U.S. Department of Health and Human Services
Longitudinal Analysis of High Cost Medicaid Children in California
Marilyn Rymer Ellwood and Elicia Herz
SysteMetrics/McGraw-Hill, Inc.
October 1990
This report was prepared under contract #HHS-100-88-0041 between the U.S. Department of Health and Human Services (HHS), Office of Family, Community and Long-Term Care Policy (now the Office of Disability, Aging and Long-Term Care Policy (DALTCP)) and SysteMetrics. For additional information about the study, you may visit the DALTCP home page at http://aspe.hhs.gov/_/office_specific/daltcp.cfm or contact the ASPE Project Officer, John Drabek, at HHS/ASPE/DALTCP, Room 424E, H.H. Humphrey Building, 200 Independence Avenue, SW, Washington, DC 20201. His e-mail address is: John.Drabek@hhs.gov.
An earlier paper in this project analyzed four State Medicaid programs to assess the extent to which they served as a "safety net" for high cost children and youth, using cross-sectional Medicaid data for one year in each State (Burwell and Herz, 1990). This study takes that analysis one step further, and examines the experience of a cohort of high cost Medicaid children over several years. In a sense, this study examines the extent to which the safety net may be temporary for some high cost children, and permanent for others.
Seven years of Medicaid data were used to analyze the experience of high cost children. The study population consisted of children and youth under age 26 with Medicaid expenditures of $25,000 or more during 1983 in California. Longitudinal Medicaid data from 1980 through 1986 were analyzed for this cohort of children. Thus, the study analyzed their retrospective and prospective experience with Medicaid. The major research questions addressed by the study were:
-
What proportion of high cost children are "new" to the Medicaid program when they experience a period of high medical expenditures? To what extent do high cost children remain enrolled in Medicaid after their period of high expenditures?
-
Have these children had high costs on Medicaid in the past? Do they have persistently high costs in the future?
-
Are there variations in the longitudinal experience of high cost Medicaid children by age, institutional status or eligibility group? What are the characteristics of high cost children who use Medicaid as a permanent safety net?
DATA SOURCES AND STUDY LIMITATIONS
The data for this study were drawn from the Tape-to-Tape data base. Tape-to-Tape is a multi-State Medicaid data base developed by the Office of Research and Demonstrations at HCFA. Tape-to-Tape includes information on every Medicaid enrollee and every claim processed by the Medicaid Management Information System (MMIS) in several States since 1980. For this study, a research file was constructed of all children and young adults up to age 26 in California who had total Medicaid payments in 1983 in excess of $25,000.1 The threshold amount of $25,000 was arbitrary and was simply used to identify children with extraordinarily high Medicaid expenditures. Study data for each child included information on their enrollment, utilization and Medicaid expenditures in 1983, plus their experience in the Medicaid program from 1980 through 1986. Thus, the research file included a total of 7 years of data for this cohort of high cost children.
A few high cost children were excluded from the study cohort. Appendix A reviews the sample selection steps and discusses other data limitations.
It should be noted that California was not a representative State with regard to its Medicaid program in 1983 or at any point over the seven year study period. From 1980 through 1986, it covered more of the Medicaid optional eligibility groups than other States. Of relevance to this analysis of children, California included the optional Medicaid group of all Ribicoff children under age 21 in its coverage throughout the study period. Ribicoff children are those residing in two-parent families. Ordinarily, children living with both parents cannot qualify for Medicaid through the AFDC program since they are not considered to be deprived of parental support or "dependent." With the Ribicoff optional group, children living with both parents can qualify for Medicaid (although their parents cannot qualify) if the family's income meets the Medicaid income eligibility standards used by the State.
California also had a medically needy program during the study period. Medically needy coverage is important since it allows children in families of any income level to qualify for Medicaid. With a medically needy program, a State can allow persons to qualify for Medicaid through "spending-down," even if their income exceeds the medically needy income level. The spend-down process allows applicants to deduct medical expenses from income in determining financial eligibility. Thus, children from families of any income level could qualify for Medicaid, assuming their medical bills were large enough.
Finally, for all its eligibility groups, California used much higher income thresholds than other States to determine financial eligibility. As shown in Table 1, its monthly payment standard for an AFDC family of 4 in 1983 was $625, compared to $368 for the median State nationwide. California's SSI income standard for a disabled person living independently was $451 in 1983, compared to $304 for the median State. Its medically needy income level for one-person was $544, with $801 for four-persons. These levels were also considerably higher than other States. All of California's financial criteria relevant to Medicaid were the highest in the continental United States throughout the seven year study period. Thus, California offered greater possibilities for Medicaid to work as a safety net for high cost children than other States.
| TABLE 1. Selected Income Eligibility Levels Relevant to Medicaid (California, 1983) | ||
| California | U.S. Median State | |
| AFDC 4-Person Family | $625 | $368 |
| Medically Needy 4-Persons | $801 | $458* |
| Federal Poverty Level 4-Person Family | $848 | |
| SSI Disabled Individual Living Independently | $451 | $304 |
| Medically Needy 1-Person | $544 | $300* |
| Federal Poverty Level for Single Individual Under Age 65 | $432 | |
| * Medically needy levels for U.S. median State are for March, 1984. | ||
HIGH COST COHORT
The study cohort consisted of 4,726 California children under age 26 who had Medicaid expenditures of $25,000 or more in 1983. As shown in Table 2, about half of the cohort (48.5%) were institutionalized (in a long-term care or inpatient psychiatric facility) during 1983, and about half (51.5%) were not.
Data in Table 2 show several differences between the noninstitutionalized high cost group and the institutional group. The vast majority of the institutional group were teenagers and young adults, while just over half of the noninstitutional group was 3 years of age or less. The predominance of older children in the institutionalized group is not surprising, since it is rare for young children to be institutionalized. The age distribution for the noninstitutional group resembles a reverse J-shape, with the lowest incidence of high costs for children in the 4-10 years age group. This age distribution pattern for the noninstitutional group follows the same general pattern shown for all high cost pediatric hospitalizations in California (Ku, 1990).
Both groups had significantly more males than females, which is also consistent with previous research on high cost children (Burwell, 1990). This pattern was somewhat stronger with the institutional group.
The vast majority of institutionalized children (89.4%) qualified for Medicaid through the SSI cash assistance group. This pattern is related to an important difference in eligibility criteria used for the noninstitutional and institutional groups. For children considered to be living at home (i.e. the noninstitutionalized), program regulations generally require that the income and resources of parents are considered in determining their eligibility for cash assistance and Medicaid. After certain disregards for earned and unearned income, parental income is compared to the AFDC, SSI or medically needy income standards (adjusted for family size) to determine whether a child will qualify or cash and/or medical assistance. However, parental income is not "deemed" to be available to institutionalized children. Thus, most disabled children in institutions are not considered to have any income, and they qualify for cash assistance under the SSI program. In 1983, these children would have received an SSI monthly payment of $25 to cover their incidental needs while in the institution. An additional 6.8% of the institutionalized group passed the SSI disability test, but were medically needy (indicating they had some income).
| TABLE 2. Selected Data on High Cost Medicaid Children Cohort (California, 1983) | |||
| Not Institutionalized | Institutionalized | Total | |
| Number of Children | 2,435 | 2,290 | 4,726 |
| Percent by Institutional Status | 51.5 | 48.5 | 100.0 |
| Age Group Distribution | |||
| 29.6 | 0.8 | 15.6 |
| 24.0 | 2.3 | 13.5 |
| 10.3 | 5.9 | 8.2 |
| 23.3 | 45.5 | 34.1 |
| 12.8 | 45.5 | 28.7 |
| 100.0 | 100.0 | 100.1 |
| Average Age (in Years) | 7.9 | 18.7 | 13.1 |
| Percent Male | 55.9 | 59.5 | 57.6 |
| Average Length of Enrollment in 1983 (in months) | 8.5 | 11.7 | 10.1 |
| Eligibility Group | |||
| 35.3 | 0.9 | 18.6 |
| 16.0 | 0.5 | 8.5 |
| 18.8 | 89.4 | 53.0 |
| 7.8 | 6.8 | 7.3 |
| 22.2 | 2.4 | 12.6 |
| 100.1 | 100.0 | 100.0 |
| Average Medicaid Expenditure Per Recipient in 1983 | $59,387 | $43,845 | $51,856 |
| Average Medicaid Expenditure Per Personyear of Enrollment in 1983 | $83,769 | $45,204 | $61,933 |
| Distribution of 1983 Expenditures by Service Category | |||
| 90.0 | 10.4 | 57.4 |
| --- | 71.8 | 29.4 |
| --- | 1.0 | 0.4 |
| --- | 14.6 | 6.0 |
| 10.0 | 2.2 | 6.8 |
| 100.0 | 100.0 | 100.0 |
A completely different eligibility profile prevailed for the non-institutionalized group. Only 26.6% of the noninstitutional group were eligible for Medicaid through the SSI disabled cash or medically needy groups. The AFDC and Ribicoff groups provided the main entry to Medicaid eligibility for noninstitutional high cost children.
The average Medicaid expenditure per high cost child in 1983 was $43,845 for the institutional group, compared to $59,387 for the noninstitutional group. Noninstitutional children incurred higher Medicaid costs, even though their average length of enrollment on Medicaid during 1983 was 8.5 months, compared to 11.7 months for institutionalized high cost children. The average expenditure per personyear of enrollment incorporates this adjustment for length of enrollment. Using personyears of enrollment as the denominator, noninstitutionalized children averaged $83,769 per recipient in 1983 Medicaid expenditures, compared to only $45,204 for institutionalized children.
Table 3 shows the distribution of expenditures per recipient for each of the study groups, and indicates there were many more very expensive children among the noninstitutional group. Ten percent of noninstitutional children had Medicaid expenditures in 1983 of $104,408 or more. The most expensive 10% of institutionalized children had expenditure levels of only $48,982 or more. Thus, there was less variance in overall 1983 Medicaid expenditure levels among the high cost institutional group.
Returning to Table 2, we see that 90% of the expenditures for the noninstitutional group were for inpatient hospital care, while only 10% of the expenditures for the institutional group were in this service category. The vast majority of Medicaid expenditures for high cost children in the institutional group were for ICF/MR and SNF care.
| TABLE 3. Distribution of Annual Medicaid Expenditures Per Recipient for High Cost Children (California, 1983) | |||
| Noninst. | Inst. | Total | |
| Average Annual Expenditure per Recipient | $59,387 | $43,845 | $51,856 |
| Annual Expenditure per Recipient at 25th Percentile | $31,481 | $39,536 | $36,085 |
| Median Annual Expenditure per Recipient | $42,666 | $42,303 | $42,330 |
| Annual Expenditure per Recipient at 75th Percentile | $66,340 | $44,403 | $49,904 |
| Annual Expenditure per Recipient at 90th Percentile | $104,408 | $48,982 | $81,761 |
| Annual Expenditure per Recipient at 95th Percentile | $151,345 | $66,241 | $111,215 |
| Highest Annual Expenditure per Recipient | $549,629 | $213,365 | $549,629 |
Table 4 shows that 6.1% of the noninstitutional group and 7.4% of the institutional group had some form of private health insurance during 1983, in addition to their Medicaid coverage. Children with private insurance coverage in the noninstitutional group had significantly lower Medicaid expenditures per recipient (using personyears of enrollment) in 1983--$77,036 compared to $84,143 for children without insurance. However, private insurance did not reduce Medicaid expenditures for the institutional group. Institutionalized children with insurance averaged $46,461 per recipient in 1983 Medicaid expenditures, compared to $44,909 for uninsured children. Since private insurance usually provides little coverage for long-term care, this result is not surprising.
| TABLE 4. High Cost Children by Private Health Insurance Status and Average Medicaid Expenditure* in 1983 | ||||
| No Insurance | Insurance | |||
| Percent | 1983 $/PYE | Percent | 1983 $/PYE | |
| Noninstitutionalized Children | 93.9 | $84,183 | 6.1 | $77,036 |
| Institutionalized Children | 92.6 | $44,909 | 7.4 | $46,461 |
| Total | 93.3 | $62,150 | 6.7 | $59,043 |
| * Using personyears of enrollment. | ||||
Table 5 presents data on the two groups by spend-down status. About 15% of the noninstitutional high cost group had a spend-down liability in 1983, compared to only 5% of the institutional group. Since parental income is not deemed to be available to institutionalized children, it is not surprising that fewer children in long-term care facilities had spend-down liabilities.
| TABLE 5: High Cost Children by Spend-down Status and Average Medicaid Expenditure* in 1983 | ||||
| No Spend-Down | Spend-Down | |||
| Percent | 1983 $/PYE | Percent | 1983 $/PYE | |
| Noninstitutionalized Children | 85.2 | $81,558 | 14.8 | $98,298 |
| Institutionalized Children | 95.0 | $43,739 | 5.0 | $45,843 |
| Total | 89.9 | $60,018 | 10.1 | $82,645 |
| * Using personyears of enrollment | ||||
Somewhat surprising, noninstitutionalized children with a spend-down contribution had higher average Medicaid expenditures than children without a spend-down--$98,298 compared $81,558. Since the spend-down children incurred costs to satisfy the spend-down liability, their total costs (the spend-down liability plus the Medicaid expenditures) would clearly exceed the Medicaid expenditure level for high cost children who did not spend-down. It is not clear why spend-down children had higher Medicaid expenditures. One possible explanation is that families may resort to the spend-down process only when the hospital costs are extraordinarily high. Another possibility is that children whose families have some income to contribute to the cost of their care may have access to more expensive or extensive services.
Table 6 shows the distribution of institutionalized and noninstitutionalized children with spenddown liabilities by the amount of their spend-down liabilities in 1983. The average annual spend-down liability was $1,296 per child for the noninstitutional group, compared to $2,171 for the Institutionalized group. Of interest, just over half of the institutional group had spend-down amounts of over $1,500 annually, compared to only 27% of the noninstitutional group. Thus, while there were fewer children with spend-down liabilities among the institutional group, they had larger spend-downs.
| TABLE 6: High Cost Children with Spend-down by Amount of Spend-down Liability in 1983 | ||
| Annual Spend-down Liability in 1983 | Percent of Noninstitutionalized Children with Spend-down | Percent of Institutionalized Children with Spend-down |
| $250 | 27.7 | 7.0 |
| $251-$500 | 14.4 | 7.8 |
| $501-$1,000 | 18.3 | 11.3 |
| $1,001-$1,500 | 12.5 | 18.3 |
| $1,501+ | 27.1 | 55.6 |
| 100.0 | 100.0 | |
| Average Annual Spend-down Liability in 1983 | $1,296n=361 | $2,171n=115 |
Reliable diagnostic information was only available for the noninstitutional group. Table 7 shows the distribution of noninstitutional high cost children by ICD-9-CM diagnosis group and age. Children were assigned to the diagnosis group in which they incurred the greatest total Medicaid expenditures during 1983. Diagnoses varied substantially by age. For infants under age 1, the vast majority had diagnoses related to conditions originating in the perinatal period (72.2%) and congenital anomalies (9%). Specific diagnoses for conditions originating in the perinatal period included short gestation period and low birthweight, respiratory distress syndrome and other respiratory conditions. Congenital anomalies included congenital hydrocephalus and other congenital anomalies of the nervous system, congenital heart defects and spinal bifida. For children ages 1-3, the most frequently occurring diagnoses were ill-defined conditions (22.6%), conditions originating during the perinatal period (17.5%), and diseases of the respiratory system (12.7%). For the three older age groups, the most frequently occurring diagnosis was in the category of injuries, accidents and poisonings.
| TABLE 7: Percent Distribution of High Cost Noninstitutionalized Children by Major Diagnostic Group and Age | ||||||
| 1 | 1-3 | 4-10 | 11-20 | 20-25 | Total | |
| Infections/Parasitic | 1.9 | 2.7 | 2.8 | 1.9 | 1.6 | 2.2 |
| Neoplasms | 0.6 | 6.3 | 17.5 | 8.1 | 7.4 | 6.3 |
| Endocrine | 1.0 | 2.4 | 5.6 | 4.0 | 5.8 | 3.1 |
| Blood/Blood Organs | 0.1 | 1.4 | 4.0 | 5.3 | 8.3 | 3.1 |
| Mental Disorder | -- | -- | -- | 1.2 | 2.9 | 0.7 |
| Nervous System/Sense | 1.4 | 5.3 | 0.8 | 6.2 | 9.6 | 5.0 |
| Circulatory System | 0.7 | 3.6 | 6.3 | 2.8 | 2.9 | 2.5 |
| Respiratory System | 4.2 | 12.7 | 4.0 | 4.4 | 2.9 | 6.7 |
| Digestive System | 3.8 | 6.5 | 10.3 | 2.8 | 2.6 | 4.2 |
| Genitourinary System | 0.1 | 1.5 | 5.2 | 2.5 | 2.6 | 1.6 |
| Pregnancy Complications | 0.4 | 0.2 | -- | 3.3 | 1.9 | 1.2 |
| Skin and Subcutaneous Tissue | -- | -- | 1.6 | 2.8 | 4.5 | 1.6 |
| Musculoskeletal/Connective | 0.3 | 0.7 | 3.2 | 4.2 | 4.2 | 2.1 |
| Congenital Anomalies | 9.0 | 0.5 | 7.9 | 3.5 | 1.6 | 8.7 |
| Perinatal Conditions | 72.2 | 17.5 | 0.8 | 9.0 | 1.0 | 29.1 |
| Ill-defined Conditions | 3.1 | 22.6 | 4.8 | 2.5 | 2.6 | 3.5 |
| Injury/Accidents Poisonings | 0.4 | 5.0 | 18.3 | 32.0 | 35.6 | 16.5 |
| Miscellaneous V Codes | 0.4 | 10.3 | 4.0 | 1.9 | 0.6 | 1.3 |
| Other, Unknown | 0.4 | 0.9 | 0.4 | 1.4 | 1.6 | 0.7 |
| 99.9n=720 | 100.1n=584 | 100.2n=252 | 99.8n=568 | 100.2n=312 | 100.1n=2436 | |
LONGITUDINAL ANALYSIS
The major impetus for this study was to better understand the longitudinal Medicaid patterns of high cost children. The first research question of interest is the extent to which high cost children were "new" to Medicaid as a result of their high cost episode. We excluded infants from this analysis since all infants were new to the program in 1983, and the data base did not provide information on the Medicaid eligibility status of their mothers.
If Medicaid is working as a safety net for children with catastrophic health needs, presumably many children over one year of age would not have been enrolled prior to the high cost episode. However, we have to keep in mind that new children (high cost or not) are always coming onto Medicaid. For example, Ellwood and Bane reported that at a point in time, approximately 21% of AFDC cases have been enrolled for less than one year (Ellwood and Bane, 1983), although this rate included families with only newborns. We also have to consider that SSI children are a portion of our high cost group. Generally the new enrollment rate for SSI children nationwide has been running about 20% annually (Staren, 1990). Although it is difficult to estimate precisely how many new high cost children would be "normal" for Medicaid each year, these rates for the AFDC and SSI programs provide some guidance.
Table 8 shows us the extent to which children in the high cost cohort were enrolled in Medicaid before and after 1983. About 66% of the noninstitutional high cost group (who were at least age 1 by 1983) were enrolled in Medicaid in 1982, compared to 96% of the institutional group. Thus, in 1983 about one-third of the noninstitutional high cost children were "new" to the program (excluding children born in 1983). The "new" entry rate to the high cost institutional group was considerably less (about 4%).
| TABLE 8: High Cost Child Cohort Percent Enrolled and Deceased by Institutional Status, 1980-1986 | |||||||
| 1980 | 1981 | 1982 | 1983 | 1984 | 1985 | 1986 | |
| NonInstitutionalized | |||||||
| 45.2** | 53.8** | 66.1** | 100.0 | 70.6 | 54.8 | 47.8 |
| -- | -- | -- | 5.0 | 2.5 | 1.5 | 0.7 |
| -- | -- | -- | 5.0 | 7.6 | 9.1 | 9.8 |
| Institutionalized | |||||||
| 90.3** | 92.8** | 96.3** | 100.0 | 96.5 | 91.5 | 88.9 |
| -- | -- | -- | 1.4 | 2.0 | 1.6 | 1.6 |
| -- | -- | -- | 1.4 | 3.4 | 5.0 | 6.6 |
| Total | |||||||
| 74.6** | 78.5** | 83.3** | 100.0 | 83.2 | 72.6 | 67.7 |
| -- | -- | -- | 3.3 | 2.3 | 1.5 | 1.2 |
| -- | -- | -- | 3.3 | 5.6 | 7.1 | 8.3 |
| * Deceased are a subset of the enrolled.** Excluded from the denominator for 1980-1982 are children in the study sample not yet born. Thus, the data for 1980 show the 1983 high cost children enrolled in Medicaid in 1980 as a percent of those who were alive in 1980. | |||||||
The "new" entry rate of 34% for noninstitutional high cost children is considerably higher than the expected AFDC rate of 21% (which would probably be lower if newborns were excluded) and the SSI rate of 20%, suggesting that California's Medicaid program did pick up a significant number of high cost children in 1983 beyond what would be expected with normal caseload turnover and increases.
The next question is the extent to which high cost children are temporary or permanent Medicaid enrollees. Again, it is important to think about the normal expected length of enrollment for children on Medicaid. For AFDC cases at a given point in time, 50% to 60% would have been enrolled for four or more years (Ellwood and Bane, 1983). For SSI children, we would expect an even longer duration. Previous research has shown that California children who became eligible for SSI cash assistance had low turnover, whereas Ribicoff and medically needy children in California had very short periods of enrollment (Rymer and Adler, 1985).
Data in Table 8 show that high cost institutionalized children have a high probability of remaining on Medicaid over time, while noninstitutionalized children show considerably greater turnover. In 1986, about 90% of the institutionalized group were still on Medicaid, and 6% were deceased. Thus, Medicaid appears to work as a permanent source of coverage for high cost institutional children. Remember that most of the institutional children are SSI cash children.
In contrast, by 1986 only about half of the noninstitutionalized high cost group were still Medicaid enrollees. Also, by the end of 1986, about 10% of this group were deceased. Thus, for about 40% of the noninstitutional group, Medicaid was working more as a catastrophic insurance program, i.e. Medicaid coverage was used during an episode of high costs, but did not continue to provide ongoing coverage over time. On the other hand, slightly more of the high cost children continued to be enrolled in 1986 than were eligible in 1980. Thus, high cost children exited the program at a somewhat slower rate than they entered.
For the noninstitutional cohort, there were age-related differences in the pre and post 1983 enrollment patterns. Younger children were more likely than older children to have been enrolled in Medicaid prior to the high cost episode. Table 9 shows the retention rates on Medicaid for the noninstitutional cohort by age group. In 1982 (the year before the high cost episode of interest), 68.5% of children ages 1-4 and 76.2% of children ages 4-10 were enrolled in Medicaid, compared to 61% of children over age 10.
| TABLE 9: Noninstitutional High Cost Child Cohort Percent Enrolled and Deceased by Age Group, 1980-1986 | |||||||
| 1980 | 1981 | 1982 | 1983 | 1984 | 1985 | 1986 | |
| 1 Years (n=720) | |||||||
| -- | -- | -- | 100.0 | 68.5 | 47.2 | 40.6 |
| -- | -- | -- | 1.2 | 1.7 | 0.6 | 0.3 |
| -- | -- | -- | 1.2 | 2.9 | 3.5 | 3.8 |
| 1-3 Years (n=584) | |||||||
| 38.2** | 57.8** | 68.5 | 100.0 | 68.3 | 56.5 | 49.9 |
| -- | -- | -- | 4.3 | 2.7 | 1.2 | 0.5 |
| -- | -- | -- | 4.3 | 7.0 | 8.2 | 8.7 |
| 4-10 Years (n=252) | |||||||
| 58.3 | 68.3 | 76.2 | 100.0 | 78.2 | 65.9 | 56.7 |
| -- | -- | -- | 4.0 | 5.1 | 4.8 | 1.6 |
| -- | -- | -- | 4.0 | 9.1 | 13.9 | 15.5 |
| 11-20 Years (n=568) | |||||||
| 44.0 | 50.5 | 61.1 | 100.0 | 72.9 | 55.1 | 47.9 |
| -- | -- | -- | 6.5 | 1.9 | 1.6 | 0.9 |
| -- | -- | -- | 6.5 | 8.4 | 10.0 | 10.9 |
| 21-25 Years (n=312) | |||||||
| 38.1 | 54.2 | 61.5 | 100.0 | 70.2 | 60.1 | 53.5 |
| -- | -- | -- | 13.1 | 3.2 | 1.6 | 1.3 |
| -- | -- | -- | 13.1 | 16.3 | 17.9 | 19.2 |
| Total Noninstitutionalized (n=2,436) | |||||||
| 45.2** | 53.8** | 66.1** | 100.0 | 70.6 | 54.8 | 47.8 |
| -- | -- | -- | 5.0 | 2.5 | 1.5 | 0.7 |
| -- | -- | -- | 5.0 | 7.6 | 9.1 | 9.8 |
| * Deceased are a subset of the enrolled.** Excluded from the denominator for 1980-1982 are children in the study sample not yet born. Thus, the data for 1980 show the 1983 high cost children enrolled in Medicaid in 1980 as a percent of those who were alive in 1980. | |||||||
However, older high cost children (in the noninstitutional cohort) were more likely to remain enrolled on Medicaid after the high cost episode than infants. Only 40.6% of infants in the high cost cohort were still on Medicaid in 1986 (three years after the high cost episode), compared to 49.9% of children ages 1-3, 56.7% of children ages 4-10, 47.9% of children ages 11-20 and 53.5% of children ages 21-25. If the denominator was adjusted for the proportion of children in the noninstitutional cohort who died, the retention rates for the older groups would be even higher. For example, by the end of the study period, 19.2% of the 21-25 year age group were deceased, compared to only 3.8% of infants.
Thus, younger children in the noninstitutionalized high cost cohort were significantly more likely to be enrolled prior to the high cost episode than older children. This suggests that the safety net may be especially important for older children, i.e. "new" enrollees were disproportionately older children. After the high cost episode, infants were less likely than other age groups to remain enrolled.
The differences in the rates of deceased children by age group are also worth noting. The rates of death by the end of 1986 were highest for children in the 4-10 year and 21-25 year age groups. Generally, the period from 4-10 years of age is a relatively healthy time, with significantly lower morbidity races than occurs for other age groups of children (Office of Technology Assessment, 1988). However, our data suggest that for Medicaid children who become sick enough to incur very high costs at this age, the mortality rate is much higher than for younger children with similarly high costs. Returning to Table 7, we see that about 18% of children in the 4-10 year age group had diagnoses related to neoplasms, and later data will show that a very high rate of death occurred for children with neoplasms. We do not have any explanation as to why the rate of death dropped to 10.9% for children in the 11-20 age group and then rose to 19.2% for children in the 21-25 age group.
Another objective of the longitudinal analysis was to analyze the Medicaid eligibility patterns for the noninstitutional high cost children group over time. Issues of interest with regard to eligibility include the extent to which high cost children use the optional eligibility groups, such as the medically needy provisions or Ribicoff coverage, to access Medicaid. Also, what proportion of high cost children have disabling conditions of sufficient severity that they eventually become eligible for Medicaid through the SSI disability provisions?
The routes to Medicaid eligibility are less of an issue for institutionalized children. The eligibility pathway for institutional children is fairly straightforward. As reported earlier, the vast majority of them qualify through the SSI cash assistance group since parental income and resources are not deemed to be available to children in an institutional setting.
Table 10 presents eligibility information for the cohort of noninstitutionalized high cost children. The first column shows the initial enrollment group under which the children in the cohort qualified.2 The second column shows their primary eligibility group for 1983 (i.e. where they had the longest period of enrollment). Then the third column shows the distribution of children by their last reported enrollment group. For some children, their entire spell of enrollment may have been limited to 1983. Other children may have been continuously enrolled from 1980 to 1986 without a change in enrollment groups. Thus, the initial and last enrollment groups can overlap with the 1983 group.
| TABLE 10: Percent Distribution of Noninstitutionalizated High Cost Children Cohort by Eligibility Group | |||
| Eligibility Group | Initial Enrollment | 1983 Enrollment | Last Enrollment |
| AFDC, Cash | 38.5 | 35.3 | 26.5 |
| AFDC, Medically Needy | 19.6 | 16.0 | 15.9 |
| SSI Disabled, Cash | 10.8 | 18.8 | 32.6 |
| SSI Disabled, Medically Needy | 5.0 | 7.8 | 6.4 |
| Ribicoff, Medically Needy | 26.1 | 22.2 | 18.6 |
| Total | 100.0 | 100.1 | 100.0 |
Two patterns are important in the longitudinal eligibility data. First, the proportion of high cost children passing the SSI disability test was only 15.8% with regard to initial eligibility, but increased to 40.0% by the last eligibility group. In 1983 when the study sample was selected, 26.6% were considered to be SSI disabled. Thus, many of the high cost children entered the Medicaid program through the AFDC (including the AFDC medically needy) or Ribicoff groups, but were sufficiently disabled that they eventually qualified for coverage through the SSI disability provisions. By the point of their last eligibility group, about 32.6% of the study sample qualified as SSI disabled children receiving cash assistance, with another 6.4% qualifying as medically needy SSI disabled children.
A second pattern to note is the importance of medically needy coverage and the Ribicoff group as pathways for initial entry to Medicaid. In 1983, both medically needy coverage and coverage of Ribicoff children through age 20 were options for States. Half (50.7%) of the high cost children cohort (noninstitutionalized) used these optional coverage provisions for their initial entry to Medicaid. Further, this coverage remained important. During 1983, 46% of the study cohort qualified for Medicaid through the optional groups. Finally, over 40% used these provisions for their last reported eligibility group. Thus, many of the noninstitutionalized high cost children would not have qualified for coverage if California's Medicaid program had not chosen to include the medically needy and Ribicoff optional coverage groups in its program. With the medically needy coverage, California opened up Medicaid eligibility to children whose family income exceeded the AFDC and SSI cash program income standards. With Ribicoff coverage, Medicaid was made available to all children under age 21 in two-parent families.
Table 11 provides further information on the longitudinal eligibility patterns for noninstitutionalized children, showing the different eligibility "pathways" used by high cost children over the 7 year study period. Children who were eligible throughout their entire period of enrollment as SSI disabled children (either cash or medically needy) averaged 4.4 years of Medicaid enrollment over the 7 year study period. Children who qualified under the SSI disability provisions for at least part of their enrollment (plus either AFDC or Ribicoff coverage) averaged 4.2 years of eligibility on Medicaid. Thus, the 40% of high cost children who eventually passed the SSI disability test had considerably longer lengths of enrollment than children qualifying under the other groups. Children whose entire eligibility was through the Ribicoff group averaged only 1.2 years of Medicaid enrollment, and children using the AFDC provisions averaged closer to 3 years. As expected, children who were sufficiently ill to pass the SSI disability test became long-term Medicaid enrollees, whereas the AFDC and Ribicoff children experienced much shorter durations of enrollment on average.
| TABLE 11: Percent Distribution of Noninstitutionalized High Cost Children by Longitudinal Eligibility Patterns | ||
| Longitudinal Eligibility Pattern | Percent of Cohort | Average Length of Enrollment: 1980-1986 |
| AFDC Only | 34.5 | 2.7 yrs. |
| Disabled Only | 14.6 | 4.4 yrs. |
| Ribicoff Only | 13.4 | 1.2 yrs. |
| Disabled and AFDC or Ribicoff | 25.9 | 4.2 yrs. |
| AFDC and Ribicoff | 11.5 | 2.9 yrs. |
| Total | 99.9 | 3.2 yrs. |
It should be emphasized, however, that these data on durations of enrollment have problems of left and right censoring. Some children in our cohort were no doubt enrolled in Medicaid prior to 1980 (the earliest year in our data set), and we expect even more children continued to be enrolled after 1986. Thus, the magnitude of difference between eligibility patterns shown in Table 11 might be even greater if we had complete information on enrollment. In particular, we expect the eligibility groups with longer lengths of enrollment may be biased downwards. For example, we suspect that the data in Table 11 may be complete for many of the children who used the Ribicoff only eligibility path to Medicaid since this is a Medicaid only group (i.e. no cash assistance). However, we expect the two groups involving disabled children would show even greater average lengths of enrollment if complete data were available. Most of the disabled children were receiving SSI cash assistance and we know this group has little turnover.
A final issue of interest is the extent to which high cost children are persistently high cost to Medicaid. Table 12 shows the proportion of children in the 1983 high cost cohort who were high cost from 1980 to 1982 and 1984 to 1986. This table uses two definitions of high cost: those children whose expenses were equal to or greater than $25,000, and those whose Medicaid expenses were $10,000 to $24,999. Other years of data were adjusted to 1983 dollars, using the medical care component of the Consumer Price Index.
| TABLE 12: High Cost Child Cohort Percent of Children with Sustained High Costs by Institutional Status | |||||||
| 1980 | 1981 | 1982 | 1983 | 1984 | 1985 | 1986 | |
| Non-Institutionalized | |||||||
| 6.8** | 8.7** | 18.8** | 100.0 | 13.8 | 6.3 | 4.2 |
| 4.7** | 8.5** | 9.8** | -- | 11.1 | 7.0 | 4.9 |
| 45.2** | 53.8** | 66.1** | 100.0 | 70.6 | 54.8 | 47.8 |
| -- | -- | -- | 5.0 | 2.5 | 1.5 | 0.7 |
| -- | -- | -- | 5.0 | 7.5 | 9.1 | 9.8 |
| Institutionalized | |||||||
| 63.2** | 79.9** | 84.4** | 100.0 | 81.9 | 74.9 | 67.1 |
| 17.6** | 4.7** | 6.2** | -- | 8.2 | 8.1 | 9.8 |
| 90.3** | 92.8** | 96.3** | 100.0 | 96.5 | 91.5 | 88.9 |
| -- | -- | -- | 1.4 | 2.0 | 1.6 | 1.6 |
| -- | -- | -- | 1.4 | 3.4 | 5.0 | 6.6 |
| Total | |||||||
| 43.5** | 53.8** | 56.2** | 100.0 | 46.7 | 39.5 | 34.7 |
| 12.8** | 6.1** | 7.7** | -- | 9.7 | 7.5 | 7.3 |
| 74.6** | 78.5** | 83.3** | 100.0 | 83.2 | 72.6 | 67.7 |
| -- | -- | -- | 3.3 | 2.3 | 1.5 | 1.2 |
| -- | -- | -- | 3.3 | 5.6 | 7.1 | 8.3 |
| * Deceased are a subset of the enrolled.** Excluded from the denominator for 1980-1982 are children in the study sample not yet born. Thus, the data for 1980 show the 1983 high cost children enrolled in Medicaid in 1980 as a percent of those who were alive in 1980. | |||||||
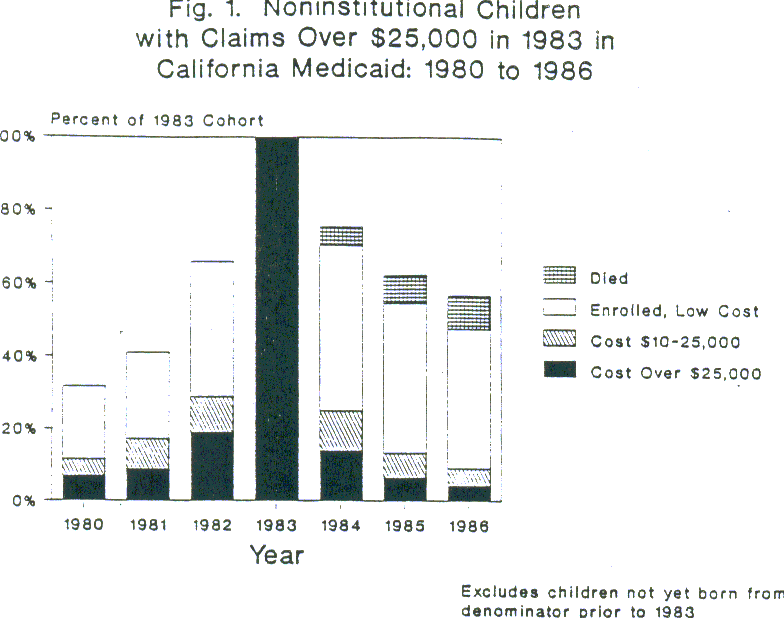
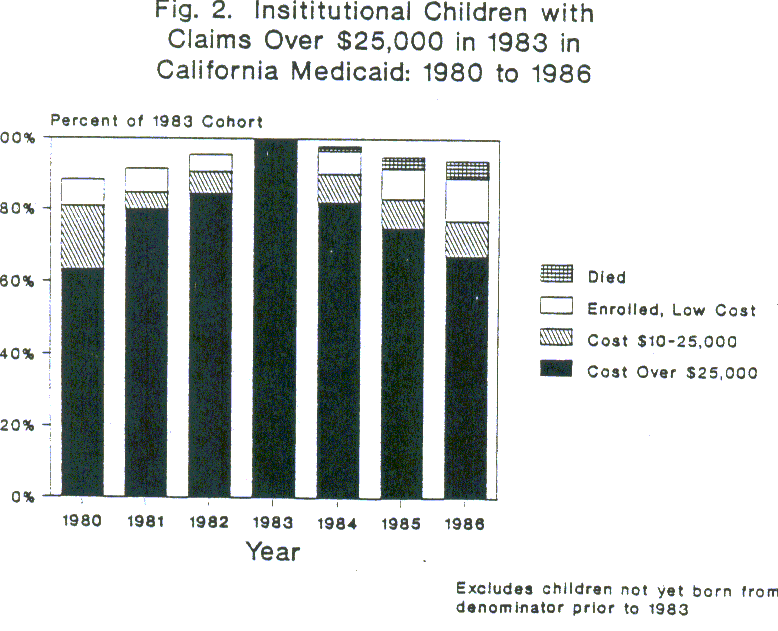
Overall, we see that just over 43% of the high cost cohort had Medicaid expenditures over $25,000 in 1980 and about 35% continued to have expenditures of this magnitude in 1986. An additional 12.8% in 1980 and 7.3% in 1986 had expenditures of $10,000 to $24,999. However, as shown in Figure 1 and Figure 2, these rates differed significantly by institutional status. In 1980, only 11.5% of the noninstitutional group were high cost (defined as over $10,000 in Medicaid expenditures), compared to 80.8% of the institutionalized. Similarly, only 9.1% of the noninstitutional group remained high cost in 1986 (or about one-fifth of those still enrolled), compared to 76.9% of the institutional group (or about 87% of those still-enrolled).
Once again, age appears to be a factor. Most institutional children were older, and Table 13 shows us that the likelihood of remaining high cost was lowest for children under age 4 in the noninstitutional high cost cohort. Only 2.6% of the 1983 high cost infant cohort (noninstitutional) continued to be high cost to Medicaid in 1986, compared to 13.6% of the 11-20 year group, and 17% of the 21-25 year group.
| TABLE 13: Noninstitutional High Cost Child Cohort Percent of Children with Sustained High Costs, 1980-1986 | |||||||
| 1980 | 1981 | 1982 | 1983 | 1984 | 1985 | 1986 | |
| 1 Years (n=720) | |||||||
| -- | -- | -- | 100.0 | 9.6 | 2.1 | 1.5 |
| -- | -- | -- | -- | 7.4 | 3.8 | 1.1 |
| 1-3 Years (n=584) | |||||||
| 2.9* | 12.7* | 21.2 | 100.0 | 11.0 | 5.7 | 1.7 |
| -- | 5.8 | 8.0 | -- | 10.6 | 7.5 | 4.3 |
| 4-10 Years (n=252) | |||||||
| 10.3 | 10.3 | 17.1 | 100.0 | 23.4 | 10.7 | 7.9 |
| 6.3 | 13.1 | 14.3 | -- | 17.1 | 14.3 | 7.5 |
| 11-20 Years (n=568) | |||||||
| 5.1 | 5.8 | 15.5 | 100.0 | 14.3 | 7.7 | 6.2 |
| 2.8 | 6.2 | 7.9 | -- | 12.5 | 5.6 | 7.4 |
| 21-25 Years (n=312) | |||||||
| 7.7 | 10.6 | 21.5 | 100.0 | 20.2 | 10.9 | 8.7 |
| 7.7 | 10.6 | 12.5 | -- | 13.1 | 9.9 | 8.3 |
| Total Non-Institutionalized (n=2,436) | |||||||
| 6.8* | 8.7* | 18.8* | 100.0 | 13.8 | 6.3 | 4.2 |
| 4.7* | 8.5* | 9.8* | -- | 11.1 | 7.0 | 4.9 |
| * Excluded from the denominator for 1980-1982 are children in the study sample not yet born. Thus, the data for 1980 show the 1983 high cost children enrolled in Medicaid in 1980 as a percent of those who were alive in 1980. | |||||||
What are some other characteristics of the persistently high cost children in the noninstitutional group? Table 14 shows that the vast majority (85.7%) of the persistently high cost children were children who had passed the SSI-related disability test. This pattern suggests that most, although not all, persistently high cost children eventually become eligible for Medicaid through the SSI provisions.
| TABLE 14: Longitudinal Eligibility Patterns of Children Continuing To Be High Cost in 1986 | |
| Longitudinal Eligibility Pattern | Percent of Children With High Costs in 1986 |
| AFDC Only | 4.9 |
| Disabled Only | 35.9 |
| Ribicoff Only | 3.1 |
| Disabled and AFDC or Ribicoff | 49.8 |
| AFDC and Ribicoff | 6.3 |
| Total | 100.0 |
What were the 1983 diagnoses of children with persistently high costs? Table 15 shows the number of high cost children in 1983 by diagnosis group and the proportion of those who were still enrolled and high cost in 1986. Forty-one percent (41.3%) of the children in the diagnostic grouping of diseases of the blood and blood-forming organs (includes sickle cell anemia) continued to be high cost to Medicaid in 1986, followed by 28.9% of children with diseases of the skin and subcutaneous tissue (includes chronic skin ulcers and bed sores). About 25% of children with endocrine, nutritional, metabolic and immunity disorders (includes diabetes and cystic fibrosis) remained high cost to Medicaid in 1986. Children with mental disorders, diseases of the genitourinary system (includes children with renal failure who probably do not qualify for End-Stage Renal Disease coverage under Medicare) and diseases of the respiratory system (includes bronchitis, pneumonia, and asthma) also had a considerably above average likelihood of continuing high cost to Medicaid. Finally, half of the children with other or unknown diagnoses continued to be high cost in 1986.
| TABLE 15: Number of High Cost Noninstitutionalized Children by Major Diagnostic Group for 1983, Percent Continuing to Be High Cost in 1986, and Percent Deceased | |||
| Number 1983 | Percent High Cost in 1986 | Percent Deceased by 1987 | |
| Infections/Parasitic | 53 | 7.5 | 11.3 |
| Neoplasms | 154 | 4.5 | 42.2 |
| Endocrine | 76 | 25.0 | 40.8 |
| Blood/Blood Organs | 75 | 41.3 | 9.3 |
| Mental Disorder | 18 | 22.2 | 5.5 |
| Nervous System/Sense | 122 | 12.3 | 5.7 |
| Circulatory System | 61 | 1.6 | 16.4 |
| Respiratory System | 164 | 18.9 | 12.2 |
| Digestive System | 103 | 9.7 | 8.7 |
| Genitourinary System | 39 | 20.5 | -- |
| Pregnancy Complications | 29 | 10.3 | 3.4 |
| Skin and Subcutaneous Tissue | 38 | 28.9 | 2.6 |
| Musculoskeletal/Connective | 50 | 16.0 | 10.0 |
| Congenital Anomalies | 212 | 5.2 | 6.1 |
| Perinatal Conditions | 708 | 2.0 | 3.8 |
| Ill-defined Conditions | 85 | 12.9 | 12.9 |
| Injury/Accidents Poisonings | 402 | 5.7 | 5.5 |
| Miscellaneous V Codes | 31 | 12.9 | 9.7 |
| Other, Unknown | 16 | 50.0 | -- |
| Total | 2,436 | 9.1 | 9.8 |
The three diagnostic groups which accounted for the greatest number of children in the high cost group in 1983--conditions originating in the perinatal period, congenital anomalies, and injuries, accidents and poisonings--had below average probabilities of continued high cost in 1986. For example, only 2% of children with problems from the perinatal period in 1983 remained high cost in 1986. Thus, most premature and low birthweight infants, as well as children involved in accidents or injuries, do not remain high cost. Instead, their need for expensive coverage under Medicaid appears to be time-limited. The children who are likely to remain high cost are those with chronic, permanent conditions.
Table 15 also shows which conditions were most likely to result in death for high cost children. By the end of 1986, 42.2% of children with neoplasms in 1983 were reported to be deceased. A very high mortality rate (40.8%) was reported for children with endocrine, nutritional, metabolic and immunity disorders. As reported above, this diagnostic group also had a very high rate of children who continued to be high cost in 1986. Other diagnostic groups with-above average death rates were diseases of the circulatory and respiratory systems (16.4% and 12.2% respectively) and ill-defined conditions (12.9%).
To complete the presentation of study data, Table 16 shows the cumulative Medicaid costs of the 1983 cohort over the 7 year period from 1980 through 1986. For the noninstitutional group, the average cumulative Medicaid expenditure per child was $100,090; however, an average of $59,387 (almost 60% of the total) was incurred in 1983. This pattern occurred for two reasons. First, many of the noninstitutional group were not enrolled prior to 1983 and only about half remained on Medicaid by 1986. Second, most of the noninstitutional group experienced high costs to Medicaid only in 1983.
| TABLE 16: Average Cumulative Medicaid Expenditure Per Child in High Cost Cohort: 1980-1986 | |||
| Average Medicaid Expenditure per Child | |||
| 1983 | Other Study Years | Total 1983-1986 | |
| Noninstitutionalized Children | $59,387 | $40,703 | $100,000 |
| Institutionalized Children | $43,845 | $284,974 | $328,819 |
| Total High Cost Children | $51,856 | $115,455 | $167,311 |
The picture for children in the institutional group is very different. Their cumulative cost to Medicaid averaged $328,819 per child over the seven year period, with only $43,845 (13% of the total) incurred in 1983. Most of the institutional children were enrolled throughout the study period, and most of them were high cost every study year. These cumulative Medicaid expenditure data underscore the persistence of enrollment and high Medicaid costs for the institutional group.
SUMMARY AND CONCLUSIONS
Study data showed several patterns with regard to the longitudinal experience of high cost Medicaid children in California in 1983:
-
About half of California's high cost children on Medicaid in 1983 were SSI children in long-term care facilities. Almost all of these institutionalized children had been high cost in the past and were high cost over the next 3 years. About 7% of this group were deceased within 3 years. Most of these children received SSI cash assistance, and their average age was 18.7 years.
-
The other half of the high cost children group, the noninstitutionalized, differed considerably. Three years following the high cost episode, only about half of the noninstitutionalized group remained on Medicaid, and 10% were deceased.
-
Most noninstitutionalized high cost children were not persistently high cost. Only about 12% of noninstitucionalized had been high cost to Medicaid 3 years prior to the high cost episode and only 9% remained high cost 3 years later.
-
Noninstitutionalized high cost children had a very different profile than institutionalized children. The average age was 7.9 years, and over half of the children were under age 4. Most of the children in this group used the AFDC cash or medically needy groups, or the Ribicoff provisions to access the Medicaid program.
-
Infants composed 30% of the noninstitutionalized high cost group. They were the age group among high cost children least likely to remain on Medicaid after 3 years. Infants were also the age group least likely to remain high cost, and the had the lowest death rate. The most frequent diagnoses for high cost infants involved conditions originating in the perinatal period and congenital anomalies. It appears that these problems were not permanently disabling, at least not to the extent that the children met the SSI disability criteria or required continued intensive medical care under Medicaid.
-
The noninstitutionalized children most likely to remain enrolled in Medicaid were those with permanent chronic conditions who became eligible under the SSI disabled provisions. SSI disabled children were also the vast majority of children with continued high cost. The diagnoses which were most likely to result in persistent high cost are: diseases of the blood and blood forming organs (includes sickle cell anemia), diseases of the skin and subcutaneous tissue (includes chronic skin ulcers and bed sores), endocrine, nutritional and metabolic disorders (includes diabetes and cystic fibrosis), mental disorders, diseases of the genitourinary system (includes kidney disease) and diseases of the respiratory system (includes bronchitis, pneumonia, and asthma).
To what extent is Medicaid working as a safety net for high cost children? Study data suggest that the number of "new" high cost children in the noninstitutional group enrolled in California during 1983 was greater than would have been expected with normal caseload turnover and growth. Further, most of these noninstitutional children did not remain high cost, and only about half were still enrolled in Medicaid three years later. This pattern suggests that California's Medicaid program was serving as catastrophic insurance for children experiencing a high cost episode. On the other hand, study data does not suggest that this catastrophic coverage was reaching middle class families with high cost children. Only 15% of the children incurred a spend-down liability (indicating their family income exceeded the medically needy level). Also, the size of the spend-down liabilities was not great. Since many of the children used the Ribicoff eligibility provisions to qualify for Medicaid, they were probably from two-parent families or the group often referred to as the working poor.
A finding of major policy significance is that about half of the high cost children (noninstitutional) used optional coverage groups (medically needy and Ribicoff coverage provisions) in order to qualify for Medicaid during the high cost episode. Without these optional coverage groups, California's safety net for high cost children would probably have been cut in half.
These results underscore the importance of optional coverage in serving high cost children--especially those who are younger and are not disabled enough to meet the SSI disability criteria. The numerous expansions to Medicaid eligibility during the 1980s to extend coverage for infants and all children living in poverty make mandatory some of the coverage groups California opted to include in its Medicaid program in 1983. However, States are still not required to have medically needy programs for children. Neither are States mandated to provide Ribicoff coverage through age 20. Finally, most States do not have income eligibility thresholds as high as those used by California.
In 1989, fifteen States did not have medically needy programs. All States now cover some Ribicoff children, although their Ribicoff coverage may only cover such children whose families meet the AFDC cash assistance financial criteria (i.e. they do not have medically needy programs). Recent Medicaid legislation mandated State coverage effective April 1990 of all children (including those in two-parent families) up to age 6 in families with incomes up to 133% of the poverty level. Nevertheless, twenty States in 1989 did not offer Ribicoff coverage to children all the way to age 18. Only twenty States in 1989 offered Ribicoff coverage to all children up to age 21, which is comparable to California's program in 1983 (National Governors' Association, 1990) .
Financial levels also continue to be low for AFDC and medically needy programs in most States. In 1989, the median AFDC benefit level in 1989 for a family of 3 was $364, which was 44% of the Federal poverty level for that size family. The Federal SSI benefit standard in 1989 for a single person was $368 which was 68% of the Federal poverty standard for a single individual under age 65 (Committee on Ways and Means, 1990). The median State medically needy threshold in 1989 for a family of 3 was $516, which was 63% of the Federal poverty level (National Governors' Association, 1990). Thus, most States Medicaid programs today would not offer the safety net available through the California program in 1983.
Another policy implication from the study results involves infants and young children. Since over half of the (noninstitutionalized) high cost group were under age 4, there is obviously an important need for catastrophic coverage to this age group. Indeed, the need for coverage to young children may be even greater now, with the spread of AIDS to children and the increased number of drug exposed infants and children. It would be interesting to update this high cost profile to see if the proportion of younger children in the high cost group has become even greater since 1983 and to determine whether the long-term patterns of high cost infants and younger children have changed, given these more recent developments. There is growing concern that drug exposed infants in particular may require prolonged medical and social assistance.
One study result regarding the catastrophic coverage of high cost infants is somewhat perplexing. Only 41% of the high cost infants in 1983 continued to be enrolled in California's Medicaid program in 1986. Further, only 3% continued to have Medicaid expenditures exceeding $10,000 annually. On the one hand, this result is reassuring in that it shows that many of these infants did not remain high cost or continue to be a burden on the Medicaid program. On the other hand, what happened to the majority of these high cost infants with regard to their ongoing health care needs? Children with major health care problems at birth are more likely to require ongoing health care throughout their lives than other children. For example, low birthweight infants are at greater risk for developing lifelong impairments such as learning disabilities, mental retardation and cerebral palsy (National Association of Children's Hospitals and Related Institutions, 1989).
Generally, we would assume these high cost infants lost Medicaid eligibility due to the improved financial circumstances of their families. However, did these high risk infants move to a source of ongoing health care coverage once they lost Medicaid eligibility? Families exiting Medicaid due to earnings often do not have a source of ongoing health care coverage. About one-third of children in working poor families in 1986 were without any health insurance (Rosenbaum, 1989). Thus, we are concerned that some of these infants may have moved to a situation of no health care coverage or inadequate coverage.
Study results showing the persistent high costs to Medicaid associated with institutionalized children underscore the importance of options available to States to provide community-based care for disabled children who would otherwise be institutionalized. Currently, 36 States are using home and community-based waivers to provide disabled children specialized services in a home or community setting. Seventeen States are using the TEFRA option to waive parental deeming of income to their children and provide them cost-effective home care (Hall, 1990). Any further steps which could be taken to assist States in providing more cost-effective care should be pursued.
Finally, it is difficult to generalize from these findings on high cost children in California to the Medicaid program as a whole. We know California's Medicaid program in 1983 offered more comprehensive benefits and used less restrictive eligibility criteria than other States. We believe that these program differences had an impact on the dynamics of Medicaid coverage for high cost children, but we do not have enough information on the longitudinal experience of high cost children in other States to say this with certainty. We also would expect that the situation in 1990 may be very different for high cost children (even in California) from what was happening in 1983. As mentioned earlier, we now have pediatric AIDS and the problems related to drug- exposed infants.
We see many needs for further research. For example, in their cross-sectional study of high cost children, Burwell and Herz reported that over 70% of the high cost group were institutionalized in Georgia, Michigan and Tennessee. Would these institutionalized children in other States show the same persistence with regard to high Medicaid costs as we saw in California? Does California provide more short-term catastrophic coverage to the noninstitutionalized than occurs in other State Medicaid programs? Do other State Medicaid programs show the same patterns with regard to high cost infants? Are high cost infants and young children more likely to remain on Medicaid and continue to be high cost than they used to be?
REFERENCES
Burwell, B. and Herz, E., Variations in the Medicaid Safety Net for Children and Youth with High Medical Costs.: A Comparison of Four States, SysteMetrics/McGraw-Hill, July, 1990. [Available at http://aspe.hhs.gov/daltcp/reports/4stvares.htm.]
Committee on Ways and Means, U.S. House of Representatives, Overview of Entitlement Programs, June, 1990.
Ellwood, D. and Bane, M.J., The Dynamics of Dependence: The Routes to Self-Sufficiency, Urban Systems Research and Engineering, Inc., 1983.
Hall, L., Medicaid Home Care Options for Disabled Children, National Governors' Association, 1990.
Ku, L., Who is Paying the Big Bills? Very High Cost Pediatric Hospitalizations in California, 1987, August, 1990. [Available at http://aspe.hhs.gov/daltcp/reports/BIGBLLES.htm.]
National Association of Children's Hospitals and Related Institutions, Inc., Profile of Child Health in the United States, 1989.
National Governors' Association, Medicaid Eligibility: Selected Program Characteristics, September 1989, March, 1990.
Office of Technology Assessment, Healthy Children: Investing in the Future, OTA-H-345, February, 1988.
Rosenbaum, S., Testimony of the Children's Defense Fund before the Subcommittee on Health and the Environment, Committee on Energy and Commerce, June 8, 1989.
Rymer, M. and Adler G., "Children and Medicaid: The Experience in Four States," Health Care Financing Review, Fall, 1987.
Staren, M., Office of Supplemental Security Income, Program Planning, Research, Analysis and Projections Branch, Social Security Administration, Personal Communication on September 18, 1990.
APPENDIX A: SAMPLE SELECTION STEPS AND DATA LIMITATIONS
Some high cost children and young adults were eliminated from the study sample based on eligibility characteristics in 1983. The original sample of persons under age 26 with total expenditures at or above $25,000 in 1983 contained 5,690 enrollee identification numbers. Of this group, the following exclusions were made:
| Number | |
| Original Sample | 5,690 |
| Excluded Groups: | |
| 499 |
| 299 |
| 42 |
| 2 |
| 2 |
| 11 |
| Sample Size After Group Exclusions | 4,835 |
| Exclusions Due to Multiple Identification Numbers | 109 |
| Final Sample Size | 4,726 |
Among the enrollees in the excluded groups, 33 persons fell into two of the six groups. Most of these enrollees (n = 30) were classified as both AFDC adults and HMO enrollees. After multiple identification numbers for the same individuals were combined, a final sample size of 4,726 was obtained. Specific reasons for eliminating certain groups of enrollees are described below.
In examining a sample of inpatient claims for high cost AFDC adults, it was evident that many identification numbers belonging to adult female enrollees had been used to bill Medicaid for both their care and their infants' care at delivery. This billing practice can extend into the first few months of life for the newborn. In many of the cases examined, mothers had significant problems during pregnancy and/or at labor and delivery (e.g., were hospitalize for fetal-pelvic disproportion, breech presentation, preterm labor, anemia of the mother). Their infants typically had significant problems as well (e.g., congenital malformations, extreme prematurity). This combination of factors undoubtedly contributed to the large total costs associated with "shared" mother-baby identification numbers. It is our belief that most of the total costs for each mother-baby case among AFDC adults were incurred by the infant rather than the mother. Because most high-cost AFDC adult cases probably represented more than one recipient, we deleted these enrollees from the study sample. More generally, the elimination of the AFDC Adult group from the study sample probably resulted in an undercount of some high cost children, especially those under the age of one and for whom a significant percentage of costly medical care occurred early in life before they received their own identification number separate from their mother's record. The exact magnitude of this problem is unknown.
Several other groups of enrollees were also eliminated from the study sample. Crossovers are those individuals who are dually enrolled in both Medicaid and Medicare. In general, claims for these enrollees are first processed and paid by Medicare. Some portion (sometimes all) of the uncovered balance of the claim is then paid by Medicaid. Because the claims information in the Tape-to-Tape files are often incomplete on crossover claims, individuals who had such claims were eliminated from our sample.
For similar reasons HMO/capitated enrollees were also deleted from the study sample. In the Tape-to-Tape files, only the monthly premium payments for these enrollees are included. These payments do not necessarily reflect the full extent of service utilization or costs associated with medical care in the same way that fee-for-service payments do. Payments for HMO/capitated enrollees are thus artifically truncated and are not directly comparable to other types of enrollees.
Finally, a small number of enrollees were eliminated from the study sample for several other reasons. Santa Barbara and Monterey county residents were dropped because the Tape-to-Tape files do not contain complete claims information on these individuals (both counties independently processed their own claims during the study period and these claims were not included in the Tape-to-Tape database). Because refugee and other Federal and State only enrollees represent very small groups who are not part of the regular Medicaid program, they were also eliminated from the study sample.
In general, the Tape-to-Tape database has certain limitations relevant to this study. First, some types of claims are not routinely part of California's Medicaid Management Information System (MMIS) from which the Tape-to-Tape files are developed. The most significant omission is EPSDT services. Only non-EPSDT preventive care and treatment services delivered to children and young adults are included in the database. However, we believe the aggregate impact of this omission is minimal in light of the fact that high costs tend to be associated with use of curative or long-term care rather than preventive services.
A second issue with the California Tape-to-Tape database is that enrollees may have multiple identification numbers over time. Assignment of new identification numbers can occur in a variety of circumstances, for example, when an enrollee moves from one county to another, when the eligibility group changes, or when new family budget units are assigned. SysteMetrics has developed a complex algorithm for linking multiple identification numbers for individual enrollees which handles the vast majority of these situations. However, it is possible that some problems of this type remain undetected and uncorrected. To the extent this is true, some children who met our criterion for high cost but whose payments were divided among unlinked identification numbers will be missing from our study sample.
NOTES
-
It is important to note that service expenditures in the Tape-to-Tape data set are based on date of service. Thus, a child with a high cost spell of illness which began in November of 1983 and continued through February of 1984 would only have been included in our sample if expenditures for services received in November and December of 1983 reached $25,000.
-
For children who qualified for Medicaid prior to 1980, data are not available on their initial enrollment group. Instead, study data use their 1980 enrollment group as the initial enrollment group.