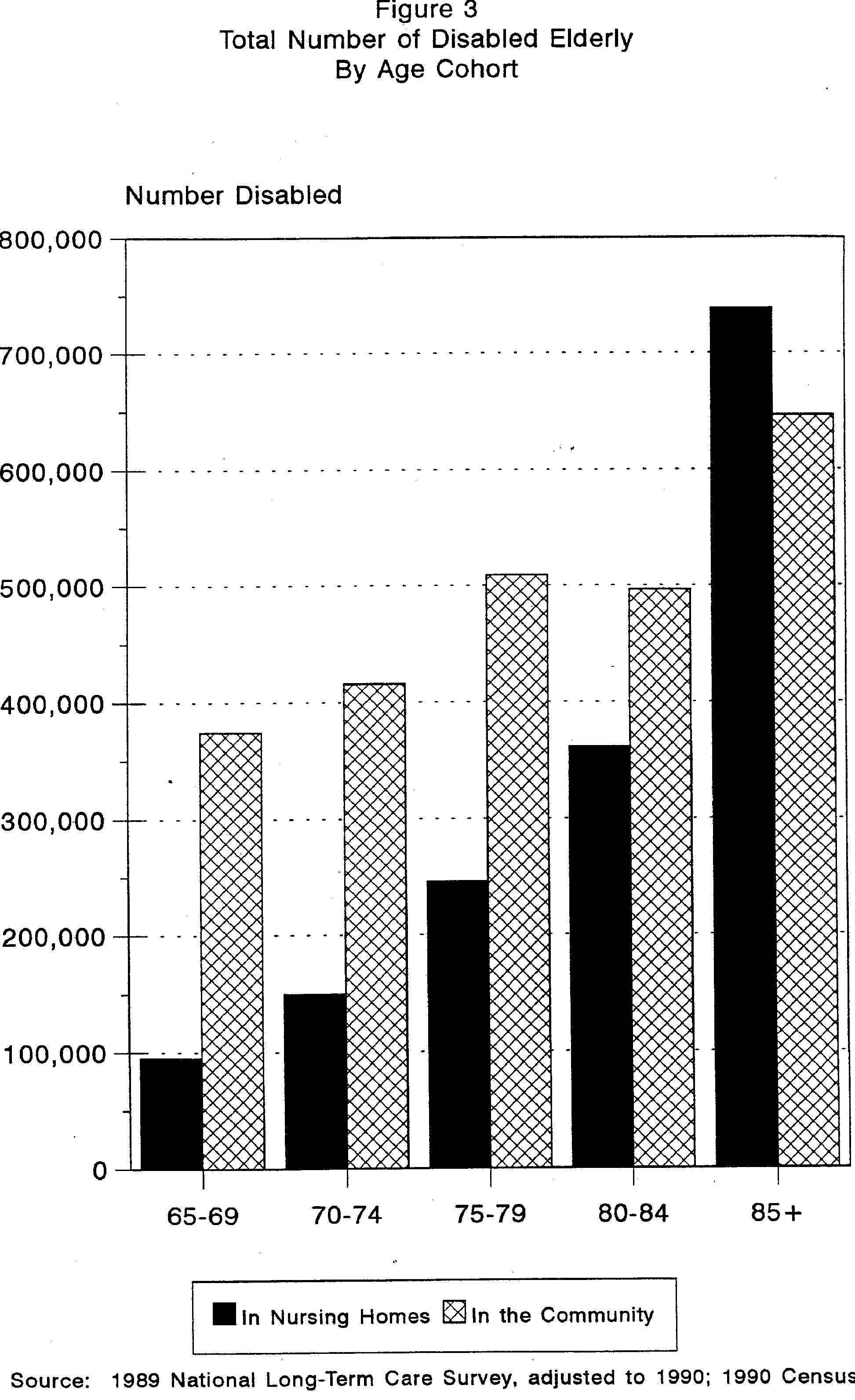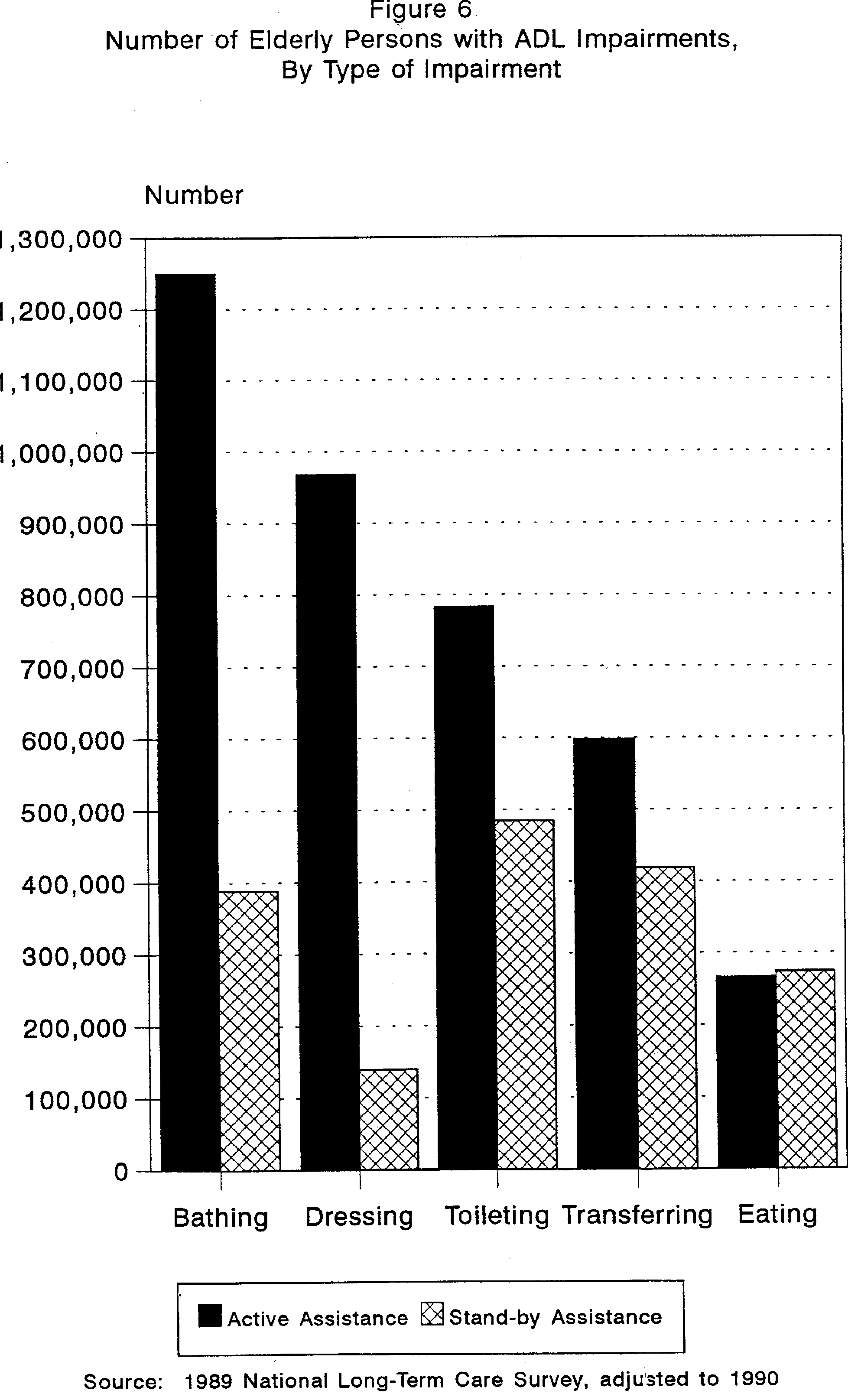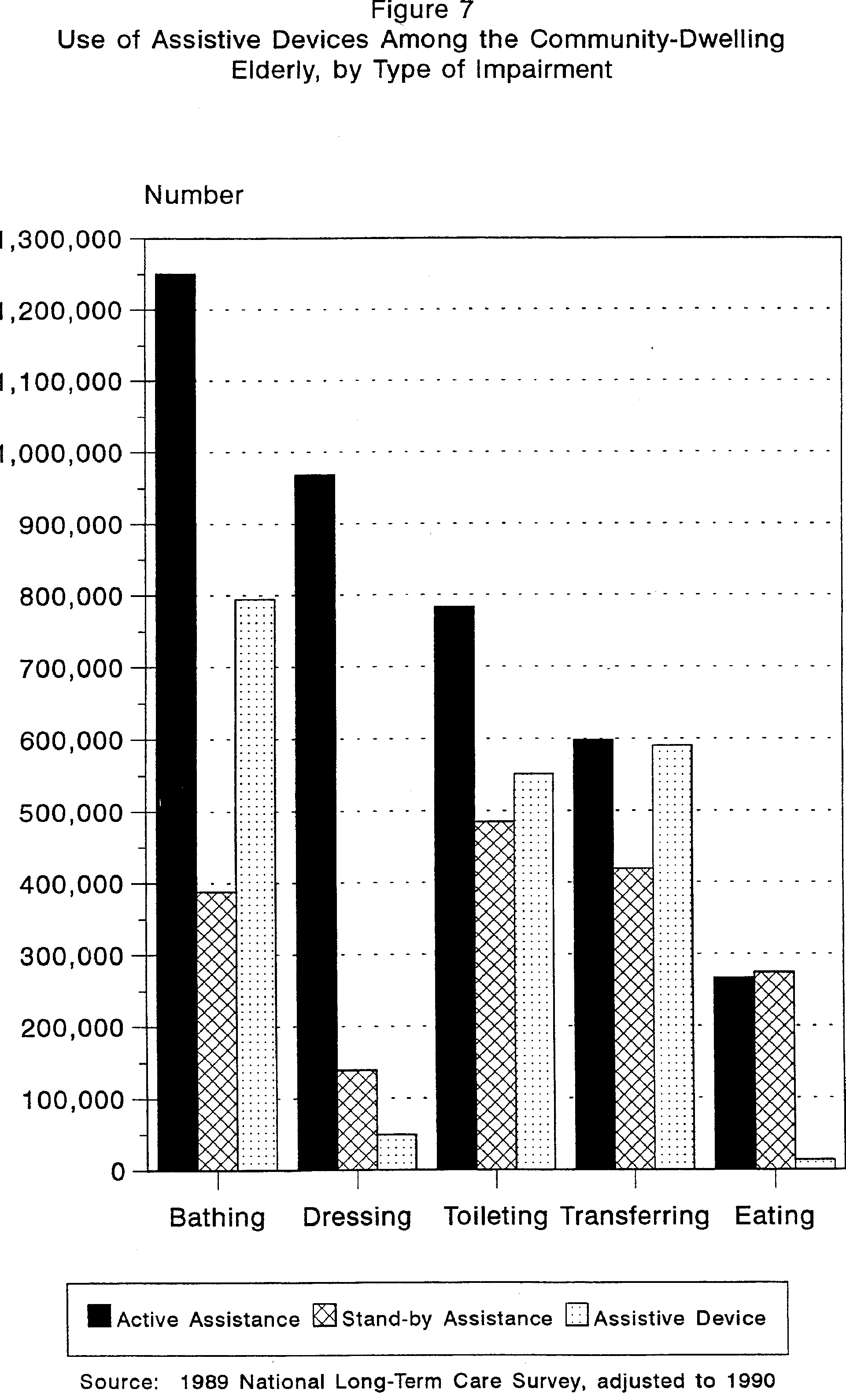U.S. Department of Health and Human Services
The Disabled Elderly and Their Use of Long-Term Care
Brian O. Burwell and Beth Jackson
SysteMetrics
July 1994
This report was prepared under contract between the U.S. Department of Health and Human Services (HHS), Office of Disability, Aging and Long-Term Care Policy (DALTCP) and SysteMetrics. For additional information about the study, you may visit the DALTCP home page at http://aspe.hhs.gov/daltcp/home.htm or contact the ASPE Project Officer, John Drabek, at HHS/ASPE/DALTCP, Room 424E, H.H. Humphrey Building, 200 Independence Avenue, SW, Washington, DC 20201. His e-mail address is: John.Drabek@hhs.gov.
The views and conclusions presented in this paper are solely those of the authors and do not necessarily reflect the views of the Department of Health and Human Services.
TABLE OF CONTENTS
THE ELDERLY POPULATION IN NEED OF LONG-TERM CARE
Defining the Elderly Disabled
Important Differences Within the Disabled Elderly Population
The Probability of Becoming Disabled
Levels of Disability Among the Elderly Living in the Community
Elderly Persons with Alzheimer's Disease and Other Cognitive Impairments
Who Uses Informal Care?
The Providers of Informal Care
The Costs of Informal Caregiving
Does Formal Home Care Substitute For Nursing Home Care?
Does Paid Care Substitute for Informal Care?
The Probability of Having to Enter a Nursing Home
Characteristics of Nursing Home Users
How Long People Stay in Nursing Homes
Persons with Long Nursing Home Stays Account for Most Nursing Home Days Used
Nursing Home Use Rates May be Declining
Continuing Care Retirement Communities
Subsidized Housing Programs with Congregate Services
Adult Foster Care
The Role of Supportive Housing In the Long-Term Care System
THE INTERSECTION OF THE ACUTE CARE AND LONG-TERM CARE SYSTEM
LIST OF FIGURES
FIGURE 1. Disability Status of the Elderly, 1990
FIGURE 2. The Percentage of Elderly Persons with Disabilities Increases Significantly with Age
FIGURE 3. Total Number of Disabled Elderly By Age Cohort
FIGURE 4. Most Disabled Elderly Are Female and Unmarried
FIGURE 5. Blacks and Other Non-Whites Have Higher Rates of Disability But Use Less Nursing Home Care
FIGURE 6. Number of Elderly Persons with ADL Impairments, By Type of Impairment
FIGURE 7. Use of Assistive Devices Among the Community-Dwelling Elderly, by Type of Impairment
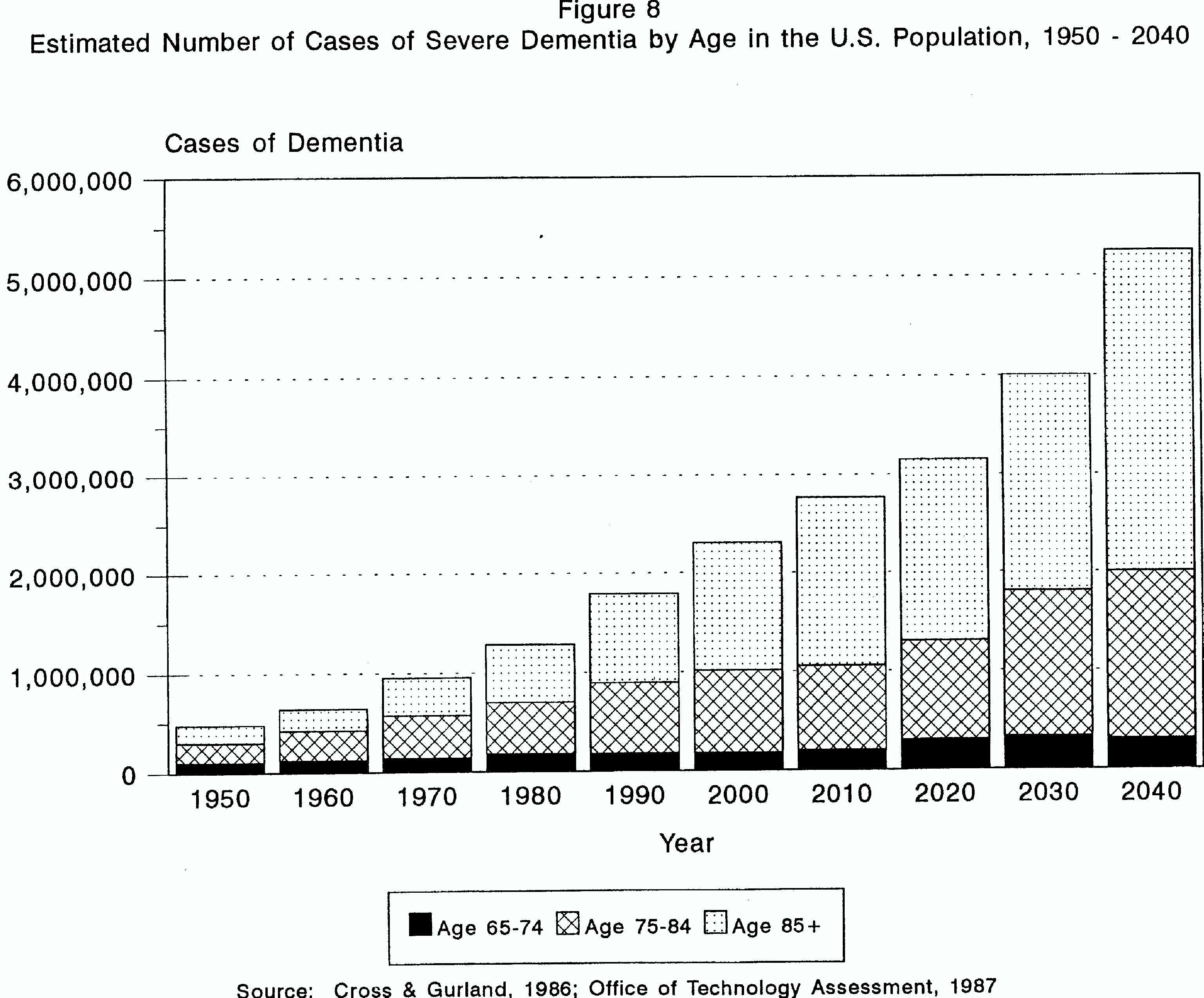
FIGURE 8. Estimated Number of Cases of Severe Dementia by Age in the U.S. Population, 1950-2040
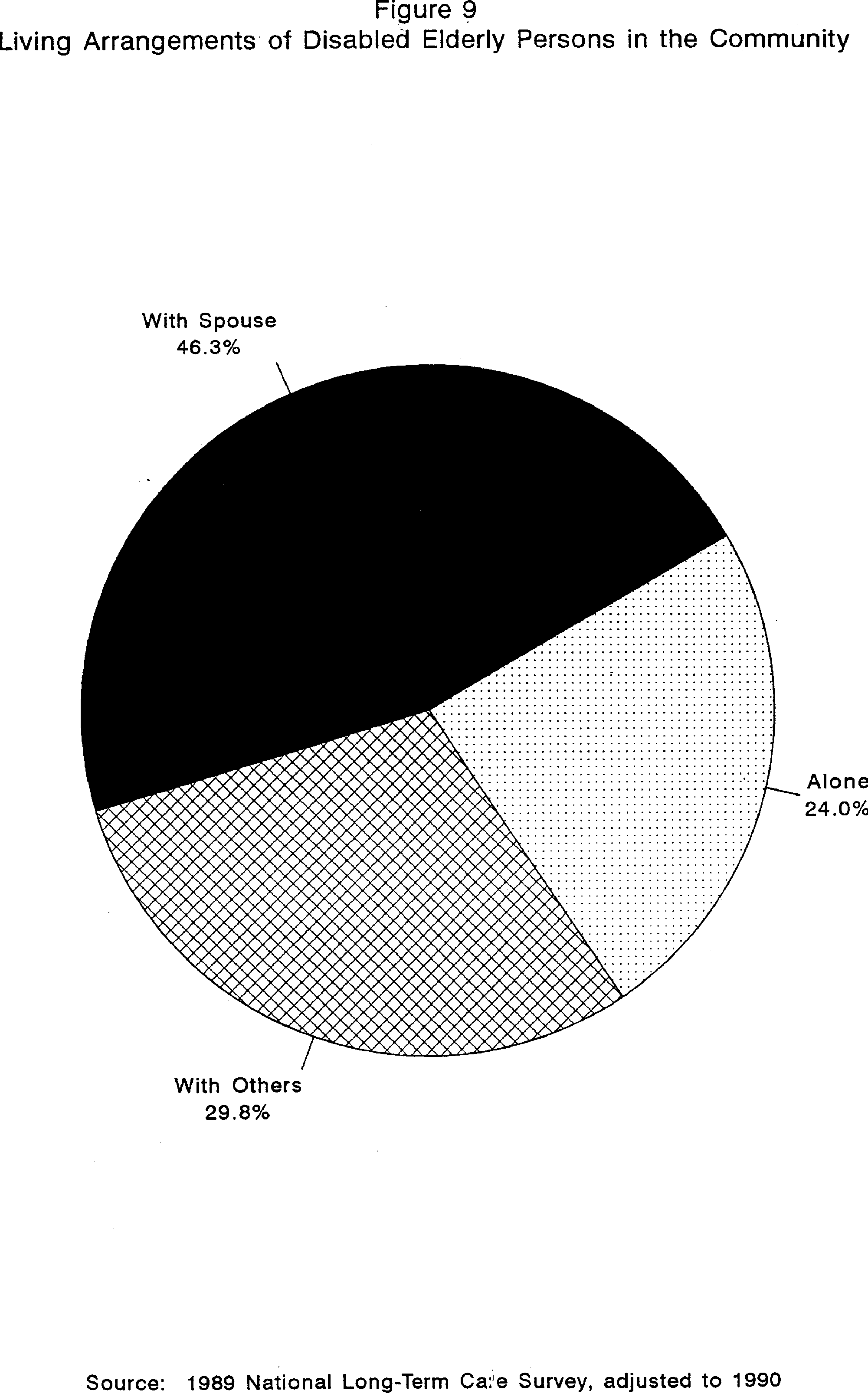
FIGURE 9. Living Arrangements of Disabled Elderly Persons in the Community
FIGURE 10. Nursing Home Residents with Long Stays Consume 70 Percent of All Days Used
TABLE 1. Length of Stay Distributions for Nursing Home Patients: Single Stays Versus Lifetime Use
TABLE 2. Change in Age-Adjusted Nursing Home Utilization Rates Per 1,000 Elderly: 1977 to 1985
INTRODUCTION
As we age, our physical and mental abilities inevitably start to decline. Although many people are able to maintain high levels of physical functioning and mental acuity to very old ages, for many others the aging process results in a reduced ability to live independently.
This loss of independence can be manifest in many ways. For some, failing eyesight and slowed motor functioning may require that they stop driving a car. Very old persons, although in relatively good health, may simply find it increasingly difficult to keep up with everyday tasks such as preparing meals, cleaning the house, doing laundry, keeping up with the maintenance of a house and yard. Persons who develop cognitive impairments as a result of Alzheimer's disease or other conditions may require increasing supervision by others to remind them what to do and ensure that they do not harm themselves. For persons with severe chronic illnesses related to heart disease, stroke, arthritis and other conditions, it may mean relying on others to help with the most routine activities of daily life...putting on clothes, getting to the bathroom, eating a meal, taking a bath. All of these persons, at different levels, require some type of long-term care.
This paper describes the elderly population which requires long-term care assistance and the services they use. Although many persons under the age of 65 also need long-term care, this paper concentrates solely on disabled individuals who are 65 years of age and over. The paper presents estimates of the number of disabled elderly, where they live, what services they use, and how services are provided.
An important theme of this paper is that elderly individuals with long-term disabilities are by no means a homogenous population. Many have mild impairments, and require only occasional help--help that is usually provided by family members. Others are in relatively good physical health, but have deficits in mental functioning that limit their ability to be independent. Still others remain mentally sharp, but develop chronic illnesses that limit their physical ability to perform the routine activities of daily life--dressing, walking, getting to the bathroom, eating a meal. Recognition of the diversity of elderly persons with functional impairments, both in their level of impairment, and in their ability to secure help without public assistance, is essential in developing policies that are responsive to the range of needs which elderly people have.
THE ELDERLY POPULATION IN NEED OF LONG-TERM CARE
Defining the Elderly Disabled
Before I die, will I be disabled? If I'm disabled, will I be a burden on my family? Will I be able to get services that will let me stay in my own home? Will I need to go to a nursing home? If I do need to go to a nursing home, how long am I likely to be there? These are some of the questions which the elderly face as they enter the later stages of life.
How does one begin to describe the elderly population that needs long-term care assistance? Although by no means clear cut, long-term care researchers have developed some common definitions to describe the disabled elderly. The most frequent approach is to define the disabled elderly as those individuals who require assistance with basic Activities of Daily Living, commonly referred to as ADLs. ADLs have become an accepted way to define and measure the long-term care population, because disability in activities of daily living is a direct indicator of the need for care.1
Functioning in five core ADLs are typically used to describe the extent of chronic disability among the elderly. These core ADLs are: (1) bathing; (2) dressing; (3) using the toilet; (4) transferring from bed to chair, and (5) feeding oneself.
In addition to functioning in core ADLs, researchers also sometimes include measures of functioning in what are called Instrumental Activities of Daily Living, or IADLs. IADLs include such activities as the ability to prepare meals, take medications properly, go grocery shopping, do housework, and manage money. Many elderly individuals do not require assistance in core ADLs, but still have impairments which prevent them from performing these IADL activities without occasional or constant help from other persons.
A distinction between ADL activities and IADL activities is that an individual can usually get by some days without performing most IADL activities (e.g. shopping) but it is extremely difficult for a person to get through a day without performing most ADL activities. Thus, persons who require IADL assistance only may not require help every single day, while persons who are ADL-disabled generally require daily assistance.
A third dimension that is often used to measure disability is cognitive functioning. Many elderly individuals, including persons with Alzheimer's disease, often are physically capable of performing ADL and/or IADL activities, but still are unable to perform them independently because they have cognitive impairments. Impairments in cognitive functioning often lead to greater assistance needs, because people who are cognitively impaired often require 24-hour supervision so they do not harm themselves or others (e.g. by forgetting to turn a stove).
Measuring impairment in ADLs and IADLs, as well as cognitive functioning, is not a straightforward matter. We generally think of people as being disabled if they cannot perform a certain activity on their own. However, not all elders with ADL limitations require the same type of assistance. Some require the active assistance of another human being to perform an activity; they absolutely cannot do it on their own. Others may be able to perform an activity with difficulty, but require another person to stand-by in case assistance is needed. Still others may be impaired in an ADL, but can perform the task with the aid of an assistive device, such as getting into a bathtub with the aid of a grab bar, or getting to the bathroom with the aid of a walker.
The most common approach, generally, is to define someone as disabled in an ADL if he or she requires the help of another person to perform the activity--with either active or stand-by help. Thus, elders who rely on assistive devices only are generally not counted in estimates of the long-term care population, because they do not require the assistance of another person. Finally, definitions of functional impairment also include a dimension of chronicity, in order to exclude individuals who may have only temporary limitations in ADLs due to acute conditions (e.g. a recent operation, the bout with the flu, etc.).
It is not surprising that estimates of the number of disabled elderly vary depending upon what definition of disability is invoked and what data source is used to derive the estimates.2,3,4 The estimates which follow employ commonly-used definitions of disability and are based on analyses of the 1984 and 1989 National Long-Term Care Surveys, the 1985 National Nursing Home Survey, and estimates from the Bureau of the Census.5 Where possible, these estimates have been adjusted to represent the population in 1990.
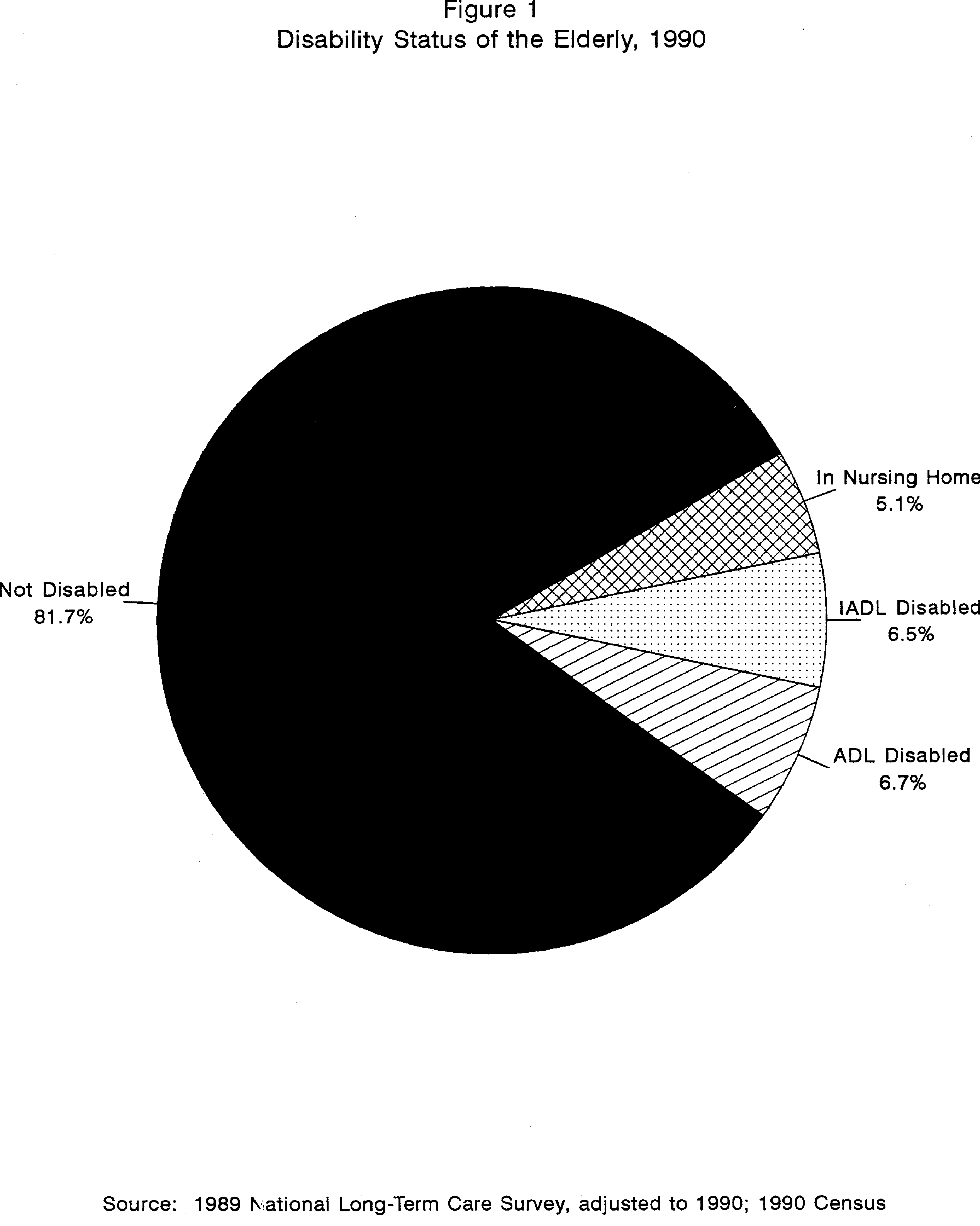
In 1990, there were about 31.2 million persons age 65 and over in the United States. Of these, about 2.1 million elderly persons living in the community were disabled in one or more of the five core ADLs (see Figure1).6 In addition, there were also approximately 2.0 million persons age 65 and over who were not impaired in ADLs but who experienced limitations in one or more Instrumental Activities of Daily Living (IADLs) such as meal preparation, grocery shopping, housework, and so on.7 These estimates exclude elderly individuals living in the community who may have difficulty performing ADL or IADL activities but who do not require human assistance because they use an assistive device. Finally, in 1990, there were about 1.6 million elderly persons living in nursing homes and other facilities that provide 24-hour residential care.
Important Differences Within the Disabled Elderly Population
The range of disability within the elderly long-term care population is extremely broad. Service programs and financing mechanisms must reflect the broad range of service needs which the disabled elderly require. For policy purposes, it is generally useful to think of the elderly disabled in three large groups:
-
There are a substantial number of elderly people (around 1.6 million) with relatively mild impairments who, as discussed above, do not require the active help of other people on a daily basis. They can generally manage their daily activities on their own (i.e. they are not disabled in any of the core ADLs) perhaps with the help of mechanical devices, although they may require the occasional assistance of other people to help with IADLs such as shopping, cleaning, doing the laundry, yardwork, preparing medications, using the telephone and so on. Many have mild impairments in mental functioning, but are not so impaired that they require continuous supervision. This group relies almost exclusively on family members and other informal caregivers for assistance.
-
At the other end of the spectrum, there is a large group of people (about 2.7 million) with multiple health problems and severe limitations in mental and/or physical functioning who require very intensive (often 24 hour) levels of care. They are generally impaired in three or more ADLs. Many are in nursing homes although almost an equal number (about 1.6 million) live in the community with the assistance of formal home care services and family-provided care. This group, in turn, is highly differentiated. Some people are severely impaired because they have recently had an acute illness (e.g. heart attack, stroke) and need intensive levels of care during their recovery period. Another group is severely impaired because they are close to death. Many people in this second group enter nursing homes for a short period of time just prior to death. A third group has chronic severe impairments over an extended period of time and require intensive levels of care for months or years. An individual in the advanced stages of Alzheimer's disease is an example of a person in this third sub-group.
-
In between these two extremes is the third group of elderly persons (about 1.6 million persons) with moderate impairments. They are functionally impaired in one or two ADLs, or have mild cognitive impairments. They generally live in the community, either in their own homes, in the homes of close relatives, or in some kind of supportive housing arrangement like a board and care home or assisted housing facility. A few live in nursing homes. These individuals are heavily dependent on informal care if family members are available to provide care, sometimes supplemented by formal services. Those who live alone are often the prime targets of public home care programs.
The Probability of Becoming Disabled
Elderly individuals become disabled for a variety of reasons, but the most dominant fact, as shown in Figure 2, is that the prevalence of disability increases dramatically with age.8,9 Among persons between the ages of 65 and 69, less than four percent are disabled in the community, and only about one percent are in nursing homes. Among persons age 85 and over, however, almost one quarter (24.0%) live in nursing homes and a little over one-fifth (21.0%) of those living in the community are disabled.
Figure 3 shows the actual number of elderly persons with disabilities in five-year age cohorts.10 One can see from Figure 3 that the actual number of disabled persons living in the community generally increases with age as well. For example, there were about 375,000 disabled elderly persons in the community between the ages of 65 and 69, but about 650,000 over the age of 85. The rise is even more dramatic in the nursing home population where there are about 100,000 persons between ages 65 and 69, but over 700,000 in the 85 and over age group.
Disabled elderly persons, both in the community and in nursing homes, are more likely to be female than male, as shown in Figure 4, and the majority do not have a living spouse. The majority of people in nursing homes are unmarried and female. This is largely due to the fact that females live longer than males. Because women live longer than men, they are more likely to develop chronic disabilities, and when disabled, they are more likely to be without a spouse. A major difference between the disabled elderly in the nursing homes and the disabled elderly in the community is that more than four out of five nursing home users do not have a living spouse, whereas almost half of all disabled elderly persons living in the community are still married.
Black and other non-white elderly persons have higher rates of disability than white elderly persons, as shown in Figure 5, but are more likely to live in the community than in nursing homes, compared to whites. Age-adjusted nursing home use rates are about 32 percent lower for non-whites than for whites. Both social and economic differences may account for these differences. Black elderly persons with disabilities tend to have larger informal caregiving networks, particularly outside direct family members, which may partially account for their lower use of nursing home care.11 On the other hand, the high cost of privately paid nursing home care may limit nursing home access for many near-poor elderly blacks who do not qualify for Medicaid, contributing to lower nursing home use rates.
Levels of Disability Among the Elderly Living in the Community
What types of functional limitations do the disabled elderly have? As shown in Figure 6, of the 2.1 million elderly who require human assistance with ADLs, the most prevalent type of disability is the need for assistance with bathing. About 1.6 million elderly in the community cannot bathe without help from other human beings. About 1.3 million require human assistance with toileting, 1.1 million with dressing, 1.0 million with transferring, and 0.5 million with eating.
Figure 6 also shows that the need for active or stand-by help varies depending upon which type of ADL is being performed. In general, people who are dependent in ADLs are more likely to require the active assistance of another person to perform the task; the only exception is in eating where slightly more than half of those disabled in this ADL require stand-by assistance. While the vast majority need active assistance in bathing and dressing, about two-fifths of those who need help in toileting and transferring require stand-by assistance.
Of course, many elderly persons are impaired in multiple ADLs, and in this regard, there is a definite hierarchy among the five ADLs. People who are dependent in eating have a high probability of also being dependent in dressing, toileting, transferring and bathing. However, people who are dependent in bathing have a much higher probability of being dependent in only one ADL. Among the 2.1 million elderly with ADL disabilities, about a third (34.7%) are disabled in only one ADL, but close to half are disabled in three or more ADLs (46.6%); and about two-thirds (65.3%) are disabled in two or more ADLs.
Assistive devices play a very important role in helping elderly individuals perform daily activities. As previously discussed, estimates of elderly persons with disabilities increase substantially if persons who rely on assistive devices only, but not human assistance, are included. As shown in Figure 7, assistive devices, such as grab bars, tub/shower stools, raised toilet seats, canes and walkers, are most frequently used to help people bathe, toilet and transfer.
While Figure 7 shows the impact that assistive devices have on estimates of elderly persons with disabilities, it also shows the potential that assistive devices can have on reducing the dependence of elderly persons with functional limitations on assistance from other people. An important policy question is the potential for further reducing the number of disabled elderly who rely on stand-by human assistance in ADLs through increased use of mechanical aids. Indeed, recent evidence indicates an increase in usage rates of assistive devices by the disabled elderly; the same research shows a concomitant decrease in the use rate of personal assistance in ADLs.12 These data underscore the point that long-term care policy must not only address the need for long-term care services, but also environmental changes and new technologies which could help to increase or maintain the independence of the elderly despite physical and mental limitations.
Elderly Persons with Alzheimer's Disease and Other Cognitive Impairments
Many elderly persons require long-term care not because they are physically impaired, but because they have impairments in mental and cognitive functioning. Most prevalent of the diseases which result in cognitive impairments is Alzheimer's disease, but there are also a variety of other conditions, including multi-infarct dementia, Pick's disease, and the dementias associated with Parkinsonism and Huntington's Chorea, to name a few, that affect cognitive abilities. They are all progressively degenerative diseases which ultimately affect not only a person's cognitive. abilities but physical capacities as well.
In the earlier stages of Alzheimer's disease, an individual may be forgetful, have poor judgment, have difficulty making calculations or handling money. Confusion, disorientation and difficulty communicating often ensue. As the disease progresses, usually over a six- to eight-year period, but up to as long as 20 years, Alzheimer's victims loose their ability to perform routine household and personal hygiene activities. Eventually they may loose control of bodily functions, become incontinent, and need to be fed. It is also not uncommon for persons with Alzheimer's to experience personality changes, become suspicious and paranoid and/or socially withdrawn, wander about aimlessly, or become quarrelsome and aggressive, have delusions and/or hallucinations and experience sleep disturbances.
It is estimated that between four and seven percent of the elderly suffer from severe dementia related to Alzheimer's disease and other dementias. Prevalence rates increase dramatically with age. Only about one percent of individuals between 65 and 74 have severe cognitive impairments, but it is estimated that persons surviving to age 80 have approximately a 30 percent risk of developing severe dementia prior to death.13,14
Given projections of substantial growth in the number of elderly persons surviving to age 80 and beyond in the decades ahead, one expected outcome is dramatic increases in the number of elderly individuals suffering from dementia. As shown in Figure 8, nearly 2.5 million cases of severe dementia among the elderly are forecast for the year 2000, and close to 5.5 million by 2040.15
Approximately two out of three persons suffering from Alzheimer's or other dementias reside in the community, thus placing substantial burdens on families and friends who assume caregiving responsibilities. It is also estimated that at least half of all elderly persons residing in nursing homes suffer from mental disorders of some type.16 These residents tend to be more disabled than their cognitively intact counterparts, to remain institutionalized longer, and to present more behavior problems to staff. In sum, insuring the health and safety of this population is a labor-intensive and costly endeavor, and one that is likely to become more costly as the nation's elderly population grows and ages.
USERS OF INFORMAL CARE
Most long-term care provided in the United States is provided by Informal caregivers: wives taking care of husbands; daughters taking care of their mothers; a neighbor mowing the lawn and buying groceries for someone who can no longer do it herself; a community group calling someone who lives alone to see if they're doing okay, or providing a ride for someone who can no longer drive himself. Informal caregivers form the bedrock of our country's long-term care system.
Although economists put dollar values on public and private expenditures for long-term care, these measured costs represent only a portion of the true cost to society of providing long-term care. The costs of providing informal care are generally not included in these measures. A large proportion of the true cost of providing long-term care is simply the time, stress and effort exerted by spouses, daughters, sons, siblings, neighbors, friends, and other unpaid caregivers who help disabled elderly persons with daily activities. The formulation of public long-term care policy must recognize the central role of these informal caregivers in the nation's long-term care system, and include strategies for ensuring that formal and informal long-term care services work in collaboration to achieve mutual objectives.17
Who Uses Informal Care?
Of the ADL disabled elderly who live in the community, a little less than two in three (64%) receive help only from informal caregivers. Another 31 percent receive help from both informal caregivers and paid caregivers, while just about five percent are cared for only by paid providers.18 When the elderly need help with activities of daily living, they overwhelmingly rely on family and friends to provide help.
Most disabled elderly persons receive help from a primary caregiver who lives with them. If married, the spouse is usually the primary caregiver; if not, it is usually an adult child, generally a daughter. As shown in Figure 9, almost half of the disabled elderly living in the community still live with their spouses (46.3%), a little less than a third live with children (29.8%), other relatives, or in some other group living arrangement (29.8%), and about 24 percent live alone.19
Informal care is the predominant source of care for those elderly with milder impairments. Compared to those elderly who receive formal home care services or nursing home care, those who receive care only from informal caregivers tend to be younger, male, nonwhite, married, lower income and less disabled. This does not mean that informal caregivers do not also care for persons with severe impairments, only that persons with less severe impairments are more likely to rely solely on care provided by family members and other informal caregivers.20
The Providers of Informal Care
In 1989, there were approximately 3.2 million primary caregivers providing ADL and/or IADL assistance to disabled elders In the community.21 Of these, about 1.4 million were spouses and about 1.1 million were children. Daughters are far more likely to be primary caregivers than sons. Overall, about 73 percent of primary informal caregivers are female.22
Many Informal caregivers are themselves elderly. In fact, the probability of becoming an informal caregiver increases with age until one reaches age 75.23 Over one third of all informal caregivers, approximately 1.5 million persons, are over the age of 65. Thus, not only does the burden of needing long-term care fall upon many elderly persons, the burden of providing informal care falls on many elderly individuals as well.24
Nearly three-quarters of the elderly who receive some assistance and who are disabled in IADLs only rely almost exclusively on informal caregivers as sources of help, but informal caregivers are also the main source of assistance for the elderly with more severe disability.25 For example, in 1989, about 1.7 million primary caregivers provided assistance to the more severely disabled elderly--persons with ADL impairments. About 45 percent were spouses, 36 percent were children, while the remaining 19% percent were other relatives or nonrelatives. The average age of spouse caregivers was about 70 years, while the average age of child caregivers was about 53 years. Slightly more than three out of four informal caregivers (78.1 %) lived with the person they were caring for, and the majority lived in lower to middle-income households (62.1%).26
The Costs of Informal Caregiving
The economic value of informally-provided care is enormous. Informal caregivers report that they spend an average of four extra hours per day performing caregiving tasks.27 Thus, over 3 billion hours of informal caregiving are provided to disabled elderly persons with ADL limitations each year.28 This fact causes concern among those who feel that the enactment of a home care entitlement program may replace informal care with publicly-financed care.
However, a common misperception is that informal care is free care. It may be free to the public treasury, but it is not free to those who provide care. To the contrary, informal caregivers are well aware of the costs associated with taking care of a disabled loved one.
Most informal caregivers take care of disabled loved ones willingly and gladly, but the stresses of caregiving are often formidable. Surveys indicate that caregivers feel particularly stressed by: (1) having to provide care when they are sick; (2) having to provide constant attention to the care-recipient; (3) experiencing financial burdens beyond what they can afford; and (4) feeling that informal caregiving has worsened their own health.29 These stresses are most strongly associated with the level of disability of the care-recipient. As the needs of the care-recipient increase, so does the stress of providing care.
Caregiving can also place stress on the nature of the relationship between caregiver and care-recipient. These relationships seem to become particularly strained when the care-recipient is cognitively impaired and cannot provide the kinds of emotional rewards that are often the prime motivators for care providers.30
For the growing number of women in the labor force, the competing demands of work and informal caregiving can be particularly difficult to juggle. About 31 percent of all primary caregivers are employed. Of those who work, many report that they cut back on their total work hours (81%), or rearranged their work schedules (42%), in order to meet their informal caregiving responsibilities.31
Since most informal care is provided by women, the contention is often made that their increased labor force participation will lead to dramatic reductions in the supply of women available to provide informal care, and a concomitant increase in the demand for formal services. Data from the 1989 National Long-Term Survey and 1989 Survey of Informal Caregivers show that care recipients of working caregivers, most of whom are women, receive 7.6 fewer hours of care per week from their primary caregivers than do care recipients of non-working primary caregivers. However, care recipients of working caregivers do not receive fewer hours of care overall, since working caregivers supplement their care with care from other sources--both informal and formal. There is no evidence to date that working women are more likely to terminate informal care or seek institutional placement for disabled elders than non-working caregivers. However, given that younger cohorts of women may join the labor force with greater commitment to careers that require full-time employment, the contention that their increased labor force participation might dramatically increase the demand for formal long-term care services is plausible. Future generations of women may be less willing to sacrifice careers by reducing their working hours to part time in order to accommodate caregiving for the elderly. If such scenarios come to pass, there may be more demand for formal long-term care services.
Other women are faced with the competing demands of caring for disabled elders and their own children at the same time.32 About one fourth of all primary caregivers have children under the age of 18 still living with them; but only five percent of all primary caregivers providing ADL assistance are also caring for children in the home.33
Policymakers have long recognized the need to support informal caregivers, and therefore researchers have tried to identify the types of caregivers who experience the most severe distress from the demands of providing care. To date, research suggests that it is usually not the competing demands of child rearing or employment which constitute the major stressors on informal caregivers. Rather, it is the demands of informal caregiving itself which usually place the greatest burden on caregivers, and these demands are closely related to the disability level of the care-receiver. Thus, public programs which target services to more severely impaired individuals are probably also targeting services to the most severely burdened caregivers.
Informal caregiving research has also demonstrated the remarkable stability of informal caregiving over time. The termination of informal caregiving is a rare event, and only occurs when caregiving demands reach exceedingly high levels. While the informal caregiving system is not crumbling, there are some trends to be noted that indicate a possible reduction, albeit small, in informal caregiving. Comparing the elderly with any ADL or IADL disability in 1982 to those in 1989, there was a modest decrease in the proportion receiving informal rare only (from 74% to 67%). At the same time there was also a moderate increase in the proportion using formal services only (from 5% to 9%). However, despite these trends that do indicate somewhat less commitment to informal caregiving, over 90% of the disabled elderly in 1989 were still receiving some care from informal sources.34,35 This fact alone demonstrates a very high level of commitment to informal caregiving on the part of children, other relatives and friends of the disabled elderly.
WHO USES PAID HOME CARE?
National survey data indicate that about 20-25 percent of elderly persons in the community with IADL or ADL disabilities, about 1.6 million elderly, receive formal home care services, either alone or in combination with informal services.36 An additional 15-20 percent of the disabled elderly receive other types of community-based services, such as attending senior centers, receiving home-delivered meals, transportation assistance, or telephone checks.37
Formal home care services encompass a broad range of skilled and non-skilled services. Medicare-certified home health agencies (HHAs) provide the most skilled home care services, but these services are generally limited to elderly persons who have time-limited needs for intensive care related to an acute illness episode.
In addition to home health agencies, there are a wide variety of commuritty-based agencies, mostly non-profit, which provide a range of supportive services to elderly persons with functional disabilities living in the community. Services provided by these agencies may Include housekeeping and chore services, personal care services, senior centers, in-home meals, congregate meals, adult day care, specialized transportation, telephone assistance and a wide variety of other supportive services. Most of these non-profit agencies rely on a mix of public and private financing sources for their operation. Indeed, it is difficult to characterize the formal home care system (other than HHAs) since a major characteristic of the system is its diversity, and its variability from state to state.
Who uses formal home care? Age and disability level are strong correlates of formal home care use. For example, only about 26 percent of persons with IADL impairments use formal home care services, compared to about 40 percent of persons disabled in three or more ADLs. Also, disabled elderly persons living alone are about 40 percent more likely to use formal home care services as persons who live with others. Thus, the availability of informal caregivers dramatically reduces formal home care use.38,39
There is also a relationship between income and use of formal home care. Both the very poor elderly who are eligible for Medicaid and upper-income elderly use formal home care services at higher rates than the elderly who are near-poor or middle class.40,41 Although being eligible for Medicaid does not guarantee someone access to home care services, since Medicaid coverage varies from state to state, it does appear to increase utilization of formal services. Thus, affordability appears to be a major barrier to the use of formal home care services.
These findings have two important implications. First, they suggest that if the price of home care services is lowered through public or private insurance, the use of formal services would increase. More persons would use formal home care if they could afford it or if they were covered through insurance. Second, these findings also suggest that many poor and near-poor elderly are receiving fewer services than they may need--they are getting by on what their informal caregivers can provide them, but this may be less than adequate care. More research needs to be conducted on the unmet needs of disabled elderly persons living in the community--a concept that is admittedly difficult to define and measure.
Of the elderly who received paid home care services in 1989, about 60 percent paid for all of their care out of their own pockets.42 The remaining 40 percent had at least some of their formal home care paid by public programs--Medicare, Medicaid, or other sources. Thus, it appears that out-of-pocket spending for home care services is more discretionary than spending for nursing home care--the elderly often elect to go without services rather than reduce spending on other household expenditures. More research is needed on the factors which determine whether, and how much, disabled elderly persons are willing to spend for formal home care services.
Does Formal Home Care Substitute For Nursing Home Care?
One question that has confronted long-term care researchers and policymakers over the years is the extent to which nursing home care and home care are substitutable services. Policymakers have been particularly interested in whether expansions in public coverage for home care services could achieve reductions in the use of nursing home care.
Unfortunately, there is little evidence to date to support the hypothesis that expanded public support of home care can be equally offset by reduced public expenditures for nursing home care. Numerous demonstrations, including the National Long-Term Care Channeling Demonstration, have shown similar results: that expanded public coverage of home care services within a target population leads to only very small reductions in nursing home use.43,44
These demonstration results do not mean that it is not possible to design cost-effective substitutes for nursing home care--only that the demonstration approaches which have been tried to date have not proven to be cost-effective. Many States continue to develop substitutes for nursing homes, such as adult foster care programs and other residential program options which can provide 24-hour care. States are developing these alternative financing and service approaches not only to find cost-effective substitutes for nursing home care, but also to simply expand the range of long-term care options from which the disabled elderly can choose. More intensive home care programs, which include overnight respite for periods when informal caregivers are in crisis, are another alternative program approach that could potentially reduce nursing home use.
The potential for developing substitutes for nursing home care also depends on the supply of nursing home beds. The possibility of achieving reductions in nursing home use is obviously greater where the supply of beds and utilization rates are higher to begin with. States continue to experiment with developing a range of long-term care settings and benefit packages to meet the diversity of needs (and preferences) of the disabled elderly.
Does Paid Care Substitute for Informal Care?
Another issue of interest to policymakers and researchers is whether expanded public coverage of home care services reduces the amount of care provided by informal caregivers. In other words, do the efforts of family caregivers decline when the availability of formal home care services increase? Research generally shows that the answer is no.45,46,47 Just as formal home care services do not appear to substitute for nursing home care, neither do they appear to substitute for the care provided by family members and other informal caregivers.
Although common sense tells us that if public home care services were expanded exponentially, informal caregiving would inevitably decline, research conducted to date shows that formal home care--as provided under existing programs and policies--leads to only marginal reductions in informal caregiving. Instead, families generally seek formal home care only when there is a significant increase in care needs--often related to a dramatic change in the health status of the care recipient. Although the introduction of formal help may redistribute the tasks of informal caregivers, their level of caregiving remains relatively constant. Formal services fill the gap caused by the increasing disability of the elder family member.
In sum, research does not support the notion that family members seek formal home care services because they are unwilling to provide care themselves. Rather, formal home care services are generally used to fill unmet needs that arise when an elderly family member becomes increasingly impaired and dependent on others for help.
USERS OF NURSING HOME CARE
The Probability of Having to Enter a Nursing Home
In planning for their future long-term care needs, many elderly want to know: What is the likelihood that I will have to go to a nursing home, and if I have to go to a nursing home, how long am I likely to be there?
Although only about five percent of the elderly were in a nursing home in 1990, this statistic should not be misinterpreted as meaning that the chances of an elderly person ever entering a nursing home are low. The percentage of elderly individuals in nursing homes at a given point in time is very different from the probability that an individual will ever require nursing home care over his or her lifetime.
In fact, recent research now indicates that the probability of an individual entering a nursing home during his or her lifetime is remarkably high. If age-adjusted nursing home use rates remain relatively constant in the future, it is estimated that between 40 to 45 percent of all persons turning age 65 in 1990 can expect to be in a nursing home at least once during their remaining lifetime.48
The risk of entering a nursing home is not the same for all people. Women have a greater likelihood of being nursing home users than men. It is currently estimated that over half of all women turning age 65 in 1990 will use nursing home care prior to death, compared to less than one third of all men.49
Age is another risk factor. The longer a person lives, the greater the chance that he or she will be a nursing home user. Living alone is another risk factor. If someone lives alone, and has no primary caregiver when they become disabled, their chances of going to a nursing home upon becoming disabled increase dramatically.50 These risk factors are also inter-related; women have a higher probability of being nursing home users largely because they live longer than men, and are more likely to live alone during their last years of life.
Of course, one's level of disability also increases the risk of entering a nursing home.51 The more disabled one becomes, and the more assistance one needs to perform activities of daily living, the more likely that 24-hour care is needed. Certain types of disabilities, or medical conditions, have also been associated with increased risk of nursing home admission. For example, people who are cognitively impaired, such as persons with Alzheimer's disease, have a greater likelihood of entering a nursing home, due to the fact that persons with severe cognitive impairments usually require constant supervision and are more difficult to care for outside of a 24-hour supervised setting.
The availability of informal caregivers (family and friends) reduces the risk of nursing home use, since informal caregivers provide much of the same kind of care that is provided in nursing homes. The availability of a healthy spouse especially reduces one's risk of entering a nursing home, since spouses are the most committed caregivers.
Other factors have also been associated with increased or decreased risk of using nursing home care. For example, some studies suggest that upper income elderly have lower rates of nursing home use services that substitute for nursing home care.52 Prior because they can better afford to purchase in-home nursing home use, and high levels of formal home care use--independent of other risk factors--have also been shown to increase the likelihood of future nursing home use. Also, a number of studies have examined more closely the role of informal caregivers in reducing the probability of nursing home entry--showing, for example, that the attitudes which families have about nursing homes strongly influence their willingness or resistance to institutionalizing an elderly family member.53
Finally, the probability of using nursing home care has also been shown to be related to where one lives. In general, nursing home utilization rates are higher in most northern States than in southern States, suggesting that hard and cold winters may play a role in the decision to seek nursing home care.54 Independent of climate, variation in the supply of nursing home beds across States and in State Medicaid policies also influence nursing home use rates. In other words, supply factors, as well as demand factors, influence the probability of nursing home use.
Characteristics of Nursing Home Users
In 1990, about 1.6 million persons age 65 and over were in nursing homes. Although the nursing home population is by no means homogeneous, the typical nursing home resident is an unmarried white female age 80 or older. Seventy-five percent of nursing home residents are female, and less than 15 percent have a living spouse.
Most users of nursing home care have multiple and severe impairments. According to the National Nursing Home Survey (NNHS), the average elderly nursing home resident in 1985 was dependent in 3.9 out of six ADLs measured in the survey (bathing, dressing, eating, transferring, using toilet room, and continence).55 Over nine of ten were dependent in bathing, almost four out of five required assistance just to get dressed, and almost three out of four could not walk without assistance, were chairbound, or bedfast. Over sixty percent required help using the toilet, and over fifty percent had difficulty controlling their bowels and/or bladders. Over sixty percent also required help getting in and out of a bed or chair and about forty percent could not eat a meal without some human assistance. More recent analyses of the 1987 National Medical Expenditure Survey (NMES) found similar levels of impairment among elderly nursing home users.56
Nursing home residents have a wide variety of acute and chronic health conditions, but the two most common diagnoses among residents are: (1) diseases of the circulatory system (heart disease and stroke); and (2) mental disorders. These two diagnoses were the primary diagnoses in over half of all nursing home residents in 1985.
Many nursing home residents have cognitive impairments. According to the 1987 National Medical Expenditures Survey, nearly 60 percent of all nursing home residents aged 65 and older have a cognitive or psychiatric problem.57 Of these, approximately 45 percent are classified as having dementia (either dementia alone or in conjunction with another mental disorder).58
One of the common difficulties involved in caring for persons with cognitive impairments is their tendency to exhibit behavior problems. Such problems may include an inability to avoid danger, wandering, yelling or noisiness that is disruptive to staff and other residents, physical abuse to self or others, dressing inappropriately, crying for long periods, stealing, hoarding, and inappropriate sexual behavior. Although cognitively intact residents may also exhibit these behaviors at one time or another, those who are cognitively impaired are much more likely to engage in these activities. The most recent estimates from the Institutional Component of the National Medical Expenditure Survey (NMES) indicate that a full 48 percent of residents evidence behavior problems at one time or another.59
How Long People Stay in Nursing Homes
The elderly not only want to know what the chances are of entering a nursing home at some point during their lifetime, but also how long they are likely to be there. The recent availability of new data sets have yielded improved estimates of lifetime use of nursing home care, although further work is still needed in this area. One important factor that affects these estimates is that about half of all people who use nursing home care have more than one nursing home stay during their lifetimes. Thus, estimates of how long an individual is likely to be in a nursing home for a single stay differ considerably from estimates of how long a nursing home user is likely to be In a nursing home over his or her entire lifetime.
This difference is evident from data presented in Table 1, which compares data on nursing home length-of-stay distributions obtained from three different data sources. The first column presents length-of-stay distributions over a single nursing home stay obtained from the 1985 National Nursing Home Survey Discharge Sample.60 These data show that most people admitted to nursing homes stay only a short while. Over 50 percent stay for less than three months, and 66 percent stay for less than six months. Only about 26 percent of all admissions stay for one year or more. Thus, many people use nursing homes for only short time periods, either to receive skilled care during recovery for an acute illness, or terminal care just prior to death.
However, the data in the first column do not account for the fact that many nursing home users are discharged and readmitted to a nursing home later on. The second through fourth columns in Table 1 present estimates of length-of-stay distributions for lifetime use of nursing home care, adjusting for multiple stays.61 These data show that when adjustments are made for multiple stays, expected lifetime use of nursing home care increases substantially. In particular, the proportion of all nursing home users with aggregate lengths of stay of three years or more increases dramatically. However, even after adjusting from multiple stays, about half of all persons who use nursing home care use less than one year of care.
| TABLE 1. Length of Stay Distributions for Nursing Home Patients: Single Stays Versus Lifetime Use | ||||
| Length of Stay | Singl Stays NNHS1 | All Stays NNHS1,2 | All Stays Connecticut1 | Lifetime Use Mortality Survey3 |
| 3 months | 51.7% | 42.6% | 34.3% | 30.3% |
| 3-6 months | 11.1% | 10.8% | 9.4% | 21.4% |
| 6-12 months | 11.0% | 11.7% | 8.8% | |
| 1-3 years | 15.1% | 17.8% | 17.6% | 31.4% |
| 3-5 years | 5.3% | 8.2% | 10.9% | |
| 5 + years | 5.8% | 8.9% | 19.0% | 16.8% |
| 100.0% | 100.0% | 100.0% | 100.0% | |
| ||||
People who use nursing home care for short periods of time are different from those who stay in nursing homes for extended periods. Short-stayers tend to be people who are discharged from hospitals, require skilled care, and either die quickly or recuperate and are discharged. Long-stayers are more likely to enter nursing homes directly from the community, have fewer medical complications, live alone prior to entering a nursing home, and are more likely to have cognitive impairments.62,63 Persons with cognitive impairments who are otherwise in relatively good physical health are often those who stay in nursing homes for three years or more.
Persons with Long Nursing Home Stays Account for Most Nursing Home Days Used
Persons with long nursing home stays account for the vast majority of all nursing home care used. Although people who stay in a nursing home for less than six months comprise about 40-50 of all admissions, these individuals account for less than 5 percent of all nursing home days used. In contrast, people who stay three years or more years or more account for less than 20 percent of all admissions, as shown in Figure 10, but about 70 percent of all nursing home consumption.64 Thus, the vast majority of public and private expenditures for nursing home care are for people who use nursing home care for extended periods of time.
Nursing Home Use Rates May be Declining
There is some evidence that nursing home utilization rates may be declining. Table 2 presents data on changes in nursing home utilization rates by age, sex and race between 1977 and 1985, based on data from the National Nursing Home Surveys. Overall, the number of nursing home residents per 1,000 elderly declined by almost 2 percent. This decline in use rates occurred even though the number of very old elderly increased substantially over this time period. Thus, more significant declines in use rates occurred within specific age cohorts, particularly among males age 65-74 and females age 65-84. Utilization rates among non-white males, on the other hand, increased by almost 20 percent.
It is not known whether this decline represents a trend that will continue into the future. It is also difficult to ascertain to what degree this decline in nursing home utilization may be due to demand factors (fewer people seeking nursing home care) or supply factors (fewer beds available to those seeking care), or both. Reduced demand for nursing home care may be attributable to such factors as: (1) declining rates of disability among the elderly; (2) increased resistance among the elderly to enter nursing homes; and/or (3) increased use of alternative service arrangements, such as assisted housing, adult day care, or in-home care. On the other hand, declining nursing home utilization rates could also be attributable to reductions in nursing home bed supply, related to State regulatory controls on the development of new nursing home beds and/or inadequate Medicaid reimbursement.
| TABLE 2. Change in Age-Adjusted Nursing Home Utilization Rates Per 1,000 Elderly: 1977 to 1985 | |||
| Nursing Home Users | Residents Per 1,000 Elderly | ||
| 1977 | 1985 | % Change | |
| All Users Over Age 65 | 47.1 | 46.2 | -1.9% |
| Males: | |||
| 65 years and Over | 30.3 | 29.0 | -4.3% |
| 65-74 | 12.6 | 10.8 | -14.3% |
| 75-84 | 44.9 | 43.0 | -4.2% |
| 85 years and Over | 146.3 | 145.7 | -0.4% |
| Females: | |||
| 65 Years and Over | 58.6 | 57.9 | -1.2% |
| 65-74 | 15.8 | 13.8 | -12.7% |
| 75-84 | 75.4 | 66.4 | -11.9% |
| 85 Years and Over | 262.4 | 250.1 | -4.7% |
| White: | |||
| Males 65 and Over | 31.1 | 29.2 | -6.1% |
| Females 65 and Over | 60.9 | 60.2 | -1.1% |
| Non-White: | |||
| Males 65 and Over | 22.9 | 27.4 | +19.6% |
| Females 65 and Over | 35.2 | 36.2 | +2.8% |
| Source: National Center for Health Statistics | |||
PAGE 36 IS MISSING...LOOK AT ORIGINAL
runaways, homeless families, and so on. Most of these homes are operated by private non-profit agencies which receive vendor payments from State and/or local governments for the cost of services, in addition to rental income obtained directly from residents. Other board and care homes, particularly those housing elderly residents, receive no public support and operate strictly on a private pay basis. Since these board and care homes are typically used as housing options by elderly persons who are poor or near-poor, the level of services provided in most of these homes is minimal.
Responsibility for the regulation of board and homes falls primarily to State governments. However, both the level of regulatory scrutiny and the range of facilities which are subject to regulation and licensure, varies widely from State to State. Given rapid growth in the board and care industry, and numerous reports of abuse and neglect in these facilities, there is growing demand to improve regulatory structures for licensing and monitoring board-and-care homes by public agencies.66 It is clear that the role of the board and care home industry as a component of the country's long-term care system will attract increasing attention in the next decade.
Continuing Care Retirement Communities
Continuing Care Retirement Communities (CCRCs), also known are Life Care Communities, are organizations that offer a range of housing, residential and health care services for elderly residents as their needs change over time. Based on the concept of self-insurance, every CCRC involves a contract between residents and the CCRC, that, at a minimum, guarantees shelter and access to various health care services for the balance of a resident's lifetime. In return, the resident pays a lump-sum entrance fee and monthly payments thereafter.
There were an estimated 700 CCRCs in operation in 1988, 99 percent of which are operated by non-profit agencies. To date, CCRCs have primarily been marketed to elderly persons with higher-than-average income and net worth.
Subsidized Housing Programs with Congregate Services
The Department of Housing and Urban Development supports a broad array of subsidized housing programs for elderly persons of low and moderate income. For example, the Section 202 Housing Program for the Elderly and Handicapped provides below-market interest loans to private non-profit sponsoring organizations for the development of subsidized housing projects for the elderly. Financially-qualified elderly tenants receive Section 8 rental assistance, and pay no more than 30 percent of their adjusted monthly income for rent.
A national survey of Section 202 projects conducted in 1988 estimated that approximately 120,000 low-income elderly persons were living in approximately 3,200 projects across the country.67 The average age of a Section 202 resident was 73.6 years in 1988, and had been steadily increasing over time. Four out of five residents were women.
Many 202 projects provide service amenities to their elderly tenants, over and above housing. The 1988 survey found that 27.3 percent of Section 202 projects provided either some kind of meal or housekeeping service, and 6.5 percent provided full congregate services, meaning assisted independent living with the availability of at least five hot meals per week and on-site housekeeping services. About 3 percent of facilities provided three meals per day. The primary funding source for support services were private payments from the residents themselves. Government programs were not generally used as sources of service funding.
Adult Foster Care
Adult foster care residences are similar to board and care homes in that they provide room and board to a small number of elderly residents (generally no more than five or six) plus personal care services, for a monthly rate. Typically, care is provided by the owner of the home, who also lives in the residence.
However, adult foster care programs are distinguished from typical board and care homes in that they are generally developed as a result of conscious policies by State governments to support alternatives to nursing homes. Therefore, they are likely to receive direct vendor payments from States, are more highly regulated and monitored by State agencies, and have less control over admission and discharge practices than board and care home operators.
For example, the State of Oregon made a major effort during the 1980s to develop adult foster care homes as alternatives to nursing homes for its for disabled senior citizens, and by the 1989, had spurred the development of 1,450 licensed homes, ranging in size from 1 to 5 residents, serving a total of almost 5,000 clients.68 Almost half of adult foster care home managers In Oregon are people who were certified nurses aids, home health aids, licensed practical nurses, or registered nurses.
The Role of Supportive Housing In the Long-Term Care System
In summary, a broader range of residential alternatives are being developed, combining housing and services for disabled elderly persons who need some assistance with daily activities but who do not require, or desire, the level of care and supervision provided by licensed nursing homes. The concept of a long-term care continuum, which allow consumers of long-term care services greater choice over where and how they live is becoming more of a reality.
Despite increasing frailty, and inevitable dependence on others for help with activities of everyday life, most elderly persons want to stay as independent as they can. Of extreme importance is the degree of control which they are able to retain over their everyday lives--to eat (or not eat) when they want and what they want, to go to bed (and get up) when they want to, to live by their own rules rather than the rules of an institution.
In the future, we are likely to witness growing diversity in the types of residential and service options available to the disabled elderly which allow them to choose a living arrangement and service package that is tailored to their own specific needs. The challenge to policy is to ensure that public and private financing mechanisms respond to this growing diversity and flexibility, so that financing mechanisms do not become a barrier to enhanced consumer choice and preference.
This is not as easy as it sounds, because public and private insurance programs must also ensure that whatever services are purchased through insurance, that adequate standards of quality are obtained. Quality is often achieved in public and private insurance programs by only providing benefits in strictly-defined settings (e.g. hospitals, nursing homes). A long-term care financing system in which consumers exercise greater control over where benefits are provided, and what the benefits themselves should be, yet which maintains adequate mechanisms monitoring and ensuring the quality of care provided, Is not an easy task.
THE INTERSECTION OF THE ACUTE CARE AND LONG-TERM CARE SYSTEM
This paper has described the characteristics of the elderly long-term care population and the services they use, but it is difficult to discuss the long-term care population and service system in isolation of the acute care system. There are many intersections between acute care and long-term care which affect who needs long-term care, how they get into the system, and how their care is paid for.
First, acute care and long-term care are clinically related. Many elderly persons with long-term care needs also have acute care needs. While they are receiving care for chronic disabilities, many are also receiving care for acute conditions. Second, many elderly persons require long-term care as a direct consequence of an acute illness episode, such as a heart attack or stroke. Indeed, the demand for long-term care has increased as a direct result of the success of new medical technologies, and better medical interventions of acute conditions. More people are surviving heart attacks and strokes and other acute medical events, but need long-term care services as a consequence of their recovery. Many long-term care patients fall into the category of requiring postacute or subacute care.
Many elderly people experience numerous transitions between the acute care system and the long-term care system. For example, data from the 1985 National Nursing Home Survey indicate that 55 percent of all nursing home patients are admitted directly from a hospital, and 35 percent of all nursing home patients are discharged to a hospital. Research has shown that a substantial number of nursing home patients discharged to hospitals experience multiple hospital admissions, and, in turn, multiple nursing home admissions.
Changes in the acute care system also have secondary impacts on the long-term care system. The most obvious example is the implementation of Medicare's hospital prospective payment system (PPS) in 1983. PPS has reduced the average hospital length-of-stay and increased the proportion of Medicare patients discharged to post-acute care. PPS also appears to have affected the type of patients being admitted to nursing homes and Medicare home health care. The number of nursing home patients with medical needs, in addition to long-term care needs, has increased substantially since PPS was adopted.
In regard to the financing of care, payers, particularly Medicare, have defined boundaries between services that are related to an acute care episode (and therefore insured by Medicare) and services that are not related to acute illness (and not insured). Thus, in regard to financing policy, the intersection of the acute care system and the long-term care system is a salient policy issue that demands operational definitions of where one system ends and the other begins.
In terms of managing patient care, the intersection between the acute care system and the long-term care system is problematic. The patient's physician assumes responsibility for managing the patient's acute care needs, but, in general, physicians are far less involved In the management of the patient's long-term care needs--no doubt related to the fact that most payers do not reimburse physicians for management of chronic care. Thus, responsibility for managing a disabled elderly person's long-term care needs often becomes diffused between family members, physicians, long-term care providers, and long-term care payers, such as Medicaid. Long-term care management, and who pays for it, is a particularly salient issue in health benefit plans, such as HMOs, in which managed care is the central focus of the plan.
LESSONS FOR POLICY
Perhaps the greatest lesson for policy which emerges from an understanding of the disabled elderly is the need for flexible responses to diverse needs. The disabled elderly are a highly diverse population. The types of assistance they need, as well as the frequency and intensity of services, is myriad. The assistance needed from formal service providers such as nursing homes, home care agencies, and personal care providers, is also a function of the resources which the elderly can draw upon in their informal support systems. Finally, we are witnessing growing diversity in the types of residential arrangements available for the elderly to choose from when the decision is made that they can no longer live at home or with family.
Federal and State programs are evolving towards becoming more flexible financing mechanisms for meeting the disabled elderly's diverse needs for long-term care, increasing opportunities for consumer choice about where, when and how services will be provided. However, many believe that there is still a long way to go.
NOTES
-
Katz, S., Ford, A., Moskowitz, R., Jackson, B., and Jaffe, M. Studies in the Illness in the Aged: The Index of ADL: A Standardized Measure of Biological and Psychosocial Function. Journal of the American Medical Association Vol. 185(12):914-919, 1963.
-
Jackson, M., Burwell, B., Clark, R. and Harahan, M. Eligibility for Publicly-Financed Home Care. Report prepared under contract to the Office of the Assistant Secretary for Planning and Evaluation, Contract No. HHS-100-88-0041, SysteMetrics/McGraw-Hill, December 1990. [Executive Summary]
-
Wiener, J., Hanley, R., Clark, R. and Van Nostrand, J. Measuring the Activities of Daily Living: Comparisons Across National Surveys. Journal of Gerontology Vol. 45(6): S229-237, 1990. [Executive Summary]
-
Stone, R. and Murtaugh, C.: The Elderly Population with Chronic Functional Disability: Implications for Home Care Eligibility. The Gerontologist Vol. 30(4): 491-494, 1990.
-
These data may lead to underestimates unrelated to the definitional issues discussed above. Many of the estimates presented are based on data obtained in the 1984 and 1989 National Long-Term Care Surveys, both based on national probability samples of households. However, household surveys may underestimate the number of disabled elderly persons living in supportive housing arrangements that are not licensed as nursing homes, such as board-and-care homes, adult foster homes, and subsidized housing programs for the elderly.
-
Disability estimates are based on the 1989 National Long-Term Care Survey. Respondents who reported that they either received hands-on assistance or stand-by assistance in a given ADL are considered disabled, as are individuals who did not perform the ADL at all. Also included in the disabled group are persons who said they needed, but were currently receiving neither human assistance nor using an assistive device in a particular ADL Only persons meeting one of these criteria who also reported that the ADL disability had lasted for three months or longer are considered chronically disabled.
-
IADL disability estimates are based on the 1989 National Long-Term Care Survey. Persons who could not perform one or more of the following tasks without human assistance were considered IADL disabled: light housework, laundry, meal preparation, grocery shopping, using transportation, going outside, money management, medication management, using the telephone.
-
In this section, the definition of the disabled elderly living in the community includes persons with one or more ADL impairments (about 2.1 million persons) and persons with no ADL impairments who have cognitive impairments which require daily human assistance (about 0.3 million). Other persons with IADL impairments are not included. All persons in nursing homes are considered disabled.
-
Estimates of disabled persons with cognitive impairments are based on the 1989 National Long-Term Care Survey. Disability criteria for persons with cognitive impairments were as follows: four or more errors (out of 10) on the Short Portable Mental Status Questionnaire (or for those with missing data on the Short Portable, judged senile by a proxy respondent or have a disability caused by mental retardation or a senile psychotic condition) AND at least one of the following: (1) a disability in at least one of the five core ADLs where human assistance is needed; (2) a disability in at least one of the cognitively-oriented IADLs of money management, medication management, or using the telephone; or (3) evidence of a behavior problem.
-
Age-, sex- and race-related disability estimates for the community-dwelling elderly were generated from 1989 National Long-Term Care Survey data. The definition of disability includes persons receiving human assistance (including stand-by assistance) in performing any of the core ADLs and/or persons identified as cognitively impaired. See footnote #9 for a description of how cognitive impairment was operationalized.
-
White-Means, S. and Thornton, M. Ethnic Differences in the Production of Informal Home Health Care. The Gerontologist Vol. 30(6):758-768, December 1990.
-
Manton, KG., Corder, L., and Stallard, E. Changes in the Use of Personal Assistive and Special Equipment from 1982 to 1989: Results from the 1982 and 1989 NLTCS. The Gerontologist 33:168-176, 1993.
-
Cross, P.S. and Gurland, B.J. Public Health Perspectives on Clinical Memory Testing of Alzheimer's Disease and Related Disorders in LW. Peon, ed., Clinical Memory Assessment, American Psychological Association, Washington, D.C., 1986.
-
Sluss, T.K., Gruenberg, E.M. and M. Kramer. The Use of Longitudinal Studies in the Investigation of Risk Factors for Senile Dementia-Alzheimers Type In J.A. Mortimer and L.M. Schuman, eds., The Epidemiologv of Dementia, New York, The Oxford University Press, 1981.
-
Cross & Gurland, 1986, op. cit.
-
Lair, T. and Lefkowitz, D. Mental Health and Functional Status of Residents of Nursing and Personal Care Homes. National Medical Expenditures Survey Research Findings 7, Agency for Health Care Policy and Research, DHHS Publication No. (PHS) 90-3470, September 1990.
-
Doty, P. Family Care of the Elderly: The Role of Public Policy. Milbank Memorial Fund Quarterly 64:34-75, 1986.
-
Ibid.
-
Ibid.
-
Ibid.
-
A primary caregiver, as defined in the 1989 Survey of Informal Caregivers, a supplement to the 1989 NLTCS, referred to a person providing either ADL or IADL assistance and who provided the most hours of unpaid help to the disabled individual. There was one exception: caregivers providing ADL assistance, even though the number of hours provided were less than another unpaid caregiver giving IADL help, the person providing the ADL assistance was identified as the primary caregiver.
-
Data from the 1989 Survey of Informal Caregivers.
-
Stone, R., Cafferta G.L and Sangi, J. Caregivers of the Frail Elderly: A National Profile, The Gerontologist, 27 (5): 616-626, 1987.
-
Data from the 1989 Survey of Informal Caregivers.
-
Ibid.
-
Ibid.
-
Stone et al., 1987, op. cit.
-
This does not include the economic value of informal care provided to persons with limitations in IADLs only.
-
Kasper, J.D., Steinbach, U. and Andrews, J. Factors Associated with Ending Caregiving Among Informal Caregivers to the Functionally and Cognitively Impaired Elderly Population. Prepared by Johns Hopkins University, Department of Health Policy and Management under Grant No. 88-ASPE-209A to the Office of the Assistant Secretary for Planning and Evaluation, Department of Health and Human Services, February 1990. [Executive Summary]
-
Miller, B. and McFall, S. Caregiver Burden and Institutionalization, Hospital Use, and Stability of Care. Prepared by the University of Illinois at Chicago under grant No. 88-ASPE-207A to the Office of the Assistant Secretary for Planning and Evaluation, Department of Health and Human Services, November 1989. [Executive Summary]
-
Data from the 1989 Survey of Informal Caregivers.
-
Boyd, S.L and Treas, J. Family Care of the Frail Elderly: A New Look at Women in the Middle. Women's Studies Quarterly 17:66-74,1989; Brody, E.M. Women In the Middle and Family Help to Older People. The Gerontologist 25:19-29, 1981.
-
Data from the 1989 Survey of Informal Caregivers.
-
Data from the 1989 National Long-Term Care Survey and/or 1989 Survey of Informal Caregivers.
-
Liu, K., Manton, K. and Liu, B.: Home Care Expenses for the Disabled Elderly. Health Care Financing Review, Vol. 7:51-57, 1985.
-
Data from the 1989 National Long-Term Care Survey.
-
Short, P. and Leon, J. Use of Home and Community-Based Services by Persons Aaes 65 and Older with Functional Difficulties. National Medical Expenditure Survey Research Findings, 5, Agency for Health Care Policy and Research, Rockville, MD, DHHS Publication No. (PHS) 90-3466, September 1990.
-
Data from the 1989 National Long-Term Care Survey.
-
However, studies indicate that the number of informal caregivers does not have an additional effect. In other words, disabled persons with three or more informal caregivers are not more or less likely to use formal home care as persons with only one informal caregiver. This finding supports the observation that most informal caregiving is provided by a single primary caregiver.
-
Short and Leon, 1990, op. cit.
-
Coughlin et al.: Home Care for the Disabled Elderly: Predictors and Expected Costs. Health Services Research 27(4): 453-479, October 1992.
-
Data from the 1989 National Long-Term Care Survey.
-
Kemper, P., Applebaum, R. and Harrigan, M.: Community Care Demonstrations: What Have We Learned? Health Care Financing Review Vol. 8(4):87-101, Summer 1987.
-
Weissert, W. Seven Reasons Why It Is So Difficult To Make Community-Based Long-Term Care Cost-Effective. Health Services Research Vol. 20(4):423-433, October 1985.
-
Christianson, J. Channeling Effects on Informal Care, Mathematica Policy Research, Princeton, NJ, 1986, pp. 266-290. [Executive Summary]
-
Edelman, P. and Hughes, S. The Impact of Community Care on Provision of Informal Care to Homebound Elderly Persons. Journal of Gerontology Vol. 45(2):S74-S84, March 1990.
-
Hanley, R. and Wiener, J. Will Paid Home Care Destroy Informal Support? Conducted for the Health Care Financing Administration under Cooperative Agreement No. 17-C-99376/3-01, The Brookings Institution, June 1990.
-
Murtaugh, C., Kemper P., and Spillman, B. "The Risk of Nursing Home Use In Later Life." Medical Care Vol. 28, No. 10: 952-962, October 1990.
-
Murtaugh et al., 1990, op. cit.
-
Branch, L and Jette, A. "A Prospective Study of Long-Term Care Institutionalization Among the Aged." Am J. Public Health Vol. 72(12):1373-1379, December 1982.
-
Liu, K., Coughlin, T. and McBride, T. "Nursing Home Utilization: Risks and Lengths of Stay." Prepared for the Health Care Financing Administration under Cooperative Agreement 99-C-98526, Urban Institute Working Paper 3876-02, December 1989.
-
Liu, K., De Vita, C., Manton, K. and Coughlin, T. Risks of Entering Nursing Homes for Long and Short Stays. Urban Institute Working Paper M-289, 1990. [Executive Summary]
-
Miller and McFall, op. cit.
-
Weissert, W. and Scanlon, W. Determinants of Institutionalization of the Aged. Urban Institute Working Paper No. 1466-21, 1983.
-
National Center for Health Statistics, E. Hing, E. Sekscenski, and G. Strahan. The National Nursing Home Survey; 1985 Summary for the United States. Vital and Health Statistics, Series 13, No. 97, DHHS Pub. No. (PHS) 89-1758, Washington, D.C., 1989.
-
Lair and Lefkowitz, 1990, op. cit.
-
Estimates from the 1987 National Medical Expenditures Survey of the number of institutionalized elders with behavior problems includes persons residing in personal care homes as well as those in nursing homes.
-
Lair and Lefkowitz, 1990, op. cit.
-
Ibid.
-
Liu, K. and Manton, K. Nursing Home Length of Stay and Spend-Down: Connecticut, 1977-1985, and Kemper, P. and Murtaugh, C. Long Term Care Financing Reform: Implications of New Evidence on Lifetime Nursing Home Use. Agency for Health Care Policy Research, January 1990. [Executive Summary]
-
Ibid.
-
Liu, K. et al., Risks of Entering Nursing Homes for Long and Short Stays. Medical Care Vol. 32, No. 4: 315-327, April 1994. [Executive Summary]
-
Ibid.
-
Spence, D. and Wiener, J. Nursing Home Length of Stay Patterns: Results From the 1985 National Nursing Home Survey. The Gerontologist, Vol. 30(l):16-20, 1990.
- x
-
Avorn, J., Dreyer, P., Connelly, K and Soumerai, S. Use of Psychoactive Medication and the Quality of Care in Rest Homes. New England Journal of Medicine Vol. 320(4):227-232, January 1989.
-
U.S. House of Representatives, Select Committee on Aging. The 1988 National Survey of Section 202 Housing for the Elderly and Handicapped. Committee Publication No. 101-36, U.S. Government Printing Office, Washington, D.C., December 1989.
-
Kane, R.A., Illston, L, Kane, R.L., and Nyman, J. Meshing Services with Housing: Lessons From Adult Foster Care and Assisted Living In Oregon. Prepared for the John A. Hartford Foundation by the Division of Health Services Research and Policy, University of Minnesota School of Public Health, May 1990.