Executive Summary
The Affordable Care Act continues to bring transparency and scrutiny to health insurance rate increases. Because of the law, the Department of Health and Human Services (HHS), along with states, is working to hold insurance companies accountable by requiring them to document, submit for review, and publicly justify rate increases of 10 percent or more. Additionally, the Affordable Care Act continues to provide states with rate review grants to enhance state efforts to review proposed increases in health insurance rates and make information and decisions about rate increases available to the public.
An analysis from the Office of the Assistant Secretary for Planning and Evaluation (ASPE) of rate review activities in calendar year (CY) 2012 shows that the rate review process saved consumers approximately $1.2 billion on their premiums when compared to the amount initially requested by insurers. These savings accrued to 6.8 million people. In the individual market, the average rate request increase dropped by 12 percent (from 8.1 percent to 7.1 percent) after rate review, saving consumers an estimated $311 million. Similarly, in the small group market, the average rate increase request declined by 19 percent (from 5.8 percent to 4.7 percent), saving consumers an estimated $866 million after rate review. This is in addition to the $500 million in medical loss ratio rebates for 2012, for a total $1.7 billion in savings in 2012.
Moreover, insurers were much less likely to submit requests for rate increases of 10 percent or more in 2012 than in previous years, and it is likely that this change in issuer behavior is a result of the Affordable Care Act policy that requires requests for increases of 10 percent or more to be justified and reviewed. In 2012, 26 percent of requests for rate increases in the individual market were for an increase of 10 percent or more, significantly lower than the 43 percent requested in 2011. This change in issuer behavior resulted in additional savings to consumers on top of the direct savings estimated above.
Introduction
This is the second Rate Review Annual Report issued by HHS. The first was issued in September 2012 and was based on data submitted by rate review grantee states from September 2011, when reporting from grantee states began, through July 2012. This Annual Report is based on the data for requested and approved rate increases submitted by grantee states for CY 2012. This report analyzes both the rate review process and rate review grant activities, which are programs initiated by the Affordable Care Act to ensure that consumers get value for their premium dollars. Due to limitations of the data submitted by certain states, this report extrapolates from an analysis of data from 39 states in the individual market and 35 states in the small group market to estimate national savings on premiums in the individual and small group markets.
Background
Rate Review Grants
The Affordable Care Act authorizes the Secretary to award grants to states for the purpose of improving their review of proposed rates in the individual and small group health insurance markets.1 The law appropriates $250 million for rate review grants for a five year period, fiscal years 2010 through 2014. Each state receiving a grant must submit data to HHS documenting all rate increases requested by issuers for major medical policies in both the individual and small group health insurance markets of that state. The Rate Review Grant Program awarded a total of $51 million to 45 states, 5 territories, and the District of Columbia through the first cycle of funding. Through the second cycle of funding, an additional $119 million was awarded to 30 states, three territories, and the District of Columbia.
Rate Requests for Increases of 10 Percent or More
Regulations implementing the Affordable Care Act also require health issuers that seek a rate increase of 10 percent or more to submit, both to their state insurance regulator and HHS, a justification of the rate increase.2 The request, justification, and determination of whether the requested increase is unreasonable, are public information posted by both HHS and the state. This report’s conclusions about rate increases that equal or exceed 10 percent are based on an analysis of the rate justification information submitted to HHS.
2012 Findings
Rate Review Grants Program
As part of the Rate Review Grants Program, HHS collects data on all rate increases, even those below 10 percent, from every state that received a grant.3 Figure 1 summarizes the results for the individual health insurance market. Figure 2 summarizes the results for the small group insurance market.
Individual Market
Based on information from 39 states from the individual market, the estimated national average rate increase implemented in the individual market in 2012 is approximately 12 percent lower than the increase originally requested by insurance companies. Based on 2012 individual market premium data for all states, this difference equates to about $311 million in savings to consumers. For the 39 states, 30.5 percent of total covered lives had rate change requests reduced or denied. Extrapolating to the total number of 11.1 million covered lives in the individual market, an estimated 3.4 million individuals had rate change requests reduced or denied.
| Individual Market Rate Change, 2012 | Requested | Implemented |
|---|---|---|
| Sources: Revised State Rate Review Grant (RRG) data and data from state websites plus data from Florida (non-grant state) | ||
| Number of rate filings in 39 states | 832 | 832 |
| Number of covered lives affected by these rate filings | 7,024,186 | 7,024,186 |
| Average rate change for 39 states | 8.1% | 7.1% |
| Average rate change when request >=10% for 39 states | 14.2% | 12.1% |
| % filings with rate change requested >=10% for 39 states | 26.1% | 21.8% |
| % covered lives with rate change requested>=10% for 39 states | 22.8% | 16.7% |
| % covered lives with rate change request reduced or denied | 30.5% | |
| Total covered lives with rate request change reduced or denied based on 11.1 million total covered lives for all states | 3.4 million | |
| Total U.S. savings based on $31.1 billion total premiums in individual and small group markets for all states | $311 million | |
Premium and covered lives data are based on the Medical Loss Ratio (MLR) annual reports4 for all 50 states and the District of Columbia, whereas the average increase in premiums is based on ASPE’s analysis of 38 states using Rate Review Grants (RRG) Program data, plus Florida, a non-grant state, using data available on Florida’s Office of Insurance Regulation website. Taking the average difference between rate changes requested and rate changes implemented, weighted by the number of covered lives, and multiplied by the estimated total U.S. premiums, this report extrapolates national savings estimates for consumers in the individual market resulting from rate review.5
Small Group Market
In the small group market, analysis of the information from 35 states indicates that the implemented rate increases are approximately 19 percent lower than the rates originally requested by insurance companies.6 This difference equates to approximately $866 million in savings to consumers based on 2012 small group market premium data. For the 35 states, 18.7 percent of total covered lives had rate requests reduced or denied. Extrapolating to the total number of 18.1 million covered lives in the small group market, an estimated 3.4 million individuals had rate requests reduced or denied.
As with the individual market data, the small group premium data are based on MLR data from 50 states and the District of Columbia,7 whereas the average difference between rate changes requested and rate changes implemented is taken from ASPE’s analysis of 35 states in the small group market using RRG data and data from Florida, a non-grant state. Again, the results were extrapolated to approximate a national savings total for the small group market as a result of rate review.
| Small Group Market Rate Change, 2012 | Requested | Implemented |
|---|---|---|
| Sources: Revised State Rate Review Grant (RRG) data and data from state websites plus data from Florida (non-grant state) | ||
| Number of rate filings in 35 states | 772 | 772 |
| Number of covered lives affected by these rate filings | 10,938,053 | 10,938,053 |
| Average rate change for 35 states | 5.8% | 4.7% |
| Average rate change when request >=10% for 35 states | 16.3% | 9.7% |
| % filings with rate change requested >=10% for 35 states | 14.0% | 11.7% |
| % covered lives with rate change requested >=10% for 35 states | 14.7% | 9.3% |
| % covered lives with rate change request reduced or denied | 18.7% | |
| Total covered lives with rate change request reduced or denied based on 18.1 million total covered lives for all states | 3.4 million | |
| Total U.S. savings based on $78.7 billion total premiums for all states | $866 million | |
Total premiums in the individual and small group markets were lower by an estimated $1.2 billion compared to the total premiums initially requested.
Rate Justification Program
The Affordable Care Act authorizes HHS to focus special attention on rate increase requests that are potentially “unreasonable.” By regulation, HHS has defined requested rate increases of 10 percent or more as the threshold triggering greater scrutiny.8 Insurance companies requesting such an increase must submit, both to HHS and their state regulator, a justification for such request. Reviewing data collected from the Rate Justification Program, HHS found that in both the individual and small group markets, approximately 28 percent of all rate increase requests of 10 percent or more were modified or rejected (see Appendix tables A-1 and A-2).
Individual Market
Approximately 28 percent of all 2012 individual market rate increase requests of 10 percent or more were modified by the issuer or rejected by the state (where the state had such authority).
Figure 3
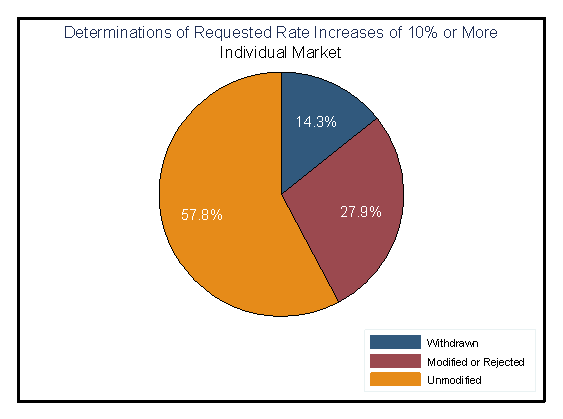
Source: Rate Review Justification data are submitted to the Center for Consumer Information and Insurance Oversight (CCIIO) for rate requests of 10 percent or more. This analysis used only adjudicated requests with effective dates between January 1, 2012 and December 31, 2012.
This trend in the individual market corroborates findings from a February 2013 ASPE issue brief based on data from 15 states. That brief showed that the proportion of rate filings for the individual market in which the requested increase was 10 percent or more declined from 75 percent in 2010 and 50 percent in 2011 to 34 percent in 2012. The average rate increases requested and implemented were 9.4 percent and 8.1 percent, respectively. Taken together, the findings from the February 2013 ASPE issue brief and this paper suggest that the rate review provisions of the Affordable Care Act result in fewer requests for large rate increases overall and in modifications or withdrawals of some proposed rate increases.9
Small Group Market
Approximately 28 percent of 2012 small group market rate increase requests of 10 percent or more were modified by the issuer or rejected by the state.
Figure 4
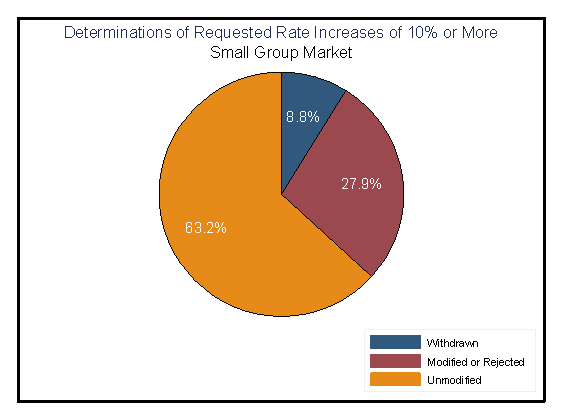
Source: Rate Review Justification data are submitted to CCIIO for rate requests of 10 percent or more. This analysis used only adjudicated requests with effective dates between January 1, 2012 and December 31, 2012.
Estimates of Savings by State for Rates Proposed at 10 Percent or Higher
In figure 5, savings by state are estimated using the Rate Review Justification (RRJ) data submitted to CCIIO for CY 2012. Note that RRJ data differs from the Rate Review Grant data in that RRJ data only includes rate increase requests of 10 percent or more and thus represents a subset of the $1.2 billion in savings previously described. The estimated savings, which include both the individual and small group markets, are calculated by taking the difference between the average requested rate increase, and the average approved rate increase, weighted by covered lives, for each filing that had a modification, rejection, or withdrawal. This method assumes that each enrollee in these plans paid the statewide average premium for the year which is a limitation of the analysis.
| Individual Market | Small Group Market | Total, Both Markets | ||||
|---|---|---|---|---|---|---|
| State | Number of Enrollees with Rate Review Savings | Estimated Premium Savings | Number of Enrollees with Rate Review Savings | Estimated Premium Savings | Number of Enrollees with Rate Review Savings | Estimated Premium Savings |
Sources: Rate Review Justification dataset for premium increase requests of 10% or more, as well as numbers of enrollees affected by each rate increase request. | ||||||
Arizona | - | - | 765 | $618,753 | 765 | $618,753 |
Arkansas | 266 | $24,279 | - | - | 266 | $24,279 |
California | 166,652 | $35,668,218 | 377 | $269,009 | 167,029 | $35,937,228 |
Colorado | 30,490 | $12,090,243 | - | - | 30,490 | $12,090,243 |
Connecticut | 163 | $10,005 | 84,799 | $6,189,943 | 84,962 | $6,199,947 |
Florida | 11,571 | $6,162,406 | 12,215 | $775,031 | 23,786 | $6,937,436 |
Illinois | 15,991 | $2,496,786 | - | - | 15,991 | $2,496,786 |
Indiana | 3,304 | $1,690,440 | 13,881 | $2,154,155 | 17,185 | $3,844,596 |
Iowa | - | - | 6,929 | $1,167,576 | 6,929 | $1,167,576 |
Kansas | - | - | 2,104 | $838,940 | 2,104 | $838,940 |
Maine | 1,105 | $413,072 | 1,105 | $413,072 | ||
Michigan | 20,503 | $3,573,777 | 61,437 | $7,352,003 | 81,940 | $10,925,781 |
Missouri | 461 | $74,294 | - | - | 461 | $74,294 |
Nevada | 7,484 | $1,074,018 | 7,484 | $1,074,018 | ||
New York | - | - | 94,991 | $22,636,478 | 94,991 | $22,636,478 |
North Carolina | - | - | 2,174 | $70,151 | 2,174 | $70,151 |
North Dakota | 4,580 | $1,710,182 | 1,416 | $507,387 | 5,996 | $2,217,568 |
Oregon | 15,554 | $2,506,854 | - | - | 15,554 | $2,506,854 |
Pennsylvania | - | - | 81,200 | $3,895,436 | 81,200 | $3,895,436 |
South Carolina | 7,684 | $1,649,812 | 1,421 | $406,381 | 9,105 | $2,056,193 |
South Dakota | 225 | $133,522 | 499 | $242,299 | 724 | $375,821 |
Utah | 3,519 | $1,075,618 | - | - | 3,519 | $1,075,618 |
Vermont | 600 | $261,378 | 2,302 | $96,164 | 2,902 | $357,542 |
Washington | 309,768 | $31,818,918 | 21,360 | $89,482 | 331,128 | $31,908,400 |
West Virginia | - | - | 221 | $197,110 | 221 | $197,110 |
Wisconsin | 286 | $108,154 | 10,350 | $4,702,400 | 10,636 | $4,810,554 |
Total | 600,206 | $102,541,976 | 398,441 | $52,208,698 | 998,647 | $154,750,674 |
Rate Review Grantee Activities
Between 2010 and 2012, 47 states, including the District of Columbia, received Rate Review Grants. States are using Rate Review Grant funds to implement extensive enhancements to their rate review programs and increase publicly-available data. One means of enhancing their programs was to institute rate review authority. Between 2010 and 2012, the number of states with prior rate review authority for their small group health insurance market products increased from 29 to 36 states.10 States with prior rate review authority for their individual health insurance market products increased from 34 to 37 states.11 While only a limited number of states made rate filings public before the Affordable Care Act (e.g., Arkansas, Florida, North Carolina, Oregon, Pennsylvania, and Wisconsin), 35 states now have rate filings or summaries of rate increases publicly available on their state insurance websites. Other examples of state activities include:
- Arkansas: The Arkansas Insurance Department created the Insurance Rate Analysis and Tracking Engine (iRATE) to automate and streamline the rate review process. The iRATE system is a customizable application that permits state officials to quickly retrieve and analyze the filing data required by their states’ rules and regulations. Upon completion in 2013, Arkansas made iRATE available to every state and territory, free of charge.
- Illinois: In 2012, the Illinois Department of Insurance used Rate Review Grant funds to develop a new rate review website with an interactive web tool displaying individual and group rate filings from 2005 to 2012.
- Maryland: Prior to July 1, 2012, the Maryland Insurance Administration only posted rate filings that proposed increases of 10 percent or more. Starting on July 1, 2012, the Maryland Insurance Administration began to publish all proposed rate filings in the individual and small group market.
- Nebraska: Nebraska developed and released a new rate review website, which permits consumers to comment online on rate filings and to learn more about the rate review process. By the end of 2012, the new website had almost 90,000 hits.
- New Jersey: In New Jersey, Rate Review Grant funds enhanced rate complaints investigations, which helped the state to institute a new tracking and consumer response system. One investigation revealed that policyholders had been overcharged due to an unintended administrative error.
- Oregon: Oregon’s Department of Consumer and Business Services (DCBS) used Rate Review Grant funds to hold live-stream rate review hearings on almost all small group and individual health benefit plan rate filings. For those who attended the hearing via live-stream, DCBS permitted phone-in testimony. After each hearing, DCBS posted the video file on its website, enabling the public to watch hearings at their convenience. During fiscal year 2012, rate review performed by the Oregon Insurance Division resulted in decreases to approximately three-quarters of the proposed rate hikes. Also, two new actuaries are helping the state to provide greater scrutiny of proposed rate hikes. In addition, Oregon has contracted with a consumer advocacy organization to represent consumers in the rate review process, participate in hearings, and develop long-term strategies to increase consumer input.
- Pennsylvania: Pennsylvania enacted a statute granting the Department of Insurance the authority to regulate commercial small group health premiums, effective March 21, 2012. Not only did this new authority permit greater scrutiny of proposed rate increases, it has also allowed the Department of Insurance to identify and halt improper rating practices by insurance companies.
- Rhode Island: Rhode Island is using its Rate Review Grant funds to expand its rate review oversight to address the underlying factors driving rate increases. By issuing and implementing “Affordability Standards” as part of its rate review process, Rhode Island is engaging health plans in delivery system transformation.
Conclusion
The rate review provisions of the Affordable Care Act are building the foundation for a health insurance marketplace where consumers can make informed choices and insurance companies are held accountable for unreasonable rate increases. Requests for rate changes are now public information, and issuers must provide a justification for requested increases of 10 percent or more. Data from 2012 suggests that rate review continues to be an important innovation that provides consumers with greater information and achieves significant savings.
Appendix
Methodology
This is the second Rate Review Annual Report issued by HHS. The first was issued in September 2012 and was based on data submitted by rate review grantee states from September 2011, when reporting from grantee states began, through July 2012. This Annual Report is based on the data for requested and approved rate increases submitted by grantee states for CY 2012.12
Rate Review Grant (RRG) Data
HHS awarded State Rate Review Grants to states in September 2011 and September 2012. States submitted data to HHS on rate increases for major medical policies in their individual and small group policies as part of their State Rate Review Grant requirements. The Rate Review Grant (RRG) database consists of state quarterly submissions, from 2011 Quarter 3 to 2013 Quarter 2, for rate increases effective for calendar years 2011, 2012, and 2013, but with only partial data for 2011 and 2013. For 2012, rate filings with a limited number of covered lives were submitted in five out of 43 states in the individual market and two out of 37 states in the small group market, and thus were excluded from the analysis. Rate filings that combined small and large groups were not included in the analysis because the rate changes and covered lives specific to the small groups are not always available. ASPE supplemented its analysis of RRG data with data from the Florida Office of Insurance Regulation website for a total of 39 states in the individual market and 35 states in the small group market for calendar year 2012.
ASPE manually cleaned the data to correct rate filings that were out of scope, or contained similar or duplicative entries, missing or incomplete filings, or incorrect data on requested and/or approved rate changes.13 ASPE then compared the cleaned RRG data with an ASPE database of individual market rate changes for 15 states (available from state websites: Arkansas, California, Connecticut, Delaware, Florida, Indiana, Maine, Minnesota, North Carolina, New Jersey, Oregon, Pennsylvania, Rhode Island, Washington, and Wisconsin). After revising the RRG data for incomplete or incorrect data and comparing the RRG data with the ASPE database, 7.5 percent of rate filings for individual policies were revised, which affected 26.6 percent of total covered lives.
ASPE does not have a database for small group rate increases but checked available data on several state websites for rate filings that had unusual entries. After cleaning the RRG data, 11.3 percent of rate filings for small group policies were revised, which affected 23.7 percent of total covered lives.
Rate Review Justification (RRJ) Data
Rate Review Justification data are submitted to the Center for Consumer Information and Insurance Oversight (CCIIO) for rate requests of 10 percent or more. This analysis used only adjudicated requests with effective dates between January 1, 2012 and December 31, 2012.
A limitation to this method for estimating savings by state is that it assumes that each affected enrollee in these plans paid the statewide average premium, which may not be likely when small numbers of enrollees are affected. Another limitation is that the savings are applied to a full year of premiums, even though many rate increases go into effect mid-year.
| State | A: Total Number of Requests Reviewed2 | B: Total Number of Requests Modified or Rejected | C: Total Number not Modified | D: Total Number Withdrawn3 |
|---|---|---|---|---|
| 1 Only includes states with at least one rate increase request of 10% or more 2 Column A=Column B + Column C + Column D 3 Includes re-submissions | ||||
Alaska | 1 | - | 1 | - |
Arizona | 9 | - | 6 | 3 |
Arkansas | 2 | 2 | - | - |
California | 9 | 6 | 3 | - |
Colorado | 6 | 2 | 3 | 1 |
Connecticut | 1 | 1 | - | - |
Florida | 6 | - | 4 | 2 |
Idaho | 5 | - | 3 | 2 |
Illinois | 9 | - | 9 | - |
Indiana | 3 | 2 | - | 1 |
Kentucky | 2 | - | 2 | - |
Louisiana | 4 | - | 4 | - |
Maine | 2 | 1 | 1 | - |
Michigan | 5 | - | 3 | 2 |
Missouri | 7 | 1 | 6 | - |
Montana | 7 | 1 | 6 | - |
Nebraska | 6 | - | 4 | 2 |
Nevada | 6 | 4 | - | 2 |
North Dakota | 6 | 2 | 4 | - |
Ohio | 4 | - | 4 | - |
Oklahoma | 1 | - | 1 | - |
Oregon | 5 | 4 | - | 1 |
South Carolina | 3 | 3 | - | - |
South Dakota | 3 | 1 | 2 | - |
Texas | 2 | - | 2 | - |
Utah | 4 | - | - | 4 |
Vermont | 1 | 1 | - | - |
Washington | 12 | 10 | - | 2 |
Wisconsin | 21 | 2 | 19 | - |
Wyoming | 2 | - | 2 | - |
Total | 154 | 43 | 89 | 22 |
State | A: Total Number of Requests | B: Total Number of Requests | C: Total Number | D: Total Number |
|---|---|---|---|---|
| 1 Only includes states with at least one rate increase request of 10% or more 2 Column A=Column B + Column C + Column D 3 Includes re-submissions | ||||
Alabama | 1 | - | 1 | - |
Alaska | 3 | - | 3 | - |
Arizona | 3 | 2 | 1 | - |
California | 9 | 1 | 8 | - |
Colorado | 1 | - | 1 | - |
Connecticut | 4 | 3 | 1 | - |
Delaware | 4 | - | 4 | - |
Florida | 9 | 1 | 8 | - |
Georgia | 1 | 1 | - | - |
Idaho | 1 | - | 1 | - |
Illinois | 4 | - | 4 | - |
Indiana | 3 | 3 | - | - |
Iowa | 5 | 4 | 1 | - |
Kansas | 4 | 2 | 2 | - |
Maine | 3 | - | 3 | - |
Maryland | 1 | - | 1 | - |
Michigan | 8 | 5 | 1 | 2 |
Mississippi | 1 | - | - | 1 |
Missouri | 2 | - | 1 | 1 |
Montana | 1 | - | 1 | - |
Nevada | 3 | - | 3 | - |
New Jersey | 6 | - | 6 | - |
New York | 4 | 4 | - | - |
North Carolina | 2 | 2 | - | - |
North Dakota | 2 | 2 | - | - |
Ohio | 6 | - | 5 | 1 |
Oklahoma | 2 | - | 2 | - |
Pennsylvania | 1 | 1 | - | - |
South Carolina | 2 | 2 | - | - |
South Dakota | 2 | 2 | - | - |
Texas | 5 | - | 3 | 2 |
Utah | 1 | - | 1 | - |
Vermont | 1 | 1 | - | - |
Washington | 6 | 1 | 5 | - |
West Virginia | 5 | 1 | 4 | - |
Wisconsin | 20 | - | 15 | 5 |
Total | 136 | 38 | 86 | 12 |
Endnotes
1 § 2794(c) of the Public Health Service Act, as added by § 1003 of the Patient Protection and Affordable Care Act, 42 U.S.C. § 18001 (2010).
2 45 C.F.R. 154.200
3 Beginning in 2014, regulations require states to report all rate increases, even though only increases of 10 percent or more are reviewed for “reasonableness.”
4 Medical Loss Ratio Data and System Resources, Public Use File for 2012, Centers for Consumer Information and Insurance Oversight, 2013. (Accessed at http://www.cms.gov/CCIIO/Resources/Data-Resources/mlr.html.)
5 Five other states submitted limited RRG data about their individual market; these data were not included in the analysis due to data limitations. See appendix for further discussion of methodology.
6 This estimate uses information submitted by 34 states through the RRG Program plus Florida (a non-grant state) and is based on the average difference between rate changes requested and rate changes implemented, weighted by the number of covered lives. Two more states submitted limited RRG data in the small group market that were not included in the analysis. As with the individual market analysis, the small group savings estimates includes data from the reporting states on all rate increases, even those below 10 percent, in the small group market and assumes that the difference will be similar in the states that did not report data. Some additional data from several state websites were used to revise the RRG data.
7 Medical Loss Ratio Data and System Resources, Public Use File for 2012, Centers for Consumer Information and Insurance Oversight, 2013. (Accessed at http://www.cms.gov/CCIIO/Resources/Data-Resources/mlr.html.)
8 42 C.F. R 154.200
9 Chu, Rose and Kronick, Richard, “Health Insurance Premium Increases in the Individual Market since the Passage of the Affordable Care Act,” ASPE Research Brief, Department of Health and Human Services, February 22, 2013. (Accessed at http://aspe.hhs.gov/health/reports/2013/rateincreaseindvmkt/rb.cfm
10 “State Statutory Authority to Review Health Insurance Rates, Small Group Plans,” The Kaiser Family Foundation, 2010 and 2012. (Accessed at http://kff.org/other/state-indicator/rate-review-small-group/#.)
11 “State Statutory Authority to Review Health Insurance Rates, Individual Plans” The Kaiser Family Foundation, 2010 and 2012. (Accessed at http://kff.org/other/state-indicator/rate-review-individual/.)
12 Savings estimates from the Annual Reports published in 2012 and 2013 are not cumulative because there is some overlap in the data.
13 For instance, if a rate filing contained documentation of an approved rate increase, but the submission did not indicate the amount of the requested increase, it was assumed that the missing rate change was the same as the rate change listed.
