U.S. Department of Health and Human Services
Summary and Policy Implications: Analyses of Medicaid Financing for Disabled and High Cost Children
Marilyn Rymer Ellwood and Leighton Ku
SysteMetrics
December 1990
This report was prepared under contract #HHS-100-88-0041 between the U.S. Department of Health and Human Services (HHS), Office of Family, Community and Long-Term Care Policy (now the Office of Disability, Aging and Long-Term Care Policy (DALTCP)) and SysteMetrics. For additional information about the study, you may visit the DALTCP home page at http://aspe.hhs.gov/_/office_specific/daltcp.cfm or contact the ASPE Project Officer, John Drabek, at HHS/ASPE/DALTCP, Room 424E, H.H. Humphrey Building, 200 Independence Avenue, SW, Washington, DC 20201. His e-mail address is: John.Drabek@hhs.gov.
PREFACE
This paper summarizes the findings and policy implications from four research reports about the health care experiences of severely disabled and high cost children, especially their participation in Medicaid. This research was completed under contract to the Office of the Assistant Secretary of Planning and Evaluation (ASPE). John Drabek was the ASPE Federal Project Officer who directed these studies. Mary Harahan of ASPE also provided considerable guidance in their development. Brian Burwell and Ellcia Herz of SysteMetrics were authors of the research studies included in this summary, in addition to Ellwood and Ku.
Copies of the detailed research reports may be obtained by writing to: Brenda Veazey, Department of Health and Human Services, Room 424E, Humphrey Building, 200 Independence Avenue, S.W., Washington, D.C. 20201.
INTRODUCTION
This paper summarizes the findings and policy implications from four research reports about the health care experiences of severely disabled and high cost children, especially their participation in Medicaid. This research was sponsored by ASPE, and relied heavily on Medicaid administrative data from the Health Care Financing Administration's Tape-to-Tape data base. The four reports included:
-
Variations in the Medicaid Safety Net for Children and Youth with High Medical Costs: A Comparison of Four States. This report analyzed the Medicaid experience of children and young adults with total Medicaid claims of $25,000 or more in California (1986), Georgia (1984), Michigan (1985) and Tennessee (1986). [Available at http://aspe.hhs.gov/daltcp/reports/4stvares.htm]
Key study questions were: Through what eligibility pathways do high-cost children and youth become enrolled in the Medicaid program? What health care utilization patterns account for their high Medicaid expenditures? How do the program characteristics of State Medicaid program affect the size and characteristics of high-cost children and youth on Medicaid?
-
SSI-Related Disabled Children and Medicaid. This report analyzed the 1984 Medicaid experience of all children passing the SSI disability test in California, Georgia and Michigan. [Available at http://aspe.hhs.gov/daltcp/reports/ssireles.htm]
Key study questions were: What are the Medicaid enrollment, utilization and expenditure patterns of SSI-related disabled children? What proportion of overall child Medicaid enrollment and expenditures do SSI-related disabled children represent? How do SSI-related disabled children fit into the overall disabled Medicaid population and expenditures? What are the disabling conditions of SSI disabled children? What differences are seen among SSI-related children by institutional status? What impact might the Supreme Court's Zebley decision have on Medicaid patterns for disabled children?
-
Longitudinal Analysis of High Cost Medicaid Children in California. This report analyzed the Medicaid experience from 1980 through 1986 of children in California who had Medicaid claims in 1983 of $25,000 or more. [Available at http://aspe.hhs.gov/daltcp/reports/cahcmces.htm]
Key study questions were: What proportion of high cost children are new to the Medicaid program when they experience a period of high medical expenditures? To what extent do high cost children remain enrolled in Medicaid after their period of high expenditures? Have these children had high costs on Medicaid in the past? Do they have persistently high costs in the future? Are there variations in the longitudinal experience of high cost Medicaid children by age, institutional status, or eligibility group? What are the characteristics of high cost children who use Medicaid as a permanent safety net?
-
Who is Paying the Big. Bills? Very High Cost Pediatric Hospitalizations in California, 1987. This report analyzed all-payor data for high cost pediatric hospitalizations (>$25,000) for all children in California in 1987, using the California All-Payor Hospital Discharge data set. [Available at http://aspe.hhs.gov/daltcp/reports/bigblles.htm]
Key study questions were: Who is paying for the hospital care for high cost child cases? How many high cost children are uninsured? What are the differences in the characteristics of very high cost cases among those who are privately insured, publicly insured and those without insurance? What are the differences in age, diagnosis, type of discharge, and length of stay?
In the following pages, we answer three questions from these reports: What did we learn? What are the policy implications? Is additional research needed? Rather than present each study separately, we have integrated the findings into major program areas.
OVERVIEW OF MEDICAID ELIGIBILITY FOR DISABLED AND HIGH COST CHILDREN
Before we present the study results, it seems appropriate to provide a brief review of the Medicaid program as it relates to severely disabled and high cost children. Medicaid is the primary public medical assistance program for low-income severely disabled children. However, Medicaid eligibility is so complicated that it is difficult to evaluate the extent to which Medicaid can be used to provide coverage to disabled and high cost children. There are numerous pathways to eligibility, and these pathways vary from State to State due to the many options available. Generally, qualifying for Medicaid can be considered to involve two steps--categorical eligibility and financial eligibility.
Categorical Eligibility. First, a child has to fit into one of the so-called categorical groups which a State covers for Medicaid:
-
Most children on Medicaid qualify through the Aid to Families with Dependent Children (AFDC) program. AFDC is our main welfare program for families in need. To qualify for AFDC, a key requirement is that a child must live in a family in which only one parent is present, although the program has recently expanded to include two-parent families with one unemployed parent. All States have to cover children receiving AFDC cash assistance under Medicaid.
-
Another pathway to Medicaid eligibility is through the Supplemental Security Income (SSI) program, a Federally administered cash assistance program for the disabled (and aged). To receive SSI benefits, a child has to pass a disability test. The SSI definition of disability is the inability to engage in substantial gainful activity by reason of any medically determinable physical or mental impairment which can be expected to result in death or has lasted or can be expected to last for a continuous period of not less than 12 months. This definition focuses on whether an adult is capable of work. For children, the SSI program is supposed to determine whether a child suffers from a condition of comparable severity. However, the Supreme Court ruled this year that SSA had been using a harsher disability test for children than had been intended by Congress. As a result, the SSI disability test for children is to be revised to include an individualized assessment for children (when necessary) with an age-appropriate functional standard. Nevertheless, many severely disabled children will not be able to pass the SSI disability test since their disabilities are acute, and they may eventually achieve recovery. Although States do not have to automatically extend Medicaid to SSI children, all but two (Connecticut and Missouri) do.
-
Ribicoff coverage is the final categorical group under which severely disabled children may qualify for Medicaid assistance only, if they are unable to qualify under the AFDC or SSI-related groups. The Ribicoff child group is named after the Connecticut Senator who sponsored the initial legislation for expanding Medicaid to all poor children, regardless of their family structure or eligibility for AFDC or SSI categorical coverage. With Ribicoff coverage, there are no categorical rules per se for children. Unlike AFDC, Ribicoff coverage includes children who live in two-parent families. Also important, there are no disability tests for children to qualify under the Ribicoff group. Instead, the Medicaid eligibility for Ribicoff children is strictly based on their financial situation.
Until recently, any Ribicoff coverage was optional to States; however, Federal legislation now requires all States to implement Ribicoff coverage for all children born on or after October 1, 1983. As a result, by the year 2002, Ribicoff coverage will be complete nationwide for all children through age 18. However, in 1989, only 30 States at their option had elected to extend Ribicoff coverage for children through age 18. Thus, in the remaining States, children born before October 1, 1983 will not qualify for Medicaid unless they can meet the AFDC or SSI categorical requirements.
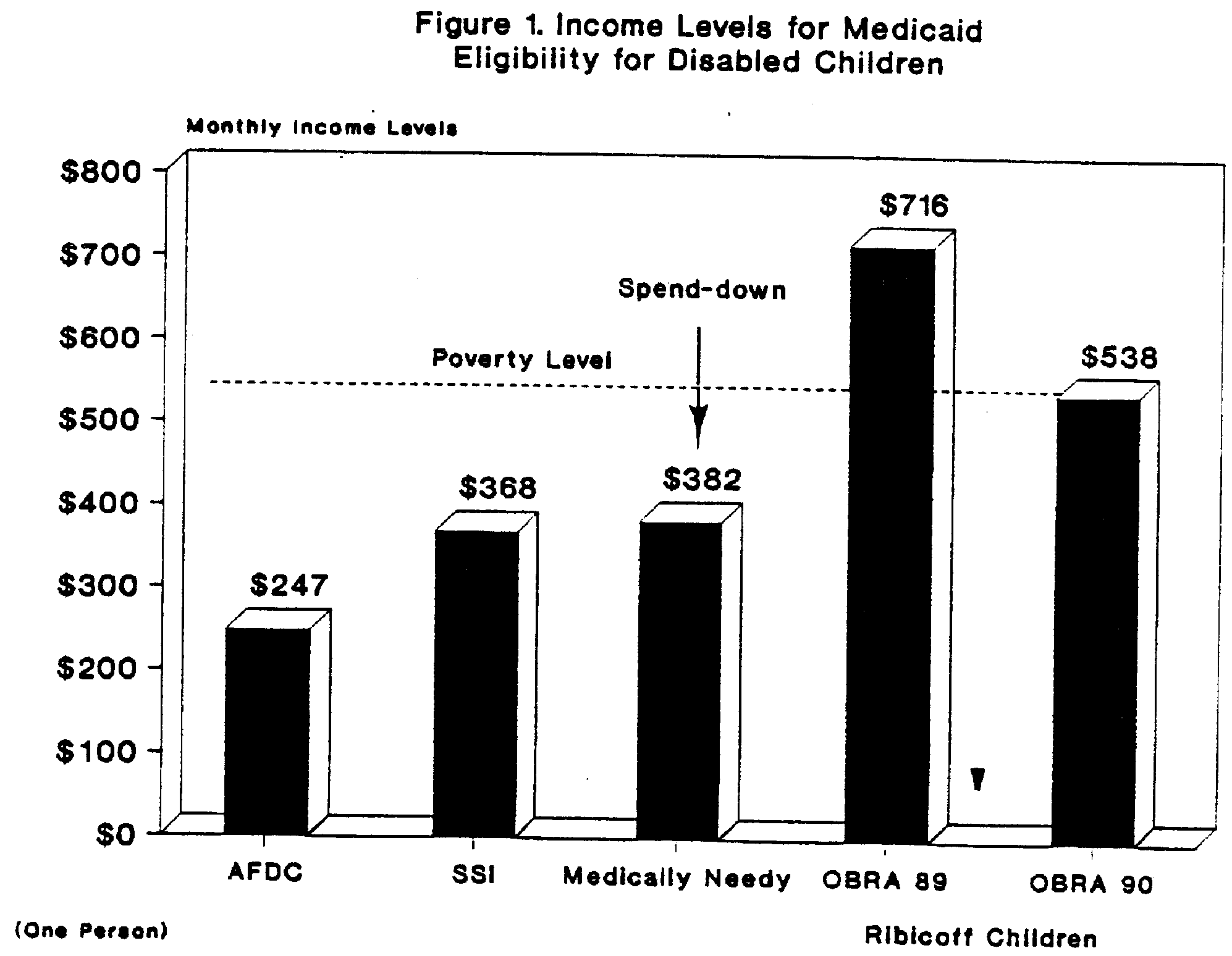
Financial Eligibility. Second, a child (or the child's family) has to pass a financial test. The financial test varies among the categorical groups and among States. For children on AFDC and SSI, financial eligibility for Medicaid is determined by the criteria used by States to determine eligibility for cash assistance. Generally, the financial thresholds for the AFDC program are quite low. In 1989, the median State used an AFDC level of $360 for a family of three, which was about 46% of the Federal poverty level. SSI financial thresholds are higher. In 1989, the median State SSI threshold for a disabled person living independently was $368 a month, 68% of the Federal poverty level.
States also have the option to adopt medically needy programs. A medically needy program allows a State to set higher income (and asset) criteria for Medicaid (only) eligibility than are used for AFDC cash assistance. Children in any of the categorical groups can qualify through the medically needy provisions. A medically needy program also requires that applicants be allowed to "spend-down" to Medicaid eligibility, even if their income exceeds the medically needy income level. The income spend-down process allows applicants to deduct incurred medical expenses from income in determining financial eligibility. Severely disabled children in States without medically needy programs are subject to the so-called Medicaid notch, whereby an additional $1 of income can mean the complete loss of Medicaid coverage. The spend-down provisions of a medically needy program mitigate this notch problem and allow children from families of any income level to qualify for Medicaid, assuming their medical bills are large enough. It is important to note that the spend-down liability only has to be incurred, not paid, by a spend-down applicant. This is different from the way Income spend-down works for Medicaid recipients in nursing homes, who always have to pay their spend-down obligation each month.
The median State medically needy level in 1989 was $382 for a one person family, about 70% of the Federal poverty level. In 1989, 36 States had medically needy programs.
Different financial eligibility levels are used for children born on or after October 1, 1983 who qualify for Medicaid under the Ribicoff coverage group. OBRA 1989 required States to provide Medicaid coverage to all children up to age 6 in families with income up to 133% of the Federal poverty level. OBRA 1990 requires States to cover all children born on or after October 1, 1983 with family income below 100% of the Federal poverty level. State medically needy financial levels are used for Ribicoff children born before October 1, 1983.
Thus, as shown in Figure 1, different financial levels are used to determine Medicaid eligibility for children, dependent on the categorical group under which they are qualifying. For Ribicoff children, age also makes a difference. Figure 1 does not represent any one State, but instead depicts in a general fashion w ere median State financial eligibility levels for children were in 1989.
It should be noted that Medicaid eligibility for children who are institutionalized works very differently than with children who are living at home with their families. Generally, the income and assets of family members with whom children are living are considered to be available to them for support and thus are counted in determining financial eligibility for Medicaid. However, children who have been institutionalized for more than one month are not "deemed' to have family income or assets available to them; only income or assets which the child may have individually are considered to be available. This approach greatly expands financial eligibility for institutionalized children, and has been criticized for providing an incentive to institutionalize children instead of caring for them at home. Although some program options and waivers are available to State Medicaid programs to waive the deeming of family income and assets for children who could be cared for appropriately and cost-effectively at home, not all States participate in these options.
STUDY RESULTS
Study analyses focused on two groups of severely disabled children served under Medicaid--children with high Medicaid costs (> $25,000 annually) and children passing the SSI disability test (called SSI-related children). Little national level data are available on either group, except the number of disabled children qualifying for cash assistance benefits under the SSI program. In December 1989, 296,293 children under age 22 were enrolled in the SSI program. SSI child enrollment has been fairly stable since 1980.
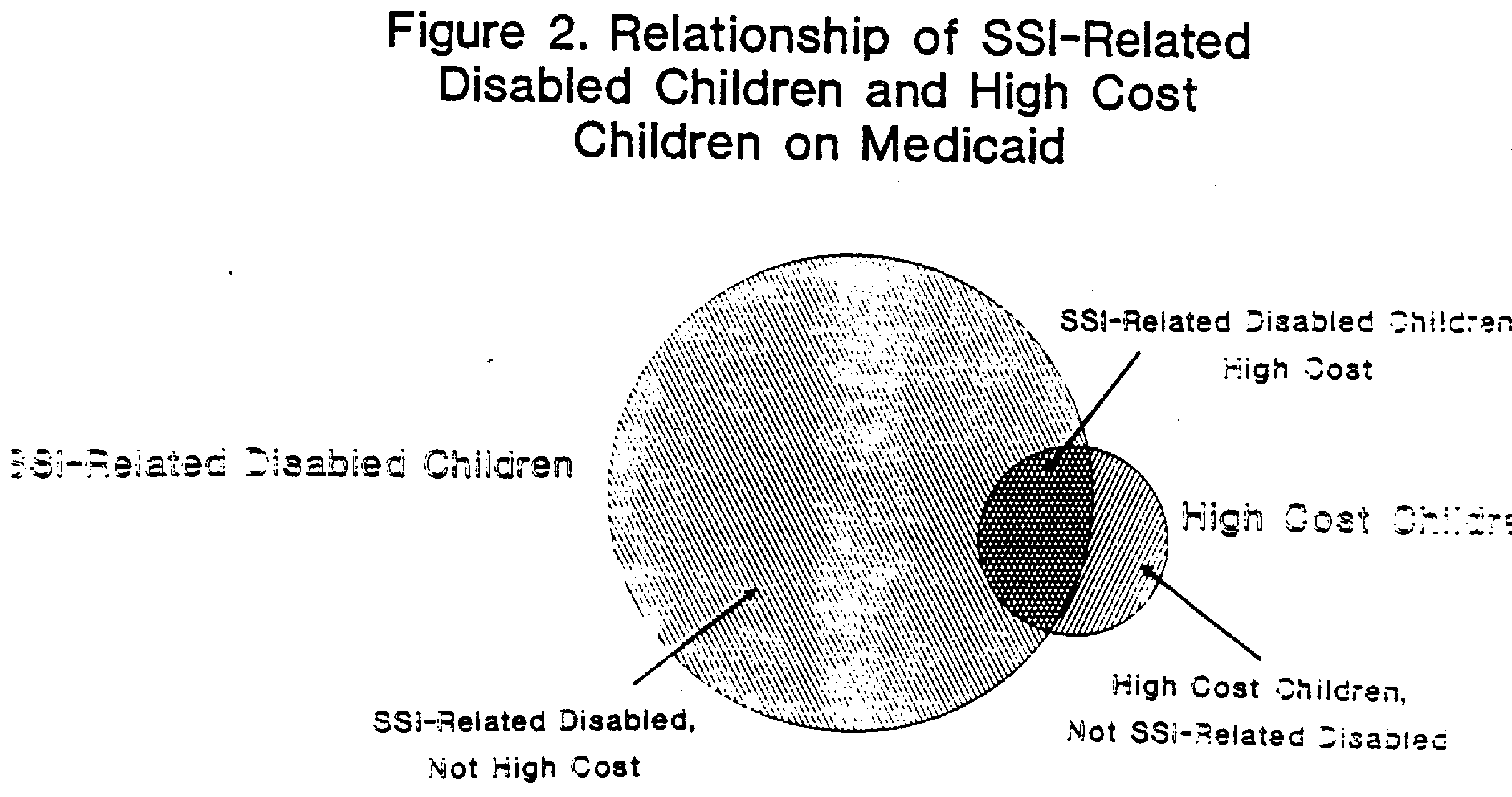
High cost Medicaid children were about 0.2% of total Medicaid recipients among the study States, while SSI-related disabled children were 1%-3%. There was some overlap between the two groups. About half of the high cost children in each State passed the SSI disability test. However, the vast majority of SSI-related children were not high cost, i.e. they did not have annual Medicaid expenditures of $25,000 a year or more. Figure 2 below shows the general relationship between high cost Medicaid children and SSI-related Medicaid children.
HIGH COST MEDICAID CHILDREN (> $25,000/Year)
Although high cost children were only about 0.2% of total Medicaid recipients among the study States in 1986, they represented 4-8% of total Medicaid expenditures, as shown in Table 1. They accounted for a greater proportion of expenditures in California and Michigan, compared to Georgia and Tennessee. Lower expenditures in Georgia and Tennessee were due to more restrictive service coverage and reimbursement policies employed in these States.
High cost children tended to fall into two major groups: 1) infants and very young children (under age 4) with high Medicaid costs related to extended hospital stays, and 2) teenagers and young adults with mental disabilities who were institutionalized.
In 3 of the 4 study States, 70% or more of high cost children were institutionalized. Most of these institutionalized children were adolescents and young adults. Most were institutionalized during the entire study year. About 60% were male. The proportion receiving ICF/MR care ranged from 50% to 97% among the study States. Most were receiving SSI cash assistance to cover their personal needs.
| TABLE 1. Selected Data on High Cost ChildrenCalifornia, Georgia, Michigan and Tennessee, 1984-1986 | ||||
| California1986 | Georgia1984 | Michigan1985 | Tennessee1986 | |
| Number of High Cost Children | 6,409 | 781 | 2,196 | 988 |
| Percent Noninstitutionalized | 61.7% | 26.4% | 29.3% | 15.8% |
| Percent Institutionalized | 38.3% | 73.6% | 70.7% | 84.2% |
| High Cost Children as Percent of Total Medicaid Recipients | 0.22% | 0.18% | 0.25% | 0.26% |
| High Cost Children as Percent of Total Medicaid Expenditures | 7.9% | 4.1% | 7.1% | 5.1% |
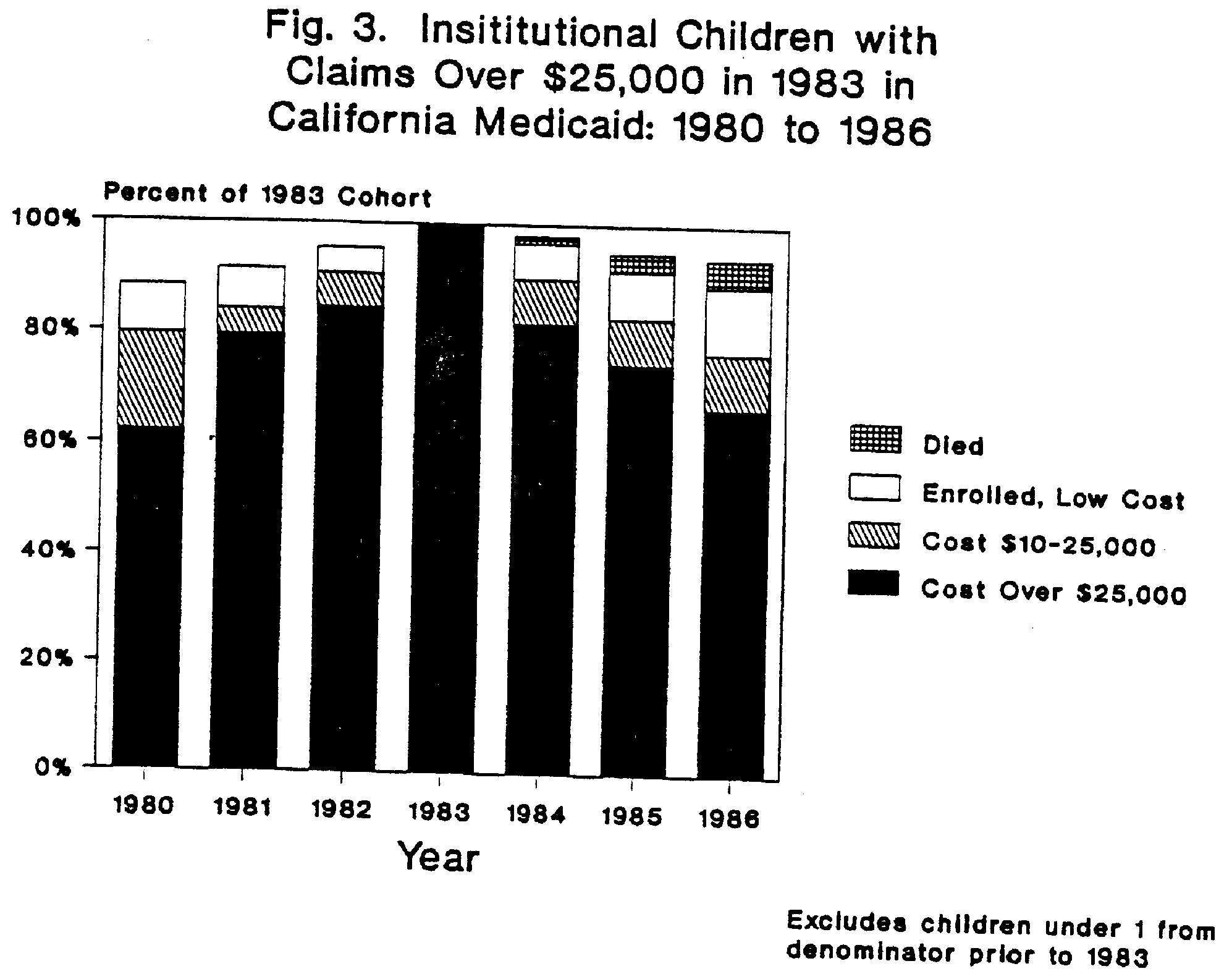
The longitudinal analysis in California showed that high cost institutionalized children were likely to main institutionalized and remain high cost, as shown in Figure 3. In 1986, about 90% of the 1983 cohort were still enrolled in Medicaid, and 67% still had Medicaid expenditures of $25,000 or more per year. The 7 year cumulative Medicaid cost (1980 through 1986) for institutionalized children who were in the high cost group in 1983 in California averaged $328,819 per child.
High cost children who were not institutionalized had a very different profile. From one-third to two-thirds were under age 4. A very high proportion were infants, suggesting that these children incurred high Medicaid costs as a result of complications of delivery and birth, such as low birth- weight.
Optional eligibility groups were critical to Medicaid coverage for many of the high cost children not in long-term care settings. The combination of full Ribicoff coverage (i.e. coverage of all low-income children up to age 21, regardless of family structure) and medically needy coverage accounted for 42% of noninstitutionalized high cost children in California, 35% in Michigan, and 26% in Tennessee. Georgia did not have Ribicoff or medically needy coverage during the study year.
Although many of the noninstitutionalized high cost children qualified for Medicaid through the medically needy and Ribicoff groups, few of the children were reported to have private insurance or spend-down liabilities. This result suggests that Medicaid coverage is not reaching many high cost children in middle class families. Instead, most of the coverage is going to children in families with income below the poverty level.
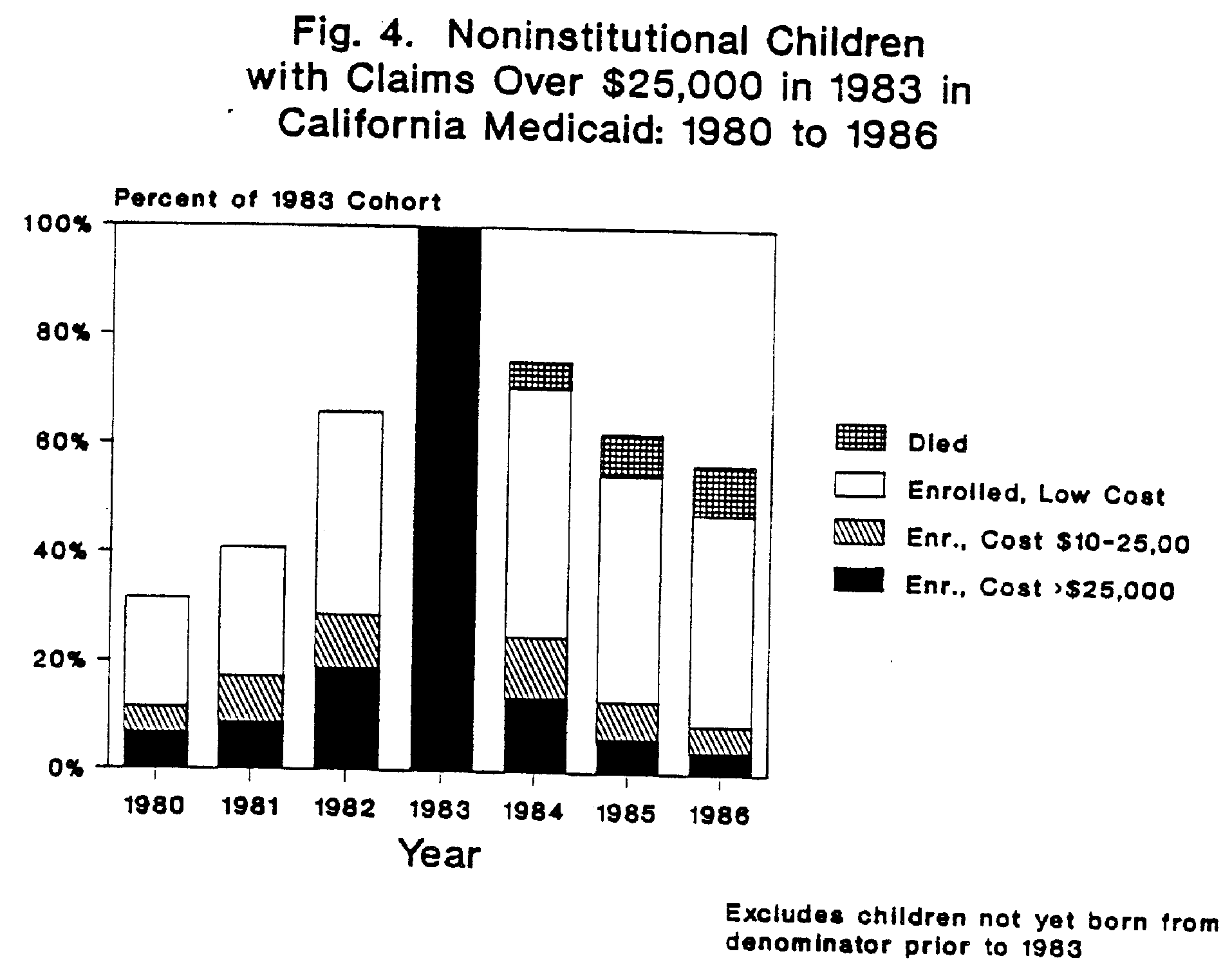
The longitudinal analysis in California showed that about one-third of the noninstitutionalized high cost children in 1983 were new entrants to Medicaid, a higher than expected rate with normal caseload turnover and growth. Figure 4 shows that only about half of these children were still enrolled in Medicaid by 1986, and about 10% were deceased. Most noninstitutionalized high cost children in 1983 were not persistently high cost. Only 9% continued to have Medicaid expenditures of $10,000 or more annually by 1986.
These results suggest that the California Medicaid program was providing transitory coverage for many noninstitutionalized high cost children. Of interest, infants were the least likely age group to remain enrolled on Medicaid, and the least likely to remain high cost. The most frequent diagnoses for high cost infants involved conditions originating in the perinatal period (such as low birth weight) and congenital anomalies. It appears that these problems were not permanently and totally disabling, since few of these infants became SSI recipients. Of the high cost infants in 1983, only 3% remained high cost to Medicaid (> $10,000 annually) three years later in 1986, compared to an overall average of 9% among high cost children.
SSI-RELATED DISABLED CHILDREN
In 1984, SSI-related disabled children were 1%-3% of overall Medicaid recipients and 3%-5% of overall Medicaid expenditures among the study States, as shown in Table 2. At least 97% of SSI-related disabled children in each State received cash assistance, so that few children passing the SSI disability test qualified through the medically needy provisions. The average age for SSI- related disabled children was about 14 years, and there were slightly more males than females. Four disease categories accounted for the vast majority of SSI children--mental retardation, disease of the nervous system and sense organs (including infantile cerebral palsy, multiple sclerosis, epilepsy and muscular dystrophy, hearing loss and blindness), mental disorders, and congenital anomalies.
| TABLE 2. Selected Data on SSI-Related Disabled ChildrenCalifornia, Georgia and Michigan, 1984 | |||
| California | Georgia | Michigan | |
| Number of SSI-Related Disabled Children | 35,645 | 12,715 | 11,255 |
| SSI-Related Disabled Children as Percent of Total Medicaid Recipients | 1.3% | 2.9% | 1.2% |
| SSI-Related Disabled Children as Percent of Total Medicaid Expenditures | 4.2% | 5.3% | 2.8% |
| Percent Receiving SSI Cash Assistance | 96.6% | 98.7% | 97.4% |
| Percent Noninstitutionalized | 90.5% | 95.3% | 91.8% |
| Percent Institutionalized | 9.5% | 4.7% | 8.2% |
| Annual Medicaid Expenditure Per Enrollee | |||
| Noninstitutionalized, Receiving SSI | $2,434 | $2,251 | $1,490 |
| Institutionalized | $28,349 | $26,792 | $31,638 |
| Noninstitutionalized, Not Receiving SSI | $12,281 | $5,037 | $3,700 |
Three subgroups of SSI-related disabled children with consistently different Medicaid enrollment and utilization patterns were identified among the study States:
-
Noninstitutionalized SSI Cash Assistance Children. The vast majority of SSI-related disabled children on Medicaid were in this group (88% to 95%). They lived at home in the community and received SSI cash assistance benefits. The annual Medicaid expenditure per child in 1984 ranged from $1,490 to $2,434, compare to an average expenditure per AFDC child of $358 to $439. However, the median expenditure per SSI-related disabled child was only $239 to $411 among the study States. A minority of these children in each State had exceptionally high expenditures, thus substantially increasing the overall average per child. About half the Medicaid expenditures for this group went to inpatient hospital care for the 11 % to 20% of children who were hospitalized during the year. Noninstitutionalized children receiving SSI accounted for 28%-39% of expenditures for SSI-related disabled children in California and Michigan. Since Georgia had little optional coverage, this group accounted for 58% of Medicaid expenditures for SSI-related disabled children in that State.
-
Institutionalized Children. About 5%-10% of SSI-related disabled children in each State were institutionalized, mainly in ICFs/MR and SNFs. The average number of institutional care days per child exceeded 300 for the year. About 17% also used inpatient hospital care during the year. The annual Medicaid expenditure per institutionalized child ranged from $26,792 to $31,638. As a result, most of these children were in the high cost group described earlier of children with annual Medicaid expenditures of $25,000 or more. Most received an SSI cash benefit each month of $25 to cover their personal needs. Institutionalized children accounted for 42% of Medicaid expenditures for SSI-related disabled children in Georgia, 58% in California, and 71% in Michigan. Institutionalized children accounted for a greater proportion of overall expenditures in Michigan because the State had a much lower average expenditure per noninstitutionalized child relative to the other study States.
-
Noninstitutionalized No Cash Children. This subgroup accounted for only 1%-2% of SSI-related disabled children among the study States, and 1%-3% of expenditures. They showed very different Medicaid utilization patterns. Their hospital user rate was relatively high (17%-26%), and they averaged many more days per hospital user than SSI cash children (noninstitutionalized). They were only enrolled for 6-7 months of the study year, compared to 10+ months for the other groups. The average Medicaid expenditure for the year ranged from $3,700 to $12,821 per child, but a small group of children had exceptionally high expenditures which greatly inflated the averages.
A major finding is that very few SSI-related disabled children living at home qualified for Medicaid through the medically needy provisions. In California, the most generous State with regard to its medically needy income threshold, only 2% of SSI-related disabled children were living at home and not receiving SSI cash assistance. Because Medicaid deems family income to be available to children living in the community, many families with disabled children have income considerably in excess of State SSI levels. Only when there is a major health crisis, such as a hospitalization, will they seek assistance from Medicaid. Several study results pointed to this pattern. SSI-related disabled children living at home and not receiving SSI had considerably higher Medicaid expenditures per enrollee when compared to the SSI cash group. They had shorter lengths of enrollment during the year. Their inpatient hospital user rates were considerably higher, and they averaged more hospital days per user.
A recent ruling by the Supreme Court (Sullivan v. Zebley, February 20, 1990) is expected to significantly increase the numbers of SSI-related disabled children on Medicaid. The court has ordered the Social Security Administration (SSA) to implement new standards for child disability determinations. The new standards will Include individualized functional assessments (when necessary) for children which will focus on the impact of a child's handicap on his/her normal daily activities. Previously, the disability assessment was limited to whether a child suffered from a condition included in (or equal to) a listing of medical impairments promulgated by SSA.
The number of new SSI awards to children has been steady at about 50,000 annually for the last few years. However, another 50,000 children are denied coverage each year, most often because of their failure to pass the disability test. Some experts have estimated that about one-third of these denials (or 17,000 children annually) may quality under the new procedures. Assuming most of the children who will qualify under the new procedures will have Medicaid expenditures similar to those of noninstitutionalized SSI cash assistance children, study results indicated that this level of expanded coverage would result in Medicaid increases of $10-$42 million a year nationally.
PRIVATE INSURANCE COVERAGE OF HIGH COST CHILDREN
Using an all-payor hospital data base, all children who had a hospital stay that cost more than $25,000 in 1987 in California were studied. Although these cases comprised only 2% of California's 1.06 million discharges for children, they comprised 35% of the $3.8 billion in total hospital charges for children in 1987. About half of the high cost children were covered by private insurance or HMOs, with another 30% covered by Medicaid. About 14% were covered by other government programs, such as CHSCN, CHAMPUS, Workers' Compensation, Medicare and various other Federal, State and local funding sources. A final 9% were reported to have no insurance.
These California data suggested government financing of a much greater proportion of high cost care for children than was expected. Altogether about 44% of the financing (30% Medicaid plus 14% other public programs) was attributable to public payors. However, since these data were limited to California, this pattern may not be representative of all States. National survey data for 1987 indicate that about two-thirds (69%) of persons under 25 had private insurance. It is not clear if the large role of public payors (especially non-Medicaid programs) in high cost care is unique to California, or if it is a broader phenomenon not previously identified due to lack of comparable data in other States.
Also of interest, the California data showed the rate of uninsurance was greatest among older adolescents and young adults, with about 30% of those 18 to 24 years of age reporting a lack of insurance. This pattern is roughly consistent with national data indicating that lack of insurance is greatest among those 18 to 24 years of age and that public insurance coverage (i.e., Medicaid, CHAMPUS, etc.) declines with the age of the child. Part of the problem is that Medicaid's coverage for children only extends through age 20. Young adults (i.e. those age 21-25) who meet Medicaid's financial requirements can only qualify for Medicaid if they have dependent children or if they pass the SSI-related disability test. A young adult, single or married, without children, has no avenue to qualifying for Medicaid if he or she has a short-term disabling condition, even if a very expensive hospitalization is involved.
The high cost uninsured were often hospitalized due to injuries or poisoning, suggesting that access for acute traumatic cases is relatively good among the uninsured. However, few hospitalized psychiatric patients were uninsured, suggesting that access to mental health services is more directly affected by insurance availability.
Another finding of importance is that as hospital stays become more expensive, the share of patients without private insurance declines. This may indicate that those without insurance have reduced access to care for serious illnesses, that hospitals are more aggressive in identifying payors for expensive cases, or that those without insurance seek less care.
If Medicaid were functioning as a good catastrophic program, we would expect the share of bills paid by Medicaid to rise as costs increased. This opposite pattern confirms the earlier conclusion that Medicaid is not reaching many high cost children in families with income just over the poverty level, even in California.
POLICY IMPLICATIONS
Generally, study results showed that although Medicaid has the potential to provide broad coverage for low-income families with disabled children, it provided only a very limited safety net in many States, with most coverage directed to severely disabled children in families poor enough to qualify for AFDC or SSI cash assistance. Even in a State like California with a relatively broad Medicaid program which extended coverage to many non-cash high cost and disabled children, it appears that Medicaid does not serve as a catastrophic insurance program for noninstitutionalized children of working class families with incomes just over the poverty level. Detailed below are some major policy implications for the Medicaid program and its coverage of severely disabled children. In some instances, the research showed that States are not exercising certain options under Medicaid which would improve their coverage of disabled and high cost children. In other instances, there are problems of program design which need to be addressed at the Federal level.
1. Ribicoff Coverage Is Critical to the Medicaid Safety Net for High Cost Children
Study results showed that the adoption of Ribicoff coverage (in conjunction with medically needy coverage) had a major effect on broadening the Medicaid safety net for severely disabled children, particularly noninstitutionalized children with extended hospital stays. During the study period, children unable to pass the SSI disability test in Georgia could only qualify for Medicaid if they were in single parent families. In 1983, 16% of high cost children in California and about 27% of the high cost children in Michigan and Tennessee qualified through the Ribicoff coverage provisions (in combination with medically needy coverage). The absence of Ribicoff coverage in Georgia in 1984 severely limited access to Medicaid coverage for high cost children in families that were not eligible for AFDC or SSI benefits.
The numerous expansions to Medicaid eligibility during the last few years to extend coverage to all infants and young children living in poverty make mandatory some of the Ribicoff children covered optionally by California, Michigan and Tennessee in 1986. OBRA 1989 required States to provide Medicaid coverage to all children up to age 6 in families with incomes up to 133% of the Federal poverty level. This coverage will be extremely important since study data showed a large proportion of infants and young children with high hospital costs. OBRA 1990 requires States to begin phasing in the coverage of all children born after September 30, 1983 whose family incomes are below 1 00% of the Federal poverty level. In effect, this will mean that eventually all States will have Ribicoff coverage for all children through age 18. Further, the income threshold will be the poverty level, not the medically needy level, which is usually well below the poverty level.
However, States are still not required to provide Ribicoff coverage for children born before October 1983. Thus, severely disabled children born before October 1983 will not qualify for Medicaid coverage in some States if they live in two-parent families and they cannot pass the SSI disability test. Full Ribicoff coverage is necessary to open up Medicaid to high cost children in two-parent families who are unable to pass the SSI disability test.
In 1989, 20 States did not offer Ribicoff coverage to children through age 17. In these States, Medicaid's coverage of severely disabled children will continue to be seriously restricted, even with the changes in OBRA 1990. The group of severely disabled children adversely affected in these States are those born before October 1983 who cannot pass the SSI disability test and who live in two-parent poor families. It is important to realize that no matter how poor the families of these children are, or how high their medical expenses are, their disabled children will not be able to qualify for Medicaid unless the State has opted to provide full Ribicoff coverage.
2. Some Provision for Buying-In to Medicaid Coverage Is Needed in All States to Replace the Medically Needy Program
Currently, the medically needy program through its spend-down provisions provides access to Medicaid for children at all Income levels, assuming they fit into one of the categorical groups and their medical expenses are high enough. However, there are several problems with the medically needy program. To start with, not all States provide medically needy coverage. In 1989, some 15 States did not have a medically needy program. In these States, no access to Medicaid (except through institutionalization) is available to otherwise eligible children born before October 1983 whose families have incomes which exceed AFDC or SSI levels. Even with the new eligibility groups Congress has implemented for younger children using income thresholds related to the poverty level, there continues to be a Medicaid notch problem. An additional $1 in family income over the poverty-related threshold can render a child completely ineligible for Medicaid in States without medically needy programs.
A second problem which exists in States with medically needy coverage is that the medically needy program is not used by very many children. Study results showed that only 2% of SSI- related children among the study States lived at home and qualified for Medicaid under the medically needy program. Participation was also low for high cost children, especially in the spend-down component of the medically needy program. Although many high cost children use the medically needy provisions to qualify for Medicaid, few children qualify by spending-down. For example, study data showed that in 1986, only 22% of California's noninstitutionalized high cost children who qualified through the medically needy provisions had a spend-down liability. Generally, for medically needy children to qualify for Medicaid without a spend-down, their family incomes must be just above AFDC or SSI levels but below medically needy levels--a fairly narrow income band. Children with family income above the medically needy level have to incur a spend-down liability to qualify for Medicaid.
Why do so few SSI-related children and families with high cost children use the spend-down provisions? Part of the problem may be that spend-down policy imposes a 100% marginal tax rate for income above the medically needy level. That means every dollar of income above the medically needy level has to be offset by incurred medical expenses. An example may help illustrate this problem. In 1986, the AFDC level in California for a four-person AFDC family was $734 monthly, compared to the medically needy level of $984. In 1986, the poverty level for a family of 4 was $933 monthly, close to California's medically needy level. Thus, a four-person family whose income was above the AFDC level but below the medically needy level (and poverty level) could have their high cost child qualify for Medicaid as medically needy without a spend-down. However, a four-person family with income above $984 a month would have to incur a spend-down liability in order for their children to become Medicaid eligible. If the family's income was $1,500 a month (or $18,000 annually), the monthly spend-down liability would be $516 ($1,500 - $984 = $516). A family with $18,000 in income would not be considered to be living on the edge of poverty. On the other hand, It is easy to imagine that such a family might not have private health coverage or only fairly limited coverage.
Although $516 is not a lot of money relative to the medical expenses for a high cost child, it would represent almost one-third of the family's monthly income. Most would agree that this is an excessive proportion of income to require for access to medical benefits. Further, this approach provides no incentive to earn additional Income. Every additional dollar of income which the family earned would have to be devoted to the spend-down liability.
Yet another problem caused by current spend-down policy involves the OBRA 1989 coverage of children through age 5 and the 1990 OBRA legislation extending coverage to all children born after September 30, 1983. Recall that OBRA 1989 mandated that all States provide Medicaid to children through age 5 whose family Income was less than 133% of poverty. A family with income just under 133% of poverty would not have to spend-down at all to obtain Medicaid coverage, providing their child was under age 6. However, if their income was 140% of poverty, they would have to spend-down to the medically needy level, not the 133% of poverty level. The OBRA 1989 legislation made no provision for spending-down to the 133% of poverty level. Neither did the OBRA 1990 legislation mention any spend-down to the 100% of poverty level.
The median State medically needy level in 1989 was only at 70% of the poverty level. As a result, in most States the disparity between the 133% of poverty level threshold for children up to age 5, the 100% of poverty level threshold for children born after September 30,1983 and the medically needy level is considerable.
Even though technically, the spend-down only has to be incurred and not paid, many families may not understand this distinction. In fact, many policymakers are surprised to learn that income spend-downs only have to be incurred. According to the Medicaid statute in Section 1903(f)(2) of the Social Security Act, medically needy applicants are supposed to be able to disregard from their income any medical expenses which they have incurred; applicants may disregard such expenses even ff they have not actually paid the bills, as long as the bills are their responsibility. There are good reasons for allowing applicants to incur spend-down costs instead of requiring that the spend-down be paid. Immediate payment of a large spend-down liability would not be possible in many circumstances. Continuing with the example above, many families would find it difficult to pay the $516 right away in order to spend-down into Medicaid. Thus, requiring only incurred costs enables applicants to collect bills, establish eligibility for Medicaid, and pay off the incurred spend-down liabilities eventually as best they can. On the other hand, if applicants are not aware that they only have to incur spend-down liabilities, or providers are not willing to let applicants incur costs, it makes little difference that the Medicaid statute does not require that the spend-down liability be paid.
We believe the spend-down provision of the medically needy program has major design flaws. The 100% marginal tax rate for some categorical groups means there is no incentive to earn additional Income. There is also a new Medicaid notch problem introduced by having some younger groups of children whose eligibility is tied to the poverty standard. Since there is no spend-down to the poverty standard, families whose income exceed the poverty threshold have to spend-down to the medically needy level to attain Medicaid eligibility for their children. Finally, although the spend-down liability only has to be incurred, not paid, this policy may not be uniformly understood or implemented. All these design problems can only be resolved by changes in Federal Medicaid policy.
The most frequently proposed solution to the spend-down problem is to replace the spend-down component of medically needy programs with an income-related Medicaid buy-in premium. The amount of the buy-in might range from 2% to 10% of family income. Consideration should be given to structuring the buy-in in such a way that there would be some incentive for additional income, perhaps similar to the sliding scale fees used for other social service programs. Using a buy-in premium paid directly to State Medicaid programs would eliminate many of the administrative problems associated with spend-down. Applicants and providers would find the buy-in concept much easier to understand than spend-down, since a buy-in would be similar to an insurance premium. Applicants would no longer have to track their medical expenses and report them to local Medicaid offices in order to successfully spend-down. Finally, applicants would no longer be dependent on the willingness of providers to extend credit before they could spend- down to achieve Medicaid eligibility.
Work is also needed on where the income threshold for Medicaid buy-in is set. The current system involves numerous income thresholds to Medicaid eligibility for children. These thresholds do not fit together logically. The differing thresholds cause substantial equity issues, as well as adverse incentives for families to increase their earned income. We ought to be able to do better in terms of structuring access to Medicaid for low-income children, especially when the children are severely disabled. Since many of the recent Congressional changes to Medicaid eligibility have involved using the poverty level as the income eligibility standard, it may be more consistent to tie State buy-in thresholds to this level as well. Currently, these changes in Medicaid program design can only be made at the Federal level. One option might be to implement these design changes only for children.
3. Controlling the Medicaid Costs of Institutionalized Children Must Continue To Be a High Priority
Study results emphasized the persistent high costs to Medicaid associated with institutionalized children. Policyrnakers might want to consider ways to encourage States to use the available options to provide community-based care for disabled children who would otherwise be institutionalized. Currently, 36 States are using home and community-based waivers to provide disabled children specialized services in a home or community setting. Seventeen States are using the TEFRA option to waive parental deeming of income to their children and provide them cost-effective home care.
Consideration could be given to further steps for encouraging States to use these options, or to develop additional incentives for States to discourage institutionalization. Institutionalized disabled children are one of the most expensive Medicaid groups. They are not likely to become ineligible for Medicaid coverage. Many are likely to remain institutionalized indefinitely. Medicaid will be covering all of their institutional care costs (which average over $30,000 annually) for as long as they live.
The good news with regard to institutionalized disabled children is that this population is not growing. This is true in spite of the fact that Medicaid eligibility policy provides incentives for institutionalization in many States. States have been successful in stabilizing or, in some instances, even lowering the number of children in ICFs/MR, for example. Thus, this is not a group of children for whom Medicaid expenditures are likely to expand.
4. Severely Disabled Children Who Qualify for Medicaid Coverage as a Result of the Supreme Courts Zebley Ruling May Not Be As Expensive to Medicaid as Expected
Study data showed that the vast majority of SSI-related disabled children were not high cost to Medicaid. Indeed, the median annual Medicaid expenditure in California and Georgia for SSI children living at home was about $550 (adjusted to 1989 dollars using the medical care price index). A minority of SSI-related children with extended hospital stays and institutionalized SSI children accounted for the vast majority of Medicaid Expenditures for SSI-related disabled children. Study data provide some parameters for estimating the costs of Medicaid expansions for disabled children under the Zebley decision. It seems likely that most children requiring institutional care are already covered under Medicaid. Thus, analysts should use the median and average costs for SSI children living at home for lower and upper bound estimates of Medicaid expansions to disabled children. This may result in lower costs than were previously predicted for adding new groups of disabled children.
RESEARCH IMPLICATIONS
Subsequent to the time period analyzed in these studies, the Federal government has imposed increased mandates on States to broaden Medicaid coverage for poor infants and children born after September 30, 1983. In addition, several States have elected to expand their coverage of children. For example, since the studies, Georgia has adopted a medically needy program and extended coverage to all Ribicoff children under age 19. Thus, it would be interesting to re- examine high-cost children in the four study States with more recent data to assess the degree to which these mandated and voluntary eligibility changes may have broadened access to Medicaid program coverage, particularly in States with more restrictive Medicaid programs in the past.
Also, the spread of AIDS to children and the increased number of drug exposed infants and children may have changed the profile of severely disabled children significantly since the study time period. An update of the high cost profile would show if the proportion of younger children in the high cost group has become even greater and whether the long-term patterns of high cost infants and younger children have changed, given these more recent developments. There is growing concern that drug exposed infants in particular may require prolonged medical and social assistance.
It would also be helpful to investigate whether the longitudinal patterns of high cost children seen in California apply to other State Medicaid programs as well. We know that California's Medicaid program in 1983 offered more comprehensive benefits and used less restrictive eligibility criteria than other States. We believe that these program differences had an impact on the dynamics of Medicaid coverage for high cost children, but we do not have enough information on the longitudinal experience of high cost children in other States to say this with certainty.
The surprising extent to which non-Medicaid government programs were financing the hospital expenses of all high cost children in California should be explored further. It would be interesting to undertake similar analyses with other State all-payor data bases, such as those in New Jersey or Florida.
Finally, one major policy issue which we were not able to address was the degree to which families are incurring out-of-pocket costs for health care for disabled children. A lot of anecdotal data have been cited which suggest these costs are substantial, but better research is needed. A special survey approach is probably necessary since childhood disability is a relatively rare event affecting only a small percentage of children in the United States.