By:
Embry Howell, Ashley Palmer, and Fiona Adams
Abstract
This review of Medicaid and CHIP risk-based managed care over 2001-2010 shows that well-established programs exist in 19 of the 20 study states. While there is substantial variation across states, all the study states have developed ways to regularly select plans, define network requirements, and monitor access and quality. There is substantial stability in the number and types of plans. HEDIS and CAHPS data suggest that preventive care use has improved and that beneficiaries are generally satisfied with their health plans. Thus, the risk-based managed care programs provide a structure to absorb the newly covered adults under the Affordable Care Act, and provide a learning laboratory and important lessons for other states. [101 PDF pages]
The authors acknowledge the advice and assistance of their project officer, Rose Chu, at the Office of the Assistant Secretary for Planning and Evaluation (ASPE)/DHHS, and of other staff at ASPE and the Centers for Medicare and Medicaid Services who provided advice and comments on the report. We also thank all of the respondents who provided time and data throughout the project; they provided almost all the information in the report. Finally, we thank our colleagues at the Urban Institute. Teresa Coughlin and Brigette Courtot conducted interviews, analyzed information, and reviewed the report. John Holahan provided guidance throughout. Vicki Chen, Matthew Carey, and Maya Joyce provided research assistance, and Eva Hruba prepared the document.
"Executive Summary
Background/Overview - Over the first decade of the 21st century, the role of risk-based managed health care for publicly insured beneficiaries has expanded substantially. This report examines this form of health care delivery in 20 states for both Medicaid and CHIP nonelderly adults and children, including people with disabilities. The 20 states were chosen because they include over 80 percent of both Medicaid and CHIP beneficiaries who are enrolled in risk-based managed care.
Findings are based on interviews with state Medicaid and CHIP officials, as well as representatives from 40 Managed Care Organizations (MCOs) serving Medicaid and CHIP beneficiaries, and 40 health care providers or provider organizations. In addition, the report contains published data from various sources, including measures of access to care, quality of care, and satisfaction with care over the study period (2001–2010).
Program Features - Medicaid and CHIP risk-based managed care programs are highly integrated in most of the study states, with only seven states separating most of the important features of administration for their Medicaid and CHIP risk-based managed care programs, such as plan selection, rate setting, and quality monitoring. Enrollment growth in risk-based MCOs was substantial during the study period, with the largest group—non-SSI Medicaid children—growing by 53 percent and other Medicaid groups—particularly SSI adults and children—experiencing even faster growth rates. Data are not available to measure the rate of CHIP enrollment growth in MCOs.
In spite of this growth, there remained at the close of the decade a substantial number of Medicaid enrollees within the study states who are not mandatorily enrolled in risk-based managed care. For example, only half the states have mandatory enrollment for TANF-related groups statewide, and only six have mandatory enrollment for SSI-related Medicaid beneficiaries statewide. Rural areas are frequently excluded from mandatory risk-based managed care in the study states due to difficulties establishing provider networks and finding plans willing to serve areas with small populations. Most study states have gradually found ways to expand into new parts of the state, with a goal of statewide mandatory enrollment over time. The exception to this pattern among the study states is Connecticut, which eliminated risk-based managed care for Medicaid and CHIP shortly after the end of the study period, citing a preference for a non–risk-based administrative service organization approach with many managed care features.
The lower rate of mandatory enrollment of SSI beneficiaries is due to conflicting opinions across states about how well MCOs can serve vulnerable groups with high mental and physical health needs. Notably, several states have incorporated such groups into risk-based managed care successfully over the entire study period, and other study states are now expanding such enrollment. Still, at the end of the study period, risk-based managed care programs in most study states continued to exclude some of the highest cost groups entirely, including many SSI beneficiaries, the elderly, and the institutionalized.
In addition, it is common to exclude certain services from MCO contracts, either carving them out to separate limited benefit plans or keeping a fee-for-service reimbursement approach. Dental services are the most frequently carved out (15 of 20 study states), and in many states informants believe that special dental plans improve access and that it is less important to integrate such services with medical services. It is also common to carve out behavioral health services (13 study states). However, this carve out is more controversial. Advocacy groups and behavioral health providers are concerned with access and utilization restrictions, although others cite the benefits of integrating physical and behavioral health services. Other common carve outs are pharmacy benefits—often because of the desire to obtain rebates, but also for administrative reasons—and transportation, among other services. When such services are carved out, the state loses some of the benefits of risk-based managed care such as care coordination and the predictability of monthly and annual expenditures for the program.
There is tremendous variation in how states design and administer their risk-based managed care programs. Some of the biggest sources of variation include:
- How states select plans. Most study states use solicitations for proposals and select a subset of bidders (although the periodicity varies), but some (8 states) use any-willing-provider contracting—whereby the state sets the terms and accepts any MCO that meets the terms (for either the Medicaid or CHIP programs, or both).
- How states set rates.
- Contractual requirements for ensuring access to adequate provider networks, with substantial variation across states in their standards, and between Medicaid and CHIP in some states.
- How plans establish and monitor provider networks.
- How states monitor plans’ provider networks.
- The types of quality monitoring conducted by states and plans.
There are trade-offs for states in deciding how many plans to include in their programs, and among the study states this varies widely from only two in some of the smallest states to over 20 in the largest. In addition to the size of the state geographically and in population, another factor is the type of contracting, with any-willing-provider states generally having more plans. States indicate that having more plans can be good, since there is adequate capacity when one or more plans leave the program. It also provides for more leverage for negotiation (for example, to persuade MCOs to operate in rural areas). On the other hand, it is administratively simpler to have fewer plans, and it may enable more frequent communication between the state and the health plans. In addition, market dynamics and negotiations between plans and providers are influenced by the number of health plans that operate in a state or region. Spreading the number of enrollees across a greater number of plans may lead to smaller (in terms of enrollees) and more financially fragile plans, and such plans may be more likely to leave the program due to financial difficulties. This is an advantage of having fewer and larger (often national) plans in the Medicaid and CHIP risk-based managed programs in the study states.
There are 189 MCOs participating in either Medicaid or CHIP risk-based managed care in the 20 study states, with most (147) participating in both programs. These plans are divided across four types: public program only/nonprofit (32.2 percent of Medicaid plans and 42.5 percent of CHIP); public program only/for-profit (20.1 percent of Medicaid plans and 14.9 percent of CHIP); some commercial enrollees/nonprofit (21.8 percent of Medicaid plans and 25.9 percent of CHIP); and some commercial/for-profit (21.8 percent of Medicaid plans and 20.7 percent of CHIP). A mix of different plan types is common across most study states, with a few exceptions. This provides, for some Medicaid and CHIP enrollees, a choice of a variety of types of plans, each with different advantages. For example, we heard that plans that only serve public enrollees often have more experience with the particular needs of low-income beneficiaries, while those with commercial enrollees have more leverage in establishing wider provider networks, among other differences.
Provider Networks - Establishing adequate provider networks can be challenging, especially in rural areas and for rare provider types (such as specialists and hospitals). Some areas have particular shortages of either primary care or specialty providers, or both. Plans use various techniques to persuade providers to participate in their Medicaid and CHIP managed care provider networks. Many providers noted that Medicaid managed care plans may pay more than fee-for-service Medicaid, depending on the location and the market dynamics. In general, we heard that Medicaid MCOs usually pay at or above fee-for-service Medicaid rates, and that CHIP plans often pay somewhat more. In spite of this, providers are often dissatisfied with risk-based managed care programs, although the opinions are not uniform. For example, there is disagreement about whether risk-based managed care improves access for Medicaid and CHIP beneficiaries, and whether it improves quality of care.
Quality of Care - Techniques for monitoring quality of care for risk-based managed care have evolved substantially over the study period. The Balanced Budget Act of 1997and its regulations (released several years later) made it easier for states to expand risk-based managed care but at the same time added requirements for additional oversight of quality of care. The development of the Healthcare Effectiveness Data and Information Set (HEDIS) and Consumer Assessment of Healthcare Providers and Systems (CAHPS) during the decade provided tools for states and plans to use in monitoring quality and satisfaction. All study states mandate that plans collect and submit HEDIS data, and all but one also collect CAHPS data, but there is tremendous variation in the variables they require and the specifications for collecting and reporting those data. Most of the variables measure health care process (e.g., utilization of services) with fewer variables on health outcomes.
We requested HEDIS and CAHPS data from all study states, and we were able to analyze a small number of variables across most states. All are measures of either use of preventive care services or of satisfaction with care. While it is difficult to compare across states and over time due to reporting differences, our analysis shows that the study states with available data have substantially varying rates of preventive care service use, and that measures of preventive care use improved over the decade for Medicaid and CHIP enrollees in risk-based managed care. While we could not measure trends in CAHPS indicators since we collected fewer measures early in the decade, we found generally high satisfaction with care (higher for children than adults). Overall satisfaction with their health plan was higher among Medicaid adults than the national adult commercial benchmark during the last five years of the study period among the 15 reporting states.
Summary - This review of Medicaid and CHIP risk-based managed care over the first decade of the 21st century shows that well-established programs exist in 19 of the 20 study states (Connecticut being the exception) and that most states are seeking to expand their programs to cover more and higher-cost enrollees. While there is substantial variation across states in approaches, all the study states have developed ways to regularly select plans, define network requirements, and monitor access and quality. In contrast to the early years of development of Medicaid managed care, there is substantial stability in the number and types of plans participating in risk-based managed care. HEDIS and CAHPS data also suggest that preventive care use has improved under risk-based managed care and that beneficiaries are generally satisfied with their health plans. Thus, the risk-based managed care programs that currently exist provide a structure to absorb the newly covered adults under the Affordable Care Act and provide a learning laboratory and important lessons for other states in how to develop an effective risk-based managed care program for Medicaid and CHIP beneficiaries.
Introduction
The past ten years have been a period of change for state Medicaid policy and have seen the continued expansion of the Children’s Health Insurance Program (CHIP). Through numerous waivers and new laws, the federal government now provides more freedom for states to experiment with alternative ways of organizing, delivering, and paying for health services. These factors have led to an expansion of comprehensive1 risk-based Medicaid and CHIP managed care programs. In such programs, health plans (Managed Care Organizations, or MCOs) receive a fixed payment per person per month to cover particular health care services, regardless of the services rendered.
Among other reasons, states often implement risk-based managed care programs to help them achieve cost-predictability and possible cost savings. The continuing financial difficulties states have faced associated with the recent recession, along with the expiration of the temporary federal fiscal relief package passed by the American Recovery and Reinvestment Act of 2009, has led states to focus more heavily on cost containment (Smith, Gifford, Ellis, Rudowitz, & Snyder, 2011).
In the past decade, some states implemented new Medicaid managed care programs, while other states expanded existing programs to new counties or populations. In particular, many disabled people were newly included in state Medicaid managed care programs during this period. It is critical to understand these recent changes to state Medicaid and CHIP programs, as enrollment in risk-based managed care is expected to further expand in 2014 as millions gain Medicaid coverage under the Affordable Care Act. This report provides a comprehensive overview of changes to 20 state Medicaid risk-based managed care programs, with a particular emphasis on comprehensive risk-based programs, during an important time in Medicaid’s history.
Evolution of Federal Medicaid Risk-Based Managed Care Policy
Risk-based Medicaid managed care has been used by some states since the 1970s and has become more common over time. Through the late 1990s, it was necessary for states that wanted to enroll Medicaid beneficiaries in risk-based managed care to obtain a waiver from the federal requirement that those beneficiaries have a "freedom of choice" of providers (when enrollment was mandated) and—if their managed care programs were limited to certain geographic areas, as most were at first—from the requirements for "statewideness." These waivers are called 1915b waivers. Another waiver authority, the 1115 waiver, allows a state to reform its Medicaid program in a more extensive way. The 1115 demonstration waivers also were often used to expand Medicaid risk-based managed care programs in the 1990s.
Generally states began their risk-based managed care programs by covering children and parents without disabilities, and states limited the programs to urban and suburban areas. Often states began with voluntary enrollment and transitioned some or all populations to mandatory enrollment in risk-based managed care over time.
Because of policymakers’ high interest in how risk-based managed care affects Medicaid enrollees’ health care outcomes and program costs, in the late 1990s numerous evaluation studies examined Medicaid managed care programs. The evaluations showed mixed findings concerning Medicaid managed care across a variety of states (Coughlin & Long, 2000; Kirby, Machlin, & Cohen, 2003; Brown, Wooldridge, Hoag, & Moreno 2001; Coughlin & Long, 2004).
An increased interest in cost-containment led to an expansion of risk-based managed care in the late 1990s and into the 21st century. Several changes to federal law allowed for such expansions. In particular, the Balanced Budget Act (BBA) of 1997 made it possible for states to implement mandatory risk-based managed care programs without regularly obtaining a federal waiver.
Because concern remained about whether enrollment in risk-based managed care might negatively affect beneficiary access to and quality of care, the BBA required access and quality monitoring of managed care programs through several provisions. These include:
- Each state must hold a service agreement with its managed care plans, in which the state specifies access requirements for provider networks, such as provider proximity to patients, the maximum time patients are expected to travel to see providers, how many providers of each type (e.g., Primary Care Providers [PCPs], specialists, hospitals) must be in the network, how providers should be credentialed, expectations about how soon appointments are available, or expected hours of operation.
- States implementing mandatory Medicaid managed care must have an annual external independent quality review of each plan. BBA regulations promulgated in 2003 required states to contract with an External Quality Review Organization (EQRO). EQROs must be independent organizations experienced with the Medicaid program, managed care, quality assessment, and statistical analysis. The EQRO must validate aggregate quality monitoring data submitted by plans. EQROs may also take on various optional activities, such as validation of encounter data, administration or validation of consumer or provider surveys, and calculation of additional performance measures.
- Generally, when risk-based Medicaid managed care is mandated, beneficiaries must be offered a choice of plans except in rural areas (called the "rural exception").
Another important managed care-related provision in the BBA is the requirement for all states to pay MCOs rates that are "actuarially sound." In particular, states are to develop rates in accordance with actuarial principles that are appropriate for the populations and services covered, and which have been certified by an actuary. The requirement for actuarially sound rates has been in federal statute since 1981, but it was not enforced strictly until the BBA regulations in 2002.
In addition to these BBA-related changes to Medicaid managed care, another source of increased managed care flexibility during the early 2000s was the Health Insurance Flexibility and Accountability (HIFA) waiver program that was introduced in 2001. HIFA originally used 1115 waiver authority to allow states to modify Medicaid benefits and cost-sharing. Savings from these modifications were then to be applied to expanding program coverage to new populations.
Increased flexibility to determine Medicaid benefit packages was later expanded to all states through the Deficit Reduction Act (DRA) of 2006, which succeeded the HIFA waiver program. The DRA allowed states to provide children and other groups with "benchmark" coverage instead of the traditional Medicaid benefit package. Benchmark benefits can be modeled after the Federal Employee Health Benefits Plan, health coverage for state employees, or the largest commercial Health Maintenance Organization (HMO) in the state. Between 2001 and 2008, more than half the states had changed their Medicaid programs through such programs (Coughlin & Zuckerman, 2008).
As a result of the many federal policy actions taken during late 1990s and early 2000s, Medicaid risk-based managed care programs expanded greatly. By 2009, 34 states and the District of Columbia had comprehensive risk-based Medicaid managed care programs, and about half of the nation’s Medicaid population received health care services through risk-based managed care (Medicaid and CHIP Payment and Access Commission [MACPAC], 2011).
The Children’s Health Insurance Program (CHIP)
The BBA of 1997 also brought about a major change in public health insurance coverage for children by creating the Children’s Health Insurance Program (CHIP), which was initially authorized and appropriated through 2007, subsequently extended in 2009. With joint federal-state funding, states are allowed to set up a program to enroll children from families with higher income levels than Medicaid into public health insurance. States may expand the Medicaid program they already have in place, create a separate CHIP program, or have a combination of both approaches. This choice affects the states’ options in terms of program administration, required benefits that must be offered, eligibility, documentation requirements for enrollees, and cost sharing. States choosing to run Medicaid expansion programs with their CHIP funding are subject to federal Medicaid rules; separate CHIP programs are subject to somewhat different federal CHIP rules. In addition, states with separate programs may cap enrollment in CHIP, while Medicaid expansion programs cannot. Finally, states received an enhanced matching rate for CHIP expenditures when compared to the Medicaid match.
Because CHIP was implemented at about the same time that risk-based managed care was being expanded widely for Medicaid-enrolled children, many states chose to use risk-based managed care as the dominant delivery model for their CHIP programs as well (Hill, Harrington, Bajaj, Black, Fasciano, Howell, et al., 2003). However, there has been little study of how managed care programs operate under CHIP.
The CHIP program was reauthorized through the Children's Health Insurance Program Reauthorization Act (CHIPRA) in 2009 and appropriated through 2015. Before CHIPRA, there was less federal oversight of CHIP risk-based managed care programs than for Medicaid. The 2009 legislation, however, brought the federal requirements of the two programs closer together by mandating, for example, the use of EQROs, a choice of MCOs, and a uniform core set of voluntary performance measures. However, some differences remain between federal Medicaid and CHIP managed care program requirements. For example, there is no mandate that capitation rates be actuarially sound under CHIP.
The Affordable Care Act
The Affordable Care Act, passed on March 23, 2010, includes unprecedented expansions in access to health coverage starting in 2014; it also mandates that most Americans have health insurance beginning in that year. The Affordable Care Act’s two primary means of expanding coverage are (1) an expansion of Medicaid to all individuals under age 65 and not enrolled in Medicare, with family incomes under 138% of the federal poverty level (FPL); and (2) establishment of a tax credit subsidy program to help individuals in the individual and small group markets with family incomes up to 400% of FPL obtain coverage through new Health Insurance Exchanges. The Affordable Care Act will lead to a large influx of enrollees into Medicaid, primarily consisting of adults who are newly eligible for the program. Estimates suggest that about 16 million newly eligible people will enroll in Medicaid or CHIP by 2019 because of the Affordable Care Act (Holahan & Headen, 2010). Given the prevalence of managed care for existing Medicaid enrollees, most Affordable Care Act expansion enrollees are likely to be enrolled in risk-based managed care programs in 2014. In some states, this new influx may cause strains on the MCOs and their associated providers, as they try to serve many new beneficiaries with unmet health needs.
Purpose of This Study
This study is designed to provide new information on the evolution of comprehensive risk-based Medicaid and CHIP managed care programs for acute care over the first decade of the 21st century, in order to develop lessons learned for states and the federal government as they jointly prepare to serve the new populations eligible for Medicaid via the Affordable Care Act expansion. This study is important because there has been less study of Medicaid risk-based managed care in the recent decade than in the 1990s, and because there has been almost no description of the risk-based managed care used by separate CHIP programs.
The study builds on results from two other recent papers describing Medicaid managed care, one by Gifford, Smith, Snipes, & Paradise (2011) and one by the Medicaid and CHIP Payment and Access Commission—MACPAC (2011). The results from this study complement those efforts. Both of those papers provide point-in-time descriptions of Medicaid managed care in 2010, while this study explores how managed care programs have evolved over the past decade and why states have chosen to design their managed care programs in the ways that they have. This study also includes CHIP, examines the perceptions of a wider range of informants (including providers and health plan representatives), and produces new data on quality of care measures in both programs. In addition, a companion report will provide information on trends in capitation rates for risk-based Medicaid and CHIP managed care programs.
The principal research questions addressed in this report are:
- How do Medicaid and CHIP risk-based managed care approaches vary across states, and how have these Medicaid and CHIP managed care approaches varied over time?
- How do Medicaid and CHIP programs monitor access to and quality of care, and what have been the results?
- Synthesizing across all study state experiences, what are the best practices in state Medicaid and CHIP managed care? What implications do these state experiences have for the 2014 Medicaid expansion included in the Affordable Care Act?
Methods
This cross-state study of Medicaid/CHIP risk-based managed care uses a case study approach to investigate changes in programs over the period 2001–10. The study is focused on risk-based Medicaid and CHIP programs in 20 states: Arizona, California, Connecticut, Delaware, Florida, Maryland, Massachusetts, Michigan, Minnesota, New Jersey, New Mexico, New York, Ohio, Pennsylvania, Rhode Island, Tennessee, Texas, Virginia, Washington, and Wisconsin.
| State | Total Medicaid MCO Enrollment (in thousands) | Percent of State Total Medicaid Enrollment | Percent of Total U.S. Medicaid MCO Enrollment |
|---|---|---|---|
|
Source: Gifford et al., 2011. Note: Medicaid includes enrollment in CHIP Medicaid expansion programs (M-CHIP). |
|||
| California | 4,079 | 55.0 | 15.3 |
| Delaware | 142 | 74.0 | 0.5 |
| Florida | 1,287 | 45.3 | 4.8 |
| Maryland | 685 | 73.9 | 2.6 |
| Massachusetts | 513 | 39.2 | 1.9 |
| Michigan | 1,251 | 68.1 | 4.7 |
| Minnesota | 477 | 66.3 | 1.8 |
| New Jersey | 974 | 95.0 | 3.6 |
| New Mexico | 335 | 68.0 | 1.3 |
| New York | 3,002 | 62.5 | 11.2 |
| Ohio | 1,730 | 85.9 | 6.5 |
| Pennsylvania | 1,222 | 58.5 | 4.6 |
| Rhode Island | 134 | 75.3 | 0.5 |
| Tennessee | 1,219 | 100.0 | 4.6 |
| Texas | 1,698 | 48.9 | 6.4 |
| Virginia | 527 | 62.1 | 2.0 |
| Washington | 627 | 54.2 | 2.3 |
| Wisconsin | 624 | 54.2 | 2.3 |
| Subtotal | 22,127 | 61.9 | 82.7 |
| All Other States | 4,613 | 25.4 | 17.3 |
| Total U.S. | 26,740 | 49.6 | 100.0 |
The study states are shown in Table 1. We primarily selected states for participation on the basis of having either a large number of people covered by risk-based Medicaid managed care programs, a large proportion of the state’s Medicaid population in risk-based managed care, or both. This allows for the inclusion of some more populous states that cover a relatively smaller proportion of the state’s Medicaid population under risk-based managed care (such as Florida and Texas, which each cover about half), as well as some less populous states that enroll a relatively large proportion of their Medicaid population in risk-based Medicaid managed care (such as Delaware, New Mexico, and Rhode Island). We also sought regional variation and have included at least four states from each of the four major census regions.
As shown in the table, the 20 study states account for just over 80 percent of the nationwide Medicaid enrollment in risk-based managed care in 2010. Across the 20 states, just over 60 percent of Medicaid enrollees are in comprehensive risk-based managed care, much higher than the non-study states, for which only 25.4 percent of their Medicaid population is enrolled in risk-based managed care.
At the time we selected states, there was not yet a source of data on the number of CHIP enrollees in risk-based managed care. When those data were published (MACPAC, 2011), it became evident that the study states report a similar proportion of CHIP enrollees in risk-based managed care as for Medicaid.
Data in this report come from five sources:
- Published Data: We obtained published data from several existing sources such as the CMS web site, state web sites, the Kaiser State Health Facts web site, the Kaiser Commission/HMA report (Gifford, et al., 2011), and the MACPAC report (2011).
- In-Person and Telephone Interviews: During January–November 2011, we conducted interviews with state Medicaid officials in person in 11 states and by telephone in nine states. For states where CHIP risk-based managed care programs are administered by a separate organization or unit of government, we interviewed those officials separately. We also conducted telephone interviews with representatives from two health plans per state and two providers or provider associations per state. Table 2 shows the number of plan and provider interviews by type of plan or provider. Thus, there were at least five interviews per state, or over 100 interviews in all. The full list of interviewees is contained in Appendix A.Interviews were conducted using a semistructured protocol, which is available on request.
| Number | ||
|---|---|---|
| Plans | Non-profit | 20 |
| For profit | 20 | |
| Total | 40 | |
| Providers | Medical Associations | 13 |
| Family Physicians Association | 1 | |
| Pediatric Association | 1 | |
| Individual Physicians | 3 | |
| Individual Dentist | 1 | |
| Hospital Associations | 13 | |
| Hospital Systems | 2 | |
| Community Health Center Associations | 6 | |
| Total | 40 | |
- Access and Quality Performance Measures: We requested and obtained Healthcare Effectiveness Data and Information Set (HEDIS)2 and Consumer Assessment of Healthcare Providers and Systems (CAHPS)3 data for at least one year, and usually multiple years, on a common cross-state set of performance measures for Medicaid and CHIP managed care programs. Some states provided plan-specific measures, which we used to create a statewide average weighted by plan enrollment.
- Model Contracts between the State and Its Health Plans: We analyzed contracts to identify state requirements regarding appointment wait times, provider/ enrollee ratios, and geographic proximity requirements.
- Medicaid Statistical Information System (MSIS): We used person-level data from the MSIS summary file to estimate enrollment in comprehensive risk-based Medicaid managed care programs by type of enrollee and year.
Key informant interviews were transcribed and the transcripts were coded with NVIVO qualitative analysis software, using a coding structure referring to the most important interview questions and topics covered, allowing for a cross-state analysis of common themes across topics. The transcripts were also used to provide selected quotes throughout the report in the voice of respondents. However, to protect respondent confidentiality, we do not directly attribute quotes or opinions to specific individuals. Factual information, either from reports or interviews, was verified with state contacts.
We obtained broad information on Medicaid and CHIP risk-based managed care programs, including limited-benefit plans (e.g., plans covering only behavioral health services or dental services) and integrated care plans that include long-term care for those dually enrolled in Medicaid and Medicare. However, due to resource and time limitations, we focus the investigation most closely on comprehensive benefit plans for acute care and programs for the nonelderly, non–dual eligible population.
Findings
Integration between Medicaid and CHIP Risk-Based Managed Care
Before describing Medicaid and CHIP risk-based managed care in the study states, it is necessary to explain the level of integration between their risk-based managed care programs. This is because in most states they are either completely or highly integrated.
There are several distinct factors that affect the degree to which risk-based managed care in the two programs is distinguishable (see Figure 1). Of the 20 study states, 6 have Medicaid expansion programs for CHIP (Maryland, Minnesota, New Mexico, Ohio, Rhode Island, and Wisconsin), and so the risk-based managed care programs are identical for Medicaid and CHIP enrollees. Tennessee (which has a combination CHIP program) does not have risk-based managed care for CHIP, though it does operate a risk-based program for Medicaid.
Figure 1: Integration between Medicaid and CHIP Risk-Based Managed Care Programs
in Study States, 2010
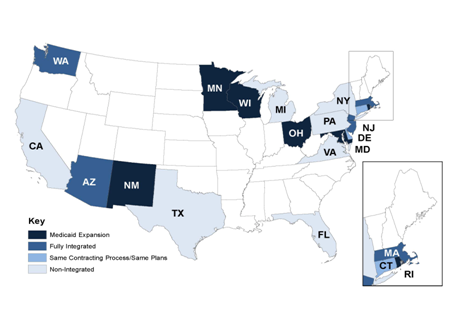
Source: Interviews with state officials.
Note: More information on the integration of Medicaid and CHIP risk-based managed care is contained in Appendix B, Table 1.
| State | Total Medicaid MCO Enrollment (in thousands) | Percent of State Total Medicaid Enrollment | Percent of Total U.S. Medicaid MCO Enrollment |
|---|---|---|---|
|
Source: Interviews with state officials. Note: More information on the integration of Medicaid and CHIP risk-based managed care is contained in Appendix B, Table 1. |
|||
| Arizona | 1,210 | 89.2 | 4.5 |
| Connecticut | 391 | 58.0 | 1.5 |
| California | 4,079 | 55.0 | 15.3 |
| Delaware | 142 | 74.0 | 0.5 |
| Florida | 1,287 | 45.3 | 4.8 |
| Maryland | 685 | 73.9 | 2.6 |
| Massachusetts | 513 | 39.2 | 1.9 |
| Michigan | 1,251 | 68.1 | 4.7 |
| Minnesota | 477 | 66.3 | 1.8 |
| New Jersey | 974 | 95.0 | 3.6 |
| New Mexico | 335 | 68.0 | 1.3 |
| New York | 3,002 | 62.5 | 11.2 |
| Ohio | 1,730 | 85.9 | 6.5 |
| Pennsylvania | 1,222 | 58.5 | 4.6 |
| Rhode Island | 134 | 75.3 | 0.5 |
| Tennessee | 1,219 | 100.0 | 4.6 |
| Texas | 1,698 | 48.9 | 6.4 |
| Virginia | 527 | 62.1 | 2.0 |
| Washington | 627 | 54.2 | 2.3 |
| Wisconsin | 624 | 54.2 | 2.3 |
| Subtotal | 22,127 | 61.9 | 82.7 |
| All Other States | 4,613 | 25.4 | 17.3 |
| Total U.S. | 26,740 | 49.6 | 100.0 |
This leaves 13 study states with either a combination CHIP program (California, Delaware, Florida, Massachusetts, Michigan, New Jersey, and Virginia) or a separate CHIP program (Arizona, Connecticut, New York, Pennsylvania, Texas, and Washington). While these 13 states all have some component of CHIP that is officially defined as "separate" from Medicaid, study results show that the risk-based managed care operations are integrated for these separate programs with Medicaid in six states (Arizona, Connecticut, Delaware, Massachusetts, New Jersey, and Washington). In these integrated states the same agency administers risk-based managed care for both CHIP and Medicaid, the contracting process is the same, and the plans are chosen together and are identical for both programs. Further, in all but two of these integrated states (Connecticut and Delaware), the capitation rates paid to plans on behalf of Medicaid and CHIP enrollees are also the same. Consequently, in the remainder of the report, we separately discuss CHIP risk-based managed care for only seven states (California, Florida, Michigan, New York, Pennsylvania, Texas, and Virginia), while findings for the CHIP risk-based managed care programs are generally integrated with those for Medicaid managed care programs in the remaining states.
| State | CHIP MCO Enrollment (in thousands) |
|---|---|
|
Source: MACPAC, 2011. Note: M-CHIP children are excluded from counts. |
|
| California | 1,175 |
| Florida | 386 |
| Michigan | 48 |
| New York | 539 |
| Pennsylvania | 273 |
| Texas | 928 |
| Virginia | 75 |
| Total | 3,424 |
Separate CHIP program risk-based managed care enrollment in these seven states is shown in Table 3. In 2010, about 3.4 million children were enrolled in risk-based MCOs in these seven states’ separate CHIP programs. This is 76 percent of all CHIP enrollees in risk-based managed care (MACPAC, 2011). Consequently, the experience of these seven states provides a good picture of how CHIP managed care programs operate when separated from Medicaid.
Voluntary and Mandatory Enrollment in Risk-Based Managed Care
re is substantial variation within and across states with regards to whether enrollment in risk-based managed care programs is mandatory or voluntary. Typically, managed care enrollment requirements vary by enrollee category.
Medicaid TANF-Related Beneficiaries. Figure 2 shows whether a state had mandatory or voluntary enrollment in risk-based Medicaid managed care for 2010 in the 20 study states for adults and children whose eligibility for Medicaid is related to their eligibility for the Temporary Assistance for Needy Families (TANF, or cash assistance) program or who meet other poverty-related eligibility criteria (called "TANF-related" enrollees throughout the remainder of the report). The figure shows states according to whether they require TANF-related groups to enroll in risk-based managed care on a statewide basis or only in certain regions, or whether risk-based Medicaid managed care enrollment is only voluntary in all of the state.
Figure 2: Type of Medicaid Enrollment in Risk-Based Managed Care for TANF and
Poverty-Related Adults and Children in Study States, 2010
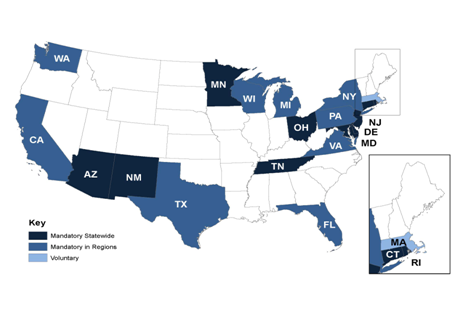
Source: Documents and interviews with state officials.
As of 2010 in the study states, risk-based managed care enrollment for TANF and poverty-related adults and children is mandatory statewide in ten (Arizona, Connecticut, Delaware, Maryland, Minnesota, New Jersey, New Mexico, Ohio, Rhode Island, and Tennessee ), mandatory by geographic region in nine (California, Florida, Minnesota, New York, Pennsylvania, Texas, Virginia, Washington, and Wisconsin ), and voluntary in one (Massachusetts). Massachusetts has chosen to allow TANF-related enrollees to select a Primary Care Case Management (PCCM)4 program as an alternative to risk-based managed care statewide, and approximately 40 percent do so.
Medicaid SSI-Related Beneficiaries. As shown in Figure 3, there is a different pattern of enrollment for non-institutionalized, nonelderly Medicaid enrollees with disabilities whose Medicaid eligibility is based on their eligibility for the Supplemental Security Income (SSI) program or who meet other disability-related eligibility criteria (called "SSI-related" throughout the report). While half the states mandate enrollment for SSI-related groups, either statewide or by region, six states (Massachusetts, Minnesota, Ohio, Texas, Washington, and Wisconsin) have voluntary enrollment for all SSI-related beneficiaries.5 In addition, four states have different enrollment requirements for SSI-related adults and children, as follows:
- Connecticut: Enrollment for SSI-related children is mandatory statewide, but SSI-related adults are excluded completely from risk-based managed care.
- Ohio: Enrollment for SSI-related children is voluntary, while SSI-related adults are mandatorily enrolled statewide.
- Texas: Enrollment for SSI-related children is voluntary, while SSI-related adults are mandatorily enrolled by region.
- Washington: SSI-related children are excluded completely, while SSI-related adults are enrolled on a voluntary basis in one county, and excluded in others.
Figure 3: Type of Medicaid Enrollment in Risk-Based Managed Care for SSI Adults and Children in Study States, 2010
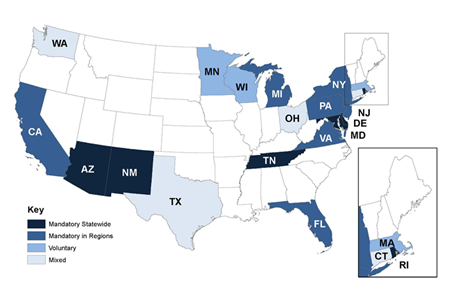
Source: Documents and interviews with state officials.
Note: 1 SSI-related children differ from adults; see text for explanation
| State | TANF Children | TANF Adults | SSI Children | SSI Adults |
|---|---|---|---|---|
|
Source: Documents and interviews with state officials. Note: SSI-related children differ from adults; see text for explanation |
||||
| Arizona | MS | MS | MS | MS |
| Connecticut | MS | MS | MS | EXCL |
| California | MR | MR | MR | MR |
| Delaware | MS | MS | MS | MS |
| Florida | MR | MR | MR | MR |
| Maryland | MS | MS | MS | MS |
| Massachusetts | V | V | V | V |
| Michigan | MR | MR | MR | MR |
| Minnesota | MS | MS | V | V |
| New Jersey | MS | MS | MR | MR |
| New Mexico | MS | MS | MS | MS |
| New York | MR | MR | MR | MR |
| Ohio | MS | MS | EXCL | MS |
| Pennsylvania | MR | MR | MR | MR |
| Rhode Island | MS | MS | MS | MS |
| Tennessee | MS | MS | MS | MS |
| Texas | MR | MR | V | MR |
| Virginia | MR | MR | MR | MR |
| Washington | MR | MR | EXCL | V |
| Wisconsin | MR | MR | V | V |
Informants in several states noted that advocacy groups play an important role in determining whether SSI-related enrollees are offered a choice regarding enrollment in risk-based Medicaid managed care. In some cases (e.g., recently in Massachusetts), advocates have been supportive of the improved coordination of care that managed care can bring, and in some (e.g., Connecticut and New Jersey) they have been opposed because of the potential for reduced access.
Advocates were concerned with managed care organizations being able to handle and understand the SSI-related population, since MCOs were more used to a commercial population. (State Official)
CHIP Beneficiaries. While not shown separately, the pattern of mandatory and voluntary enrollment for CHIP children follows that of TANF-related Medicaid enrollees in most study states. The seven states cited above with very separate Medicaid and CHIP risk-based managed care programs all mandate enrollment in CHIP managed care on a statewide basis, except for Virginia, where mandatory enrollment follows the Medicaid pattern geographically. Two of the states (California and Florida) exclude children with special health care needs from mandatory enrollment, but the others do not.
Trends in Enrollment in Risk-Based Managed Care
Figure 4 shows the growth in comprehensive risk-based Medicaid managed care enrollment in the 20 study states from 2001 to 2010 for children and nonelderly adults, separately for TANF-related and SSI-related enrollees. Since there are no uniform nationally available published statistics on enrollment in MCOs for these four groups, we estimated enrollment using data from the Medicaid Statistical Information System, which provides an annual estimate of spending on managed care services for individuals. Enrollment in comprehensive risk-based managed care is estimated by counting everyone enrolled in Medicaid in the year, according to their age and eligibility group, who had managed care expenditures of $2006 or greater for the year.
Figure 4: Enrollment in comprehesive Risk-Based Managed Care
in Study States, 2001-2010 (in millions)
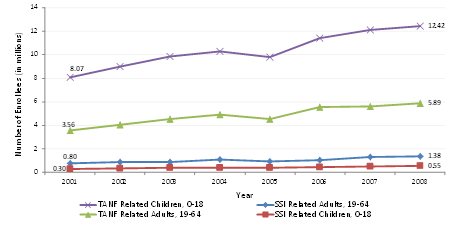
Source: Medical Statistical Information System.
Note: Excludes M-CHIP. More information on enrollment is contained in appendix B, table 2.
Enrollment in risk-based Medicaid managed care grew throughout the study period. The largest group is TANF-related children, with 8.1 million enrollees at the beginning of the period and 12.4 million by 2008, a 53 percent increase (in contrast to only a 29 percent increase in children’s enrollment in Medicaid overall—data not shown). The increase for TANF-related adults was even greater, 64 percent, and especially high for the SSI- related groups at 82 percent for children and 73 percent for adults. However, the increases for SSI-related groups are from a small base and their enrollment remains small relative to TANF-related enrollment.
In each of the study states, Medicaid mandatory risk-based managed care enrollment began in the 1990s or before but generally only in certain parts of the state, and it most often was mandatory only for TANF-related groups initially. There were exceptions, however. For example, Arizona, Delaware, New Mexico, and Tennessee operated statewide programs and enrolled the disabled on a mandatory basis from the beginning. Several other states (Maryland, Minnesota, Pennsylvania, and Virginia) began only in selected geographic areas, but they included the disabled in mandatory risk-based managed care from the beginning of the program.
Study informants observed that one reason their state began with the TANF-related population is that these groups of adults and children tend to have fewer and more predictable health needs, and thus it is easier to set capitation rates correctly, which leads to fewer problems financially for the plans. Informants noted that early on in Medicaid managed care, plans generally did not have the right types and mix of providers to adequately care for individuals with more complex mental and physical health needs. One state (Tennessee) noted that it is also more politically palatable to begin managed care with a TANF-related population. The main reason for not beginning statewide was that it was difficult to find plans willing to serve in rural areas. Informants in some states reported that this is still a problem.
While the SSI-related population enrolled in Medicaid risk-based managed care remains very small relative to TANF-related and poverty-related groups—even by the end of the study period—it is a group that is of high policy interest because of high health needs, high needs for care coordination, and high cost. Informants noted that early on in Medicaid managed care, plans generally did not have the right types and mix of providers to adequately care for individuals with more complex mental and physical health needs, but gradually plans have learned how better to address those needs. We also heard that the care coordination functions that MCOs adopt often improve the care process for SSI enrollees, over and above the fee-for-service delivery system. It is notable that we did not hear of any serious problems concerning incorporating SSI groups into Medicaid managed care in the 20 study states during the study period, although we did not interview beneficiaries or advocacy groups.
Most state officials indicated that they began at a small scale and gradually expanded their Medicaid risk-based managed care programs. Most state officials expressed a goal of expanding their programs statewide. For example, in New York mandatory risk-based managed care enrollment began in New York City and spread upstate, first for TANF-related and then for SSI-related groups. The state is nowin the process of moving to statewide mandatory risk-based managed care for all program enrollees including those dually eligible for Medicare and Medicaid and those receiving institutional services, both groups that generally have been excluded from Medicaid managed care nationwide in the past.
This process of expansion of risk-based Medicaid managed care is continuing today in each of the study states but one (Connecticut), a major exception to the pattern of continued expansion of Medicaid risk-based managed care. Connecticut gradually dismantled its Medicaid risk-based managed care program over the past few years by carving out more and more services (beginning with behavioral health in 2006, then pharmacy and dental services in 2008) and has completely replaced risk-based managed care with an Administrative Services Organization (ASO) model as of January 2012. Under this new approach, Connecticut outsources claims processing and contracts with a health plan on a non-risk basis for utilization management, disease management, and member services functions. The state is also planning to establish medical homes, and eventually accountable care organizations, as part of its approach. According to informants, many factors were at play in the state’s decision. These included a desire to achieve cost savings through administrative efficiencies, criticism of the risk-based managed care program’s ability to coordinate care for beneficiaries with complex needs, a strong advocacy community that viewed the program as a means for MCOs to profit by denying care, and a weak relationship between providers and MCOs. Moreover, the state had already adopted the ASO model for carved-out services (e.g., behavioral health) and described that move as very successful.
Two states that implemented mandatory statewide risk-based managed care for both TANF- and SSI-related Medicaid enrollees from the beginning of their program, Arizona and Tennessee, have had contrasting experiences. Arizona has a long-running risk-based Medicaid managed care program dating back to 1982 (McCall, 1997). The state has sustained the original program structure for over 25 years, and state officials attribute its continuity to a collaborative approach with plans and the availability of good data to be used for rate setting and monitoring, among other factors.
In contrast, Tennessee began statewide enrollment in risk-based Medicaid managed care for all Medicaid enrollees in 1994. While an early evaluation showed some positive outcomes for enrollees at the start of the program (Ku, Ellwood, Hoag, Ormond, & Wooldridge, 2000), according to state officials, by the late 1990s the program began to experience financial difficulties, caused by a higher cost per person than budgeted. There were other factors leading to problems retaining plans, including the state’s and the health plans’ lack of experience with managed care and numerous legal actions. Consequently, Tennessee discontinued the risk-based component of their Medicaid program for five years from 2002 to 2007, gradually moving from full-risk to partial-risk, then no-risk, and back to partial- and full-risk; the program is now reinstituted statewide as of January 2009. State officials express the opinion now that it would have been better to start implementation more slowly, which they did when they began to phase risk-based managed care back to Medicaid, beginning with Tennessee’s middle region in 2007.
Even when a state fully intends to move to statewide mandatory enrollment in risk-based managed care, there are several groups that present particular difficulty according to study informants, including the following:
- The rural population: States have struggled to develop an interest on the part of plans in including residents of very rural areas. Many states have areas that are not served by an MCO. This is because it is difficult to develop an adequate provider network there, especially for specialists. Some states—e.g., Arizona, California (CHIP), Florida (CHIP), Michigan, New Mexico, and Tennessee—have succeeded in including such areas, but most other states are not yet doing so.
- Children with special health care needs: Often, seriously emotionally disturbed and other disabled children, as well as foster care children, are excluded because of their specialized needs.
- Dual enrollees: Those entitled to both Medicare and Medicaid are difficult to include because their primary payer is Medicare for most acute-care services, so it is more difficult to establish an accurate capitation rate for Medicaid services only.
- Long-term institutionalized enrollees: It is hard to reap the benefits of risk-based managed care through deinstitutionalization and home-based services once someone has been in an institution and has given up their home.
- Spend-down enrollees: These individuals must spend a certain amount per month before they are eligible for Medicaid to cover their remaining health expenses in the month. Because of the way they obtain Medicaid coverage, it can be difficult to develop an appropriate capitation rate for such individuals.
- New enrollees: For a short period of time just after enrolling in Medicaid but before plan enrollment, it is necessary to pay for services for these individuals on a fee-for-service basis, unless the state has a waiver of retroactive eligibility and enrolls persons into plans as soon as they become eligible.
- Pregnant women: Pregnancy is a high-cost, short-term condition. Also, many women are enrolled only for their pregnancy. Many states have chosen to pay for such services on a fee-for-service basis or with a special capitated fee.
- American Indians: Many American Indians are entitled to services from the Indian Health Service and typically are not included in states’ Medicaid managed care efforts.
Most of these excluded groups have high average costs to Medicaid. Generally (but with some exceptions), these small but high-cost groups remain excluded, even in these 20 states with the most experience with risk-based managed care. This, combined with the lack of mandatory enrollment of the SSI-related groups in many states, has meant that states have yet to bring most of the highest cost groups into risk-based managed care.
Program Services Included in Risk-Based Managed Care
In addition to great variety in the populations and geographies that are mandatorily and voluntarily enrolled in risk-based managed care, another way that state programs vary is in the services that are included in comprehensive risk-based MCOs.7 In particular, states may carve out services from their risk-based managed care contracts. These services are then either contracted out to a separate, limited benefit plan or provided through fee-for-service arrangements.
States may vary the geographies or populations for which these carve-outs apply. For example, a state may carve out dental services in certain regions of the state, while elsewhere dental services are "carved in" to MCO’s contracts. Or a state may carve out the pharmacy benefit for the SSI-related population but not for the TANF-related population. Also, the state may give the health plan the option of "carving in" a particular service to their contract or leaving it out (in which case the beneficiary usually receives the service through fee-for-service). Capitation rates are adjusted accordingly.
The most commonly carved out services in Medicaid managed care programs include dental services, behavioral health (mental health and substance abuse treatment), drugs, and transportation (Gifford et al., 2011). Among the 20 study states, for Medicaid:
- Fifteen carve out dental services.
- Thirteen carve out inpatient behavioral health (but only eight carve out detoxification).
- Eleven carve out outpatient behavioral health.
- Ten carve out non-emergency transportation.
- Nine carve out prescription drugs.
Among the seven separate risk-based managed care CHIP programs in the study states:
- Five carve out dental services.
- One carves out behavioral health.
There are some other carve-outs that are more variable in definition and less common, such as for personal care services, therapies, and transplants. In addition to these carve-outs, some services (such as adult dental services) may be excluded from Medicaid coverage altogether. That is, an MCO may not include a benefit not because of a carve-out but simply because the state does not offer it as a covered Medicaid benefit. This applies to Early Periodic Screening, Diagnosis, and Testing (EPSDT)8 benefits, mandated for Medicaid but not for CHIP, which are excluded from separate CHIP MCO contracts but included for Medicaid MCO contracts.
| Service | Reasons to Carve Out | Reasons to Carve In |
|---|---|---|
| Source: Interviews with state officials. | ||
| Dental |
|
|
| Prescription Drugs |
|
|
| Behavioral Health |
|
|
Table 4 summarizes some of the reasons cited in conversations with states regarding their decisions to carve in or carve out dental services, behavioral health, or pharmacy services. Many factors are considered by states deciding whether to carve services out of or into MCO contracts. Carving in services may facilitate better care coordination (for example, coordination between physical and mental health needs). On the other hand, when services are carved out to a separate plan, quality of care may improve when the organization has more experience providing the service.
Dental Services.
The most common services that states reporting carving out are dental services. Consistently states that carve out dental services stated that the primary reason is to improve service provision since MCOs typically do not have experience with these services.
Dental wasn’t necessarily the MCO’s core competency, so we carved it out, and it’s been running well. (State Official)
We had problems with access for dental services for kids, so we engaged a third-party administrator to focus on dental. We think it is better managed as a single program with a single vendor. (State Official)
Behavioral Health.
Study states have experimented with a variety of arrangements for behavioral health. For example, it is common to use a "partial carve-out." In that circumstance, a certain number of visits or inpatient days are included in the risk-based managed care contract, and the rest are carved out to a special plan or to fee-for-service. For example, in the state of Washington, 20 outpatient mental health visits may be covered by the MCO, and any use beyond that is carved out. In several states (e.g., California and Michigan) the behavioral carve out is diagnosis driven, with conditions that can be treated in a primary care office being carved in, but other more serious conditions (e.g., Serious Emotional Disturbance) being carved out to a limited-benefit behavioral health plan. The advantages of this are expressed by a state official below concerning children’s mental health needs.
If there are mental health needs that the plan physician determines may not be seriously emotionally disturbed (SED), the plan provides the service. If the child is SED, then they send the child to county mental health services. (State Official)
According to those with whom we spoke, carving in some mental health services can improve access to mental health services for those with mild and moderate conditions.
One of the major reasons for having SSI-related adults in managed care for mental health services is that there was such a paucity of access in fee-for-service. There was no access for people who didn’t have serious mental health needs. When we carved mental health in, that became one of the big winners. (State Official)
On the other hand, we heard the countervailing opinion that carving in mental health services could restrict access, especially for those with intensive needs.
I think that historically there has been concern with the plans’ ability to treat more vulnerable, high-intense behavioral health populations. There are some [local] facilities that feel that managed care and their process of authorizing and denying care is not conducive to these populations and their needs. They have lobbied very strongly for these populations to be carved out. (State Official)
This opinion is associated with political pressure by state and local authorities who are concerned that their behavioral health programs may lose clients and potential funding.
We’re trying to get over the political hurdles of those in the community who want to make sure all the dollars go to behavioral health authorities. (State Official)
The political will has not been there to expand behavioral health as a managed care model because the community mental health centers want to get fee-for-service patients. (State Official)
However, carving out behavioral health, especially when it is paid fee-for-service, is another factor in limiting a state’s ability to use risk-based managed care as a cost-control mechanism, according to study informants.
I want to put the incentive on the plan for them to manage people that are high cost and high need who are going in and out of hospitals and institutions. (State Official)
Prescription Drugs.
Another common carve-out from risk-based managed care is prescription drugs. Until this year, states have carved out prescription drugs to fee-for-service to collect the manufacturers’ drug rebates. Pre–Affordable Care Act federal law stipulates that drug manufacturers that want their drugs covered by Medicaid must give rebates to federal and state governments. At the state level, these rebates were previously only allowed to be collected for drugs purchased on a fee-for-service basis; drugs covered by Medicaid managed care organizations were not eligible for rebates. The Affordable Care Act authorizes Medicaid Drug Rebate Equalization, which became effective in April 2010. This provision potentially extends drug rebates to MCOs. State officials in several states (e.g., Delaware, New Jersey, New York, Ohio, and Texas) indicated that consequently they are considering carving pharmacy back into their contracts with MCOs and adjusting capitation rates accordingly.
When pharmacy is carved out, it is frequently carved out to a pharmacy benefits manager (which may or may not take on risk) or to fee-for-service. In addition, certain specific types of drugs may be carved out from MCO contracts; examples include behavioral health drugs and HIV/AIDS drugs. Another reason to carve out pharmacy services is to have a single preferred drug list for the state’s Medicaid program. This simplifies the prescribing process for providers, who then only have to refer to a single list of preferred drugs.
Contracting with Managed Care Organizations
States have developed a variety of ways to contract with the MCOs that serve their Medicaid and CHIP enrollees. Generally, state officials indicate that they strive to ensure that:
- Beneficiaries have a choice of plans
- There is competition among plans
- Plans have enough enrollees and are stable financially
- Plans provide high-quality services
- All beneficiaries have adequate access geographically to all contracted services
The list of participating plans is relatively stable over time, so that state officials and plans can develop a good, collaborative working relationship.
Informants acknowledge that meeting all these criteria is very difficult, and finding the right number and mix of plans is challenging. This is especially true for states with a small enrollee base and for rural areas where plans do not have a large number of providers from which to build a network. However, representatives from the study states on the whole express satisfaction with the MCOs with which they contract.
Procurement Approaches.
Federal requirements are not very specific concerning how Medicaid or CHIP programs select their risk-based MCOs. Study results reveal that states have developed two basic contrasting methods (with variations on these two themes). The first is competitive contracting, whereby states have a periodic solicitation for plans, request proposals, and select plans to participate based on these proposals. A plan’s response to the state’s solicitation may be both a technical response and a price bid, or only a technical response (in which case the state would set or negotiate the plan’s capitation rate). For example, the technical response would specify which parts of the state and populations the plan proposes to serve and how it will meet the state’s quality and network adequacy standards. States do not necessarily take all bidders with this approach.
A second approach is any-willing-provider contracting. With this approach, the state provides the contract terms and requirements, and sets an actuarially sound rate range of rates within rate cells such as age groups or geographic regions. Any health plan meeting those requirements and willing to provide the contracted services within the rate range may do so.
Appendix B, Table 3 indicates which of the study states are using each type of contracting approach for their Medicaid and CHIP programs in 2011. The competitive approach is used in all but five study states (Florida, Maryland, Minnesota, New Jersey, and Virginia) for Medicaid. California also uses a competitive process except for its County Organized Health System (COHS) counties.9 Wisconsin uses a competitive approach only in one region of the state, with any-willing-provider contracting elsewhere. One state (Ohio) procures MCOs separately for the TANF-related and SSI-related populations.
In most states, the contracting approach is identical for Medicaid and for CHIP. However, in California, Florida, Michigan, and Pennsylvania, Medicaid and CHIP programs use different approaches. The CHIPRA provision that mandates a choice of plans poses new challenges to these separate CHIP programs that must now cover the whole state, including rural areas, with at least two plans when risk-based enrollment is mandated.
While generally the bidding process when it is competitive is behind closed doors, two states use a remarkably open process. For example, in the Florida CHIP program, bidders who have met the minimum requirements in the RFP present their proposals to a committee composed of state staff from multiple agencies. These presentations are open to the public, including the plan’s competitors. After the contracts have been awarded, all proposals as well as the scoring tools used in the grading of those proposals become public documents. Similarly, in Arizona, the scoring tools used to assess each bidder during the selection process are made publicly available on the state agency’s web site after contracts have been awarded.
Early in Medicaid risk-based managed care contracting, several state officials said that a competitive process was often used to obtain a "price bid," and plans with the lowest bids were selected. However, with the requirement from the BBA to have actuarially sound rates , this approach is less common (although bids are taken and sometimes negotiated within the actuarially sound rate range). The federal requirement for actuarially sound rates does not apply to CHIP, so separate CHIP programs may still use the price-bid approach, especially in times of economic stringency in the state.
Appendix B, Table 3also shows the periodicity with which states have solicited proposals over the past decade when they have a competitive approach. Solicitations are relatively rare; only three states have solicited three times: Florida (CHIP only), Michigan (Medicaid only), and New Mexico. All other states have solicited only once or twice in the decade. Some state officials indicate a preference for less frequent procurements because of the staff resources needed to solicit and review proposals, and because it takes time to develop a collaborative relationship with plans.
It can take a while to bring a new contractor up— it takes them a while and then when they get comfortable, it’s time to rebid already…. I wish it would be longer than a four-year contract period. I would be very comfortable with six years. (State Official)
| Advantages | Disadvantages | |
|---|---|---|
| Source: Interviews with state officials. | ||
| Competitive |
|
|
| Any Willing Provider |
|
|
Medicaid and CHIP officials described the inherent advantages and disadvantages to competitive and any-willing-provider contracting. Some of these are summarized in Table 5. On the one hand, a competitive process increases the state’s ability to control the number, quality, and geographic distribution of health plans serving program enrollees across the state. The process can also provide a vehicle through which the state can assert more quality control via requirements specified in the RFP. One state official commented on why the state switched from any-willing-provider to competitive contracting:
An impetus [for switching to competitive procurement] was that the quality measures in one area were not as high as the rest of the state, so we were looking for ways to raise that area up to improve its performance compared to others. (State Official)
The main advantage of any-willing-provider contracting is greater initial administrative simplicity. The process of releasing an RFP, reviewing proposals, and selecting health plans is burdensome, requiring a significant investment of staff time for both the state and plans. Another advantage of this approach is that it can encourage new entrants into the program, an advantage if there are too few plans to assure continuity if plans leave the program.
Number of Plans.
States report there being a "sweet spot" in the number and distribution of MCOs in the state, statewide and in specific geographic regions. States use competitive contracting in an attempt to award contracts to obtain the number of plans they feel is needed in each geographic area: not too few (assuring choice of plans, especially in rural areas) and not too many (so that beneficiaries are not distributed too thinly across too many plans, which could lead to financial problems for small plans). Too many health plans also means a greater administrative burden for the state in terms of management and oversight.
When there are too many plans, it may be difficult for competing plans to solicit providers for their network without paying a premium, especially for "rare" providers such as hospitals and specialists.
Each plan has to have a broad provider network, particularly as it relates to hospitals. As we have gained more plans, hospitals are gaining an advantage because they know the plans have to have an adequate hospital network. So now the hospitals are ending up having a better negotiating position, because they know the plans need them. That’s an unintended consequence that’s making us think, "Gee, we need to look at this more." (State Official)
Having an adequate number of plans is viewed as an important safeguard for the state in case a plan leaves the market or goes out of business. Having this occur without an adequate fallback could be potentially disruptive for program beneficiaries. In addition, having a sizeable number of plans is also viewed by several states as a good way to instill a sense of competition among plans.
We have also added some plans because we thought it would be good to introduce more competition because some of the plans were giving us a lot of pushback, and we wanted to make sure that we had other options. (State Official)
On the other hand, a large number of small (and potentially financially fragile) plans may be a possible disadvantage of any-willing-provider contracting. Too many plans can mean that there is "not enough business to go around," in that there are too few covered lives available for each health plan. When there is no guaranteed market share for health plans, this can discourage plans from participating.
We don’t get them a set amount of lives, which they might like to have. Some plans have chosen not to come in because they needed a lot more lives than we were able to give them. (State Official)
In order to help new plans add enrollees, some states have used the auto-assignment process, whereby beneficiaries who do not select a Primary Care Provider within a specified period of time after enrollment are assigned to one of the smaller, new plans.
Figure 5 shows that the number of Medicaid risk-based managed care enrollees in a state is directly related to the number of Medicaid MCOs. For example, most states have from four to nine plans, with smaller states in terms of both Medicaid enrollment and geographic area (e.g., Connecticut, Delaware, and Rhode Island) having fewer. Five states (California, Florida, New York, Texas, and Wisconsin) contract with 14 or more MCOs. These states all have either (1) very large Medicaid risk-based managed care enrollment (California and New York); (2) a large geographic area to cover (Texas); or (3) any-willing-provider contracting (Florida and Wisconsin).
Figure 5: Number of Medicaid MCOs by Risk-Based Managed Care Enrollment
in Study states, 2010

| State | Total MCO Enrollment (in millions) | Number of Medicaid managed care plans |
|---|---|---|
| Sources: (1) Gifford et al., 2011; (2) Review of state documents. | ||
| Arizona | 1.210 | 9 |
| Connecticut | 0.391 | 3 |
| California | 4.079 | 19 |
| Delaware | 0.142 | 2 |
| Florida | 1.287 | 18 |
| Maryland | 0.685 | 7 |
| Massachusetts | 0.513 | 5 |
| Michigan | 1.251 | 9 |
| Minnesota | 0.477 | 8 |
| New Jersey | 0.974 | 4 |
| New Mexico | 0.335 | 4 |
| New York | 3.002 | 21 |
| Ohio | 1.730 | 7 |
| Pennsylvania | 1.222 | 9 |
| Rhode Island | 0.134 | 2 |
| Tennessee | 1.219 | 4 |
| Texas | 1.698 | 14 |
| Virginia | 0.527 | 5 |
| Washington | 0.627 | 7 |
| Wisconsin | 0.624 | 17 |
Plan Characteristics
States contract with a wide mix of types of plans. Two important traits are (1) whether the plan enrolls only public beneficiaries, or commercial enrollees as well; and (2) whether the plan is nonprofit or for-profit.
Medicaid Plans.
Figure 6shows the distribution of the Medicaid MCOs in study states, according to these two criteria. (State-by-state detail is provided in Appendix B, Table 4.) The dominant type of plan serving Medicaid risk-based managed care enrollees in the study states is a nonprofit plan that serves only publicly funded enrollees, accounting for 32.2 percent of the plans. However, there are substantial numbers of other plans, with about one-fourth being nonprofit plans that have both public and commercial enrollees, and the remainder being for-profit, evenly distributed between public-only and public and commercial.
Figure 6: Types of Managed Care Organizations Participating in Medicaid in Study States, 2010
The plan-type pattern is different across states. Most states, except the smallest, have a mix of at least three plan types. However, two states (Massachusetts and Minnesota10) were contracted only with nonprofit plans in 2010, and Tennessee was contracted only with for-profits. All states but Delaware contract with at least one or more plans with some commercial enrollment.
There is a substantial presence of large, national managed care companies in the study states. As evidence, we generally interviewed (as one of two MCOs interviewed) the largest health plan in the state in terms of Medicaid managed care enrollment. Of the 40 plans representatives interviewed, 16 (40 percent) are from one of the following MCOs: Aetna, Amerigroup, Anthem/WellPoint, Centene, Molina Healthcare, or United Healthcare. Some of these large national MCOs are public-only, and some have commercial enrollment.
CHIP Plans.
In the seven states with CHIP risk-based managed care programs that are not fully integrated with Medicaid, there is a somewhat different mix of plans to that of Medicaid (see Figure 7 and Appendix B, Table 5), with more nonprofit public-only plans for CHIP in those states.
Figure 7: Types of Managed Care Organizations Participationg In CHIP
Programs in Seven Study States, 2010
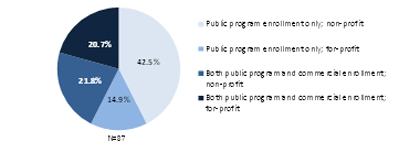
Source: review of state documents.
Note: State-specific details are provided in appendix B, Table 5
Despite this difference, there is substantial overlap in the plans that participate in both Medicaid and CHIP. Of the 189 plans participating in either program in the 20 study states, fully 147 participate in both Medicaid and CHIP with 15 participating only in CHIP and the remaining 27 participating only in Medicaid (see Figure 8). There are only three states without a very substantial overlap in the two programs’ plans (see Appendix B, Tables 4 and 5).
Figure 8: Number of Managed care Organizations with Medicaid
or CHIP Enrollment in study states, 2010
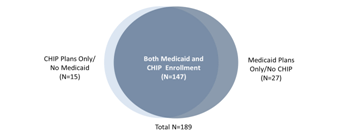
Source: Review of state documents
Advantages of Different Plan Types.
In the opinion of state officials, plans with a national presence have many advantages. One advantage is that they have experience in other states, particularly experience with a variety of administrative standards and requirements.
If they can adopt basically the same standards that are the highest out of all their markets, then everybody gets the benefit. (State Official)
On the other hand, state officials said that it is critical for large, national plans to establish a local presence and to learn about the communities they are serving. For instance, one state representative expressed the importance of a local presence for national plans.
There is a way for them to invest in the area that they are serving. They may have their national headquarters outside of the state, but they can still be connected here.
(State Official)
Large MCOs are viewed as often having the infrastructure in place to provide services efficiently, such as a good IT infrastructure. They also can spread their risk across markets and many covered lives.
Even if you’re not making it in [this state] you may be making it somewhere else. You get to cover part of your fixed administrative costs over a large range of lives [by virtue of operating in several states]. (State Official)
By contrast, smaller plans are viewed as possibly suffering from high administrative costs because they cannot benefit from the economies of scale of a large insurer.
Plan representatives from larger plans, especially those with commercial enrollees, expressed the opinion that they have more leverage with providers than smaller plans do because they are able to take advantage of their existing provider networks. One health plan stated that its decision to enter the Medicaid managed care market came from this ability to provide ready access to care through the strength of its provider network.
Plans with commercial enrollees often create a Medicaid-only subsidiary to operate Medicaid managed care. This may evolve through purchasing a previously (sometimes local) public-only plan. Several reasons were given for setting up such a subsidiary. One informant claimed that subsidiaries are formed in Medicaid managed care because of provider taxes by the state on plans.
There is an MCO tax, which is subject only to the Medicaid gross revenues. [By having a separate Medicaid subsidiary] they shelter all the additional sources of revenue that they may have. (State Official)
While large national commercial plans have created Medicaid-only subsidiaries, they may brand them as a national plan in preparation for implementation of the Affordable Care Act.
They are anticipating people moving across different products once the health exchange is up and running; [large insurer] wants to maintain brand identity so they don’t lose people [who move between Medicaid and the exchange plans]. (State Official)
Changes in Number and Type of Plans over the Decade
Most state officials indicate that they have had substantial stability over the decade in the number and mix of MCOs with which they contract, which in turn has brought stability to their programs and beneficiaries. This stability is in sharp contrast to the 1990s, when several of the states experienced more turmoil in their risk-based managed care programs, with plans exiting and entering the programs more frequently.
Connecticut, Delaware, and Tennessee represent exceptions to this pattern of plan stability during the first decade of the 21st century. All experienced difficulties with plan participation during the study period, resulting in Tennessee suspending risk-based managed care for five years, Delaware reverting to a state-administered plan that was essentially a fee-for-service arrangement, and Connecticut transitioning to a non–risk-based arrangement. Both Tennessee and Delaware have recently returned to statewide risk-based managed care. Though Connecticut also returned to a risk-based model in 2009, this arrangement did not last long, as the state decided to replace risk-based managed care with an ASO model (described above) beginning in January 2012.
In spite of this general stability, the Medicaid and CHIP risk-based managed care market in the study states slowly continues to consolidate. Most states report that, while they have retained their largest plans, there has been some decline in the number of smaller plans and some shift toward national plans. Much of this shift is due to the acquisition of smaller, local plans by larger national plans. The trend was more pronounced in the first half of the decade, with more stability in the latter half of the 2000s.
States continue to work toward achieving full geographic coverage, especially in rural areas. Several states report that throughout the past decade there have been shifts in where plans operate. The mobility is affected by where the plans feel capitation rates are sufficient, where there are enough enrollees, and where they can obtain a reasonable provider network. Over time the states may be able to persuade plans to reenter the counties they left.
It was a business decision to choose the [counties we are in] for Medicaid. We are making an investment in infrastructure. We look at where membership is, and where take-up is by other plans. A county with many plans already would mean slow enrollment. (Plan Representative)
We are reentering the counties that we left now. The state did make some rate increases—they wised up…They understood it was not a joke. We also got better at our work—more creative, more collaborative, and more partnership-oriented. That produced some results. (Plan Representative)
We got out because we had serious problems with one of the major providers there. We were losing too much money, so we pulled out. (Plan Representative)
In addition, in some states the requirements to maintain more substantial financial reserves, and/or to obtain licensure as an HMO, have tightened over time and hospital or provider-based plans have left the Medicaid market because they were unable to maintain these reserves.
States may perceive plan decisions to leave the market as a lack of willingness to undertake the effort needed to survive in the Medicaid managed care market.
Some plans have left because they have not been able to get efficient enough to make a decent return on their investment based on the rates we’re providing. (State Official)
There are some [health plans] that have had difficulties maintaining the networks, the right number of Primary Care Providers. I mean, when this happens it's because they're either not paying claims, or they're doing other things….internally to not run a sound plan. (State Official)
Provider Networks
Once states have selected plans to participate in their Medicaid and CHIP risk-based managed care programs, they then delegate (as specified in contractual requirements) the responsibility for selecting a network of service providers. This provider network defines which providers a Medicaid/CHIP enrollee can access: Primary Care Providers (their first point of contact), specialists, hospitals, or other service providers. Thus the size and composition of the provider networks (by provider type and geographical location) are largely responsible for the degree of access to care that beneficiaries have under risk-based managed care.
Network Standards.
The Balanced Budget Act requires that Medicaid programs generally provide adequate access to care, but states have wide latitude in how this broad requirement is translated into the standards they impose on their MCOs. We reviewed a model Medicaid and CHIP MCO contract for each study stateto determine the provider network requirements that states impose on their plans. Table 6 shows the requirements for appointment wait times (routine and urgent), the maximum number of enrollees allowed per Primary Care Provider (PCP), and any requirements for geographic proximity to a PCP in the study states. State-by-state detail on these requirements is contained in Appendix B, Table 6.
| Standard | Minimum | Maximum | Mode | Number of States with Standard |
|---|---|---|---|---|
|
Source: Review of state contracts. Note: See Appendix B, Table 6 for state-specific detail. |
||||
| Appointment Wait Times | ||||
| Routine (days) | 7 | 45 | 30 | 17 |
| Urgent (days) | 1 | 2 | 1 | 18 |
| Maximum Number of Enrollees to Each Primary Care Provider | 750 | 2500 | 1500 | 14 |
| Geographic Proximity for Primary Care Providers | ||||
| Urban Areas (miles) | 5 | 30 | 30 | 19 |
| Rural Areas (miles) | 15 | 60 mins | 30 | 17 |
There is considerable variation in the number and strength of the standards states impose on MCOs for Medicaid. Standards for routine appointment wait times (an appointment for a condition that is not urgent) vary from only 7 days in Florida to 45 days in Massachusetts and Minnesota, with the mode being about 30 days among the 17 states with a standard specified in their model contract. Three states do not impose a standard for Medicaid. The standard for urgent appointments is much shorter, 1–2 days, among the 18 study states that impose this standard. Similarly, the range in the number of enrollees allowed per PCP varies widely, from 750 to 2,500 per PCP. Six states do not have such a standard in their model contract. Finally, the standard for geographic proximity to PCPs ranges from 5 to 30 miles (or 30 minutes) in urban areas and from 15 miles to 60 minutes in rural areas. All but three states have such standards for Medicaid.
The access standards for CHIP MCOs differ from Medicaid standards in all of the seven states that separately administer their Medicaid and CHIP risk-based managed care programs, except for Texas, where the standards are the same across all the access measures in Table 6, and New York, where the standards are very similar for Medicaid and CHIP. In the remaining five states, there is no clear pattern to differences in the strictness of access standards for Medicaid and CHIP plans. Sometimes standards are stricter for CHIP plans than Medicaid plans, and sometimes the reverse is true. For example, in Virginia routine appointment wait times must be within 30 days for Medicaid and within only 15 days for CHIP. On the other hand, PCPs must be within 15 miles for Medicaid enrollees but within a longer distance, 30 miles, for CHIP.
Equally important is whether and how plans monitor these standards to assure network adequacy. We asked both state officials and plan representatives about how they monitor their provider network requirements. As with the standards themselves, there is wide variation in how states enforce their provider network standards. Half the states require plans to submit monthly or quarterly reports concerning their networks (although the content of reports varies widely), but others require less frequent reporting. Another common method is "secret shopper calling," whereby the states call providers in the plan’s network to request an appointment, posing as a plan enrollee.
We have staff that take the plan’s most current provider directory, and they make calls. They make calls to see if the provider is actually participating in the plan. (State Official)
The frequency, type, and methods of these calls vary within and across states. For example, New York noted that they called everyone in the plan’s most current provider directory twice a year to determine provider participation, and in Pennsylvania monitoring staff are required to complete 55 survey calls quarterly.
We asked states whether their monitoring of access requirements has varied over time. More intensive monitoring over time can occur when there are access concerns for a particular plan.
[Speaking of monitoring intensity and frequency] Some of it is monthly, some of it is quarterly, and some of it is every six months. That’s what we use to monitor the activity and make sure they stay on track. There are quarterly or monthly grievance reports; there are quarterly or monthly claims dashboards. It just depends on how well the health plan is performing and how well they do on all the different types of oversight that we do. (State Official)
However, some states said that state budget restrictions have reduced the size of their monitoring staff and therefore limited what they can do.
One representative of a national-level plan indicated that there is a wide range of sophistication in the type of monitoring states do. While he generally expressed admiration for the most experienced states’ monitoring programs (mentioning Arizona, New York, Tennessee, and Wisconsin specifically), he indicated it can lead to challenges for the plan.
It makes it challenging for the contractor because the states are so well run and they understand their data and our performance pretty well. So it creates a twofold problem [laughs]—(1) they are a great state [i.e. at monitoring] and (2) they are a great state [i.e. at pointing out the plans’ flaws].
Plans also do monitoring of their network providers’ availability in a variety of ways, as illustrated by the following examples:
We have a very comprehensive access program, including mapping [our plan’s provider requirements] against state requirements, secret shopper calls for open/closed practice and availability, and close monitoring of any access grievances that come in.
(Plan Representative)
Through our quality department, we do appointment availability audits for routine, emergent, and urgent appointments. We also do after hours audits for availability, to check that they are actually able to get in contact with a provider (in Spanish also).
(Plan Representative)
As for open panels—we monitor quarterly. We’ll address [the problem] if we have areas that have a higher rate of closed panels. We have people checking when panels are opening or closing. This is the same for appointment waiting times; we survey regularly.
(Plan Representative)
This latter comment highlights an issue that was discussed in interviews with both state and plan representatives. The provider network size may appear to be adequate, but the list of providers can include providers that have closed their panels. For example, there may be providers who serve existing Medicaid patients but will not take new patients. Provider access is also reflected in how long it takes an individual to make an appointment, especially a new patient.
We do monitoring of our providers for the next available appointments to ensure there is access, which is why we went out and expanded community-based providers.
(Plan Representative)
We asked both plan and provider representatives about their impressions of the adequacy of the size of provider networks maintained by Medicaid and CHIP MCOs. While the plans generally asserted that the size of their networks is adequate, providers often had a countervailing opinion. Three provider association representatives thought that their state overestimated the number of providers participating in MCO networks.
It’s hard to get to [the number of providers required by the state]…. In [our state] there are laws that require an adequate network so it’s not in the plan’s best interest to reveal that they don’t have enough. (Provider Association Representative)
In another state, a provider representative said that their state often double-counts the total number of participating providers statewide, counting them once for each plan with which they contract.
The size of provider networks has either remained stable or grown according to the plan representatives that we interviewed. Fifteen said that they have expanded their networks, and the same number said the size has remained essentially stable over the study period. The main reason for expansion is either growth in enrollment or the plan’s expansion into new geographic areas of the state. Only two plans said that the size of their networks has declined. (The remaining eight plans did not discuss this issue in the interview.)
There is a trade-off between having a wide network in order to assure access and being selective about which providers are in the network. We did not hear of plans that have regularly eliminated providers from their network based on findings from quality monitoring, such as their HEDIS scores.
We didn’t pare our network down yet. There is an opportunity to be more selective over time. As we monitor care and access, and when we ensure we have appropriate access, then we can talk about the quality of providers. (Plan Representative)
Plan and Provider Negotiations.
In establishing their networks, plans interact with potential providers in a health care marketplace that typically serves both public and commercial enrollees. Each MCO and each provider faces a different dynamic in such negotiations, which can vary a great deal by type of provider or region of the state.
The number of MCOs in a region is important, because when there are several MCOs establishing networks in areas where providers of certain types are scarce (for example, specialists or hospitals) the providers have more bargaining power than in an area where the provider supply is greater or where Medicaid is the dominant payer.
For example, there may be only a single group of a certain type of specialist or a single hospital. When these entities negotiate with the various plans, they may hold out their agreement to participate in the plan’s network for higher payments or other benefits. Indeed, as mentioned earlier, an unintended consequence of the requirement for a choice of plans in the BBA and CHIPRA is to exacerbate this situation in certain circumstances.
If a hospital or hospital system is essentially a monopoly in an area, they can demand largely whatever rate increases that they want to demand. (State Official)
We heard that establishing an adequate network of specialists is particularly difficult, especially when all the specialists of a particular type practice and negotiate as a group.
They may have to pay the specialty pediatric cardiologist at 150% of the [Medicaid fee-for-service] rate, and they might have to pay a dermatology provider much more, because there’s a lack of that specialty. (State Official)
Larger provider groups (for example, a multi-specialty clinic) or networks have greater bargaining power. For example, the Provider Service Networks in Florida are groups of providers that contract with the state (on either a risk or fee-for-service basis) to provide all care to a group of beneficiaries.
There are legal limits on the size and structure of such provider networks for negotiating with plans.
When negotiating, I negotiate independently for each provider in our system. They do not get the same rates across the board. So even though there is one system, the Federal Trade Commission prohibits that kind of bulk contracting. (Provider Representative)
Physicians have taken steps to enhance their negotiating power, which happens more often in areas that are dominated by Medicaid patients or when there are excess numbers of providers of different types. Such providers may want to participate but may be excluded completely from Medicaid if they are not included in one of the MCO networks, especially when risk-based managed care is mandatory. This situation could be one underlying reason that some of the provider representatives felt that MCO networks should be larger.
A lot of the pediatricians, they kind of have to participate in Medicaid, because so many kids are on Medicaid. (State Official)
Provider Shortages.
We asked state officials, plans, and provider representatives whether they perceived provider shortages or excess provider capacity and of what type. In five states (Florida, New Jersey, Texas, Virginia, and Washington), we consistently heard of shortages from all three types of informants, while in other states there was less consistency. Indeed, some informants commented on the need for more accurate information on this important topic.
When there are shortages, states have devised various strategies to expand the number of providers participating in MCO networks. Several states reported on their efforts to use mid-level practitioners to enhance the supply of PCPs in geographic areas with shortages of PCPs, such as rural areas.
We’ve been using more physician extenders—nurse practitioners—in the rural areas. It’s been more prevalent now than ten years ago. (Plan Representative)
However, state licensing laws determine whether the scope of practice for nurse practitioners, physician assistants, or nurse midwives allows them to be a PCP.
The state has mandated more practice rights for physician extenders like nurse practitioners and physician assistants. (Plan Representative)
The model that we believe works best is physician-led primary care practice where mid-levels, including nurse practitioners and physician assistants, practice as part of an enabled team. We do have nurse-managed sites in our program, and the ones we have do extremely well, so we believe that that’s an additional capacity that we’re going to need going forward to 2014. (Plan Representative)
This latter comment reflects a heightened awareness of the potential for provider shortages— particularly PCP shortages—with the implementation of the Affordable Care Act. At the same time, there is some evidence that new providers are participating in Medicaid managed care in anticipation of the changes in 2014.
There are some reasons why a doctor or a hospital might say "Wow, I’d prefer not to work with Medicaid but maybe I should." (Plan Representative)
Factors Contributing to Provider Participation in MCOs.
Provider representatives noted many factors which contribute to a provider’s decision to participate in Medicaid managed care networks. While the plan’s reimbursement rates are the most critical factor (discussed further below), providers noted several other important factors.
Administrative issues were often mentioned as inhibiting physician participation in Medicaid/CHIP managed care. These include issues such as utilization review and prior authorization standards; a lack of procedural standardization among health plans (for example, insurance verification can be done by some health plans online, but not others); and state systems that are infrequently updated to reflect a patient’s insurance status and their insurer. Providers also complained about the credentialing process, which has to be completed separately for each health plan.
A strategy to increase provider participation used by some states and health plans is to take advantage of the enhanced bargaining power of plans with both public and commercial enrollees. As shown earlier in Figures 6 and 7, these plans represent almost half of both the Medicaid and CHIP MCOs in study states.
Rhode Island includes a "mainstreaming clause" in its standard contract. Providers that serve commercial enrollees in a plan must also accept Medicaid/CHIP patients in the plan. State officials noted that provider participation in Medicaid/CHIP MCOs increased substantially after they added this clause. (None of the other states mentioned imposing this requirement on their plans.) Rhode Island’s experience is consistent with research by Adams and Herring (2008) that found that nationally, higher Medicaid commercial HMO penetration in a geographic area led to higher odds of physician participation in Medicaid.
Even if this is not a state requirement, plans with commercial enrollees may use their increased market power to increase provider participation in their Medicaid/CHIP networks, since they can require (or encourage) their providers for commercial enrollees to accept Medicaid patients. Generally, we heard that plans with both public and commercial enrollees maintain separate Medicaid and commercial provider networks, but often with considerable overlap.
Our rule is 80 percent overlap with our commercial plan. There are some challenges with specialties that don’t want to take Medicaid no matter what. We have offered them more than any commercial plan is paying, and they just don’t want to take Medicaid. (Plan Representative)
There is quite a bit of overlap. For example, [in our Medicaid network] we might have 100 providers in our commercial plan network and another 50 that aren’t in the commercial network. (Plan Representative)
While there is reluctance among some providers to participate in Medicaid/CHIP, some physicians and physician associations that we interviewed express a preference for working with plans which concentrate on serving public enrollees. They indicated that such plans are more focused on the Medicaid/CHIP population and can provide better quality care.
There are plans that only do public programs, and they have a different reputation and perception in the community than commercial plans that also do Medicaid… Lots of attention is paid to provider retention and community outreach. They are not distracted by commercial business. (Provider Representative)
They [i.e., providers] realize that we understand the issues they’re going to face dealing with Medicaid populations, and we give lots of support that a commercial plan wouldn’t have for dealing with these populations. (Plan Representative)
Provider Reimbursement.
As mentioned, provider reimbursement is the most critical factor contributing to provider participation in MCOs. While federal legislation mandates that Medicaid health plans must be paid an actuarially sound rate,11 there is no requirement that plans pay their providers in a particular way or at a particular level. In addition, there is no existing quantitative data on the amount that Medicaid/CHIP MCOs reimburse their providers, or how those rates compare to Medicaid fee-for-service, Medicare, or commercial insurance rates.
When we asked states what their plans pay providers, most state officials said that they take a hands-off approach to provider reimbursement for MCOs. In addition, most do not even know how or how much their plans reimburse providers. Most state officials feel that, as long as health plans meet provider network standards, payment arrangements negotiated between health plans and their providers are between those parties, and the state prefers not get involved.
From the plan’s point of view, their market power with providers is the factor that determines whether they can negotiate a lower rate than, for example, Medicaid fee-for-service rates, with certain providers.
We can negotiate under the fee-for-service schedule sometimes if they accept it. (Plan Representative)
Plans may also negotiate a capitation rate with providers, thus pushing the risk down to the provider level.
In contrast to this general pattern of lack of involvement by the state in what plans pay their providers, four of the study states (Arizona, Connecticut, Maryland, and New Mexico) do have minimum provider reimbursement requirements. Even without any such requirements, officials in several states said they expect their health plans are usually benchmarking from Medicaid fee-for-service. In four states (California, Maryland, Ohio, and Pennsylvania), provider representatives thought that the rates that MCOs pay their providers might actually be somewhat higher than fee-for-service for some services, although there is uncertainty about how prevalent this pattern is.
Even when the state uses risk-based managed care and takes a hands-off approach to provider reimbursement, it cannot avoid political controversy or litigation surrounding the issue of adequate provider reimbursement by health plans. This can occur when the state cuts fee-for-service payment rates (for example, as happened recently in California), leading to a reduction in the capitation rate, and in turn to what plans can pay providers.
Specific comments on how CHIP plans pay their providers were rare, since as noted most study states operate risk-based managed care programs seamlessly. In one of the states with separate administration, a provider association noted that CHIP reimbursement rates are higher than for Medicaid. Generally state CHIP officials were unable to make an informed comparison, but their opinion is that CHIP MCOs pay their providers either the same rate, or potentially a higher rate, than for Medicaid.
As states move more and more Medicaid and CHIP beneficiaries into risk-based managed care, there are fewer people in the fee-for-service system, so fee-for-service rates become only a hypothetical benchmark for provider rate-setting. For example, in Arizona, there are only small, specialized subgroups in fee-for-service.
From the point of view of most provider representatives, Medicaid MCO provider reimbursement rates are too low—often at cost or below cost. Some doctors also feel that the plans are not paying an adequate rate given what plans receive as capitation rates from the state.
Our Medicaid fee-for-service rates are below our costs. We continue to take cuts and managed care plans continue to get increases on a per member per month amount based on "actuarial soundness." (Provider Representative)Some providers, those with more market power, may judge that the rates offered by the plans are insufficient and consequently decide not to participate in the network.
When I negotiate, we will not sign a contract for less than 100% Medicaid fee-for-service schedules. Plans try to come in at 85–90%, and we do not sign anything.
(Provider Representative)
But some providers do not have that option, depending on the market dynamics they face.
The money that comes in is barely covering our costs. We are barely surviving. But we don’t want to leave here. We like what we are doing here; we are making a difference. (Provider Representative)
The issue of low provider reimbursement by MCOs has become more acute in some places recently. Due to the budgetary constraints imposed on states by the recent recession, many of our provider informants (for example, in Arizona, California, Connecticut, Massachusetts, Michigan, Minnesota, and Texas) reported that their states have reduced fee-for-service provider payment rates. Since states adjust their capitation rates to reflect such provider payment cuts, capitation rates have also decreased. Only one provider informant (in Tennessee) noted that Medicaid payments have improved in recent years, in part due to the state’s previous experience with risk-based managed care in which rates were viewed as too low to sustain adequate participation by plans and providers. This situation is somewhat less severe for providers who negotiate with health plans for both commercial and Medicaid enrollees, since they can potentially cross-subsidize by having a mix of commercial and Medicaid reimbursement.
Quality Monitoring
Concerns that risk-based managed care could harm beneficiaries (through incentives to reduce care or provide substandard care) have gradually led to more intensive monitoring of quality of care for Medicaid and CHIP managed care programs. The federal government and states have adopted a broad definition of quality to include utilization of appropriate services, outcomes, and beneficiary satisfaction. A major advantage of the managed care delivery system is that it facilitates the measurement of health care quality, through improved information systems and a population-based approach to quality measurement.
Quality Standards.
The BBA requires that states develop quality standards for their Medicaid health plans and monitor compliance with those standards. States are required to have an ongoing quality strategy and must also arrange for annual external quality reviews. They must validate performance measures and performance improvement programs. Although the BBA ensures that quality monitoring occurs, it does not specify or define how quality of care should be measured. The result is a wide range in approaches with many common features.
Through the passage of the CHIPRA and ACA legislation, the federal government is increasingly engaged in an effort to improve quality measurement in risk-based managed care. Both laws call for the development of standard measures of quality for adults (the ACA) and children (CHIPRA). While this effort is already influencing how and what states collect and require of their plans, during the study period for this report (2001–2010) those new metrics had not yet been disseminated. Consequently, the information in this report generally predates those efforts.12
Without a strong federal role in mandating how states monitor quality during the study period, the development of quality monitoring standards and methods has been greatly facilitated by the National Committee for Quality Assurance (NCQA), which has undertaken special initiatives to develop approaches for state Medicaid agencies in their quality monitoring programs. Since 2007, the Centers for Medicare and Medicaid Services has participated in NCQA committees to provide input on quality measurement approaches. NCQA not only publishes standards, measurement metrics, and methods, but also has an accreditation program for health plans. Achieving NCQA accreditation assures that the plan must meet a uniform set of nationwide quality monitoring standards that are applied to all MCOs, regardless of the populations they serve (commercial or public). The accreditation process further investigates plans’ utilization management, provider credentialing, and member communication processes. Accreditation is voluntary on the part of plans in most of the study states. However, in 2010 six states (New Mexico, Ohio, Rhode Island, Tennessee, Texas, and Virginia) required all Medicaid MCOs to achieve NCQA accreditation. Two (Florida and Michigan) required plans to achieve accreditation from one of three bodies: NCQA, the Joint Commission on Accreditation of Healthcare Organizations, or URAC. Both the Joint Commission and URAC perform similar functions to that of NCQA in terms of accreditation of health plans. Of the remaining states, six (Arizona, California, Massachusetts, Pennsylvania, Washington, and Wisconsin) do not require accreditation but may use the results of accreditation in selecting and monitoring plans (NCQA, 2010).
The role of NCQA was described by one state representative in an interview:
[Before the BBA] we used NCQA standards to guide both our contract specifications as well as our monitoring activities. So we would go out on an annual basis and monitor each of our health plans and produce a report based on NCQA standards. In 2003, the BBA went into effect, and BBA mirrored in many ways, in my opinion, NCQA standards, but it didn’t include any kind of instructions about how you monitor against those standards. (State Official)
One of the most commonly used tools that have been developed by NCQA for quality monitoring is the Healthcare Effectiveness Data and Information Set (HEDIS), a tool that, according to NCQA, is used by more than 90 percent of health plans to measure performance. The HEDIS is a uniform set of quality measures, along with very detailed instructions for how to analyze data in a uniform way to compute the measures. Every health plan that is NCQA accredited must collect currently recommended HEDIS measures according to NCQA specifications. Most other plans (including those that are not accredited) also collect and report on some HEDIS measures, and all study states currently require reporting of some HEDIS measures periodically to the state. Most have required HEDIS reporting throughout the study period. However, this apparent uniformity in reporting masks tremendous variation across states in which measures they require, how the measures are computed, and how they are reported (discussed further below).
An additional tool—the Consumer Assessment of Healthcare Providers and Systems (CAHPS)—is also used by all study states for measuring beneficiary satisfaction with care provided by health plans and providers in their networks. This tool was developed by the Agency for Healthcare Research and Quality (AHRQ), which serves a similar role to NCQA, in terms of developing and promulgating measures and methods for the CAHPS. In contrast to HEDIS measures, which are generally computed either from claims/encounter or medical record data, the CAHPS measures come from periodic surveys of beneficiaries. There are separate surveys for adults and parents (reporting on their child’s care). For children’s care, six states (Arizona, California, Florida, New York, Pennsylvania, and Texas ) report data separately for CHIP programs for HEDIS and four (California, Florida, Texas, and Washington) report CAHPS separately. Similarly to HEDIS, there is tremendous variation in what states require, as well as in how often the surveys are done and who administers the survey. All study states but Arizona13 currently require some CAHPS reporting, but (as with HEDIS) measures differ across states and over time. Usually CAHPS reporting started later than HEDIS reporting.
There is considerable variation in who collects the HEDIS and CAHPS data. Fifteen of the study states require plans to collect and report HEDIS data, but five states oversee the collection directly (for example, by an NCQA-certified vendor contracted by the state). There is more diversity in who collects the CAHPS data than for HEDIS. Plans are required to do the survey in only five states, with the state taking the responsibility through various types of vendors in the others. This may differ for the adult and child surveys.
Plans do the adult CAHPS, and we do the child CAHPS. NCQA only requires the adult CAHPS, but we wanted the child CAHPS so we pay for it. (State Official)
NCQA plays an important role in CAHPS reporting through its certification of the vendors that collect the data. However, NCQA and AHRQ do not mandate certain critical things such as the response rates to the surveys, which vary across states and from vendor to vendor. One state reported that a vendor hired by one plan had a 28 percent response rate, while another vendor achieved a 45 percent response rate. In general, response rates are relatively low—under 50 percent—for most plans for the CAHPS.
Variations in Reporting CAHPS and HEDIS. We requested HEDIS and CAHPS data for the full study period from the 10 largest study states —in terms of Medicaid risk-based managed care enrollment—and one recent year of HEDIS and CAHPS data for the remaining 10 states. This process, along with information gathered in interviews, revealed tremendous variation in data collection and reporting for these quality measures. Remarkably, our review of HEDIS/CAHPS data for the first four states that submitted data to us revealed 202 distinct HEDIS-type measures for which definitions differed in some way over the study period. The types of variations include:
- Wide variations in definitions for HEDIS quality measures; for example across the study states we found 10 different childhood immunization measures (e.g., different combinations, periodicity, or age groups) being used at some time in the study period.
- Variations in who collects data, and variation in which approach is used to compute HEDIS measures. Some states use only administrative (claims/encounter) data to compute measures, and some use a hybrid of administrative and medical record data. Some states leave the choice of method up to their plans (see Table 7). Since the hybrid method is known to produce higher rates than using administrative data alone, there is a lack of comparability of measures across plans and states, and over time, depending on the data collection method used for the particular HEDIS measure.
| Type of Data Collection | Timeliness of Prenatal Care | Well-Child Visits | Childhood Immunizations | Breast Cancer Screening | Cervical Cancer Screening | HbA1c Screening |
|---|---|---|---|---|---|---|
| Source: Review of state documents and interviews with state officials. | ||||||
| Administrative Data Only | 4 | 4 | 0 | 18 | 4 | 2 |
| Hybrid Method | 10 | 10 | 11 | 0 | 8 | 11 |
| Plan Choice | 5 | 5 | 4 | 0 | 5 | 4 |
| Not Collected | 1 | 1 | 5 | 2 | 3 | 3 |
| Total | 20 | 20 | 20 | 20 | 20 | 20 |
- In terms of CAHPS, though the questionnaires and sampling methods are recommended by AHRQ, the methods are not mandated, and there are differences in data collection, as well as in how data are analyzed and reported.
An additional issue leading to a lack of uniformity in reporting is one of scale. Small plans may not have a sufficient sample size to meet HEDIS reporting specifications, especially for measures that are for smaller groups of enrollees such as diabetics. Many of these and other issues with variability and quality of reporting of data are documented in a recent report from the NCQA (2010).
External Quality Review Organizations (EQROs). Under the BBA, as required in 2003 regulations, states must use an EQRO to assist them in independently monitoring the quality of care provided by MCOs. More recently, under CHIPRA states are also required to use an EQRO to assist in monitoring CHIP quality of care. The functions of the EQROs vary from state to state. For example, some EQROs monitor the aggregate HEDIS and CAHPS data that plans submit for quality, some receive encounter data and compute HEDIS measures from those data, some do the CAHPS survey and process the data, and some perform other quality functions such as annual site visits.
We have an EQRO assessment of our plans’ operations. Every plan goes through that. It’s an exhaustive process. (State Official)
CHIP-related EQRO functions are still evolving for the states that manage their Medicaid and CHIP quality monitoring programs separately. They generally (with the exception of Florida) have hired the same EQRO for Medicaid and CHIP. The Centers for Medicare and Medicaid Services has recently released protocols for how EQROs should monitor access and quality under both programs. This process is bringing the quality monitoring process for Medicaid and CHIP MCOs closer together in most of the states where it has previously been separated (see Appendix B, Table 1).
The role of the EQRO is more important in oversight of quality monitoring in those states that do not require NCQA plan accreditation. In such states, the EQRO often takes on the function of periodic auditing of HEDIS data to assure that the data are correctly extracted and computed according to state specifications. In contrast, when a plan is NCQA-accredited this oversight function is performed by auditors hired by NCQA. Still, NCQA oversight does not completely eliminate the need for state and EQRO oversight. For example, states often design their own measures, or other quality processes, which must be separately monitored.
Encounter Data.
Anothertool that was frequently mentioned as being essential to quality monitoring and other administrative oversight is the collection and analysis of claims/encounter data. These administrative data contain a record for each service provided by the provider. Every study state requires plans to submit encounter data, and most use the data both for quality monitoring and rate setting. The art and science of maintaining and using good encounter data has evolved over the past decade to the point where most study states are now confident that their encounter data provide useful information for program management and quality oversight of plans. States are increasingly analyzing the data internally, rather than solely relying on the plans to analyze the data and provide aggregate reports.
However, encounter data still have limitations in completeness and accuracy. There are three critical factors that contribute to how complete a state’s encounter data will be. First, when plans use "sub-capitation" (paying providers a capitated rate) there is less incentive for the provider to submit complete data, leading to underreporting. A second critical factor is whether encounter data are used in setting capitation rates. When plans are paid a higher rate when they serve a sicker population (as judged from encounter data), the data will be more complete. A final important factor is the level of experience the plans have with managing encounter data. More years of experience with collecting and reporting encounters improves the chances that an MCO will have the structures and incentives in place to ensure data quality.
States have found that they must continually monitor the quality of encounter data and provide feedback to plans, and they are becoming more sophisticated in how they do the monitoring.
It takes 1–3 years to master reporting encounters to the state. (State Official)
Two of three CEOs came in to meet with us specifically about the methodologies for how we collect our data and how we report the data, and that resulted in them applying appropriate resources, making sure their data and encounters were correct, and really paying attention to detail. (State Official)
One of the things we found is that they [the health plans] could send data, but it was missing key components, and there wasn’t a good process of ensuring that it got corrected and resubmitted. We put in a front-end editing system that can deny claims individually that come in. (State Official)
Performance Improvement Programs.
The BBA requires that states develop performance improvement programs, but this broad requirement permits states to choose the topics and methods for their programs.Performance goals are set by the state and passed on to the plans, usually as contractual requirements. A state may collaborate with its plans in defining topics and methods and some have established a quality improvement collaborative for this purpose. For example, in Virginia the collaborative includes both plans and the medical society.
Many states have taken their performance improvement programs one step further, by providing financial incentives to achieve a defined target. For example, 12 study states have established at least one pay-for-performance program, whereby a state provides financial incentives for improved HEDIS quality measures (see Table 8). Usually the incentive is a small portion of the capitation rate (most typically reported to be 1 percent or less, although one state offered up to 5 percent) as a bonus (or withhold). In most programs, that amount is initially withheld from the capitation rate and awarded retrospectively to those plans that reach a predetermined threshold. In addition to these financial incentives, another important reward that can be used is auto-assignment of new enrollees to plans with the highest scores.
| State | Timeliness of Prenatal Care | Childhood Immunizations | Well-Child Visits | Breast Cancer Screening | Cervical Cancer Screening | HbA1c Screening | Type of Incentive Offered |
|---|---|---|---|---|---|---|---|
|
Source: Review of state documents and interviews with state officials. Note: Other study states do not have Medicaid HEDIS-based pay-for-performance programs. |
|||||||
| Maryland | — | — | X | — | X | — | Withhold/Bonus |
| Massachusetts | Pay-for-performance but not for these measures. | Withhold/Bonus | |||||
| Michigan | X | X | X | X | X | X | Withhold/Bonus |
| Minnesota | Pay-for-performance but not for these measures. | Withhold | |||||
| New Mexico | X | X | X | X | — | X | Withhold |
| New York | — | — | X | X | X | — | Bonus |
| Ohio | Pay-for-performance but not for these measures. | Bonus | |||||
| Pennsylvania | X | — | — | X | X | — | Bonus |
| Rhode Island | X | X | X | X | X | Bonus | |
| Tennessee | — | — | X | X | — | X | Withhold/Bonus |
| Texas | Pay-for-performance but not for these measures. | Bonus | |||||
| Wisconsin | — | X | — | — | — | X | Withhold/Bonus |
Choosing the correct quality measures for rewarding good performance is challenging. States must be strategic in choosing measures, because both health plans and providers are likely to be focused on those aspects of their performance that are most closely monitored and assessed, particularly if they are provided incentive payments based on the metrics. Because of concern that plans and providers may respond to the incentives by neglecting quality of care in non-incentivized areas, some states rotate the measures included in the pay-for-performance program on a regular basis.
What we’ve found is that if we said it was immunization, mammography, cervical cancer screening, the plans focus on those specific areas and nothing else, so that they could get the quality incentive. (State Official)As with other aspects of quality monitoring, the table illustrates wide variety across states in the measures they focus on, and whether they use only bonuses, or both withholds and bonuses, in their programs. For example, five states use both withholds and bonuses, while two use only withholds and five use only bonuses.
In addition to these HEDIS-based pay-for-performance programs, states use pay-for-performance programs to reward a variety of other quality-related functions. Examples include payments (or withholds) for high-quality encounter data, reporting timely information, statewide coverage by the plan, broad provider networks, electronic prescribing, use of safety-net providers in health plan networks, use of electronic medical records, lower emergency room usage, and lower medically preventable hospital admissions or readmissions.
Because such programs involve winners and losers, implementing pay-for-performance is potentially controversial. Two states mentioned having a pay-for-performance program that was eliminated for political reasons, and one state has been unable to secure legislative approval for a proposed pay-for-performance program.
Some health plans have adopted pay-for-performance for their providers, since the plan itself relies on the performance of providers in achieving the state’s quality goals. These are often based on the HEDIS data, though some plans also look at provider credentials, member satisfaction, and emergency room visits. One health plan noted that it offers an incentive for doctors to open their offices after hours so that people are not using the emergency room unnecessarily. The plans also use non-financial incentives for their providers.
The best doctors are recognized in the local paper. We give them a gift and have a dinner to recognize them. The providers really like it, and it helps our relationship with them, too. (Plan Representative)
Changing beneficiary behavior is also critical to achieving certain targets such as improving preventive care use and reducing emergency room use. For this reason, some plans offer incentives to their enrollees as well as their providers.
I firmly believe that if you can get the patient to participate in their own health care then you go a long way to managing things. (Plan Representative)
Because the delivery of medicine is both pieces—the doctor can only do so much without the member, and the member can only do so much without the doctor. (Plan Representative)
Other Quality Initiatives
everal other quality improvement initiatives are a part of the "quality tool kit," although there is even more diversity in approaches for these various initiatives. Some of these are defined by NCQA accreditation requirements, which have been adopted by many states. For example, to establish a basic standard of provider quality, NCQA requires that all health providers be credentialed. For physicians, the credentialing process involves verifying licensure and hospital privileges, review of provider sanctions and malpractice history, and conducting a structured review of the provider’s office, among other things.
Another critical aspect of NCQA accreditation is that complaints and grievances should be addressed quickly with a standardized approach, and that the data from this process should be analyzed to identify patterns. Our respondents did not provide concrete information on how this is done, or how frequently, but it was mentioned by several states as an important quality monitoring tool (e.g., in California, Florida, and Texas).
If we’ve got items that escalated to complaints and you start seeing a trend to the complaints, same HMO, same providers, or same class or grouping of people [we are concerned]. (State Official)
Another important quality improvement tool is intensive care coordination for high risk groups, in order to assure appropriate health services. This can take a variety of forms. For example, one health plan hired pharmacists to identify those members that were taking more than six drugs, and to identify possible contraindications of particular groups of medications. They contacted the enrollee and his or her doctor to determine whether all of the medications were necessary. In addition, some plans offer social services in addition to health services to high-cost users. The medical home model is a special case of this increased emphasis on care coordination. For example, Arizona is considering whether to provide financial incentives for plans that establish medical homes.
Another quality improvement approach is to use advice lines to assure ready access to physician advice after hours, along with electronic medical records that provide the consulting physician or nurse with ready access to information.
We created a service for 24-hour physician calls… and we have technology to make sure they have access to the medical records. The doctor can really talk to you and the doctor knows something about your child and knows what medicines/ diagnoses [he has]. (Plan Representative)
A final example of a quality improvement tool mentioned by study states is the "report card" or "dashboard" approach. While the formats and methods vary widely, at a minimum states may post the HEDIS/CAHPS scores on their web site. Some states, such as Maryland, have taken a more proactive approach. Maryland’s EQRO creates an easy-to-read chart which ranks health plans according to their scores for access to care, doctor communication, service, preventive health care, and diabetes care. This chart is then sent with enrollment materials to help new enrollees choose their health plans.
Similarly, health plans may choose to compare their contracted physicians in a similar manner, and to share the results with all providers.
We have quality reports to share with providers that indicate usage of medicines and proper protocols and who is practicing outside the norm of their peers. (Plan Representative)
Impressions of Quality Monitoring under Risk-Based Managed Care
States, providers, and plans give somewhat contrasting impressions of the effectiveness of the quality monitoring initiatives that have been adopted in their states for Medicaid/CHIP risk-based managed care enrollees. State representatives generally expressed positive opinions about their programs, but providers were more negative in their assessments as shown by these opinions.
I don’t see managed care for Medicaid as being the driver of quality improvement just because they are tracking the data. (Provider Representative)
I think Medicaid managed care has helped some, but has it sufficiently addressed the opportunity to improve health? I don’t think so. (Provider Representative)
Plan representatives gave a more mixed assessment, reflecting an impression that the "cup is half empty and half full." On the positive side:
We have been proud of the fact that our principal focus is on the quality side and "patients first" side, and the finance piece follows second. (Plan Representative)
We take pride in the fact that we provide high-quality care even within the constraints of limited Medicaid funding. (Plan Representative)
[Speaking of quality improvement] We work hard to improve our results. Are there problems? Sure. But I think overall we get good quality. (Plan Representative)
However, one plan representative thought that the heavy emphasis on HEDIS as a quality improvement tool is misplaced.
I don’t think HEDIS drives quality; [it uses] very old, superficial metrics.
(Plan Representative)
And another plan representative admitted that quality of care may suffer when rates are cut.
We don’t want to admit that it [reimbursement cuts] affects quality, but we are certainly stretched. (Plan Representative)
Trends in Quality-of-Care Measures
An initial goal of this project was to obtain a set of comparable HEDIS and CAHPS data for all study states, to track the change in measures over time, and to compare measures across states. The data were to be aggregated to the state level for as many years as possible.
We obtained data for all study states, but the variability in definitions of the measures has severely limited the number of measures that can be compared across time and across states. The effort to identify comparable measures resulted in six comparable HEDIS measures and eight comparable CAHPS measures. They are:
HEDIS Measures
- Percent of pregnant women with timely prenatal care (a visit in the first trimester)
- Percent of children age 3–6 with a well-child visit in the past year
- Percent of children age 2 with up-to-date immunizations (Combination 214)
- Percent of adult women with a breast cancer screen in the past two years (ages vary by state)
- Percent of women age 21–64 with a cervical cancer screen in past three years
- Percent of adult diabetics with an HbA1c test in the past year
CAHPS Measures
- Overall satisfaction with health plan (adults)
- Overall satisfaction with health care (adults)
- Overall satisfaction with personal doctor (adults)
- Overall satisfaction with specialist (adults)
- Overall satisfaction with health plan (children)
- Overall satisfaction with health care (children)
- Overall satisfaction with personal doctor (children)
- Overall satisfaction with specialist (children)
Notably, all of the common HEDIS measures are measures of preventive care services. There are no commonly reported measures of health outcomes (for example, the outcomes from screening tests) across the time period. In addition, there are not enough study states reporting CAHPS measures in the first half of the decade for a cross-state analysis.
Even for these commonly reported measures, not all 20 states collected data in a common way across the time period. Appendix C contains a set of figures showing state-by-state data for all of these measures for the earliest year in the study period for which the state reported data and for the most recent year.
All states reported some HEDIS data for the six common measures, although no study states reported on all of them. Between 17 to 19 states reported on each of the six HEDIS measures for Medicaid (depending on the measure). The most commonly reported measure was well-child visits (19 states for Medicaid). Separate reporting for CHIP was less common; only six states reported separately on well-child visits, and only three reported separately on up-to-date childhood immunizations (Combination 2).
Eighteen states reported any CAHPS data for 2006–2010. In addition, the way that CAHPS data are reported varies by state. For example, on a satisfaction scale of 1 to 10, some report the percent scoring 7–10, some report the percent scoring 8–10, and some report the percent scoring 9–10, all very different measures. So even in the 20 states with the longest-established and largest risk-based managed programs, a very limited set of quality measures are available with common definitions for cross-state analysis. In addition to the limited number of quality and satisfaction measures for comparison, the different measurement approaches mentioned above and variations in definitions over time limit the comparability of data.15
With these limitations in mind, we created box plots to illustrate the level and range of quality/satisfaction measures for the most commonly reported HEDIS and CAHPS measures as shown in Figures 9–12. These figures demonstrate considerable variability in both HEDIS and CAHPS quality/satisfaction measures. The first box plot (Figure 9) shows variation in three pregnancy/pediatric HEDIS measures: timeliness of prenatal care, well-child visits, and immunizations (Combination 2). The mid-point of each box plot (represented by a triangle) is the median across all the states with data. The box plots also indicate the extreme values and the 25th (Q1) and 75th (Q3) percentiles. For well-child visits and immunizations, HEDIS Medicaid and CHIP measures are both included, since there are not enough CHIP measures to analyze separately. For all three measures, we present data for the first half of the study period (2001–2005) and the second half of the study period (2006–2010).
The range of values for these quality measures varies considerably across states and over time. For example, the percent of pregnant women with timely prenatal care varies from 56 to 82 percent during the first half of the study period (median = 74 percent), rising to from 68 to 91 percent (median = 84 percent). The improvement in this measure is impressive, and the median for the second time period is very similar to the rate for all women in the United States in 2007 at 82 percent (National Center for Health Statistics [NCHS], 2011), and higher than for African American women in that year (75 percent). In addition, the median rate is slightly higher than the Medicaid average for plans that are either NCQA accredited or that voluntarily report data, at 81.5 percent in 2007. However, it is substantially below the rate for commercial enrollees (91.5 percent) as reported by NCQA in the same year (NCQA, 2011).
The figure shows that there has been substantial improvement in both of the child HEDIS measures (well-child visits and immunizations) among the states reporting over the decade. In addition, the study states reporting data compare favorably to both Medicaid and commercial enrollees reporting data to NCQA. For example, the median percent with a well-child visit for study states was 73 percent, and 65 percent (Medicaid) and 68 percent (commercial) for plans reporting to NCQA for 2007. The NCQA rates both rose to about 70 percent by 2010. All the caveats suggested earlier in this report should be kept in mind in making these comparisons, including the variations in how quality measures are developed and reported, and how intensively the quality of data is reviewed (for example, by EQROs).
Turning to adult HEDIS measures, Figure 10 shows the range and trends in rates of screening for diabetes among diabetics, and cervical and breast cancer among adult women. The adult rates of use of these preventive care services are slightly lower than for the obstetric/pediatric preventive care services, and the range is generally greater across states. However, as with children, there is an improved trend over time for diabetic screening and cervical cancer screening. The NCQA (2011) found rates of 65 percent (Medicaid) and 82 percent (commercial) for cervical cancer screening nationally in 2007, which compares to a median of 67 percent among study states. Breast cancer screening rates are lower for study states and for NCQA, and have not shown substantial improvement over the decade in either case. For example, for NCQA reporting plans the rate was only 50 percent for Medicaid women in 2007 (69 percent for commercial women). This compares to a median of 54 percent among the 18 study states reporting on all their plans, essentially the same throughout the study period.
Figures 11 and 12 show satisfaction with various aspects of care for children and adults, as reported in CAHPS surveys. The range across the limited number of states that report CAHPS data is much less than for the HEDIS measures. For example, for the child CAHPS, the percent of parents who report they are highly satisfied with their child’s health plan varies from 77 percent to 90 percent with a median of 82 percent. The median values for the other child CAHPS measures are very similar (83 percent for health care, 86 percent for personal doctor, and 82 percent for specialist satisfaction). The ranges in these values across states are no more than 7 percentage points. Unfortunately there were not enough study states reporting CAHPS data in the first half of the time period (only three states reported), so it is not possible to discern a trend in satisfaction over time.
The levels of satisfaction for adults are consistently lower for adults than for children. While this pattern could be due to some measurement differences of various types (such as which states are included in the figure), it appears from this limited information that adults are less satisfied with their own care under risk-based Medicaid managed care than parents are with their children’s care. This could be due to many factors, including differences in the types of providers used and the fact that adults are in worse health, on average, than children.
The median percentage of adults who are satisfied with their health plan (reporting a satisfaction level of 8–10 on a scale of 0–10), across the nine reporting states, is similar at 75 percent to the percent for Medicaid adults reporting to NCQA at 72 percent. These rates of satisfaction for Medicaid enrollees are higher than satisfaction of commercial enrollees reporting to NCQA at 64 percent (NCQA, 2011).
Conclusions
Program Features - The past decade has seen rapid growth in risk-based managed care in public health insurance programs for low income nonelderly adults and children. In the 20 study states, comprising over 80 percent of the risk-based Medicaid managed care nationally, enrollment in risk-based MCOs rose substantially for all Medicaid groups. Rising from a small base early in the decade, growth was at a faster rate for the non-institutionalized SSI population than for TANF-related and poverty-related Medicaid beneficiaries (see Figure 4).
Medicaid and CHIP risk-based managed programs, even for separate programs, are highly integrated, with the exception of a few notable states. While data on trends in CHIP enrollment in risk-based managed care are not available, the CHIP risk-based managed care programs that are administered separately from Medicaid began early in the decade, so likely the growth rate for CHIP enrollment in risk-based managed care—which was already high early in the program—has not been as great as for Medicaid children during this period.
All of the study states have almost a decade of experience using risk-based managed care as a means of delivering care for Medicaid and CHIP beneficiaries, including for at least a portion of their SSI enrollees. As an indication of general political support for risk-based managed care as an alternative to fee-for-service Medicaid and CHIP care delivery, all the study states but one are on a path to expand their risk-based managed care programs to new populations and/or new parts of the state. The notable exception is Connecticut, which discontinued risk-based managed care just after the end of the study period. Reasons given were a perceived lack of cost savings from the program, and a preference for alternative models of care coordination and quality improvement. The two other study states that experienced disruptions in their risk-based managed care programs—Delaware and Tennessee—have returned to risk-based managed care enthusiastically.
In spite of this general trend toward expansion, there are still many populations and geographic areas that are not yet under mandatory risk-based managed care (see Figures 2 and 3). Almost no states included several high-cost groups, such as dual enrollees and institutionalized enrollees, during the study period. In addition, in most study states enrollment remains voluntary in some parts of the state, most often rural areas. The most important reason for this is that it has been difficult to establish a choice of plans with adequate provider networks in the most rural areas, where some counties do not have specialists of various types, for example. In contrast, some states have incorporated very rural areas without extreme difficulty (examples are Arizona and New Mexico).
Even when they have moved to mandatory enrollment for TANF- and poverty-related groups, some states have maintained voluntary enrollment for either SSI adults, children, or both. The continued use of voluntary enrollment means that there remains the possibility of "risk selection" into Medicaid MCOs by individuals who are in better health than those in fee-for-service.
CHIP programs, in contrast, have had less difficulty mandating statewide risk-based managed care enrollment. Until the passage of CHIPRA, there was no requirement for a choice of plans under CHIP risk-based managed care, so most study states have been able to recruit at least one plan for rural areas under separate CHIP programs.
In addition to variations in the populations covered by risk-based managed care, the study states vary widely in how they design and administer their programs. We learned from talking to state officials, plan representatives, and provider organizations that there is no one-size-fits-all way to design a risk-based managed care program.
One source of important variation is the degree to which states carve out certain services from the acute-care services MCOs are required to provide (almost none yet include long-term care). The most common carve-out is for dental services, and there is a general consensus that a dental carve-out is efficient, since traditionally commercial MCOs have not provided dental services. While pharmacy and behavioral health services are also common carve-outs, there is more controversy about whether these carve-outs are helpful for improving access or quality, or for reducing costs (see Table 4).
An additional source of variation across states is in the methods states use to select participating MCOs. A majority of states use a competitive RFP process for selecting plans (see Table 5 and Appendix B, Table 3). The RFP process gives a state more flexibility in meeting their goals for the number and type of plans to have in various parts of the state. The alternative to a competitive process is to use any-willing-provider contracting, which generally yields more participating plans. Having more plans can be good, since beneficiaries have more choice, and there is always back-up capacity for expansion or when plans drop out. However, this can result in numerous smaller plans which do not have the economies of scale of larger plans.
The number and type of MCOs in study states has stabilized in most places compared to the 1990s. We heard in interviews with states that a great advantage of such relative stability is that states have been able to establish more trust and a more a collaborative working relationship with their plans. Closer communication can be helpful when changes (for example, benefits changes) are needed that must be communicated to beneficiaries, or when there are any problems identified with quality or satisfaction. While we did not collect data on the number of plans by year, it appears that the number of plans has gone down over time due to consolidation through mergers, plans exiting the Medicaid managed care market, and states selecting fewer plans.16 In addition there is an apparent trend toward more participation in more states by several national MCOs, such as UnitedHealthcare, Aetna, and others. These plans bring large national enrollment and economies of scale, as well as experience from a variety of states in how to design programs and monitor quality. On the other hand they may lack a local presence. This has often been solved by acquiring a local plan.
Provider Networks - Another source of variation across and within states is the way that plans select and maintain their provider networks. All study states have requirements concerning the size and other characteristics of networks, but these standards vary widely across states, as does the enforcement of standards by states and plans (see Table 6). Larger plans, particularly those with commercial enrollees, have more market power in negotiations with individual providers. In contrast, rarer providers (such as hospitals and specialists but not primary care as often) have substantial market power in negotiating with plans. This means that such providers likely have higher reimbursement rates, at least in some geographic areas, than they did under fee-for-service arrangements, while the general pattern seems to be a norm of provider reimbursement at approximately the level of state fee-for-service rates in most places. Thus it is not clear that providers are substantially worse off under Medicaid and CHIP risk-based managed care than under fee-for-service, at least financially, although they are subject to more scrutiny and have some additional administrative burden.
An important factor in how risk-based managed care programs can be designed and implemented has to do with scale. Small states, with fewer enrollees, have more difficulty attracting as many health plans, and the plans inevitably have smaller enrollment in those states. This can also transfer to the plans themselves, who in turn (if they are small) may have trouble attracting participating providers. These difficulties are compounded in rural areas where few Medicaid/CHIP enrollees live, and which have very few providers. This in large measure explains the growth of national plans, which span the borders of states and can spread risk over a larger number of covered lives. In addition, commercial plans have a greater ability to attract providers because of a larger enrollment base, among other reasons. While the commercial and Medicaid/CHIP networks differ to some extent, there is usually substantial overlap. The larger plans also bring a broader experience base, particularly with information systems. It remains to be seen whether the trend toward larger and fewer plans might lead to higher cost for states (through the increased bargaining power of plans), to less innovation, or to poorer quality.
Quality Monitoring - Due to concerns by policymakers that risk-based managed care might affect access, quality, and satisfaction, there has been a pronounced trend during the study period (2001–2010) toward more intensive monitoring of health plans. The BBA required such monitoring but did not provide much specific guidance. This gap has to a large extent been filled by the NCQA, with help from the AHRQ in the design of the CAHPS survey. This has led to a reliance on HEDIS and CAHPS measures as the backbone of Medicaid/CHIP monitoring of quality and satisfaction. This greater uniformity in methods, and particularly the outside scrutiny brought in by NCQA when plans are required to obtain accreditation, likely has standardized access, quality, and satisfaction measurement with positive consequences for beneficiaries.
In spite of this pattern, we have documented a continued diversity in how quality monitoring is implemented across states. In addition, most of the measures that have been used most heavily by states to date are measures of the health care process (e.g., utilization of preventive care services) rather than measures of health outcomes. Some study informants—especially providers—expressed skepticism about the effectiveness of the quality improvement processes that have been used to date for Medicaid/CHIP risk-based managed care programs. It is perhaps best to consider these programs as still under development, with the many states and plans around the country functioning as a laboratory for new methods. In the meantime, the limited data we were able to collect suggests that preventive care use has improved for adults and children under risk-based Medicaid managed care during the study period, but that there is substantial variation across states in these patterns.
The recent recession and states’ needs to save money through reduced capitation rates have brought increased financial pressures on plans and their providers. We heard that the requirement for actuarial soundness of rates mitigates this to some extent. For example, the legislature cannot make an across-the-board capitation rate reduction. (This is not a factor when CHIP rates are set separately from Medicaid, since there is no actuarial soundness requirement.) Budget stringency also affects the size of state staff and so can have an impact on, for example, the quality monitoring process. We did not speak with beneficiaries or measure changes in beneficiary access or satisfaction during the recession, so it is not possible to know whether recent budget pressure has resulted in negative beneficiary experiences under Medicaid/CHIP risk-based managed care. We can only state that there was no evidence from our study of such changes, but that more research is needed, and that most states and plans feel strongly that risk-based managed care provides a more cost-effective approach to care delivery.
All respondents are looking to the implementation of the Affordable Care Act as a major milestone for risk-based Medicaid managed care because of the large number of new Medicaid enrollees who will enter MCOs. There is already change under way in many states, particularly around issues of establishing an exchange, although this varies according, in large part, to the political party of the governor and legislative majority. This expected enrollment growth has led to concerns about whether the number of plans, and especially the number of providers, is adequate to maintain access and quality. Without a large number of new participating providers, it seems inevitable that some states will relax the standards (or enforcement) they impose on plans for the size of their networks. This is another important area for additional research as ACA implementation approaches.
The medical home and Accountable Care Organization provisions of the ACA were highlighted by some state officials as providing opportunities for enhancing care co-ordination and quality of care for people with disabilities. As an example, New Mexico, which has mandatory statewide enrollment for SSI groups, is encouraging health plans to obtain NCQA certification as a medical home.
Summary - Risk-based managed care has grown, and study states are poised to continue the expansion as the implementation of the ACA approaches (with the notable exception of Connecticut). The results of this study suggest that the risk-based managed care infrastructure is in place to absorb these new beneficiaries in 19 of the 20 study states, but that expansion of the provider supply is necessary in some places. The development of more refined techniques for monitoring access, quality, and satisfaction should continue in order to assure that Medicaid and CHIP enrollees’ care does not suffer under the expansion.
References
Adams, K.E., & Herring, B. (2007). Medicaid HMO penetration and its mix: Did increased penetration affect physician participation in urban markets? Health Services Research, 43(1), Part II, 363-383.
Brown, R., Wooldrige, J., Hoag, S., & Moreno, L. (2001). Reforming Medicaid: The experiences of five pioneering states with mandatory managed care and eligibility expansions. Princeton, NJ: Mathematica Policy Research, Inc.
Coughlin, T., & Long, S. (2000). Effects of Medicaid managed care on adults. Medical Care, 38(4), 433-446.
Coughlin, T., & Long, S. (2004). Moving to Medicaid managed care: Lessons from state experiences under the section 1115 waiver authority. Washington, DC: The Urban Institute.
Coughlin, T., & Zuckerman, S. (2008). State responses to new flexibility in Medicaid. The Milbank Quarterly, 86(2), 209-240.
Felt-Lisk, S. & Yang, S. (1997). Changes in health plans serving Medicaid, 1993-1996. Health Affairs, 16(5), 125-133.
Gifford, K., Smith, V.K., Snipes, D., & Paradise, J. (2011). A profile of Medicaid managed care programs in 2010: Findings from a 50-state survey. Washington, DC: The Kaiser Commission on Medicaid and the Uninsured.
Hill, I., Harrington, M., Bajaj, R., Black, W., Fasciano, N., Howell, E., et al. (2003). Congressionally mandated evaluation of the State Children’s Health Insurance Program: Final cross-cutting report on the findings from ten state site visits. Washington, DC: Mathematica Policy Research.
Holahan, J., & Headen, I. (2010). Medicaid coverage and spending in health reform: National and state-by-state results for adults at or below 133% FPL. Washington, DC: The Kaiser Commission on Medicaid and the Uninsured.
Kaiser Family Foundation State Health Facts. Monthly CHIP enrollment tables. Retrieved from Kaiser State Health Facts website
Kirby, J., Machlin, S., & Cohen, J. (2003). Has the increase in HMO enrollment within the Medicaid population changed the pattern of health service use and expenditures? Medical Care, 41(7 Suppl), III24-III34.
Ku, L., Ellwood, M., Hoag, S., Ormond, B., & Wooldridge, J. (2000). Evolution of Medicaid managed care systems and eligibility expansions. Health Care Financing Review, 22(2), 7-27.
McCall, N. (1997). Lessons from Arizona’s Medicaid managed care program. Health Affairs, 16(4), 1994-199.
Medicaid and CHIP Payment and Access Commission. (2011). Report to the congress: The evolution of managed care in Medicaid. Washington, DC: Author.
National Center for Health Statistics. (2011). Health, United States, 2010: With special feature on death and dying. Hyattsville, MD: Author.
National Committee for Quality Assurance. (2010). Medicaid managed care quality benchmarking project: Final report. Washington, DC: Author.
Smith, V., Gifford, K., Ellis, E., Rudowitz, R., & Snyder, L. (2011). Moving ahead amid fiscal challenges. A look at Medicaid spending, coverage and policy trends: Results from a 50 state Medicaid budget survey for state fiscal years 2011 and 2012. Washington, DC: The Kaiser Commission on Medicaid and the Uninsured.
Endnotes
1 Comprehensive risk-based managed care does not include Primary Care Case Management (PCCM) or managed care plans covering limited benefits such as dental and behavioral health benefits.
2 For more information on HEDIS, see NCQA website at http://www.ncqa.org/tabid/59/default.aspx.
3 For more information on CAHPS, see AHQR website at http://www.ahrq.gov/cahps/.
4 Such programs require enrollees to select a Primary Care Provider, who manages their care for a fee but is not at risk.
5 Sometimes states (such as Wisconsin) automatically enroll SSI-related beneficiaries into MCOs and then allow them to voluntarily opt out. This approach is categorized as voluntary.
6 In 2001 constant dollars. Prior to 2006, the MSIS did not have a flag to indicate comprehensive risk-based managed care enrollment. However, we compared the counts of enrollees by type using both methods (the $200 inflation-adjusted premium payments and the managed care enrollment flags) for 2008 and found very similar counts nationally and for the two largest states (California and New York), both in total and by enrollment group. For example, in 2008 using premium payment indicators, there were 20.2 million people enrolled in Medicaid comprehensive risk-based managed care nationally and using enrollment flags there were 21.0 million.
7 Comprehensive programs include at a minimum ambulatory and inpatient hospital services among others.
8 EPSDT services are mandatory for Medicaid children; any health problems identified in these routine screenings (including behavioral, dental, and vision services) must be referred for treatment, which must in turn be covered by Medicaid.
9 California counties with Medicaid managed care choose one of three approaches. In the COHS model, the state contracts with selected counties to provide care for all Medicaid enrollees in the county for a fixed capitation rate.
10 Minnesota requires HMOs to be nonprofit and to participate in Medicaid managed care as a condition of licensure.
11 This requirement does not pertain to CHIP MCOs.
12 The ACA required the development of voluntary quality measures for Medicaid adults. An initial set of measures was released on January 4, 2012, and states are encouraged to adopt the measures. CHIPRA required the development of voluntary quality measures for children.
13 Arizona required CAHPS reporting prior to 2001 and will be reinstituting it in 2013.
14 Four DTaP/DT, three IPV, one MMR, three H influenza type B, three hepatitis B, and one chicken pox vaccination.
15 See Appendix D for more detail on changes in NCQA-specified HEDIS definitions during the study period.
16 In 1996, Felt-Lisk and Yang (1997) found 355 health plans participating in risk-based managed care in 15 states, but by 2010 we found only 174 such plans in the 20 states with over 80 percent of Medicaid risk-based managed care enrollment nationwide.
Appendix A: List of State Agencies, Health Plans, and Providers/Provider Organizations Interviewed.
| State | State Agencies | Health Plans | Providers/Provider Organizations |
|---|---|---|---|
|
Arizona |
-Arizona Health Care Cost Containment System |
-Care1st -UnitedHealthcare |
-Arizona Association of Community Health Centers -Arizona Medical Association |
|
California |
-Department of Health Care Services -Managed Risk Medical Insurance Board |
-Anthem/WellPoint -CalOptima |
-California Medical Association -California Hospital Association |
|
Connecticut |
-Department of Social Services |
-Aetna Better Health -Community Health Network |
-American Academy of Pediatrics (Connecticut) -Connecticut Medical Society |
|
Delaware |
-Department of Health and Social Services |
-UnitedHealthcare -Delaware Physicians Care/Aetna |
-Medical Society of Delaware -Delaware Healthcare Association |
|
Florida |
-Agency for Health Care Administration -Healthy Kids Corporation |
-UnitedHealthcare -Amerigroup |
-Florida Academy of Family Physicians -Florida Hospital Association |
|
Maryland |
-Department of Health and Mental Hygiene |
-Medstar Family Choice -Priority Partners |
-Healthcare for the Homeless -Individual Provider (Pediatrician) |
|
Massachusetts |
-Department of Health and Human Services |
-Neighborhood Health Plan -Boston Medical Center Health Plan |
-Massachusetts League of Community Health Centers -Massachusetts Hospital Association |
|
Michigan |
-Department of Community Health |
-Molina Healthcare -Priority Health |
-Michigan Health and Hospital Association -Individual Provider (Pediatrician) |
|
Minnesota |
-Department of Human Services |
-Blue Plus -Medica |
-Minnesota Medical Association -Minnesota Hospital Association |
|
New Jersey |
-Department of Human Services |
-UnitedHealthcare -Horizon NJ Health |
-New Jersey Primary Care Association -Individual Provider (Dentist) |
|
New Mexico |
-Department of Human Services |
-Molina Healthcare -Presbyterian |
-White Sands Health Care System -Individual Provider (Pediatrician) |
|
New York |
-Department of Health |
-Fidelis Care -MetroPlus |
-New York Hospital Association -New York Medical Association |
|
Ohio |
-Department of Job and Family Services |
-CareSource -Paramount Advantage |
-Ohio Hospital Association -Ohio State Medical Association |
|
Pennsylvania |
-Department of Public Welfare -Pennsylvania Insurance Department |
-Gateway -Keystone Mercy/AmeriHealth |
-Hospital and Health System Association of Pennsylvania -Pennsylvania Medical Society |
|
Rhode Island |
-Department of Human Services |
-Neighborhood Health Plan -UnitedHealthcare |
-Rhode Island Medical Association -Hospital Association of Rhode Island |
|
Tennessee |
-Department of Finance & Administration |
-UnitedHealthcare -Amerigroup |
-Tennessee Medical Association -Tennessee Hospital Association |
|
Texas |
-Health and Human Services Commission |
-Texas Children's Plan -Superior/Centene |
-Texas Medical Association -Texas Association of Community Health Centers |
|
Virginia |
-Department of Medical Assistance Services |
-Virginia Premier -Anthem/WellPoint |
-Medical Society of Virginia -INOVA Health System |
|
Washington |
-Department of Social and Health Services |
-Group Health Cooperative -Molina Healthcare |
-Washington Association of Community and Migrant Health Centers -Washington Hospital Association |
|
Wisconsin |
-Department of Health Services |
-Dean Health Plan -Independent Care |
-Wisconsin Hospital Association -Wisconsin Medical Society |
Appendix B: Tables
| Study States | CHIP Program Type | Contracting Processing the Same | Capitation Rates the Same | Intentional Contracting with all of the Same Health Plans | Quality Monitoring Done The Same | Administered by the Same Agency | Integration Category for Figure 1 |
|---|---|---|---|---|---|---|---|
|
Source: Interviews with state officials. Notes: (1) Excludes M-CHIP. Annual premium spending of $200+ is considered an indicator of enrollment in a comprehensive risk-based managed care plan. (2) TANF related includes those enrolled in TANF and non-SSI poverty related adults and children. |
|||||||
| Arizona | Separate | x | x | x | x | x | Fully Integrated |
| California | Combination | Non-Integrated | |||||
| Connecticut | Separate | x | x | x | x | Same Contracting Process/Same Plans | |
| Delaware | Combination | x | x | x | x | Same Contracting Process/Same Plans | |
| Florida | Combination | Non-Integrated | |||||
| Maryland | Medicaid Expansion | x | x | x | x | x | Medicaid Expansion |
| Massachusetts | Combination | x | x | x | x | x | Fully Integrated |
| Michigan | Combination | x | Non-Integrated | ||||
| Minnesota | Medicaid Expansion | x | x | x | x | x | Medicaid Expansion |
| New Jersey | Combination | x | x | x | x | x | Fully Integrated |
| New Mexico | Medicaid Expansion | x | x | x | x | x | Medicaid Expansion |
| New York | Separate | x | x | Non-Integrated | |||
| Ohio | Medicaid Expansion | x | x | x | x | x | Medicaid Expansion |
| Pennsylvania | Separate | Non-Integrated | |||||
| Rhode Island | Medicaid Expansion | x | x | x | x | x | Medicaid Expansion |
| Tennessee | Combination | No Risk-Based Managed Care for CHIP | |||||
| Texas | Separate | x | x | x | Non-Integrated | ||
| Virginia | Combination | x | x | Non-Integrated | |||
| Washington | Separate | x | x | x | x | x | Fully Integrated |
| Wisconsin | Medicaid Expansion | x | x | x | x | x | Medicaid Expansion |
| Population | Annual Premium Spending | 2001 | 2002 | 2003 | 2004 | 2005 | 2006 | 2007 | 2008 |
|---|---|---|---|---|---|---|---|---|---|
| Source: Medical Statistical Information System, data as analyzed by the Urban Institute. | |||||||||
| TANF-Related Children, 0–18 | $200+ | 8,066,530 | 9,002,211 | 9,863,270 | 10,300,518 | 9,792,777 | 11,443,596 | 12,134,827 | 12,421,974 |
| $1 - $199 | 1,252,472 | 1,516,179 | 1,750,735 | 2,158,071 | 1,742,405 | 2,251,106 | 2,305,968 | 2,302,435 | |
| $0 | 4,778,619 | 4,655,603 | 4,970,293 | 5,179,497 | 3,135,783 | 4,444,444 | 3,463,632 | 3,494,558 | |
| Total | 14,097,621 | 15,173,993 | 16,584,298 | 17,638,086 | 14,670,965 | 18,139,146 | 17,904,427 | 18,218,967 | |
| TANF-Related Adults, 19–64 | $200+ | 3,562,013 | 4,034,708 | 4,522,326 | 4,925,755 | 4,557,851 | 5,534,074 | 5,609,745 | 5,888,751 |
| $1 - $199 | 576,904 | 774,515 | 725,822 | 854,207 | 702,012 | 780,770 | 848,575 | 928,866 | |
| $0 | 4,518,237 | 5,401,340 | 5,708,322 | 5,770,149 | 3,848,267 | 5,702,396 | 5,445,033 | 5,453,200 | |
| Total | 8,657,154 | 10,210,563 | 10,956,470 | 11,550,111 | 9,108,130 | 12,017,240 | 11,903,353 | 12,270,817 | |
| SSI-Related Children, 0–18 | $200+ | 304,035 | 348,049 | 380,567 | 386,141 | 419,763 | 467,876 | 524,778 | 552,918 |
| $1 - $199 | 72,988 | 63,058 | 69,710 | 76,854 | 78,498 | 71,819 | 80,504 | 84,062 | |
| $0 | 323,044 | 295,705 | 289,470 | 313,140 | 259,605 | 299,422 | 251,653 | 257,417 | |
| Total | 700,067 | 706,812 | 739,747 | 776,135 | 757,866 | 839,117 | 856,935 | 894,397 | |
| SSI-Related Adults, 19–64 | $200+ | 800,418 | 874,763 | 903,692 | 1,083,570 | 923,109 | 1,056,139 | 1,310,641 | 1,381,426 |
| $1 - $199 | 307,727 | 312,978 | 335,095 | 338,966 | 344,730 | 342,829 | 421,596 | 442,844 | |
| $0 | 987,485 | 970,364 | 989,855 | 1,510,263 | 781,612 | 898,775 | 716,437 | 770,310 | |
| Total | 2,095,630 | 2,158,105 | 2,228,642 | 2,932,799 | 2,049,451 | 2,297,743 | 2,448,674 | 2,594,580 | |
| All Populations | $200+ | 12,732,996 | 14,259,731 | 15,669,855 | 16,695,984 | 15,693,500 | 18,501,685 | 19,579,991 | 20,245,069 |
| $1 - $199 | 2,210,091 | 2,666,730 | 2,881,362 | 3,428,098 | 2,867,645 | 3,446,524 | 3,656,643 | 3,758,207 | |
| $0 | 10,607,385 | 11,323,012 | 11,957,940 | 12,773,049 | 8,025,267 | 11,345,037 | 9,876,755 | 9,975,485 | |
| Total | 25,550,472 | 28,249,473 | 30,509,157 | 32,897,131 | 26,586,412 | 33,293,246 | 33,113,389 | 33,978,761 | |
| State3 | Type (2010)1 | Calendar Years of Competitive (RFP) Procurements in 2001–20102 |
|---|---|---|
|
Source: Review of state documents and interviews with state officials. 1Competitive contracting: not all health plans are necessarily selected to participate; this approach may or may not include a competitive price bid. Any-willing-provider contracting: the state sets a rate, possibly within a rate range, provides contract terms and requirements, and any health plan that meets those requirements is allowed to participate. |
||
| Arizona | Competitive | 2003, 2008 |
| California | ||
| Medicaid | Competitive in some counties | Every five years; staggered by counties |
| CHIP | Competitive | 2005 |
| Connecticut | Competitive | 2008, 2009 |
| Delaware | Competitive | 2003, 2006 |
| Florida | ||
| Medicaid | Any Willing Provider | N/A |
| CHIP | Competitive | 2002, 2006, 2010 |
| Maryland | Any Willing Provider | N/A |
| Massachusetts | Competitive | 2008 |
| Michigan | ||
| Medicaid | Competitive | 2002, 2004, 2009 |
| CHIP | Any Willing Provider | N/A |
| Minnesota | Any Willing Provider | N/A |
| New Jersey | Any Willing Provider | N/A |
| New Mexico | Competitive | 2001, 2004, 2007 |
| New York | Competitive | 2002, 2007 |
| Ohio | Competitive | 2006 (statewide), 2009 (for some regions) |
| Pennsylvania | ||
| Medicaid | Competitive | Every five years; staggered by region |
| CHIP | Any Willing Provider | N/A |
| Rhode Island | Competitive | 2004, 2010 |
| Tennessee (Medicaid only) | Competitive | 2007 (Middle), 2008 (West), 2009 (East) |
| Texas | Competitive | 2008 |
| Virginia | Any Willing Provider | One RFP in 2001; since then Any Willing Provider |
| Washington | Competitive | 2002 |
| Wisconsin | Competitive in one region; Any Willing Provider in rest of state | 2010 (for one region) |
| State | Number of Participating Plans (Comprehensive Medical Service Plans Only)1 | |||||
|---|---|---|---|---|---|---|
| Total | Serves Public Enrollees Only | Serves Public and Commercial Enrollees | Also participate in CHIP | |||
| Nonprofit | For-profit | Nonprofit | For-profit | |||
|
Sources: (1) Gifford et al., 2011; (2) Review of state documents. 1Excludes limited-benefit, specialized plans such as those that deliver only behavioral health care, dental care, or long-term care. |
||||||
| Arizona | 9 | 2 | 2 | 3 | 2 | 9 |
| Connecticut | 3 | 1 | 0 | 0 | 2 | 3 |
| California | 19 | 13 | 1 | 2 | 3 | 18 |
| Delaware | 2 | 0 | 2 | 0 | 0 | 2 |
| Florida | 18 | 1 | 9 | 1 | 7 | 7 |
| Maryland | 7 | 3 | 2 | 2 | 0 | 7 |
| Massachusetts | 5 | 2 | 0 | 3 | 0 | 5 |
| Michigan | 9 | 3 | 1 | 3 | 2 | 5 |
| Minnesota | 8 | 4 | 0 | 4 | 0 | 8 |
| New Jersey | 4 | 0 | 1 | 2 | 1 | 4 |
| New Mexico | 4 | 0 | 1 | 2 | 1 | 4 |
| New York | 21 | 12 | 3 | 6 | 0 | 18 |
| Ohio | 7 | 4 | 1 | 1 | 1 | 7 |
| Pennsylvania | 9 | 1 | 1 | 3 | 4 | 5 |
| Rhode Island | 2 | 1 | 0 | 0 | 1 | 2 |
| Tennessee | 4 | 0 | 1 | 0 | 3 | 0 |
| Texas | 14 | 6 | 3 | 2 | 3 | 14 |
| Virginia | 5 | 1 | 1 | 1 | 2 | 5 |
| Washington | 7 | 1 | 2 | 4 | 0 | 7 |
| Wisconsin | 17 | 1 | 4 | 6 | 6 | 17 |
| Total | 174 | 56 | 35 | 45 | 38 | - |
| Percent | 100.0 | 32.2 | 20.1 | 25.9 | 21.8 | - |
| State | Number of Participating Plans (Comprehensive Medical Service Plans Only)1 | |||||
|---|---|---|---|---|---|---|
| Total | Serves Public Enrollees Only | Serves Public and Commercial Enrollees | Also participate in Medicaid | |||
|
Nonprofit |
For-Profit |
Nonprofit |
For-Profit |
|||
| Source: Review of state documents. 1Excludes limited-benefit, specialized plans such as those that deliver only behavioral health care, dental care, or long-term care. |
||||||
| California | 21 | 15 | 1 | 1 | 4 | 18 |
| Florida | 9 | 3 | 2 | 2 | 2 | 7 |
| Michigan | 9 | 2 | 2 | 3 | 2 | 5 |
| New York | 19 | 9 | 3 | 6 | 1 | 18 |
| Pennsylvania | 9 | 1 | 1 | 3 | 4 | 5 |
| Texas | 15 | 6 | 3 | 3 | 3 | 14 |
| Virginia | 5 | 1 | 1 | 1 | 2 | 5 |
| Total | 87 | 37 | 13 | 19 | 18 | - |
| Percent | 100.0 | 42.5 | 14.9 | 21.8 | 20.7 | - |
| Appointment Wait Times | Maximum Number of Enrollees to Each Provider | Required Geographic Proximity for PCPs | ||||
|---|---|---|---|---|---|---|
| State | Routine Care (days) | Urgent Care (days) | Urban Areas (miles) | Rural Areas (miles) | ||
|
Source: Review of state model contracts. * These contracts specify that a PCP must be available to serve Medicaid patients 40 hours a week in order to qualify. Providers who are available for a fraction of the time will qualify as a fraction of a participating provider. |
||||||
| Arizona | 21 | 2 | No Standard | 5 | No Standard | |
| Connecticut | 10 | 2 | No standard | 15 | 15 | |
| California | ||||||
| Medicaid | No Standard | 2 | 1,200* | 10 | 10 | |
| CHIP | 10 | 2-4 | 1,200 | 15 | 15 | |
| Delaware | 21 | 2 | 2,500* | 30 | 30 | |
| Florida | ||||||
| Medicaid | 7 | 1 | 1,500* | 30 mins | 60 mins | |
| CHIP | 28 | 1 | No Standard | 20 mins | 20 mins | |
| Maryland | 30 | 2 | 2,000 | 10 | 30 | |
| Massachusetts | 45 | 2 | 1,500 | 15 | 15 | |
| Michigan | ||||||
| Medicaid | No Standard | No Standard | 750 | 30 | 30 | |
| CHIP | No Standard | No Standard | No Standard | No Standard | No Standard | |
| Minnesota | 45 | 1 | No | 30 | 30 | |
| New Jersey | 28 | 1 | 2,000* | 15 | 15 | |
| New Mexico | 30 | No Standard | 1,500 | 30 | 45 | |
| New York | ||||||
| Medicaid | 28 | 1 | 1,500 | 30 | No Standard | |
| CHIP | 28 | 1 | 1,500 | 30 mins | 30 mins | |
| Ohio | 42 | 1 | 2,000 | 20 | 45 | |
| Pennsylvania | ||||||
| Medicaid | 30 | 1 | No Standard | 30 mins | 60 mins | |
| CHIP | No Standard | No Standard | 2,000 | 20 | 45 | |
| Rhode Island | 30 | 1 | 1,500 | No Standard | No Standard | |
| Tennessee | 21 | 2 | 2,500 | 20 | 30 | |
| Texas | ||||||
| Medicaid | 14 | 1 | No Standard | 30 | 30 | |
| CHIP | 14 | 1 | No Standard | 30 | 30 | |
| Virginia | ||||||
| Medicaid | 30 | 1 | 1,500 | 15 | 30 | |
| CHIP | 14 | 1 | 1,500* | 30 | 60 | |
| Washington | 10 | 2 | No Standard | 10 | 25 | |
| Wisconsin | No Standard | 1 | No Standard | 20 | 20 | |
Appendix C: HEDIS and CAhps Data
Figure 1: Percent with Timely Prenatal Care
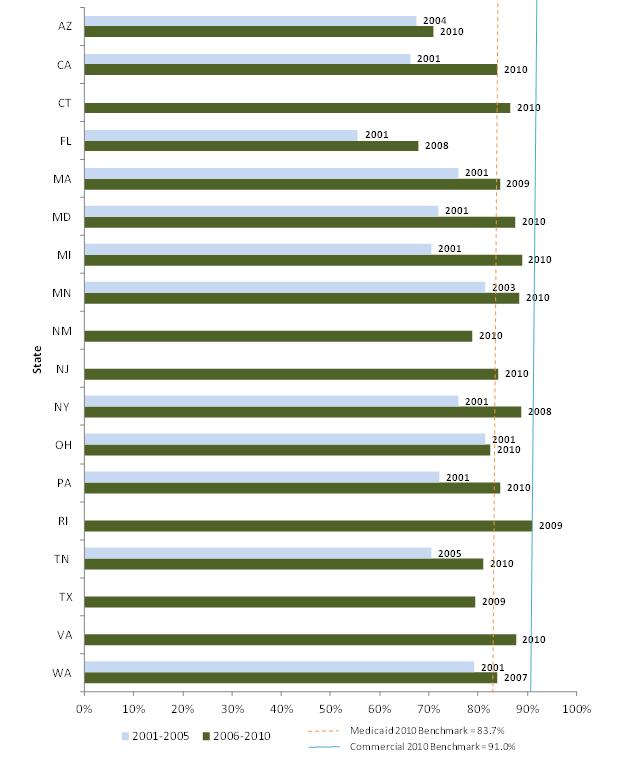
Source: Aggregate state data.
Note: All states use the HEDIS definition: percent of deliveries that received a prenatal care visit as a member of the organization in the first trimester of with in 42 days of enrollment in the organization.
Figure 2: Percent with Well Child Visit
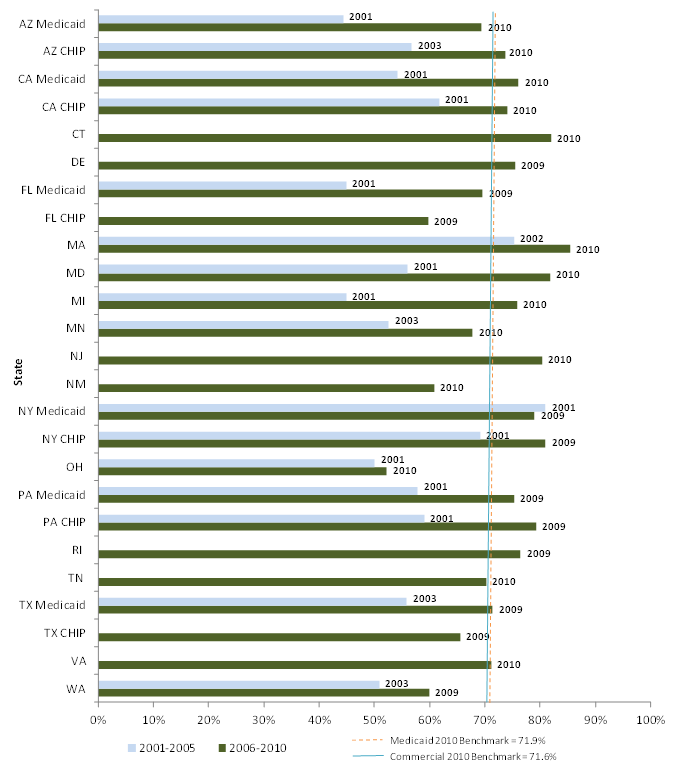
Source: Aggregate state data
Note: States use the HEDIS definition: percent of members 3-6 years of age who received one or more well-child visits with a primary care provider during the measurement year. Data are for Medicaid and CHIP unless otherwise specified.
| State | 2001-2005 | Year Reporting | 2006-2010 | Year Reporting | |
|---|---|---|---|---|---|
|
Source: Aggregate state data Note: States use the HEDIS definition: percent of members 3-6 years of age who received one or more well-child visits with a primary care provider during the measurement year. Data are for Medicaid and CHIP unless otherwise specified. Not reported: MD, PA, VA, WI |
|||||
| WA | 51% | 2003 | 59.90% | 2009 | * |
| VA | 71.17% | 2010 | |||
| TX CHIP | 65.52% | 2009 | |||
| TX Medicaid | 55.87% | 2003 | 71.38% | 2009 | This measure relies on specific provider specialty codes, and the state believes that it is likely inflated from the lifting of provider constraints. |
| TN | 70.23% | 2010 | * | ||
| RI | 76.50% | 2009 | * | ||
| PA CHIP | 59.00% | 2001 | 79.31% | 2010 | |
| PA Medicaid | 57.80% | 2001 | 75.35% | 2010 | |
| OH | 50.10% | 2001 | 52.20% | 2010 | U |
| NY CHIP | 69.20% | 2001 | 81% | 2009 | |
| NY Medicaid | 81.00% | 2001 | 79% | 2009 | * |
| NM | 60.85% | 2010 | * | ||
| NJ | 80.33% | 2010 | * | ||
| MN | 52.63% | 2003 | 67.83% | 2010 | * |
| MI | 44.90% | 2001 | 75.90% | 2010 | ? |
| MD | 56.00% | 2001 | 81.80% | 2010 | |
| MA | 75.30% | 85.50% | 2010 | * | |
| FL CHIP | 59.73% | 2009 | |||
| FL Medicaid | 44.92% | 2001 | 69.64% | 2009 | * |
| DE | 75.52% | 2009 | U | ||
| CT | 82% | 2010 | * | ||
| CA CHIP | 61.70% | 2001 | 74.00% | 2010 | |
| CA Medicaid | 54.20% | 2001 | 76.10% | 2010 | * |
| AZ CHIP | 56.8% | 2003 | 73.70% | 2010 | |
| AZ Medicaid | 44.40% | 69.40% | 2010 | * | |
Figure 3: Percent of Children with Up-to-Date Immunizations
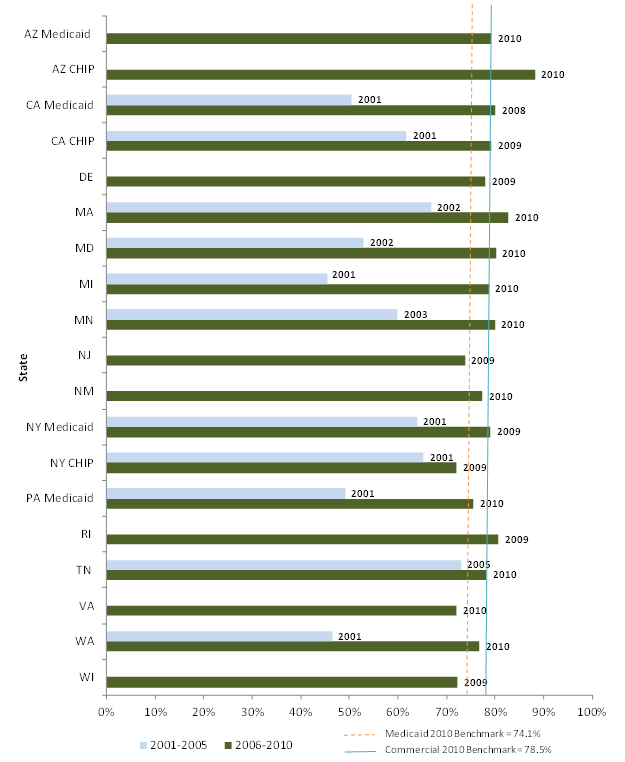
Source: Aggregate state data.
Note: States use the HEDIS definition: percent of children two years of age who had four DTaP/DT, three IPV, one MMR, three H infuenza typeB, three hepatitis B, and one chicken pox vaccine (VZV) by their second birthday. Data are for Medicaid and CHIP unless otherwise specified.
| State | 2001-2005 | Year Reporting | 2006-2010 | Year Reporting | HEDIS |
|---|---|---|---|---|---|
|
Source: Aggregate state data. Note: States use the HEDIS definition: percent of children two years of age who had four DTaP/DT, three IPV, one MMR, three H infuenza typeB, three hepatitis B, and one chicken pox vaccine (VZV) by their second birthday. Data are for Medicaid and CHIP unless otherwise specified. Not reported: AZ, CT, FL, NY, OH, PA, TX |
|||||
| AZ Medicaid | 79.30% | 2009 | * | ||
| AZ CHIP | 88.20% | 2010 | * | ||
| CA Medicaid | 50.50% | 2001 | 80.10% | 2010 | U |
| CA CHIP | 61.70% | 2001 | 79.30% | 2010 | * |
| DE | 78.00% | 2009 | * | ||
| MA | 66.80% | 2002 | 82.70% | 2010 | |
| MD | 53% | 2002 | 80.20% | 2009 | |
| MI | 45.60% | 2001 | 79% | 2009 | |
| MN | 59.93% | 2003 | 79.97% | 2010 | * |
| NJ | 73.81% | 2009 | * | ||
| NM | 77.46% | 2010 | * | ||
| NY Medicaid | 63.90% | 2001 | 79% | 2010 | U |
| NY CHIP | 65% | 2001 | 72% | 2010 | * |
| PA Medicaid | 49.10% | 2001 | 75.50% | 2010 | * |
| RI | 80.70% | 2009 | U | ||
| TN | 73.00% | 2005 | 78.17% | 2009 | |
| VA | 72% | 2008 | * | ||
| WA | 46.43% | 2001 | 76.72% | 2010 | |
| WI | 72.20% | 2010 | * | ||
Figure 4: Percent with Breast Cancer Screening
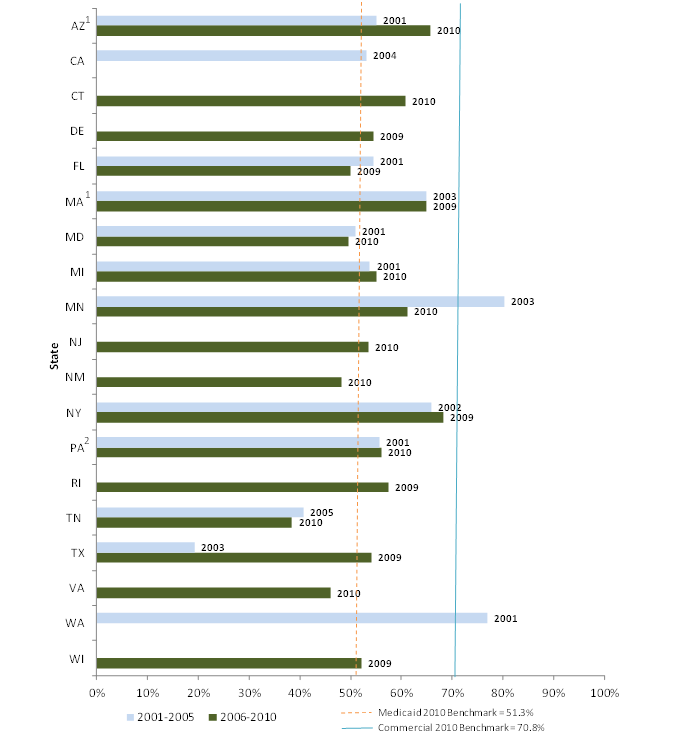
Source: Aggregate state data.
Notes: Unless noted, states use the HEDIS definition: percent of women aged 40 through 69 years of age who had a mammogram in the prior two years.
1Percent of women aged 52-69 who had a mammogram in the prior two years.
2Percent of women aged 40-64 who had a mammogram in the prior two years.
| State | 2001-2005 | Year Reporting | 2006-2010 | Year Reporting | HEDIS |
|---|---|---|---|---|---|
|
Source: Aggregate state data. Notes: Unless noted, states use the HEDIS definition: percent of women aged 40 through 69 years of age who had a mammogram in the prior two years. 1Percent of women aged 52-69 who had a mammogram in the prior two years. |
|||||
| AZ | 55.00% | 2001 | 65.70% | 2010 | Percentage of women aged 52-69 years of age who had a mammogram in the prior two years |
| CA | 53.10% | 2004 | * | ||
| CT | 60.70% | 2010 | * | ||
| DE | 54.40% | 2009 | U | ||
| FL | 54.48% | 2001 | 50.01% | 2009 | * |
| MA | 65% | 2003 | 64.90% | 2009 | * (percentage of women aged 52 through 69 years of age who had a mammogram in the prior two years in 2003) |
| MD | 51% | 2001 | 49.50% | 2010 | % of women aged 40- 69 who had a mammogram |
| MI | 53.80% | 2001 | 55.10% | 2010 | U |
| MN | 80.28% | 2003 | 61.15% | 2010 | * |
| NM | 48.14% | 2010 | * | ||
| NJ | 53.43% | 2010 | * | ||
| NY | 66% | 2002 | 68% | 2009 | * |
| PA | 55.60% | 2001 | 56.11% | 2010 | % of women aged 40- 64 who had a mammogram to screen for breast cancer |
| RI | 57.50% | 2009 | * | ||
| TN | 40.70% | 38.45% | * | ||
| TX | 19.22% | 2003 | 54.12% | 2009 | * |
| VA | 46% | 2010 | U | ||
| WI | 52.20% | 2009 | * | ||
| WA | 76.90% | 2001 | U | ||
Figure 5: Percent with Cervical Cancer Screening
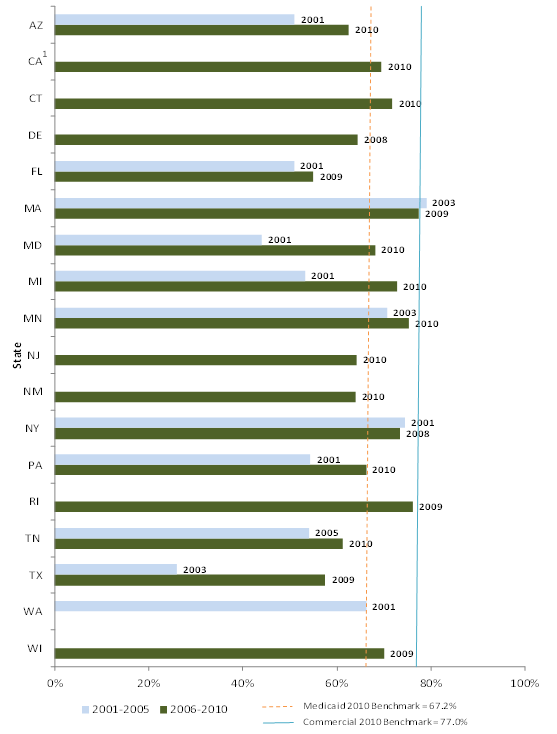
Source: Aggregate state data.
Notes: Unless noted, states use the HEDIS definition: percent of women aged 21-64 who received one or more PAP tests to screen for cervical cancer in prior three years.
1Percentage of women aged 21-64 who received one or more Pap tests within the prior three years.
| State | 2001-2005 | Year Reporting | 2006-2010 | Year Reporting | HEDIS |
|---|---|---|---|---|---|
|
Source: Aggregate state data. Notes: Unless noted, states use the HEDIS definition: percent of women aged 21-64 who received one or more PAP tests to screen for cervical cancer in prior three years. 1Percentage of women aged 21-64 who received one or more Pap tests within the prior three years. |
|||||
| AZ | 51.00% | 70% | 2009 | * | |
| CA | 2001 | U | |||
| CT | 2003 | 57.55% | 2009 | * | |
| DE | 2005 | 61.30% | 2010 | * | |
| FL | 50.92% | 76.20% | 2009 | * | |
| MA | 79% | 2001 | 66.24% | 2010 | * |
| MD | 44% | 2001 | 73.40% | 2008 | * |
| MI | 53.20% | 63.92% | 2010 | * | |
| MN | 70.63% | 64.29% | 2010 | * | |
| NJ | 2003 | 75.27% | 2010 | * | |
| NM | 2001 | 72.70% | 2010 | U | |
| NY | 74.50% | 2001 | 68.10% | 2010 | * |
| PA | 54.40% | 2003 | 77.40% | 2009 | * |
| RI | 2001 | 55.00% | 2009 | * | |
| TN | 54.10% | 64.41% | 2008 | U | |
| TX | 25.97% | 71.80% | 2010 | * | |
| WA | 66.20% | 69.50% | 2010 | Percentage of women 21-64 years of age who received one or more Pap tests within the prior three years | |
| WI | 2001 | 62.60% | 2010 | * | |
Figure 6: Percent of Diabetics with HbA1c Test
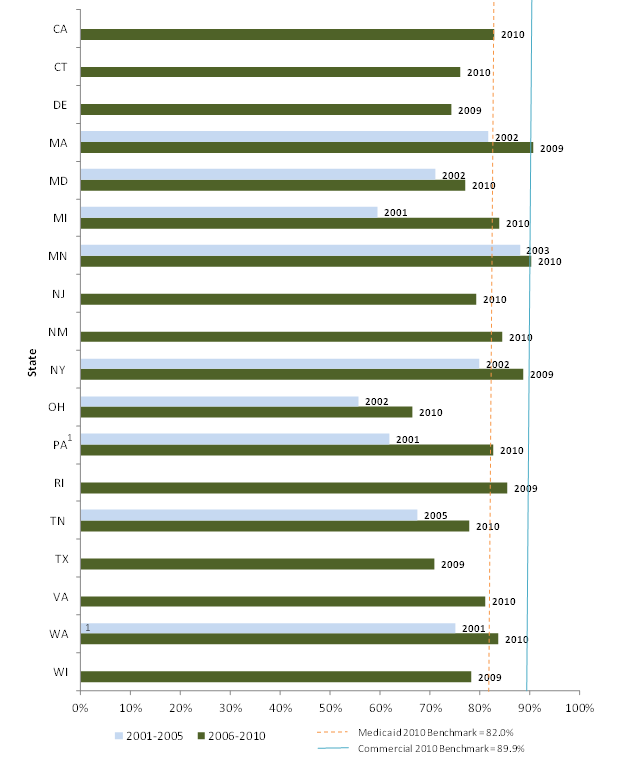
Source: Aggregate state data.
Notes: Unless noted, states use the HEDIS definition: percent of members aged 18-75 with diabetes who had one or more HbA1c test(s) during the measurement year.
| State | 2001-2005 | Year Reporting | 2006-2010 | Year Reporting | HEDIS |
|---|---|---|---|---|---|
|
Source: Aggregate state data. Notes: Unless noted, states use the HEDIS definition: percent of members aged 18-75 with diabetes who had one or more HbA1c test(s) during the measurement year. |
|||||
| CA | 82.80% | 2010 | * | ||
| CT | 76.10% | 2010 | * | ||
| DE | 74.25% | 2009 | U | ||
| MA | 81.60% | 2002 | 90.70% | 2009 | * |
| MD | 71% | 2002 | 77.10% | 2010 | * |
| MI | 59.50% | 2001 | 83.90% | 2010 | U |
| MN | 87.98% | 2003 | 90.29% | 2010 | * |
| NJ | 79.23% | 2010 | * | ||
| NM | 84.53% | 2010 | * | ||
| NY | 79.90% | 2002 | 89% | 2009 | * |
| OH | 55.70% | 2002 | 66.50% | 2010 | U |
| PA | 61.90% | 2001 | 82.74% | 2010 | The percentage of members 19-64 years of age with diabetes (type 1 and type 2) who had HbA1c testing |
| RI | 85.40% | 2009 | * | ||
| TN | 67.40% | 2005 | 77.93% | 2010 | * |
| TX | 70.83% | 2009 | * | ||
| VA | 81% | 2010 | U | ||
| WA | 75.10% | 2001 | 83.67% | 2010 | * |
| WI | 78.30% | 2009 | * | ||
Figure 7: Perents’ Overall satisfaction with Health Plan for Children
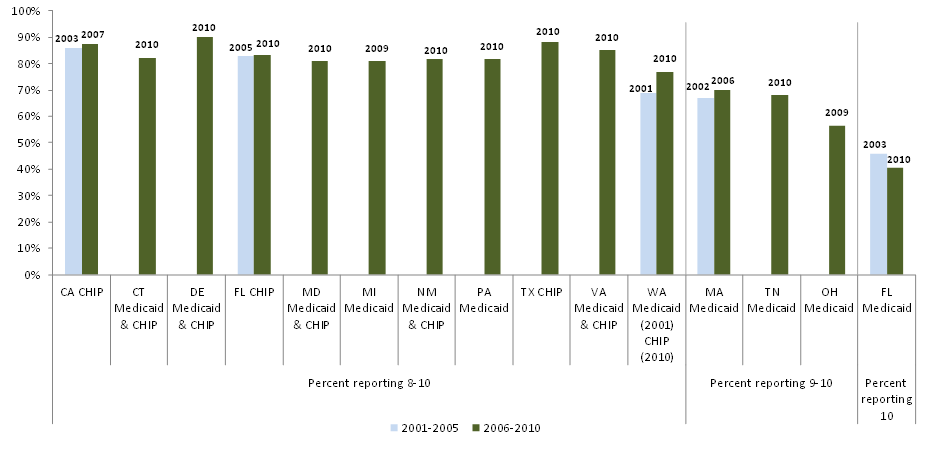
| State | 2001-2005 | Year reporting | 2006-2010 | Year Reporting | Percent Reported | Population |
|---|---|---|---|---|---|---|
|
Source: Aggregate state data. Note: CAHPS question is: "On a scale from 0 to 10, with 10 being the highest, over, how satisfied are you with your health plan?" |
||||||
| CT | 74.40% | 2010 | % reporting 8-10 | Adult | ||
| DE | 77.30% | 2010 | % reporting 8-10 | Adult and Children | ||
| MD | 76% | 2010 | % reporting 8-10 | Adult | ||
| MI | 72% | 2003 | 77% | 2010 | % reporting 8-10 | Adult |
| NM | 76.84% | 2010 | % reporting 8-10 | Adult | ||
| NY | 72.20% | 2001 | 67% | 2009 | % reporting 8-10 | Adults and Children |
| PA | 77.18% | 2010 | % reporting 8-10 in 2010 | Adult | ||
| VA | 78% | 2010 | % reporting 8-10 | |||
| MA | 56% | 2002 | 57% | 2006 | % reporting 9 or 10 | Adults |
| MN | 59% | 2009 | % reporting 9 or 10 | Adults and Children | ||
| NJ | 58% | 2009 | % reporting 9 or 10 | Adults | ||
| OH | 59.7% | 2009 | % reporting 9 or 10 | Adult | ||
| RI | 55.84% | 2010 | % reporting 9 or 10 | Adult | ||
| TN | 65.04% | 2010 | % reporting 9 or 10 | Adult | ||
| WA | 52% | 2007 | % reporting 9-10 in 2007 | Adults | ||
Figure 8: Parents’ Overall Satisfaction with Heath Care for Children
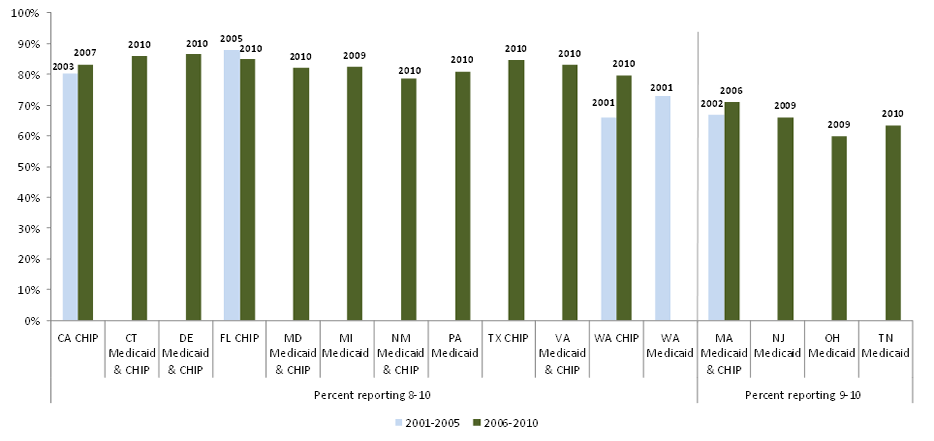
Source: Aggregate state data.
Note: CAHPS question is: "On a scale from 0 to 10, with 10 being the highest, overall, how satisfied are you with your health care?"
| State | 2001-2005 | Year Reporting | 2006-2010 | Year Reporting | Percent Reported | Population |
|---|---|---|---|---|---|---|
|
Source: Aggregate state data. Note: CAHPS question is: "On a scale from 0 to 10, with 10 being the highest, overall, how satisfied are you with your health care?" |
||||||
| CA | 80.26% | 2003 | 83.10% | % reporting 8-10 | CHIP | |
| CT | 85.90% | 2010 | % reporting 8-10 | Medicaid and CHIP | ||
| DE | 86.50% | 2010 | 8to10 | Medicaid and CHIP | ||
| FL | 87.80% | 2005 | 85.10% | 2010 | % reporting 8-10 | CHIP |
| MD | 82% | 2010 | % reporting 8-10 | Medicaid and CHIP | ||
| MI | 82.40% | 2009 | % reporting 8-10 | |||
| NM | 78.70% | 2010 | % reporting 8-10. | Medicaid and CHIP | ||
| PA | 80.91% | 2010 | % reporting 8-10 | Medicaid | ||
| TX | 84.62% | 2010 | % reporting 8-10 | CHIP | ||
| VA | 83.00% | 2010 | % reporting 8-10 | |||
| WA | 66% | 2001 | 79.60% | 2010 | % reporting 8-10 | CHIP |
| WA | 73% | 2001 | % reporting 8-10 | Medicaid | ||
| MA | 67% | 2002 | 71% | 2006 | % reporting 9-10 | Medicaid and CHIP |
| NJ | 66% | 2009 | % Reporting 9-10 | Medicaid | ||
| OH | 59.90% | 2009 | % Reporting 9-10 | Medicaid | ||
| TN | 63.30% | 2010 | % reporting 9-10 | Medicaid | ||
Figure 9: Parents’ Overall Satisfaction with Personal Doctor for Children
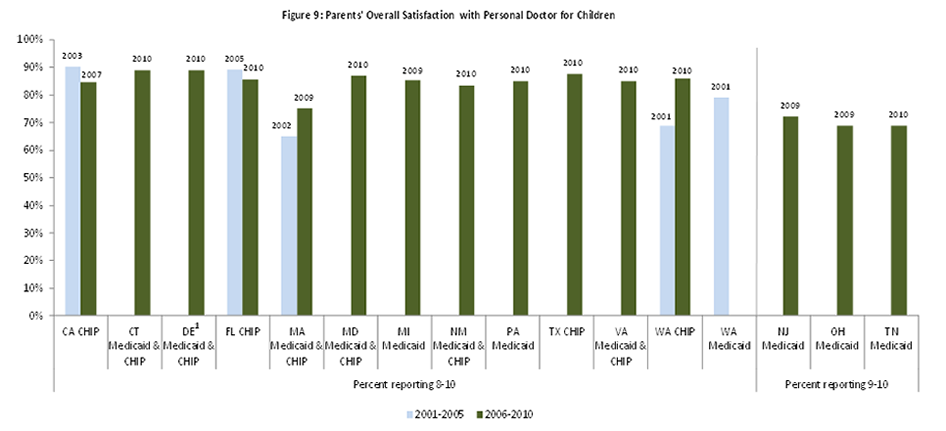
Source: Aggregate state data.
Note: CAHPS question is: "On a scale from 0 to 10, with 10 being the highest, overall, how satisfied are you with your personal doctor?"
| Statistic | Timeliness of Prenatal Care 2001-2005 (M=12) | Timeliness of Prenatal Care 2006-2010 (M=18) | Well Child Visits 2001-2005 (M=11, C=4) | Well Child Visits 2006-2010(M=19, C=6) | Childhood Immunization 2001-2005 (M=9, C=2) | Childhood Immunization 2006-2010 (M=16, C=3) |
|---|---|---|---|---|---|---|
|
Source: Aggregate state data. Note: CAHPS question is: "On a scale from 0 to 10, with 10 being the highest, overall, how satisfied are you with your personal doctor?" |
||||||
| Q1 | 0.72 | 0.81 | 0.51 | 0.67 | 0.50 | 0.76 |
| Min | 0.56 | 0.68 | 0.45 | 0.52 | 0.46 | 0.72 |
| Median | 0.74 | 0.84 | 0.56 | 0.73 | 0.60 | 0.79 |
| Max | 0.82 | 0.91 | 0.81 | 0.86 | 0.73 | 0.88 |
| Q3 | 0.80 | 0.88 | 0.64 | 0.79 | 0.65 | 0.80 |
| N | 16.00 | 12.00 | 14.00 | 13.00 | 4.00 | 13.00 |
Figure 10: Parents’ Overall Satisfaction with Specialist Care for Children
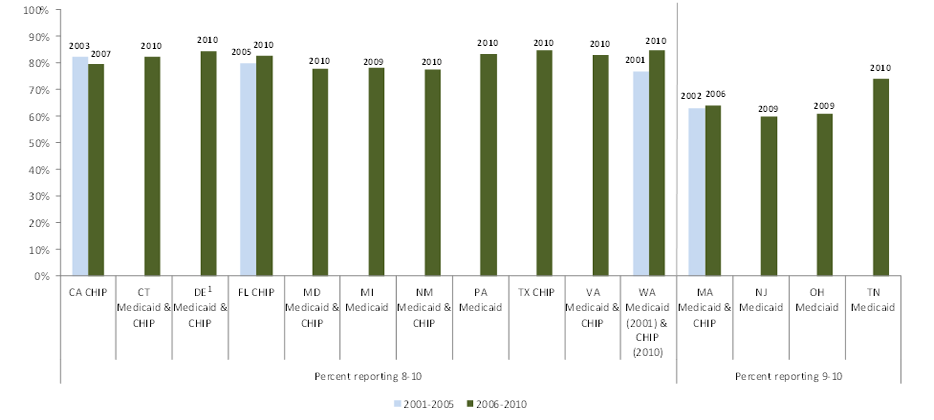
Source: Aggregate state data.
Note: CAHPS question is: "On a scale from 0 to 10, with 10 being the highest, overall, how satisfied are you with your specialist care?"
| Statistic | HbA1c 2001-2005 (N=9) | HbA1c 2006-2010 (N=18) | Cervical Cancer Screening 2001-2005 (N=12) | Cervical Cancer Screening 2006-2010 (N=16) | Breast Cancer Screening 2001-2005 (N=12) | Breast Cancer Screening 2006-2010 (N=18) |
|---|---|---|---|---|---|---|
|
Source: Aggregate state data. Note: CAHPS question is: "On a scale from 0 to 10, with 10 being the highest, overall, how satisfied are you with your specialist care?" |
||||||
| Q1 | 0.61 | 0.77 | 0.51 | 0.64 | 0.53 | 0.51 |
| Min | 0.56 | 0.67 | 0.26 | 0.55 | 0.19 | 0.38 |
| Median | 0.69 | 0.82 | 0.54 | 0.67 | 0.55 | 0.54 |
| Max | 0.88 | 0.91 | 0.79 | 0.77 | 0.80 | 0.68 |
| Q3 | 0.76 | 0.84 | 0.69 | 0.73 | 0.65 | 0.60 |
| N | 16.00 | 12.00 | 14.00 | 13.00 | 4.00 | 13.00 |
Figure 11: Overall Satisfaction with Health Plan for Adults

Source: Aggregate state data.
Note: CAHPS question is: "On a scale from 0 to 10, with 10 being the highest, overall, how satisfied are you with your health plan?"
1Population includes children.
| State | 2001-2005 | Reporting Year | 2006-2010 | Reporting Year | Reported | Population |
|---|---|---|---|---|---|---|
|
Source: Aggregate state data. Note: CAHPS question is: "On a scale from 0 to 10, with 10 being highest, overall, how satisfied are you with your health plan?" 1Population includes children. |
||||||
| CT | 72.70% | 2010 | % reporting 8-10 | Adults | ||
| DE1 | 77.35% | 2010 | % reporting 8 to 10 | Adults and Children | ||
| MD | 67.00% | 2010 | % reporting 8,9, 10 | Adults | ||
| MI | 61% | 2003 | 69.40% | 2010 | % reporting 8 to 10 | Adults |
| NM | 79.77% | 2010 | % reporting 8 to 10 | Adults | ||
| NY1 | 69.90% | 2001 | 69.00% | 2009 | % reporting 8,9, or 10 | Adults and Children |
| PA | 76.17% | 2010 | in 2010, measure is % reporting 8-10 | Adults | ||
| VA | 75.00% | 2010 | % reporting 8 to 10 | Adults | ||
| WI1 | 83.20% | 2002 | 82.40% | 2008 | % reporting 8 to 10 | Adults and Children |
| MA | 56.00% | 2002 | 53.00% | 2006 | % reporting 9 or 10 | Adults |
| MN1 | 55.00% | 2009 | % reporting 9 or 10 | Adults and Children | ||
| OH | 44.60% | 2008 | % reporting 9 or 10 | Adults | ||
| RI | 59.60% | 2010 | % reporting 9 or 10 | Adults | ||
| TN | 53.76% | 2010 | % reporting 9 or 10 | Adults | ||
| WA | 46.00% | 2007 | % reporting 10 in 2001, % reporting 9-10 in 2007 | Adults | ||
| FL | 40.73% | 2003 | 37.51% | 2010 | % reporting 10 | Adults |
Figure 12: Overall Satisfaction with Health Care for Adults
Source: Aggregate state data.
Note: CAHPS question is: "On a scale from 0 to 10, with 10 being the highest, overall, how satisfied are you with your health care?"
1Population includes children.
| State | 2001-2005 | Year Reported | 2006-2010 | Year Reported | Percent Reporting | Population |
|---|---|---|---|---|---|---|
|
Source: Aggregate state data. Note: CAHPS question is: "On a scale from 0 to 10, with 10 being the highest, overall,how satisfied are you with your health care?" 1Population includes children. |
||||||
| CT | 69.80% | % reporting 8-10 | Adult | |||
| DE1 | 74.95% | % reporting 8-10 | Adults and Children | |||
| MD | 66% | % reporting 8,9, 10 | Adult | |||
| MI | 66% | 66.40% | % reporting 8-10 | Adult | ||
| NM | 72.36% | % reporting 8-10 | Adult | |||
| NY | 69% | 65% | % reporting 8,9, or 10 | Adults | ||
| PA | 70.16% | measure is % reporting 8-10 | Adult | |||
| VA | 67.00% | % reporting 8-10 | Adults | |||
| WI1 | 85.90% | 86.20% | % reporting 8-10 | Adults and Children | ||
| MA | 56% | 55% | % reporting 9 or 10 | Adults | ||
| MN1 | 48% | % reporting 9 or 10 | Adults and Children | |||
| NJ | 44% | % reporting 9 or 10 | Adults | |||
| OH | 42.90% | % reporting 9 or 10 | Adults | |||
| RI | 50.22% | % reporting 9 or 10 | Adult | |||
| TN | 47.98% | % reporting 9 or 10 | Adult | |||
| WA | 42% | % reporting 9-10 in 2007 | Adults | |||
Figure 13: Overall Satisfaction with Personal Doctor for Adults
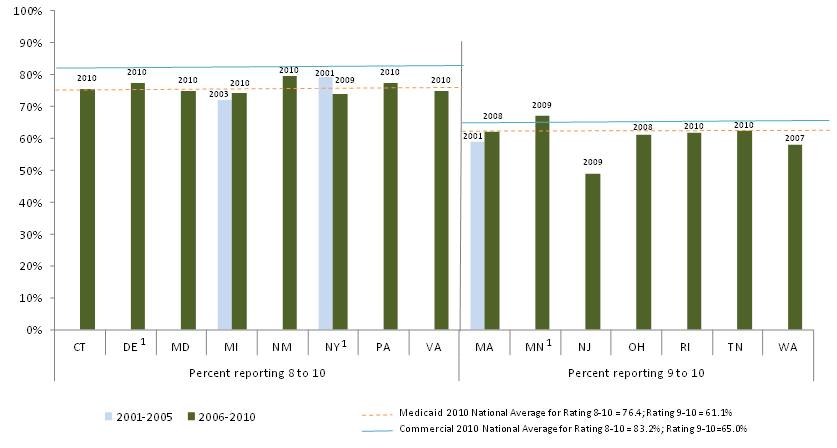
Source: Aggregate state data.
Note: CAHPS question is: "On a scale from 0 to 10, with 10 being the highest, overall, how satisfied are you with your personal doctor?"
1Population includes children.
| State | 2001-2005 | Year Reported | 2006-2010 | Year Reported | Percent Reporting | Population |
|---|---|---|---|---|---|---|
|
Source: Aggregate state data. Note: CAHPS question is: "On a scale from 0 to 10, with 10 being the highest, overall, how satisfied are you with your personal doctor?" 1Population includes children. |
||||||
| CT | 75.50% | 2010 | % reporting 8-10 | Adult | ||
| DE1 | 77.30% | 2010 | % reporting 8-10 | Adults and Children | ||
| MD | 75% | 2010 | % reporting 8-10 | Adult | ||
| MI | 72% | 2003 | 74.20% | 2010 | % reporting 8-10 | Adult |
| NM | 79.71% | 2010 | % reporting 8-10 | Adult | ||
| NY1 | 79.20% | 2001 | 74% | 2009 | % reporting 8-10 | Adults and Children |
| PA | 77.26% | 2010 | % reporting 8-10 | Adult | ||
| VA | 75% | 2001 | % reporting 8-10 | Adults | ||
| MA | 59% | 2001 | 62% | 2008 | % reporting 9 or 10 | Adults |
| MN1 | 67% | 2009 | % reporting 9 or 10 | Adults and Children | ||
| NJ | 49% | 2009 | % reporting 9 or 10 | Adults | ||
| OH | 61% | 2008 | % reporting 9 or 10 | Adults | ||
| RI | 61.80% | 2010 | % reporting 9 or 10 | Adult | ||
| TN | 62.33% | 2010 | % reporting 9 or 10 | Adult | ||
| WA | 58% | 2007 | % reporting 9-10 in 2007 | Adults | ||
Figure 14: Overall Satisfaction with Specialist Care for Adults
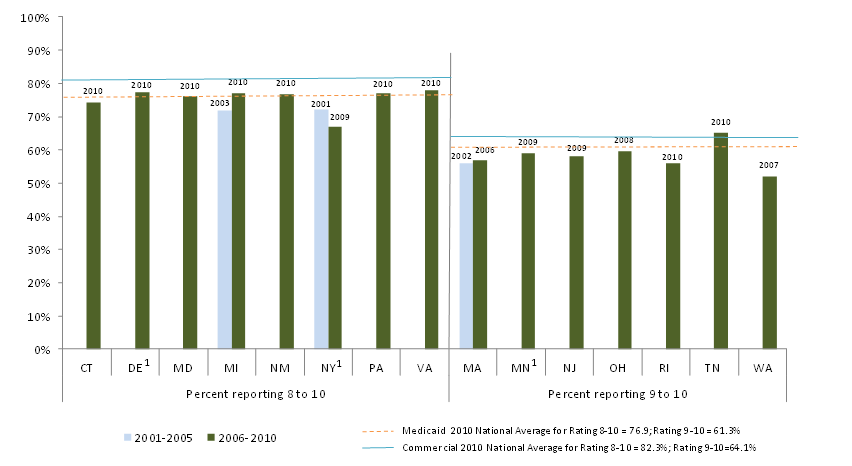
Source: Aggregate state data.
Note: CAHPS question is: "On a scale from 0 to 10, with 10 being the highest, overall, how satisfied are you with your specialist care?"
1Population includes children.
| State | 2001-2005 | Year reporting | 2006-2010 | Year Reporting | Percent Reported | Population |
|---|---|---|---|---|---|---|
|
Source: Aggregate state data. Note: CAHPS question is: "On a scale from 0 to 10, with 10 being the highest, overall, how satisfied are you with your specialist care?" 1Population includes children. |
||||||
| CT | 74.40% | 2010 | % reporting 8-10 | Adult | ||
| DE | 77.30% | 2010 | % reporting 8-10 | Adult and Children | ||
| MD | 76% | 2010 | % reporting 8-10 | Adult | ||
| MI | 72% | 2003 | 77% | 2010 | % reporting 8-10 | Adult |
| NM | 76.84% | 2010 | % reporting 8-10 | Adult | ||
| NY | 72.20% | 2001 | 67% | 2009 | % reporting 8-10 | Adults and Children |
| PA | 77.18% | 2010 | % reporting 8-10 in 2010 | Adult | ||
| VA | 78% | 2010 | % reporting 8-10 | |||
| MA | 56% | 2002 | 57% | 2006 | % reporting 9 or 10 | Adults |
| MN | 59% | 2009 | % reporting 9 or 10 | Adults and Children | ||
| NJ | 58% | 2009 | % reporting 9 or 10 | Adults | ||
| OH | 59.7% | 2009 | % reporting 9 or 10 | Adult | ||
| RI | 55.84% | 2010 | % reporting 9 or 10 | Adult | ||
| TN | 65.04% | 2010 | % reporting 9 or 10 | Adult | ||
| WA | 52% | 2007 | % reporting 9-10 in 2007 | Adults | ||
Appendix D: Trends in NCQA HEDIS Requirements, 2001-2010
Timeliness of Prenatal Care
2002
Revised to ensure that measures share the same denominator as Frequency of Ongoing Prenatal Care. Measure was clarified to include visits to physician assistants and nurse practitioners.
2010
Added a practitioner requirement to the Postpartum Care numerator for the Hybrid Specification
Well-Child Visits
No changes
Childhood Immunizations
2007
Deleted "documented history of illness" and "seropositive test result" as numerator evidence for DTaP, IPV, HiB, and pneumococcal conjugate. These were infrequent, and likely to affect plans equally. They were deleted due to small impact and measure and burden for reporting. Four acellular pertussis vaccines for the DTaP atigen were required.
2008
Revised the required number of doses for the HiB vaccine, per ACIP recommendations to defer to the third HiB booster during vaccine shortage.
2010
Increased HiB dose requirement from 2 to 3.
Breast Cancer Screening
2005
Hybrid methodology was retired for this method.
2006
Changed age range from 50–69 to 40–69. Plans reported three rates: Total; 40–49; 50–69.
2008
Measure changed to one age band of 40–69.
Cervical Cancer Screening
2006
The lower age limit was raised to 21 years of age from 18 years of age.
Comprehensive Diabetes Care (HbA1c)
2004
Removed glycohemoglobin from the HbA1c screening and control indicators. Added new LOINC codes.
2005
Added an administrative method to the measure.
Source: Personal communication with Alan Hoffman, NCQA, 2011.
Disclaimer
This study was conducted by the Urban Institute under contract number HHSP23320095654WC, task order number HHSP23337015T, with the HHS’s Office of Assistant Secretary for Planning and Evaluation. The authors take full responsibility for the accuracy of material presented herein. The views expressed are those of the authors and should not be attributed to ASPE or HHS.
