Monday, August 1, 2016
Clinical Services Subcommittee Federal Update
Ellen Blackwell, MSW
Goal Two: Enhance Care Quality and Efficiency
National Quality Forum
The Neurology Standing Committee issued a draft report for public comment that closed July 27. It evaluated 26 measures against NQF's standard evaluation criteria: nine measures were recommended for endorsement and one measure was recommended for Approval for Trial Use:
- 2111 Antipsychotic Use in Persons with Dementia (Pharmacy Quality Alliance): Recommended
- Description: The percentage of individuals 65 years of age and older with dementia who are receiving an antipsychotic medication without evidence of a psychotic disorder or related condition. This process measure was originally endorsed in 2013 and is planned for use in accountability programs including Medicare Part D
- 2872 Dementia- Cognitive Assessment (Physician Consortium for Performance Improvement): Recommended for Approval for Trial Use
- Description: Percentage of patients, regardless of age, with a diagnosis of dementia for whom an assessment of cognition is performed and the results reviewed at least once within a 12 month period. This new process eMeasure was reviewed for consideration in the NQF Approval for Trial Use Program. It is currently in use in the CMS PQRS and Meaningful Use Stage 2
(Strategy 2.D) Neurology Project: http://www.qualityforum.org/Neurology_Project_2015-2016.aspx
Health Care Innovation AwardsRound One Update
- In May CMS published the 2nd annual independent evaluation reports
- These illustrate a wide range of experiences that have resulted in tangible benefits for beneficiaries, and informed CMS
- This morning's presentations show that there is much to learn from new payment and service delivery models!
- The independent CMS Office of the Actuary has certified that expansion of a Round One project - the Diabetes Prevention Program - would reduce net Medicare spending, and the expansion was also determined by CMS to improve the quality of beneficiary care without limiting coverage/benefits
- This is the first time that a preventive service model from the CMS Innovation Center has become eligible for expansion into Medicare
(Strategy 2.E) https://innovation.cms.gov/initiatives/Health-Care-Innovation-Awards/
Transforming Clinical Practice Initiative (TCPI) Support and Alignment Networks 2.0
- In June CMS announced launched the second round of the Support and Alignment Networks under TCPI
- The opportunity will provide up to $10 million over the next three years to leverage primary and specialist activities including coaching and technical assistance
- The Support and Alignment Networks 2.0 will also help clinicians prepare for the proposed two paths of the new Quality Payment Program, the Merit-based Incentive Payment System (MIPS), and Advanced Alternative Payment Models (APMs)
- Awards will be announced in Fall 2016
(Strategy 2.E) https://innovation.cms.gov/initiatives/Transforming-Clinical-Practices/
Medicaid's Innovation Accelerator Program Physical-Mental Health Integration
- In May, CMS held kick-off webinars with selected states and one territory (NV, NH, NJ, PR, and WA)
- The Agency will provide ten months of individualized technical support to improve mental and physical health integration approaches
- HI, ID, IL, and MA are also participating in a facilitated integration strategy workgroup to incentivize primary care providers to deliver more integrated care to Medicaid beneficiaries
- To date, no state has focused on ADRD in the physical-mental health integration area
Comprehensive Primary Care + Update
- In April CMS announced CPC+, a five-year multi-payer model that begins in January, 2017 and will include more than 20,000 clinicians
- Enrolled beneficiaries with complex needs (e.g. cognitive impairment, chronic conditions, frailty) will be better able to achieve their goals and become engaged in care, have 24 hour access, and receive preventive services and care coordination
- CMS will publicize the CPC+ regions soon, and solicit applications from practices within them
- CMS posted an updated FAQ sheet in May
(Strategy 2.E) https://innovation.cms.gov/initiatives/comprehensive-primary-care-plus
Medicare Physician Fee Schedule (PFS)
- In July CMS issued proposed 2017 changes to the PFS including:
- The Diabetes Prevention Program
- A PFS billing code set that more accurately recognizes the work of primary care and other cognitive specialties to accommodate the changing needs of Medicare beneficiaries
- Separate payments for certain existing Current Procedural Terminology (CPT) codes describing non-face-to-face prolonged evaluation and management services
- Revaluation of existing CPT codes describing face-to-face prolonged services
- Separate payments using new codes to describe the comprehensive assessment and care planning for beneficiaries with cognitive impairment (e.g., dementia)
- Advance Care Planning delivered through telehealth
- Separate payments using new codes to pay primary care practices that use interprofessional care management resources for beneficiaries with behavioral health conditions -- some codes describe integrated services like the Collaborative Care model that involves care coordination between a behavioral health specialist and the primary care clinician
Medicare Proposed 2017 PFS Continued
- Separate payments using new codes to recognize the increased resource costs of furnishing visits to beneficiaries with mobility-related impairments, relevant for Medicare-Medicaid enrollees
- Separate payments for codes describing Chronic Care Management for beneficiaries with greater complexity
- Changes to reduce administrative burden associated with furnishing/billing the Chronic Care Management codes
- Comment period closes September 6, 2016
Goal Three: Expand Supports for People with Alzheimer's Disease and their Families
National Partnership to Improve Dementia Care Antipsychotic Medication Use Trend Update
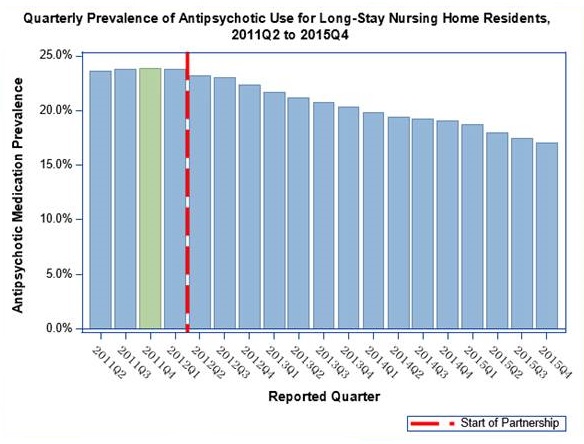
- Since the start of the National Partnership to Improve Dementia Care in 2012, there has been a 28.8% reduction in the national use of antipsychotic medications among long-stay nursing home residents
- In 2012 23.9% of long-stay residents were on antipsychotic medications. By the end of 2015, the percentage dropped to 17.0%
- Success has varied by state and CMS region, with some states and regions recording greater reductions
Antipsychotic Use Quarterly Prevalence
 |
Goal Four: Enhance Public Awareness and Engagement
Innovative Approaches to Palliative Care, Dementia Care, and Data Analysis - Grand Rounds
- In June CMS hosted a "Grand Rounds" monthly educational event on dementia and palliative care
- These educate health care professionals on the evidence-based practice of medicine and provide the latest scientific information on selected topics
- Presenters included HCIA Round One and Two awardees
- A playback of the session is available at: https://www.cms.gov/Medicare/Quality-Initiatives-Patient-Assessment-Instruments/QualityMeasures/CCSQGrandRoundsContinuingEducationSeries.html
(Strategy 4A)
"Addressing Neuropsychiatric Symptoms in Patients with Dementia"
- In June CMS sponsored a Medscape continuing education opportunity for professionals presented by Shari Ling and Laura Gitlin -- both Advisory Council members - and Sharon Inouye and Constantine Lyketsos, also expert in ADRD
- The program provides a summary of treatment goals for comprehensive dementia care, addresses neuropsychiatric symptom management including a DICE (describe, investigate, create, evaluate) approach to difficult behaviors, provides for acute hospital management, and lists clinical and administrative resources
- The focus is on improving and maintaining quality of life of people with dementia, including support for families and caregivers across settings of care
- Continuing Medication Education Credit is valid through 06/09/2017
(Strategy 4A) http://www.medscape.org/viewarticle/863605?src=acdmpart_hhs_863605
Health Resources & Services Administration Updates
- Alzheimer's Disease and Related Dementias Curriculum
- Expected release: October, 2016
- Medscape Article: Bidirectional Impact of Alzheimer's Disease and Common Comorbid Conditions: Managing Patients
- Expected release: October, 2016
QUESTIONS?
Ellen Blackwell
ellen.blackwell@cms.hhs.gov
Shari Ling
shari.ling@cms.hhs.gov
