational practices and guides.
The Head Start Bureau, located within the Administration on Children, Youth and Families (ACYF) under the Administration for Children and Families (ACF), supports local Head Start programs in implementing the Head Start Program Performance Standards related to health (which is broadly defined to include medical, dental, mental health and nutrition); promoting preventive health practices; and striving to improve health services delivery to Head Start children and families through coordination and collaboration with other Federal programs serving low-income children and families. The Bureau periodically sends health information to Head Start grantee and delegate agencies on a variety of topics, such as immunizations, Medicaid, and child nutrition.
The topic of asthma is generally or specifically discussed in two training guides developed through contract by ACF. Activities in the guides are intended for use by Head Start front line staff, management teams, and Head Start parents. Asthma is generally discussed in the guide Sustaining a Healthy Environment. The issue of second hand smoke and air pollution and its impact on young children is discussed in the guide. Asthma is specifically addressed in the training guide: Caring for Children with Chronic Diseases. This guide builds on staff capacity to make Head Start a safe, welcoming place to learn and play for children with chronic illness and their families, and offers skill building activities on individual planning to meet the special health needs of children with chronic conditions. After discussing the impact of chronic illness on the family and the principles of family-centered care, the guide puts into practice the information and skills learned by focusing on children with asthma.
Administration For Children, Youth and Families -- Child Care Bureau
The Child Care Bureau is dedicated to enhancing the quality, affordability, and supply of child care available for all families. The Child Care Bureau administers Federal funds to States, Territories, and Tribes to assist low income families in accessing quality child care for children while parents work or participate in education or training.
The health of children in child care is a top priority of the Child Care Bureau(CCB). One of the major initiatives that the CCB has undertaken to promote healthy development of children is through its "Healthy Child Care America Campaign." The "Healthy Child Care America Campaign (HCCAC)" is a collaborative initiative between the Child Care Bureau and the Maternal and Child Health Bureau in partnership with the American Academy of Pediatrics to support linkages between child care and health in communities across the country to improve health and safety in child care. Forty-eight States, the District of Columbia, Puerto Rico and Palau have successfully launched Healthy Child Care America Campaigns. States and communities involved in these partnerships are developing innovative approaches to ensure the health of children, including utilizing the child care setting as an opportunity to provide preventive health services. Technical assistance is provided to States and communities through an agreement with the American Academy of Pediatrics.
The HCCAC Blueprint for Action outlines 10 steps that States and communities can take to either expand existing public and private services and resources or to create new services to link child care and health. One of the 10 steps specifically focuses on providing support to child care providers caring for children with special health care needs, including asthma.
The Child Care Bureau's National Child Care Information Center (NCCIC) disseminates information to the child care community on children's health related information. Earlier this year multiple copies of the Sesame Street: "A is for Asthma" video was disseminated to each State Child Care Administrator. The NCCIC website features health and safety resources and also "hotlinks" to health related organizations.
AHRQ supports research designed to improve the quality of health care, reduce its cost, and broaden access to essential services. AHRQ's broad programs of research bring practical, science-based information to medical practitioners and to consumers and other health care purchasers. Here are highlighted several asthma-related projects supported by the agency.
Research
Health Services and Outcome
AHRQ supports research on the quality and outcomes of asthma care. The AHRQ asthma program evaluates the efficacy and cost effectiveness of asthma management programs. AHRQ also supports the development of outcome measures to monitor the quality of asthma care delivered, quality of life, and patient satisfaction with the health care received.
AHRQ's principal efforts in asthma research are grants to study and improve the quality of care delivered to patients with asthma. The "Pediatric Asthma Patient Outcome Research Team (PORT) II" is a 5-year randomized clinical trial that will test the cost-effectiveness of the Guidelines designed to reduce asthma morbidity among children. AHRQ is sponsoring several other research projects to assess whether specific quality improvement approaches, being implemented in real-world clinical settings, are effective in helping clinicians better manage childhood and adult asthma in accordance with the Guidelines. One study is comparing the effects of an opinion leader training program to an organizational change intervention in managed care plans; another is comparing a continuous quality improvement approach in office-based care to routine care; a third is looking at guideline implementation in emergency care; and another is studying disease management strategies for adult asthmatics in Medicaid HMOs. Cost-effectiveness is being examined in several of these studies, which are also testing health outcome measures, such as number of symptom-free days, to identify how treatments affect children's daily lives. Another strategy for improving asthma care is to update aspects of the Guidelines that have been addressed by recent research. An AHRQ-supported Evidence-based Practice Center is examining recent research in five Guidelines areas.
In another effort, "Measuring Quality of Life in Children with Asthma," researchers are examining the relationship between a general multi-dimensional approach and a disease-specific approach to measuring quality of life in children with asthma.
The mission of ATSDR is to prevent exposure and adverse human health effects and diminished quality of life associated with exposure to hazardous substances from waste sites, unplanned releases, and other sources of pollution present in the environment. To specifically address asthma, the Agency does on-site investigations of communities where exposures have occurred to toxic substances which are known or suspected as contributing to asthma morbidity; it also conducts epidemiological studies to increase understanding of the effects of these toxic substances and provides education and outreach to communities and health care providers.
Research
Risk Factors/Triggers
ATSDR's research activities in the area of asthma fall into two broad program areas. The first is the investigation of human health effects in communities where citizens have been exposed to hazardous substances released from hazardous waste sites or other environmental sources. Communities have been expressing growing concern about perceived increases in asthma. Often atmospheric releases of hazardous pollutants include substances that are known or hypothesized contributors to asthma morbidity. For example, one recently completed investigation examined whether ambient emissions from a large municipal landfill (characterized by levels of hydrogen sulfide and odor) were associated with an increase in respiratory symptoms and a decrease in respiratory function among persons with asthma who live near the landfill. Another investigation examined the occurrence of asthma among children exposed to airborne emissions of toluene diisocyanate from a foam manufacturing facility. Enhanced ambient air monitoring in another community with multiple sources of high hydrogen sulfide emissions has enabled ATSDR to examine the relationship between hydrogen sulfide and hospital visits for asthma and other respiratory conditions.
The second broad program area is the conduct of epidemiologic studies to address important gaps in our understanding of the relationship between hazardous substances and seven priority health conditions. Lung and respiratory diseases, including asthma, are included among these seven priority health conditions. (The other conditions are: birth defects and reproductive disorders; cancer; immune function disorders; kidney dysfunction; liver dysfunction; and neurotoxic disorders). Two recently initiated projects, one with the Utah Department of Health and the other with the Massachusetts Department of Health, are examining the relationship between childhood asthma and exposure to hazardous substances. ATSDR also is supporting two projects with the New York State Department of Health to examine the relationship between asthma and toxic air pollution; one is specifically focused on asthma among children.
ATSDR supported health investigations typically involve a close partnership among ATSDR and the local and state health departments, state and Federal environmental agencies, and community groups and citizens. Through cooperative agreements with 23 state health departments, ATSDR is working to build the capacity of state health departments to address concerns related to specific Superfund sites. Often community health concerns include asthma. For several health investigations, local Community Assistance Panels have been established as a mechanism to establish open and ongoing communications with residents of the community.
Many ATSDR products and services contribute to professional and public education regarding hazardous substances that have been associated with asthma. ATSDR has published toxicologic profiles that present critical assessments of current knowledge and emerging science relevant to hazardous wastes. Two that have focused on substances recognized as respiratory irritants include sulfur dioxide and hydrogen sulfide.
ATSDR and its partners have educated more than 4,000 primary care providers at 108 Superfund sites to diagnose, treat, and counsel people who may have been exposed to hazardous substances. The agency's health education and promotion activities have included continuing medical education for physicians on the relationship between asthma and the environment. Recent agency efforts have focused on the development of guidelines for the clinical evaluation of children who may have been exposed to hazardous substances. Asthma is one of several health endpoints of interest. In addition, a case study in environmental medicine is under development which focuses specifically on environmental asthma.
Other agency activities contribute to the reduction in human exposure to hazardous substances and thus potentially to the primary or secondary prevention of asthma. Public health assessments and related activities evaluate data and information on the release of hazardous substances into the environment to assess any current or future impact on public health, develop health advisories or other health recommendations, and identify studies or actions needed to mitigate or prevent human health effects.
The Centers for Disease Control and Prevention (CDC) is responsible for promoting health and quality of life by preventing and controlling disease, injury, and disability. In its half-century of successes working with partners across the nation and the world, CDC has been a leader and pioneer in detecting and investigating health problems, conducting research to enhance prevention, developing and advocating sound health policies, implementing prevention strategies, promoting healthy behaviors, fostering safe and healthy environments, and providing leadership and training in public health.
National Center for Chronic Disease and Health Promotion-Division of Adolescent and School Health
The vision of the National Center for Chronic Disease Prevention and Health Promotion is to enable all people in an increasingly diverse society to lead long, healthy, satisfying lives. The Center's mission is to: prevent death and disability from chronic disease; promote maternal, infant, and adolescent health; promote healthy personal behaviors; and to accomplish these goals in partnership with health and education agencies, major voluntary associations, the private sector, and other federal agencies.
CDC is committed to promoting the most effective means the nation might use to prevent the major health and social problems that affect school-aged children and adolescents. It is estimated that more than 4 million children have asthma. This disease is one of the leading causes of school absenteeism, accounting for over 10 million missed school days per year. CDC's Division of Adolescent and School Health (DASH) has an existing framework that includes approximately 55 state and territorial departments of education and partnerships with 35 national nongovernmental organizations and their constituents who have the capacity to help schools implement effective school health programs. While the program does not currently focus on asthma, its partnerships are relevant to school based asthma initiatives.
National Center for Environmental Health
The mission of the NCEH is to provide national leadership, through science and service, to promote health and quality of life by preventing and controlling disease, birth defects, disability, and death resulting from interactions between people and their environment. Program highlights include a comprehensive ZAP Asthma program and related projects, building state infrastructure and capacity to enhance programs in asthma, as well as research on the effects of air pollution in Mexico City.
Research
Risk Factors/Triggers
NCEH has supported a variety of studies examining the effects of various air pollutants on the health of children in Mexico City, both asthmatic children and those not diagnosed with the disease. Different studies have varied their methods: one measures daily respiratory symptoms and peak flow, while others observed episodes of respiratory illness through diary questionnaires. Respiratory health and pulmonary function of the children studied were compared in all cases with air quality, especially levels of ozone and inhalable suspended particulates.
Asthma Management [Related topics: Community-based partnership and Outreach]
Environmental Control
ZAP Asthma, Atlanta, Georgia, seeks to show that a comprehensive approach to controlling asthma (access to quality medical care, reductions in allergens and patient education) will reduce the number of asthma hospitalizations for children. The program includes an intensive evaluation component; a physicians' advisory committee to improve clinician practices in diagnosing and treating asthma; community level health education efforts; and applied research. Unique features of the project are the extensive partnerships (public and private) formed to carry out the project and the hiring of local community health workers. Seventeen partners are involved--including the American Lung Association of Georgia, the City of Atlanta, health insurance companies, and Emory University.
Surveillance
In 1999, state health departments had the option of including a standard series of questions in the Behavioral Risk Factor Surveillance System to determine the prevalence of asthma among adults. This surveillance system uses the random digit dialing technique to provide state level information for a variety of health conditions and health related behaviors. In 2000, the questions on asthma prevalence will be asked in all states.
With funding from NIH and EPA, CDC has provided grants to four state health departments and two city health departments to devise model asthma surveillance systems, including uses of these data for program development and evaluation.
To foster family and patient education in asthma, NCEH has funded the Asthma Intervention and Welfare Reform Project in Wisconsin. The purpose of this project is to bring public health expertise on asthma and welfare reform together to provide asthma education and management techniques to enable families enrolled in the welfare-to-work program to finish job training, enter and stay in the work force, and improve their quality of life.
Other -- State Capacity Building
In late 1997, CDC requested each state health officer to identify an individual in the health department (or health agency for some jurisdictions) to serve as the focal point for asthma activities in the health department. These individuals, known as asthma contacts, now number 55 and include officials from every state, the District of Columbia, two city health departments and two territorial health departments. During the first year of the program, CDC staff mailed material on asthma epidemiology, surveillance, treatment, and control at approximately monthly intervals. In February 1999 and February 2000, conferences were convened to identify appropriate asthma surveillance and control strategies and to share experiences in efforts to reduce the burden of asthma.
National Center for Health Statistics
The mission of the NCHS is to provide statistical information that will guide actions and policies to improve the health of the American people. As the Nation's principal health statistics agency, NCHS leads the way with accurate, relevant, and timely data. NCHS contributes to the body of asthma research through various national surveys of the American population.
Surveillance
The National Center for Health Statistics has a number of health information systems that provide data to monitor the impact of asthma on the American people. The purpose of these systems is to monitor a number of health issues; information on asthma is obtained as one of a broad range of adverse health conditions. The following are descriptions of the major data systems.
The main objective of the National Health Interview Survey (NHIS) is to monitor the health of the United States population through the collection and analysis of data on a broad range of health topics. This survey can display these health characteristics by many demographic and socioeconomic characteristics. The Basic Module, which is asked on one sample adult and one sample child in the household, contains specific questions that address asthma. Additional information that is available includes: information on household composition and sociodemographic characteristics; information for matches to administrative databases; and basic indicators of health status and utilization of health care services.
The goals of the National Health and Nutrition Examination Survey (NHANES) program are: to estimate the number and percent of persons in the U.S. population and designated subgroups with selected diseases or risk factors for selected diseases, to study the relationship between diet, nutrition and health, and to explore emerging public health issues. Respiratory diseases have been an important component of NHANES since the first survey was fielded in the 1960's. A medical history of respiratory and allergic symptoms, as well as previous diagnoses of asthma, have been included in the sample person questionnaire. In addition, lung function is assessed through spirometric testing in a mobile examination center. Auxiliary data on exercise, diet, occupation, tobacco use, and medication use are collected. In some surveys, allergic responses and exposure to tobacco smoke have also been assessed. The NHANES is designed to provide estimates in selected racial and ethnic populations.
One survey (National Hospital Discharge Survey) studies inpatient utilization of hospitals, including information on diagnoses, procedures, length of stay, expected source of payment, and patterns of use of care in hospitals. This survey has been used to monitor hospitalizations due to asthma among young and old. Another survey (National Ambulatory Medical Care Survey) collecting data on hospital care provides information on demographic characteristics of patients, patients' complaints, medication therapy, and types of health care professionals seen, among other factors. Some mortality surveys (National Mortality Followback Survey; National Vital Statistics System: Mortality Files) have focused on deaths attributed to asthma and have provided an opportunity to study socioeconomic differentials in mortality, associations between risk factors and cause of death, disability, and access and utilization of health care facilities in the last year of life. The NCHS has collected and published information on deaths and causes of death since the early 1930's. Monitoring the trend in asthma mortality among various age, racial and ethnic groups, and genders has been an important signal to alert the public health community to the increasing problem of asthma in the American population.
National Institute of Occupational Safety and Health
NIOSH is responsible for conducting research and making recommendations for the prevention of work-related illnesses and injuries. Asthma that is either initiated or significantly worsened by job environments is a major focus of the NIOSH research and surveillance program.
Research
Natural History of the Disease
Asthma is one of the top priorities for research in the U.S. over the next decade, as defined by the National Occupational Research Agenda (NORA). Recent investigations of work-related asthma include health hazard evaluations of workplaces in which the new onset of asthma has been reported in relation to airborne and dermal exposures from chemicals, metals, animal and vegetable products, as well as organic composts and metal working fluids (both of which often are contaminated by biological agents). Additional studies are evaluating the incidence, risk factors, and natural history of asthma in groups of workers working in exposure settings with a previously recognized asthma risk, such as aluminum reduction, wood products manufacturing, insect rearing, and health care (natural rubber latex). Exposures to many of the implicated workplace agents are also common in the home and other settings, although at generally lower levels. Exposure-response relationships in the workplace may be more easily investigated due to the larger range of exposures and more accurate classification of exposure levels. Multiple reports in the occupational literature document that timely and adequate control of exposures in individuals with work-related asthma can at times result in complete cessation of asthma symptoms and findings. To further delineate the conditions required for asthma onset and cessation, NIOSH has ongoing investigations addressing improved methods for characterizing and quantifying exposures to chemical sensitizers (e.g. isocyanates and certain metals), protein antigens (natural rubber latex, insect and crab proteins), and other organic materials, such as endotoxins.
Pathogenesis and Mechanisms (also risk factors/triggers)
NIOSH is currently investigating the pathobiological mechanisms of asthma, including markers of responses, utilizing in vitro preparations, in vivo animal models of asthma, and observational studies of exposed workers and their blood and nasal fluids. Both dermal and inhalation exposures to natural rubber latex and isocyanates are under investigation in the laboratory, also in conjunction with observational studies in exposed workers.
Prevention
A large scale intervention trial is evaluating primary asthma prevention in health care facilities through a comprehensive program of reduction in worker exposures to powdered natural latex gloves, with concurrent monitoring of several health outcomes, as well as skin and airborne antigen exposures. Methods for medical screening, and early detection of asthma are being investigated in groups of workers with various potential asthma-inducing exposures, as secondary prevention methods.
Surveillance
Components of several ongoing NIOSH activities involve surveillance of asthma. The Health Hazard Evaluation Program responds to requests from workers and managers for workplace investigations, and in recent years, multiple complaints related to asthma symptoms have been investigated. NIOSH has funded state-based demonstration projects for occupational asthma surveillance systems. Data collection from this surveillance is ongoing, and assists in the identification of high risk exposures and the recognition of new environmental causes of asthma. Additionally, currently funded projects are addressing population-based asthma surveillance and evaluating the role of occupational environments and other exposures in asthma incidence, prevalence, and severity.
NIOSH has ongoing involvement in the development of asthma management guidelines. Institute representatives continue active involvement with the National Asthma Education and Prevention Program and the American Thoracic Society in the development of professional guidelines for the evaluation and management of asthma, with emphasis on the recognition and management of occupational and environmental exposures. Certain
NIOSH publications also offer management guidelines for asthma in relation to specific workplace exposures, including natural rubber latex, isocyanates, and laboratory animals.
Clinician Education
Limited programmatic support is currently offered to a health care provider association for the development of clinician education and print/electronic information resources, to assist providers in the recognition and management of occupational and environmental triggers in asthma patients.
FDA is a public health agency, charged with protecting American consumers by enforcing the Federal Food, Drug, and Cosmetic Act and several related public health laws. FDA examines the results of studies done on products by the manufacturer, and ensures that these products meet certain safety standards. The FDA has programs investigating allergy and asthma-related devices, drugs, and diagnostic and therapeutic allergen vaccines.
Center for Drug Evaluation and Research
Policy/Regulatory
Asthma Management -- Pharmacotherapy
CDER, primarily through the Division of Pulmonary Drug Products, works in partnership with pharmaceutical sponsors to facilitate the timely development and approval of safe, effective, and high quality drug products for the treatment and/or prevention of asthma. CDER also is involved in facilitating the development and approval of drugs such as: the first non-chlorofluorocarbon (CFC) propelled metered-dose inhaler (MDI) for the treatment of asthma, and three new multi-dose dry powder inhalers (DPIs) for the treatment of asthma. Efforts also include the improvement of drug labeling for children.
Center for Biologics Evaluation and Research
Policy/Regulatory
Risk Factors/Triggers
Allergens found in house dust emanating from cats and dogs, cockroach, molds, rodent allergens, and house dust mites are recognized as important sensitizers/triggers of asthma in allergic individuals. Extracts from these source allergens are currently FDA approved both for use in diagnosis of asthma triggers/sensitizers by means of allergy skin testing and asthma treatment by means of allergy injections to reduce airway reactivity to the allergen trigger identified. The Public Health Service Act requires allergens licensed by the FDA to meet potency standards. To date, in compliance with the Act, CBER research initiatives have developed U.S. Standards of Potency for house dust mites and cat. These standardized allergenic extracts are licensed by CBER for sale in the U.S. for diagnosis and immunotherapy of hypersensitive asthmatics whose symptoms are elicited following exposure to these allergens. Licensed allergenic extracts are accompanied by adequate directions for use in diagnosis and treatment via FDA approved package inserts and labeling. Standardization increases the value of information available to patients and physicians, reduces the risk of incorrect dosing, reduces the risk of inadvertent allergen overdose and serious side effects. Standardization also permits scientific studies that are predictable, replicable, and can be extrapolated. In contrast to standardized allergenic extracts of cat and house dust mite, allergen extracts licensed by FDA of cockroach, dog, mold, and rodent allergens are currently nonstandardized.
CBER is planning to develop U.S. Standards of Potency for cockroach and mold. CBER will support the conduct clinical trials using cockroach and/or mold allergen vaccines meeting U.S. Standards of Potency to determine their safety and efficacy in the diagnosis and immunotherapy of cockroach- and mold-induced asthma.
HCFA is the federal agency that administers Medicare, Medicaid, and the State Children's Health Insurance Programs. HCFA's asthma work includes research and monitoring of care provided to Medicare beneficiaries through Medicare Peer Review Organizations. The goal of these activities is to improve access to care and outcomes of health services delivery for patients using HCFA's services.
Research
Using Medicaid and Medicare data, HCFA's extramural and intramural research related to asthma includes: tracking: the disease, the frequency of services, risk factors, and other factors involved in a person's medical and environmental history of asthma treatment, and assessing the quality of asthma-care provided to program beneficiaries. Also, when feasible, the analyses include comparisons with other populations. The data sets being analyzed are Medicare administrative claims files and the Medicare Current Beneficiary Survey (MCBS); and the Medicaid eligibility and claims files, and certain medical records. When feasible, HCFA's research uses the Guidelines for Diagnosis and Management of Asthma (NHLBI: Expert Panel Report 2, "Guidelines") as a framework for studies, and in other instances, as criteria for quality of care measurement.
HCFA funded a substantial portion of the RAND work in the development of global quality of care, asthma-related indicators for women under fifty years of age and for children who receive their services through a managed care environment. The indicators were completed in 1999.
Quality and Outcome of Care HCFA's program on quality of care for Medicaid children with asthma includes access to care factors and proxies. This aspect of HCFA's research program on asthma is based on the theory that if Medicaid children have adequate and timely access, then their severity and repetition of acute episodes may decrease, and the outcomes of their care improve.
HCFA has a small program on quality and outcomes of care among Medicaid children with allergic asthma. This asthma program is part of HCFA's assurance that its beneficiaries receive appropriate and timely health and illness care.
Two HCFA Medicare Peer Review Organizations participate in the Agency's asthma program through a state-wide project aimed to verify that physicians treating asthma in Medicare patients do so in accordance with the Guidelines.
Family/Patient Education
The Medicare Peer Review Organizations also aim to verify that patient education is being provided for proper administration and use of prescribed medication, and the use of peak flow meter home monitoring in accordance with the Guidelines.
-Quality of Delivery Systems
HCFA and AHRQ funded an NCQA Pediatric Health Plan Assessment Task Force that identified gaps in HEDIS quality performance measures. The work was completed in 1999. The new HEDIS asthma measure, which now includes children and adults, is being tested. Managed care organizations with contracts to provide services to Medicaid beneficiaries are among the entities responding to NCQA during this testing phase. Also, HCFA participates in the NCQA Committee on Performance Measurement with input into the HEDIS measures.
HRSA directs national health programs which improve the health of the Nation by assuring quality health care to underserved, vulnerable and special-need populations and by promoting appropriate health professions workforce capacity and practice, particularly in primary care and public health. HRSA programs are designed to promote comprehensive primary care education and practice, and to support the Nation's public health infrastructure. The management of asthma is addressed through several programs which provide resources and services for broad health improvement, especially in vulnerable groups.
Research
General
The Bureau of Primary Health Care (BPHC) collaborates with AHRQ on the development of health center practice based research networks. One of the practice based research projects focuses on asthma. There are four phases to this research: descriptive studies, epidemiological studies, clinical outcome studies and intervention trials. Currently, the project is beginning the second phase of work.
Health Services and Outcomes
BPHC has developed an evaluation and research strategy to measure health outcomes in the underserved population through health center effectiveness studies, and it has developed a quality improvement strategy to improve health outcomes and disseminate breakthrough changes (see section on "Access to Quality Care.")
Health Services
Clinician Education
The Bureau of Health Professions provides support for major training programs in general internal medicine, general pediatrics, family medicine, geriatrics, advanced nurse/nurse practitioner education, and for physician assistants; and for interdisciplinary training through rural health and area health education centers. All of these efforts include management of patients with asthma in the context of comprehensive primary care services.
Access to Quality Care
BPHC supports several major programs to increase access to comprehensive primary and preventive health care for underserved and vulnerable populations. Critical health professional provider needs of underserved areas are addressed through the National Health Service Corps. Essential health services for vulnerable populations of homeless, migrant farm workers, public housing residents, and others, are targeted through the Consolidated Health Centers Program. Although not specific to asthma, these activities forge community-based partnerships and encourage outreach to manage acute and chronic health problems.
Comprehensive primary care services in Health Centers include the treatment of asthma. In addition to providing both primary care, appropriate specialty referral, and hospitalization for these patients, health centers provide critical enabling services that are key for asthma care. These services include case management, environmental health risk reduction, health education, outreach, transportation, and interpretation and translation services. In addition, health centers operate over 200 primary care sites in schools, and most health centers provide pharmacy services.
BPHC, in collaboration with the Institute for Healthcare Improvement (IHI), the Environmental Protection Agency (EPA), the Agency for Toxic Substances and Disease Registry (ATSDR) and public and private agencies, has launched an aggressive, innovative program to address the growing health disparities and a changing market place. Beginning in February 2000, 20-25 health centers, including school based health centers and free standing National Health Service Corps will participate in a Health Status and Performance Improvement on Providing More Effective Care for Adults and Children with Asthma. This effort seeks to 1) generate and document improved health outcomes for the underserved population with asthma 2) transfer knowledge about how to promote positive breakthrough changes; and 3) develop infrastructure, expertise, and leadership to support and drive improved health, access, and cost outcomes.
Health Centers participating in the Collaborative select teams to attend three learning sessions and they receive ongoing support from IHI to make accelerated improvements in the care they give to patients with asthma. Examples of measures include, symptom free days, reduction in certain environmental exposures, emergency department visits for asthma, and treatment with maintenance anti-inflammatory medication.
The collaborative emphasizes team cooperation to obtain optimal patient care outcomes. Teams submit monthly reports which 1) document their performance on key patient care measures, and 2) assess their progress as a team. Attainment of these goals depends upon continual learning, improvement, change, and expansion of partnerships at the local, state, and national levels.
Community-based Outreach
The Maternal and Child Health Bureau provides block grants to the States and administers discretionary grants to support the Nation's maternal and child health infrastructure. Of special relevance to management of asthma patients, and community-based partnerships and outreach, are two program areas. One supports the development of systems of care and services for children with special health care needs, including those at risk for or suffering from chronic illness and disabilities. The other comprises interdisciplinary training of professional health personnel, including working through pediatric pulmonary centers to improve community-based care for children with chronic respiratory diseases (such as asthma) and their families.
The mission of the IHS is to raise the physical, mental, social, and spiritual health of American Indians and Alaska Natives to the highest level. IHS aims to assure that comprehensive, culturally acceptable personal and public health services are available and accessible to American Indian and Alaska Native people. The bulk of IHS's asthma-related activity is in clinical care, but another important aspect of their activity is in fostering asthma research. IHS plays a critical role in collaboration with outside researchers looking at conditions that affect specific tribes.
Research
General
The function of IHS regarding research is to serve as a liaison between outside researchers, which are mostly academic institutions (e.g. University of New Mexico, University of Arizona, University of Washington, the Strong Heart Study), and tribes. In addition to bringing together tribal communities, IHS (with individual and tribal approval) assists the researchers with clinical health data to be integrated into the research. IHS also provides a unique dimension to the Institutional Review Board (IRB) process. Not only does it serve to protect individual subjects; the IHS IRB also requires that research is approved by the tribes served by IHS facilities involved in research. In these ways, the IHS provides in-kind support promoting research to the extent that it will benefit the tribes. Working with a number of universities, IHS has provided assistance in respiratory research affecting tribal populations, and in surveillance documenting long term increasing trends in asthma incidence in tribal communities in New Mexico, Arizona, Washington State and Alaska.
Health Services
Community-Based Partnership/Outreach
The bulk of IHS's asthma-related activity is in delivery of health care to tribes. In addition to providing asthma treatment as part of standard care, IHS has helped to establish several specialty clinics focused on asthma. For example, Children's Medical Services of New Mexico developed special community-based asthma clinics and a Children's Hospital-based family education program for families of Indian children with asthma. The University of Washington is working with several health centers serving
American Indian and Alaska Native communities to promote excellence in clinical asthma services.
The mission of the National Institutes of Health (NIH) is to uncover new knowledge that will lead to better health for everyone. NIH works toward that mission by: conducting research in its own laboratories; supporting the research of non-Federal scientists in universities, medical schools, hospitals, and research institutions throughout the country and abroad; helping in the training of research investigators; and fostering communication of biomedical information.
National Heart, Lung, and Blood Institute
NHLBI plans, conducts, fosters, and supports an integrated and coordinated program of basic research, clinical investigations and trials, observational studies, and demonstration and education projects. NHLBI has many programs directly targeting asthma; the Institute conducts and sponsors extensive research efforts aimed at understanding all aspects of the disease, including mechanisms, genetics, environmental and other factors, and drug therapy. There is also a strong emphasis on Demonstration and Education. The National Asthma Education and Prevention Program, coordinated by NHLBI, has published the widely distributed "Guidelines for the Diagnosis and Management of Asthma." and undertakes extensive education and outreach efforts to help translate the latest scientific understanding of asthma into practice.
Research
Natural History of the Disesase
Epidemiological studies funded by the NHLBI include longitudinal studies focused on identifying the risk factors associated with the development of asthma and asthma-like-symptoms during childhood and young adulthood. Such research has helped identify phenotypes, or characteristics of asthma among populations, that may reveal new hypotheses about the mechanisms of asthma. Recent studies of young children, for example, raise new questions about the role of respiratory infection in the onset of asthma. There is a well established association of respiratory viral illness and exacerbations of asthma, and it has long been thought to be a cause of asthma in all ages and particularly in young children.
Current epidemiologic studies indicate that there are two different patterns of wheezing with viral illness in young children--many of whom do not have continued asthma symptoms after 6 years of age. The data support the intriguing suggestion that rather than causing the onset of asthma, some respiratory viruses may protect some young children. In this view, asthma may be a result of an altered developmental pattern of both the lungs and the immune system. Two major research initiatives undertaken by NHLBI in FY98 are exploring the role of respiratory infections in asthma and the mechanisms underlying risk factors of the onset of asthma in early life.
Other epidemiologic studies supported by the NHLBI are identifying the factors, such as environmental exposures, that influence the rate of decline in pulmonary function and increased hyperresponsiveness in older adults. Epidemiologic studies are also assessing the separate and interactive effects of asthma severity, job characteristics, psychosocial and other factors on asthma disability.
Epidemiologic studies on the natural history of asthma focus on identifying factors that are associated with the risk of severe asthma and asthma related death. Recent statistics on asthma morbidity and mortality underscore that African-Americans and Puerto-Rican Hispanics have a disproportionately high risk of asthma related hospitalizations and deaths. Socioeconomic factors and access-to-health care factors are most likely involved, but research on how genetic, immunologic, and environmental factors contribute --either independently or together -- to asthma onset and severity will elucidate other risk factors for these populations.
Pathogenesis and Mechanisms
A major portion of NHLBI supported research in asthma is devoted to identifying and examining the underlying pathogenesis and basic mechanisms of the disease. Through this research, appropriate targets for treatment to stop, and ultimately reverse, the asthmatic process can be developed. A major focus of studies is the dissection of the cellular and molecular events which appear to initiate, direct, and perpetuate the development of airway inflammation in response to both immunologic and non-immunologic stimuli. For example, studies are examining specific inflammatory cells such as thymus-derived lymphocyte (T-Cell) abnormalities and their interaction with each other and with resident airway cells such as cytokines and inflammatory mediators. This research will define the mechanisms that underlie the selective migration of inflammatory cells to the airways. Research is also directed at establishing the mechanisms of neural control of bronchoconstriction and airways, hyper-responsiveness in asthma, as well as the mechanism involved in the integrated regulation of airway and blood vessels in the lung by neural reflex control. Studies are also determining the sequence of biochemical events generating and regulating hypersecretion in inflamed airways, a common feature of asthma.
Genetically engineered murine models are being developed and used to explore immune and inflammatory responses in the lung that are relevant to asthma. This research exploits the findings that a number of proteins including cytokines, adhesion products, growth factors, and membrane ion channels act as pivotal elements in asthma. Since the ability to address questions in a mechanistic manner and to manipulate the system in humans are limited, many studies are performed with mammalian models alongside clinical studies.
Another promising area of NHLBI supported research are studies directed at understanding the cellular and molecular mechanisms regulating the function of receptors found in the walls of the airways (e.g. beta-adrenergic receptors) and other receptors. For example, evidence suggests that a defect in beta-adrenergic receptors could contribute to the development of asthma and may lead to a more severe clinical course for the disease.
Research into the mechanisms contributing to the persistence, or chronicity, of asthma is focused on the nature of the repair process in the airway wall and the remodeling of the airway epithelium and airway smooth muscle.
Neuroregulation of the airway is another mechanism that influences the nature and severity of asthma. Immunological and neural factors have been investigated independently, but now research indicates that these two processes are interrelated. It appears that stimulation of sensory nerve endings within the airways leads to production and release of substances that cause inflammation. Moreover, stress has been shown to play an important role in asthma but its role is not well understood. Intriguing early studies suggest that interdisciplinary research in the pscyho-immuno-neurological aspects of asthma may reveal new insights about the mechanisms of asthma. Further studies in both epidemiologic and basic research are assessing the importance of stress in terms of the timing of disease onset, potential interactions with allergens, and interaction with other factors that may influence the onset of the disease and how it is expressed. In addition, investigation of the role of neural and immunologic factors in chronobiology of asthma, including nocturnal asthma may lead to a better understanding of risk factors of asthma related death, since studies suggest that there is an association between asthma that worsens at night and asthma severity and deaths.
The NHLBI supports six Specialized Centers of Research in the Cellular and Molecular Mechanisms of Asthma. Through multidisciplinary basic and clinical investigations, these centers are poised to provide major scientific advances in understanding the interaction and integration of various inflammatory, immunologic, and neural process and how they cause the clinical syndrome of asthma.
Genetics
Currently, a genome-wide search, sponsored by the NHLBI with participation of the NIAID, is underway to identify all the various genes that confer susceptibility to asthma, with the NHLBI-supported Mammalian Genotyping Service involved in defining the chromosomal regions influencing the complex phenotypes in asthma in humans. Early findings from these studies confirm that multiple genes may be involved in asthma and that they may vary between ethnic/racial groups. Examination of known candidate genes in the regions of linkage support the concept that the pathophysiology of asthma may involve genetically determined changes in inflammatory pathways and T cell signaling.
With the support of the NHLBI, researchers have identified individual genes affecting airway hyperresponsiveness in bred mouse strains. Also, studies of human pedigrees using a candidate gene approach, have reported evidence for specific genes influencing asthma or atopy.
Additional genetics research supported by the NHLBI include the fine mapping of initial linked regions found to influence asthma and positional cloning to characterize the precise alleles that confer risk. The goal is to delineate the genes and mutations involved in the development of allergy and asthma and to explore specific gene-environment interactions that lead to asthma and different clinical manifestations of the disease
An exciting new area of research supported by NHLBI is pharmacogenetics research, in which genetically determined factors influence individual response to pharmacologic therapy. For example, current studies are exploring the role of beta-adrenergic polymorphisms in a diminished response to beta-agonist medication.
Prevention
Primary prevention of asthma should be achievable. As noted in the "Natural History and Epidemiology" and "Pathogenesis and Mechanisms" sections, recent studies supported by the NHLBI are leading to insights into the mechanism of asthma and risk factors for the onset of asthma that will suggest promising avenues for future research. Two large research initiatives launched by the NHLBI in FY 1998 will promote identification of the most promising targets for future interventions to prevent the onset of asthma. These are Request For Application (RFA): "Role of Respiratory Infections in the Development of Childhood Asthma," which is co-sponsored by NIAID, and RFA: "Origins of Asthma in Early Life." The research will include studies that: investigate at what point in the cellular events can the chain of inflammatory events be interrupted; use animal models to explore the interaction of viruses and antigen sensitization; and help identify if there is a "preasthma" state in early childhood during which exposure to respiratory infection or environmental allergens bring about asthma in genetically predisposed, at-risk individuals.
Asthma Management
The NHLBI supports a variety of studies that investigate new drug therapies, evaluate the effectiveness of existing therapies, both pharmacologic and non-pharmacologic (e.g. environmental control measures), on asthma management, and explore the effect of therapies on the course of the disease. The studies include clinical research and demonstration and education research.
Environmental control
The NHLBI supports several studies that assess the effectiveness of reducing exposure to known allergens and environmental tobacco smoke on reducing asthma symptoms, emergency department visits, and hospitalizations. Current studies focus on reducing exposures among children with asthma, especially children in low income urban areas since such exposures have been associated with disproportionately more severe disease in these areas.
Pharmacotherapy
The NHLBI supports several large clinical research programs devoted to studying the long term effects of asthma medications and to examining the potential effectiveness of novel new treatments. The Childhood Asthma Management Program, a multi center clinical trial with over 1,000 children will provide critical information about the long term effects and safety of three key therapies in childhood asthma.
The Asthma Clinical Research Network provides an infrastructure for the rapid completion of multiple therapeutic trials in well characterized populations of patients with asthma and for the timely communication of results to the medical community. This research of the Network helps resolve current clinical controversies in asthma management.
In partnership with other Institutes within NIH, including NICHD, NHLBI supports clinical trials among women with asthma to identify the treatments that will lead to the both effective management of asthma during pregnancy and healthy pregnancy outcomes.
Several clinical studies build on the results of studies on the basic mechanisms of asthma. For example, the recent development of anti-leukotrienne medications, the first new class of medication to become available in over 10 years, is based on basic research that identified the critical role of leukotriennes in the inflammatory process of asthma.
Monitoring
Investigations supported by the NHLBI are examining the relative merits of peak flow monitoring or symptom monitoring for guiding day-to-day therapeutic decisions. There is some evidence that a subgroup of people with asthma may be at greater risk of severe and even life-threatening asthma exacerbations because they are unable to perceive symptoms of increasing airflow obstruction. Ongoing studies are attempting to define factors that contribute to poor symptom perception (e.g., gender, neurologic, psychosocial, physiologic, circadian rhythms), and what factors may be amenable to intervention.
Education and Outreach
NHLBI demonstration and education (D&E) research evaluates educational and behavioral approaches and environmental and organization strategies that may improve the prevention or management of asthma. D&E studies have demonstrated the effectiveness of teaching self-management strategies to patients of all ages. Current research focuses on identifying what elements of the education are most essential and what methods or combination of methods will promote the most efficient use of patient and clinician efforts: group vs. individual education, use of interactive multi-media, separate asthma education vs. education that is integrated into routine primary medical care; and adjunctive education in the community setting. Research is also underway to determine more effective ways to promote a partnership between the health care professional and the patient, especially in the managed care environment. A related issue is research on training health care professionals and disseminating the new advances in asthma management throughout the medical community.
A major thrust of recent D&E research has been on identifying appropriate strategies for extending the benefits of asthma management strategies to populations that have been traditionally harder to reach, for example, minorities and economically disadvantaged children. These are the populations that are at greatest risk for more serious disability due to asthma and asthma related death. Outreach educational programs using non-medical settings --the school, community neighborhood centers, an peer education-home visitors are testing the use of culturally sensitive behavior change strategies for children with asthma and their families. Others studies evaluate specific asthma management interventions, for example, programs to reduce smoking among parents of children with asthma and programs to promote continuous, comprehensive management of asthma rather than episodic emergency care.
Because children under 18 years of age have experienced a dramatic increase in asthma prevalence and morbidity in the last 10 years, and children with asthma miss twice as much school as the national average, the NHLBI has launched a new initiative "Interventions to Improve Asthma Management and Prevention at School" to develop and evaluate innovative asthma management and prevention programs that incorporate all components of a comprehensive school health program.
The NIH has established programs to translate the findings of NHLBI-supported research into effective tools to educate health providers, patients, and the public. The National Asthma Education and Prevention Program (NAEPP), coordinated by the National Heart, Lung, and Blood Institute (NHLBI), is responsible for translating research on asthma into practical health education materials and tools for use by health professional, patients, and the public. The NAEPP was initiated in March 1989 to address the growing problem of asthma. The goal of the NAEPP is to reduce asthma-related morbidity and mortality and to enhance the quality of life of asthma patients.
The NAEPP works with a wide range of organizations to conduct asthma educational interventions. A group of 38 professional, voluntary health, lay, and governmental organizations involved with asthma form the NAEPP Coordinating Committee. The coordinating committee advises the program and the members assist in activities to achieve the goal of the program. These coordinating committee organizations help communicate to their members the key messages the NAEPP is trying to convey.
The NAEPP designed a model web-based system to improve the diagnosis and management of asthma. The site provides virtually all the scientific literature on chronic asthma that has ever been published, as well as practical information for clinicians, patients, and public health professionals. See www.nhlbi.nih.gov.
Management Guidelines
The first major activity of the NAEPP was the development of Guidelines for the Diagnosis and Management of asthma in 1991. Subsequently, the NAEPP has been working with its partners to implement the guideline recommendations and to disseminate education materials and programs based on those guidelines, particularly to health care professionals and asthma patients. An update of those guidelines was produced in 1997--Expert Panel Report 2: Guidelines for the Diagnosis and Management of Asthma. Major attention is now devoted to promoting use of the Guidelines, including in managed care organizations.
Clinician Education
The NAEPP Coordinating Committee has organized a series of partnership activities to facilitate the implementation of the new guideline recommendations in various clinical settings. The NAEPP has enlisted its members to become actively involved in not only disseminating the new treatment guidelines, but also in encouraging clinicians to adopt the guideline recommendations and use them in caring for their patients. For example, the NAEPP is working with the American Academy of Allergy, Asthma, and Immunology (AAAAI) to develop a multi-faceted program to help all clinicians who care for children with asthma learn about and adopt the recommendations in the updated guidelines. A summary guide, based on the 1997 Expert Panel Report 2 Clinical Practice Guidelines, but tailored to the needs of primary care physicians, is being sent to pediatricians, family physicians, and nurses practitioners around the country. The practical guide will be the centerpiece for numerous continuing education programs.
The NAEPP and the American College of Chest Physicians organized a conference on asthma management for managed care organizations (MCO), especially those receiving Medicaid funding. As a result of this partnership effort, a number of organizations have agreed to participate in a year-long process to improve asthma outcomes using the guidelines and to document their results. Further examples of partnership activities to promote dissemination and adoption of Clinical Practice Guidelines includes projects with the National Medical Association to develop pocket guides for resident trainees, development of a nurses guide for managing asthma, and a guide delineating the role of pharmacists in asthma care.
Future plans in clinician education include replicating successful strategies in additional managed care organizations, as well as public health organizations and other communities. Activities at the local, State, and national levels will facilitate the adoption and use by health care providers of the most effective therapies available for the management of asthma and thereby help to improve the quality of life of asthma patients and their families.
Family/Patient Education
The NAEPP has produced an extensive array of patient and public education materials in both English and Spanish to help patients and their families increase their asthma self-management skills.
Public Education
The NHLBI continues to implement a strong, vibrant public education campaign to increase awareness of warning signs and symptoms of undiagnosed asthma. The campaign's key message focuses on encouraging those who experience signs and symptoms of asthma to see their doctor or health care provider for treatment. Future campaigns will emphasize the expectations patients with asthma should have for their asthma to be well-controlled. The public health education efforts are accentuated by far-reaching partnerships with the private sector, advertising media and radio networks, as well as local governments to disseminate critical and life-saving messages of the NAEPP mass media campaign.
School-Based Education
The NAEPP has developed a comprehensive set of materials to promote appropriate management of asthma in the school setting. A guide for school personnel delineates activities that each member of the school team perform in order to help students with asthma follow their asthma management plans and participate fully in school activities. A video and accompanying pamphlet provides guidance to teachers and physical education instructors to enable and encourage children with asthma to be physically active. Policy statements, prepared in partnership with the American Association of School Board Administrators and the American Association of School Health have been produced outlining measures to assure student access to medications and a school environment that is "asthma friendly" --i.e. supportive of the students with asthma.
Community-Based Partnership/Outreach
The NAEPP is collaborating with local community-based asthma coalitions to get the messages of the new guidelines disseminated and used at the local public health level. The NHLBI has supported the development of several community based coalitions on asthma, and is currently working with a variety of community groups around the country that deal directly with asthma problems at the local level and strive to coordinate community efforts to address the problems. In this work, the NAEPP provides technical assistance and a vital network for exchanging information and advice on organizing and maintaining community coalitions for asthma. The coalitions are composed of members from local public health departments, local hospital/medical centers, schools, community recreation centers, concerned parents groups, lung associations, and local media. The NAEPP and the coalitions will jointly develop public education objectives and implement a strategic plan to not only increase public awareness, but also to increase asthma management skills of patients and their families. Such efforts will provide synergy and will increase the penetration of important asthma education messages to communities at high risk of asthma morbidity and mortality.
Quality of Delivery Systems
The NAEPP, in partnership with the National Commission on Quality Assurance and the American College of Chest Physicians, provides conferences and training programs in the development of quality improvement disease management programs. Based on the work of the NAEPP Cost Effectiveness Task Force, the partnership efforts are developing performance measures for health care purchasers to use in evaluating asthma care services.
National Institute of Allergy and Infectious Diseases
NIAID provides the major support for scientists conducting research aimed at developing better ways to diagnose, treat and prevent the many infectious, immunologic and allergic diseases that afflict people worldwide. NIAID has a broad-based program aimed at understanding the pathogenesis of asthma and developing improved methods for preventing and treating asthma. NIAID research emphasizes the key role in the pathogenesis of the disease of certain allergens and viruses. NIAID supports a network of asthma research centers which also have a demonstration and outreach component for translation to the public. NIAID has provided long-term support for the Inner-City Asthma Study, which aims to reduce asthma morbidity among inner-city children.
Research
Natural history [Related topics: Risk factors/triggers and Genetics]
NIAID is funding a multi-center national program to study the natural history of allergy and asthma in early childhood, and the effects of exposure to cockroach, mold, house dust mite and other indoor allergens, and respiratory syncytial virus, on the course of disease. The studies are intended to develop approaches for the primary prevention of asthma (i.e., identifying individuals at high risk of developing asthma, and intervening in early childhood to prevent asthma from ever appearing). Several studies in this program are now co-funded with NIEHS.
In addition to the above program of the natural history in early childhood, the Inner-City Asthma Study (co-funded by NIEHS) supports studies on the natural history of asthma among 4-10 year old children.
Pathogenesis and Mechanisms: [Related topics: Risk factors/triggers]
A major thrust of NIAID supported research in asthma is devoted to the study of basic cellular and molecular mechanisms resulting in manifestations of asthma, including bronchoconstriction, mucus secretion, IgE antibody production, inflammation, airways hyperreactivity, and fibrosis and remodeling of lung tissue. The long-term goal of this research is to identify new targets for prevention and treatment of asthma.
Some research studies focus on the role of T lymphocytes in asthma, and investigate the differences in signaling pathways between two subsets of these cells. Other research focuses on cell surface receptors and intracellular signaling pathways in T and B lymphocytes that regulate IgE production. Other studies evaluate the functions and migration of eosinophils and other inflammatory cells that are prominent in asthmatic inflammation. Animal models, as well as combined genetic and molecular studies in animals, are contributing to studies of asthma pathogenesis.
Genetics
In addition to the genome-wide search for asthma-related genes described by NHLBI, NIAID supports a program to identify candidate genes associated with allergy and asthma, and to search for linkages of homologous candidate genes in mouse models of allergy and asthma. This program was the first to identify a linkage of high IgE levels (i.e., high allergic response) to a region of human chromosome 5, near genes for IL-4 and other cytokines.
Risk Factors/Triggers
Allergens, Infections, and Irritants
Many studies focus on allergens relevant to asthma, since IgE antibodies to certain indoor allergens (cockroach, house dust mite, dog and cat, other) increase the risk of asthma exacerbation, and preliminary data indicate that exposure to these allergens in early childhood may induce the onset of asthma. Both molecular and cellular approaches are used to identify regions of the allergen molecule that are critical to T and B cell recognition. Control of the effects of allergens is critical to asthma management. While one approach is to reduce environmental exposure, another approach is to develop vaccines or other reagents which prevent patients from making IgE antibodies to the allergens.
A substantial portion of this NIAID- supported research program is within a network of 12 extramural, and 1 intramural, Asthma, Allergic and Immunologic Diseases Cooperative Research Centers. Three of these Centers have their primary focus on environmental aspects of asthma and allergy, including the role of indoor allergens; two are co-funded by NIEHS. One of these is studying the mechanisms whereby polyaromatic hydrocarbons from diesel exhaust particulates induce IgE responses and act synergistically with inhaled allergen in stimulating immune responses. The second Center is studying the role of indoor allergens and respiratory syncytial virus (RSV) in inducing asthma in children, and determining methods of altering the responses to allergen by combinations of reduced exposure and reduced immune responses. A third Center studies the role of viruses, in conjunction with allergens, in both human and rodent models of asthma.
Risk Factors/Triggers
Infections
NHLBI and NIAID have funded a program on the role in respiratory infections in the development of childhood asthma. The NIAID-funded portion of this program investigates the epidemiology and genetic susceptibility to asthma in relation to early respiratory syncytial virus (RSV) infections, the molecular basis of immune responses induced by RSV and rhinoviruses, and the effects of viral infections on modifying the balance between allergen sensitization versus tolerance.
NIAID also supports a related program, on the mechanisms by which viruses induce inflammation and exacerbate asthma. RSV infection in young children, and rhinovirus infection in older children and adults, induce exacerbations of asthma. The interactions of viruses with epithelial cells, endothelial cells, and inflammatory cells, and the induction of cytokines and adhesion molecules, as well as synergistic actions of viruses and allergens, are of particular interest.
Asthma Management [Related Topics: Community-based partnerships and outreach]
Environmental Control, Allergens, Irritants, Strategies for secondary prevention
NIAID supports a network of 7 Cooperative Inner City Asthma Centers and a Data Coordinating Center. This program, now co-funded by NIEHS, represents an effort begun in 1991, to reduce asthma morbidity in populations which have disproportionately high asthma morbidity: namely, inner-city, predominantly African-American and Hispanic, children. The present study is testing effects on asthma morbidity of two interventions. The first is a comprehensive environmental intervention, to reduce levels of indoor allergens such as cockroach, house dust mite and mold. The second is a physician education intervention, to improve medical care via providing regular feedback on the clinical and laboratory status of children under the care of community primary care physicians. In collaboration with the U.S. Environmental Protection Agency, the Inner City Asthma Study is now evaluating the effects of indoor and outdoor pollutants on asthma morbidity.
The objective of this cooperative study is to develop, implement, and evaluate a culturally-appropriate, comprehensive, and cost-effective intervention program aimed at reducing asthma morbidity by modifying those potentially reversible factors, such as allergens and environmental tobacco smoke shown to contribute to asthma morbidity. The core protocol includes all of the following elements: medical treatment for asthma delivered in a health care facility, self-management by asthmatics and their families, and indoor environmental interventions including studies to measure, monitor, and improve indoor allergens and environmental tobacco smoke exposure.
Asthma Management/ Education and Outreach
NIAID supports a Demonstration and Education Research Program targeted toward medically under-served, predominantly inner city Hispanic and African-American populations. Many of the components of this program are funded as part of the Asthma, Allergic and Immunologic Diseases Cooperative Research Centers. This Demonstration and Education Research Program includes a multi-center study to test the effectiveness of dust mite allergen avoidance on asthma severity. The program also funds school-based studies to identify children with asthma and to use combinations of environmental control (to avoid allergens) and school-based asthma counselors to reduce asthma severity. Related studies include the identification of, and thus early intervention in very young children with asthma in a Head Start program. For example, one study utilizes nurse home visitors for self-management training and environmental intervention in high risk infants with wheezing; another study has developed a unique computer-based medical and self-management training program for families of children with asthma.
The aforementioned network of Research Centers (see Natural history and Risk factors/ Triggers) has public health efforts as well as research. Each center includes a Demonstration and Education outreach research project to test interventions for asthma in underserved populations; all but one asthma project focus on children.
National Institute of Child Health and Human Development -- Center for Research for Mothers and Children
NICHD seeks to assure that every individual is born healthy, is born wanted, and has the opportunity to fulfill his or her potential for a healthy and productive life unhampered by disease or disability. In pursuit of this mission, the NICHD conducts and supports laboratory, clinical, and epidemiological research on the reproductive, neurobiologic, developmental, and behavioral processes that determine and maintain the health of children, adults, families, and populations. The Institute conducts research on asthma in pregnant women, in infants and in children.
Research
Natural History of the Disease
NICHD's asthma research program is divided into two project areas: asthma in pregnancy and asthma in infants (less than 2 years of age). Because of the diverse nature of the projects, they are described separately below.
The first project, co-sponsored by NHLBI, is a prospective cohort study of the effects of asthma during pregnancy and treatment regimens on perinatal outcome. The objective of this study is to compare the frequency of very premature births among moderate and severe pregnant asthmatics with that of normal controls, to track asthma severity with regard to maternal morbidity and neonatal outcome, and to investigate the effects of degree of asthma control and medications with other demographic and social factors on differences on perinatal outcome. Outcome measures include small for gestational age, low birth weight, perinatal morbidity and mortality, and preterm delivery rate less than 37 weeks.
Asthma Management -- Pharmacotherapy
The second project, co-sponsored by NHLBI involves a randomized clinical trial of theophylline versus inhaled beclomethasone. The objective of this study is to determine if prolonged anti-inflammatory therapy with inhaled corticosteroids will result in better control of moderate asthma in pregnancy as compared to control with a non-anti-inflammatory drug (theophylline). Another research effort involves the NICHD Pediatric Pharmacology Research Network's evaluation of medications which are frequently used in pharmacotherapy of asthma in infants and children. This network offers an opportunity to evaluate both old therapies, as well as new chemical entities, which are being introduced by the pharmaceutical industry without any evaluation in infants and children. The network is already undertaking a study of albuterol (medication used for immediate relief of asthma symptoms) in infants and children under two years of age.
National Institute of Environmental Health Sciences
Human health and human disease result from three interactive elements: environmental factors, individual susceptibility and age. The mission of NIEHS is to reduce the burden of human illness and dysfunction from environmental causes by understanding each of these elements and how they interrelate. Highlighted activities which are co-sponsored by NIEHS include the Environmental Genome Project, the National Allergen Survey, and the Inner-City Asthma Study.
Research
Pathogenesis and Mechanisms (also Natural History of the Disease)
Poor air quality and aeroallergens can cause airway inflammation and are known risk factors for asthma development, morbidity and mortality. Developing insights into the fundamental cellular and molecular mechanisms of the respiratory system and understanding how environmental agents perturb this complex system is critical in designing effective and novel strategies for disease prevention and intervention.
NIEHS's pulmonary pathobiology research encompasses four areas: airway cell biology, inflammation, mechanisms of toxicity of pollutants, and translational research/clinical studies. This research is intended to lead to the prevention of, or intervention in, the environmental components of airway diseases, especially asthma. Research at all levels is targeted towards prevention and intervention and other translational activities. Examples include large-scale population-based studies which define risks and consequences; mechanism-based studies which use sophisticated molecular biological approaches to examine disease pathogenesis; and genetic studies which seek to identify populations that are particularly susceptible to certain environmental factors, is targeted towards prevention and intervention and other translational activities.
Genetics [Related topic: Risk factors/triggers]
NIEHS is expanding its research program on genetic susceptibility to environmentally- associated diseases through the new Environmental Genome Project initiative. This project, which will make use of technology developed by the NIH Human Genome Project, is aimed at: identifying allelic variants (polymorphisms) of environmental disease susceptibility genes in the U.S. population, developing a central database of polymorphisms for these genes, and fostering population-based studies of gene-environment interaction in disease etiology.
The NIEHS Environmental Genome Project is a multi-disciplinary, collaborative effort, involving several other NIH institutes as well as the Department of Energy (DOE) and other federal agencies. Environmental response genes that will be included in the Environmental Genome Project include, among many others, genes that mediate the immune and inflammatory responses such as those involved in asthma.
An example of this type of research is an epidemiologic study being conducted at NIEHS. DNA has been collected from children in 12 communities in Southern California to evaluate the relationship between asthma and exposure to ozone, particulate matter, acid aerosols, and nitrogen oxides. An examination of genes that may be involved in susceptibility to the respiratory effects of ozone will be conducted. Similar research by the same investigators is proposed for populations in China and Mexico.
Given the disturbingly high morbidity and mortality data from asthma seen in African-Americans and certain Hispanic populations, a genetic predisposition for asthma in these groups is a viable theory. Asthma will certainly be a disease of major interest to the Environmental Genome Project.
Risk Factors [Related topic: Natural History of the Disease]
Triggers
Although existing, smaller allergen studies have provided important data on the relationship between allergens and disease in selected groups, they have not permitted estimates of allergen exposure in the population, addressed the magnitude of allergen problems, or evaluated demographic characteristics with regard to allergen exposure. In response to these data gaps, NIEHS has joined with the Department of Housing and Urban Development (HUD) to conduct the first National Allergen Survey. The major objective of this program is to conduct a descriptive study of allergen types and levels in floor and bedding dust in the nation's housing to provide estimates of allergen exposure in the U.S. population. The secondary objective is to collect relevant data on housing conditions, demographic factors, and climate, in order to facilitate evaluation of regional, ethnic, socioeconomic, and housing characteristics and their relationship to allergen types and levels.
NIAID is funding grants, one of which is co-funded by NIEHS, on the natural history of allergy and asthma in early childhood, and the effect on the course of disease of exposure to allergens. All of these studies are intended to develop approaches for the primary prevention of asthma. More detail is provided in the "Natural History" section under NIAID's program descriptions.
Prevention
NIEHS and EPA have awarded grants to Centers that will develop multidisciplinary basic and applied research in combination with community-based prevention research projects in order to: support studies on the causes and mechanisms of children's disorders having an environmental etiology, identify relevant environmental exposures, intervene to reduce hazardous exposures and their adverse health effects, and eventually decrease the prevalence, morbidity, and mortality of environmentally related childhood diseases. One purpose of these Centers for Children's Environmental Health and Disease Prevention Research is to provide for multidisciplinary interactions among basic, clinical, and behavioral scientists interested in establishing outstanding, state-of-the-art research programs addressing environmental contributions to children's health and disease, including but not limited to asthma.
Primary Prevention
NIEHS has developed the Environmental Intervention in the Primary Prevention of Asthma in Children Study (EIPPAC) to investigate the effectiveness of persistent allergen avoidance in preventing allergen sensitization, reducing asthma prevalence, and improving lung function in high risk, lower socioeconomic status children. This interventional study will provide important information concerning the role of environmental intervention in the primary prevention of asthma in children and will provide insight into basic immunologic mechanisms operative during allergen sensitization and the expression of allergic diseases.
Secondary Prevention
NIAID and the NIEHS cooperatively fund the Inner-City Asthma Study (ICAS). Details of this study can be found under "Asthma Management/Environmental Control" in NIAID's program descriptions.
The NIEHS and the Office of Behavioral and Social Sciences Research (OBSSR) have invited research grant applications addressing development of community-based strategies aimed at prevention and intervention activities in economically disadvantaged and/or underserved populations adversely impacted by an environmental contaminant. The purpose of awards in this program of Community-Based Prevention/Intervention Research in Environmental Health Sciences is to: 1) stimulate further advances in the design and implementation of prevention and intervention methods that are appropriately applied to environmental health, 2) develop community-based public health research approaches to diseases and health conditions--including asthma--having an environmentally related etiology and determine the impact of these methods, and 3) bridge the gaps between basic and clinical research in environmental health science as well as gaps between institutional researchers and community members.
The long-range goal of this program is to improve the knowledge and behavior of disadvantaged or underserved community members regarding prevention, detection, and treatment of environmentally related diseases and health conditions, and thereby reduce incidence and mortality rates of such diseases and conditions.
Other
The purpose of the Environmental Justice program is to strengthen NIEHS support of research aimed at achieving environmental justice for socioeconomically disadvantaged and medically underserved populations in the United States. The main objective of this initiative is to establish methods for linking members of a community, who are directly affected by adverse environmental conditions, with researchers and health care providers. This will ensure that the community: is aware of basic environmental health concepts, issues, and resources; has a role in identifying and defining problems and risks related to environmental exposures; is included in the dialogue shaping potential future research approaches to the problem; and actively participates with researchers and health care providers in developing responses and setting priorities for intervention strategies.
National Institute of Nursing Research
The NINR supports clinical and basic research to establish a scientific basis for the care of individuals across the life span--from management of patients during illness and recovery to the reduction of risks for disease and disability and the promotion of healthy lifestyles. According to its broad mandate, the Institute seeks to understand and ease the symptoms of acute and chronic illness such as asthma through interventions at various levels, and to improve the clinical settings in which care is provided.
Research
Prevention
NINR sponsors interventions emphasizing prevention at three levels. These include interventions targeting: the general population, particular high risk groups (such as children with family members who smoke), and those who already have asthma.
Asthma Management -- Education and Outreach
Inaccurate perceptions of symptom severity are believed to be a major reason for delays in asthma treatment, and contribute to morbidity and mortality. Nursing investigators are testing symptom-monitoring interventions in a clinical trial involving children with asthma and their parents. Results of the clinical trial will provide information on the relative benefits of the monitoring interventions and their effects on physiological, functional, and psychosocial factors. Relative use of the healthcare system will also be ascertained. Descriptive data will be developed concerning both parents' and children's views about monitoring and their adherence to the monitoring regimens.
Young, inner city children are disproportionately affected by asthma. Although asthma education programs either in the home or in clinics have been shown to increase families' effective management of asthma symptoms, the problem has repeatedly been one of ensuring attendance of low-income parents. Researchers are studying self-care management of asthma in African-American school-aged children. The research is aimed at verifying that better self-management practices coupled with nurse home visits will improve quality of life, reduce symptoms associated with asthma attacks, and decrease the number of medical visits.
NINR is supporting research to examine the effectiveness of computer-based asthma education for children 7 to 12 years old. Adherence to the education model, use of health care resources, health and quality of life will be examined. Using adult subjects, researchers are also testing the effectiveness of a 30-minute asthma education intervention to be provided in the context of the usual medical care appointment. .
National Library of Medicine
The National Library of Medicine (NLM), on the campus of the National Institutes of Health in Bethesda, Maryland, is the world's largest medical library. The Library collects materials in all areas of biomedicine and health care, as well as works on biomedical aspects of technology, the humanities, and the physical life, and social sciences. The collections stand at 5.3 million items-books, journals, technical reports, manuscripts, microfilms, photographs, and images. Housed within the Library is one of the world's finest medical history collections of old and rare medical texts and manuscripts. The Library's collections may be consulted in the reading room or requested on interlibrary loan. NLM is a national resource for all U.S. health science libraries through a National Network of Libraries of Medicine.
The National Library of Medicine, in collaboration with the National Heart, Lung, and Blood Institute (NHLBI), the National Institute of Allergy and Infectious Diseases (NIAID), and the National Institute of Environmental Health Services (NIEHS) developed an exhibition that highlights the history of asthma, the experiences of people with asthma, and contemporary research and management efforts to control the disease. The exhibit, entitled "Breath of Life," opened with a gala reception in the rotunda of the National Library of Medicine on the grounds of the National Institutes of Health in Bethesda, MD on March 22, 1999 and runs through May, 2000. Following the exhibit's debut in the nation's capital, it will travel to cities throughout the United States and Europe carrying its message to the public in a variety of forums, via the Internet, in museums, and in places where the public gather. In addition, the Institutes are developing a broad range of supplemental programs to expand "Breath of Life's" outreach to the public about how to prevent, identify, and treat asthma.
OPHS serves as the focal point for leadership and coordination across the Department in public health and science; provides direction to program offices within OPHS; and provides advice and counsel on public health and science issues to the Secretary.
Office of Minority Health
The Office of Minority Health (OMH) was established by DHHS in 1985. It advises the Secretary and the Office of Public Health and Science on public health program activities affecting American Indian and Alaska Native, African American, Asian American and Pacific Islander, and Hispanic populations. Its goal is to promote improved health among these racial and ethnic minority populations.
Disparities in the impacts of asthma are striking among different ethnic populations. For example, rates of death and hospitalizations due to asthma are significantly higher in African Americans than in whites. The purpose of the Office of Minority Health Asthma Attack Avoidance Education Program is to establish a community-based, parent-child focused program designed to increase identification of potential asthma attack-triggering factors among minority urban children, and to ensure appropriate referral for medical care.
Office of Women's Health
The mission of the Office of Women's Health (OWH) is to improve the health of women across the life-span by directing, developing, stimulating, and coordinating women's health research, health care services, and public and health professional education and training across the agencies and offices of the DHHS; and with other government agencies, public and private organizations, and consumer and health care professional groups. The Office also advises the Secretary and Assistant Secretary for Health of DHHS on the scientific, medical, ethical and policy issues related to the advancement of women's health in the United States and internationally.
Research
While asthma prevalence has been a very immediate issue for all populations, there are certain populations which are particularly affected by the disease. Among these special concerns is women. Many reports have agreed that while males are treated for asthma more than twice as much as females up to the age of 10, after this age, the trend reverses. In addition, several issues concerning women--such as pregnancy, differences in hormones, and intake of aspirin and other antinflammatory drugs--serve as complicating factors for their asthma. Another concern is adult onset of asthma, especially in women at the start of menopause.
OWH coordinates, collaborates, develops partnerships, convenes appropriate people to address issues related to women's health. OWH often focuses on diseases for which severity, incidence, diagnosis, and treatment may be different because of gender and tries to ensure that those differences are not glossed over in the approaches being used by health care practitioners, researchers, patients, etc. OWH also helps sponsor academic centers for excellence in women's health. There are many women-centered issues which are of particular concern to people with asthma. While widespread and increasing across age groups and gender lines, the disease is becoming a growing concern in the specific field of women's health.
Region I
In Region I (Boston), DHHS and the public health commissioners from the six New England states are collaborating with the region's major managed care organizations to address asthma. Also, the Environmental Protection Agency (EPA), DHHS and the Department of Housing and Urban Development (HUD) are convening a summit meeting of federal and state environment, public health and housing officials to develop a joint strategy to help reduce the burden of asthma in New England.
Region II
Region II has developed a multi-faceted asthma initiative with components of technical assistance/consultation, grant support, and inter-departmental collaboration. The Regional Office has worked with New York City Department of Health in their implementation of a broad based community initiative with clinical, school, and home based modules. It has also awarded grants to the New York and New Jersey State Health Departments to develop community based partnerships. DHHS, the Environmental Protection Agency, and the Department of Housing and Urban Development have begun to shape coordinated asthma initiatives under the Region II Federal Regional Council. The agencies are compiling a data base and identifying geographic areas within the region exhibiting high incidence rates of asthma.
The Clinical Directors Network of Region II in collaboration with EPA and HRSA is conducting an evaluation of home environmental and medical interventions in four HRSA-funded community health centers serving minority and low-income areas. The project will measure outcomes from both interventions in 200 children.
Region III
In Region III (Philadelphia), DHHS and EPA officials are working with state and local agencies and organizations to coordinate activities and develop a strategic plan for addressing asthma in the mid-Atlantic states.
Region V
For the first time, Illinois has the highest rate of African Americans who die of asthma in the U.S., according to CDC data released in April, 1998. To address this problem, DHHS is working with EPA, the Chicago Asthma Consortium and several public, private and community organizations to develop a community-based project to reduce the morbidity and mortality due to asthma in the Chicago area. This project involves the community as a co-researcher and the professional as a co-learner. The definition of community-based for the purposes of this project are that community members are involved in laying the ground work, the design, review, implementation and interpretation of the results. This model for participatory/action research draws on the strengths and knowledge of communities to aid in disease management and the design of systems to improve health outcomes.
Appendix F: Asthma Programs Outside of DHHS
U.S. Olympic gold-medalist Jackie Joyner-Kersee encourages fellow asthma sufferers, "I control my asthma every day. So can you." Olympic gold medalist swimmers Amy Van Dyken and Tom Dolan, as well as NBA All-Star Dennis Rodman also devote time and resources to carrying the message that asthma should not prevent people from pursuing their dreams--even in top-level athletic competition.
Organizations involved in community outreach and education include corporations, professional societies, government agencies, and state and local coalitions. These same groups also conduct research. They often work in collaboration with each other and with federal agencies.
This appendix gives examples of activities undertaken by organizations in six broad categories. Its purpose is to highlight the depth and breadth of work on asthma beyond DHHS in order to stimulate thinking about how DHHS funded activities can best complement and support activities by other organizations. It is by no means exhaustive. More information on asthma activities in the U.S. and overseas can be found at the NHLBI web site: www.nhlbi.nih.gov.
Professional Societies
Several professional societies sponsor asthma programs that support research, distribution of information to physicians and other health care professionals, and education of asthma patients. Research support includes both seed money and longer-term funding for clinical and epidemiological studies examining, for example, treatment options and implementation of the Asthma Management Guidelines in different health care settings.
Professional societies also distribute information on asthma to physicians and the public. Recent examples include a forum for physicians and scientists from around the world who work in pulmonary and critical care medicine, and a speaker's bureau to assist in providing speakers and funding on topics related to asthma. Several organizations sponsor programs for continuing education to update health care providers on the diagnosis and treatment of asthma including an on-line resource for physicians and other health professionals. Several groups provide information resources for the public as well, via hotlines, pamphlets, booklets, and newsletters on asthma.
Non-Governmental Organizations
Non-governmental organizations (NGOs) also play a vital role in educating the public about asthma. Some are well-established, well-funded groups; others are newer and work with modest budgets. At the national level, and often through local chapters, NGOs have raised awareness about asthma and supported effective education and outreach efforts. They have developed innovative, interactive teaching curricula that bring together children with asthma, their families, and community volunteers in school settings. To reach younger children with asthma, NGOs have prepared educational kits and television programs geared toward pre-schoolers and their families. These materials are disseminated during presentations at health fairs, meetings of support groups, schools, to industry, government, and community organizations. They are used at asthma camps--where children learn about managing their asthma while also building friendships through shared activities--and in direct delivery of care: NGO supported clinics on wheels regularly deliver state-of-the-art care to schools in the inner city. NGOs are also involved in research, and make available results of population-based studies and surveys to companies or others investing in the care of people with asthma.
Private Industry
Insurance and managed care companies are active in education and outreach through classes, workshops, and programs on asthma-related topics such as maintaining a healthy lifestyle, smoking cessation, and chronic disease management. One program designed for members and their physicians to better manage asthma integrates comprehensive education in asthma self-management and instruction in the use of asthma management equipment designed for home use.
The pharmaceutical industry is active in asthma outreach as well. Several companies provide educational materials directly to asthma patients. Others fund educational services carried out by other groups. Easy-to-read pamphlets developed by the industry provide helpful tips and updates on asthma control. Research by the pharmaceutical industry includes drug development as well as investigations--usually in conjunction with other groups--of the effectiveness of various methods of outreach or treatment.
Other Federal Agencies
A number of Federal agencies other than DHHS support research, public education and outreach programs related to asthma. The Environmental Protection Agency (EPA) conducts and supports research on the respiratory health effects of air pollutants and sets regulatory standards that control their emissions. In partnership with the National Institute of Environmental Health Sciences, EPA supports an innovative research centers program on children's environmental health and disease prevention, including asthma. EPA supports research and dissemination of information relating to the health effects associated with exposure to environmental tobacco smoke. It also supports education and outreach programs in schools and communities related to environmental aspects of asthma through such programs as Childhood Champions and Tools for Schools. In fiscal 2000, the Department of Education, together with EPA, plans to expand school-based programs that teach parents and children how to identify and avoid allergens that trigger asthma attacks. NIEHS and the Department of Housing and Urban Development are developing a National Allergen Survey to provide estimates of allergen exposure in the U.S. population. The study will also facilitate evaluation of regional, ethnic, socioeconomic, and housing characteristics and their relationship to allergen types and levels.
State and Local Governments and Coalitions
State and local governments, often in cooperation with coalitions of various kinds of organizations, support a variety of programs to reverse increasing rates of asthma and reduce the burden of the disease. State health departments and Medicaid agencies educate the public about effective asthma care and support health services delivery. For example, Virginia substantially reduced hospitalizations and emergency room visits by providing Medicaid physicians with asthma patients six hours of training in appropriate asthma treatment. State and local environmental agencies set and enforce air pollution standards established to reduce risk of exacerbation of asthma and other health effects. In addition, many state environmental agencies conduct education and outreach on reducing exposure to environmental factors that can aggravate asthma.
State and local coalitions working on asthma include groups of concerned patients or parents, representatives from community recreation centers, schools, hospitals and clinics, and members of the medical community, among others. They are a relatively new phenomenon--sixty three percent of the 43 coalitions identified by the NIH-coordinated National Asthma Education and Prevention Program (NAEPP) are less than two years old--but they are proving to be powerful and effective mechanisms for addressing asthma. Examples of activities include encouraging local primary care physicians and other health care professionals to adopt clinical practice guidelines, developing culturally competent and appropriate outreach programs to inner-city and other high risk communities, and establishing partnerships with local schools.
International Initiatives
In 1992, the National Heart, Lung and Blood Institute and the World Health Organization initiated a collaborative project--the Global Health Initiative for Asthma (GINA)--to address asthma as a global health problem. It is now estimated that over 150 million people worldwide have been diagnosed with asthma, and there is evidence that prevalence is increasing in most countries, especially in children. GINA's objectives are to decrease asthma morbidity and mortality by developing and implementing optimal strategies for the management and prevention of asthma, to increase public awareness, and to stimulate research into the causes of the increasing prevalence of the disease.
Member Organizations of the National Asthma Education and Prevention Program Coordinating Committee
Many of the organizations outside DHHS active in asthma (as well as several DHHS agencies) are represented on NAEPP's Coordinating Committee, which provides input to strategies and materials developed by NAEPP.
- Agency for Healthcare Research and Quality
- Allergy and Asthma Network/Mothers of Asthmatics, Inc.
- American Academy of Allergy, Asthma, and Immunology
- American Academy of Family Physicians
- American Academy of Pediatrics
- American Academy of Physician Assistants
- American Association of Respiratory Care
- American Association of Occupational Health Nurses
- American College of Allergy, Asthma, and Immunology
- American College of Chest Physicians
- American College of Emergency Physicians
- American Lung Association
- American Medical Association
- American Nurses Association, Inc.
- American Pharmaceutical Association
- American Public Health Association
- American School Health Association
- American Society of Health-System Pharmacists
- American Thoracic Society
- Association of State and Territorial Directors of Health
- Asthma and Allergy Foundation of America
- National Association of School Nurses
- National Black Nurses Association, Inc.
- National Center for Chronic Disease and Health Promotion
- National Center for Environmental Health
- National Center for Health Statistics
- National Institute for Occupational Safety and Health
- National Heart Lung and Blood Institute Ad Hoc Committee on Minority Populations
- National Heart Lung and Blood Institute
- National Institute of Allergy and Infectious Disease
- National Institute of Environmental Health Sciences
- National Medical Association
- Society for Academic Emergency Medicine
- Society for Public Health Education
- U.S. Department of Education
- U.S. Environmental Protection Agency
- U.S. Food and Drug Administration
- U.S. Public Health Service
Appendix G: Healthy People 2010 Objectives
Goal
Promote respiratory health through better prevention, detection, treatment, and education.
Overview
Asthma, chronic obstructive pulmonary disease (COPD), and obstructive sleepapnea (OSA) are a significant public health burden to the United States.1 Specific methods of detection, intervention, and treatment exist that may reduce this burden. Several behaviors and diseases that affect the respiratory system, such as tuberculosis, acquired immunodeficiency syndrome (AIDS), pneumonia, occupational lung disease, lung cancer, and smoking, are covered in other focus area chapters. Certain other important respiratory diseases, such as respiratory distress syndromes, sarcoidosis, and chronic sinusitis, which are difficult to define, detect, prevent, or treat, are not discussed in this chapter. Their omission, however, is not a reflection on the magnitude of the health problems associatedwith them.
Asthma and COPD are among the 10 leading chronic conditions causing restricted activity. After chronic sinusitis, asthma is the most common cause of chronic illness in children.2 Methods are available to treat these respiratory diseases and promote respiratory health.
Asthma
Issues and Trends
Asthma is a serious and growing health problem. An estimated 14.9 million persons in the United States have asthma.3 The number of people with asthma increased by 102 percent between 1979-80 and 1993-94.4
Asthma is responsible for about 500,000 hospitalizations,3 5,000 deaths,3 and 134 million days5 of restricted activity a year. Yet most of the problems caused by asthma could be averted if persons with asthma and their health care providers managed the disease according to established guidelines. Effective management of asthma comprises four major components: controlling exposure to factors that trigger asthma episodes, adequately managing asthma with medicine, monitoring the disease by using objective measures of lung function, and educating asthma patients to become partners in their own care.2, 6 Such prevention efforts are essential to interrupt the progression from disease to functional limitation and disability and to improve the quality of life for persons with asthma.
In 1996, asthma was the 10th most common principal diagnosis in emergency department (ED) visits. 3, 7 Among diseases commonly seen in outpatient departments, asthma was the ninth most frequent diagnosis in 1996.8 In 1995, some 9 million physician office visits were made for asthma.8 From 1990 to 1992, persons with asthma spent an estimated 64 million days in bed because of asthma, ranking asthma as the fourth highest chronic condition.5 The proportion of people with asthma who are limited in activity increased slightly from 19.4 percent in 1986-88 to 19.6 percent in 1994-96.9
Direct medical expenditures for asthma amounted to $3.64 billion in 1990, and indirect economic losses accounted for an additional $2.6 billion.10 Of direct medical care costs, approximately 57 percent was spent on hospitalizations ($1.6 billion), outpatient hospital visits ($190 million), and emergency department visits ($295 million). Physician-related services accounted for 14 percent of the total expenditures, including $347 million for outpatient services. Prescription medications represented 30 percent of direct medical costs. Such facts highlight the significant cost of hospital care for asthma, compared to the more frequently used and less costly outpatient and pharmaceutical services.
Indirect costs—nonmedical economic losses such as days missed from work or school, caregiver costs, travel and waiting time, early retirement due to disability, and premature death—account for slightly less than 50 percent of the total costs of asthma. Data suggest that the uneven distribution of costs of asthma relates to nonscheduled acute or emergency care, indicating poor asthma management and suboptimal outcomes.11, 12
Environmental and occupational factors contribute to illness and disability from asthma. Decreases in lung function and a worsening of asthma have been associated with exposure to allergens, indoor pollutants (for example, tobacco smoke), and ambient air pollutants (for example, ozone, sulfur dioxide, nitrogen dioxide, acid aerosols, and particulate matter).13, 14 Approximately 25 percent of children in the United States live in areas that exceed the Federal Government’s standard for ozone.15 Occupational factors cause or trigger asthma episodes in 5 to 30 percent of adults with the disease.16 Environmental factors are associated with upper respiratory infections, which contribute to illness and disability in children and adults.17 (See Focus Area 8. Environmental Health.)
Disparities
Within the U.S. population, the health, economic, and social burdens of asthma vary. Disproportionate rates of death, hospitalization, emergency room use, and disability from asthma occur in specific age, gender, racial, and ethnic groups.
While the number of adults with asthma is greater than the number of children with asthma, the asthma rate is rising more rapidly in preschool-aged children than in any other group.1 In 1995, the rate of self-reported asthma among children and adolescents under age 18 years was 7.5 percent, compared to 5.7 percent among the general population. The rates were higher in boys under age 18 years than in girls in the same age group. The rates of self-reported asthma were higher for women (6.7 percent) than men (5.2 percent) and higher for African Americans (6.7 percent) than whites (5.6 percent).1 Among adults, women of all races have higher rates of illness and death from asthma than men.18
Death from asthma is 2 to 6 times more likely to occur among African Americans and Hispanics than among whites.1 Although the number of deaths annually from asthma is low compared to other chronic diseases, the death rate for children aged 5 to 14 years and young adults aged 15 to 24 years doubled from 1979-80 to 1993-95 (from 1.5 to 3.7 deaths per million children aged 5 to 14 years and 2.8 to 6.3 deaths per million persons aged 15 to 34 years, respectively).4 In 1993-95, death rates are slightly higher overall in women than in men.4
Rates of hospitalization for asthma demonstrate similar variations. Rates for African Americans are almost triple those for whites. Rates are higher among women than among men.1 Asthma hospitalization rates have increased dramatically among children under age 5 years. From 1980 to 1993, the rate increased from 36 to 65 children hospitalized per 10,000 children under age 1 year. Some of this increase may be related to changes in diagnostic practices and changes in coding
and reimbursement, but a large portion represents a true increase in illness and
disability.
In the inner city, patients frequently use EDs for asthma care. In 1993 and 1994, African Americans were 4 times more likely than whites to visit an ED because of asthma.1 Asthma patients in general and high-risk inner-city patients—in particular, those with a history of severe asthma who were hospitalized or visited the ED for asthma within the previous 2 years—need to be able to recognize the signs and symptoms of uncontrolled asthma and know how to respond appropriately.
The economic burden of asthma disproportionately affects patients with severe disease. Socioeconomic status, particularly poverty, appears to be an important contributing factor to asthma illness, disability, and death. In the United States, the rate of asthma cases for nonwhites is only slightly higher than for whites, yet the death, hospitalization, and ED visit rates for nonwhites are more than twice those for whites.1 Although reasons for these differences are unclear, they likely result from multiple factors: high levels of exposure to environmental tobacco smoke, pollutants, and environmental allergens (for example, house dust mites, cockroach particles, cat and dog dander, and possibly rodent dander and mold); a lack of access to quality medical care; and a lack of financial resources and social support to manage the disease effectively on a long-term basis.19 Research into the role of socioeconomic factors is needed to identify additional prevention opportunities.
Opportunities
Scientific research has led to greater asthma control than was available in the early 1980s.6 Effective management of asthma includes four components: avoiding or controlling the factors that may make asthma worse (for example, environmental and occupational allergens and irritants), taking appropriate medications tailored to the severity of the disease, objective monitoring of the disease by the patient and the health care professional, and actively involving the patient in managing the disease.6 Effective asthma management reduces the need for hospitalizations and urgent care visits (in either an ED or physician’s office) and enables patients to enjoy normal activities.14, 20
Advances in human genetics related to asthma are expected to provide better information about the contribution of genetic variation to the development of disease when people are exposed to certain environmental factors. The use of this genetic information will improve targeted disease prevention and health management strategies for respiratory diseases.
Patient education is one of four components of effective asthma management. 6 Patients who are taught asthma self-management skills are able to manage and control their disease better than patients who do not receive education. 6 Patients need to learn to work with health care providers to optimize asthma care. Thus, both patients and health care providers need to be trained and educated on effective asthma management. Health outcomes for asthma—illness, disability, quality of life, and death—are related directly to the actions of health care professionals and patients. The National Asthma Education and Prevention Program (NAEPP) provides guidelines for diagnosis and management which should be incorporated into the curricula of health professional schools.6, 21 Currently, there are no national data systems for tracking the training of health care providers in asthma management. Therefore, the issue is not covered in this focus area’s objectives. It represents an important research and data collection agenda for the coming decade. In addition, research to identify the primary causes of development of asthma is a high priority. Such research can provide a scientific basis for efforts to prevent the development of asthma.
To control asthma effectively, asthma patients, particularly those on daily medication, need an Aasthma action plan developed under their physician’s guidance. The plan spells out when and how to take medicines correctly, as well as what to do when asthma worsens. The treatment of persistent asthma emphasizes daily long-term therapy aimed at the underlying inflammation and preventing symptoms, rather than relying solely on treating symptoms with short-acting inhaled medication, such as a short-acting beta agonist medication. Use of more than one canister of the medication per month is an indication of uncontrolled asthma and the need to start or increase long-term preventive therapy. Patients also need to work with health care providers during followup visits, particularly after being hospitalized, to make sure they understand and are able to follow the long-term management plan.
Working with local community groups to mobilize community resources for a comprehensive, culturally and linguistically competent approach to controlling asthma among high-risk populations is a priority. From a community-based perspective, States need to track occupational and environmental factors that cause or trigger asthma episodes. Such surveillance efforts should include collecting State-based data on the proportion of the population with asthma and monitoring occupational and environmental exposures and their impact on illness and disability related to asthma. Efforts directed to improving the environmental management of asthma also include reducing exposure to allergens and irritants, such as environmental tobacco smoke, and outdoor air pollution from ozone, sulfur dioxide, and particulate diesel matter. (See Focus Area 8. Environmental Health.)
Professional organizations, lay volunteer groups, Federal agencies, and the private sector have worked together and with NAEPP to implement a spectrum of asthma programs at national and local community levels. For example, numerous publications, media campaigns, and conferences target different audiences. Intensified efforts are planned to reach primary care providers, patients, and school personnel.18, 21 A high-level work group convened by the U.S. Department of Health and Human Services in 1997 assessed the most urgent needs for tackling the growing problem of asthma. The work group’s department-wide strategic plan, Action Against Asthma, identified opportunities and presented a coordinated approach for improving asthma prevention and management.18
Chronic Obstructive Pulmonary Disease
Issues and Trends
COPD includes chronic bronchitis and emphysema—both of which are characterized by irreversible airflow obstruction and often exist together. Similar to asthma, COPD may be accompanied by an airway hyper responsiveness. Most patients with COPD have a history of cigarette smoking. COPD worsens over time with continued exposure to a causative agent—usually tobacco smoke or sometimes a substance in the workplace or environment.
COPD occurs most often in older people. As much as 10 percent of the population 65 years of age and over is estimated to have COPD.2 COPD has a major impact on health care, illness, disability, and death in the older population, and the magnitude of the problem is growing. Since 1980, the prevalence and age-adjusted death rate for COPD increased more than 30 percent.2, 22, 23 Most of the increase occurred in people over age 65 years. Taking into account the expected aging of the U.S. population over the next 10 to 30 years as well as the improved management of other smoking-related diseases, any decline in the proportion of persons with COPD is unlikely without substantial changes in risk factors, mainly reductions in cigarette smoking. This is important for both men and women, given
the modest decline in cigarette smoking rates from 1990 to 1995.23
Between 80 and 90 percent of COPD is attributable to cigarette smoking. However, not all smokers develop COPD, and not all patients with COPD are smokers or have smoked in the past.24, 25 Individual susceptibility to the adverse health effects of cigarette smoke on the lung appears to vary within the general population. Some 10 to 15 percent of smokers show a rate of decline in lung function that will result in COPD with severe disability. Smoking cessation is the only treatment that slows the decline. Susceptible smokers who stop smoking do not regain lost lung function,26 but the rate of loss will return to what is normal for a nonsmoker.
How cigarette smoking causes COPD is an active area of research. The development of COPD—in particular, emphysema—is thought to be due to a chemical imbalance in the lungs caused by cigarette smoke.27 In some individuals, emphysema occurs because of a genetic deficiency. Emphysema due to genetic deficiency, called familial emphysema, occurs even in nonsmokers, but smoking hastens its occurrence. Familial emphysema probably accounts for less than 5 percent of all cases of COPD. 28
Smoking and occupational exposures together cause respiratory diseases and lung cancer.29, 30 Miners, firefighters, metal workers, grain handlers, cotton workers, paper mill workers, agricultural workers, construction workers who handle cement, and others employed in occupations associated with prolonged exposure to dusts, fumes, or gases develop significant airflow obstruction, coughing, phlegm, dyspnea, wheezing, and reduced lung function.28, 30, 31
Population studies have shown that chronic exposure to air pollution has an independent adverse effect on lung function.32, 33 A multi-year study of the respiratory effects of long-term exposure to environmental tobacco smoke and air pollution reported that both long-term ozone and childhood exposure to maternal tobacco smoke were associated with diminished lung function in college students.34 Viral infections also may contribute to susceptibility to COPD, and they are considered to play a role in the onset of airflow obstruction.
The direct costs of health care services and indirect costs through loss of productivity related to COPD amounted to $26 billion in 1998.27 About 14 million persons in the United States have COPD—about 12.5 million have chronic bronchitis and 1.9 million have emphysema.28 Emphysema has not increased, but since 1980, cases of chronic bronchitis increased 75 percent.28
Because national data systems will not be available in the first half of the decade for tracking progress, two subjects of interest concerning respiratory diseases are not addressed in this focus area’s objectives. Representing a research and data collection agenda for the coming decade, the topics cover cultural competence and early detection. The first topic addresses increasing the proportion of primary care providers who are trained to provide culturally competent health services to racial and ethnic groups seeking care for chronic obstructive pulmonary disease. The second involves increasing the proportion of primary care providers who are trained to use appropriate lung function tests to recognize the early signs of chronic obstructive pulmonary disease before the disease becomes serious and disabling.
Disparities
Reliable statistics are not as available for COPD total cases, illness, disability, or death in African Americans, Hispanics, and other ethnic groups as for whites.35, 36 From 1982 to 1984, the proportion of adults with COPD was 6.2 percent among whites and 3.2 percent among African Americans. In 1982, the age-adjusted COPD death rate for whites was 16.6 deaths per 1,000 population and 12.8 deaths per 1,000 for African Americans. Among the Hispanic groups studied, Puerto Ricans demonstrated a higher proportion of chronic bronchitis (2.9 percent) than Mexican Americans (1.7 percent) or Cuban Americans (1.7 percent).35, 36
In 1995, the proportion of the population with COPD was 5 percent in men aged 45 to 64 years and 11 percent in men aged 65 years or older. The proportion was 10 percent in women aged 45 to 64 years and 9 percent in women aged 65 to 74 years.
Death from COPD is more common in men than in women, and the death rate increases steeply with age.28, 37 Men and women have similar COPD death rates before age 55 years, but the rate for men rises thereafter. At age 70 years, the rate for men is more than double that for women, and at age 85 years and older, the COPD death rate for men is 3.5 times that for women.38 The proportion was 8 percent for whites aged 45 to 64 years and 10 percent for whites aged 65 years and older. The proportion of African Americans with COPD was 6 percent for those aged 45 to 64 years and 8 percent for those aged 65 years and older.2 COPD death rates were lower in the Hispanic groups than in non-Hispanic whites; however, these rates have been increasing for Hispanics.35
Women might be more susceptible than men to developing COPD when exposed to risk factors such as tobacco smoke.39 The beneficial effects of stopping smoking on the rate of lung function decline may be greater for women than men.40
Opportunities
Primary care physicians are in a key position to provide optimal care to patients with COPD and to provide counseling during clinical or health center visits to patients who smoke. Effective tests are available to screen patients for COPD, and primary care physicians need to be trained in the latest methods to detect and treat the disease.
Obstructive Sleep Apnea
Issues and Trends
Some 18 million persons in the United States were estimated to have OSA in 1993.41 OSA affects all races, ages, and socioeconomic and ethnic groups.42 Because OSA causes serious disturbances in normal sleep patterns, patients experience excessive daytime sleepiness and impaired performance. Common consequences of OSA range from personality changes and sexual dysfunction to falling asleep at work or while driving.41, 42
OSA symptoms include many repeated involuntary breathing pauses during sleep. The breathing pauses often are accompanied by choking sensations that may wake the patient. Other symptoms include intermittent snoring, awakening from sleep (poor sleep), early morning headaches, and excessive daytime sleepiness.
OSA can increase the seriousness of other lung diseases that decrease airflow, such as asthma and COPD. Cardiovascular deaths alone due to OSA have been estimated at 38,000 a year.41 Individuals with OSA often do not recognize reductions in alertness, diminished productivity, and discord in interpersonal relationships as part of the syndrome. Persons affected by OSA, for example, are seven times more likely to be involved in multiple vehicular crashes.43 In children, OSA can disrupt sleep. OSA also may cause daytime behavioral problems that affect workplace performance and affect their learning ability in school.
Infants with siblings or parents who have OSA inherit an increased risk of sudden infant death syndrome (SIDS).44 This tragic sleep-related breathing disorder takes the lives of more infants than all other causes combined.
Disparities
OSA is prevalent particularly in men over age 50 years and in postmenopausal women, when hormonal changes appear to increase risk. The risk of OSA also is increased in certain racial and ethnic groups. Among young African Americans, the likelihood of experiencing OSA symptoms is twice that of young whites.45 Nearly 50 percent of OSA patients have high blood pressure.46, 47, 48
Opportunities
A major factor in the pervasiveness of OSA’s effects on health and society has been the failure to educate Americans - and especially health care practitioners - about the disorder. A wide range of behavioral, mechanical, and surgical treatments can be used to manage OSA symptoms. Providing persons at risk with culturally and linguistically appropriate information about OSA could enable them to prevent or lessen the effects of OSA. Improved awareness of OSA symptoms represents a major public health challenge.
Primary care providers are an important barometer of OSA awareness because they are a first stop for patients who are seeking appropriate diagnosis and treatment. However, only 79 cases of sleep disorder were diagnosed in a sample of 10 million patient records from 1989 and 1990.41 In 1990 about a third of the medical schools in the United States offered no training in sleep medicine, and another third provided less than 2 hours on average for all sleep topics.49 Data systems to track the training of health care providers in OSA over the decade are not currently available, and therefore the issue is not addressed in this focus area’s objectives. However, it represents an important research and data collection agenda. In the absence of strong educational models for physicians, the risk remains high that OSA will be misdiagnosed and mismanaged.
The National Commission on Sleep Disorders Research41 was established by the U.S. Congress in 1988 to assess the societal and economic impact of sleep disorders and the resources available to promote the prevention, diagnosis, and treatment of such disorders. In a 1994 report to Congress, the Commission concluded that even though the science of sleep disorders is not fully developed, such disorders can be prevented. The commission recommends that research on the natural history of sleep disorders be made an urgent national concern. Epidemiologic studies must be conducted to evaluate risk factors that lead to sleep disorders and to determine which sleep disorders lead to other serious health problems.
Interim Progress Toward Year 2000 Objectives
For the three objectives specific to asthma in Healthy People 2000, available data indicate movement away from the targets as the rate of hospitalizations and activity limitation increase and a movement toward the target for increasing the proportion of persons with asthma who receive patient education. There were no objectives in Healthy People 2000 for COPD and OSA.
Healthy People 2010—Summary of Objectives
Respiratory Diseases
Goal: Promote respiratory health through better prevention, detection, treatment, and education.
| Number | Objective |
|---|---|
| Asthma | |
| 24-1 | Deaths from asthma |
| 24-2 | Hospitalizations for asthma |
| 24-3 | Hospital emergency department visits for asthma |
| 24-4 | Activity limitations |
| 24-5 | School or work days lost |
| 24-6 | Patient education |
| 24-7 | Appropriate asthma care |
| 24-8 | Surveillance systems |
| Chronic Obstructive Pulmonary Disease (COPD) | |
| 24-9 | Activity limitations due to chronic lung and breathing problems |
| 24-10 | Deaths from COPD |
| Obstructive Sleep Apnea (OSA) | |
| 24-11 | Medical evaluation and followup |
| 24-12 | Vehicular crashes related to excessive sleepiness |
Healthy People 2010 Objectives
Asthma
24-1. Reduce asthma deaths.
Target and baseline:
| Objective | Age Group | 1998 Baseline* | 2010 Target |
|---|---|---|---|
| Rate per Million | |||
| 24-1a. | Children under age 5 years | 1.7 | 1.0 |
| 24-1b. | Children aged 5 to 14 years | 3.2 | 1.0 |
| 24-1c. | Adolescents and adults aged 15 to 34 years | 5.9 | 3.0 |
| 24-1d. | Adults aged 35 to 64 years | 17.0 | 9.0 |
| 24-1e. | Adults aged 65 years and older | 87.5 | 60.0 |
| *Preliminary data. | |||
| Target setting method: Better than the best. Data source: National Vital Statistics System (NVSS), CDC, NCHS. | |||
| Select Age Groups, 1997* | Asthma Deaths | ||||
|---|---|---|---|---|---|
| 24-1a. Children Under Age 5 Years | 24-1b. Children Aged 5 to 14 Years | 24-1c. Persons Aged 15 to 34 Years | 24-1d. PersonsAged 35to 64 Years | 24-1e. Persons Aged 65 Years and Older | |
| Rate per Million | |||||
| TOTAL | 1.8 | 3.1 | 6.2 | 18.9 | 85.9 |
| Race and ethnicity | |||||
| American Indian or Alaska Native | DSU | DSU | DSU | DSU | DSU |
| Asian or Pacific Islander | DSU | DSU | DSU | 22.3 | 141.2 |
| Asian | DSU | DSU | DSU | DSU | DSU |
| Native Hawaiian and other Pacific Islander | DSU | DSU | DSU | DSU | DSU |
| Black or African American | 7.6 | 9.7 | 17.4 | 52.7 | 120.2 |
| White | DSU | 1.8 | 4.3 | 14.3 | 81.5 |
| Hispanic or Latino | DSU | DSU | 4.8 | 17.1 | 81.8 |
| Not Hispanic or Latino | 2.2 | 3.4 | 6.4 | 19.1 | 86.1 |
| Black or African American | 7.8 | 10.1 | 18.1 | 54.6 | 122.7 |
| White | DSU | 1.9 | 4.2 | 13.8 | 81.0 |
| Gender | |||||
| Female | DSU | 2.8 | 5.2 | 23.5 | 99.5 |
| Male | 2.3 | 3.3 | 7.2 | 14.2 | 66.3 |
| Education (aged 25 to 64 years) | |||||
| Less than high school | NA | NA | 12.5 | 30.6 | NA |
| High school graduate | NA | NA | 10.5 | 23.4 | NA |
| At least some college | NA | NA | 4.3 | 11.1 | NA |
| DNA = Data have not been analyzed. DNC = Data are not collected. DSU = Data are statistically unreliable. NA = Not applicable. *New data for population groups will be added when available. | |||||
24-2. Reduce hospitalizations for asthma.
Target and baseline:
| Objective | Age Group | 1997 Baseline Rate p | 2010 Target er 10,000 |
|---|---|---|---|
| 24-2a. | Children under age 5 years | 60.9 | 25 |
| 24-2b. | Children and adults aged 5 to 64 years* | 13.8 | 8 |
| 24-2c. | Adults aged 65 years and older* | 19.3 | 10 |
| *Age adjusted to the year 2000 standard population. | |||
| Target setting method: Better than the best. Data source: National Hospital Discharge Survey (NHDS), CDC, NCHS. | |||
| Select Age Groups, 1997 | Asthma Hospitalizations | ||
|---|---|---|---|
| 24-2a. Children Under Age 5 Years | 24-2b. Persons Aged 5 to 64 Years* | 24-2c. Persons Aged 65 Years and Older* | |
| Rate per 10,000 | |||
| TOTAL | 60.9 | 13.8 | 19.3 |
| Race and ethnicity | |||
| American Indian or Alaska Native | DSU | DSU | DSU |
| Asian or Pacific Islander | DSU | DSU | DSU |
| Asian | DNC | DNC | DNC |
| Native Hawaiian and other Pacific Islander | DNC | DNC | DNC |
| Black or African American | 125.6 | 26.4 | 26.5 |
| White Hispanic or Latino | 33.3 DSU | 9.3 DSU | 15.4 DSU |
| Not Hispanic or Latino | DSU | DSU | DSU |
| Black or African American | DSU | DSU | DSU |
| White | DSU | DSU | DSU |
| Gender | |||
| Female | 45.3 | 17.3 | 24.7 |
| Male | 75.9 | 10.2 | 11.7 |
| DNA = Data have not been analyzed.DNC = Data are not collected.DSU = Data are statistically unreliable. *Age adjusted to the year 2000 standard population. | |||
24-3. Reduce hospital emergency department visits for asthma.
Target and baseline:
| Objective | Age Group | 1995-97 Baseline Rate per 1 | 2010 Target 0,000 |
|---|---|---|---|
| 24-3a. | Children under age 5 years | 150.0 | 80 |
| 24-3b. | Children and adults aged 5 to 64 years | 71.1 | 50 |
| 24-3c. | Adults aged 65 years and older | 29.5 | 15 |
| Target setting method: Better than the best. Data source: National Hospital Ambulatory Medical Care Survey (NHAMCS) CDC, NCHS. | |||
| Age Groups, 1995–97 | Hospital Emergency Department Visits for Asthma | ||
|---|---|---|---|
| 24-3a. Children Under Age 5Years | 24-3b. Persons Aged 5 to 64 Years | 24-3c. Persons Aged 65 Years and Older | |
| Rate per 10,000 | |||
| TOTAL | 150.0 | 71.1 | 29.5 |
| Race and ethnicity | |||
| American Indian or Alaska Native | DSU | DSU | DSU |
| Asian or Pacific Islander | DSU | DSU | DSU |
| Asian | DNC | DNC | DNC |
| Native Hawaiian and other Pa- cific Islander | DNC | DNC | DNC |
| Black or African American | 407.2 | 191.7 | 90.8 |
| White | 101.7 | 53.4 | 23.1 |
| Hispanic or Latino | DSU | DSU | DSU |
| Not Hispanic or Latino | DSU | DSU | DSU |
| Black or African American | DSU | DSU | DSU |
| White | DSU | DSU | DSU |
| Gender | |||
| Female | 103.0 | 83.6 | 37.8 |
| Male | 195.5 | 57.9 | 17.9 |
24-4. Reduce activity limitations among persons with asthma.
Target: 10 percent.
Baseline: 19.5 percent of persons with asthma in 1994-96 (age adjusted to the year 2000 standard population).
Target setting method: Better than the best.
Data source: National Health Interview Survey (NHIS), CDC, NCHS.
| Persons With Asthma, 1994–96 | Activity Limitations Percent |
|---|---|
| TOTAL | 19.5 |
| Race and ethnicity | |
| American Indian or Alaska Native | DSU |
| Asian or Pacific Islander | DSU |
| Asian | DSU |
| Native Hawaiian and other Pacific Islander | DSU |
| Black or African American | 26.3 |
| White | 18.3 |
| Hispanic or Latino | 22.4 |
| Not Hispanic or Latino | 19.2 |
| Black or African American | 26.0 |
| White | 17.8 |
| Gender | |
| Female | 20.9 |
| Male | 17.3 |
| Family income level | |
| Poor | 28.2 |
| Near poor | 20.0 |
| Middle/high income | 16.4 |
| DNA = Data have not been analyzed. DNC = Data are not collected. DSU = Data are statistically unreliable. Note: Age adjusted to the year 2000 standard population. | |
24-5. (Developmental) Reduce the number of school or work days missed by persons with asthma due to asthma.
Potential data source: National Health Interview Survey (NHIS), CDC, NCHS.
24-6. Increase the proportion of persons with asthma who receive formal patient education, including information about community and self-help resources, as an essential part of the management of their condition.
Target: 30 percent.
Baseline: 6.4 percent of persons with asthma received formal patient education in 1998 (preliminary data; age adjusted to the year 2000 standard population).
Target setting method: Better than the best.
Data source: National Health Interview Survey (NHIS), CDC, NCHS.
| Persons With Asthma, 1993* | Patient Education Percent |
|---|---|
| TOTAL | 10 |
| Race and ethnicity | |
| American Indian or Alaska Native | DSU |
| Asian or Pacific Islander | DSU |
| Asian | DSU |
| Native Hawaiian and other Pacific Islander | DSU |
| Black or African American | DSU |
| White | 10 |
| Hispanic or Latino | DSU |
| Not Hispanic or Latino | 11 |
| Black or African American | DSU |
| White | 11 |
| Gender | |
| Female | 11 |
| Male | 9 |
| Family income level | |
| Poor | DSU |
| Near poor | DSU |
| Middle/high income | 11 |
| DNA = Data have not been analyzed. DNC = Data are not collected. DSU = Data are statistically unreliable. Note: Age adjusted to the year 2000 standard population. *New data for population groups will be added when available. | |
24-7. (Developmental) Increase the proportion of persons with asthma who receive appropriate asthma care according to the NAEPP Guidelines.
24-7a. Persons with asthma who receive written asthma management plans from their health care provider.
24-7b. Persons with asthma with prescribed inhalers who receive instruction on how to use them properly.
24-7c. Persons with asthma who receive education about recognizing early signs and symptoms of asthma episodes and how to respond appropriately, including instruction on peak flow monitoring for those who use daily therapy.
24-7d. Persons with asthma who receive medication regimens that prevent the need for more than one canister of short-acting inhaled beta agonists per month for relief of symptoms.
24-7e. Persons with asthma who receive followup medical care for long-term management of asthma after any hospitalization due to asthma.
24-7f. Persons with asthma who receive assistance with assessing and reducing exposure to environmental risk factors in their home, school, and work environments.
Potential data source: National Health Interview Survey (NHIS), CDC, NCHS.
24-8. (Developmental) Establish in at least 15 States a surveillance system for tracking asthma death, illness, disability, impact of occupational and environmental factors on asthma, access to medical care, and asthma management.
Potential data sources: Council of State and Territorial Epidemiologists; Association of Schools of Public Health.
Chronic Obstructive Pulmonary Disease
24-9. Reduce the proportion of adults whose activity is limited due to chronic lung and breathing problems.
Target: 1.5 percent.
Baseline: 2.2 percent of adults had activity limitations due to chronic lung and breathing problems in 1997 (age adjusted to the year 2000 standard population).
Target setting method: Better than the best.
Data source: National Health Interview Survey (NHIS), CDC, NCHS.
| Adults Aged 45 Years and Older, 1997 | Chronic Obstructive Pulmonary Disease Cases Percent |
|---|---|
| TOTAL | 2.2 |
| Race and ethnicity | |
| American Indian or Alaska Native | DSU |
| Asian or Pacific Islander | DSU |
| Asian | DSU |
| Native Hawaiian and other Pacific Islander | DSU |
| Black or African American | 2.3 |
| White | 2.3 |
| Hispanic or Latino | 1.7 |
| Not Hispanic or Latino | 2.3 |
| Black or African American | 2.2 |
| White | 2.3 |
| Gender | |
| Female | 2.1 |
| 45 to 64 years | 1.6 |
| 65 years and older | 3.0 |
| Male | 2.5 |
| 45 to 64 years | 1.6 |
| 65 years and older | 4.1 |
| Family income level | |
| Poor | 5.2 |
| Near poor | 4.0 |
| Middle/high income | 1.8 |
| DNA = Data have not been analyzed. DNC = Data are not collected. DSU = Data are statistically unreliable. Note: Age adjusted to the year 2000 standard population. | |
24-10. Reduce deaths from chronic obstructive pulmonary disease (COPD) among adults.
Target: 18 deaths per 100,000 adults.
Baseline: 120.9 deaths from COPD per 100,000 persons aged 45 years and older in 1998 (preliminary data; age adjusted to the year 2000 standard population).
Target setting method: 85 percent improvement.
Data source: National Vital Statistics System (NVSS), CDC, NCHS.
| Adults Aged 45 Years and Older, 1997* | Chronic Obstructive Pulmonary Disease Deaths Rate per 100,000 |
|---|---|
| TOTAL | 117.4 |
| Race and ethnicity | |
| American Indian or Alaska Native | 75.9 |
| Asian or Pacific Islander | 55.1 |
| Asian | DNC |
| Native Hawaiian and other Pacific Islander | DNC |
| Black or African American | 82.4 |
| White | 122.2 |
| Hispanic or Latino | 55.3 |
| Not Hispanic or Latino | 120.8 |
| Black or African American | 84.2 |
| White | 125.3 |
| Gender | |
| Female | 107.4 |
| Male | 134.9 |
| Education (ages 25 to 64 years) | |
| Less than high school | 18.8 |
| High school graduate | 12.9 |
| At least some college | 4.6 |
| DNA = Data have not been analyzed. DNC = Data are not collected. DSU = Data are statistically unreliable. Note: Age adjusted to the year 2000 standard population. *New data for population groups will be added when available. | |
Obstructive Sleep Apnea
24-11. (Developmental) Increase the proportion of persons with symptoms of obstructive sleep apnea whose condition is medically managed.
24-11a. Persons with excessive daytime sleepiness, loud snoring, and other signs associated with obstructive sleep apnea who seek medical evaluation.
24-11b. Persons with excessive daytime sleepiness, loud snoring, and other signs associated with obstructive sleep apnea who receive followup medical care for long-term management of their condition.
Potential data source: National Health Interview Survey (NHIS), CDC, NCHS.
24-12. (Developmental) Reduce the proportion of vehicular crashes caused by persons with excessive sleepiness.
Potential data sources: National Health Interview Survey (NHIS), CDC, NCHS; Fatal Accident Reporting System (FARS), U.S. Department of Transportation, National Highway Traffic Safety Administration.
Related Objectives From Other Focus Areas
1. Access to Quality Health Services
1-10. Delay or difficulty in getting emergency care
7. Educational and Community-Based Programs
7-8. Satisfaction with patient education
7-10. Culturally appropriate community health promotion
8. Environmental Health
8-1. Harmful air pollutants
8-2. Alternative modes of transportation
8-3. Cleaner alternative fuels
8-4. Airborne toxins
8-14. Toxic pollutants
8-16. Indoor allergens
8-17. Office building air quality
8-20. School policies to protect against environmental hazards
8-23. Substandard housing
8-26. Information systems used for environmental health
8-27. Monitoring environmentally related diseases
8-28. Local agencies using surveillance data for vector control
11. Health Communication
11-6. Satisfaction with providers’ communication skills
15. Injury and Violence Prevention
15-15. Deaths from motor vehicle crashes
15-17. Nonfatal motor vehicle injuries
20. Occupational Safety and Health
20-1. Work-related injury deaths
20-2. Work-related injuries
20-4. Pneumoconiosis deaths
22. Physical Activity and Fitness
22-6. Moderate physical activity in young persons
22-7. Vigorous physical activity in young people
23. Public Health Infrastructure
23-2. Public access to information and surveillance data
23-6. Data for all population groups
23-6. National tracking of Healthy People 2010 objectives
23-7. Timely release of data on objectives
23-10. Continuing education and training by public health agencies
23-16. Data on public health expenditures
23-17. Prevention research
27. Tobacco Use
27-1. Adult tobacco use
27-2. Adolescent tobacco use
27-3. Initiation of tobacco use
27-4. Age at first use of tobacco
27-5. Smoking cessation by adults
27-6. Smoking cessation during pregnancy
27-7. Smoking cessation by adolescents
27-8. Insurance coverage of cessation treatment
27-9. Exposure to tobacco smoke at home among children
27-10. Exposure to environmental tobacco smoke
27-11. Smoke-free and tobacco-free schools
27-12. Worksite smoking policies
27-13. Smoke-free indoor air laws
27-14. Enforcement of illegal tobacco sales to minors laws
27-15. Retail license suspension for sales to minors
27-16. Tobacco advertising and promotion targeting adolescents and young adults
27-17. Adolescent disapproval of smoking
27-18. Tobacco control programs
27-19. Preemptive tobacco control laws
27-20. Tobacco product regulation
27-21. Tobacco tax
Terminology
(A listing of all abbreviations and acronyms used in this publication appears in Appendix K.)
Ambulatory care: Medical care provided at hospital emergency rooms and outpatient departments.
Asthma: A lung disease characterized by airway constriction, mucus secretion, and chronic inflammation, resulting in reduced airflow and wheezing, coughing, chest tightness, and difficulty breathing.
Chronic bronchitis: A lung disease characterized by the presence of chronic productive cough most days for 3 months in each of 2 successive years.
Chronic obstructive pulmonary disease (COPD): A lung disease characterized by airflow obstruction due to chronic bronchitis and emphysema, two diseases that often occur together. COPD is one of the most common respiratory conditions among adults worldwide and is the fourth leading cause of death in the United States.
Dyspnea: Shortness of breath.
Emphysema: Abnormal permanent enlargement of the airspaces in the lungs accompanied by coughing and difficulty breathing.
Epidemiologic studies: Studies of disease occurrence.
Obstructive sleep apnea (OSA): An illness characterized by snoring, partial or complete cessation of breathing during sleep, reductions in blood oxygen levels, severe sleep disruptions, and excessive daytime sleepiness. OSA is a chronic breathing problem with serious effects on individual health and productivity, including an inheritable risk of sudden infant deaths, behavior and learning disturbances, injury from accidents, and reduced quality of life.
Rate: The basic measure of disease occurrence that most clearly expresses the probability of risk of disease in a defined population over a specified period of time. A rate is defined as:
References
1. Mannino, D.M.; Homa, D.M.; Pertowski, C.A.; Ashizawa, A.; Nixon, L.L.; Johnson, C.A.; et al. Surveillance for asthma—United States, 1960-1995. Morbidity and Mortality Weekly Report CDC Surveillance Summaries 47:1-27, 1998.
2. National Center for Health Statistics (NCHS). Current estimates from the National Health Interview Survey, 1995. National Center for Health Statistics. Vital and Health Statistics, Series 10(199), 1998.
3. National Heart, Lung, and Blood Institute. Data Fact Sheet. Asthma Statistics. Bethesda, MD: National Institutes of Health, Public Health Service, January 1999.
4. Mannino, D.M.; Homa, D.M.; Pertowski, C.A.; et al. Surveillance for asthma—United States, 1960-1995. Morbidity and Mortality Weekly Report CDC Surveillance Summaries 47(1):1-27, April 24, 1998.
5. NCHS. Current estimates from the National Health Interview Survey, 1990-92. National Center for Health Statistics. Vital and Health Statistics, Series 10(194), 1997.
6. National Asthma Education and Prevention Program. Expert Panel Report 2: Guidelines for the Diagnosis and Management of Asthma. NIH Pub. No. 97-4051. Bethesda, MD: National Institutes of Health, 1997.
7. Panhuysen, C.I.; Vonk, J.M.; Koeter, G.H.; Schouten, J.P.; van Altena, R.; Bleecker, E.R.; et al. Adult patients may outgrow their asthma: A 25-year follow-up study [published erratum appears in American Journal of Respiratory and Critical Care Medicine 156(2, Pt 1):674]. American Journal of Respiratory and Critical Care Medicine 155:1267-1272, 1997.
8. NCHS. Ambulatory care visits to physicians’ offices, hospital outpatient departments, and emergency departments: United States, 1996. National Center for Health Statistics. Vital and Health Statistics, Series 13(134), 1998.
9. NCHS. Healthy People 2000 Review, 1998-99. Hyattsville, MD: Public Health Service, 1999.
10. Weiss, K.B.; Gergen, P.J.; and Hodgson, T.A. An economic evaluation of asthma in the United States. New England Journal of Medicine 326:862-866, 1992.
11. Sullivan, S.; Elixhauser, S.; Buist, A.S.; Luce, B.R.; Eisenberg, J.; and Weiss, K.B. National Asthma Education and Prevention Program working group report on the cost effectiveness of asthma care. American Journal of Respiratory and Critical Care Medicine 154(3, Pt. 2):584-595, September 1996.
12. Glaxco Canada. The Costs of Asthma in Canada. Princeton, NJ: Communications Media for Education, 1993.
13. Koren, H.S. Environmental risk factors in atopic asthma. International Archives of Allergy and Immunology 113:65-68, 1997.
14. Becklake, M.R., and Ernst, P. Environmental factors. Lancet 350(suppl. 2):10-13, 1997.
15. Office of Air Quality Planning and Standards, Environmental Protection Agency. National Air Quality and Emissions Report, 1997. CPA Pub. No. EPA 454/R-98-016. Research Triangle Park, NC: Environmental Protection Agency, 1998.
16. Schwartz, D.A., and Peterson, M.W. Occupational lung disease. Advances in Internal Medicine 42:269-312, 1997.
17. Busse, W.W.; Gern, J.E.; and Dick, E.C. The role of respiratory viruses in asthma. Ciba Foundation Symposium 206:208-213, 1997.
18. U.S. Department of Health and Human Services. Action Against Asthma: A strategic plan for the Department of Health and Human Services. Washington, DC, draft March 22, 1999.
19. Wade, S.; Weil, C.; Holden, G.; Mitchell, H.; Evans, R.; Kruszon-Moran, D.; et al. Psycho social characteristics of inner-city children with asthma: A description of the NCICAS psychosocial protocol. National Cooperative Inner-City Asthma Study. Pediatric Pulmonology 24:263-276, 1997.
20. Evans, D.; Mellins, R.; Lobach, K.; Ramos-Bonoan, C.; Pinkett-Heller, M.; Wiesemann, S.; et al. Improving care for minority children with asthma: Professional education in public health clinics. Pediatrics 99:157-164, 1997.
21. National Heart, Lung, and Blood Institute. National Asthma Education and Prevention Program Summary Report. Bethesda, MD: National Institutes of Health, March 1999.
22. NCHS. Health United States. Prevalance of Selected Chronic Conditions. Hyattsville, MD: NCHS, 1986.
23. NCHS. Health United States, with Health and Aging Chartbook. Hyattsville, MD: NCHS, 1999.
24. Bone, R.C.; Dantzker, D.R.; and George, R.B. Pulmonary and Critical Care Medicine. Chapter G-1. St. Louis, MO: Mosby Year Book, 1993.
25. Sherril, D.L.; Lebowitz, M.D.; and Burrows, B. Epidemiology of COPD. Clinical Chest Medicine 11:375-388, 1990.
26. Fletcher, C., and Peto, R. The natural history of COPD. British Medical Journal 1:1645-1648, 1977.
27. Fishman, A.P. Pulmonary Diseases and Disorders. 2nd ed. New York, NY: McGraw-Hill, Inc., 1994.
28. National Heart, Lung, and Blood Institute. Morbidity and Mortality: 1998 Chartbook on Cardiovascular, Lung and Blood Diseases. Bethesda, MD: National Institutes of Health, October 1998.
29. Schwartz, D.A., and Peterson, M.W. Occupational lung disease. Disease-A-Month 44:41-84, 1998.
30. Wynder, E.L., and Hoffmann, D. Tobacco and health: a societal challenge. New England Journal of Medicine 300:894-903, 1979.
31. Bakke, S.; Baste, V.; Hanoa, R.; and Gulsvik, A. Prevalence of obstructive lung disease in a general population: Relation to occupational title and exposure to some airborne agents. Thorax. 46(12):863-870, 1991.
32. Souza, M.B.; Saldiva, P.H.; Pope, III, C.A.; and Capelozzi, V.L. Respiratory changes due to long-term exposure to urban levels of air pollution: a histopathologic study in humans. Chest 113:1312-1318, 1998.
33. Dockery, D.W., and Brunekreef, B. Longitudinal studies of air pollution effects on lung function. American Journal of Respiratory and Critical Care Medicine 154(6, Pt 2):S250-S256, 1996.
34. Galizia, A., and Kinney, P.L. Long-term residence in areas of high ozone: associations with respiratory health in a nationwide sample of nonsmoking young adults. Environmental Health Perspectives 107(8):675-679, 1999.
35. Coultas, D.B.; Gong, Jr., H.; Grad, R.; et al. Respiratory diseases in minorities of the United States. American Journal of Respiratory and Critical Care Medicine 149:S93-S131, 1993.
36. Gibson, K.F.; Aguayo, S.M.; Flowers, J.C.; et al. NHLBI special report. Respiratory diseases disproportionately affecting minorities. Chest 108:1380-1392, 1995.
37. Higgins, M.W., and Keller, J.B. Trends in COPD morbidity and mortality in Tecumseh, Michigan. Annual Review of Respiratory Diseases 140:S42-S48, 1989.
38. Feinlieb, M.; Rosenburg, H.M.; Collins, J.G.; et al. Trends in COPD morbidity and mortality in the United States. American Journal of Respiratory Diseases 140:S9-S18, 1989.
39. Tashkin, D.P.; Altose, M.F.; Bleecker, E.R.; et al. The Lung Health Study: Airway responsiveness to inhaled methacholine in smokers with mild to moderate airflow limitation. American Review of Respiratory Diseases 145:301-310, 1992.
40. Anthonisen, N.R.; Connell, J.E.; Kiley, J.P.; et al. Effects of smoking intervention and the use of an inhaled anticholinergic bronchodilator on the rate of decline of FEV1: The Lung Health Study. Journal of the American Medical Association 272:1497-1505, 1994.
41. Anonymous. Wake Up America: A National Sleep Alert, Report of the National Commission on Sleep Disorders Research to the U.S. Congress and Department of Health and Human Services. Bethesda, MD: National Institute on Aging, 1994.
42. Redline, S., and Strohl, K.P. Recognition and consequences of obstructed sleep apnea hypopnea syndrome. Clinical Chest Medicine 19:1-19, 1998.
43. Young, T.; Blustein, J.; Finn, L.; and Palta, M. Sleepdisordered breathing and motor vehicle accidents in a population-based sample of employed adults. Sleep 20:608-613, 1997.
44. Tischler, P.V.; Redline, S.; Ferrette, V.; Hans, M.G.; et al. The association of sudden unexpected infant death with obstructive sleep apnea. American Journal of Respiratory and Critical Care Medicine 153:1857-1863, 1996.
45. Redline, S. Epidemiology of sleep disordered breathing. Seminars in Respiratory and Critical Care Medicine 19(2):113-122.
46. Fletcher, E.C.; DeBehunke, R.D.; Lovoi, M.S.; and Gorin, A.B. Undiagnosed sleep apnea in patients with essential hypertension. Annals of Internal Medicine 103:190-195, 1995.
47. Guilleminault, H.C.; Tilkian, A.; and Dement, W.C. The sleep apnea syndromes. Annual Review of Medicine 27:465-484, 1976.
48. Carlson, J.T.; Hedner, J.A.; Ejnell, H.; and Peterson, L.E. High prevalence of hypertension in sleep apnea patients independent of obesity. American Journal of Respiratory and Critical Care Medicine 150:72-77, 1994.
49. Rosen, R.C.; Rosekind, M.; Rosevear, C.; Cole, W.E.; and Dement, W.C. Physician education in sleep and sleep disorders: A national survey of U.S. medical schools. Sleep 16:249-254, 1993
Appendix H: Clearing the Air
National Academy Press • 2101 Constitution Avenue, N.W. • Washington, D.C.
NOTICE: The project that is the subject of this report was approved by the Governing Board of the National Research Council, whose members are drawn from the councils of the National Academy of Sciences, the National Academy of Engineering, and the Institute of Medicine. The members of the committee responsible for the report were chosen for their special competences and with regard for appropriate balance.
Support for this study was provided by the U.S. Environmental Protection Agency (contract no. X825863-01-3). The views presented in the book are those of the Institute of Medicine Committee on Asthma and Indoor Air and are not necessarily those of the funding organization.
Clearing the Air: Asthma and Indoor Air Exposures is available for sale from the National Academy Press, 2101 Constitution Avenue, N.W., Box 285, Washington, DC 20055. Call 800-624-6242 (202-334-3313 in the Washington DC metropolitan area) or visit the NAP’s on-line bookstore at www.nap.edu.
Copyright 2000 by the National Academy of Sciences. All rights reserved.
Printed in the United States of America.
The serpent has been a symbol of long life, healing, and knowledge among almost all cultures and religions since the beginning of recorded history. The image adopted as a logotype by the Institute of Medicine is based on a relief carving from ancient Greece, now held by the Staatliche Museen in Berlin.
Committee on the Assessment of Asthma and Indoor Air
Richard B. Johnston, Jr., M.D. (Chair), Professor, Department of Pediatrics, University of Colorado School of Medicine, National Jewish Medical & Research Center, Denver, CO
Harriet A. Burge, Ph.D., Associate Professor of Environmental Health, Department of Environmental Health, Harvard School of Public Health, Boston, MA
William J. Fisk, M.S., P.E., Staff Scientist/Group Leader, Indoor Environment Department, Lawrence Berkeley National Laboratory, Berkeley, CA
Diane R. Gold, M.D., M.P.H., Assistant Professor of Medicine, Harvard Medical School, Assistant Professor, Environmental Health, Harvard School of Public Health, Boston, MA
Leon Gordis, M.D., Dr.P.H., Professor of Epidemiology, School of Hygiene and Public Health, The Johns Hopkins University, Baltimore, MD
Michael M. Grunstein, M.D., Ph.D., Professor, Department of Pediatrics, Children’s Hospital of Philadelphia, Philadelphia, PA
Patrick L. Kinney, Sc.D., Associate Professor, Division of Environmental Health Sciences, Columbia School of Public Health, New York, NY
Herman E. Mitchell, Ph.D., Adjunct Professor of Biostatistics, University of North Carolina, School of Public Health, Senior Research Scientist, Rho Federal Systems Division, Chapel Hill, NC
Dennis R. Ownby, M.D., Professor of Pediatrics, Medical College of Georgia, Augusta, GA
Thomas A. E. Platts-Mills, M.D., Ph.D., Professor, Department of Medicine and Microbiology, Chief, Division of Allergy, Asthma, and Clinical Immunology, University of Virginia Health Sciences Center, Charlottesville, VA
Sampson B. Sarpong, M.B.B.Ch., Assistant Professor of Pediatrics, The University of Chicago Children’s Hospital, Chicago, IL
Sandra Wilson, Ph.D., Senior Staff Scientist and Chair, Department of Health Services Research, Palo Alto Medical Foundation, Palo Alto, CA
Project Staff
DAVID A. BUTLER, Study Director
JAMES A. BOWERS, Research Assistant
JENNIFER A. COHEN, Research Assistant
ROSE MARIE MARTINEZ, Director, Division of Health Promotion and Disease Prevention (as of December 1999)
KATHLEEN R. STRATTON, Director, Division of Health Promotion and Disease Prevention (through November 1999)
DONNA D. DUNCAN, Division Assistant
ANDREA COHEN, Financial Associate
The National Academies
The National Academy of Sciences is a private, nonprofit, self-perpetuating society of distinguished scholars engaged in scientific and engineering research, dedicated to the furtherance of science and technology and to their use for the general welfare. Upon the authority of the charter granted to it by the Congress in 1863, the Academy has a mandate that requires it to advise the federal government on scientific and technical matters. Dr. Bruce M. Alberts is president of the National Academy of Sciences.
The National Academy of Engineering was established in 1964, under the charter of the National Academy of Sciences, as a parallel organization of outstanding engineers. It is autonomous in its administration and in the selection of its members, sharing with the National Academy of Sciences the responsibility for advising the federal government. The National Academy of Engineering also sponsors engineering programs aimed at meeting national needs, encourages education and research, and recognizes the superior achievements of engineers. Dr. William A. Wulf is president of the National Academy of Engineering.
The Institute of Medicine was established in 1970 by the National Academy of Sciences to secure the services of eminent members of appropriate professions in the examination of policy matters pertaining to the health of the public. The Institute acts under the responsibility given to the National Academy of Sciences by its congressional charter to be an adviser to the federal government and, upon its own initiative, to identify issues of medical care, research, and education. Dr. Kenneth I. Shine is president of the Institute of Medicine.
The National Research Council was organized by the National Academy of Sciences in 1916 to associate the broad community of science and technology with the Academy’s purposes of furthering knowledge and advising the federal government. Functioning in accordance with general policies determined by the Academy, the Council has become the principal operating agency of both the National Academy of Sciences and the National Academy of Engineering in providing services to the government, the public, and the scientific and engineering communities. The Council is administered jointly by both Academies and the Institute of Medicine. Dr. Bruce M. Alberts and Dr. William A. Wulf are chairman and vice chairman, respectively, of the National Research Council.
Executive Summary
The statistics are disturbing.
The Centers for Disease Control and Prevention (CDC) estimates that asthma affected about 17.3 million individuals in the United States in 1998. It is the most common chronic illness among children in the United States and one of the most common chronic illnesses overall in the country. Although by many measures the health of Americans is improving, CDC notes the self-reported prevalence rate for asthma increased 75% from 1980 to 1994. Studies show that asthma mortality is disproportionately high among African Americans and in urban areas that are characterized by high levels of poverty and minority populations. Nor is the phenomenon limited to the United States. The prevalence of asthma in some other parts of the world—including Australia, New Zealand, Ireland, and the United Kingdom—exceeds that of the United States.
Researchers have wondered whether the indoor environment may play a role in the increasing asthma problem. There is ample justification for this speculation. We know, for example, that individuals spend nearly all of their time indoors—most of it in their own homes—and that many of the exposures thought to be associated with asthma occur predominately indoors. If the indoor environment plays a role, then interventions to limit or eliminate exposures there have the potential to help asthmatics and perhaps result in primary prevention of the illness.
Against this backdrop, the U.S. Environmental Protection Agency (EPA) is developing an outreach strategy focused on reducing asthma-related morbidity and mortality potentially associated with exposure to indoor environments. To help ensure that such efforts are based on sound science, EPA requested that the National Academies undertake an assessment of asthma and its relationship to indoor air quality. The EPA charged the
committee with two primary objectives:
- To provide the scientific and technical basis for communications to the public on the health impacts of indoor pollutants related to asthma, and mitigation and prevention strategies to reduce these pollutants.
- To help determine what research is needed in these areas. This report presents the results of that assessment.
Organization and Framework
The content of this report reflects the committee’s goal to speak to a wide-ranging audience of science, health, and engineering professionals; government officials; and interested members of the public. The material presented thus covers a broad range of topics in order to establish a common base of knowledge for the reader. The scope of this material is far too vast for any one book to deal with comprehensively. Other publications, cited throughout the report, go into greater detail on specific issues.
The major topics addressed in the report are the following:
- the definition of asthma and the characteristics of its clinical presentation (Chapter 1);
- methodologic issues in evaluating the evidence regarding indoor air exposures and asthma, including the categorizations used to summarize the evidence and the framework for considering exposure to indoor sources (Chapter 2);
- patterns of asthma morbidity and mortality (Chapter 3);
- the pathophysiology of asthma—that is, the molecular mechanisms that underlie the structural and functional changes in the lungs and airways of asthmatics (Chapter 4);
- the committee’s review of the state of the scientific literature regarding indoor air exposures and the exacerbation and development of asthma—Table ES-1 lists the biologic and chemical exposures addressed in this report. (Chapters 5–7);
- the scientific literature on general exposures in indoor environments (Chapters 8–9); and
- how indoor exposures to pollutants associated with the incidence or symptoms of asthma are affected by building ventilation and particle air cleaning (Chapter 10).
Table ES-1 Indoor Exposures Addressed in This Report
| Biological | |
| Animals | Fungi or molds |
| Cats | Houseplants |
| Dogs | Pollen |
| Rodents | Infectious agents |
| Cows and horses | Rhinovirus |
| Domestic birds | Respiratory syncytial virus |
| Cockroaches | Chlamydia trachomatis |
| House dust mites | Chlamydia pneumoniae |
| Endotoxins | Mycoplasma pneumoniae |
| Chemical | |
| NO2, NOX (nitrogen oxides) | Plasticizers |
| Pesticides | Volatile organic compounds |
| Ozone* | Formaldehyde |
| Particulate matter with sources other than ETS* | Fragrances |
| SO2 , SOX (sulfur oxides)* | Environmental Tobacco Smoke (ETS) |
| *an outdoor air pollutants potentially associated with asthma that can penetrate the indoor environment and that may in some cases have indoor sources. Since the committee’s mandate was to address indoor air pollutants, the discussion of this agent is less detailed than others in the report and no conclusions are drawn concerning indoor exposures and asthma outcomes. | |
The committee faced a significant challenge in conducting its review—research on asthma is burgeoning and significant new papers are constantly being published. Although the committee did its best to paint an accurate picture of the state of the science at the time the report was completed, it is inevitable that research advances will overtake its conclusions.
Conclusions About the Relationship Between Indoor Exposures and Asthma
The committee used a uniform set of categories to summarize its conclusions regarding the association between exposure to an indoor agent and asthma development and exacerbation, and the effectiveness of exposure mitigation and prevention measures. Box ES-1 lists the definitions of these categories. The distinctions among categories reflect the committee’s judgment of the overall strength, quality, and persuasiveness of the scientific literature evaluated. Chapter 2 details the methodologic considerations underlying the categorizations and their definitions.
The sections below are a synopsis of the committee’s findings. Chapters 5 through 10 address the reasoning underlying the conclusions and present the findings in greater detail.
Exposure Settings
The indoor exposures considered in this report are highly dependent on the characteristics of the outdoor and indoor environment and its occupants. For example, house dust mites are a very common exposure in temperate and humid regions. They are found primarily within residences, concentrated in the bedroom. Cockroaches, which also thrive in temperate and humid regions, are an important exposure in some urban environments. They are found primarily near food sources. Fungi are ubiquitous and have been the primary source of allergen for several studied populations. Endotoxins may be found in humidifiers and in bacteria from other indoor, as well as outdoor sources. In some environments, exposure to animal allergens; molds; environmental tobacco smoke (ETS); indoor combustion products; and chemicals used in cleaning, building materials, and furnishings may be important. Many of these pollutants are also present in outdoor air, and indoor exposures can result from the infiltration of outdoor air into buildings.
Sufficient Evidence of a Causal Relationship
Evidence is sufficient to conclude that a causal relationship exists between the action or agent and the outcome. That is, the evidence fulfills the criteria for “Sufficient Evidence of an Association” below and in addition satisfies criteria regarding the strength of association, biologic gradient (dose–response effect), consistency of association, biologic plausibility and coherence, and temporality used to assess causality.
Sufficient Evidence of an Association
Evidence is sufficient to conclude that there is an association. That is, an association between the action or agent and the outcome has been observed in studies in which chance, bias, and confounding can be ruled out with reasonable confidence. For example, if several small studies that are free from bias and confounding show an association that is consistent in magnitude and direction, there may be sufficient evidence of an association.
Limited or Suggestive Evidence of an Association
Evidence is suggestive of an association between the action or agent and the outcome but is limited because chance, bias, and confounding cannot be ruled out with confidence. For example, at least one high-quality study shows a positive association, but the results of other studies are inconsistent.
Inadequate or Insufficient Evidence to Determine Whether or Not an Association Exists
The available studies are of insufficient quality, consistency, or statistical power to permit a conclusion regarding the presence or absence of an association; or no studies exist that examine the relationship. For example, available studies have failed to adequately control for confounding or have inadequate exposure assessment.
Limited or Suggestive Evidence of No Association
Several adequate studies are mutually consistent in not showing an association between the action or agent and the outcome. A conclusion of “no association” is inevitably limited to the conditions, level of exposure, and length of observation covered by the available studies. In addition, the possibility of a very small elevation in risk at the levels of exposure studied can never be excluded.
Indoor Air Exposures and Asthma Exacerbation
Studies of asthma can be divided into those dealing with factors leading to the development of asthma and those dealing with factors that exacerbate the illness in known asthmatics. Most of the research on this topic addresses “asthma exacerbation,” the onset or worsening of symptoms—some combination of shortness of breath, cough, wheezing, and chest tightness—in someone who already has developed asthma.
Epidemiologic investigations, challenge studies, and clinical experience have yielded solid information on the potential for many indoor exposures to exacerbate asthma. The committee found sufficient evidence to conclude that there is a causal relationship between
- exposure to the allergens produced by cats, cockroaches, and house dust mites, and exacerbations of asthma in sensitized individuals; and
- ETS exposure and exacerbations of asthma in preschool-aged children.
There is sufficient evidence of an association between several exposures and exacerbations of asthma. Dog allergen exposure is associated with exacerbation of asthma in individuals specifically sensitized to these allergens. Fungal exposure is associated with exacerbation in sensitized asthmatics and may be associated with nonspecific chest symptoms. Research indicates that rhinovirus infection is associated with wheezing and exacerbations in asthmatics. There is also sufficient evidence to conclude that brief high-level1 exposures to NO2 and increased airway responses among asthmatic subjects to both nonspecific chemical irritants and inhaled allergens.
Damp conditions are associated with the presence of symptoms considered to reflect asthma; symptom prevalence among asthmatics is also related to dampness indicators. The factors related to dampness that may actually lead to asthma exacerbation are not yet confirmed, but probably relate to dust mite and fungal allergens. There is sufficient evidence that some nonresidential buildings provide exposures that exacerbate asthma. However, the specific agents responsible for such exacerbations are as yet unstudied.
Limited or suggestive evidence was found for an association between exposures to domestic birds and exacerbation of asthma, although it is unclear what portion of this association is attributable to an allergic asthmatic response to the mites harbored by these birds. There is also limited or suggestive evidence of a relationship between
- exposure to the infectious agents respiratory syncytial virus (RSV), Chlamydia pneumoniae, and Mycoplasma pneumoniae, and exacerbation of asthma;
- chronic ETS exposure and exacerbation of asthma in older children and adults;
- acute ETS exposure and exacerbation of asthma in individuals responsive to this exposure;
- nonacute, nonoccupational formaldehyde exposure and wheezing and other respiratory symptoms; and
- exposure to certain fragrances and the manifestation of respiratory symptoms in asthmatics sensitive to such exposures.
Inadequate or insufficient information was identified to determine whether or not exacerbations of asthma result from nonacute, nonoccupational exposures to cow, horse, and rodent allergens; endotoxins; houseplants2 or cut flowers; the bacterial agent Chlamydia trachomatis; pesticides; plasticizers; and volatile organic compounds (VOCs) other than formaldehyde. Some of these same agents do or may play a role in asthma resulting from exposures in occupational settings, a topic outside the purview of this study.
Although there is sufficient evidence to conclude that pollen exposure is associated with exacerbation of existing asthma in sensitized individuals, and pollen allergens have been documented in both dust and indoor air, there is inadequate or insufficient information to determine whether indoor exposure to pollen is associated with exacerbations of asthma.
These findings are summarized in Table ES-2.
Table ES-2 Summary of Findings Regarding the Association between Indoor Biologic and Chemical Exposures and the Exacerbation of Asthma in Sensitive Individuals
| Biological Agents | Chemical Agents |
|---|---|
| Sufficient Evidence of a Causal Relationship | |
| Cat | ETS (in preschool-aged children) |
| Cockroach | |
| House Dust Mite | |
| Sufficient Evidence of an Association | |
| Dog | a NO2, NOX (high-level exposures ) |
| Fungi or molds | |
| Rhinovirus | |
| Limited or Suggestive Evidence of an Association | |
| Domestic birds | ETS (in school-aged and older children, and in |
| Chlamydia pneumoniae | adults) |
| Mycoplasma pneumoniae | Formaldehyde |
| Respiratory Syncytial Virus (RSV) | Fragrances |
| Inadequate or Insufficient Evidence to Determine Whether or Not an Association Exists | |
| Cow and horse | Pesticides |
| Rodents (as pets or feral animals) | Plasticizers |
| Chlamydia trachomatis | VOCs |
| Endotoxins | |
| Houseplants | |
| Pollen exposure in indoor environments | |
| Insects other than cockroaches | |
| Limited or Suggestive Evidence of No Association | |
| (no agents met this definition) | |
| At concentrations that may occur only when gas appliances are used in poorly ventilated kitchens. | |
Indoor Air Exposures and Asthma Development
The second outcome reviewed by the committee was the development of asthma—the initial onset of the illness. Asthma is defined by the manifestation of a set of symptoms rather than by any one objective test. With asthma symptoms ranging from clearly episodic to nearly continuous, from mild to severe, and from coughing without other respiratory symptoms to a loud wheeze, the initial diagnosis of the illness can be complicated and subject to controversy. It is thus difficult to study the determinants of and influences on asthma development. An additional complication stems from the fact that some of the most provocative evidence regarding development comes from studies of infants. Prior to the age of approximately 3, children may exhibit symptoms that are characteristic of asthma, but they may not exhibit persistent asthmatic symptoms or other related conditions such as bronchial reactivity or allergy later in life. Chapter 2 discusses the definitions of asthma and the characteristics of its clinical presentation.
Saying that a particular agent may be associated with the development of asthma does not mean it is the sole factor determining whether an individual will manifest the illness. Most scientists believe that some individuals have a prior, underlying predisposition that permits the evolution of clinical asthma. The development of this predisposition to asthma is dependent on a complex—and at present poorly understood—combination of factors, which are partially inherited and partially acquired later in life.
After careful consideration of the scientific literature, the committee concluded there is sufficient evidence of a causal relationship between exposure to house dust mite allergen and the development of asthma in susceptible children. This conclusion was based on the preponderance of several lines of evidence, including the results of clinical studies and population-based, case-control, and prospective epidemiologic investigations; the consistency of the association in different racial and ethnic groups; and the presence of a dose–response relationship between exposure to dust mite allergen and sensitization. Chapter 5 delineates the reasoning underlying this conclusion in greater detail.
There is sufficient evidence to conclude that there is an association between ETS exposure and the development of asthma in younger children. In the limited number of studies that have been able to separate the effects of maternal active smoking during pregnancy from the effects of ETS exposure after birth, evidence suggests that—although both exposures are detrimental—maternal smoking during pregnancy has the stronger adverse effect.
Limited or suggestive evidence exists for associations between
- cockroach allergen exposure and development of asthma in preschool-aged children; and
- infection with RSV and development of asthma in preschool-aged children.
The impact of exposure to these agents has been the subject of great research interest in the past few years, and efforts presently underway may clarify their role in asthma development.
Published case reports, public health surveillance of physician reporting, and cross-sectional studies of building occupants with indoor air quality complaints also provide limited or suggestive evidence of an association between aspects of the nonindustrial indoor environment and the development of asthma, with a building occupancy-related pattern of symptoms and in some instances objective abnormalities. What is lacking for the most part, however, is knowledge of specific etiologic agents in these nonindustrial indoor environments that might be responsible for new work-related asthma cases.
Inadequate or insufficient evidence exists to determine whether or not the other indoor exposures listed in Table ES-1 are associated with the development of asthma. This lack of information points to a gap in present-day knowledge concerning asthma—one that will be challenging to resolve.
There is limited or suggestive evidence of no association between infection with rhinovirus—the medical term for the large and ubiquitous group of viruses responsible for a variety of respiratory infections including those referred to as “the common cold”—and asthma development.
Table ES-3 summarizes these findings.
Table ES-3 Summary of Findings Regarding the Association Between Indoor Biologic and Chemical Exposures and the Development of Asthma
| Biologic Agents | Chemical Agents |
|---|---|
| Sufficient Evidence of a Causal Relationship | |
| House dust mite | (no agents met this definition) |
| Sufficient Evidence of an Association | |
| (no agents met this definition) | ETS (in preschool-aged children) |
| Limited or Suggestive Evidence of an Association | |
| Cockroach (in preschool-aged children) | (no agents met this definition) |
| Respiratory Syncytial Virus (RSV) | |
| Inadequate or Insufficient Evidence to Determine Whether or Not an Association Exists | |
| Cat | NO2, NOX |
| Cow and horse | Pesticides |
| Dog | Plasticizers |
| Domestic birds | VOCs |
| Rodents | Formaldehyde |
| Cockroaches (except for preschool-aged children) | Fragrances |
| Endotoxins Fungi or molds | ETS (in school-aged and older children, and in adults) |
| Chlamydia pneumoniae | |
| Chlamydia trachomatis | |
| Mycoplasma pneumoniae | |
| Houseplants | |
| Pollen | |
| Limited or Suggestive Evidence of No Association | |
| Rhinovirus (adults) | (no agents met this definition) |
Effectiveness of Indoor Environmental Interventions in Limiting Exposures and Affecting Asthma Outcomes
Patients with asthma and the parents of children with asthma need reliable information on which measures are likely to be most effective for improving indoor air quality. Specific recommendations are found in each chapter but there are general principles that should be kept in mind. Agents that can exacerbate asthma may generally be thought of in two categories: specific allergens and non-specific respiratory tract irritants. Exposure to non-specific irritants, such as cigarette smoke, may lead to asthma symptoms in any person with asthma; while allergens are only problems for individuals who are allergic to them. For example, if a person with asthma is allergic to cats, exposure to cats may cause wheezing; but if that person is not allergic to cats, exposure to them will not cause any problems. Therefore, reducing indoor airborne exposure to irritants is likely to help all asthmatic individuals to some degree while reductions in allergen exposure would only be expected to help individuals who are allergic to the allergens being reduced.
While the report identifies a number a mitigation strategies that are or may be effective in reducing exposure to potentially problematic agents, the committee found only a small number for which there is presently evidence that proper implementation of the strategy results in an improvement of symptoms or lung function in asthmatics. It is important to remember, though, that the absence of evidence does not mean an absence of effect. The science regarding indoor environmental interventions, exposure limitation, and effects on asthma outcomes is not nearly as well developed as that regarding the health effects of exposures. Exposure assessment3 is often the weakest link in environmental health studies because it is difficult to do and is given inadequate attention by many researchers.
Nonetheless, the committee was able to identify well-conducted, rigorous studies on which to base conclusions.
Sufficient evidence of an association was found between the use of a combination of physical measures and a reduction in indoor dust mite allergen levels in dust samples. As detailed in Chapter 5, strategies for the effective control of mite growth vary by climate. Such measures have been shown to be effective at reducing symptoms in controlled trials and should be part of normal management of asthma in mite-allergic individuals. Several studies now underway are evaluating whether aggressive allergen avoidance regimes have an effect on the subsequent development of asthma. The results of these and other studies will inform the question of whether primary prevention of dust mite-induced asthma is possible. Two related issues that will have to be addressed are (1) the feasibility of implementing such comprehensive interventions and (2) whether these interventions result in lower rates of sensitization to a particular exposure or all exposures.
The committee found limited or suggestive evidence that the combined use of cockroach extermination and control of potential reservoirs of allergen in beds, carpets, furnishings, and clothing through cleaning can achieve a short-term decrease in cockroach allergen levels in indoor environments. Extermination alone appears ineffective because significant allergen levels remain in settled dust; cleaning alone in the absence of complete extermination does not eliminate the sources of the allergen. There was inadequate or insufficient evidence to determine whether or not an association exists between any cockroach mitigation or prevention strategy and transient or long-term improvement of symptoms or lung function in cockroach-allergic asthmatics. However, since evidence does suggest that dust mite mitigation strategies result in improvement of symptoms or lung function, mitigation of cockroach exposures would appear to be a sensible course of action in the absence of more definitive information.
Although the strategy may be unpopular, there is limited or suggestive evidence of an association between removal of a cat from the home and improvement of symptoms or lung function in cat-allergic asthmatics. Concomitant removal or isolation of known reservoirs of cat allergen (carpets, upholstery, mattresses, pillows) may be required to diminish allergen levels to those commonly measured in homes without cats. Limited or suggestive evidence indicates that some measures short of removal (e.g.,, washing the animal) may result in transient reduction in allergen levels. However, there is inadequate or insufficient evidence to determine whether or not an association exists between measures short of removal of a cat from the home and improvement in symptoms in cat-allergic asthmatics. Data on the effectiveness of interventions for other animals are too sparse to draw informed conclusions.
It is possible to physically remove accessible growing fungi from indoor environments. The entry of fungal spores from outdoors can be substantially reduced in mechanically ventilated buildings by pressurizing them and filtering incoming air; closing windows should also reduce indoor concentrations from outdoor sources. Although there is limited or suggestive evidence that such steps may result in a reduction in the levels of fungi in the indoor environment, the health impact of such reduction has not been studied. Fungi are difficult to kill, and dead fungal material probably contains allergens that can become airborne, although this has not been thoroughly tested. There is relatively little information on the impact of ventilation and air-cleaning measures on indoor pollen levels, although it is clear that shutting windows and other measures that generally limit the entry rate of unfiltered outdoor air can be effective.
No general conclusions about means of altering exposure to low levels of endotoxin can be made at the present time. However, avoiding the use of cool mist humidifiers would appear to be a simple and effective means of eliminating risk of high-level exposure to endotoxin at home as well as exposure to organisms associated with hypersensitivity pneumonitis.
Source control—that is, stopping smoking—appears to be the only reliably effective means of preventing environmental tobacco smoke exposure. There is sufficient evidence to conclude that increased ventilation is technologically capable of reducing the indoor concentration of ETS particles and gases, and that particle air-cleaning methods are technologically capable of reducing the indoor concentration of ETS particles. However, evidence is lacking on whether interventions designed to encourage the use of the requisite ventilation and air cleaning methods would be associated with a reduction in asthma development or exacerbation.
Control options for chemical and particulate pollutants in indoor environments include source modification (removal, substitution, or emission reduction), ventilation (exhaust or dilution), or pollutant removal (filtration). The various forms of pollutant source modification are usually the most effective. For most gaseous pollutants—NO2 for example—removal via air cleaning is not presently practical.
No intervention studies clearly document that any form of dampness control works effectively to reduce symptoms or to reduce the chances of asthma development. However, given its relationship to factors (such as dust mites and fungal growth) associated with asthma, steps to reduce dampness may be appropriate. For homes, these measures include powered mechanical ventilation to remove or dilute occupant-generated moisture, proper installation of vapor barriers, channeling ground water away from foundations, sealing below-ground walls to prevent water intrusion, protecting ground-level concrete slabs from moisture intrusion, and constructing crawl spaces to prevent water intrusion.
There are both theoretical evidence and limited empirical data indicating that feasible modifications in ventilation rates can decrease or increase4 concentrations of some of the indoor pollutants associated with asthma by up to approximately 75%. Limited or suggestive evidence exists to indicate that particle air cleaning is associated with a reduction in the exacerbation of asthma symptoms. Theoretical and limited empirical data indicate that particle air cleaners are most likely to be effective in reducing the exacerbation of asthma symptoms associated with particles smaller than approximately 2 μm, such as ETS particles5 and some airborne cat allergen. There is insufficient evidence to determine whether or not the use of particle air cleaners is associated with decreased asthma development. It should also be noted that microorganisms can grow on some air-cleaning equipment such as filter media; thus, improperly maintained air cleaners are also a potential source of indoor pollutants.
Inadequate or insufficient information was available regarding several other interventions. These are discussed in Chapters 5 through 10.
It is difficult to draw general conclusions regarding effective indoor environmental interventions. However, the committee is able to offer some observations. For many allergens, effective strategies consist of integrated approaches consistently applied over time. The two primary components of an integrated approach are (1) removal or cleaning of allergen reservoirs and (2) control of new sources of exposure. Source removal—where it is possible—is typically the most effective control measure and may be the only effective measure for some agents.
Avoidance of exposure through source removal, substitution, or emission reduction is usually the most successful approach for chemical agents.
General Research Recommendations and Conclusions
Asthma is a complex illness. The many variables that determine its development and severity defy simple summary. Although great strides have been made over the past few years in elucidating mechanisms and understanding the role of environmental and genetic influences, much work remains to be done. Importantly, we still do not know whether or to what extent the reported increases in asthma can be attributed to indoor exposures.
Subsequent chapters of this report contain specific recommendations for further research on the biologic and chemical agents addressed and on the characteristics of indoor environments that may influence asthma outcomes. A digest of these recommendations is contained in Chapter 11. Some general observations are offered below.
The factors that determine the predisposition to sensitivity to certain agents and lead to the development of asthma are still not well understood. There is a great need for studies that rigorously examine the role of prenatal exposure and whether the age of first exposure influences the development of sensitization. The interaction of different environmental exposures with genetic susceptibilities—a topic of great interest but little research progress—also has to be pursued.
A major problem in choosing and implementing an intervention to mitigate an exposure is the generally limited data available. The limitations exist in regard to both the quantity and the quality of research data. Many of the studies reported are not based on rigorous protocols. Definition of clinical outcome (especially in infants), measurement of exposure, rigorous study design, appropriate population selection, and generalizability of the findings are among the issues that are often not adequately addressed. Indoor environments typically include exposures to multiple potentially problematic agents—dust mites and fungi, for example, are ubiquitous. It has proven difficult to assess the individual roles of the factors implicated in existing studies because complete characterization of exposures has not been done. Therefore, it is often not possible to determine with confidence whether any effects noted are indeed the results of specific exposures studied or of confounders.
The poor and inner city residents are vulnerable populations for asthma development, morbidity, and mortality. As such, there is great interest in identifying effective means to address prevalent exposure problems. Although some research on interventions has been directed at these populations, some of the strategies tried may not be practical to implement unless the subjects are part of an organized protocol providing guidance and funds. Further, individuals living in public or rental housing, or in multifamily units, may not have control over parts of their indoor environment that would be desirable to modify, such as carpeting, excessive moisture, and comprehensive pest management. Future research has to address more effectively the feasibility and generalizability of intervention programs on target populations.
Finally, to date there has been little connection between the scientific literature regarding asthma and the scientific literature regarding the characteristics of healthy indoor environments (for example, building design and operation; and sources, transport, control methods, and exposures to indoor pollutants). Relatively little of the existing medical and epidemiologic literature on asthma quantifies indoor environmental conditions such as humidity, ventilation, and pollutant concentrations or exposures in sufficient detail. The effectiveness of exposure limitation strategies in reducing exposures and asthma development or exacerbation has, in general, been inadequately studied. These are areas of research that have the potential to impact public health significantly. The committee believes that better communication between medical, public health, behavioral science, engineering, and building professionals is likely to result in more informed studies on the causes of asthma and the means to limit problematic exposures. The committee encourages efforts to bring these groups together to educate one another on their areas of expertise. Although considerable work has been done and is being done on asthma per se, increased research efforts are needed to address the characteristics of healthy indoor environments. Asthma research clearly needs interdisciplinary involvement—not only of clinicians, immunologists, and researchers in related biologic areas—but also of engineers, architects, materials manufacturers and others who are responsible for the design and function of indoor environments. Collaborations should be fostered, and consideration should be given to formulating model research protocols that include indoor environmental characteristics.
References
Benson V, Marano MA. 1998. Current estimates from the National Health Interview Survey, 1995. National Center for Health Statistics. Vital Health Statistics Series 10 No. 199. DHHS Publication PHS 98-1527.
Carr W, Zeitel L, Weiss K. 1992. Variations in asthma hospitalizations and deaths in New York City. American Journal of Public Health 82:59–65.
Lang DM, Polansky M. 1994. Patterns of asthma mortality in Philadelphia from 1969 to 1991. New England Journal of Medicine 331:1542–1546.
Mannino DM, Homa DM, Pertowski CA, Ashizawa A, Nixon LL, Johnson CA, Ball LB, Jack E, Kang DS. 1998. Centers for Disease Control and Prevention. Surveillance for Asthma Prevalence—United States, 1960–1995. Morbidity and Mortality Weekly Report. 47(no. SS-1):1–28.
National Academy of Sciences (NAS). 1994. Science and Judgement in Risk Assessment. National Academy Press: Washington, DC.
Rappaport S, Boodram B. 1998. Forecasted state-specific estimates of self-reported asthma prevalence—United States, 1998. Morbidity and Mortality Weekly Report 47(47):1022–1025.
1 At concentrations that may occur only when gas appliances are used in poorly ventilated kitchens.
2 Mites and fungi associated with houseplants could be involved in asthma outcomes but no studies document this connection.
3 Classically, “exposure assessment” involves specifying the population that might be exposed to the agent of concern; identifying the routes through which exposure can occur, and estimating the magnitude, duration, and timing of the dose that individuals might receive as a result of their exposure (NAS, 1994).
4 The indoor concentrations of some pollutants from outdoors—particulate matter and ozone, for example—may increase with the ventilation rate.
5 Particle air cleaners are not effective in reducing concentrations of the gaseous components of ETS.
