U.S. Department of Health and Human Services
U.S. Department of Health and Human Services
Study of Medicare Home Health Practice Variations: Final Report
Angela G. Brega, Ph.D., Robert E. Schlenker, Ph.D., Kamal Hijjazi, Ph.D., Susannah Neal, M.A., Elaine S. Belansky, Ph.D., Sylvia Talkington, R.N., Anne K. Jordan, Ph.D., Jeff Bontrager, B.A., and Colleen Tennant, M.S.P.H.
University of Colorado, Center for Health Policy Research
August 2002
This report was prepared under contract #HHS-100-95-0045 between the U.S. Department of Health and Human Services (HHS), Office of Disability, Aging and Long-Term Care Policy (DALTCP) and University of Colorado. For additional information about the study, you may visit the DALTCP home page at http://aspe.hhs.gov/daltcp/home.htm or contact the ASPE Project Officer, Andreas Frank, at HHS/ASPE/DALTCP, Room 424E, H.H. Humphrey Building, 200 Independence Avenue, SW, Washington, DC 20201. His e-mail address is: Andreas.Frank@hhs.gov.
This report was produced as part of the "Study of Medicare Home Health Practice Variations," funded by the Office of the Assistant Secretary for Planning and Evaluation (ASPE), Department of Health and Human Services (Contract No. 100-95-0045). This document represents the final report for the study and integrates several project deliverables (13.2a, 13.2b, 13.2c, 13.4, 14.9, 14.10, 14.11, 14.12, 14.13, 14.14, 14.15, and 14.16).
TABLE OF CONTENTS
- I. INTRODUCTION
- A. Background
- B. Overview of Methods
- State, Agency, and Patient Selection
- Quantitative and Qualitative Methods
- C. Report Overview
- II. METHODS
- A. State, Agency, and Patient Selection
- Selection of State Sample
- Selection of Home Care Agencies
- Selection of Study Patients
- B. Data Collection Procedures
- Quantitative Methods
- Qualitative Methods
- C. Data Management and Analysis Procedures
- Data Management Procedures
- Data Analysis Procedures
- Identification of Important Variables
- Missing Data
- III. DESCRIPTIONS OF STUDY STATES, AGENCIES, CARE PROVIDERS, AND PATIENTS
- A. Description of Study States
- B. Description of Study Agencies
- Overview of Study Agencies
- AQ Descriptive Statistics
- C. Description of Study Care Providers
- D. Description of Study Patients
- IV. PRACTICE AND PRACTICE VARIATIONS IN HOME HEALTH CARE
- A. Practices in Home Health Care
- B. Causes of Practice Variation in Home Health Care
- Influence of Patient Factors on Home Care Practices
- Influence of Provider Factors on Home Care Practices
- Influence of Agency Factors on Home Care Practices
- Influence of Market/Regulatory Factors on Home Care Practices
- C. Effect of Practice Patterns on Home Health Episode Length
- D. Patient Outcome of Home Health Care
- V. PRACTICE AND DECISION MAKING IN HOME HEALTH CARE
- A. Focus Group Interviews
- Patient and Caregiver Factors
- Actors
- Agency Factors
- External Factors
- Medicare Coverage Rules
- B. Case Study Interviews
- Key Characteristics of the Episodes of Care
- Services Provided in Home Health Care
- Care Planning and Coordination
- Content of the Skilled Nursing Visit
- C. Conclusions
- What is the Actual Practice of Home Health Care?
- How are Decisions About Care Made in Light of Medicare Coverage Rules?
- VI. PROVIDER PERSPECTIVES ON THE INTERIM PAYMENT SYSTEM AND CHANGES IN HOME HEALTH CARE
- A. State Home Care Association Interviews
- Overview of Findings
- State-Specific Findings
- B. Administrator Interviews
- How Has IPS Affected Your Administrative and Staffing Practices?
- In What Ways Has IPS Affected the Structure of Care That You Provide?
- How Have the Reduction in Visit Cost Limits and the New Per-Beneficiary Limits Specifically Affected Your Agency?
- How is Your Agency Preparing for Prospective Payment?
- C. Focus Group Interviews
- Case Mix
- Patient Education
- Caregiver Education
- Goals of Care
- Quality of Care
- D. Case Study Interviews
- VII. SUMMARY AND CONCLUSIONS
- A. Practice and Decision Making in Home Health Care
- Quantitative Findings
- Qualitative Findings
- B. Provider Perspectives on the Interim Payment System (IPS) and Changes in Home Health Care
- C. Implications
- Implications for Clinical Practice Guidelines
- Implications for Medicare Home Health Coverage Rules
- D. Conclusions
- APPENDICES
- APPENDIX A: Study Questionnaires
- APPENDIX B: Focus Group Materials
- APPENDIX C: Case Study Materials
- APPENDIX D: Supplemental Information on the Study States
- APPENDIX E: Administrator Questionnaire Descriptive Statistics and Write-in Responses
- APPENDIX F: Multivariate Analysis Variable List
- LIST OF TABLES AND FIGURES
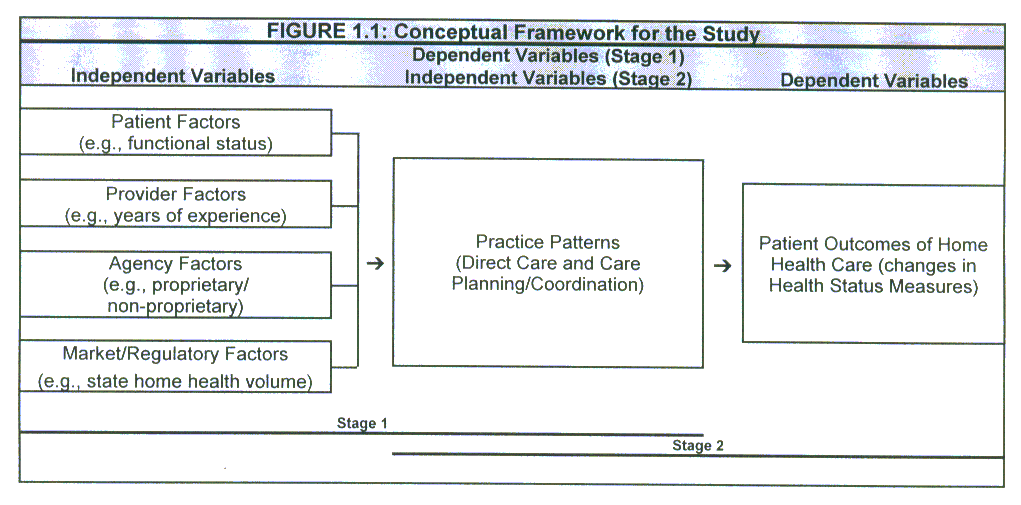
- Figure 1.1: Conceptual Framework for the Study
- Table 1.1: Major Home Health Provisions of and Amendments to the Balanced Budget Act of 1997
- Table 2.1: Factors Influencing Agency Attrition
- Table 2.2: Summary of Qualitative Methods
- Table 2.3: Administrator Interview Questions and Probes
- Table 2.4: Administrator Interviews by State Volume Group and Agency Ownership Categories
- Table 2.5: State Home Care Association Interview Questions and Probes
- Table 2.6: Design for Agency Selection for the Focus Groups and Case Studies
- Table 2.7: Focus Group Participant Demographic Characteristics (N=43 Participants)
- Table 3.1: Average Medicare Home Health Visits per Patient for the Study States
- Table 3.2: Selected Demographic and Economic Measures for the Study States
- Table 3.3: Selected Elderly Health Care Coverage Measures for the Study States
- Table 3.4: Selected Health Care Resource and Use Measures for the Study States
- Table 3.5: Selected Medicare and Medicaid Expenditure Measures for the Study States
- Table 3.6: Selected Medicare and Medicaid Home Health Expenditure Measures for the Study States
- Table 3.7: Agency Ownership and Type Distribution of Study Agencies
- Table 3.8: Descriptive Information Regarding Study Care Providers
- Table 3.9: Patient Case Mix at Start of Episode by Condition
- Table 4.1: Care Provided During the Study Episodes
- Table 4.2: Effect of Patient, Provider, Agency, and Market/Regulatory Factors on Practice Patterns
- Table 4.3: Effect of Practice Patterns on Episode Length, Controlling for Patient, Provider, Agency, and Market/Regulatory Factors
- Table 4.4: Effect of Practice Patterns on Patient Outcome, Controlling for Patient, Provider, Agency, and Market/Regulatory Factors
- Table 5.1: Key Episode Characteristics by State Volume, Agency Ownership, and Agency Type
- Table 5.2: Service Utilization by Case Study Patient
- Table 5.3: Skilled Nursing Activities
- Table 5.4: Assistance Provided by Family Members
- Table 5.5: Activities of Patient Assessment and Treatment
- Table 6.1: Home Health Market Changes in the Eight Study States
- Table 6.2: Recent Changes to Home Health Care
EXECUTIVE SUMMARY
A. Background
The main goal of this study was to examine how patient, provider, agency, and market/regulatory factors relate to variations in home health care practices and how practice patterns relate to outcomes for Medicare beneficiaries. Five important aspects of home health practice, covering both direct care provision and care coordination, were selected for examination. The four measures of direct care investigated were (1) the average number of visits provided to a patient per day (i.e., visit intensity), (2) the duration of the home health episode (length of stay), (3) the total number of disciplines involved in patient care, and (4) the number of alternative services provided during the episode of care.1 The amount of feedback received by the primary home care provider from other agency personnel regarding a patient's care plan and discharge was examined as a measure of care coordination.2 The three key research questions were:
- What is the actual practice of home health care, in terms of type, amount, and decision making (e.g., care planning, care coordination)?
- How are decisions about care made in light of Medicare coverage rules?
- What elements of practice are associated with long lengths of stay in the Medicare home health benefit?
In addition, although the study was not originally intended to address issues related to the Balanced Budget Act (BBA) of 1997, the timing of the project allowed for an examination of the impact of the Interim Payment System (IPS) and other policy changes that occurred prior to the implementation of the Medicare home health Prospective Payment System (PPS) in October 2000.
The objective of this report is to summarize the findings from the quantitative and qualitative methods used to answer the key study questions. The report provides a description of the states, agencies, and patients that participated in the study. Quantitative data are used to (1) examine the influence of patient, provider, agency, and market/regulatory factors on practice patterns, (2) explore the impact of practice patterns on length of stay, and (3) identify the effect of practice patterns on patient outcomes. Practice patterns and decision making in home health care are explored using data from focus group and case study interviews. Finally, qualitative data regarding provider perspectives on IPS, a major provision of the BBA, and other changes in the field of home health care are summarized.
B. Findings
1. Key Features of Study States, Agencies, and Patients
Study States: Eight states were chosen for participation in the study on the basis of their home health visit volume, defined as the average number of visits per Medicare beneficiary receiving home care per year in 1995. Four low-volume and four high-volume states were selected. The four low-volume states selected were Minnesota, New Jersey, Oregon, and Pennsylvania and the four high-volume states were Georgia, Massachusetts, Mississippi, and Texas.
Descriptive information about the states shows variation within each state volume group, but greater variation between the two groups. Further, although visit volume (visits per beneficiary per year) has decreased in both the low- and high-volume states, the percentage reduction in visit volume is only slightly higher in high-volume states than low-volume states. Some key differences between the states in the high-and low-volume groups are the following:
- On average, a slightly larger percentage of the population is 65 years old or older in the low-volume than the high-volume states.
- In low-volume states, a slightly smaller percentage of the age 65 and older population lives in poverty than in the high-volume states. Likewise, a smaller percentage of Medicare patients are covered by Medicaid in the low-volume than the high-volume states.
- A larger number of people aged 65 and older per 1000 has difficulties with mobility/self-care in the high-volume than the low-volume states.
- The high-volume study states have many more home health users per 1000 among their Medicare beneficiaries than do the low-volume states.
Study Agencies: Agencies were randomly sampled from the eight states and invited to participate in the study until the target agency sample of 56 agencies was reached. During the course of data collection, several agencies discontinued their participation in the study (often due to the greater financial stringency under IPS) or failed to submit useable longitudinal data. Of the 56 agencies recruited for participation in the study, 44 contributed data to the final sample used for analysis purposes.
The study agencies reflected a variety of important agency-level factors, providing a cross-section with regard to three factors that were hypothesized to play a critical role in the practice of home health care:
- The final sample of 44 agencies had good representation of agencies in both the high-volume and low-volume states (41% and 59%, respectively).
- More than half of the agencies were nonproprietary or government agencies (66%). The remaining 34% were proprietary agencies.
- The sample had nearly equal representation of hospital-based and freestanding agencies (48% and 52%, respectively).
Study Patients: The final patient sample included 684 patients, contributing a total of 732 complete episodes of care. Patients enrolled in the study reflected a variety of important variations in their conditions and living situations.
- The study patients were quite elderly, with an average age of 78 years.
- The majority of patients were White and female.
- Despite their age, 80% of the study patients lived in their own homes.
- Nearly all patients had family members or other persons who provided them with some assistance.
- Slightly over 81% of patients had been discharged from an inpatient facility within two weeks of beginning home care.
- The majority of patients (95%) had only a single episode of care during their time in the study.
2. Practice Variations in Home Health Care
Quantitative analyses were conducted on longitudinal data for congestive heart failure (CHF) and diabetes mellitus patient episodes to examine (1) the effect of patient, provider, agency, and market/regulatory factors on home care practices, (2) the influence of practice patterns on episode length, and (3) the impact of home care practices on patient outcome. The following are the key findings from the multivariate analyses:
- Patient complexity, functional status, and diagnoses were important predictors of visit frequency, the number of disciplines and alternative services included in the patient's care, episode length, and the amount of feedback a care provider receives from other agency personnel about the patient's care plan.
- Care providers with more years of experience in home health care tended to have patients with significantly longer episode lengths than did less experienced providers.
- Agency ownership and type were strong predictors of home care practices. Proprietary agencies appeared to counterbalance visit intensity and length of stay, providing their patients with more frequent visits over shorter episodes than did nonproprietary agencies. These agencies also made greater use of alternative services.
- Freestanding agencies provided both more frequent visits and longer episodes of care than did hospital-based agencies.
- States that had been identified based on 1995 data as providing a large number of home care visits per patient appeared to continue to utilize home care resources more heavily than did states with lower visit volume (e.g., more frequent visits, more disciplines involved).
- Agencies appeared to counterbalance frequency of visits and length of stay, such that episodes involving more frequent visits were significantly shorter than episodes with less frequent visits.
- Episodes of care that involved more disciplines were significantly longer than those involving fewer home health disciplines.
- Patients receiving more frequent visits experienced marginally better outcomes of home care than did patients with less frequent visits.
3. What is the Actual Practice of Home Health Care?
The focus group and case study interviews were conducted to examine home health care in greater depth than was possible with the primary data sample. Key findings regarding service provision, and care planning and coordination are summarized here.
Service Provision:
- Often, elderly recipients of Medicare home care services are complex patients, many having been recently discharged from hospital care. According to focus group participants, patients just released from the hospital often are sicker than other home care recipients and frequently require complex or high-tech services.
- Home care nurses engage in a wide variety of activities as part of providing skilled nursing care, including assessment of patients' medical conditions and needs, education of patients and their families, development of the care plan, management of the medications, completion of required forms, documentation, coordination of the patients' support networks, psychological counseling, and coordination of care across disciplines.
- The family support system is of great importance to elderly home care patients. Family members provide assistance with activities of daily living (ADLs), instrumental activities of daily living (IADLs), environmental support, and psychological support. In addition, they often are heavily involved in the patients' home health care activities (e.g., present at visits, involved in the development of the plan of care). The presence of a family support system is an important factor affecting nurses' decisions about the frequency of visits a patient needs.
- Patients and/or their families often refuse to accept the services of home health aides and medical social workers. Usually, patients who refuse services have family members who are willing and able to provide for the patients' needs.
Care Planning and Coordination:
- The role of the primary nurse in the process of developing the patient's care plan varies from agency to agency. At some of the case study agencies, primary nurses have a great deal of control over a patient's care plan. However, many agencies involve nursing supervisors in the development of patients' care plans. Although the sample size was small, the case study interviews suggest that primary nurses have greater control over the development of their patients' care plans in low-volume states and in nonproprietary agencies. Administrator Questionnaire data corroborate these findings and also suggest that primary nurses have greater control over their patients' care plans in hospital-based than freestanding agencies.
- Physician involvement in home care appears to be minimal in most cases. Generally, the patient's plan of care is developed independently by home care agency staff based on their initial assessment of the patient's needs. The care plan often has little resemblance to the physician's initial referral, which rarely specifies the types of visits needed and the frequency with which they should occur. Nurses usually communicate with their patients' physicians only at milestone time points, such as recertification and discharge, or when the patient's condition changes. Contact between home care nurses and physicians is nearly always made indirectly through the physician's nursing staff.
- Home health agency case conferences are a main mechanism through which home care providers of different disciplines stay in contact about their patients.
- Discharge planning begins very early in the home care episode, often at the first visit. Nurses cited a number of factors they consider in determining a patient's readiness for discharge: homebound status and other Medicare eligibility requirements, stability of the patient's medical condition and medication regimen, attainment of educational goals, the patient's endurance, and the patient's ability to manage his or her medications.
- In preparation for discharge, primary nurses work to identify resources to assist with the patient's continuing needs following discharge, such as transportation and meal preparation.
4. How are Decisions About Care Made in Light of Medicare Coverage Rules?
The focus group and case study interviews also provided important information about the decision-making process in home health care. This section highlights some key findings from these interviews.
- Recertification and discharge decisions are based on a number of factors, including patient factors (e.g., living environment), agency factors (e.g., supervision of decision-making process), and external factors (e.g., IPS, coverage rules).
- The patient's primary nurse usually makes the decisions about the care plan, although some agencies involve nursing supervisors and a multi-disciplinary team in the review of each patient's care plan. Nurses in low-volume states appear to have greater control over the decision-making process than do nurses in high-volume states. Supervisory staff appear to be more involved in the development of the patient's care plan in proprietary than nonproprietary agencies.
- There appears to be considerable confusion surrounding Medicare coverage rules. Nurses often are uncertain about the definition of "homebound," about what constitutes skilled nursing care, and about the appropriate use of Management and Evaluation (M&E). Nurses suggested that physicians seem to struggle with these concepts as well, sometimes referring patients who are not eligible for Medicare home health services.
- However, the focus group and case study interviews produced no evidence that the lack of clarity in coverage rules encourages home care providers to continue to provide services to patients who may be ready for discharge. Indeed, there was some suggestion from the interviews that this ambiguity may actually result in shorter episodes of care. Fear of Medicare review leads some nurses to opt for discharging a patient for whom it is unclear whether discharge or recertification is the correct approach. Further, it appears that agencies may avoid the use of services for which the coverage rules are ambiguous, such as M&E.
5. Provider Perspectives on the Interim Payment System (IPS)
This study was not originally intended to examine the impact of recent regulatory changes related to home health care. However, because the BBA was implemented prior to the major data acquisition phase of the project, the opportunity arose to obtain information about the impact of IPS and other recent changes in home health care. A number of important themes emerged across several methods used to examine provider perceptions of IPS and concurrent changes:3
- Interview participants reported that home care patients receive fewer services and are on service for shorter periods of time than they once were.
- The focus on reducing home health utilization has led to the identification and increased involvement of community and other outside resources early in patients' episodes of care.
- According to agency administrators, this increased emphasis on community resources has expanded the role of social workers in patient care. However, this finding is not consistent with recent work conducted by Abt Associates (1999), which indicated that more agencies have decreased (8.4%) than increased (4.2%) the involvement of social workers.
- Patient education intended to help patients and their families to provide for their own needs has become an increasingly important aspect of home care. According to many providers, this education must take place in an increasingly short period of time.
- Interview participants reported that agencies sometimes refuse high-need patients, such as chronic, complex, or rural patients. In particular, the respondents contend that access to home care services has been reduced for diabetic patients and patients who need daily wound care. Other studies have reported similar findings.
- Many interview participants noted that a large number of home care agencies have closed or merged with other agencies during the past few years.
- Many agencies have instituted cost saving measures, laid off staff, instituted additional case management procedures, increased nurse productivity standards, and changed their geographic service areas in an attempt to respond to IPS and other regulatory changes.
- Many agencies are pursuing ways to diversify their payer sources, seeking to shift their case load more toward Medicaid and managed care and away from Medicare.
- Agency administrators noted a reduction in physician referrals to home care.
C. Conclusions
The field of home health care has seen dramatic changes over the past several years. Since the collection of the data used in this study, several major regulations have been implemented that are expected to have a powerful impact on the practice of home health care. The implementation of the home health PPS in October 2000 has provided agencies with strong incentives to reduce the number of visits provided to patients and to find other means of minimizing the cost of care. These incentives have the potential to lead to underservice and poor patient outcomes. On the other hand, the 1999 implementation of OASIS data collection and transmission requirements and the more recent generation of case mix, adverse event, and outcome reports focus agency attention on the quality of care they provide, perhaps lessening the likelihood of underutilization of care. The findings from this study provide a baseline of information on practice patterns during the IPS period, allowing researchers to identify the impact of the implementation of PPS and other recent federal regulations.
PREFACE AND ACKNOWLEDGMENTS
This study was designed to use quantitative and qualitative data and methods to examine how patient, provider, agency, and market/regulating factors influence variations in home health care practices and how practices influence outcomes for Medicare beneficiaries. Although the study was not originally intended to examine the effects of the Balanced Budget Act (BBA) of 1997, the study data were collected during the early BBA period (i.e., under the Interim Payment System, IPS) and thereby provide a baseline against which future trends under the Prospective Payment System (PPS) can be assessed.
Floyd Brown, the ASPE Project Officer, provided constructive oversight during the final phase of the project, which we greatly appreciate. In addition, Kamal Hijjazi and Bob Clark, former Project Officers, provided valuable input and guidance to this study. We acknowledge and thank the following individuals for their careful review of an earlier version of this report: Floyd Brown, Pamela Doty, John Drabek, Jennie Harvell, and Kamal Hijjazi from the Office of the Assistant Secretary for Planning and Evaluation (ASPE); Tricia Davis, Heidi Gelzer, Ann Meadow, and Kathleen Walsh from the Centers for Medicare & Medicaid Services; Sharon Bee and Sally Kaplan from the Medicare Payment Advisory Commission (MedPAC); and Barbara Gage from Health Economics Research.
The Research Center Project Director is Peter Shaughnessy. In addition to the authors of this report, other former and current project team members and Research Center staff contributing to the study work are Blythe Allen, Lanee Bounds, Amy Bush, Cynthia Eby, María Fernández-Fletcher, Natasha Floersch, Colleen Homedale, Karis May, Delores Smyth, Helen Tabachny, and Jennifer Wolgemuth.
I. INTRODUCTION
A. Background
The growth of the elderly population and changes in Medicare policy have led to dramatic increases in the volume and costs of home health care during the late 1980s and early 1990s. In light of this recent growth, it has become increasingly important to understand the actual practice of home health care and how health care providers interpret Medicare policies. This study was intended to explore several important dimensions of home health care, with particular emphasis on the delivery and outcome of care in the context of current Medicare policies and regulations. The information collected in the study is intended to contribute to the knowledge base of government agencies in dealing with current and future issues surrounding home health care.
The main goal of this study, conducted for the Office of the Assistant Secretary for Planning and Evaluation (ASPE), was to examine factors related to variations in the care practices of Medicare-certified home health care providers. During the 1990s, dramatic variations in the provision of home health care became apparent. In 1995, the Office of the Inspector General (OIG) identified wide variation in reimbursement rates per beneficiary at agencies across the country (OIG 1995a). Using 1993 data, OIG found that one-third of all home health agencies received 51.5% of all Medicare reimbursement for home health services. Although the average reimbursement per visit was similar across agencies, the number of visits provided varied dramatically. Agencies with the highest level of reimbursement provided an average of five times more visits per beneficiary than did agencies with the lowest level of reimbursement (141 vs. 27 visits).
Agencies that received high levels of reimbursement differed from low-reimbursement agencies in several important respects (OIG 1995a). Agencies with high reimbursement levels tended to be proprietary and freestanding. Further, these agencies had larger numbers of employees, especially home health aides, than did agencies with lower reimbursement rates per beneficiary. Agencies with high reimbursement rates provided seven times the number of home health aide visits than did agencies with lower average per-beneficiary reimbursement.
Large differences in average reimbursement rates per beneficiary did not seem to be explained by patient characteristics (OIG 1995a). A comparison of reimbursement rates for the 15 principal diagnostic codes with the highest reimbursement amounts indicated that average reimbursement rates per beneficiary varied dramatically even within specific diagnostic groups. Further, beneficiary age, gender, race, and Medicare-eligibility category were quite similar across agencies of varying reimbursement levels. Contrary to what one might expect, patients in the care of high-reimbursement agencies were slightly more likely to die while on service than were patients in the care of agencies with lower levels of reimbursement per beneficiary. However, this difference was quite small and might suggest that high-reimbursement agencies care for patients with more severe illness.
OIG also examined the relationship between average reimbursement per beneficiary and quality of care (1995a). In the absence of true outcome measures, agency-level measures were used as proxies for service quality (i.e., number of deficiencies and complaints recorded by the Health Care Financing Administration (HCFA) Survey and Certification Branch and accreditation status).4 Agencies with high reimbursement rates per beneficiary did not have fewer deficiencies and complaints than agencies with lower average reimbursement rates per beneficiary. They were, however, less likely to be accredited (this may be related to the fact that these agencies are less likely to be affiliated with hospitals, skilled nursing facilities, or other medical service organizations).
In 1994, Schore found striking regional variations in the use of home health services. Examining utilization of home health services in nine multi-state regions, corresponding to regional categories typically used by HCFA, Schore found that the mean number of visits provided per home care episode was much lower in the Pacific region (Alaska, California, Hawaii, Oregon, and Washington) and Middle Atlantic region (New Jersey, New York, and Pennsylvania) than in the East South Central and West South Central regions (East: Alabama, Kentucky, Mississippi, and Tennessee; West: Arkansas, Louisiana, Oklahoma, and Texas). The mean numbers of visits per episode were 28 in the Pacific region and 30 in the Middle Atlantic region. In the East and West South Central regions, on the other hand, the mean numbers of visits per home health episode were 95 and 64, respectively. Regional variations in episode length followed this same pattern. The Pacific and Middle Atlantic regions had much shorter mean lengths of stay in the home health benefit (60 and 66 days, respectively) than did the East and West South Central regions (180 and 121 days, respectively). OIG (1995b) also reported that states in the Southeastern region of the country (Alabama, Florida, Georgia, Kentucky, Mississippi, North Carolina, South Carolina, and Tennessee) provide more visits per beneficiary than other states.
According to Schore (1994), the types of visits provided also varied somewhat by geographic region. Although there was little regional variability in the inclusion of skilled nursing visits in the episodes of care, the inclusion of home health aide visits, therapy visits, and social work visits was subject to greater regional variability. Home health aides provided at least one visit in 37% of the episodes in the Pacific region and 52% in the East South Central region. The percentages of episodes in a region that included at least one therapy visit ranged from 26% (West North Central region: Iowa, Kansas, Minnesota, Missouri, Nebraska, North Dakota, and South Dakota) to 46% (Pacific region). Medical social workers provided at least one visit in 8% of the episodes of care in the New England region (Connecticut, Maine, Massachusetts, New Hampshire, Rhode Island, and Vermont) and 32% of the episodes in the Pacific region.
Importantly, in the Schore study (1994), patient outcomes (measured through claims data) appeared to vary somewhat by geographic region. Patients in the Pacific region had the lowest rates of inpatient admission within 30 days of the end of their home health episodes, home health readmission between 31 and 60 days after the end of their episodes, and home health readmission between 31 and 60 days after the end of their episodes for the same diagnostic group as the original episode. Patients in the East South Central region had the highest rates of these outcomes and also the highest death rate within 30 days of the end of a home health episode.
Schore's results (1994) suggest that high utilization does not necessarily enhance patient outcomes, as one might expect. On the contrary, the region with the highest utilization rates had the highest occurrence of negative outcomes on four of the six outcome measures, whereas the region with the lowest utilization had the lowest occurrence of three of the six outcomes. However, it is clear from this study that the characteristics of home health markets, agencies, and patients in these different regions were quite distinct. The South Central agencies tended to operate in nonmetropolitan areas with high rates of poverty and few alternative resources. A large proportion of the home health episodes in these regions were provided by proprietary and freestanding agencies. Agencies in the Pacific and Middle Atlantic regions were more likely to be located in large metropolitan areas where the elderly population was less impoverished and alternative resources were more widely available. Most of the episodes of care in these regions were provided by non-proprietary home health agencies.
Further, the two South Central regions, both of which had high utilization rates, appeared to have a particularly frail and chronically ill patient population. Agencies in the Pacific and Middle Atlantic regions, on the other hand, appeared to serve more post-acute care patients and fewer chronically ill patients. As a result of this variability in agency and patient characteristics, it appeared that agencies in the South Central regions were using home health care as a type of long-term care, providing relatively extensive home health aide services and relatively few therapy services, to a caseload of very frail patients. The Pacific and Middle Atlantic regions, on the other hand, used the home health benefit mainly for short-term rehabilitation following acute care. Patients in these regions received relatively more therapy and social work visits than patients in other regions. However, even after controlling for patient and agency characteristics (e.g., type of control), regional variation in home health utilization remained.
Together, the reports prepared by OIG (1995a) and Schore (1994) demonstrated striking variations in the utilization of home health care services across the country. According to these studies, certain patient, agency, and market characteristics influence the use of home health care. Although, this OIG report suggested that patient characteristics such as age, gender, and race had little association with utilization rates, Schore reported that race and certain diagnostic categories were related to an increase in the number of visits provided. Both studies demonstrated an association between high utilization and certain agency characteristics (i.e., proprietary control, freestanding type). Further, the findings from the Schore study suggest that certain characteristics of the local health care markets influence the utilization of home health care (i.e., poverty rate, alternative resources available, urban/rural nature of community). Both studies report a paradoxical relationship between utilization and outcomes. In the Schore report, low-use regions had fewer inpatient admissions, home health readmissions, and post-discharge deaths than did high-use regions. Similarly, the OIG report found a slight inverse relationship between average reimbursement rates per beneficiary and patient death while on service, although this indicator was not intended as an outcome measure. Further, the authors of the OIG report indicated that agencies with higher average reimbursement rates per beneficiary were less likely to be accredited, a proxy measure of service quality, than were agencies with lower reimbursement rates.
Many questions remain unanswered regarding practice variations in home health care. Because the OIG (1995a) and Schore (1994) studies were based entirely on secondary data, they were limited in the kinds of relationships that could be explored and the kinds of conclusions that could be drawn. Neither project was able to identify causal relationships between patient, agency, and market characteristics and practice patterns, nor between practice patterns and patient outcomes. Further, the data with which patient and agency characteristics and patient outcomes could be examined were limited. For example, patient characteristics that might have a powerful influence on home health utilization, such as specific details about the patient's medical condition, his or her ability to learn, compliance with the medical regimen, assistance provided by the family support system, and willingness to accept certain home health services, are not accessible through secondary data sources. Information about agency-specific policies, such as case management, supervision of nursing decisions, and productivity standards, also are not readily available. Further, these studies were able to examine the outcomes or quality of care only to a limited degree.
The current study was designed to examine practice variations in home health care through the collection of primary longitudinal data. Figure 1.1 presents the conceptual framework for the study. In Stage 1, several sets of independent variables (patient, provider, agency, and market/regulatory factors) are hypothesized to influence practice patterns. In Stage 2, practice patterns are hypothesized to affect patient outcomes. The main emphasis in this study was on Stage 1, although quantitative analyses were conducted to examine how variations in practice patterns relate to patient outcomes (after controlling for patient, provider, agency, and market/regulatory factors).
Three main research questions were identified for the study:
- What is the actual practice of home health care, in terms of type, amount, and decision making (e.g., care planning, care coordination)?
- How are decisions about care made in light of Medicare coverage rules?
- What elements of practice are associated with long lengths of stay in the Medicare home health benefit?
The first question focuses on the direct care Medicare home care patients receive, such as the number and frequency of skilled nurse and home health aide visits, the types of services provided during a skilled nursing visit (e.g., teaching, assessment), and the amount and type of care planning and coordination organized by the home care provider. Of particular importance is how such practice patterns are related to patient, provider, agency, and market/regulatory factors. To answer the second question, methods were developed to examine care provider variation in interpretation of Medicare home health care coverage rules (e.g., the definition of homebound status and the need for skilled care), and to investigate how care providers interpret coverage rules when making decisions to discharge or recertify patients in situations in which either choice may be reasonable. Finally, the third question focuses on identifying care provider practices that relate to shorter versus longer lengths of stay for similar patients (e.g., amount of teaching, coordination of alternative or community services to assist the patient, care planning with physicians). An important issue associated with all three questions is whether practice differences are related to differences in patient outcomes. Thus, the linkage between practice patterns and outcomes was also explored in the study.
A study of practice patterns in home health care is particularly important at this time in view of the major changes that have occurred over the past several years in the utilization of Medicare home health services, as well as in government policies designed to constrain spending on Medicare home health care. Several factors have resulted in an increase in the magnitude and cost of the Medicare home health benefit. In 1980, the Omnibus Reconciliation Act (P.L. 96-499) eliminated the limit on the number of visits a home care patient could receive each year (U.S. General Accounting Office [GAO] 1999). Further, after the Prospective Payment System (PPS) for acute care hospitals was implemented in 1984, Medicare spending on home health services began to increase dramatically (Liu, Harvell & Gage 2000; Schore 1994). Since the hospital PPS provides hospitals with the incentive to reduce the lengths of their patients' inpatient stays, many patients who might have spent additional time in the hospital prior to PPS began to be discharged to their homes and to home health care services instead.
Utilization of Medicare home health services also increased as a result of the 1988 lawsuit, Duggan vs. Bowan, which prompted the clarification of Medicare home health regulations and the broadening of eligibility criteria for the Medicare home health benefit. Among other changes that resulted from Duggan vs. Bowan, a patient with a chronic disease or long-term care needs could no longer be denied Medicare home health coverage so long as he or she had a demonstrated need for skilled care (Schore 1994).
Other factors contributed to the increase in home health utilization. Agencies' increased ability to provide high-technology care, such as infusion therapy, parenteral nutrition, and ventilator care, increased the number of patients they were able to serve. As well, according to GAO, many states instituted Medicare maximization policies designed to encourage providers to utilize the Medicare home health benefit for dually eligible home care recipients (GAO 1998). Finally, many believe that Medicare reimbursement policy, by which agencies were paid on the basis of their costs up to pre-established limits for each visit type, did not provide agencies with any incentive to provide care in a cost-effective manner.
Although the number of home health claims increased dramatically as a result of these factors, Medicare oversight of home care agencies did not. Between 1989 and 1995, the percentage of claims that were reviewed dropped from approximately 12% to 2%, although the number of claims nearly tripled (GAO 1999). The reduction in oversight of home health agencies may have contributed to the number of inaccurate and fraudulent claims filed.
Together, these factors dramatically increased the number of home care providers as well as Medicare home health expenditures. Between 1989 and 1996, Medicare home health expenditures rose from $2.5 billion to $16.8 billion (GAO 1998). During this same time period, the number of certified home health care agencies grew from approximately 5,700 to more than 10,000. According to OIG (1999a), the increase in the number of agencies was concentrated among certain agency types. The number of freestanding and urban agencies doubled, and the number of proprietary agencies tripled. The increase in Medicare home health expenditures during the early 1990s was due largely to the increase in the number of users and visits per user (Komisar & Feder 1998). The duration of home health episodes also increased. Whereas 14% of home care episodes lasted 166 days or more in 1990, 20% lasted 166 days or more in 1995 (OIG 1999a).
The provision of home care services that did not meet Medicare coverage and/or eligibility rules and fraudulent billing practices contributed to the tremendous increase in Medicare home health care expenditures during the 1980s and 1990s. Beginning in 1995, the anti-fraud initiative Operation Restore Trust (ORT) was implemented to address concerns over growing Medicare expenditures for home health care, nursing home care, hospice care, and durable medical equipment (OIG 1997b). ORT focused on five states (California, Florida, Illinois, New York, and Texas) that account for a large percentage of the nation's Medicare population. In a 1997 audit of home health claims in four of these states (all but Florida), OIG estimated that 40% of services billed in a sample of Medicare home health claims did not meet Medicare reimbursement requirements. The majority of these improperly billed services were deemed not to be reasonable and necessary, were for patients that were not homebound, or were not accompanied by valid physician orders. OIG estimated that Medicare expenditures for these unallowable claims totaled $2.6 billion, approximately 38.8% of the entire Medicare expenditures for home health care in these four states.5
According to another OIG report (1997a), more than 25% of the home health agencies in the five ORT states were "problem providers" (i.e., they had abused or defrauded Medicare or misappropriated Medicare funds). These problem agencies received nearly 45% of all Medicare home health care expenditures in these five states. Although 50% of the nation's Medicare-certified home health care agencies were proprietary, 80% of the problem agencies were proprietary. The average reimbursement per patient for these agencies was nearly 50% more than the average reimbursement per patient for non-proprietary problem agencies.
To stem the dramatic rise in Medicare home health care expenditures, both those resulting from legitimate increases in utilization and those resulting from fraud and abuse, the Federal Government implemented new regulations to control home health expenditures and to improve the oversight of the home health industry. As mentioned previously, the anti-fraud initiative ORT was implemented in 1995 in the five states with the largest share of the Medicare beneficiary population. Agencies providing an unusually large number of Medicare services were reviewed to identify improper and/or fraudulent home health claims (GAO 1999). In 1997, ORT was expanded to include 12 additional states as well as additional care providers (e.g., psychiatric hospitals). In the same year, the Wedge Project was established in 14 high-utilization states to identify invalid claims and to recover Medicare funds. Also in 1997, Medicare participation rules were revised to screen out agencies that might become problem providers (GAO 1999; OIG 1999a). The Health Insurance Portability and Accountability Act (HIPAA, P.L. 104-191), which was implemented in August 1996, established a monetary penalty for any physician who falsely certifies the need for Medicare-covered home health services.
Of particular interest in this study are changes in home care resulting from the Balanced Budget Act (BBA) of 1997 (P.L. 105-33). This legislation incorporated a number of cost-containment measures for home care, with the goal of reducing home care expenditures by $16 billion over a five-year period (1998-2002). The major provisions of the BBA related to home health care are summarized in Table 1.1. In an attempt to reduce the utilization of home health services, the legislation mandated the transition from a cost-based system of payment for home health care to a prospective payment structure. The BBA resulted in the implementation of the Interim Payment System (IPS) and laid the foundation for the PPS for home health care.
IPS was the system of payment for home health services that was designed to be in effect from the time the BBA was passed to the time PPS went into effect. Its major component was a new annual per-beneficiary reimbursement limit that was based on 1994 visits per-beneficiary data. This limit placed stringent reimbursement constraints on most home health providers. The BBA also constrained and clarified home health eligibility criteria. Patients with the need for venipuncture services only were no longer considered eligible for Medicare home health services. In addition, the BBA clarified coverage requirements for part-time or intermittent nursing care and home health aide services.
In each year following the implementation of IPS, actual reductions in home health expenditures exceeded the projected reductions. According to estimates generated by the Congressional Budget Office (CBO), spending on Medicare home health services declined by nearly 45% between 1997 and 1999 (NAHC 2000). Primarily for this reason, subsequent legislation was passed that provided some relief to home health care agencies. Table 1.1 identifies major amendments that have occurred to the original provisions of the BBA.
| TABLE 1.1: Major Home Health Provisions of and Amendments to the Balanced Budget Act (BBA) of 1997 |
| ORIGINAL PROVISIONS |
Establishment of the Interim Payment System (IPS)
|
Establishment of Prospective Payment System (PPS)
|
| Payment based on geographic location where services are provided |
Modification of Part A home health benefit for individuals enrolled in Part B
|
| Clarification of coverage requirements for part-time or intermittent nursing and home health aide services |
| Establishment of research on definition of homebound status |
| Elimination of venipuncture as an eligibility criteria for home health services |
| Submission of reports to Congress regarding home health cost containment |
| Establishment of surety bond requirement for home health agencies |
| AMENDMENTS |
| PPS effective date was changed from October 1998 to October 1, 2000 |
| As a result of the Medicare, Medicaid, and SCHIP Balanced Budget Refinement Act (BBRA) of 1999, agencies that fall below the national median on per-beneficiary limit receive a 2% increase in their per-beneficiary limits starting in fiscal year 2000 |
| The BBRA restored $1.3 billion to the Medicare home health benefit |
| The BBRA delayed the 15% reduction in payment limits until one year following the implementation of the PPS |
| Bills in the House and Senate (H.R. 2361 and S. 2766) during the 106th Congress proposed the possible elimination of the 15% automatic reduction in Medicare home health outlays |
| The BBRA mandated that durable medical equipment can be billed by suppliers rather than home health agencies |
| The BBRA established that home health agencies must have a bond for the lower of $50,000 or 10% of the aggregate amount of Medicare and Medicaid payments to the agency that year, and that agencies may have a single bond to cover both Medicare and Medicaid business (replaced the BBA surety bond requirement) |
Although this study was not originally intended to address issues related to the BBA, the timing of the project allowed for an examination of the impact of recent policy changes on the field of home health care. For instance, the decrease in the per-visit cost limits and the addition of per-beneficiary limits under IPS have affected many home health agencies. Information on care practices under IPS can provide a baseline for later assessments of the impacts of PPS, implemented in the Fall of 2000 (HCFA 1999b).
B. Overview of Methods
This section provides a brief overview of the methods used in the study. Detailed information about the research design is presented in Chapter 2.
1. State, Agency, and Patient Selection
Because a major dimension on which home care practice varies is visit volume per home health care user, the main study sample was designed to include a substantial degree of variation in visit volume. The 48 contiguous states were categorized by volume based on the average number of visits per Medicare beneficiary. Those states in the highest and lowest quartiles with regard to volume were identified. Four states from the high-volume (Georgia, Massachusetts, Mississippi, Texas) and four states from the low-volume quartiles (Minnesota, New Jersey, Oregon, Pennsylvania) were chosen as the focus of the study.
According to the agency sampling protocol described in Chapter 2, 56 home health care agencies were recruited to participate in the study. Twenty-nine of these agencies were located in the four low-volume states and 27 agencies were located in the four high-volume states. Clinical staff at each of the 56 recruited agencies received training regarding data collection instruments and protocols. Training took place on site at each agency and was conducted by a nurse researcher from the Center for Health Policy Research.
During the course of data collection, several agencies discontinued their participation in the study. Twelve agencies formally withdrew from the study and an additional six agencies failed to submit useable patient data. Of the agencies that formally withdrew, half submitted at least some useable data prior to withdrawing from the study. Therefore, of the 56 agencies recruited for participation in the study, 44 contributed data to the final sample used for analysis purposes.
Because one of the main goals of the study was to identify practice patterns associated with long lengths of stay in the Medicare home health benefit, it was important to collect data on a patient population for which long home health episodes are not uncommon. For this reason, the sample was limited to patients having primary or secondary diagnoses of congestive heart failure (CHF) or diabetes mellitus. In order to be considered eligible for the study, a patient also had to be age 65 years or older, covered by Medicare, and living in the state in which his or her home care agency was located. Using these criteria, a total of 1,217 patients were enrolled in the study.
In the final patient sample, only patients with complete assessment data at the episode level were included. The final patient sample for the study included 684 patients. Of these patients, 292 were diagnosed with CHF, 246 with diabetes mellitus, and 146 with both conditions. Across the 684 patients, complete assessment data were available for 732 episodes of care.
2. Quantitative and Qualitative Methods
Data were collected using both quantitative and qualitative methods. Primary quantitative data were collected to examine patient, provider, and agency factors related to practice patterns and outcomes in home health care. Specifically, Outcome and Assessment Information Set (OASIS) and Care Provider Questionnaire (CPQ) data were collected longitudinally to assess important patient factors that might influence care practices and eventual patient outcomes. Care Provider Profile (CPP) data were collected for each home care provider caring for a study patient. The CPP assessed important characteristics of the care providers, such as years of experience and education. At the time each agency was recruited to participate in the study, the agency's administrator was asked to complete the Administrator Questionnaire (AQ). This instrument was designed to elicit information related to agency factors that may affect the practice of home health care (e.g., licensing and accreditation, reimbursement, caseload, changes due to venipuncture regulations, use of nurse productivity standards, case management and supervision).
Information about market/regulatory factors likely to affect practice patterns in home health care was obtained primarily from secondary sources. Although the AQ provided some market/regulatory information, other data relevant to market/regulatory factors were obtained through publicly available data sets, such as OSCAR, the Area Resource File (ARF), and through publications of the American Association of Retired Persons (AARP).
Practice patterns were measured primarily through billing data, which provided information about the number and kinds of visits conducted during an episode of care. Some additional practice pattern variables, such as variables reflecting the use of alternative resources and oversight of clinicians' decisions regarding patient care were calculated from CPQ data items.
The study also involved a number of qualitative data collection methods designed to address the main study questions and/or the impact of IPS and other policy changes. The administrators of the study agencies were interviewed to collect information about how IPS had affected the agencies participating in the study. In addition, interviews were conducted with representatives of home care associations in the eight study states to identify how home health care practices had changed in response to the implementation of IPS.
Focus group interviews, involving several nurses each, were conducted at eight agencies to explore how home care decisions are made in light of Medicare coverage rules. In order to assess whether the ambiguity of Medicare coverage rules encourages providers to increase the amount of care provided by lengthening patients' episodes of care, the focus groups were designed to facilitate discussions among home health care providers regarding the decision to recertify or to discharge a patient. During the focus group interviews, two vignettes illustrating common clinical situations were presented. The vignettes, which described patients for whom the appropriateness of recertification or discharge was somewhat unclear, provided context for discussing the interpretation of coverage rules and the process for justifying a need for home health services. In this report, data from the focus group interviews are used to explore the role of the following factors influencing the decision-making process in home health care: (1) patient and caregiver factors (e.g., living situation), (2) the actors involved in the decision-making process (e.g., nurses, physicians), (3) agency factors (e.g., supervision of the decision-making process), (4) external factors (e.g., managed care), and (5) Medicare coverage rules (e.g., homebound status).
Case study interviews, conducted with one nurse from each of seven agencies, were conducted to provide a description of the practice of home health care by exploring the treatment episodes of seven recently discharged patients (one per nurse). To control for practice variation due to the condition being treated, the case studies were limited to CHF patients. The information gathered during the course of the case study interviews was used to explore the following aspects of home health care: (1) key characteristics of home care episodes (e.g., length, disciplines involved), (2) services provided by various disciplines and the family support system, (3) care planning and coordination (e.g., development and documentation of the care plan), and (4) content of the skilled nursing visit (e.g., teaching, direct care).
As noted earlier, the initial design work for this study took place prior to the passage of the BBA and the subsequent implementation of the changes it mandated, such as IPS. To capture information on the impact of the BBA, the final design for the administrator interviews, state home care association interviews, focus groups, and case studies was shaped to be relevant under IPS and the forthcoming move to PPS. Each of these interview methods included components to obtain information on industry stakeholders' perceptions of changes in home health care provision resulting from recent policy changes, particularly those under the BBA.
C. Report Overview
This document represents the final report for the Study of Medicare Home Health Practice Variations. The report presents the findings from both the quantitative and qualitative methods designed to answer the three key study questions and to examine the impact of policy changes resulting from the BBA. The topics covered in many of the following chapters were first presented in separate draft reports, which subsequently were consolidated into this report.
Chapter 2 provides a more detailed description of the study's quantitative and qualitative methods. The procedures for selecting study states, study agencies, and study patients are described. In addition, the methods used to conduct the administrator, state home care association, focus group, and case study interviews are outlined. The processes employed in the management and analysis of the study data are also described.
Chapter 3 provides descriptive information regarding the states, agencies, and patients involved in the study. Demographic, economic, health system, and beneficiary health status indicators are presented for each study state. The AQ data are used to provide a description of the agencies that contributed data to the final sample. Finally, the start of care case mix of the patients enrolled in the study is presented using OASIS and CPQ data. Descriptive information is presented across all patient episodes and also separately for episodes involving patients with the two tracer conditions, CHF and diabetes mellitus.
Chapter 4 presents the bulk of the quantitative analyses conducted as part of the study. In this chapter, the care provided during the study episodes is described and the impact of patient, provider, agency and market/regulatory factors on home care practices is summarized. The affect of practice patterns on the length of the episodes of care also is discussed. Finally, in this chapter, the relationship between practice patterns and patient functional outcomes is assessed.
The findings from the focus group and case study interviews are presented in Chapter 5. The analysis of the focus group data concentrates on factors that influence the decision to recertify or discharge home care patients. This chapter also provides a description of the case study episodes of care, including information about the services provided by the various disciplines. The content of the skilled nursing visits conducted with these patients is described, as is the process by which agency personnel plan, coordinate, and document their patients' care.
Chapter 6 presents information about provider perspectives on IPS and other changes in home health care. Findings are based on four different qualitative methods used to gather information about provider perspectives: (1) state home care association interviews, (2) administrator interviews, (3) focus group interviews, and (4) case study interviews.
Chapter 7 provides a summary of the information and findings contained in this final report. Specifically, the process for selecting states and agencies is reviewed, and a brief description of the agency sample is given. Key findings with regard to practice and decision making in home health care are highlighted. In addition, the chapter provides a summary of provider perspectives on IPS, as well as a brief discussion of the findings from other studies, focusing on the impact of policy changes in the field of home health care. Finally, this chapter contains a discussion of the implication of the study findings for clinical practice and Medicare coverage regulations.
The report includes five appendices. Appendix A contains copies of all study questionnaires. Appendix B contains materials related to the focus group interviews. The focus group protocol and a copy of the Participant Demographic Form, which each participating nurse completed, are provided. Appendix C contains the written protocol used for the case study interviews. Supplemental information on the eight study states is provided in Appendix D and is intended to provide some additional descriptive information regarding state demographic, economic, and health care system features. Appendix E contains descriptive statistics for all AQ items, as well as all responses to the open-ended AQ items. Finally, Appendix F contains a list of the variables included in the multivariate analyses.
II. METHODS
This chapter summarizes the methods used to answer the three key study questions identified in Chapter 1 and to examine the impact of policy changes on the field of home health care. Section A of this chapter presents the methods used for selecting the states, home care agencies, and patients involved in the study. The data collection procedures designed to (1) address the key study questions and (2) assess the impact of IPS are described in Section B. Section C provides information about the procedures employed in managing and analyzing the quantitative study data.
A. State, Agency, and Patient Selection
1. Selection of State Sample
States were categorized by volume based on their average number of visits per Medicare beneficiary receiving home care in 1995. State volume group was identified through Online Survey Certification and Reporting System (OSCAR) data maintained by the Centers for Medicare & Medicaid Services (CMS). Excluding Alaska and Hawaii, the highest and lowest quartiles (12 states each) were identified. To obtain a cross-section of states in each volume category, four states were selected in each of the two quartiles. The selection process was a collaborative effort between the Office of the Assistant Secretary for Planning and Evaluation (ASPE) and the Center for Health Policy Research (the Research Center), with the final selection made by ASPE. The four low-volume states selected were Minnesota, New Jersey, Oregon, and Pennsylvania and the four high-volume states were Georgia, Massachusetts, Mississippi, and Texas.
The objective in the state-selection process was to select states in each volume category that reflected the entire category reasonably well in terms of state-level variables such as Medicaid home and community-based care expenditures, percentage of Medicare beneficiaries enrolled in managed care plans, and home health agency ownership and type distribution.6 Four states were selected per volume category so that variation in state characteristics could be obtained while at the same time including data from several agencies within each state. To avoid having any given state dominate a volume category, the goal was to obtain approximately equal numbers of agencies and patients from each state.
2. Selection of Home Care Agencies
The original design for agency selection called for a random sample of Medicare-certified home care agencies; seven agencies were to be randomly selected from each of the eight study states. The random-sampling approach was constrained for practical reasons by the implementation of three eligibility criteria: (1) agencies were required to have at least 150 annual admissions, (2) agencies could not be participating in other Research Center studies, and (3) agencies must have been in operation for at least one year prior to becoming involved in the study. Once agencies were randomly selected, agency administrators received recruitment materials by mail and were contacted by telephone and encouraged to participate in the study.
Sampling and recruitment of study agencies was complicated by the implementation of IPS. Agency administrators' concerns regarding the potential impact of IPS along with IPS-inspired changes in agency policies and staffing (e.g., more stringent productivity standards, downsizing of administrative staff) hindered the process of agency recruitment. Administrators of some randomly selected agencies were not willing to enroll their agencies in the study as a result of increasingly tight staffing and a general sense of concern about the future of their agencies. In order to recruit the target number of agencies, two of the eligibility criteria were relaxed. Agencies were required to have at least 100 annual admissions instead of 150, and agencies now were allowed to be involved in other Research Center studies.
During recruitment, agencies were offered a number of incentives to participate in the study. All agencies were offered one complimentary set of case mix and outcome reports to be produced after a minimum of one year of OASIS data on all agency patients had been submitted. Such reports were produced for 17 study agencies. In addition, agencies were offered the use of OASIS Genie software free of charge during the data collection phase of the study. Agencies that did use OASIS Genie received free technical assistance throughout their involvement in the study. Finally, all agencies were offered financial compensation for completion of important study milestones (e.g., the completion of data collection on thirty patients, participation in a focus group). The maximum possible payment for participating agencies was $1,500.
As a result of challenges to agency recruitment, random selection of agencies was not possible. Instead, agency administrators in the eight study states were contacted and invited to participate in the study with the goal of obtaining a sample of agencies that was representative of the home health market in the high- and low-volume states, which would provide approximately equal numbers of agencies and patients from each of the eight states, and include proprietary and non-proprietary, as well as hospital-based and freestanding agencies in each state sample.
As agency recruitment proceeded, it became apparent that a disproportionate number of participating agencies were hospital-based. Therefore, in order to ensure the recruitment of a sufficient number of freestanding agencies in the study, subsequent recruiting efforts emphasized freestanding agencies. (In addition, administrators of freestanding agencies were asked to enroll ten additional study patients each if possible.) The distribution of agencies within state volume categories was monitored for the hospital-based/freestanding and proprietary/non-proprietary splits.
These revised recruitment procedures resulted in the successful recruitment of the targeted 56 agencies for the study. Twenty-nine agencies were located in the four low-volume states and twenty-seven agencies were located in the four high-volume states. Detailed descriptive information about the study agencies is presented in Chapter 3.
Agency Training: Clinical staff at each of the 56 recruited agencies received training regarding data collection instruments and protocols. Training took place on site at each agency and was conducted by a nurse researcher from the Research Center. Each agency clinician who attended training received a reference manual containing detailed information about study goals and procedures. One staff member at each agency was designated as the Data Collection Coordinator (DCC).7 The DCC, who participated in a one-on-one training session with a Research Center nurse researcher on site at his or her agency, was responsible for identifying patients that were eligible for participation in the study, tracking study patients and ensuring that data were collected according to the study protocol, informing clinical staff of the need to obtain informed consent and collect study data on eligible patients, and acting as the liaison between the agency and the Research Center.
Agencies were allowed to submit patient data in hardcopy form or electronically. For those agencies that submitted data electronically, a Data Entry Clerk (DEC) was identified at each site and was responsible for entry and electronic transmission of study data. For agencies using OASIS Genie software to enter and transmit data, the DEC participated in a telephone training session with technical assistance personnel from the Research Center. DECs from agencies using other data entry software were trained in the transmission of study data only. Technical assistance was provided as needed for the duration of the data collection phase of the study.
Because of high staff turnover at many study agencies during the data collection phase of the study, it was important for agencies to train clinical staff who had not been present for the original on-site training. In order to meet agency needs for periodic retraining, a professionally produced training video was developed and provided to each agency. This video contained complete training sessions for clinicians and DCCs. New DECs were trained over the telephone as needed.
Agency Attrition: During the course of data collection, several agencies discontinued their participation in the study. Twelve agencies formally withdrew from the study and an additional six agencies failed to submit useable longitudinal patient data. Of the agencies that formally withdrew, half submitted at least some useable data prior to withdrawing from the study. Therefore, of the 56 agencies recruited for participation in the study, 44 contributed data to the final sample used for analysis purposes.
Administrators of agencies that withdrew from the study cited a number of reasons for discontinuing their participation, many of which may have been related to the challenge of coping with new federal regulations and a new Medicare payment system for home health care. (The study data were collected entirely under IPS.) Table 2.1 identifies the main reasons agency administrators identified for discontinuing their participation in the study. Administrators cited multiple barriers to continued participation. Five agencies experienced changes in ownership and three agencies closed or underwent bankruptcy proceedings during the data collection phase of the study. Seven agencies had a change in location or coverage area and six experienced reductions in staff and/or the number of branch offices. Staff turnover and/or shortages influenced administrators' decisions to withdraw from the study at ten agencies. A shortage of staff often resulted in an agency's DCC assuming additional clinical, administrative, or clerical responsibilities, often interfering with his or her ability to coordinate study-related activities at the agency. In addition, staff turnover resulted in a shortage of study-trained clinicians and the need to retrain staff at five agencies. Other changes, such as changes in referral patterns and patient census, contributed to the withdrawal of six agencies. The transition to a new software system made study participation challenging for eight agencies. Finally, three agencies withdrew from the study in part because of the burden of OASIS data collection and of preparing for the then-upcoming implementation of PPS.
Agency attrition was greater for some categories of agencies than others. Of the 12 agencies that withdrew from the study, the majority was located in the high-volume states. Fifty-eight percent of the agencies that discontinued their participation in the study were located in states with high visit volume per beneficiary. Three quarters of agencies that withdrew from the study were proprietary and 83% were freestanding. These patterns held true for the six agencies that never formally withdrew from the study, but failed to submit useable study data.
This pattern of agency attrition suggests that agencies in the high-volume states, as well as proprietary and freestanding agencies, had greater difficulty adjusting to the changes brought about by the BBA. As discussed in Chapter 3, agencies in high-volume states showed a more dramatic decline in visit volume per beneficiary after the implementation of IPS than did agencies in low-volume states. These agencies, as well as proprietary and freestanding agencies, which may have been less parsimonious in their provision of services prior to the implementation of IPS, may have had to reduce service utilization more substantially than other agencies to adjust to the changing home care environment. Indeed, according to the GAO (1999), agency closures between October 1997 and January 1999 were more common among agencies in high-utilization states, and among proprietary and freestanding agencies.
| TABLE 2.1: Factors Influencing Agency Attrition | ||||||||||
| Agency | Change in Ownership | Closure and/or Bankruptcy | Relocation and/or Change in Coverage Area | Downsizing of Staff and/or Branches | Staff Turnover/ Shortage | Increased DCC Responsibilities or New DCC | Other Changes (Referral Sources, Administrator, Patient Census, Admission Diagnosis) | Software Changes | OASIS Data Collection | PPS Preparation |
| A | 3 | 3 | 3 | 3 | 3 | 3 | 3 | |||
| B | 3 | 3 | 3 | 3 | 3 | 3 | 3 | |||
| C | 3 | 3 | 3 | |||||||
| D | 3 | 3 | 3 | 3 | 3 | |||||
| E | 3 | 3 | 3 | 3 | ||||||
| F | 3 | 3 | 3 | 3 | 3 | 3 | 3 | 3 | ||
| G | 3 | 3 | 3 | 3 | ||||||
| H | 3 | 3 | 3 | 3 | ||||||
| I | 3 | |||||||||
| J | 3 | 3 | 3 | 3 | 3 | 3 | ||||
| K | 3 | 3 | 3 | 3 | 3 | 3 | ||||
| L | 3 | 3 | 3 | 3 | ||||||
| TOTAL | 5 | 3 | 7 | 6 | 10 | 8 | 6 | 8 | 3 | 3 |
3. Selection of Study Patients
Because one of the main goals of the study was to identify practice patterns associated with long lengths of stay in the Medicare home health benefit, it was important to collect data on a patient population for which long home health episodes are not uncommon. For this reason, the sample was limited to patients having primary or secondary diagnoses of congestive heart failure (CHF) or diabetes mellitus.8 In order to be considered eligible for the study, a patient also had to be age 65 years or older, covered by Medicare, and live in the state where the home care agency was located. Using these criteria, a total of 1,217 patients were enrolled in the study.
In the final patient sample, only patients with complete assessment data at the episode level were included. That is, in order to be included in the final sample, a patient was required to have complete OASIS and CPQ data both for the beginning and the ending of the episode of care. Patients were eliminated from the final patient sample for a variety of other reasons as well. Thirteen patients who were nonresponsive at start of care, died during the course of their episodes of care, or had large amounts of missing data were not included in the final sample because several important measures, including outcome measures could not be calculated for these individuals. In addition, 14 patients were found to be ineligible for the study (e.g., had only one home health visit, were under that age of 65, did not have either requisite diagnosis).
The final patient sample for the study included 684 patients.9 Of these patients, 292 were diagnosed with CHF, 246 with diabetes mellitus, and 146 with both conditions. Across the 684 patients, complete assessment data were available for 732 episodes of care.
B. Data Collection Procedures
Data were collected using a variety of methods and instruments. Both quantitative and qualitative data were collected. Primary quantitative data were collected to examine patient, provider, and agency factors related to practice patterns and outcomes in home health care. Secondary data were used to measure important market/regulatory characteristics. Qualitative data were collected to explore practice and decision making in home health care and to assess provider perspectives regarding the impact of regulatory changes on the field of home health care. This section provides detailed information about the procedures employed in collecting the study data.
1. Quantitative Methods
This section identifies the data sources and describes the data collection procedures employed to collect quantitative data regarding patient factors, provider factors, agency factors, market/regulatory factors, practice patterns, and patient outcomes. The quantitative data analysis techniques employed as part of the study are described in Section C of this chapter.
Patient Factors: Beginning in February 1999 and ending in August 2000,10 study patients were followed longitudinally, from start of care up to 260 days or study discharge, whichever occurred first.11 Study discharge occurred when a patient was discharged from his or her home care agency and did not resume services within 14 days.12
Information on patient condition and care practices was collected every 60 days using the Outcome and Assessment Information Set (OASIS-B1) and the newly created Care Provider Questionnaire (CPQ). OASIS data items focus on sociodemographic attributes, home environment, family support, health status, and functional status. Three versions of the OASIS instrument were used, one for start of care, one for follow-up, and one for discharge visits. The CPQ contained questions related to patient homebound status, Medicare authorization of services, assistance provided by the family/support system, and services provided by the agency. Two versions of the CPQ were created, one to be used for start of care, resumption of care, or readmission visits and one for recertification or discharge visits. At the episode level, 684 patients had complete assessment data. Episode-level data were considered complete if a patient had both a CPQ and an OASIS assessment for both the beginning (i.e., start of care, resumption of care, readmission) and ending (i.e., discharge, transfer) of the home care episode. Across these 684 patients, there were 732 complete episodes. Copies of the OASIS and CPQ are provided in Appendix A.
Provider Factors: One of the goals of the study was to identify attributes of care providers that are related to variations in practice patterns. Information about the providers caring for study patients was collected primarily using the Care Provider Profile (CPP). This newly developed instrument contained questions regarding the educational background, experience, and expertise of the care providers involved in the study. The CPP was to be completed by all care providers expected to collect study data. Completed CPPs were available for 678 of the 732 study episodes. A copy of the CPP is included in Appendix A. Additional information about the home care providers and physicians caring for study patients was obtained from the CPQ.
Agency Factors: At the time each agency was recruited to participate in the study, the agency's administrator was asked to complete the Administrator Questionnaire (AQ). This instrument was designed to elicit information related to agency factors that may affect the practice of home health care (e.g., licensing and accreditation, reimbursement, caseload, changes due to venipuncture regulations, use of nurse productivity standards, case management and supervision). (Administrators' responses to the AQ items were not independently verified.) Completed AQs were received from 42 of the 44 study agencies included in the final sample and were completed between November 1998-October 1999. Appendix A contains a copy of the AQ. Additional information about the study agencies was obtained through the CPQ.
Market/Regulatory Factors: Information about market/regulatory factors that may affect practice patterns in home health care was obtained primarily from secondary sources. Although the AQ provided some market/regulatory information, other data relevant to market/regulatory factors were obtained through publicly available data sets, such as OSCAR, the Area Resource File (ARF), and through publications of the American Association of Retired Persons (AARP).
Practice Patterns: Many of the practice pattern measures used as part of the study were calculated based on billing data. Participating agencies submitted billing records (e.g., UB-92 data) for each of their study patients. From these records, practice pattern measures such as visits by discipline and total visits were calculated. In the calculation of practice pattern measures, such as the number of visits per discipline, all non-Medicare and non-billable visits were excluded. Some additional practice pattern variables, such as those variables reflecting the use of alternative resources and oversight of clinicians' decisions regarding patient care were calculated from CPQ data items.
Patient Outcome: Patient functional outcome was assessed using OASIS data. An aggregate measure of functional outcome was calculated, representing the percentage of the 27 standard improvement scores reported by CMS in nationally available outcome-based quality improvement (OBQI) reports on which a patient improved. The denominator for this calculation was the number of improvement scores for which a patient had valid data. Each improvement score was calculated only if a patient had the possibility of improving. If a patient was at the most independent level at start of care for a given measure, an improvement score could not be calculated.
2. Qualitative Methods
The study involved a number of qualitative data collection methods designed to address the study questions and/or the impact of IPS. The impact of IPS as perceived by the home care industry was examined through interviews with the administrators of the study agencies and through interviews with representatives of the home care associations in each of the eight study states. Focus groups composed of several nurses each were conducted on site at eight of the study agencies to gather information regarding decision making in home health care. Case study interviews designed to examine practice and decision making in home health care were conducted with one nurse from each of seven agencies. The focus groups and case studies also provided insight into provider perspectives on IPS and changes in the field of home health care. The procedures, samples, and analytic techniques used as part of these qualitative methods are presented in the following sections and are summarized in Table 2.2.
| TABLE 2.2: Summary of Qualitative Methods | ||||
| Administrator Interviews | State Association Interviews | Focus Group Interviews | Case Study Interviews | |
| Number of Interviews Conducted | 54 | 8 | 8 | 7 |
| Parties Interviewed | Administrators of study agencies | Representatives of home care associations in each of the eight study states | Nurses from eight study agencies | Nurses from seven study agencies |
| Number of Participants per Interview | 1 | 1 | 4-7 per focus group | 1 |
| Method of Interview | Conducted either by telephone or in person | Conducted by telephone | Conducted in person | Conducted by telephone |
| Location of Interview | In-person interviews were conducted at agencies | NA | Interviews were conducted at agencies | NA |
| Timing of Interviews | February to September 1999 | July to November 1999 | July to October 1999 | October to November 1999 |
Administrator Interviews: Interviews were conducted with the administrators of 54 of the original 56 study agencies in order to collect information about how home health practice patterns have changed in response to IPS (the remaining two administrators declined to be interviewed). Because the data from the administrator interviews were analyzed and reported in an interim deliverable before the composition of the final agency sample was known, the summary of the results from these interviews that is presented in Chapter 6 includes all 54 agencies for which interviews were completed. The interviews, which took place between February and September 1999, were conducted by Research Center staff either over the telephone (19 interviews) or on site at each of the agencies (35 agencies). A standardized interview protocol was used that consisted of four questions and standard probes within each question (shown in Table 2.3). A copy of the protocol was made available to each administrator prior to the interview. The interviews lasted approximately 20 minutes and the responses were recorded by the interviewer directly into a laptop or desktop computer.
| TABLE 2.3: Administrator Interview Questions and Probes |
1. How has IPS affected your agency's administrative and staffing practices? Probes:
|
2. In what ways has IPS affected the structure of care that you provide? Probes:
|
| 3. How have the reduction in per-visit cost limits and the new per-beneficiary limits specifically affected your agency? |
| 4. How is your agency preparing for prospective payment? |
The responses from the administrator interviews were sorted by question into the following four agency categories for analysis: proprietary agencies in low-volume states, proprietary agencies in high-volume states, non-proprietary agencies in low-volume states, and non-proprietary agencies in high-volume states. Agency sample sizes by category are shown in Table 2.4.
| TABLE 2.4: Administrator Interviews by State Volume Group and Agency Ownership Categories | |||
| Agency Ownership Category | State Volume Group | ||
| Low Volume | High Volume | Total | |
| Non-proprietary | 21 | 10 | 31 |
| Proprietary | 7 | 16 | 23 |
| TOTAL | 28 | 26 | 54 |
The first step of the thematic analysis involved categorizing the data into discrete themes by question and agency category. These themes were recorded with the agency identification number and, if a theme appeared more than once, the additional agency numbers were recorded for that theme. Appropriate quotes also were recorded. The next step of the thematic analysis involved analyzing the discrete themes for broader patterns within each question and across volume and ownership categories. A research assistant conducted the data reduction coding. Ten percent of the interviews also were coded by a research associate to ensure reliability and quality assurance in the coding procedure. The remaining portion of the thematic analysis was conducted by a research associate and was reviewed by a nurse researcher for quality assurance.
State Home Care Association Interviews: To identify how IPS impacted the field of home health care in the eight study states, telephone interviews were conducted with representatives of the state home care associations in each state. These interviews were conducted between July and November 1999. Like the administrator interviews, the more unstructured state home care association interviews focused on how IPS had impacted the administrative and care practices of agencies in the study states. The following themes were explored during the course of the interviews: staffing changes, cost shifting, agency closures and mergers, changes in case mix and services offered, and reduction in access to home care. Table 2.5 contains the three questions included in the state home care association interviews. Qualitative analyses of the data collected during the state home care association interviews was conducted by a research associate following the same steps of thematic analysis used in the analysis of the administrator interviews.
| TABLE 2.5: State Home Care Association Interview Questions and Probes |
| 1. How has the BBA of 1997 affected agencies (e.g., IPS; venipuncture; reimbursement based on location of patient, not agency; sequential billing)? |
| 2. As a result of IPS and the BBA of 1997, what is going on in your state that we should let policy makers know about? |
| 3. Are agencies relying more on the state for reimbursement now that IPS has gone into effect? |
Focus Groups and Case Studies: Focus group and case study interviews were designed to examine practice and decision making in home health care. As a condition of involvement in this study, agencies agreed to participate in the focus groups and case studies. Eight agencies (one agency from each of the eight states involved in the study) were selected to participate in the focus group and case study interviews.13 These eight agencies were selected to maximize the diversity of the focus group and case study samples. Therefore, four of the agencies were from states with high visit volume, and four agencies were from states with low visit volume. Within each state volume group, equal numbers of agencies from each of the agency ownership and agency type categories were selected for participation. Table 2.6 presents the 2X2 design for agency selection. The same agencies were selected for participation in both the focus groups and the case studies.
| TABLE 2.6: Design for Agency Selection for the Focus Groups and Case Studies | ||
| Agency Ownership Category | State Volume Categorya | |
| Low Volume | High Volume | |
| Proprietary | Minnesota (hospital-based)Pennsylvania (freestanding) | Georgia (hospital-based)Massachusetts (freestanding) |
| Non-proprietary | New Jersey (hospital-based)Oregon (freestanding) | Texas (hospital-based)bMississippi (freestanding) |
| ||
The focus group interviews were conducted on site at each of the eight selected agencies between July and October 1999. Each focus group involved several nurses. Prior to participating in a focus group, nurses signed a consent form and completed the Participant Demographic Form (Appendix B contains the Focus Group Protocol and Participant Demographic Form). As Table 2.7 indicates, the number of participants involved in the focus group interviews ranged from four to seven, with an average of five participants per group. The majority of participants was female (93.0%), White (81.4%), and between 32 and 54 years of age (74.4%). With the exception of a single participant who failed to indicate her educational background, all of the participants were RNs. Although 54.8% of the focus group participants had been in home care for more than five years, 72.1% had been with their agencies for five years or less.
A nurse researcher from the Research Center facilitated the focus groups. The main purpose of the focus groups was to facilitate discussions among home health care providers regarding the decision to recertify or to discharge a patient. During the focus group interviews, two vignettes illustrating common clinical situations were presented. The vignettes, which describe patients for which the appropriateness of recertification or discharge is somewhat unclear, provided context for discussing the interpretation of coverage rules and the process of justifying a need for home health services.
The focus group discussion was audiotaped and also recorded by a note taker from the Research Center. The notes from the focus groups (augmented by the audiotape information) were transcribed and imported into a qualitative analysis software package, NUD*IST (Non-numeric Unstructured Data, Index Searching and Theorizing). NUD*IST was used by the analysis team (consisting of both clinical and analysis staff) to code the focus group data (i.e., text) into analytic themes. The first step of the thematic analysis involved categorizing the data into themes related to the research and policy questions that the focus group interviews were designed to address. Data related to each theme were examined for patterns associated with state volume, agency ownership, agency type, and patient vignette. Although the sample was too small to identify differences between agencies in the different state volume, agency ownership, and agency type categories, participants' responses often were specific to one vignette or the other. Vignette-specific information is reported when appropriate.
| TABLE 2.7: Focus Group Participant Demographic Characteristics(N=43 Participants) | ||||||||||
| State | Total | Percent | ||||||||
| GA | PA | MA | MN | TX | OR | MS | NJ | |||
| SEX | ||||||||||
| Male Female | 15 | 05 | 05 | 04 | 05 | 24 | 05 | 07 | 340 | 7.0%93.0% |
| RACE | ||||||||||
| African AmericanWhiteMissing | 060 | 050 | 032 | 040 | 140 | 060 | 500 | 070 | 6352 | 14.0%81.4%4.6% |
| AGE | ||||||||||
| 20-3132-4243-5455+ | 1230 | 3020 | 0221 | 1111 | 0500 | 1230 | 0140 | 0223 | 615175 | 14.0%34.9%39.5%11.6% |
| DISCIPLINE | ||||||||||
| Registered Nurse Licensed Practical Nurse Missing | 600 | 500 | 500 | 400 | 500 | 600 | 500 | 601 | 4201 | 97.7%0.0%2.3% |
| YEARS IN HOME HEALTH CARE | ||||||||||
| 5 Year or Less 6-10 Years 11-15 Years 16+ Years | 5001 | 1210 | 1310 | 3010 | 3200 | 1410 | 1400 | 4120 | 191661 | 45.2%38.1%14.3%2.4% |
| YEARS WITH THIS AGENCY | ||||||||||
| 5 Year or Less 6-10 Years 11-15 Years 16+ Years | 6000 | 4100 | 5000 | 3010 | 5000 | 2310 | 3200 | 3130 | 31750 | 72.1%16.3%11.6%0.0% |
The eight agencies that participated in the focus groups also were selected for participation in the case study interviews. These interviews were conducted between October and November 1999. Personnel at each of the eight agencies were asked to identify each patient fitting the following criteria:
- 65 years of age or older;
- Medicare as the primary payer;
- Primary diagnosis of CHF;14
- Discharged after January 1, 1999; and
- Not discharged due to death or admission to an inpatient facility.
For each patient fitting the five criteria, agency personnel provided information about the patient's start of care and discharge dates, the number of visits the patient received from the various disciplines (e.g., aides, physical therapy), date of birth, level of family involvement, diagnoses, level of independence in activities of daily living (ADLs) and instrumental activities of daily living (IADLs), and services provided outside of the agency. Research Center staff used this information to identify a single patient at each agency on which the case study interview would focus. When more than one patient met all of the eligibility criteria, patients were chosen based on their episode lengths. Because it might have been difficult to obtain long-stay patients in states with a low number of visits per patient on average, we attempted to select short-stay patients in low-volume states and long-stay patients in high-volume states. We were able to identify patients with episodes of 120 days or longer (the definition of long stay used for the case study) in only two states (both high-volume states). The remaining case study patients were on service less than 60 days.
After the patient-selection process was complete, informed consent was received from both the selected patients and their primary nurses. A research associate at the Research Center then conducted case study interviews with the primary nurses (Appendix C contains the protocol for the case study interviews). In one case, the patient's primary nurse was no longer working at the agency. The nursing supervisor, who had been in daily contact with the primary nurse about this patient, took part in the case study interview. It was clear that the supervisor was well acquainted with the patient and the details of the episode of care.
At one of the eight agencies, agency personnel were able to identify only a single patient who met the patient-eligibility criteria. This patient had been discharged from home care and subsequently died prior to the time that the case study interviews were conducted. Agency personnel were unwilling to contact the patient's family to obtain consent for the patient's nurse to participate in a case study interview. Therefore, Research Center staff was unable to conduct a case study interview with this agency.
The case study interviews were audiotaped and transcribed. Similar to the analysis of the focus group data, themes relevant to the key research questions were identified in the case study data. Due to the small number of participants involved, the classification of the case study data into thematic categories was conducted manually (rather than using software such as NUD*IST).
C. Data Management and Analysis Procedures
This section of the report summarizes procedures used in managing and assuring the quality of the study data as well as the statistical techniques employed in analyzing the quantitative data.
1. Data Management Procedures
Study-related data were received at the Research Center either in hardcopy or in electronic format. Agencies were permitted to submit OASIS and CPQ data in either format, whereas all other data (e.g., AQ, CPP, billing records) were submitted in hardcopy. Data that were submitted in hardcopy were data entered by Research Center staff. Ten percent of CPQ and OASIS data were entered two times each to identify typos and/or systematic errors in data entry. The accuracy rate for CPQ and OASIS data entry was 99.5%.
Several measures were taken to ensure the quality of the study data. All hardcopy data underwent "up-front review," whereby a research assistant reviewed the data for any obvious data quality problems prior to the data being entered (e.g., missing responses). If problems were identified, the research assistant contacted the agency's DCC for clarification. Further, during the data collection phase of the study, a clinician from the Research Center contacted DCCs regularly (usually biweekly) to clarify data collection procedures and to follow-up on data collection and quality issues. All data were subjected to a variety of quality checks, such as checks to identify out of range or extreme values, to ensure that skip patterns were followed appropriately, and to identify and remove patient assessment data collected more than 14 days after the visit date. In addition, data that violated the data collection protocol or patient eligibility requirements were eliminated from the study database.
All OASIS and CPQ data were processed through an extensive series of electronic data quality checks. These checks were designed to identify inappropriately missing data or cross-item inconsistency in responses (e.g., reporting that there is no family support system on one data item and that the family support system provides assistance with activities of daily living [ADLs] on another item). When missing data or inconsistencies were apparent in an agency's data, a Data Quality Report (DQR) outlining the problems was sent to the DCC along with a request for clarification. After the data collection phase of the study ended, all questionnaire responses for which clarification had not been received were set to missing.
After all data quality activities were completed, longitudinal data files were generated. As a first step, OASIS and CPQ assessments were matched to each other to establish complete assessment data for a given assessment time point for a patient. Then, episodes of care were established separately for OASIS and CPQ data. That is, each OASIS start of care and resumption of care assessment was matched to the next chronological discharge or transfer assessment. Likewise, each start of care, resumption of care, and readmission CPQ was matched to the next chronological discharge CPQ assessment.15 These separate OASIS and CPQ episodes were then matched to each other. Episodes with complete matching OASIS and CPQ data were retained for final analysis.
2. Data Analysis Procedures
This section of the report contains summary information regarding the analytic techniques used as part of the study. Information is provided regarding techniques for conducting descriptive analyses, two-group comparisons, and multivariate analyses of practice patterns and patient outcomes.
Descriptive Analyses: In Chapter 3 and Chapter 4 of the report, basic descriptive statistics are presented to provide an overview of the study care providers, agencies, and patterns of home care practice. The descriptive statistics presented differ for continuous and categorical variables. For continuous variables, the mean, median, minimum, and maximum values are presented. For categorical variables, the percentage of agencies, care providers, or patients for which each response was selected is identified. The N is reported for all variables. Also in Chapter 3, secondary data are presented describing the market/regulatory characteristics of the eight study states.
Chapter 3 includes a summary of the sample of patients enrolled in the study. Descriptive statistics and two-group comparisons are presented to provide a picture of the patients at the start of each episode of care. (These analyses were conducted at the episode, rather than the patient level.16) For each variable, the mean value or the percentage of episodes having each response is presented. In addition, the degree to which the responses differ by tracer condition (i.e., CHF or diabetes mellitus) is reported. For categorical variables for which the minimum expected cell frequency was less than or equal to 20, two-tailed Fisher's exact tests were conducted to determine the significance of the differences between the responses of patients with CHF and diabetes mellitus. When the minimum expected cell frequency was larger than 20, the significance value reported was the p-value associated with the continuity-adjusted Chi-Square.
For items with continuous response options, the Kolmogorov-Smirnov test of normality and the N for each sample were used to determine which two-group test should be employed. When both samples sizes were larger than 120, the t-test was used, regardless of the results of the Kolmogorov-Smirnov test. When either sample size was less than 30, the Wilcoxon Rank-Sum test was used regardless of the Kolmogorov-Smirnov results. When either sample size was between 30 and 120, the test used depended on the results of Kolmogorov-Smirnov test. If the Kolmogorov-Smirnov test was not significant at the .10 level (indicating normality), the t-test was used, whereas if the Kolmogorov-Smirnov test was significant at the .10 level (indicating nonnormality), the Wilcoxon Rank-Sum test was used.
Multivariate Analyses: The bulk of the quantitative analyses for the study are presented in Chapter 4. In addition to the descriptive statistics based on practice pattern variables mentioned previously, Chapter 4 includes three sets of multivariate analyses respectively designed to assess the impact of (1) patient, provider, agency, and market/regulatory factors on practice patterns (e.g., length of stay), (2) practice patterns on episode length, and (3) practice patterns on patient outcomes. In the latter two sets of analyses, important patient, provider, agency, and market/regulatory factors were controlled.17
The multivariate analyses were conducted using ordinary least squares (OLS) regression. For each of the three sets of analyses identified above, the analysis procedure involved two steps. Step 1 focused on the identification of important independent variables to be retained in the final regression model for a particular dependent variable (i.e., Step 2). In the first set of analyses listed above, four regression models were conducted for each practice pattern dependent variable, identifying important patient, provider, agency, and market/regulatory factors, respectively. Independent variables showing a significant or marginal relationship with the dependent variable (p.10) were identified for inclusion in the final model. Certain patient, provider, agency, and market/regulatory variables were designated as "required variables." These variables, such as patient age, agency ownership, and state volume group, were considered important enough theoretically to be retained in the final regression model, regardless of the significance value associated with their relationships with the dependent variable. Step 2 involved a single model in which all significant and marginal independent variables, as well as all required variables, were combined into a single regression model predicting the dependent variable.
The second set of analyses described above was conducted using a similar process. In this case, however, the Step 1 models were used to identify important patient, provider, agency, and market/regulatory variables to be included as covariates when examining the relationship between practice patterns and episode length. Again, all independent variables from the four Step 1 models that were significant or marginal, or were considered too important theoretically to eliminate, were included in the final Step 2 model along with the practice pattern independent variables, to predict length of stay for home care practices.
The third set of analyses described above was conducted in similar fashion. Four Set 1 models were conducted to identify important patient, provider, agency, and market/regulatory factors needing to be controlled in the final regression model. The significant/marginal and required variables were included in the final Step 2, along with the practice pattern independent variables, to predict patient functional outcome from care practices.
3. Identification of Important Variables
A large amount of data was collected during the course of the study. Consequently, there were far more variables available than reasonably could be analyzed. Prior to conducting multivariate analyses, the variables that would be included in the Step 1 regression models were designated. After identifying the variables of greatest theoretical value, preliminary descriptive and correlation analyses were conducted to assist in the identification of the most important variables. Some potential independent variables were eliminated from the multivariate analyses as a result of large amounts of missing data and/or a lack of sufficient variability. Others were removed because of strong correlations with other important independent variables. As mentioned above, of those variables retained for use as independent variables in the Step 1 regression models, some were identified as being of particular importance (i.e., the required variables).18Appendix F contains a list of the variables selected for inclusion as independent variables in the multivariate analyses. The variables designated as required variables are identified.
4. Missing Data
Because of the small size of the final episode-level sample, it was important to retain as many records as possible when conducting the multivariate analyses. Therefore, missing values for each independent variable identified for inclusion in the regression models were substituted with the variable's cross-sample mean. Of the thirty-six variables for which some records had missing values, none of those variables had more than 10% missing data. All but eight variables had less than 5% missing data.
III. DESCRIPTION OF STUDY STATES, AGENCIES, CARE PROVIDERS, AND PATIENTS
This chapter provides descriptive information regarding the states, agencies, and patients participating in the study. Section A provides a detailed description of the eight study states. For each state, information is provided about economic measures, demographic characteristics, and health care resources and expenditures. Section B presents descriptive information regarding the agency sample based on Administrator Questionnaire (AQ) data. In Section C, information about the study patients' physicians and home care staff is summarized. Data from the Care Provider Profile (CPP) and the Care Provider Questionnaire (CPQ) are used to describe the background, expertise, and level of involvement of the care providers. Section D summarizes the start of care case mix of the study patients. Descriptive analyses using OASIS and CPQ data are presented across the sample and by tracer condition (i.e., CHF and diabetes mellitus) and differences in case mix between the patients in the two tracer groups are described.19
A. Description of Study States
As indicated previously, states were categorized into high- and low-volume groups based on their average number of Medicare home health visits per beneficiary per year. Data from 1995 were used to categorize states into volume groups. To ensure that the volume categorizations were appropriate for later years during which the study data were collected, visit volume by state was compared for 1995, 1996, 1997, and 1998. Examining the data for these years was especially important given the major changes brought about by IPS.
Table 3.1 presents information regarding visits per patient for each study state and volume category for the four years. These data show the dramatic reduction in visits per patient in all states between 1997 and 1998 (the first full year of IPS). The reduction in the average number of visits was greater for the high-volume than for the low-volume states (averaging 36 visits versus 11 visits, respectively). As one would expect, these findings suggest that agencies in states where visits were provided in a parsimonious fashion prior to IPS might have had fewer discretionary services that could be eliminated than did agencies in states where visits were provided in higher volume. However, in percentage terms, the reduction in the high-volume states was not much greater than in the low-volume states (32.0% versus 25.3%, respectively). Thus, even with the dramatic reductions in visit volume in 1998, fairly large and consistent differences in visits per patient between high- and low-volume states continued under IPS. Whereas high-volume states provided an average of 2.65 times the number of visits per patient in 1997 than did low-volume states, they provided 2.44 times the average number of visits per patient in 1998.
| TABLE 3.1: Average Medicare Home Health Visits per Patient for the Study States | ||||||
| Visits/Patient | 1997-98 Decrease in Visits/Patient | |||||
| 1995a | 1996b | 1997c | 1998d | Number | Percent | |
| LOW VOLUME | ||||||
| Minnesota | 43 | 46 | 47 | 34 | 13 | 27.7 |
| New Jersey | 43 | 43 | 43 | 35 | 8 | 18.6 |
| Oregon | 38 | 35 | 34 | 24 | 10 | 29.4 |
| Pennsylvania | 46 | 46 | 47 | 36 | 11 | 23.4 |
| Average of Low-Volume States | 42 | 42 | 43 | 32 | 11 | 25.6 |
| HIGH VOLUME | ||||||
| Georgia | 108 | 104 | 99 | 64 | 35 | 35.4 |
| Massachusetts | 94 | 96 | 97 | 65 | 32 | 33.0 |
| Mississippi | 128 | 126 | 120 | 88 | 32 | 26.7 |
| Texas | 117 | 130 | 141 | 95 | 46 | 32.6 |
| Average of High-Volume States | 112 | 114 | 114 | 78 | 36 | 31.6 |
| NATIONAL | 72 | 74 | 73 | 51 | 22 | 30.1 |
| ||||||
Demographic, economic, health system, and health status indicators also were compared between the state volume groups using available secondary data. Selected statistics are presented in Tables 3.2-3.6. It should be noted that the data presented in these tables pertain to periods prior to the implementation of IPS. (Additional summary information is presented by state in Appendix D.) In the tables, data are presented for each state, along with averages for the four states in each state volume group, and for the nation. The differences between the volume group averages often are not large, and in some cases, the differences among states within a volume group are greater than the differences between the groups. Nevertheless, taken together, the various differences suggest the general patterns described below.
Demographic and economic statistics are presented in Table 3.2. Comparing the two state volume groups, low-volume relative to high-volume states have higher per capita incomes than high-volume states. However, there is considerable variation within each volume group, particularly the high-volume group in which per capita income ranges from a low of $18,300 in Mississippi to a high of $31,500 in Massachusetts (the lowest and second highest per capita incomes for all eight study states). Although the low-volume group has a higher average percentage of the population in the 65 and over age group, a lower percentage of that age group is in poverty (as measured by the percentage at or below 135% of the federally established poverty rate). In both state groups, approximately the same percentage of the elderly population lives alone, but the low-volume group has a lower rate of elderly with mobility or self-care difficulties. (The highest rate is in the high-volume state of Mississippi, where over one-quarter of the elderly population reported such difficulties in 1990.)
| TABLE 3.2: Selected Demographic and Economic Measures for the Study States | |||||
| Personal Per Capita Income (in $1,000s),1997a | Population 65+ (%),1998a | Persons 65+ at 135% of Poverty (%),1995-96a | Persons 65+ Living Alone (%),1990b | Persons 65+ per 1,000 with Difficulty in Mobility or Self-Care,1990b | |
| LOW VOLUME | |||||
| Minnesota | 26.8 | 12.3 | 26.4 | 30.5 | 165.1 |
| New Jersey | 32.7 | 13.5 | 19.2 | 26.5 | 198.0 |
| Oregon | 24.4 | 13.8 | 16.6 | 27.7 | 169.1 |
| Pennsylvania | 26.1 | 15.7 | 20.1 | 28.8 | 201.9 |
| Average of Low-Volume States | 27.5 | 13.8 | 20.6 | 28.4 | 183.5 |
| HIGH VOLUME | |||||
| Georgia | 24.1 | 9.9 | 23.6 | 28.3 | 246.8 |
| Massachusetts | 31.5 | 13.8 | 20.2 | 29.7 | 189.6 |
| Mississippi | 18.3 | 12.2 | 29.9 | 30.6 | 276.9 |
| Texas | 23.7 | 10.4 | 28.1 | 27.5 | 215.8 |
| Average of High-Volume States | 24.4 | 11.6 | 25.5 | 29.0 | 232.3 |
| NATIONAL | 25.6 | 12.7 | 21.7 | 28.2 | 201.1 |
| |||||
Selected health care coverage statistics are presented in Table 3.3. Relative to the high-volume state group, the low-volume group has a higher percentage of elderly with private health insurance and a higher percentage of Medicare beneficiaries enrolled in Risk Health Management Organizations (HMOs). The state volume groups are similar with regard to regulations specifying whether elderly persons in poverty qualify for full Medicaid benefits, but the low-volume group has a lower average percentage of Medicare beneficiaries covered by Medicaid. This finding is consistent with the data in Table 3.2 indicating that a lower percentage of elderly persons in the low-volume states are in poverty.
| TABLE 3.3: Selected Elderly Health Care Coverage Measures for the Study Statesa | ||||
| Persons Age 65+ with Private Health Insurance (%),1995-96 | Medicare Enrollment in Risk HMOs (as % of total beneficiaries),1998 | Persons Age 65+ in Poverty Quality for Full Medicaid Benefits,1998 | Medicare Beneficiaries Covered by Medicaid (%),1995-96 | |
| LOW VOLUME | ||||
| Minnesota | 69.7 | 8.9 | NO | 11.2 |
| New Jersey | 72.3 | 11.7 | YES | 9.2 |
| Oregon | 76.4 | 28.2 | NO | 11.8 |
| Pennsylvania | 75.1 | 24.5 | YES | 77.8 |
| Average of Low-Volume States | 73.4 | 18.3 | 50% YES | 11.0 |
| HIGH VOLUME | ||||
| Georgia | 59.8 | 3.9 | NO | 17.1 |
| Massachusetts | 67.3 | 21.4 | YES | 11.5 |
| Mississippi | 64.3 | 0.0 | YES | 22.5 |
| Texas | 59.8 | 13.7 | NO | 18.5 |
| Average of High-Volume States | 62.8 | 9.8 | 50% YES | 17.4 |
| NATIONAL | 67.4 | 15.4 | 20% YES | 13.7 |
| ||||
Table 3.4 provides selected information on health care resources and utilization. The low-volume states generally have greater availability of physician generalists and geriatricians (in terms of rates per population and per elderly, respectively). Although the numbers of geriatricians are small, the difference in rates between the low- and high-volume groups indicates the availability of about one-third more geriatricians per elderly person in the low-volume state group. The pattern for physician visits per Medicare beneficiary is consistent with the differences in physician availability, with generally higher visit rates in the low-volume states.
The low-volume states tend to use less of both institutional and noninstitutional long-term care per elderly than do the high-volume states. The rate of nursing home residents per 1,000 elderly persons is slightly lower in the low-volume states, despite the fact that Minnesota has by far the highest rate of all eight study states. The mean number of Medicare beneficiaries per 1,000 receiving home health care also is lower in the low- than the high-volume states. Because the selection of states was based on visits per home health user, the data on home health users per beneficiary indicate a positive correlation at the state level between home health use rates (i.e., number of beneficiaries receiving Medicare home health care per 1,000) and visits per user.
| TABLE 3.4: Selected Health Care Resource and Use Measures for the Study States | |||||
| Physician Generalists per 100,000 Population,1996a | Geriatricians per 10,000 Person Age 65+,1997a | Routine Physician Office Visits per Medicare Beneficiary,1997a | Nursing Home Residents per 1,000 65+ Population(1996 est.)b | Medicare Home Health Users per 1,000 Beneficiaries,1997b | |
| LOW VOLUME | |||||
| Minnesota | 48 | 5 | 4.1 | 72.2 | 72 |
| New Jersey | 18 | 4 | 6.1 | 39.5 | 97 |
| Oregon | 31 | 2 | 5.3 | 26.6 | 94 |
| Pennsylvania | 31 | 5 | 5.9 | 45.3 | 125 |
| Average of Low-Volume States | 32 | 4 | 5.4 | 45.9 | 97 |
| HIGH VOLUME | |||||
| Georgia | 24 | 2 | 5.5 | 48.6 | 110 |
| Massachusetts | 18 | 5 | 5.2 | 55.6 | 152 |
| Mississippi | 25 | 2 | 4.7 | 45.6 | 153 |
| Texas | 26 | 2 | 4.9 | 44.0 | 134 |
| Average of High-Volume States | 23 | 3 | 5.1 | 48.4 | 137 |
| NATIONAL | 28 | 3 | 5.5 | 43.7 | 109 |
| |||||
Further information on Medicare and Medicaid expenditures, particularly for long-term care, is presented in Table 3.5. The two groups of states have contrasting expenditure patterns, with the low-volume group characterized by lower Medicare but higher Medicaid payments per beneficiary or enrollee than the high-volume group. Medicaid long-term care expenditures show considerable variation in total program size among the states, reflected by differences in the number of recipients, services provided, and payment rates. Both volume groups include relatively small (Oregon and Mississippi) as well as relatively large (Pennsylvania and Texas) Medicaid long-term care expenditure components. The allocation of long-term care expenditures by service category reveals differences among states within each volume group and between volume groups. On average, the low-volume group devotes a slightly lower percentage of Medicaid long-term care expenditures to nursing home care than does the high-volume group, but this is largely due to the very low percentage for Oregon. Both the lowest and highest percentages are in the low-volume group, with 34.1% for Oregon and 76.4% for Minnesota. All other states devote between one-half and three-quarters of their long-term care expenditures to nursing home care.
Comparing the averages of the low- and high-volume state groups, the low-volume group has slightly lower personal care and home health expenditure percentages but a higher home and community-based services waiver percentage. However, the group averages are highly influenced by individual state percentages. In particular, Oregon devotes nearly half (45.3%) of its Medicaid long-term care expenditures to waiver programs. At the opposite extreme, Mississippi (in the high-volume group) spends less than 1% of its long-term care expenditures on waiver programs. Thus, the distribution of long-term care Medicaid expenditures varies considerably among states and no clear pattern emerges that distinguishes between the two volume groups.
| TABLE 3.5: Selected Medicare and Medicaid Expenditure Measures for the Study States | |||||||
| Medicare Payments per Beneficiary,1996a,b | Medicaid Payments per Elderly Disabled Enrollee,1995a | Long-Term Care Medicaid Expenditures (in $1000s),1996c | Percent of Long-Term Care Medicaid Expenditures, 1996c,d | ||||
| Nursing Home | Personal Care | Home Health | Home and Community-Based Services Waiver | ||||
| LOW VOLUME | |||||||
| Minnesota | $3,856 | $15,088 | $1,278,531 | 76.4 | 2.0 | 1.1 | 6.1 |
| New Jersey | 5,353 | 12,855 | 1,933,232 | 58.7 | 6.3 | 5.1 | 11.2 |
| Oregon | 3,999 | 10,191 | 483,830 | 34.1 | 4.4 | 0.1 | 45.3 |
| Pennsylvania | 5,333 | 9,690 | 3,195,571 | 70.8 | 0.0 | 2.4 | 9.4 |
| Average of Low-Volume States | 4,635 | 11,956 | 1,722,791 | 60.0 | 3.2 | 2.2 | 18.0 |
| HIGH VOLUME | |||||||
| Georgia | 5,081 | 6,335 | 915,199 | 70.5 | 0.0 | 5.3 | 10.4 |
| Massachusetts | 6,266 | 11,953 | 1,961,987 | 63.2 | 6.0 | 4.3 | 12.3 |
| Mississippi | 5,299 | 5,175 | 411,639 | 70.8 | 0.0 | 3.5 | 0.9 |
| Texas | 5,905 | 7,522 | 2,453,962 | 51.9 | 12.0 | 1.7 | 10.8 |
| Average of High-Volume States | 5,638 | 7,746 | 1,435,697 | 64.1 | 4.5 | 3.7 | 8.6 |
| NATIONAL | 5,048 | 9,167 | 1,006,418 | 60.6 | 5.6 | 4.0 | 11.0 |
| |||||||
Table 3.6 provides another perspective on Medicare and Medicaid home health expenditures. The table provides information on Medicare and Medicaid home health expenditures in total and per enrollee for 1995 (enrollees include both users and non-users of home care). The Medicaid home care expenditures include the various categories listed in Table 3.5 above (i.e., personal care, home care, and waiver services). The table generally confirms the pattern noted earlier of low-volume states as a group having lower Medicare but higher Medicaid expenditures per enrollee than high-volume states. The state rankings shown in the Table 3.6 are consistent with this pattern. Thus, to some extent, the lower use of Medicare home health care in the low-volume states is somewhat offset, at least for those eligible for Medicaid, by greater use of Medicaid home health care.
| TABLE 3.6: Selected Medicare and Medicaid Home Health Expenditure Measures for the Study Statesa | ||||||
| Medicare, 1995 | Medicaid, 1995 | |||||
| Total(millions) | Per Enrolleeb | Total(millions) | Per Enrolleeb | |||
| LOW VOLUME | ||||||
| Minnesota | $100 | $195 | (49) | $127 | $399 | (14) |
| New Jersey | 330 | 293 | (40) | 399 | 454 | (9) |
| Oregon | 101 | 310 | (38) | 235 | 484 | (8) |
| Pennsylvania | 779 | 401 | (27) | 372 | 187 | (31) |
| Average of Low-Volume States | 328 | 300 | (39) | 306 | 381 | (16) |
| HIGH VOLUME | ||||||
| Georgia | 595 | 711 | (10) | 128 | 104 | (43) |
| Massachusetts | 629 | 742 | (8) | 577 | 716 | (4) |
| Mississippi | 419 | 1,055 | (2) | 13 | 24 | (49) |
| Texas | 1,910 | 986 | (5) | 317 | 110 | (41) |
| Average of High-Volume States | 888 | 874 | (6) | 184 | 238 | (34) |
| NATIONAL | 16,961 | 516 | NA | 9,701 | 237 | NA |
| ||||||
B. Description of Study Agencies
1. Overview of Study Agencies
Forty-four home care agencies contributed complete assessment data to the final patient sample.20 Administrators of 42 of these agencies completed the AQ. Therefore, the AQ descriptive statistics presented in this chapter are based on a sample of 42 agencies across the eight study states.21 Despite agency attrition, the number of agencies per state remained relatively comparable. Each of the eight states contributed between four and eight agencies to the final sample. On average, six agencies were located in each state.22
| TABLE 3.7: Agency Ownership and Type Distribution of Study Agencies | |||
| Agency Ownership | Agency Type | Total | |
| Freestanding | Hospital-Based | ||
| Non-Proprietary | 10 | 19 | 29 |
| Visiting Nurse Association | 5 | ||
| Government | 2 | ||
| Private | 1 | ||
| Other | 2 | ||
| Proprietary | 13 | 2 | 15 |
| Total Agencies | 23 | 21 | 44a |
| |||
The study agencies reflected a variety of important agency-level factors. Importantly, the agencies provided a cross-section with regard to three factors that may play a critical role in the practice of home health care: state volume, agency ownership, and agency type. Slightly more than half of the agencies (59.1%) were located in states with low visit volume per patient. The remaining 40.9% of the agencies were located in high-volume states. Sixty-six percent of the agencies were non-proprietary or government agencies (see Table 3.7). The remaining 34% were proprietary agencies. The agency sample had nearly equal representation of hospital-based and freestanding agencies (48% and 52%, respectively). As is typically the case, the hospital-based agencies are primarily non-proprietary. In the freestanding category, more agencies are proprietary than non-proprietary; the non-proprietary category includes Visiting Nurse Association (VNA), government, and private non-profit agencies.
2. AQ Descriptive Statistics
Table E.1 in Appendix E contains descriptive statistics for each AQ item (Appendix A contains a copy of the AQ). For continuous variables, the mean, median, minimum and maximum values are presented. For categorical variables, the percentage of agencies for which each response was selected is identified. The number of agencies having data for each item also is reported. The final two items in the AQ (items 69 and 70) were excluded from the table. These items, which elicit information about staff attendance at study training sessions and identifying information about each agency's Data Collection Coordinator, respectively, were designed for internal Research Center use only. Therefore, responses to these items have not been included in this report. For a number of questions on the AQ, agency administrators were allowed to provide open-ended responses. These responses are compiled by question in Table E.2 in Appendix E. Items with open-ended responses contained in the Appendix are identified in Table E.1.
The main objective of the following comments is to provide basic descriptive information about the study agencies using the AQ data. Appendix E provides descriptive statistics for each AQ item so that the reader can concentrate on specific areas of interest. Therefore, only a few summary narrative comments are included here. Most study agencies (95.2%) were located in states requiring licensure (AQ item 7). Among the study agencies, the majority was accredited (76.2%), most by JCAHO (73.8%). Only 2.4% of the study agencies were accredited by the Community Health Assessment Program (CHAP), the only other accrediting organization mentioned by study agency administrators (AQ item 8).
Medicare patients represented a large percentage of the caseload for most study agencies. On average, 74.1% of the agencies' patients were Medicare patients (AQ item 13). However, the range in Medicare caseload was considerable -- from as little as 10% to 100% of the caseload. Slightly less than half of the agencies were operating over the Medicare per-visit cost limits (42.9%) (AQ item 11). One-third was operating over their annual per-beneficiary limits as well (33.3%) (AQ item 12).
Most agencies had standards with regard to nurse productivity, but not with regard to the assignment of a home health aide. Of the responding agencies, 40.5% had unwritten nurse productivity standards and another 45.2% maintained written nurse productivity standards (AQ item 23). On average, nurses were required to make 5.6 patient visits per day (AQ item 24). The number of visits required was as low as four at some agencies and as high as eight at others. The majority (76.2%) of the agencies did not use standards for the assignment of home health aide services (AQ item 39).
In most agencies, primary care providers made important decisions about the care patients receive. The nurse who performed the initial assessment of a patient was almost always the person responsible for making the initial decision regarding the number of visits that patient would receive (93.8% of the time) (AQ item 35). Further, the provider who saw the patient at start of care was usually responsible for completing the HCFA-485 (78.6% of the time) (AQ item 48). Administrators from most agencies (81.0%) indicated that it was most frequently the primary care provider who made decisions regarding recertification (AQ item 51).
However, in most agencies, care providers received supervision in their decision making. At the majority of the agencies (85.7%), nurses met with their supervisors at least weekly (AQ item 46). At more than half of the agencies (60.9%), therapists met with their supervisors at least weekly, as well. At 69.0% of the agencies, interdisciplinary case conferences (at which patients' cases were reviewed) occurred at least twice a month (AQ item 47). At nearly half of the agencies (47.6%), these case conferences occurred at least once a week. Administrators at 90.5% of the agencies reported that staff other than the primary care provider regularly verified patient eligibility for home health care services (AQ item 38).
Further, the care that home care workers provided often was guided by their agencies' critical pathways. More than 40% of agency administrators indicated that their agencies use standardized care plans or critical pathways (AQ item 25). These agencies had diagnosis-specific pathways for several important conditions. The majority of these agencies use pathways for chronic obstructive pulmonary disease (COPD), CHF, myocardial infarction (MI) and other cardiac conditions, pressure ulcers, other wounds, fractured hip, total hip replacement, total knee replacement, cerebral vascular accident (CVA), diabetes mellitus, and osteoarthritis (AQ item 27).
Administrators reported few changes in the delivery of services at their agencies as a result of the then newly implemented venipuncture regulations (AQ item 28). Most agencies had experienced no changes in their service areas (86.5%) or in the amount of time spent on care planning (76.9%). However, many agencies (65.4%) had decreased the number of visits they provided to their patients.
C. Description of Study Care Providers
Table 3.8 provides descriptive information based on CPP and CPQ data about the home care providers and physicians caring for the study patients. Because the home care provider conducting the start of care visit plays a vital role in determining a patient's plan of care, most of the information provided in the table reflects the characteristics of the providers conducting the start of care visits for each of the 732 episodes of care.23 However, a few variables from the CPQ are presented based on discharge data (i.e., the physician's care plan role, level of input, overall physician awareness and involvement). Because these variables are based on home care provider perception, it seemed that care providers would be better able to assess the role of the physician at the end, rather than the beginning, of the episode.
Across the 732 episodes of care, the vast majority of the start of care visits was conducted by registered nurses (98.7%). Physical therapists and speech therapists conducted the remaining start of care visits (1.2% and 0.1%, respectively). The majority of the providers conducting these visits was full-time agency staff (71.8%), and nearly all were employees of their agencies (i.e., not contracted staff; 95.4%). Most had traveled less than half an hour to conduct the start of care visit (84.5%).
Of the 678 providers for whom data were available at the start of care, nearly half had an Associate's degree as their highest level of education (43.5%), 30.2% had a Bachelor's degree, and 19.8% had a high school diploma. Only 6.1% of the care providers had a Master's degree. Most of the providers indicated they had specific areas of health care expertise (e.g., special certification or strong experience). Most commonly, the providers noted having special expertise in treating patients with medical/surgical conditions (50.1%). A substantial percentage of the care providers reported having expertise or experience in the care of patients with the two medical conditions targeted for this project. Forty-three percent had experience treating cardiovascular problems and 32.7% had expertise in treating diabetes. Slightly over one-third of the care providers had expertise in IV therapy and wound management (33.6% and 35.4%, respectively). Other areas of expertise were less commonly reported.
The care providers conducting the start of care visits had quite a bit of experience in home health care. More than half of the providers (54.4%) had six or more years of experience in the home health industry. Only 13.4% of the providers were relatively new to home health care, having been in the business less than two years. Perhaps partly because of the experience of the care providers, the majority of visits were conducted without the use of a standardized care plan (62.4%). Indeed, there is a small, but significant correlation between these variables, suggesting that more experienced care providers were less likely to use standardized care plans (r=-0.135, p=0.0004).
| TABLE 3.8: Descriptive Information Regarding Study Care Providers | |||
| Provider Variables | Provider Variables | ||
| Discipline (n=678) | |||
| RN | 98.7% | LPN | 0.0% |
| PT | 1.2% | SLP/ST | 0.1% |
| OT | 0.0% | MSW | 0.0% |
| Contract Status (n=668) | |||
| No | 95.4% | Yes | 4.6% |
| Travel Time (n=724) | |||
| 10 minutes or less | 31.2% | 11-20 minutes | 33.3% |
| 21-30 minutes | 30.0% | 31-40 minutes | 9.0% |
| 41-50 minutes | 3.6% | 51-60 minutes | 1.7% |
| Over one hour | 1.2% | ||
| Years of Home Health Experience (n=677) | |||
| Less than 2 years | 13.4% | 2 to 5 years | 32.2% |
| 6 to 10 years | 31.2% | More than 10 years | 23.2% |
| Standardized Care Plan Used for Visit (n=728) | |||
| No | 62.4% | Yes | 37.6% |
| Highest Level of Education (n=672) | |||
| LPN/LVN Education | 0.0% | Diploma | 19.8% |
| Associate's degree | 43.5% | Bachelor's degree | 30.2% |
| Master's degree | 6.1% | Other | 0.4% |
| Specific Areas of Expertise (n=672) | |||
| Cardiovascular | 43.0% | Diabetes | 32.7% |
| Infectious Diseases | 11.2% | IV Therapy | 33.6% |
| Medical/Surgery | 50.1% | Neurology | 6.7% |
| Nutrition/Diet | 12.4% | Orthopedic | 7.7% |
| Psychiatric | 2.5% | Rehabilitation | 10.7% |
| Respiratory | 14.3% | Speech | 0.4% |
| Strength/Endurance Training | 2.1% | Would Management | 35.4% |
| Other | 17.0% | None of the above | 10.3% |
| Part-Time/Full-Time Status (n=677) | |||
| Part time | 28.2% | Full time | 71.8% |
| Familiarity with Patient (n=725) | |||
| Once | 6.2% | Two to five times | 31.6% |
| Six to ten times | 26.3% | More than ten | 35.9% |
| Did Care Provider Conducting DC Assessment Also Conduct SOC? (n=732) | |||
| No | 30.7% | Yes | 69.3% |
| Physician | |||
| Frequency of SN Visits Suggested (n=684) | Home Health Aide Services Were Ordered (n=684) | ||
| NoYes | 80.4%19.6% | NoYes | 83.9%16.1% |
| Evaluation of Need for Aide Services was Requested (n=685) | Care Plan Rolea (n=731) | ||
| NoYes | 76.9%23.1% | MajorModerateMinor | 27.1%54.0%18.9% |
| Physician Inputa (n=731) | Physician Awareness of Care Provided by Agencya (n=726) | ||
| Not enoughRight amountMore input than needed | 9.2%87.1%3.7% | More than adequateAdequateInadequate | 39.5%58.3%2.2% |
| Physician Suggested that Home Health Services be Terminateda (n=727) | |||
| NoYes | 85.6%14.4% | ||
| |||
The 732 episodes of care appear to have been characterized by considerable continuity of care. In the majority of the cases, the care providers who conducted the start of care visit also conducted the discharge visit (69.3%). By the time of discharge, 62.2% of the care providers had seen their respective patients six or more times over the course of the episodes.
Information about the physicians overseeing the care of the study patients was provided by the home health care providers in response to questions on the start of care and discharge versions of the CPQ. Prior to the beginning of the home care episodes, few physicians provided home care agency staff with specific recommendations regarding the type and frequency of home care services to be provided. In only 19.6% of the study episodes did the patients' physicians recommend a specific frequency with which nursing visits should occur. Only 16.1% of the physicians ordered home health aide services, and 23.1% requested an evaluation for the need for aide services.
During the episode, many physicians maintained a relatively low level of involvement. Only 27.1% of the home care providers completing the discharge CPQ for a given episode of care indicated that the physician overseeing the episode had a major role (i.e., was actively involved) in the development of the patient's care plan. In most cases (54.0%), the physician was perceived as being moderately involved. In these cases, the physician mainly responded to suggestions from the home care staff as to how a patient's care should be handled rather than actively making suggestions regarding the care plan. In 18.9% of the cases, the physicians were perceived as having no involvement in care planning other than signing the HCFA-485 and other orders. In the vast majority of cases (85.6%), discharge came at the recommendation of the home care staff rather than the physicians.
Although the physicians did not always play a major role in the development of the care plan, the home care personnel appear to have been comfortable with the level of physician involvement throughout the episodes of care. Although only slightly over one-quarter of home care providers indicated that the physician was actively involved in the development of the patient's care plan, the majority of home care providers considered the level of physician input to be sufficient (87.1%) and nearly all (97.8%) felt that the physicians were aware of the care being provided.
D. Description of Study Patients
The final patient sample included 684 patients. Of these patients, 292 were diagnosed with CHF, 246 with diabetes mellitus, and 146 with both conditions.24 Only patients with complete assessment data for one or more episodes of care were retained in the final sample. Assessment data were considered complete if a patient had OASIS and CPQ data for both the beginning and the ending of an episode of care.
Across the 684 patients, complete assessment data were available for 732 episodes of care. The vast majority of patients had only one episode of care in the final sample (94.7%). An additional 4.1% of patients had two episodes, and 1.1% had three or more.25 The number of episodes per patient is similar for those patients with CHF and those with diabetes mellitus. Among CHF patients, 93.8% had only a single episode, whereas 5.0% had two episodes, and 1.1% had three or more. Likewise, 94.9% of diabetes mellitus patients had only a single episode of care, whereas 3.3% had two episodes, and 1.8% had three or more episodes.
Table 3.9 provides descriptive information about the start of care case mix of the patients treated during the 732 study episodes. This information is provided across episodes and also separately by tracer condition. The degree to which the patients in the two condition groups differ is reported. (The episodes for the 146 patients diagnosed with both conditions are included in both the CHF and the diabetes mellitus groups.) Given that a patient's condition can vary drastically from episode to episode, analyses were conducted at the episode level rather than the patient level. Therefore, for patients with multiple episodes of care, start of care information from each episode was included in the analyses.
Patients enrolled in the study were quite elderly. Although patients age 65 and older were eligible for participation, at the start of care, the average age of study subjects across conditions was 78.4 years of age. Patients diagnosed with CHF were significantly older than those diagnosed with diabetes mellitus (80.2 versus 76.4, respectively). Not surprising for such an elderly population, the majority of subjects in both the CHF and diabetes mellitus groups was female. In both condition groups, the majority of the study participants was White.
| TABLE 3.9: Patient Case Mix at Start of Episode by Conditiona | |||||||
| Across Conditions | CHF | Diabetes Mellitus | Sigc | ||||
| Nb | Mean or % | Nb | Mean or % | Nb | Mean or % | ||
| DEMOGRAPHICS | |||||||
| Age (average in years) | 732 | 78.8 | 474 | 80.2 | 423 | 76.4 | ** |
| Gender (%) - Female - Male | 732732 | 60.139.9 | 474474 | 58.042.0 | 423423 | 61.538.5 | |
| Race (%) - White - Black or African-American - Other | 713 713713 | 84.313.32.5 | 465465465 | 83.913.62.6 | 410410410 | 82.214.93.2 | |
| PAYMENT SOURCE | |||||||
| Any Medicaid (%) | 732 | 7.2 | 474 | 7.0 | 423 | 8.3 | |
| Any Third Party (%) | 732 | 8.9 | 474 | 10.1 | 423 | 8.5 | |
| Any HMO (%) | 732 | 10.7 | 474 | 10.6 | 423 | 10.9 | |
| Medicare HMO (%) | 732 | 9.3 | 474 | 9.3 | 423 | 9.7 | |
| LIVING ENVIRONMENT | |||||||
| Current Residence (%) - Living in own home - Living in family member's home | 724724 | 80.013.0 | 469469 | 78.313.9 | 416416 | 81.511.3 | |
| Current Living Situation (%) - Living alone - Living with family member (unpaid) - Living with friend (unpaid) - Living with paid help | 730730730730 | 29.764.40.75.5 | 472472472472 | 30.163.80.65.7 | 423423423423 | 29.164.80.55.2 | |
| Structural barriers limiting independent mobility in home (%) | 732 | 46.2 | 474 | 46.2 | 423 | 46.3 | |
| Safety hazards in home (%) | 732 | 10.0 | 474 | 10.1 | 423 | 9.7 | |
| HOMEBOUND STATUS | |||||||
| Absences from Home (%) - Infrequent - For periods of relatively short duration - Attributable to the need to receive medical treatment | 731731731 | 54.336.374.1 | 473473473 | 53.134.075.5 | 423423423 | 55.339.074.9 | |
| Requirements to Leave Home (%) - Aid of supportive devices - Use of special transportation - Assistance of another person - None of the above | 731731731731 | 63.612.087.14.4 | 473473473473 | 64.311.487.73.6 | 423423423423 | 65.514.087.55.2 | |
| Leaving the Home is Medically Contraindicated (%) | 732 | 13.7 | 474 | 13.5 | 423 | 14.2 | |
| Difficulty Receiving Services Outside the Home (%) - Very difficult - Somewhat difficult - Not at all difficult | 732732732 | 48.046.25.9 | 474474474 | 49.845.44.9 | 423423423 | 46.846.36.9 | |
| FAMILY/SUPPORT SYSTEM | |||||||
| Patient has a Family/Support System (%) | 710 | 97.2 | 463 | 98.1 | 408 | 96.8 | |
| Assistance Provided by Family/Support System (%) - ADL assistance - IADL assistance - Assistance with wounds and/or equipment - Psychosocial support - Advocacy or facilitation of appropriate medical care - Transportation | 658684671692685689 | 64.997.521.098.394.692.0 | 437452437453452450 | 64.397.818.198.796.293.3 | 375391387398392395 | 66.498.225.198.093.490.6 | *** |
| People Providing Assistance to the Patient (%) - Spouse or significant other - Daughter or son - Other family member - Friend, neighbor, or community/church member - Paid help other than above | 335553302257207 | 12.25.121.926.837.2 | 195361198173134 | 88.795.881.379.868.7 | 217318175142122 | 87.194.773.164.154.1 | ***** |
| Assisting Persons (%) - Person residing in home - Person residing outside of home | 731 731 | 52.5 58.0 | 473 473 | 50.3 58.8 | 423 423 | 54.9 58.9 | |
| Primary Caregiver (%) - No one person - Spouse or significant other - Daughter or son - Other family member - Friend, neighbor, or community/church member - Paid help other than above | 700700700700700700 | 9.734.637.97.01.76.4 | 460460460460460460 | 10.231.140.78.01.56.7 | 403403403403403403 | 9.737.734.76.51.76.7 | |
| Frequency of Assistance Provided by Primary Caregiver (1-6, scale average)d | 728 | 4.2 | 470 | 4.2 | 422 | 4.1 | |
| CAREGIVER INVOLVEMENT IN CARE PLAN | |||||||
| Involvement of Primary Caregiver in Care Plan (%) - Very/somewhat involved - Minimally involved | 597597 | 76.423.6 | 392392 | 77.622.5 | 347347 | 73.226.8 | |
| Primary Caregiver's Ability to Learn (%) - Excellent - Good - Fair - Poor | 567 567 567 567 | 44.8 43.2 10.9 1.1 | 370 370 370 370 | 45.7 42.4 10.3 1.6 | 330 330 330 330 | 44.2 42.7 12.4 0.6 | |
| Caregiver is knowledgeable about Medicare Home Health Benefit (%) | 549 | 87.4 | 356 | 89.9 | 316 | 85.8 | |
| Primary Caregiver Willing for Patient to Receive Needed Aide Services (%) | 307 | 86.3 | 219 | 85.8 | 167 | 89.2 | |
| PATIENT INVOLVEMENT IN CARE PLAN | |||||||
| Patient Involvement in Care Plan (%) - Very/somewhat involved - Minimally involved | 694694 | 59.540.5 | 451451 | 58.141.9 | 403403 | 60.839.2 | |
| Patient Ability to Learn (%) - Excellent - Good - Fair - Poor | 730730730730 | 12.251.226.89.7 | 472472472472 | 11.250.229.78.9 | 423423423423 | 12.853.023.610.6 | |
| Patient is knowledgeable about Medicare Home Health Benefit (%) | 695 | 75.1 | 446 | 77.1 | 406 | 74.6 | |
| Patient Willing to Accept Needed Aide Services (%) | 363 | 77.7 | 258 | 77.5 | 196 | 80.1 | |
| COMPLEXITY/SEVERITY OF CONDITION | |||||||
| Medical regimen change within 14 days of SOC (%) | 731 | 88.0 | 473 | 88.0 | 423 | 88.7 | |
| Inpatient DC within 14 Days of SOC (%) - Hospital - Rehabilitation Facility - Nursing Home | 730730730 | 69.06.75.6 | 473473473 | 73.44.75.5 | 422422422 | 65.28.85.5 | **** |
| Patient Requires Complex Management (%) | 731 | 55.5 | 473 | 53.1 | 423 | 61.0 | ** |
| Patient Has Greater than Average Functional Assistance Needs (%) | 730 | 36.4 | 472 | 37.7 | 423 | 35.5 | |
| Overall Prognosis (%) - Good/fair - Poor | 714714 | 89.410.6 | 462462 | 87.013.0 | 413413 | 90.69.4 | |
| Rehabilitative prognosis (%) - Good - Guarded | 710710 | 67.932.1 | 456456 | 63.836.2 | 413413 | 71.428.6 | ** |
| Number of High Risk Factors (average) | 702 | 0.3 | 450 | 0.3 | 406 | 0.3 | |
| Nutritional Status (%) - Excellent - Adequate - Probably inadequate - Very poor | 731731731731 | 23.058.715.92.5 | 473473473473 | 20.161.715.62.5 | 423423423423 | 26.258.213.22.4 | |
| CURRENT ADL DISABILITIES | |||||||
| Grooming (0-3, scale average) | 732 | 0.8 | 474 | 0.8 | 423 | 0.7 | ** |
| Dress upper body (0-2, scale average) | 732 | 0.8 | 474 | 0.9 | 423 | 0.8 | |
| Dress lower body (0-3, scale average) | 732 | 1.0 | 474 | 1.0 | 423 | 1.0 | |
| Bathing (0-5, scale average) | 732 | 2.1 | 474 | 2.1 | 423 | 2.1 | |
| Toileting (0-4, scale average) | 731 | 0.5 | 473 | 0.5 | 423 | 0.5 | |
| Transferring (0-5, scale average) | 732 | 0.7 | 474 | 0.7 | 423 | 0.7 | |
| Ambulation (0-5, scale average) | 732 | 1.2 | 474 | 1.2 | 423 | 1.2 | |
| Eating (0-5, scale average) | 731 | 0.3 | 473 | 0.3 | 423 | 0.3 | |
| Mild ADL disabilities (0-8)e | 730 | 3.9 | 472 | 4.0 | 423 | 3.9 | |
| Moderate ADL disabilities (0-8)e | 730 | 1.6 | 472 | 1.6 | 423 | 1.6 | |
| Severe ADL disabilities (0-8)e | 730 | 0.4 | 472 | 0.4 | 423 | 0.4 | |
| CURRENT IADL DISABILITIES | |||||||
| Light meal preparation (0-2, scale average) | 732 | 1.0 | 474 | 1.0 | 423 | 0.9 | * |
| Transportation (0-2, scale average) | 732 | 1.0 | 474 | 1.0 | 423 | 1.0 | |
| Laundry (0-2, scale average) | 732 | 1.6 | 474 | 1.7 | 423 | 1.6 | |
| Housekeeping (0-4, scale average) | 732 | 2.9 | 474 | 3.0 | 423 | 2.9 | |
| Shopping (0-3, scale average) | 732 | 2.2 | 474 | 2.3 | 423 | 2.2 | ** |
| Phone use (0-5, scale average) | 722 | 0.7 | 468 | 0.8 | 415 | 0.7 | |
| Management of oral medications (0-2, scale average) | 728 | 0.9 | 471 | 1.0 | 422 | 0.9 | ** |
| Mild IADL Disabilities (0-6)f | 722 | 4.7 | 468 | 4.8 | 415 | 4.6 | * |
| Severe IADL Disabilities (0-6)f | 722 | 2.0 | 468 | 2.1 | 415 | 2.0 | |
| MEDICATION/EQUIPMENT MANAGEMENT | |||||||
| Management inhalant/mist meds (0-2, scale average) | 190 | 0.7 | 133 | 0.7 | 103 | 0.6 | |
| Management of injectable meds (0-2, scale average) | 230 | 1.1 | 102 | 1.2 | 215 | 1.0 | |
| Patient management of equipment (0-4, scale average) | 171 | 2.2 | 140 | 2.2 | 79 | 2.2 | |
| RESPIRATORY STATUS | |||||||
| Dyspnea (0-4, scale average) | 732 | 1.7 | 474 | 1.9 | 423 | 1.5 | ** |
| SENSORY STATUS | |||||||
| Vision impairment (0-2, scale average) | 731 | 0.4 | 473 | 0.4 | 423 | 0.4 | |
| PAIN | |||||||
| Pain interfering with activity (0-3, scale average) | 731 | 0.9 | 474 | 0.8 | 422 | 0.9 | |
| Intractable pain (%) | 731 | 9.3 | 474 | 9.3 | 422 | 10.7 | |
| INTEGUMENTARY STATUS | |||||||
| Presence of wound/lesion (%) | 732 | 26.5 | 474 | 21.7 | 423 | 34.3 | ** |
| Surgical wound(s) present (%) | 732 | 13.1 | 474 | 7.6 | 423 | 18.9 | ** |
| Stasis ulcer(s) present (%) | 732 | 2.3 | 474 | 2.1 | 423 | 2.4 | |
| Pressure ulcer(s) present (%) | 732 | 5.3 | 474 | 4.6 | 423 | 7.1 | |
| Stage 2-4 ulcer(s) present (%) | 732 | 4.2 | 474 | 3.0 | 423 | 6.2 | ** |
| Stage 3-4 ulcer(s) present (%) | 732 | 0.8 | 474 | 0.8 | 423 | 1.2 | |
| ELIMINATION STATUS | |||||||
| UTI within past 14 days (%) | 725 | 8.4 | 469 | 7.3 | 419 | 8.8 | |
| Urinary incontinence/catheter (%) | 732 | 23.5 | 474 | 24.3 | 423 | 21.5 | |
| Bowel incontinence (0-5, scale average) | 717 | 0.2 | 467 | 0.2 | 414 | 0.2 | |
| NEUROLOGIC/EMOTIONAL/BEHAVIORAL STATUS | |||||||
| Behavior problems (% > twice a week) | 731 | 4.0 | 474 | 3.6 | 422 | 4.7 | |
| Severe anxiety level (%) | 732 | 16.8 | 474 | 17.3 | 423 | 15.4 | |
| Moderate cognitive disability (%) | 732 | 10.9 | 474 | 11.6 | 423 | 9.7 | |
| Severe confusion disability (%) | 732 | 10.7 | 474 | 10.3 | 423 | 10.6 | |
| Psychiatric nursing services (%) | 732 | 0.7 | 474 | 0.4 | 423 | 1.0 | |
| DIAGNOSES FOR WHICH PATIENTS ARE RECEIVING HOME CARE | |||||||
| Neoplasms (%) | 732 | 3.0 | 474 | 2.5 | 423 | 3.1 | |
| Endocrine/nutritional/metabolic (%) | 732 | 57.5 | 474 | 36.9 | 423 | 92.9 | ** |
| Blood diseases (%) | 732 | 7.1 | 474 | 8.4 | 423 | 5.2 | * |
| Mental diseases (%) | 732 | 6.1 | 474 | 6.1 | 423 | 6.2 | |
| Nervous system diseases (%) | 732 | 4.8 | 474 | 3.6 | 423 | 5.9 | |
| Circulatory system diseases (%) | 732 | 83.7 | 474 | 96.2 | 423 | 74.5 | ** |
| Respiratory system diseases (%) | 732 | 25.4 | 474 | 30.2 | 423 | 21.3 | ** |
| Digestive system diseases (%) | 732 | 9.2 | 474 | 9.5 | 423 | 8.5 | |
| Genitourinary system diseases (%) | 732 | 12.3 | 474 | 12.7 | 423 | 14.2 | |
| Skin/subcutaneous diseases (%) | 732 | 7.1 | 474 | 5.3 | 423 | 9.7 | ** |
| Musculoskeletal system diseases (%) | 732 | 16.3 | 474 | 16.5 | 423 | 15.6 | |
| Ill-defined conditions (%) | 732 | 15.3 | 474 | 16.2 | 423 | 15.6 | |
| Fractures (%) | 732 | 2.2 | 474 | 1.7 | 423 | 2.6 | |
| Other injury (%) | 732 | 3.4 | 474 | 1.9 | 423 | 4.5 | ** |
| Iatrogenic conditions (%) | 732 | 1.4 | 474 | 0.8 | 423 | 1.4 | |
| THERAPIES RECEIVED AT HOME | |||||||
| IV/infusion therapy (%) | 732 | 1.5 | 474 | 1.9 | 423 | 1.9 | |
| Parenteral nutrition (%) | 732 | 0.0 | 474 | 0.0 | 423 | 0.0 | |
| Enteral nutrition (%) | 732 | 0.5 | 474 | 0.6 | 423 | 0.7 | |
| Oxygen (%) | 731 | 20.0 | 474 | 26.8 | 422 | 14.7 | ** |
| Ventilator (%) | 731 | 0.1 | 474 | 0.2 | 422 | 0.2 | |
| Continuous positive airway pressure (%) | 731 | 0.5 | 474 | 0.4 | 422 | 0.5 | |
| |||||||
Although all of the patients enrolled in the study were Medicare patients, few patients had additional health care coverage. Only 7.6% of patients were covered by Medicaid and 9.4% were covered by third party insurance carriers. Most patients were not covered by managed care organizations. Only 10.7% of patients across condition groups had health insurance through a Health Maintenance Organization (HMO). Most of these patients had Medicare managed care as a current payment source.
Despite their age, the majority of patients involved in the study lived in their own homes (79.8% across the two condition groups). Although the majority of the subjects lived with an unpaid family member, nearly one-third lived alone. Few study subjects had safety hazards in their homes, such as inadequate heating/cooling, unsafe floor coverings, and lead-based paint. However, nearly half had structural barriers limiting independent mobility within their homes.
Consistent with Medicare home health coverage rules, the study patients were homebound. Although leaving home was medically contraindicated for only a small percentage of patients, it was challenging for all patients. For approximately three-quarters of the study subjects, absences from home were attributable solely to the need to obtain medical care. More than half of the patients left their homes only rarely and for slightly over one-third of the patients, these absences were of short duration.
Most patients needed assistance to leave their homes. Commonly, patients needed the assistance of another person or the aid of supportive devices. Only a small percentage of patients (less than 5%) was able to leave home without some sort of assistance. As expected, for nearly all patients, receiving medical care outside of the home was very or somewhat difficult. For a small percentage of patients (5.8%), the home care providers conducting the start of care assessments indicated that it was not difficult at all for the patients to receive services outside of the home. It appears that some episodes, representing slightly under 2% of the total episode sample, may not have met the requirements of the Medicare coverage rules related to homebound status. Patients treated during 14 episodes were rated by their care providers as having no difficulty receiving services outside of the home and requiring no assistance to leave home. For 50.0% of these patients, absences from home were not infrequent, for 42.9% these absences were not of short duration, and for 78.6% absences from home were not attributable to the need to receive medical care.
Informal, unpaid caregivers are of great significance in home care. Nearly all study patients had family members or other persons who provided them with assistance of one kind or another. The vast majority of patients (98.0%) received assistance with instrumental activities of daily living (IADLs), such as light meal preparation, transportation, and housekeeping. Further, almost all patients received psychosocial support, transportation, and advocacy of their medical care. Patients were less likely to receive assistance with activities of daily living (ADLs), such as grooming, bathing, and toileting (65.3%). Only a minority of patients received assistance with wounds or medical equipment from members of their family support systems.
Patients with CHF and those with diabetes mellitus were quite similar in the kinds of assistance received from their family/support systems. There was only one area in which these groups differed significantly. Diabetic patients were significantly more likely to receive assistance with wounds or medical equipment (which may be a reflection of the fact that diabetic patients were more likely than CHF patients to have surgical wounds). Although the majority of patients in both groups had informal caregivers who helped to facilitate appropriate medical care, CHF patients were marginally more likely to receive assistance in this area.
The majority of patients received assistance from a variety of people. Most commonly, patients were helped by one or more of their children (95.3%). Nearly 90% were assisted by their spouses or significant others. However, at times, assistance provided by a Medicare patient's spouse or partner can be problematic in that the informal caregiver may be just as frail and elderly as the patient him- or herself. Approximately, one-third of the patients received assistance from other family members or from friends, neighbors, or community/church members. Over 61% also received assistance from paid help. CHF patients were significantly more likely than diabetic patients to receive assistance from paid help and from friends, neighbors, or community/church members. Likewise, they were marginally more likely to receive assistance from family members other than their spouses/significant others and their children. Slightly over half of the patients were assisted by a person or persons residing in their home.
Most patients had a single person who assumed the lead responsibility for providing/managing the patient's care and providing the most frequent assistance among all informal caregivers. For slightly over one-third of the patients, the spouse or significant other fulfilled this role. For another one-third, one of the patient's children was the "primary caregiver." For 15.6% of the sample, this role fell to other members of the family/support group.
On average, study patients received some form of assistance from the primary caregiver on a daily basis. However, primary caregivers differed in their level of involvement in care planning and their ability to assist in patient care. Although three-quarters of primary caregivers were very or somewhat involved in the development of the patients' care plans (e.g., asking questions, making suggestions, identifying needs), nearly 25% were only minimally involved, showing little interest in and making little contribution to the patient's care plan. In most cases, the home care provider completing the start of care assessment felt that the primary caregiver had either an excellent or good ability to learn, which is critical to his or her ability to assist with the patient's home care regimen. Slightly over 12% of primary caregivers were rated as having only a fair or poor ability to learn. In such cases, home care providers may be concerned that the primary caregiver may not be able to follow the patient's care plan accurately. Nearly 90% of primary caregivers were perceived by the home care providers to have a good understanding of the services and eligibility requirements associated with the Medicare home health benefit.
As will be discussed in the summary of the findings from the case study interviews (Chapter 5), it is not uncommon for patients and/or their families to refuse certain types of home care services, most commonly aide services. For cases in which the assistance of a home health aide was needed, 87.3% of the primary caregivers were willing for the patient to receive the recommended services. The remaining 12.7%, however, were unwilling to have an aide assist the patients. In these cases, it is possible that the primary caregiver felt that these services could or should be provided by members of the family/support system.
Patients tended to be less involved in the development of their care plans and less capable of assisting in their care than were their primary caregivers. Only slightly over 59% of the patients were very or somewhat involved in their care plans. More than 40% were only minimally involved. Patients also were less capable of learning than were their primary caregivers. Only 12.0% of patients were believed by their home care providers to have an excellent ability to learn and slightly over half had a good ability to learn. A full 36.5% were believed to have only a fair or poor ability to learn. Likewise, a smaller percentage of patients than caregivers were perceived to be knowledgeable regarding the Medicare home health benefit. These data emphasize the great importance of informal caregivers in the delivery of home health care. In many cases, the primary caregiver may be more capable of representing the patient's interests and providing the necessary care than the patient him- or herself.
Of the study patients, 88.3% had experienced a medical regimen change and 81.6% had been discharged from an inpatient facility within 14 days of the beginning of their home care episodes. Nearly 70% of the patient episodes began following an hospital discharge. Another 6.6% of episodes began following a discharge from a rehabilitation facility and 5.5% followed a nursing home discharge. CHF patients were significantly more likely than diabetic patients to have been discharged from the hospital within 14 days of their home care start of care date, whereas diabetic patients were significantly more likely than CHF patients to have been discharged from a rehabilitation facility within that time period.
A variety of measures of complexity and severity were available from the OASIS and CPQ data. On most of these measures, it appeared that the study patients were in relatively good health. On average, patients had few high-risk factors, such as smoking, obesity, or alcohol/drug dependency, and over 80% had adequate or excellent nutritional status. Although 56.8% of the patients were believed by the home care providers to require complex management (e.g., procedures more than once a day, coordination of multiple providers, educational instruction at each visit),26 only one-third of patients were perceived to have greater than average functional assistance needs. Further, most of the patients seemed to have good prognoses. Nearly 90% of patients were rated as having good or fair overall prognoses and nearly 70% were rated has having good rehabilitative prognoses.
Aggregate ADL and IADL disability measures provide an overview of the functional impairment of the study patients.27 Out of the eight ADLs on which the aggregate ADL disability measures were calculated, the typical patient had at least a mild disability on four of those measures. Most patients were at least moderately disabled in one or two ADLs and were severely disabled in less than one of the eight ADLs. The average patient was at least mildly disabled in four of the six IADL measures included in the calculation of the aggregate measures, and severely disabled in two.
Patients with CHF and patients with diabetes mellitus did not differ greatly in their functional disabilities. None of the aggregate functional disability measures showed significant differences between patients in the two groups and only a small number of individual ADL and IADL measures showed such differences. Although CHF patients were significantly more impaired than diabetes patients in the areas of grooming, shopping, and management of oral medications, the two groups did not differ significantly on any of the other 12 ADLs and IADLs.
Patients did not appear to be severely impaired in the management of oral medications and equipment. However, the average patient did require some assistance (e.g., doses prepared in advance or reminders given by another person) in administering inhalant/mist and injectable medications. With regard to the management of equipment, such as oxygen or intravenous therapy equipment, the average patient required considerable assistance, but was capable of completing some equipment management tasks independently.
The remainder of Table 3.9 provides detailed information about the physiologic and neurologic condition of the patients enrolled in the study. Rather than summarizing all of the data thoroughly, the findings of greatest significance are reported here. On average, patients tended to experience shortness of breath (dyspnea) while performing activities requiring moderate exertion, such as dressing and walking short distances. As one would expect, CHF patients were more likely than their diabetic counterparts to experience dyspnea.
Sensory impairments were not common in the patient sample. Despite their age, the average patient had either normal or mildly impaired vision. Interestingly, diabetic patients were not more likely than patients with CHF to have impaired vision. Pain did not appear to be a major problem for the study patients either; the average patient experienced pain less often than daily and less than 10% experienced pain that was not easily relieved.
Integumentary problems were not unusual in the study sample. Slightly under one-third of the sample entered home care with a wound or lesion. For 12.9% of the patients, one or more surgical wounds were present. A smaller percentage of patients experienced pressure and stasis ulcers. Diabetic patients were more likely than their counterparts with CHF to have any kind of wound or lesion, surgical wounds, and stage 2-4 ulcers.
Incontinence is often a problem for elderly home care patients. Twenty-three percent of the study patients had bladder incontinence or had been catheterized to manage problems with incontinence. However, few patients had problems with bowel incontinence or urinary tract infections. Elimination status did not differ by tracer condition.
Neurologic, emotional, and behavior problems did not appear to affect a large number of study patients. Behavior problems appeared to be rare in this sample, with only 4.1% of patients experiencing behavior problems more than twice a week. Moderate cognitive disability and severe confusion disability each affected approximately 10% of the patients in the sample. Severe anxiety was a problem for approximately 16% of the sample.
Patients were receiving home care to treat a variety of conditions, with the majority being treated for circulatory and endocrine/nutritional/metabolic diseases. As one would expect, CHF patients were more likely than diabetic patients to be receiving home care for circulatory problems and diabetes patients were more likely than CHF patients to be treated for endocrine/nutritional/metabolic diseases. Over one-quarter of all patients were receiving care related to their respiratory problems. Understandably, CHF patients were more likely to be receiving such care. Slightly more than 20% of the patients received oxygen therapy at home, a treatment that was much more common for the CHF patients than the diabetes patients.
IV. PRACTICE AND PRACTICE VARIATIONS IN HOME HEALTH CARE
The study was designed primarily to examine the causes and consequences of practice variations in home health care. Data collected as part of the study were used to identify the patient, provider, agency, and market/regulatory factors that influence the practice of home health care. Further, the effect of practice patterns on patient outcomes was examined.
In this chapter, the quantitative analyses regarding practice patterns and patient outcomes are presented. The chapter includes four sections. Section A presents descriptive information regarding the care provided to the study patients (e.g., length of stay, number of visits per discipline, care coordination activities). In Section B, the results of multivariate analyses examining the influence of patient, provider, agency, and market/regulatory factors on practice patterns are discussed. Section C focuses on the influence of practice patterns on length of stay in the Medicare home health benefit. In Section D, the effect of practice patterns on patient outcomes is examined. For all sections, analyses were conducted at the episode level with a total of 732 episodes. For those patients with more than one episode of care, each episode was used in the analyses. All data were collected under the Interim Payment System (IPS).
A. Practices in Home Health Care
This section provides descriptive information about the care provided to the study patients. Table 4.1 presents information on both direct care and care coordination activities. Direct care was represented by length of stay, discipline mix, visits per discipline, total visits across disciplines, visit intensity by discipline (i.e., visits per day on service), visit intensity across disciplines, resource consumption, activities performed at each visit, and alternative services provided during the episode of care.
The mean length of stay was 41.9 days, with a median of 30.0 days. The six disciplines commonly involved in home health care are nurses, physical therapists, occupational therapists, speech-language pathologists, medical social workers, and home care aides. In the study sample, care usually was provided by one or two disciplines, most commonly by nurses, followed by home care aides and physical therapists. Other disciplines were involved less frequently.
Nurses made 15.4 visits per episode on average, followed by home care aides (6.9 visits), and physical therapists (2.8 visits). The mean total number of visits across the six disciplines was 26.5 per episode, with a median of 15.0. Visit intensity represents the frequency with which visits were provided (i.e., the number of visits provided per day). Nurses had the highest level of visit intensity, averaging 0.4 visits per day. The mean overall visit intensity across disciplines was 0.6 visits per day, with a median of 0.5.
| TABLE 4.1: Care Provided During the Study Episodes | |||
| Practice Patterns | Practice Patterns | ||
| DIRECT CARE | |||
| Episode Length (n=687) | mean=41.9median=30.0minimum=2.0maximum=252.0 | ||
| Discipline Mix (n=687) | |||
| Skilled Nursing | 98.0% | Total Number of Disciplines (n=687) 1 2 3 4 5 6 | 43.5%29.0%15.9%9.0%2.5%0.1% |
| Physical Therapy | 33.8% | ||
| Occupational Therapy | 12.5% | ||
| Speech-Language Pathology | 2.0% | ||
| Medical Social Services | 16.9% | ||
| Home Care Aide | 35.2% | ||
| Number of Visits Per Discipline (n=687) | |||
| Skilled Nursing | mean=15.4 median=9.0 minimum=0.0 maximum=224.0 | Physical Therapy | mean=2.8median=0.0minimum=0.0maximum=51.0 |
| Occupational Therapy | mean=0.8median=0.0 minimum=0.0 maximum=37.0 | Speech-Language Pathology | mean=0.3median=0.0minimum=0.0maximum=43.0 |
| Medical Social Services | mean=0.3median=0.0minimum=0.0 maximum=11.0 | Home Care Aide | mean=6.9median=0.0minimum=0.0 maximum=171.0 |
| Total Number of Visits Across Six Disciplines (n=687) | mean=26.5median=15.0minimum=1.0maximum=316.0 | ||
| Visit Intensity (visits per day) (n=687) | |||
| Skilled Nursing | mean=0.4median=0.3minimum=0.0maximum=2.0 | Physical Therapy | mean=0.1median=0.0minimum=0.0maximum=1.0 |
| Occupational Therapy | mean=0.0median=0.0minimum=0.0maximum=0.4 | Speech-Language Pathology | mean=0.0median=0.0minimum=0.0maximum=0.4 |
| Medical Social Services | mean=0.0median=0.0minimum=0.0maximum=0.3 | Home Care Aide | mean=0.1median=0.0minimum=0.0maximum=1.9 |
| Overall Intensity | mean=0.6median=0.5minimum=0.1maximum=3.9 | ||
| Resource Consumption (RC) | |||
| RC Intensity (cost per day) (n=687) | mean=$54.20median=$43.93minimum=$5.98maximum=$328.36 | Total RC (cost per episode) (n=687) | mean=$2201.22median=$1329.44minimum=$94.96maximum=$25658.79 |
| Visit Activities at Start of Care (n=731) | |||
| Skilled Observation and Assessment | 99.3% | Total Number of Activities (n=731) 1 2 3 4 5 6 7 | 1.4%4.4%16.1%35.3%28.9%12.9%1.1% |
| Procedures | 39.3% | ||
| Teaching | 96.6% | ||
| Coordination of Care | 64.7% | ||
| Care Planning | 89.54% | ||
| Management & Evaluation of Care Plan | 34.3% | ||
| Other | 38.0% | ||
| Provision of Alternative Services (n=727) | |||
| Meals on Wheels | 8.9% | Food Bank/Meal Services (other than Meals on Wheels) | 1.5% |
| Outpatient Rehab | 1.4% | Transportation Assistance | 11.4% |
| Assisted Living Facility | 3.9% | Foster Care Services | 1.7% |
| Respite Services | 0.6% | Homemaker Services | 12.2% |
| Personal Care Services | 8.4% | Friendly Visitor/ Companion Services | 3.9% |
| Adult Day Care | 0.3% | Mental Health Services | 0.6% |
| Legal/Protective Services | 0.0% | Emergency Response Services | 5.0% |
| Case Management (such as placement or referral services) | 1.9% | Environmental/Home Modifications | 1.4% |
| Volunteer Services | 0.7% | Other | 6.9% |
| None of the Above | 57.6% | Unknown | 0.8% |
| Number of Alternative Services Provided at Discharge (n=727) | mean=0.7median=0.0minimum=0.0maximum=6.0 | ||
| CARE COORDINATION | |||
| Frequency of Interdisciplinary Case Conferences for Medicare Patients (N=700) | |||
| More than once a week | 18.3% | Weekly | 26.0% |
| Twice monthly | 20.6% | Monthly | 34.0% |
| Quarterly | 0.0% | Less than quarterly | 1.1% |
| Number of Care Coordination Communications at Start of Care (n=712) | mean=3.8median=3.8minimum=0.0maximum=20.0 | Time Spent on Care Coordination at Start of Care (minutes) (n=711) | mean=31.2median=20.0minimum=0.0maximum=800.0 |
| Percent of Providers Receiving Feedback Regarding Care Plan | |||
| Feedback from Other Agency | Overall Level of Feedbacka (n=732) | mean=0.4median=0.3minimum=0.0maximum=1.0 | |
| Personnel about Frequency of RN Visits (n=667) | 42.6% | ||
| Personnel about Home Health Aide Services (n=680) | 26.0% | ||
| Personnel about Discharge (n=727) | 54.9% | ||
| |||
Resource consumption reflects the total cost of the visits provided to a patient during an episode of care and was calculated by multiplying the number of visits per discipline by the average cost per visit by discipline28 and summing the cost of all disciplines. Total resource consumption averaged $2201.22 per episode, with a median of $1329.44. Resource consumption intensity, or the average cost per day on service, averaged $54.20, with a median of $43.93.
Care providers engaged in a number of different activities at patients' start of care visits. On average, providers conducted four or five different activities at the initial visit. These activities included (ranging from highest to lowest rate) observation and assessment, teaching, care planning, coordination of care, procedures, other activities, and management and evaluation of the care plan.
Alternative services represent those services coordinated by an agency, but provided by another organization in the community. On the discharge Care Provider Questionnaire (CPQ), the home health provider identified which alternative services, out of 18 listed, were provided to the patient. Examples of such services include meals on wheels, outpatient rehabilitation, transportation services, homemaker or personal care services, adult day care, and mental health services. Of the 18 services listed, the mean number of alternative services provided to study patients was 0.7, ranging from zero to six services. The most common alternative services provided were homemaker services (provided during 12.2% of all study episodes), transportation assistance (11.4%), meals on wheels (8.9%), and personal care services (8.4%). A majority of patients did not receive any alternative services (57.6%).
Care coordination was measured by frequecy of interdisciplinary case conferences, number of care coordination communications, time spent on care coordination, and feedback regarding a patient's care plan.29 At most agencies, interdisciplinary case conferences occurred once a month. The number of care coordination communications that occurred between the receipt of the original referral and the start of care visit averaged 3.8. On average, the nurse or therapist spent 31.2 minutes coordinating with other care providers involved with a given patient. It was not uncommon for a care provider to receive feedback from other agency personnel regarding a patient's care plan. Specifically, care providers received feedback on the frequency with which skilled nursing visits should be provided (42.6% of providers received such input), the necessity for home health aide services (26%), and the appropriateness of discharging the patient (54.9%). The mean overall level of feedback was 0.4, on a scale from zero to one.
B. Causes of Practice Variation in Home Health Care
In this section of the report, the influence of patient, provider, agency, and market/regulatory factors on practice patterns is summarized. Five important aspects of home health practice, covering direct care provision and care coordination, were selected for examination. Four measures of direct care investigated were (1) the average number of visits provided per day (i.e., visit intensity), (2) the duration of the home health episode (length of stay),30 (3) the total number of disciplines involved in patient care, and (4) the number of alternative services provided during the episode of care. The amount of feedback received by the primary home care provider from other agency personnel regarding a patient's care plan and discharge was examined as a measure of care coordination.
As described in detail in Chapter 2, the analyses assessing the impact of patient, provider, agency, and market/regulatory factors on home health agency practices were conducted using ordinary least squares (OLS) regression. For each practice pattern variable, four preliminary OLS models were conducted to identify the patient, provider, agency, and market/regulatory factors, respectively, that significantly or marginally effect each practice pattern. These variables were then combined into a single final OLS model, examining the impact of all factors simultaneously.31Table 4.2 presents the results of the five final OLS models investigating the effect of patient, provider, agency, and market/regulatory factors on the five practice patterns of interest.
1. Influence of Patient Factors on Home Care Practices
Patient, provider, agency, and market/regulatory variables had an important effect on the four measures of direct patient care. As one would expect, patient factors were particularly strong predictors of home health practices. Patient demographic characteristics were important influences on some of the practice patterns. Although age was not a significant predictor of three of the four direct care measures, it was significantly related to visit intensity. Contrary to what one might expect, however, older patients received significantly fewer visits per day on average than younger patients. This effect is likely a result of the particular characteristics of the older patients in the study. Although these patients were more functionally impaired than their younger counterparts, their medical conditions tended to be less complex. Older patients were significantly less likely to be rated by their care providers as requiring complex management than were younger patients. Further, these patients had significantly fewer comorbid conditions, calculated as the number of diagnoses severe enough to affect daily functioning for which home care was being provided. In addition, older patients were significantly or marginally less likely to have certain conditions or receive certain therapies that might result in more frequent visits (e.g., open wounds or lesions, infusion therapy, enteral nutrition, ventilator therapy). Some, but not all of these variables were controlled in the multivariate analyses.
| TABLE 4.2: Effect of Patient, Provider, Agency, and Market/Regulatory Factors on Practice Patterns | ||||||||||
| Visit Intensity | Episode Length | No. of Disciplines | No. of Alternative Services | Amount of Feedback | ||||||
| Coeff. | Sig. | Coeff. | Sig. | Coeff. | Sig. | Coeff. | Sig. | Coeff. | Sig. | |
| Patient Variables | ||||||||||
| Age at start of care | -0.006 | ** | 0.001 | -0.003 | 0.002 | -0.001 | ||||
| Female | -0.036 | 0.064 | -0.048 | 0.074 | 0.007 | |||||
| White | -0.002 | -0.254 | ** | -0.168 | 0.219 | * | -0.014 | |||
| Any Medicaid payor source | -0.022 | 0.065 | -0.108 | 0.361 | ** | 0.034 | ||||
| Medicare HMO payor source | -0.031 | -0.164 | -0.139 | 0.329 | ** | 0.003 | ||||
| No financial factors limiting health | -- | -- | -- | -- | -0.085 | ** | ||||
| Patient lives alone | 0.121 | ** | -0.068 | 0.177 | ** | 0.214 | ** | 0.076 | ** | |
| Limitation in absences from home | -- | 0.045 | -- | -- | -- | |||||
| Difficulty receiving services outside home | -- | -- | -- | -0.192 | ** | -- | ||||
| Frequency of caregiver assistance | -- | -- | -- | -0.090 | ** | -- | ||||
| Patient needs aide services | 0.253 | ** | -- | 0.855 | ** | 0.198 | ** | -- | ||
| Requires complex management | 0.063 | ** | 0.079 | 0.135 | * | -- | 0.073 | ** | ||
| Number of conditions affecting functioning | -- | -- | -- | -- | -- | |||||
| Hospital discharge within 14 days of start of care | 0.058 | 0.098 | 0.237 | ** | -0.039 | -0.038 | ||||
| Nursing home/rehab facility discharge within 14 days of start of care | 0.121 | ** | 0.504 | ** | 0.953 | ** | -- | -- | ||
| Good rehabilitative prognosis | -- | -- | 0.135 | * | -- | -- | ||||
| Level of functional disability | 0.567 | ** | 0.093 | 0.956 | ** | 0.608 | ** | 0.166 | ** | |
| Dyspnea | -- | -- | -0.066 | ** | -- | -- | ||||
| Incontinent or has catheter | -- | -- | -- | -- | -- | |||||
| Any surgical wound | -- | -- | -0.167 | -- | -- | |||||
| At least one stage 1-4 ulcer | 0.235 | ** | -- | 0.349 | ** | 0.116 | ** | |||
| Mental diseases | 0.090 | -- | 0.229 | -0.324 | ** | -- | ||||
| Nervous system diseases | -- | -- | 0.330 | ** | -- | -- | ||||
| Respiratory system diseases | -- | -- | -- | -- | -- | |||||
| Musculoskeletal system diseases | -- | -- | 0.319 | ** | -- | 0.056 | * | |||
| Ill-defined conditions | -- | -- | -- | -- | -- | |||||
| Fractures | -- | -- | 0.494 | ** | -- | -- | ||||
| Other injury | -- | -- | -- | 0.208 | -- | |||||
| Patient has CHF | -0.031 | 0.162 | * | -0.037 | 0.034 | 0.015 | ||||
| Patient has diabetes mellitus | 0.050 | 0.122 | -0.032 | 0.043 | -0.013 | |||||
| Cognitive/mental/behavioral problem | -- | 0.062 | -- | -- | -- | |||||
| Provider Variables | ||||||||||
| Standardized care plan used for start of care visit | -- | 0.083 | -- | -- | 0.086 | ** | ||||
| Highest level of provider education | -0.021 | -0.034 | -- | -- | -0.012 | |||||
| Years of home health experience | -- | 0.108 | ** | -- | -- | -- | ||||
| Physician involvement | 0.124 | ** | -- | -- | -- | 0.031 | ||||
| Agency Variables | ||||||||||
| Proprietary agency | 0.172 | ** | -0.207 | ** | 0.043 | 0.316 | ** | 0.115 | ** | |
| Hospital-based agency | -0.063 | * | -0.233 | ** | 0.057 | 0.289 | ** | 0.034 | ||
| Number of years in operation | -- | -- | -- | 0.057 | ** | -- | ||||
| Over Medicare per-visit limit | -- | -0.349 | ** | -- | 0.100 | -0.057 | * | |||
| Over Medicare per-beneficiary limit | -- | 0.251 | ** | -- | -- | -- | ||||
| % caseload that is Medicare | -0.003 | ** | 0.005 | ** | -- | -- | -- | |||
| Agency has nurse productivity standards | -- | 0.277 | ** | -- | -- | -- | ||||
| Agency uses standardized care plans | -- | 0.176 | ** | -- | 0.248 | ** | 0.054 | ** | ||
| Recertification decisions made by nurse/therapist (1) or supervisor/ quality assurance staff (2) | -0.051 | -- | -0.076 | -0.156 | -- | |||||
| Location of patients (1=rural, 2=mixed, 3=urban) | -0.030 | -- | -- | -- | -0.067 | ** | ||||
| Frequency of interdisciplinary case conferences | -- | -- | -- | -- | -0.025 | ** | ||||
| Total admissions (1998) | -- | -- | -- | -0.000 | ** | -- | ||||
| Market Variables | ||||||||||
| State volume group (high/low) | 0.215 | ** | 0.013 | 0.151 | * | -0.161 | * | 0.112 | ** | |
| Per capita income | 0.003 | -0.025 | ** | 0.003 | -- | -0.008 | * | |||
| County is an MSA | -- | -0.078 | -- | -- | -0.011 | |||||
| Number of community resources available | 0.020 | ** | -- | 0.060 | ** | 0.030 | -- | |||
| Nursing home/board & care beds per 1000 elderly | 0.000 | -- | -0.002 | -0.004 | ** | - | ||||
| * p .10, ** p .05, dashes indicate that the variable did not meet the criteria to be included in a specific final model. | ||||||||||
Although gender did not appear to influence care practices, race was an important predictor of length of stay and the number of alternative services provided.32 White patients had significantly shorter home care episodes and were provided with a marginally larger number of alternative services than were non-White patients. These two effects could be closely linked to one another. That is, patients who receive a large number of alternative services - services that are likely to continue after a patient's discharge from the home care agency - may be ready for discharge earlier than other patients because their remaining needs are met by outside organizations and do not need to be met by the home care agency itself.
With regard to the effect of race on length of stay and the receipt of alternative services, White study patients might have been more likely to live in those geographic regions where alternative services were more likely to be available. Further, these patients might have entered home care as a result of more acute, rather than chronic, illness. Indeed, White study patients were marginally less likely than non-White patients to be rated by their care providers as requiring complex management.
Payment issues appeared to have little impact on all but one of the practice pattern variables. Whether a patient was covered by Medicaid or by a Medicare Health Maintenance Organization (HMO) was only predictive of the provision of alternative services. Patients with Medicaid or a Medicare HMO as a payer were more likely to receive services from organizations outside of the home care agency. These effects likely are due to different mechanisms.
Medicaid patients may receive more alternative services for a variety of reasons. States that provide coverage for home health care through their respective Medicaid programs may be more likely to make other services available as well. Therefore, patients living in these states may have a larger array of services available to them than patients living in states with less generous Medicaid programs. Further, agency personnel may more actively attempt to coordinate alternative services for those patients they know will not be able to fund such care independently. It may be especially important for agency staff to establish these services for patients with limited financial resources than for patients who would be able to locate and pay for these services themselves.
Patients receiving care through a Medicare HMO also received more alternative services than other patients. HMOs of all varieties are known for their parsimonious use of medical resources and their involvement of case managers in determining appropriate patient care. It is possible that agency staff caring for Medicare HMO patients were more likely to coordinate alternative services in order to compensate for agency services that the HMO had not approved or might not approve.
Although financial factors limiting patients' ability to meet basic health needs did not appear to influence direct care provision, they did influence care coordination. Care providers received significantly more feedback from other agency personnel about the patient care plan when the patient had financial factors limiting his or her ability to meet basic health needs than when no financial limitations were present. Patients with more problems, including financial problems, appear to have required greater coordination among care providers.
Patient living situation was an important predictor of home care practices. Living alone was a particularly important predictor of both direct care provision and care coordination. Patients who lived alone received significantly more frequent visits, had significantly more home care disciplines involved in their care (and significantly greater feedback among these providers), and received significantly more alternative services. Although patients living alone were significantly less functionally impaired than those living with others (likely the reason they were able to live alone in the first place), they were marginally older, had significantly fewer types of people in their informal support systems providing them with assistance,33 received significantly less frequent assistance from their primary caregivers, and thus had significantly more unmet needs at start of care. Similarly, controlling for living situation, patients who received less frequent assistance from their primary caregivers were provided with a significantly larger number of alternative services to compensate for this missing assistance. These findings emphasize the importance of a patient's family/support system in determining the care provided by a home health agency.
CPQ data were used to assess the degree to which a study patient was homebound. A patient's limitations in leaving the home and in receiving medical care outside the home were used to predict care practices. Although the former variable did not appear to influence care practices, while controlling for other important patient, provider, agency, and market/regulatory variables, difficulty receiving services outside of the home did predict the number of alternative services provided. Patients for whom it was more difficult to receive services outside of the home received significantly more alternative services during their episodes of care. Again, agency staff may be using alternative services to compensate for services the patient would be unlikely to receive if he or she had to leave the home to obtain them.
Patients requiring aide services had significantly more frequent visits, more disciplines involved in their care, and more alternative services provided. It is possible that patients needing aide services received care from more disciplines and more frequent visits simply because they received care from both nurses and aides, whereas many patients received care from only a single discipline (43.5%). However, patients identified by their primary care providers at start of care as needing aide services had significantly more complex needs and more serious functional disabilities than did those patients who did not require aide services. For example, patients needing aide services were significantly older, more likely to have financial problems limiting their ability to meet their basic health needs, required significantly more assistance to leave the home, had significantly more unmet needs at start of care, and had a significantly larger number of comorbid conditions impacting their daily functioning. Likewise, regardless of the need for aide services, patients identified as requiring complex management received significantly more frequent visits, had marginally more disciplines involved in their care, and thus required significantly more feedback about their care among their care providers, than did less complex patients.34
A recent inpatient discharge appeared to strongly influence care practices. Patients discharged from a hospital within 14 days of the beginning of their home health episodes were likely to receive care from a significantly larger number of disciplines than were other patients. Those discharged from a nursing home or rehabilitation facility within 14 days of start of home care received significantly more frequency visits, had significantly longer episodes, and received care from a significantly larger number of disciplines. It appears that patients recently discharged from an inpatient facility may have particularly complex needs, requiring frequent care by a number of home health care providers. Episode lengths may be elongated not only as a result of this complexity, but also as a result of the need to educate the patient and family caregivers about new conditions that may have been the cause of inpatient admission, and new medical treatments and medication regimens that were developed during those inpatient stays. Nurses interviewed during the case studies (see Chapter 5) commented on the particular frailty of newly discharged hospital patients and the need to strengthen these patients physically before they will be able learn about their conditions and treatments. These nurses also noted that hospital patients do not always receive adequate education prior to being discharged.
As one would expect, functional status and rehabilitative prognosis were important predictors of care practices. Patients with greater functional disability received significantly more frequent visits, and received care from a significantly larger number of disciplines and alternative services, and thus required greater feedback amongst their care providers regarding their care plans.35 Contrary to what one might expect, patients with a poor rehabilitative prognosis received care from marginally fewer disciplines than did patients with a better rehabilitative outlook. It is likely, however, that home care nurses recommend the involvement of physical or occupational therapists for those patients they perceive as having the possibility of rehabilitative improvement. Indeed, nurses involved in the case study interviews summarized in Chapter 5 reported that they do not order therapy for all patients who might need it, but instead for those patients they perceive will benefit from and are motivated to participate in such care.
Patient diagnoses and conditions influenced the kind of care received, particularly the number of disciplines involved in care. Specifically, patients having at least one stage 1-4 ulcer, nervous system diseases, musculoskeletal system diseases, and patients with fractures received care from significantly more disciplines than did patients not having these conditions.36 Patients with at least one stage 1-4 ulcer also received significantly more frequent visits. For these patients as well as patients with musculoskeletal system diseases, care providers received significantly more feedback from other care agency personnel about the patients' care plans. Presumably, the impact of ulcers on care visit intensity and number of disciplines results from the use of home health aides to assist with wound care and dressing changes. Patients with congestive heart failure (CHF) had marginally longer episode lengths than did patients without CHF. Patients with mental diseases received significantly fewer alternative resources than did other patients. It is possible that patients with serious mental disorders are less capable of identifying and expressing their needs, and that home care nurses are therefore less likely to attempt to coordinate services to meet these needs.
2. Influence of Provider Factors on Home Care Practices
Characteristics of the medical care providers were much less strongly associated with care practices. The use of a standardized care plan at the start of care visit and the home care provider's highest level of education did not predict any of the direct care measures. However, the use of a standardized care plan was significantly related to the amount of feedback a care provider received from other agency personnel regarding a patient's care plan. Specifically, for patients with which a standardized care plan was used at the start of care visit, providers reported having received significantly more feedback from other agency personnel about the patient's plan of care than did providers who had not used a standardized care plan at the start of care visit. This relationship may reflect a general acceptance of feedback and assistance in care planning among a certain group of care providers. Nurses (or therapists) who are willing to use a standardized care plan, rather than relying solely on their own judgment, may also be more willing to seek and/or receive the input of other care providers about a case.
The years of experience of the home care provider conducting the start of care visit and the involvement of the patient's physician in the care plan did have some impact on care practices. Patients whose start of care assessments were conducted by a care provider who had been involved in home care for many years had significantly longer lengths of stay than did patients whose start of care assessments were conducted by less experienced care providers.37 Two possible explanations for this effect exist. First, it is reasonable to expect that more experienced care providers might be assigned to more challenging patients, requiring treatment that is more complex and longer episodes of care. (Although many patient factors are controlled in these analyses, patient complexity may not be completely captured.) However, there is little evidence that this is the case. Years of home health experience is not correlated with patient need for complex management, number of comorbid conditions, or other measures that can be used to examine patient complexity.
The second, and seemingly more likely, explanation for the effect of care provider experience on length of stay relates to style of practice. Care providers who have been in the home health business for a number of years learned how to provide home care during a time of greater home health prosperity and lesser concern regarding financial issues. Nurses (and therapists) who were in practice during the 1980s and early 1990s may focus on doing what they consider to be best for the patient with little consideration for cost. They also may proceed with planning and implementing care in a more autonomous manner, as might have been more common prior to the rise in prevalence of managed care organizations and case management techniques. Indeed, it appears that care providers with more years of experience in home health care are less likely than their less experienced counterparts to use standardized care plans and more likely to report that the patient's physician is only minimally involved in the patient's care, implying that the care plan has been primarily or solely the responsibility of the home care provider.
As mentioned previously, physician involvement also is related to some extent to care practices. Specifically, the more involved the patient's physician, the more frequently visits are provided to the patient.38 It is possible that this effect is a result of patient complexity that is not fully accounted for in the regression model. That is, patients with particularly complex needs may receive more visits from their home care agencies, while also receiving more supervision of this care from their physicians.
3. Influence of Agency Factors on Home Care Practices
Agency factors were more prominent predictors of practice patterns than were provider factors.39 Agency ownership and type were particularly influential. Controlling of other patient, provider, agency, and market/regulatory factors, proprietary agencies had significantly higher visit intensity, shorter length of stay, more use of alternative services, and a higher level of feedback among agency personnel about patient care. It may be that these agencies attempt to restrict episode lengths without restricting services dramatically by providing services over a shorter period of time, resulting in higher visit intensity. It also is possible that proprietary agencies specifically select acute care patients, who may need more frequent services in the short run, but who can be discharged after fairly short episodes. Proprietary agencies involved in the study appear to have made use of alternative services more so than did nonproprietary agencies. Perhaps proprietary agencies attempt to cut costs by outsourcing the care for certain of their patients' needs. It is possible that care providers receive a good deal of input from other agency personnel as a result of identifying the need for and coordinating these alternative services.
Hospital-based agencies also made use of alternative services provided in the community, significantly more so than did freestanding agencies. Further, hospital-based agencies had significantly shorter lengths of stay and marginally lower visit intensity than their freestanding counterparts. Unlike proprietary agencies, hospital-based agencies do not appear to counterbalance episode length and visit frequency. This effect also could be a result of patient case mix that is not fully accounted for by the patient variables included in the regression models.
Agencies in operation for a longer period of time tended to use significantly more alternative services in the care of their patients than did newer agencies. It may be that staff at long-standing agencies are simply more aware of the resources available in the surrounding community and therefore are more likely to take advantage of them.
Whether or not an agency was over or under the Medicare per-visit and per-beneficiary cost limits was predictive of length of stay. Agencies that were over the per-visit limit had significantly shorter episode lengths than did agencies that were under the limit. Further, care providers in these agencies reported receiving marginally less feedback from other agency personnel than did care providers in agencies not over the per-visit limit. It appears that agencies over the per-visit limit may have attempted to cut costs by keeping episodes relatively short, thus providing fewer visits. The shorter episode lengths may reduce the likelihood of substantial feedback being shared amongst care providers. Conversely, agencies that were over their per-beneficiary limits had significantly longer home care episodes than agencies that were not over their limits. It may be that a tendency to keep patients on service for long periods of time was the reason that these agencies were over their per-beneficiary limits in the first place and that these agencies had not yet adjusted to the new cost limits by reducing utilization.
The percentage of an agency's caseload that is represented by Medicare patients had a strong impact on length of stay and visit intensity. Agencies with a larger percentage of Medicare patients provided significantly longer home care episodes and significantly fewer visits per day. Given that Medicare patients are likely to be older and more chronically ill than non-Medicare patients, it may be that these patients require regular care over a longer period of time. Younger patients may be more likely to have acute problems, such as surgical wounds, requiring frequent care over a short period of time.
Standards regarding nurse productivity and care planning tend to increase length of stay. Agencies that had nurse productivity standards specifying the number of visits a nurse should conduct during the course of a day provided their patients with significantly longer episodes of care than did agencies without nurse productivity standards in place. It is possible that agencies are counterbalancing episode length with visit length. In order to make the required number of patient visits each day, home care nurses may have to constrain the length of time they spend with each patient. (Nurses involved in the case study interviews noted that increased burdens in terms of documentation and productivity standards often reduced the amount of time they were able to spend with a given patient.) In order to provide the needed care to a patient, while keeping each visit short, providers may need to see the maintain the patient on service over a longer episode.
Agencies that use standardized care plans when planning and providing patient care also had significantly longer episode lengths than did agencies without such standards. At first glance, this effect may seem unexpected. One might assume that care plans are intended, in part, to reduce unnecessary utilization of services. However, these care plans also may serve to ensure that nurses provide appropriate care, regardless of utilization. The use of a standardized care plan may prevent both inappropriate over- and underutilization of services. Agencies that used standardized care plans also tended to have significantly more feedback amongst care providers about care provision. Both the use of care plans and the frequency of provider feedback may result from a general atmosphere of team decision making, rather than a focus on the supremacy of the "primary nurse" for making all care plan decisions.
Although the rural/urban location of patients and the frequency of interdisciplinary communication had no impact on direct care, each of these variables significantly influenced the amount of feedback a care provider received about his or her patient's care plan.40 Agencies caring primarily for patients living in rural areas had significantly more feedback among care providers than did agencies treating a more urban patient population. Perhaps the remote location of rural patients and agencies required more communication among care providers in order to assure proper care coordination. As one would expect, care providers in agencies in which interdisciplinary communication occurs more frequently reported receiving significantly more feedback about their patients' care plans than did providers in agencies which less frequent cross-provider communication.
Finally, agencies with a larger number of annual admissions provided their patients with significantly fewer alternative services than did agencies with fewer admissions. It is likely that agencies with a larger number of admissions are larger agencies, with more substantial staff resources. Alternative services may not be utilized by such agencies because they may be able to provide all of these services through the agency.
4. Influence of Market/Regulatory Factors on Home Care Practices
Market/regulatory variables also were important in predicting variations in home health practices. Agencies in high-volume states provided significantly more frequent visits to their patients, and involved a marginally larger number of disciplines and a marginally smaller number of alternative services in the care of their patients than did agencies in the low-volume states. (Likely as a result of the increased number of care providers and alternative services involved, providers in these agencies reported significantly more feedback from other agency personnel about their patients' care plans.) As state trends in per patient visit volume demonstrate (see Chapter 3), agencies in the low-volume states have long provided care in a more parsimonious manner than have agencies in the high-volume states. Controlling for many patient, provider, agency, and other market/regulatory factors, it appears that the study agencies continue to follow these patterns. The marginally more frequent use of alternative services in the low-volume states may reflect an attempt by agencies to reduce their utilization further by obtaining care for their patients through other community organizations.
Although living in an MSA had no impact on the care a patient received, state per capita income was significantly related to length of stay and amount of feedback received by the care provider from other agency personnel. Specifically, patients in states with higher per capita incomes tended to be on service for shorter periods of time. Likely as a result of these shorter episodes, there was significantly less feedback from other agency personnel about the patients' care plans in states with high per capita incomes. In these areas, communities may have more resources, reducing the necessity for patients to rely on the Medicare home health benefit. Patients themselves may be more affluent and may have the ability to obtain services in other ways. Further, as discussed in Chapter 1, previous research (Schore 1994) has demonstrated that certain regions of the country have both a more impoverished and a more chronically ill population, whereas certain regions are more affluent and have mainly patients with more acute needs. It is possible that patients in more impoverished states do not receive medical assistance until their needs become relatively severe, explaining the longer lengths of stay in states with lower per capita incomes.
Community resources also were fairly strong predictors of home care practices. The number of resources available within an agency's community was significantly related to both visit intensity and number of disciplines involved in care.41 In communities in which a larger number of community resources were available, patients received significantly more frequent visits and care was provided by significantly more disciplines. Again, these results may be tied to community affluence and patient case mix. Patients in geographic areas that can afford to provide a large number of alternative services may require high intensity, but short-term care (e.g., wound care following surgery). Likewise, in areas with a large number of nursing home beds per elderly person, significantly fewer alternative services were provided to home care patients. It may be that fewer alternative resources are available as a result of a focus on providing accessible nursing home care in these areas.
C. Effect of Practice Patterns on Home Health Episode Length
One of the key study goals was to identify practice patterns leading to long or short lengths of stay in home health care. Table 4.3 presents the results of the OLS regression model used to examine the influence of direct care (i.e., visit intensity, number of disciplines, alternative services, and amount of feedback received from other care providers regarding the patient's care plan) and care coordination on episode duration. Important patient, provider, agency, and market/regulatory factors were included in this model to control for these other influences on length of stay.42
| TABLE 4.3: Effect of Practice Patterns on Episode Length, Controlling for Patient, Provider, Agency, and Market/Regulatory Factors | |||||
| Coeff. | Sig. | Coeff. | Sig. | ||
| Patient Variables | Agency Variables | ||||
| Age at start of care | -0.003 | Proprietary agency | -0.188 | ** | |
| Female | 0.036 | Hospital-based agency | -0.323 | ** | |
| White | -0.202 | ** | Over Medicare per-visit limit | -0.361 | ** |
| Any Medicaid payor source | 0.085 | Over Medicare per-beneficiary limit | 0.293 | ** | |
| Medicare HMO payor source | -0.167 | * | % caseload that is Medicare | 0.003 | ** |
| Patient lives alone | -0.085 | Agency has nurse productivity standards | 0.234 | ** | |
| Hospital discharge within 14 days from start of care | 0.067 | Agency uses standardized care plans | 0.147 | ** | |
| Nursing home/rehab discharge within 14 days from start of care | 0.262 | ** | Market Variables | ||
| Level of functional disability | 0.199 | State volume group (high/low) | 0.136 | * | |
| Patient has CHF | 0.151 | ** | Per capita income | -0.032 | ** |
| Patient has diabetes mellitus | 0.178 | ** | Practices | ||
| Provider Variables | Visit intensity (visits per day) | -0.659 | ** | ||
| Years of home health experience | 0.107 | ** | Number of disciplines involved | 0.294 | ** |
| Number of alternative services provided | 0.043 | ||||
| Feedback regarding care plan | 0.113 | ||||
| * p .10, ** p .05. | |||||
In the model, two of the four practice patterns significantly influenced length of stay. Patients who received more frequent visits had significantly shorter episode lengths than did patients with less frequent visits. As discussed above, it may be that some agencies counterbalance episode length with visit frequency (i.e., visit intensity). Depending on staff resources, some agencies may be better able to handle cases requiring more frequent visits, whereas other agencies may be better able to adjust their staff resources to meet the demands of long episodes with less frequent visits. For example, agencies with smaller staffs may be less able to provide frequent visits to their patients. To compensate for less frequent visits, agency personnel may lengthen patient episodes to ensure all the patients' needs are met.
The inverse relationship between visit intensity and length of stay also may result from patient case mix differences that are not completely controlled by the patient factor variables included in the model. As suggested previously, patients with acute medical problems (e.g., patients requiring wound care following inpatient hospitalization) may require frequent visits to accommodate their immediate health care needs. However, their acute needs may be met and these patients may be ready for discharge after only a short time on service with their home health care agencies. A more chronically ill patient may require less frequent visits over a longer period of time to allow home care staff to monitor and manage his or her chronic illness. Further, such patients may require more extensive education than patients with short-term medical needs.
The number of disciplines involved in a patient's care also was associated with episode length. Episodes that involved more disciplines were significantly longer than episodes with a smaller number of disciplines involved. Again, this finding could be a result of patient case mix differences that are not fully controlled in the regression model. Patients of greater complexity may require both the services of multiple disciplines and longer episodes of home health care.
On the other hand, the relationship between the number of disciplines and length of stay may represent a general practice culture of high or low utilization. Controlling for case mix, certain agencies may be prone to providing patients with a large number of services over a long period of time. Other agencies may have a more parsimonious approach to care provision. Previous research has suggested that, even after controlling for substantial variations in case mix, large regional variations in home health practice still exist (OIG 1995a; Schore 1994). It appears that such variations continued under the Interim Payment System (IPS).
Controlling for important patient, provider, agency, and market/regulatory factors, the number of alternative services provided to a patient did not predict length of stay. One might have expected that agencies might coordinate alternative services in order to allow for earlier discharge of their patients. Although findings discussed in Section B suggest that agency personnel may attempt to cut costs by coordinating alternative services rather than having those services provided by the agencies themselves, it does not appear that agencies are able to discharge patients more quickly as a result.
The amount of feedback a care provider received from other agency personnel about a patient's care plan also did not predict length of stay. It was expected that nurses (and therapists) might receive feedback from case managers or others whose objective was to ensure that resources were not overutilized during the course of an episode of care. Such feedback might lead care providers to discharge patients earlier than they might have otherwise. However, this did not appear to be the case. Controlling for patient, provider, agency, market/regulatory, and other practice pattern variables, feedback appeared to have no impact on length of stay. Perhaps the feedback received by care providers was primarily from other care providers whose focus was on the quality of the care plan rather than on utilization of services. As noted in Chapter 5, some of the nurses involved in the case study interviews reported that, although their agency administrators were focused on financial issues, the nursing staff was allowed to plan and provide care based on patient need rather than cost concerns.
D. Patient Outcome of Home Health Care
Another important goal of the study was to examine the relationship between agency practices and patient outcome. Patient outcome was measured as the percentage of the standard improvement measures reported on the Centers for Medicare & Medicaid Services (CMS) outcome reports on which a patient improved.43Table 4.4 presents the results of an OLS regression model predicting patient outcome from practice patterns, while controlling for important patient, provider, agency, and market/regulatory variables.
As is evident from Table 4.4, practice patterns were not strong predictors of patient outcome. Notably, length of stay, the number of disciplines involved in care, and the number of alternative services provided did not appear to influence outcome for the study patients. Two other variables did marginally predict patient outcome. Visit intensity, or the number of visits provided per day, was marginally related to patient outcome, such that the more frequently visits were provided, the better the patient outcome. This effect was apparent even after important patient factors such as rehabilitative prognosis, complexity, and comorbidities were controlled in the model, suggesting that visit intensity had an independent impact on the outcome of home care patients. It appears that more frequent visits may allow care providers to maintain a more accurate understanding of a patient's condition and to be made quickly aware of any changes or declines in patient condition.
The amount of feedback a care provider received from other agency personnel about a patient's care plan had an unexpected relationship with patient outcome. Controlling for important patient, provider, agency, market/regulatory, and other practice pattern variables, more feedback received by a care provider was marginally related to worse patient outcome. Again, although many patient factors were accounted for in the model, this finding might suggest that patients who were sicker to begin with both were the subject of more discussion among care providers, and were less likely to achieve positive outcomes as a result of care.
| TABLE 4.4: Effect of Practice Patterns on Patient Outcome, Controlling for Patient, Provider, Agency, and Market/Regulatory Factors | |||||
| Coeff. | Sig. | Coeff. | Sig. | ||
| Patient Variables | Agency Variables | ||||
| Age at start of care | -0.341 | ** | Proprietary agency | 8.589 | ** |
| Female | -1.177 | Hospital-based agency | -0.206 | ||
| White | -4.785 | Over Medicare per-visit limit | -3.746 | ||
| Any Medicaid payor source | 5.967 | Over Medicare per-beneficiary limit | 8.187 | ** | |
| Medicare HMO payor source | 0.808 | Recertification decisions made by nurse/ therapist (1) or supervisor/quality assurance staff (2) | -4.686 | ||
| Patient lives alone | 3.257 | Market Variables | |||
| Limitations in absences from home | -1.911 | State volume group (high/low) | 2.165 | ||
| Hospital discharge within 14 days of start of care | 9.639 | ** | Per capita income | 0.568 | |
| Level of functional disability | 1.912 | Practices | |||
| Anxiety level | 4.893 | ** | Episode Length | -0.974 | |
| Patient has CHF | -4.740 | Visit intensity (visits per day) | 6.602 | * | |
| Patient has diabetes mellitus | 0.211 | Number of disciplines involved | -0.055 | ||
| Provider Variables | Number of alternative services provided | -1.646 | |||
| Standardized care plan used for start of care visit | 5.629 | ** | Feedback regarding care plan | -6.906 | * |
| Years of home health experience | -1.555 | ||||
| * p .10, ** p .05. | |||||
V. PRACTICE AND DECISION MAKING IN HOME HEALTH CARE
As noted in Chapter 1, the study was designed in part to examine practice and decision making in home health care. Focus group and case study interviews were two methods used to gather qualitative data to address these topics. The focus group interviews were designed primarily to explore how home care decisions are made in light of Medicare coverage rules. Focus group discussion concentrated on issues surrounding the decision to recertify or discharge two hypothetical patients. The case study interviews, on the other hand, were designed primarily to provide a description of the practice of home health care by interviewing nurses regarding recently completed patient episodes. During the case study interviews, the care patterns and care coordination activities for seven actual CHF patients were reviewed. Although the focus group and case study interviews were designed primarily to elicit information on different topics (i.e., decision making and practice, respectively), these methods overlapped to some degree in the issues they addressed. Information about provider perspectives on IPS and changes in home health care also was collected during the focus group and case study interviews. This information is summarized in Chapter 6.
It is important to note that the findings from the focus group and case study interviews are necessarily limited by the size and composition of their samples. Focus groups were conducted with four to seven individuals at each of eight home care agencies. Case study interviews were conducted with a single person at each of seven agencies. The participants in both sets of interviews were home health care nurses. As stakeholders in the industry, home health nurses may feel negatively toward new federal policies and regulations designed to restrain the dramatic growth in home health utilization and spending. Further, because their focus is on providing care to patients, many home care nurses may not be fully aware of the historical context and goals underpinning new policies and payment structures.
A. Focus Group Interviews
The eight focus groups were designed to examine decision making in home health care, focusing specifically on how decisions are made in light of Medicare coverage rules. In this section, the data from the focus group interviews are used to explore several factors that influence the process of decision making in home health care: (1) patient and caregiver factors (e.g., living environment), (2) the actors involved in the decision-making process (e.g., primary nurses, Fiscal Intermediaries [FIs]), (3) agency factors (e.g., supervision of the decision-making process), (4) external factors (e.g., managed care), and (5) Medicare coverage rules.
Data related to each of the factors that influence decision making in home health care were examined for patterns associated with state volume, agency ownership, agency type, and patient vignette. No differences were found between agencies in the different volume, ownership, and type categories. However, some of the focus group responses were related to the specific circumstances of the two hypothetical patients presented in the patient vignettes. Vignette-specific information is reported when appropriate. Vignette 1 and Vignette 2, which are shown in their entirety in Appendix B, are summarized below.
1. Patient and Caregiver Factors
Patient factors play an important role in the decision-making process regarding recertification and discharge. The patient factors most often mentioned by focus group participants included the following: (a) homebound status and the need for skilled services, (b) medication management, (c) alternative resources, (d) patient knowledge, (e) living environment, (f) financial status, (g) patient health status, and (h) caregiver factors. Participants' comments regarding each of these factors are summarized below.
Homebound Status and the Need for Skilled Services: Participants in all of the focus groups acknowledged that decisions to recertify or discharge a patient rest on the patient's homebound status and need for skilled services. Nurses mentioned these two factors in their discussion of patient factors, agency factors, and Medicare coverage rules. Therefore, the discussion of homebound status and the need for skilled services is consolidated under item 5 (Medicare Coverage Rules) of this section.
Medication Management: A patient's ability to manage his or her medication regimen was described by focus group participants at all eight agencies as an important factor in assessing the patient's readiness for discharge. A primary role of the home health nurse is to provide medication management education to the patient and his or her caregiver. As cognitive functioning is critical to the ability to perform medication management, the focus group participants highlighted the need for care providers to assess the cognitive ability of the patient and caregiver. This assessment of education and skills includes examining the patient or caregiver's ability to correctly read a glucometer, fill syringes and/or pillboxes, and recognize important signs and symptoms of medication complications. Several nurses indicated that patient or caregiver independence in these activities is very important because some of these activities (e.g., filling pillboxes) are not considered skilled services and thus patients cannot be recertified on the basis of these needs alone.
Alternative Resources: The identification of alternative resources was considered important by the members of each of the focus groups. The majority of the focus group participants indicated that one of their primary responsibilities as home care nurses is to find alternative resources for their patients. They do so by locating people, such as neighbors and volunteers, who can help with the patient's needs (e.g., grocery shopping) as well as by utilizing social work services to assist in assessing patient needs and making appropriate referrals. A few nurses indicated that they might recertify a patient for a short time until alternative services were in place. However, such recertifications are quite rare as planning for these services normally begins the very first day of a home health care episode and is accomplished long before the recertification decision is made.
Patient Knowledge: The role of patient education in home health care was a primary point of discussion at all of the focus groups. The nurses described the teaching process as a skilled service that involves educating the patient about the disease process, risk factors, signs and symptoms of complications, how to manage symptoms, and when to call a nurse or physician. When changes occur in a patient's condition or care plan (e.g., new diagnoses or medications), the teaching process often has to be repeated. The need for additional education resulting from such changes was considered a reason for recertification.
Educational priorities are dependent on the specific needs of each patient. With regard to hypothetical patient Mrs. Smith, the focus group participants emphasized the need to educate her about the signs and symptoms of acute exacerbation of CHF and when to call for help. In Mr. Lucas' case, a major goal of home health care is to stabilize his blood sugar. Home care providers would accomplish this goal by teaching him what to eat, how to measure his insulin, and how to recognize signs and symptoms of high and low blood sugar.
Living Environment: Nurses at all eight agencies emphasized the importance of a patient's living environment. For example, the focus group participants expressed concern about Mrs. Smith because she does not have heat and she may be at risk of falling down the stairs in her home. Most participants indicated that concerns about a patient's living environment are not necessarily justification for recertification. However, the participants suggested that a social worker should be contacted or community resources (e.g., a 24-hour care service) identified for a patient with unresolved safety issues in the home. The focus group participants indicated that safety and living environment issues generally are addressed early in a home health care episode and are resolved before recertification decisions are made. For this reason, it is unusual to recertify a patient solely on the basis of an unsafe living environment. However, it might be necessary to do so for a short time until community resources are identified to address the patient's needs.
Financial Status: Participants in five of the focus groups stated that the patient's financial status is a factor that home care nurses consider when making decisions about recertification and discharge. However, it was noted that a patient's financial difficulties alone cannot justify recertification. The participants indicated that, prior to discharge, home health agencies should use the services of a social worker to identify community organizations that can provide financial assistance.
Health Status: Focus group participants at each of the agencies reported that the patient's health status is one of the most important factors nurses consider in making decisions about recertification and discharge. The participants focused primarily on the patient's physical health and cognitive functioning.
Participants discussed a number of important indicators of a patient's physical health. They emphasized that a patient's medical condition must be stable before discharge. Such stability denotes that the patient no longer is in need of skilled nursing services. Many participants reported that they would recertify a patient whose medical condition had worsened since the start of care. Participants also stressed (as noted earlier) the importance of a patient's ability to manage his or her own medications. With regard to both of the patient vignettes, participants reported that they would use the following indicators of the patients' physical condition to assess readiness for discharge: presence of edema or swelling, skin breakdown and ulceration, weight gain or loss, and ability to ambulate.
When discussing the importance of a patient's physical health in the decision-making process, participants focused on many aspects of health that were specific to the two patient vignettes and the medical conditions represented in them. The physical health indicators discussed for each hypothetical patient and medical condition are detailed below.
- Lightheadedness
- Shortness of breath (e.g., oxygen use, oxygen saturations)
- Coughing, wheezing, crackling
- Dizziness
- Hearing
- Vision
- Ability to dress herself (need for assistive equipment)
- Energy conservation, increased fatigue
- Increased abdominal girth
- Waking up often at night
- Vision and presence of retinopathy
- Presence of peripheral vascular disease secondary to diabetes mellitus
- Need for assistive devices
- Blood sugar stable
- Need for and ability to use compression hose
- Cardiac problems associated with diabetes mellitus
- Diabetic foot care
- Nutrition and hydration
- Ability to use glucometer
- Ability to self-administer insulin
Participants also expressed concern about the hypothetical patients' cognitive functioning. Cognitive functioning was viewed as important not only for medication management, but also for other personal care and safety. Other concerns about recent cognitive changes were case-specific. Because hypothetical patient Mrs. Smith recently has begun to forget to take her medications, the participants expressed some concern that she might need a cognitive evaluation. Some of the participants suggested the need for community services to assist Mrs. Smith should she have a cognitive deficit. However, if Mrs. Smith's cognition were not impaired, many focus group participants felt she would have to be discharged given the stability of her other symptoms.
Participants believed that hypothetical patient Mr. Lucas should undergo a cognitive evaluation because of his recent inability to process instructions. Because cognitive difficulties are sometimes the result of infection, many of the focus group participants suggested that specific blood work should be performed. Participants recommended checking for a urinary tract infection and other kidney problems, as diabetics are at high risk for such complications.
Caregiver Factors: Caregiver factors were discussed by participants during each of the focus groups. Nurses stressed the importance of caregiver availability and burden, as well as education and ability to learn. The availability of a caregiver was a topic of discussion at all of the focus groups. As mentioned above, some of the focus group participants noted that they might recertify a patient until a caregiver could be found or community services coordinated. A few participants suggested that the two hypothetical patients must have had help in the past and that the previous caregivers might be able to assist the patients after discharge.
With regard to the two patient vignettes, participants at five agencies discussed the difficulties involved in having family members perform caregiving duties. For example, Mrs. Smith's daughter lives out of state and therefore is unavailable to assist her mother. Mr. Lucas' daughter is a single mother raising three pre-teen boys and cannot afford to cut back on her work hours. In both cases, participants recommended that other people (e.g., other family members, neighbors, fellow church members) or alternative community services be identified. To further ease the burden on caregivers, participants suggested that social workers or caregiver support groups might be of help. Some participants noted that the patients may need to live with their families if other resources are not available, a proposition that may or may not be acceptable to the patients, caregivers, and other family members.
Participants at six agencies suggested that it is important to educate the caregiver about a patient's condition and care plan. They felt that the caregiver should know the signs and symptoms associated with the patient's disease, how to manage medications, and what to do in case of an emergency. Participants emphasized the importance of assessing the caregiver's ability and willingness to learn about the patient's condition and needs.
2. Actors
The focus group interviews elicited information about the influence exerted by different "actors" involved in the process of making decisions about recertification and discharge. Important actors include the patient's primary nurse, physician, the patient himself or herself, caregivers, the agency's FI, and payers (Medicaid, private insurance companies, managed Medicare contractors).
The focus group participants indicated that all decisions are made following the guidelines of Medicare and the FI. The primary decision makers are the physicians and home health nurses. Often, there is extensive dialogue between the physician ordering home health services and the nurse making the home visits. Participants suggested that home health nurses have less influence in decisions regarding recertification and discharge than they once did. Now, the physician makes the final decisions about a patient's care. The nurse's role in this process is to inform the physician about the patient's home situation. Participants indicated that they report information to the patient's physician about patient noncompliance with medications, cognitive impairments of caregivers, and medical instability. The physician often is unaware of these circumstances unless informed by the home health nurse.
Some focus group participants reported that there is agency-wide fear of Medicare review. One participant stated that "there is almost a sense of paranoia dealing with Medicare now." Participants perceived a very low tolerance for mistakes and a lack of trust between Medicare and home health nurses. One nurse suggested that "it just seems so wrong that something done in such good faith is investigated so closely." Some participants suggested that fear of Medicare review has resulted in patients being discharged more readily than they once were.
The patient's influence over and involvement in the decision to recertify or discharge varies. Most of the participants reported that they make recommendations to patients based on the patients' expectations and the guidelines of Medicare home health coverage. Communication with a patient about eventual discharge occurs early in the home health episode and helps the nurse plan alternative resources as well as education for the patient and/or caregiver. Some patients attempt to influence the decisions their nurses make in the hopes of lengthening their episodes of care.
3. Agency Factors
Focus group participants reported that there are no agency rules specific to recertification or discharge. However, participants at each of the focus groups reported that their agencies have developed processes through which recertification and discharge decisions are overseen. To promote adherence to Medicare coverage rules, agencies have the unwritten expectation that nurses will work with a clinical supervisor and/or through a case conference model (often multidisciplinary) as they make recertification/discharge decisions. Agencies generally support the decisions of the primary nurse provided that he or she is able to demonstrate a patient's need for services through this process. For example, participants at one of the focus groups indicated that their agency's policy is for recertification and discharge decisions to be made based on case conferences and discussions between the primary nurse and the nursing supervisor. It is expected that the supervisor will provide feedback on what services are appropriate based on the patient's needs and Medicare coverage rules.
4. External Factors
Several external factors were identified as influential in the decision-making process: (a) the IPS, (b) managed care, (c) the ORT, and (d) other factors affecting agency case mix.
Interim Payment System (IPS): Although IPS is an external factor known to influence agencies' practice patterns, focus group participants from only one agency specifically referred to IPS. Since the focus group participants were nurses providing direct patient care (not clinical supervisors or managers), they might not have in-depth information about IPS and its implications. Although agency expectations and policies may be influenced by IPS, care providers are not exposed to the direct cause/effect relationship. It is not clear from the focus group data how many of the eight groups of participants had been informed about IPS. At best, the participants had been provided with information through newsletters, inservices, and/or informational meetings.
Despite the lack of direct mention of IPS, several issues likely to be associated with IPS were identified in the focus group data: reduction of patient services, documentation and nurse productivity, and refusal of patients. Some focus group participants indicated that the services they are able to provide to their patients have been reduced. Participants at one agency specifically referred to the impact of IPS and the forthcoming PPS. These participants reported that they are unable to offer as many services to their patients as they once did. This is partly because they have been encouraged to "get in and get out" of the home quickly and keep the number of visits low. As one participant explained, the patient can only have so many visits "because there are only so many dollars." Another group of participants noted that their agency has limited social work visits to two per patient.
Focus group participants frequently reported an increase in the burden of and changes in the means of documenting patient care. For some agencies, paperwork has doubled. At one agency, nurses reported that they must complete 25 pages of documentation for an admission visit. Another agency has transitioned to computer documentation as a result of IPS. Nurses from two other agencies discussed the increase in paperwork, but did not specifically link these circumstances to IPS. Participants at three agencies indicated that additional paperwork, including collection of OASIS data (which is not a provision of IPS), have led to a reduction in time spent with patients.
Focus group participants from one agency reported that they are taking more work home with them at the end of their long workdays. As expressed by one participant, "we're stretched out." Participants at a different agency predicted that the amount of face-to-face contact with patients would continue to diminish. Productivity, as well as time spent with patients, is affected primarily by nurses spending more time doing paperwork, assuming clerical or support duties, tracking and obtaining supplies, and contacting physicians and others to obtain authorization for care and coordination of services.
Nurses from one agency linked IPS to the refusal of patients. These nurses reported that they complete forms every month to estimate the number of visits that will be needed for a patient. "High-need" patients sometimes are turned away because the services needed for these patients exceed the per-beneficiary or per-visit cost limits.
Managed Care: Nurses at five of the eight agencies indicated that managed care was an external factor affecting decision making. Participants reported that they care for more managed care (including Medicare managed care) and insurance patients than they did five years ago. The nurses expressed a general belief that managed care companies want participants to discontinue home care services as quickly as possible.
Participants reported spending considerably more time than they once did obtaining required authorization from managed care companies. The focus group participants reported that obtaining approval for visits and/or services was the major focus of all contacts with managed care companies. In addition, participants in all of the focus groups reported having experienced difficulty contacting managed care case managers to discuss patient care needs and decisions. Some nurses noted that authorization decisions vary depending on the particular case manager contacted. Some are lenient, whereas others require extensive justification for patient services. Nurses' workload is further increased because contacting managed care case managers often necessitates additional calls to physicians.
Although some of the focus group participants feel that they generally have control over the decision-making process, they do not believe they have autonomy in making decisions about their managed care patients. The primary nurse, physician, and other agency personnel can make recommendations about patients' care plans. However, the managed care company has the final say about the services to be provided. Nurses at one agency noted that even physicians can be overruled by the managed care company. One participant lamented, "our hands are tied."
Some of the focus group participants commented on the restrictions that managed care places on home care providers. One participant was familiar with a managed care organization that does not approve any medical social work visits, even for Medicare managed care patients. Another participant noted that a particular managed care company was known to approve more visits for patients who have been recently hospitalized, regardless of their diagnoses or symptoms. One nurse commented that "with Medicare HMOs, it's very limited what can be provided and length of services."
The focus group participants emphasized that managed care has forced nurses to teach patients and families more information in a shorter period of time. Many reported that managed care companies do not allow the duration of home care services necessary for instruction to be completed, especially in the case of patients with complicated care needs. Some focus group participants equated this situation with elder abuse. "Insurance companies are on our back about 'Why can't you teach them to do it. How come they can't learn? What's wrong?' We're trying to teach 85 year old spouses how to administer [intravenous] drugs with dangerous side effects."
Additionally, the focus group participants expressed suspicion and mistrust of managed care companies. One participant reported knowledge of a case worker at a managed care company who received a bonus for cutting back on patient visits. Another participant stated that managed care is "unsafe, I don't feel good about it. It's affecting our seniors."
Operation Restore Trust (ORT): Participants at two of the focus groups specifically referred to the anti-fraud initiative, ORT. At one agency, participants suggested that all agencies, not just those that have submitted fraudulent claims, are being monitored as part of ORT. However, participants at this agency reported that they do not worry about ORT. These nurses suggested that ORT does not influence the decisions they make about their patients' care. In their view, they simply provide patients with the care that they need. "There is no fraud here," was a typical respondent comment.
At the other agency, a participant had been told that home care was being regulated because agencies tried to maximize visits. Participants felt strongly about this issue, noting that "we're suffering so much from agencies that were charging fraudulently. There were rumors about the FBI sending nurses and physicians to jail. There are so many things you can do for people, but because we're suffering for those who were fraudulent, we can't do it."
Other Factors Affecting Agency Case Mix: Focus group participants noted that patients are coming out of the hospital sicker than they once did. The first visit for these patients can be especially long and difficult. These complex patients require a great deal of attention and often require high-technology care, such as infusion therapy, parenteral nutrition, and ventilator care. The focus group participants noted that many home care nurses do not have the skills needed to care for these patients, nor are they able to manage the productivity and documentation requirements associated with these complex cases. At one agency, the change in case mix is reflected as a larger caseload of Medicaid and Medicare managed care patients. Although the nurses felt that this change promoted their autonomy in decision making, it also necessitated more responsibility, more paperwork, and more contact with physicians. There was agreement that this added stress is a factor in decision making.
5. Medicare Coverage Rules
Focus group participants at each of the eight agencies discussed the influence of Medicare coverage rules on decisions regarding recertification and discharge. Several factors associated with Medicare coverage rules emerged as important themes in the focus group data: (a) homebound status, (b) skilled nursing services, (c) management and evaluation (M&E), (d) ambiguity of coverage rules, (e) documentation, and (f) effect on patient care.
Homebound Status: The results of the focus group interviews indicate that, although a patient's homebound status is critical to the decision to recertify or discharge, the definition of "homebound" is ambiguous and subjective. Nurses agreed that they would need the following information to make a determination about a patient's homebound status: how often and why the patient leaves the home, the degree of difficulty the patient has in getting to the car, who drives the patient, and how long it takes the patient to recover from a trip.
However, the definition of "homebound" differed substantially among nurses. Some participants interpret homebound to mean that a patient cannot leave his or her home under any circumstances. Other nurses reported that a homebound patient is one who is able to leave the home only with taxing effort. One participant suggested that, to be considered homebound, a patient could not leave the home for socialization or shopping, but that attendance at church, doctor's visits, and appointments with the hairdresser were acceptable. This nurse stated that a patient does not "have to be stretched out in bed to be considered homebound." Participants agreed that patients who are able to drive are not homebound, even if there are medical contraindications, the patient's disease process is uncontrolled, or there are influencing psychosocial factors. The nurses indicated that patients who can drive would be discharged, regardless of such factors. Note that, according to Medicare coverage rules, the ability to drive is not a definitive indication that a patient is not homebound.
When discussing Mrs. Smith's case, most participants stated that her visit to the hairdresser does not disqualify her from being considered homebound. One participant, however, said that she would discharge Mrs. Smith because her trip to the hairdresser indicates that her CHF is under control and that she should be considered stable and no longer in need of skilled services.
Skilled Nursing Services: The need for skilled nursing services is the determining factor in the decision-making process. If a patient does not meet skilled care criteria, he or she is not eligible for Medicare coverage. Some nurses noted that physicians are not always clear about what constitutes a need for skilled nursing care. The participants in one focus group reported that physicians sometimes refer patients for home care who do not have a skilled need. At times, this agency has tried to find some type of skilled service need in order to retain the physician's continued referral. Nurses did point out that patients with unskilled needs had the option of paying for private services. Further, two of the study states have state waiver programs to which patients needing only unskilled services are referred.
In examining Mrs. Smith's case, participants discussed the possibility of pre-pouring her medication. However, according to Medicare coverage rules, pre-pouring of medications is not a skilled service. Without a skilled need, Mrs. Smith cannot be recertified. In examining Mr. Lucas' case, one participant stated that she would not have admitted Mr. Lucas. She did not believe he had a need for skilled care to begin with. However, other participants suggested that he might qualify for skilled services. There were different points of view about whether his wound care should be considered a skilled service. Some noted that if the wound was healed, Medicare would not allow continued home care and the patient would have to be discharged. If Mr. Lucas could not self-administer insulin because of neuropathy or blindness, Medicare would cover such visits. It was noted that Mr. Lucas may have social issues as well, but that social issues are not indicative of a need for skilled services.
Participants expressed concern that families in situations similar to Mrs. Smith's or Mr. Lucas' tend to expect that aide services will continue even after nursing care is no longer needed. In such cases, care providers must explain that Medicare will not cover continued aide services when a patient no longer requires skilled nursing care.
Management and Evaluation (M&E): Skilled nursing visits for M&E of a patient's care plan are covered by Medicare in cases in which only an RN can assure the complex and necessary care that an unstable patient receives from nonskilled caregivers is successfully maintaining the patient's medical condition. The focus group data suggest that nurses are uncertain what the M&E treatment code is and when it can be used. M&E arose as a topic of discussion at six of the eight focus groups. Five of the eight agencies participating in the focus group interviews do not use M&E. Nurses at one additional agency reported that they had been told not to use the M&E treatment code, although it had been used at their agency in the past. Nurses' explanations of M&E were strikingly different across these six agencies.
Nurses at an agency at which M&E never has been used explained that this treatment code applies to complex patients, especially those who are forgetful. These nurses believed that M&E also could involve managing a patient's medications, especially if a caregiver is responsible for medication management. The participants from this agency emphasized that the nurse must make sure that caregivers are appropriately caring for the patient. According to these participants, M&E requires detailed documentation and requires the nurse to visit the patient monthly. Home health aides can be ordered more frequently.
Nurses from a different agency reported that Medicare no longer covers M&E. "It can't be done." One participant explained that this was true because M&E was linked to intravenous (IV) therapy and venipuncture, in particular monthly protimes. However, she expected that M&E could apply to a patient with a central (IV) line if the family was unable to manage it appropriately.
When examining the hypothetical patient scenarios presented to them, participants from three agencies suggested that M&E would not apply to Mr. Lucas' case or similar cases. There was disagreement as to the appropriateness of M&E with respect to Mrs. Smith's case. Nurses from one agency felt M&E could apply to her situation. They described M&E as the ability to recertify a patient for the purpose of long-term planning and establishing care plans for complex patients. They suggested that the following needs could be listed as skilled services to justify coverage: observation, assessment, and management of caregivers. Nurses from another agency indicated that M&E would not apply to Mrs. Smith. Their interpretation was that a patient had to have complex needs, have multiple caregivers, and need a large number of hours for the necessary care. Apparently, Mrs. Smith did not qualify under their definition. Another group of participants did not think their agency had a specific policy for situations such as Mrs. Smith's. However, they were certain that M&E required specific training of nurses and that M&E is one of the "four skilled services" in home care. It requires different criteria for documentation and is used for short-term periods while community resources are located for a patient.
Ambiguity: Participants in three of the focus groups referred to the ambiguity of Medicare coverage rules. One agency's participants noted that it was difficult to understand the HIM-11 (the Medicare manual on home health). One participant stated that she does not "understand [the HIM-11], it's kind of vague. You have to be a lawyer because it's difficult to understand." Nurses at another agency noticed differing interpretations of the coverage rules when their agency had a change in FI. These nurses reported a sense of not knowing the rules until they get broken.
Discussion of Mr. Lucas' case at one agency revealed one participant's misinformation concerning the coverage rules. She believed that to justify a patient's need for B12 injections, she would have to document the patient's need for monthly venipuncture. She was unaware that venipuncture is no longer a qualifying service for Medicare home health care. This participant and others believed that the venipuncture regulations applied only to venipuncture for lab work to measure prothrombin time ("protime"). As discussed previously, the confusion surrounding venipuncture may contribute to nurses misunderstanding of the M&E treatment code.
Documentation: Documentation is the key to justification of services and must support the need for skilled nursing care. It must be specific and concrete. Participants made it clear that there has been an increase in the amount of paperwork in home care, including more forms to complete and more repetitive documentation. Some nurses expressed a sense of paranoia based on the documentation requirements that every "i" must be dotted and every "t" crossed. Others believed that documentation should not cause added worry so long as patients are given the care they need. If agencies are not submitting fraudulent claims and nurses provide the needed care, the documentation (485s and 488s) should speak for itself.
Participants reported that omissions or a lack of clarity in documentation have led to denials of recertification. Nurses reported that the FIs ask for more records than they once did, which has resulted in an increased need for staff education on coverage rules and appropriate documentation. One participant observed that nurses may fail to document teaching as a skilled service. As a result, agencies may receive requests for additional documentation, each of which requires the completion of the 488 form in response.
Among the focus group participants, there was support for the 485 as the best form for standardization. Together, the 485 and 488 are adequate for substantiating care needs. Participants at one agency reported that there are certain terms that their FI does not like to see in the 485s (e.g., "monitor," "stable"). However, they indicated that their documentation is not determined by what they think Medicare or the FI wants. Documentation should explain the activities of the care provider. As one participant put it, "you want to paint a picture so that when they ask for the records everything is clear. They can look at your documentation and tell exactly what is going on and if there is a need."
When discussing documentation, participants also identified the following vignette-specific information that they would include in their reports to justify skilled care:
- Fluid/weight gain and other active signs and symptoms of CHF
- Medication changes and patient responses
- Safety/risk for falls (what has been done to reduce risk and why services are still needed)
- Ability to manage personal hygiene
- Eating habits/ability to cook
- Medication compliance/ability to take medications
- Mentation/cognition (forgetfulness), increased anxiety, depression, apathy
- Discussions with daughter/caregivers (availability and willingness to help)
- Deterioration/declines
- Inability to recognize and report acute symptoms to medical provider
- Reports of findings from other assessments as applicable (county assessor for evaluating the home's safety/heat/fire risk)
Specific phrases that would be used to assure coverage in this case include: "Patient unable to verbalize three symptoms of CHF." "Patient lives in unsafe environment" (followed by detailed description). "Patient is forgetful, weekly pill count revealed only 2 of 7 days medications taken." "Medication management is poor secondary to inability to process new information." "New medications prescribed. Side effects observed within 24 hours."
- Any deterioration in physical or mental status (e.g., skin and wound condition)
- Diet, ability to cook and manage meals
- Appropriateness of medications, changes in medications
- Blood glucose levels and trends, out-of-range measurements
- Presence of hypoglycemic or hyperglycemic symptoms and measures used to correct or prevent
- Integrity of feet, foot care practices, proper shoes
- Self-care ability, personal hygiene
- Independent/dependent abilities and potential to regain independence
- Medication management including ability to self-administer insulin, manage and read glucometer
- Cognitive level including ability to understand instruction, especially regarding safety
- Specifics of what was taught and the patient's response
- Specifics of what was done to address other problems
Specific phrases that would be used to assure coverage include: "Knowledge deficit for " "Unable to manage " "Minimal skills for " "No survival skills for " "Ineffective long term plan."
Effect on Patient Care: Participants noted that federal regulations are always a factor in decision making in home health care. They worry that coverage rules have shifted the focus of care from the patient to money. Participants discussed the effect that coverage rules have had on patient care. Nurses expressed the general belief that non-medical people are setting guidelines for home health care, not truly understanding how their decisions impact the quantity and quality of the services provided. One agency's nurses felt that the changes in coverage rules have affected what services agencies can provide and patients can receive. For example, a patient may need more education "than the guidelines dictate." The nurses suggested that Medicare wants patient and family education to be achieved in a shorter period of time in an effort to discharge patients sooner. The participants felt that Medicare policy-makers do not have a realistic view of the patient education process.
B. Case Study Interviews
The case study interviews were designed primarily to examine the practice of home health care. In this chapter, the qualitative information gathered during the case study interviews is used to describe the care provided during seven episodes of care. Specifically, information is summarized concerning the following aspects of care: (1) key characteristics of the episodes of care (e.g., length, disciplines involved), (2) services provided by home care personnel and the family support system, (3) care planning and coordination (e.g., development and documentation of the care plan), and (4) content of the skilled nursing visit (e.g., assessment, teaching). The small sample of nurses involved in the case study interviews made it difficult to identify differences between agencies in different state volume, agency ownership, and agency type groups. However, nurses' responses with regard to certain aspects of home care did appear to differ depending on volume, ownership, and type. These differences are described when appropriate.
1. Key Characteristics of the Episodes of Care
In order to examine factors that may be related to variations in lengths of stay in the Medicare home health benefit, patients with either long or short episodes of care were identified. The seven patients whose care was examined during the case study interviews were on service with their home health agencies an average of 102.3 days, with a range of 19 to 441. However, because two patients had very lengthy stays, the median number of days on service across the seven patients was much smaller (26.0 days). Because of the presence of these two outliers, median rather than mean values will be used throughout this chapter to describe the services provided in home health care.
Table 5.1 presents length of stay, number of disciplines, number of skilled nursing visits, and total number of visits for the case study patients by state volume group, agency ownership, and agency type. The small sample size for the case study limits our ability to draw conclusions based on these data. Therefore, information regarding the key characteristics of the case study episodes of care is presented for descriptive purposes only. Because we attempted to identify long-stay patients in the high-volume states and short-stay patients in the low-volume states, the differences in length of stay and the number of visits between the patients treated in the two state groups is not surprising.
| TABLE 5.1: Key Episode Characteristics by State Volume, Agency Ownership, and Agency Typea | ||||||
| State Volume | Agency Ownership | Agency Type | ||||
| High Volume (n=3) | Low Volume (n=4) | Proprietary (n=4) | Non- Proprietary (n=3) | Hospital- Based (n=3) | Free- standing (n=4) | |
| Episode length (days) | 120.0 | 28.5 | 44.5 | 26.0 | 31.0 | 39.5 |
| # Disciplines Involved | 2.0 | 1.5 | 1.0 | 2.0 | 1.0 | 2.0 |
| # Skilled Nursing Visits | 28.0 | 8.5 | 11.5 | 9.0 | 9.0 | 11.5 |
| Total # Visits (all disciplines) | 28.0 | 10.5 | 20.0 | 22.0 | 22.0 | 20.0 |
| ||||||
Lengths of stay for the case study patients appeared to be somewhat related to agency ownership and type. Case study patients on service with proprietary agencies tended to have longer lengths of stay than did patients on service with non-proprietary agencies (44.5 versus 26.0 days). Patients of freestanding home health agencies tended to be on service slightly longer than did patients of hospital-based agencies (39.5 versus 31.0 days).
Agencies typically involved two disciplines in the care of each patient. The actual number of disciplines involved ranged from one to four. The disciplines involved in treating the seven case study patients were the following: skilled nursing (seven patients), physical therapy (PT) (three patients), home health aide (two patients), social work (one patient), and occupational therapy (OT) (one patient). Nurses from two of the case study agencies mentioned that they would have involved PT, but they felt that their patients were too weak to receive benefit from these services. In one of these cases, the nurse also believed the patient to be unmotivated to engage in PT. Agencies in the different state volume, agency ownership, and agency type groups did not appear to differ in their involvement of different home care disciplines.
The services of some disciplines were offered by home care agencies, but refused by the patients. In fact, five of the seven case study patients refused a recommended service. Two patients refused to accept the services of a social worker, and three others refused to accept the services of a home health aide. Table 5.2 provides service utilization information for each of the seven case study patients.
| TABLE 5.2: Service Utilization by Case Study Patient | ||||||
| Patient | Episode Length (days) | Skilled Nursing Visits | Physical Therapy Visits | Occupational Therapy Visits | Medical School Work Visits | Home Health Aide Visits |
| 1 | 120 | 28 | 0 | 0 | 0 | Patient refused |
| 2 | 21 | 10 | 7 | 1 | Patient refused | 9 |
| 3 | 31 | 8 | 0 | 0 | 0 | Patient refused |
| 4 | 441 | 150 | 1 | 0 | 0 | Patient refused |
| 5 | 26 | 9 | 3 | 0 | Patient refused | 10 |
| 6 | 19 | 4 | 0 | 0 | 1 | 0 |
| 7 | 58 | 13 | 0 | 0 | 0 | 0 |
The case study nurses were asked whether there were any services they would have liked to provide for their patients, but that were not available. None of the nurses indicated there were services that they were unable to provide for the case study patients. However, speaking in general terms, two nurses reported that they frequently are unable to obtain certain services for their patients. One nurse remarked that respite care is a chronic need in home care. Suggesting that "one sick person can kill ten healthy people," this nurse commented that respite care is of critical importance because "if we don't take care of [the caregivers], they are going to end up costing us more money in the long run.... The caregivers give out, especially a spouse that is the same age." A second nurse commented on the lack of community resources in her county. In the rural Southern town where this nurse's agency is located, no senior activity centers, community or public transportation systems, or volunteer programs are available to help elderly patients. The agency itself is currently working to set up a volunteer program in the community to meet some of these needs.
The findings regarding the number of skilled nursing visits mirror those regarding episode length. Patients received a median of ten skilled nursing visits during the course of their home care episodes. The actual number of such visits varied drastically across patients, with a range from four to 150. Patients of proprietary agencies received a slightly larger median number of skilled nursing visits than did patients of non-proprietary agencies (11.5 versus 9.0). Freestanding agencies provided slightly more frequent skilled nursing visits for their patients than did hospital-based agencies (11.5 versus 9.0).
The median total number of visits (across disciplines) that the case study patients received was 22.0, with a range from five to 151. The total number of visits across disciplines differed only slightly by agency ownership and type. Non-proprietary agencies provided slightly more visits than proprietary agencies (22.0 versus 20.0), and hospital-based agencies provided slightly more visits than freestanding agencies (22.0 versus 20.0).
2. Services Provided in Home Health Care
Five disciplines were involved in the care of the seven case study patients. Each discipline provided a unique set of services to these patients. The services provided by skilled nursing staff, physical therapists, occupational therapists, medical social workers, home health aides, and the family support system are summarized in this section.
Skilled Nursing: Home care nurses provide a variety of services to their patients (see Table 5.3). Assessment represents one of the nurses' major activities. In five of the seven cases, the primary nurses admitted the patients, conducting the initial assessments of their needs (in two cases, patients were admitted by an admission nurse and the on-call nurse, respectively). In the initial assessments, the patients' conditions, needs, and eligibility for services were examined as well as the patients' social and home environment. These assessments provide a basis for the development of the care plan.
| TABLE 5.3: Skilled Nursing Activities | ||
|
|
|
Throughout the episodes of care, the nurses continued to assess their patients. These assessments comprised a major component of each visit. Indeed, three nurses indicated that assessment was one of the most time-consuming activities they engage in during their visits. In coordination with the nurses' regular assessments of the patients, nurses managed their patients' medications. They identified medication side effects, set up pill boxes to enhance the patients' ability to take medications correctly, and at some visits drew lab work to assess the appropriateness of medication doses.
The case study nurses indicated that education was one of their most time-consuming and important activities. All of the nurses noted that the focus of home care activities has increasingly turned from the direct provision of services by medical personnel to teaching patients and their families how to provide those services for themselves. According to three case study nurses, home care providers "are being told to get in and get out" of their patients' homes as quickly as possible. To shorten their patients' duration in home care, the nurses reported the need to educate patients to the point that they are capable of caring for themselves independently. Nurses educated patients about the signs and symptoms of their medical conditions, their medication regimens (e.g., purposes, doses, side effects, use of a pill box), their diets, home safety, use of medical equipment, use of weight or diabetic diaries, and changes in condition that would require medical attention.
Four of the nurses commented that it can be a struggle to teach elderly patients the information they need to know to care for themselves. In two cases, the patients had great difficulty understanding and remembering the details of their medication regimens. In one of these cases, the patient was never able to understand his medication regimen, whereas in the other case, the patient learned very slowly. The nurse in this latter case commented that, in her agency, the nurses "are told to try to get in and get out, but that's not always possible because people learn at different paces." In another case, the nurse reported that her patient was simply not receptive to learning about his medical condition.
The nurses engaged in a number of other activities on their patients' behalf. Three of the nurses indicated that one of their most time-consuming activities in caring for their patients was coordinating care among various care providers. According to one nurse, "orchestrating, organizing, making sure everyone was on the same page" was a major component of the work she performed while caring for her patient. Four nurses commented that the completion of mandated forms and the documentation of their care plans comprised a major component of their workload with regard to the case study patients. Two nurses indicated that they spent a major portion of their time just talking to the patients, building rapport, and trying to identify the patients' needs and concerns. In addition, as mentioned above, one nurse emphasized the importance of the psychological services that primary nurses often provide. Another nurse suggested that helping the patient to establish a network of friends and family members to assist him was an important part of her work with this patient.
Physical and Occupational Therapy: Three of the case study patients received PT during the course of their home health care episodes. In all cases, PT was ordered because the patients were weak or unsteady on their feet. In one case, the physical therapist conducted an evaluation only, concluding that the patient did not actually require PT. In the other two cases, physical therapists worked with patients on their balance as well as their walking and stair-climbing abilities.
OT was involved in the care of only one of the case study patients. In this case, OT was ordered by the patient's physician. However, at the time of the initial OT evaluation, the occupational therapist determined that the patient was not in need of these services.
Medical Social Work: Three of the seven case study nurses believed that their patients needed the services of a social worker. In two cases, the nurses hoped a social worker could identify resources outside of the home health agency. In one case, the patient, whose elderly wife was having trouble driving, was in need of transportation to and from medical appointments. In the other case, the patient was being evicted from her home and needed assistance finding new housing for herself and her developmentally-impaired son and daughter-in-law. In the third case, a social worker was recommended because the primary nurse believed the patient needed psychological help to address her anxiety and fear that she was incapable of caring for her terminally ill significant other.
Although a social worker was recommended to three patients, only one patient accepted such services. A social worker completed a single visit with the patient in need of new housing. She then contacted a state caseworker that arranged for new housing and state-run nursing services for this patient. In the other two cases, the patients refused social work services, "as patients often do." These refusals put the nurses in the position of having to provide services that ideally would be provided by another discipline. The nurse caring for the patient who was experiencing anxiety over her ability to care for her terminally ill significant other had to take on the role of a social worker, both helping the patient and her family to identify outside resources (e.g., hospice care), and providing psychological counseling. Although immersed in the role of counselor more so in this situation than she normally would be, this nurse commented that psychological counseling is not an uncommon activity for primary nursing staff. Indeed, it is "one of the most important things [nurses] do in home health care. The head and the body are not disconnected."
Home Health Aide: Five of the seven case study nurses recommended home health aide services to their patients. In two cases, home health aides assisted patients two or three times a week with a variety of activities including showering, skin care, meal preparation, bedroom and bathroom cleaning, laundry, and shopping. Aides also have responsibilities associated with the assessment of the patients. For example, the aides in one of these cases weighed the patient and reminded her to take her medications. Further, aides report any changes in a patient's condition immediately to the primary nurse. In this way, they serve as another set of eyes for the nursing staff.
As with the services of a social worker, the case study patients often refused home health aide services. In three of the five cases in which aides were recommended, the patients refused to accept these services. In two of these cases, aide services were refused because the patients' family members were able and committed to helping the patients with these activities. The third patient did not have such family assistance, but still would not accept help from an aide. Some patients may be uncomfortable having a stranger help them with the very personal activities in which aides are often involved (e.g., bathing assistance).
The case study nurses often indicated that those patients who do accept home health aide services greatly appreciate these services. One nurse noted that the patients "love [the aides], they become part of their families." Indeed, patients often become overly dependent on the aides who care for them. In both cases in which patients received aide services, the patients did not want to discontinue these services. One nurse commented on the need to "wean" patients from aide services. In this case, the nurse initially provided the patient with the minimum number of weekly aide visits she thought the patient might need. She commented that it was easier to increase than to reduce the number of weekly visits provided. In addition, the nurse progressively cut back on the services the aides provided. Although the aides continued to see the patient with equal frequency throughout the episode of care, they performed fewer and fewer services at each visit. Near the end of the episode of care, the aides were in the house primarily to provide a sense of comfort and security to the patient as she became increasingly capable of caring for her own needs. This same nurse noted that, more recently, she has begun to reduce not only the services provided by the aides across the episode of care, but the number of weekly visits as well.
Family Support System: The family support system is of critical importance to home health care patients. Each of the case study patients had at least one family member who assisted them. Four patients relied on two or more family members on a regular basis. Five of the patients received a great deal of assistance from their family support systems. The other two patients had a single involved family member who provided minimal assistance. In both of these cases, the family member involved was elderly. In one case, the patient's brother ran some errands for him. In the other, the patient's wife, who drove the patient to the doctor and did some cleaning around the house, was quite ill herself with a cardiac condition. Her ability to assist the patient was quite limited. Among the five patients with highly involved family support systems, the patients' wives were the main caregivers in two cases and the patients' children were the main caregivers in three cases. In one case, the patient's son and daughter-in-law, who were both cognitively impaired, struggled to help the patient check her blood sugar and to understand and follow the medication regimen.
Family members of the case study patients provided assistance with ADLs, IADLs, environmental support, and psychosocial support. In addition, family members were quite active in the patients' home care. Table 5.4 identifies the activities that family members performed for patients. Family members were somewhat active in assisting patients with their ADLs. Of the case study patients, three received help in bathing and personal care from the members of their families. In one other family, the patient was assisted by her son and daughter-in-law in grooming, transferring, and feeding. Families were frequently involved in patients' IADLs. Five of the seven families took an active role in helping the patients manage their medications. Family members picked up patients' medications, learned about medication side effects and schedules, set up pillboxes with the patients' daily doses of medications, and reminded patients to take their medications.
For elderly patients for whom managing varying schedules for multiple medications can be a real challenge, the assistance of family members in the management of medications was invaluable. Four patients relied on family members for transportation, and three patients had family assistance with meal preparation. Members of two families took on housekeeping and shopping responsibilities. Family members assisted one patient in doing the laundry.
| TABLE 5.4: Assistance Provided by Family Members | |
| Number of Patients for Whom FamilyMembers Provided this Service | |
| Activities of Daily Living (ADLs) | |
| Bathing and personal care Grooming Transferring Feeding | 3111 |
| Instrumental Activities of Daily Living (IADLs) | |
| Management of medications Meal preparation Transportation Housekeeping Shopping Laundry | 533221 |
| Participation in Home Care | |
| Present at skilled nursing visits Weighing and recording weight of patient Helping patient check and record blood sugar Change dressings Care for medical equipment (IV pump, central line) | 62111 |
| Psychosocial Support | |
| Companionship | 1 |
| Environmental Support | |
| Yard work | 1 |
Family members took an active role in the patients' home care activities as well. In all but one of the seven cases, family members were present at most or all of the skilled nursing visits. Family members often were involved in the development of the patients' care plans. In some cases, family members even requested and refused services for the patients. One nurse commented that the family of her patient was less involved in determining the care plan than it otherwise might have been because the patient herself was alert and capable of making decisions on her own.
Family members participated in the patients' care in several additional ways. Family members of two patients weighed the patients every day, recording these measurements in a weight log. These individuals had been educated about the importance of weight changes, and instructed as to when they should contact the patients' physicians in response to a weight change. One patient had family assistance in conducting and recording the results of her regular blood sugar tests. The wife of one patient was responsible for learning how to use her husband's IV pump, setting up and turning on/off her husband's IV medication, and caring for his central line.
Clearly, family members provide substantial assistance to elderly home care patients. The nurses for some of the case study patients indicated that certain services (e.g., transportation, aide services) were unnecessary for their patients because the family support system was so strong. Indeed, in two of the three cases in which patients refused the services of a home health aide, they did so specifically because they had family members who were willing and able to take over those functions. Nurses often commented that their educational activities are targeted at family members as well as the patients. In some cases, the patients were so weak at the beginning of their episodes of care that the families were the primary targets of initial education activities, until the patients became stronger and more capable of involvement in their own medical care. One nurse commented that elderly home care patients are "just out of luck unless they have family to help them."
3. Care Planning and Coordination
Development of the Care Plan: The original referral from a patient's physician marks the starting point for the provision of home health care. The referrals for the seven case study patients varied in content and specificity. In four of the seven cases, the physicians ordered skilled nursing care only. In the remaining three cases, the physicians ordered visits by multiple disciplines including PT (three cases), aide services (two cases), and OT (one case). Rarely did physicians specify the frequency or duration of visits. In only two of the seven cases did the referring physicians indicate the frequency with which visits should occur. None of the physicians indicated an expected duration for the home care episode.
After the original referrals were received by the home care agencies, agency nurses completed their initial assessments of the condition and needs of the case study patients. For the three patients whose physicians had ordered PT and/or OT, the initial PT and/or OT assessments were conducted at this time. During the course of their evaluations of the case study patients, the nurses and therapists developed recommendations as to the appropriate care plans. The nurses and therapists identified the patients' problems, worked with the patients to establish treatment goals with expected achievement dates, laid out education topics, and pinpointed other disciplines that might be needed. At this time, the nurses identified the expected duration of the episode of care and the frequency with which the skilled nursing and aide visits should occur. The therapists identified the expected frequency and duration of their services.
In three cases, the nurses indicated that it is the primary nurse who makes decisions about the patient's care plan. At two agencies, the primary nurse and supervisor both were involved in the development of the care plan. In one of these cases, the supervisor and the nurse met to establish the care plan. In the other case, the supervisor reviewed the care plan that the primary nurse developed independently. In this latter case, the approved care plan was then sent to the "chart review committee" at the agency's home office for final approval. In one case in which the primary nurse had not conducted the initial assessment with the patient, the primary and admission nurses met together to establish the care plan. In only two cases did nurses note the involvement of the physicians in the development of the care plan. In one case, the nurse reported that she generated the care plan, which was then approved (with no changes) by the physician. In the other case, the nurse stressed that her findings from the initial assessment simply provided information to the physician as he developed the patient's care plan.
The case study nurses also commented on the involvement of the patients and the family in care planning decisions. By virtue of the fact that patients must be motivated to achieve the goals laid out in the care plan, nurses work closely with the patients to identify appropriate goals and achievement dates. Patients and their family members also are involved in determining what services are provided and with what frequency. As previously described, patients and/or their families often refuse services that are recommended by the primary nurse. Patients also have to approve the frequency of visits that the care providers recommend. Sometimes, patients and their families request services that the nurses perceive to be unnecessary. In two cases, patients and their families wanted additional aide services, another patient and her family wanted to receive as many services as possible, and another patient did not want to discontinue home care.
Consistent with the Administrator Questionnaire findings described in Chapter 3, agencies in the different state volume and agency ownership groups appeared to differ somewhat in the actors involved in the development of a patient's care plan. Nurses in the low-volume states appear to have greater influence over the decision-making process than do nurses in high-volume states. Among the four nurses from agencies in low-volume states, three reported that the primary nurse was responsible for the development of the care plans, and the fourth reported that she generated care plan recommendations that were then approved by the physician. The nurses from the agencies in high-volume states reported having less control over their patients' care plans. Two of these three nurses reported that the care plans were developed in conjunction with or were approved by nursing supervisors. In one case, the care plan was approved by the chart review committee at the agency's home office as well. The third nurse from a high-volume state reported that the physician, not the nurse, created the care plan.
Supervisory staff appears to be more involved in the development of patient care plans in proprietary than non-proprietary agencies. Two of the four nurses from proprietary agencies reported that their supervisors and/or chart review committees were involved in the development or approval of the case study patients' care plans. None of the nurses from the non-proprietary agencies reported the involvement of such staff.
Although the physician's referral is the starting place for identifying what services a patient will receive, these original orders generally only provide a glimpse of what a patient's final care plan will include. As mentioned above, the physicians usually left decisions about the kind, frequency, and duration of care a patient should receive up to the home care nurses and therapists. Even when the physicians made suggestions regarding the kinds and frequency of services that should be provided, the nurses and therapists in six of these seven cases were allowed ample leeway to alter the plans laid out in the original referral.
Indeed, in all but one case, the services offered to the patients were different from those recommended in the original referral. One nurse commented that she does "not usually go by the original referral [as] the doctor ... may not know about the patient's other needs," having little knowledge of the patient's social and home environment. In several cases, patients were offered services that were not recommended in the physicians' original referrals. Although none of the physicians ordered the services of a social worker in their original referrals, home care nurses offered these services to three of the case study patients. Whereas physicians ordered aide services in two cases, three additional patients were offered these services by their home care nurses.
In other cases, patients were not offered all the services that the physicians had recommended. Two nurses reported that physicians sometimes write orders for services for which their patients are not eligible or that their patients do not need. Indeed, in two cases, physicians recommended services that agency personnel considered to be unnecessary. In one of the three cases in which a physician ordered PT for a patient, the physical therapist who evaluated the patient believed that there was no need for these services. In the only case in which a patient's physician ordered OT, the therapist assessed that the patient was not in need of such therapy. On a general note, one nurse reported that physicians "may automatically write down 'home health aide'" in their orders, even when their patients do not really need these services. In these situations, the nurses inform the physicians that the patients are not eligible for or do not need these services.
Nurses identified a number of factors that influenced their decisions and recommendations about the frequency with which skilled nursing services should be provided to the case study patients. Most commonly, nurses reported that the stability or instability of their patients' medical conditions was a factor considered in the decision-making process. Three nurses reported that they felt their patients, each of whom had just been discharged from the hospital, needed fairly frequent nursing visits (i.e., three times a week at the start of care) because their conditions were quite unstable. In another case, the nurse reported that she would have recommended more frequent visits than she did had the patient been more unstable.
The presence of a family support system also had an important impact on nurses' decisions about the frequency of care to provide. Two nurses specifically mentioned that they would have visited their patients more frequently if it were not for the availability of the patients' family members. Three nurses reported that a family member's ability to learn was a major influence on their decisions about the frequency with which skilled nursing visits should be provided. One nurse reported visiting the patient more frequently at the start of care than might have been necessary because the family was confused about the patient's medication regimen. Another nurse reported that her perception of the patient's ability to learn also contributed to her decisions about frequency.
Three nurses indicated that the activities they would need to perform at their skilled nursing visits helped them determine how frequently those visits should occur. In each case, the nurses suggested that they did not need to see their patients very frequently because their activities in the house would be restricted to assessment and teaching. If their patients required wound care or other hands-on treatment, the visits would have been more frequent.
Issues related to the patients' medications also were mentioned by nurses as factors considered in the decision-making process. One nurse visited the patient more frequently than she might have otherwise because he had recently been placed on a number of new medications. This new and more complicated medication regimen required the nurse to engage in immediate education of the patient and to watch the patient closely to evaluate the appropriateness of the doses and the presence of side effects. Another nurse timed her visits to occur on the three days each week that the patient's wife would administer the patient's IV medication. One nurse felt compelled to visit her patient more frequently because it was clear that he was not in compliance with his medication regimen.
Documentation of the Care Plan: Home care providers document their patients' care plans in a variety of ways. The two primary approaches to documenting patient care plans are to use nursing notes or care plan forms to record information about a patient's case. In four cases, the case study nurses indicated that their patients' care plans are documented in nursing notes, which are stored in the patients' charts. These notes document information about the patient's condition, care plan, and progress at each visit. Nurses from the other three agencies indicated that they use a specific form for documenting the care plan. At two agencies, this document -- called the "Care Plan Form" and the "Nursing Treatment Plan," respectively -- contains extensive information about the patient's medical condition, needs, treatment plan, goals, and prognosis as well as the orders for the patient. At one agency, the care plan documents also contain a checklist of activities that should be performed at each visit and a "plan of focus" for the next visit. The third agency that uses a specific form for documenting the care plan uses a "Problem List." This form is less detailed than the care plan documents at the other two agencies, containing only information about the patient's problems and short- and long-term goals. The form does not include any information about the interventions planned for the patient.
In addition to care plan documents and progress notes, the case study nurses reported additional ways in which the care plan for a patient is documented. Nurses from three agencies indicated that their comprehensive assessment tools (OASIS in two cases) represent a component of their documentation process. Two agencies use the orders for a patient as part of their documentation. A nurse from one of these agencies indicated that her agency no longer uses written care plan documents because all the needed information is contained in the orders. Discontinuing the use of a care plan form has cut down on repetitive documentation for the nursing staff. Two agencies use teaching guides as part of their care plans. These guides, copies of which are given to patients, also serve as a documented teaching plans for the nurses. One nurse indicated that her hospital-based agency has clinical pathways that often serve as documentation of the care plan for patients with specific conditions.
Communication Among Home Care Providers: One important aspect of home care is the coordination of the many care providers involved in patient care. The primary nurse is in regular contact with the patient's physician, aides, and therapists throughout the course of the episode of care. Nurses generally communicate with the patients' physicians at milestone time points in their patients' care. The nurses provide the physicians with the care plan following the start of care visit and inform the physicians of their intentions to discharge. All of the nurses indicated that they are in contact with the physicians when there are any changes to the patients' conditions or care plan. Two nurses reported that they contact physicians with information about patients' lab values. One additional nurse reported that she contacts the physician to clarify orders, to request an extension to the duration of care she had recommended in her original care plan, and to follow up after the patient's scheduled clinic visits.
Contact with the physician is nearly always indirect. With the exception of one nurse who met with her patient's physician at least once or twice a week, all of the nurses reported communicating with the physicians by leaving telephone messages with the doctors' nurses.44 One nurse commented that "you never get the doctor, never, never...when I do, I get startled!" Two of the case study nurses specifically reported that they never interacted with their patients' physicians directly. In two cases, nurses indicated that they had tried to contact the physicians multiple times about changes in patient condition or discharge plans without ever receiving a return call. One nurse lamented that, unlike hospital nurses, home care nurses have little access to their patients' physicians.
Communication between the primary nurses and the other disciplines involved in patient care appears to involve more regular and direct interaction. Nurses are in frequent contact with the aides caring for their patients. In both cases in which home health aide services were provided, the nurses did an orientation at the beginning of the aides' involvement. At one agency, this orientation is carried out either over the phone or at the patient's home. At the other agency, the orientation always takes place during the aide's first visit to the home. At both agencies, the nurse accompanied the aide on a visit to the home every 14 days. Nurses in both cases indicated that they were in contact with the aides at least weekly, and that the aides frequently called with questions or new information. One nurse indicated that, in her small agency, the communication between herself and the aides can be quite informal. She just "sees them around" the office. The other nurse indicated that aides complete a checklist of their activities at each visit and send it to the nurse once a week.
Case conferences are an important method of communication between home care nurses and other disciplines. Three of the four nurses who coordinated other disciplines on behalf of their patients indicated that they communicated with other care providers through this mechanism. At one agency, the patient's case was presented at an interdisciplinary case conference every other week. The other two nurses reported that their patients were presented at case conferences at start of care, recertification, discharge, and when problems arose. Two nurses reported that therapists and social workers inform the primary nurses of their plans of care after completing their initial evaluation visits and upon their decision to discontinue services to the patient. One nurse noted the importance of progress notes in providing a means of communication among disciplines. Another nurse identified a more informal mechanism for her communications with the agency social worker: "I sit right next to her!"
Discharge Planning: All of the case study nurses reported that discharge planning begins very early in a patient's episode of care. Six of the seven nurses indicated that they began thinking about discharge at their first visit with the case study patients. Two nurses specifically commented that a plan for discharge is included in the care plan document that is completed at the start of care assessment. As one nurse put it, home care providers "have a road map from the very beginning."
The nurses cited numerous factors they considered in assessing the case study patients' readiness for discharge. All but two of the nurses cited more than one reason they considered their patients ready for discharge. Most of the nurses (five of seven) indicated that their patients were discharged because they were medically stable. Three nurses reported that they discharged their patients in part because they had reached their educational goals in terms of their knowledge of CHF, their medications, and diets. Two nurses noted that their patients were no longer homebound. Although both nurses reported that they would have liked to keep their patients on service, they felt obligated to discharge their patients because of their homebound status. The nurses specifically noted that any further services provided to these patients would not be covered by Medicare. Two nurses each reported that their patients had become ready for discharge by virtue of the fact that their endurance had increased, they or their family members were able to manage their medications, and/or their medication regimens had stabilized (most of the case study patients experienced changes in their medications and doses during the course of their episodes of care). In determining the case study patients' readiness for discharge, the following factors were considered by one nurse each: household safety issues had been resolved, the patient had become more independent in her IADLs, the patient was able to manage diet or dressing changes, or the patient moved out of the nurse's service area.
As mentioned previously, two nurses noted that they discharged their patients because they were no longer homebound. One nurse commented on the subjective nature of determinations of homebound status. She indicated that all of the nurses in her agency have their own personal definitions of the concept of homebound. This nurse reported that the definition of "homebound" according to Medicare is that a patient leaves home infrequently, and does so only with taxing effort and assistance. Her personal definition is that a patient leaves home less than weekly, needs the assistance of a device and/or a person to leave the house, and is exhausted the next day. The other nurse who discharged her patient because of his homebound status reported that she did not consider her patient homebound because he was able to go to the doctor's office once every three weeks with the assistance of his wife. Clearly, these two nurses define this important concept somewhat differently.
The case study nurses engaged in a variety of activities in preparation for discharging their patients. Most commonly, the nurses made arrangements for their patients' continuing needs to be met. Three nurses established plans for their patients' future transportation needs by arranging with friends and family members to assist the patients in this way. Another nurse arranged for family members to help the patient with meal preparation and shopping. One nurse commented that "in home care, you try to establish the support system -- who is going to do what -- [these systems] often fall apart and the patient ends up back in home care." Two nurses made arrangements for their patients to begin attending an outpatient clinic or lab for continuing medical care or lab work. Another ensured that the IV company working with the patient was aware of the discharge and that the IV company nurses would continue to follow up with the patient. Two nurses established plans for their patients to receive non-agency nursing care after their discharge from home care (i.e., state Medicaid nurse, private nurse). One nurse provided her patient with information about arranging for private aide services after discharge.
The nurses prepared for discharge in other ways as well. Three nurses mentioned that they warn their patients about eventual discharge very early in the episode of care (two nurses talked with their patients about discharge at the start of care visit). The patients need to know that the nurse "is not going to be here forever" and that they "are going to need to be independent." One nurse indicated that she mentioned discharge at every visit with her patient.
Communicating with other agency personnel and the patients' physicians was an important part of the discharge planning process for the case study patients. Four of the seven nurses indicated that their patients' cases were presented at interdisciplinary case conferences prior to discharge. All of the disciplines involved in a patient's care, other agency nurses, and sometimes nursing supervisors and quality assurance (QA) personnel attend these conferences during which patient cases are reviewed and readiness for discharge is discussed. In addition, five of the seven nurses specifically mentioned that they prepared for discharge by communicating their intentions to discharge with the patients' physicians.
There are a number of actors who took part in the discharge planning process for the case study patients. Each of the seven nurses indicated that a patient's primary care nurse is an important player in the discharge decision-making process. However, the agencies varied in how much power is afforded to the primary nurse. At two of the seven agencies, the nurses indicated that the primary nurse has the ultimate power to make discharge decisions. One nurse commented that she "consider[s] this a nursing decision." Three other nurses reported that the decision to discharge is left primarily up to the primary nurse and the patient's physician. Two of these nurses noted that their supervisors have important influence on these decisions as well. One nurse reported that the primary nurse and the nursing supervisor are responsible for making the decision to discharge. At this agency, the branch manager or QA staff are brought into the decision-making process when the primary decision makers are in doubt about the best course of action. As mentioned previously, four of the agencies conduct case conferences as part of the discharge planning process. At these sites, all disciplines involved with a patient and other agency nurses provide input into discharge decisions.
4. Content of the Skilled Nursing Visit
Skilled care home visits are comprised of two main components: (1) assessment and (2) teaching. Each of the seven case study nurses mentioned participating in these activities at each visit with their patients. A nurse's assessment of a patient involves a careful examination of numerous aspects of the patient's condition and care plan. Assessment activities fall into five main categories. At each visit, the case study nurses assess their patients' general medical condition, mobility level, medication issues, home environment, and compliance with the care plan (see Table 5.5). Most of the nurses noted that their initial visits were longer and more involved than subsequent visits. Certain activities take place mainly or only at the start of care visit: explaining the care plan, establishing the treatment goals, obtaining the patient's medical history, and completing the start of care paperwork. In addition, the initial assessment focuses on every aspect of a patient's condition, "from head to toe," whereas subsequent assessments focus mainly on a patient's problem areas. One nurse commented that the time spent on assessment decreases as the episode of care progresses because patients tend to become more stable with each visit.
| TABLE 5.5: Activities of Patient Assessment and Treatment | |
| Assessment of General Medical Condition Vital signs (blood pressure, pulse, temperature) Weight (check weight, review weight log) Skin condition Edema Cardiovascular condition Pulmonary condition Bowel condition Homebound status Review diabetic diary | Assessment of Medication Issues Identify medication side effects Evaluate need for adjustment of medication doses Fill pill box |
| Assessment of Home Environment Utilities working Safety Cleanliness | |
| Assessment of Mobility Level Activity level Walking/transferring ability Shortness of breath/endurance Falls | Assessment of Compliance with Care Plan Medications Diet Attending scheduled doctor's appointments |
| Provision of Care Lab draws Dressing changes | |
As time spent on assessment decreases, time spent on the other major component of the skilled nursing visit (teaching) tends to increase across the episode of care. Each of the nurses indicated that teaching is one of the major activities of their visits. Nurses educate patients about their medical conditions (signs and symptoms, when they should contact the physicians), their care plans (treatment plans and goals), their medications (purposes, schedules, doses, side effects, use of the IV equipment), and diet restrictions. According to many of the case study nurses, the topics the nurses teach change across the episode of care. Some nurses indicated that they taught their patients the information of greatest necessity or new information early in the episode of care. For example, after beginning to infuse her patient with his IV medication for the first time at the start of care visit, one nurse focused on teaching her patient how to disconnect from the IV pump when his six-hour infusion was complete. Another nurse noted that she began by teaching her patient information about his new medications and conditions, and then proceeded to teach information the patient was weak on. Two nurses indicated that they changed their teaching activities toward the end of their patients' episodes of care to emphasize the information that the patients needed to know to successfully care for themselves after discharge. According to these nurses, as a patient nears discharge, it is of particular importance that he or she know the signs and symptoms for which medical treatment should be sought.
Nurses frequently commented on the need to develop rapport with their patients. They suggested that the provision of medical care inside a patient's home requires the careful fostering of a relationship between the care provider and the patient. One nurse commented that "if [the patients] don't trust you, they don't tell you anything." To this end, three of the nurses indicated that an important activity during their home care visits is simply to talk to their patients. One nurse reported that this is especially important with an elderly population: "This generation of people are not complainers, they are brave people, stoic, so it often takes a while to identify what all of their problems are."
C. Conclusions
The focus group and case study interviews were designed to address two of the key questions identified for the study:
- What is the actual practice of home health care, in terms of type, amount, and decision making (e.g., care planning, care coordination)?
- How are decisions about care made in light of Medicare coverage rules?
In this section, key findings from the focus group and case study interviews are discussed in relation to these questions.
1. What is the Actual Practice of Home Health Care?
Services Provided: Medicare home health care involves skilled nursing; physical, occupational, and speech therapy; medical social work; and aide services. Nurses are the central providers in the home health care system. The primary responsibilities of the home care nurses are to assess the patients' medical condition and needs, and to educate the patient and family about the patients' illnesses and treatment regimens. Patients' primary nurses engage in numerous other activities as well. The nurse plays an important role in determining a patient's care plan (e.g., frequency of visits, disciplines involved), managing the patient's medications, completing required forms, documenting the patient's case, organizing a support network for the patient, performing psychological counseling, and ensuring that care providers from different disciplines are "on the same page."
Care providers from other disciplines provide important services for patients in home health care. PT was provided to three of the seven case study patients to help the patients improve their strength and balance. Some patients were believed by their nurses to be too weak or unmotivated to benefit from PT.
The primary role of medical social workers is to identify community resources to assist home care patients. For two case study patients, a social worker was needed to identify resources for the patients (e.g., new housing, transportation). In a third case, the primary nurse had hoped the social worker could assist the patient with her anxiety about not being capable of caring for her dying significant other. Importantly, two of the three patients refused to accept the services of a social worker, leaving the primary nurses in the position of having to provide these services themselves.
Home health aides assisted two case study patients with showering, skin care, meal preparation, cleaning, laundry, and shopping. Aides also reminded the patients to take their medications, monitored the patients' weights, and reported changes in the patients' conditions immediately to the primary nurses. Three case study patients refused aide services, "as they often do."
Factors Affecting Services Provided: The nurses participating in the focus group and case study interviews identified a number of factors affecting services provided to Medicare home care beneficiaries. Often, elderly patients receiving home care services through Medicare are complex patients, many having been recently discharged from hospital care. According to focus group participants, patients just released from the hospital often are sicker than other home care recipients and frequently require complex or high-tech services. These complex cases involve more vigilant attention from the nurses, as well as more frequent communication between disciplines, and documentation that is more excessive.
Although the family support network is important for all recipients of home health care, a number of the focus group and case study participants noted the special importance of family members for elderly home care recipients. Patients may have great difficulty caring for themselves and may need assistance in multiple domains of their daily lives. Focus group participants indicated that they consider the availability of caregivers in their decisions to recertify or discharge patients. Family members of the case study patients commonly provided assistance with ADLs, IADLs, medication management, and were frequently involved directly in the patients' care (e.g., accepting or refusing services, attending nursing visits, weighing the patients). One case study participant commented that these patients "are just out of luck unless they have family to help them." Interview participants emphasized that some home care patients are cared for by spouses or other family members who may be as old and frail as the patients themselves.
Care Planning and Coordination: Substantial variation in the process of care planning and coordination was found among agencies in both the focus groups and case studies. The role of the primary nurse in the process of developing the patient's care plan varies from agency to agency. At some of the case study agencies, nurses reported that they have a great deal of control over a patient's care plan. Although the referring physician must approve the care plan at all agencies, several nurses indicated that the primary nurse develops the care plan and writes the orders. The physician simply approves the nurse's plan.
However, according to a number of focus group and case study participants, many agencies involve supervisors in the development of patients' care plans. They either approved the plans laid out by the primary nurses or worked with the primary nurses to jointly develop the plan. Although not definitive due to small sample size, the case study interviews suggested that primary nurses have greater control over the development of their patients' care plans in low-volume states and in non-proprietary agencies.
Agencies also differ in the procedure for documenting a patient's care plan. Most commonly, the case study nurses indicated that a patient's care plan is documented in the nursing notes or care plan forms developed by the agencies. Nurses noted that a patient's care plan can be documented through the assessment forms, orders, teaching guides, and clinical pathways as well.
Communication among care providers appears to be fairly consistent across agencies. The focus group participants indicated that the process of coordinating care for patients begins immediately at the start of care. The case study nurses reported that they generally communicate with their patients' physicians only at milestone time points in the episodes of care. Nurses communicate with physicians at the start of care and as the patient approaches recertification or discharge. In between these time points, nurses tend to contact the physicians only when changes occur in a patient's condition or treatment plan. Contact with physicians is nearly always made indirectly through the physician's nursing staff. "You never get the doctor, never, never," one nurse reported. Some of the case study nurses reported having difficulty getting return calls from their patients' physicians.
Communication between the primary nurses and other care providers is fairly regular and direct. The case study nurses reported being in contact with their patients' aides at least weekly. In addition, the nurses made home visits with the aides every two weeks. The nurses also indicated that the aides frequently call with questions or new information about a patient.
Case conferences are a main mechanism through which care providers of different disciplines stay in contact regarding their patients. Most of the case study nurses who coordinated other disciplines on behalf of their patients were in contact with those other providers at case conferences. Generally, patients are presented at conferences at the start of care, recertification, discharge, and when problems arise. In addition, therapists and social workers generally contact the primary nurse once they have developed their own care plans for a patient.
Discharge planning begins very early in the home care episode, usually at the first visit. Nurses cited a number of factors that they consider in determining a patient's readiness for discharge: patient is medically stable, the educational goals have been reached, the patient is no longer homebound, services will no longer be covered by Medicare, the patient's medication regimen has been stabilized, the patient has increased endurance, and the patient is able to manage his or her medications.
Nurses engage in a variety of activities in planning for a patient's discharge. Most commonly, nurses make arrangements for the patient's continuing needs to be met after discharge (e.g., identify resources to assist with transportation, meal preparation). Communicating with other care providers through case conferencing and other methods of interaction is an important component of the discharge-planning process.
2. How Are Decisions About Care Made In Light Of Medicare Coverage Rules?
The focus group and case study interviews provided important information about the decision-making process in home health care. Recertification and discharge decisions are based on a number of factors, including patient factors (e.g., living environment), agency factors (e.g., supervision of decision-making process), and external factors (e.g., IPS).
A lack of clarity in and failure to fully understand federal regulations has a major impact on the decision-making process in home health care. The nurses who participated in the focus group and case study interviews indicated that some of the critical concepts of the Medicare coverage rules are unclear. Specifically, nurses referred to the difficulty they and others have understanding the HIM-11, the concept of "homebound," what constitutes skilled nursing care, and what M&E is and when it can be used. One nurse suggested that "you have to be a lawyer" to understand the regulations.
Focus group and case study nurses alike reported that the definition of "homebound," a critical feature of the Medicare coverage rules, is unclear. Interview participants suggested that the definition is quite subjective. When asked what the definition of "homebound" is, one case study nurse asked "do you mean the definition of homebound, or my definition of homebound." This nurse reported that all of the nurses in her agency have their own personal definitions of this concept. Although the nurses involved in the focus group interviews differed in their interpretations of homebound status as well, they agreed that a patient who drives cannot be considered homebound. It is important to note that, according to Medicare coverage rules, the ability to drive per se does not make a patient ineligible for Medicare home health services.
Some of the focus group participants indicated that there is uncertainty in the field about what constitutes skilled nursing care. In discussing the patient vignettes, the nurses disagreed about whether the services needed by these patients represented skilled care. In particular, the nurses were uncertain whether wound care represented a skilled need. Further, it appears that nurses are not the only members of the medical community who are unclear about what constitutes skilled nursing care. Nurses reported that physicians often refer patients to home care who do not need skilled nursing services.
M&E also appears to be an elusive concept. Focus group participants' understanding of M&E differed widely from agency to agency. Some nurses indicated that M&E applied to patients with IV therapy and family members who were not able to learn the medication regimen. Other nurses suggested that M&E was appropriate only for complex patients with multiple caregivers, needing many hours of service. A few nurses even thought that M&E requires special training for nurses.
The focus group and case study interviews produced no evidence that the lack of clarity in coverage rules encourages home care providers to continue to provide services to patients who may be ready for discharge. Despite the wide variation in their understanding of the concept of "homebound," the nurses participating in these interviews did not appear to use the ambiguity of this concept to their advantage. In fact, two of the case study patients were discharged before the nurses felt they were ready specifically because the nurses no longer considered the patients to be homebound. The focus group participants reported that patients who drive cannot be considered homebound. Because of this misinterpretation of the Medicare coverage rules, these nurses may discharge patients who might legitimately be considered homebound.
Not only was there no evidence that ambiguity in coverage rules leads to the provision of unnecessary services, there was some suggestion in the focus group and case study data that this ambiguity may actually result in shorter episodes of care. One focus group participant indicated that "in a case where you might be borderline on discharging or making another visit, [her agency] would lean toward not making another visit for fear of Medicare review."
The focus group interviews produced some evidence that agencies may avoid the use of services for which the coverage rules are ambiguous. Many focus group participants appear to be uncertain what M&E is and when it can be used. During most of the focus group interviews, nurses simply indicated that M&E is not used at their agencies. Although none of the participants specifically made this suggestion, it may be that agencies have eliminated the use of M&E due to concerns that these services will not be covered. Uncertainty about the meaning of the coverage rules with regard to M&E may have encouraged agencies to avoid the practice altogether.
A number of the focus group and case study participants noted that the additional documentation required under the new federal regulations has increased the pressure on home care nurses. Several nurses involved in the focus groups indicated that they feel a sense of paranoia about the patient documentation process. Some reported that every "i" has to be dotted and every "t" has to be crossed in documenting a patient's case. If documentation is vague or incomplete, visits will be denied. One nurse reported that "it makes [her] nervous to think that what [she] writes in the notes will determine whether the agency will get paid" for her services. In the face of more careful scrutiny of the field of home health care and a lack of clarity in the coverage rules, nurses seem to prefer to discharge a patient rather than take the chance that their services will not be covered.
VI. PROVIDER PERSPECTIVES ON THE INTERIM PAYMENT SYSTEM AND CHANGES IN HOME HEALTH CARE
The study was not originally intended to assess the impact of the Interim Payment System (IPS). However, the timing of the project allowed for the acquisition and synthesis of information from several sources on how this and other policy changes have affected the field of home health care. As noted previously, the impact of IPS, as perceived by the home care industry, was examined through interviews of state home care association representatives and study agency administrators, as well as through focus group and case study interviews with home care nurses. The findings from each of these qualitative methods are summarized in this chapter.
Although these four interview methods provided valuable qualitative information regarding the effects of recent policy changes on home health care, it is important to note that the data gathered through these methods are not based on a random sample of home care providers, administrators, and state association representatives. The information that this sample of participants provided with regard to the impact of the Balanced Budget Act of 1997 (BBA) on their states and agencies thus may not be an accurate reflection of the impact that the BBA has had on home health care nationwide. Further, as noted earlier, home health nurses, administrators, and state association representatives are stakeholders in the industry and may feel negatively toward new federal policies that restrict the growth of spending on the Medicare home health benefit. Some of these individuals also may not be fully informed about the historical context and goals underpinning new policies and payment structures.
A. State Home Care Association Interviews
1. Overview of Findings
This section provides a general overview of the findings from the state home care association interviews, followed by state-specific information. Although state association representatives varied somewhat in their responses, their overall message was one of increased financial stringency under Medicare. This included not only IPS, but also related policy initiatives such as Operation Restore Trust (ORT)45 and the surety bond provisions of the BBA of 1997. As a consequence, some associations indicated a trend among agencies to provide fewer Medicare services, shift to Medicaid and managed care, and avoid high-cost Medicare patients. Agency closures, downsizing, and mergers were frequently noted, as was the perception that home care providers, particularly nurses, are leaving the field. Although definitive data on access were not obtained from these interviews, several respondents suggested that these changes have created access problems for Medicare patients (especially rural patients), resulting in the provision of fewer services than needed to those who are able to obtain care. Responses were similar between high-volume and low-volume states.
OSCAR data maintained by HCFA provide additional information about changes in the home care market as a result of the implementation of IPS and other regulatory changes. Table 6.1 presents the number of active agencies, the number of newly certified agencies, and the number of agency closures in the eight study states and nationally during 1997, 1998, and 1999.46 In 1997, the year the BBA was passed, there were 10,071 home health care agencies in the country approved to provide Medicare/Medicaid services. Nearly 9% of those agencies originally received their Medicare/Medicaid certifications in that year. Slightly over 5% of active agencies closed during 1997. In five of the eight study states, more agencies received Medicare/Medicaid certification than closed that year.
The pattern of agency certifications and closures was quite different in 1998 (the first full year of IPS) and 1999. Less than 2% of active agencies in 1998 were newly certified, whereas more than 14% of active agencies closed in that year. All but one of the study states had more agency closures than new certifications in 1998. The pattern of market changes was quite similar in 1999.
The 1998 and 1999 agency closure percentages varied considerably between and within the state volume groups. The percentage of agencies that closed was considerably higher in the high-volume than the low-volume states. However, this difference is primarily due to the large number and percentage of closures in Texas in both years. Within the low-volume group, Oregon experienced a relatively large percentage of agency closures in 1998 and 1999. In the high-volume group, Georgia experienced a fairly small percentage of closures. Thus, no clear difference in the closure pattern was evident between the two state volume groups.
| TABLE 6.1: Home Health Market Changes in the Eight Study Statesa | |||||||||
| 1997 | 1998 | 1999 | |||||||
| Total # Active Agencies | New Agenciesb (% of total) | Agency Closures (% of total) | Total # Active Agencies | New Agencies (% of total) | Agency Closures (% of total) | Total # Active Agencies | New Agencies (% of total) | Agency Closures (% of total) | |
| LOW-VOLUME STATES | |||||||||
| Minnesota | 261 | 8(3.1%) | 6(2.3%) | 263 | 6(2.3%) | 9(3.4%) | 260 | 2(0.8%) | 6(2.3%) |
| New Jersey | 55 | 2(3.6%) | 0(0.0%) | 57 | 1(1.8%) | 3(5.3%) | 55 | 0(0.0%) | 1(1.8%) |
| Oregon | 92 | 2(2.2%) | 5(5.4%) | 89 | 1(1.1%) | 18(20.2%) | 72 | 1(1.4%) | 12(16.7%) |
| Pennsylvania | 378 | 16(4.2%) | 15(4.0%) | 379 | 11(2.9%) | 32(8.4%) | 358 | 6(1.7%) | 25(7.0%) |
| Total for Low-Volume States | 786 | 28(3.6%) | 26(3.3%) | 788 | 19(2.4%) | 62(7.9%) | 745 | 9(1.2%) | 44(5.9%) |
| HIGH-VOLUME STATES | |||||||||
| Georgia | 85 | 20(23.5%) | 9(10.6%) | 96 | 5(5.2%) | 2(2.1%) | 99 | 2(2.0%) | 2(2.0%) |
| Massachusetts | 202 | 12(5.9%) | 16(7.9%) | 198 | 2(1.0%) | 23(11.6%) | 177 | 2(1.1%) | 22(12.4%) |
| Mississippi | 107 | 3(2.8%) | 13(12.1%) | 97 | 0(0.0%) | 15(15.5%) | 82 | 0(0.0%) | 17(20.7%) |
| Texas | 1,687 | 338(20.0%) | 104(6.2%) | 1,921 | 26(1.4%) | 398(20.7%) | 1,549 | 34(2.2%) | 463(29.9%) |
| Total for High-Volume States | 2,081 | 373(17.9%) | 142(6.8%) | 2,312 | 33(1.4%) | 438(18.9%) | 1,907 | 38(2.0%) | 504(26.4%) |
| National | 10,071 | 875(8.7%) | 532(5.3%) | 10,414 | 187(1.8%) | 1,518(14.6%) | 9,083 | 161(1.8%) | 1,314(14.5%) |
| |||||||||
2. State-Specific Findings
This section summarizes, for each state, the comments made by state association representatives with regard to changes that have occurred in the field of home health care as a result of the implementation of IPS. Although the data are presented here by state volume group, the general trends were similar across all states. Quantitative statements by respondents were not verified or checked against any other data sources. Therefore, they should be considered primarily a reflection of the views on IPS that are held by provider associations and their members.
Low-Volume States: Minnesota home care agencies have adjusted to reduced Medicare revenues, increased administrative expenses due to OASIS data collection and IPS, and the pervasive attitude that the industry is full of fraud and abuse. According to the state association representative, a major impact that IPS has had in rural parts of Minnesota is a reduction in access to care. There have been some agency closures, but mostly mergers and downsizing. In addition, there is a general trend across the whole state to provide fewer Medicare services. This reduction is occurring in home care agencies, hospitals, and county boards. When possible, home care agencies are billing Medicaid rather than Medicare. Agencies are refusing to admit certain types of patients, especially Medicare and/or long-stay patients. Minnesota residents appear willing and able to pay privately for services. The number of home health licenses that are not Medicare certified is increasing, as is the number of new assisted living facilities.
Compared to other states, New Jersey appears to be impacted less strongly by IPS. According to the state association representative, there are staff shortages due to layoffs at the middle management level. However, there has not been a large number of agency closures. It has been difficult to hire home care aides due to the strong economy in New Jersey. Some agencies are not accepting certain types of patients (e.g., those with high-technology needs, severe wounds, those requiring more than one visit per day and/or longer than average visits). The state has a Medicare maximization program; therefore, cost shifting to Medicaid is not occurring.
Although Oregon agencies are predominantly hospital-based, most of the agencies that have closed in Oregon have been freestanding proprietary agencies. Oregon is considered at low risk for fraud, and ORT has not had an impact on agency closures. Hospital-based agencies have managed to remain open and avoid problems with patient access, although if these agencies were to close, rural patients might have a difficult time obtaining home care services. According to the state association representative, most patients in Oregon needing home health care receive some visits, although perhaps not as many as they need. Currently, only a few agencies (mostly freestanding proprietary agencies) are turning away long-term and/or high-utilization patients.
Agencies in Oregon are challenged to reduce overhead administrative costs due to the new per-beneficiary and per-visit cost limits. Oregon's historically low utilization has caused increasing difficulty in absorbing costs over a small number of visits. The significant presence of managed care in Oregon also has caused agencies to downsize and cut costs.
The market for home care staff is tightening and there is a perception that nurses are leaving home care for other industries. This movement of nurses out of home care may be in part due to the increase in the burden of paperwork. Home care agencies have had difficulty retaining nurses hired from hospital settings because of the heavier documentation burden in home care.
Since 1997, Pennsylvania has seen a substantial number of agency closures. According to the state association representative, the average home care agency is unable to stay under cap limits and will lose $275,000 under IPS, forcing agencies to find ways of cutting losses. Twelve thousand jobs in Pennsylvania were lost from downsizing alone, not counting agency closures. No Pennsylvania agencies were surveyed as part of ORT, and only four Pennsylvania agencies have "been in trouble" with HCFA over the past 13 years.
The average number of visits in Pennsylvania in 1997 was 44, compared with 72 nationally. The state association representative reported that visits in the state are down 30%, and suggested that patients may be experiencing difficulty gaining access to home health services. Providers do not take high-need and long-term patients, reducing access to care for such patients. In addition, agencies are attempting to rely on state programs in which access has become restricted as well. New state programs, in development before IPS, have yet to be implemented.
In addition to IPS, agencies have struggled with other recent policy changes, such as the surety bond regulation, the implementation of OASIS, and the fifteen-minute billing requirement. According to this state association representative, "There is just a parade of regulatory burdens of greater or lesser degree of merit that agencies have to bear when reimbursement is being decreased."
High-Volume States: In Georgia, the biggest impact of IPS has been on patients living in rural areas. The Georgia state home care association representative indicated that home care was serving as a stopgap to prevent medium- to long-stay patients from being admitted to nursing homes. Now, those same patients are going to high-cost modalities of care such as the emergency room and long-term care facilities. Other patients are not getting the care they need.
Home care agencies are trying to shift costs to Medicaid; however, the program does not have sufficient funds. Georgia has a community care Medicaid waiver program but it is operating at nearly full capacity. There are not enough slots remaining to absorb patients who have been discharged from home health care. Agencies have reduced their workforce by a third. The Georgia Association of Home Health Agencies has closed its Atlanta office, laid off its executive director, and experienced a significant cut in membership.
At the same time that agencies in Massachusetts have been adjusting to the new payment system, they also have been recovering from ORT. The state association representative noted that a large number of closures and mergers has caused some hospital discharge staff to experience difficulties in referring patients to home care agencies. There is concern that if Medicaid reimbursement rates do not increase or Medicare policy does not change, more agency closures will occur.
The state association representative stated that referrals to personal care services have increased but that patients who have received the maximum allowable personal care services through the state and who do not qualify for Medicare services are "falling through the cracks." It is unclear what is happening to this group of patients with respect to receiving assistance. Beneficiaries are unwilling to purchase private pay personal care services since they expect the Federal Government to provide that care. Home care agencies are putting more emphasis on educating family caregivers so that they can play a larger role in providing care.
The state has a Medicare maximization program and, therefore, is not experiencing cost shifting to Medicaid. Because Medicaid reimbursement rates are lower than Medicare reimbursement rates, agencies are motivated to obtain payment from Medicare. In addition, because eligibility requirements are the same for Medicare and Medicaid, a patient who does not qualify for Medicare services also will not qualify for Medicaid services. If cost shifting is occurring, it is happening in hospitals.
The state association representative from Massachusetts expressed that many home care agencies are operating at a loss and are using endowments in order to remain in operation. Before the BBA went into effect, home health aides were one of the fastest growing classes of workers in the state. However, as the Massachusetts economy continues to strengthen, it is becoming more and more difficult to attract home health workers. Agencies are competing with department stores and the fast food industry for home health aide staff.
Medicare recipients are confused about the Medicare home care benefit. Although the services and coverage rules have largely remained the same, the reimbursement rate has dropped and therefore, the volume of services has decreased. The lack of public awareness regarding this policy change has left home health agencies with the responsibility of educating patients about changes in policy. According to the state association representative, patients are not aware of recent regulatory changes affecting home health agencies and think that the decrease in services is driven by profit.
The state of Mississippi has not experienced a large number of agency closures. However, some branch offices have closed and/or declared bankruptcy. According to the Mississippi association representative, patients with chronic conditions (e.g., stroke, paraplegia) are reaching the per-beneficiary limit and are not getting all of the services they need.47 For many agencies, there are not enough short-term patients to offset the costs of long-term patients. As a result, according to the association representative, agencies are not accepting very sick patients. Because Medicaid funding is limited and the program approves few visits, agencies have not attempted to shift costs from Medicare to Medicaid.
The Texas home care association representative indicated that the state has experienced dramatic changes in the delivery of home health care. There has been a large decrease in the number of parent and branch home care agencies, particularly in rural areas. Prior to the BBA going into effect, there were 18 counties with no home care agencies and less than six counties with only one agency per county. According to the association representative, as of July 1999, there were 43 counties in which no home care agencies were located and 53 counties in which only one agency each was located. The majority of counties that are underserved are in the panhandle and western parts of Texas. There is one county in western Texas that has 350 Medicare beneficiaries. The county covers 6,000 square miles and has not had a home health agency for two years. All of the agencies in surrounding counties have closed as well. Many beneficiaries in rural areas no longer have choices among home health agencies, since at most there is only one agency serving an area. Anecdotal information suggests that the census in nursing homes located in the panhandle and western part of the state has increased, but that the facilities are unable to keep up with the demand.
The Texas association representative suggested that therapy services for rural patients may have become more limited under the tighter reimbursement of the IPS period. The provision of care to rural patients is particularly challenging in Texas, a large state with a sizable rural population. The respondent noted further that therapists have been unwilling to drive long distances under the current reimbursement system. Thus, needed therapy services often are not provided. Patients are confused about why they are not getting services for which they are eligible.
Although Texas has one of the largest home and community-based waiver programs in the country, the funding is capped. From August 1998 through June 1999, enrollment in the program was closed and no beneficiaries were enrolled. Currently, the program serves approximately 23,000 people but there are approximately 9,000 people on the waiting list.
B. Administrator Interviews
Interviews were conducted with the administrators of 54 of the 56 study agencies in order to collect information about how home health practice patterns have changed in response to IPS.48 This section of the report summarizes the interview findings. The findings are presented under subheadings that correspond to the interview questions as they were asked of the agency administrators. (Chapter 2 contains a list of the questions asked during the administrator interviews.) To the extent possible, the qualitative findings were compared between the high- and low-volume states and between proprietary and non-proprietary agencies. (No comparisons were made between hospital-based and freestanding agencies, due largely to the similarities in responses across all agencies, which are described in the following discussion.)
1. How Has IPS Affected Your Administrative and Staffing Practices?
Agency administrators in all ownership and volume categories reported that IPS has affected the administrative and staffing practices their agencies. The changes most commonly reported are reductions in operating expenses and staff (administrative and clinical). Those agencies least affected by IPS either made changes just prior to IPS or are still not prepared for IPS (e.g., one administrator did not yet know the per-beneficiary limit for the agency). The following subsections of the report describe the findings from the administrative and staffing practice questions that were included in the interview protocol. These questions focused on approaches that agencies might take in an effort to cut costs or increase non-Medicare revenues in response to tighter Medicare fiscal constraints.
Using Licensed Practical Nurses (LPNs) Rather Than Registered Nurses (RNs): Agencies in all categories reported that they are not using licensed practical nurses (LPNs), primarily because LPNs cannot do OASIS assessments, have limited clinical roles, and require supervision. For these reasons, agency administrators stated that it is not cost-effective to hire LPNs or to keep them on staff. Agencies that had LPNs on staff are reassigning them to office positions and not filling position vacancies. Unlike other agencies, administrators from a few rural agencies stated that LPNs are not available in their area and that they might consider hiring one or two to do follow-up visits if they were available.
Productivity Standards: Approximately equal numbers of agency administrators reported increasing productivity standards as those that reported no change in standards. This finding is consistent across agency categories. The average productivity standard quoted is approximately five visits per day. High-volume proprietary agencies require approximately seven visits per day. Administrators who reported no change in standards often stated that they had increased productivity standards at their agencies prior to the implementation of IPS and therefore did not need to make any further changes. Non-proprietary agencies in public health settings (such as county health departments) did not increase standards because nurses have various teaching responsibilities and it is difficult to enforce fair standards for all staff.
Agencies that have increased standards have used a variety of strategies to decrease office time: requiring staff to call in for pre-approval of overtime, using peer assessments of productivity, adjusting productivity standards on a daily basis, and using point of service computer systems. Administrators from the proprietary agencies in high-volume states reported that productivity is constantly monitored and all staff members are carrying a heavier workload than they once did. One administrator reported that increasing productivity standards at this time represents a "catch 22" situation because OASIS implementation requires more time to complete paperwork.
Unexpectedly, administrators from two agencies reported lowering productivity standards. A non-proprietary agency in the low-volume state group lowered productivity standards during OASIS implementation, but now standards are back to the same level. A proprietary agency in a high-volume state lowered productivity standards on a more long-term basis. This particular agency has been unable to recruit experienced bilingual home health nurses and, therefore, has hired nurses with no home health experience. For this agency, maintaining quality bicultural/bilingual care remains a priority above productivity standards and documentation deadlines.
Standardized Care Plans: The use of standardized care plans is mixed across the state volume and agency ownership categories. Administrators from most proprietary agencies in high-volume states reported using standardized care plans. Changes have not been made to these care plans as a result of IPS. However, a few such agencies do not use care plans at all and a few others use teaching guides but not care plans. There are no strong themes represented among the non-proprietary agencies in either the low-volume or the high-volume states. The responses from the administrators of these agencies were mixed with respect to use of care plans; some agencies use them, others do not. However, these agencies generally use care plans less frequently than do high-volume proprietary agencies. Few of these agencies have made changes to their care plan protocols as a result of IPS.
Contracts with Managed Care Organizations (MCOs): The extent to which agencies have contracts with MCOs appears to vary by agency ownership and state volume. These differences are summarized by category below.
- Proprietary Agencies in High-Volume States: Proprietary agencies in high-volume states are increasing managed care contracts as a result of IPS. They are seeking and obtaining more contracts in order to have a diversity of payers. Administrators from some agencies reported wanting to decrease their Medicare caseload and to increase private payers. The only exceptions are the proprietary agencies in high-volume rural southern states, where managed care contracts are not available.
- Non-proprietary Agencies in High-Volume States: These agencies generally do not have contracts with MCOs and this has not changed due to IPS. The administrators of these agencies stated that they receive less reimbursement per visit from managed care and that working with managed care companies is very time consuming.
- Proprietary Agencies in Low-Volume States: The proprietary agencies in low-volume states also do not have many MCO contracts, but they are split equally in their desire to obtain such contracts. Some agencies are actively seeking contracts, whereas others are not.
- Non-proprietary Agencies in Low-Volume States: These agencies have contracts with MCOs, but these contracts have not changed due to IPS. A few of these agencies are trying to obtain more MCO contracts, and a few others are trying to renegotiate their contracts. Administrators from these agencies also noted that working with MCOs is problematic with regard to quality of care and reimbursement.
Administrative Costs: Administrators of agencies in all state volume and agency ownership categories reported making significant cuts in administrative costs and "doing more for less." These cutbacks include staff decreases, hiring freezes, decreases in salaries and benefits, reduced (or eliminated) mileage reimbursement, cuts in continuing education and staff training, reduction in overhead expenses, and merging of administrative positions (i.e., "wearing ten different hats"). The administrator of one high-volume proprietary agency reported a 25% staff decrease. Some agencies can no longer afford to maintain JCAHO certification and most agencies are no longer providing supplies to patients. Although decreases in administrative costs have occurred in all categories of agencies, administrators of a few low-volume non-proprietary agencies noted that they have not cut clinical staff. This, however, does not appear to be true for the majority of agencies.
Billing/Accounting: Few of the agencies in the four categories reported a substantial change in billing/accounting practices. Of those that have made changes, some have installed or upgraded their computerized billing systems, and others are spending more time on cross-checking accounting data with back-up documentation. One administrator said this cross-checking process has been a "Goliath." A few agencies have restructured their staff (added or deleted positions), and several agencies noted that incremental billing was very problematic when it was required. In contrast to most of the administrators' comments, one administrator reported that the changes resulting from IPS have been good for the agency and have enhanced efficiency with authorization and verification.
2. In What Ways Has IPS Affected the Structure of Care That You Provide?
Types of Patients: The majority of home health agencies are seeing more patients with complex and acute care needs since the implementation of IPS. According to the administrators interviewed, patients are frequently discharged from the hospital sooner than they once were and many of these patients require complex acute care, often with specialized technology. Some home health agencies are choosing not to accept these patients, whereas most agencies are committed to not refusing care to anyone. According to the administrators of agencies that do not refuse care, agency closures in rural areas often result in special needs patients who must be seen at long distances.
As mentioned above, although the majority of agencies in all subgroups do not refuse patients, there are a few agencies that do report refusing service to long-stay patients, wound care patients, and patients that require more than one visit per day. Some of these agencies also refuse patients who require complex care involving specialized technologies. There is no evidence from the interview data that certain types of agencies are more likely to refuse care.
The agencies that accept all referrals are experiencing other changes in their case mix. These changes differ by state volume group, as summarized below.
- Agencies in High-Volume States: Administrators from agencies in high-volume states (both proprietary and non-proprietary) report that they do not refuse patients regardless of cost, acuity, or required visit intensity. However, these agencies are seeking a balance of short-stay and long-stay patients and are working with physicians to improve their referral case mix, including targeting physicians and clinics with short-stay patients. Some agencies in the high-volume states have had a decrease in their overall census since the changes in venipuncture coverage. Administrators from other non-proprietary agencies in high-volume states are concerned about financial losses incurred when their agencies exceed their per-beneficiary limits and per-visit cost limits.
- Agencies in Low-Volume States: Administrators of agencies in the low-volume states reported receiving complex patients that have been turned away by other agencies or that have been discharged early from the hospital. Given the changes in the nursing home industry, it also has become more difficult for these agencies to place patients in long-term care facilities. Some agencies are working with hospital social workers to improve assessment of patients for nursing homes. Other agencies are cutting back on the number of chronic patients they will admit and are referring more patients to waiver programs. The administrator of one low-volume non-proprietary agency expressed concern about going out of business due to financial losses incurred from treating chronic and complex patients.
Finally, several agencies across all ownership and volume categories appear to be experiencing changes in the referral patterns of home health patients from physicians. Some agencies have had an increase in referrals from new physicians with whom they have never before worked. These agencies do not necessarily accept these new referrals, particularly if the physician does not refer short-stay patients. Other agencies report that physicians do not refer patients to home health as often as they once did because the physicians are frightened by HCFA warnings regarding fraud and abuse or they do not think the patient will be accepted by the home health agency.
Geographic Location of Patients: Most agencies in all subgroups have maintained their geographic service area. Of those agencies that have made changes to their geographic area, some have decreased it due to increased mileage expenses and are no longer serving long-distance patients. Other agencies have increased their coverage areas in order to serve rural patients who are no longer served by other agencies. The administrator of one such agency reported that if a nurse travels a long distance, the visit often is much longer than average, especially just before a weekend. In this way, the shifts in geographical coverage may result in changes to home health visit intensity. However, it is unclear from these data if this pattern is widespread or if access to home health care for rural patients has been significantly affected at this time.
Types of Visits Provided (e.g., Aide vs. Skilled): Administrators of agencies in all subgroups report providing fewer aide visits and more social work visits than they did prior to the implementation of IPS. As noted below in the discussion of alternative services, this escalation in the provision of social work services likely results from an increased focus on identifying community resources for patients. In addition, all agencies, except high-volume proprietary agencies, report a decrease in PT visits (high-volume proprietary agencies have increased the number of PT visits). Most agencies continue to provide the types of services that patients need and emphasize that patient care remains their priority. However, one low-volume non-proprietary agency no longer provides services requiring complex technology.
Content of Visit: Agencies in all subgroups reported either a greater emphasis on teaching and care coordination or no change in the content of visits. Many administrators stated that helping the patient achieve independence is more of a focus now and that safety and medication management issues are addressed early in the episode of care. Teaching and coordination activities are intensified early in the episode of care, a process that was described as "cramming" and "concentrating" services in the first few visits with a patient. Agencies also are getting families involved in caregiving earlier in the episode. Many administrators reported that families are willingly taking on these increased responsibilities.
Volume of Visits: The total volume of visits provided has decreased across all subgroups. The patterns associated with this decrease include reduced referrals from physicians, decreases associated with loss of patients who need only venipuncture services, reduced aide visits, and concentration of skilled nursing visits early in the treatment episode. Most administrators report that this decrease is distributed across all types of patients. However, at one high-volume proprietary agency, visit volume has decreased for chronic patients, but increased for acute patients.
Length of Stay: Length of stay in home health has decreased for agencies in all subgroups with the exception of a few agencies in each category that have had no change in episode length. The administrators that reported no change in length of stay usually also stated that they have enough short-stay patients in their case mix to offset the long-stay patients. Otherwise, the majority of administrators reported decreases in their lengths of stay, reductions that appear to be distributed across all types of patients with the exception of two proprietary agencies. Administrators from these two proprietary agencies reported reduced length of stay only for chronic patients. Some administrators reported being concerned that patients are sometimes discharged too soon from home health care and that this might result in increased rehospitalizations or readmissions to home care.
Intensity: As discussed in Chapter 3, the average number of visits per patient decreased in both high- and low-volume states following the implementation of IPS (see Table 3.1). Although the percent of reduction in the average number of visits per patient was only slightly larger in the high- than the low-volume states, agency administrators from the high-volume states reported greater changes in the intensity of services provided (number of visits per week) than did their counterparts in the low-volume states. According to their administrators, most agencies in the high-volume states are providing fewer visits per week and providing visits earlier in the treatment episode. These agencies also have increased care coordination activities to determine the patient's individual needs for care and services. Administrators in low-volume states reported that visit intensity has not changed greatly at their agencies and that they continue to base the number of visits provided on patient needs. However, these administrators reported that their agencies provide more visits earlier in the episode and provide more visits per week after a patient returns home from a rehospitalization.
Alternative Services: Study agency administrators reported having increased patient referrals to community resources for care and homemaking services. This trend was apparent across all categories of agencies, but was particularly pronounced for agencies in high-volume states. These agencies have increased time spent coordinating care, use more community resources, utilize social work services earlier in the treatment episode, and work more closely with physicians to develop alternative strategies for patients. Agencies in low-volume states also have begun to involve social workers and community resources more heavily, although they already were using alternative resources fairly extensively prior to the implementation of IPS.
3. How Have the Reduction in Visit Cost Limits and the New Per-Beneficiary Limits Specifically Affected Your Agency?
The responses to this question in many ways echo the responses to the previous questions and no new issues were raised. However, administrators' responses to this question emphasize the financial impact of IPS. Many administrators discussed cash flow problems, payback plans, anticipated future losses, and the need to become more cost efficient. In addition, non-proprietary agencies in both volume groups are trying to decrease the number of repeat patients because the per-beneficiary limits are problematic, especially for agencies in low-volume states. On the other hand, administrators from proprietary agencies in the high-volume states reported less difficulty with the per-beneficiary limits and more concern with staying under the per-visit cost limits.
4. How Is Your Agency Preparing for Prospective Payment?
The responses to this question were very specific to each agency but there were four common themes across all categories of agencies:
- Increasing the use of standardized care plans for prospective payment,
- Continuing to monitor current volume and costs in preparation for implementation of PPS,
- Increasing staff education regarding policy issues, and
- Waiting to prepare for PPS until more is known.
Administrator attitudes about PPS are mixed. Some are looking forward to PPS and think that it will be an improvement over IPS. Others are pessimistic and fear that PPS could put their agencies out of business. The following are some examples of the variety of perceptions expressed by the administrators regarding PPS:
- "We are trying not to panic."
- "I can't do anything. I will do what I have to do, but am not doing anything in particular now. We will be okay because we don't provide excessive services."
- "I'm not sure if PPS went into effect tomorrow that we would make it."
- "We're as lean and mean as we can get. Home health is not as fluffy as it used to be."
- "The BBA overreacted. The industry needed some changes, but most people did not understand the impact of BBA. Now it's like turning a battleship around."
- "PPS might be an improvement and provide more opportunity to plan."
C. Focus Group Interviews
At the beginning of each focus group interview, participants were asked how the field of home care has changed during their years in practice. Many of the responses to this question were not specific to IPS. Nurses reported important changes in the following five areas: (1) case mix, (2) patient education, (3) caregiver education, (4) goals of patient care, and (5) quality of care.
1. Case Mix
Several factors affecting agency case mix already have been noted. In particular, participants reported that patients admitted to home care are sicker and more complex than they once were. Many patients have acute problems or persisting active symptoms of their disease. Patient complexity has increased, with many patients requiring high-technology treatment (e.g., advanced wound care, IV administration of drugs with increased risk of complications and side effects, chemotherapy, chest tubes, and the operation or management of equipment with risk for patient injury or complication). Because of this increase in the number of patients with high-tech needs, there has been an increasing need for nurses with high-tech skills. Nurses also reported that these complicated patients require more immediate care and attention.
Participants from all agencies suggested that home care patients are sicker than they once were because they are discharged from hospital care earlier than in the past. Nurses from one agency reported that hospital social workers, who are responsible for coordinating hospital discharge to home, may not be well informed about the patients' conditions and needs. Participants at two of the focus groups suggested that patients often are discharged without proper self-care instructions and are not prepared to be at home.
2. Patient Education
According to the focus group participants, patient education is an important part of home health care. Nurses from six of the eight agencies confirmed that patient education has become increasingly important, particularly education concerning medication management. The problem-oriented teaching that is necessary for complex patients is especially detailed and time-consuming. Despite the increase in the importance of education, participants suggested that their ability to provide adequate and appropriate teaching has declined in recent years. As stated previously, participants indicated that they are attempting to teach patients with increasingly complex needs in a shorter period of time than in years past. Nurses at one agency suggested that insurance companies (including Medicare HMOs) do not allow home care for the duration necessary for nurses to provide instruction about complex conditions and treatment regimens. Historically, nurses often repeated their teachings to ensure that patients gained a full understanding of the information provided. However, because of shortened episode lengths, nurses reported that they must try to educate their patients quickly, often teaching the entire disease process in a single visit.
The focus group participants suggested that hospitals also struggle to educate their patients. One nurse suggested that even a normal, non-hospitalized person requires teaching up to six times before information is retained. In some situations, a patient's hospital discharge occurs before he or she is able to remember all that was taught. One nurse noted that hospitals are trying to do a better job of educating patients, but that some patients are still missed.
The focus group participants had particularly strong sentiments regarding the teaching of elderly patients. Many noted that it can be especially difficult for elderly patients, as well as their often elderly caregivers, to learn and retain information about complex medical conditions, medications, and treatment regimens. One participant expressed great frustration with the need to educate patients quickly by saying, "Giving a compromised senior citizen a dissertation on their disease in one sitting, asking if they understand and documenting they verbalized understanding....they don't even know what they had for breakfast."
3. Caregiver Education
All participants reported that the involvement and education of family caregivers is an important focus of their practice. Participants noted that family members try to help elderly home care patients, but that they often are busy and may not be available or able to learn about the patients' conditions and needs. Even when family members are available, some patients do not want to rely on their families for assistance.
The focus group participants suggested that they often do not have enough time to get to know and instruct patients' family members, especially in the cases of more complicated patients. Participants believe that payers do not allow them the number of visits they need to teach caregivers, who are often elderly themselves, how to manage technically difficult wound care and complicated IV therapies that may have potentially serious side effects. The need to educate caregivers quickly about complicated treatment regimens was equated by one nurse with elder abuse. Other nurses provided examples of cases in which they felt they did not have enough time to educate caregivers properly. One nurse spoke of an 85 year old woman who had to be taught how to manage her husband's IV therapy. Another nurse recounted the story of having to teach an elderly woman how to administer adrenaline in the event that her spouse had a reaction to his intravenous antibiotic. Several nurses emphasized that some patients are themselves caregivers for other ill family members. With regard to hypothetical patient vignette #2 (Mr. Lucas), it was suggested that diabetic ulcers rarely heal in 45 days and nurses would have to get families involved immediately. (The patient vignettes discussed at the focus groups are presented in Appendix B.) The family would be told at the admission visit that they must find someone willing and able to take over the wound care as soon as possible.
4. Goals of Care
Nurses from all of the agencies reported changes in the goals of care. Participants described how case mix, payer source, reductions in staff, and documentation requirements have shifted the focus of care. Many felt that paperwork has overshadowed patient goals. Nurses from all agencies were outspoken that the goal of care is to "get in and get out," especially if a patient is considered stable. One nurse even suggested that it "seems like we're pushed to say someone is stable."
Many providers are initiating more services at the time of admission than in the past for the purpose of identifying ancillary services to provide for their patients' needs. Visits are increased early in an episode in an effort to get all services the patient needs in place, especially medication management education. The underlying goal is to promote the transition out of home care. If home health aide services are needed, the goal is to move the patient to community programs, waiver programs, or private pay as quickly as possible. Families become involved early in care planning and care provision activities in order to promote a quick transition out of home care. Families are warned that the patients' nurses will be available only for a short time and that other caregivers will have to help the patient.
Some participants felt that financial concerns have become a more important factor in home care than patient goals. As one participant stated, "You work hard to get clients taken care of because the money's going to be cut off fast. It's cut off anyway, well or not, dead or alive." Focus group participants at one agency felt relieved to have state waiver programs to which they can refer patients. For them, transfer to waiver programs is a common goal. At other agencies, discharge to community resources or private pay is the goal.
When examining Mrs. Smith's case, participants stated that discharge planning would begin immediately upon admission. This planning would involve trying to find someone other than home care providers to help with the patient's needs. Participants suggested that they would only attempt to address Mrs. Smith's major acute problems. "The goal is to have the patient be well and independent. The longer you're in there, the more dependent they become."
Some nurses reported that, in the past, patients such as hypothetical patient Mr. Lucas often received home care for more than two years. Diabetic goals of care were to draw fasting blood glucose levels, pre-fill insulin syringes weekly, check morning glucose monitoring, and administer insulin. The goal of care was to maintain the patient, keeping him or her stable and out of the hospital. Nurse visits continued and were justified until the patient's wounds were healed and did not recur. The presence of a willing and able family member (or other caregiver) often influenced the frequency of the services provided in the home. Nurses indicated that there has been a shift in the treatment of patients such as Mr. Lucas. The goal of care now focuses to a greater degree on increasing family involvement and coordinating alternative resources to assist the patient to become independent and ready for discharge.
5. Quality of Care
Participants perceived a change in the quality of home care. They stated that quality of care increasingly is influenced by non-medical people (e.g., insurance company personnel). Participants expressed frustration that people without clinical experience often are in a position to provide home care agencies with rules and guidelines for patient care. According to the focus group participants, managed care case managers often rely on information gleaned from voice messages and phone conversations to make decisions about authorizing visits. Participants felt that home health quality of care has been negatively affected by such procedures.
Many of the focus group participants suggested that ongoing home care could prevent costly hospitalizations. Many of these nurses believe that agency and regulatory factors often require nurses to discharge patients before they are ready. Premature discharge, they believe, contributes to a cycle of rehospitalizations and readmission to home care. The participants reported feeling helpless, that their hands are tied.
Participants also felt that they are unable to spend enough time with patients and families due to financial pressures. One participant stated, "You don't have time to help them, you're rushing people. Dollars have changed. Medicare has gotten so strict, it's very unusual for anyone to recertify. It's a colder environment and worse for seniors."
At one agency, the focus group participants were nurse specialists with advanced education/certification in the care of CHF patients. These nurses reported that their productivity requirements have increased dramatically and that their patient visits have become more complicated. Further, they reported that they must now accomplish more in fewer visits, and that their patients have little opportunity to receive the quality of care these specialists are capable of providing.
D. Case Study Interviews
To obtain provider perspectives on changes that have occurred in home health care as a result of federal policy changes, the case study nurses were asked to identify how the practice of home care has changed in their agencies as a result of new federal policies and regulations, such as the implementation of IPS.49 The case study nurses perceived several changes in the practice of home care (see Table 6.2). Generally, these direct care nurses tended to have little exposure to the financial and policy aspects of home care, and therefore often were unable to identify the causes of these changes. When nurses specifically tied these changes to federal policies, this is indicated.
The case study nurses identified a number of ways in which the practice of home care at their agencies has changed in recent years. Two nurses indicated that their agencies have instituted cost saving measures. One agency has closed branch offices, discontinued incentive and yearly bonuses, cut the mileage reimbursement rate, and increased nurse productivity standards. This nurse indicated that her agency had been preparing for IPS for the past three years and had been losing money for several years. She reported that "It has been a very difficult last three years with all the downsizing and rearranging. Changes, changes, changes. We are all saying prayers." Another agency has developed a case management system for tracking patient costs as a result of IPS. When patients are referred to this agency, a case manager estimates how much the patient will cost the agency. If the cost is over a certain "goal" value, the agency may refuse the patient.
| TABLE 6.2: Recent Changes to Home Health Care |
| Cost-Saving Measures |
| Closure of branch offices Discontinuation of staff bonuses Reduction in mileage reimbursement Increase nurse productivity standards More careful tracking of patient costs Greater scrutiny of patient medical status prior to admission |
| Changes to Home Care Nursing |
Provide less nursing care Increased documentation requirements Increased pressure on RNs
|
| Changes to Agency Personnel |
Staffing Cuts:
Decreased availability of aides Many nurses have quit home care |
| Consideration of Cost and Coverage in Decision Making about Patient Care |
| Decisions are based partially on coverage Perception that some patients are discharged too early |
| Changes to Patient Care |
Fewer patients recertified Refusal of high-need patients:
Refusal of patients in need of maintenance care:
|
| Impact on Patients |
| Venipuncture regulation is difficult for patients Patients put in nursing homes who do not require nursing home care Hard for patients to get medications without coverage |
Nurses noted a number of changes to home care nursing. Although nurses from two agencies indicated that the services provided to patients have not changed since IPS went into effect, a nurse from another agency indicated that patients are provided with less nursing care than they once were. Two nurses commented on the increase in the paperwork they must complete for each patient. When asked what they spent the most time doing when they were working on these cases outside of the patients' homes, three additional nurses indicated that they spent most of their time completing paperwork and documenting the cases. Three nurses suggested that the changes in home care have placed increased pressure on agency nurses. One nurse noted that the "hurry to discharge" patients leaves nurses feeling uncertain about their patients' readiness for discharge. Nurses are left wondering "was I too hasty?" Two nurses suggested that the need for more thorough documentation of patient cases puts pressure on the primary care nurses. One nurse noted that the new federal policies "are probably more cost-effective, but definitely double the paperwork and double the stress." Another nurse noted that "it makes [her] nervous to think that what [she] writes in the notes will determine whether the agency will get paid" for her services. Two nurses also noted that home care nurses spend more time than in the past requesting needed services from HMOs and Medicare. One of these nurses lamented that home care nurses can no longer "just talk to the doctor and go from there."
A few of the case study nurses commented on changes in agency personnel in the recent past. Nurses from two agencies indicated that there have been lay-offs at their agencies. In one case, a large number of administrative and an entire level of management staff have been fired. The nurse commented that this agency is trying to "cut costs without affecting patient care." At one agency, all LPNs have been laid off. A nurse from another agency indicated that there has been a substantial decrease in the availability of home health aides at her agency. Sometimes, patients do not receive the aide services they need because of this shortage. One nurse reported that many nurses are leaving home care and taking positions in hospital settings. She suggested that these nurses have left home care because "the paperwork is phenomenal."
Five of the seven case study nurses commented on the extent to which coverage issues are considered in the process of making decisions about patient care. Nurses from three agencies indicated that coverage rules do not enter into decisions about patient care. One of these nurses reported that she is "pleased to say that [her] agency's policy is to provide for the patients' needs whether or not it goes over the limits." She suggested that her supervisors "probably think about the money issues a lot more than [she] does," but that she has not been made to feel that she has to consider finances when she makes decisions about a patient's care. She noted that she would "love to not ever have to think about finances at all." Nurses from two other agencies indicated that coverage is an important factor considered in decision making about patient care. Two nurses felt that some patients are discharged from home care sooner than they should be.
The case study nurses reported several changes to patient care in their agencies. Nurses from three agencies reported that substantially fewer patients are recertified in their agencies than in earlier years. Frequently, nurses expressed that they have been told that they have to "get in and get out" of patients' homes. In addition, four of the seven case study nurses indicated that their agencies often turn away certain types of patients. Two agencies frequently refuse high-need patients. Although the agencies do not have hard-and-fast rules about refusing these cases, the nurses indicated that their agencies often will not take patients needing daily aide or nursing services, patients with high estimated costs, diabetic patients, or wound care patients. Nurses from two agencies noted that their agencies are no longer able to care for patients who need only infrequent nursing care. Nurses from three agencies indicated that their agencies do not refuse any kinds of patients. A nurse from one of these agencies qualified this statement, reporting that her agency does not refuse any patients, provided they are teachable or have teachable caregivers.
Four case study nurses suggested that Medicare patients have been affected negatively by recent changes in home health care. Two nurses believe that the venipuncture regulation represents a difficult "double bind" for patients. These nurses noted that, although many elderly patients have difficulty getting to the hospital or doctor's office, they no longer are able to have necessary labs drawn at home. These comments may reflect a fundamental misunderstanding of Medicare coverage rules (i.e., venipuncture is a covered service for patients who are in need of skilled nursing care). Some nurses commented that restrictions on home care services may be resulting in patients being discharged before they should be or in patients being relegated to nursing homes when they may not need this level of care. One nurse commented that she thinks "it is very unfair that people work all their lives and when they need care, they are shoved to the side because someone has told us that we need to get in and get out." Two nurses indicated that the lack of Medicare coverage for medications represents a hardship for patients. One nurse suggested that, without supplemental insurance, many patients are unable to get the medications they need. Another nurse wondered how long patients will take medications that they must pay for themselves. In discussing recent changes to the home health industry, one nurse suggested that "it makes [her] fear getting old."
The case study nurses frequently commented on a general sense of mistrust between home health payers and providers. Although the nurses understand the need to eradicate abuse in the industry, they perceive that payers do not trust home care providers. One nurse commented, "we really do work in home health," referring to her sense that policymakers have a perception to the contrary. The case study nurses also expressed concern that the payers do not have a clear understanding of all of the issues involved in caring for elderly patients in their homes. One nurse wondered if "policymakers [are] just out of touch with elderly people and their obstacles." A number of nurses suggested that agencies that fund home health care do not understand how critical the education component of home care is and how difficult it can be to teach elderly patients complex information about their conditions and treatments. Case study nurses also expressed concern about the motives of payers. One nurse mentioned that she had heard that HMOs give bonuses to their case managers for refusing services. Another nurse commented that she is "not sure which is worse anymore, HMOs or Medicare." HMOs pay for medications, but the patients and their nurses have little control over the care provided.
VII. SUMMARY AND CONCLUSIONS
The Study of Medicare Home Health Practice Variations was designed to examine the following key study questions:
- What is the actual practice of home health care, in terms of type, amount, and decision making (e.g., care planning, care coordination)?
- How are decisions about care made in light of Medicare coverage rules?
- What elements of practice are associated with long lengths of stay in the Medicare home health benefit?
In addition, although the project was not initially intended to explore the impact of recent policy changes on the field of home health care, the timing of the study allowed for an examination of provider perspectives on regulatory changes in home health care.
This final report summarizes the findings from the quantitative and qualitative methods used to answer the key study questions. Specifically, the report summarizes the study methods and sample, explores the causes of practice variations in home health care, examines the relationship between practices and patient outcome, summarizes qualitative findings regarding practice and decision making in home health care, and explores provider perspectives on the changes in home health care resulting primarily from the implementation of the Balanced Budget Act (BBA) of 1997.
A. Practice and Decision Making in Home Health Care
1. Quantitative Findings
Quantitative analyses were conducted on longitudinal data to examine (1) the effect of patient, provider, agency, and market/regulatory factors on home care practices, (2) the influence of practice patterns on episode length, and (3) the impact of home care practices on patient outcome. Five important aspects of home health practice, covering both direct care provision and care coordination, were selected for examination. The four measures of direct care investigated were (1) the average number of visits provided to a patient per day (i.e., visit intensity), (2) the duration of the home health episode (length of stay), (3) the total number of disciplines involved in patient care, and (4) the number of alternative services provided during the episode of care.50 The amount of feedback received by the primary home care provider from other agency personnel regarding a patient's care plan and discharge was examined as a measure of care coordination.51
Effect of Patient, Provider, Agency, and Market/Regulatory Factors on Practice Patterns: Results of the multivariate analyses reported in Chapter 4 suggest that home care practice under IPS was heavily influenced by patient condition, as it should be. Patient complexity, functional status, and diagnoses were important predictors of the practice pattern measures of frequency of visits a patient would receive, the number of disciplines and alternative services that would be included in the patient's care, the patient's length of stay, and the amount of feedback a care provider would receive from other agency personnel about the patient.
Factors other than patient condition, however, also impacted home care practices. Although care provider characteristics were not extremely important statistically, they did have some effect on practice patterns. Notably, even after controlling for patient characteristics, care providers with many years of experience in home health care tended to have patients with significantly longer episode lengths than did less experienced providers. It appears that these providers, having been in home health care prior to the implementation of the BBA, may have experienced more difficulty adjusting to a new era characterized by significant constraints on the cost and utilization of Medicare home health care services.
Despite the implementation of BBA regulations to curb home health spending and to reduce unnecessary variations in practice patterns, it appears that such variations may still exist. After controlling for patient, provider, market/regulatory, and other agency factors, agency ownership and type were strong predictors of home care practices. Proprietary agencies appeared to counterbalance visit intensity and length of stay, providing their patients with more frequent visits over shorter episodes than did nonproprietary agencies. These agencies also made greater use of alternative services in the community, perhaps attempting to reduce agency costs by outsourcing the care for some of their patient's needs.
Freestanding agencies appeared to be higher utilizers than their hospital-based counterparts. After controlling for patient case mix, as well as provider, market/regulatory, and other agency factors, freestanding agencies provided both more frequent visits and longer episodes of care than did hospital-based agencies. These findings are consistent with previous research indicating that freestanding agencies experienced greater hardship in attempting to adjust to the demands of IPS (GAO 1999). Freestanding agencies were more likely than hospital-based agencies to close during the IPS period.
Variation in practices continued to follow state-level patterns. In this study, states that had been identified based on 1995 data as providing a large number of home care visits per patient appeared to continue to utilize home care resources more heavily than did states with lower visit volume. Specifically, after controlling for patient factors, episodes occurring in high-volume states involved significantly more frequent visits and more disciplines than those occurring in low-volume states. Holding patient and other factors constant, it appears that certain states continue to provide a setting in which high utilization of home health resources is the norm.
Effect of Practice Patterns on Episode Length: Controlling for patient case mix, as well as important provider, agency, and market/regulatory factors, visit intensity and the number of disciplines involved in patient care both were associated with the length of a patient's home health episode. Agencies appeared to counterbalance frequency of visits and length of stay, such that episodes involving more frequent visits were significantly shorter than episodes with less frequent visits. Episodes of care that involved more disciplines were significantly longer than those involving fewer home health disciplines, even after controlling for patient, provider, agency, and market/regulatory factors.
Effect of Practice Patterns on Patient Outcome: The practice patterns examined in this study were not strong predictors of patient outcome. Of particular interest was the relationship between visit intensity and patient outcome. After controlling for patient, provider, agency, and market/regulatory factors, and other practice patterns, patients receiving more frequent visits experienced marginally better outcomes of home care than did patients with less frequent visits. Length of stay, however, did not predict patient outcome. It is possible that frequent visits allow care providers to monitor a patient's condition more carefully and thus provide that patient with care that is more timely and is based on a clearer understanding of the patient's needs.
2. Qualitative Findings
The focus group and case study interviews were designed to identify the actual practice of home health care and to examine how decisions about care are made in light of Medicare coverage rules. In this section, key findings from the focus group and case study interviews related to the actual practice of home health care are discussed. Information regarding Medicare coverage rules is discussed in Section C below. The findings both augment and extend into areas beyond those covered by the quantitative analyses. All information was gathered during the IPS period.
Services Provided: Medicare home health care involves skilled nursing; physical, occupational, and speech therapy; medical social work; and aide services. Nurses are the central providers in the home health care system. The primary responsibilities of the home care nurses are to assess the patients' medical condition and needs, and to educate the patient and family about the patients' illnesses and treatment regimens. A patient's primary nurse also plays an important role in determining a patient's care plan (e.g., frequency of visits, disciplines involved), managing the patient's medications, completing required forms, documenting the patient's case, organizing a support network for the patient, performing psychological counseling, and ensuring that care providers from different disciplines are "on the same page."
Care providers from other disciplines provide important services for patients in home health care. Physical therapy is provided to help the patients improve their strength and balance. Primary nurses often do not order physical therapy for patients they consider too unmotivated to benefit from these services. The primary role of medical social workers is to identify community resources and to assist home care patients with their psychological needs. Importantly, two of three case study patients for which a social work consultation was requested refused to accept these services, leaving the primary nurses in the position of having to provide these services themselves. Home health aides assist patients with showering, skin care, meal preparation, cleaning, laundry, and shopping. Aides also remind the patients to take their medications, monitor the patients' weights, and report changes in the patients' conditions immediately to the primary nurses. Three case study patients refused aide services.
Factors Affecting Services Provided: The nurses participating in the focus group and case study interviews identified a number of factors affecting services provided to Medicare home care beneficiaries. According to focus group participants, patients just released from the hospital often are sicker than other home care recipients and frequently require complex or high-tech services. These complex cases involve more vigilant attention from the nurses, as well as more frequent communication between disciplines, and documentation that is more excessive.
Although the family support network is important for all recipients of home health care, a number of the focus group and case study participants noted the special importance of family members for elderly home care recipients. Patients may have great difficulty caring for themselves and may need assistance in multiple domains of their daily lives. Focus group participants indicated that they consider the availability of caregivers in their decisions to recertify or discharge patients. Family members of the case study patients commonly provided assistance with ADLs, IADLs, medication management, and were frequently involved directly in the patients' care (e.g., accepting or refusing services, attending nursing visits, weighing the patients). Interview participants emphasized that some home care patients are cared for by spouses or other family members who may be as old and frail as the patients themselves.
Care Planning and Coordination: Substantial variation in the process of care planning and coordination was found among agencies in both the focus groups and case studies. The role of the primary nurse in the process of developing the patient's care plan varied from agency to agency. At some of the case study agencies, nurses reported that they have a great deal of control over a patient's care plan. Although the referring physician must approve the care plan at all agencies, several nurses indicated that the primary nurse develops the care plan and writes the orders. The physician simply approves the nurse's plan.
According to a number of focus group and case study participants, many agencies involve supervisors in the development of patients' care plans. They either approve the plans laid out by the primary nurses or worked with the primary nurses to jointly develop the plan. Although not definitive due to small sample size, the case study interviews suggested that primary nurses have greater control over the development of their patients' care plans in low-volume states and in non-proprietary agencies.
Communication among care providers appears to be fairly consistent across agencies. The focus group participants indicated that the process of coordinating care for patients begins immediately at the start of care. The case study nurses reported that they generally communicate with their patients' physicians only at milestone time points in the episodes of care. Nurses communicate with physicians at the start of care and as the patient approaches recertification or discharge. In between these time points, nurses tend to contact the physicians only when changes occur in a patient's condition or treatment plan. Contact with physicians is nearly always made indirectly through the physician's nursing staff.
Communication between the primary nurses and other care providers is fairly regular. The case study nurses reported being in contact with their patients' aides at least weekly. In addition, the nurses made home visits with the aides every two weeks. The nurses also indicated that the aides frequently call with questions or new information about a patient.
Case conferences are an important mechanism through which care providers of different disciplines stay in contact regarding their patients. Most of the case study nurses who coordinated other disciplines on behalf of their patients were in contact with those other providers at case conferences. Generally, patients are presented at conferences at the start of care, recertification, discharge, and when problems arise. In addition, therapists and social workers generally contact the primary nurse once they have developed their own care plans for a patient.
Discharge planning begins very early in the home care episode, usually at the first visit. Nurses cited a number of factors that they consider in determining a patient's readiness for discharge: patient is medically stable, the educational goals have been reached, the patient is no longer homebound, services will no longer be covered by Medicare, the patient's medication regimen has been stabilized, the patient has increased endurance, and the patient is able to manage his or her medications.
Nurses engage in a variety of activities in planning for a patient's discharge. Most commonly, nurses make arrangements for the patient's continuing needs to be met after discharge (e.g., identify resources to assist with transportation, meal preparation). Communicating with other care providers through case conferencing and other methods of interaction is an important component of the discharge-planning process.
B. Provider Perspectives on the Interim Payment System (IPS) and Changes in Home Health Care
This study was not originally intended to examine the impact of recent regulatory changes related to home health care. However, since the 1997 BBA was implemented prior to the major data acquisition phase of the project, it was possible to investigate provider perspectives on the impact of the provisions of the BBA and other regulatory changes during the IPS period on home health care. Four qualitative methods were used to explore provider perspectives on IPS and other changes in home health care. The impact of these regulatory changes was examined through (1) interviews with administrators of the study agencies, (2) interviews with representatives of home care associations in each of the eight study states, as well as (3) focus groups, and (4) case study interviews with home health care nurses at the study agencies. These methods provided valuable qualitative information regarding the effects of IPS and related policy changes on home health care. This information can serve as a baseline against which home health practices under PPS can be compared in the future.
It is important to note that the data gathered through these methods were not based on a random sample of home care providers, administrators, and state association representatives. Therefore, the information that this sample of participants provided with regard to the impact that the BBA had (prior to the implementation of PPS) on their states and their agencies may not be an accurate reflection of the impact that the BBA had on home health care nationwide. Further, these individuals may not have been fully aware of the provisions of the BBA and probably were not unbiased toward federal policies and regulations designed to restrict the growth of home health utilization.
Several important themes emerged across the four methods used to examine provider perceptions of IPS and concurrent regulatory changes. Participants in the focus group, case study, and state home care association interviews reported that home care providers were more restricted in the services they were able to offer to their patients under IPS than prior to IPS. In addition, many participants suggested that patients were on service for shorter periods of time than they once were and that some patients were discharged before they should be. The pressure to discharge patients quickly led to the identification and involvement of community and other outside resources early in patients' episodes of care. According to agency administrators, this increased emphasis on community resources resulted in the expansion of the role of social workers in patient care.
Participants involved in all four of the interview methods reported that some agencies had begun to refuse high-need patients, such as chronic, complex, or rural patients in an attempt to avoid expensive patients whose care needs might substantially exceed the agencies' per-beneficiary limits. Most commonly, participants suggested that access to home care services had been reduced for diabetic patients and patients who needed daily wound care. These data suggest that some high-need patients may have experienced reduced access to home health care as a result of the increasingly stringent admissions practices of some home care agencies under IPS.
Participants in the administrator, focus group, and case study interviews suggested that education had become an increasingly important aspect of home care. Patients and their families were required to develop an understanding of the patients' conditions and needs and to provide for those needs themselves. Interview participants noted that this education had to take place in an increasingly short period of time, as nurses often were told to "get in and get out" of their patients' homes. Several focus group and case study nurses suggested that policymakers did not understand how difficult it was to teach an elderly patient or an elderly spouse the things they needed to know to take over the services that agency personnel provide.
Changes occurred at the agency level as well. Interview participants noted that many home care agencies in their states had closed or merged with other agencies. Other agencies had instituted cost-saving measures, laid off staff, reduced staff benefits, and instituted additional case management procedures. Agencies had increased nurse productivity standards, were providing less nursing care overall, and had changed their geographic service areas in an attempt to respond to the pressures imposed by IPS and other regulatory changes. A number of participants noted that many nurses had left home care and that there was a shortage of home health aides, circumstances that often impacted patient care. According to agency administrators, even when aides were available, fewer aide visits were provided than once were. Participants in the state home care association and administrator interviews agreed that many agencies were pursuing ways to diversify their payer sources, seeking to shift their case mix more toward Medicaid and managed care and away from Medicare. Agency administrators also noted a reduction in physician referrals to home care.
Other studies designed to assess the impact of BBA provisions, IPS in particular, corroborate many of this study's findings. In the current study, agency representatives reported reducing the level of services and the number of visits provided to their patients, as well as reducing the duration of their patients' episodes of care. Similarly, in a report prepared for the Medicare Payment Advisory Commission (MedPAC), Abt Associates (1999) reported that 71% of agencies surveyed had decreased the number of visits provided to Medicare patients. Proprietary agencies (76%) and agencies of medium to large size (more than 75%) were most likely to have reduced the number of visits they provide. Smith, Maloy, and Hawkins (1999) also reported a reduction in the level of services provided, the number of visits provided, and a reduction in the length of stabilization periods for home care patients. These effects may be a result of IPS, as well as agencies' more careful determination that patients were only on service so long as they meet Medicare eligibility criteria.
In the current study, many interview participants reported that agencies had changed the mix of visit types provided to their patients. Specifically, they suggested that patients received fewer aide visits and less nursing care than they did prior to the implementation of IPS and other changes, but that social workers were more likely to be involved in patient care than they once were. These findings were only partially corroborated by other research. As in the current study, the Abt Associates study (1999) indicated that many agencies provided fewer aide visits (28.1%) than they once did. Further, 14.5% of agencies surveyed provided less skilled nursing care than they did prior to IPS. Representatives of 8.4% of agencies, however, reported providing more skilled nursing care under IPS. The additional 77.1% of the agencies reported no change in the provision of skilled nursing care. Contrary to the current study's findings, the MedPAC report prepared by Abt Associates (1999) suggested that social workers may, in fact, have been less involved in patient care than they once were. In that study, more agency representatives reported decreasing (8.4%) than increasing (4.2%) the involvement of social workers. However, most agencies (87.4%) made no changes in their utilization of social work services.
Some interview participants in the current study reported that home care agencies were actively seeking to change their case mix by reducing the number of Medicare patients they served. Likewise, in 1999, Abt Associates reported that more than half of the 1,054 agencies at which interviews were conducted experienced a decline in their Medicare caseload following the implementation of IPS. Proprietary agencies and VNAs were most likely to report declines in their Medicare caseload. Smith and her colleagues (1999) reported a 21% decline in the number of Medicare beneficiaries admitted to the home care agencies involved in their study under IPS. However, a report from the GAO (1998) suggested that the shift away from Medicare patients may not have been universal. In that study, more than half of the hospital discharge planners and many of the representatives of local aging organizations that were interviewed had not seen a reduction in the willingness or ability of home health agencies in their states to accept Medicare patients.
Participants in the administrator interviews, state home care association interviews, focus group interviews, and case study interviews suggested that some agencies had begun to screen patients more selectively at admission to maintain a desired case mix. A number of other studies support this finding (Abt Associates 1999; GAO 1998; GAO 1999; MedPAC 2000; OIG 1999a; Smith et al. 1999). In 1999, Abt Associates reported that 38.9% of home care agency representatives interviewed indicated that, as a result of IPS, certain types of patients were no longer admitted to their agencies. Agency control, size, and reimbursement appeared to influence the likelihood that an agency would turn away a potential patient. Representatives of 52% of the proprietary agencies reported not admitting certain patients, compared with 30% of the representatives of VNAs and government agencies. Representatives of smaller agencies were more likely to report IPS-related refusals compared with those of larger agencies. In addition, a greater proportion of agencies expecting to exceed their per-beneficiary limits or per-visit limits refused to admit certain types of patients than did agencies that were not expecting to exceed these limits (per-beneficiary limits: 47% vs. 33%; per-visit limits: 45% vs. 31%).
As suggested in the current study, other studies provided evidence that particular types of patients may have experienced reduced access to home health care as a result of agencies' more stringent admission practices. Although 85% of hospital discharge planners interviewed as part of an OIG study (1999a) reported that Medicare patients had access to home health care when they needed it, more than half of those interviewed reported that certain kinds of patients had become more difficult to place (i.e., those needing care for chronic illnesses or Alzheimer's/dementia, IV care, high-cost care, intensive care, or dialysis). In 1998, GAO concluded that, overall, IPS had not had a negative impact on Medicare beneficiaries' access to home health care. However, hospital discharge planners and representatives of local organizations for the aged who participated in that study reported that beneficiaries who were likely to be expensive were more difficult to place than were other types of patients. In a 1999 report, GAO noted that some agencies were reluctant to admit wound patients and diabetics unable to self-administer insulin. In addition, representatives of national advocacy groups and Area Agencies on Aging interviewed reported having received complaints about a lack of access for patients with chronic illness, Alzheimer's disease, multiple sclerosis, quadriplegia, and long-term care needs. Approximately two-thirds of discharge planners and more than one-third of organization representatives reported having difficulty placing patients with intensive skilled nursing needs and patients needing large numbers of visits and long episodes of care. Abt Associates (1999) reported that patients with long-term care needs or chronic disease, diabetes or wound care patients, and patients with expensive care needs were most commonly mentioned by agency representatives as patients who might no longer be admitted to their home care agencies. In their interviews with agency representatives, Smith and her colleagues (1999) also found that patients who required high-cost treatments, intensive skilled nursing care, frequent visits, or long episodes of care may have experienced reduced access to home health care. On the other hand, low-cost patients may actually have experienced improved access to care as a result of IPS-related incentives to reduce per-patient costs.52 Many agencies had seen a substantial shift away from long-stay and toward short-stay patients in response to IPS.
The possibility of access problems for certain patient types also was found in an OIG study (OIG 2000) that examined Medicare claims data for the top 12 diagnosis related groups (DRGs) discharged to home care. For only one of these DRGs was there a substantial decrease between the pre- and post-IPS periods in the percentage of hospital patients admitted to home care (DRG 106, coronary bypass). However, it is important to note that the OIG report did not examine the DRGs used to categorize patients with primary diagnoses of diabetes mellitus (i.e., DRGs 294 and 295). Since many reports have suggested that diabetes patients might have experienced a reduction in access to home health care, it would be informative to examine the impact of IPS on home health access for these DRGs directly.53
Participants in the current study reported many agency-level changes related to IPS and other policy changes. Many participants reported that their agencies had laid off staff and reduced staff benefits. Similarly, Abt Associates (1999) reported that 75% of agencies had reduced their staff or staff hours. Proprietary agencies (82%), large agencies (86%), and agencies expecting to exceed their per-beneficiary limits (83%) and per-visit limits (80%) were more likely than other agencies to have reduced the size of their staffs overall. Smith and her colleagues (1999) also reported significant staffing changes as a result of IPS. Between 1994 and 1999, skilled nursing staff had been reduced by 23% and aide staff had been reduced by 43%. Administrative staff also had been cut dramatically (Abt Associates 1999; Smith et al. 1999). Clinical staff had seen increased administrative responsibility as a result of the reductions in the size of agencies' administrative staffs (Smith et al. 1999). As in the current study, Abt Associates (1999) reported that many agencies (55%) had reduced staff benefits.
The current study suggests that under IPS, agencies had developed a greater focus on efficiency. Agencies had instituted more careful case management and supervisory procedures, and had increased their focus on patient independence as a result of IPS. Nurses in the focus groups and case studies commented on the increased role of nursing supervisors, multidisciplinary team conferences, and other oversight mechanisms in the decision-making process in home health care. Nurses emphasized the increasing importance of education in home health care as a means of enabling patients and/or their caregivers to become capable of providing for the patients' needs independently. Smith et al. (1999) also reported these changes in agency practice. As a result of IPS, agencies in that study began to make greater use of case managers and to focus more extensively on the goal of patient independence than they had in the pre-IPS period. GAO (1999) also found that agencies attempted to educate patients earlier in the episodes of care than they once had.
Many interview participants in the current study commented on the closure of home care agencies or branch offices as a result of regulatory changes affecting home health care (e.g., IPS, ORT). Between October 1, 1997, when IPS was implemented, and January 1, 1999, 14% of home care agencies closed their doors (GAO 1999). However, some studies suggested that these closures might have been a market correction following a period of tremendous growth in the number of home health care agencies. Many of these agency closures had occurred in states that had the largest growth in the number of agencies and high utilization rates prior to the implementation of IPS (GAO 1999). Further, the agencies that closed following the implementation of IPS were similar in many ways to the agencies that opened in the early 1990s, when home health utilization grew dramatically. These agencies were disproportionately of proprietary control, freestanding, and urban (GAO 1999; Liu, Harvell, Gage 2000). They also were newer, had smaller Medicare caseloads, and provided 44% more visits per beneficiary than did agencies that remained open following the implementation of IPS (GAO 1999). In addition to agency closures, Abt Associates (1999) reported that 40% of the agencies involved in that survey had shut down branch offices in response to IPS. Proprietary agencies (53%) were more likely than non-proprietary (31%) and government agencies (22%) to close branches. Agencies that were expected to exceed their cost limits were more likely than those agencies not expected to exceed their limits to close branch offices (per-beneficiary limit: 47% vs. 35%; per-visit limit: 44% vs. 33%).
According to GAO (1999), access to home health care was not negatively impacted by agency closures. By 1999, the utilization of home health services had declined to 1994 levels. Although 1994 was not the peak of home health utilization, it was a period of relatively high utilization. Further, as intended, regional variations in the utilization of home health services had declined following the implementation of IPS. Most representatives of state survey organizations interviewed by GAO indicated that beneficiary access was not reduced by agency closures. Even in rural counties that lost their only home health agencies, hospital discharge planners and managers of nearby agencies reported that beneficiaries were able to obtain care from agencies in other counties or branch locations within their own county. Although utilization decreased slightly in counties without any home health agencies, it remained above the national average.
The current study identified a decline in physician referrals to home health care. Similarly, Abt Associates (1999) reported that 77% of agency representatives surveyed had noticed a reluctance of physicians to refer patients for Medicare home care services. According to Smith and her colleagues (1999), changing referral patterns might have been a result of the failure of physicians to understand Medicare eligibility criteria. Other physicians no longer referred patients to home care out of fear of becoming the target of a physician review by their Medicare Fiscal Intermediary (FI). In addition to these concerns, the Health Insurance Portability and Accountability Act (HIPAA), which went into effect in August 1996, likely had been the impetus behind some of the reduction in physician referrals. HIPAA established a monetary penalty for any physician who falsely certifies the need for Medicare-covered home health services.
C. Implications
Implications of the study's quantitative and qualitative findings for clinical practice guidelines and Medicare home health coverage rules are considered in this section. Since the study pertains to the IPS period, it will be important for future work to reassess the validity of the implications under PPS.
1. Implications for Clinical Practice Guidelines
Quantitative analyses confirm that patient factors are predominant in predicting practice patterns in home health care. Patient care plans clearly are designed largely based on patients' medical conditions and needs. Despite an increasing focus on cost of care, agency staffs have maintained their focus on providing care tailored to the individual needs of their patients.
It is clear, however, that other factors continue to influence practice decisions. Notably, certain characteristics of the care providers, agencies, and home care markets influence care planning and provision, regardless of patient condition. Care providers with more years of experience in home health care do not appear to have adjusted their style of practice to incorporate a consideration of cost in addition to a focus on the good of the patient. Although length of stay was not found to predict patient outcome, episodes of care involving care providers with more years of experience were significantly longer than episodes involving less experienced providers (controlling for patient, agency, market/regulatory, and other agency factors). This finding suggests that more experienced care providers may be continuing to utilize services as they had prior to the increase in concern over the cost of home health care, but that their higher use of services does not appear to benefit their patients. It could be helpful for agencies to educate their care providers to a greater extent about concerns related to overutilization of care. Emphasizing that patient outcome is the priority, it may be possible to encourage providers to incorporate a secondary focus on cost that could reduce unnecessary utilization of services without reducing the effectiveness of the care provided. Under PPS, financial incentives to reduce utilization are quite strong, so this trend may occur naturally.
Agency and market/regulatory factors also influenced practice patterns, even after controlling for patient case mix and other important factors. It appears that specific types of agencies and specific states provide an environment in which high levels of utilization are the norm. Freestanding agencies, for example, provide more frequent visits and longer episodes of care than their hospital-based counterparts, even after controlling for patient case mix. Although more frequent visits were marginally related to more positive patient outcome, length of stay was not. It may be that patients treated by freestanding agencies receive appropriate visit frequency, while experiencing longer than necessary episodes of care.
Likewise, states identified as high utilizers based on 1995 data, appeared to maintain this status under IPS. Controlling for patient case mix and other factors, agencies in high-volume states provided significantly higher visit intensity and involved more disciplines in care. It appears that these agencies might be able to reduce their utilization of home health care services without diminishing their patients' outcomes of care. Utilization of services under PPS should be monitored with regard to patient outcomes.
Analyses examining patient outcome revealed that higher visit intensity was marginally related to better patient outcomes. As noted earlier, it is possible that more frequent visits, particularly early on in a patient's episode of care, may help the patient achieve more positive outcomes. The care plan may be more accurate in episodes in which the patient is seen frequently. Further, providers are likely to become aware of problems or changes in condition very quickly under such circumstances. Although more frequent visits have a positive impact on outcome, it does not necessarily follow that frequent visits require an increased level of utilization. The quantitative analyses suggested that many agencies counterbalance visit intensity with length of stay, providing visits more frequently over shorter episodes of care. Further, and more importantly, it appears that this pattern may have positive results for home care patients. Indeed, proprietary agencies, which provided more frequent visits over shorter episodes of care, were found to have significantly better patient outcomes than did nonproprietary agencies (see Table 4.4). A focus on visit intensity rather than length of stay may be appropriate for some types of patients.
2. Implications for Medicare Home Health Coverage Rules
The focus groups and case study interviews revealed that a lack of clarity regarding home health regulations has a major impact on home health practice. Some of the critical concepts of the Medicare coverage rules are unclear to many providers. Specifically, nurses involved in the focus group and case study interviews referred to the difficulty they and others have understanding the concept of "homebound," what constitutes skilled nursing care, and what management and evaluation (M&E) is and when it can be used.
Focus group and case study nurses alike reported that the definition of "homebound," a critical feature of the Medicare coverage rules, is unclear. Interview participants suggested that the definition is quite subjective and that most home care nurses have their own personal definitions of this concept.
Some of the focus group participants indicated that there is uncertainty in the field about what constitutes skilled nursing care. In discussing the patient vignettes, the nurses disagreed about whether the services needed by these patients represented skilled care. In particular, the nurses were uncertain whether wound care represented a skilled need. Further, it appeared that nurses were not the only members of the medical community who were unclear about this concept. Nurses reported that physicians often referred patients to home care who do not need skilled nursing services, apparently maintaining an incorrect understanding what does and does not constitute skilled care.
Management and evaluation (M&E) also appeared to be an elusive concept. Focus group participants' understanding of M&E differed widely from agency to agency. Some nurses indicated that M&E applied to patients with IV therapy and family members who were not able to learn the medication regimen. Other nurses suggested that M&E was appropriate only for complex patients with multiple caregivers, needing many hours of service. A few nurses even thought that M&E required special training for nurses.
The lack of clarity in coverage rules did not appear to encourage home care providers to continue to provide services to patients ready for discharge. Despite the wide variation in their understanding of the concept of homebound, the nurses participating in these interviews did not appear to use this lack of conceptual clarity to their advantage. In fact, some of the nurses reported discharging patients before they were thought to be ready because the patients were believed to no longer meet the criteria for homebound status. In cases in which nurses held inaccurate views of the kinds of activities a homebound patient should not be able to participate in (e.g., driving), patients who might legitimately be considered homebound could have been prematurely discharged as a result of the nurses' misunderstanding of the regulations.
Not only was there no evidence that ambiguity in coverage rules lead to the provision of unnecessary services, there was some suggestion in the focus group and case study data that this ambiguity may actually have resulted in shorter episodes of care. One focus group participant indicated that "in a case where you might be borderline on discharging or making another visit, [her agency] would lean toward not making another visit for fear of Medicare review." Further, the focus group interviews produced some evidence that agencies may avoid the use of services for which the coverage rules are ambiguous. During most of the focus group interviews, nurses indicated that M&E is not used at their agencies. Uncertainty about the meaning of the coverage rules with regard to M&E may have encouraged agencies to avoid the practice altogether.
Lack of clarity with regard to the Medicare coverage rules appeared to have a strong impact on decision making in home health care. Evidence from the focus group and case study interviews suggest that home care nurses often may misinterpret the rules and that, at times, such misinterpretations may result in inappropriate underutilization of services for certain patients. Efforts to clarify the regulations and educate care providers should ensure that patients receive the care they need and for which they are eligible.
D. Conclusions
The field of home health care has seen dramatic changes over the past several years. Since the collection of the data used in this study, several major changes have been implemented that are expected to have a powerful impact on the practice of home health care. The implementation of PPS in October 2000 and the resulting major shift in financial incentives facing agencies has been mentioned several times. Under PPS, agencies have strong incentives to minimize visits and otherwise constrain costs. Such incentives could result in inappropriate underutilization of care and declining patient outcomes.
A possibly countervailing change is the 1999 implementation of the Outcome and Assessment Information Set (OASIS) data collection and transmission requirement for all Medicare-certified home health agencies and the generation of case mix, adverse event, and outcome reports for these agencies. (The outcome reports became available in early 2002.) Outcome reports can be a powerful tool for outcome-based quality improvement (OBQI) by home health care providers (Shaughnessy, Crisler, Hittle, Schlenker 2002a; Shaughnessy, Hittle, Crisler, Powell 2002b) and may help offset the possibly negative consequences of PPS for patient outcomes. The findings from this study will provide a useful baseline of information on practice patterns during the IPS period, allowing researchers to identify the impact of the implementation of PPS and other recent federal regulations.
NOTES
-
Alternative services represent those services coordinated by an agency, but provided by another organization in the community.
-
This variable reflects whether the primary care provider received feedback from other agency personnel regarding (1) the appropriate frequency of skilled nursing visits, (2) whether aide services should be provided, and (3) when discharge should occur.
-
The methods that obtained information on provider perceptions, noted earlier, were the focus group and case study interviews as well as interviews of state home care association representatives and study agency administrators.
-
The Health Care Financing Administration (HCFA) changed its name to the Centers for Medicare & Medicaid Services (CMS) in June 2001. Both names (and acronyms) are used in this report, depending on context.
-
A follow-up audit conducted by the OIG (1999b) found that ORT and other anti-fraud initiatives have had a potent effect on error rates in home health claims. The error rate dropped to 19% during the nine-month period ending on September 30, 1998, from 40% during the 15-month period ending on March 31, 1996. This reduction was primarily due to a reduction in the number of claims for services that were not reasonable and necessary, for services without valid physician orders, and for beneficiaries who were not homebound.
-
The terminology for characteristics such as ownership, type, and volume varies across studies. In this report, "ownership" is used to designate proprietary or non-proprietary ownership and control. Government agencies are included in the non-proprietary category. "Type" is used to designate hospital-based or freestanding agencies. "Volume" refers to the average number of visits per patient, based on 1995 data. This variable is defined at the state level as opposed to the agency level. Therefore, volume is an indicator of home health utilization practices in a given state, rather than a measure of a single agency's practice patterns. Volume itself is determined by, and is a proxy for, a multitude of market factors that may influence the provision of home health care at the agency level (e.g., availability of alternative resources, case mix).
-
A small number of agencies had two employees that shared the role of DCC.
-
Subjects were identified as having CHF or diabetes mellitus based on the ICD-9 codes provided on the OASIS start of care assessment form and/or on the Notification of Study Admission (NSA) form, which agency personnel submitted upon enrollment of a new patient in the study. To be eligible for participation, patients were required to have an ICD-9 code representing CHF (i.e., 398.91, 428.0, 428.1, 428.9, 402.01, 402.11, 402.91, 404.01, 404.03, 404.11, 404.13, 404.91, 404.93, 429.4) or diabetes mellitus (i.e., 250.0 through 250.9). Some patients had ICD-9 codes reflecting both CHF and diabetes mellitus.
-
With allowance for attrition and incomplete data, the target analysis sample was 1,152 patients--the equivalent of 48 agencies with 24 patients per agency. Greater than expected agency attrition and missing patient assessment data resulted in a smaller than expected final patient sample.
-
Data collection was ended in August 2000 to ensure that the data would not be confounded by the implementation of the Prospective Payment System (PPS). Thus, the data examined as part of this study reflect practice patterns and patient outcomes under IPS only.
-
The data collection protocol specified that data collection was to be discontinued 240 days after a patient's original start of care date. However, as many long-stay patients are discharged and admitted multiple times during the course of their care, it is common for the timing of their recertification periods to differ from the timing one would expect based on their initial start of care dates in the study. In order to retain as many complete episodes as possible, all recertification, transfer, and discharge data collected through 260 days were retained. However, data representing the beginning of a new episode of care (i.e., start of care, resumption of care, and readmission assessments) were collected only through 240 days from the original start of care date.
-
Patients who were discharged from their agencies and resumed services within 14 days of discharge were readmitted to the study. This definition of discharge was meant to control for variability in agency-specific policies regarding inpatient facility admission. Some agencies discharge patients at the time of admission to inpatient facilities, whereas others discharge patients after a certain number of hospital days. Using 14 days after agency discharge as the definition of study discharge allowed for the collection of equivalent data for those patients who were and were not discharged at the time of their inpatient facility admissions.
-
The eight agencies selected to participate in the focus groups and case studies all are included in the final sample of 44 agencies.
-
To avoid introducing excessive variation in the case study data, which might have made thematic analysis of the data from this small sample difficult, the case study sample was restricted to patients with a single tracer condition, CHF.
-
Assessment time points differed slightly on the OASIS and the CPQ. On the OASIS, an assessment at the beginning of an episode is identified as either a start of care assessment or as a resumption of care following an inpatient stay during which the patient was not discharged from the agency. At the end of an episode, a patient is discharged, transferred to an inpatient facility with or without agency discharge, or dies at home. On the CPQ, an assessment at the beginning of an episode is identified as a start of care assessment (equivalent to a start of care on OASIS), a resumption of care after an inpatient stay during which the patient was not discharged from the agency (equivalent to an OASIS resumption of care), or a readmission to the agency within 14 days of agency discharge (equivalent to an OASIS start of care). At the end of a CPQ episode, a patient is discharged. There is no option for transfer on the CPQ. For this reason, at transfer, only OASIS data were collected.
-
Because analyses were conducted at the episode level, patients with multiple episodes of care were represented more than once in the analyses.
-
All multivariate analyses were conducted across the final sample of patient episodes, rather than separately by tracer condition.
-
Some patient factor variables were designated as "required" because they reflect areas in which patients with CHF and diabetes mellitus differed. In pooling these two groups in the multivariate analysis, we controlled for the conditions themselves as well as those patient factor variables related to the conditions.
-
Some patients were diagnosed with both CHF and diabetes mellitus. These patients are included in both tracer condition groups.
-
The final patient sample was composed of patients having complete assessment data for one or more episodes of care. Assessment data were considered complete if a patient had both OASIS and CPQ data for both the beginning and ending of an episode.
-
It is important to note that, although we attempted to sample agencies randomly, participation in the study was voluntary. Therefore, the descriptive information presented in this section is intended to provide a general description of the agency sample rather than precise estimates of population characteristics.
-
The number of agencies located in each of the eight study states was as follows: Georgia (5), Massachusetts (4), Minnesota (6), Mississippi (4), New Jersey (6), Oregon (8), Pennsylvania (6), Texas (5).
-
Of the 732 episodes of care, CPP data were available for 678 of the care providers conducting the start of care/readmission/resumption of care visits.
-
Patients were identified as having one or both tracer conditions using ICD-9 codes. Codes were obtained through OASIS start of care data (data items M0230 and M0240) and through the Notification of Study Admission (NSA) form that DCCs used to report the enrollment of new patients in the study. The NSA is included in Appendix A.
-
The calculation of the number of episodes per patient is based on those episodes for which complete episode-level assessment data were available. Episodes for which either the OASIS and/or the CPQ was missing for either the beginning or ending of the episode are not included.
-
Diabetic patients were significantly more likely than CHF patients to be rated as requiring complex management.
-
Each ADL and IADL data item was transformed into a number of dichotomous variables. The three dichotomies created for each ADL data item identified whether a patient was mildly, moderately, or severely disabled. The two IADL dichotomies reflected whether a patient was mildly or severely disabled with regard to a given IADL. In general, the mild dichotomy split the original scale at the lowest level at which a patient required human supervision or assistance. The severe dichotomy split the scale at the other end, differentiating patients who were totally dependent from those who were capable of participating or assisting in a given task (e.g., eating) to some extent. The moderate dichotomy split each scale at an intermediate level that was considered to be clinically meaningful, but was different from scale to scale. The dichotomies then were summed to identify the number of disabilities at a given level (e.g., number of mild ADL disabilities). Note that the disability measures are not exclusive. That is, if a patient is completely dependent in grooming, the mild, moderate, and severe dichotomies for this ADL each will reflect this disability.
-
The cost per visit data used in these calculations were published in the Prospective Payment System for Home Health Agencies; Final Rule (HCFA 2000).
-
Feedback regarding the care plan represented the amount of input a care provider received from other agency personnel regarding a patient's care plan. This variable was calculated as the average of three dichotomous (yes/no) CPQ variables indicating whether the primary care provider received feedback from other agency personnel regarding (1) the appropriate frequency of skilled nursing visits, (2) whether aide services should be provided, and (3) when discharge should occur. Values have a possibility range of zero to one, with larger numbers reflecting greater feedback from other agency personnel.
-
Because length of stay data often are skewed, length of stay was log transformed (natural log) to normalize the distribution. Note that the total number of visits provided to a patient over the course of an episode was not examined in these analyses because of that variable's strong correlation with length of stay.
-
In addition to including all significant (p.05) and marginal (p.10) variables in the final OLS models, ten variables were considered vital enough to be included in the final models whether or not they were significant in the preliminary models. Table F.1 in Appendix F identifies all variables included in these multivariate analyses and identify these "required" variables.
-
Because only a small percentage of patients were not White, the race variable used in the multivariate analyses was a dichotomous variable identifying whether a patient was White or not.
-
This refers to the number of types of people in the family/support system who provide assistance to the patient out of the following: (1) spouse/significant other, (2) daughter or son, (3) other family member, (4) friend, church or community member, and (5) paid help other than from the home care agency.
-
Controlling for the other patient, provider, agency, and market/regulatory factors, the number of comorbid conditions impacting daily functioning for which home health care was being provided did not influence care practices.
-
Functional disability was calculated by standardizing and computing the mean of the eight activities of daily living (ADLs) and six instrumental activities of daily living (IADLs) from the OASIS.
-
Unexpectedly, patients with more severe dyspnea received care from significantly fewer disciplines than did patients with less severe shortness of breath. It is possible that these patients were cared for primarily by nursing staff, with little involvement from other disciplines.
-
The care provider conducting the start of care visit is particularly important in that he or she is likely to develop the patient's plan of care and to conduct the majority of the visits with the patient throughout the episode of care.
-
Physician involvement was calculated as the average of three CPQ variables: (1) C730, (2) C740, and (3) C750. Items C730 and C750 were reverse coded prior to calculating the average. Therefore, larger numbers reflect greater physician involvement in the care plan and awareness of the services provided.
-
Although most of the agency factor variables predicted care practices in some way, one agency variable, the staff making recertification decisions (i.e., primary nurse or therapist [1] or supervisor/quality assurance staff [2]) did not impact any of the practice patterns under investigation.
-
The variable reflecting the frequency of interdisciplinary communication was collected as part of the Administrator Questionnaire. In the response scale, larger numbers reflect less frequent communication.
-
The variable assessing the availability of community resources was based on Administrator Questionnaire item number 52 and is a sum of the community resources identified by each agency's administrator.
-
The same patient, provider, agency, and market/regulatory factor variables were included in this regression model as were included in the previously described model predicting length of stay from these factors alone.
-
There are 27 dichotomous improvement measures reported by CMS that specify whether or not a patient improved on a given construct over the course of the episode of care (e.g., improvement in ambulation). For each study patient, these 27 improvement measures were calculated. However, when a patient was at the highest level of functioning for a given construct at the start of care (i.e., he or she could not possibly improve), an improvement score was not derived. The aggregate measure representing the percentage of improvement measures on which a patient improved was calculated as the number of measures on which improvement occurred over the number of measures on which a given patient had the possibility of improving.
-
The one nurse who communicated with her patient's physician in person noted that she did so to encourage him to continue to refer patients to her agency.
-
ORT was instituted as a demonstration project in 1995 by the Department of Health and Human Services. The project was designed to reduce health care fraud in five states (California, Florida, Illinois, New York, and Texas), focusing on three high-growth specialty areas: home health care, nursing home care, and durable medical equipment. Since that time, the initiative has been expanded to include all 50 states and to focus on additional specialty areas (e.g., hospice care).
-
The number of active agencies for a given year reflects the number of agencies certified to provide Medicare/Medicaid services as of January 1 of that year.
-
This reflects a misinterpretation of the limit. It is not intended to be applied to individual cases, but rather is applied as an average to all cases combined.
-
Differences between this interview sample and the sample of 52 Administrator Questionnaire (AQ) respondents reported on in Chapter 3 are: (a) two proprietary agencies in the interview sample (one from each volume group) are not in the AQ sample, and (b) in the non-proprietary category, one AQ respondent is not in the interview sample while one of the interview sample agencies is not in the AQ sample (both are from the high-volume group).
-
Two of the nurses interviewed were fairly new to home health care. They each indicated that they might not be aware of all the changes that have occurred in the field in recent years.
-
Alternative services represent those services coordinated by an agency, but provided by another organization in the community.
-
This variable reflects whether the primary care provider received feedback from other agency personnel regarding (1) the appropriate frequency of skilled nursing visits, (2) whether aide services should be provided, and (3) when discharge should occur.
-
In addition to more stringent screening practices at admission, representatives of some agencies involved in other studies reported discharging high-cost patients at the time of the implementation of IPS. Abt Associates (1999) reported that 31.1% of agencies had discharged patients as a result of IPS. Smith et al. (1999) reported that 18% of agencies had discharged high-cost patients upon the implementation of IPS.
-
Patients are categorized into DRGs based on their primary diagnoses. Therefore, patients with secondary diagnoses of diabetes might be included in the 12 DRGs examined in the OIG report. However, patients with primary diagnoses of diabetes would be included in the DRGs 294 and 295, neither of which were examined in the OIG report.
REFERENCES
Abt Associates, Inc. (1999). Survey of Home Health Agencies. Final Report prepared for the Medicare Payment Advisory Commission (MedPAC), Washington, DC, under contract no. T-814143343. Cambridge, MA.
Bectel, RW, NG Tucker, eds. (1998). Across the States 1998: Profiles of Long-Term Care Systems, Third Edition. Washington, DC: American Association of Retired Persons (AARP).
Birnbaum, M (1998). Health Policy for Low-Income People in Pennsylvania. Washington, DC: The Urban Institute.
Bovbjerg, RR, JA Marsteller (1998). Health Care Market Competition in Six States: Implications for the Poor. Washington, DC: The Urban Institute.
Bovbjerg, RR, F Ullman, A Evans, J Holahan, S Flanagan (1998). Health Policy for Low-Income People in New Jersey. Washington, DC: The Urban Institute.
Coughlin, TA, S Rajan, S Zuckerman, JA Marsteller (1998). Health Policy for Low-Income People in Minnesota. Washington, DC: The Urban Institute.
Health Care Financing Administration (HCFA), U.S. Department of Health and Human Services (US DHHS) (1997). Medicare and Medicaid Statistical Supplement, 1997. Baltimore, MD: US DHHS.
Health Care Financing Administration (HCFA), U.S. Department of Health and Human Services (US DHHS) (1998). Data Compendium, 1998. Baltimore, MD: US DHHS.
Health Care Financing Administration (HCFA), U.S. Department of Health and Human Services (US DHHS) (1999a). Medicare and Medicaid Statistical Supplement, 1999. Baltimore, MD: US DHHS.
Health Care Financing Administration (HCFA), U.S. Department of Health and Human Services (US DHHS) (1999b). Medicare Program; Prospective Payment System for Home Health Agencies; Proposed Rule. Federal Register 64(208):58134-58209 (October 28).
Health Care Financing Administration (HCFA), U.S. Department of Health and Human Services (US DHHS) (2000). Medicare Program; Prospective Payment System for Home Health Agencies; Final Rule. Federal Register 65(128):41184 (July 3).
Holahan, J, R Bovbjerg, A Evans, J Wiener, S Flanagan (1998). Health Policy for Low-Income People in Massachusetts. Washington, DC: The Urban Institute.
Holahan, J, J Wiener, S Wallin (1998). Health Policy for the Low-Income Population: Major Findings from the Assessing the New Federalism Case Studies. Washington, DC: The Urban Institute.
Kenney, GM, S Rajan, S Soscia (1998). State spending for Medicare and Medicaid home care programs. Health Affairs, 17(1):201-212.
Komisar, HL, J Feder (1998). The Balanced Budget Act of 1997: Effects on Medicare's Home Health Benefit and Beneficiaries Who Need Long-Term Care. Georgetown University: Institute for Health Care Research and Policy.
Ku, L, A Berkowitz, F Ullman, M Regenstein (1998). Health Policy for Low-Income People in Mississippi. Washington, DC: The Urban Institute.
Lamphere, J, N Brangan, S Bee, R Semansky (1998). Reforming the Health Care System: State Profiles 1998. Washington, DC: American Association of Retired Persons (AARP).
Liu, K, J Harvell, B Gage (2000). Post-Acute Care Issues for Medicare: Interviews with Provider and Consumer Groups, and Researchers and Policy Analysts. Report prepared for the Office of Disability, Aging, and Long-Term Care Policy, Office of the Assistant Secretary for Planning and Evaluation, U.S. Department of Health and Human Services under Contract #100-97-0010. [Full Report]
Medicare Payment Advisory Commission (MedPAC) (2000). Report to the Congress: Medicare Payment Policy. Washington, DC. March 2000.
National Association for Home Care (NAHC) (2000). NAHC Report No. 853. Washington, DC: National Association for Home Care. March 17.
Office of Inspector General (OIG), U.S. Department of Health and Human Services (1995a). Variation Among Home Health Agencies in Medicare Payments for Home Health Services, Report No. OEI-04-93-00260, July.
Office of Inspector General (OIG), U.S. Department of Health and Human Services (1995b). Geographical Variation in Visits Provided by Home Health Agencies, Report No. OEI-04-93-00262, September.
Office of Inspector General (OIG), U.S. Department of Health and Human Services (1997a). Home Health: Problem Providers and Their Impact on Medicare, Report No. OEI-09-96-00110, July.
Office of Inspector General (OIG), U.S. Department of Health and Human Services (1997b). Results of the Operation Restore Trust Audit of Medicare Home Health Services in California, Illinois, New York and Texas, Report No. A-04-96-02121, July.
Office of Inspector General (OIG), U.S. Department of Health and Human Services (1999a). Medicare Beneficiary Access to Home Health Agencies, Report No. OEI-02-99-00530, October.
Office of Inspector General (OIG), U.S. Department of Health and Human Services (1999b). Review of Medicare Home Health Services in California, Illinois, New York, and Texas, Report No. A-04-99-01194, October.
Office of Inspector General (OIG), U.S. Department of Health and Human Services (2000). Medicare Beneficiary Access to Home Health Agencies: 2000, Report No. OEI-02-00-00320, September.
Schore, J (1994). Patient, Agency, and Area Characteristics Associated with Regional Variation in the Use of Medicare Home Health Services. Princeton, NJ: Mathematica Policy Research, Inc., September.
Shaughnessy, PW, KS Crisler, DF Hittle, RE Schlenker, with KS Conway, LR West, MC Powell, AA Richard (2002a). Volume 1, Policy and Program Overview from the report series OASIS and Outcome-Based Quality Improvement in Home Health Care: Research and Demonstration Findings, Policy Implications, and Considerations for Future Change. Denver, CO: Center for Health Services Research, University of Colorado Health Sciences Center, February.
Shaughnessy, PW, DF Hittle, KS Crisler, MC Powell, with AA Richard, AM Kramer, RE Schlenker, JS Steiner, NS Donelan-McCall, JM Beaudry, K Engle, KS Conway, LR West (2002b). Volume 2, Research and Technical Overview from the report series OASIS and Outcome-Based Quality Improvement in Home Health Care: Research and Demonstration Findings, Policy Implications, and Considerations for Future Change. Denver, CO: Center for Health Services Research, University of Colorado Health Sciences Center, February.
Smith, BM, KA Maloy, DJ Hawkins (1999). An Examination of Medicare Home Health Services: A Descriptive Study of the Effects of the Balanced Budget Act Interim Payment System on Access to and Quality of Care. Washington, DC: Center for Health Services Research and Policy, The George Washington University Medical Center, September.
Sparer, MS (1999). Health Policy for Low-Income People in Oregon. Washington, DC: The Urban Institute.
Ullman, F (1998). Health Policy for Low-Income People in Georgia. Washington, DC: The Urban Institute.
U.S. General Accounting Office (GAO), Health, Education, and Human Services Division (HEHS) (1998). Medicare Home Health Benefit: Impact of Interim Payment System and Agency Closures on Access to Services, Publication No. GAO/HEHS-98-238, Washington, DC: GAO.
U.S. General Accounting Office (GAO), Health, Education, and Human Services Division (HEHS) (1999). Medicare Home Health Agencies: Closures Continue, With Little Evidence Beneficiary Access is Impaired, Publication No. GAO/HEHS-99-120, Washington, DC: GAO.
Wiener, JM, A Evans, C Kuntz, M Sulvetta (1998). Health Policy for Low-Income People in Texas. Washington, DC: The Urban Institute.
APPENDIX A. STUDY QUESTIONNAIRES
This appendix contains the Outcome and Assessment Information Set (OASIS), as well as the five questionnaires developed specifically for this study:
- The OASIS-B1 (October 1998) was used for collection of patient health and functional status information. The start/resumption of care, follow-up, and discharge/transfer versions of the OASIS are included in this appendix.
- The Administrator Questionnaire (AQ), which was completed by agency administrators at the beginning of the study, elicits information related to agency factors that may affect the practice of home health care (e.g., licensing and accreditation, reimbursement, caseload, changes due to venipuncture regulations, use of nurse productivity standards, case management, and supervision).
-
Administrator Questionnaire [PDF File]
-
- The Care Provider Profile (CPP) was used to collect information about all care providers conducting assessment visits with the study patients. This questionnaire elicits information regarding provider discipline, education, and experience, among other factors.
-
Care Provider Profile [PDF File]
-
- Two versions of the Care Provider Questionnaire (CPQ), which contain questions related to patient homebound status, Medicare authorization of services, assistance provided by the family/support system, services provided by the agency, physician involvement in care planning, and care coordination. The first version was completed at start of care, resumption of care, or readmission, and the second version was completed at recertification or discharge.
- The Notification of Study Admission (NSA) was completed by home care agency personnel upon admission of a patient into the study. This form served to provide staff at the Center for Health Policy Research with information about each newly enrolled patient, including identifying information, start of care date, and diagnostic information.
-
Notification of Study Admission [PDF File]
-
APPENDIX B. FOCUS GROUP MATERIALS
This appendix contains the Focus Group materials developed specifically for this study:
- The Focus Group Protocol identifies the questions asked during the focus group interviews as well as the two hypothetical patient vignettes that the participants were asked to discuss.
-
Focus Group Protocol [PDF File]
-
- The Participant Demographic Form, which all focus group participants completed prior to participating in the interviews, was used to obtain information about participant characteristics such as age, gender, and years of home health care experience.
-
Focus Group Participant Demographic Form [PDF File]
-
APPENDIX C. CASE STUDY MATERIALS
This appendix contains the Case Study Protocol. This document identifies the questions that were asked of the nurses participating in the case study interviews.
- Case Study Protocol [PDF File]
APPENDIX D. SUPPLEMENTAL INFORMATION ON THE STUDY STATES
This appendix contains additional information about the demographic, economic, and health system characteristics of the eight states selected for involvement in the study.
A. Introduction
This appendix supplements Chapter 3 and is drawn primarily from reports by the American Association of Retired Persons (AARP) and the Urban Institute (UI). The sources are listed in Table D.1; full citations are in the References section following the main text.
| TABLE D.1: Source Materials for Study State Information | |
| Low Volume | |
| Minnesota | UI: Bovbjerg and Marsteller 1998; Coughlin, Rajan, Zuckerman, and Marsteller 1998; Holahan, Wiener, and Wallin 1998. |
| New Jersey | UI: Bovbjerg, Ullman, Evans, Holahan, and Flanagan 1998; Holahan, Wiener, and Wallin 1998. |
| Oregon | UI: Sparer 1999. |
| Pennsylvania | UI: Birnbaum 1998. |
| High Volume | |
| Georgia | UI: Ullman 1998. |
| Massachusetts | UI: Holahan, Bovbjerg, Evans, Wiener, and Flanagan 1998; Bovbjerg and Marsteller 1998; Holahan, Wiener, and Wallin 1998. |
| Mississippi | UI: Ku, Berkowitz, Ullman, and Regenstein 1998; Holahan, Wiener, and Wallin 1998. |
| Texas | UI: Wiener, Evans, Kuntz, and Sulvetta 1998; Bovbjerg and Marsteller 1998. |
| All States | |
| AARP: Lamphere et al. 1998. AARP: Bectel and Tucker 1998. | |
The following sections, which provide brief comments on each study state, are intended to provide some additional descriptive information on state demographic, economic, and health care system features. Many of the points are based on data in the tables presented in Chapter 3. (The AARP reports listed in Table D.1 are the sources for most of the information about the states contained in Chapter 3.)
B. Low-Volume States
1. Minnesota
Demographic-Economic Characteristics: Minnesota is enjoying a strong economy and a low unemployment rate. However, the poverty level among the elderly is above average. The population overall has good health status. For example, compared to the other study states, there are fewer elderly people with difficulty in mobility or self care.
Health Care System Features: Minnesota has one of the lowest uninsured rates in the country and a greater than average number of physician generalists. The Medicaid program appears to be quite generous. Minnesota is attempting to increase the use of managed care through MinnesotaCare Acts of 1992. It is also trying to increase third-party revenues such as Medicare. Compared to other states, there is a high level of HMO penetration. However, the level of Medicare enrollment in Risk HMOs is below the national average.
2. New Jersey
Demographic-Economic Characteristics: New Jersey is the most urbanized and densely populated of all states in the nation. New Jersey has a high per capita income ($32,700 compared to $25,600 nationally in 1997) and more of the state's elderly are insured than average. Of the study states, New Jersey has the lowest rate of persons 65 years or older living alone.
Health Care System Features: New Jersey's large Medicaid program comprises about one-fourth of the state's budget, and is moving toward managed care and home and community-based care instead of institutional care. Despite relatively high Medicaid expenditures on home and community-based care, 84 percent of New Jersey's Medicaid long-term care expenditures go to nursing homes. Widespread interest in home and community-based care expansion has targeted existing nursing home spending for budget cuts. Medicaid spends an average of nearly $4,000 more per elderly enrollee than the national average. New Jersey has a low rate of physician generalists and a low rate of nursing home residents per 1000 elderly. Of the study states, New Jersey has the lowest rate of Medicare beneficiaries covered by Medicaid.
3. Oregon
Demographic-Economic Characteristics: Throughout the 1990's, Oregon's population growth rate was twice the national average, and a successfully diversified economy led to economic growth and wage increases. From 1990 to 1998, Oregon experienced a seven percent drop in the number of uninsured residents, leaving only 11 percent without insurance. However, this number has recently begun to increase as the state's economy has somewhat weakened. Oregon's population is comprised of 6.4 percent ethnic and racial minorities, well under the 17.4 percent national average. Of all the study states, Oregon has the lowest percentage of elderly persons living below the poverty line.
Health Care System Features: As in Pennsylvania and a handful of other states, Oregon requires all Medicaid beneficiaries to enroll in managed care. This is one provision of the Oregon Health Plan (OHP) enacted in 1989, which also expands Medicaid eligibility to the poor and requires employers to provide insurance to their workers. Oregon is the only study state spending more Medicaid dollars on home and community-based health services than on institutional care provided in nursing homes. Most elderly Medicaid beneficiaries in Oregon are enrolled in a managed care plan, and traditional long-term care services such as physical therapy and home health are covered by this plan. Of the study states, Oregon has the lowest number of nursing home beds, and is one of only two states in the nation to have had a decline in this number.
4. Pennsylvania
Demographic-Economic Characteristics: Pennsylvania's economy is the sixth largest in the nation (as measured by gross state product). The economy is characterized by service industries, which have replaced manufacturing as the predominant source of output. Roughly 16 percent of Pennsylvania's residents are over 65 years of age, second only to Florida. Of the low-volume study states, Pennsylvania has the highest rate of elderly having difficulty in mobility or self care.
Health Care System Features: Pennsylvania's large elderly population and the extensive penetration of managed care distinguish the state's health care system from other states, and are reflected in Pennsylvania's large Medicaid program. Between 1990 and 1996, Medicaid spending on long-term care and acute care services for the elderly increased by 140 percent, well above the national average (80 percent). Pennsylvania has increased its enrollment of Medicaid beneficiaries in managed care during the past decade. Overall enrollment of Medicaid beneficiaries in some form of managed care programs increased from 12 percent in 1991 to 70 percent in August 1998. Though experiencing financial challenges, Pennsylvania's mandatory Medicaid HMO enrollment program, Healthshares, has been implemented in Philadelphia and Pittsburgh, and will be introduced throughout the state in 2000.
C. High-Volume States
1. Georgia
Demographic-Economic Characteristics: The population in Georgia is rapidly growing and the state's economy is strong. About one-third of the state's population is African-American (compared to 12.5 percent for the nation as a whole). Of all the study states, Georgia has the lowest elderly population percentage (9.9 percent aged 65 and over in 1998). Despite this, compared to other states, residents of Georgia do not fare as well on many indicators of health status. For example, Georgia has a higher rate of premature death and of elderly having difficulty in mobility or self care than all the study states other than Mississippi.
Health Care System Features: Although the Medicaid program in Georgia is considered to be generous, the rate of growth for Medicaid programs for the elderly is below the national average. For example, long-term care spending per elderly Medicaid recipient is significantly less than the national average. Most long-term care spending (70.5 percent) is for institutional care. Compared to other states, there are fewer nursing facility beds available in Georgia and a lower nursing home utilization rate. Currently, the state has very low Medicare enrollment in Risk HMOs (3.9 percent of Medicare beneficiaries in 1998).
2. Massachusetts
Demographic-Economic Characteristics: Massachusetts differs from the other high-volume states in many characteristics. It has a largely urbanized population with a relatively high percentage of elderly (13.8 percent, the highest of the high-volume states). Per capita income is approximately $6,000 higher in Massachusetts compared to the national average and individuals tend to have good scores on standard measures of health (e.g., low premature death rates). In addition, the number of persons aged 65 and over with difficulty in mobility or self-care is substantially lower compared to the other high-volume study states.
Health Care System Features: Massachusetts is characterized as having a very generous Medicaid program. The Medicaid program is expanding its managed care component and is substituting community-based long-term care services for institutional services whenever possible. There are twice as many Medicaid home health recipients per 1000 recipients compared to the other high-volume study states. The state is regarded as successful in shifting Medicaid long-term care expenditures to Medicare (i.e., Medicaid bills Medicare for home health and nursing home care when possible). Compared to other states, Massachusetts is very concerned about "Medicaid Estate Planning" (i.e., individuals who provide misleading information about their financial situation in order to qualify for Medicaid).
Over one-fifth (21.4 percent) of Medicare beneficiaries are enrolled in Risk HMOs, a figure that is above average for the nation and roughly twice as high as the average HMO penetration rate for the four high-volume study states. Of the four high-volume study states, Massachusetts also has the highest percentage of individuals covered by private insurance.
3. Mississippi
Demographic-Economic Characteristics: The majority of Mississippi's population is classified as living in rural areas, and approximately two-fifths of the population is African-American. Mississippi's economy has experienced recent growth, partly due to an increase in legalized gambling revenues. The state is one of the poorest in the nation, with a high unemployment rate and low per capita income. Mississippi's poverty rate is the highest of all the study states, and is eight percentage points higher than the national average (29.9 percent versus 21.7 percent). Mississippi residents have relatively poor health status, and the state has the highest number of persons 65 years or older per thousand that have difficulty in mobility or self-care of all study states, a figure about 38 percent higher than the national average (276.9 percent versus 201.1 percent).
Health Care System Features: Managed care has only recently entered Mississippi and has faced physician shortages in creating provider networks. As a result, HMO penetration is low; about two percent of Mississippi residents (compared to 23 percent nationally) receive health services from an HMO. Compared to other study states and the nation, there is a small number of nursing facility beds in Mississippi, and nursing homes have a 99 percent occupancy rate. Mississippi's Medicaid program accounted for 22 percent of total state expenditures in 1995 and the federal Medicaid matching rate is the highest in the country at 77.2 percent. The Medicaid program has a high rate of expenditure growth but does not spend as much as the national average on long-term care services such as home health. This is due to a strict certificate-of-need policy restricting capacity. Additionally, the Medicaid program continues to utilize mostly institutional care more than home and community-based care, which is relatively sparse and dominated by Medicare.
4. Texas
Demographic-Economic Characteristics: Compared to other study states, the Texas population is characterized by higher rates of poverty and uninsured individuals, and the majority of its 254 counties are considered rural. In addition, the proportion of Hispanics in Texas is high relative to the rest of the nation. With respect to several indicators of health status and the percentage of elderly living alone, Texans are similar to the rest of the nation.
Health Care System Features: Texas is a politically conservative state with a strong anti-tax philosophy (as illustrated by the fact that Texas does not have an income tax). The state is described as taking "a minimalist approach to health and social welfare programs, funding little beyond what is required to draw down federal matching payments" (Wiener et al., 1998). Medicaid eligibility requirements are restrictive though the program is growing (mainly because the state is trying to obtain the highest level of federal matching funds possible). The state has a large home and community-based services program, and it has the highest Medicaid expenditure percentage for personal care (12.0 percent) of all study states. The movement toward managed care is growing; most HMOs in the state are proprietary organizations.
APPENDIX E. ADMINISTRATOR QUESTIONNAIRE DESCRIPTIVE STATISTICS AND WRITE-IN RESPONSES
This appendix contains information gathered using the Administrator Questionnaire (AQ).
- Table E.1 presents descriptive statistics for each AQ item. For continuous variables, the mean, median, minimum, and maximum values are presented. For categorical variables, the percentage of agencies for which each response was selected is identified. The number of agencies responding to each item also is reported. The final two items in the AQ (items 69 and 70) have been excluded from Table E.1. These items were designed for internal Research Center use only.
-
Table E.1: Descriptive Statistics for the Administrator Questionnaire Items [PDF File]
-
- Table E.2 contains the responses to AQ items in which administrators were allowed to provide additional or open-ended information. Administrators' responses to some items (AQ18 and AQ27_4SP) were reformatted so that like responses could be combined. For example, for AQ item 18, the responses "GBA Palmetto," "Palmetto," "PGBA," and other variations all were categorized as "Palmetto Government Benefits Administrators." Generally, for the other items in this appendix, administrators' responses are presented as they were written. Only minor corrections of spelling were made to these responses.
-
TABLE E.2: Administrator Questionnaire Write-in Responses [PDF File]
-
APPENDIX F. MULTIVARIATE ANALYSIS VARIABLE LIST
This appendix contains the list of independent variables included in the multivariate analyses, which are summarized in Chapter 4. As described in Chapter 2, this list (Table F.1) includes the patient, provider, agency, market/regulatory, and practice pattern variables of greatest theoretical interest. Some potential independent variables were eliminated from the multivariate analyses as a result of large amounts of missing data and/or a lack of sufficient variability. Others were removed because of strong correlations with other important independent variables. Some of the independent variables presented in Table F.1 were identified as being of particular theoretical importance. These "required variables" were included in the final multivariate analysis models, regardless of their degree of statistical significance in the preliminary models. The variables designated as required are identified in the table. (The procedure for conducting the multivariate analyses is described in detail in Chapter 2.)
- Table F.1: Variables Included in Multivariate Analyses Reported in Chapter 4 [PDF File]