Overview
Prevention is an investment opportunity in our nation's future: for individuals, for community groups, for businesses, and for government. When we have this kind of opportunity to make a difference, it is incumbent upon us to embrace it wholeheartedly and take action.
Tommy G. Thompson
Secretary, HHS
On June 20, 2002, President George W. Bush announced his HealthierUS Initiative, calling on government officials, business leaders, communities, health care providers, churches and civic organizations, to come together as partners in helping Americans live longer, better and healthier lives. HealthierUS identifies four key health-protection objectives for a healthier America: increased physical activity, responsible dietary habits, increased use of preventive health screenings, and healthy choices concerning alcohol, tobacco, drugs and safety.
The U.S. Department of Health and Human Services (HHS) took up the President's challenge and Secretary Thompson launched Steps to a HealthierUS, a bold initiative that mobilizes the resources of HHS in collaboration with outside organizations to promote healthy habits and chronic disease prevention. Prevention: A Blueprint for Action, the latest activity in the HHS Steps Initiative, outlines simple steps that individuals and interested groups can take to promote healthy lifestyles and encourage healthy behavior.
The Steps initiative is founded on a growing body of research showing that small, simple steps can often prevent or control chronic diseases. Its goal is to reverse the growth in the number of people suffering from diseases like asthma, diabetes, cancer, heart disease and stroke, as well as factors that contribute to them such as obesity and tobacco use. The intent of Steps to a HealthierUS is to reach the broadest number of Americans by using multiple approaches and involving groups and organizations to foster health, physical activity and good nutrition. To date, these approaches have focused on communities, businesses and organizations, and the actions that they can take to influence individuals’ choices and actions to improve health. The HHS prevention effort and Steps to a HealthierUS have many components:
- Grants to Communities: As the cornerstone of the Steps initiative, HHS currently provides a total of $13.7 million for twelve cooperative agreements to establish community-wide partnerships to improve the health and well-being of individuals by encouraging people to maintain physically active lifestyles and make healthy lifestyle choices.
- Roundtable Discussions: The Secretary hosted a series of Roundtable discussions, which brought together interested stakeholders including academia, insurers, business executives, health care providers, and researchers. The purpose of these roundtables was to highlight the importance of prevention and specifically discuss best approaches to stem the tide of chronic diseases and encourage healthy lifestyles - regular physical activity and balanced diets. The roundtables also identified obstacles to adopting healthy habits.
- Prevention Town hall: The Secretary hosted a Prevention Town hall in Austin, Texas in 2003. The goal of the town hall was to engage stakeholders in a discussion of the importance of health promotion and disease prevention. Featured experts identified successful approaches to foster healthy behaviors.
- Secretary’s Challenge--Steps to a HealthierHHS: This is a HHS worksite health promotion program encouraging department employees to become more physically active. This voluntary initiative promotes the benefits of a healthy lifestyle by challenging employees to be on the move -- at least 30 minutes a day, five days a week for six weeks. Nearly 800 employees participated and 25 percent completed the pilot program in the Washington, DC area. The Secretary plans to take this challenge to all HHS employees and other federal departments soon.
- Prevention Summit: Held on April 15-16, 2003 in Baltimore, Maryland, the Steps to a HealthierUS: Putting Prevention First Summit focused attention on the urgency of prevention and on promising approaches for tackling key challenges. At this inaugural conference, the Secretary laid out his priorities and programs for Steps to a HealthierUS. The second annual summit was held on April 29-30, 2004 in Baltimore, Maryland.
- Awards for Innovation: Another component of the Steps initiative is the Steps Innovation in Prevention Awards Program. In December 2003, HHS awarded eight Steps Innovation Awards in seven categories, to groups and organizations recognizing their accomplishments and highlighting the concrete health improvements that each has achieved.
- Partnerships: Another aspect of the Steps initiative is the Partnerships program where HHS seeks to work with other public and private sector organizations to support and promote healthier living. It is designed to encourage other organizations to follow the lead of the Innovation Award recipients.
- Secretarial Workgroups and the Blueprint for Action: While recognizing the importance of many other diseases such as cancer, cardiovascular disease, and asthma, the Secretary established five senior staff workgroups on specific areas that were identified as presenting particular opportunities for cross-Departmental coordination and that are central to advancing health promotion and disease prevention: overweight and obesity, diabetes, tobacco, media and messages, and health literacy. This work provided the basis for the Blueprint for Action.
- Initial Preventive Physical Examination and Other New Medicare Benefits: The Medicare Prescription Drug, Improvement, and Modernization Act (MMA) of 2003 establishes coverage of a one-time “Welcome to Medicare Physical Examination” within 6 months of a beneficiary’s first coverage under Part B, with the goal of health promotion and disease detection. The benefit covers a physical exam (including measurement of height, weight and blood pressure, and an electrocardiogram) and includes education, counseling and referral with respect to screening and other preventive services. The effective date is January 1, 2005, for new beneficiaries whose coverage period under Medicare Part B begins on or after such date. The MMA also adds coverage for cardiovascular and diabetes screening for Medicare beneficiaries, which also begin on January 1, 2005.
This report provides an overview of these efforts. First, it highlights the problems and challenges in these areas. Then, based on a series of roundtable discussions between the Secretary and various interested stakeholders, it delineates specific action steps that individuals, communities, insurers, employers, healthcare providers, and other public and private entities can take. Finally, it profiles HHS activities that address these challenges, reports on progress and accomplishments, and identifies opportunities for additional action. This Blueprint for Action will create a template for collaborative efforts to improve the health and well-being of all Americans.
Scope of the Problem
As the latest element of the Steps initiative, the Secretary established five HHS workgroups on specific areas that are central to advancing health promotion and disease prevention: diabetes, overweight and obesity, smoking cessation, media and messages, and health literacy. Overweight and obesity, lack of physical activity, and smoking greatly increase the risk of developing serious diseases, such as diabetes, heart disease, stroke, and cancer, accounting for much of the morbidity and mortality in the U.S., and the enormous direct and indirect costs associated with them. In large part, these disorders stem from, and are exacerbated by, individual behaviors and, thus, are preventable. The Department’s efforts to promote health and prevent such disorders depend in part on developing effective messages that are appropriate for individuals and groups in ways that they can understand and act on. The goals of these workgroups were to evaluate current HHS programs and activities; recommend ways to better coordinate these efforts; and identify areas of opportunities for new initiatives.
Overweight and Obesity
Facts and Figures on Overweight and Obesity
- In 1999-2000, 64 percent of U.S. adults were overweight, an increase from 56 percent when surveyed in 1988-1994; 30 percent of adults were obese, an increase from 23 percent in the earlier survey [2].
- Dramatic increases in the prevalence of overweight and obesity have occurred in children and adolescents of both sexes, with approximately 15.3 percent of children aged 6 to 11 years and 15.5 percent of adolescents aged 12 to 19 years considered to be overweight [3].
- Overweight and obesity are associated with increased morbidity and mortality. An estimated 300,000 deaths per year may be attributed to obesity, and overweight and obesity increase the risk for coronary heart disease, Type 2 diabetes, and certain cancers [4].
- The total economic cost of obesity in the U.S. is up to $117 billion per year, including more than $60 billion in avoidable medical costs, more than 5 percent of total annual health care expenditures [5].
- The prevalence of overweight and obesity varies by gender, age, socioeconomic status, and race and ethnicity. For example, although overweight has increased among all children, the prevalence of overweight and obesity is significantly higher among non-Hispanic black and Mexican-American adolescents than among non-Hispanic white teens (12-19 years old) [3]. A majority of non-Hispanic black women over 40 are overweight or obese [2].
The nation is currently facing a major long-term public health crisis. In recent years, unprecedented numbers of Americans of all ages have become either overweight or obese (Figure 1). This trend toward overweight and obesity has accelerated during the past decade and is well documented by numerous scientific analyses (see Facts and Figures on Obesity). Unfortunately, this trend toward obesity shows no signs of abating. If it is not reversed, the gains in life expectancy and quality of life resulting from modern medicine’s advances on disease will erode, and more health-related costs will burden the nation. It is estimated that almost half of the annual costs of obesity reflects indirect costs, such as loss of productivity caused by absenteeism, disability, and premature death [1]. Obesity and overweight are preventable conditions for most Americans. The increasing prevalence in obesity-related illnesses must be reversed.
Figure 1. Prevalence of Obesity by Age, 1999 - 2000
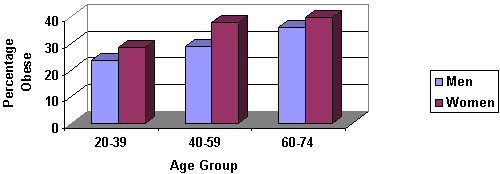
Source: NHANES Continuous, 1999-2000 (JAMA 2002; 288(14):1723-27)
Health care providers can play a vital role in helping patients with obesity. The US Preventive Service Task Force (USPSTF) recently recommended that clinicians screen for obesity on all adult patients using the Body Mass Index (BMI), calculated as weight in kilograms divided by height in meters squared. People with a BMI between 25 and 29.9 are considered overweight, and those with a BMI of more than 30 are considered obese. An online BMI calculator can be found at www.cdc.gov/nccdphp/dnpa/bmi/calc-bmi.htm. The USPSTF also recommended that clinicians offer obese patients intensive counseling and behavioral interventions to promote sustained weight loss or refer them to other clinicians for these services.
Poor diet and physical inactivity, resulting in an energy imbalance (an imbalance between the calories consumed and the calories expended), are two of the most important factors contributing to the increase in obesity. Other contributing factors include psychological considerations and motivations, education level, time constraints, and even cooking skills.
Changes in food intake and energy expenditure.
Substantial changes in food intake and physical activity have occurred over the last 20 years in the U.S. Changes in food intake are better documented than changes in physical activity, since they have been easier to measure in research studies. Some examples of changes in food consumption and purchasing include:
- Research has shown that when adolescents eat on their own and not with their families, they are less likely to eat healthy food, including fruits and vegetables [6].
- Soft drink consumption, which consists of both sodas and juice-based drinks, increased by over 60 percent between 1972 and 1992 [7], and accounts for over 10 percent of the average adolescent’s daily caloric intake [8]. While such drinks can be enjoyed in moderation, for many they may substitute inappropriately for water, nonfat or low fat milk, and lower-calorie drinks.
- An increased variety of products are available in supermarkets [9].
- People are eating outside the home more than ever [10]. The proportion of the food budget spent on food consumed outside the home has grown from approximately one third in the late 1970s to almost one half in the late 1990s, and over this same time period, portion sizes of foods consumed both outside and in the home have increased substantially [11, 12].
Although each of these shifts has been associated with an increase in food intake, none has clearly been linked to the onset of obesity. It is the imbalance between food intake and energy expended, however, that leads to weight gain. Calculations of the caloric content of fat suggest that an excess of 50 calories per day may produce as much as five pounds excess weight gain per year. (This is roughly the equivalent of one small cookie, per day.) Therefore, modest uncompensated changes in energy intake or expenditure over years may produce significant weight gains.
Behavior and weight management.
Many factors contribute to behaviors that lead to overeating, insufficient activity, and weight gain in contemporary American culture. There are intricate biological systems that regulate human hunger and satiety. It has been argued that humans are biologically programmed to prefer foods that are dense in fat, sugar and protein as a mechanism to assure adequate nutrition and healthy existence, particularly in times of scarce food. Additionally, human biology allows easy storage of nutrients in times of excess to provide a reserve for times of need. The biologic signals for satiety, or fullness, are often subtle, and are not perceived quickly or intensely. In ordinary circumstances, it is easy to eat more than is necessary to stop hunger anxiety signals. Eating food quickly furthers the likelihood of overshooting the satiety signal. The human predisposition toward conserving physical energy increases demand for inventions and technologies that help people increase productivity and reduce physical expenditure. For some individuals, exercising may run counter to the instinct to conserve physical energy.
The American social environment greatly facilitates the biologic and psychological predispositions toward eating, often contributing to repeated overeating. Social interactions and connectivity are important factors in interpersonal success and mental well-being. Food is a central component of many social gatherings. For most of the population, an abundance of food is readily available. Grocery stores and other kinds of stores offer increasingly large varieties of food, including heavily marketed and already prepared items. Many grocery stores even offer convenient home deliveries. As consumers eat more of their meals outside the home, restaurants play a bigger role in shaping ideas on appropriate portion sizes and balance of nutrients.
Diabetes
Facts and Figures on Diabetes
- In 2002, an estimated 6.3 percent of the population, or some 18.2 million persons, had diabetes in the U.S.[13].
- About 70 percent are aware of their disease (13.0 million) compared to 30 percent (5.2 million) who are unaware [13].
- Diabetes affects various sociodemographic groups unequally. Persons aged 65 years and over make up almost 40 percent of all the persons with diagnosed diabetes, and this age group has a prevalence rate over 10 times that of persons under 45 years of age [17]. Minority populations also are disproportionately affected, with the prevalence of diabetes generally 1.5 to 4 times higher in those groups than in the majority population (Figure 2) [17, 18]. A higher prevalence in adults is associated with a lower educational level; adults with less than a high school education are more than twice as likely to have diabetes than college graduates [20].
- Rates of diabetes among adults also vary by geography; in 2001, prevalence ranged from 5.0 percent in Minnesota to 10.5 percent in Alabama [20]. The highest reported diabetes prevalence in the world (over 50 percent) is among the Pima Indians of the southwestern U.S. [21].
- Diabetes also imposes a tremendous economic burden, estimated at $132 billion in 2002 in the U.S. Most of this is spent on medical care for those affected ($92 billion) but a substantial proportion is also due to disability, work loss, and premature mortality ($40 billion) [13]. Unemployment and reduced productivity may also be manifestations of disability. The work disability rate is over three times as high for persons with diabetes as for those without the disease (26 percent versus 8 percent) [22]. Generally, diabetes results in the loss of about one third of a year’s earnings.
An increasingly large proportion of people in the U.S. have diabetes (Figure 2). High health care costs are associated with this condition, and the consequences to individuals, families and society in terms of quality of life are even more staggering. Diabetes is a disease in which blood glucose (sugar) levels are elevated either because of the body’s failure to make adequate amounts of the hormone insulin and/or failure of cells to respond to insulin. There are several types of diabetes:
- Type 1 diabetes, often called “insulin-dependent diabetes mellitus” or juvenile-onset diabetes, develops when the body’s immune system destroys pancreatic beta cells, the cells in the body that make the hormone insulin that regulates blood glucose. Thus, the pancreas can no longer produce insulin. This form of diabetes usually strikes children and young adults, but it may occur at any age, and requires individuals to take several insulin injections a day or use a pump to survive. Type 1 diabetes may account for 5 to 10 percent of all diagnosed cases of diabetes. [13, 14]
- Type 2 diabetes, formerly termed “adult-onset diabetes” is “non-insulin dependent diabetes mellitus,” even though some affected individuals require insulin for control of the disease. Type 2 diabetes usually begins as insulin resistance, a disorder in which cells do not use insulin properly. As it progresses, the pancreas gradually loses its ability to produce insulin. Type 2 diabetes often appears after age 40, although it is now being diagnosed increasingly in children and adolescents. This form of diabetes accounts for 90 to 95 percent of all diagnosed cases of diabetes. [13, 14] .
- Gestational diabetes mellitus (GDM) is a form of diabetes that affects between 2.5 percent and 4 percent of women in the U.S. during pregnancy. This type of diabetes results from the body's resistance to the action of insulin. The increased resistance during pregnancy is caused by hormones produced in the placenta. Gestational diabetes usually ends after the baby is born, but women with gestational diabetes have up to a 45 percent risk of recurrence with the next pregnancy and up to a 63 percent risk of developing type 2 diabetes later in life [15].
- Prediabetes is a condition that affects millions of people. It is defined as impaired fasting glucose or impaired glucose tolerance (IGT) or both. People with prediabetes are at high risk for developing full-blown diabetes and are also at risk of developing other serious health problems such as heart attack and stroke. Recently, the Expert Committee on the Diagnosis and Classification of Diabetes Mellitus of the American Diabetes Association lowered the blood glucose level threshold for diagnosis of impaired fasting glucose from 110mg/dl to 100mg/dl in order to provide a more reliable means of identifying persons at risk for developing diabetes [16]. This lowered threshold for impaired fasting glucose doubled the number persons identified as having prediabetes. As estimated in the CDC’s National Diabetes Fact Sheet, over 40 million Americans aged 40-74 years have prediabetes.[13]
Figure 2. Prevalence of Diabetes: Diagnosed and Undiagnosed
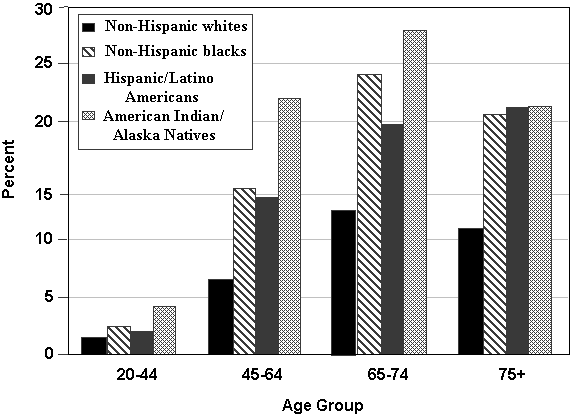
Source: Centers for Disease Control and Prevention. Diabetes Surveillance System. Atlanta, GA,
U.S. Department of Health and Human Services.
Available at http://www.cdc.gov/diabetes/statistics/index.htm.
Over the last half century there has been a 4- to 8-fold increase in the prevalence of diagnosed diabetes in the U.S. [17, 18] . Projections of diabetes into the 21st century are not comforting (Figure 3). A 165 percent increase in persons with diabetes in the U.S. is projected between 2000 and 2050, a rise from 11 to 29 million diagnosed persons of all ages [19] . Those aged over 75 years are expected to have the largest increases (271 percent in women and 437 percent in men). Among racial and ethnic groups, African Americans are expected to have a larger increase (363 percent for males and 217 percent for females) than Caucasians (148 percent for males and 107 percent for females).
Figure 3. Prevalence of Diagnosed Diabetes in the United States
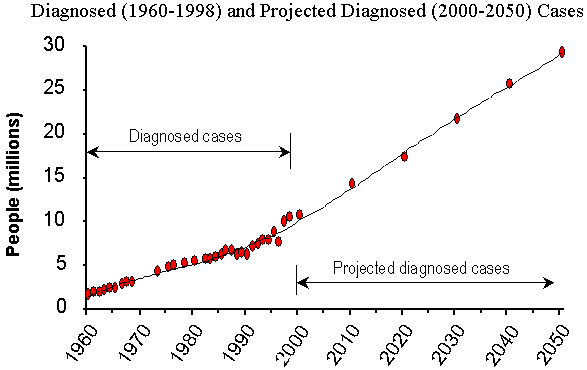
Source: Data for 1960-1998 from the National Health Interview Survey, NCHS, CDC
Projected data for 2000-2050 from the Behavioral Risk Factor Surveillance System, Division of Diabetes Translation, CDC
Diabetes can have a major impact on both the quality and length of life. Acute complications, such as dangerously low blood glucose levels, called hypoglycemia, could be life-threatening. Chronic complications--such as eye disease leading to blindness, kidney disease leading to kidney failure, lower extremity nerve disease leading to amputations, and premature cardiovascular disease leading to heart disease and stroke-- are ultimately the main causes for reductions in the quality and also the length of life of persons with diabetes (Table 1).
|
Condition |
Annual Number of Cases Associated with Diabetes |
|---|---|
| Blindness | 12,000 – 24,000 |
| Kidney failure | 42,813 |
| Amputations | 82,000 |
| Cardiovascular disease deaths | 130,000 |
Diabetes is the major cause of kidney failure, lower limb amputations and adult-onset blindness. Diabetes increases cardiovascular disease risk 2-4 fold.
Among the elderly, diabetes-related cognitive impairment or dementia is also well recognized. Diabetes is the sixth leading cause of death and lowers average life expectancy by up to 15 years [23] .
High quality of care for diabetes is based on ensuring that people with diabetes have needed tests that can help them and their providers manage their condition. All people with diabetes should obtain these services, which are relatively inexpensive to provide. However, only 20.7 percent of patients reported having received all five major tests for diabetes within the past 2 years. [24]
Many factors have affected the upward trends in the prevalence of diabetes, including changes in diagnostic criteria, enhanced detection, decreasing general mortality, changes in population demographics (e.g., aging and growth in minority populations who experience higher prevalence rates), and increased incidence. Demographic changes in the population such as increases in minority populations at higher risk (37 percent), increasing prevalence rates (36 percent), and population growth (27 percent) have increased the diabetes burden. The concomitant rise in obesity and the elevated risk it presents for type 2 diabetes are also major contributors to these increases. The prevalence of overweight or obesity significantly increased from 1988-94 to 1999-2000 (from 55.9 percent to 64.5 percent); and obesity also rose (from 22.9 percent to 30.5 percent) [2] . The prevalence of overweight in children has doubled and in adolescents has tripled since 1970 (rising from 11 percent in 1988-94 to 15 percent in 1999-2000) [3].
While it is not yet possible to prevent type 1 diabetes, findings from major clinical trials have demonstrated that the onset of type 2 diabetes can be prevented or delayed in high-risk groups, including minority groups, who carry a disproportionately heavy burden of this disease. Clinical research has identified risk factors that place individuals at high-risk for this disease. Because over 5 million people are currently undiagnosed in the U.S., and because more intensive treatment of hypertension and hyperlipidemia is recommended for people with diabetes to reduce their increased risk of cardiovascular disease, the U.S. Preventive Services Task Force recommends that people with elevated levels of blood lipids (such as cholesterol and triglycerides) or high blood pressure be screened for type 2 diabetes [25] .
Tobacco
Facts and Figures on Tobacco [30]
- An estimated 71.5 million Americans reported current use (past month use) of a tobacco product in 2002, a prevalence rate of 30.4 percent for the population aged 12 or older.
- Among that same population, 61.1 million (26.0 percent of the total population aged 12 or older) smoked cigarettes, 12.8 million (5.4 percent) smoked cigars, 7.8 million (3.3 percent) used smokeless tobacco, and 1.8 million (0.8 percent) smoked tobacco in pipes.
- Young adults aged 18 to 25 continued to report the highest rate (45.3 percent) of use of tobacco products. Past month rates of use for this age group were 40.8 percent for cigarettes, 11.0 percent for cigars, 4.8 percent for smokeless tobacco, and 1.1 percent for pipes.
- By age group, the prevalence of cigarette use was 13.0 percent among 12 to 17 year olds, 40.8 percent among young adults aged 18 to 25 years, and 25.2 percent among adults aged 26 or older.
- Higher proportion of males than females aged 12 or older smoked cigarettes in 2002 (28.7 vs. 23.4 percent). However, among youths aged 12 to 17, girls were slightly more likely than boys to smoke (13.6 vs. 12.3 percent)
- In 2002, 17.3 percent of pregnant women aged 15 to 44 smoked cigarettes in the past month compared with 31.1 percent of nonpregnant women of the same age group.
- Current cigarette smoking rates among persons aged 12 or older were 37.1 percent among American Indians/Alaska Natives, 35.0 percent among persons reporting two or more races, 26.9 percent among whites, 25.3 percent among blacks, 23.0 percent for Hispanics, and 17.7 percent for Asians.
- The prevalence of cigarette smoking decreased with increasing levels of education. Among adults aged 18 or older in 2002, college graduates were the least likely to report smoking cigarettes (14.5 percent) compared with 35.2 percent of adults who lacked a high school diploma.
- The annual toll on the nation’s health and economy is staggering: 440,000 deaths, 8.6 million people suffering from at least one serious illness related to smoking, $75 billion in direct medical costs, $82 billion in lost productivity, and 5.6 million years of potential lives lost [31,32,33].
Perhaps the most impressive recent accomplishment has been the decline in smoking among adolescents after nearly a decade (during the 1990s) of rising smoking rates among youth (Figure 4). Although more than one in four U.S. high school students currently smokes cigarettes, smoking among this group has been falling since 1997.
Tobacco use remains the leading preventable cause of death and disease in the U.S. and continues to pose a formidable challenge to the public health community. The downward trend in adult smoking is far too slow, particularly among people with lower education and income levels; declines in smoking among middle-school students appear to have stalled; and the long-term success rate for smokers who try to quit each year is still under 5 percent [34].
Figure 4. Percentage of High School Students Who Reported Current Cigarette Smoking*—United States, 1991–2001
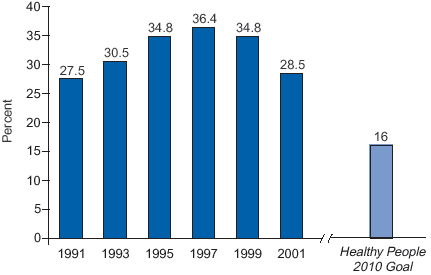
*Smoked cigarettes on 1 or more of the 30 days preceding the survey.
Source: CDC, Youth Risk Behavior Surveillance System (MMWR 2002;51(19):409–12).
Compounding these challenges is the current fiscal condition in several states that threatens successful statewide comprehensive tobacco control programs. The amount of money states are spending on tobacco prevention dropped by 28 percent over the past two years [35].
Over the past four decades, the scientific knowledge about the health consequences of tobacco use has expanded greatly. Much of this knowledge is the outgrowth of research that HHS has conducted or sponsored. It is now well documented that smoking cigarettes causes heart disease, lung cancer and many other cancers, chronic lung disease, and a wide range of other diseases and conditions affecting virtually every organ of the body. Cigar smoking and smokeless tobacco use have also been found to increase the risk of certain types of cancer and are not safe alternatives to smoking cigarettes. In addition to these conventional tobacco products, a new generation of nicotine products that purport to be less harmful has emerged, such as cigarettes that promise fewer carcinogens, and tobacco lozenges. However, establishing any claim of harm reduction requires extensive independent research on the products themselves and their impact on human health.
The health hazards of tobacco use extend beyond the actual users. Exposure to secondhand smoke increases nonsmokers’ risk for cancer (particularly lung cancer), other respiratory diseases, and heart disease. Among children, secondhand smoke increases the risk of developing serious respiratory problems, including asthma, pneumonia, and bronchitis. Additionally, substantial evidence now links secondhand smoke with sudden infant death syndrome and low birth weight.
The burden of tobacco use is not evenly distributed within the U.S. population. Specific population groups differ in the risk, incidence, morbidity, mortality, exposure, and burden of tobacco–related illness, as well as in their access to resources. For example, American Indians and Alaska Natives smoke at higher rates than any other ethnic/racial group.
Media and Messages
The dangers of risky behaviors – poor eating habits, lack of exercise, and smoking – and their potential effects on health are well known to many. We know many steps that can be taken to help reduce these behaviors and other risk factors, and to help promote healthy behaviors. The NICHD Back to Sleep campaign is an example of successfully conveying a health promotion message to the public. Research has shown that after this campaign was undertaken, the prevalence of infants placed in the prone sleep position declined by 66 percent between 1992 and 1996. Although causality cannot be proved, Sudden Infant Death Syndrome rates declined approximately 38 percent during this period [36]. Yet clinically based science is not always communicated in a meaningful way that engages individuals, communities, States and Federal agencies.
Health communications and health messaging can contribute to taking what we know from science and clinical experience to support what is done at the personal, community, State, and National levels to prevent illness and disability.
The challenge is to make health promotion and disease prevention messages as effective as possible. A variety of factors have been identified that may limit the effectiveness of messages:
- Failure to deliver the right messages to the right segments of the audience at the right times.
- Reluctance to combine service programs with public affairs/communications initiatives; neither alone may be sufficient to change behavior.
- A “health problem at a time” approach creates multiple messages that can compete with each other for the same audiences and generate confusing “noise.”
- Insufficient collaboration and coordination can limit the reach of prevention efforts.
- The absence of a unified theme across prevention communication and programs that can create a strategic framework for partnerships.
When it comes to communicating prevention messages or undertaking prevention-oriented programs at the community level, there are several key guidelines:
- Whether addressing diabetes or lung cancer, heart disease or drug addiction, the underlying message is about taking action to reduce the factors that might lead to long-term illnesses and to encourage the adoption of behaviors, attitudes and lifestyles that decrease the risks.
- The readiness to receive and act on a prevention message varies. People have different levels of awareness and knowledge about their health, and these may vary with age, gender, geographic location, education, and race/ethnicity. Readiness, along with many other factors, must be assessed, target audience by target audience, so that messages will be appropriate for them.
- Prevention messaging should not be an isolated incident or a one-time effort intended to reach all Americans. It is better to work with the intended audience segments to identify the most appropriate messages that will motivate action.
- Over time, many prevention messages must change to reflect a changing society. When advertising has helped create a demand for a product, it shifts its orientation to selling that product. To keep the product fresh in the eyes of the consumer, the sales messages change over time – sometimes targeting different audiences, sometimes repositioning the product in the market. The same is true for prevention messaging. Static messages often become unheard messages over time; they must remain current as levels of awareness and readiness for behavior change increase.
- It is more effective to communicate messages through multiple channels. No one channel works for every audience or all members of a particular audience.
- Effective prevention messaging begins with assessments of the intended audiences for the prevention activity and ends with evaluation of successful efforts and activities.
- Coordination and collaboration can help to reduce the “noise” of competing prevention messages and to leverage resources. Too much information, too many requests for behavior change in different arenas, absent an underlying theme, can lead to indecision about what to do in any one area or, worse, can result in a “turn off.”
- Prevention messages should be integrated with prevention programs.
- The effectiveness of messages promoting prevention needs to be evaluated to inform new directions. Is the message reaching the target audiences? Are they learning from and using the message?
Health Literacy
The innovations produced by the healthcare and public health systems often are poorly matched with the day-to-day information and services that the public needs to lead longer, healthier lives. This gap between what science has discovered and the public’s ability to put health information, messages and recommendations to appropriate use, may be explained in large part by limited understanding. Prevention often requires individuals to understand the effects of their behavior. Efforts to increase prevention often require significant resources. Realizing the benefits of investments in prevention requires that individuals have the capacity to take responsibility for making health-related choices and that policy makers and health professionals take responsibility for supporting and coordinating the information, resources and programs that foster healthy behaviors and prevent disease.
It is critical that individuals have access to health information in a way they can understand to make appropriate health decisions. The corollary is that health professionals must provide useful information and be able to communicate clearly and effectively. The ability to access, understand and apply health information is known as “health literacy.” Information encompasses traditional print brochures, discussions between patients and healthcare providers, public health messages on the Internet, television and other mass media, instructions on food and medication labels, and forms to apply for insurance programs or provide informed consent. Efforts to promote health literacy continue to evolve.
The basic definitions of literacy and health literacy are widely known and generally agreed upon. The National Literacy Act of 1991 defines functional literacy as
The ability to read, write, speak, and compute and solve problems at levels of proficiency necessary to function on the job and in society, to achieve one’s goals, and develop one’s knowledge and potential.
The following definition of health literacy was first used in a 1999 National Library of Medicine bibliography. It has since been widely adopted, and adapted.
Health literacy is the degree to which individuals have the capacity to obtain, process and understand basic health information and services needed to make appropriate health decisions.
Health literacy is not a set of skills specific to a health topic but basic communication capacities that consumers, patients, and providers bring to bear on many different types of health situations. The core of the health literacy concept is “understanding,” and the core of the health literacy problem is the mismatch between the public’s functional health literacy and the complexity of health terminology, recommendations, instructions, forms, healthcare systems and public health services. The mismatch is even more critical for individuals with limited literacy skills and multiple health conditions. Too often they have the greatest health burdens, limited access to relevant health information and limited abilities to understand the information.
The concept of health literacy derives from the general idea of literacy as a set of functional skills that are applied in different situations or contexts. Thus, “health literacy” is typically described as literacy in health settings. There has not been sufficient research, however, to determine if health situations or contexts require skills in addition to or different from those described as basic literacy skills. Moreover, the research literature as well as HHS’s program operations and research projects indicate that “health literacy” refers not only to an individual’s or group’s capacities to understand information but also to their knowledge of a specific set of health-related facts, e.g., the acceptable range for blood pressure, the number and types of fruits and vegetables that a person should eat every day, or the frequency of a medication dose. The Agency for Healthcare Research and Quality (AHRQ) recently released a report on Literacy and Health Outcomes that provides new information on health literacy skills.
Currently, national data on general literacy skills are used to assess health literacy. Data from the 1992 National Adult Literacy Survey (NALS) from the U.S. Department of Education indicate that approximately one-half of the adult English-speaking population has what researchers consider “limited literacy skills.” [37] HHS collaborated with the Department of Education to develop a module on health literacy for the 2003 National Assessment of Adult Literacy, that will provide the first-ever population-based assessment of health literacy. The data from this national population sample will be available in 2005.
Consumers and patients increasingly manage their own health. Reading, writing, speaking, listening, and interpreting proficiencies are necessary to interact with the modern health care system. Moreover, health treatment and prevention services are more effective if they are geared toward different literacy levels and native languages, life stages, and nature and severity of illnesses. Health literacy is broader than general reading and writing skills, and includes abilities to: comprehend quickly “on your feet,” comprehend complex vocabulary and concepts relevant to health (e.g., medical terms or probability and risk), share personal information with providers about health history and symptoms, make decisions about basic healthy behaviors, such as healthy eating and exercise, and engage in self-care and chronic disease management. These health literacy skills enable consumers to identify and understand health risks, evaluate different health promotion, treatment, and intervention options, and follow specific health care recommendations.
Health care providers and health information professionals need to communicate effectively with individuals with a variety of skills, from those with limited levels of understanding to those who have the skills to comprehend complex information and recommendations. Limitations and a mismatch of skills on both sides can hamper the effectiveness of prevention messages, health information, and health care.
The nation's estimated 90 million adults with lower-than-average reading skills are less likely than other Americans to get potentially life-saving screening tests such as mammograms and Pap smears, to get flu and pneumonia vaccines, and to take their children for well child care visits, according to the recently released AHRQ literacy report. Research suggests that the consequences of low health literacy are poorer health because consumers, patients and their families are less likely to understand how to prevent disease and disability, and to benefit from health care advances. Research has linked limited health literacy with poorer self-management of chronic diseases [38-40]; less knowledge of healthy behaviors [41-44]; higher rates of hospitalizations [45, 46]; and overall poorer health [47, 48]. Low literacy also plays an important role in health disparities and may contribute to lower quality care and even medical errors.
Opportunities for Action
During his tenure, Secretary Thompson has hosted many roundtable discussions and listening sessions with different stakeholders and interested parties. Drawing on these meetings, research and other information, this section suggests actions that specific stakeholders can take to promote health and prevent chronic disease in all Americans. These steps are not meant to be prescriptive but rather to identify starting points for individuals, families, communities and other interested constituencies as they begin to work for better health and wellness.
Action Steps for Individuals and Families
Individuals and families are the heart of healthy communities and provide the foundation for a strong and vibrant America. Individuals and families must adopt healthy habits and assume responsibility for living a healthy lifestyle.
- Be physically active. Strive for at least 30 minutes of physical activity for adults and 60 minutes for children each day. Play and be active as a family. Decrease time spent in sedentary activities such as watching television.
- Eat a healthy diet. Consume 5 to 9 servings of fruits and vegetables each day. Consume fat and sugar in moderation.
- Educate yourself about health and risk factors for disease and chronic conditions such as obesity. Become a student of healthy habits. Learn what constitutes a healthy diet and how to read and use food labels.
- Set an example for your children by being physically active and eating a healthy diet. Instill healthy habits in children (e.g., play actively and eat healthy foods). Teach your children about the importance of exercise and a healthy diet.
- Avoid risky behaviors. Limit alcohol intake. If you smoke, quit; if you do not smoke, don’t start.
- Get recommended screenings (such as pap smears and mammograms) and immunizations (such as influenza vaccinations).
Action Steps for Communities
Communities are the cornerstones for promoting healthy behaviors of their residents. Partnerships within and among local private sector constituencies and stakeholders can promote and reinforce healthy habits and environments for individuals and families.
- Engage individuals, families, policy makers, and community organizations in a process to enhance their understanding of the importance of healthy diets and regular physical activity. Raise consumer awareness about the adverse impact of inactivity and poor diets on overall health and well-being. Highlight community programs that support healthful food and physical activity.
- Acting through community coalitions and partnerships, explore the creation of more community-based health promotion and disease prevention programs and initiatives for individuals and families. Empower individuals and families to manage weight and health through community programs that encourage skill-building, active parenting and behavioral management.
- Consider providing for active lifestyles when planning and engineering community development and creating safe environments for physical activity, such as biking and walking trails, sidewalks, and playgrounds.
Action Steps for Schools
Schools are an especially critical site for encouraging healthy behaviors in youth. Most children spend a large portion of their time in school. In many cases, life-long habits and behaviors, good and bad, are formed during the elementary and middle school years. Schools, therefore, offer an opportunity to engage children in healthy eating and regular physical activity and to reinforce important health messages including those regarding avoidance of risky behaviors. Schools can also provide a bridge to eliciting parental involvement in shaping children’s habits and attitudes about healthy lifestyle choices.
- Encourage cooperation among teachers, coaches, nurses, and food service staff to educate students about the importance of proper nutrition and regular physical activity to lifelong healthy weight maintenance.
- Reinforce healthy habits by examples set by role models including teachers, coaches, and other school personnel.
- Engage parents in a process to enhance their understanding of the importance of healthy diets and the benefits of exercise and engage them to reinforce this message in their homes.
- Provide age-appropriate extracurricular physical activity and organized sports programs.
- Provide elementary school students with daily recess periods for unstructured supervised play.
- Encourage regular physical activity for all children (pre-school through 12th grade) in order to develop the knowledge, skills, attitudes, behaviors, and confidence to sustain life-long physically active lifestyles.
- Explore the possibility of creating “before the bell” and after school physical fitness and nutrition programs for students.
- Provide age-appropriate and culturally appropriate instruction in health education.
- Provide healthy food and snack options in school cafeterias and vending machines.
- Incorporate health-related tasks, materials and examples in regular everyday instruction for preschool to grade 12 education, including the topics of nutrition and the balance between calories consumed and calories expended in physical activity.
Action Steps for Employers
Working adults spend many of their waking hours at their worksite. Thus, the worksite is an important and convenient environment in which to foster healthier habits. Moreover, companies are beginning to recognize that the health of the individual employee is inseparable from the ‘health’ of the corporation. Employees with chronic diseases and/or conditions, which may be prevented or attenuated by diet and exercise, often have higher rates of absenteeism and health care usage than healthy employees without chronic ailments. Thus, worksite programs designed to promote health and prevent chronic disease are a wise investment for employers.
- Design worksites and work schedules to provide opportunities for regular physical activity, including simple and readily available activities such as stair climbing.
- Ensure that healthy food options are available for employees.
- Consider creating exercise facilities at the worksite or providing incentives for employees to join local fitness centers.
- Consider providing health promotion or wellness programs and disease management programs for employees as part of their health benefits.
- Offer incentives to employees to adopt documentable healthy behaviors (e.g., miles walked or weight goals attained, obtaining recommended screenings, completion of a medically supervised smoking cessation treatment program). [See Appendix F.]
- Engage employees in a process to enhance their understanding of the importance of a healthy lifestyle.
- Actively partner with community and other local entities/stakeholders to develop and implement community health promotion and disease prevention initiatives.
- Examine the cost and benefits of worksite health promotion and disease prevention efforts.
- Request health insurers to develop appropriate information for employees to enhance health literacy.
- Include health literacy measures in quality of care and outcomes assessments.
Action Steps for Health Insurers
Health insurers can play a significant role in promoting health and preventing or lessening the consequences of chronic diseases and conditions for individuals. Insurers can design and offer innovative and comprehensive preventative services benefit packages based on scientific evidence. In addition, insurers can disseminate educational information about the importance of prevention to their customers/consumers.
- Offer insurance products that include preventative services, disease management and wellness programs.
- Engage consumers in a process to enhance their understanding of the importance of healthy habits and avoidance of risky behavior.
- Encourage research evaluating the efficacy and cost/benefit of strategies to change behavior and translate research into clinical practice. Share this information with employers and other purchasers of health care.
- Create incentives to encourage individuals to adopt healthy behaviors. [See Appendix F.]
- Partner with communities and other entities to promote and encourage healthy lifestyles.
- Include health literacy in quality of care and outcomes assessments.
Action Steps for Health Care Providers and Professionals
Health care providers/professionals are key for promoting healthy lifestyles and reducing the impact of chronic diseases and conditions. In any year, most Americans will interact with the health care system. Thus, health care providers are strategically poised to intervene and influence individuals to adopt healthy behaviors. Health care professionals can also provide critical leadership to communities, state and local governments, schools and other interested stakeholders to guide and catalyze health promotion and disease prevention efforts.
- Lead by example; live a healthy lifestyle.
- Accrue and maintain state-of-the-art knowledge about best practices and behavioral interventions to promote healthy habits and reduce risky behaviors.
- Inform and educate individuals (patients, parents, students, community leaders, other health professionals, etc.) about the importance of healthy eating, regular physical activity, recommended disease screening, and avoidance of risky behaviors (such as tobacco use) to promote health and prevent chronic disease.
- Implement effective weight reducing initiatives and smoking cessation programs.
- Direct or participate in studies to explore the effectiveness of approaches to weight loss and healthy weight maintenance and smoking cessation.
- Explore partnerships between health care providers/professionals and schools, communities, faith-based organizations, local and state governments, and other interested parties to develop and implement health promotion and disease prevention initiatives.
- Seek out training in health literacy and effective provider-patient communication.
- Practice evidence-based prevention—adhere to evidence-based recommendations of the US Preventive Services Task Force (USPSTF) on whether a clinical preventive service should be routinely delivered www.preventiveservices.ahrq.gov.
- Identify individuals who are ready to make important changes and take maximum advantage of the “teachable moment” that often occurs in clinical care (e.g., counseling individuals who have just had a heart attack or chest pain to quit smoking).
- Harness the power of health information technology systems, including decision support systems, to remind clinicians and patients when preventive services are needed. HHS has supported much of the research that demonstrates the effectiveness of these systems to improve the use of clinical preventive services.
Action Steps for Researchers and Health Professions Educators
Progress in health promotion and disease prevention necessarily depends on continued research and knowledge generation and dissemination. Therefore, researchers and health professions educators are critical in furthering our understanding of the etiology of chronic conditions such as obesity and effective approaches for prevention and treatment of these conditions. In addition, successful health promotion and disease prevention requires translation and dissemination of scientific findings into effective clinical practices to reach all individuals.
- Continue research into the pathogenesis, etiology, epidemiology, prevention and treatment of chronic diseases and conditions including obesity. Continue to explore optimal methods to translate research findings into clinical practice to change human behavior and foster healthy habits.
- Develop outcome measures for health promotion and disease prevention activities, services, and practices.
- Encourage and adopt an interdisciplinary approach to address chronic conditions such as obesity.
- Develop and assess innovative methods to engage the public about the importance of health promotion and disease prevention and the link between the risk for chronic conditions and personal behaviors and choices such as physical activity and diet choices. Information, communication, and education should encompass the lifespan beginning in early childhood and continuing into older age.
- Focus on identifying effective ways to improve the health literacy of all individuals to reinforce the importance of health promotion and disease prevention for all segments of the population.
- Seek partnerships with community, public or private entities to promote research and educational initiatives regarding health promotion and disease prevention. Develop a multi-pronged community approach involving all stakeholders to reach all individuals.
- Design curricula and testing for health professionals (undergraduate and graduate) that comprehensively cover the science of health promotion and disease prevention and that examine and teach effective approaches to change individual behaviors. Integrate health professional education and training across disciplines.
Action Steps for Media
The power of the media should be harnessed to educate the public by disseminating health information and to promote effective strategies to improve dietary and exercise habits.
- Promote/conduct public awareness campaigns of the health benefits of energy balance through regular physical activity, and a healthy diet to maintain a healthy weight.
- Partner with medical professionals, federal, state and local governments, and private sector and community entities to help the public understand the importance of preventive screenings.
- Develop and disseminate appropriate messages that encourage healthy habits and avoidance of risky behaviors in youth.
- Showcase successful initiatives and programs that promote health and prevent disease.
- Conduct or participate in consumer research to study the appropriateness and effectiveness of media messages promoting healthy lifestyles and avoidance of risky behaviors.
- Consider use of public access networks to broadcast local conferences or training videos on various health topics (e.g., exercise class for seniors).
Action Steps for State, Local, and Tribal Governments
State, local, and tribal governments can play a key role in coordinating an approach to encourage healthy habits and prevent chronic diseases. State, local and tribal governments can partner with, and provide guidance to, other organizations and entities to facilitate health promotion initiatives. They can also act as a bridge between Federal programs and community activities providing the necessary infrastructure and support needed to maximize and coordinate efforts among stakeholders. In addition, state, local, and tribal governments can create and implement policies that encourage healthy behaviors.
- Review and design policies to ensure that health promotion and disease prevention are priorities.
- Partner with communities and other entities to create environments and implement initiatives that encourage healthy lifestyles and habits.
- Disseminate audience-appropriate information about the importance of healthy lifestyles and avoidance of risky behaviors. Foster a consistent age and culturally appropriate message to the public, especially high-risk groups, about the consequences of unhealthy lifestyles and practices.
- Identify high-risk groups for targeting prevention initiatives and activities.
- Provide guidance and support for research on the efficacy of different interventions to prevent and treat obesity, diabetes, and other chronic conditions and tobacco use.
Action Steps for HHS/Overweight and Obesity
HHS has a large number of current initiatives and programs underway to address obesity and overweight. They include programs in education, communication and outreach, intervention, diet and nutrition, physical activity and fitness, disease surveillance, research, clinical preventive services and therapeutics, and policy and web-based tools. The programs are targeted to a variety of populations including infants and breastfeeding mothers, children and adolescents, women, minorities, the elderly, the disabled, rural, and the general population. Additional areas to target initiatives may include:
- Design and implement programs that work with children and parents to prevent and treat obesity, since the best opportunity to slow the U.S. obesity ‘epidemic’ may be in childhood.
- Evaluate effectiveness of treatment and preventive programs to build a practical evidence base for new interventions. Relevant research questions may include:
- Do certain populations (e.g., gender or age-related, racial/ethnic populations) benefit more from certain therapies?
- What is the optimum amount of time to treat, and what is the optimum level of weight loss to target?
- What evidence exists to support long-term weight loss and weight-maintenance, e.g., over one year or five years?
- What is the safety and efficacy of certain therapies?
- What risks are associated with weight loss, especially for certain populations such as the elderly, for example, who generally are at high risk for osteoporosis?
- Explore ways to increase awareness and knowledge, especially in certain populations, about obesity and interventions that may reduce obesity and promote healthy energy balance.
- Develop interventions that address needs of special populations.
- Focus further research on the psychological and motivational aspects of weight maintenance, and on identifying any demonstrable benefits for private or public health insurance programs.
- Enhance food labels to display calorie count more prominently and to use meaningful serving sizes.
- Evaluate and recommend the types of health communication activities that would most effectively support the "Calories Count" message.
- Encourage restaurants to provide meaningful nutritional information to consumers.
- Step up enforcement actions concerning accuracy of food labels.
- Revise FDA guidance for developing drugs to treat obesity.
- Work cooperatively with other government agencies, non-profit organizations, industry, and academia on obesity research.
- Incorporate the findings from the recently released reports on health literacy from the Institute of Medicine and AHRQ into overweight and obesity information and communication activities.
Action Steps for HHS/Diabetes
HHS agencies are pursuing vigorous programs in prevention that include basic research, clinical trials, community health efforts, educational programs, translating research into practice, efforts in special populations, and providing a new Medicare benefit for diabetes testing. Through these comprehensive programs, HHS agencies are continuing to pursue prevention studies to optimize and identify additional intervention strategies. HHS also is improving methods to disseminate and implement effective strategies into diverse community settings. Particular opportunities for HHS action involve underserved or vulnerable populations and include:
- To focus attention on the long-term implications of gestational diabetes mellitus (GDM), the National Diabetes Information Clearinghouse of the NIDDK/NIH will produce a new booklet entitled, “What I Need to Know about Gestational Diabetes,” which will incorporate messages based on diabetes prevention research. The National Diabetes Education Program’s Small Steps. Big Rewards. Prevent Type 2 Diabetes campaign will also be expanded to include a specific focus on GDM.
- · To analyze the effects of treatment and ascertain the durability of these effects over time, a Diabetes Prevention Program follow-up study of women with a history of GDM is in progress.
- Enhance the focus on women with GDM in community health centers and Indian Health Service programs, and through AHRQ’s Integrated Delivery System Research Network and Practice Based Research Networks.
- Since there is a disproportionate risk for the development of type 2 diabetes in persons with serious mental illness, in general, and treatment with antipsychotic medications predispose individuals to gain weight [49-54] , examine and apply evidence-based lifestyle interventions in mental health settings that would reduce the rate of obesity and prevent the development of type 2 diabetes in Americans with serious mental illness.
- Since American Indians and Alaska Natives have a higher incidence of diabetes, determine if diabetes prevention activities previously demonstrated to be efficacious under well-controlled conditions (such as the NIDDK-sponsored Diabetes Prevention Program study) can be implemented with fidelity in a variety of Indian health settings and through community-based human services providers.
- Evaluate whether a comprehensive health system intervention delivered through Indian health programs can reduce risk factors for cardiovascular disease in individuals with diabetes and/or the metabolic syndrome ( characterized by insulin resistance and the presence of obesity, abdominal fat, high blood sugar and triglycerides, high blood cholesterol, and high blood pressure).
- Implement evidenced-based interventions to prevent diabetes as part of the Primary Prevention of Diabetes Initiative in 25-30 Health Service/Tribal/Urban (I/T/U) community sites of varying sizes and types.
- Implement, as part of the Cardiovascular Disease Risk Reduction Initiative, a comprehensive health system intervention consisting of patient-, provider-, systems- and community-level components in 25-30 clinical sites that participate in the IHS Diabetes Care and Outcomes Audit.
- Consider utilizing the community health center program Diabetes Prevention Collaborative and Health Disparity Collaborative strategy and models to translate and disseminate the results of Diabetes Prevention Program pilot into clinical practice.
- Incorporate the findings from the recently released reports on health literacy from the Institute of Medicine and AHRQ into diabetes information and communication activities.
- CMS should assess utilization of the new Medicare benefits (beginning in 2005) establishing coverage of an initial preventive physical exam, and diabetes and cardiovascular disease screening tests, to ensure beneficiaries are taking advantage of these services and getting the care they need to better manage their diabetes.
Action Steps for HHS/Tobacco
Prevention of the ill effects of tobacco is an essential part of the HHS mission, and HHS is committed to working in a coordinated, comprehensive, and effective manner to protect the public’s health from the harmful effects of tobacco use. In 2000, HHS launched a roadmap for improving the health of all people in the U.S. during the first decade of the 21st century, including objectives for reducing the death and disease caused by tobacco use. In addition, the Secretary’s Steps to a HealthierUS has as one of its major components avoiding risky behaviors, such as using tobacco products, to promote good health and save lives. There are many opportunities for strategic collaboration among agencies to further reduce the health and economic impact of tobacco-related diseases.
- Consider opportunities for encouraging smoking cessation activities in a variety of programs and areas, such as: the Federal workplace; among hospitalized cardiac patients; among Americans who receive their health care through or with financing from the Federal Government (Veteran’s Administration, Medicaid, Medicare, Older Americans Act services provider network, Department of Defense, Indian Health Service); or in the HRSA prevention collaborative.
- Examine ways to encourage use of the Web site, www.smokefree.gov, which offers science-driven tools, information, and other resources that have been found effective in helping smokers quit.
- Consider opportunities for incorporating tobacco use prevention messages into community-based shelters for runaway and homeless youth and their families; and the National Youth Sports Program youth camps for middle-school-aged, low-income youth.
- Examine opportunities for tobacco use prevention and smoking cessation among Head Start and Early Head Start staff and parents.
- Examine opportunities to enhance the delivery of technical assistance on tobacco control through SAMHSA’s Center for Substance Abuse Prevention (CSAP) Center for the Application of Prevention Technologies.
- Consider opportunities to deliver tobacco use and prevention messages to young people through sports and entertainment media campaigns.
- Examine opportunities to enhance SAMHSA Best Practices via the National Registry of Effective Prevention Programs to include tobacco prevention programs.
- Examine opportunities to expand the number of materials on tobacco prevention and control that are available through the National Clearinghouse for Alcohol and Drug Information.
- Consider research that examines the toxicity of current and new tobacco products.
- Incorporate the findings from the recently released reports on health literacy from the Institute of Medicine and AHRQ into tobacco information and communication activities.
- Highlight community-based programs that provide rewards for young people who do not smoke.
- Evaluate and disseminate the results of the Medicare Stop Smoking Program (a pilot currently underway in seven states).
Action Steps for HHS/ Media and Messages
HHS has a vast number of individual initiatives, products and messages designed to promote healthy behaviors and reduce illness and disability, such as the national nutrition program, 5 A Day for Better Health Program, the Small Steps program, and its accompanying advertising campaign (Healthy Lifestyles and Disease Prevention), which encourages American families to take small, manageable steps to ensure effective, long-term weight control.
- Identify a standard for clear and effective communication for all information, forms, materials and communication from HHS with the public.
- Update and change prevention messages to maintain ‘freshness’ and reflect the state-of-the-art practices and information.
- Research the information and communication needs, characteristics, preferences, and environments to develop effective messages.
- Coordinate prevention messages to reduce the ‘noise’ of competing messages and to leverage resources.
- Integrate prevention messages with prevention programs.
Action Steps for HHS/Health Literacy
Health literacy and messaging are important aspects of HHS research and program activities focusing on prevention. The Department’s agencies are engaged in a variety of health literacy activities. HHS agencies are beginning to include health literacy as a consideration in their research, assessment, training, program operations, and communication with the public, but there are opportunities for improvement.
- Continue research on multiple aspects of health literacy including: the impact of limited health literacy on health disparities; the nature and extent of limited health literacy in different populations and for different topics and contexts; the interaction of limited health literacy with other factors, such as age and disabilities; the most effective health literacy interventions for different segments of the population; and the impact of limited health literacy on the quality, access and outcomes of health care and public health services.
- Develop health and program information in a variety of languages.
- Emphasize the need to pre-test publications designed for wide-spread dissemination with the target audience prior to publication.
- Support the development of an evidence-based approach to training a broad spectrum of healthcare and public health professionals to communicate effectively with different types of patients, including those with limited literacy.
- Develop and validate measures of successful health literacy approaches.
- Provide leadership to identify and build consensus for outcome measures needed to improve health literacy across the population, in particular for the most vulnerable groups.
- Advise agencies to assess their information, communication, and programmatic activities with their intended audiences, particularly low literacy audiences.
Acronyms
| Acronyms | |
|---|---|
| AHRQ | Agency for Healthcare Research and Quality |
| AI/AN | American Indians/Alaska Natives |
| AoA | Administration on Aging |
| CDC | Centers for Disease Control and Prevention |
| CMS | Centers for Medicare and Medicaid Services |
| CSAP | Center for Substance Abuse Prevention |
| FDA | Food and Drug Administration |
| GDM | Gestational Diabetes Mellitus |
| HHS | U.S. Department of Health and Human Services |
| HRSA | Health Resources and Services Administration |
| IHS | Indian Health Service |
| I/T/U | Indian Health Service/Tribal/Urban |
| NCI | National Cancer Institute |
| NIA | National Institute on Aging |
| NICHD | National Institute of Child Health and Human Development |
| NIDA | National Institute on Drug Abuse |
| NIDDK | National Institute of Diabetes and Digestive and Kidney Diseases |
| NIH | National Institutes of Health |
| SAMHSA | Substance Abuse and Mental Health Services Administration |
| USPSTF | US Preventive Service Task Force |
Resources
Overweight and Obesity
NIH Obesity Research
http://www.obesityresearch.nih.gov/
NIDDK Weight Loss and Control
http://www.niddk.nih.gov/health/nutrit/nutrit.htm
NHLBI Aim for a Healthy Weight
http://www.nhlbi.nih.gov/health/public/heart/obesity/lose_wt/index.htm
NLM Medline Plus
http://www.nlm.nih.gov/medlineplus/nutrition.html
USDA Center for Nutrition Policy and Promotion
http://www.usda.gov/cnpp/
Nutrition and Your Health: Dietary Guidelines for Americans
http://www.health.gov/dietaryguidelines
Exercise: A Guide from the National Institute on Aging
http://www.niapublications.org/exercisebook/index.asp
Exercise: A Video from the National Institute on Aging
http://www.nia.nih.gov/exercisevideo/
FDA Guidance on How To Understand and Use the Nutrition Facts Panel on Food Labels
http://www.cfsan.fda.gov/~dms/foodlab.html
Healthfinder® Gateway to Reliable Consumer Health Information on the Internet
http://www.healthfinder.gov
Diabetes
National Institute of Diabetes and Digestive and Kidney Diseases
http://www.niddk.nih.gov
National Diabetes Education Program
http://www.ndep.nih.gov/
National Diabetes Information Clearinghouse
http://diabetes.niddk.nih.gov/
CDC Diabetes Public Health Resource
http://www.cdc.gov/diabetes/
IHS National Diabetes Program
http://www.ihs.gov/MedicalPrograms/diabetes/index.asp
HRSA Health Disparities Collaborative
http://bphc.hrsa.gov/programs/HDCProgramInfo.htm
AHRQ Preventive Services Task Force
http://www.preventiveservices.ahrq.gov/
Conquering Diabetes: A Strategic Plan for the 21st Century
http://www.niddk.nih.gov/federal/dwg/fr.pdf
Medicare Coverage of Diabetes Related Supplies and Services
http://www.medicare.gov/Health/Diabetes.asp
Tobacco
Centers for Disease Control and Prevention. Annual Smoking-Attributable Mortality, Years of Potential Life Lost, and Economic Costs --- United States, 1995--1999. MMWR 2003; 52: 300-303.
Centers for Disease Control and Prevention. Best Practices for Comprehensive Tobacco Control Programs. Atlanta: Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health, 1999.
Centers for Disease Control and Prevention. Cigarette smoking among adults—United States, 2001. Morbidity and Mortality Weekly Report 2003a;52(40):953–6.
Centers for Disease Control and Prevention. Cigarette smoking-attributable morbidity—United States, 2000. Morbidity and Mortality Weekly Report 2003b;52(35):842–4.
Centers for Disease Control and Prevention. Early release of selected estimates from the National Health Interview Survey (NHIS). Available at http://www.cdc.gov/nchs/about/major/nhis/released200312.htm.
Centers for Disease Control and Prevention. State-Specific Prevalence of Current Cigarette Smoking Among Adults- United States, 2002. MMWR 2004; 52: 1276-1280.
Centers for Disease Control and Prevention. Tobacco Use Among Middle and High School Students-United States, 2002. MMWR 2003; 52: 1096-1098.
Centers for Disease Control and Prevention. Trends in Cigarette Smoking Among High School Students — United States, 1991–2001. Morbidity and Mortality Weekly Report 2002;51(19) 409–12.
National Cancer Institute, Centers for Disease Control and Prevention & American Cancer Society. You Can Quit Smoking Now!. http://www.smokefree.gov.
Substance Abuse and Mental Health Services Administration, Center for Substance Abuse Prevention. State Synar Non-Compliance Rate Table,
FFY 1997 - FFY 2003. http://prevention.samhsa.gov/tobacco/01synartable.asp
Substance Abuse and Mental Health Services Administration, U.S. Dept of Health and Human Services (HHS), “Overview of Findings from 2002 National Survey on Drug Use and Health (NSDUH),” 2002. Available at http://www.samhsa.gov/oas/nhsda/2k2nsduh/Overview/2k2Overview.htm#toc.
U.S. Department of Health and Human Services. Reducing Tobacco Use: A Report of the Surgeon General. Atlanta, Georgia: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health, 2000.
U.S. Preventive Services Task Force. Counseling to Prevent Tobacco Use and Tobacco-Related Diseases: Recommendation Statement. November 2003. Agency for Healthcare Research and Quality, Rockville, MD. http://www.ahrq.gov/clinic/3rduspstf/tobacccoun/tobcounrs.htm.
Health Literacy
Dynamic search of the health literacy literature indexed in Medline. Available online at http://phpartners.org/hp/health_comm.html. Last viewed March 4, 2004.
HRSA health literacy Web pages. Available online at http://www.hrsa.gov/quality/healthlit.htm. Last viewed March 4, 2004.
NIDCD health literacy Web pages. Available online at http://www.nidcd.nih.gov/health/education/news/improving_health_literacy.asp. Last viewed March 4, 2004.
U.S. Department of Health and Human Services. Health literacy action plan. In Communicating Health: Priorities and Strategies for Progress. Washington, D.C. July 2003. Available online at http://odphp.osophs.dhhs.gov/projects/HealthComm/. Last viewed March 4, 2004.
AHRQ report on Literacy and Health Outcomes. A summary is available online at www.ahrq.gov/clinic/epcsums/litsum.htm and the full report can be downloaded from www.ahrq.gov/clinic/evrptfiles.htm#literacy.
National Library of Medicine. Understanding health literacy and its barriers. Bethesda, MD. Available May 2004 at http://www.nlm.nih.gov/pubs/cbm/healthliteracybarriers.html.
Appendix A - Key HHS Activities
Obesity Activities
Cross-cutting focus at NIH and the Food and Drug Administration.
As the problems of overweight and obesity have grown, the need for new action and research has become more evident. In response, NIH assembled a Task Force to identify areas for new research across its many institutes. In March 2004, NIH released the draft of its Strategic Plan for NIH Obesity Research (www.obesityresearch.nih.gov). This report identifies key areas of research need, priorities among those areas, a road map for advancing these research priorities, and the establishment of a committee for monitoring progress in addressing the issues and problems relating to overweight and obesity.
Similarly, the Food and Drug Administration (FDA) established an Obesity Working Group to advise the agency on innovative ways to deal with the increase in obesity and to identify ways to help consumers lead healthier lives through better nutrition. In March 2004, the working group released its report with a focus on the message, "calories count." The group’s long- and short-term proposals are based on the scientific fact that weight control is mainly a function of the balance between calories consumed and calories expended. That is, calories in must equal calories out. The report includes recommendations to strengthen food labeling, to educate consumers about maintaining a healthy diet and weight and to encourage restaurants to provide calorie and nutrition information. It also recommends increasing enforcement efforts to ensure food labels accurately portray serving size, revising and reissuing guidance on developing obesity drugs and strengthening coordinated scientific research to reduce obesity and to develop foods that are healthier and low in calories.
Dietary guidelines.
HHS is collaborating with the U.S. Department of Agriculture to review the Dietary Guidelines that were published in 2000 and to draft new 2005 Dietary Guidelines for Americans. In light of the growing number of overweight and obese Americans, a major focus of the new guidelines will be providing guidance to the public on maintaining a healthy weight, and creating lifestyles that balance the number of calories eaten with the number of calories expended. These guidelines must (1) contain nutritional and dietary information and guidelines for the general public, (2) be based in the preponderance of scientific and medical knowledge current at the time of publication, and (3) be promoted by each Federal agency in carrying out and Federal food, nutrition, or health program.
5 a Day for Better Health.
One of the most recognizable efforts to promote good nutrition and healthy eating habits has been the 5 A Day for Better Health Program. This national nutrition program seeks to increase to 5 or more the number of daily servings Americans eat of fruits and vegetables. In addition to its widely known slogan, the 5 A Day program reaches many individuals through health care provider networks, the internet, and print media to provide information about the health benefits of eating more fruits and vegetables, as well as easy steps for adding more of them into daily eating patterns.
Administration on Aging action.
The Administration on Aging’s (AoA) National Policy and Resource Center on Nutrition, Physical Activity and Aging was created for the purpose of increasing and improving food and nutrition services to older Americans through their caregivers at home, with community-based service providers, and in long-term care systems. The Center focuses on linking proper nutrition and physical activity as key themes in the healthy aging process. One strategy for making this link has been the development and publication of, You Can! Steps to Healthier Aging, a community guide detailing a 12-week program to help older Americans “eat better” and “move more.” The Center is awarding 10 mini-grants to local communities to implement the You Can! Program in 2004.
AoA provides funding to states to implement health promotion and disease prevention activities. Educational information is disseminated through Senior Centers, congregate meal sites and home-delivered meal programs. Health screening and risk assessment activities including hypertension, glaucoma, hearing, nutrition screening, cholesterol, vision, diabetes, bone density and others are also provided. Physical activity and fitness programs are provided along with education about the prevention and reduction of alcohol, substance abuse, and smoking. Further, the importance of appropriately managing medications is emphasized.
VERB. It’s what you do.
Since the problem of overweight and obesity has also reached America’s young people, the youth media campaign, VERB. It’s what you do. was created. VERB’s goal is to promote social norms that support physical activity and portray fitness as fun and healthy. In order to reach tweens and motivate their participation, HHS/CDC has enlisted partner organizations in the campaign, such as 4-H, Boys and Girls Clubs and the National Hockey League (NHL), to brand the VERB message and make it appealing to its audience. VERB also reaches out to parents and other adults influential to young people, encouraging them to support and participate in physical activity with tweens.
The President’s Council on Physical Fitness and Sports (PCPFS).
Although it is an independent agency, the PCPFS is headquartered at HHS. It promotes physical activity for all ages, backgrounds and abilities with information and publications (www.fitness.gov) and physical activity/fitness motivational awards programs (www.presidentschallenge.org).
Diabetes Activities
The Diabetes Prevention Program demonstrated that prevention of type 2 diabetes is possible in high-risk adults, including adults from minority populations who are at disproportionately increased risk [55] .
The Diabetes Prevention Program clinical trial compared three approaches in overweight people with impaired glucose tolerance (IGT) to test whether type 2 diabetes could be delayed or prevented:
- lifestyle modification [56]
- treatment with the insulin-sensitizing drug metformin
- standard medical advice
The Diabetes Prevention Program demonstrated that diet and exercise that achieved a 5-7 percent weight loss reduced diabetes incidence by 58 percent in participants randomized to the study's lifestyle intervention group. Participants in this group exercised at moderate intensity. The lifestyle intervention was effective in both men and women and in all of the racial/ethnic groups. Lifestyle intervention worked particularly well in people over age 60, reducing the development of diabetes by 71 percent in this group. Volunteers randomly assigned to treatment with metformin had a 31 percent lower incidence of type 2 diabetes over the 2.9 year average duration of participation in the trial. Metformin was most effective in younger and heavier study participants. About twice as many people in the lifestyle group compared to placebo regained normal glucose tolerance, showing that diet and exercise can reverse IGT.
Following the dramatic and positive results of the Diabetes Prevention Program, in 2002 the American Diabetes Association and the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) published a position paper on “The Prevention or Delay of Type 2 Diabetes” [57] . In addition, a subsequent National Institutes of Health (NIH) and CDC co-sponsored study showed that the lifestyle and metformin interventions were cost-effective and could be implemented in routine clinical practice [58] . Ongoing follow-up studies of the Diabetes Prevention Program patient population are currently examining the durability of the interventions in preventing or delaying diabetes onset as well as their effects on cardiovascular disease and other diabetes complications.
National Diabetes Education Program.
The successful and well-recognized National Diabetes Education Program, a partnership of the NIDDK, the CDC, and more than 200 public and private organizations, was established to disseminate information about the importance of glucose control in those individuals with diabetes following a successful NIDDK-supported trial. Following announcement of the Diabetes Prevention Program results, this well-established program was expanded to launch the primary prevention campaign, Small Steps, Big Rewards, Prevent Type 2 Diabetes, in November 2002. The Small Steps educational material contains a “Game Plan” for health care providers and patients that gives information about implementing a program to prevent or delay disease onset. The Game Plan also includes a “fat and calorie counter” as well as a “food and activity tracker” so individuals can more easily monitor food intake and physical activity level. The Small Steps, Big Rewards, Prevent Type 2 Diabetes campaign has reached millions of people.
Diabetes Prevention Prototype Collaborative.
A pilot with five HRSA-funded health centers was initiated in November 2002 to translate the results of the Diabetes Prevention Program into practice, utilizing the Health Disparity Collaborative strategy and models. The Health Resources and Services Administration (HRSA), CDC, NIDDK/NIH, and the MedStar Research Institute support the Diabetes Prevention Prototype Collaborative. Health Disparity Collaboratives represent a multi-pronged approach to improve quality that includes a care model, a system improvement model, and a model of learning and sharing that allows for systematic spread of quality improvements. Health Centers participate in year-long intense learning and quality improvement activities that involve attending learning sessions and a final meeting to disseminate outcomes. Health Centers report the results of nationally shared measures while disseminating successful changes throughout their system of care through uniform, nationally recognized process and outcome measures.
As part of the Diabetes Prevention Collaborative pilot, teams have tested and implemented successful strategies to identify persons at-risk for diabetes, and screen them. As of November 2003, 3,167 high-risk persons have been identified; 903 (28.5 percent) have been screened, resulting in 276 (30.6 percent) prediabetes patients in the registry and 155 (17.2 percent) newly diagnosed persons with diabetes. Thirty-four patients (16.6 percent) have met the goal of 7 percent or greater average weight loss.
Efforts in American Indian Populations.
American Indians and Alaska Natives (AI/AN) have the highest prevalence rate of diabetes in the U.S. Diabetes mortality in AI/AN is increasing, as are the rates of diabetes in children and youth. In 1979, Congress established the Indian Health Service (IHS) National Diabetes Program to address the epidemic of diabetes in American Indians/Alaska Natives (AI/AN). The mission of the National Diabetes Program is to develop, document, and sustain a public health effort to prevent and control diabetes in AI/AN people. The agency promotes collaborative strategies for the prevention of diabetes and its complications in the 12 IHS Administrative Service Areas (regions) through coordination of a network of 19 Model Diabetes Programs and 12 Area Diabetes Consultants.
The Special Diabetes Program for Indians grant program, first established in1997 and now extended through 2008, distributes over 96 percent of its funds through grants awarded to 318 programs under 286 administrative organizations within the 12 IHS Areas in 35 states. Nationally, 67 percent of the new grant programs are focused on primary and secondary diabetes prevention.
Medicare Disease Management Initiatives
Section 721 of the Medicare Prescription Drug, Improvement, and Modernization Act (MMA) of 2003 establishes the Chronic Care Improvement Program, a population-based approach to helping people with chronic diseases, such as diabetes, manage their illness. CMS also has several disease management demonstrations to help people with diabetes and other chronic conditions better manage their disease and prevent complications. A demonstration established by the Medicare, Medicaid, and SCHIP Benefits Improvement and Protection Act of 2000 provides disease management services and a comprehensive prescription drug benefit to 30,000 beneficiaries living in California, Arizona, and parts of Louisiana and Texas. The Coordinated Care Demonstration established by the Balanced Budget Act of 1997, currently operating in 15 sites, is testing whether case management and disease management approaches are clinically effective and cost-effective.
Tobacco Activities
Tobacco use cessation.
A recent accomplishment is the Public Health Service document, Treating Tobacco Use and Dependence: Clinical Practice Guideline, which identifies treatments with demonstrated effectiveness in helping smokers quit. This resource will be a tremendous aid to Americans trying to quit tobacco use. It is available online at: http://www.surgeongeneral.gov/tobacco.
The FDA approves drugs intended for smoking cessation and has approved over-the-counter use for several of them. These steps have been instrumental in helping people quit smoking. Cessation materials across the Department also have been tailored to more effectively reach specific populations and decrease tobacco-related health disparities. Examples include the National Cancer Institute’s (NCI) La guía para dejar de fumar, a smoking cessation guide written in Spanish, and CDC’s Pathways to Freedom, a smoking cessation guide tailored to the African American community. This CDC guide provides education and guidance for individuals who smoke, helps friends and families be part of the solution, and provides strategies for community members who want to educate people about the dangers of tobacco.
The Centers for Medicare and Medicaid Services’ (CMS) Medicare Stop Smoking Program is a demonstration project on the most effective and cost-effective ways to help Medicare beneficiaries quit smoking. Findings from this project may affect a substantial proportion of the country, and have implications for health plans and other populations.
Programs from across the Department collectively create a comprehensive approach to promoting smoking cessation among women, particularly pregnant women. While women who smoke during pregnancy comprise a small percentage of the overall population, cessation efforts for these women are critical to protect the health and well being of future generations, including opportunities to continue smoking cessation following pregnancy and childbirth. Examples include the National Partnership to Help Pregnant Smokers Quit, a coalition of more than 50 federal, national, state, and local organizations that has developed guiding strategies around issues critical for pregnant women; several National Institute of Nursing Research-funded research projects; and CDC’s Dispelling the Myths About Tobacco: A Community Toolkit for Reducing Tobacco Use Among Women (www.cdc.gov/tobacco/sgr/sgr_forwomen/sgrtool.htm). These studies and programs seek to identify effective cessation and relapse prevention techniques, and to provide timely and relevant tools for community programs, including mass media and print materials. These efforts are critical to ensure that women who quit smoking during pregnancy continue to not smoke.
Examples of successful collaboration among U.S. public health agencies and organizations include: the development of the National Blueprint for Disseminating and Implementing Evidence-based Clinical and Community Strategies to Promote Tobacco use Cessation, a practical guideline for implementation of cessation strategies with demonstrated effectiveness; and the National Blueprint for Action, developed by the Youth Tobacco Cessation Collaborative to guide future research on cessation strategies for youth. NCI has a toll-free “Smoking Quitline” that will connect individuals with information specialists to answer smoking-related questions in English or Spanish.
The Synar program is one example of an effective collaboration between HHS and State governments to effectively prohibit the sale of tobacco products to minors. As a result, the rate at which retailers are willing to sell tobacco products to minors has decreased from a high of 41 percent in 1996 to approximately 14.5 percent in the most recent surveys in 2003.
In February 2004, Secretary Thompson announced plans for a new toll-free telephone number that will serve as a single access point to the national network of “quitlines.” By providing one easy-to-remember number, smokers in every state will have access to the tools they need to quit smoking. The program has three main components: (1) States with existing “quitlines” will receive increased funding to enhance existing state “quitline” services. States could use these supplements to expand their hours of operation, hire bilingual counselors, build referral linkages with local health care systems, or promote “quitlines” to more individuals. (2) States that do not have “quitlines” will receive grants to establish them to provide their residents the tools that they need to quit smoking. (3) HHS' National Cancer Institute (NCI) Cancer Information Service telephone counselors will provide assistance to individuals in states without “quitlines.”
HHS and its partner organizations also have helped state tobacco control programs through the creation of Smokefree.gov, the Web-based cessation tool provided by NCI with support from CDC and others, as well as by providing access to low-cost mass media materials and delivering relevant technical assistance and training through CDC’s Media Campaign Resource Center.
HHS agencies will continue monitoring youth tobacco-related behaviors through such programs as the following. The successful, ongoing surveillance of this ever-changing population through established tools, such as the National Institute on Drug Abuse (NIDA) Monitoring the Future Study, CDC’s Youth Risk Behavior Survey, and the Substance Abuse and Mental Health Services Administration’s (SAMHSA) National Survey on Drug Use and Health, has been vital to determine trends and focus efforts at the federal, state, and local levels. The Synar Regulation, which is implemented and monitored by SAMHSA's Center for Substance Abuse Prevention, and requires States, the District of Columbia and Territories to enact and enforce tobacco access laws that restrict the availability of tobacco products to youth under 18 years of age, has been demonstrated to be effective in reducing illegal sales to minors.
Tobacco research.
The simple facts about tobacco use – that it causes death and disease and results in a tremendous social and economic burden – are well documented. There is still a great deal to be known. NIH is conducting research aimed at better understanding the biological, genetic, and behavioral aspects of nicotine addiction, which will aid in the development of more effective pharmacological and behavioral treatments.
As new tobacco products and cessation aids become available, many questions arise regarding their efficacy and health effects.
Data collection on youth and adult knowledge, attitudes, and behaviors is conducted through a multi-factorial surveillance system for both adults and youth by CDC, NIH, and SAMHSA. This surveillance remains critical to understanding the impact of tobacco use over time, and to monitor trends in tobacco use among specific populations.
The Department supports an extensive training network to provide technical assistance and expertise to State and local tobacco control program staff to implement the findings of Department-wide research. Examples include the National Conference on Tobacco or Health, CDC’s Annual Leadership Forum, Community Guide Workshops, and Disparities Pilot Training Programs. Through coordinated efforts across the agencies, communication campaigns disseminate key information to the public regarding effective cessation treatments, the hazards of exposure to secondhand smoke, and other prevention messages.
Health Literacy Activities
Research.
HHS agencies conduct and sponsor research on the prevalence of low health literacy among specific populations and for specific topic areas; the barriers, skills and needs of low literacy audiences; different audiences’ health attitudes, knowledge, preferences, sources of information, and behaviors; and the health effects of low literacy and low health literacy. Most of this research is ongoing and part of broad programs in health communication research; specific topic areas, such as cancer, oral health, or dietary practices; or assessment of program operations, such as the National Medicare Education Program. Examples of health literacy research include:
- First-ever national assessment of health literacy as part of the 2003 National Assessment of Adult Literacy (NAAL), in partnership with the U.S. Department of Education. Data will be available in 2005.
- An evidence-based practice report on literacy and health outcomes was released in April 2004 by AHRQ. (A summary of Literacy and Health Outcomes is available online at www.ahrq.gov/clinic/epcsums/litsum.htm.)
- The Institute of Medicine report, Health Literacy: A Prescription to End Confusion, sponsored in part by the National Cancer Institute, was released in April 2004.
Guidelines and tools to improve communication with the public.
HHS agencies have developed a large number of guidelines and tools to apply to HHS programs and communication. They address how to develop materials for print, video and Web sites to improve audiences’ understanding. Most of the agency-developed tools and guidelines are not specific to working with low literacy audiences. Some are based on plain language principles, and others promote well-recognized good health communication practices. Examples of guidelines and tools that can be used to improve public understanding include:
- Scientific and Technical Information: Simply Put – a guide to communicating in plain language from the CDC http://www.cdc.gov/communication/resources/resource_idea.htm
- HORIZONS Project – a communication toolkit that provides information on demographic research, tip sheets and sample prototype communication products for working with minority populations from CMS.
- Research-based web design and usability guidelines from the NCI http://usability.gov/guidelines/
- Research-based web design and usability guidelines for older adults from the National Institute on Aging (NIA) http://nihseniorhealth.gov/about.html
Training and skill building.
The Department supports training in clear and effective communication or plain language training for staff, grantees, and health professionals or intermediaries, such as lay community workers. CDC has a broad-based agency training program in health communication, health literacy, and effective Web-based communication. Other training activities in the department are individual efforts related to increasing health professionals’ knowledge of how to communicate about a specific health topic or with culturally diverse audiences, increasing translators’ and lay workers’ competence, or broad health communication and health literacy training. Examples of training and skill building include:
- Agency and nationwide health communication, health literacy and risk communication training through the health communication certificate program and CDCynergy CDRom modules from CDC.
- Training of healthcare providers in plain language, clear and effective communication, and health literacy through Area Health Education Centers, funded by HRSA.
- NIH Plain Language Initiative and Award program – NIH requires the use of plain language in all new documents for the public, government entities and staff, and provides annual awards to staff for the effective use of plain language.
Appendix B - Steps Community Grants
In 2003, HHS awarded 12 communities with five-year grants to implement effective community-based chronic disease prevention and control programs. Twelve communities were selected for their innovative proposals to improve the health of their target populations. (For more information, visit: www.healthierus.gov/steps/grants.html.)
The ultimate goal of these Steps Community grants is to improve the health of individuals in the communities. They do this by working to decrease risk factors for chronic diseases, to prevent the occurrence of these diseases, and to decrease their consequences in people’s lives. Each community focuses on three areas--asthma, diabetes and obesity—and, given the emphasis on prevention, each community also works to address the factors that put individuals at risk for these diseases, such as nutrition, physical activity, and preventive health screenings.
Each grantee has assembled a community partnership that is charged with improving both the broader public’s health, as well as the health of specific target groups. These partnerships pursue interventions that address the community and the environment by:
-
Using media and information technology to educate and foster healthy behaviors;
-
Influencing the environment in ways that support and promote health and healthy lifestyles;
-
Fostering social support healthy behaviors and choices; and
-
Improving access to and quality of health care services.
They also address the school environment by:
-
Establishing full-time health coordinators or councils;
-
Providing physical education for students;
-
Implementing staff wellness programs;
-
Ensuring the availability of healthy food choices in the schools; and
-
Establishing tobacco-free environments.
| Grantees | |
|---|---|
|
Tribe |
Large Cities/Urban Communities |
|
State-Coordinated Small Cities/Rural Communities |
|
Appendix C - Steps Innovation Awards
Innovation on the part of local groups and businesses is a central focus of the Steps Initiative. Secretary Thompson recently recognized eight organizations, in seven separate categories, for their creativity in helping Americans stay healthy in one or more of the following areas: asthma, cancer, diabetes, heart disease and stroke, obesity, physical activity, poor nutrition, and tobacco use. These eight Innovation Award recipients have modeled the Department’s ideals of partnership and individual action, and serve as examples for other groups and organizations:
Faith Based Organization--The Church Health Center (Memphis, TN) was recognized for reaching more than 5,000 people each month, in its efforts to provide health care for the uninsured and prevention services to the community at large.
Health Care Delivery System—The Southeast Kentucky Community Access Program [SKYCAP] (Hazard, KY) was recognized for its innovative “patient navigators” program, which trains local residents to be advocates for the care and rehabilitation of individuals suffering from chronic diseases and other health conditions.
Healthy Workplace/Small Employer---The Waco-McLennan County Public Health District Worksite Wellness Training Program (Waco, TX) was recognized for supporting and encouraging employees to set personal fitness goals and to establish flexible exercise routines. The program offers workers paid time to exercise and record their progress, which has resulted in greater physical activity, lower body weight and improved health statistics for participants.
Healthy Workplace/Large Employer— The Johnson & Johnson (New Brunswick, NJ) was recognized for the success of its health and wellness program, which integrates disabilities management, employee assistance and occupational health into a comprehensive wellness approach that has reduced health risk among employees and saves approximately $9 million annually in medical expenses and administrative costs.
Healthy Workplace/Large Employer—The Union Pacific Railroad (Omaha, NB) was recognized for its Health Index and Health Track programs. These comprehensive programs provide at-risk employees and work groups with opportunities to establish health goals and to monitor their progress toward improving their health.
Schools (K-12)—The American Cancer Society’s Healthy Kids Network was recognized for its success in educating and mobilizing parents on how to promote healthier habits among children. Their efforts have brought about changes in school policies and educational materials, as well as improved the quality of school health programs in 19 States.
Public Sector—The Seattle-King County Healthy Homes Project (Seattle, WA) was recognized for its success in using community health workers to educate families on how to maintain “asthma-friendly” homes, as well as to educate public housing officials and builders on how to reduce “asthma triggers” in public housing and new construction.
Non-Profit—The Campuses Organized & United for Good Health [COUGH], California Youth Advocacy Network [CYAN] (Sacramento, CA) was recognized for its success in fostering a campaign to establish healthy environments for students, ultimately making it possible for State Universities to create 20-foot no smoking zones around buildings and entrances.
For more information: http://www.healthierus.gov/steps
Appendix D - The President’s Challenge
The President’s Challenge is a physical activity and fitness awards program—a long-standing program of the President’s Council on Physical Fitness and Sports that is designed to motivate Americans of all ages, backgrounds and abilities to be physically active every day. To advance this goal, individuals are challenged to build a personal “Active Lifestyle Plan” that includes meeting an activity goal of exercising at least 5 days a week, for a total of 6 weeks, in order to Get Fit! Participants in the program are encouraged to track their activities and record their progress on paper or through an interactive website. The website, www.presidentschallenge.org, offers participants, as well as groups, the opportunity to collect useful health and fitness information, to tailor their Active Lifestyle Plans to their own personal characteristics, such as age, gender and current level of fitness, and to challenge and support others in achieving their fitness goals. Since its inception, the President’s Challenge has helped to motivate millions of people each year to be physically active. There are currently four President’s Challenge programs: 1) Active Lifestyle Program—helping Americans ages 6 years and up become active, 2) Presidential Champions Program—encouraging already-active individuals to strive for even greater fitness improvements, 3) Physical Fitness Program—helping educators and community leaders plan events to assess the physical fitness of young people and recognize their achievements, and 4) Health Fitness Program—recognizing students who achieve a healthy level of fitness. This motivational, interactive tool has attracted corporations, community groups, schools, and state governors who are adopting the President’s Challenge to track physical activity within diverse venues.
Appendix E - Medicare Preventive Benefits
New Medicare Benefits in 2005
- “Welcome to Medicare” visit (initial preventive exam)
- Diabetes screening
- Cardiovascular disease screening
Immunizations & Vaccinations
- Influenza
- Pneumococcal
- Hepatitis B
Screening & Detection
- Mammography
- Pap test & pelvic exam
- Colon cancer screening tests
- PSA test & rectal exam
- Bone density measurements
- Glaucoma testing
Chronic Disease Management
- Diabetes self-management
- Medical nutrition therapy
Appendix F - Incentives for Healthy Behavior
Employers and health plans may have questions about how the Health Insurance Portability and Accountability Act of 1996, and the Americans with Disabilities Act, apply to wellness programs and incentives for their employees or enrollees. In particular, they may want to know whether these laws prevent employers and health insurers from providing incentives for healthy behaviors or imposing penalties for unhealthy behavior.
Health Insurance Portability and Accountability Act (HIPAA)
Under HIPAA, group health insurance plans generally may not charge similarly situated individuals different premiums or contributions, based on a health factor. 1 For example, people whose body mass index is lower may not be charged a different premium or contribution from those having a higher body mass index, based on the body mass differential. However, group health insurance plans are not prohibited from establishing premium discounts or rebates, or modifying otherwise applicable copayments or deductibles in return for “adherence to programs of health promotion and disease prevention.” 2 Such programs are often referred to as “bona fide wellness programs.” 3
A proposed regulation laying out the parameters for such “wellness” programs has been issued 4 ; a final rule is expected to be published in 2005. Until then, the proposed rule indicated that group plans and issuers can currently rely on the proposed requirements in the proposed regulation in establishing bona fide wellness plans. 5 The proposed rule stipulates that, if a program’s reward is contingent upon satisfying a standard related to a health factor:
- The rewards that are offered to an individual must be limited.
- The program must be reasonably designed to promote good health or prevent disease for the individuals in the program, and must give eligible individuals the opportunity to qualify for the reward at least once per year.
- The reward must be available to all similarly situated individuals, and a reasonable alternative standard must be made available for any individual for whom, due to a health factor, it would be unreasonably difficult to meet the initial standard (or for whom it is medically inadvisable to attempt to satisfy that standard).
- All plan materials that describe the terms of the wellness program must disclose the availability of a reasonable alternative standard. 6
Finally, a wellness program that merely provides reimbursement for a health club membership or merely provides a health benefit, regardless of health status, does not have to satisfy the above requirements of a “bona fide wellness program,” because it does not require satisfaction of a standard related to a health factor and since it provides no rewards or penalties. 7
The Americans with Disabilities Act (ADA): Nothing in the Americans with Disabilities Act (ADA) prohibits employers or health insurers from implementing wellness programs that are geared at promoting good health and disease prevention. The ADA prohibits covered entities from denying, on the basis of disability, qualified individuals with disabilities an equal opportunity to participate in, or receive benefits under, programs or activities conducted by those entities. 8
Whether a wellness program that offers rewards or discounts to employees for weight loss or maintaining a certain body mass index violates the ADA will depend on how the program is designed and implemented. Under the proposed HIPAA nondiscrimination regulations, employers are permitted to offer discounts or rebates in return for employees’ adherence to programs of health promotion and disease prevention. The proposed HIPAA regulations for wellness programs describe a wide range of wellness programs that comply with the HIPAA nondiscrimination requirements without having to satisfy any additional standards. 9 In addition, employers would have flexibility to design wellness programs, other than those listed in the proposed regulations, that would also comply with HIPAA’s nondiscrimination requirements, if certain requirements are met. One of the proposed requirements is the reasonable alternative standard. The reasonable alternative standard would require employers to make an alternative standard available to individuals for whom it is unreasonably difficult to meet the initial standard (or for whom it is medically inadvisable to do so).
Under the proposed HIPAA regulations for wellness programs, employers and health plans have considerable flexibility in designing wellness programs. That flexibility would also be useful to them in designing wellness programs that would be permissible under the ADA. However, employers and health plans should be aware that compliance with the proposed HIPAA wellness program requirements is not determinative of compliance with the ADA. 10 Therefore, they should consider the applicability of the ADA to their wellness programs and may want to seek legal guidance in designing and implementing such programs to ensure that they comply with ADA nondiscrimination requirements.
Conclusion
While in general these laws do not prohibit wellness programs, their bearing on specific employer or health plan incentives for health and wellness is a matter of legal interpretation. Therefore, employers and health plans may want to seek legal guidance in designing and implementing wellness programs.
1 45 C.F.R. § 146.121(c); 42 U.S.C. 300gg-1(b)(1).
2 42 U.S.C. 300-gg-1(b)(2)(B)
3 45 C.F.R. § 146.121(c)(3); 66 FR 1421, 1422.
4 66 FR at 1421.
5 66 FR at 1422.
6 45 C.F.R. § 146.121(f), as proposed at 66 FR at 1434.
7 66 FR 1421, 1422.
8 42 U.S.C. § 12101.
9 45 C.F.R. § 146.121(f)(1), as proposed at 66 FR at 1434.
10 45 C.F.R. § 146.121(b) and (h).
References
- The Surgeon General's call to action to prevent and decrease overweight and obesity 2001. [Rockville, MD]: U.S. Dept. of Health and Human Services, Public Health Service, Office of the Surgeon General. 2001.
- Flegal KM, Carroll MD, Ogden CL, Johnson CL: Prevalence and trends in obesity among US adults, 1999-2000. JAMA. 2002;288(14):1723-7.
- Ogden CL, Flegal KM, Carroll MD, Johnson CL. Prevalence and trends in overweight among US children and adolescents, 1999-2000. JAMA. 2002; 288(14): 1728-1732.
- Mokdad A, Marks J, Stroup D, Gerberding J. Actual Causes of Death in the United States, 2000. JAMA. 2004; 291(10): 1238-1245.
- HHS/NIDDK. Statistics related to overweight and obesity. NIH Publication No. 03-4158, July 2003. www.niddk.nih.gov/health/nutrit/pubs/statobes.htm
- Videon TM, Manning CK. Influences on adolescent eating patterns: The importance of family meals. Journal of Adolescent Health. 2003; 32(5):365-373.
- Federation of American Societies for Experimental Biology, Life Sciences Research Office. Third Report on Nutrition Monitoring in the United States: Executive Summary. U.S. Government Printing Office, Washington, DC; 1995.
- CDC/NCHS. Third National Health and Nutrition Examination Survey (NHANES III), unpublished data. Available at www.cdc.gov/nchs/nhanes.htm
- Food Institute Report. New products slip a trifle in ’97. Food Institute Report, 2/2/1998.
- Lin, B-H, Frazao E, Guthrie J. Away-From-Home Foods Increasingly Important to Quality of American Diet. Washington, DC, U.S. Department of Agriculture, Agriculture Information Bulletin #749. 1999.
- Young LR, Nestle M.. The contribution of expanding portion sizes to the US obesity epidemic. American Journal of Public Health. 2002; 92(2), 246-249.
- Nielsen SJ, Popkin, BM. Patterns and trends in food portion sizes, 1977-1998. JAMA. 2003; 289, 450-453
- Centers for Disease Control and Prevention. National diabetes fact sheet: general information and national estimates on diabetes in the United States, 2003. Rev. ed. Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, 2004. Available at http://www.cdc.gov/diabetes/pubs/factsheet.htm.
- Report of the Expert Committee on the Diagnosis and Classification of Diabetes Mellitus. Diabetes Care.1997;20(7):1183-97.
- CDC. Diabetes and Women's Health Across the Life Stages: A Public Health Perspective Fact Sheet. http://www.cdc.gov/diabetes/pubs/women/index.htm
- Genuth S, Alberti KG, Bennett P, Buse J, Defronzo R, Kahn R, Kitzmiller J, Knowler WC, Lebovitz H, Lernmark A, Nathan D, Palmer J, Rizza R, Saudek C, Shaw J, Steffes M, Stern M, Tuomilehto J, Zimmet P: Follow-up report on the diagnosis of diabetes mellitus. Diabetes Care. 2003;26(11):3160-7.
- Centers for Disease Control and Prevention. Diabetes Surveillance System. Atlanta, GA, U.S. Department of Health and Human Services. Available at http://www.cdc.gov/diabetes/statistics/index.htm.
- Kenny SJ, Aubert RE, Geiss LS: Prevalence and incidence of non-insulin-dependent diabetes, in Harris MI, Cowie CC, Stern MP, Boyko EJ, Reiber GE, Bennett PH (eds): Diabetes in America, 2nd Edition. Bethesda, MD, National Institutes of Health, 1995, pp 47-68.
- Boyle JP, Honeycutt AA, Narayan KM, Hoerger TJ, Geiss LS, Chen H, Thompson TJ: Projection of diabetes burden through 2050: impact of changing demography and disease prevalence in the U.S. Diabetes Care. 2001;24(11):1936-40.
- Mokdad AH, Ford ES, Bowman BA, Dietz WH, Vinicor F, Bales VS, Marks JS: Prevalence of obesity, diabetes, and obesity-related health risk factors, 2001. JAMA. 2003;289(1):76-9.
- Knowler WC, Saad MF, Pettitt DJ, Nelson RG, Bennett PH: Determinants of diabetes mellitus in the Pima Indians. Diabetes Care 1993;16(1):216-27.
- Mayfield JA, Deb P, Whitecotton L: Work disability and diabetes. Diabetes Care. 1999;22(7):1105-9.
- Anderson RN, Minino AM, Hoyert DL, Rosenberg HM: Comparability of cause of death between ICD-9 and ICD-10: preliminary estimates. Natl Vital Stat Rep. 2001;49(2):1-32.
- HHS/AHRQ. National Healthcare Quality Report, 2003. Available at http://www.ahrq.gov/qual/nhqr03/nhqrsum03.htm
- United States Preventive Services Task Force. Guide to Clinical Preventive Services, Third Edition: Periodic Updates, 2003., Available at http://www.ahrq.gov/clinic/3rduspstf/preface.htm.
- Substance Abuse and Mental Health Services Administration. 2001 National Household Survey on Drug Abuse: Trends in Initiation of Substance Abuse. Rockville, MD: Substance Abuse and Mental Health Services Administration, 2003. Available at: http://www.samhsa.gov/oas/NHSDA/2k1NHSDA/vol1/Chapter5.htm. Date of Access: August 26, 2003.
- Centers for Disease Control and Prevention. Cigarette smoking-attributable mortality and years of potential life lost — United States, 1990. Morbidity and Mortality Weekly Report. 1993;42(33):645-8.
- National Health Interview Surveys, 1965,1966, 19701974, 1978, 1979, 1980, 1983, 1985, 1987, 1988, 1990, 1991, 1992, 1993, 1994, 1995, 1997, 1998, 1999, 2000.
- Centers for Disease Control and Prevention. Tobacco Use Among Middle and High School Students—United States, 2002. Morbidity and Mortality Weekly Report. 2003; 52 (45): 1096-1098.
- Substance Abuse and Mental Health Services Administration. (2003). Results from the 2002 National Survey on Drug Use and Health: National Findings (Office of Applied Studies, NHSDA Series H-22, DHHS Publication No. SMA 03–3836). Rockville, MD.
- Centers for Disease Control and Prevention. Annual Smoking-Attributable Mortality, Years of Potential Life Lost, and Economic Costs --- United States, 1995--1999. Morbidity and Mortality Weekly Report. 2003; 52(14): 300-303.
- Centers for Disease Control and Prevention. Cigarette smoking among adults—United States, 2001. Morbidity and Mortality Weekly Report. 2003a;52(40):953–6.
- Centers for Disease Control and Prevention. Annual Smoking-Attributable Mortality, Years of Potential Life Lost, and Economic Costs — United States, 1995–1999 Morbidity and Mortality Weekly Report. 2002, 51(14).
- CDC/National Center for Health Statistics. National Health Interview Survey: 2000
- CDC/National Center for Chronic Disease Prevention and Health Promotion. State Highlights 2002: Impact and Opportunity
- Willinger M; Hoffman HJ; Wu K-T; Hou J-R; Kessler RC; Ward SL; Keens TG; Corwin MJ Factors Associated With the Transition to Nonprone Sleep Positions of Infants in the United States: The National Infant Sleep Position Study. JAMA. 1998;280(4):329-35.
- Kirsch IS, Jungeblut A, Jenkins L, Kolstad A. Adult literacy in America: A first look at the findings of the National Adult Literacy Survey. National Center for Education Statistics, U.S. Department of Education. 1993. Available online at http://nces.ed.gov/pubsearch/pubsinfo.asp?pubid=93275. Last viewed March 4, 2004.
- Schillinger D, Grumbach K, Piette J, et al. Association of health literacy with diabetes outcomes. JAMA. 2002; 288(4):475-82.
- Williams MV, Baker DW, Honig EG, et al. Inadequate literacy is a barrier to asthma knowledge and self-care. Chest. 1998; 114(4):1008-15.
- Williams MV, Baker DW, Parker RM, et al. Relationship of functional health literacy to patients’ knowledge of their chronic disease. A study of patients with hypertension and diabetes. Arch Int Med. 1998; 158(2):166-72.
- Davis TC, Arnold C, Berkel HJ, et al. Knowledge and attitude on screening mammography among low-literate, low-income women. Cancer.1996; 78(9):1912-20.
- Lindau ST, Tomori C, Lyons T, et al. The association of health literacy with cervical cancer prevention knowledge and health behaviors in a multiethnic cohort of women. Am J Obstet Gynecol. 2002; 186(5):938-43.
- TenHave TR, Van Horn B, Kumanyika S, et al. Literacy assessment in a cardiovascular nutrition education setting. Patient Educat Counsel. 1997: 31(2):139-50.
- Arnold CL, Davis TC, Berkel HJ, et al. Smoking status, reading level, and knowledge of tobacco effects among low-income pregnant women. Prevent Med. 2001; 32(4):313-20.
- Baker DW, Gazmararian JA, Williams MV, et al. Functional health literacy and the risk of hospital admission among Medicare managed care enrollees. Am J Pub Health. 2002; 92(8):1278-83.
- Baker, DW, Parker RM, Williams MV, et al. Health literacy and the risk of hospital admission. J Gen Int Med. 1998: 13(12):791-8.
- Baker DW, Parker RM, Williams MV, et al. The relationship of patient reading ability to self-reported health and use of health services Am J Pub Health. 1997; 87(6):1027-30.
- Gazmararian JA, Baker DW, Williams MV, et al. Health literacy among Medicare enrollees in a managed care organization. JAMA. 1999; 281(6):545-51.
- Keck, Buse J, Dagogo-Jack, D'Alessio, Daniels, Sernyak, Wirshing, Wirshing: Managing Metabolic Concerns in Patients with Severe Mental Illness, Postgraduate Medicine Special. December, 2003.
- Narrow WE: One-year prevalence of depressive disorders among adults 18 and over in the U.S.: NIMH ECA prospective data, Population estimates based on U.S. Census estimated residential population age 18 and over on July 1, 1998.
- McIntyre RS, Trakas K, Lin D, Balshaw R, Hwang P, Robinson K, Eggleston A: Risk of weight gain associated with antipsychotic treatment: results from the Canadian National Outcomes Measurement Study in Schizophrenia. Can J Psychiatry. 2003;48(10):689-94.
- Murray, Lopez: The Global Burden of Disease, Harvard University Press, 1990.
- Regier DA, Narrow WE, Rae DS, Manderscheid RW, Locke BZ, Goodwin FK: The de facto US mental and addictive disorders service system. Epidemiologic catchment area prospective 1-year prevalence rates of disorders and services. Arch Gen Psychiatry.1993;50(2):85-94.
- U.S. Census Bureau Website, U.S. Population estimate data from June 2003, Available at http://www.census.gov/.
- Knowler WC, Barrett-Connor E, Fowler SE, Hamman RF, Lachin JM, Walker EA, Nathan DM: Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med. 2002;346(6):393-403.
- The Diabetes Prevention Program (DPP): Description of lifestyle intervention. Diabetes Car. 2002;25(12):2165-71.
- The prevention or delay of type 2 diabetes. Diabetes Care. 2002;25(4):742-9.
- Herman WH, Brandle M, Zhang P, Williamson DF, Matulik MJ, Ratner RE, Lachin JM, Engelgau MM: Costs associated with the primary prevention of type 2 diabetes mellitus in the diabetes prevention program. Diabetes Care. 2003;26(1):36-47.
