Burton D. Dunlop, Ph.D., and James A. Wells, Ph.D.
Project HOPE, Center for Health Affairs
"This report was prepared under grant #ASPE210A between the U.S. Department of Health and Human Services (HHS), Office of Family, Community and Long-Term Care Policy (now known as the Office of Disability, Aging and Long-Term Care Policy) and Project HOPE. For additional information about the study, you may visit the DALTCP home page at http://aspe.hhs.gov/daltcp/home.shtml or contact the ASPE Project Officer, Pamela Doty, at HHS/ASPE/DALTCP, Room 424E, H.H. Humphrey Building, 200 Independence Avenue, SW, Washington, DC 20201. Her e-mail address is: Pamela.Doty@hhs.gov.
SECTION 1: OVERVIEW AND SIGNIFICANCE
Use of nursing home care is typically a last resort for both the disabled elderly individual and the individual's family (Stone et al., 1987; Doty, 1986; Soldo and Manton, 1985; Dunlop, 1980). Attempts to substitute formal home-based care consisting of skilled nursing and personal care, homemaking, and chore services for nursing home care have been disappointing. Higher costs associated with use of formal services, with little or no offsetting reduction in nursing home admissions, reflect largely additional services provided to persons who would not have entered a nursing home even in the absence of the in-home services program (Thornton et al., 1988; Kemper et al., 1987; Weissert, 1986; 1985). Hughes et al. (1987) did find that in-home services reduce use of lighter care nursing homes. Branch et al. (1988) found that the key predictors of nursing home admissions are quite different from those for use of medical home care.
To date, however, home-based care has been evaluated only broadly, with little attention to potential variability in outcomes according to specific caregiving arrangements. A very small number of studies have attempted to assess differences in outcomes among experimental subpopulations, but these efforts have been inconsistent and plagued by small sample sizes (Kemper et al. 1987). Probably the most careful analysis of differential impacts on subpopulations was carried out in the evaluation of the Channeling Demonstration. Overall, impacts did not vary by subpopulation in any clear cut pattern.
Theory, notably by Litwak (1985), suggests that some sources of caregiving or combinations of caregiving sources may work better than others. Staging theories of health care utilization imply that if informal support or care were available, ill persons would seldom reach formal care. Applied to a very old, disabled population, however, this theory would predict at best only a delay in formal care use rather than its prevention. Extended further, this line of reasoning also would predict postponement of death for those with informal care.
The specific aim of the study reported here is to determine whether home-based care, when provided by certain types of caregivers or by particular combinations of caregiver types, is more efficacious than other home-based care arrangements in preventing or delaying mortality and admission to a nursing home for elderly persons with dependencies in activities of daily living. The comparison groups examined include functionally impaired elderly receiving help vs. no help, paid vs. unpaid help, and help from immediate family vs. help from more distant relatives or nonrelatives, as well as help from paid and unpaid sources vs. help from unpaid sources alone. If some caregiving arrangements rather than others result in improved outcomes, policy makers will be in a better position to target resources for home-based care where those more effective arrangements exist or can be created.
The analyses relied on data from the Longitudinal Study of Aging, consisting of elderly aged 70 years and older, living in the community, originally interviewed in 1984, and followed through 1986. Outcomes derive from linkages to the National Death Index (mortality) and the Medicare Part A data (nursing home admissions). Statistical methods appropriate to a prospective cohort design are used to analyze the data, viz., survival analysis and logistic regression of dichotomous outcomes.
1.1 Background and Hypotheses
The prevalence of impaired functioning in carrying out Activities of Daily Living (ADL) appears to progress in an monotonic pattern over the life course of the elderly population in the U.S. Analyzing data from the 1984 Supplement on Aging of the National Health Interview Survey, Dunlop and Wells (1988), found that elderly persons 65-69 years of age experience, on average, 0.3 ADL dependencies, while those 95-99 report 2.1 ADL dependencies. Consequently, barring unforeseen medical breakthroughs, the number of persons in the population with ADL dependencies will increase as the number of older elderly individuals continues to rise.
Meeting these needs with a medical service model over the long-term often is inappropriate, and institutionalization may be expensive and may lead to more rapid functional or physiological decline by encouraging the dependency characteristic of institutional environments. As is now widely recognized, many impaired elderly individuals already receive help from friends, neighbors, and especially relatives (Stone et al., 1987a, 1987b; Doty, 1986; Doty et al., 1985); and this help may be at least as efficacious as the help provided by institutions or even paid home care providers.
In 1982, formally provided services in the home from home health or homemaker agencies constituted less than 15 percent of all "helper days of care" (Doty et al., 1985). Overall, families tend to use a lower volume of formal services than professional assessors judge they need (Stoller and Pugliesi, 1988; Noelker and Townsend, 1987). All of the available evidence strongly suggests that, except for some emotional support and chore and errand services provided by friends and neighbors, formal in-home service use tends to supplement informal care and does not replace it (e.g., Christianson, 1988; Moscovice et al., 1988; Noelker and Townsend, 1987). Use of formal services, in fact, can be a good predictor (though not necessarily a cause), of both institutionalization and death (Newman and Struyk, 1990; Hanley et al., 1990), perhaps because these services often are used in conjunction with informal care only after the care recipient has become very ill or incapacitated. This phenomenon means that in any assessment of impact of formal service provision on these outcomes, health status needs to be carefully controlled for.
Informal caregivers, usually family members, may experience worsening mental health and decreased social involvement (George, 1987). There is some indication that they also may experience financial difficulties and physical illness as a result of the burden of providing care. The utilization of part-time paid help amounts to almost half of all community services utilized by caregivers (George, 1987). Thus, there is a corollary (often implicit) argument among those who advocate expansion of formal home-based care as a means of reducing institutionalization and of improving the quality of life of the impaired elderly. It is that paid help relieves or lessens the caregiving burden for unpaid caregivers, so that they are able to provide better care for a longer period of time (Noelker and Toensend, 1987). Although it is hypothesized in this study that unpaid help is better than paid help alone in reducing institutionalization and death (because it is better suited to the provision of continuous or "demand" assistance), some combination of paid and unpaid help may be more effective than either alone or than even some other tandem configurations of caregiving in delaying institutionalization or death.
The potential direct effect of formal home care on mortality is undoubtedly less obvious than that on nursing home admission. However, formal home care may affect mortality in one or more of several ways. When professional caregivers are present, conditions needing medical attention may be recognized more quickly. This attention may be especially important for the elderly lacking informal caregivers. In the joint caregiving situation, informal caregivers may find more time to provide additional care or emotional support to the recipient, thereby potentially enhancing the recipient's well-being and "will to live". Litwak suggests that joint provision, when complementary, (i.e., with the formal sources providing the skilled or routine care and the family the emotional and nonuniform care) would comprise the optimal arrangement. Then too, formal caregivers, especially when they are skilled professionals, may teach the family better techniques of providing quasi-skilled care (e.g., cleansing catheter, use of oxygen for those with COPD), thereby improving the recipient's physical condition and, perhaps, preventing a traumatic hospital admission. They also may convince the family which has been providing excessive care to let the patient do more for himself or herself, thereby reducing the patient's dependency and enhancing self-efficacy and "will to live" (Ulbrich and Warheit, 1989).
On the other hand, the joint caregiving situation, with each party vying to be useful or to control the situation, could end up administering excessive care and induce more rapid functional and physiological decline of the impaired elder. Such induced dependency or sense of loss of control or autonomy could contribute to loss of the "will to live", as well; or formal service provision may somehow contribute to the reduction of interaction with friends and the emotional support and well-being that these friendships provide. One or more of these processes may help explain recent findings in a number of studies that use of formal home care services is a good predictor of institutionalization (Hanley et al., 1990; Newman et al., 1990). The more obvious explanation that persons receiving formal services are sicker is possible, of course, although these analyses just cited included specific controls for health and functional status.
According to Litwak and other group theorists, primary social relationships are characterized by face-to-face contact, emphasize small groups with diffuse ties, and are based on affection and long-term commitment. Such contacts typically involve relatives and friends. They also may include, to a lesser degree, neighbors, workmates or schoolmates. These relationships may be contrasted with formal relationships, especially insofar as the latter are specialized, economically motivated, and lack long-term commitment.
Litwak (1985) argues that due, in part, to their flexibility, primary group networks overall are better suited structurally than are formal organizations for providing personal services, such as those required by persons with ADLs or IADL deficits. Litwak's theory also posits that these nonuniform tasks are primary group-specific, such that some tasks appropriate for spouses or children are not appropriate for friends or neighbors or even for other more distant relatives. Litwak also argues that tasks which are uniform and require expertise are best provided by formal organizations. This group structure theory turns on the notion of optimizing the fit between the provider's capabilities (determined by structure) and the recipient's needs (the tasks required). A better fit should mean a greater provision of services over a longer period. In the end, better fit of services should be reflected in improved long-term outcomes such as avoidance of institutionalization and greater longevity for the care recipient.
Thus, once it is established that some type of help with significant functional debility is better than none, this theory would seem to argue: 1) that unpaid (primary group) help is better than paid (formal group) help; 2) that unpaid help from close relatives, because of the presence of more intense feelings of affection and commitment, is better than unpaid help supplied by more distant relatives; and 3) that help from both formal and informal sources is better than help from either alone because the joint caregiving arrangement provides a balance in functions. The informal meets the idiosyncratic, unpredictable and simple care needs while the formal provides the skilled, uniform, and predictable services the client requires.
1.2 Hypotheses
-
For persons with ADLs or IADLs, primary groups are better than formal organizations for providing personal services, and this will be reflected in outcomes such as reduced institutionalization in nursing homes or mortality. Primary groups, themselves, may be arrayed on a continuum from marital dyad to friends and neighbors.
1a. Mortality and institutionalization will be greater among those with no help versus those with some help.
1b. Mortality and institutionalization will be greater among those with only paid help versus those with some unpaid help (because the provision of paid help by itself will be shaped by the bureaucratic imperatives of the service agency, unmitigated by the influence and informal oversight of unpaid caregivers).
1c. Mortality and institutionalization will be greater among those receiving unpaid help only from distant relatives (other than spouse or child) or nonrelatives than among those receiving assistance from close relatives (spouse or adult child).
-
Among persons with ADLs or IADLs, multiple sources of help may imply an optimal caregiving arrangement, including caregiver respite, and should result in better outcomes (i.e., lower rates of mortality and institutionalization). Thus, mortality and institutionalization will be greater among those with only unpaid help versus those with both paid and unpaid help.
SECTION 2: METHODS
2.1 Survey Sampling and Data Collection
This analysis employs data from the Longitudinal Study on Aging (LSOA) an offshoot of the National Health Interview survey (NHIS) jointly sponsored by the National Center for Health Statistics (NCHS) and the National Institute on Aging (NIA). The LSOA is an extended follow-up of elderly persons originally sampled in 1984. For the present analysis, we are using data on outcomes from the follow-up wave of 1986 and baseline data from the first wave. We have constructed two working data files: one for the analysis of mortality (N=4571) and one for the analysis of institutionalization in nursing homes (N=4184). Each data set contains information on the outcome plus baseline data on caregiving arrangements, social and demographic characteristics, and health status.
The baseline data constitute the 1984 Supplement on Aging (SOA) to the NHIS. Investigators at NCHS designed this supplement to answer some of the concerns among policy makers and researchers regarding the increasing proportion of older people in the U.S. population and the need for alternatives to institutionalization.
The sample is based on NHIS procedures. The NHIS employs a multistage probability sample design that permits a continuous sampling of the civilian non-institutionalized population of the United States. Geographical areas of the country are clustered into strata having similar characteristics. From each strata one small area is sampled and a small cluster of housing units is selected to be contacted. In a selected household, all family members are included in the sample. In 1984, 41,471 eligible households were in the NHIS sample. Interviews were conducted in 39,996 of these households, yielding data on 105,290 persons of all ages who resided in them at the time of the interview (Kovar and Poe, 1985). The SOA sampled all persons aged 65 years and over (as well as half those aged 55-64). The final results of the sampling produced 11,497 interviews with persons aged 65 and over.
In general, the survey sought information about each person that would be reported most reliably by the sample person. Self-response is the rule in the SOA. However, for cases in which the sample person was physically or mentally unable to respond, the field staff accepted as a proxy an adult, preferably living in the household (Fitti and Kovar, 1987).
The LSOA design proposes to follow persons in the SOA through 1992, with NCHS conducting re-interviews at two-year intervals, ascertaining mortality, and linking data to Medicare utilization files. In 1986, the re-interview sample consisted of all black elderly over 70 years of age, half of all white elderly aged 70-79, and all white elderly aged 80 years or older. The 1986 follow-up interview used computer-assisted telephone interviewing (CATI). During the baseline contact, interviewers had asked respondents for a telephone number and address for themselves and a contact person. A letter explaining the study preceded the telephone call. This allowed persons who could not answer for themselves to discuss the information with proxy respondents. The field staff sent a self-administered mail questionnaire to respondents who could not be reached by telephone. The staff also administered a decedent follow-up questionnaire to the contact person or next-of-kin of respondents who had died. This interview ascertained date and place of death, hospitalization or nursing home use in the last year of life.
The eligible population for follow-up was 5151, of which the field staff ascertained the vital status of 4734 (91.9%). Among these, 604 people, or 11.7% of eligible respondents, were deceased. The field staff completed interviews with 99.6 percent of living eligible respondents or their proxies, and with 90.7 percent of the contacts for deceased eligible people.
2.2 Measures
The questionnaire employed for the Supplement on Aging was developed by a work group at NCHS in extensive consultation with other federal agencies and individuals with expertise in the suggested topic areas. These persons reviewed the literature and questionnaires previously employed among the elderly and participated in conferences on issues of aging. A draft questionnaire was developed in October of 1982 and pre-tested in Bradenton, Florida in June of 1983 and again in Wilmington, Delaware in September of 1983. Based upon these pre-tests, the final questionnaire was determined. The revised questionnaire, included sections on: disability and caregiving; living arrangements; social contacts; conditions and impairments; health opinions; health conditions, and demographic background.
Outcomes: In this study we have measured two outcomes, mortality and institutionalization in a nursing home. As noted above, the field staff ascertained the vital status of the people who had been contacted at baseline: 604 sample, people had died since the earlier interview. We created a working file with mortality information as well as caregiving arrangements, social and demographic characteristics, and health status. We have complete information on these variables for 537 individuals who died and 4,034 individuals alive at follow up. This data set contains 96.6 percent of persons whose vital status at follow-up was known.
The interviewers ascertained whether or not the individual had experienced a nursing home stay during the follow-up period. They also asked about nursing home stays as part of the decedent follow-up for those individuals who had died during the intervening period. The investigators found that 138 individuals were in a nursing home at the time of the follow-up. They were able to interview 126 of these persons. Another 59 individuals reported a nursing home stay since 1984. Finally, the decedent follow-up study ascertained that an additional 113 individuals had experienced a nursing home stay in the last year of life. This results in 298 individuals who were in a nursing home some time during the follow-up period. Our final data set includes 273 individuals with complete information on outcome, caregiving arrangements, sociodemographics, and health status.
In all, 11.7 percent of the initial sample died during the follow up period. Also, 6.5 percent of the initial sample were institutionalized at some time during the follow up period. About 40 percent of those who entered a nursing home in the follow-up period also died during that period.
Caregiving: We based the measure of caregiving arrangements on responses reported at baseline. In the LSOA interview caregiving is ascertained in the context of reports of decrements in activities of daily living and instrumental activities of daily living. In the baseline interview seven activities of daily living are ascertained: bathing or showering, dressing, eating, getting in and out of the bed or chair, walking, getting outside, and using or getting to the toilet. Six instrumental activities of daily living are included: preparing one's own meal, shopping for personal items, managing money, using the telephone, doing heavy housework, and doing light housework. Respondents were asked whether they had difficulty with a particular activity or instrumental activity of daily living, for example: "Do you have difficulty bathing or showering?" If the individual said "yes" they were asked what level of difficulty they experienced: "some," "a lot," or "unable to do." Then respondents were asked whether they received help from another person; and if, again, they responded in the affirmative, they were asked whether or not the person giving help was a relative or non-relative, whether or not the person lived in the household, and whether or not the person was paid for this service. It was assumed that spouse, child, and parent helpers were not paid.
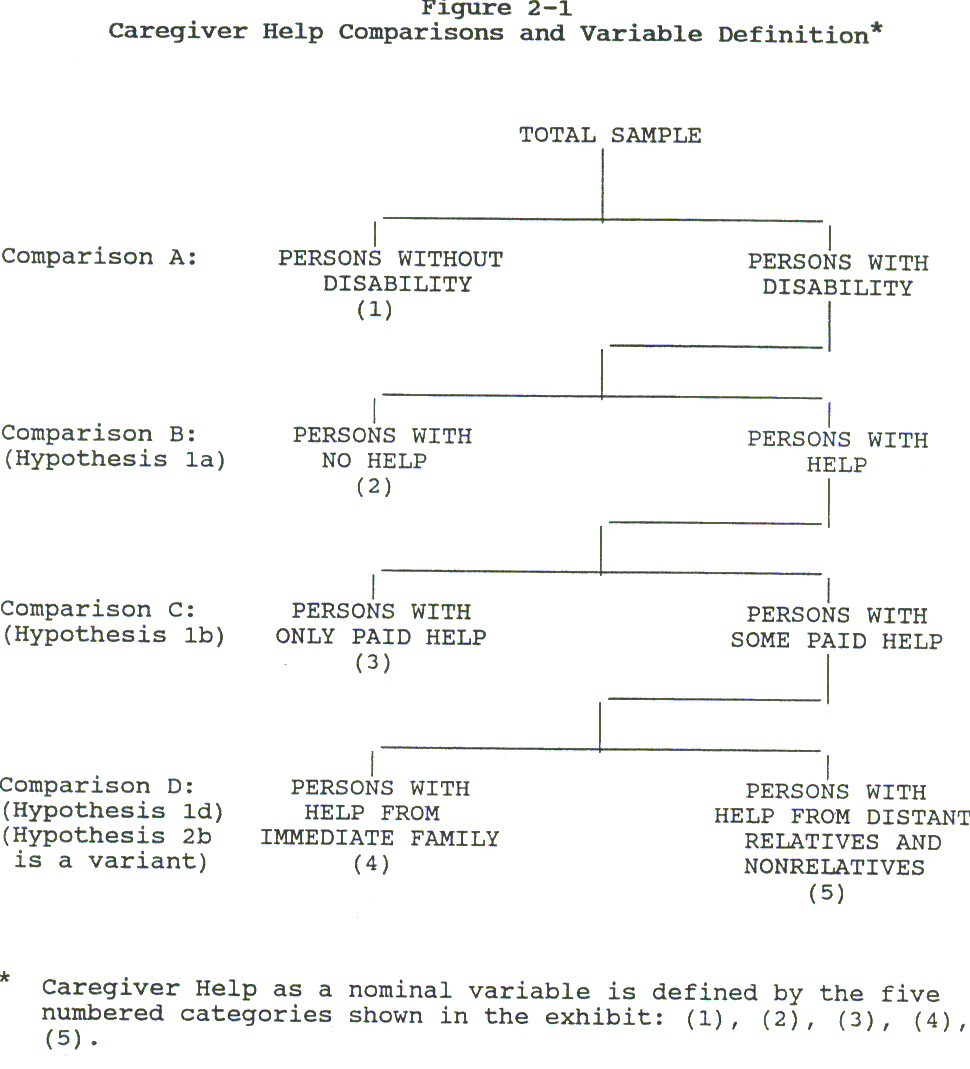
Using these data elements, we constructed a set of orthogonal comparisons among a variety of categories of responses. The comparisons correspond to our hypotheses as only persons with at least one ADL or an IADL deficit were asked the questions about receiving help. Our first comparison was between those with a disability and those without. only among those with a disability (ADL or IADL impairment) is it meaningful to differentiate persons receiving help from those not receiving help. Because the help versus no help distinction is not made within the no disability category, then the two comparisons, disability versus no disability, and help versus no help are uncorrelated. This is an analytic advantage in that if both are related to an outcome, for example, to increased mortality, then the estimated effects are statistically independent. We have simply capitalized on the hierarchical and nested structure of the caregiving questions to develop analyses that provide independent assessments of our hypotheses. Following our discussion of hypotheses, we have constructed two forms of our orthogonal contrasts. Both are identical in having disability versus no disability and help versus no help as the initial contrasts. Figure 2-1 presents a tree diagram illustrating the logic of these contrasts.
We created the next differentiation among persons who obtained help. One contrast compares those who have any kind of unpaid help with those who only have paid help. Then, within those with any kind of unpaid help, we contrast those who have unpaid help provided by immediate family members (spouse or child) to those who have unpaid help provided by others. An alternative set of contrasts compares persons who received only unpaid help to those who received some paid and some unpaid help. Within the former category, we then distinguish between those who received all unpaid help from close family members versus those who received all unpaid help, but from other than their close family.
 |
Orthogonal coding is a class of dummy variable coding. We simply have taken a mutually exclusive and exhaustive set of categories and developed a set of dummy variables. Typically we think of dummy variables as being coded 1 or 0 to identify the appropriate comparison. In this case we can think of the appropriate comparisons as being coded 1 or -1, say for disability versus no disability. Similarly, help could be coded as 1 and no help as -1, but all the persons without a disability would then not have a code. In this instance they are coded 0. A further complication occurs because we would like the logistic regression coefficients to be expressed as the logarithm of the odds ratio. This would work only if we had a balanced design i.e., one having the same number of cases in each of the categories of caregiving. We overcome this problem by weighting the codes according to the numbers of persons observed in the categories. This is explained in Appendix A. In the end, the orthogonal contrasts represent individual tests of the hypotheses we stated earlier. The test of the significance of the logistic regression coefficient associated with each contrast, or its antilog, the odds ratio, is a test of the significance of the hypothesis.
Other Measures: The remaining measures employed in this study fall into two categories: social and demographic characteristics and health status. In this section we will briefly introduce these measures. These variables represent potential confounders that past research suggests could influence the strength of association between caregiving and the outcome variables.
Social and Demographic Measures: This category of confounders includes measures of age, sex, race/ethnicity, education, income, living arrangements, social contactsf volunteering, and perceived control over health. Table 2-1 reports the distribution of these variables in the two analytic data sets. Age, sex, and race/ethnicity are self-reported. race/ethnicity reflects the group that the respondent felt best reflected his or her origin or ancestry. Hispanic refers to any person, black or white, whose family originated in a Spanish-speaking country. The categories, White and Black, reflect nonSpanish speakers. The other category contains largely native Americans and Asians. Education reflects the highest grade in school ever attended. We recoded this to eighth grade or less, some high school or high school graduate, and some college or college graduate. Income originally reported in broad categories is coded as follows: below poverty; poverty to $9,999; $10,00019,999; $20,000-29,999; and $30,000 or more. The poverty level is based on family size, number of children under eighteen years of age, and family income, using the 1983 poverty levels by the Census Bureau published in August 1984 (NCHS, 1984). An indicator is also included for persons refusing to report their income.
| TABLE 2-1. Distribution of Confounding Variables in the Mortality and Institutionalization Data Sets | ||
|---|---|---|
| Variable | Data Set | |
| Mortality | Institutionalization | |
| No. of cases | 4571 | 4184 |
| Proxy Yes No | 8.3% 97.1 | 8.2% 91.8 |
| Age (yrs.) | 78.0 | 77.9 |
| Sex Female Male | 63.5 36.5 | 63.6 36.4 |
| Race White Black Hispanic Other | 85.8 10.2 2.8 1.2 | 86.4 9.8 2.71.1 |
| Education Grade School High School College | 41.8 40.8 17.4 | 41.1 41.0 17.9 |
| Income Missing <Poverty >Poverty, <$10,000 $10,000-19,000 $20,000-34,000 <$35,000 | 16.4 15.5 23.1 26.8 12.6 5.6 | 15.9 15.3 22.9 27.3 12.9 5.7 |
| Living Arrangements Lives w/Spouse Lives Alone Lives w/Other Persons | 44.6 37.5 17.9 | 45.4 36.7 17.9 |
| Social Contacts (#/2 wks) | 4.0 | 4.1 |
| Volunteers in Community Yes No | 14.3 85.7 | 14.9 85.1 |
| Control Over Health A lot Some Little None Unknown (proxy) | 30.3 41.1 8.0 6.5 14.1 | 30.4 41.9 7.8 6.1 13.8 |
| Health Status Excellent Very Good Good Fair Poor | 15.9 20.7 30.8 21.3 11.3 | 15.9 21.1 30.9 21.0 11.1 |
| Activities of Daily Living (#) | 0.4 | 0.4 |
| Instrumental Activities of Daily Living (#) | 0.6 | 0.6 |
| Confusion Yes No | 3.9 96.1 | 3.9 96.1 |
| Alzheimer's Yes No | 0.5 99.5 | 0.6 99.4 |
| Urinary Incontinence Yes No | 9.6 90.4 | 9.5 90.5 |
| Bowel Incontinence Yes No | 6.7 93.3 | 6.6 93.4 |
| Cancer Yes No | 12.0 88.0 | 12.2 87.8 |
| Heart Disease Yes No | 17.0 83.0 | 16.3 83.7 |
| Cerebrovascular Accident (Stroke) Yes No | 7.3 92.7 | 7.2 92.8 |
| Osteoporosis Yes No | 3.4 96.6 | 3.4 96.6 |
| Hip Fracture Yes No | 4.9 95.1 | 4.9 95.1 |
| Fell 2 or More Times Yes No | 10.8 89.2 | 10.8 89.2 |
| Fell Because of Dizziness Yes No | 4.3 95.7 | 4.2 95.8 |
| Nursing Home Stay Prior to 1st Interview Yes No | 2.6 97.4 | 2.4 97.6 |
| Hospital Inpatient Stays (# Stays/yr) | 0.3 | 0.3 |
Living arrangements differentiate persons living alone from those living with their spouse and those living with someone other than a spouse. To measure social contacts we combined in an additive scale seven questions that were included in the baseline questionnaire: interaction with relatives (in person or by telephone), interaction with friends (in person or by telephone), attendance at church, attendance at public or social functions, and volunteering for organized groups. We separately include the measure of volunteering for organized groups, because in previous research (Wells and Dunlop), we found this component of an index of social contact to be the most discriminating predictor of survival. Self-reported belief in control over future health is categorized according to responses: "a great deal," "some," "a little," or "none at all". Because proxies could not appropriately answer this question, we include an indicator of proxy response.
Health Measures: A second set of confounding variables includes health variables: self-reported health status, activities of daily living, instrumental activities of daily living, impairments and chronic conditions, and prior utilization in hospital or nursing home. The categories of self-reported health status are "excellent", "very good", "good", "fair or poor". Methods of ascertaining ADLs and IADLs are described above in introducing our measures of caregiving. Here, however, we include an additive scale of the number of each type of dependency the respondent reported. Impairments and chronic conditions include the presence of or a history of mental confusion, Alzheimer's, urinary and bowel incontinence, cancer, heart disease, cerebrovascular accident, osteoporosis, hip fracture, having fallen twice or more, or having fallen because of dizziness. Prior utilization measures include an indicator of a nursing home stay prior to the baseline interview, and the number of hospital inpatient stays in the year prior to the baseline interview.
2.3 Data Analysis
The analysis is straightforward. For each outcome we estimate the bivariate association between each indicator of caregiving arrangements (indicating one of the analytic hypotheses) and the outcome. Our estimate of association is the odds ratio:
| OR = P(O) / X = CARE P(O) / X = NO CARE | |
| where | X = an indicator of caregiving 0 = an outcome |
In a simple logistic regression of outcome on the caregiving indicator, the estimated regression coefficient will be the logarithm of the odds ratio 1n(OR). The odds ratio is obtained through a simple transformation. The significance test of 1n(OR), a z-test based on the ratio 1n(OR) over its standard error, is equivalent to the significance test of OR.
We then employ a multivariate analysis to determine whether any of the set of confounders appreciably alters the estimated association between caregiving arrangements and outcome. In the case of multivariate logistic regression the 1n(OR) and OR associated with caregiving is a net value adjusted for the other variables in the equation.
Because there were many potential confounders, we undertook several analytic steps to trim their number. First we regressed the outcome on the set of health variables. We eliminated variables that were not significantly related to the outcome. We tested to assure that the deletion of the predictors did not significantly diminish the model chi-square. We repeated these steps for the social and demographic variables. We then combined the trimmed social and health models and trimmed this model. This was done for both mortality and institutionalization with differing results.
SECTION 3: RESULTS
Table 3-1 shows the results for mortality in each of the equation models: health variables only, social variables only, and the first and second trimmed models. Adjusted for age and sex, the following variables are significant: self-reported health status, activities of daily living, instrumental activities of daily living, cancer, cerebrovascular accident, and hospital inpatient stays. Persons reporting poor health were 2.59 times more likely to die in the follow-up period as those reporting excellent health status. Those reporting fair health status are nearly twice as likely to die. Each activity of daily living or instrumental activity of daily living increases the odds of mortality by about 1.1 or 10 percent. Cancer and cerebrovascular accident increase the odds of dying by 1.42 and each hospital stay increases the likelihood of dying by 38 percent. Among the social variables, in addition to age and sex, social contacts and control over health were the only variables significantly related to mortality. For each social contact the person is about 0.87 times as likely to die; that is, the more social contacts, the lower the odds of dying. Those saying that they have some, little or no control over health are significantly more likely to have died than those who said they have a great deal of control over their health. The association is especially strong for those with proxy reporting. In combining these models, only instrumental activities of daily living falls out of the equation. The final model includes age, sex, social contacts, control over health, self-reported health status, activities of daily living, cancer, cerebrovascular accident, and hospital inpatient stays. The overall chi-square is 3,419.49, which is significant.
| TABLE 3-1. Odds of Dying During Two-Year Follow-Up As A Function of Social and Health Status at Baseline | |||||
|---|---|---|---|---|---|
| Crude Odds Ratios | Net Odds Ratios | ||||
| Health Variables Only | Social Variables Only | First Trimmed Model3 | Second Trimmed Model4 | ||
| Proxy | 3.68** | 1.58* | 1.05 | ||
| Age2 | 1.07** | 1.06** | 1.05** | 1.05** | 1.06** |
| Sex | .56** | .49** | .53** | .52** | .53** |
| Race1 Black Hispanic Other | .78 .77 1.49 | .79 .64 1.34 | |||
| Education1 High School College | .74** .63** | 1.03 .91 | |||
| Income1 Missing >Poverty, <$10,000 $10,000-19,000 $20,000-34,000 >$35,000 | .97 .97 .88 .96 1.06 | .90 1.05 .91 .98 1.01 | |||
| Living Arrangements1 Lives Alone Lives w/Other Persons | .90 1.48** | 1.08 1.21 | |||
| Social Contacts | .76** | .87** | .92* | .91* | |
| Volunteers in Community | .37** | .71 | |||
| Control Over Health1 Some Little None Unknown (Proxy) | 1.43* 2.16** 1.87* 3.89** | 1.34* 1.80* 1.59* 1.92* | 1.14 1.26 1.16 1.56* | 1.14 1.26 1.17 1.76* | |
| Health Status1 Very Good Good Fair Poor | 1.18 1.48* 2.50** 5.20** | 1.14 1.36 1.90** 2.59** | 1.13 1.29 1.77* 2.37** | 1.13 1.30 1.80* 2.45** | |
| Activities of Daily Living2 | 1.43** | 1.12* | 1.11* | 1.15** | |
| Instrumental Activities of Daily Living2 | 1.43** | 1.11* | 1.06 | ||
| Confusion | 1.53* | 1.06 | |||
| Alzheimer's | 3.56* | 1.21 | |||
| Urinary Incontinence | 2.29** | 1.06 | |||
| Bowel Incontinence | 2.59** | 1.08 | |||
| Cancer | 1.84** | 1.42* | 1.45* | 1.45* | |
| Heart Disease | 1.60** | .96 | |||
| Cerebrovascular Accident (stroke) | 2.67** | 1.42* | 1.40* | 1.42* | |
| Osteoporosis | .89 | .70 | |||
| Hip Fracture | 2.07** | 1.32 | |||
| Fell 2 or More Times | 1.86** | .95 | |||
| Fell Because of Dizziness | 2.37** | 1.24 | |||
| Nursing Home Stay Prior to 1st Interview | 2.59** | 1.37 | |||
| Hospital Inpatient Stays2 | 1.68** | 1.38** | 1.38** | 1.38** | |
| Model CHI Square | 3408.74 | 3281.32 | 3421.19 | 3419.49 | |
* = significant at <0.05; ** = significant at <0.001 | |||||
Table 3-2 shows the results for institutionalization in a nursing home. Following the same procedures, the health variables related to institutionalization, in addition to age and sex, are: self-reported health status, instrumental activities of daily living, Alzheimers, heart disease, having fallen twice or more, having fallen because of dizziness, and a prior nursing home stay. Especially strong associations are exhibited by prior nursing home stays, where persons who have had a prior stay are four times as likely to enter a nursing home as those without a prior stay. Persons with Alzheimers are 3.2 times more likely to enter a nursing home. Those with self-reported fair or poor health are about twice as likely, as are those who have fallen because of dizziness or who have fallen two or more times. Heart disease is inversely related to entering a nursing home, the odds ratio being 0.69.
Among the social variables, education, living arrangements, social contacts, and perceived control over health are significantly related to entering a nursing home. Those with some high school or a high school diploma are about 1.6 times as likely as those with education less than eighth grade to enter a nursing home. Those with education beyond high school graduation are not significantly different than those with an education of eighth grade or less. Persons living alone are twice as likely to enter a nursing home. Persons with more social contacts are less likely to enter a nursing home, the odds decreasing 28 percent for each additional social contact. Those expressing little control over health are 2.76 times as likely to enter a nursing home as those expressing a lot of control over health. Persons expressing some or no control over health are also more likely to enter a nursing home. When the health and social variables are combined, the inverse association of heart disease with entering a nursing home drops out, as does the association between instrumental activities of daily living and entering a nursing home. Although the odds ratio for Alzheimers disease is not statistically significant, it is of such substantial magnitude, 2.45, that we have left it in the equation. The overall chi-square for this model, 4171.99, is significant.
| TABLE 3-2. Odds of Entering a Nursing Home During Two-Year Follow-Up As A Function of Social and Health Status at Baseline | |||||
|---|---|---|---|---|---|
| Crude Odds Ratios | Net Odds Ratios | ||||
| Health Variables Only | Social Variables Only | First Trimmed Model4 | Second Trimmed Model5 | ||
| Proxy | 4.02** | 1.67 | |||
| Age2 | 1.15** | 1.12** | 1.11** | 1.11** | 1.11** |
| Sex | 1.24 | 1.04 | .93 | ||
| Race1 Black Hispanic Other | .05* .61 1.30 | .59 .69 1.17 | |||
| Education1 High School College | .96 .75 | 1.53* 1.18 | 1.60* 1.17 | 1.60* 1.17 | |
| Income1 Missing >Poverty, <$10,000 $10,000-19,000 $20,000-34,000 >$35,000 | 1.03 .87 .56** .64 .86 | 1.08 1.01 .78 .78 1.05 | |||
| Living Arrangements1 Lives Alone Lives w/Other Persons | 2.46** 2.74** | 2.08** 1.38 | 1.99** 1.22 | 1.98** 1.25 | |
| Social Contacts | .70** | .78** | .81** | .80** | |
| Volunteers in Community | .36** | .93 | |||
| Control Over Health Some Little None Unknown (Proxy) | 1.74* 3.20** 2.74** 5.43** | 1.73* 2.76** 2.33* 2.30* | 1.53* 2.01* 1.77 2.04* | 1.54* 2.09* 1.83* 2.27** | |
| Health Status1 Very Good Good Fair Poor | 1.58 1.74* 3.07** 3.95** | 1.56 1.64 2.30* 1.93* | 1.53 1.61 2.21* 1.99* | 1.52 1.61 2.20* 2.05* | |
| Activities of Daily Living2 | 1.41** | 1.03 | |||
| Instrumental Activities of Daily Living2 | 1.51** | 1.14* | 1.08 | ||
| Confusion | 2.31** | 1.67 | |||
| Alzheimer's3 | 8.73** | 3.20* | 2.23 | 2.45 | |
| Urinary Incontinence | 2.30** | .97 | |||
| Bowel Incontinence | 2.61** | .88 | |||
| Cancer | 1.57** | 1.11 | |||
| Heart Disease | 1.08 | .69* | .77 | ||
| Cerebrovascular Accident (stroke) | 2.56** | 1.43 | |||
| Osteoporosis | 1.18 | .84 | |||
| Hip Fracture | 3.34** | 1.37 | |||
| Fell 2 or More Times | 3.52** | 1.71* | 1.72* | 1.73* | |
| Fell Because of Dizziness | 4.93** | 2.00* | 1.99* | 1.96* | |
| Nursing Home Stay Prior to 1st Interview | 10.40** | 4.09** | 4.10** | 4.36** | |
| Hospital Inpatient Stays2 | 1.30** | 1.13 | |||
| Model CHI Square | 4122.73 | 4090.21 | 4176.40 | 4171.99 | |
* = significant at <0.05; ** = significant at <0.001 | |||||
3.1 Crude Associations of Caregiving with Outcomes
We calculated the crude odds of dying and the crude odds of institutionalization in a nursing home, given the various caregiving arrangements. Table 3-3 reports results for mortality. Under the heading of caregiving arrangements we list 6 comparisons pertaining to our hypotheses. For each level of the comparison we list the number of persons alive at follow-up, the number of persons who had died, and then calculate a crude odds ratio of mortality.
| TABLE 3-3. Odds of Dying During Two-Year Follow-Up by Characteristics of Disability and Caregiving | |||
|---|---|---|---|
| Caregiving Arrangements | Number Alive | Number Dead | Crude Odds Ratio |
| Disability vs. No Disability | 1,013 3,021 | 250 287 | 2.60** |
| Help vs. No Help | 859 154 | 237 13 | 3.27** |
| Any Unpaid Help vs. All Paid Help | 675 174 | 203 34 | 1.52* |
| Any Close Family Unpaid Help vs. No Close Family Unpaid Help | 269 416 | 61 142 | 0.66 |
| All Unpaid Help vs. Some Paid, Some Unpaid | 139 546 | 43 160 | 1.06 |
| All Unpaid Help, Close Family vs. All Unpaid Help, Not Close Family | 77 62 | 19 24 | 0.64 |
| * = significant at <0.05; ** = significant at <0.001 | |||
Given that having a disability is a necessary condition for receiving help under our operationalization, we include a comparison of disabled and non-disabled persons. Among 1,263 persons disabled at baseline, 250 had died; whereas among 3,308 non-disabled persons at baseline, 287 had died. This results in an odds ratio of 2.60 that is significant at p<.001. The odds ratio indicates that a person disabled at baseline is 2.6 times as likely to die as one not disabled.
The next comparison is that between persons with a disability who received help versus those with a disability who received no help. Among 1,096 of the former, 237 died during the follow up period, whereas among 167 of the latter, 13 had died. This results in a crude odds ratio of 3.27, indicating that disabled persons receiving help were 3.27 times more likely to die over the follow-up period than those receiving no help. Is receiving help a risk factor for mortality? Probably we should not rule out these explanations, although one would expect to be given help in proportion to need. In later analyses we will control for severity of illness, which may be a distorter variable in this instance.
The remaining four comparisons distinguish among types of help received. Persons who received any unpaid help versus only paid help were 1.52 times more likely to die over the follow-up period. When we compare unpaid help from close family members to unpaid help from more distant relatives or non-relatives the crude odds ratio is 0.66 and is not statistically significant. The next caregiving comparison places all unpaid help opposite persons receiving some paid and some unpaid help: the odds ratio is 1.06 and not significant. Finally, receiving all unpaid help from close family members compared to all unpaid help from more distant relatives and non-relatives results in a crude odds ratio of 0.64, also not statistically significant.
Table 3-4 presents the association between caregiving arrangements and entering a nursing home during the two-year follow up. Among 1,053 disabled persons, 163 entered a nursing home; whereas among 3,031 non-disabled persons, 110 experienced a nursing home admission. Thus, the crude odds ratio is 4.37, indicating that disabled persons are 4.37 times as likely as non-disabled to enter a nursing home in a two-year period. This odds ratio is statistically significant, p<.001. Disabled persons receiving help are 1.73 times as likely to enter a nursing home as those disabled persons without help. Though not statistically significant, this is a fairly sizable odds ratio and, once again, may reflect the association between receiving help and illness severity on one hand and illness severity and entering a nursing home on the other hand. Among those who receive help, those receiving any unpaid versus all paid help are 1.24 times as likely to enter a nursing home, though the odds ratio is not significant. Those with unpaid help from any close family members versus unpaid help from distant relatives and non-relatives have similar odds of entering a nursing home. Persons receiving all unpaid help versus some paid and some unpaid help were 1.41 times as likely to enter a nursing home. Among the former, those with unpaid help all from close family members were 1.36 times as likely to enter a nursing home as those with all unpaid help from more distant relatives or non-relatives.
| TABLE 3-4. Odds of Entering a Nursing Home During Two-Year Follow-Up by Characteristics of Disability and Caregiving | |||
|---|---|---|---|
| Caregiving Arrangements | Number Alive | Number Dead | Crude Odds Ratio |
| Disability vs. No Disability | 990 2,921 | 163 110 | 4.37** |
| Help vs. No Help | 861 129 | 150 13 | 1.73 |
| Any Unpaid Help vs. All Paid Help | 696 165 | 126 24 | 1.24 |
| Any Close Family Unpaid Help vs. No Close Family Unpaid Help | 260 436 | 48 78 | 1.03 |
| All Unpaid Help vs. Some Paid, Some Unpaid | 135 561 | 32 94 | 1.41 |
| All Unpaid Help, Close Family vs. All Unpaid Help, Not Close Family | 70 65 | 19 13 | 1.36 |
| * = significant at <0.05; ** = significant at <0.001 | |||
In summary, disability has a positive association with both mortality and institutionalization in a nursing home. In both cases this is statistically significant, although it is stronger for mortality. Receiving help for a disability is also positively associated with both of these outcomes, although it not statistically significant for entering a nursing home. Receiving any unpaid help versus all paid help is positively associated with mortality and is statistically significant.
For the remaining caregiving comparisons the associations are much weaker and are not statistically significant. Illness severity and social resources also may be related to caregiving arrangements. Therefore, controlling for these confounders may result in our observing stronger and statistically significant associations between caregiving arrangements and outcomes. Before taking these steps we turn to analysis of the associations of confounder variables with the outcomes.
3.2 Potential Confounding Variables
A confounder variable may affect the estimated relationship between two other variables. In the present analysis we are interested in the association between caregiving arrangements and the outcomes of mortality or entering a nursing home. We may observe two kinds of confounding. one is a situation in which there is a significant bi-variate association between caregiving arrangements and the outcomes. For example, receiving help is related to mortality and entering a nursing home. If a confounding variable were associated with both caregiving arrangements and with the outcomes, then in a multivariate analysis where all the variables are included so that caregiving and outcomes are adjusted for the presence of the confounder, the original association might disappear or even be reversed. In the case of receiving help and mortality, controlling for severity of illness should cause the positive association between help and mortality to disappear. That is to say, there would be no true association between receiving help and dying; rather, both help and mortality are a reflection of an underlying progression of disease.
A second kind of confounder is a suppressor variable. This describes a situation in which there is no observed bivariate association between caregiving arrangements and the outcomes. This we have observed for most of the caregiving variables. In this instance, a variable that is associated with caregiving and with the outcomes in opposite ways could result in an observed association between caregiving and the outcomes when the confounder is included in a multivariate analysis. For example, if income decreased the likelihood of mortality, yet increased the likelihood of unpaid help, then the association between unpaid help and mortality may be seen to be positive after adjustment for income.
As described in our methods section, we have two major categories of confounding variables: social variables -- including demographic, socioeconomic, and social network variables -- and health status variables. Our analyses of confounders identified the sets of these variables that are related to mortality and to entering a nursing home, respectively.
As we have noted, for a confounder to affect the association of caregiving and either of the outcomes, it must be related both to the outcomes and to the caregiving. Thus, for each of caregiving comparisons we might determine which of the confounders that are related to mortality or entering a nursing home are also related to that particular caregiving arrangement. By doing this, we would have a unique set of confounders for each pair of caregiving arrangements and outcomes. To avoid the inefficiency of such an approach, however, we have decided to use all of the predictors related to each of the outcomes. As it turns out, each of the confounders is related to at least one of the caregiving arrangements, making it reasonable to include all of them. An additional rationale for keeping in a predictor related to the outcomes even though it is not related to the caregiving arrangements is for precision of estimation (Kleinbaum et al., 1980). We have included in Appendix B a table of associations between the confounder variables and the caregiving arrangements. The odds ratios in the table indicate the strengths of the associations. Although the associations differ slightly between the mortality and the institutionalization analyses because of the differing number of cases, the two sets of associations are nearly identical. Thus, we have reported only those for the mortality data set, the larger data set of the two.
3.3 Multivariate Analysis
The next step in our analytic strategy, then, is to control for the set of confounders while evaluating the association between caregiving arrangements and the outcome. Thus we can estimate an adjusted odds ratio that takes into account social and health variables related to the outcomes. Table 3-5 reports the results for mortality. The table includes the crude odds ratio between caregiving arrangements and mortality. It also includes the odds ratio after adjusting only for social, then only for health variables, and finally, for both social and health variables. The table illustrates how confounders can affect the association between two variables. For example, the association between disability and, finally, mortality is decreased by adjusting for social variables. Nonetheless, there remains a significant association between disability and mortality. (The odds ratio falls from 2.60 to 1.83). However, after controlling for health variables, only a trivial association between disability and mortality remains, an odds ratio of 1.11. Controlling for both health and social variables (Column 4) results-in an odds ratio very close to 1, meaning no association. This indicates that, in large part, the apparent excess mortality associated with disability was really related to severity of illness. Considering only the adjustment for health variables, the association between receiving help and mortality also is, in part, a function of illness severity. After controlling for health variables the odds ratio dropped from 3.27 to 2.56. However, this odds ratio is still statistically significant, indicating that the health confounders did not account entirely for the associations of help with mortality. Adding in the social variables decreases the odds ratios further to 2.48. It is conceivable that the health variables measured here simply are not as sensitive to illness severity as the measure of receiving help itself is. Conversely, we might conclude that receiving help is, in fact, a risk factor for mortality.
| TABLE 3-5. Odds of Dying During Two-Year Follow-Up by Characteristics of Disability and Caregiving | ||||
|---|---|---|---|---|
| Caregiving Arrangements | Crude Odds Ratio | Net Odds Ratios Controlling for: | ||
| Social Variables | Health Variables | Both Health and Social | ||
| Disability vs. No Disability | 2.60** | 1.83** | 1.11 | 1.02 |
| Help vs. No Help | 3.27** | 4.69** | 2.56* | 2.48* |
| Any Unpaid Help vs. All Paid Help | 1.52* | 1.22 | 1.19 | 1.09 |
| Any Close Family Unpaid Help vs. No Close Family Unpaid Help | 0.66 | 0.76 | 0.86 | 0.93 |
| All Unpaid Help vs. Some Paid, Some Unpaid | 1.06 | 1.04 | 0.68 | 0.73 |
| All Unpaid Help, Close Family vs. All Unpaid Help, Not Close Family | 0.64 | 0.77 | 1.21 | 1.29 |
| * = significant at <0.05; ** = significant at <0.001 | ||||
In assessing the association between the contrast, any unpaid help versus all paid help, and mortality, we find that the association decreases substantially and becomes insignificant when controlling for either social variables or health variables. It approaches no association, an odds ratio of 1.09, when both sets of variables are controlled. A similar pattern is seen for receiving unpaid help from close family members versus only distant or non-relatives.
In contrast, the crude odds ratio for all unpaid help versus some paid and some unpaid help is close to 1 and remains unchanged after controlling for social confounders. However, after controlling for health confounders, this association becomes much stronger, having an odds ratio of 0.68. This illustrates a classic suppressor effect. In this instance more severe illness is positively related to mortality but negatively related to receiving all unpaid help. This makes it appear that all unpaid help is unrelated to mortality, whereas, in reality, receiving all unpaid help is negatively related to mortality. Those receiving all unpaid help are 47 percent less likely to die than those receiving some paid and some unpaid help. However, the association, though moderate in magnitude, is not statistically significant. This may be a function of small numbers of individuals in these categories.
A distorter effect is observed for the subset of all unpaid help from close family members versus distant relatives or non-relatives. The crude odds ratio is 0.64 indicating that help from close family members is associated with a lower odds of dying in the follow-up period. However, after controlling for health variables, the odds ratio becomes positive, 1.21, indicating that those receiving unpaid help from close family members are more likely to die than those receiving unpaid help from others.
| TABLE 3-6. Odds of Entering a Nursing Home During Two-Year Follow-Up by Characteristics of Disability and Caregiving | ||||
|---|---|---|---|---|
| Caregiving Arrangements | Crude Odds Ratio | Net Odds Ratios Controlling for: | ||
| Social Variables | Health Variables | Both Health and Social | ||
| Disability vs. No Disability | 4.37** | 2.15** | 2.00** | 1.58* |
| Help vs. No Help | 1.73 | 1.36 | 1.19 | 1.12 |
| Any Unpaid Help vs. All Paid Help | 1.24 | 1.02 | 1.01 | 1.04 |
| Any Close Family Unpaid Help vs. No Close Family Unpaid Help | 1.03 | 1.05 | 1.16 | 1.03 |
| All Unpaid Help vs. Some Paid, Some Unpaid | 1.41 | 1.21 | 1.30 | 1.12 |
| All Unpaid Help, Close Family vs. All Unpaid Help, Not Close Family | 1.36 | 1.65 | 2.02 | 1.80 |
| * = significant at <0.05; ** = significant at <0.001 | ||||
We also performed a similar analysis for entering a nursing home. In Table 3-6 a pattern of classical confounders is observed for the association of disability with entering a nursing home. After controlling for both health and social behaviors, the odds ratio falls from 4.37 to 1.58. The odds ratio remains statistically significant. In most instances the odds ratio falls from a larger association to a smaller association after controlling for social health variables or both. The exception to the rule in this pattern is for the last comparison of persons receiving all unpaid help from close members versus receiving all unpaid help from distant relative and non-relatives. The crude odds ratio is 1.36. This increases slightly after control for social variables and increases even more after control for health variables, reaching an odds ratio of 2.02. Together, the adjustment for health and social variables results in odds ratios of 1.8. Such an odds ratio is not trivial in terms of its substantive importance. However, because of the small number of cases in this analysis, it is not statistically significant.
3.4 Additional Considerations
Both mortality and entering a nursing home are events that were distributed over the follow-up period. Thus, we might be concerned with estimating a time-to-event function rather than the relative odds of the occurrence of the events. A statistical technique which allows such an event history approach is the Cox proportional hazards regression. Unfortunately, the user data set produced by the National Center for Health Statistics did not include all of the dates necessary to record nursing home entry. However, the data set did include dates of death, allowing the application of this method to the mortality data.
| TABLE 3-7. Comparison of Adjusted1 Odds Ratio and Hazard Ratio for Estimating the Impact of Caregiving Arrangements on Dying During Two-Year Follow-Up | ||
|---|---|---|
| Caregiving Arrangements | Odds Ratio | Hazard Ratio |
| Disability vs. No Disability | 1.02 | 1.07 |
| Help vs. No Help | 2.48* | 2.33* |
| Any Unpaid Help vs. All Paid Help | 1.09 | 1.08 |
| Any Close Family Unpaid Help vs. No Close Family Unpaid Help | 0.93 | 0.91 |
| All Unpaid Help vs. Some Paid, Some Unpaid | 0.73 | 0.76 |
| All Unpaid Help, Close Family vs. All Unpaid Help, Not Close Family | 1.29 | 1.33 |
* = significant at <0.05 | ||
Table 3-7 shows the results of a comparison of adjusted odds ratios and hazard ratios for estimating the impact for caregiving arrangements on mortality during the two-year follow-up period. The results in the table indicate that the hazard ratio is nearly identical to the odds ratio. The estimate of the instantaneous hazard of dying is almost identical to the relative odds of dying over the entire period. After adjusting for social and health status variables, only receiving help is significantly associated with death. The odds ratio is 2.48 and the hazard ratio is 2.33. These results indicate that no information is being lost by ignoring the timing of death over the follow-up period. This may change even in these data as the follow-up period is extended. However, two years of follow-up is quite short for measuring an event like mortality. Thus, the potential differences in findings between the two techniques would not be likely to show up over such a short interval. Differences could be expected to widen over an extended follow-up period.
We were also interested in the potential for interaction effects between caregiving and living arrangements. Potentially, caregiving arrangements may have heterogeneous effects on the outcomes, depending upon the kind of household in which the respondent lives. We know that persons living alone are much more likely to use paid care than are those living with others. (For example, see Tennestadt et al., 1990). Therefore, we re-estimated the associations between caregiving arrangements and the outcomes for each of the three living arrangement categories: living alone, living with others, that is, other than spouse, and living with spouse. We were especially interested in finding whether some of the associations that we found not significant turn out to be significant only for one or the other of the living arrangements.
Table 3-8 shows the results for mortality. Among persons living alone, those receiving help are twice as likely to die in the follow-up period. In particular, those receiving all unpaid help are half as likely to die as those receiving a combination of paid and unpaid help, the odds ratio equaling 0.48. In contrast, among those receiving all unpaid help, those receiving it from close family members are 1.8 times as likely to die during the follow-up period as those receiving it from someone else. Overall, caregiving arrangements have very small effects on mortality among those living with others. Among those living with spouse, receiving help is strongly and significantly related to mortality, an odds ratio of 4.43. Odds ratios contrasting various combinations of help, however, are not particularly large and they are not statistically significant. While these findings may be suggestive, especially for persons living alone, and are difficult to interpret for those living with a spouse, they generally do not contradict the results from the overall analysis.
Table 3-9 shows the same results for entering a nursing home. Most of the effects are quite small, especially for those who live alone. Among those who live with others, there is an association between receiving unpaid help from close family members and mortality, with an odds ratio of 2.18; but it is not statistically significant. The same association is even larger among persons living with a spouse (odds ratio 2.38). The only significant association in the table is for those with disabilities who live with a spouse. They are 2.33 times more likely than those without a disability to enter a nursing home. Once again, there are some interesting contrasts between receiving unpaid help from close family members versus others, but the associations are not significant and the results remain quite similar to those derived from the overall analysis.
| TABLE 3-8. Adjusted Odds of Dying After Two-Year Follow-Up by Characteristic of Caregiving and Living Arrangements | |||
|---|---|---|---|
| Caregiving Arrangements | Mortality | ||
| Lives Alone OR | Lives w/ Others OR | Lives w/ Spouse OR | |
| Disability vs. No Disability | 1.02 | 1.32 | .85 |
| Help vs. No Help | 2.10 | 1.14 | 4.43* |
| Any Unpaid Help vs. All Paid Help | 1.06 | .84 | 1.26 |
| Any Close Family Unpaid Help vs. No Close Family Unpaid Help | 1.21 | .65 | .84 |
| All Unpaid Help vs. Some Paid, Some Unpaid | .48 | .93 | .74 |
| All Unpaid Help, Close Family vs. All Unpaid Help, Not Close Family | 1.77 | .59 | 1.57 |
| * = significant at <0.05 | |||
| TABLE 3-9. Adjusted Odds of Entering a Nursing Home After Two-Year Follow-Up by Characteristics of Caregiving and Living Arrangements | |||
|---|---|---|---|
| Caregiving Arrangements | Institutionalization | ||
| Lives Alone OR | Lives w/ Others OR | Lives w/ Spouse OR | |
| Disability vs. No Disability | 1.39 | 1.24 | 2.33* |
| Help vs. No Help | 1.76 | 0.80 | 0.84 |
| Any Unpaid Help vs. All Paid Help | 1.12 | 0.61 | 1.52 |
| Any Close Family Unpaid Help vs. No Close Family Unpaid Help | 1.01 | 1.49 | 0.40 |
| All Unpaid Help vs. Some Paid, Some Unpaid | 1.12 | 1.23 | 0.79 |
| All Unpaid Help, Close Family vs. All Unpaid Help, Not Close Family | 1.00 | 2.18 | 2.38 |
| * = significant at <0.05 | |||
SECTION 4: DISCUSSION
4.1 Mortality
The fact that help is associated with death would make great sense in the absence of adjustors for severity of illness. However, we have controlled for a wide range of health status indicators and still obtain this result; i.e., disabled persons receiving help with daily living activities, irrespective of severity of illness, are nearly two and one-half times as likely to die as those persons who received no help.
At least two explanations for this seemingly anomalous result are possible. one is that despite our efforts, some key dimension of condition severity is left uncontrolled in our multivariate analysis. Considerable discussion has emerged in the recent literature of the appropriate way to measure functional deficits (e.g., Weiner et al., 1990). However, no consensus has yet emerged and there exists no compelling empirical findings to suggest that our additive scale of ADLs is not the best way of capturing functional decrements. Stone and Murtaugh (1990), Kasper (1990), and Coughlin et al. (1989) have argued the need to include measures of cognitive status and behavior. Jackson and Burwell (1990), on the other hand, argue that most persons with cognitive impairments will be counted by measuring ADL and IADL deficits. We measured both ADL and IADL and we included indices of Alzheimer and confusion. The LSOA contains no clear indices of behavior, per se.
We cannot rule out the possibility, as well, that some help may be deleterious, leading to accelerated decline in functioning and even physiological integrity. This may happen because too much help induces dependency, loss of automony and "the will to live."
Receipt of help, as it turns out, is predictive of death only for those living with spouse. Perhaps those living with spouse (or their proxies) reported help only when it came from someone other than the spouse; that is, they assumed the interviewer perceived help from the spouse as a given and was inquiring only about other help. Individuals receiving this "external" help, undoubtedly, would tend to be very ill with medical conditions which acted to impair their functioning.
We controlled for a number of major medical conditions; and, in fact, both cancer and stroke prove to be strong predictors of mortality. However, our controls for terminal illnesses are undoubtedly incomplete so that the variable indexing receipt of help, in fact, may reflect care needs related to other terminal medical conditions. With one exception, none of the other caregiving arrangements appears to have any effect on the risk of dying. Although not quite significant (at the .05 level), persons receiving all unpaid help were only 73 percent as likely to die over the two-year period as those receiving both unpaid and paid help. This runs counter to the direction hypothesized and could reflect unmeasured illness severity or, perhaps, deterioration owing to induced dependency or loss of emotional support from friends.
A number of effects of confounding variables are quite interesting. Not surprisingly, the likelihood of death increases with age and is lower for females. Social contacts reduce the risk of death, a consistent finding in a number of rigorous studies dating back to Berkman and Syme (1979). Health status as reported by respondents proves to be the most powerful predictor of death. Persons appear to have a rather accurate sense of their total physiological well-being. Three other health status indices also are significant predictors of death. Number of ADL deficits, cancer, and stroke all have been found in previous studies to be rather powerful predictors of mortality. Number of hospital inpatients stays, categorized in much research as a measure of health status, also positively predicts death.
4.2 Institutionalization
Reported difficulty with or inability to do an ADL or IADL, even after controlling for a continuous scale of ADL and IADL deficits, positively predicted admission to a nursing home among the LSOA population. Those (or their proxies) reporting such an impairment were one and one-half times as likely to be institutionalized over a two-year period. This finding is consistent with past research.
We found little support in our data for the remainder of our hypotheses. Except for our measure of the impact of close family caregiving as opposed to unpaid caregiving from more distant unpaid sources, the particular care arrangement seems to make little difference. For the close versus distant unpaid care arrangements, the impact appears to be opposite from that hypothesized, although it is not statistically significant. Persons receiving unpaid help all from close family were almost two times (1.8) more likely to have been institutionalized as those receiving all of their unpaid help from more distant relatives. Perhaps disabled persons receiving help all from close family are more impaired than their counterparts and the services they receive are more intensive than those services received from more distant relatives. This would suggest the need to measure the specific kind and intensity of help received.
Another explanation may be that close relatives provide inappropriate or too much care, contributing to the impaired relative's deterioration. In the latter case, deterioration may result in increased dependency and loss of control. We controlled for perceived control over health, but this may be too narrow a measure, or the sense of total control felt may not get articulated by the respondent. In the former case, care simply may not meet the need; for example, care may be of the unskilled variety when skilled care is needed.
Finally, Litwak (1985) has argued that joint caregiving by paid and unpaid sources is optimal in meeting the needs of impaired elders. We did not find any such effect in our test.
However, it is not clear that we measured the tandem care arrangement that Litwak has in mind. According to his formulation, the situation is ideal when the formal and the informal caregivers function in complementary fashion, i.e., when the unpaid caregiver performs the nonuniform tasks and the paid sources provide the routinized or skilled tasks. It may be that our joint caregivers in many instances were competing to carry out the same tasks or to meet the same needs. When the potential for this situation exists, Litwak argues, the formal and primary groups must adapt by developing buffering arrangements. There is no guarantee, of course, that this happened nor any information in our data which would allow us to assess this precisely. As is, however, our findings show no benefit of the joint arrangement in terms of reducing risk of institutionalization.
As with the mortality outcome, a number of interesting independent effects of the confounding variables on risk of institutionalization are worth noting. Age, as has been found in numerous previous studies, including our own, is positively related. Each year above 65 increases the risk by 11%. Interestingly, the effect of education proves to be curvilinear, with those with a high school education the most likely to enter a nursing home. College education seems to have no added salutary impact in terms of likelihood of nursing home admission beyond what a grade school education provides.
As has been uncovered in previous research, persons living alone are at a significantly elevated risk of entering a nursing home relative to those who live with a spouse or other persons. As with mortality, social contacts reduce the risk of nursing home admission substantially. Each additional contact reduces a disabled person's risk of institutionalization by 25 percent.
A person's sense of control over his or her health, independently of ADL status, is negatively related to risk of nursing home admission. Relative to persons reporting a great deal of control, persons perceiving themselves as possessing only some control were 50 percent more likely to enter a nursing home over a two-year period. Those reporting little or no control are approximately twice as likely to be institutionalized. Likewise, those reporting fair or poor health status are two times more likely to enter a nursing home over a two-year period than are those reporting excellent health.
As with mortality, several specific medical conditions predicted admission to a nursing home, although these conditions are different than the ones that predict death. Persons with Alzheimers and persons with a history of falling at least twice or falling as a result of dizziness are roughly two times more likely to be admitted to a nursing home than those not experiencing these conditions.
Instead of number of prior hospital stays, which was a very powerful predictor of death, having experienced any nursing home stay prior to the respondent interview turned out to be a very powerful predictor of nursing home admission over the subsequent two-year period. Persons with such a history were over four times more likely to be institutionalized again.
4.3 Conclusions
Overall, differences in caregiving arrangements do not seem to affect the likelihood of death or institutionalization over a two-year period for disabled elderly who receive help from others in carrying out their daily activities. Being disabled itself distinguishes those with a significantly higher risk of entering a nursing home, and receipt of help among those who are disabled further distinguishes those with a greater risk of dying over a subsequent two-year period.
Perhaps if we had been able to separate short-term or transitory nursing home admissions from long-term or permanent nursing home stays, differences in caregiving arrangements might have shown more impact. Because the dates surrounding nursing home stays were missing from the data base, we were unable to ascertain the length of these stays. Being able to distinguish more finely among close family (i.e., spouse vs. adult child) or possibly among gradations of more distant relatives might have made a difference as well. However, small cell sizes did not permit such fine distinctions.
Still another factor may have seriously limited our ability to discern effects of even the broader care arrangements we tested with the data at hand. Health among persons 70 and over all too frequently can decline precipitously and without much warning. This sudden failure of major physiological systems and the abrupt onslaught of care needs which accompany it may overwhelm the capacity of any caregiving arrangements outside of an inpatient setting to adjust to these needs. Litwak, as well as others (Doty, 1986; Harkins, 1985) have made just such a point. Perhaps, treating caregiving arrangements as condition-specific would help in this regard. Conditions, for example, which call for the application of substantial skilled or medical care may well be more difficult to cope with or arrange for than conditions calling only for significantly increased personal care.
Comparisons of condition-focused care arrangements notwithstanding, it is becoming increasingly clear that a steady decline in functioning as people age is not the norm. This is the pattern that most of us have assumed, however. we have been lured into committing the "ecological fallacy" by looking too many times at tables and graphs of the functional status of the elderly in the aggregate. From such aggregate data, as we noted in our introductory section, we observe a monotonic pattern of functional diminution when we look at 70 year old versus 80 year old versus 90 year old populations. Aggregate patterns so often observed do not represent a simple agglomeration of individuals' health experiences, however. They reflect a "smoothing" of the data, a statistical phenomenon. At the individual level, declines in health status are often abrupt and they are not infrequently reversible (Whitehall, 1990). Our faulty assumption has gotten in the way of designing data collection which captures these abrupt discontinuities. A discontinuity or catastrophic perspective would lead us, at the least, to try harder to measure health status over more frequent intervals, certainly shorter than 24 months.
SECTION 5: BIBLIOGRAPHY
Allison, P.D. Event History Analysis: Regression for Longitudinal Event Data. Beverly Hills: Sage Publications, 1985.
Bass, D.M., Noelker, L.S. "Influence of Family Caregivers on Elder's Use of In-Home Services: An expanded Conceptual Framework." Journal of Health and Social Behavior, Vol. 23, June, 1987.
Benjamin, A.E. "Determinants of State Variations in Home Health Utilization and Expenditures Under Medicare." Medical Care, June 1986, Vol. 24, No. 6.
Benjamin, A.E. "In-Home Health and Supportive Services for Older Persons: Background and Perspective." The Institute of Health and Aging, University of CA, San Francisco, March 1, 1990.
Berkman, L. and Syme, L. "Social Networks, Host Resistance and Mortality: a nine year follow-up study of Almeda County residents." American Journal of Epidemiology 190: 1986-204, 1979.
Blazer, D.G. "Social Support and Morbidity in Elderly Community Population" American Journal of Epidemiology 115, 1982.
Branch, L.G., Jette, A.M. "A Prospective Study of Long-Term Care Institutionalization Among the Aged." American Journal of Public Health, Vol. 72, No. 12, December 1982.
Branch, L. et al. "A Prospective Study of Incident Comprehensive Medical Home Care Use Among the Elderly." American Journal of Public Health 78, 1988.
Branch, L. et al. "Transition Probabilities to Dependency, Institutionalization, and Death Among the Elderly Over a Decade." Journal of Aging and Health, Vol. 1 No. 3, August 1989.
Cohen, J. Statistical Power Analysis for the Behavioral Sciences, New York: Academic Press, 1977.
Cohen, J. and Cohen, P. Applied Multiple Regression/Correlation Analysis for the Behavioral Sciences. Lawrence Erlbaum Associates, 1975.
Coughlin, T.A., McBride, T.D., and Liu, K. Determinants of Transitory and Permanent Nursing Home Admissions. The Urban Institute. Working Paper, January, 1989.
Doty, P., Liu, K., and Wiener, J. "An Overview of Long-Term Care." Health Care Financing Review, Vol. 6 No. 3, Spring 1985.
Doty, P. "Family Care of the Elderly: The Role of Public Policy." The Millbank Quarterly, Vol. 64, No. 1, 1986.
Dunlop, B. "Expanded Home-Based Care for the Impaired Elderly: Solution or Pipe Dream?" American Journal of Public Health 70, 1980.
Dunlop, B.D.; Wells, J.A. and DeFilippes, P. "Social Contacts of the Elderly--Distribution and Demographic Correlates." Presented at the 40th Scientific Meeting of the Gerontological Society of America, Washington, D.C., 1987.
Dunlop, B. and Wells, J. Social Isolation and Health Care Utilization Among the Elderly: The Role of Informal Contacts in the Use of Services in Later Life. Draft Final Report to The Travelers Companies Foundation, May 12, 1988.
Dunlop, B.D.; Wells, J.A. and Wilensky, G.R. "The Influence of Source of Insurance Coverage on the Health Care Utilization of the Elderly." Journal of Health and Human Resources Administration 11, 1989.
Feinstein, A.R. Clinical Epidemiology. Philadelphia: W.B. Saunders, 1985.
Fitti, J.E. and Kovar, M.G. The Supplement of Aging to the 1984 National Health Interview Survey. Vital and Health Statistics. Series 1, No. 21. DHHS Publication No. (PHS)87-1323. Washington, D.C. U.S. Government Printing Office, 1987.
Freeman, D.H. Jr. "Sample Size Determination in Comparative Studies." in Bracken, M.B. (ed.) Perinatal Epidemilogy. New York: Oxford University Press, 1984.
George, L. "Easing Caregiver Burden; The Role of Informal and Formal Supports" pp.113-158 in Ward R. and S. Tobin (eds.) Health In Aging: Sociological Issues and Policy Directions. New York: Springer Publishing Company, 1987.
Greene, V.L. and Ondricj, J.I. "Risk Factors for Nursing Home Admissions and Exits: A Discrete-Time Hazard Function Approach." Journal of Gerontology, 1990, Vol. 45, No. 6.
Greene, V.L. et al. "Reducing Nursing Home Use Through Community-Based Long-Term Care: An Optimization Analysis." The All-University Gerontology Center, The Maxwell School of Citizenship and Public Affairs, Syracuse, NY, October, 1989. [Executive Summary]
Hanley, R.J., Alecxih, L.S., Wiener, J. and Kednnell D. "Predicting Elderly Nursing Home Admissions." Research on Aging, Vol. 12, No. 2, June, 1990.
Harkus, E. Family Support and Costs of Sources for the Frail Elderly: Final Report. Richmond: Virginia Center on Aging, Virginia Commonwealth University.
Hennessy, C.A. "Autonomy and Risk: The Role of Client Wishes in Community-Based Long-Term Care." The Gerontologist, Vol. 29, No. 5, 1989.
Hedrick, S.C., Koepsell, T.D., and Inui, T. "Meta-analysis of Home-Care Effects on Mortality and Nursing-Home Placement." Medical Care, November 1989, Vol. 27, No. 11.
House, J.S., Robbins, C. and Metzner, H.L. "The Association of Social Relationships and Activities with Mortality: Prospective Evidence from the Tecumseh Community Health Study. American Journal of Epidemiology 116:123-140, 1982.
Hughes, S., R. Applebaum, and Ms. Harrigan. "Impact of Long-Term Care on Hospital and Nursing Home Use and Cost" Health Services Research 22:19-47, 1987.
Hughes, S.L., Conrad, K.J., Manheim, L.M., and Edelman, P.L. "Impact of Long-Term Home Care on Mortality, Functional Status, and Unmet Needs." Health Services Research, 23:2 (June 1989).
Jackson, M.E. and Burwell, B. "Alternative Estimates of the Number of Community-Dwelling Disabled Elderly in 1990." SysteMetrics/McGraw-Hill, June 25, 1990.
Kasper, J.D. "Cognitive Impairment Among Functionally Limited Elderly People in the Community: Future Considerations for Long-Term Care Policy." Forthcoming in the Millbank Quarterly Vol. 68, No. 1, 1990.
Kemper, P. et al. "Community Care Demonstrations: What Have We Learned" Health Care Financing Review 3:87:99, 1987.
Kovar, M.G. and Poe, G.S. The National Health Interview Survey Design, 1973-1984, and Procedures, 1975-1983. Vital and Health Statistics. Series 1, No. 18, DHHS Publication No. (PHS)85-1320. Washington, D.C. U.S. Government Printing Office, 1985.
Kleinbaum, D.G., Kupper, L.L. and Morgenstern, H. Epidemiologic Research: Principles and Quantitative Methods. New York: Van Nostrand Reinhold Company, 1982.
Litwak, E. Helping the Elderly, New York: Guilford Press, 1985.
Litwak, E., and Messeri, P. "Social Supports and Mortality Rates: A Disease Specific Formulation." In Steinmetz, S.K. (ed.) Family and Social Support Systems Across the Life Span. New York: Plenum Press, 1988.
Moscovice, I., Davidson, G. and McCaffrey, D. Substitution of Formal and Informal Care for the Community-Based Elderly. Medical Care, October 1988, Vol. 26, No. 10.
Newman, S.J., and Struyk, R., with Wright, P., and Rice, M. "Overwhelming Odds: Caregiving and the Risk of Institutionalization." Journal of Gerontology: Social Sciences 1990, Vol. 45, No. 5. [Executive Summary]
National Center for Health Statistics. Supplement on Aging, Person Level Use File. Hyattsville, MD: NCHS, 1984.
Penning, M.J. "Receipt of Assistance by Elderly People: Hierarchical Selection and Task Specificity." The Gerontologist, Vol. 30, No. 2, 1990.
Rosenberg, M. The Logic of Survey Analysis. New York: Basic Books, 1968.
Seeman, T., and Berkman, L. "Structural Characteristics of Social Networks and Their Relationship with Social Support in the Elderly: Who Provides Support." Social Science and Medicine 26(3), 1988.
Shapiro, E., and Tate, R. "Who is Really At Risk of Institutionalization?" The Gerontologist, Vol. 28, No. 2, 1988.
Soldo, B., and Manton, K. "Health status and service needs of the oldest old: current patterns and future trends." Millbank Memorial Fund Quarterly: Health and Society 63, 1985.
Soldo, B.J., Agree, E.M., and Wolf, D.A. "The Balance Between Formal and Informal Care." Aging and Health Care, 1989.
Stoller, E.P., and Pugliesi, K.L. "Informal Networks of Community-Based Elderly, Changes in Composition over Time." Research on Aging, Vol. 10, No. 4, December 1988.
Stone, R., and Maurtaugh, C.M. "The Elderly Population with Chronic Functional Disability: Implications for Home Care Eligibility." The Gerontological Society of America, Vol. 30, No. 4, 1990.
Stone, R., and Short, P. "The Competing Demands of Employment and Informal Caregiving to Disabled Elders." Medical Care. Vol. 8, No. 6, June 1990.
Stone, R., and Kemper, P. "Spouses and Children of Disabled Elders: How Large a Constituency for Long-term Care Reform?" The Millbank Quarterly, Vol. 67, Nos. 3-4, 1989.
Stone, R., Cofferata, G., and Sangl, J. "Caregivers of the Frail Elderly: A National Profile." The Gerontologist 27(1), 1987.
Susser, M. Causal Thinking in the Health Sciences Concepts and Strategies of Epidemiology. New York: Oxford University Press, 1978.
Tennstedt, S., Sullivan, L.M., McKinlay, J.B., and D'Agostino, R. "How Important is Functional Status as a Predictor of Service Use by Older People?" Journal of Aging and Health, Vol. 2, No. 4, November 1990.
Travis, S.S., and McAuley, W.J. "Simple Counts of the Number of Basic ADL Dependencies for Long-Term Care Research and Practice." Health Services Research, 25:2, June 1990.
U.S. House of Representatives, Select Committee on Aging. "Exploding the Myths: Caregiving in America" Commercial Publication No. 99-611. Washington, DC: U.S. Government.
Whitelaw, N.A. "Who Are the Frail Elderly: Comparing Different Definitions of Frailty." Unpublished Paper, October 12, 1990.
Wiener, J.M., Hanley, R., Clark, R., and Van Nostrand, J. "Measuring the Activities of Daily Living: Comparisons Across National Surveys." Journal of Gerontology: Social Sciences, 1990, Vol. 45, No. 6.
Weissert, W. "Seven Reasons Why it is so Difficult to Make Community-Based Long-Term Care Cost-Effective." Health Services Research, Vol. 20, 1985.
Weissert, W. "Hard Choices: Targeting Long-Term Care to the At Risk Aged?" Journal of Health Politics, Policy and Law, 11:463-481, Fall 1986.
Weissert, W., and Scanlon, W. "Determinants of Institutionalization of the Aged." The Urban Institute, July 1983.
Wells, J.A., and Dunlop, B.D. "Social Isolation of the Elderly Predicts Lack of Contacts with Physicians." Presented to the Ninth Annual Meeting of the Society of Behavioral Medicine, Boston, MA, 1988.
Wells, J.A., and Dunlop, B.D. "Social Networks and Mortality: A Natural Sample Two-Year Follow-up." (In preparation.)
Wells, J.A. "The Role of Social Support Groups in Stress Coping in Organizational Settings." In Sethi, A.S., and Schuler, R.S. (eds.) Cambridge, MA: The Handbook of Organizational Stress Coping Strategies. Ballinger Publishing Company, 1984.
APPENDIX A: ORTHOGONAL CODING OF DUMMY VARIABLES
Dummy variables representing the comparisons are designed by coding one category in each comparison as 1 and the other category as -1. For the five categories of help shown in the following table, four comparisons are possible. To be orthogonal, i.e., uncorrelated, they must fulfill the criteria that the mean of each contrast equals zero and the cross-products of any pair of contrasts equal zero. If the number of cases in each category is equal, then the orthogonal criteria will hold. otherwise the values in the table must be weighted according to the proportion of cases observed in the categories.
| Comparison | Caregiver Help Category | ||||
|---|---|---|---|---|---|
| Without Disability (1) | Disability Without Help (2) | With Only Paid Help (3) | Some Unpaid Help: Family (4) | Some Unpaid Help: Other (5) | |
| (A) | 1 | -1/4 | -1/4 | -1/4 | -1/4 |
| (B) | 0 | 1 | -1/3 | -1/3 | -1/3 |
| (C) | 0 | 0 | 1 | -1/2 | -1/2 |
| (D) | 0 | 0 | 0 | 1 | -1 |
In comparison (D), for example, if the latter categories have 50 and 25 cases respectively, then the comparison will have weights 2/3 (50/75) and 1/3 (25/75), respectively. Note that [50 cases x 1 (the code) x 1/3 (the weight)] + [25 cases x -1 (the code) x 2/3 (the weight)] = 0. Weights differ depending on the outcome analyzed since the mortality and nursing home data sets differ in number of cases. The weights used in this report are shown in Table A.1 and Table A.2.
| TABLE A.1. Weights for Orthogonal Contrasts Among Caregiving Categories: Mortality Data Set | ||||||||
|---|---|---|---|---|---|---|---|---|
| Hypothesis | Caregiver Help Category | |||||||
| Without Disability (1) | Disability Without Help (2) | With Only Paid Help (3) | Some Unpaid Help: Family (4) | Some Unpaid Help: Other (5) | With Only Unpaid Help (6) | Some Paid Help: Family (7) | Some Paid Help: Other (8) | |
| (0) | .7237 | -.2763 | -.2763 | -.2763 | -.2763 | N/A | N/A | N/A |
| (1A) | 0 | .1322 | -.8678 | -.8678 | -.8678 | N/A | N/A | N/A |
| (1B) | 0 | 0 | .1898 | -.8102 | -.8102 | N/A | N/A | N/A |
| (1C) | 0 | 0 | 0 | .6284 | -.3716 | N/A | N/A | N/A |
| (2B) | 0 | 0 | N/A | N/A | N/A | .7970 | -.2050 | -.2050 |
| (2C) | 0 | 0 | N/A | N/A | N/A | 0 | .4725 | -.5275 |
| TABLE A.2. Weights for Orthogonal Contrasts Among Caregiving Categories: Nursing Home Data Set | ||||||||
|---|---|---|---|---|---|---|---|---|
| Hypothesis | Caregiver Help Category | |||||||
| Without Disability (1) | Disability Without Help (2) | With Only Paid Help (3) | Some Unpaid Help: Family (4) | Some Unpaid Help: Other (5) | With Only Unpaid Help (6) | Some Paid Help: Family (7) | Some Paid Help: Other (8) | |
| (0) | .7244 | -.2756 | -.2756 | -.2756 | -.2756 | N/A | N/A | N/A |
| (1A) | 0 | .1232 | -.8768 | -.8768 | -.8768 | N/A | N/A | N/A |
| (1B) | 0 | 0 | .1869 | -.8131 | -.8131 | N/A | N/A | N/A |
| (1C) | 0 | 0 | 0 | .6253 | -.3747 | N/A | N/A | N/A |
| (2B) | 0 | 0 | N/A | N/A | N/A | .7968 | -.2032 | -.2032 |
| (2C) | 0 | 0 | N/A | N/A | N/A | 0 | .4671 | -.5329 |
APPENDIX B: ASSOCIATIONS BETWEEN CAREGIVING ARRANGEMENTS AND CONFOUNDING VARIABLES
| TABLE B.1. Associations Between Caregiving Arrangements and Confounding Variables: Mortality | ||||||
|---|---|---|---|---|---|---|
| Disability | Help | Any Unpaid Help | Any Close Family Unpaid Help | All Unpaid Help | All Unpaid Help, Close Family | |
| Age | 1.10* | 1.11* | 1.11* | 1.09* | 1.12* | 1.12* |
| Sex | 1.78* | 1.92* | 0.72 | 2.00* | 2.07* | 2.19 |
| Race Black Hispanic Other |
1.37* 1.09 1.03 |
0.78 0.97 - |
1.06 1.27 1.53 |
1.75* 0.84 1.06 |
0.40* 0.88 0.70 |
4.34 0.59 - |
| Education High School College |
0.73* 0.70* |
1.13 1.30 |
0.62* 0.43* |
1.36* 1.16 |
1.61* 1.70* |
1.49 0.95 |
| Income Missing >Poverty, <$10,000 $10,000-$19,000 $20,000-$34,000 >$35,000 |
1.08 0.99 0.74* 0.84 0.95 |
1.34 1.87 0.89 1.74 2.53 |
0.98 0.66* 1.02 0.88 2.89* |
1.48* 1.16 0.57* 0.63* 0.32* |
1.91* 1.06 0.71 1.13 0.99 |
1.29 1.12 0.60 1.19 1.06* |
| Living Arrangements Lives Alone Lives w/Other Persons |
0.97 2.30* |
0.76 2.51* |
0.26* 3.73* |
5.18* 0.67* |
1.82* 0.71 |
3.44* 1.01 |
| Social Contacts | 0.68* | 0.69* | 0.67* | 0.76* | 0.71* | 0.77* |
| Volunteers in Community | 0.30* | 0.79 | 0.72* | 1.50 | 0.88 | 2.80 |
| Control Over Health Some Little None Unknown (Proxy) |
0.74* 2.10* 2.06* 3.59* |
0.73 0.73 1.05 2.40* |
0.72* 0.68 0.99 3.22* |
2.01* 1.50 1.11 0.31* |
0.63* 1.30 1.22 1.17 |
2.19* 1.30 1.53 0.28* |
| Health Status Very Good Good Fair Poor |
1.44* 0.52* 2.13* 9.59* |
0.96 0.61* 1.46* 1.26 |
0.45* 1.32 1.03 1.39 |
1.51 1.04 1.15 0.64* |
0.56 0.91 0.86 1.38 |
2.86 1.15 1.06 0.57 |
| Activities of Daily Living | NA | 1.38* | 4.02* | 1.53* | 1.94* | 1.60* |
| Institutional Activities of Daily Living | NA | 8.69* | 13.85 | 1.80* | 2.21* | 1.88* |
| Confusion | 2.74* | 1.61 | 0.76 | 1.29 | 0.91 | 7.86 |
| Alzheimer's | 10.63* | 2.93 | 4.28 | 0.64 | 4.03* | 0.43 |
| Urinary Incontinence | 4.92* | 2.28* | 1.24 | 1.09 | 1.69* | 0.73 |
| Bowel Incontinence | 6.46* | 2.00* | 0.87 | 1.16 | 2.16* | 0.73 |
| Cancer | 1.45* | 1.65 | 0.80 | 0.73 | 1.02 | 0.88 |
| Heart Disease | 2.44* | 1.34 | 0.99 | 1.12 | 1.28 | 1.23 |
| Cerebrovascular Accident (Stroke) | 4.52* | 1.78* | 1.60* | 0.55* | 1.64* | 0.53 |
| Osteoporosis | 2.55* | 1.54 | 0.64 | 0.92 | 2.24* | 0.41 |
| Hip Fracture | 3.42* | 2.35* | 1.00 | 1.04 | 2.10* | 0.59 |
| Fell 2 or More Times | 4.16* | 1.24 | 1.16 | 1.04 | 0.99 | 0.87 |
| Fell Because of Dizziness | 5.25* | 1.06 | 1.86* | 0.76 | 0.73 | 0.67 |
| Nursing Home Stay Prior to 1st Interview | 5.52* | 2.38 | 0.79 | 1.41 | 1.99* | 1.26 |
| Hospital Inpatient Stays | 1.86* | 1.90* | 1.73* | 1.35* | 1.50* | 1.27* |
| * = significant at <.05 NA = disability outcome is defined on basis of ADLs and IADLs. |
||||||
| TABLE B.2. Associations Between Caregiving Arrangements and Confounding Variables: Institutionalization Data Set (Odds Ratios) | ||||||
|---|---|---|---|---|---|---|
| Disability | Help | Any Unpaid Help | Any Close Family Unpaid Help | All Unpaid Help | All Unpaid Help, Close Family | |
| Age | 1.10* | 1.11* | 1.11* | 1.09* | 1.12* | 1.10* |
| Sex | 1.75* | 1.95* | 0.71 | 1.87* | 2.06* | 1.98 |
| Race Black Hispanic Other |
1.29* 1.03 1.04 |
0.72 1.37 - |
1.07 2.03 2.79 |
1.70 0.88 1.20 |
0.39 0.93 0.78 |
7.61 0.58 -- |
| Education High School College |
0.72* 0.67* |
1.12 1.22 |
0.60* 0.40* |
1.35* 1.14 |
1.64* 1.61 |
1.37 0.93 |
| Income Missing >Poverty, <$10,000 $10,000-$19,000 $20,000-$34,000 >$35,000 |
1.07 0.97 0.76* 0.83 1.00 |
1.53 1.00 0.82 1.46 2.25 |
0.94 0.74 0.98 0.76 2.74* |
1.57* 1.15 0.58* 0.65 0.33* |
1.91* 1.09 0.68 1.17 1.05 |
1.40 1.27 0.61 0.96 0.16* |
| Living Arrangements Lives Alone Lives w/Other Persons |
0.97 2.34* |
0.80 2.57* |
0.27* 3.46* |
5.24* 0.66* |
1.64* 0.78 |
3.57* 0.99 |
| Social Contacts | 0.68* | 0.69* | 0.66* | 0.75* | 0.69* | 0.76* |
| Volunteers in Community | 0.31* | 0.70 | 0.48* | 1.55 | 0.92 | 2.75 |
| Control Over Health Some Little None Unknown (Proxy) |
0.75* 2.12* 2.05* 3.68* |
0.72 0.73 1.04 3.18* |
0.68 0.80 1.00 3.31* |
1.97* 1.58* 1.18 0.31* |
0.63* 1.33 1.30 1.14* |
2.03 1.43 1.58 0.31* |
| Health Status Very Good Good Fair Poor |
0.44* 0.54* 2.12* 10.00* |
0.91 0.61* 1.16* 1.22 |
0.41* 1.29 0.98 1.64* |
1.36 1.07 1.16 0.66* |
0.50 0.92 0.90 1.34 |
2.13 1.33 1.04 0.59 |
| Activities of Daily Living | NA | 1.39* | 4.18* | 1.52* | 1.92* | 1.58* |
| Institutional Activities of Daily Living | NA | 7.81* | 15.65* | 1.78* | 2.17* | 1.84* |
| Confusion | 3.01* | 1.38 | 0.68 | 1.39 | 1.03 | 1.83 |
| Alzheimer's | 10.14* | 2.56 | 3.97 | 0.69 | 3.61* | 0.51 |
| Urinary Incontinence | 4.92* | 1.97* | 1.38 | 1.04 | 1.62* | 0.70 |
| Bowel Incontinence | 6.21* | 1.87* | 0.96 | 1.11 | 2.02* | 0.69 |
| Cancer | 1.48* | 1.77 | 0.75 | 0.73 | 1.07 | 0.93 |
| Heart Disease | 2.38* | 1.22 | 0.99 | 1.16 | 1.37 | 1.29 |
| Cerebrovascular Accident (Stroke) | 4.58* | 1.69 | 1.74* | 1.61* | 1.57* | 2.50 |
| Osteoporosis | 2.50* | 1.48 | 0.59 | 1.1 | 2.81* | 0.40 |
| Hip Fracture | 3.66* | 2.00 | 1.01 | 0.90 | 2.12* | 0.47 |
| Fell 2 or More Times | 4.11* | 1.24 | 1.24 | 0.96 | 0.89 | 0.64 |
| Fell Because of Dizziness | 5.54* | 1.13 | 1.67 | 0.77 | 0.70 | 0.46 |
| Nursing Home Stay Prior to 1st Interview | 6.15* | 3.34* | 0.80 | 1.30 | 1.77 | 1.14 |
| Hospital Inpatient Stays | 1.90* | 1.93* | 1.76* | 1.36* | 1.50* | 1.31* |
| * = significant at <.05 NA = disability outcome is defined on basis of ADLs and IADLs. |
||||||
