Final Report
Prepared by:
Neeraj Sood, Arkadipta Ghosh, and Jose J. Escarse
September, 2007
Prepared for:
Office of the Assistant Secretary for Planning and Evaluation (ASPE)
U.S. Department of Health and Human Services (HHS)
This report was produced under the direction of Donald Cox, Project Officer, Office of the Assistant Secretary for Planning and Evaluation (ASPE), Office of Health Policy. The findings and conclusions of this report are those of the authors and do not necessarily represent the views of ASPE or HHS.
1. Introduction
The rate of growth in health care spending in the U.S. has outpaced the growth rate in the gross domestic product (GDP), inflation, and population for many years. Between 1940 and 1990, the annual rate of growth in real health spending per capita ranged from 3.6% in the 1960s to 6.5% in the 1990s. Correspondingly, the share of GDP accounted for by health care spending rose from 4.5% in 1940 to 12.2% in 1990. In 2005 health care spending was nearly $2 trillion, or $6,697 per capita, which represents 16% of GDP (Catlin et al., 2007). The sustained increase in U.S. health spending over the previous four and half decades is likely to continue, and total spending on health is projected to reach $4 trillion, 20% of GDP, by 2015.
Figure 1: Richer Countries Spend More on Health Care: the United States Is a Clear Outlier
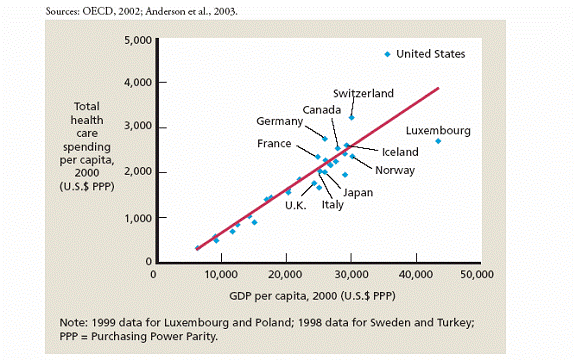
Total health care spending per capita, 2000 (U.S.$ PPP),0--3900 versus GDP per capita,2000 (U.S.$PPP), 6,000--45,000. Uk--1900/25,000;Italy--2,000/25,000;Japan--2,000/26,000; France---2200/26,000; Germany---2500/26,000; Canada--2300/28,000;Iceland---2400/28,000;Norway--2200/30,000; Luxemburg--2500/42,000; Switzerland--3200/30,000; United States--4700/35,000.Note: 1999 data for Luxemburg and Polan; 1998 data for Sweden and Turkey; PPP=Purchasing Power parity.
These figures make the U.S. a clear outlier in international comparisons of health care spending. For example, per capita spending in the U.S. exceeds the level in the next closest country by more than 50% (Figure 1). Similarly, the share of GDP devoted to health care in the U.S. surpasses that in other developed nations by a wide margin.1
This sustained increase and high level of spending on health care in the United States has been the subject of discussion and scrutiny for several decades. Concern has intensified recently as both research studies and anecdotal reports suggest that continued rapid growth in spending may harm the U.S. economy.
Investigating this potential link is not a straightforward effort. Health care spending affects the economy in diverse and complex ways, and effects may differ across sectors of the economy and population groups. For example, commentators have noted that although health care spending may hamper broad economic growth, it may also stimulate economic growth and prosperity in certain sectors of the economy. Understanding how health care spending affects economic growth requires an assessment of these numerous dimensions.
This report presents findings from an evaluation of the effect of health care cost growth on the U.S. economy, based on – 1) a thorough and systematic review of the existing literature, anecdotal evidence and survey findings, and 2) limited quantitative analyses of available secondary data sources. We examine key indicators of economic well-being including per capita GDP and employment; we also describe the effects of health care costs growth on two other sectors of the economy - employers/businesses and government. Our discussion is organized as follows.
- Section 2 presents various perspectives on how growth in health care spending affects the US economy.
- Section 3 summarizes the review of the literature, focusing on the mechanisms through which health care spending could affect the U.S. economy, including aggregate economic outcomes, employers, the government, households, and local economies.
- In section 4, available state-level data are used to analyze the effects of health care cost growth on aggregate economic indictors, industries, and state governments. Section 5 summarizes the main findings.
2. Conceptual Overview of Potential Mechnisms Through Which Health Care Inflation Could Affect the Us Economy
Not surprisingly, the dramatic increases in health care spending and the share of GDP devoted to health care have raised concerns about the negative impact of health care cost inflation on the U.S. economy. In an era of global economic markets, these concerns are reinforced by the status of the U.S. as a spending outlier among competing nations. The major concern is that rapid increases in health care spending can affect major economic indicators such per capita GDP, employment and inflation. The effects are likely to occur across all sectors of the economy – governments, businesses and households – as all these interrelated sectors play an important role in the provision, financing and consumption of health care in the US. For example, Federal, state and local governments collect taxes from businesses and households to finance public health insurance programs and to directly provide health care to households. Businesses provide employment to US households and also provide health insurance to their employees. Households are the final consumers of health care and also bear some incidence of health care costs. In this report we separately identify the effects of health care costs on the aggregate economy and on each one of these interrelated sectors. However, it is important to note that the effects of health care costs on one sector are likely to affect outcomes in other sectors. For example, faced with rising health care costs governments might attempt to reduce health spending by reducing eligibility for public health insurance, consequently increasing uninsurance rates among households. The increase in health care costs might also prompt governments to raise taxes, increase borrowing or reduce investments in other critical sectors such as education and infrastructure, suppressing economic growth and affecting both businesses and households. Similarly, US companies faced with rapidly growing health care costs might reduce employment and investments in the US economy. Rising health care costs could also fuel inflation in the U.S. and make U.S. goods and services less competitive in international markets over time, because increasing health care costs might eventually be reflected in higher product prices. Since most other nations do not have employer-sponsored health insurance, companies in those nations may be better able to keep prices low.2 Finally, high health care costs could reduce access to health care, bankrupt consumers and deplete retirement savings.
However, the view that rapidly rising health care spending harms the U.S. economy is not without dissenters, and some prominent economists view increases in health spending as having a neutral, or perhaps even a positive, economic effect. For example, Pauly (2003) has argued that rising health care spending naturally results in rapid growth in the health care and related sectors, and in employment and incomes for workers in those sectors. Notably, health care firms are largely U.S.-owned. A related argument is that as total per capita GDP rises, consumers may choose to spend a higher portion of their income on health care consequently improving population health and productivity.
To summarize, rapidly rising health care spending could harm the economy by lowering GDP and employment, and increasing inflation (ASPE, 2005). But a contrary view suggests that health care spending has a neutral or positive effect on the economy by raising incomes and employment for workers in the health sector and by increasing the labor market productivity of workers. These and other potential mechanisms for the economic effects of health care spending are summarized in Table 1 below. The next section summarizes the peer-reviewed literature, anecdotal evidence, and survey findings that bear on both aggregate and sector-specific effects.
| Mechanisms Underlying Positive Effect on the Economy |
Mechanisms Underlying Negative Effect on the Economy |
|---|---|
|
|
3. Literature Review
This section presents findings from a systematic review of peer-reviewed academic papers, anecdotal evidence published in the popular press, and findings from secondary data published by government agencies and other research institutions. The literature review was carried out in the following three steps – developing key words or search terms, initial literature scan, and detailed review. Each of these three steps is described below.
ASPE published a background paper on the effects of health care spending growth on the economy (ASPE, 2005). This paper cites several other research papers, reports and newspaper articles. These papers and articles were reviewed to identify index terms or keywords for the literature review. Next, additional keywords or search terms were added to prepare a master list of keywords. A list of keywords and their combinations used for the literature search is provided in Appendix 1 at the end of this report. In the second step, these keywords were used to search the Medline, EconLit and Lexis–Nexis databases. In addition to searches within these databases, online searches were also conducted with Google using various combinations of keywords developed in step 1. Any relevant articles obtained through these searches were “reference mined,” i.e., the reference lists were reviewed for additional articles. Finally, all papers identified in the literature scan were examined for relevance and relevant papers were reviewed and summarized for inclusion in this report.
Overall, the literature review suggests that rapid growth in health care spending could affect the U.S. economy through several plausible mechanisms. It also shows that even though prior work has examined several aspects of the effect of rising health care costs on the economy and its sectors, several gaps remain. The main findings from this review are summarized below.
3.1 Effect on Aggregate Economic Outcomes
Negative Effects
There are no large scale studies that directly examine the detrimental effect of health care cost growth on aggregate economic outcomes such as per capita income, inflation, and unemployment rate. However, there is evidence of a negative effect on employment, which we discuss in a subsequent sub-section.
Anecdotal evidence from several newspaper reports suggests that rapid increase in health care costs negatively affects the economy. Prominent examples include the following:
- For each mid-size car Daimler Chrysler AG builds at one of its U.S. plants, the company pays about $1,300 to cover employee health care costs - more than twice the cost of the sheet metal in the vehicle. In comparison, when it builds an identical car across the border in Canada, the health care cost is negligible (Downey, 2004). Politicians have claimed that auto worker jobs have been moving from Michigan to Ontario in response to lower health care costs in Canada (Harper, 2007). A recent report suggests that faced with shrinking markets and billions of dollars in future health care liabilities, Detroit’s Big Three automakers – General Motors, Ford Motor and Chrysler Group – have expressed interest in exploring an arrangement with the United Auto Workers whereby the latter would assume responsibility for billions of dollars of retiree health care costs (Carty, 2007).
- Government data, industry surveys and interviews with employers big and small indicate that many businesses remain reluctant to hire full-time employees because health insurance, which now costs the nation's employers an average of about $3,000 a year for each worker, has become one of the fastest-growing costs for companies. Health premiums are eroding corporate balance sheets even more than the rising cost of energy (Porter, 2004).
- Starbucks reports that they spent more on health insurance than they did to buy the raw materials to produce their coffee (NCHC, 2006). Wal-Mart, which employs more than 1.2 million U.S. workers and is an industry trendsetter, says it spends $4.7 billion a year on health care and retirement benefits for employees (Hall, 2006).
Positive Effects
Increased spending on health could stimulate job growth in certain sectors. Pauly (2003) argues that rising health care spending naturally results in rapid growth in the health care and related sectors, and in employment and incomes for workers in those sectors. Anecdotal evidence supports this hypothesis. For example, a recent Business Week article reports that since 2001, 1.7 million new jobs have been added in the health care sector, which includes related industries such as pharmaceuticals and health insurance; in contrast, the number of private sector jobs outside of health care is no higher than it was five years ago. With expenditures of more than $2 trillion, health care supports local job markets in the northeast, midwest, and south – the regions hit hardest by globalization and the collapse of manufacturing.
Increased spending improves health and productivity. Murphy and Topel (2003) estimate that between 1970 and 2000, increased longevity added about $3.2 trillion per year to national wealth, an unaccounted value equal to about half of average annual GDP over the period. To the extent that some of these gains resulted from increased health care spending, it is possible that increased spending has dramatically increased the welfare of U.S. citizens.
Similarly, a RAND study found that, between 1970 and 1999, survival gains and reduction in number of work days missed due to health added $1.5 trillion to the value of the labor market human capital. It is likely that a significant proportion of these gains were due to increased capabilities of health care to improve health outcomes (Bhattacharya and Lakdawalla, 2006).
Reverse Causation
Rising income leads to higher expenditures on health. Hall and Jones (2004) show that the rising share of health care in GDP may reflect the natural course of economic growth: as individuals get richer, one of the most valuable and productive opportunities for spending is to purchase better health and longer lives.
Several macroeconomic studies show a link between per capita GDP and per capita health care costs. Using data from a sample of 13 developed countries, Newhouse (1977) estimates the income elasticity of national medical care expenditure to be greater than one—that is with rising incomes health care spending rises faster than per capita GDP. Gerdtham et al. (1992) find that the elasticity of health care expenditure with respect to per capita income was significantly above one in a cross-sectional study of OECD countries, while Hitiris and Posnett (1992) estimate the income elasticity to be at or around unity for the same countries.3 Di Matteo and Di Matteo (1998) find per capita income to be a crucial determinant of Canadian provincial government health expenditures.
This reverse causation could negatively bias estimates of the effect of health care costs on GDP if the true causal effect of health care costs is to suppress GDP. In other words, we might underestimate the harmful effects of health care cost growth on aggregate economic indicators if higher costs are the product of past increases in income.
Is Increased Spending on Health Care Sustainable?
By 2014, 18.7% of GDP could be spent on health care (Heffler et al., 2005); this could rise to 27% of GDP by 2040 (Warshawsky, 1999). Is such a high share of spending on health care affordable or sustainable?
Research suggests that health care spending growth is sustainable only up to a one percentage point gap between the growth rates of health spending and GDP. Follette & Sheiner (2005) propose that health care spending growth is sustainable if increases in health care spending do not lead to an absolute decline in real per capita non-health care consumption. They use a simple macroeconomic model to forecast health care and non-health care consumption under alternative assumptions about the growth of health care spending. In their simulations they assume that the growth rate of GDP, government expenses, current account balance, and gross investments follow historical trends. The baseline scenario assumes that per capita health care spending grows one percentage point faster than per capita GDP. Under this assumption, health care spending growth is sustainable for the next 75 years. However, per capita health care spending that grows two percentage points faster than per capita GDP will lead to a decline in non-health consumption by 2040 and will leave no resources for non health care consumption in 75 years. Chernew, Hirth and Cutler (2003) reach similar conclusions - a one percentage point gap between real per capita growth in health care costs and growth in GDP would be affordable through 2075, and a two percentage point gap would be affordable through 2039.
Summary
Anecdotal evidence suggests that rising health care costs have a negative effect on the U.S. economy. However, there are no empirically rigorous studies that have examined the causal impact of health care cost growth on aggregate economic outcomes. Studies that examine the association between per capita income or GDP and health care costs almost always find a positive relationship. This is possibly because economic growth is accompanied by a rising share of health care in GDP. While some economists believe that rising health care costs could improve health and consequently improve labor productivity, empirical evidence in favor of this view is limited.
3.2 Effect on Employers
In the U.S., the private sector bears a large part of the burden of rapidly rising health care costs because about three-fifths of all Americans have employer-sponsored health insurance. The popularity of employer provided insurance in the US partly stems from the fact that employer contributions to health insurance premiums are exempt from income and payroll taxes. Higher health insurance premiums may erode profits. In fact, some employers now view increasing premiums for health insurance as important to their profitability as rising energy costs and broader economic trends (Business Roundtable, 2004). For example, according to the chairman of Associated Industries of Massachusetts, where virtually all members provide health benefits, health care costs have been the number one concern over the past 15 years (Wroe, 2007). Similarly, a recent survey by the National Federation of Independent Business (NFIB) shows that rising cost of health care is the top health care concern of the nation's small businesses, but small business owners do not support sweeping health care reforms (BNA, 2007).
To preserve profits, firms faced with rising health care premiums may cut employment, reduce health benefits, raise prices, and reduce other expenses, including investments that may enhance future productivity. There is some research on the effects of rising health care costs on employment and benefits. However, we found very little research on how health care costs affect profits, revenues, output, or competitiveness of U.S. employers. Below, we summarize some of the main findings from the literature on the effect of health care cost growth on employers or private businesses.
Health care cost growth has no effect on employers if workers bear incidence of the costs. The traditional economic model of wage-benefit tradeoff implies that workers bear most of the burden of health care costs as long as workers value health insurance at its cost (Summers, 1989). There is some evidence that increase in the cost of fringe benefits results in a decrease in wages with no effect on employment (Gruber 1994). In this standard model, health care cost growth would result in a one-for-one decrease in wages with little or no effect on employer profits, output, employment, and employee cost sharing. However, recent evidence suggests that rising employee costs are prompting employers to reduce benefits, change health care providers, and move to high deductible, consumer-driven health plans4. Recent reports also suggest that employers are showing greater interest in cost-containment measures such as adopting workplace wellness programs, and offering financial incentives to workers to pay closer attention to their health (Butler, 2007; Shea, 2007; Race, 2007).
If employers bear some incidence of health care costs, then cost growth will lead to higher prices and lower output, less employment, and lower profits. The standard economic view, as described above, runs contrary to the general perception that employers bear a significant fraction of health care costs. Under this popular view, health care cost growth is likely to lead to higher prices and lower output, less employment, and lower profits.
Sommers (2005) and Baicker and Chandra (2005) offer potential explanations to reconcile the opposing views of the economic model and the view expressed by employers about the effect of health care costs. Sommers (2005) shows that an economic model where nominal wages do not decline in response to rising employment costs (a situation known as ‘sticky wages’) predicts that rapid health care inflation will lead to (1) lower profits, (2) higher prices, (3) lower output, and (4) higher employee contributions. These effects are more pronounced for employers facing low general inflation and a high benefit to wage ratio.
Baicker and Chandra (2005) suggest that institutional constraints such as minimum wage laws and IRS non-discriminatory provisions might limit firms’ ability to offset increases in health care costs by lowering wages or reducing benefits. They exploit variation in medical malpractice payments across states to estimate the causal effect of health insurance premiums on labor market outcomes. They estimate that a 10% increase in health insurance premiums reduces the probability of being employed by 1.6%, reduces hours worked by 1%, and increases the probability of part-time work by 1.9%. For workers covered by health insurance, this increase in premiums leads to a 2.3% reduction in wages. They find no effect on the employee cost of health insurance.
Cutler and Madrian (1998) show that when health insurance costs increase, firms have an incentive to reduce employment but increase hours worked per employee. They estimate that increases in health insurance costs in the 1980s led to a 3% increase in hours worked for those with employer provided health insurance relative to those without insurance. They argue that health insurance being a fixed cost, employers substitute greater hours per employee for the number of workers when insurance costs rise. However, Baicker and Chandra’s (2005) findings suggest that employers might also substitute full time workers by part time workers (without benefits), which results in a reduction in hours of work. The exact mechanism chosen by an employer would of course depend on a range of factors including the legal or institutional environment within which a firm operates.
Summary
There is little empirical research on how health care costs affect profits, revenues, output, or competitiveness of U.S. employers. There is some evidence that rising health care costs can lead to a decline in employment.Economists are divided in their opinion as to how health spending growth affects wages, employment, and output. While traditional economic models suggest that health care cost growth has no effect on employers if workers bear the costs, others have argued that cost growth will lead to higher prices and lower output, less employment, and lower profits if employers bear some of the increased burden from rising health care costs.
3.3 Effect on Federal and State Government
For many years, the public sector has faced health care costs that are rising more rapidly than revenues. This exerts pressure on government to increase revenues by raising taxes or increasing borrowing and to curb other discretionary spending. Higher taxes reduce the amount of income that firms and households are able to spend on other goods and services, save, or invest; higher taxes also create incentives to engage in activities to avoid taxes (Pauly, 2003). Similarly, increased government borrowing to pay for health care leads to higher interest rates, which raises the cost of capital and reduces the ability of firms and households to obtain resources to invest in other productive activities. Below we summarize key findings from the literature on the effect of rising health care costs on government.
The share of health care expenditures financed by public sources (federal, state, and local governments) has risen steadily over the last decade. Data from the National Health Expenditure Accounts show that the share of health care costs financed by public sources increased from 40.2% in 1990 to 45.4% in 2005.
Effects also appear at state and local levels. As a result of rapidly rising health care costs, state and local health care spending as percent of state and local revenues rose from 14% in 1987 to 22% in 2000 (Cowan et al., 2002). For example, a recent news report suggests that health care costs of the Nassau county in New York are rising at an unsustainable level and will consume nearly 40 percent of all property tax revenues, and 11 percent of the annual budget - by 2010 (Epstein, 2007).
Rising costs increase pressure to cut state medical spending. As a result of this increased burden, there has been mounting pressure at both Federal and state levels to curb spending on health care in several ways, including reducing physician reimbursement, increasing beneficiary cost sharing and reducing eligibility for public insurance programs such as Medicaid. For example, in 2005, eight states reduced or restricted Medicaid eligibility and seven reduced program benefits (Smith et al. 2005).
Rising health care costs also increase pressure to cut spending in other sectors—for example, transportation and education, that are necessary for sustained economic growth. Pressure on the government to curb other discretionary spending can result in reduced investment in publicly-funded activities that are ultimately necessary for sustained economic growth, such as transportation, infrastructure, and education. Reduced spending on education is also part of a more general increase in intergenerational wealth transfers from younger to older segments of the population that results from rapid growth in health spending. For example, a news report in the San Francisco Chronicle suggests that rising retiree health benefit costs were a major financial strain for the school district, leaving little room for increasing resources devoted to the classroom (Knight, 2006). Similarly, Kane and Orszag (2003) estimate that each new dollar in Medicaid spending crowds out 6 to 7 cents of higher education appropriations. However, more research is needed to understand the relationship between health care costs and state spending in other areas.
Rising health insurance costs and changing demographics are the two main reasons for the financial woes of the Medicare program. The annual report by the Medicare Board of Trustees states that “Medicare’s financial difficulties come sooner and are much more severe than those confronting Social Security. While both programs face demographic challenges, the impact is more severe for Medicare because health care costs increase at older ages. Moreover, underlying health care costs per enrollee are projected to rise faster than the wages per worker on which payroll tax is paid.”
Rising health care costs might also increase public insurance coverage if private employers drop coverage. Not many studies have examined this relationship. However, Chernew et al. (2003) find that rising premiums for employer provided coverage are not associated with any change in public insurance coverage.
Summary
The share of health care expenditures borne by federal, state and local governments has increased over time. There is some evidence that governments are cutting down on health expenditures by reducing reimbursement to providers, increasing patient cost sharing, reducing eligibility and generosity of public insurance and reducing expenditures on other sectors of the economy. However, more research is needed to systematically analyze the effects of rising health care expenditures on government budgets and expenditures.
3.4 Effect on Households
Rapid growth in health insurance premiums also affects households. Firms faced with rising health care costs may limit wage increases, reduce health insurance benefits or require employees to pay a greater share of costs, or increase the number of hours worked (Goldman, Sood & Leibowitz, 2005; Cutler and Madrian 1996). Goldman, Sood & Leibowitz (2005) estimate that when health insurance premiums rise, companies finance about two-thirds of the premium increase by reducing wages and the remaining one-third by reducing benefits. In 2002, the average household spent $2,350, or 4.8% of income, on health care, an increase from 1999, when average household health care spending was $1,959, or 4.5% of income. As more costs are shifted to consumers, they may drop health insurance coverage or reduce their demand for other goods and services.5
If companies are unable to offset increases in health care premiums by adjusting wages, benefits, or hours of work, they may reduce employment or at least cut back on full-time employees who are eligible for benefits, replacing them with part-time employees or temporary workers who are not eligible. Many firms also face quickly rising costs of providing health insurance to retirees. Below we summarize the key findings about how health care cost growth affects households, including recent trends.
Recent trends: Data from the Kaiser/HRET survey show that employer health care premiums increased by 73% between 2000 and 2005 (KFF, 2006). Employee contributions for individual and family plans increased at similar rates while the proportion of premiums paid by employees remained relatively stable since 2000 (16% for individual coverage and 27% for family coverage. Nearly all large firms offer health insurance, and the proportion of large firms offering health benefits remained virtually unchanged between 2000 (99%) and 2005 (98%). However, offer rates by small firms declined from 68% in 2000 to 59% in 2005. The proportion of employees with health coverage from their own employer fell by 4 percentage points. The rate of those without insurance for the whole year has grown 1.5 percentage points during 2000 – 2004 (Gould, 2005).
Rising health care costs could increase the percentage of the population that is uninsured. Chernew et al., (2005) analyze data on two cohorts (1989-1991 and 1998-2000) of non-elderly Americans residing in 64 large Metropolitan Statistical Areas to estimate the relationship between rising health insurance costs and probability of being insured. During the study period, insurance coverage fell by 3.1 percentage points and premiums increased by 53%. They find that over half of the decline in coverage rates experienced over the 1990s is attributable to the increase in health insurance costs. They project that the number of uninsured could increase by 1.9 million to 6.3 million in the next decade if growth in real per capita costs outpaced growth in per capita GDP by 1 to 3 percentage points. Data from Kaiser/HRET survey show that the proportion of large employers offering retiree health insurance declined from 66% in 1988 to 33% in 2005 (KFF, 2006). Fronstin (2005) estimates that the percentage of early retirees with health benefits dropped from 39.2% in 1997 to 28.7% in 2002. The proportion of Medicare eligible retirees with health benefits dropped from 28.1% to 25.5%. Gilmer and Kronick (2005) estimate that if current trends continue, the number of uninsured Americans will grow from 45 million in 2003 to 56 million in 2013.
Cutler (2003) analyzes data from the CPS (1988, 1993, 2001) and the Kaiser/HRET surveys to estimate the relationship between employee share of health care costs and take-up rates. He finds that despite the tax exempt status of employer contributions to health insurance premiums, employers have been increasing employee contributions towards health insurance premiums. In fact, the rising employee share of costs can explain 75% of the decline in take-up rates during this period. He posits that the most likely reason for higher employee costs is the underlying trend of rising medical care costs. He also analyzes data on overall insurance rates and estimates that the decline in take-up rather than changes in offer and eligibility rates can explain roughly 60% of the decline in employer provided coverage. Cooper and Schone (1997) reach similar conclusions. They show that most of the decline in employer provided insurance between 1987 and 1996 can be explained by a decline in take-up rates. A recent issue brief by the Kaiser Family Foundation uses the two most recent years of data from the Kaiser/HRET employee benefits survey and finds a negative relationship between employee share of premiums and take-up rates for health insurance (KFF, 2007).6
Rising health care costs could lead to less generous health plans for households. Faced with growing health insurance costs, employers might switch to low-premium, high-deductible plans for their workers. For example, Wal-Mart Stores Inc. intends to make its primary health coverage a low-premium, high-deductible plan. Under its new health plan, new hires will have small premiums deducted from their paychecks, about $10 a week, and will face higher deductibles when paying for medical care. They will be offered special health savings accounts in which they can set aside money in interest-bearing accounts to save for medical needs. (McClatchy Newspapers, 2006). Such changes in health plans offered by employers can potentially force households to forego needed medical care and treatments.
Rising health care costs could increase consumer debt and reduce access to care. Data from the 2003 Commonwealth Fund Biennial Health Insurance Survey show that an estimated 77 million (37%) Americans age 19 and older have difficulty paying medical bills, have accrued medical debt, or both. Nearly two thirds of people with a medical bill or debt problem went without needed care because of cost – nearly three times the rate of those without these financial problems (Doty et al., 2005). Medical debt is also related to having subsequent housing problems. For example, in a recent survey of low and middle income households, 50% reported having medical debt and a quarter of those reported subsequent housing problems as a result of the debt (Seifert, 2005). Himmelstein et al. (2005) surveyed personal bankruptcy filers in five federal courts and found that about half cited medical reasons as a cause of their bankruptcy. Among those whose illnesses led to bankruptcy, out-of-pocket costs averaged $11,854 since the start of illness.
A recent report released by the Access Project documents how low and middle income households are turning to credit cards to pay for medical care (Zeldin and Rukavina, 2007). Based on a national telephone survey of over 1,100 low and middle income households, the report shows that nearly a third (29%) of the respondents reported that medical expenses contributed to their current level of credit card debt. In households with medical debt, the average credit card debt was significantly higher (46%) than in those households without medical expenses as a contributing factor in their overall credit card debt. Although uninsured respondents had the highest levels of credit card debt, even respondents with health insurance were not completely shielded from the medical debt problem.
The Access Project also carried out some community-specific studies on the problem of medical debt. For example, Kohn et al. (2005) examine the scope and consequences of medical debt for people in Kansas, and find that medical bills can exhaust family savings, health insurance can fail to protect families from crushing debt problems, and that medical debt can create barriers to people’s access to future medical services. Another report from Massachusetts shows that people can accumulate medical debt that causes them to forgo further care, damages their credit, and creates housing and employment problems (Pryor and Gurewich, 2004).
Rising health insurance costs could affect labor market outcomes. As mentioned before, Baicker and Chandra (2005) estimate that a 10% increase in health insurance premiums reduces the probability of being employed by 1.6%, and conditional on employment, increases the probability of part-time work by 1.9%. Johnson et al. (2003) find that insurance costs significantly reduce retirement rates for workers aged 51 to 61.
Rising health care costs mean less money for non health care consumption, other benefits, and retirement. Johnson and Penner (2004) estimate that in 2030, out-of-pocket health care costs will take up roughly one third of after-tax income for older adults, up from roughly 16% in 2000. Follette & Sheiner (2005) estimate that a 2 percentage point excess growth in per capita health care spending relative to per capita GDP will lead to decline in non-health consumption by 2040 and will leave no resources for non-health care consumption within 75 years. A recent report suggests that a 65-year-old couple retiring in 2007 will need about $215,000 to cover medical costs in retirement, up 7.5 percent from the previous year. For about 40 percent of the retirees whose primary source of income is Social Security, health expenses could eat up as much as half of their retirement benefits (Hamilton, 2007).
Goldman, Sood and Leibowitz (2005) show that employees facing an increase in the price of health insurance respond by lowering their level of insurance coverage. However, employees do not completely shift increases in expenditures away from health insurance—in fact, increases in prices lead to increases in health insurance expenditures. These increases are accommodated by reducing both take-home income and other benefits such as life insurance, disability insurance, dental insurance, and retirement benefits. For example, they estimate that a $1 increase in premiums leads to a 52-cent increase in health insurance expenditures. Approximately 2/3 of this increase is financed through reduced wages and 1/3 through other benefits. These results suggest that rising health insurance prices not only reduce resources for current consumption but also lower insurance purchases against a variety of risks.
Consumers are concerned about rising health care costs. Rising costs of health insurance create uneasiness among voters. Results from the annual health confidence survey suggest more than half of those surveyed were dissatisfied with health insurance costs. Results from an ABC/Washington Post poll found that 75% of the people would prefer to have employer-sponsored health insurance rather than a $6,700 raise (Alonso-Zaldivar, 2006).
Summary
There is some evidence that rising health care expenditures have led to a rise in uninsurance rates among U.S. households. Evidence from recent surveys also indicates that a significant proportion of consumers, especially the uninsured, are burdened by debt due to medical bills and sometimes forego needed medical care and other spending due to high medical care costs. Finally, recent studies have shown that rising health care costs can also affect labor market outcomes and reduce non-health consumption as well as other non-wage benefits.
3.5 Effect on Local Economies
As spending on health care accounts for a higher percentage of GDP, the health sector is a major and rapidly growing source of employment for U.S. workers. According to the Bureau of Labor Statistics (2006), and as shown in Table 2 below, the health care sector employed over 10 million workers in 2006. Over the period 1998 to 2006, employment in the health care sector grew by a staggering 21%. In contrast during this period of rising health care costs, employment across all occupations grew by only 6%. Further, according to projections made by the Bureau of Labor Statistics (BLS), home health aides are likely to be the fastest growing occupation category over the next decade growing by as much as 56% between 2004 and 2014 (Hecker, 2005). Hence, the healthcare sector can have a major impact on the local economy. For example, a recent Business Week article reports that since 2001, 1.7 million new jobs have been added in the health care sector, which includes related industries such as pharmaceuticals and health insurance; in contrast, the number of private sector jobs outside of health care is no higher than it was five years ago. With expenditures of more than $2 trillion, health care supports local job markets in the northeast, midwest, and south – the regions hit hardest by globalization and the collapse of manufacturing.
Conversely, researchers have found that government deficit spending, e.g. to finance public health expenditures, disproportionately harms export and capital goods industries, whereas payroll tax financing disproportionately harms consumer service industries (Monaco and Phelps, 1995).
| Year | Healthcare Practitioners and Technical Occupations |
Healthcare Support Occupations |
Total Healthcare |
Total All Occupations |
Healthcare as a percentage of total employment |
|---|---|---|---|---|---|
| 1998 | 5,831,260 | 2,562,280 | 8,393,540 | 124,704,600 | 6.73% |
| 1999 | 6,001,950 | 2,970,780 | 8,972,730 | 127,274,000 | 7.05% |
| 2000 | 6,041,210 | 3,039,430 | 9,080,640 | 129,738,980 | 7.00% |
| 2001 | 6,118,970 | 3,122,870 | 9,241,840 | 127,980,410 | 7.22% |
| 2002 | 6,185,020 | 3,173,400 | 9,358,420 | 127,523,760 | 7.34% |
| 2003 | 6,173,760 | 3,208,770 | 9,382,530 | 127,567,910 | 7.35% |
| 2004 | 6,359,380 | 3,271,350 | 9,630,730 | 128,127,360 | 7.52% |
| 2005 | 6,547,350 | 3,363,800 | 9,911,150 | 130,307,840 | 7.61% |
| 2006 | 6,713,780 | 3,483,270 | 10,197,050 | 132,604,980 | 7.69% |
| Source: Occupational Employment Statistics, Bureau of Labor Statistics, U.S. Department of Labor Available at: http://www.bls.gov/oes/oes_dl.htm | |||||
4. Empirical Analysis
This section analyzes how health care cost growth affects the economy using available secondary data from a variety of sources. The quantitative analysis described below examines effects on three sectors: aggregate economic indicators, industries, and state governments. The analyses involving aggregate economic indicators and state government finances are carried out at the state-year level, while the analysis on industries is at the industry-year level. Typically, data from multiple sources were combined to carry out each of these analyses. The data were merged at the state-year or industry-year level depending on the particular analysis. The data sources along with descriptions of the variables used in the various analyses are provided in Appendix 2 at the end of this report.
4.1 Effect on Aggregate Economic Indicators
First, state level data across several years are used to investigate the effect of rising health care costs on aggregate economic indicators. The measure of health care cost is per capita health expenditure, and the specific outcomes examined are per capita gross state product and state unemployment rate.
Cross-Sectional Analysis Using State-Level Data
We first use data on all 50 states for the year 2004 (the most recent year for which these data are available) and examine the association between health care costs and aggregate economic indicators including per capita gross state product (GSP) and unemployment rate. Table 3 provides descriptive statistics for these variables.
Differences in aggregate economic indicators between states with high versus low health care costs are examined. A state was coded as having high health care cost if the per capita health expenditure for that state exceeded the median per capita health expenditure ($5,260) for all states in 2004. The simple comparisons presented in Table 4 suggest that states with high health cost tend to have higher per capita GSP, and lower unemployment rate. For example, states with higher than median health care expenditures had a per capita GSP in 2004 of $40,430. In contrast, states with lower than median expenditures had a per capita GSP in 2004 of only $36,770. This difference in per capita GSP is statistically significant at the 10% level and suggests a positive association between health care costs and per capita GSP.
| Variable | Mean | Std. Dev. | Min | Max |
|---|---|---|---|---|
| Per capita health care expenditure (thousands of dollars) |
5.33 | 0.68 | 4.04 | 7.07 |
Per capita GSP (thousands of dollars) |
38.60 | 6.94 | 26.58 | 63.00 |
Unemployment rate (percent) |
5.17 | 0.97 | 3.30 | 7.40 |
| Variable | States with low health care cost |
States with high health care cost |
t-statistic (p-value) |
|---|---|---|---|
| Per capita GSP (thousands of dollars) | 36.77 | 40.43 | -1.91 (0.06) |
Unemployment rate (percent) |
5.37 | 4.96 | 1.48 (0.14) |
Next, mean values of the indicators are plotted against the quartiles of per capita health expenditure to further investigate possible correlations between high health care costs and these outcomes. Figure 2 also suggests a positive correlation between per capita health expenditure and per capita GSP, with little or no correlation between health expenditure and the unemployment rate.
The cross-sectional analysis described above does not establish that higher health care costs lead to an increase in per capita income. It merely establishes that richer states spend more on health care. In addition, the positive correlation between GSP and health expenditure could also arise due to state-specific attributes that lead some states to have both higher levels of income as well as higher health care costs. Therefore, a longitudinal analysis with the same data follows, which accounts for state specific attributes as well as national time trends that could affect health care costs and aggregate economic indicators.
Figure 2: Average Values of Aggregate Economic Indicators in 2004:
By Quartiles of Per Capita Health Expenditure
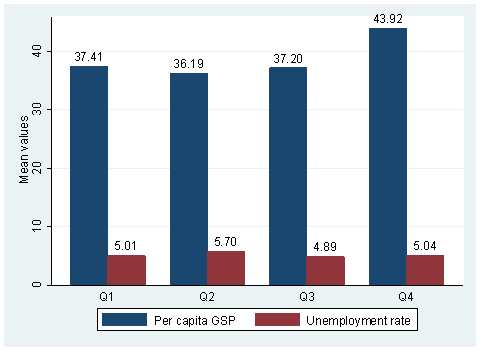
Note: Per capita GSP in thousands of dollars; unemployment rate in percent.
Q1,mean values: per capita GSP--37.41, unemployment---5.01; Q2,mean value: per capita GSP--36.19, unemployment---5.70; Q3,mean values: per capita GSP--37.20, unemployment---4.89; Q4,mean values: per capita GSP--43.92, unemployment---5.04.
Longitudinal Analysis Using State Level Data
For the longitudinal analysis, data on all 50 states over a period of 20 years (1985-2004) are used to examine how the increase in per capita health expenditure affects per capita GSP and unemployment rate. Table 5 provides descriptive statistics for these variables.
| Variable | Mean | Std. Dev. | Min | Max |
|---|---|---|---|---|
| Per capita health care expenditure (thousands of dollars) |
3.13 | 1.18 | 1.11 | 7.07 |
Per capita GSP (thousands of dollars) |
26.62 | 8.17 | 11.82 | 63.00 |
Unemployment rate (percent) |
5.44 | 1.65 | 2.30 | 13.40 |
Next, the average change in each variable over these 20 years is computed separately for each state, and these mean changes over time (averaged across all 50 states) are presented below in Table 6.
| Variable | Obs. | Mean | Std. Dev. | Min | Max |
|---|---|---|---|---|---|
| Change in per capita health care expenditure (thousands of dollars) | 50 | 0.20 | 0.03 | 0.14 | 0.27 |
Change in per capita GSP (thousands of dollars) |
50 | 1.13 | 0.27 | 0.29 | 2.19 |
Change in unemployment rate (percentage point) |
50 | -0.10 | 0.09 | -0.43 | 0.08 |
These changes over time in various outcomes are now compared with the change over time in per capita health care expenditure. Specifically, the average change over time for each outcome is plotted against quartiles of the change in per capita health expenditure (Figure 3) over the same period.
Figure 3: Average Change in Aggregate Economic Indicators:
By Quartiles of Change in Per Capita Health Expenditure
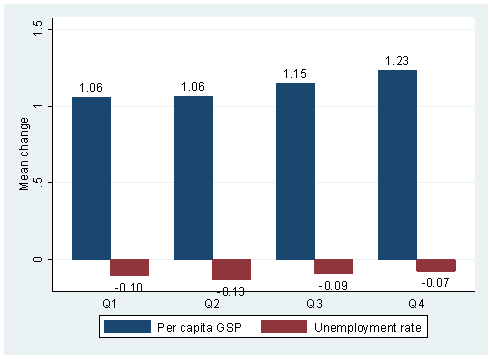
Note: Changes in thousands of dollars (per capita GSP), and in percentage points (unemployment rate)
Q1,mean change: per capita GSP--1.06, unemployment--- -0.10; Q2,mean change: per capita GSP--1.06, unemployment--- -0.13; Q3,mean change: per capita GSP--1.15, unemployment--- -0.09; Q4,mean change: per capita GSP--1.23, unemployment--- -0.07
Figure 3 suggests that states that experienced greater increases in per capita health expenditure during 1985-2004 also experienced higher growth in per capita GSP. For example, while the growth in per capita GSP is $1,060 in the bottom two quartiles of the change in per capita health expenditure, it is over $1,200 in the top quartile. For unemployment, we do not find such a clear pattern, although states in the upper two quartiles of increase in per capita health expenditure do seem to have experienced a smaller decline in unemployment.
Finally, multivariable regression models are estimated using longitudinal data. .The regression models include state and year fixed effects that respectively control for time invariant state-level heterogeneity and national trends in health care costs and outcomes. Table 7 reports results from these regressions for each outcome. All regressions are estimated with Huber-Eicker-White (HEW) or robust standard errors to account for possible heteroskedasticity in the data (White, 1980). The regressions are estimated in levels as well as in logs, and the results from both specifications are reported in Table 7.
| (1)Per capita GSP (thousands of dollars) |
(2)Unemp. rate |
(3)Log of per capita GSP (thousands of dollars) |
(4)Log of unemp. rate |
|
|---|---|---|---|---|
| Per capita health expenditure | 1.842*** | 0.608*** | ||
| [0.419] | [0.152] | |||
| Log of per capita health expenditure | 0.101** | 0.096 | ||
| [0.044] | [0.105] | |||
| Constant | 14.486*** | 6.153*** | 2.777*** | 1.878*** |
| [0.829] | [0.307] | [0.018] | [0.048] | |
| Observations | 1000 | 999 | 1000 | 999 |
| Number of States | 50 | 50 | 50 | 50 |
| R-squared | 0.93 | 0.53 | 0.96 | 0.54 |
|
Robust standard errors in parentheses; * significant at 10%;
|
||||
The estimates in Table 7 suggest a statistically significant and positive relationship between per capita health expenditure and per capita GSP, even after controlling for state and year fixed effects. Specifically, the estimate from the log specification suggests that a ten percent increase in per capita health expenditure leads to a one percent increase in per capita GSP. The results for unemployment rate are somewhat mixed with the estimate from the log specification showing no significant relationship.
In general, these results might suggest that higher health care expenditure was beneficial to economic growth; however, one needs to be careful in interpreting the findings. As reported in the literature review, rising health care costs can have both a positive and a negative impact on the economy, and the results above are possibly due to reverse causation, whereby rising incomes over time lead to a higher proportion of GDP being spent on health care. Several macroeconomic studies have indeed shown such a link between per capita GSP and health care costs. Consequently, this analysis might underestimate the harmful effects of health care cost growth on aggregate economic indicators, if higher incomes do lead to increased expenditure on health care. Therefore, these findings do not rule out the possibility that health care cost growth has a negative effect on the economy, but the evidence so far is insufficient to reach any firm conclusion.
4.2 Effect on Private Business / Industry
Standard economic models predict that an increase in employee health care costs would be financed by an equivalent reduction in cash wages (Summers, 1989; Gruber, 1994). In this model, total compensation remains unchanged even if health care costs rise, and health care cost inflation has no effect on employment or output.
However, this view is contrary to popular wisdom. One approach to reconciling the economic model with popular wisdom is to assume that cash wages are “sticky” (that is, firms have limited ability to reduce wages in response to rising health care costs) and that rising health care costs lead to a less than one-for-one reduction in cash wages. In this case, rising health care costs will increase total compensation. The increase in total compensation creates incentives to reduce employment, since employment costs have risen but labor productivity has remained the same. The reduction in employment will also lead to a reduction in output and an increase in prices.
The extent to which an increase in health care costs affects output and employment in different industries depends on how much total compensation rises due to health care cost inflation. Industries where health care benefits are a larger share of total employee compensation will experience a larger increase in total compensation, consequently leading to a larger reduction in employment and output. For example, a 10% increase in health care costs will lead to a 5% increase in total compensation for industries with a benefit share of 50%, but only a 1% increase in total compensation for industries with a benefit share of 10%.
This section investigates how health care cost growth affects specific industries. It analyzes whether industries where benefits are a larger share of total compensation were hit harder by rising health care costs. The analysis covers the period 1987 – 2005. Since the classification of industries changed in 1997 (from SIC to NAICS), industry definitions from the SIC classification (1987-1997) were matched to those in the NAICS classification (1998-2005) using definitions that were consistent across the two time periods.7 The final dataset consists of 39 industries (matched across the two periods) over these 19 years, yielding a total of 741 observations. The share of benefits in 1987 was adopted as a baseline measure of the degree to which various industries might be affected by growth in health care costs. The rise in health care costs over time is captured by the medical care price index;8 the specific outcomes studied are employment, gross output, and value added to GDP, for each industry. Appendix 2 describes the data sources for each of the variables in the analysis. Table 8 provides summary statistics of the variables used in this analysis.
| Variable | Mean | Std. Dev. | Min | Max |
|---|---|---|---|---|
| Share of benefits in total compensation in 1987 (percent) |
17.62 | 3.98 | 12.41 | 31.14 |
| Real medical care price index | 1.43 | 0.15 | 1.15 | 1.65 |
| Unionization (percent) | 15.30 | 8.84 | 1.20 | 35.25 |
| Value added per worker (thousands of dollars) |
100.52 | 116.40 | 19.36 | 1246.70 |
| Employment (thousands) | 2148 | 3462 | 52 | 22434 |
| Gross output (millions of dollars) | 283706 | 309919 | 15499 | 2300601 |
| Value added to GDP (millions of dollars) | 151448 | 206822 | 6413 | 1578378 |
Descriptive Analysis
It is expected that industries with a larger share of benefits in total compensation will be affected more by the growth in health care costs. Table 9 provides a detailed list of industries by quartiles of the benefit share in total compensation in 1987.
Next, the average changes (percentage) in output and employment over this 19-year period (1987 – 2005) are plotted against the benefit share in 1987 9. The rationale behind this exercise is to explore whether industries that had a higher share of benefits in total compensation initially perform worse than others when health care costs rise over time.
There is a significant pattern in these graphs – industries with a higher share of benefits in 1987 do seem to have worse performance than others in subsequent years. Specifically, industries with a higher initial benefit share had less or even negative growth in employment and output over time (Figures 4 – 6).
| Q1 (benefit share <= 14.25%) |
Q2 (benefit share between 14.25 & 17.29%) |
Q3 (benefit share between 17.29 & 18.75%) |
Q4 (benefit share above 18.75%) |
|---|---|---|---|
| Agriculture, forestry, and fishing |
Construction | Oil and gas extraction | Mining, except oil and gas |
| Wholesale trade | Miscellaneous manufacturing | Wood products | Primary metals |
| Retail trade | Textiles, apparel and leather | Furniture and fixtures | Fabricated metal products |
| Depository and nondepository institutions |
Paper products | Nonmetallic mineral products | Machinery |
| Insurance carriers and related activities |
Plastics and rubber products | Electronic and other electric equipment |
Motor vehicles and equipment |
| Real estate | Transit and ground passenger transportation |
Other transportation equipment | Food and beverage and tobacco products |
| Legal services | Communications | Chemical products | Petroleum and coal products |
| Amusement and recreation services |
Motion pictures | Air transportation | Rail transportation |
| Accommodation | Educational services | Utilities | Water transportation |
| Other services | Health and social services | Trucking and warehousing |
Figure 4: Average Change (Percentage) in Employment:
Against Benefit Share in 1987
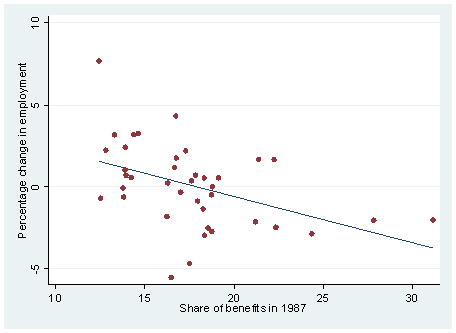
1987 share benefits,(12.5--31)/average percentage change in employment,(1--(-4)), respectively.
Figure 5: Average Change (Percentage) in Gross Output:
Against Benefit Share in 1987
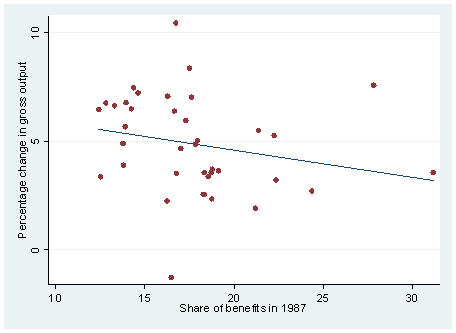
1987 share benefits,(12.--31)/ percentage change in gross output(6--4), respectively.
Figure 6: Average Change (Percentage) in Value Added to GDP:
Against Benefit Share in 1987
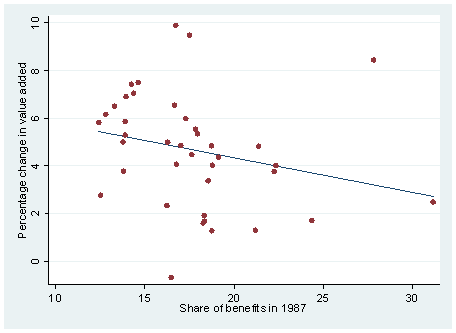
1987 share benefits,(12.5--31)/ percentage change in value added(5--3), respectively.
Regression Analysis
To further build upon the graphical analysis presented above, multivariate regression models were estimated. The key explanatory variable in the model is the interaction between the log of medical care price index and benefit share in 1987. A negative coefficient on this variable implies that industries that provided a larger share of compensation as benefits experienced a larger decline (or smaller increase) in output or employment due to rising prices. The regressions also include year and industry fixed effects that control for secular time trends and time invariant observed and unobserved industry characteristics respectively. Since benefit share in 1987 does not vary within the same industry, its main effect is not identified in these models with industry fixed effects. Similarly, the main effect of medical care price index is not identified since it does not vary across industries in the same year and our models control for year fixed effects. In alternate models controls for sector- specific time trends and also changes in unionization status and labor productivity were included. As before, the regressions were carried out in levels as well as in logs. The results from the log specification are presented and discussed in this report.10 All models were estimated with Huber-Eicker-White (HEW) or robust standard errors to account for possible heteroskedasticity in the data (White, 1980).
In the first set of regressions, industry and year fixed effects are included apart from the interaction between the log of medical care price index and benefit share in 1987 among explanatory variables. Columns (1) – (3) in Table 10 report results from these models. The coefficient estimate on the interaction between medical care prices and share of benefits is negative and significant for all outcomes. Thus, the estimates suggest that industries with higher benefit shares were hit harder by rising health care costs.
Note that the level of unionization within an industry could affect the share of benefits, and also affect employment and output. Similarly, labor productivity could affect aggregate output and employment. Omitting these variables could therefore bias the regression estimates. Hence, additional controls for unionization (measured by percentage of workers who are affiliated to unions) and labor productivity (measured by value added per worker) are now included into the model. Unionization is measured at the sectoral level, and productivity is measured at the level of the specific industry. These results are reported in columns (4) – (6) of Table 10.
Even after controlling for unionization and productivity, rising health care costs still seem to have a sustained adverse effect on industries that provide a larger share of compensation as benefits. In addition, unionization seems to be positively associated with employment growth although it has no significant effect on output or value added. Labor productivity has a small but significant negative effect on employment, and a small yet significant positive effect on output and value added.
Another source of bias is that sectors of the economy with high benefit shares might be experiencing an economic downturn for external reasons but this downturn coincided with rising medical care prices. To account for this source of bias, additional regressions are estimated that control for sector-specific time trends. Five such sectors were defined – (1) manufacturing, (2) finance and services, (3) wholesale and retail trade, (4) transportation, communications and utilities, and (5) agriculture, mining and construction. These results are reported in columns (7) – (9) of Table 10. The results clearly show that even after taking sector specific time trends into account, industries with a higher share of benefits suffer greater employment and output loss due to rising medical prices. Once again, labor productivity has a significant negative effect on employment, and a significant positive effect on output. The estimates also show a significant and negative effect of unionization on employment and output.11
Overall, the regression results indicate that industries that bear a larger burden of the rise in health care costs due high benefit shares were hit harder by rising health care costs. It is likely that the labor contracts that led to high benefit shares of these industries were negotiated during a period when health care costs were not rising significantly. Consequently, these industries did not anticipate the rapid increase in health care costs when negotiating these contracts that promised large benefits. In addition, the tax exempt status of employer contributions towards health insurance premiums implied that employers were reluctant to reduce benefits in times of moderate health care cost inflation.12 Some industries are now realizing the adverse effect of these high benefit shares and are renegotiating labor contracts to reduce benefits and thus mitigate the adverse economic consequences of health care cost inflation. For example, General Motors is currently negotiating an arrangement with the United Auto Workers whereby the latter would assume responsibility for billions of dollars of retiree health care costs (Carty, 2007). Thus, in the long run some of the adverse economic consequences of health care cost inflation might be mitigated as industries reduce benefits and wages to pass some of the burden of health care cost inflation to their employees.
| (1)Log of employment |
(2)Log of gross Output |
(3)Log of value added to GDP |
(4)Log of employment |
(5)Log of gross Output |
(6)Log of value added to GDP |
(7)Log of employment |
(8)Log of gross Output |
(9)Log of value added to GDP |
|
|---|---|---|---|---|---|---|---|---|---|
| Benefit share in 87* Log of medical care price index |
-0.158*** | -0.097*** | -0.113*** | -0.130*** | -0.101*** | -0.112*** | -0.065*** | -0.062*** | -0.066*** |
| [0.018] | [0.014] | [0.016] | [0.020] | [0.015] | [0.017] | [0.018] | [0.016] | [0.017] | |
| Unionization | 0.009** | 0.000 | 0.003 | -0.020*** | -0.018*** | -0.017*** | |||
| [0.004] | [0.004] | [0.004] | [0.007] | [0.006] | [0.006] | ||||
| Labor productivity (value added per worker) |
-0.001*** | 0.000*** | 0.000** | -0.001*** | 0.001*** | 0.001*** | |||
| [0.000] | [0.000] | [0.000] | [0.000] | [0.000] | [0.000] | ||||
| Constant | 7.369*** | 11.899*** | 11.191*** | 7.218*** | 11.885*** | 11.105*** | 7.600*** | 12.078*** | 11.320*** |
| [0.054] | [0.041] | [0.046] | [0.121] | [0.115] | [0.116] | [0.142] | [0.120] | [0.127] | |
| Observations | 741 | 741 | 741 | 741 | 741 | 741 | 741 | 741 | 741 |
| Number of Industries | 39 | 39 | 39 | 39 | 39 | 39 | 39 | 39 | 39 |
| R-squared | 0.15 | 0.69 | 0.63 | 0.26 | 0.70 | 0.64 | 0.35 | 0.73 | 0.68 |
|
Robust standard errors in brackets. * significant at 10%; |
|||||||||
Predictions
Finally, the estimates from the full model (reported in columns (7) – (9) of Table 10) are used to predict the percentage changes in employment and value added that would have occurred for a slower (zero growth) or faster (3% per annum) growth in health care costs compared to the actual, observed growth of 2% per annum. These predictions are generated for four different industries – agriculture, communications, chemical products, and automobiles – that belong to four different quartiles (from lowest to highest) of the benefit share in total compensation during 1987. The predicted changes are shown in Figures 7 & 8 – for both employment and value added to GDP.13
The analysis shows that industries in all four quartiles would have benefited if health care costs had remained constant over time; in addition, the positive effects would have been larger for industries with a higher benefit share in 1987. Similarly, with a faster (3%) increase in health care costs, industries in all four quartiles would suffer losses in employment and value added, with greater losses accruing to industries that had higher benefit shares to start with. For example, the automobile industry, in the highest benefit share bracket in 1987, would have been hardest hit – suffering a 7% loss in both employment and value added for a faster cost growth scenario. The corresponding estimate for agriculture – in the lowest benefit share bracket – is 4%.
Using average employment and value added for each of these industries over this 19-year period, the predicted changes are interpreted in real terms and reported in Table 11. The numbers suggest that industries would have suffered significant gains (losses) from a slower (faster) cost growth scenario. For example, the automobile industry would have suffered losses of 71,000 employees and more than 6 billion dollars in value added if health care costs had grown at 3% per annum. The corresponding estimates for the communication industry are 69,000 employees and nearly 11 billion dollars.
Figure 7: Percent Change in Employment for Alternative Cost Growth Scenarios:
For Industries in Different Quartiles (Lowest to Highest) of Benefit Share in 1987
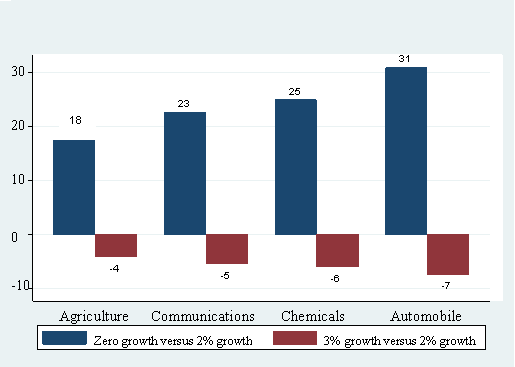
Agriculture--(zero growth versus 2% growth,18),(3% growth versus 2% growth,-4);Communications--(zero growth versus 2% growth,23),(3% growth versus 2% growth,-5);Chemicals--(zero growth versus 2% growth,25),(3% growth versus 2% growth,-6); Automobile--(zero growth versus 2% growth,31),(3% growth versus 2% growth,-7.
Figure 8: Percent Change in Value Added for Alternative Cost Growth Scenarios:
For Industries in Different Quartiles (Lowest to Highest) of Benefit Share in 1987
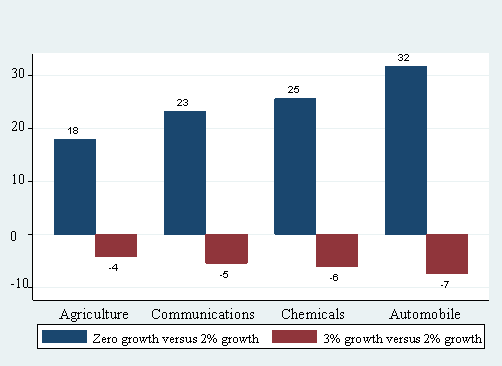
Agriculture--(zero growth versus 2% growth,18),(3% growth versus 2% growth,-4);Communications--(zero growth versus 2% growth,23),(3% growth versus 2% growth,-5);Chemicals--(zero growth versus 2% growth,25),(3% growth versus 2% growth,-6); Automobile--(zero growth versus 2% growth,32),(3% growth versus 2% growth,-7.
| Employment (in thousands) | Value added (in millions of dollars) | |||||
|---|---|---|---|---|---|---|
| Industry | Average | Gain from zero growth | Loss from 3% growth | Average | Gain from zero growth | Loss from 3% growth |
| Agriculture | 1748 | 297 | -70 | 107544 | 19358 | -4302 |
| Communications | 1373 | 316 | -69 | 215502 | 49566 | -10775 |
| Chemicals | 1008 | 252 | -61 | 143477 | 35869 | -8609 |
| Automobile | 1011 | 314 | -71 | 88031 | 28170 | -6162 |
| Note: Predicted gains/losses are based on observed averages in the data and predicted percentage changes in employment and value added from regressions using the full model. | ||||||
4.3 Effect on State Government
Finally, state level data across several years are used to investigate how rising health care costs affect state government finances. As for the analysis involving aggregate economic indicators, the measure of health care cost is per capita health expenditure, and the specific outcomes examined are per capita state government expenditures on health and other sectors, total expenditures, and per capita state government debt. Details on the construction and sources of these variables are provided in the data appendix at the end of this document.
Cross-Sectional Analysis Using State-Level Data
First, a cross-sectional analysis is carried out using data from all 50 states for the year 2004 – the most recent year for which data are available on the variables in the analysis. Table 12 provides descriptive statistics for these variables.
As before, the analysis differentiates between states with high versus low health care costs. A state was defined as having high health care cost if the per capita health expenditure for that state exceeded the median per capita health expenditure ($5,260) for all states in 2004. This analysis therefore examine whether states with high health care expenditures fare worse than others in terms of various indicators. The simple comparisons presented in Table 13 suggest that states with high health cost tend to have significantly higher per capita state government health expenditure and debt.
| Variable | Obs. | Mean | Std. Dev. | Min | Max |
|---|---|---|---|---|---|
| Per capita health care expenditure | 50 | 5.33 | 0.68 | 4.04 | 7.07 |
| Per capita state government health expenditure |
50 | 0.74 | 0.20 | 0.36 | 1.52 |
| Per capita state government all other expenditures |
50 | 4.26 | 1.30 | 2.91 | 11.43 |
| Per capita state government total expenditure |
50 | 5.00 | 1.38 | 3.44 | 12.30 |
| Per capita state government debt |
50 | 2.81 | 1.73 | 0.61 | 8.71 |
| Note: All variables are in thousands of dollars. | |||||
| Variable | States with low health care cost |
States with high health care cost |
t-statistic (p-value) |
|---|---|---|---|
| Per capita state government health expenditure |
0.68 | 0.79 | -2.03 (0.05) |
| Per capita state government all other expenditures |
4.01 | 4.52 | -1.39 (0.17) |
| Per capita state government total expenditure |
4.69 | 5.31 | -1.61 (0.11) |
| Per capita state government debt |
2.13 | 3.49 | -3.01 (0.00) |
| Note: All variables are in thousands of dollars | |||
Next, the means of various outcomes are plotted against quartiles of per capita health expenditure to further investigate possible correlations between high health care costs and the outcomes. These relationships, shown in Figure 9, once again seem to suggest a positive correlation between per capita health expenditure and per capita state government expenditures on health, on other sectors, and per capita state government debt.
The cross-sectional analysis is helpful in uncovering the correlation between health care costs and state government finances. However, the analysis is limited by the fact that such correlations could arise due to state-specific attributes that lead to some states having both higher government expenditures and higher health care costs.
Therefore, the same data is now utilized for a longitudinal analysis that allows better controls for state-specific attributes as well as for periodic shocks to health care costs and outcomes.
Figure 9: Average Per Capita State Government Expenditure & Debt in 2004:
By Quartiles of Per Capita Health Expenditure
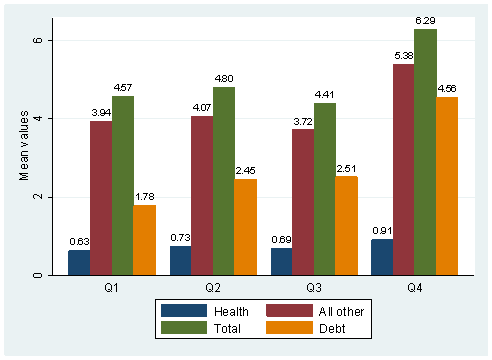
Note: All variables are in thousands of dollars
Q1,mean values: health--.63, debt--1.78, all other--3.94, total--4.57; Q2,mean values: health--.73, debt--2.45, all other--4.07, total--4.80; Q3,mean values: health--.69, debt--2.51, all other--3.72, total--4.41; Q4,mean values: health--.91, debt--4.56, all other--5.38, total--6.29.
Longitudinal Analysis Using State Level Data
Per capita measures of state government expenditures are used to investigate how per capita health expenditure affects state government finances for the period 1992-2004. Table 14 provides descriptive statistics for these variables.
The changes over time in the outcomes and also in per capita health care expenditure are now analyzed for each of the 50 states. The average change in each variable over these 13 years is calculated for each state, and the mean changes over time (computed across all 50 states) are presented in Table 15.
| Variable | Obs. | Mean | Std. Dev. | Min | Max |
|---|---|---|---|---|---|
| Per capita health care expenditure | 650 | 3.77 | 0.94 | 1.94 | 7.07 |
| Per capita state government health expenditure |
650 | 0.54 | 0.19 | 0.19 | 1.52 |
| Per capita state government all other expenditures |
650 | 3.26 | 1.23 | 1.61 | 11.59 |
| Per capita state government total expenditure |
650 | 3.80 | 1.34 | 1.91 | 12.52 |
| Per capita state government debt |
650 | 2.17 | 1.54 | 0.19 | 8.99 |
| Note: All variables are in thousands of dollars | |||||
| Variable | Obs. | Mean | Std. Dev. | Min | Max |
|---|---|---|---|---|---|
| Change in per capita health care expenditure | 50 | 0.22 | 0.04 | 0.14 | 0.31 |
| Change in per capita state govt. health expenditure |
50 | 0.03 | 0.01 | 0.01 | 0.06 |
| Change in per capita state govt. all other expenditures |
50 | 0.15 | 0.04 | 0.06 | 0.25 |
| Change in per capita state govt. total expenditure |
50 | 0.18 | 0.04 | 0.07 | 0.28 |
| Change in per capita state govt. debt |
50 | 0.08 | 0.06 | -0.01 | 0.33 |
| Note: All variables are in thousands of dollars | |||||
Next, the changes over time in various outcomes are compared against the change over time in per capita health care expenditure. Specifically, the average change over time for each outcome is plotted against quartiles of the change in per capita health expenditure (Figure 10).
Figure 10 suggests weak positive correlation between the average increase in per capita state government expenditure on health and change in per capita health expenditure.14 There appears to be somewhat stronger correlation between increase in per capita health expenditure and the average increase in per capita state government expenditure on all other categories. Specifically, per capita state government expenditure on all other categories registers an increase of $130 in the first quartile and a somewhat higher increase of $170 in the fourth quartile of the change in per capita health expenditure. The same holds true for per capita state government debt that increases by $70-80 in the first three quartiles, and by $100 in the fourth quartile of the change in per capita health expenditure.
Figure 10: Average Change in Per Capita State Government Expenditures &
Debt By Quartiles of Change in Per Capita Health Expenditure
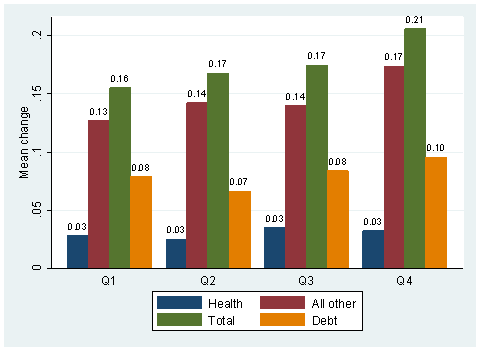
Note: All variables are in thousands of dollars
Q1,mean change: health-.03, debt-.08, all other-.13, total-.16; Q2,mean change: health--.03, debt--.07, all other--.14, total-.17; Q3,mean change: health--.03, debt--.08, all other--.14, total-.17; Q4,mean change: health--.03, debt--.10, all other--.17, total-.21.
This descriptive evidence seems to suggest that state government expenditures on health and on other sectors tend to move together over time. This could be because sectors such as health and education compete for funding so an increase in health expenditures is accompanied by a similar increase in several other sectors. Alternatively, this relationship could reflect unobserved state-specific factors. For example, states with rising per capita income would have larger increases in per capita health expenditures, and also have faster increases in various categories of state government expenditures, including health.
To further investigate this issue, a regression analysis is now carried out that incorporates state and year fixed effects. The regressions also control for state-specific factors that vary over time, e.g., per capita income, per capita state government revenue, and unemployment rate. As before, all regressions were estimated with HEW or robust standard errors to account for heteroskedasticity in the data (White, 1980). Results from both specifications – in levels and in logs – are reported in Table 16.
The regression analysis suggests a significant positive relationship between per capita health expenditure and state government expenditures on health and other sectors (columns (1) and (2) of Table 16). State government expenditures on health (as well as on most other sectors) tend to move together with increase in total spending on health; in addition, the growth rates of state government expenditures on health exceed the rate of increase in population so that the per capita measures keep rising over time.
There is no evidence that rising health expenditure crowds out other components of state expenditure. On the contrary, there is some evidence that the government’s total expenditure and debt increase over time (columns (3) and (4) of Table 16) as health care costs and state government expenditures rise in tandem. However, while all other changes are significant even in percentage terms (or, in terms of elasticity with respect to per capita health expenditure), change in government debt is not significant in percentage terms when we look at the results from the log specification in column (5) – (8). Further investigation revealed that the level of debt in 1992 was positively correlated with increase in health care costs. So, even though states in the fourth quartile of the change in per capita health expenditure experienced the largest increase in debt (Figure 11), it was a small increase in percentage terms because these states already had high debt.
| (1)Per capita state govt. health expenditure |
(2)Per capita state govt. other expenditure |
(3)Per capita state govt. total expenditure |
(4)Per capita state govt. debt |
(5)Log of per capita state govt. health expenditure |
(6)Log of per capita state govt. other expenditure |
(7)Log of per capita state govt. total expenditure |
(8)Log of per capita state govt. debt |
|
|---|---|---|---|---|---|---|---|---|
| Per capita health expenditure | 0.078***] | 0.487*** | 0.565*** | 0.491*** | ||||
| [0.017] | [0.074] | [0.078] | [0.130] | |||||
| Log of per capita health expenditure | 0.452*** | 0.277*** | 0.297*** | -0.093 | ||||
| [0.096] | [0.075] | [0.073] | [0.167] | |||||
| Per capita gross state product | 0.000 | 0.011* | 0.01 | 0.005 | -0.001 | 0.003* | 0.002 | -0.012*** |
| [0.001] | [0.006] | [0.007] | [0.015] | [0.002] | [0.002] | [0.001] | [0.004] | |
| Unemployment rate | -0.009*** | 0.005 | -0.004 | -0.024 | -0.004 | 0.014*** | 0.011*** | 0.038*** |
| [0.003] | [0.014] | [0.014] | [0.022] | [0.005] | [0.004] | [0.004] | [0.012] | |
| Per capita state govt. revenue | 0.004 | 0.042 | 0.046 | -0.096* | 0.000 | 0.024*** | 0.022*** | 0.008 |
| [0.004] | [0.034] | [0.036] | [0.053] | [0.007] | [0.007] | [0.007] | [0.012] | |
| Constant | 0.226*** | 0.792*** | 1.018*** | 0.858* | -1.407*** | 0.370*** | 0.528*** | 0.430* |
| [0.062] | [0.246] | [0.264] | [0.502] | [0.115] | [0.085] | [0.082] | [0.224] | |
| Observations | 649 | 649 | 649 | 649 | 649 | 649 | 649 | 649 |
| Number of States | 50 | 50 | 50 | 50 | 50 | 50 | 50 | 50 |
| R-squared | 0.87 | 0.92 | 0.93 | 0.55 | 0.91 | 0.94 | 0.95 | 0.66 |
| Robust standard errors in brackets | ||||||||
|
* significant at 10%; Note: There was missing information on unemployment rate for Connecticut in 1999, and this resulted in 649 observations in the regressions instead of 650. |
||||||||
5. Conclusion
Rising health care costs have generated concerns that continued growth could adversely affect the nation’s economy, as well as pose problems for particular sectors of the economy, such as employers and households. This report evaluated how increased spending on health care affected aggregate economic indicators and individual sectors. As a basis for this investigation, a thorough and detailed review of the literature was conducted that included anecdotal evidence, survey findings and the peer reviewed literature. The literature review highlighted the economic effects of health care cost growth, and identified possible mechanisms through which cost growth could affect the aggregate economy, as well as government, households and business. The main findings from the review of the empirical literature were as follows.
- Negative Effect on Economy: Anecdotal evidence cited in newspapers and the popular media suggests that rising health care costs have a negative effect on the U.S. economy. However, no large scale and empirically rigorous studies have been conducted to determine the causal impact of health care cost growth on aggregate economic outcomes such as per capita income and inflation. Studies that examine the association between per capita income or GDP and health care costs almost always find a positive relationship. This is possibly because economic growth leads to greater spending on health care.
- Positive Effect on Economy: Several economists believe that rising health care costs could improve health and consequently improve labor productivity. However, no large scale and empirically rigorous studies have established that rising health care costs have increased labor productivity in the U.S.
- Effect on employers: There is very little rigorous empirical research on how health care costs affect profits, revenues, output, or competitiveness of U.S. employers. Some evidence suggests that rising health care costs have led to a decline in employment.While traditional economic models suggest that health care cost growth has no effect on employers if workers bear the costs, others have argued that cost growth will lead to higher prices and lower output, less employment, and lower profits if employers bear some of the increased burden from rising health care costs. For example, one study finds that a 10% increase in health insurance premiums reduces the probability of being employed by 1.6%, reduces hours worked by 1%, and increases the probability of part-time work by 1.9%. The current literature in this area could be improved by investigating into the causal link between employers’ share of the growing burden of health care costs and firm employment and output.
- Effect on governments: The share of health care expenditures borne by federal, state and local governments has increased over time. There is some evidence that governments are cutting down on health expenditures by reducing reimbursement to providers, increasing patient cost sharing, reducing eligibility and generosity of public insurance and reducing expenditures on other sectors of the economy. For example, in 2005, eight states reduced or restricted Medicaid eligibility and seven reduced program benefits. Also, one study found that each new dollar in Medicaid spending crowds out 6 to 7 cents of higher education appropriations. However, more research is needed to systematically analyze the effects of rising health care expenditures on government budgets and expenditures. Given that most of the literature in this area is based on anecdotal reports or descriptive evidence, there is significant scope for improving the current methods by using longitudinal data and more rigorous empirical analysis.
- Effects on consumers: There is some evidence that rising health care expenditures have led to a rise in uninsurance rates among U.S. households. Evidence from recent surveys also indicates that a significant proportion of consumers, especially the uninsured, are burdened by debt due to medical bills and sometimes forego needed medical care and other spending due to high medical care costs.
In summary, although prior work has examined several aspects of the effect of rising health care costs on the economy and its sectors, several gaps remain. Available data from various sources were therefore analyzed in an attempt to answer some of the most pressing gaps in the literature – (1) What is the impact of rising health care spending on aggregate economic indicators?, (2) What is the impact on businesses and do the effects vary by industry?, (3) What is the impact on government budgets and expenditures? The main findings from this analysis are described below.
- There is a significant and positive relationship between per capita health expenditure and per capita GSP. Although available evidence suggests that health care costs can have both a positive and a negative impact on the economy, our finding of a positive association between health care expenditures and per capita GSP is most likely due to reverse causation – states with high or rising incomes spend more on health care and experience a faster increase in health care expenditures. This finding is consistent with several macroeconomic studies that have shown such a link between per capita income and per capita health care costs. Hence, the positive relationship between health care cost growth and per capita GSP does not rule out the possibility that health care cost growth has a negative effect on the economy.
- Rising health care costs had a larger negative effect on employment and output of industries where benefits constitute a higher share of compensation. Standard economic models predict that an increase in employee health care costs would be financed by an equivalent reduction in cash wages. Thus, rising health care costs should have no effect on employment or output. However, if rising health care costs lead to a less than one-for-one reduction in cash wages then rising health care costs will increase total compensation, consequently reducing employment and output. Thus, industries where health care benefits are a larger share of total employee compensation will experience a larger increase in total compensation, consequently leading to a larger reduction in employment and output. Our empirical findings are consistent with this hypothesis and show that employment and output in industries where benefits were a larger share of compensation were hit harder by health care cost inflation.
- There is a significant positive correlation between per capita health expenditure and state government expenditures on health as well as on other sectors. The empirical findings from this analysis show that state government expenditures on various sectors including health care seem to rise together with rising health care costs. This could be because sectors such as health and education compete for allocation of funds so that an increase in health expenditures is accompanied by a similar increase in several other sectors. We do not find any evidence that rising health expenditure crowds out other components of state expenditure. On the contrary, we find evidence that government’s total expenditure and debt increase over time as health care costs and state government expenditures rise in tandem.
The literature review and empirical analysis highlighted various mechanisms through which rising health expenditures could affect the economy and its various sectors. The range of mechanisms identified in this report, together with the empirical evidence on the effects of cost increases, lay a strong foundation for carrying out a more comprehensive model-based analysis that simultaneously models all potential mechanisms to predict the long term impact of rising health care costs on the U.S. economy. Such an analysis is beyond the scope of this report but would be an important avenue for future research.
References
Alonso-Zaldivar, R. Health care costs magnify voter unease on economy. Los Angeles Times. October 25, 2006.
Assistant Secretary for Planning and Evaluation (ASPE). Effects of Health Care Spending on the U.S. Economy. U.S. Department of Health and Human Services (HHS): Washington, D.C., 2005.
Available at: http://aspe.hhs.gov/health/costgrowth/report.pdf
Baicker, K., and A. Chandra. The labor market effects of rising health insurance premiums. NBER working paper # 11160. National Bureau of Economic Research: Cambridge, 2005.
Bhattacharya, J. and D.N. Lakdawalla. The labor market value of health improvements. Forum for Health Economics and Policy, Forum: Biomedical Research and the Economy: Article 2, 2006. http://www.bepress.com/fhep/biomedical_research/
Blomqvist, A.G., and R.A.L. Carter. Is health care really a luxury? Journal of Health Economics, 16, 1997.
Bureau of Labor Statistics (BLS), U.S. Department of Labor, 2006.
http://www.bls.gov/oes/current/oes290000.htm
Bureau of National Affairs (BNA). Rising costs biggest health care concern of small businesses, federation survey finds. BNA, 12(98), May 22, 2007. Available at:http://www.aapd-dc.org/News/health/070523bna2.htm
Business Roundtable. December 2004. CEO Economic Outlook Survey.
Butler, K.M. A more convenient truth. Employee Benefit News, June 1, 2007.
Catlin, A., C. Cowan, S. Heffler, B. Washington, and the National Health Expenditure Accounts Team. National health spending in 2005: the slowdown continues. Health Affairs, 26(1), 2007.
Carty, S.S. Big 3, UAW tackle health care; Goodyear could be model for union-run fund. USA Today, July 10, 2007.
Chernew, M.E., R.A. Hirth, D.M. Cutler. Increased spending on health care: how much can the United States afford? Health Affairs, 22(4), 2003.
Chernew, M., D. Cutler and P.S. Keenan. Increasing health insurance costs and the decline in insurance coverage. ERIU working paper 8. Economic Research Initiative on the Uninsured: Ann Arbor, 2005.
Cooper, P.F. and B.S. Schone. More offers, fewer takers for employment-based health insurance: 1987 and 1996. Health Affairs, 16(6), 1997.
Cowan, C.A., P.A. McDonnell, K.R. Levit and M.A. Zezza. Burden of health care costs: businesses, households, and governments, 1987-2000. Health Care Financing Review, 23(3), 2002.
Cutler, D.M. Employee costs and the decline in health insurance coverage. Forum for Health Economics and Policy, Frontiers in health policy research, vol. 6, article 3, 2003.
Cutler, D.M., and B.C. Madrian. Labor market responses to rising health insurance costs: evidence on hours worked. The RAND Journal of Economics, 29(3), 1998.
Di Matteo, L., and R. Di Matteo. Evidence on the determinants of Canadian provincial government health expenditures: 1965-1991. Journal of Health Economics, 17, 1998.
Doty, M.M., J.N. Edwards, A.L. Holmgren. Seeing red: Americans driven into debt by medical bills. Issue brief. The Commonwealth Fund, August 2005.
Downey, K. A heftier dose to swallow: Rising cost of health care in U.S. gives other developed countries an edge in keeping jobs. Washington Post, March 6, 2004.
Emanuel, E.J., and Fuchs, V.R. Beyond health-care band-aids. The Washington Post, February 7, 2007.
Epstein, R.J. Nassau struggling to keep up with health care costs. Newsday (New York), June 19, 2007, Nassau and Suffolk edition.
Follette, G., and L. Sheiner. The Sustainability of Health Spending Growth. Staff working paper. Federal Reserve Board: Washington, D.C., 2005.
Fronstin, P. The impact of the erosion of retiree health benefits on workers and retirees. Issue brief no. 279. Employee Benefit Research Institute: Washington, D.C., 2005.
Gerber, A. The health care crisis. The Washington Times, March 18, 2007.
Gerdtham, U-G., J. Sogaard, F. Andersson, and B. Jonsson. An econometric analysis of health care expenditure: a cross-section study of the OECD countries. Journal of Health Economics, 11, 1992.
Getzen, T.E. Health care is an individual necessity and a national luxury: applying multilevel decision models to the analysis of health care expenditures. Journal of Health Economics, 19, 2000.
Getzen, T.E. Aggregation and the measurement of health care costs. Health Services Research, 41(5), 2006.
Gilmer, T. and R. Kronick. It’s the premiums, stupid: projections of the uninsured through 2013. Health Affairs, April 2005.
Goldman, D.P., N. Sood, and A. Leibowitz. Wage and benefit changes in response to rising health insurance. Forum for Health Economics & Policy, Frontiers in health policy research, vol. 8, article 3, 2005. http://www.bepress.com/fhep/8/3
Gould, E. Prognosis worsens for workers’ health care: fourth consecutive year of decline in employer-provided insurance coverage. Briefing paper. Economic Policy Institute, Washington, D.C., 2005.
Gruber, J. The incidence of mandated maternity benefits. American Economic Review, 84(3), 1994.
Hall, Kevin G. Health care, wages, energy costs put squeeze on middle class. McClatchy
Newspapers, Oct 17, 2006.
Hall, R.E. and C.I. Jones. The value of life and the rise in health spending. NBER Working paper # 10737. National Bureau of Economic Research: Cambridge, 2004.
Hamilton, M.M. Health-care trends you dare not forget. The Washington Post, April 1, 2007.
Harper, T. Clinton links health care, jobs; New York senator says Canada’s universal system an ‘excuse’ to move quality jobs north of the border. Toronto Star, June 20, 2007.
Hecker, D.E. Occupational employment projections to 2014. Monthly Labor Review, 128, November 2005.
Heffler, S., S. Smith, S. Keehan, C. Borger, et al. U.S. health spending projections for 2004-2014. Health Affairs, 24, Jan-Jun 2005.
Himmelstein, D.U., E. Warren, D. Thorne and S. Woolhandler. Market watch: illness and injury as contributors to bankruptcy. Health Affairs, February 2005.
Hitiris, T., and J. Posnett. The determinants and effects of health expenditure in developed countries. Journal of Health Economics, 11, 1992.
Johnson, R.W., A.J. Davidoff and K. Perese. Health insurance costs and early retirement decisions. Industrial and Labor Relations Review, 56(4), 2003.
Johnson, R.W. and R.G. Penner. Will health care costs erode retirement security? Issue brief no. 23. Center for Retirement Research: Boston College, October 2004.
Kaiser Family Foundation. 2005 Kaiser/HRET Employer Health Benefit Survey. Kaiser Family Foundation, 2006.
Kaiser Family Foundation. Insurance premium cost-sharing and coverage take-up. Issue brief, Kaiser Family Foundation, February 2007.
Kane, T.J., P.R. Orszag, and D.L. Gunter. State fiscal constraints and higher education spending: the role of medicaid and the business cycle. Discussion Paper no. 11. The Urban Institute: Washington, D.C., 2003.
Kohn, N.B., D. Cash and K.L. Brown. Heartache in the heartland: Kansans speak about the burden of medical debt. The Access Project: Boston, 2005.
Knight, H. The dollars don’t add up: falling enrollments, rising health care costs squeeze district’s budget. San Francisco Chronicle, June 1, 2006.
Krugman, P. The health care racket. The New York Times, February 16, 2007.
Lalonde, R.J., G. Marschke, and K. Troske. Using longitudinal data on establishments to analyze the effects of union organizing campaigns in the United States. Annales D'Economie Et De Statistique. n41-42: 155-85, 1996.
Lopes, G. Small firms find few insurers. The Washington Times, May 25, 2007.
Monaco, R.M., and J.H. Phelps, Health Care Prices, the Federal Budget and Economic Growth, Health Affairs, Vol.14, No. 2, 1995, pp. 248-259.
Murphy, K.M. and R.H. Topel. The value of health and longevity. Journal of Political Economy, 114(5), 2006.
National Coalition on Health Care (NCHC). The Impact of Rising Health Care Costs on the Economy: Effects on Business Operations. National Coalition on Health Care: Washington D.C., 2006.
Newhouse, J.P. Medical-care expenditure: a cross-national survey. The Journal of Human Resources, 12(1), 1977.
Newhouse, J.P. Medical Care Costs: How Much Welfare Loss. Journal of Economic Perspectives, 6(3):3-21, 1993.
Parkin, D., A. McGuire, and B. Yule. Aggregate health care expenditures and national income: is health care a luxury good? Journal of Health Economics, 6, 1987.
Pauly, M.V. Should we be worried about high real medical spending growth in the United States? Health Affairs, Jan-Jun 2003, Web Exclusives: W3-15-27.
Porter, E. Rising costs of health benefits cited as factor in slump of jobs. The New York Times, Aug 19, 2004.
Pryor, C. and D. Gurewich. Getting care but paying the price: how medical debt leaves many in Massachusetts facing tough choices. The Access Project: Boston, 2004.
Quinn, R.D. The health care crisis: not about coverage, but cost. Employee Benefit News, May 1, 2007.
Race, T. Health costs push companies to set targets for workers. The New York Times, June 11, 2007.
Samuelson, R.J. Let’s not hide health costs. Newsweek, February 5, 2007.
Seifert, R.W. Home sick: how medical debt undermines housing security. The Access Project: Boston, 2005.
Shea, B. Stuck on health costs; efforts to slow growth stalled at 6 percent a year, local survey says. Crain’s Detroit Business, May 14, 2007.
Smith V., K. Gifford, E. Ellis, et al. Medicaid Budgets, Spending and Policy Initiatives in State Fiscal Years 2005 and 2006: Results from a 50-state Survey. Kaiser Commission on Medicaid and the Uninsured: Washington, D.C., 2005.
Sommers, B.D. Who really pays for health insurance? The incidence of employer-provided health insurance with sticky nominal wages. International Journal of Health Care Finance and Economics, 5, 2005.
Summers, L.H. Some simple economics of mandated benefits. The American Economic Review, 79(2), 1989.
U.S. Chamber of Commerce. Employee Benefits Study 2006. U.S. Chamber of Commerce: Washington D.C., 2007.
Vedder, R., and L. Gallaway. The economic effects of labor unions revisited. Journal of Labor Research, 23(1): 105-30, 2002.
Warshawsky, M.J. An enhanced macroeconomic approach to long-range projections of health care and social security expenditures as a share of GDP. Journal of Policy Modeling, 21(4), 1999.
White, H. A heteroskedasticity-consistent covariance matrix estimator and a direct test for heteroskedasticity. Econometrica, 48, 1980.
Wroe, T. Containing the cost of health care. The Boston Globe, March 16, 2007.
Zeldin, C. and M. Rukavina. Borrowing to stay healthy: how credit card debt is related to medical expenses. Demos: New York & The Access Project: Boston, 2007.
Appendix 1: List of Keywords and Their Combinations Used for the Literature Search
- Health care costs + U.S. economy
- Rising costs + health + economy
- Health care sector + role + U.S. economy
- Rise + health care spending + U.S.
- Health care costs + economic growth
- Health care costs + GDP
- Health spending + impact
- Health spending + GDP
- Health spending + employment
- Health spending growth + productivity
- Health care costs + state spending
- Health care costs + households
- Health care expenditures + macroeconomic effect
- Price + employers + health insurance decisions
- Health costs + low wage + workers
- Employer provided insurance + wage benefit tradeoff
- Health spending + local economies
- Manufacturing firms + health insurance
- Health care costs + strategies + small business
- Labor market + health insurance premiums
- Medical care costs + welfare loss
- Health care prices + budget + economic growth
- Technological change + medicine + costs benefits
- High medical spending + growth + United States
- Health spending + projections + United States
- Carmakers + retiree + health care costs
- Employment-based benefits + uninsured
- Employer + health insurance costs
- Companies + rising health costs
- Rising costs + health benefits + jobs
- Employer-sponsored health benefits + survey
- Retiree health benefits + survey
- Economic contribution + hospitals
- Economic impact + hospitals
- Federal health spending + metropolitan economies
- Economics + mandated benefits
- Substitution + wage + non-wage benefits
- Compensation + health insurance + premium increase
- Labor market responses + health insurance costs
- Employer-provided insurance + workers’ compensation
- Trade-offs + medical bills + family finances
- Rising health costs + medical debt
- High cost + medical care + consumers
Appendix 2: Description of Variables and Data Sources
| Variable | Unit of measurement |
Source | Comments |
|---|---|---|---|
| State population | Number | Bureau of Economic Analysis |
|
| Per capita health expenditure |
Thousands of current dollars |
CMS | Total personal health care expenditure divided by state population |
| Per capita GSP | Thousands of current dollars |
Bureau of Economic Analysis |
Gross state product divided by state population |
Unemployment rate |
Percentage | Bureau of Labor Statistics |
By state |
| Per capita state government health expenditure |
Thousands of current dollars |
Census Bureau, CMS |
State expenditures on health and hospitals added to state Medicaid expenditure. Total divided by state population. |
| Per capita state government all other expenditures |
Thousands of current dollars |
Census Bureau | State expenditure divided by state population |
| Per capita state government total expenditure |
Thousands of current dollars |
Census Bureau | State expenditure divided by state population |
Per capita state government debt |
Thousands of current dollars |
Census Bureau | State debt at the end of fiscal year divided by state population |
| Share of benefits in total compensation in 1987 |
Percentage | Bureau of Economic Analysis |
Benefits or supplements to wages and salaries as a percent of total compensation to employees |
Medical care price index |
Number | Bureau of Labor Statistics |
Consumer price index (U.S. city average) for medical care; base period: 1982-84 = 100 |
| Share of employee contribution to premiums |
Percentage | Medical Expenditure Panel Survey |
Percent of total premiums contributed by employees enrolled in single coverage at private-sector establishments offering insurance |
Unionization (percent) |
Percentage | Bureau of Labor Statistics |
Union members as a percent of total employed workers |
Labor productivity: value added per worker |
Thousands of current dollars |
Bureau of Economic Analysis |
Value added by an industry divided by its total number of employees |
Employment |
Thousands of workers |
Bureau of Economic Analysis |
By industry |
Gross output |
Millions of current dollars |
Bureau of Economic Analysis |
By industry |
Value added to GDP |
Millions of current dollars |
Bureau of Economic Analysis |
By industry |
Footnotes
- Recent estimates suggest that the U.S. spends $98 billion in excess administrative costs and $66 billion in excess drug costs, compared to other nations with a single-payer system (Krugman, 2007).
- For example, in 1971, both the U.S. and Canada spent 7-8 percent of their GDP on health care. With the adoption of its single-payer health care system 25 years ago, Canada's ratio rose to 9.6 percent in 2006, while the U.S. with its largely employer-sponsored insurance coverage now spends 16 percent of its GDP on health care (Gerber, 2007).
- However, there is some dispute as to whether health care is a luxury good, i.e., whether the true income elasticity of health care expenditure is greater than one or not (Parkin et al., 1987; Blomqvist and Carter, 1997). Getzen (2000) reconciles the two opposing views by pointing out that a particular finding depends on the level of analysis. While micro analyses typically find that individual income elasticities were small, analysis at the macro level tends to support the “luxury good” hypothesis. He further demonstrates that the correlation of income with health expenditures becomes larger as the level of aggregation becomes larger, so much so, that for nations, differences in per capita income explain over 90 percent of the variation in health care expenditure (Getzen 2006).
- http://www.inc.com/news/briefs/200707/0724benefits.html
- Given the rapid rise in health care costs and the growing number of uninsured, there have been a number of recent health care proposals that aim to provide insurance to the estimated 47 million uninsured Americans (Samuelson, 2007). However, commentators argue that broader coverage would follow once the problem of high health care costs were resolved, while expanding coverage without addressing inefficiency or long-term cost control would in fact lead to even higher costs, health care rationing, and a greater number of uninsured in the future (e.g., see Emanuel and Fuchs, 2007; Quinn, 2007).
- Since the Kaiser/HRET employee benefits survey focuses on employer-sponsored health benefits, information on the use of medical care is not available from this survey. Hence, it is not known whether the reported decline in take-up rates of health insurance is also associated with lower medical care use.
- Some industries that could not be consistently matched across the two time periods were omitted. However, the final dataset consists of industries from all the major sectors and hence is representative of all industry types over 1987-2005.
- The medical care price index was divided by the consumer price index (CPI) to arrive at changes in real medical care prices over time. This deflated medical care price index registered an average increase of 2% per annum during this time period.
- Note that percentage change is more meaningful in this context rather than change in levels, since various industries would have very different levels of output and employment to start with.
- Since the coefficient estimates in the log specification is the percentage change in a particular outcome as opposed to change in levels (in the specification without logs), the estimates from the log specification are more appropriate for interpreting the results.
- The results for the effect of unionization are in broad agreement with previous findings in the literature that indicate that greater unionization typically leads to a decline in employment and output (Lalonde et al. 1996, Vedder and Gallaway 2002).
- A separate analysis was performed looking at the effect of employee cost sharing on industrial employment and output. While the results suggested that greater employee cost sharing could potentially mitigate the adverse impact of rising health care costs for industries with a higher benefit share, this analysis could only be carried out at the sectoral level in the absence of comparable data at a more disaggregated level, and as such, these results lacked precision due to a significantly smaller sample size. Hence, those results are not reported, but are available on request.
- Since these predictions are based on the regression models estimated above, all factors that affect employment and output other than the rate of health care cost growth are held constant in generating the predictions for different cost growth scenarios. Therefore, these are only meant to provide an easier way of interpreting the main results from the regressions, and to compare employment and output under the different scenarios, given the model assumptions.
- While it appears that the increase in per capita state government expenditure on health was around $30 in all four quartiles, this is due to rounding up to 2 decimal places. The average increase was actually between $25 – $28 in the bottom two quartiles, and around $33 – $34 in the upper two quartiles of the change in per capita health expenditure.
