U.S. Department of Health and Human Services
Risk of Institutionalization: 1977-1985
William G. Weissert, PhD, and Jennifer M. Elston, MHSAUniversity of Michigan, Ann Arbor
Gary G. Koch, PhDUniversity of North Carolina, Chapel Hill
July 24, 1990
This report was prepared under grant #88ASPE206A between the U.S. Department of Health and Human Services (HHS), Office of Social Services Policy (now known as the Office of Disability, Aging and Long-Term Care Policy) and the University of North Carolina. For additional information about the study, you may visit the DALTCP home page at http://aspe.hhs.gov/_/office_specific/daltcp.cfm or contact the office at HHS/ASPE/DALTCP, Room 424E, H.H. Humphrey Building, 200 Independence Avenue, SW, Washington, DC 20201. The e-mail address is: webmaster.DALTCP@hhs.gov. The DALTCP Project Officer was Floyd Brown.
Opinions are those of the authors only and do not necessarily reflect the views of the Federal Government.
Dr. Weissert is Professor of Health Services Management and Policy in the School of Public Health and Research Scientist at the Institute of Gerontology at the University of Michigan in Ann Arbor. Ms. Elston is a doctoral student in Health Services Organization and Policy in the School of Public Health at the University of Michigan in Ann Arbor. Dr. Koch is Professor of Biostatistics in the School of Public Health at The University of North Carolina at Chapel Hill.
TABLE OF CONTENTS
- INDIVIDUAL-LEVEL ANALYSIS
- Analysis
- Variable Definitions
- Simultaneity
- Statistical Model and Hypotheses
- Results
- STATE-LEVEL ANALYSIS
- Variable Definitions
- Analysis
- Results
- LIST OF TABLES
- TABLE 1: Logistic Regression Results: Population Inflation Factor
- TABLE 2: Diagnostic Categories
- TABLE 3: 1985 Weighted Logistic Regression Model: Individual Level Analysis
- TABLE 4: 1977 Weighted Logistic Regression Model: Individual Level Analysis
- TABLE 5: Percent Distribution of Demographic, Social, Dependency, and Diagnostic Characteristics of Elderly Individuals by Residency Status and Year
- TABLE 6: State Level Multiple Regression Paired Comparison Test: 1976 versus 1985
- TABLE 7: Weighted Least Squares and Weighted Two-Stage Least Squares Regression Results: State Nursing Home Use Rates, 1986
ABSTRACT
States which endeavor to cut their Medicaid outlays by more effectively targeting home care services to individuals at high risk of becomming long-term nursing homes residents find a critical need for effective models to predict institutional residency.
Given a variety of Medicaid and Medicare policy changes since the mid-1970s, we hypothesized that some risk factors for nursing home residency might have changed. Using two national cohorts of institutionalized and noninstitutionalized aged, we estimated weighted logistic regression models to identify individual factors which differentiated nursing home residents from the noninstitutionalized elderly in 1985 compared to 1977.
To test whether state sociodemographic and Medicaid policy variables differentially affected statewide nursing home use rates between 1986 and 1976, we estimated a multiple regression paired comparison model. We also estimated a two stage weighted least squares regression model of state-to-state nursing home use rate variation for 1986.
Results showed considerable resilency across the two study years in individual indicators of need, including dependency in activities of daily living, mental disorders, lack of social support, poverty age and race. Prior nursing home use and Alzheimer's disease newly evaluated in the 1985 model proved to be important additions to the model. Dignoses, other than specific mental illnesses, ceased to be important predictors of nursing home residency.
State-level analysis of the change in nursing home use rates detected no differences in the predictors between the two study years. Variation in use in 1955 was positively associated with the supply of nursing home beds, the percent of the state's population that was aged 85 and over, and broader and more generous Medicaid coverage policies. Use declined as the state's total population and its population aged 65 and over increased, and as the average price of nursing home care increased.
INTRODUCTION
Targeting home and community care services to applicants at high risk of nursing home entry is an essential requirement for cost effectiveness of home care (Weissert and Cready, 1989) and is required of states in providing services under the Medicaid Home and Community Care Act (Title XIX, Section 1915 [c][1] of the Social Security Act. For states trying to use their nursing home pre-admission screening programs and similar assessment opportunities to accomplish such targeting, valid algorithms for predicting institutionalization are essential.
While there is considerable agreement in previous research on the important variables to include in such preadmission screening instruments, the continued importance of these predictors has not been tested in nationally representative data collected after the introduction of a large number of Medicaid and Medicare policy changes which were implemented during the late 70s and early 80s.
This analysis compares predictors of institutional residency in 1977 and 1985 among two national cohorts of individuals who responded to national surveys of nursing home and community-dwelling elderly persons. A state-level analysis of change in predictors of state nursing home use rates for 1976 and 1986 was also conducted using aggregate state sociodemographic and Medicaid policy variables. Finally, a model was estimated to predict state-to-state variation in nursing home use in 1986.
PREVIOUS RESEARCH
Over the past two decades factors associated with institutionalization have been the subject of numerous multivariate research efforts. Some have been cross-sectional in design, comparing noninstitutionalized and institutionalized elderly at a particular time. Others have used longitudinal designs, and therefore are able to assess, assuming appropriate theoretical underpinnings, which factors cause nursing home institutionalization. The overriding concern with all of these studies is what characteristics put a person at high risk for institutionalization.
Nursing home residency has been found to be positively associated with advanced age (Chiswick, 1976; Vicente, Wiley and Carrington, 1979; McCoy and Edwards, 1981; Branch and Jette, 1982; Brock and O'Sullivan, 1985; Shapiro and Tate, 1985; Cohen, Tell and Wallack, 1986; Weissert and Cready, 1989), being female (Greenberg and Ginn, 1979; Shapiro and Tate, 1985), and being white (Palmore, 1976; McCoy and Edwards, 1981; Weissert and Cready, 1989). However, many have found no relationship between gender and institutional residency (Vicente, Wiley and Carrington, 1979; McCoy and Edwards, 1981; Branch and Jette, 1982; Cohen, Tell and Wallack, 1986 and Weissert and Cready, 1989).
Institutional residency also has been found to vary positively with income (Chiswick, 1976; and Greenberg and Ginn, 1979) and with receipt of public assistance (Cohen, Tell and Wallack, 1986; Weissert and Cready, 1989).
Availability of social support, variously measured, has been shown to be negatively correlated with nursing home use. Currently, single (e.g. widowed) elderly are more likely to reside in a nursing home (Greenberg and Ginn, 1979; Vincente, Wiley and Carrington, 1979; Cohen, Tell, and Wallack, 1985; and Weissert and Cready, 1989), as are those living alone (Vincente, Wiley, and Carrington, 1979; McCoy and Edwards, 1981; and Branch and Jette, 1982), living without a spouse (Shapiro and Tate, 1985), living with a nonrelative (McCoy and Edwards, 1981) or living in senior housing (Shapiro and Tate, 1985). Likewise, lacking a social support network (Brock and O'Sullivan, 1985), or having few social contacts (McCoy and Edwards, 1981 and Shapiro and Tate, 1985) have been shown to be positively associated with institutionalization.
Various health related conditions have also been shown to be related to institutionalization. These include mental impairment (Branch and Jette, 1982; Shapiro and Tate, 1985; Weissert and Cready, 1989), physical functioning dependency (Greenberg and Ginn, 1979; McCoy and Edwards, 1981; Branch and Jette, 1982; Shapiro and Tate, 1985; Cohen, Tell and Wallack, 1986; Weissert and Cready, 1989), and certain diagnoses, such as cancer, stroke and diseases of the nervous system (Greenberg and Ginn, 1979; Weissert and Cready, 1989). Attitudinal factors have also been shown to play a role. Perceived poor health status has been positively associated with institutional residency (Evashwich et al, 1984; Shapiro and Tate, 1985; Cohen, Tell, and Wallack, 1986), as has favorable attitudes towards nursing home placement (Greenberg and Ginn, 1979).
Other patient level factors associated with institutionalization include being in a hospital (McCoy and Edwards 1981; and Shapiro and Tate, 1985), not seeing a physician regularly (Evaswhick, et al., 1984), having few formal service contacts (Branch and Jette, 1982), and taking medications (Greenberg and Ginn, 1979).
In addition to individual characteristics, community characteristics or contextual variables also have been shown to significantly affect nursing home use. These include region of residency (McCoy and Edwards, 1981), although Cohen, Tell, and Wallack (1986) found no regional effect, and the availability of nursing home beds (which varies by region), which has been found to positively affect nursing home use (Scanlon, 1980; McCoy and Edwards, 1981; and Weissert and Cready, 1989).
Findings on the effect of the level of urbanization have been mixed. Some (Chiswick, 1976; McCoy and Edwards, 1981; and Shapiro and Tate, 1985) have found no significant difference in nursing home use rates by urbanicity, while others (Dunlop, 1976; and Scanlon, 1980) have found a positive relationship.
The percentage of households residing in poverty has been found to negatively affect rates of institutionalization (Scanlon, 1980; and McCoy and Edwards, 1981), while income has been found to positively affect rates (Scanlon, 1980; and McCoy and Edwards, 1981). Finally, private pay price has been found to vary inversely with rates of nursing home use (Scanlon, 1980).
Thus, despite varying methods and data sources, the results of research conducted on data from the late 1970s have shown considerable agreement regarding what factors place an individual at risk of nursing home residency. Drawing from these previous works, a model of nursing home residency can be conceptualized as follows:
Institutionalization = f[Sociodemographic Characteristics (e.g., age, sex, race, income, etc.), Social Support (e.g., living arrangement, marital status, etc.), Functional Status (e.g., activities of daily living dependencies, mobility dependencies, etc.), Mental Impairments and Diagnoses (e.g., cancer, nervous system disorder, etc.), Prior Health Care Use (e.g., recent hospitalization, previous nursing home admission, etc.), Perceptions/Attitudes (e.g., perceived health status, attitude towards nursing home placement, etc.), and Community Characteristics (e.g., region, supply of beds, etc.)].
Because data limitations precluded us from estimating one model which contained both individual characteristics and contextual factors, we developed both an individual- and a state-level model. Each is described in detail below.
DATA SOURCES AND METHODOLOGY
For the 1985 individual-level analysis data were drawn from two national surveys: the 1984 National Health Interview's supplement on Aging (SOA) (which we aged as described below) and the 1985 National Nursing Home Survey. The 1977 analysis, used the 1977 National Nursing Home Survey merged with the 1977 Health Interview Survey.
For the state-level analysis data were drawn from a variety of sources: the 1986 Area Resource File System (ARF); the 1984 Medicaid 2082 data set; 1976 and 1986 Medicare Enrollment Statistics; 1980 and 1989 Statistical Abstract of the United States; 1984 and 1986 Analysis of State Medicaid Program Characteristics; and the 1986 Inventory of Long Term Care Places.
The 1984 SOA, based on a multistage area probability sample, provides self-reported characteristics (such as conditions and impairments, and functional abilities) for 11,497 civilian noninstitutionalized people aged 65 and over. A more detailed description of the survey is provided by Fitti and Kovar (1987).
The 1985 NNHS is a stratified two-stage probability sample of nursing and related care homes, their residents and their staff, which contains sociodemographic, diagnostic, and functional status data for 5,243 current nursing home residents. Data were obtained via interviews with staff most familiar with the resident's medical record, and supplemented with phone interviews with the resident's family members. A more detailed description is provided by Hing (1987).
For the state-level analysis data were drawn from the 1986 Area Resource File System (ARF) and the 1986 Inventory of Long Term Care Places, as well as a variety of government publications. The ARF is a county-specific data base containing more than 7,000 variables concerning a wide range of social, economic, and health resource characteristics, and is described in detail elsewhere (Area Resource File, 1987).
Medicaid 2082 data sets contain annually compiled state-level data pertaining to Amount of Medicaid spending and number of recipients. The data are categorized by eligibility and service type.
The 1986 Inventory of Long Term Care Places (U.S. Department of Health Services, 1987a) was designed to provide a current sampling frame for nursing and related-care homes (and facilities for the mentally retarded) for the 1987 National Expenditure Survey, and therefore provides a comprehensive listing of nursing homes in the United States. It is also described in detail elsewhere (National Center for Health Statistics, 1987).
Medicare Enrollment Statistics were used as estimates of the elderly population. Enrollment data by age, sex, and race for each state and county in the United States are available from the Bureau of Data Management and Strategy at the Health Care Financing Administration (Medicare Enrollment Statistics, 1985).
Data were also compiled from Statistical Abstracts of the United States (U.S. Bureau of the Census 1982; 1987), and 1984 and 1986 Analysis of State Medicaid Program Characteristics (U.S. Department of Health and Human Services, 1985; 1987b).
INDIVIDUAL-LEVEL ANALYSIS
Analysis
Two national cohorts of institutionalized and noninstitutionalized aged were used for the individual level analyses. Analysis on the 1977 cohort was previously conducted and is described in detail elsewhere (Weissert and Cready, 1989).
For the later year anlysis the 1984 SOA and the 1985 NNHS were used to develop a weighted-logistic regression model to estimate the likelihood of institutional residency--that is being a resident of an institution at a given point in time, not of being admitted to an institution. Because data relate to a cross sectional sample of nursing home residents, they are more reflective of long-term stayers in nursing homes than short-term stayers. This is so, because while turnover rates tend to be high in nursing homes, the proportion of long stayers in a home at any given time greatly exceeds the proportion of short stayers (Keeler, Kane, and Solomon, 1981; and Lui and Manton, 1984). For the purposes of identifying characteristics of individuals who actually become nursing home residents and consume most nursing home resources, this type of sample is greatly superior to an admission cohort, which is dominated by short stay patients.
To conduct the analysis the SOA and the NNHS were concatenated. Because both surveys were designed to be representative samples of their corresponding populations, it was possible to devise a weighting strategy allowing for estimation which is representative of the nation (exclusive of Hawaii and Alaska).
The strategy bad to account for three factors. First, because the two surveys were collected at different sampling rates, the weights had to account for the "oversampling" of nursing home residents relative to their presence in the population. Additionally, the complex nature of the survey design on both data sets and the inconsistency in survey years between the two data sets had to be taken into account. To account for these three factors we developed three weighting procedures and a population inflation factor.
The first procedure normalizes the provided survey weight variable separately within each of the two data sets (the NNHS and the SOA) to sum to the actual sample size of each data set. Under such a weighting procedure appropriate coefficient estimates are produced for all parameters of interest except the intercept, and standard errors produced are equivalent to those produced with simple random sampling.
The second procedure has two parts. The first part normalizes the provided survey weight variable for the NNHS to sum to the actual sample size for the NNHS. The second part accounts for the oversampling of the nursing home population by multiplying the SOA weight from part one by the ratio of the true size of the nursing home sample to the size of the nursing home sample population. The parameter estimates produced with this procedure are equivalent to those produced under the first procedure, except for the intercept which is now correct.
The problem is that to account for the "oversampling" of the nursing home population the noninstitutionalized population is inflated, thus producing overstated significance levels and standard errors somewhat smaller than are appropriate. However, more appropriate standard errors can be calculated by multiplying the standard errors produced under this second procedure by an inflation factor composed of the median ratio of the standard errors produced under the first procedure to those produced under this procedure.
The third procedure accounts for the complex nature of the survey resign. The inflated standard error--produced from calculations combining the first and second procedure as described above--is adjusted relative to the mean square error (MSE) from a SAS supported procedure called RTILOGIT (Shah et al., 1984). This procedure uses the primary sampling unit and strata to account for the complex nature of the sampling design. (While the primary sampling unit was avaiable on both the public. use tapes, and the stratum was available on the SOA, we were forced to construst the strata for the NNHS.)
In summary, by adjusting standard errors produced under the second procedure by the inflation factor (median ratio of the standard errors produced under the first procedure to those produced under the second procedure), and by the ratio of the MSE from RTILOGIT relative to the second procedure, results which are compatible with the structure of the two samples are obtained.
Finally, because of the inconsistency in years between the SOA (1984) and the NNHS (1985) a population inflation factor was needed for the SOA. The purpose of the population inflation factor is to adjust the weights for the 1984 SOA data, making the weighted data set representative of the 1985 noninstitutionalized elderly population, and thus compatible with the 1985 NNHS.
Two data sets were used to construct the inflation factor: the 1984 SOA and the 1985 Health Interview Survey (National Center for Health Statistics, 1986). Comparing population estimates produced on the two allows for calculation of the rate of change in the noninstitutionalized population between 1984 and 1985. Growth rates were compared by age, sex, race, and region by fitting a logistic regression model that included age, sex, race, and region to a binary dependent variable indicating from which survey an individual came (see Table 1).
Results showed that rates of growth did not vary significantly by age, sex, race, or region, thus indicating that a single inflation factor (1.0231) could be used to reweight the 1984 SOA. After reweighting, the SOA was merged with the NNHS. It was this merged data set on which the later year individual-level analysis was conducted. The SAS procedure PROC LOGIT (SAS Institute Inc., 1985) was used in combination with the three weighting procedures as described above to develop the logistic regression model.
Combined, the data sets represent substantially the entire aged population in the coterminous United States, excluding persons who reside in long-term institutional facilities other than nursing homes. (Predominant among these would be mental institutions and board and care homes.) Thus, results are in general representative of the national elderly population.
Variable Definitions
The dependent variable for the analysis, residency status, was coded '1' for nursing home residents and '0' for SOA respondents. Merger of the two data sets required construction of a single set of comparable variables. While identical variable definitions were available on both data sets for the majority of explanatory variables, in a few instances comparable constructs had to be developed.
Sociodemographics, Prior Nursing Home Use, and Geographic Residency. With minimal recoding age, gender, race, marital status, having living children, having previously resided in a nursing home, residence in a metropolitan area, and residence in the midwest were identically available on both data sets. Age was coded as a continuous variable that reflected age at interview and ranged from 65 to 108. The others were each coded as dichotomous variables with males, whites, those not currently married, those having living children, those having previously resided in a nursing home, those residing in a metropolitan area, and those residing in the Midwest coded 1; others were coded 0.
Functional Dependency. Dependency in activities of daily living was also available on both data sets. Dichotomous variables were created for each of six activities of daily living (ADLs): bathing, dressing, toileting, continence, transferring, and eating. Bathing and transferring were coded 1 if the respondent currently received human assistance in performing the activity, and 0 otherwise. Dressing, toileting, and eating were coded 1 if the respondent currently received human assistance in performing the activity or did not engage in the activity, and 0 otherwise. Last, a dichotomous variable was created for incontinence status. If the respondent received human assistance with a device (such as a catheter or ostomy), or was bowel or bladder incontinent once a week or more, the incontinent variable was coded 1; otherwise it was coded 0.
In addition to these six dichotomous variables four dependency recodes were constructed for use in the analysis. The first was a count of how many activities in which the respondent was dependent (coded 0 to 6). The second was a dichotomous variable reflecting whether or not the respondent was dependent in any of five (bathing, dressing, toileting, transferring, or eating) activities (coded 1 if dependent in any of the five; 0 otherwise).
Finally individuals were classified by their most severe functional dependency into one of two mutually exclusive groups. In order of severity the groups were: (1) receives human assistance toileting or eating, or both and (2) receives human assistance bathing or dressing, or both, but does not receive human assistance toileting or eating. Each of the two variables was coded 1 to reflect dependency, and 0 otherwise.
An additional third level, mobility dependency, was added to the severity pair. Individuals who were neither toileting or eating dependent, nor bathing or dressing dependent were coded 1 if they received human assistance in walking or transferring, or if they were bedfast or chairfast; otherwise they were coded 0.
In addition a separate variable, regardless of other functional dependencies, indicating whether or not the individual was bedfast or chairfast was constructed. For respondents from both the NNHS and the SOA individuals were coded 1 if they were bedfast or chairfast, or both, and 0 otherwise.
Poverty Status. Poverty, also a dichotomous variable, was coded 1 for those determined to be living in poverty, and 0 for all others. However, for this variable identical constructs were not available on both data sets.
For respondents to the SOA residing in poverty was defined by a poverty index which was available on the public use data set. The index is based on family size, number of children under 18 years of age and family income using 1983 poverty levels published by the Census Bureau in August of 1984. For several respondents this item was missing. Therefore, for any respondent for which the poverty index was missing, but for whom household size was known and household income was known to be greater than or equal to $20,000 the poverty variable also was coded 0. This was a justifiable imputation, because cross tabulations of $20,000 income indicator variable and the household size variable indicated that each of the respondents with household income greater than or equal to $20,000 fell well above 1983 federal poverty levels given household size (U.S. Census Bureau, 1987).
For respondents to the NNHS no direct measure of income was available. Instead individuals were classified as living in poverty if any of their charges during their month of admission were paid by Medicaid, other state funded indigent care, other government assistance (excluding Medicare) or welfare, or if the payment source was undetermined.
The lack of comparability for the poverty status variable as defined on both data sets is unavoidable. Persons supported by Medicaid or other government assistance or welfare can, and perhaps often do, have incomes above the poverty line. However, they still represent the lower portion of the income distribution.
Mental Impairment and Diagnoses. Dichotomous variables were also developed for a series of diagnositic categories. For each diagnositic category the individual was coded 1 if they currently had at least one of the diagnoses included in the category.
For nursing home residents (1985 NNHS) current primary and other diagnoses were taken from the medical record. The 1985 NNHS used the Ninth Revision of the International Classification of Diseases (ICD-9) to code diagnoses.
For noninstitutionalized elderly (1984 SOA) diagnostic categories were generated from conditions listed in the Diagnostic Recode B file of the survey. This file primarily contains conditions mentioned in response to other questions on the SOA. Over 90 percent of the conditions were listed in response to questions regarding activity limitations, doctor's visits, hospitalizations or restricted activity days.
Although the 1984 SOA used specially created diagnostic codes, they are fully computable with ICD-9 codes for the level of diagnostic detail we desired. Thus, from these codes and the ICD-9 codes on the NNHS, we developed diagnostic categories which are comparable for both data sets. The diagnositic categories and their defining ICD-9 codes are shown in Table 2.
Simultaneity
Because of the cross sectional nature of the data set it is possible that characteristics which distinguish aged individuals in nursing homes from those in the community reflect the effects of institutional life rather than the cause of institutionalization. This is not of concern if our purpose is to discuss the correlates of nursing home residency or factors which awe indicative of residency status. However, if the model is to be used prospectively simultaneity becomes an important issue.
This is of particular concern with the poverty status variable and the functional dependency variables. To overcome this problem for the poverty status variable we used payer source upon admission. This should eliminate the simultaneity problem caused by the fact that many people become poor after they enter a nursing home and "spend down" their resources, prior to becoming Medicaid eligible (Burwell, Adams, and Meiners, 1988).
To evaluate the potential effects of simultaneity from the functional status variables we replaced these variables and corresponding interaction terms with instruments. Neither significance levels nor conclusions were found to be altered substantially by such a replacement.
Statistical Model and Hypotheses
Given the variables available on both data sets we hypothesized that residency status is a function of Sociodemographic Characteristics (age, sex, race, and poverty status), Social Support (marital status and living children), Functional Status (activities of daily living dependencies, mobility dependency, and bed/chair fast), Mental Impairment, Diagnoses (cancer, nervous system disorder, arthritis, cerebrovascular disorder, circulatory disorder, diabetes, hypertension, injuries, and respiratory disorder), Prior Health Care Use (previous nursing home admission), and Community Characteristics (region, and urbanization). Specifically we hypothesized that the likelihood of nursing home residency would increase with age, and was higher for females; whites; unmarried individuals; functionally dependent individuals; individuals with each system disorder; individuals residing in poverty, the midwest, and urban areas; and those who have previously been in a nursing home.
Results
Weighted logistic regression results are presented in Table 3. The model was statistically significant (X2=3981.28 with 19 df, p<.0001). The probability that the i-th individual resided in a nursing home is specified as
| Pi = exp(bo + XiB) / 1 + exp(bo + XiB) |
| where: Pi is the predicted probability for the i-th indiviudalexp is the exponential functionbo is an intercept termXi is a vector of explanatory variables, andB is a vector of coefficients. |
The final model included age, sex, race, marital status, children, prior nursing home use, poverty status, residing in the midwest, residing in a metropolitan area, being ADL dependent, number of ADL dependencies, being bed or chairfast, having arthritis, having Alzheimer's disease, having a mental diagnosis, having a disorder of the nervous system, and having cancer. Each of the explanatory variables except for gender were found to be significantly related (p <.05) to the likelihood of nursing home use. Although gender has sometimes been shown to affect nursing home use, it was not a significant factor in our model.
All pairwise interactions were tested, and only two were found to be significant: being ADL dependent interacted with prior nursing home residency and being ADL dependent interacted with having a mental disorder. The final model therefore consisted of all significant main effects, gender, and the two significant pairwise interactions.
Because the constructed poverty status variable was not available for a number of respondents on both data sets (11.6 percent of all respondents), we evaluated the similarity of missing respondents to individuals of known poverty status. Comparisions were made through cross tabulations of poverty status with each of the other variables in the model, as well as through logistic regression analysis. The latter was done by adding a third category to the poverty status variable, unknown poverty status. Results from both sets of analyses indicated that individuals of unknown poverty status are similar to those who are not in poverty, and similar in a manner which causes them to have a smaller likelihood of being a nursing home resident. Furthermore, logistic regression results did not significantly change when the unknown poverty category was collapsed with the not-in-poverty category. Because the results did not significantly change and because of the similarity of respondents with unknown poverty status to those known not to be in poverty, we elected to combine individuals with unknown poverty status with those known not to be in poverty. All results are reported using this combination.
Table 3 ranks by type--dichotomous and continuous/ordinal--each variable in descending order by estimated odds ratio (far right column). The odds ratio indicates the relative risk of institutionalization associated with a given trait. For a dichotomous variable the odds ratio represents the extent to which the chance of institutionalization is greater for an elderly person with the trait relative to one without the trait. For example, an individual who has a mental disorder has a 91.73:1 greater chance of nursing home residency than one who does not have a mental disorder, or an individual who is not married has a 5.09:1 greater chance of residing in a nursing home than an individual who is married. For a continuous variable the odds ratio represents the increased likelihood of nursing home residency for each additional unit of the trait held. For example, with each increasing year (i.e., age) the likelihood of institutional residency increases by 1.10.
Main effects with large positive odds ratios were mental disorder, ADL dependency and prior nursing home use. However, the effect of ADL dependency was found to differ by whether individuals had previously been in a nursing home and whether they had a mental disorder. Similarly the effects of prior nursing home use and mental disorders were found to vary by ADL dependency. Regardless of the level of those significant interaction variables, ADL dependency, prior nursing home use and mental disorder all had an odds ratio greater than one. Increases in the likelihood of nursing home residency also were associated with being not married, white, having Alzheimer's disease, living in the midwest, and living in a metropolitan area. An increase in the number of ADLs and age also produced substantial increases in the likelihood of nursing home residency. All other variables had a small negative effect on the likelihood of residency, including having cancer, being bedridden or chairfast, not being in poverty, having arthritis or rheumatism, and having a nervous disorder.
Since the model is based on cross-sectional data it does not imply causal relationships, but instead describes the similarity of an elderly individual to nursing home residents. Stemming from this is the potential problem of simultaneity, or that the distinguishing characteristics are not causes of institutional residency but in fact the effects of institutionalization.
Furthermore, due to the lack of availability of certain data items, the equation omits several important variables. In particular these include perceived health status and attitudes towards nursing home placement. Additionally, while a region and urbanicity variable were entered in the model, privacy concerns prevented us from other including other community variables such as the availability of nursing home beds, which are known to affect nursing home use rates. Interpretation of the estimated coefficients therefore must be undertaken cautiously since the importance of each may be distorted because the coefficient for any included variable is influenced by any omitted variables that are correlated with it (Kennedy, 1989).
1985 VS 1977 COMPARISON
Results from the 1977 individual-level analysis, including odds ratios, are presented in Table 4. Differences between those and the 1985 results are primarily among three sets of measures: mental illness; poverty; and other diagnoses. Though precise odds ratio comparison across the years are not appropriate due to differences in samples, variable definitions, and model specification, the substantial changes in the odds ratios for these three sets of variables warrant investigation.
Three types of explanations appear to be important: changes in variable definitions; changes in model specification; and true changes in the residency status of elderly individuals with a particular trait. Changes due to different samples should be minimal given that all four of the data sets used are nationally representative and used similar sampling frames in each year.
But some variable definition options changed in both surveys between the two years. For example, both used the ICD-9 codes in 1985 to collect diagnostic information. Data item collected also increased on both surveys. Living children and prior nursing home use, which were not available in 1977, were added in 1985. On the other hand, geographic identifiers were not available for the later data set, precluding addition of state-specific variables to patient records as was done in 1977.
Real changes are indicated by higher or lower proportions of the population residing in nursing homes in the two years after definitional differences have been controlled. Table 5 presents prevalence rates by residency for the two years under the 1977 definition. Also shown are the prevalence rates by residency in 1985 for the variables which were not available in 1977 or for which an altered definition was found to improve the 1985 model fit.
Residents with a mental disorder as defined using the 1977 definition were about as likely to reside in nursing homes in 1985 as they were in 1977: roughly 40 percent were nursing home residents in both years. However, using the 1985 definition--which excludes senility--, almost two thirds of individuals with mental disorders resided in nursing homes. In other words, when the disorder was specific or serious enough to be labeled something other than senility, the individual had about a two-thirds chance of residing in a nursing home in 1985, accounting for its greater importance as a predictor. Had the more precise definition been available in 1977, mental disorders might have been more important in the 1977 model.
Similarly, a more precise definition of poverty became available in 1985. Because of the potential simultaneity problems associated with poverty (i.e., elderly individuals often become poor upon admission to a nursing home), we elected to use payor status upon admission to reflect poverty status for nursing home residents in 1985, an option that was not available in 1977. (The previous analysis had available only current payor status.) Because the variable has been reversed (i.e., coded one reflects poverty in 1977 and not in poverty in 1985), appropriate odds ratio comparisons can be made by taking the inverse of one of the odds ratios. Thus, residing in poverty, which had an odds ratio of 3.36 in 1977, had an odds ratio of 5.26 (1/0.19) in 1985, meaning that being in poverty increased the likelihood of nursing home residency by more in 1985 than in 1977.
In comparison to mental disorders and poverty, the importance of other diagnoses appear to have diminished between the two years. Each of the diagnoses variables which were available for inclusion in the 1977 model were also available for inclusion in the 1985 model. However, many were found to no longer be significant (e.g., diabetes, circulatory diseases, respiratory disease, and injuries), or to have diminished in importance (e.g., nervous system disorders, cancer, and arthritis), regardless of the definition employed. In fact the nervous system disorders variable found to produce the best fit in the 1985 model was a broader one than the one used in 1977. In 1977 it included only Parkinson's disease, multiple sclerosis, and epilepsy, but, in the later year it included all nervous system disorders including sensory impairments and a variety of other problems likely to be noteworthy to a community resident but not important enough to list as a diagnosis in a nursing home chart filled with multiple disabling disorders. This probably explains its drop in odds ratio to less than one, indicating a small negative association with nursing home residency.
Nonetheless, prevalence rates for seven disorders did change substantially suggesting that individuals with those problems were treated differently in 1985 versus 1977. Five conditions less likely to be associated with nursing home residence in 1985 compared to 1977 were (Table 5): arthritis/rheumatism; circulatory disease; diabetes; and a multiple disease category called cancer, anemia, kidney and digestive disease. Although individuals with an injury were more likely to be nursing home residents in 1985 than in 1977, the presence of an injury was not a significant predictor of nursing home residency when controlling for other factors in 1985.
Beyond these three domains (mental illness, poverty and other diagnoses) little substantial change was found between the years. Although the importance of marital status appeared to decline, some of the explanation almost certainly lies in the presence in the 1985 model of another variable measuring social support: living children.
Prior nursing home use, which was available for inclusion in the 1985 model and not in the 1977 model, is likely to be an indirect indicator of poor social support, and in capturing some of variation which in 1977 was attributed to social support.
Taken together, these results indicate that what is most important in differentiating residents from nonresidents is functional ability, both physical and mental. Both the drop in predictive power of most diagnoses and the sorting out of mental disorders leads to the conclusion that institutionalization was best predicted in 1985 by focusing on behavioral rather than clinical indicators of need. Nursing home residents in 1985, as they did in 1977, suffered a multiplicity of breakdowns including physical and mental functioning, social support, mental disorders and financial resources. However, the importance of diagnoses other than mental disorders apparently diminished, while mental disorders, functional dependency, old age and social support continued to be important. Prior nursing home use which was found to be important in 1985, would most likely would have been important in 1977 had a measure been available for the model, and the significance of region and metropolitan area in 1985 probably reflected the continued importance of both the nursing home bed supply and style of practice variation.
STATE-LEVEL ANALYSIS
Variable Definitions
Candidate explanatory variables for analysis of change in predictors of statewide nursing home use rates included aggregate measures of each state's population, including age, sex, and race structure, socioeconomic status, and death rate; nursing home bed supply; and a variety of Medicaid policy variables (Table 6). Dollar values for the earlier year variables were adjusted for inflation with the Historical Consumer Price Index for All Urban Consumers (U.S. Department of Labor, 1987), and for both years for regional cost of living differences with average hourly earnings data from the U.S. Bureau of Labor Statistics (U.S. Bureau of the Census, 1987).
Our state-level conceptual model paralleled the individual level model. Thus, we expected nursing home use rates to be higher among states in which the population was older (ELDERLY POP, 75+ POP, 85+ POP), a greater percent of whom were white (WHITE) and female (FEMALE). Per capita income (INCOME) was expected to vary positively with use rates, while the number of Supplemental Security Income recipients (SSI RECPTS) was expected to vary inversely with nursing home use rates.
Use was expected to increase with broadened Medicaid eligibility. Hence, the ratio of the Medicaid eligible population to the poverty population (MCAID ELIGIBLES) was expected to vary positively with use rates, while status as a 209 B state (209B) was expected to decrease use rates. Additional indicators of Medicaid generosity, the average Medicaid payment per elderly recipient (MCAID PAY/RCPT) and the average Medicaid Home health care payment (MCAID HH PAY/RCPT), were also expected to vary positively with the nursing home use rate.
In addition, the level of urbanization in the state (METRO POP) was expected to vary positively with nursing home use. As was the supply of nursing home beds (NH BEDS), which varies regionally and within region by level of urbanization.
Because private pay price is not readily available for nursing home care we used the Medicaid state average per them payment to nursing homes (MCAID ICF, MCAID SNF) as a proxy for private pay price. Although Medicaid payments are always less than private pay charges, State Medicaid programs are mandated to set rates in accordance with actual costs, and may also account for private pay prices when establishing reimbursement rates (Harrington and Swan, 1984). We therefore hypothesized that nursing-home use rates would decrease as the Medicaid payment rate increased--an indication that the demand for nursing home care is price elastic, or downward sloping.
Although direct measures of the prevalence of functional dependency are not available at the state-level, functional dependency has been shown to be effectively modeled among the noninstitutionalized population by age, race and sex (Unger and Weissert, 1988; Elston, Koch and Weissert, forthcoming). As mentioned above, all three proxies are included in the model. Nor were direct measures of the prevalence of specific diseases available at the state-level. Instead, we used the death rate for persons age 65 and over (DEATH RATE) as a proxy.
Unfortunately, due to data constraints a number of variables were not available for entry in our state-level model. These included the availability of social support, and consumer preferences or the population's general attitude towards nursing home placement.
Analysis
Initially we conducted a multiple regression paired comparison test to determine whether contextual factors affecting nursing home use rates had changed significantly between 1976 and 1986. The paired multiple regression comparison test was in the form of
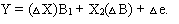 |
The dependent variable was the change in the number of nursing home residents per 1000 elderly state residents between 1986 and 1976. The explanatory variables in such a model are entered in pairs: both the later year (1986) and the change between the two years (1986's value less 1976's value). Because the coefficient on the later year reflects the change in the coefficient between the two years, this approach allows for the statistical testing of which of several policy factors differentially affected rates of state nursing home residency between 1976 and 1986.
As a result of the paired entry of explanatory variables (e.g., the later year and the change variables), results tend to be unstable due to the high degree of multicollinearity present. We therefore elected to use the multiple regression paired comparison test as a means only to test whether significant differences existed between the two years, and to fit a separate ordinary least squares regression model to determine what factors affected nursing home use rates in 1986.
Each of these two models was checked for violations of the assumptions necessary for ordinary least squares regression such as heteroskedasticity, correlated error terms, and non-normality of errors. To correct for heteroskedasticity weighted least squares regression was used for both analyses. Weights were constructed by taking the inverse of the variance estimate pooled over both years. Cases found to be overly influential in either of the two models were individually dropped from the analysis, but subsequently reincluded because results and conclusions were not significantly altered by their elimination.
Results
Using the multiple regression paired comparison test, changes in the coefficients between the two years were evaluated for statistical significance. Results indicated that none of the coefficients changed significantly between the two years (Table 7). How much of this inability to detect a change is due to the exclusion of important variables such as a direct measure of the prevalence of ADL dependency, precise measures of changes in the adoption and effectiveness of a variety of health policy variables, such as pre-admission screening programs and nursing home payment methodology we cannot say. That fact that Medicare's hospital Prospective Payment System (PPS) apparently had no effect on rates of institutionalization may reflect the fact that only a relatively small proportion of nursing home residents could have been affected by PPS in 1985 (Hing, 1989).
The model found to best fit the 1985 data is shown in Table 8. Nursing home use rates increased as the percent of the state's elderly population over the age of 85 increased, as the percent of the poverty population covered by Medicaid increased, as the supply of nursing home beds increased, and as the average Medicaid payment per elderly Medicaid recipient increased. On the other hand use rates decreased as the ICF rate (a proxy for private price) increased, as the state's total population increased, and as the percent of the state's population over 65 increased. Per capita income was found not to significantly affect nursing home use rates. This model fit expectations quite well.
However, possible endogeneity exists with the Medicaid ICF rate, as well as with the Medicaid average payment, and the supply of nursing home beds. To adjust for these effects, we re-estimated the 1986 model using weighted two-stage least squares regression using the SAS procedure PROC SYSLIN.
Two-stage least squares regression requires the specification of instrumental variables which can be substituted for each included endogenous variable in the system of equations. In the first stage each endogenous variable (e.g., Medicaid ICF rate, Medicaid average payment rate, and nursing home bed supply) was regressed on all exogenous variables in the system. In the second stage, the estimated values generated in the first stage for each of the endogenous variables were substituted for the actual values in the regression equation.
The weighted two stage least squares results are shown in Table 7. As expected results did not differ substantially from the weighted ordinary least squares estimation. Each of the variables remained significant (p<.10), except the per capita income variable which remained nonsignificant. Furthermore, none of the estimated coefficients for the significant variables changed substantially in magnitude, and none changed in sign.
DISCUSSION
Recent reviews of the risk of institutionalization literature by Kane and Kane (1987) and Shapiro and Roos (1989) have shown that despite differences in the definitions of measures used, and varying study populations and research methodologies, age, social support, mental impairment, and functional dependency have continually been shown to be significantly associated with nursing home placement. However, all of the studies reviewed were conducted using pre-1980 data, and thus, it is reasonable to question whether the same factors predict nursing home placement today.
Using both individual- and state-level, mid-1980 data, the purpose of this study was to determine what factors affect nursing home residency status, and to examine how these factors have changed over the past decade. Findings here confirm the resiliency of previously confirmed risk factors at both the individual- and state-level. Specifically, our findings confirm that the likelihood of nursing home residency continues to be greater with the presence of a mental disorder, functional dependency, lack of social support, and increasing age. Additionally, we found the likelihood of nursing home residency to be greater if an individual had previously been in a nursing home, had Alzheimers disease, was poor, or resided in the Midwest.
Changes, to the limited extent that there were any, generally suggest an increasing focus in the more recent year on behavioral indicators of need rather than clinical diagnoses. In state-level analysis, however, no significant changes were detected between the two years. But, the 1985 state-level nursing home use model produced results generally supportive of the 1985 individual level model.
The apparent resiliency of these nursing home risk factors lends support for their inclusion in nursing home and home care preadmission screening (PAS) instruments which are intended to identify likely nursing home users. Furthermore, results across the two years appear to be similar. The relative importance of several highly predictive measures: ADL dependency, mental disorder, lack of social support, and age, has not changed substantially. Likewise, race, poverty and region remained moderately important. But, diagnoses, other than specific mental disorders, became much less important. Prior nursing home use, an addition to the model in 1985, proved to be an important positive predictor of nursing home residency.
This finding of little shift in importance of the major predictors is an especially important finding because while there is substantial agreement in the field on which variables are predictors, the field has seen continued discrepancy in the relative weights assigned to these risk factors in predicting nursing home residency. In this study, which used nationally representative data sets for two widely separated time periods and estimated different models, the most important predictors proved robust in relative as well as overall importance.
The authors gratefully acknowledge the assistance of Professor Willard Manning, Department of Health Services Management and Policy, School of Public Health, University of Michigan for early assistance in specification of the multiple regression paired comparison model used to evaluate change in state use rates. Errors, if any, are the responsibility of the authors.
REFERENCES
Area Resource File (ARF) System. (February 1987) ODAM Report No. 4-87, Department of Health and Human Services. Baltimore.
Booth T. (1986) "Institutional Regimes and Induced Dependency in Homes for the Aged." The Gerontologist. 26(4):418-423
Branch, LG and AM Jette. (1982) "A Prospective Study of Long-term Care institutionalization Among the Elderly." American Journal of Public Health. 72(12):1373-1379.
Brock, AM and P O'Sullivan. (1985) "A Study to Determine What Variables Predict Institutionalization of Elderly People." Journal of Advanced Nursing. 10:555-557.
Burwell, B, EK Adams, and M Meiners. (November 1988) "Spend-Down of Assets Prior to Medicaid Eligibility Among Nursing Home Recipients in Michigan." SysteMetrics/McGraw-Hill.
Chiswick, B. (1976) "The Demand for Nursing Home Care: An Analysis of the Substitution Between Institutional and Non-institutional Care." Health Care Financing Review. 1(4):47-63.
Cohen, MA, EJ Tell and SS Wallack. (1986) "Client-Related Risk Factors of Nursing Home Entry Among Elderly Adults." Journal of Gerontology. 41(6):785-792.
Dunlop, B. (1976) "Determinants of Long-term Care Facility Utilization by the Elderly: An Empirical Analysis." Working Paper 963-35. Washington, DC: Urban Institute.
Evashwick, C, G Rowe, P Diehr, and L Branch. (1984) "Factors Explaining the Use of Health Care Services by the Elderly." Health Services Research 19(3):357-382.
Fitti, JE and MG Kovar. (1987) "The Supplement on Aging to the 1984 National Health Interview Survey." Vital and Health Stat. 1(21). U.S. Government Printing Office, Washington, DC.
Greenberg, JN and A Ginn. (1979) "A Multivariate Analysis of the Predictors of Long-term Care Placement." Home Health Care Services Quarterly. l(l):75-79.
Harrington, C and JH Swan. (1984) "Medicaid Nursing Home Reimbursement Policies, Rates, and Expenditures." Health Care Financing Review. 6(l):39-49.
Hing, E. (May 14, 1987) "Use of Nursing Homes by the Elderly: Preliminary Data from the 1985 National Nursing Home Survey." Advanced Data, National Center for Health Statistics, No. 135.
Hing, E. (March, 1989) "Effects of the Prospective Payment System on Nursing Homes" Vital and Health Stat. 13(95). U.S. Government Printing Office; Washington, DC.
Kane, RA and RL Kane. (1987) Long-Term care: Principles, Programs and Policies. Springer Publishing Company: New York.
Keeler, E, R Kane, and D Solomon. (1981) "Short- and Long-Term Residents of Nursing Homes." Medical Care 11:363-.
Kennedy, P. (1989) A Guide to Econometrics. The MIT Press: Cambridge.
Liu, K and KG Manton. (1984) "The Characteristics and Utilization Patterns of an Admission Cohort of Nursing Home Patients (II)." The Gerontologist 24:70-76.
Medicare Enrollment Statistics. (1976 and 1986) Table AE10 Hospital and/or Medical Insurance for Persons by Age, Race, Sex, and Place of Residence as of 07/01/76 and 07/01/86. The Health Care Financing Administration (Medicare) BDMS, SSIB DIA.
McCoy JL and BE Edwards. (1981) "Contextual and Demographic Antecedents of Institutionalization Among Aged Welfare Recipients." Medical Care 19(9):907-921.
National Center for Health Statistics. (1986) "Public Use Data Tape Dsocumentation: National Health Interview Survey 1985." Hyattsville, MD.
National Center for Health Statistics. (1987) "Public Use Data Tape Documentation: 1986 Inventory of Long-Term Care Places." Hyattsville, MD.
National Center for Health Statistics. (198?) "1985 NNHS Microdata Tape Documentation"
Palmore, E. (1976). "Total chance of Institutionalization Among the Aged." The Gerontologist 16(6):504-507.
SAS Institute Inc. (1985) Sas Users Guide: Statistics, Version 5 Edition. Cary, NC: SAS INstitute Inc.
Shah, BV, RE Folsom, FE Harrell, and CN Dillard. (1984) Survey Data Analysis Software for Logistic Regression. Research Triangle Institute. Research Triangle Park, NC.
Shapiro E, and NP Roos. (1989) "Predictors and Patterns of Nursing Home and Home Care Use." in MD Peterson and DL White, eds. Health Care of the Elderly. Sage Publications: Newbury Park.
Scanlon, WJ. (1980) "A Theory of the Nursing Home Market." Inquiry 17:25-41.
Shapiro, E and RB Tate. (1985) "Predictors of Long-term Care Facility Use Among the Elderly." Canadian Journal on Aging. 4(1):11-19.
Swan, JH, and C Harrington. (1987) "Estimating Undersupply of Nursing Home Beds in States." Health Services Research. 21(l):57-83.
U.S. Bureau of the Census. (1982) Statistical Abstract of the United States: 1982. U.S. Government Printing Office, Washington D.C.
U.S. Bureau of the Census. (1987) Statistical Abstract of the United States: 1987. U.S. Government Printing Office, Washington D.C.
U.S. Department of Health and Human Services. (1985). Analysis of State Medicaid Program Characteristics, 1984. HCFA Pub. No. 03204
U.S. Department of Health and Human Services. (1987a). Analysis of State Medicaid Program Characteristics, 1986. HCFA Pub. No. 03249
U.S. Department of Health and Human Services. (1987b) Public Use Data Tape Documentation: 1986 Inventory of Long-Term Care Places.
U.S. Department of Labor, Bureau of Labor Statistics. (April 1987) CPI Detailed Report. Washington.
Vicente, L, JA Wiley and RA Carrington. (1979) "The Risk of Institutionalization Before Death." The Gerontologist. 19:361-367.
Weissert, WG and CM Cready. (1989) "Towards a Model for Improved Targeting of Aged at Risk of Institutionalization." Health Services Research. 24:4:475-510.
TABLES
| TABLE 1. Logistic Regression Results: Population Inflation FactorDependent Variable = Survey Year (1984/1985) | ||||
| Variable | Estimate | Standard Error | Chi- Square | Prob.a |
| Age 75 or older | -.001888 | .0138504 | 0.02 | 0.8916 |
| Female | -.005491 | .0136951 | 0.16 | 0.6885 |
| Black | .001937 | .0247138 | 0.01 | 0.9375 |
| Northeast | -.026077 | .0240842 | 1.17 | 0.2789 |
| Midwest | .010491 | .0235058 | 0.20 | 0.6554 |
| West | -.022385 | .0216505 | 1.07 | 0.3012 |
| Intercept | .073837 | .0256233 | 8.30 | 0.0040 |
SOURCE: 1984 Supplement on Aging and 1985 Health Interview Survey
|
||||
| TABLE 2. Diagnostic Categories | |
| Category | Corresponding ICD-9 Codes |
| Alzheimer's Disease | 331 |
| Arthritis/Rheumatism | 710-729 |
| Neoplasms | 140-239 |
| Malignant Neoplasms | 140-208 |
| Cerebrovascular Disorder | 430-438 |
| Circulatory Disorders | 390-459 |
| Ischemic/Pulm./Stroke/Art | 410-448 |
| Diabetes Mellitus | 250 |
| Hypertensive Disease | 401-405 |
| Injuries and Adverse Effects | 800-999 |
| Fractures | 800-829, 885-7, 895-7 |
| Ischemic Heart Disease/Myocardial Infraction/Agina | 410-414 |
| Mental Disorder/Alzheimer's | 290-319, 331 |
| Mental Disorder/Senility | 290-319, 797 |
| Mental Disorders | 290-319 |
| Cent. & Periph. Nervous System | 320-359 |
| Nervous System Disorders | 320-389 |
| Parkinson/MS/Epilepsy | 332, 340, 345 |
| Pneumonia/Influenza/Chronic Obs. Pulmonary Disease | 480-6, 490-6 |
| Respiratory Disorders | 460-519 |
| Bronchitis/Pneum./Other Resp. | 466, 480-519 |
| TABLE 3. 1985 Weighted Logistic Regression Model: Individual Level Analysis(1984 Supplement on Aging and 1985 Nursing Home Survey)a | ||||
| Independent Variable | Mean | Estimated Coefficient | Odds Ratio | |
| Confidence Intervalb | Point Estimate | |||
| DICHOTOMOUS | ||||
| Mental disorder | 0.03 | 4.5189 | 52.40-160.59 | 91.73 |
| ADL dependent | 0.11 | 4.4211 | 54.91-126.03 | 83.19 |
| Prior NH residency | 0.04 | 2.9062 | 10.20-32.80 | 18.29 |
| Not married | 0.47 | 1.6269 | 3.80-6.81 | 5.09 |
| White | 0.91 | 1.4240 | 2.74-6.30 | 4.15 |
| Alzheimers | 0.01 | 1.3816 | 2.45-6.48 | 3.98 |
| Midwest region | 0.26 | 0.8471 | 1.83-2.97 | 2.33 |
| Metropolitan area | 0.63 | 0.4065 | 1.19-1.89 | 1.50 |
| Male | 0.40 | 0.2824c | 1.03-1.71 | 1.33 |
| Has living children | 0.82 | -0.6135 | 0.42-0.69 | 0.54 |
| Cancer | 0.12 | -1.2240 | 0.20-0.43 | 0.29 |
| Bedridden or chairfast | 0.06 | -1.4046 | 0.18-0.33 | 0.25 |
| Not in poverty | 0.86 | -1.6724 | 0.15-0.24 | 0.19 |
| Arthritis/rheumatism | 0.50 | -1.7271 | 0.14-0.22 | 0.18 |
| Nervous system disorders | 0.52 | -2.6884 | 0.05-0.09 | 0.07 |
| CONTINUOUS/ORDINAL | ||||
| Number of ADL's | 0.40 | 0.6801 | 1.81-2.15 | 1.97 |
| Age | 73.76 | 0.0931 | 1.08-1.11 | 1.10 |
| ADL dep. * Prior NH | 0.02 | -1.7217 | 0.09-0.34 | 0.18 |
| ADL dep. * Mental disorder | 0.02 | -2.5671 | 0.04-0.15 | 0.08 |
| Intercept | -13.7782 | |||
|
||||
| TABLE 4. 1977 Weighted Logistic Regression Model: Individual Level Analysis(1977 Health Interview Survey and 1977 Nursing Home Survey)a | ||||
| Independent Variable | Mean | Estimated Coefficient | Odds Ratio | |
| Confidence Intervalb | Point Estimate | |||
| DICHOTOMOUS | ||||
| Toileting/Feeding dependent | 0.05 | 4.3097 | 54.25-102.07 | 74.42 |
| Bathing/Dressing dependent | 0.05 | 3.5137 | 24.99-45.10 | 33.57 |
| Mental disorder | 0.07 | 2.7786 | 12.45-20.81 | 16.10 |
| Cancer/anemia/kidney/digestive disease | 0.05 | 2.2505 | 6.95-12.96 | 9.49 |
| Circulatory disease | 0.22 | 2.0645 | 6.16-10.08 | 7.88 |
| Not married | 0.47 | 1.8395 | 4.57-8.67 | 6.29 |
| White | 0.91 | 1.5038 | 2.99-6.77 | 4.50 |
| Poverty | 0.23 | 1.2111 | 2.63-4.28 | 3.36 |
| Nervous system disease | 0.01 | 0.9926 | 1.34-5.4 | 2.70 |
| Injury | 0.04 | 0.9903 | 1.84-3.93 | 2.69 |
| Diabetes | 0.03 | 0.9138 | 1.63-3.81 | 2.49 |
| Respiratory disease | 0.05 | 0.6705 | 1.26-3.03 | 1.96 |
| Arthritis/Rheumatism | 0.11 | 0.5938 | 1.37-2.40 | 1.81 |
| Mobility dependent | 0.06 | 0.5438 | 1.24-2.39 | 1.72 |
| Male | 0.41 | 0.1195c | 0.86-1.47 | 1.13 |
| CONTINUOUS | ||||
| Age | 73.47 | 0.0358 | 1.02-1.05 | 1.04 |
| Unoccupied N.H. beds | 7.11 | 0.0197 | 1.01-1.03 | 1.02 |
| Heating-degree days | 4,772.62 | 0.0001 | 1.00-1.00 | 1.00 |
| Intercept | -13.7611 | |||
Reprinted from Weissert, W.G. and Cready, C.M. "Toward a Model for Improved Targeting of Aged at Risk of Institutionalization." Health Services Research, October 1989, Vol. 24 No. 4. pp 485-510. |
||||
| TABLE 5. Percent Distribution of Demographic, Social, Dependency, and Diagnostic Characteristics of Elderly Individuals by Residency Status and Year | ||||
| 1977 | 1985 | |||
| Nursing Home Residents | Community Residents | Nursing Home Residents | Community Residents | |
| Age | ||||
| 65-74 | 1.5% | 98.5% | 1.3% | 98.7% |
| 75+ | 10.3 | 89.7 | 9.6 | 90.4 |
| Gender | ||||
| Male | 3.1 | 96.9 | 2.9 | 97.1 |
| Female | 6.0 | 94.0 | 5.8 | 94.2 |
| Race | ||||
| Nonwhite | 3.6 | 96.4 | 3.4 | 96.6 |
| White | 5.0 | 95.0 | 4.8 | 95.2 |
| Marital Status | ||||
| Married | 1.1 | 98.9 | 1.1 | 98.9 |
| Unmarried | 9.1 | 90.9 | 8.5 | 91.5 |
| Living Children | ||||
| No | NA | NA | 8.12 | 91.9 |
| Yes | NA | NA | 3.64 | 96.4 |
| Poverty | ||||
| No | 2.9 | 97.1 | 3.0 | 97.0 |
| Yes | 14.5 | 85.5 | 15.0 | 85.0 |
| Prior Nursing Home Use | ||||
| No | NA | NA | 2.7 | 97.3 |
| Yes | NA | NA | 47.8 | 52.2 |
| Level of Dependency | ||||
| No human ADL or mobility help needed | 0.4 | 99.6 | 0.4 | 99.6 |
| Human help needed in mobility | 2.4 | 97.6 | 0.6 | 99.4 |
| Human help needed in bathing/dressing | 35.9 | 64.1 | 22.0 | 78.0 |
| Human help needed in toileting/feeding | 63.3 | 36.7 | 55.5 | 44.5 |
| Bed or Chairfast | NA | NA | 35.1 | 64.9 |
| Diagnostic Groups | ||||
| Respiratory disease | 7.7 | 92.3 | 10.3 | 89.7 |
| Arthritis/Rheumatism | 11.7 | 88.3 | 2.0 | 98.0 |
| Injury | 17.9 | 82.1 | 25.6 | 74.4 |
| Circulatory disease | 18.4 | 81.6 | 5.0 | 95.0 |
| Diabetes | 22.2 | 77.8 | 5.8 | 94.2 |
| Parkinson's/MS/Epilepsy | 24.9 | 75.1 | 28.0 | 72.0 |
| Nervous system disease1 | NA | NA | 6.9 | 93.1 |
| Parkinson's/MS/Epilepsy | 24.9 | 75.1 | 28.0 | 72.0 |
| Cancer, anemia, kidney trouble and/or digestive disease | 37.3 | 62.7 | 6.3 | 93.7 |
| Cancer1 | NA | NA | 2.4 | 97.6 |
| Mental disorder | 42.6 | 57.4 | 39.8 | 60.2 |
| Mental disorder excluding senility1 | NA | NA | 60.2 | 36.0 |
| Alzheimer's1 | NA | NA | 38.2 | 61.8 |
| All Elderly | 4.8 | 95.2 | 4.6 | 95.4 |
|
||||
| TABLE 6. State Level Multiple Regression Paired Comparison Test: 1976 Versus 1985a | ||
| Variable | Coefficient | Prob >ITI |
| POPULATION | ||
| Changeb | -0.000186 | .18 |
| 1985 | 0.000005 | .73 |
| ELDERLY POP | ||
| Change | -0.732379 | .59 |
| 1985 | 0.419336 | .60 |
| 85+ POP | ||
| Change | 1.296995 | .28 |
| 1986 | -0.394605 | .56 |
| MCAID ELIGIBLES | ||
| Change | 0.016124 | .58 |
| 1982 | 0.002266 | .95 |
| INCOME | ||
| Change | -0.001243 | .01 |
| 1985 | 0.000287 | .24 |
| MCAID ICF RATE | ||
| Change | 0.046686 | .75 |
| 1985 | -0.104051 | .30 |
| MCAID PAY/RCPT | ||
| Change | 0.000531 | .32 |
| 1984 | 0.000026 | .97 |
| NH BEDS | ||
| Change | 0.825419 | .00 |
| 1986 | -0.081002 | .12 |
| Intercept | 5.535780 | |
|
||
| TABLE 7. Weighted Least Squares and Weighted Two-Stage Least Squares Regression Results: State Nursing Home Use Rates, 1986a | ||||
| Variable | Weighted Least Squaresb | Two-Stage Least Squaresc | ||
| Coefficient | Prob>ITI | Coefficient | Prob>ITI | |
| POPULATION | -0.000017 | .014 | -0.000018 | .005 |
| ELDERLY POP | -0.616963 | .045 | -0.774862 | .047 |
| 85+ POP | 0.713436 | .006 | 0.840121 | .015 |
| MCAID ELIGIBLES | 0.073529 | .000 | 0.071500 | .004 |
| INCOME | -0.000025 | .870 | 0.000003 | .989 |
| MCAID ICF RATE* | -0.152053 | .003 | -0.166272 | .056 |
| MCAID PAY/RCPT* | 0.000579 | .010 | 0.000633 | .086 |
| NH BEDS* | 0.789043 | .000 | 0.767625 | .001 |
| Intercept | 7.876152 | 9.537790 | ||
* For these variables the two-stage estimates represent estimated coefficients using predicted values, not actual values. |
||||
