Final Report
July 2004
Prepared for:
U.S. Department of Health and Human Services
Assistant Secretary for Planning and Evaluation
Prepared by:
The Lewin Group
and its subcontractor
The Nelson A. Rockefeller Institute of Government
Contract No.: 282-98-0016; Task Order 34
"Executive Summary
Social welfare programs strive to improve the well-being of needy and vulnerable populations. The fact that states spend different amounts on these programs is well known, but why they do so is less understood, including the extent to which differences are affected by states' relative fiscal capacity, defined as their ability to raise revenue through taxation. The federal government has long played an important role in offsetting state fiscal disparities. However, recent changes in federal grant programs might have affected poor and rich states in different ways.
This study was conducted for the Office of the Assistant Secretary for Planning and Evaluation, U.S. Department of Health and Human Services, by The Lewin Group and the Nelson A. Rockefeller Institute of Government. It addresses how a state's fiscal capacity affects its spending on social welfare, how states differ in their "packaging" of services for low-income populations, how economic conditions affect state spending on social welfare, and how the poorest states have adjusted to their relative economic austerity. The study also looks at factors in addition to fiscal capacity and federal grants that might influence state spending, including state needs for social welfare spending, as measured by poverty and unemployment rates and political and institutional factors, including state budget processes.
For the purpose of this report, we measure fiscal capacity-and thus distinguish between rich and poor states-using states' real per capita income. By social welfare spending, we mean per capita state spending on programs intended to support lower-income households, usually programs that are means tested. These programs might include cash assistance programs such as Aid to Families with Dependent Children (AFDC) or cash payments under AFDC's replacement, Temporary Assistance for Needy Families (TANF); health programs such as Medicaid and state child health insurance programs (SCHIP); and a wide variety of non-health service programs providing child care, foster care, low-income energy assistance, and social services to the physically disabled and programs funded by the Social Services Block Grant (SSBG).1
The Study
Conducted over 21 months, the study involved two major activities:
Analysis of expenditures across 50 states. Our analysis examined variation in spending patterns across the 50 states and the District of Columbia. Our team analyzed 24 years of data on state and local social welfare spending patterns for four categories of social welfare spending and a residual category of all other state and local spending. These categories encompassed cash assistance; Medicaid; non-health social services, such as child care, child welfare, energy assistance, and services to the aged and disabled; public hospitals; and all other non-social welfare spending.
We approached the analysis of spending in three ways: (1) employing descriptive data to analyze trends and patterns, (2) developing and estimating econometric models of state spending to estimate how differences in states' fiscal capacity affect spending, and (3) using the results from the descriptive and econometric analysis to better understand the spending variations we observed between rich and poor states.
Case studies. We collected and analyzed qualitative and quantitative data from six states- Arizona, Louisiana, Mississippi, New Mexico, South Carolina, and West Virginia-selected for their high needs relative to their fiscal capacities. Findings from the econometric analysis were used to compare states on their propensities to spend on certain types of social welfare. Comparisons were drawn between rich states (i.e., states with high fiscal capacity) and poor states (i.e., states with low fiscal capacity) and among the six states selected for case studies.
To obtain in-depth information about how state fiscal capacity affects state spending on social programs, we conducted site visits to case study states. Four questions guided our interviews:
- How do states with the greatest needs and the least resources make financial decisions regarding their social welfare programs?
- How do these states respond to short-term financial challenges, such as the recent state fiscal crises?
- Why do some poor states spend more on social welfare programs than other poor states? And why did some spend more on certain programs and less on others?
Our analyses cover spending from 1977 through 2003, though the econometric study ends in 2000.
What We Found
Several important findings emerged from the project:
- Finding #1: States of LESS fiscal capacity spent LESS PER CAPITA on social welfare programs than states with HIGHER per capita incomes. Federal grants did not reduce absolute spending differences between rich and poor states. Average federal grants to the wealthiest states were actually higher in dollar terms when compared to states with lower fiscal capacity. However, because state own-source spending was much lower in poor states, federal intergovernmental grants constituted a larger share of the social welfare budgets of poor states than of rich states.
- Finding #2: State fiscal capacity bore a stronger relationship to spending on non-health social welfare programs than on health-related programs. Between 1977 to 2000, differences between rich and poor states were greatest for spending on cash assistance and non-health social services (such as child care, child welfare, energy assistance, transportation assistance, and programs for the homeless). Differences between rich and poor states were smaller for health-related programs, such as per capita spending on Medicaid and payments to public hospitals.
- Finding #3A: Between 1977 and 2000, state spending on social welfare changed in major ways. Even after controlling for the higher levels of inflation found in health services, spending on Medicaid greatly increased throughout this period, most rapidly in the late 1980s and early 1990s. Spending on non-health social services rose gradually throughout this period. Average state spending on cash assistance rose in the late 1980s and early 1990s but fell dramatically after the mid-1990s.
- Finding #3B: These trends varied greatly between rich and poor states. Medicaid grew substantially for all states, but the growth was strongest among those of low fiscal capacity. The correlation between state fiscal capacity and per capita spending on Medicaid declined over time, as per capita spending by poor states climbed to levels only exceeded by the wealthiest states, while Medicaid spending in wealthier states grew slowly or stalled during the late 1990s. Wealthier states reduced their cash assistance spending during the middle and late 1990s, while poor states on average showed little change in their per capita spending on cash assistance throughout the last two and a half decades. By contrast, differences grew between rich and poor states in their spending on non-health social service programs, as growth in spending on these non-health services lagged behind in the poorest states.
- Finding #3C: These changes produced major shifts in the composition of social welfare budgets in rich and poor states. States of all fiscal capacity have greatly increased the proportion of their spending devoted to Medicaid while reducing the proportion spent on cash assistance. Poor states, unlike rich states, also reduced the proportion of their budgets spent on non-health services. The packages of benefits offered by poor states have thus changed markedly in recent years, toward health care and away from non-health services.
- Finding #4: Econometric analyses found that different factors influenced different social programs. Spending on cash assistance was increased by federal grants, unemployment, and greater population density. Medicaid spending was increased by fiscal capacity, grants, and unemployment. However, the effects of federal grants were particularly strong for Medicaid spending, and population density had an effect opposite to its impact on cash assistance, with higher levels of spending found in comparatively rural states. Finally, non-health social services was most affected by overall state income. It was strongly and consistently related to state fiscal capacity and federal grants for non-social-welfare programs.
- Finding #5A: The econometric models were most successful in explaining spending differences and changes among wealthy states; the models fared less well in accounting for spending in poor states Most of the variables-including fiscal capacity, unemployment, and federal grants-showed relatively strong effects among the wealthier states. In poorer states, fiscal capacity, unemployment, and federal grants showed little or no effects. One important exception was Medicaid. Spending on Medicaid was significantly and strongly affected by federal grant dollars in poor states.
- Finding #5B: There were substantial differences among poor states in their long-run propensities to spend on programs (as captured in the "state effects" of the econometric model). In particular, there were different propensities for spending on cash assistance and health-related programs (Medicaid and public hospitals). Some poor states (mostly rural southern states) spent very little on cash assistance but relatively more on health-related programs, while other poor states (mostly in the West) had larger cash assistance programs and spent less on Medicaid. This trade-off between health and cash assistance programs was not found among wealthier states. Wealthier states were, in general, less likely than poor states to display negative correlations between their long-run propensities to spend on different program functions. Thus, poor states showed greater specialization and variation in their spending "packages" when compared to wealthier states.
- Finding #6: Case studies of six states of low fiscal capacity and high social needs indicated that the basic trends in spending found among poor states before 2000 continued after that year. Spending on Medicaid grew in most of the poor states despite fiscal downturns. Large cut-backs in Medicaid eligibility and basic services were uncommon; in fact, some major program expansions occurred. Nor did cash assistance spending decline-in fact, some increases were found in spending on TANF cash assistance. Major cuts were most often imposed on non-health social services and administrative expenses, especially staffing.
- Finding #7: The case studies visits also revealed that, at least among poor states, spending in different program areas were typically determined by different political and administrative processes. Spending on cash assistance programs were most affected by the interaction between caseload levels and the rules and benefit levels determined (and not often revised) by state legislatures. Choices affecting cash assistance spending seemed to be more influenced by the ideological views of elected officials. By contrast, Medicaid policies and expenditures were, especially in the rural southern states, strongly affected by the active political involvement of service providers, federal match rates, and federal mandates. Together, these factors have helped to sustain Medicaid spending in poor states despite recent fiscal pressures to cut expenditures. Finally, non-health social services were typically of low political salience and administrators were often given significant discretion over how to allocate funds across different services. State resources, increasing program flexibility (partly attributable to the TANF block grant), and executive priorities seemed more important in determining how much was spent on these non-health services and which services were funded and which were not.
One intriguing implication of this last finding is that price effects-determined largely by federal matching rates-might vary depending on other factors or characteristics of the states. When a program has strong and active constituencies that support greater spending, such as Medicaid, an attractive match rate might suffice to expand spending during boom times and prevent major cutbacks during recessions. If, however, a program enjoys no such strong political advocates, even the same federal match rate might fail to prevent major cuts in services during fiscal downturns.
By connecting econometric estimation with intensive analyses of particular states, this study discerned the different processes affecting different types of social welfare spending and how those processes interacted with state fiscal capacity and other state characteristics. The result is a deeper and more discriminating understanding of the enormous changes in the level and composition of state social welfare expenditures, and their complex relations to fiscal capacity, in the American states.
Endnote
1 Because we are interested in the effects of state fiscal capacity on social welfare spending, we consider only spending that goes through the budgets of state and local governments, not direct expenditures by the federal government. Thus, we do not analyze the federal Earned Income Tax Credit (EITC), the Food Stamp Program (FSP), or, with some exceptions, Supplemental Security Income (SSI).
Key Findings
How does a state’s fiscal capacity affect its spending on social welfare programs? Do “poor states” (i.e., states with low fiscal capacity as measured by per capita personal income) differ from richer states in how much they spend on social welfare programs or how they allocate expenditures across cash assistance, Medicaid, and social services for low-income populations? And how do economic downturns and recent changes in federal policy affect state social welfare spending?
To address these questions, the Office of the Assistant Secretary for Planning and Evaluation (ASPE) of the U.S. Department of Health and Human Services (HHS) sponsored a study of the relationship between state fiscal capacity and social welfare spending in the U.S. from the late 1970s through the early 2000s. The study was conducted by the Lewin Group and the Nelson A. Rockefeller Institute of Government of the State University of New York. Our research included econometric analyses of more than two decades of state social welfare spending and case studies of six states with low-fiscal capacities and high needs for social welfare services. This brief presents key findings from the research. More information on the econometric models and the poor-state analyses may be found in the project’s final report.
What Is Social Welfare Spending? And What Is State Fiscal Capacity?
For the purposes of the study, we defined social welfare spending as programs that supported lower-income households, typically, though not exclusively, programs with means tests. These programs included health initiatives such as Medicaid and state child health insurance programs (SCHIP); cash assistance programs such as Aid to Families with Dependent Children (AFDC) or cash payments under AFDC’s replacement, Temporary Assistance for Needy Families (TANF); and a wide variety of other service programs providing child care, foster care, low-income energy assistance, services to the homeless and those funded by the Social Services Block Grant (SSBG). Because the study was designed to understand the effects of state fiscal capacity on social welfare spending, we included in the analyses only spending that went through the budgets of state and local governments. Direct expenditures by the federal government — such as the federal Earned Income Tax Credit (EITC), Food Stamp Program (FSP) benefits, and the federal portion of Supplemental Security Income (SSI) for poor elderly and disabled people — were excluded from direct examination.
Although the study used spending data on specific programs, such as Medicaid and TANF, at several points in the analysis, most of the quantitative research in the project was based on state and local spending data collected annually by the U.S. Census Bureau (Census Bureau) since 1977. One of the largest expenditure categories in the Census of Governments (Census) data was termed public welfare expenditures, amounting to $233 billion in fiscal year (FY) 2000. To determine whether fiscal capacity affected different types of social welfare spending in different ways, the study organized the 10 subcategories under public welfare expenditures into three basic types of spending:
- Cash assistance, which included AFDC, TANF cash assistance, general assistance, and state supplements to SSI;
- Medicaid, which was found to be closely related to one of the Census categories, “Payments to Medical Vendors”; and
- Non-health social services, which included a wide variety of services and in-kind benefits, such as child welfare services, child care subsidies, energy assistance programs, shelters for the homeless, and many others.
Because some Medicaid dollars flowed to public hospitals and such hospitals serviced many low-income families, we also analyzed a Census category called Public Hospitals at several points in the study, though the analyses were usually done separately. Exhibit 1 details these categories, showing the spending levels in many of the subcategories for FY 2000 (the most recent data available). Health care expenditures constituted the largest part of total spending on social welfare, with Medicaid and Public Hospitals being the largest and second largest categories of spending. States spent a total of $230.2 billion on these two functions in 2000. Non-health Social Services made up the third largest category ($58 billion), and Cash Assistance came in fourth ($20.7 billion).
| Spending Category | Detailed Item in Census Data | FY 2000 $ (billions) |
Definition |
|---|---|---|---|
| Cash Assistance | E67 Federal Categorical Assistance |
17.7 | Includes AFDC or TANF cash assistance; federal Supplemental Security Income (SSI) when it passes through state accounts; and state SSI supplements.
Note: The only federal SSI funds that pass through state accounts are retroactive federal payments reimbursing the state for payments made to individuals under state supplement programs; the total amounts are small |
| E68 Other Cash Assistance |
3.0 |
Includes cash assistance programs not under federal categorical programs (e.g., general assistance, refugee assistance, home relief, and emergency relief) | |
| Medicaid | E74 Vendor Payments for Medical Care |
155.0 | Includes payments made directly to private vendors for medical assistance and hospital and health care (payments consist mostly of Medicaid/SCHIP) |
| Non-health Social Services | E75 Vendor Payments for Other Purposes |
2.1 | Includes payments made directly to private vendors for services and commodities other than medical, hospital, and health care |
| E77, F77, G77 Welfare Institutions |
1.2 | Includes payments for provision, construction, and maintenance of nursing homes and welfare institutions owned and operated by a government for the benefit of needy persons | |
| E79, F79, G79 Other Public Welfare |
54.4 | Includes operational payments for public employees in the sphere of public welfare; and payments for welfare programs such as child care, child welfare, adoption assistance, foster care, low-income energy assistance and weatherization, social services to the physically disabled, SSBG-funded programs, welfare-related community action programs, and temporary shelters and other services for the homeless | |
| Public Hospitals | E36, F36, G36 Own Hospitals (except federal veterans) |
75.2 | Includes payments for hospital facilities providing in-patient medical care and institutions primarily for the care and treatment of the disabled that are directly administered by a government as well as direct payments for acquisition or construction of hospitals |
| Non-social Welfare | All Other Spending | 1,309.0 | Includes primarily elementary and secondary education, higher education, highways and public mass transit, police protection, financial administration, housing and community development, utilities (water supply and electric power), and sewerage |
We measured state fiscal capacity using states’ real per capita personal income. Per capita personal income relates in many ways to the resources that state and local governments may tax to pay for social welfare as well as non-social welfare spending — and the availability of such resources might affect overall levels of spending. We considered and compared other measures of fiscal capacity, but real per capita personal income was strongly correlated with other indicators, and it had the virtue of being available annually throughout the time period our analyses covered.
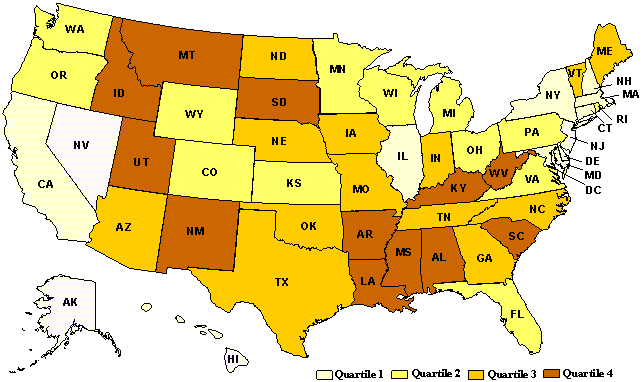
To compare changes in spending patterns for rich and poor states over time, we classified all of the states plus the District of Columbia into four quartiles with respect to their fiscal capacity, as measured by real per capita income averaged over the 24-year period. Exhibit 2 displays, in map form, the states in each of the quartiles, from the richest states in Quartile 1 to the poorest in Quartile 4.
Exhibit 2.
States by Fiscal Capacity Quartile,
Measured by Average Real Per Capita Personal Income, 1977–2000
| Selected Characteristics | Quartile 1 | Quartile 2 | Quartile 3 | Quartile 4 |
|---|---|---|---|---|
| Mean per capita personal income, 1977–2000 (2000 dollars) | $24,794 | $21,387 | $19,242 | $17,058 |
| Mean percentage of people under federal poverty level, 1977–2000 | 11.0 | 11.0 | 13.2 | 17.1 |
| Median population density (population per square mile), 1977–2000 | 338 | 89 | 57 | 52 |
The map shows that the poorest states come from two areas of the country. One group of states in Quartile 4 includes several southern states. Another group of poor states is located in the West, from New Mexico to Montana and South Dakota. We chose states for the case studies in part to represent this regional variation. West Virginia and South Carolina were selected among the eastern states; Mississippi and Louisiana were selected among the states in the central South; and New Mexico and Arizona were selected among the western states. As we note below, regional differences among the poor states were correlated with major differences in how they allocated funding among different social welfare programs.
Exhibit 2 also displays information about the states in these different quartiles, including average real per capita income, poverty rates, and population density. States in different quartiles differed in income; low-fiscal capacity states also had higher poverty rates and lower population densities (i.e., they were generally more rural).
Major Findings
Study findings emerged from several methods and data sources, including analyses of spending trends, econometric models of state spending on different types of social welfare functions, and the case studies of the six poor states (Arizona, Louisiana, Mississippi, New Mexico, South Carolina, and West Virginia). Five of the six case study states were in the fourth, or poorest, quartile. The sixth state (Arizona) was at the bottom of the third quartile. All had high social needs as measured by poverty and unemployment rates. The states also showed important differences in geography and recent changes in fiscal capacity and need. The case studies relied on discussions with public officials, administrative data on program spending and caseloads, and state budgets, reports, policy information, and other public documents.
The study’s major findings are as follows:
- States of less fiscal capacity spent less per capita on social welfare than states with higher per capita incomes. These differences between rich and poor states resulted largely from differences in states’ spending from their own sources of revenue. The distribution of federal funds neither greatly diminished nor greatly increased state differences in spending.
Poor states spent less per capita than rich states did on social welfare programs. As the chart at the top of Exhibit 3 shows, when averaged over the entire period of 1977 to 2000, per capita spending on social welfare was positively correlated with state fiscal capacity. The wealthiest 13 states (Quartile 1) spent an average of $639 per capita on social welfare programs over this time period, after expenditures were adjusted for inflation. The poorest 12 states (Quartile 4) spent only $408 per capita.
This $231 difference resulted largely from differences in states’ spending of their own tax revenues. Federal grants did not reduce absolute spending differences between rich and poor states. Average federal grants to the wealthiest states were $371, higher than the average grants to the other three quartiles, including the poorest states, which received an average of $339. However, because poor states spent less money overall on social welfare, that $339 constituted a large proportion (83 percent) of their total spending on such programs. By contrast, the $371 per capita from federal sources spent by the richest quartile of states made up a much smaller share (58 percent) of their total social welfare budgets. That is, more federal money went to rich states than to poor states, but poor states relied more heavily on the federal government to support their social programs.
Exhibit 3. Per Capita Spending on Social Welfare and Non-social Welfare Functions,
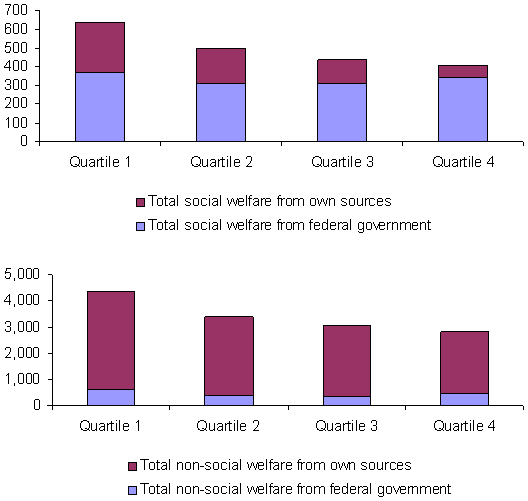
The chart at the bottom of Exhibit 3 shows that state fiscal capacity was also positively correlated with state spending on non-social welfare functions. The differences across quartiles again were due to how much states spent of their own revenues. However, federal spending played a smaller role in this component of state budgets. Although federal spending averaged over two-thirds (69 percent) of state spending on social welfare functions, federal grants typically made up only about one-eighth (13 percent) of total state spending on non-social welfare functions.
The study’s econometric models generally confirmed the importance of state fiscal capacity for spending on social welfare. State fiscal capacity was related to overall spending on social welfare even after controlling for other variables, such as social need (measured by per capita unemployment and poverty), federal grants per capita, population density, year effects, and long-run “state effects.”1 State fiscal capacity was even more strongly related to spending on non-social welfare functions after controlling for these other factors, perhaps because states relied more on their own-source revenues in supporting non-social welfare functions.
- State fiscal capacity bore a stronger relationship to spending on non-health programs than on health-related programs.
When we broke total social welfare spending down into more specific categories, the relationships between state fiscal capacity and state spending varied greatly. As the chart at the top of Exhibit 4 demonstrates, states of lower fiscal capacity showed consistently lower levels of per capita spending on cash assistance and non-health social services when compared to wealthier states. Spending on health-related functions showed a weaker relationship to fiscal capacity than spending on non-health functions. Levels of spending on Medicaid were highest for the richest quartile of states, and spending levels were lower for Quartiles 2 through 4. Yet Medicaid spending showed no differences among Quartiles 2, 3, and 4, indicating a weaker relationship to fiscal capacity than found for cash assistance and non-health services. In the case of payments to public hospitals, the relationship was the inverse of what was found for social welfare spending. The poorest states spent the most per capita on public hospitals.
Exhibit 4.
Spending Per Capita and Per Poor Person on Different Types of Social Welfare Functions,
Averages for Fiscal Capacity Quartiles, 1977–2000
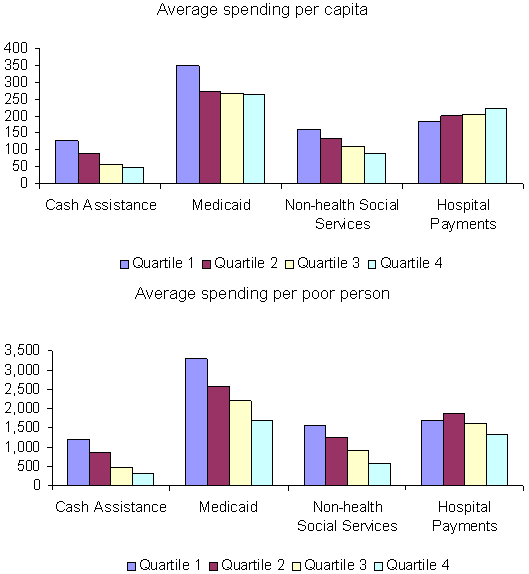
Because most social programs targeted low-income people, per capita spending levels failed to capture differences in the degree to which states met social needs. To understand spending from that perspective, we compared state spending per poor person. Differences between rich and poor states were more consistent, as shown in the chart at the bottom of Exhibit 4. Disparities between the top and bottom quartiles were even greater for spending on cash assistance and non-health social services, while spending on Medicaid and public hospitals showed positive though weaker relationships to fiscal capacity. For example, the poorest states spent only one-fourth the amount that the richest states spent on cash assistance, while the ratio of spending on Medicaid in poor to rich states was about one-half.
- Between 1977 and 2000, state spending on social services changed in major ways, and the changes differed between rich and poor states.
As Exhibit 5 shows, Medicaid spending grew rapidly among all states in the late 1980s and early 1990s, even after controlling for the high rates of inflation in health care services. But the strongest growth occurred among the poorest states, those in Quartile 4, probably a consequence in part of federal Medicaid expansions in eligible populations, services, and special funding for health care providers during those years. In the middle and late 1990s, Medicaid spending growth slowed or even stalled among the wealthier states — not surprisingly, given the strong economy and possible downward pressures on Medicaid caseloads exerted by welfare reforms. But the poorest states continued to show increases in spending even in the late 1990s. By 2000, differences between the richest and poorest states in per capita spending on Medicaid had narrowed substantially.
Exhibit 5.
Changes in Average Per Capita Spending on Medicaid,
by State Fiscal Capacity, 1977–2000
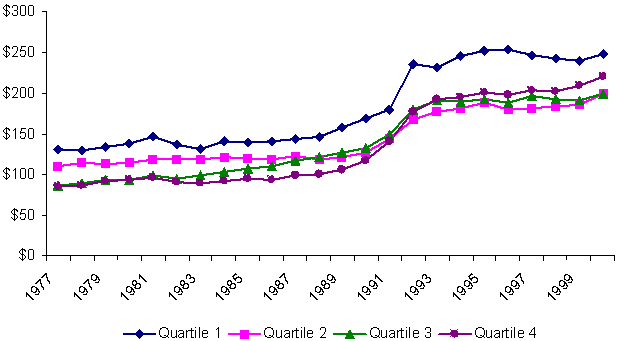
Changes in real per capita spending on cash assistance varied even more across states, as Exhibit 6 illustrates. In the wealthier states of Quartiles 1 and 2, spending on cash assistance either declined slowly or remained static until the late 1980s, when spending began to grow. Spending then declined in the middle and late 1990s as caseloads dropped due to welfare reform and economic growth. Richer states thus reaped substantial fiscal savings in late 1990s from reductions in spending on cash assistance.
Exhibit 6.
Changes in Average Per Capita Spending on Cash Assistance,
by State Fiscal Capacity, 1977–2000
(adjusted with GDP price deflator)
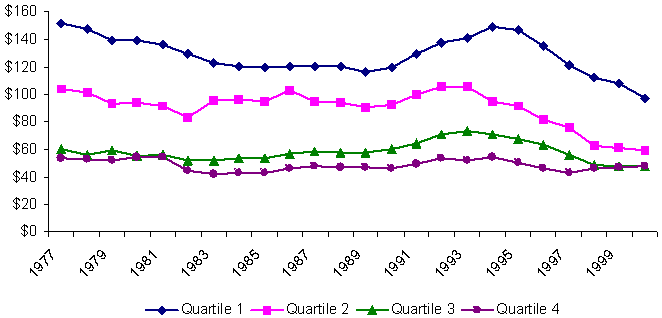
By contrast, spending on cash assistance was already low in poor states, so even large caseload declines in the late 1990s yielded small fiscal savings. State fiscal capacity became less correlated with spending on cash assistance programs at the end of the 1990s when compared to the early 1990s and before. In contrast to the upward convergence of states with respect to spending on Medicaid, states of different fiscal capacities converged downward in their spending on cash assistance after the early 1990s.
Spending on non-health social services programs, by contrast, showed growing divergence among states of different fiscal capacities, as Exhibit 7 shows. All quartiles gradually increased their spending on non-health social services between 1977 and 2000. But growth was faster among the wealthiest states, especially during the late 1990s, while spending growth on services in the poorest states (Quartile 4) lagged behind.
Exhibit 7.
Changes in Average Per Capita Spending on Non-health Social Services Programs,
by State Fiscal Capacity, 1977–2000
(adjusted with GDP price deflator)
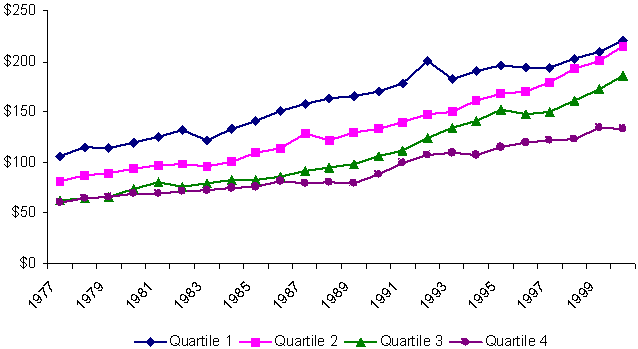
These different trends produced enormous changes in the composition of social welfare expenditures — and in the relationship between state fiscal capacity and how states allocated their dollars across social welfare functions. Exhibit 8 shows these shifts by tracking the percentage of total public welfare spending for different program functions in the wealthiest and the poorest quartiles (Quartiles 1 and 4) during the years 1980, 1990, and 2000. Over these two decades, Medicaid came to absorb a much larger share of the budgets of both rich and poor states. Cash assistance spending shrank as percentage of total social welfare spending in all states, though most precipitously in rich states, thereby reducing differences between rich and poor states.
Exhibit 8.
Average Percentage of Total Public Welfare Spending on Different Functions,
by State Fiscal Capacity (Quartiles 1 and 4), 1980, 1990, and 2000
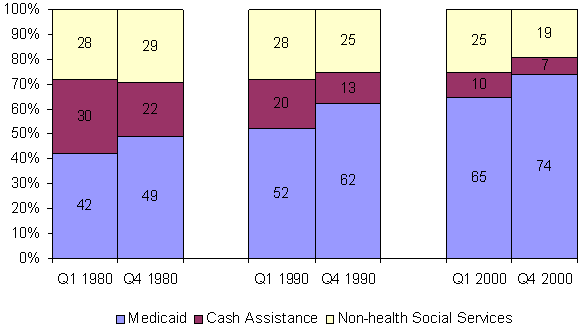
One striking change was the growing disparity between rich and poor states in their spending on non-health social services. In 1980, poor states spent a slightly larger percentage of their social welfare budgets on such programs than did rich states. By 2000, poor states were spending a much smaller percentage of their social welfare budgets on non-health services. Most of the remainder of their social welfare budgets — nearly three out of every four dollars — was devoted to Medicaid.
- Econometric analyses found that different factors influenced different social programs.
Based on estimations of econometric models of state spending on different social programs in all states from 1977 to 2000, we found different types of programs to be influenced by different state characteristics. State fiscal capacity was positively related to Medicaid spending (i.e., rich states spent more than poor states, other things equal). We also found that Medicaid expenditures were positively related to unemployment. Medicaid spending responded strongly to federal grants for social welfare, perhaps reflecting the attractiveness to the states in matching federal Medicaid dollars. The regression equations also indicated that Medicaid spending was higher in states with lower population densities.
Unlike Medicaid, cash assistance spending was negatively related to state fiscal capacity.2 Spending on cash assistance, however, was significantly and positively related to unemployment and federal grants. Thus, like Medicaid, cash assistance spending rose with unemployment, other things equal; and, though less strongly as Medicaid, cash assistance spending was encouraged by federal spending. Unlike Medicaid, however, cash assistance expenditures were higher among states with high population densities than among rural states.
Non-health social services — mostly services such as child care, child welfare, and energy assistance, programs serving the homeless, and a wide variety of others — responded to a different set of factors. State fiscal capacity and federal grants for non-social welfare programs strongly affected spending on these diverse services; also, spending was higher in low population density states. Spending on non-health social services was not sensitive to unemployment, like other program areas. In fact, a negative, albeit insignificant, relationship occurred between unemployment and service spending, other things equal. A negative, though significant, relationship also appeared between such spending and the percentage of people in poverty. These relationships suggest that a state’s total economic resources were critical in understanding spending for non-health social services.
In sum, the multivariate econometric analyses suggested the following:
- Unemployment pushed up spending on cash assistance and Medicaid but not on non-health social services.
- Growth in state per capita income enhanced spending on Medicaid and non-health social services but not necessarily on cash assistance.
- Rural states spent less of their money on cash assistance programs and more on health and non-health social services.
- States were especially responsive to federal grants for Medicaid.
- States of different fiscal capacity responded to different factors — or responded to the same factors in different ways. Wealthy states, for example, were more affected than poor states by economic cycles, fiscal capacity, and federal spending on social welfare programs.
By estimating regression equations for states of different fiscal capacities (i.e., for each of the four quartiles), we found that our general model of spending fit wealthy states more closely than poor states. In other words, poor states showed weaker relationships between the independent variables in the equations and all types of social welfare spending. For example, fiscal capacity, federal grants, unemployment, and population density were all significantly related to spending on cash assistance for the rich states in Quartile 1. Yet, only population density showed a significant relationship to cash assistance spending for the poor states in Quartile 4. Also, unemployment was positively and significantly related to Medicaid spending among Quartile 1 states, but the same coefficient was insignificant when the regression was estimated for Quartile 4 states. Similar differences in the degree of fit were found in equations for non-health social services, payments to public hospitals, and non-social welfare services.
But we found important exceptions. For Medicaid, federal spending for social welfare was at least as important for poor states in affecting state spending as it was for wealthier states. Population density was also important in many of the equations for poor states. Finally, our analyses of state effects revealed that poor states showed long-run differences in the ways they allocated their social welfare budgets, especially between cash assistance and health care programs, including Medicaid and payments to public hospitals. For example, poor western states showed higher levels of spending on cash assistance programs than did poor southern states, and they also showed lower levels of per capita spending on Medicaid. Poor states thus seemed to undergo smaller short-run changes in their spending patterns but did vary from one another based on relatively stable attributes, such as population density, region, and demographic composition of the state’s population.
- Case studies of six states of low fiscal capacity and high social needs indicated that the basic trends in spending found among poor states before 2000 continued after that year.
When we examined what happened in the six poor states after 2000 — and through 2003, when the case studies were completed — we found that the trends identified between 1977 and 2000 generally continued. Per capita Medicaid spending increased in most states between federal FYs 2000 and 2003, and the growth was greater among the six poor states in our sample than for all states. Using administrative data from the federal agency responsible for Medicaid, we found, as the graph at the top of Exhibit 9 shows, that the average nominal growth in spending among the six poor states between 2000 and 2003 was slightly higher than the average growth in Medicaid spending for all states.
Exhibit 9.
Per Capita Spending on Medicaid and TANF Basic Assistance,
Averages for the Six Poor States and for All States
Per capita spending on Medicaid, 1997–2003.
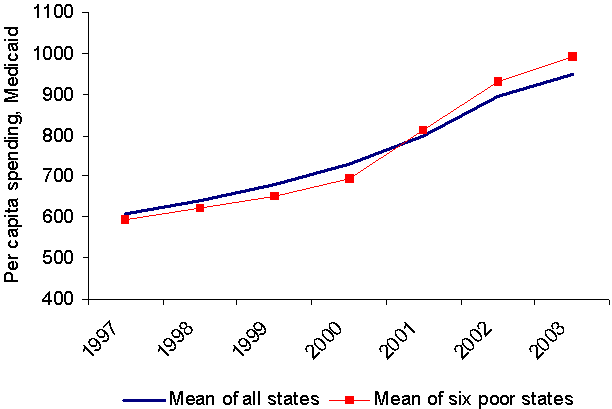
Per capita spending on TANF basic assistance, 1998–2002
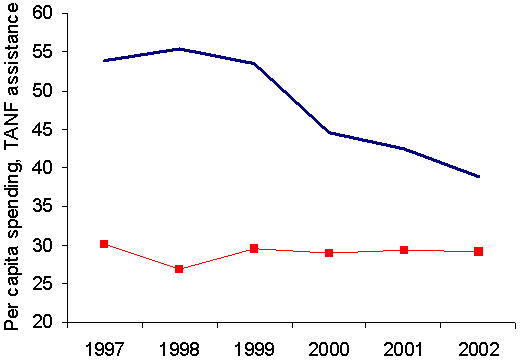
Some of this growth was due to the fact that some of the poor states (notably New Mexico and Arizona) that had spent relatively little on Medicaid in the late 1990s greatly expanded their programs in the early 2000s. The most striking change occurred in Arizona. State voters overrode years of legislative opposition to Medicaid expansion in 2000 by enacting a citizen’s initiative, Proposition 204, that greatly expanded Medicaid coverage to include households up to 100 percent of the federal poverty level. Enrollment grew from 575,000 in January 2001 to 902,500 in January 2003. Louisiana also expanded eligibility for children and aged and disabled people in FY 2003, and it increased eligibility among pregnant women to include all those under 200 percent of the federal poverty level. Other major factors driving up Medicaid costs — and noted by our respondents — included expansions in enrollments due to the weakened economy and SCHIP outreach efforts and the substantial increases in prescription drug costs.
In recent years, TANF basic assistance constituted an important part of the cash assistance component of the Census data. Spending on this assistance continued to drop among all states between federal FYs 2000 and 2002, with an average decline of 13 percent, as the graph at the bottom of Exhibit 9 shows. However, as was also true before 2000, no average decline occurred among poor states in cash assistance spending. Mean cash assistance expenditures remained comparatively static among these states, as before 2000.
The econometric analyses indicated that non-health social services were most likely to show a cyclical effect (i.e., be vulnerable to cuts when government revenues declined). Our case studies confirmed that the greatest pressures on spending in the poor states were imposed on non-health social services and expenses. Administrative expenditures were often severely curtailed during the recent state fiscal crises. South Carolina’s department of social services saw a 26 percent reduction in staff between FYs 2001 and 2003. Arizona reduced its human service workforce despite substantial increases in Medicaid and cash assistance caseloads. Administrative cutbacks were greater among poor states than among others. For example, TANF administrative costs per capita declined by 22 percent among the six states between FYs 2000 and 2002, while the average decline for all states was only 5 percent.
Legislatures often cut state spending on child welfare programs, including staffing and payments for protective services, foster care, and adoption. However, the effects of some of these cuts were sometimes mitigated by the greater use of federal TANF dollars to support such programs. A number of programs deemed less critical to basic agency goals were cut or eliminated, including parenting and fatherhood programs, employment services, job development positions, and pregnancy prevention programs. Some discretionary cuts in child care were imposed. However, because most of these states put small amounts of state money into their child care programs, only the two states that had put larger sums of TANF or state money into their subsidy programs in the 1990s (Arizona and Louisiana) made major reductions in their child care spending.
- Case studies found that, in poor states, different processes influenced spending on different social programs.
The case studies of the six poor states revealed important differences in the processes affecting spending on different social welfare functions. Cash assistance spending in low fiscal capacity states was largely determined by policies established through state legislation. These policies were changed infrequently in the six case study states. A flurry of policymaking around AFDC waivers and TANF cash assistance occurred in these and many other states in the middle and late 1990s. By 2003, however, TANF and its policies drew little attention from legislators in these six states and changes in earned income disregards, maximum benefits, time limits, and sanction policies had changed little since the late 1990s. For example, maximum benefit levels for AFDC and TANF assistance had changed only once or twice in most of the six states during the last 20 years. Debates over these policies also seemed more ideologically and racially charged than most other social policy questions.
Our site visits indicated that Medicaid spending processes were vastly different. Federal mandates, considerations of federal match rates, and active participation of organized provider groups that served as advocates for various parts of the program often dominated Medicaid spending. Perhaps because of the involvement of such groups, Medicaid was also a more politically salient program area. Unlike “welfare,” even the post-reform versions, health programs regularly engaged the attention of elected officials, including legislators, governors, and top administrators.
Among the six poor states in our sample, organized providers were especially strong in the four rural and southern states where Medicaid played a major role in the health care industry and local economy. In these states, hospitals and other health institutions played a large economic role; nursing home residents were more likely to rely on Medicaid; and a greater proportion of births, often more than half, were paid for by Medicaid. Also, most health institutions in these states relied on Medicaid, making it more of a universalistic program, in contrast to the situation in wealthy states, where some institutions depended heavily on Medicaid, while many did not.
Attractive federal match rates were often noted in debates over Medicaid budgets in poor states, especially during periods of budgetary stress. By themselves, however, match rates appeared to constitute insufficient conditions for understanding levels of support for Medicaid in poor states because equally strong match rates had been available under AFDC and were still available under child welfare programs, though with much less expansive effects. However, the combination of attractive match rates, federal minimum requirements, and strong constituencies seemed critical and meant that, even in poor and conservative states, medical assistance programs could enjoy substantial support.
Other factors might have bolstered support for Medicaid. In most of the states, the agencies that administered Medicaid were separated from those that administered welfare and non-health social services, and that separation insulated health programs from the often negative views about social service agencies held among legislators.
Our case studies indicated that, for the most part, non-health service programs elicited less political interest. These programs did not evoke the ideological divisions affecting cash assistance programs. Nor did they elicit participation of major provider groups in these low-fiscal capacity states. As a result, decisions in poor states about what programs to support in this diverse category of non-health social services were often delegated to and controlled by state administrators rather than legislators and governors. Choices regarding non-health services were more likely to reflect a sort of technocratic politics. Decisions were often made on the basis of state administrators’ assessments about the relative merits of different programs and their centrality in achieving major goals.
However, though administrators had some control over which programs grew and which were cut, they had little control over general fiscal constraints, and these changing constraints often dominated recent budgetary processes for this group of programs. Since the last recession, legislatures and governors typically instructed social service agencies in the six case study states how much they must cut from their total budgets, not precisely where to reduce services. Administrators often made cuts based on judgments about what services were critical to major agency goals, what programs were successful in terms of performance standards, what programs were needed to create or maintain a coherent “package” of benefits or services, what programs involved high stakes (e.g., “life or death” issues), and how and whether programs can be administered with fewer staff.
Conclusions
This study sought to understand how state fiscal capacity affected spending on social welfare programs. It found that low fiscal capacity states spent less on social welfare programs than did high fiscal capacity states and that these differences were greater for cash assistance and non-health social services than for health-related programs.
We also found that the level and composition of social welfare spending changed enormously in the last two and a half decades. Medicaid spending grew much faster than overall social welfare expenditures, particularly since the late 1980s. Cash assistance spending was more volatile — rising in the early 1990s and falling in the late 1990s — though the general tendency was down. Non-health social services grew more steadily throughout the period. These trends produced a major shift in the basic structure of state social welfare budgets, away from cash assistance and toward health care services. At the same time, a major realignment occurred in the relationship between the composition of social welfare services and state fiscal capacity. Per capita expenditures on Medicaid and cash assistance by rich and poor states converged, especially since the middle 1990s. By contrast, per capita spending on non-health social services diverged, with rich states spending much more than poor states on these programs.
These shifting patterns of spending are partly understandable in light of our findings that different social programs respond to different factors and that states of different fiscal capacity vary in their responsiveness to the same variables. Unemployment, for example, changes the mix of expenditures, as higher unemployment increases Medicaid spending and fails to boost non-health social services. Increases in state per capita personal income tend to push up Medicaid and non-health social services while showing an inconsistent effect on cash assistance.
Our case studies also suggested that different institutional processes characterize different program areas. Although these findings are limited to these six poor states, they also indicate the possibility of dramatically different dynamics across program areas. The greater role of ideology and demographic characteristics in decisions affecting cash assistance expenditures; the importance of federal match rates, minimum requirements, and organized providers in Medicaid politics; and the significance of overall state resources and flexibility in non-health social services all suggest that the mix of social welfare programs is likely to continue to change.
Endnotes
1 “State effects” are separate intercepts estimated in the regression models for each of the 50 states (plus the District of Columbia). They may be viewed as average differences in state spending over the entire period (1977-2000), after controlling for the linear effects of the included variables, such as fiscal capacity and unemployment. State effects may, for example, be the result of differences in state political cultures, which were not directly measured in this study. “Year effects” are dummy or binary variables representing each year of the time series. A year effect indicates an average difference in spending across all states compared to some baseline year. A significant year effect may result from a national policy change or some other factor operating on all states but not fully measured by the independent variables included in the regression.
2 However, when the equations were estimated for each fiscal capacity quartile, only the wealthiest quartile (Quartile 1) showed a negative and significant relationship.
Chapter I: Introduction
Social welfare programs strive to improve the well-being of needy and vulnerable populations. Government spending on social welfare programs, although not a guarantee that programs will meet this goal, nonetheless constitutes important tangible evidence of state policies and commitment to social welfare programs. Certainly, a low level of state social welfare spending in poor states relative to a high level of need would constitute cause for concern among policymakers.
States vary enormously in their need for social welfare services and their capacity to finance the services. Presumably, states that have higher proportions of individuals living in poverty have a greater need for programs that provide cash benefits, health care, employment supports, and other services. Often, however, these states bring in fewer tax revenues.
In addition, worsening economic conditions increase the need for these types of services but reduce tax revenue to fund them. Entitlement programs, which provide pre-established benefit levels to all individuals meeting the eligibility criteria, provide some protection to ensure increased funding when the economy worsens. States determine the benefit levels and eligibility criteria based, in part, on the long-term fiscal capacity of the state. Nevertheless, programs that include a state match, such as Medicaid, can place great stress on state budgets as they expand to satisfy needs while state revenues are declining.
This study, produced for the U.S. Department of Health and Human Services (HHS) Office of the Assistance Secretary for Planning and Evaluation (ASPE) by The Lewin Group and the Rockefeller Institute of Government, examines the extent to which fiscal capacity affects state social welfare spending. First, we reviewed the relevant literature regarding this topic. Then, we analyzed spending patterns across the 50 states and over time using Census of Governments (Census) data. Finally, we conducted site visits to six low fiscal capacity states and used qualitative and quantitative information to describe the differences among these states in their spending on social programs.
This report is organized into four major sections plus two appendixes. Section I, Introduction, presents information on the project, policy context, research questions, and a brief literature review. Section II, Approach, describes our methodology for analyzing the spending data as well as our methodology for selecting the six states for field visits and the data collection and analysis. Section III, Findings and Results, lays out the detailed findings from primarily the cross-state spending analysis. Section IV, A Closer Look at Poor States, describes the integrated analysis using the results from the Census data spending analysis and the quantitative and qualitative data collected in the field visits. Lastly, Section V, Final Observations and Conclusions, summarizes and comments on the projects major findings. The two appendixes provide additional information on the econometric modeling (Appendix A) and the six states visited (Appendix B).
A. Policy Context
The fact that states spend differing amounts per capita on social welfare is well known; the extent to which these differences relate to differences in state fiscal capacity is less understood. The federal government has long played an important role in offsetting state fiscal disparities. However, significant changes have occurred in federal grant programs and eligibility requirements that impact differentially poor and rich states. Other factors in the state environment in addition to fiscal capacity and federal grants influence state spending, including various determinants of state need for social welfare spending such as poverty and unemployment. Finally, political and institutional factors, including the state budget process, affect state spending.
The federal government can offset state fiscal disparities through federal reimbursement for Medicaid and foster care under a formula more generous to low-income states than to high-income states. In addition, the federally funded Supplemental Security Income (SSI), Food Stamps, and Earned Income Tax Credit (EITC) programs provide assistance to all eligible individuals and require no state funds.2 Thus, a state with a relatively high share of low-income individuals presumably has a high share of residents receiving federal benefits, regardless of the states low-fiscal capacity.
Significant changes in federal cash assistance have also occurred. In 1996, the Personal Responsibility and Work Opportunity Reconciliation Act (PRWORA) transferred some of the responsibility for social programs, and the fiscal risk, from the federal government to states. Under the earlier AFDC program, states and the federal government shared the risk of increased entitlement welfare spending. Under the TANF program, which replaced AFDC, states bear the full cost of spending increases above the value of their federal block grant and reap the full savings of spending reductions as long as maintenance-of-effort (MOE) and certain other requirements are satisfied. In some ways, these reforms reduced the incentives for poorer states to increase spending on social welfare programs, even if their needs increased, because their increased spending is not matched with increases in federal support.
Around this time, the Medicaid program3 was experiencing explosive growth, placing more stress on state budgets. In fact, the Medicaid program increased nearly 150 percent, from $91.5 billion in 1991 to $228 billion in 2001 (Snell, Eckl, & Williams, 2003). Several factors contributed to the increase in expenditures, including the early 1990s recession, which increased the number of families eligible for Medicaid; extensions in the Medicaid program to cover more of the uninsured, working poor; demographic trends that increased the share of enrollees who were disabled and required more medical services; and increases in the overall costs for medical services.
Some have expressed concern that spending on Medicaid will crowd out state spending on other social welfare programs, such as cash assistance (e.g., see Steuerle & Mermin, 1997; Ladenheim, 2002). Given states increased flexibility in funding cash assistance, changed incentives, and increasing Medicaid costs, understanding how fiscal capacity, especially in poorer states, might affect state policy choices about social welfare programs is important.
B. Research Questions
In an effort to understand the relationship between fiscal capacity and state spending on social welfare programs, this study addresses several research questions:
- How does a state's fiscal capacity affect the proportion of total state spending on social welfare programs? Does a significant difference occur between rich and poor states? Have increases in spending for other services come at the expense of social welfare services, and vice versa?
- How have states decided to package their services for their low-income populations, including expenditures on cash assistance, Medicaid, child care, child welfare, and other social services?
- How have economic downturns and booms affected state social welfare spending? What social welfare programs were most affected by economic downturns?
- How does a states fiscal capacity affect the availability of social welfare services? Do benefit levels and eligibility requirements for social welfare services, including cash assistance, child care, employment, Medicaid, and child welfare, vary based on state fiscal capacity?
- How have changes in federal program requirements, particularly the adoption of TANF and changes in Medicaid policies, affected states ability to provide social services to low-income populations?
- Is there a relationship between a states fiscal capacity and the size of its low-income population?
- How have states with the lowest fiscal capacity adjusted their spending patterns in responses to changes in economic conditions, federal funding, and legislative provisions?
C. Review of Related Literature
The following literature review touches on the highlights of prior literature on trends in social welfare spending, issues in measurement of state fiscal capacity, and determinants of state and local spending on social welfare, including state fiscal capacity, need for services, and political and institutional factors.
1. Trends in Spending on Social Welfare Programs
Researchers have tracked changes in spending over time. According to Census data, total real general expenditures on social welfare increased from about $2,000 to about $2,600 per capita from 1988 to 1997, a 30 percent increase. Almost half of the increase in state spending resulted from increased spending for social welfare. Merriman (2000a) found that this increase in social welfare spending was due primarily to growth in federal Medicaid expenditures.
Boyd et al. (2003) analyzed state spending on social service programs other than Medicaid between state fiscal years (FY) 1995 and 1999 in 16 states (Arizona, California, Colorado, Connecticut, Louisiana, Maryland, Michigan, Minnesota, New York, Ohio, Oregon, Rhode Island, Tennessee, Texas, Virginia, and Wisconsin) and the District of Columbia and found that spending on cash assistance declined sharply. In contrast, state spending on child care and work support services increased in all study states and the District of Columbia. State spending on child welfare also increased in 14 study states and the District of Columbia.
The reduction in state spending on cash assistance was generally consistent with the dramatic reductions in welfare caseloads. The caseload decline began in 1994, before welfare reform at the federal level was enacted in 1996. This decline accelerated after 1996, and, as of September 2003, caseloads were 54 percent lower than in 1996. These savings allowed states to undertake new programs designed to move people to work, improve child well-being, or accomplish other objectives of the welfare law.4 Boyd et al. also found that states with higher cash assistance benefits had greater cash assistance savings per person in poverty because they saved more per case that left the welfare roles. These high-benefit states generally had higher per capita income than the low-benefit states.
2. Measuring Fiscal Capacity
The term fiscal capacity can be measured several ways, although this term is generally used to represent a states potential to raise revenue and not the actual fiscal choices made. Common ways for measuring fiscal capacity include the following:
- Per capita personal income (PCPI). This measure represents the total personal income of the states residents (e.g., wages and salaries, interest income, social security benefits, SSI, AFDC/TANF cash assistance and pensions, but not Food Stamps, housing vouchers, and EITC) divided by the states total population. PCPI is widely used to measure fiscal capacity because data are readily available and because it is a relatively good indicator of residents ability to pay taxes, which, in turn, can fund services. It is also used in determining the federal match for Medicaid reimbursement. One shortcoming of this approach is that it ignores the extent to which states can impose tax burdens on nonresidents.5 PCPI data are available from the Bureau of Economic Analysis for 1929 through 2001.
- Representative tax system (RTS). To measure state tax capacity, the Advisory Commission on Intergovernmental Relations (ACIR) applies the average tax rate on income, consumption, and real property over all states to each states tax bases. The ACIR produced the RTS between 1962 and 1991.
- Total taxable resources (TTR). This measure, which has been calculated by the U.S. Department of Treasury since 1992, captures a states ability to raise revenues. It is equal to the states Gross State Product increased by residents income earned out of state, federal transfers, and accrued capital gains less federal taxes paid and depreciation.
Of the three measures, only the PCPI data are available from FYs 1977 through 2000, the period examined for this study. Generally, states that rank low on one measure also rank low on the other measures. However, some states are ranked differently. For example, Alaska is ranked the 17th highest state using the PCPI, the 3rd highest using the RTS, and the 5th highest using the TTR. These differences can be explained, for the most part, by the fact that a large portion of the income produced in Alaska is earned from oil and natural gas production (Compson & Navratil, 1997) by individuals residing outside Alaska.
3. Determinants of Social Welfare Spending
We hypothesized that three factors drive state spending on social welfare programs: fiscal capacity, need, and political and institutional factors. Prior literature has attempted to explain the connection between these factors and spending.
a. Fiscal Capacity
Overall, research has found a positive association between fiscal capacity and social welfare spending. One study (Mogull, 1978) found that primarily fiscal resources, measured by per capita personal income and federal aid, determined state and local expenditures on antipoverty programs. Other studies (Jennings, 1980; Orr, 1976; Plotnick & Winters, 1985; Dye, 1969) came to similar conclusions.
Although a strong association appears to exist between fiscal capacity and social welfare spending, Mogull (1989) notes that this correlation fails to explain the causal basis for the association. Most researchers, however, contend that the higher the taxpayers income, the better able the state is to fund the additional services. This higher per capita income reduces the financial burden on the state.
Another factor to consider is the role that federal funding plays. Douglas and Flores (1998) found that federal government grants target states with the least ability to pay and the highest need for services. Without considering federal spending, in 1995, high-ability states (i.e., 10 states with the highest levels of personal income per poor child) spent 4.3 times as much as low- ability states (i.e., 10 states with the lowest levels). When federal funding is included, high-ability states spend only 1.82 times as much.
b. Need
It is hypothesized that the higher the poverty and other indicators of need, the more the state will spend on programs benefiting the poor. Mogull (1989) suggests that poverty affects expenditures in two ways. First, high levels of poverty increase the pool of eligible persons. Second, increased visibility of concentrations of poor people can increase social and political activism, which in turn, leads to increased spending.
Some research has shown this positive association between poverty and social welfare expenditures. Mogull (1993) found that indicators of need, such as unemployment rates, were estimated to exert a significant effect on social welfare spending, presumably by expanding the pool of eligible families. Similarly, Hicks and Swank (1983) found a direct impact of need on welfare caseloads.
Other research has shown an inverse relationship between poverty and social welfare spending. For example, Tannenwald (1999) examined the diversity across states in preferences for the size of state and local government, given their fiscal need. If preferences for levels of state and local public services were similar across states, one would expect states with low levels of fiscal comfort (i.e., low ratio of tax capacity to need) to raise relatively more revenue from their tax bases by taxing more intensively.6 However, only a handful of states (i.e., California, Michigan, Mississippi, and New Mexico) had low fiscal comfort and above-average tax effort. Most states exhibit both low tax effort and low comfort or high tax effort and high comfort. A number of states had both high comfort and low effort. Overall, the correlation coefficient between effort and comfort was negative and statistically insignificant. This finding suggests that many low fiscal comfort states prefer lower levels of government than their fiscally more comfortable counterparts.
Another study (Jennings, 1980) examining welfare expenditures from 1964 to 1971 found an inverse association between poverty and welfare expenditures. This study found that increases in the percentage in poverty were negatively related to increases in the percentage change in welfare spending from both state funds and federal funds. However, as the authors note, this might reflect the inability of poor states to meet the needs of their poor residents given their low per capita incomes. Fry and Winters (1970) examined the effect of poverty on the ratio of expenditure benefits to revenue burdens for the three lowest income classes (the net redistributive impact). The authors hypothesized that the larger the proportion of low income families in the state, the greater the perceived need for redistribution through state revenue and expenditure policies. The study found, however, that the proportion of families with less than $3,000 annual income was negatively related to redistribution. We should note that these two studies examined a much earlier time period than our study.
c. Political and Institutional Determinants
State political cultures and institutions might also affect state spending on social welfare programs. But prior research often showed unstable results, and it failed to cover the wide range of program areas dealt with in this study. In political science, the investigation into the effects of political and institutional factors on redistributive policies and expenditures began with V.O. Keys study of southern politics (1949), where Key argued that one party dominance in the South limited political competition for voters and thus incentives to mobilize low-income families. Also, intra-party divisions made enacting major policy initiatives more difficult for parties once in power. The result, Key hypothesized, was a lack of real responsiveness to the interests of the have nots. This argument inspired a series of studies, beginning in the late 1950s, which attempted to isolate the roles of party competition, party control, and other institutional or political variables on redistributive policies or expenditures (often Aid to Families with Dependent Children [AFDC] spending) while controlling for the effects of state wealth or fiscal resources, state need, and federal grants (Dye, 1966; Dye, 1979).
In the earlier studies, the estimated effects of political and institutional variables proved small or nonexistent. Mogulls (1989) review of the literature found that neither party competition, hypothesized to create incentives to mobilize lower income strata, nor government control by the Democratic Party, viewed as more supportive of spending on social welfare programs, corresponded consistently to state welfare spending in multivariate analyses.
More recent studies amended these conclusions by using more refined models and measures that attempted to isolate the conditions under which political and institutional variables were likely to exert impacts. Brown (1995) claimed that inconsistent and weak effects of party on welfare and other redistributive policies might be due to differences across states in party coalitions. Where parties were divided by class, party control over government was more likely to influence state and local AFDC spending. Brown found that the effects of Democratic Party control of state government were greater where parties were class based. He also found, like other studies, that welfare effort was reduced by the percentage of the states population that was black.
Plotnick and Winters (1985; 1990) argued that the effects of political variables were underestimated because total welfare spending, the dependent variable typically used in the early studies, was not controlled by governors and legislators. State officials determined such policies as benefit and eligibility levels. Once these factors were established by law, demographic and economic changes interacted with policies to produce total expenditures. Using a measure of income guarantee for the dependent variable-the cash value of AFDC, Food Stamp, and Medicaid benefits for a nonworking family of four-they found that the size of the guarantee was significantly and directly related to interest group strength, measured by per capita memberships of liberal interest groups in the state, and inter-party competition but that Democratic Party control over state governments and local cost-sharing arrangements exerted no impact. They also found that the population density of the poor was positively related to the size of the guarantee, while smaller guarantees were associated with large numbers of illegitimate births in the state and high proportions of non-white families on welfare.
Other studies followed Plotnick and Winters lead and focused on choices under state control. Gais and Weaver (2002) examined state policy choices under welfare reform and also found that the racial composition of the welfare caseloads and a measure of state conservatism were associated with stronger sanction policies, shorter time limits, and immediate work activity requirements for welfare recipients. Kousser (2002) found that Democratic control of the legislature had strong and positive effects on changes in discretionary spending under Medicaid-but not on mandatory spending. Like other studies, he also found that the size of a states minority population was weakly though significantly related to lower levels of spending. Kousser found that the party of the governor had no impact on spending, nor did a measure of state ideology.
The literature as a whole suggests that political and institutional factors might influence state policies and expenditures on social programs. However, the estimated effects have been unstable across the studies. Some of the instability seems to be due to differences in the measurement of dependent variables (e.g., results are more consistent when dependent variables measure actual state choices, such as eligibility criteria and benefit levels, rather than total spending). But some of the instability still seems inexplicable, perhaps because of little real analysis in the studies of how states make decisions. Another weakness in the literature is that, with few exceptions (Kousser, 2002; Barrilleaux & Miller, 1988), most of the empirical analyses have focused on traditional cash welfare benefits, while the theories have usually treated social or redistributive policies as an undifferentiated whole. Thus, little theoretical or empirical work has been done on whether and how different kinds of social welfare programs-whether health or non-health, cash or services-might be affected by different institutional or political processes or conditions. Finally, no research has been conducted on how state fiscal capacity might interact with political and institutional variables in affecting social welfare spending. Yet such interactions would seem likely, because low fiscal capacity, almost by definition, would appear to limit the range of state political choices.
Endnotes
2 The Food Stamp Program requires a state match for administrative costs.
3 Medicaid is a program that pays for medical assistance for certain individuals and families with low incomes and resources. This program became law in 1965 and is jointly funded by the Federal and State governments (including the District of Columbia and the Territories) to assist States in providing medical long-term care assistance to people who meet certain eligibility criteria. Medicaid is the largest source of funding for medical and health-related services for people with limited income. Source: <http://www.cms.hhs.gov/medicaid/>
4 Section 401 (a) of the Social Security Act says that the purpose of TANF is to increase flexibility of States in operating a program designed to: 1) Provide assistance to needy families so that children may be cared for in their own homes or in the homes of relatives; 2) End the dependence of needy parents on government benefits by promoting job preparation, work, and marriage; 3) Prevent and reduce the incidence of out-of-wedlock pregnancies and establish annual numerical goals for preventing and reducing the incidence of these pregnancies; and 4) Encourage the formation and maintenance of two-parent families.
5 Two commonly cited examples are states that impose severance and property taxes on oil, gas, and coal companies for extracting fossil fuels and states that derive large amounts of sales tax and fee revenue from a substantial tourist trade. Also, it fails to count the income of nonresident commuters (e.g., New Jersey and Connecticut residents who work in New York).
6 Tannenwald (1998) calculates each state's "fiscal comfort" by dividing its index of RTS tax capacity by its index of fiscal need. The fiscal need is based on how much is required to provide a standard level of services in the state. Tax effort is measured by the ratio of state tax collections to the taxes it would have collected under the RTS.
Chapter II: Approch
A. Overview
To answer the research questions identified in the Introduction, first we analyzed spending trends and patterns over 24 years for the 50 states plus the District of Columbia by using sample means from Census data and an econometric model estimated from the pooled time series and cross-section data. We supplemented this analysis with site visits and further analysis of qualitative and quantitative data from six states, selected as having high needs relative to their fiscal capacity. The econometric model estimates were used to identify states exhibiting a high propensity to spend on certain types of social welfare. Employing this information, we drew comparisons between rich states and poor states in general and also among the six states for which we had additional case study data.
B. Fifty-State Analysis
1. Overview of Analysis
Our analysis of Census spending data involved both examining time trends and patterns across states and estimating an econometric model. The analysis of trends and patterns entailed primarily the study of time trends and cross-state patterns for different components of spending. We developed the econometric model to give insight into the determinants of state and local spending on social welfare and to provide useful input for the analysis of spending decisions between rich and poor states in general and in the six poor states we visited. As explained below, the model specification is based on a linear expenditure function derived from a behavioral theory of state and local spending decisions subject to a budget constraint. The model attempts to identify causal factors that explain variation in spending patterns. The explanatory factors include state fiscal capacity, federal grant amounts, indicators of need for social welfare programs (e.g., poverty and unemployment), time effects (e.g., dummy variables for year), and state effects (e.g., dummy variables for state). We did not intend the model to capture all factors responsible for variation in spending. Indeed, to help us understand variation in spending across states, we relied on measures of "state effects," which are effects associated with particular states after controlling for the effects of included explanatory variables.
a. Analysis of Trends and Patterns
Our analysis of time trends and cross-state patterns in social welfare spending involved examining Census data on per capita spending by state and local governments for the period 1977 to 2000 for each of the 50 states plus the District of Columbia. In subsection IIC below, we describe in detail the data examined. A central focus of the trends and patterns analysis was to identify important differences in real state and local spending by category of social welfare (e.g., cash assistance, Medicare, and non-health social welfare) and non-social welfare spending and by states grouped into quartiles based on average per capita personal income. This essentially descriptive analysis of the data served as a prelude to developing a model to identify causal factors related to state and local spending on social welfare and non-social welfare functions.
b. Linear Expenditure Models
Following McGuire (1978) for the basic theoretical model, we assumed that the decision-maker is the combined state and local system. This approach allowed us to model state and local spending on both public and private goods in a consistent way. The budget constraint consists of state fiscal capacity augmented by federal grants. The state and local governments then make spending and taxation choices subject to this budget constraint. States that have preferences for public spending over private consumption tend to raise more from their citizens in taxes and allocate such tax revenue to public spending. The theoretical foundation for the linear expenditure model used in this report is described more fully in McGuire (1978) and Appendix A to this report.
i) Dependent Variable: Spending Per Capita
The dependent variable in the regression was total state and local spending per capita on public functions defined for five general areas: (1) cash assistance, (2) Medicaid,7 (3) other non-health social services (e.g.,foster care, child care, low-income energy assistance), (4) spending on public hospitals8; and (5) non-social welfare (e.g., education, transportation, law enforcement).9 The total state and local spending for particular categories includes the federal grants that the state and localities spend. However, such federal grants are not reported in the Census of Governments at the same level of detail as is the spending activity. Federal grants are reported only for social welfare spending as a whole, which fails to include public hospitals, and for non-social welfare spending. This practice makes measuring spending impossible from state and local sources at the higher levels of disaggregation for which we report types of social welfare spending. The price deflators used in the analysis depended on the type of spending. For cash assistance and other non-health social welfare spending, we used the general gross domestic product (GDP) price deflator. For Medicaid and public hospitals, we used the Consumer Price Index (CPI) for health care, which we believe better captures price trends in the health sector than does the overall deflator.
ii) Explanatory Variables
The explanatory, or independent, variables in the regression models included a measure of fiscal capacity, measures of the need for social welfare spending, state effect dummy variables, and year dummy variables. In addition, some but not all models attempted to capture price effects of federal grants using a McGuire-type analysis (see Appendix A).
Fiscal Capacity
We considered the possibility of creating a consistent data series incorporating some or all of the elements of the PCPI, RTS, and TTR approaches, as discussed in the Introduction. However, the PCPI model is the easiest and most reliable to implement because consistent data are available across states from the Bureau of Economic Analysis (BEA). Therefore, in our models, state and local resources (i.e., fiscal capacity) are measured by state per capita personal income, deflated by the implicit price deflators of the general GDP relative to 1996.
Federal Grants
Federal grant amounts for social welfare and non-social welfare functions as measured by the Census data on intergovernmental revenues appear as explanatory variables in the model. Because both variables enter the "budget constraint" for the public decision-makers, the effects of federal grants might be thought comparable to the effects of personal income. However, research on public expenditures has identified what has been termed the "flypaper effect" (i.e., money sticks where it hits) through which federal grant money exerts a greater stimulatory effect on public spending than increases in private income on public spending (Gramlich, 1977; Hines & Thaler, 1995; Gamkhar & Oates, 1996). We accommodated the likelihood of a flypaper effect by introducing grants into the model as explanatory variables separately from our measure of state fiscal capacity. We also adjusted federal grants for inflation using the general GDP price deflator.
Need Variables
As measures of the (relative) need for spending on social welfare in the core model, we included:
- Number of poor persons per capita,
- Number of unemployed persons per capita, and
- Population density.
These variables are thought to capture need for social welfare spending for several reasons. First, families in poverty are more likely to qualify for cash assistance and also need social services. Second, unemployment captures economic downturns and also economic hardship associated with involuntary unemployment. Third, population density is a variable that has in other studies been correlated with government spending. It undoubtedly captures a number of effects, including urbanization and special resource costs associated with a high population density.
A number of additional factors might influence state spending. We have chosen the three variables identified above because poverty, unemployment, and population density are thought to proxy in slightly different ways for the need for social welfare spending. We considered adding poverty for various subgroups, such as children and elderly, but the data were unavailable over a sufficient time period. We also experimented with per capita number of persons in urban areas, but this variable was highly correlated with population density, and population density seemed more strongly associated with per capita spending than urbanization.
State Effect Variables
The state effect variables, as described above, were dummy variables defined as one for a particular state and zero otherwise. Inclusion of such variables in the regression allowed us to estimate separate intercepts for each state.10 These state effects were useful in assessing how much of the spending on certain categories of social welfare was due to explanatory variables, such as per capita personal income, per capita federal grants, or need variables, and how much was due to an inherent willingness of the state to spend on the particular function. The state effect variables were important in our analysis of spending patterns in the six states selected for more in-depth study and in comparing spending among rich and poor states in general.
Time Trends
We captured time trends in the models primarily by dummy variables for year. The magnitude of the coefficients on the year dummies indicated whether spending increased or decreased following certain seminal policy initiatives or shifts, such as welfare reform or expansion in Medicaid eligibility. We did not interact the year dummies with the state dummies in general because we had no specific hypotheses to test state by state. However, we estimated the quartile regressions with and without the year dummies, essentially estimating different time trends for rich and poor states.
c. Cyclical Models
An important question is how state and local spending responds to changes in the level of overall economic activity such as booms and recessions and changes in state labor market conditions. To some extent, the unemployment variable in the need analysis incorporates the effects of unemployment on state and local spending. In addition, we developed other models that examined the effect of the state unemployment rate alone and in conjunction with other variables, such as per capita personal income, on per capita spending. We expected that any negative effect on spending of increased state unemployment would occur at least in significant part through the reduction in state per capita personal income that occurs when unemployment rises. Our models allowed us to test this hypothesis.
2. Overview of Data Sources and How the Data Were Used
We considered several data sources on state spending for estimating the 50-state econometric model, including data from the U.S. Census Bureau (Census Bureau), the National Association of State Budget Officers (NASBO), the National Conference of State Legislatures (NCSL), and federal departments. No data source provides comprehensive, detailed measures of social services spending comparable across states and time. In addition, other sources are available for a limited number of states or covering limited periods of time. We relied primarily on the Census of Governments for data on spending by states and localities and estimated federal grants through intergovernmental revenues. Below, we summarize the primary data sources used in our analysis.
The Census Bureau collects finance data from state and local governments and aggregates these data for each state and year at the state level, providing information on revenue and expenditures of state government, revenue and expenditures for all local governments in aggregate within a state, and for state and local governments combined. The state and local expenditure data include state and local spending with federal grants. One of the largest and broadest expenditure categories, public welfare expenditure, amounted to $233 billion in state and local expenditures in fiscal year 2000.11
To measure social welfare spending, we aggregated several Census data categories. Exhibit II-1 breaks 2000 public welfare spending, in billions of dollars, into its detailed components, using the Census Bureau's codes and also shows how we aggregated the Census categories.
| Spending Category | Detailed Item in Census Data | FY 2000 $ (billions) |
Definition |
|---|---|---|---|
| Cash Assistance | E67 Federal Categorical Assistance |
17.7 | Includes AFDC or TANF cash assistance; federal Supplemental Security Income (SSI) when it passes through state accounts; and state SSI supplements Note: The only federal SSI funds that pass through state accounts are retroactive federal payments reimbursing the state for payments made to individuals under state supplement programs; the total amounts are small |
| E68 Other Cash Assistance |
3.0 | Includes cash assistance programs not under federal categorical programs (e.g., general assistance, refugee assistance, home relief, and emergency relief) | |
| Medicaid | E74 Vendor Payments for Medical Care |
155.0 | Includes payments made directly to private vendors for medical assistance and hospital and health care (payments consist mostly of Medicaid/SCHIP) |
| Non-health Social Services | E75 Vendor Payments for Other Purposes |
2.1 | Includes payments made directly to private vendors for services and commodities other than medical, hospital, and health care |
| E77, F77, G77 Welfare Institutions | 1.2 | Includes payments for provision, construction, and maintenance of nursing homes and welfare institutions owned and operated by a government for the benefit of needy persons | |
| E79, F79, G79 Other Public Welfare | 54.4 | Includes operational payments for public employees in the sphere of public welfare; and payments for welfare programs such as child care, child welfare, adoption assistance, foster care, low-income energy assistance and weatherization, social services to the physically disabled, SSBG-funded programs, welfare-related community action programs, and temporary shelters and other services for the homeless | |
| Public Hospitals | E36, F36, G36 Own Hospitals (except federal veterans) | 75.2 | Includes payments for hospital facilities providing in-patient medical care and institutions primarily for the care and treatment of the disabled that are directly administered by a government as well as direct payments for acquisition or construction of hospitals |
| Non-social Welfare | All Other Spending | 1,309.0 | Includes primarily elementary and secondary education, higher education, highways and public mass transit, police protection, financial administration, housing and community development, utilities (water supply and electric power), and sewerage |
As shown in Exhibit II-1, there are six major categories of social welfare spending as defined in the Census as well as Own Hospitals, or state-run hospitals, which the Census does not count as part of social welfare spending. To estimate the model, we combined several categories of data. Federal Categorical Assistance and Other Cash Assistance were combined into a single Cash Assistance variable.12 Vendor Payments for Medical Care (chiefly Medicaid) served as its own category.13 The remaining three Census categories (Vendor Payments for Other Purposes, Welfare Institutions, and Other Public Welfare) were combined into a single Non-health Social Services category.14 Additionally, we created two more categories of spending from Census data, one for Public Hospitals shown in Exhibit II-1 as Own Hospitals and a residual category of all other spending that we called Non-social Welfare.
Per capita personal income was taken from BEA data and adjusted for inflation using the price deflator from the National Income Accounts. We measured the need variables by Bureau of Labor Statistics data (unemployment) and Bureau of Census data (poverty and population density).
C. Site Visits
1. Purpose
The study included site visits to six states for in-depth answers to questions about how state fiscal capacity affects state spending on social programs. We visited states with low fiscal capacity and high social needs to understand how such states coped with this seeming imbalance. Three questions were of particular interest:
- How did states with the greatest needs and the least resources make financial decisions regarding their social welfare programs?
- How did such states respond to short-run financial challenges, such as the recent state fiscal crises?
- Why did some poor states spend more on needy populations than other poor states? And why did some spend more on certain programs and less on others?
Thus, we devised a research plan to (1) discern variation in spending levels and program emphases among poor states, (2) identify the processes of decision-making that affected spending on social programs as well as influences on those processes, (3) use this information to assess the credibility of hypotheses about differences in spending by poor states, and (4) examine how state decisions were affected by economic expansions and contractions, such as the recent downturn in state revenues in FYs 2001 and 2002.
2. Approach
The site visits consisted of discussions with state officials in each of six states about state budget processes and choices involving major social programs, including TANF cash and non-cash assistance, child care subsidies, child welfare, Medicaid, SCHIP, SSBG, and others. We met with high-level agency administrators responsible for these programs, legislative aides involved in the budget process, executive budget officials, and gubernatorial staff.
Though the conversations were relatively unstructured, we began the site visits with a list of topics to be addressed:
- Budget formulation and implementation. Do budget procedures affect budget outcomes for social programs? These states vary in the roles performed by governors, legislatures, and agency administrators. Do these differences affect spending choices? Also, under what constraints do these persons and institutions make choices (e.g., federal mandates, court directives, citizen initiatives, and revenue projections)? And, how do non-social welfare programs, such as education and corrections, impinge on budget choices for social programs? Can some programs operate with a deficit? What is done when such deficits occur?
- Policies and spending. State policies regarding program eligibility, benefit levels, services, and time limits affect state spending on social welfare services. Yet how do these policy choices relate to the budget process (i.e., what drives what)? Are such policies routinely altered during the budget process? Or, are major policy changes made only every few years in a particular program?
- State response to federal programs. How do changes at the federal level in major programs, such as TANF, Medicaid, child care, and child welfare, affect state funding decisions? What, for example, was the effect of greater flexibility under the TANF block grant on state budget decision-making? What weight is given to federal match rates and maintenance of effort requirements in state choices? How do work participation requirements and other performance requirements affect funding decisions?
- Program constituencies. How important in funding decisions for social programs are organized and active constituencies, such as interest groups, industries, private service providers, public employee unions, professional organizations, or even recipients? How salient are different program areas to the media and the public-and with what effects?
- State spending during economic booms and downturns. How did the recent economic downturn and preceding boom affect state spending on social welfare programs? How did the state use its flexibility in the TANF block grant to weather the downturn? What programs or areas of the state budget were exempt from cuts? And what programs or categories of spending were slashed?
To help answer these questions, we also collected budget documents and other materials describing the state's social programs, the agencies administering them, and budget procedures and rules. Finally, to help trace changes in state spending and make comparisons across states, we compiled and analyzed administrative data on major state programs, such as TANF, Medicaid, and the Child Care and Development Fund (CCDF).
3. Selection of Poor States
Selected for site visits through a three-step process, the six states were Arizona, Louisiana, Mississippi, New Mexico, South Carolina, and West Virginia. First, we ranked all states by an index composed of state fiscal incapacity (i.e., per capita personal income, inversely scored) and social needs (i.e., federal poverty rates) and eliminated the two lower quartiles. Second, we scored the states on several other indicators of need and resources (e.g., children without health insurance, unemployment rates, and alternative measures of fiscal incapacity) and eliminated states that showed several discrepancies (i.e., indicators of wealth or low needs). Third, we reviewed the remaining 12 states to ensure that they fit the basic criteria while still offering useful variation for comparisons. When selected, the six states seemed to divide into three main groupings:
- Louisiana and Mississippi. Especially poor with large needy populations and traditions of providing few benefits to low income families, both Louisiana and Mississippi were also hit by the economic slowdown early, with unemployment levels increasing after 1999. Louisiana (population 4.48 million, 2000) is more liberal and Democratic than Mississippi and other southern states. On measures of fiscal capacity, Louisiana also varies more than most states. It is especially low on PCPI, but, due to its oil and natural gas industries, its TTR fiscal capacity ranking is about average. Mississippi (population 2.87 million, 2000) also has a high poverty rate, though it is especially low on all fiscal capacity measures. Nonetheless, its poverty rate has declined significantly in recent years, from 24.4 percent in 1990 to 15.8 percent in 2000. Until this year, Mississippi was controlled by Democrats, but it has long shown conservative tendencies in national voting.
- West Virginia and New Mexico. Although poor with large needy populations, as well, West Virginia and New Mexico demonstrate traditions of greater benefits to low income families. West Virginia (population 1.80 million, 2000) has low fiscal capacity and great needs on all measures. Poverty is high, but it has declined substantially since 1992. Unemployment has fallen in the last decade. Despite a large and important decline in the coal industry, employment, largely low-wage services, has grown. Still, West Virginia's labor participation rate remains low, in part due to an aging population. The state's political culture is more liberal than other poor border states. New Mexico (population 1.86 million, 2000) exhibits the highest poverty rate in the nation and is extremely low on all measures of fiscal capacity, though it differs from other poor states. A southwestern state, its politics and policies are less conservative than those in the poor southern states. For example, New Mexico's TANF maximum cash benefit level is more than twice that of Louisiana and Mississippi.
- Arizona and South Carolina. With greater fiscal capacity though substantial needs, Arizona and South Carolina face severe short-run fiscal problems due to large recent increases in unemployment, population, and revenue shortfalls. Arizona (population 5.46 million, 2000) is higher than the national average on overall poverty and unemployment and lower than average on per capita personal income, but it is not among the neediest states on these indicators. It does have particularly high levels of child poverty. The most striking characteristic of Arizona has been the growth of demands for social programs due to population increases. Its population increase of 23 percent between 1995 and 2002 tops all states. South Carolina (population 4.11 million, 2000) has also suffered from substantial increases in social needs in recent years. The state's unemployment rate has increased significantly, as did welfare caseloads (17 percent between 2000 and 2002). Population growth has been moderately high, with a 9.6 percent increase between 1995 and 2002. And FYs 2001 and 2002 showed a 3.1 percent drop in revenues, a relatively large decline for poor states.
These states offered sufficient variation in spending levels, program emphases, political cultures, budget processes, constituencies, and other factors to give us leverage in generating plausible hypotheses about influences (i.e., how the effects of fiscal capacity might play out under different governmental, economic, and cultural conditions).
D. Integrated Analysis Between Econometric Model and Site Visit Data
We designed our field research in part to help interpret the estimated econometric models and extend the range of factors whose influences might be assessed. At the most general level, the analyses of the econometric data posed and sharpened the questions for the site visits and related analyses of the six states.
First, the site visits were used to weigh the credibility of different explanations of the estimated regression coefficients. For example, the econometric models found that population density exerted positive effects on cash assistance expenditures and negative effects on health-related spending. The site visits suggested hypotheses, consistent with a wide array of quantitative and qualitative data, as to why these differences might occur, at least in poor states.
Second, the econometric models estimated state effects for total as well as different types of social welfare spending. Intercepts estimated for each state,15 these coefficients represented an average level of spending for a particular state after controlling for the effects of all included variables, such as fiscal capacity, unemployment, and poverty. Because these state-effect estimates stripped off the linear effects of economic and demographic variables, they varied greatly among the six poor states and helped sharpen our analyses of institutional and political factors. For example, though Mississippi's spending on medical assistance could not be considered high in an absolute sense, it was sizeable after controlling for the state's fiscal capacity and other significant variables. Thus, the econometric analysis changed the question from why the state's spending on medical assistance was so low to why it was higher than we had expected, given the state's economy and demographics.
Third, the estimated state effects allowed us to examine with greater precision how states varied in the ways they combined, or failed to combine, different types of social welfare expenditures. For example, we found a fundamental division between poor states (i.e., between states that put enormous emphasis on medical assistance and other states whose long-run spending tendencies were more balanced between different functions). We estimated these different configurations, or packages, of spending through the econometric analysis and posed important questions for the site visits.
Fourth, the six state case studies allowed us to assess findings from the econometric analyses in light of state spending changes after fiscal year 2000, the last year for which Census Bureau spending data were available. For example, the models indicated that spending on cash assistance and Medicaid went up during recessions and down during economic booms, other things being equal, while non-health social services showed the opposite pattern. Because the states we studied were, for the most part, experiencing severe fiscal pressures after several years of economic growth, we could draw on quantitative and qualitative data in the case studies to tests these and other expectations.
We also estimated separate econometric models for each of the six states in the field research sample, and we thought these separate estimates would clarify other important differences and similarities among these states. However, with few exceptions, these separate models also turned out to be hard to interpret because of instability, we suspect, due to small degrees of freedom. Thus, we do not present these models in the current report.
Endnotes
7 The Census defines this category, which is primarily Medicaid spending, as "payments to medical vendors."
8 Census does not consider spending on state run hospitals social welfare spending because the patients at such hospitals might not be predominantly low-income. However, some part of the federal grants, which we measured by Census intergovernmental revenues, goes to support public hospitals primarily through the Medicare and Medicaid Disproportionate Share Hospital (DSH) program. Therefore, examining how spending on public hospitals varied across states was important. Unfortunately, Census considers grants for public hospitals to be grants for non-social welfare and fails to disaggregate grant amounts by detailed function. So, we were unable to identify federal grants for public hospitals and thus were unable to separate public hospital spending into a federal share component and a state and local share component as we could do for overall Census social welfare spending. Nonetheless, we used spending per capita on public hospitals as a dependent variable in most of our regression analyses where we did not have to identify separately the federal and state and local funding components.
9 Definitions for these five categories in the Census data used in our analysis appear in Exhibit II-1.
10 The coefficients on the explanatory variables were not allowed to vary across states in our general model, but we did estimate the regression separately for each quartile defined in terms of average per capita personal income. These quartile regressions estimated the coefficients separately for each quartile. However, the estimated state effects used in our cross-state analysis (see subsection III .B.4.) came from the regression estimated over all states. These state effects captured differences in state spending unexplained by the variables in the fixed coefficient model. Some part of these effects could be due to the fact that states had different responses (i.e., variable coefficients) to the explanatory variables.
11 Public welfare expenditure includes all of the categories shown in Exhibit II-1, except Public Hospitals. The Census views spending on state-run public hospitals as outside its social welfare category. However, we included spending on public hospitals as a variable of interest, partly because state-run public hospitals receive Medicaid funding and also because low-income individuals might receive services in the public hospitals.
12 The Federal Categorical Assistance category (E67) tracks federally funded programs and includes AFDC cash assistance, TANF cash assistance, or both, to the extent it passes through state accounts; federal Supplemental Security Income (SSI); plus state supplements. The only federal SSI included in E67 is retroactive federal payments to reimburse the state for payments made to individuals under state supplement programs. The Other Cash Assistance Programs category (E68) includes cash assistance programs not under federal categorical programs.
13 As noted, Vendor Payments for Medical Care is the largest category by far and consists mostly of Medicaid.
14 The Other Public Welfare category (E79) includes operational payments for administrative workers and payments for programs such as child care, foster care, low-income energy assistance, social services to the physically disabled, and programs funded by the Social Services Block Grant.
15 The "state effect" for each state was computed by adding the intercept to the coefficient of the dummy variable for the state.
Chapter III: Findings and Results
Organized into two subsections, section III, Findings and Results, lays out the report's findings. Subsection A provides an overview of trends and patterns in social welfare spending observed over the period from 1977 to 2000, based primarily on Census data. Subsection B presents the results from the 50-state econometric model.
A. Historical and Cross-State Perspective: Trends and Patterns
The connections between state fiscal capacity and spending on social welfare have undergone vast changes in recent years. Between 1977 and 2000, major shifts occurred in how much was spent on social welfare programs, how states allocated funding across different social welfare functions, and how state fiscal capacity was related to these developments. To compare changes in spending patterns for rich and poor states over time, we classified all of the states plus the District of Columbia into four quartiles with respect to their fiscal capacity, as measured by real per capita income averaged over the 24-year period. Exhibit III-1 shows a map indicating the states in each of the quartiles, from the richest states in Quartile 1 (shown as the lightest colors) to the poorest in Quartile 4 (shown as the darkest colors). States with the lowest per capita income are generally found in the South and the West, while the wealthier states are located in the Northeast, around the Great Lakes, and on the Pacific Coast.
Exhibit III-1.
States by Fiscal Capacity Quartile
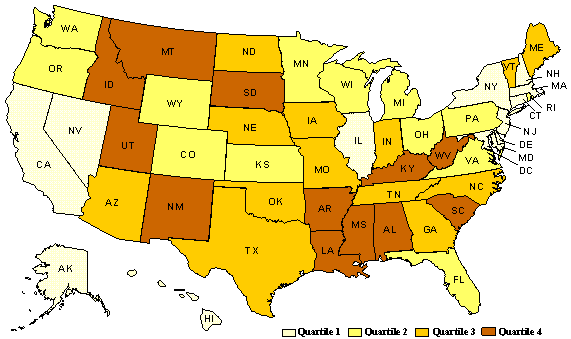
| Selected Characteristics | Quartile 1 | Quartile 2 | Quartile 3 | Quartile 4 |
|---|---|---|---|---|
| Mean per capita personal income, 1977-2000 (2000 dollars) | $24,794 | $21,387 | $19,242 | $17,058 |
| Mean percentage of people under federal poverty level, 1977-2000 | 11.0 | 11.0 | 13.2 | 17.1 |
| Mean percentage of population unemployed, 1977-2000 | 3.1 | 3.0 | 2.7 | 3.2 |
| Median population density (persons per square mile), 1977-2000 | 338 | 89 | 57 | 52 |
Exhibit III-1 also displays information about states in these different quartiles, including average real per capita income, poverty rates, unemployment (per capita), and population density-all characteristics included in the econometric models as independent variables. As well as differing in income levels, these poor states also had higher poverty rates and lower population densities (they were generally more rural) though, surprisingly, they did not have much higher per capita unemployment rates.16
This classification is simplistic. If one calculated fiscal capacity quartiles every year, some states would shift from one to the other over time. However, these simple four-level rankings showed unexpected stability. Most of the states would not shift quartiles even if allowed, and where changes did occur, the changes were nearly always to an adjacent quartile, not a jump of two or three.
1. State Fiscal Capacity and Average Spending on Social Welfare
When averaged over the entire period from 1977 to 2000, per capita spending on social welfare was positively correlated with state fiscal capacity, as shown in the chart at the top of Exhibit III-2.17 A similar pattern exists for spending per poor person, shown at the bottom of Exhibit III-2. When public hospital payments were included, the wealthiest 13 states (Quartile 1) spent an average of $825 per capita (in 2000 dollars) over this time period, while the poorest 12 states (Quartile 4) spent $630 per capita. When payments to public hospitals were excluded, mean per capita spending by states in the wealthiest quartile was $639, while average spending by states in the poorest quartile was $407.
Exhibit III-2.
Spending Per Capita and Per Poor Person on Social Welfare, With and Without Hospital Payments, Averages by Fiscal Capacity Quartiles, 1977-2000
Average spending per capita
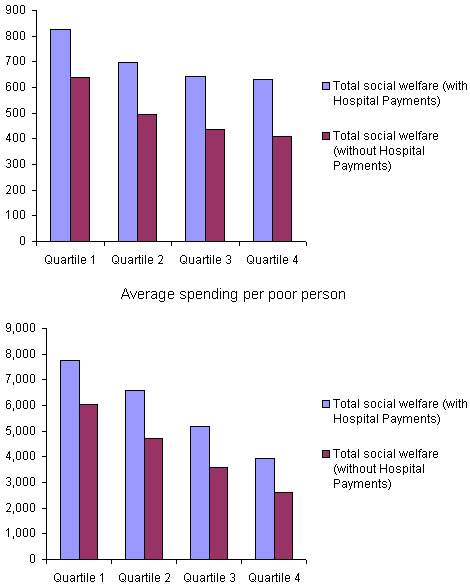
This difference in spending between rich and poor states resulted largely from differences in states' spending of their own tax revenues, as shown in the chart at the top of Exhibit III-3. Federal grants exerted a complex effect on inequalities in state spending. In dollar terms, federal funding actually increased state differences with respect to fiscal capacity because the Quartile 1 received higher grants per capita than the other quartiles. The richest quartile of states, for example, spent an average $371 per capita from federal sources, while the poorest quartile spent $339 (when public hospital payments are included). However, because poor states spent less money overall on social welfare, that $339 constituted a large proportion (83 percent) of their total spending on such programs. By contrast, the $371 per capita from federal sources spent by the richest quartile of states made up a much smaller share (58 percent) of their total social welfare budgets. That is, more federal money went to rich states than to poor states, but poor states relied more heavily on the federal government to support their social programs.
The chart at the bottom of Exhibit III-3 also shows that state fiscal capacity bore a similar relationship to state spending on non-social welfare functions. Again, the differences were due to how much of their own revenues states spent. However, federal spending played a smaller role in this component of state budgets. Although federal spending averaged over two-thirds (69%) of all spending on social welfare functions, federal grants typically made up only about one-eighth (13%) of total state spending on non-social welfare functions.
Exhibit III-3.
Per Capita Spending on Social Welfare and Non-social Welfare Functions, Averages for Fiscal Capacity Quartiles, 1977-2000
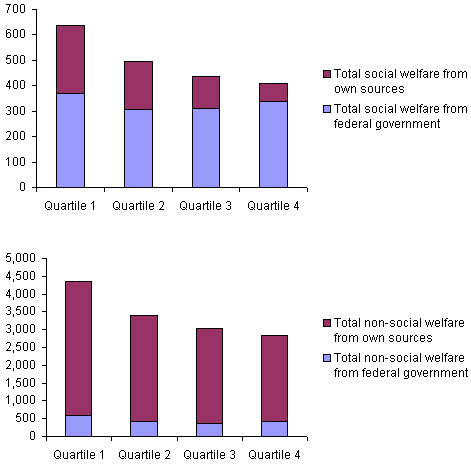
When we disaggregated social welfare spending into more specific categories, the relationships between state fiscal capacity and state spending became more complex. As the chart at the top of Exhibit III-4 demonstrates, the poorest states (Quartile 4) showed much lower levels of spending on cash assistance and non-health social services than did wealthier states.18 Levels of spending on Medicaid were also highest for the rich states in Quartile 1; spending levels were lower, albeit similar, across Quartiles 2 through 4. By contrast, the poorest states spent the most per capita on public hospitals. State fiscal capacity was, in sum, strongly related to spending on cash assistance, moderately correlated with spending on non-health social services, and least correlated (even negative for hospital payments) with spending on health or medical assistance.
Exhibit III-4.
Spending Per Capita and Per Poor Person on Different Types of Social Welfare Functions, Averages for Fiscal Capacity Quartiles, 1977-2000
Average spending per capita
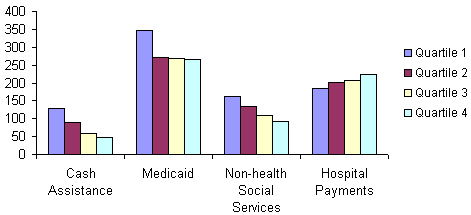
Average spending per poor person
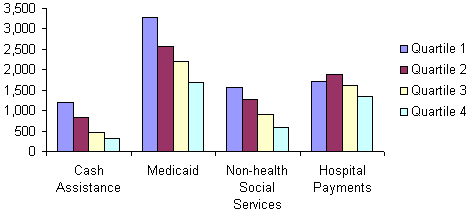
Because social programs were intended mostly to help low-income people, per capita spending levels might fail to capture differences in the degree to which states met social needs. To understand spending from this perspective, we compared spending levels per poor person in each state. Using this measure, differences among rich and poor states were greater and more consistent, as shown in the chart at the bottom of Exhibit III-4. Disparities between the top and bottom quartiles were even larger for spending on cash assistance and other non-health social services; and Medicaid expenditures and public hospital payments showed stronger and positive relationships to fiscal capacity.
2. Changes Over Time
Averages over time cannot show changes in the relationships between state fiscal capacity and spending on social welfare programs. Yet those relationships changed enormously between 1977 and 2000. To see these developments, we traced changes in average spending levels in each of these quartiles and for each category of social welfare spending.
Exhibit III-5 compares trends in spending for cash assistance, Medicaid, and non-health social services, with spending levels adjusted for inflation using the GDP price deflator. Per capita spending on cash assistance was lowest in the poorest quartile of states throughout the 24-year period, as shown in the graph at the top of Exhibit III-5. However, states with different fiscal capacities began to converge in their spending on cash assistance in the mid-1990s. This convergence came about as cash assistance spending in richer states (i.e., states in Quartiles 1, 2, and 3) declined, while states in Quartile 4 saw virtually no change in their already low spending levels. State fiscal capacity thus became less correlated with spending on cash assistance programs at the end of the 1990s when compared to the early 1990s and especially the late 1970s.
The 1990s also produced major changes in state spending on Medicaid, as depicted in the graph in the middle of Exhibit III-5. At the beginning of the decade, Medicaid payments grew rapidly for states in all quartiles, though the greatest growth occurred among poor states. By 2000, per capita spending in Quartile 4 was about 10 percent higher than per capita spending in Quartiles 2 and 3. The relationship between state fiscal capacity and spending on Medicaid thus declined in strength. Like the trends for cash assistance, spending levels of rich and poor states converged. But unlike cash assistance, spending on medical assistance programs saw an upward convergence as previous low spenders joined high spenders, not a downward convergence as high spending states came down to the level of low spending states.
Per capita spending on non-health social services showed no such convergence, as illustrated in the graph at the bottom of Exhibit III-5. Instead, it revealed growing differences between states of different fiscal capacities. The poorest states showed the lowest per capita spending throughout, since 1980. Yet the real separation occurred in the 1990s. Although spending on other social welfare grew in all states during the 1990s, the wealthier states in the top three quartiles showed rapid growth in such spending from 1997 through 2000 at the same time states in the poorest quartile increased their spending much more slowly. Non-health social services include expenditures for child welfare, child care, energy assistance, and many other social services, as well as the costs to public agencies of administering such programs, cash assistance, and Medicaid.
The strong growth in Medicaid spending might result in part from higher levels of inflation for health services. To gauge the importance of health-specific inflation rates, Exhibit III-6 shows trends in spending for medical assistance using the CPI for health care. With this inflationary adjustment, average per capita spending on Medicaid still rose, though less strongly, as illustrated in the graph at the top of Exhibit III-6. Spending on public hospitals actually declined over this period for the three wealthier quartiles, as depicted in the graph at the bottom of Exhibit III-6. However, the poorest quartile showed a slight increase in per capita expenditures. Thus, as was the case for Medicaid, the poorest states increased their spending on health-related functions more than wealthier states did in the 1990s.
Exhibit III-5.
Changes in Average Per Capita Spending on Different Social Welfare Functions, by State Fiscal Capacity, 1977-2000
Average Per Capita Spending on Cash Assistance Adjusted with GDP Price Deflator over Time by Income Quartile
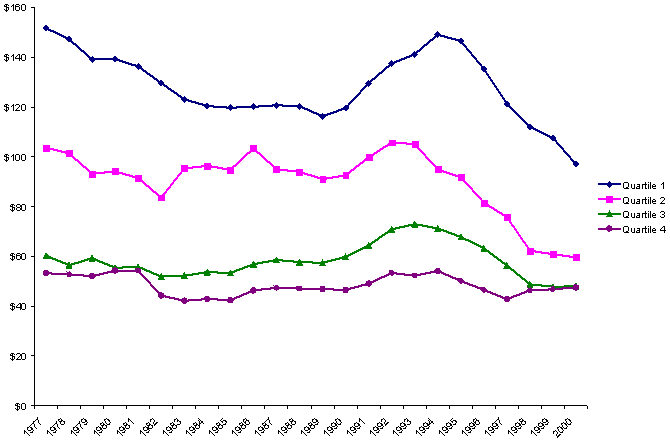
Average Per Capita Spending on Cash Assistance Adjusted with GDP Price Deflator over Time by Income Quartile
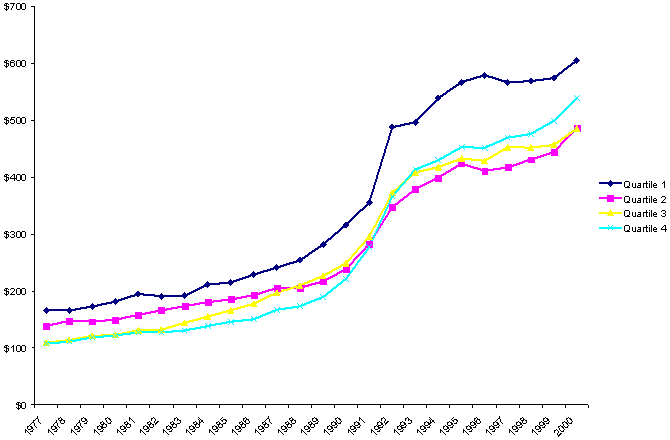
Average Per Capita Spending on Non-health Social Services Adjusted with GDP Price Deflator over Time by Income Quartile
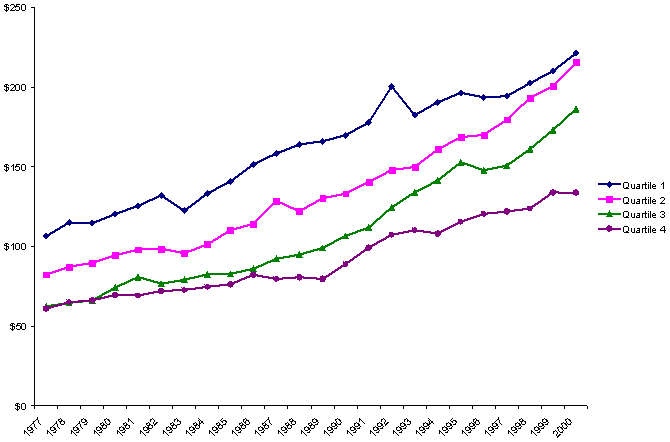
Exhibit III-6.
Changes in Average Per Capita Spending on Health-Related Functions, by State Fiscal Capacity, 1977-2000
Average Per Capita Spending on Public Hospitals Adjusted with CPI Medical Index over Time by Income Quartile
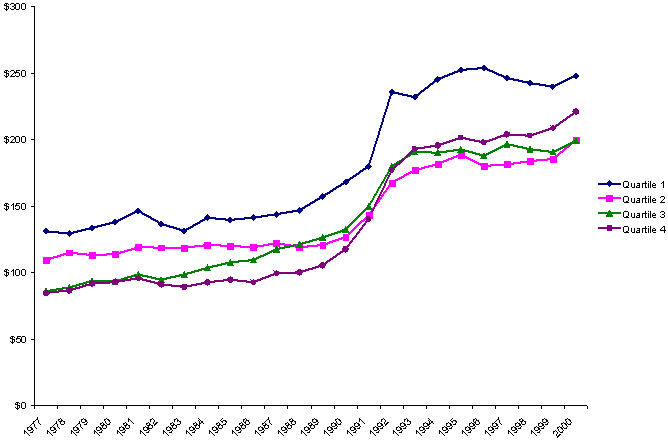
Average Per Capita Spending on Public Hospitals Adjusted with CPI Medical Index over Time by Income Quartile
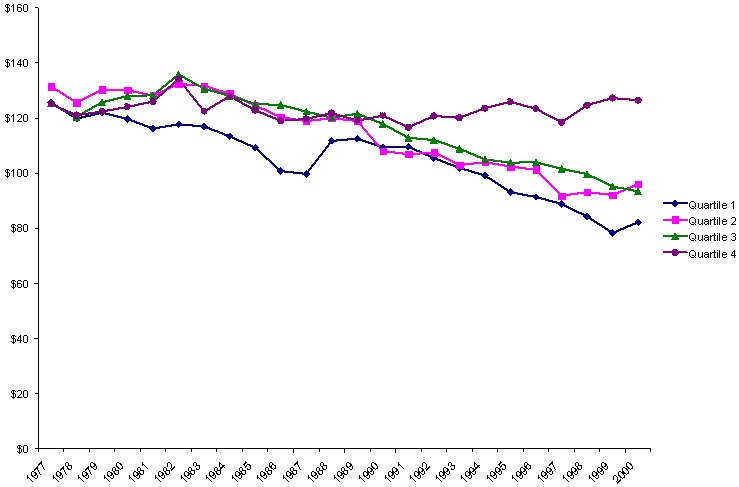
These increasingly complex relationships between state fiscal capacity and various forms of social welfare spending were not found in trends and patterns for non-social welfare spending, as indicated in Exhibit III-7. Throughout the 24-year period, spending per capita outside the social welfare area was greatest in the richest states and lowest in the poorest states, and growth in spending after adjusting for inflation showed none of the dramatic short-run changes found in cash assistance and Medicaid.
Exhibit III-7.
Changes in Average Per Capita Spending on Non-social Welfare Functions, by State Fiscal Capacity, 1977-2000
Average Per Capita Spending on Non Social Welfare Adjusted with GDP Price Deflator Over Time by Income Quartile
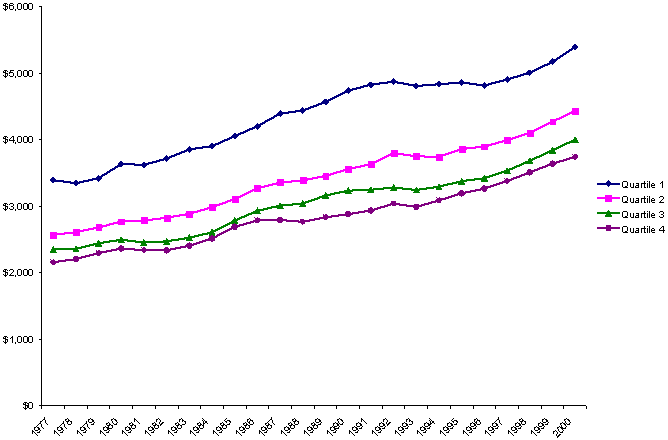
Finally, states have changed how they spend their social welfare dollars as well as the way they fund those functions. Exhibit III-8 indicates the percentage of social welfare spending supported from state and local governments' own-source revenues rather than federal grants. Over the entire period, states in all quartiles showed a long-run decline in their reliance on own-source revenues. But the declines were greatest among the wealthier states, which, at any point, relied less on federal grants and more on their own-source revenues than did poor states. Thus, some convergence occurred, especially in the 1990s, as poor states in Quartile 4 slightly increased their proportionate use of own-source revenues, while the richer states decreased their reliance on such sources and increased their dependence on federal dollars.
Exhibit III-8.
Percentage of Total Social Welfare Spending From State and Local Sources, by Fiscal Capacity Quartile (public hospital spending not included)
Percent of Spending From State/Local Sources over Total Social Welfare Spending By Income Quartile
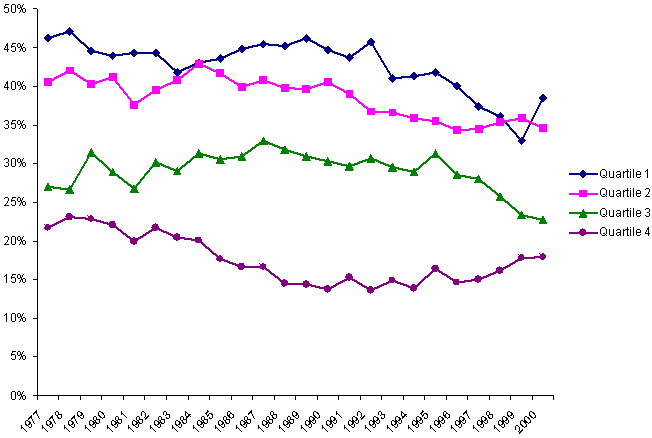
These many changes combined to produce major realignments in a relatively brief period in the spending profiles of rich and poor states. Exhibit III-9 shows evidence of these shifts by tracking the percentage of total public welfare spending in different program functions in the wealthiest and the poorest quartiles (Quartiles 1 and 4). Medicaid absorbed a much larger share of the budgets of both rich and poor states. Cash assistance spending fell in all states, though most precipitously in rich states, thereby reducing differences between rich and poor states between 1980 and 2000.
Non-health social services declined slightly as a component of overall social welfare spending in all states. But the biggest change with respect to this category of mostly non-health social services was the growing disparity between rich and poor states. Although poor states spent slightly more on such services as a percentage of their total social welfare budgets in 1990, by 2000, they had spent a much smaller percentage of their budget on these non-health social services. In just 2 decades, the components of state social welfare budgets changed in fundamental ways. They moved away from cash assistance and toward health services, and poor and rich states became increasingly different in the role of non-health social services in their total social service budgets.
These findings reinforce the need to estimate different econometric models for different types of social welfare spending, because each type shows distinct dynamics. They also pose a challenge: the relationship between state fiscal capacity and spending on different public goods seems to be mutable, suggesting a need to dig deeper after the econometric analysis and determine what dynamics are accounted for by the models and what changes are not. Finally, the trends show that poor states in particular have seen a radical transformation in the package of social welfare functions they support, a development that argues for special attention to their social welfare budgets and the factors affecting them.
Exhibit III-9.
Changes in Percentage of Total Social Welfare Spending for Three Major Functions, Comparing Rich and Poor States, 1980, 1990, and 2000
Rich states (Q1) are those in the 1st or highest quartile on fiscal capacity; poor states (Q4) are those in the 4th or lowest quartile
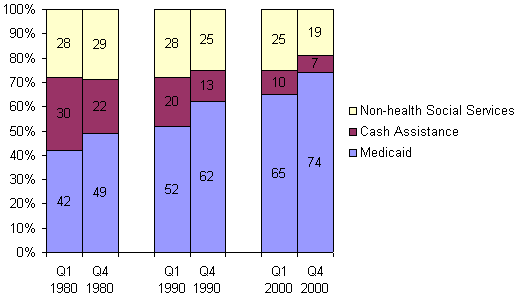
B. Overall Results of Econometric Analysis
Using conventional ordinary least squares, we estimated the 50-state econometric model on pooled time series and cross-section data on state and local spending for the 24 years from 1977 to 2000. We conducted standard tests for auto-correlation of residuals, which sometimes constitutes an issue for time series analysis.19
The model and its estimates had two general purposes. First, the model estimates allowed us to assess the magnitude and statistical significance of variables of interest, such as state fiscal capacity as measured by per capita personal income, federal grants, and other determinants of state and local spending. Second, the model estimated state effects used in the comparisons among rich and poor states in general and among the six poor states selected for further analysis. We report an overview of the results in the text of this report. More detailed estimation results appear in Appendix A.
We estimated a number of models,20 but for purposes of this discussion we will focus on a single preferred model in which we allow for flypaper effects by including both state personal income and federal grants as separate variables, and we attempt to measure state and local needs through the poverty, unemployment, and population density variables. Both state and year dummies are included.
Below, we present the results, first for the regressions estimated over all states and then for the regressions estimated separately for each quartile defined by the historical average of real PCPI.
1. Results for All States
Exhibit III-10 displays the regression results for the five regressions with dependent variables defined as respective categories of per capita state and local spending (CA - cash assistance, M - Medicaid, NSS - non-health social services, PH - public hospitals, and non-social welfare - NW) for all states.21 Below the estimated coefficients, t-statistics appear in parentheses. A t-value greater than approximately 1.96 indicates statistical significance at the .05 level, and a t-value greater than approximately 2.44 indicates statistical significance at the .01 level.
| Variable | CA | M | NSS | PH | NSWS |
|---|---|---|---|---|---|
| Adjusted R-Squared | 0.87 | 0.91 | 0.87 | 0.89 | 0.96 |
| Constant | 61.09** (3.12) |
-79.00** (3.57) |
-52.70* (2.13) |
155.96** (8.05) |
2356.25** (8.20) |
| Per capita personal income | -0.0039** (6.89) |
0.0033** (5.24) |
0.0060** (8.47) |
0.0003 (0.50) |
0.1236** (15.07) |
| Federal grants for non-social welfare | 0.0049 (0.64) |
-0.0017 (0.20) |
0.0543** (5.71) |
0.0396** (5.32) |
-0.1222 (1.11) |
| Federal grants for social welfare | 0.0943** (8.82) |
0.3278** (27.18) |
0.0052 0.3800 |
0.0843** (7.99) |
0.0280 0.1800 |
| Population Density | 0.06** (5.89) |
-0.05** (4.89) |
-0.09** (7.21) |
-0.06** (6.59) |
0.65** (4.48) |
| Unemployment per capita | 836.09** (7.13) |
702.63** (5.31) |
-84.84 (0.57) |
193.19 (1.67) |
8295.98** (4.83) |
| Poverty per capita (moving average) | -30.10 (1.05) |
-95.68** (2.95) |
-45.79 (1.26) |
-76.00** (2.67) |
320.19 (0.76) |
| CA means Cash Assistance, M means Medicaid, NSS means Non-health Social Services, PH means Public Hospital Spending, and NSWS means Non-Social Welfare Spending. T-statistics are in parentheses. ** Significant at the 1% level. * Significant at the 5% level. |
|||||
As shown in Exhibit III-10, the linear effects of per capita personal income on per capita social welfare spending after we control for federal grants and need are positive, and statistically significant for Medicaid and non-health social services. However, the effects are negative and statistically significant for cash assistance and statistically insignificant for public hospital spending.22 The impact of per capita personal income on per capita non-social welfare spending is larger, but we expected this outcome because non-social welfare spending is much larger than the individual components of social welfare spending.23
When we examine the effects of federal grants on the components of social welfare spending for all states in Exhibit III-10, we find, unsurprisingly, that grants for non-social welfare exert weak and statistically insignificant effects on cash assistance and Medicaid spending, but such grants exert much stronger and statistically significant effects on non-health social services and public hospital spending. This result might constitute evidence of a positive income effect of non-social welfare grants24 on the latter two categories of non-health social services and hospital spending. The federal grants for social welfare have strong, positive, and generally statistically significant effects on spending for cash assistance, Medicaid, and public hospitals. The effect of federal grants on Medicaid is particularly strong, indicating the attractiveness to the states in matching federal Medicaid dollars.
Exhibit III-10 also shows the results for the three main indicators of need for social welfare spending (i.e., poverty per capita, unemployment per capita, and population density) for all states. The negative signs on the poverty variable seem surprising and difficult to explain. Possibly the measures of fiscal capacity and federal grants are insufficient to capture the state's perceived resources and poverty proxies for available resources (in a negative direction). Also, high poverty states might resist spending because of an omitted unobserved variable correlated with poverty. The poverty variable was statistically significant and negative only for Medicaid and public hospital spending.
Unemployment per capita had the expected positive sign for all categories of social welfare spending except non-health social services, and the effect was statistically significant for cash assistance, Medicaid, and public hospitals. Population density was statistically significant for all categories of social welfare spending, including public hospitals, but was positive for cash assistance and negative for Medicaid, non-health social services, and public hospitals.
2. Results by Quartile
Exhibit III-11 shows results for the same regression model estimated separately for each of the 4 quartiles defined by mean real per capita personal income. Below, we summarize the general findings from this analysis by quartile and spending category for the explanatory variables of greatest interest: (1) fiscal capacity, (2) federal grants, (3) need variables, (4) state unemployment rates, and (5) state effects.
| Variable | Q 1 CA |
Q 2 CA |
Q 3 CA |
Q 4 CA |
Q 1 M |
Q 2 M |
Q 3 M |
Q 4 M |
|---|---|---|---|---|---|---|---|---|
| Adjusted R-Squared | 0.90 | 0.74 | 0.87 | 0.37 | 0.93 | 0.88 | 0.89 | 0.89 |
| Constant | 231.38** (6.22) |
-288.79** (3.21) |
-156.30** (5.23) |
77.23 (1.49) |
-38.83 (0.82) |
42.12 (0.53) |
-202.85** (3.42) |
-164.18* (2.22) |
| Per Capita Personal Income | -0.0078** (9.07) |
0.0068** (2.84) |
0.0012 (1.14) |
-0.0042 (1.88) |
0.0032** (2.93) |
0.0001 (0.03) |
0.0053** (2.54) |
0.0084** (2.62) |
| Federal Grants for Non-social Welfare | 0.0284** (2.66) |
0.0119 (0.41) |
0.0222 (1.80) |
-0.0339 (1.53) |
-0.0077 (0.56) |
0.0081 (0.32) |
0.0161 (0.66) |
0.0311 (0.99) |
| Federal Grants for Social Welfare | 0.1547** (7.33) |
0.0527 (1.78) |
0.1526** (10.19) |
-0.0275 (1.70) |
0.3545** (13.21) |
0.2074** (8.01) |
0.3467** (11.65) |
0.3422** (14.77) |
| Population Density | 0.054** (4.10) |
0.40** (3.43) |
1.13** (8.75) |
1.01** (3.04) |
-0.04* (2.38) |
-0.04 (0.36) |
0.35 (1.36) |
-0.04 (0.07) |
| Unemployment Per Capita | 841.88** (3.17) |
1277.17** (4.28) |
386.67** (2.78) |
139.93 (0.59) |
1081.63** (3.20) |
77.50 (0.30) |
451.51 (1.64) |
382.24 (1.14) |
| Poverty Per Capita (moving average) | -42.40 (1.01) |
499.69** (3.50) |
164.87** (3.50) |
94.24 (1.51) |
-130.43* (2.44) |
94.71 (0.76) |
84.89 (0.91) |
-4.42 (0.05) |
| Q means Quartiles CA means Cash Assistance, M means Medicaid, NSS means Non-health Social Services, PH means Public Hospital, NSWS means Non-social Welfare. T-statistics are in parentheses. ** Significant at the 1% level. * Significant at the 5% level. |
||||||||
| Variable | Q 1 NSS |
Q 2 NSS |
Q 3 NSS |
Q 4 NSS |
Q 1 PH |
Q 2 PH |
Q 3 PH |
Q 4 PH |
Q 1 NSWS |
Q 2 NSWS |
Q 3 NSWS |
Q 4 NSWS |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Adjusted R-Squared | 0.86 | 0.87 | 0.86 | 0.80 | 0.87 | 0.90 | 0.89 | 0.95 | 0.95 | 0.94 | 0.96 | 0.95 |
| Constant | 98.43 (1.78) |
-100.50 (1.13) |
25.85 (0.39) |
100.31* (1.95) |
43.61 (1.17) |
367.17** (5.71) |
-91.59 (1.48) |
-221.98** (4.69) |
405.14 (0.47) |
4118.30** (5.39) |
2099.03** (5.48) |
1797.11** (3.68) |
| Per Capita Personal Income | 0.0063** (4.89) |
0.0097** (4.10) |
0.0049* (2.09) |
0.0048* (2.14) |
0.0025** (2.94) |
-0.0056** (3.29) |
-0.0007 (0.33) |
0.0024 (1.18) |
0.1496** (7.57) |
0.0529** (2.62) |
0.0798** (5.86) |
0.0050 (0.23) |
| Federal Grants for Non-social Welfare | 0.0307* (1.93) |
0.0063 (0.22) |
0.1842** (6.75) |
-0.0155 (0.70) |
0.0415** (3.87) |
-0.0017 (0.08) |
0.0308 (1.21) |
-0.0303 (1.50) |
-0.4988* (2.03) |
-0.3084 (1.27) |
0.5041** (3.19) |
0.7086** (3.40) |
| Federal Grants for Social Welfare | 0.0401 (1.28) |
0.0406 (1.39) |
0.1402** (4.22) |
-0.0461** (2.85) |
0.805** (3.80) |
0.0561** (2.65) |
0.1205** (3.88) |
0.0281 (1.89) |
-0.3581 (0.74) |
0.7400** (2.95) |
0.0314 (0.16) |
0.0767 (0.50) |
| Population Density | -0.07** (3.39) |
-0.31** (2.71) |
-1.59** (5.54) |
-0.34 (1.03) |
-0.06** (4.90) |
-0.30** (3.59) |
0.32 (1.18) |
2.87** (9.39) |
0.81** (2.69) |
2.00* (2.05) |
0.88 (0.53) |
17.17** (5.45) |
| Unemployment Per Capita | 310.34 (0.79) |
94.33 (0.32) |
196.59 (0.64) |
-452.51 (1.93) |
-218.42 (0.82) |
594.61** (2.79) |
-420.39 (1.46) |
372.15 (1.73) |
15519.00** (2.54) |
11648.00** (4.60) |
5923.35** (3.32) |
-5225.86* (2.35) |
| Poverty Per Capita (moving average) | -64.62 (1.03) |
40.52 (0.29) |
-258.74** (2.47) |
89.02 (1.43) |
-36.41 (0.86) |
13.34 (0.13) |
-69.47 (0.71) |
56.02 (0.98) |
1461.13 (1.51) |
29.16 (0.02) |
-2192.36** (3.62) |
162.03 (0.28) |
| Q means Quartiles CA means Cash Assistance, M means Medicaid, NSS means Non-health Social Services, PH means Public Hospital, NSWS means Non-social Welfare. T-statistics are in parentheses. ** Significant at the 1% level. * Significant at the 5% level. |
||||||||||||
d. Fiscal Capacity Effects
From Exhibit III-11, we can see that when the states are separated by quartiles based on average per capita personal income, differences across quartiles in the estimated effects emerge. For example, for cash assistance and non-health social services, the effect of personal income for the richer states (Quartiles 1 and 2) is statistically significant25, while for the poorer states (Quartile 3 and 4), the effect is nearer zero for both categories and statistically insignificant for cash assistance. The reverse occurs with respect to effects on Medicaid, for which the effects of personal income is near zero for the richer states, although statistically significant and positive for Quartile 1, and larger and statistically significant for the poorer states. For public hospitals, the effect of personal income is positive and statistically significant only for the richest states.
In general, the regression analysis confirmed that personal income was an important factor in causing social welfare spending disparities among rich and poor states. These disparities based on sample means were reported, for example, in Exhibit III-2. When we controlled for the effects of non-income explanatory variables, the differences in per capita spending on social welfare across rich and poor states narrowed but did not disappear. For example, if Quartile 1 states were assigned the same average income as those in Quartiles 2, 3 and 4, the regression model for Quartile 1 predicted that Quartile 1 per capita spending on social welfare would fall by $60, $98, and $137, respectively. This amounted to reductions of 7 percent, 12 percent, and 17 percent.
e. Federal Grant Effects
When we estimated the regression separately for each quartile, the signs of the effects of federal grants reverse or the coefficients are estimated with less statistical significance for the poorest states (Quartile 4), indicating weak grant income effects for those states, as shown in Exhibit III-11. In particular, for the social welfare spending categories, federal grants have positive and statistically significant effects only for Medicaid, suggesting a substitution toward Medicaid spending as federal grant income rises.26 For the other quartiles, the results are mixed, as also shown in Exhibits III-11; however, the effect of social welfare grants on Medicaid is generally large, positive, and statistically significant.
f. Need Effects
When we repeated the regressions separately by quartile, poverty continued to exert consistently negative signs only for the richest states (Quartile 1) and generally had more positive signs for the other quartiles. However, the only statistically significant and positive effects of the poverty variable occurred for cash assistance in quartiles 2 and 3.
The effect of unemployment per capita on the various categories of social welfare spending was positive and statistically significant generally only for the richer states (Quartiles 1 and 2), although an exception is cash assistance in Quartile 3. For the richer states, the unemployment effects were positive and statistically significant for cash assistance and Medicaid in Quartile 1 and for cash assistance and public hospitals in Quartile 2.
The strongest unemployment effect occurred in the cash assistance category for which we observed statistically significant and positive effects for Quartiles 1, 2, and 3. This result might constitute a kind of "caseload effect," but it does not occur in Quartile 4, perhaps because the spending levels are so low they decline no further with lower unemployment.27 But the spending for Quartile 4 apparently also declines no further as unemployment increases. Instead, the spending levels seem "stuck" and independent of the state of the economy.
The effects of population density seem mixed with positive and statistically significant signs on the effects for cash assistance for all quartiles and statistically significant and negative signs on the effects for the remaining categories of social welfare spending, including public hospitals in the richer states (Quartiles 1 and 2). The results were more mixed for Quartiles 3 and 4 with no particular pattern discernable.
3. Cyclical Models
To confirm that the effects estimated for the unemployment per capita variable were truly state labor market effects and to get a better sense of how spending changed in response to unemployment changes alone, we estimated simple linear relationships between spending per capita in each category and the state unemployment rate with and without per capita personal income as an additional explanatory variable. In the regressions of per capita spending on the state unemployment rate alone (but including state effect dummies) for all states, as shown in Exhibit III-12, spending for cash assistance and public hospitals was positively related to unemployment, in other words an anti-cyclical effect,28 but spending on Medicaid and other social welfare was negatively related to unemployment, a pro-cyclical effect.
| Variable | Overall | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| CA | M | NSS | PH | NSWS | ||||||
| Adjusted R-Squared | 0.83 | 0.83 | 0.56 | 0.76 | 0.68 | 0.85 | 0.86 | 0.87 | 0.84 | 0.95 |
| Constant | 22.23** (4.46) |
57.91** (7.10) |
158.15** (14.15) |
-178.30** (12.95) |
161.04** (18.85) |
-120.92** (12.54) |
241.19** (49.31) |
305.19** (39.40) |
5577.77** (45.42) |
937.94** (8.45) |
| State Unemployment Rate | 3.07** (8.29) |
1.66** (3.70) |
-11.34** (13.67) |
2.03** (2.69) |
-10.70** (16.87) |
0.51 (0.96) |
3.66** (10.07) |
1.11** (2.62) |
-156.62** (17.17) |
27.86** (4.57) |
| Per Capita Personal Income | -0.00** (5.49) |
0.01** (30.68) |
0.01** (36.72) |
-0.00** (10.37) |
0.17** (52.47) |
|||||
| Q means Quartiles CA means Cash Assistance, M means Medicaid, NSS means Non-health Social Services, PH means Public Hospital, NSWS means Non-social Welfare. T-statistics are in parentheses. ** Significant at the 1% level. * Significant at the 5% level. |
||||||||||
To see how much of the effect of unemployment was operating through the per capita personal income variable, we included per capita personal income in the regression. These results can be seen also in Exhibit III-12. Over all states, the unemployment rate exerted a positive effect on spending for all categories of social welfare spending, and the effect was statistically significant for all categories except non-health social services. Thus, the presence of the per capita personal income variable has eliminated the negative effect for Medicaid and non-health social services spending observed in the regression on the unemployment rate alone. The fact that unemployment and personal income are negatively correlated suggests the negative effects observed in Exhibit III-12 are due to the absence of a control for income. Across all states, then, unemployment seems to do an effective job of picking up positive need effects on spending, except for other non-health social welfare, with personal income held constant. This finding is generally consistent with the results reported in Exhibit III-10 with other explanatory factors (e.g., poverty, population density, federal grants, and year dummy variables) in addition to personal income included in the regression.
4. State Effects: Long-Run Differences in State Spending on Social Welfare
One result of the 50-state model was the estimation of unexplained variance in spending across different states. These state effects were estimated intercepts or constant terms for each of the states in the econometric models. They may be interpreted as general dispositions of states-averaged across the entire period, 1977-2000-to support certain types of spending after controlling for the linear effects of fiscal capacity, social needs, federal grants, and population density.29
In their original form, the state intercepts, or effects, were difficult to interpret. To make them easier to understand, we standardized them with respect to the mean and standard deviation of the state effects. That is, for each set of estimated state effects-one set of 50 for each dependent variable, such as cash assistance or Medicaid-the mean of the 50 state effects was set at zero and the standard deviation was set at 100. Thus, if a state's effect for Medicaid was 2 standard deviations above the mean of the 50 state effects that particular effect was scored as 200. If the state's effect for cash assistance was 1/4 of a standard deviation below the mean for all states, then that effect was scored -25.
Exhibit III-13 shows the standardized versions of the estimated state effects for all of the states. The larger and more positive the number, the greater the tendency of the state to spend on that particular category of public function over the entire time period, 1977-2000, after controlling for the linear effects of the other independent variables, including per capita personal income, per capita grants, and the various need variables. For example, even after controlling for these factors, Alaska shows a strong additional propensity to spend on cash assistance and non-social welfare and a tendency to spend less on Medicaid and public hospitals relative to other states. New York and Minnesota, however, show additional propensities (again, compared to other states) to spend more than predicted by the econometric model on all social programs.
Despite the good fit of the models to the data, these state effects show variation in their spending on different types of social programs. For example, the difference between the 25th and 75th percentiles in the state effect estimates for cash assistance is $49 per capita, a large amount compared to the mean per capita spending for all states (averaged over all years, 1977-2000) of $82.
| Cash Assistance | Medicaid | Non-heath Social Services | Public Hospitals | Non-social Welfare | ||
|---|---|---|---|---|---|---|
| Quartile 1 | Alaska | 273 | -171 | 19 | -190 | 611 |
| California | 275 | -47 | -2 | 30 | -18 | |
| Connecticut | 123 | 92 | -14 | 52 | -106 | |
| Delaware | -24 | -141 | 75 | -96 | 9 | |
| Hawaii | 207 | -39 | -122 | -57 | 33 | |
| Illinois | 102 | 1 | 14 | -52 | -62 | |
| Maryland | 27 | 85 | -51 | -48 | -63 | |
| Massachusetts | 79 | 292 | 152 | 48 | -64 | |
| Nevada | -59 | -98 | -140 | 64 | -10 | |
| New Hampshire | -10 | 77 | 115 | -134 | -61 | |
| New Jersey | -43 | 190 | 117 | 39 | -95 | |
| New York | 189 | 110 | 309 | 133 | 38 | |
| Quartile 2 | Colorado | -3 | -109 | -16 | -30 | -3 |
| Florida | -64 | 12 | -107 | 55 | -39 | |
| Kansas | -3 | -47 | -93 | 23 | -9 | |
| Michigan | 147 | -79 | 122 | 8 | -27 | |
| Minnesota | 125 | 169 | 129 | 46 | 18 | |
| Ohio | 44 | 48 | 45 | -23 | -61 | |
| Oregon | -10 | -167 | -19 | -63 | 35 | |
| Pennsylvania | 72 | -43 | 232 | -74 | -56 | |
| Rhode Island | 4 | 260 | 208 | 1 | -70 | |
| Virginia | 32 | -25 | -112 | -1 | -51 | |
| Washington | 88 | -58 | -49 | -34 | 54 | |
| Wisconsin | 46 | 107 | 94 | -65 | -1 | |
| Wyoming | -59 | -116 | -173 | 210 | 140 | |
| Quartile 3 | Arizona | -36 | -21 | -77 | -85 | 34 |
| Georgia | 6 | 52 | -103 | 221 | -31 | |
| Indiana | -97 | 48 | -44 | 55 | -61 | |
| Iowa | -3 | -6 | 56 | 90 | -7 | |
| Maine | 32 | 128 | 96 | -156 | -16 | |
| Missouri | -34 | -50 | -93 | -16 | -68 | |
| Nebraska | -34 | -43 | 24 | 66 | 75 | |
| North Caroline | -20 | -61 | -49 | 52 | -27 | |
| North Dakota | -92 | 37 | 61 | -134 | 47 | |
| Oklahoma | -48 | -3 | -37 | 37 | -32 | |
| Tennessee | -101 | 8 | -35 | 72 | -7 | |
| Texas | -52 | -43 | -122 | 35 | -33 | |
| Vermont | 39 | -98 | 52 | -197 | 30 | |
| Quartile 4 | Alabama | -71 | 12 | -117 | 181 | -24 |
| Arkansas | -129 | 37 | -40 | -10 | -53 | |
| Idaho | -85 | -68 | -58 | -3 | -23 | |
| Kentucky | -78 | 85 | 17 | -87 | -32 | |
| Louisiana | -125 | -39 | -33 | 153 | -15 | |
| Mississippi | -169 | 30 | -37 | 172 | -23 | |
| Montana | -92 | -116 | -21 | -145 | 36 | |
| New Mexico | -52 | -98 | -5 | -7 | 43 | |
| South Carolina | -113 | 15 | -33 | 137 | -17 | |
| South Dakota | -59 | -68 | -54 | -125 | 16 | |
| Utah | -31 | -83 | -58 | -81 | 68 | |
| West Virginia | -111 | 41 | -21 | -68 | -17 |
When these estimated state effects are analyzed, they show that state fiscal capacity interacts with program area (i.e., the relationship with fiscal capacity varies with program area). Exhibit III-14 shows these variations by displaying the average state effects, in their standardized versions, for states of different fiscal capacities, using our basic four quartiles. The relationship between state effects and fiscal capacity are compared across four different program areas: cash assistance, Medicaid, non-health social services, and public hospitals. We should note that the differences in state effects are most important, not the absolute values (e.g., whether they are negative or positive, that is, above or below the average state effects across all states).
Exhibit III-14 indicates that states of different fiscal capacities still vary in their long-run spending patterns even after controlling for the linear effects of annual changes in states' per capita personal income, as the 50-state model does. For example, the wealthiest states (Quartile 1) spent on average about $180 more per capita per year on cash assistance than did the poorest quartile (Quartile 4). A consistent and positive, albeit weaker, relationship between fiscal capacity and average state effects is also evident in spending on non-health social services.
Exhibit III-14.
Average State Effects for Different Types of Social Welfare Spending, by State Fiscal Capacity, Based on Data From 1977-2000
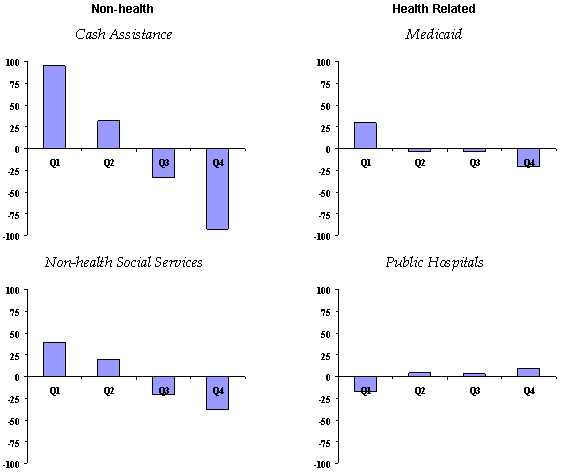
Health-related expenditures show a different pattern. With respect to Medicaid, the average state effects for the richest states were higher than for states in the other quartiles, but the differences among the three less wealthy quartiles were small. The relationship between fiscal capacity and spending on public hospitals was actually reversed. Per capita spending was lowest among the richest states and highest among the poorest states. After controlling for the linear effects of annual changes in fiscal capacity and other variables, as the 50-state model does, poor states still spent less on cash assistance and other social welfare, while their spending on health-related programs was not much lower and sometimes higher than the amount wealthier states spent.
Poor states, on average, thus revealed greater support for spending on health-related programs than for spending on non-health programs. One possible consequence of this pattern was a weaker statistical relationship among poor states in their support across different program areas. Among non-poor states (i.e., states in the first three quartiles for fiscal capacity), tendencies to spend on different social welfare functions were, for the most part, either positively correlated with each other or not correlated at all, suggesting that no major tradeoff existed among these states between their financial support for one type of social welfare and their support for another.
We can see these relationships in the first column of Exhibit III-15, which shows the bivariate correlation coefficients between the state effect estimates for cash assistance, Medicaid, non-health social services, and public hospitals. For the 38 states in the first three quartiles of fiscal capacity, the correlations were generally either positive or especially small. The strongest correlation was between Medicaid and non-health social services, though a moderate relationship also existed between cash assistance and non-health social services. Only the state effects for public hospitals showed a slight negative relationship to state effects for other types of spending.
| Types of Spending | Pearson correlations between estimated state effects for different types of spending, by state fiscal capacity |
|
|---|---|---|
| Non-poor States | Poor States | |
| Cash Assistance vs. Non-health Social Services | .33 | -.15 |
| Cash Assistance vs. Medicaid | -.01 | -.51 |
| Cash Assistance vs. Public Hospitals | -.23 | -.51 |
| Non-health Social Services vs. Medicaid | .50 | .13 |
| Non-health Social Services vs. Public Hospitals | -.22 | -.40 |
| Medicaid vs. Public Hospitals | .17 | .33 |
| Number of cases | 38 | 12 |
By contrast, among the 12 poorest states, the correlations among these spending tendencies were more likely to be negative. Cash assistance was negatively correlated with both types of health-related functions, Medicaid and public hospitals. Non-health social services was also negatively related to spending on public hospitals and, albeit weakly, cash assistance. On the other hand, the poor states showed a slightly stronger relationship between the two types of health program areas. We can see an example of the contrasting structure of these relationships in Exhibit III-16, which shows the scatterplots between the state effects for cash assistance and Medicaid-separately for poor and non-poor states. No correlation existed between the estimated state effects for non-poor states, but a clear negative relationship existed among the poor states.
Exhibit III-16.
Scatterplots Between State Effects for Payments to Medicaid and Cash Assistance, Based on Model Estimated for Years 1977-2000
Scatterplot between state effects estimated for Medicaid and cash assistance, only states in Quartiles 1, 2, and 3 in fiscal capacity (i.e., wealthier 75%)
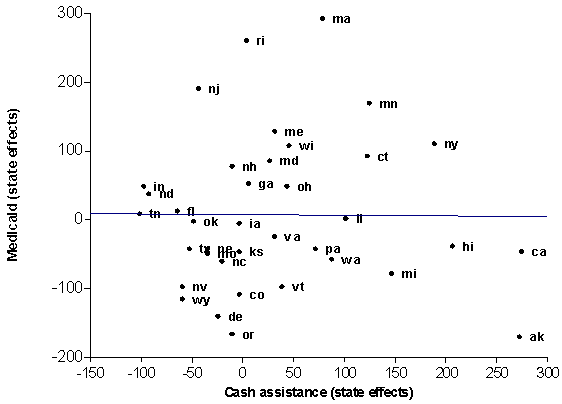
Scatterplot between state effects estimated for Medicaid and cash assistance, only states in Quartile 4 in fiscal capacity (plus Arizona, because it is one of the study states and is near the cutoff point between Quartiles 3 and 4)
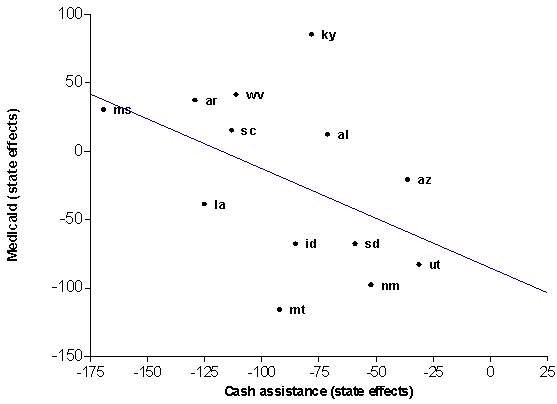
More generally, low fiscal capacity states divided between those that put money into health programs and little else and those that put money into other programs, especially cash assistance. As Exhibit III-16 shows, the former were southern and border states, including Mississippi, Arkansas, West Virginia, and South Carolina. Poor western states, including Utah and New Mexico, showed greater levels of support for cash assistance. Whatever the reasons for these differences among poor states, such states clearly showed divisions in their spending patterns across different functions. Poor states, unlike wealthy states, seemed to choose or specialize in one or another type of social program area. Their packages of social programs were, thus, more particularized as well as smaller. Although knowing how much a wealthy state spent in one social program area often helped us know how much it spent in another area, the same was untrue for poor states.
5. Conclusions from Econometric Analysis
i) Effects of Fiscal Capacity
Although per capita income generally had the expected positive effect on spending, notable differences occurred between rich and poor states. When we analyzed the sample separately by quartile, we found the income effects on cash assistance, non-health social services, and public hospitals much more consistently larger and statistically significant for the rich states than for the poorer states. On the other hand, the income effects on Medicaid were larger and more positive for the poorer states than for the richer states. This finding suggests that when personal income rises in the richer states, the states are more likely to increase social welfare spending across the board, and when income rises in the poorer states, spending is likely to occur largely on Medicaid.
ii) Effects of Federal Grants
Although federal grants largely increased state and local spending on social welfare, the effects on federal grants were hardly noticeable for the poorest states (Quartile 4), except for a positive effect on Medicaid. The grant effects were most apparent on payments to Medicaid, suggesting the importance of the Medicaid matching funds.
iii) Effects of Need Variables, Including Unemployment
Estimating a stable needs function that would predict well state and local spending proved impossible. That poverty seemed negatively correlated with spending in a number of spending categories was puzzling, particularly for the richest states. Although the sign on the per capita unemployment was much more likely to be positive than the sign on the poverty variable, the statistically significant positive unemployment effects on spending seemed generally confined to the richer states. The strongest positive effects of unemployment occurred on cash assistance spending. This result might constitute a kind of caseload effect, but it fails to occur in Quartile 4 for the poorest states. The effects of population density on social welfare spending were generally mixed, but we estimated a number of coefficients to be statistically significant.
The poorer states seem to have less protection against adverse unemployment effects, and their needs are more likely to go unmet in a downturn. When we more closely evaluated the effect of state unemployment on spending using the state unemployment rate, we found that cash assistance and Medicaid spending were positively related to the unemployment rate with no income control, particularly for the richer states. However, for non-health social services, the coefficient on unemployment was consistently negative and statistically significant across quartiles and largely statistically insignificant for public hospital spending. We conclude that the total effect of a rise in unemployment is likely to be a cutback in spending for non-health social services across all states with increases in spending for cash assistance and Medicaid in richer states.
iv) State Effects
Stable differences among states in their spending patterns persisted even after controlling for the linear effects of fiscal capacity, need, federal grant, and other independent variables. These propensities to spend (i.e., estimated state effects) suggested that state fiscal capacity was more strongly related to non-health expenditures than to health-related expenditures. They also suggested that the basic structure of expenditures was different in rich and poor states. In wealthier states, spending on each social welfare function was more likely to be positively related or largely independent of spending on other social welfare functions. In the poorest states, however, spending on each social welfare function, such as Medicaid, was more likely to be negatively related to spending on other functions, such as cash assistance. These negative relationships between expenditures by poor states result in some interesting differences among the states with respect to their spending patterns, one difference being the regional split between western and southern states in their relative emphasis on cash assistance and Medicaid. This is discussed further in the next section.
In sum, the multivariate econometric analyses suggested the following:
- Unemployment pushed up spending on cash assistance and Medicaid but not on non-health service spending.
- Growth in state per capita incomes enhanced spending on Medicaid and non-health social services but not necessarily on cash assistance.
- Rural states spent less of their money on cash assistance programs and more on health and non-health social services.
- States were especially responsive to federal grants for Medicaid.
Endnotes
16 Unemployment rates per capita are lower than unemployment rates usually reported. The former rate is the number of unemployed divided by the total population in the state, while the latter is the number of unemployed divided by the number of persons seeking jobs.
17 Social welfare spending in this analysis includes no spending on public hospitals.
18 The Non-health Social Services category includes support activities, such as operational payments for administrative workers; payments for child care, foster care, low-income energy assistance, and social services for the physically disabled programs; Social Services Block Grant-funded programs; and temporary shelters and services for the homeless. The category also includes direct payments to private vendors for non-health services and commodities and for the provision, construction, and maintenance of governmentally owned and operated welfare institutions and nursing homes.
19 The Durbin Watson statistics indicated some autocorrelation but insufficient, in our opinion, to adjust the analysis.
20 The model structures are described in Appendix A. Generally, we estimated three generic models with sub-models within each model. In Model 1D, we introduced need variables into the structure for Model 1C. Model 1D is the model described in the body of this report. Models 2 and 3 experimented with specifications that explicitly introduced price effects of federal grants using the method McGuire (1978) recommended. . For reasons related to both the lack of appropriate data to estimate price effects, econometric difficulties related to the same variable appearing on both sides of the equations, and the model statistical results being weak and inconsistent (including many "wrong" signs), we focus primarily on Model 1. Although no explicit grant price effects occur in Model 1, we expect the combination of state and year dummies to pick up much of the variation of grant price effects across states and over time.
21 For definitions of these variables in terms of Census categories, see Exhibit II-1 and the accompanying discussion.
22 The relationship between fiscal capacity and spending on cash assistance seems to be more complex, however. When the equations were estimated for each fiscal capacity quartile, only the wealthiest quartile (Quartile 1) showed a significant and negative relationship. Also, when we examined the estimated state effects from the cash assistance equation, we found the state effects were positively correlated with our four quartiles of states, quartiles that reflected long-run differences in state fiscal capacity. One possible interpretation of these inconsistencies was that our indicator of fiscal capacity-per capita personal income-had two counteracting effects on cash assistance: one long-run effect and one short-run effect. Higher state income in the long run might have encouraged states to adopt more generous cash assistance policies (in terms of higher maximum benefits and need standards, greater earnings disregards, and less stringent asset limits). However, in the short run, increases in per capita income during economic downturns would have decreased welfare rolls as recipients left voluntarily for jobs or became disqualified because their incomes were too high. This latter dynamic (the wage effect) might have been particularly strong among richer states because they tended to have more generous benefit policies, and their cash assistance rolls were thus more likely to include large numbers of working families, whose income fluctuations exerted a greater, countercyclical effect on state spending. (Maximum benefit levels, one indicator of the relative generosity of cash assistance policies, averaged $575 for a three-person family in 2000 for the states in Quartile 1 (the wealthiest). The median maximum benefit levels for Quartiles 2, 3, and 4 were $429, $292, and $277 respectively.)
23 For example, the means of the variables are cash assistance ($82), Medicaid ($151), non-health social services ($125), public hospitals ($115), and other non-social welfare ($3,422). The small relative value for cash assistance spending leads to the odd result that the coefficient on PCPI for cash assistance spending is close to zero but nonetheless statistically significant because its standard error is also extremely small.
24 We should note, however, that the non-social welfare federal grants (i.e., intergovernmental revenue) include federal grants for the public hospital category of spending because the Census classifies public hospital spending as spending for non-social welfare. Census data do not permit disaggregating federal grants in more detail than the broad categories of federal grants for social welfare spending and other federal grants.
25 It should be noted, however, that the effect is negative in quartile 1 for cash assistance. This mirrors the negative impact of personal income on cash assistance found in the overall regression, as reported in Exhibit III-10.
26 The large positive effect might also reflect the increase in federal spending for Medicaid in response to increases in state matching funds. McGuire (1978) reviews the arguments why federal grants can be viewed as exogenous in a model such as this one. However, his major assumption is that the federal government acts through its grants to induce a target level of state spending, implying that if state matching funds increase, no resultant change in federal spending would occur as a result because the state behavior was anticipated. This assumption might prove untrue in practice, and reverse causality effects might occur.
27 One possibility is that in the poorest states, less movement on and off cash assistance occurs as the state of the economy improves or worsens.
28 A pro-cyclical effect means spending moves in the general direction of the economy. When the economy improves, so does spending and vice versa. Conversely, an anti-cyclical effect occurs when spending moves contrary to the direction of the economy.
29 For more on state effects, see footnote 7 in subsection II.B.1.
Chapter IV: A Closer Look at Poor States
The econometric models support the claim that state fiscal capacity exerts positive effects on total spending for social programs as well as spending for major components of social welfare budgets, such as cash assistance, medical assistance, and other public welfare programs. However, the models raise two sets of new questions:
- Why do the significance and weights of the variables vary across different types of social welfare spending? Fiscal capacity is most strongly related to spending on non-health social services, while its relationship to spending on public hospitals is insignificant. Population density is negatively related to spending on health-related functions but directly related to spending on cash assistance. Unemployment pushes up cash assistance and Medicaid spending but not non-health social services. These differences do not undermine the basic model, but the underlying general theory of state spending does not account for them.
- Why do the models find large, unexplained differences among states in their propensities to spend on different social welfare functions? Although the linear effects of fiscal capacity, unemployment, federal grants, and population density account for a major part of state variation in spending on social programs, another large part of the variance is "explained" by state effects. These state effects are average spending levels for individual states after controlling for the effects of variables in the model. These estimated state effects vary greatly among states. Thus, they represent long-run differences in state spending levels that might be attributable to factors not included in the model, such as differences in political systems, other indicators of social needs, or even nonlinear effects of included variables such as fiscal capacity.
The econometric models, therefore, fail to fully explain important differences across program areas and states, though the models narrow and focus the explanatory problems.
The remainder of this analysis explores these unexplained differences among states and program areas in three ways. First, we examine the estimated state effects from the econometric models among the six case study states, all of which have high social needs and low fiscal-capacity. How do these state effects relate to each other? Do we find clusters of states with similar spending patterns?
Second, after we identify state differences in spending patterns based on the econometric models, we determine whether those findings are consistent with changes in state spending after 2000, the last year in the Census data, in our six case study states. These states, along with nearly all states in the U.S., experienced fiscal difficulties after the economic downturn of 2001 and 2002. And we consider whether our statistical findings are consistent with or depart from the spending decisions these poor states made in the years after 2000, including the fiscal crises. Although we have no comparable Census data for these years, we can examine changes in roughly comparable spending based on administrative data on program expenditures and on reports of decisions from interviews and documents obtained during site visits in middle and late 2003.
Third, we use the site visits and especially the discussions with state officials to understand how spending choices are made in different program areas and what factors influence those choices. We want to understand what decision-making processes might generate the statistical relationships found in the econometric models, how and whether these processes vary across program areas, and what state characteristics affect those processes. Succinctly stated, we found that spending decisions in different program areas are made in different ways; that these different modes of decision-making respond to different state characteristics; and that these differences in processes and influences might help explain why certain variables are important, or unimportant, in the econometric analyses and why poor states vary in their spending patterns. These findings might also help us understand some of the trends in state spending on social programs noted in subsection IIIA. And, they hold important implications for the broader questions posed in this study about federal influence over state spending, packages of social programs, and effects of economic cycles.
A. Differences Among the Six Poor States Selected for Case Studies
The division among the poor states we noted in section III was also found among the six poor states selected for site visits. Exhibit IV-1 shows the estimated state effects for cash assistance, Medicaid, non-health social services, public hospitals, and non-social welfare. Again, these state effect scores were scaled to equal zero for the mean state effect and 100 (or -100) for a state effect one standard deviation above, or below, the mean.
| Cash Assistance | Medicaid | Non-health Social Services | Public Hospitals | Non-social Welfare | |
|---|---|---|---|---|---|
| New Mexico | -52 | -98 | -5 | -7 | 43 |
| Arizona | -36 | -21 | -77 | -85 | 34 |
| West Virginia | -111 | 41 | -21 | -68 | -17 |
| South Carolina | -113 | 15 | -33 | 137 | -17 |
| Louisiana | -125 | -39 | -33 | 153 | -15 |
| Mississippi | -169 | 30 | -37 | 172 | -23 |
New Mexico and Arizona were higher than the southern states on cash assistance spending but lower on Medicaid and public hospitals. Mississippi, Louisiana, South Carolina, and West Virginia were all low on cash assistance as well as spending on non-social welfare. Yet they were relatively high on payments to medical vendors or public hospitals. Spending on non-health services was less clearly related to other expenditures. It was high in New Mexico but low in Arizona; high for West Virginia but lower in Mississippi, Louisiana, and South Carolina.
These basic differences among poor states also seemed to be reflected in spending changes from 1977 to 2000, as displayed in Exhibit IV-2. Because the spending patterns of the two western states generally differed from those found among the four southern and border states, we divided the states into those two groupings for the purpose of comparing trends. Thus, the left side of Exhibit IV-2 shows the changes in spending on cash assistance, Medicaid, and non-health social services for New Mexico and Arizona, while the right side traces those changes for Mississippi, Louisiana, South Carolina, and West Virginia.
Exhibit IV-2.
Trends in Spending on Social Welfare Programs Among Six Poor States, 1977-2000
| Arizona and New Mexico Medicaid 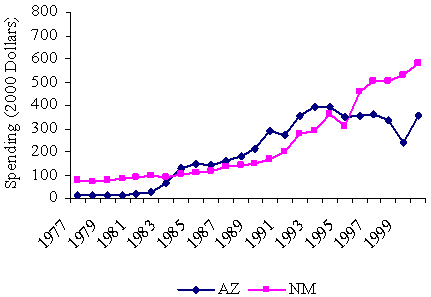 |
Louisiana, Mississippi, South Carolina, and West Virginia Medicaid 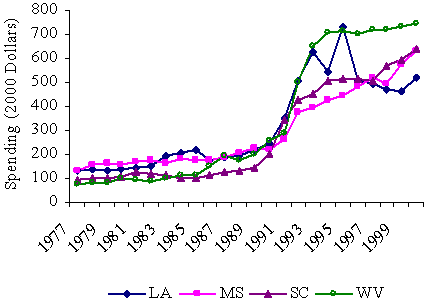 |
Cash Assistance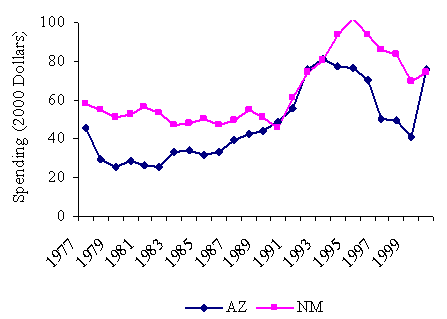 |
Cash Assistance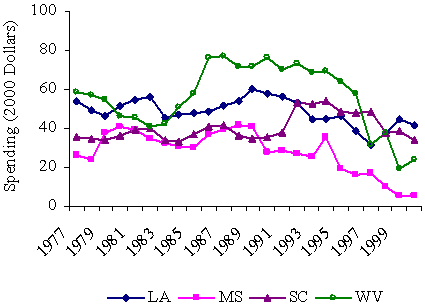 |
Non-health Social Services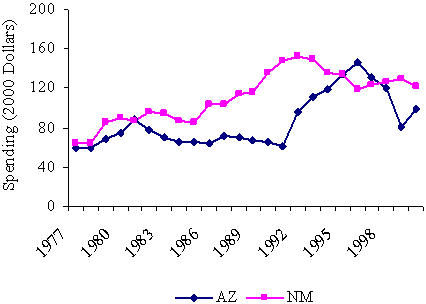 |
Non-health Social Services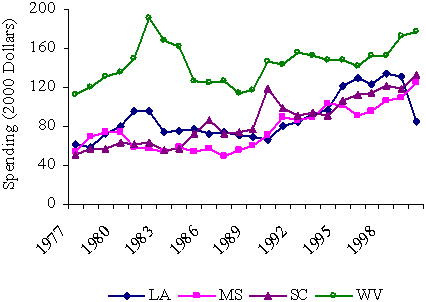 |
The most consistent pattern in spending changes across all states was the strong growth of Medicaid in the early 1990s. Most of the states continued to show growth or at least stability for the remainder of the decade. The two exceptions were Arizona and Louisiana, which showed some decline in real spending on Medicaid in the late 1990s.
Most states also showed a marked decline in spending on cash assistance from the middle 1990s onward, due presumably to a combination of welfare reforms and economic growth. However, the western states differed from the others in that this decline came after a substantial increase in spending on cash assistance in the early 1990s. The southern states experienced no such increase. In fact, Mississippi and Louisiana were already seeing declines in real spending on cash assistance before the bigger drops in spending of the middle and late 1990s. Changes in non-health social services spending were typically less dramatic. Most states showed overall though slow increases in spending over these years, with the western states and West Virginia showing more volatility than the southern states.
Perhaps the most striking finding from these data involves the different linkages between spending trends in each state. In Arizona and New Mexico, spending changes in cash assistance, Medicaid, and non-health social services showed a rough correspondence, with slow change before the 1990s, strong growth in the early 1990s, and some stalling or even a decline in real spending in the late 1990s. Arizona, for example, showed strong increases in all three forms of spending in the early 1990s, reversals in the late 1990s, and an uptick in 2000. In contrast, spending changes in other states showed less linkage or even negative relationships. In Mississippi and South Carolina, Medicaid and non-health social services grew rapidly while spending on cash assistance grew slowly or fell. West Virginia and Louisiana showed little linkage in spending trends across functional areas.
Thus, the dynamic patterns of spending reflected some of the state differences we found in the estimated state effects. Arizona and New Mexico treated all three major functional spending areas in roughly similar ways-to some extent, like the wealthier states did. Their spending on cash assistance was not extremely low, nor did it show secular decline. The other states showed a sharp divergence between long-run staticity or decline in cash assistance spending and rapid growth in spending on Medicaid, starting in the early 1990s. In these latter states, other public welfare spending also grew, though usually more fitfully and less strongly. Thus, at least among the southern states, little evidence of a linked package of social welfare programs emerged. In fact, different program areas showed some indications of negative relationships over time.
B. Recent State Spending Patterns and State Fiscal Crises
Although we have no Census data after 2000, we can draw from the site visits and administrative spending data on selected programs to determine whether these six poor states continued or departed from prior trends and differences. Subsection IVB examines recent changes in spending among the six states and finds, for the most part, that the state trends and differences noted in the Census data through FY 2000 continued with some modifications after that year. Before we trace those spending changes, however, we must put them into context by briefly discussing the most important change in the recent fiscal environment, the state fiscal crises and especially the revenue shortfalls of 2001 and thereafter.
1. The State Fiscal Crisis and Low Fiscal Capacity States
At the time of our site visits, all six states were experiencing difficult fiscal problems. Yet these problems varied between rich and poor states as well as among these six states. The crisis was driven largely by a sharp drop in revenues in 2001 and 2002 (Boyd 2003). The declines were greatest among the comparatively wealthy states in the Northeast and Far West. They were less severe in the Middle Atlantic and Rocky Mountain states, while the declines were smallest among states in the Great Lakes area, the South, and the Plains states.
One behind this geographical variation was the source of states' tax revenues. Because the greatest decline in revenues occurred in individual and corporate income taxes, states that relied heavily on consumption taxes saw no extreme declines in revenues. In general, the poor states in our sample relied more heavily on sales taxes. For example, in FY 2003, Arizona, Mississippi, and New Mexico each received about half of their tax revenues from sales taxes. Of these six states, only West Virginia, which received 34 percent of its tax revenues from this source, relied less on sales taxes than the median state (which received 37 percent of its tax revenues from consumption). In addition, smaller revenue declines occurred in states without many wealthy residents, since much of the revenue decline stemmed from losses in income from capital gains after the stock market bubble of the 1990s burst in late 2001. Because these low fiscal capacity states did not reap large revenue gains from the bubble, they did not greatly suffer from its abrupt termination.
Exhibit IV-3 shows changes in tax revenues in these six poor states, and for all states, for the years 1998 to 2003, standardized to equal 100 during the revenue peak of 2001. Though four of the states experienced declines in tax revenues after 2001, two states continued to see growth. Thus, except for the two western states, which tracked national averages closely, the poor states, when compared to the rest of the country, saw smaller increases in revenues in the late 1990s as well as smaller declines after 2001.
| 1998 | 1999 | 2000 | 2001 | 2002 | 2002 | |
|---|---|---|---|---|---|---|
| Arizona | 80 | 91 | 97 | 100 | 94 | 96 |
| New Mexico | 77 | 82 | 87 | 100 | 99 | 97 |
| South Carolina | 87 | 96 | 98 | 100 | 97 | 98 |
| Louisiana | 88 | 88 | 91 | 100 | 101 | 98 |
| Mississippi | 86 | 93 | 97 | 100 | 102 | 105 |
| West Virginia | 92 | 96 | 97 | 100 | 104 | 107 |
| All States | 83 | 87 | 96 | 100 | 95 | 96 |
Some short-run factors alleviated state revenue problems in poor as well as wealthy states. Two of the most important were money from the tobacco settlement and state fiscal relief from the federal government in 2003. Nonetheless, social welfare programs in low fiscal capacity states were hit hard in other ways, largely as a result of increasing needs. Food Stamp recipients-one measure of need roughly comparable across states-grew an average of 38.5 percent among the six poor states between FYs 2000 and 2003, while the average growth among all states was 24.9 percent. Low fiscal capacity states also saw no significant decline in TANF caseloads between 2000 and 2003, while higher fiscal capacity states did (Gais, Burke, & Corso, 2003).
Unemployment rates among the six poor states generally did not rise faster than the rates in the U.S. as a whole, but their rates were already higher than the U.S. average, as Exhibit IV-4 demonstrates. Unemployment levels rose in most of the six states between 1999 and 2002. South Carolina, Louisiana, and Mississippi saw the largest increases. The southern states also experienced relatively early increases in unemployment: Mississippi and Louisiana's unemployment rates began to rise in 2000 and South Carolina's as early as 1999.
Exhibit IV-4.
Unemployment Rates in the Six Poor States and in the U.S. as a Whole, 1995-2003
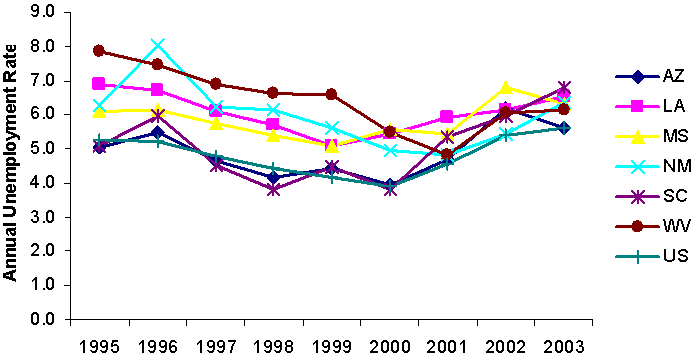
Other factors compounded the short-run fiscal problems in these states while alleviating them in others. For example, although West Virginia experienced no decline in revenues, neither had it participated in the boom of the 1990s. It, thus, had few reserves to draw on in managing its fiscal crisis. In fact, West Virginia's fiscal problems were compounded by unfunded liabilities in the state's workers' compensation and retirement programs-spending that was enforced by the courts. South Carolina also saw slow growth in revenues for some years, compounded by its large increases in unemployment; indeed, budget shortfalls and cuts have plagued the state since 2000.
New Mexico was exceptional in suffering little from the recession. The state was able to rely on revenues from minerals, oil, and gas as well as many services. Because it had tried to keep 5 percent of recurring appropriations in reserves, the general fund entered the recession with an operating reserve and had no deficit, even in fiscal year (SFY) 2004.
Despite this variation, these six states have generally faced substantial increases in needs since the beginning of the decade, while their tax revenues grew slowly or even declined. All of the states were, thus, under some fiscal pressure, and how they handled that pressure revealed much about influences on state choices in social welfare programs.
2. Recent Changes in Spending on Health Care: Medicaid
The site visits largely indicated that the spending trends and state differences found before 2000 continued even through the recession. Perhaps the clearest example was the continued growth of Medicaid in these states. In most of the six poor states, the growth in spending on Medicaid before 2000-indicated by increases in the Census Bureau's Vendor Payments for Medical Care category-continued through 2003, despite budget pressures in the states.
Exhibit IV-5 illustrates changes in per capita spending on Medicaid, including federal as well as state expenditures, from federal FYs 1997 to 2003. These data come not from the Census Bureau but from Medicaid administrative data on program spending. The data series include the six case study states plus the mean of all states in the U.S. as well as the mean of the six poor states.
Exhibit IV-5.
Per Capita Spending on Medicaid in Six Poor States, 1997-2003 (federal and state)
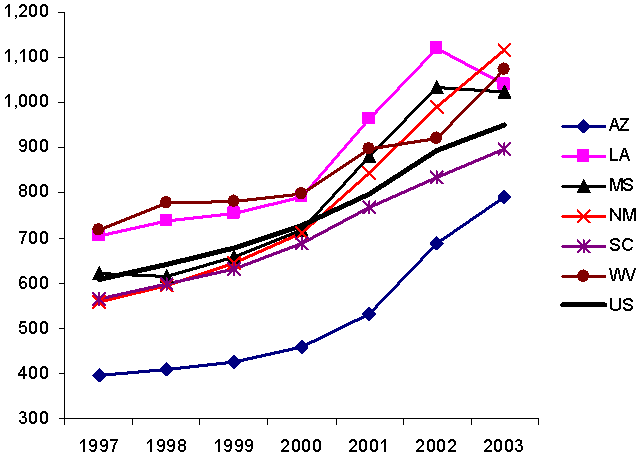
As the graph shows, spending on Medicaid among the six poor states typically grew faster than the average per capita spending among all states in the U.S. Although not shown in the graph, the average per capita spending among the six poor states was slightly below the national state average from 1997 through 2000. By 2001, however, the poor state per capita average was higher than the national average and remained so through 2003.
Four of the states (i.e., South Carolina, Arizona, New Mexico, and West Virginia) showed continued or even accelerated growth in nominal spending after 2000. Growth was especially strong in New Mexico and Arizona. Only Louisiana, which had spent the most per capita on its Medicaid program in 2002, substantially reduced its spending in 2003, while Mississippi showed little change.
Spending growth in Medicaid in recent years was especially high among the two western states, Arizona and New Mexico. Although Arizona's per capita spending remained well below that of other states throughout this period, New Mexico's per capita spending on Medicaid exceeded that of the other five states and was well above the national average by 2003. The large regional differences among these states in their per capita expenditures on Medicaid thus declined in recent years.
The reasons for this continued growth in spending and growing convergence among the poor states were many, but some factors were widespread. The economic cycle and the growing costs of pharmaceutical drugs and home/personal care services were widely cited in site visits as forcing up spending. Another major force was the expansion of Medicaid enrollments in recent years as a byproduct of child health insurance program (CHIP) outreach activities in the late 1990s and early 2000s. In one state, for example, administrators thought that two Medicaid participants were found and added for every new CHIP enrollee.
Respondents also indicated that Medicaid programs in their states were limited to begin with. Large parts of their budgets were driven by mandatory services rather than optional services or optional groups. Major cutbacks in eligibility were, thus, often impossible without federal cutbacks.
Yet some of the growth resulted from major program expansions since 2000. The most striking change occurred in Arizona. State voters overrode years of legislative opposition to Medicaid expansion in 2000 by enacting a citizen's initiative, Proposition 204 that greatly expanded Medicaid coverage to include households up to 100 percent of the federal poverty level. Enrollment grew from 575,000 in January 2001 to 902,500 in January 2003. The state also took advantage of the Health Insurance Flexibility and Accountability (HIFA) initiative, which allowed eligible working parents of children enrolled in the SCHIP program to qualify for coverage. Louisiana expanded eligibility, as well, for children, aged, and disabled in FY 2003, and it increased eligibility among pregnant women to include all those under 200 percent of the federal poverty level.
Some of the growth in Medicaid spending seemed attributable to a lack of fiscal pressures in some states. New Mexico, as noted already, was little affected by the recession and was able to cover its substantial increases in Medicaid costs with its large operating reserves. Officials attributed some of the program growth in recent years to delayed efforts to institute cost-saving measures, such as preferred drug lists.
When cuts were made, they were generally reductions in services or reimbursements, not new restrictions on eligibility. In Louisiana, Medicaid prescriptions were limited to eight per month; upfront payments to hospitals for outpatient services were reduced; and subsidies for the state's charity hospitals were cut. South Carolina lowered ceilings on the number of office visits, prescription drugs, and home health visits, and it reduced reimbursement rates for physicians, though not for hospitals and nursing homes. In general, however, these cuts were marginal and were not expected to greatly slow Medicaid spending.30
3. Recent Changes in Spending: TANF Benefits
Spending on cash assistance has declined sharply in most states over the last several years, especially since the implementation of welfare reform (Boyd et al., 2003). As noted above, the declines in cash assistance spending through 2000 were steep for wealthy states but smaller for poor states.
Although the categories we combined and labeled Cash Assistance under the Census Bureau definitions might include state SSI and federal SSI that passes through state accounts, state and local general assistance programs, and some other programs, for these six poor states, most of the spending in the cash assistance category seems to be TANF benefits.31 Before 2000, per capita spending on cash assistance dropped in all of these six states. Some of the declines, especially among the southern states, began long before state welfare reforms were implemented, with the western states showing more volatility.
The graph at the top of Exhibit IV-6 shows changes in per capita TANF benefits from 1997 through 2002. Among the six poor states, cash assistance spending typically changed little, continuing the dominant trend among states in the lowest fiscal capacity quartile before 2000. New Mexico was an exception among the poor states: its cash assistance spending continued to fall. But declines after 2000 were not found among the other low fiscal capacity states. Louisiana, Mississippi, and South Carolina saw little change through 2002. Some of the poor states saw increases in cash assistance spending: our site visits indicated that Louisiana's spending on TANF benefits increased dramatically between FY 2002 and 2003, and Arizona's spending on assistance increased, as well. West Virginia was more volatile, dropping steeply through 1999, rising in 2000, and then falling and rising again. Thus, through 2002, most of the poor states either stayed close to the already low levels of spending on cash assistance they had reached by 2000, or their spending began to creep up. The regional differences between states in their cash assistance spending, evident in the 1977-2000 Census data, continued through the early 2000s, as South Carolina, Louisiana, and Mississippi's TANF per capita expenditures remained lower than the other states through 2002.
Exhibit IV-6.
Changes in TANF Spending and Caseloads, 1997-2002
TANF Per Capita Expenditures
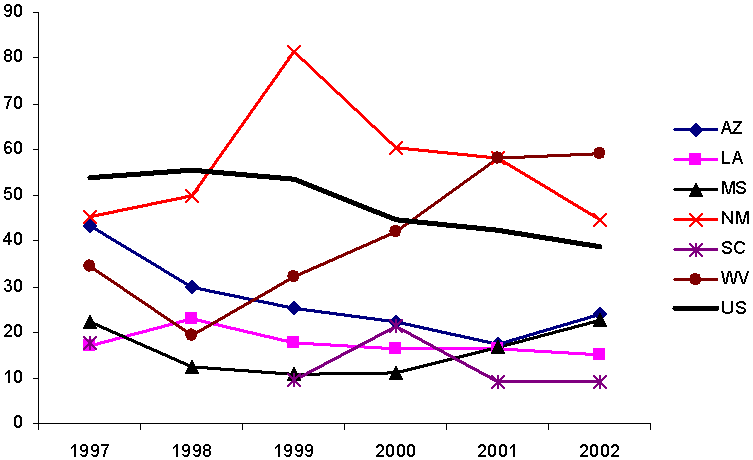
Number of TANF Cases Per Capita
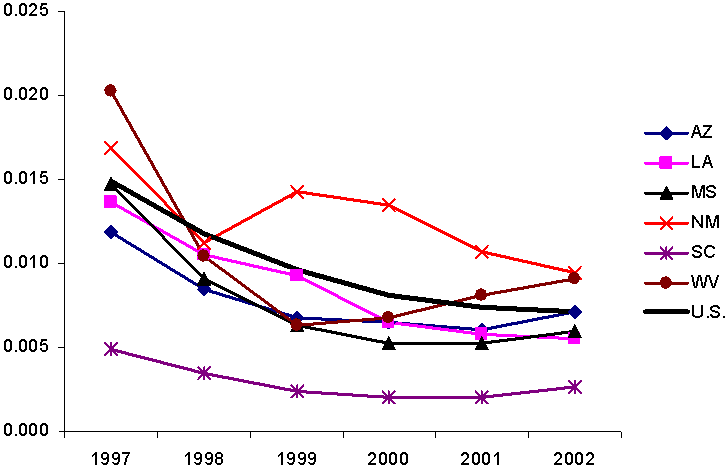
The flat spending levels for TANF benefits among the poor states contrasted with changes in other, mostly wealthier, states, where drops in spending on assistance continued past 2000. In the nation as a whole, the average state's TANF per capita spending declined between 2000 and 2002, as shown in the graph at the top of Exhibit IV-6, freeing some money for services and other programs. The trend in Census data toward convergence in per capita spending on cash assistance between rich and poor states before 2000 thus also appeared in the expenditure data for TANF cash assistance, even after 2000.
Changes in TANF spending roughly reflected changes in TANF caseloads among the poor states, which are displayed in graph at the bottom of Exhibit IV-6 as the number of TANF cases per capita. After the large and widespread caseload declines through 1999, caseloads in most of the six states began to hold steady or climb. New Mexico and, to a lesser extent, Louisiana were exceptions; their caseloads fell through 2002. The other states either showed little change or drifted upwards. West Virginia's caseloads rose sharply from 2000 through 2002, while Arizona, Mississippi, and South Carolina's cases grew more slowly and later.
One reason spending on assistance tracked caseload changes was that, with few exceptions, these six states made few major changes in their cash assistance benefits, eligibility criteria, or other policies since 2000. Exhibit IV-7 shows AFDC/TANF benefits levels (based on the amount a three-person family would receive if it had no other income), adjusted for inflation, between 1980 and 2001. These six states rarely changed their benefit levels, producing a long-run downward trend in benefit levels due to inflation. Exceptions included Mississippi, which used its TANF surplus to raise its maximum benefits for a three-person family in the late 1990s, the state's first increase in benefits in more than two decades. West Virginia increased its benefits in 2000 to pay recipients the equivalent of a minimum wage for their hours in the state's work experience program (required under the rules of the Fair Labor Standards Act). And New Mexico raised and then lowered its maximum benefits between 1998 and 2000. As these exceptions indicate, most of the change among these states was upward, not downward, with respect to cash assistance benefits.
Exhibit IV-7.
AFDC/TANF Maximum Benefit Levels in Six Poor States, Adjusted for Inflation, 1980-2000
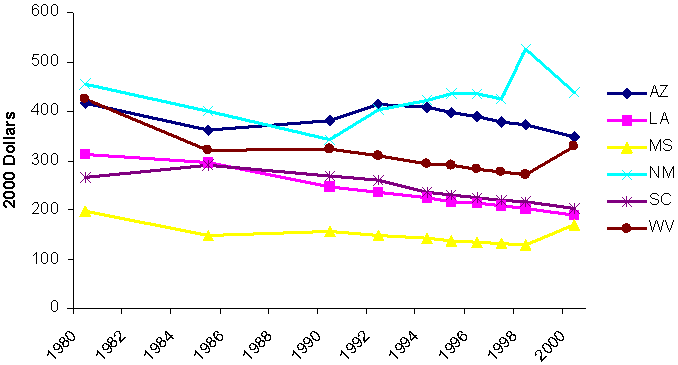
Only West Virginia made substantial cuts in its assistance program through other policy changes: it reduced its earned income disregard and child support pass-through in 2002.32 But the remaining states made few changes in other TANF policies, including their income disregards, time limits on assistance, and sanctions for noncompliance with work activities. The interviews with state officials revealed little interest in making these rules less generous during a recession.33
4. Changes in Non-health Social Services: TANF "Non-assistance," Child Care, Child Welfare, and Others
Because Medicaid spending was not cut substantially in these states and, in fact, continued to grow in most states and because spending on cash assistance programs remained essentially flat, offering few opportunities for savings, fiscal pressures during state budget crises fell mostly on non-health social services programs. This outcome was especially true because other budget pressures to maintain or increase spending in non-social welfare were strong in these states. The greatest external pressures came from education programs, which were the top priorities of elected officials in South Carolina and Louisiana and were high priorities elsewhere. However, states had some flexibility in dealing with these pressures due to two factors: the large "surpluses" in TANF spending that states had accumulated since 1997 and the wide array of programs that might be funded under TANF non-assistance.
One way in which states responded to fiscal pressures was to spend down their TANF surpluses. Most poor states were fiscally conservative in 1997 and 1998 in using their federal TANF dollars and typically spent less than three-fourths of their grants on current program needs. Their total spending grew rapidly, but the surpluses they built gave them a cushion they drew on to support their basic assistance programs in later years.
Exhibit IV-8 tracks these changes by displaying the percentage of federal TANF grants spent by states from 1998 through 2002, averaged for each quartile of state fiscal capacity. State spending of federal dollars in the poorest quartile as a percentage of states' annual grants was low in 1998, only 57 percent. All but the wealthiest quartile of states increased their spending of federal TANF funds in 1999, at least partly in response to the flexibility offered by the federal government's "non-assistance rule" (see below; also see Plein (2001)). Spending continued to grow after 1999 among states in the poorest quartile until average spending of federal TANF funds exceeded 111 percent of states' annual TANF grants in 2002. Between 2001 and 2002, when the recession began to hit most states, TANF spending increased in all quartiles, probably reflecting growing fiscal pressures due to revenue shortfalls and growing needs.
Exhibit IV-8.
Average of TANF Spending as a Percentage of the State's Annual Grant, by State Fiscal Capacity, 1998-2002 (federal dollars only)
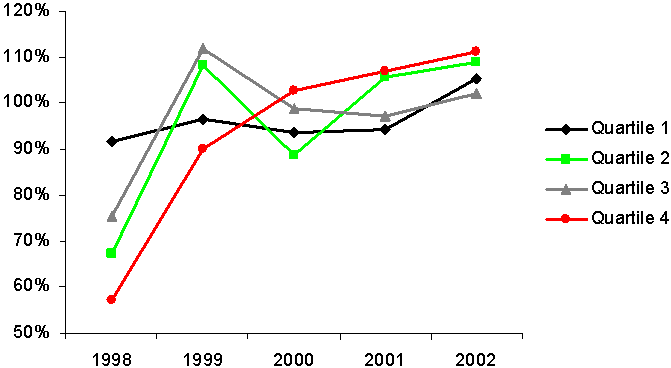
Carry-over funds accumulated for most states, though they were especially large among the poor states, despite the small size of their grants relative to their needy populations (Gais & Weaver, 2002). The federal TANF law required states to use their carry-over funds only for "basic assistance," or benefits to meet a family's "ongoing basic needs," such as food, clothing, and shelter or supportive services such as transportation or child care for families whose heads were unemployed (U.S. House of Representatives 2000, p. 355). Because most low fiscal capacity states had small cash assistance programs-and states tended to refrain from expanding such benefits-such states were more constrained in using their surpluses than were others. Nonetheless, the TANF surpluses relieved fiscal pressures on the states in our sample; they typically used their surpluses to fund their current basic assistance needs, thereby freeing current TANF grant funds for other, non-assistance programs.
A second source of flexibility was the wide range of services and programs that could be funded with federal TANF and required state MOE funds. Especially important was the broad definition of TANF non-assistance, which was clarified by the federal government in its rulemaking in 1999. Non-assistance could include any non-recurrent, short-term benefits, work subsidies, and supportive services to employed families. Exhibit IV-9 shows that per capita spending on non-assistance was generally lower and grew less rapidly among the six poor states when compared to the average for all states in the U.S. These differences in per capita spending on TANF non-assistance between the poorest states and other states seemed to continue the trends we noted in the Census data on state spending on non-health social services during the late 1990s. Nonetheless, TANF non-assistance spending rose in most of these states after 1999, most notably in West Virginia. Thus, even the poor states, with their relatively small TANF grants, had a new source of funding for non-health social services.
Exhibit IV-9.
Per Capita Spending on TANF Non-assistance, Six Poor States and U.S. State Average, 1997-2002
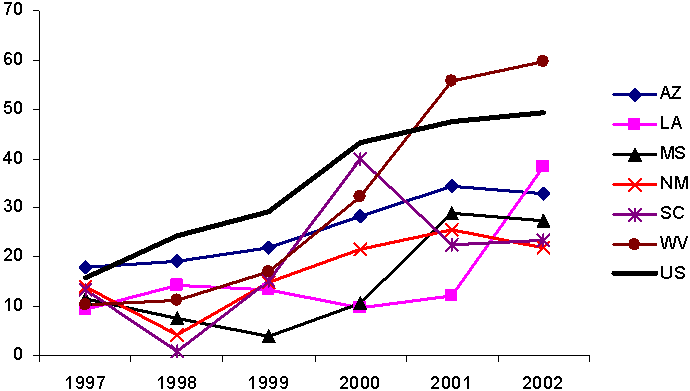
How did the states use their flexibility under TANF to deal with their fiscal crises? And what happened to their spending on non-health social services? Considerable variation occurred among these six states, but a few generalizations applied to most.
First, we found a growing variety of programs funded with TANF dollars, as administrators and elected officials sought funding for high-priority services. Administrators viewed as critical many of these programs that otherwise faced cuts. South Carolina and West Virginia were using a growing share of their TANF grants to support child welfare programs, including protective services, foster care, emergency shelters, and others that administrators regarded as involving high stakes. TANF thus allowed these states to mitigate cuts in funding for their child welfare programs, despite large reductions in state matching funds under Title IV-E. Still, cuts occurred in South Carolina in staffing and payments for protective services, foster care, and adoption in the late 1990s and early 2000s. These cuts suggest an intriguing puzzle for fiscal federalism theory because major parts of IV-E used the same attractive open-ended match rate as Medicaid. To make room in TANF for these child welfare funding needs, which administrators viewed as involving "life and death" issues, they eliminated a number of employment services that had been funded under TANF.
The greater importance of TANF dollars in funding a wider array of programs also seemed to be pushed by drops in federal aid. For example, the nominal and constant-dollar decline in federal support for the Social Services Block Grant has left some of these states scrambling for dollars for child welfare, child care, and a number of other basic services-a deficiency that TANF non-assistance dollars seemed to address.
Other changes in the composition of TANF non-assistance spending resulted less from stress than surplus. Louisiana's large TANF surplus led the state to set up a nearly universal pre-Kindergarten (pre-K) program with TANF dollars. But even though the TANF surplus declined substantially in recent years-and although the state's transportation, child care, and employment services programs were poorly funded-the popularity of the pre-K program prevented legislators from cutting it or even requiring the program to be supported with general revenue funds. Another state noted how it drew on TANF dollars to launch a school readiness program. Several states also began to use a wider range of programs to meet their MOE requirements. Because of cuts in state programs previously included under MOE, state TANF agencies searched for current public expenditures in other agencies and public institutions that might fit within the fairly broad definition of MOE spending, even if the programs had had little or no connection with TANF in the past. Such processes led, for example, to counting several university scholarship programs as MOE dollars.34
We found, thus, an expanding range of programs supported under TANF and its MOE requirements, sometimes because money could be found nowhere else and sometimes because the programs, often educational in nature and serving a larger population, were more politically popular than programs that exclusively served the poor. We are not suggesting that this expanded range of programs represents "supplantation," or improper shifting of program funds from state to federal sources. Yet it does suggest that states have learned to exercise greater flexibility in using the block grant, just as they did after the promulgation of the non-assistance rule in 1999. Gauging the aggregate effects of these program shifts was difficult. To the extent, however, that TANF and MOE funds were redirected to support child welfare, education, and other programs, fewer funds were perhaps available for income and work supports.
Second, we found that state flexibility under TANF allowed policymakers and especially administrators to weigh and adjust programs already funded under the block grant. In general, programs were cut that served goals considered less critical or that were thought to have less immediate impacts. In most states, for example, few child care programs were cut. Child care programs were perceived in most of these states as already under-funded, yet valuable, because the child care subsidies constituted one of the few significant services with immediate and widespread importance for low-income families. These programs were also regarded as serving multiple goals. Transitional child care encouraged people to move off of cash assistance, and child care subsidies for foster parents, many of whom worked, were considered essential to the foster care program. Some discretionary cuts in child care were imposed, though since most of these states did not put large amounts of state money into their child care programs, only the two states that had put larger sums of TANF or state money into their subsidy programs in the 1990s (Arizona and Louisiana) made major reductions in their child care spending. For all these reasons, child care programs outside Arizona and Louisiana did not bear the brunt of cuts even through FY 2004.
Some programs, however, were considered less essential, though states varied in what they thought essential. Pregnancy prevention programs, fatherhood programs, parenting classes (e.g., in Mississippi, involving a charitable choice initiative), and job services contracts were often seen as inconsequential in the short-run to meet basic performance criteria and fared less well in these states. In South Carolina, for example, many job development positions and their functions were eliminated in FY 2004. There were exceptions. A TANF advisory board in West Virginia recommended the elimination of the state's "marriage bonus," a cash grant to people who wed while on assistance, but the state eventually decided to keep the provision. Also, Louisiana saw its TANF priorities as including pregnancy prevention programs. For the most part, however, TANF services were often weighed in terms of their immediate importance. In several states, agency administrators also said they used performance measures to decide which programs to cut and which to sustain-or which contracts to eliminate.
Third, we found that administrative expenses, especially staff, were often severely cut in social service agencies. South Carolina's Department of Social Services saw a 26 percent reduction in staff between FYs 2001 and 2003. Arizona has made major reductions in its human service workforce since the beginning of the decade, despite the state's large increase in Medicaid workloads after the passage of Proposition 204. Louisiana has refrained from cutting staff much in the last year, but it reduced positions in its state administered welfare system substantially in FY 2002. Plans to improve information systems were widely postponed or cancelled altogether in most of the six states. These administrative cutbacks seemed greater among poor states than among others: TANF administrative costs per capita declined 22 percent among these six states between FYs 2000 and 2002, while the average decline in all states was only 5 percent over the same period.
Administrative expenses have been reduced in other funding streams, too, or at least they have failed to keep up with caseloads. Food Stamp administrative expenses were generally split equally between the federal and state governments. But despite substantial increases in the number of households on Food Stamps in recent years, states were sometimes unwilling to pull down additional federal dollars to support Food Stamp Program (FSP) administration. As Exhibit IV-10 indicates, federal dollars for administrative expenses per FSP household recently declined. For example, although South Carolina, Mississippi, and especially Arizona have seen large increases in their Food Stamp caseloads in recent years, they have either refrained from increasing or have cut their state matches and, thus, the amounts they get from the federal government to support the program's administration.
Exhibit IV-10.
Federal Share of State Administrative Expenses in the Food Stamp Program in the Six Poor States (dollars per FSP household)
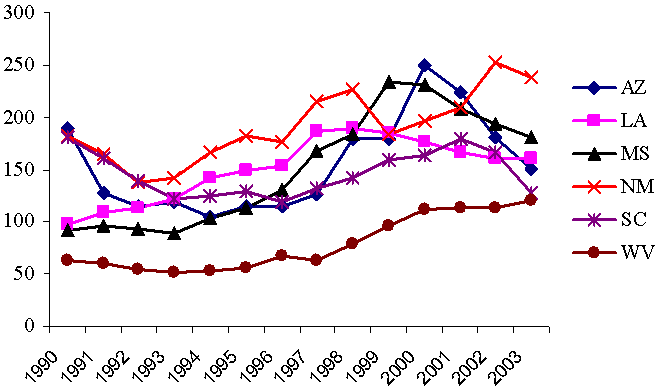
5. Influences on Spending and Explanations of State Differences
These six states varied in their spending patterns, both before and after FY 2000, though we found that some regional differences in spending patterns of poor states before 2000 have declined in strength in recent years. For the most part, spending trends evident among the poor states before 2000 continued after that year: medical assistance expanded; cash assistance spending remained low and fairly static; and non-health social services programs grew slowly or, in states where fiscal problems were most acute, not at all.
What accounts for these patterns of change and differences across states? We explored several factors in the site visits. But our major finding was that the state differences and the trends in various program functions stemmed in part from differences in how states made decisions in major program areas. Each of the major functional areas in social services- cash assistance, Medicaid, and non-health social services-were dominated by a distinct mode of decision-making. These modes varied by who participated in or controlled the decisions, the frequency of major choices, and the criteria brought to bear on decisions. These distinct decision-making styles might help account for different decision outcomes and changes over time.
C. Medicaid
The site visits indicated that decisions about Medicaid were more likely than other social program areas to involve active and highly organized constituencies, especially service providers, and to engage the attention of elected officials, including legislators and sometimes governors and their staff or top appointees. Medicaid budgets and policies were thus highly salient to elected officials and often assessed as much for their economic effects on health industries and jobs as for their effects on clients. Our respondents singled out nursing homes and hospitals as having especially powerful lobbies in several of our states. Developmental disability programs were also viewed as having effective advocates among institutions as well as community-based providers. Doctors were typically seen as less effective, and their reimbursements were more likely to be cut or less likely to be increased. Drug companies, dentists, and others also became active from time to time in state legislatures if and when relevant cuts or expanded services were under consideration. Even child advocacy organizations in these states were more interested and active on CHIP and Medicaid issues than in other social programs; indeed, some were service providers themselves because many were directly involved in CHIP outreach.
| Hospital beds per 100,000 population, 2001 |
Percentage of Nursing Facility Residents Using Medicaid, 2001 |
|
|---|---|---|
| Mississippi | 430 | 82.3 |
| Louisiana | 396 | 79.1 |
| West Virginia | 384 | 73.0 |
| South Carolina | 271 | 74.5 |
| Arizona | 210 | 63.1 |
| New Mexico | 195 | 69.5 |
The direct involvement of service providers or industry representatives in the budget process might help account for some of the geographical differences found in state spending on payments to medical vendors. Southern and rural states have more hospitals and nursing homes per capita than other states, and the health industry plays a larger role in these states' economies. As Exhibit IV-10 demonstrates, Mississippi and Louisiana had about twice the hospital beds per unit population than did Arizona and New Mexico, and nursing home industries in southern states depended more on Medicaid patients than in the western states. The nursing home data suggest another important difference between poor southern and border states and others: although hospitals and other health care institutions in many states tend to split between some that rely heavily on Medicaid and many that do not, such divisions are less common among poor rural states (i.e., most institutions get substantial support from Medicaid). Most births, for example, are paid for by Medicaid in these states. In such states, Medicaid is more likely perceived as a universalistic program-one that helps many, if not most, communities and populations.
Political support for Medicaid was more than simply a matter of organized providers. It was also one of the few major programs where legislators knew some of the clients and viewed them sympathetically. Officials regarded many nursing home residents as coming from middle or working class families. Also, one legislative aide noted that experienced legislators in his state knew every one of the families in their districts who relied on the Continuum of Care program under Medicaid that paid for expensive and intensive services to families caring for dependents with multiple and severe problems. The prevalent view that these and other health-related problems were not the clients' fault, the fact that some clients relied so intensively on these programs that they often contacted legislators if problems occurred, and the widespread distribution of such cases throughout the state were all characteristics that enhanced political support in state legislatures, which often dominated budget decisions, especially in the southern states.
Federal requirements and incentives were also critical. Many of these poor states had minimal Medicaid programs, covering relatively few optional services and populations. Thus, increases in federal minimum requirements, which grew dramatically in the early 1990s, strongly affected these states. Also, unquestionably, the poor states are willing to spend money on Medicaid due to the high federal match rate for low fiscal capacity states and the ability of states to use a number of strategies to maximize their draw of federal dollars under Medicaid. The attractive "prices" of Medicaid in these states were indeed important factors in maintaining state support for the program, especially during a recession. Medicaid match rates, which were based on states' per capita personal income, ranged among these states from more than 3:1 for Mississippi to 2:1 for Arizona, and they were even higher for CHIP. Health care administrators and other advocates used these rates widely as arguments in budget battles that any cut in state spending produces a much larger cut in total spending.
But though the fiscal formula might prove a necessary condition for Medicaid's fiscal robustness, it seems to be an insufficient condition. The same match was available for child welfare programs, and the results were much less expansive. As a matter of fact, child welfare programs have had such problems obtaining state matching funds in recent years, some state administrators have used their discretion over the TANF block grant to support such programs, even though the fiscal price of TANF dollars was much higher. Attractive matching formulae would seem to exert a contingent effect on spending: they can constitute powerful political arguments in budget battles when the arguments are backed up by strong, organized constituencies.
That states, and especially poor states, support Medicaid strongly because they can use certain strategies to maximize their draw of federal resources might also be argued. Again, the site visits revealed that poor states employ these strategies, and they surely exert some impact on support for the program. The two most common methods of maximizing federal dollars among these states relied on Medicaid expenditures for disproportionate share hospital (DSH) programs and upper payment limit (UPL) programs (for details on these expenditure programs and their use in maximization strategies, see Coughlin and Zuckerman, 2002). For example, Louisiana has relied a great deal on DSH programs to increase its federal payments under Medicaid, while South Carolina has relied more on UPL. DSH and UPL programs have allowed states to make large Medicaid payments to health providers, payments which the state has in turn used to claim federal matching dollars. Sometimes these state payments to providers under DSH or UPL are made in response to large payments by providers to the state (through, for example, intergovernmental transfers or donations). In such instances, the health care providers are usually reimbursed for their donations or intergovernmental transfers by the state, while the state gets, in effect, a higher federal match rate as it uses its transactions with health care providers to pull down federal dollars.
Yet such strategies do not account for much of the Medicaid program in these states. Nor do they provide much help in explaining recent program expansions.
As Exhibit IV-11 demonstrates, DSH payments constitute a small part of the Medicaid budgets in most of these states. Only Louisiana and South Carolina rely more than the national average on DSH payments as a percentage of their total Medicaid expenditures, and some of the states receive little DSH money. Also, these payments have declined over the years as the federal government imposed limits on their use in the middle 1990s, so such strategies cannot account for the growth in spending among poor states on Medicaid in the late 1990s and early 2000s. Again, Medicaid maximization strategies might well contribute to the growth of the program, but by themselves they cannot explain its dynamics and widespread support. Such strategies are probably more powerful when they are backed up by more concrete motivations, such as important constituencies. For example, the extensive use of DSH in Louisiana might reflect formalized concerns about supporting parts of the state's health industry: Louisiana has a statutory provision that requires it to keep rural hospitals viable.
Exhibit IV-11.
DSH Payments as a Percentage of Total Medicaid Spending, Six Poor States and Average for All States, 1993-2003
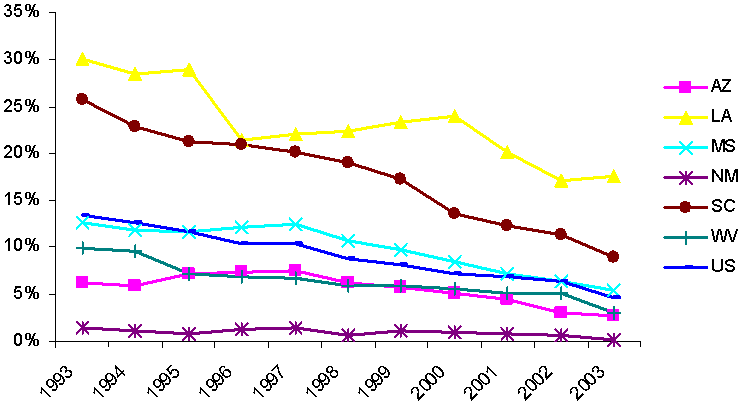
Other factors might have increased support for Medicaid. In most of the states, the agencies that administered Medicaid were separated from those that administered welfare and non-health social services, and that separation insulated health programs from the often negative views about social service agencies held among legislators. As Exhibit IV-12 shows, the most consistent divide in agency responsibilities in these six states was between health programs and all non-health social services and income support programs. Only in West Virginia did the same agency that handled "welfare" also manage Medicaid.
| TANF | Child Care | Child Welfare | Medicaid | SCHIP | |
|---|---|---|---|---|---|
| West Virginia | Department of Health and Human Services | Department of Administration | |||
| Arizona | Department of Economic Security | Arizona Health Care Cost Containment System | |||
| Louisiana | DSS and Governor's Office | Department of Social Services | Department of Health and Hospitals | ||
| Mississippi | Department of Human Services | Office of the Governor | State and Public School Employees Health Ins Mgt Brd | ||
| New Mexico | Human Services Department | Children, Youth, and Families Department | Human Services Department | ||
| South Carolina | Department of Social Services | Department of Health and Human Services | Department of Social Services | Department of Health and Human Services | |
Perhaps reflecting while also reinforcing the strong political support for health programs, political and administrative leadership were frequently more stable among health agencies and legislative committees dealing with health issues, while other human service agencies often saw rapid turnover. Sometimes, as in South Carolina, the decades-long involvement of a single senator was seen by respondents as a critical factor in ensuring stable support for Medicaid. But though that situation might not be the case in every state, such stability in leadership was much less common in other social program areas.
D. Cash Assistance
We found a different type of decision-making in TANF cash assistance programs. Medicaid was a high visibility program that sometimes commanded the attention of governors and often drew the attention of legislators and organized lobbyists, but TANF cash assistance programs drew attention only sporadically from legislators and from few others outside the state bureaucracies. Although many changes were made in Medicaid rates, service coverage, eligibility levels, and other elements in annual state budget processes, policies governing cash assistance changed much less often.
As already noted, most of these states had low maximum benefit levels, especially in the southern states. Other rules governing cash assistance also tended to be stricter among these states. Time limits were more likely to be shorter than required by federal law. Sanctions were usually stricter, applying to the entire household. Earnings disregards were in all but one case time dependent (i.e., they became less generous or disappeared altogether after 4 to 12 months of working while on assistance.) That provision is atypical among the non-poor states, most of which had earnings disregards that remained the same indefinitely.
These benefit levels and other rules were changed infrequently. Until 2000, Mississippi had not changed its nominal benefits for more than 2 decades. Nor had most of these states revisited many of their newer, welfare-reform rules-such as sanction policies or earnings disregards-that they had established when they enacted their AFDC waivers or TANF programs in the middle 1990s. West Virginia was, as noted, one exception. It did reduce its earnings disregard in the face of budget pressures but took that action only after a special advisory board was established to recommend changes. In the normal course of budget politics, these rules were not reconsidered. In fact, there was considerable reluctance to revisit them.
The rules, benefit levels, and eligibility standards that applied to cash assistance were usually established by legislation, and in these states, some deference was shown to the legislature on such matters. One state, where the agency administering TANF benefits believed it had the authority to change the maximum benefits, refused to do so on its own even though agency officials believed an increase was overdue. State decision-making about cash assistance was thus dominated by the legislative process, and changes occurred occasionally rather than regularly as a part of the budget process.
The lack of change in cash assistance policies in some of the case study states appeared to reflect a reluctance to engage in a policy discussion that was often ideologically and racially divisive. The intertwined issue of race and welfare was brought up during a number of the site visits, although usually indirectly. For example, officials spoke of the poor reputation of the state departments of social services (DSS)-"welfare agencies"-in the state legislatures, and how some of this poor reputation was attributable to negative views of their clients. In some instances, the political problems faced by cash assistance programs appeared to be reinforced by restrictive policies, which limited the number of participants in the program to the neediest families in the state. According to a DSS report from a state with low maximum benefits, only 2 percent of families in the state received cash assistance, and 86 percent of these recipients were African American.
As noted in our literature review, several studies of social welfare spending found that welfare spending was influenced by the racial composition of the state population or the state welfare caseload.35 Consistent with this literature, among the six states studied, the lowest levels of spending on cash assistance, the lowest benefit levels, and the strictest regulations were found among three states with the highest proportions of assistance caseloads composed of African Americans. This relationship held more generally with poor states, not just those in our sample. As Exhibit IV-13 demonstrates, the relationship between the proportion of African Americans in a state and the estimated state effects for cash assistance was negative for states in the lowest quartile for fiscal capacity. The proportion of African-Americans in a state may be a proxy for other demographic and economic variables, and it is interesting to note that his relationship failed to appear among wealthier states (those in the first three quartiles of fiscal capacity). There also was little relationship between the proportion of African Americans in a state and estimated state effects for either Medicaid or non-health social services. This supports our belief that there are distinct decision-making modes for each of the major functional areas in social services - cash assistance, Medicaid, and non-health social services.
Exhibit IV-4.
Relationship Between State Effects for Cash Assistance and Average Percentage of African American Population, Lowest Quartile for State Fiscal Capacity

E. Non-health Social Services
A third mode of decision-making was prominent when we examined choices about non-health social services in these states, including TANF non-assistance, child care subsidies, and child welfare. Although decisions about Medicaid funding were strongly affected by provider interests and state funding needs and decisions about the critical parameters in cash assistance were influenced by political ideologies, choices regarding non-health social services more likely reflected a sort of technocratic politics. Decisions were made on the basis of assessments by state administrators about the relative merits of different programs and their centrality in achieving major goals.
However, these decisions were constrained by the availability of resources, and in recent years, those resources have been limited. Administrators were given flexibility in deciding what services to support, but the flexibility often looked like a delegation by the legislature, and sometimes the governor, of difficult choices between competing needs. That is, in recent years, many of the social service agencies among these six states were instructed by their legislatures not precisely where to reduce services but how much they had to cut from their total budgets. There were exceptions: sometimes governors or legislators championed particular services or programs, and these programs served as additional constraints. In these six states, such programs were usually some relatively popular educational initiative, such as Louisiana's pre-K program.
This manner of decision-making in part resulted from the low political salience of these non-health social service programs. Although many of the services, such as child care or child welfare, involved private providers, the providers were rarely organized and active in advocating these programs in state legislatures. Nor were child and other advocacy organizations as involved with these programs as they were in Medicaid or CHIP.
This political flexibility was augmented in recent years by the availability of the TANF block grant and fairly loose constraints as to what service and benefit programs might be included under TANF non-assistance and the state's MOE. In fact, sometimes this flexibility was as much a "burden" as a "blessing," as one administrator told us. Because the state legislature viewed the social services agency as having so much discretion in managing the block grant, agency officials perceived the legislature as unconcerned about imposing major cuts in state funding of agency programs because "they thought we could cover critical shortfalls with our 'slush fund'" (i.e., TANF block grant).
As noted above, within these constraints, administrators often made decisions based on judgments about which services were critical to major agency goals, which programs were successful in terms of performance standards, which programs were needed to create or maintain a coherent package of benefits or services, which programs involved high stakes (e.g., life or death issues), and how and whether programs can be administered with fewer staff. These were unenviable decisions in most of the states because state funds were scarce, TANF surpluses declined rapidly, and some block grants that provided greater per capita support to poor states, such as SSBG, were reduced in size. But, unquestionably, state officials had more control over the mix of services the state could offer than they had just a decade ago.
F. Conclusions
Our analyses of estimated state effects and site visits to poor states suggest several basic conclusions:
- Poor states differ from one another in the ways they distribute funds across different program areas. Although state spending on various social programs-after controlling for fiscal capacity, social need, and the other variables included in the 50-state model-tend to be correlated with one another among non-poor states, poor states show a regional divide between those that have small cash assistance programs and devote the great bulk of their social program resources to Medicaid and those that have retained significant cash assistance programs and put fewer resources into Medicaid.
- Since 2000, spending trends in programs among poor states continued some of the trends evident before 2000 and diverged from others. Spending on Medicaid continued to rise, even during the recession and slightly faster among the poor states than in the nation as a whole. In fact, Medicaid spending rose especially quickly among poor states that traditionally had spent little on Medicaid, thereby reducing some of the regional differences among poor states. Spending on cash assistance generally remained flat among these poor states, though some saw modest increases in cash assistance expenditures while wealthier states continued to see declines in cash assistance spending. Knowing whether non-health social services programs were rising or falling in these six poor states was difficult, but the site visits suggested that many of these non-health social services functions, especially administrative spending, bore the brunt of state budget cuts.
- These patterns of change might reflect differences in how decisions were made in different program areas. We found, for example, that budget choices about Medicaid in these states were often dominated by strong and active provider institutions-a politics of organized interests, frequently involving the legislature as well as the governor, that was absent in the rest of social welfare system. Spending on health programs was, thus, sensitive to the role of the health industry in the state's economy and the industry's reliance on public programs, and spending growth in Medicaid continued despite the fiscal pressures of the 2001-2002 recession.
- Cash assistance spending was more directly affected by relatively infrequent changes in policies, set largely by the legislature, and their interactions with the economy. When policies were established, they appeared to reflect ideological viewpoints found among state elected officials.
- Decisions about non-health social services were less politically salient and, thus, more likely to involve choices by administrators about what programs were of higher priority and more effective. Their choices were strongly affected by short-run budget constraints, such as declines in tax revenues, availability of funding through various grant programs, flexibility administrators had in drawing on these funds as well as governors and state administrators' priorities and judgments in exercising their flexibility.
These different modes of decision-making might help account for some of the findings from the 50-state models of various forms of social welfare spending, though we cannot say so with certainty. Cash assistance, for example, was found to be strongly related to unemployment, a finding which makes sense in light of our conclusion that policies were infrequently changed in this area, except during major periods of reform, as in the early and middle 1990s, and spending changes were usually driven by caseloads. Medicaid spending was negatively related to state population density, a finding that made sense if health providers in rural states were particularly active politically in supporting Medicaid because they constituted a larger part of the economy or they depended more on public funds to sustain themselves. Our conclusions might also help explain the fact that unemployment failed to increase spending on non-health social services and that federal grants to non-social welfare tended to increase spending on such functions. The site visits suggested that overall state revenue levels strongly affected spending on these non-health social services, which were more discretionary in the short-run than other programs. And it was reasonable to assume that these overall revenues were negatively related to unemployment rates and positively related to sources of federal dollars.
More generally, our findings suggest the importance of state and local constituencies in understanding why some programs thrive, even during difficult budgetary conditions, and why others fail to thrive, even when the different programs offer similar fiscal federalism incentives. In these states, constituencies-mostly service providers-were active and strong on health issues, while they were largely absent from state budgetary politics on other social welfare matters, a fact consistent with spending trends among poor states as well as with state differences. If constituencies are, in fact, critical and if they continue to be skewed toward the health industry, low fiscal capacity states might face a long-term squeeze on non-health social services unless social welfare spending can obtain a larger share of the state budget. Given the strong pressures from other program areas outside social welfare, from education, to prisons, to highways and roads, the latter option is unlikely.36 Thus, non-health social services might well continue to constitute a smaller and smaller share of state budgets.
Endnotes
30 In 2004, after the case studies were completed, Mississippi enacted program changes that may eliminate eligibility for 65,000 Medicaid recipients, mostly elderly and disabled people. Although most of these recipients were eligible for Medicare benefits, some estimates indicated that about 5,000 were not. However, the strong political reaction to the cuts led the state House and its leadership to seek to rescind the changes soon after passage. As of mid-June 2004, the final resolution was still unclear.
31 Of these six states, only South Carolina offered more than a negligible SSI state supplementation benefit (U.S. House Ways and Means Committee 2000, pp. 266-267).
32 "Earned income disregard" refers to the amount of earnings excluded when determining a family's eligibility for cash benefits or the size of the benefit. Under AFDC, states disregarded $120 plus one-third of the remaining earnings for the first four months on a job when calculating benefits. For the next 8 months, the disregard was reduced to $120, and thereafter (after 12 months) to $90. Most states increased their earned income disregards under TANF; most (i.e., 30 out of 51) also eliminated the time-dependency of earnings disregards in calculating benefits. Of the six states in our sample, earnings disregards in calculating benefits are reduced after a person is on assistance for several months in Louisiana, Mississippi, New Mexico, and South Carolina (Administration for Children and Families 2003). "Child support pass-through policies" refers to the amount of child support money a state passes along to a family on welfare. Although the family receives TANF benefits, the state might retain current support and arrearages it collects up to the cumulative amount of TANF benefits that have been paid to the family. Under AFDC, states had to pay, or pass through, the first $50 of collections to the family.
33 Time limits either restrict the number of months a family may receive assistance before work requirements begin, or they limit the number of months a family may receive assistance regardless of their employment status. Arizona, Mississippi, South Carolina, and West Virginia required family heads to work immediately, and New Mexico required them to work after 3 months on assistance-all lower than the 24 months required under federal law. Arizona, Louisiana, and South Carolina also had special "intermittent" time limits that precluded families' receiving assistance for more than 24 months during some overall time period (i.e., either 60 or 120 months). "Sanctions" refer to the loss of benefits if the family head or heads fail to comply with TANF work requirements. Full family sanctions (i.e., the complete elimination of the benefit) are imposed at the first violation in Mississippi and South Carolina for 1 to 2 months, and partial sanctions lasting at least 3 months are imposed for the first violation in Louisiana and West Virginia. The more typical initial sanctions, sometimes full though usually partial, are imposed until compliance (i.e., there is no minimum period) (Administration for Children and Families 2003).
34 TANF Maintenance of Effort (TANF-MOE) requirements were, in general, not particularly constraining for these six low fiscal capacity states. TANF-MOE provisions impose financial penalties on states for failing to spend state funds on low-income children and families at a level equal to at least 80 percent of their FY 1994 level (or 75 percent if they meet the minimum work participation rates). However, in low fiscal capacity states, the required TANF-MOE spending levels tend to be low. For example, in the six poor states, the minimal (75 percent) MOE requirements constituted, on average, only 30.5 percent of the states' federal TANF grants (FY 2001). For all states, the same average was 61.4 percent. In wealthy states, such as New York and Massachusetts, the MOE spending requirements were equal to their TANF grants (i.e., these states had to spend state funds at least 100 percent of their TANF grant to satisfy the MOE requirement). Since TANF grants were also typically smaller on a per capita basis in the low fiscal capacity states, TANF-MOE requirements were generally easier to meet in poor states than in wealthy states.
35 As noted in the literature review in the first section of the report, this literature includes studies by Brown (1995), Plotnick and Winters (1985; 1990), Gais and Weaver (2002), and Kousser (2002).
36 Although social welfare spending, based on the Census data, increased more rapidly than non-social welfare spending in the late 1980s and early 1990s in the six poor states analyzed here, little change occurred in the ratio during the middle and late 1990s. The average percentage of total state and local expenditures going to social welfare, not including the public hospital category, was about 18 percent from 1977 to 1989. It then rose to 26 percent by 1993, after which it drifted slightly downward to just under 25 percent in 2000. The highest percentages were in the southern and border states, which ranged between 27 percent (West Virginia) to 31 percent (Mississippi) in 2000. Arizona (14 percent) and New Mexico (21 percent) invested much smaller parts of their total budgets to social welfare spending.
Chapter V: Final Observations and Conclusions
Our econometric analyses and case studies of six poor states led us to several conclusions regarding state fiscal capacity and state spending on social welfare:
Finding #1: States of LESS fiscal capacity spent LESS PER CAPITA on social welfare programs than states with HIGHER per capita incomes. Federal grants did not reduce absolute spending differences between rich and poor states. Average federal grants to the wealthiest states were actually higher in dollar terms when compared to states with lower fiscal capacity. However, because state own-source spending was much lower in poor states, federal intergovernmental grants constituted a larger share of the social welfare budgets of poor states than of rich states.
Finding #2: State fiscal capacity bore a stronger relationship to spending on non-health social welfare programs than on health-related programs. Between 1977 to 2000, differences between rich and poor states were greatest for spending on cash assistance and non-health social services (such as child care, child welfare, energy assistance, transportation assistance, and programs for the homeless). Differences between rich and poor states were smaller for health-related programs, such as per capita spending on Medicaid and payments to public hospitals.
Finding #3A: Between 1977 and 2000, state spending on social welfare changed in major ways. Even after controlling for the higher levels of inflation found in health services, spending on Medicaid greatly increased throughout this period, most rapidly in the late 1980s and early 1990s. Spending on non-health social services rose gradually throughout this period. Average state spending on cash assistance rose in the late 1980s and early 1990s but fell dramatically after the mid-1990s.
Finding #3B: These trends varied greatly between rich and poor states. Medicaid grew substantially for all states, but the growth was particularly strong among those of low fiscal capacity. The correlation between state fiscal capacity and per capita spending on Medicaid declined over time, as per capita spending by poor states climbed to levels only exceeded by the wealthiest states, while Medicaid spending in wealthier states grew slowly or stalled during the late 1990s.
States of different fiscal capacities also converged in their spending on cash assistance programs. Wealthier states reduced their spending during the middle and late 1990s, while poor states on average showed little change in their per capita spending on cash assistance throughout the last two and a half decades.
By contrast, differences grew between rich and poor states in their spending on non-health social service programs, especially in the late 1990s. Growth was fairly consistent among wealthier states through the 1980s and 1990s; growth in spending on these non-health services was much weaker, however, among the poorest states.
Finding #3C: These changes produced major shifts in the composition of social welfare budgets in rich and poor states. States of all fiscal capacity have greatly increased the proportion of their spending devoted to Medicaid while reducing the proportion spent on cash assistance. Poor states, however, unlike rich states, have also reduced the proportion of their budgets spent on non-health social services. Thus, the package of benefits offered by poor states has changed markedly in recent years, toward health care and away from non-health services.
Finding #4: Econometric analyses found that different factors influenced different social programs. Spending on cash assistance was increased by federal grants, and unemployment. Spending on cash assistance was also greater in urban states, i.e., those with higher population densities. There was a negative relationship between spending on cash assistance and state fiscal capacity. This negative effect not well understood, and could be related to the positive effect of wages on personal income and the negative effect of wages on cash assistance rolls.
Medicaid spending was increased by personal income, federal grants, and unemployment. However, the effects of federal grants (measured by federal grants for social welfare programs) were particularly strong for Medicaid spending, and population density had an effect opposite to its impact on cash assistance. Medicaid spending was greater, other things equal, in comparatively rural states, i.e., those with lower population densities.
Non-health social services was most affected by overall state income. It was strongly and consistently related to state fiscal capacity. It was also significantly related to federal grants for non-social-welfare programs. Like Medicaid (and public hospital payments), it was also higher in states with lower population densities.
Thus, some variables shaped the composition and dynamics of state social welfare spending. States with higher population densities spent more on cash assistance, while rural states with low population densities spent more on Medicaid, public hospitals, and non-health social services. Unemployment, an indicator of changing social needs, increased spending on cash assistance and Medicaid but not on non-health services or public hospitals.
Finding #5A: The econometric models were most successful in explaining spending differences and changes among wealthy states; the models fared less well in accounting for spending in poor states Most of the variables — including fiscal capacity, unemployment, and federal grants — showed relatively strong effects among the wealthier states. In poorer states, fiscal capacity, unemployment, and federal grants showed little or no effects. One important exception was Medicaid. Spending on Medicaid was significantly and strongly affected by federal grant dollars in poor states.
Finding #5B: There were substantial differences among poor states in their long-run propensities to spend on programs (as captured in the “state effects of the econometric model). In particular, there were different propensities for spending on cash assistance and health-related programs (Medicaid and public hospitals). Some poor states (mostly rural southern states) spent very little on cash assistance but relatively more on health-related programs, while other poor states (mostly in the West) had larger cash assistance programs and spent less on Medicaid. This trade-off between health and cash assistance programs was not found among wealthier states. Wealthier states were, in general, less likely than poor states to reveal negative correlations between their long-run propensities to spend on different program functions. Thus, poor states showed greater specialization in their spending “packages when compared to wealthier states.
Finding #6: Case studies of six states of low fiscal capacity and high social needs indicated that the basic trends in spending found among poor states before 2000 continued after that year. Spending on Medicaid grew in most of the poor states despite fiscal downturns. Large cut-backs in Medicaid eligibility and basic services were uncommon; in fact, some major program expansions occurred. Nor did cash assistance spending decline — in fact, some increases were found in spending on TANF assistance.
Major cuts were most often imposed on non-health social services and administrative expenses, especially staffing. This may have been a departure from previous recessions, when government employment was usually not strongly affected by revenue downturns. But our case studies revealed large reductions in front-line personnel, supervisors, and managers — and sometimes the elimination of entire local offices. Cuts were also made in employment services; transportation and other work supports; fatherhood, parenting, and pregnancy prevention programs; and child welfare services. Child care subsidies were reduced substantially in the two states that had devoted considerable state revenues to such subsidies in the past.
Finding #7: The case studies visits also revealed that, at least among poor states, spending in different program areas were typically determined by different political and administrative processes. Cash assistance programs were affected by the interaction between caseload levels and the rules and benefit levels determined (and not often revised) by state legislatures. Choices affecting cash assistance spending seemed to be more influenced by racial and ideological divisions in the state.
By contrast, Medicaid policies and expenditures were, especially in the rural southern and border states, strongly affected by the active political involvement of service providers, such as nursing homes, hospitals, physicians, and many others — resulting in a relatively bipartisan politics of institutionalized interests. This public-private interdependence was especially strong in the rural southern states and may help account for their relatively higher levels of Medicaid spending.
To be sure, the generous federal matching rates for Medicaid in poor states were also critical in state budget and policy processes; and poor states were strongly affected by federal changes in mandated eligible populations or minimal services, changes which were frequent in the Medicaid program during the late 1980s and early 1990s. However, these factors alone did not seem sufficient in accounting for Medicaid’s robust support during the recent state fiscal crises. Our case studies suggested that when a program has strong and active constituencies that supported greater spending, an attractive match rate may suffice to expand spending during boom times and prevent major cutbacks during recessions. If, however, a program (such as many in the child welfare area) does not have such strong political advocates, even the same federal match rate may not prevent major services during fiscal downturns.
Finally, non-health social services were typically of low political salience and administrators were often given significant discretion over how to allocate funds across different services. State resources, program flexibility, and executive priorities seemed more important in determining how much was spent on these non-health services and which services were funded and which were not.
Recent changes in federal programs affected the ability of poor states to support and control their non-health services to low-income people. For example, TANF surpluses and the block grant’s flexibility offered administrators and other officials greater control in determining spending priorities among these services, when they needed to make cuts. This flexibility — and the observed tendency of states to fund a wider range of programs under TANF and MOE — also created a more wide-ranging competition for resources among many services that probably had not competed before.
In sum, fiscal capacity remains an important factor in understanding state spending on social services. The most remarkable findings of the study, however, concern the different influences on spending across program areas and states. These differences suggest important dynamics in state spending on social welfare. Because different states and program areas are subject to different influences, we may continue to see — as we did find in the period from 1977 through 2003 — major shifts in the levels, composition, and distribution of state spending on various social welfare functions.
References
Barrilleaux, C. J., & Miller, M. E. (1988). The political economy of state Medicaid policy. American Political Science Review, 82, 1089 107.
Boyd, D., Billen, P., Rockefeller Institute of Government, Dearborn, P., & Brookings Institution. (2003). The fiscal effects of welfare reform: State social service spending before and after welfare reform (Final Report). Albany, NY: Rockefeller Institute of Government.
Boyd, Donald. 2003. “The Current State Fiscal Crisis and Its Aftermath. Paper prepared for the Kaiser Commission on Medicaid and the Uninsured. The Henry J. Kaiser Family Foundation.
Bradford, D. F., & Oates, W. E. (1971). The analysis of revenue sharing in a new approach to collective fiscal decisions. Quarterly Journal of Economics, 85(3), 416-39.
Brown, R. D. (1995). Party cleavages and welfare effort in the American states. American Political Science Review, 89, 23-32.
Compson, M., & Navratil, J. (1997). An improved method for estimating the total taxable resources of the states (Research Paper No. 9702). Washington, D.C.: U.S. Department of the Treasury, Office of Economic Policy.
Coughlin, T., & Zuckerman, S. (2002). States use of Medicaid maximization strategies to tap federal revenues: Program implications and consequences. Washington, D.C.: The Urban Institute.
Douglas, T., & Flores, K. (1998). Federal and state funding of children’s programs (Occasional Paper No. 5). Washington, DC: Urban Institute.
Dye, T. R. (1966). Politics, Economics, and the Public Policy in Outcomes in the American States. Chicago, IL: Rand McNally.
Dye, T. R. (1969). Politics in States and Communities. Englewood Cliffs, NJ: Prentice-Hall.
Dye, T. R. (1979). Politics vs. economics: The development of the literature on policy determinism. Policy Studies Journal, 7, 652 2.
Ellwood, J., & Boyd, D. (2000). Changes in state spending on social services since the implementation of welfare reform: a preliminary report (p. 35). Albany, NY: Rockefeller Institute of Government.
Fry, B. R., & Winters, R. F. (1970). The politics of redistribution. American Political Science Review, 64, 508 2.
Gais, T., & Weaver, R. K. (2002). State policy choices under welfare reform (Policy Brief No. 22). In I. Sawhill et al. (Eds.), Welfare reform and beyond: The future of the safety net. Washington, DC: The Brookings Institution.
Gamkhar, S., & Oates, W. (1996). Asymmetries in the response to increases and decreases in intergovernmental grants: Some empirical findings. National Tax Journal, 49(4), 501 2.
Gramlich, E. M. (1977). Intergovernmental grants: A review of the empirical literature. In W. Oats (Ed.), The political economy of fiscal federalism, 219 9.
Hicks, A., & Swank, D. H. (1983). Civil disorder, relief mobilization, and AFDC caseloads: A reexamination of the Piven and Cloward thesis. American Journal of Political, Science, 27, 695 16.
Hicks, A., & Swank, D. H. (1992). Politics, institutions, and welfare spending in industrial democracies, 1960 982. American Political Science Review, 86, 658 74.
Hines, J. R., Jr., & Thaler, R. H. (1995). The flypaper effect. Journal of Economic Perspectives, 9(4), 217 26.
Hirsch, B. T. (1985). Poverty, transfers, and economic growth. Public Finance Quarterly, 13, 81 8.
Jennings, E. T., Jr. (1980). Urban riots and the growth of state welfare expenditures. Policy Studies Journal, 9, 34 0.
Key, V. O., Jr. (1949). Southern Politics. New York, NY: Alfred Knopf.
Kousser, T. (2002). The politics of discretionary Medicaid spending, 1980 993. Journal of Health Politics, Policy and Law, 27, 639-671.
Ladenheim, K. (2002). Medicaid Cost Containment: A Legislator's Tool Kit. NCSL.
McGuire, M. (1978). A method for estimating the effect of subsidy on the receiver's resource constraint: With an application to U.S. local governments 1964 971. Journal of Public Economics, 10, 25 4.
Merriman, D. (2000a). What Accounts for the Growth of State Government Budgets in the 1990s? (Policy Brief No. A-39). Washington, D.C.: The Urban Institute.
Merriman, D. (2000b). Sources of Data about State Government Revenues and Expenditures. Washington, D.C.: The Urban Institute.
Mogull, R. G. (1978). State and local antipoverty expenditures. Public Finance Quarterly, 6 (3), 287 03.
Mogull, R. G. (1989). Determinants of state welfare spending. Mankind Quarterly, 30 (1/2), 39 5.
Mogull, R. G. (1993). Determinants of states' welfare expenditures. Journal of Socio-Economics, 22 (3), 259 77.
Orr, L. L. (1976). Income transfers as a public good: An application to AFDC. American Economic Review, 66, 359 1.
Plein, L. C. (2001). Welfare reform in a hard place: The West Virginia experience. (Rockefeller Report No. 13.) Albany, NY: Rockefeller Institute of Government.
Plotnick, R. D., & Winters, R. F. (1985). A politico-economic theory of redistribution. American Political Science Review, 79: 458 3.
Plotnick, R. D., & Winters, R. F. (1990). Party, political liberalism, and redistribution: An application to the American states. American Politics Quarterly, 18, 430 58.
Snell, R. K., Eckl, C., & Williams, G. (2003). State Spending in the 1990s. National Conference of State Legislatures.
Steuerle, C. E., & Mermin, G. (1997). Devolution as seen from the budget. Washington, DC: Urban Institute.
Tannenwald, R. (1998). Come the devolution, will states be able to respond? New England Economic Review, May/June, 53 3.
Tannenwald, R. (1999). Fiscal disparity among the states revisited. New England Economic Review, July/August, 3 5.
U.S. House of Representatives (2000). Background Material and Data on Programs within the Jurisdiction of the Committee
Appendix A
[This appendix is only available in a PDF version (Adobe's Portable Document Format).
If you want a printed copy or need help with accessibility, please contact us.]
Appendix B: Field Visit Documentation
Field Visit Documentation
The study "Spending on Social Welfare Programs in Rich and Poor States" examined the policies, institutions, and processes of six states with low fiscal capacity and high social needs to better understand how these states make decisions in funding social welfare programs, and to identify factors that influence their social welfare spending. The six states selected for analysis were Arizona, Louisiana, Mississippi, New Mexico, South Carolina, and West Virginia. This Appendix includes a brief discussion of the fiscal capacity and need measures for the six states examined and the methodology used for this study component. Also included are narratives that briefly describe significant features of each state's budget process, its reaction to federal welfare reform, and trends in non-Temporary Assistance for Need Families (TANF) federal programs that influence state social welfare spending decisions.
Fiscal Capacity and Need Measures
Per capita personal income data suggest that the six states selected for analysis have less potential to raise revenue than most states. As noted in Exhibit Appendix B-1, Mississippi and West Virginia rank the lowest in ability to raise revenue in 1995 and 2001, 50 and 49 respectively, using per capita personal income as the measure of fiscal capacity. New Mexico, Louisiana, and South Carolina rank in the lowest quartile of states, and Arizona falls in one of the bottom two quartiles depending on the year analyzed.
| 1995 | 2001 | |||
|---|---|---|---|---|
| PCPI | State Ranking | PCPI | State Ranking | |
| Mississippi | 16,984 | 50 | 21,750 | 50 |
| West Virginia | 17,882 | 49 | 22,881 | 49 |
| New Mexico | 18,435 | 47 | 23,155 | 47 |
| Louisiana | 19,314 | 40 | 24,535 | 44 |
| South Carolina | 19,221 | 41 | 24,886 | 41 |
| Arizona | 20,050 | 36 | 25,872 | 38 |
| United States | 23,255 | 30,472 | ||
| Source: Per capita personal income levels developed by Rockefeller Institute staff using U.S. Department of Commerce, Bureau of Economic Analysis and Census Bureau data. The levels are in current dollars and were developed by dividing total personal income by total mid-year population estimates. | ||||
The six states also rank low in fiscal capacity using other measures such as representative tax system and total taxable resources. Exceptions are Louisiana and New Mexico, which rank somewhat higher using total taxable resources. This can probably be explained, for the most part, by income from oil and natural gas production that may not be captured by other measures.
| 1995 | 2001 | |||
|---|---|---|---|---|
| Rate | State Ranking | Rate | State Ranking | |
| New Mexico | 25.5% | 1 | 17.4% | 2 |
| Louisiana | 21.9% | 2 | 16.7% | 3 |
| Mississippi | 21.3% | 3 | 16.6% | 4 |
| Arizona | 18.2% | 4 | 13.3% | 12 |
| West Virginia | 17.6% | 6 | 15.3% | 5 |
| South Carolina | 15.6% | 14 | 12.7% | 14 |
| United States | 13.2% | 11.1% | ||
| Source: Poverty rates developed by Rockefeller Institute staff using U.S. Department of Commerce, Census Bureau data. The rates are three-year averages calculated using the number of poor people and total population: for example, the poverty rate for 2000 is equal to the average of the number of poor people in 1999, 2000, and 2001 divided by the total population in 2000. | ||||
Poverty and unemployment data suggest that the six study states have high social needs when compared to the rest of nation. As noted in Exhibit Appendix B-2, all of the selected states have poverty rates above the national rate. New Mexico, Louisiana, Mississippi, Arizona, and West Virginia had poverty rates in 1995 that were among the highest in the nation. Although poverty rates in general improved from 1995 to 2001, Arizona's improvement was somewhat greater than other states, moving from the fourth highest rate in the nation in 1995 to the twelfth highest in 2001. Four of the states selected for further analysis, Louisiana, Mississippi, New Mexico, and West Virginia, had unemployment rates higher than the national rate from 1995 to 2003 (see Exhibit Appendix B-3). Although unemployment declined in general from 1995 to about 2000, West Virginia's decline was greater than other study states, falling from 7.9 percent in 1995 to 4.8 percent in 2001. Arizona's unemployment rate remained close to the nation's average rate from 1995 to 2001. South Carolina's rate was also about average until about 2000 when it increased more rapidly.
Exhibit Appendix B-3:
State Social Need - Unemployment Rates
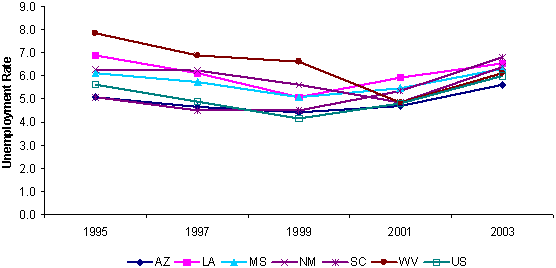
Source: Calendar year unemployment rates calculated by Rockefeller Institute staff using U.S. Department of Commerce, Bureau of Labor Statistics seasonally adjusted data.
Methodology
As noted in Section II.C., Arizona, Louisiana, Mississippi, New Mexico, South Carolina, and West Virginia were selected for further analysis using a three-step process that examined measures of state fiscal capacity and need for social welfare services. Staff from the Rockefeller Institute of Government and The Lewin Group spent approximately three days in each state interviewing executive budget and program officials; legislators and staff; and high-level agency staff responsible for the state's TANF, Medicaid, child welfare, welfare employment, and child care programs. The site visits took place from August to November 2003. Project researchers visited West Virginia and Arizona in August, South Carolina and New Mexico in September, and Louisiana and Mississippi in November.
Interview questions covered state budget formulation and implementation; social welfare policies and spending; state response to changes in federal programs; program constituencies; and state support of social welfare programs during the recent economic boom and downturn. Project researchers also reviewed public documents including state social welfare legislation and regulations; federally required state plans, performance reports and expenditure data for large social programs; federal and state agency reports; state budget bills and summaries; newspaper articles; and, where available, previous work completed by Rockefeller Institute and other researchers.
The six states selected for further analysis have fiscal years that begin July 1. All have annual budget cycles except for Arizona, which has a biennial cycle. Each state had enacted its state fiscal year (SFY) 2003-04 budget prior to the project's site visit and state officials were in the process of developing their SFY 2004-05 budget proposals when visits were completed. The governors of three study states, Arizona, New Mexico, and South Carolina, were in their first year of office when interviews were completed. Two study states, Louisiana and Mississippi, have sworn in new governors since the site visits were completed. The narratives for Louisiana and Mississippi that follow include information on the goals and priorities of the new governors where possible.
For each state, we use National Association of State Budget Officers (NASBO) 2002 data to provide information on total state expenditures, TANF expenditures, and Medicaid expenditures. There are interesting observations when comparing spending patterns for the six states selected for further analysis to the nation. For example, Arizona, Louisiana, Mississippi, and South Carolina spent a lower proportion of their total expenditures on TANF compared to the nation, whereas New Mexico and West Virginia spent a higher proportion of their total expenditures on TANF. Arizona, New Mexico, and West Virginia spent a lower proportion of their total expenditures on Medicaid compared to the nation, whereas Louisiana, Mississippi, and South Carolina spent a higher proportion of their total expenditures on Medicaid.
State Narratives
Arizona
Population (July 2003): 5.6 Million
Total State Expenditures - SFY 2002: $18,983 Million (US Total: $1,073,816 Million)
TANF Expenditures - SFY 2002 (% of total): 0.7% (US: 1.3%)
Medicaid Expenditures - SFY 2002 (% of total): 19% (US: 20.8%)
(Source: U.S. Department of Commerce, Census Bureau and NASBO 2002 State Expenditure Report)
Arizona's per capita personal income is lower than the national average, although higher than any of the other five states in the case study. As noted earlier, in 1995 and 2001, Arizona, while not in the bottom quartile, was in the second to bottom quartile when ranking states using this measure. Data from the state's Joint Legislative Budget Committee indicate that 95 percent of Arizona's state revenue comes from sales, personal income, and corporate taxes. The state relies heavily on sales tax with 52 percent of its revenue in 2003 coming from this source. The committee is projecting revenue from the three taxes to continue to recover in 2004 and 2005 after either declines or declining growth from 1999 to 2002. Information from the Center on Budget and Policy Priorities suggests that Arizona faces a significant budget deficit of approximately $1.1 billion for SFY 2005.
Arizona's overall poverty rate is higher than the national average. Arizona's rapid growth in population from 1995 to 2003, over one million new citizens or a 25 percent increase, has put pressure on the state budget by increasing need from all government services. The state has also experienced an increase in cash assistance and Medicaid caseloads. Arizona's cash assistance caseload increased 53 percent from January 2001 to June 2003, compared to a 5 percent decline for all states. Medicaid caseload has also increased due to an expansion in eligibility from a voter-driven initiative discussed below.
State Budget Development and Implementation
Arizona slowly transitioned from an annual to biennial budget in the 1990s. In 2002, the state returned to an annual budget cycle for larger state agencies including the Department of Economic Security (TANF, Food Stamps, child care, child welfare, adoption, foster care, and child support enforcement) and the Arizona Health Care Cost Containment System (Medicaid and State Child Health Insurance Plus (SCHIP)).
Arizona's budget process begins with the governor providing funding targets to state agencies for the upcoming fiscal year. State agencies submit their budget requests to the Governor's Office of Strategic Planning and Budget (OSPB) in September. OSPB shares these requests with staff of the Joint Legislative Budget Committee (JLBC). The governor presents his or her budget proposal in January. The legislature presents a separate budget that can be very different from the executive proposal. The state Constitution and statute impose a balanced budget requirement on both the executive and legislative branches of government, although there is authority to incur up to $350,000 in debt. Arizona does not have a consensus revenue forecast requirement.
The Arizona legislature has been characterized as the most powerful branch of government in the state in budget development. The state's Constitution gives the legislature authority to develop, amend, and pass budget bills for the governor's signature. A state official interviewed indicated that it can be difficult for the executive to get the legislature to incorporate the governor's priorities in its budget. The executive must lobby the legislature by way of the Governor's state of the state address, appropriations hearings, and other avenues.
Governors can direct state spending through the threat and use of their veto authority that includes the ability to veto specific items or the entire budget bill. Governor Janet Napolitano, who took office in 2003, is currently being sued by members of the legislature over 13 line-item vetoes to the legislature's SFY 2004 budget. The vetoes delayed $75 million in payments on a class action tax lawsuit and restored more than $31 million in legislative cuts to state agencies, social services, and education. The legislature argues that Governor Napolitano's vetoes violated the separation of powers between the executive and legislative branches of government and intruded on the legislature's appropriation authority. The outcome could impact the governor's power in future budget cycles.
Citizen-driven initiatives limit the ability of the legislature to raise revenue and direct spending. Successful ballot measures that impose significant restraints include:
- Proposition 108-Limits the ability of the legislature to raise revenue by requiring a two-thirds vote by the legislature to enact a tax or fee increase. The same two-thirds vote is necessary to eliminate or reduce a tax deduction or exemption.
- Proposition 204-Expanded eligibility for the state's Medicaid program and allocated state tobacco settlement funds to this effort.
- Proposition 105-Limits the legislature's ability to amend citizen-driven initiatives by requiring three-fourths vote by the legislature to amend a proposition and only when the action furthers the proposition's purpose.
Arizona's Response to Federal Welfare Reform(1)
Arizona initiated its welfare reform efforts in late 1995 through waivers from the federal government. The state's EMPOWER program, (Employing and Moving People Off Welfare and Encouraging Responsibility), included requirements under consideration for federal welfare reform including time-limited cash assistance, automatic sanctions for not meeting JOBS work requirements, a family benefit cap, transitional medical and child care assistance, restricted eligibility for unwed minor parents, and individual development accounts.
The state legislature began work on Arizona's second round of reform efforts in 1996 by holding a series of meetings and hearings to gather information on the EMPOWER program. The legislature heard from state agency officials, local officials, welfare advocates, welfare recipients, and others. The two houses of the state legislature ultimately presented welfare reform packages that differed significantly. The state senate, the more conservative body, was skeptical about the incentives in the existing state bureaucracy to reduce caseload and supported the complete privatization of the new welfare program. The state's house (and executive) favored restructuring Arizona's welfare agency to meet the goals of federal welfare reform. A compromise was reached to privatize eligibility and job services decisions in a limited number of sites, for a limited time, and with an evaluation requirement.
Empower Redesign, the state's TANF program, went into effect in August 1997. The new program built upon earlier efforts to establish a more employment focused "work first" client flow, require Personal Responsibility Agreements, institute progressive reductions in monthly cash assistance benefits including a full-family sanction for not complying with requirements of the Personal Responsibility Agreement, and elimination of exemptions from work requirements.
Due to the block grant structure of TANF and the decline in Arizona's welfare caseload in the late 1990s, the state accumulated a surplus of federal TANF funds. In SFYs 1999 and 2000, Arizona used TANF to implement new programs including Wheels-to-Work, Character Education Training, Young Fathers, Employment Transition Program, Domestic Violence Training, Post-Employment Education Program, and Technical Assistance to Business. These programs were eliminated to meet demands for cash assistance payments when Arizona's TANF caseload began to increase shortly after the recent economic downturn. Several programs providing child protective services, substance abuse services, and grant diversion payments, implemented with TANF funds, survived the initial round of cutbacks.
Other Federal Social Welfare Programs
The impact of Proposition 204 on Arizona's Medicaid program was the most significant issue for non-TANF social welfare programs when we interviewed state officials. The citizen initiative expanded Medicaid eligibility from 36 percent of the 1992 federal poverty level to 100 percent of the current federal poverty level, and allocated tobacco settlement money to support the newly eligible population, although these funds have not covered all non-federal costs and state general fund dollars have been used. Shortly after passage of the ballot measure, the legislature shifted responsibility for determining eligibility for many of Arizona's healthcare programs from the counties to the state Department of Economic Security.
OSPB and JLBC projections suggest that Proposition 204 will increase enrollment in the state's Medicaid program by approximately 188,300 to 211,400 individuals by SFY 2004, and will cost over $1.1 billion in federal and state funding. The state general fund will support approximately $187 to $195 million of the increased costs. Critics of Proposition 204 suggest that the increased costs associated with the ballot measure, make services that are not voter protected more vulnerable to budget cuts, especially in an economic downturn.
Louisiana
Population (July 2003): 4.5 Million
Total State Expenditures - SFY 2002: $17,608 Million (US Total: $1,073,816 Million)
TANF Expenditures - SFY 2002 (% of total): 0.8 % (US: 1.3%)
Medicaid Expenditures - SFY 2002 (% of total): 26.8% (US: 20.8%)
(Source: U.S. Department of Commerce, Census Bureau and NASBO 2002 State Expenditure Report)
Louisiana has low fiscal capacity as measured by per capita personal income and representative tax system (43rd on both). It ranks 26th if fiscal capacity is measured by total taxable resources, which are largely based on goods and services produced in the state, and reflect the value of oil production. Louisiana holds almost 10 percent of U.S. oil reserves, making it the country's third largest producer of petroleum. It also has large reserves of natural gas, producing over one-quarter of all U.S. supplies.
Although Louisiana's poverty rate declined in the 1990s, its level has remained high. 2001's 16.7 percent poverty rate is among the highest in the nation, exceeded only by Arkansas and New Mexico. In 2000, 51.5 percent of Louisiana's children lived in households at or below 200 percent of the federal poverty rate and 13.4 percent of those children had no health insurance, placing Louisiana second highest nationwide after New Mexico. Unemployment is above average, as well, increasing 5.1 percent in 1999 to 6.6 percent in 2003.
State Budget Development and Implementation
In 1987, Louisiana moved from line item budgeting to program budgeting, and since 1997, it has implemented a performance-based budgeting system. The governor's office sets priorities and budget strategies. The legislature is not an independent body by practice, and is influenced by the governor, who carries line-item veto power. Political parties do not represent the major political divisions in Louisiana, and the governor's party has less impact on how the legislature reacts than in many other states. In general, Louisiana state government is more divided along policy lines.
The revenue forecast is adopted by the Revenue Estimation Conference, comprised of the governor, the president of the Senate, the Speaker of the House of Representatives (or their respective designees), and a faculty member from a public or private university in the state. The state constitution forbids the legislature from adopting a budget that exceeds the Conference's adopted revenue forecast. The budget originates in the Division of Administration (DOA), the central budget agency for the governor, which prepares the general budget guidelines for executive agencies. From August to December, the executive agencies prepare and submit budget requests to the DOA. The DOA then reviews the requests and prepares an executive budget for the legislature. Prior to the regular legislative session, the general appropriations bill is introduced, putting the governor's executive budget recommendations into a legislative proposal. This bill originates in the House, and, if passed, it is sent to the Senate. Once the bill is introduced in the Senate, it is referred to the Senate's Committee on Finance. After the Committee hearings, the Senate votes on the bill, and if passed, it is returned to the House for concurrence. The House then sends the bill to the governor for review and signature.
According to the Center on Budget and Policy Priorities, Louisiana faces a projected budget shortfall of $500 million in SFY 2005. Although Louisiana did not make any cuts after the budget was passed in SFY 2002, Louisiana reduced the SFY 2003 budget by $100 million mid-year. Louisiana has also been cutting state agency positions. Between SFYs 2001 and 2002, its full-time equivalent positions were reduced by 17.5 percent, including state administered welfare system positions.
Several areas of the state budget are considered non-discretionary and not subject to budget cuts, including natural resources programs, debt services, and the Minimum Foundation Program. Social services programs, however, are discretionary and subject to cuts. Higher education and economic development recently have been given higher priority in the budget process through efforts by the governor.
Louisiana's Response to Federal Welfare Reform
Louisiana's TANF and childcare programs are administered by the Office of Family Support within the Department of Social Services (DSS) and the state's child welfare, adoption, and foster care programs are administered by the Office of Community Services, also within the DSS. In 2001, the TANF Executive Office of Oversight and Evaluation was established within the Division of Administration to oversee the state's TANF initiatives.
In January 1997, Louisiana implemented two principal TANF programs: Family Independence Temporary Assistance Program (FITAP) and Family Independence Work Program (FIND Work) both administered by the DSS. FITAP provides time-limited cash grants to needy families. FIND Work (the work component of the state TANF program) provides job preparation, work, and support services to place recipients in jobs or in educational, training, and other work-related activities. In March 2000 Louisiana implemented another TANF program - Kinship Care Subsidy Program - which provides assistance to children residing with relatives other than their parents.
Louisiana's welfare caseloads fell by 66 percent from 1993 to 1999. In the same period, the poverty rate decreased 27 percent (to 19 percent). Louisiana limits cash assistance to twenty-four months in a sixty-month period. According to DSS reports, two percent of Louisiana families receive cash assistance. Seventy-seven percent of welfare recipients are children, nearly all of whom live in households headed by females, and 86 percent of welfare recipients are African-American. Louisiana's maximum TANF benefit level is low; from 1985 to 2000, the maximum benefit for a three-person family was $190. In 2001, the state increased its benefit level for a family of three to $220.
During the initial years of FITAP and FIND Work, Louisiana accumulated a large surplus of unspent federal TANF block grant funds, partially due to declining welfare rolls. In addition, the state was slow to respond to the increased flexibility afforded by welfare reform. In 2001, Louisiana began using TANF funds for a variety of programs, referred to as TANF Initiatives, to focus on the broader low-income population. The TANF Initiatives included 22 different service initiatives for low-income families in 11 agencies.2 For example, the state's pre-kindergarten program was created to provide high quality early childhood services for low-income 4-year-olds, and is funded with federal TANF funds. To help oversee this broad range of diverse programs, the TANF Executive Office of Oversight and Evaluation was established in 2001 within the Division of Administration to oversee and evaluate TANF initiatives. The TANF Office is involved in (1) developing, approving, and monitoring performance measurement and accountability standards; (2) TANF budget development and approval; (3) capacity building and technical assistance; and (4) evaluation of FITAP and FIND Work services. The TANF Office also funded a number of research projects including a needs assessment of low-income families, a mapping of poverty indicators, a fragile families study, a teen pregnancy prevention study, and a welfare leavers' study. Allocations for TANF initiatives grew from $89 million in FFY 2002 to $154 million in FFY 2003, but declined to $117 million in FFY 2004. However, FFY 2004 is the last "big year" for TANF initiatives, since the unexpended funds from prior years will be exhausted in FFY 2005. According to state officials' projections, only $37 million will be available for funding TANF initiatives in FFY 2005 due to the reduction in TANF funds transferred to CCDF. Most of Louisiana's TANF expenditures during this period have been for non-assistance service initiatives to low-income populations.
Other Federal Social Welfare Programs
Louisiana's Medicaid and LaCHIP (Louisiana's SCHIP program) programs are administered by the Department of Health and Hospitals (DHH). The number of Medicaid enrollees including LaCHIP, increased 17 percent from 1997 to 2002. This enrollment increase was primarily for children, due to the successful outreach efforts to enroll them in LaCHIP. In SFY 2003, Louisiana's Medicaid program was further expanded for children, aged, and the disabled. Changes were also made for pregnant women by expanding the program in January 2003 to cover those under 200 percent of federal poverty level (after a 15 percent income disregard).
Louisiana also has a high disproportionate share hospital (DSH) cap. The availability of these large DSH funds allows the state, primarily through the state charity hospital system administered by the Louisiana State University Health Care Services Division, to provide medical care to approximately 800,000 uninsured citizens in Louisiana. DHH continues to explore ways to provide more primary care through DSH funding.
Health care comprises almost a third of the Louisiana's total budget. The state is projected to receive $3.6 billion in federal Medicaid funds for FY 2004. In SFY 2003, federal fiscal relief reduced the severity of originally planned long-term care and pharmacy cuts that had been proposed to reduce state Medicaid funding.
The SFY 2004 budget adopted by the legislature included a significant policy change affecting the operation of the state's charity hospitals. Louisiana State University (LSU) was granted more power to manage the public (charity) hospitals that it operates for the state. This allowed them to cut hospital spending by up to 35 percent of a previous year's actual expenses without legislative approval, as opposed to the up-to-10 percent previously allowed by law. Hospitals will be allowed to charge non-emergency patients whose incomes are at least twice the poverty level. Governor Blanco and the DHH secretary discussed several short-term improvements that involved (1) enrolling as many eligible children as possible into Children's Health Insurance Program and, (2) increasing the number of federally qualified health centers.
The programs administered by the DHH have a powerful lobby, unlike the ones administered by the DSS. The Nursing Home Association is one of the most powerful lobby groups in Louisiana. Other influential advocacy groups include the Area Health Education Consortium, groups representing Mental Retardation Developmental Disability (MR/DD), and drug industry associations.
Louisiana's Office of Family Support within the Department of Social Services is the lead agency for the Child Care and Development Fund (CCDF). According to federal administrative data, Louisiana's total CCDF expenditures decreased from $128 million in FFY 2001 to $33 million in FFY 2002, or by 74%. This decrease is largely due to an 82 percent decline in discretionary spending, from $104 million in FFY 2001 to $19 million in FFY 2002. From FFY 2001 to FFY 2002, the TANF transfer to CCDF was cut by 25.7%. In Louisiana, recent childcare policy changes include increased co-payments, restrictions on the number of eligible families, and an increase in the number of hours parents must work to qualify for childcare assistance.
Mississippi
Population (July 2003): 2.9 Million
Total State Expenditures - SFY 2002: $10,521 Million (US Total: $1,073,816 Million)
TANF Expenditures - SFY 2002 (% of total): 0.7 % (US: 1.3%)
Medicaid Expenditures - SFY 2002 (% of total): 26% (US: 20.8%)
(Source: U.S. Department of Commerce, Census Bureau and NASBO 2002 State Expenditure Report)
Mississippi has the lowest fiscal capacity in the nation based on per capita personal income, representative tax system, and total taxable resources. Its poverty rate of 16.6 percent for 2001 is among the highest, exceeded only by New Mexico and Louisiana in the six sample states. However, in 2000 the proportion of children without health insurance was only slightly above the national average: 7.7 percent of children below 200 percent of the federal poverty level did not have health insurance, compared to an average state rate in the U.S. of 6.8 percent. Mississippi thus resembles South Carolina and West Virginia-whose percentages of children without health insurance are also near the national average-rather than New Mexico, Louisiana, and Arizona, where the percentages of children without insurance are much higher.
Although the state's poverty rate remains high, it declined greatly in the 1990s, from 25.6 percent in 1991 to 15.6 percent in 1999. Unemployment also dropped from 8.8 percent in 1991 to 5.1 percent in 1999, after which it rose to 6.8 percent in 2002. Major industries in the state have included automobiles, poultry, timber, and gambling casinos (on the river). The state's population grew more slowly than the national average: 5.5 percent between 1995 and 2002. Unlike most states, tax revenues grew every year between FY 2000 and FY 2003, though the rate of increase declined after 2000. The state has had a series of budget shortfalls due to rising needs as well as slow revenue growth.
State Budget Development and Implementation
The governorship has traditionally been weak in Mississippi. The office has no line item veto power. Thus, even though the state legislature only meets 90 days per session in the early spring, the legislature has long played the dominant role in developing and enacting the budget. However, the governor has significant control over its implementation and adjustments in the budget if revenues are lower than expected.
The state budget process lasts about one year. For the SYF 2005-06 budget the Legislative and Executive budget offices solicit budget requests from agencies beginning in July 2004. These requests will be submitted to both budget offices by August 1, 2004. Beginning September 2004 the Joint Legislative Budget Committee conducts budget hearings with top agency officials to review the requests. The Governor will submit the executive budget in November of 2004. The legislative budget recommendation will be released and published in November and December 2004. The legislative session begins in January 2005 and the appropriation bills for the FY2006 budget will be finalized and passed by April 2005.
The governor and legislature adopt a consensus revenue estimate drawing on (though not constrained by) revenue estimates provided by the Revenue Estimating Committee, composed of people from the executive and legislative branches as well as institutions of higher learning. Division directors develop budget requests based on what services are mandated and what services may be funded with what remains. By statute, the legislature can only appropriate 98 percent of projected revenue.
The governor has the authority to manage the budget during the fiscal year to ensure expenditures do not exceed revenues. Should revenue come in more than two percent short of projections through the current month, the governor must adjust spending to stay within projected revenues. The governor can make selective cuts to agency budgets of up to five percent to stay within revenue projections. State statute exempts several agencies from these cuts. Cuts exceeding 5% must be administered across the board.
The Department of Human Services (DHS) administers TANF, CCDF, Social Services Block Grant (SSBG), child welfare, and most other social welfare programs. Prior to FY 2005 DHS also determined eligibility for Medicaid and SCHIP programs. However, Medicaid and SCHIP are administered by the Division of Medicaid operating within the Office of the Governor. Until 1992, the Department was largely governed by an advisory board. But the legislature disbanded the board in that year and the governor was given greater and more direct control over DHS, including appointment of its director.
Nonetheless, legislators retain significant control over the Department's actions. The budget is very specific on programs, especially those they care about, such as Medicaid. Separate appropriation bills must be passed for each agency. Legislators also limit DHS's discretion over policies. Some state officials consider Mississippi's Medicaid program to be the most codified in the U.S., with reimbursement and coverage policies detailed in law-governing, for example, how many office visits as well as prescriptions are permitted per year.
DHS and its administration of major social programs are centralized. Most programs are administered by state officials through local state offices, not through counties or other local governments.
In recent years, as needs grew due to expanded enrollments in social programs and revenue growth slowed, the budget process became quite contentious between the legislature and the governor, even though both branches were controlled by Democrats from early 2000 to early 2004. A major source of uncertainty was Medicaid. Since SFY 2002, the Medicaid budget has faced recurrent deficits. At first, the shortfalls were covered with tobacco funds, but then some cuts were made in reimbursement rates to providers. More recently, Medicaid deficits have been alleviated by increases in the federal matching rate (FMAP) and last year's one-time federal grant to states. Medicaid has generally been protected from major cuts. Along with health care programs, other programs protected from significant budget reductions include economic development programs and, most of all, education, which takes up 62 percent of state general revenues.
Compounding the budget controversies has been the tendency of the legislature and the former governor to use different revenue projections. The former governor, for example, advocated reducing the revenue estimating committee's projection of SFY 2002 revenue growth to one percent, while the legislature adopted an estimate of 3.7 percent. In the 2003 session, most observers thought that legislators knew they had padded or overstated the budget. Over-projection of revenue forced the governor to cut agencies only after the legislature enacted the budget.
Mississippi's Response to Federal Welfare Reform
Mississippi began to reform its welfare programs with passage of a bill in late 1992, though its AFDC waiver request was not approved by U.S. Department of Health and Human Services until mid-1995. The waivers involved two programs, Work First and Work Encouragement. Work First, the larger program, made benefits contingent on fulfilling work requirements and introduced new mandatory processes for applicants. After the enactment of TANF at the federal level, the Mississippi legislature passed its TANF program, called the TANF Work Program (TWP), in early 1997. The debates over the early AFDC reforms and the TANF program were very divisive, especially along racial lines (Breaux, et al. 2000) and in the early 1990s, when the state legislature focused on out-of-wedlock births and marriage.
Mississippi's TANF program features immediate work requirements, time limits, full family sanctions, a family cap, and transitional child care and transportation services. Maximum cash benefits for a three-person family are $170 per month, which was increased from $120 in 2000, the only increase in the stipend in the last 26 years. In determining benefits, Mississippi disregards all income for some families for up to six months; otherwise, it disregards $90 of earnings. Its asset rules are somewhat more liberal than average: it disregards the entire value of one vehicle and $2,000 in assets beyond that. The state's sanctions are strict, however. Its first sanction for non-compliance with work requirements is imposed for two months, a longer than average duration for full family sanctions. The state does not have a diversion program. Its lifetime time limits (60 months) follow the federal law.
The low benefits, the severity of the sanctions, and early problems of implementation (such as complex applications processes involving multiple local agencies) probably contributed to the very large caseload declines of the 1990s-72 percent between 1995 and 2000. Since 2000, caseloads rose 23 percent through 2003. Yet, even with the caseload increases, TANF assistance plays a relatively small role in Mississippi's safety net. Only 1.3 percent of the Mississippi population received TANF assistance in 2001, compared, for example, to 10.7 percent of the population who received Food Stamps. Federal spending on Food Stamp benefits was 9.4 times greater in 2001 than total TANF assistance payments (Mississippi Department of Human Services 2003).
Mississippi's large decline in caseloads and its low benefits meant that it was able to accumulate large TANF surpluses. By 2000, the state could pay very little of its current year TANF grant on assistance. In fact, by 2001, it spent none of its current-year TANF grant on cash assistance. The surplus allowed the state, by 2000, to transfer the maximum amounts from TANF to CCDF and SSBG (30 percent of the grant in FFY 2002), and to increase other non-cash spending. In FFY 2002, major categories of spending under TANF included work subsidies, education, and training (25 percent); child care (37 percent, including the 20 percent transferred to CCDF); transportation and other supportive services (19 percent); and transfers to SSBG (10 percent).
In the last two fiscal years, however, moderate increases in caseloads have pushed up spending on TANF assistance, including cash payments, child care (for persons on assistance), and transportation services. The TANF block grant has also been used to fund additional programs while it pulled back from others. TANF thus serves as a "cushion" that agencies have used to fund high-priority items. For example, in FY 2004, about $26 million (about 27 percent of the annual block grant) was allocated to child welfare programs. Despite the attractive match rate for such programs (usually the same as under Medicaid), the state reduced its appropriations for this already cash-strapped, high-stakes service area-and TANF was used to compensate. By contrast, TANF funding was reduced or eliminated for several other programs in FY 2004, including fatherhood programs, SSBG, an adolescent offender program, some child care programs (not CCDF), education programs, and programs under the Attorney General.
During these tight budget years, the state has also struggled to satisfy its Maintenance of Effort (MOE) requirement. Among other things, they moved assistance families with two parents into a separate state program funded with MOE dollars (thus freeing $2 million in TANF), and they identified dollars spent in existing state programs that they could count as MOE. Such programs included certain university scholarships for low-income families, after-school programs, and mental health services.
Although TANF supports a wide array of services, "welfare" is still not a popular program in the state. The program is identified with minorities and the public perception is still that people do not want to work. Even state child advocacy organizations pay little attention to TANF per se. However, there have been effective advocacy efforts for child care, e.g., the Low Income Child Care Institute, run by a former director of the state Office of Children and Youth.
Other Federal Social Welfare Programs
Prior to FY 2005 the DHS's Division of Economic Assistance administered the Medicaid Program. However, the Division of Medicaid operating within the office of the Governor determines the Medicaid eligibility for the poverty level aged and disabled and for nursing home residents. Mississippi's spending per Medicaid enrollee is below the national average for all categories of enrollees, with the exception of nonelderly, nondisabled adults. The state's Medicaid eligibility standards are close to federal minimums; therefore, cuts in Medicaid enrollment or benefits are difficult. Tobacco settlement funds were used to fund the SCHIP program and eligibility expansions for the aged and disabled, allowing small expansions of benefits and increases in some provider payment rates.
Political support for Medicaid and SCHIP is strong. First, the programs have strong and organized proponents, such as hospitals, nursing homes, and doctors. Nursing homes, for example, beat back a recent legislative threat to reduce nursing home coverage. Among child advocates, SCHIP is the primary focus. The strong lobbying has been one reason why the Medicaid program is so "codified" and the executive director of the Medicaid division has so little control over the program.
Second, many people are enrolled in the programs: 25 percent of the population is on Medicaid; 57 percent of the children are enrolled in Medicaid or SCHIP. Outreach for SCHIP expanded enrollment in the regular Medicaid program (every child in SCHIP brought two children into Medicaid).
Third, the Medicaid program's match rate (3 to 1) is very attractive. One administrator makes the argument that the program is an economic development issue. Mississippi has also used intergovernmental transfers with Disproportionate Share Hospitals (DSH) funding to maximize federal dollars. In FY 2000, intergovernmental transfers constituted over 40 percent of the state share. The state share is funded through intergovernmental transfers and participating hospitals keep a fixed percentage of the revenues thus generated. The state began a new Upper Payment Limit (UPL) program for hospital reimbursement in 2000.
For all these reasons, Governors pay much more attention to Medicaid than to other human services, and legislators generally have a good relationship with Medicaid officials. (By contrast, Human Services has had three directors in the last three years and has not had a good relationship with the state legislature.) In 1999, Mississippi was the first state to establish a health care trust fund with money from the state's tobacco settlement. Mississippi's tobacco settlement funds are all targeted for health, about two-thirds of which is allocated to Medicaid.
Although Medicaid has been fairly well protected through SFY 2004, the legislature made some modifications and cuts in reimbursements. Some reductions were made in benefits, such as those involving eyeglasses and prescription drugs. In SFY 2004, the state faced a $90 million deficit, which was helped by an increase by the federal government in the state's FMAP rate.
It has been hard for Mississippi to hold spending down in Medicaid. There is a growing number of elderly in the state, especially those over 85. Expenditures per enrollee have grown, largely among recipients who cannot be dropped, including the elderly, the blind and disabled, and cash assistance children. The state is still doing SCHIP outreach, which brings in Medicaid applicants.
Pharmacy costs have also grown enormously, though some cost containment efforts have been underway. Other major sources of growth in costs include nursing homes, outpatient hospital services, hospices, and home and community based waiver programs. The state's managed care initiative was not very effective in holding down costs.
As a result of Medicaid's protection and growing costs, the program's spending has taken a growing share of the state's human services budget. Its share of the budget grew from 69 percent in 1998 to 75 percent in 2003.
The SSBG is federally funded and gets little attention from legislators, according to an administrator. It is largely used to support protective services, family planning, mental health services among other programs. The grants go to the agencies rather than the particular programs-so the block grant, like TANF, has provided state officials greater flexibility in shaping their package of social programs. However, the SSBG has declined even in nominal terms, from $23.4 million in 1998, to $16.4 million in 2004. As noted above, 10 percent of the TANF grant is transferred to SSBG, all of which goes to programs aimed at child neglect and abuse.
The CCDF is, as noted above, partly funded with TANF dollars. Before recent cutbacks, the program was able to support low-income working parents or students below 85 percent of the state's median income. But the eligibility level has been lowered to 50 percent of median income. Child care for TANF clients is automatic for those who are working, and there is one-year transitional benefit. There are extensive waiting lists for child care subsidies, about 12 thousand in the fall of 2003.
The state relies very heavily on federal dollars for child care, either from the CCDF or the TANF grant. Although CCDF allows states to put up state matches and draw down additional dollars, Mississippi has never been able to draw down the entire match. To increase the state's match, the agency (Office of Children and Youth) has used expenditures for Mississippi's lunch programs, reading programs, and others as MOE expenditures for TANF and CCDF. Child care does have some effective advocates, but legislators have mixed attitudes, and few pay any attention to developmental or quality issues.
Of the several divisions in the Department of Human Services, only a few rely significantly on state funding. Youth Services gets 68 percent of its funds from state general revenues; Economic Assistance gets 26 percent from general revenues; Family and Children's Services get 13 percent; while all the other divisions get less than 10 percent of their funds from the state. Thus, this low fiscal capacity state is very vulnerable to changes in federal spending.
Spending pressures from Medicaid will continue and probably grow with the increasing number of elderly people in the state. Since education spending is also strongly supported, pressures will fall on nonhealth services and administrative expenses in the human service system if revenues fail to expand as fast as overall spending. The state's child welfare system is strained already, yet there are few prospects for additional support. Mississippi's funding of nonhealth services will continue to rely heavily on federal funding.
New Mexico
Population (July 2003): 1.9 Million
Total State Expenditures - SFY 2002: $8,981 Million (US Total: $1,073,816 Million)
TANF Expenditures - SFY 2002 (% of total): 1.8% (US: 1.3%)
Medicaid Expenditures - SFY 2002 (% of total): 19.4% (US: 20.8%)
(Source: U.S. Department of Commerce, Census Bureau and NASBO 2002 State Expenditure Report)
Although New Mexico's per capita personal income is one of the lowest in the nation, the state does a good job raising revenue. The state's general fund recurring revenue collections are expected to increase by 8.1 percent in SFY 2004. Nearly 16 percent
of New Mexico's general fund revenues come from oil and gas production.
New Mexico has weathered the recent economic downturn well, experiencing only minor declines in revenue later than most states and maintaining an operating reserve well above five percent. The Department of Finance and Administration projects reserve balances will reach 9.6 percent of total recurring appropriations at the end of SFY 2004. State general fund revenues are expected to increase by 4.2 percent from SFY 2004 to 2005 due to abnormally high oil and gas prices as well as improvements in gross receipts, personal income, and corporate income tax collections. Projections suggest New Mexico's revenue will flatten from 2006 to 2008 as oil and gas prices decline and recent reductions in personal income taxes are phased in.
As noted earlier, New Mexico had one of the highest poverty rates in the nation in 2001, with approximately 17 percent of the state's population living in poverty, compared to 11 percent for the nation. New Mexico's unemployment rate is typically higher than most states. However, New Mexico performed better than the nation and most states during the recent economic downturn. In 2002, New Mexico's unemployment rate fell below the national rate and in 2003 and the first few months of 2004, unemployment rates in New Mexico have been only slightly above the national level. New Mexico employment growth has consistently been among the top five among all western states during the last year.
State Budget Development and Implementation
New Mexico's budget cycle begins with the executive budget agency sending funding targets to state agencies for their budget requests. The executive budget proposal typically includes agency budget recommendations by functional category. The Legislative Finance Committee, the fiscal arm of the state legislature, releases its budget proposal at the same time the governor releases the executive proposal. The executive budget agency and staff of the Legislative Finance Committee present their budget proposals to members of the state legislature in public hearings. State legislators then negotiate and pass a budget bill that is sent to the governor for signature.
Several characteristics of New Mexico's budget process provide the governor significant authority in budget development. Many state officials cited the governor's line item veto authority, which in New Mexico includes the ability to veto selected lines and items in any bill that appropriates funds, as the primary source of the governor's authority. For Governor Johnson, New Mexico's governor from 1995 to 2003, this authority was enhanced by his ability to sustain vetoes from legislative overrides. Johnson vetoed more than 700 bills while in office, including budget bills and social welfare proposals. Several state officials interviewed characterized Johnson as a "fiscal conservative" who used his veto authority to suppress social welfare spending. For example, the governor vetoed a 2002-03 budget bill because it did not sufficiently control Medicaid spending, among other reasons.
New Mexico's treatment of federal funds in the budget process also provides the state's governor increased authority over spending decisions. New Mexico is one of few states that does not appropriate all federal funds, thus limiting the legislature's ability to influence spending decisions. Additionally, the governor has authority to spend unanticipated federal funds without the legislature's approval.
The New Mexico Human Services Department administers the state's TANF, Medicaid, and SCHIP programs. Other public welfare programs such as child care, child welfare, adoption, and foster care are administered by the Children, Youth and Families Department, a separate state agency.
New Mexico's Response to Federal Welfare Reform
Welfare reform in New Mexico was a legal and philosophical struggle between the executive and legislative branches of government. The Johnson administration started work on its welfare reform proposal before the federal government enacted the Personal Responsibility and Work Opportunity Reconciliation Act of 1996. The administration's first proposal included several "work first" requirements that the federal government was considering for federal welfare reform including a lifetime limit on receipt of cash benefits, job search requirements, and a limit on the amount of education and training a recipient could apply toward work requirements. Johnson's "work first" reform bill died in committee in early 1996.
The Johnson administration began implementing its reform package in October 1996 without the legislature's approval by using regulatory changes. The first measure to go into effect required welfare applicants to register for work with the state's Department of Labor. Additional requirements implemented by regulations in July 1997 include a three-year lifetime limit on the receipt of cash assistance, requiring recipients to be in a work activity within 60 days of receiving assistance, and new income eligibility requirements such as counting federal housing subsidies and the income of all household members, including those not in the assistance unit, when determining eligibility.
The legislature responded by passing welfare reform legislation that softened several of the measures scheduled to go into effect in July 1997. For example, the legislative proposal included a five-year lifetime limit on the receipt of benefits, instead of the administration's three-year limit, and gave recipients two years to find employment before participating in mandatory work activities or facing penalties. The legislature also tried to stop the administration's reform efforts by inserting language into budget bills that tied the state's $35 million general fund appropriation for welfare to passage of the legislature's welfare reform bill. Governor Johnson ultimately vetoed the legislature's proposals.
In late 1997, New Mexico's Supreme Court ruled in favor of three state legislators and others who argued that Governor Johnson violated the state Constitution's separation of powers provisions when he implemented his welfare reform policies without the legislature's consent. This ruling required the administration to suspend implementation of its reform regulations. The administration ultimately reverted back to the state's pre-TANF welfare program. This ruling was the catalyst that brought the governor and legislature to agree upon a reform package that was enacted in February 1998. This agreement looked much like the federal law. The executive and legislature's struggle over welfare reform did not end with passage of the 1998 act. It continued in the budget process where the legislature pursued expansions to the state's welfare benefits and spending, and the executive pursued fiscally conservative policies.
Other Federal Social Welfare Programs
When research staff interviewed state officials for this project in September 2003, many cited New Mexico's growing Medicaid program as the most pressing issue for the state's social welfare programs. In 2002, Medicaid was one of the largest programs in the state budget, second only to k-12 education spending. In that same year, the program provided health care coverage to one of every five people in New Mexico. The state's general fund spending for Medicaid increased 55 percent from $263 million in 2000 to $407 million in 2004. During that period, New Mexico's Medicaid costs periodically exceeded projections in enacted budgets requiring additional appropriations during the state fiscal year. State officials noted that the cost drivers for New Mexico's program are the same as the rest of the nation including pharmacy costs, personal care services, facility based services, and others. Several officials indicated that New Mexico has not kept pace with others states in instituting measures to control Medicaid costs.
According to Governor Richardson's 2005 executive budget proposal (Richardson took office in January 2003), "without additional cost containment measures and revenue enhancement measures in SFY 2005, the New Mexico Medicaid program will require $115 million of General Fund over what is required for SFY 2004. This increase is greater than the current consensus revenue estimate of increased General Fund revenue for all of state government in SFY 2005." The executive proposal recommended a $54.7 million increase in state funding for Medicaid; $25.7 million in revenue enhancements including bed assessments for nursing homes and hospitals, and increasing the medical insurance premium tax from three to four percent; and cost saving strategies such as a reduction in benefits, increased co-payments, and re-certifying program eligibility every six months rather than every 12 months. Governor Richardson's proposals to increase the premium tax and assess a surcharge on nursing home and hospital beds were passed by the 2004 Legislature and signed by the governor.
Governor Richardson is also spearheading an effort to reform the state's healthcare system to extend coverage to the uninsured through a pooling system. Also noteworthy are the administration's efforts to consolidate children's behavioral health services, which include collapsing funding from many sources for multiple services into one "super" request for proposals.
South Carolina
Population (July 2003): 4.1 Million
Total State Expenditures - SFY 2002: $14,894 Million (US Total: $1,073,816 Million)
TANF Expenditures - SFY 2002 (% of total): 0.2 % (US: 1.3%)
Medicaid Expenditures - SFY 2002 (% of total): 22.6% (US: 20.8%)
(Source: U.S. Department of Commerce, Census Bureau and NASBO 2002 State Expenditure Report)
South Carolina has low fiscal capacity as measured by per capita personal income, representative tax system, and total taxable resources. Its poverty rates have been above average-12.7 percent in 2001, compared to 11.1 percent in the U.S. as a whole-though they have not been as high as most of the other poor states in the site visit sample (e.g., New Mexico, West Virginia, Mississippi, and Louisiana all have poverty rates in 2001 well over 15 percent). The proportion of children without health insurance was close to the national average in 2000.
But the state has suffered more than other low fiscal capacity states from recent increases in social needs. Between 2000 and 2003, the state's average monthly unemployment rate increased by 80 percent, from 3.8 percent to 6.8 percent, the largest increase among these six states. Welfare caseloads increased 17 percent between 2000 and 2002. Population growth has been moderately high, with a 9.6 percent increase between 1995 and 2002. The state's population is also aging more rapidly than other states (a change that puts great demands on Medicaid spending). Fiscal years 2001 and 2002 showed a 3.1 percent drop in revenues, a large decline for poor states.
State Budget Development and Implementation
South Carolina's budget process is dominated by the legislature. The governorship is one of the weakest in the nation. Until 1977, governors served only one term, so legislators were around much longer and exerted greater influence. In 1993, the Restructuring Act created eight appointed cabinet positions (the positions were elective before then). The state's governor submitted a budget for the first time in 1993.
Nonetheless, the legislature routinely ignores the executive budget. The budget process really begins with hearings with agency officials before the subcommittees of the House Ways and Means Committee. The subcommittees then get together and make recommendations to the full committee, which sends the budget to the full House. The chamber typically makes few changes in the committee's recommendations before passing the budget. The Senate develops its own budget more or less autonomously and in parallel. Differences between the two chambers-often large-are worked out in conference sessions.
The Senate is generally more supportive of social services than the House, partly due to the longtime leadership of the Senate Finance Committee chairperson, who has long been a strong supporter of Medicaid. His influence reflects another difference between the two chambers: the Senate tends to be dominated by seniority and individual senators, while the House is more controlled by committees and subcommittees. The greater role of subcommittees and committees in the House may account for its reported tendency to delve into greater budgetary detail than the Senate. For example, the House was said to look at performance measures more than the Senate. In recent years, the House also is reputed to ask more questions, look at more options, question Medicaid officials more skeptically, and look for evidence of fraud, abuse, or waste. Nearly all lobbying regarding social programs and the budget is directed at the legislature, not at the executive.
For the first time in the state's history, the government is entirely controlled by the Republican Party. Republicans won the House in 1994, the Senate in 2000, and the governorship in 2002.
The Department of Health and Human Services (DHHS) is the single state agency designated to administer Medicaid and SCHIP. The Department of Social Services (DSS) administers TANF, Food Stamps, child welfare services, foster care, child care licensing and regulation, adoption, adult and child protective services, and child support enforcement, CCDF, and SSBG. When the budget process involves budget cuts, agencies are generally instructed what percentage of their budgets must be cut, not exactly where, though this is less true for Medicaid, whose details are of greater interest to legislators. Mid-year cuts have been frequent in recent years; instructions specify a percentage to cut in agencies' budgets. Education and Medicaid traditionally have been exempted from mid-year reductions, though Medicaid is no longer exempt. Medicaid, unlike most other social programs, is allowed to run a deficit. Large and unexpected Medicaid deficits in recent years have hurt DHHS's reputation for management, though they have been paid.
Both DHHS and DSS administer contracts or agreements with other agencies to implement programs using funding streams they administer, especially Medicaid and TANF. Medicaid provides funding to 12 other agencies or institutions, the largest sums going to the Department of Disabilities and Special Needs, the Department of Mental Health, the Department of Education, and the Department of Social Services. DSS administers its programs through a variety of governmental entities. TANF, child and adult protective services, and foster care are administered by counties, while central or regional offices handle adoptions, licensing, and child support enforcement.
South Carolina's Response to Federal Welfare Reform
South Carolina's welfare reform program - known as the Family Independence Program (FIP) - was implemented in October 1996 as an AFDC waiver. The waiver remained in effect until September 2003. The cash assistance program is limited in duration to 24 months out of 10 years and no more than 60 months in a lifetime. To qualify, a family of two must have income less than $480 per month (or only $5,800 per year); once a family's earnings exceed the income limit ( the equivalent of 30 hours per week at minimum wage for a family of two), it is no longer eligible to receive assistance. Maximum benefits are only $204 per month for a family of three, an amount that has not changed in 15 years. Families who leave welfare due to earnings may receive up to two years of child care, transportation assistance, and other work-related expenses. The state's welfare caseload declined sharply after FIP was implemented-by 39 percent between 1998 and 2000. However, between 2000 and 2003, the average number of families per month increased by 25 percent.
Under the waiver, South Carolina could exempt recipients who were not "determined able to engage in work" and who were not provided transportation and child care services. They could count a wider variety of activities as meeting the participation requirement than they can under TANF. Officials expect service spending to go up as a result of the lapsed waiver.
The legislature was involved in establishing time limits, reasons for exemptions, extensions, and other such policies. But once welfare reform was completed, legislators lost most interest in TANF. In recent years, relatively minor changes were made as DSS promulgated regulations, which the legislature would review and pass, often with little debate. One exception to the general tendency of the legislature to show little interest in TANF occurred when it recently directed DSS to spend part of the TANF grant on abstinence-only pregnancy prevention programs.
Other than these actions, however, the legislature has given DSS discretion in using the TANF block grant to meet the purposes of the TANF program. The TANF surplus grew during the period of 1996 through 1998. Beginning in 1999, an increasing variety of programs were funded under the block grant, such as "First Steps," a school readiness program that provided services to pre-first-grade children and their families (this program also received general fund dollars).
In response to the economic downturn, the legislature severely cut the DSS budget. The DSS "base budget" was first reduced from $119 million to $102 million between SFYs 2001 and 2002. It declined further to $94 million in SFY 2003 and then to $78 million with the recently enacted budget for SFY 2004. These cuts were largely dealt with by cutting a variety of service contracts; by eliminating an agency that administered pregnancy prevention and after-school programs; and by reducing staff in the department. Positions were cut by 33 percent between January 2001 and June 2004-and by using TANF where allowable to cover the costs of "high-stakes" programs involving children-at-risk, such as foster care and emergency shelters. DSS also instituted a two-week mandatory unpaid furlough for all staff for the fiscal year ending June 2004.
South Carolina transfers a comparatively small share of its federal TANF grant and state MOE dollars to child care programs (about $4 million to CCDBG annually). It typically transfers a larger share to SSBG. Currently, TANF does little contracting for services. Virtually no legislative lobbying occurs on TANF issues.
Other Federal Social Welfare Programs
The state's Medicaid program plays a central role in South Carolina. It provides benefits to 20 percent of the population-including 40 percent of all children-and pays for 50 percent of all births. One-third of the state's senior citizens receive support from the program, and 75 percent of all nursing home beds are paid for by Medicaid.
Although 74 percent of the people eligible for Medicaid are low-income families, children, and pregnant women and infants, only 36 percent of the expenditures are for such categories. Elderly and especially disabled people are much more expensive to treat. Thus, though they constitute only 26 percent of the eligibles, their total expenditures make up 64 percent of the Medicaid budget.
Medicaid spending increases have closely correlated with changes in the number of recipients over time. Both spending and recipients rose modestly from 1994 to 1997 but grew more rapidly thereafter, even through 2003. There has also been some increase in spending per case, due to increases in pharmaceutical costs and the proportion of clients who are elderly.
The lobby for Medicaid is extensive, including representatives of hospitals (association and individual hospitals), nursing homes, doctors, the pharmaceutical industry, AARP, and other advocacy organizations. Strong grass roots support also exists, especially for programs that provide intensive services to families (such as Continuum of Care, which supports severely disturbed children).
Two other factors also protect the Medicaid program from major cuts: the state has an attractive match rate (about 70/30), and the program is "not an elaborate one," as one official noted. Although the state's program provides some optional services and supports some optional groups, many of the services are either mandatory or provided to hard-to-cut groups. As legislative staff noted, "It's hard to cut nursing beds and maternity services. The constituencies would come out of the woodwork."
The programs funded by state's CCDF constitute a centralized, voucher-based system. It relies much more on federal than on state dollars and was thus not much affected by the economic downturn. It supports foster care working parents, child-protective services families under certain conditions, Head Start, TANF and transitional child care for welfare leavers, and teens going back to school. Slots for the non-TANF (and nontransitional) working poor are well below need levels: only 3,000 slots can be funded, compared to 80,000 eligibles. Despite the fact that child care has not been cut to date, there were discussions about reducing transitional assistance from two years to one after families leave TANF. But the cuts have been resisted partly because child care is viewed as one of the few significant benefits provided to TANF families. Like TANF, there are few advocates for child care, and the program is not on the legislature's "radar screen."
The Social Services Block Grant gets 10 percent of the TANF grant and focuses on mandated services: child and adult protective services, foster care, and various support services. Federal funding has declined in real as well as nominal levels since the mid-1990s. To deal with the declines, staffing and administration were cut, and programs were eliminated that were local in coverage (rather than statewide) and that had weaker performance records.
As noted above, child welfare programs were cut by the legislature in recent years-one of the larger items being foster care board payments and therapeutic provider rates. As a result of these cuts, DSS is using TANF funds to meet Title IVA-EA costs to the maximum extent allowable.
South Carolina's Medicaid spending is likely to grow well into the future, as its population is aging more quickly than in other states. Greater competition for TANF funds is also likely. Since the state's AFDC waiver expired and the state was forced to restrict countable activities to work, work-experience, and community service, demands for job services and child care were likely to increase. State tax revenues have begun to grow again in SFY 2004. But the state's reliance on consumption taxes may dampen long-run revenue growth as the shift from goods to services and to purchases through the Internet reduce the base for such taxes. Education programs are a very high priority among elected officials, and such programs may, along with Medicaid, crowd out nonhealth social programs.
West Virginia
Population (July 2003): 1.8 Million
Total State Expenditures - SFY 2002: $8,150 Million (US Total: $1,073,816 Million)
TANF Expenditures - SFY 2002 (% of total): 2.5 % (US: 1.3%)
Medicaid Expenditures - SFY 2002 (% of total): 19.8 % (US: 20.8%)
(Source: U.S. Department of Commerce, Census Bureau and NASBO 2002 State Expenditure Report)
West Virginia's per capita personal income has been one of the lowest in the nation for the past twenty years. West Virginia did not benefit as much as other states from the economic boom of the late 1990s probably because its personal income tax is not as heavily dependent on the stock market. The recent projected state budget deficits for SFYs 2004 and 2005 have forced state officials to make difficult cuts.
West Virginia is also a high need state by most standards. The state's poverty rate has been one of the highest in the nation since 1995. Unemployment in West Virginia has also been consistently higher than the national rate, although it has decreased from 6.6 percent in 1998 to 4.8 percent in 2001, and again increased to 6.1 percent in 2003. West Virginia's labor force participation rate is especially low, ranging from 50 to 55 percent since 1995, compared to 63 to 65 percent for the nation. This may reflect large number of unemployed individuals who have stopped looking for work, as well as an aging population.
State Budget Development and Implementation
West Virginia's executive budgeting model provides the governor and executive agencies with much authority in budget development and implementation. Significant gubernatorial authority includes sole responsibility for establishing revenue estimates, line item veto, and the ability to extend the legislature's regular session if they do not enact a state budget before the new state fiscal year. The state's budget process begins with the governor's central budgeting agency releasing guidelines for agency budget requests for the upcoming fiscal year. These guidelines have included cuts of three to ten percent across agencies due to recent declines in state revenue. The governor's budget proposal is a compilation of agency budget requests developed to meet the executive's goals.
The legislature's authority in the budget process is limited by legal prohibitions to changing the governor's revenue projections and creating a deficit. The legislature's changes to the executive budget proposal must be cost neutral - an increase in funding in one area must be accompanied by an equivalent cut in another area. Limited staff to examine the governor's budget proposal and track agency administration of programs also restricts the legislature's influence.
The Department of Health and Human Resources administers a range of public welfare programs including TANF, child care, child welfare, adoption, and foster care. In West Virginia Medicaid and SCHIP are administered by two different agencies: Medicaid is administered by the Bureau of Medical Services within the Department of Health and Human Resources, whereas SCHIP is administered by the Children's Health Insurance Agency within the Department of Administration.
Two factors have converged to provide the Department of Health and Human Resources influence and autonomy in developing and implementing the state's social welfare budget. First, the governor's executive budgeting agency and legislature have limited staff to oversee the Department and must rely heavily on the expertise of Department staff during all phases of the budget process. Second, the state's budget typically appropriates funds at a broad level rather than itemizing funding in detailed appropriations, which are legal mandates restricting flexibility in budget implementation. This approach gave the Department significant authority to allow a large surplus of TANF funds to accumulate when caseloads plummeted in the late 1990s and to allocate the state's surplus TANF funds to programs and services when West Virginia started to spend down these dollars.
West Virginia's Response to Federal Welfare Reform(3)
West Virginia's response to federal welfare reform encompassed three phases. In the first phase, West Virginia officials designed the state's early TANF program to reduce caseloads to minimize financial risks associated with the new block grant structure of TANF and federal penalties for not meeting federal work participation rates. The state experienced a dramatic 71 percent decline in caseload from 1995 to 1999, compared to 45 percent for the nation. Specific policies that contributed to this decline included 1) more restrictive income eligibility guidelines (reducing the state's monthly eligibility threshold from $498 to $420 a month and counting SSI as income - the SSI requirement was later overturned by court and legislative action), 2) changes in administrative procedures requiring AFDC recipients to re-certify eligibility in early 1998 and instituting a more complicated application process, and 3) clear "work first" signals including a full-family sanction for non-compliance with work requirements.
Like most states, West Virginia amassed a surplus of federal TANF funds due to the block grant structure of the program and caseload decline. By the spring of 2000, the state's $160 million TANF surplus exceeded its $110 million annual federal block grant. This surplus of federal funds coupled with the flexibility in the final TANF regulations, provided incentive for the state to expand its TANF program, the second phase. Significant changes to West Virginia's TANF program during this period included: 1) an increase in income disregard rates from 40 to 60 percent, 2) a gradual, $200 increase in monthly cash assistance payments, 3) more generous diversion payment of up to four months of cash assistance payments, and 4) new supportive services to TANF recipients and others at risk of TANF recipiency. In addition to efforts to expand eligibility and services, West Virginia sought ways to use its federal TANF funds to support TANF-eligible services in its foster care and child protective services programs that had been funded with state funds. The state's TANF caseload began to increase during this period, earlier than in most states, yet it remained approximately half the 1995 pre-TANF level of 39,231 cases.
The third phase of West Virginia's TANF program was marked by budget deficits and the need to limit program expansion. In early 2001, the West Virginia Department of Health and Human Resources announced a projected $90 million deficit in the state's TANF program for federal fiscal year 2003. This announcement and subsequent efforts to restrain spending attracted media attention.
The state used an open process to tackle the projected deficit which included a TANF advisory council of non-profit stakeholders, advocates, and state officials appointed by Governor Bob Wise to recommend a cost reduction plan. The Council recommended a series of cuts to TANF funded benefits and services, giving priority to fund those services that were more closely aligned with goals one and two of the federal TANF program - to assist needy families and promote employment. Changes recommended by the Council that have been enacted include reducing the state's 1) earned income disregard rate from 60 to 40 percent, its previous level, 2) child support pass-through from $50 to $25 a month, and 3) eligibility for services to individuals not in receipt of TANF from 185 to 150 percent of federal poverty level. The following recommendations have met resistance from stakeholders and have either been taken off the table or scaled back 1) use non-TANF funds to support $43 million in foster care and other services provided by the Bureau of Social Services - these services were previously funded by a TANF transfer 2) discontinue $27 million in contracts with mostly community-based organizations for supportive services, 3) reduce eligibility for child care services, and 4) eliminate the state's marriage incentive of $100 a month.
Other Federal Social Welfare Programs
West Virginia spends more on its Medicaid program than any other single area of the state budget except for elementary and secondary education. Several state officials characterized the Medicaid program as an integral part of the West Virginia's health care system. It funds approximately 55 percent of the state's births. West Virginia's Medicaid program has been plagued with budget shortfalls. In general, the governor and legislature have been hesitant to cut coverage preferring instead to rely periodically on state funds set aside for changes in federal programs, funds from the state's tobacco tax, and attempts to control utilization. West Virginia has a Health Care Provider Tax that dates back to 1993. This tax continues to be a source of contention between the state and the various health care providers that are taxed.
The start-up and administration of West Virginia's SCHIP has been a source of contention. The state was slow to ramp up its SCHIP program due to problems inherent to starting a new program and fear that SCHIP would expand the state's already costly Medicaid program. From July 1998 to October 2000, West Virginia expanded its program to cover all children in households with income from 150 to 200 percent of the federal poverty level. SCHIP became a high profile item when Governor Bob Wise campaigned on a platform that included improving the program's enrollment. West Virginia's SCHIP program was one of only a few spared from the executive's directive to cut SFY 2005 state agency funding requests by 9 percent.
Endnotes
1 Information in this section is from Nelson A. Rockefeller Institute of Government field reports written by John Hall et. al. (1997 and 2002) , public documents, and interviews with state officials.
2 The eleven agencies are: Department of Corrections, Department of Education, Department of Economic Development, Department of Health and Hospitals, Department of Social Services, Governor's Office of the Workforce Commission, Louisiana Community and Technical College System, Governor's Office of Women's Services, Supreme Court, Governor's Office of Community Programs, and Louisiana State University. The TANF initiatives are targeted towards programs and services involving literacy, employment and family stability.
3 Information in this section is from a Nelson A. Rockefeller Institute of Government field report written by Chris Plein (2002), public documents, and interviews with state officials.
