June 2001
Joanne Rawlings-Sekunda, Deborah Curtis, and Neva Kaye
National Academy for State Health Policy
Produced for the
U.S. Department of Health and Human Services (HHS)
Office of the Assistant Secretary for Planning and Evaluation (ASPE)
Acknowledgments
This document could not have been produced without the support of the U.S. Department of Health and Human Services, Office of the Assistant Secretary for Planning and Evaluation (HHS/ASPE). Special thanks go to Jennifer Tolbert for her direction and encouragement.
Thanks also go to the many state officials who participated in interviews and reviewed the draft:
- Kimberly Davis Allen and Jacqueline Gray of Alabama
- Maresa Corder of Florida
- Dennis Janssen, Diana Kading, and Dann Stevens of Iowa
- Deborah Blanchette, Katherine Levasseur, Brenda McCormick, and Gino Nalli of Maine
- Denise Levis, Jeffrey Simms and Torlen Wade of North Carolina
- Nancy Austin, Charlene Benson, Melinda Jones, and Rebecca Pasternik-Ikard of Oklahoma
- Jill Melton, Susan Milam, Dee Sportsman,and Cynthia Walker of the state of Texas, and Carla Barnes, Vicki Jones, Ann Prescott, and Sandy Tyler of Birch and Davis (the plan administrator for Texas' PCCM program)
- Scott Cannady of Virginia
Finally, the authors would like to thank the physicians who agreed to be interviewed for the report:
- Roger Hofford, M.D., of Virginia
- Burtt Richardson, M.D., of Maine
We appreciate that these individuals took time from their very busy schedules in order to help us better understand their primary care case management programs. We salute them for their hard work in developing and administering these innovative programs.
Executive Summary
Primary care case management (PCCM) is a system of managed care used by state Medicaid agencies in which a primary care provider is responsible for approving and monitoring the care of enrolled Medicaid beneficiaries, typically for a small monthly case management fee in addition to fee-for-service reimbursement for treatment. States began enrolling beneficiaries in their PCCM programs by the mid-1980s to increase access and reduce inappropriate emergency room and other high cost care. State use of PCCM grew steadily during the 1990s.
In many ways, early PCCM programs were more like traditional fee-for-service Medicaid than their managed care counterpart, risk-based programs. Some states developed PCCM as a stepping stone to risk-based managed care, and therefore considered their MCO contracts as the predominant managed care system. That emphasis has been shifting, however, in those states that are experiencing a decrease in contractors as MCOs choose to exit Medicaid managed care.
PCCM programs have evolved significantly over time. Each state has taken a slightly different approach, depending in part on the state's particular managed care environment. The eight states studied for this paper (Alabama, Florida, Iowa, Maine, North Carolina, Oklahoma, Texas, and Virginia) were chosen for the range of strategies used in their PCCM programs. What these states have in common is a desire for increased accountability among their provider networks, in order to ensure high quality care for Medicaid beneficiaries.
As PCCM programs have matured, state goals have changed from simply expanding access to better management of the quality of care provided. To this end, case-study states are using strategies in managing their PCCM programs that are similar to network management principles used by MCOs. The case-study states are employing innovative strategies in the areas of:
- Organizational structure and administration, such as use of a plan administrator to implement the state's policies and decisions (Texas), programs focusing on population management (North Carolina), and a demonstration project geared to Medicaid beneficiaries who are receiving long-term care services at home (Maine).
- Provider recruitment and retention, including a greater focus on supporting participating providers through specially designated provider outreach staff (Alabama, Florida, Virginia, Texas), provider hotlines (Alabama, Iowa, Maine, North Carolina, Oklahoma, Texas, Virginia), feedback mechanisms such as provider profiling (Maine, Alabama, Texas), and strategies to gain providers' input and suggestions (nearly all case-study states).
- Quality activities, such as disease management programs (Florida, North Carolina, Oklahoma), use of HEDIS or other measures to gauge PCP performance (Iowa, Maine, North Carolina, Oklahoma, Texas), individual and community health needs assessments (Maine, Texas), community-based preventive health educational campaigns (Maine, Texas), and nurse advice lines (Oklahoma, Texas).
- Finance modifications, such as incentive payment systems (Maine, Oklahoma) and capitating primary/preventive services (Oklahoma).
- Service management, such as care coordinators within PCP offices for people eligible to receive long-term care services at home (Maine) and health needs assessments (Maine, North Carolina).
- Enrollment functions, such as targeted processes used to facilitate the enrollment of populations with special needs (Alabama, Oklahoma).
Chapter 1: Introduction
Primary care case management (PCCM) is a system of managed care used by state Medicaid agencies in which a primary care provider (PCP) is responsible for approving and monitoring the care of enrolled Medicaid beneficiaries, typically for a small monthly case management fee in addition to fee-for-service reimbursement for treatment. The Health Care Financing Administration (HCFA(now known as CMS)) in the Department of Health and Human Services (DHHS), defines PCCM services as "case management-related services, including the locating, coordinating, and monitoring of health care services provided by a physician, physician group practice, or an entity employing or having other arrangements with physicians (including nurse practitioners, certified nurse midwives, and physician assistants at the state's option), under a PCCM contract with the state." 1 As of June 30, 1998, 29 states had Medicaid PCCM programs.
PCCM programs have evolved significantly since HCFA(now known as CMS) first authorized implementation in 1981. The purposes of this paper are to examine this evolution and illustrate the current practices in PCCM programs in eight states that have developed a broad range of implementation strategies.
National Academy for State Health Policy (NASHP) staff utilized several methods to study PCCM programs during October/November 2000:
- A review was completed of the available literature on PCCM programs and their evolution. This included an analysis of trends in the state use of Medicaid PCCM from NASHP's Medicaid Managed Care: A Guide for States (Fourth Edition). 2
- Telephone interviews were conducted with Medicaid officials and others implementing PCCM programs in seven states: Alabama, Florida, Iowa, North Carolina, Oklahoma, Texas, and Virginia. Officials in the eighth state, Maine, were interviewed in person. NASHP staff spoke with a total of 24 people in one-and-a-half-hour interviews. Interviewees discussed the major features of their programs, program evolution, strengths and weaknesses, and lessons learned.
- Physicians in two states were interviewed by telephone. These interviews lasted approximately half an hour and focused on the physicians' motivations for participating in the program and what they viewed as strengths and weaknesses.
Studied States
The eight states studied (Alabama, Florida, Iowa, Maine, North Carolina, Oklahoma, Texas, and Virginia) were chosen for the range of strategies used in their PCCM programs. These programs vary in age (from one to ten years) and size (from several pilot sites to statewide). What also varies is the place of PCCM within the Medicaid managed care picture: some states implemented these programs with the intent that they would continue indefinitely, while others planned to phase them out in favor of Managed Care Organizations (MCOs). A few states still intend to reduce or eliminate the PCCM system for MCO-based programs, while others are moving in the opposite direction. What these states have in common is a desire for increased accountability among their provider networks, in order to ensure high quality care for Medicaid beneficiaries. The PCCM programs studied are
- Alabama's Patient 1st, initiated in 1997, operates statewide for TANF, SOBRA children, Aged/Blind/Disabled Medicaid beneficiaries, and CHIP beneficiaries.
- Florida's MediPass, initiated in 1992, operates statewide for poverty-related and Blind/Disabled Medicaid beneficiaries, CHIP beneficiaries, and children in foster care. It includes disease management programs throughout the state and a provider service network in two counties.
- Iowa's MediPASS, started in 1990, operates in 92 of the state's 99 counties and covers poverty-related Medicaid beneficiaries and CHIP beneficiaries. The Medicaid program also contracts with a behavioral health organization for all Medicaid beneficiaries.
- Maine PrimeCare, started in 1994, became operational statewide in January 2001; it covers poverty-related Medicaid beneficiaries and CHIP (Medicaid expansion) beneficiaries. MaineNET/Partnership, started in 2000, operates in three pilot PCP sites and covers Medicaid beneficiaries who are either adults with disabilities or elderly. MaineNET participants obtain primary and acute services from their PCP. Partnership participants are people who are receiving long-term care services in the community; in addition to obtaining primary/acute services from their PCP, they also work with a care coordinator.
- North Carolina ACCESS I, started in 1991, is a standard PCCM model that operates in 99 of the state's 100 counties and covers poverty-related and Aged/Blind/Disabled Medicaid beneficiaries. ACCESS II and III, both begun in 1998, are enhanced case management demonstration projects that build on ACCESS I and share its features. ACCESS II has six locally integrated networks and one statewide physician network; ACCESS III includes two countywide plans. Networks typically include physicians, hospitals, public health departments, and other providers. Both ACCESS II and III focus on the development of a local infrastructure that is responsible for an enrolled population and improved quality of care.
- Oklahoma's SoonerCare Choice PCCM Model, begun in 1996, operates in 61 counties (as of January, 2001) and serves poverty-related and Aged/Blind/Disabled Medicaid beneficiaries and CHIP (Medicaid expansion) beneficiaries. Primary/preventive care and case management services are capitated, and specialty services are paid fee-for-service; PCPs also receive a bonus for meeting EPSDT screening goals.
- Texas Health Network, started in 1993 as part of the state's STAR (Medicaid managed care) program, operates in six of the state's eight service areas (in 37 counties); it serves poverty-related Medicaid beneficiaries. STAR+PLUS has operated since 1998 in the Harris Service Area (containing Houston); it serves SSI children and people who meet certain eligibility criteria of the Department of Mental Health and Mental Retardation. The El Paso region has a partially capitated PHP that is being phased out.
- Virginia's MEDALLION, started in 1992, operates in 66 counties and 26 cities. It serves poverty-related and Aged/Blind/Disabled Medicaid beneficiaries and CHIP beneficiaries.
Endnotes
1. HCFA(now known as CMS), letter from Sally K. Richardson, Director, Center for Medicaid and State Operations, PCCM Services Without Waiver, Jan. 21, 1998.
2. Neva Kaye, Cynthia Pernice, Helen Pelletier (Editor), Medicaid Managed Care: A Guide for
Chapter 2: Background: Evolution of PCCM
First Wave
The Omnibus Budget Reconciliation Act (OBRA) of 1981 allowed state Medicaid programs to implement both PCCM and risk-based managed care programs, pending HCFA(now known as CMS) waiver approval. HCFA(now known as CMS) approval required that the state satisfy two requirements.
- The case management restrictions must not "substantially impair access" to primary care services of "adequate quality where medically necessary;" and
- The case management restrictions must be "cost effective."3
Many states focused their first efforts in managed care on PCCM programs, with the goal of moving to risk-based contracting later.
Intent
States began enrolling beneficiaries in their PCCM programs by the mid-1980s. In 1986, seven states had implemented PCCM programs, 4 and by 1990, 19 states had such programs. 5 Several factors motivated decisions to implement PCCM programs.
- States wanted to increase access to care. First, by offering physicians a small payment, state officials hoped more providers would accept Medicaid beneficiaries. Then each beneficiary would choose or be assigned to a participating physician, rather than needing to locate a provider who would accept Medicaid on his/her own; this would serve as his/her "medical home."
- States hoped to save money by reducing inappropriate emergency room (ER) and specialist use and other high-cost care. With continuity of care established, the member would presumably contact this medical home, rather than the emergency room, when health problems arose. Moreover, continuity of care would, in all likelihood, lead to better quality of care as well as more preventive care.
- States felt PCCM would be more palatable to physicians than risk-based managed care.
- States believed PCCM was better suited than MCOs in certain areas, such as rural regions where it would be difficult for MCOs to maintain an adequate population base for financial viability.
Characteristics
In typical PCCM programs, the PCP is paid a monthly case management fee for each enrolled Medicaid beneficiary, in addition to fee-for-service reimbursement for all non-emergency primary care services that he/she provides. In return, the PCP is responsible for providing primary care and for prior authorizations to hospitals and specialty care providers.6 Hospitals and specialists are also paid fee-for-service, as long as prior authorization has been obtained.
In many ways, early PCCM programs were more like traditional fee-for-service Medicaid than their managed care counterpart, risk-based programs. For example, a 1995 NASHP study of PCCM programs found that provider requirements were usually very minimal, PCP selection was non-competitive, and most states maintained existing fee-for-service payment rules (such as prior authorization and hospital pre-admission review) but added the requirement that a specified set of services must either be provided or authorized by the PCP.7
Impact
PCCM programs have been successful in increasing the access of Medicaid beneficiaries to primary care physicians and creating medical homes, but the impact on costs is more mixed. In certain studies, access and utilization of primary care were noticeably improved, due largely to these provider-patient relationships. While some states showed reduced costs (including New York, 8 and Arkansas 9, no reduction was found in others (including Maryland,10 11 Missouri,12 and Utah).13 In some of the latter states, utilization patterns for emergency rooms, specialty care, and prescription drugs remained unchanged. Possible explanations for this include:
- Traditionally-run PCCM programs usually provide little incentive for either physicians or beneficiaries to change their behavior. Since services are reimbursed fee-for-service, more services equal greater reimbursement. The referral process for specialty and hospital care, by itself, does not cut down on this care. In some states, such as Utah, procedures do not exist for denying reimbursement for a Medicaid beneficiary receiving unauthorized services, so specialists and emergency rooms have no economic incentive to deny care to patients who self-refer.14
- With greater access to primary care, it is possible that more health problems that require additional care, such as prescription drugs or specialty care, may be detected.
Evolution
As of 1998, 13 percent of all Medicaid beneficiaries (4.1 million people) were served through PCCM providers in 29 states. 15 Although the number of states has fallen from a high of 33 in 1994 (see Chart A), the number of beneficiaries since that time has risen (from 2.4 million in 1994).16
The National Academy for State Health Policy (NASHP) has conducted four surveys of state Medicaid managed care programs since 1990. The information collected from all 50 states and the District of Columbia gives a strong sense of the evolution of PCCM programs. The information in this section is taken from the most recent edition of Medicaid Managed Care: A Guide for States.17
Chart A.
Use of PCCM by Population
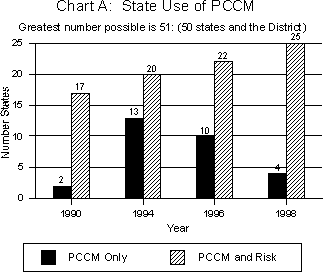
Since 1990, states have primarily used PCCM programs to enroll people in the following Medicaid categories of eligibility: AFDC/TANF, poverty level pregnant women, and poverty level children. Medicaid use of PCCM programs for these populations has been fairly stable and very high. Also relatively stable is the use of PCCM for institutionalized populations as a percentage of states with PCCM programs; this has remained fairly low. As Chart B illustrates, states' use of PCCM programs to enroll other populations has fluctuated between 1990 and 1998. Among the states that operate PCCM programs, the number choosing to enroll SSI children increased dramatically; those choosing to enroll SSI adults living in the community dropped and then gained ground.
Subpopulations excluded or exempted from PCCM programs have remained fairly constant. Most frequently excluded/exempted are: Medicare dual eligibles (excluded in 83 percent of the 29 states operating PCCM programs in 1998), people receiving long-term care in institutions (excluded in 79 percent in 1998) or in the community (excluded in 69 percent in 1998), and people with other insurance (excluded/exempted in 69 percent in 1998). Other subpopulations excluded/exempted from state PCCM programs included: children in foster care (in 62 percent of the states), children with special health care needs (in 31 percent), and American Indians/Alaska Natives (in 28 percent).
Chart B:
Enrollment Policies
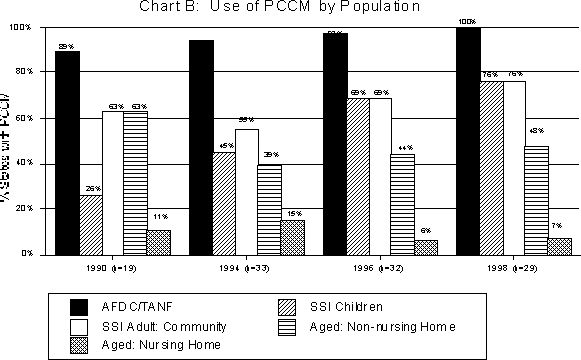
States are increasingly mandating enrollment in PCCM for their Medicaid beneficiaries. As Chart C illustrates, in 1990, 63 percent of the 19 states with PCCM programs (a total of 12 states) mandated enrollment; 47 percent (nine states) made enrollment voluntary. (These add up to over 100 percent, as states may use both mandatory and voluntary enrollment, depending on geographic region, population group, or some other factor.) By 1998, 93 percent of the 29 states operating PCCM programs (a total of 27 states) mandated enrollment; 17 percent (five states) made enrollment voluntary.
Chart C:
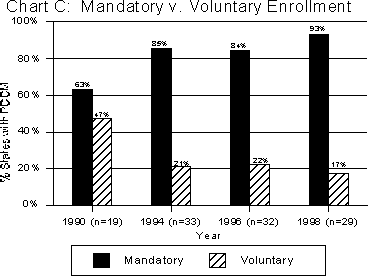
States have increasingly used enrollment brokers for their PCCM programs, from 10 states in 1996 to 16 in 1998 — a 40 percent increase. Five states (17 percent of the 29 states with PCCM programs) reported involving community-based organizations in informing and outreach for PCCM in 1998, although the most common venue for informing was the welfare/social service agency (used in 20 states). Other commonly used venues include: the beneficiary's home (18 states), point of service/provider locations (17 states), health fairs (14 states), and community-sponsored events (13 states). Brochures/flyers mailed directly to the beneficiary were the most common way to inform; phone calls were another common informing technique. In most states, beneficiaries were allowed to phone in their PCP selection in order to make enrollment more convenient
Chart D:
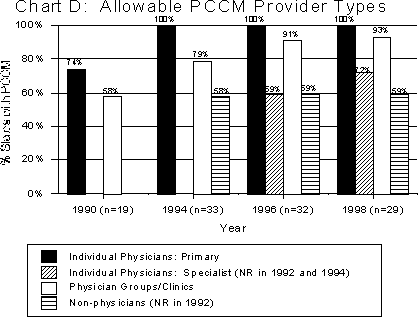
Providers
Allowable PCCM primary care providers (PCPs) are typically those who can provide the full range of Medicaid primary care services. All states with PCCM programs allow individual primary care physicians (MDs or DOs) to serve as PCPs (the chart on the previous page); nearly all (27 states, or 93 percent of the 29 states with PCCM programs in 1998) allow physician groups or clinics (including Federally Qualified Health Centers, Community Health Centers, Rural Health Centers, local public health departments, Maternal and Child Health clinics, Indian Health Service clinics and tribal clinics) to do so. As Chart D indicates, states are increasingly allowing specialists to participate as PCPs, as long as they can provide the required services. This may reflect the increase in the number of states enrolling SSI populations, many of whom may already have established relationships with specialists who act as their PCPs. More than half the states with PCCM programs are also allowing physician extenders (nurse practitioners, physician assistants, and nurse midwives) as PCPs. This may relate, in part, to the use of PCCM in rural areas, where physicians may be more scarce.
Chart D:

Services
Chart E:
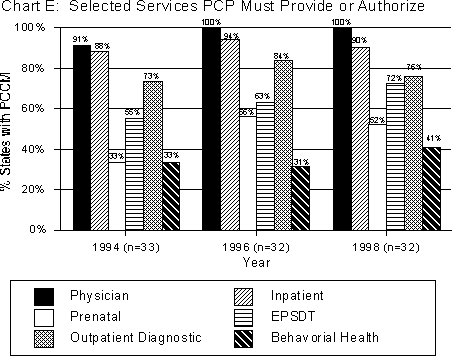
States require PCPs to directly provide, or authorize through referral, a full range of Medicaid primary care services. Chart E illustrates services commonly provided or authorized by the PCP. Not surprisingly, the most commonly provided/authorized services are physician, inpatient hospitalization, and outpatient diagnostic.
Quality Activities
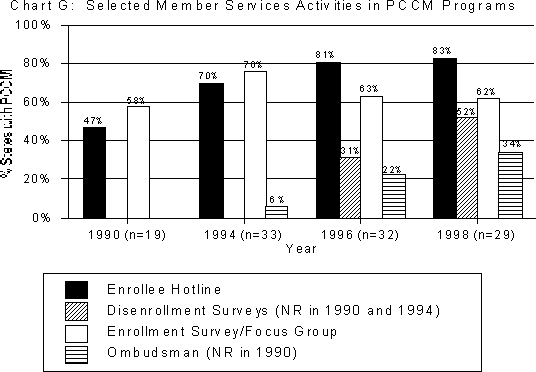
States are increasingly monitoring quality of care in PCCM programs using multiple strategies. As evidenced in Charts F and G, the strategies with the greatest increased use by states include: spot-checking 24-hour availability of PCPs (from 11 states or 58 percent of the 19 states with PCCM programs in 1990 to 25 states or 86 percent of the 29 states with programs in 1998); member survey/focus groups (from 13 states or 68 percent in 1990 to 25 states or 86 percent in 1998); member hotlines (from nine states or 47 percent in 1990 to 24 states or 83 percent in 1998); and random medical record review (from 13 states or 68 percent in 1990 to 24 states or 83 percent in 1998). Other methods include focused studies, PCCM provider performance feedback, monitoring voluntary disenrollments of members, provider hotlines, disenrollment surveys, on-site state reviews/audits, desk reviews/audits, and ombudsman programs.
Chart F:
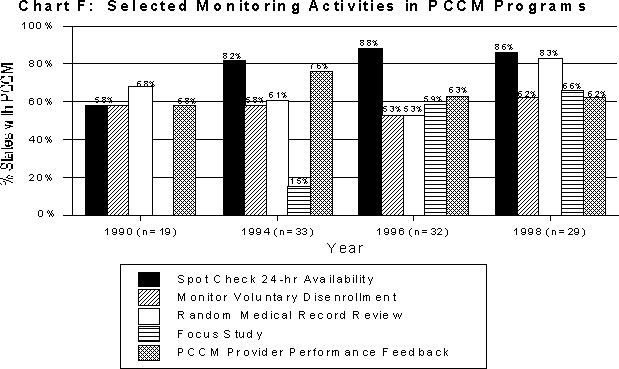
Chart G:
External Drivers for Evolving PCCM Programs
Both external and internal factors have driven the evolution of states' PCCM programs. The most significant external factors are the Balanced Budget Act and the changing marketplace for risk-based MCOs.
Balanced Budget Act (BBA)
The Balanced Budget Act of 1997 included provisions specifically affecting PCCM programs. For example, states can now require Medicaid beneficiaries to enroll in managed care, including PCCM programs, by amending their state plans rather than seeking a waiver. The only populations excluded from this state plan option are certain children with special needs (including SSI children), beneficiaries dually eligible for Medicare and Medicaid, and American Indians/Alaska Natives.18
In our study of eight states (Alabama, Florida, Iowa, Maine, North Carolina, Oklahoma, Texas and Virginia), the most frequently stated impact of the BBA is the "prudent lay person standard" for emergency room utilization, prohibiting the need for prior authorization of coverage. This requirement was specified in a letter from HCFA(now known as CMS) to state Medicaid programs, stating that PCCM programs are required to pay for emergency services that meet the prudent layperson standard.19
State officials struggle with the lack of an operational definition of prudent lay person. Prior to the BBA, many states had determined whether services were emergency or non-emergency (non-emergency meaning not being reimbursable without prior authorization from a PCP); the new regulations no longer allow such classifications. Thus, a major tool for managing care and costs in PCCM programs is no longer available to Medicaid programs.
In response, several states are developing methods to reduce inappropriate emergency room use through educational efforts.
- Texas created an Emergency Room/Urgent Care Subcommittee, which drafted a common set of protocols for voluntary emergency room use. The Texas Medicaid program is now presenting these protocols to emergency rooms across the state.
- Maine is focusing its efforts on member education strategies.
- The state's quality management nurses send letters to PCCM members (or their families) who seek services within an emergency room at least twice per quarter for such issues as earaches, coughs, sore throats, or colds (identified through diagnostic codes in medical records). The letter encourages the member to visit his/her PCP for these issues; attached to the letter is a card that lists steps to managing the symptoms at home. If the member's emergency room use does not change, one of the nurses sends a more forceful letter. If the second letter has no impact, one of the nurses actively manages the member; however, the program has not been in place long enough for any beneficiaries to reach this last stage.
- The state recently implemented a system for PCPs to refer patients for education. A physician sends a completed Member Education Request Form, which lists the area for education (including appropriate emergency room use), to the PCCM program's enrollment broker. The broker sends an educational flier that contains information about the requested topic area to the member. If this has no discernable impact, the enrollment broker can contact the member by telephone.
The effectiveness of states' efforts to influence physician or patient behavior solely through education -- without the availability of incentives or disincentives -- is limited. One official noted that emergency rooms in some of that state's rural areas are considered gathering places on weekends; patient and provider education has not been effective in changing utilization patterns.
A related issue is the states' ability to promote communication between the emergency room and the PCP. One PCP interviewed for this study expressed frustration that without information about his patients' use of the emergency room, he lacks the ability to effectively oversee his patients. Several states, including Alabama and North Carolina, encourage emergency room physicians to contact the beneficiary's PCP with a description of the encounter. However, such notification depends on the individual emergency room physician's inclination.
Other BBA requirements affecting PCCM programs, such as access standards or lock-in provisions, did not appear to impact these eight states, possibly because they already have these standards in place.
Changes in the MCO Marketplace
A study of 15 states with the greatest number of Medicaid managed care members found annual MCO withdrawal rates of 18 percent in 1997 and 15 percent in 1998, compared with 7 to 8 percent each year from 1994 to 1996.20 In 1998, on average, one commercial MCO entered the Medicaid market for every six MCOs that exited; in 1997, the ratio was closer to one entering for every two exiting.21 With fewer MCOs in the market, PCCM programs have become a long-term managed care alternative, even for states that originally intended to move all their Medicaid populations to risk-based MCO programs.
Several of the eight case-study states mentioned concerns about the MCO marketplace as a factor in their considerations about the role of PCCM in their Medicaid managed care programs. For example, the MaineNET/Partnership program's original approach called for contracting with an MCO, but the absence of potential bidders in the state called for the revised, PCCM approach. Iowa officials reported that they expect PCCM to take a larger role in the near future, due to the withdrawal of one MCO from Medicaid and the concerns that another may withdraw. Oklahoma officials noted that their original vision of eventually enrolling Medicaid beneficiaries throughout the state in MCOs was not realistic, especially in rural areas.
Internal Drivers for Evolving PCCM Programs
As PCCM programs have matured, states have turned their focus from simply expanding access to developing methods for better management of their providers. States have learned many network management principles from MCOs, and are increasingly seeking to use these principles in managing their PCCM programs. Ensuring that Medicaid beneficiaries receive quality care is becoming a particularly important activity, as states put tighter language into their PCP contracts and dedicate staff to monitoring compliance with the stricter standards. Programs now often include strict provider credentialing, member surveys, care coordinated across multiple providers and conditions, 24-hour member services, selective provider contracting, HEDIS reporting, member education, disciplined utilization management, disease management programs, complaint log reviews, GeoAccess provider network analytic tools, provider profiles, and other approaches typically associated with MCOs.22
North Carolina is a good example of this expansion of focus. The goal of the original ACCESS program (started in 1991) was to increase access to primary and preventive care. ACCESS II and III (started in 1998) have an additional goal: to help physicians with large Medicaid populations manage their patients in order to improve the quality of care provided, as well as to increase access and cost effectiveness. Further, the state seeks to promote community-based systems of care by retaining dollars in the local delivery system and developing an ongoing commitment to community needs and values.
Components and Innovations in Current PCCM Programs
The bulk of this paper focuses on current innovations in eight states' PCCM programs. The areas with the most frequent activities are described first.
Endnotes
3. Deborah A. Freund, Medicaid Reform: Four Studies of Case Management (Washington, DC: American Enterprise Institute, 1984).
4. Maren D. Anderson, Peter D. Fox, "Lessons Learned from Medicaid Managed Care Approaches," Health Affairs 6, no. 1 (Spring 1987): 71-88.
5. See Note 2.
6. Originally, prior authorizations were typically required for emergency room use as well, but this practice is now prohibited by the BBA (see below).
7. Neva Kaye, "PCCM Contracting and Quality Monitoring", Medicaid Managed Care: A Guide for States (Second Edition) (Portland, ME: National Academy for State Health Policy, 1995), 115-135.
8. T.C. Rosenthal et al., "Medicaid Primary Care Services in New York State: Partial Capitation vs. Full Capitation," Journal of Family Practice 42, no. 4 (April 1996): 362-368.
9. A. Muller, J.A. Baker, "Evaluation of the Arkansas Medicaid Primary Care Physician Management Program," Health Care Financing Review 17, no. 4 (Summer 1996): 117-133.
10. J.A. Schoenmann, W. N. Evans, C. L. Schur, "Primary Care Case Management for Medicaid Recipients: Evaluation of the Maryland Access to Care Program," Inquiry 34, no. 2 (Summer 1997): 155-170.
11. A. Gadomski, P. Jenkins, M. Nichols, "Impact of a Medicaid Primary Care Provider and Preventive Care on Pediatric Hospitalization," Pediatrics 101, no. 3 (March 1998): E1.
12. Robert E. Hurley, J.E. Paul, Deborah A. Freund, "Going into Gatekeeping: an Empirical Assessment," Quality Review Bulletin 15, no. 10 (Oct. 1989): 306-314.
13. Stephen H. Long, Russell F. Settle, "An Evaluation of Utah's Primary Care Case Management Program for Medicaid Recipients," Medical Care 26, no. 11 (Nov. 1988): 1021-1032.
14. See Note 13.
15. See Note 2.
16. See Note 2.
17. See Note 2.
18. Complete information about the BBA and Medicaid managed care, including the actual text and a series of letter to states from HCFA(now known as CMS) regarding the BBA, is available at http://www.hcfa.gov/medicaid/bbahmpg.htm.
19. According to the letter from Timothy Westmoreland (Director, HCFA(now known as CMS) Center for State and Medicaid Operations) dated April 18, 2000, an emergency medical condition is "a medical condition manifesting itself by acute symptoms of sufficient severity (including severe pain) such that a prudent layperson, who possesses an average knowledge of health and medicine, could reasonably expect the absence of immediate medical attention to result in placing the health of the individual (or, with respect to a pregnant woman, the health of the woman or her unborn child) in serious jeopardy, serious impairment to bodily functions, or serious dysfunction of any bodily organ or part."
20. M. Gold, et al., Medicare Managed Care: Preliminary Analysis of Trends in Benefits and Premiums, 1997-1999. (Washington, DC: Mathematica Policy Research Inc., 1999).
21. Susan Felt-Lisk, The Changing Medicaid Managed Care Market: Trends in Commercial Plans' Participation. (Washington, DC: Mathematica Policy Research Inc., 1999).
22. Charles Milligan, "States Building Second-Generation Primary Care Case Management Programs in Medicaid Managed Care, Competing Against HMOs," News and Strategies for Managed Medicare and Medicaid 6, no. 8 (Feb. 28, 2000): 6-7.
Chapter 3: Organizational Structure and Administration
Several of the case-study states have made significant changes in the administration of their PCCM programs, creating organizational arrangements that more closely resemble contracted managed care networks. Whether state-administered or through contract agreements, these states have identified distinct functions for administration, such as enrollment, member services, provider network development, quality improvement, and medical management. In many instances, states are choosing to contract out for these program functions instead of administering them internally. The result is that PCCM programs have gained a new level of sophistication and importance as managed care delivery systems in state Medicaid programs. Chart H shows the range of delivery systems used in the case-study states.
| State | Program | Model |
|---|---|---|
| Alabama | Patient 1st | Mandatory |
| Florida | MediPass | 1/3 of Medicaid beneficiaries in PCCM, 1/3 in MCOs, 1/3 institutional/other; PCCM members in 6 counties also enrolled in BHO |
| Iowa | MediPASS | PCCM in 92 (of state's 99) counties; choice of MCO or PCCM in 43 counties; behavioral health organization (BHO) |
| Maine | Maine PrimeCare | PCCM is the only managed care delivery system (as of December 2000) — will be statewide by 2001 |
| MaineNET/ Partnership | MaineNET: PCCM; Partnership: PCCM with external care coordination entity | |
| North Carolina | ACCESS I |
1 county - mandatory MCO; 5 counties - choose between MCO/PCCM (default to PCCM); rest of 99 counties - PCCM only ACCESS II and III build upon ACCESS I, have all ACCESS I features |
| ACCESS II | ||
| ACCESS III | ||
| Oklahoma | SoonerCare Choice PCCM Model | PCCM in rural areas; MCO in urban areas |
| Texas | Texas Health Network | In STAR, can choose between MCO or PCCM (Texas Health Network); one area has BHO; one area has partially capitated PHP being phased out |
| STAR+PLUS | Choose between MCO/PCCM | |
| Virginia | MEDALLION | PCCM and MCO in different areas (PCCM in more rural areas) |
Third Party Contracting
Six of the eight case-study states contract with private entities to perform enrollment functions for PCCM. Alabama and North Carolina retain that function within their state and county governments. In each of the six states, the enrollment broker provides services for MCO enrollment as well. Maine's enrollment broker is also responsible for provider recruitment and member services. State officials in Maine combined these functions because they felt that it provided an opportunity for the broker to develop a comprehensive understanding of the community as the state rolls out its PCCM program from county to county. The broker learns the dynamics of the local delivery system as it recruits PCPs to participate. It then has a better knowledge and understanding of the community when it begins enrollment of Medicaid beneficiaries.
As Chart I illustrates, each of the eight states operates its PCCM program a bit differently from the way the other states do, illustrating considerable variability in administration. For example, rather than having its enrollment broker conduct provider recruitment for PCCM, as Maine does, Florida has it fiscal agent provide that service. Oklahoma contracts with a separate entity to provide a 24-hour nurse advice line for members but has combined this function with those of the enrollment broker in one contract. Four of the states (North Carolina, Oklahoma, Texas, and Virginia) contract with independent entities to conduct quality improvement activities for PCCM Programs in Texas, North Carolina, and Maine provide three different examples of how states have structured the administration of their PCCM programs.
| State | Program | Functions |
|---|---|---|
| Alabama | Patient 1st | None |
| Florida | MediPass | Fiscal agent, enrollment, pharmacy management, disease management |
| Iowa | MediPASS | Fiscal agent |
| Maine | Maine PrimeCare | Enrollment, policy institute at university does program development and evaluation |
| MaineNET/ Partnership | Medical eligibility, enrollment, care coordination, policy institute at university does program development and evaluation | |
| North Carolina | ACCESS I |
Quality improvement |
| ACCESS II | ||
| ACCESS III | ||
| Oklahoma | SoonerCare Choice PCCM Model | Enrollment, nurse advice line, quality improvement, encounter data verification |
| Texas | Texas Health Network |
Plan administrator to manage network and member services, enrollment, fiscal agent, quality improvement |
| STAR+PLUS | ||
| Virginia | MEDALLION | Enrollment, prior authorizations, quality improvement |
State Variations in PCCM Administration
Texas: Texas Health Network
Texas STAR program, the state's Medicaid managed care program, is comprised of three models: MCO, PHP and PCCM (Texas Health Network). The administration of Texas Health Network program resembles that of a managed care organization. According to state officials, the PCCM program is a state-administered health plan. The state has entered into several contracts for program operation but does not require its contractors to assume any financial risk. The state Medicaid agency has developed what they describe as an enhanced PCCM model, featuring increased member services, significant case management, improved services to providers, and linkages between services. Texas Health Network began as a pilot program and has gradually expanded to six service areas in the state. The state now has the following four separate contracts for the administration of the program:
- plan administration;
- enrollment;
- claims processing; and
- certain quality improvement activities.
Originally, claims processing was included in the plan administrator's responsibilities, but state officials subsequently decided that there would be better checks and balances if the functions were not combined.
The core of Texas Health Network is the contracted plan administrator. This contractor is responsible for provider network development and contracting, provider services, member services, case management, utilization management, and health and wellness education. Field staff are located in the six regional service areas in which the STAR program has implemented the PCCM model, where they can provide information and assistance directly to both members and network providers. In addition to negotiating contracts with PCPs, the plan administrator has the authority to negotiate state contracts with hospitals. Using claims data that is provided through the fiscal agent, the contractor sets hospital payment rates for PCCM members.
State staff maintain that having a plan administrator is a great asset to the program, because it allows for greater flexibility in managing the resources dedicated to the program and, ultimately, better program support. The plan administrator can provide adequate staffing and resources to the program, without state limitations on personnel and on the transfer of funds between categories. Staff note that the burden is on the state to ensure that sufficient funds are in the contract so that the administrator can do the work required. State Medicaid agency staff work closely with plan administrator staff, viewing the contractor as the state's administrator of the PCCM program. The state retains the authority for policy development and decisions. Financial goals are set for the plan administrator, and the contract is monitored quarterly through selected financial measures, required reporting, and state contract oversight.
North Carolina: ACCESS
North Carolina has embraced the concept of state and local partnerships in the development and implementation of its PCCM program. State agency officials view the development of infrastructure at the local level to be one of the most important aspects of their successful PCCM initiatives. The state began Carolina ACCESS as a small PCCM demonstration in 1991, and expanded by county, achieving statewide coverage in 1999. The Medicaid agency funds a position at the regional level to work with both members and providers. Known as a managed care representative, this individual is based at the regional social services office and provides a link with the various providers and services in the community. By taking a gradual county-by-county approach and providing representation and accountability within the community, state officials believe that their agency built credibility and an acceptance of the ACCESS program, as well as preparing each region prior to implementation.
The ACCESS II and III programs began with the state issuing a letter in 1997 to the 35 provider groups in the state that had the largest number of Medicaid patients, to gauge their interest in participating in a PCCM program that focused on quality as well as access, in exchange for a greater case management fee. The response was overwhelmingly positive, so the state issued a Request for Proposals (RFP), asking respondents to propose how they would partner with the other providers in their area to manage the care of their members. ACCESS II and III are network-driven, combining physicians, hospitals, public health, social services, and other community-based services.
Currently, there are seven ACCESS II sites serving local regions, with the exception of a large provider network that spans 32 counties. The two ACCESS III sites are countywide networks composed of physicians, hospitals, health departments, departments of social services, and other community providers. The ACCESS II and III networks are paid an enhanced case management fee of $5.00 per member per month. The PCP receives the usual monthly $2.50 case management fee per patient 23, and the remaining $2.50 goes to the network's administrative entity for case management and administrative functions related to the network's enrolled population. With this network approach to PCCM, case management is an expectation of not only the individual PCP but also of the ACCESS II and III networks. In addition, the networks are expected to build a community service delivery infrastructure and promote collaboration among providers.
North Carolina has invested in the development of local infrastructures with each of the ACCESS programs. The state has promoted an enhanced model of PCCM and has helped the networks build service delivery collaboration at the local level to avoid duplication. State officials firmly believe that partnerships — both within communities and between the state and local providers — are essential to the long-term success and sustainability of North Carolina's PCCM system.
Maine: MaineNET/Partnership
MaineNET is a voluntary PCCM program for Maine's elderly and disabled adults. A second component of the program, the MaineNET/Partnership, serves Medicaid beneficiaries who are receiving long-term care at home through the state's Home and Community-based Waiver (HCBS) program. MaineNET/Partnershipis a program of the Maine Department of Human Services (DHS), but it is a complex program that involves multiple agencies, both state and private, in its administration.
Within DHS, the Medicaid agency is responsible for the overall administration of the program and the state unit on aging is responsible for policy development and implementation. The enrollment broker under contract with the Medicaid agency conducts enrollment, as it does for Maine PrimeCare. The state unit on aging administers two separate contracts for services related to Medicaid members who are eligible for long-term care services, including those beneficiaries who are eligible for the Partnership component of MaineNET. One contract is responsible for the determination of medical eligibility for long-term care services; the other arranges long-term care services for those found eligible. In the case of Partnership members, this contractor (the Health Care Coordinating Agency [HCCA]) provides a care coordinator who manages the member's home- and community-based long-term care services.
The Medicaid agency contracts with selected physician practices to participate as MaineNET/Partnership PCPs. These practices are selected based on the high number of patients in the Home and Community Based Services (HCBS) waiver program. The practices develop collaborative agreements with HCCA so that a care coordinator can be located at the MaineNET/Partnership practice.
Endnote
23. The PCP receives $3.00 for the first 250 patients on his/her panel and $2.50 per patient thereafter.
Chapter 4: Primary Care Providers
Primary care providers are the heart of a PCCM program. All eight case-study states emphasized the importance of establishing adequate networks of PCPs and of developing relationships with those providers. As one official noted, states must take providers seriously and know how to support and serve them in order to have a successful PCCM program.
The contract requirements and expectations of PCPs are similar across PCCM programs. Generally, the PCP is expected to
- provide and/or arrange for the delivery of a certain set of services, defined by the state;
- provide 24-hour, 7 day-a-week coverage through an arrangement that meets the state's requirements;
- follow the state's authorization procedures when referring a patient to specialty care;
- accept all enrollees who either choose or are assigned to his/her panel;
- provide education to the PCCM member about how to seek care;
- not disenroll a patient from the panel unless certain criteria are met; and
- review utilization reports, if available, to ensure that his/her patients are receiving appropriate care.
Who Can Be a Primary Care Provider?
Generally, PCPs in PCCM programs are those physicians who practice primary care, such as pediatricians, family practitioners, general practitioners, internists, and in some instances, obstetricians and gynecologists. States also contract with providers in those settings where many Medicaid beneficiaries customarily seek care: Federally Qualified Health Centers (FQHCs), Rural Health Centers (RHCs), and local public health departments. In Oklahoma, contracting with Indian Health Service PCPs has been explored and is currently under review by HCFA(now known as CMS). All eight case-study states allow some of these providers to serve as PCPs. Chart J shows the range of state policies in this area.
In an effort to maximize access to primary care and to build a network of providers, states also turn to physician extenders to be PCPs. In five of the case-study states (Florida, Maine, North Carolina, Oklahoma, and Texas), nurse practitioners and/or physician assistants are allowed to enroll as PCPs. North Carolina and Texas also include nurse midwives as PCPs. In all instances, state officials comment that using these practitioners as PCPs is essential for increasing access to consistent primary care in their PCCM programs. Although several officials note that the inclusion of physician assistants and nurse practitioners is particularly important in providing access to care in rural areas where there may not be enough physicians, others report that it is equally important in urban areas where physicians cannot accommodate additional patients.
| State | Program | # Providers Participating (Latest Figures) |
Allowable Provider Types |
|---|---|---|---|
| Alabama | Patient 1st | 1500 (both solo and group practices) | GP, family practitioner, internist, pediatrician, OB/GYN, FQHC, RHC, specialist approved case by case |
| Florida | MediPass | 5000 (in 3000 practices) plus disease mgmt. orgs. and provider svc. network | GP, family practitioner., internist, pediatrician, OB/GYN, FQHC, RHC, specialist approved case by case |
| Iowa | MediPASS | 1400 providers | GP, family practitioner., internist, pediatrician, OB/GYN, FQHC, RHC, specialist approved case by case |
| Maine | Maine PrimeCare | 1215 PCPs at 420 sites | GP, family practitioner, internist, pediatrician, OB/GYN, FQHC, RHC, NP, PA |
| MaineNET/ Partnership | 15 | GP, family practitioner, internist, NP, PA, specialists if part of a pilot practice site and doing primary care | |
| North Carolina | ACCESS I | 1500 sites (not individual physicians) |
GP, family practitioner, internist, pediatrician, OB/GYN, FQHC, RHC, NP, PA, nurse midwife, PH department |
| ACCESS II | 139 practices (April) | ||
| ACCESS III | |||
| Oklahoma | SoonerCare Choice PCCM Model | 610 | GP, family practitioner, internist, pediatrician, OB/GYN, FQHC, RHC, NP, PA |
| Texas | Texas Health Network | 2,554 |
GP, family practitioner, internist, pediatrician, OB/GYN, FQHC, RHC, NP, nurse midwife, psychiatrist or other specialist approved case by case |
| STAR+PLUS | 806 | ||
| Virginia | MEDALLION | 2042 (active providers) | GP, family practitioner, internist, pediatrician, OB/GYN, FQHC, RHC, local PH depts., specialists approved case by case |
States have varying criteria as to when they allow specialists to serve as PCPs. Among the case-study states, Alabama, Florida, Iowa, Texas, Virginia, and the MaineNET/Partnership program in Maine approve specialists as PCPs on a case-by-case basis. Officials in states that include persons with special needs in their managed care programs note the importance of identifying the provider who can best serve as the medical home for the member. For example, a pediatrician may remain the PCP for an individual with mental retardation who transitions to adulthood, or a specialist who has been caring for a child with cerebral palsy may be identified as the appropriate PCP when the child enrolls in managed care. Some states make provisions for a specialist to act as the PCP on a time-limited basis if the member's medical needs are better met by that physician for the duration of an illness or condition. The MaineNET program, which enrolls aged and disabled adults, will approve a specialist as the PCP if that physician also provides primary care.
Provider Recruitment
Provider participation is one of the cornerstones of a PCCM program. States with successful PCCM programs have worked hard to gain that participation. The case-study states report that they have learned that the time initially invested in educating physicians and practice office staff during the recruitment process pays off in physician participation later. State provider relations staff, or their contracted designees, visit individual practices, conduct regional orientation and training, and provide follow-up contact prior to finalizing a contract with the provider. Face-to-face contact seems to be extremely important in communicating state program expectations to physicians; according to state officials it cannot be done solely through memos and manuals. Case-study states that have implemented their PCCM programs gradually emphasize the benefits of this approach in attaining physician buy-in. Officials in states such as Iowa, Maine, and North Carolina note the importance of gaining sufficient participation of providers in a given area before activating beneficiary enrollment.
Increasingly, state Medicaid agencies are contracting with provider groups and hospital-owned practices instead of individual physicians. They are also focusing their recruitment activities on traditional Medicaid providers so that members can maintain continuity of care.
- Three of the case-study states (North Carolina, Texas, and Florida) contract with provider service networks in certain areas of the state, in addition to individual PCPs and practices. In these instances, the networks are responsible for the recruitment of PCPs as well as other providers.
- In the MaineNET/Partnership, the state has identified three primary care physician practices to serve as PCPs for MaineNET members. These practices were selected because of the large numbers of their patients who are enrolled in the Home and Community-based Services waiver program.
Case study state officials repeatedly noted the importance of clarifying the expectations of the PCP during the recruitment process. PCPs must understand the contract requirements and their responsibilities in order to avoid problems of misunderstandings or compliance. Some state agency staff acknowledge that initial recruitment was focused largely on getting sufficient provider participation to make the program operational. Now that they have adequate networks, state agency staff feel that they need to focus on improving the performance and caliber of the participating physicians. They want physicians to understand that being a PCP is more than business as usual in the Medicaid program.
Provider Retention
Many of the state officials interviewed emphasized that the development of relationships with participating physicians is critical to keeping physicians enrolled and active in the program. Generally, case-study states reported that physicians accept the PCCM system and often prefer it over an MCO network. One of the physicians interviewed said that he likes the simple logic of PCCM -- linking the patient directly with a PCP. The case management fee is an incentive for the PCP to establish that relationship with his or her patients. As Chart K demonstrates, the case-study states cultivate this willingness to participate by providing information, support, and opportunities for physician input.
| State | Program | Services |
|---|---|---|
| Alabama | Patient 1st | Provider hotline, utilization performance feedback, outreach and education unit provide on-site education for providers who request, or who the state feels need it; will be doing provider profiling as of Spring 2001 |
| Florida | MediPass | Provider focus groups/surveys (esp. in rural areas), utilization performance feedback, newsletter, outreach through disease management organizations |
| Iowa | MediPASS | Hotline, utilization performance feedback, newsletter, advisory committee includes physician from each of six regions |
| Maine | Maine PrimeCare | Newsletter, provider help line, utilization performance feedback (part of incentive payment system), physician advisory committee |
| MaineNET/ Partnership | Case manager coordinates long-term care svcs.; pharmacy profiling report | |
| North Carolina | ACCESS I | Quarterly utilization reports, (moving toward risk-adjusted utilization reports) targeted services reports, referral reports (all shown to doctors), regional consultants (state employees) serve as resources |
| ACCESS II | rovider hotline, utilization performance feedback/provider profile, state staff follow up with members to keep appointments, members can sign up with a practice, providers contract with 24-hour-a-day nurse phone service (can make referrals or authorize services), website | |
| ACCESS III | ||
| Oklahoma | SoonerCare Choice PCCM Model | Toll-free phone line, provider relations staff, specialty care work group, provider trainings (CEUs), nurse advice line for 24-7 coverage, allow provider groups to contract as a whole, follow-up on high ER users, language line, provider updates (on standards), on-site training soon, Exceptional Needs Coordinators (ENCs) |
| Texas | Texas Health Network | Regional advisory committees and function-specific work groups include doctors, customize national standards to reflect unique needs of local populations, provider hotline, utilization performance feedback, network administrator staff follow up with members on missed appointments, network administrator's provider relations staff do outreach with PCCM offices and recruit new providers, annual provider survey, educational workshops/meetings/in-service trainings |
| STAR+PLUS | ||
| Virginia | MEDALLION | Provider hotline, provider relations staff, fiscal agent has dedicated provider service staff, regional provider advisory committees, dedicated quality assurance review analysts |
Training and Education
All case-study states report that provider education is an ongoing process. It does not end with the approval of the contract, nor can it be limited to the physician only; it must include other health professionals and office staff within the practice. Four of the eight case-study states issue periodic newsletters to inform providers about various policy and financial issues related to PCCM. Specific examples of training/education efforts include:
- Field staff for Florida's MediPass program go to provider offices to deliver training and technical assistance, as do MEDALLION provider relations staff in Virginia. They also conduct regional trainings.
- Iowa's enrollment broker conducts training for the PCPs, including providing information about how to coordinate their patients' care with the state's behavioral health plan.
- In Texas, provider relations representatives employed by the plan administrator are based in the six service areas for PCCM STAR. They conduct provider education, contract compliance sessions, and in-service training routinely and upon request.
Support
States also provide support services to PCPs to assist them with their daily practices and contract responsibilities. Most states maintain a hotline that can assist providers with questions about member eligibility, covered services, authorization requirements, and other issues. Field staff help PCPs work with members who may not understand the program and help problem-solve contract compliance issues.
- Oklahoma provides a toll-free information line for providers and a nurse-advice line that offers 24-7 fill-in coverage, that is, 24 hours a day, 7 days a week, for the PCP so that he/she can meet the contract requirements of a PCP. Staff within the nurse-advice service also follow up with members who appear to be using the emergency room excessively. Exceptional Needs Coordinators (ENCs) have been hired by Oklahoma's Medicaid agency to assist persons with special needs in managed care. One of their functions is to assist PCPs with arranging specialty care that the special needs member may require. They have also provided training to providers about the special needs populations that are required to enroll in managed care. The ENCs work in partnership with provider relations staff, providing a team approach to addressing the physician's concerns.
- Primary care physicians participating in North Carolina's ACCESS II and III initiatives have found the case management provided to their patients by the network to be an asset to their practice. Case managers at the network level, supported by the network's portion of the case management fee, help the physicians coordinate the care of their patients.
Feedback to PCPs
As PCCM programs have evolved, some states have developed reporting mechanisms to provide participating providers with information about the costs and service utilization of their patients. These reports vary in the level of detail that they provide; some simply provide aggregate information about service utilization of the physician's panel, while others compare utilization of the practice with that of other providers. A few states also include lists of services that individual patients have obtained to provide a comprehensive picture of the members' utilization histories.
- North Carolina produces a quarterly utilization report for PCPs in ACCESS, including such targeted service reports as emergency room use. This gives the PCP information about where patients are seeking services. The PCP can then work with the local managed care representative to do some follow-up with patients who appear to have used services inappropriately. Physicians participating in ACCESS II and III receive similar utilization reports, with the addition of data from the initial risk assessments that are conducted with all ACCESS II and III members.
- The Maine PrimeCare program produces the quarterly Maine Primary Provider Profile. The report provides information on cost and utilization in a number of areas, comparing the experience of the physician's Maine PrimeCare members and fee-for-service patients with those statewide in his/her specialty. In addition to member per month costs and utilization rates, the report also provides lists of the PCP's Maine PrimeCare members who have used the emergency room or been hospitalized within the quarter. The information in the quarterly report is used to determine incentive payments in the Primary Care Provider Incentive Payment system. (Please refer to the sections on Quality Improvement and Finance for more details.)
Feedback to the PCP is one of the key elements of provider satisfaction, according to the physicians interviewed for this report. One physician is very pleased with the utilization reports he receives from the state and likes how his practice information is compared to that of other physicians within his specialty. He believes that these reports help him and his colleagues manage their patients appropriately. He adds, however, that it is up to the PCP to respond to the comparative information and change his/her practice, if necessary. The other physician interviewed practices in a state that does not currently provide reports to the PCP on patient utilization. He would like to see data on his patients' utilization of services and would like to know how he compares to his peers. He is particularly concerned about his patients' use of the ER. He feels that this is the information that can make the difference between a PCCM program and a traditional fee-for-service program.
Input from PCPs
Many states establish both formal and informal mechanisms by which providers have input into the program. They conduct provider satisfaction surveys, hold focus groups, and organize work groups to address specific program issues. Several states have provider advisory committees for their managed care programs as well as other forums for provider input so that they can maintain ongoing communication with the provider community.
- Alabama has formed the Patient 1st Advisory Council, composed of ten physicians who serve as policy advisors to the Agency. One of their first recommendations was to tighten the contract language to encourage compliance with PCP requirements, particularly in the area of 24-7 coverage.
- Iowa has a Managed Health Care Advisory Committee, composed of six physicians from the state's service regions who provide input to the state on both the MCO and PCCM programs.
- Maine formed a Physician Advisory Committee in June 2000 so that physicians can have ongoing input into the Maine PrimeCare program. The committee is co-chaired by the state Medicaid agency's medical director and the Maine PrimeCare director.
- Oklahoma schedules periodic regional meetings for physicians so that they can give their feedback to the Medicaid agency about various managed care program issues.
- North Carolina has asked physicians to define best practices for the purpose of developing quality improvement measures for the ACCESS II and III programs. The physicians have chosen their own performance measures and, according to state officials, have probably set higher standards for themselves than the state program would have.
Physician satisfaction surveys and anecdotal reports indicate that physicians are generally happy with their participation in PCCM programs. After some initial skepticism, they are satisfied with the case management fee and find that it adds a significant monthly payment to their practice for prevention and patient education activities. They are also glad to be in charge of their patients and not be required to go through an intermediate authorization process. From state officials' comments, physicians seem to want to work with their states to improve the quality of their respective PCCM programs.
Chapter 5: Quality Improvement
States are increasingly active in monitoring and encouraging quality improvements in PCCM; many are using methods similar to those used within MCOs or to those used to manage their MCO contractors. Many of the case-study states have developed processes for monitoring quality and for passing this information back to PCPs in order that they can improve their performances. Some use HEDIS measures; some compare across PCCM and MCO programs or across Medicaid and commercial populations. Also, states are implementing a greater number of strategies for serving members, such as member help lines, nurse advice lines, greater educational efforts, and health assessments.
Member Services
Services designed to facilitate membership are essential components of high quality health care. Some member services are offered in all the case-study states - complaint and grievance processes, member help lines run internally or by enrollment brokers, enrollee interpreter/translation services, new member handbooks and materials, and the provision of lists of participating PCPs to new members. Chart N lists some of the member services offered in the case-study states.
| State | Program | Member Services Included |
|---|---|---|
| Alabama | Patient 1st | Member hotline, grievance/complaint process, targeted case management for medically at-risk or non-compliant patients, enrollee interpreter/translation services |
| Florida | MediPass | Member hotline, grievance/complaint process, disease management, enrollee interpreter/translation services |
| Iowa | MediPASS | Member hotline, grievance/complaint process, newsletter mailings, member handbook and Medicaid guide routinely sent to members, enrollee interpreter/translation services |
| Maine | Maine PrimeCare | Member hotline, grievance/complaint process, enrollee interpreter/translation services |
| MaineNET/ Partnership | MaineNET: PRA-Plus screen, preventive health screen complaint/grievance process, enrollee interpreter/translation services Partnership: above, plus local care coordinator works with physician |
|
| North Carolina | ACCESS I | Member hotline, grievance/complaint process, local managed care representative serves as resource for each county, enrollee interpreter/translation services |
| ACCESS II | Incentives for members to see PCCMs, member hotline, grievance/complaint process, local managed care representative serves as resource for each county, enrollee interpreter/translation services | |
| ACCESS III | ||
| Oklahoma | SoonerCare Choice PCCM Model | Member services department, nurse advice hotline, grievance/ complaint process, case management, member handbook, enrollee hotline, information mailings on benefits and preventive health topics, enrollee interpreter/translation services |
| Texas | Texas Health Network | Nurse advice hotline, customer service help line, prenatal care line for new pregnant members, utilization management help line, grievance/complaint process, ombudsman program (Harris service area only), case management, outreach workers link with health-related and socioeconomic community resources, community-based member health education, community I&R database, case management staff coordinate care for all members who meet criteria, member education materials, newsletter, enrollee interpreter/translation services |
| STAR+PLUS | ||
| Virginia | MEDALLION | Member hotline, grievance/complaint process, enrollee interpreter/translation services |
Additional efforts made by the case-study states include:
- Special hotlines: Oklahoma and Texas have 24-hour/7-day nurse advice lines, in addition to member services hotlines. In Oklahoma, members calling the hotline to determine whether to seek emergency room care are triaged by the nurse, who faxes the state a copy of the recommendation he/she made to the caller. Oklahoma's nurse advice line also calls 10 percent of new members monthly to orient new members; the state plans to increase this to 100 percent of new members in Spring 2001. Oklahoma has a specially dedicated member services department. In Texas, the nurse advice line promotes coordination of care through a faxed summary of the call to the PCP for members who are triaged to emergent or urgent care. Texas also has a 24-hour/7-day utilization management help line for precertification and authorization and a prenatal care line to facilitate appointment setting for newly enrolled pregnant women.
- Incentives: Some of the networks in North Carolina's ACCESS II and III programs offer incentives for members to make and keep appointments. These incentives include diapers and gasoline coupons. Oklahoma has an EPSDT bonus payment system (discussed in greater detail in the Finance section of this report).
- Newsletters: Iowa, Maine, and Texas send quarterly newsletters to all PCCM members. These newsletters include healthy promotion messages; Texas' (which is printed in English and Spanish) includes a cartoon character designed to appeal to children. Iowa also sends letters to beneficiaries to provide education about the appropriate use of the health care system. Maine's enrollment broker distributes the newsletter as well as handles member requests for information.
- Special education efforts: In both the Texas Health Network and STAR+PLUS, Texas gears educational efforts to the needs of the community (as identified in the annual health needs assessment). Outreach staff employed by the plan administrator in each service area conduct new member orientations, EPSDT education, and follow up when a member is overdue for a screen or has sought services inappropriately from an ER. Outreach and education activities occur in places frequented by Medicaid beneficiaries, including their homes. These staff also work with community based organizations to link members to nonmedical services, such as GED classes, housing, child care, and donated housewares. One current project is the Reach Out and Read Program, which distributes books through PCPs' offices. Maine's enrollment broker conducts community outreach and education efforts to increase members' understanding of managed care and EPSDT.
Oklahoma does extensive outreach to newly eligible Aged/Blind/Disabled (ABD) Medicaid beneficiaries, including outbound telephone calls, direct mail, and enrollment fairs. Exceptional Needs Coordinators and other state medical staff complete health profiles of these new members whenever possible. Each profile is sent to the enrollee's chosen PCP, in order to provide that PCP with a medical history of his/her new patient
- Ombudsman program: In the Harris County service area of Texas, STAR+PLUS members can obtain help from the Client Advocate program. The program is designed to represent the beneficiary's interests and facilitates communication between the beneficiary and the provider. Special attention is given to SSI members.
Quality Monitoring
The case-study states conduct a variety of activities related to quality monitoring and improvement, many of which have traditionally been associated with MCOs. As Chart L indicates, all eight states conduct member satisfaction surveys (often the CAHPS survey) and/or focus groups. All monitor 24-hour access; most monitor utilization. Six (Florida, Iowa, North Carolina, Oklahoma, Texas, and Virginia) conduct focused studies (on such state-chosen topics as asthma, immunization [either children or older adults], prenatal care and pregnancy outcomes, access for populations with special needs, hypertension, diabetes, dementia, and EPSDT screening); Maine has contracted an NCQA reviewer to improve methods for designing, tracking, and reporting these studies. Oklahoma is nearing completion on an encounter data validation study for their capitated PCCMs. Five (Florida, North Carolina, Oklahoma, Texas, and Virginia) have contracted with external quality review organizations (EQROs) to conduct reviews of medical records; 24 three of these states (Florida, Texas, and Virginia) also conduct medical records reviews internally. Iowa and Maine also conduct internal medical records reviews.
| State | Program | Quality Activities Included |
|---|---|---|
| Alabama | Patient 1st | Claims data examined for utilization (Medicaid agency), computer generated survey on Medicaid beneficiaries based on services received (e.g., ER use), monitoring 24-hour access |
| Florida | MediPass | Random medical records reviews (independent agency and Medicaid), disease management, focused studies, member surveys/focus groups, monitoring 24-hour access |
| Iowa | MediPASS | Focused studies, member surveys/focus groups, monitoring 24-hour access, HEDIS measurements, random medical record review, Managed Health Care Advisory Committee review and oversight of all quality activities |
| Maine | Maine PrimeCare | Random medical records reviews (Medicaid agency), CAHPS surveys, 24-hour access monitoring |
| MaineNET/ Partnership | PCP must do annual preventive screen, results sent to be used as quality indicator | |
| North Carolina | ACCESS I | Random medical records reviews (PRO), focused studies, member surveys/focus groups, HEDIS (generated from claims data), monitoring 24-hour access |
| ACCESS II | Uniform standards of care, standard set of performance measures, local responsibility for quality (work with providers on-site), uses NCQA to credential PCCM in some networks, pediatric asthma care and diabetes care quality measurement projects | |
| ACCESS III | ||
| Oklahoma | SoonerCare Choice PCCM Model | PRO review (random medical records reviews), uses HEDIS to compare PCCM and MCOs in urban areas, focused studies surveys/focus groups, QARI and modified QISMC, quality assurance committee, encounter data validation study in process, monitoring 24-hour access, enrollee surveys |
| Texas | Texas Health Network | PCCMs credentialed and recredentialed every 2 years using QARI, Texas Dept. of Health, and NCQA standards, random medical records reviews (independent agency and Medicaid), member surveys/focus groups, focused studies, Quality Management/ Improvement Committee meets quarterly, special project on diabetes, complaints, appeals, auditing 24-hour access, annual community health needs assessments |
| STAR+PLUS | ||
| Virginia | MEDALLION | Random medical records reviews (PRO and Medicaid), disease management program evaluates health outcomes, focused studies, member surveys, drafting provider profiling reports, monitoring 24-hour access |
Iowa's Birth Outcomes Study is an example of a focused study. The goal of the study was to compare risk-adjusted quality of care provided to Medicaid mothers and babies in fee-for-service, PCCM, and MCOs. All included records were of mothers who were enrolled for at least 18 months of Medicaid eligibility, including during the pregnancy, and enrolled in the same MCO during the last two months of pregnancy. The study was performed in two stages: comparing outcomes of PCCM and MCO programs in 1999, and MCO and fee-for-service in 2000. In 1999, the sample included 741 PCCM members and 532 MCO members. Conclusions included: PCCM neonates had longer lengths of stay for very low birth weights, but MCO neonates had longer stays for low birth weights; slightly less than 50 percent of mothers in both payment systems had received adequate prenatal care; and maternal and neonatal mortality outcome scores in both programs were better than national averages.
Some states have implemented certain program components/features that are showing success in quality monitoring and improvement.
- Provider profiling: Maine uses provider profiling as part of its incentive payment system for physicians in the PCCM program. On a quarterly basis, pediatricians, family practices/group practices, internists, and OB/GYNs receive scores for measures related to each of the goals shown in Chart M. They are then ranked with other members of their provider group. Quarterly payments are made to physicians within the top 20th percentile within each provider group. (For more information on the payment structure, please see the Finance section of this report.) Although in cases of group practices or physicians working for hospitals, the physicians may not see the payments; the profile reports are sent directly to each physician. Both state officials and a physician interviewed for this study agreed that physicians appreciate obtaining this information. State officials noted that PCPs pay close attention to the scores and rankings; the state receives approximately 25 calls after each profile is released from physicians seeking ways to improve their scores.
- Texas also distributes provider profiles, which are risk-adjusted and have peer group comparisons, to providers. Outliers are identified and education performed. Alabama will begin distributing provider profiles in Spring 2001. MaineNET monitors practice profiles in demographics, clinical practice, quality indicators, utilization, and cost; however, this information is for state use only. Virginia and North Carolina are currently determining the indicators to be included in future provider profiles. A physician from a state without provider profiling who was interviewed for this study asserted that he would appreciate having the opportunity to compare his performance with that of his peers.
| Goal | Weight | Measures |
|---|---|---|
| Reduce disincentives to having higher Medicaid patient panels | 40% |
|
| Reduce inappropriate emergency room utilization |
30% |
|
| Increase the utilization of preventive services | 30% |
|
- Local accountability: North Carolina's ACCESS II and III networks are required to follow uniform standards founded on evidence-based best practices measured through a standard set of performance measures. Each network is responsible for quality monitoring and improvement; state staff work on-site with these networks to facilitate a rapid cycle quality improvement process. 25 Local networks define and select performance measures. Examples of quality improvement initiatives include: identifying and decreasing inappropriate emergency room use, improving processes for referrals and prescriptions, managing inpatient admissions through education and follow-up, developing a health screening process to identify members needing case management, and program-wide asthma and diabetes disease management programs.
- Use of HEDIS/other measures: Iowa, Maine, North Carolina, and Oklahoma use HEDIS measures to monitor PCCM providers. Oklahoma uses this data to compare its PCCM and MCO Medicaid programs in urban areas. Maine compares PCCM, MCO, and fee-for-service Medicaid programs, as well as commercial programs, across 15 measures. Iowa uses HEDIS for internal analysis; the first series of results were provided through an independent organization in August 2000.
Oklahoma formerly used QARI and now relies on modified QISMC standards to compare PCCM and MCOs. Texas uses QARI standards. Oklahoma will soon begin on-site reviews with a sample of providers; focus areas will include finance, care management, professional services, and member services.
- Advisory committees: Alabama, Iowa, Maine, and Texas have quality improvement committees, usually composed of participating physicians. Oklahoma's newly formed committee looks at all forms of Medicaid (fee-for-service, PCCM, and MCO) and has a physician participating in PCCM. Maine PrimeCare has a physician advisory committee; MaineNET/Partnership has a clinical advisory group which requires the participation of at least one PCP from each pilot site. These advisory committees deal with issues other than those strictly of quality, such as confidentiality concerns. (For more information on these committees, see the Primary Care Providers section of this report.)
- Community health needs assessments: Texas counties conduct annual community health needs assessments in six regions, surveying both members and physicians. These assessments form the basis for planning educational efforts. Educational topics resulting from these assessments include pediatric illnesses, otitis media, and sexually transmitted diseases (STDs).
- Targeted surveys (in addition to all-member satisfaction surveys): Alabama generates a list (from computer databases) of Medicaid beneficiaries who have used specific services (e.g., emergency room) and sends surveys to the people on this list. This survey asks four or five questions on such issues as patient wait times and satisfaction. State officials use the survey as a concentrated way to determine specific needs for a doctor or service.
Florida, Virginia, Texas, and Maine conduct periodic provider surveys to gauge their satisfaction with the PCCM program; Maine surveys both PCPs and office staff. Maine PrimeCare is in the process of piloting a FAACT survey to assess the delivery of care to children up to the age of four and will be surveying adolescent members using a tool also developed by FAACT.
- Pharmacy management: Florida, Oklahoma, Texas, and Maine have pharmacy management structures in place for their Medicaid managed care programs, including PCCM. Florida limits the number of brand-name pharmaceuticals (for which a generic equivalent exists) to four in both the PCCM and fee-for-service Medicaid programs, after which the PCP must get prior authorization. Texas identifies overutilizers of pharmacy services and performs outreach, often linking the member with plan services that include member education and case management. All MaineNET PCPs must participate in the MaineNET Pharmacy Management Program, which focuses on polypharmacy and medication review, appropriate prescribing within targeted chronic conditions, and cost-effective prescribing within targeted major drug categories, through information provided by the Medicaid Physician Directed Drug Initiative. The state provides ongoing pharmacy reports for each MaineNET member to his/her PCP, including all prescriptions filled. The Maine Medicaid agency's narcotics project for pain management has a physician to oversee the pharmacy use of beneficiaries (including Maine PrimeCare members) who have large numbers of pain prescriptions, such as oxycontin.
Disease Management
Disease management strategies can be seen as both a form of quality improvement and a type of member services. The system is better served through appropriate utilization of services leading to lower overall costs; the chronically ill person is better served by having systematic health care that is state-of-the-art for his/her particular illness.
Three case-study states (Florida, North Carolina, and Oklahoma) have developed formalized disease management structures and approaches. Florida has chosen to contract with disease management organizations; sites in North Carolina's ACCESS II and III programs and Oklahoma's program have chosen to develop internal programs. Texas has implemented a special project on diabetes as a pre-curser to a formal disease management program. The Virginia Medicaid agency has a disease management program, but this is considered separate from its PCCM program; the two programs intersect if the PCCM member happens to require disease management assistance.
Florida has hired disease management organizations (DMOs) to serve patients with six chronic illnesses.
- HIV/AIDS (one vendor covers all but two counties; second vendor covers remaining two counties)
- Hemophilia (two providers)
- End stage renal disease (ESRD) (one provider)
- Congestive heart failure (one provider currently under contract; state is negotiating with second provider)
- Diabetes (statewide)
- Asthma (one provider)
Each contractor must guarantee the state 6.5 percent annual savings compared to adjusted baseline per member per month spending for PCCM members with these illnesses.
Approximately 100,000 Floridian PCCM members qualify for one of these DM programs. On a monthly basis, the Medicaid agency analyzes the claims of PCCM members to identify CPT codes that relate to the six illnesses listed above. The state created a claims analysis hierarchy with the first cut for HIV/AIDS, the second for hemophilia, and on down the list. Therefore, a person with both HIV/AIDS and asthma will be served by the HIV/AIDS DMO. The names of individuals with these CPT codes are sent to the appropriate DMOs, which are required to send letters within 30 days informing these individuals about the program. These individuals are automatically enrolled unless they choose to opt out. The DMOs are required to work with the individuals' PCPs. Many DMOs offer additional benefits to participants, such as glucometers for people with diabetes.
The Florida HIV/AIDS DMO distributed to physicians a CD-ROM with state-of-the-practice protocols and guidelines. It provides a comprehensive source of the most up-to-date information for the medical community and a baseline of information in support of the DM initiative. 26
All North Carolina's ACCESS II and III sites have implemented internal asthma disease management programs. One site is currently running diabetes disease management programs; all sites will have such programs within the next year. The sites chose asthma as the first DM initiative based on the following principles: 27
- There are enough Medicaid members with the disease to obtain a return on investment.
- Evidence exists that best practices lead to predictable and improved outcomes.
- Appropriate evidenced-based practice guidelines are available.
- Physicians will support the process.
- Patient education and support can improve outcomes.
- Best practices and outcomes are measurable, reliable, and relevant.
- There is room for improvement — a gap exists between best practice and everyday practice.
- The ability exists to measure baseline and thus to be able to measure improvement.
The core elements of the Asthma Disease Management Program were developed by the sites themselves with the help of state staff. The four core elements are listed below and further detailed in Appendix B.
- Build capacity for routine assessment of asthma.
- Reduce unintended variation of care and establish consistency of care.
- Build capacity to educate patients, families, and school personnel about asthma.
- Regularly report outcomes and process measures to all providers and staff.
With these core elements in place, the participating sites implemented a number of asthma management initiatives.
- A health risk assessment process;
- An asthma action/management plan;
- A process to ensure that a copy of the asthma action plan goes to the patient and family, PCP, and local school/day care;
- An arrangement with durable medical equipment providers to stock and provide peak flow meters and spacers to Medicaid beneficiaries while they are in the PCP's office;
- Patient education materials on asthma management;
- Home and environment assessments on the at-risk asthma population;
- Provider and provider staff education sessions;
- Asthma management forms for the PCP and medical records that coordinate care and ease the burden of paperwork; and
- Shared office processes and best practices.
The group also developed quarterly performance measures for the Asthma Disease Management Program. These take into account both outcomes (e.g., emergency room use rate for asthma) and process (e.g., proportion of asthma patients with an asthma management plan). Outcome information is gathered from claims data. Process information is obtained through chart reviews.
In Oklahoma, participating physicians assess their practices related to diagnosis and treatment. They are expected to follow the National Asthma Education and Prevention (NAEP) guidelines recommended by the National Heart, Lung, and Blood Institute. The state offers on-site assistance, patient education, and monitoring materials. Physicians benefit from participation because they are able to apply what they learn, along with the program materials (encounter forms, self-assessment and action plans, patient education brochures) to their entire asthma patient population. Oklahoma is also considering a collaborative on depression and a diabetes disease management program.
Endnotes
24. Maine used an EQRO in the past; these reviews are now conducted by state staff.
25. The model of rapid cycle quality improvement was developed by the Institute for Healthcare Improvement. It focuses on the processes of "plan, do, study, and act", and stresses setting aims, establishing measures, and making system changes to remove barriers to care.
26. Vernon K. Smith, Terrisca Des Jardins, and Karin A. Peterson, Exemplary Practices in Primary Care Case Management: A Review of State Medicaid PCCM Programs (Princeton, NJ: Center for Health Care Strategies, Inc., 2000), 62.
27. Bulleted North Carolina information in this section taken from: Department of Health and Human Services, "ACCESS II and III Plans Asthma Disease Management Program", ACCESS II and III Update no. 2 (July 2000), 1-8.
Chapter 6: Finance
Early PCCM programs were implemented when Medicaid reimbursement rates to physicians were extremely low compared to the rates of other payers. Many Medicaid agencies were concerned about retaining sufficient provider participation to offer adequate access to primary and preventive care. As a result, contracted PCPs were not asked to accept any financial risk for provision of care. Until recently there were only two major forms of reimbursement among state PCCM programs.
- Fee-for-service payment for all services provided to members, plus a case management fee. In 1998, 26 of the 29 states (90 percent) with PCCM programs used this method.28
- Fee-for-service payment for all services, including an enhanced rate for routine office visits by PCPs, with no care coordination fee. In 1998, 4 of the 29 states (14 percent) used this method. 29
It was thought that continuing fee-for-service payments would create an incentive for PCPs to see their members on a regular basis. The 1998 data also showed that two states (California and New York) shared any savings generated by the PCCM program with contracted PCPs, in addition to one of the standard forms of reimbursement, to create an incentive for PCPs to closely manage referrals and specialty care. Recently, some states have begun applying such financial strategies as capitation or bonus payments, used by MCOs, to their PCCM programs.
Case Management Fees
Paying a case management fee plus fee-for-service is the dominant payment method among the eight case-study states. Only one, Oklahoma, did not use this reimbursement method, since it pays a capitated rate. (This system is detailed later in this section.)
Among the seven case-study states that pay case management fees, $3 per person per month is the most common fee.
- Alabama, Florida, Maine (Maine PrimeCare), Texas (both Texas Health Network and STAR+PLUS), and Virginia all pay $3 per person per month.
- Iowa pays $2 per person per month.
- North Carolina pays
- all PCPs $3 per person per month for the first 250 members and then $2.50 per person per month for the remainder; and
- the sponsor network an additional $2.50 per person per month for each member in the ACCESS II and III programs
- Maine pays all PCPs in its MaineNET program $5 per person per month. If the member is also a member of the Partnership program, the practice to which the PCP belongs receives a $20 per person per month case management fee (instead of $5).
Three PCCM programs in two case-study states (ACCESS II and III in North Carolina and MaineNET/Partnership in Maine) have begun to extend the case management fee method of payment to providers other than the PCCM provider. All three programs serve people with disabilities and the elderly.30 In all three programs, this method of payment is extended to other entities that play a large role in providing the type of care that PCCM members need.
All three programs pay an additional fee to an organization that supports the PCP's ability to practice.
- In North Carolina's ACCESS II and III programs the case management fee is extended to the network to which the PCP belongs. The networks use this fee to perform care management activities, including conducting risk assessments to identify members at greatest risk, operating targeted disease management initiatives, and hiring care managers who work with the PCP to coordinate care delivered to individual members. (Please see the Service Management section for more information on these positions.)
- Physicians participating in the MaineNET/Partnership receive a $5 case management fee for MaineNET members and a $20 case management fee for Partnership members. This fee is to compensate the practice for the time needed to coordinate the care of members, all of whom have very complex needs.
The MaineNET/Partnership is a separate contract between the Medicaid agency and a contractor that manages the care of all beneficiaries in the state who need community long-term care services. This contractor is paid $100 per member per month for eligible beneficiaries who are receiving Home and Community Based Services (HCBS) waiver services (regardless of their participation in Partnership). Care coordinators arrange, but do not pay, for the long-term care services a member needs to remain in the community. This contract is discussed here because the Partnership must co-locate one of their care coordinators at each MaineNET/Partnership physician's practice. The co-location of care coordinators enables the member to have both medical and long-term care needs addressed at a single location and often in a single visit. This arrangement is also an advantage for the physician, who gains the expertise of the care coordinator to help provide better care for patients with the most complex needs.
Capitation
The BBA's definition of a PCCM provider31 does not exclude providers who are capitated for providing services, thus creating a new class of capitated PCCM programs. HCFA(now known as CMS), however, also considers PCPs in capitated PCCM programs to be either PHPs or MCOs (depending on the package of capitated services) and regulates them as such.
Among the case-study states only Oklahoma pays PCPs using capitation. The capitation rates ($15.90 for TANF and $23.26 for ABD) cover primary, preventive, and case management services (including lab and X-ray services). Oklahoma Medicaid representatives reported taking this approach for two reasons.
- They believe paying a capitation for primary, preventive, and case management services emphasizes the medical home concept; and
- The state legislature mandated the use of capitated models to assure greater budget predictability. Creating a capitated PCCM was a means of achieving that goal in areas where sufficient MCO participation might not occur.
At first, some providers expressed concern with a capitated approach. The Medicaid agency, therefore, piloted the program for a few months in three counties. Providers in those counties successfully managed the primary and preventive services under the budget imposed by the capitation. Word of this success encouraged other providers to join the program.
Oklahoma also requires PCPs to serve those with complex needs, such as the aged and those with disabilities. Providers were concerned about taking on the additional risk of serving those populations under a capitated arrangement. The Medicaid agency successfully allayed those concerns by instituting a bridge payment under which the agency agreed to pay any difference in cost between the capitation payment and the cost, in the fee-for-service system, of serving those with complex needs. This payment was retroactively calculated based on the fee-for-service cost of all capitated services (as reported in encounter data) actually provided to the member.
Financial Incentives for Performance
As reported in other National Academy for State Health Policy work,32 states have begun to create financial incentives for good MCO performance. Two case-study states have extended this concept to their PCCM programs. Both use bonus payments to enhance the medical home concept by rewarding PCPs who provide the best access to key primary care services.
- Maine established a $3 million per year fund for bonus payments to the Maine PrimeCare PCPs who show the best performance on a series of measures related to access, emergency room utilization, and prevention/quality. (See the Quality Improvement section of this report for more details on these measures).
- Oklahoma offers a bonus payment to PCCM providers who exceed expected performance in provision of EPSDT screens to members. The bonus amount increases in proportion to performance.
Maine's system is the more extensive of the two, and has been in place since July 1998. For purposes of calculating this payment, PCPs are grouped by specialty and panel size so that physicians compete only with their closest peers. Those providers whose performance is in the top 20 percent of their group receive a bonus payment. Those who perform better receive larger bonuses. The specific amount of an individual provider's bonus payment depends on provider specialty and overall performance.
Maine Medicaid staff report satisfaction with this system. Based on calls from physicians regarding their performances, state staff also believe that this system does encourage physicians to improve their performances, although it is not always clear how much of the concern with improving performance results from simply knowing where they rank against other practices versus from the potential bonus payment. Some physicians in group practices may not realize that they receive a bonus payment, as it may go directly to the practice's business office. Maine Medicaid staff are working to develop a way to make the physicians aware of the payment without creating accounting problems within the billing office.
Savings
All of the case-study states reported that their PCCM programs produce savings when compared to fee-for-service programs. Some concern was expressed, however, about what impact the BBA requirements for emergency room usage would have on future savings. As discussed in the Evolution of PCCM section, the BBA requires Medicaid agencies to pay hospitals and physicians for emergency room visits using the prudent layperson standard. All but one of the case-study states (Virginia) indicated that they believed this new language essentially required them to pay for all emergency room visits. Some case-study states reported that PCPs also believed that the new language hampered their ability to manage their patients' emergency room usage. Given that much of the savings from PCCM programs results from improved state and PCP management to prevent inappropriate emergency room visits, they felt this new language would reduce the amount of cost savings that PCCM programs produce.
Endnotes
28. See Note 2 for source of all 1998 information.
29. California reported using both methods and is, therefore, counted twice in these statistics.
30. In the case of MaineNET/Partnership, the program serves only those Medicaid beneficiaries who also receive Medicare, live in the community, and require a level of care that would normally require placement in a nursing home, effectively limiting the program to serving those elderly who have the most complex needs. The complex needs of the populations enrolled also account for the higher than standard case management fee paid to PCPs for MaineNET/Partnership members.
31. Please refer to the Evolution of PCCM section for the full BBA definition.
32. Neva Kaye and Michael Bailit, Innovations in Payment Strategies to Improve Plan Performance (Portland, ME: National Academy for State Health Policy, 1999).
Chapter 7: Service Management
States require PCPs to directly provide or authorize through referral a full range of Medicaid services. Chart O illustrates services commonly provided or authorized by the PCP in the eight case-study states. These states uniformly include primary and preventive services; however, several states allow Medicaid beneficiaries to obtain EPSDT services, immunizations, OB/GYN services, and family planning services from providers other than their PCPs without a referral. These states commonly exclude dental, mental health/substance abuse services, residential care, and long-term care services.
| State | Program | Services |
|---|---|---|
| Alabama | Patient 1st | Physician, services, excluding dental and family planning, outpatient hospital services |
| Florida | MediPass | Hospital, lab, x-ray, EPSDT, immunization, family planning |
| Iowa | MediPASS | Physician, hospital, lab, x-ray, EPSDT (no authorization required), immunization, home health, durable medical equipment (DME), hearing |
| Maine | Maine PrimeCare | Physician, hospital, lab, x-ray, chiropractic, audiology, DME, EPSDT, home health, optometry, physical/occupational/speech therapy, podiatry |
| MaineNET/ Partnership | All Medicaid services (including pharmacy, mental health) | |
| North Carolina | ACCESS I | Physician, hospital, lab, x-ray, skilled nursing, EPSDT, immunization, family planning, durable medical equipment, hearing, hospice |
| ACCESS II | ||
| ACCESS III | ||
| Oklahoma | SoonerCare Choice PCCM Model | Physician, lab, x-ray, EPSDT, immunization, case management |
| Texas | Texas Health Network | Physician, hospital, lab, x-ray, case management, skilled nursing facility, EPSDT, immunization, family planning, home health, mental health (no referral or prior authorization needed except for inpatient psychiatric) |
| STAR+PLUS | ||
| Virginia | MEDALLION | Physician, hospital, lab, x-ray, home health, EPSDT, DME, OB/GYN (no referral required) |
Referral Policies
Referral policies can impact PCCM programs in several ways. First, case-study states reported that the more rigorous the policies, the more accountability is built into the system. On the other hand, more rigorous policies can create obstacles for PCPs as well as their patients, which may discourage the PCPs' continued participation in the program.
Referral policies vary among the eight case-study states, ranging from a requirement for paper referrals (which can be faxed to the state) prior to authorization to phone referrals with documented follow-up. State officials working solely with paper referrals noted that this is the largest source of complaints among PCPs; however, a physician interviewed noted that MCOs often have the same requirements, so it has become standard procedure.
Several states expressed concerns that specialists or emergency room physicians were using referral authorization numbers repeatedly and without the PCP's knowledge. A recent study on PCCM programs found that Florida requires its new fiscal intermediary to implement a system to provide a unique number for each specialist referral. Upon need, the provider will place a call to an 800 number, where an automated system will generate a unique referral authorization number valid for 90 days.33 Several states, such as Maine and North Carolina, send out periodic utilization reports showing referrals; the state follows up incidents with the specialist or emergency room staff in cases where the PCP claims not to have made a referral. Iowa reports on emergency room utilization and pharmacy utilization by members.
Florida officials noted that they are tightening the prior authorization process by creating disincentives for PCPs to make frequent referrals. They are concurrently increasing their interaction with PCPs in order to make the system more user-friendly.
Florida also manages pharmacy costs by imposing a four-drug limit on brand-name drugs that have generic counterparts. PCPs wishing to override this limit must seek authorization from the state's pharmacy benefits manager. State officials are pleased with the results of this policy.
Iowa has a behavioral health organization (BHO) contracted to serve Medicaid beneficiaries, called the Iowa Plan. PCPs can provide mental health services to patients up to 12 times per year without authorization from the Iowa Plan; after the twelfth session, they must obtain this authorization. The state has worked to educate PCPs about the Iowa Plan in the hope that they will make referrals to the plan before the patient's twelfth visit. The state also encourages the Iowa Plan to coordinate with the PCP, since services that it provides may impact the general health of the member.
Health Needs Assessments
In Maine, MaineNET and Partnership staff perform initial and annual assessments on each member. Initial assessments use the PraPlus tool34, designed to identify people at high risk of hospitalizations unless they obtain additional medical or social support services to lower their risk, as well as to identify needs for cognitive or dementia follow-up. The questionnaire is completed over the phone with the member by the enrollment broker for MaineNET members and the care coordinator for Partnership members. The enrollment broker reviews all questionnaires and calculates a score, which is relayed to the PCP. MaineNET developed its Periodic Preventive Screen with recommendations taken from the U.S. Preventive Task Force. It includes questions on level of function, need for assistance, current service utilization, medical history, preventive screens and immunizations, and follow-up needs. PCPs or care coordinators are to conduct this assessment with each member at least annually; a copy is sent to the state, as well as kept in the medical record.
ACCESS II and III sites in North Carolina complete health needs assessments on all new members. These are frequently completed by care coordinators working with members. Oklahoma has also implemented health needs assessments to better coordinate care for newly enrolled ABD beneficiaries (as referenced in the Quality Improvement section, earlier in this report).
Care Coordination
Several case-study states have designated care coordinators to assist Medicaid beneficiaries in PCCM programs. North Carolina officials reported that care management, targeted appropriately, has been critical to the success of ACCESS II and III. Many networks have hired their own care managers and developed individual care management initiatives. PCPs appreciate the functions undertaken by care coordinators, including conducting health needs assessments with all new members. For example, care coordinators in sites participating in the asthma disease management initiative35 have
- implemented a screening process to identify those members who would most benefit from case management;
- reinforced compliance in managing asthma;
- performed home visits for environmental assessments and patient education;
- provided outreach and follow-up for PCP visits for checking compliance with home monitoring;
- managed and coordinated referrals;
- educated provider staff and implemented educational activities within the PCP's practice; and
- assisted individual practices in implementing quality improvement activities.36
Oklahoma has three Exceptional Need Coordinators (ENCs) serving all Aged/Blind/Disabled Medicaid beneficiaries in PCCM in rural areas. The state is currently seeking to hire one more ENC and also mandates MCOs to employ ENCs in contract requirements. Two ENCs are RNs and the other is a social worker with extensive field experience; state officials are pleased with the combination of skills embodied in these three individuals. ENCs primarily serve Medicaid beneficiaries in PCCM or fee-for-service but also assist the ENCs within MCOs, as needed. PCPs call the state provider representative for their area in order to initiate contact with the ENCs; members can self-refer, or PCPs can call ENCs directly.
In Texas, regional case managers employed by the plan administrator coordinate medical care (working with the PCP) and non-medical care for certain PCCM members. These workers link with health-related and socioeconomic community resources, working from community-specific information-and-referral databases that can be accessed through the state's web site. Case management staff, employed by the plan administrator, coordinate care for members who meet certain criteria.
Iowa has 250 providers enrolled in a program in which they receive a periodic list of their members who are due for immunizations and EPSDT screening examinations. The Department of Human Services contracts with the Department of Public Health to provide such notification to all other PCCM members.
MaineNET's Partnership program serves people who are eligible to receive long-term care services in the community. Upon voluntarily joining the program, these individuals work with a care coordination organization and the PCP to develop a care plan for long-term care services, including necessary social and community services. An employee of the care coordination organization, typically an RN or LSW, is located in the PCP's office. While members do have a choice of PCP, they work with the care coordinator assigned to that PCP's office. The care coordinator works with the member and PCP to implement the care plan through telephone coordination and in-home case management, coordinating services among providers as needed, as well as administering yearly risk screens. The care coordinator also serves as a resource to the PCP and staff, sharing knowledge of long-term care programs and informal services available. The PCP continues to provide primary and acute services and collaborates with the care coordinator on the care plan as necessary; the care coordinator may even attend office visits with the approval of both the PCP and the member. Average caseload per care coordinator is 50-60 clients; potential practice sites are considered for inclusion in the program if their practices have at least 50 potential Partnership clients who would support a full-time care coordinator. The state is currently developing performance measures for the care coordination piece of this program.
Endnotes
33. See Note 27.
34. The Pra Plus tool is designed to identify older adults at high risk medical risk within the next four years, particularly those at highest risk for inpatient care (Pra = Probability of Repeat Admissions). Copyright 1996 by the Regents of the University of Minnesota.
35. For more information on this initiative, see the Quality section of this report.
36. North Carolina Department of Health and Human Services, "ACCESS II and III Plans Asthma Disease Management Program", ACCESS II and III Update no. 2 (2000), 7.
Chapter 8: Enrollment
Populations Enrolled
State Medicaid programs include several eligibility groups in their PCCM programs. With the exception of the MaineNET/Partnership program, the eight case-study states require mandatory participation of certain eligibility groups. Most states selected AFDC/TANF eligibles and related eligibility categories for initial enrollment in their Medicaid managed care initiatives. As they developed more experience, states added those populations considered to be more challenging for a managed care environment. Among the eight case-study states, six include eligibility groups in addition to TANF/related in mandatory enrollment. These eligibility categories include SSI disabled children and adults, aged beneficiaries, and children in foster care. Under the BBA, states are permitted to mandate managed care enrollment as a state option for most beneficiaries without obtaining 1915(b) or 1115 waivers. States must still seek a waiver from HCFA(now known as CMS) if they require mandatory enrollment of certain Medicare beneficiaries, American Indians/Alaska Natives, and special needs children.37 Since the advent of the State Children's Health Insurance Program (SCHIP), all of the study states except North Carolina and Texas have incorporated CHIP members into their PCCM programs. North Carolina provides CHIP coverage outside the Medicaid program. Chart P lists the populations included in mandatory managed care enrollment, as well as total numbers of people enrolled.
| State | Program | Total Enrolled (Latest Figures) |
Populations Included in Mandatory Managed Care Enrollment |
|---|---|---|---|
| Alabama | Patient 1st | 355,000 (Oct 1) | TANF38, SOBRA children, SSI, Aged, CHIP |
| Florida | MediPass | 580,000 (Oct 1) | TANF, SSI, foster care children, CHIP |
| Iowa | MediPASS | 47,000 (Oct 1) | TANF, CHIP |
| Maine | Maine PrimeCare | 71,677 (Oct 1) | TANF and related, CHIP (Medicaid expansion) |
| MaineNET/ Partnership | MaineNET: 40; Partnership: 40 (Oct 1) | Enrollment not mandatory | |
| North Carolina | ACCESS I | 413,702 (Oct 1) | TANF, SSI, Aged/Blind/Disabled (ABD) |
| ACCESS II | 137,305 (Oct 1) | ||
| ACCESS III | 28,112 (Oct 1) | ||
| Oklahoma | SoonerCare Choice PCCM Model | 140,336 (Oct 1) | TANF, SSI, Aged, CHIP (Medicaid expansion) |
| Texas | Texas Health Network | 209,000 (Oct 1) | TANF |
| STAR+PLUS | 6,000 (Oct 1) | SSI children, certain MH/MR | |
| Virginia | MEDALLION | 127,828 (Aug 31) | TANF, SSI, Aged, CHIP |
The MaineNET/Partnership is a voluntary program for Medicaid beneficiaries in the SSI and Aged eligibility categories. If they receive long-term care services at home as part of the Home and Community-based Services (HCBS) waiver program, they are eligible to receive Partnership services as well. Beneficiaries who reside in a nursing home or a facility for people with mental retardation, or who are enrolled in the HCBS waiver for persons with mental retardation, are excluded from enrollment.
States often make exceptions to their mandatory enrollment requirements for certain individuals and groups who may be better served outside the state's managed care delivery system. These individuals may enroll in the PCCM program but are not required to do so. Alabama, Florida, Maine, Iowa, and Virginia exempt persons with special needs and medical conditions on a case-by-case basis if it appears that their health needs can be better met in a fee-for-service system. American Indians/Alaska Natives are not exempt from participation in the Maine PrimeCare program, North Carolina ACCESS, and Texas Health Network, because they may receive their health care from providers (such as the Indian Health Service) who do not participate in the state's PCCM program. Maine enrolls pregnant women with primary care providers and tells the women that they can choose their own providers for pregnancy-related OB care. North Carolina makes participation voluntary for pregnant women.
States also identify a range of Medicaid eligibility groups who are excluded from participating in their managed care programs. These are often populations who, because of medical or residential needs, or their dual eligibility status, would be difficult to serve effectively in a managed care environment. States commonly exclude dual eligibles (Medicaid beneficiaries who are also eligible for Medicare), children who are in the state's foster care and subsidized adoption programs, and those individuals who reside in nursing facilities or other residential care. (Please refer to Appendix C for a complete listing of enrollment exemptions and exclusions in the case-study states.)
Enrollment Process
The enrollment process is fairly standard from state to state, and PCCM programs face similar issues and challenges in developing systems that provide adequate information and notification to members. States are increasingly using private vendors to conduct enrollment and other functions for their managed care programs. Six of the eight case-study states contract with an enrollment broker; Alabama and North Carolina do not. Several of these states (Florida, Virginia, and Iowa) initially conducted enrollment services internally, then converted to contracting with an outside vendor for this function. Maine used an enrollment broker for the first year and a half of its managed care programs, then brought the enrollment function into the state agency using welfare to work participants as enrollment staff. The state subsequently decided to contract with an enrollment broker again; the current contractor has hired some of these workers.
Among the states using enrollment brokers, officials appear to be satisfied with the performance of their contractors and the collaborative relationships they have developed. They report that they work with their respective contractors on a nearly daily basis, thereby preventing problems before they occur.
Regardless of whether a state uses an enrollment broker or retains enrollment as a state-administered function, there are certain issues that are intrinsic to Medicaid managed care enrollment. Informing prospective members about Medicaid managed care and its requirements is one of the most challenging tasks, according to state officials, yet one of the most critical for the success of the program. As one state official noted, the top issue is whether members really understand and agree/comply with what it means to enroll with a PCP and how to access services. States use a variety of strategies to inform beneficiaries about their managed care choices, including
- informational materials and instructions about how to enroll;
- group educational sessions;
- 1-800 help lines; and
- individual face-to-face counseling, in some instances.
In general, enrollment staff, whether employed by the state agency or by an enrollment broker, have limited personal contact with the prospective member unless the member calls for further information. Maine has tried to counter that limited contact with phone outreach to prospective members. The state's enrollment broker works with the regional eligibility determination staff to get the most current telephone numbers of Medicaid beneficiaries in order to call and encourage them to choose a PCP. State staff believe that their voluntary choice rate of 85 percent is due, in part, to their success in reaching prospective members by telephone.
Several Medicaid staff commented that they would like to see the agency responsible for Medicaid eligibility determination take a role in educating the beneficiary about managed care. Iowa provides training about its managed care programs to income maintenance workers who determine eligibility in the county offices so that they can reinforce managed care information for new members. In Maine, state eligibility workers previously provided information about PCCM to TANF beneficiaries during their orientation, but the Bureau of Family Independence (the state agency responsible for eligibility determination) decided to eliminate this task from the workers' duties. According to state Medicaid staff, this change in policy has resulted in new members not knowing anything about PCCM when asked to choose a provider. They often call their caseworkers at the Bureau for Family Independence for information about the program, creating more work for eligibility staff.
States also struggle with the challenge of enrolling new members in managed care as soon as possible after their initial Medicaid eligibility determination. Officials comment that they often lose contact and continuity with prospective members between the time they are found eligible for Medicaid and the time they are asked to enroll in PCCM; the mobility of Medicaid beneficiaries presents a considerable challenge. Maine enrolls PCCM members on either the 1st or the 15th of the month, whichever gives the new member at least a five-day notice. The state previously did daily enrollment, but this constant flow of information was too difficult for physician practices to administer. Virginia is in the process of reducing the window for prospective members to select a managed care option from 60 days to 30 days. Staff believe that the longer time frame resulted in many missed opportunities to provide appropriate health care, particularly for pregnant women.
Several of the case-study states have implemented lock-in requirements, mandating that the member stay with a PCP for a certain period of time. The case-study states, including those without lock-in provisions, report minimal disenrollment in their PCCM programs; few members elect to change their PCP when given the opportunity.
- Florida has a 12 month lock-in provision for both its PCCM and MCO systems.
- Iowa has the Extended Participation Program, which requires members to stay with their PCP in the PCCM program or their MCO for six months.
- Virginia also has a six-month lock-in provision, but state officials note that members are permitted to change their PCP within the lock-in period. When they have legitimate reasons for requesting a different PCP, their requests are approved.
- Oklahoma initially had a lock-in requirement but, as of July 1999, permits members to change their PCP up to four times a year.
Enrollment of Special Needs Populations
A few of the case-study states have made specific accommodations in their enrollment processes for special needs populations. The practices of Alabama and Oklahoma are of particular interest.
Alabama pays close attention to the enrollment of individuals with special needs. As the state proceeds with enrollment county by county, it works with community agencies in the particular county to identify subpopulations of individuals with special needs. The state makes sure that specific providers who serve persons with special needs are recruited as PCPs before proceeding with mandatory enrollment. When bringing on a county with a fairly large population of Russian Medicaid beneficiaries, state agency staff contacted a physician in the community who speaks Russian and serves the population. The physician assisted the state by helping prospective members understand the program and how to enroll.
Oklahoma began enrolling the Aged, Blind, and Disabled (ABD) populations in its PCCM and MCO programs in January 2000. The state adopted several strategies to facilitate the enrollment of these individuals.
- Staff education: The Medicaid agency worked closely with regional eligibility determination staff to educate them about the particular needs and concerns of the ABD members and about their managed care options.
- Enrollment fairs: The Medicaid agency staff (including Exceptional Needs Coordinators) conducted health fairs and informational events at sites accessible to the targeted populations to help them understand how their health care delivery was going to change.
- Transportation: The state enlisted the transportation contractor to transport prospective members to the enrollment fairs. The state ensured that the contractor was aware of the particular needs of the ABD populations.
- Exceptional needs coordinators (ENCs): The state has identified nurses and social workers with case management experience to serve as ENCs for the PCCM members. (The state has required its contracted MCOs to hire ENCs for their special needs members as well.) The ENCs work with community service agencies and other providers to coordinate resources and services for special needs members.
- Targeted outreach: During initial enrollment of the ABD populations, the ENCs make phone calls to those Medicaid beneficiaries who have high utilization of services, based on their claims history. The purpose of the phone call is to inform members about upcoming changes in their coverage, explain managed care, and to complete a profile to identify their outstanding health needs. The ENC also helps the prospective member select a PCP who can best meet their needs. The health information about the member is then forwarded to the selected PCP so that the provider is aware of the new member's health needs.
Endnotes
37. Specifically, the BBA exempts the following populations from mandatory enrollment in Medicaid managed care; dual Medicare-Medicaid eligibles; American Indians/Alaska Natives who are members of federally recognized tribes; and children who are eligible for SSI, in home and community-based settings, in foster care or other out-of-home placement, receiving foster or adoption assistance, or receiving services through a family-centered, community-based coordinated care system receiving Title V grant funds.
38. In general, TANF refers to other poverty-related populations in addition to TANF beneficiaries. However, Alabama makes a distinction between SOBRA women and SOBRA children; SOBRA children are mandatorily enrolled; SOBRA adults are not eligible.
Chapter 9: Lessons Learned: State Perspectives
Those who participated in the interviews conducted for this report provided a wealth of information on how their Medicaid PCCM programs have evolved and the actions they have taken to get their programs to their present incarnations. These state officials had a myriad of advice to share with states looking to replicate the innovations they have implemented.
Overall Advice
The most frequent advice given by case-study states is to use the principles and tools of MCOs, such as prior authorization, performance standards, benchmarks, and quality strategies. This was asserted by the majority of case-study states. Other advice includes
- Know what the desired accomplishments are, from day one; have specific goals and steps for reaching them; and communicate these goals and steps to key players (including providers).
- To work well, the program must be both provider- and beneficiary-focused.
- Evolve slowly: start small and learn from pilot sites before expanding.
- Keep building a base of political support for the program.
Organizational Structure
Advice on organizational structure emphasized the need for sufficient state investment of personnel and resources:
- The state investment must be long-term for the PCCM project to show results; building the right infrastructure is an ongoing process and was often more difficult than expected.
- Dedicate significant internal resources with multiple staff who can respond to questions and concerns from members and providers. Locating these staff at the local level will increase buy-in, as their knowledge of community services makes them more effective resources for providers and members.
- Consider how local communities can be empowered to change the service delivery system. Partnering with localities takes a long time and creates a great deal of work, but the resulting program can be very successful.
- In contracting with a plan administrator, include an adequate reimbursement rate in order to be able to expect best practices.
Providers
Case study state officials agreed that provider commitment is the key to their success. Their advice stressed identifying and implementing ways to obtain the buy-in of a wide variety of providers.
- Meet with medical societies and other key players who can positively influence providers to participate in the program.
- Face-to-face communication with providers (both PCPs and practice staff) is key to good state-provider relations.
- Set expectations for providers from the beginning; make clear that this is not just another fee-for-service program.
- Do your homework in communities before beginning to recruit providers: physically inspect offices and meet with all practice staff.
- It is critical for state staff to support providers on an ongoing basis, to take their concerns seriously, and to develop new ways to better serve them.
- Allow providers to police themselves; second-guessing their decisions does not work. The state's job is to provide the tools to facilitate that process (e.g., utilization review, provider profiling, information on best practices) and to work with outliers to get their practices in line with state expectations.
- Work with providers to modify inappropriate patient behaviors (e.g., emergency room use).
Quality Activities
Case-study states have implemented a broad range of mechanisms to ensure high quality care for members. Therefore, their advice covers a wide range of issues.
- Have a plan, from the start, for quality improvement processes.
- Use multiple methods for obtaining beneficiary and provider feedback.
- Include physicians on advisory committees so that messages and recommendations are more palatable to their peers and greater PCP buy-in for program policies can be obtained.
- Provide a base for member outreach and education activities; conduct such activities on an ongoing basis.
- Hands-on beneficiary education can promote appropriate emergency room use and facilitate access to timely preventive care.
- Disease management programs are beneficial for the state, PCPs, and beneficiaries.
Finance
States with incentive payment systems noted that these systems can be very effective in reinforcing the state's key program goals.
Service Management
States with active care coordination components to their PCCM programs reported that providers and beneficiaries found them very helpful. Other recommendations included
- Recognize that the referral process is key to managing services
- Make prior authorization and other state-required procedures as hassle-free as possible for providers.
- Employ care coordinators who are familiar with the community and available resources. Collaborate with existing services (e.g., WIC).
Enrollment
State advice on enrollment focused mostly on additional roles a contracted enrollment broker can play.
- Use the enrollment broker to recruit providers, in order to learn the area before starting member enrollment.
- Use the enrollment broker for member education.
- Do not try to enroll a great number of people into a mandatory program all at once; providers prefer to have new patients trickle in, rather than adding 100 new patients on any given day.
Conclusions
As Medicaid managed care has evolved during the past decade, states have balanced the development of their PCCM programs with the growth and/or decline of risk-based managed care. Each state has taken a slightly different approach, depending in part on the state's particular managed care environment. Some states developed PCCM as a stepping stone to risk-based managed care, and therefore considered their MCO contracts as the predominant managed care system. That emphasis has been shifting, however, in those states that are experiencing a decrease in contractors as MCOs choose to exit Medicaid managed care. State officials in several of the case-study states commented that their states' initial expectations for the growth of managed care contracting have not been realized, and therefore, they are focusing more on PCCM as the major form of Medicaid managed care. Others, however, continue to anticipate expanding their risk-based programs.
Many states use the PCCM model of managed care in rural areas where there is not sufficient population density to support a contract with an MCO. Among the case-study states, Virginia and Oklahoma, in particular, have developed separate managed care initiatives to serve distinct areas of their respective states. PCCM is the managed care system in the states' rural areas, and MCO contracts are limited to urban areas. Several state officials note that physicians in rural areas are reluctant to join an MCO network, and prefer the PCCM model for serving their patients.
Among the eight case-study states, Alabama, Maine, and North Carolina rely almost exclusively on PCCM for their Medicaid managed care delivery systems. Alabama and Maine expected to see managed care contracting develop into the principal managed care system in their states, but in both instances that has not been the case. Alabama retains MCO contracting in pockets of urban areas but Patient 1st is its major managed care initiative. Maine had one contract with an MCO to serve certain areas of the state, but the state Medicaid agency discontinued that contract in December 2000 and is transitioning all members to Maine PrimeCare. In North Carolina, only one county has a mandatory MCO program; five counties have a choice between an MCO and North Carolina ACCESS; and in the remaining 93 counties, ACCESS is the mandatory managed care program.
Seeing PCCM as a significant piece of a long-term managed care strategy has led many case study state Medicaid agencies to make changes in their approaches. As PCCM programs have matured, state goals have evolved from simply expanding access to better management of the quality of care provided. States learned many network management principles from MCOs, and are increasingly using these strategies in managing their PCCM programs. The case-study states are employing innovative strategies in the areas of:
- Organizational structure and administration, such as use of a plan administrator to implement the state's policies and decisions (Texas), programs focusing on population management (North Carolina), and a demonstration project geared to Medicaid beneficiaries who are receiving long-term care services at home (Maine).
- Provider recruitment and retention, including a greater focus on supporting participating providers through specially designated provider outreach staff (Alabama, Florida, Virginia, Texas), provider hotlines (Alabama, Iowa, Maine, North Carolina, Oklahoma, Texas, Virginia), feedback mechanisms such as provider profiling (Maine, Alabama, Texas), and strategies to gain providers' input and suggestions (nearly all case-study states).
- Quality activities, such as disease management programs, use of HEDIS or other measures to gauge PCP performance, individual and community health needs assessments, community-based preventive health educational campaigns, and nurse advice lines.
- Finance modifications, such as incentive payment systems (Maine, Oklahoma) and capitating primary/preventive services (Oklahoma).
- Service management, such as care coordinators within PCP offices for people eligible to receive long-term care services at home (Maine) and health needs assessments (Maine, North Carolina).
- Enrollment functions, such as targeted processes used to facilitate the enrollment of populations with special needs (Alabama, Oklahoma).
Appendices
Appendix A: Case Study States' Contacts
Charlene J. Benson
Director, Medicaid Care Management
Oklahoma Health Care Authority
4545 North Lincoln Suite 124
Oklahoma City, OK 73105
405-522-7366
bensonc@ohca.state.ok.us
Scott F. Cannady
Managed Care Unit Supervisor
Department of Medical Assistance Services
P.O. Box 537
Richmond, VA 23204
804-786-5445
SCannady@dmas.state.va.us
Maresa Corder, RN, MPA
RN Consultant
Agency for Health Care Administration
2727 Mahan Drive
Fort Knox Building 3, Mailstop 20
Tallahassee, FL 32308
850-488-9287
Vicki Huff
Director
Alabama Medicaid Agency, Medical Services
501 Dexter Avenue, P. O. Box 5624
Montgomery, AL 36103-5624
334-242-5000
vhuff@medicaid.state.al.us
Dennis Janssen
Manager
Managed Care & Clinical Services
Division of Medical Services
Iowa Department of Human Services, Division of Medical Services
Hoover State Office Building, 5th Floor South
Des Moines, IA 50319-0114
515-281-8747
djansse@dhs.state.ia.us
Denise Levis
ACCESS II & III Program Consultant
North Carolina Foundation for Advanced Healthcare
311 Ashe Avenue, Cooke Building
Raleigh, NC 27606
919-733-2040 or 919-715-1088
denise.levis@ncmail.net
Brenda McCormick
Human Services
Bureau of Medical Services
249 Western Avenue
Augusta, ME 04333
207-287-1774
Gino Nalli
Assistant Research Professor
Edmund S. Muskie School of Public Service, University of Southern Maine
P.O. Box 9300
96 Falmouth Street, 5th Floor
Portland, ME 04104-9300
207-780-4237
gnalli@usm.maine.edu
(Conducts program development and evaluation for MaineNET/Partnership)
Ann Prescott
Director, Provider/Member Services
Birch & Davis Health Management Corporation (BDHMC)
6987 N IH 35
Austin, TX 78752
512-421-3012
aprescott@txbirchdavis.com
(BDHMC administers the Texas Health Network)
Dee Sportsman
Acting Bureau Chief, Bureau of Managed Care
Division Director, Customer Services
Texas Department of Health
1100 W. 49th Street, Y-980
Austin, TX 78756
512-794-5164
dee.sportsman@tdh.state.tx.us
Appendix B: North Carolina Access II & III Core Elements of the Asthma Disease Management Program
Build Capacity for Routine Assessment of Asthma
- Adopt the NIH (National Institute of Health) guidelines.
- Develop a method for identifying and recruiting asthma patients in the participating provider network.
- Develop and implement a simple questionnaire that allows providers to quickly stage the severity of an asthmatic patient.
- Develop a method to record severity staging on a regular basis.
- Establish peak flow meter readings as a tool for all asthma patients, and the peak flow at all appropriate times and in all appropriate settings.
- Record each patient's personal best peak flow in the medical record and/or the care management plan.
- Stock peak flow meters and spacers in all providers' practices and care settings to assure availability and ease in dispensing to patients.
- Use spacers/holding chambers, when appropriate.
- Identify one staff person per practice as the "asthma QI champion."
Reduce Unintended Variation in Care and Establish Consistency of Care
- Educate all medical personnel regarding the proper use of anti-inflammatory medications.
- Use anti-inflammatones and/or inhaled corticosteroids for stage II, III and IV asthmatics.
- Focus educational effort on clinicians not using the correct medications when appropriate.
- Educate all medical personnel regarding the step approach to asthma management based on NIH guidelines.
- Offer physician profiling as a part of this effort. Conduct detailed visits with staff and physicians to review each practice's prescribing histories, including a case-by-case discussion of diagnoses and recommended medications.
- Utilize case managers to coordinate information gathering, transfer, and care delivery as appropriate.
- Assess home environment for smoking, allergenic materials, and other known asthma triggers. Coordinate sharing of this information with all care givers.
- Educate all medical personnel to stage asthmatics appropriately and write an asthma action plan accordingly.
Build Capacity to Educate Patients, Families and School Personnel About Asthma
- Develop and implement simple asthma management plans that include the patient performing and monitoring peak flows.
- Develop the capacity to teach each child and family how to properly use peak flow meters, inhalers, spacers and/or holding chambers.
- When possible, collaborate with school nurses, teachers, administrators, and day care personnel to assure appropriate education, assessment, and treatment for school-age children with asthma.
- Encourage self management of diseases.
- For young children who cannot use peak flow meters — educate family on symptom-based management.
Appendix C
| Alabama | Florida | Iowa | Maine | North Carolina | Oklahoma | Texas | Virginia | |||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Patient 1st | MediPass | MediPASS | Maine Prime-Care | Maine-NET/ Partnership | ACCESS I | ACCESS II | ACCESS III | SoonerCare Choice PCCM Model | Texas Health Network | STAR+ PLUS | MEDALLION | |
| Populations included in mandatory enrollment (in managed care) | TANF1, SOBRA children, SSI, Aged, CHIP | TANF, SSI, foster care children, CHIP | TANF, CHIP | TANF & related, CHIP (Medicaid expan-sion) | --- | TANF, SSI, ABD | TANF, SSI, Aged, CHIP (Medicaid expansion) | TANF | SSI children, certain MH/MR | TANF, SSI, Aged, CHIP | ||
| Populations included in voluntary enrollment | Exemp-tions for medical reasons are granted case-by-case | Have other insurance, enrolled in another mgd care prgm, "grand-fathered" SSI (enrolled pre-1993) | Special needs | American Indian/ Alaska Natives, hospice, Medicaid pregnant women, special needs | SSI, Aged | Dual eligibles, foster care children, subsidized adoption, American Indian/Alaska Natives, Medicaid pregnant women | --- | American Indian/ Alaska Natives, ABD | Special needs | |||
| Populations not eligible | Medicare, reside in nursing facility or ICF/MR or thera-peutic group home, SOBRA adults, enrolled in another mgd care prgm., foster care children, retro-active eligibility/ eligibility less than 3 mos. | Aged, reside in nursing facility or ICF/MR, participate in HCBS waiver, medically needy, incar-cerated | SSI, dual eligibles foster care children, subsidized adoption, reside in nursing facility or ICF/MR, participate in HCBS waiver, have other insurance, enrolled in another mgd care prgm, short-term medical, long-term medical in com-munity, spend down | SSI, dual eligibles, foster care children, subsidized adoption, other insurance, enrolled in another mgd care prgm, long-term mental health, participate in HCBS waiver, special needs adults | Reside in nursing facility or ICF/MR | CHIP, reside in nursing facilities or ICF/MR, long-term medical in the community, long-term mental health, retroactive eligibility/eligibility under 3 mos., refugees, spend down | Medicare, foster care children, reside in nursing facility or ICF/MR, enrolled in another mgd care prgm, participate in HCBS waiver, travel more than 45 miles or 45 minutes, children in custody, subsidized adoption | Medicare, foster care children, reside in nursing facility or ICF/MR, hospice, medically needy | TANF, foster care children, CHIP, partici-pate in HCBS waiver, QMB, SLMB, participate in nursing facility waiver | Medicare, foster care children, subsidized adoption, other insurance, enrolled in another mgd care prgm, reside in nursing facility or ICF/MR, participate in HCBS waiver, long term medical in community, long-term mental health, retro-active elig./elig. under 3 mos., refugees, hospice, spend down | ||
Endnote
1. In general, "TANF" refers to other poverty-related populations in addition to TANF beneficiaries. However, Alabama makes a distinction between SOBRA women and SOBRA children; SOBRA children are mandatorily enrolled, while SOBRA adults are not eligible.
